Treatment of edentulous patients by means of
|
|
|
- Stephany Atkinson
- 6 years ago
- Views:
Transcription
1 Rehabilitation of Patients With Severely Resorbed Maxillae by Means of Implants With or Without Bone Grafts. A 1-Year Follow-up Study Göran Widmark, LDS, Odont Dr*/Bernt Andersson, LDS, Odont Dr**/ Bengt Andrup, LDS***/Gunnar E. Carlsson, LDS, Odont Dr, Dr Odont hc****/ Carl-Johan Ivanoff, LDS*****/Ann Marie Lindvall, LDS, Odont Dr****** Forty-three patients with severely resorbed maxillae who had been referred for implant treatment were assigned to one of three treatment groups: bone grafting and implant placement (graft group); modified implant placement but no bone grafting (trial group); or optimized complete dentures (no-implant group). Sixteen, 20, and 7 patients, respectively, were assigned to the three groups. At the 1-year follow-up, 10% of the implants had been lost. Only a few of the failures (3/22) occurred after prosthesis placement. The cumulative success rates were 83% in the graft group and 96% in the trial group. A substantial reduction of the grafted bone, especially of the onlay grafts, occurred in many patients. During the period from prosthesis connection to the 1-year follow-up, marginal peri-implant bone loss was on average 0.5 mm. Despite the often demanding procedures involved, all but one patient in each implant group said that they would undergo the treatment again. Most patients were very satisfied with the treatment outcome and their improved masticatory ability. Those who had renounced implant treatment appeared modestly adapted to their optimized dentures, but reported retention problems and less satisfaction with mastication. (INT J ORAL MAXILLOFAC IMPLANTS 1998;13: ) Key words: bone resorption, bone transplant, dental implants, oral radiography, osseointegration Treatment of edentulous patients by means of implant-supported prostheses according to the osseointegration concept has proved to be a very successful method. Success in the treatment of jaws with ******Head, Department of Oral and Maxillofacial Surgery, Bohus County Public Dental Service, Mölndal Hospital, Mölndal, Sweden. ******Head, Clinic of SIM-Prosthetic Dentistry, Bohus County Public Dental Service, Mölndal Hospital, Mölndal, Sweden. ******Senior Prosthodontist, Clinic of SIM-Prosthetic Dentistry, Bohus County Public Dental Service, Mölndal Hospital, Mölndal, Sweden. ******Professor Emeritus, Department of Prosthetic Dentistry, Göteborg University, Göteborg, Sweden. ******Oral Surgeon, Department of Oral and Maxillofacial Surgery, Bohus County Public Dental Service, Mölndal Hospital, Mölndal, Sweden. ******Head, Department of Oral Radiology, Bohus County Public Dental Service, Mölndal Hospital, Mölndal, Sweden. Reprint requests: Dr Göran Widmark, Department of Oral and Maxillofacial Surgery, Bohus County Public Dental Service, Mölndal Hospital, SE Mölndal, Sweden. little to moderate resorption has led to attempts to rehabilitate jaws with more extensive bone loss. Even severely resorbed edentulous mandibles can be treated in a predictable way. 1 3 However, the results of implant treatment in the maxilla under similar conditions have not always been as satisfactory. Conventional implant procedures have thus been considered inappropriate for the treatment of severely reduced maxillary bone. 4 7 To compensate for severe maxillary resorption, two principally different types of treatment have been proposed: (a) augmentation techniques, eg, bone grafting (for a review, see Tolman 8 ), and (b) modifications of the conventional implant method, eg, a modified drilling technique or placement of implants in the maxillary tuberosity. 5,9 A variety of reconstructive procedures combining bone grafting with endosseous implants have therefore been developed The results available today of most of the presented methods are primarily short-term. In a recent extensive review, Tolman concluded that detailed follow-up studies are necessary for continued advancement of bone graft techniques utilizing implants. 8p Volume 13, Number 4, 1998
2 The aims of this study were to evaluate, both clinically and radiographically, the results of implant treatment in patients with severely resorbed maxillae with and without bone grafting, and to compare the use of bone grafting with other modifications of the conventional implant technique. This investigation reports the 1-year outcome with respect to implant and bone graft survival, peri-implant bone resorption, prosthodontic rehabilitation, and patient assessment of the treatment. Materials and Methods The patients in this study were selected from those who, during a specified time period, were referred to the Clinic of SIM-Prosthetic Dentistry, Mölndal, Sweden, for implant treatment in the maxilla. After radiographic examination, all patients who were judged to have insufficient bone for conventional implant placement were presented with three treatment options: a grafting procedure combined with implants (graft group), modified implant placement but no bone grafting (trial group), or optimized complete denture (no-implant group). Detailed information about the various treatment possibilities and risks was given to all patients, who were then invited to discuss their preferences with the specialists involved (oral surgeon and prosthodontist). The radiologist s evaluation of the maxillary bone anatomy with regard to the prerequisites for the alternatives was included in the information provided. After these discussions, 16 patients were assigned to the graft group and 20 to the trial group; the remaining 7 renounced any implant treatment and were assigned to the no-implant group. The age and gender distributions of the patients are presented in Table 1. The distribution of the patients according to the opposing dentition is given in Table 2. The majority of the patients had natural teeth in the mandible, even though the dentition often was reduced. A few had various types of prosthetic restorations (Table 2). The study was designed according to the Declaration of Helsinki and accepted by the Ethical Committee, Medical Faculty, Göteborg University. Radiographic Examination. A radiographic examination of all patients was performed preoperatively using intraoral, lateral, and panoramic radiographs and serial tomography with either spiral movement or with the Scanora technique. 13 The maxillary bone was examined with respect to pathologic changes and shape of the jawbone. The following measurements were performed for evaluation of the residual bone quantity: (1) the distance from the nasal floor to the crest of the ridge in the anterior region; (2) the bone height from the nasal or sinus floor to a Table 1 Age and Gender Distribution of the Patients in the Three Treatment Groups Treatment group Graft Trial No implant Age (y) M F M F M F Total > Total M = male; F = female. Table 2 Patient Distribution According to Opposing Dentition Treatment group Natural teeth FISP CD Graft (n = 16) 15* 1 Trial (n = 20) 13** 7 No implant (n = 7) 06 1 FISP = fixed full-arch implant-supported prosthesis; CD = complete denture. *Two patients also had a removable partial denture. **One patient also had a fixed partial implant-supported prosthesis. Three patients also had a removable partial denture; two patients also had a fixed partial implant-supported prosthesis. level where the bone had a width of 4 mm in a buccopalatal direction; and (3) the horizontal distance from the most anterior sinus wall to the midline (if this distance was less than 13 mm, it was recorded as short). The postoperative radiographic examination included all of these techniques except tomography, supplemented with oblique lateral views, one from each side. The postoperative exam was performed after bone grafting, after placement of the implants, after abutment connection, immediately after placement of the prosthesis, and at the 1-year follow-up. Reduction of the height and width of the bone graft was evaluated. The marginal bone level was measured in relation to the junction between the implant and the abutment. The marginal peri-implant bone loss was defined as the difference between the level at the time of prosthesis placement and at the 1-year follow-up. Surgical Procedure. The maxillary jawbone was exposed through an incision in the buccal sulcus of the patients to have onlay grafting (Fig 1); otherwise, a crestal incision was used. In the one-stage procedure, the graft was fixed and the implants were placed simultaneously. The graft was held in place manually and with consecutively placed guide indicators (Nobel Biocare, Göteborg, Sweden). In the two- The International Journal of Oral & Maxillofacial Implants 475
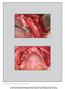
