Implant Site Development Part II
|
|
|
- Elaine Bennett
- 5 years ago
- Views:
Transcription
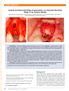
1 IJCID REVIEW ARTICLE 1 Umang Nayar, 2 Shankar Iyer 1 Consultant, Dental Surgeon and Periodontist at Max Health Care, New Delhi, Professor and Head, Department of Periodontics Harsarn Dass Dental College, Ghaziabad, Uttar Pradesh, India 2 Director, The Center for Reconstructive Dentistry, Elizabeth, New Jersey, USA Correspondence: Umang Nayar, 145 Shivalik Apartment, Alaknanda, New Delhi , India, umangsnayar@rediffmail.com ABSTRACT The internal and external architecture of bone determines positioning of dental implants in partially and fully edentulous patients. A deficient jaw bone creates a new demand for bone reconstruction before or during implant therapy. The second part of the review discusses various surgical reconstructive modalities to improve bone support for placement of implant in prosthetically driven position to restore the natural position and to emulate the natural emergence of a tooth from soft tissues. Surgical procedures that have been developed to deal with problems of insufficient alveolar ridge width or height include extraction site bone grafting, ridge augmentation using principles of GBR with block grafts or particulate materials and protective barriers, grafting with bone harvested from both extraoral and intraoral donor sites, use of platelet rich plasma and growth factors etc. Bone augmentation allows clinicians to reconstruct alveolar bone deficiencies, preserve alveolar dimensions and replace missing teeth with dental implants in a prosthetically driven position with natural appearance and function. Keywords: Bone augmentation, Block grafts, Particulate materials, Protective barriers, GBR (guided bone regeneration), PRP (platelet rich plasma), Growth factors, Intraoral and extraoral donor, Autogenous donor grafts. BONE AUGMENTATION FOR IMPROVING THE IMPLANT SITE 1,2,4 Bone Grafting for Implant Placement: Applications and Principles Following an extraction, there is 25% decrease in width and 4 mm decrease in height of the alveolar bone during the first year. Bone loss following an extraction can have negative cosmetic, hygienic, prosthetic and structural consequences. Preservation of bone contour for dental implants, pontic design, denture stability, soft tissue esthetics, and maintaining periodontal status of adjacent teeth are important considerations following an extraction. To reduce or eliminate potential problems, extraction site grafting can be commonly employed by the general dental practice. Fig. 1: Radiograph showing endodontic failure with 24 Extraction Site Bone Grafting (Figs 1 to 6) The keys to bone grafting in extraction sites (Misch): Atraumatic tooth removal Asepsis and complete removal of granulomatous tissue An evaluation of the remaining walls of bone following the extraction and evaluation of the size of defect Ensuring adequate blood supply to the graft site Graft containment and soft tissue closure Choice of the appropriate graft material Insuring adequate time for healing. Fig. 2: Clinical picture showing failing 24 International Journal of Clinical Implant Dentistry, January-April 2010;2(1):
2 Umang Nayar, Shankar Iyer Fig. 3: Postextraction socket Fig. 5: Resorbable membrane placed over the grafted site 14 Fig. 4: Bone graft placed in the socket Atraumatic Tooth Removal Atraumatic extraction of teeth can be achieved with the use of periotomes, tooth sectioning, orthodontic therapy and minimum forceps rotation. When all the walls of bone surrounding a tooth are left intact, the grafting material is better contained and immobilized and osteoprogenitor cells are more readily recruited. When walls of bone are missing (i.e. the loss of facial plate as a consequence of periodontal disease or the extraction process), the graft procedure is more complicated. Asepsis and Removal of Granulomatous Tissue Before an extraction site can receive a graft, any granulomatous tissue present must be removed. Ideally, bone remodels through cell-mediated resorption. If infection is present in an extraction site, the graft will undergo solution-mediated resorption due to the lower (acidic) ph, and bone will not form. An Evaluation of the Size of the Defect Once a tooth is removed, first the remaining walls of socket are evaluated. The greater the number of walls of bone Fig. 6: Primary closer achieved by suturing remaining, the more predictable will be the ridge preservation procedure. The choice of grafting material, the need for a membrane, provisionalization of the graft area, and healing time are all affected. Once the tooth is removed, the walls of remaining bone can be used to classify the area as a 2, 3, 4 or 5 wall defect. A 5-wall defect contains all possible walls of bone, offering the greatest predictability. When a large facial wall of bone is missing, a barrier membrane should be used to contain the graft material. Use of the barrier can prevent fibrous tissue ingrowth. Ensuring Adequate Blood Supply to the Graft Site A bone graft requires blood supply to provide osteoprogenitor cells and associated growth factors. While blood supply from the soft tissue does supply blood to the graft site, osteoprogenitor cells will be supplied only from adjacent bone, or in a limited fashion from the periosteum. To ensure the presence of these critical cells, the bone adjacent to a graft site must be traumatized in a nonpathological fashion. This has been called a regional acceleratory phenomenon (RAP) by Frost. A tooth extraction also provides a RAP, and the periodontal membrane complex provides an excellent blood supply to the JAYPEE
3 IJCID extraction site. If little or no bleeding exists, decortication of the bone beyond the apex with a round bur using sterile saline for cooling is suggested. This decortication also allows for an improved physical integration of the graft material. Graft Containment and Soft Tissue Closure When the extraction site is an optimal 5-wall defect, the surrounding walls of bone will contain and immobilize the graft. Grafting bone into a 5-wall defect usually requires only coverage of the graft site with a rapidly resorbing collagen membrane stabilized with sutures. If the extraction site has 4 walls or less, use of a barrier membrane to contain the graft material and to exclude fibrous cells. Also, primary soft tissue closure to minimize bacterial contamination of the membrane in larger defects is suggested (Fig 7). Choice of Appropriate Graft Material The choice of graft material is based on the number of remaining walls of bone and prosthetic treatment plan. As a general rule, more the missing walls of bone, more the autogenous bone should be part of extraction site grafting. The terms osteogenic, osteoconductive and osteoinductive are useful to explain the different types of grafts. Osteogenesis is the growth of bone from cells transferred within a graft. An osteogenic material will promote growth of bone in ectopic tissue. Osteoconduction is growth of bone from surrounding bone. Osteoconductive materials act as a biocompatible scaffold. Osteoconductive materials are biocompatible, but will not grow bone without the presence of cells that will form bone. Fig. 7: Clinical picture showing barrier membrane for guided tissue regeneration and to contain the particulate bone graft in position Osteoinduction induces bone growth from osteoprogenitor cells created by the influence of inducing agents from the host bone matrix. There are four types of grafting materials available for use in the oral cavity: Autogenous bone is the only source of osteogenic bone. Allograft bone (demineralized) Xenograft bone Alloplastic Autogenous bone is the gold standard for bone grafting, since it contains both osteoprogenitor cells and scaffolding. It can be obtained from an intraoral or extraoral source. Common intraoral sites for socket grafting include the mandibular symphysis, mandibular ramus, and maxillary tuberosity. The advantages of autogenous bone include: Only osteogenic material available A source of the bone proteins Cost effective and predictable Fastest bone regeneration material. And the disadvantages are: Need for a second surgical site Possibly postoperative discomfort Potential limitations on the amount of graft material that can be harvested. As a general rule, however, the more walls of the socket that are missing, greater consideration should be given to the use of an autogenous graft. Allograft bone is from the same species but a different genotype (individual). This is a donor bone obtained by FDA-regulated tissue banks, and is both tested for infection (donor) and processed. Allograft bone has been used extensively in dentistry for more than two decades. Allograft bone is available as: Particles in different sizes: Cortical fibers, putty forms have various proprietary carriers, such as glycerin and cellulose. The handling characteristics differ for the different preparations and the choices dependent on the clinical situation and the clinician. Cortical bone (versus medullary bone) as the source of allograft material offers advantages for extraction site grafting. These advantages include ease of handling, increased containment in the graft site, and an increase in the osteoinductive effect. There are two types of allograft material; mineralized and demineralized forms. When allograft bone is demineralized, it is processed with an acid solution. This process dissolves the mineral component (hydroxyapatite) and exposes collagen and organic constituents, believed to include bone morphogenic proteins (BMPs). Although allograft bone may contain these International Journal of Clinical Implant Dentistry, January-April 2010;2(1):
