Thoracic outlet syndrome (TOS) results from compression
|
|
|
- Gervais Marshall
- 6 years ago
- Views:
Transcription
1 Safety and Efficacy of the Supraclavicular Approach to Thoracic Outlet Decompression Thomas S. Maxey, MD, T. Brett Reece, MD, Peter I. Ellman, MD, Curtis G. Tribble, MD, Nancy Harthun, MD, Irving L. Kron, MD, and John A. Kern, MD Division of Thoracic and Cardiovascular Surgery, University of Virginia Health Science Center, Charlottesville, Virginia Background. Thoracic outlet syndrome (TOS) is a clinical diagnosis encountered by both thoracic and vascular surgeons. The goal of surgical therapy involves relieving compression of the neurovascular structures at the superior thoracic aperture. The traditional approach to thoracic outlet decompression has been transaxillary; however more centers are moving toward a more tailored approach through a supraclavicular incision. Methods. The medical records of 67 patients who underwent surgical decompression between 1993 and 2001 for TOS were retrospectively reviewed. Patient demographics and early outcome were assessed through clinic follow-up. Results. Seventy-two thoracic outlet decompressions were performed on 67 patients with the diagnosis of TOS. Five patients underwent bilateral thoracic outlet decompression. All operations in this time period were safely accomplished through a supraclavicular approach. The syndromes associated with thoracic outlet compression were neurogenic (n 59), venous (n 10), and arterial (n 3). Forty-six of 72 (63.9%) operations resulted in complete resolution of symptoms, 17 cases (23.6%) had partial resolution, and 9 patients (12.5%) had no resolution. There were no deaths and morbidity was minimal with 6 complications (8.3%). Conclusions. The supraclavicular approach is a safe and effective technique in managing all forms of thoracic outlet compression. (Ann Thorac Surg 2003;76: ) 2003 by The Society of Thoracic Surgeons Thoracic outlet syndrome (TOS) results from compression of the neurovascular structures at the superior thoracic aperture. The syndrome has been attributed to cervical ribs, long transverse processes, first thoracic ribs, compression by the scalene muscles, clavicle fractures, and tumors at the thoracic outlet [1]. Regardless of the etiology, external compression can occur upon the subclavian artery, subclavian vein or brachial plexus and produce myriad symptoms. The various syndromes and presentations of TOS are related to which structure or structures are compressed. The role of operative intervention for TOS is controversial and not well established. Indications for operative management include both subjective and objective evidence of neurovascular compression at the thoracic outlet. There is also a difference of opinion as to which patients are candidates for operation, with some believing physical therapy is adequate treatment [2 4]. Despite these differences surgery is often performed to treat TOS. The surgical procedure to manage TOS has continued to evolve from a posterior approach [5] to the transaxillary approach [1, 6]. In more recent years the supraclavicular incision and exposure has become a popular technique for thoracic decompression. For the past decade we have decompressed all forms of Presented at the Forty-ninth Annual Meeting of the Southern Thoracic Surgical Association, Miami, FL, Nov 7 9, Address reprint requests to Dr Kern, University of Virginia Health Science Center, Box , Charlottesville, VA 22908; jak3r@virginia.edu. TOS using supraclavicular exposure. To assess the safety and efficacy of this approach we reviewed our institutional experience with the surgical management of TOS through a supraclavicular approach. Patients and Methods The medical records of patients surgically managed for TOS between June 1993 and June 2001 were retrospectively reviewed. All patients were decompressed through a supraclavicular incision. Early outcomes (14 to 24 months) were assessed through follow-up clinic visits and were categorized as complete response (no residual symptoms, complete range of motion, and able to return to all previous activities without restriction), partial response (some residual symptoms but able to return to most activities), or no response (no change from preoperative state). Operative Technique All patients are operated upon using general anesthesia. A supraclavicular incision is made one fingerbreadth above the clavicle extending 5 to 7 cm. The platysma is divided and subplatysmal flaps are created. The omohyoid is divided and the scalene fat pad is dissected and retracted laterally. For all patients with neurogenic or arterial TOS, first rib resection is carried out in the following manner. The phrenic nerve is carefully mobilized and retracted medially. The anterior scalene is divided 1 cm above its insertion onto the first rib. The 2003 by The Society of Thoracic Surgeons /03/$30.00 Published by Elsevier Inc PII S (03)
2 Ann Thorac Surg MAXEY ET AL 2003;76: THORACIC OUTLET DECOMPRESSION subclavian artery is mobilized and encircled with vessel loops. Any abnormalities in the artery requiring repair mandates further dissection and mobilization of the artery. The brachial plexus is dissected from surrounding tissues medially and laterally and the middle scalene laterally and the first rib medially are identified. The middle scalene is divided lateral to the plexus with care to avoid injury to the long thoracic nerve. The medial and lateral edges of the first rib are palpated and the intercostal muscle attachments are divided bluntly and sharply. The rib is then divided posteriorly with a rongeur just distal to the transverse process. The intercostal muscle attachments are divided from the inferolateral aspect of the rib and the rib is transected anteriorly under the clavicle. This results in a small fragment of the most anterior segment of the first rib remaining. This small segment plays no role in neurogenic or arterial compression and is left in place. Any arterial reconstruction is carried out at this point. Cervical ribs are easily resected through this same incision, and are identified just superior to the posterior aspect of the first thoracic rib. Patients with venous TOS undergo a more tailored approach. A supraclavicular incision is made as described above. Patients without previous clavicular trauma, and evidence of a normal vein (documented by venogram after thrombolysis), undergo first rib resection as described above. The remaining most anterior segment of the first rib is removed through an infraclavicular incision. Symptomatic patients with venous TOS requiring more extensive subclavian vein reconstruction may require clavicular resection. This technique decompresses as well as exposes the entire subclavian vein for reconstruction. Once the clavicle is resected the subclavian vein is easily dissected out from the axillary vein and its branches laterally to the junction with the internal jugular vein medially. The vein is then opened, thrombus is removed, and if needed, venous reconstruction is carried out. The venotomy is closed with a vein patch. Results This cohort was composed of 67 patients. Five of these patients required bilateral thoracic outlet decompression bringing the total number of cases to 72. There were 41 women (mean age 34.1 years) and 25 men (mean age 37.7 years). Fifty-nine (82%) of the cases were neurogenic in origin, 3 (4.2%) had arterial symptoms, and 10 (13.8%) had venous thrombosis (Fig 1). Complete resolution was obtained in 46 of 72 (63.9%) of cases, partial resolution in 17 (23.6%), and no resolution in 9 (12.5%). The no resolution group was comprised entirely of neurogenic TOS. Sixty-six percent of the no resolution group had previous neck or shoulder injuries. Twenty-two percent of the no resolution cohort had undergone at least one previous surgery to the neck or shoulder girdle or both. Fifty-four percent of our entire cohort were laborers, whereas 78% of the no resolution group were laborers. All patients with arterial or venous compression had at least partial resolution with 75% of them having complete resolution Fig 1. Incidence of compressive syndromes included in the study. Solid section arterial; dotted section neurogenic; shaded section venous. (Fig 2) Within the entire cohort a supraclavicular incision safely allowed for 14 cervical rib resections, 64 first thoracic rib resections, 5 claviculectomies, and 7 vascular procedures. A supraclavicular incision alone was used in all but 3 cases, and in these 3 cases an infraclavicular counter incision was used to gain access to the most medial aspect of the first rib for completed decompression of the subclavian vein. There were no deaths and morbidity was 8.3%. Complications consisted of 2 pneumothoracies, 2 hematomas, 1 temporary phrenic nerve palsy, and 1 traction injury to the brachial plexus. Comment The three clinical entities of TOS arise from neural, venous, or arterial compression. These entities sometimes coexist but more often occur independently. The diagnosis and workup of TOS is fairly straightforward; however the management decisions are not uniform and can be challenging. Surgery is often considered the primary treatment yet the surgical approach has been questioned. Compression of the subclavian artery represents fewer than 5% TOS and may result in ischemia and aneurysmal dilation and may even be limb threatening. Arterial compression at the thoracic outlet is almost always asso- Fig 2. Overall outcome (response to thoracic decompression) of each compressive syndrome. Solid bars arterial; dotted bars neurogenic; shaded bars venous. 397 GENERAL THORACIC
