Research Article UV Photofunctionalization Effect on Bone Graft in Critical One-Wall Defect around Implant: A Pilot Study in Beagle Dogs
|
|
|
- Gyles Laurence O’Connor’
- 6 years ago
- Views:
Transcription
1 Hindawi Publishing Corporation BioMed Research International Volume 2016, Article ID , 9 pages Research Article UV Photofunctionalization Effect on Bone Graft in Critical One-Wall Defect around Implant: A Pilot Study in Beagle Dogs Min-Young Kim, 1 Hyunmin Choi, 1 Jae-Hoon Lee, 1 Jee-Hwan Kim, 1 Han-Sung Jung, 2 Jae-Hong Kim, 3 Young-Bum Park, 1 and Hong-Seok Moon 1 1 Department of Prosthodontics, Oral Science Research Center, BK21 PLUS Project, Yonsei University College of Dentistry, Seoul, Republic of Korea 2 Division in Anatomy and Developmental Biology, Department of Oral Biology, Oral Science Research Center, BK21 PLUS Project, Yonsei University College of Dentistry, Seoul, Republic of Korea 3 Department of Dental Technology, School of Medical and Public Health, Kyungdong University, Wonju, Gangwon-do, Republic of Korea Correspondence should be addressed to Hong-Seok Moon; hsm5@yuhs.ac Received 19 August 2016; Revised 3 November 2016; Accepted 1 December 2016 Academic Editor: Wei-Jen Chang Copyright 2016 Min-Young Kim et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. The purpose of this study was to compare and evaluate, through histomorphometric and radiological analysis, the effects of UV photofunctionalization on an implant placed over a critical defect area with and without a bone graft. Four female beagle dogs were first divided into control and bone graft groups. Each group was then subdivided into UV-treated and UV-untreated groups. The mandibular premolars in each dog were extracted. 12 weeks after extraction, implants were placed according to the condition of each group. Four and 12 weeks after implantation on left and right mandible, the dogs were sacrificed. The specimens were prepared for histomorphometric and micro-computed tomographic analysis. In both 4-week and 12-week groups, UV-treated implant surfaces showed better osseointegration than SA implant surfaces. Also, with implant surfaces placed over the critical defect with bone graft, UV photofunctionalization increased bone-to-implant contact (BIC) and new bone formation at the initial stage (4 weeks). Based on the results of this study, it can be suggested that UV photofunctionalization on the surface of implants placed over large critical defects with bone graft aids initial osseointegration and osteogenesis. 1. Introduction In modern implant dentistry, implant therapy is known as the most effective treatment for edentulous patient and is regarded as the first treatment of choice for missing teeth. The success of dental implants depends on how directly new bone formation occurs on titanium surface after implant placement [1]. The initial amounts of osseointegration and osteogenesis are crucial factors in the success rate of implant therapy [2, 3]. In recent studies, Ogawa et al. researched the effects of UV photofunctionalization on titanium surface and concluded that conversion of implant surface from bioinert to bioactive yielded better osseointegration and osteogenesis on titanium surface [4 6]. The success of implant therapy also depends on bone condition of the surgical site during implant placement, as surgery is not always under ideal conditions. When there is insufficient bone support from the surrounding bones and surfaces are not fully covered with bones, this may lead to a failure of the surgery in the long term. In the case of a large bone defect area, a bone graft may be used along with an implant placement and the bone graft becomes a scaffold around the implant. It was reported that migration of osteoblastandosteoinductivematerialstotheimplantsurface increases the probability of implant success in the long term [7 9]. On the other hand, however, some reported that bone graft materials arrested new bone formation at the outset by blocking proliferation of osteoblast [10 12]. Nevertheless, it is
2 2 BioMed Research International generally accepted that once grafting materials are absorbed and eventually disappear, the space is filled with new bone so that the level of osseointegration and osteogenesis eventually increases [13, 14]. Since there already exists previous study regarding positive effects of UV photofunctionalization on implant surfaces under insufficient bone condition [5], the purpose of this study was to compare and evaluate the effects of UV photofunctionalization on an implant placed over a critical defect area that did not heal over the duration of the study with and without a bone graft through histomorphometric and radiological analysis. 2. Materials and Methods 2.1. Experimental Animals. In this study, four female beagle dogs of twelve months old (weighing approximately 10 kg) were used. As a prestudy preparation, scaling and plaque control were performed for periodontal health. After treatment, they were fed with liquid foods to prevent masticatory trauma during healing. Animal selection, management, surgical protocol, and all experiments were reviewed and approved by theanimalcareandusecommittee,yonseimedicalcenter, Seoul, Korea (Approval number ) Experimental Implants. Atotalof32sandblastingwith alumina and acid etching (SA) surface-treated internal type implants (Osstem implant system, TS II SA Fixture, Busan, Korea) being 3.5 mm in diameter and 8.5 mm in length were used in this study. All implants used in the experiment were manufactured simultaneously and stored in a sealed container, being kept minimally exposed to the air immediately before placement Ultraviolet Photofunctionalization. Photofunctionalization was performed by treating implants with UV light for 15 minutes using a photo device (TheraBeam Affiny, Ushio Inc., Tokyo, Japan) immediately before implantation according to manufacturer s recommendation [1, 4 6] (Figure 1). Details specifications of a photo device were as follows: input voltage (AC 100 to 240 V ± 10%), input current (2.2 A max), temperature (15 Cto30 C), humidity (20% to 70% RH), and altitude (below 2,000 m) Graft Materials. Demineralized freeze dried bone allograft (DFDBA) (SureOss-D, Demineralized Cortical Bone Powder,HansBiomedCorp.,Seoul,Korea) μm in particle size was used for grafting at bone defect Experimental Groups Design. First, all implant placement sites were divided into bone graft groups and control groups, with each group then subdivided again into UV-treated group and UV untreated group. The UV untreated group with bone graft was set to Group 2 (BG only), the UV-treated group with bone graft was set to Group 4 (UV/BG), the UV-treated group without bone graft was set to Group 3 (UV only), and finally the UV untreated group without bone graft was set to Group 1 (control). Eight SA surface implants were used for Group 4, eight SA surface implants for Group 2, four SA surface implants for Group 3, and lastly twelve SA surface implants for Group 1. In this study, the sample sizes of Group 3 were reduced since the UV photofunctionalization effect has already been proven in many previous studies [1, 5, 6, 15, 16]. Implants were placed symmetrically to reduce differences in the sites by matching the initial states. Four implants were placedfromposteriorareaofthe1stpremolarintheright and left side of mandible (Figure 2). The distance between each implant was 10 mm and the experiment was carried out using a split-mouth design to minimize the interindividual variability from the estimates of the treatment effect [17]. The implants placed in the left side of mandible had a healing period of four weeks (4-week group) and the other implants placed in the right side of mandible had a healing period of twelve weeks (12-week group) (Figure 3) Surgical Procedure. All of the surgical treatments were carried out under general anesthesia. Both mandibular premolars (from first to fourth premolar) were extracted atraumatically. 12 weeks after the extraction of four teeth (P1, P2, P3, and P4) on right side of mandible, sequential drilling for implant placement was performed. The distance between centers of implants was 10 mm. A one-wall bony defect in cuboid shape was then formed for each group. Those defects were uniformly 3 mm in depth and 5 mm in width (buccolingual and mesiodistal). The center of implant was then placed on the edge of the cuboid (Figure 4). Photofunctionalization of implants was performed for 15 minutes using a photo device immediately before implantation cc DFDBA was gently packed into each bone defect until it filled the entire cavity (Figure 5). One week after the surgical procedure, stitching out was done. The same processes were executed on left side of mandible eight weeks later. The beagle dogs were sacrificed after 4 weeks Fabrication of Histologic Specimens. After buffering of the tissue samples with neutral formalin fixation for two weeks, micro-ct was taken. Next, the samples were dehydrated in increasing grades of ethanol and subsequently infiltrated in Technovit 7200 resin (Heraeus Kulzer, Dormagen, Germany). Following the embedding in the acrylic resin, the blocks were polymerized and sectioned in the mesiodistal plane using a cutting-grinding unit (Exakt Exakt 300, Heraeus Kulzer, Norderstedt, Germany). The tissue samples were processed for ground sectioning according to methods described by Donath and Breuner and the sections were stained in H&E (hematoxylin and eosin) for light microscopic examination [18] Micro-Computed Tomographic Analysis. A microcomputed tomography scanner (SkyScan 1076, SkyScan, Aartselaar, Belgium) was used to measure the percentage of the amount of new bone formation around implants. The new region of interest (ROI), the area most prone to be affected by the UV photofunctionalization and bone grafting, was set up in a rectangular parallelepiped 3.5 mm in width (mesiodistal) from the center of implant, 3.0 mm in length (buccolingual), and 3.0 mm in height. The amount of bone was measured in this area (Figure 6).
3 BioMed Research International 3 (a) (b) Figure 1: Photofunctionalization of implant fixture surface by ultraviolet light. (a) TheraBeam Affiny device (TheraBeam Affiny, Ushio, Tokyo, Japan). (b) Process of UV treatment on implant fixture during 15 minutes. Right Posterior Left Right Posterior Left Beagle 1 Beagle 2 Anterior Anterior Right Posterior Left Right Posterior Left Beagle 3 Beagle 4 Anterior Anterior Control BG UV UV/BG Figure 2: Experimental schematic diagrams.
