Pathology and Diagnosis of Inflammatory Bowel Disease (IBD)
|
|
|
- Heather Sutton
- 5 years ago
- Views:
Transcription
1 Inflammatory Bowel Disease Pathology and Diagnosis of Inflammatory Bowel Disease (IBD) JMAJ 45(2): 45 54, 2002 Takashi SHIMOYAMA Director, Department of Gastroenterology, Hyogo College of Medicine Abstract: Intractable inflammatory bowel diseases (IBD) include ulcerative colitis ( UC hereinafter) and Crohn s disease ( CD ). The patients with IBD are on the increase each year in Japan. In 1973, the Ministry of Health & Welfare designated 2 non-specific inflammatory bowel diseases whose causes were unknown and against which no radical treatment existed as intractable diseases, and organized a group to study the causes of and treatment against these diseases. This is a study group to investigate intractable inflammatory bowel disorders, so-called diseases specified by the Ministry of Health & Welfare. So long as the number of patients remained 50,000 or less, it was decided for the government to shoulder the medical expenses of the patients who cooperated in the study. However, the number of UC patients increased from 9,193 in 1984 to about 60,000 in 1999, indicating an increase of 6 times or more within the 15 years. On the other hand, the number of CD patients increased from 2,174 in 1984 to 17,000 in the year 1999, showing an increase of 8 times or more, that is an increase by 15% each year. A significant relation between the psychological stress (worries) and the onset of UC, and that between the increased ingestion of sugar, fast food such as hamburger, etc. and CD were indicated by a study of pre-onset conditions. Furthermore, the improved health environment decreased infection with parasite, etc. and caused changes in intestinal flora. As a result, the immune response in the host has also been changed to provide a favorable environment for the onset of these diseases. Key words: IBD; UC; CD; Individual survey card of specified disease Intractable inflammatory bowel diseases include ulcerative colitis ( UC hereinafter) and Crohn s disease ( CD ). The Patients with Inflammatory Bowel Disease (IBD) Are on the Increase. Twenty-eight years ago from now, in 1973, the Ministry of Health & Welfare designated 2 This article is a revised English version of a paper originally published in the Journal of the Japan Medical Association (Vol. 124, No. 9, 2000, pages ). The Japanese text is a transcript of a lecture originally aired on October 9, 2000, by the Nihon Shortwave Broadcasting Co., Ltd., in its regular program Special Course in Medicine. JMAJ, February 2002 Vol. 45, No. 2 45
2 T. SHIMOYAMA non-specific inflammatory bowel diseases whose causes were unknown and against which no radical treatment existed as intractable diseases, and organized a group to study the causes of and treatment for these diseases. It was a study group to investigate intractable inflammatory bowel disorders, so-called diseases specified by the Ministry of Health & Welfare. So long as the number of patients remain 50,000 or less, it was decided for the government to shoulder the medical expenses of the patients who cooperate in the study. It was I 1984 when the Ministry of Health and Welfare registered the recipients of the state medical expense nationwide. However, the number of UC patients that was 9,193 in 1984 went up to about 60,000 in 1999, indicating an increase by 6 times or more within the 15 years. On the other hand, the number of CD patients increased from 2,174 in 1984 to 17,000 in the year 1999, showing an increase by 8 times or more. The extent of increase in the latter is higher than that in the former. That is, the number of CD patients is showing a 15% increase each year. As the reasons for such sharp increase will be given in detail in another report, it is simply mentioned here that a significant relation between the psychological stress (worries) and the onset of UC, and that between the increased ingestion of sugar, fast food such as hamburger, etc. and CD were indicated by a study of pre-onset conditions. Furthermore, the improved health environment decreased parasite infection cases, etc. and thereby causing changes in the intestinal flora. As a result, the immune response in the host has also been changed to provide a favorable environment for the onset of these diseases. From the next year onward, the patients with intractable diseases including UC and CD will be electronically registered in each prefecture in the forms shown in Tables 1 and 2. Definition, Concept 1. UC UC is a diffuse non-specific inflammation of large intestine that mainly invades the mucosa and submucosa, frequently forming erosion or ulcer there. According to CI-MOS of WHO (1973), Though UC frequently occurs in adults aged under 30 years old, the onset of this disease is also noted in children and those aged older than 50. The cause is unknown but the involvement of immunopathological mechanism and psychological factors is conceivable. In general, bloody stools and diarrhea occur, demonstrating various degree of systemic symptoms. When the disease invades all of large intestine for a long term, a tendency of canceration may be observed. As the complications, there are necrotic pyoderma, nodular erythema, sclerotic cholangitis, arthritis, iritis, etc. 2. CD The study group investigating the intractable inflammatory bowel disorders as the diseases specified by the Ministry of Health & Welfare, partially revised the concept established by WHO and re-defined the disease as transmular inflammatory colitis of unknown cause in young people in their teens to 20 s. The symptoms include edema and ulcer as well as granular inflammation accompanied with fibrosis that mainly occur in the ileum and large intestine. The lesion may be found in any site of digestive tract from oral cavity through stomach, duodenum, small intestine, large intestine to anus. The disease is characterized by inconsecutive longitudinal ulcer and sporadic appearance of cobble stone. The sclerosis of intestinal wall appears in asymmetrical form. Though major symptoms are abdominal pain, diarrhea and nutritive disorder, there are also fever and anemia. Systemic complications including arthritis, iritis and hepatic disorder also occur in this disease. 46 JMAJ, February 2002 Vol. 45, No. 2
3 PATHOLOGY AND DIAGNOSIS OF IBD Clinical Symptoms 1. UC The major symptom is bloody stools. It is said that UC is always accompanied with bloody stools but, in rare cases, patients are not aware of bloody stools because the quantity is negligible. However, the more extensive and the severer the lesion, the more bleeding generally occurs. Sometimes mucous and purulent fluid is excreted. Diarrhea also becomes more frequent and more watery when the lesion becomes more extensive. However, constipation occurs in the initial stage of cure in the case of proctitis whose lesion is limited. Without evacuation and gas excretion, toxic megacolon results in paralytic ileus. Abdominal pain spreads all over the abdomen in some cases but patients often complain of strong pain like the gripes in the lower left abdomen before evacuation. Fever, tachycardia, anemia and leukocytosis are the signs observed in severe cases and fulminant cases. 2. CD Unlike UC, fever accompanied with body weight decrease occurs in addition to diarrhea and abdominal pain in CD patients. The abdominal pain often extends all over the abdomen but gripping pain is caused if there is a stenosis. Due to frequent diarrhea and resultant poor digestion and absorption, malnutrition is observed in the patient. Diarrhea that occurs 6 times or more a day suggests extensive lesion in the small intestine. Fever is caused by inflammation and complicated abscess. The fever of 38 C or higher indicates severe condition. Digestive tract bleeding and hematochezia are observed less in comparison with UC. The presence of extensive lesion or deep ulcer in the large intestine results in severe bloody stools and bloody diarrhea, causing anemia. Sometimes tumor is tactile in the abdomen. Stenosis, fistula or abscess are often found there. In such case, tenderness is observed. As described hereinafter, the body weight decrease and malnutrition are used as indices of severity in CD. The digestion and absorption are disturbed by the presence of an extensive lesion in the small intestine, resulting in malnutrition. The symptoms characteristic to CD are fistula formation, and anal fistula and anal lesion. Fistula occurs between the intestines, between the intestine and bladder or vagina. Sometimes anal fistula triggers CD. The anal fistula of CD is characteristically complicated and intractable. Pathology 1. UC As the lesion generally becomes diffuse starting from the rectum, the pathology is classified by the spread of lesion. 1) Spread of lesion: Pancolitis, left sided colitis, proctitis, right sided or segmental colitis 2) Disease stage: Classified into active stage and remission stage. Remission refers to the disappearance of hemorrhagic tendency, erosion and ulcer in the mucosa, and improvement to a condition in which vessels are fluoroscopically observed at least in some mucosa. 3) Endoscopic findings of active stage: The active stage is classified into mild, moderate, and severe. Extensive ulcer formation and marked spontaneous bleeding are noted in the severe stage while the rubor and small yellow dots in the mucosa characterize the mild stage in which vessels are not detectable by fluoroscopy and the mucosa become microgranular. Other inflammatory findings indicate moderate stage. The details are described in the Draft for revision of diagnostic criteria, pp released by the study group investigating the intractable inflammatory bowel disorders, that is, the diseases specified by the Ministry of Health & Welfare. 4) Clinical course: The clinical course is classified into the initial onset type, acute fulminant type, recurrent remissive type, and chronically JMAJ, February 2002 Vol. 45, No. 2 47
