A Preliminary Clinical Comparison of the Use of Fascia Lata
|
|
|
- Junior Clarke
- 5 years ago
- Views:
Transcription
1 ORIGINAL PAPERS Adv Clin Exp Med 2016, 25, 3, DOI: /acem/44849 Copyright by Wroclaw Medical University ISSN Wojciech Bednarz 1, A, C E, Jacek Żurek 2, A D, Thomas Gedrange 3, C F, Marzena Dominiak4, C F A Preliminary Clinical Comparison of the Use of Fascia Lata Allograft and Autogenous Connective Tissue Graft in Multiple Gingival Recession Coverage Based on the Tunnel Technique 1 Specialistic Outpatient Medical Clinic MEDIDENT, Gorlice, Poland 2 Specialist Medical Practice, Tarnowskie Góry, Poland 3 Dresden University of Technology, Germany 4 Department of Oral Surgery, Wroclaw Medical University, Poland A research concept and design; B collection and/or assembly of data; C data analysis and interpretation; D writing the article; E critical revision of the article; F final approval of article Abstract Background. The most effective method for treating gingival recessions (GR) is with an autogenous connective tissue graft (CTG) via flap surgery. Often, however, the amount of CTG that can be grafted is insufficient to cover all of a patient s gingival recessions at one time. Objectives. The objective of this study was to provide a 6-month comparative assessment of the results of covering multiple Miller Class I and II gingival recessions with a Fascia Lata Allograft (FL) and a CTG harvested from palatal mucosa. Material and Methods. The study comprised a total of 30 people who underwent multiple gingival recession (GR) procedures using a modified, coronally advanced tunnel technique (MCAT). The patients were divided into two groups of 15 according to the type of materials used for gingival augmentation purposes: FL for the test group and CTG for the control group. A clinical assessment was made at baseline, as well as 3 and 6 months following surgery. The following factors were assessed: recession depth, recession width, probing depth, clinical attachment level, height of keratinized tissue (HKT), distance between the cemento-enamel junction and the muco-gingival junction (CEJ-MGJ), API, SBI. The following values were calculated: average root coverage (ARC), complete root coverage (CRC). Results. No statistically significant differences were observed between the groups in terms of clinical parameters assessed after 6 months, apart from CRC, which was ± 0.14 mm in the control group and ± 0.20 mm in the study group (p = 0.034). The average HKT in the control group after 6 months amounted to 2.86 ± 1.60 mm, and in the test group to 3.09 ± 0.95 mm, which translates into an increase in comparison to the baseline values of 0.73 mm (p < 0.001) and 0.48 mm (p = 0.017), respectively. Conclusions. FL Allografts may serve as an alternative to autogenous CTG in multiple gingival recession coverage procedures based on the tunnel technique (Adv Clin Exp Med 2016, 25, 3, ). Key words: gingival recession, connective tissue, autograft, allograft, fascia lata. Comprehensive treatment of gingival recessions primarily involves eliminating as many known recession risk factors as possible, in particular through optimal oral hygiene, then surgical coverage of recessions and long-term maintenance of results achieved during the maintenance phase. The techniques employed to cover gingival reces- sions are surgical-based and include coronal or lateral flap displacement, tunnel methods, autogenous (FGG, CTG), allogenous, and xenogenous grafts as well as guided tissue regeneration [1]. The best and most documented gingival recession coverage method involves the grafting of autogenous connective tissue harvested from hard palate
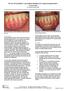
2 588 mucosa [2, 3]. Over a 5-year observation period the technique achieved statistically significantly higher complete (CRC) and average (ARC) root coverage percentages than procedures involving the exclusive use of various flaps and/or an acellular dermal matrix (ADM), platelet rich fibrin (PRF) or a resorbable membrane [2, 4]. While the grafting of autogenous connective tissue ensures predictability, it also entails the need for two operating fields in both the donor and recipient sites. For anatomic-histological reasons graft donor sites are restricted to the area between the canine and the second molar, the clinical attachment on the palatal side of these teeth and the position of the palatine neurovascular bundle [5]. Therefore, the scope of the procedure in the recipient site must correspond to the potential size of the graft which can be harvested from the donor site. In the case of multiple gingival recession coverage, a multi-stage procedure is necessary, one that involves harvesting multiple grafts from the same donor sites. According to Harris [6], the minimum thickness of palatal mucosa in the donor site to ensure optimal coverage of the subepithelial connective tissue must be 3 mm. If the thickness is less than this, the epithelial tissue, by forming characteristic rete pegs, penetrates deep into the stromal connective tissue, thereby making it impossible to harvest a graft without the presence of keratinocytes. The presence of a larger volume of epithelial cells in a connective tissue graft placed in the supraperiosteal space of recipient sites increases the risk of it becoming separated or even of cysts forming [7, 8]. For this very reason, alternative methods that make use of connective tissue graft substitutes are increasingly being sought. Most studies have focused on acellular dermal matrix [9 13], while recently xenogenous Mucograft has also been considered [14 17]. Admittedly, connective tissue grafting remains the gold standard procedure. However, when multiple gingival recession coverage is required, the acellular dermal matrix technique may offer an alternative approach to harvesting autogenous connective tissue [11 13, 18]. To date, the available literature does not include any study on the use of a different allogenous material as coverage for multiple gingival recessions. The objective of the study was to provide a 6-month comparative assessment of the results of covering multiple Miller Class I and II gingival recessions with both Fascia Lata Allografts (FL) and CTGs harvested from palatal mucosa. Material and Methods W. Bednarz et al. A total of 30 people of both sexes took part in the study, 27 of whom were women. They were aged and had at least two Miller Class I and II gingival recessions neighboring one another. The patients were divided at random into two 15-person groups. In the Test Group the gingival recessions were covered with Fascia Lata Allografts using a modified coronally advanced tunnel technique (MCAT/FL), while in the Control Group MCAT recessions were covered with connective tissue grafts (MCAT/CTG). Consent for the study was obtained from the Bioethics Committee of Medical University of Silesia in Katowice (No KNW/0022/KB1/107/12) and from the Bioethics Committee of Wroclaw Medical University (No. KB-104/2014). All the patients were informed of the details of the experimental treatment and gave their consent to take part in it. The biostatic fascia lata grafts were harvested in compliance with Polish law (The Harvesting and Grafting of Cells, Tissue and Organs Act Journal of Laws 2005, no. 169, item 1411) and the European Union Directive 2004/23/WE of which set the standards for the quality, safety, commissioning, grafting, testing, processing, preservation, storage and distribution of human tissues and cells. Directly after the tissue was harvested it was frozen and deposited in the Tissue Bank at the Regional Blood Donation and Hemotherapy Centre in Katowice (Poland), where it underwent a histopathological examination. The donor s blood serum was tested with the aim of detecting any antigens against Treponema Pallidum was also subject to screening tests for HCVAb, HBsAg, HBcAb total HBsAg, HIV1.2Ab/Ag. After appropriate preparation, conservation and sterilisation with gamma radiation the allograft can be stored for 18 months at a temperature of C. Patient Selection To participate in the study a patient had to be at least 17 years of age, have at least two neighboring Miller Class I or II gingival recessions, a gingival recession height of 2 mm and the following indicators: API no greater than 25% and SBI no greater than 15% (Fig. 1). The following criteria excluded patients from the study: pregnancy, breast feeding, systemic diseases (diabetes, autoaggression diseases, primary and secondary immunodeficiency diseases, severe infectious diseases), no identifiable CEJ (fillings
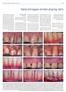
3 FLA and CTG in Gingival Recession Coverage 589 Fig. 1. Patient Ś-G.A. Multiple gingival recessions before MCAT/CTG surgery present, non-carious lesions), earlier gingival recession coverage procedures, smoking (over 10 cigarettes a day). Clinical Parameters The state of the gingival recessions was assessed prior to the procedure as well as 3 and 6 months later, using the following parameters: 1. RD height of gingival recession distance between the gingival margin and CEJ measured midbuccally (mm); 2. RW width of gingival recession mesiodistal distance of gingival margins measured at the CEJ level of tooth (mm); 3. HKT height of keratinized gingiva (mm); 4. PD probing depth (mm); 5. CAL clinical attachment level measured on midbuccal side (mm); 6. Gingival recession class according to the Miller scale; 7. ARC mean percentage of vertical coverage of gingival recessions measured after 3 and 6 months (%); 8. CRC percentage of total gingival recession coverage measured after 3 and 6 months (%); 9. CEJ MGJ distance of cemento-enamel junction from muco-gingival junction (mm). The RD, RW HKT, PD and CAL parameters were measured with a periodontal probe calibrated every 1 mm (UNC 15 Hu-Friedy USA). In addition, Aproximal Plaque Index (API) and Sulcus Bleeding Index (SBI) were assessed at baseline as well as 3 and 6 months after the surgery. The results were recorded on a special test card that a member of the study team filled out at different observation periods. Surgical Procedures Surgical procedures were performed in outpatient conditions under local anesthesia using a 4% articaine solution with adrenaline (Ubistesin Forte 3M Germany). In both groups the tunnel was formed in the recipient site in the same way. The tunnel was created by connecting together individual supraperiosteal envelopes formed by each of the teeth covered by the procedure. Only groove incisions (microsurgery blade no 69) were made, while a tunneling tool (Tunnelling Knives, Helmut Zepf, Germany) was used for further delamination of the flap on the alveolar ridge surface as well as under the interdental papillae (Fig. 2). After appropriate mobilization of the split thickness flap the CTG or FL was inserted in the space thus formed (Fig. 3, 4). After it has been removed from the packaging, the Allograft was placed in a physiological saline solution for approximately 5 10 min. Then it was cut down to the necessary size and inserted in the supraperiosteal tunnel using 2 lace sutures. To ensure the graft is placed at CEJ level and the split thickness flap is advanced to a height of 2 mm more coronally than CEJ level, individual sling sutures were used for each tooth (Fig. 5). The flap was advanced coronally in a similar way in the control group and the CTG inserted and stabilized in the recipient site (Fig. 6). It was harvested from the palatal masticatory mucosa by making a single incision running parallel to the Fig. 2. Creating the supraperiosteal tunnel in the recipient site Fig. 3. Insertion of connective tissue graft in the tunnel thus formed