3 Fig 1 Thin maxilla before grafting. Fig 2 Buccal onlay graft placed with microscrews. Fig 3 Buccal onlay graft packed with cancellous bone chips. stage procedure, the graft was held in place with microscrews (Leibinger, Würzburg, Germany) in the onlay patients (Figs 2 and 3), and with a stainless steel wire in the patients having sinus or nasal inlays. The grafting operations were performed under general anesthesia, supplemented with local anesthesia (Lidocain Adrenalin 2%, Astra, Södertälje, Sweden). Most of the patients in the trial group were under local anesthesia with sedation during surgery (Diazepam Stesolid, 0.3 mg/kg body weight). The bone harvesting from the iliac crest was performed as described by Isaksson and Alberius, 14 but involved the medial corner of the crest, including a cm bone portion containing both cortical and spongeous bone. The graft was placed with its compact part cranially in sinus or nasal inlay situations, and with its v shape placed caudally over the crest when the onlay technique was used. In the two-stage procedure, a healing time of 3 to 4 months was allowed prior to implant placement. A patient presentation of the two-stage procedure is shown in Figs 4a to 4f. In the trial group, the maxillary bone was exposed, and the crest was prepared for implant placement and for unconventional approaches, such as the acceptance of free implant threads to be covered with bone chips and membranes for guided tissue regeneration; for unusual implant positions, eg, buccal to the incisive canal; and for small-diameter implants. The types and sizes of the implants placed are presented in Table 3. In 15 of the patients, the implants were placed in the second premolar, canine, and central incisor regions, while the lateral incisor region was used instead of the central incisor region in the remaining 5 patients. One patient had one implant placed in a second molar region instead of the premolar region. One-stage grafting procedures were most common. In 11 patients, the graft and implants were placed simultaneously (10 onlay and 1 onlay + bilateral sinus inlay). A two-stage procedure was performed in 5 patients (3 unilateral sinus inlays, 1 unilateral onlay, 1 nasal inlay + bilateral sinus inlay). Of the 221 implants placed, 201 were placed at the time of bone grafting, and 20 were placed secondarily in the consolidated grafts (3 to 4 months after grafting). The distribution of bone quality and quantity is shown in Table 4. Prosthodontic Procedure. After surgery, the patients who had undergone bone grafting were not allowed to wear their dentures for 8 weeks, after which they were provided with a new maxillary denture. Patients in the trial group were without dentures for 2 weeks prior to resumption of the use of their original dentures relined with a tissue conditioner. The soft tissues and dentures were checked regularly during the healing period, and when neces- 476 Volume 13, Number 4, 1998
4 Figs 4a to 4f Presentation of maxillary grafting combined with implants. Fig 4a Buccal onlay graft fixed with microscrews. Fig 4b Remodeling of graft after 4 months. Fig 4c (Above) Implant placement in the graft after a 4-month healing period. Fig 4d (Right) Radiographic view of the implants. Fig 4e Status after abutment placement, 6 months after implant placement. Fig 4f Prosthetic reconstruction with an implant-supported fixed partial denture in the maxilla. The International Journal of Oral & Maxillofacial Implants 477
5 Table 3 Distribution of Placed Brånemark Implants with Respect to Diameter, Type, Length, and Failure Graft group Trial group Length (mm) Placed Failed Placed Failed Diameter (mm) Self-tapping Mark II Total Table 4 Distribution in the Treatment Groups of Bone Quality and Quantity According to Lekholm and Zarb 17 Bone quantity Treatment group Bone quality B C D E Total Graft 1 2 1* ** 5 9 Total Trial Total No implant Total *6/6 implants lost. **6/28 implants lost. 5/35 implants lost. 2/38 implants lost. 7/67 implants lost. 478 Volume 13, Number 4, 1998
6 sary, the dentures were adjusted and/or relined. Abutment connection was performed 6 to 8 months after implant placement in all patients in both groups. The prosthetic treatment was started about 1 week later and primarily followed the standard protocol of the Brånemark system. 15 The aim was to provide the patients with a fixed implant-supported prosthesis, but when the situation was unsuitable, for example because of an insufficient number of implants and/or unfavorable implant location, an overdenture was chosen. Fixed prostheses were more common among the implant-supported reconstructions than overdentures (13:3 in the graft group and 15:5 in the trial group). The fixed prostheses were made with a cast gold alloy frame and acrylic resin teeth and bases (Fig 4f). The overdentures were fabricated of acrylic resin and a cast cobalt-chromium framework. The retention system consisted of bars between the implants and clip attachments (Nobel Biocare) placed in the dentures. A balanced occlusion concept was the goal, as far as possible, for the overdentures, while a group contact occlusion without balancing side contacts was applied for the fixed prostheses. Examinations. Patients in the implant groups were clinically examined according to a specified protocol at the time of connection of the prosthesis and at the follow-up each year thereafter. Clinical recordings comprised assessment of soft tissues around the implants, bleeding on probing, occlusion and wear of the artificial teeth, and any failures and/or complications related to implants and prostheses. At the 1- year follow-up, patients were asked to answer a few questions about treatment outcome. Pretreatment and current masticatory ability were assessed by means of a visual analog scale (VAS) graded 0 to 10. The follow-up examination was performed by a specialist in prosthodontics who had not participated in the treatment. Patients in the no-implant group were not clinically examined after 1 year, but interviewed by telephone using the same questionnaire given to the implant patients. When evaluating success and failure, the criteria suggested by Albrektsson et al 16 were followed. Results Evaluation of Bone Quality and Quantity. The radiographic evaluation showed that only 1 patient in the trial group and none in the graft group had an anterior residual ridge with a dimension large enough to accommodate a 7-mm implant. A bone height from the nasal floor to a level where the bone was 4 mm in the buccopalatal direction was extremely reduced (less than 4 mm) in 1 patient in the trial group and in 11 patients in the graft group. In 3 patients (2 in the trial and 1 in the graft group), the distance from the anterior wall of the sinus to the midline was very small (less than 13 mm). The classification of the quality and quantity of the maxillary bone according to Lekholm and Zarb 17 (Table 4) showed that the patients in the graft group, on average, exhibited more severe bone loss than those in the trial group (median values D 4 and D 3, respectively). Implant Survival. At the 1-year follow-up, 22 (10%) of 221 placed implants had failed, 17 (17%) in the graft group and 5 (4%) in the trial group. Most of the failures were observed at the time of abutment operation, and only 3 implants were lost after connection of the prosthesis. The life table analysis showed the cumulative success rate (CSR) to be 83% in the graft group and 96% in the trial group. Failure rates of the implants placed in the one-stage and twostage procedures in the graft group were 5% (10 of 201) and 20% (4 of 20), respectively. Failures in the graft group occurred in 4 patients. One patient in the graft group lost all 6 implants, but had a new operation in which 7 implants were placed. Two patients in the trial group have been treated with bone grafts after implant losses. Most failures involved shorter implants (Table 3). All implant losses occurred in D and E quality bone (Table 4). Bone Graft. Marked reduction of the volume of the bone grafts occurred in all grafted patients (Figs 4a and 4b). This was first observed during the period immediately following grafting surgery. At the 1-year follow-up, more than one half the height of the graft had disappeared in 9 of the 12 patients with onlays. In 4 of these patients, no or only minor parts of the graft remained. A similarly extensive loss of bone was seen from the buccal side. The bone loss of inlay grafts was less extensive; 4 of the 5 patients with inlays had two thirds or more of the graft left at the 1-year follow-up. One patient completely lost his bilateral sinus inlays. Marginal Bone Level and Peri-implant Bone Loss. The bone level was on average 2.9 mm apical to the implant-abutment junction at the time of prosthesis placement, without any significant difference between the graft and trial group. The range was large in both groups (0.5 to 10.0 and 0.5 to 8.0 mm, respectively). The marginal bone loss during the observation period, which did not differ between the groups, was on average 0.5 mm (range 0 to 2.0 and 0 to 3.0 mm in the graft and trial group, respectively). Prosthesis Stability. All patients (except the patient who lost all implants) have been wearing their implant-supported prostheses continuously. Questionnaire. The patients evaluated their masticatory ability as much improved after the treatment; similar values were recorded in the two groups The International Journal of Oral & Maxillofacial Implants 479