4 Umang Nayar, Shankar Iyer growth factors, it is not considered osteogenic. Preparation techniques vary among manufacturers, resulting in proprietary differences in handling characteristics and relative amounts of growth factors (Figs 8 to 11). Demineralized bone allograft is a composite of collageneous proteins and bone growth factors following the mineral extraction of bone by a chemical preparatory process. Fig. 11: Puros allograft Fig. 8: Allograft from bone bank Xenograft bone is from a different species (e.g. bovine), contains the inorganic portion of bone (hydroxyapatite) and is available in various particulate sizes. These grafts are osteoconductive, without having any osteoinductive properties. These grafts create a biocompatible scaffold. The osteoprogenitor cells are provided by the recipient. Xenografts can be added to allografts to improve the mineralization potential (Fig 12). Fig. 12: Xenograft from bovine Fig. 9: Demineralized bone matrix and cancellous putty Fig. 10: Rocky mountain bone allograft Alloplastic materials are synthetic products, and include ceramic and acrylic materials. They can be resorbable or nonresorbable. Nonresorbable material should only be used when an implant will not be placed in the location of the graft. The nonresorable material cannot attach to the implant surface or grow into the thread or macro design of the implant. Insuring Adequate Time for Healing To allow a graft to mature into lamellar bone, adequate time for healing is needed. The time required is dependent on factors, such as the patient s age, the patient s healing capacity, residual infection in the graft site, and size of the defect. In general, the time for a graft to heal varies between 4 and 6 months when autogenous bone is a part of the graft. 16 JAYPEE
5 IJCID Figs 13A to C: Socket repair membranes Osteoblasts, cementoblasts and periodontal ligament cells are then afforded the opportunity to regenerate a new periodontal attachment (new bone and new connective tissue fibers inserted in newly formed cementum). Guided bone regeneration (GBR) employed the same principles of specific tissue exclusion and regenerated single tissue, namely bone by use of barrier membranes. Requirement Biologic Requirements for Bone Regeneration 3 Blood supply Stabilization Osteoblasts Confined space Space maintenance Wound coverage Fig. 14: Recombinant growth factor Surgical procedure Cortical perforations Fixation screws, membrane tacks Autogenous bone (Graft or recipient site) Barrier membrane Tenting screws, bone graft materials Flap management, tension free suturing Biologic Properties of Various Bone Graft Materials 3 Source Osteoconductive Osteoinductive Osteogenic Alloplast Yes No No Xenograft Yes No No Allograft Yes Yes/No No Autograft Yes Yes Yes Guided Bone Regeneration (Figs 13A to 17) Historically, augmentation or regeneration of alveolar bone lost as a result of tooth extraction, resorption or trauma was a challenge. Extraction sites healed with fibrous connective tissue or scar formation leaving an anatomic deficiency. Guided tissue regeneration (GTR) principle employs exclusion of fast growing epithelium, and connective tissue from periodontal wound for six to eight weeks, allows slower tissues to occupy the space adjacent to the tooth. Ideal Properties of Barrier Membranes Biocompatibility Space maintenance Cell occlusiveness Good handling properties Resorbability Nonresorbable Membranes Latex Teflon (Expanded poly tetrafluoroethylene eptfe, Gore tex peridontal and bone regenerative membranes, Gore and associate, Flagstff, Ariz) Titanium reinforced membranes (TR) Resorbable Barrier Membranes Copolymers of polylactide and polyglycolide (PLA/ PGA) Collagen Membranes for guided bone regeneration 3 act as a biological barrier to protect underlying bone graft. They also provide matrix for formation of new keratinized tissue. Platelet Rich Plasma 5,7 Clinical implications: PRP has proved to be effective at improving surgical results in the field of oral and maxillofacial surgery and periodontal regenerative therapy. Using platelet rich plasma (PRP), is a way to accelerate and enhance the body s natural wound-healing mechanisms. Platelets primarily are involved in wound healing through clot formation and release of growth factors that initiate and International Journal of Clinical Implant Dentistry, January-April 2010;2(1):
6 Umang Nayar, Shankar Iyer support wound healing. Using PRP involves taking a sample of a patient s blood preoperatively, concentrating autologous platelets and applying the resultant gel to the surgical site. Surgical sites enhanced with PRP have been shown to heal at rates two to three times that of normal surgical sites. 6 Growth Factors 5,7 It is now known that platelets also actively extrude several growth factors involved in initiating and sustaining wound repair. The two most important of these growth factors are 18 Fig. 15: Bioguide membrane Fig. 16: Alloderm Fig. 17: Collatape platelet-derived growth factor (PDGF) (Fig. 14) and transforming growth factor-ß (TGF-ß). PDGF is chemotactic for polymorphonucleocytes, macrophages, fibroblasts and smooth muscle cells. PDGF also stimulates cell replication of important stem cells for fibroblasts and endothelial cells (increasing budding of new capillaries), stimulates production of fibronectin a cell adhesion molecule. With hyaluronic acid, it helps bring about wound contraction and remodeling. TGF-ß stimulates fibroblast chemotaxis and the production of collagen and fibronectin by cells, while inhibiting collagen degradation by decreasing proteases and increasing protease inhibitors, all of which favor fibrogenesis. The topical application of these growth factors to healing sites can accelerate repair and wound maturation. Future Directions: To date, the greatest commercial interest has been in rhbmp-2 and rhbmp-7. Many different carriers have been used to deliver BMPs, i.e. collagen sponge impregnated with BMP. Also demineralized bone matrix (DBM) has been incorporated in various carriers, such as collagen or selected polymers. DBM can be used as a bone expander. INTRAORAL AUTOGENOUS DONOR GRAFTS FOR DENTAL IMPLANT A primary diagnostic consideration for implant placement is the available bone in the edentulous span. If inadequate bone exists, the morphology of a bony defect is an important consideration in the selection of a method for ridge augmentation. Although allografts and guided tissue regeneration techniques have been used bone repair, these methods have limitations in treatment of larger bone defects. The use of autologous bone grafts with osseointegrated implants was originally discussed by Branemark et al 1975 and continues to be a gold standard for jaw reconstruction. With exception of alveolar bone, the maxilla and body of mandible develop intramembraneously while condyles develop from endochonral bone formation. These grafts show less resorption and revascularize more rapidly than endochondral bone grafts. An intraoral donor site (Figs 18 to 32) offers several advantages: Convenient surgical access Only require one operational field, which decreases the surgical and anesthetic time Proximity of donor and recipient site No cutaneous scar associated with extraoral donor sites Minimal discomfort and reduced morbidity Offers favorable results. Block grafts offering large amount of bone are harvested from: mandibular symphysis (Figs 20 to 30), body or ramus (Figs 31 and 32). JAYPEE