4 590 W. Bednarz et al. Fig. 4. Insertion of Fascia Lata Allograft in the supraperiosteal tunnel Fig. 7. Harvesting of connective tissue graft from the palatal masticatory mucosa Fig. 5. Stabilisation of allograft and split thickness flap using single sling sutures Fig. 8. Primarily closure of the wound in the donor site using cross mattress sutures Post-Surgical Management The control group sutures were removed 14 days after the operation while the study group sutures were removed 3 weeks after the operation. The healing process was checked 1, 7 and 14 days after the procedure. Post-operative instructions for the study group included taking 500 mg of amoxicillin orally three times a day for 7 days, starting 24 h before surgery, as well as pain killers if a patient experienced any discomfort. Fig. 6. The clinical situation direct after multiple gingival recession coverage using modified coronally advanced tunnel technique with connective tissue graft dental arch from the canine up to the second molar and no closer than 2 mm from the gingival margin (Fig. 7). A lyophilized collagen sponge was placed in the wound in the donor site and closed primarily with cross mattress sutures (Fig. 8). Soft surgical dressings (Reso-pac, Hager&Werken, Duisburg, Germany) were applied to all the operating sites Statistics The t Student test for paired samples was used to determine similarities between the mean continuous parameters in particular groups. To determine whether the study groups had similar parameters we used ANOVA variance analysis for groups with homogeneity of variance or the Wilcoxon non-parametric test (homogeneity of variance measured using the Bartlett test). The statistical analysis of the API and SBI indices was based
5 FLA and CTG in Gingival Recession Coverage 591 on the Mann Whitney U test. Statistical significance was set at p < The statistical analysis was performed with STATISTICA 10 v statistical software ( ). Results The gingival recession distribution for both groups, taking into account the sex of the patients and location in the mandible or maxilla, is presented for individual groups of teeth in Tables 1 and 2. Table 3 shows the division (number, percentage) Table 1. Number of gingival recession at particular groups of teeth by gender in the test group groups of teeth Test group No. maxilla mandible females I C P M into classes of gingival recession based on the Miller scale, taking into account sex and topography in both groups. A total of 97 gingival recessions were covered in the study group, all in women patients, of which 75 were located in the maxilla and 22 in the mandible (Table 1). On the other hand, a total of 40 gingival recessions were covered in the control group, including 34 in women patients. Of this total, 23 were located in the maxilla and 17 in the mandible (Table 2). In total 137 gingival recessions were covered, including 125 Miller Class I and 12 Miller Class II recessions (Table 3). The smaller number of gingival recessions covered in the control group was due to problems with harvesting the correct amount of autogenous connective tissue graft from the palatal mucosa (Fig. 9). An assessment of the clinical parameters revealed that the mean baseline values in an intergroup comparison did not differ in any statistically significant way, apart from RD and PD (Table 4). The average RD at baseline in the control group was significantly higher than in the test group. After six months the height of the recession in both groups was comparable. Amount I incisors; C canines; P premolars; M molars. Table 2. Number of gingival recession at particular groups of teeth by gender in the control group Control group groups of teeth No. maxilla mandible females males I C P M Amount I incisors; C canines; P premolars; M molars. Fig. 9. Comparing the size of the autogeuous connective tissue graft and Fascia Lata Allograft Table 3. Miller s class division of gingival recession defects (number, percentage) in both groups, by gender and topography Miller s class Test group Control group in all maxilla mandible females in all maxilla mandible females males I % % % % % % % % % II % % % % % % % % % Amount
6 592 W. Bednarz et al. Table 4. The comparison beetwen control group and test group in values of clinical parameters at baseline, 3- and 6-month after surgery Clinical parameters x SD p-value Fascia Lata Allograft Connective Tissue Graft Fascia Lata Allograft Connective Tissue Graft ARC3 (%) ,059 ARC6 (%) CRC3 (%) * CRC6 (%) * RD0 (mm) * RD3 (mm) * RD6 (mm) RW0 (mm) RW3 (mm) RW6 (mm) PD0 (mm) < 0.001* PD3 (mm) * PD6 (mm) * CAL0 (mm) CAL3 (mm) CAL6 (mm) HKT0 (mm) HKT3 (mm) HKT6 (mm) CEJ-MGJ0 (mm) CEJ-MGJ3 (mm) CEJ-MGJ6 (mm) ARC average root coverage; CRC complete root coverage; RD recession depth; RW recession width; PD probing depth; CAL clinical attachment level; HKT height of keratinized tissue; CEJ-MGJ distance of cemento-enamel junction from muco-gingival junction, (0 at baseline, 3 3-months, 6 6-months after surgery); x average; SD standard deviation; p significance factor; * statistical significance The initial mean value of PD in the control group was significantly less than in the study group. After 3 and 6 months the differences between the groups were also statistically significant. On the other hand, the intergroup analysis revealed that the mean PD value for the control group was not significantly higher either after 3 months or after 6 months in relation to the initial value. The mean PD value for the study group at baseline was significantly higher than after 3 months as well as after 6 months. In the case of the other clinical parameters, no statistically significant differences were noted in the intergroup comparison (Table 4). After 3 months the mean RW value for the control group had declined significantly, and in the case of the test group it had dropped (Table 4 6). After 3 months average CAL had dropped and these results were statistically significant in both groups compared with the baseline. After 6 months the average HKT was significantly higher, which represents a significant increase of 0.73 mm for the control group and 0.48 mm for the test group, compared to the baseline. The mean CEJ-MGJ values after 6 months had declined significantly compared to the baseline about 1.64 mm in the control group and about 1.56 mm in the test group.
7 FLA and CTG in Gingival Recession Coverage 593 Table 5. Values of clinical parameters at baseline, 3- and 6-month after surgery in test group Test group N = 97 x M SD 0 vs. 3 (p) 0 vs. 6 (p) 3 vs. 6 (p) ARC 3 (%) ,0 0, * ARC 6 (%) ,20 CRC3 (%) , CRC6 (%) RD0 (mm) < 0.001* < 0.001* RD3 (mm) RD6 (mm) RW0 (mm) < 0.001* < 0.001* 0.028* RW3 (mm) RW6 (mm) PD0 (mm) < 0.001* < 0.001* PD3 (mm) PD6 (mm) CAL0 (mm) < 0.001* < 0.001* CAL3 (mm) CAL6 (mm) HKT0 (mm) < 0.001* < 0.001* HKT3 (mm) HKT6 (mm) CEJ-MGJ0 (mm) < 0.001* < 0.001* CEJ-MGJ3 (mm) CEJ-MGJ6 (mm) ARC average root coverage; CRC complete root coverage; RD recession depth; RW recession width; PD probing depth; CAL clinical attachment level; HKT height of keratinized tissue; CEJ-MGJ distance of cemento-enamel junction from muco-gingival junction, (0 at baseline, 3 3-months, 6 6-months after surgery); x average; M median; SD standard deviation; p significance factor; * statistical significance. CRC after 3 months was 90% in the control group and about 97% in the test group and it was significantly higher. After 6 months CRC had increased to above 94.24% for the control group, but had fallen to 94.87% for the test group and the difference between the groups was statistically significant. The 3-month observation revealed an ARC of 94% for the control group and about 98% for the study group. After 6 months ARC had increased slightly in the control group to about 96%, but had fallen sharply to about 94% in the test group (Fig. 1, 10 12). A comparison of the mean API and SBI values (Tables 7, 8) shows that the value of these indicators for both groups were similar and baseline and after 6 months. Discussion The allogeneic fascia lata used in the study is a highly cross-linked hydrated collagen matrix containing collagen types I and III. The fascia lata is built out of dense connective tissue, the main components of which are collagen fiber bundles surrounded by a small amount of loose connective tissue with elastin fibers. A small number of fibroblasts are linearly distributed between the collagen bundles. The fascia is weakly vascularized and in-
8 594 W. Bednarz et al. Table 6. Values of clinical parameters at baseline, 3- and 6-month after surgery in control group Control group n= 40 x M SD p (0 vs. 3) p (0 vs. 6) p (3 vs. 6) ARC3 (%) ARC6 (%) CRC3 (%) * CRC6 (%) RD0 (mm) < 0.001* < 0.001* 0.029* RD3 (mm) RD6 (mm) RW0 (mm) < 0.001* < 0.001* RW3 (mm) RW6 (mm) PD0 (mm) PD3 (mm) PD6 (mm) CAL0 (mm) < 0.001* < 0.001* CAL3 (mm) CAL6 (mm) HKT0 (mm) * 0.017* HKT3 (mm) HKT6 (mm) CEJMGJ0 (mm) < 0.001* < 0.001* CEJ-MGJ3 (mm) CEJ-MGJ6 (mm) ARC average root coverage; CRC complete root coverage; RD recession depth; RW recession width; PD probing depth; CAL clinical attachment level; HKT height of keratinized tissue; CEJ-MGJ distance of cemento-enamel junction from muco-gingival junction, (0 at baseline, 3 3-months, 6 6-months after surgery); x average; M median; SD standard deviation; p significance factor; * statistical significance. Table 7. Values of API, SBI in test group at baseline (0), 3 and 6 months after surgery x M SD p (0 vs. 3) p (0 vs. 6) p (3 vs. 6) API 0 (%) * < 0.001* API 3 (%) API 6 (%) SBI 0 (%) < 0.001* < 0.000* SBI 3 (%) SBI 6 (%) API Approximal Plaque Index; SBI Sulcus Bleeding Index, (0 at baseline, 3 3-months, 6 6-months after surgery); x average; M median; SD standard deviation; p significance factor; * statistical significance.
9 FLA and CTG in Gingival Recession Coverage 595 Fig. 10. Patient Ś-G.A. Clinical situation 6 months after surgery with CTG Fig. 11. Patient L.E. Multiple gingival recessions before MCAT/FL surgery Fig. 12. Patient L.E. Clinical situation 6 months after surgery using Fascia Lata Allograft nervated. The limited immunogenicity of this tissue is due to its histological structure. The right conservation methodology makes a further reduction of the immunogenicity of the allogeneic material possible while preserving the physiochemical parameters [19, 20]. The local immune response, although visible, has no effect on the incorporation of the allogeneic graft. A commonly applied conservation method is irradiation of the fascia in a physiological salt solution with 33 kgy [21]. Based on nine randomized clinical studies featuring 208 subjects and 858 gingival recessions Graziani et al. [22] discussed the effectiveness of periodontal plastic procedures in covering multiple gingival recession defects. The restorations assessed in their study had to have had a minimum observation period of no less than 6 months. CRC ranged between 24% and 89%, depending on the operating technique assessed, and the average root coverage percentage was 86.27%. Based on their meta-analysis the authors claim that it is not possible to state which is the best method for treating multiple gingival recessions. However, in their opinion the most predictable method appears to be the coronally positioned flap and tunnel technique with simultaneous placement of a connective tissue graft. Dembowska and Drozdzik [23] employed the tunnel technique with a connective tissue graft to cover 48 multiple Miller Class I and II gingival recessions in 18 patients. Complete root coverage 6 months after surgery was achieved in 78.6% of all Class I gingival recessions and in 60% of all Class II recessions according to the Miller scale, and the mean root coverage was 97% and 96.6%, respectively. Modaressi et al. [24] used the tunnel technique with ADMA to cover Miller Class I and II multiple gingival recessions. After 6 months the mean root coverage was equal to 58.67%. The multiple gingival recession coverage technique employed in the present study was based on Table 8. Values of API, SBI in control group at baseline (0), 3 and 6 months after surgery x M SD p (0 vs. 3) p (0 vs. 6) p (3 vs. 6) API 0 (%) < 0.001* < 0.001* API 3 (%) API 6 (%) SBI 0 (%) < 0.001* < 0.001* SBI 3 (%) SBI 6 (%) API approximal plaque index; SBI sulcus bleeding index, (0 at baseline, 3 3-months, 6 6-months after surgery); x average; M median; SD standard deviation; p significance factor; * statistical significance.
