The long-term clinical stability of implants placed with ridge splitting technique
|
|
|
- Cameron Griffin Robertson
- 6 years ago
- Views:
Transcription
1 대한치과이식 ( 임프란트 ) 학회지 2011;30(1):1-8 1 The long-term clinical stability of implants placed with ridge splitting technique 1 Department of Periodontology, National health insurance corporation, Ilsan hospital, Goyang, Korea 2 Department of Periodontology, Research Institute for Periodontal Regeneration, Yonsei University College of Dentistry, Seoul, Korea Jae-Min Yoon 1, Young-taek Kim 1, Yong-ju Jang 2, Jung-chul Park 2, Seong-ho Choi 2, Kyoo-sung Cho 2, Chang-sung Kim 2 INTRODUCTION After the loss of teeth, the vertical and horizontal absorption of alveolar bone is in progress 1). If a tooth is extracted due to severe periodontitis, physical trauma, or vertical root fracture or if the facial bone plate suffers a traumatic injury during extraction, the apparent absorption of alveolar bone occurs horizontally and vertically, making ideal implant placement impossible 2). When the implant cannot be placed in an ideal location due to absorption of alveolar bone, there will be a the negative effect on emergence profile, bucco-palatal relationship, and embrasure space, which can affect the future of implant-supported restorations in esthetics and function 2-3). There must be at least 1mm bone surrounding the implant for a favorable clinical outcome 4). Therefore, the evaluation of the residual ridge dimension must be performed through preoperative clinical and radiographic examination. If there is lack of the width of the residual ridge for implant placement, the clinicians should determine the surgical procedures to overcome the insufficient ridge dimension before implant surgery 5). There are several procedures that have been suggested for lateral augmentation of the residual ridge, for example guided bone regeneration (GBR), onlays of bone grafting material, and distraction osteogenesis. These methods have several drawbacks. The drawbacks Corresponding author: Dr. Chang- Sung Kim Department of Periodontology, Research Institute for Periodontal Regeneration, College of Dentistry, Yonsei University, 134 Shinchon- Dong, Seodaemun-gu, Seoul , South Korea. Tel: , Fax: dentall@yuhs.ac Received Apr18,2011 Revised May20,2011 Accepted Jun10,2011 of GBR procedures are membrane collapse, membrane exposure, increased treatment cost to the use of membrane and delayed implant treatment time 6-9). The drawbacks of bone grafting are a morbidity of the autogenous bone donor site, absorption of graft materials and delayed treatment time 8). Use of distraction osteogenesis for lateral bone augmentation, which requires a device to improve bone defects, is faced with unavoidable elevated treatment cost a limited area on which to apply this technique. In addition to these methods, ridge splitting is used for expansion of insufficient width of residual ridge. Crestal osteotomy is performed first on the residual ridge crest for ridge splitting by surgical blade, hand instrument, microsaw 10), or ultrasonic device 9). After crestal osteotomy, the ridge expansion is performed with an osteotome, bone chisel, and bone spreader. When the width of ridge is properly expanded, implant placement is done simultaneously. Generally, the type of implant used with ridge splitting technique is a submerged implant. Ridge splitting was firstly introduced by Tatum (1986) 11). Subsequently, the clinical application of modified ridge splitting techniques have been reported by many researchers 9-10, 12-15). Therefore, the ridge splitting technique has been mentioned as a ridge expansion, bone spreading, osteotome technique 5). The ridge splitting technique, unlike the GBR and bone graft procedures, enables implant placement simultaneously, thereby shortening treatment time 5). The healing between separated bone plates is similar to that of a bone fracture, so additional bone grafts or barrier membrane applications on furrows is not always necessary when the 13, 16). ridge splitting technique is applied The evaluation of vertical and horizontal bone change around the implant is regarded as an important measure
2 2 J M Yoon, Y T Kim, Y J Jang, J C Park, S H Choi, K S Cho, C S Kim of implant success 17-18). The success criteria of the Br anemark implant was suggested to be that marginal bone loss is less than 1mm at the 1st year after implant installation and thereafter less than 0.2 mm marginal bone resorption annually 19). With regard to ITI implant (non-submerged implant), marginal bone resorption in the first year after placement was reported as 0.8 mm on average 20). However, reports about long-term marginal bone change around implants placed with the ridge splitting technique have been limited. The purpose of this study is to evaluate the long-term clinical stability of the ridge splitting technique, through the investigation of the survival rate and marginal bone loss of implants. MATERIALS AND METHODS Inclusion criteria and demographics From October 2000 to July 2004, the patients who underwent implant placement at the Department of Periodontology, College of Dentistry, Yonsei University, were selected. The inclusion criteria were as followed: (1) ridge splitting technique was performed to place implants; (2) a minimum follow-up period of 1 year after implant placement; (3) a prosthetic procedure was done on the implants; (4) graft material, type of implant used, occurrence of complication during procedure were clearly recorded. According to inclusion criteria, the total number of patients was 20 (7 males and 13 females) with 34 implants placed (Table 1). Table 1. Demographic description. Subjects 20 patients (34 implants) Gender Male:Female = 7:13 Mean age (years) 33 (range: 17~62) Mean follow up period (years) 4.2±2.1 Br anemark MKIII (Nobel Biocare, Goteborg, Sweden), ITI (Straumann Dental Implants; Institute Straumann AG, Waldenberg, Switzerland), Replace (Nobel Biocare, Goteborg, Sweden), and 3i Osseotite (Implant innovations, Palm Beach Gardens, FL, USA) were used in this study. Twenty, eight, four and two implants of those types were placed, respectively. ITI implants were placed with a non-submerged approach. The other system implants were placed with a submerged approach. A second surgery was performed on submerged implants for healing abutment connection after average of 5.3±3.7 months of healing period. A prosthetic procedure was performed at an average of 7.9±3.0 months after placement. The average follow-up period was 4.2±2.1 years. The mean diameter of the implants placed in this study was 3.95 ± 0.37 mm (3.3 mm~5.0 mm). A 4 mm diameter implant (n=18) was used most frequently. The mean length of the implants placed in this study was 11.87±1.26 mm (8.5 mm~13 mm). A 12mm long implant (n=18) was used most frequently (Table 2). Table 2. Distribution of implant diameter and length. Diameter (mm) No. of implant Length (mm) No. of implant The distribution of implants was as follows: (1) 18 implants were placed at the maxilla (13 implants were placed in the anterior region and 5 implants in the posterior region). (2) 16 implants were placed at the mandible (8 implants were placed in the anterior region Table 3. Site distribution of the ridge splitting technique according to jaw. Mx Right Left Mn Right Left Central incisor 2 2 Central incisor 1 3 Lateral incisor 4 3 Lateral incisor 2 1 Canine 1 1 Canine 1 1 st premolar st premolar nd premolar nd premolar st molar 1 st molar nd molar 2 nd molar 1
3 The long-term clinical stability of implants placed with ridge splitting technique 3 Table 4. Complications during procedures. Distribution Complication Type ofimplant Treatment modality for (tooth number) system managing complications #11 Buccal fenestration Replace Bone graft #11 Buccal fenestration Br anemark MKⅢ Bone graft #15 Buccal dehiscence 3i Osseotite Bone graft #25 Buccal dehiscence 3i Osseotite Bone graft #22 Buccal bone plate fracture Br anemark MKⅢ GBR and 8 implants in the posterior region). Overall, the number of implants placed in the anterior region was larger than in posterior region (21 out of 34 implants) (Table 3). In this study, complications during procedures occurred with 5 implants. Dehiscence occurred with 2 implants, penestration with 2 implants, buccal bone plate fracture with 1 implant (Table 4). Surgical procedure In all patients, prophylactic antibiotics were given before surgery. Local anesthesia was achieved by infiltrating lidocaine 2% containing 1:100,000 epinephrine. A soft tissue incision was made to create a full and partial-thickness flap in the surgical sites (Fig. 2A). If necessary, an anterior and posterior vertical releasing incision was made. Crestal osteotomy was performed at residual ridge with various surgical instruments, for example an oscillating surgical bur, rotary instrument, a guide drill and a number 15 surgical blade (Figs. 1A and 2B). In some cases, vertical osteotomy at the adjacent remaining tooth area was made in order to facilitate the expansion of the residual ridge and to prevent the fracture of the buccal bone plate during expansion. A bone chisel (Stoma, Germany), bone spreader (Meisinger, USA), and osteotome (3i, Implant Innovations, Palm Beach Garden, FL, USA) were applied sequentially to expand the residual ridge through the induction of a green stick fracture of the buccal bone plate (Figs. 1B and 2C). After the residual ridge was expanded appropriately, osteotomy for the implant placement was done with drills and an osteotome. Then, implants were placed (Figs. 1C and 2D). If complications, like dehiscence, penestration, and bone fracture, occurred at the surgical area during implant placement, GBR and bone graft were applied to cope with the complications. The flap was replaced and sutured in a tension free state (Fig. 1D). Stitches were removed after 10~14 days postoperative (Fig. 2E). Patients were asked to rinse with chlorhexidine 0.12% three times daily for 2 weeks postoperative. In submerged implants, a few months healing period was allowed prior to the second surgery. A B C D Fig. 1. Submerged implants were placed at #35, 36, 37. (A) After crestal osteotomy. (B) After Ridge expansion was performed. (C) Implants were placed into expanded ridge. (D) After suturing. A Fig. 2. Non-submerged implants were placed at #32, 33, 34. (A) Flap was opened. (B) Crestal osteotomy with bone chisel. (C) Ridge widening with bone spreader. (D) Implant was placed. (E) After stitches were removed. B C D E