7 Table 5 Self-Assessed (VAS) Masticatory Ability (Mean ± SD)* Before treatment After treatment Treatment group Mean SD Mean SD Graft (n = 16) Trial (n = 20) No implant (n = 7) *Questions asked: How was your chewing function before treatment? and How is your chewing function now? (Table 5). The mean values for all patients according to the VAS assessment was 3.0 before and 8.3 at the 1-year follow-up. Sixty percent in the graft group and 29% in the trial group reported residual phonetic problems at the 1-year examination. Answers to questions pertaining to the esthetic results of treatment and whether oral hygiene procedures were difficult to perform did not differ significantly between the groups. All but one patient in each group expressed willingness to undergo the treatment again even when knowing the difficulties and problems involved. Clinical Examinations. Gingival bleeding around implants was recorded at a few sites in nine patients. There was no gingival bleeding observed in 63% of the patients in the graft group and in 82% of those in the trial group. The dental wear was more marked in the trial group than in the graft group, in which the great majority (88%) had no or minimal wear. One quarter of the patients in both groups had a prenormal jaw relationship. One patient in the graft group had a postnormal (Angle Class II) jaw relationship, while the remaining patients had normal jaw relationships. Donor Site. The occurrence of hip donor site morbidity was low, and only one patient had a prolonged period (greater than 2 weeks) of postoperative pain. This patient also had a disturbance of the lateral cutaneous nerve of the thigh. The paresthesia resolved completely within 2 months. Complications. Two of the four patients in the graft group who lost implants also lost the entire grafted bone block. Most probably, the one who had an onlay graft lost the bone block because of traumatic occlusion from the opposite jaw combined with an infection of the graft through a dehiscence of the mucosa. The graft sequestrated and was lost. The other loss was in a heavy smoker who lost bilateral sinus inlays and still had an oroantral fistula on one side. Primarily minor prosthodontic problems were encountered and managed by means of routine clinical and laboratory procedures. No-Implant Group. The patients who renounced implant treatment assessed their mean masticatory ability as 5.8 (SD 1.6) according to the VAS at the 1-year follow-up. Six of seven reported retention problems with their complete dentures. Nevertheless, two said their mastication functioned well, three said it functioned fairly well, and only one said it was problematic. One did not wish to answer these questions. These patients reasons for refraining from implant treatment varied, but fear and hesitation for the complicated, time-consuming, and expensive treatment necessary were most often mentioned. Five of these patients said they would still renounce implant treatment today, one was uncertain, and one would now like to have implants. Discussion All patients in this study had lost so much maxillary bone that conventional implant treatment was judged to be impossible. The treatment options available at the clinic at that time were presented to the patients, who took part in the decision and had an influence on the chosen method. However, besides patient preferences, the clinical and radiographic evaluation also influenced the decision. A retrospective comparison of the bone quality and quantity between the groups suggests that the graft group exhibited more severe residual ridge resorption than the trial group (Table 4). It is probable that the amount of ridge resorption, as manifested in the radiographic examinations, to some extent affected the placement of the patients in the different groups. Thus, this is not a randomized study, and the results must be evaluated with caution. At the start of this study, the knowledge of alternative treatment for severely resorbed maxillae was insufficient for proper decision-making. A fully randomized study was therefore difficult to design and motivate patients for. Nevertheless, it was considered valuable to evaluate the outcome of the various treatments by carefully registering clinical and radiographic observations as well as patient views at regular follow-ups. The necessity for more research in this field was one of the conclusions of an extensive review of grafting techniques in implant treatment of severely resorbed jaws. 8 The implant survival in this study compares well with that reported in studies using similar procedures. 2,11,12,18 20 The implant survival rate is higher than that presented by Nyström et al 20 for the development group in their study. Their patients, however, all belonged to classes V and VI according to the classification system proposed by Cawood and Howell, 21 and were probably more severely affected in general 480 Volume 13, Number 4, 1998
8 than patients in the present study, some of whom had less severe bone resorption according to the Lekholm and Zarb classification system 17 (Table 4). Varying success rates have been reported in comparisons of one- and two-stage procedures. 8 This study suggested that the results were better with the one-stage than with the two-stage procedure. However, the number of patients and implants in the latter group was too small for the results to be conclusive. In a recent study with a larger number of patients, it was concluded that the results were more predictable when the implants were placed in a secondary stage 6 to 9 months after the time of bone grafting rather than simultaneously. 10 The two-stage procedure is said to allow the bone time to heal before implant placement. If a postoperative infection develops, it is easier to manage when only the bone graft is involved. In a one-stage procedure, healing can be complicated by the implants placed in the grafted bone. Even if a loss of bone volume because of infection occurs in the two-stage procedure, enough bone often remains to allow placement of implants. As a consequence of such considerations, it is a tendency today, at least in Sweden, to prefer a two-stage procedure. Rapid graft resorption has been reported in several studies of bone grafting techniques. 1,19 In a study using computed tomography to measure the fate of the bone graft, a 2.0-mm reduction in height and a 3.6-mm reduction in width were found at a 2-year postoperative follow-up. 22 Most of this reduction took place during the first few months. In a recent study by Widmark et al 23 using localized bone grafts from the mandible in the anterior maxilla for singletooth implants, 25% had been resorbed after 4 months and 60% after 10 months. These findings, that in many patients grafts are substantially reduced and that this occurs primarily in the initial postoperative period, are corroborated by the present study. It can be speculated that this rapid initial resorption may be a consequence of excessive augmentation beyond the limits of normal anatomy in the grafted region. It should be emphasized, however, that in spite of the severe reduction of the bone graft, the grafting procedure provided enough bone to enable implant placement with total bony coverage. The mean marginal peri-implant bone loss of 0.5 mm up to the 1-year follow-up is remarkably small with respect to the amount of remodeling that the graft undergoes. One interpretation is that the bone adjacent to the implants is maintained as a result of proper stimulation, while the more peripheral portions are resorbed because of inadequate stimulation. Despite the complexity of the treatment in the graft group, including harvesting of the graft from the iliac bone with often reported short-term complications, overall the patients were very satisfied with the treatment and its outcome. In fact, donor site morbidity in these patients was rare, which verifies findings in a recent study also using bone harvesting from the anterior iliac crest. 24 Patient satisfaction was also demonstrated by the fact that practically all said that they would undergo the treatment again. On average, those who had refrained from implants reported lower self-assessed masticatory ability than those with implant-supported prostheses. Nevertheless, they exhibited a modest level of adaptation to their optimized complete dentures, albeit with a sigh of resignation. It was probably appropriate from a psychologic aspect that these patients were given the opportunity to be examined and informed and to participate in the evaluation of possibilities, limitations, and risk of implant treatment. Most of them renounced implant treatment because they thought it would be too tiring, time-consuming, and/or expensive with an uncertain outcome. Conclusion Implant treatment in patients with severely resorbed maxillae is a demanding procedure, but it can be successful, in the short-term perspective, with both bone grafting procedures and modified placement of implants without bone grafts. However, the success rate and implant survival are lower, and the complication rate is higher than for implants placed in maxillae with better bone quality and quantity. The choice of appropriate treatment in borderline cases bone grafting, modified conventional implant treatment, or optimized complete dentures is difficult and influenced by many factors. It is clearly advantageous to include the patients, after careful presentation of information, in the choice of treatment options. This was especially obvious for the group that declined implant treatment, but reached a level of modest adaptation to their optimized complete dentures. Acknowledgments The authors would like to thank Ms Berit Lithner, Nobel Biocare, Göteborg, Sweden, for compiling and analyzing the data. The study has been supported by Nobel Biocare. The International Journal of Oral & Maxillofacial Implants 481
