A Review of Survival Rates for Implants Placed in Grafted Maxillary Sinuses Using Meta-analysis
|
|
|
- Annabella Jefferson
- 6 years ago
- Views:
Transcription
1 A Review of Survival Rates for Implants Placed in Grafted Maxillary Sinuses Using Meta-analysis Darryl C. Tong, BDS*/Kim Rioux**/Mark Drangsholt, DDS, MPH***/ O. Ross Beirne, DMD, PhD**** A variety of materials and procedures are used to create adequate bone volume in the maxillary sinus for placement of endosseous implants in the posterior atrophic maxilla. This review used the structured method of metaanalysis to evaluate the survival of the implants placed into various materials that have been used in the maxillary sinus with the sinus lift procedure. A MEDLINE computer search of the English literature yielded 28 studies that reported using the maxillary sinus augmentation procedure to increase bone volume for placement of endosseous implants; only 10 of these met the inclusion criteria for meta-analysis. Data regarding immediate or delayed placement of implants were combined to simplify analysis. Implant survival was 90% for autogenous bone (484 implants in 130 patients followed for 6 to 60 months), 94% for the combination of hydroxyapatite (HA) and autogenous bone (363 implants in 104 patients followed for 18 months), 98% for the combination of demineralized freeze-dried bone (DFDB) and HA (215 implants in 50 patients followed for 7 to 60 months), and 87% for HA alone (30 implants in 11 patients followed for 18 months). The results for autogenous bone were based on six reports, for the combination of autogenous bone and HA on three reports, and for DFDB/HA and HA alone on one study each. The results of single studies cannot be weighted as heavily as the results combining several studies; however, the analysis of these studies suggests that implant survival rates were similar for autogenous bone, HA/autogenous bone mix, HA/DFDB, and HA alone. (INT J ORAL MAILLOFAC IMPLANTS 1998;13: ) Key words: implants, maxillary sinus augmentation, meta-analysis, review, sinus lift ****Resident, Department of Oral and Maxillofacial Surgery, School of Dentistry, University of Washington, Seattle, Washington. ****Student Research Fellow, School of Dentistry, University of Washington, Seattle, Washington. ****Instructor Department of Oral Medicine, School of Dentistry, and Senior Fellow, Department of Epidemiology, School of Public Health and Community Medicine, University of Washington, Seattle, Washington. ****Professor and Director of Residency Training, Department of Oral and Maxillofacial Surgery, University of Washington, Seattle, Washington. Reprint requests: Dr O. Ross Beirne, Department of Oral and Maxillofacial Surgery, School of Dentistry, University of Washington, Box , Seattle, Washington Fax: (206) The edentulous posterior maxillary ridge with a large pneumatized maxillary sinus poses a difficult challenge for the placement of endosseous implants. Recently, clinicians have recommended augmenting the maxillary sinus to facilitate placement of endosseous implants in the severely atrophic posterior maxilla. 1 While various surgical techniques and materials have been used to augment the maxillary sinus, data examining short-term and long-term outcomes have been scarce and have been reported for only a limited number of patients. The objective of this review was to compare the survival of implants placed in the different materials used to increase bone volume in the maxillary sinus. Meta-analysis offers a structured method to systematically identify, review, and analyze all published reports examining the outcome of implants placed in maxillary sinuses augmented using the sinus lift procedure. 2 Using meta-analysis, the data available from different studies were reviewed, statistically compared, and used to form opinions and draw conclusions. The International Journal of Oral & Maxillofacial Implants 175
2 Table 1 Studies Included in the Meta-analysis Overall No. of Delayed vs No. of Follow-up survival Study Material* implants immediate patients (mo) (%) Wheeler et al 28 HA alone 30 Immediate/delayed HA/autogenous bone 36 Immediate/delayed Chiapasco and Ronchi 5 HA/autogenous bone 124 Delayed Tidwell et al 26 HA/autogenous bone 203 Delayed Lundgren et al 18 Autogenous bone 30 Delayed Zinner and Small 30 HA/DFDB 215 Immediate Kent and Block 15 Autogenous bone 54 Immediate Bloomqvist et al 3 Autogenous bone 171 Immediate Hall and McKenna 8 Autogenous bone 70 Delayed Raghoebar et al 22 Autogenous bone 93 Immediate/delayed Keller et al 14 Autogenous bone 66 Immediate *HA = hydroxyapatite; DFDB = demineralized freeze-dried bone. Table 2 Studies Excluded From the Meta-analysis and the Basis for Exclusion Not a Inadequate no. Inadequate root-form Duplicate Study of patients reporting implant patient data* Misch and Dietsh 19 Jensen et al 10 Jensen and Greer 13 Wagner 27 GaRey et al 7 Jensen and Sindet-Petersen 11 Smiler et al 25 Moy et al 20 Nishibori et al 21 Jensen et al 12 Fugazzotto 6 Smiler and Holmes 24 Boyne and James 4 Leder et al 16 Wood and Moore 29 Small et al 23 Loukota et al 17 Hürzeler et al 9 *See Table 1. Materials and Methods An exhaustive MEDLINE computer search was undertaken to identify all studies in the English literature reporting the outcomes of implants placed in the augmented maxillary sinus between 1980 and Multiple strategies to identify key words, such as sinus lift, implants, and augmentation, were used to search the database. A total of 28 studies was identified for consideration Four examiners screened and selected articles according to the following criteria: (1) at least 10 patients participated in the study; (2) all patients received root-form endosseous implants; (3) less than 5% of the patients were lost to follow-up over a 6-month period; (4) patient followup was no less than 6 months; and (5) data regarding survival of implants were reported. A log of excluded studies and the reasons for their exclusion was kept, while the identified reports were evaluated in detail. The key variables were abstracted and placed in tabular form. A variety of outcome measures was reported. Because it was consistently reported in the articles, implant survival was the outcome measure used for analysis. The proportion of surviving implants was calculated by dividing the number of surviving implants by the total number of implants placed into grafted maxillary sinuses. A Kaplan-Meier (life table) analysis could not be done because most of the reports did not provide the precise follow-up period for each patient. Instead, 95% confidence intervals were calculated using the normal approximation to the binomial probability distribution. 31 Confidence intervals were also calculated using the length of follow-up when 176 Volume 13, Number 2, 1998
3 Table 3 Mean Survival Rates and Confidence Intervals for the 10 Studies Included in 95% No. of Total no. of No. of implant Rate of Confidence Graft material studies implants failures survival (%)* interval Autogenous bone HA alone HA/autogenous bone HA/DFDB *Survival rate calculated by combining the data at the longest follow-up evaluation reported in each article. The study by Wheeler et al 28 used both HA alone and in combination with autogenous bone. the data were included in the report. Chi-square analysis was used to test statistical significance. 31 Results Of the 28 identified by the literature search, 10 studies 3,5,8,14,15,18,22,26,28,30 met the inclusion criteria for meta-analysis (Table 1). The reasons for excluding the other 18 studies from the analysis are reported in Table 2. The studies that were included in the analysis represented a 7-year period from 1989 to 1996 and consisted of both retrospective and prospective follow-up reports of implants placed into augmented maxillary sinuses. No randomized controlled trials were identified. Six of the 10 studies reported using autogenous bone alone. 3,8,13,14,18,22 Bone was harvested from the anterior iliac crest in five studies 3,8,13,14,22 and from the mandibular symphysis in one study. 18 A total of 484 implants were placed in 130 patients followed for 6 to 60 months. The combined average implant survival rate for autogenous bone alone at 18 months of follow-up was 90%. Three studies reported using a combination of hydroxyapatite (HA) autogenous bone in 61 patients followed for 12 to 60 months. 5,25,28 The compiled mean survival rate for 363 implants in 104 patients using HA/autogenous bone was 94% at 18 months. One study used a 1:1 ratio of HA demineralized freeze-dried bone (DFDB) to augment the maxillae of 50 patients, and reported 98% implant survival for 215 implants with 7 to 60 months of follow-up. 30 In addition to the patients who received HA/autogenous bone, Wheeler et al 28 described 11 patients who had 30 implants placed in sinuses augmented with HA alone; the survival rate was 87% at 18 months. The mean survival rates, along with confidence intervals for each of the 10 studies, are reported in Table 3 and Fig 1. These studies could not be statistically compared in detail because the augmentation and implant techniques used were significantly different and the outcomes were reported at different follow-up times. Survival (%) Autogenous bone HA only HA autogenous bone Graft type HA/DFDB Fig 1 Mean implant survival at 18 months of follow-up. Survival is reported as the percent of the total number of implants surviving after 18 months. Bars represent the 95% confidence intervals. Delayed placement of implants was reported in four studies, 5,8,18,25 immediate implant placement was reported in four studies, 3,13,14,30 and both immediate and delayed implant placement were reported in two studies 22,28 (Table 1). Some studies used cortical block grafts, while others used particulate grafts. Some clinicians used press-fit implants, while others used screwfit implants. Some implants were titanium, while others were coated with HA. Although implant survival rates for the various types of materials were not identical, the differences were not great, and the confidence intervals overlapped each other (Fig 1). The effect of inconsistent follow-up in the 10 studies was examined by calculating confidence limits for each study. The 95% confidence limits for implant survival were examined relative to the length of follow-up for each study (Table 4 and Fig 2). There were no statistically significant differences in The International Journal of Oral & Maxillofacial Implants 177