4 Family history of Crohn s disease No 1 Yes 2 Internal treatment T. SHIMOYAMA Form No. 2 (12) Table 1 Individual Survey Card of Specified Disease (new/update) Name of patient Male 1 / Female 2 Date of birth / / Address Occupation at Office worker 1 Civil servant 2 Student 3 Patient No. at the institution the time of onset No occupation 4 Other 5 ( ) Diagnosis Ulcerative colitis Estimated onset time year month day Date of first examination year month day Treatment Hospitalization 1 (beginning at year month day) receiving status Regular visit to outpatient clinic 2 Irregular visit to outpatient clinic 3 No visit 4 Prior clinic None 1 Yes 2 (name of medical institution/name of attending physician/tel) Clinical course Frequency of hospitalization Pathology (for updating, indicate the current status only) Initial attack 1 Relapse, remission 2 Chronic, persistent (initial time 3, relapse 4 ) Acute, fulminant 5 Unknown 6 Total times ( times at the present institution, times at other institution) Intractable or not No 1 Yes (6 months of active stage 2 Relapse of 2 times/year 3 ) Disease stage, severity (for updating, indicate the current status only) Severity at the time of first onset (at the first examination) Mild 1 Moderate 2 Severe 3 Fulminant 4 Unknown 5 Severity at the worst time year month day Mild 1 Moderate 2 Severe 3 Fulminant 4 Unknown 5 Current severity year month day Mild 1 Moderate 2 Severe 3 Fulminant 4 Unknown 5 Remission 6 Spread of lesion Site of lesion at the time of first Rectum 1 Colon (sigmoid 2, descending 3, transverse 4, ascending 5 ) onset (at the first examination) Cecum 6 Ileum 7 Unknown 8 Site of maximum lesion Rectum 1 Colon (sigmoid 2, descending 3, transverse 4, ascending 5 ) year month day Cecum 6 Ileum 7 Unknown 8 Site of current lesion Rectum 1 Colon (sigmoid 2, descending 3, transverse 4, ascending 5 ) year month day Cecum 6 Ileum 7 Unknown 8 Intestinal complication No 1 Yes 2 ( ) Extraintestinal complication No 1 Yes 2 ( ) Family history of ulcerative colitis No 1 Yes 2 Tel: At the severest time Steroid No 1 Yes 2 IVH No 1 Yes 2 Other At present Steroid No 1 Yes 2 IVH No 1 Yes 2 Other 5-ASA No 1 Yes 2 Immunosuppressant No 1 Yes 2 Adverse reaction of drug No 1 Yes 2 (symptom or finding: ) Surgical treatment Reason for operation Bleeding 1 Megacolon 2 Cancer 3 Perforation 4 Intractable 5 Extraintestinal complication 6 ( ) Other 7 ( ) Date of operation 1. year month day 2. year month day Surgical technique Post-operative complication No 1 Yes 2 ( ) 48 JMAJ, February 2002 Vol. 45, No. 2
5 PATHOLOGY AND DIAGNOSIS OF IBD Item Table 1 Individual Survey Card of Specified Disease (new/update) (Continued) Recent findings Clinical symptoms and findings Findings obtained at the severest time Recent findings Height cm cm Body weight kg kg 1. Main symptoms year year 3. Barium enema year year months months month month (1) Frequency of time/day time/day Conduct of test No 1 Yes 2 No 1 Yes 2 evacuation (2) Description of stools Bleeding Severe 1, Severe 1, (1) Continuous lesion (2) Disappearance of houstra No 1 No 1 Yes 2 Yes 2 No 1 No 1 Yes 2 Yes 2 Moderate 2, Moderate 2, (3) Coarse surface of Mild 3, Mild 3, mucosa No 1 Yes 2 No 1 Yes 2 None 4 None 4 (4) Erosion, ulcer No 1 Yes 2 No 1 Yes 2 Description Watery 1, Watery 1, (5) Pseudopolyposis No 1 Yes 2 No 1 Yes 2 Muddy 2 Muddy 2 4. Endoscopy year year (3) Abdominal pain month month (Spontaneous pain) No 1 Yes 2 No 1 Yes 2 (Site) ( ) ( ) (4) Body temperature C C Conduct of test No 1 Yes 2 No 1 Yes 2 (5) Pulse rate /min /min (1) Vascular fluoroscopy No 1 Yes 2 No 1 Yes 2 (2) Hemarrhagic tendency No 1 Yes 2 No 1 Yes 2 2. Blood test year year (3) Microgranular mucosa No 1 Yes 2 No 1 Yes 2 months months (4) Erosion, ulder No 1 Yes 2 No 1 Yes 2 (5) Pseudopolyposis No 1 Yes 2 No 1 Yes 2 Conduct of test No 1 Yes 2 No 1 Yes 2 (6) Inconsecutive lesion No 1 Yes 2 No 1 Yes 2 (1) RBC /mm 3 /mm 3 5. Pathological findings year year (2) Hb g/dl g/dl 5. of biopsy month month (3) WBC /mm 3 /mm 3 (4) Erythrocyte sedimentation Conduct of test No 1 Yes 2 No 1 Yes 2 (1 hour) mm mm (1) Neutrophil infiltration No 1 Yes 2 No 1 Yes 2 (5) CRP mg/dl mg/dl (2) Crypt abscess No 1 Yes 2 No 1 Yes 2 (6) Total protein g/dl g/dl (3) Decreased goblet cells No 1 Yes 2 No 1 Yes 2 (7) Albumin g/dl g/dl (4) Abnormal glandular (8) 2 -globulin % % alignment No 1 Yes 2 No 1 Yes 2 (9) -globulin % % (5) Dysplasia No 1 Yes 2 No 1 Yes 2 Detection of pathogenic microorganism in stools ( year month day) No 1 Yes 2 (name of microorganism ) Other (comment of attending physician on the severity certification) Item Findings obtained at the severest time I have diagnosed the patient as in the above. Date: year month day Address of medical institution Name: Tel: Name of physician (seal) JMAJ, February 2002 Vol. 45, No. 2 49
6 T. SHIMOYAMA Form No. 2 (17) Table 2 Individual Survey Card of Specified Disease (new/update) Name of patient Male 1 / Female 2 Date of birth / / Address Occupation at Office worker 1 Civil servant 2 Student 3 Patient No. at the institution the time of onset No occupation 4 Other 5 ( ) Diagnosis Crohn s disease Estimated onset time year month day Date of first examination year month day Treatment Hospitalization 1 ( times) Regular visit to outpatient clinic 2 receiving status Irregular visit to outpatient clinic 3 No visit 4 Prior clinic None 1 Yes 2 (name of medical institution/name of attending physician/tel) Pathology (for updating, indicate the current status only) Site of lesion at the time of Esophagus 1 Stomach 2 Duodenum 3 Jejunum 4 Ileum 5 Cecum 6 first onset (first examination) Colon 7 Rectum 8 Anus 9 Other 10 ( ) Unknown 11 Site of maximum lesion Esophagus 1 Stomach 2 Duodenum 3 Jejunum 4 Ileum 5 Cecum 6 year month day Colon 7 Rectum 8 Anus 9 Other 10 ( ) Unknown 11 Site of current lesion Esophagus 1 Stomach 2 Duodenum 3 Jejunum 4 Ileum 5 Cecum 6 year month day Colon 7 Rectum 8 Anus 9 Other 10 ( ) Unknown 11 None 12 Severity at the time of first onset (at the first examination) Severity at the worst time year month day Current severity year month day IOIBD scores: points IOIBD scores: points IOIBD scores: points Refer to Note Intestinal complication No 1 Yes 2 ( ) Extraintestinal complication No 1 Yes 2 ( ) Family history of ulcerative colitis No 1 Yes 2 Family history of Crohn s disease No 1 Yes 2 Hyperalimentation method At the severest time (kcal/day) IVH 1 HPN 2 Enteral 3 HEN 4 Other 5 At present (kcal/day) IVH 1 HPN 2 Enteral 3 HEN 4 Other 5 Drug therapy At the severest time Steroid No 1 Yes 2 5-ASA preparation No 1 Yes 2 (kcal/day) Immunosuppressant No 1 Yes 2 Other No 1 Yes 2 ( ) At present Steroid No 1 Yes 2 5-ASA preparation No 1 Yes 2 Immunosuppressant No 1 Yes 2 Other No 1 Yes 2 ( ) Adverse reaction of drug No 1 Yes 2 (symptom or finding: ) Reason for operation Surgical treatment (description from the recent operation) Tel: Intestinal stenosis 1 Fistula 2 Anal lesion 3 Perforation 4 Extraintestinal complication 5 ( ) Other 6 ( ) Date of operation 1. year month day 2. year month day 3. year month day Surgical technique Post-operative complication No 1 Yes 2 ( ) 50 JMAJ, February 2002 Vol. 45, No. 2
7 PATHOLOGY AND DIAGNOSIS OF IBD Table 2 Individual Survey Card of Specified Disease (new/update) (Continued) Clinical symptoms and findings Item Findings Findings Recent Recent obtained at Item obtained at findings findings the severest time the severest time Height cm cm Body weight kg kg 1. Main symptoms year year 3. Barium enema year year month month month month (1) Abdominal pain No 1 Yes 2 No 1 Yes 2 Esophagus 1 Esophagus 1 (2) 6 times/day of No 1 Yes 2 No 1 Yes 2 Stomach 2 Stomach 2 diarrhea or mucous Small intestine 3 Small intestine 3 & bloody stools Large intestine 4 Large intestine 4 (3) Anal lesion No 1 Yes 2 No 1 Yes 2 Conduct of test No 1 Yes 2 No 1 Yes 2 (4) Fistula No 1 Yes 2 No 1 Yes 2 (1) Inconsecutive lesion No 1 Yes 2 No 1 Yes 2 (5) Other complication No 1 Yes 2 No 1 Yes 2 (2) Cobblestone (content of appearance No complication) ( ) ( ) Yes 2 No 1 Yes 2 (3) Longitudinal ulcer No 1 Yes 2 No 1 Yes 2 (6) Abdominal tumor No 1 Yes 2 No 1 Yes 2 (4) Aphtha, small ulcer No 1 Yes 2 No 1 Yes 2 (7) Decreased body (5) Stenosis, narrowing No 1 Yes 2 No 1 Yes 2 weight No 1 Yes 2 No 1 Yes 2 (6) Fissure No 1 Yes 2 No 1 Yes 2 (8) 38 C or higher fever No 1 Yes 2 No 1 Yes 2 (7) Fistula No 1 Yes 2 No 1 Yes 2 (9) Abdominal tenderness No 1 Yes 2 No 1 Yes 2 4. Endoscopy findings year year 2. Blood test month month year year months months Esophagus 1 Esophagus 1 Stomach 2 Stomach 2 Conduct of test No 1 Yes 2 No 1 Yes 2 Small intestine 3 Small intestine 3 (1) Hb g/dl g/dl Large intestine 4 Large intestine 4 (2) RBC /mm 3 /mm 3 (3) WBC /mm 3 /mm 3 Conduct of test No 1 Yes 2 No 1 Yes 2 (4) Platelet 10 4 /mm /mm 3 (1) Inconsecutive lesion No 1 Yes 2 No 1 Yes 2 (2) Cobblestone (5) Erythrocyte mm mm appearance No 1 Yes 2 No 1 Yes 2 sedimentation (3) Longitudinal ulcer No 1 Yes 2 No 1 Yes 2 (1 hour) (4) Aphtha, small ulcer No 1 Yes 2 No 1 Yes 2 (6) CRP mg/dl mg/dl (5) Stenosis, narrowing No 1 Yes 2 No 1 Yes 2 (7) Total protein g/dl g/dl (6) Fissure No 1 Yes 2 No 1 Yes 2 (8) Albumin g/dl g/dl (7) Fistula No 1 Yes 2 No 1 Yes 2 (9) Cholesterol mg/dl mg/dl 5. Istopathological year year findings month month Conduct of test No 1 Yes 2 No 1 Yes 2 Non-caseous epithelioid granuloma No 1 Yes 2 No 1 Yes 2 (detected site) ( ) ( ) Tuberculosis reaction: mm Date: year month day mm Detection of pathogenic microorganism in stools ( year month day) No 1 Yes 2 (name of microorganism ) Other (comment of attending physician on the severity certification) I have diagnosed the patient as in the above. Date: year month day Address of medical institution Name: Tel: Name of physician (seal) (Note) IOIBD score: The major symptoms from (1) to (9) and Hb of 10 g/dl are calculated by giving 1 point to each item. JMAJ, February 2002 Vol. 45, No. 2 51