9 References 01. Breine U, Brånemark P-I. Reconstruction of alveolar jaw bone. An experimental and clinical study of immediate and performed autologous bone grafts in combination with osseointegrated implants. Scand J Plast Reconstr Surg 1980;14: Adell R, Lekholm U, Gröndahl K, Brånemark P-I, Lindström J, Jacobsson M. Reconstruction of severely resorbed edentulous maxillae using osseointegrated fixtures in immediate autogenous bone grafts. Int J Oral Maxillofac Implants 1990;5: Zarb GA, Schmitt A. The edentulous predicament II: The longitudinal effectiveness of implant-supported overdentures. J Am Dent Assoc 1996;127: Jaffin RA, Berman CL. The excessive loss of Brånemark fixtures in type IV bone. A 5-year analysis. J Periodontol 1991;62: Bahat O. Osseointegrated implants in the maxillary tuberosity: Report on 45 consecutive patients. Int J Oral Maxillofac Implants 1992;7: Jemt T, Book K, Lindén B, Urde G. Failures and complications in 92 consecutively inserted overdentures supported by Brånemark implants in severely resorbed edentulous maxillae: A study from prosthetic treatment to first annual check up. Int J Oral Maxillofac Implants 1992;7: Gunne J, Nyström E, Kahnberg K-E. Bone grafts and implants in the treatment of the severely resorbed maxillae: A 3-year follow-up of the prosthetic restoration. Int J Prosthodont 1995;8: Tolman DE. Reconstructive procedures with endosseous implants in grafted bone: A review of the literature. Int J Oral Maxillofac Implants 1995;10: Balshi TJ, Lee HY, Hernandez RE. The use of pterygomaxillary implants in the partially edentulous patient: A preliminary report. Int J Oral Maxillofac Implants 1995;10: Nyström E. Onlay bone grafts and implants in the reconstruction of severely resorbed maxillae. A 1-stage procedure [thesis]. Umeå, Sweden, Umeå Univ, Köndell PÅ, Nordenram Å, Moberg LE, Eliasson S, Nyberg B. Reconstruction of the resorbed edentulous maxilla using autogenous rib grafts and osseointegrated implants. Clin Oral Implants Res 1996;7: Triplett RG, Schow SR. Autologous bone grafts and endosseous implants: Complementary techniques. J Oral Maxillofac Surg 1996;54: Gröndahl K, Ekestubbe A, Gröndahl H-G. Radiography in Oral Endosseous Prosthetics. Göteborg: Nobel Biocare AB, Isaksson S, Alberius P. Maxillary alveolar ridge augmentation with onlay bone-grafts and immediate endosseous implants. J Craniomaxillofac Surg 1992;20: Zarb GA, Jansson T. Prosthodontic procedures. In: Brånemark P-I, Zarb GA, Albrektsson T (eds). Tissue-Integrated Prostheses: Osseointegration in Clinical Dentistry. Chicago: Quintessence, 1985: Albrektsson T, Zarb G, Worthington P, Eriksson AR. The long-term efficacy of currently used dental implants: A review and proposed criteria of success. Int J Oral Maxillofac Implants 1986;1: Lekholm U, Zarb GA. Patient selection and preparation. In: Brånemark P-I, Zarb GA, Albrektsson T (eds). Tissue- Integrated Prostheses: Osseointegration in Clinical Dentistry. Chicago: Quintessence, 1985: Nord PG, Åstrand P. Implantatbehandling vid kraftigt resorberade käkar. Metodbeskrivning och preliminärt resultat. Tandläkartidningen 1992;84: Isaksson S. Evaluation of three bone grafting techniques for severely resorbed maxillae in conjunction with immediate endosseous implants. Int J Oral Maxillofac Implants 1994;9: Nyström E, Kahnberg K-E, Gunne J. Bone grafts and Brånemark implants in the treatment of the severely resorbed maxilla: A 2-year longitudinal study. Int J Oral Maxillofac Implants 1993;8: Cawood JI, Howell RA. A classification of the edentulous jaw. Int J Oral Maxillofac Surg 1988;17: Nyström E, Legrell PE, Forssell Å, Kahnberg K-E. Combined use of bone grafts and implants in the severely resorbed maxilla. Postoperative evaluation by computed tomography. Int J Oral Maxillofac Surg 1995;24: Widmark G, Andersson B, Ivanoff CJ. Mandibular bone graft in the anterior maxilla for single-tooth implants. Presentation of a surgical method. Int J Oral Maxillofac Surg 1997;26: Beirne JC, Barry NJ, Brady FA, Morris VB. Donor site morbidity of the anterior iliac crest following cancellous bone harvest. Int J Oral Maxillofac Surg 1996;25: Volume 13, Number 4, 1998
Implant treatment in patients with severely
 Rehabilitation of Patients with Severely Resorbed Maxillae by Means of Implants With or Without Bone Grafts: A 3- to 5-Year Follow-up Clinical Report Göran Widmark, LDS, Odont Dr 1 /Bernt Andersson, LDS,
Rehabilitation of Patients with Severely Resorbed Maxillae by Means of Implants With or Without Bone Grafts: A 3- to 5-Year Follow-up Clinical Report Göran Widmark, LDS, Odont Dr 1 /Bernt Andersson, LDS,
The Brånemark osseointegration method, using titanium dental implants (fixtures)
 Early Failures in 4,641 Consecutively Placed Brånemark Dental Implants: A Study From Stage 1 Surgery to the Connection of Completed Prostheses Bertil Friberg, DDS/Torsten Jemt, DDS, PhD/Ulf Lekholm, DDS,
Early Failures in 4,641 Consecutively Placed Brånemark Dental Implants: A Study From Stage 1 Surgery to the Connection of Completed Prostheses Bertil Friberg, DDS/Torsten Jemt, DDS, PhD/Ulf Lekholm, DDS,
Survival Analysis of Endosseous Implants in Grafted and Nongrafted Edentulous Maxillae
 Survival Analysis of Endosseous Implants in Grafted and Nongrafted Edentulous Maxillae Jonas P. Becktor, DDS 1 /Sten Isaksson, MD, DDS, PhD 2 /Lars Sennerby, DDS, PhD 3 Purpose: The aim of this study was
Survival Analysis of Endosseous Implants in Grafted and Nongrafted Edentulous Maxillae Jonas P. Becktor, DDS 1 /Sten Isaksson, MD, DDS, PhD 2 /Lars Sennerby, DDS, PhD 3 Purpose: The aim of this study was
PALATAL POSITIONING OF IMPLANTS IN SEVERELY RESORBED POSTERIOR MAXILLAE F. Atamni, M.Atamni, M.Atamna, Private Practice Tel-aviv Israel
 PALATAL POSITIONING OF IMPLANTS IN SEVERELY RESORBED POSTERIOR MAXILLAE F. Atamni, M.Atamni, M.Atamna, Private Practice Tel-aviv Israel Abstract: Objectives: To evaluate an alternative treatment for rehabilitation
PALATAL POSITIONING OF IMPLANTS IN SEVERELY RESORBED POSTERIOR MAXILLAE F. Atamni, M.Atamni, M.Atamna, Private Practice Tel-aviv Israel Abstract: Objectives: To evaluate an alternative treatment for rehabilitation
Osseointegrated dental implant treatment generally
 Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
During the last 30 years, endosseous oral
 Influence of Variations in Implant Diameters: A 3- to 5-Year Retrospective Clinical Report Carl-Johan Ivanoff, DDS*/Kerstin Gröndahl, DDS, PhD**/Lars Sennerby, DDS, PhD***/ Christina Bergström, MSc****/Ulf
Influence of Variations in Implant Diameters: A 3- to 5-Year Retrospective Clinical Report Carl-Johan Ivanoff, DDS*/Kerstin Gröndahl, DDS, PhD**/Lars Sennerby, DDS, PhD***/ Christina Bergström, MSc****/Ulf
Treatment planning in a case of restoration of the maxilla and mandible using osseointegrated implants with four types of bone graft
 227 Journal of Oral Science, Vol. 45, No. 4, 227-232, 2003 Case report Treatment planning in a case of restoration of the maxilla and mandible using osseointegrated implants with four types of bone graft
227 Journal of Oral Science, Vol. 45, No. 4, 227-232, 2003 Case report Treatment planning in a case of restoration of the maxilla and mandible using osseointegrated implants with four types of bone graft
The use of endosseous implants is currently a routine
 Evaluation of 31 Zygomatic Implants and 74 Regular Dental Implants Used in 16 Patients for Prosthetic Reconstruction of the Atrophic Maxilla with Cross-Arch Fixed Bridges Jonas P. Becktor, DDS;* Sten Isaksson,
Evaluation of 31 Zygomatic Implants and 74 Regular Dental Implants Used in 16 Patients for Prosthetic Reconstruction of the Atrophic Maxilla with Cross-Arch Fixed Bridges Jonas P. Becktor, DDS;* Sten Isaksson,
The majority of the early research concerning
 Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
Osseointegrated implants are a very reliable means
 Tridimensional Reconstruction of Knife-Edge Edentulous Maxillae by Sinus Elevation, Onlay Grafts, and Sagittal Osteotomy of the Anterior Maxilla: Preliminary Surgical and Prosthetic Results Matteo Chiapasco,
Tridimensional Reconstruction of Knife-Edge Edentulous Maxillae by Sinus Elevation, Onlay Grafts, and Sagittal Osteotomy of the Anterior Maxilla: Preliminary Surgical and Prosthetic Results Matteo Chiapasco,
Prosthetic Options in Implant Dentistry. Hakimeh Siadat, DDS, MSc Associate Professor
 Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Placement of Posterior Mandibular and Maxillary Implants in Patients with Severe Bone Deficiency: A Clinical Report of Procedure
 Placement of Posterior Mandibular and Maxillary Implants in Patients with Severe Bone Deficiency: A Clinical Report of Procedure Leonard Krekmanov, DDS, PhD 1 The purpose of this investigation was to modify
Placement of Posterior Mandibular and Maxillary Implants in Patients with Severe Bone Deficiency: A Clinical Report of Procedure Leonard Krekmanov, DDS, PhD 1 The purpose of this investigation was to modify
Young-Jin Park, DDS,* and Sung-Am Cho, DDS, MS, PhD
 J Oral Maxillofac Surg 68:1338-1344, 2010 Retrospective Chart Analysis on Survival Rate of Fixtures Installed at the Tuberosity Bone for Cases With Missing Unilateral Upper Molars: A Study of 7 Cases Young-Jin
J Oral Maxillofac Surg 68:1338-1344, 2010 Retrospective Chart Analysis on Survival Rate of Fixtures Installed at the Tuberosity Bone for Cases With Missing Unilateral Upper Molars: A Study of 7 Cases Young-Jin
Dental Implants: A Predictable Solution for Tooth Loss. Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor
 Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
Moderately to severely resorbed edentulous
 The Zygomatic Implant: Preliminary Data on Treatment of Severely Resorbed Maxillae. A Clinical Report Edmond Bedrossian, DDS, FACD, FACOMS 1 /Lambert Stumpel III, DDS 2 / Michael Beckely, DDS 3 /Thomas
The Zygomatic Implant: Preliminary Data on Treatment of Severely Resorbed Maxillae. A Clinical Report Edmond Bedrossian, DDS, FACD, FACOMS 1 /Lambert Stumpel III, DDS 2 / Michael Beckely, DDS 3 /Thomas
Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis
 CASE REPORT Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis Dr Ashish Yadav 1, Dr Aratee Gupta 2, Dr Archana Singh 3, 1,3-
CASE REPORT Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis Dr Ashish Yadav 1, Dr Aratee Gupta 2, Dr Archana Singh 3, 1,3-
Endosseous dental implants initially showed very
 Five-mm-Diameter Implants without a Smooth Surface Collar: Report on 98 Consecutive Placements Franck Renouard, DDS*/Jean-Pierre Arnoux, DDS**/David P. Sarment, DDS*** In recent years, indications for
Five-mm-Diameter Implants without a Smooth Surface Collar: Report on 98 Consecutive Placements Franck Renouard, DDS*/Jean-Pierre Arnoux, DDS**/David P. Sarment, DDS*** In recent years, indications for
A Prospective Randomized Study of 1- and 2-Stage Sinus Inlay Bone Grafts: 1-Year Follow-up
