Evaluation of Titanium Implants Placed into Simulated Extraction Sockets: A Study in Dogs
|
|
|
- Roland Scott
- 5 years ago
- Views:
Transcription
1 Evaluation of Titanium Implants Placed into Simulated Extraction Sockets: A Study in Dogs Ken Akimoto, DDS, MS*/William Becker, DDS, MS**/ Rutger Persson, DDS, Odont Dr***/David A. Baker, DDS, MS*/ Michael D. Rohrer, DDS, MS****/Robert B. O Neal, DDS, MS***** The purpose of this study was to evaluate the effect of gap width on bone healing around implants placed into simulated extraction socket defects of varying widths in 10 mongrel dogs. All premolars were removed and the alveolar ridges were reduced to a width of 7 mm. Nine weeks later, a total of 80 implants, 10 mm long by 3.3 mm wide, were placed into osteotomy sites prepared to 3 different diameters in the coronal half, simulating extraction sockets. Three experimental sites, with gap sizes of 0.5 mm, 1.0 mm, and 1.4 mm, were created; the control sites had no gap. The depth of each defect was measured at the time of implant placement. All implants were stable at the time of placement. The dogs were euthanized 12 weeks after implant placement, and blocks containing the implants and adjacent bone were submitted for histologic evaluation. Clinically, all control and test sites healed, with complete bone fill in the defect. Percentages of bone-to-implant contact were measured histologically. As the gap widened, the amount of bone-to-implant contact decreased, and the point of the highest bone-to-implant contact shifted apically. These changes were statistically significant (P <.001). No statistically significant differences in bone-to-implant contact were found between the sites when the apical 4 mm of implants were compared. Within the limits of this study, the simulated extraction socket defects healed clinically, with complete bone fill, regardless of the initial gap size. However, the width of the gap at the time of implant placement had a significant impact on the histologic percentage and the height of bone-to-implant contact. (INT J ORAL MAXILLOFAC IMPLANTS 1999;14: ) Key words: gap, gap width, histomorphometry, immediate placement, implant, osseointegration The use of titanium dental implants ad modum Brånemark to replace missing teeth has been shown to be predictable. 1 The placement of implants at the time of extraction has recently been *****Resident, Department of Periodontics, School of Dentistry, University of Washington, Seattle, Washington. *****Visiting Professor, Department of Periodontics, School of Dentistry, University of Washington, Seattle, Washington. *****Professor, Department of Periodontics, School of Dentistry, University of Washington, Seattle, Washington. *****Professor, Hard Tissue Research Laboratory, University of Oklahoma, Oklahoma City, Oklahoma. *****Associate Professor, Department of Periodontics, School of Dentistry, University of Washington, Seattle, Washington. Reprint requests: Dr Robert B. O Neal, University of Washington, School of Dentistry, Department of Periodontics, D570 Health Sciences Center, Box , Seattle, WA Fax: advocated as a means of reducing the time needed for healing. 2 Excellent rates of survival with these immediately placed implants, ranging from 93.6% to 100%, have been reported in the literature. 3 6 When implants are placed at the time of tooth extraction, there is often a gap between the walls of the extraction socket and the implant. This gap is usually widest in the coronal aspect of the socket. Various techniques and materials have been used to encourage bone growth within these sockets at the time of implant placement, including barrier membranes, 3,7 9 autogenous bone grafts, 4 demineralized or mineralized freeze-dried bone allografts (DFDBA and FDBA), and hydroxyapatite (HA). 13,14 Most of these studies report complete bone fill of the gaps clinically. The question that remains unanswered is: does the newly formed bone truly osseointegrate with the implant surface? The International Journal of Oral & Maxillofacial Implants 351
2 Several studies have been published to date in an effort to answer this question. In 1988, Carlsson et al 15 placed titanium rods of varying widths into the tibias of rabbits. After 6 and 12 weeks of healing, when the initial gap between bone and implant had been larger than 0.35 mm, histologic evaluation revealed no direct bone-to-implant contact in 10 of 13 implants. Knox et al 16 then compared the height and the percentage of direct bone-to-implant contact in simulated extraction sockets in dogs. Titanium grit-blasted press-fit implants, 3.25 mm long and varying in diameter from 3.25 to 7.25 mm, were placed into the osteotomy sites. The results indicated that gaps larger than 1 mm resulted in a smaller amount of direct bone-to-implant contact. In a recent study, Stentz et al 17,18 examined the healing of mm-diameter titanium implants placed into mm osteotomies in dogs. The gaps received expanded polytetraflouroethylene (e-ptfe) membranes alone or in combination with DFDBA. The researchers found no evidence of direct contact between bone and titanium implants in the area within the defect, regardless of the treatment rendered. The lack of statistical power and inaccurate simulation of the clinical situation lead to difficulties in the interpretation of these studies. The purpose of the present study was to evaluate the effect of gap width on bone healing around implants placed into simulated extraction socket defects of various widths when no additional materials or techniques are used to promote bone formation during healing. Materials and Methods Animal Model and Surgical Procedures. The study protocol was approved by the University of Washington Animal Care Committee. Ten adult mongrel dogs weighing 25 to 30 kg each were used. The dogs were given general anesthesia, and the first, second, third, and fourth premolars (P1, P2, P3, P4) were extracted from both sides of the mandible. At this time, the ridge height was reduced to achieve a uniform, 7-mm ridge width. Nine weeks postextraction, the dogs were premedicated with amoxicillin 15 mg/kg and anesthetized with appropriate general anesthetic agents. The fields of surgery received block and infiltration anesthesia (2% xylocaine 1:100,000 epinephrine) (Astra, Westborough, MA). Crestal incisions were made extending from the canine to first molar. Full-thickness mucoperiosteal flaps were reflected, and the mental nerve was visualized. Implant sites were not randomized. Table 1 summarizes the drilling sequence. Standard drilling procedures were used to prepare 4 osteotomy sites 2.7 mm wide and 10 mm long in the right and left mandible. Drilling was performed under a copious stream of sterile saline. In 9 of 10 dogs, sites were prepared from first molar to canine in the following order: control, site I, site II, and site III. In one dog, the order was reversed, ie, the control site was adjacent to the canines. Control sites (n = 20) received standard countersink preparations and 3.3-mm narrow-platform, selftapping implants (Nobel Biocare, Westmont, IL). In test sites, the coronal 6 mm was enlarged to various specified diameters using commercially available drills, as summarized in Table 1. Three different sizes were created for test sites. Site I (n = 20) was enlarged to 4.3 mm wide by 6 mm deep. Site II (n = 20) was enlarged to 5.25 mm wide by 6 mm deep, and site III (n = 20) was enlarged to 6 mm wide by 6 mm deep (Fig 1a). Sixty commercially pure titanium implants 3.3 mm in diameter (Nobel Biocare) were placed into the test sites. All implants were stable at the time of placement (Fig 1b). The resulting gap between the bone and the implant for each control site was 0 mm. The gaps for the test sites were 0.5 mm, 1.0 mm, and 1.4 mm, for sites I, II, and III, respectively. At the mesial aspect of the implants, 2 clinical measurements were taken using calibrated 15- mm University of North Carolina periodontal probes (HuFriedy, Chicago, IL). The measurements were: (1) the distance from the top of the implant rim to the ridge crest (CR-RM); and (2) the distance from the ridge crest to the bottom of the defect (CR-BD) (Fig 2). In site I defects, the gap (0.5 mm) was too narrow to accommodate a probe between the implant and the bony wall; therefore, the depth of the osteotomy (6 mm) was used as the distance from the ridge crest to the bottom of the defect (CR-BD). Clinical photographs were taken of all sites. Cover screws were secured onto the top of the implants, and the flaps were coapted with 4-0 chromic gut using horizontal mattress and interrupted sutures (Johnson and Johnson, Sommerville, NJ). The dogs were given amoxicillin orally (15 mg/kg every 12 hours) for 7 days and buprenorphine (.02 mg/kg) as needed for pain as determined by their activity. The dogs were examined daily for the first postoperative week and once per week thereafter. Twelve weeks after implant placement, the dogs were euthanized with an overdose of pentobarbital. Clinical photographs were taken of the specimens, and the bone blocks were defleshed. After the cover screws were removed, the implants were 352 Volume 14, Number 3, 1999