10 596 W. Bednarz et al. the tunnel method devised by Azzi et al. [25] together with autogenous connective tissue harvested from palatal masticatory mucosa and fascia lata Allografts. No vertical incisions were made. Instead, access to the tunnel was achieved via groove incisions. In this way the graft was inserted by the tooth with the greatest gingival recession or by the tooth located in the center of the operating field. The fascia lata Allograft was positioned at the margin of the CEJ, while the flap itself was positioned 2 mm coronally in relation to the CEJ. At each treated tooth single sling mattress sutures were placed. They were removed 2 weeks afterwards in the case of the control group just as in Ayub et al. [26], Koudale et al. [27], and after 3 weeks in the case of the test group. A comparison of multiple gingival recession coverage procedures performed with the tunnel method using fascia lata Allograft as well as autogenous connective tissue graft indicates that similar clinical results were achieved at the end of a 6-month observation period. The mean API and SBI values for both groups at baseline and in the study after 3 and 6 months were similar and confirmed that the hygiene measures prior to procedures were correct and periodontal maintenance care was optimal. After 6 months CRC was ± 0.14% for the control group and ± 0.20% for the study group and the difference was statistically significant. In the case of the other clinical parameters assessed after 6 months no significant differences between the groups were evident. ARC was ± 0.11% for the control group and ± 0.20% for the test group. These observations are in accordance with other papers comparing the use of ADMA and CTG in cases of both individual and multiple gingival recession coverage using different operating techniques [27 29]. On the other hand, they contradict other studies which showed statistically better results when a connective tissue graft was applied [11, 30]. Rahmani et al. [30] observed mean root coverage of 70% for SCTG and 70% for the ADMA group. Similarly, Koudale et al. [27] did not observe any statistically significant differences 6 months after multiple gingival recession coverage procedures using CPF with ADMA and CTG. In this case, the mean percent root coverage achieved was 94% and 97%, respectively. Hirsch et al. [30] reported 97.8% root coverage for an SCTG group and 95.9% for an ADMA group and the difference between the groups was statistically significant. In a randomized controlled study, Thombre et al. [12] compared the clinical effects of 43 multiple gingival recession coverage procedures in 20 patients who were divided into 2 groups that underwent coronally positioned flap procedures either with or without ADMA. Average gingival recession coverage 6 months after the procedures was 90% for the ADMA group and in the group without ADMA the percentage was 66% for the group without ADMA. Complete root coverage after 6 months was 64% and 24%, respectively. These differences were statistically significant. Significantly higher growth in the keratinized gingiva zone was noted in both groups in relation to the baseline 1.3 ± 0.4 mm in the test group, compared with 1.0 ± 0.6 mm in the control group (CPF alone). In the authors own research the keratinized gingiva zone was widened by just under 0.5 mm in the MCAT/FL group. Perhaps a different location for the allograft would have improved this result. This is because Ayub et al. [26] showed that the positioning of the acellular dermal matrix allograft (ADMA) 1mm apically and the flap 1 mm coronally in relation to the CEJ results in statistically better widening of the keratinized gingiva than when the allograft is positioned at CEJ level. The significant reduction in CEJ-MGJ observed in relation to baseline is due to the coverage of the gingival recession via coronal repositioning of the flap together with its muco-gingival junction. The position of MGJ is genetically determined. If the displacement is too great it may result in it returning to its original position and thus in relapse of gingival recessions. In view of this fact it is especially important, therefore, to achieve a stable position for the MGJ after the procedure, as the authors noted in their own observations after 3 and 6 months. In a 5-year study Dominiak et al. [2] reported a stable reduction in the CEJ-MGJ distance and this reduction was greater in the case of coronally advanced flap procedures, namely a double lateral bridging flap (DLBF) and guided tissue regeneration with collagen membrane (GTR-CM), than it was for CPF-CTG. The latter study also noted the biggest increase in keratinized gingiva width, which may be explained by the fact that this group had the most stable value throughout the entire 5-year observation period, i.e. 5 mm. The values for the other two groups increased marginally, which is also in line with the findings of the authors own study. For the FL group this value increased slightly by 0.07 mm in the 3 6 month observations and for the CTG group by 0.02 mm. Longer observation periods are vital for assessing this parameter. Thombre et al. (2013) reported a mean CAL of 3. 9 ± 0. 9 mm at baseline and 1.9 ± 1.1 mm after 6 months (the mean CAL gain was 2.0 ± 0.9 mm) in CPF alone and 4.1 ± 0.9 mm at baseline and 1.0 ± 0.7 mm after 6 months, respectively, for the group with ADMA (the mean CAL gain was
11 FLA and CTG in Gingival Recession Coverage ± 1.0 mm) and the difference between the groups was statistically significant. In the authors own study the absence of any significant differences between the CTG group and fascia lata in terms of CAL indicates similar possibilities for its effective reconstruction using both grafts, with PD values not increasing at the same time. Ahmedbeyli et al. [18] compared clinical and aesthetic results 12 months after multiple gingival recession coverage procedures using a coronal flap displacement method alone and CPF as well as an acellular dermal matrix allograft in 48 patients. ARC in the ADM group was 94.84% and in the CPF alone group ACR was 74.99%. CRC was equal to 83.33% and 50.00%, respectively. The differences between the groups were statistically significant. The situation was similar with regard to the increase in the height of the keratinized tissue and the GT value. A positive correlation was also observed between GT and average root coverage. The authors stress that ADM may be used successfully in both cases of multiple gingival recession coverage and in cases where the periodontal biotype is thin. The results of the study confirm that fascia lata Allografts and autogenous connective tissue grafts harvested from palatal mucosa are similarly effective in covering multiple gingival recession defects. The unlimited amount of this allogeneic material can make it an interesting alternative to the multistage application of CTG harvested from the same palatal masticatory mucosa sites during extensive gingival augmentation procedures. Not creating a second operating field should shorten the operating time, reduce post-operative pain and in this way help increase the patient s comfort. Further studies should be carried to confirm these observations. Acknowledgments. The authors would like to thank the Chair of Periodontal and Mucous Membrane Diseases Clinic of Conservative Dentistry with Endodontics of the Medical University of Silesia in Katowice as well as the Chair of the Department of Conservative Dentistry at Wroclaw Medical University for making this study possible. References [1] Dominiak M, Gedrange T: New perspectives in the diagnostic of gingival recession. Adv Clin Exp Med 2014, 23, 6, [2] Dominiak M, Konopka T, Lompart H, Kubasiewicz P: Comparative research concerning clinical efficiency of three surgical methods of periodontium recessions treatment in five-year observations. Adv Med Sci 2006, 51, Suppl 1, [3] Zucchelli G, Mounssif I, Mazzotti C, Stefanini M, Marzadori M, Petracci E, Montebugnoli L: Coronally advanced flap with and without connective tissue graft for the treatment of multiple gingival recessions: A comparative short- and long-term controlled randomized clinical trial. J Clin Periodontol 2014, 41, [4] Hofmänner P, Alessandri R, Laugisch O, Aroca S, Salvi GE, Stavropoulos A, Sculean A: Predictability of surgical techniques used for coverage of multiple adjacent gingival recessions. A systematic review. Quintessence Int 2012, 43, [5] Benninger B, Andrews K, Carter W: Clinical measurements of hard palate and implications for subepithelial connective tissue grafts with suggestions for palatal nomenclature. J Oral Maxillofacial Surg 2012, 70, [6] Harris RJ: Histologic Evaluation of Connective Tissue Grafts in Humans. Int J Periodontics Restorative Dent 2003, 23, [7] Harris RJ: Formation of a cyst-like area after a connective tissue graft for root coverage. J Periodontol 2002, 73, [8] Wei P-Ch, Geivelis M: A gingival Cul-de-Sac following a root coverage procedure with a subepithelial connective tissue submerged graft. J Periodontol 2003, 74, [9] Harris RJ: Gingival augmentation with an acellular dermal matrix: Human histologic evaluation of a case-placement of the graft on periosteum. Int J Periodontics Restorative Dent 2004, 24, [10] Mahn DH: Use of the tunnel technique and an acellular dermal matrix in the treatment of multiple adjacent teeth with gingival recession in the esthetic zone. Int J Periodontics Restorative Dent 2010, 30, [11] Schlee M, Esposito M: Human dermis graft versus autogenous connective tissue grafts for thickening soft tissue and covering multiple gingival recessions: 6-month results from a preference clinical trial. Eur J Oral Implant 2011, 4, [12] Thombre V, Somnath B, Koudale SB, Manohar L, Bhongade ML: Comparative evaluation of the effectiveness of coronally positioned flap with or without Acellular Dermal Matrix Allograft in the treatment of multiple marginal gingival recession defects. Int J Periodontics Restorative Dent 2013, 33, e88 e94. [13] Gholami GA, Saberi A, Kadkhodazadeh M, Amid R, Karami D: Comparison of the clinical outcomes of connective tissue and acellular dermal matrix in combination with double papillary flap for root coverage: A 6 month trial. Dent Res J 2013, 10, [14] Cardaropoli D, Tamagnone L, Roffredo A, Gaveglio L: Treatment of gingival recession defects using coronally advanced flap with a porcine collagen matrix compared to coronally advanced flap with connective tissue graft: A randomized clinical trial. J Periodontol 2012, 83,
