The False-positive Rate of Thoracic Outlet Syndrome Shoulder Maneuvers in Healthy Subjects Michael C. Plewa, MD, Mark Delingel; MD
|
|
|
- Beatrix Dean
- 5 years ago
- Views:
Transcription
1 Thoracic Outlet Syndrome Shoulder Maneuvers, Plewa, Delinger 337 The False-positive Rate of Thoracic Outlet Syndrome Shoulder Maneuvers in Healthy Subjects Michael C. Plewa, MD, Mark Delingel; MD I... ABSTRACT Objective: To estimate the incidence of false-positive findings of thoracic outlet syndrome (TOS) shoulder maneuvers, Adson s test (AT), costoclavicular maneuver (CCM). elevated arm stress test (EAST), and supraclavicular pressure (SCP) in healthy subjects. Methods: A cross-sectional, observational study was performed in a medical school and affiliated emergency medicine residency program setting. Participants included healthy adult volunteers without symptoms of TOS. The shoulder maneuvers AT, CCM, EAST, and SCP were performed in randomized order for 30 sec, 30 sec, 3 min, and 30 sec, respectively. Pulse quality and the presence and timing of pain or paresthesias were assessed. Results: 53 subjects were enrolled, including 27 women, aged 29.7 & 6.4 years (range years). AT, CCM, EAST, and SCP resulted in an altered pulse in 11%. 11%. 62%. and 21%; pain in 0%. 0%, 21%, and 2%; and paresthesias in 11%, 15%, 36%, and 15% of cases, respectively. The following outcomes had reasonable false-positive rates (upper 95% confidence limit): pain with the AT (7%). CCM (7%), SCP (lo%), or any 2 TOS shoulder maneuvers (10%); discontinuing the EAST because of symptoms (16%); or any symptom with 3 (13%) or 4 (7%) TOS shoulder maneuvers. Conclusions: In a study of TOS shoulder maneuvers in healthy subjects, the outcomes of pulse alteration or paresthesias were unreliable in general. However, TOS shoulder maneuvers have reasonably low false-positive rates when a positive outcome is defined as pain after AT, CCM, or SCP; discontinuation of the EAST secondary to pain; pain in the same arm with 22 maneuvers; or any symptom in the same arm with 23 maneuvers. Key words: physical examination; thoracic outlet syndrome; pain; paresthesia; perfusion; upper extremity. Acad. Emerg. Med. 1998; 5: I Emergency physicians (EPs) should consider thoracic outlet syndrome (TOS) in the differential diagnosis during the evaluation of patients with upper-extremity symptoms of pain, weakness, numbness, or paresthesias. TOS can result from compression of the neurovascular bundle by the first rib, a cervical rib, congenital fibrous bands, or the anterior scalene muscle. There are several variants of TOS, depending on the site of compression, although all classically result in pain exacerbated with the arm in the... From Sr. Vincent Mercy Medical Center/The Toledo Hospital Emergency Medicine Residency Program (MCP, MD): and the Medical Colleae -., of Ohio. Toledo. OH. Demrtmeni of - Suraerv -. (MCP). Received: June 3, 1997; revision received: September 30, 1997: accepted: October 5, 1997; updaied: October 31, Prior presentation: SAEM annual meeting. Washington, DC, May 1997, and the 7th Annual Midwest Regional Emergency Medicine Research Symposium. Akron, OH. April elevated position. Vascular forms of TOS are rare, and can occur following venous compression in 4% of TOS cases, resulting in upper-extremity swelling, fatigue, venous distention, and cyanosis, or may be due to arterial compression in 1% of TOS cases, resulting in upper-extremity pallor, coolness, claudication, and eventually ulceration and gangrene. More than 95% of patients with TOS will have symptoms related to compression of the brachial plexus, including numbness, pain, or paresthesias, typically in the ulnar distribution but occasionally radiating to the chest and neck, and eventual weakness in the hand grip, triceps, and hand interosseous muscles. The diagnostic evaluation of TOS should focus on excluding other disorders such as myocardial ischemia, arthritis, fibromyalgia, cervical disk disease, spinal stenosis, rotator cuff injury, reflex sympathetic dystrophy, multiple sclerosis, causalgia, carpal tunnel syndrome, Pancoast tumor, and arteritis. Although cervical spine and chest radiographs are recommended, evidence supporting their diagnostic utility is lacking. The rare case of complete Address for correspondence and reprinis: Michael C. Plewa. MD. Si. Vincent Mercy Medical Cenrec 2213 Cherry Streei, Toledo, OH vascular is codhned by Doppler studies, ve- Fax: ; mcpiewa@msn.com nography, or arteriography. Patients with neurologic find-
2 338 ACADEMIC EMERGENCY MEDICINE APR 1998 VOL 5/NO 4 ings such as weakness and muscle atrophy (especially in the intrinsic hand muscles) may also have electrophysiologic abnormalities on electromyographic, somatosensory evoked potential, or nerve conduction velocity (NCV) st~dies..~ NCV findings classically include low-amplitude median motor responses and ulnar sensory action potentials, and normal ulnar motor responses and median sensory re~ponses ~ and are also useful in excluding nerve entrapment disorders such as carpal tunnel and ulnar entrapment syndrome. The utility of MRI is accepted in excluding cervical disk disease and spinal stenosis, but is uncertain in the evaluation of neurovascular compression in the thoracic ~utlet. ~ The diagnostic standard for TOS is controversial. Many author^"^" suggest the diagnosis of TOS can be made with the following criteria: 1) the presence of typical I FIGURE 1. Demonstration of the TOS shoulder maneuvers. A. Adson s rest (AT) involves full inspiration with the neck extended and turned to either side for 30 seconds. B. For the cosrocluviculur maneuver, both shoulders are pulled downward and backward, in an exaggerated military position. for 30 seconds. C. The elevated urn srress test (EAST) involves extension of both shoulders with opening and closing of both fists for 3 minutes. D. Suprucluviculur pressure (SCP) is performed with both thumbs at the lowest portion of the anterior scalene muscle near the first rib for 30 seconds.
3 ~ ~~ Thoracic Outlet Syndrome Shoulder Maneuvers, Plewu, Delinger 339 upper-extremity symptoms exacerbated by arm elevation, 2) positive findings on TOS shoulder maneuvers, and 3) the absence of other disorders. Others refute the existence of neurogenic TOS in the absence of objective physical (muscle wasting) or electrophysiologic findings, and have labeled this disputed neurogenic TOS.3-8 Regardless of the final diagnosis, it is important for EPs to be familiar with the various provocative TOS shoulder maneuvers necessary in the diagnostic evaluation of this syndrome. Schukla and Carlton have noted that 98% of TOS patients were missed during their initial ED evaluations, in the majority of these instances because TOS maneuvers were not performed. Several bedside physical maneuvers have been described to aid in the diagnosis of TOS, including Adson s test (AT)? the hyperabduction test, the elevated arm stress test (EAST), the costoclavicular maneuver (CCM), and supraclavicular pressure (SCP) (the Methods section and Figure 1 provide further descriptions regarding these techniques). These TOS shoulder maneuvers have been used with variable test performance Although several authors state that TOS shoulder maneuvers are unreliable and result in high percentages of false positives in normal subject^,"-^^ these articles refer to the AT, hyperabduction test, and CCM, which were initially defined as positive if there was loss of the radial pulse. Most a~thors *~* - ~*~~ now suggest that positive TOS maneuvers, especially the EAST and SCP, should result in reproduction of the patient s symptoms rather than pulse alteration. The false-positive rate of TOS maneuvers defined by pain and paresthesias, however, has been inadequately studied. Our objective was to estimate the incidence of false-positive findings of TOS shoulder maneuvers in healthy subjects. I METHODS... Study Design: A cross-sectional, observational study was performed to estimate the incidence of abnormal TOS shoulder maneuvers in healthy volunteers. The study was approved by the Institutional Review Board of the St. Vincent Mercy Medical Center. Setting and Population: The study was performed in a medical school and affiliated (EM) residency program setting during November and December Subjects included healthy adult volunteers who did not have a known history of previous clavicle, neck, or shoulder fracture, carpal tunnel syndrome, cervical disk disease, fibromyalgia, reflex sympathetic dystrophy, or symptoms (such as neck, shoulder or arm pain, or paresthesias) compatible with TOS. Interventions and Measurements: The shoulder maneuvers AT, CCM, EAST, and SCP were performed on one arm at a time (except for the EAST, which was with both arms simultaneously) in each subject in a randomized order (according to a computer-generated random number list) for 30 sec, 30 sec, 3 min. and 30 sec, respectively, with an approximately 60-second rest period between maneuvers. See Figure 1 for details regarding these maneuvers. The hyperabduction test was not studied because this position is incorporated into the EAST. Adson s test (AT) involves sitting in the upright position with shoulders back and hands on the lap, taking a deep inspiration and extending the neck and the chin toward the affected side. This increases the tension of the anterior and middle scalene muscles, and decreases the interscalene space. This test has poor sensitivity, being positive in as few as 2% of patients with TOS. For the elevated arm stress test (EAST), both hands are opened and closed into fists for 3 minutes with both arms in the hyperabduction position, which closes the costoclavicular space and compresses the neurovascular bundle under the pectoralis minor muscle. A positive EAST, including reproduction of symptoms of pain and paresthesias in the arm, shoulder, chest, or neck and discontinuation with dropping of the arm for relief of pain, is considered the most reliable test with regard to sensitivity. The costocluviculur maneuver (CCM) involves pulling the shoulders downward and backwards in an exaggerated military position. This closes the space between the clavicle and the first rib. For suprucluviculur pressure (SCP), the observer s thumb is pressed in the supraclavicular fossa over the medial scalene muscle for at least 30 seconds. This indirectly presses on the brachial plexus, and a positive test results in not only tenderness but reproduction of symptoms in the upper extremity. The palpated radial pulse quality (present, absent, or diminished in comparison with previous pulse amplitude) and the presence, location, and time of onset of pain or paresthesias were recorded individually by an EM attending and a fourth-year medical student trained in these maneuvers. Measurements were neither repeated in the same subject (reproducibility) nor repeated with different observers (reliability). Pain was self-reported, but not quantified on a scale, and defined as any discomfort in the upper extremity, neck, or head on the involved side. Paresthesias were defined as any tingling, burning, pins and needles, or otherwise funny sensation. The percentage of positive tests for each maneuver represents the number of positive tests present in either extremity over the total number of subjects. Data Analysis: Data were described with 95% confidence intervals (CIS). A sample size of 50 subjects was chosen to obtain an estimated precision of 510% if the percentage of subjects with a negative test is 85% or higher.