4 4 BioMed Research International 12 wks healing duration Table 1: The mean of micro-ct value ratios at 4 and 12 weeks. 4 wks healing duration Group Micro CT value ratio 4weeks 12weeks ± ± ± ± ± ± ± ± 0.13 Extraction Implantation on Rt. Mn. Implantation on Lt. Mn. Sacrifice 0 weeks 12 weeks 20 weeks 24 weeks Figure 3: Diagram of experimental design protocol. 3 mm 5 mm 10 mm 5 mm Figure 4: Schematic diagram of experimental design Histomorphometric Analysis. The stained histologic specimens were scanned and captured using optical microscopy at 12.5x and 50x magnification and then histomorphometrically measured using ImagePro Plus 4.5 (Media Cydernetrics, Silver Spring, Maryland, USA). At first, the actual zone of formed defect was set as ROI, the area most prone to be affected by the UV photofunctionalization and bone grafting, by sectionalizing the region on histologic specimens. Then, the ratio for bone-to-implant contact (BIC, %), new bone area formed in defect area (new bone area, %), remaining graft material area in defect area (graft material area, %), and resorption area in defect area (resorption area, %) were calculated in ROI. BIC was measured at three consecutivethreadsinroi.newbonearearatioandremaininggraft material area ratio were calculated as a percentage of the area occupied by each one in ROI. Lastly, resorption area ratios were obtained as a percentage of the area in which bone filling did not occur in ROI (Figure 7) Statistical Analysis. The ratios for BIC, new bone area, remaining graft material area, resorption area, and micro- CT value were compared to verify the difference between Groups 1 and 3. The same measurements were carried out forgroups2and4.thewilcoxonranksumtestwasused as a nonparametric statistical method to evaluate the data duetothesmallsamplesizeandlargestandarddeviations. All calculations were performed using a specific statistical program (SPSS ver. 18.0, IBM Co., Somers, NY, USA), and thelevelofsignificancewassetat5%. 3. Results 3.1. Micro-Computed Tomographic Findings. For the comparison of cases without bone graft, in Groups 1 and 3, micro-ct bone volume ratio was measured in ROI (Figures 8 and 9). The mean value and standard deviation were then calculated (Table 1). Group 3 showed significantly increased micro-ct bone volume at 12 weeks compared to that of Group 1 (p < 0.05). However, for the comparison of cases with bone graft, in Groups 2 and 4, Group 4 displayed significantly increased micro-ct bone volume at 4 weeks compared to that of Group 2(p < 0.05) (Figure 10) Histomorphometric Findings. In Groups 1 and 3, BIC ratio was calculated. Although increased BIC ratio was identified in Group 3, there was no significant difference in BIC ratio between the two groups at either time point (4 weeks and 12 weeks). Also, no significant difference in BIC was identified between Groups 2 and 4 at either time point (Table 2 and Figure 11). Regarding new bone area ratio, a greater new bone area was identified in Group 3 than in Group 1. However, there was no significant difference in new bone area ratio between Groups 1 and 3. Also, in Groups 2 and 4, the similar results were identified but with no significant difference identified between two groups. Also, the remaining graft material area ratio was calculated and there was no significant difference between Group 2 and Group 4. Although no significant difference was found, there was much reduced resorption area ratio observed in Group 3comparedtothatinGroup1at12weeks.Evenwhenbone graft materials was used, decreased resorption area ratio was identifiedingroup4comparedtothatingroup2.however, no statistically significant difference was found. 4. Discussion The purpose of this study was to compare and evaluate, through histomorphometric and radiological analysis, the effects of UV photofunctionalization on an implant placed over a critical defect area with and without a bone graft. A large critical bone defect 5 mm in width was designed for the present study as the term Critical Size Defect (CSD) was defined in animal research as the size of a defect that will not heal over the duration of the study [19]. First, measurements for BIC ratio in ROI of each group were compared. The groups of implants placed over bone defect without graft yielded the similar BIC ratios at 4 weeks regardless of the presence of UV treatment. Conversely,
5 BioMed Research International 5 (a) (b) UV/BG BG UV Control (c) (d) Figure 5: Clinical views of surgical procedure. (a) Forming the standardized defects. (b) Drilling for implant placement and forming the defects. (c) Implants placed with bone graft (Group 4, Group 2, Group 3, and Group 1). (d) Wound closure with suture. 3 mm 3 mm Figure 6: Bone volume measuring range in micro-ct image. Table 2: The mean value of each ratio at 4 and 12 weeks. Group 1 Group 2 Group 3 Group 4 4 weeks 12 weeks 4 weeks 12 weeks 4 weeks 12 weeks 4 weeks 12 weeks BIC ratio ± ± ± ± ± ± ± ± New bone area ratio 32 ± ± ± ± ± ± ± ± 3.2 Remaining graft material area ratio 9.78 ± ± ± ± 6.31 Resorption area ratio ± ± ± ± ± ± ± ± 17.66
6 6 BioMed Research International (a) (b) Figure 7: Histologic images showing experimental site, red box ROI. (a) H&E stained image showing experimental site ( 12.5), purple zone new bone area or remaining graft material area, and yellow zone resorption area. (b) BIC in ROI, (H&E stained, 50.0). (a) (b) (c) (d) Figure 8: The representative micro-ct images of each group at 4 weeks. Red box ROI in experimental site. (a) Group 1, (b) Group 2, (c) Group 3, and (d) Group 4. (a) (b) (c) (d) Figure 9: The representative micro-ct images of each group at 12 weeks. Red box ROI in experimental site. (a) Group 1, (b) Group 2, (c) Group 3, and (d) Group 4. in the group of implants placed over bone defect with graft, BIC ratios of UV-treated implant surfaces were greater than those at 4 weeks but lower than those at 12 weeks although there was no statistically significant difference in BIC ratio between UV-treated group and UV-untreated group. BIC values in Group 4 at 4 weeks were actually more than twice the BIC values in Group 2. On the other hand, BIC values in Group 4 at 12 weeks showed little difference from BIC values in Group 2. These results suggest that BIC of implant surfaces was increased by UV photofunctionalization for bone defects with a bone graft at the initial stage of the implant placement. The decrease in BIC values at 12 weeks could possibly be attributable to the characteristics of female beagle dogs, including concerns that they are more variable than males due to cyclical reproductive hormones [20], which may lead to a larger variation among the individuals. This can be related to the one of the limitations of the present study: relatively high standard deviation. A small number of sample sizes may also have resulted in such high standard deviation. To resolve these issues in further research and to further evaluate the effect of experimental intervention prior to the application in clinic, it may be necessary to use a larger number of male dogs. Next, the new bone area ratio was measured in ROI. The mean of groups with UV photofunctionalization was slightly higher at both 4 and 12 weeks when the implant
7 BioMed Research International Group 1 Group weeks 12 weeks Group 3 Group Figure 10: The mean of micro-ct value ratios at 4 and 12 weeks. Red star indicates that there was a significant difference (p < 0.05) weeks 12 weeks 4 weeks 12 weeks 4 weeks 12 weeks 4 weeks 12 weeks BIC ratio New bone area ratio Remaining graft material area ratio Resorption area ratio Group 1 Group 2 Group 3 Group 4 Figure 11: The mean value of each ratio at 4 and 12 weeks. was placed without a bone graft, yet with no statistically significant difference. As UV photofunctionalization affected the bone defect area itself, more new bone might have been formed. Group 4 at 4 weeks had a greater new bone area ratio values than those of Group 2, which may indicate that the UV photofunctionalization had again a positive influence on early new bone formation for bone defect with a bone graft. However, Group 2 measurements at 12 weeks were higher than those in Group 4, which is in accordance with the results from the BIC ratio at 12 weeks and can be explained in the same extent. The area of the remaining graft material ratio in ROI was measured for comparisons. The higher the remaining graft material ratio is, the more the graft material remained in the defect area and thus the greater the volume of the defect is maintained. Because the grafted, demineralized materials were absorbed rapidly, there were questions whether they could serve as a scaffold for a long time. In fact, Group 2 showed greater measurements at 4 weeks than at 12 weeks. Group 4 showed less remaining grafting material at 12 weeks. Based on comparisons of the actual measurements of each group, values were inconsistent and had large standard deviations at 12 weeks. In fact, it was previously reported that, in a one-wall defect, it is important to prevent dissipation of graft materials [21, 22]. In the present study, however, no membrane or any other methods for maintenance of graft material were used and this may have resulted in inconsistent and large standard deviation at 12 weeks. Therefore, subsequent experiments may yield more reliable results if any methods for maintaining graft material are used. The resorption area ratio reflected the degree of defect volume maintenance. In the