Research Article Root Coverage for Single Deep Gingival Recessions: Outcomes Based on a Decision-Making Algorithm
|
|
|
- Rodger Kenneth Whitehead
- 5 years ago
- Views:
Transcription
1 International Journal of Dentistry Volume 2019, Article ID , 9 pages Research Article Root Coverage for Single Deep Gingival Recessions: Outcomes Based on a Decision-Making Algorithm João B. César Neto, 1 Marília C. Cavalcanti, 1 Ricardo T. Sekiguchi, 1 Claudio M. Pannuti, 1 Giuseppe A. Romito, 1 and Dimitris N. Tatakis 2 1 Division of Periodontology, College of Dentistry, University of São Paulo, São Paulo, Brazil 2 Division of Periodontology, College of Dentistry, The Ohio State University, Columbus, OH, USA Correspondence should be addressed to João B. César Neto; jbcesarneto@usp.br Received 6 August 2018; Revised 1 December 2018; Accepted 10 December 2018; Published 22 January 2019 Academic Editor: Tommaso Lombardi Copyright 2019 João B. César Neto et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Aim. The aim of this study is to report root coverage outcomes in single deep gingival recessions (GR) following a proposed decision-making algorithm. Materials and Methods. A retrospective, practice-based study included single deep ( 5 mm) Miller Class II and III defects. The step-by-step decision-making algorithm led to a choice among three different flap designs(coronally advanced flap(caf), double papilla envelope flap(dpe) or modified lateral sliding flap(lsf)) used with a connective tissue graft. Recession depth (RD) at 6 months follow-up and the corresponding root coverage (RC) were the primary outcomes assessed. Results. Sixteen GR defects were included, with baseline RD of 6.7 ± 1.8 mm. Six months postoperatively, RD was significantly reducedto1.2±0.8mm(p<0.05).meanrcwas81.7±13.0%,withoutsignificantdifferencesbetweenmillerclassii(87.1±9.2%; n 9) and Class III (74.6±14.5%; n 7) GRs (p 0.07). Postoperatively, keratinized tissue width increase was greater for LSF (3.5±1.1)andDPE(4.2±1.4mm)thanforCAF(1.9±0.9mm).Conclusions.Followingtheproposeddecision-makingalgorithm, root coverage outcomes for GR defects 5 mm were comparable to outcomes reported for shallow defects. Prospective clinical trials are needed to validate the proposed approach and techniques. Practical Implications. The proposed algorithm allows the clinician to select the appropriate surgical technique for treatment of single deep gingival recessions with good predictability. 1.Introduction Gingival recession(gr) is a common periodontal condition that can negatively impact esthetics, plaque control, and hypersensitivity [1]. Furthermore, the exposed root surfaces are susceptible to root caries and noncarious cervical lesion development [2, 3]. In patients with good oral hygiene, longitudinal evidence indicates that untreated GR defects tend to increase in depth over time [4]. The outcomes of available GR treatment modalities have been analyzed through several systematic reviews, which conclude that use of subepithelial connective tissue graft (CTG) provides the best results for predictable and longlasting root coverage (RC) [5 7]. However, GR treatment outcomes may be modulated by defect characteristics, such as defect dimensions (depth, width), site (maxilla, mandible), defect number (single, multiple), soft tissue anatomy (keratinized tissue quality/quantity; papilla height/width; frenum/muscle pull; vestibular depth), and tooth position [7 10]. Despite the extensive literature on GR treatment, adequate evidence is lacking on outcomes at specific sites other than maxillary canines and premolars or on the effect of site characteristics, such as root prominence and vestibular depth [9]. Most of the existing literature has explored treatment of 2 4 mm deep GRs, providing limited evidence on deeper defects. Evidence indicates that deeper GR defects represent more of an aesthetic concern for patients and is one of the reasons for which they seek treatment[11]. The definition of a deep GR defect varies widely in the literature: authors have used subjective assessment[12], depth 3 mm[13 15], >3mm [16], 4mm [10, 17 19], 5mm [20], or>5mm [21, 22]. Despite thelackof consensus on the definitionof a deep GR defect, evidence indicates that increasing GR
2 2 InternationalJournalofDentistry depth negatively affects RC outcomes [7]. To overcome the challenges of treating deep GR defects, diverse CTG-based surgical approaches have been proposed; these combine CTG with envelope flap or lateral sliding flap (LSF) or coronally advanced flap (CAF) [21]. Close attention to confounding anatomical factors, such as increased defect width and shallow residual vestibular depth, is needed when dealing with deep GR defects [21]. Therefore, the decisionmaking process for treatment of deep GR defects is complex, requiring careful consideration of additional anatomical parameters. The aim of this retrospective, practice-based case series study is to evaluate the outcomes of treating deep ( 5mm) GR defects when following a step-by-step clinical decisionmaking algorithm which incorporates assessment of GR dimension, residual vestibular depth, and potential compromising factors. 2.Materials and Methods 2.1. Patient and Site Selection. The records of adult and systemically healthy patients who were referred to a private periodontal practice(sorocaba-sp, Brazil) for GR evaluation and treatment were reviewed. Patients treated between October 2009 and May 2016 for a single deep ( 5mm in depth) and Miller Class II or III [23] defect were included. All patients were given detailed information on surgical procedures, materials, medications, anticipated outcomes, potential complications, side effects, and alternative treatment options; all provided informed consent prior to surgery. Eligibility criteria were adult ( 18 years old), nonsmoker, nonsignificant and noncontributory medical history, no systemic medications, periodontally healthy, single deep GR defect treated, at least 6-months of postoperative follow-up, and documentation of clinical parameters reported below. The study protocol was approved by the Ethics Review Board of College of Dentistry (USP) (ERB approval n ) Preoperative Patient and Site Management. Patients received oral hygiene instructions, prophylaxis, or scaling and root planing, as needed, prior to surgery. Surgical procedures were not scheduled until patients achieved satisfactory oral hygiene levels (plaque score <20%, plaquefree GR site and adjacent teeth, and negative for bleeding on probing (BOP)) Clinical Parameters. Clinical parameters were recorded immediately preoperatively (baseline) and six months postoperatively(tables 1 and 2). Evaluated parameters were plaque score; BOP; recession depth (RD; cementoenamel junction (CEJ) to gingival margin (GM)); recession width (RW) at the CEJ level; GR classification [23]; probing depth (PD); clinical attachment level(cal); and keratinized tissue width (KTW; GM to mucogingival junction(mgj)). Plaque and BOP were recorded at 6 sites per tooth on all teeth present. The remaining parameters were measured on the midbuccal aspect of the study tooth and recorded to the nearest 0.5 mm. Parameters were measured using a periodontal probe (UNC-15 probe, Hu-Friedy, Chicago, IL, USA) by the same operator (JBCN) who performed the procedures. Root coverage (RC, in percentage) was calculated by the following formula: baseline RD 6-months RD 100. (1) baseline RD 2.4. Decision Tree. In the course of treating deep GR defects, the primary author (JBCN) has been following a defined step-by-step decision-making algorithm(figure 1). The first step is to determine the anticipated GM displacement necessary to cover the defect in relation to the remaining vestibular depth. The decision tree considers that the necessary GM displacement should allow RD coverage and postoperative GM positioning 1 mm coronal to CEJ; therefore, the anticipated GM displacement (in mm) equals RD + 1. The relation between anticipated GM displacement and residual vestibular depth modulates flap design choice. This is because as RD increases, the distance between GM (RD site) and vestibular fornix (VF) depth (GM-VF distance) decreases, thus resulting in reduced tissue length available for coronal displacement (Figure 2). Hence, a formula was created to facilitate interpretation of the clinical parameters that guide the decision-making. To measure the GM-VF distance, a lip retractor was used to gently retract the tissues to allow visualization of the VF. Meanwhile, the patient was asked to keep the mouth slightly open(about10mm),toavoidtensiononthelowerlip.then, the periodontal probe, positioned along the long axis of the tooth and resting against the buccal surface of the tooth/ alveolar process, was used to measure the distance from GM tovf.todeterminewhentheprobetiptouchedthevf,the probewasviewedfromanapproximate45 horizontalangle relative to the buccal surface of the tooth. When RD+1<(GM-VF) 1.1, a coronally advanced flap plus CTG (CAF+CTG) design was used (Figure 1). Otherwise, alternative designs were adopted. In borderline cases, where the flap design choice was deemed ambivalent, the CAF design was chosen. The use of the multiplication factor ( 1.1) ensures that the remaining buccal tissue height (GM-VF) is at least 10% greater than the anticipated gingival margin displacement (RD + 1), a needed condition that became apparent from working on and analyzing cases of RD 5mm. Whenever CAF+CTG was rejected, the choice of flap design was either double papilla envelope flap(dpe + CTG) or lateral sliding flap (LSF+CTG) (Figure 1). The second stepofthedecisiontreewastochoosebetweendpeandlsf (Figure 1). The primary factor determining this decision was RW, classified as narrow ( 3.5mm) or wide (>3.5mm) [24,25].DPEwasemployedinnarrowdefects,andLSFwas chosen for wide defects (Figure 1). This decision step was modified by additional factors, considered as potentially compromising the treatment outcome. Such factors included buccal tooth position, root prominence, proximity of
3 InternationalJournalofDentistry 3 Flap design Table 1: Individual patient data and descriptive statistics for RD, RW, GR reduction, and RC. Patient Tooth Miller class Baseline RW (mm) Baseline RW (mm) 6-month RD (mm) RD reduction (mm) 6-month RC (%) 1 6 III III CAF+CTG 3 11 II III II Mean ± SD 4.9 (±0.8) 5.5 (±0.7)A 1.3 (±0.7)B 4.2 (±0.3) 77.2 (±9.4) 6 25 III II DPE+CTG 8 26 III II II III Mean ± SD 3.6 (±0.9) 6.3 (±1.9)A 1.0 (±1.0)B 5.3 (±2.5) 82.3 (±18.2) II III LSF+CTG II II II Mean ± SD 3.6 (±1.3) 8.2 (±1.5)A 1.2 (±0.8)B 7 (±1.5) 85.3 (±9.6) Overall mean ± SD 4.0 (±1.1) 6.7 (±1.8)A 1.2 (±0.8)B 5.5 (±2.0) 81.7 (±13.0) RD recession depth; RW recession width; GR gingival recession; RC root coverage; CAF coronally advanced flap; DPE double papilla envelope; LSF lateral sliding flap; CTG connective tissue graft; different upper cases indicate statistically significant intragroup differences. Table 2: Individual patient data and descriptive statistics for KTW. Flap design Patient Tooth Miller class Baseline KTW (mm) 6-month KTW (mm) KTW change (mm) 1 6 III III CAF+CTG 3 11 II III II Mean ± SD 0.5 (±0.5)A 2.4 (±1.1)B 1.9 (±0.9) 6 25 III II DPE+CTG 8 26 III II II III Mean ± SD 0.1 (±0.2)A 4.3 (±1.5)B 4.2 (±1.4) II III LSF+CTG II II II Mean ± SD 0 (±0)A 3.5 (±1.1)B 3.5 (±1.1) Overall mean ± SD 0.2 (±0.4)A 3.4 (±1.4)B 3.3 (±1.5) KTW keratinized tissue width; CAF coronally advanced flap; DPE double papilla envelope; LSF lateral sliding flap; CTG connective tissue graft; different upper cases indicate statistically significant intragroup differences. vital structures (e.g., mental nerve), and deep bone dehiscence. The presence of compromising factors led to LSF use even in narrow GR defects (Figure 1). The third step in the decision process was concerning CTG length (mesiodistal dimension), which varied by flap design and compromising factor presence (Figure 1). With CAF+CTG approach, CTG length equaled RW+6mm (3mmoneithersideoftheGR).WithDPE+CTGapproach, CTG length equaled RW plus width of two adjacent teeth. With LSF+CTG choice, CTG length varied depending on the absence/presence of compromising factors; in the absence of compromising factors, CTG length equaled RW plus width of one adjacent tooth (the tooth associated with the tunnel). When compromising factors were present, CTG length equaled RW plus width of two adjacent teeth. In all cases, CTG height (apicocoronal dimension) was as close to RD as possible; when donor site dimensions permitted, CTG height was RD+2mm.
