Survival of dental implants in patients with oral cancer treated by surgery and radiotherapy: a retrospective study
|
|
|
- Duane Sullivan
- 6 years ago
- Views:
Transcription
1 Pompa et al. BMC Oral Health 2015, 15:5 RESEARCH ARTICLE Open Access Survival of dental implants in patients with oral cancer treated by surgery and radiotherapy: a retrospective study Giorgio Pompa, Matteo Saccucci *, Gabriele Di Carlo, Edoardo Brauner, Valentino Valentini, Stefano Di Carlo, Tina Gentile, Giorgio Guarino and Antonella Polimeni Abstract Background: The aim of this retrospective study was to evaluate the survival of dental implants placed after ablative surgery, in patients affected by oral cancer treated with or without radiotherapy. Methods: We collected data for 34 subjects (22 females, 12 males; mean age: 51 ± 19) with malignant oral tumors who had been treated with ablative surgery and received dental implant rehabilitation between 2007 and Postoperative radiation therapy (less than 50 Gy) was delivered before implant placement in 12 patients. A total of 144 titanium implants were placed, at a minimum interval of 12 months, in irradiated and non-irradiated residual bone. Results: Implant loss was dependent on the position and location of the implants (P = ). Moreover, implant survival was dependent on whether the patient had received radiotherapy. This result was highly statistically significant (P < 0.01). Whether the implant was loaded is another highly significant (P < 0.01) factor determining survival. We observed significantly better outcomes when the implant was not loaded until at least 6 months after placement. Conclusions: Although the retrospective design of this study could be affected by selection and information biases, we conclude that a delayed loading protocol will give the best chance of implant osseointegration, stability and, ultimately, effective dental rehabilitation. Keywords: Dental implants, Osseointegration, Radiation Background Head-and-neck cancer is the most common cancer worldwide with an estimated global incidence of 500,000 new cases annually, three-quarters of which are in underdeveloped countries. The vast majority (approximately 90%) of head-and-neck cancers are squamous cell carcinomas [1]. According to a recent review, in the United States the 5- year survival rate of head and neck cancer is 57% [2]. Patients with oral cancer are commonly treated by a combination of radiotherapy and ablative surgery. After radical cancer surgery, the oral rehabilitation of a patient is a demanding procedure. Following radiation and surgical resection, most patients suffer from soft and hard tissue defects resulting in functional disabilities and esthetic deformity [3]. Dental rehabilitation using conventional * Correspondence: matteo.saccucci@uniroma1.it Department of Oral and Maxillofacial Science, Sapienza University of Rome, Via Caserta 272/A, Rome, Italy prostheses may be compromised or precluded by disadvantageous changes in oral anatomy, and radiotherapy can produce mucositis, xerostomia and disruption of bone healing processes [3]. In this situation, dental implants can potentially result in a more effective oral rehabilitation in terms of mastication, esthetics and speech function. However, even implant treatment in oral cancer patients is challenging because the bone into which the dental implants are placed has often been within the field of irradiation, or is grafted. Implant failure increases when they are placed in irradiated bone [3], in part because radiotherapy can result in progressive fibrosis of vessels and soft tissue, leading to diminished healing capacity. In addition radiations impedes the osseointegration of implants by reducing bone vascularity, clinically expressed as osteoradionecrosis. The interaction between ionizing radiation and tissue causes damage to the bone, periosteum, and connective tissue of the mucosa and the endothelium 2015 Pompa et al.; licensee BioMed Central. This is an Open Access article distributed under the terms of the Creative Commons Attribution License ( which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly credited. The Creative Commons Public Domain Dedication waiver ( applies to the data made available in this article, unless otherwise stated.
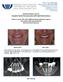
2 Pompa et al. BMC Oral Health 2015, 15:5 Page 2 of 6 of the vessels, which at later stages leads to hypoxia, hypocellularity and hypovascularity in the affected tissues, and the loss of resistance against infection and trauma [4,5]. Tissue dehiscence and osteoradionecrosis can occur, and often leads to implant loss. Implant treatment of irradiated patients is dependent upon issues like the timing of implant placement in relation to the radiation therapy, the anatomic site chosen for implant placement, the radiation dosage at that site and the consequent risk of osteoradionecrosis [6,7]. The aim of the present study, we evaluate the survival of dental implants in patients affected by oral cancer, treated with surgical and radiotherapy. Methods This study was conducted as a retrospective study at the Department of Oral and Maxillofacial Science, Sapienza University of Rome. Data were collected for a period between 2007 and The study comprised 34 subjects (22 females, 12 males) with malignant oral tumors (22 in the mandible/floor of the mouth, 12 in the maxilla) who underwent dental implant rehabilitation. The patients had undergone ablative surgery with or without adjunctive radiation therapy. The study was approved by the Ethics Committee at Sapienza University of Rome (ref. n 3452). All subjects gave their signed informed consent to medical and surgical procedure and to the use of data in this research. The mean age of the patients at the time of surgery was 51 ± 19 years. Patients with certain systemic disease (uncontrolled diabetes mellitus) and smokers were excluded [8]. The most prevalent tumor diagnosed was squamous cell carcinoma (n = 16). Other tumor types were: ameloblastoma (n = 6); osteosarcoma (n = 4); pleomorphic adenoma (n = 4); fibrous dysplasia (n = 2); and nasopharyngeal angiofibroma (n = 2). Orofacial defects in 26 patients were reconstructed microsurgically using a range of revasculated flap techniques (Figure 1). A total of 168 titanium implants were placed in irradiated or nonirradiated residual bone, with a minimum interval of 12 months between irradiation and implant placement. This procedure was performed by an experienced oral surgeon (G.P). The minimum implant length was 10 mm. In this study, indirectly irradiated bone was considered as non-irradiated. The time interval between radical oral cancer surgery, radiation therapy and implant placement, respectively, ranged from months. After implant placement patients underwent to a routine follow-up at 1 month, 3 months, 6 and 12 months performing an intraoral radiograph.. Based on the histological findings, post-operative radiotherapy was set in accordance with the NCCN guidelines [9]. Considering this, postoperative radiation therapy (less than 50 Gy) was delivered before implant placement to 12 patients and was delivered in fractions of 2 Gy given daily for 5 days each week (Table 1). The OSSEOTITE implants (3i Biomet, Palm Beach Figure 1 Patient affected by squamous cell carcinoma. a) intraoral image of the squamous cell carcinoma, b) ortopanoramic radiograph after ablative surgery. Gardens, FL, USA) were made from commercially pure titanium (grade IV) treated with a specific, proprietary dual acid-etching protocol. The acid-etch protocol does not include the coronal 3 mm of the titanium surface, which is machined instead. All implants (n = 168) were placed in jaws affected by surgical resection. There were 152 and 16 implants inserted into non irradiated and irradiated bone, respectively. The implant primary stability was evaluated measuring the torque at the moment of insertion. The torque level was not superior of 40 Nm. We have planned to use these implants as abutments for removable overdentures (12 patients), screw-retained fixed dentures (11 Table 1 Patients and radiation characteristics Patient Radiotherapy dose (Gy) Standard fractionation therapy (2 Gy daily)/hyperfractioned therapy 1 50 Standard fractionation therapy 2 50 Standard fractionation therapy 3 44 Standard fractionation therapy 4 48 Standard fractionation therapy 5 48 Standard fractionation therapy 6 44 Standard fractionation therapy 7 48 Standard fractionation therapy 8 44 Standard fractionation therapy 9 50 Standard fractionation therapy Standard fractionation therapy Standard fractionation therapy Standard fractionation therapy
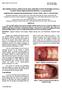
3 Pompa et al. BMC Oral Health 2015, 15:5 Page 3 of 6 patients) and cement-retained implant-supported prostheses (11 patients). Implant survival was evaluated within five different subgroups: location (maxilla vs. mandible); implant site (anterior vs. posterior); gender (male vs. female); radiotherapy (irradiated vs. non-irradiated); and time after initial loading (immediate, <6 months, 6 months, and >6 months) (Figure 2). Regarding the perio conditions, patients were followed by an Oral Hygienist before surgical procedures, where the patients received instructions to maintain oral health and care. The dental elements parodontally compromised were extracted as well. After surgery an Oral Hygiene follow up was performed every 3 months in the first year after implantation and every 6 months thereafter. Patients were evaluated at each review by clinical and radiographic examination. Implants were considered to be successful when there were no patient complaints, implant mobility, peri-implantitis [7]. Survival time was measured from initial implantation to either the failure (removal) or the last review of the implant. In the present study, we considered aesthetics and functional characteristics for each patient to optimize the results of the final implant-prosthetic rehabilitation. We Figure 2 Patient after implant-supported prosthesis rehabilitation. a) implants placed in the jaw after revasculated flap reconstruction, b) final panoramic radiograph with ossointegrated implants, c) implant-supported prosthesis. used patients existing removable partial or complete dentures as templates for implant planning. As a consequence, our implant treatment was prosthetically driven. The observation mean period after radiation therapy was 39,5 months with a standard deviation of 22,8 months. Moreover, the mean observation period after implant placement is 22,9 months with a SD of 15.5 months. Statistical analysis Implant survival was evaluated within the subgroups listed above. The null hypothesis of independence between implant survival and