4 the survival rates (P >.05). Most implant failures occurred in the first 6 months after placement, while only a few losses occurred after the initial healing period. Discussion Several surgical techniques, including onlay grafts and Le Fort I osteotomies, have been described for augmenting the atrophic maxilla. 1,32,33 Recently, augmentation of the maxillary sinus floor through the lateral sinus wall has been recommended for augmenting the atrophic posterior maxilla. The technique has had only minor modifications 1 since it was described by Boyne and James 4 in Initially, a vestibular incision is made approximately 6 mm superior to the attached gingival margin, extending from the canine to the zygomatic buttress. The incision is carried to the bone, and soft tissue and periosteum are reflected to expose the lateral wall of the maxillary sinus, which can be extremely thin (Fig 3). If implants are placed simultaneously with the graft, the incision is made from the tuberosity to the canine 2 to 5 mm palatal to the crest of the alveolar ridge, and Table 4 Proportion of Implants Surviving at Various Periods of Follow-Up* Period of follow-up Graft material/study 0 to 6 Months 7 to 12 Months 13 to 18 Months > 18 Months Autogenous bone alone Keller et al 14 (66) ( ) 98.5 ( ) 98.5 ( ) 92.4 ( ) Hall and McKenna 8 (70) 90.0 ( ) Raghoebar et al 22 (93) 94.6 ( ) 94.6 ( ) 94.6 ( ) Bloomqvist et al 3 (171) 82.5 ( ) Lundgren et al 18 (30) 100 ( ) Kent and Block 15 (54) ( ) ( ) Mean survival 97.6 ( ) 97.2 ( ) 90.0 ( ) HA/autogenous bone Tidwell et al 26 (203) 93.5 ( ) 93.8 ( ) 93.8 ( ) Chiapasco and Ronchi 5 (124) 98.4 ( ) 93.5 ( ) Wheeler et al 28 (36) ( ) 97.1 ( ) 97.1 ( ) Mean survival 98.7 ( ) 94.2 ( ) 94.2 ( ) HA/DFDB Zinner and Small 30 (215) 99.1 ( ) 98.1 ( ) 97.2 ( ) 97.2 ( ) HA alone Wheeler et al 28 (30) 93.1 ( ) 89.7 ( ) 89.7 ( ) 86.2 ( ) *Data reported as percentage survival, followed by the 95% confidence interval in parentheses. Number in parentheses is the total number of implants in the study Survival (%) Autogenous HA/autogenous HA/DFDB HA alone > 18 Follow-up period (months) Fig 2 Mean implant survival at various lengths of follow-up. Survival is reported as the percent of the total number of implants surviving at each follow-up period. Bars represent the 95% confidence intervals for the number of studies reporting data for the time period (see Table 4). 178 Volume 13, Number 2, 1998
5 the lateral maxillary sinus wall is exposed by elevating the flap to the buccal (Figs 4 and 5). Using a rotary instrument and a large round bur, or a combination of a rotary instrument and osteotomes, a bony window is created through the lateral sinus wall, and care is taken to leave the underlying Schneiderian mucosal membrane intact. Boyne and James 4 recommended removing the bone from the window; however, recent reports describe scoring a series of perforations along the superior margin of the bony window and infracturing the bone medially into the sinus (Fig 3). 1 In either case, the underlying mucosa is lifted intact from the sinus floor. Augmentation material is packed into the space created by infracturing the bone and elevating the mucous membrane (Fig 5). If the sinus membrane is torn during the procedure, clinicians have recommended various techniques to repair the defect, including suturing, no treatment, and guided tissue regeneration. 1,34 The soft tissues incisions are closed over bone. Both immediate and delayed placement of implants have been reported Immediate implant placement into single corticocancellous bone blocks, 14 into corticocancellous struts placed superiorly 35 to sandwich the augmentation material, and into areas that have adequate residual bone to stabilize the implants, have been described. Various augmentation materials have been used to augment the maxillary sinus. 1,3 30 Autogenous bone can be harvested from many areas, eg, the anterior iliac crest, the symphysis of the mandible, the maxillary tuberosity, the calvarium, and the external oblique ridge of the mandible (Fig 6). 36 The advantages of using autogenous bone are that it is not immunogenic, it is both osteoinductive and osteoconductive, and it is a source of osteoprogenitor cells. The disadvantage is the need for a second surgical site (with the increased morbidity and surgical time). In addition, a short hospital stay, which adds to the overall cost and inconvenience to the patient, may be required. Fig 3 A vestibular incision is made and a buccal window outlined with a rotary instrument prior to infracture and elevation of the sinus membrane. Maxillary sinus Nasal cavity Maxillary sinus lining Buccal cortex of maxilla Edentulous maxillary alveolar ridge Fig 4 Periosteal flap used to expose the maxillary alveolar ridge and buccal cortex. Fig 5 The buccal cortex is elevated intact with the sinus membrane, and the augmentation material is placed into the maxillary sinus. The International Journal of Oral & Maxillofacial Implants 179
6 Outer table of the calvarium Anterior iliac crest Fig 6 Autogenous bone can be harvested from many sites, eg, symphysis of the mandible; outer table of the calvarium; maxillary tuberosity; external oblique ridge of the mandible; anterior iliac crest. Maxillary tuberosity Symphysis of the mandible External oblique ridge of the mandible Hydroxyapatite alone and in combination with other materials has been used to augment the maxillary sinus. 5,9,24 26 Various forms of hydroxyapatite are available, including resorbable and nonresorbable and particulate or block material; moreover, the particles and blocks can be solid or porous. The advantages of using HA are that a second surgical site is not needed and HA is biocompatible and forms a direct bond with bone. 3 The disadvantages of HA are that it is not osteoinductive and does not contain osteoprogenitor cells. Demineralized freeze-dried bone has been used for sinus augmentation because of its osteoinductive as well as osteoconductive potential. 32 In addition, like HA, DFDB eliminates the need for a second surgical site. However, the osteoinductive properties of DFDB may be altered by harvesting, sterilization, and storage techniques. 37 While many different materials are used to augment the maxillary sinus for the placement of endosseous implants, it is not clear whether the various materials are equally capable of supporting implants. This review attempted to systematically identify all of the published studies reporting survival rates for implants placed in augmented maxillary sinuses. Because most reports include only a small number of patients and implants, the authors had hoped that data could be combined for analysis and comparison of the different augmentation materials. However, no clinical studies comparing the different augmentation materials were identified. Therefore, data analysis was done using studies that met simple criteria. Meta-analysis has significant limitations. The validity of the analysis depends on the quality and the similarity of the studies. None of the studies analyzed was a randomized clinical trial, and the patient populations in the reports were probably dissimilar with respect to age, gender, medical problems, and so forth. The outcome measures, criteria for success, and surgical techniques varied from study to study, and included such uncontrolled variables as different survival criteria and implant type, delayed versus immediate implant placement, variable healing time before loading, and disparate management of the autogenous graft. Meta-analyses are affected not only by the quality of the reported data, but also by publication bias. If investigators are unwilling to submit studies reporting implant failures, or if the publisher rejects articles that report negative results, only favorable studies will be identified for analysis. Such publication bias would distort the results of this review toward favorable as opposed to unfavorable outcomes. Because of the limitations of the meta-analysis, very conservative conclusions can be drawn. Hypothesis testing cannot be done because of the limitations of the analysis and the quality of the reports that were identified. However, even with its limitations, this review shows that implant survival in maxillary sinuses augmented with autogenous bone, HA/autogenous bone, HA/DFDB, and HA alone appears to be relatively stable after a period of 6 months (Table 4, Fig 2). Tidwell et al 26 and Bloomqvist et al 3 observed that 180 Volume 13, Number 2, 1998