3 Table 1 Size of Osteotomy and Drills Implant Osteotomy Size of Site diameter (mm) diameter (mm) gap (mm) Drills used Control Drill kit, mm twist, 2 Counter sink 3 Site I Above plus 3 mm twist, 4 3/4.3 mm pilot, mm twist drill 6 Site II Above plus 4.25/5.25 mm pilot, mm twist drill 8 Site III Above plus 5/6 mm pilot, 9 modified 5/6 mm pilot 10 1 SDIA 557 (Nobel Biocare), 2 SDIA 444 (Nobel Biocare), 3 SDIA 463 (Nobel Biocare), 4 SDIC 003 (Nobel Biocare), 5 SDIC291 (Nobel Biocare), 6 SDIA496 (Nobel Biocare), 7 DC600 (Implant Innovations, Palm Beach, Gardeus, FL), 8 DT528 (Implant Innovations), 9 PD600 (Implant Innovations), 10 PD600 (Implant Innovations) modified with tip removed to work as a 6-mm drill. Fig 1a Prepared osteotomy sites. Left to right: control, site I, site II, site III. The diameter of the osteotomy in the coronal 6 mm is 2.7 mm, 4.3 mm, 5.25 mm, and 6 mm, respectively. Fig 1b Four identical 3.3-mm-diameter titanium implants were placed into the osteotomy sites. The apical portion of the osteotomy enabled initial stability of the implants. Fig 2 Two clinical measurements were taken at the mesial aspect of each implant: the ridge crest to the implant rim (CR- RM), and the ridge crest to the bottom of the defect (CR-BD). These measurements were taken at the time of implant placement and again at reentry. examined for stability by applying pressure apically and laterally with cotton pliers. Clinical measurements were repeated at the mesial aspect of each implant. Each block of bone containing an implant was reduced to approximately 8 mm wide by 12 mm long. The blocks were placed into neutral buffered formalin. Histologic Processing. Blocks of specimens containing the implants were sent to the Hard Tissue Research Laboratory at the University of Oklahoma College of Dentistry. Each block was sectioned mesiodistally through the center of the implant. The sections were fixed in 10% neutral buffered formalin for an additional 24 hours; this was followed by dehydration in a graded series of alcohols for 9 days. Following dehydration, the specimens were infiltrated with a light-curing embedding resin (Technovit 7200 VLC, Kulzer, Wehrheim, Germany). Following 30 days of infiltration with constant shaking at normal atmospheric pressure, the specimens were embedded and polymerized by a 450 nm light, with the temperature of the specimens never exceeding 40 C. The specimens were then prepared by the cutting/grinding method of Donath. 19,20 The specimens were cut to a thickness of 150 µm on the Exakt cuttinggrinding system (Exakt Apparatebau, Norderstedt, Germany) using a precision parallel control oscillating specimen mounting system. Three sections The International Journal of Oral & Maxillofacial Implants 353
4 Table 2 No. of Implants and Dogs Clinical evaluation Histologic evaluation Initial No. of No. of No. of dogs with No. of dogs with No. of No. of implants retrieved implants integrated Site implants dogs retrieved implants integrated implants Control Site I Site II Site III were made of each implant. Each section was polished to a thickness of 50 µm using a series of polishing discs (800 to 2400 grit) on the Exakt microgrinding system, followed by a final polish with 0.3-µm alumina. The final slides were stained with Stevenel s blue and van Gieson s picric fuchsin. Histomorphometric Measurements. Three mesiodistal sections from each block were available for evaluation. The section that was cut most perpendicular to the implant was selected for measurement. The coronal and apical 4 mm of each implant were examined separately to avoid possible bias. First, an opaque mask was laid over the apical part of the slide, leaving only the coronal 4 mm available for evaluation. A photomicrograph was taken at 2:1 magnification using a microscope fitted with a single-lens reflex camera (BX40 and SC35, Olympus America, Melville, NY). The opaque mask was then removed and placed coronally, exposing only the apical 4 mm of the implant. Photomicrographs were taken at the same magnification. The photographic slides were scanned at 600 dots per inch (dpi) using a slide scanner (Dimage Scan Dual, Minolta, Tokyo, Japan). The photographic slides were coded and evaluated by a blinded examiner, who took measurements using a microcomputer and a Windowsbased software program (NIH Image for PC, Scion, Fredrick, MD). The measurements were made in pixels and converted to millimeters (136 pixels per millimeter). Two measurements were taken on each slide, which was masked to show only the coronal 4 mm of the implant. First, the length of the implant surface and the sum of boneto-implant contact were calculated, and the percentage of bone-to-implant contact was determined. Second, the linear distance from the rim to the highest point of bone-to-implant contact was measured. Then the slide was masked to show only the apical 4 mm of the implant, and the percentage of bone-to-implant contact was determined. In the coronal 4 mm, both the mesial and distal sides of the implant were measured and averaged. In the apical 4 mm, the total surface of the implant, including the apex, was used for the measurement. Reproducibility of Measurements. On 10 randomly selected samples, histomorphometric measurements were repeated after 2 weeks. All measurements of bone-to-implant contact, both in the coronal and apical 4 mm were within 5% of initial measurements, with the exception of 1 measurement, which differed by 6%. All measurements of the highest bone-to-implant contact were within 0.2 mm of the initial measurements. Eight of 10 measurements were exactly the same. Statistical Analysis. The data were analyzed with statistical software (StatView Version 4.5 for Windows, Berkeley, CA) on an IBM-compatible microcomputer. For clinical measurements, analysis of variance (ANOVA) for block design was used to compare results between the sites. For histomorphometric measurements, a nonparametric Friedman rank test for block design was employed because of nonnormal distribution of the data. Post hoc multiple comparisons were done using Bonferroni method for significant ANOVA and Friedman rank tests. An alpha level of.05 was used to determine the statistical significance. Results There were no postoperative complications, and healing was uneventful. Of the 80 implants placed, 79 were successfully retrieved. One site III implant was missing. All retrieved implants were clinically immobile. All implants, except the one that was not found at the time of sacrifice, were included in the analysis of clinical outcome. Upon histologic examination, 2 control group implants and 7 implants in site III were found to be completely encapsulated within connective tissue. These implants were not included in the histomorphometric analysis. When implants from both the left and right sides with the same gap 354 Volume 14, Number 3, 1999
5 Table 3 Results Per Animal and Sites Clinical data (mm) Histomorphometric data Preoperatively Postoperatively Bone-implant contact (%) Ridge crest Ridge crest Ridge crest Ridge crest Implant rim to rim to bottom Defect to rim to bottom Residual to bone Animal of implant of defect depth of implant of defect defect Defect fill Coronal Apical (mm) Remarks Control # # NA NA NA A # # # # # # # # Site I # # # # # # # # # # Site II # # # # # # # # # # Site III # B # # NA NA NA A # B # B # C # NA NA NA A # # # A = both implants not integrated; B = 1 implant not integrated; C = 1 implant missing at the time of retrieval. size were encapsulated in fibrous tissue, no data were reported for that gap size from that animal. If 1 of the implants was available, that implant was used to represent the animal. This reduced the number of animals available for histomorphometric analysis to 9 for the control and 8 for site III (Table 2). Both clinical and histomorphometric data are presented in Table 3. Clinical Outcomes. The clinical outcomes for control and test sites are presented in Table 4. Most of the implants in the test sites healed with no signs of residual defect (Fig 3). Clinically, it was impossible to distinguish test sites from controls. The mean clinical bone fill for site I (0.5- mm gap), site II (1.0-mm gap), and site III (1.4- mm gap), were 4.6 ± 0.4 mm, 4.6 ± 0.8 mm, and The International Journal of Oral & Maxillofacial Implants 355
6 Table 4 Results of Clinical Measurements (mm)* Initial measurements Final measurements Ridge crest to Rim of implant to Depth of Ridge crest to Rim of implant to Residual Site rim of implant bottom of defect defect rim of implant bottom of defect defect Bone fill Control 1.1 ± ± ± ± ± ± ± 0.4 (n=10) Site I 1.4 ± ± ± ± ± ± ± 0.4 (n=10) Site II 2.2 ± ± ± ± ± ± ± 0.8 (n=10) Site III 2.1 ± ± ± ± ± ± ± 0.9 (n=10) *Mean values and standard deviation. Significant difference between sites (P <.001; ANOVA); all pairwise differences were significant except control versus site I and site II versus site III (P <.05; Bonferroni). No significant difference between any sites (P =.22; ANOVA). Figs 3a and 3b Clinical photographs taken at the time of sacrifice after the cover screws were removed. Left to right: control, site I, site II, and site III implants. No residual defect can be observed clinically. All implants were stable when tested with cotton pliers. Amount of bone fill (mm) Control Site I Site II Site III Fig 4 Graph indicating mean amount of clinical bone fill and standard deviation for all sites. 4.9 ± 0.9 mm, respectively (Fig 4). At the time of implant placement, there were significant differences among sites for the distance from the bone crest to the implant rim (P <.001). When residual defect depths were compared, no significant differences were found. Histomorphometric Outcomes. Table 5 summarizes the results of the histomorphometric measurements. When the coronal 4 mm of the implants were examined, the control sites had the highest mean percentage of bone-to-implant contact (38.8%), followed by site I (22.9%), site II (11.0%), and site III (2.7%) (Fig 5). The differences were statistically significant (P <.0001). In the apical 4 mm of the implants, no statistical differences in percentage of bone-to-implant contact were found. When the linear distance from the implant rim to the highest position of direct bone contact was measured, the control sites had the shortest dis- 356 Volume 14, Number 3, 1999