7 IJCID Particulate autografts are harvested from (a) maxillary tuberosity, (b) zygoma, extraosseus tori (Figs 18 and 19), (c) residual ridge osteoplasty, (d) implant osteotomy, (e) extraction sites and (f) bone collection devices. Comparison of Mandibular Donor Site 4 Symphysis Ramus Tuberosity Surgical access Good Fair to good Good to fair Patient cosmetic High Low Low Concerns Graft shape Thicker block Thinner veneer Porous block Graft morphology Cortiocancellous Cortical Cancellous Graft size (cm 3 ) > 1 cm 3 < 1 cm 3 < 1 cm 3 Graft resorption Minimal Minimal Moderate Healed bone quality D1, D2 D1, D2 D3 MANDIBULAR SYMPHYSEAL GRAFT Fig. 18: Clinician view of mandibular tori Procedure (Figs 20 to 32) Fig. 19: Bone fragments retrieved from a tori Fig. 21: Deficient areas are exposed, assessed and decorticated Fig. 20: X-rays are used to evaluate the existence of bone deterioration issues and clearly reveal to the patient what areas may require treatment Fig. 22: Mandibular symphyseal region exposed Donor Site Complications Postoperative pain/edema Moderate Minimal to moderate Minimal Neurosensory-teeth Common (temporary) Uncommon None Neurosensory-tissue Common (temporary) Uncommon Uncommon Incision dehiscence Occasional (vestibular) Uncommon Uncommon Sinus perforation None None Occasional International Journal of Clinical Implant Dentistry, January-April 2010;2(1):
8 Umang Nayar, Shankar Iyer Fig. 23: Once these anatomical sites are identified, small perforations are made to outline the graft margins. Then perforations are connected, the appropriate sized area of needed bone is removed. Pieso surgery is also being used nowadays Fig. 26: Demineralized freeze-dried bone and bovine bone can also be used. This is a painless procedure with bone filling in the area through self-regeneration in a few short months Fig. 24: Bone is harvested from the mandibular symphyseal region Fig. 27: Particulate graft may also be used to fill the donor site Fig. 25: Small holes are drilled in the bone for a titanium screw that affixes the bone to the desired surgical site. Titanium screws are small and will be removed at the next stage of surgery during implant placement EXTRAORAL AUTOGENOUS DONOR BONE GRAFTS FOR IMPLANTS General Considerations An extraoral origin for autogenous graft is necessary for large atrophic regions of the jaws. Extraoral donor sites 20 Fig. 28: A primary closure is achieved are iliac crest, tibia, cranium, rib and fibula. An advantage of corticocancellous solid block graft is to permit contouring and adaptation to the recipient bed anatomy, maintains greater volume and allows rigid fixation. The cortical bone on outside of the graft acts like a barrier similar to membranes used in GTR. JAYPEE
9 IJCID Fig. 29: Healed ridge, 3 months postoperatively Fig. 32: This block is shaped and screwed onto the desired recepient site with best possible adaptation Fig. 30: Bone crusher is used to create a compound of prepared bone material (patient s own) that is used to fill in the spaces Mandibular Ramus Bone Graft A Fig. 31: Posterior mandibular region is exposed and, similar to graft taken from the symphysis region, an island of bone is removed B Extraoral Donor Sites (Figs 33A and B) Originally reported by Kratochil and Boyne in 1972, this area provides large volume of graft, permits shaping of 2/3rd of mandible or maxilla or filling larger bony voids. Outer portion is cortical with abundant cancellous bone Figs 33A and B: (A) Anatomical position and relations of iliac crest bone graft donor site, (B) steps to harvest and contour the block graft underneath in the extraoral autogenous graft bone. Easy access and harvesting, safe well-accepted procedure makes it popular. International Journal of Clinical Implant Dentistry, January-April 2010;2(1):
10 Umang Nayar, Shankar Iyer Rapid resorption of 30 to 50% of the grafts is reported when conventional dentures are placed, but placement of the implants in the grafted bone has modified, resorption rates similar to host bone. Vascularized Bone Grafts Ilium microvascular grafts are more often indicated when blood supply is severely compromized or when recipient bed is scarred, i.e. cancer patient who has undergone radiation therapy, post-trauma, postsurgery. This graft consists of a portion of iliacus and gluteus medius muscles, anterior and medial aspect of the iliac crest and the deep circumflex iliac artery and variable veins. Distraction Osteogenesis It is the formation of new bone between vascular bone surfaces created by an osteotomy and separated by gradual distraction. Maxillary Sinus Lifts and Sinus Graft Surgery 8 The maxillary sinus may be elevated and subantral bone regenerated to improve implant height. There are two main approaches for implant site development using sinus lift: 1. Indirect sinus lift done using various techniques like osteotome technique, balloon technique 9 etc. 2. Direct sinus lift; tantum lateral wall approach. Sinus membrane elevation and subantral augmentation with a mixture of autogenous bone and/or allograft material is placed into the area previously occupied by the sinus cavity. This helps gain height for immediate or subsequent implant placement. The advent of biomaterials and advances in reconstructive techniques have contributed to increased application of dental implants in the restoration of partial and completely edentulous patients. Often, in these patients, soft and hard tissue defects create an anatomically less favorable foundation for ideal implant placement. For prostheticdriven dental implant therapy, reconstruction of the alveolar bone through a variety of regenerative surgical procedures has become predictable; it may be necessary prior to implant placement or simultaneously at the time of implant surgery to provide a restoration with a good longterm prognosis. REFERENCES 1. Block MS. Team management of atrophic edentulous with autogenous inlay, veneer and split grafts with endosseous implants. In: Block MS, Kent JN, Guerra LR. Implants in dentistry. WB Saunders Co 1997: Babbush CA. Dental Implants: The art and science. 3. Klokkevold PR, Jovanovic SA. Advanced implant surgery and bone grafting techniques. In: Newmann MC, Takei HH, Carranza FA 2003;(9th ed): Misch CE. Implant dentistry (2nd ed) Carlson NE, Roach RB. Platelet rich plasma: Clinical applications in dentistry. JADA 2002;133: Farsirotu S. Porous-surface dental implants placed in grafted sinuses with irradiated cancellous bone and platelet rich plasma. Journal Dentaire Du Quebec 2001;38: Garg AK. The use of platelet rich plasma to enhance the success of bone grafts around dental implants. Dental implantology update 2000;11(3). 8. Stephen S Wallace, Stuart J Froum. Effect of maxillary sinus augmentation on the survival of endosseous dental implants. A systematic review. Annals of Periodontology Dec 2003; 8(1): Sultan M, Smiler DG. Antral membrane balloon elevation. J Oral Implantol 2005;31(2): CONCLUSION Umang Nayar umangsnayar@rediffmail.com 22 JAYPEE
Multi-Modality Anterior Extraction Site Grafting Increased Predictability for Aesthetics Michael Tischler, DDS
 Page 1 of 5 Issue Date: March 2003, Posted On: 8/1/2005 Multi-Modality Anterior Extraction Site Grafting Increased Predictability for Aesthetics Michael Tischler, DDS The extraction of teeth creates a
Page 1 of 5 Issue Date: March 2003, Posted On: 8/1/2005 Multi-Modality Anterior Extraction Site Grafting Increased Predictability for Aesthetics Michael Tischler, DDS The extraction of teeth creates a
BONE AUGMENTATION AND GRAFTING
 1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
Dental Implants: A Predictable Solution for Tooth Loss. Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor
 Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
Case Study. Case # 1 Author: Dr. Suheil Boutros (USA) 2013 Zimmer Dental, Inc. All rights reserved. 6557, Rev. 03/13.
 Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
Bone Grafting for Socket Preservation
 Bone Grafting for Socket Preservation Dr. Karl R. Koerner Normal extraction facial bone loss. Excessive force. Commonly the thickness of facial bone. Hussain, A. et al. Ridge preservation comparing a nonresorbable
Bone Grafting for Socket Preservation Dr. Karl R. Koerner Normal extraction facial bone loss. Excessive force. Commonly the thickness of facial bone. Hussain, A. et al. Ridge preservation comparing a nonresorbable
Contemporary Implant Dentistry
 Contemporary Implant Dentistry C H A P T ER 1 4 O F C O N T E M P OR A R Y O R A L A N D M A X I L L OFA C IA L S U R G E RY B Y : D R A R A S H K H O J A S T EH Dental implant is suitable for: completely
Contemporary Implant Dentistry C H A P T ER 1 4 O F C O N T E M P OR A R Y O R A L A N D M A X I L L OFA C IA L S U R G E RY B Y : D R A R A S H K H O J A S T EH Dental implant is suitable for: completely
More than bone regeneration. A total solution.
 More than bone regeneration. A total solution. More than a dental implant company. A total solution. When it comes to treatment options, your patients want positive results both functionally and esthetically.
More than bone regeneration. A total solution. More than a dental implant company. A total solution. When it comes to treatment options, your patients want positive results both functionally and esthetically.