3 398 MAXEY ET AL Ann Thorac Surg THORACIC OUTLET DECOMPRESSION 2003;76: ciated with a cervical rib [7]. The 3 patients with arterial compression in this series had bilateral cervical ribs. Longstanding arterial compression leads to stenosis at the thoracic outlet. These changes can cause fibrosis and often manifest as poststenotic dilation. None of our patients manifested any aneurysmal changes; however all had evidence of thrombosis, distal embolization and ischemia. The treatment of arterial complications secondary to compression at the thoracic outlet is surgery. During surgery one must be prepared to address and treat the three anatomic components of this disease process: arterial compression, arterial lesions, and distal emboli. The ideal surgical approach to thoracic decompression with associated arterial disease is one that allows complete exposure for cervical and first rib resection as well as the ability to address associated arterial lesions. We believe the ability to address the key issues associated with arterial compression are more easily accomplished through a supraclavicular rather than the standard transaxillary approach. In our series cervical and first rib resections as well as arterial repairs were safely and successfully accomplished through a supraclavicular approach. All patients had resolution of their arterial symptoms. Primary axillary-subclavian vein thrombosis or Paget- Schroetter syndrome typically afflicts younger patients and constitutes only 4% to 12% of thoracic outlet symptoms in most reports and only 13.9% of our review [8]. Historically the treatment of subclavian vein thrombosis was rest and anticoagulation. It was not until investigators understood the underlying physiology of primary thrombosis (venous compression at the thoracic outlet) that advances in therapy were made. Today it is well accepted that the optimal treatment of subclavian vein thrombosis requires early restoration of luminal patency and surgical removal of any extrinsic compression, usually a first rib resection [9]. Venous TOS often results from more medial compression, either by the anteromedial portion of the first rib or by the costoclavicular ligament. Extensive first rib resection can not be achieved through a supraclavicula incision alone and the addition of an infraclavicular incision is frequently required. The additional exposure provided by this counter incision allows for complete decompression of the vein through division of the subclavious muscle and costoclavicular ligament as well as complete resection of the most medial aspect of the first rib. Through these two incisions the entire subclavian vein can be decompressed and any external venolysis of adhesions can easily be carried out. Three of the 10 patients with venous disease underwent this operation. Occasionally patients are encountered who require more extensive subclavian vein reconstruction. This is usually associated with unsuccessful thrombolysis or significant intraluminal defects after lysis. We have found clavicular resection not only decompresses the vein but also provides excellent exposure to the entire subclavian vein for reconstruction. This technique is particularly useful for patients with previous clavicular fractures and bony pannus growth as a cause for their venous obstruction. For these patients, of whom there were 5, the supraclavicular incision was extended laterally and the clavicle was exposed. Medially the clavicle is disarticulated from the manubrium and the lateral dissection is carried out to the acromion. Once the decision is made to remove the clavicle and repair the vein, there is no need for rib resection as the vein is now decompressed. We believe a common mistake is to not remove enough clavicle. All patients in our cohort who had resection of their clavicles (n 5) have returned to their prior employment with no significant disability related to the clavicle resection. Of note is that 1 of these patients is a welder and another is a lumberjack. Venous compression at the thoracic outlet can be challenging. The flexibility offered by the supraclavicular approach easily allows us to tailor our technique, even intraoperatively, to each patient s needs. Eight of 10 patients (80%) with venous thrombosis had complete resolution of symptoms and 20% had partial resolution. This subgroup of patients has maintained a 100% vein patency rate and no morbidity. Perhaps no subject generates more controversy in cardiothoracic and vascular surgery circles than the diagnosis and treatment of neurogenic thoracic outlet syndrome. The majority of thoracic outlet cases reported in the literature as well as in our study fall within the disputed neurologic classification. The incidence of neurogenic TOS is controversial. Some authors [10, 11] quote an incidence of 8% of the general population while others [12] doubt its existence entirely. Eighty-two percent of our cohort was classified as having neurogenic TOS. The affect of blunt chest and shoulder trauma on brachial plexus neuropathies is not well defined. In our series a history of shoulder or neck trauma was noted in 49% of patients surgically managed for neurogenic TOS with 24% of those having at least one previous neck or shoulder surgery or both. Neck and shoulder trauma is the most common predisposing factor for neurogenic TOS with a reported incidence near 80% [13]. In our series previous trauma appears to be a predictor of poor outcome after surgical decompression. Fifty-five percent of previously injured patients in our series had a less than complete response. The symptoms in this subset of patients may be attributed to direct muscle injury, traction injury to nerve roots, or simply arthritic changes and have no component of neurovascular compression at the thoracic outlet. Evaluation of this group of patients may require a more thorough, multidisciplinary approach as well as a more prolonged course of conservative therapy. In our series the neurogenic subset of patients had the poorest outcome. Seventeen percent of this cohort had no resolution of symptoms. These outcomes are consistent with other similar series evaluating a transaxillary approach [14, 15]. The difference in outcome observed in neurogenic compression compared with vascular forms of TOS is notable. Only 9 patients (12.5%) of our cohort had no resolution of symptoms after thoracic decompression. This subset consisted solely of patients with the preoperative diagnosis of neurogenic TOS. Seven of 9 (78%) were laborers, all but 1 of whom was previously
4 Ann Thorac Surg MAXEY ET AL 2003;76: THORACIC OUTLET DECOMPRESSION 399 injured and had been unsuccessfully treated for shoulder or neck injuries. Three of these 7 patients had at least one surgery for these injuries before being evaluated for TOS. Despite these results there is an acceptable rate of success from supraclavicular thoracic decompression for neurogenic TOS. Seventy-eight percent of patients surgically treated for neurogenic TOS had improved symptoms, with 56% demonstrating complete resolution. Clearly accurate patient selection is essential for excellent operative outcome and minimal morbidity. When evaluating patients referred with the suspected diagnosis of neurogenic TOS one can not be too cautious. No one protocol or battery of test is appropriate for all patients. Thoroughly considering the patients history (previous shoulder-neck injury or surgery, noninvasive therapy, and previous diagnostics) we tailor our workup to each patients. Understanding that no one diagnostic modality is 100% sensitive and specific for neurogenic compression at the thoracic outlet, these measures are used only to strengthen our clinical diagnosis. Thoracic outlet syndrome is one of the most controversial symptom complexes in surgery. The surgical approach has been altered over the last several decades with variable results. Our experience with the supraclavicular approach has provided excellent results and outcomes comparable with those of groups using a transaxillary approach (Fig 3). In our experience the exposure provided by this technique is safe and superior to that of other approaches and allows for a wide range of surgical maneuvers required to manage all forms of thoracic outlet syndrome. GENERAL THORACIC References Fig 3. Response to decompression using a supraclavicular approach compared with similar reports of thoracic decompression using a transaxillary approach. (Dotted bars Leffert; vertical striped bars Sharp; shaded bars Lingren; horizontal striped bars supraclavicular approach.) 1. Urschel HC, Razzuk MA. Neurovascular compression of the thoracic outlet: changing management over 50 years. Ann Surg 1998;228: Lindgren K. Conservative treatment of thoracic outlet syndrome: a 2-year follow up. Arch Phys Med Rehabil 1997;78: Walsh MT. Therapist management of thoracic outlet syndrome. J Hand Ther 1994;7: Kenny RA, Traynor GB, Withington D, Keegan DJ. Thoracic outlet syndrome: a useful exercise option. Am J Surg 1993; 165: Clagett OT. Presidential address: research and prosearch. J Thorac Cardiovasc Surg 44: Roos DB. Thoracic outlet syndrome. Arch Surg 1966;93: Blank RH, Connar RG. Arterial complications associated with thoracic outlet syndrome. Ann Thorac Surg 1994;17: Machleder H. Veno-occlusive disorders of the upper extremity. Curr Prob Surg 1988;25: Urshcel HC Jr, Razzuk MA. Improved management of the Paget-Schroetter syndrome secondary to thoracic outlet compression. Ann Thorac Surg 1991;52: Urschel HC Jr, Razzuk MA. Neurovascular compression in the thoracic outlet. Ann Surg 1998;228: Roos DR. Thoracic outlet syndrome is underdiagnosed. Muscle Nerve 1999;22: Wilbourn AJ. The thoracic outlet syndrome is overdiagnosed. Arch Neurol 1990;47: Sanders R. Results of the surgical treatment for thoracic outlet syndrome. Semin Thorac Cardiovasc Surg 1996;8: Leffert RD, Perlmutter GS. Thoracic outlet syndrome: results of 282 transaxillary first rib resections. Clin Orthop 1999;228: Lindgren KA, Oksala I. Long-term outcome of surgery for thoracic outlet syndrome. Am J Surg 1995;169: DISCUSSION DR HAROLD C. URSCHEL, JR (Dallas, TX): I would like to congratulate Dr Maxey on an excellent preparation of his data and clear presentation to us here. One of the points that he mentioned is that this approach is good for all types of thoracic outlet syndrome. Our principle has always been that anybody operating should know all the approaches technically, be familiar with them, and able to perform them. What he chooses to do is what he is most comfortable with and safest, as you have done here, and I think that is excellent. I had the opportunity of reading Dr Maxey s paper. The 7 cases that did not respond quite possibly had an error in diagnosis since they did not get better and then get worse, such as with scarring. I would like to ask you what your opinion is of those 7 cases, whether they had carpal tunnel or any other type of compression, a multiple crush syndrome, ala Mackinnon, or what do you think is the reason they did not get a response, because your operations are done very well and anatomically correct as far as I can see? The total claviculectomy was the operation done when I started in thoracic outlet syndrome by Lord, and we reported actually 40 cases together at one time. This is a wonderful approach if you are going to patch the vein. If you take the clavicle off, you get wonderful exposure of the vein, which is much more difficult through the transaxillary approach. We do not do any thrombectomies. We have not for about 15 years, so that we are comfortable still through the transaxillary approach. I think this is a much better incision for the thrombectomy or the patching vein procedure.