4 4 InternationalJournalofDentistry Decision tree for recessions 5mm RD+1 < (GM-VF) 1.1 < RD+1 CAF DPE or LSF Narrow RW 3.5mm Wide RW > 3.5mm No compromising factors Compromising factors present No compromising factors Compromising factors present DPE CTG-3 teeth LSF CTG-3 teeth LSF CTG-2 teeth LSF CTG-3 teeth Figure 1: Graphic illustration of the decision-making process. When the GM-VF distance is clearly greater than RD, CAF + CTG should be adopted. In borderline cases (gray color), CAF + CTG was adopted. When CAF is rejected, narrow recessions should be treated with DPE+CTG and wide recessions should be treated with LSF+CTG. The presence of compromising factors in narrow defects moves the decision towards LSF + CTG. In addition, 3-teeth length is recommended for CTG in the presence of compromising factors (see text for extended explanation). RD recession depth; GM gingival margin; VF vestibule fornix; CAF coronally advanced flap; DPE double papilla envelope; LSF lateral sliding flap; CTG connective tissue graft; RW recession width. (a) (b) (c) (d) Figure 2: Clinical images illustrating the relationship between RD and GM-VF distance. From (a d), it is possible to note that as RD increases, the GM-VF distance decreases. This affects the availability of tissue to displace coronally and the possible muscular tension on the flap. For abbreviations, see Figure 1 caption. 2.5.SurgicalProtocols. CAF+CTG(Figure3)isbasedonthe original trapezoidal flap design of Langer and Langer [26]. Horizontal incisions were performed, mesial and distal to CEJ, leaving the papillae intact and were connected by a sulcular incision on the buccal aspect of the defect (Figure 3(a)). Vertical releasing incisions were then performed, delineating the trapezoidal flap (Figure 3(b)). Fullthickness elevation was performed to the MGJ followed by split-thickness elevation(sharp dissection(15c scalpel blade, Swann-Morton, Sheffield, England)) apical to MGJ (Figure 3(b)). Papillae were deepithelialized and appropriately sized CTG (see above section) was positioned at CEJ and secured by one interrupted suture (Vycril 6 0, Ethicon, Johnson and Johnson, São José dos Campos, SP, Brasil) at each papilla (Figure 3(c)). Trapezoidal flap was then advanced to 1mm coronal to CEJ and secured with
5 International Journal of Dentistry 5 (a) (b) (d) (c) (e) Figure 3: Clinical images illustrating the CAF + CTG technique used. (a) Line shows design of horizontal incisions at CEJ level and sulcular incision; (b) vertical releasing incisions resulting in a trapezoidal flap; (c) CTG secured at CEJ level by interrupted single sutures; (d) CAF sutured 1 mm coronal to CEJ; (e) 6-month follow-up. For abbreviations, see Figure 1 caption. suspensory suture (Figure 3(d)). Vertical incisions were sutured using interrupted sutures (Figure 3(d)). DPE + CTG (Figure 4) is based on the envelope flap design [27] modified to include elevation and approximation of adjacent papillae [28, 29]. A sulcular incision was made first on the buccal aspect of the defect, extending to both adjacent papillae (Figure 4(a)). Subsequently, a fullthickness flap was reflected to create an envelope extending 5 mm apical to RD and encompassing the two adjacent teeth (Figure 4(b)). Appropriately sized CTG (see above) was placed in the envelope (Figure 4(c)), positioned at CEJ level whenever possible and stabilized by two interrupted sutures, one at either end of the envelope flap and a suspensory suture around the defect site tooth (Figure 4(d)). Subsequently, interrupted sutures, spaced 2 mm apart, were used to approximate the mesial and distal margins of the recession defect starting at apical end and finishing with a suture connecting the 2 elevated papillae (Figure 4(e)). Lastly, a suspensory suture penetrating the flap 3 mm apical to GM (of the adjacent tooth), at the level of the proximal aspect of each adjacent tooth, was applied to stabilize the flap (Figure 4(e)). LSF + CTG (Figure 5) is based on the original LSF design [24, 25, 30] combining elements of the pouch approach [31]. Full-thickness flap including papillae was elevated on the distal of the defect up to the distal of adjacent distal tooth (Figure 5(a)). This was followed by a tunnel preparation on the opposite (mesial) defect aspect, i.e., in the area of the adjacent mesial tooth (Figure 5(b)). Subsequently, a movable flap (LSF) covering 2-3 teeth was created by performing a releasing incision on the elevated flap starting at the distal of adjacent distal tooth (Figure 5(c)). Split-thickness elevation may be performed apical to MGJ to provide additional flap mobility (Figure 5(c)). When potentially encroaching on the mental foramen, releasing incisions are placed distal to the foramen (Figure 5(c)). Appropriately sized CTG (see above) was positioned inside the prepared tunnel mesially with the remaining portion covering the defect area. CTG was stabilized by two simple interrupted sutures, one on the prepared tunnel and one on the opposite papilla of the defect site (Figure 5(d)). The LSF recipient site (marginal area of prepared tunnel) was deepithelialized (Figure 5(d)), and the mobilized flap was then laterally positioned and secured with suspensory sutures (one per tooth; to immobilize flap) and simple interrupted sutures (to approximate defect margins and secure LSF margin on recipient site) (Figure 5(e)). CTG harvesting. CTG was harvested using the parallel incisions technique [29]. Following harvesting, a collagen sponge (Hemospon, Technew, Rio de Janeiro, RJ, Brasil) was placed at the donor site and the wound was sutured Postoperative Protocol. Dressing was not applied. Patients were instructed to stop all mechanical plaque control in the surgical area for 3 weeks. They received prescriptions for antimicriobial rinse (chlorhexidine gluconate 0.12%, 60 seconds twice daily, 21 days) and analgesic (paracetamol 750 mg, 4x/day, 3 days). Donor and recipient site sutures were removed at 7 and 21 days, respectively. Thereafter, a postsurgical toothbrush was dispensed, to be used at the treated area for the next 20 days. Subsequently, patients were instructed to resume regular soft toothbrush use (Stillman s modified technique).
6 6 International Journal of Dentistry FIGURE 4: Clinical images illustrating the DPE + CTG technique used. (a) Line represents the design of sulcular and papillary incisions; (b) dotted line represents flap extension; (c) area highlighted by line and light white shading represents CTG position; (d) CTG positioned and stabilized by sutures (single interrupted suture at each end and sling suture at CEJ level; (e) single interrupted sutures used to approximate papillae (arrows); (f ) 6-month follow-up. For abbreviations, see Figure 1 caption. (a) (b) (c) (d) (e) (f ) Figure 5: Clinical images illustrating the LSF + CTG technique used. (a) Line represents sulcular and papilla incision design; (b) dotted line outlines tunneled region that will receive CTG; (c) combined full- and split-thickness flap elevated. Continuous line outlines split-thickness portion and dotted line indicates where releasing incision can be performed. Area of mental nerve emergence is noted (arrows), where incision must be avoided. (d) CTG placed in pouch and secured by interrupted sutures at edge and at papilla region. Note also the deepithelialized region (pouch margin) that will receive LSF; (e) LSF, covering CTG and recipient bed, secured by sling suture at recession area and single sutures in the remaining portions. (f ) 6-month follow-up. For abbreviations, see Figure 1 caption Statistical Analysis. Normality of the data (Kolmogorov Smirnov test) and homogeneity of variances (Levene test) were confirmed before further analysis. Descriptive data were recorded as mean ± standard deviation (SD). Paired Student s t-test was used to compare baseline values and 6-month outcomes. Paired t-test was used to verify intragroup RD changes. Independent samples t-test was used to compare different Miller Class defects (II or III) and different RW (narrow or wide) regarding %RC, GR reduction, and KTW change. Pearson correlation coefficient (PCC) was used to
7 InternationalJournalofDentistry 7 measure correlation between GR reduction and baseline RD or RW. Statistical significance was set at p< Results 3.1. Study Population. Records of sixteen (11 females) healthy nonsmoking adults, aged 41.6 ± 10.8 years (range: years), met the inclusion criteria. Each patient had a single deep GR treated. Of the 16 (10 mandibular) treated teeth, 14 were anterior (8 mandibular), and two were posterior (mandibular premolar and molar). Nine defects were Miller Class II and 7 were Miller Class III Baseline Clinical Parameters. Individual patient data, by surgical approach, for RD, RW, GR reduction and RC are shown in Table 1 and for KTW in Table 2. Baseline RD was 6.7±1.8mm (range: 5 10mm) and RW was 4.0±1.1mm (range: mm) (Table 1), with 9 defects classified as wide.ktwaveraged0.2±0.4mm(range:0-1mm)(table2). PDatall surgicalsiteswas 3mm.CALrangewas6 13mm. All sites were BOP-negative and plaque-free at surgery time Clinical Outcomes: Entire Study Population. All procedures were completed uneventfully, and no postoperative complications were noted or reported by patients during the early( 1 month) healing period. During subsequent followup, all patients reported that their chief complaint was resolved. At 6 months postoperatively, all sites were BOP-negative and presented PD 3mm. RD was 1.2±0.8mm (range: mm), significantly different from baseline (p < 0.05). GR reduction was 5.5±2.0mm (range: 3 10mm) and RC was81.7±13.0%(table1);twositeshadcompleterc.miller Class II defect RC (87.1 ± 9.2%; range: %) compared to Miller Class III defect RC (74.6±14.5%; range: %) approached but did not reach statistical significance (p 0.07). No significant differences in RC (p 0.21) or GR reduction (p 0.80) were detected when comparing narrow (86.4±13.0%; 5.6±1.6mm) versus wide defects (78.0±12.6%; 5.4±2.4mm) at 6 months. Regarding KTW, a significant increase was noted from baseline to 6 months (Table 2). GR reduction was strongly and positively correlated with baseline RD (r 0.91; p<0.0001) Clinical Outcomes by Surgical Approach. CAF + CTG. Individualpatient(cases1,2,3,4,and5)andgroupdataare presented in Table 1. Figure 3(e) illustrates the 6-month follow-up of a case treated with this technique. DPE+CTG. Individual patient (cases 6, 7, 8, 9, 10, and 11) and group data are presented in Table 1. Figure 4(f) illustrates the 6-month follow-up of a case treated with this technique. LSF+CTG.Individualpatient(cases12,13,14,15,and16) and group data are presented in Table 1. Figure 5(f) illustrates the 6-month follow-up of a case treated with this technique. 