12 598 W. Bednarz et al. [15] Aroca, S, Molnar B, Windisch P, Gera I, Salvi GE, Nikolidakis D, Sculean A: Treatment of multiple adjacent Miller class I and II gingival recessions with a modified coronally advanced tunnel (MCAT) technique and a collagen matrix or palatal connective tissue graft: A randomized, controlled clinical trial. J Clin Periodontol 2013, 40, [16] Jepsen K, Jepsen S, Zucchelli, G, Stefanini M, desanctis M, Baldini N, Greven B, Heinz B, Wennström J, Cassel B, Vignoletti F, Sanz M: Treatment of gingival recession defects with a coronally advanced flap and a xenogeneic collagen matrix: A multicenter randomized clinical trial. J Clin Periodontol 2013, 40, [17] Dominiak M, Mierzwa-Dudek D, Puzio M, Gedrange T: Clinical evaluation of the effectiveness of using collagen matrix (Mucograft prototype) in gingival recession coverage a pilot study. J Stomat 2012, 65, [18] Ahmedbeyli C, İpçi SD, Cakar G, Kuru BE, Yılmaz S: Clinical evaluation of coronally advanced flap with or without acellular dermal matrix graft on complete defect coverage for the treatment of multiple gingival recessions with thin tissue biotype. J Clin Periodontol 2014, 41, [19] Defrere J, Franckart A: Freeze-dried fascia lata allografts in the reconstruction of anterior cruciate ligament defects. A two- to seven-year follow-up study. Clin Orthop Relat Res 1994, 303, [20] Dufrane D, Cornu O, Delloye C, Schneider YJ: Physical and chemical processing for a human dura mater substitute. Biomaterials 2002, 23, [21] Kamiński A, Gut G, Marowska J, Lada-Kozłowska M, Biwejnis W, Zasacka M: Mechanical properties of radiation sterilised human Bone-Tendon-Bone grafts preserved by different methods. Cell Tissue Bank 2009, 10, [22] Graziani F, Gennai S, Roldan S, Discepoli N, Buti J, Madianos P, Herrera D: Efficacy of periodontal plastic procedures in the treatment of multiple gingival recessions. J Clin Periodontol 2014, 41, Suppl 15, [23] Dembowska E, Drozdzik A: Subepithelial connective tissue graft in the treatment of multiple gingival recession. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2007, 104, e1 e7. [24] Modaressi M, Wang HL: Tunneling procedure for root coverage using acellular dermal matrix: A case series. Int J Periodontics Restorative Dent 2009, 29, [25] Azzi R, Etienne D, Takei H, Fenech P: Surgical thickening of the existing gingiva and interdental papillae around imlant-supported restorations. Int J Periodontics Rest Dent 2002, 22, [26] Ayub LG, Ramos UD, Reino DM, Grisi MFM, Taba Jr M, Souza SLS, Palioto DB, Novaes Jr AB: A Randomized comparative clinical ctudy of two surgical procedures to improve root coverage with the acellular dermal matrix graft. J Clin Periodontol 2012, 39, [27] Koudale SB, Pretti A, Charde PA, Bhongade ML: A comparative clinical evaluation of acellular dermal matrix allograft and subepithelial connective tissue graft for the treatment of multiple gingival recessions. J Indian Soc Periodontol 2012, 16, [28] Gapski R, Parks CA, Wang HL: Acellular dermal matrix for mucogingival surgery: A meta-analysis. J Periodontol 2005, 76, [29] Rahmani ME, Mohammed A, Rigi Lades ME, Lades MA: Comparative clinical evaluation of Acellular Dermal Matrix Allograft and connective tissue graft for the treatment of gingival recession. J Contemp Dent Prac 2006, 2, [30] Hirsch A, Goldstein M, Goultschin J, Boyan BD, Schwartz Z: A 2-year follow-up of root coverage using subpedicle acellular dermal matrix allograft and subepithelial connective tissue graft autograft. J Periodontol 2005, 76, Address for correspondence: Wojciech Bednarz Specialistic Outpatient Medical Clinic MEDIDENT ul. Okulickiego Gorlice Poland wojcie_ch@poczta.onet.pl Conflict of interest: None declared Received: Revised: Accepted:
Alarge number of sound clinical
 Volume 83 Number 5 Long-Term 8-Year Outcomes of Coronally Advanced Flap forrootcoverage Giovanpaolo Pini-Prato,* Debora Franceschi,* Roberto Rotundo,* Francesco Cairo,* Pierpaolo Cortellini, and Michele
Volume 83 Number 5 Long-Term 8-Year Outcomes of Coronally Advanced Flap forrootcoverage Giovanpaolo Pini-Prato,* Debora Franceschi,* Roberto Rotundo,* Francesco Cairo,* Pierpaolo Cortellini, and Michele
The Use of DynaMatrix Extracellular Membrane for Gingival Augmentation: A Case Series Dr. Stephen Saroff, DDS
 The Use of DynaMatrix Extracellular Membrane for Gingival Augmentation: A Case Series Dr. Stephen Saroff, DDS LOCALIZED RECESSION ON TOOTH #25 DUE TO BONE RECESSION (PRE OP) Introduction Tissue grafting
The Use of DynaMatrix Extracellular Membrane for Gingival Augmentation: A Case Series Dr. Stephen Saroff, DDS LOCALIZED RECESSION ON TOOTH #25 DUE TO BONE RECESSION (PRE OP) Introduction Tissue grafting
Management of millers class III marginal tissue recession associated with endodontic lesion: Report of two cases managed using second stage surgery
 CASE SERIES 1 OPEN ACCESS Management of millers class III marginal tissue recession associated with endodontic lesion: Report of two cases managed using second stage surgery Sangeeta ABSTRACT Introduction:
CASE SERIES 1 OPEN ACCESS Management of millers class III marginal tissue recession associated with endodontic lesion: Report of two cases managed using second stage surgery Sangeeta ABSTRACT Introduction:
The Treatment of Gingival Recession Associated with Deep Corono-Radicular Abrasions (CEJ step) a Case Series
 CLINICAL AND RESEARCH REPORT The Treatment of Gingival Recession Associated with Deep Corono-Radicular Abrasions (CEJ step) a Case Series Giovanpaolo Pini-Prato, Carlo Baldi, Roberto Rotundo, Debora Franceschi,
CLINICAL AND RESEARCH REPORT The Treatment of Gingival Recession Associated with Deep Corono-Radicular Abrasions (CEJ step) a Case Series Giovanpaolo Pini-Prato, Carlo Baldi, Roberto Rotundo, Debora Franceschi,
Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report
 Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
A 2-Year Follow-Up of Root Coverage Using Subpedicle Acellular Dermal Matrix Allografts and Subepithelial Connective Tissue Autografts
 J Periodontol August 2005 A 2-Year Follow-Up of Root Coverage Using Subpedicle Acellular Dermal Matrix Allografts and Subepithelial Connective Tissue Autografts A. Hirsch,* M. Goldstein,* J. Goultschin,*
J Periodontol August 2005 A 2-Year Follow-Up of Root Coverage Using Subpedicle Acellular Dermal Matrix Allografts and Subepithelial Connective Tissue Autografts A. Hirsch,* M. Goldstein,* J. Goultschin,*
Michael K. McGuire* and E. Todd Scheyer*
 Long-Term Results Comparing Xenogeneic Collagen Matrix and Autogenous Connective Tissue Grafts With Coronally Advanced Flaps for Treatment of Dehiscence-Type Recession Defects Michael K. McGuire* and E.
Long-Term Results Comparing Xenogeneic Collagen Matrix and Autogenous Connective Tissue Grafts With Coronally Advanced Flaps for Treatment of Dehiscence-Type Recession Defects Michael K. McGuire* and E.
A Porcine Collagen Matrix (Mucograft ) vs Connective Tissue Graft in the Treatment of Multiple Gingival Recessions: A Comparative Clinical Study
 ORIGINAL RESEARCH Porcine Collagen Matrix (Mucograft 10.5005/jp-journals-10015-1548 ) vs Connective Tissue Graft A Porcine Collagen Matrix (Mucograft ) vs Connective Tissue Graft in the Treatment of Multiple
ORIGINAL RESEARCH Porcine Collagen Matrix (Mucograft 10.5005/jp-journals-10015-1548 ) vs Connective Tissue Graft A Porcine Collagen Matrix (Mucograft ) vs Connective Tissue Graft in the Treatment of Multiple
botiss dental bone & tissue regeneration biomaterials mucoderm 3D-Regenerative Tissue Graft strictly biologic
 dental bone & tissue regeneration botiss biomaterials 3DRegenerative Tissue Graft strictly biologic mucoderm Soft Tissue Graft Indications mucoderm is a collagen tissue matrix derived of animal dermis
dental bone & tissue regeneration botiss biomaterials 3DRegenerative Tissue Graft strictly biologic mucoderm Soft Tissue Graft Indications mucoderm is a collagen tissue matrix derived of animal dermis
Case Series. BK Somnath, Pretti Charde, ML Bhongade
 Case Series Evaluation of Effectiveness of Acellular Dermal Matrix Allograft and Subepithelial Connective Tissue Graft in Combination with Coronally Positioned Flap in Treatment of Mutiple Gingival Recession
Case Series Evaluation of Effectiveness of Acellular Dermal Matrix Allograft and Subepithelial Connective Tissue Graft in Combination with Coronally Positioned Flap in Treatment of Mutiple Gingival Recession
MUCOGINGIVAL THERAPY PERIODONTAL PLASTIC SURGERY
 MUCOGINGIVAL THERAPY PERIODONTAL PLASTIC SURGERY DR.H.Gharati Periodontist & Dental Implant Specialist Assistant Professor, School Of Dentistry Friedman(1957): DEFINITION Mucogingival surgery, Surgical
MUCOGINGIVAL THERAPY PERIODONTAL PLASTIC SURGERY DR.H.Gharati Periodontist & Dental Implant Specialist Assistant Professor, School Of Dentistry Friedman(1957): DEFINITION Mucogingival surgery, Surgical
REGENERATIONTIME. A Case Report by. Geistlich Mucograft for the treatment of multiple adjacent recession defects: A more palatable option
 A Case Report by Dr. Daniel Gober Geistlich Mucograft for the treatment of multiple adjacent recession defects: A more palatable option The Situation A 35 year old male presented in my practice with a
A Case Report by Dr. Daniel Gober Geistlich Mucograft for the treatment of multiple adjacent recession defects: A more palatable option The Situation A 35 year old male presented in my practice with a
DENTAL TRIBUNE ISRAEL 12/2017
 8 1 Thin periodontal biotype Lindhe piercing Glossary of Periodontal Terms CEJ :1 :1 thickperiodontal biotype :Emdogain 6 : : 31 41 9 DENTAL TRIBUNE ISRAEL 12/2017 2 Free soft tissue graft ( Coronally
8 1 Thin periodontal biotype Lindhe piercing Glossary of Periodontal Terms CEJ :1 :1 thickperiodontal biotype :Emdogain 6 : : 31 41 9 DENTAL TRIBUNE ISRAEL 12/2017 2 Free soft tissue graft ( Coronally
TWO-STEP SURGICAL PROCEDURE FOR ROOT COVERAGE (FREE GINGIVAL GRAFT AND CORONALLY POSITIONED FLAP) - A CASE REPORT
