Lia Kosmidou, DDS, MS*/Joseph A. Toljanic, DDS**/ William J. Moran, DMD, MD, FACS***/William R. Panje, MD, FACS****
|
|
|
- Anis King
- 5 years ago
- Views:
Transcription
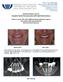
1 The Use of Percutaneous Implants for the Prosthetic Rehabilitation of Orbital Defects in Irradiated Cancer Patients: A Report of Clinical Outcomes and Complications Lia Kosmidou, DDS, MS*/Joseph A. Toljanic, DDS**/ William J. Moran, DMD, MD, FACS***/William R. Panje, MD, FACS**** This retrospective study evaluated the use of percutaneous craniofacial implants for the prosthetic rehabilitation of patients with a history of orbital exenteration and irradiation for oncologic tumors of the head and neck. A total of 24 implants were placed in six patients. All implants were determined to be osseointegrated at the time of uncovering. Three implants were subsequently resubmerged beneath the soft tissue because of positional interferences with prosthesis fabrication. The remaining 21 implants were ultimately used to retain six orbital prostheses. Two implants failed to maintain osseointegration during the follow-up period and were subsequently removed without complications. This represents an overall integration success rate of 90.5% over a mean followup period of 32.8 months (range = 11 to 68 months). The significance of these findings and their relationship to comparable reports in the literature are discussed. (INT J ORAL MAXILLOFAC IMPLANTS 1998;13: ) Key words: craniofacial implants, orbital defect, osseointegration, radiation therapy Since their introduction in 1977 for use with bone conduction hearing aids, percutaneous craniofacial implants have found more extensive applications in maxillofacial prosthetic rehabilitation. 1 These implants have been shown to effectively retain a wide variety of removable prostheses for individuals with defects of the face resulting from congenital malformation, surgery, or trauma (Fig 1). Craniofacial implants offer significant advantages over traditional ****Former Fellow, Maxillofacial Prosthetics, University of Chicago, Zoller Dental Clinics, Chicago, Illinois. ****Associate Professor of Clinical Surgery, Chief of Prosthetics, University of Chicago, Zoller Dental Clinics, Chicago, Illinois. ****Staff Surgeon, Section of Otolaryngology-Head and Neck Surgery, Lutheran General Hospital, Park Ridge, Illinois. ****Professor and Chief, Head and Neck Reconstruction and Skull Base Surgery, Rush Medical Center, Chicago, Illinois. Reprint requests: Dr Joseph A. Toljanic, University of Chicago, MC-2108, 5841 S. Maryland Avenue, Chicago, Illinois means of retaining facial prostheses, including the use of medical-grade adhesives, the engaging of anatomic undercuts within the confines of the defect, and eyeglasses. 2 Implants provide improved retention while avoiding the tissue and prosthesis damage that can be associated with adhesives. In this manner, craniofacial implants can help to provide a convenient, comfortable, and emotionally satisfactory prosthesis with excellent long-term functional and cosmetic results (Figs 2 and 3). Based on these successes, craniofacial implants are now being placed with increasing frequency in patients who have undergone radiotherapy for oncologic lesions of the head and neck, in spite of the well-documented adverse biologic changes that occur when osseous tissues are exposed to ionizing radiation. These changes include alterations in the cellular components of bone involving a significant reduction in the number of viable osteoblasts and osteocytes, as well as the development of areas of fatty degeneration within the marrow spaces. In addition, the vasculature undergoes progressive endarteritis, hyalin- The International Journal of Oral & Maxillofacial Implants 121
2 Fig 1 Right orbital defect with four screw-retained transdermal implant abutments in place. Note screwattached cast-metal alloy framework with three retentive magnets. Fig 2 Implant-retained right orbital prosthesis. Fig 3 Orbital prosthesis as viewed from tissue surface. Note three magnets incorporated within prosthesis for retention. Table 1 Reported Integration Success Rates (%) for Orbital Sites in Irradiated and Nonirradiated Populations Irradiated Nonirradiated Parel and Tjellstrom Roumanas et al Tolman and Taylor Jacobsson et al Mean ization, and fibrosis, resulting in regional ischemia. 3 Following such changes, irradiated sites would presumably be at significant risk for tissue necrosis and integration failure if subjected to implant surgery. As a result, the appropriateness of using craniofacial implants in the rehabilitation of facial defects in this population subset has been questioned. A number of recent articles have raised such concerns by describing significantly decreased survival rates when implants were placed in irradiated craniofacial bones as compared to nonirradiated sites. Pearl and Tjellstrom 4 described integration success rates as reported from multiple sites within the United States and Sweden. By pooling all data presented, the results indicate overall success rates of 61.3% and 95.9% for irradiated and nonirradiated populations, respectively. Roumanas et al 5 found a similar disparity in results describing integration success rates of 68.4% and 85.3% for irradiated versus nonirradiated patients. Tolman and Taylor 6 described a success rate of 85% and 97% for irradiated and nonirradiated patients, respectively. Most recently, Eckert et al 7 described their experience with endosseous implants placed in multiple irradiated locations, including craniofacial sites. While only two patients were described in this report and the radiation histories were unclear, 7 of the 13 craniofacial implants failed, resulting in an integration success rate of 46%. The literature also suggests that craniofacial implant integration may be site-dependent. When multiple reports are cumulatively examined for irradiated versus nonirradiated orbital sites alone, the data demonstrate a combined integration success rate of 59.1% and 80.2%, respectively (Table 1). 4 6,8 This appears to indicate that the irradiated orbit presents a poor site for craniofacial implant placement. The purpose of this study was to review an experience with craniofacial implants used in the retention of facial prostheses for patients with orbital defects and a history of irradiation for oncologic tumors of the head and neck. These findings were then compared to similar reports in the current literature. 122 Volume 13, Number 1, 1998
3 Table 2 Demographic Data and Oncologic Treatment Performed RT dose Diagnosis and to implant Patient Age/race/sex tumor location Surgery performed sites (Gy) 1 40/white/m Adenoid cystic cancer, left antrum Maxillectomy, orbital exenteration /white/f Scca* left maxillary and ethmoid sinus Maxillectomy, orbital exenteration /white/f Poorly differentiated cancer, left ethmoid sinus Orbital exenteration /white/f Scca* left ethmoid and maxillary sinus Ethmoidectomy, orbital exenteration /black/f Scca* right antrum Maxillectomy, orbital exenteration /white/f Lymphoma, right orbit Orbital exenteration 45.0 *Squamous cell carcinoma. Radiation therapy Table 3 Craniofacial Implant Treatment Data Surgery/RT time No. of Implant Healing No. of implants Patient interval (mo)* implants location period (mo) integrated Superior rim Superior rim Superior rim Inferior rim Superior rim Superior rim Inferior rim Superior rim 9 3 *Time interval between radiotherapy and implantation. Materials and Methods Six consecutive patients treated at the University of Chicago, Zoller Dental Clinics for postoncologic orbital defects, were included in this review. All data were obtained from patient medical and dental charts. Table 2 presents selected demographic data and oncologic treatment performed. Each patient history was significant for surgical exenteration of an orbit and postoperative adjuvant radiotherapy. Two patients underwent hyperbaric oxygen (HBO) therapy as an adjunctive means to address unanticipated postoperative wound healing complications unrelated to subsequent implant rehabilitation. Patient 1 developed necrosis and bleeding in the area of the left cavernous sinus. He received HBO therapy prior to and after base of skull reconstruction. Patient 2 was given adjunctive HBO for treatment of osteomyelitis of the medial wall of the orbital defect. A variable time interval was allowed to elapse after irradiation before implant placement because of individual patient desires for rehabilitation (Table 3). After a thorough clinical and radiographic evaluation, each patient underwent craniofacial implant placement in the operating room under general anesthesia employing surgical techniques as described by Tjellstrom et al. 9 The superior orbital rim was typically the implantation site of choice because of the availability of adequate bony volume. However, for two patients, four implants were placed in the inferior orbital rim (Table 3). Postoperative healing progressed uneventfully for all patients. Stage-two implant uncovering proceeded 9 to 12 months following implantation. At that time, the subcutaneous tissues were thinned and transdermal healing abutments were screwed into place. Following adequate healing, orbital prosthesis fabrication was initiated following standard clinical and laboratory procedures. 10 Retention was obtained in all patients through the use of magnets incorporated into retentive frameworks (Shiner Magnets, Preat Corp, San Mateo, CA). All patients were instructed in appropriate home care, which included daily use of soap and water at the implant sites as well as mechanical debridement of the abutments and retentive bar with the use of floss. Patients typically presented for follow-up at 1- and 3-month intervals after prosthesis placement. Subsequently, 6-month follow-up appointments were routinely scheduled. At each examination, the retentive frameworks were removed and cleaned and soft tissue health at the implant sites was evaluated. The The International Journal of Oral & Maxillofacial Implants 123