 A Prospective Randomized Study of 1- and 2-Stage Sinus Inlay Bone Grafts: 1-Year Follow-up Karin Wannfors, DDS, PhD 1 /Björn Johansson, DDS 2 /Mats Hallman, DDS 3 /Tomas Strandkvist, DDS 3 The purpose
A Prospective Randomized Study of 1- and 2-Stage Sinus Inlay Bone Grafts: 1-Year Follow-up Karin Wannfors, DDS, PhD 1 /Björn Johansson, DDS 2 /Mats Hallman, DDS 3 /Tomas Strandkvist, DDS 3 The purpose
Bone Reduction Surgical Guide for the Novum Implant Procedure: Technical Note
 Bone Reduction Surgical Guide for the Novum Implant Procedure: Technical Note Stephen M. Parel, DDS 1 /Steven L. Ruff, CDT 2 /R. Gilbert Triplett, DDS, PhD 3 /Sterling R. Schow, DMD 4 The Novum System
Bone Reduction Surgical Guide for the Novum Implant Procedure: Technical Note Stephen M. Parel, DDS 1 /Steven L. Ruff, CDT 2 /R. Gilbert Triplett, DDS, PhD 3 /Sterling R. Schow, DMD 4 The Novum System
Oral Health and Dentistry
 Page 107 to 118 Volume 1 Issue 2 2017 Case Report Oral Health and Dentistry ISSN: 2573-4989 Full Mouth Implants Rehabilitation of a Patient with Ectodermal Dysplasia After 3-Ds Ridge Augmentation and Bilateral
Page 107 to 118 Volume 1 Issue 2 2017 Case Report Oral Health and Dentistry ISSN: 2573-4989 Full Mouth Implants Rehabilitation of a Patient with Ectodermal Dysplasia After 3-Ds Ridge Augmentation and Bilateral
The Use of Alpha-Bio Tec's Narrow NeO Implants with Cone Connection for Restoration of Limited Width Ridges
 Case Study 48 The Use of Alpha-Bio Tec's Narrow NeO Implants with Cone Connection for Restoration of Limited Width Ridges Dr. Amir Gazmawe DMD, Specialist in Prosthodontics, Israel Dr. Amir Gazmawe graduated
Case Study 48 The Use of Alpha-Bio Tec's Narrow NeO Implants with Cone Connection for Restoration of Limited Width Ridges Dr. Amir Gazmawe DMD, Specialist in Prosthodontics, Israel Dr. Amir Gazmawe graduated
Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study
 Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study Henny J. A. Meijer, DDS, PhD 1 /Rutger H. K. Batenburg, DDS,
Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study Henny J. A. Meijer, DDS, PhD 1 /Rutger H. K. Batenburg, DDS,
Dental Implant Treatment with Diffe Title for Sinus Floor Elevation-A Case Re. Sekine, H; Taguchi, T; Seta, S; Tak Author(s) T; Kakizawa, T
 Dental Implant Treatment with Diffe Title for Sinus Floor Elevation-A Case Re Sekine, H; Taguchi, T; Seta, S; Tak Author(s) T; Kakizawa, T Journal Bulletin of Tokyo Dental College, 4 URL http://hdl.handle.net/10130/200
Dental Implant Treatment with Diffe Title for Sinus Floor Elevation-A Case Re Sekine, H; Taguchi, T; Seta, S; Tak Author(s) T; Kakizawa, T Journal Bulletin of Tokyo Dental College, 4 URL http://hdl.handle.net/10130/200
Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Abstract Purpose: Materials and methods Results:
 Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Bum-Soo Kim 1, Young-Kyun Kim 1, Pil-Young Yun 1, Yang-Jin Lee 2, Hyo-Jeong Lee 3, Su-Gwan Kim 4 1Department of
Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Bum-Soo Kim 1, Young-Kyun Kim 1, Pil-Young Yun 1, Yang-Jin Lee 2, Hyo-Jeong Lee 3, Su-Gwan Kim 4 1Department of
1- Implant-supported vs. implant retained distal extension mandibular partial overdentures and residual ridge resorption. Abstract Purpose: This
 1- Implant-supported vs. implant retained distal extension mandibular partial overdentures and residual ridge resorption. Abstract Purpose: This retrospective study in male patients sought to examine posterior
1- Implant-supported vs. implant retained distal extension mandibular partial overdentures and residual ridge resorption. Abstract Purpose: This retrospective study in male patients sought to examine posterior
MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION
 Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
Many of the problems reported by conventional
 Maxillary Overdentures Retained by Splinted and Unsplinted Implants: A Retrospective Study Timo O. Närhi, DDS, PhD 1 /Miluska Hevinga, DDS 2 / Ralph A. C. A. Voorsmit, DDS, PhD 3 /Warner Kalk, DDS, PhD
Maxillary Overdentures Retained by Splinted and Unsplinted Implants: A Retrospective Study Timo O. Närhi, DDS, PhD 1 /Miluska Hevinga, DDS 2 / Ralph A. C. A. Voorsmit, DDS, PhD 3 /Warner Kalk, DDS, PhD
John P. Zarb, BA, DDS George A. Zarb, BChD, DDS, MS, MS, FRCD(C)
 C L I N I C A L P R A C T I C E Implant Prosthodontic Management of Anterior Partial Edentulism: Long-Term Follow-Up of a Prospective Study John P. Zarb, BA, DDS George A. Zarb, BChD, DDS, MS, MS, FRCD(C)
C L I N I C A L P R A C T I C E Implant Prosthodontic Management of Anterior Partial Edentulism: Long-Term Follow-Up of a Prospective Study John P. Zarb, BA, DDS George A. Zarb, BChD, DDS, MS, MS, FRCD(C)
RESTORATION OF A FULLY EDENTULOUS PATIENT UTILIZING SIMPLE TECHNIQUES FOR IMPRESSION AND FABRICATION OF A HYBRID BRIDGE
 Case Report International Journal of Dental and Health Sciences Volume 02,Issue 01 RESTORATION OF A FULLY EDENTULOUS PATIENT UTILIZING SIMPLE TECHNIQUES FOR IMPRESSION AND FABRICATION OF A HYBRID BRIDGE
Case Report International Journal of Dental and Health Sciences Volume 02,Issue 01 RESTORATION OF A FULLY EDENTULOUS PATIENT UTILIZING SIMPLE TECHNIQUES FOR IMPRESSION AND FABRICATION OF A HYBRID BRIDGE
The surgical placement of dental implants has
 Flapless Implant Surgery: A 10-year Clinical Retrospective Analysis Luis Dominguez Campelo, DDS 1 /Jose R. Dominguez Camara, MD, DDS 2 Purpose: This article is a retrospective clinical analysis of implants
Flapless Implant Surgery: A 10-year Clinical Retrospective Analysis Luis Dominguez Campelo, DDS 1 /Jose R. Dominguez Camara, MD, DDS 2 Purpose: This article is a retrospective clinical analysis of implants
Immediate implant placement in the Title central incisor region: a case repo. Journal Journal of prosthodontic research,
 Immediate implant placement in the Title central incisor region: a case repo Author(s) Sekine, H; Taguchi, T; Yamagami, M; Alternative Takanashi, T; Furuya, K Journal Journal of prosthodontic research,
Immediate implant placement in the Title central incisor region: a case repo Author(s) Sekine, H; Taguchi, T; Yamagami, M; Alternative Takanashi, T; Furuya, K Journal Journal of prosthodontic research,
Osseointegrated implant-supported
 CLINICAL SCREWLESS FIXED DETACHABLE PARTIAL OVERDENTURE TREATMENT FOR ATROPHIC PARTIAL EDENTULISM OF THE ANTERIOR MAXILLA Dennis Flanagan, DDS This is a case report of the restoration of a partially edentulous
CLINICAL SCREWLESS FIXED DETACHABLE PARTIAL OVERDENTURE TREATMENT FOR ATROPHIC PARTIAL EDENTULISM OF THE ANTERIOR MAXILLA Dennis Flanagan, DDS This is a case report of the restoration of a partially edentulous
Endosseous cylindric implants are well accepted
 Soft Tissue Exposure of Endosseous Implants Between Stage I and Stage II Surgery as a Potential Indicator of Early Crestal Bone Loss Joseph A. Toljanic, DDS*/Mark L. Banakis, DDS**/Leslee A. K. Willes,
Soft Tissue Exposure of Endosseous Implants Between Stage I and Stage II Surgery as a Potential Indicator of Early Crestal Bone Loss Joseph A. Toljanic, DDS*/Mark L. Banakis, DDS**/Leslee A. K. Willes,
A Novel Technique for the Management of a Maxillary Anterior Alveolar Defect with an Implant-retained Fixed Prosthesis: A Clinical Report
 Neenu M Varghese et al Case Report 10.5005/jp-journals-10012-1148 A Novel Technique for the Management of a Maxillary Anterior Alveolar Defect with an Implant-retained Fixed Prosthesis: A Clinical Report
Neenu M Varghese et al Case Report 10.5005/jp-journals-10012-1148 A Novel Technique for the Management of a Maxillary Anterior Alveolar Defect with an Implant-retained Fixed Prosthesis: A Clinical Report
Case study 2. A Retrospective Multi-Center Study on the Spiral Implant
 Case study 2 A Retrospective Multi-Center Study on the Spiral Implant Benny Karmon DMD, Jerry Kohen DMD, Ariel Lor DMD, Yiftach Gratciany DMD, Zvi Laster DMD, Gideon Hallel DMD MPA, Tsvia Karmon A Retrospective
Case study 2 A Retrospective Multi-Center Study on the Spiral Implant Benny Karmon DMD, Jerry Kohen DMD, Ariel Lor DMD, Yiftach Gratciany DMD, Zvi Laster DMD, Gideon Hallel DMD MPA, Tsvia Karmon A Retrospective
A Long-term Retrospective Analysis of Survival Rates of Implants in the Mandible
 A Long-term Retrospective Analysis of Survival Rates of Implants in the Mandible Thomas J. Balshi, DDS, PhD, FACP 1 /Glenn J. Wolfinger, DMD, FACP 2 / Brett E. Stein 3 /Stephen F. Balshi, MBE 4 Purpose:
A Long-term Retrospective Analysis of Survival Rates of Implants in the Mandible Thomas J. Balshi, DDS, PhD, FACP 1 /Glenn J. Wolfinger, DMD, FACP 2 / Brett E. Stein 3 /Stephen F. Balshi, MBE 4 Purpose:
Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report
 Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
CHAPTER. 1. Uncontrolled systemic disease 2. Retrognathic jaw relationship
 CHAPTER 7 Immediate Implant Supported Restoration of the Edentulous Arch Stephen G. Alfano and Robert M. Laughlin Department of Oral and Maxillofacial Surgery, Naval Medical Center San Diego, San Diego,
CHAPTER 7 Immediate Implant Supported Restoration of the Edentulous Arch Stephen G. Alfano and Robert M. Laughlin Department of Oral and Maxillofacial Surgery, Naval Medical Center San Diego, San Diego,
Retreatment: Fractured Implants Due To Biomechanical Overload
 Glenn J. Wolfinger, DMD, FACP Retreatment: Fractured Implants Due To Biomechanical Overload Thomas J. Balshi, DDS, FACP he strength of osseointegration, T the biologic and biomechanical union of bone to
Glenn J. Wolfinger, DMD, FACP Retreatment: Fractured Implants Due To Biomechanical Overload Thomas J. Balshi, DDS, FACP he strength of osseointegration, T the biologic and biomechanical union of bone to
Brånemark System Facts & Figures
 Brånemark System Facts & Figures Brånemark System is synonymous with the revolution in dental care by the introduction of safe and effective implants. Professor Brånemark, its inventor, always put the