 TWO-STEP SURGICAL PROCEDURE FOR ROOT COVERAGE (FREE GINGIVAL GRAFT AND CORONALLY POSITIONED FLAP) - A CASE REPORT Dr Prashant Bhusari*, Dr Apoorva Saxena**, Dr Jaya Jain***,Dr Rashmi Rathore***, Dr Aditi
TWO-STEP SURGICAL PROCEDURE FOR ROOT COVERAGE (FREE GINGIVAL GRAFT AND CORONALLY POSITIONED FLAP) - A CASE REPORT Dr Prashant Bhusari*, Dr Apoorva Saxena**, Dr Jaya Jain***,Dr Rashmi Rathore***, Dr Aditi
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Case Report Bridge Flap: A Sine Qua Non For Mucogingival Deformities Debajyoti Mondal, Anju L, Rajul Choradia, Somen
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Case Report Bridge Flap: A Sine Qua Non For Mucogingival Deformities Debajyoti Mondal, Anju L, Rajul Choradia, Somen
CLINICAL. Free gingival grafts to manage recession when and how? Matthew B M Thomas CLINICAL
 CLINICAL CLINICAL Free gingival grafts to manage recession when and how? Matthew B M Thomas Gingival recession results from displacement of the gingival margin below the cemento-enamel junction leading
CLINICAL CLINICAL Free gingival grafts to manage recession when and how? Matthew B M Thomas Gingival recession results from displacement of the gingival margin below the cemento-enamel junction leading
ijcrr Vol 04 issue 12 Category: Case Report Received on:22/04/12 Revised on:07/05/12 Accepted on:22/05/12
 SURGICAL RECONSTRUCTION OF INTERDENTAL PAPILLA USING AN INTERPOSED SUBEPITHELIAL CONNECTIVE TISSUE GRAFT: A CASE REPORT ijcrr Vol 04 issue 12 Category: Case Report Received on:22/04/12 Revised on:07/05/12
SURGICAL RECONSTRUCTION OF INTERDENTAL PAPILLA USING AN INTERPOSED SUBEPITHELIAL CONNECTIVE TISSUE GRAFT: A CASE REPORT ijcrr Vol 04 issue 12 Category: Case Report Received on:22/04/12 Revised on:07/05/12
Over the years, mucogingival surgery
 The Use of DynaMatrix Extracellular Membrane for Gingival Augmentation and Root Coverage: A Case Series Saroff Stephen Andrew Saroff, DDS, MSD 1 Abstract Over the years, mucogingival surgery has developed
The Use of DynaMatrix Extracellular Membrane for Gingival Augmentation and Root Coverage: A Case Series Saroff Stephen Andrew Saroff, DDS, MSD 1 Abstract Over the years, mucogingival surgery has developed
The Internatonal Journal of Periodontics & Restoraive Dentistry
 The Internatonal Journal of Periodontics & Restoraive Dentistry 3 Incisive Vessel Based Palatal Flap for the Reconstruction of Anterior Maxillary Soft Tissues [Au: Text has been edited heavily. Please
The Internatonal Journal of Periodontics & Restoraive Dentistry 3 Incisive Vessel Based Palatal Flap for the Reconstruction of Anterior Maxillary Soft Tissues [Au: Text has been edited heavily. Please
ELIMINATE POCKETS. Periodontal pocket is the consequence of periodontal infection But also a major risk factor for the further progression of disease
 ELIMINATE POCKETS Periodontal pocket is the consequence of periodontal infection But also a major risk factor for the further progression of disease CONSEQUENTLY Periodontal pockets should be eliminated
ELIMINATE POCKETS Periodontal pocket is the consequence of periodontal infection But also a major risk factor for the further progression of disease CONSEQUENTLY Periodontal pockets should be eliminated
SUBEPITHELIAL CONNECTIVE TISSUE GRAFT A PREDICTABLE INDICATOR FOR ROOT COVERAGE
 SUBEPITHELIAL CONNECTIVE TISSUE GRAFT A PREDICTABLE INDICATOR FOR ROOT COVERAGE Munishwar Singh* * 201 Military Dental Centre, C/o 99 APO, India Keywords: Gingival recession, Root coverage procedure, Connective
SUBEPITHELIAL CONNECTIVE TISSUE GRAFT A PREDICTABLE INDICATOR FOR ROOT COVERAGE Munishwar Singh* * 201 Military Dental Centre, C/o 99 APO, India Keywords: Gingival recession, Root coverage procedure, Connective
Management of miller class II gingival recession by laterally positioned pedicle flap revised technique
 Management of miller class II gingival by laterally positioned pedicle flap revised technique Received: 2/4/206 Accepted: 3/0/206 Dildar Abdullah Othman* Abstract Background and objective: Gingival is
Management of miller class II gingival by laterally positioned pedicle flap revised technique Received: 2/4/206 Accepted: 3/0/206 Dildar Abdullah Othman* Abstract Background and objective: Gingival is
BONE AUGMENTATION AND GRAFTING
 1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
Many techniques have been proposed for root coverage:
 Case Series Localized Gingival Recessions Treated With the Original Envelope Technique: A Report of 50 Consecutive Patients Jaime A. Vergara* and Raul G. Caffesse Background: The surgical techniques used
Case Series Localized Gingival Recessions Treated With the Original Envelope Technique: A Report of 50 Consecutive Patients Jaime A. Vergara* and Raul G. Caffesse Background: The surgical techniques used
Gum Graft? Patient Need a. Does My. 66 JANUARY 2017 // dentaltown.com. by Dr. Brian S. Gurinsky
 by Dr. Brian S. Gurinsky Dr. Brian S. Gurinsky was born in Dallas and attended college at the University of Texas at Austin. He continued his education at Baylor College of Dentistry in Dallas, where he
by Dr. Brian S. Gurinsky Dr. Brian S. Gurinsky was born in Dallas and attended college at the University of Texas at Austin. He continued his education at Baylor College of Dentistry in Dallas, where he
Masking Buccal Plate Remodeling in the Esthetic Zone with Connective Tissue Grafts: Concepts and Techniques with Immediate Implants
 Peer-Reviewed and Indexed Annual Implant Issue Masking Buccal Plate Remodeling in the Esthetic Zone with Connective Tissue Grafts: Concepts and Techniques with Immediate Implants of Continuing Education
Peer-Reviewed and Indexed Annual Implant Issue Masking Buccal Plate Remodeling in the Esthetic Zone with Connective Tissue Grafts: Concepts and Techniques with Immediate Implants of Continuing Education
Connective Tissue Graft for Gingival Recession in Mandibular Incisor Area: A Case Report
 Bull Tokyo Dent Coll (2017) 58(3): 155 162 Case Report doi:10.2209/tdcpublication.2016-0038 Connective Tissue Graft for Gingival Recession in Mandibular Incisor Area: A Case Report Masahiro Egawa 1), Satoru
Bull Tokyo Dent Coll (2017) 58(3): 155 162 Case Report doi:10.2209/tdcpublication.2016-0038 Connective Tissue Graft for Gingival Recession in Mandibular Incisor Area: A Case Report Masahiro Egawa 1), Satoru
Surgical reconstruction of lost papilla around implant with a modified technique: A case report
 Journal of Periodontology & Implant Dentistry Case Report Surgical reconstruction of lost papilla around implant with a modified technique: A case report Mahdi Faraji* Andre Van Zyl University of Pretoria,
Journal of Periodontology & Implant Dentistry Case Report Surgical reconstruction of lost papilla around implant with a modified technique: A case report Mahdi Faraji* Andre Van Zyl University of Pretoria,
Avita Rath, 1 Smrithi Varma, 2 and Renny Paul Case Presentation. 1. Background
 Case Reports in Dentistry Volume 2016, Article ID 9289634, 5 pages http://dx.doi.org/10.1155/2016/9289634 Case Report Two-Stage Mucogingival Surgery with Free Gingival Autograft and Biomend Membrane and
Case Reports in Dentistry Volume 2016, Article ID 9289634, 5 pages http://dx.doi.org/10.1155/2016/9289634 Case Report Two-Stage Mucogingival Surgery with Free Gingival Autograft and Biomend Membrane and
Case Report Esthetic Root Coverage with Double Papillary Subepithelial Connective Tissue Graft: A Case Report
 Case Reports in Dentistry, Article ID 509319, 5 pages http://dx.doi.org/10.1155/2014/509319 Case Report Esthetic Root Coverage with Double Papillary Subepithelial Connective Tissue Graft: A Case Report
Case Reports in Dentistry, Article ID 509319, 5 pages http://dx.doi.org/10.1155/2014/509319 Case Report Esthetic Root Coverage with Double Papillary Subepithelial Connective Tissue Graft: A Case Report
Townie Guest Editorial. Gingival Attachment Loss: Evaluation and Surgical Options. Daniel J. Melker, DDS. fig. 1
 Gingival Attachment Loss: Evaluation and Surgical Options Daniel J. Melker, DDS Attached connective tissue (a.k.a. attached tissue) in the simplest terms is the body s only barrier between the underlying
Gingival Attachment Loss: Evaluation and Surgical Options Daniel J. Melker, DDS Attached connective tissue (a.k.a. attached tissue) in the simplest terms is the body s only barrier between the underlying
Findings and Conclusions: Clinical parameters mean at baseline at post-surgery were:
 Barros R, Novaes AB, Grisi M, et al. A 6 month comparative clinical study of a conventional and a new surgical approach for root coverage with acellular dermal matrix. J Periodontol 2004;75:1350-56. (29
Barros R, Novaes AB, Grisi M, et al. A 6 month comparative clinical study of a conventional and a new surgical approach for root coverage with acellular dermal matrix. J Periodontol 2004;75:1350-56. (29
Free Gingival Graft as a Single Step Procedure for Treatment of Mandibular Miller Class I and II Recession Defects
 12 Gingival graft in mandibular defect Original Article Free Gingival Graft as a Single Step Procedure for Treatment of Mandibular Miller Class I and II Recession Defects Lata Goyal1*, Narender Dev Gupta2,
12 Gingival graft in mandibular defect Original Article Free Gingival Graft as a Single Step Procedure for Treatment of Mandibular Miller Class I and II Recession Defects Lata Goyal1*, Narender Dev Gupta2,
Principles of Periodontal flap surgery. Dr.maryam khosravi
 Principles of Periodontal flap surgery Dr.maryam khosravi Goals of periodontal SURGICAL phase 1 - Controlling or eliminating periodontal disease. 2 Correcting anatomic conditions that may a. favor periodontal
Principles of Periodontal flap surgery Dr.maryam khosravi Goals of periodontal SURGICAL phase 1 - Controlling or eliminating periodontal disease. 2 Correcting anatomic conditions that may a. favor periodontal
Pouch and tunnel technique: Minimally invasive periodontal plastic surgery for root coverage
 www.edoriumjournals.com case Series OPEN ACCESS Pouch and tunnel technique: Minimally invasive periodontal plastic surgery for root coverage Sangeeta Singh ABSTRACT Introduction: The indications for root
www.edoriumjournals.com case Series OPEN ACCESS Pouch and tunnel technique: Minimally invasive periodontal plastic surgery for root coverage Sangeeta Singh ABSTRACT Introduction: The indications for root