4 Table 4 Implant Treatment Complications Prostheses Implants Implants Soft tissue Patient in place (mo) removed submerged complications Soft tissue infection treated with antibiotics 6 31 Soft tissue infection treated with antibiotics status of implant integration was determined by digitally torquing the abutment using the appropriate hand-held driver. The prostheses were also evaluated for adequacy of fit and function. Results A total of 24 implants were placed in six patients. All implants were clinically determined to be integrated at the time of stage-two uncovering. Three of the integrated, asymptomatic implants were subsequently resubmerged beneath the soft tissues prior to concluding prosthetic treatment because of anticipated prosthetic treatment interferences secondary to implant location as determined by a maxillofacial prosthodontist (Table 4). Each submerged implant has remained in place without complication as of the time of this report. Of the 21 implants available for prosthetic restoration, two were subsequently removed because of loss of integration and concomitant complaints of pain and tenderness (Table 4). Both implants were located in the inferior orbital rim of Patient 3. The first implant was removed during prosthesis fabrication. The second implant required removal 16 months after uncovering while the prosthesis was in function. Each implant was removed without complication, and healing proceeded uneventfully. Retention of the prosthesis was effectively maintained using the remaining implants in the superior orbital rim. As of the time of this report, the remaining 19 implants continue in function, and all six patients have successfully worn their orbital prostheses without interruption throughout the period under review. This represents an integration rate of 90.5% over a mean postprosthesis placement follow-up interval of 32.8 months (range = 11 to 68 months). In addition, two episodes of soft tissue infection were encountered during the evaluation period. Patients 5 and 6 each developed one episode of periimplant soft tissue erythema and swelling. Purulent exudate was noted upon probing. Each situation was treated successfully with antibiotics and reinforcement of home care without the need for surgical intervention. The implants at these sites remain integrated and in function as of the writing of this report. Discussion In the current study, the percentage of successful implant integration in irradiated orbital sites for six patients was found to be 90.5% over a mean followup period of 32.8 months (range = 11 to 68 months). The results are consistent with those reported by Wolfaardt et al, 11 who described an integration success rate of 96.4% for this population subset over a follow-up period that ranged from 12 to 48 months. These findings lend support to the placement of craniofacial implants in irradiated sites. However, the results are at significant variance with a number of other reports (Table 1). These variations in described integration outcomes pose serious difficulties when attempting to interpret the data or draw appropriate conclusions for selecting patient treatment. While differences between centers with regard to treatment techniques and duration of patient follow-up may play a role in reported integration success, perhaps an interaction between patient-specific factors heretofore undetermined, compounded with biologic changes associated with irradiation, may prove to be the principal factors for integration success. The ability to identify and assess these factors with sufficient accuracy so as to make meaningful predictions of outcome then appears to be the major challenge to be addressed in the future. One such factor under investigation is the relationship of the time interval between irradiation and surgical manipulation of the bone. The importance of long time intervals between irradiation and surgery has been suggested by some authors. An improvement in the bone-healing capacity by a factor of almost 2.5 during a 12-month period following irradi- 124 Volume 13, Number 1, 1998
5 ation was found using animal models. 12 Conversely, Marx and Johnson 13 recommend that reconstructive surgery should be performed within a shorter time interval ranging from 1 to 6 months postirradiation. This was based on findings of late progressive loss of vascular perfusion and healing capacity over time following radiation therapy. In the current study, issues unrelated to implant treatment planning resulted in a postirradiation implantation time frame that ranged from 15 to 149 months. This variation in timing for implant placement typically was dictated by overall patient health factors, as well as delays in ultimately accepting and proceeding with treatment. The uncontrolled manner in which the time frame evolved, as well as the small population size, limits the ability to draw conclusions from this study regarding when to place implants in irradiated craniofacial sites. The ideal time period for proceeding with implantation following radiation therapy awaits further elucidation. Hyperbaric oxygen therapy has also been recommended as a means to improve regional vascularity and to heighten implant integration success. 12,14 HBO therapy is known to stimulate angiogenesis, resulting in neovascularization and an increase in cellular oxygen tension to support new osteoblast and fibroblast proliferation. 15 In the current study, no patient underwent preplanned HBO in preparation for craniofacial implant placement. Two patients received HBO therapy to address postoncologic treatment-healing complications. Therapy was initiated in each patient prior to implant surgery without the direct intention of improving the implant integration potential. These results do not permit the drawing of conclusions, as the data were obtained from a relatively small population. However, the results suggest that the application of HBO may not be a universal requirement for successful craniofacial implantation in an irradiated population. Further, the data as found in this review and described by others demonstrate little postoperative morbidity associated either with implantation or integration failure and implant removal. This would indicate that an irradiated craniofacial population may be at minimal risk for serious treatment complications such as osteoradionecrosis. Perhaps larger trials will be required to adequately assess these risks. In addition to the two implant integration failures in Patient 3, peri-implant soft tissue complications were noted for two patients in this study. Each patient experienced one episode of pain and tenderness along with soft tissue erythema and purulent drainage. Each was successfully treated empirically with antibiotics and by encouraging proper home maintenance without further complications. While each episode of infection was effectively treated using conservative measures, these findings demonstrate the potential for other complications that may be encountered in this population. Such complications, if left untreated, may pose serious risks that need to be addressed aggressively. The presence of enteric and hemolytic streptococcal organisms apparently existing as part of the normal microflora in the peri-implant crevicular space has been documented. 16 These opportunistic pathogens are commonly associated with significant infection that could lead to implant failure. Regular follow-up examinations and closely supervised home care appear to be warranted. Conclusion A retrospective review was undertaken to evaluate the use of percutaneous craniofacial implants placed in irradiated osseous tissues for the retention of orbital prostheses. Over a mean follow-up period of 32.8 months, 19 of a total of 21 integrated implants placed into function remained integrated, representing an overall success rate of 90.5%. While this result supports the use of implants in irradiated craniofacial sites, it is at variance with data reported by others in the literature, suggesting that the factors that determine integration success in this patient population are not clearly understood. Further study is needed to determine the appropriate time interval between the conclusion of radiotherapy and implant placement. In addition, both the role of HBO in maximizing osseointegration and the effects of the resident crevicular microflora in long-term maintenance need to be further assessed. References 1. Brånemark PI, Albrektsson T. Titanium implants permanently penetrating human skin. Scand J Plast Reconstr Surg 1982;16: Del Valle V, Faulkner G, Wolfaardt J, Rangert B, Tan HK. Mechanical evaluation of craniofacial osseointegration retention systems. Int J Oral Maxillofac Implants 1995;10: Marx RE. Osteoradionecrosis: A new concept of its pathophysiology. J Oral Maxillofac Surg 1983;41; Parel SM, Tjellstrom A. The United States and Swedish experience with osseointegration and facial prostheses. Int J Oral Maxillofac Implants 1991;6: Roumanas E, Nishimura R, Beumer J, Moy P, Weinlander M, Lorant J. Craniofacial defects and osseointegrated implants: Six-year follow-up report on the success rates of craniofacial implants at UCLA. Int J Oral Maxillofac Implants 1994;9: Tolman D, Taylor PF. Bone anchored craniofacial prosthesis study. Int J Oral Maxillofac Implants 1996;11: Eckert SE, Desjardins RP, Keller EE, Tolman DE. Endosseous implants in an irradiated tissue bed. J Prosthet Dent 1996;76: The International Journal of Oral & Maxillofacial Implants 125