Brånemark System Facts & Figures Brånemark System is synonymous with the revolution in dental care by the introduction of safe and effective implants. Professor Brånemark, its inventor, always put the
The influence of radiotherapy on osseointegration
 Experience with Osseointegrated Implants Placed in Irradiated Tissues in Japan and the United States Atsushi Niimi, DDS, DMSc*/Minoru Ueda, DDS, PhD**/ Eugene E. Keller, DDS, PhD***/Philip Worthington,
Experience with Osseointegrated Implants Placed in Irradiated Tissues in Japan and the United States Atsushi Niimi, DDS, DMSc*/Minoru Ueda, DDS, PhD**/ Eugene E. Keller, DDS, PhD***/Philip Worthington,
Endosseous Implants and Bone Augmentation in the Partially Dentate Maxilla: An Analysis of 17 Patients with a Follow-up of 29 to 101 Months
 Endosseous Implants and Bone Augmentation in the Partially Dentate Maxilla: An Analysis of 17 Patients with a Follow-up of 29 to 101 Months Jonas P. Becktor, DDS, PhD 1 / Sten Isaksson, MD, DDS, PhD 2
Endosseous Implants and Bone Augmentation in the Partially Dentate Maxilla: An Analysis of 17 Patients with a Follow-up of 29 to 101 Months Jonas P. Becktor, DDS, PhD 1 / Sten Isaksson, MD, DDS, PhD 2
Samantha W. Chou, D.M.D N. Southport Ave. Chicago, Illinois Phone: Fax:
 Samantha W. Chou, D.M.D. 2325 N. Southport Ave. Chicago, Illinois 60614 Phone: 312-608-6881 Fax: 773-296-0601 Samanthawchou@gmail.com What is our role as the dentist? "We live in a culture in which people
Samantha W. Chou, D.M.D. 2325 N. Southport Ave. Chicago, Illinois 60614 Phone: 312-608-6881 Fax: 773-296-0601 Samanthawchou@gmail.com What is our role as the dentist? "We live in a culture in which people
Conus Concept: A Rewarding Complete Denture Treatment
 Conus Concept: A Rewarding Complete Denture Treatment Complete dentures have largely become the domain of the denturist due to the dissatisfaction general dentists feel with this treatment. Multiple visits,
Conus Concept: A Rewarding Complete Denture Treatment Complete dentures have largely become the domain of the denturist due to the dissatisfaction general dentists feel with this treatment. Multiple visits,
Fixed full-arch implant-supported acrylic resin prostheses
 Tooth Fractures in Fixed Full-Arch Implant-Supported Acrylic Resin Prostheses: A Retrospective Clinical Study Javier Ventura, PhD, DMD 1 /Emilio Jiménez-Castellanos, PhD, DMD 2 / José Romero, PhD, DMD
Tooth Fractures in Fixed Full-Arch Implant-Supported Acrylic Resin Prostheses: A Retrospective Clinical Study Javier Ventura, PhD, DMD 1 /Emilio Jiménez-Castellanos, PhD, DMD 2 / José Romero, PhD, DMD
In spite of the great advances made by the osseointegration concept 1 in the oral rehabilitation of
 Placement of Screw-Type Implants in the Pterygomaxillary-Pyramidal Region: Surgical Procedure and Preliminary Results Jesús Fernández Valerón, MD, DDS/José Fernández Velázquez, MD, DDS A surgical technique
Placement of Screw-Type Implants in the Pterygomaxillary-Pyramidal Region: Surgical Procedure and Preliminary Results Jesús Fernández Valerón, MD, DDS/José Fernández Velázquez, MD, DDS A surgical technique
EFFECTIVE DATE: 04/24/14 REVISED DATE: 04/23/15, 04/28/16, 06/22/17, 06/28/18 POLICY NUMBER: CATEGORY: Dental
 MEDICAL POLICY SUBJECT: DENTAL IMPLANTS PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including an Essential
MEDICAL POLICY SUBJECT: DENTAL IMPLANTS PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including an Essential
It has been proposed that partially edentulous maxillectomy
 CLASSICAL ARTICLE Basic principles of obturator design for partially edentulous patients. Part II: Design principles Mohamed A. Aramany, DMD, MS* Eye and Ear Hospital of Pittsburgh and University of Pittsburgh,
CLASSICAL ARTICLE Basic principles of obturator design for partially edentulous patients. Part II: Design principles Mohamed A. Aramany, DMD, MS* Eye and Ear Hospital of Pittsburgh and University of Pittsburgh,
Implant osseointegration and successful restoration
 Prosthodontic Complications in a Prospective Clinical Trial of Single-stage Implants at 36 Months Jacqueline P. Duncan, DMD, MDSc 1 /Elena Nazarova, DMD, PhD 2 /Theodora Vogiatzi, DDS 1 / Thomas D. Taylor,
Prosthodontic Complications in a Prospective Clinical Trial of Single-stage Implants at 36 Months Jacqueline P. Duncan, DMD, MDSc 1 /Elena Nazarova, DMD, PhD 2 /Theodora Vogiatzi, DDS 1 / Thomas D. Taylor,
Contemporary Implant Dentistry
 Contemporary Implant Dentistry C H A P T ER 1 4 O F C O N T E M P OR A R Y O R A L A N D M A X I L L OFA C IA L S U R G E RY B Y : D R A R A S H K H O J A S T EH Dental implant is suitable for: completely
Contemporary Implant Dentistry C H A P T ER 1 4 O F C O N T E M P OR A R Y O R A L A N D M A X I L L OFA C IA L S U R G E RY B Y : D R A R A S H K H O J A S T EH Dental implant is suitable for: completely
Radiographic Stent for Simplified Placement of Implants in the Mandible
 10.5005/jp-journals-10026-1086 CASE REPORT Radiographic Stent for Simplified Placement of Implants in the Mandible ABSTRACT This article aims to present a modified yet simple technique for the placement
10.5005/jp-journals-10026-1086 CASE REPORT Radiographic Stent for Simplified Placement of Implants in the Mandible ABSTRACT This article aims to present a modified yet simple technique for the placement
EssentialSmile Ped 221 Schedule of Benefits
 EssentialSmile Ped 221 Schedule of Benefits P.O. Box 9 Plantation, FL 33318 Telephone: 877 760 2247 Fax: 954 370 1701 www.mysolstice.net Members can search for a Network Provider atwww.solsticecare.com/provider
EssentialSmile Ped 221 Schedule of Benefits P.O. Box 9 Plantation, FL 33318 Telephone: 877 760 2247 Fax: 954 370 1701 www.mysolstice.net Members can search for a Network Provider atwww.solsticecare.com/provider
BUILDING A. Achieving total reconstruction in a single operation. 70 OCTOBER 2016 // dentaltown.com
 BUILDING A MANDI Achieving total reconstruction in a single operation by Dr. Fayette C. Williams Fayette C. Williams, DDS, MD, FACS, is clinical faculty at John Peter Smith Hospital in Fort Worth, Texas,
BUILDING A MANDI Achieving total reconstruction in a single operation by Dr. Fayette C. Williams Fayette C. Williams, DDS, MD, FACS, is clinical faculty at John Peter Smith Hospital in Fort Worth, Texas,
Columbia Dental Review
 Columbia Dental Review groper appliance in a pediatric patient: a case report and review of the literature periapical cemental dysplasia and an adjacent compound odontoma successful osseointegration and
Columbia Dental Review groper appliance in a pediatric patient: a case report and review of the literature periapical cemental dysplasia and an adjacent compound odontoma successful osseointegration and
Newport News Public Schools Summary Schedule of Services Delta Dental PPO EPO Plan
 Newport News Public Schools Summary of Services Delta Dental PPO EPO Plan Services In-Network Out-of-Network PPO Premier All Other Diagnostic & Preventive Oral Exams & Teeth Cleanings Fluoride Applications
Newport News Public Schools Summary of Services Delta Dental PPO EPO Plan Services In-Network Out-of-Network PPO Premier All Other Diagnostic & Preventive Oral Exams & Teeth Cleanings Fluoride Applications
BONE AUGMENTATION AND GRAFTING
 1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
Frequency of the Various Classes of Removable Partial Dentures and Selection of Major Connectors and Direct/Indirect Retainers
 Turk J Med Sci 31 (2001) 445-449 TÜB TAK Filiz KEYF Frequency of the Various Classes of Removable Partial Dentures and Selection of Major Connectors and Direct/Indirect Retainers Received: November 30,
Turk J Med Sci 31 (2001) 445-449 TÜB TAK Filiz KEYF Frequency of the Various Classes of Removable Partial Dentures and Selection of Major Connectors and Direct/Indirect Retainers Received: November 30,
The severely resorbed edentulous maxilla presents
 Rehabilitation of Severely Resorbed Maxillae with Zygomatic Implants: An Evaluation of Implant Stability, Tissue Conditions, and Patients Opinion Before and After Treatment Payam Farzad, DDS, MSc 1 /Lars
Rehabilitation of Severely Resorbed Maxillae with Zygomatic Implants: An Evaluation of Implant Stability, Tissue Conditions, and Patients Opinion Before and After Treatment Payam Farzad, DDS, MSc 1 /Lars
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 3 Influence of the 3-D Bone-to-Implant Relationship on Esthetics Ueli Grunder, DMD* Stefano Gracis, DMD** Matteo Capelli, DMD** There are
The International Journal of Periodontics & Restorative Dentistry 3 Influence of the 3-D Bone-to-Implant Relationship on Esthetics Ueli Grunder, DMD* Stefano Gracis, DMD** Matteo Capelli, DMD** There are
While the protocol for direct bone-to-implant
 Immediate Functional Loading of Brånemark System Implants in Edentulous Mandibles: Clinical Report of the Results of Developmental and Simplified Protocols Glenn J. Wolfinger, DMD 1 / Thomas J. Balshi,
Immediate Functional Loading of Brånemark System Implants in Edentulous Mandibles: Clinical Report of the Results of Developmental and Simplified Protocols Glenn J. Wolfinger, DMD 1 / Thomas J. Balshi,
LIST OF COVERED DENTAL SERVICES
 LIST OF COVERED DENTAL SERVICES The following is a complete list of those dental Services which will be considered for payment by Constitution Life Insurance Company after the expiration of any applicable
LIST OF COVERED DENTAL SERVICES The following is a complete list of those dental Services which will be considered for payment by Constitution Life Insurance Company after the expiration of any applicable
A retrospective study on separate single-tooth implant restorations to replace two or more consecutive. maxillary posterior teeth up to 6 years.