the various factors were tested by Pearson s chi-squared test [10]. We also used Fisher s Exact Test [11] for count data, as the chi-squared test can be misleading when the frequency in a single cell is less than 5 units. Results Sixteen implants (9.5%) failed over the study period: six during the healing phase, two during the loading phase and eight due to recurrence of the cancer. In the mandible, 96 implants were inserted: 28 anteriorly and 68 posteriorly. In the maxilla, 72 implants were inserted: 26 anteriorly and 46 posteriorly. In 34 patients, the initial prosthodontic treatment was maintained throughout the observation period. Two patients had recurrence of their cancer, which required a second surgical intervention during which all eight mandibular implants were removed. Dehiscence with disturbed wound healing occurred in four irradiated patients, while dehiscence and oroantral communication was observed in two irradiated patients. The frequency and distribution of implant lost among the population is shown in Table 2. Descriptive analysis of these factors is shown in Tables 3, 4, 5 and 6. Overall, implant survival was not dependent on whether the implant was placed in the maxilla or mandible (Table 3; p > 0.1). However, there was a significant correlation between the rate of mandibular implant loss and implant position, with all failing implants being in a posterior position (Table 3; p = ). In contrast, there was no correlation in either the maxilla or the mandible between an implant surviving and its placement position (Table 4; p > 0.8). Furthermore, implant survival was significantly linked with radiotherapy (p < 0.01): implants in non-irradiated bone predominantly survived, whereas more implants in irradiated bone failed (Table 5). Finally, implant survival is highly dependent on the interval period before loading. (Table 6; p < 0.01). Discussion Dental implants play a crucial role in the therapy of patients affected by malignancies in the head-and-neck region. The goal of implant rehabilitation is to improve the quality of life of these patients by allowing proper retention of removable prostheses and a reduction in the load
4 Pompa et al. BMC Oral Health 2015, 15:5 Page 4 of 6 Table 2 Frequency and distribution of implant lost among the population Less More 60 Total Frequency F M Total Percentage F 0,0% 0,0% 62,5% 62,5% M 0,0% 12,5% 25,0% 37,5% Total 0,0% 12,5% 87,5% 100,0% placed on vulnerable soft tissues [12]. Several factors influence implant survival, especially when patients undergo surgical removal of the malignancies. Indeed, the experience of the surgeon, bone quality, and technical aspects such as implant length, diameter and primary stability each play pivotal roles. After oral cancer surgery, additional factors influence implant osseointegration, such as bone topography and applied radiation dose [13]. Moreover, poor general health, diminished oral hygiene, smoking and alcohol abuse all reduce implant survival. Radiation therapy is often the first line of therapy for patients with head and neck cancer and is often used as an adjunct to surgical excision. There are three different types of radiotherapy: external beam radiation, brachytherapy, and radioisotope therapy. For the treatment of head-and-neck cancer, external beam methods are most commonly used [13]. Radiation guidelines are variable depending on the method of radiotherapy selected as well as the type, location, and stage of the cancer. Therapeutic radiation protocols for head-and-neck tumors commonly consist of Gy [14]. Usually, the radiation dose is given in fractions of 2 Gy given either once a day (standard fractionation therapy) or twice a day (hyperfractionated therapy) for a defined time period. According to Anderson et al., fractions can be administered every day for 25 days or for 5 days a week for a 5 7-week period [15]. Table 3 Implants by survival (yes or no) and location (mandible, maxilla), Odds ratio: , p-value = Mandible Maxilla Total Yes 84 (50,0%) 68 (40,5%) 152 (90,5%) No 12 (7,1%) 4 (2,4%) 16 (9,5%) Total 96 (57,1%) 72 (42,9%) 168 (100,0%) Anterior Posterior Total Odds ratio: , p-value = Below, lost implants by location (mandible, maxilla) and position (anterior, posterior). Odds ratio = 0 p-value = Table 4 Survived implants by location (mandible, maxilla) and position (anterior, posterior) Anterior Posterior Total Mandible Maxilla Total Anterior Posterior Total Mandible 18,40% 36,80% 55,30% Maxilla 15,80% 28,90% 44,70% Total 34,20% 65,80% 100,00% Odds ratio: p-value = Our results indicate that implant survival is strongly influenced by radiotherapy, confirming previous findings [16] demonstrating that radiotherapy is an important factor in implant failure. Ihde et al. [17] report that implant failure is a more significant risk (up to 12 times greater) in irradiated bone rather than in non-irradiated bone. Yerit et al. [4], using a comparable protocol of irradiation to that used here, found that mandibular implants were significantly less likely to survive in irradiated bone than in non-irradiated bone. Although our findings indicate that radiotherapy is an important factor in implant failure, the impact of the position of implant placement within irradiated bone remains contentious. There is much variation in the reported success rates of implant rehabilitation. Recently, De La Plata et al. [3] reported that the overall 5-year survival rate in irradiated patients was 92.6%, although irradiated patients had a slightly but significantly higher rate of implant loss than non-irradiated patients. Linsen et al. [13] reported implant success rates of over 89% in irradiated bone at 1-, 5-, and 10-year follow-up. However, although these findings suggest a smaller influence of radiation on implant survival than we found here, this discrepancy may be explained by differences between their radiation protocol and our own. Dosage protocol is a crucial factor with regard to radiation therapy. There is no literature consensus regarding Table 5 Implants by survival (yes or no) and radiotherapy (not irradiated, irradiated bone) Not irradiated Irradiated Total Yes No Total Not irradiated Irradiated Total Yes 67,30% 23,20% 90,50% No 2,40% 7,10% 9,50% Total 69,60% 30,40% 100,00% Odds ratio: p-value =
5 Pompa et al. BMC Oral Health 2015, 15:5 Page 5 of 6 Table 6 Implants by survival (yes or no) and number of implants loaded at different time (immediate, less than 6 months, 6 months, more than 6 months) Immediate Less than 6 months 6 months More than 6 months Total Yes No Total Immediate Less than 6 months 6 months More than 6 months Total Yes 26,20% 10,10% 31,00% 23,20% 90,50% No 2,40% 4,80% 2,40% 0,00% 9,50% Total 28,60% 14,90% 33,30% 23,20% 100,00% the radiation dosage at which implants begin to experience increased risk of failure. Indeed, Javed et al. [18] observed that dental implants showed up to 100% osseointegration when exposed to radiation dosages up to 65 Gy, and suggested that radiation dosages between Gy do not negatively influence osseointegration. Conversely, several authors [4,19,20] concluded that a total dose less than 50 Gy is necessary to minimize the negative effects of radiotherapy. In conclusion, it seems realistic to assume that full-course radiotherapy (50 65 Gy) is not an absolute contraindication to implant surgery, but that determination of the absolute risk of implant survival must take into account the other contributory factors, as described here. The optimal timing of implant placement in radiotherapy patients is controversial [21]. Some authors recommend the insertion of implants following the ablative procedure [21-24]. This is advantageous because initial implant healing (osseointegration) takes place before irradiation and there is a reduced risk of late complications, such as the development of osteoradionecrosis [20-22]. However, there is a risk of inappropriate implant positioning, which makes subsequent prosthodontic treatment more complex [13,18,19]. There is also a risk that early tumor recurrence will negate the benefits of the implant therapy [25]. In this study, we opted for delayed implant insertion to avoid these complications. However, there is also little consensus on the optimal time interval between irradiation and implant placement. Although implant placement is performed generally no earlier than 6 months after irradiation, Ganström et al. suggest that implant therapy should be complete by 6 18 months after radiation [19]. However, Sammartino et al. [8] recommend waiting at least 12 months to achieve the best clinical results. It is important to note that the risk of osteoradionecrosis after radiotherapy in head-and-neck cancer patients does not diminish over time because it is underpinned by the progressive and irreversible loss of capillaries [16]. Moreover, immediate implant insertion can be problematic because ablative surgery alters bone anatomy extensively. In our study, the time interval from radical oral cancer surgery through radiation therapy until implant placement ranged from months (mean: 39.58). For the rehabilitative implant-supported prosthesis, we aimed to achieve group function as an occlusal scheme and no mucosal contact, to minimize the risk of mucosal complications. The reduction of mucosal contact is important because fragile mucosa and severe mucositis are common manifestations observed long after radiation therapy. This increases the risk that prosthetic pressure lesions will result in septic osteoradionecrosis [26,27]. There was a highly significant relationship between the time of loading and the success of the implant in irradiated bone. Good results were obtained with an implant loading protocol of 6 months, and no implants were lost when the period of healing was greater than 6 months. These data support those of Dholam et al. [28], who commented on the importance of bone healing and the slow rate of osseointegration in irradiated bone. These data thus do not support immediate loading [28], and we would recommend a period of 6 months or more before loading implants in irradiated bone. We found no relationship between implant survival and the location of placement (maxilla vs. mandible).we did find a stark discrepancy in implant failure in terms of positioning. Implants in the posterior mandible were much more frequently lost than in other positions. This finding is in disagreement with the conclusions of a recent review [20] that reported better outcomes in the mandible. We are unclear why this contradiction occurred. Regarding the influence of prosthetic rehabilitation on implants survivals, it is important to underline that no standard prosthetic appliance is described in the literature. This is due to the large interindividual variability regarding the topography and dimension of the defects. Nevertheless, in this study as well as in a previous study [8] no specific superstructure was found to be particularly favorable in terms of implant survival. Conclusions Irradiated bone is a challenging environment for implant placement. Successful rehabilitation of irradiated patients with implant-supported prostheses is