5 400 MAXEY ET AL Ann Thorac Surg THORACIC OUTLET DECOMPRESSION 2003;76: Finally, I would just like to recognize one of these young guys on my left here who sat through that last paper of Osler Abbott and Tiki. His name is Dr Daughtry. He is one of the founding members of this organization, the eighth president and the oldest living president. DR MAXEY: Thank you, Dr Urschel, for your comments. I will start with the patients who did not respond to surgical decompression. Those were 7 patients all with neurogenic thoracic outlet syndrome. Using the supraclavicular approach we aim to resect as much of the first rib as possible as well as perform an anterior scalenectomy and neurolysis of the plexus. These patients often have other more distal compressive syndromes, such as ulnar nerve compression and/or carpal tunnel syndrome. We have become much more conservative with patients with the presumed diagnosis of neurogenic compression, and are very attentive to other possible etiologies of their symptoms. To address the issue of our claviculectomy patients, we had five clavicle resections: four of those patients were men, two of whom were welders and lumberjacks. We had no significant morbidity; similar to the experience you and Lord described several years back. Your point is well taken; however, that a thin, young female requiring claviculectomy may have more of a cosmetic concern than that we typically experience with more muscular males. DR JOSEPH I. MILLER (Atlanta, GA): Just a couple of comments. In Georgia, to my knowledge there are only three surgeons performing this operation: myself, Dr Mansour, and one of our vascular surgeons. Between Dr Mansour and myself, we have done a few more than 110 cases, not anything like Dr Urschel has previously reported, and that has been in a 29-year period. We have done these all through the transaxillary approach, and our results have essentially been the same as you have reported. We have had two reoperations for bleeding. My questions concerning the supraclavicular approach are as follows. We have tended to utilize that approach only for the upper plexus syndrome previously reported by Dr Hal Urschel in the Annals of Thoracic Surgery and think it works well with that but we have been unable to do a complete resection of the first rib through the supraclavicular approach. It may be due to our inexperience, but also our vascular surgeon, who is pretty well experienced in this, has been unable to excise completely the first rib. But you stated in your talk that you were able to do a complete resection of the first rib. My questions are, firstly, what percentage of your patients have no objective measurable index and only physical findings of thoracic outlet syndrome that I guess you would call them traumatic, but that is, they have no measurable index either through Doppler, ulnar nerve conduction, EMG or whatever type study, and you are only going on physical findings? Secondly, how do you manage complete resection of the entire first rib through the supraclavicular approach? At times that I have done that, I have found it quite difficult, and I have previously discussed with Drs Mackinnon and Patterson at Washington University, and they do not feel that they can resect the entire rib, but they resect the pathologic area of involvement, which has been more parallel with our experience. DR MAXEY: Those are excellent points. As far as first rib resection through the supraclavicular approach, there is no problem whatsoever resecting the most posterior, lateral aspect of the first rib. Gaining access to the most medial portion of the anterior first rib is what provides us difficulty. Leaving a small portion of the most medial aspect of the first rib has no effect whatsoever in patients with neurogenic and arterial disease and the supraclavicular approach is more than adequate. Patients that we do need access to the most medial aspect of that first rib are those patients with Paget-Schroetters. In these circumstances, we use the counterincision, which I described. This incision adds no more morbidity yet provides tremendous exposure to allow us to completely decompress the vein. As far as patients and their diagnostic workup, certainly arterial and venous diseases are fairly straightforward. We typically rely first on noninvasive studies followed by an angiogram or venogram. These techniques are usually highly sensitive and specific for arterial and venous compression. The controversy arises with the neurogenic patients. These are patients who oftentimes have been worked up to the hilt from their primary care doctors, physical therapists, and chiropractors. Certainly in these complicated patients we do a very detailed history and physical examination, but do not hesitate to get more precise imaging modalities, CT scan, MRI, to rule out any disk disease or cervical stenosis, and I think the role of conduction studies is quite evident from Dr Urschel s published work. You do, however, need to rule out more distal entrapment syndromes. That is, make sure the ulnar nerve is not entrapped and no evidence of carpal tunnel syndrome is present. I think utilizing all of these modalities decreases one s chances of operative failure from thoracic decompression by allowing one to choose the correct patient most likely to have excellent results.
Compression of neural or vascular structures within the
 Thoracic Outlet Syndrome: Transaxillary Approach Margaret Clarke Tracci, MD, JD Compression of neural or vascular structures within the constrained space of the thoracic outlet may give rise to 3 separate
Thoracic Outlet Syndrome: Transaxillary Approach Margaret Clarke Tracci, MD, JD Compression of neural or vascular structures within the constrained space of the thoracic outlet may give rise to 3 separate
THORACIC OUTLET SYNDROME: A FREQUENT CAUSE OF NON-DISCOGENIC BRACHIALGIA
 THORACIC OUTLET SYNDROME: A FREQUENT CAUSE OF NON-DISCOGENIC BRACHIALGIA Debora Garozzo Brachial Plexus and Peripheral Nerve Surgery Unit Neurospinal Hospital Dubai, United Arab Emirates THE THORACIC OUTLET
THORACIC OUTLET SYNDROME: A FREQUENT CAUSE OF NON-DISCOGENIC BRACHIALGIA Debora Garozzo Brachial Plexus and Peripheral Nerve Surgery Unit Neurospinal Hospital Dubai, United Arab Emirates THE THORACIC OUTLET
Thoracic Outlet Syndrome
 Disclosures None relevant to this discussion The Management of Thoracic Outlet Syndrome: Acute Charles Eichler MD Professor, Department of Surgery Division of Vascular and Endovascular Surgery University
Disclosures None relevant to this discussion The Management of Thoracic Outlet Syndrome: Acute Charles Eichler MD Professor, Department of Surgery Division of Vascular and Endovascular Surgery University
THORACIC OUTLET SYNDROME (T.O.S.) Prof J van Marle
 THORACIC OUTLET SYNDROME (T.O.S.) Prof J van Marle 1. Definition Clinical syndrome caused by compression of the neurovascular bundle as it passes through the thoracic outlet, a narrow space bordered by
THORACIC OUTLET SYNDROME (T.O.S.) Prof J van Marle 1. Definition Clinical syndrome caused by compression of the neurovascular bundle as it passes through the thoracic outlet, a narrow space bordered by
THORACIC OUTLET DECOMPRESSION
 THORACIC OUTLET DECOMPRESSION Thesis Submitted in partial fulfillment of the degree of M.D. in general surgery By Abd El Aty Mohammed Sakr Supervised by Prof. Dr. Amr Ahmed Gad Prof. of vascular surgery
THORACIC OUTLET DECOMPRESSION Thesis Submitted in partial fulfillment of the degree of M.D. in general surgery By Abd El Aty Mohammed Sakr Supervised by Prof. Dr. Amr Ahmed Gad Prof. of vascular surgery
The supraclavicular approach to scalenectomy and first rib resection: Description of technique
 The supraclavicular approach to scalenectomy and first rib resection: Description of technique Richard J. Sanders, M.D., and Susan Raymer, Denver, Colo. Supraclavicular first rib resection has been performed
The supraclavicular approach to scalenectomy and first rib resection: Description of technique Richard J. Sanders, M.D., and Susan Raymer, Denver, Colo. Supraclavicular first rib resection has been performed
4/3/2014. Disclosures. Venous Thoracic Outlet Syndrome: Our Approach and Results. Paget Schroetter Syndrome. Paget Schroetter Syndrome.