4 ~~~~ 340 ACADEMIC EMERGENCY MEDICINE APR 1998 VOL 5/NO 4 I RESULTS Fifty-three subjects were enrolled, including 27 women and 26 men, aged years (range years). The incidence of abnormal TOS shoulder maneuvers is listed in Table 1. Pulse alterations were observed in some patients with all maneuvers, but were most common with the EAST in comparison with other maneuvers. Paresthesias were also more common with the EAST, were present only in the upper extremity, and did not radiate into the neck, head, or chest in any case. Pain was absent in cases with the AT and CCM maneuvers, and was present in 1 case with SCP. Although discomfort was more likely with the EAST, it resulted in discontinuation of the maneuver in only 3 (6%; 1-16%) subjects who dropped the arm at sec, 2 because of pain and 1 from fatigue. Pulse alteration, pain, and paresthesias with at least 1 maneuver were present in 74% (60435%). 21% (11-34%) and 47% (33-61%) of subjects, respectively. although no subject had positive findings with all maneuvers. Table 2 lists the outcomes of altered pulse, pain, or paresthesias into the same extremity with >1 shoulder maneuver. Pain occurred with the EAST in the shoulder in 1 case, the forearm and hand in 6, the hand in 3, and the thumb in 1. Pain occurred with SCP in the hand and arm in 1 case each. Pain did not follow the classic ulnar distribution in any case. Pain intensity was described as mild in all cases except for 1 subject, who described pain associated with EAST as severe. Although subjects were allowed to discontinue any TOS shoulder maneuver if necessary because of pain, only 2 individuals discontinued during the EAST because of pain. Paresthesias occurred with the AT in the hand and small finger in 1 case each; with the CCM in the forearm in 2 cases and the hand in 6; with the EAST in the arm in 1 case, the forearm in 4, the forearm and hand in 4, the hand in 7, the small finger in 1, the thumb in 1, and all fingers in 1; with the SCP in the shoulder in 1 case, the arm in 2, the forearm in 4, and the hand in 1. Paresthesias were in the ulnar distribution in 5 cases, 3 in the forearm and 2 in the small finger. In all cases the pares- I TABLE 1 Abnormal TOS Shoulder Maneuver Findings* Maneuver Altered Pulse Pain Paresthesias Time (set)? AT 11% 0% 11% CCM (3-1945) 11% (0-14%) 0% (3-19%) 15% EAST (3-198) 62% (0-14%) 21% (5-2596) 36% 89 t 45 SCP (49-75%) 21% (0-32%) (0-32%) 2% (0-696) (23-49%) 15% (5-258) 18 k 6 *95% CI in parentheses. tdenotes average time of onset of altered symptoms. thesias were mild and described as a tingling or "pins and needles' ' sensation rather than burning or pain. I DISCUSSION There has been controversy regarding the accuracy of these shoulder maneuvers in the diagnosis of TOS because of varying definitions. When based on findings of a diminished radial pulse, these maneuvers are thought to be ~nreliable'~-~ since pulse alterations may be found in a high percentage of asymptomatic individuals. Using photoplethysmographic recordings, Gergoudis and Barnes" noted significant arterial obstruction (defined as 275% reduction in the digital pulse amplitude) in 51%. 14%. and 9% of cases using the Adson's, costoclavicular, and hyperabduction maneuvers, respectively. Telford and Mottenhead'' noted diminished radial pulses in approximately 50% of healthy medical students with the costoclavicular or hyperabduction maneuvers. Vin et al.'" described reasonable specificities for the maneuvers in 150 normal subjects, with pulse obliteration in no subjects with the Adson's test, and in 1-17% with hyperabduction between 45" and 180". Warrens and Heatonz3 described false positives in 58% of cases with at least 1 maneuver, 27% with the costoclavicular test, 15% with Adson's test, and 14% with the hyperabduction test. Wright noted hyperabduction of the arms obliterated the radial pulse in 83% of 150 young, healthy adult volunteer^.'^ Our results are consistent with these in that the majority of patients (74%) had alteration in pulse with at least 1 maneuver; however, we did find that diminished pulse was less common with AT and CCM than most previous reports. Whereas previous studies have not addressed pulse alterations with EAST and SCP, we found a diminished pulse in the majority of subjects following EAST (62%) and in a significant percentage of subjects following SCP (21%). Positive findings on TOS shoulder maneuvers should include reproduction or exacerbation of the patient's symptoms,'."*2' although several authors criticizing the poor specificity of these maneuvers have not commented on production of pain or paresthesias with these test^.'^'^^'^ The few prior studies to prospectively evaluate the falsepositive rate of TOS maneuvers in healthy subjects with regard to pain or paresthesias have addressed the hyperabduction maneuver1' and the EAST,= and not the AT, CCM, or SCP. In the study described by Wright,I7 only 2 of 150 normal volunteers noted neurologic symptoms of pain or paresthesias with shoulder hyperabduction. Novak et a1.26 found 10 of 300 normal persons developed sensory symptoms within 2-4 minutes after arm elevation. In the study by Costigan and Wilb~urn?~ the EAST produced discomfort in 74% of control subjects, although none of these discontinued the maneuver secondary to pain. Similarly, we found that discontinuing the test because of pain, argued by ROOS' as being essential for a
5 Thoracic Outlet Syndrome Shoulder Maneuvers, Pfewa, Definger 341 positive test, was quite uncommon (3%), and EAST elicited pain or paresthesias in 21% to 36% of subjects. Also, since many of our subjects did not develop symptoms until beyond 90 seconds, it is likely that the specificity of EAST might be improved by limiting the test to 90 seconds duration. Supraclavicular pressure, described by Roos as one of the most helpful tests in the diagnosis of TOS, has been the least studied of all the physical maneuvers. Costigan and Wilbourn noted supraclavicular tenderness in only 4% of controls and did not describe reproduction of symptoms in any of these healthy volunteers. We also found the SCP maneuver rarely caused pain, although paresthesias were present in 15%. Our results suggest that resultant pain may be the most specific finding during TOS shoulder maneuvers, since pain was present in no subject during the AT or CCM tests, and in a single subject during SCP. In general, the incidence of false-positive findings of pain with the AT, CCM, and SCP were lower than with EAST and lower than findings of paresthesias with these maneuvers. Using the results of several shoulder maneuvers in combination may also improve the specificity for TOS, since paresthesias or pulse alterations in the same arm with 22 tests were uncommon (1 1 %), and pain in the same arm with 22 tests was rare (2%). Although some authors have discounted the TOS maneuvers as being nonspecific, they remain an integral component of the diagnosis of TOS. For example, Lindgren uses a TOS index defined as at least 3 of 4 criteria, including history of symptoms aggravated with arm elevation, paresthesias along the C8-T1 distribution, supraclavicular tenderness over the brachial plexus, and a positive EAST. Our results suggest that TOS shoulder maneuvers have reasonable specificity when they result in pain after AT, CCM, or SCP, discontinuation of the EAST secondary to pain, pain in the same arm with 22 maneuvers, or any symptom with 23 maneuvers. Positive TOS maneuvers in the patient with arm pain, numbness, paresthesias, or weakness aggravated in the elevated position should suggest TOS as a possible diagnosis. Further workup should rule out other causes listed previously. Since the majority of patients with TOS can be managed with conservative measures such as simple analgesics, physical therapy, shoulder girdle and cervical spine mobility exercises, psychosocial intervention, and avoidance of precipitating factors, most patients can be managed by their primary care physician with possible referral to physical medicine and rehabilitation, neurology, rheumatology, and orthopedic or vascular surgery specialists, as necessary. Rarely, surgical transaxillary first rib resection * will be indicated for cases with documented aneurysm, arterial or venous insufficiency, or true neurologic TOS with muscle weakness and atrophy, or cases refractory to conservative measures. I TABLE 2 Abnormal Findings in the Same Arm with a Combination of TOS Shoulder Maneuvers* Number of Maneuvers Altered Pulse Pain Paresthesias W O 6% (4-23%) 2% (9-10%) 21% (11-34%) Three 4% (0-13%) 0% (0-7%) 4% 0-13%) Four 0% (0-7%) O%(O-7%), 0% (0-7%) *95% CI in parentheses. I LIMITATIONS AND FUTURE QUESTIONS... This study has several limitations that deserve discussion. Because of the small sample size, the confidence intervals around specificity estimates were wide. There were only 2 observers performing the TOS shoulder maneuvers, and observations were not repeated on the same subjects; therefore, the interrater variability could not be determined. The pressure was not measured during the CCM or SCP maneuvers, but was estimated to be approximately 10 pounds. In addition, we did not measure pain intensity, such as with a linear analog pain score, although many subjects described their discomfort as mild. It is possible