4 4 J M Yoon, Y T Kim, Y J Jang, J C Park, S H Choi, K S Cho, C S Kim Analysis methods Measuring of marginal bone loss Implant marginal bone loss around the implant was evaluated using periapical radiographs that were taken on the day of the implant placement and on the followup visit. The distance from a reference point at the implant to the most coronal point where the marginal bone contacts the implant was measure. Measurements were made mesially and distally of each implant. In order to calibrate dimensional magnitude, the apparent dimension of each implant was measured in the radiograph and compared with the real implant length 21). For submerged implants, the fixture-abutment junction, plat-top of implant, was used as the reference point 22). For ITI implants, the margin of rough surface was used as the reference 23) (Fig. 6). ITI implants were inserted with the margin between the rough and smooth surface level with the alveolar crest. However, this margin was not discernible on radiographs. Measurement was performed at the shoulder of implant. The margin between the rough and smooth surface was situated 2.8 mm from the shoulder of the implant (1.8 mm for the standard plus ITI implants). Therefore, the marginal bone loss of ITI implants was determined by subtracting the distance of the smooth surface (2.8 mm or 1.8 mm) from the calibrated measurements. The periapical radiographs were converted to JPEG image files using the PACS system of the dental hospital of Yonsei University to measure the distance from the reference point of the implant to the first visible marginal bone contact on computer monitor (Fig. 3). The marginal bone loss was measured in 0.1 mm increments. B A Fig. 3. Periapical radiographs of implants. (A) Submerged implant (Left: the day of surgery, Right: 6.4 years after implant placement). Marginal bone loss of distal side of #36 implant was 1.41 mm. (B) Non-submerged implant. Marginal bone loss of distal side of #33 implant was not occurred (Left: the day of surgery, Right: 7 years after implant placement). (arrow: reference point, dotted arrow: most coronal point of bone to implant contact). Evaluation of implant survival rate In this study, the criteria for implant survival were used as proposed by Buser et al. (1990) 24). The criteria are as followed: (1) Absence of persistent subjective complaints, such as pain, foreign body sensation, or dysanaesthesia; (2) Absence of a recurrent peri-implant infection with suppuration; (3) Absence of mobility; and (4) Absence of a continuous radiolucency around the implant. Statistical evaluation For statistical evaluation, the paired T-test was performed using the EXEL program (Microsoft, USA): (1) between non-submerged implants and submerged implants; and (2) between implants that had complications during the procedure and implants that had no complications. A P-value < 0.05 was considered to be statistically significant. For review of implant survival rate, the Keplan-Meier survival analysis was assessed. RESULTS Marginal bone loss of implants The mean marginal bone loss of implants in this study was 1.57±1.44 mm at the mesial side and 1.42±1.48 mm at the distal side. In the non-submerged ITI implants (n=8), the mean marginal bone loss was 1.17 ±0.76 mm and 0.70±0.82 mm on the mesial and the distal sides, respectively. In the submerged implants (n=26) the loss was 1.74±1.40 mm and 1.59±1.41 mm on the mesial and the distal sides, respectively. The difference between the two groups was not statistically significant (P>0.05) (Table 5). In complicated implants (n=5), the mean marginal bone loss was 1.73±1.24 mm and 1.90±1.22 mm on the mesial and the distal sides, respectively. In non-complicated implants, the mean marginal bone loss was 1.57±1.31 mm and 1.26 ±1.35 mm on the mesial and the distal sides, respectively. The difference between the two groups was not statistically significant (P>0.05) (Table 6). Survival rate of implants The implant survival rate during an average follow-up period of 4.2±2.1 years was 100% regardless of the implant system and complications (Table 7).
5 The long-term clinical stability of implants placed with ridge splitting technique 5 DISCUSSION The ridge splitting technique is a useful approach for implant placement in sites where the width of the residual ridge is insufficient due to progressed bone resorption. Since first reported in 1986 by Tatum 11), various modified procedures have been reported. Simion et al. (1992) reported the split crest technique in 5 patients 12). They were able to gain 1~4 mm of the alveolar ridge width by a split-ridge crest technique and guided tissue regeneration at the same time. Scipioni et al. (1994) reported the ridge expansion technique 13). In that study, the ridge expansion technique involved a partial thickness flap, crestal and vertical osteotomy, and buccal displacement of the buccal cortical plate, including a portion of the underlying cancellous bone. Implants were placed in the expanded ridge and allowed to heal for 4~5 months. They installed 329 implants in 170 patients and found that the survival rate of implant over 5 years was 98.8%. But, they did not report the marginal bone loss around implants. Sethi et al. (2000) placed 449 implants in 150 patients in the narrow edentulous ridge of the maxilla by the ridge expansion technique 15). After crestal osteotomy was done, they used an osteotome and D-shaped ridge expander for ridge expansion. The implants were followed up for 5 years after the placement. They found that the implant survival rate was 97%. Blus et al. (2006) used the piezosurgery for the ridge splitting 9). They placed 220 implants in 57 patients and evaluated the implant survival rate with life table analysis. After 3 years of functional loading, the cumulative implant survival rate was 100%. In this study, 34 implants in 20 patients were placed with the ridge splitting technique. During an average follow-up period of 4.2 years, the cumulative survival rate was 100%. These results are similar to other previous studies. The ridge splitting technique, unlike guided bone regeneration and bone graft, allows the implant to be placed at the same time. The placed implant with the ridge splitting technique is covered with a split ridge (dense bone plate), and the healing of the furrow between the split plates is similar to that of fractured bone 25). If primary closure of the flap is obtained over the furrow, a bone graft into the furrow is not necessary. At least 3mm of the residual ridge is needed for the ridge splitting technique because cancellous bone must exist between cortical bone plates for bone expansion 5, 10). To maintain the vitality of the separated buccal bone plate through the ridge splitting procedure, an adequate blood supply is essential. If the blood supply from buccal periosteal flap and endosteal blood supply to the split buccal bone plate are blocked at the same time, the resorption of the buccal bone plate may be unavoidable even though a bone graft is applied into the furrow area. Thus, for successful clinical outcomes, it is necessary to minimize the amount of full-thickness flap on the buccal side 26). Using the development of osseointegration to judge the ridge splitting technique is not an appropriate method. If apical fixation of implant occurs, the osseointegration between ridge splitting and bone graft is same. Therefore, in order to evaluate the width expansion success, the assessment of marginal bone resorption is a proper measure 26). The assessment of marginal bone dimension around implants placed by the osteotome technique, like ridge splitting or ridge expansion, has been performed 27). They used Osseotite, Frialit-2, Tiolox, and ITI implant systems. The total number of patients was 22, with 22 implants placed in their study. During the healing period of 6 months after placement, the mean loss of marginal bone was 0.8 mm. Then 6 months after functional loading, the marginal bone around the implants were reduced on average by 1mm. In another study, evaluation of the marginal bone dimension of ITI TE implants, which were placed with ridge splitting technique and the submerged approach, was performed. During the 6 months after functional loading, the mean loss of marginal bone was 2.0 mm 9). Evaluation of the marginal bone stability using 3 different flap approaches for the ridge splitting technique was performed 26). Full-thickness flap, partialthickness flap, and osteoperiosteal flap were applied with ridge splitting technique for widening the narrow ridges. Osteoperiosteal flap was flap reflection was performed on the crestal area only. A total of 81 implants were placed, of which 4 lost osseointegration. 45 implants were placed with partial-thickness flap reflection, 12 implants with full-thickness flap, and 20 implants with osteoperiosteal flap. Bone sounding with a probe and explorer was used to assess marginal bone stability. The assessment was performed 2 years after placement. Buccal bone loss of 2 mm or more was seen in 11 implants, 10 implants of which used the full-thickness flap reflection and 1 implant used an osteoperiosteal flap reflection. These results show that marginal bone stability is influenced by blood supply on different flap approaches and suggests that full thickness flap should not be reflected when ridge splitting is done.