group without bone graft, UV treatment showed little effect at 4 weeks. With time, the resorption area ratio decreased in Group 3. This maybe resulted from the large amount of new bone as well as from less resorption of bone itself. The differences in bone volume measured using micro-ct surely account for the differences in resorption area ratio. The amount of new bone was measured in three dimensions with a micro-ct scanner whereas the resorption area was measured in one plane with a light microscopy. These differences must be considered in calculating each measurement and may underlie limitations in calculating the resorption area using micro-ct measurements. For this reason, the implant placement position was considered the major cause of differences in resorption area ratio at 12 weeks. Further study should be required to employ more subdivided positions for implant placement in order to enable greater uniformity of placement. The resorption area ratio in Group 4 was less than in Group 2 at 4 weeks. This may be attributed to the greater amount of new bone and remaining graft material in Group 4 than in Group 2. Similarly, the resorption area ratio in Group 4 was less than in Group 2 at 12 weeks, a consequence of the difference in resorption rates due to posterior implant placement. Due to the difference in resorption rate caused by implant placement position, the amount of remaining graft material in Group 4 exceeded that of Group 2 and this may also explain the relatively reduced resorption area ratio in Group 4. Regarding amount of new bone in ROI measured by micro-ct, in the group without bone graft, although the similar patterns in histomorphometric measurements at 4 weeks are identified, Group 3 measurements were about twice higher than those of Group 1 at 12 weeks. There was also statistically significant difference identified. These distinctions may be due to differences between measurement with light microscopy and micro-ct scanner as mentioned above.inthebonegraftgroups,group4scoredhigherinnew bone volume measurements than Group 2 at an early stage (4 weeks). This agrees with the pattern of new bone formation measurements using a light microscopy. Within the limitation of the present study, based on aforementioned results, it can be concluded that UV photofunctionalization had a positive effect on new bone formation of bone defect with bone graft in the early stage. However, the
8 8 BioMed Research International results of each group in a late stage (12 weeks) were not significantly correlated with the presence of UV treatment and this may be partly attributed to the fact that the results of these experiments do not completely rule out the effect of implant location. Therefore, further study will be required to maintain uniform implant conditions including placement location as much as possible by increasing the number of sample sizes and by subdividing the location of implant placement. Disclosure Young-Bum Park is co-corresponding author for supervising overall animal study. This paper is a part of Min-Young Kim s thesis. Competing Interests The authors declare that they have no competing interests. Authors Contributions Min-Young Kim and Hyunmin Choi equally contributed to the works described in this manuscript. Acknowledgments This research was supported by a faculty research grant of Yonsei University College of Dentistry ( ), Basic Science Research Program, through the National Research Foundation of Korea (NRF) funded by the Ministry of Education (NRF-2016R1D1A1B ) and Institute for Information & Communications Technology Promotion (IITP) grant funded by the Korea Government (MSIP) (no. R ). References [1] T. Ogawa, Ultraviolet photofunctionalization of titanium implants, The International journal of oral & maxillofacial implants,vol.29,no.1,pp.e95 102,2014. [2] T.Berglundh,I.Abrahamsson,N.P.Lang,andJ.Lindhe, De novo alveolar bone formation adjacent to endosseous implants: a model study in the dog, Clinical Oral Implants Research,vol. 14, no. 3, pp , [3] J. E. Davies, Mechanisms of endosseous integration, International Journal of Prosthodontics, vol. 11, no. 5, pp , [4] H. Aita, N. Hori, M. Takeuchi et al., The effect of ultraviolet functionalization of titanium on integration with bone, Biomaterials,vol.30,no.6,pp ,2009. [5] A. Funato and T. Ogawa, Photofunctionalized dental implants: a case series in compromised bone, The International journal of oral & maxillofacial implants,vol.28,no.6,pp ,2013. [6] A. Funato, M. Yamada, and T. Ogawa, Success rate, healing time, and implant stability of photofunctionalized dental implants, The International Journal of Oral & Maxillofacial Implants,vol.28,no.5,pp ,2013. [7]D.Buser,V.Chappuis,M.M.Bornstein,J.-G.Wittneben,M. Frei, and U. C. Belser, Long-term stability of contour augmentation with early implant placement following single tooth extraction in the esthetic zone: a prospective, cross-sectional study in 41 patients with a 5- to 9-year follow-up, Journal of Periodontology,vol.84,no.11,pp ,2013. [8] G. E. Friedlaender, Bone grafts. The basic science rationale for clinical applications, The Journal of Bone & Joint Surgery American Volume,vol.69,no.5,pp ,1987. [9] R. E. Jung, N. Fenner, C. H. F. Hämmerle, and N. U. Zitzmann, Long-term outcome of implants placed with guided bone regeneration (GBR) using resorbable and non-resorbable membranes after years, Clinical Oral Implants Research,vol.24, no.10,pp ,2013. [10] A. Stavropoulos, L. Kostopoulos, J. R. Nyengaard, and T. Karring, Deproteinized bovine bone (Bio-Oss) and bioactive glass (Biogran) arrest bone formation when used as an adjunct to guided tissue regeneration (GTR): an experimental study in the rat, Journal of Clinical Periodontology,vol.30,no.7,pp , [11] D. Carmagnola, T. Berglundh, M. Araújo, T. Albrektsson, and J. Lindhe, Bone healing around implants placed in a jaw defect augmented with Bio-Oss. An experimental study in dogs, Journal of Clinical Periodontology, vol.27,no.11,pp , [12] F.A.Santos,M.T.Pochapski,M.C.Martins,E.G.Zenóbio,L.C. Spolidoro, and E. Marcantonio Jr, Comparison of biomaterial implants in the dental socket: histological analysis in dogs, Clinical Implant Dentistry and Related Research, vol.12,no.1, pp.18 25,2010. [13] M.MarcoDegidi,A.Piattelli,V.Perrotti,andG.Iezzi, Histologic and histomorphometric evaluation of an implant retrieved 8 years after insertion in a sinus augmented with anorganic bovine bone and anorganic bovine matrix associated with a cell binding peptide, The International Journal of Periodontics & Restorative Dentistry, vol. 32, pp , [14] A. Philipp, W. Duncan, M. Roos, C. H. Hämmerle, T. Attin, and P. R. Schmidlin, Comparison of SLA or SLActive implants placed in the maxillary sinus with or without synthetic bone graft materials an animal study in sheep, Clinical Oral Implants Research,vol.25,no.10,pp ,2014. [15] T.Ueno,M.Yamada,N.Hori,T.Suzuki,andT.Ogawa, Effect of ultraviolet photoactivation of titanium on osseointegration in a rat model, The International Journal of Oral & Maxillofacial Implants,vol.25,no.2,pp ,2010. [16] T. Ueno, M. Yamada, T. Suzuki et al., Enhancement of bonetitanium integration profile with UV-photofunctionalized titanium in a gap healing model, Biomaterials, vol. 31, no. 7, pp , [17] J. C. de Vicente, O. Recio, L. Martín-Villa, L. M. Junquera, and J. S. López-Arranz, Histomorphometric evaluation of guided bone regeneration around implants with SLA surface: an experimental study in beagle dogs, International Journal of Oral and Maxillofacial Surgery,vol.35,no.11,pp ,2006. [18] K. Donath, Equipment and methodical performance, in Preparation of Histologic Sections, EXAKT-Kulzer-Publication, Norderstedt, Germany, [19] A. K. Gosain, L. Song, P. Yu et al., Osteogenesis in cranial defects: reassessment of the concept of critical size and the expression of TGF-β isoforms, Plastic and Reconstructive Surgery,vol.106,no.2,pp ,2000. [20] I. Zucker and A. K. Beery, Males still dominate animal studies, Nature,vol.465,no.7299,p.690,2010. [21] J. Sakata, H. Abe, A. Ohazama et al., Effects of combined treatment with porous bovine inorganic bone grafts and bilayer
9 BioMed Research International 9 porcinecollagenmembraneonrefractoryone-wallintrabony defects, International Journal of Periodontics and Restorative Dentistry,vol.26,no.2,pp ,2006. [22] J.-I. Park, C. Yang, Y.-T. Kim et al., Space maintenance using crosslinked collagenated porcine bone grafted without a barrier membrane in one-wall intrabony defects, Journal of Biomedical Materials Research B Applied Biomaterials, vol.102,no.7,pp , 2014.
Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs
 Current Applied Physics 5 (2005) 507 511 www.elsevier.com/locate/cap Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs Ui-Won Jung a, Hee-Il
Current Applied Physics 5 (2005) 507 511 www.elsevier.com/locate/cap Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs Ui-Won Jung a, Hee-Il
BONE AUGMENTATION AND GRAFTING
 1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
( ) 2009;28(2):89-94
 ( ) 2009;28(2):89-94 Osseointegration is important in the functional aspect, however, esthetics is also important, especially in the maxillary anterior region. An adequate surgical technique is necessary
( ) 2009;28(2):89-94 Osseointegration is important in the functional aspect, however, esthetics is also important, especially in the maxillary anterior region. An adequate surgical technique is necessary
The Original remains unique.