Cytoflex Barrier Membrane Clinical Evaluation
 Cytoflex Barrier Membrane Clinical Evaluation Historical Background Guided tissue regeneration is a well established concept in the repair of oral bone defects. The exclusion of soft tissue epithelial
Cytoflex Barrier Membrane Clinical Evaluation Historical Background Guided tissue regeneration is a well established concept in the repair of oral bone defects. The exclusion of soft tissue epithelial
Socket Treatment. Procedure Guide
 Socket Treatment Procedure Guide www.implantdirect.com 888.649.6425 Extraction Healing and Ridge Resorption The Why Working with patients to educate them on the benefits of bone maintenance post extraction
Socket Treatment Procedure Guide www.implantdirect.com 888.649.6425 Extraction Healing and Ridge Resorption The Why Working with patients to educate them on the benefits of bone maintenance post extraction
Management of a complex case
 2 Soft- and hard-tissue reconstruction of a severely deficient site prior to implant placement: a case report Management of a complex case Younes Khosroshahy, DDS, MFDS RCS (Eng), Dip Imp Dent RCSEd, Blue
2 Soft- and hard-tissue reconstruction of a severely deficient site prior to implant placement: a case report Management of a complex case Younes Khosroshahy, DDS, MFDS RCS (Eng), Dip Imp Dent RCSEd, Blue
A WIDE RANGE OF REGENERATIVE SOLUTIONS
 A WIDE RANGE OF REGENERATIVE SOLUTIONS INDICATIONS: 1/ SOCKET AND RIDGE PRESERVATION 2/ FILLING OF EXTRACTION SOCKETS Biomaterials offers portfolio of regenerative materials for implantology, aimed at
A WIDE RANGE OF REGENERATIVE SOLUTIONS INDICATIONS: 1/ SOCKET AND RIDGE PRESERVATION 2/ FILLING OF EXTRACTION SOCKETS Biomaterials offers portfolio of regenerative materials for implantology, aimed at
Clinical Case Reports using Cytoplast GTR Barrier Membranes
 Clinical Case Reports using Cytoplast GTR Barrier Membranes Barry K. Bartee, DDS, MD The Cytoplast Technique: Extraction Site Grafting Without Primary Closure 1. 1. Preoperative view. To maximize the result
Clinical Case Reports using Cytoplast GTR Barrier Membranes Barry K. Bartee, DDS, MD The Cytoplast Technique: Extraction Site Grafting Without Primary Closure 1. 1. Preoperative view. To maximize the result
A Novel Technique for the Management of a Maxillary Anterior Alveolar Defect with an Implant-retained Fixed Prosthesis: A Clinical Report
 Neenu M Varghese et al Case Report 10.5005/jp-journals-10012-1148 A Novel Technique for the Management of a Maxillary Anterior Alveolar Defect with an Implant-retained Fixed Prosthesis: A Clinical Report
Neenu M Varghese et al Case Report 10.5005/jp-journals-10012-1148 A Novel Technique for the Management of a Maxillary Anterior Alveolar Defect with an Implant-retained Fixed Prosthesis: A Clinical Report
Versatile grafting Solutions
 Versatile grafting Solutions A Canadian company serving Canadian dentists since 1997 Here s why your colleagues are calling us for their bone regeneration needs Founded in 1997 Citagenix has been providing
Versatile grafting Solutions A Canadian company serving Canadian dentists since 1997 Here s why your colleagues are calling us for their bone regeneration needs Founded in 1997 Citagenix has been providing
P105 Predictable Bone Grafting for Site Preparation for Implants and Prosthetics Workshop JAMES GRISDALE, DDS THURSDAY, FEBRUARY 26
 P105 Predictable Bone Grafting for Site Preparation for Implants and Prosthetics Workshop JAMES GRISDALE, DDS THURSDAY, FEBRUARY 26 Please complete the speaker evaluation form in the Midwinter Meeting
P105 Predictable Bone Grafting for Site Preparation for Implants and Prosthetics Workshop JAMES GRISDALE, DDS THURSDAY, FEBRUARY 26 Please complete the speaker evaluation form in the Midwinter Meeting
Contemporary Periodontal Surgery
 Contemporary Periodontal Surgery Chris van Kesteren, D.D.S. CPCC Dental Hygiene Program October 18, 2011 Surgical Management of Periodontitis Periodontal Plastic Surgery Soft tissue and esthetics Dental
Contemporary Periodontal Surgery Chris van Kesteren, D.D.S. CPCC Dental Hygiene Program October 18, 2011 Surgical Management of Periodontitis Periodontal Plastic Surgery Soft tissue and esthetics Dental
Socket preservation in the daily practice: A clinical case report
 Clinical Socket preservation in the daily practice: A clinical case report Rabih Abi Nader 1 and Carine Tabarani 2 Abstract Soft tissue contour depends on the underlying bone anatomy. Following tooth extraction,
Clinical Socket preservation in the daily practice: A clinical case report Rabih Abi Nader 1 and Carine Tabarani 2 Abstract Soft tissue contour depends on the underlying bone anatomy. Following tooth extraction,
Extraction with Immediate Implant Placement and Ridge Preservation in the Posterior
 Extraction with Immediate Implant Placement and Ridge Preservation in the Posterior by Timothy F. Kosinski, DDS, MAGD The following case presentation illustrates the diagnosis, planning and treatment for
Extraction with Immediate Implant Placement and Ridge Preservation in the Posterior by Timothy F. Kosinski, DDS, MAGD The following case presentation illustrates the diagnosis, planning and treatment for
( ) 2009;28(2):89-94
 ( ) 2009;28(2):89-94 Osseointegration is important in the functional aspect, however, esthetics is also important, especially in the maxillary anterior region. An adequate surgical technique is necessary
( ) 2009;28(2):89-94 Osseointegration is important in the functional aspect, however, esthetics is also important, especially in the maxillary anterior region. An adequate surgical technique is necessary
Vertical and Horizontal Ridge Augmentation of a Severely Resorbed Ridge in the Anterior Maxilla
 CASE REPORT Vertical and Horizontal Ridge Augmentation of a Severely Resorbed Ridge in the Anterior Maxilla Alberto Monje,* Florencio Monje, Fernando Suarez,* Raúl González-García, Laura Villanueva-Alcojol,
CASE REPORT Vertical and Horizontal Ridge Augmentation of a Severely Resorbed Ridge in the Anterior Maxilla Alberto Monje,* Florencio Monje, Fernando Suarez,* Raúl González-García, Laura Villanueva-Alcojol,
Implant Site Development Part I
 REVIEW ARTICLE Implant Site Development Part I 1 Umang Nayar, 2 Shankar Iyer IJCID Implant Site Development Part I 1 Consultant, Dental Surgeon and Periodontist at Max Health Care, New Delhi, Professor
REVIEW ARTICLE Implant Site Development Part I 1 Umang Nayar, 2 Shankar Iyer IJCID Implant Site Development Part I 1 Consultant, Dental Surgeon and Periodontist at Max Health Care, New Delhi, Professor
Case Report. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
 Case Report RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
Case Report RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis
 CASE REPORT Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis Dr Ashish Yadav 1, Dr Aratee Gupta 2, Dr Archana Singh 3, 1,3-
CASE REPORT Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis Dr Ashish Yadav 1, Dr Aratee Gupta 2, Dr Archana Singh 3, 1,3-
Limited bone availability makes implant placement challenging
 Bone Grafting: Essential Indications and Techniques in Implant Dentistry Limited bone availability makes implant placement challenging and sometimes unpredictable. Candidates for implant therapy must have
Bone Grafting: Essential Indications and Techniques in Implant Dentistry Limited bone availability makes implant placement challenging and sometimes unpredictable. Candidates for implant therapy must have
Horizontal bone augmentation by means of guided bone regeneration
 Periodontology 2000, Vol. 66, 2014, 13 40 2014 John Wiley & Sons A/S. Published by John Wiley & Sons Ltd Printed in Singapore. All rights reserved PERIODONTOLOGY 2000 Horizontal bone augmentation by means
Periodontology 2000, Vol. 66, 2014, 13 40 2014 John Wiley & Sons A/S. Published by John Wiley & Sons Ltd Printed in Singapore. All rights reserved PERIODONTOLOGY 2000 Horizontal bone augmentation by means
INTERNATIONAL MEDICAL COLLEGE
 INTERNATIONAL MEDICAL COLLEGE Joint Degree Master Program: Implantology and Dental Surgery (M.Sc.) Specialized Modules: List of individual modules Specialized Module 1 Basic principles of implantology
INTERNATIONAL MEDICAL COLLEGE Joint Degree Master Program: Implantology and Dental Surgery (M.Sc.) Specialized Modules: List of individual modules Specialized Module 1 Basic principles of implantology
Biomaterials Line. MIS Corporation. All Rights Reserved.
 7. Biomaterials Line MIS Corporation. All Rights Reserved. 6. MIS s Quality System complies with international quality standards: ISO 13485: 2003 - Quality Management System for Medical Devices, ISO 9001:
7. Biomaterials Line MIS Corporation. All Rights Reserved. 6. MIS s Quality System complies with international quality standards: ISO 13485: 2003 - Quality Management System for Medical Devices, ISO 9001:
The Sandwich Bone Augmentation Technique. Jia-Hui Fu* and Hom-Lay Wang*
 CASE REPORT The Sandwich Bone Augmentation Technique Jia-Hui Fu* and Hom-Lay Wang* Introduction: Horizontal ridge width reduction after tooth extraction is a common clinical scenario. As such, when implant-supported
CASE REPORT The Sandwich Bone Augmentation Technique Jia-Hui Fu* and Hom-Lay Wang* Introduction: Horizontal ridge width reduction after tooth extraction is a common clinical scenario. As such, when implant-supported
Guided Tissue and Bone Regeneration
 Guided Tissue and Bone Regeneration One toolbox for your needs! Tefguide 9000 742 401 12x24 mm pc 1 Osgide 9000 701 520 15 x 20 mm pc 1 Osbone 9000 800 255 250-1000 μm 0.25 cc 5 Product Specifications
Guided Tissue and Bone Regeneration One toolbox for your needs! Tefguide 9000 742 401 12x24 mm pc 1 Osgide 9000 701 520 15 x 20 mm pc 1 Osbone 9000 800 255 250-1000 μm 0.25 cc 5 Product Specifications
Thick vs. Thin Gingival Biotypes: A Key Determinant in Treatment Planning for Dental Implants
 r s Thick vs. Thin Gingival Biotypes: A Key Determinant in Treatment Planning for Dental Implants richard t. kao, dds, phd; mark c. fagan, ms, dds; and gregory j. conte, ms, dmd abstract During the treatment
r s Thick vs. Thin Gingival Biotypes: A Key Determinant in Treatment Planning for Dental Implants richard t. kao, dds, phd; mark c. fagan, ms, dds; and gregory j. conte, ms, dmd abstract During the treatment
The Original remains unique.