7 Table 5 Results of Histomorphometric Measurements * Percentage of bone to implant contact (%) Distance from rim to highest Site Coronal 4 mm Apical 4 mm point of bone contact (mm) Control (n = 9) 38.8 ± ± ± 0.4 Site I (n = 10) 22.9 ± ± ± 0.8 Site II (n = 10) 11.0 ± ± ± 0.9 Site III (n = 8) 2.7 ± ± ± 0.9 * Mean values and standard deviation. Significant difference between sites (P <.0001; Friedman rank test); all pairwise differences were significant except site I versus site II and site II versus site III (P <.05; Bonferroni). No significant difference (P <.29; Friedman rank test). Significant difference between sites (P <.001; Friedman rank test); all pairwise differences except control versus site I and site II versus site III (P <.05; Bonferroni). Percentage of contact Control Site I Site II Site III Distance (mm) Control Site I Site II Site III Fig 5 Graph indicating mean percentages (and standard deviation) of bone-to-implant contact in the coronal 4 mm of each group of implants. Fig 6 Graph indicating mean distance (and standard deviation) from the implant rim to the highest point of bone contact. tance. This distance increased as the size of the gap increased (Fig 6), with statistically significant differences (P <.001). Descriptive Histology. The control specimens generally had good bone-to-implant contact for the entire implant length (Fig 7). Enlarged marrow spaces (fatty and/or fibrous) were seen in many sections. In control specimens, bone-to-implant contact frequently extended to the implant rim. In many of the test sections, a space occupied by connective tissue was observed between the implant surface and bone. A bundle of connective tissue fibers running parallel to the implant surface separated the bone and the implant. Epithelial cells contacting the implants were not observed in any specimens. In 2 of the implants in the control and 7 in site III, the implants contacted the canine root. In all of these implants, fibrous tissue was observed encapsulating the implants (Fig 8). The formation of cementum on the titanium surface was not observed. Discussion The clinical outcomes of this study demonstrated that in most of the test sites, the defects filled completely with bone. At retrieval, all implants were also clinically immobile. In terms of residual defects, there were no differences between control and test sites. These results corroborate with reports related to bone fill and clinical success associated with implants placed at the time of tooth extraction. 2,4,21 Complete fill of the defect was achieved without the addition of any type of alloplast, allograft, autograft, or barrier membrane. The circumferential defect morphology may have allowed for formation of a more stabilized blood clot, which uneventfully filled with bone. As the gap distance increased, the implants were unintentionally submerged slightly further below the crest. The presence of a defect around the implant at the time of placement made it more difficult for the surgeon to control the depth of The International Journal of Oral & Maxillofacial Implants 357
8 Fig 7 One of the control implants. Bone is in direct contact with the implant up to the rim. Note good boneto-implant contact for the entire length of the implant. Fig 8 Site III implant, which was placed in contact with the canine root (right). Note the complete fibrous encapsulation, without any direct bone-to-implant contact. No cementum is seen on the implant surface. Fig 9 Site II implant. In the coronal portion, where the gap was created at the time of placement, connective tissue can be seen between the implant and bone. In the apical portion of the implant, good bone-to-implant contact is observed. placement. Placing implants slightly below the ridge crest has been suggested as an appropriate procedure for implants placed at the time of extraction 3 and may have positively influenced the results in test sites. At the time of retrieval, mobility could not be detected in any of the implants when they were tested with cotton pliers. However, 9 of 79 implants were not osseointegrated when examined histologically. The failure to detect implant mobility clinically at initial uncovering may be the result of the narrowness of the zone of connective tissue between the bone and the implants (Fig 8). Also, it might have been easier to detect mobility if healing abutments were connected. Adell et al 1 have reported that some implants, which seemed to be integrated at the time of second-stage surgery, developed mobility later. The nonintegrated implants in this study may belong to this category. Histomorphometric measurements were made only in the coronal and apical 4 mm of the implants because in all specimens, the coronal and apical 4 mm were in only the defect or the host bone, respectively. The middle 2 mm were not used for measurement, since this portion of the implant was either in the defect or the host bone, depending on the specimen. By masking the apical or coronal portion during measurement, examiner bias was also minimized. In the coronal 4 mm, bone-to-implant contact ranged between 0 and 71.7%, with the highest mean percentage occurring in controls and the lowest in site III. Of the integrated implants, 1 (5%) in site I, 5 (25%) in site II, and 6 (50%) in site III were found to have absolutely no bone-to-implant contact in the coronal 4 mm (Fig 9). None of the 18 control implants had 0% contact in this area. In this model, the gap at the time of implant placement had a negative effect on bone-to-implant contact, confirming the findings by Carlsson et al, 15 who indicated that histologically, as the initial gap increases, the amount of bone-to-implant contact diminishes. Barzilay et al 22 reported similar percentages of bone-to-implant contact when immediate and control implants in monkeys were compared. In their study, 3.75-mm-diameter implants were placed into extraction sockets of lateral incisors, mesial root sockets of mandibular first molars, distal root sockets of mandibular first premolars, and the palatal root socket of maxillary first molars. This resulted in almost no initial gap between the implants and the host bone. The authors propose 358 Volume 14, Number 3, 1999
9 that the present study model with a defined gap better represents the clinical situation of immediate implant placement. The lack of gap, as well as different experimental animal models and healing, may explain the differing results of this study and other studies. A recently published human case report 23 confirms this decrease in bone-to-implant contact as the initial gap widens. The histologic evaluation of healing apparently conflicted with clinical findings. The controls healed with the smallest distance from the implant rim to the first contact of bone. As the initial gap widened, the first bone contact moved apically, with statistically significant differences related to the initial gap distance. Because the residual defect was narrow (Fig 9), it may be that the residual gaps were not possible to detect clinically. It is important to recognize that the clinical bone fill may not indicate true histologic integration of bone to implant. In the apical 4 mm of the implants, good bone-to-implant contact was observed, with no significant differences between control and test sites. Although the placement of implants was not randomized, the results indicate that in all areas, good bone-to-implant contact could be achieved regardless of the coronal gap. Large marrow spaces were noted in many sections. The significance of this finding is unknown and may be related to the species model. When specimens were observed at higher magnification, no epithelial cells were found in any of the sections. In this model, primary closure of the wound apparently resulted in the exclusion of epithelium without the use of any additional devices. One of the problems with this study is a lack of randomization in the position of implants. Initially, an attempt was made to randomize implant placement; however, when the implants were placed into wide defects created adjacent to the molars, initial stability was very difficult to achieve. This may have been the result of the presence of wide marrow spaces in the molar areas. As a result of this problem, 18 of 20 site III (1.4-mm gap) defects were created adjacent to the mandibular canines. In 9 sites, the implants were inadvertently placed into or very close to the canine roots. Histologic evaluation demonstrated that when the implants contacted the root surface, connective tissue always interposed between the implants and adjacent bone, resulting in lack of osseointegration (Fig 8). These findings differ somewhat from those reported by others, 24 who found cementum deposited onto titanium plasma-sprayed implant surfaces when the implants were placed in close approximation to root surfaces. Conclusions In this study, titanium implants were placed into simulated extraction socket defects of varying gap width (0 to 1.4 mm); they healed with complete clinical bone fill, and the initial gap width did not influence the stability of the implants at the time of retrieval. When healing was examined histologically in the coronal 4 mm of implant, however, the percentage of bone-to-implant contact diminished as the gap distance increased. Additionally, the highest point of bone-to-implant contact moved apically as the initial gap widened, but the coronal gap did not influence