 The Original remains unique. Geistlich leading regeneration 2A, 2B Geistlich is the world leader in regenerative dentistry. We transform natural biomaterials into safe and reliable treatment methods that
The Original remains unique. Geistlich leading regeneration 2A, 2B Geistlich is the world leader in regenerative dentistry. We transform natural biomaterials into safe and reliable treatment methods that
SalvinOss Xenograft Bone Graft Material In Vivo Testing Summary
 SalvinOss Xenograft Bone Graft Material In Vivo Testing Summary Summary of In Vivo Use Of Bioresorbable Xenograft Bone Graft Materials In The Treatment Of One-Walled Intrabony Defects In A Canine Model
SalvinOss Xenograft Bone Graft Material In Vivo Testing Summary Summary of In Vivo Use Of Bioresorbable Xenograft Bone Graft Materials In The Treatment Of One-Walled Intrabony Defects In A Canine Model
Socket preservation in the daily practice: A clinical case report
 Clinical Socket preservation in the daily practice: A clinical case report Rabih Abi Nader 1 and Carine Tabarani 2 Abstract Soft tissue contour depends on the underlying bone anatomy. Following tooth extraction,
Clinical Socket preservation in the daily practice: A clinical case report Rabih Abi Nader 1 and Carine Tabarani 2 Abstract Soft tissue contour depends on the underlying bone anatomy. Following tooth extraction,
REGENERATIONTIME. A Case Report by. Ridge Augmentation and Delayed Implant Placement on an Upper Lateral Incisor
 A Case Report by Dr. Daniele Cardaropoli Ridge Augmentation and Delayed Implant Placement on an Upper Lateral Incisor The Situation An adult female patient presented with an endodontic/prosthetic failure
A Case Report by Dr. Daniele Cardaropoli Ridge Augmentation and Delayed Implant Placement on an Upper Lateral Incisor The Situation An adult female patient presented with an endodontic/prosthetic failure
Guided Tissue and Bone Regeneration
 Guided Tissue and Bone Regeneration One toolbox for your needs! Tefguide 9000 742 401 12x24 mm pc 1 Osgide 9000 701 520 15 x 20 mm pc 1 Osbone 9000 800 255 250-1000 μm 0.25 cc 5 Product Specifications
Guided Tissue and Bone Regeneration One toolbox for your needs! Tefguide 9000 742 401 12x24 mm pc 1 Osgide 9000 701 520 15 x 20 mm pc 1 Osbone 9000 800 255 250-1000 μm 0.25 cc 5 Product Specifications
Case Study. Case # 1 Author: Dr. Suheil Boutros (USA) 2013 Zimmer Dental, Inc. All rights reserved. 6557, Rev. 03/13.
 Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
SOCKET WHETHER TO PRESERVE IT NOW OR TO CREATE LATER? - A CASE REPORT
 MAVEN CASE REPORT SOCKET WHETHER TO PRESERVE IT NOW OR TO CREATE LATER? - A CASE REPORT Dr. Parthasarathi Biswas 1, Dr. Debajyoti Mondal 1, Dr. B Praveena Devi 1, Dr. Indrasri Das 2, Dr. Somen Bagchi 3,
MAVEN CASE REPORT SOCKET WHETHER TO PRESERVE IT NOW OR TO CREATE LATER? - A CASE REPORT Dr. Parthasarathi Biswas 1, Dr. Debajyoti Mondal 1, Dr. B Praveena Devi 1, Dr. Indrasri Das 2, Dr. Somen Bagchi 3,
Evaluation of a Combination Allograft Material Compared to DFDBA in Alveolar Ridge Preservation. Sanju P. Jose
 Evaluation of a Combination Allograft Material Compared to DFDBA in Alveolar Ridge Preservation by Sanju P. Jose B.S., University of Maryland Baltimore County, 2008 D.D.S., University of Maryland School
Evaluation of a Combination Allograft Material Compared to DFDBA in Alveolar Ridge Preservation by Sanju P. Jose B.S., University of Maryland Baltimore County, 2008 D.D.S., University of Maryland School
MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION
 Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
More than bone regeneration. A total solution.
 More than bone regeneration. A total solution. More than a dental implant company. A total solution. When it comes to treatment options, your patients want positive results both functionally and esthetically.
More than bone regeneration. A total solution. More than a dental implant company. A total solution. When it comes to treatment options, your patients want positive results both functionally and esthetically.
Socket preservation using deproteinized horsederived
 Research Article J Periodontal Implant Sci 2010;40:227-231 doi: 10.5051/jpis.2010.40.5.227 Socket preservation using deproteinized horsederived bone mineral Jang-Yeol Park, Ki-Tae Koo, Tae-Il Kim, Yang-Jo
Research Article J Periodontal Implant Sci 2010;40:227-231 doi: 10.5051/jpis.2010.40.5.227 Socket preservation using deproteinized horsederived bone mineral Jang-Yeol Park, Ki-Tae Koo, Tae-Il Kim, Yang-Jo
Dental Implants: A Predictable Solution for Tooth Loss. Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor
 Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
Contemporary Implant Dentistry
 Contemporary Implant Dentistry C H A P T ER 1 4 O F C O N T E M P OR A R Y O R A L A N D M A X I L L OFA C IA L S U R G E RY B Y : D R A R A S H K H O J A S T EH Dental implant is suitable for: completely
Contemporary Implant Dentistry C H A P T ER 1 4 O F C O N T E M P OR A R Y O R A L A N D M A X I L L OFA C IA L S U R G E RY B Y : D R A R A S H K H O J A S T EH Dental implant is suitable for: completely
Years of research and advancement in
 Immediate Implants with Guided Bone Regeneration Using Titanium Mesh and Alloplast in an Infected Site: A Case Report Mahesh et al Dr. Lanka Mahesh 1 Dr. Ajay Bibra 2 Dr. Vishal Gupta 3 Abstract Years
Immediate Implants with Guided Bone Regeneration Using Titanium Mesh and Alloplast in an Infected Site: A Case Report Mahesh et al Dr. Lanka Mahesh 1 Dr. Ajay Bibra 2 Dr. Vishal Gupta 3 Abstract Years
Alveolar Ridge Augmentation with Titanium Mesh and Particulate Allograft A Case Report
 Alveolar Ridge Augmentation with Titanium Mesh and Particulate Allograft A Case Report Dr. Pratibha Borasi, Dr. Praneeta Kamble Department of Periodontics, Nair Hospital Dental College, Mumbai, Maharashtra,
Alveolar Ridge Augmentation with Titanium Mesh and Particulate Allograft A Case Report Dr. Pratibha Borasi, Dr. Praneeta Kamble Department of Periodontics, Nair Hospital Dental College, Mumbai, Maharashtra,
Purpose: To assess the long term survival of sites treated by GTR.
 Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
The International Journal of Periodontics & Restorative Dentistry
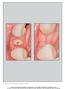 The International Journal of Periodontics & Restorative Dentistry 67 Efficacy Evaluation of a New Buccal Bone Plate Preservation Technique: A Pilot Study Federico Brugnami, DDS* Alfonso Caiazzo, DDS**
The International Journal of Periodontics & Restorative Dentistry 67 Efficacy Evaluation of a New Buccal Bone Plate Preservation Technique: A Pilot Study Federico Brugnami, DDS* Alfonso Caiazzo, DDS**
Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report
 C A S E R E P O R T Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report Rhoodie Garrana 1 and Govindrau Mohangi
C A S E R E P O R T Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report Rhoodie Garrana 1 and Govindrau Mohangi
Patient's Guide to Dental Implants. an investment for a lifelong smile
 Patient's Guide to Dental Implants an investment for a lifelong smile Introduction Genicore is a specialized products and service provider to dental professionals in the United States. Genicore strategically
Patient's Guide to Dental Implants an investment for a lifelong smile Introduction Genicore is a specialized products and service provider to dental professionals in the United States. Genicore strategically
Clinical cases by Dr. Fernando Rojas-Vizcaya. botiss. dental bone & tissue regeneration. biomaterials. strictly biologic
 Clinical cases by Dr. Fernando Rojas-Vizcaya dental bone & tissue regeneration botiss biomaterials strictly biologic botiss BTR system: BONE biologic potential bovine block & granules: pure bone mineral
Clinical cases by Dr. Fernando Rojas-Vizcaya dental bone & tissue regeneration botiss biomaterials strictly biologic botiss BTR system: BONE biologic potential bovine block & granules: pure bone mineral
Vertical and Horizontal Augmentation Using Guided Bone Regeneration. Ph.D. Thesis. Dr. med. dent. et univ. Istvan Urban
 Vertical and Horizontal Augmentation Using Guided Bone Regeneration Ph.D. Thesis Dr. med. dent. et univ. Istvan Urban Supervisor: Prof. Dr. Katalin Nagy, DDS, PhD Faculty of Dentistry, University of Szeged
Vertical and Horizontal Augmentation Using Guided Bone Regeneration Ph.D. Thesis Dr. med. dent. et univ. Istvan Urban Supervisor: Prof. Dr. Katalin Nagy, DDS, PhD Faculty of Dentistry, University of Szeged
Inion GTR Biodegradable Membrane System
 Inion GTR Biodegradable Membrane System The concept of GTR/GBR Intended use The Inion GTR Biodegradable Membrane System is intended to be used as a barrier membrane in dental guided tissue regeneration
Inion GTR Biodegradable Membrane System The concept of GTR/GBR Intended use The Inion GTR Biodegradable Membrane System is intended to be used as a barrier membrane in dental guided tissue regeneration
Socket Treatment. Procedure Guide
 Socket Treatment Procedure Guide www.implantdirect.com 888.649.6425 Extraction Healing and Ridge Resorption The Why Working with patients to educate them on the benefits of bone maintenance post extraction
Socket Treatment Procedure Guide www.implantdirect.com 888.649.6425 Extraction Healing and Ridge Resorption The Why Working with patients to educate them on the benefits of bone maintenance post extraction
Immediate Implant Placement:
 Immediate Implant Placement: Parameters Influencing Tissue Remodeling Bernard Touati, DDS and Mario Groisman, DDS In esthetic implant therapy, the patient s objective is to obtain an imperceptible, natural-looking
Immediate Implant Placement: Parameters Influencing Tissue Remodeling Bernard Touati, DDS and Mario Groisman, DDS In esthetic implant therapy, the patient s objective is to obtain an imperceptible, natural-looking
Scientific & Clinical Evidence Jason membrane
 Scientific & Clinical Evidence Jason membrane Pericardium GBR/GTR Membrane Facts - CE since 2009 - so far no serious clinical complication or objection - approx. 250.000 successful clinical treatments
Scientific & Clinical Evidence Jason membrane Pericardium GBR/GTR Membrane Facts - CE since 2009 - so far no serious clinical complication or objection - approx. 250.000 successful clinical treatments
Sang-Sun Han, 1 Kwang-Min Lee, 2 and Kee-Deog Kim Introduction
 BioMed Research International Volume 2015, Article ID 808625, 5 pages http://dx.doi.org/10.1155/2015/808625 Research Article Availability of Software-Based Correction of Mandibular Plane for the Vertical
BioMed Research International Volume 2015, Article ID 808625, 5 pages http://dx.doi.org/10.1155/2015/808625 Research Article Availability of Software-Based Correction of Mandibular Plane for the Vertical
Hyun-Jae Cho, Kun-Soo Jang, Ki-Hyun Jeong, Jae-Yun Jeon, Kyung-Gyun Hwang, Chang-Joo Park
 Vol. 33 No. 1, March 2014 Peri-implant gingival tissue changes following immediate placement of maxillary anterior single implant with a collagen-coated xenograft: A 1-year follow-up result Hyun-Jae Cho,
Vol. 33 No. 1, March 2014 Peri-implant gingival tissue changes following immediate placement of maxillary anterior single implant with a collagen-coated xenograft: A 1-year follow-up result Hyun-Jae Cho,
Case Report. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
 Case Report RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
Case Report RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
Cerasorb M DENTAL. O:\Zulassung\Cerasorb Dental Kanada 2013\Texte\Cerasorb M Dental final IFU docx
 Cerasorb M DENTAL Resorbable, pure-phase beta-tricalcium phosphate matrix with interconnecting porosity for bone regeneration for use in dental and maxillofacial surgery DESCRIPTION: Cerasorb M DENTAL
Cerasorb M DENTAL Resorbable, pure-phase beta-tricalcium phosphate matrix with interconnecting porosity for bone regeneration for use in dental and maxillofacial surgery DESCRIPTION: Cerasorb M DENTAL
Sinus Augmentation Studies Methods and Definition
 FDA approved indications for Infuse Bone Graft in the Maxillofacial Skeleton Alveolar Ridge Augmentation (Buccal Wall Defects) in the Maxilla Maxillary Sinus Floor augmentation Sinus Augmentation Studies
FDA approved indications for Infuse Bone Graft in the Maxillofacial Skeleton Alveolar Ridge Augmentation (Buccal Wall Defects) in the Maxilla Maxillary Sinus Floor augmentation Sinus Augmentation Studies
The Use of Freeze-Dried Bone Allograft as an Alternative to Autogenous Bone Graft in the Atrophic Maxilla: A 3-Year Clinical Follow-up
 643 The Use of Freeze-Dried Bone Allograft as an Alternative to Autogenous Bone Graft in the Atrophic Maxilla: A 3-Year Clinical Follow-up Marco Aurélio Bianchini, DDS, MSc, PhD 1 André R. Buttendorf,
643 The Use of Freeze-Dried Bone Allograft as an Alternative to Autogenous Bone Graft in the Atrophic Maxilla: A 3-Year Clinical Follow-up Marco Aurélio Bianchini, DDS, MSc, PhD 1 André R. Buttendorf,
Bringing you Geistlich biocompatibility with improved application and handling benefits. Your combination for success
 Bringing you Geistlich biocompatibility with improved application and handling benefits Your combination for success Geistlich Combi-Kit Collagen: Combining ease and predictablility Geistlich Combi-Kit
Bringing you Geistlich biocompatibility with improved application and handling benefits Your combination for success Geistlich Combi-Kit Collagen: Combining ease and predictablility Geistlich Combi-Kit
INTERNATIONAL MEDICAL COLLEGE
 INTERNATIONAL MEDICAL COLLEGE Joint Degree Master Program: Implantology and Dental Surgery (M.Sc.) Specialized Modules: List of individual modules Specialized Module 1 Basic principles of implantology
INTERNATIONAL MEDICAL COLLEGE Joint Degree Master Program: Implantology and Dental Surgery (M.Sc.) Specialized Modules: List of individual modules Specialized Module 1 Basic principles of implantology
Bone augmentation with biomaterials
 Patient information dental bone & tissue regeneration botiss biomaterials Bone augmentation with biomaterials established safe natural X100 Implantation stability is crucial for success Atrophy of the
Patient information dental bone & tissue regeneration botiss biomaterials Bone augmentation with biomaterials established safe natural X100 Implantation stability is crucial for success Atrophy of the
The anatomic limitations of the. Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD*
 CASE REPORT Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD* The anatomic limitations of the residual alveolar bone may cause problems for
CASE REPORT Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD* The anatomic limitations of the residual alveolar bone may cause problems for
Bone augmentation with maxgraft
 Patient information bone & tissue regeneration botiss biomaterials Bone augmentation with maxgraft established safe X100 natural Implantation stability is crucial for success Atrophy of the jaw bone loss
Patient information bone & tissue regeneration botiss biomaterials Bone augmentation with maxgraft established safe X100 natural Implantation stability is crucial for success Atrophy of the jaw bone loss
Excellent Choice for a Beautiful Smile - OSSTEM IMPLANT
 Excellent Choice for a Beautiful Smile - OSSTEM IMPLANT About Implants 01. What if a tooth is lost and the toothless area is left alone? 02. Do you want to restore the confidence in your appearance? 03.
Excellent Choice for a Beautiful Smile - OSSTEM IMPLANT About Implants 01. What if a tooth is lost and the toothless area is left alone? 02. Do you want to restore the confidence in your appearance? 03.
Immediate Implant Placement Along With Guided Bone Regeneration In Mandibular Anterior Region A Case Report.
 IMMEDIATE IMPLANT PLACEMENT ALONG WITH GUIDED BONE REGENERATION IN MANDIBULAR ANTERIOR REGION A CASE REPORT. Dr.C.P.Dhivakar 1, Dr.T.Saravanan 2, Dr.A.Aniz 3 1) Department of Periodontics, Karpaga Vinayaga
IMMEDIATE IMPLANT PLACEMENT ALONG WITH GUIDED BONE REGENERATION IN MANDIBULAR ANTERIOR REGION A CASE REPORT. Dr.C.P.Dhivakar 1, Dr.T.Saravanan 2, Dr.A.Aniz 3 1) Department of Periodontics, Karpaga Vinayaga
Periimplant Regeneration Fenestration
 Indication Sheet PIR Periimplant Regeneration Fenestration Treatment concept of Dr. Jean-Pierre Gardella (surgeon) and Dr. Christian Richelme (prosthodontist), Marseille, France > Filling of a peri-implant
Indication Sheet PIR Periimplant Regeneration Fenestration Treatment concept of Dr. Jean-Pierre Gardella (surgeon) and Dr. Christian Richelme (prosthodontist), Marseille, France > Filling of a peri-implant
A WIDE RANGE OF REGENERATIVE SOLUTIONS
 A WIDE RANGE OF REGENERATIVE SOLUTIONS INDICATIONS: 1/ SOCKET AND RIDGE PRESERVATION 2/ FILLING OF EXTRACTION SOCKETS Biomaterials offers portfolio of regenerative materials for implantology, aimed at
A WIDE RANGE OF REGENERATIVE SOLUTIONS INDICATIONS: 1/ SOCKET AND RIDGE PRESERVATION 2/ FILLING OF EXTRACTION SOCKETS Biomaterials offers portfolio of regenerative materials for implantology, aimed at
The Use of Alpha-Bio Tec's Narrow NeO Implants with Cone Connection for Restoration of Limited Width Ridges
 Case Study 48 The Use of Alpha-Bio Tec's Narrow NeO Implants with Cone Connection for Restoration of Limited Width Ridges Dr. Amir Gazmawe DMD, Specialist in Prosthodontics, Israel Dr. Amir Gazmawe graduated
Case Study 48 The Use of Alpha-Bio Tec's Narrow NeO Implants with Cone Connection for Restoration of Limited Width Ridges Dr. Amir Gazmawe DMD, Specialist in Prosthodontics, Israel Dr. Amir Gazmawe graduated
Consensus Statements and Recommended Clinical Procedures Regarding Loading Protocols
 Group 3 Consensus Statements Consensus Statements and Recommended Clinical Procedures Regarding Loading Protocols Hans-Peter Weber, DMD, Dr Med Dent 1 /Dean Morton, BDS, MS 2 /German O. Gallucci, DMD,
Group 3 Consensus Statements Consensus Statements and Recommended Clinical Procedures Regarding Loading Protocols Hans-Peter Weber, DMD, Dr Med Dent 1 /Dean Morton, BDS, MS 2 /German O. Gallucci, DMD,
Consensus Report Tissue augmentation and esthetics (Working Group 3)
 B. Klinge Thomas F. Flemmig Consensus Report Tissue augmentation and esthetics (Working Group 3) Members of working group: Matteo Chiapasco Jan-Eirik Ellingsen Ronald Jung Friedrich Neukam Isabella Rocchietta
B. Klinge Thomas F. Flemmig Consensus Report Tissue augmentation and esthetics (Working Group 3) Members of working group: Matteo Chiapasco Jan-Eirik Ellingsen Ronald Jung Friedrich Neukam Isabella Rocchietta
Alveolar ridge preservation techniques
 Alveolar ridge preservation techniques Semmelweis University, Department of Periodontology, Budapest Dr. Windisch Péter Head of Department of Periodontology Changes of the alveolar ridge dimensions after
Alveolar ridge preservation techniques Semmelweis University, Department of Periodontology, Budapest Dr. Windisch Péter Head of Department of Periodontology Changes of the alveolar ridge dimensions after
Implant Placement in Maxillary Anterior Region Along with Soft and Hard Tissue Grafting- A Case Report.