6 6 J M Yoon, Y T Kim, Y J Jang, J C Park, S H Choi, K S Cho, C S Kim In this study, during an average 4.2 year observation period after implant placement, the mean marginal bone loss around the implants was 1.57 mm and 1.42 mm at the mesial and the distal sides, respectively. In another study, the marginal bone loss around ITI and Br anemark implants was evaluated. Implants were typically placed in partially edentulous maxilla. For the Br anemark implants, the fixture-abutment junction (plat top of implant) was used as the reference point for measurement. After 3 years of functional loading, the mean marginal bone loss from reference point was 1.8 mm on ITI implants and 1.3 mm on Br anemark implants 22). The result was similar to this study. The comparison of marginal bone loss between the non-submerged ITI implant and submerged implants was performed in this study. In the non-submerged ITI implants (n=8), the mean marginal bone loss was 1.17 mm and 0.70 mm at the mesial and the distal sides, respectively. In submerged implants (n=26), 1.74 mm and 1.59 mm at the mesial and the distal sides, respectively. The difference between the two groups was not statistically significant. Commonly, a submerged implant is used with the ridge splitting technique. However, the results of this study showed that nonsubmerged implants placed with the ridge splitting technique did not have a disadvantage of absorption of marginal bone loss. These results mean that if the initial stability of the implant is achievable and a primary flap closure can be obtained, the ridge splitting technique may be applied with non-submerged implant placement. In this study, complications during implant placement occurred with 5 implants. Buccal dehiscence occurred with 2 implants, buccal bone fenestrations with 2 implants, and buccal bone fracture with 1 implant. The marginal bone loss of complicated implants was also investigated. In complicated implants, the mean marginal bone loss was 1.73 mm and 1.90 mm on the mesial and the distal sides, respectively. In non-complicated implants, the mean marginal bone loss was 1.57 mm and 1.26 mm on the mesial and the distal sides, respectively. The difference between complicated and noncomplicated implants was not statistically significant. The reason may be that bone graft and barrier membrane were used to cope with complications. Considering the results of this study, the ridge splitting technique is a predictable method to place implants at a narrow alveolar ridge. However, this study has the limitations that the number of implants investigated in this study is small, the follow-up period is not longer than other studies, and the study design is retrospective. Therefore, more researches are needed for evaluation the long-term stability of the ridge splitting technique. Conclusion 1. During an average follow up period of 4.2years, the cumulative survival rate of implants placed with the ridge splitting technique was 100%. 2. The mean marginal bone loss of implants in this study was 1.57 ± 1.44mm at mesial side and 1.42 ± 1.48mm at distal side. 3. In non-submerged ITI implants (n = 8), the mean marginal bone loss was 1.17±0.76mm and 0.70± 0.82mm on the mesial and the distal sides, respectively. In submerged implants (n = 26) the loss was 1.74± 1.40mm and 1.59±1.41mm on the mesial and the distal sides, respectively. The difference between the two groups was not statistically significant (p >0.05). 4. In complicated implants (n=5), the mean marginal bone was 1.73±1.24mm and 1.90±1.22mm on the mesial and the distal sides, respectively. In noncomplicated implants, the mean marginal bone was 1.57 ±1.31mm and 1.26±1.35mm on the mesial and the distal sides, respectively. The difference between the two groups was not statistically significant (p > 0.05). 5. Considering the results of this study, the ridge splitting technique is a predictable method to place implants at a narrow alveolar ridge. Acknowledgement This work was supported by a faculty research grant of Yonsei University College of Dentistry for 2010( ). REFERENCES 1. Schropp L, Wenzel A, Kostopoulos L, Karring T. Bone healing and soft tissue contour changes following single-tooth extraction: a clinical and radiographic 12- month prospective study. Int J Periodontics Restorative Dent 2003;23(4): Ferrigno N, Laureti M. Surgical advantages with ITI TE implants placement in conjunction with split crest technique. 18-month results of an ongoing prospective study. Clin Oral Implants Res 2005;16(2): Mecall RA, Rosenfeld AL. Influence of residual ridge resorption patterns on fixture placement and tooth position, Part III: Presurgical assessment of ridge
7 The long-term clinical stability of implants placed with ridge splitting technique 7 augmentation requirements. Int J Periodontics Restorative Dent 1996;16(4): Nedir R, Bischof M, Briaux JM, Beyer S, Szmukler- Moncler S, Bernard JP. A 7-year life table analysis from a prospective study on ITI implants with special emphasis on the use of short implants. Results from a private practice. Clin Oral Implants Res 2004;15(2): Misch CM. Implant site development using ridge splitting techniques. Oral Maxillofac Surg Clin North Am 2004;16(1):65-74, vi. 6. Nystrom E, Ahlqvist J, Kahnberg KE, Rosenquist JB. Autogenous onlay bone grafts fixed with screw implants for the treatment of severely resorbed maxillae. Radiographic evaluation of preoperative bone dimensions, postoperative bone loss, and changes in soft-tissue profile. Int J Oral Maxillofac Surg 1996;25(5): Nevins M, Mellonig JT. Enhancement of the damaged edentulous ridge to receive dental implants: a combination of allograft and the GORE-TEX membrane. Int J Periodontics Restorative Dent 1992;12(2): Chiapasco M, Abati S, Romeo E, Vogel G. Clinical outcome of autogenous bone blocks or guided bone regeneration with e-ptfe membranes for the reconstruction of narrow edentulous ridges. Clin Oral Implants Res 1999;10(4): Blus C, Szmukler-Moncler S. Split-crest and immediate implant placement with ultra-sonic bone surgery: a 3-year life-table analysis with 230 treated sites. Clin Oral Implants Res 2006;17(6): Suh JJ, Shelemay A, Choi SH, Chai JK. Alveolar ridge splitting: a new microsaw technique. Int J Periodontics Restorative Dent 2005;25(2): Tatum H, Jr. Maxillary and sinus implant reconstructions. Dent Clin North Am 1986;30(2): Simion M, Baldoni M, Zaffe D. Jawbone enlargement using immediate implant placement associated with a split-crest technique and guided tissue regeneration. Int J Periodontics Restorative Dent 1992;12(6): Scipioni A, Bruschi GB, Calesini G. The edentulous ridge expansion technique: a five-year study. Int J Periodontics Restorative Dent 1994;14(5): Engelke WG, Diederichs CG, Jacobs HG, Deckwer I. Alveolar reconstruction with splitting osteotomy and microfixation of implants. Int J Oral Maxillofac Implants 1997;12(3): Sethi A, Kaus T. Maxillary ridge expansion with simultaneous implant placement: 5-year results of an ongoing clinical study. Int J Oral Maxillofac Implants 2000;15(4): Coatoam GW, Mariotti A. The segmental ridge-split procedure. J Periodontol 2003;74(5): Albrektsson T, Isidor F. Consensus report in Session V. In: Lang NP, Karring T, editors. Proceedings of the 1st European Workshop on Periodontology. London: Quintessence; Roos J, Sennerby L, Lekholm U, Jemt T, Grondahl K, Albrektsson T. A qualitative and quantitative method for evaluating implant success: a 5-year retrospective analysis of the Br anemark implant. Int J Oral Maxillofac Implants 1997;12(4): Albrektsson T, Zarb G, Worthington P, Eriksson AR. The long-term efficacy of currently used dental implants: a review and proposed criteria of success. Int J Oral Maxillofac Implants 1986;1(1): Bragger U, Hafeli U, Huber B, Hammerle CH, Lang NP. Evaluation of postsurgical crestal bone levels adjacent to non-submerged dental implants. Clin Oral Implants Res 1998;9(4): Ferrigno N, S. DS, Fanali S. Conventional and computed tomography in dental implantation surgery. Proceedings of the 1st World Congress of Osseointegration. Venice; p Astrand P, Engquist B, Anzen B, Bergendal T, Hallman M, Karlsson U, et al. A three-year follow-up report of a comparative study of ITI Dental Implants and Br anemark System implants in the treatment of the partially edentulous maxilla. Clin Implant Dent Relat Res 2004;6(3): Kang NW, Jung UW, Choi SH, Chai JK, Kim CK, Kim CS. Bone added osteotome sinus elevation with simultaneous placement of Br anemark Ti-Unite and ITI SLA implants. Journal of Periodontal and Implant Science 2005;35: Buser D, Warrer K, Karring T. Formation of a periodontal ligament around titanium implants. J Periodontol 1990;61(9): Scipioni A, Bruschi GB, Giargia M, Berglundh T, Lindhe J. Healing at implants with and without primary bone contact. An experimental study in dogs. Clin Oral Implants Res 1997;8(1): Jensen OT, Cullum DR, Baer D. Marginal bone stability using 3 different flap approaches for alveolar split expansion for dental implants: a 1-year clinical study. J Oral Maxillofac Surg 2009;67(9): Strietzel FP, Nowak M, Kuchler I, Friedmann A. Peri-implant alveolar bone loss with respect to bone quality after use of the osteotome technique: results of a retrospective study. Clin Oral Implants Res 2002;13(5):
8 8 J M Yoon, Y T Kim, Y J Jang, J C Park, S H Choi, K S Cho, C S Kim 치조능분리술을이용해식립된임프란트의장기간의임상적안정성 윤재민 1, 김영택 1, 장용주 2, 박정철 2, 최성호 2, 조규성 2, 김창성 2 1 국민건강보험공단일산병원치주과 2 연세대학교치과대학치주과학교실, 치주조직재생연구소 Purpose: The purpose of this study is to evaluate the clinical stability of implants placed with a ridge splitting technique through the investigation of the survival rate and marginal bone loss of implants. Methods: 34 implants were placed in 20 patients with the ridge splitting technique. 8 out of 34 implants were placed with the nonsubmerged approach. 26 out of 34 implants were placed with the submerged approach. Guided bone regeneration (GBR) and bone graft were applied in 13 implants. Results: A prosthetic procedure was performed on average 7.9 æ 3.0 months after placement. The average follow up period was 4.2 æ 2.1 years. During the follow up, the cumulative survival rate of implants was 100%. The mean marginal bone loss of implants was 1.57 æ 1.44 mm at the mesial side and 1.42 æ 1.48 mm at the distal side. In non-submerged implants, the mean marginal bone loss was 1.17 mm and 0.70 mm on the mesial and the distal sides, respectively. In submerged implants, the loss was 1.74 mm and 1.59 mm on the mesial and the distal sides, respectively. The difference between the two groups was not statistically significant (P > 0.05). Complications during implant placement surgery, buccal bone dehiscence, fenestration, and buccal bone plate fracture, occurred with 5 implants. In those implants, the mean marginal bone loss was 1.73 mm and 1.90 mm on mesial and distal sides, respectively. In implants without complications, the mean marginal bone loss was 1.57 mm and 1.26 mm on the mesial and the distal side, respectively. The difference between the two groups was not statistically significant (P>0.05). Conclusions: Within limits of this study, considering the results of this study, the ridge splitting technique has a long-term clinical stability to place the implant at the narrow alveolar ridge. [THE JOURNAL OF THE KOREAN ACADEMY OF IMPLANT DENTISTRY 2011;30(1):1-8] Keywords: Dental implant, Alveolar bone loss, Bone regeneration,ridge splitting technique.
Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis
 CASE REPORT Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis Dr Ashish Yadav 1, Dr Aratee Gupta 2, Dr Archana Singh 3, 1,3-
CASE REPORT Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis Dr Ashish Yadav 1, Dr Aratee Gupta 2, Dr Archana Singh 3, 1,3-
Ridge Split Procedure
 Ridge Split Procedure in the Atrophic Maxilla Udatta Kher B.D.S., M.D.S. Loss of teeth causes extensive resorption of the alveolar ridge. In the maxilla the resorption pattern occurs towards the midline,
Ridge Split Procedure in the Atrophic Maxilla Udatta Kher B.D.S., M.D.S. Loss of teeth causes extensive resorption of the alveolar ridge. In the maxilla the resorption pattern occurs towards the midline,
Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report
 C A S E R E P O R T Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report Rhoodie Garrana 1 and Govindrau Mohangi
C A S E R E P O R T Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report Rhoodie Garrana 1 and Govindrau Mohangi
MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION
 Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
Immediate Implant Placement With Ridge Split in A Siebert's Class 1 Defect - A Case Report
 Immediate Implant Placement With Ridge Split in A Siebert's Class 1 Defect - A Case Report Arjun. M. R 1, Nandini Manjunath 2 1, 2 Department of Periodontics, A. J. Institute of Dental Sciences, India
Immediate Implant Placement With Ridge Split in A Siebert's Class 1 Defect - A Case Report Arjun. M. R 1, Nandini Manjunath 2 1, 2 Department of Periodontics, A. J. Institute of Dental Sciences, India
Retrospective radiographic study of marginal bone changes of 88 implants placed with split crest technique in the maxillary latero-posterior area
 Retrospective radiographic study of marginal bone changes of 88 implants placed with split crest technique in the maxillary latero-posterior area S. Longoni 1, I. Maroni 2, A. Baldini 3, M. Sartori 4 1
Retrospective radiographic study of marginal bone changes of 88 implants placed with split crest technique in the maxillary latero-posterior area S. Longoni 1, I. Maroni 2, A. Baldini 3, M. Sartori 4 1
A simple approach to preserve keratinized mucosa around implants using a pre-fabricated implantretained stent: a report of two cases
 Case Report J Periodontal Implant Sci 2010;40:194-200 doi: 10.5051/jpis.2010.40.4.194 A simple approach to preserve keratinized mucosa around implants using a pre-fabricated implantretained stent: a report
Case Report J Periodontal Implant Sci 2010;40:194-200 doi: 10.5051/jpis.2010.40.4.194 A simple approach to preserve keratinized mucosa around implants using a pre-fabricated implantretained stent: a report
Consensus Report Tissue augmentation and esthetics (Working Group 3)
 B. Klinge Thomas F. Flemmig Consensus Report Tissue augmentation and esthetics (Working Group 3) Members of working group: Matteo Chiapasco Jan-Eirik Ellingsen Ronald Jung Friedrich Neukam Isabella Rocchietta
B. Klinge Thomas F. Flemmig Consensus Report Tissue augmentation and esthetics (Working Group 3) Members of working group: Matteo Chiapasco Jan-Eirik Ellingsen Ronald Jung Friedrich Neukam Isabella Rocchietta
Osseointegrated dental implant treatment generally
 Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Case Study. Case # 1 Author: Dr. Suheil Boutros (USA) 2013 Zimmer Dental, Inc. All rights reserved. 6557, Rev. 03/13.
 Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
BONE SPREADING TECHNIQUE A CASE REPORT. simultaneous implant placement and is an alternative Summer s osteotome both clinical use as well as the
 BONE SPREADING TECHNIQUE A CASE REPORT AUTHORS: Renato Sussumu Nishioka, DDS, PhD*, João Carlos Paixão** ABSTRACT: Bone spreading technique (BST) is horizontal augmentation with minimal trauma for simultaneous
BONE SPREADING TECHNIQUE A CASE REPORT AUTHORS: Renato Sussumu Nishioka, DDS, PhD*, João Carlos Paixão** ABSTRACT: Bone spreading technique (BST) is horizontal augmentation with minimal trauma for simultaneous
Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report
 Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
The anatomic limitations of the. Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD*
 CASE REPORT Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD* The anatomic limitations of the residual alveolar bone may cause problems for
CASE REPORT Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD* The anatomic limitations of the residual alveolar bone may cause problems for
Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs
 Current Applied Physics 5 (2005) 507 511 www.elsevier.com/locate/cap Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs Ui-Won Jung a, Hee-Il
Current Applied Physics 5 (2005) 507 511 www.elsevier.com/locate/cap Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs Ui-Won Jung a, Hee-Il
Case Report. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
 Case Report RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
Case Report RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
Vertical and Horizontal Augmentation Using Guided Bone Regeneration. Ph.D. Thesis. Dr. med. dent. et univ. Istvan Urban
 Vertical and Horizontal Augmentation Using Guided Bone Regeneration Ph.D. Thesis Dr. med. dent. et univ. Istvan Urban Supervisor: Prof. Dr. Katalin Nagy, DDS, PhD Faculty of Dentistry, University of Szeged
Vertical and Horizontal Augmentation Using Guided Bone Regeneration Ph.D. Thesis Dr. med. dent. et univ. Istvan Urban Supervisor: Prof. Dr. Katalin Nagy, DDS, PhD Faculty of Dentistry, University of Szeged
Dental Implants: A Predictable Solution for Tooth Loss. Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor
 Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
BONE AUGMENTATION AND GRAFTING
 1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
Prosthetic Options in Implant Dentistry. Hakimeh Siadat, DDS, MSc Associate Professor
 Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Years of research and advancement in
 Immediate Implants with Guided Bone Regeneration Using Titanium Mesh and Alloplast in an Infected Site: A Case Report Mahesh et al Dr. Lanka Mahesh 1 Dr. Ajay Bibra 2 Dr. Vishal Gupta 3 Abstract Years
Immediate Implants with Guided Bone Regeneration Using Titanium Mesh and Alloplast in an Infected Site: A Case Report Mahesh et al Dr. Lanka Mahesh 1 Dr. Ajay Bibra 2 Dr. Vishal Gupta 3 Abstract Years
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 3 Influence of the 3-D Bone-to-Implant Relationship on Esthetics Ueli Grunder, DMD* Stefano Gracis, DMD** Matteo Capelli, DMD** There are
The International Journal of Periodontics & Restorative Dentistry 3 Influence of the 3-D Bone-to-Implant Relationship on Esthetics Ueli Grunder, DMD* Stefano Gracis, DMD** Matteo Capelli, DMD** There are
Mechanical and technical risks in implant therapy.
 Mechanical and technical risks in implant therapy. Salvi GE, Brägger U. Int J Oral Maxillofac Implants. 2009;24 Suppl:69-85. Department of Periodontology, School of Dental Medicine, University of Bern,
Mechanical and technical risks in implant therapy. Salvi GE, Brägger U. Int J Oral Maxillofac Implants. 2009;24 Suppl:69-85. Department of Periodontology, School of Dental Medicine, University of Bern,
Staged ridge split evaluated using cone beam computed tomography and peri implant plastic surgery in the mandibular arch
 CASE REPORT Staged ridge split evaluated using cone beam computed tomography and peri implant plastic surgery in the mandibular arch Nikhil Vasant Jain, Purva H. Shinde, Gaurav R. Poplai 2, Affaf A. Gharatkar
CASE REPORT Staged ridge split evaluated using cone beam computed tomography and peri implant plastic surgery in the mandibular arch Nikhil Vasant Jain, Purva H. Shinde, Gaurav R. Poplai 2, Affaf A. Gharatkar
Immediate implant placement in the Title central incisor region: a case repo. Journal Journal of prosthodontic research,
 Immediate implant placement in the Title central incisor region: a case repo Author(s) Sekine, H; Taguchi, T; Yamagami, M; Alternative Takanashi, T; Furuya, K Journal Journal of prosthodontic research,
Immediate implant placement in the Title central incisor region: a case repo Author(s) Sekine, H; Taguchi, T; Yamagami, M; Alternative Takanashi, T; Furuya, K Journal Journal of prosthodontic research,
Osseointegrated implants are a very reliable means
 Tridimensional Reconstruction of Knife-Edge Edentulous Maxillae by Sinus Elevation, Onlay Grafts, and Sagittal Osteotomy of the Anterior Maxilla: Preliminary Surgical and Prosthetic Results Matteo Chiapasco,
Tridimensional Reconstruction of Knife-Edge Edentulous Maxillae by Sinus Elevation, Onlay Grafts, and Sagittal Osteotomy of the Anterior Maxilla: Preliminary Surgical and Prosthetic Results Matteo Chiapasco,