 Disclosures No relevant financial relationships with commercial interests Venous Thoracic Outlet Syndrome: Our Approach and Julie A. Freischlag, M.D. Vice Chancellor for Human Health Sciences Dean of the
Disclosures No relevant financial relationships with commercial interests Venous Thoracic Outlet Syndrome: Our Approach and Julie A. Freischlag, M.D. Vice Chancellor for Human Health Sciences Dean of the
Most patients with neurologic thoracic outlet syndrome
 ORIGINAL ARTICLES: GENERAL THORACIC Upper Plexus Thoracic Outlet Syndrome: Optimal Therapy Harold C. Urschel, Jr, MD, and Maruf A. Razzuk, MD Division of Thoracic and Cardiovascular Surgery, The University
ORIGINAL ARTICLES: GENERAL THORACIC Upper Plexus Thoracic Outlet Syndrome: Optimal Therapy Harold C. Urschel, Jr, MD, and Maruf A. Razzuk, MD Division of Thoracic and Cardiovascular Surgery, The University
Emergency Approach to the Subclavian and Innominate Vessels
 Emergency Approach to the Subclavian and Innominate Vessels Joseph J. Amato, M.D., Robert M. Vanecko, M.D., See Tao Yao, M.D., and Milton Weinberg, Jr., M.D. T he operative approach to an acutely injured
Emergency Approach to the Subclavian and Innominate Vessels Joseph J. Amato, M.D., Robert M. Vanecko, M.D., See Tao Yao, M.D., and Milton Weinberg, Jr., M.D. T he operative approach to an acutely injured
Thoracic outlet syndrome: first rib resection
 Review rticle Page 1 of 7 Thoracic outlet syndrome: first rib resection ornelis G. Vos 1, Çag das Ünlü 1, Michiel T. Voûte 2, Rob H. W. van de Mortel 3, Jean-Paul P. M. de Vries 3 1 Department of Surgery,
Review rticle Page 1 of 7 Thoracic outlet syndrome: first rib resection ornelis G. Vos 1, Çag das Ünlü 1, Michiel T. Voûte 2, Rob H. W. van de Mortel 3, Jean-Paul P. M. de Vries 3 1 Department of Surgery,
D E L L O N I N S T I T U T E S F O R P E R I P H E R A L N E R V E S U R G E R Y
 Thoracic Outlet (TOS), Winged Scapula, Brachial Plexus Compression 12 D E L L O N I N S T I T U T E S F O R P E R I P H E R A L N E R V E S U R G E R Y 1122 KENILWORTH DRIVE, SUITE 18, TOWSON, MARYLAND
Thoracic Outlet (TOS), Winged Scapula, Brachial Plexus Compression 12 D E L L O N I N S T I T U T E S F O R P E R I P H E R A L N E R V E S U R G E R Y 1122 KENILWORTH DRIVE, SUITE 18, TOWSON, MARYLAND
Vascular Injuries in the Throwing Shoulder MLB Winter Meeting 2015
 Neurovascular Problems in the Throwing Athlete s Shoulder Professor, Department of Orthopedics Head, Section of Shoulder and Elbow Surgery Team Physician, Chicago White Sox and Bulls Chief Medical Editor,
Neurovascular Problems in the Throwing Athlete s Shoulder Professor, Department of Orthopedics Head, Section of Shoulder and Elbow Surgery Team Physician, Chicago White Sox and Bulls Chief Medical Editor,
Richard Dobrusin DO FACOFP
 Richard Dobrusin DO FACOFP Define Thoracic Outlet Syndrome (TOS) Describe the Mechanisms of Dysfunction List Diagnostic tests for (TOS) Understand (TOS) referral patterns Discuss Treatment Options Definition:
Richard Dobrusin DO FACOFP Define Thoracic Outlet Syndrome (TOS) Describe the Mechanisms of Dysfunction List Diagnostic tests for (TOS) Understand (TOS) referral patterns Discuss Treatment Options Definition:
Thoracic Outlet Syndrome
 Thoracic Outlet Syndrome Cristina Sola, BSN, RN-BC Nurse Manager Department of Cardiothoracic and Vascular Surgery McGovern Medical School The University of Texas Science Center at Houston Memorial Hermann
Thoracic Outlet Syndrome Cristina Sola, BSN, RN-BC Nurse Manager Department of Cardiothoracic and Vascular Surgery McGovern Medical School The University of Texas Science Center at Houston Memorial Hermann
Paget-Schrötter Syndrome and the Thoracic Outlet. Carl Aschkenasi September 6, 2001
 Paget-Schrötter Syndrome and the Thoracic Outlet Carl Aschkenasi September 6, 2001 1 Our Patient: Acute onset left arm pain J.B. is a 44 yo male lawyer Has had a hx of occasional mild L arm pain on exertion
Paget-Schrötter Syndrome and the Thoracic Outlet Carl Aschkenasi September 6, 2001 1 Our Patient: Acute onset left arm pain J.B. is a 44 yo male lawyer Has had a hx of occasional mild L arm pain on exertion
University Journal of Medicine and Medical Specialities
 ISSN 2455-2852 2018, Vol. 4(5) Imaging Assessment of Vascular Thoracic Outlet Syndrome BALAJI A AYYAMPERUMAL Department of Radio Diagnosis,MADRAS MEDICAL COLLEGE AND GOVERNMENT GENERAL HOSPITAL Abstract
ISSN 2455-2852 2018, Vol. 4(5) Imaging Assessment of Vascular Thoracic Outlet Syndrome BALAJI A AYYAMPERUMAL Department of Radio Diagnosis,MADRAS MEDICAL COLLEGE AND GOVERNMENT GENERAL HOSPITAL Abstract
Upper Plexus Thoracic Outlet Syndrome
 Neurol Med Chir (Tokyo) 42, 237 241, 2002 Upper Plexus Thoracic Outlet Syndrome Case Report Takeshi MATSUYAMA, KazuoOKUCHI, andkazuogoda* Department of Emergency and Critical Care Medicine, Nara Medical
Neurol Med Chir (Tokyo) 42, 237 241, 2002 Upper Plexus Thoracic Outlet Syndrome Case Report Takeshi MATSUYAMA, KazuoOKUCHI, andkazuogoda* Department of Emergency and Critical Care Medicine, Nara Medical
Outcome of Surgical Treatment for Arterial Thoracic Outlet Syndrome
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 6 Ver. IV (June. 2017), PP 09-13 www.iosrjournals.org Outcome of Surgical Treatment for Arterial
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 6 Ver. IV (June. 2017), PP 09-13 www.iosrjournals.org Outcome of Surgical Treatment for Arterial
The treatment of Paget-Schroetter syndrome or effort
 Reoperations After Failed Transaxillary First Rib Resection to Treat Paget-Schroetter Syndrome Patients J. Ernesto Molina, MD Division of Cardiothoracic Surgery, University of Minnesota, Medical School,
Reoperations After Failed Transaxillary First Rib Resection to Treat Paget-Schroetter Syndrome Patients J. Ernesto Molina, MD Division of Cardiothoracic Surgery, University of Minnesota, Medical School,
SAMPLE CHAPTERS UNESCO-EOLSS MANAGEMENT OF SUBCLAVIAN VEIN THROMBOSIS KNOWN AS PAGET-SCHROETTER SYNDROME
 MANAGEMENT OF SUBCLAVIAN VEIN THROMBOSIS KNOWN AS PAGETSCHROETTER SYNDROME J. Ernesto Molina University of Minnesota, Minneapolis, Minnesota, U.S.A. Keywords: Thoracic outlet, Venous disease Contents 1.
MANAGEMENT OF SUBCLAVIAN VEIN THROMBOSIS KNOWN AS PAGETSCHROETTER SYNDROME J. Ernesto Molina University of Minnesota, Minneapolis, Minnesota, U.S.A. Keywords: Thoracic outlet, Venous disease Contents 1.
Video-assisted thoracoscopic surgery for intrathoracic first rib resection in thoracic outlet syndrome
 Original Article Video-assisted thoracoscopic surgery for intrathoracic first rib resection in thoracic outlet syndrome Jinwook Hwang, Byung-Ju Min, Won-Min Jo, Jae Seung Shin Department of Thoracic and
Original Article Video-assisted thoracoscopic surgery for intrathoracic first rib resection in thoracic outlet syndrome Jinwook Hwang, Byung-Ju Min, Won-Min Jo, Jae Seung Shin Department of Thoracic and
Pseudothrombosis of the Subclavian Vein
 416507JDMXXX10.1177/8756479311416507Wash ko et al.journal of Diagnostic Medical Sonography Pseudothrombosis of the Subclavian Vein Journal of Diagnostic Medical Sonography 27(5) 231 235 The Author(s) 2011
416507JDMXXX10.1177/8756479311416507Wash ko et al.journal of Diagnostic Medical Sonography Pseudothrombosis of the Subclavian Vein Journal of Diagnostic Medical Sonography 27(5) 231 235 The Author(s) 2011
Objective Diagnosis (Ulnar Nerve Conduction Velocity) and Current Therapy of the Thoracic Outlet Syndrome
 Objective Diagnosis (Ulnar Nerve Conduction Velocity) and Current Therapy of the Thoracic Outlet Syndrome Harold C. Urschel, Jr., M.D., Maruf A. Razzuk, M.D., Richard E. Wood, M.D., Manaharlal Parekh,
Objective Diagnosis (Ulnar Nerve Conduction Velocity) and Current Therapy of the Thoracic Outlet Syndrome Harold C. Urschel, Jr., M.D., Maruf A. Razzuk, M.D., Richard E. Wood, M.D., Manaharlal Parekh,
Alexander C Vlantis. Selective Neck Dissection 33
 05 Modified Radical Neck Dissection Type II Alexander C Vlantis Selective Neck Dissection 33 Modified Radical Neck Dissection Type II INCISION Various incisions can be used for a neck dissection. The incision
05 Modified Radical Neck Dissection Type II Alexander C Vlantis Selective Neck Dissection 33 Modified Radical Neck Dissection Type II INCISION Various incisions can be used for a neck dissection. The incision
Subclavian vein obstruction without thrombosis
 Subclavian vein obstruction without thrombosis Richard J. Sanders, MD, a and Sharon L. Hammond, MD, a,b Denver, Colo Background: Unilateral arm swelling caused by subclavian vein obstruction without thrombosis
Subclavian vein obstruction without thrombosis Richard J. Sanders, MD, a and Sharon L. Hammond, MD, a,b Denver, Colo Background: Unilateral arm swelling caused by subclavian vein obstruction without thrombosis
Resection of malignant tumors invading the thoracic inlet
 Resection of Superior Sulcus Tumors: Anterior Approach Marc de Perrot, MD, MSc Resection of malignant tumors invading the thoracic inlet represents a technical challenge because of the complex anatomy
Resection of Superior Sulcus Tumors: Anterior Approach Marc de Perrot, MD, MSc Resection of malignant tumors invading the thoracic inlet represents a technical challenge because of the complex anatomy
thoracic outlet syndrome
 29 thoracic outlet syndrome N. Garcia-Henriquez, K.A. Illig Thoracic outlet syndrome (TOS) is a term describing one or more patterns of symptoms as a result of compression of the neurovascular bundle at
29 thoracic outlet syndrome N. Garcia-Henriquez, K.A. Illig Thoracic outlet syndrome (TOS) is a term describing one or more patterns of symptoms as a result of compression of the neurovascular bundle at
2 Aortic Arch Debranching UCSF Vascular Symposium /14/16. J Endovasc Ther 2002;9:suppl 2; II98 105
 How I Do It: Aortic Arch Debranching Exposures, Tunnels and Techniques Warren Gasper MD Assistant Professor of Surgery UCSF Vascular Surgery No disclosures 2 Aortic Arch Debranching UCSF Vascular Symposium
How I Do It: Aortic Arch Debranching Exposures, Tunnels and Techniques Warren Gasper MD Assistant Professor of Surgery UCSF Vascular Surgery No disclosures 2 Aortic Arch Debranching UCSF Vascular Symposium
THORACIC OUTLET SYNDROME AND THE OVERHEAD ATHLETE LISA PIROPATO, PT, DPT, ATC NORTHEAST INDIANA SPORTS MEDICINE SYMPOSIUM MARCH 25, 2017
 THORACIC OUTLET SYNDROME AND THE OVERHEAD ATHLETE LISA PIROPATO, PT, DPT, ATC NORTHEAST INDIANA SPORTS MEDICINE SYMPOSIUM MARCH 25, 2017 LEARNING OBJECTIVES Explain the etiologies of thoracic outlet syndrome.