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 10 Ver. XII (October. 2016), PP 68-73 www.iosrjournals.org Implant Placement in Maxillary Anterior
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 10 Ver. XII (October. 2016), PP 68-73 www.iosrjournals.org Implant Placement in Maxillary Anterior
Vertical Augmentation
 Indication Sheet V Dr. Mauro Merli Vertical Augmentation Vertical alveolar ridge augmentation by means of the fence technique with Geistlich biomaterials > Original publication of the technique on PubMed;
Indication Sheet V Dr. Mauro Merli Vertical Augmentation Vertical alveolar ridge augmentation by means of the fence technique with Geistlich biomaterials > Original publication of the technique on PubMed;
Alveolar Ridge Preservation:
 Alveolar Ridge Preservation: Preserving and Building up the Bony Structures after Extraction» By: Prof. Roland Hille Konigsallee 49c, 41747 Viersen, Germany E-mail: dr-hille@t-online.de» Prof. Rolf Vollmer
Alveolar Ridge Preservation: Preserving and Building up the Bony Structures after Extraction» By: Prof. Roland Hille Konigsallee 49c, 41747 Viersen, Germany E-mail: dr-hille@t-online.de» Prof. Rolf Vollmer
Guided surgery as a way to simplify surgical implant treatment in complex cases
 52 STARGET 1 I 12 StraUMaNN CareS r ry vincenzo MiriSOLA Di TOrreSANTO AND LUCA COrDArO Guided surgery as a way to simplify surgical implant treatment in complex cases Background A 41-year-old woman with
52 STARGET 1 I 12 StraUMaNN CareS r ry vincenzo MiriSOLA Di TOrreSANTO AND LUCA COrDArO Guided surgery as a way to simplify surgical implant treatment in complex cases Background A 41-year-old woman with
The Essential Choice. With the Benefits of Biologic Predictability
 The Essential Choice With the Benefits of Biologic Predictability Documented, Reliable, Experienced is the essential choice for your daily regenerative needs. Throughout our long history and dedication
The Essential Choice With the Benefits of Biologic Predictability Documented, Reliable, Experienced is the essential choice for your daily regenerative needs. Throughout our long history and dedication
We Want to Keep You Smiling. Bone Regeneration with Geistlich Bio-Oss and Geistlich Bio-Gide
 We Want to Keep You Smiling Bone Regeneration with Geistlich Bio-Oss and Geistlich Bio-Gide Strong Bone for a Healthier Smile Strong and healthy teeth provide a feeling of well-being, self-confidence and
We Want to Keep You Smiling Bone Regeneration with Geistlich Bio-Oss and Geistlich Bio-Gide Strong Bone for a Healthier Smile Strong and healthy teeth provide a feeling of well-being, self-confidence and
From planning to surgery: a totally digital working flow for Leone implants placement
 Dr. Giancarlo Romagnuolo Roma, Italy From planning to surgery: a totally digital working flow for Leone implants placement Keywords guided surgery, 3D implant planning, single missing tooth, delayed immediate
Dr. Giancarlo Romagnuolo Roma, Italy From planning to surgery: a totally digital working flow for Leone implants placement Keywords guided surgery, 3D implant planning, single missing tooth, delayed immediate
We want to keep you smiling. Bone regeneration with Geistlich Bio-Oss and Geistlich Bio-Gide
 We want to keep you smiling Bone regeneration with Geistlich Bio-Oss and Geistlich Bio-Gide Strong bone for a healthier smile Strong and healthy teeth provide a feeling of well-being, self-confidence and
We want to keep you smiling Bone regeneration with Geistlich Bio-Oss and Geistlich Bio-Gide Strong bone for a healthier smile Strong and healthy teeth provide a feeling of well-being, self-confidence and
Horizontal bone augmentation by means of guided bone regeneration
 Periodontology 2000, Vol. 66, 2014, 13 40 2014 John Wiley & Sons A/S. Published by John Wiley & Sons Ltd Printed in Singapore. All rights reserved PERIODONTOLOGY 2000 Horizontal bone augmentation by means
Periodontology 2000, Vol. 66, 2014, 13 40 2014 John Wiley & Sons A/S. Published by John Wiley & Sons Ltd Printed in Singapore. All rights reserved PERIODONTOLOGY 2000 Horizontal bone augmentation by means
Resorbable bilayer synthetic membrane Biomimetic tissue-engineered matrix for GBR and GTR
 Resorbable bilayer synthetic membrane Biomimetic tissue-engineered matrix for GBR and GTR Patented Jet-Spraying technology: Full barrier effect during 4 weeks, and complete resorption in 6 months PATENTED
Resorbable bilayer synthetic membrane Biomimetic tissue-engineered matrix for GBR and GTR Patented Jet-Spraying technology: Full barrier effect during 4 weeks, and complete resorption in 6 months PATENTED
The Essential Choice. With the Benefits of Biologic Predictability
 The Essential Choice With the Benefits of Biologic Predictability Documented, Reliable, Experienced is the essential choice for your daily regenerative needs. Throughout our long history and dedication
The Essential Choice With the Benefits of Biologic Predictability Documented, Reliable, Experienced is the essential choice for your daily regenerative needs. Throughout our long history and dedication
Augmentation of Peri-implant Bone Defects with Different Bone Grafts and Guided Bone Regeneration: A Pilot Experimental Study in the Dog
 Original J.Hard Tissue Biology.15(3): 82-88,2006 Journal of Hard Tissue Biology 15[3] (2006) p82-88 2006The Society for Regenerative Hard Tissue Biology Printed in Japan, All rights reserved. CODEN-JHTBFF,
Original J.Hard Tissue Biology.15(3): 82-88,2006 Journal of Hard Tissue Biology 15[3] (2006) p82-88 2006The Society for Regenerative Hard Tissue Biology Printed in Japan, All rights reserved. CODEN-JHTBFF,
Cytoflex Barrier Membrane Clinical Evaluation
 Cytoflex Barrier Membrane Clinical Evaluation Historical Background Guided tissue regeneration is a well established concept in the repair of oral bone defects. The exclusion of soft tissue epithelial
Cytoflex Barrier Membrane Clinical Evaluation Historical Background Guided tissue regeneration is a well established concept in the repair of oral bone defects. The exclusion of soft tissue epithelial
Periimplant Regeneration Fenestration
 Indication Sheet PIR-1 Periimplant Regeneration Fenestration Treatment concept of Dr. Jean-Pierre Gardella (surgeon) and Dr. Christian Richelme (prosthodontist), Marseille, France > Filling of a peri-implant
Indication Sheet PIR-1 Periimplant Regeneration Fenestration Treatment concept of Dr. Jean-Pierre Gardella (surgeon) and Dr. Christian Richelme (prosthodontist), Marseille, France > Filling of a peri-implant
botiss dental bone & tissue regeneration biomaterials collacone max Innovative composite matrix socket preservation form-fitting resorbable composite
 dental bone & tissue regeneration botiss biomaterials socket preservation Innovative composite matrix form-fitting resorbable composite 1 botiss regeneration system maxresorb flexbone* collacone.. max
dental bone & tissue regeneration botiss biomaterials socket preservation Innovative composite matrix form-fitting resorbable composite 1 botiss regeneration system maxresorb flexbone* collacone.. max
Contents HIOSSEN IMPLANT
 SMARTbuilder Contents HIOSSEN IMPLANT SMARTbuilder Lateral 3 Key Features 4 Pore Specifications 5 Surgical Procedure 7 Clinical Cases 9 Suggested Application by Type 10 Products Specficiations 11 Components
SMARTbuilder Contents HIOSSEN IMPLANT SMARTbuilder Lateral 3 Key Features 4 Pore Specifications 5 Surgical Procedure 7 Clinical Cases 9 Suggested Application by Type 10 Products Specficiations 11 Components
Vertical Bone Augmentation for Implant Placement in the Mandible a Systematic. Review
 Vertical Bone Augmentation for Implant Placement in the Mandible a Systematic Review A dissertation submitted to the University of Manchester for the degree of Master of Science in Dentistry (Oral and
Vertical Bone Augmentation for Implant Placement in the Mandible a Systematic Review A dissertation submitted to the University of Manchester for the degree of Master of Science in Dentistry (Oral and
Redefining Regeneration
 Redefining Regeneration Taking Volume to the MAX One Product, One Treatment, Real VOLUME Buccal Bone Loss Socket Preservation Lateral / Vertical Augmentation Grafting Material Scaffold Barrier (4-6 months)
Redefining Regeneration Taking Volume to the MAX One Product, One Treatment, Real VOLUME Buccal Bone Loss Socket Preservation Lateral / Vertical Augmentation Grafting Material Scaffold Barrier (4-6 months)