The surgical placement of dental implants has
 Flapless Implant Surgery: A 10-year Clinical Retrospective Analysis Luis Dominguez Campelo, DDS 1 /Jose R. Dominguez Camara, MD, DDS 2 Purpose: This article is a retrospective clinical analysis of implants
Flapless Implant Surgery: A 10-year Clinical Retrospective Analysis Luis Dominguez Campelo, DDS 1 /Jose R. Dominguez Camara, MD, DDS 2 Purpose: This article is a retrospective clinical analysis of implants
PALATAL POSITIONING OF IMPLANTS IN SEVERELY RESORBED POSTERIOR MAXILLAE F. Atamni, M.Atamni, M.Atamna, Private Practice Tel-aviv Israel
 PALATAL POSITIONING OF IMPLANTS IN SEVERELY RESORBED POSTERIOR MAXILLAE F. Atamni, M.Atamni, M.Atamna, Private Practice Tel-aviv Israel Abstract: Objectives: To evaluate an alternative treatment for rehabilitation
PALATAL POSITIONING OF IMPLANTS IN SEVERELY RESORBED POSTERIOR MAXILLAE F. Atamni, M.Atamni, M.Atamna, Private Practice Tel-aviv Israel Abstract: Objectives: To evaluate an alternative treatment for rehabilitation
The Use of Alpha-Bio Tec's Narrow NeO Implants with Cone Connection for Restoration of Limited Width Ridges
 Case Study 48 The Use of Alpha-Bio Tec's Narrow NeO Implants with Cone Connection for Restoration of Limited Width Ridges Dr. Amir Gazmawe DMD, Specialist in Prosthodontics, Israel Dr. Amir Gazmawe graduated
Case Study 48 The Use of Alpha-Bio Tec's Narrow NeO Implants with Cone Connection for Restoration of Limited Width Ridges Dr. Amir Gazmawe DMD, Specialist in Prosthodontics, Israel Dr. Amir Gazmawe graduated
MODIFIED SINGLE ROLL FLAP APPROACH FOR SIMULTANEOUS IMPLANT PLACEMENT AND GINGIVAL AUGMENTATION
 Journal of IMAB ISSN: 1312-773X https://www.journal-imab-bg.org https://doi.org/10.5272/jimab.2017233.1667 Journal of IMAB - Annual Proceeding (Scientific Papers). 2017 Jul-Sep;23(3): Case report MODIFIED
Journal of IMAB ISSN: 1312-773X https://www.journal-imab-bg.org https://doi.org/10.5272/jimab.2017233.1667 Journal of IMAB - Annual Proceeding (Scientific Papers). 2017 Jul-Sep;23(3): Case report MODIFIED
SPLIT CREST: IMMEDIATE EXPANSION RIM TECHNIQUE FOR REHABILITATION OF ATROPHIC MAXILLA A CASE REPORT
 Vol.13,n.2,pp.15-19 (Dec 2015 Feb 2016) Brazilian Journal of Surgery and Clinical Research- SPLIT CREST: IMMEDIATE EXPANSION RIM TECHNIQUE FOR REHABILITATION OF ATROPHIC MAXILLA A CASE REPORT DEISE KERSTEN
Vol.13,n.2,pp.15-19 (Dec 2015 Feb 2016) Brazilian Journal of Surgery and Clinical Research- SPLIT CREST: IMMEDIATE EXPANSION RIM TECHNIQUE FOR REHABILITATION OF ATROPHIC MAXILLA A CASE REPORT DEISE KERSTEN
Narrow-diameter implants in premolar and molar areas
 2 Long-term follow-up of 2.5mm NDIs supporting a fixed prosthesis Narrow-diameter implants in premolar and molar areas EDUARDO ANITUA, DDS, MD, PHD¹,² A narrow-diameter implant (NDI) is an implant with
2 Long-term follow-up of 2.5mm NDIs supporting a fixed prosthesis Narrow-diameter implants in premolar and molar areas EDUARDO ANITUA, DDS, MD, PHD¹,² A narrow-diameter implant (NDI) is an implant with
TOPICS. T O P I C S Day 1. Implant Locations. Implant Placement in the Posterior Maxilla. Anatomy and risk factors Option 1: Short implants
 T O P I C S Day 1 Factors influencing the long-term stability of dental implants Surgical procedures in posterior sites: Standard implant placement with or without flap elevation Surgical procedures in
T O P I C S Day 1 Factors influencing the long-term stability of dental implants Surgical procedures in posterior sites: Standard implant placement with or without flap elevation Surgical procedures in
GUIDED BONE & TISSUE REGENERATION 2-DAY MASTERCLASS (CHOOSE LONDON OR PARIS) DR. ISABELLA ROCCHIETTA & DR. DAVID NISAND
 GUIDED BONE & TISSUE REGENERATION DR. ISABELLA ROCCHIETTA & DR. DAVID NISAND 2-DAY MASTERCLASS (CHOOSE LONDON OR PARIS) This hands-on course will be delivered in small group workshops and will equip the
GUIDED BONE & TISSUE REGENERATION DR. ISABELLA ROCCHIETTA & DR. DAVID NISAND 2-DAY MASTERCLASS (CHOOSE LONDON OR PARIS) This hands-on course will be delivered in small group workshops and will equip the
Immediate Implant Placement:
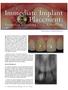 Immediate Implant Placement: Parameters Influencing Tissue Remodeling Bernard Touati, DDS and Mario Groisman, DDS In esthetic implant therapy, the patient s objective is to obtain an imperceptible, natural-looking
Immediate Implant Placement: Parameters Influencing Tissue Remodeling Bernard Touati, DDS and Mario Groisman, DDS In esthetic implant therapy, the patient s objective is to obtain an imperceptible, natural-looking
Esthetic management of multiple missing anterior teeth A Case report
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 13, Issue 1 Ver. II (Jan. 2014), PP 97-101 Esthetic management of multiple missing anterior teeth A
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 13, Issue 1 Ver. II (Jan. 2014), PP 97-101 Esthetic management of multiple missing anterior teeth A
Contemporary Implant Dentistry
 Contemporary Implant Dentistry C H A P T ER 1 4 O F C O N T E M P OR A R Y O R A L A N D M A X I L L OFA C IA L S U R G E RY B Y : D R A R A S H K H O J A S T EH Dental implant is suitable for: completely
Contemporary Implant Dentistry C H A P T ER 1 4 O F C O N T E M P OR A R Y O R A L A N D M A X I L L OFA C IA L S U R G E RY B Y : D R A R A S H K H O J A S T EH Dental implant is suitable for: completely
Young-Jin Park, DDS,* and Sung-Am Cho, DDS, MS, PhD
 J Oral Maxillofac Surg 68:1338-1344, 2010 Retrospective Chart Analysis on Survival Rate of Fixtures Installed at the Tuberosity Bone for Cases With Missing Unilateral Upper Molars: A Study of 7 Cases Young-Jin
J Oral Maxillofac Surg 68:1338-1344, 2010 Retrospective Chart Analysis on Survival Rate of Fixtures Installed at the Tuberosity Bone for Cases With Missing Unilateral Upper Molars: A Study of 7 Cases Young-Jin
Surgical reconstruction of lost papilla around implant with a modified technique: A case report
 Journal of Periodontology & Implant Dentistry Case Report Surgical reconstruction of lost papilla around implant with a modified technique: A case report Mahdi Faraji* Andre Van Zyl University of Pretoria,
Journal of Periodontology & Implant Dentistry Case Report Surgical reconstruction of lost papilla around implant with a modified technique: A case report Mahdi Faraji* Andre Van Zyl University of Pretoria,
Dental Implant Treatment with Diffe Title for Sinus Floor Elevation-A Case Re. Sekine, H; Taguchi, T; Seta, S; Tak Author(s) T; Kakizawa, T
 Dental Implant Treatment with Diffe Title for Sinus Floor Elevation-A Case Re Sekine, H; Taguchi, T; Seta, S; Tak Author(s) T; Kakizawa, T Journal Bulletin of Tokyo Dental College, 4 URL http://hdl.handle.net/10130/200
Dental Implant Treatment with Diffe Title for Sinus Floor Elevation-A Case Re Sekine, H; Taguchi, T; Seta, S; Tak Author(s) T; Kakizawa, T Journal Bulletin of Tokyo Dental College, 4 URL http://hdl.handle.net/10130/200
( ) 2009;28(2):89-94
 ( ) 2009;28(2):89-94 Osseointegration is important in the functional aspect, however, esthetics is also important, especially in the maxillary anterior region. An adequate surgical technique is necessary
( ) 2009;28(2):89-94 Osseointegration is important in the functional aspect, however, esthetics is also important, especially in the maxillary anterior region. An adequate surgical technique is necessary
Sinus elevation with short implant
 Sinus elevation with short implant Authors: Prof. Dr Mauro Marincola, Prof. Dr Dr Rolf Ewers, Prof. Giorgio Lombardo (University of Verona) & Prof. Miguel Simancas Pallares (University of Cartagena), Austria/Italy/Colombia
Sinus elevation with short implant Authors: Prof. Dr Mauro Marincola, Prof. Dr Dr Rolf Ewers, Prof. Giorgio Lombardo (University of Verona) & Prof. Miguel Simancas Pallares (University of Cartagena), Austria/Italy/Colombia
A Novel Technique for the Management of a Maxillary Anterior Alveolar Defect with an Implant-retained Fixed Prosthesis: A Clinical Report
 Neenu M Varghese et al Case Report 10.5005/jp-journals-10012-1148 A Novel Technique for the Management of a Maxillary Anterior Alveolar Defect with an Implant-retained Fixed Prosthesis: A Clinical Report
Neenu M Varghese et al Case Report 10.5005/jp-journals-10012-1148 A Novel Technique for the Management of a Maxillary Anterior Alveolar Defect with an Implant-retained Fixed Prosthesis: A Clinical Report
Nabil Nadji A THESIS SUBMITTED IN PARTIAL FULFILLMENT OF THE REQUIREMENTS FOR THE DEGREE OF MASTER OF SCIENCE
 CLINICAL OUTCOMES OF SHORT IMPLANTS PLACED IN THE POSTERIOR MAXILLA WITH THE INDIRECT SINUS ELEVATION TECHNIQUE AND IN THE POSTERIOR MANDIBLE: A RETROSPECTIVE STUDY WITH UP TO 5-YEAR FOLLOW-UP. by Nabil
CLINICAL OUTCOMES OF SHORT IMPLANTS PLACED IN THE POSTERIOR MAXILLA WITH THE INDIRECT SINUS ELEVATION TECHNIQUE AND IN THE POSTERIOR MANDIBLE: A RETROSPECTIVE STUDY WITH UP TO 5-YEAR FOLLOW-UP. by Nabil