8 T. SHIMOYAMA persistent type. 5) Disease type classification by macroscopic finding of lesion: The disease type is classified into pseudopolyposis type and atrophic colitis type. 6) Clinical severity: The severity is assessed by the 6 items including 1) evacuation frequency, 2) hematochezia, 3) fever, 4) tachycardia, 5) anemia, and 6) erythrocyte sedimentation rate as follows. 1) Evacuation frequency: Six times or more/a day severe, 4 times or less/a day mild 2) Hematochezia: Bloody diarrhea severe, irregular bloody stools mild 3) Fever: 37.5 C or higher severe, no fever mild 4) Tachycardia: Ninety or more beats/minute severe, no tachycardia mild 5) Anemia: Ten g/dl or less Hb severe, no anemia mild 6) Erythrocyte sedimentation rate: Thirty mmhg/h or higher severe, normal rate mild When 1) and 2) are assessed as severe, either 3 or 4 is assessed severe, and 4 of the 6 items are assessed as severe, the case is diagnosed as severe. The condition between mild and severe is moderate. 2. CD 1) Classified by the site of lesion Small intestine type: The lesion is in the small intestine. As the lesion mainly exists in the ileum, this type is also called ileitis type. Large intestine type: The lesion is limited to the large intestine. Small & large intestine type: The lesion exists both in the small and large intestine. However, the lesion is mainly observed in the small intestine during the longer clinical course. 2) Clinical severity of CD Crohn s Disease Activity Index (CDAI) is used in Europe and USA but assessment in Japan is often made according to the criteria of IOIBD (International Organization of Inflammatory Bowel Diseases) employed in Europe. The assessment is based on 10 items of 1) abdominal pain, 2) 6 times or more/day of evacuation, 3) anal lesion, 4. fistula, 5) complication, 6) abdominal tumor, 7. body weight decrease, 8) fever of 38 C or higher, 9) abdominal tenderness, and 10) 10 g/dl or less Hb. The presence of each of these items is expressed as a point and the total points are expressed as the IOIBD scores. 3) Active stage and remission stage The criteria of remission are normalized erythrocyte sedimentation rate and CRP, disappearance of inflammatory finding, decrease in the above IOIBD scores to 1 point or less, and no subjective symptom. The initial treatment of UC and CD is targeted at remission. Once remission is reached, attention is focused on the management and treatment to maintain the remission. Diagnosis Criteria and Procedure When inflammatory bowel disease (IBD) is suspected from the symptom of patient, that is, when diarrhea, abdominal pain or fever is noted, it is necessary to first of all cross out the likelihood of infectious colitis. If severe bloody stools are observed, consider UC. If fistula, anal lesion, and fistula are observed, consider CD. Then cross out the possibility of infectious colitis such as bacterial or amebic dysentery, salmonella colitis, campyrobacter colitis, and intestinal tuberculosis. As the next step, it is also necessary to cross out the possibility of radiation-caused colitis, drug-caused colitis, ischemic colitis, intestinal type Bhecet s disease, intestinal lymphoid follicle proliferation. Then, the diagnosis of UC or CD is given by the following procedure depending on which is more strongly suspected. 1. Diagnostic procedure of UC In addition to a) in the following, one of the items of b as well as c have to be satisfied for definite diagnosis of UC. 52 JMAJ, February 2002 Vol. 45, No. 2
9 PATHOLOGY AND DIAGNOSIS OF IBD Table 3 Severity Certification Criteria (draft) a) UC severity certification criteria (draft) 1. Moderate and severe cases with 6 months or more of persisting active stage 2. Cases of ileocystitis persisting for 6 months or more after radical resection of large intestine 3. Fulminant cases 4. Severe cases requiring operation (including severe cases with a likelihood of operation) b) CD severity certification criteria (draft) 1. Cases that suffer permanent small intestine function disorder due to the extensive CD lesion or extensive intestinal resection and that always require central intravenous hyperalimentation or enteral hyperalimentation of 1,200 kcal/day or more because nutritive maintenance is difficult despite the drug therapy 2. Cases that have stoma, external fistula or intractable complex hemorrhoid and that always require central intravenous hyperalimentation or enteral hyperalimentation 3. Cases that require intestinal operation due to intestinal complications (advanced stenosis, fistula/ulcer formation, perforation, mass bleeding, severe anal lesion, etc.) or extraintestinal complications (necrotic pyoderma, etc.) 4. Cases that have growth disorder accompanied with secondary minor disorder Note 1: Nutritive maintenance is difficult means the body weight decrease rate in the recent 3 months is 10% or more or serum albumin concentration of 3.2 g/dl or less despite the treatment with drugs. Note 2: The duration for certification is limited to the year of operation. a) Clinical symptoms Presence of persistent or repeated mucous bloody stools or bloody diarrhea, or history thereof. b) Test findings (1) Endoscopy 1) Diffuse invasion of mucosa, vessels in the mucosa undetectable by fluoroscopy, coarse or microgranular mucosa. Fragile mucosa that becomes easily hemorrhagic (contact bleeding) and attachment of mucous, bloody and purulent secrete. 2) Multiple erosion and ulcer or pseudopolyposis. (2) X-ray by barium enema 1) Coarse or microgranular changes in the surface of mucosa 2) Multiple erosion and ulcer 3) Pseudopolyposis In addition, disappearance of houstra (lead pipe figure) as well as narrowing and curtailment of intestinal tract are observed. c) Histological examination by biopsy Diffuse inflammatory cell infiltration is noted in the whole mucosal layer in the active stage. Also observed are crypt abscess and advanced goblet cell depletion. Abnormal alignment (undulation, bifurcation) and atrophy of glandular tube remain in the remission stage. These changes are generally observed continuously from the rectum to oral side. 2. Diagnostic procedure of CD Please refer to the report made in 1997 by the study group investigating the intractable inflammatory bowel disorders, the diseases specified by the Ministry of Health & Welfare. The findings used for diagnostic criteria are as follows. JMAJ, February 2002 Vol. 45, No. 2 53
10 T. SHIMOYAMA a) Major findings (1) Longitudinal ulcer (2) Cobblestone appearance (3) Non-caseous epithelioid granuloma b) Auxiliary findings (1) Longitudinal irregular ulcer or aphtha (2) Irregular ulcer or aphtha observed in both the superior and inferior digestive tract A. For definite diagnosis, the following criteria have to be satisfied. 1. The cases that correspond to (1) or (2) of major findings (refer to Note 1 and 2). 2. The cases that correspond to (3) of major findings and any one of auxiliary findings. B. Suspected cases should satisfy the following criteria 1. The cases that correspond to any one of auxiliary findings (refer to Note 3). 2. The cases that demonstrate only the major finding (3) (refer to Note 4). 3. The cases that correspond to (1) or (2) of major findings but that cannot be differentiated from ischemic colitis and ulcerative colitis. Note 1: It is necessary to exclude the likelihood of ischemic colitis and ulcerative colitis if only (1) longitudinal ulcer is present. Note 2: It is necessary to exclude the likelihood of ischemic colitis if only (2) cobblestone appearance is present. Note 3: When the case is considered as a suspected case based on the auxiliary finding (2) alone, it is necessary that the finding should be persistent for 3 months. Note 4: It is necessary to cross out the likelihood of inflammatory diseases including intestinal tuberculosis complicated with granuloma. Lastly, for your reference, the certification criteria (draft) of severe cases established by the Ministry of Health & Welfare for the government to shoulder the whole medical expenses are summarized in Table 3 for UC and CD separately. 54 JMAJ, February 2002 Vol. 45, No. 2
What do we need for diagnosis of IBD
 What do we need for diagnosis of IBD Kaichun Wu Dept. of Gastroenterology, Xijing Hospital Fourth Military Medical University Xi an an,, China In China UC 11.6/10 5,CD 1.4/10 5 Major cause of chronic diarrhea
What do we need for diagnosis of IBD Kaichun Wu Dept. of Gastroenterology, Xijing Hospital Fourth Military Medical University Xi an an,, China In China UC 11.6/10 5,CD 1.4/10 5 Major cause of chronic diarrhea
INFLAMMATORY BOWEL DISEASE
 National University Faculty of Medicine INFLAMMATORY BOWEL DISEASE Gehan M. Osman, MD. MBBS Pediatrician Jaffar Ibn Auf Specialized Hospital EDUCATIONAL OBJECTIVES Definitions and spectrum of (IBD) Epidemiology
National University Faculty of Medicine INFLAMMATORY BOWEL DISEASE Gehan M. Osman, MD. MBBS Pediatrician Jaffar Ibn Auf Specialized Hospital EDUCATIONAL OBJECTIVES Definitions and spectrum of (IBD) Epidemiology
Surgical Management of IBD. Val Jefford Grand Rounds October 14, 2003
 Surgical Management of IBD Val Jefford Grand Rounds October 14, 2003 Introduction Important Features Clinical Presentation Evaluation Medical Treatment Surgical Treatment Cases Overview Introduction Two
Surgical Management of IBD Val Jefford Grand Rounds October 14, 2003 Introduction Important Features Clinical Presentation Evaluation Medical Treatment Surgical Treatment Cases Overview Introduction Two
INFLAMMATORY BOWEL DISEASE. Jean-Paul Achkar, MD Center for Inflammatory Bowel Disease Cleveland Clinic
 INFLAMMATORY BOWEL DISEASE Jean-Paul Achkar, MD Center for Inflammatory Bowel Disease Cleveland Clinic WHAT IS INFLAMMATORY BOWEL DISEASE (IBD)? Chronic inflammation of the intestinal tract Two related
INFLAMMATORY BOWEL DISEASE Jean-Paul Achkar, MD Center for Inflammatory Bowel Disease Cleveland Clinic WHAT IS INFLAMMATORY BOWEL DISEASE (IBD)? Chronic inflammation of the intestinal tract Two related
Treatment of Inflammatory Bowel Disease. Michael Weiss MD, FACG
 Treatment of Inflammatory Bowel Disease Michael Weiss MD, FACG What is IBD? IBD is an immune-mediated chronic intestinal disorder, characterized by chronic or relapsing inflammation within the GI tract.