Peri-implant Augmentation
 Indication Sheet PIR3 Peri-implant Augmentation Early implantation with simultaneous GBR for contour augmentation using the technique by Prof. Daniel Buser and Prof. Urs Belser, University of Berne, Switzerland
Indication Sheet PIR3 Peri-implant Augmentation Early implantation with simultaneous GBR for contour augmentation using the technique by Prof. Daniel Buser and Prof. Urs Belser, University of Berne, Switzerland
Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Abstract Purpose: Materials and methods Results:
 Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Bum-Soo Kim 1, Young-Kyun Kim 1, Pil-Young Yun 1, Yang-Jin Lee 2, Hyo-Jeong Lee 3, Su-Gwan Kim 4 1Department of
Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Bum-Soo Kim 1, Young-Kyun Kim 1, Pil-Young Yun 1, Yang-Jin Lee 2, Hyo-Jeong Lee 3, Su-Gwan Kim 4 1Department of
GUIDED BONE & TISSUE REGENERATION 2-DAY MASTERCLASS (CHOOSE LONDON OR PARIS) DR. ISABELLA ROCCHIETTA & DR. DAVID NISAND
 GUIDED BONE & TISSUE REGENERATION DR. ISABELLA ROCCHIETTA & DR. DAVID NISAND 2-DAY MASTERCLASS (CHOOSE LONDON OR PARIS) This hands-on course will be delivered in small group workshops and will equip the
GUIDED BONE & TISSUE REGENERATION DR. ISABELLA ROCCHIETTA & DR. DAVID NISAND 2-DAY MASTERCLASS (CHOOSE LONDON OR PARIS) This hands-on course will be delivered in small group workshops and will equip the
One-year Re-entry Results of Guided Bone Regeneration around Immediately Placed Implants with Immediate or Conventional Loading: A Case Series
 Journal of the International Academy of Periodontology 2012 14/3:62-68 One-year Re-entry Results of Guided Bone Regeneration around Immediately Placed Implants with Immediate or Conventional Loading: A
Journal of the International Academy of Periodontology 2012 14/3:62-68 One-year Re-entry Results of Guided Bone Regeneration around Immediately Placed Implants with Immediate or Conventional Loading: A
The Influence of Controlled Occlusal Overload on Peri-implant Tissue. Part 3: A Histologic Study in Monkeys
 The Influence of Controlled Occlusal Overload on Peri-implant Tissue. Part 3: A Histologic Study in Monkeys Takashi Miyata, DDS, DDSc 1 /Yukinao Kobayashi, DDS 2 /Hisao Araki, DDS, DDSc 3 / Takaichi Ohto,
The Influence of Controlled Occlusal Overload on Peri-implant Tissue. Part 3: A Histologic Study in Monkeys Takashi Miyata, DDS, DDSc 1 /Yukinao Kobayashi, DDS 2 /Hisao Araki, DDS, DDSc 3 / Takaichi Ohto,
(Images are at the end of article)
 Long term provisionalization during periodontal surgery and extraction site tissue grafting: A Case Review Michael Tischler, DDS Diplomate American Board Of Oral Implantology/Implant Dentistry (Images
Long term provisionalization during periodontal surgery and extraction site tissue grafting: A Case Review Michael Tischler, DDS Diplomate American Board Of Oral Implantology/Implant Dentistry (Images
GUIDED BONE & TISSUE REGENERATION 2-DAY LIVE COURSE DR. ISABELLA ROCCHIETTA & DR. DAVID NISAND
 GUIDED BONE & TISSUE REGENERATION DR. ISABELLA ROCCHIETTA & DR. DAVID NISAND 2-DAY LIVE COURSE Soft tissue management is the key to achieve aesthetic success. Periodontal and peri-implant soft tissue management
GUIDED BONE & TISSUE REGENERATION DR. ISABELLA ROCCHIETTA & DR. DAVID NISAND 2-DAY LIVE COURSE Soft tissue management is the key to achieve aesthetic success. Periodontal and peri-implant soft tissue management
Puros Cancellous Particulate Allograft & Puros Block Allograft
 Puros Cancellous Particulate Allograft & Puros Block Allograft Puros Cancellous Particulate Allograft The Natural Choice For Healthy 1 Bone Growth. 1. Proven, Predictable Regeneration Acts as an osteoconductive
Puros Cancellous Particulate Allograft & Puros Block Allograft Puros Cancellous Particulate Allograft The Natural Choice For Healthy 1 Bone Growth. 1. Proven, Predictable Regeneration Acts as an osteoconductive
Clinical Case Reports using Cytoplast GTR Barrier Membranes
 Clinical Case Reports using Cytoplast GTR Barrier Membranes Barry K. Bartee, DDS, MD The Cytoplast Technique: Extraction Site Grafting Without Primary Closure 1. 1. Preoperative view. To maximize the result
Clinical Case Reports using Cytoplast GTR Barrier Membranes Barry K. Bartee, DDS, MD The Cytoplast Technique: Extraction Site Grafting Without Primary Closure 1. 1. Preoperative view. To maximize the result
Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report
 Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
botiss biomaterials bone & tissue regeneration collacone max Innovative composite matrix socket preservation form-fitting resorbable composite
 bone & tissue regeneration botiss biomaterials socket preservation Innovative composite matrix form-fitting resorbable composite 1 Socket preservation safeguarding your sockets collacone.. max flexbone*
bone & tissue regeneration botiss biomaterials socket preservation Innovative composite matrix form-fitting resorbable composite 1 Socket preservation safeguarding your sockets collacone.. max flexbone*
Clinical presentation of a horse-derived biomaterial and its Biocompatibility: A Clinical Case Report
 Case report J Korean Acad Periodontol 2009;39:287-291 Clinical presentation of a horse-derived biomaterial and its Biocompatibility: A Clinical Case Report Ki-Tae Koo, Jang-Yeol Park, Jun-Seok Park, Tae-Il
Case report J Korean Acad Periodontol 2009;39:287-291 Clinical presentation of a horse-derived biomaterial and its Biocompatibility: A Clinical Case Report Ki-Tae Koo, Jang-Yeol Park, Jun-Seok Park, Tae-Il
TOPICS. T O P I C S Day 1. Implant Locations. Implant Placement in the Posterior Maxilla. Anatomy and risk factors Option 1: Short implants
 T O P I C S Day 1 Factors influencing the long-term stability of dental implants Surgical procedures in posterior sites: Standard implant placement with or without flap elevation Surgical procedures in
T O P I C S Day 1 Factors influencing the long-term stability of dental implants Surgical procedures in posterior sites: Standard implant placement with or without flap elevation Surgical procedures in
Regeneration Bone Grafting & Soft Tissue Management
 Regeneration Bone Grafting & Soft Tissue Management OSTEON TM II Table of Contents Bone Graft Material OSTEON TM II Collagen 04 OSTEON TM Collagen 06 OSTEON TM II 08 OSTEON TM 12 ORTHOPEDIC OSTEON TM 14
Regeneration Bone Grafting & Soft Tissue Management OSTEON TM II Table of Contents Bone Graft Material OSTEON TM II Collagen 04 OSTEON TM Collagen 06 OSTEON TM II 08 OSTEON TM 12 ORTHOPEDIC OSTEON TM 14
Strong bone for beautiful teeth. Patient Information I Bone reconstruction with Geistlich Bio-Oss and Geistlich Bio-Gide
 Strong bone for beautiful teeth Patient Information I Bone reconstruction with Geistlich Bio-Oss and Geistlich Bio-Gide Contents Smiling is the most beautiful way to show your teeth 3 What are the causes
Strong bone for beautiful teeth Patient Information I Bone reconstruction with Geistlich Bio-Oss and Geistlich Bio-Gide Contents Smiling is the most beautiful way to show your teeth 3 What are the causes
Symbios Xenograft Granules Porcine Bone Graft Material
 Symbios Xenograft Granules Porcine Bone Graft Material 32671122-USX-1607_Symbios Highlight Brochure.indd 1 2016-09-27 12:12 Symbios Xenograft Granules Porcine bone graft material Symbios Xenograft Granules
Symbios Xenograft Granules Porcine Bone Graft Material 32671122-USX-1607_Symbios Highlight Brochure.indd 1 2016-09-27 12:12 Symbios Xenograft Granules Porcine bone graft material Symbios Xenograft Granules
Benefits of CBCT in Implant Planning
 10.5005/jp-journals-10012-1032 CLINICAL SCIENCE 1 Gregori M Kurtzman, 2 Douglas F Dompkowski 1 Private General Practice in Silver Spring, Maryland, USA 2 Private Periodontal Practice in Bethesda, Maryland,
10.5005/jp-journals-10012-1032 CLINICAL SCIENCE 1 Gregori M Kurtzman, 2 Douglas F Dompkowski 1 Private General Practice in Silver Spring, Maryland, USA 2 Private Periodontal Practice in Bethesda, Maryland,
Case Report Total CAD/CAM Supported Method for Manufacturing Removable Complete Dentures
 Case Reports in Dentistry Volume 2016, Article ID 1259581, 5 pages http://dx.doi.org/10.1155/2016/1259581 Case Report Total CAD/CAM Supported Method for Manufacturing Removable Complete Dentures Arthur
