Journal of Dental Biomaterials. 2015;2(3) Raoofi S. a, Sabagh S. a, Shabahangfar MR. a, Mozafari Gh. a, GhoraishiAbhari M. b
|
|
|
- Claire Cunningham
- 5 years ago
- Views:
Transcription
1 Guided tissue regeneration therapy following the use of d-ptfe membrane Journal of Dental Biomaterials. 2015;2(3) Original Article Histomorphometric Analysis of Periodontal Tissue Regeneration by the Use of High Density Polytetrafluoroethylen Membrane in Grade II Furcation Defects of Dogs Raoofi S. a, Sabagh S. a, Shabahangfar MR. a, Mozafari Gh. a, GhoraishiAbhari M. b a Department of Periodontology, School of Dentistry, Shiraz University of Medical Sciences, Shiraz, Iran b Department of Endodontics, School of Dentistry, Shiraz University of Medical Sciences, Shiraz, Iran ARTICLE INFO Article History Received 8 May 2015 Accepted 17 August 2015 Key words: Furcation involvement GTR Barrier membrane d-ptfe (n-ptfe) membrane Corresponding Author: Ghazaleh Mozafari Department of Periodontology, School of Dentistry, Shiraz University of Medical Sciences, Shiraz, Iran Tel: ghazaal.mozafari@yahoo.com Abstract Statement of Problem: There are limited histomorphometric studies on biologic efficacy of high density tetrafluoroethylen (d-ptfe) membrane. Objectives: To investigate the healing of surgically induced grade II furcation defects in dogs following the use of dense polytetrafluoroethylene as the barrier membrane and to compare the results with the contra lateral control teeth without the application of any membrane. Materials and Methods: Mandibular and maxillary 3rd premolar teeth of 18 young adult male mongrel dogs were used for the experiment. The furcation defects were created during the surgery. 5 weeks later, regenerative surgery was performed. The third premolar teeth were assigned randomly to control and test groups. In the test group, after a full thickness flap reflection, the d-ptfe membrane was placed over furcation defects. In the control group, no membrane was placed over the defect. 37 tissue blocks containing the teeth and surrounding hard and soft tissues were obtained three months post-regenerative surgery. The specimens were demineralized, serially sectioned, mounted and stained with Hematoxylin and Eosin staining technique. From each tissue block, sections of 10 µm thickness within 60µm interval captured the entire surgically created defect. The histological images were transferred to computer and then the linear measurement ranges of the defects area, interadicular alveolar bone, epithelial attachment and coronal extension of the new cementum were done. Then, the volume and area of aforementioned parameters were calculated considering the thickness and interval of the sections. To compare the parameters between the control and test teeth, we calculated the amount of each one proportionally to the original amount of defects. Results: The mean interradicular root surface areas of original defects covered with new cementum was 74.46% and 29.59% for the membrane and control defects, respectively (p < ). Corresponding values for epithelial attachment were 16.03% and 48.93% for the membrane and control defects, respectively (p < 0.005). The mean volume of the new bone formed in the inter-radicular defects was 61.80% and 35.93% for the membrane and control defects, respectively (p < 0.02). Conclusions: The present study provided a biological rationale for high density polytetrafluoroethylen (d-ptfe, n-ptfe) as a barrier membrane for enhancement of the bone and cementum regeneration in grade II furcation defects subjected to regeneration therapy. Cite this article as: Raoofi S, Sabagh S, ShabahangfarMR,MozafariGh, GhoraishiAbhari M.Histomorphometric Analysis of Periodontal Tissue Regeneration by the Use of High Density Polytetrafluoroethylen Membrane in Grade II Furcation Defects of Dogs.J Dent Biomater, 2015;2(3): Jdb.sums.ac.irJ Dent Biomater2015; 2(3) 110
2 Raoofi S. et al. Introduction One of the inflammatory diseases is periodontitis that leads to alveolar bone and periodontal ligament destruction. There are different approaches to treatment of this kind of disease. In recent years, however, the use of regenerative procedures has become more common, aiming at restoring the lost periodontal support. It has been documented that for the formation of a new connective tissue attachment, the progenitor cells reside in the periodontal ligament [1]. Consequently, it should be expected that a new connective tissue attachment would be predictably achieved if such cells aggregate in the root surface during healing. During GTR, a membrane is placed over the defect to prevent epithelial cells, connective tissue cells and bone cells from contacting the root surface and also to provide a space for in-growth of periodontal ligament tissue [2,3]. Different types of membranes have been introduced for the regenerative therapy. The first non-resorbable membrane ever used was made of expanded polytetrafluoroethylene(e- PTFE). It is a biocompatible polymer that resists against enzymatic and microbiological attack [4,5]. Ingrowth of bacteria occurs due to the highly porous structure of eptfe when the membrane is exposed in the mouth [6]. Exposure results in high rates of infection; this frequently requires an early removal of the device. The highly porous structure allows the soft tissue ingrowth, which complicates the removal. So the removal of the membrane needs sharp dissection and extensive surgery. Expanded PTFE must be completely buried and the primary closure must be maintained to ensure the predictability of regenerative surgery [7]. Other non-resorbable membrane which is made of 100% non-porous, dense, non-expanded and non-permeable PTFE is high-density polytetrafluoroethylene membrane (n-ptfe, d- PTFE). The primary advantage of the dense PTFE is the ability to remain exposed in the mouth while protecting the underlying defect and the bone graft. Since the n-ptfe membrane is soft and flexible, it is easy to handle. Primary closure is not required, and if the membrane is exposed, it may be removed without the need to second surgery. If the primary closure technique is used, the membrane may be easily removed through a small incision in a flapless technique [8,9]. Dense PTFE is also available with titanium reinforcement. It can increase the stiffness of the material for use in defects where space-making is required. The embedded titanium framework allows the membrane to be shaped to fit with a variety of defects without rebounding. It also provides extra stability in large, non-space-making osseous defects [10,11]. Bioabsorbable membranes have been introduced to avoid a second surgery for the membrane removal. The main disadvantage of bioabsorbable membranes is the unpredictable resorption period. The primary closure is also needed when using bioabsobable membranes in regenerative surgery [12-15]. There are different ways to assess the GTR therapy outcome. The most valid one is histologic method. One of the disadvantages of histologic studies is the use of linear measurement. By the use of histomorphometric method, the area of attachment and the volume of regenerated tissue can be measured. There are few studies in the literature using d-ptfe membrane in which histomorphometric method has been used [16]. In 2003 Stephan et al. compared porous and nonporous teflon membrane in treatment of vertical osseous defect. They used clinical reentry method to assess the amount of regenerated tissues and found no statistically significant difference between the two groups [17]. In 2008, Hoffmann et al. used d-ptfe membrane for socket preservation. 12 month after the extraction, evaluation showed significantly higher amounts of bone regeneration following the use of d-ptfe membrane [18]. The only study in which the d-ptfe membrane was used for class II furcation treatment was the one conducted by James et al. in They compared porous (e-ptfe) and non- porous (d-ptfe) membrane and used clinical reentry method for assessing the tissue regeneration. They concluded that there was no statistically significant difference between the two groups [7]. The aim of this study was to evaluate the periodontal regeneration histomorphometrically after using the high-density polytetrafluoroethylene membrane in grade II furcation involvement in Mongrel dogs. 111 Jdb.sums.ac.irJ Dent Biomater2015; 2(3)
3 Guided tissue regeneration therapy following the use of d-ptfe membrane Materials and Methods In the current study, 18 one year old Mongrel dogs, each weighing approximately 22 kg were included. The third premolars in each jaw of the dogs were selected for study and the following indices were assessed: plaque index, gingival index and probing depth, amount of gingival recession and width of attached gingival on the buccal aspect of the third premolars measured by Williams periodontal probe. All surgical procedures were carried out under general anesthesia. 