MODIFIED SINGLE ROLL FLAP APPROACH FOR SIMULTANEOUS IMPLANT PLACEMENT AND GINGIVAL AUGMENTATION
 Journal of IMAB ISSN: 1312-773X https://www.journal-imab-bg.org https://doi.org/10.5272/jimab.2017233.1667 Journal of IMAB - Annual Proceeding (Scientific Papers). 2017 Jul-Sep;23(3): Case report MODIFIED
Journal of IMAB ISSN: 1312-773X https://www.journal-imab-bg.org https://doi.org/10.5272/jimab.2017233.1667 Journal of IMAB - Annual Proceeding (Scientific Papers). 2017 Jul-Sep;23(3): Case report MODIFIED
soft tissue mucoderm botiss native stable 3-dimensional 3D-Regenerative Tissue Graft Handling, Clinical Application and Cases
 dental bone & tissue regeneration botiss biomaterials mucoderm 3D-Regenerative Tissue Graft Handling, Clinical Application and Cases by PD Dr. med. dent. Adrian Kasaj soft tissue native stable 3-dimensional
dental bone & tissue regeneration botiss biomaterials mucoderm 3D-Regenerative Tissue Graft Handling, Clinical Application and Cases by PD Dr. med. dent. Adrian Kasaj soft tissue native stable 3-dimensional
A Promising Periodontal Procedure for the Treatment of Adjacent Gingival Recession Defects. Tolga Fikret Tözüm, DDS, PhD
 C L I N I C A L P R A C T I C E A Promising Periodontal Procedure for the Treatment of Adjacent Gingival Recession Defects Tolga Fikret Tözüm, DDS, PhD A b s t r a c t Various clinical reports on the reconstruction
C L I N I C A L P R A C T I C E A Promising Periodontal Procedure for the Treatment of Adjacent Gingival Recession Defects Tolga Fikret Tözüm, DDS, PhD A b s t r a c t Various clinical reports on the reconstruction
A Fantastic Aprroach for Multiple Recession Coverage: Vestibular Incision Subperiosteal Tunnel Access Technique (Vista)-A Case Report
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 2 Ver. I (Feb. 2016), PP 52-56 www.iosrjournals.org A Fantastic Aprroach for Multiple Recession
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 2 Ver. I (Feb. 2016), PP 52-56 www.iosrjournals.org A Fantastic Aprroach for Multiple Recession
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Case Report The Vestibular Incision Subperiosteal Tunnel Access (VISTA) for Treatment of Maxillary Anterior Gingival
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Case Report The Vestibular Incision Subperiosteal Tunnel Access (VISTA) for Treatment of Maxillary Anterior Gingival
Root Coverage with an Acellular Dermal Matrix Graft [Alloderm ] A Case Report
![Root Coverage with an Acellular Dermal Matrix Graft [Alloderm ] A Case Report Root Coverage with an Acellular Dermal Matrix Graft [Alloderm ] A Case Report](/thumbs/77/75855545.jpg) IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 13, Issue 12 Ver. VI (Dec. 2014), PP 39-43 www.iosrjournals.org Root Coverage with an Acellular Dermal
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 13, Issue 12 Ver. VI (Dec. 2014), PP 39-43 www.iosrjournals.org Root Coverage with an Acellular Dermal
Efficacy of Lateral Pedicle Graft in the Treatment of Isolated Gingival Recession Defects
 International Journal of Pharmaceutical Science Invention ISSN (Online): 2319 6718, ISSN (Print): 2319 670X Volume 3 Issue 1 January 2014 PP.46-50 Efficacy of Lateral Pedicle Graft in the Treatment of
International Journal of Pharmaceutical Science Invention ISSN (Online): 2319 6718, ISSN (Print): 2319 670X Volume 3 Issue 1 January 2014 PP.46-50 Efficacy of Lateral Pedicle Graft in the Treatment of
Geistlich Fibro-Gide. The Alternative Soft-Tissue Graft
 Geistlich Fibro-Gide The Alternative Soft-Tissue Graft Geistlich Fibro-Gide shows comparable results to connective tissue grafts in terms of change in soft-tissue volume over time., This demonstrates that
Geistlich Fibro-Gide The Alternative Soft-Tissue Graft Geistlich Fibro-Gide shows comparable results to connective tissue grafts in terms of change in soft-tissue volume over time., This demonstrates that
SURGICAL TREATMENT OF GINGIVAL RECESSION WITH SOFT TISSUE GRAFT PROCEDURE
 Journal of IMAB ISSN: 1312-773X https://www.journal-imab-bg.org https://doi.org/10.5272/jimab.2018243.2149 Journal of IMAB - Annual Proceeding (Scientific Papers). 2018 Jul-Sep;24(3) Literature review
Journal of IMAB ISSN: 1312-773X https://www.journal-imab-bg.org https://doi.org/10.5272/jimab.2018243.2149 Journal of IMAB - Annual Proceeding (Scientific Papers). 2018 Jul-Sep;24(3) Literature review
Consensus Report Tissue augmentation and esthetics (Working Group 3)
 B. Klinge Thomas F. Flemmig Consensus Report Tissue augmentation and esthetics (Working Group 3) Members of working group: Matteo Chiapasco Jan-Eirik Ellingsen Ronald Jung Friedrich Neukam Isabella Rocchietta
B. Klinge Thomas F. Flemmig Consensus Report Tissue augmentation and esthetics (Working Group 3) Members of working group: Matteo Chiapasco Jan-Eirik Ellingsen Ronald Jung Friedrich Neukam Isabella Rocchietta
Surgical Therapy. Tuesday, April 2, 13. Alessan"o Geminiani, DDS, MS
 Surgical Therapy Alessan"o Geminiani, DDS, MS Periodontal Flap: a surgical procedure in which incisions are made in the gingiva or mucosa to allow for separation of the epithelium and connective tissues
Surgical Therapy Alessan"o Geminiani, DDS, MS Periodontal Flap: a surgical procedure in which incisions are made in the gingiva or mucosa to allow for separation of the epithelium and connective tissues
Rescuing Tooth with Regenerative Technique: A Case Report. Women,, Suraram Mainroad, Ghmc Quthbullapur, Hyderabad , Telangana.
 ISSN- O: 2458-868X, ISSN P: 2458 8687 Index Copernicus Value: 49. 23 PubMed - National Library of Medicine - ID: 101731606 SJIF Impact Factor: 4.956 International Journal of Medical Science and Innovative
ISSN- O: 2458-868X, ISSN P: 2458 8687 Index Copernicus Value: 49. 23 PubMed - National Library of Medicine - ID: 101731606 SJIF Impact Factor: 4.956 International Journal of Medical Science and Innovative
Advanced Probing Techniques
 Module 21 Advanced Probing Techniques MODULE OVERVIEW The clinical periodontal assessment is one of the most important functions performed by dental hygienists. This module begins with a review of the
Module 21 Advanced Probing Techniques MODULE OVERVIEW The clinical periodontal assessment is one of the most important functions performed by dental hygienists. This module begins with a review of the
W J C C. World Journal of Clinical Cases. Gingival unit transfer using in the Miller Ⅲ recession defect treatment. Abstract INTRODUCTION CASE REPORT
 W J C C World Journal of Clinical Cases Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.12998/wjcc.v3.i2.199 World J Clin Cases 2015 February
W J C C World Journal of Clinical Cases Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.12998/wjcc.v3.i2.199 World J Clin Cases 2015 February
Clinical Abstract Review
 Multi-study Meta-Analysis Acellular Dermal Matrix for Mucogingival Surgery: A Meta-Analysis Ricardo Gapski, Christopher Allen Parks, and Hom-Lay Wang Background: Many clinical studies revealed the effectiveness
Multi-study Meta-Analysis Acellular Dermal Matrix for Mucogingival Surgery: A Meta-Analysis Ricardo Gapski, Christopher Allen Parks, and Hom-Lay Wang Background: Many clinical studies revealed the effectiveness
The alternative to connective tissue grafts. Geistlich Fibro-Gide
 The alternative to connective tissue grafts Geistlich Fibro-Gide CONTENTS From Then to Now 2 Geistlich Fibro-Gide in a Nutshell 4 Treatment Concepts Staged Approach After Implant Placement 8 Interview
The alternative to connective tissue grafts Geistlich Fibro-Gide CONTENTS From Then to Now 2 Geistlich Fibro-Gide in a Nutshell 4 Treatment Concepts Staged Approach After Implant Placement 8 Interview
Michael K. McGuire* and Martha Nunn
 Volume 74 Number 8 Evaluation of Human Recession Defects Treated with Coronally Advanced Flaps and Either Enamel Matrix Derivative or Connective Tissue. Part 1: Comparison of Clinical Parameters Michael
Volume 74 Number 8 Evaluation of Human Recession Defects Treated with Coronally Advanced Flaps and Either Enamel Matrix Derivative or Connective Tissue. Part 1: Comparison of Clinical Parameters Michael
Classifications for Gingival Recession: A Mini Review
 Galore International Journal of Health Sciences and Research Vol.3; Issue: 1; Jan.-March 2018 Website: www.gijhsr.com Review Article P-ISSN: 2456-9321 Classifications for Gingival Recession: A Mini Review
Galore International Journal of Health Sciences and Research Vol.3; Issue: 1; Jan.-March 2018 Website: www.gijhsr.com Review Article P-ISSN: 2456-9321 Classifications for Gingival Recession: A Mini Review
Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report
 C A S E R E P O R T Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report Rhoodie Garrana 1 and Govindrau Mohangi
C A S E R E P O R T Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report Rhoodie Garrana 1 and Govindrau Mohangi
Gingival recession causes periodontal
 J Periodontol October 2005 Factors Affecting the Outcomes of Coronally Advanced Flap Root Coverage Procedure Lien-Hui Huang,* Rodrigo E.F. Neiva, and Hom-Lay Wang Background: The coronally advanced flap
J Periodontol October 2005 Factors Affecting the Outcomes of Coronally Advanced Flap Root Coverage Procedure Lien-Hui Huang,* Rodrigo E.F. Neiva, and Hom-Lay Wang Background: The coronally advanced flap
Free Gingival Autograft: A Case Report
 CASE REPORT Free Gingival Autograft: A Case Report Veena Ashok. P. MDS, Bhargav Neetha BDS Abstract: Gingival recession is defined as Displacement of soft tissue margin apical to the cemento-enamel junction
CASE REPORT Free Gingival Autograft: A Case Report Veena Ashok. P. MDS, Bhargav Neetha BDS Abstract: Gingival recession is defined as Displacement of soft tissue margin apical to the cemento-enamel junction
MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION
 Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
The use of platelet-rich plasma in combination with connective tissue grafts following treatment of gingival recessions
 RESEARCH REPORT 63 Sasha M Jankovic, Aleksic M Zoran, Lekovic M Vojislav, Dimitrijevic S Bozidar, Barry E Kenney The use of platelet-rich plasma in combination with connective tissue grafts following treatment