 The Original remains unique. Geistlich leading regeneration 2A, 2B Geistlich is the world leader in regenerative dentistry. We transform natural biomaterials into safe and reliable treatment methods that
The Original remains unique. Geistlich leading regeneration 2A, 2B Geistlich is the world leader in regenerative dentistry. We transform natural biomaterials into safe and reliable treatment methods that
Consensus Report Tissue augmentation and esthetics (Working Group 3)
 B. Klinge Thomas F. Flemmig Consensus Report Tissue augmentation and esthetics (Working Group 3) Members of working group: Matteo Chiapasco Jan-Eirik Ellingsen Ronald Jung Friedrich Neukam Isabella Rocchietta
B. Klinge Thomas F. Flemmig Consensus Report Tissue augmentation and esthetics (Working Group 3) Members of working group: Matteo Chiapasco Jan-Eirik Ellingsen Ronald Jung Friedrich Neukam Isabella Rocchietta
THE NEW STANDARD OF EXCELLENCE IN BIOMATERIALS. Collagenated heterologous cortico-cancellous bone mix + TSV Gel GTO I N S P I R E D B Y N A T U R E
 GTO THE NEW STANDARD OF EXCELLENCE IN BIOMATERIALS Collagenated heterologous cortico-cancellous bone mix + TSV Gel R E G E N E R A T I O N S C I E N C E I N S P I R E D B Y N A T U R E A unique biotechnology
GTO THE NEW STANDARD OF EXCELLENCE IN BIOMATERIALS Collagenated heterologous cortico-cancellous bone mix + TSV Gel R E G E N E R A T I O N S C I E N C E I N S P I R E D B Y N A T U R E A unique biotechnology
REFERENCES for PLATELET RICH PLASMA (PRP)
 REFERENCES for PLATELET RICH PLASMA (PRP) Daif ET. Autologous blood injection as a new treatment modality for chronic recurrent temporomandibular joint dislocation. Oral Surg Oral Med Oral Pathol Oral
REFERENCES for PLATELET RICH PLASMA (PRP) Daif ET. Autologous blood injection as a new treatment modality for chronic recurrent temporomandibular joint dislocation. Oral Surg Oral Med Oral Pathol Oral
Bone augmentation with maxgraft
 Patient information bone & tissue regeneration botiss biomaterials Bone augmentation with maxgraft established safe X100 natural Implantation stability is crucial for success Atrophy of the jaw bone loss
Patient information bone & tissue regeneration botiss biomaterials Bone augmentation with maxgraft established safe X100 natural Implantation stability is crucial for success Atrophy of the jaw bone loss
REGENERATIONTIME. A Case Report by. Ridge Augmentation and Delayed Implant Placement on an Upper Lateral Incisor
 A Case Report by Dr. Daniele Cardaropoli Ridge Augmentation and Delayed Implant Placement on an Upper Lateral Incisor The Situation An adult female patient presented with an endodontic/prosthetic failure
A Case Report by Dr. Daniele Cardaropoli Ridge Augmentation and Delayed Implant Placement on an Upper Lateral Incisor The Situation An adult female patient presented with an endodontic/prosthetic failure
Vertical Bone Augmentation for Implant Placement in the Mandible a Systematic. Review
 Vertical Bone Augmentation for Implant Placement in the Mandible a Systematic Review A dissertation submitted to the University of Manchester for the degree of Master of Science in Dentistry (Oral and
Vertical Bone Augmentation for Implant Placement in the Mandible a Systematic Review A dissertation submitted to the University of Manchester for the degree of Master of Science in Dentistry (Oral and
Sinus Augmentation Studies Methods and Definition
 FDA approved indications for Infuse Bone Graft in the Maxillofacial Skeleton Alveolar Ridge Augmentation (Buccal Wall Defects) in the Maxilla Maxillary Sinus Floor augmentation Sinus Augmentation Studies
FDA approved indications for Infuse Bone Graft in the Maxillofacial Skeleton Alveolar Ridge Augmentation (Buccal Wall Defects) in the Maxilla Maxillary Sinus Floor augmentation Sinus Augmentation Studies
Alveolar Ridge Augmentation with Titanium Mesh and Particulate Allograft A Case Report
 Alveolar Ridge Augmentation with Titanium Mesh and Particulate Allograft A Case Report Dr. Pratibha Borasi, Dr. Praneeta Kamble Department of Periodontics, Nair Hospital Dental College, Mumbai, Maharashtra,
Alveolar Ridge Augmentation with Titanium Mesh and Particulate Allograft A Case Report Dr. Pratibha Borasi, Dr. Praneeta Kamble Department of Periodontics, Nair Hospital Dental College, Mumbai, Maharashtra,
The Use of Freeze-Dried Bone Allograft as an Alternative to Autogenous Bone Graft in the Atrophic Maxilla: A 3-Year Clinical Follow-up
 643 The Use of Freeze-Dried Bone Allograft as an Alternative to Autogenous Bone Graft in the Atrophic Maxilla: A 3-Year Clinical Follow-up Marco Aurélio Bianchini, DDS, MSc, PhD 1 André R. Buttendorf,
643 The Use of Freeze-Dried Bone Allograft as an Alternative to Autogenous Bone Graft in the Atrophic Maxilla: A 3-Year Clinical Follow-up Marco Aurélio Bianchini, DDS, MSc, PhD 1 André R. Buttendorf,
Vertical and Horizontal Augmentation Using Guided Bone Regeneration. Ph.D. Thesis. Dr. med. dent. et univ. Istvan Urban
 Vertical and Horizontal Augmentation Using Guided Bone Regeneration Ph.D. Thesis Dr. med. dent. et univ. Istvan Urban Supervisor: Prof. Dr. Katalin Nagy, DDS, PhD Faculty of Dentistry, University of Szeged
Vertical and Horizontal Augmentation Using Guided Bone Regeneration Ph.D. Thesis Dr. med. dent. et univ. Istvan Urban Supervisor: Prof. Dr. Katalin Nagy, DDS, PhD Faculty of Dentistry, University of Szeged
FDBA(Freeze Dried Bone Allograft) SureOss Cortical Bone - Powder / Chip. OsteOss Cortical with Cancellous Bone - Powder / Chip
 PERIODONTAL Bone & Skin Allograft Products FDBA(Freeze Dried Bone Allograft) SureOss - Powder / Chip OsteOss Cortical with - Powder / Chip DFDBA(Demineralized Freeze Dried Bone Allograft) SureOss -D Demineralized
PERIODONTAL Bone & Skin Allograft Products FDBA(Freeze Dried Bone Allograft) SureOss - Powder / Chip OsteOss Cortical with - Powder / Chip DFDBA(Demineralized Freeze Dried Bone Allograft) SureOss -D Demineralized
botiss dental bone & tissue regeneration biomaterials collacone max Innovative composite matrix socket preservation form-fitting resorbable composite
 dental bone & tissue regeneration botiss biomaterials socket preservation Innovative composite matrix form-fitting resorbable composite 1 botiss regeneration system maxresorb flexbone* collacone.. max
dental bone & tissue regeneration botiss biomaterials socket preservation Innovative composite matrix form-fitting resorbable composite 1 botiss regeneration system maxresorb flexbone* collacone.. max
Clinical Report The Use of Autogenous Bone Grafting With Platelet-Rich Plasma for Alveolar Ridge Reconstruction: A Clinical Report
 The Use of Autogenous Bone Grafting With Platelet-Rich Plasma for Alveolar Ridge Reconstruction: A Ziv Simon, DMD, MSc, and Joseph Friedlich, DDS Abstract Implant dentistry has become an effective and
The Use of Autogenous Bone Grafting With Platelet-Rich Plasma for Alveolar Ridge Reconstruction: A Ziv Simon, DMD, MSc, and Joseph Friedlich, DDS Abstract Implant dentistry has become an effective and
Clinical cases by Dr. Fernando Rojas-Vizcaya. botiss. dental bone & tissue regeneration. biomaterials. strictly biologic
 Clinical cases by Dr. Fernando Rojas-Vizcaya dental bone & tissue regeneration botiss biomaterials strictly biologic botiss BTR system: BONE biologic potential bovine block & granules: pure bone mineral
Clinical cases by Dr. Fernando Rojas-Vizcaya dental bone & tissue regeneration botiss biomaterials strictly biologic botiss BTR system: BONE biologic potential bovine block & granules: pure bone mineral
Osseointegrated dental implant treatment generally
 Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Clinical UM Guideline
 Clinical UM Guideline Subject: Bone Grafts for Dental and Oral Surgical Services Guideline #: 04-201 Current Effective Date: 03/24/2017 Status: Revised Last Review Date: 02/08/2017 Description This document