bone-to-implant contact in the apical 4 mm of any implant. Intimate contact between bone and implant at the time of placement seems to be an important factor in obtaining maximum bone-to-implant contact following healing. The clinical significance of these findings for long-term implant stability requires further investigation. Acknowledgments The authors would like to thank Dr Frank Roberts for the generous use of his time and facilities for this study. The authors would like to acknowledge the expert help of research assistant Hari Prasad and senior histology technician Towm Sprowl of the Hard Tissue Research Laboratory at the University of Oklahoma. The authors would also like to thank Nobel Biocare for providing implant components. This study was supported in part by the Osseointegration Foundation Implant Research Grant and the Hack Endowment of the Department of Periodontics, University of Washington. References 01. Adell R, Eriksson B, Lekholm U, Brånemark P-I, Jemt T. Long-term follow-up study of osseointegrated implants in the treatment of totally edentulous jaws. Int J Oral Maxillofac Implants 1990;5: Lazzara RJ. Immediate implant placement into extraction sites: Surgical and restorative advantages. Int J Periodontics Restorative Dent 1989;9: Becker W, Dahlin C, Becker BE, Lekholm U, van Steenberghe D, Higuchi K, Kultje C. The use of e-ptfe barrier membranes for bone promotion around titanium implants placed into extraction sockets: A prospective multicenter study. Int J Oral Maxillofac Implants 1994;9: Becker W, Becker BE, Polizzi G, Bergström C. Autogenous bone grafting of bone defects adjacent to implants placed into immediate extraction sockets in patients: A prospective study. Int J Oral Maxillofac Implants 1994;9: Rosenquist B, Grenthe B. Immediate placement of implants into extraction sockets: implant survival. Int J Oral Maxillofac Implants 1996;11: Becker BE, Becker W, Ricci A, Geurs N. A prospective clinical trial of endosseous screw-shaped implants placed at the time of tooth extraction without augmentation. J Periodontol 1998;69: The International Journal of Oral & Maxillofacial Implants 359
10 07. Brägger U, Hammerle CH, Lang NP. Immediate transmucosal implants using the principle of guided tissue regeneration (II). A cross-sectional study comparing the clinical outcome 1 year after immediate to standard implant placement. Clin Oral Implants Res 1996;7: Lang NP, Brägger U, Hammerle CH, Sutter F. Immediate transmucosal implants using the principle of guided tissue regeneration. I. Rationale, clinical procedures and 30- month results. Clin Oral Implants Res 1994;5: Augthun M, Yildirim M, Spiekermann H, Biesterfeld S. Healing of bone defects in combination with immediate implants using the membrane technique. Int J Oral Maxillofac Implants 1995;10: Gher ME, Quintero G, Assad D, Monaco E, Richardson AC. Bone grafting and guided bone regeneration for immediate dental implants in humans. J Periodontol 1994;65: Shanaman RH. A retrospective study of 237 sites treated consecutively with guided tissue regeneration. Int J Periodontics Restorative Dent 1994;14: Gelb DA. Immediate implant surgery: Three-year retrospective evaluation of 50 consecutive cases. Int J Oral Maxillofac Implants 1993;8: Watzek G, Haider R, Mensdorff-Pouilly N, Haas R. Immediate and delayed implantation for complete restoration of the jaw following extraction of all residual teeth: A retrospective study comparing different types of serial immediate implantation. Int J Oral Maxillofac Implants 1995;10: Block MS, Kent JN. Placement of endosseous implants into tooth extraction sites. J Oral Maxillofac Surg 1991;49: Carlsson L, Rostlund T, Albrektsson B, Albrektsson T. Implant fixation improved by close fit. Cylindrical implantbone interface studied in rabbits. Acta Orthop Scand 1988; 59: Knox R, Caudill R, Meffert R. Histologic evaluation of dental endosseous implants placed in surgically created extraction defects. Int J Periodontics Restorative Dent 1991;11: Stentz WC, Mealey BL, Nummikoski PV, Gunsolley JC, Waldrop TC. Effects of guided bone regeneration around commercially pure titanium and hydroxyapatite-coated dental implants. I. Radiographic analysis. J Periodontol 1997;68: Stentz WC, Mealey BL, Gunsolley JC, Waldrop TC. Effects of guided bone regeneration around commercially pure titanium and hydroxyapatite-coated dental implants. II. Histologic analysis. J Periodontol 1997;68: Donath K, Breuner G. A method for the study of undecalcified bones and teeth with attached soft tissues. The Sage- Schliff (sawing and grinding) technique. J Oral Pathol 1982;11: Rohrer MD, Schubert CC. The cutting-grinding technique for histologic preparation of undecalcified bone and boneanchored implants. Improvements in instrumentation and procedures. Oral Surg Oral Med Oral Pathol 1992;74: Becker W, Urist M, Becker BE, Jackson W, Parry DA, Bartold M, et al. Clinical and histologic observations of sites implanted with intraoral autologous bone grafts or allografts. 15 human case reports. J Periodontol 1996;67: Barzilay I, Graser GN, Iranpour B, Natiella JR, Proskin HM. Immediate implantation of pure titanium implants into extraction sockets of Macaca fascicularis. Part II: Histologic observations. Int J Oral Maxillofac Implants 1996; 11: Wilson TG, Schenk R, Buser D, Cochran D. Implants placed in immediate extraction sites: A report of histologic and histometric analyses of human biopsies. Int J Oral Maxillofac Implants 1998;13: Buser D, Warrer K, Karring T. Formation of a periodontal ligament around titanium implants. J Periodontol 1990;61: Volume 14, Number 3, 1999
Osseointegrated dental implant treatment generally
 Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION
 Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
Case Study. Case # 1 Author: Dr. Suheil Boutros (USA) 2013 Zimmer Dental, Inc. All rights reserved. 6557, Rev. 03/13.
 Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
The surgical placement of dental implants has
 Flapless Implant Surgery: A 10-year Clinical Retrospective Analysis Luis Dominguez Campelo, DDS 1 /Jose R. Dominguez Camara, MD, DDS 2 Purpose: This article is a retrospective clinical analysis of implants
Flapless Implant Surgery: A 10-year Clinical Retrospective Analysis Luis Dominguez Campelo, DDS 1 /Jose R. Dominguez Camara, MD, DDS 2 Purpose: This article is a retrospective clinical analysis of implants
Years of research and advancement in
 Immediate Implants with Guided Bone Regeneration Using Titanium Mesh and Alloplast in an Infected Site: A Case Report Mahesh et al Dr. Lanka Mahesh 1 Dr. Ajay Bibra 2 Dr. Vishal Gupta 3 Abstract Years
Immediate Implants with Guided Bone Regeneration Using Titanium Mesh and Alloplast in an Infected Site: A Case Report Mahesh et al Dr. Lanka Mahesh 1 Dr. Ajay Bibra 2 Dr. Vishal Gupta 3 Abstract Years
Successful Bone Formation at Immediate Transmucosal Implants: A Clinical Report
 Successful Bone Formation at Immediate Transmucosal Implants: A Clinical Report Christoph H.F. Hämmerle, PD Dr med dent*/urs Brägger, Prof Dr med dent*/ Bruno Schmid, Dr med dent**/niklaus P. Lang, Prof
Successful Bone Formation at Immediate Transmucosal Implants: A Clinical Report Christoph H.F. Hämmerle, PD Dr med dent*/urs Brägger, Prof Dr med dent*/ Bruno Schmid, Dr med dent**/niklaus P. Lang, Prof
Dental Implants: A Predictable Solution for Tooth Loss. Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor
 Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
Endosseous cylindric implants are well accepted
 Soft Tissue Exposure of Endosseous Implants Between Stage I and Stage II Surgery as a Potential Indicator of Early Crestal Bone Loss Joseph A. Toljanic, DDS*/Mark L. Banakis, DDS**/Leslee A. K. Willes,
Soft Tissue Exposure of Endosseous Implants Between Stage I and Stage II Surgery as a Potential Indicator of Early Crestal Bone Loss Joseph A. Toljanic, DDS*/Mark L. Banakis, DDS**/Leslee A. K. Willes,
Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs
 Current Applied Physics 5 (2005) 507 511 www.elsevier.com/locate/cap Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs Ui-Won Jung a, Hee-Il
Current Applied Physics 5 (2005) 507 511 www.elsevier.com/locate/cap Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs Ui-Won Jung a, Hee-Il
There is a paucity of postmortem histologic
 Postmortem Histologic Evaluation of Mandibular Titanium and Maxillary Hydroxyapatite-Coated Implants from 1 Patient Michael D. Rohrer, DDS, MS*/Randall R. Sobczak, DDS, FAGD**/ Hari S. Prasad, BS, MDT***/Harold
Postmortem Histologic Evaluation of Mandibular Titanium and Maxillary Hydroxyapatite-Coated Implants from 1 Patient Michael D. Rohrer, DDS, MS*/Randall R. Sobczak, DDS, FAGD**/ Hari S. Prasad, BS, MDT***/Harold
Case Report. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
 Case Report RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
Case Report RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
Immediate implant placement in the Title central incisor region: a case repo. Journal Journal of prosthodontic research,
 Immediate implant placement in the Title central incisor region: a case repo Author(s) Sekine, H; Taguchi, T; Yamagami, M; Alternative Takanashi, T; Furuya, K Journal Journal of prosthodontic research,
Immediate implant placement in the Title central incisor region: a case repo Author(s) Sekine, H; Taguchi, T; Yamagami, M; Alternative Takanashi, T; Furuya, K Journal Journal of prosthodontic research,
BONE AUGMENTATION AND GRAFTING
 1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
Implant Placement in Maxillary Anterior Region Along with Soft and Hard Tissue Grafting- A Case Report.