6 8. Jacobsson M, Tjellstrom A, Fine L, Andersson H. A retrospective study of osseointegrated skin-penetrating titanium fixtures used for retaining facial prostheses. Int J Oral Maxillofac Implants 1992;7: Tjellstrom A, Rosenhall U, Lindstrom J, Hallen O, Albrektsson T, Brånemark PI. Five-year experience with skinpenetrating bone-anchored implants in the temporal bone. Acta Otolaryngol 1983;95: Moran WJ, Toljanic JA, Panje WR. Implant-retained prosthetic rehabilitation of orbital defects. Arch Otolaryngol Head Neck Surg 1996;122: Wolfaardt JF, Wilkes GH, Parel SM, Tjellstrom A. Craniofacial osseointegration: The Canadian experience. Int J Oral Maxillofac Implants 1993;8: Granstrom G, Jacobsson M, Tjellstrom A. Titanium implants in irradiated tissue. Int J Oral Maxillofac Implants 1992;7: Marx RE, Johnson RP. Studies in the radiobiology of osteoradionecrosis and their clinical significance. Oral Surg Oral Med Oral Pathol 1987;64: Larsen PE, Stroncjek MJ, Beck FM, Rohrer M. Osseointegration of implants in radiated bone with and without adjunctive hyperbaric oxygen. J Oral Maxillofac Surg 1993;51: Consensus Development Conference on Oral Complications of Cancer Therapies: Diagnosis, Prevention, and Treatment. NCI Monograph. Bethesda: National Institute for Health, 1990;9: Toljanic JA, Morello JA, Moran WJ, Panje WR, May EF. Microflora associated with percutaneous craniofacial implants used for the retention of facial prostheses: A pilot study. Int J Oral Maxillofac Implants 1995;10: Volume 13, Number 1, 1998
The influence of radiotherapy on osseointegration
 Experience with Osseointegrated Implants Placed in Irradiated Tissues in Japan and the United States Atsushi Niimi, DDS, DMSc*/Minoru Ueda, DDS, PhD**/ Eugene E. Keller, DDS, PhD***/Philip Worthington,
Experience with Osseointegrated Implants Placed in Irradiated Tissues in Japan and the United States Atsushi Niimi, DDS, DMSc*/Minoru Ueda, DDS, PhD**/ Eugene E. Keller, DDS, PhD***/Philip Worthington,
Treatment Outcome of Bone-Anchored Craniofacial Prostheses after Tumour Surgery
 Treatment Outcome of Bone-Anchored Craniofacial Prostheses after Tumour Surgery Pieter J Schoen Gerry M Raghoebar Robert P van Oort Harry Reintsema Bernard FAM van der Laan Fred R Burlage Jan LN Roodenburg
Treatment Outcome of Bone-Anchored Craniofacial Prostheses after Tumour Surgery Pieter J Schoen Gerry M Raghoebar Robert P van Oort Harry Reintsema Bernard FAM van der Laan Fred R Burlage Jan LN Roodenburg
Many papers have reported on histologic
 Histologic Evaluation of Clinically Successful Osseointegrated Implants Retrieved from Irradiated Bone: A Report of 2 Patients Hidetaka Nakai, DDS*/Atsushi Niimi, DDS, DMSc**/Minoru Ueda, DDS, PhD*** The
Histologic Evaluation of Clinically Successful Osseointegrated Implants Retrieved from Irradiated Bone: A Report of 2 Patients Hidetaka Nakai, DDS*/Atsushi Niimi, DDS, DMSc**/Minoru Ueda, DDS, PhD*** The
Endosseous cylindric implants are well accepted
 Soft Tissue Exposure of Endosseous Implants Between Stage I and Stage II Surgery as a Potential Indicator of Early Crestal Bone Loss Joseph A. Toljanic, DDS*/Mark L. Banakis, DDS**/Leslee A. K. Willes,
Soft Tissue Exposure of Endosseous Implants Between Stage I and Stage II Surgery as a Potential Indicator of Early Crestal Bone Loss Joseph A. Toljanic, DDS*/Mark L. Banakis, DDS**/Leslee A. K. Willes,
Osseointegrated dental implant treatment generally
 Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
In Scandinavia, malignant tumors in the maxillofacial
 Oral Implant Rehabilitation in Irradiated Patients Without Adjunctive Hyperbaric Oxygen Gunilla Andersson, DDS, PhD*/Lars Andreasson, MD, PhD**/Göran Bjelkengren, MD*** In 15 patients treated for malignant
Oral Implant Rehabilitation in Irradiated Patients Without Adjunctive Hyperbaric Oxygen Gunilla Andersson, DDS, PhD*/Lars Andreasson, MD, PhD**/Göran Bjelkengren, MD*** In 15 patients treated for malignant
Bone Reduction Surgical Guide for the Novum Implant Procedure: Technical Note
 Bone Reduction Surgical Guide for the Novum Implant Procedure: Technical Note Stephen M. Parel, DDS 1 /Steven L. Ruff, CDT 2 /R. Gilbert Triplett, DDS, PhD 3 /Sterling R. Schow, DMD 4 The Novum System
Bone Reduction Surgical Guide for the Novum Implant Procedure: Technical Note Stephen M. Parel, DDS 1 /Steven L. Ruff, CDT 2 /R. Gilbert Triplett, DDS, PhD 3 /Sterling R. Schow, DMD 4 The Novum System
Head and Neck Surgery, University of Groningen and University Medical Center Groningen, Groningen, The Netherlands.
 ORIGINAL ARTICLE Recommendations for implant-retained nasal prostheses after ablative tumor surgery: Minimal surgical aftercare, high implant survival, and satisfied patients Anke Korfage, DDS, 1 * Gerry
ORIGINAL ARTICLE Recommendations for implant-retained nasal prostheses after ablative tumor surgery: Minimal surgical aftercare, high implant survival, and satisfied patients Anke Korfage, DDS, 1 * Gerry
Case Report Prosthetic Rehabilitation of Primary Osteosarcoma of the Orbit - A Clinical Report
 Cronicon OPEN ACCESS Bharat Mirchandani, Binit Shrestha and Sita Thaworanunta* Department of Prosthodontics, Mahidol University, Thailand Received: April 03, 2015; Published: April 08, 2015 DENTAL SCIENCE
Cronicon OPEN ACCESS Bharat Mirchandani, Binit Shrestha and Sita Thaworanunta* Department of Prosthodontics, Mahidol University, Thailand Received: April 03, 2015; Published: April 08, 2015 DENTAL SCIENCE
The majority of the early research concerning
 Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
CHAPTER. 1. Uncontrolled systemic disease 2. Retrognathic jaw relationship
 CHAPTER 7 Immediate Implant Supported Restoration of the Edentulous Arch Stephen G. Alfano and Robert M. Laughlin Department of Oral and Maxillofacial Surgery, Naval Medical Center San Diego, San Diego,
CHAPTER 7 Immediate Implant Supported Restoration of the Edentulous Arch Stephen G. Alfano and Robert M. Laughlin Department of Oral and Maxillofacial Surgery, Naval Medical Center San Diego, San Diego,
The Brånemark osseointegration method, using titanium dental implants (fixtures)
 Early Failures in 4,641 Consecutively Placed Brånemark Dental Implants: A Study From Stage 1 Surgery to the Connection of Completed Prostheses Bertil Friberg, DDS/Torsten Jemt, DDS, PhD/Ulf Lekholm, DDS,
Early Failures in 4,641 Consecutively Placed Brånemark Dental Implants: A Study From Stage 1 Surgery to the Connection of Completed Prostheses Bertil Friberg, DDS/Torsten Jemt, DDS, PhD/Ulf Lekholm, DDS,
THREE-DIMENSIONAL COMPUTED TOMOGRAPIDC ANALYSIS FOR PLACEMENT OF MAXILLOFACIAL IMPLANTS AFTER MAXILLECTOMY
 Nagoya J. Med. Sci. 56. 69-79,1993 THREE-DIMENSIONAL COMPUTED TOMOGRAPIDC ANALYSIS FOR PLACEMENT OF MAXILLOFACIAL IMPLANTS AFTER MAXILLECTOMY MINORU VEDA, YOSHIHIRO SAWAKI, and TOSHIO KANEDA Department
Nagoya J. Med. Sci. 56. 69-79,1993 THREE-DIMENSIONAL COMPUTED TOMOGRAPIDC ANALYSIS FOR PLACEMENT OF MAXILLOFACIAL IMPLANTS AFTER MAXILLECTOMY MINORU VEDA, YOSHIHIRO SAWAKI, and TOSHIO KANEDA Department
University of Groningen. Dental implants in maxillofacial prosthodontics Korfage, Anke
 University of Groningen Dental implants in maxillofacial prosthodontics Korfage, Anke DOI: 10.1016/j.bjoms.2014.05.013 10.1016/j.ijom.2013.04.003 10.1002/hed.24053 IMPORTANT NOTE: You are advised to consult
University of Groningen Dental implants in maxillofacial prosthodontics Korfage, Anke DOI: 10.1016/j.bjoms.2014.05.013 10.1016/j.ijom.2013.04.003 10.1002/hed.24053 IMPORTANT NOTE: You are advised to consult
Much has been written about the success of various
 Simplified Guide for Precise Implant Placement: A Technical Note Brent D. Kennedy, MD, DDS*/Thomas A. Collins, Jr, DDS**/ Patrick C. W. Kline, DMD, MD** Ideal implant placement is ultimately determined
Simplified Guide for Precise Implant Placement: A Technical Note Brent D. Kennedy, MD, DDS*/Thomas A. Collins, Jr, DDS**/ Patrick C. W. Kline, DMD, MD** Ideal implant placement is ultimately determined
Basic information on the. Straumann Pro Arch TL. Straumann Pro Arch TL
 Basic information on the Straumann Pro Arch TL Straumann Pro Arch TL Contents 1. Introduction 2 1.1 Discover more treatment options with the 4 mm Short Implant 2 2. Technical information 3 3. Step-by-step
Basic information on the Straumann Pro Arch TL Straumann Pro Arch TL Contents 1. Introduction 2 1.1 Discover more treatment options with the 4 mm Short Implant 2 2. Technical information 3 3. Step-by-step
Ninety percent of oral cancers are epidermoid
 Dental Prosthetic Reconstruction of Osseointegrated Implants Placed in Irradiated Bone Véronique Brogniez*/Patrice Lejuste**/Alain Pecheur***/Hervé Reychler**** Nineteen patients who were treated for oncologic