 Original Article A retrospective study on separate single-tooth implant restorations to replace two or more consecutive maxillary posterior teeth up to 6 years follow up Myat Nyan Department of Prosthodontics,
Original Article A retrospective study on separate single-tooth implant restorations to replace two or more consecutive maxillary posterior teeth up to 6 years follow up Myat Nyan Department of Prosthodontics,
EssentialSmile Ped 221 Schedule of Benefits
 EssentialSmile Ped 221 Schedule of Benefits P.O. Box 19199 Plantation, FL 33318 Telephone: 877-760-2247 Fax: 954-370-1701 www.mysolstice.net Members can search for a Network Provider at www.solsticecare.com/provider-search.aspx
EssentialSmile Ped 221 Schedule of Benefits P.O. Box 19199 Plantation, FL 33318 Telephone: 877-760-2247 Fax: 954-370-1701 www.mysolstice.net Members can search for a Network Provider at www.solsticecare.com/provider-search.aspx
Areview of recent studies concerning molar. Single Molar Replacement with a Progressive Thread Design Implant System: A Retrospective Clinical Report
 Single Molar Replacement with a Progressive Thread Design Implant System: A Retrospective Clinical Report George E. Romanos, Dr med dent 1 /Georg H. Nentwig, Prof Dr med dent 2 Many clinical studies have
Single Molar Replacement with a Progressive Thread Design Implant System: A Retrospective Clinical Report George E. Romanos, Dr med dent 1 /Georg H. Nentwig, Prof Dr med dent 2 Many clinical studies have
Vertical and Horizontal Augmentation Using Guided Bone Regeneration. Ph.D. Thesis. Dr. med. dent. et univ. Istvan Urban
 Vertical and Horizontal Augmentation Using Guided Bone Regeneration Ph.D. Thesis Dr. med. dent. et univ. Istvan Urban Supervisor: Prof. Dr. Katalin Nagy, DDS, PhD Faculty of Dentistry, University of Szeged
Vertical and Horizontal Augmentation Using Guided Bone Regeneration Ph.D. Thesis Dr. med. dent. et univ. Istvan Urban Supervisor: Prof. Dr. Katalin Nagy, DDS, PhD Faculty of Dentistry, University of Szeged
Benefits of CBCT in Implant Planning
 10.5005/jp-journals-10012-1032 CLINICAL SCIENCE 1 Gregori M Kurtzman, 2 Douglas F Dompkowski 1 Private General Practice in Silver Spring, Maryland, USA 2 Private Periodontal Practice in Bethesda, Maryland,
10.5005/jp-journals-10012-1032 CLINICAL SCIENCE 1 Gregori M Kurtzman, 2 Douglas F Dompkowski 1 Private General Practice in Silver Spring, Maryland, USA 2 Private Periodontal Practice in Bethesda, Maryland,
University of Groningen. Dental implants in maxillofacial prosthodontics Korfage, Anke
 University of Groningen Dental implants in maxillofacial prosthodontics Korfage, Anke DOI: 10.1016/j.bjoms.2014.05.013 10.1016/j.ijom.2013.04.003 10.1002/hed.24053 IMPORTANT NOTE: You are advised to consult
University of Groningen Dental implants in maxillofacial prosthodontics Korfage, Anke DOI: 10.1016/j.bjoms.2014.05.013 10.1016/j.ijom.2013.04.003 10.1002/hed.24053 IMPORTANT NOTE: You are advised to consult
Dental Implant Planning using Cone Beam CT imaging: a pictorial guide.
 Dental Implant Planning using Cone Beam CT imaging: a pictorial guide. Poster No.: C-1970 Congress: ECR 2015 Type: Educational Exhibit Authors: S. R. Rice, G. Price, S. Morley, T. Beale; London/UK Keywords:
Dental Implant Planning using Cone Beam CT imaging: a pictorial guide. Poster No.: C-1970 Congress: ECR 2015 Type: Educational Exhibit Authors: S. R. Rice, G. Price, S. Morley, T. Beale; London/UK Keywords:
Case Report. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
 Case Report RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
Case Report RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
Senior Dental Insurance Scheduled Allowance
 Senior Dental Insurance Scheduled Allowance LIST OF COVERED DENTAL SERVICES The following is a complete list of those dental services which will be considered for payment by The American Progressive Life
Senior Dental Insurance Scheduled Allowance LIST OF COVERED DENTAL SERVICES The following is a complete list of those dental services which will be considered for payment by The American Progressive Life
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 141 Screw Spreading: Technical Considerations and Case Report Renato Sussumu Nishioka, DDS, PhD, MSc* Alberto Noriyuki Kojima, DDS, PhD,
The International Journal of Periodontics & Restorative Dentistry 141 Screw Spreading: Technical Considerations and Case Report Renato Sussumu Nishioka, DDS, PhD, MSc* Alberto Noriyuki Kojima, DDS, PhD,
Brånemark System Facts & Figures
 Brånemark System Facts & Figures Brånemark System is synonymous with the revolution in dental care by the introduction of safe and effective implants. Professor Brånemark, its inventor, always put the
Brånemark System Facts & Figures Brånemark System is synonymous with the revolution in dental care by the introduction of safe and effective implants. Professor Brånemark, its inventor, always put the
Mandibular implant-supported hybrid prostheses
 Occlusal Contacts of Edentulous Patients with Mandibular Hybrid Dentures Opposing Maxillary Complete Dentures Tetsuya Suzuki, DDS, PhD*/Hiroshi Kumagai, DDS, PhD**/ Nobuyuki Yoshitomi, DDS, PhD***/Edwin
Occlusal Contacts of Edentulous Patients with Mandibular Hybrid Dentures Opposing Maxillary Complete Dentures Tetsuya Suzuki, DDS, PhD*/Hiroshi Kumagai, DDS, PhD**/ Nobuyuki Yoshitomi, DDS, PhD***/Edwin
م.م. طارق جاسم حممد REMOVABLE PARTIAL DENTURE INTRODUCTION
 Lec.1 م.م. طارق جاسم حممد REMOVABLE PARTIAL DENTURE INTRODUCTION االسنان طب Prosthodontics is the branch of dentistry pertaining to the restoration and maintenance of oral function, comfort, appearance,
Lec.1 م.م. طارق جاسم حممد REMOVABLE PARTIAL DENTURE INTRODUCTION االسنان طب Prosthodontics is the branch of dentistry pertaining to the restoration and maintenance of oral function, comfort, appearance,
Utilizing Digital Treatment Planning and Guided Surgery in Conjunction with Narrow Body Implants. by Timothy F. Kosinski, DDS, MAGD
 Utilizing Digital Treatment Planning and Guided Surgery in Conjunction with Narrow Body Implants by Timothy F. Kosinski, DDS, MAGD Implant dentistry is undergoing some amazing transformations. With the
Utilizing Digital Treatment Planning and Guided Surgery in Conjunction with Narrow Body Implants by Timothy F. Kosinski, DDS, MAGD Implant dentistry is undergoing some amazing transformations. With the
Long-term success for osteointegrated
 CASE REPORT Symphyseal Bone Cylinders Tapping With the Dental Implant Into Insufficiency Bone Situated Esthetic Area at One-Stage Surgery: A Case Report and the Description of the New Technique Umut Tekin,
CASE REPORT Symphyseal Bone Cylinders Tapping With the Dental Implant Into Insufficiency Bone Situated Esthetic Area at One-Stage Surgery: A Case Report and the Description of the New Technique Umut Tekin,
Rehabilitation of a Patient with Completely Edentulous Maxillary Arch using All on 4 Concept of Implantation
 IJopRD K Harshakumar et al CASE REPORT 10.5005/jp-journals-10019-1179 Rehabilitation of a Patient with Completely Edentulous Maxillary Arch using All on 4 Concept of Implantation 1 K Harshakumar, 2 Nimisha
IJopRD K Harshakumar et al CASE REPORT 10.5005/jp-journals-10019-1179 Rehabilitation of a Patient with Completely Edentulous Maxillary Arch using All on 4 Concept of Implantation 1 K Harshakumar, 2 Nimisha
The Application of Cone Beam CT Image Analysis for the Mandibular Ramus Bone Harvesting
 44 The Application of Cone Beam CT Image Analysis for the Mandibular Ramus Bone Harvesting LivingWell Institute of Dental Research Lee, Jang-yeol, Youn, Pil-sang, Kim, Hyoun-chull, Lee Sang-chull Ⅰ. Introduction
44 The Application of Cone Beam CT Image Analysis for the Mandibular Ramus Bone Harvesting LivingWell Institute of Dental Research Lee, Jang-yeol, Youn, Pil-sang, Kim, Hyoun-chull, Lee Sang-chull Ⅰ. Introduction
DELTA DENTAL PPO EPO PLAN DESIGN CP070
 DELTA DENTAL PPO EPO PLAN DESIGN CP070 SCHEDULE OF BENEFITS AND The benefits shown below are performed as deemed appropriate by the attending Dentist subject to the limitations and exclusions of the program.
DELTA DENTAL PPO EPO PLAN DESIGN CP070 SCHEDULE OF BENEFITS AND The benefits shown below are performed as deemed appropriate by the attending Dentist subject to the limitations and exclusions of the program.