0.5 mg/kg acepromazin 2% was injected intra-muscularly half an hour before the surgery. Induction of the general anesthesia was done by 20 mg/kg sodium pentobarbital. After the intubation, general anesthesia was maintained by 2% halotan and 50% oxygen during the procedure. Creation of furcation involvement After the induction of general anesthesia, a sulcular incision was done on the buccal aspect of the third premolars and a full thickness flap was elevated. After removing the supracrestal periodontal tissue, the distance between CEJ and alveolar bone was measured. This distance on different teeth was mm. A grade II furcation involvement was created by the high speed rotary instrument and bur in width and height of 4mm. For preventing the reattachment of periodontal ligament to the root surface denuded from the alveolar bone, impression paste was placed in the space created in advance. After one week, the stitches were removed. Impression paste was maintained in the area for 5 weeks. After 5 weeks since the creation of furcation defect, the plaque and gingival indices were measured again. Afterwards, the impression paste was removed. Supra-gingival scaling was performed by ultrasonic instrument. Brushing was done every other day during the following week after removal of the impression paste. GTR surgical procedure One week after the plaque control program, GTR surgery was performed. A full thickness flap was reflected after induction of general anesthesia. Then, debridment and root planning were carried out. The depth and width of the furcation defects were assessed and mm increase in defects was found. For having a reference as the primary level of the bone to future microscopic assessment, a groove was created next to the most coronal part of the alveolar bone. Up to this stage, the procedure was the same between the test and control teeth. After creation of the groove, one of the third premolars of the jaws was selected as the control and the other one in the same jaw was chosen as the test randomly. In the control teeth, the flap was returned to its place and sutured. In the test teeth, the membrane (industrial d-ptfe sheets were used after sterilization) was placed over the defect so that it covered the defect completely and also 4-5 mm of the alveolar bone. Then the flap was returned to its place and sutured. After the surgery, oral amoxicilline was prescribed 1gr per day for 7 days.10 days after the surgery, the stitches were removed. In the test teeth, the membranes were maintained for 5 weeks. During this period, the plaque control was done by 0.2% chlorhexidine mouthwash. Chlorhexidine was applied on the teeth and gingiva by the cotton pellet. For removing the membranes, no incision was needed and they were removed easily by a forceps. Three months after the regenerative surgery, the dogs were sacrificed by extra dose of anesthetic drug. The third premolar teeth with the surrounding tissue were removed with two vertical dissections at the mesial and distal parts of the teeth and one horizontal dissection. The samples were kept in formalin for 72 hours and then in formic acid for 21 days to be decalcified. After that, the blocks were formed with paraffin. Mesial-distal serial sections were provided from each block in 10 micron width and 60 micron interval sections from each block were prepared for the microscopic assessment. Finally, histomorphometrican analysis was carried out. The histologic images of histological sections were transferred with the computerized image analysis Axio-Vision (Carl Zeiss, Germany) to the computer. Then, linear measurements of the defects area range, interadicular alveolar bone range, epithelial attachment range and coronal extension of the new cementum were done. Then, volumetric measurements of the aforementioned parameters Jdb.sums.ac.irJ Dent Biomater2015; 2(3) 112
4 Raoofi S. et al. Table 1: The mean, standard deviation and P-value of BN,NC,E,V,CT in the test and control teeth in the lower jaw using Paired T-test P-value Standard deviation Mean Parameters BN T BN C NC T NC C E T E C V T V C CT T CT C were calculated by considering the thickness of histologic sections and interval of these sections. To compare the afore-mentioned parameters between the test and control teeth, the amount of each one was calculated proportional to the volume and area of original defects. The following parameters were assessed in the defect zone: - Ratio of the volume of the new bone formation (BN) - Ratio of the area of the root covered with the new cementum (NC) - Ratio of the area of the root with epithelial attachment (E) - Ratio of the area of the root with the connective tissue attachment without new cementum formation (CT) - Ratio of the area of the root without any attach- ment(v) Results The test and control teeth in each jaw were compared according to the new bone formation (BN), new cementum (NC), the length of the root with the connective tissue attachment without cementum formation (CT), epitheial attachment (E), and the length of the root in the defect area without any attachment (V). The test and the control teeth were compared by the afore-mentioned factors in both jaws. For this analysis, paired T-test and Wilcoxon signed rank test were used. In the lower jaw, the volume of the new bone formation was greater in the test teeth in comparison with the control ones but the difference was not statistically significant (p = 0.114). No significant difference was Table 2: The mean, standard deviation and P-value of BN,NC,E,V,CT in the test and control teeth in the upper jaw using Paired T-test P-value Standard deviation Mean Parameters BN T BN C NC T NC C E T E C V T V C CT T CT C 113 Jdb.sums.ac.irJ Dent Biomater2015; 2(3)
5 Guided tissue regeneration therapy following the use of d-ptfe membrane Table 3: The mean, standard deviation and P-value of BN,NC,E,V,CT in the test and control teeth in both jaws using Paired T-test P-value Standard deviation mean Parameters BN T BN C NC T NC C E T E C V T V C CT T CT C also found in V (p = 0.63) and CT (p = 0.811). The new cementum formation was significantly higher in the test teeth (p = 0.002). On the contrary, the epithelial attachment was more in the control teeth (p = 0.003). In both paired T-test and Wilcoxon signed ranks test, the results for these factors were the same (Tables 1 and 4). In the upper jaw, the new cementum formation in the test teeth was considerably more compared to the control teeth (p = 0.010). On the other hand, the amount of the root surface in the defect area had no attachment and the root surface with epithelial attachment was more in the control teeth. There was no significant difference in the other factors. (p-value for V was and for E was 0.299) (Table 2). As shown in Table 3, the comparison of the contr- ol and test teeth in both jaws revealed that the volume of the new bone and cementum formation in the test teeth was greater compared to the control teeth (pvalue for NC was and for BN it was 0.017). There was no significant difference in the V and CT. (p-value for V was and for CT it was 0.513). The amount of epithelial attachment was greater in the control teeth (p = 0.005). Moreover, the control and test teeth in the upper and lower jaws were compared. The results obtained from all factors were the same in the control and test teeth in the lower and upper jaws, except for the amount of the root s lack of attachment which was greater considerably in the control teeth in the upper jaw compared to the control teeth in the lower jaw (p = 0.028). Table 4: Data obtained from comparing the control and test teeth in each jaw using Wilcoxon signed ranks test (T and C represent test and control teeth and L and U represent lower and upper jaws) P-value Parameters BN TL -BN CL NC TL -NC CL E TL -E CL V TL -V CL 1.00 CT TL -CT CL BN TU -BN CU NC TU -NC CU E TU -E CU V TU -V CU CT TU -CT CU Jdb.sums.ac.irJ Dent Biomater2015; 2(3) 114
6 Raoofi S. et al. Discussion The ultimate goal of periodontal therapy is regeneration of perioduntium. One of the methods believed to have predictable results in treatment of periodontal defects including grade II furcation involvement is GTR. In several studies, it has been shown that the teeth undergoing GTR treatments have gained more clinical attachment compared to the controlled teeth. There are several factors that affect GTR treatment. They include meticulous plaque control, prevention of barrier membrane infection and bacterial accumulation and provision of an adequate and stable space under the barrier membrane [16]. Several materials have been introduced to be used as barrier membranes. The gold standard for GTR materials is e-ptfe. But as mentioned earlier, there are several problems with e-ptfe including bacterial contamination due to its high porosity, need for the primary closure and the complicated removal [6,7,19]. Another non-resorbable membrane is n-ptfe which is less porous. This membrane is believed to have better handling properties and does not need any primary closure. This membrane can also be easily removed through a flapless surgery [18]. Also, different types of bioabsorbable membranes have been introduced. The main advantage of these membranes is that they permit a single- step procedure, thus alleviating patient discomfort and expenses for a second procedure, and avoiding the risk of additional morbidity and tissue damage. The main disadvantage of resorbable membranes is unpredictable resorption time. These membranes also need primary closure [14]. n-ptfe membranes are less costly compared to e-ptfe and resobable membranes. According to the results of this study, n-ptfe led to an increased regeneration of the bone and cementum in grade II furcation defects in the maxillary and mandibular third premolars in dogs (p < 0.05). The means of bone regeneration in the test and control teeth were 61.8% and 35.9% of the primary defects, respectively. The mean of cementum regeneration in the test and control teeth were 74.5% and 29.6% of the root surfaces lack of tissue attachment in primary defects. The non-significant results of bone regeneration in each jaw can be explained by inadequate number of the teeth in each jaw, so when the teeth of the maxilla and mandible were assessed, this difference was significant. In many histologic sections of the test teeth, bone formation was still in an active phase. So it can be assumed if more time had been given for the bone to be generated, more amounts of bone would have been regenerated and more differences between the test and control teeth would have been observed. It was not possible to perform optimum oral hygiene during the healing phase after regenerative surgery. This could lead to gingival inflammation and release of the inflammatory mediators which