Dental Prosthetic Reconstruction of Osseointegrated Implants Placed in Irradiated Bone Véronique Brogniez*/Patrice Lejuste**/Alain Pecheur***/Hervé Reychler**** Nineteen patients who were treated for oncologic
The proven effectiveness of prosthetic treatment
 Multicenter Experience with Maxillary Prostheses Supported by Brånemark : A Clinical Report Koichiro Ihara, DDS*/Masaaki Goto, DDS, PhD**/Akira Miyahara, DDS***/ Junichiro Toyota, DDS*/Takeshi Katsuki,
Multicenter Experience with Maxillary Prostheses Supported by Brånemark : A Clinical Report Koichiro Ihara, DDS*/Masaaki Goto, DDS, PhD**/Akira Miyahara, DDS***/ Junichiro Toyota, DDS*/Takeshi Katsuki,
AO Certificate in Implant Dentistry Certificate
 AO Certificate in Implant Dentistry Certificate The AO Certificate in Implant Dentistry provides an opportunity for AO members to demonstrate that they have attained a level of education and experience
AO Certificate in Implant Dentistry Certificate The AO Certificate in Implant Dentistry provides an opportunity for AO members to demonstrate that they have attained a level of education and experience
Conus Concept: A Rewarding Complete Denture Treatment
 Conus Concept: A Rewarding Complete Denture Treatment Complete dentures have largely become the domain of the denturist due to the dissatisfaction general dentists feel with this treatment. Multiple visits,
Conus Concept: A Rewarding Complete Denture Treatment Complete dentures have largely become the domain of the denturist due to the dissatisfaction general dentists feel with this treatment. Multiple visits,
Implant osseointegration and successful restoration
 Prosthodontic Complications in a Prospective Clinical Trial of Single-stage Implants at 36 Months Jacqueline P. Duncan, DMD, MDSc 1 /Elena Nazarova, DMD, PhD 2 /Theodora Vogiatzi, DDS 1 / Thomas D. Taylor,
Prosthodontic Complications in a Prospective Clinical Trial of Single-stage Implants at 36 Months Jacqueline P. Duncan, DMD, MDSc 1 /Elena Nazarova, DMD, PhD 2 /Theodora Vogiatzi, DDS 1 / Thomas D. Taylor,
Surgical treatment of malignancies involving the
 Oral Implants in Radiated Patients: A Systematic Review Giuseppe Colella, MD, DDS 1 /Rosangela Cannavale, DDS 2 /Monica Pentenero, DDS, MSc 3 / Sergio Gandolfo, MD, DDS 4 Purpose: Oral malignancy is often
Oral Implants in Radiated Patients: A Systematic Review Giuseppe Colella, MD, DDS 1 /Rosangela Cannavale, DDS 2 /Monica Pentenero, DDS, MSc 3 / Sergio Gandolfo, MD, DDS 4 Purpose: Oral malignancy is often
ISSN: Volume 4 Issue Faciomaxillary prosthesis in rehabilitation. After maxillectomy. A clinical study
 ISSN: 2250-0359 Volume 4 Issue 4 2014 Faciomaxillary prosthesis in rehabilitation After maxillectomy A clinical study Prasad c Parimala V Vijjaykanth M Sivakumar P Department of Dental Surgery Govt. Stanley
ISSN: 2250-0359 Volume 4 Issue 4 2014 Faciomaxillary prosthesis in rehabilitation After maxillectomy A clinical study Prasad c Parimala V Vijjaykanth M Sivakumar P Department of Dental Surgery Govt. Stanley
Contemporary Implant Dentistry
 Contemporary Implant Dentistry C H A P T ER 1 4 O F C O N T E M P OR A R Y O R A L A N D M A X I L L OFA C IA L S U R G E RY B Y : D R A R A S H K H O J A S T EH Dental implant is suitable for: completely
Contemporary Implant Dentistry C H A P T ER 1 4 O F C O N T E M P OR A R Y O R A L A N D M A X I L L OFA C IA L S U R G E RY B Y : D R A R A S H K H O J A S T EH Dental implant is suitable for: completely
Implants- immediate restoration of postextraction edentation both esthetically and functionally
 Implants- immediate restoration of postextraction edentation both esthetically and functionally Otilia Stana (Gag), LileIoana Elena, Freiman Paul, Mugur Popescu, Elisei Gabriela, Sebesan Voicu, Vincze
Implants- immediate restoration of postextraction edentation both esthetically and functionally Otilia Stana (Gag), LileIoana Elena, Freiman Paul, Mugur Popescu, Elisei Gabriela, Sebesan Voicu, Vincze
Maxillofacial prosthetics is a subspecialty of
 Invited Article Maxillofacial Prosthesis: A Review of Treatment Concepts for Better Prosthesis Prognosis Sanjay Prasad 1 ABSTRACT Maxillofacial prosthesis currently finds itself experiencing more change
Invited Article Maxillofacial Prosthesis: A Review of Treatment Concepts for Better Prosthesis Prognosis Sanjay Prasad 1 ABSTRACT Maxillofacial prosthesis currently finds itself experiencing more change
Young-Jin Park, DDS,* and Sung-Am Cho, DDS, MS, PhD
 J Oral Maxillofac Surg 68:1338-1344, 2010 Retrospective Chart Analysis on Survival Rate of Fixtures Installed at the Tuberosity Bone for Cases With Missing Unilateral Upper Molars: A Study of 7 Cases Young-Jin
J Oral Maxillofac Surg 68:1338-1344, 2010 Retrospective Chart Analysis on Survival Rate of Fixtures Installed at the Tuberosity Bone for Cases With Missing Unilateral Upper Molars: A Study of 7 Cases Young-Jin
Featured Patient Case #1: Complete Mouth Reconstruction with Hybrid Restorations
 Philip L. Fava II, DMD, MDSc Robert A. Levine, DDS, FCPP, FISPPS 9880 Bustleton Ave, Suite 211 Philadelphia, PA 19115 PADentalImplants.com 215-677-8686 Featured Patient Case #1: Complete Mouth Reconstruction
Philip L. Fava II, DMD, MDSc Robert A. Levine, DDS, FCPP, FISPPS 9880 Bustleton Ave, Suite 211 Philadelphia, PA 19115 PADentalImplants.com 215-677-8686 Featured Patient Case #1: Complete Mouth Reconstruction
Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report
 Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
It has been proposed that partially edentulous maxillectomy
 CLASSICAL ARTICLE Basic principles of obturator design for partially edentulous patients. Part II: Design principles Mohamed A. Aramany, DMD, MS* Eye and Ear Hospital of Pittsburgh and University of Pittsburgh,
CLASSICAL ARTICLE Basic principles of obturator design for partially edentulous patients. Part II: Design principles Mohamed A. Aramany, DMD, MS* Eye and Ear Hospital of Pittsburgh and University of Pittsburgh,
In 1977, Lew1 developed a passive
 CLINICAL AN OVERVIEW OF THE LEW ATTACHMENT: CLINICAL REPORTS Jack Piermatti, DMD Sheldon Winkler, DDS KEY WORDS Lew attachment Atrophic mandible Subperiosteal implant Root form implant Although the Lew
CLINICAL AN OVERVIEW OF THE LEW ATTACHMENT: CLINICAL REPORTS Jack Piermatti, DMD Sheldon Winkler, DDS KEY WORDS Lew attachment Atrophic mandible Subperiosteal implant Root form implant Although the Lew
Specialty Dentistry. Dentistry has nine specialty fields recognized by the American Dental Association
 Specialty Dentistry Dentistry has nine specialty fields recognized by the American Dental Association Dental Public Health Endodontics Oral and Maxillofacial Pathology Oral and Maxillofacial Radiology
Specialty Dentistry Dentistry has nine specialty fields recognized by the American Dental Association Dental Public Health Endodontics Oral and Maxillofacial Pathology Oral and Maxillofacial Radiology
Use of osseointegrated oral implants for orbital prosthesis: a clinical case
 Use of osseointegrated oral implants for orbital prosthesis: a clinical case Borgia Gonzalo 1, Ravecca Tabaré 2, Fumero Miriam 3, Pebé Pablo 4 1 Assistant Prof. Oral-maxillofacial Prostheses Service, Professor
Use of osseointegrated oral implants for orbital prosthesis: a clinical case Borgia Gonzalo 1, Ravecca Tabaré 2, Fumero Miriam 3, Pebé Pablo 4 1 Assistant Prof. Oral-maxillofacial Prostheses Service, Professor
TITLE: Immediate Osseointegrated Implants for Cancer Patients: A Review of Clinical and Cost-Effectiveness
 TITLE: Immediate Osseointegrated Implants for Cancer Patients: A Review of Clinical and Cost-Effectiveness DATE: 13 January 2015 CONTEXT AND POLICY ISSUES According to the World health Organization, the
TITLE: Immediate Osseointegrated Implants for Cancer Patients: A Review of Clinical and Cost-Effectiveness DATE: 13 January 2015 CONTEXT AND POLICY ISSUES According to the World health Organization, the
Long-term success of osseointegrated implants
 Against All Odds A No Bone Solution Long-term success of osseointegrated implants depends on the length of the implants used and the quality and quantity of bone surrounding these implants. As surgical
Against All Odds A No Bone Solution Long-term success of osseointegrated implants depends on the length of the implants used and the quality and quantity of bone surrounding these implants. As surgical
Dental and Surgical Applications of Selective Laser Melting
 Dental and Surgical Applications of Selective Laser Melting Dr. Richard Bibb Rapid Manufacturing The following examples adhere to this conference s definition of RM They are end use parts, made directly
Dental and Surgical Applications of Selective Laser Melting Dr. Richard Bibb Rapid Manufacturing The following examples adhere to this conference s definition of RM They are end use parts, made directly
EFFECTIVE DATE: 04/24/14 REVISED DATE: 04/23/15, 04/28/16, 06/22/17, 06/28/18 POLICY NUMBER: CATEGORY: Dental
 MEDICAL POLICY SUBJECT: DENTAL IMPLANTS PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including an Essential
MEDICAL POLICY SUBJECT: DENTAL IMPLANTS PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including an Essential
A retrospective study on separate single-tooth implant restorations to replace two or more consecutive. maxillary posterior teeth up to 6 years.