THORACIC OUTLET SYNDROME AND THE OVERHEAD ATHLETE LISA PIROPATO, PT, DPT, ATC NORTHEAST INDIANA SPORTS MEDICINE SYMPOSIUM MARCH 25, 2017 LEARNING OBJECTIVES Explain the etiologies of thoracic outlet syndrome.
Surgical approach for DVT. Division of Vascular Surgery Department of Surgery Seoul National University College of Medicine
 Surgical approach for DVT Seung-Kee Min Division of Vascular Surgery Department of Surgery Seoul National University College of Medicine Treatment Options for Venous Thrombosis Unfractionated heparin &
Surgical approach for DVT Seung-Kee Min Division of Vascular Surgery Department of Surgery Seoul National University College of Medicine Treatment Options for Venous Thrombosis Unfractionated heparin &
Treatment of acute thrombosis of axillo-subclavian vein
 Treatment of acute thrombosis of axillo-subclavian vein Yang Jin Park Vascular Surgery, Samsung Medical Center Sungkyunkwan University School of Medicine CASE A 32-year-old male patient 3-day history of
Treatment of acute thrombosis of axillo-subclavian vein Yang Jin Park Vascular Surgery, Samsung Medical Center Sungkyunkwan University School of Medicine CASE A 32-year-old male patient 3-day history of
The Brachial Plexus and Thoracic Outlet Syndrome
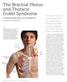 The Brachial Plexus and Thoracic Outlet Syndrome Understanding Signs and Symptoms By Joseph E. Muscolino, DC The brachial plexus of nerves and the subclavian/axillary artery and vein comprise a neurovascular
The Brachial Plexus and Thoracic Outlet Syndrome Understanding Signs and Symptoms By Joseph E. Muscolino, DC The brachial plexus of nerves and the subclavian/axillary artery and vein comprise a neurovascular
Karl A. Illig, MD, and Mathew Wooster, MD
 Neurogenic Thoracic Outlet Syndrome Karl A. Illig, MD, and Mathew Wooster, MD Perhaps no condition treated by vascular surgeons has been associated with more confusion, subjectivity, and nihilism than
Neurogenic Thoracic Outlet Syndrome Karl A. Illig, MD, and Mathew Wooster, MD Perhaps no condition treated by vascular surgeons has been associated with more confusion, subjectivity, and nihilism than
Michael Meuse, M.D. Vascular and Interventional Radiology
 Michael Meuse, M.D. Vascular and Interventional Radiology Iliac Vein Compression Syndrome Left CIV compressed by right CIA Virchow 1851: DVT L>R May and Thurner 1954: venous spurs Cockett and Thomas 1965:
Michael Meuse, M.D. Vascular and Interventional Radiology Iliac Vein Compression Syndrome Left CIV compressed by right CIA Virchow 1851: DVT L>R May and Thurner 1954: venous spurs Cockett and Thomas 1965:
Management of Brachial Plexus & Peripheral Nerves Blast Injuries. First Global Conflict Medicine Congress
 Management of Brachial Plexus & Peripheral Nerves Blast Injuries Joseph BAKHACH First Global Conflict Medicine Congress Hand & Microsurgery Department American University of Beirut Medical Centre Brachial
Management of Brachial Plexus & Peripheral Nerves Blast Injuries Joseph BAKHACH First Global Conflict Medicine Congress Hand & Microsurgery Department American University of Beirut Medical Centre Brachial
Tumors of the thoracic apex, even when benign,
 Anterior Cervical Transsternal Approach for Resection of Benign Tumors at the Thoracic Inlet George Ladas, MD, Peter H. Rhys-Evans, FRCS, and Peter Goldstraw, FRCS Department of Thoracic Surgery, Royal
Anterior Cervical Transsternal Approach for Resection of Benign Tumors at the Thoracic Inlet George Ladas, MD, Peter H. Rhys-Evans, FRCS, and Peter Goldstraw, FRCS Department of Thoracic Surgery, Royal
Case 1. Your diagnosis
 Case 1 44-year-old midwife presented with intermittent pins and needles in the little and ring fingers with blanching. Symptoms were exacerbated by cold exposure. Your diagnosis Diagnosis Hypothenar syndrome
Case 1 44-year-old midwife presented with intermittent pins and needles in the little and ring fingers with blanching. Symptoms were exacerbated by cold exposure. Your diagnosis Diagnosis Hypothenar syndrome
Thoracic Outlet Syndrome
 Thoracic Outlet Syndrome Part 1: The Scalene Triangle TOS: Vascular Symptom Presentation Venous persistent/intermittent edema heaviness and fatigue deep pain in neck/shoulder increased pain at night warm
Thoracic Outlet Syndrome Part 1: The Scalene Triangle TOS: Vascular Symptom Presentation Venous persistent/intermittent edema heaviness and fatigue deep pain in neck/shoulder increased pain at night warm
Critical Upper Limb Ischemia Due to Brachial Tourniquet in Misdiagnosed Thoracic Outlet Syndrome after Carpal Tunnel Decompression: A.
 2 Upper limb ischemia in misdiagnosed TOS Case Report Critical Upper Limb Ischemia Due to Brachial Tourniquet in Misdiagnosed Thoracic Outlet Syndrome after Carpal Tunnel Decompression: A Case Report Cesare
2 Upper limb ischemia in misdiagnosed TOS Case Report Critical Upper Limb Ischemia Due to Brachial Tourniquet in Misdiagnosed Thoracic Outlet Syndrome after Carpal Tunnel Decompression: A Case Report Cesare
Supraclavicular approach for outlet decompression. thoracic. Linda M. Reilly, MD, and Ronald J. Stoney, MD, San Francisco, Calif.
 Supraclavicular approach for outlet decompression thoracic Linda M. Reilly, MD, and Ronald J. Stoney, MD, San Francisco, Calif. Supraclavicular decompression of the thoracic outlet was performed in 40
Supraclavicular approach for outlet decompression thoracic Linda M. Reilly, MD, and Ronald J. Stoney, MD, San Francisco, Calif. Supraclavicular decompression of the thoracic outlet was performed in 40
Subclavian and Axillary Artery Aneurysms
 Subclavian and Axillary Artery Aneurysms April 2008 Francesco A Aiello, M.D. Assistant Professor of Surgery Division of Vascular Endovascular Surgery University of Massachusetts Medical School None DISCLOSURES
Subclavian and Axillary Artery Aneurysms April 2008 Francesco A Aiello, M.D. Assistant Professor of Surgery Division of Vascular Endovascular Surgery University of Massachusetts Medical School None DISCLOSURES
Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi
 Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi For the purpose of anatomical description the neck is sub divided into two major triangles, the Anterior and the Posterior by muscle bellies
Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi For the purpose of anatomical description the neck is sub divided into two major triangles, the Anterior and the Posterior by muscle bellies
The Upper Limb III. The Brachial Plexus. Anatomy RHS 241 Lecture 12 Dr. Einas Al-Eisa
 The Upper Limb III The Brachial Plexus Anatomy RHS 241 Lecture 12 Dr. Einas Al-Eisa Brachial plexus Network of nerves supplying the upper limb Compression of the plexus results in motor & sensory changes
The Upper Limb III The Brachial Plexus Anatomy RHS 241 Lecture 12 Dr. Einas Al-Eisa Brachial plexus Network of nerves supplying the upper limb Compression of the plexus results in motor & sensory changes
10/14/2018 Dr. Shatarat
 2018 Objectives To discuss mediastina and its boundaries To discuss and explain the contents of the superior mediastinum To describe the great veins of the superior mediastinum To describe the Arch of
2018 Objectives To discuss mediastina and its boundaries To discuss and explain the contents of the superior mediastinum To describe the great veins of the superior mediastinum To describe the Arch of
Thoracic Outlet Syndrome
 Thoracic Outlet Syndrome The Coraco-Pectoral Loop Environmental Stress Reinforcers Culture Behavioral Sick Role somatization Biological Genetics Physiology Psychological Emotional deficit Cog. Tendency
Thoracic Outlet Syndrome The Coraco-Pectoral Loop Environmental Stress Reinforcers Culture Behavioral Sick Role somatization Biological Genetics Physiology Psychological Emotional deficit Cog. Tendency
Outcomes of Mitral Valve Repair for Mitral Regurgitation Due to Degenerative Disease
 Outcomes of Mitral Valve Repair for Mitral Regurgitation Due to Degenerative Disease TIRONE E. DAVID, MD ; SEMIN THORAC CARDIOVASC SURG 19:116-120c 2007 ELSEVIER INC. PRESENTED BY INTERN 許士盟 Mitral valve
Outcomes of Mitral Valve Repair for Mitral Regurgitation Due to Degenerative Disease TIRONE E. DAVID, MD ; SEMIN THORAC CARDIOVASC SURG 19:116-120c 2007 ELSEVIER INC. PRESENTED BY INTERN 許士盟 Mitral valve
Peel-Apart Percutaneous Introducer Kits for
 Bard Access Systems Peel-Apart Percutaneous Introducer Kits for Table of Contents Contents Page Bard Implanted Ports Hickman*, Leonard*, Broviac*, Tenckhoff*, and Groshong* Catheters Introduction....................................