7 implant survival in adjacent nongrafted bone was similar to implant survival in grafted maxillary sinuses. In addition, the survival rates identified in this review were greater than those identified for implants placed in the posterior maxilla with poorquality bone. Jaffin and Berman 38 reported a 40% implant failure rate in the posterior maxilla with poor-quality bone. The highest failure rate in the maxillary sinus grafted with autogenous bone alone, 17.5%, was reported by Bloomqvist et al. 3 The failure rates for autogenous bone/ha and DFDB/HA were also much lower than reported for the posterior maxilla with poor-quality bone. Some clinicians have harvested core biopsy specimens when placing implants several months after augmenting the maxillary sinus. 13,18,20,24,28 It is encouraging that all of the specimens, including the ones harvested from sites grafted with HA alone, contained new bone, and that the amount of bone appears to increase with time. Wheeler et al 28 reported, however, that implant survival did not correlate with the quantity of bone in the graft site. Conclusions This review reveals that implants placed in maxillary sinuses augmented with autogenous bone alone, HA/autogenous bone, HA/DFDB, and HA alone had similar survival rates. However, only one study each demonstrated the efficacy of HA alone and HA/DFDB. From this analysis of the literature, it is reasonable to say that the gold standard for bone graft material remains autogenous bone; however, with sound surgical technique, appropriate patient selection, and proper postoperative care, the survival rates identified in this review indicate that HA alone or in combination with DFDB or autogenous bone can be placed in the maxillary sinus to create support for endosseous implants. It is also interesting to note that the rate of implant survival in the augmented posterior maxillary sinus appears to be better than that in the posterior maxilla with bone of poor quality, but adequate quantity for implant placement. However, additional randomized clinical trials and/or follow-up studies are needed before final conclusions can be drawn concerning the long-term safety and efficacy of these augmentation materials. Acknowledgments This study was supported in part by the National Institute of Dental Research Grant No. T35 DE References 01. Hochwald DA, Davis WH. Bone grafting in the maxillary sinus floor. In: Worthington P, Brånemark P-I (eds). Advanced Osseointegration Surgery: Application in Maxillofacial Region. Chicago: Quintessence, 1992: Ingelfinger JA. Biostatistics in Clinical Medicine. New York: McGraw-Hill, 1994: Bloomqvist JE, Alberius P, Isaksson S. Retrospective analysis of one-stage maxillary sinus augmentation with endosseous implants. Int J Oral Maxillofac Implants 1996;11: Boyne PJ, James RA. Grafting of the maxillary sinus floor with autogenous marrow and bone. J Oral Surg 1980;38: Chiapasco M, Ronchi P. Sinus lift and endosseous implants preliminary surgical and prosthetic results. Eur J Prosthodont Rest Dent 1994;3: Fugazzotto PA. Maxillary sinus grafting with and without simultaneous implant placement: Technical considerations and case reports. Int J Periodont Rest Dent 1994;14: GaRey DJ, Whittaker JM, James RA, Lozada JL. The histologic evaluation of the implant interface with heterograft and allograft materials an eight-month autopsy report, Part II. J Oral Implantol 1991;17: Hall HD, McKenna SJ. Bone graft of the maxillary sinus floor for Brånemark implants. Oral Maxillofac Surg Clinics North Am 1991;3: Hürzeler MB, Kirsch A, Ackermann K-L, Quiñones CR. Reconstruction of the severely resorbed maxilla with dental implants in the augmented maxillary sinus: A 5-year clinical investigation. Int J Oral Maxillofac Implants 1996;11: Jensen J, Simonsen EK, Sindet-Pedersen S. Reconstruction of the severely resorbed maxilla with bone grafting and osseointegrated implants: A preliminary report. J Oral Maxillofac Surg 1990;48: Jensen J, Sindet-Petersen S. Autogenous mandibular bone grafts and osseointegrated implants for reconstruction of the severely atrophied maxilla: A preliminary report. J Oral Maxillofac Surg 1991;49: Jensen J, Sindet-Petersen S, Oliver AJ. Varying treatment strategies for reconstruction of maxillary atrophy with implants: Results in 98 patients. J Oral Maxillofac Surg 1994;52: Jensen OT, Greer R. Immediate placement of osseointegrated implants into the maxillary sinus augmented with mineralized cancellous allograft and Gore-Tex: Second-stage surgical and histological findings. In: Laney WR, Tolman DE (eds). Tissue Integration in Oral, Orthopedic, and Maxillofacial Reconstruction. Chicago: Quintessence, 1990: Keller EE, Eckert SE, Tolman DE. Maxillary antral and nasal one-stage inlay composite bone graft: Preliminary report on 30 recipient sites. J Oral Maxillofac Surg 1994;52: Kent JN, Block MS. Simultaneous maxillary sinus floor bone grafting and placement of hydroxyapatite-coated implants. J Oral Maxillofac Surg 1989;47: Leder AJ, McElroy J, Deasy MJ. Reconstruction of the severely atrophic maxilla with autogenous iliac bone graft and hydroxylapatite decalcified freeze-dried bone allograft in the same patient: A preliminary report. Periodont Clin Invest 1993;15: Loukota RA, Isaksson SG, Linner J, Bloomqvist. A technique for inserting endosseous implants in the atrophic maxilla in a single stage procedure. Br J Oral Maxillofac Surg 1992;30: The International Journal of Oral & Maxillofacial Implants 181
8 18. Lundgren S, Moy P, Johansson C, Nilsson H. Augmentation of the maxillary sinus floor with particulate mandible: A histological and histomorphometric study. Int J Oral Maxillofac Implants 1996;11: Misch CE, Dietsh F. Endosteal implants and iliac crest grafts to restore severely resorbed totally edentulous maxillae A retrospective study. J Oral Implantol 1994;20: Moy PK, Lundgren S, Holmes RE. Maxillary sinus augmentation: Histomorphometric analysis of graft materials for maxillary sinus floor augmentation. J Oral Maxillofac Surg 1993;51: Nishibori M, Betts NJ, Salama H, Listgarten MA. Short-term healing of autogenous and allogenic bone grafts after sinus augmentation: A report of 2 cases. J Periodontol 1994;65: Raghoebar GM, Brouwer TJ, Reintsema H, Van Oort RP. Augmentation of the maxillary sinus floor with autogenous bone for the placement of endosseous implants: A preliminary report. J Oral Maxillofac Surg 1993;51: Small SA, Zinner ID, Panno FV, Shapiro HJ, Stein JI. Augmenting the maxillary sinus for implants: Report of 27 patients. Int J Oral Maxillofac Implants 1993;8: Smiler DG, Holmes RE. Sinus lift procedure using porous hydroxyapatite: A preliminary clinical report. J Oral Implantol 1987;13: Smiler DG, Johnson PW, Lozada JL, Misch C, Rosenlicht JL, Tatum OH Jr, et al. Sinus lift grafts and endosseous implants. Treatment of the atrophic posterior maxilla. Dent Clin North Am 1992;36: Tidwell JK, Blijdorp PA, Stoelinga PJW, Brouns JB, Hinderks F. Composite grafting of the maxillary sinus for placement of endosteal implants a preliminary report of 48 patients. Int J Oral Maxillofac Surg 1992;21: Wagner JR. A 3 1/2 year clinical evaluation of resorbable hydroxylapatite OsteoGen (HA Resorb) used for sinus lift augmentation in conjunction with the insertion of endosseous implants. J Oral Implantol 1991;17: Wheeler SL, Holmes RE, Calhoun CJ. Six-year clinical and histologic study of sinus-lift grafts. Int J Oral Maxillofac Implants 1996;11: Wood RM, Moore DL. Grafting of the maxillary sinus with intraorally harvested autogenous bone prior to implant placement. Int J Oral Maxillofac Implants 1988;3: Zinner ID, Small SA. Sinus-lift graft: Using the maxillary sinuses to support implants. J Am Dent Assoc 1996;127: Fleiss JL. Statistical Methods for Rates and Proportions, ed 2. New York: Wiley and Sons, Sailer HF. A new method of inserting endosseous implants in totally atrophic maxillae. J Craniomaxillofac Surg 1989;17: Krekmanov L. A modified method of simultaneous bone grafting and placement of endosseous implants in the severely atrophic maxilla. Int J Oral Maxillofac Implants 1995;10: Tucker MR. Ambulatory Preprosthetic Reconstructive Surgery. In: Peterson LJ, Indresano AT, Marciani RD, Roser SM (eds). Principles of Oral & Maxillofacial Surgery, vol II. Philadelphia: Lippincott, 1992: Momtaheni DM, Schweitzer K, Muenchinger F. Technique for stabilization of autogenous cancellous bone growth in sinus lift procedures. Oral Surg Oral Med Oral Path 1994;78: Misch CM. Ridge augmentation using mandibular ramus bone grafts for the placement of dental implants: Presentation of a technique. Pract Periodontics Aesthet Dent 1996;8: Becker W, Urist M, Tucker LM, Ochsenbein C. Human demineralized freeze-dried bone: Inadequate bone formation in athymic mice. J Periodont 1995;66: Jaffin RA, Berman CL. The excessive loss of Brånemark fixtures in type IV bone. A 5 year analysis. J Periodontol 1991;62: Volume 13, Number 2, 1998
Effectively restoring a grossly atrophic maxilla
 Augmentation Grafting of the Maxillary Sinus and Simultaneous Implant Placement in Patients with 3 to 5 mm of Residual Alveolar Bone Height Michael Peleg, DMD*/Ziv Mazor, DMD**/Arun K. Garg, DMD*** This
Augmentation Grafting of the Maxillary Sinus and Simultaneous Implant Placement in Patients with 3 to 5 mm of Residual Alveolar Bone Height Michael Peleg, DMD*/Ziv Mazor, DMD**/Arun K. Garg, DMD*** This
BONE AUGMENTATION AND GRAFTING
 1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
Survival Analysis of Endosseous Implants in Grafted and Nongrafted Edentulous Maxillae
 Survival Analysis of Endosseous Implants in Grafted and Nongrafted Edentulous Maxillae Jonas P. Becktor, DDS 1 /Sten Isaksson, MD, DDS, PhD 2 /Lars Sennerby, DDS, PhD 3 Purpose: The aim of this study was