 Original Article A retrospective study on separate single-tooth implant restorations to replace two or more consecutive maxillary posterior teeth up to 6 years follow up Myat Nyan Department of Prosthodontics,
Original Article A retrospective study on separate single-tooth implant restorations to replace two or more consecutive maxillary posterior teeth up to 6 years follow up Myat Nyan Department of Prosthodontics,
Dental Implants: A Predictable Solution for Tooth Loss. Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor
 Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
م.م. طارق جاسم حممد REMOVABLE PARTIAL DENTURE INTRODUCTION
 Lec.1 م.م. طارق جاسم حممد REMOVABLE PARTIAL DENTURE INTRODUCTION االسنان طب Prosthodontics is the branch of dentistry pertaining to the restoration and maintenance of oral function, comfort, appearance,
Lec.1 م.م. طارق جاسم حممد REMOVABLE PARTIAL DENTURE INTRODUCTION االسنان طب Prosthodontics is the branch of dentistry pertaining to the restoration and maintenance of oral function, comfort, appearance,
INCREASED RETENTION OF A PARTIAL DENTURE MAXILLARY OBTURATOR USING DENTAL IMPLANT
 INCREASED RETENTION OF A PARTIAL DENTURE MAXILLARY OBTURATOR USING DENTAL IMPLANT N. Yunus1, Z.A.A. Rahman 2. Increased retention of a partial denture maxillary obturator using dental implant. Annal Dent
INCREASED RETENTION OF A PARTIAL DENTURE MAXILLARY OBTURATOR USING DENTAL IMPLANT N. Yunus1, Z.A.A. Rahman 2. Increased retention of a partial denture maxillary obturator using dental implant. Annal Dent
Stability measurements of craniofacial implants by means of resonance frequency analysis. A clinical pilot study
 The Journal of Larvngologv and Otology June 1998, Vol. 112, pp. 57-52 Stability measurements of craniofacial implants by means of resonance frequency analysis. clinical pilot study S. J. HEO*,**, L. SENNERBY,*t,.
The Journal of Larvngologv and Otology June 1998, Vol. 112, pp. 57-52 Stability measurements of craniofacial implants by means of resonance frequency analysis. clinical pilot study S. J. HEO*,**, L. SENNERBY,*t,.
A Long-term Retrospective Analysis of Survival Rates of Implants in the Mandible
 A Long-term Retrospective Analysis of Survival Rates of Implants in the Mandible Thomas J. Balshi, DDS, PhD, FACP 1 /Glenn J. Wolfinger, DMD, FACP 2 / Brett E. Stein 3 /Stephen F. Balshi, MBE 4 Purpose:
A Long-term Retrospective Analysis of Survival Rates of Implants in the Mandible Thomas J. Balshi, DDS, PhD, FACP 1 /Glenn J. Wolfinger, DMD, FACP 2 / Brett E. Stein 3 /Stephen F. Balshi, MBE 4 Purpose:
doi: /aedj PROSTHETIC REHABILITATION OF A PATIENT WITH ACQUIRED AURICULAR DEFECT USING SILICONE BIOMATERIAL -A CASE REPORT.
 doi:105368/aedj20135352 PROSTHETIC REHABILITATION OF A PATIENT WITH ACQUIRED AURICULAR DEFECT USING SILICONE BIOMATERIAL -A CASE REPORT 1 Nikhil sood 2 Niti sood 3 Vikas punia 1 2 3 Senior Lecturer 1 Department
doi:105368/aedj20135352 PROSTHETIC REHABILITATION OF A PATIENT WITH ACQUIRED AURICULAR DEFECT USING SILICONE BIOMATERIAL -A CASE REPORT 1 Nikhil sood 2 Niti sood 3 Vikas punia 1 2 3 Senior Lecturer 1 Department
Devoted to the Advancement of Implant Dentistry
 Devoted to the Advancement of Implant Dentistry Devoted to the Advancement of Implant Dentistry Our ultimate goal is to provide you and your patients with the highest standards in implant case planning
Devoted to the Advancement of Implant Dentistry Devoted to the Advancement of Implant Dentistry Our ultimate goal is to provide you and your patients with the highest standards in implant case planning
Module 2 Introduction to immediate full arch fixed implant treatment - surgical options
 Module 2 Introduction to immediate full arch fixed implant treatment - surgical options First Name Last Name Objectives Identify the need and opportunity to treat full arch patients with fixed detachable
Module 2 Introduction to immediate full arch fixed implant treatment - surgical options First Name Last Name Objectives Identify the need and opportunity to treat full arch patients with fixed detachable
A Novel Technique for the Management of a Maxillary Anterior Alveolar Defect with an Implant-retained Fixed Prosthesis: A Clinical Report
 Neenu M Varghese et al Case Report 10.5005/jp-journals-10012-1148 A Novel Technique for the Management of a Maxillary Anterior Alveolar Defect with an Implant-retained Fixed Prosthesis: A Clinical Report
Neenu M Varghese et al Case Report 10.5005/jp-journals-10012-1148 A Novel Technique for the Management of a Maxillary Anterior Alveolar Defect with an Implant-retained Fixed Prosthesis: A Clinical Report
Implant Restorations: A Step-By-Step Guide
 Implant Restorations: A Step-By-Step Guide Drago, Carl DDS, MS ISBN-13: 9780813828831 Table of Contents Contributors. Foreword. Acknowledgments. Chapter 1. Introduction To Implant Dentistry. 1. Introduction.
Implant Restorations: A Step-By-Step Guide Drago, Carl DDS, MS ISBN-13: 9780813828831 Table of Contents Contributors. Foreword. Acknowledgments. Chapter 1. Introduction To Implant Dentistry. 1. Introduction.
The use of endosseous implants is currently a routine
 Evaluation of 31 Zygomatic Implants and 74 Regular Dental Implants Used in 16 Patients for Prosthetic Reconstruction of the Atrophic Maxilla with Cross-Arch Fixed Bridges Jonas P. Becktor, DDS;* Sten Isaksson,
Evaluation of 31 Zygomatic Implants and 74 Regular Dental Implants Used in 16 Patients for Prosthetic Reconstruction of the Atrophic Maxilla with Cross-Arch Fixed Bridges Jonas P. Becktor, DDS;* Sten Isaksson,
Maxillofacial rehabilitation after rhinectomy using two different treatment options: clinical reports
 Journal of Oral Rehabilitation 2007 34; 311 315 Maxillofacial rehabilitation after rhinectomy using two different treatment options: clinical reports L. CIOCCA*, P. MAREMONTI, B. BIANCHI & R. SCOTTI* *Section
Journal of Oral Rehabilitation 2007 34; 311 315 Maxillofacial rehabilitation after rhinectomy using two different treatment options: clinical reports L. CIOCCA*, P. MAREMONTI, B. BIANCHI & R. SCOTTI* *Section
Use of Anatomical Undercut in Adhesive Retained Orbital Prosthesis: An Alternative to Osseointegration to Improve Retention and Reduce Margin Gap
 British Journal of Medicine & Medical Research 6(8): 841-847, 2015, Article no.bjmmr.2015.258 ISSN: 2231-0614 SCIENCEDOMAIN international www.sciencedomain.org Use of Anatomical Undercut in Adhesive Retained
British Journal of Medicine & Medical Research 6(8): 841-847, 2015, Article no.bjmmr.2015.258 ISSN: 2231-0614 SCIENCEDOMAIN international www.sciencedomain.org Use of Anatomical Undercut in Adhesive Retained
Implant Placement in Maxillary Anterior Region Along with Soft and Hard Tissue Grafting- A Case Report.