6 Pompa et al. BMC Oral Health 2015, 15:5 Page 6 of 6 multifactorial. Although the retrospective design of this study could be affected by selection and information biases our results, leads us to believe that immediate [29] and progressive [30] loading protocols are not advisable in irradiated patients. We conclude that a delayed loading protocol will give the best chance of implant osseointegration, stability and, ultimately, effective dental rehabilitation. Competing interests The authors declare that they have no competing interests. Authors contributions GP and EB were the principal investigators of this study they made substantial contributions to conception and design, as well as the acquisition, analysis and interpretation of data and gave final approval of the version to be published; MS, AP and GDC were involved in drafting the manuscript and in analysis, interpretation of data; SDC, VV, GG and TG participated in drafting and revision of the manuscript. All authors have read and approved the manuscript. Acknowledgements We thank Prof. Livia Ottolenghi (Department of oral and maxillofacial science Sapienza University of Rome) for discussions and help. She made substantial contributions in revising the manuscript for important intellectual content. We also thank Edanz Group for the English professional editing. Received: 23 June 2014 Accepted: 14 January 2015 Published: 20 January 2015 References 1. Garg A, Guez G. Head and neck cancer, dental implants, and dental oncology. Dent Implantol Update. 2011;13: Oral cancer foundation. Oral Cancer Facts org/facts/. 3. De la Plata M, Gías LN, Díez PM, Muñoz-Guerra M, González-García R, Lee GY, et al. Osseointegrated implant rehabilitation of irradiated oral cancer patients. J Oral Maxillofac Surg. 2012;70: Yerit KC, Posch M, Seemann M, Hainich S, Dörtbudak O, Turhani D, et al. Implant survival in mandibles of irradiated oral cancer patients. Clin Oral Implants Res. 2006;17: Marx RE, Johnson RP. Studies in the radiobiology of osteoradionecrosis and their clinical significance. Oral Surg Oral Med Oral Pathol. 1987;64: Jacobsson M, Tjellstrom A, Thomsen P. Integration of implants in irradiated bone. Histologic and clinical study. Ann Otol Rhinol Laryngol. 1988;97: Van Steenberghe D. Outcomes and their measurements in clinical trials of endosseus oral implants. Ann Periodontol. 1997;2: Sammartino G, Marenzi G, Cioffi I. Implant therapy in irradiated patients. J Craniofac Surg. 2011;22: NCCN Guidelines. f_guidelines.asp#site. 10. Agresti A. An Introduction to Categorical Data Analysis. 2nd ed. New York: John Wiley & Sons; Fisher RA. Confidence limits for a cross-product ratio. Aust J Stat. 1962;4: Schiegnitz E, Al-Nawas B, Kämmerer PW, Grötz KA. Oral rehabilitation with dental implants in irradiated patients: a meta-analysis on implant survival. Clin Oral Investig. 2014;18: Linsen SS, Martini M, Stark H. Long-term results of endosteal implants following radical oral cancer surgery with and without adjuvant radiation therapy. Clin Implant Dent Relat Res. 2012;14: Harrison J, Stratemann S, Redding SW. Dental implants for patients who have had radiation treatment for head and neck cancer. Spec Care Dentist. 2003;23: Anderson L, Meraw S, Al-Hezaimi K, Wang HL. The influence of radiation therapy on dental implantology. Implant Dent. 2013;22: Zheng M, Li L, Tang Y, Liang XH. How to improve the survival rate of implants after radiotherapy for head and neck cancer? J Periodontal Implant Sci. 2014;44: Ihde S, Kopp S, Gundlach K, Konstantinović VS. Effects of radiation therapy on craniofacial and dental implants: a review of the literature. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2009;107: Javed F, Al-Hezaimi K, Al-Rasheed A, Almas K, Romanos GE. Implant survival rate after oral cancer therapy: a review. Oral Oncol. 2010;46: Ganström G. Radiotherapy, osseointegration and hyperbaric oxygen therapy. Periodontol ;33: Schoen PJ, Reintsema H, Raghoebar GM, Vissink A, Roodenburg JLN. The use of implant retained mandibular prostheses in the oral rehabilitation of head and neck cancer patients. A review and rationale for treatment planning. Oral Oncol. 2004;40: Colella G, Cannavale R, Pentenero M, Gandolfo S. Oral implants in radiated patients: a systematic review. Int J Oral Maxillofac Implants. 2007;22: Barber AJ, Butterworth CJ, Rogers SN. Systematic review of primary osseointegrated dental implants in head and neck oncology. Br J Oral Maxillofac Surg. 2011;49: Schepers RH, Slagter AP, Kaanders JH, Van den Hoogen FJ, Merkx MA. Effect of postoperative radiotherapy on the functional result of implants placed during ablative surgery for oral cancer. Int J Oral Maxillofac Surg. 2006;35: Korfage A, Schoen PJ, Raghoebar GM, Roodenburg JLN, Vissink A, Reintsema H. Benefits of dental implants installed during ablative tumor surgery in oral cancer patients: a prospective 5-years clinical trial. Clin Oral Implants Res. 2010;21: De Ceulaer J, Magremanne M, Van Veen A. Squamous cell carcinoma recurrence around dental implants. J Oral Maxillofac Surg. 2010;68: Visch LL, Van Waas MA, Schmitz PI, Levendag PC. A clinical evaluation of implants in irradiated oral cancer patients. J Dent Res. 2002;81: Weischer T, Mohr C. Ten-year experience in oral implant rehabilitation of cancer patients: treatment concept and proposed criteria for success. Int J Oral Maxillofac Implants. 1999;14: Dholam KP, Gurav SV. Dental implants in irradiated jaws: a literature review. J Cancer Res Ther. 2012;8 Suppl 1: Misch CE. Progressive Bone Loading. In: Misch CE, editor. Dental Implant Prosthetics. St Louis: Elsevier Mosby MO; p Misch CE, Scortecci GM. Immediate Load Application in Implant Dentistry. In: Misch CE, editor. Dental Implant Prosthetics. St Louis: Elsevier Mosby MO; p doi: / Cite this article as: Pompa et al.: Survival of dental implants in patients with oral cancer treated by surgery and radiotherapy: a retrospective study. BMC Oral Health :5. Submit your next manuscript to BioMed Central and take full advantage of: Convenient online submission Thorough peer review No space constraints or color figure charges Immediate publication on acceptance Inclusion in PubMed, CAS, Scopus and Google Scholar Research which is freely available for redistribution Submit your manuscript at
TITLE: Immediate Osseointegrated Implants for Cancer Patients: A Review of Clinical and Cost-Effectiveness
 TITLE: Immediate Osseointegrated Implants for Cancer Patients: A Review of Clinical and Cost-Effectiveness DATE: 13 January 2015 CONTEXT AND POLICY ISSUES According to the World health Organization, the
TITLE: Immediate Osseointegrated Implants for Cancer Patients: A Review of Clinical and Cost-Effectiveness DATE: 13 January 2015 CONTEXT AND POLICY ISSUES According to the World health Organization, the
University of Groningen. Dental implants in maxillofacial prosthodontics Korfage, Anke
 University of Groningen Dental implants in maxillofacial prosthodontics Korfage, Anke DOI: 10.1016/j.bjoms.2014.05.013 10.1016/j.ijom.2013.04.003 10.1002/hed.24053 IMPORTANT NOTE: You are advised to consult
University of Groningen Dental implants in maxillofacial prosthodontics Korfage, Anke DOI: 10.1016/j.bjoms.2014.05.013 10.1016/j.ijom.2013.04.003 10.1002/hed.24053 IMPORTANT NOTE: You are advised to consult
The effect of radiotherapy on survival of dental implants in head and neck cancer patients
 Journal section: Implantology Publication Types: Review doi:10.4317/jced.52346 http://dx.doi.org/10.4317/jced.52346 The effect of radiotherapy on survival of dental implants in head and neck cancer patients
Journal section: Implantology Publication Types: Review doi:10.4317/jced.52346 http://dx.doi.org/10.4317/jced.52346 The effect of radiotherapy on survival of dental implants in head and neck cancer patients
The influence of radiotherapy on osseointegration
 Experience with Osseointegrated Implants Placed in Irradiated Tissues in Japan and the United States Atsushi Niimi, DDS, DMSc*/Minoru Ueda, DDS, PhD**/ Eugene E. Keller, DDS, PhD***/Philip Worthington,
Experience with Osseointegrated Implants Placed in Irradiated Tissues in Japan and the United States Atsushi Niimi, DDS, DMSc*/Minoru Ueda, DDS, PhD**/ Eugene E. Keller, DDS, PhD***/Philip Worthington,
Osseointegrated dental implant treatment generally
 Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
In Scandinavia, malignant tumors in the maxillofacial
 Oral Implant Rehabilitation in Irradiated Patients Without Adjunctive Hyperbaric Oxygen Gunilla Andersson, DDS, PhD*/Lars Andreasson, MD, PhD**/Göran Bjelkengren, MD*** In 15 patients treated for malignant
Oral Implant Rehabilitation in Irradiated Patients Without Adjunctive Hyperbaric Oxygen Gunilla Andersson, DDS, PhD*/Lars Andreasson, MD, PhD**/Göran Bjelkengren, MD*** In 15 patients treated for malignant
Viability of dental implants in head and neck irradiated patients: A systematic review
 CLINICAL REVIEW David W. Eisele, MD, Section Editor Viability of dental implants in head and neck irradiated patients: A systematic review Edson Virgılio Zen Filho, DDS, MSc, 1 Elen de Souza Tolentino,
CLINICAL REVIEW David W. Eisele, MD, Section Editor Viability of dental implants in head and neck irradiated patients: A systematic review Edson Virgılio Zen Filho, DDS, MSc, 1 Elen de Souza Tolentino,
BIOMECHANICS AND OVERDENTURES
 Proceedings of the 6th International Conference on Mechanics and Materials in Design, Editors: J.F. Silva Gomes & S.A. Meguid, P.Delgada/Azores, 26-30 July 2015 PAPER REF: 5734 BIOMECHANICS AND OVERDENTURES
Proceedings of the 6th International Conference on Mechanics and Materials in Design, Editors: J.F. Silva Gomes & S.A. Meguid, P.Delgada/Azores, 26-30 July 2015 PAPER REF: 5734 BIOMECHANICS AND OVERDENTURES
Surgical treatment of malignancies involving the
 Oral Implants in Radiated Patients: A Systematic Review Giuseppe Colella, MD, DDS 1 /Rosangela Cannavale, DDS 2 /Monica Pentenero, DDS, MSc 3 / Sergio Gandolfo, MD, DDS 4 Purpose: Oral malignancy is often
Oral Implants in Radiated Patients: A Systematic Review Giuseppe Colella, MD, DDS 1 /Rosangela Cannavale, DDS 2 /Monica Pentenero, DDS, MSc 3 / Sergio Gandolfo, MD, DDS 4 Purpose: Oral malignancy is often
A retrospective study on separate single-tooth implant restorations to replace two or more consecutive. maxillary posterior teeth up to 6 years.