4.Discussion This retrospective case series documented clinical outcomes when a novel clinical decision-making algorithm was followed to treat single deep ( 5mm) GRs. The use of this concept resulted in>80% RC and>5mm GR reduction in Miller Class II and III GR defects with mean baseline RD>6.5mm. These findings suggest that deep GRs can be treated with predictability similar to shallow and moderate GRs when using CTG [7] if the proposed surgical approaches are followed. To the best of our knowledge, this is the first study that proposes different flap designs, taking into consideration defect anatomy, GRs 5 mm deep, and the first study on outcomes of LSF+CTG. The lack of studies on treatment of 5mm deep GRs along with the evidence of poorer RC outcomes with increasing RD [7], makes it challenging for practitioners to treat such defects. Similarly, despite evidence that treatment of Class III defects can achieve good results[7], treatment of a Class III deep GR is often fraught with challenges. Use of the proposed algorithm, which aimed to facilitate decisionmaking and improve treatment predictability for challenging defects, allows a more detailed assessment of relevant anatomical factors, including residual vestibular depth; the latter has not been previously objectively included in a decision tree. Consistent with the evidence of the best RC outcomes,eveninclassiiidefects,whenusingctg[7],the algorithm guides the use of CTG-flap approaches that support CTG nutrition and flap stabilization. The biological basis for these choices may have favored the positive study outcomes. Although there is no directly comparable study(different CTG-flap combinations, GR defects 5 mm deep) available, some literature data allow for limited comparisons with the present results. In a study comparing bilaminar technique versus GTR in Miller class I and II GRs, the CAF+CTG group had 18 patients with recessions 5 mm(mean baseline RD 5.6mm), and achieved 93.5±8.6% RC [20]. Differences in outcomes may be partly explained by inclusion of Class III GRs, absence of Class I GRs, deeper mean baseline RD (6.7 mm), and inclusion of mostly mandibular teeth in the present study. In a case series treating single and multiple GRs using DPE+CTG, Nelson [28] treated 20 teeth with deep RD (range: 7 10mm) and achieved 88% mean RC. Although Nelson s results are similar to the present study results, inclusion of multiple defects and lack of Miller Class information limit comparability between studies. Present study limitations include the retrospective, nonrandomized design, and the small sample size per individual surgical technique; the latter precluded analysis of intergroup differences in outcomes. According to a meta-analysis of individual patient data by Chambrone et al. [32] including 320 patients from 22 trials the mean baseline RD for included defects was 3.3±1.1mm.ThisresultillustratesthatmostofRCliterature has focused on shallow/moderate defects. Evaluation of baseline data of 43 studies investigating CTG-based procedures included in the Chambrone and Tatakis [7] systematic review corroborates the previous finding; the mean
8 8 InternationalJournalofDentistry baselinerdformillerclassiandiidefectswas3.3mmand 2.3mm for Miller Class III GRs. The corresponding compiled results of these CTG-based studies indicated mean RC of 86.9% and 69.9% for Miller Class I/II and for Class III, respectively[7]; the present study RC outcomes for deep GR defects compare favorably with outcomes obtained in shallow/moderate defects. The lack of evidence evaluating deep ( 5mm) GRs highlights the need for studies on this clinical scenario. Given the evidence that RD increases with time in untreated GRs, use of a predictable treatment approach could improve the long-term outlook for teeth with such deep GR defects [4]. Despite the extensive evidence on CTG-based approaches, mainly CAF-associated [7], and the availability of few studies on LSF alone[33, 34], the literature lacks studies on LSF+CTG combination. Only two recent case reports using LSF+CTG are available [35, 36]. The present study results suggest that in deep and wide GRs LSF+CTG can provide RC outcomes similar to the ones expected from CAF + CTG in shallow/moderate defects [7]. Comparing the decision-aid model proposed by Bouchard et al. [21] with the present decision tree, there are some critical differences. First, and most important, the algorithm described herein is for single GRs with RD 5mm, while the Bouchard model referred to single, multiple, shallow (<3mm), moderate (3 5mm) and deep (>5mm)defects.RegardingdeepGRs,Bouchardetal.[21] suggested previously described flap designs, while the present decision tree includes novel flap approaches. In shallow vestibule cases, Bouchard et al. [21] advise use of Envelope+CTG as the main choice, considering LSF a second option for single defects; in deep vestibule cases, both CAF+CTG and Envelope+CTG may be used. Although Bouchard et al. [21] used vestibular depth as an important reference for decision-making, classification of vestibular depth was not addressed. This lack of standardization can lead to subjective decision-making and mayhindertranslationintopractice;thepresentalgorithm is based on proportion of RD in relation to residual vestibule, overcoming this limitation. Bouchard et al. [21] did not consider RW as a decision parameter for flap design choice indeep defects or use ofdpe+ctg orlsf+ctg; in contrast, the present decision tree incorporates RW as a determinantfortheprimaryselectionbetweendpe+ctg andlsf+ctg,twotechniquesatthecoreoftheproposed approach. The presented algorithm, which represents an initial reference for the practitioner when dealing with similar deep GR defects, was based on biological rationale. Nevertheless, biologyisnotanexactscience,anduseofanequation(such as the proposed one) may not adequately fit every case. Prospective investigations are necessary to validate and possibly improve this decision-making approach. 5.Conclusions Following a decision-making algorithm to treat deep gingival recessions resulted in significantly positive root coverage outcomes. The proposed algorithm allows the clinician to select the appropriate surgical technique for treatment of single deep gingival recessions with good predictability. Data Availability The data used to support the findings of this study are included within the article. Conflicts of Interest The authors declare that there are no conflicts of interest regarding the publication of this paper. Acknowledgments The authors thank Marcelo Sirolli Ferreira for imaging support. This study was financed in part by the Coordenação de Aperfeiçoamento de Pessoal de Nível Superior-Brasil (CAPES)-Finance Code 001. The study was supported by the Division of Periodontology, College of Dentistry, UniversityofSãoPaulo,SãoPaulo,Brazil,andbytheDivisionof Periodontology, College of Dentistry, The Ohio State University, Columbus, Ohio, USA. References [1] P. Cortellini and G. Pini Prato, Coronally advanced flap and combination therapy for root coverage. Clinical strategies based on scientific evidence and clinical experience, Periodontology 2000, vol. 59, no. 1, pp , [2] M. Goldstein, E. Nasatzky, J. Goultschin, B. D. Boyan, and Z. Schwartz, Coverage of previously carious roots is as predictable a procedure as coverage of intact roots, Journal of Periodontology, vol. 73, no. 12, pp , [3] I. Bignozzi, C. Littarru, A. Crea, G. Vittorini Orgeas, and L. Landi, Surgical treatment options for grafting areas of gingival recession association with cervical lesions: a review, Journal of Esthetic and Restorative Dentistry, vol. 25, no. 6, pp , [4] L. Chambrone and D. N. Tatakis, Long-term outcomes of untreated buccal gingival recessions: a systematic review and meta-analysis, Journal of Periodontology, vol. 87, no. 7, pp , [5] J. Buti, M. Baccini, M. Nieri, M. La Marca, and G. P. Pini- Prato, Bayesian network meta-analysis of root coverage procedures: ranking efficacy and identification of best treatment, Journal of Clinical Periodontology, vol. 40, no. 4, pp , [6] F. Cairo, M. Nieri, and U. Pagliaro, Efficacy of periodontal plastic surgery procedures in the treatment of localized facial gingival recessions. A systematic review, Journal of Clinical Periodontology, vol. 41, no. 15, pp. S44 S62, [7] L. Chambrone and D. N. Tatakis, Periodontal soft tissue root coverage procedures: a systematic review from the AAP regeneration workshop, Journal of Periodontology, vol. 86, no. 2, pp. S8 S51, [8] G. Zucchelli and I. Mounssif, Periodontal plastic surgery, Periodontology 2000, vol. 68, no. 1, pp , [9] D. N. Tatakis, L. Chambrone, E. P. Allen et al., Periodontal soft tissue root coverage procedures: a consensus report from the AAP regeneration workshop, Journal of Periodontology, vol. 86, no. 2, pp. S52 S55, 2015.