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 10 Ver. XII (October. 2016), PP 68-73 www.iosrjournals.org Implant Placement in Maxillary Anterior
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 10 Ver. XII (October. 2016), PP 68-73 www.iosrjournals.org Implant Placement in Maxillary Anterior
Simulation Training in Implant Restorative Care for Single- Tooth Sites and Implant Overdenture Prosthetic Rehabilitation
 Original Publication Simulation Training in Implant Restorative Care for Single- Tooth Sites and Implant Overdenture Prosthetic Rehabilitation Joseph A. Toljanic, DDS*, Preetha P. Kanjirath, Ryan R. Vahdani,
Original Publication Simulation Training in Implant Restorative Care for Single- Tooth Sites and Implant Overdenture Prosthetic Rehabilitation Joseph A. Toljanic, DDS*, Preetha P. Kanjirath, Ryan R. Vahdani,
UNDERSTANDING DENTAL IMPLANTS Comfort and Confidence Again
 502 Jefferson Highway N. Champlin, MN 55316 763 427-1311 www.moffittrestorativedentistry.com UNDERSTANDING DENTAL IMPLANTS Comfort and Confidence Again NEW TEETH FOR A NEW SMILE Do you avoid laughing aloud,
502 Jefferson Highway N. Champlin, MN 55316 763 427-1311 www.moffittrestorativedentistry.com UNDERSTANDING DENTAL IMPLANTS Comfort and Confidence Again NEW TEETH FOR A NEW SMILE Do you avoid laughing aloud,
Oral and maxillofacial rehabilitation of head and neck cancer patients Schoen, Pieter Jan
 University of Groningen Oral and maxillofacial rehabilitation of head and neck cancer patients Schoen, Pieter Jan IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if
University of Groningen Oral and maxillofacial rehabilitation of head and neck cancer patients Schoen, Pieter Jan IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if
Failures in implant therapy. Biological and mechanical complications. Their prevention management. Dr. Katalin Csurgay Dr.
 Failures in implant therapy. Biological and mechanical complications. Their prevention management. Dr. Katalin Csurgay Dr. Tatiana Shkolnik Complications could be: Doctor related Patient related Early
Failures in implant therapy. Biological and mechanical complications. Their prevention management. Dr. Katalin Csurgay Dr. Tatiana Shkolnik Complications could be: Doctor related Patient related Early
While the protocol for direct bone-to-implant
 Immediate Functional Loading of Brånemark System Implants in Edentulous Mandibles: Clinical Report of the Results of Developmental and Simplified Protocols Glenn J. Wolfinger, DMD 1 / Thomas J. Balshi,
Immediate Functional Loading of Brånemark System Implants in Edentulous Mandibles: Clinical Report of the Results of Developmental and Simplified Protocols Glenn J. Wolfinger, DMD 1 / Thomas J. Balshi,
Moderately to severely resorbed edentulous
 The Zygomatic Implant: Preliminary Data on Treatment of Severely Resorbed Maxillae. A Clinical Report Edmond Bedrossian, DDS, FACD, FACOMS 1 /Lambert Stumpel III, DDS 2 / Michael Beckely, DDS 3 /Thomas
The Zygomatic Implant: Preliminary Data on Treatment of Severely Resorbed Maxillae. A Clinical Report Edmond Bedrossian, DDS, FACD, FACOMS 1 /Lambert Stumpel III, DDS 2 / Michael Beckely, DDS 3 /Thomas
BUILDING A. Achieving total reconstruction in a single operation. 70 OCTOBER 2016 // dentaltown.com
 BUILDING A MANDI Achieving total reconstruction in a single operation by Dr. Fayette C. Williams Fayette C. Williams, DDS, MD, FACS, is clinical faculty at John Peter Smith Hospital in Fort Worth, Texas,
BUILDING A MANDI Achieving total reconstruction in a single operation by Dr. Fayette C. Williams Fayette C. Williams, DDS, MD, FACS, is clinical faculty at John Peter Smith Hospital in Fort Worth, Texas,
PALATAL POSITIONING OF IMPLANTS IN SEVERELY RESORBED POSTERIOR MAXILLAE F. Atamni, M.Atamni, M.Atamna, Private Practice Tel-aviv Israel
 PALATAL POSITIONING OF IMPLANTS IN SEVERELY RESORBED POSTERIOR MAXILLAE F. Atamni, M.Atamni, M.Atamna, Private Practice Tel-aviv Israel Abstract: Objectives: To evaluate an alternative treatment for rehabilitation
PALATAL POSITIONING OF IMPLANTS IN SEVERELY RESORBED POSTERIOR MAXILLAE F. Atamni, M.Atamni, M.Atamna, Private Practice Tel-aviv Israel Abstract: Objectives: To evaluate an alternative treatment for rehabilitation
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 827 Thirty-Two Year Success of Dental Implants in Periodontally Compromised Dentition Thomas J. Balshi, DDS, PhD, FACP 1 Glenn J. Wolfinger,
The International Journal of Periodontics & Restorative Dentistry 827 Thirty-Two Year Success of Dental Implants in Periodontally Compromised Dentition Thomas J. Balshi, DDS, PhD, FACP 1 Glenn J. Wolfinger,
MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION
 Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
Telescopic Retainers: An Old or New Solution? A Second Chance to Have Normal Dental Function
 Telescopic Retainers: An Old or New Solution? A Second Chance to Have Normal Dental Function Joseph B. Breitman, DMD, FACP, 1,2 Scott Nakamura, DMD, 3 Arnold L. Freedman, DDS, 4 & Irving L. Yalisove, DDS
Telescopic Retainers: An Old or New Solution? A Second Chance to Have Normal Dental Function Joseph B. Breitman, DMD, FACP, 1,2 Scott Nakamura, DMD, 3 Arnold L. Freedman, DDS, 4 & Irving L. Yalisove, DDS
All authors abide by the Association for Medical Ethics (AME) ethical rules of disclosure.
 Fogli V, Michele C, Lauritano D, Carinci F. Intraoraly welded titanium bar for immediate restoration in maxilla: Case report and review of the literature. Annals of Oral & Maxillofacial Surgery 2014 Mar
Fogli V, Michele C, Lauritano D, Carinci F. Intraoraly welded titanium bar for immediate restoration in maxilla: Case report and review of the literature. Annals of Oral & Maxillofacial Surgery 2014 Mar
Frequency and Type of Prosthetic Complications Associated with Interim, Immediately Loaded Full-Arch Prostheses: A 2-Year Retrospective Chart Review
 Frequency and Type of Prosthetic Complications Associated with Interim, Immediately Loaded Full-Arch Prostheses: A 2-Year Retrospective Chart Review Carl Drago, DDS, MS, FACP 1,2,3 1 Department of Dental
Frequency and Type of Prosthetic Complications Associated with Interim, Immediately Loaded Full-Arch Prostheses: A 2-Year Retrospective Chart Review Carl Drago, DDS, MS, FACP 1,2,3 1 Department of Dental
BEN C. TAYLOR, MD TRAUMA FELLOW GRANT MEDICAL CENTER
 Evaluation of Primary Total Knee Arthroplasty Incision Closure with the Use of Continuous Bidirectional SCOTT STEPHENS, MD RESIDENT PHYSICIAN MOUNT CARMEL MEDICAL CENTER JOEL POLITI, MD DEPARTMENT OF ORTHOPEDIC
Evaluation of Primary Total Knee Arthroplasty Incision Closure with the Use of Continuous Bidirectional SCOTT STEPHENS, MD RESIDENT PHYSICIAN MOUNT CARMEL MEDICAL CENTER JOEL POLITI, MD DEPARTMENT OF ORTHOPEDIC
During the last 30 years, endosseous oral
 Influence of Variations in Implant Diameters: A 3- to 5-Year Retrospective Clinical Report Carl-Johan Ivanoff, DDS*/Kerstin Gröndahl, DDS, PhD**/Lars Sennerby, DDS, PhD***/ Christina Bergström, MSc****/Ulf
Influence of Variations in Implant Diameters: A 3- to 5-Year Retrospective Clinical Report Carl-Johan Ivanoff, DDS*/Kerstin Gröndahl, DDS, PhD**/Lars Sennerby, DDS, PhD***/ Christina Bergström, MSc****/Ulf
Mechanical and technical risks in implant therapy.