 Original Article A retrospective study on separate single-tooth implant restorations to replace two or more consecutive maxillary posterior teeth up to 6 years follow up Myat Nyan Department of Prosthodontics,
Original Article A retrospective study on separate single-tooth implant restorations to replace two or more consecutive maxillary posterior teeth up to 6 years follow up Myat Nyan Department of Prosthodontics,
Oral and maxillofacial rehabilitation of head and neck cancer patients Schoen, Pieter Jan
 University of Groningen Oral and maxillofacial rehabilitation of head and neck cancer patients Schoen, Pieter Jan IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if
University of Groningen Oral and maxillofacial rehabilitation of head and neck cancer patients Schoen, Pieter Jan IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if
Implant survival in patients with oral cancer: A 5-year follow-up
 Journal section: Oral Surgery Publication Types: Research doi:0.47/jced.5497 http://dx.doi.org/0.47/jced.5497 Implant survival in patients with oral cancer: A 5-year follow-up Rafael Flores-Ruiz, Lizett
Journal section: Oral Surgery Publication Types: Research doi:0.47/jced.5497 http://dx.doi.org/0.47/jced.5497 Implant survival in patients with oral cancer: A 5-year follow-up Rafael Flores-Ruiz, Lizett
4. What about age? There is no age limit. After puberty, anyone can get dental implants.
 Dental Implants 1. What are Osseointegrated implants? Osseointegrated implants are a new generation of dental implants in Rio de Janeiro, introduced in the 1960 s, they come in different shapes and sizes.
Dental Implants 1. What are Osseointegrated implants? Osseointegrated implants are a new generation of dental implants in Rio de Janeiro, introduced in the 1960 s, they come in different shapes and sizes.
The Brånemark osseointegration method, using titanium dental implants (fixtures)
 Early Failures in 4,641 Consecutively Placed Brånemark Dental Implants: A Study From Stage 1 Surgery to the Connection of Completed Prostheses Bertil Friberg, DDS/Torsten Jemt, DDS, PhD/Ulf Lekholm, DDS,
Early Failures in 4,641 Consecutively Placed Brånemark Dental Implants: A Study From Stage 1 Surgery to the Connection of Completed Prostheses Bertil Friberg, DDS/Torsten Jemt, DDS, PhD/Ulf Lekholm, DDS,
Purpose: To assess the long term survival of sites treated by GTR.
 Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
Implant-prosthetic rehabilitation after radiation treatment in head and neck cancer patients: a case-series report of outcome
 9 research article Implant-prosthetic rehabilitation after radiation treatment in head and neck cancer patients: a case-series report of outcome Jasna Cotic 1, Jure Jamsek 1, Milan Kuhar 1,2, Natasa Ihan
9 research article Implant-prosthetic rehabilitation after radiation treatment in head and neck cancer patients: a case-series report of outcome Jasna Cotic 1, Jure Jamsek 1, Milan Kuhar 1,2, Natasa Ihan
م.م. طارق جاسم حممد REMOVABLE PARTIAL DENTURE INTRODUCTION
 Lec.1 م.م. طارق جاسم حممد REMOVABLE PARTIAL DENTURE INTRODUCTION االسنان طب Prosthodontics is the branch of dentistry pertaining to the restoration and maintenance of oral function, comfort, appearance,
Lec.1 م.م. طارق جاسم حممد REMOVABLE PARTIAL DENTURE INTRODUCTION االسنان طب Prosthodontics is the branch of dentistry pertaining to the restoration and maintenance of oral function, comfort, appearance,
EFFECTIVE DATE: 04/24/14 REVISED DATE: 04/23/15, 04/28/16, 06/22/17, 06/28/18 POLICY NUMBER: CATEGORY: Dental
 MEDICAL POLICY SUBJECT: DENTAL IMPLANTS PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including an Essential
MEDICAL POLICY SUBJECT: DENTAL IMPLANTS PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including an Essential
Prosthetic Options in Implant Dentistry. Hakimeh Siadat, DDS, MSc Associate Professor
 Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
 A New Procedure Reduces Laboratory Time to 6 Hours for the Elaboration of Immediate Loading Prostheses with a Titanium Frame Following Implant Placement Huard C, Bessadet M, Nicolas E, Veyrune JL * International
A New Procedure Reduces Laboratory Time to 6 Hours for the Elaboration of Immediate Loading Prostheses with a Titanium Frame Following Implant Placement Huard C, Bessadet M, Nicolas E, Veyrune JL * International
ORAL IMPLANT PROCEDURES
 ORAL IMPLANT PROCEDURES Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and
ORAL IMPLANT PROCEDURES Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and
Re-growth of an incomplete discoid lateral meniscus after arthroscopic partial resection in an 11 year-old boy: a case report
 Bisicchia and Tudisco BMC Musculoskeletal Disorders 2013, 14:285 CASE REPORT Open Access Re-growth of an incomplete discoid lateral meniscus after arthroscopic partial resection in an 11 year-old boy:
Bisicchia and Tudisco BMC Musculoskeletal Disorders 2013, 14:285 CASE REPORT Open Access Re-growth of an incomplete discoid lateral meniscus after arthroscopic partial resection in an 11 year-old boy:
Treatment Outcome of Bone-Anchored Craniofacial Prostheses after Tumour Surgery
 Treatment Outcome of Bone-Anchored Craniofacial Prostheses after Tumour Surgery Pieter J Schoen Gerry M Raghoebar Robert P van Oort Harry Reintsema Bernard FAM van der Laan Fred R Burlage Jan LN Roodenburg
Treatment Outcome of Bone-Anchored Craniofacial Prostheses after Tumour Surgery Pieter J Schoen Gerry M Raghoebar Robert P van Oort Harry Reintsema Bernard FAM van der Laan Fred R Burlage Jan LN Roodenburg
Narrow-diameter implants in premolar and molar areas
 2 Long-term follow-up of 2.5mm NDIs supporting a fixed prosthesis Narrow-diameter implants in premolar and molar areas EDUARDO ANITUA, DDS, MD, PHD¹,² A narrow-diameter implant (NDI) is an implant with
2 Long-term follow-up of 2.5mm NDIs supporting a fixed prosthesis Narrow-diameter implants in premolar and molar areas EDUARDO ANITUA, DDS, MD, PHD¹,² A narrow-diameter implant (NDI) is an implant with
Osseointegrated implant-supported
 CLINICAL SCREWLESS FIXED DETACHABLE PARTIAL OVERDENTURE TREATMENT FOR ATROPHIC PARTIAL EDENTULISM OF THE ANTERIOR MAXILLA Dennis Flanagan, DDS This is a case report of the restoration of a partially edentulous
CLINICAL SCREWLESS FIXED DETACHABLE PARTIAL OVERDENTURE TREATMENT FOR ATROPHIC PARTIAL EDENTULISM OF THE ANTERIOR MAXILLA Dennis Flanagan, DDS This is a case report of the restoration of a partially edentulous
Utilizing Digital Treatment Planning and Guided Surgery in Conjunction with Narrow Body Implants. by Timothy F. Kosinski, DDS, MAGD
 Utilizing Digital Treatment Planning and Guided Surgery in Conjunction with Narrow Body Implants by Timothy F. Kosinski, DDS, MAGD Implant dentistry is undergoing some amazing transformations. With the
Utilizing Digital Treatment Planning and Guided Surgery in Conjunction with Narrow Body Implants by Timothy F. Kosinski, DDS, MAGD Implant dentistry is undergoing some amazing transformations. With the
Contemporary Implant Dentistry
 Contemporary Implant Dentistry C H A P T ER 1 4 O F C O N T E M P OR A R Y O R A L A N D M A X I L L OFA C IA L S U R G E RY B Y : D R A R A S H K H O J A S T EH Dental implant is suitable for: completely
Contemporary Implant Dentistry C H A P T ER 1 4 O F C O N T E M P OR A R Y O R A L A N D M A X I L L OFA C IA L S U R G E RY B Y : D R A R A S H K H O J A S T EH Dental implant is suitable for: completely
Creating emergence profiles in immediate implant dentistry