Treatment of Inflammatory Bowel Disease Michael Weiss MD, FACG What is IBD? IBD is an immune-mediated chronic intestinal disorder, characterized by chronic or relapsing inflammation within the GI tract.
Patho Basic Chronic Inflammatory Bowel Diseases. Jürg Vosbeck Pathology
 Patho Basic Chronic Inflammatory Bowel Diseases Jürg Vosbeck Pathology General Group of chronic relapsing diseases with chronic bloody or watery diarrhea Usually ulcerative colitis (UC) or Crohn s disease
Patho Basic Chronic Inflammatory Bowel Diseases Jürg Vosbeck Pathology General Group of chronic relapsing diseases with chronic bloody or watery diarrhea Usually ulcerative colitis (UC) or Crohn s disease
Ulcerative Colitis. ulcerative colitis usually only affects the colon.
 Ulcerative Colitis Introduction Ulcerative colitis is an inflammatory bowel disease. It is one of the 2 most common inflammatory bowel diseases. The other one is Crohn s disease. Ulcerative colitis and
Ulcerative Colitis Introduction Ulcerative colitis is an inflammatory bowel disease. It is one of the 2 most common inflammatory bowel diseases. The other one is Crohn s disease. Ulcerative colitis and
Mohamed EL-hemaly Gastro- intestinal surgical center, Mansoura University.
 Mohamed EL-hemaly Gastro- intestinal surgical center, Mansoura University. Chronic transmural inflammatory process of the bowel & affects any part of the gastro -intestinal tract from the mouth to the
Mohamed EL-hemaly Gastro- intestinal surgical center, Mansoura University. Chronic transmural inflammatory process of the bowel & affects any part of the gastro -intestinal tract from the mouth to the
... Inflammatory disorder of the colon that occurs as a complication of antibiotic treatment.
 Definition Inflammatory disorder of the colon that occurs as a complication of antibiotic treatment. " Epidemiology Humans represent the main reservoir of Clostridium difficile, which is not part of the
Definition Inflammatory disorder of the colon that occurs as a complication of antibiotic treatment. " Epidemiology Humans represent the main reservoir of Clostridium difficile, which is not part of the
SURGICAL MANAGEMENT OF ULCERATIVE COLITIS
 SURGICAL MANAGEMENT OF ULCERATIVE COLITIS Cary B. Aarons, MD Associate Professor of Surgery Division of Colon & Rectal Surgery University of Pennsylvania AGENDA Background Diagnosis/Work-up Medical Management
SURGICAL MANAGEMENT OF ULCERATIVE COLITIS Cary B. Aarons, MD Associate Professor of Surgery Division of Colon & Rectal Surgery University of Pennsylvania AGENDA Background Diagnosis/Work-up Medical Management
What is Crohn's disease?
 What is Crohn's disease? Crohn's disease is a chronic inflammatory disorder that causes inflammation of the digestive tract. It can affect any area of the GI tract, from the mouth to the anus, but it most
What is Crohn's disease? Crohn's disease is a chronic inflammatory disorder that causes inflammation of the digestive tract. It can affect any area of the GI tract, from the mouth to the anus, but it most
Supplementary Online Content
 Supplementary Online Content Tran AH, Ngor EWM, Wu BU. Surveillance colonoscopy in elderly patients: a retrospective cohort study. JAMA Intern Med. Published online August 11, 2014. doi:10.1001/jamainternmed.2014.3746
Supplementary Online Content Tran AH, Ngor EWM, Wu BU. Surveillance colonoscopy in elderly patients: a retrospective cohort study. JAMA Intern Med. Published online August 11, 2014. doi:10.1001/jamainternmed.2014.3746
How do I choose amongst medicines for inflammatory bowel disease. Maria T. Abreu, MD
 How do I choose amongst medicines for inflammatory bowel disease Maria T. Abreu, MD Overview of IBD Pathogenesis Bacterial Products Moderately Acutely Inflamed Chronic Inflammation = IBD Normal Gut Mildly
How do I choose amongst medicines for inflammatory bowel disease Maria T. Abreu, MD Overview of IBD Pathogenesis Bacterial Products Moderately Acutely Inflamed Chronic Inflammation = IBD Normal Gut Mildly
IBD 101. Ronen Stein, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition
 IBD 101 Ronen Stein, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition Objectives Identify factors involved in the development of inflammatory bowel
IBD 101 Ronen Stein, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition Objectives Identify factors involved in the development of inflammatory bowel
What is ulcerative colitis?
 What is ulcerative colitis? Ulcerative colitis is a disease that causes inflammation and sores, called ulcers, in the lining of the rectum and colon. Ulcers form where inflammation has killed the cells
What is ulcerative colitis? Ulcerative colitis is a disease that causes inflammation and sores, called ulcers, in the lining of the rectum and colon. Ulcers form where inflammation has killed the cells
Inflammatory Bowel Disease When is diarrhea not just diarrhea?
 Inflammatory Bowel Disease When is diarrhea not just diarrhea? Jackie Kazik, MA, PA C CME Resources CAPA Annual Conference, 2011 Inflammatory Bowel Disease Objectives Discuss what is known about the pathophysiology
Inflammatory Bowel Disease When is diarrhea not just diarrhea? Jackie Kazik, MA, PA C CME Resources CAPA Annual Conference, 2011 Inflammatory Bowel Disease Objectives Discuss what is known about the pathophysiology
Inflammatory Bowel Disease Ischemic bowel disease
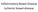 Inflammatory Bowel Disease Ischemic bowel disease Inflammatory Bowel Disease The two disorders that comprise IBD are: ulcerative colitis Crohn disease The distinction between ulcerative colitis and Crohn
Inflammatory Bowel Disease Ischemic bowel disease Inflammatory Bowel Disease The two disorders that comprise IBD are: ulcerative colitis Crohn disease The distinction between ulcerative colitis and Crohn
WHAT IS ULCERATIVE COLITIS?
 235 60th Street, West New York, NJ 07093 T: (201) 854-4646 F: (201) 854-4647 810 Main Street, Hackensack, NJ 07601 T: (201) 488-0095 Ulcerative Colitis WHAT IS ULCERATIVE COLITIS? Ulcerative colitis is
235 60th Street, West New York, NJ 07093 T: (201) 854-4646 F: (201) 854-4647 810 Main Street, Hackensack, NJ 07601 T: (201) 488-0095 Ulcerative Colitis WHAT IS ULCERATIVE COLITIS? Ulcerative colitis is
A Case of Crohn s Disease with Mesalazine Allergy that was Difficult to Differentiate from Comorbid Ulcerative Colitis
 doi: 10.2169/internalmedicine.1607-18 http://internmed.jp CASE REPORT A Case of Crohn s Disease with Mesalazine Allergy that was Difficult to Differentiate from Comorbid Ulcerative Colitis Rumiko Tsuboi,
doi: 10.2169/internalmedicine.1607-18 http://internmed.jp CASE REPORT A Case of Crohn s Disease with Mesalazine Allergy that was Difficult to Differentiate from Comorbid Ulcerative Colitis Rumiko Tsuboi,
The Spectrum of IBD. Inflammatory Bowel Disease. Symptoms. Epidemiology. Tests for IBD. CD or UC? Inflamatory Bowel Disease. Fernando Vega, M.D.
 The Spectrum of IBD Inflammatory Bowel Disease Fernando Vega, M.D. Epidemiology CD and UC together 1:400 UC Prevalence 1:500 UC Incidence 6-12K/annum CD Prevalence 1:1000 CD Incidence 3-6K/annum Symptoms
The Spectrum of IBD Inflammatory Bowel Disease Fernando Vega, M.D. Epidemiology CD and UC together 1:400 UC Prevalence 1:500 UC Incidence 6-12K/annum CD Prevalence 1:1000 CD Incidence 3-6K/annum Symptoms
Colon Cancer , The Patient Education Institute, Inc. oc Last reviewed: 05/17/2017 1
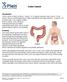 Colon Cancer Introduction Colon cancer is fairly common. About 1 in 15 people develop colon cancer. Colon cancer can be a life threatening condition that affects the large intestine. However, if it is
Colon Cancer Introduction Colon cancer is fairly common. About 1 in 15 people develop colon cancer. Colon cancer can be a life threatening condition that affects the large intestine. However, if it is
IBD 101. Ronen Stein, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition
 IBD 101 Ronen Stein, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition Objectives Identify factors involved in the development of inflammatory bowel
IBD 101 Ronen Stein, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition Objectives Identify factors involved in the development of inflammatory bowel
Crohn's Disease. What causes Crohn s disease? What are the symptoms?