that the pain intensities are quite different between subjects with and without TOS. Since a complete radiographic and electrophysiologic evaluation of subjects was not performed, it is possible that positive shoulder maneuvers identified individuals with asymptomatic carpal tunnel syndrome or cervical disk disease, or predisposition to TOS in the future. Several other tests were not evaluated, such as the hyperabduction test, the cervical rotation lateral flexion test, Tinel s sign (tenderness to percussion over the brachial plexus and supraclavicular fossa), and the scalene muscle block. It is possible that any of these could have better specificity than the 4 TOS shoulder maneuvers studied here. The most serious study limitation was that our population of normal subjects does not reflect those patients presenting to the ED with symptoms suggestive of TOS. We did not address the false-positive rate of TOS shoulder maneuvers in patients with cervical disk disease, fibromyalgia, reflex sympathetic dystrophy, carpal tunnel syndrome, or other disorders mimicking TOS. In fact, Costigan and Wilbourn have found positive findings with the SCP and EAST in 23% and 92%. respectively, of patients with carpal tunnel syndrome. We also did not attempt to duplicate the typical 3: 1 female-to-male ratio found in TOS cases. In addition, this study did not assess the sensitivities of these TOS shoulder maneuvers in symptomatic ED patients. In fact, prior studies have infrequently reported the sensitivity of these TOS shoulder maneuvers because they are usually included in the definition of TOS. Future study should address the following issues: 1)
6 342 ACADEMIC EMERGENCY MEDICINE APR 1998 VOL 5/NO 4 the optimal force required for the SCP and CCM maneuvers, 2) the interobserver variability of the various TOS maneuvers, 3) the utility of chest and cervical radiographic screening in patients with TOS symptoms, and 4) the optimal TOS shoulder maneuvers with regard to sensitivity and specificity in a prospective evaluation of patients presenting to the ED with symptoms suggestive of TOS. I CONCLUSION In a study of TOS shoulder maneuvers in healthy subjects, which did not address sensitivity, we found outcomes of pulse alteration or paresthesias to be unreliable in general. However, TOS shoulder maneuvers have reasonably low false-positive rates when a positive outcome is defined as pain after AT, CCM, or SCP; discontinuation of the EAST secondary to pain; pain in the same arm with 2 2 maneuvers; or any symptom in the same arm with 23 maneuvers. The authors thank Nancy Fenn Buderer. MS, for her statistical assistance and Brooke Thibert for manuscript preparation. I REFERENCES 1. Roos DB. Congenital anomalies associated with thoracic outlet syndrome. Anatomy, symptoms, diagnosis, and treatment. Am J Surg. 1976; 132~ Schukla PC, Carlton FB Jr. Diagnosis of thoracic outlet syndrome in the emergency department. South Med J. 1996; 89: Pang D, Wessel HB. Thoracic outlet syndrome. Neurosurgery. 1988; 22: Smith T, Trojaborg W. Diagnosis of horacic outlet syndrome. Value of sensory and motor conduction studies and quantitative electromyography. Arch Neurol. 1987; 44: Panegyres PK, Moore N, Gibson R. Rushworth G, Donaghy M. Thoracic outlet syndromes and magnetic resonance imaging. Brain. 1993; 116: Poole GV, Thomae KR. Thoracic outlet syndrome reconsidered. Am Surg. 1996; 4: Lindgren K-A. Conservative treatment of thoracic outlet syndrome: a 2-year follow-up. Arch Phys Med Rehabil. 1997; 78: Wilbourn AJ. The thoracic outlet syndrome is overdiagnosed. Arch Neurol. 1990; 47: Adson AW, Coffey JR. Cervical rib: a method of anterior approach for relief of symptoms by division of the scalenus anticus. Ann Surg. 1927; 85: Thomas GI, Jones TW, Stavney LS, Manhas DR. Thoracic outlet syndrome. Am Surg. 1978; 44: Roos DB. New concepts of thoracic outlet syndrome that explain etiology, symptoms, diagnosis, and treatment. J Vasc Surg. 1979; 13: Sanders M, Monsour JW, Gerber WF, Adams WR, Thompson N. Scalenectomy versus first rib resection for treatment of thoracic outlet syndrome. Surgery. 1979; 85: Gilroy J, Meyer JS. Compression of the subclavian artery as a cause of ischaemic brachial neuropathy. Brain. 1963; 86: Vin F, Koskas F, Levy D. GoEau-Brissonnibre 0, Bacourt F. Thoracic outlet syndrome. Value of non-invasive arterial exploratory methods. Presse Med. 1986; 15: Stallworth JM, Home JB. Diagnosis and management of thoracic outlet syndrome. Arch Surg. 1984; 119: Sellke FW, Kelly TR. Thoracic outlet syndrome. Am J Surg. 1988; Wright IS. The neurovascular syndrome produced by hyperabduction of the arms. Am Heart J. 1945; 29:l Sanders M, Mounsour JW, Baer SB. Transaxillary first rib resection for the thoracic outlet syndrome. Arch Surg. 1968; 97: Telford ED, Mottershead S. Pressure at the cervico-brachial junction: an operative and anatomical study. J Bone Joint Surg Br. 1948; 30: Silver D. Thoracic outlet syndrome. Mo Med. 1980; 77: Crawford FA. Thoracic outlet syndrome. Surg Clin North Am : Gergoudis R, Barnes RW. Thoracic outlet compression: prevalence in normal persons. Angiology. 1980; Warrens AN, Heaton JM. Thoracic outlet compression syndrome: the lack of reliability of its clinical assessment. Ann R Coll Surg Engl. 1987; 69~ Falconer MA, Weddell G. Costoclavicular compression of the subclavian artery and vein. Lancet. 1943; ii: Costigan DA, Wilbourn AJ: The elevated arm stress test: specificity in the diagnosis of the thoracic outlet syndrome [abstract]. Neurology. 1985; 35(s~ppl 1): Novak CB, Mackinnon SE, Patterson GA. Evaluation of patients with thoracic outlet syndrome. J Hand Surg. 1993; 18A Urschel HC Jr, Razzuk MA. Upper plexus thoracic outlet syndrome: optimal therapy. Ann Thorac Surg. 1997; 63:935-9.
Richard Dobrusin DO FACOFP
 Richard Dobrusin DO FACOFP Define Thoracic Outlet Syndrome (TOS) Describe the Mechanisms of Dysfunction List Diagnostic tests for (TOS) Understand (TOS) referral patterns Discuss Treatment Options Definition:
Richard Dobrusin DO FACOFP Define Thoracic Outlet Syndrome (TOS) Describe the Mechanisms of Dysfunction List Diagnostic tests for (TOS) Understand (TOS) referral patterns Discuss Treatment Options Definition:
THORACIC OUTLET SYNDROME (T.O.S.) Prof J van Marle
 THORACIC OUTLET SYNDROME (T.O.S.) Prof J van Marle 1. Definition Clinical syndrome caused by compression of the neurovascular bundle as it passes through the thoracic outlet, a narrow space bordered by
THORACIC OUTLET SYNDROME (T.O.S.) Prof J van Marle 1. Definition Clinical syndrome caused by compression of the neurovascular bundle as it passes through the thoracic outlet, a narrow space bordered by
THORACIC OUTLET SYNDROME: A FREQUENT CAUSE OF NON-DISCOGENIC BRACHIALGIA
 THORACIC OUTLET SYNDROME: A FREQUENT CAUSE OF NON-DISCOGENIC BRACHIALGIA Debora Garozzo Brachial Plexus and Peripheral Nerve Surgery Unit Neurospinal Hospital Dubai, United Arab Emirates THE THORACIC OUTLET
THORACIC OUTLET SYNDROME: A FREQUENT CAUSE OF NON-DISCOGENIC BRACHIALGIA Debora Garozzo Brachial Plexus and Peripheral Nerve Surgery Unit Neurospinal Hospital Dubai, United Arab Emirates THE THORACIC OUTLET
The Brachial Plexus and Thoracic Outlet Syndrome
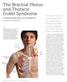 The Brachial Plexus and Thoracic Outlet Syndrome Understanding Signs and Symptoms By Joseph E. Muscolino, DC The brachial plexus of nerves and the subclavian/axillary artery and vein comprise a neurovascular
The Brachial Plexus and Thoracic Outlet Syndrome Understanding Signs and Symptoms By Joseph E. Muscolino, DC The brachial plexus of nerves and the subclavian/axillary artery and vein comprise a neurovascular
Thoracic Outlet Syndrome
 Thoracic Outlet Syndrome Part 1: The Scalene Triangle TOS: Vascular Symptom Presentation Venous persistent/intermittent edema heaviness and fatigue deep pain in neck/shoulder increased pain at night warm
Thoracic Outlet Syndrome Part 1: The Scalene Triangle TOS: Vascular Symptom Presentation Venous persistent/intermittent edema heaviness and fatigue deep pain in neck/shoulder increased pain at night warm
THORACIC OUTLET DECOMPRESSION
 THORACIC OUTLET DECOMPRESSION Thesis Submitted in partial fulfillment of the degree of M.D. in general surgery By Abd El Aty Mohammed Sakr Supervised by Prof. Dr. Amr Ahmed Gad Prof. of vascular surgery
THORACIC OUTLET DECOMPRESSION Thesis Submitted in partial fulfillment of the degree of M.D. in general surgery By Abd El Aty Mohammed Sakr Supervised by Prof. Dr. Amr Ahmed Gad Prof. of vascular surgery
Thoracic Outlet Syndrome
 Discussion paper prepared for The Workplace Safety and Insurance Appeals Tribunal January 2000 Prepared by: Dr. J.F.R. Fleming Professor Emeritus, Division of Neurosurgery University of Toronto The Toronto
Discussion paper prepared for The Workplace Safety and Insurance Appeals Tribunal January 2000 Prepared by: Dr. J.F.R. Fleming Professor Emeritus, Division of Neurosurgery University of Toronto The Toronto
THORACIC OUTLET SYNDROME AND THE OVERHEAD ATHLETE LISA PIROPATO, PT, DPT, ATC NORTHEAST INDIANA SPORTS MEDICINE SYMPOSIUM MARCH 25, 2017
 THORACIC OUTLET SYNDROME AND THE OVERHEAD ATHLETE LISA PIROPATO, PT, DPT, ATC NORTHEAST INDIANA SPORTS MEDICINE SYMPOSIUM MARCH 25, 2017 LEARNING OBJECTIVES Explain the etiologies of thoracic outlet syndrome.