 Creating emergence profiles in immediate implant dentistry AUTHORS Dr. Daniel Capitán Maraver Dr. Manuel Fuentes Ortiz Visiting lecturers in the Master s Degree in Clinical Practice in Implantology and
Creating emergence profiles in immediate implant dentistry AUTHORS Dr. Daniel Capitán Maraver Dr. Manuel Fuentes Ortiz Visiting lecturers in the Master s Degree in Clinical Practice in Implantology and
SCD Case Study. Implant-supported overdentures
 SCD Case Study Implant-supported overdentures An implant-retained overdenture may be indicated in patients with changed anatomy, neuromuscular disorders, significant gag reflex or considerable ridge resorption
SCD Case Study Implant-supported overdentures An implant-retained overdenture may be indicated in patients with changed anatomy, neuromuscular disorders, significant gag reflex or considerable ridge resorption
AO Certificate in Implant Dentistry Certificate
 AO Certificate in Implant Dentistry Certificate The AO Certificate in Implant Dentistry provides an opportunity for AO members to demonstrate that they have attained a level of education and experience
AO Certificate in Implant Dentistry Certificate The AO Certificate in Implant Dentistry provides an opportunity for AO members to demonstrate that they have attained a level of education and experience
CHAPTER 1. General Introduction
 CHAPTER 1 General Introduction Chapter 1 The loss of remaining natural teeth and provision of artificial removable dentition is a major and irreversible procedure for the patient. The main limitations
CHAPTER 1 General Introduction Chapter 1 The loss of remaining natural teeth and provision of artificial removable dentition is a major and irreversible procedure for the patient. The main limitations
Long-term success of osseointegrated implants
 Against All Odds A No Bone Solution Long-term success of osseointegrated implants depends on the length of the implants used and the quality and quantity of bone surrounding these implants. As surgical
Against All Odds A No Bone Solution Long-term success of osseointegrated implants depends on the length of the implants used and the quality and quantity of bone surrounding these implants. As surgical
Use of Implant Retained Overdenture in Atrophic Mandible - A Case Report
 Case report AODMR Use of Implant Retained Overdenture in Atrophic Mandible - A Case Report Sheren Fatima 1, Rajarshi Basu 2, Neelkamal Hallur 3, Aaisha Siddiqua 4, Syed Zakaullah 4, Sumaiyya 2, Chaitanya
Case report AODMR Use of Implant Retained Overdenture in Atrophic Mandible - A Case Report Sheren Fatima 1, Rajarshi Basu 2, Neelkamal Hallur 3, Aaisha Siddiqua 4, Syed Zakaullah 4, Sumaiyya 2, Chaitanya
Consensus Statements and Recommended Clinical Procedures Regarding Contemporary Surgical and Radiographic Techniques in Implant Dentistry
 Group 1 and Recommended Clinical Procedures Regarding Contemporary Surgical and Radiographic Techniques in Implant Dentistry Michael M. Bornstein, PD Dr Med Dent 1 /Bilal Al-Nawas, Prof Dr Med, Dr Med
Group 1 and Recommended Clinical Procedures Regarding Contemporary Surgical and Radiographic Techniques in Implant Dentistry Michael M. Bornstein, PD Dr Med Dent 1 /Bilal Al-Nawas, Prof Dr Med, Dr Med
Conus Concept: A Rewarding Complete Denture Treatment
 Conus Concept: A Rewarding Complete Denture Treatment Complete dentures have largely become the domain of the denturist due to the dissatisfaction general dentists feel with this treatment. Multiple visits,
Conus Concept: A Rewarding Complete Denture Treatment Complete dentures have largely become the domain of the denturist due to the dissatisfaction general dentists feel with this treatment. Multiple visits,
In 1977, Lew1 developed a passive
 CLINICAL AN OVERVIEW OF THE LEW ATTACHMENT: CLINICAL REPORTS Jack Piermatti, DMD Sheldon Winkler, DDS KEY WORDS Lew attachment Atrophic mandible Subperiosteal implant Root form implant Although the Lew
CLINICAL AN OVERVIEW OF THE LEW ATTACHMENT: CLINICAL REPORTS Jack Piermatti, DMD Sheldon Winkler, DDS KEY WORDS Lew attachment Atrophic mandible Subperiosteal implant Root form implant Although the Lew
Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis
 CASE REPORT Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis Dr Ashish Yadav 1, Dr Aratee Gupta 2, Dr Archana Singh 3, 1,3-
CASE REPORT Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis Dr Ashish Yadav 1, Dr Aratee Gupta 2, Dr Archana Singh 3, 1,3-
Many papers have reported on histologic
 Histologic Evaluation of Clinically Successful Osseointegrated Implants Retrieved from Irradiated Bone: A Report of 2 Patients Hidetaka Nakai, DDS*/Atsushi Niimi, DDS, DMSc**/Minoru Ueda, DDS, PhD*** The
Histologic Evaluation of Clinically Successful Osseointegrated Implants Retrieved from Irradiated Bone: A Report of 2 Patients Hidetaka Nakai, DDS*/Atsushi Niimi, DDS, DMSc**/Minoru Ueda, DDS, PhD*** The
A Novel Technique for the Management of a Maxillary Anterior Alveolar Defect with an Implant-retained Fixed Prosthesis: A Clinical Report
 Neenu M Varghese et al Case Report 10.5005/jp-journals-10012-1148 A Novel Technique for the Management of a Maxillary Anterior Alveolar Defect with an Implant-retained Fixed Prosthesis: A Clinical Report
Neenu M Varghese et al Case Report 10.5005/jp-journals-10012-1148 A Novel Technique for the Management of a Maxillary Anterior Alveolar Defect with an Implant-retained Fixed Prosthesis: A Clinical Report
Mechanical and technical risks in implant therapy.
 Mechanical and technical risks in implant therapy. Salvi GE, Brägger U. Int J Oral Maxillofac Implants. 2009;24 Suppl:69-85. Department of Periodontology, School of Dental Medicine, University of Bern,
Mechanical and technical risks in implant therapy. Salvi GE, Brägger U. Int J Oral Maxillofac Implants. 2009;24 Suppl:69-85. Department of Periodontology, School of Dental Medicine, University of Bern,
Devoted to the Advancement of Implant Dentistry
 Devoted to the Advancement of Implant Dentistry Devoted to the Advancement of Implant Dentistry Our ultimate goal is to provide you and your patients with the highest standards in implant case planning
Devoted to the Advancement of Implant Dentistry Devoted to the Advancement of Implant Dentistry Our ultimate goal is to provide you and your patients with the highest standards in implant case planning
Basic information on the. Straumann Pro Arch TL. Straumann Pro Arch TL
 Basic information on the Straumann Pro Arch TL Straumann Pro Arch TL Contents 1. Introduction 2 1.1 Discover more treatment options with the 4 mm Short Implant 2 2. Technical information 3 3. Step-by-step
Basic information on the Straumann Pro Arch TL Straumann Pro Arch TL Contents 1. Introduction 2 1.1 Discover more treatment options with the 4 mm Short Implant 2 2. Technical information 3 3. Step-by-step
Featured Patient Case #1: Complete Mouth Reconstruction with Hybrid Restorations
 Philip L. Fava II, DMD, MDSc Robert A. Levine, DDS, FCPP, FISPPS 9880 Bustleton Ave, Suite 211 Philadelphia, PA 19115 PADentalImplants.com 215-677-8686 Featured Patient Case #1: Complete Mouth Reconstruction
Philip L. Fava II, DMD, MDSc Robert A. Levine, DDS, FCPP, FISPPS 9880 Bustleton Ave, Suite 211 Philadelphia, PA 19115 PADentalImplants.com 215-677-8686 Featured Patient Case #1: Complete Mouth Reconstruction
MULTIDIRECTIONAL APPROACH OF ORAL REHABILITATION WITH IMPLANTS IN A PATIENT WITH LIMITED MOUTH OPENING: A CASE REPORT
 ISSN: 0976-2876 (Print) ISSN: 2250-0138 (Online) MULTIDIRECTIONAL APPROACH OF ORAL REHABILITATION WITH IMPLANTS IN A PATIENT WITH LIMITED MOUTH OPENING: A CASE REPORT ROMESH SONI a, HARAKH CHAND BARANWAL