Guided surgery as a way to simplify surgical implant treatment in complex cases
 52 STARGET 1 I 12 StraUMaNN CareS r ry vincenzo MiriSOLA Di TOrreSANTO AND LUCA COrDArO Guided surgery as a way to simplify surgical implant treatment in complex cases Background A 41-year-old woman with
52 STARGET 1 I 12 StraUMaNN CareS r ry vincenzo MiriSOLA Di TOrreSANTO AND LUCA COrDArO Guided surgery as a way to simplify surgical implant treatment in complex cases Background A 41-year-old woman with
Vertical and horizontal alveolar ridge augmentation
 CLINICAL SIMULTANEOUS VERTICAL GUIDED BONE REGENERATION AND GUIDED TISSUE REGENERATION IN THE POSTERIOR MAXILLA USING RECOMBINANT HUMAN PLATELET-DERIVED GROWTH FACTOR: A CASE REPORT Istvan Urban, DMD,
CLINICAL SIMULTANEOUS VERTICAL GUIDED BONE REGENERATION AND GUIDED TISSUE REGENERATION IN THE POSTERIOR MAXILLA USING RECOMBINANT HUMAN PLATELET-DERIVED GROWTH FACTOR: A CASE REPORT Istvan Urban, DMD,
Extraction with Immediate Implant Placement and Ridge Preservation in the Posterior
 Extraction with Immediate Implant Placement and Ridge Preservation in the Posterior by Timothy F. Kosinski, DDS, MAGD The following case presentation illustrates the diagnosis, planning and treatment for
Extraction with Immediate Implant Placement and Ridge Preservation in the Posterior by Timothy F. Kosinski, DDS, MAGD The following case presentation illustrates the diagnosis, planning and treatment for
Role of flap tension in primary wound closure of mucoperiosteal flaps: a prospective cohort study
 R. Burkhardt N. P. Lang Role of flap tension in primary wound closure of mucoperiosteal flaps: a prospective cohort study Authors affiliation: R. Burkhardt, N. P. Lang, The University of Hong Kong, Hong
R. Burkhardt N. P. Lang Role of flap tension in primary wound closure of mucoperiosteal flaps: a prospective cohort study Authors affiliation: R. Burkhardt, N. P. Lang, The University of Hong Kong, Hong
REGENERATIONTIME. A Case Report by. Ridge Augmentation and Delayed Implant Placement on an Upper Lateral Incisor
 A Case Report by Dr. Daniele Cardaropoli Ridge Augmentation and Delayed Implant Placement on an Upper Lateral Incisor The Situation An adult female patient presented with an endodontic/prosthetic failure
A Case Report by Dr. Daniele Cardaropoli Ridge Augmentation and Delayed Implant Placement on an Upper Lateral Incisor The Situation An adult female patient presented with an endodontic/prosthetic failure
The Brånemark osseointegration method, using titanium dental implants (fixtures)
 Early Failures in 4,641 Consecutively Placed Brånemark Dental Implants: A Study From Stage 1 Surgery to the Connection of Completed Prostheses Bertil Friberg, DDS/Torsten Jemt, DDS, PhD/Ulf Lekholm, DDS,
Early Failures in 4,641 Consecutively Placed Brånemark Dental Implants: A Study From Stage 1 Surgery to the Connection of Completed Prostheses Bertil Friberg, DDS/Torsten Jemt, DDS, PhD/Ulf Lekholm, DDS,
03 Best combination for thin ridge
 MILAkit TM BonEx kit TM 03 Best combination for thin ridge Joel A. Gonzales RDA Product Specialist Email: Cell: joelg@megagenus.com (480) 440-3927 Thor MEGAGEN Implant 28 29 Why Thor? 1. Simple & Strong
MILAkit TM BonEx kit TM 03 Best combination for thin ridge Joel A. Gonzales RDA Product Specialist Email: Cell: joelg@megagenus.com (480) 440-3927 Thor MEGAGEN Implant 28 29 Why Thor? 1. Simple & Strong
Interproximal Papilla Levels Following Early Versus Delayed Placement of Single-Tooth Implants: A Controlled Clinical Trial
 Interproximal Papilla Levels Following Early Versus Delayed Placement of Single-Tooth Implants: A Controlled Clinical Trial Lars Schropp, DDS, PhD /Flemming Isidor, DDS, PhD, Dr Odont /Lambros Kostopoulos,
Interproximal Papilla Levels Following Early Versus Delayed Placement of Single-Tooth Implants: A Controlled Clinical Trial Lars Schropp, DDS, PhD /Flemming Isidor, DDS, PhD, Dr Odont /Lambros Kostopoulos,
Minimal invasive horizontal ridge augmentation using subperiosteal tunneling technique
 Kim et al. Maxillofacial Plastic and Reconstructive Surgery (2016) 38:41 DOI 10.1186/s40902-016-0087-8 Maxillofacial Plastic and Reconstructive Surgery RESEARCH Open Access Minimal invasive horizontal
Kim et al. Maxillofacial Plastic and Reconstructive Surgery (2016) 38:41 DOI 10.1186/s40902-016-0087-8 Maxillofacial Plastic and Reconstructive Surgery RESEARCH Open Access Minimal invasive horizontal
Vertical Augmentation
 Indication Sheet V Dr. Mauro Merli Vertical Augmentation Vertical alveolar ridge augmentation by means of the fence technique with Geistlich biomaterials > Original publication of the technique on PubMed;
Indication Sheet V Dr. Mauro Merli Vertical Augmentation Vertical alveolar ridge augmentation by means of the fence technique with Geistlich biomaterials > Original publication of the technique on PubMed;
Labial and lingual/palatal bone thickness of maxillary and mandibular anteriors in human cadavers in Koreans
 Research Article J Periodontal Implant Sci 2011;41:60-66 doi: 10.5051/jpis.2011.41.2.60 Labial and lingual/palatal bone thickness of maxillary and mandibular anteriors in human cadavers in Koreans Ji Young
Research Article J Periodontal Implant Sci 2011;41:60-66 doi: 10.5051/jpis.2011.41.2.60 Labial and lingual/palatal bone thickness of maxillary and mandibular anteriors in human cadavers in Koreans Ji Young
Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Abstract Purpose: Materials and methods Results:
 Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Bum-Soo Kim 1, Young-Kyun Kim 1, Pil-Young Yun 1, Yang-Jin Lee 2, Hyo-Jeong Lee 3, Su-Gwan Kim 4 1Department of
Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Bum-Soo Kim 1, Young-Kyun Kim 1, Pil-Young Yun 1, Yang-Jin Lee 2, Hyo-Jeong Lee 3, Su-Gwan Kim 4 1Department of
Endosseous dental implants initially showed very
 Five-mm-Diameter Implants without a Smooth Surface Collar: Report on 98 Consecutive Placements Franck Renouard, DDS*/Jean-Pierre Arnoux, DDS**/David P. Sarment, DDS*** In recent years, indications for
Five-mm-Diameter Implants without a Smooth Surface Collar: Report on 98 Consecutive Placements Franck Renouard, DDS*/Jean-Pierre Arnoux, DDS**/David P. Sarment, DDS*** In recent years, indications for
Alveolar Ridge Preservation:
 Alveolar Ridge Preservation: Preserving and Building up the Bony Structures after Extraction» By: Prof. Roland Hille Konigsallee 49c, 41747 Viersen, Germany E-mail: dr-hille@t-online.de» Prof. Rolf Vollmer
Alveolar Ridge Preservation: Preserving and Building up the Bony Structures after Extraction» By: Prof. Roland Hille Konigsallee 49c, 41747 Viersen, Germany E-mail: dr-hille@t-online.de» Prof. Rolf Vollmer
Implant Placement in Maxillary Anterior Region Along with Soft and Hard Tissue Grafting- A Case Report.
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 10 Ver. XII (October. 2016), PP 68-73 www.iosrjournals.org Implant Placement in Maxillary Anterior
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 10 Ver. XII (October. 2016), PP 68-73 www.iosrjournals.org Implant Placement in Maxillary Anterior
Minimally invasive implant dentistry with short or narrow implants Ridge splitting and crestal and internal sinus lift
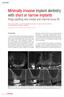 Minimally invasive implant dentistry with short or narrow implants Ridge splitting and crestal and internal sinus lift Prof. Mauro Marincola 1, Dr Daniel Hernández-González 1, Dr Jaime Guzmán-De Ávila
Minimally invasive implant dentistry with short or narrow implants Ridge splitting and crestal and internal sinus lift Prof. Mauro Marincola 1, Dr Daniel Hernández-González 1, Dr Jaime Guzmán-De Ávila
GUIDED BONE & TISSUE REGENERATION 2-DAY LIVE COURSE DR. ISABELLA ROCCHIETTA & DR. DAVID NISAND
 GUIDED BONE & TISSUE REGENERATION DR. ISABELLA ROCCHIETTA & DR. DAVID NISAND 2-DAY LIVE COURSE Soft tissue management is the key to achieve aesthetic success. Periodontal and peri-implant soft tissue management
GUIDED BONE & TISSUE REGENERATION DR. ISABELLA ROCCHIETTA & DR. DAVID NISAND 2-DAY LIVE COURSE Soft tissue management is the key to achieve aesthetic success. Periodontal and peri-implant soft tissue management
Factors influencing ridge alterations following immediate implant placement into extraction sockets
 Jorge Ferrus Denis Cecchinato E. Bjarni Pjetursson Niklaus P. Lang Mariano Sanz Jan Lindhe Factors influencing ridge alterations following immediate implant placement into extraction sockets Authors affiliations:
Jorge Ferrus Denis Cecchinato E. Bjarni Pjetursson Niklaus P. Lang Mariano Sanz Jan Lindhe Factors influencing ridge alterations following immediate implant placement into extraction sockets Authors affiliations:
Case study 2. A Retrospective Multi-Center Study on the Spiral Implant