 Crohn's Disease Crohn s disease is an ongoing disorder that causes inflammation of the digestive tract, also referred to as the gastrointestinal (GI) tract. Crohn s disease can affect any area of the GI
Crohn's Disease Crohn s disease is an ongoing disorder that causes inflammation of the digestive tract, also referred to as the gastrointestinal (GI) tract. Crohn s disease can affect any area of the GI
NON INVASIVE MONITORING OF MUCOSAL HEALING IN IBD. THE ROLE OF BOWEL ULTRASOUND. Fabrizio Parente
 NON INVASIVE MONITORING OF MUCOSAL HEALING IN IBD. THE ROLE OF BOWEL ULTRASOUND Fabrizio Parente Gastrointestinal Unit, A.Manzoni Hospital, Lecco & L.Sacco School of Medicine,University of Milan - Italy
NON INVASIVE MONITORING OF MUCOSAL HEALING IN IBD. THE ROLE OF BOWEL ULTRASOUND Fabrizio Parente Gastrointestinal Unit, A.Manzoni Hospital, Lecco & L.Sacco School of Medicine,University of Milan - Italy
The Third Department of Internal Medicine, Tohoku University School of Medicine, Sendai 980
 Tohoku J. exp. Med., 1977, 123, 197-213 Clinical Observations on Ulcerative Colitis HIKARU WATANABE, NOBUO HIWATASHI and SHOICHI YAMAGATA The Third Department of Internal Medicine, Tohoku University School
Tohoku J. exp. Med., 1977, 123, 197-213 Clinical Observations on Ulcerative Colitis HIKARU WATANABE, NOBUO HIWATASHI and SHOICHI YAMAGATA The Third Department of Internal Medicine, Tohoku University School
Inflammatory Bowel Disease
 Inflammatory Bowel Disease Objectives: NOT FOUND. Team Members: Shrouq alsomali + Basel almeflh + Alaa alaqeel + Raneem alghamdi Team Leader: Haneen Alsubki Revised By: Maha AlGhamdi Resources: 435 team
Inflammatory Bowel Disease Objectives: NOT FOUND. Team Members: Shrouq alsomali + Basel almeflh + Alaa alaqeel + Raneem alghamdi Team Leader: Haneen Alsubki Revised By: Maha AlGhamdi Resources: 435 team
Diseases of the Colon. Jack Bragg, D.O., F.A.C.O.I.
 Diseases of the Colon Jack Bragg, D.O., F.A.C.O.I. I have no disclosures I work for the Curators of the University of Missouri Inflammatory Bowel Disease ULCERATIVE COLITIS CROHN S DISEASE Transmural Inflammation
Diseases of the Colon Jack Bragg, D.O., F.A.C.O.I. I have no disclosures I work for the Curators of the University of Missouri Inflammatory Bowel Disease ULCERATIVE COLITIS CROHN S DISEASE Transmural Inflammation
X-Plain Sigmoidoscopy Reference Summary
 X-Plain Sigmoidoscopy Reference Summary Introduction Colon diseases are common. A sigmoidoscopy is a test that can help detect colon diseases. If your doctor recommends that you have a sigmoidoscopy, the
X-Plain Sigmoidoscopy Reference Summary Introduction Colon diseases are common. A sigmoidoscopy is a test that can help detect colon diseases. If your doctor recommends that you have a sigmoidoscopy, the
CROHN S DISEASE. The term "inflammatory bowel disease" includes Crohn's disease and the other related condition called ulcerative colitis.
 CROHN S DISEASE What does it consist of? Crohn s disease is an inflammatory process that affects mostly to the intestinal tract, although it can affect any other part of the digestive apparatus from the
CROHN S DISEASE What does it consist of? Crohn s disease is an inflammatory process that affects mostly to the intestinal tract, although it can affect any other part of the digestive apparatus from the
Surgical Treatment of Inflammatory Bowel Disease (IBD)
 Surgical Treatment of Inflammatory Bowel Disease (IBD) JMAJ 45(2): 55 62, 2002 Tetsuichiro MUTO Vice-Director, Cancer Institute Hospital Abstract: IBD, especially ulcerative colitis (UC) and Crohn s disease
Surgical Treatment of Inflammatory Bowel Disease (IBD) JMAJ 45(2): 55 62, 2002 Tetsuichiro MUTO Vice-Director, Cancer Institute Hospital Abstract: IBD, especially ulcerative colitis (UC) and Crohn s disease
Implementation of disease and safety predictors during disease management in UC
 Implementation of disease and safety predictors during disease management in UC DR ARIELLA SHITRIT DIGESTIVE DISEASES INSTITUTE SHAARE ZEDEK MEDICAL CENTER JERUSALEM Case presentation A 52 year old male
Implementation of disease and safety predictors during disease management in UC DR ARIELLA SHITRIT DIGESTIVE DISEASES INSTITUTE SHAARE ZEDEK MEDICAL CENTER JERUSALEM Case presentation A 52 year old male
FY 2016 MCRCEDP Approved ICD-10 Code List
 Approved List C18.0 Malignant neoplasm of cecum C18.1 Malignant neoplasm of appendix C18.2 Malignant neoplasm of ascending colon C18.3 Malignant neoplasm of hepatic flexure C18.4 Malignant neoplasm of
Approved List C18.0 Malignant neoplasm of cecum C18.1 Malignant neoplasm of appendix C18.2 Malignant neoplasm of ascending colon C18.3 Malignant neoplasm of hepatic flexure C18.4 Malignant neoplasm of
IBD. Crohn s. Outline. Ulcerative colitis versus Crohn s disease: is biopsy useful? UC vs. Crohn s? Is it easy? Biopsy settings 21/07/2017 IBD
 Outline Ulcerative colitis versus Crohn s disease: is biopsy useful? Roger Feakins Colorectal biopsies Ileal and upper GI biopsies Special situations New techniques Summary Inflammatory bowel disease (IBD)
Outline Ulcerative colitis versus Crohn s disease: is biopsy useful? Roger Feakins Colorectal biopsies Ileal and upper GI biopsies Special situations New techniques Summary Inflammatory bowel disease (IBD)
Listed below are some of the words that you might come across concerning diseases and conditions of the bowels.
 Listed below are some of the words that you might come across concerning diseases and conditions of the bowels. Abscess A localised collection of pus in a cavity that is formed by the decay of diseased
Listed below are some of the words that you might come across concerning diseases and conditions of the bowels. Abscess A localised collection of pus in a cavity that is formed by the decay of diseased
Crohn's disease CAUSES COURSE OF CROHN'S DISEASE TREATMENT. Sulfasalazine
 Crohn's disease Crohn's disease is an inflammatory condition of the digestive tract that affects children and adults. Common features of Crohn's disease include mouth sores, diarrhea, abdominal pain, weight
Crohn's disease Crohn's disease is an inflammatory condition of the digestive tract that affects children and adults. Common features of Crohn's disease include mouth sores, diarrhea, abdominal pain, weight
Diarrhea may be: Acute (short-term, usually lasting several days), which is usually related to bacterial or viral infections.
 Pediatric Gastroenterology Conditions Evaluated and Treated Having a child suffer with abdominal pain, chronic eating problems, or other gastrointestinal disorders can be a very trying time for a parent.
Pediatric Gastroenterology Conditions Evaluated and Treated Having a child suffer with abdominal pain, chronic eating problems, or other gastrointestinal disorders can be a very trying time for a parent.
The Role of Ultrasound in the Assessment of Inflammatory Bowel Disease
 The Role of Ultrasound in the Assessment of Inflammatory Bowel Disease Dr. Richard A. Beable Consultant Gastrointestinal Radiologist Queen Alexandra Hospital Portsmouth Hospitals NHS Trust Topics for Discussion
The Role of Ultrasound in the Assessment of Inflammatory Bowel Disease Dr. Richard A. Beable Consultant Gastrointestinal Radiologist Queen Alexandra Hospital Portsmouth Hospitals NHS Trust Topics for Discussion
UNDERSTANDING X-RAYS: ABDOMINAL IMAGING THE ABDOMEN
 UNDERSTANDING X-RAYS: ABDOMINAL IMAGING THE ABDOMEN Radiology Enterprises radiologyenterprises@gmail.com www.radiologyenterprises.com STOMACH AND SMALL BOWEL STOMACH AND SMALL BOWEL Swallowed air is a
UNDERSTANDING X-RAYS: ABDOMINAL IMAGING THE ABDOMEN Radiology Enterprises radiologyenterprises@gmail.com www.radiologyenterprises.com STOMACH AND SMALL BOWEL STOMACH AND SMALL BOWEL Swallowed air is a
Small Bowel and Colon Surgery
 Small Bowel and Colon Surgery Why Do I Need a Small Bowel Resection? A variety of conditions can damage your small bowel. In severe cases, your doctor may recommend removing part of your small bowel. Conditions
Small Bowel and Colon Surgery Why Do I Need a Small Bowel Resection? A variety of conditions can damage your small bowel. In severe cases, your doctor may recommend removing part of your small bowel. Conditions
Treating Crohn s and Colitis in the ASC
 Treating Crohn s and Colitis in the ASC Kimberly M Persley, MD Texas Digestive Disease consultants TASC Meeting Outline IBD 101 Diagnosis Treatment Burden of Disease Role of ASC Inflammatory Bowel Disease
Treating Crohn s and Colitis in the ASC Kimberly M Persley, MD Texas Digestive Disease consultants TASC Meeting Outline IBD 101 Diagnosis Treatment Burden of Disease Role of ASC Inflammatory Bowel Disease
Schistosome life cycle.
 Schistosomiasis infects approximately 200 million persons and kills approximately 280,000 annually. Most of the mortality comes from hepatic granulomas and fibrosis Schistosoma japonicum and Schistosoma
Schistosomiasis infects approximately 200 million persons and kills approximately 280,000 annually. Most of the mortality comes from hepatic granulomas and fibrosis Schistosoma japonicum and Schistosoma
2015 복영증례 51/M C.C. Past Hx: DM, HTN (1998), Lab: WBC (11500/ μl ), CRP (0.71 mg/dl) 순천향서울병원황지영, 홍성숙 APCT (HAD #1) APCT (HAD#1) APCT (HAD #15)
 Case 1 2015 복영증례 순천향서울병원황지영, 홍성숙 51/M C.C Abdominal pain and chilling (1 week ago) Diarrhea (a month ago) Past Hx: DM, HTN (1998), Alcoholic liver disease (2008) Lab: WBC (11500/ μl ), CRP (0.71 mg/dl)
Case 1 2015 복영증례 순천향서울병원황지영, 홍성숙 51/M C.C Abdominal pain and chilling (1 week ago) Diarrhea (a month ago) Past Hx: DM, HTN (1998), Alcoholic liver disease (2008) Lab: WBC (11500/ μl ), CRP (0.71 mg/dl)
3/22/2011. Inflammatory Bowel Disease. Inflammatory Bowel Disease Objectives: Appendicitis. Lemone and Burke Chapter 26
 Inflammatory Bowel Disease Lemone and Burke Chapter 26 Inflammatory Bowel Disease Objectives: Discuss etiology, patho and clinical manifestations of Appendicitis Peritonitis Ulcerative Colitis Crohn s
Inflammatory Bowel Disease Lemone and Burke Chapter 26 Inflammatory Bowel Disease Objectives: Discuss etiology, patho and clinical manifestations of Appendicitis Peritonitis Ulcerative Colitis Crohn s
Increasing Trend in the Incidence of Colorectal Cancer in Japan
 Cancer Increasing Trend in the Incidence of Colorectal Cancer in Japan JMAJ 46(6): 251 256, 2003 Susumu KODAIRA Professor, Department of Surgery, Teikyo University School of Medicine Abstract: Malignant
Cancer Increasing Trend in the Incidence of Colorectal Cancer in Japan JMAJ 46(6): 251 256, 2003 Susumu KODAIRA Professor, Department of Surgery, Teikyo University School of Medicine Abstract: Malignant
X-Plain Colostomy Reference Summary
 X-Plain Colostomy Reference Summary Introduction Diseases of the colon and intestines are common. When diseases of the intestines are treated with surgery, it sometimes results in a colostomy or an ileostomy.