ISSN: 0976-2876 (Print) ISSN: 2250-0138 (Online) MULTIDIRECTIONAL APPROACH OF ORAL REHABILITATION WITH IMPLANTS IN A PATIENT WITH LIMITED MOUTH OPENING: A CASE REPORT ROMESH SONI a, HARAKH CHAND BARANWAL
Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report
 Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
A new score predicting the survival of patients with spinal cord compression from myeloma
 Douglas et al. BMC Cancer 2012, 12:425 RESEARCH ARTICLE Open Access A new score predicting the survival of patients with spinal cord compression from myeloma Sarah Douglas 1, Steven E Schild 2 and Dirk
Douglas et al. BMC Cancer 2012, 12:425 RESEARCH ARTICLE Open Access A new score predicting the survival of patients with spinal cord compression from myeloma Sarah Douglas 1, Steven E Schild 2 and Dirk
CHAPTER. 1. Uncontrolled systemic disease 2. Retrognathic jaw relationship
 CHAPTER 7 Immediate Implant Supported Restoration of the Edentulous Arch Stephen G. Alfano and Robert M. Laughlin Department of Oral and Maxillofacial Surgery, Naval Medical Center San Diego, San Diego,
CHAPTER 7 Immediate Implant Supported Restoration of the Edentulous Arch Stephen G. Alfano and Robert M. Laughlin Department of Oral and Maxillofacial Surgery, Naval Medical Center San Diego, San Diego,
Immediate Complete Denture: A Case Report
 Human Journals Case Report July 2018 Vol.:10, Issue:1 All rights are reserved by Ruby et al. Immediate Complete Denture: A Case Report Keywords: immediate denture, dental prosthesis ABSTRACT Ruby*, Manish
Human Journals Case Report July 2018 Vol.:10, Issue:1 All rights are reserved by Ruby et al. Immediate Complete Denture: A Case Report Keywords: immediate denture, dental prosthesis ABSTRACT Ruby*, Manish
Diagnostics and treatment planning. Dr. Attila Szűcs DDS
 Diagnostics and treatment planning. Dr. Attila Szűcs DDS Considering both surgical Aim and prosthetic aspects in the planning of implant prosthetics Arrangements for implant therapy Preliminary examinations
Diagnostics and treatment planning. Dr. Attila Szűcs DDS Considering both surgical Aim and prosthetic aspects in the planning of implant prosthetics Arrangements for implant therapy Preliminary examinations
A PERIO-PROSTHETIC. with the BIO-GLASS. DR. Mirko Paoli (DDS) DT. Roberto Fabris ABUTMENT SYSTEM
 A PERIO-PROSTHETIC with the TREATMENT use of ABUTMENT SYSTEM BIO-GLASS DR. Mirko Paoli (DDS) DT. Roberto Fabris 110 SUMMER 2015 The implant therapy in dentistry has allowed the modification of prosthetic
A PERIO-PROSTHETIC with the TREATMENT use of ABUTMENT SYSTEM BIO-GLASS DR. Mirko Paoli (DDS) DT. Roberto Fabris 110 SUMMER 2015 The implant therapy in dentistry has allowed the modification of prosthetic
Specialty Dentistry. Dentistry has nine specialty fields recognized by the American Dental Association
 Specialty Dentistry Dentistry has nine specialty fields recognized by the American Dental Association Dental Public Health Endodontics Oral and Maxillofacial Pathology Oral and Maxillofacial Radiology
Specialty Dentistry Dentistry has nine specialty fields recognized by the American Dental Association Dental Public Health Endodontics Oral and Maxillofacial Pathology Oral and Maxillofacial Radiology
BONE AUGMENTATION AND GRAFTING
 1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report
 C A S E R E P O R T Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report Rhoodie Garrana 1 and Govindrau Mohangi
C A S E R E P O R T Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report Rhoodie Garrana 1 and Govindrau Mohangi
What You Should Know About Dental Implants: The Process of Care Applies
 Learn how the process of care model can apply to dental implants and empower decisions for providing quality care for clients. Starting with assessing the need for implants, the process covers documentation,
Learn how the process of care model can apply to dental implants and empower decisions for providing quality care for clients. Starting with assessing the need for implants, the process covers documentation,
Occlusal Rehabilitation in a Partially Edentulous Patient with Lost Vertical Dimension Using Dental Implants: A Clinical Report
 Occlusal Rehabilitation in a Partially Edentulous Patient with Lost Vertical Dimension Using Dental Implants: A Clinical Report Azam Sadat Madani, DDS, MS; Amir Moeintaghavi, DDS, MS; Maryam Rezaeei, DDS,MS
Occlusal Rehabilitation in a Partially Edentulous Patient with Lost Vertical Dimension Using Dental Implants: A Clinical Report Azam Sadat Madani, DDS, MS; Amir Moeintaghavi, DDS, MS; Maryam Rezaeei, DDS,MS
Oral Health and Dentistry
 Page 107 to 118 Volume 1 Issue 2 2017 Case Report Oral Health and Dentistry ISSN: 2573-4989 Full Mouth Implants Rehabilitation of a Patient with Ectodermal Dysplasia After 3-Ds Ridge Augmentation and Bilateral
Page 107 to 118 Volume 1 Issue 2 2017 Case Report Oral Health and Dentistry ISSN: 2573-4989 Full Mouth Implants Rehabilitation of a Patient with Ectodermal Dysplasia After 3-Ds Ridge Augmentation and Bilateral
University of Groningen. Dental implants in maxillofacial prosthodontics Korfage, Anke
 University of Groningen Dental implants in maxillofacial prosthodontics Korfage, Anke DOI: 10.1016/j.bjoms.2014.05.013 10.1016/j.ijom.2013.04.003 10.1002/hed.24053 IMPORTANT NOTE: You are advised to consult
University of Groningen Dental implants in maxillofacial prosthodontics Korfage, Anke DOI: 10.1016/j.bjoms.2014.05.013 10.1016/j.ijom.2013.04.003 10.1002/hed.24053 IMPORTANT NOTE: You are advised to consult
A 42-year-old patient presenting with femoral
 Kanda et al. Journal of Medical Case Reports 2015, 9:17 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access A 42-year-old patient presenting with femoral head migration after hemiarthroplasty performed
Kanda et al. Journal of Medical Case Reports 2015, 9:17 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access A 42-year-old patient presenting with femoral head migration after hemiarthroplasty performed
Endosseous cylindric implants are well accepted
 Soft Tissue Exposure of Endosseous Implants Between Stage I and Stage II Surgery as a Potential Indicator of Early Crestal Bone Loss Joseph A. Toljanic, DDS*/Mark L. Banakis, DDS**/Leslee A. K. Willes,
Soft Tissue Exposure of Endosseous Implants Between Stage I and Stage II Surgery as a Potential Indicator of Early Crestal Bone Loss Joseph A. Toljanic, DDS*/Mark L. Banakis, DDS**/Leslee A. K. Willes,
Product Information. Straumann SLActive Performance beyond imagination. A new magnitude of healing power.
 Product Information Straumann SLActive Performance beyond imagination. A new magnitude of healing power. 10 YEARS OF CLINICAL SUCCESS AND PROVEN PREDICTABILITY IMMEDIATE LOADING High predictability in
Product Information Straumann SLActive Performance beyond imagination. A new magnitude of healing power. 10 YEARS OF CLINICAL SUCCESS AND PROVEN PREDICTABILITY IMMEDIATE LOADING High predictability in
Implant Restorations: A Step-By-Step Guide
 Implant Restorations: A Step-By-Step Guide Drago, Carl DDS, MS ISBN-13: 9780813828831 Table of Contents Contributors. Foreword. Acknowledgments. Chapter 1. Introduction To Implant Dentistry. 1. Introduction.
Implant Restorations: A Step-By-Step Guide Drago, Carl DDS, MS ISBN-13: 9780813828831 Table of Contents Contributors. Foreword. Acknowledgments. Chapter 1. Introduction To Implant Dentistry. 1. Introduction.