Survival Analysis of Endosseous Implants in Grafted and Nongrafted Edentulous Maxillae Jonas P. Becktor, DDS 1 /Sten Isaksson, MD, DDS, PhD 2 /Lars Sennerby, DDS, PhD 3 Purpose: The aim of this study was
Osseointegrated implants are a very reliable means
 Tridimensional Reconstruction of Knife-Edge Edentulous Maxillae by Sinus Elevation, Onlay Grafts, and Sagittal Osteotomy of the Anterior Maxilla: Preliminary Surgical and Prosthetic Results Matteo Chiapasco,
Tridimensional Reconstruction of Knife-Edge Edentulous Maxillae by Sinus Elevation, Onlay Grafts, and Sagittal Osteotomy of the Anterior Maxilla: Preliminary Surgical and Prosthetic Results Matteo Chiapasco,
A Prospective Randomized Study of 1- and 2-Stage Sinus Inlay Bone Grafts: 1-Year Follow-up
 A Prospective Randomized Study of 1- and 2-Stage Sinus Inlay Bone Grafts: 1-Year Follow-up Karin Wannfors, DDS, PhD 1 /Björn Johansson, DDS 2 /Mats Hallman, DDS 3 /Tomas Strandkvist, DDS 3 The purpose
A Prospective Randomized Study of 1- and 2-Stage Sinus Inlay Bone Grafts: 1-Year Follow-up Karin Wannfors, DDS, PhD 1 /Björn Johansson, DDS 2 /Mats Hallman, DDS 3 /Tomas Strandkvist, DDS 3 The purpose
The utilization of dental implants in the rehabilitation
 Maxillary Sinus Augmentation Prior to Placement of Endosseous Implants: A Histomorphometric Analysis Oliver Hanisch, DMD, MS*/Jaime L. Lozada, DDS**/Ralph E. Holmes, MD***/ Christopher J. Calhoun, MBA****/Joseph
Maxillary Sinus Augmentation Prior to Placement of Endosseous Implants: A Histomorphometric Analysis Oliver Hanisch, DMD, MS*/Jaime L. Lozada, DDS**/Ralph E. Holmes, MD***/ Christopher J. Calhoun, MBA****/Joseph
Effects of Maxillary Sinus Graft on the Survival of Endosseous Implants: A 10-Year Retrospective Study
 University of Pennsylvania ScholarlyCommons Departmental Papers (Dental) Penn Dental Medicine 8-2008 Effects of Maxillary Sinus Graft on the Survival of Endosseous Implants: A 10-Year Retrospective Study
University of Pennsylvania ScholarlyCommons Departmental Papers (Dental) Penn Dental Medicine 8-2008 Effects of Maxillary Sinus Graft on the Survival of Endosseous Implants: A 10-Year Retrospective Study
Treatment planning in a case of restoration of the maxilla and mandible using osseointegrated implants with four types of bone graft
 227 Journal of Oral Science, Vol. 45, No. 4, 227-232, 2003 Case report Treatment planning in a case of restoration of the maxilla and mandible using osseointegrated implants with four types of bone graft
227 Journal of Oral Science, Vol. 45, No. 4, 227-232, 2003 Case report Treatment planning in a case of restoration of the maxilla and mandible using osseointegrated implants with four types of bone graft
Crestal Sinus Augmentation: A Simplified Approach to Implant Placement in the Posterior Maxilla
 IJOICR 10.5005/jp-journals-10012-1036 RECENT TECHNICAL ADVANCES Crestal Sinus Augmentation: A Simplified Approach to Implant Placement in the Posterior Maxilla Crestal Sinus Augmentation: A Simplified
IJOICR 10.5005/jp-journals-10012-1036 RECENT TECHNICAL ADVANCES Crestal Sinus Augmentation: A Simplified Approach to Implant Placement in the Posterior Maxilla Crestal Sinus Augmentation: A Simplified
PALATAL POSITIONING OF IMPLANTS IN SEVERELY RESORBED POSTERIOR MAXILLAE F. Atamni, M.Atamni, M.Atamna, Private Practice Tel-aviv Israel
 PALATAL POSITIONING OF IMPLANTS IN SEVERELY RESORBED POSTERIOR MAXILLAE F. Atamni, M.Atamni, M.Atamna, Private Practice Tel-aviv Israel Abstract: Objectives: To evaluate an alternative treatment for rehabilitation
PALATAL POSITIONING OF IMPLANTS IN SEVERELY RESORBED POSTERIOR MAXILLAE F. Atamni, M.Atamni, M.Atamna, Private Practice Tel-aviv Israel Abstract: Objectives: To evaluate an alternative treatment for rehabilitation
Oral Health and Dentistry
 Page 107 to 118 Volume 1 Issue 2 2017 Case Report Oral Health and Dentistry ISSN: 2573-4989 Full Mouth Implants Rehabilitation of a Patient with Ectodermal Dysplasia After 3-Ds Ridge Augmentation and Bilateral
Page 107 to 118 Volume 1 Issue 2 2017 Case Report Oral Health and Dentistry ISSN: 2573-4989 Full Mouth Implants Rehabilitation of a Patient with Ectodermal Dysplasia After 3-Ds Ridge Augmentation and Bilateral
The International Journal of Periodontics & Restorative Dentistry
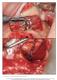 The International Journal of Periodontics & Restorative Dentistry 413 Schneiderian Membrane Perforation Rate During Sinus Elevation Using Piezosurgery: Clinical Results of 100 Consecutive Cases Stephen
The International Journal of Periodontics & Restorative Dentistry 413 Schneiderian Membrane Perforation Rate During Sinus Elevation Using Piezosurgery: Clinical Results of 100 Consecutive Cases Stephen
Dental Implant Treatment with Diffe Title for Sinus Floor Elevation-A Case Re. Sekine, H; Taguchi, T; Seta, S; Tak Author(s) T; Kakizawa, T
 Dental Implant Treatment with Diffe Title for Sinus Floor Elevation-A Case Re Sekine, H; Taguchi, T; Seta, S; Tak Author(s) T; Kakizawa, T Journal Bulletin of Tokyo Dental College, 4 URL http://hdl.handle.net/10130/200
Dental Implant Treatment with Diffe Title for Sinus Floor Elevation-A Case Re Sekine, H; Taguchi, T; Seta, S; Tak Author(s) T; Kakizawa, T Journal Bulletin of Tokyo Dental College, 4 URL http://hdl.handle.net/10130/200
The placement of endosseous implants may be difficult
 Measurement of Maxillary Sinus Volume Using Computerized Tomographic Images Yuki Uchida, DDS, PhD*/Masaaki Goto, DDS, PhD**/ Takeshi Katsuki, DDS, PhD***/Yoshikazu Soejima, DDS, PhD**** This study measured
Measurement of Maxillary Sinus Volume Using Computerized Tomographic Images Yuki Uchida, DDS, PhD*/Masaaki Goto, DDS, PhD**/ Takeshi Katsuki, DDS, PhD***/Yoshikazu Soejima, DDS, PhD**** This study measured
Endosseous Implants and Bone Augmentation in the Partially Dentate Maxilla: An Analysis of 17 Patients with a Follow-up of 29 to 101 Months
 Endosseous Implants and Bone Augmentation in the Partially Dentate Maxilla: An Analysis of 17 Patients with a Follow-up of 29 to 101 Months Jonas P. Becktor, DDS, PhD 1 / Sten Isaksson, MD, DDS, PhD 2
Endosseous Implants and Bone Augmentation in the Partially Dentate Maxilla: An Analysis of 17 Patients with a Follow-up of 29 to 101 Months Jonas P. Becktor, DDS, PhD 1 / Sten Isaksson, MD, DDS, PhD 2
Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis
 CASE REPORT Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis Dr Ashish Yadav 1, Dr Aratee Gupta 2, Dr Archana Singh 3, 1,3-
CASE REPORT Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis Dr Ashish Yadav 1, Dr Aratee Gupta 2, Dr Archana Singh 3, 1,3-
Management of a complex case
 2 Soft- and hard-tissue reconstruction of a severely deficient site prior to implant placement: a case report Management of a complex case Younes Khosroshahy, DDS, MFDS RCS (Eng), Dip Imp Dent RCSEd, Blue
2 Soft- and hard-tissue reconstruction of a severely deficient site prior to implant placement: a case report Management of a complex case Younes Khosroshahy, DDS, MFDS RCS (Eng), Dip Imp Dent RCSEd, Blue
Augmentation of the Maxillary Sinus with Calcium Sulfate: One-Year Clinical Report from a Prospective Longitudinal Study
 Augmentation of the Maxillary Sinus with Calcium Sulfate: One-Year Clinical Report from a Prospective Longitudinal Study Dario De Leonardis, DDS*/Gabriele E. Pecora, MD, DDS** The aim of the present investigation
Augmentation of the Maxillary Sinus with Calcium Sulfate: One-Year Clinical Report from a Prospective Longitudinal Study Dario De Leonardis, DDS*/Gabriele E. Pecora, MD, DDS** The aim of the present investigation
Dental Implants: A Predictable Solution for Tooth Loss. Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor
 Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
Maxillary sinus augmentation without any graft material- A case Report
 A CASE REPORT ISSN: 2321-4988 D.Shiva kumar et al. /JPR:BioMedRx: An International Journal 2013,1(8), Available online through www.jpronline.info Maxillary sinus augmentation without any graft material-
A CASE REPORT ISSN: 2321-4988 D.Shiva kumar et al. /JPR:BioMedRx: An International Journal 2013,1(8), Available online through www.jpronline.info Maxillary sinus augmentation without any graft material-
Annals of Dental Research
 P a g e 1 ADR 7 (1), 1-6, 2017 Journal Homepage: www.hgpub.com/ojs2/index.php/adr Direct Sinus Lift with Putty Alloplastic Bone Substitute for Simultaneous Implant Placement A Case Report Chander Prakash*,
P a g e 1 ADR 7 (1), 1-6, 2017 Journal Homepage: www.hgpub.com/ojs2/index.php/adr Direct Sinus Lift with Putty Alloplastic Bone Substitute for Simultaneous Implant Placement A Case Report Chander Prakash*,
Alveolar Ridge Augmentation with Titanium Mesh and Particulate Allograft A Case Report
 Alveolar Ridge Augmentation with Titanium Mesh and Particulate Allograft A Case Report Dr. Pratibha Borasi, Dr. Praneeta Kamble Department of Periodontics, Nair Hospital Dental College, Mumbai, Maharashtra,
Alveolar Ridge Augmentation with Titanium Mesh and Particulate Allograft A Case Report Dr. Pratibha Borasi, Dr. Praneeta Kamble Department of Periodontics, Nair Hospital Dental College, Mumbai, Maharashtra,
The International Journal of Periodontics & Restorative Dentistry
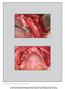 The International Journal of Periodontics & Restorative Dentistry 141 Screw Spreading: Technical Considerations and Case Report Renato Sussumu Nishioka, DDS, PhD, MSc* Alberto Noriyuki Kojima, DDS, PhD,