THORACIC OUTLET SYNDROME AND THE OVERHEAD ATHLETE LISA PIROPATO, PT, DPT, ATC NORTHEAST INDIANA SPORTS MEDICINE SYMPOSIUM MARCH 25, 2017 LEARNING OBJECTIVES Explain the etiologies of thoracic outlet syndrome.
Thoracic Outlet Syndrome
 Thoracic Outlet Syndrome Cristina Sola, BSN, RN-BC Nurse Manager Department of Cardiothoracic and Vascular Surgery McGovern Medical School The University of Texas Science Center at Houston Memorial Hermann
Thoracic Outlet Syndrome Cristina Sola, BSN, RN-BC Nurse Manager Department of Cardiothoracic and Vascular Surgery McGovern Medical School The University of Texas Science Center at Houston Memorial Hermann
A Patient s Guide to Ulnar Nerve Entrapment at the Wrist (Guyon s Canal Syndrome)
 A Patient s Guide to Ulnar Nerve Entrapment at the Wrist (Guyon s Canal Syndrome) Introduction The ulnar nerve is often called the funny bone at the elbow. However, there is little funny about injury to
A Patient s Guide to Ulnar Nerve Entrapment at the Wrist (Guyon s Canal Syndrome) Introduction The ulnar nerve is often called the funny bone at the elbow. However, there is little funny about injury to
 Nerve Compression Syndromes Median Nerve Carpal Tunnel Syndrome Pronator Syndrome Ulnar Nerve Cubital Tunnel Syndrome Ulnar Tunnel Syndrome TOS www.fisiokinesiterapia.biz Carpal Tunnel Syndrome (CTS) Definition
Nerve Compression Syndromes Median Nerve Carpal Tunnel Syndrome Pronator Syndrome Ulnar Nerve Cubital Tunnel Syndrome Ulnar Tunnel Syndrome TOS www.fisiokinesiterapia.biz Carpal Tunnel Syndrome (CTS) Definition
Paget-Schrötter Syndrome and the Thoracic Outlet. Carl Aschkenasi September 6, 2001
 Paget-Schrötter Syndrome and the Thoracic Outlet Carl Aschkenasi September 6, 2001 1 Our Patient: Acute onset left arm pain J.B. is a 44 yo male lawyer Has had a hx of occasional mild L arm pain on exertion
Paget-Schrötter Syndrome and the Thoracic Outlet Carl Aschkenasi September 6, 2001 1 Our Patient: Acute onset left arm pain J.B. is a 44 yo male lawyer Has had a hx of occasional mild L arm pain on exertion
Thoracic Outlet Syndrome
 James J. Lehman, DC, MBA, FACO Associate Professor of Clinical Sciences Director Health Sciences Postgraduate EducaCon University of Bridgeport Diagnosis is the key to successful treatment James J. Lehman,
James J. Lehman, DC, MBA, FACO Associate Professor of Clinical Sciences Director Health Sciences Postgraduate EducaCon University of Bridgeport Diagnosis is the key to successful treatment James J. Lehman,
Upper Plexus Thoracic Outlet Syndrome
 Neurol Med Chir (Tokyo) 42, 237 241, 2002 Upper Plexus Thoracic Outlet Syndrome Case Report Takeshi MATSUYAMA, KazuoOKUCHI, andkazuogoda* Department of Emergency and Critical Care Medicine, Nara Medical
Neurol Med Chir (Tokyo) 42, 237 241, 2002 Upper Plexus Thoracic Outlet Syndrome Case Report Takeshi MATSUYAMA, KazuoOKUCHI, andkazuogoda* Department of Emergency and Critical Care Medicine, Nara Medical
Pain Assessment Patient Interview (location/nature of symptoms), Body Diagram. Observation and Examination: Tests and Measures
 Examination of Upper Quarter Neurogenic Pain Jane Fedorczyk, PT, PhD, CHT Thomas Jefferson University, Philadelphia, PA Center of Excellence for Hand and Upper Limb Rehabilitation I. History Mechanism
Examination of Upper Quarter Neurogenic Pain Jane Fedorczyk, PT, PhD, CHT Thomas Jefferson University, Philadelphia, PA Center of Excellence for Hand and Upper Limb Rehabilitation I. History Mechanism
Most patients with neurologic thoracic outlet syndrome
 ORIGINAL ARTICLES: GENERAL THORACIC Upper Plexus Thoracic Outlet Syndrome: Optimal Therapy Harold C. Urschel, Jr, MD, and Maruf A. Razzuk, MD Division of Thoracic and Cardiovascular Surgery, The University
ORIGINAL ARTICLES: GENERAL THORACIC Upper Plexus Thoracic Outlet Syndrome: Optimal Therapy Harold C. Urschel, Jr, MD, and Maruf A. Razzuk, MD Division of Thoracic and Cardiovascular Surgery, The University
Symptoms and Referred Pain from Myofascial Trigger Points in the Anterior Scalene Muscle or Scalenus Anterior
 Symptoms and Referred Pain from Myofascial Trigger Points in the Anterior Scalene Muscle or Scalenus Anterior picture Symptoms and signs Aching or throbbing in the lateral forearm extending to thumb and
Symptoms and Referred Pain from Myofascial Trigger Points in the Anterior Scalene Muscle or Scalenus Anterior picture Symptoms and signs Aching or throbbing in the lateral forearm extending to thumb and
1. Which branch of the brachial plexus is most commonly involved in thoracic outlet syndrome compression?
 1 1. Which branch of the brachial plexus is most commonly involved in thoracic outlet syndrome compression? a. Musculocutaneous nerve b. Radial nerve c. Ulnar nerve d. Median nerve 2. Sensory symptoms
1 1. Which branch of the brachial plexus is most commonly involved in thoracic outlet syndrome compression? a. Musculocutaneous nerve b. Radial nerve c. Ulnar nerve d. Median nerve 2. Sensory symptoms
5 minutes: Attendance and Breath of Arrival. 50 minutes: Problem Solving Torso
 5 minutes: Attendance and Breath of Arrival 50 minutes: Problem Solving Torso Punctuality- everybody's time is precious: o o Be ready to learn by the start of class, we'll have you out of here on time
5 minutes: Attendance and Breath of Arrival 50 minutes: Problem Solving Torso Punctuality- everybody's time is precious: o o Be ready to learn by the start of class, we'll have you out of here on time
Lowe Plastic Surgery (LPS)
 Lowe Plastic Surgery (LPS) PATIENT EDUCATION FOR: CUMULATIVE TRAUMA DISORDER THE PROBLEM: There has been a remarkable increase in what is termed cumulative trauma disorder (CTD) in the last 20 years. Other
Lowe Plastic Surgery (LPS) PATIENT EDUCATION FOR: CUMULATIVE TRAUMA DISORDER THE PROBLEM: There has been a remarkable increase in what is termed cumulative trauma disorder (CTD) in the last 20 years. Other
Arm Pain, Numbness, and Tingling: Etiologies and Treatment
 Arm Pain, Numbness, and Tingling: Etiologies and Treatment Steve Fowler MD Confluence Health Department of Physiatry Education Medical School: University of Utah Residency: Mayo Clinic Work Confluence
Arm Pain, Numbness, and Tingling: Etiologies and Treatment Steve Fowler MD Confluence Health Department of Physiatry Education Medical School: University of Utah Residency: Mayo Clinic Work Confluence
82a Orthopedic Massage! Introduction - Thoracic Outlet"
 82a Orthopedic Massage! Introduction - Thoracic Outlet" 82a Orthopedic Massage! Introduction - Thoracic Outlet! Class Outline" 5 minutes" "Attendance, Breath of Arrival, and Reminders " 10 minutes "Lecture:"
82a Orthopedic Massage! Introduction - Thoracic Outlet" 82a Orthopedic Massage! Introduction - Thoracic Outlet! Class Outline" 5 minutes" "Attendance, Breath of Arrival, and Reminders " 10 minutes "Lecture:"
Critical Upper Limb Ischemia Due to Brachial Tourniquet in Misdiagnosed Thoracic Outlet Syndrome after Carpal Tunnel Decompression: A.