Clinical UM Guideline Subject: Bone Grafts for Dental and Oral Surgical Services Guideline #: 04-201 Current Effective Date: 03/24/2017 Status: Revised Last Review Date: 02/08/2017 Description This document
Bone augmentation with biomaterials
 Patient information dental bone & tissue regeneration botiss biomaterials Bone augmentation with biomaterials established safe natural X100 Implantation stability is crucial for success Atrophy of the
Patient information dental bone & tissue regeneration botiss biomaterials Bone augmentation with biomaterials established safe natural X100 Implantation stability is crucial for success Atrophy of the
A new approach with an in-situ self-hardening grafting material
 74 Bone grafting with simultaneous early implant placement A new approach with an in-situ self-hardening grafting material MINAS LEVENTIS 1,2, PHD; PETER FAIRBAIRN 1,3, BDS; ORESTIS VASILIADIS 2,4, DDS
74 Bone grafting with simultaneous early implant placement A new approach with an in-situ self-hardening grafting material MINAS LEVENTIS 1,2, PHD; PETER FAIRBAIRN 1,3, BDS; ORESTIS VASILIADIS 2,4, DDS
botiss dental bone & tissue regeneration biomaterials mucoderm 3D-Regenerative Tissue Graft strictly biologic
 dental bone & tissue regeneration botiss biomaterials 3DRegenerative Tissue Graft strictly biologic mucoderm Soft Tissue Graft Indications mucoderm is a collagen tissue matrix derived of animal dermis
dental bone & tissue regeneration botiss biomaterials 3DRegenerative Tissue Graft strictly biologic mucoderm Soft Tissue Graft Indications mucoderm is a collagen tissue matrix derived of animal dermis
MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION
 Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
SOCKET WHETHER TO PRESERVE IT NOW OR TO CREATE LATER? - A CASE REPORT
 MAVEN CASE REPORT SOCKET WHETHER TO PRESERVE IT NOW OR TO CREATE LATER? - A CASE REPORT Dr. Parthasarathi Biswas 1, Dr. Debajyoti Mondal 1, Dr. B Praveena Devi 1, Dr. Indrasri Das 2, Dr. Somen Bagchi 3,
MAVEN CASE REPORT SOCKET WHETHER TO PRESERVE IT NOW OR TO CREATE LATER? - A CASE REPORT Dr. Parthasarathi Biswas 1, Dr. Debajyoti Mondal 1, Dr. B Praveena Devi 1, Dr. Indrasri Das 2, Dr. Somen Bagchi 3,
Puros Cancellous Particulate Allograft & Puros Block Allograft
 Puros Cancellous Particulate Allograft & Puros Block Allograft Puros Cancellous Particulate Allograft The Natural Choice For Healthy 1 Bone Growth. 1. Proven, Predictable Regeneration Acts as an osteoconductive
Puros Cancellous Particulate Allograft & Puros Block Allograft Puros Cancellous Particulate Allograft The Natural Choice For Healthy 1 Bone Growth. 1. Proven, Predictable Regeneration Acts as an osteoconductive
Revisions for CDT 2016
 Revisions for CDT 2016 This document was developed from preliminary actions of the Code Maintenance Committee (CMC). This document has been compared to the CMC meeting notes and the ASCII file. This document
Revisions for CDT 2016 This document was developed from preliminary actions of the Code Maintenance Committee (CMC). This document has been compared to the CMC meeting notes and the ASCII file. This document
Oral Health and Dentistry
 Page 107 to 118 Volume 1 Issue 2 2017 Case Report Oral Health and Dentistry ISSN: 2573-4989 Full Mouth Implants Rehabilitation of a Patient with Ectodermal Dysplasia After 3-Ds Ridge Augmentation and Bilateral
Page 107 to 118 Volume 1 Issue 2 2017 Case Report Oral Health and Dentistry ISSN: 2573-4989 Full Mouth Implants Rehabilitation of a Patient with Ectodermal Dysplasia After 3-Ds Ridge Augmentation and Bilateral
Periimplant Regeneration Fenestration
 Indication Sheet PIR-1 Periimplant Regeneration Fenestration Treatment concept of Dr. Jean-Pierre Gardella (surgeon) and Dr. Christian Richelme (prosthodontist), Marseille, France > Filling of a peri-implant
Indication Sheet PIR-1 Periimplant Regeneration Fenestration Treatment concept of Dr. Jean-Pierre Gardella (surgeon) and Dr. Christian Richelme (prosthodontist), Marseille, France > Filling of a peri-implant
botiss biomaterials bone & tissue regeneration collacone max Innovative composite matrix socket preservation form-fitting resorbable composite
 bone & tissue regeneration botiss biomaterials socket preservation Innovative composite matrix form-fitting resorbable composite 1 Socket preservation safeguarding your sockets collacone.. max flexbone*
bone & tissue regeneration botiss biomaterials socket preservation Innovative composite matrix form-fitting resorbable composite 1 Socket preservation safeguarding your sockets collacone.. max flexbone*
Inion GTR Biodegradable Membrane System
 Inion GTR Biodegradable Membrane System The concept of GTR/GBR Intended use The Inion GTR Biodegradable Membrane System is intended to be used as a barrier membrane in dental guided tissue regeneration
Inion GTR Biodegradable Membrane System The concept of GTR/GBR Intended use The Inion GTR Biodegradable Membrane System is intended to be used as a barrier membrane in dental guided tissue regeneration
Periimplant Regeneration Fenestration
 Indication Sheet PIR Periimplant Regeneration Fenestration Treatment concept of Dr. Jean-Pierre Gardella (surgeon) and Dr. Christian Richelme (prosthodontist), Marseille, France > Filling of a peri-implant
Indication Sheet PIR Periimplant Regeneration Fenestration Treatment concept of Dr. Jean-Pierre Gardella (surgeon) and Dr. Christian Richelme (prosthodontist), Marseille, France > Filling of a peri-implant
Surgical Therapy. Tuesday, April 2, 13. Alessan"o Geminiani, DDS, MS
 Surgical Therapy Alessan"o Geminiani, DDS, MS Periodontal Flap: a surgical procedure in which incisions are made in the gingiva or mucosa to allow for separation of the epithelium and connective tissues
Surgical Therapy Alessan"o Geminiani, DDS, MS Periodontal Flap: a surgical procedure in which incisions are made in the gingiva or mucosa to allow for separation of the epithelium and connective tissues
Maryland AGD AE and Socket Grafting 2015
 The Goodacre Study 5 year retrospective study looked at Crown & Bridge Caries Single crowns 1% FPD abutments 17% Periodontal Involvement Single crowns
The Goodacre Study 5 year retrospective study looked at Crown & Bridge Caries Single crowns 1% FPD abutments 17% Periodontal Involvement Single crowns
Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report
 Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
SHELL TECHNIQUE WITH ALLOGENIC CORTICAL STRUTS
 bone & tissue regeneration botiss biomaterials maxgraft cortico SHELL TECHNIQUE WITH ALLOGENIC CORTICAL STRUTS Surgical guide innovative efficient hard tissue atraumatic 1 Content maxgraft cortico Surgical
bone & tissue regeneration botiss biomaterials maxgraft cortico SHELL TECHNIQUE WITH ALLOGENIC CORTICAL STRUTS Surgical guide innovative efficient hard tissue atraumatic 1 Content maxgraft cortico Surgical
botiss maxgraft bonering botiss maxgraft bonebuilder Because one option is not enough. PROCESSED ALLOGENIC BONERING
 Product Information Allograft Biomaterials@Straumann Because one option is not enough. botiss maxgraft bonering PROCESSED ALLOGENIC BONERING botiss maxgraft bonebuilder CUSTOMIZED ALLOGENIC BONE BLOCK
Product Information Allograft Biomaterials@Straumann Because one option is not enough. botiss maxgraft bonering PROCESSED ALLOGENIC BONERING botiss maxgraft bonebuilder CUSTOMIZED ALLOGENIC BONE BLOCK
hard tissue maxgraft cortico Surgical guide botiss biomaterials innovative efficient atraumatic Prefabricated allogenic bone plate
 bone & tissue regeneration botiss biomaterials maxgraft cortico Prefabricated allogenic bone plate Surgical guide innovative efficient hard tissue atraumatic 1 Content maxgraft cortico Surgical guide 1.
bone & tissue regeneration botiss biomaterials maxgraft cortico Prefabricated allogenic bone plate Surgical guide innovative efficient hard tissue atraumatic 1 Content maxgraft cortico Surgical guide 1.