9 InternationalJournalofDentistry 9 [10] C. R. Richardson, E. P. Allen, L. Chambrone et al., Periodontal soft tissue root coverage procedures: practical applications from the AAP regeneration workshop, Clinical Advances in Periodontics, vol. 5, no. 1, pp. 2 10, [11] M.Nieri,G.P.PiniPrato,M.Giani,N.Magnani,U.Pagliaro, and R. Roberto, Patient perceptions of buccal gingival recessions and requests for treatment, Journal of Clinical Periodontology, vol. 40, no. 7, pp , [12] H. C. Sullivan and J. H. Atkins, Free autogenous gingival grafts. III. Utilization of grafts in the treatment of gingival recession, Periodontics, vol. 6, no. 4, pp , [13] P. Bertrand and R. Dunlap, Coverage of deep, wide gingival clefts with free gingival autografts: root planing with and without citric acid demineralization, International Journal of Periodontics and Restorative Dentistry, vol. 8, no. 1, pp , [14] A. Scabbia and L. Trombelli, Long-term stability of the mucogingival complex following guided tissue regeneration in gingival recession defects, Journal of Clinical Periodontology, vol. 25, no. 12, pp , [15] G. Zucchelli, M. Marzadori, I. Mounssif, C. Mazzotti, and M. Stefanini, Coronally advanced flap + connective tissue graft techniques for the treatment of deep gingival recession in the lower incisors. A controlled randomized clinical trial, Journal of Clinical Periodontology, vol. 41, no. 8, pp , [16] H. Corn and M. H. Marks, Ginigival grafting for deep-wide recession a status report. Part I. Rationale, case selection, and root preparation, Compendium of Continuing Education in Dentistry, vol. 4, no. 1, pp , [17] L.Trombelli,D.N.Tatakis,A.Scabbia,andG.J.Zimmermar, Comparison of mucogingival changes following treatment with coronally positioned flap and guided tissue regeneration procedures, International Journal of Periodontics and Restorative Dentistry, vol. 17, no. 5, pp , [18] L. Trombelli and A. Scabbia, Healing response of gingival recession defects following guided tissue regeneration procedures in smokers and non-smokers, Journal of Clinical Periodontology, vol. 24, no. 8, pp , [19] F. Cangini, R. Cornelini, and S. Andreana, Simultaneous treatment of multiple, bilateral, deep buccal recession defects with bioabsorbable barrier membranes: a case report, Quintessence International, vol. 34, no. 1, pp , [20] G. Zucchelli, C. Clauser, M. De Sanctis, and M. Calandriello, Mucogingival versus guided tissue regeneration procedures in the treatment of deep recession type defects, Journal of Periodontology, vol. 69, no. 2, pp , [21] P. Bouchard, J. Malet, and A. Borghetti, Decision-making in aesthetics: root coverage revisited, Periodontology 2000, vol. 27, no. 1, pp , [22] K. L. Pasquinelli, The histology of new attachment utilizing a thick autogenous soft tissue graft in an area of deep recession: a case report, International Journal of Periodontics and Restorative Dentistry, vol. 15, no. 3, pp , [23] P. D. Miller Jr., A classification of marginal tissue recession, International Journal of Periodontics and Restorative Dentistry, vol. 5, no. 2, pp. 8 13, [24] E. A. Guinard and R. G. Caffesse, Treatment of localized gingival recessions: Part I. Lateral sliding flap, Journal of Periodontology, vol. 49, no. 7, pp , [25] E. A. Guinard and R. G. Caffesse, Treatment of localized gingival recessions: Part III. Comparison of results obtained with lateral sliding and coronally repositioned flaps, Journal of Periodontology, vol. 49, no. 9, pp , [26] B. Langer and L. Langer, Subepithelial connective tissue graft technique for root coverage, Journal of Periodontology, vol. 56, no. 12, pp , [27] J. F. Bruno, Connective tissue graft technique assuring wide root coverage, International Journal of Periodontics and Restorative Dentistry, vol. 14, no. 12, pp , [28] S. W. Nelson, The subpedicle connective tissue graft, Journal of Periodontology, vol. 58, no. 2, pp , [29] R. J. Harris, The connective tissue and partial thickness double pedicle graft: a predictable method of obtaining root coverage, Journal of Periodontology, vol. 63, no. 5, pp , [30] H.E.GrupeandR.F.Warren, Repairofgingivaldefectsbya sliding flap operation, Journal of Periodontology, vol. 27, no. 2, pp , [31] P. B. Raetzke, Covering localized areas of root exposure employing the envelope technique, Journal of Periodontology, vol. 56, no. 7, pp , [32] L.Chambrone,C.M.Pannuti,Y.-K.Tu,andL.A.Chambrone, Evidence-based periodontal plastic surgery. II. An individual data meta-analysis for evaluating factors in achieving complete root coverage, Journal of Periodontology, vol. 83, no. 4, pp , [33] R. B. Santana, M. B. Furtado, C. M. L. Mattos, E. de Mello Fonseca, and S. Dibart, Clinical evaluation of single-stage advanced versus rotated flaps in the treatment of gingival recessions, Journal of Periodontology, vol. 81, no. 4, pp , [34] G. Zucchelli, M. Marzadori, M. Mele, M. Stefanini, and L. Montebugnoli, Root coverage in molar teeth: a comparative controlled randomized clinical trial, Journal of Clinical Periodontology, vol. 39, no. 11, pp , [35] F. S. Ribeiro, J. A. de Morais-Camillo, J. M. Fernandes, J. R. Pires, E. P. Zuza, and A. E. Pontes, Multiple marginal tissue recession treated with a simplified lateral sliding flap technique, Case Reports in Dentistry, vol. 2014, Article ID , 5 pages, [36] G. Lecio, F. R. Cirano, M. Z. Casati, F. V. Ribeiro, R. C. V. Casarin, and S. P. Pimentel, Multidisciplinary therapeutic approach for a severe mucogingival deformity, Clinical Advances in Periodontics, vol. 5, no. 4, pp , 2015.
10 Publishing Corporation Advances in Preventive Medicine Advances in Public Health The Scientific World Journal International Journal of Dentistry Scientifica Case Reports in Medicine Case Reports in Dentistry Submit your manuscripts at International Journal of Biomaterials Pain Research and Treatment Journal of Environmental and Public Health Computational and Mathematical Methods in Medicine Advances in Orthopedics Radiology Research and Practice Surgery Research and Practice BioMed Research International International Journal of Endocrinology Advances in Medicine Anesthesiology Research and Practice Journal of Drug Delivery
Alarge number of sound clinical
 Volume 83 Number 5 Long-Term 8-Year Outcomes of Coronally Advanced Flap forrootcoverage Giovanpaolo Pini-Prato,* Debora Franceschi,* Roberto Rotundo,* Francesco Cairo,* Pierpaolo Cortellini, and Michele
Volume 83 Number 5 Long-Term 8-Year Outcomes of Coronally Advanced Flap forrootcoverage Giovanpaolo Pini-Prato,* Debora Franceschi,* Roberto Rotundo,* Francesco Cairo,* Pierpaolo Cortellini, and Michele
The Treatment of Gingival Recession Associated with Deep Corono-Radicular Abrasions (CEJ step) a Case Series
 CLINICAL AND RESEARCH REPORT The Treatment of Gingival Recession Associated with Deep Corono-Radicular Abrasions (CEJ step) a Case Series Giovanpaolo Pini-Prato, Carlo Baldi, Roberto Rotundo, Debora Franceschi,
CLINICAL AND RESEARCH REPORT The Treatment of Gingival Recession Associated with Deep Corono-Radicular Abrasions (CEJ step) a Case Series Giovanpaolo Pini-Prato, Carlo Baldi, Roberto Rotundo, Debora Franceschi,
Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report
 Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
Case Report Esthetic Root Coverage with Double Papillary Subepithelial Connective Tissue Graft: A Case Report
 Case Reports in Dentistry, Article ID 509319, 5 pages http://dx.doi.org/10.1155/2014/509319 Case Report Esthetic Root Coverage with Double Papillary Subepithelial Connective Tissue Graft: A Case Report
Case Reports in Dentistry, Article ID 509319, 5 pages http://dx.doi.org/10.1155/2014/509319 Case Report Esthetic Root Coverage with Double Papillary Subepithelial Connective Tissue Graft: A Case Report
TWO-STEP SURGICAL PROCEDURE FOR ROOT COVERAGE (FREE GINGIVAL GRAFT AND CORONALLY POSITIONED FLAP) - A CASE REPORT
 TWO-STEP SURGICAL PROCEDURE FOR ROOT COVERAGE (FREE GINGIVAL GRAFT AND CORONALLY POSITIONED FLAP) - A CASE REPORT Dr Prashant Bhusari*, Dr Apoorva Saxena**, Dr Jaya Jain***,Dr Rashmi Rathore***, Dr Aditi
TWO-STEP SURGICAL PROCEDURE FOR ROOT COVERAGE (FREE GINGIVAL GRAFT AND CORONALLY POSITIONED FLAP) - A CASE REPORT Dr Prashant Bhusari*, Dr Apoorva Saxena**, Dr Jaya Jain***,Dr Rashmi Rathore***, Dr Aditi
Many techniques have been proposed for root coverage:
 Case Series Localized Gingival Recessions Treated With the Original Envelope Technique: A Report of 50 Consecutive Patients Jaime A. Vergara* and Raul G. Caffesse Background: The surgical techniques used
Case Series Localized Gingival Recessions Treated With the Original Envelope Technique: A Report of 50 Consecutive Patients Jaime A. Vergara* and Raul G. Caffesse Background: The surgical techniques used
Gingival recession causes periodontal
 J Periodontol October 2005 Factors Affecting the Outcomes of Coronally Advanced Flap Root Coverage Procedure Lien-Hui Huang,* Rodrigo E.F. Neiva, and Hom-Lay Wang Background: The coronally advanced flap
J Periodontol October 2005 Factors Affecting the Outcomes of Coronally Advanced Flap Root Coverage Procedure Lien-Hui Huang,* Rodrigo E.F. Neiva, and Hom-Lay Wang Background: The coronally advanced flap
Avita Rath, 1 Smrithi Varma, 2 and Renny Paul Case Presentation. 1. Background
 Case Reports in Dentistry Volume 2016, Article ID 9289634, 5 pages http://dx.doi.org/10.1155/2016/9289634 Case Report Two-Stage Mucogingival Surgery with Free Gingival Autograft and Biomend Membrane and
Case Reports in Dentistry Volume 2016, Article ID 9289634, 5 pages http://dx.doi.org/10.1155/2016/9289634 Case Report Two-Stage Mucogingival Surgery with Free Gingival Autograft and Biomend Membrane and
MUCOGINGIVAL THERAPY PERIODONTAL PLASTIC SURGERY
 MUCOGINGIVAL THERAPY PERIODONTAL PLASTIC SURGERY DR.H.Gharati Periodontist & Dental Implant Specialist Assistant Professor, School Of Dentistry Friedman(1957): DEFINITION Mucogingival surgery, Surgical
MUCOGINGIVAL THERAPY PERIODONTAL PLASTIC SURGERY DR.H.Gharati Periodontist & Dental Implant Specialist Assistant Professor, School Of Dentistry Friedman(1957): DEFINITION Mucogingival surgery, Surgical
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Case Report Bridge Flap: A Sine Qua Non For Mucogingival Deformities Debajyoti Mondal, Anju L, Rajul Choradia, Somen
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Case Report Bridge Flap: A Sine Qua Non For Mucogingival Deformities Debajyoti Mondal, Anju L, Rajul Choradia, Somen
Treatment of multiple gingival recessions using subepithelial connective tissue grafting with a single-incision technique
 317 Journal of Oral Science, Vol. 51, No. 2, 317-321, 2009 Case Report Treatment of multiple gingival recessions using subepithelial connective tissue grafting with a single-incision technique Jun-Beom
317 Journal of Oral Science, Vol. 51, No. 2, 317-321, 2009 Case Report Treatment of multiple gingival recessions using subepithelial connective tissue grafting with a single-incision technique Jun-Beom
A 2-Year Follow-Up of Root Coverage Using Subpedicle Acellular Dermal Matrix Allografts and Subepithelial Connective Tissue Autografts
 J Periodontol August 2005 A 2-Year Follow-Up of Root Coverage Using Subpedicle Acellular Dermal Matrix Allografts and Subepithelial Connective Tissue Autografts A. Hirsch,* M. Goldstein,* J. Goultschin,*
J Periodontol August 2005 A 2-Year Follow-Up of Root Coverage Using Subpedicle Acellular Dermal Matrix Allografts and Subepithelial Connective Tissue Autografts A. Hirsch,* M. Goldstein,* J. Goultschin,*
Efficacy of Lateral Pedicle Graft in the Treatment of Isolated Gingival Recession Defects
 International Journal of Pharmaceutical Science Invention ISSN (Online): 2319 6718, ISSN (Print): 2319 670X Volume 3 Issue 1 January 2014 PP.46-50 Efficacy of Lateral Pedicle Graft in the Treatment of
International Journal of Pharmaceutical Science Invention ISSN (Online): 2319 6718, ISSN (Print): 2319 670X Volume 3 Issue 1 January 2014 PP.46-50 Efficacy of Lateral Pedicle Graft in the Treatment of
A Promising Periodontal Procedure for the Treatment of Adjacent Gingival Recession Defects. Tolga Fikret Tözüm, DDS, PhD
 C L I N I C A L P R A C T I C E A Promising Periodontal Procedure for the Treatment of Adjacent Gingival Recession Defects Tolga Fikret Tözüm, DDS, PhD A b s t r a c t Various clinical reports on the reconstruction