 Case study 2 A Retrospective Multi-Center Study on the Spiral Implant Benny Karmon DMD, Jerry Kohen DMD, Ariel Lor DMD, Yiftach Gratciany DMD, Zvi Laster DMD, Gideon Hallel DMD MPA, Tsvia Karmon A Retrospective
Case study 2 A Retrospective Multi-Center Study on the Spiral Implant Benny Karmon DMD, Jerry Kohen DMD, Ariel Lor DMD, Yiftach Gratciany DMD, Zvi Laster DMD, Gideon Hallel DMD MPA, Tsvia Karmon A Retrospective
The effect of peri-implant bone exposure on soft tissue healing and bone loss in two adjacent implants
 Research Article J Periodontal Implant Sci 2012;42:20-24 http://dx.doi.org/10.5051/jpis.2012.42.1.20 on soft tissue healing and bone loss in two adjacent implants Seung-Yun Shin 1, Seung-Boem Kye 1, Jongrak
Research Article J Periodontal Implant Sci 2012;42:20-24 http://dx.doi.org/10.5051/jpis.2012.42.1.20 on soft tissue healing and bone loss in two adjacent implants Seung-Yun Shin 1, Seung-Boem Kye 1, Jongrak
FIVE-YEAR FOLLOW-UP OF IMPLANTS PLACED SIMULTANEOUSLY WITH INFERIOR ALVEOLAR NERVE LATERALISATION OR TRANSPOSITION
 original articles FIVE-YEAR FOLLOW-UP OF IMPLANTS PLACED SIMULTANEOUSLY WITH INFERIOR ALVEOLAR NERVE LATERALISATION OR TRANSPOSITION Stefan Peev 1, Borislav Ivanov 2, Elitsa Sabeva 1, Tihomir Georgiev
original articles FIVE-YEAR FOLLOW-UP OF IMPLANTS PLACED SIMULTANEOUSLY WITH INFERIOR ALVEOLAR NERVE LATERALISATION OR TRANSPOSITION Stefan Peev 1, Borislav Ivanov 2, Elitsa Sabeva 1, Tihomir Georgiev
Management of a complex case
 2 Soft- and hard-tissue reconstruction of a severely deficient site prior to implant placement: a case report Management of a complex case Younes Khosroshahy, DDS, MFDS RCS (Eng), Dip Imp Dent RCSEd, Blue
2 Soft- and hard-tissue reconstruction of a severely deficient site prior to implant placement: a case report Management of a complex case Younes Khosroshahy, DDS, MFDS RCS (Eng), Dip Imp Dent RCSEd, Blue
Implant Site Development Part I
 REVIEW ARTICLE Implant Site Development Part I 1 Umang Nayar, 2 Shankar Iyer IJCID Implant Site Development Part I 1 Consultant, Dental Surgeon and Periodontist at Max Health Care, New Delhi, Professor
REVIEW ARTICLE Implant Site Development Part I 1 Umang Nayar, 2 Shankar Iyer IJCID Implant Site Development Part I 1 Consultant, Dental Surgeon and Periodontist at Max Health Care, New Delhi, Professor
THE PERIODONTAL ASPECT OF IMPLANT THERAPY Prof. Dr. Windisch Péter
 THE PERIODONTAL ASPECT OF IMPLANT THERAPY Prof. Dr. Windisch Péter Periodontal aspects of implant therapy 1) Comprehensive perioprosthodontic treatment by utilizing implants on perio-patients. 2) Anatomical
THE PERIODONTAL ASPECT OF IMPLANT THERAPY Prof. Dr. Windisch Péter Periodontal aspects of implant therapy 1) Comprehensive perioprosthodontic treatment by utilizing implants on perio-patients. 2) Anatomical
Analysis of Short-term Success Rate and Healing Patterns of Implantium Implant
 Analysis of Short-term Success Rate and Healing Patterns of Implantium Implant Gyung-Joon Chae 1, Sung-Min Chung 2, Ui-Won Jung 1, Kyoo-Sung Cho 1, Jung-Kyu Chai 1, Chong-Kwan Kim 1, Seong-Ho Choi 1, and
Analysis of Short-term Success Rate and Healing Patterns of Implantium Implant Gyung-Joon Chae 1, Sung-Min Chung 2, Ui-Won Jung 1, Kyoo-Sung Cho 1, Jung-Kyu Chai 1, Chong-Kwan Kim 1, Seong-Ho Choi 1, and
The International Journal of Periodontics & Restorative Dentistry
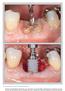 The International Journal of Periodontics & Restorative Dentistry 89 Pre-extractive Interradicular Implant Bed Preparation: Case Presentations of a Novel Approach to Immediate Implant Placement at Multirooted
The International Journal of Periodontics & Restorative Dentistry 89 Pre-extractive Interradicular Implant Bed Preparation: Case Presentations of a Novel Approach to Immediate Implant Placement at Multirooted
Socket preservation in the daily practice: A clinical case report
 Clinical Socket preservation in the daily practice: A clinical case report Rabih Abi Nader 1 and Carine Tabarani 2 Abstract Soft tissue contour depends on the underlying bone anatomy. Following tooth extraction,
Clinical Socket preservation in the daily practice: A clinical case report Rabih Abi Nader 1 and Carine Tabarani 2 Abstract Soft tissue contour depends on the underlying bone anatomy. Following tooth extraction,
Working together as a team, the periodontist
 The Team Approach to Esthetic Immediate Implant Placement Bobby L. Butler, DDS; and Greggory Kinzer, DDS Working together as a team, the periodontist and restorative dentist can provide an increased level
The Team Approach to Esthetic Immediate Implant Placement Bobby L. Butler, DDS; and Greggory Kinzer, DDS Working together as a team, the periodontist and restorative dentist can provide an increased level
Cumulative survival rate of Astra Tech implants: a retrospective analysis
 Research Article Journal of Periodontal J Periodontal Implant Sci 2011;41:86-91 doi: 10.5051/jpis.2011.41.2.86 Cumulative survival rate of Astra Tech implants: a retrospective analysis Jung-Soo Kim 1,
Research Article Journal of Periodontal J Periodontal Implant Sci 2011;41:86-91 doi: 10.5051/jpis.2011.41.2.86 Cumulative survival rate of Astra Tech implants: a retrospective analysis Jung-Soo Kim 1,
A new approach with an in-situ self-hardening grafting material
 74 Bone grafting with simultaneous early implant placement A new approach with an in-situ self-hardening grafting material MINAS LEVENTIS 1,2, PHD; PETER FAIRBAIRN 1,3, BDS; ORESTIS VASILIADIS 2,4, DDS
74 Bone grafting with simultaneous early implant placement A new approach with an in-situ self-hardening grafting material MINAS LEVENTIS 1,2, PHD; PETER FAIRBAIRN 1,3, BDS; ORESTIS VASILIADIS 2,4, DDS
CASE REPORT. CBCT-Assisted Treatment of the Failing Long Span Bridge with Staged and Immediate Load Implant Restoration
 Computer Aided Implantology Academy Newsletter - Newsletter 20 - July 2009 CASE REPORT CBCT-Assisted Treatment of the Failing Long Span Bridge with Staged and Immediate Load Implant Restoration Case Report
Computer Aided Implantology Academy Newsletter - Newsletter 20 - July 2009 CASE REPORT CBCT-Assisted Treatment of the Failing Long Span Bridge with Staged and Immediate Load Implant Restoration Case Report
Consensus Statements and Recommended Clinical Procedures Regarding Contemporary Surgical and Radiographic Techniques in Implant Dentistry
 Group 1 and Recommended Clinical Procedures Regarding Contemporary Surgical and Radiographic Techniques in Implant Dentistry Michael M. Bornstein, PD Dr Med Dent 1 /Bilal Al-Nawas, Prof Dr Med, Dr Med
Group 1 and Recommended Clinical Procedures Regarding Contemporary Surgical and Radiographic Techniques in Implant Dentistry Michael M. Bornstein, PD Dr Med Dent 1 /Bilal Al-Nawas, Prof Dr Med, Dr Med
BONE SPREADER TECHNIQUE: APRELIMINARY 3-YEAR STUDY Renato Sussumu Nishioka, DDS, MSc, PhD; Francisley Avila Souza, DDS, MSc
 RESEARCH BONE SPREADER TECHNIQUE: APRELIMINARY 3-YEAR STUDY Renato Sussumu Nishioka, DDS, MSc, PhD; Francisley Avila Souza, DDS, MSc The purpose of this study was to observe the clinical outcome of bone
RESEARCH BONE SPREADER TECHNIQUE: APRELIMINARY 3-YEAR STUDY Renato Sussumu Nishioka, DDS, MSc, PhD; Francisley Avila Souza, DDS, MSc The purpose of this study was to observe the clinical outcome of bone
GBR membrane for ideal regeneration
 GBR membrane for ideal regeneration 1) i-gen Lingual Extension should be considered for a large defect. Need to have at least 1mm of space above the platform of a fixture: Make this space with a pre-existing
GBR membrane for ideal regeneration 1) i-gen Lingual Extension should be considered for a large defect. Need to have at least 1mm of space above the platform of a fixture: Make this space with a pre-existing
A retrospective study on separate single-tooth implant restorations to replace two or more consecutive. maxillary posterior teeth up to 6 years.
 Original Article A retrospective study on separate single-tooth implant restorations to replace two or more consecutive maxillary posterior teeth up to 6 years follow up Myat Nyan Department of Prosthodontics,
Original Article A retrospective study on separate single-tooth implant restorations to replace two or more consecutive maxillary posterior teeth up to 6 years follow up Myat Nyan Department of Prosthodontics,
Benefits of CBCT in Implant Planning
 10.5005/jp-journals-10012-1032 CLINICAL SCIENCE 1 Gregori M Kurtzman, 2 Douglas F Dompkowski 1 Private General Practice in Silver Spring, Maryland, USA 2 Private Periodontal Practice in Bethesda, Maryland,
10.5005/jp-journals-10012-1032 CLINICAL SCIENCE 1 Gregori M Kurtzman, 2 Douglas F Dompkowski 1 Private General Practice in Silver Spring, Maryland, USA 2 Private Periodontal Practice in Bethesda, Maryland,
Immediate Implant Placement Along With Guided Bone Regeneration In Mandibular Anterior Region A Case Report.