Patient's Guide to Dental Implants. an investment for a lifelong smile
 Patient's Guide to Dental Implants an investment for a lifelong smile Introduction Genicore is a specialized products and service provider to dental professionals in the United States. Genicore strategically
Patient's Guide to Dental Implants an investment for a lifelong smile Introduction Genicore is a specialized products and service provider to dental professionals in the United States. Genicore strategically
Pre op Failed endodontic treatment with sinus involvement.
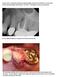 Case #1 of 10 consecutive extraction sockets grafted with Socket Graft Putty, covered with Socket Seal and sealed with Periacryl. I D # HEU This patient is a 66 year old female. Pre op Failed endodontic
Case #1 of 10 consecutive extraction sockets grafted with Socket Graft Putty, covered with Socket Seal and sealed with Periacryl. I D # HEU This patient is a 66 year old female. Pre op Failed endodontic
BUILDING A. Achieving total reconstruction in a single operation. 70 OCTOBER 2016 // dentaltown.com
 BUILDING A MANDI Achieving total reconstruction in a single operation by Dr. Fayette C. Williams Fayette C. Williams, DDS, MD, FACS, is clinical faculty at John Peter Smith Hospital in Fort Worth, Texas,
BUILDING A MANDI Achieving total reconstruction in a single operation by Dr. Fayette C. Williams Fayette C. Williams, DDS, MD, FACS, is clinical faculty at John Peter Smith Hospital in Fort Worth, Texas,
PRP Usage in Today's Implantology
 Volume 1, December 2004 www.implant.co.il PRP Usage in Today's Implantology by Dr. R. Shapira Introduction: Treating patients suffering from hematological disorders or using anticoagulant medications always
Volume 1, December 2004 www.implant.co.il PRP Usage in Today's Implantology by Dr. R. Shapira Introduction: Treating patients suffering from hematological disorders or using anticoagulant medications always
Alpha-Bio's GRAFT complete portfolio bone substitutes resorbable membranes best combination of quality & value with efficient, easy-to-use products
 Alpha-Bio Tec, a world leader in advanced implantology solutions, is proud to present its growing biomaterials product line: Alpha-Bio's GRAFT, which has taken a leading position in the global dental biomaterials
Alpha-Bio Tec, a world leader in advanced implantology solutions, is proud to present its growing biomaterials product line: Alpha-Bio's GRAFT, which has taken a leading position in the global dental biomaterials
Implant Placement in Maxillary Anterior Region Along with Soft and Hard Tissue Grafting- A Case Report.
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 10 Ver. XII (October. 2016), PP 68-73 www.iosrjournals.org Implant Placement in Maxillary Anterior
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 10 Ver. XII (October. 2016), PP 68-73 www.iosrjournals.org Implant Placement in Maxillary Anterior
The International Journal of Periodontics & Restorative Dentistry
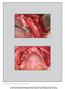 The International Journal of Periodontics & Restorative Dentistry 141 Screw Spreading: Technical Considerations and Case Report Renato Sussumu Nishioka, DDS, PhD, MSc* Alberto Noriyuki Kojima, DDS, PhD,
The International Journal of Periodontics & Restorative Dentistry 141 Screw Spreading: Technical Considerations and Case Report Renato Sussumu Nishioka, DDS, PhD, MSc* Alberto Noriyuki Kojima, DDS, PhD,
RPC. Surgical Solutions USA Regenerative Product Catalog
 RPC Surgical Solutions USA Regenerative Product Catalog RESORBABLE COLLAGEN MEMBRANES (BOVINE) CYTOPLAST RTM Collagen Resorption time of 26-38 weeks RTM1520 $185 15mm x 20mm Membranes per box: 2 RTM2030
RPC Surgical Solutions USA Regenerative Product Catalog RESORBABLE COLLAGEN MEMBRANES (BOVINE) CYTOPLAST RTM Collagen Resorption time of 26-38 weeks RTM1520 $185 15mm x 20mm Membranes per box: 2 RTM2030
Innovative Range of Regenerative Solutions
 TM Innovative Range of Regenerative Solutions MIS Implant Technologies Ltd. All rights reserved. Optimal volumes and quality of hard and soft tissue are required to satisfy the goals of oral rehabilitation
TM Innovative Range of Regenerative Solutions MIS Implant Technologies Ltd. All rights reserved. Optimal volumes and quality of hard and soft tissue are required to satisfy the goals of oral rehabilitation
A Retrospective Analysis of Maxillary Sinuses and Implant Survival after Lateral Window Sinus Augmentation. Marlon Foote, DDS Periodontics
 A Retrospective Analysis of Maxillary Sinuses and Implant Survival after Lateral Window Sinus Augmentation Marlon Foote, DDS Periodontics Boyne, 1980 Maxillary Sinus Augmentations Maxillary sinus augmentation,
A Retrospective Analysis of Maxillary Sinuses and Implant Survival after Lateral Window Sinus Augmentation Marlon Foote, DDS Periodontics Boyne, 1980 Maxillary Sinus Augmentations Maxillary sinus augmentation,
Surgical Solutions USA Regenerative Product Catalog USA
 RPC Surgical Solutions Regenerative Product Catalog RESORBABLE COLLAGEN MEMBRANES (BOVINE) CYTOPLAST RTM Collagen Resorption time of 26-38 weeks RTM1520 $185 15mm x 20mm Membranes per box: 2 RTM2030 $230
RPC Surgical Solutions Regenerative Product Catalog RESORBABLE COLLAGEN MEMBRANES (BOVINE) CYTOPLAST RTM Collagen Resorption time of 26-38 weeks RTM1520 $185 15mm x 20mm Membranes per box: 2 RTM2030 $230
EDI Journal. Augmentation Techniques the Basis of Aesthetic Success in Implant Dentistry. European Journal for Dental Implantologists
 EDI Journal European Journal for Dental Implantologists Augmentation Techniques the Basis of Aesthetic Success in Implant Dentistry A Contribution by Dr. Claudio Cacaci, Munich, Germany Kindly offered
EDI Journal European Journal for Dental Implantologists Augmentation Techniques the Basis of Aesthetic Success in Implant Dentistry A Contribution by Dr. Claudio Cacaci, Munich, Germany Kindly offered
Study Cases: Ride Augmentation Bone by Grafting and PRP/Preparation for Dental Implants Placement
 Cronicon OPEN ACCESS EC DENTAL SCIENCE Case Report Study Cases: Ride Augmentation Bone by Grafting and PRP/Preparation for Dental Implants Placement Farzat Alksiri* Implantologist, German Board of Oral
Cronicon OPEN ACCESS EC DENTAL SCIENCE Case Report Study Cases: Ride Augmentation Bone by Grafting and PRP/Preparation for Dental Implants Placement Farzat Alksiri* Implantologist, German Board of Oral
Predictable Synthetic Bone Grafting Procedures for Implant Reconstruction: Part Two
 CLINICAL ARTICLE IJCID Predictable Synthetic Bone Grafting Procedures for Implant Reconstruction: Part Two Predictable Synthetic Bone Grafting Procedures for Implant Reconstruction: Part Two 1 Scott D
CLINICAL ARTICLE IJCID Predictable Synthetic Bone Grafting Procedures for Implant Reconstruction: Part Two Predictable Synthetic Bone Grafting Procedures for Implant Reconstruction: Part Two 1 Scott D
Posterior mandible and vertical augmentation
 CASE REPORT Bilateral Vertical Ridge Augmentation With Block Grafts and Guided Bone Regeneration in the Posterior Mandible: A Case Report Maria A. Peñarrocha* Jose A. Vina Laura Maestre David Peñarrocha-Oltra
CASE REPORT Bilateral Vertical Ridge Augmentation With Block Grafts and Guided Bone Regeneration in the Posterior Mandible: A Case Report Maria A. Peñarrocha* Jose A. Vina Laura Maestre David Peñarrocha-Oltra
Techniques for the use of autogenous bone grafting to minimize morbidity and increase treatment outcome
 Front Cover Bone Symposium 2014 Dear Colleague, I want to personally invite you to attend the Pikos Institute sponsored Bone Symposium 2014. This one of a kind program will feature 12 of the world s master
Front Cover Bone Symposium 2014 Dear Colleague, I want to personally invite you to attend the Pikos Institute sponsored Bone Symposium 2014. This one of a kind program will feature 12 of the world s master
Long-term success for osteointegrated