Osteoradionecrosis of Jaw in Head and Neck Cancer Patient Treated with Free Iliac Bone and Umbilical Fat Pad Graft
 Maxillofac Plast Reconstr Surg 2014;36(2):62-66 http://dx.doi.org/10.14402/jkamprs.2014.36.2.62 ISSN 2288-8101(Print) ISSN 2288-8586(Online) Case Report Osteoradionecrosis of Jaw in Head and Neck Cancer
Maxillofac Plast Reconstr Surg 2014;36(2):62-66 http://dx.doi.org/10.14402/jkamprs.2014.36.2.62 ISSN 2288-8101(Print) ISSN 2288-8586(Online) Case Report Osteoradionecrosis of Jaw in Head and Neck Cancer
Lia Kosmidou, DDS, MS*/Joseph A. Toljanic, DDS**/ William J. Moran, DMD, MD, FACS***/William R. Panje, MD, FACS****
 The Use of Percutaneous Implants for the Prosthetic Rehabilitation of Orbital Defects in Irradiated Cancer Patients: A Report of Clinical Outcomes and Complications Lia Kosmidou, DDS, MS*/Joseph A. Toljanic,
The Use of Percutaneous Implants for the Prosthetic Rehabilitation of Orbital Defects in Irradiated Cancer Patients: A Report of Clinical Outcomes and Complications Lia Kosmidou, DDS, MS*/Joseph A. Toljanic,
Reconstruction with fibular osteocutaneous free flap in patients with mandibular osteoradionecrosis
 Kim et al. Maxillofacial Plastic and Reconstructive Surgery (2015) 37:7 DOI 10.1186/s40902-015-0007-3 RESEARCH ARTICLE Open Access Reconstruction with fibular osteocutaneous free flap in patients with
Kim et al. Maxillofacial Plastic and Reconstructive Surgery (2015) 37:7 DOI 10.1186/s40902-015-0007-3 RESEARCH ARTICLE Open Access Reconstruction with fibular osteocutaneous free flap in patients with
Invisalign technique in the treatment of adults with pre-restorative concerns
 Mampieri and Giancotti Progress in Orthodontics 2013, 14:40 REVIEW Open Access Invisalign technique in the treatment of adults with pre-restorative concerns Gianluca Mampieri * and Aldo Giancotti Abstract
Mampieri and Giancotti Progress in Orthodontics 2013, 14:40 REVIEW Open Access Invisalign technique in the treatment of adults with pre-restorative concerns Gianluca Mampieri * and Aldo Giancotti Abstract
Saudi Journal of Oral and Dental Research. DOI: /sjodr. ISSN (Print) Dubai, United Arab Emirates Website:
 DOI:10.21276/sjodr Saudi Journal of Oral and Dental Research Scholars Middle East Publishers Dubai, United Arab Emirates Website: http://scholarsmepub.com/ ISSN 2518-1300 (Print) ISSN 2518-1297 (Online)
DOI:10.21276/sjodr Saudi Journal of Oral and Dental Research Scholars Middle East Publishers Dubai, United Arab Emirates Website: http://scholarsmepub.com/ ISSN 2518-1300 (Print) ISSN 2518-1297 (Online)
Pathological mandibular fracture: A severe complication of periimplantitis
 Journal section: Implantology Publication Types: Case Report doi:10.4317/jced.52305 http://dx.doi.org/10.4317/jced.52305 Pathological mandibular fracture: A severe complication of periimplantitis Luis
Journal section: Implantology Publication Types: Case Report doi:10.4317/jced.52305 http://dx.doi.org/10.4317/jced.52305 Pathological mandibular fracture: A severe complication of periimplantitis Luis
The anatomic limitations of the. Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD*
 CASE REPORT Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD* The anatomic limitations of the residual alveolar bone may cause problems for
CASE REPORT Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD* The anatomic limitations of the residual alveolar bone may cause problems for
Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study
 Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study Henny J. A. Meijer, DDS, PhD 1 /Rutger H. K. Batenburg, DDS,
Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study Henny J. A. Meijer, DDS, PhD 1 /Rutger H. K. Batenburg, DDS,
MEDICAL UNIVERSITY OF VARNA FACULTY OF DENTAL MEDICINE DEPARTMENT OF PROSTHETIC DENTAL MEDICINE GOVERNMENT EXAMINATION SYLLABUS
 MEDICAL UNIVERSITY OF VARNA FACULTY OF DENTAL MEDICINE DEPARTMENT OF PROSTHETIC DENTAL MEDICINE GOVERNMENT EXAMINATION SYLLABUS OF PROSTHETIC DENTAL MEDICINE ACADEMIC YEAR 2016/2017 1 1. Biomechanics of
MEDICAL UNIVERSITY OF VARNA FACULTY OF DENTAL MEDICINE DEPARTMENT OF PROSTHETIC DENTAL MEDICINE GOVERNMENT EXAMINATION SYLLABUS OF PROSTHETIC DENTAL MEDICINE ACADEMIC YEAR 2016/2017 1 1. Biomechanics of
Saudi Dental Licensure Examination Content Outline
 Saudi Dental Licensure Examination Content Outline This outline provides a common organization of SDLE content. SDLE central committee continually reviews the outline to ensure content is relevant to the
Saudi Dental Licensure Examination Content Outline This outline provides a common organization of SDLE content. SDLE central committee continually reviews the outline to ensure content is relevant to the
AMERICAN ACADEMY OF IMPLANT DENTISTRY
 AMERICAN ACADEMY OF IMPLANT DENTISTRY 211 East Chicago Ave., Suite 750, Chicago IL 60611-2616 312/335-1550 GUIDELINES FOR CASE REPORTS FOR FELLOW MEMBERSHIP* General Information Each Fellow candidate must
AMERICAN ACADEMY OF IMPLANT DENTISTRY 211 East Chicago Ave., Suite 750, Chicago IL 60611-2616 312/335-1550 GUIDELINES FOR CASE REPORTS FOR FELLOW MEMBERSHIP* General Information Each Fellow candidate must
All authors abide by the Association for Medical Ethics (AME) ethical rules of disclosure.
 Fogli V, Michele C, Lauritano D, Carinci F. Intraoraly welded titanium bar for immediate restoration in maxilla: Case report and review of the literature. Annals of Oral & Maxillofacial Surgery 2014 Mar
Fogli V, Michele C, Lauritano D, Carinci F. Intraoraly welded titanium bar for immediate restoration in maxilla: Case report and review of the literature. Annals of Oral & Maxillofacial Surgery 2014 Mar
Multi-Modality Anterior Extraction Site Grafting Increased Predictability for Aesthetics Michael Tischler, DDS
 Page 1 of 5 Issue Date: March 2003, Posted On: 8/1/2005 Multi-Modality Anterior Extraction Site Grafting Increased Predictability for Aesthetics Michael Tischler, DDS The extraction of teeth creates a
Page 1 of 5 Issue Date: March 2003, Posted On: 8/1/2005 Multi-Modality Anterior Extraction Site Grafting Increased Predictability for Aesthetics Michael Tischler, DDS The extraction of teeth creates a
JD Implant: 10 reasons for the best choice
 JD Implant: 10 reasons for the best choice The implant system for all your needs 100% Made in Italy [1 st reason: 100% Made in Italy] JDEvolution is 100% Made in Italy. It is manufactured in Modena, in
JD Implant: 10 reasons for the best choice The implant system for all your needs 100% Made in Italy [1 st reason: 100% Made in Italy] JDEvolution is 100% Made in Italy. It is manufactured in Modena, in
Dental Implants: A Predictable Solution for Tooth Loss. Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor
 Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
INTERNATIONAL MEDICAL COLLEGE
 INTERNATIONAL MEDICAL COLLEGE Joint Degree Master Program: Implantology and Dental Surgery (M.Sc.) Specialized Modules: List of individual modules Specialized Module 1 Basic principles of implantology
INTERNATIONAL MEDICAL COLLEGE Joint Degree Master Program: Implantology and Dental Surgery (M.Sc.) Specialized Modules: List of individual modules Specialized Module 1 Basic principles of implantology
MALO CLINIC PROTOCOL IMMEDIATE-FUNCTION CONCEPT UPPER AND LOWER JAW REHABILITATION: A CLINICAL REPORT
 MALO CLINIC PROTOCOL IMMEDIATE-FUNCTION CONCEPT UPPER AND LOWER JAW REHABILITATION: A CLINICAL REPORT PURPOSE Rehabilitation case with an implant-supported rehabilitation with immediate function implants.
MALO CLINIC PROTOCOL IMMEDIATE-FUNCTION CONCEPT UPPER AND LOWER JAW REHABILITATION: A CLINICAL REPORT PURPOSE Rehabilitation case with an implant-supported rehabilitation with immediate function implants.
REMOVABLE PROSTHODONTICS
 REMOVABLE PROSTHODONTICS UnitedHealthcare Dental Coverage Guideline Guideline Number: DCG020.03 Effective Date: January 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE...1 BENEFIT CONSIDERATIONS...1
REMOVABLE PROSTHODONTICS UnitedHealthcare Dental Coverage Guideline Guideline Number: DCG020.03 Effective Date: January 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE...1 BENEFIT CONSIDERATIONS...1
THREE-DIMENSIONAL COMPUTED TOMOGRAPIDC ANALYSIS FOR PLACEMENT OF MAXILLOFACIAL IMPLANTS AFTER MAXILLECTOMY
 Nagoya J. Med. Sci. 56. 69-79,1993 THREE-DIMENSIONAL COMPUTED TOMOGRAPIDC ANALYSIS FOR PLACEMENT OF MAXILLOFACIAL IMPLANTS AFTER MAXILLECTOMY MINORU VEDA, YOSHIHIRO SAWAKI, and TOSHIO KANEDA Department
Nagoya J. Med. Sci. 56. 69-79,1993 THREE-DIMENSIONAL COMPUTED TOMOGRAPIDC ANALYSIS FOR PLACEMENT OF MAXILLOFACIAL IMPLANTS AFTER MAXILLECTOMY MINORU VEDA, YOSHIHIRO SAWAKI, and TOSHIO KANEDA Department
Prosthodontic Rehabilitation of a Partially Edentulous Hemiglossectomy Patient: A Clinical Report
 case report 10.5005/jp-journals-10031-1067 Prosthodontic Rehabilitation of a Partially Edentulous Hemiglossectomy Patient: A Clinical Report 1 Ragini Sudhakar Sanaye, 2 Sabita M Ram, 3 Naisargi Shah, 4
case report 10.5005/jp-journals-10031-1067 Prosthodontic Rehabilitation of a Partially Edentulous Hemiglossectomy Patient: A Clinical Report 1 Ragini Sudhakar Sanaye, 2 Sabita M Ram, 3 Naisargi Shah, 4
Instructions for Use for dental implant
 Instructions for Use for dental implant 1. Disclaimer of liability This product is part of the Cortex Dental Implant System and may only be used in conjunction with the corresponding original components
Instructions for Use for dental implant 1. Disclaimer of liability This product is part of the Cortex Dental Implant System and may only be used in conjunction with the corresponding original components
Implants are a part of IMPLANT TREATMENT IN AN URBAN GENERAL DENTISTRY RESIDENCY PROGRAM: A7-YEAR RETROSPECTIVE STUDY CLINICAL
 CLINICAL IMPLANT TREATMENT IN AN URBAN GENERAL DENTISTRY RESIDENCY PROGRAM: A7-YEAR RETROSPECTIVE STUDY Clifford B. Starr, DMD Mohamed A. Maksoud, DMD KEY WORDS Dental implants General dentistry Resident
CLINICAL IMPLANT TREATMENT IN AN URBAN GENERAL DENTISTRY RESIDENCY PROGRAM: A7-YEAR RETROSPECTIVE STUDY Clifford B. Starr, DMD Mohamed A. Maksoud, DMD KEY WORDS Dental implants General dentistry Resident
The majority of the early research concerning
 Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
Module 2 Introduction to immediate full arch fixed implant treatment - surgical options
 Module 2 Introduction to immediate full arch fixed implant treatment - surgical options First Name Last Name Objectives Identify the need and opportunity to treat full arch patients with fixed detachable
Module 2 Introduction to immediate full arch fixed implant treatment - surgical options First Name Last Name Objectives Identify the need and opportunity to treat full arch patients with fixed detachable
Plastic Surgery: An International Journal
 Plastic Surgery: An International Journal Vol. 2013 (2013), Article ID 874416, 29 minipages. DOI:10.5171/2013.874416 www.ibimapublishing.com Copyright 2013 Akira Saito, Noriko Saito, Emi Funayama and Hidehiko
Plastic Surgery: An International Journal Vol. 2013 (2013), Article ID 874416, 29 minipages. DOI:10.5171/2013.874416 www.ibimapublishing.com Copyright 2013 Akira Saito, Noriko Saito, Emi Funayama and Hidehiko
Head and Neck Surgery, University of Groningen and University Medical Center Groningen, Groningen, The Netherlands.