In Scandinavia, malignant tumors in the maxillofacial
 Oral Implant Rehabilitation in Irradiated Patients Without Adjunctive Hyperbaric Oxygen Gunilla Andersson, DDS, PhD*/Lars Andreasson, MD, PhD**/Göran Bjelkengren, MD*** In 15 patients treated for malignant
Oral Implant Rehabilitation in Irradiated Patients Without Adjunctive Hyperbaric Oxygen Gunilla Andersson, DDS, PhD*/Lars Andreasson, MD, PhD**/Göran Bjelkengren, MD*** In 15 patients treated for malignant
Pre prosthetic surgery
 Pre prosthetic surgery The surgical procedures designed to facilitate fabrication of a prosthesis or to improve the prognosis of prosthodontics care. AIMS OF PRE PROSTHETIC SURGERY 1-provide adequate bony
Pre prosthetic surgery The surgical procedures designed to facilitate fabrication of a prosthesis or to improve the prognosis of prosthodontics care. AIMS OF PRE PROSTHETIC SURGERY 1-provide adequate bony
JOMI on CD-ROM, 1990 Mar ( ): The Applicability of Osseointegrated Oral Imp
 The Applicability of Osseointegrated Oral Implants in the Rehabilitation of Partial Edentulism: A Prospective Multicenter Study on 558 Fixtures Daniel van Steenberghe, MD, PhD/Ulf Lekholm, DDS, PhD/Charles
The Applicability of Osseointegrated Oral Implants in the Rehabilitation of Partial Edentulism: A Prospective Multicenter Study on 558 Fixtures Daniel van Steenberghe, MD, PhD/Ulf Lekholm, DDS, PhD/Charles
Bernt Andersson, DDS, Odont Dr/PhD;* Sibel Bergenblock, DDS; Björn Fürst, DDS; Torsten Jemt, DDS, Odont Dr/PhD
 Long-Term Function of Single-Implant Restorations: A 17- to 19-Year Follow-Up Study on Implant Infraposition Related to the Shape of the Face and Patients Satisfactioncid_381 1..10 Bernt Andersson, DDS,
Long-Term Function of Single-Implant Restorations: A 17- to 19-Year Follow-Up Study on Implant Infraposition Related to the Shape of the Face and Patients Satisfactioncid_381 1..10 Bernt Andersson, DDS,
Prosthodontic Rehabilitation with Overdenture Using Modified Impression Technique: A Case Report
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 10 Ver.VII (Oct. 2015), PP 102-107 www.iosrjournals.org Prosthodontic Rehabilitation with Overdenture
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 10 Ver.VII (Oct. 2015), PP 102-107 www.iosrjournals.org Prosthodontic Rehabilitation with Overdenture
The restoration of partially and completely
 CLINICAL MANAGEMENT OF DENTAL IMPLANT FRACTURES. ACASE HISTORY Firas A. M. AL Quran, PhD, MSc Med; Bashar A. Rashan, MS; Ziad N. AL-Dwairi, PhD The widespread use of endosseous osseointegrated implants
CLINICAL MANAGEMENT OF DENTAL IMPLANT FRACTURES. ACASE HISTORY Firas A. M. AL Quran, PhD, MSc Med; Bashar A. Rashan, MS; Ziad N. AL-Dwairi, PhD The widespread use of endosseous osseointegrated implants
Management of a complex case
 2 Soft- and hard-tissue reconstruction of a severely deficient site prior to implant placement: a case report Management of a complex case Younes Khosroshahy, DDS, MFDS RCS (Eng), Dip Imp Dent RCSEd, Blue
2 Soft- and hard-tissue reconstruction of a severely deficient site prior to implant placement: a case report Management of a complex case Younes Khosroshahy, DDS, MFDS RCS (Eng), Dip Imp Dent RCSEd, Blue
Intramembranous autogenous bone graft is the gold
 CASE LETTER CBCT Morphologic Analysis of Edentulous Posterior Mandible for Mandibular Body Bone Graft Jae-Min Song, DDS, MSD, PhD 1 Jae-Yeol Lee, DDS, MSD, PhD 1,2 Yong-Deok Kim, DDS, MSD, PhD 2,3 * INTRODUCTION
CASE LETTER CBCT Morphologic Analysis of Edentulous Posterior Mandible for Mandibular Body Bone Graft Jae-Min Song, DDS, MSD, PhD 1 Jae-Yeol Lee, DDS, MSD, PhD 1,2 Yong-Deok Kim, DDS, MSD, PhD 2,3 * INTRODUCTION
Guided surgery as a way to simplify surgical implant treatment in complex cases
 52 STARGET 1 I 12 StraUMaNN CareS r ry vincenzo MiriSOLA Di TOrreSANTO AND LUCA COrDArO Guided surgery as a way to simplify surgical implant treatment in complex cases Background A 41-year-old woman with
52 STARGET 1 I 12 StraUMaNN CareS r ry vincenzo MiriSOLA Di TOrreSANTO AND LUCA COrDArO Guided surgery as a way to simplify surgical implant treatment in complex cases Background A 41-year-old woman with
In 1977, Lew1 developed a passive
 CLINICAL AN OVERVIEW OF THE LEW ATTACHMENT: CLINICAL REPORTS Jack Piermatti, DMD Sheldon Winkler, DDS KEY WORDS Lew attachment Atrophic mandible Subperiosteal implant Root form implant Although the Lew
CLINICAL AN OVERVIEW OF THE LEW ATTACHMENT: CLINICAL REPORTS Jack Piermatti, DMD Sheldon Winkler, DDS KEY WORDS Lew attachment Atrophic mandible Subperiosteal implant Root form implant Although the Lew
/TLv/ A classification of the edentulous jaws. Trauma; Preprosthetic Surgery. iiiii!iii!iii! ] BASAL
![/TLv/ A classification of the edentulous jaws. Trauma; Preprosthetic Surgery. iiiii!iii!iii! ] BASAL /TLv/ A classification of the edentulous jaws. Trauma; Preprosthetic Surgery. iiiii!iii!iii! ] BASAL](/thumbs/72/66558540.jpg) Trauma; Preprosthetic Surgery A classification of the edentulous jaws J. I. awood ~ and R. A. Howell 2 ~Maxillofacial Unit, Royal Infirmary, hester, UK, 2Liverpool Dental Hospital, Liverpool, UK J. L awood
Trauma; Preprosthetic Surgery A classification of the edentulous jaws J. I. awood ~ and R. A. Howell 2 ~Maxillofacial Unit, Royal Infirmary, hester, UK, 2Liverpool Dental Hospital, Liverpool, UK J. L awood
Zygomaticus Implants: A New Treatment Modality for the Edentulous Maxilla
 Zygomaticus Implants: A New Treatment Modality for the Edentulous Maxilla Thomas Salinas, DDS*/Avishai Sadan, DMD **/Tom Peterson, CDT, MDT***/ Bundhit Jirajariyavej, DDS, MSc****/Michael Block, DMD*****
Zygomaticus Implants: A New Treatment Modality for the Edentulous Maxilla Thomas Salinas, DDS*/Avishai Sadan, DMD **/Tom Peterson, CDT, MDT***/ Bundhit Jirajariyavej, DDS, MSc****/Michael Block, DMD*****
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Case Report Rehabilitating Anterior Ridge Defect with Implant Supported Prosthesis Using Bone Graft and Customized Abutment
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Case Report Rehabilitating Anterior Ridge Defect with Implant Supported Prosthesis Using Bone Graft and Customized Abutment
Jonas P. Becktor, DDS, PhD,* Hadar Hallström, LDS, Sten Isaksson, MD, DDS, PhD, and Lars Sennerby, DDS, PhD
 J Oral Maxillofac Surg 66:780-786, 2008 The Use of Particulate Bone Grafts From the Mandible for Maxillary Sinus Floor Augmentation Before Placement of Surface-Modified Implants: Results From Bone Grafting
J Oral Maxillofac Surg 66:780-786, 2008 The Use of Particulate Bone Grafts From the Mandible for Maxillary Sinus Floor Augmentation Before Placement of Surface-Modified Implants: Results From Bone Grafting
Long-term success of osseointegrated implants
 Against All Odds A No Bone Solution Long-term success of osseointegrated implants depends on the length of the implants used and the quality and quantity of bone surrounding these implants. As surgical
Against All Odds A No Bone Solution Long-term success of osseointegrated implants depends on the length of the implants used and the quality and quantity of bone surrounding these implants. As surgical
Initially, Brånemark System (Nobel Biocare AB,
 Clinical Application of Narrow Brånemark System Implants for Single-Tooth Restorations Giovanni Polizzi, MD, DDS*/Sandro Fabbro, MD**/Marco Furri, DDS**/ Irene Herrmann, DDS***/Sergio Squarzoni, MD****
Clinical Application of Narrow Brånemark System Implants for Single-Tooth Restorations Giovanni Polizzi, MD, DDS*/Sandro Fabbro, MD**/Marco Furri, DDS**/ Irene Herrmann, DDS***/Sergio Squarzoni, MD****
Rehabilitation of Resorbed Mandibular Ridge with Implant Supported Overdenture- A Clinical Report
 Rehabilitation of Resorbed Mandibular Ridge with Implant Supported Overdenture- A Clinical Report 1 2 1 1 Mittal R, Saxena D, Rao S, Kumar M Abstract: Statement of Problem: Complete denture rehabilitation
Rehabilitation of Resorbed Mandibular Ridge with Implant Supported Overdenture- A Clinical Report 1 2 1 1 Mittal R, Saxena D, Rao S, Kumar M Abstract: Statement of Problem: Complete denture rehabilitation
INSIGHT & INNOVATION. Restorative Considerations for the Immediate-Load Transitional Prosthesis The predictability of successful osseointegrated
 SAJ JIVRAJ BDS MSED 32 INSIGHT & INNOVATION Restorative Considerations for the Immediate-Load Transitional Prosthesis The predictability of successful osseointegrated implant rehabilitation of the edentulous
SAJ JIVRAJ BDS MSED 32 INSIGHT & INNOVATION Restorative Considerations for the Immediate-Load Transitional Prosthesis The predictability of successful osseointegrated implant rehabilitation of the edentulous
Implant Placement in Maxillary Anterior Region Along with Soft and Hard Tissue Grafting- A Case Report.
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 10 Ver. XII (October. 2016), PP 68-73 www.iosrjournals.org Implant Placement in Maxillary Anterior
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 10 Ver. XII (October. 2016), PP 68-73 www.iosrjournals.org Implant Placement in Maxillary Anterior
Fixed Partial Dentures /FPDs/, Implant Supported. in implant prosthodontics
 Fixed Partial Dentures /FPDs/, Implant Supported Prosthesis/ISP/ in implant prosthodontics Prof.dr.Tamas Divinyi Semmelweis University, Faculty of Dentistry Department of Oral and Maxillofacial Surgery
Fixed Partial Dentures /FPDs/, Implant Supported Prosthesis/ISP/ in implant prosthodontics Prof.dr.Tamas Divinyi Semmelweis University, Faculty of Dentistry Department of Oral and Maxillofacial Surgery
Implant Site Development Part I
 REVIEW ARTICLE Implant Site Development Part I 1 Umang Nayar, 2 Shankar Iyer IJCID Implant Site Development Part I 1 Consultant, Dental Surgeon and Periodontist at Max Health Care, New Delhi, Professor
REVIEW ARTICLE Implant Site Development Part I 1 Umang Nayar, 2 Shankar Iyer IJCID Implant Site Development Part I 1 Consultant, Dental Surgeon and Periodontist at Max Health Care, New Delhi, Professor