RESEARCH REPORT 63 Sasha M Jankovic, Aleksic M Zoran, Lekovic M Vojislav, Dimitrijevic S Bozidar, Barry E Kenney The use of platelet-rich plasma in combination with connective tissue grafts following treatment
Over the years, mucogingival surgery
 The Use of DynaMatrix Extracellular Membrane for Gingival Augmentation and Root Coverage: A Case Series Saroff Stephen Andrew Saroff, DDS, MSD 1 Abstract Over the years, mucogingival surgery has developed
The Use of DynaMatrix Extracellular Membrane for Gingival Augmentation and Root Coverage: A Case Series Saroff Stephen Andrew Saroff, DDS, MSD 1 Abstract Over the years, mucogingival surgery has developed
Alveolar ridge preservation techniques
 Alveolar ridge preservation techniques Semmelweis University, Department of Periodontology, Budapest Dr. Windisch Péter Head of Department of Periodontology Changes of the alveolar ridge dimensions after
Alveolar ridge preservation techniques Semmelweis University, Department of Periodontology, Budapest Dr. Windisch Péter Head of Department of Periodontology Changes of the alveolar ridge dimensions after
A Clinical Evaluation of Anatomic Features of Gingiva in Dental Students in Tabriz, Iran
 Received 26 October 2007; Accepted 11 February 2008 A Clinical Evaluation of Anatomic Features of Gingiva in Dental Students in Tabriz, Iran Adileh Shirmohammadi 1 Masoumeh Faramarzie 1 * Ardeshir Lafzi
Received 26 October 2007; Accepted 11 February 2008 A Clinical Evaluation of Anatomic Features of Gingiva in Dental Students in Tabriz, Iran Adileh Shirmohammadi 1 Masoumeh Faramarzie 1 * Ardeshir Lafzi
Treatment of multiple gingival recessions using subepithelial connective tissue grafting with a single-incision technique
 317 Journal of Oral Science, Vol. 51, No. 2, 317-321, 2009 Case Report Treatment of multiple gingival recessions using subepithelial connective tissue grafting with a single-incision technique Jun-Beom
317 Journal of Oral Science, Vol. 51, No. 2, 317-321, 2009 Case Report Treatment of multiple gingival recessions using subepithelial connective tissue grafting with a single-incision technique Jun-Beom
S John Wiley & Sons A/S. Published by John Wiley & Sons Ltd. Spain; 2 University of Milano, Milan, Italy
 J Clin Periodontol 2014; 41 (Suppl. 15): S92 S97 doi: 10.1111/jcpe.12215 Surgical techniques on periodontal plastic surgery and soft tissue regeneration: Consensus Report of Group 3 of the 10th European
J Clin Periodontol 2014; 41 (Suppl. 15): S92 S97 doi: 10.1111/jcpe.12215 Surgical techniques on periodontal plastic surgery and soft tissue regeneration: Consensus Report of Group 3 of the 10th European
A mucogingival technique for the treatment of multiple recession defects in the
 A mucogingival technique for the treatment of multiple recession defects in the mandibular anterior region: a case series with two-year follow-up. Nicola Bethaz, DDS* Federica Romano, DDS** Francesco Ferrarotti,
A mucogingival technique for the treatment of multiple recession defects in the mandibular anterior region: a case series with two-year follow-up. Nicola Bethaz, DDS* Federica Romano, DDS** Francesco Ferrarotti,
Delta Dental of Virginia Clinical Policy # 402
 Delta Dental of Virginia Clinical Policy # 402 Subject Mucogingival Surgery and Soft Tissue Grafting Originating Department Clinical Professional Services Signature Authority Dental Director Type: New
Delta Dental of Virginia Clinical Policy # 402 Subject Mucogingival Surgery and Soft Tissue Grafting Originating Department Clinical Professional Services Signature Authority Dental Director Type: New
Clinical Application of Modified Apically Repositioned Flap in Class III/IV Gingival Recession Cases
 J Harjeet Singh et al SE REPORT 10.5005/jp-journals-10031-1200 linical pplication of Modified pically Repositioned Flap in lass III/IV Gingival Recession ases 1 Harjeet Singh, 2 Manab Kosala, 3 Vivek apurao
J Harjeet Singh et al SE REPORT 10.5005/jp-journals-10031-1200 linical pplication of Modified pically Repositioned Flap in lass III/IV Gingival Recession ases 1 Harjeet Singh, 2 Manab Kosala, 3 Vivek apurao
Derma S O F T T I S S U E A U G M E N TAT I O N. Acellular dermal matrix
 Derma A XENOGENIC GRAFT FOR S O F T T I S S U E A U G M E N TAT I O N Acellular dermal matrix A xenogenic graft for soft tissue augmentation CHARACTERISTICS Obtained from derma of porcine origin, using
Derma A XENOGENIC GRAFT FOR S O F T T I S S U E A U G M E N TAT I O N Acellular dermal matrix A xenogenic graft for soft tissue augmentation CHARACTERISTICS Obtained from derma of porcine origin, using
Gingival Unit Graft Versus Free Gingival Graft for Treatment of Gingival Recession: A Randomized Controlled Clinical Trial
 Original Article Gingival Unit Graft Versus Free Gingival Graft for Treatment of Gingival Recession: A Randomized Controlled Clinical Trial Niloofar Jenabian 1, Mohadese Yazdanpanah Bahabadi 2, Ali Bijani
Original Article Gingival Unit Graft Versus Free Gingival Graft for Treatment of Gingival Recession: A Randomized Controlled Clinical Trial Niloofar Jenabian 1, Mohadese Yazdanpanah Bahabadi 2, Ali Bijani
Papilla and pontic area regeneration in patient with gingival smile: A clinical case
 Journal section: Esthetic Dentistry Publication Types: Case Report doi:10.4317/jced.54859 http://dx.doi.org/10.4317/jced.54546 Papilla and pontic area regeneration in patient with gingival smile: A clinical
Journal section: Esthetic Dentistry Publication Types: Case Report doi:10.4317/jced.54859 http://dx.doi.org/10.4317/jced.54546 Papilla and pontic area regeneration in patient with gingival smile: A clinical
Pre-orthodontic gingival augmentation with an acellular dermal matrix allograft: a case report
 CLINICAL REPORT 99 Publication Randy R Fitzgerald, Swati Y Rawal, Ann W Walters, John D Walters Pre-orthodontic gingival augmentation with an acellular dermal matrix allograft: a case report Randy R Fitzgerald
CLINICAL REPORT 99 Publication Randy R Fitzgerald, Swati Y Rawal, Ann W Walters, John D Walters Pre-orthodontic gingival augmentation with an acellular dermal matrix allograft: a case report Randy R Fitzgerald
Soft-Tissue Success with the. Clinical Success. Proven Matrix. with the Proven. Geistlich Mucograft Geistlich Mucograft Seal
 Soft-Tissue Success with the Clinical Success Proven Matrix with the Proven Bone Geistlich Mucograft Substitute Seal The Softer Side of Geistlich Innovation Decades of collagen expertise leads naturally
Soft-Tissue Success with the Clinical Success Proven Matrix with the Proven Bone Geistlich Mucograft Substitute Seal The Softer Side of Geistlich Innovation Decades of collagen expertise leads naturally
Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports
 0 Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports R.G. Caffesse, B.A. Smith/ B. Duff, E.C. Morrison, D. Merrill/ and W. Becker In the cases reported here, the response
0 Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports R.G. Caffesse, B.A. Smith/ B. Duff, E.C. Morrison, D. Merrill/ and W. Becker In the cases reported here, the response
Treatment of dental recessions in the esthetic zone by gingival and osseous recontouring. A multidisciplinary perio-prosthodontic case report.
 European International Journal of Science and Technology Vol. 6 No. 5 July 2017 Treatment of dental recessions in the esthetic zone by gingival and osseous recontouring. A multidisciplinary perio-prosthodontic
European International Journal of Science and Technology Vol. 6 No. 5 July 2017 Treatment of dental recessions in the esthetic zone by gingival and osseous recontouring. A multidisciplinary perio-prosthodontic
Management of Thin Gingival Biotype with Hard and Soft Tissue Augmentation Post Orthodontic Treatment: A Case Report
 Open Journal of Dentistry and Oral Medicine 3(2): 53-58, 2015 DOI: 10.13189/ojdom.2015.030204 http://www.hrpub.org Management of Thin Gingival Biotype with Hard and Soft Tissue Augmentation Post Orthodontic
Open Journal of Dentistry and Oral Medicine 3(2): 53-58, 2015 DOI: 10.13189/ojdom.2015.030204 http://www.hrpub.org Management of Thin Gingival Biotype with Hard and Soft Tissue Augmentation Post Orthodontic
Patient Satisfaction With Acellular Dermal Matrix Graft In The Treatment Of Multiple Gingival Recession Defects - A Clinical Study
 Article ID: WMC00458 2046-1690 Patient Satisfaction With Acellular Dermal Matrix Graft In The Treatment Of Multiple Gingival Recession Defects - A Clinical Study Corresponding Author: Dr. Ajay Mahajan,
Article ID: WMC00458 2046-1690 Patient Satisfaction With Acellular Dermal Matrix Graft In The Treatment Of Multiple Gingival Recession Defects - A Clinical Study Corresponding Author: Dr. Ajay Mahajan,
Original Article Reconstruction of attached soft tissue around dental implants by acelluar dermal matrix grafts and resin splint
 Int J Clin Exp Med 2014;7(12):4666-4676 www.ijcem.com /ISSN:1940-5901/IJCEM0002921 Original Article Reconstruction of attached soft tissue around dental implants by acelluar dermal matrix grafts and resin
Int J Clin Exp Med 2014;7(12):4666-4676 www.ijcem.com /ISSN:1940-5901/IJCEM0002921 Original Article Reconstruction of attached soft tissue around dental implants by acelluar dermal matrix grafts and resin
Coronally advanced flap with Platelet Rich Fibrin- An effective mode of treating gingival recession: A case report
 Case Report Coronally advanced flap with Platelet Rich Fibrin- An effective mode of treating gingival recession: A case report Vijendra Pal Singh 1,*, Sangeeta Umesh Nayak 2, Dipen Shah 3 1 Associate Professor,
Case Report Coronally advanced flap with Platelet Rich Fibrin- An effective mode of treating gingival recession: A case report Vijendra Pal Singh 1,*, Sangeeta Umesh Nayak 2, Dipen Shah 3 1 Associate Professor,
Soft-Tissue Solutions from The Collagen Expert. Clinical Success with the Proven. Geistlich Mucograft Geistlich Mucograft Seal Geistlich Fibro-Gide
 Soft-Tissue Solutions from The Collagen Expert Clinical Success with the Proven Bone Geistlich Mucograft Substitute Geistlich Mucograft Seal Geistlich Fibro-Gide Documented More than 1,000 publications
Soft-Tissue Solutions from The Collagen Expert Clinical Success with the Proven Bone Geistlich Mucograft Substitute Geistlich Mucograft Seal Geistlich Fibro-Gide Documented More than 1,000 publications