The International Journal of Periodontics & Restorative Dentistry 141 Screw Spreading: Technical Considerations and Case Report Renato Sussumu Nishioka, DDS, PhD, MSc* Alberto Noriyuki Kojima, DDS, PhD,
Puros Cancellous Particulate Allograft & Puros Block Allograft
 Puros Cancellous Particulate Allograft & Puros Block Allograft Puros Cancellous Particulate Allograft The Natural Choice For Healthy 1 Bone Growth. 1. Proven, Predictable Regeneration Acts as an osteoconductive
Puros Cancellous Particulate Allograft & Puros Block Allograft Puros Cancellous Particulate Allograft The Natural Choice For Healthy 1 Bone Growth. 1. Proven, Predictable Regeneration Acts as an osteoconductive
Osseointegrated dental implant treatment generally
 Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION
 Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
The influence of radiotherapy on osseointegration
 Experience with Osseointegrated Implants Placed in Irradiated Tissues in Japan and the United States Atsushi Niimi, DDS, DMSc*/Minoru Ueda, DDS, PhD**/ Eugene E. Keller, DDS, PhD***/Philip Worthington,
Experience with Osseointegrated Implants Placed in Irradiated Tissues in Japan and the United States Atsushi Niimi, DDS, DMSc*/Minoru Ueda, DDS, PhD**/ Eugene E. Keller, DDS, PhD***/Philip Worthington,
The use of endosseous implants is currently a routine
 Evaluation of 31 Zygomatic Implants and 74 Regular Dental Implants Used in 16 Patients for Prosthetic Reconstruction of the Atrophic Maxilla with Cross-Arch Fixed Bridges Jonas P. Becktor, DDS;* Sten Isaksson,
Evaluation of 31 Zygomatic Implants and 74 Regular Dental Implants Used in 16 Patients for Prosthetic Reconstruction of the Atrophic Maxilla with Cross-Arch Fixed Bridges Jonas P. Becktor, DDS;* Sten Isaksson,
Consensus Report Tissue augmentation and esthetics (Working Group 3)
 B. Klinge Thomas F. Flemmig Consensus Report Tissue augmentation and esthetics (Working Group 3) Members of working group: Matteo Chiapasco Jan-Eirik Ellingsen Ronald Jung Friedrich Neukam Isabella Rocchietta
B. Klinge Thomas F. Flemmig Consensus Report Tissue augmentation and esthetics (Working Group 3) Members of working group: Matteo Chiapasco Jan-Eirik Ellingsen Ronald Jung Friedrich Neukam Isabella Rocchietta
Assessment of the autogenous bone graft for sinus elevation
 ORIGINAL ARTICLE http://dx.doi.org/10.5125/jkaoms.2013.39.6.274 pissn 2234-7550 eissn 2234-5930 Assessment of the autogenous bone graft for sinus elevation Wang Peng, Il-Kyu Kim, Hyun-Young Cho, Sang-Pill
ORIGINAL ARTICLE http://dx.doi.org/10.5125/jkaoms.2013.39.6.274 pissn 2234-7550 eissn 2234-5930 Assessment of the autogenous bone graft for sinus elevation Wang Peng, Il-Kyu Kim, Hyun-Young Cho, Sang-Pill
A Novel Technique for the Management of a Maxillary Anterior Alveolar Defect with an Implant-retained Fixed Prosthesis: A Clinical Report
 Neenu M Varghese et al Case Report 10.5005/jp-journals-10012-1148 A Novel Technique for the Management of a Maxillary Anterior Alveolar Defect with an Implant-retained Fixed Prosthesis: A Clinical Report
Neenu M Varghese et al Case Report 10.5005/jp-journals-10012-1148 A Novel Technique for the Management of a Maxillary Anterior Alveolar Defect with an Implant-retained Fixed Prosthesis: A Clinical Report
Moderately to severely resorbed edentulous
 The Zygomatic Implant: Preliminary Data on Treatment of Severely Resorbed Maxillae. A Clinical Report Edmond Bedrossian, DDS, FACD, FACOMS 1 /Lambert Stumpel III, DDS 2 / Michael Beckely, DDS 3 /Thomas
The Zygomatic Implant: Preliminary Data on Treatment of Severely Resorbed Maxillae. A Clinical Report Edmond Bedrossian, DDS, FACD, FACOMS 1 /Lambert Stumpel III, DDS 2 / Michael Beckely, DDS 3 /Thomas
Stefan Peev 1, Tihomir Georgiev 2, Elitsa Sabeva 1, Georgi Papanchev 2, Vladimir Panov 3.
 DOI: 1018044/Medinform.201631.370 Sinus floor elevation with lateral approach and five-year follow-up Stefan Peev 1, Tihomir Georgiev 2, Elitsa Sabeva 1, Georgi Papanchev 2, Vladimir Panov 3. 1. Department
DOI: 1018044/Medinform.201631.370 Sinus floor elevation with lateral approach and five-year follow-up Stefan Peev 1, Tihomir Georgiev 2, Elitsa Sabeva 1, Georgi Papanchev 2, Vladimir Panov 3. 1. Department
One in four sinus lift procedures can be
 11 Volume 5, Issue 1: Summer 2017 Inspyred: The alternative EAO voice Handling perforations of the sinus membrane A new approach using advanced platelet-rich fi brin (A-PRF) One in four sinus lift procedures
11 Volume 5, Issue 1: Summer 2017 Inspyred: The alternative EAO voice Handling perforations of the sinus membrane A new approach using advanced platelet-rich fi brin (A-PRF) One in four sinus lift procedures
Vertical Bone Augmentation for Implant Placement in the Mandible a Systematic. Review
 Vertical Bone Augmentation for Implant Placement in the Mandible a Systematic Review A dissertation submitted to the University of Manchester for the degree of Master of Science in Dentistry (Oral and
Vertical Bone Augmentation for Implant Placement in the Mandible a Systematic Review A dissertation submitted to the University of Manchester for the degree of Master of Science in Dentistry (Oral and
Socket Treatment. Procedure Guide
 Socket Treatment Procedure Guide www.implantdirect.com 888.649.6425 Extraction Healing and Ridge Resorption The Why Working with patients to educate them on the benefits of bone maintenance post extraction
Socket Treatment Procedure Guide www.implantdirect.com 888.649.6425 Extraction Healing and Ridge Resorption The Why Working with patients to educate them on the benefits of bone maintenance post extraction
Young-Jin Park, DDS,* and Sung-Am Cho, DDS, MS, PhD
 J Oral Maxillofac Surg 68:1338-1344, 2010 Retrospective Chart Analysis on Survival Rate of Fixtures Installed at the Tuberosity Bone for Cases With Missing Unilateral Upper Molars: A Study of 7 Cases Young-Jin
J Oral Maxillofac Surg 68:1338-1344, 2010 Retrospective Chart Analysis on Survival Rate of Fixtures Installed at the Tuberosity Bone for Cases With Missing Unilateral Upper Molars: A Study of 7 Cases Young-Jin
Predictable Synthetic Bone Grafting Procedures for Implant Reconstruction: Part Two
 CLINICAL ARTICLE IJCID Predictable Synthetic Bone Grafting Procedures for Implant Reconstruction: Part Two Predictable Synthetic Bone Grafting Procedures for Implant Reconstruction: Part Two 1 Scott D
CLINICAL ARTICLE IJCID Predictable Synthetic Bone Grafting Procedures for Implant Reconstruction: Part Two Predictable Synthetic Bone Grafting Procedures for Implant Reconstruction: Part Two 1 Scott D
The Use of Freeze-Dried Bone Allograft as an Alternative to Autogenous Bone Graft in the Atrophic Maxilla: A 3-Year Clinical Follow-up
 643 The Use of Freeze-Dried Bone Allograft as an Alternative to Autogenous Bone Graft in the Atrophic Maxilla: A 3-Year Clinical Follow-up Marco Aurélio Bianchini, DDS, MSc, PhD 1 André R. Buttendorf,
643 The Use of Freeze-Dried Bone Allograft as an Alternative to Autogenous Bone Graft in the Atrophic Maxilla: A 3-Year Clinical Follow-up Marco Aurélio Bianchini, DDS, MSc, PhD 1 André R. Buttendorf,
Multi-Modality Anterior Extraction Site Grafting Increased Predictability for Aesthetics Michael Tischler, DDS
 Page 1 of 5 Issue Date: March 2003, Posted On: 8/1/2005 Multi-Modality Anterior Extraction Site Grafting Increased Predictability for Aesthetics Michael Tischler, DDS The extraction of teeth creates a
Page 1 of 5 Issue Date: March 2003, Posted On: 8/1/2005 Multi-Modality Anterior Extraction Site Grafting Increased Predictability for Aesthetics Michael Tischler, DDS The extraction of teeth creates a
Endosseous cylindric implants are well accepted
 Soft Tissue Exposure of Endosseous Implants Between Stage I and Stage II Surgery as a Potential Indicator of Early Crestal Bone Loss Joseph A. Toljanic, DDS*/Mark L. Banakis, DDS**/Leslee A. K. Willes,
Soft Tissue Exposure of Endosseous Implants Between Stage I and Stage II Surgery as a Potential Indicator of Early Crestal Bone Loss Joseph A. Toljanic, DDS*/Mark L. Banakis, DDS**/Leslee A. K. Willes,
Guided surgery as a way to simplify surgical implant treatment in complex cases
 52 STARGET 1 I 12 StraUMaNN CareS r ry vincenzo MiriSOLA Di TOrreSANTO AND LUCA COrDArO Guided surgery as a way to simplify surgical implant treatment in complex cases Background A 41-year-old woman with
52 STARGET 1 I 12 StraUMaNN CareS r ry vincenzo MiriSOLA Di TOrreSANTO AND LUCA COrDArO Guided surgery as a way to simplify surgical implant treatment in complex cases Background A 41-year-old woman with
Maxillary Sinus Floor Elevation: Review of Anatomy and Lateral Sinus Lift Technique
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 1 Ver. IV (Jan. 2016), PP 29-33 www.iosrjournals.org Maxillary Sinus Floor Elevation: Review
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 1 Ver. IV (Jan. 2016), PP 29-33 www.iosrjournals.org Maxillary Sinus Floor Elevation: Review
Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report
 Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
The Application of Cone Beam CT Image Analysis for the Mandibular Ramus Bone Harvesting
 44 The Application of Cone Beam CT Image Analysis for the Mandibular Ramus Bone Harvesting LivingWell Institute of Dental Research Lee, Jang-yeol, Youn, Pil-sang, Kim, Hyoun-chull, Lee Sang-chull Ⅰ. Introduction
44 The Application of Cone Beam CT Image Analysis for the Mandibular Ramus Bone Harvesting LivingWell Institute of Dental Research Lee, Jang-yeol, Youn, Pil-sang, Kim, Hyoun-chull, Lee Sang-chull Ⅰ. Introduction
Crestal Window Sinus Lift, minimally invasive, predictable, and systematic approach to sinus grafting.