X-Plain Colostomy Reference Summary Introduction Diseases of the colon and intestines are common. When diseases of the intestines are treated with surgery, it sometimes results in a colostomy or an ileostomy.
The focus of this week s lab will be pathology of the gastrointestinal and hepatobiliary systems.
 GASTROINTESTINAL AND HEPATOBILIARY SYSTEMS The focus of this week s lab will be pathology of the gastrointestinal and hepatobiliary systems. GASTROINTESTINAL SYSTEM AND HEPATOBILIARY SYSTEM We will examine
GASTROINTESTINAL AND HEPATOBILIARY SYSTEMS The focus of this week s lab will be pathology of the gastrointestinal and hepatobiliary systems. GASTROINTESTINAL SYSTEM AND HEPATOBILIARY SYSTEM We will examine
Crohn s Disease. Resident Lecture 1/17/19
 Crohn s Disease Resident Lecture 1/17/19 Objectives Features/Classification of Crohn s Disease Medical Treatment Surgical Indications Surgical Considerations 2 Case 25 yo F presents to your office with
Crohn s Disease Resident Lecture 1/17/19 Objectives Features/Classification of Crohn s Disease Medical Treatment Surgical Indications Surgical Considerations 2 Case 25 yo F presents to your office with
Case Discussion. Nutrition in IBD. Rémy Meier MD. Ulcerative colitis. Crohn s disease
 26.08.2017 Case Discussion Nutrition in IBD Crohn s disease Ulcerative colitis Rémy Meier MD Case Presentation 30 years old female, with diarrhea for 3 months Shool frequency 3-4 loose stools/day with
26.08.2017 Case Discussion Nutrition in IBD Crohn s disease Ulcerative colitis Rémy Meier MD Case Presentation 30 years old female, with diarrhea for 3 months Shool frequency 3-4 loose stools/day with
Billing Guideline. Subject: Colorectal Cancer Screening Exams (Invasive Procedures) Effective Date: 1/1/14 Last revision effective 4/16
 Billing Guideline Subject: Colorectal Cancer Screening Exams (Invasive Procedures) Effective Date: 1/1/14 Last revision effective 4/16 Florida Hospital Care Advantage plans include full coverage of in-network
Billing Guideline Subject: Colorectal Cancer Screening Exams (Invasive Procedures) Effective Date: 1/1/14 Last revision effective 4/16 Florida Hospital Care Advantage plans include full coverage of in-network
Digestion: Small and Large Intestines Pathology
 Digestion: Small and Large Intestines Pathology Dr. Ritamarie Loscalzo Medical Disclaimer: The information in this presentation is not intended to replace a one onone relationship with a qualified health
Digestion: Small and Large Intestines Pathology Dr. Ritamarie Loscalzo Medical Disclaimer: The information in this presentation is not intended to replace a one onone relationship with a qualified health
HCPCS Codes (Alphanumeric, CPT AMA) ICD-9-CM Codes Covered by Medicare Program
 HCPCS s (Alphanumeric, CPT AMA) 82272 Blood, occult, by peroxidase activity (e.g., guaiac), qualitative, feces, 1-3 simultaneous determinations, performed for other than colorectal neoplasm screening ICD-9-CM
HCPCS s (Alphanumeric, CPT AMA) 82272 Blood, occult, by peroxidase activity (e.g., guaiac), qualitative, feces, 1-3 simultaneous determinations, performed for other than colorectal neoplasm screening ICD-9-CM
Certain genes passed on from parent to child increase the risk of developing Crohn's disease, if the right trigger occurs.
 Topic Page: Crohn's disease Definition: Crohn's disease from Benders' Dictionary of Nutrition and Food Technology Chronic inflammatory disease of the bowel, commonly the terminal ileum, of unknown aetiology,
Topic Page: Crohn's disease Definition: Crohn's disease from Benders' Dictionary of Nutrition and Food Technology Chronic inflammatory disease of the bowel, commonly the terminal ileum, of unknown aetiology,
PEDIATRIC INFLAMMATORY BOWEL DISEASE
 PEDIATRIC INFLAMMATORY BOWEL DISEASE Alexis Rodriguez, MD Pediatric Gastroenterology Advocate Children s Hospital Disclosers Abbott Nutrition - Speaker Inflammatory Bowel Disease Chronic inflammatory disease
PEDIATRIC INFLAMMATORY BOWEL DISEASE Alexis Rodriguez, MD Pediatric Gastroenterology Advocate Children s Hospital Disclosers Abbott Nutrition - Speaker Inflammatory Bowel Disease Chronic inflammatory disease
The Digestive System
 The Digestive System Identify the Structure and Function. Mesentery of the Large Intestine The mesentery functions to connect the visceral organs to the abdominal wall. Identify the Structure. Nasal Cavity
The Digestive System Identify the Structure and Function. Mesentery of the Large Intestine The mesentery functions to connect the visceral organs to the abdominal wall. Identify the Structure. Nasal Cavity
INVESTIGATIONS OF GASTROINTESTINAL DISEAS
 INVESTIGATIONS OF GASTROINTESTINAL DISEAS Lecture 1 and 2 دز اسماعيل داود فرع الطب كلية طب الموصل Radiological tests of structure (imaging) Plain X-ray: May shows soft tissue outlines like liver, spleen,
INVESTIGATIONS OF GASTROINTESTINAL DISEAS Lecture 1 and 2 دز اسماعيل داود فرع الطب كلية طب الموصل Radiological tests of structure (imaging) Plain X-ray: May shows soft tissue outlines like liver, spleen,
Standard of care Inflammatory Bowel Disease (IBD)
 Standard of care Inflammatory Bowel Disease (IBD) Inflammatory bowel disease (IBD) Tens of thousands of Australians live with the debilitating symptoms of Crohn s disease or ulcerative colitis the two
Standard of care Inflammatory Bowel Disease (IBD) Inflammatory bowel disease (IBD) Tens of thousands of Australians live with the debilitating symptoms of Crohn s disease or ulcerative colitis the two
Medical therapies and IBD
 Medical therapies and IBD Although there is no cure for IBD, there are many treatment options available. There is no standard treatment for IBD that is effective in all situations or for all patients,
Medical therapies and IBD Although there is no cure for IBD, there are many treatment options available. There is no standard treatment for IBD that is effective in all situations or for all patients,
Understanding Your Benefits and Risks
 IBD Treatment Options Understanding Your Benefits and Risks benefit risk assessment tool Understand your options. Improve your health... and life. Inflammatory bowel disease (IBD) is two, separate disorders
IBD Treatment Options Understanding Your Benefits and Risks benefit risk assessment tool Understand your options. Improve your health... and life. Inflammatory bowel disease (IBD) is two, separate disorders
THE DIGESTIVE SYSTEM THE FOUR STEPS OF DIGESTION
 THE DIGESTIVE SYSTEM WHAT IS THE DIGESTIVE SYSTEM? the digestive system is a long, muscular tube The entire system is approximately 9m in length and is usually a one way tract WHY DO WE NEED A DIGESTIVE
THE DIGESTIVE SYSTEM WHAT IS THE DIGESTIVE SYSTEM? the digestive system is a long, muscular tube The entire system is approximately 9m in length and is usually a one way tract WHY DO WE NEED A DIGESTIVE
Understanding Learning is the first step to getting help.