can decrease the rate of new bone formation. This can have more effects on the test teeth as a result of barrier membrane presence. On the other hand, the dog teeth have very short root trunk and there is not an adequate space between CEJ and furcation. This can lead to lack of optimum adaptation of the membrane that influences the result of GTR treatment [16]. So we can suggest that the GTR surgery with d-ptfe membrane might yield better results in human. There are several means for assessment of the periodontal regeneration. In most studies [5,7,9,17,18,19, 20], the outcome of regenerative periodontal surgery was evaluated by measuring the attachment level using periodontal probe, radiographic analysis or reentry operations. However, such methods did not provide any reliable proof for the attachment (i.e. formation of the cementum with inserting collagen fibers coronal to the attachment level before treatment). The most valid means of assessment of the periodontal regeneration is histological method. As this method is invasive and hard to be done, the usage of this method is limited. One of the drawbacks of the histologic measurement is the use of linear measurement instead of measuring the area of attachment and volume of the regenerated tissue [16]. With the use of histomorphometric method, the attachment area and volume of the regenerated tissue can be measured [16,21]. But as histomorphometric studies are time-consuming and difficult to perform, there are few previous studies using this method especially in grade II furcation defects. Treatment of furcation defects is very challenging because it is usually hard to obtain thorough membrane adaptation and optimal oral hygiene [16]. 115 Jdb.sums.ac.irJ Dent Biomater2015; 2(3)
7 Guided tissue regeneration therapy following the use of d-ptfe membrane The review of the literature revealed that most of the studies found no difference or no statically significant difference between e-ptfe and d-ptfe membranes [4,5,7,17,18,19,20]. In 1995, Bartee et al. evaluated n-ptfe (d-ptfe) membrane as a barrier material to facilitate guided tissue regeneration in the rat mandibles. They created bilateral through-and-through defects in the mandibular angle of 12 rats. The experimental sites were covered by n-ptfe and the opposite defects served as the control sites. After 10 weeks, complete ossification was observed on the d-ptfe treated sites by histological evaluation while little osseous regeneration was observed on the control defects [9]. In 2001, Lamb et al. compared porous and non-porous teflon membranes in class II furcation defects using clinical reentry evaluation method. 24 patients with periodontitis and one class II furcation defect were included in this study and randomly divided into two groups. In one of the groups, porous Teflon membrane was used during GTR surgery and in the other one non-porous Teflon membrane was used. 9 months after the initial surgery, the second surgery for evaluation of healing outcome was performed. No statistically significant difference was found between the two groups [7]. In 2003, Walters et al. conducted a study relatively similar to Lamb et al. s research. They included 24 patients with periodontitis and divided them into two groups. Also, they used reentry method for evaluation of regenerative surgery outcome to compare porous and non-porous teflon membrane with this difference that they used the membranes to treat vertical osseous defects. They found no statistically significant difference between the two groups [17]. In 2007, Macedo et al. evaluated the possibility to obtain guided bone regeneration with two types of physical barriers (calcium sulfate and PTFE nonporous barrier) in surgical defects created in the rat parietal bones. After 7,14, 30 and 45 days, four animals were sacrificed in each period and microscopic analysis was done. They found that PTFE barrier was more effective when compared to calcium sulfate during bone regeneration, involving transcortical shallow defects [22]. In 2008, Hoffmann et al. used d- PTFE membrane to preserve the alveolar bone after tooth extraction. 276 extraction sites were evaluated. Measurements were taken post-extraction and 12 months after the surgery. The distance from the cemento-enamel junction of the adjacent teeth to the bone level was measured. Hard tissue biopsies were taken from 10 representative cases during implant placement 12 months after the socket preservation. The results of this study showed that the use of a d- PTFE membrane allowed for a significant regeneration of the volume of the sockets following tooth extraction. Histologic evaluation indicated that the newly formed tissue in the extraction sites was mainly regular trabecular bone with areas of bone marrow and typical cells. The authors mentioned absence of a control group as a limitation of this study [18]. In 2000, Marouf compared e-ptfe and d-ptfe effectiveness in guided bone regeneration surgery. They used elderly rabbits as the experimental animals. Two non-self-healing defects were created in each rabbit calvarium. One of the 2 defects was fully covered with e-ptfe membrane and the other one was covered with d-ptfe. The specimens were obtained at 4,8 and 16 weeks and examined with light microscopy. They observed greater speed and quantity of bone regeneration in the defects covered with e-ptfe. However, in the defects covered with d-ptfe, marginal bone regeneration was observed, so it can be postulated that if more time had been given, more bone regeneration would have been observed and the difference would have been less significant between the two groups. [6] Conclusions As this study showed, with the use of d-ptfe membrane in guided tissue regeneration surgery, an increase of periodontal tissue regeneration was gained in comparison to the control teeth. This can provide a biologic reason for using this type of membrane in GTR surgery. References 1. Nyman S, Gottlow J, Karring T, et al. The regenerative potential of the periodontal ligament. J Clin Periodontol. 1982;9: Aukhil I, Pettersson E, Suggs C. Guided Tissue Regeneration: An Experimental Procedure in Beagle Jdb.sums.ac.irJ Dent Biomater2015; 2(3) 116
8 Raoofi S. et al. Dogs. J Periodontol. 1986;57: Shanaman RH. The use of guided tissue regeneration to facilitate ideal prosthetic placement of implants.int J Periodontics Restorative Dent.1991;12: Bartee BK. The use of high-density polytetrafluoroethylene membrane to treat osseous defects: clinical reports. Implant Dent. 1995;4: Bartee BK. Evaluation of new polytetrafluoroethyleneguided tissue regeneration membrane in healing extraction sites. Compendium. 1998;19: Marouf HA, El-Guindi HM. Efficacy of high-density versus semipermeable PTFE membranes in an elderly experimental model.oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2000;89: Lamb III JW, Greenwell H, Drisko C, et al. A comparison of porous and non-porous teflon membranes plus demineralized freeze-dried bone allograft in the treatment of class II buccal/lingual furcation defects: A clinical reentry study. J Periodontol. 2001;72: Fotek PD, Neiva RF, Wang H-L. Comparison of dermal matrix and polytetrafluoroethylene membrane for socket bone augmentation: a clinical and histologic study. J Periodontol. 2009;80: Bartee BK, Carr J. Evaluation of a high-density polytetrafluoroethylene (n-ptfe) membrane as a barrier material to facilitate guided bone regeneration in the rat mandible. J Oral Implantol. 1995;21: Carbonell J, Martín IS, Santos A, et al. High-density polytetrafluoroethylene membranes in guided bone and tissue regeneration procedures: a literature review. Int J Oral Maxillofac Surg. 2014;43: Eickholz P, Kim TS, Holle R. Regenerative periodontal surgery with non resorbable and biodegradable barriers: results after 24 months. J Clin Periodontol. 1998;25: Takata T, Wang HL, Miyauchi M. Attachment, proliferation and differentiation of periodontal ligament cells on various guided tissue regeneration membranes. J Periodontal Res. 2001;36: Hürzeler MB, Kohal RJ, Naghshbandl J, et al. Evaluation of a new bioresorbable barrier to facilitate guided bone regeneration around exposed implant threads: An experimental study in the monkey. Int J Oral Maxillofac Surg.1998;27: Eickholz P, Lenhard M, Benn DK, et al. Periodontal surgery of vertical bony defects with or without synthetic bioabsorbable barriers. 12-month results. J Periodontol. 1998;69: MacDonald ES, Nowzari H, Contreras A, et al. Clinical and microbiological evaluation of a bioabsorbable and a nonresorbable barrier membrane in the treatment of periodontal intraosseous lesions. J Periodontol. 1998; 69: Lang NP, Lindhe J. Clinical periodontology and implant dentistry: John Wiley & Sons; Walters SP, Greenwell H, Hill M, et al. Comparison of porous and non-porous teflon membranes plus a xenograft in the treatment of vertical osseous defects: a clinical reentry study. J Periodontol. 2003; 74: Hoffmann O, Bartee BK, Beaumont C, et al. Alveolar bone preservation in extraction sockets using nonresorbable dptfe membranes: a retrospective nonrandomized study. J Periodontol. 2008;79: Barboza EP, Stutz B, Ferreira VF, et al. Guided bone regeneration using nonexpanded polytetrafluoroethylene membranes in preparation for dental implant placements a report of 420 cases. Implant Dent. 2010;19: Floriano JF. Estudos sistemáticos de biocompatibilidade e potencial osteogênico de membranas bioativas em coelhos machos Cortellini P, Prato GP, Tonetti MS. Periodontal regeneration of human infrabony defects. II. Re-entry procedures and bone measures. J Periodontol. 1993; 64: demacedo NL, de Macedo LGS, MonteiroAdSF. Calcium sulfate and PTFE nonporous barrier for regeneration of experimental bone defects. CEP. 2008; 12245: Jdb.sums.ac.irJ Dent Biomater2015; 2(3)
Purpose: To assess the long term survival of sites treated by GTR.
 Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports
 0 Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports R.G. Caffesse, B.A. Smith/ B. Duff, E.C. Morrison, D. Merrill/ and W. Becker In the cases reported here, the response
0 Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports R.G. Caffesse, B.A. Smith/ B. Duff, E.C. Morrison, D. Merrill/ and W. Becker In the cases reported here, the response
Surgical Procedure in Guided Tissue Regeneration with the. Inion GTR Biodegradable Membrane System
 Surgical Procedure in Guided Tissue Regeneration with the Inion GTR Biodegradable Membrane System 1 Introduction This presentation familiarizes you with the basic steps how to use the Inion GTR membrane
Surgical Procedure in Guided Tissue Regeneration with the Inion GTR Biodegradable Membrane System 1 Introduction This presentation familiarizes you with the basic steps how to use the Inion GTR membrane
Minimally invasive techniques for periodontal regeneration
 2016; 2(12): 230-234 ISSN Print: 2394-7500 ISSN Online: 2394-5869 Impact Factor: 5.2 IJAR 2016; 2(12): 230-234 www.allresearchjournal.com Received: 04-10-2016 Accepted: 05-11-2016 Dr. Rizwan M Sanadi Professor,
2016; 2(12): 230-234 ISSN Print: 2394-7500 ISSN Online: 2394-5869 Impact Factor: 5.2 IJAR 2016; 2(12): 230-234 www.allresearchjournal.com Received: 04-10-2016 Accepted: 05-11-2016 Dr. Rizwan M Sanadi Professor,
SalvinOss Xenograft Bone Graft Material In Vivo Testing Summary
 SalvinOss Xenograft Bone Graft Material In Vivo Testing Summary Summary of In Vivo Use Of Bioresorbable Xenograft Bone Graft Materials In The Treatment Of One-Walled Intrabony Defects In A Canine Model
SalvinOss Xenograft Bone Graft Material In Vivo Testing Summary Summary of In Vivo Use Of Bioresorbable Xenograft Bone Graft Materials In The Treatment Of One-Walled Intrabony Defects In A Canine Model
Cytoflex Barrier Membrane Clinical Evaluation
 Cytoflex Barrier Membrane Clinical Evaluation Historical Background Guided tissue regeneration is a well established concept in the repair of oral bone defects. The exclusion of soft tissue epithelial
Cytoflex Barrier Membrane Clinical Evaluation Historical Background Guided tissue regeneration is a well established concept in the repair of oral bone defects. The exclusion of soft tissue epithelial
RELIABLE WHEN IT COUNTS. The unique collagenase-resistant membrane protects bone graft and supports treatment success even when exposed 4
 RELIABLE WHEN IT COUNTS 1 RELIABLE WHEN IT COUNTS RESISTANT TO EXPOSURE The unique collagenase-resistant membrane protects bone graft and supports treatment success even when exposed 4 RELIABLE BARRIER
RELIABLE WHEN IT COUNTS 1 RELIABLE WHEN IT COUNTS RESISTANT TO EXPOSURE The unique collagenase-resistant membrane protects bone graft and supports treatment success even when exposed 4 RELIABLE BARRIER
Surgical Therapy. Tuesday, April 2, 13. Alessan"o Geminiani, DDS, MS
 Surgical Therapy Alessan"o Geminiani, DDS, MS Periodontal Flap: a surgical procedure in which incisions are made in the gingiva or mucosa to allow for separation of the epithelium and connective tissues
Surgical Therapy Alessan"o Geminiani, DDS, MS Periodontal Flap: a surgical procedure in which incisions are made in the gingiva or mucosa to allow for separation of the epithelium and connective tissues
Contemporary Periodontal Surgery
 Contemporary Periodontal Surgery Chris van Kesteren, D.D.S. CPCC Dental Hygiene Program October 18, 2011 Surgical Management of Periodontitis Periodontal Plastic Surgery Soft tissue and esthetics Dental
Contemporary Periodontal Surgery Chris van Kesteren, D.D.S. CPCC Dental Hygiene Program October 18, 2011 Surgical Management of Periodontitis Periodontal Plastic Surgery Soft tissue and esthetics Dental
The Original remains unique.
 The Original remains unique. Geistlich leading regeneration 2A, 2B Geistlich is the world leader in regenerative dentistry. We transform natural biomaterials into safe and reliable treatment methods that
The Original remains unique. Geistlich leading regeneration 2A, 2B Geistlich is the world leader in regenerative dentistry. We transform natural biomaterials into safe and reliable treatment methods that
Guided bone regeneration using two types of non-resorbable barrier membranes
 DOI:10.5125/jkaoms.2010.36.4.275 Guided bone regeneration using two types of non-resorbable barrier membranes Ji-Young Lee 1, Young-Kyun Kim 1, Pil-Young Yun 1, Ji-Su Oh 2, Su-Gwan Kim 2 1 Department of
DOI:10.5125/jkaoms.2010.36.4.275 Guided bone regeneration using two types of non-resorbable barrier membranes Ji-Young Lee 1, Young-Kyun Kim 1, Pil-Young Yun 1, Ji-Su Oh 2, Su-Gwan Kim 2 1 Department of
The anatomic limitations of the. Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD*
 CASE REPORT Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD* The anatomic limitations of the residual alveolar bone may cause problems for
CASE REPORT Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD* The anatomic limitations of the residual alveolar bone may cause problems for
ELIMINATE POCKETS. Periodontal pocket is the consequence of periodontal infection But also a major risk factor for the further progression of disease
 ELIMINATE POCKETS Periodontal pocket is the consequence of periodontal infection But also a major risk factor for the further progression of disease CONSEQUENTLY Periodontal pockets should be eliminated
ELIMINATE POCKETS Periodontal pocket is the consequence of periodontal infection But also a major risk factor for the further progression of disease CONSEQUENTLY Periodontal pockets should be eliminated
Dental Research Journal
 Dental Research Journal Case Report Treatment strategy for guided tissue regeneration in various class II furcation defect: Case series Pushpendra Kumar Verma 1, Ruchi Srivastava 1, K. K. Gupta 2, T. P.
Dental Research Journal Case Report Treatment strategy for guided tissue regeneration in various class II furcation defect: Case series Pushpendra Kumar Verma 1, Ruchi Srivastava 1, K. K. Gupta 2, T. P.
Socket preservation in the daily practice: A clinical case report
 Clinical Socket preservation in the daily practice: A clinical case report Rabih Abi Nader 1 and Carine Tabarani 2 Abstract Soft tissue contour depends on the underlying bone anatomy. Following tooth extraction,
Clinical Socket preservation in the daily practice: A clinical case report Rabih Abi Nader 1 and Carine Tabarani 2 Abstract Soft tissue contour depends on the underlying bone anatomy. Following tooth extraction,
The Treatment of Gingival Recession Associated with Deep Corono-Radicular Abrasions (CEJ step) a Case Series
 CLINICAL AND RESEARCH REPORT The Treatment of Gingival Recession Associated with Deep Corono-Radicular Abrasions (CEJ step) a Case Series Giovanpaolo Pini-Prato, Carlo Baldi, Roberto Rotundo, Debora Franceschi,
CLINICAL AND RESEARCH REPORT The Treatment of Gingival Recession Associated with Deep Corono-Radicular Abrasions (CEJ step) a Case Series Giovanpaolo Pini-Prato, Carlo Baldi, Roberto Rotundo, Debora Franceschi,
More than bone regeneration. A total solution.
 More than bone regeneration. A total solution. More than a dental implant company. A total solution. When it comes to treatment options, your patients want positive results both functionally and esthetically.
More than bone regeneration. A total solution. More than a dental implant company. A total solution. When it comes to treatment options, your patients want positive results both functionally and esthetically.
Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs
 Current Applied Physics 5 (2005) 507 511 www.elsevier.com/locate/cap Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs Ui-Won Jung a, Hee-Il
Current Applied Physics 5 (2005) 507 511 www.elsevier.com/locate/cap Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs Ui-Won Jung a, Hee-Il
BONE AUGMENTATION AND GRAFTING
 1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Case Report Bridge Flap: A Sine Qua Non For Mucogingival Deformities Debajyoti Mondal, Anju L, Rajul Choradia, Somen
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Case Report Bridge Flap: A Sine Qua Non For Mucogingival Deformities Debajyoti Mondal, Anju L, Rajul Choradia, Somen
Case Study. Case # 1 Author: Dr. Suheil Boutros (USA) 2013 Zimmer Dental, Inc. All rights reserved. 6557, Rev. 03/13.
 Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
( ) 2009;28(2):89-94
 ( ) 2009;28(2):89-94 Osseointegration is important in the functional aspect, however, esthetics is also important, especially in the maxillary anterior region. An adequate surgical technique is necessary
( ) 2009;28(2):89-94 Osseointegration is important in the functional aspect, however, esthetics is also important, especially in the maxillary anterior region. An adequate surgical technique is necessary
Advanced Probing Techniques
 Module 21 Advanced Probing Techniques MODULE OVERVIEW The clinical periodontal assessment is one of the most important functions performed by dental hygienists. This module begins with a review of the
Module 21 Advanced Probing Techniques MODULE OVERVIEW The clinical periodontal assessment is one of the most important functions performed by dental hygienists. This module begins with a review of the
Clinical Case Reports using Cytoplast GTR Barrier Membranes
 Clinical Case Reports using Cytoplast GTR Barrier Membranes Barry K. Bartee, DDS, MD The Cytoplast Technique: Extraction Site Grafting Without Primary Closure 1. 1. Preoperative view. To maximize the result
Clinical Case Reports using Cytoplast GTR Barrier Membranes Barry K. Bartee, DDS, MD The Cytoplast Technique: Extraction Site Grafting Without Primary Closure 1. 1. Preoperative view. To maximize the result
Horizontal bone augmentation by means of guided bone regeneration
 Periodontology 2000, Vol. 66, 2014, 13 40 2014 John Wiley & Sons A/S. Published by John Wiley & Sons Ltd Printed in Singapore. All rights reserved PERIODONTOLOGY 2000 Horizontal bone augmentation by means
Periodontology 2000, Vol. 66, 2014, 13 40 2014 John Wiley & Sons A/S. Published by John Wiley & Sons Ltd Printed in Singapore. All rights reserved PERIODONTOLOGY 2000 Horizontal bone augmentation by means
Socket Treatment. Procedure Guide
 Socket Treatment Procedure Guide www.implantdirect.com 888.649.6425 Extraction Healing and Ridge Resorption The Why Working with patients to educate them on the benefits of bone maintenance post extraction
Socket Treatment Procedure Guide www.implantdirect.com 888.649.6425 Extraction Healing and Ridge Resorption The Why Working with patients to educate them on the benefits of bone maintenance post extraction
a closer look at Cytoplast High Density PTFE performance predictability efficacy High-Density PTFE (dptfe)
 a closer look at Cytoplast High Density PTFE High-Density PTFE (dptfe) SEM 500X SEM 20,000X performance A B SEM 1,500X (Inset: SEM at 100X) SEM 20,000X (Inset: SEM at 6,000X) SEM views of Cytoplast TXT-200
a closer look at Cytoplast High Density PTFE High-Density PTFE (dptfe) SEM 500X SEM 20,000X performance A B SEM 1,500X (Inset: SEM at 100X) SEM 20,000X (Inset: SEM at 6,000X) SEM views of Cytoplast TXT-200
Working together as a team, the periodontist
 The Team Approach to Esthetic Immediate Implant Placement Bobby L. Butler, DDS; and Greggory Kinzer, DDS Working together as a team, the periodontist and restorative dentist can provide an increased level
The Team Approach to Esthetic Immediate Implant Placement Bobby L. Butler, DDS; and Greggory Kinzer, DDS Working together as a team, the periodontist and restorative dentist can provide an increased level
The regeneration of the tooth supporting structures
 Position Paper Periodontal Regeneration* Untreated periodontal disease leads to tooth loss through destruction of the attachment apparatus and toothsupporting structures. The goals of periodontal therapy
Position Paper Periodontal Regeneration* Untreated periodontal disease leads to tooth loss through destruction of the attachment apparatus and toothsupporting structures. The goals of periodontal therapy
Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of
 Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of peri-implantitis I: microbiological outcomes. Clin Oral Imp Res 2006;
Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of peri-implantitis I: microbiological outcomes. Clin Oral Imp Res 2006;
Evidence-based decision making in periodontal tooth prognosis
 Clin Dent Rev (2017) 1:3 https://doi.org/10.1007/s41894-017-0004-2 TREATMENT Evidence-based decision making in periodontal tooth prognosis Carlos Ernesto Nemcovsky 1 Received: 12 April 2017 / Accepted:
Clin Dent Rev (2017) 1:3 https://doi.org/10.1007/s41894-017-0004-2 TREATMENT Evidence-based decision making in periodontal tooth prognosis Carlos Ernesto Nemcovsky 1 Received: 12 April 2017 / Accepted:
Clinical Case Reports using Cytoplast GTR Barrier Membranes
 Clinical Case Reports using Cytoplast GTR Barrier Membranes S I M P L E P R E D I C TA B L E P R A C T I C A L C L I N I C A L E D U C A T I O N 4620 71st Street Lubbock, Texas 79424 888.796.1923 www.osteogenics.com
Clinical Case Reports using Cytoplast GTR Barrier Membranes S I M P L E P R E D I C TA B L E P R A C T I C A L C L I N I C A L E D U C A T I O N 4620 71st Street Lubbock, Texas 79424 888.796.1923 www.osteogenics.com
The ultimate goal in periodontal
 Volume 71 Number 4 Interleukin-1 Gene Polymorphisms and Long-Term Stability Following Guided Tissue Regeneration Therapy* Massimo De Sanctis and Giovanni Zucchelli Background: Specific interleukin (IL)-1
Volume 71 Number 4 Interleukin-1 Gene Polymorphisms and Long-Term Stability Following Guided Tissue Regeneration Therapy* Massimo De Sanctis and Giovanni Zucchelli Background: Specific interleukin (IL)-1
Management of a complex case
 2 Soft- and hard-tissue reconstruction of a severely deficient site prior to implant placement: a case report Management of a complex case Younes Khosroshahy, DDS, MFDS RCS (Eng), Dip Imp Dent RCSEd, Blue
2 Soft- and hard-tissue reconstruction of a severely deficient site prior to implant placement: a case report Management of a complex case Younes Khosroshahy, DDS, MFDS RCS (Eng), Dip Imp Dent RCSEd, Blue
Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report
 C A S E R E P O R T Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report Rhoodie Garrana 1 and Govindrau Mohangi
C A S E R E P O R T Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report Rhoodie Garrana 1 and Govindrau Mohangi
The treatment of destructive periodontal disease, due to specific periodontopathic
 1 1 INTRODUCTION The treatment of destructive periodontal disease, due to specific periodontopathic bacteria, aims at the regeneration of a periodontal attachment composed of new cementum, alveolar bone
1 1 INTRODUCTION The treatment of destructive periodontal disease, due to specific periodontopathic bacteria, aims at the regeneration of a periodontal attachment composed of new cementum, alveolar bone
SOCKET WHETHER TO PRESERVE IT NOW OR TO CREATE LATER? - A CASE REPORT
 MAVEN CASE REPORT SOCKET WHETHER TO PRESERVE IT NOW OR TO CREATE LATER? - A CASE REPORT Dr. Parthasarathi Biswas 1, Dr. Debajyoti Mondal 1, Dr. B Praveena Devi 1, Dr. Indrasri Das 2, Dr. Somen Bagchi 3,
MAVEN CASE REPORT SOCKET WHETHER TO PRESERVE IT NOW OR TO CREATE LATER? - A CASE REPORT Dr. Parthasarathi Biswas 1, Dr. Debajyoti Mondal 1, Dr. B Praveena Devi 1, Dr. Indrasri Das 2, Dr. Somen Bagchi 3,
Tooth Retained Implant: No More an Oxymoron
 بنام خدا بنام خدا OPEN ACCESS Freely Available Online Original Hypothesis Tooth Retained Implant: No More an Oxymoron Divya Bhat a Abstract a Department of Periodontics, D.A.P.M.R.V. Dental College, Karnataka,
بنام خدا بنام خدا OPEN ACCESS Freely Available Online Original Hypothesis Tooth Retained Implant: No More an Oxymoron Divya Bhat a Abstract a Department of Periodontics, D.A.P.M.R.V. Dental College, Karnataka,
REGENERATIONTIME. A Case Report by. Ridge Augmentation and Delayed Implant Placement on an Upper Lateral Incisor
 A Case Report by Dr. Daniele Cardaropoli Ridge Augmentation and Delayed Implant Placement on an Upper Lateral Incisor The Situation An adult female patient presented with an endodontic/prosthetic failure
A Case Report by Dr. Daniele Cardaropoli Ridge Augmentation and Delayed Implant Placement on an Upper Lateral Incisor The Situation An adult female patient presented with an endodontic/prosthetic failure
Alarge number of sound clinical
 Volume 83 Number 5 Long-Term 8-Year Outcomes of Coronally Advanced Flap forrootcoverage Giovanpaolo Pini-Prato,* Debora Franceschi,* Roberto Rotundo,* Francesco Cairo,* Pierpaolo Cortellini, and Michele
Volume 83 Number 5 Long-Term 8-Year Outcomes of Coronally Advanced Flap forrootcoverage Giovanpaolo Pini-Prato,* Debora Franceschi,* Roberto Rotundo,* Francesco Cairo,* Pierpaolo Cortellini, and Michele
Esthetic Crown Lengthening for Upper Anterior Teeth: Indications and Surgical Techniques
 I J Pre Clin Dent Res 2014;1(2):49-53 April-June All rights reserved International Journal of Preventive & Clinical Dental Research Esthetic Crown Lengthening for Upper Anterior Teeth: Indications and
I J Pre Clin Dent Res 2014;1(2):49-53 April-June All rights reserved International Journal of Preventive & Clinical Dental Research Esthetic Crown Lengthening for Upper Anterior Teeth: Indications and
botiss dental bone & tissue regeneration biomaterials mucoderm 3D-Regenerative Tissue Graft strictly biologic
 dental bone & tissue regeneration botiss biomaterials 3DRegenerative Tissue Graft strictly biologic mucoderm Soft Tissue Graft Indications mucoderm is a collagen tissue matrix derived of animal dermis
dental bone & tissue regeneration botiss biomaterials 3DRegenerative Tissue Graft strictly biologic mucoderm Soft Tissue Graft Indications mucoderm is a collagen tissue matrix derived of animal dermis
Multi-Modality Anterior Extraction Site Grafting Increased Predictability for Aesthetics Michael Tischler, DDS