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 10 Ver. XII (October. 2016), PP 68-73 www.iosrjournals.org Implant Placement in Maxillary Anterior
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 10 Ver. XII (October. 2016), PP 68-73 www.iosrjournals.org Implant Placement in Maxillary Anterior
The Brånemark osseointegration method, using titanium dental implants (fixtures)
 Early Failures in 4,641 Consecutively Placed Brånemark Dental Implants: A Study From Stage 1 Surgery to the Connection of Completed Prostheses Bertil Friberg, DDS/Torsten Jemt, DDS, PhD/Ulf Lekholm, DDS,
Early Failures in 4,641 Consecutively Placed Brånemark Dental Implants: A Study From Stage 1 Surgery to the Connection of Completed Prostheses Bertil Friberg, DDS/Torsten Jemt, DDS, PhD/Ulf Lekholm, DDS,
Identification of Stability Changes for Immediately Placed Dental Implants
 Identification of Stability Changes for Immediately Placed Dental Implants Jason D. West, DDS, MS 1 /Thomas W. Oates, DMD, PhD 2 Purpose: To evaluate the changes in stability of immediately placed implants
Identification of Stability Changes for Immediately Placed Dental Implants Jason D. West, DDS, MS 1 /Thomas W. Oates, DMD, PhD 2 Purpose: To evaluate the changes in stability of immediately placed implants
The healing of an extraction socket often produces
 Immediate One-Stage Postextraction Implant: A Human Clinical and Histologic Case Report Roberto Cornelini, MD, DDS 1 /Antonio Scarano, DDS 2 /Ugo Covani, MD, DDS 3 / Giovanna Petrone, DDS 2 /Adriano Piattelli,
Immediate One-Stage Postextraction Implant: A Human Clinical and Histologic Case Report Roberto Cornelini, MD, DDS 1 /Antonio Scarano, DDS 2 /Ugo Covani, MD, DDS 3 / Giovanna Petrone, DDS 2 /Adriano Piattelli,
Dental Implant Treatment with Diffe Title for Sinus Floor Elevation-A Case Re. Sekine, H; Taguchi, T; Seta, S; Tak Author(s) T; Kakizawa, T
 Dental Implant Treatment with Diffe Title for Sinus Floor Elevation-A Case Re Sekine, H; Taguchi, T; Seta, S; Tak Author(s) T; Kakizawa, T Journal Bulletin of Tokyo Dental College, 4 URL http://hdl.handle.net/10130/200
Dental Implant Treatment with Diffe Title for Sinus Floor Elevation-A Case Re Sekine, H; Taguchi, T; Seta, S; Tak Author(s) T; Kakizawa, T Journal Bulletin of Tokyo Dental College, 4 URL http://hdl.handle.net/10130/200
Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis
 CASE REPORT Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis Dr Ashish Yadav 1, Dr Aratee Gupta 2, Dr Archana Singh 3, 1,3-
CASE REPORT Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis Dr Ashish Yadav 1, Dr Aratee Gupta 2, Dr Archana Singh 3, 1,3-
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 3 Influence of the 3-D Bone-to-Implant Relationship on Esthetics Ueli Grunder, DMD* Stefano Gracis, DMD** Matteo Capelli, DMD** There are
The International Journal of Periodontics & Restorative Dentistry 3 Influence of the 3-D Bone-to-Implant Relationship on Esthetics Ueli Grunder, DMD* Stefano Gracis, DMD** Matteo Capelli, DMD** There are
Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports
 0 Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports R.G. Caffesse, B.A. Smith/ B. Duff, E.C. Morrison, D. Merrill/ and W. Becker In the cases reported here, the response
0 Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports R.G. Caffesse, B.A. Smith/ B. Duff, E.C. Morrison, D. Merrill/ and W. Becker In the cases reported here, the response
Endosseous dental implants initially showed very
 Five-mm-Diameter Implants without a Smooth Surface Collar: Report on 98 Consecutive Placements Franck Renouard, DDS*/Jean-Pierre Arnoux, DDS**/David P. Sarment, DDS*** In recent years, indications for
Five-mm-Diameter Implants without a Smooth Surface Collar: Report on 98 Consecutive Placements Franck Renouard, DDS*/Jean-Pierre Arnoux, DDS**/David P. Sarment, DDS*** In recent years, indications for
Vertical and Horizontal Augmentation Using Guided Bone Regeneration. Ph.D. Thesis. Dr. med. dent. et univ. Istvan Urban
 Vertical and Horizontal Augmentation Using Guided Bone Regeneration Ph.D. Thesis Dr. med. dent. et univ. Istvan Urban Supervisor: Prof. Dr. Katalin Nagy, DDS, PhD Faculty of Dentistry, University of Szeged
Vertical and Horizontal Augmentation Using Guided Bone Regeneration Ph.D. Thesis Dr. med. dent. et univ. Istvan Urban Supervisor: Prof. Dr. Katalin Nagy, DDS, PhD Faculty of Dentistry, University of Szeged
During the last 30 years, endosseous oral
 Influence of Variations in Implant Diameters: A 3- to 5-Year Retrospective Clinical Report Carl-Johan Ivanoff, DDS*/Kerstin Gröndahl, DDS, PhD**/Lars Sennerby, DDS, PhD***/ Christina Bergström, MSc****/Ulf
Influence of Variations in Implant Diameters: A 3- to 5-Year Retrospective Clinical Report Carl-Johan Ivanoff, DDS*/Kerstin Gröndahl, DDS, PhD**/Lars Sennerby, DDS, PhD***/ Christina Bergström, MSc****/Ulf
Treatment planning in a case of restoration of the maxilla and mandible using osseointegrated implants with four types of bone graft
 227 Journal of Oral Science, Vol. 45, No. 4, 227-232, 2003 Case report Treatment planning in a case of restoration of the maxilla and mandible using osseointegrated implants with four types of bone graft
227 Journal of Oral Science, Vol. 45, No. 4, 227-232, 2003 Case report Treatment planning in a case of restoration of the maxilla and mandible using osseointegrated implants with four types of bone graft
Factors influencing ridge alterations following immediate implant placement into extraction sockets
 Jorge Ferrus Denis Cecchinato E. Bjarni Pjetursson Niklaus P. Lang Mariano Sanz Jan Lindhe Factors influencing ridge alterations following immediate implant placement into extraction sockets Authors affiliations:
Jorge Ferrus Denis Cecchinato E. Bjarni Pjetursson Niklaus P. Lang Mariano Sanz Jan Lindhe Factors influencing ridge alterations following immediate implant placement into extraction sockets Authors affiliations:
Esthetic management of multiple missing anterior teeth A Case report
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 13, Issue 1 Ver. II (Jan. 2014), PP 97-101 Esthetic management of multiple missing anterior teeth A
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 13, Issue 1 Ver. II (Jan. 2014), PP 97-101 Esthetic management of multiple missing anterior teeth A
An osseointegrated oral implant is characterized
 Mobility Assessment with the Periotest System in Relation to Histologic Findings of Oral Implants Flemming Isidor, DDS, PhD, Dr Odont* The relationship between mobility assessment with the Periotest system
Mobility Assessment with the Periotest System in Relation to Histologic Findings of Oral Implants Flemming Isidor, DDS, PhD, Dr Odont* The relationship between mobility assessment with the Periotest system
GBR membrane for ideal regeneration
 GBR membrane for ideal regeneration 1) i-gen Lingual Extension should be considered for a large defect. Need to have at least 1mm of space above the platform of a fixture: Make this space with a pre-existing
GBR membrane for ideal regeneration 1) i-gen Lingual Extension should be considered for a large defect. Need to have at least 1mm of space above the platform of a fixture: Make this space with a pre-existing
Narrow-diameter implants in premolar and molar areas
 2 Long-term follow-up of 2.5mm NDIs supporting a fixed prosthesis Narrow-diameter implants in premolar and molar areas EDUARDO ANITUA, DDS, MD, PHD¹,² A narrow-diameter implant (NDI) is an implant with
2 Long-term follow-up of 2.5mm NDIs supporting a fixed prosthesis Narrow-diameter implants in premolar and molar areas EDUARDO ANITUA, DDS, MD, PHD¹,² A narrow-diameter implant (NDI) is an implant with
Contemporary Implant Dentistry
 Contemporary Implant Dentistry C H A P T ER 1 4 O F C O N T E M P OR A R Y O R A L A N D M A X I L L OFA C IA L S U R G E RY B Y : D R A R A S H K H O J A S T EH Dental implant is suitable for: completely
Contemporary Implant Dentistry C H A P T ER 1 4 O F C O N T E M P OR A R Y O R A L A N D M A X I L L OFA C IA L S U R G E RY B Y : D R A R A S H K H O J A S T EH Dental implant is suitable for: completely
Purpose: To assess the long term survival of sites treated by GTR.
 Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report
 C A S E R E P O R T Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report Rhoodie Garrana 1 and Govindrau Mohangi
C A S E R E P O R T Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report Rhoodie Garrana 1 and Govindrau Mohangi
Masking Buccal Plate Remodeling in the Esthetic Zone with Connective Tissue Grafts: Concepts and Techniques with Immediate Implants
 Peer-Reviewed and Indexed Annual Implant Issue Masking Buccal Plate Remodeling in the Esthetic Zone with Connective Tissue Grafts: Concepts and Techniques with Immediate Implants of Continuing Education
Peer-Reviewed and Indexed Annual Implant Issue Masking Buccal Plate Remodeling in the Esthetic Zone with Connective Tissue Grafts: Concepts and Techniques with Immediate Implants of Continuing Education
The Influence of Controlled Occlusal Overload on Peri-implant Tissue. Part 3: A Histologic Study in Monkeys
 The Influence of Controlled Occlusal Overload on Peri-implant Tissue. Part 3: A Histologic Study in Monkeys Takashi Miyata, DDS, DDSc 1 /Yukinao Kobayashi, DDS 2 /Hisao Araki, DDS, DDSc 3 / Takaichi Ohto,
The Influence of Controlled Occlusal Overload on Peri-implant Tissue. Part 3: A Histologic Study in Monkeys Takashi Miyata, DDS, DDSc 1 /Yukinao Kobayashi, DDS 2 /Hisao Araki, DDS, DDSc 3 / Takaichi Ohto,
The anatomic limitations of the. Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD*
 CASE REPORT Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD* The anatomic limitations of the residual alveolar bone may cause problems for
CASE REPORT Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD* The anatomic limitations of the residual alveolar bone may cause problems for
Dental implants offer a predictable treatment
 Histologic evaluation of a 12-year-old threaded hydroxyapatite-coated implant placed in conjunction with subantral augmentation procedure: A clinical report Periklis Proussaefs, DDS, MS, a Henry-Savajol
Histologic evaluation of a 12-year-old threaded hydroxyapatite-coated implant placed in conjunction with subantral augmentation procedure: A clinical report Periklis Proussaefs, DDS, MS, a Henry-Savajol
The majority of the early research concerning
 Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report
 Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
GBR membrane for ideal regeneration. i-gen TM. 2mm. >2.5mm. Lingual Extension. >100 blunt angle
 REGENERATION 02/03 Design Concept GBR membrane for ideal regeneration i-gen TM Description Single A type Small IG1W4509 Single A type Regular IG1W5510 Single A type Wide IG1W6511 Single B type Small IG2W0918
REGENERATION 02/03 Design Concept GBR membrane for ideal regeneration i-gen TM Description Single A type Small IG1W4509 Single A type Regular IG1W5510 Single A type Wide IG1W6511 Single B type Small IG2W0918
Rigid Fixation by Means of Titanium Mesh in Edentulous Ridge Expansion for Horizontal Ridge Augmentation in the Maxilla
 Rigid Fixation by Means of Titanium Mesh in Edentulous Ridge Expansion for Horizontal Ridge Augmentation in the Maxilla Luciano Malchiodi, MD, DDS*/Antonio Scarano, DDS**/Manlio Quaranta, MD, DDS***/ Adriano
Rigid Fixation by Means of Titanium Mesh in Edentulous Ridge Expansion for Horizontal Ridge Augmentation in the Maxilla Luciano Malchiodi, MD, DDS*/Antonio Scarano, DDS**/Manlio Quaranta, MD, DDS***/ Adriano
The International Journal of Periodontics & Restorative Dentistry
 The nternational Journal of Periodontics & Restorative Dentistry 2009 BY QUNTESSENCE PUBLSHNG CO, NC. PRNTNG OF THS DOCUMENT S RESTRCTED TO PERSONAL USE ONLY. NO PART OF THS ARTCLE 549 Time Sequence of
The nternational Journal of Periodontics & Restorative Dentistry 2009 BY QUNTESSENCE PUBLSHNG CO, NC. PRNTNG OF THS DOCUMENT S RESTRCTED TO PERSONAL USE ONLY. NO PART OF THS ARTCLE 549 Time Sequence of
Clinical Perspectives
 Clinical Perspectives Inside This Issue: Revised Drilling Guidelines For Parallel Walled Implants Case Presentation By: Pär-Olov Östman, DDS, PhD, MD Volume 8, Issue 1 Recommended Drilling Guidelines For
Clinical Perspectives Inside This Issue: Revised Drilling Guidelines For Parallel Walled Implants Case Presentation By: Pär-Olov Östman, DDS, PhD, MD Volume 8, Issue 1 Recommended Drilling Guidelines For
Periimplant Regeneration Fenestration
 Indication Sheet PIR Periimplant Regeneration Fenestration Treatment concept of Dr. Jean-Pierre Gardella (surgeon) and Dr. Christian Richelme (prosthodontist), Marseille, France > Filling of a peri-implant
Indication Sheet PIR Periimplant Regeneration Fenestration Treatment concept of Dr. Jean-Pierre Gardella (surgeon) and Dr. Christian Richelme (prosthodontist), Marseille, France > Filling of a peri-implant
Management of a complex case
 2 Soft- and hard-tissue reconstruction of a severely deficient site prior to implant placement: a case report Management of a complex case Younes Khosroshahy, DDS, MFDS RCS (Eng), Dip Imp Dent RCSEd, Blue
2 Soft- and hard-tissue reconstruction of a severely deficient site prior to implant placement: a case report Management of a complex case Younes Khosroshahy, DDS, MFDS RCS (Eng), Dip Imp Dent RCSEd, Blue
Advanced Probing Techniques
 Module 21 Advanced Probing Techniques MODULE OVERVIEW The clinical periodontal assessment is one of the most important functions performed by dental hygienists. This module begins with a review of the
Module 21 Advanced Probing Techniques MODULE OVERVIEW The clinical periodontal assessment is one of the most important functions performed by dental hygienists. This module begins with a review of the
Enhancing implant stability with osseodensification a case report with 2-year follow-up
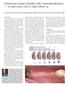 Enhancing implant stability with osseodensification a case report with 2-year follow-up Dr. Salah Huwais discusses how osseodensification facilitates ridge expansion with enhanced implant stability Introduction
Enhancing implant stability with osseodensification a case report with 2-year follow-up Dr. Salah Huwais discusses how osseodensification facilitates ridge expansion with enhanced implant stability Introduction
Alveolar Ridge Preservation:
 Alveolar Ridge Preservation: Preserving and Building up the Bony Structures after Extraction» By: Prof. Roland Hille Konigsallee 49c, 41747 Viersen, Germany E-mail: dr-hille@t-online.de» Prof. Rolf Vollmer
Alveolar Ridge Preservation: Preserving and Building up the Bony Structures after Extraction» By: Prof. Roland Hille Konigsallee 49c, 41747 Viersen, Germany E-mail: dr-hille@t-online.de» Prof. Rolf Vollmer
Evaluation of implant stability and crestal bone loss around the implant prior to prosthetic loading: A six month study
 Original Article Evaluation of implant stability and crestal bone loss around the implant prior to prosthetic loading: A six month study P. Singh, H. G. Garge*, V. S. Parmar, M. Viswambaran*, M. M. Goswami*