 Crestal Window Sinus Lift, minimally invasive, predictable, and systematic approach to sinus grafting. Samuel Lee, DDS*, Grace Kang-Lee, DDS, Kwang-Bum Park, DDS, MS, PhD, Thomas Han, DDS, MS Abstract
Crestal Window Sinus Lift, minimally invasive, predictable, and systematic approach to sinus grafting. Samuel Lee, DDS*, Grace Kang-Lee, DDS, Kwang-Bum Park, DDS, MS, PhD, Thomas Han, DDS, MS Abstract
A Technique for Utilizing Upper Lid Blepharoplasty Full thickness Skin for Peri-Implant Keratinized Tissue Grafting *,y
 A Technique for Utilizing Upper Lid Blepharoplasty Full thickness Skin for Peri-Implant Keratinized Tissue Grafting *,y George R. Deeb D.D.S., M.D. i, Bach T. Le D.D.S., M.D. ii, Brett A. Ueeck D.M.D iii,
A Technique for Utilizing Upper Lid Blepharoplasty Full thickness Skin for Peri-Implant Keratinized Tissue Grafting *,y George R. Deeb D.D.S., M.D. i, Bach T. Le D.D.S., M.D. ii, Brett A. Ueeck D.M.D iii,
Nasal floor elevation combined with dental implant placement
 1 Nasal floor elevation combined with dental implant placement Ziv Mazor, DMD * Adi Lorean, DMD ** Eitan Mijiritsky Liran Levin, DMD * Private Practice, Ra anana, Israel ** Private Practice, Tiberius,
1 Nasal floor elevation combined with dental implant placement Ziv Mazor, DMD * Adi Lorean, DMD ** Eitan Mijiritsky Liran Levin, DMD * Private Practice, Ra anana, Israel ** Private Practice, Tiberius,
Jonas P. Becktor, DDS, PhD,* Hadar Hallström, LDS, Sten Isaksson, MD, DDS, PhD, and Lars Sennerby, DDS, PhD
 J Oral Maxillofac Surg 66:780-786, 2008 The Use of Particulate Bone Grafts From the Mandible for Maxillary Sinus Floor Augmentation Before Placement of Surface-Modified Implants: Results From Bone Grafting
J Oral Maxillofac Surg 66:780-786, 2008 The Use of Particulate Bone Grafts From the Mandible for Maxillary Sinus Floor Augmentation Before Placement of Surface-Modified Implants: Results From Bone Grafting
Implant Site Development Part II
 IJCID REVIEW ARTICLE 1 Umang Nayar, 2 Shankar Iyer 1 Consultant, Dental Surgeon and Periodontist at Max Health Care, New Delhi, Professor and Head, Department of Periodontics Harsarn Dass Dental College,
IJCID REVIEW ARTICLE 1 Umang Nayar, 2 Shankar Iyer 1 Consultant, Dental Surgeon and Periodontist at Max Health Care, New Delhi, Professor and Head, Department of Periodontics Harsarn Dass Dental College,
Placement of Posterior Mandibular and Maxillary Implants in Patients with Severe Bone Deficiency: A Clinical Report of Procedure
 Placement of Posterior Mandibular and Maxillary Implants in Patients with Severe Bone Deficiency: A Clinical Report of Procedure Leonard Krekmanov, DDS, PhD 1 The purpose of this investigation was to modify
Placement of Posterior Mandibular and Maxillary Implants in Patients with Severe Bone Deficiency: A Clinical Report of Procedure Leonard Krekmanov, DDS, PhD 1 The purpose of this investigation was to modify
Augmentation in Two Stages of Atrophic Alveolar Bone Prior to Dental Rehabilitation: A Case Report
 Augmentation in Two Stages of Atrophic Alveolar Bone Prior to Dental Rehabilitation: A Case Report Abstract Aim: The aim of this report is to describe a significantly deficient case of alveolar bone that
Augmentation in Two Stages of Atrophic Alveolar Bone Prior to Dental Rehabilitation: A Case Report Abstract Aim: The aim of this report is to describe a significantly deficient case of alveolar bone that
Socket preservation in the daily practice: A clinical case report
 Clinical Socket preservation in the daily practice: A clinical case report Rabih Abi Nader 1 and Carine Tabarani 2 Abstract Soft tissue contour depends on the underlying bone anatomy. Following tooth extraction,
Clinical Socket preservation in the daily practice: A clinical case report Rabih Abi Nader 1 and Carine Tabarani 2 Abstract Soft tissue contour depends on the underlying bone anatomy. Following tooth extraction,
Subantral Augmentation Utilizing the Zimmer. Sinus Lift Balloon Technique
 Copyright 2010 by Zimmer Dental Inc. Subantral Augmentation Utilizing the Zimmer Sinus Lift Balloon Technique Geraldo Nicolau Rodrigues, Americo Yuti Katayama, Ronald F. Cardoso The edentulous posterior
Copyright 2010 by Zimmer Dental Inc. Subantral Augmentation Utilizing the Zimmer Sinus Lift Balloon Technique Geraldo Nicolau Rodrigues, Americo Yuti Katayama, Ronald F. Cardoso The edentulous posterior
Deep-Frozen Allogeneic Onlay Bone Grafts for Reconstruction of Atrophic Maxillary Alveolar Ridges: A Preliminary Study
 J Oral Maxillofac Surg 67:1300-1306, 2009 Deep-Frozen Allogeneic Onlay Bone Grafts for Reconstruction of Atrophic Maxillary Alveolar Ridges: A Preliminary Study Antonio Barone, DDS, PhD, MSc,* Paolo Varanini,
J Oral Maxillofac Surg 67:1300-1306, 2009 Deep-Frozen Allogeneic Onlay Bone Grafts for Reconstruction of Atrophic Maxillary Alveolar Ridges: A Preliminary Study Antonio Barone, DDS, PhD, MSc,* Paolo Varanini,
Comparison of Peri-Implant Bone Loss and Survival of Maxillary Intrasinus and Extrasinus Implants After 2 Years
 Original Article Comparison of Peri-Implant Bone Loss and Survival of Maxillary Intrasinus and Extrasinus Implants After 2 Years AR. Rokn 1,2, AAR. Rasouli Ghahroudi 3,4, S. Hemati 5, A. Soolari 6 1 Associate
Original Article Comparison of Peri-Implant Bone Loss and Survival of Maxillary Intrasinus and Extrasinus Implants After 2 Years AR. Rokn 1,2, AAR. Rasouli Ghahroudi 3,4, S. Hemati 5, A. Soolari 6 1 Associate
Case Study. Case # 1 Author: Dr. Suheil Boutros (USA) 2013 Zimmer Dental, Inc. All rights reserved. 6557, Rev. 03/13.
 Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
A WIDE RANGE OF REGENERATIVE SOLUTIONS
 A WIDE RANGE OF REGENERATIVE SOLUTIONS INDICATIONS: 1/ SOCKET AND RIDGE PRESERVATION 2/ FILLING OF EXTRACTION SOCKETS Biomaterials offers portfolio of regenerative materials for implantology, aimed at
A WIDE RANGE OF REGENERATIVE SOLUTIONS INDICATIONS: 1/ SOCKET AND RIDGE PRESERVATION 2/ FILLING OF EXTRACTION SOCKETS Biomaterials offers portfolio of regenerative materials for implantology, aimed at
Vertical and Horizontal Ridge Augmentation of a Severely Resorbed Ridge in the Anterior Maxilla
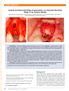 CASE REPORT Vertical and Horizontal Ridge Augmentation of a Severely Resorbed Ridge in the Anterior Maxilla Alberto Monje,* Florencio Monje, Fernando Suarez,* Raúl González-García, Laura Villanueva-Alcojol,
CASE REPORT Vertical and Horizontal Ridge Augmentation of a Severely Resorbed Ridge in the Anterior Maxilla Alberto Monje,* Florencio Monje, Fernando Suarez,* Raúl González-García, Laura Villanueva-Alcojol,
Puros Cancellous Particulate Allograft & Puros Block Allograft
 Puros Cancellous Particulate Allograft & Puros Block Allograft Puros Cancellous Particulate Allograft The Natural Choice For Healthy 1 Bone Growth. 1. Proven, Predictable Regeneration Acts as an osteoconductive
Puros Cancellous Particulate Allograft & Puros Block Allograft Puros Cancellous Particulate Allograft The Natural Choice For Healthy 1 Bone Growth. 1. Proven, Predictable Regeneration Acts as an osteoconductive
Case Report. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
 Case Report RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
Case Report RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
Ridge Split Procedure
 Ridge Split Procedure in the Atrophic Maxilla Udatta Kher B.D.S., M.D.S. Loss of teeth causes extensive resorption of the alveolar ridge. In the maxilla the resorption pattern occurs towards the midline,
Ridge Split Procedure in the Atrophic Maxilla Udatta Kher B.D.S., M.D.S. Loss of teeth causes extensive resorption of the alveolar ridge. In the maxilla the resorption pattern occurs towards the midline,
/TLv/ A classification of the edentulous jaws. Trauma; Preprosthetic Surgery. iiiii!iii!iii! ] BASAL
![/TLv/ A classification of the edentulous jaws. Trauma; Preprosthetic Surgery. iiiii!iii!iii! ] BASAL /TLv/ A classification of the edentulous jaws. Trauma; Preprosthetic Surgery. iiiii!iii!iii! ] BASAL](/thumbs/72/66558540.jpg) Trauma; Preprosthetic Surgery A classification of the edentulous jaws J. I. awood ~ and R. A. Howell 2 ~Maxillofacial Unit, Royal Infirmary, hester, UK, 2Liverpool Dental Hospital, Liverpool, UK J. L awood
Trauma; Preprosthetic Surgery A classification of the edentulous jaws J. I. awood ~ and R. A. Howell 2 ~Maxillofacial Unit, Royal Infirmary, hester, UK, 2Liverpool Dental Hospital, Liverpool, UK J. L awood