 Page 1 of 5 Issue Date: March 2003, Posted On: 8/1/2005 Multi-Modality Anterior Extraction Site Grafting Increased Predictability for Aesthetics Michael Tischler, DDS The extraction of teeth creates a
Page 1 of 5 Issue Date: March 2003, Posted On: 8/1/2005 Multi-Modality Anterior Extraction Site Grafting Increased Predictability for Aesthetics Michael Tischler, DDS The extraction of teeth creates a
We Want to Keep You Smiling. Bone Regeneration with Geistlich Bio-Oss and Geistlich Bio-Gide
 We Want to Keep You Smiling Bone Regeneration with Geistlich Bio-Oss and Geistlich Bio-Gide Strong Bone for a Healthier Smile Strong and healthy teeth provide a feeling of well-being, self-confidence and
We Want to Keep You Smiling Bone Regeneration with Geistlich Bio-Oss and Geistlich Bio-Gide Strong Bone for a Healthier Smile Strong and healthy teeth provide a feeling of well-being, self-confidence and
Bone Levels - From Hypothesis To Facts
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 6, Issue 5 (May.- Jun. 2013), PP 19-23 Bone Levels - From Hypothesis To Facts Savitha B 1, Priyanka
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 6, Issue 5 (May.- Jun. 2013), PP 19-23 Bone Levels - From Hypothesis To Facts Savitha B 1, Priyanka
Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report
 Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
Maryland AGD AE and Socket Grafting 2015
 The Goodacre Study 5 year retrospective study looked at Crown & Bridge Caries Single crowns 1% FPD abutments 17% Periodontal Involvement Single crowns
The Goodacre Study 5 year retrospective study looked at Crown & Bridge Caries Single crowns 1% FPD abutments 17% Periodontal Involvement Single crowns
Resorbable bilayer synthetic membrane Biomimetic tissue-engineered matrix for GBR and GTR
 Resorbable bilayer synthetic membrane Biomimetic tissue-engineered matrix for GBR and GTR Patented Jet-Spraying technology: Full barrier effect during 4 weeks, and complete resorption in 6 months PATENTED
Resorbable bilayer synthetic membrane Biomimetic tissue-engineered matrix for GBR and GTR Patented Jet-Spraying technology: Full barrier effect during 4 weeks, and complete resorption in 6 months PATENTED
Management of millers class III marginal tissue recession associated with endodontic lesion: Report of two cases managed using second stage surgery
 CASE SERIES 1 OPEN ACCESS Management of millers class III marginal tissue recession associated with endodontic lesion: Report of two cases managed using second stage surgery Sangeeta ABSTRACT Introduction:
CASE SERIES 1 OPEN ACCESS Management of millers class III marginal tissue recession associated with endodontic lesion: Report of two cases managed using second stage surgery Sangeeta ABSTRACT Introduction:
Inion GTR Biodegradable Membrane System
 Inion GTR Biodegradable Membrane System The concept of GTR/GBR Intended use The Inion GTR Biodegradable Membrane System is intended to be used as a barrier membrane in dental guided tissue regeneration
Inion GTR Biodegradable Membrane System The concept of GTR/GBR Intended use The Inion GTR Biodegradable Membrane System is intended to be used as a barrier membrane in dental guided tissue regeneration
Prosthetic Options in Implant Dentistry. Hakimeh Siadat, DDS, MSc Associate Professor
 Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Case Report. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
 Case Report RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
Case Report RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
골내결손부에서의치주조직재생 : 증례보고
 ISSN 1229-5418 Implantology 2015; 19(4): 228~232 골내결손부에서의치주조직재생 : 증례보고 김설희, 김태일서울대학교치의학대학원치주과학교실 Periodontal Regeneration in Intrabony Defects: A Case Report Sul-hee Kim, Tae-il Kim Department of Periodontology,
ISSN 1229-5418 Implantology 2015; 19(4): 228~232 골내결손부에서의치주조직재생 : 증례보고 김설희, 김태일서울대학교치의학대학원치주과학교실 Periodontal Regeneration in Intrabony Defects: A Case Report Sul-hee Kim, Tae-il Kim Department of Periodontology,
Dental Research Journal
 Dental Research Journal Original Article Clinical and biometrical evaluation of socket preservation using demineralized freeze dried bone allograft with and without the palatal connective tissue as a biologic
Dental Research Journal Original Article Clinical and biometrical evaluation of socket preservation using demineralized freeze dried bone allograft with and without the palatal connective tissue as a biologic
A New Papilla Preservation Technique for Periodontal Regeneration of Severely Compromised Teeth. Jose A. Moreno Rodríguez and Raúl G.
 A New Papilla Preservation Technique for Periodontal Regeneration of Severely Compromised Teeth Jose A. Moreno Rodríguez and Raúl G. Caffesse Introduction: Periodontal regeneration of hopeless teeth represents
A New Papilla Preservation Technique for Periodontal Regeneration of Severely Compromised Teeth Jose A. Moreno Rodríguez and Raúl G. Caffesse Introduction: Periodontal regeneration of hopeless teeth represents
Alveolar Ridge Preservation:
 Alveolar Ridge Preservation: Preserving and Building up the Bony Structures after Extraction» By: Prof. Roland Hille Konigsallee 49c, 41747 Viersen, Germany E-mail: dr-hille@t-online.de» Prof. Rolf Vollmer
Alveolar Ridge Preservation: Preserving and Building up the Bony Structures after Extraction» By: Prof. Roland Hille Konigsallee 49c, 41747 Viersen, Germany E-mail: dr-hille@t-online.de» Prof. Rolf Vollmer
Bone augmentation with biomaterials
 Patient information dental bone & tissue regeneration botiss biomaterials Bone augmentation with biomaterials established safe natural X100 Implantation stability is crucial for success Atrophy of the
Patient information dental bone & tissue regeneration botiss biomaterials Bone augmentation with biomaterials established safe natural X100 Implantation stability is crucial for success Atrophy of the
ALVEOLAR RIDGE AUGMENTATION UTILIZING PLATELET RICH FIBRIN IN COMBINATION WITH DEMINERALIZED FREEZE-DRIED BONE ALLOGRAFT A CASE REPORT
 ALVEOLAR RIDGE AUGMENTATION UTILIZING PLATELET RICH FIBRIN IN COMBINATION WITH DEMINERALIZED FREEZE-DRIED BONE ALLOGRAFT A CASE REPORT * Mishal Piyush Shah 1 and Sheela Kumar Gujjari 2 1 Department of
ALVEOLAR RIDGE AUGMENTATION UTILIZING PLATELET RICH FIBRIN IN COMBINATION WITH DEMINERALIZED FREEZE-DRIED BONE ALLOGRAFT A CASE REPORT * Mishal Piyush Shah 1 and Sheela Kumar Gujjari 2 1 Department of
The International Journal of Periodontics & Restorative Dentistry
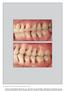 The International Journal of Periodontics & Restorative Dentistry 395 Clinical Case Report on Treatment of Generalized Aggressive Periodontitis: 5-Year Follow-up Kai-Fang Hu, DDS, MD 1 /Ya-Ping Ho, DDS,
The International Journal of Periodontics & Restorative Dentistry 395 Clinical Case Report on Treatment of Generalized Aggressive Periodontitis: 5-Year Follow-up Kai-Fang Hu, DDS, MD 1 /Ya-Ping Ho, DDS,
Scientific & Clinical Evidence Jason membrane
 Scientific & Clinical Evidence Jason membrane Pericardium GBR/GTR Membrane Facts - CE since 2009 - so far no serious clinical complication or objection - approx. 250.000 successful clinical treatments
Scientific & Clinical Evidence Jason membrane Pericardium GBR/GTR Membrane Facts - CE since 2009 - so far no serious clinical complication or objection - approx. 250.000 successful clinical treatments
Principles of Periodontal flap surgery. Dr.maryam khosravi
 Principles of Periodontal flap surgery Dr.maryam khosravi Goals of periodontal SURGICAL phase 1 - Controlling or eliminating periodontal disease. 2 Correcting anatomic conditions that may a. favor periodontal
Principles of Periodontal flap surgery Dr.maryam khosravi Goals of periodontal SURGICAL phase 1 - Controlling or eliminating periodontal disease. 2 Correcting anatomic conditions that may a. favor periodontal
The International Journal of Periodontics & Restorative Dentistry
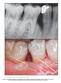 The International Journal of Periodontics & Restorative Dentistry 257 Minimally Invasive Surgical Technique and Enamel Matrix Derivative in Intrabony Defects: 2. Factors Associated with Healing Outcomes
The International Journal of Periodontics & Restorative Dentistry 257 Minimally Invasive Surgical Technique and Enamel Matrix Derivative in Intrabony Defects: 2. Factors Associated with Healing Outcomes
Periodontal Regeneration
 Periodontal Regeneration Regeneration The most ideal treatment Attempts to recreate the tissues destroyed by periodontitis Cement, bone and ligament Reduces the risk for recession and sensitivity (could
Periodontal Regeneration Regeneration The most ideal treatment Attempts to recreate the tissues destroyed by periodontitis Cement, bone and ligament Reduces the risk for recession and sensitivity (could
Derma S O F T T I S S U E A U G M E N TAT I O N. Acellular dermal matrix
 Derma A XENOGENIC GRAFT FOR S O F T T I S S U E A U G M E N TAT I O N Acellular dermal matrix A xenogenic graft for soft tissue augmentation CHARACTERISTICS Obtained from derma of porcine origin, using
Derma A XENOGENIC GRAFT FOR S O F T T I S S U E A U G M E N TAT I O N Acellular dermal matrix A xenogenic graft for soft tissue augmentation CHARACTERISTICS Obtained from derma of porcine origin, using
The Use of DynaMatrix Extracellular Membrane for Gingival Augmentation: A Case Series Dr. Stephen Saroff, DDS
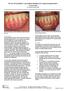 The Use of DynaMatrix Extracellular Membrane for Gingival Augmentation: A Case Series Dr. Stephen Saroff, DDS LOCALIZED RECESSION ON TOOTH #25 DUE TO BONE RECESSION (PRE OP) Introduction Tissue grafting