Original Article Evaluation of implant stability and crestal bone loss around the implant prior to prosthetic loading: A six month study P. Singh, H. G. Garge*, V. S. Parmar, M. Viswambaran*, M. M. Goswami*
Socket preservation using deproteinized horsederived
 Research Article J Periodontal Implant Sci 2010;40:227-231 doi: 10.5051/jpis.2010.40.5.227 Socket preservation using deproteinized horsederived bone mineral Jang-Yeol Park, Ki-Tae Koo, Tae-Il Kim, Yang-Jo
Research Article J Periodontal Implant Sci 2010;40:227-231 doi: 10.5051/jpis.2010.40.5.227 Socket preservation using deproteinized horsederived bone mineral Jang-Yeol Park, Ki-Tae Koo, Tae-Il Kim, Yang-Jo
The Sandwich Bone Augmentation Technique. Jia-Hui Fu* and Hom-Lay Wang*
 CASE REPORT The Sandwich Bone Augmentation Technique Jia-Hui Fu* and Hom-Lay Wang* Introduction: Horizontal ridge width reduction after tooth extraction is a common clinical scenario. As such, when implant-supported
CASE REPORT The Sandwich Bone Augmentation Technique Jia-Hui Fu* and Hom-Lay Wang* Introduction: Horizontal ridge width reduction after tooth extraction is a common clinical scenario. As such, when implant-supported
Surgery All at Once : Socket preservation and immediate placement of an implant in an infected site in the anterior region a Case Report
 Surgery All at Once : Socket preservation and immediate placement of an implant in an infected site in the anterior region a Case Report W.P. van der Schoor*, A.R.M. van der Schoor Tooth extraction followed
Surgery All at Once : Socket preservation and immediate placement of an implant in an infected site in the anterior region a Case Report W.P. van der Schoor*, A.R.M. van der Schoor Tooth extraction followed
Platform switching for marginal bone preservation around dental implants: a systematic review and meta-analysis.
 Platform switching for marginal bone preservation around dental implants: a systematic review and meta-analysis. Atieh MA, Ibrahim HM, Atieh AH. J Periodontol. 2010 Oct;81(10):1350-66. BACKGROUND: Platform
Platform switching for marginal bone preservation around dental implants: a systematic review and meta-analysis. Atieh MA, Ibrahim HM, Atieh AH. J Periodontol. 2010 Oct;81(10):1350-66. BACKGROUND: Platform
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Case Report The Socket Science of Immediate Implants - Case Report Sanjay Kaul 1**, Shantipriya Reddy 2*, Soumya Kambali
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Case Report The Socket Science of Immediate Implants - Case Report Sanjay Kaul 1**, Shantipriya Reddy 2*, Soumya Kambali
One-year Re-entry Results of Guided Bone Regeneration around Immediately Placed Implants with Immediate or Conventional Loading: A Case Series
 Journal of the International Academy of Periodontology 2012 14/3:62-68 One-year Re-entry Results of Guided Bone Regeneration around Immediately Placed Implants with Immediate or Conventional Loading: A
Journal of the International Academy of Periodontology 2012 14/3:62-68 One-year Re-entry Results of Guided Bone Regeneration around Immediately Placed Implants with Immediate or Conventional Loading: A
Extraction with Immediate Implant Placement and Ridge Preservation in the Posterior
 Extraction with Immediate Implant Placement and Ridge Preservation in the Posterior by Timothy F. Kosinski, DDS, MAGD The following case presentation illustrates the diagnosis, planning and treatment for
Extraction with Immediate Implant Placement and Ridge Preservation in the Posterior by Timothy F. Kosinski, DDS, MAGD The following case presentation illustrates the diagnosis, planning and treatment for
The influence of radiotherapy on osseointegration
 Experience with Osseointegrated Implants Placed in Irradiated Tissues in Japan and the United States Atsushi Niimi, DDS, DMSc*/Minoru Ueda, DDS, PhD**/ Eugene E. Keller, DDS, PhD***/Philip Worthington,
Experience with Osseointegrated Implants Placed in Irradiated Tissues in Japan and the United States Atsushi Niimi, DDS, DMSc*/Minoru Ueda, DDS, PhD**/ Eugene E. Keller, DDS, PhD***/Philip Worthington,
Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Abstract Purpose: Materials and methods Results:
 Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Bum-Soo Kim 1, Young-Kyun Kim 1, Pil-Young Yun 1, Yang-Jin Lee 2, Hyo-Jeong Lee 3, Su-Gwan Kim 4 1Department of
Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Bum-Soo Kim 1, Young-Kyun Kim 1, Pil-Young Yun 1, Yang-Jin Lee 2, Hyo-Jeong Lee 3, Su-Gwan Kim 4 1Department of
Developing Keratinized Mucosa Around Nonsubmerged Dental Implants. Part I: The Use of Vascularized Flaps
 CLINICAL AND RESEARCH REPORTS Developing Keratinized Mucosa Around Nonsubmerged Dental Implants. Part I: The Use of Vascularized Flaps Jay R. Beagle Despite the continued debate regarding the need for
CLINICAL AND RESEARCH REPORTS Developing Keratinized Mucosa Around Nonsubmerged Dental Implants. Part I: The Use of Vascularized Flaps Jay R. Beagle Despite the continued debate regarding the need for
Annals of Dental Research
 P a g e 1 ADR 7 (1), 1-6, 2017 Journal Homepage: www.hgpub.com/ojs2/index.php/adr Direct Sinus Lift with Putty Alloplastic Bone Substitute for Simultaneous Implant Placement A Case Report Chander Prakash*,
P a g e 1 ADR 7 (1), 1-6, 2017 Journal Homepage: www.hgpub.com/ojs2/index.php/adr Direct Sinus Lift with Putty Alloplastic Bone Substitute for Simultaneous Implant Placement A Case Report Chander Prakash*,
Clinical Case Reports using Cytoplast GTR Barrier Membranes
 Clinical Case Reports using Cytoplast GTR Barrier Membranes Barry K. Bartee, DDS, MD The Cytoplast Technique: Extraction Site Grafting Without Primary Closure 1. 1. Preoperative view. To maximize the result
Clinical Case Reports using Cytoplast GTR Barrier Membranes Barry K. Bartee, DDS, MD The Cytoplast Technique: Extraction Site Grafting Without Primary Closure 1. 1. Preoperative view. To maximize the result
The International Journal of Periodontics & Restorative Dentistry
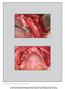 The International Journal of Periodontics & Restorative Dentistry 141 Screw Spreading: Technical Considerations and Case Report Renato Sussumu Nishioka, DDS, PhD, MSc* Alberto Noriyuki Kojima, DDS, PhD,
The International Journal of Periodontics & Restorative Dentistry 141 Screw Spreading: Technical Considerations and Case Report Renato Sussumu Nishioka, DDS, PhD, MSc* Alberto Noriyuki Kojima, DDS, PhD,
Periimplant Regeneration Fenestration
 Indication Sheet PIR-1 Periimplant Regeneration Fenestration Treatment concept of Dr. Jean-Pierre Gardella (surgeon) and Dr. Christian Richelme (prosthodontist), Marseille, France > Filling of a peri-implant
Indication Sheet PIR-1 Periimplant Regeneration Fenestration Treatment concept of Dr. Jean-Pierre Gardella (surgeon) and Dr. Christian Richelme (prosthodontist), Marseille, France > Filling of a peri-implant
CASE REPORT MEGAGEN IMPLANT. AnyRidge. CLINICAL CASE REPORT Davide Farronato, DDs, PhD, PD, AP