Michael K. McGuire,* E. Todd Scheyer,* and Martha Nunn
 J Periodontol November 2012 Evaluation of Human Recession Defects Treated With Coronally Advanced Flaps and Either Enamel Matrix Derivative or Connective Tissue: Comparison of Clinical Parameters at 10
J Periodontol November 2012 Evaluation of Human Recession Defects Treated With Coronally Advanced Flaps and Either Enamel Matrix Derivative or Connective Tissue: Comparison of Clinical Parameters at 10
Therapeutic Outcomes for Gingival Recession Defects in the Esthetic Zone: A Systematic Review
 Review Article imedpub Journals http://www.imedpub.com/ Periodontics and Prosthodontics ISSN DOI: 10.21767/.100012 Abstract Therapeutic Outcomes for Gingival Recession Defects in the Esthetic Zone: A Systematic
Review Article imedpub Journals http://www.imedpub.com/ Periodontics and Prosthodontics ISSN DOI: 10.21767/.100012 Abstract Therapeutic Outcomes for Gingival Recession Defects in the Esthetic Zone: A Systematic
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 345 A Mucogingival Technique for the Treatment of Multiple Recession Defects in the Mandibular Anterior Region: A Case Series with a 2-Year
The International Journal of Periodontics & Restorative Dentistry 345 A Mucogingival Technique for the Treatment of Multiple Recession Defects in the Mandibular Anterior Region: A Case Series with a 2-Year
Nicholas Caplanis DMD MS 6/13/2012
 Considerations In The Esthetic Zone Nick Caplanis DMD MS Private Practice Periodontics and Implant Surgery Mission Viejo, California Nick@drcaplanis.com Assistant Professor Loma Linda University Anatomic
Considerations In The Esthetic Zone Nick Caplanis DMD MS Private Practice Periodontics and Implant Surgery Mission Viejo, California Nick@drcaplanis.com Assistant Professor Loma Linda University Anatomic
Michael K. McGuire,* E. Todd Scheyer,* and Mark B. Snyder
 J Periodontol October 2014 Evaluation of Recession Defects Treated With Coronally Advanced Flaps and Either Recombinant Human Platelet-Derived Growth Factor-BB Plus b-tricalcium Phosphate or Connective
J Periodontol October 2014 Evaluation of Recession Defects Treated With Coronally Advanced Flaps and Either Recombinant Human Platelet-Derived Growth Factor-BB Plus b-tricalcium Phosphate or Connective
Clinical Comparison of Subepithelial Connective Tissue Grafts and Coronally Advanced Flaps with Emdogain in the Treatment of Gingival Recessions
 Original Article Clinical Comparison of Subepithelial Connective Tissue Grafts and Coronally Advanced Flaps with Emdogain in the Treatment of Gingival Recessions F. Haghighati 1,2, AA. Khoshkhoonejad 3,
Original Article Clinical Comparison of Subepithelial Connective Tissue Grafts and Coronally Advanced Flaps with Emdogain in the Treatment of Gingival Recessions F. Haghighati 1,2, AA. Khoshkhoonejad 3,
Department of Periodontology & Oral Implantology, Genesis Institute of Dental Sciences and Research, Ferozepur, Punjab, India
 Original Article Comparison of semilunar coronally advanced flap alone and in combination with button technique in the treatment of Miller s Class I and II gingival recessions: A Pilot Study Ranjit Singh
Original Article Comparison of semilunar coronally advanced flap alone and in combination with button technique in the treatment of Miller s Class I and II gingival recessions: A Pilot Study Ranjit Singh
Bone augmentation with maxgraft
 Patient information bone & tissue regeneration botiss biomaterials Bone augmentation with maxgraft established safe X100 natural Implantation stability is crucial for success Atrophy of the jaw bone loss
Patient information bone & tissue regeneration botiss biomaterials Bone augmentation with maxgraft established safe X100 natural Implantation stability is crucial for success Atrophy of the jaw bone loss
Modified Pedicle Grafting: A Novel Noninvasive Technique for Soft Tissue Augmentation Around Maxillary Dental Implants
 Original Article Modified Pedicle Grafting: A Novel Noninvasive Technique for Soft Tissue Augmentation Around Maxillary Dental Implants Seyed Hossein Mohseni Salehi 1, Afshin Khorsand 2, Sahar Chokami
Original Article Modified Pedicle Grafting: A Novel Noninvasive Technique for Soft Tissue Augmentation Around Maxillary Dental Implants Seyed Hossein Mohseni Salehi 1, Afshin Khorsand 2, Sahar Chokami
Management of a complex case
 2 Soft- and hard-tissue reconstruction of a severely deficient site prior to implant placement: a case report Management of a complex case Younes Khosroshahy, DDS, MFDS RCS (Eng), Dip Imp Dent RCSEd, Blue
2 Soft- and hard-tissue reconstruction of a severely deficient site prior to implant placement: a case report Management of a complex case Younes Khosroshahy, DDS, MFDS RCS (Eng), Dip Imp Dent RCSEd, Blue
Practical Advanced Periodontal Surgery
 Practical Advanced Periodontal Surgery Serge Dibart Blackwell Munksgaard Chapter 8 Papillary Construction After Dental Implant Therapy Peyman Shahidi, DOS, MScD, Serge Dibart, DMD, and Yun Po Zhang, PhD,
Practical Advanced Periodontal Surgery Serge Dibart Blackwell Munksgaard Chapter 8 Papillary Construction After Dental Implant Therapy Peyman Shahidi, DOS, MScD, Serge Dibart, DMD, and Yun Po Zhang, PhD,
Regaining Your Gum Tissue. Soft-Tissue Regeneration With Geistlich Mucograft
 Regaining Your Gum Tissue Soft-Tissue Regeneration With Geistlich Mucograft Why is Healthy Gum Tissue So Important? Gum tissue can recede due to grinding of the teeth, thin insufficient gum tissue, as
Regaining Your Gum Tissue Soft-Tissue Regeneration With Geistlich Mucograft Why is Healthy Gum Tissue So Important? Gum tissue can recede due to grinding of the teeth, thin insufficient gum tissue, as
Biology of soft tissue wound healing and regeneration consensus report of Group 1 of the 10th European Workshop on Periodontology
 Zurich Open Repository and Archive University of Zurich Main Library Strickhofstrasse 39 CH-8057 Zurich www.zora.uzh.ch Year: 2014 Biology of soft tissue wound healing and regeneration consensus report
Zurich Open Repository and Archive University of Zurich Main Library Strickhofstrasse 39 CH-8057 Zurich www.zora.uzh.ch Year: 2014 Biology of soft tissue wound healing and regeneration consensus report
Clinical Case Reports using Cytoplast GTR Barrier Membranes
 Clinical Case Reports using Cytoplast GTR Barrier Membranes Barry K. Bartee, DDS, MD The Cytoplast Technique: Extraction Site Grafting Without Primary Closure 1. 1. Preoperative view. To maximize the result
Clinical Case Reports using Cytoplast GTR Barrier Membranes Barry K. Bartee, DDS, MD The Cytoplast Technique: Extraction Site Grafting Without Primary Closure 1. 1. Preoperative view. To maximize the result
WHAT IS THE PURPOSE OF WHAT WE DO? TEAM PERIODONTICS: WORKING TOGETHER TO IMPROVE PATIENT CARE YOU ARE THE PERIODONTISTS IN YOUR PRACTICE!
 Setter Periodontics 2075 SW 1 st Ave #2L Portland, OR 97201 503-222-9961 michael@setterperio.com WHAT IS THE PURPOSE OF WHAT WE DO? Gum Gardeners Study Club 2.27.17 TEAM PERIODONTICS: WORKING TOGETHER
Setter Periodontics 2075 SW 1 st Ave #2L Portland, OR 97201 503-222-9961 michael@setterperio.com WHAT IS THE PURPOSE OF WHAT WE DO? Gum Gardeners Study Club 2.27.17 TEAM PERIODONTICS: WORKING TOGETHER
REGENERATIONTIME. A Case Report by. Ridge Augmentation and Delayed Implant Placement on an Upper Lateral Incisor
 A Case Report by Dr. Daniele Cardaropoli Ridge Augmentation and Delayed Implant Placement on an Upper Lateral Incisor The Situation An adult female patient presented with an endodontic/prosthetic failure
A Case Report by Dr. Daniele Cardaropoli Ridge Augmentation and Delayed Implant Placement on an Upper Lateral Incisor The Situation An adult female patient presented with an endodontic/prosthetic failure
Esthetic Crown Lengthening for Upper Anterior Teeth: Indications and Surgical Techniques
 I J Pre Clin Dent Res 2014;1(2):49-53 April-June All rights reserved International Journal of Preventive & Clinical Dental Research Esthetic Crown Lengthening for Upper Anterior Teeth: Indications and
I J Pre Clin Dent Res 2014;1(2):49-53 April-June All rights reserved International Journal of Preventive & Clinical Dental Research Esthetic Crown Lengthening for Upper Anterior Teeth: Indications and
Multi-Modality Anterior Extraction Site Grafting Increased Predictability for Aesthetics Michael Tischler, DDS
 Page 1 of 5 Issue Date: March 2003, Posted On: 8/1/2005 Multi-Modality Anterior Extraction Site Grafting Increased Predictability for Aesthetics Michael Tischler, DDS The extraction of teeth creates a
Page 1 of 5 Issue Date: March 2003, Posted On: 8/1/2005 Multi-Modality Anterior Extraction Site Grafting Increased Predictability for Aesthetics Michael Tischler, DDS The extraction of teeth creates a
INTRODUCTION. long-term results in the restoration of both totally and partially
 CLINICAL RESTORATION OF THE SOFT-TISSUE MARGIN IN SINGLE-TOOTH IMPLANT IN THE ANTERIOR MAXILLA Jamil Awad Shibli, DDS, MS, PhD Susana d Avila, DDS, MS KEY WORDS Dental implants Subepithelial connective
CLINICAL RESTORATION OF THE SOFT-TISSUE MARGIN IN SINGLE-TOOTH IMPLANT IN THE ANTERIOR MAXILLA Jamil Awad Shibli, DDS, MS, PhD Susana d Avila, DDS, MS KEY WORDS Dental implants Subepithelial connective
RESEARCH REVIEW. Gingival recession: a proposal for a new classification ISSN :
 RESEARCH REVIEW Gingival recession: a proposal for a new classification Shantipriya Reddy, Sanjay Kaul, Prasad M.G.S., Jaya Agnihotri, Amudha D., Soumya Kambali ABSTRACT An accurate diagnosis is often
RESEARCH REVIEW Gingival recession: a proposal for a new classification Shantipriya Reddy, Sanjay Kaul, Prasad M.G.S., Jaya Agnihotri, Amudha D., Soumya Kambali ABSTRACT An accurate diagnosis is often
All Dentistry is Cosmetic Betsy Bakeman, DDS Arkansas State Dental Association
 All Dentistry is Cosmetic Betsy Bakeman, DDS Arkansas State Dental Association Patients have traditionally sought treatment when concerned with the way their teeth look, function or feel. Over the past
All Dentistry is Cosmetic Betsy Bakeman, DDS Arkansas State Dental Association Patients have traditionally sought treatment when concerned with the way their teeth look, function or feel. Over the past