The Use of DynaMatrix Extracellular Membrane for Gingival Augmentation: A Case Series Dr. Stephen Saroff, DDS LOCALIZED RECESSION ON TOOTH #25 DUE TO BONE RECESSION (PRE OP) Introduction Tissue grafting
Surgical reconstruction of lost papilla around implant with a modified technique: A case report
 Journal of Periodontology & Implant Dentistry Case Report Surgical reconstruction of lost papilla around implant with a modified technique: A case report Mahdi Faraji* Andre Van Zyl University of Pretoria,
Journal of Periodontology & Implant Dentistry Case Report Surgical reconstruction of lost papilla around implant with a modified technique: A case report Mahdi Faraji* Andre Van Zyl University of Pretoria,
Years of research and advancement in
 Immediate Implants with Guided Bone Regeneration Using Titanium Mesh and Alloplast in an Infected Site: A Case Report Mahesh et al Dr. Lanka Mahesh 1 Dr. Ajay Bibra 2 Dr. Vishal Gupta 3 Abstract Years
Immediate Implants with Guided Bone Regeneration Using Titanium Mesh and Alloplast in an Infected Site: A Case Report Mahesh et al Dr. Lanka Mahesh 1 Dr. Ajay Bibra 2 Dr. Vishal Gupta 3 Abstract Years
Masking Buccal Plate Remodeling in the Esthetic Zone with Connective Tissue Grafts: Concepts and Techniques with Immediate Implants
 Peer-Reviewed and Indexed Annual Implant Issue Masking Buccal Plate Remodeling in the Esthetic Zone with Connective Tissue Grafts: Concepts and Techniques with Immediate Implants of Continuing Education
Peer-Reviewed and Indexed Annual Implant Issue Masking Buccal Plate Remodeling in the Esthetic Zone with Connective Tissue Grafts: Concepts and Techniques with Immediate Implants of Continuing Education
Evaluation of a Combination Allograft Material Compared to DFDBA in Alveolar Ridge Preservation. Sanju P. Jose
 Evaluation of a Combination Allograft Material Compared to DFDBA in Alveolar Ridge Preservation by Sanju P. Jose B.S., University of Maryland Baltimore County, 2008 D.D.S., University of Maryland School
Evaluation of a Combination Allograft Material Compared to DFDBA in Alveolar Ridge Preservation by Sanju P. Jose B.S., University of Maryland Baltimore County, 2008 D.D.S., University of Maryland School
Townie Guest Editorial. Gingival Attachment Loss: Evaluation and Surgical Options. Daniel J. Melker, DDS. fig. 1
 Gingival Attachment Loss: Evaluation and Surgical Options Daniel J. Melker, DDS Attached connective tissue (a.k.a. attached tissue) in the simplest terms is the body s only barrier between the underlying
Gingival Attachment Loss: Evaluation and Surgical Options Daniel J. Melker, DDS Attached connective tissue (a.k.a. attached tissue) in the simplest terms is the body s only barrier between the underlying
MODIFIED SINGLE ROLL FLAP APPROACH FOR SIMULTANEOUS IMPLANT PLACEMENT AND GINGIVAL AUGMENTATION
 Journal of IMAB ISSN: 1312-773X https://www.journal-imab-bg.org https://doi.org/10.5272/jimab.2017233.1667 Journal of IMAB - Annual Proceeding (Scientific Papers). 2017 Jul-Sep;23(3): Case report MODIFIED
Journal of IMAB ISSN: 1312-773X https://www.journal-imab-bg.org https://doi.org/10.5272/jimab.2017233.1667 Journal of IMAB - Annual Proceeding (Scientific Papers). 2017 Jul-Sep;23(3): Case report MODIFIED
REGENERATIONTIME. A Case Report by. Geistlich Mucograft for the treatment of multiple adjacent recession defects: A more palatable option
 A Case Report by Dr. Daniel Gober Geistlich Mucograft for the treatment of multiple adjacent recession defects: A more palatable option The Situation A 35 year old male presented in my practice with a
A Case Report by Dr. Daniel Gober Geistlich Mucograft for the treatment of multiple adjacent recession defects: A more palatable option The Situation A 35 year old male presented in my practice with a
Pre op Failed endodontic treatment with sinus involvement.
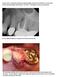 Case #1 of 10 consecutive extraction sockets grafted with Socket Graft Putty, covered with Socket Seal and sealed with Periacryl. I D # HEU This patient is a 66 year old female. Pre op Failed endodontic
Case #1 of 10 consecutive extraction sockets grafted with Socket Graft Putty, covered with Socket Seal and sealed with Periacryl. I D # HEU This patient is a 66 year old female. Pre op Failed endodontic
Socket preservation using deproteinized horsederived
 Research Article J Periodontal Implant Sci 2010;40:227-231 doi: 10.5051/jpis.2010.40.5.227 Socket preservation using deproteinized horsederived bone mineral Jang-Yeol Park, Ki-Tae Koo, Tae-Il Kim, Yang-Jo
Research Article J Periodontal Implant Sci 2010;40:227-231 doi: 10.5051/jpis.2010.40.5.227 Socket preservation using deproteinized horsederived bone mineral Jang-Yeol Park, Ki-Tae Koo, Tae-Il Kim, Yang-Jo
Redefining Regeneration
 Redefining Regeneration Taking Volume to the MAX One Product, One Treatment, Real VOLUME Buccal Bone Loss Socket Preservation Lateral / Vertical Augmentation Grafting Material Scaffold Barrier (4-6 months)
Redefining Regeneration Taking Volume to the MAX One Product, One Treatment, Real VOLUME Buccal Bone Loss Socket Preservation Lateral / Vertical Augmentation Grafting Material Scaffold Barrier (4-6 months)
More than regeneration.
 Straumann Product Emdogain Information More than regeneration. Patient comfort. Straumann Emdogain More than regeneration. Peace of mind. Tooth Preservation with Straumann Emdogain Periodontitis is associated
Straumann Product Emdogain Information More than regeneration. Patient comfort. Straumann Emdogain More than regeneration. Peace of mind. Tooth Preservation with Straumann Emdogain Periodontitis is associated
Bone Grafting for Socket Preservation
 Bone Grafting for Socket Preservation Dr. Karl R. Koerner Normal extraction facial bone loss. Excessive force. Commonly the thickness of facial bone. Hussain, A. et al. Ridge preservation comparing a nonresorbable
Bone Grafting for Socket Preservation Dr. Karl R. Koerner Normal extraction facial bone loss. Excessive force. Commonly the thickness of facial bone. Hussain, A. et al. Ridge preservation comparing a nonresorbable
Esthetic Crown Lengthening for Upper Anterior Teeth: Indications and Surgical Techniques
 Esthetic Crown Lengthening for Upper Anterior Teeth: Indications and Surgical Techniques Mohammad Assaf Assistant Professor, Faculty of Dentistry, Al-Quds University, Jerusalem, Palestine. ABSTRACT Correspondence
Esthetic Crown Lengthening for Upper Anterior Teeth: Indications and Surgical Techniques Mohammad Assaf Assistant Professor, Faculty of Dentistry, Al-Quds University, Jerusalem, Palestine. ABSTRACT Correspondence
Thick vs. Thin Gingival Biotypes: A Key Determinant in Treatment Planning for Dental Implants
 r s Thick vs. Thin Gingival Biotypes: A Key Determinant in Treatment Planning for Dental Implants richard t. kao, dds, phd; mark c. fagan, ms, dds; and gregory j. conte, ms, dmd abstract During the treatment
r s Thick vs. Thin Gingival Biotypes: A Key Determinant in Treatment Planning for Dental Implants richard t. kao, dds, phd; mark c. fagan, ms, dds; and gregory j. conte, ms, dmd abstract During the treatment
A Clinical Evaluation of Anatomic Features of Gingiva in Dental Students in Tabriz, Iran
 Received 26 October 2007; Accepted 11 February 2008 A Clinical Evaluation of Anatomic Features of Gingiva in Dental Students in Tabriz, Iran Adileh Shirmohammadi 1 Masoumeh Faramarzie 1 * Ardeshir Lafzi
Received 26 October 2007; Accepted 11 February 2008 A Clinical Evaluation of Anatomic Features of Gingiva in Dental Students in Tabriz, Iran Adileh Shirmohammadi 1 Masoumeh Faramarzie 1 * Ardeshir Lafzi
Contemporary Implant Dentistry
 Contemporary Implant Dentistry C H A P T ER 1 4 O F C O N T E M P OR A R Y O R A L A N D M A X I L L OFA C IA L S U R G E RY B Y : D R A R A S H K H O J A S T EH Dental implant is suitable for: completely
Contemporary Implant Dentistry C H A P T ER 1 4 O F C O N T E M P OR A R Y O R A L A N D M A X I L L OFA C IA L S U R G E RY B Y : D R A R A S H K H O J A S T EH Dental implant is suitable for: completely
Ridge Preservation. Selection of Applicable Abstracts and Posters. Cytoplast Technique
 Ridge Preservation Selection of Applicable Abstracts and Posters Cytoplast Technique Laurito D, Lollobrigida M, Gianno F, Bosco S, Lamazza L, De Biase A. Alveolar Ridge Preservation with nc-ha and d-ptfe
Ridge Preservation Selection of Applicable Abstracts and Posters Cytoplast Technique Laurito D, Lollobrigida M, Gianno F, Bosco S, Lamazza L, De Biase A. Alveolar Ridge Preservation with nc-ha and d-ptfe
Educational Training Document
 Educational Training Document Table of Contents Part 1: Resource Document Disclaimer Page: 2 Part 2: Line Item Grade Sheets Page: 3 Release: 11/2016 Page 1 of 6 Part 1: Resource Document Disclaimer The
Educational Training Document Table of Contents Part 1: Resource Document Disclaimer Page: 2 Part 2: Line Item Grade Sheets Page: 3 Release: 11/2016 Page 1 of 6 Part 1: Resource Document Disclaimer The
Osseointegrated dental implant treatment generally
 Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Guided surgery as a way to simplify surgical implant treatment in complex cases
 52 STARGET 1 I 12 StraUMaNN CareS r ry vincenzo MiriSOLA Di TOrreSANTO AND LUCA COrDArO Guided surgery as a way to simplify surgical implant treatment in complex cases Background A 41-year-old woman with
52 STARGET 1 I 12 StraUMaNN CareS r ry vincenzo MiriSOLA Di TOrreSANTO AND LUCA COrDArO Guided surgery as a way to simplify surgical implant treatment in complex cases Background A 41-year-old woman with
Which reconstructive procedures are effective for treating the periodontal intraosseous defect?