BONE SPREADING TECHNIQUE A CASE REPORT. simultaneous implant placement and is an alternative Summer s osteotome both clinical use as well as the
 BONE SPREADING TECHNIQUE A CASE REPORT AUTHORS: Renato Sussumu Nishioka, DDS, PhD*, João Carlos Paixão** ABSTRACT: Bone spreading technique (BST) is horizontal augmentation with minimal trauma for simultaneous
BONE SPREADING TECHNIQUE A CASE REPORT AUTHORS: Renato Sussumu Nishioka, DDS, PhD*, João Carlos Paixão** ABSTRACT: Bone spreading technique (BST) is horizontal augmentation with minimal trauma for simultaneous
FIVE-YEAR FOLLOW-UP OF IMPLANTS PLACED SIMULTANEOUSLY WITH INFERIOR ALVEOLAR NERVE LATERALISATION OR TRANSPOSITION
 original articles FIVE-YEAR FOLLOW-UP OF IMPLANTS PLACED SIMULTANEOUSLY WITH INFERIOR ALVEOLAR NERVE LATERALISATION OR TRANSPOSITION Stefan Peev 1, Borislav Ivanov 2, Elitsa Sabeva 1, Tihomir Georgiev
original articles FIVE-YEAR FOLLOW-UP OF IMPLANTS PLACED SIMULTANEOUSLY WITH INFERIOR ALVEOLAR NERVE LATERALISATION OR TRANSPOSITION Stefan Peev 1, Borislav Ivanov 2, Elitsa Sabeva 1, Tihomir Georgiev
Prosthetic Options in Implant Dentistry. Hakimeh Siadat, DDS, MSc Associate Professor
 Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Long-term success for osteointegrated
 CASE REPORT Symphyseal Bone Cylinders Tapping With the Dental Implant Into Insufficiency Bone Situated Esthetic Area at One-Stage Surgery: A Case Report and the Description of the New Technique Umut Tekin,
CASE REPORT Symphyseal Bone Cylinders Tapping With the Dental Implant Into Insufficiency Bone Situated Esthetic Area at One-Stage Surgery: A Case Report and the Description of the New Technique Umut Tekin,
Sandwich bone graft for vertical augmentation of the posterior maxillary region: a case report with 9-year follow-up
 Tanaka et al. International Journal of Implant Dentistry (2017) 3:20 DOI 10.1186/s40729-017-0063-9 International Journal of Implant Dentistry CASE REPORT Sandwich bone graft for vertical augmentation of
Tanaka et al. International Journal of Implant Dentistry (2017) 3:20 DOI 10.1186/s40729-017-0063-9 International Journal of Implant Dentistry CASE REPORT Sandwich bone graft for vertical augmentation of
MASTERS SERIES 2010 ACCELERATED IMPLANT DENTISTRY EDUCATION. San Francisco April-September Miami March-August CREDIT HOURS
 MASTERS SERIES 2010 Level II Implant Continuum Advanced Continuum Miami March-August 2010 San Francisco April-September 2010 ACCELERATED IMPLANT DENTISTRY EDUCATION 120 CREDIT HOURS Arun K. Garg, D.M.D.
MASTERS SERIES 2010 Level II Implant Continuum Advanced Continuum Miami March-August 2010 San Francisco April-September 2010 ACCELERATED IMPLANT DENTISTRY EDUCATION 120 CREDIT HOURS Arun K. Garg, D.M.D.
Comparison of implant survival with implants placed in acceptable and compromised bone: a literature review
 J Maxillofac Oral Surg 8(1):1 7 COMPARATIVE STUDY Comparison of implant survival with implants placed in acceptable and compromised bone: a literature review Stefan Ihde 1 Sigmar Kopp 2 Thomas Maier 3
J Maxillofac Oral Surg 8(1):1 7 COMPARATIVE STUDY Comparison of implant survival with implants placed in acceptable and compromised bone: a literature review Stefan Ihde 1 Sigmar Kopp 2 Thomas Maier 3
An aging world population and a progressive
 Evaluation of the Use of Iliac Cancellous Bone and Anorganic Bovine Bone in the Reconstruction of the Atrophic Maxilla with Titanium Mesh: A Clinical and Histologic Investigation Carlo Maiorana, MD, DDS
Evaluation of the Use of Iliac Cancellous Bone and Anorganic Bovine Bone in the Reconstruction of the Atrophic Maxilla with Titanium Mesh: A Clinical and Histologic Investigation Carlo Maiorana, MD, DDS
Vertical and horizontal alveolar ridge augmentation
 CLINICAL SIMULTANEOUS VERTICAL GUIDED BONE REGENERATION AND GUIDED TISSUE REGENERATION IN THE POSTERIOR MAXILLA USING RECOMBINANT HUMAN PLATELET-DERIVED GROWTH FACTOR: A CASE REPORT Istvan Urban, DMD,
CLINICAL SIMULTANEOUS VERTICAL GUIDED BONE REGENERATION AND GUIDED TISSUE REGENERATION IN THE POSTERIOR MAXILLA USING RECOMBINANT HUMAN PLATELET-DERIVED GROWTH FACTOR: A CASE REPORT Istvan Urban, DMD,
Vertical and Horizontal Augmentation Using Guided Bone Regeneration. Ph.D. Thesis. Dr. med. dent. et univ. Istvan Urban
 Vertical and Horizontal Augmentation Using Guided Bone Regeneration Ph.D. Thesis Dr. med. dent. et univ. Istvan Urban Supervisor: Prof. Dr. Katalin Nagy, DDS, PhD Faculty of Dentistry, University of Szeged
Vertical and Horizontal Augmentation Using Guided Bone Regeneration Ph.D. Thesis Dr. med. dent. et univ. Istvan Urban Supervisor: Prof. Dr. Katalin Nagy, DDS, PhD Faculty of Dentistry, University of Szeged
Consensus Statements and Recommended Clinical Procedures Regarding Loading Protocols
 Group 3 Consensus Statements Consensus Statements and Recommended Clinical Procedures Regarding Loading Protocols Hans-Peter Weber, DMD, Dr Med Dent 1 /Dean Morton, BDS, MS 2 /German O. Gallucci, DMD,
Group 3 Consensus Statements Consensus Statements and Recommended Clinical Procedures Regarding Loading Protocols Hans-Peter Weber, DMD, Dr Med Dent 1 /Dean Morton, BDS, MS 2 /German O. Gallucci, DMD,
INTERNATIONAL MEDICAL COLLEGE
 INTERNATIONAL MEDICAL COLLEGE Joint Degree Master Program: Implantology and Dental Surgery (M.Sc.) Specialized Modules: List of individual modules Specialized Module 1 Basic principles of implantology
INTERNATIONAL MEDICAL COLLEGE Joint Degree Master Program: Implantology and Dental Surgery (M.Sc.) Specialized Modules: List of individual modules Specialized Module 1 Basic principles of implantology
Dental implants offer a predictable treatment
 Histologic evaluation of a 12-year-old threaded hydroxyapatite-coated implant placed in conjunction with subantral augmentation procedure: A clinical report Periklis Proussaefs, DDS, MS, a Henry-Savajol
Histologic evaluation of a 12-year-old threaded hydroxyapatite-coated implant placed in conjunction with subantral augmentation procedure: A clinical report Periklis Proussaefs, DDS, MS, a Henry-Savajol
Pre-operative evaluation of the volume of bone graft in sinus lifts by means of CompuDent
 Journal section: Oral Surgery Publication Types: Research doi:0.7/medoral..e Pre-operative evaluation of the volume of bone graft in sinus lifts by means of CompuDent Oscar Arias-Irimia, Cristina Barona-Dorado,
Journal section: Oral Surgery Publication Types: Research doi:0.7/medoral..e Pre-operative evaluation of the volume of bone graft in sinus lifts by means of CompuDent Oscar Arias-Irimia, Cristina Barona-Dorado,
PLACEMENT OF DENTAL IMPANT IN POSTERIOR MAXILLARY RIDGE USING INDIRECT SINUS LIFT TECHNIQUE WITHOUT GRAFT: A CASE REPORT
 CSE REPORT PLCEMENT OF DENTL IMPNT IN POSTERIOR MXILLRY RIDGE USING INDIRECT SINUS LIFT TECHNIQUE WITHOUT GRFT: CSE REPORT S.P.S Sooch 1, Puja 2, Seema ggarwal 3 (e) ISSN Online: 2321-9599 (p) ISSN Print:
CSE REPORT PLCEMENT OF DENTL IMPNT IN POSTERIOR MXILLRY RIDGE USING INDIRECT SINUS LIFT TECHNIQUE WITHOUT GRFT: CSE REPORT S.P.S Sooch 1, Puja 2, Seema ggarwal 3 (e) ISSN Online: 2321-9599 (p) ISSN Print:
In 1977, Lew1 developed a passive
 CLINICAL AN OVERVIEW OF THE LEW ATTACHMENT: CLINICAL REPORTS Jack Piermatti, DMD Sheldon Winkler, DDS KEY WORDS Lew attachment Atrophic mandible Subperiosteal implant Root form implant Although the Lew
CLINICAL AN OVERVIEW OF THE LEW ATTACHMENT: CLINICAL REPORTS Jack Piermatti, DMD Sheldon Winkler, DDS KEY WORDS Lew attachment Atrophic mandible Subperiosteal implant Root form implant Although the Lew
Columbia Dental Review
 Columbia Dental Review groper appliance in a pediatric patient: a case report and review of the literature periapical cemental dysplasia and an adjacent compound odontoma successful osseointegration and
Columbia Dental Review groper appliance in a pediatric patient: a case report and review of the literature periapical cemental dysplasia and an adjacent compound odontoma successful osseointegration and
Revisions for CDT 2016
 Revisions for CDT 2016 This document was developed from preliminary actions of the Code Maintenance Committee (CMC). This document has been compared to the CMC meeting notes and the ASCII file. This document
Revisions for CDT 2016 This document was developed from preliminary actions of the Code Maintenance Committee (CMC). This document has been compared to the CMC meeting notes and the ASCII file. This document
More than bone regeneration. A total solution.