 CASE REPORT Symphyseal Bone Cylinders Tapping With the Dental Implant Into Insufficiency Bone Situated Esthetic Area at One-Stage Surgery: A Case Report and the Description of the New Technique Umut Tekin,
CASE REPORT Symphyseal Bone Cylinders Tapping With the Dental Implant Into Insufficiency Bone Situated Esthetic Area at One-Stage Surgery: A Case Report and the Description of the New Technique Umut Tekin,
Maxillary sinus augmentation without any graft material- A case Report
 A CASE REPORT ISSN: 2321-4988 D.Shiva kumar et al. /JPR:BioMedRx: An International Journal 2013,1(8), Available online through www.jpronline.info Maxillary sinus augmentation without any graft material-
A CASE REPORT ISSN: 2321-4988 D.Shiva kumar et al. /JPR:BioMedRx: An International Journal 2013,1(8), Available online through www.jpronline.info Maxillary sinus augmentation without any graft material-
BioVin Collagen Membrane
 BioVin Collagen Membrane Resorbable cross-linked collagen membrane BioVin Bovine Bone Bovine Bone Substitute OToss Synthetic Bone Synthetic Resorbable Biphasic Calcium Phosphate OToss Synthetic Bone Inject
BioVin Collagen Membrane Resorbable cross-linked collagen membrane BioVin Bovine Bone Bovine Bone Substitute OToss Synthetic Bone Synthetic Resorbable Biphasic Calcium Phosphate OToss Synthetic Bone Inject
CASE REPORT. CBCT-Assisted Treatment of the Failing Long Span Bridge with Staged and Immediate Load Implant Restoration
 Computer Aided Implantology Academy Newsletter - Newsletter 20 - July 2009 CASE REPORT CBCT-Assisted Treatment of the Failing Long Span Bridge with Staged and Immediate Load Implant Restoration Case Report
Computer Aided Implantology Academy Newsletter - Newsletter 20 - July 2009 CASE REPORT CBCT-Assisted Treatment of the Failing Long Span Bridge with Staged and Immediate Load Implant Restoration Case Report
Developments in bone grafting in veterinary orthopaedics part one
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk Developments in bone grafting in veterinary orthopaedics part one Author : John Innes, Peter Myint Categories : Vets Date
Vet Times The website for the veterinary profession https://www.vettimes.co.uk Developments in bone grafting in veterinary orthopaedics part one Author : John Innes, Peter Myint Categories : Vets Date
Alveolar Ridge Preservation:
 Alveolar Ridge Preservation: Preserving and Building up the Bony Structures after Extraction» By: Prof. Roland Hille Konigsallee 49c, 41747 Viersen, Germany E-mail: dr-hille@t-online.de» Prof. Rolf Vollmer
Alveolar Ridge Preservation: Preserving and Building up the Bony Structures after Extraction» By: Prof. Roland Hille Konigsallee 49c, 41747 Viersen, Germany E-mail: dr-hille@t-online.de» Prof. Rolf Vollmer
OSSIX PLUS The Resorbable Collagen Membrane Instructions for Use for OSSIX PLUS
 OSSIX PLUS The Resorbable Collagen Membrane Instructions for Use for OSSIX PLUS DESCRIPTION OSSIX PLUS is a biodegradable and biocompatible collagen membrane intended for use during the process of guided
OSSIX PLUS The Resorbable Collagen Membrane Instructions for Use for OSSIX PLUS DESCRIPTION OSSIX PLUS is a biodegradable and biocompatible collagen membrane intended for use during the process of guided
Bone Grafting and Immediate Implant Placement in the Anterior
 Bone Grafting and Immediate Implant Placement in the Anterior by Timothy F. Kosinski, DDS, MAGD Whether a consequence of periodontal disease, caries or trauma to the root, losing an anterior tooth is psychologically
Bone Grafting and Immediate Implant Placement in the Anterior by Timothy F. Kosinski, DDS, MAGD Whether a consequence of periodontal disease, caries or trauma to the root, losing an anterior tooth is psychologically
Symbios Xenograft Granules Porcine Bone Graft Material
 Symbios Xenograft Granules Porcine Bone Graft Material 32671122-USX-1607_Symbios Highlight Brochure.indd 1 2016-09-27 12:12 Symbios Xenograft Granules Porcine bone graft material Symbios Xenograft Granules
Symbios Xenograft Granules Porcine Bone Graft Material 32671122-USX-1607_Symbios Highlight Brochure.indd 1 2016-09-27 12:12 Symbios Xenograft Granules Porcine bone graft material Symbios Xenograft Granules
Inion BioRestore. Bone Graft Substitute. Product Overview
 Inion BioRestore Bone Graft Substitute Product Overview Inion BioRestore Introduction Inion BioRestore is a synthetic bone graft substitute, which remodels into bone and is easy to use. Inion BioRestore
Inion BioRestore Bone Graft Substitute Product Overview Inion BioRestore Introduction Inion BioRestore is a synthetic bone graft substitute, which remodels into bone and is easy to use. Inion BioRestore
Innovative Treatment Concepts IN ORAL AND MAXILLOFACIAL SURGERY
 Innovative Treatment Concepts IN ORAL AND MAXILLOFACIAL SURGERY LEADING REGENERATION CLINICAL CASES Dr. J. Aranda Onlay grafting for horizontal augmentation 8 Prof. Dr. D. Buser et al. Onlay grafting for
Innovative Treatment Concepts IN ORAL AND MAXILLOFACIAL SURGERY LEADING REGENERATION CLINICAL CASES Dr. J. Aranda Onlay grafting for horizontal augmentation 8 Prof. Dr. D. Buser et al. Onlay grafting for
(Images are at the end of article)
 Long term provisionalization during periodontal surgery and extraction site tissue grafting: A Case Review Michael Tischler, DDS Diplomate American Board Of Oral Implantology/Implant Dentistry (Images
Long term provisionalization during periodontal surgery and extraction site tissue grafting: A Case Review Michael Tischler, DDS Diplomate American Board Of Oral Implantology/Implant Dentistry (Images
Guided surgery as a way to simplify surgical implant treatment in complex cases
 52 STARGET 1 I 12 StraUMaNN CareS r ry vincenzo MiriSOLA Di TOrreSANTO AND LUCA COrDArO Guided surgery as a way to simplify surgical implant treatment in complex cases Background A 41-year-old woman with
52 STARGET 1 I 12 StraUMaNN CareS r ry vincenzo MiriSOLA Di TOrreSANTO AND LUCA COrDArO Guided surgery as a way to simplify surgical implant treatment in complex cases Background A 41-year-old woman with
Citagenix Catalogue 2017 ALLOGRAFTS BONE SUBSTITUTES BONE GRANULES & BLOCKS RESORBABLE MEMBRANES
 Citagenix Catalogue 2017 ALLOGRAFTS BONE SUBSTITUTES BONE GRANULES & BLOCKS RESORBABLE MEMBRANES 100% Allograft Hydratable Inductive Matrix NEW Create your customized osteoinductive graft by combining
Citagenix Catalogue 2017 ALLOGRAFTS BONE SUBSTITUTES BONE GRANULES & BLOCKS RESORBABLE MEMBRANES 100% Allograft Hydratable Inductive Matrix NEW Create your customized osteoinductive graft by combining
The healthy natural tooth AMODIFIED SOCKET SEAL SURGERY WITH COMPOSITE GRAFT APPROACH CLINICAL
 CLINICAL fil AMODIFIED SOCKET SEAL SURGERY WITH COMPOSITE GRAFT APPROACH Carl E. Misch, DDS, MDS Francine Dietsh-Misch, DDS, MDS Craig M. Misch, DDS, MDS KEY WORDS Bone contour Socket seal Composite graft
CLINICAL fil AMODIFIED SOCKET SEAL SURGERY WITH COMPOSITE GRAFT APPROACH Carl E. Misch, DDS, MDS Francine Dietsh-Misch, DDS, MDS Craig M. Misch, DDS, MDS KEY WORDS Bone contour Socket seal Composite graft
Clinical UM Guideline
 Clinical UM Guideline Subject: Biological Materials to Aid in Soft and Hard Tissue Grafting Guideline #: 03-401 Current Effective Date: 03/24/2017 Status: New Last Review Date: 02/08/2017 Description This
Clinical UM Guideline Subject: Biological Materials to Aid in Soft and Hard Tissue Grafting Guideline #: 03-401 Current Effective Date: 03/24/2017 Status: New Last Review Date: 02/08/2017 Description This
The International Journal of Periodontics & Restorative Dentistry
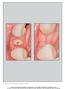 The International Journal of Periodontics & Restorative Dentistry 67 Efficacy Evaluation of a New Buccal Bone Plate Preservation Technique: A Pilot Study Federico Brugnami, DDS* Alfonso Caiazzo, DDS**
The International Journal of Periodontics & Restorative Dentistry 67 Efficacy Evaluation of a New Buccal Bone Plate Preservation Technique: A Pilot Study Federico Brugnami, DDS* Alfonso Caiazzo, DDS**