C L I N I C A L P R A C T I C E A Promising Periodontal Procedure for the Treatment of Adjacent Gingival Recession Defects Tolga Fikret Tözüm, DDS, PhD A b s t r a c t Various clinical reports on the reconstruction
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 345 A Mucogingival Technique for the Treatment of Multiple Recession Defects in the Mandibular Anterior Region: A Case Series with a 2-Year
The International Journal of Periodontics & Restorative Dentistry 345 A Mucogingival Technique for the Treatment of Multiple Recession Defects in the Mandibular Anterior Region: A Case Series with a 2-Year
Free Gingival Graft as a Single Step Procedure for Treatment of Mandibular Miller Class I and II Recession Defects
 12 Gingival graft in mandibular defect Original Article Free Gingival Graft as a Single Step Procedure for Treatment of Mandibular Miller Class I and II Recession Defects Lata Goyal1*, Narender Dev Gupta2,
12 Gingival graft in mandibular defect Original Article Free Gingival Graft as a Single Step Procedure for Treatment of Mandibular Miller Class I and II Recession Defects Lata Goyal1*, Narender Dev Gupta2,
Management of miller class II gingival recession by laterally positioned pedicle flap revised technique
 Management of miller class II gingival by laterally positioned pedicle flap revised technique Received: 2/4/206 Accepted: 3/0/206 Dildar Abdullah Othman* Abstract Background and objective: Gingival is
Management of miller class II gingival by laterally positioned pedicle flap revised technique Received: 2/4/206 Accepted: 3/0/206 Dildar Abdullah Othman* Abstract Background and objective: Gingival is
ijcrr Vol 04 issue 12 Category: Case Report Received on:22/04/12 Revised on:07/05/12 Accepted on:22/05/12
 SURGICAL RECONSTRUCTION OF INTERDENTAL PAPILLA USING AN INTERPOSED SUBEPITHELIAL CONNECTIVE TISSUE GRAFT: A CASE REPORT ijcrr Vol 04 issue 12 Category: Case Report Received on:22/04/12 Revised on:07/05/12
SURGICAL RECONSTRUCTION OF INTERDENTAL PAPILLA USING AN INTERPOSED SUBEPITHELIAL CONNECTIVE TISSUE GRAFT: A CASE REPORT ijcrr Vol 04 issue 12 Category: Case Report Received on:22/04/12 Revised on:07/05/12
Free Gingival Autograft: A Case Report
 CASE REPORT Free Gingival Autograft: A Case Report Veena Ashok. P. MDS, Bhargav Neetha BDS Abstract: Gingival recession is defined as Displacement of soft tissue margin apical to the cemento-enamel junction
CASE REPORT Free Gingival Autograft: A Case Report Veena Ashok. P. MDS, Bhargav Neetha BDS Abstract: Gingival recession is defined as Displacement of soft tissue margin apical to the cemento-enamel junction
SUBEPITHELIAL CONNECTIVE TISSUE GRAFT A PREDICTABLE INDICATOR FOR ROOT COVERAGE
 SUBEPITHELIAL CONNECTIVE TISSUE GRAFT A PREDICTABLE INDICATOR FOR ROOT COVERAGE Munishwar Singh* * 201 Military Dental Centre, C/o 99 APO, India Keywords: Gingival recession, Root coverage procedure, Connective
SUBEPITHELIAL CONNECTIVE TISSUE GRAFT A PREDICTABLE INDICATOR FOR ROOT COVERAGE Munishwar Singh* * 201 Military Dental Centre, C/o 99 APO, India Keywords: Gingival recession, Root coverage procedure, Connective
Connective Tissue Graft for Gingival Recession in Mandibular Incisor Area: A Case Report
 Bull Tokyo Dent Coll (2017) 58(3): 155 162 Case Report doi:10.2209/tdcpublication.2016-0038 Connective Tissue Graft for Gingival Recession in Mandibular Incisor Area: A Case Report Masahiro Egawa 1), Satoru
Bull Tokyo Dent Coll (2017) 58(3): 155 162 Case Report doi:10.2209/tdcpublication.2016-0038 Connective Tissue Graft for Gingival Recession in Mandibular Incisor Area: A Case Report Masahiro Egawa 1), Satoru
Classifications for Gingival Recession: A Mini Review
 Galore International Journal of Health Sciences and Research Vol.3; Issue: 1; Jan.-March 2018 Website: www.gijhsr.com Review Article P-ISSN: 2456-9321 Classifications for Gingival Recession: A Mini Review
Galore International Journal of Health Sciences and Research Vol.3; Issue: 1; Jan.-March 2018 Website: www.gijhsr.com Review Article P-ISSN: 2456-9321 Classifications for Gingival Recession: A Mini Review
REGENERATIONTIME. A Case Report by. Geistlich Mucograft for the treatment of multiple adjacent recession defects: A more palatable option
 A Case Report by Dr. Daniel Gober Geistlich Mucograft for the treatment of multiple adjacent recession defects: A more palatable option The Situation A 35 year old male presented in my practice with a
A Case Report by Dr. Daniel Gober Geistlich Mucograft for the treatment of multiple adjacent recession defects: A more palatable option The Situation A 35 year old male presented in my practice with a
Delta Dental of Virginia Clinical Policy # 402
 Delta Dental of Virginia Clinical Policy # 402 Subject Mucogingival Surgery and Soft Tissue Grafting Originating Department Clinical Professional Services Signature Authority Dental Director Type: New
Delta Dental of Virginia Clinical Policy # 402 Subject Mucogingival Surgery and Soft Tissue Grafting Originating Department Clinical Professional Services Signature Authority Dental Director Type: New
A mucogingival technique for the treatment of multiple recession defects in the
 A mucogingival technique for the treatment of multiple recession defects in the mandibular anterior region: a case series with two-year follow-up. Nicola Bethaz, DDS* Federica Romano, DDS** Francesco Ferrarotti,
A mucogingival technique for the treatment of multiple recession defects in the mandibular anterior region: a case series with two-year follow-up. Nicola Bethaz, DDS* Federica Romano, DDS** Francesco Ferrarotti,
W J C C. World Journal of Clinical Cases. Gingival unit transfer using in the Miller Ⅲ recession defect treatment. Abstract INTRODUCTION CASE REPORT
 W J C C World Journal of Clinical Cases Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.12998/wjcc.v3.i2.199 World J Clin Cases 2015 February
W J C C World Journal of Clinical Cases Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.12998/wjcc.v3.i2.199 World J Clin Cases 2015 February
Clinical Application of Modified Apically Repositioned Flap in Class III/IV Gingival Recession Cases
 J Harjeet Singh et al SE REPORT 10.5005/jp-journals-10031-1200 linical pplication of Modified pically Repositioned Flap in lass III/IV Gingival Recession ases 1 Harjeet Singh, 2 Manab Kosala, 3 Vivek apurao
J Harjeet Singh et al SE REPORT 10.5005/jp-journals-10031-1200 linical pplication of Modified pically Repositioned Flap in lass III/IV Gingival Recession ases 1 Harjeet Singh, 2 Manab Kosala, 3 Vivek apurao
Michael K. McGuire* and Martha Nunn
 Volume 74 Number 8 Evaluation of Human Recession Defects Treated with Coronally Advanced Flaps and Either Enamel Matrix Derivative or Connective Tissue. Part 1: Comparison of Clinical Parameters Michael
Volume 74 Number 8 Evaluation of Human Recession Defects Treated with Coronally Advanced Flaps and Either Enamel Matrix Derivative or Connective Tissue. Part 1: Comparison of Clinical Parameters Michael
Michael K. McGuire* and E. Todd Scheyer*
 Long-Term Results Comparing Xenogeneic Collagen Matrix and Autogenous Connective Tissue Grafts With Coronally Advanced Flaps for Treatment of Dehiscence-Type Recession Defects Michael K. McGuire* and E.
Long-Term Results Comparing Xenogeneic Collagen Matrix and Autogenous Connective Tissue Grafts With Coronally Advanced Flaps for Treatment of Dehiscence-Type Recession Defects Michael K. McGuire* and E.
The use of platelet-rich plasma in combination with connective tissue grafts following treatment of gingival recessions
 RESEARCH REPORT 63 Sasha M Jankovic, Aleksic M Zoran, Lekovic M Vojislav, Dimitrijevic S Bozidar, Barry E Kenney The use of platelet-rich plasma in combination with connective tissue grafts following treatment
RESEARCH REPORT 63 Sasha M Jankovic, Aleksic M Zoran, Lekovic M Vojislav, Dimitrijevic S Bozidar, Barry E Kenney The use of platelet-rich plasma in combination with connective tissue grafts following treatment
Gingival Unit Graft Versus Free Gingival Graft for Treatment of Gingival Recession: A Randomized Controlled Clinical Trial
 Original Article Gingival Unit Graft Versus Free Gingival Graft for Treatment of Gingival Recession: A Randomized Controlled Clinical Trial Niloofar Jenabian 1, Mohadese Yazdanpanah Bahabadi 2, Ali Bijani
Original Article Gingival Unit Graft Versus Free Gingival Graft for Treatment of Gingival Recession: A Randomized Controlled Clinical Trial Niloofar Jenabian 1, Mohadese Yazdanpanah Bahabadi 2, Ali Bijani
RESEARCH REVIEW. Gingival recession: a proposal for a new classification ISSN :
 RESEARCH REVIEW Gingival recession: a proposal for a new classification Shantipriya Reddy, Sanjay Kaul, Prasad M.G.S., Jaya Agnihotri, Amudha D., Soumya Kambali ABSTRACT An accurate diagnosis is often
RESEARCH REVIEW Gingival recession: a proposal for a new classification Shantipriya Reddy, Sanjay Kaul, Prasad M.G.S., Jaya Agnihotri, Amudha D., Soumya Kambali ABSTRACT An accurate diagnosis is often
Management of millers class III marginal tissue recession associated with endodontic lesion: Report of two cases managed using second stage surgery
 CASE SERIES 1 OPEN ACCESS Management of millers class III marginal tissue recession associated with endodontic lesion: Report of two cases managed using second stage surgery Sangeeta ABSTRACT Introduction:
CASE SERIES 1 OPEN ACCESS Management of millers class III marginal tissue recession associated with endodontic lesion: Report of two cases managed using second stage surgery Sangeeta ABSTRACT Introduction:
Advanced Probing Techniques
 Module 21 Advanced Probing Techniques MODULE OVERVIEW The clinical periodontal assessment is one of the most important functions performed by dental hygienists. This module begins with a review of the
Module 21 Advanced Probing Techniques MODULE OVERVIEW The clinical periodontal assessment is one of the most important functions performed by dental hygienists. This module begins with a review of the
botiss dental bone & tissue regeneration biomaterials mucoderm 3D-Regenerative Tissue Graft strictly biologic
 dental bone & tissue regeneration botiss biomaterials 3DRegenerative Tissue Graft strictly biologic mucoderm Soft Tissue Graft Indications mucoderm is a collagen tissue matrix derived of animal dermis
dental bone & tissue regeneration botiss biomaterials 3DRegenerative Tissue Graft strictly biologic mucoderm Soft Tissue Graft Indications mucoderm is a collagen tissue matrix derived of animal dermis
Michael K. McGuire,* E. Todd Scheyer,* and Martha Nunn
 J Periodontol November 2012 Evaluation of Human Recession Defects Treated With Coronally Advanced Flaps and Either Enamel Matrix Derivative or Connective Tissue: Comparison of Clinical Parameters at 10
J Periodontol November 2012 Evaluation of Human Recession Defects Treated With Coronally Advanced Flaps and Either Enamel Matrix Derivative or Connective Tissue: Comparison of Clinical Parameters at 10
Tina M. Beck, DDS, MS
 The Pinhole Surgical Technique: A Clinical Perspective and Treatment Considerations From a Periodontist Tina M. Beck, DDS, MS ABSTRACT Multiple treatment options exist when considering therapeutic approaches
The Pinhole Surgical Technique: A Clinical Perspective and Treatment Considerations From a Periodontist Tina M. Beck, DDS, MS ABSTRACT Multiple treatment options exist when considering therapeutic approaches
Michael K. McGuire,* E. Todd Scheyer,* and Mark B. Snyder
 J Periodontol October 2014 Evaluation of Recession Defects Treated With Coronally Advanced Flaps and Either Recombinant Human Platelet-Derived Growth Factor-BB Plus b-tricalcium Phosphate or Connective
J Periodontol October 2014 Evaluation of Recession Defects Treated With Coronally Advanced Flaps and Either Recombinant Human Platelet-Derived Growth Factor-BB Plus b-tricalcium Phosphate or Connective
Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports
 0 Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports R.G. Caffesse, B.A. Smith/ B. Duff, E.C. Morrison, D. Merrill/ and W. Becker In the cases reported here, the response
0 Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports R.G. Caffesse, B.A. Smith/ B. Duff, E.C. Morrison, D. Merrill/ and W. Becker In the cases reported here, the response
Treatment of dental recessions in the esthetic zone by gingival and osseous recontouring. A multidisciplinary perio-prosthodontic case report.