 ORIGINAL ARTICLE Recommendations for implant-retained nasal prostheses after ablative tumor surgery: Minimal surgical aftercare, high implant survival, and satisfied patients Anke Korfage, DDS, 1 * Gerry
ORIGINAL ARTICLE Recommendations for implant-retained nasal prostheses after ablative tumor surgery: Minimal surgical aftercare, high implant survival, and satisfied patients Anke Korfage, DDS, 1 * Gerry
Minimally Invasive Implant Dentistry Using Narrow, Shorter and Mini Implants
 Minimally Invasive Implant Dentistry Using Narrow, Shorter and Mini Implants Jose Luis Ruiz DDS, FAGD Statistics show that 69% of adults ages 35 to 44 have lost at least one permanent tooth to an accident,
Minimally Invasive Implant Dentistry Using Narrow, Shorter and Mini Implants Jose Luis Ruiz DDS, FAGD Statistics show that 69% of adults ages 35 to 44 have lost at least one permanent tooth to an accident,
INCREASED RETENTION OF A PARTIAL DENTURE MAXILLARY OBTURATOR USING DENTAL IMPLANT
 INCREASED RETENTION OF A PARTIAL DENTURE MAXILLARY OBTURATOR USING DENTAL IMPLANT N. Yunus1, Z.A.A. Rahman 2. Increased retention of a partial denture maxillary obturator using dental implant. Annal Dent
INCREASED RETENTION OF A PARTIAL DENTURE MAXILLARY OBTURATOR USING DENTAL IMPLANT N. Yunus1, Z.A.A. Rahman 2. Increased retention of a partial denture maxillary obturator using dental implant. Annal Dent
Case Report Soft Tissue Management and Prosthetic Rehabilitation in a Tongue Cancer Patient
 Case Reports in Dentistry Volume 2013, Article ID 475186, 5 pages http://dx.doi.org/10.1155/2013/475186 Case Report Soft Tissue Management and Prosthetic Rehabilitation in a Tongue Cancer Patient Umberto
Case Reports in Dentistry Volume 2013, Article ID 475186, 5 pages http://dx.doi.org/10.1155/2013/475186 Case Report Soft Tissue Management and Prosthetic Rehabilitation in a Tongue Cancer Patient Umberto
BUILDING A. Achieving total reconstruction in a single operation. 70 OCTOBER 2016 // dentaltown.com
 BUILDING A MANDI Achieving total reconstruction in a single operation by Dr. Fayette C. Williams Fayette C. Williams, DDS, MD, FACS, is clinical faculty at John Peter Smith Hospital in Fort Worth, Texas,
BUILDING A MANDI Achieving total reconstruction in a single operation by Dr. Fayette C. Williams Fayette C. Williams, DDS, MD, FACS, is clinical faculty at John Peter Smith Hospital in Fort Worth, Texas,
Esthetic management of multiple missing anterior teeth A Case report
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 13, Issue 1 Ver. II (Jan. 2014), PP 97-101 Esthetic management of multiple missing anterior teeth A
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 13, Issue 1 Ver. II (Jan. 2014), PP 97-101 Esthetic management of multiple missing anterior teeth A
PDF of Trial CTRI Website URL -
 Clinical Trial Details (PDF Generation Date :- Sat, 07 Jul 2018 14:19:46 GMT) CTRI Number Last Modified On 04/07/2012 Post Graduate Thesis Type of Trial Type of Study Study Design Public Title of Study
Clinical Trial Details (PDF Generation Date :- Sat, 07 Jul 2018 14:19:46 GMT) CTRI Number Last Modified On 04/07/2012 Post Graduate Thesis Type of Trial Type of Study Study Design Public Title of Study
The Canadian contribution to the otolaryngology literature: a five year bibliometric analysis
 Gurberg et al. Journal of Otolaryngology - Head and Neck Surgery 2014, 43:47 ORIGINAL RESEARCH ARTICLE Open Access The Canadian contribution to the otolaryngology literature: a five year bibliometric analysis
Gurberg et al. Journal of Otolaryngology - Head and Neck Surgery 2014, 43:47 ORIGINAL RESEARCH ARTICLE Open Access The Canadian contribution to the otolaryngology literature: a five year bibliometric analysis
Case Report Prosthodontic Rehabilitation of the Patient with Severely Worn Dentition: A Case Report
 Case Reports in Dentistry Volume 2012, Article ID 961826, 4 pages doi:10.1155/2012/961826 Case Report Prosthodontic Rehabilitation of the Patient with Severely Worn Dentition: A Case Report Mahnaz Hatami,
Case Reports in Dentistry Volume 2012, Article ID 961826, 4 pages doi:10.1155/2012/961826 Case Report Prosthodontic Rehabilitation of the Patient with Severely Worn Dentition: A Case Report Mahnaz Hatami,
Prosthodontic Management of Combination Syndrome Case with Metal Reinforced Maxillary Complete Denture and Mandibular Teeth supported Overdenture
 Case Report imedpub Journals www.imedpub.com Periodontics and Prosthodontics DOI: 10.21767/2471-3082.100041 Prosthodontic Management of Combination Syndrome Case with Metal Reinforced Maxillary Complete
Case Report imedpub Journals www.imedpub.com Periodontics and Prosthodontics DOI: 10.21767/2471-3082.100041 Prosthodontic Management of Combination Syndrome Case with Metal Reinforced Maxillary Complete
Pharmacologyonline 2: (2008) Young Researchers Gavasova and Budev EPULIS FISSURATUM CLINICAL APPEARANCE AND TREATMENT. Dr G.Gavasova, Dr I.
 EPULIS FISSURATUM CLINICAL APPEARANCE AND TREATMENT Dr G.Gavasova, Dr I.Budev Medical University, Faculty of Dental Medicine Oral Surgery Department Head: Prof. Dr D. Atanasov, Ph.D, MD. Summary Continuous
EPULIS FISSURATUM CLINICAL APPEARANCE AND TREATMENT Dr G.Gavasova, Dr I.Budev Medical University, Faculty of Dental Medicine Oral Surgery Department Head: Prof. Dr D. Atanasov, Ph.D, MD. Summary Continuous
EVERYONE I M P L A N T C O M P A N Y
 A SMILE FOR EVERYONE I M P L A N T C O M P A N Y WHAT IS AN IMPLANT? A dental implant is an effective alternative to the root of a tooth. It consists of a titanium screw only a few millimetres in size.
A SMILE FOR EVERYONE I M P L A N T C O M P A N Y WHAT IS AN IMPLANT? A dental implant is an effective alternative to the root of a tooth. It consists of a titanium screw only a few millimetres in size.
A Long-term Retrospective Analysis of Survival Rates of Implants in the Mandible
 A Long-term Retrospective Analysis of Survival Rates of Implants in the Mandible Thomas J. Balshi, DDS, PhD, FACP 1 /Glenn J. Wolfinger, DMD, FACP 2 / Brett E. Stein 3 /Stephen F. Balshi, MBE 4 Purpose:
A Long-term Retrospective Analysis of Survival Rates of Implants in the Mandible Thomas J. Balshi, DDS, PhD, FACP 1 /Glenn J. Wolfinger, DMD, FACP 2 / Brett E. Stein 3 /Stephen F. Balshi, MBE 4 Purpose:
The clinical use of endosseous implants has
 A Prospective Multicenter Clinical Trial of 3i Machined-Surface Implants: Results After 6 Years of Follow-up Dietmar Weng, DDS, Dr Med Dent 1 /Zhimon Jacobson, DDS 2 /Dennis Tarnow, DDS 3 / Markus B. Hürzeler,
A Prospective Multicenter Clinical Trial of 3i Machined-Surface Implants: Results After 6 Years of Follow-up Dietmar Weng, DDS, Dr Med Dent 1 /Zhimon Jacobson, DDS 2 /Dennis Tarnow, DDS 3 / Markus B. Hürzeler,