 Understanding Inflammatory Bowel Disease (IBD) Learning is the first step to getting help. This booklet has been created through an educational grant provided by Fulford India Ltd., A subsidiary of Schering-Plough
Understanding Inflammatory Bowel Disease (IBD) Learning is the first step to getting help. This booklet has been created through an educational grant provided by Fulford India Ltd., A subsidiary of Schering-Plough
The Digestive System. Chapter
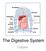 The Digestive System Chapter 15.1 Functions: mechanical and chemical breakdown of food *absorption of nutrients Consists of alimentary canal and accessory organs Wall of the Alimentary Canal 15.2 Characteristics
The Digestive System Chapter 15.1 Functions: mechanical and chemical breakdown of food *absorption of nutrients Consists of alimentary canal and accessory organs Wall of the Alimentary Canal 15.2 Characteristics
Diarrhoea on the AMU. Dr Chris Roseveare
 Diarrhoea on the AMU Dr Chris Roseveare The Society for Acute Medicine, Spring Meeting, Radisson Blu Hotel, Dublin 3-4 May 2012 Acute diarrhoea in developed countries adult populations Mainly a primary
Diarrhoea on the AMU Dr Chris Roseveare The Society for Acute Medicine, Spring Meeting, Radisson Blu Hotel, Dublin 3-4 May 2012 Acute diarrhoea in developed countries adult populations Mainly a primary
Terumitsu; Nagayasu, Takeshi
 NAOSITE: Nagasaki University's Ac Title Author(s) Citation A rare case of segmental ulcerative Tominaga, Tetsuro; Nonaka, Takashi; Shuichi; Kunizaki, Masaki; Sumida, Terumitsu; Nagayasu, Takeshi Acta medica
NAOSITE: Nagasaki University's Ac Title Author(s) Citation A rare case of segmental ulcerative Tominaga, Tetsuro; Nonaka, Takashi; Shuichi; Kunizaki, Masaki; Sumida, Terumitsu; Nagayasu, Takeshi Acta medica
Diagnostic and Therapeutic Approaches to Dysplasia in Inflammatory Bowel Diseases
 Diagnostic and Therapeutic Approaches to Dysplasia in Inflammatory Bowel Diseases Parakkal Deepak, M.B.B.S., M.S. Assistant Professor of Medicine Division of Gastroenterology John T. Milliken Department
Diagnostic and Therapeutic Approaches to Dysplasia in Inflammatory Bowel Diseases Parakkal Deepak, M.B.B.S., M.S. Assistant Professor of Medicine Division of Gastroenterology John T. Milliken Department
Ulcerative Colitis after Multidisciplinary Treatment for Colorectal Cancer with Multiple Liver Metastases : A Case Report
 Showa Univ J Med Sci 29 3, 315 319, September 2017 Case Report Ulcerative Colitis after Multidisciplinary Treatment for Colorectal Cancer with Multiple Liver Metastases : A Case Report Kodai TOMIOKA 1
Showa Univ J Med Sci 29 3, 315 319, September 2017 Case Report Ulcerative Colitis after Multidisciplinary Treatment for Colorectal Cancer with Multiple Liver Metastases : A Case Report Kodai TOMIOKA 1
Pouchitis and Cuffitis A bloody mess. Sze-Lin Peng Colorectal Surgeon Counties Manukau District Health Board
 Pouchitis and Cuffitis A bloody mess Sze-Lin Peng Colorectal Surgeon Counties Manukau District Health Board Ileal-pouch anal anastomosis https://www.pennmedicine.org/for-health-care-professionals/for-physicians/physician-education-and-resources/clinicalbriefings/2018/february/total-proctocolectomy-with-jpouch-reconstruction-for-ulcerative-colitis
Pouchitis and Cuffitis A bloody mess Sze-Lin Peng Colorectal Surgeon Counties Manukau District Health Board Ileal-pouch anal anastomosis https://www.pennmedicine.org/for-health-care-professionals/for-physicians/physician-education-and-resources/clinicalbriefings/2018/february/total-proctocolectomy-with-jpouch-reconstruction-for-ulcerative-colitis
GRANULOMATOUS COLITIS: SIGNIFICANCE OF INVOLVEMENT OF THE TERMINAL ILEUM
 GASTROENTEROLOGY 64: 1071-1076, 1973 Copyright 1973 by The Williams & Wilkins Co. Vol. 64, No.6 Printed in U.S.A. GRANULOMATOUS COLITIS: SIGNIFICANCE OF INVOLVEMENT OF THE TERMINAL ILEUM JAMES A. NELSON,
GASTROENTEROLOGY 64: 1071-1076, 1973 Copyright 1973 by The Williams & Wilkins Co. Vol. 64, No.6 Printed in U.S.A. GRANULOMATOUS COLITIS: SIGNIFICANCE OF INVOLVEMENT OF THE TERMINAL ILEUM JAMES A. NELSON,
children Crohn s disease in MR enterography for GI Complications Microscopy Characterization Primary sclerosing cholangitis Anorectal fistulae
 MR enterography for Crohn s disease in children BOAZ KARMAZYN, MD PEDIATRIC RADIOLOGY ASSOCIATE PROFESSOR Characterization Crohn disease Idiopathic chronic transmural IBD Increasing incidence Age 7/100,000
MR enterography for Crohn s disease in children BOAZ KARMAZYN, MD PEDIATRIC RADIOLOGY ASSOCIATE PROFESSOR Characterization Crohn disease Idiopathic chronic transmural IBD Increasing incidence Age 7/100,000
ד"ר דוד ירדני המכון לגסטרואנטרולוגיה ומחלות כבד מרכז רפואי סורוקה
 ד"ר דוד ירדני המכון לגסטרואנטרולוגיה ומחלות כבד מרכז רפואי סורוקה Presentaion: S.A is 38 years old. Referred for rectal bleeding investigation. Describes several occasions of bleeding and abdominal pain.
ד"ר דוד ירדני המכון לגסטרואנטרולוגיה ומחלות כבד מרכז רפואי סורוקה Presentaion: S.A is 38 years old. Referred for rectal bleeding investigation. Describes several occasions of bleeding and abdominal pain.
Inflammatory Bowel Disease. Your Illness and Its Treatment
 Inflammatory Bowel Disease Your Illness and Its Treatment What Is Inflammatory Bowel Disease? Inflammatory bowel disease (IBD) is inflammation (irritation and swelling) of the digestive tract. Your digestive
Inflammatory Bowel Disease Your Illness and Its Treatment What Is Inflammatory Bowel Disease? Inflammatory bowel disease (IBD) is inflammation (irritation and swelling) of the digestive tract. Your digestive
An Unusual Complication of Crohn s Disease. Dr Gerald Busuttil Mr Debono s Firm Surgical Grand Round 25 th November 2008
 An Unusual Complication of Crohn s Disease Dr Gerald Busuttil Mr Debono s Firm Surgical Grand Round 25 th November 2008 Case Presentation 70 year old lady k/c of Crohns disease h/o of Hartmann s procedure
An Unusual Complication of Crohn s Disease Dr Gerald Busuttil Mr Debono s Firm Surgical Grand Round 25 th November 2008 Case Presentation 70 year old lady k/c of Crohns disease h/o of Hartmann s procedure
The ABCs of Inflammatory Bowel Disease. Jennifer Choi, M.D. Associate Director March 31, 2012
 The ABCs of Inflammatory Bowel Disease Jennifer Choi, M.D. Associate Director March 31, 2012 What Will This Talk Cover? What is IBD? What causes it? What are complications of it? How do I find out if I
The ABCs of Inflammatory Bowel Disease Jennifer Choi, M.D. Associate Director March 31, 2012 What Will This Talk Cover? What is IBD? What causes it? What are complications of it? How do I find out if I
The London Gastroenterology Partnership CROHN S DISEASE
 CROHN S DISEASE What is Crohn s disease? Crohn s disease is a condition, in which inflammation develops in parts of the gut leading to symptoms such as diarrhoea, abdominal pain and tiredness. The inflammation
CROHN S DISEASE What is Crohn s disease? Crohn s disease is a condition, in which inflammation develops in parts of the gut leading to symptoms such as diarrhoea, abdominal pain and tiredness. The inflammation
Management of the Hospitalized IBD Patient. Drew DuPont MD
 Management of the Hospitalized IBD Patient Drew DuPont MD Ulcerative Colitis: Indications for Admission Severe ulcerative colitis Frequent loose bloody stools ( 6 per day) Severe cramps Systemic toxicity:
Management of the Hospitalized IBD Patient Drew DuPont MD Ulcerative Colitis: Indications for Admission Severe ulcerative colitis Frequent loose bloody stools ( 6 per day) Severe cramps Systemic toxicity:
Mucosal Healing in Crohn s Disease. Geert D Haens MD, PhD University Hospital Gasthuisberg University of Leuven Leuven, Belgium
 Mucosal Healing in Crohn s Disease Geert D Haens MD, PhD University Hospital Gasthuisberg University of Leuven Leuven, Belgium Mucosal Lesions in CD: General Features CD can affect the entire GI tract
Mucosal Healing in Crohn s Disease Geert D Haens MD, PhD University Hospital Gasthuisberg University of Leuven Leuven, Belgium Mucosal Lesions in CD: General Features CD can affect the entire GI tract
IMAGING GUIDELINES - COLORECTAL CANCER
 IMAGING GUIDELINES - COLORECTAL CANCER DIAGNOSIS The majority of colorectal cancers are diagnosed on colonoscopy, with some being diagnosed on Ba enema, ultrasound or CT. STAGING CT chest, abdomen and
IMAGING GUIDELINES - COLORECTAL CANCER DIAGNOSIS The majority of colorectal cancers are diagnosed on colonoscopy, with some being diagnosed on Ba enema, ultrasound or CT. STAGING CT chest, abdomen and
Guided by Dr. Michal Amitai Head of Abdominal Imaging Department of Diagnostic Imaging Sheba Medical Center Sackler School of Medicine, Tel Aviv
 Guided by Dr. Michal Amitai Head of Abdominal Imaging Department of Diagnostic Imaging Sheba Medical Center Sackler School of Medicine, Tel Aviv University 1 SHARE study My year Collaboration between gastroenterology
Guided by Dr. Michal Amitai Head of Abdominal Imaging Department of Diagnostic Imaging Sheba Medical Center Sackler School of Medicine, Tel Aviv University 1 SHARE study My year Collaboration between gastroenterology
F A M N O P R S ! D !
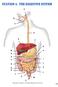 A B C D E F A M N O P Q G H I J R S T U V 595 W http://www.encognitive.com/images/digestive-system-2.jpg K L M A N B C O P D E F G D Q R H S I J K http://apbrwww5.apsu.edu/thompsonj/anatomy%20&%20physiology/2020/2020%20exam%20reviews/exam%203/colon%20diagram.jpgd
A B C D E F A M N O P Q G H I J R S T U V 595 W http://www.encognitive.com/images/digestive-system-2.jpg K L M A N B C O P D E F G D Q R H S I J K http://apbrwww5.apsu.edu/thompsonj/anatomy%20&%20physiology/2020/2020%20exam%20reviews/exam%203/colon%20diagram.jpgd
Original Article Etiologic and clinical analysis of chronic complex anal and rectal inflammation in children less than 3 years old
 Int J Clin Exp Med 2014;7(11):4016-4023 www.ijcem.com /ISSN:1940-5901/IJCEM0002461 Original Article Etiologic and clinical analysis of chronic complex anal and rectal inflammation in children less than
Int J Clin Exp Med 2014;7(11):4016-4023 www.ijcem.com /ISSN:1940-5901/IJCEM0002461 Original Article Etiologic and clinical analysis of chronic complex anal and rectal inflammation in children less than
Surgery and Crohn s. Crohn s Disease 70 % Why Operate? Complications of Disease. The Gastrointestinal Tract. Surgery for Inflammatory Bowel Disease
 The Gastrointestinal Tract Surgery for Inflammatory Bowel Disease Jonathan Chun, MD The regon Clinic Gastrointestinal and Minimally Invasive Surgery Crohn s Disease Can affect anywhere in the GI tract,
The Gastrointestinal Tract Surgery for Inflammatory Bowel Disease Jonathan Chun, MD The regon Clinic Gastrointestinal and Minimally Invasive Surgery Crohn s Disease Can affect anywhere in the GI tract,
This is the portion of the intestine which lies between the small intestine and the outlet (Anus).