Bard Access Systems Peel-Apart Percutaneous Introducer Kits for Table of Contents Contents Page Bard Implanted Ports Hickman*, Leonard*, Broviac*, Tenckhoff*, and Groshong* Catheters Introduction....................................
Upper Extremity Venous Duplex. Michigan Sonographers Society Fall Ultrasound Symposium October 15, 2016
 Upper Extremity Venous Duplex Michigan Sonographers Society Fall Ultrasound Symposium October 15, 2016 Patricia A. (Tish) Poe, BA RVT FSVU Director of Quality Assurance Navix Diagnostix Patricia A. Poe
Upper Extremity Venous Duplex Michigan Sonographers Society Fall Ultrasound Symposium October 15, 2016 Patricia A. (Tish) Poe, BA RVT FSVU Director of Quality Assurance Navix Diagnostix Patricia A. Poe
Review Article Understanding Thoracic Outlet Syndrome
 Scientifica, Article ID 248163, 6 pages http://dx.doi.org/10.1155/2014/248163 Review Article Understanding Thoracic Outlet Syndrome Julie Freischlag 1 and Kristine Orion 2 1 Division of Vascular Surgery,
Scientifica, Article ID 248163, 6 pages http://dx.doi.org/10.1155/2014/248163 Review Article Understanding Thoracic Outlet Syndrome Julie Freischlag 1 and Kristine Orion 2 1 Division of Vascular Surgery,
82a Orthopedic Massage! Introduction - Thoracic Outlet"
 82a Orthopedic Massage! Introduction - Thoracic Outlet" 82a Orthopedic Massage! Introduction - Thoracic Outlet! Class Outline" 5 minutes" "Attendance, Breath of Arrival, and Reminders " 10 minutes "Lecture:"
82a Orthopedic Massage! Introduction - Thoracic Outlet" 82a Orthopedic Massage! Introduction - Thoracic Outlet! Class Outline" 5 minutes" "Attendance, Breath of Arrival, and Reminders " 10 minutes "Lecture:"
Normal ulnar nerve conduction velocity across the thoracic outlet: comparison of two measuring techniques
 Journal of Neurology, Neurosurgery, and Psychiatry, 1975, 38, 756-760 Normal ulnar nerve conduction velocity across the thoracic outlet: comparison of two measuring techniques GARY W. LONDON' From the
Journal of Neurology, Neurosurgery, and Psychiatry, 1975, 38, 756-760 Normal ulnar nerve conduction velocity across the thoracic outlet: comparison of two measuring techniques GARY W. LONDON' From the
Saphenous Vein Autograft Replacement
 Saphenous Vein Autograft Replacement of Severe Segmental Coronary Artery Occlusion Operative Technique Rene G. Favaloro, M.D. D irect operation on the coronary artery has been performed in 180 patients
Saphenous Vein Autograft Replacement of Severe Segmental Coronary Artery Occlusion Operative Technique Rene G. Favaloro, M.D. D irect operation on the coronary artery has been performed in 180 patients
T treat empyema, although modern day thoracic
 The Schede and Modern Thoracoplasty Benjamin J. Pomerantz, Joseph C. Cleveland, Jr, and Marvin Pomerantz THORACOPLASTY-GENERAL CONSIDERATIONS horacoplasty evolved as a procedure designed to T treat empyema,
The Schede and Modern Thoracoplasty Benjamin J. Pomerantz, Joseph C. Cleveland, Jr, and Marvin Pomerantz THORACOPLASTY-GENERAL CONSIDERATIONS horacoplasty evolved as a procedure designed to T treat empyema,
ORIGINAL ARTICLE. Spectrum of Thoracic Outlet Syndrome Presentation in Adolescents
 ORIGINAL ARTICLE Spectrum of Thoracic Outlet Syndrome Presentation in Adolescents Kevin Chang, BA; Emma Graf; Kylie Davis; Jasmine Demos, CRNP; Taylor Roethle; Julie Ann Freischlag, MD Objective: To study
ORIGINAL ARTICLE Spectrum of Thoracic Outlet Syndrome Presentation in Adolescents Kevin Chang, BA; Emma Graf; Kylie Davis; Jasmine Demos, CRNP; Taylor Roethle; Julie Ann Freischlag, MD Objective: To study
Comprehensive Management of Subclavian Vein Effort Thrombosis
 44 Comprehensive Management of Subclavian Vein Effort Thrombosis Robert W. Thompson, M.D. 1, 2 1 The Center for Thoracic Outlet Syndrome and the Department of Surgery, Section of Vascular Surgery 2 Radiology,
44 Comprehensive Management of Subclavian Vein Effort Thrombosis Robert W. Thompson, M.D. 1, 2 1 The Center for Thoracic Outlet Syndrome and the Department of Surgery, Section of Vascular Surgery 2 Radiology,
Subclavian artery Stenting
 Subclavian artery Stenting Etiology Atherosclerosis Takayasu s arteritis Fibromuscular dysplasia Giant Cell Arteritis Radiation-induced Vascular Injury Thoracic Outlet Syndrome Neurofibromatosis Incidence
Subclavian artery Stenting Etiology Atherosclerosis Takayasu s arteritis Fibromuscular dysplasia Giant Cell Arteritis Radiation-induced Vascular Injury Thoracic Outlet Syndrome Neurofibromatosis Incidence
Paget-Schroetter syndrome, or effort thrombosis of
 ORIGINAL ARTICLES: GENERAL THORACIC Paget-Schroetter Syndrome: What Is the Best Management? Harold C. Urschel, Jr, MD, and Maruf A. Razzuk, MD Division of Thoracic and Cardiovascular Surgery, The University
ORIGINAL ARTICLES: GENERAL THORACIC Paget-Schroetter Syndrome: What Is the Best Management? Harold C. Urschel, Jr, MD, and Maruf A. Razzuk, MD Division of Thoracic and Cardiovascular Surgery, The University
Sign up to receive ATOTW weekly -
 1 SUBCLAVIAN PERIVASCULAR BRACHIAL PLEXUS BLOCK ANAESTHESIA TUTORIAL OF THE WEEK 156 19 th OCTOBER 2009 Dr. Martin Herrick Department of Anaesthesia, Addenbrooke s Hospital, Cambridge, U.K. Correspondence
1 SUBCLAVIAN PERIVASCULAR BRACHIAL PLEXUS BLOCK ANAESTHESIA TUTORIAL OF THE WEEK 156 19 th OCTOBER 2009 Dr. Martin Herrick Department of Anaesthesia, Addenbrooke s Hospital, Cambridge, U.K. Correspondence
Anatomy Lecture #19 AN INTRODUCTION TO THE THORAX April 3, 2012
 Page 1 بسم الله الرحمن الرحيم The Thoracic Wall Firstly, when we talk about thorax, we should begin with the thorax wall which means not only bones that construct the thorax but also the muscles which
Page 1 بسم الله الرحمن الرحيم The Thoracic Wall Firstly, when we talk about thorax, we should begin with the thorax wall which means not only bones that construct the thorax but also the muscles which
James Lawrence Guzzo, MD, Kevin Chang, BA, Jasmine Demos, CRNP, CPNP, James H. Black, MD, and Julie A. Freischlag, MD, Baltimore, Md
 From the Southern Association for Vascular Surgery Preoperative thrombolysis and venoplasty affords no benefit in patency following first rib resection and scalenectomy for subacute and chronic subclavian
From the Southern Association for Vascular Surgery Preoperative thrombolysis and venoplasty affords no benefit in patency following first rib resection and scalenectomy for subacute and chronic subclavian
The anatomy of the thoracic inlet is an important determinant
 Anterior Approach to Superior Sulcus Tumors Philippe Dartevelle and Steven J. Mentzer The anatomy of the thoracic inlet is an important determinant of the radiographic appearance and clinical syndrome
Anterior Approach to Superior Sulcus Tumors Philippe Dartevelle and Steven J. Mentzer The anatomy of the thoracic inlet is an important determinant of the radiographic appearance and clinical syndrome
Anatomy of the Thorax
 Anatomy of the Thorax A) THE THORACIC WALL Boundaries Posteriorly by the thoracic part of the vertebral column Anteriorly by the sternum and costal cartilages Laterally by the ribs and intercostal spaces
Anatomy of the Thorax A) THE THORACIC WALL Boundaries Posteriorly by the thoracic part of the vertebral column Anteriorly by the sternum and costal cartilages Laterally by the ribs and intercostal spaces
Clinical Study Early versus Late Surgical Treatment for Neurogenic Thoracic Outlet Syndrome
 ISRN Neurology Volume 2013, Article ID 673020, 6 pages http://dx.doi.org/10.1155/2013/673020 Clinical Study Early versus Late Surgical Treatment for Neurogenic Thoracic Outlet Syndrome Jasem Yousef Al-Hashel,
ISRN Neurology Volume 2013, Article ID 673020, 6 pages http://dx.doi.org/10.1155/2013/673020 Clinical Study Early versus Late Surgical Treatment for Neurogenic Thoracic Outlet Syndrome Jasem Yousef Al-Hashel,
Paget-Schroetter syndrome (PSS), or effort thrombosis
 Surgery Remains the Most Effective Treatment for Paget-Schroetter Syndrome: 50 Years Experience Harold C. Urschel, Jr, MD, and Amit N. Patel, MD Cardiovascular and Thoracic Surgical Education, Research
Surgery Remains the Most Effective Treatment for Paget-Schroetter Syndrome: 50 Years Experience Harold C. Urschel, Jr, MD, and Amit N. Patel, MD Cardiovascular and Thoracic Surgical Education, Research
Brachial plexus blockade within the interscalene groove involves local anesthetic
 Interscalene Brachial Plexus Block- How I do it. Part 1 of a 2 part discussion on technique. Stuart Grant Professor of Anesthesiology Duke University Medical Center Durham NC Brachial plexus blockade within
Interscalene Brachial Plexus Block- How I do it. Part 1 of a 2 part discussion on technique. Stuart Grant Professor of Anesthesiology Duke University Medical Center Durham NC Brachial plexus blockade within
5/5/15. Overview. Deep vein thrombosis of the upper extremity (UEDVT) Classification of UEDVT Epidemiology. Primary UEDVT.