 2 Upper limb ischemia in misdiagnosed TOS Case Report Critical Upper Limb Ischemia Due to Brachial Tourniquet in Misdiagnosed Thoracic Outlet Syndrome after Carpal Tunnel Decompression: A Case Report Cesare
2 Upper limb ischemia in misdiagnosed TOS Case Report Critical Upper Limb Ischemia Due to Brachial Tourniquet in Misdiagnosed Thoracic Outlet Syndrome after Carpal Tunnel Decompression: A Case Report Cesare
TECHNOLOGY AND HOW WE USE IT TO DAMAGE OURSELVES WILLIAM A. DELP, DO ASSISTANT PROFESSOR OF OMM GA PCOM
 TECHNOLOGY AND HOW WE USE IT TO DAMAGE OURSELVES WILLIAM A. DELP, DO ASSISTANT PROFESSOR OF OMM GA PCOM OBJECTIVES Understand how we interact with technology new and old Understand how injury occurs Texting
TECHNOLOGY AND HOW WE USE IT TO DAMAGE OURSELVES WILLIAM A. DELP, DO ASSISTANT PROFESSOR OF OMM GA PCOM OBJECTIVES Understand how we interact with technology new and old Understand how injury occurs Texting
The Upper Limb III. The Brachial Plexus. Anatomy RHS 241 Lecture 12 Dr. Einas Al-Eisa
 The Upper Limb III The Brachial Plexus Anatomy RHS 241 Lecture 12 Dr. Einas Al-Eisa Brachial plexus Network of nerves supplying the upper limb Compression of the plexus results in motor & sensory changes
The Upper Limb III The Brachial Plexus Anatomy RHS 241 Lecture 12 Dr. Einas Al-Eisa Brachial plexus Network of nerves supplying the upper limb Compression of the plexus results in motor & sensory changes
University Journal of Medicine and Medical Specialities
 ISSN 2455-2852 2018, Vol. 4(5) Imaging Assessment of Vascular Thoracic Outlet Syndrome BALAJI A AYYAMPERUMAL Department of Radio Diagnosis,MADRAS MEDICAL COLLEGE AND GOVERNMENT GENERAL HOSPITAL Abstract
ISSN 2455-2852 2018, Vol. 4(5) Imaging Assessment of Vascular Thoracic Outlet Syndrome BALAJI A AYYAMPERUMAL Department of Radio Diagnosis,MADRAS MEDICAL COLLEGE AND GOVERNMENT GENERAL HOSPITAL Abstract
D E L L O N I N S T I T U T E S F O R P E R I P H E R A L N E R V E S U R G E R Y
 Thoracic Outlet (TOS), Winged Scapula, Brachial Plexus Compression 12 D E L L O N I N S T I T U T E S F O R P E R I P H E R A L N E R V E S U R G E R Y 1122 KENILWORTH DRIVE, SUITE 18, TOWSON, MARYLAND
Thoracic Outlet (TOS), Winged Scapula, Brachial Plexus Compression 12 D E L L O N I N S T I T U T E S F O R P E R I P H E R A L N E R V E S U R G E R Y 1122 KENILWORTH DRIVE, SUITE 18, TOWSON, MARYLAND
Compression of neural or vascular structures within the
 Thoracic Outlet Syndrome: Transaxillary Approach Margaret Clarke Tracci, MD, JD Compression of neural or vascular structures within the constrained space of the thoracic outlet may give rise to 3 separate
Thoracic Outlet Syndrome: Transaxillary Approach Margaret Clarke Tracci, MD, JD Compression of neural or vascular structures within the constrained space of the thoracic outlet may give rise to 3 separate
Otoshi K 1, Kaga T 1, Sato R 2, Igari T 2, Shishido H 2, Konno S 2, Itoh Y 3, Furushima K 3, Koga R 3
 35 th SITEMSH congress The prevalence and characteristics of TOS in high school baseball players Otoshi K 1, Kaga T 1, Sato R 2, Igari T 2, Shishido H 2, Konno S 2, Itoh Y 3, Furushima K 3, Koga R 3 1.
35 th SITEMSH congress The prevalence and characteristics of TOS in high school baseball players Otoshi K 1, Kaga T 1, Sato R 2, Igari T 2, Shishido H 2, Konno S 2, Itoh Y 3, Furushima K 3, Koga R 3 1.
Evaluation of Tingling and Numbness in the Upper Extremities
 Evaluation of Tingling and Numbness in the Upper Extremities DR. W. ANTHONY FRISELLA M.D. ADVANCED BONE & JOINT, ST CHARLES MO MONA 2018 Overview Polyneuropathy Compressive nerve lesions Carpal tunnel
Evaluation of Tingling and Numbness in the Upper Extremities DR. W. ANTHONY FRISELLA M.D. ADVANCED BONE & JOINT, ST CHARLES MO MONA 2018 Overview Polyneuropathy Compressive nerve lesions Carpal tunnel
A simple MRI technique for the assessment of thoracic outlet compression syndrome (TOCS)
 A simple MRI technique for the assessment of thoracic outlet compression syndrome (TOCS) Poster No.: C-3128 Congress: ECR 2010 Type: Scientific Exhibit Topic: Vascular Authors: E. Fanou, M. Cowling; Stoke-on-Trent/UK
A simple MRI technique for the assessment of thoracic outlet compression syndrome (TOCS) Poster No.: C-3128 Congress: ECR 2010 Type: Scientific Exhibit Topic: Vascular Authors: E. Fanou, M. Cowling; Stoke-on-Trent/UK
thopaedic Science Diagnosis and treatment of thoracic outlet syndrome* Instructional lecture
 J Orthop Sci (1997) 2:119-127 ~ Journal of thopaedic Science The Japanese Orthopaedic Association Instructional lecture Diagnosis and treatment of thoracic outlet syndrome* MASATAKA ABE, TADASHI SHIMAMURA,
J Orthop Sci (1997) 2:119-127 ~ Journal of thopaedic Science The Japanese Orthopaedic Association Instructional lecture Diagnosis and treatment of thoracic outlet syndrome* MASATAKA ABE, TADASHI SHIMAMURA,
Dr Ng Swee Cheng Senior Consultant Khoo Teck Puat Hospital
 Dr Ng Swee Cheng Senior Consultant Khoo Teck Puat Hospital 1. Soft Tissue Rheumatism 2. Myofascial Pain 3. Neurovascular compression Syndromes 4. Complex Regional Pain Syndromes Tendinitis, tenosynovitis
Dr Ng Swee Cheng Senior Consultant Khoo Teck Puat Hospital 1. Soft Tissue Rheumatism 2. Myofascial Pain 3. Neurovascular compression Syndromes 4. Complex Regional Pain Syndromes Tendinitis, tenosynovitis
Official Definition. Carpal tunnel syndrome, the most common focal peripheral neuropathy, results from compression of the median nerve at the wrist.
 Mod 2 MMT Course Official Definition Carpal tunnel syndrome, the most common focal peripheral neuropathy, results from compression of the median nerve at the wrist. epidemiology Affects an estimated 3
Mod 2 MMT Course Official Definition Carpal tunnel syndrome, the most common focal peripheral neuropathy, results from compression of the median nerve at the wrist. epidemiology Affects an estimated 3
CNS & PNS Entrapment. Disclosure - Nothing
 Peripheral Nerve Entrapments That Mimic Spinal Pathology: Evaluation And Treatment Both Medical And Surgical Michel Kliot MD Clinical Professor UCSF Department of NeuroSurgery Director Center For Evaluation
Peripheral Nerve Entrapments That Mimic Spinal Pathology: Evaluation And Treatment Both Medical And Surgical Michel Kliot MD Clinical Professor UCSF Department of NeuroSurgery Director Center For Evaluation
Sick Call Screener Course
 Sick Call Screener Course Musculoskeletal System Upper Extremities (2.7) 2.7-2-1 Enabling Objectives 1.46 Utilize the knowledge of musculoskeletal system anatomy while assessing a patient with a musculoskeletal
Sick Call Screener Course Musculoskeletal System Upper Extremities (2.7) 2.7-2-1 Enabling Objectives 1.46 Utilize the knowledge of musculoskeletal system anatomy while assessing a patient with a musculoskeletal
Thoracic Outlet Syndrome
 Thoracic Outlet Syndrome The Coraco-Pectoral Loop Environmental Stress Reinforcers Culture Behavioral Sick Role somatization Biological Genetics Physiology Psychological Emotional deficit Cog. Tendency
Thoracic Outlet Syndrome The Coraco-Pectoral Loop Environmental Stress Reinforcers Culture Behavioral Sick Role somatization Biological Genetics Physiology Psychological Emotional deficit Cog. Tendency
Normal ulnar nerve conduction velocity across the thoracic outlet: comparison of two measuring techniques
 Journal of Neurology, Neurosurgery, and Psychiatry, 1975, 38, 756-760 Normal ulnar nerve conduction velocity across the thoracic outlet: comparison of two measuring techniques GARY W. LONDON' From the
Journal of Neurology, Neurosurgery, and Psychiatry, 1975, 38, 756-760 Normal ulnar nerve conduction velocity across the thoracic outlet: comparison of two measuring techniques GARY W. LONDON' From the
American College of Occupational and Preventive Medicine 2011 Annual Meeting, Orlando, Florida, November 1, 2011
 CARPAL TUNNEL SYNDROME AN EVIDENCE-BASED PROTOCOL CARPAL TUNNEL SYNDROME Entrapment of the median nerve at the wrist Causing paresthesias, pain and occasional paralysis ICD-9 354.0 Patricia Meyer, D.O.,
CARPAL TUNNEL SYNDROME AN EVIDENCE-BASED PROTOCOL CARPAL TUNNEL SYNDROME Entrapment of the median nerve at the wrist Causing paresthesias, pain and occasional paralysis ICD-9 354.0 Patricia Meyer, D.O.,
RESEARCH IDEAS. Cervical Traction in Conservative Management of Thoracic Outlet Syndrome
 RESEARCH IDEAS Cervical Traction in Conservative Management of Thoracic Outlet Syndrome Mehmet Ali Taskaynatan Birol Balaban Evren Yasar Ahmet Ozgul Tunc Alp Kalyon ABSTRACT. Objective: The aim of this
RESEARCH IDEAS Cervical Traction in Conservative Management of Thoracic Outlet Syndrome Mehmet Ali Taskaynatan Birol Balaban Evren Yasar Ahmet Ozgul Tunc Alp Kalyon ABSTRACT. Objective: The aim of this
Introduction to Neurosurgical Subspecialties:
 Introduction to Neurosurgical Subspecialties: Spine Neurosurgery Brian L. Hoh, MD 1 and Gregory J. Zipfel, MD 2 1 University of Florida, 2 Washington University Spine Neurosurgery Spine neurosurgeons treat
Introduction to Neurosurgical Subspecialties: Spine Neurosurgery Brian L. Hoh, MD 1 and Gregory J. Zipfel, MD 2 1 University of Florida, 2 Washington University Spine Neurosurgery Spine neurosurgeons treat
Outcome of Surgical Treatment for Arterial Thoracic Outlet Syndrome
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 6 Ver. IV (June. 2017), PP 09-13 www.iosrjournals.org Outcome of Surgical Treatment for Arterial
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 6 Ver. IV (June. 2017), PP 09-13 www.iosrjournals.org Outcome of Surgical Treatment for Arterial
Objective Diagnosis (Ulnar Nerve Conduction Velocity) and Current Therapy of the Thoracic Outlet Syndrome
 Objective Diagnosis (Ulnar Nerve Conduction Velocity) and Current Therapy of the Thoracic Outlet Syndrome Harold C. Urschel, Jr., M.D., Maruf A. Razzuk, M.D., Richard E. Wood, M.D., Manaharlal Parekh,
Objective Diagnosis (Ulnar Nerve Conduction Velocity) and Current Therapy of the Thoracic Outlet Syndrome Harold C. Urschel, Jr., M.D., Maruf A. Razzuk, M.D., Richard E. Wood, M.D., Manaharlal Parekh,
Brachial Plexopathy in a Division I Football Player
 www.fisiokinesiterapia.biz Brachial Plexopathy in a Division I Football Player Brachial Plexus Injuries in Sport Typically a transient neurapraxia - 70% of injured players said they did not always report
www.fisiokinesiterapia.biz Brachial Plexopathy in a Division I Football Player Brachial Plexus Injuries in Sport Typically a transient neurapraxia - 70% of injured players said they did not always report
Manual therapy approach to the Patient with Carpal Tunnel Syndrome.