 Mechanical and technical risks in implant therapy. Salvi GE, Brägger U. Int J Oral Maxillofac Implants. 2009;24 Suppl:69-85. Department of Periodontology, School of Dental Medicine, University of Bern,
Mechanical and technical risks in implant therapy. Salvi GE, Brägger U. Int J Oral Maxillofac Implants. 2009;24 Suppl:69-85. Department of Periodontology, School of Dental Medicine, University of Bern,
KAREN O. From Failure to Fantastic
 KAREN O From Failure to Fantastic THE Pi TEAM THOMAS J. BALSHI, DDS, PhD, FACP GLENN J. WOLFINGER, DMD, FACP JAMES R. BOWERS, DDS IAN SMITH, DMD KAREN O Karen suffered from painful and swollen gum tissue
KAREN O From Failure to Fantastic THE Pi TEAM THOMAS J. BALSHI, DDS, PhD, FACP GLENN J. WOLFINGER, DMD, FACP JAMES R. BOWERS, DDS IAN SMITH, DMD KAREN O Karen suffered from painful and swollen gum tissue
4. What about age? There is no age limit. After puberty, anyone can get dental implants.
 Dental Implants 1. What are Osseointegrated implants? Osseointegrated implants are a new generation of dental implants in Rio de Janeiro, introduced in the 1960 s, they come in different shapes and sizes.
Dental Implants 1. What are Osseointegrated implants? Osseointegrated implants are a new generation of dental implants in Rio de Janeiro, introduced in the 1960 s, they come in different shapes and sizes.
Abstract The field of maxillofacial prosthetics is embracing the rapid explosion of technology.use of retention
 Review Article An Update on Retentive Aids in Maxillofacial Rehabilitation Anchala Sarke 1, Himanshu Gupta 2, Roshika Sudan 3, Ranjan Singh 4 1 Post Graduate Student, 2 Reader, 3 Senior Lecturer, Department
Review Article An Update on Retentive Aids in Maxillofacial Rehabilitation Anchala Sarke 1, Himanshu Gupta 2, Roshika Sudan 3, Ranjan Singh 4 1 Post Graduate Student, 2 Reader, 3 Senior Lecturer, Department
Revisions for CDT 2016
 Revisions for CDT 2016 This document was developed from preliminary actions of the Code Maintenance Committee (CMC). This document has been compared to the CMC meeting notes and the ASCII file. This document
Revisions for CDT 2016 This document was developed from preliminary actions of the Code Maintenance Committee (CMC). This document has been compared to the CMC meeting notes and the ASCII file. This document
Screw hole-positioning guide and plate-positioning guide: A novel method to assist mandibular reconstruction
 Journal of Dental Sciences (2012) 7, 301e305 Available online at www.sciencedirect.com journal homepage: www.e-jds.com CASE REPORT Screw hole-positioning guide and plate-positioning guide: A novel method
Journal of Dental Sciences (2012) 7, 301e305 Available online at www.sciencedirect.com journal homepage: www.e-jds.com CASE REPORT Screw hole-positioning guide and plate-positioning guide: A novel method
The restoration of partially and completely
 CLINICAL MANAGEMENT OF DENTAL IMPLANT FRACTURES. ACASE HISTORY Firas A. M. AL Quran, PhD, MSc Med; Bashar A. Rashan, MS; Ziad N. AL-Dwairi, PhD The widespread use of endosseous osseointegrated implants
CLINICAL MANAGEMENT OF DENTAL IMPLANT FRACTURES. ACASE HISTORY Firas A. M. AL Quran, PhD, MSc Med; Bashar A. Rashan, MS; Ziad N. AL-Dwairi, PhD The widespread use of endosseous osseointegrated implants
4766 Research Dr. San Antonio, TX insightdentalsystems.com
 OVERVIEW OF THE INSIGHT DENTAL IMPLANT DELIVERY SYSTEM The IDS system comes in a unit dose implant system where its advantage provides sterile instrumentation in one single-use kit. It is organized to
OVERVIEW OF THE INSIGHT DENTAL IMPLANT DELIVERY SYSTEM The IDS system comes in a unit dose implant system where its advantage provides sterile instrumentation in one single-use kit. It is organized to
History of Anaplastology. Objectives ANAPLASTOLOGY. Abstract. Conflict of Interest? Types of Prostheses. 2) Enumerate the steps
 Abstract ANAPLASTOLOGY Changing Appearances/Changing Lives Sharon Jamison, RN, CORLN We all have imperfections in our faces and bodies that we would like to change. Consider, though, the cancer patient
Abstract ANAPLASTOLOGY Changing Appearances/Changing Lives Sharon Jamison, RN, CORLN We all have imperfections in our faces and bodies that we would like to change. Consider, though, the cancer patient
 A New Procedure Reduces Laboratory Time to 6 Hours for the Elaboration of Immediate Loading Prostheses with a Titanium Frame Following Implant Placement Huard C, Bessadet M, Nicolas E, Veyrune JL * International
A New Procedure Reduces Laboratory Time to 6 Hours for the Elaboration of Immediate Loading Prostheses with a Titanium Frame Following Implant Placement Huard C, Bessadet M, Nicolas E, Veyrune JL * International
A Study of Classification Systems for Maxillectomy Defects
 A Study of Classification Systems for Maxillectomy Defects Zubair Durrani FFDRCS, FRCS, FRCS (OMFS)* Syed Ghazanfar Hassan FFDRCS** Shomaila Ameer Alam BDS*** * Associate Professor & Consultant Oral and
A Study of Classification Systems for Maxillectomy Defects Zubair Durrani FFDRCS, FRCS, FRCS (OMFS)* Syed Ghazanfar Hassan FFDRCS** Shomaila Ameer Alam BDS*** * Associate Professor & Consultant Oral and
Disclosures. The Expanding Role of Microvascular Reconstruction. Overview. Things they are a Changing. Surgical Advisory Board, Genentech Corp
 Disclosures Surgical Advisory Board, Genentech Corp The Expanding Role of Microvascular Reconstruction P. Daniel Knott, MD FACS Associate Professor Director, Facial Plastic and Reconstructive Surgery UCSF
Disclosures Surgical Advisory Board, Genentech Corp The Expanding Role of Microvascular Reconstruction P. Daniel Knott, MD FACS Associate Professor Director, Facial Plastic and Reconstructive Surgery UCSF
NIPPLE SPARING PRE-PECTORAL BREAST RECONSTRUCTION
 NIPPLE SPARING PRE-PECTORAL BREAST RECONSTRUCTION 42 yo female healthy athlete Right breast mass. Past medical history: none Family history: aunt with Breast cancer Candidates for nipple-sparing mastectomy
NIPPLE SPARING PRE-PECTORAL BREAST RECONSTRUCTION 42 yo female healthy athlete Right breast mass. Past medical history: none Family history: aunt with Breast cancer Candidates for nipple-sparing mastectomy
Summary of Benefits Dental Coverage - New Dental Option
 Summary of Benefits Dental Coverage - New Dental Option Managed Dental Plan MET225 - Texas Code Description Co-Payment Diagnostic Treatment D0120 Periodic Oral Evaluation established patient $0 D0150 Comprehensive
Summary of Benefits Dental Coverage - New Dental Option Managed Dental Plan MET225 - Texas Code Description Co-Payment Diagnostic Treatment D0120 Periodic Oral Evaluation established patient $0 D0150 Comprehensive
A Clinical Study of the Efficacy of Gold-Tite Square Abutment Screws in Cement-Retained Implant Restorations. Carl J.