 THE COLON This is the portion of the intestine which lies between the small intestine and the outlet (Anus). 3 4 5 This part is responsible for formation of stool. The large intestine (colon- coloured
THE COLON This is the portion of the intestine which lies between the small intestine and the outlet (Anus). 3 4 5 This part is responsible for formation of stool. The large intestine (colon- coloured
Mucosal healing: does it really matter?
 Oxford Inflammatory Bowel Disease MasterClass Mucosal healing: does it really matter? Professor Jean-Frédéric Colombel, New York, USA Oxford Inflammatory Bowel Disease MasterClass Mucosal healing: does
Oxford Inflammatory Bowel Disease MasterClass Mucosal healing: does it really matter? Professor Jean-Frédéric Colombel, New York, USA Oxford Inflammatory Bowel Disease MasterClass Mucosal healing: does
Bleeding in the Digestive Tract
 Bleeding in the Digestive Tract National Digestive Diseases Information Clearinghouse National Institute of Diabetes and Digestive and Kidney Diseases NATIONAL INSTITUTES OF HEALTH U.S. Department of Health
Bleeding in the Digestive Tract National Digestive Diseases Information Clearinghouse National Institute of Diabetes and Digestive and Kidney Diseases NATIONAL INSTITUTES OF HEALTH U.S. Department of Health
ABC of Colorectal Diseases
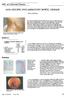 ABC of Colorectal Diseases NON-SPECIFIC INFLAMMATORY BOWEL DISEASE S Pettit, M H Irving Non-specific inflammatory bowel diseases are those for which there is no discernible aetiological agent. The two
ABC of Colorectal Diseases NON-SPECIFIC INFLAMMATORY BOWEL DISEASE S Pettit, M H Irving Non-specific inflammatory bowel diseases are those for which there is no discernible aetiological agent. The two
Kids Like to Break the Rules: Gastrointestinal Pathology in Children
 Kids Like to Break the Rules: Gastrointestinal Pathology in Children Jeffrey Goldsmith MD Director of Surgical Pathology, Beth Israel Deaconess Medical Center; Consultant in Gastrointestinal Pathology,
Kids Like to Break the Rules: Gastrointestinal Pathology in Children Jeffrey Goldsmith MD Director of Surgical Pathology, Beth Israel Deaconess Medical Center; Consultant in Gastrointestinal Pathology,
Title: Author: Journal:
 IMPORTANT COPYRIGHT NOTICE: This electronic article is provided to you by courtesy of Ferring Pharmaceuticals. The document is provided for personal usage only. Further reproduction and/or distribution
IMPORTANT COPYRIGHT NOTICE: This electronic article is provided to you by courtesy of Ferring Pharmaceuticals. The document is provided for personal usage only. Further reproduction and/or distribution
A. Incorrect! The esophagus connects the pharynx and the stomach.
 Human Physiology - Problem Drill 19: Digestive Physiology and Nutrition Question No. 1 of 10 Instructions: (1) Read the problem and answer choices carefully, (2) Work the problems on paper as 1. This organ
Human Physiology - Problem Drill 19: Digestive Physiology and Nutrition Question No. 1 of 10 Instructions: (1) Read the problem and answer choices carefully, (2) Work the problems on paper as 1. This organ
The Morphologic Profile of Inflammatory Bowel Disease and the Diagnostic Problem of Crohn s Disease versus TB Colitis A Case Series
 OPEN ACCESS CASE REPORT The Morphologic Profile of Inflammatory Bowel Disease and the Diagnostic Problem of Crohn s Disease versus TB Colitis A Case Series Maria Lourdes Tilbe, Francia Victoria De Los
OPEN ACCESS CASE REPORT The Morphologic Profile of Inflammatory Bowel Disease and the Diagnostic Problem of Crohn s Disease versus TB Colitis A Case Series Maria Lourdes Tilbe, Francia Victoria De Los
Endoscopy in IBD. F.Hartmann K.Kasper-Kliniken (St.Marienkrankenhaus) Frankfurt/M.
 F.Hartmann K.Kasper-Kliniken (St.Marienkrankenhaus) Frankfurt/M. F.Hartmann@em.uni-frankfurt.de Indications for endoscopy Diagnosis Management Surveillance Diagnosis Single most valuable tool: ileocolonoscopy
F.Hartmann K.Kasper-Kliniken (St.Marienkrankenhaus) Frankfurt/M. F.Hartmann@em.uni-frankfurt.de Indications for endoscopy Diagnosis Management Surveillance Diagnosis Single most valuable tool: ileocolonoscopy
Chapter 32 Gastroenterology General Pathophysiology General Risk Factors for GI emergencies: Excessive Consumption Excessive Smoking Increased
 1 2 3 4 5 6 7 Chapter 32 Gastroenterology General Pathophysiology General Risk Factors for GI emergencies: Excessive Consumption Excessive Smoking Increased Ingestion of Caustic Substances Poor Bowel Habits
1 2 3 4 5 6 7 Chapter 32 Gastroenterology General Pathophysiology General Risk Factors for GI emergencies: Excessive Consumption Excessive Smoking Increased Ingestion of Caustic Substances Poor Bowel Habits
Pitfalls in the Diagnosis of Inflammatory Bowel Disease
 Pitfalls in the Diagnosis of Inflammatory Bowel Disease Robert H Riddell MD Mt Sinai Hospital Toronto Prof of Lab. Medicine and Pathobiology University of Toronto Atypical gross / endoscopic distribution
Pitfalls in the Diagnosis of Inflammatory Bowel Disease Robert H Riddell MD Mt Sinai Hospital Toronto Prof of Lab. Medicine and Pathobiology University of Toronto Atypical gross / endoscopic distribution
For the past 40 years, it has been standard practice to obtain
 ORIGINAL ARTICLE: GASTROENTEROLOGY Good Agreement Between Endoscopic Findings and Biopsy Reports Supports Limited Tissue Sampling During Pediatric Colonoscopy Michael A. Manfredi, Hongyu Jiang, Lawrence
ORIGINAL ARTICLE: GASTROENTEROLOGY Good Agreement Between Endoscopic Findings and Biopsy Reports Supports Limited Tissue Sampling During Pediatric Colonoscopy Michael A. Manfredi, Hongyu Jiang, Lawrence
CASE STUDY: ULCERATIVE COLITIS. Sammi Montag Dietetic Intern
 CASE STUDY: ULCERATIVE COLITIS Sammi Montag Dietetic Intern 2013-2014 PATIENT (CK) INTRODUCTION 26 year old female Chief complaint: bloody diarrhea and abdominal pain Admitting diagnosis: Ulcerative colitis
CASE STUDY: ULCERATIVE COLITIS Sammi Montag Dietetic Intern 2013-2014 PATIENT (CK) INTRODUCTION 26 year old female Chief complaint: bloody diarrhea and abdominal pain Admitting diagnosis: Ulcerative colitis
NCD for Fecal Occult Blood Test
 NCD for Fecal Occult Blood Test Applicable CPT Code(s): 82272 Blood, occult, by peroxidase activity (e.g., guaiac), qualitative, feces, 1-3 simultaneous determinations, performed for other than colorectal
NCD for Fecal Occult Blood Test Applicable CPT Code(s): 82272 Blood, occult, by peroxidase activity (e.g., guaiac), qualitative, feces, 1-3 simultaneous determinations, performed for other than colorectal
Colon Cancer Surgery
 Colon Cancer Surgery Introduction Colon cancer is a life-threatening condition that affects thousands of people. Doctors usually recommend surgery for the removal of colon cancer. If your doctor recommends
Colon Cancer Surgery Introduction Colon cancer is a life-threatening condition that affects thousands of people. Doctors usually recommend surgery for the removal of colon cancer. If your doctor recommends
Inflammatory Bowel Diseases (IBD) Clinical aspects Nitsan Maharshak M.D., IBD Center, Department of Gastroenterology and Liver Diseases Tel Aviv Soura
 Inflammatory Bowel Diseases (IBD) Clinical aspects Nitsan Maharshak M.D., IBD Center, Department of Gastroenterology and Liver Diseases Tel Aviv Sourasky Medical Center Tel Aviv, Israel IBD- clinical features
Inflammatory Bowel Diseases (IBD) Clinical aspects Nitsan Maharshak M.D., IBD Center, Department of Gastroenterology and Liver Diseases Tel Aviv Sourasky Medical Center Tel Aviv, Israel IBD- clinical features
Inflammatory Bowel Disease and Surgery: What You Should Know
 Inflammatory Bowel Disease and Surgery: What You Should Know Ask the Experts March 9, 2019 Kristen Blaker, MD Colon and Rectal Surgery MetroHealth Medical Center Disclosures None Outline Who undergoes
Inflammatory Bowel Disease and Surgery: What You Should Know Ask the Experts March 9, 2019 Kristen Blaker, MD Colon and Rectal Surgery MetroHealth Medical Center Disclosures None Outline Who undergoes
The Digestive System. Chapter 25
 The Digestive System Chapter 25 Introduction Structure of the digestive system A tube that extends from mouth to anus Accessory organs are attached Functions include Ingestion Movement Digestion Absorption
The Digestive System Chapter 25 Introduction Structure of the digestive system A tube that extends from mouth to anus Accessory organs are attached Functions include Ingestion Movement Digestion Absorption
What is Crohn's disease?
 What is Crohn's disease? Crohn s disease is an ongoing disorder that causes inflammation of the digestive tract, also referred to as the gastrointestinal (GI) tract. Crohn s disease can affect any area
What is Crohn's disease? Crohn s disease is an ongoing disorder that causes inflammation of the digestive tract, also referred to as the gastrointestinal (GI) tract. Crohn s disease can affect any area