 Manual therapy approach to the Patient with Carpal Tunnel Syndrome www.fisiokinesiterapia.biz Symptoms and Signs Thumb, index, middle, and radial aspect of ring finger Hand Pain Paresthesia Numbness Pins
Manual therapy approach to the Patient with Carpal Tunnel Syndrome www.fisiokinesiterapia.biz Symptoms and Signs Thumb, index, middle, and radial aspect of ring finger Hand Pain Paresthesia Numbness Pins
Pseudothrombosis of the Subclavian Vein
 416507JDMXXX10.1177/8756479311416507Wash ko et al.journal of Diagnostic Medical Sonography Pseudothrombosis of the Subclavian Vein Journal of Diagnostic Medical Sonography 27(5) 231 235 The Author(s) 2011
416507JDMXXX10.1177/8756479311416507Wash ko et al.journal of Diagnostic Medical Sonography Pseudothrombosis of the Subclavian Vein Journal of Diagnostic Medical Sonography 27(5) 231 235 The Author(s) 2011
Thoracic outlet syndrome (TOS) results from compression
 Safety and Efficacy of the Supraclavicular Approach to Thoracic Outlet Decompression Thomas S. Maxey, MD, T. Brett Reece, MD, Peter I. Ellman, MD, Curtis G. Tribble, MD, Nancy Harthun, MD, Irving L. Kron,
Safety and Efficacy of the Supraclavicular Approach to Thoracic Outlet Decompression Thomas S. Maxey, MD, T. Brett Reece, MD, Peter I. Ellman, MD, Curtis G. Tribble, MD, Nancy Harthun, MD, Irving L. Kron,
SOME OBSERVATIONS CONCERNING PAIN IN THE NECK, UPPER CHEST, AND ARMS
 SOME OBSERVATIONS CONCERNING PAIN IN THE NECK, UPPER CHEST, AND ARMS JOHN TUCKER, M.D. Division of Internal Medicine The diagnosis of the specific neurologic lesion that produces pain in the neck and arm
SOME OBSERVATIONS CONCERNING PAIN IN THE NECK, UPPER CHEST, AND ARMS JOHN TUCKER, M.D. Division of Internal Medicine The diagnosis of the specific neurologic lesion that produces pain in the neck and arm
Chapter 2 Diagnostic Algorithms. 4 Traumatic Neck Pain Algorithm
 Chapter 2 Diagnostic Algorithms 4 Traumatic Neck Pain Algorithm Patient presents with a traumatic onset of neck pain. In general, radiographs should be ordered with a history of recent, significant trauma.
Chapter 2 Diagnostic Algorithms 4 Traumatic Neck Pain Algorithm Patient presents with a traumatic onset of neck pain. In general, radiographs should be ordered with a history of recent, significant trauma.
Common Upper Extremity Neuropathies (Not Carpal Tunnel Syndrome)
 Common Upper Extremity Neuropathies (Not Carpal Tunnel Syndrome) Nerve Compressions Common in adults, rare in children Frequently cause missed days of work and sleepless nights CDC 2001 26,794 cases of
Common Upper Extremity Neuropathies (Not Carpal Tunnel Syndrome) Nerve Compressions Common in adults, rare in children Frequently cause missed days of work and sleepless nights CDC 2001 26,794 cases of
Vascular Injuries in the Throwing Shoulder MLB Winter Meeting 2015
 Neurovascular Problems in the Throwing Athlete s Shoulder Professor, Department of Orthopedics Head, Section of Shoulder and Elbow Surgery Team Physician, Chicago White Sox and Bulls Chief Medical Editor,
Neurovascular Problems in the Throwing Athlete s Shoulder Professor, Department of Orthopedics Head, Section of Shoulder and Elbow Surgery Team Physician, Chicago White Sox and Bulls Chief Medical Editor,
Thoracic Outlet Syndrome, Part 1: New proposed classification system
 Thoracic Outlet Syndrome, Part 1: New proposed classification system Written by: Dr. Bahram Jam, PT Advanced Physical Therapy Education Institute (APTEI), Thornhill, ON, Canada January 3, 2017 Article
Thoracic Outlet Syndrome, Part 1: New proposed classification system Written by: Dr. Bahram Jam, PT Advanced Physical Therapy Education Institute (APTEI), Thornhill, ON, Canada January 3, 2017 Article
Case 1. Your diagnosis
 Case 1 44-year-old midwife presented with intermittent pins and needles in the little and ring fingers with blanching. Symptoms were exacerbated by cold exposure. Your diagnosis Diagnosis Hypothenar syndrome
Case 1 44-year-old midwife presented with intermittent pins and needles in the little and ring fingers with blanching. Symptoms were exacerbated by cold exposure. Your diagnosis Diagnosis Hypothenar syndrome
Distal chronic spinal muscular atrophy involving the hands
 Journal ofneurology, Neurosurgery, and Psychiatry, 1978, 41, 653-658 Distal chronic spinal muscular atrophy involving the hands D. J. O'SULLIVAN AND J. G. McLEOD From St Vincent's Hospital, and Department
Journal ofneurology, Neurosurgery, and Psychiatry, 1978, 41, 653-658 Distal chronic spinal muscular atrophy involving the hands D. J. O'SULLIVAN AND J. G. McLEOD From St Vincent's Hospital, and Department
Use of First Rib Mobilization and Muscle Energy Techniques to Treat a Patient with Thoracic Outlet Syndrome: A Case Report
 Use of First Rib Mobilization and Muscle Energy Techniques to Treat a Patient with Thoracic Outlet Syndrome: A Case Report Cody Moldenhauer, SPT & Thomas Pahnke, MS, PT, ATC Abstract Title: Use of First
Use of First Rib Mobilization and Muscle Energy Techniques to Treat a Patient with Thoracic Outlet Syndrome: A Case Report Cody Moldenhauer, SPT & Thomas Pahnke, MS, PT, ATC Abstract Title: Use of First
INTRODUCTION Cubital Tunnel Syndrome
 INTRODUCTION Cubital Tunnel Syndrome Diagram of the ulnar nerve supplying the muscles of forearm and hand Cubital Tunnel is a condition that refers to the ulnar nerve being compressed around the elbow.
INTRODUCTION Cubital Tunnel Syndrome Diagram of the ulnar nerve supplying the muscles of forearm and hand Cubital Tunnel is a condition that refers to the ulnar nerve being compressed around the elbow.
Case Report. Annals of Rehabilitation Medicine INTRODUCTION CASE REPORT
 Case Report Ann Rehabil Med 2013;37(6):896-900 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2013.37.6.896 Annals of Rehabilitation Medicine Thoracic Outlet Syndrome Caused by Schwannoma
Case Report Ann Rehabil Med 2013;37(6):896-900 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2013.37.6.896 Annals of Rehabilitation Medicine Thoracic Outlet Syndrome Caused by Schwannoma
Physical examination protocol in the study of VPT and nerve conduction in working women with and without chronic pain
 Physical examination protocol in the study of VPT and nerve conduction in working women with and without chronic pain ID number General health OK Affected Height cm Weight kg Heart OK Arrhythmia Murmurs
Physical examination protocol in the study of VPT and nerve conduction in working women with and without chronic pain ID number General health OK Affected Height cm Weight kg Heart OK Arrhythmia Murmurs
Electrodiagnostics for Back & Neck Pain. Steven Andersen, MD Providence Physiatry Clinic
 Electrodiagnostics for Back & Neck Pain Steven Andersen, MD Providence Physiatry Clinic Electrodiagnostics Electromyography (EMG) Needle EMG exam (NEE) Nerve conduction studies (NCS) Motor Sensory Late
Electrodiagnostics for Back & Neck Pain Steven Andersen, MD Providence Physiatry Clinic Electrodiagnostics Electromyography (EMG) Needle EMG exam (NEE) Nerve conduction studies (NCS) Motor Sensory Late
#SPECIALTESTFRIDAY- Roos Test Friday 8 th May Roos Test Friday 15 th May Adsons Test Friday 22 nd May
 #PODCASTTUESDAY W/C 11.4.15 AM Problem Solving Shoulders part 3 Anju Jaggi and Prof Ginn #AHPSPodcasts W/C 18.5.15 AM Problem Solving Biomechanics and pain: The ongoing dilemma with Greg Lehman Shoulders
#PODCASTTUESDAY W/C 11.4.15 AM Problem Solving Shoulders part 3 Anju Jaggi and Prof Ginn #AHPSPodcasts W/C 18.5.15 AM Problem Solving Biomechanics and pain: The ongoing dilemma with Greg Lehman Shoulders
Physical Examination of the Shoulder
 General setup Patient will be examined in both the seated and supine position so exam table needed 360 degree access to patient Expose neck and both shoulders (for comparison); female in gown or sports
General setup Patient will be examined in both the seated and supine position so exam table needed 360 degree access to patient Expose neck and both shoulders (for comparison); female in gown or sports
Work Related Musculoskeletal Disorders
 Work Related Musculoskeletal Disorders Upper Extremity Disorders Carpel tunnel syndrome Cubital tunnel syndrome Thoracic outlet syndrome Raynaud s syndrome (white finger) Rotator cuff syndrome DeQuervain
Work Related Musculoskeletal Disorders Upper Extremity Disorders Carpel tunnel syndrome Cubital tunnel syndrome Thoracic outlet syndrome Raynaud s syndrome (white finger) Rotator cuff syndrome DeQuervain
American Board of Physical Medicine & Rehabilitation. Part I Curriculum & Weights
 American Board of Physical Medicine & Rehabilitation Part I Curriculum & Weights Neurologic Disorders 30% Stroke Spinal Cord Injury Traumatic Brain Injury Neuropathies a) Mononeuropathies b) Polyneuropathies
American Board of Physical Medicine & Rehabilitation Part I Curriculum & Weights Neurologic Disorders 30% Stroke Spinal Cord Injury Traumatic Brain Injury Neuropathies a) Mononeuropathies b) Polyneuropathies
Interesting Case Series. Posterior Interosseous Nerve Compression
 Interesting Case Series Posterior Interosseous Nerve Compression Jeon Cha, BMedSci, MBBS, Blair York, MBChB, and John Tawfik, MBBS, BPharm, FRACS The Sydney Hospital Hand Unit, Sydney Hospital and Sydney
Interesting Case Series Posterior Interosseous Nerve Compression Jeon Cha, BMedSci, MBBS, Blair York, MBChB, and John Tawfik, MBBS, BPharm, FRACS The Sydney Hospital Hand Unit, Sydney Hospital and Sydney
Hand and wrist emergencies
 Chapter1 Hand and wrist emergencies Carl A. Germann Distal radius and ulnar injuries PEARL: Fractures of the distal radius and ulna are the most common type of fractures in patients younger than 75 years.