 Periodontology 2000, Vol. 37, 2005, 88 105 Printed in Denmark. All rights reserved Copyright Ó Blackwell Munksgaard 2005 PERIODONTOLOGY 2000 Which reconstructive procedures are effective for treating the
Periodontology 2000, Vol. 37, 2005, 88 105 Printed in Denmark. All rights reserved Copyright Ó Blackwell Munksgaard 2005 PERIODONTOLOGY 2000 Which reconstructive procedures are effective for treating the
Surgery All at Once : Socket preservation and immediate placement of an implant in an infected site in the anterior region a Case Report
 Surgery All at Once : Socket preservation and immediate placement of an implant in an infected site in the anterior region a Case Report W.P. van der Schoor*, A.R.M. van der Schoor Tooth extraction followed
Surgery All at Once : Socket preservation and immediate placement of an implant in an infected site in the anterior region a Case Report W.P. van der Schoor*, A.R.M. van der Schoor Tooth extraction followed
The majority of the early research concerning
 Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
Coverage of gingival recession defe Titletissue regeneration with and withou enamel matrix derivative in
 Coverage of gingival recession defe Titletissue regeneration with and withou enamel matrix derivative in a dog m Author(s) Fujita, T; Yamamoto, S; Ota, M; Shi Alternative Yamada, S International journal
Coverage of gingival recession defe Titletissue regeneration with and withou enamel matrix derivative in a dog m Author(s) Fujita, T; Yamamoto, S; Ota, M; Shi Alternative Yamada, S International journal
Patient s Presenting Complaint V.C. presented with discomfort and mobility from the crowned maxillary left central incisor tooth. Fig 1.
 Patient s Presenting Complaint V.C. presented with discomfort and mobility from the crowned maxillary left central incisor tooth. Fig 1. A longitudinal root fracture was suspected and confirmed when the
Patient s Presenting Complaint V.C. presented with discomfort and mobility from the crowned maxillary left central incisor tooth. Fig 1. A longitudinal root fracture was suspected and confirmed when the
RADIOLOGY. Head & Neck IMAGING. Iranian Journal of
 Head & Neck IMAGING Iran J Radiol. 2012;9(2):83-87. DOI: 10.5812/iranjradiol.7732 Iranian Journal of RADIOLOGY RADIOLOGYwww.iranjradiol.com Determination of Vertical Interproximal Bone Loss Topography:
Head & Neck IMAGING Iran J Radiol. 2012;9(2):83-87. DOI: 10.5812/iranjradiol.7732 Iranian Journal of RADIOLOGY RADIOLOGYwww.iranjradiol.com Determination of Vertical Interproximal Bone Loss Topography:
Immediate Implant Placement Along With Guided Bone Regeneration In Mandibular Anterior Region A Case Report.
 IMMEDIATE IMPLANT PLACEMENT ALONG WITH GUIDED BONE REGENERATION IN MANDIBULAR ANTERIOR REGION A CASE REPORT. Dr.C.P.Dhivakar 1, Dr.T.Saravanan 2, Dr.A.Aniz 3 1) Department of Periodontics, Karpaga Vinayaga
IMMEDIATE IMPLANT PLACEMENT ALONG WITH GUIDED BONE REGENERATION IN MANDIBULAR ANTERIOR REGION A CASE REPORT. Dr.C.P.Dhivakar 1, Dr.T.Saravanan 2, Dr.A.Aniz 3 1) Department of Periodontics, Karpaga Vinayaga
One-year Re-entry Results of Guided Bone Regeneration around Immediately Placed Implants with Immediate or Conventional Loading: A Case Series
 Journal of the International Academy of Periodontology 2012 14/3:62-68 One-year Re-entry Results of Guided Bone Regeneration around Immediately Placed Implants with Immediate or Conventional Loading: A
Journal of the International Academy of Periodontology 2012 14/3:62-68 One-year Re-entry Results of Guided Bone Regeneration around Immediately Placed Implants with Immediate or Conventional Loading: A
Journal of Periodontology & Implant Dentistry. Research Article
 Journal of Periodontology & Implant Dentistry Research Article Clinical and Radiographic Evaluation of the Effect of Bovinederived Hydroxyapatite (Bio-Oss ) and A Synthetic HA/β-TCP (Osteon ) in the Treatment
Journal of Periodontology & Implant Dentistry Research Article Clinical and Radiographic Evaluation of the Effect of Bovinederived Hydroxyapatite (Bio-Oss ) and A Synthetic HA/β-TCP (Osteon ) in the Treatment
Guided Tissue and Bone Regeneration
 Guided Tissue and Bone Regeneration One toolbox for your needs! Tefguide 9000 742 401 12x24 mm pc 1 Osgide 9000 701 520 15 x 20 mm pc 1 Osbone 9000 800 255 250-1000 μm 0.25 cc 5 Product Specifications
Guided Tissue and Bone Regeneration One toolbox for your needs! Tefguide 9000 742 401 12x24 mm pc 1 Osgide 9000 701 520 15 x 20 mm pc 1 Osbone 9000 800 255 250-1000 μm 0.25 cc 5 Product Specifications
Management of miller class II gingival recession by laterally positioned pedicle flap revised technique
 Management of miller class II gingival by laterally positioned pedicle flap revised technique Received: 2/4/206 Accepted: 3/0/206 Dildar Abdullah Othman* Abstract Background and objective: Gingival is
Management of miller class II gingival by laterally positioned pedicle flap revised technique Received: 2/4/206 Accepted: 3/0/206 Dildar Abdullah Othman* Abstract Background and objective: Gingival is
Alveolar Ridge Augmentation with Titanium Mesh and Particulate Allograft A Case Report
 Alveolar Ridge Augmentation with Titanium Mesh and Particulate Allograft A Case Report Dr. Pratibha Borasi, Dr. Praneeta Kamble Department of Periodontics, Nair Hospital Dental College, Mumbai, Maharashtra,
Alveolar Ridge Augmentation with Titanium Mesh and Particulate Allograft A Case Report Dr. Pratibha Borasi, Dr. Praneeta Kamble Department of Periodontics, Nair Hospital Dental College, Mumbai, Maharashtra,
Clinical literature for therapeutic indications. Straumann Emdogain
 Clinical literature for therapeutic indications Straumann Emdogain Table of contents 1 Basic principles of periodontal regeneration with 2 Enamel Matrix Proteins 2 Straumann Emdogain in intrabony defects
Clinical literature for therapeutic indications Straumann Emdogain Table of contents 1 Basic principles of periodontal regeneration with 2 Enamel Matrix Proteins 2 Straumann Emdogain in intrabony defects
Periodontal Disease. Radiology of Periodontal Disease. Periodontal Disease. The Role of Radiology in Assessment of Periodontal Disease
 Radiology of Periodontal Disease Steven R. Singer, DDS srs2@columbia.edu 212.305.5674 Periodontal Disease! Includes several disorders of the periodontium! Gingivitis! Marginal Periodontitis! Localized
Radiology of Periodontal Disease Steven R. Singer, DDS srs2@columbia.edu 212.305.5674 Periodontal Disease! Includes several disorders of the periodontium! Gingivitis! Marginal Periodontitis! Localized