 A Clinical Study of the Efficacy of Gold-Tite Square Abutment Screws in Cement-Retained Implant Restorations Carl J. Drago, DDS, MS 1 Purpose: The purpose of this study was to record the effectiveness
A Clinical Study of the Efficacy of Gold-Tite Square Abutment Screws in Cement-Retained Implant Restorations Carl J. Drago, DDS, MS 1 Purpose: The purpose of this study was to record the effectiveness
Consensus Statements and Recommended Clinical Procedures Regarding Risk Factors in Implant Therapy
 Consensus Statements and Recommended Clinical Procedures Regarding Risk Factors in Implant Therapy David L. Cochran, DDS, MS, PhD, MMSci 1 /Søren Schou, DDS, PhD, Dr Odont 2 / Lisa J. A. Heitz-Mayfield,
Consensus Statements and Recommended Clinical Procedures Regarding Risk Factors in Implant Therapy David L. Cochran, DDS, MS, PhD, MMSci 1 /Søren Schou, DDS, PhD, Dr Odont 2 / Lisa J. A. Heitz-Mayfield,
Building a Strong Team for the Dental Implant Practice
 Building a Strong Team for the Dental Implant Practice Samuel M. Strong, DDS Stephanie Strong, RDH, BS Course Synopsis This course deals with the organization and training to successfully complete restorative
Building a Strong Team for the Dental Implant Practice Samuel M. Strong, DDS Stephanie Strong, RDH, BS Course Synopsis This course deals with the organization and training to successfully complete restorative
Management of a complex case
 2 Soft- and hard-tissue reconstruction of a severely deficient site prior to implant placement: a case report Management of a complex case Younes Khosroshahy, DDS, MFDS RCS (Eng), Dip Imp Dent RCSEd, Blue
2 Soft- and hard-tissue reconstruction of a severely deficient site prior to implant placement: a case report Management of a complex case Younes Khosroshahy, DDS, MFDS RCS (Eng), Dip Imp Dent RCSEd, Blue
The surgical placement of dental implants has
 Flapless Implant Surgery: A 10-year Clinical Retrospective Analysis Luis Dominguez Campelo, DDS 1 /Jose R. Dominguez Camara, MD, DDS 2 Purpose: This article is a retrospective clinical analysis of implants
Flapless Implant Surgery: A 10-year Clinical Retrospective Analysis Luis Dominguez Campelo, DDS 1 /Jose R. Dominguez Camara, MD, DDS 2 Purpose: This article is a retrospective clinical analysis of implants
The Bulletin Spring 2000
 The Bulletin Spring 2000 Spring Meeting - Friday March 31, 2000 Joint Symposium: Northeastern Society of Periodontists and Northeastern Gnathological Society New York Marriott Marquis Hotel 1535 Broadway
The Bulletin Spring 2000 Spring Meeting - Friday March 31, 2000 Joint Symposium: Northeastern Society of Periodontists and Northeastern Gnathological Society New York Marriott Marquis Hotel 1535 Broadway
Limited To Endodontics Newsletter. Limited To Endodontics A Practice Of Endodontic Specialists July Volume 2
 Limited To Endodontics Newsletter LTE Limited To Endodontics A Practice Of Endodontic Specialists July 1 2009 Volume 2 Endodontic Treatment For The Compromised Tooth The goal of endodontic therapy is to
Limited To Endodontics Newsletter LTE Limited To Endodontics A Practice Of Endodontic Specialists July 1 2009 Volume 2 Endodontic Treatment For The Compromised Tooth The goal of endodontic therapy is to
An Alternative Prosthetic Approach for Rehabilitation of Two Edentulous Maxillectomy Patients: Clinical Report
 An Alternative Prosthetic Approach for Rehabilitation of Two Edentulous Maxillectomy Patients: Clinical Report Murat Yenisey, DDS, PhD, Şafak Külünk, DDS, PhD, & Necati Kaleli, DDS, PhD Department of Prosthodontics,
An Alternative Prosthetic Approach for Rehabilitation of Two Edentulous Maxillectomy Patients: Clinical Report Murat Yenisey, DDS, PhD, Şafak Külünk, DDS, PhD, & Necati Kaleli, DDS, PhD Department of Prosthodontics,
Immediate Implant Placement in Deficient Bone Sites
 clinical Raj Chopra BSc, DDS Immediate Implant Placement in Deficient Bone Sites THIS ARTICLE HAS BEEN PEER-REVIEWED. Introduction The presence of a low-lying sinus floor and inadequate bone volume often
clinical Raj Chopra BSc, DDS Immediate Implant Placement in Deficient Bone Sites THIS ARTICLE HAS BEEN PEER-REVIEWED. Introduction The presence of a low-lying sinus floor and inadequate bone volume often
PROSTHETIC REHABILITATION OF MAXILLARY DEFECTS: A REVIEW
 Review Article International Journal of Dental and Health Sciences Volume 01,Issue 04 PROSTHETIC REHABILITATION OF MAXILLARY DEFECTS: A REVIEW Sanjeeva Rao Olepu 1, Mithilesh Kumar 2,Ramu Rajesh Babu 3,Tanvi
Review Article International Journal of Dental and Health Sciences Volume 01,Issue 04 PROSTHETIC REHABILITATION OF MAXILLARY DEFECTS: A REVIEW Sanjeeva Rao Olepu 1, Mithilesh Kumar 2,Ramu Rajesh Babu 3,Tanvi
An Introduction to Dental Implants
 An Introduction to Dental Implants Aims: This article provides an introduction to dental implants, outlining the categories of dental implants, the phases involved in implant dentistry and assessing a
An Introduction to Dental Implants Aims: This article provides an introduction to dental implants, outlining the categories of dental implants, the phases involved in implant dentistry and assessing a
A Technique for Utilizing Upper Lid Blepharoplasty Full thickness Skin for Peri-Implant Keratinized Tissue Grafting *,y
 A Technique for Utilizing Upper Lid Blepharoplasty Full thickness Skin for Peri-Implant Keratinized Tissue Grafting *,y George R. Deeb D.D.S., M.D. i, Bach T. Le D.D.S., M.D. ii, Brett A. Ueeck D.M.D iii,
A Technique for Utilizing Upper Lid Blepharoplasty Full thickness Skin for Peri-Implant Keratinized Tissue Grafting *,y George R. Deeb D.D.S., M.D. i, Bach T. Le D.D.S., M.D. ii, Brett A. Ueeck D.M.D iii,
Frame designed partial prosthesis for the rehabilitation of a maxillectomy patient
 VARIA Frame designed partial prosthesis for the rehabilitation of a maxillectomy patient Sorin Popºor, Lia Maria Coman Târgu Mureº, Romania Summary This article is a case report and it describes a technique
VARIA Frame designed partial prosthesis for the rehabilitation of a maxillectomy patient Sorin Popºor, Lia Maria Coman Târgu Mureº, Romania Summary This article is a case report and it describes a technique
Laser Assembled and CAD/CAM Prosthetic Frameworks for the Debilitated Mandible. Robert Schneider, DDS, MS
 Laser Assembled and CAD/CAM Prosthetic Frameworks for the Debilitated Mandible Robert Schneider, DDS, MS University of Iowa Hospitals and Clinics Hospital Dentistry Institute Division of Maxillofacial
Laser Assembled and CAD/CAM Prosthetic Frameworks for the Debilitated Mandible Robert Schneider, DDS, MS University of Iowa Hospitals and Clinics Hospital Dentistry Institute Division of Maxillofacial
CHAPTER 1. General Introduction
 CHAPTER 1 General Introduction Chapter 1 The loss of remaining natural teeth and provision of artificial removable dentition is a major and irreversible procedure for the patient. The main limitations
CHAPTER 1 General Introduction Chapter 1 The loss of remaining natural teeth and provision of artificial removable dentition is a major and irreversible procedure for the patient. The main limitations
Prosthodontic Surgery Interactions in Head and Neck Cancer Patients Tailored for Surgeons
 LECTURE AND COURSE PROGRAM Prosthodontic Surgery Interactions in Head and Neck Cancer Patients Tailored for Surgeons Wednesday, September 5 th, 2018 Clinic for Maxillofacial Surgery, 8 Dr Subotica Street
LECTURE AND COURSE PROGRAM Prosthodontic Surgery Interactions in Head and Neck Cancer Patients Tailored for Surgeons Wednesday, September 5 th, 2018 Clinic for Maxillofacial Surgery, 8 Dr Subotica Street
Dentatus ANEW Narrow Diameter Implants. Expanding Implantology with More Treatment Options
 Dentatus ANEW Narrow Diameter Implants Expanding Implantology with More Treatment Options The Versatility of Dentatus ANEW LONG-TERM RESTORATIONS INTERIM SOLUTIONS LONG-TERM RESTORATIONS Many dentists
Dentatus ANEW Narrow Diameter Implants Expanding Implantology with More Treatment Options The Versatility of Dentatus ANEW LONG-TERM RESTORATIONS INTERIM SOLUTIONS LONG-TERM RESTORATIONS Many dentists
IQ IMPLANTS Smart Choice PRODUCT C ATA L O G
 IQ IMPLANTS Smart Choice PRODUCT C ATA L O G www.iqimplants.com info@iqimplants.com 2 TABLE OF CONTENTS GENERAL Company Profile 3 IMPLANTS 5 PROSTHETICS 13 TOOLS 27 3 COMPANY PROFILE IQ Implants Ltd. reflects
IQ IMPLANTS Smart Choice PRODUCT C ATA L O G www.iqimplants.com info@iqimplants.com 2 TABLE OF CONTENTS GENERAL Company Profile 3 IMPLANTS 5 PROSTHETICS 13 TOOLS 27 3 COMPANY PROFILE IQ Implants Ltd. reflects
Then and Now. Implant Therapy:
 Implant Therapy: Then and Now by Timothy F. Kosinski, DDS, MAGD Implant dentistry has come a long way since blade and subperiostal implants were widely used. Improvements in implant design and site preparation
Implant Therapy: Then and Now by Timothy F. Kosinski, DDS, MAGD Implant dentistry has come a long way since blade and subperiostal implants were widely used. Improvements in implant design and site preparation