 More than bone regeneration. A total solution. More than a dental implant company. A total solution. When it comes to treatment options, your patients want positive results both functionally and esthetically.
More than bone regeneration. A total solution. More than a dental implant company. A total solution. When it comes to treatment options, your patients want positive results both functionally and esthetically.
Procedure Manual and Catalog
 Procedure Manual and Catalog TM Why SynthoGraft? SynthoGraft offers a unique structure which provides stability, while its micro-porosity allows for rapid vascularization and subsequent resorption. Although
Procedure Manual and Catalog TM Why SynthoGraft? SynthoGraft offers a unique structure which provides stability, while its micro-porosity allows for rapid vascularization and subsequent resorption. Although
Bone Morphogenic Proteins
 Bone Morphogenic Proteins Science, Techniques, and Clinical Applications with Hands on Workshop Course Dates: Dallas - December 18, 2010 Philadelphia - November 13, 2010 Phoenix - January 22, 2011 Atlanta
Bone Morphogenic Proteins Science, Techniques, and Clinical Applications with Hands on Workshop Course Dates: Dallas - December 18, 2010 Philadelphia - November 13, 2010 Phoenix - January 22, 2011 Atlanta
In spite of the great advances made by the osseointegration concept 1 in the oral rehabilitation of
 Placement of Screw-Type Implants in the Pterygomaxillary-Pyramidal Region: Surgical Procedure and Preliminary Results Jesús Fernández Valerón, MD, DDS/José Fernández Velázquez, MD, DDS A surgical technique
Placement of Screw-Type Implants in the Pterygomaxillary-Pyramidal Region: Surgical Procedure and Preliminary Results Jesús Fernández Valerón, MD, DDS/José Fernández Velázquez, MD, DDS A surgical technique
Clinical Case Reports using Cytoplast GTR Barrier Membranes
 Clinical Case Reports using Cytoplast GTR Barrier Membranes Barry K. Bartee, DDS, MD The Cytoplast Technique: Extraction Site Grafting Without Primary Closure 1. 1. Preoperative view. To maximize the result
Clinical Case Reports using Cytoplast GTR Barrier Membranes Barry K. Bartee, DDS, MD The Cytoplast Technique: Extraction Site Grafting Without Primary Closure 1. 1. Preoperative view. To maximize the result
In the moderately to severely atrophic maxilla,
 Staged Sinus Floor Elevation Using the Crestal Core Elevation (CCE) Procedure: A Review of the Technique Michael, DDS Abstract In the moderately to severely atrophic maxilla, trephined cores measuring
Staged Sinus Floor Elevation Using the Crestal Core Elevation (CCE) Procedure: A Review of the Technique Michael, DDS Abstract In the moderately to severely atrophic maxilla, trephined cores measuring
Sandwich osteotomy of the atrophic posterior mandible prior to implant placement
 CASE REPORT Sandwich osteotomy of the atrophic posterior mandible prior to implant placement Luan Mavriqi 1, Egresa Baca 2 & Ariona Demiraj 3 1 Departament of Periodontology, Albanian University and Private
CASE REPORT Sandwich osteotomy of the atrophic posterior mandible prior to implant placement Luan Mavriqi 1, Egresa Baca 2 & Ariona Demiraj 3 1 Departament of Periodontology, Albanian University and Private
THE USE OF TEMPORARY ANCHORAGE DEVICES FOR MOLAR INTRUSION & TREATMENT OF ANTERIOR OPEN BITE By Eduardo Nicolaievsky D.D.S.
 THE USE OF TEMPORARY ANCHORAGE DEVICES FOR MOLAR INTRUSION & TREATMENT OF ANTERIOR OPEN BITE By Eduardo Nicolaievsky D.D.S. Skeletal anchorage, the concept of using the facial skeleton to control tooth
THE USE OF TEMPORARY ANCHORAGE DEVICES FOR MOLAR INTRUSION & TREATMENT OF ANTERIOR OPEN BITE By Eduardo Nicolaievsky D.D.S. Skeletal anchorage, the concept of using the facial skeleton to control tooth
Much has been written about the success of various
 Simplified Guide for Precise Implant Placement: A Technical Note Brent D. Kennedy, MD, DDS*/Thomas A. Collins, Jr, DDS**/ Patrick C. W. Kline, DMD, MD** Ideal implant placement is ultimately determined
Simplified Guide for Precise Implant Placement: A Technical Note Brent D. Kennedy, MD, DDS*/Thomas A. Collins, Jr, DDS**/ Patrick C. W. Kline, DMD, MD** Ideal implant placement is ultimately determined
Buccal Corticotomy for Closure of Oroantral Openings: Case Report
 Turk J Med Sci 34 (2004) 409-414 TÜB TAK SHORT REPORT Buccal Corticotomy for Closure of Oroantral Openings: Case Report Bedrettin Cem fiener, Hasan GAR P, Faysal U URLU, Kamil GÖKER Department of Oral
Turk J Med Sci 34 (2004) 409-414 TÜB TAK SHORT REPORT Buccal Corticotomy for Closure of Oroantral Openings: Case Report Bedrettin Cem fiener, Hasan GAR P, Faysal U URLU, Kamil GÖKER Department of Oral
Bone Grafting for Socket Preservation
 Bone Grafting for Socket Preservation Dr. Karl R. Koerner Normal extraction facial bone loss. Excessive force. Commonly the thickness of facial bone. Hussain, A. et al. Ridge preservation comparing a nonresorbable
Bone Grafting for Socket Preservation Dr. Karl R. Koerner Normal extraction facial bone loss. Excessive force. Commonly the thickness of facial bone. Hussain, A. et al. Ridge preservation comparing a nonresorbable
Reconstruction and rehabilitation
 CLINICAL Minimally Invasive Subnasal Elevation and Antral Membrane Balloon Elevation Along With Bone Augmentation and Implants Placement Efraim Kfir, DMD 1 Vered Kfir, DMD 2 Moshe Goldstein, DMD 3 Ziv
CLINICAL Minimally Invasive Subnasal Elevation and Antral Membrane Balloon Elevation Along With Bone Augmentation and Implants Placement Efraim Kfir, DMD 1 Vered Kfir, DMD 2 Moshe Goldstein, DMD 3 Ziv
Horizontal bone augmentation by means of guided bone regeneration
 Periodontology 2000, Vol. 66, 2014, 13 40 2014 John Wiley & Sons A/S. Published by John Wiley & Sons Ltd Printed in Singapore. All rights reserved PERIODONTOLOGY 2000 Horizontal bone augmentation by means
Periodontology 2000, Vol. 66, 2014, 13 40 2014 John Wiley & Sons A/S. Published by John Wiley & Sons Ltd Printed in Singapore. All rights reserved PERIODONTOLOGY 2000 Horizontal bone augmentation by means
The Brånemark osseointegration method, using titanium dental implants (fixtures)
 Early Failures in 4,641 Consecutively Placed Brånemark Dental Implants: A Study From Stage 1 Surgery to the Connection of Completed Prostheses Bertil Friberg, DDS/Torsten Jemt, DDS, PhD/Ulf Lekholm, DDS,
Early Failures in 4,641 Consecutively Placed Brånemark Dental Implants: A Study From Stage 1 Surgery to the Connection of Completed Prostheses Bertil Friberg, DDS/Torsten Jemt, DDS, PhD/Ulf Lekholm, DDS,
Gingivectomy, excision gingival, each quadrant Gingivoplasty, each quadrant
 Dental in Nature Oral Surgery Effective CDT D3410 surgery - anterior D3421 surgery bicuspid (first root) D3425 surgery molar (first root) D3426 D3427 surgery (each additional root) Periradicular surgery
Dental in Nature Oral Surgery Effective CDT D3410 surgery - anterior D3421 surgery bicuspid (first root) D3425 surgery molar (first root) D3426 D3427 surgery (each additional root) Periradicular surgery
EFFECTIVE DATE: 04/24/14 REVISED DATE: 04/23/15, 04/28/16, 06/22/17, 06/28/18 POLICY NUMBER: CATEGORY: Dental
 MEDICAL POLICY SUBJECT: DENTAL IMPLANTS PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including an Essential
MEDICAL POLICY SUBJECT: DENTAL IMPLANTS PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including an Essential
Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs
 Current Applied Physics 5 (2005) 507 511 www.elsevier.com/locate/cap Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs Ui-Won Jung a, Hee-Il
Current Applied Physics 5 (2005) 507 511 www.elsevier.com/locate/cap Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs Ui-Won Jung a, Hee-Il
IJCMR 73. REVIEW ARTICLE Maxillary Sinus Floor Elevation Surgeries: An Overview
 IJCMR 73 REVIEW ARTICLE Maxillary Sinus Floor Elevation Surgeries: An Overview Riddhi Katara, 1 D. Gopalakrishnan, 2 Tuhina Tyagi, 1 Disha Kataria, 1 Gurbani Kaur, 1 Archana Singh 3 ABSTRACT Maxillary
IJCMR 73 REVIEW ARTICLE Maxillary Sinus Floor Elevation Surgeries: An Overview Riddhi Katara, 1 D. Gopalakrishnan, 2 Tuhina Tyagi, 1 Disha Kataria, 1 Gurbani Kaur, 1 Archana Singh 3 ABSTRACT Maxillary