 European International Journal of Science and Technology Vol. 6 No. 5 July 2017 Treatment of dental recessions in the esthetic zone by gingival and osseous recontouring. A multidisciplinary perio-prosthodontic
European International Journal of Science and Technology Vol. 6 No. 5 July 2017 Treatment of dental recessions in the esthetic zone by gingival and osseous recontouring. A multidisciplinary perio-prosthodontic
PRACTICAL APPLICATIONS
 Enhancing Periodontal Health Through Regenerative Approaches Periodontal Soft Tissue Root Coverage Procedures: Practical Applications From the AAP Regeneration Workshop Christopher R. Richardson,* Edward
Enhancing Periodontal Health Through Regenerative Approaches Periodontal Soft Tissue Root Coverage Procedures: Practical Applications From the AAP Regeneration Workshop Christopher R. Richardson,* Edward
Surgical reconstruction of lost papilla around implant with a modified technique: A case report
 Journal of Periodontology & Implant Dentistry Case Report Surgical reconstruction of lost papilla around implant with a modified technique: A case report Mahdi Faraji* Andre Van Zyl University of Pretoria,
Journal of Periodontology & Implant Dentistry Case Report Surgical reconstruction of lost papilla around implant with a modified technique: A case report Mahdi Faraji* Andre Van Zyl University of Pretoria,
Double Papillary Flap - A Treatment for Gingival Recession
 World Journal of Medical Sciences 10 (2): 117-121, 2014 ISSN 1817-3055 IDOSI Publications, 2014 DOI: 10.5829/idosi.wjms.2014.10.2.82175 Double Papillary Flap - A Treatment for Gingival Recession 1 1 1
World Journal of Medical Sciences 10 (2): 117-121, 2014 ISSN 1817-3055 IDOSI Publications, 2014 DOI: 10.5829/idosi.wjms.2014.10.2.82175 Double Papillary Flap - A Treatment for Gingival Recession 1 1 1
Practical Advanced Periodontal Surgery
 Practical Advanced Periodontal Surgery Serge Dibart Blackwell Munksgaard Chapter 8 Papillary Construction After Dental Implant Therapy Peyman Shahidi, DOS, MScD, Serge Dibart, DMD, and Yun Po Zhang, PhD,
Practical Advanced Periodontal Surgery Serge Dibart Blackwell Munksgaard Chapter 8 Papillary Construction After Dental Implant Therapy Peyman Shahidi, DOS, MScD, Serge Dibart, DMD, and Yun Po Zhang, PhD,
Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report
 C A S E R E P O R T Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report Rhoodie Garrana 1 and Govindrau Mohangi
C A S E R E P O R T Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report Rhoodie Garrana 1 and Govindrau Mohangi
Clinical Comparison of Subepithelial Connective Tissue Grafts and Coronally Advanced Flaps with Emdogain in the Treatment of Gingival Recessions
 Original Article Clinical Comparison of Subepithelial Connective Tissue Grafts and Coronally Advanced Flaps with Emdogain in the Treatment of Gingival Recessions F. Haghighati 1,2, AA. Khoshkhoonejad 3,
Original Article Clinical Comparison of Subepithelial Connective Tissue Grafts and Coronally Advanced Flaps with Emdogain in the Treatment of Gingival Recessions F. Haghighati 1,2, AA. Khoshkhoonejad 3,
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Case Report The Vestibular Incision Subperiosteal Tunnel Access (VISTA) for Treatment of Maxillary Anterior Gingival
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Case Report The Vestibular Incision Subperiosteal Tunnel Access (VISTA) for Treatment of Maxillary Anterior Gingival
Principles of Periodontal flap surgery. Dr.maryam khosravi
 Principles of Periodontal flap surgery Dr.maryam khosravi Goals of periodontal SURGICAL phase 1 - Controlling or eliminating periodontal disease. 2 Correcting anatomic conditions that may a. favor periodontal
Principles of Periodontal flap surgery Dr.maryam khosravi Goals of periodontal SURGICAL phase 1 - Controlling or eliminating periodontal disease. 2 Correcting anatomic conditions that may a. favor periodontal
Rescuing Tooth with Regenerative Technique: A Case Report. Women,, Suraram Mainroad, Ghmc Quthbullapur, Hyderabad , Telangana.
 ISSN- O: 2458-868X, ISSN P: 2458 8687 Index Copernicus Value: 49. 23 PubMed - National Library of Medicine - ID: 101731606 SJIF Impact Factor: 4.956 International Journal of Medical Science and Innovative
ISSN- O: 2458-868X, ISSN P: 2458 8687 Index Copernicus Value: 49. 23 PubMed - National Library of Medicine - ID: 101731606 SJIF Impact Factor: 4.956 International Journal of Medical Science and Innovative
Surgical Therapy. Tuesday, April 2, 13. Alessan"o Geminiani, DDS, MS
 Surgical Therapy Alessan"o Geminiani, DDS, MS Periodontal Flap: a surgical procedure in which incisions are made in the gingiva or mucosa to allow for separation of the epithelium and connective tissues
Surgical Therapy Alessan"o Geminiani, DDS, MS Periodontal Flap: a surgical procedure in which incisions are made in the gingiva or mucosa to allow for separation of the epithelium and connective tissues
ELIMINATE POCKETS. Periodontal pocket is the consequence of periodontal infection But also a major risk factor for the further progression of disease
 ELIMINATE POCKETS Periodontal pocket is the consequence of periodontal infection But also a major risk factor for the further progression of disease CONSEQUENTLY Periodontal pockets should be eliminated
ELIMINATE POCKETS Periodontal pocket is the consequence of periodontal infection But also a major risk factor for the further progression of disease CONSEQUENTLY Periodontal pockets should be eliminated
Consensus Report Tissue augmentation and esthetics (Working Group 3)
 B. Klinge Thomas F. Flemmig Consensus Report Tissue augmentation and esthetics (Working Group 3) Members of working group: Matteo Chiapasco Jan-Eirik Ellingsen Ronald Jung Friedrich Neukam Isabella Rocchietta
B. Klinge Thomas F. Flemmig Consensus Report Tissue augmentation and esthetics (Working Group 3) Members of working group: Matteo Chiapasco Jan-Eirik Ellingsen Ronald Jung Friedrich Neukam Isabella Rocchietta
SURGICAL TREATMENT OF GINGIVAL RECESSION WITH SOFT TISSUE GRAFT PROCEDURE
 Journal of IMAB ISSN: 1312-773X https://www.journal-imab-bg.org https://doi.org/10.5272/jimab.2018243.2149 Journal of IMAB - Annual Proceeding (Scientific Papers). 2018 Jul-Sep;24(3) Literature review
Journal of IMAB ISSN: 1312-773X https://www.journal-imab-bg.org https://doi.org/10.5272/jimab.2018243.2149 Journal of IMAB - Annual Proceeding (Scientific Papers). 2018 Jul-Sep;24(3) Literature review
Gum Graft? Patient Need a. Does My. 66 JANUARY 2017 // dentaltown.com. by Dr. Brian S. Gurinsky
 by Dr. Brian S. Gurinsky Dr. Brian S. Gurinsky was born in Dallas and attended college at the University of Texas at Austin. He continued his education at Baylor College of Dentistry in Dallas, where he
by Dr. Brian S. Gurinsky Dr. Brian S. Gurinsky was born in Dallas and attended college at the University of Texas at Austin. He continued his education at Baylor College of Dentistry in Dallas, where he
Findings and Conclusions: Clinical parameters mean at baseline at post-surgery were:
 Barros R, Novaes AB, Grisi M, et al. A 6 month comparative clinical study of a conventional and a new surgical approach for root coverage with acellular dermal matrix. J Periodontol 2004;75:1350-56. (29
Barros R, Novaes AB, Grisi M, et al. A 6 month comparative clinical study of a conventional and a new surgical approach for root coverage with acellular dermal matrix. J Periodontol 2004;75:1350-56. (29
CITRIC ACID ROOT BIOMODIFICATION IN RECESSION COVERAGE WITH LATERAL PEDICLE FLAP TECHNIQUE- A CASE REPORT
 Case Report International Journal of Dental and Health Sciences Volume 02, Issue 05 CITRIC ACID ROOT BIOMODIFICATION IN RECESSION COVERAGE WITH LATERAL PEDICLE FLAP TECHNIQUE- A CASE REPORT Mamta Singh
Case Report International Journal of Dental and Health Sciences Volume 02, Issue 05 CITRIC ACID ROOT BIOMODIFICATION IN RECESSION COVERAGE WITH LATERAL PEDICLE FLAP TECHNIQUE- A CASE REPORT Mamta Singh
Periosteal fenestration: A single stage surgical procedure for root coverage along with vestibular deepening
 2017; 3(2): 14-18 ISSN Print: 2394-7489 ISSN Online: 2394-7497 IJADS 2017; 3(2): 14-18 2017 IJADS www.oraljournal.com Received: 05-02-2017 Accepted: 06-03-2017 Dr. Hoti Lal Gupta MDS, Professor and Head
2017; 3(2): 14-18 ISSN Print: 2394-7489 ISSN Online: 2394-7497 IJADS 2017; 3(2): 14-18 2017 IJADS www.oraljournal.com Received: 05-02-2017 Accepted: 06-03-2017 Dr. Hoti Lal Gupta MDS, Professor and Head
Esthetic Crown Lengthening for Upper Anterior Teeth: Indications and Surgical Techniques
 I J Pre Clin Dent Res 2014;1(2):49-53 April-June All rights reserved International Journal of Preventive & Clinical Dental Research Esthetic Crown Lengthening for Upper Anterior Teeth: Indications and
I J Pre Clin Dent Res 2014;1(2):49-53 April-June All rights reserved International Journal of Preventive & Clinical Dental Research Esthetic Crown Lengthening for Upper Anterior Teeth: Indications and
Effect of Periodontal Parameters on Root Coverage
 Journal of the International Academy of Periodontology 2016 18/3: 86 93 Effect of Periodontal Parameters on Root Coverage Thaís Ribeiral Vieira 1, Dhelfeson Willya Douglas de Oliveira 1, Frederico Santos
Journal of the International Academy of Periodontology 2016 18/3: 86 93 Effect of Periodontal Parameters on Root Coverage Thaís Ribeiral Vieira 1, Dhelfeson Willya Douglas de Oliveira 1, Frederico Santos