 Deep vein thrombosis of the upper extremity (UEDVT) Hong H. Keo, MD, MSc Angiologie Kantonsspital Aarau 07.05.2015 06. Symposium venöse Insuff. und arterielle Gefässerkr. Glarus Overview Epidemiology Classification/Risk
Deep vein thrombosis of the upper extremity (UEDVT) Hong H. Keo, MD, MSc Angiologie Kantonsspital Aarau 07.05.2015 06. Symposium venöse Insuff. und arterielle Gefässerkr. Glarus Overview Epidemiology Classification/Risk
KNEE DISLOCATION. The most common injury will be an anterior dislocation, and this usually results from a hyperextension mechanism.
 KNEE DISLOCATION Introduction Dislocation of the knee is a severe injury associated with major soft tissue injury and a high incidence of damage to the popliteal artery. There is displacement of the tibia
KNEE DISLOCATION Introduction Dislocation of the knee is a severe injury associated with major soft tissue injury and a high incidence of damage to the popliteal artery. There is displacement of the tibia
Adult Brachial Plexus Injuries: Introduction and the Role of Surgery
 Adult Brachial Plexus Injuries: Introduction and the Role of Surgery Tim Hems Scottish National Brachial Plexus Injury Service Department of Orthopaedic Surgery, Queen Elizabeth University Hospital, GLASGOW.
Adult Brachial Plexus Injuries: Introduction and the Role of Surgery Tim Hems Scottish National Brachial Plexus Injury Service Department of Orthopaedic Surgery, Queen Elizabeth University Hospital, GLASGOW.
Orthopedics - Dr. Ahmad - Lecture 2 - Injuries of the Upper Limb
 The shoulder and the upper arm Fractures of the clavicle 1. Fall on the shoulder. 2. Fall on outstretched hand. In mid shaft fractures, the outer fragment is pulled down by the weight of the arm and the
The shoulder and the upper arm Fractures of the clavicle 1. Fall on the shoulder. 2. Fall on outstretched hand. In mid shaft fractures, the outer fragment is pulled down by the weight of the arm and the
Prof. Nabil CHAKFE et coll.
 Prof. Nabil CHAKFE et coll. For the Department of Vascular Surgery and Kidney Transplantation University Hospital of Strasbourg, FRANCE Popliteal artery entrapment: misdiagnosed Epidemiology Prevalence:
Prof. Nabil CHAKFE et coll. For the Department of Vascular Surgery and Kidney Transplantation University Hospital of Strasbourg, FRANCE Popliteal artery entrapment: misdiagnosed Epidemiology Prevalence:
Official Definition. Carpal tunnel syndrome, the most common focal peripheral neuropathy, results from compression of the median nerve at the wrist.
 Mod 2 MMT Course Official Definition Carpal tunnel syndrome, the most common focal peripheral neuropathy, results from compression of the median nerve at the wrist. epidemiology Affects an estimated 3
Mod 2 MMT Course Official Definition Carpal tunnel syndrome, the most common focal peripheral neuropathy, results from compression of the median nerve at the wrist. epidemiology Affects an estimated 3
A Patient s Guide to Ulnar Nerve Entrapment at the Wrist (Guyon s Canal Syndrome)
 A Patient s Guide to Ulnar Nerve Entrapment at the Wrist (Guyon s Canal Syndrome) Introduction The ulnar nerve is often called the funny bone at the elbow. However, there is little funny about injury to
A Patient s Guide to Ulnar Nerve Entrapment at the Wrist (Guyon s Canal Syndrome) Introduction The ulnar nerve is often called the funny bone at the elbow. However, there is little funny about injury to
Early View Article: Online published version of an accepted article before publication in the final form.
 : Online published version of an accepted article before publication in the final form. Journal Name: Journal of Case Reports and Images in Medicine Type of Article: Case Report Title: Use of new oral
: Online published version of an accepted article before publication in the final form. Journal Name: Journal of Case Reports and Images in Medicine Type of Article: Case Report Title: Use of new oral
Surgery has been proven to be beneficial for selected patients
 Thoracoscopic Lung Volume Reduction Surgery Robert J. McKenna, Jr, MD Surgery has been proven to be beneficial for selected patients with severe emphysema. Compared with medical management, lung volume
Thoracoscopic Lung Volume Reduction Surgery Robert J. McKenna, Jr, MD Surgery has been proven to be beneficial for selected patients with severe emphysema. Compared with medical management, lung volume
Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman
 Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman Breast anatomy: Breast conserving surgery: The aim of wide local excision is to remove all invasive and in situ
Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman Breast anatomy: Breast conserving surgery: The aim of wide local excision is to remove all invasive and in situ
Tracheal Trauma: Management and Treatment. Kosmas Iliadis, MD, PhD, FECTS
 Tracheal Trauma: Management and Treatment Kosmas Iliadis, MD, PhD, FECTS Thoracic Surgeon Director of Thoracic Surgery Department Hygeia Hospital, Athens INTRODUCTION Heterogeneous group of injuries mechanism
Tracheal Trauma: Management and Treatment Kosmas Iliadis, MD, PhD, FECTS Thoracic Surgeon Director of Thoracic Surgery Department Hygeia Hospital, Athens INTRODUCTION Heterogeneous group of injuries mechanism
Gateway to the upper limb. An area of transition between the neck and the arm.
 Gateway to the upper limb An area of transition between the neck and the arm. Pyramidal space inferior to shoulder @ junction of arm & thorax Distribution center for the neurovascular structures that serve
Gateway to the upper limb An area of transition between the neck and the arm. Pyramidal space inferior to shoulder @ junction of arm & thorax Distribution center for the neurovascular structures that serve
OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function
 The root of the neck Jeff Dupree, Ph.D. e mail: jldupree@vcu.edu OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function READING ASSIGNMENT: Moore and
The root of the neck Jeff Dupree, Ph.D. e mail: jldupree@vcu.edu OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function READING ASSIGNMENT: Moore and
thopaedic Science Diagnosis and treatment of thoracic outlet syndrome* Instructional lecture
 J Orthop Sci (1997) 2:119-127 ~ Journal of thopaedic Science The Japanese Orthopaedic Association Instructional lecture Diagnosis and treatment of thoracic outlet syndrome* MASATAKA ABE, TADASHI SHIMAMURA,
J Orthop Sci (1997) 2:119-127 ~ Journal of thopaedic Science The Japanese Orthopaedic Association Instructional lecture Diagnosis and treatment of thoracic outlet syndrome* MASATAKA ABE, TADASHI SHIMAMURA,
Axial Skeleton: Vertebrae and Thorax
 Axial Skeleton: Vertebrae and Thorax Function of the vertebral column (spine or backbone): 1) 2) 3) Composition of Vertebral column The vertebral column is formed by 33 individual vertebrae (some of which
Axial Skeleton: Vertebrae and Thorax Function of the vertebral column (spine or backbone): 1) 2) 3) Composition of Vertebral column The vertebral column is formed by 33 individual vertebrae (some of which
Matt Woronczak Advanced Practice Musculoskeletal Physiotherapist Emergency Department, Dandenong Hospital
 Matt Woronczak Advanced Practice Musculoskeletal Physiotherapist Emergency Department, Dandenong Hospital Only joint holding the upper limb to the rest of the skeleton Classified as a diarthroidal saddle
Matt Woronczak Advanced Practice Musculoskeletal Physiotherapist Emergency Department, Dandenong Hospital Only joint holding the upper limb to the rest of the skeleton Classified as a diarthroidal saddle
Indications: following: embolization. artery that has diseases 5. The evaluation. of suspected. such entities. a cold hand. biopsy
 Peripheral Arterial Ultrasound Protocol Using Color and Spectral Doppler Reviewed by: Mark Yuhasz, MD Last Review Date: January 2015 Contact: (866) 761 4200, Option 1 Indications: The indications for peripheral
Peripheral Arterial Ultrasound Protocol Using Color and Spectral Doppler Reviewed by: Mark Yuhasz, MD Last Review Date: January 2015 Contact: (866) 761 4200, Option 1 Indications: The indications for peripheral
Thoracic Outlet Syndrome
 Discussion paper prepared for The Workplace Safety and Insurance Appeals Tribunal January 2000 Prepared by: Dr. J.F.R. Fleming Professor Emeritus, Division of Neurosurgery University of Toronto The Toronto
Discussion paper prepared for The Workplace Safety and Insurance Appeals Tribunal January 2000 Prepared by: Dr. J.F.R. Fleming Professor Emeritus, Division of Neurosurgery University of Toronto The Toronto
Otoshi K 1, Kaga T 1, Sato R 2, Igari T 2, Shishido H 2, Konno S 2, Itoh Y 3, Furushima K 3, Koga R 3
 35 th SITEMSH congress The prevalence and characteristics of TOS in high school baseball players Otoshi K 1, Kaga T 1, Sato R 2, Igari T 2, Shishido H 2, Konno S 2, Itoh Y 3, Furushima K 3, Koga R 3 1.