 IMMEDIATE IMPLANT PLACEMENT ALONG WITH GUIDED BONE REGENERATION IN MANDIBULAR ANTERIOR REGION A CASE REPORT. Dr.C.P.Dhivakar 1, Dr.T.Saravanan 2, Dr.A.Aniz 3 1) Department of Periodontics, Karpaga Vinayaga
IMMEDIATE IMPLANT PLACEMENT ALONG WITH GUIDED BONE REGENERATION IN MANDIBULAR ANTERIOR REGION A CASE REPORT. Dr.C.P.Dhivakar 1, Dr.T.Saravanan 2, Dr.A.Aniz 3 1) Department of Periodontics, Karpaga Vinayaga
The Sandwich Bone Augmentation Technique. Jia-Hui Fu* and Hom-Lay Wang*
 CASE REPORT The Sandwich Bone Augmentation Technique Jia-Hui Fu* and Hom-Lay Wang* Introduction: Horizontal ridge width reduction after tooth extraction is a common clinical scenario. As such, when implant-supported
CASE REPORT The Sandwich Bone Augmentation Technique Jia-Hui Fu* and Hom-Lay Wang* Introduction: Horizontal ridge width reduction after tooth extraction is a common clinical scenario. As such, when implant-supported
Flapless, Immediate Implantation & Immediate Loading with Socket Preservation in the Esthetic Area Using the Alpha-Bio Tec's NeO Implants
 Flapless Surgery Case Study 48 Flapless, Immediate Implantation & Immediate Loading with Socket Preservation in the Esthetic Area Using the Alpha-Bio Tec's NeO Implants Dr. Gadi Schneider DMD, Specialist
Flapless Surgery Case Study 48 Flapless, Immediate Implantation & Immediate Loading with Socket Preservation in the Esthetic Area Using the Alpha-Bio Tec's NeO Implants Dr. Gadi Schneider DMD, Specialist
The International Journal of Periodontics & Restorative Dentistry
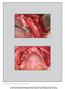 The International Journal of Periodontics & Restorative Dentistry 141 Screw Spreading: Technical Considerations and Case Report Renato Sussumu Nishioka, DDS, PhD, MSc* Alberto Noriyuki Kojima, DDS, PhD,
The International Journal of Periodontics & Restorative Dentistry 141 Screw Spreading: Technical Considerations and Case Report Renato Sussumu Nishioka, DDS, PhD, MSc* Alberto Noriyuki Kojima, DDS, PhD,
Periimplant Regeneration Fenestration
 Indication Sheet PIR Periimplant Regeneration Fenestration Treatment concept of Dr. Jean-Pierre Gardella (surgeon) and Dr. Christian Richelme (prosthodontist), Marseille, France > Filling of a peri-implant
Indication Sheet PIR Periimplant Regeneration Fenestration Treatment concept of Dr. Jean-Pierre Gardella (surgeon) and Dr. Christian Richelme (prosthodontist), Marseille, France > Filling of a peri-implant
Sandwich bone graft for vertical augmentation of the posterior maxillary region: a case report with 9-year follow-up
 Tanaka et al. International Journal of Implant Dentistry (2017) 3:20 DOI 10.1186/s40729-017-0063-9 International Journal of Implant Dentistry CASE REPORT Sandwich bone graft for vertical augmentation of
Tanaka et al. International Journal of Implant Dentistry (2017) 3:20 DOI 10.1186/s40729-017-0063-9 International Journal of Implant Dentistry CASE REPORT Sandwich bone graft for vertical augmentation of
Enhancing implant stability with osseodensification a case report with 2-year follow-up
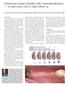 Enhancing implant stability with osseodensification a case report with 2-year follow-up Dr. Salah Huwais discusses how osseodensification facilitates ridge expansion with enhanced implant stability Introduction
Enhancing implant stability with osseodensification a case report with 2-year follow-up Dr. Salah Huwais discusses how osseodensification facilitates ridge expansion with enhanced implant stability Introduction
Oral Health and Dentistry
 Page 107 to 118 Volume 1 Issue 2 2017 Case Report Oral Health and Dentistry ISSN: 2573-4989 Full Mouth Implants Rehabilitation of a Patient with Ectodermal Dysplasia After 3-Ds Ridge Augmentation and Bilateral
Page 107 to 118 Volume 1 Issue 2 2017 Case Report Oral Health and Dentistry ISSN: 2573-4989 Full Mouth Implants Rehabilitation of a Patient with Ectodermal Dysplasia After 3-Ds Ridge Augmentation and Bilateral
Successful Bone Formation at Immediate Transmucosal Implants: A Clinical Report
 Successful Bone Formation at Immediate Transmucosal Implants: A Clinical Report Christoph H.F. Hämmerle, PD Dr med dent*/urs Brägger, Prof Dr med dent*/ Bruno Schmid, Dr med dent**/niklaus P. Lang, Prof
Successful Bone Formation at Immediate Transmucosal Implants: A Clinical Report Christoph H.F. Hämmerle, PD Dr med dent*/urs Brägger, Prof Dr med dent*/ Bruno Schmid, Dr med dent**/niklaus P. Lang, Prof
Alveolar Ridge Augmentation with Titanium Mesh and Particulate Allograft A Case Report
 Alveolar Ridge Augmentation with Titanium Mesh and Particulate Allograft A Case Report Dr. Pratibha Borasi, Dr. Praneeta Kamble Department of Periodontics, Nair Hospital Dental College, Mumbai, Maharashtra,
Alveolar Ridge Augmentation with Titanium Mesh and Particulate Allograft A Case Report Dr. Pratibha Borasi, Dr. Praneeta Kamble Department of Periodontics, Nair Hospital Dental College, Mumbai, Maharashtra,
Maxillary sinus augmentation without any graft material- A case Report
 A CASE REPORT ISSN: 2321-4988 D.Shiva kumar et al. /JPR:BioMedRx: An International Journal 2013,1(8), Available online through www.jpronline.info Maxillary sinus augmentation without any graft material-
A CASE REPORT ISSN: 2321-4988 D.Shiva kumar et al. /JPR:BioMedRx: An International Journal 2013,1(8), Available online through www.jpronline.info Maxillary sinus augmentation without any graft material-
Clinical Case Reports using Cytoplast GTR Barrier Membranes
 Clinical Case Reports using Cytoplast GTR Barrier Membranes Barry K. Bartee, DDS, MD The Cytoplast Technique: Extraction Site Grafting Without Primary Closure 1. 1. Preoperative view. To maximize the result
Clinical Case Reports using Cytoplast GTR Barrier Membranes Barry K. Bartee, DDS, MD The Cytoplast Technique: Extraction Site Grafting Without Primary Closure 1. 1. Preoperative view. To maximize the result
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/31632 holds various files of this Leiden University dissertation. Author: Mensink, Gertjan Title: Bilateral sagittal split osteotomy by the splitter-separator
Cover Page The handle http://hdl.handle.net/1887/31632 holds various files of this Leiden University dissertation. Author: Mensink, Gertjan Title: Bilateral sagittal split osteotomy by the splitter-separator
Management of peri-implant recession associated with bone fenestration and dehiscence in the anterior region
 CLINICAL REPORT 269 George Nikou, Dimitris Nikolidakis, Peter Thoolen, Anton Sculean Management of peri-implant recession associated with bone fenestration and dehiscence in the anterior region KEY WORDS
CLINICAL REPORT 269 George Nikou, Dimitris Nikolidakis, Peter Thoolen, Anton Sculean Management of peri-implant recession associated with bone fenestration and dehiscence in the anterior region KEY WORDS
GBR membrane for ideal regeneration. i-gen TM. 2mm. >2.5mm. Lingual Extension. >100 blunt angle
 REGENERATION 02/03 Design Concept GBR membrane for ideal regeneration i-gen TM Description Single A type Small IG1W4509 Single A type Regular IG1W5510 Single A type Wide IG1W6511 Single B type Small IG2W0918
REGENERATION 02/03 Design Concept GBR membrane for ideal regeneration i-gen TM Description Single A type Small IG1W4509 Single A type Regular IG1W5510 Single A type Wide IG1W6511 Single B type Small IG2W0918
Buccal Bone Resorption Around Posterior Implants After Surgery: A 1-Year Prospective Study
 Buccal Bone Resorption Around Posterior Implants After Surgery: A 1-Year Prospective Study Toshio Takuma, DDS 1,2 /Keiji Oishi, DDS, PhD 3 /Tomofusa Manabe, DT 2 / Satoshi Yoneda, DDS, PhD 4 /Toshihiko
Buccal Bone Resorption Around Posterior Implants After Surgery: A 1-Year Prospective Study Toshio Takuma, DDS 1,2 /Keiji Oishi, DDS, PhD 3 /Tomofusa Manabe, DT 2 / Satoshi Yoneda, DDS, PhD 4 /Toshihiko
Evaluation of a Combination Allograft Material Compared to DFDBA in Alveolar Ridge Preservation. Sanju P. Jose
 Evaluation of a Combination Allograft Material Compared to DFDBA in Alveolar Ridge Preservation by Sanju P. Jose B.S., University of Maryland Baltimore County, 2008 D.D.S., University of Maryland School
Evaluation of a Combination Allograft Material Compared to DFDBA in Alveolar Ridge Preservation by Sanju P. Jose B.S., University of Maryland Baltimore County, 2008 D.D.S., University of Maryland School
01/05/2014. Background. Minimally invasive tooth extraction. Thomas Dietrich Professor of Oral Surgery University of Birmingham, School of Dentistry
 Background Remodelling of alveolar bone following extraction Minimally invasive tooth extraction Thomas Dietrich Professor of Oral Surgery University of Birmingham, School of Dentistry 2 weeks 4 weeks
Background Remodelling of alveolar bone following extraction Minimally invasive tooth extraction Thomas Dietrich Professor of Oral Surgery University of Birmingham, School of Dentistry 2 weeks 4 weeks
Periimplant Regeneration Fenestration
 Indication Sheet PIR-1 Periimplant Regeneration Fenestration Treatment concept of Dr. Jean-Pierre Gardella (surgeon) and Dr. Christian Richelme (prosthodontist), Marseille, France > Filling of a peri-implant
Indication Sheet PIR-1 Periimplant Regeneration Fenestration Treatment concept of Dr. Jean-Pierre Gardella (surgeon) and Dr. Christian Richelme (prosthodontist), Marseille, France > Filling of a peri-implant