Case Reports in Dentistry Volume 2016, Article ID 1259581, 5 pages http://dx.doi.org/10.1155/2016/1259581 Case Report Total CAD/CAM Supported Method for Manufacturing Removable Complete Dentures Arthur
Comparison of Peri-Implant Bone Loss and Survival of Maxillary Intrasinus and Extrasinus Implants After 2 Years
 Original Article Comparison of Peri-Implant Bone Loss and Survival of Maxillary Intrasinus and Extrasinus Implants After 2 Years AR. Rokn 1,2, AAR. Rasouli Ghahroudi 3,4, S. Hemati 5, A. Soolari 6 1 Associate
Original Article Comparison of Peri-Implant Bone Loss and Survival of Maxillary Intrasinus and Extrasinus Implants After 2 Years AR. Rokn 1,2, AAR. Rasouli Ghahroudi 3,4, S. Hemati 5, A. Soolari 6 1 Associate
Maxillary sinus augmentation without any graft material- A case Report
 A CASE REPORT ISSN: 2321-4988 D.Shiva kumar et al. /JPR:BioMedRx: An International Journal 2013,1(8), Available online through www.jpronline.info Maxillary sinus augmentation without any graft material-
A CASE REPORT ISSN: 2321-4988 D.Shiva kumar et al. /JPR:BioMedRx: An International Journal 2013,1(8), Available online through www.jpronline.info Maxillary sinus augmentation without any graft material-
Oral Rehabilitation with CAMLOG implants after loss of dentition due to an accident
 Case Report 13 2011 Oral Rehabilitation with CAMLOG implants after loss of dentition due to an accident Dr Hitoshi Minagawa Tokyo, Japan Prosthetics Dr Hitoshi Minagawa successfully completed his studies
Case Report 13 2011 Oral Rehabilitation with CAMLOG implants after loss of dentition due to an accident Dr Hitoshi Minagawa Tokyo, Japan Prosthetics Dr Hitoshi Minagawa successfully completed his studies
THE NEW STANDARD OF EXCELLENCE IN BIOMATERIALS. Collagenated heterologous cortico-cancellous bone mix + TSV Gel GTO I N S P I R E D B Y N A T U R E
 GTO THE NEW STANDARD OF EXCELLENCE IN BIOMATERIALS Collagenated heterologous cortico-cancellous bone mix + TSV Gel R E G E N E R A T I O N S C I E N C E I N S P I R E D B Y N A T U R E A unique biotechnology
GTO THE NEW STANDARD OF EXCELLENCE IN BIOMATERIALS Collagenated heterologous cortico-cancellous bone mix + TSV Gel R E G E N E R A T I O N S C I E N C E I N S P I R E D B Y N A T U R E A unique biotechnology
The Application of Cone Beam CT Image Analysis for the Mandibular Ramus Bone Harvesting
 44 The Application of Cone Beam CT Image Analysis for the Mandibular Ramus Bone Harvesting LivingWell Institute of Dental Research Lee, Jang-yeol, Youn, Pil-sang, Kim, Hyoun-chull, Lee Sang-chull Ⅰ. Introduction
44 The Application of Cone Beam CT Image Analysis for the Mandibular Ramus Bone Harvesting LivingWell Institute of Dental Research Lee, Jang-yeol, Youn, Pil-sang, Kim, Hyoun-chull, Lee Sang-chull Ⅰ. Introduction
Implant Site Development Part I
 REVIEW ARTICLE Implant Site Development Part I 1 Umang Nayar, 2 Shankar Iyer IJCID Implant Site Development Part I 1 Consultant, Dental Surgeon and Periodontist at Max Health Care, New Delhi, Professor
REVIEW ARTICLE Implant Site Development Part I 1 Umang Nayar, 2 Shankar Iyer IJCID Implant Site Development Part I 1 Consultant, Dental Surgeon and Periodontist at Max Health Care, New Delhi, Professor
ALVEOLAR RIDGE AUGMENTATION UTILIZING PLATELET RICH FIBRIN IN COMBINATION WITH DEMINERALIZED FREEZE-DRIED BONE ALLOGRAFT A CASE REPORT
 ALVEOLAR RIDGE AUGMENTATION UTILIZING PLATELET RICH FIBRIN IN COMBINATION WITH DEMINERALIZED FREEZE-DRIED BONE ALLOGRAFT A CASE REPORT * Mishal Piyush Shah 1 and Sheela Kumar Gujjari 2 1 Department of
ALVEOLAR RIDGE AUGMENTATION UTILIZING PLATELET RICH FIBRIN IN COMBINATION WITH DEMINERALIZED FREEZE-DRIED BONE ALLOGRAFT A CASE REPORT * Mishal Piyush Shah 1 and Sheela Kumar Gujjari 2 1 Department of
Distribution of the maxillary artery related to sinus graft surgery for implantation
 42 Distribution of the maxillary artery related to sinus graft surgery for implantation LvingWell Dental Hospital LivingWell Institute of Dental Research Jang-yeol Lee, Hyoun-chull Kim, Il-hae Park, Sang-chull
42 Distribution of the maxillary artery related to sinus graft surgery for implantation LvingWell Dental Hospital LivingWell Institute of Dental Research Jang-yeol Lee, Hyoun-chull Kim, Il-hae Park, Sang-chull
Procedure Manual and Catalog
 Procedure Manual and Catalog TM Why SynthoGraft? SynthoGraft offers a unique structure which provides stability, while its micro-porosity allows for rapid vascularization and subsequent resorption. Although
Procedure Manual and Catalog TM Why SynthoGraft? SynthoGraft offers a unique structure which provides stability, while its micro-porosity allows for rapid vascularization and subsequent resorption. Although
RELIABLE WHEN IT COUNTS. The unique collagenase-resistant membrane protects bone graft and supports treatment success even when exposed 4
 RELIABLE WHEN IT COUNTS 1 RELIABLE WHEN IT COUNTS RESISTANT TO EXPOSURE The unique collagenase-resistant membrane protects bone graft and supports treatment success even when exposed 4 RELIABLE BARRIER
RELIABLE WHEN IT COUNTS 1 RELIABLE WHEN IT COUNTS RESISTANT TO EXPOSURE The unique collagenase-resistant membrane protects bone graft and supports treatment success even when exposed 4 RELIABLE BARRIER
DIOnavi. Brochure Ver.2. Product Introduction: DIOnavi. Clinical Case Report
 DIOnavi. Brochure Ver.2 Product Introduction: DIOnavi. Clinical Case Report Evolved for Precision and Stability Digital Navigation Implant 04 Product Introduction: DIOnavi. One-Step Protocol 10 Clinical
DIOnavi. Brochure Ver.2 Product Introduction: DIOnavi. Clinical Case Report Evolved for Precision and Stability Digital Navigation Implant 04 Product Introduction: DIOnavi. One-Step Protocol 10 Clinical
BONE GRAFTING. Product Catalog
 BONE GRAFTING Product Catalog PRODUCT LINE Titanium Mesh Surgitime Titanium Titanium Foil Surgitime Titanium Seal Polytetraflouroethylene Membrane Surgitime PTFE Bone Screws Fixation Set We innovate to
BONE GRAFTING Product Catalog PRODUCT LINE Titanium Mesh Surgitime Titanium Titanium Foil Surgitime Titanium Seal Polytetraflouroethylene Membrane Surgitime PTFE Bone Screws Fixation Set We innovate to
Regeneration Bone Grafting & Soft Tissue Management
 Regeneration Bone Grafting & Soft Tissue Management Human Histology OSTEON II 26.5 months Regeneration Products information Table of contents Bone Graft Material OSTEON II OSTEON OSTEON II Collagen OSTEON
Regeneration Bone Grafting & Soft Tissue Management Human Histology OSTEON II 26.5 months Regeneration Products information Table of contents Bone Graft Material OSTEON II OSTEON OSTEON II Collagen OSTEON
THE NEXT FRONTIER OF BONE REGENERATION
 THE NEXT FRONTIER OF BONE REGENERATION where Technology meets Nature swiss made SmartBone is new composite bone substitute specifically developed for bone regeneration in oral and maxillofacial reconstructive
THE NEXT FRONTIER OF BONE REGENERATION where Technology meets Nature swiss made SmartBone is new composite bone substitute specifically developed for bone regeneration in oral and maxillofacial reconstructive
Since the report of Adell and associates, 1 well-documented
 Immediate Loading of an Implant Following Implant Site Development Using Forced Eruption: A Case Report Young-Seok Park, DDS, MSD 1 /Ki-Young Yi, DDS 2 /Seong-Cheol Moon, DDS, MSD, PhD 3 / Young-Chul Jung,
Immediate Loading of an Implant Following Implant Site Development Using Forced Eruption: A Case Report Young-Seok Park, DDS, MSD 1 /Ki-Young Yi, DDS 2 /Seong-Cheol Moon, DDS, MSD, PhD 3 / Young-Chul Jung,
Clinical Success. with the Proven. Clinical Success. with the Proven Bone Substitute Products
 Clinical Success with the Proven Bone Substitute Products Clinical Success with the Proven Bone Geistlich Bio-Oss Substitute Geistlich Bio-Oss Collagen Geistlich Bio-Oss Pen Documented More than 1,000
Clinical Success with the Proven Bone Substitute Products Clinical Success with the Proven Bone Geistlich Bio-Oss Substitute Geistlich Bio-Oss Collagen Geistlich Bio-Oss Pen Documented More than 1,000
Safety and esthetics with
 Safety and esthetics with dental implants A guide for patients Dear reader, Implant restorations follow nature's example. You can have the functions of natural teeth completely restored and thus maintain
Safety and esthetics with dental implants A guide for patients Dear reader, Implant restorations follow nature's example. You can have the functions of natural teeth completely restored and thus maintain