Department of Periodontology & Oral Implantology, Genesis Institute of Dental Sciences and Research, Ferozepur, Punjab, India
 Original Article Comparison of semilunar coronally advanced flap alone and in combination with button technique in the treatment of Miller s Class I and II gingival recessions: A Pilot Study Ranjit Singh
Original Article Comparison of semilunar coronally advanced flap alone and in combination with button technique in the treatment of Miller s Class I and II gingival recessions: A Pilot Study Ranjit Singh
soft tissue mucoderm botiss native stable 3-dimensional 3D-Regenerative Tissue Graft Handling, Clinical Application and Cases
 dental bone & tissue regeneration botiss biomaterials mucoderm 3D-Regenerative Tissue Graft Handling, Clinical Application and Cases by PD Dr. med. dent. Adrian Kasaj soft tissue native stable 3-dimensional
dental bone & tissue regeneration botiss biomaterials mucoderm 3D-Regenerative Tissue Graft Handling, Clinical Application and Cases by PD Dr. med. dent. Adrian Kasaj soft tissue native stable 3-dimensional
A Fantastic Aprroach for Multiple Recession Coverage: Vestibular Incision Subperiosteal Tunnel Access Technique (Vista)-A Case Report
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 2 Ver. I (Feb. 2016), PP 52-56 www.iosrjournals.org A Fantastic Aprroach for Multiple Recession
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 2 Ver. I (Feb. 2016), PP 52-56 www.iosrjournals.org A Fantastic Aprroach for Multiple Recession
Coronally Positioned Flap for Root Coverage: Comparison between Smokers and Nonsmokers
 Coronally Positioned Flap for Root Coverage: Comparison between Smokers and Nonsmokers Bhaumik Nanavati 1, Neeta V Bhavsar 2, Jaydeepchandra Mali 3 1 Senior Lecturer, Department of Peridontology, College
Coronally Positioned Flap for Root Coverage: Comparison between Smokers and Nonsmokers Bhaumik Nanavati 1, Neeta V Bhavsar 2, Jaydeepchandra Mali 3 1 Senior Lecturer, Department of Peridontology, College
Pouch and tunnel technique: Minimally invasive periodontal plastic surgery for root coverage
 www.edoriumjournals.com case Series OPEN ACCESS Pouch and tunnel technique: Minimally invasive periodontal plastic surgery for root coverage Sangeeta Singh ABSTRACT Introduction: The indications for root
www.edoriumjournals.com case Series OPEN ACCESS Pouch and tunnel technique: Minimally invasive periodontal plastic surgery for root coverage Sangeeta Singh ABSTRACT Introduction: The indications for root
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 573 Technique to Identify and Reconstruct the ementoenamel Junction Level Using ombined Periodontal and Restorative Treatment of Gingival
The International Journal of Periodontics & Restorative Dentistry 573 Technique to Identify and Reconstruct the ementoenamel Junction Level Using ombined Periodontal and Restorative Treatment of Gingival
Case Report Esthetic Rehabilitation of a Severely Compromised Anterior Area: Combined Periodontal and Restorative Approach
 Case Reports in Dentistry, Article ID 658790, 6 pages http://dx.doi.org/10.1155/2014/658790 Case Report Esthetic Rehabilitation of a Severely Compromised Anterior Area: Combined Periodontal and Restorative
Case Reports in Dentistry, Article ID 658790, 6 pages http://dx.doi.org/10.1155/2014/658790 Case Report Esthetic Rehabilitation of a Severely Compromised Anterior Area: Combined Periodontal and Restorative
Decellularized Dermis Allograft
 Decellularized Dermis Allograft Treatment of Human Gingival Recession Defects With Decellularized Dermis Matrix and Enamel Matrix Derivative Using Coronally Advanced Flaps. Stephen C. Wallace, M.H.S. 2525
Decellularized Dermis Allograft Treatment of Human Gingival Recession Defects With Decellularized Dermis Matrix and Enamel Matrix Derivative Using Coronally Advanced Flaps. Stephen C. Wallace, M.H.S. 2525
Surgical treatment of localized gingival recessions using coronally advanced flaps with or without subepithelial connective tissue graft
 Journal section: Oral Surgery Publication Types: Research doi:10.4317/medoral.21043 http://dx.doi.org/doi:10.4317/medoral.21043 Surgical treatment of localized gingival recessions using coronally advanced
Journal section: Oral Surgery Publication Types: Research doi:10.4317/medoral.21043 http://dx.doi.org/doi:10.4317/medoral.21043 Surgical treatment of localized gingival recessions using coronally advanced
The Use of DynaMatrix Extracellular Membrane for Gingival Augmentation: A Case Series Dr. Stephen Saroff, DDS
 The Use of DynaMatrix Extracellular Membrane for Gingival Augmentation: A Case Series Dr. Stephen Saroff, DDS LOCALIZED RECESSION ON TOOTH #25 DUE TO BONE RECESSION (PRE OP) Introduction Tissue grafting
The Use of DynaMatrix Extracellular Membrane for Gingival Augmentation: A Case Series Dr. Stephen Saroff, DDS LOCALIZED RECESSION ON TOOTH #25 DUE TO BONE RECESSION (PRE OP) Introduction Tissue grafting
Evaluation of the effect of dosedependent
 Original Article http://dx.doi.org/10.1590/1678-7757-2017-0278 Evaluation of the effect of dosedependent platelet-rich fibrin membrane on treatment of gingival recession: a randomized, controlled clinical
Original Article http://dx.doi.org/10.1590/1678-7757-2017-0278 Evaluation of the effect of dosedependent platelet-rich fibrin membrane on treatment of gingival recession: a randomized, controlled clinical
Prosthetic Options in Implant Dentistry. Hakimeh Siadat, DDS, MSc Associate Professor
 Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Case Series. BK Somnath, Pretti Charde, ML Bhongade
 Case Series Evaluation of Effectiveness of Acellular Dermal Matrix Allograft and Subepithelial Connective Tissue Graft in Combination with Coronally Positioned Flap in Treatment of Mutiple Gingival Recession
Case Series Evaluation of Effectiveness of Acellular Dermal Matrix Allograft and Subepithelial Connective Tissue Graft in Combination with Coronally Positioned Flap in Treatment of Mutiple Gingival Recession
Therapeutic Outcomes for Gingival Recession Defects in the Esthetic Zone: A Systematic Review
 Review Article imedpub Journals http://www.imedpub.com/ Periodontics and Prosthodontics ISSN DOI: 10.21767/.100012 Abstract Therapeutic Outcomes for Gingival Recession Defects in the Esthetic Zone: A Systematic
Review Article imedpub Journals http://www.imedpub.com/ Periodontics and Prosthodontics ISSN DOI: 10.21767/.100012 Abstract Therapeutic Outcomes for Gingival Recession Defects in the Esthetic Zone: A Systematic
WHAT IS THE PURPOSE OF WHAT WE DO? TEAM PERIODONTICS: WORKING TOGETHER TO IMPROVE PATIENT CARE YOU ARE THE PERIODONTISTS IN YOUR PRACTICE!
 Setter Periodontics 2075 SW 1 st Ave #2L Portland, OR 97201 503-222-9961 michael@setterperio.com WHAT IS THE PURPOSE OF WHAT WE DO? Gum Gardeners Study Club 2.27.17 TEAM PERIODONTICS: WORKING TOGETHER
Setter Periodontics 2075 SW 1 st Ave #2L Portland, OR 97201 503-222-9961 michael@setterperio.com WHAT IS THE PURPOSE OF WHAT WE DO? Gum Gardeners Study Club 2.27.17 TEAM PERIODONTICS: WORKING TOGETHER
Gingival Recession and Various Root Coverage Procedures: A Review
 REVIEW ARTICLE www.ijcmr.com and Various Root Coverage Procedures: A Review Mamta Singh 1, Kratee Sharma 2, Manvi Chandra Agarwal 3, Pranav Gupta 4 ABSTRACT Esthetics is of prime concern in today s sophisticated
REVIEW ARTICLE www.ijcmr.com and Various Root Coverage Procedures: A Review Mamta Singh 1, Kratee Sharma 2, Manvi Chandra Agarwal 3, Pranav Gupta 4 ABSTRACT Esthetics is of prime concern in today s sophisticated
CASE REPORT MANAGEMENT OF MILLER S CLASS III GINGIVAL RECESSION USING FREE CONNECTIVE TISSUE GRAFTS - THE USE OF TWO DIFFERENT TECHNIQUES
 (e) ISSN Online: 2321-9599 Rao J et al. Free connective tissue grafts in Miller s class III defects. (p) ISSN Print: 2348-6805 CASE REPORT MANAGEMENT OF MILLER S CLASS III GINGIVAL RECESSION USING FREE
(e) ISSN Online: 2321-9599 Rao J et al. Free connective tissue grafts in Miller s class III defects. (p) ISSN Print: 2348-6805 CASE REPORT MANAGEMENT OF MILLER S CLASS III GINGIVAL RECESSION USING FREE
CLINICAL. Free gingival grafts to manage recession when and how? Matthew B M Thomas CLINICAL
 CLINICAL CLINICAL Free gingival grafts to manage recession when and how? Matthew B M Thomas Gingival recession results from displacement of the gingival margin below the cemento-enamel junction leading
CLINICAL CLINICAL Free gingival grafts to manage recession when and how? Matthew B M Thomas Gingival recession results from displacement of the gingival margin below the cemento-enamel junction leading
DENTAL TRIBUNE ISRAEL 12/2017
 8 1 Thin periodontal biotype Lindhe piercing Glossary of Periodontal Terms CEJ :1 :1 thickperiodontal biotype :Emdogain 6 : : 31 41 9 DENTAL TRIBUNE ISRAEL 12/2017 2 Free soft tissue graft ( Coronally
8 1 Thin periodontal biotype Lindhe piercing Glossary of Periodontal Terms CEJ :1 :1 thickperiodontal biotype :Emdogain 6 : : 31 41 9 DENTAL TRIBUNE ISRAEL 12/2017 2 Free soft tissue graft ( Coronally
Over the years, mucogingival surgery
 The Use of DynaMatrix Extracellular Membrane for Gingival Augmentation and Root Coverage: A Case Series Saroff Stephen Andrew Saroff, DDS, MSD 1 Abstract Over the years, mucogingival surgery has developed
The Use of DynaMatrix Extracellular Membrane for Gingival Augmentation and Root Coverage: A Case Series Saroff Stephen Andrew Saroff, DDS, MSD 1 Abstract Over the years, mucogingival surgery has developed
Purpose: To assess the long term survival of sites treated by GTR.
 Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
Esthetic Crown Lengthening for Upper Anterior Teeth: Indications and Surgical Techniques
 Esthetic Crown Lengthening for Upper Anterior Teeth: Indications and Surgical Techniques Mohammad Assaf Assistant Professor, Faculty of Dentistry, Al-Quds University, Jerusalem, Palestine. ABSTRACT Correspondence
Esthetic Crown Lengthening for Upper Anterior Teeth: Indications and Surgical Techniques Mohammad Assaf Assistant Professor, Faculty of Dentistry, Al-Quds University, Jerusalem, Palestine. ABSTRACT Correspondence
Influence of Periodontal Parameters on Root Coverage: A Longitudinal Study
 Journal of the International Academy of Periodontology 2018 20/1: 25 31 Influence of Periodontal Parameters on Root Coverage: A Longitudinal Study Thaís Ribeiral Vieira 1, Dhelfeson Willya Douglas-de-Oliveira
Journal of the International Academy of Periodontology 2018 20/1: 25 31 Influence of Periodontal Parameters on Root Coverage: A Longitudinal Study Thaís Ribeiral Vieira 1, Dhelfeson Willya Douglas-de-Oliveira
Townie Guest Editorial. Gingival Attachment Loss: Evaluation and Surgical Options. Daniel J. Melker, DDS. fig. 1
 Gingival Attachment Loss: Evaluation and Surgical Options Daniel J. Melker, DDS Attached connective tissue (a.k.a. attached tissue) in the simplest terms is the body s only barrier between the underlying
Gingival Attachment Loss: Evaluation and Surgical Options Daniel J. Melker, DDS Attached connective tissue (a.k.a. attached tissue) in the simplest terms is the body s only barrier between the underlying
Case Report Coverage of Gingival Fenestration Using Modified Pouch and Tunnel Technique: A Novel Approach
 Case Reports in Dentistry Volume 2013, Article ID 902585, 5 pages http://dx.doi.org/10.1155/2013/902585 Case Report Coverage of Gingival Fenestration Using Modified Pouch and Tunnel Technique: A Novel
Case Reports in Dentistry Volume 2013, Article ID 902585, 5 pages http://dx.doi.org/10.1155/2013/902585 Case Report Coverage of Gingival Fenestration Using Modified Pouch and Tunnel Technique: A Novel
A combined approach to non-carious cervical lesions associated with gingival recession
 Case report ISSN 2234-7658 (print) / ISSN 2234-7666 (online) A combined approach to non-carious cervical lesions associated with gingival recession SungEun Yang 1 *, HyeJin Lee 1, Sung-Ho Jin 2 1 Department
Case report ISSN 2234-7658 (print) / ISSN 2234-7666 (online) A combined approach to non-carious cervical lesions associated with gingival recession SungEun Yang 1 *, HyeJin Lee 1, Sung-Ho Jin 2 1 Department
The Internatonal Journal of Periodontics & Restoraive Dentistry
 The Internatonal Journal of Periodontics & Restoraive Dentistry 3 Incisive Vessel Based Palatal Flap for the Reconstruction of Anterior Maxillary Soft Tissues [Au: Text has been edited heavily. Please
The Internatonal Journal of Periodontics & Restoraive Dentistry 3 Incisive Vessel Based Palatal Flap for the Reconstruction of Anterior Maxillary Soft Tissues [Au: Text has been edited heavily. Please
Periodontal Disease. Radiology of Periodontal Disease. Periodontal Disease. The Role of Radiology in Assessment of Periodontal Disease
 Radiology of Periodontal Disease Steven R. Singer, DDS srs2@columbia.edu 212.305.5674 Periodontal Disease! Includes several disorders of the periodontium! Gingivitis! Marginal Periodontitis! Localized
Radiology of Periodontal Disease Steven R. Singer, DDS srs2@columbia.edu 212.305.5674 Periodontal Disease! Includes several disorders of the periodontium! Gingivitis! Marginal Periodontitis! Localized
S John Wiley & Sons A/S. Published by John Wiley & Sons Ltd. Spain; 2 University of Milano, Milan, Italy
 J Clin Periodontol 2014; 41 (Suppl. 15): S92 S97 doi: 10.1111/jcpe.12215 Surgical techniques on periodontal plastic surgery and soft tissue regeneration: Consensus Report of Group 3 of the 10th European
J Clin Periodontol 2014; 41 (Suppl. 15): S92 S97 doi: 10.1111/jcpe.12215 Surgical techniques on periodontal plastic surgery and soft tissue regeneration: Consensus Report of Group 3 of the 10th European
A comparison of the effectiveness of two suturing techniques for the coronally positioned tunnel procedure with an acellular dermal matrix allograft.
 University of Louisville ThinkIR: The University of Louisville's Institutional Repository Electronic Theses and Dissertations 8-2010 A comparison of the effectiveness of two suturing techniques for the
University of Louisville ThinkIR: The University of Louisville's Institutional Repository Electronic Theses and Dissertations 8-2010 A comparison of the effectiveness of two suturing techniques for the
Dental Morphology and Vocabulary
 Dental Morphology and Vocabulary Palate Palate Palate 1 2 Hard Palate Rugae Hard Palate Palate Palate Soft Palate Palate Palate Soft Palate 4 Palate Hard Palate Soft Palate Maxillary Arch (Maxilla) (Uppers)
Dental Morphology and Vocabulary Palate Palate Palate 1 2 Hard Palate Rugae Hard Palate Palate Palate Soft Palate Palate Palate Soft Palate 4 Palate Hard Palate Soft Palate Maxillary Arch (Maxilla) (Uppers)
FRENECTOMY WITH LATERALLY DISPLACED FLAP: A CASE REPORT
 FRENECTOMY WITH LATERALLY DISPLACED FLAP: A CASE REPORT Dr. Minu.P. Mathew, Dr.R.Saravanakumar, Dr.Pratebha.B, Dr.Jannani.M, ABSTRACT An aberrant Maxillary labial frenum is capable of creating diastema
FRENECTOMY WITH LATERALLY DISPLACED FLAP: A CASE REPORT Dr. Minu.P. Mathew, Dr.R.Saravanakumar, Dr.Pratebha.B, Dr.Jannani.M, ABSTRACT An aberrant Maxillary labial frenum is capable of creating diastema
Clinical sessions in recession coverage at teeth and implants
 Clinical sessions in recession coverage at teeth and implants Main sponsors: Clinical sessions in recession coverage at teeth and implants It is an honour for us to present this joint SEPA-SIdP symposium,
Clinical sessions in recession coverage at teeth and implants Main sponsors: Clinical sessions in recession coverage at teeth and implants It is an honour for us to present this joint SEPA-SIdP symposium,
The International Journal of Periodontics & Restorative Dentistry
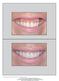 The International Journal of Periodontics & Restorative Dentistry 433 Lip Repositioning for Reduction of Excessive Gingival Display: A Clinical Report Ari Rosenblatt, DMD, DDS* Ziv Simon, DMD, MSc* Excessive
The International Journal of Periodontics & Restorative Dentistry 433 Lip Repositioning for Reduction of Excessive Gingival Display: A Clinical Report Ari Rosenblatt, DMD, DDS* Ziv Simon, DMD, MSc* Excessive
Minimally invasive techniques for periodontal regeneration
 2016; 2(12): 230-234 ISSN Print: 2394-7500 ISSN Online: 2394-5869 Impact Factor: 5.2 IJAR 2016; 2(12): 230-234 www.allresearchjournal.com Received: 04-10-2016 Accepted: 05-11-2016 Dr. Rizwan M Sanadi Professor,
2016; 2(12): 230-234 ISSN Print: 2394-7500 ISSN Online: 2394-5869 Impact Factor: 5.2 IJAR 2016; 2(12): 230-234 www.allresearchjournal.com Received: 04-10-2016 Accepted: 05-11-2016 Dr. Rizwan M Sanadi Professor,
Maintenance. Periodontics & Restorative. Naoshi Sato. A Clinical Atlas
 Naoshi Sato Periodontics & Restorative Maintenance A Clinical Atlas London, Berlin, Chicago, Tokyo, Barcelona, Beijing, Istanbul, Milan, Moscow, New Delhi, Paris, Prague, São Paulo, Seoul and Warsaw Preface
Naoshi Sato Periodontics & Restorative Maintenance A Clinical Atlas London, Berlin, Chicago, Tokyo, Barcelona, Beijing, Istanbul, Milan, Moscow, New Delhi, Paris, Prague, São Paulo, Seoul and Warsaw Preface
Subepithelial connective tissue graft for root coverage: clinical case reports and histologic evaluation
 Romanian Journal of Morphology and Embryology, ():793 797 CASE REPORTS Subepithelial connective tissue graft for root coverage: clinical case reports and histologic evaluation ALEXANDRA ROMAN ), R. CÂMPIAN
Romanian Journal of Morphology and Embryology, ():793 797 CASE REPORTS Subepithelial connective tissue graft for root coverage: clinical case reports and histologic evaluation ALEXANDRA ROMAN ), R. CÂMPIAN
Contemporary Periodontal Surgery
 Contemporary Periodontal Surgery Chris van Kesteren, D.D.S. CPCC Dental Hygiene Program October 18, 2011 Surgical Management of Periodontitis Periodontal Plastic Surgery Soft tissue and esthetics Dental
Contemporary Periodontal Surgery Chris van Kesteren, D.D.S. CPCC Dental Hygiene Program October 18, 2011 Surgical Management of Periodontitis Periodontal Plastic Surgery Soft tissue and esthetics Dental
Connective tissue graft associated or not with low laser therapy to treat gingival recession: randomized clinical trial
 J Clin Periodontol 2015; 42: 54 61 doi: 10.1111/jcpe.12328 Connective tissue graft associated or not with low laser therapy to treat gingival recession: randomized clinical trial Stephanie B. Fernandes-Dias
J Clin Periodontol 2015; 42: 54 61 doi: 10.1111/jcpe.12328 Connective tissue graft associated or not with low laser therapy to treat gingival recession: randomized clinical trial Stephanie B. Fernandes-Dias
A Clinical Evaluation of Anatomic Features of Gingiva in Dental Students in Tabriz, Iran
 Received 26 October 2007; Accepted 11 February 2008 A Clinical Evaluation of Anatomic Features of Gingiva in Dental Students in Tabriz, Iran Adileh Shirmohammadi 1 Masoumeh Faramarzie 1 * Ardeshir Lafzi
Received 26 October 2007; Accepted 11 February 2008 A Clinical Evaluation of Anatomic Features of Gingiva in Dental Students in Tabriz, Iran Adileh Shirmohammadi 1 Masoumeh Faramarzie 1 * Ardeshir Lafzi