35 th SITEMSH congress The prevalence and characteristics of TOS in high school baseball players Otoshi K 1, Kaga T 1, Sato R 2, Igari T 2, Shishido H 2, Konno S 2, Itoh Y 3, Furushima K 3, Koga R 3 1.
Suprascapular Nerve: How to identify when it is a problem and what to do? Speaker Disclosure
 Suprascapular Nerve: How to identify when it is a problem and what to do? Eric C. McCarty, MD Associate Professor Chief of Sports Medicine and Shoulder Surgery University of Colorado School of Medicine
Suprascapular Nerve: How to identify when it is a problem and what to do? Eric C. McCarty, MD Associate Professor Chief of Sports Medicine and Shoulder Surgery University of Colorado School of Medicine
In 1980, Bex and associates 1 first introduced the initial
 Technique of Aortic Translocation for the Management of Transposition of the Great Arteries with a Ventricular Septal Defect and Pulmonary Stenosis Victor O. Morell, MD, and Peter D. Wearden, MD, PhD In
Technique of Aortic Translocation for the Management of Transposition of the Great Arteries with a Ventricular Septal Defect and Pulmonary Stenosis Victor O. Morell, MD, and Peter D. Wearden, MD, PhD In
Lung cancer or primary malignant tumors of the mediastinum
 Technique of Superior Vena Cava Resection for Lung Carcinomas David R. Jones, MD Division of Thoracic and Cardiovascular Surgery, Department of Surgery, University of Virginia School of Medicine, Charlottesville,
Technique of Superior Vena Cava Resection for Lung Carcinomas David R. Jones, MD Division of Thoracic and Cardiovascular Surgery, Department of Surgery, University of Virginia School of Medicine, Charlottesville,
Pathologic abnormality of the sternoclavicular joint (SCJ)
 Surgical Management of the Infected Sternoclavicular Joint Rubie Sue Jackson, MD, Yvonne M. Carter, MD, and M. Blair Marshall, MD Pathologic abnormality of the sternoclavicular joint (SCJ) is rare. The
Surgical Management of the Infected Sternoclavicular Joint Rubie Sue Jackson, MD, Yvonne M. Carter, MD, and M. Blair Marshall, MD Pathologic abnormality of the sternoclavicular joint (SCJ) is rare. The
Introduction to Neurosurgical Subspecialties:
 Introduction to Neurosurgical Subspecialties: Spine Neurosurgery Brian L. Hoh, MD 1 and Gregory J. Zipfel, MD 2 1 University of Florida, 2 Washington University Spine Neurosurgery Spine neurosurgeons treat
Introduction to Neurosurgical Subspecialties: Spine Neurosurgery Brian L. Hoh, MD 1 and Gregory J. Zipfel, MD 2 1 University of Florida, 2 Washington University Spine Neurosurgery Spine neurosurgeons treat
Anatomical Study of Pectoral Nerves and its Implications in Surgery
 DOI: 10.7860/JCDR/2014/8631.4545 Anatomy Section Original Article Anatomical Study of Pectoral Nerves and its Implications in Surgery Prakash KG 1, Saniya K 2 ABSTRACT Introduction: This anatomical study
DOI: 10.7860/JCDR/2014/8631.4545 Anatomy Section Original Article Anatomical Study of Pectoral Nerves and its Implications in Surgery Prakash KG 1, Saniya K 2 ABSTRACT Introduction: This anatomical study
Thoracoscopic left upper lobectomy with systematic lymph nodes dissection under left pulmonary artery clamping
 GCTAB Column Thoracoscopic left upper lobectomy with systematic lymph nodes dissection under left pulmonary artery clamping Yi-Nan Dong, Nan Sun, Yi Ren, Liang Zhang, Ji-Jia Li, Yong-Yu Liu Department
GCTAB Column Thoracoscopic left upper lobectomy with systematic lymph nodes dissection under left pulmonary artery clamping Yi-Nan Dong, Nan Sun, Yi Ren, Liang Zhang, Ji-Jia Li, Yong-Yu Liu Department
Proximal Humerus Fractures
 Proximal Humerus Fractures Trafford General Hospital, June 2010 Nehmat Singh, Jawad Sultan Anatomy of the Proximal Humerus Consists of four parts: humeral head, surgical neck and greater and lesser tubercles
Proximal Humerus Fractures Trafford General Hospital, June 2010 Nehmat Singh, Jawad Sultan Anatomy of the Proximal Humerus Consists of four parts: humeral head, surgical neck and greater and lesser tubercles
Lecture 2: Clinical anatomy of thoracic cage and cavity II
 Lecture 2: Clinical anatomy of thoracic cage and cavity II Dr. Rehan Asad At the end of this session, the student should be able to: Identify and discuss clinical anatomy of mediastinum such as its deflection,
Lecture 2: Clinical anatomy of thoracic cage and cavity II Dr. Rehan Asad At the end of this session, the student should be able to: Identify and discuss clinical anatomy of mediastinum such as its deflection,
BRACHIAL PLEXUS INJURY INVESTIGATION, LOCALIZATION AND TREATMENT. Presented By : Dr.Pankaj Jain
 BRACHIAL PLEXUS INJURY INVESTIGATION, LOCALIZATION AND TREATMENT Presented By : Dr.Pankaj Jain EMBRYOLOGY l Brachial plexus (BP) is developed at 5 weeks of gestation l Afferent fibers develop from neuroblast
BRACHIAL PLEXUS INJURY INVESTIGATION, LOCALIZATION AND TREATMENT Presented By : Dr.Pankaj Jain EMBRYOLOGY l Brachial plexus (BP) is developed at 5 weeks of gestation l Afferent fibers develop from neuroblast
5 minutes: Attendance and Breath of Arrival. 50 minutes: Problem Solving Torso
 5 minutes: Attendance and Breath of Arrival 50 minutes: Problem Solving Torso Punctuality- everybody's time is precious: o o Be ready to learn by the start of class, we'll have you out of here on time
5 minutes: Attendance and Breath of Arrival 50 minutes: Problem Solving Torso Punctuality- everybody's time is precious: o o Be ready to learn by the start of class, we'll have you out of here on time
PLEURAE and PLEURAL RECESSES
 PLEURAE and PLEURAL RECESSES By Dr Farooq Aman Ullah Khan PMC 26 th April 2018 Introduction When sectioned transversely, it is apparent that the thoracic cavity is kidney shaped: a transversely ovoid space
PLEURAE and PLEURAL RECESSES By Dr Farooq Aman Ullah Khan PMC 26 th April 2018 Introduction When sectioned transversely, it is apparent that the thoracic cavity is kidney shaped: a transversely ovoid space
Thyroidectomy. Siu Kwan Ng. Modified Radical Neck Dissection Type II 47
 06 Thyroidectomy Siu Kwan Ng Modified Radical Neck Dissection Type II 47 Thyroidectomy STEP 1. EXPOSING THE THYROID GLAND The collar incision Figure 1 (curvilinear skin crease incision) is made at 1.5-2
06 Thyroidectomy Siu Kwan Ng Modified Radical Neck Dissection Type II 47 Thyroidectomy STEP 1. EXPOSING THE THYROID GLAND The collar incision Figure 1 (curvilinear skin crease incision) is made at 1.5-2
Copyright 2010 Pearson Education, Inc.
 E. VERTEBRAL COLUMN 1. The vertebral column extends from the skull to the pelvis and forms the vertical axis of the skeleton. 2. The vertebral column is composed of vertebrae that are separated by intervertebral
E. VERTEBRAL COLUMN 1. The vertebral column extends from the skull to the pelvis and forms the vertical axis of the skeleton. 2. The vertebral column is composed of vertebrae that are separated by intervertebral
thoracic cage inlet and outlet landmarks of the anterior chest wall muscles of the thoracic wall sternum joints ribs intercostal spaces diaphragm
 Thoracic Wall Lecture Objectives Describe the shape and outline of the thoracic cage including inlet and outlet. Describe the anatomical landmarks of the anterior chest wall. List various structures making
Thoracic Wall Lecture Objectives Describe the shape and outline of the thoracic cage including inlet and outlet. Describe the anatomical landmarks of the anterior chest wall. List various structures making
Appendix. Suggested Forms to Gather Information from Patients with TOS
 Appendix Suggested Forms to Gather Information from Patients with TOS Three forms seem to be most useful for patients with thoracic outlet syndrome, and we urge all who treat this disorder to use them
Appendix Suggested Forms to Gather Information from Patients with TOS Three forms seem to be most useful for patients with thoracic outlet syndrome, and we urge all who treat this disorder to use them