Chapter1 Hand and wrist emergencies Carl A. Germann Distal radius and ulnar injuries PEARL: Fractures of the distal radius and ulna are the most common type of fractures in patients younger than 75 years.
An Osteopathic Approach to Upper Extremity Pain Syndromes. Laura Griffin, D.O. FAAO American Academy of Osteopathy OMED 2014
 An Osteopathic Approach to Upper Extremity Pain Syndromes Laura Griffin, D.O. FAAO American Academy of Osteopathy OMED 2014 Outline Differential diagnosis for upper extremity pain Clinical presentations
An Osteopathic Approach to Upper Extremity Pain Syndromes Laura Griffin, D.O. FAAO American Academy of Osteopathy OMED 2014 Outline Differential diagnosis for upper extremity pain Clinical presentations
Bilateral arterial thoracic outlet syndrome with intermittent subclavian artery occlusion
 Case Report Bilateral arterial thoracic outlet syndrome with intermittent subclavian artery occlusion Arterial thoracic outlet syndrome presentation is frequently misdiagnosed because of its varied clinical
Case Report Bilateral arterial thoracic outlet syndrome with intermittent subclavian artery occlusion Arterial thoracic outlet syndrome presentation is frequently misdiagnosed because of its varied clinical
Nerves of Upper limb. Dr. Brijendra Singh Professor & Head Department of Anatomy AIIMS Rishikesh
 Nerves of Upper limb Dr. Brijendra Singh Professor & Head Department of Anatomy AIIMS Rishikesh 1 Objectives Origin, course & relation of median & ulnar nerves. Motor & sensory distribution Carpal tunnel
Nerves of Upper limb Dr. Brijendra Singh Professor & Head Department of Anatomy AIIMS Rishikesh 1 Objectives Origin, course & relation of median & ulnar nerves. Motor & sensory distribution Carpal tunnel
Department of Anesthesia, Critical Care and Pain Medicine Massachusetts General Hospital, Boston, Mass
 Feature article Neurogenic thoracic outlet syndrome: An often overlooked but treatable condition Rely primarily on a patient s history and your physical examination findings in considering the diagnosis.
Feature article Neurogenic thoracic outlet syndrome: An often overlooked but treatable condition Rely primarily on a patient s history and your physical examination findings in considering the diagnosis.
Dynamic Neuromobilization for the Treatment of Thoracic Outlet Syndrome Courtney Convey and Dr. Erickson
 Dynamic Neuromobilization for the Treatment of Thoracic Outlet Syndrome Courtney Convey and Dr. Erickson Abstract Title: Dynamic Neuromobilization for the Treatment of Thoracic Outlet Syndrome Background:
Dynamic Neuromobilization for the Treatment of Thoracic Outlet Syndrome Courtney Convey and Dr. Erickson Abstract Title: Dynamic Neuromobilization for the Treatment of Thoracic Outlet Syndrome Background:
Is This Really a Musculoskeletal Problem?
 Is This Really a Musculoskeletal Problem? UCSF Orthopedics Primary Care Sports Medicine Anthony Luke MD, MPH Annual Review in Family Medicine 2015 Disclosures Founder, RunSafe Founder & CEO, SportZPeak
Is This Really a Musculoskeletal Problem? UCSF Orthopedics Primary Care Sports Medicine Anthony Luke MD, MPH Annual Review in Family Medicine 2015 Disclosures Founder, RunSafe Founder & CEO, SportZPeak
Upper extremity paraesthesia: Clinical assessment and reasoning
 Journal of Bodywork and Movement Therapies (2008) 12, 268 273 Journal of Bodywork and Movement Therapies www.intl.elsevierhealth.com/journals/jbmt CASE REVIEW Upper extremity paraesthesia: Clinical assessment
Journal of Bodywork and Movement Therapies (2008) 12, 268 273 Journal of Bodywork and Movement Therapies www.intl.elsevierhealth.com/journals/jbmt CASE REVIEW Upper extremity paraesthesia: Clinical assessment
Sign up to receive ATOTW weekly -
 1 SUBCLAVIAN PERIVASCULAR BRACHIAL PLEXUS BLOCK ANAESTHESIA TUTORIAL OF THE WEEK 156 19 th OCTOBER 2009 Dr. Martin Herrick Department of Anaesthesia, Addenbrooke s Hospital, Cambridge, U.K. Correspondence
1 SUBCLAVIAN PERIVASCULAR BRACHIAL PLEXUS BLOCK ANAESTHESIA TUTORIAL OF THE WEEK 156 19 th OCTOBER 2009 Dr. Martin Herrick Department of Anaesthesia, Addenbrooke s Hospital, Cambridge, U.K. Correspondence
Assessment of the Brachial Plexus EMG Course CNSF Halifax Fraser Moore, Canadian Society of Clinical Neurophysiology McGill University
 Assessment of the Brachial Plexus EMG Course CNSF Halifax 2018 Fraser Moore, Canadian Society of Clinical Neurophysiology McGill University Angela Scott, Association of Electromyography Technologists of
Assessment of the Brachial Plexus EMG Course CNSF Halifax 2018 Fraser Moore, Canadian Society of Clinical Neurophysiology McGill University Angela Scott, Association of Electromyography Technologists of
CARPAL TUNNEL SYNDROME (CTS)
 CARPAL TUNNEL SYNDROME (CTS) CTS: why does it matter? Fairly prevalent Early detection may prevent permanent impairment 1 To review: Learning Objectives Signs/symptoms Causes Management prevention treatment
CARPAL TUNNEL SYNDROME (CTS) CTS: why does it matter? Fairly prevalent Early detection may prevent permanent impairment 1 To review: Learning Objectives Signs/symptoms Causes Management prevention treatment
Osteopathic Considerations in Shoulder Pain. Kristen Brusky DO February 22, 2018
 Osteopathic Considerations in Shoulder Pain Kristen Brusky DO February 22, 2018 Overview Importance of pectoral girdle Ligaments, ligaments tensegrity Bones, joints, muscles Neurovasculature Innervation
Osteopathic Considerations in Shoulder Pain Kristen Brusky DO February 22, 2018 Overview Importance of pectoral girdle Ligaments, ligaments tensegrity Bones, joints, muscles Neurovasculature Innervation
Multiple variations involving all the terminal branches of the brachial plexus and the axillary artery a case report
 SHORT REPORT Eur J Anat, 10 (3): 61-66 (2006) Multiple variations involving all the terminal branches of the brachial plexus and the axillary artery a case report K. Ramachandran, I. Kanakasabapathy and
SHORT REPORT Eur J Anat, 10 (3): 61-66 (2006) Multiple variations involving all the terminal branches of the brachial plexus and the axillary artery a case report K. Ramachandran, I. Kanakasabapathy and
STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 5. September 30, 2011
 STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 5 September 30, 2011 PART l. Answer in the space provided. (12 pts) 1. Identify the structures. (2 pts) EXAM NUMBER A. Suprascapular nerve B. Axillary nerve
STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 5 September 30, 2011 PART l. Answer in the space provided. (12 pts) 1. Identify the structures. (2 pts) EXAM NUMBER A. Suprascapular nerve B. Axillary nerve
Making sense of Nerve conduction & EMG
 Making sense of Nerve conduction & EMG Drs R Arunachalam Consultant Clinical Neurophysiologist Wessex Neurological Centre Southampton University Hospital EMG/NCS EMG machine For the assessment of patients
Making sense of Nerve conduction & EMG Drs R Arunachalam Consultant Clinical Neurophysiologist Wessex Neurological Centre Southampton University Hospital EMG/NCS EMG machine For the assessment of patients
OMM for the Family Physician OMED 2014 Seattle Washington
 OMM for the Family Physician OMED 2014 Seattle Washington Kevin D. Treffer, D.O., FACOFP Associate Professor Interim Chair, Department of OMM KCUMB-COM Objectives At the end of the session the attendee
OMM for the Family Physician OMED 2014 Seattle Washington Kevin D. Treffer, D.O., FACOFP Associate Professor Interim Chair, Department of OMM KCUMB-COM Objectives At the end of the session the attendee
Referral Criteria: Carpal Tunnel Syndrome Feb
 Referral Criteria: Carpal Tunnel Syndrome Feb 2019 1 5.2. Carpal Tunnel Syndrome Background Carpal tunnel syndrome present with non-traumatic tingling of the fingers due to compression of the median nerve
Referral Criteria: Carpal Tunnel Syndrome Feb 2019 1 5.2. Carpal Tunnel Syndrome Background Carpal tunnel syndrome present with non-traumatic tingling of the fingers due to compression of the median nerve
SPECTRUM NEUROLOGY GROUP
 SPECTRUM NEUROLOGY GROUP On-Site Diagnostic Testing Patient Care with Quality About Spectrum Neurology Group... Patient Care With Quality Spectrum Neurology Group (SNG), leaders in diagnostic testing,
SPECTRUM NEUROLOGY GROUP On-Site Diagnostic Testing Patient Care with Quality About Spectrum Neurology Group... Patient Care With Quality Spectrum Neurology Group (SNG), leaders in diagnostic testing,
Common Elbow Problems
 Common Elbow Problems Duncan Ferguson FRACS Knee and Shoulder Specialist Elbow Instability Common 10-25% of elbow injuries Median age 30 yrs Most simple dislocations are stable after reduction recurrence
Common Elbow Problems Duncan Ferguson FRACS Knee and Shoulder Specialist Elbow Instability Common 10-25% of elbow injuries Median age 30 yrs Most simple dislocations are stable after reduction recurrence
Inhibition Associated with somatic dysfunctions, no matter which components are impaired Implies consideration of all components in treatment planning
 Somatic Dysfunction Impaired or altered function of related components of the somatic system including the skeletal, arthrodial, myofascial structures and their related vascular, lymphatic and neural elements.
Somatic Dysfunction Impaired or altered function of related components of the somatic system including the skeletal, arthrodial, myofascial structures and their related vascular, lymphatic and neural elements.
Diagnosis of Neck & Upper Extremity Pain
 Diagnosis of Neck & Upper Extremity Pain David B. Bumpass, MD Assistant Professor, Spine Surgery UAMS Depts. of Orthopaedic Surgery & Neurosurgery May 12, 2018 Disclosures Medtronic Spine speaking fees
Diagnosis of Neck & Upper Extremity Pain David B. Bumpass, MD Assistant Professor, Spine Surgery UAMS Depts. of Orthopaedic Surgery & Neurosurgery May 12, 2018 Disclosures Medtronic Spine speaking fees
Peripheral Vascular Examination. Dr. Gary Mumaugh Western Physical Assessment
 Peripheral Vascular Examination Dr. Gary Mumaugh Western Physical Assessment Competencies 1. Inspection of upper extremity for: size symmetry swelling venous pattern color Texture nail beds Competencies
Peripheral Vascular Examination Dr. Gary Mumaugh Western Physical Assessment Competencies 1. Inspection of upper extremity for: size symmetry swelling venous pattern color Texture nail beds Competencies
Elbow. Chapter 2 LISTEN. Mechanism of Injury (If Applicable) Pain
 Chapter 2 Elbow LISTEN Mechanism of Injury (If Applicable) Patient usually remembers their position at the time of injury Certain mechanisms of injury result in characteristic patterns Fall on outstretched
Chapter 2 Elbow LISTEN Mechanism of Injury (If Applicable) Patient usually remembers their position at the time of injury Certain mechanisms of injury result in characteristic patterns Fall on outstretched
Current Developments in the Prevention and Treatment of Repetitive Motion Injuries of the Upper Extremity
 Current Developments in the Prevention and Treatment of Repetitive Motion Injuries of the Upper Extremity D. Mowry 1 Mowry, D. 1995. Current Development in the Prevention and Treatment of Repetitive Motion
Current Developments in the Prevention and Treatment of Repetitive Motion Injuries of the Upper Extremity D. Mowry 1 Mowry, D. 1995. Current Development in the Prevention and Treatment of Repetitive Motion
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Acetaminophen, in neck pain, 505 506 Acupuncture, chi and, 524 for mechanical neck disorders, 525 in neck pain, 524 525 safety of, 525 Adson
Note: Page numbers of article titles are in boldface type. A Acetaminophen, in neck pain, 505 506 Acupuncture, chi and, 524 for mechanical neck disorders, 525 in neck pain, 524 525 safety of, 525 Adson
Thoracic Spine Applied Anatomy. Jason Zafereo, PT, OCS, FAAOMPT
 Thoracic Spine Applied Anatomy Jason Zafereo, PT, OCS, FAAOMPT Clinical i l Orthopedic Rehabilitation ti Education 1 Objectives Discuss red flag signs for the thoracic region Apply key concepts from the
Thoracic Spine Applied Anatomy Jason Zafereo, PT, OCS, FAAOMPT Clinical i l Orthopedic Rehabilitation ti Education 1 Objectives Discuss red flag signs for the thoracic region Apply key concepts from the
4/3/2014. Disclosures. Venous Thoracic Outlet Syndrome: Our Approach and Results. Paget Schroetter Syndrome. Paget Schroetter Syndrome.
 Disclosures No relevant financial relationships with commercial interests Venous Thoracic Outlet Syndrome: Our Approach and Julie A. Freischlag, M.D. Vice Chancellor for Human Health Sciences Dean of the
Disclosures No relevant financial relationships with commercial interests Venous Thoracic Outlet Syndrome: Our Approach and Julie A. Freischlag, M.D. Vice Chancellor for Human Health Sciences Dean of the
Upper Extremity Venous Duplex. Michigan Sonographers Society Fall Ultrasound Symposium October 15, 2016
 Upper Extremity Venous Duplex Michigan Sonographers Society Fall Ultrasound Symposium October 15, 2016 Patricia A. (Tish) Poe, BA RVT FSVU Director of Quality Assurance Navix Diagnostix Patricia A. Poe
Upper Extremity Venous Duplex Michigan Sonographers Society Fall Ultrasound Symposium October 15, 2016 Patricia A. (Tish) Poe, BA RVT FSVU Director of Quality Assurance Navix Diagnostix Patricia A. Poe
Eco-color-doppler of the upper extremity: technique, indications and semeiotics
 Eco-color-doppler of the upper extremity: technique, indications and semeiotics Poster No.: C-0029 Congress: ECR 2012 Type: Educational Exhibit Authors: S. Pollice, P. Pollice, R. Stanzione, P. Maggi,
Eco-color-doppler of the upper extremity: technique, indications and semeiotics Poster No.: C-0029 Congress: ECR 2012 Type: Educational Exhibit Authors: S. Pollice, P. Pollice, R. Stanzione, P. Maggi,
Peet etal 1 first used the term thoracic
 Review Article Thoracic Outlet Syndrome John E. Kuhn, MD George F. Lebus V, MD Jesse E. Bible, MD Abstract Thoracic outlet syndrome is a well-described disorder caused by thoracic outlet compression of
Review Article Thoracic Outlet Syndrome John E. Kuhn, MD George F. Lebus V, MD Jesse E. Bible, MD Abstract Thoracic outlet syndrome is a well-described disorder caused by thoracic outlet compression of
Clinical examination of the wrist, thumb and hand
 Clinical examination of the wrist, thumb and hand 20 CHAPTER CONTENTS Referred pain 319 History 319 Inspection 320 Functional examination 320 The distal radioulnar joint.............. 320 The wrist.......................
Clinical examination of the wrist, thumb and hand 20 CHAPTER CONTENTS Referred pain 319 History 319 Inspection 320 Functional examination 320 The distal radioulnar joint.............. 320 The wrist.......................
RECIPES FOR RATINGS !!! A. FIBROMYALGIA: 0% WPI P. 569 B. THORACIC OUTLET SYNDROME 0% WPI P. 569 C. MYOFASCIAL PAIN SYNDROME 0% WPI P.
 RECIPES FOR RATINGS 1. THE "0% WPI" RATINGS A. FIBROMYALGIA: 0% WPI P. 569 B. THORACIC OUTLET SYNDROME 0% WPI P. 569 C. MYOFASCIAL PAIN SYNDROME 0% WPI P. 569 D. TENDINITIS OF UPPER EXTREMITY 0% WPI P.
RECIPES FOR RATINGS 1. THE "0% WPI" RATINGS A. FIBROMYALGIA: 0% WPI P. 569 B. THORACIC OUTLET SYNDROME 0% WPI P. 569 C. MYOFASCIAL PAIN SYNDROME 0% WPI P. 569 D. TENDINITIS OF UPPER EXTREMITY 0% WPI P.
IAIABC 2003 Upper Extremity Impairment Guides Part 3 of the Supplemental Impairment Rating Guides
 IAIABC 2003 Upper Extremity Impairment Guides Part 3 of the Supplemental Impairment Rating Guides Draft 11-03 IAIABC Executive Office 5610 Medical Circle, Suite 14 Madison, WI 53719 Phone: (608) 663-6355
IAIABC 2003 Upper Extremity Impairment Guides Part 3 of the Supplemental Impairment Rating Guides Draft 11-03 IAIABC Executive Office 5610 Medical Circle, Suite 14 Madison, WI 53719 Phone: (608) 663-6355
The supraclavicular approach to scalenectomy and first rib resection: Description of technique
 The supraclavicular approach to scalenectomy and first rib resection: Description of technique Richard J. Sanders, M.D., and Susan Raymer, Denver, Colo. Supraclavicular first rib resection has been performed
The supraclavicular approach to scalenectomy and first rib resection: Description of technique Richard J. Sanders, M.D., and Susan Raymer, Denver, Colo. Supraclavicular first rib resection has been performed
Brachial plexus blockade within the interscalene groove involves local anesthetic
 Interscalene Brachial Plexus Block- How I do it. Part 1 of a 2 part discussion on technique. Stuart Grant Professor of Anesthesiology Duke University Medical Center Durham NC Brachial plexus blockade within
Interscalene Brachial Plexus Block- How I do it. Part 1 of a 2 part discussion on technique. Stuart Grant Professor of Anesthesiology Duke University Medical Center Durham NC Brachial plexus blockade within