 AnyRidge CLINICAL CASE REPORT Davide Farronato, DDs, PhD, PD, AP AnyRidge Clinical Case Ⅰ. Dr. Davide Farronato Baseline - fractured tooth Baseline - fractured tooth #25 Rx view Atraumatic avulsion technique
AnyRidge CLINICAL CASE REPORT Davide Farronato, DDs, PhD, PD, AP AnyRidge Clinical Case Ⅰ. Dr. Davide Farronato Baseline - fractured tooth Baseline - fractured tooth #25 Rx view Atraumatic avulsion technique
Immediate Implant Placement:
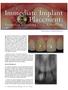 Immediate Implant Placement: Parameters Influencing Tissue Remodeling Bernard Touati, DDS and Mario Groisman, DDS In esthetic implant therapy, the patient s objective is to obtain an imperceptible, natural-looking
Immediate Implant Placement: Parameters Influencing Tissue Remodeling Bernard Touati, DDS and Mario Groisman, DDS In esthetic implant therapy, the patient s objective is to obtain an imperceptible, natural-looking
Bone Reduction Surgical Guide for the Novum Implant Procedure: Technical Note
 Bone Reduction Surgical Guide for the Novum Implant Procedure: Technical Note Stephen M. Parel, DDS 1 /Steven L. Ruff, CDT 2 /R. Gilbert Triplett, DDS, PhD 3 /Sterling R. Schow, DMD 4 The Novum System
Bone Reduction Surgical Guide for the Novum Implant Procedure: Technical Note Stephen M. Parel, DDS 1 /Steven L. Ruff, CDT 2 /R. Gilbert Triplett, DDS, PhD 3 /Sterling R. Schow, DMD 4 The Novum System
In 1981, Dr. Albrektsson, a member of
 Osseodensification facilitates ridge expansion with enhanced implant stability in the maxilla: part II case report with 2-year follow-up Drs. Ann Marie Hofbauer and Salah Huwais offer another case study
Osseodensification facilitates ridge expansion with enhanced implant stability in the maxilla: part II case report with 2-year follow-up Drs. Ann Marie Hofbauer and Salah Huwais offer another case study
SalvinOss Xenograft Bone Graft Material In Vivo Testing Summary
 SalvinOss Xenograft Bone Graft Material In Vivo Testing Summary Summary of In Vivo Use Of Bioresorbable Xenograft Bone Graft Materials In The Treatment Of One-Walled Intrabony Defects In A Canine Model
SalvinOss Xenograft Bone Graft Material In Vivo Testing Summary Summary of In Vivo Use Of Bioresorbable Xenograft Bone Graft Materials In The Treatment Of One-Walled Intrabony Defects In A Canine Model
The Use of Alpha-Bio Tec's Narrow NeO Implants with Cone Connection for Restoration of Limited Width Ridges
 Case Study 48 The Use of Alpha-Bio Tec's Narrow NeO Implants with Cone Connection for Restoration of Limited Width Ridges Dr. Amir Gazmawe DMD, Specialist in Prosthodontics, Israel Dr. Amir Gazmawe graduated
Case Study 48 The Use of Alpha-Bio Tec's Narrow NeO Implants with Cone Connection for Restoration of Limited Width Ridges Dr. Amir Gazmawe DMD, Specialist in Prosthodontics, Israel Dr. Amir Gazmawe graduated
Successful osseointegration of implants has been
 Therapeutic Management for Immediate Implant Placement in Sites with Periapical Deficiencies Where Coronal Bone Is Present: Technique and Case Report Cyril I. Evian, DMD 1 /Ahmed Al-Momani, BDS 2 /Edwin
Therapeutic Management for Immediate Implant Placement in Sites with Periapical Deficiencies Where Coronal Bone Is Present: Technique and Case Report Cyril I. Evian, DMD 1 /Ahmed Al-Momani, BDS 2 /Edwin
Sinus elevation with short implant
 Sinus elevation with short implant Authors: Prof. Dr Mauro Marincola, Prof. Dr Dr Rolf Ewers, Prof. Giorgio Lombardo (University of Verona) & Prof. Miguel Simancas Pallares (University of Cartagena), Austria/Italy/Colombia
Sinus elevation with short implant Authors: Prof. Dr Mauro Marincola, Prof. Dr Dr Rolf Ewers, Prof. Giorgio Lombardo (University of Verona) & Prof. Miguel Simancas Pallares (University of Cartagena), Austria/Italy/Colombia
Limited bone availability makes implant placement challenging
 Bone Grafting: Essential Indications and Techniques in Implant Dentistry Limited bone availability makes implant placement challenging and sometimes unpredictable. Candidates for implant therapy must have
Bone Grafting: Essential Indications and Techniques in Implant Dentistry Limited bone availability makes implant placement challenging and sometimes unpredictable. Candidates for implant therapy must have
Ridge Split Procedure
 Ridge Split Procedure in the Atrophic Maxilla Udatta Kher B.D.S., M.D.S. Loss of teeth causes extensive resorption of the alveolar ridge. In the maxilla the resorption pattern occurs towards the midline,
Ridge Split Procedure in the Atrophic Maxilla Udatta Kher B.D.S., M.D.S. Loss of teeth causes extensive resorption of the alveolar ridge. In the maxilla the resorption pattern occurs towards the midline,
Immediate implants at fresh extraction sockets: bone healing in four different implant systems
 J Clin Periodontol 2009; 36: 705 711 doi: 10.1111/j.1600-051X.2009.01427.x Immediate implants at fresh extraction sockets: bone healing in four different implant systems de Sanctis M, Vignoletti F, Discepoli
J Clin Periodontol 2009; 36: 705 711 doi: 10.1111/j.1600-051X.2009.01427.x Immediate implants at fresh extraction sockets: bone healing in four different implant systems de Sanctis M, Vignoletti F, Discepoli
JMSCR Vol 06 Issue 07 Page July 2018
 www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v6i7.101 Immediate Implant Following
www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v6i7.101 Immediate Implant Following
CASE REPORT. CBCT-Assisted Treatment of the Failing Long Span Bridge with Staged and Immediate Load Implant Restoration
 Computer Aided Implantology Academy Newsletter - Newsletter 20 - July 2009 CASE REPORT CBCT-Assisted Treatment of the Failing Long Span Bridge with Staged and Immediate Load Implant Restoration Case Report
Computer Aided Implantology Academy Newsletter - Newsletter 20 - July 2009 CASE REPORT CBCT-Assisted Treatment of the Failing Long Span Bridge with Staged and Immediate Load Implant Restoration Case Report
The effect of peri-implant bone exposure on soft tissue healing and bone loss in two adjacent implants
 Research Article J Periodontal Implant Sci 2012;42:20-24 http://dx.doi.org/10.5051/jpis.2012.42.1.20 on soft tissue healing and bone loss in two adjacent implants Seung-Yun Shin 1, Seung-Boem Kye 1, Jongrak
Research Article J Periodontal Implant Sci 2012;42:20-24 http://dx.doi.org/10.5051/jpis.2012.42.1.20 on soft tissue healing and bone loss in two adjacent implants Seung-Yun Shin 1, Seung-Boem Kye 1, Jongrak
Maxillary sinus augmentation without any graft material- A case Report
 A CASE REPORT ISSN: 2321-4988 D.Shiva kumar et al. /JPR:BioMedRx: An International Journal 2013,1(8), Available online through www.jpronline.info Maxillary sinus augmentation without any graft material-
A CASE REPORT ISSN: 2321-4988 D.Shiva kumar et al. /JPR:BioMedRx: An International Journal 2013,1(8), Available online through www.jpronline.info Maxillary sinus augmentation without any graft material-
Implants- immediate restoration of postextraction edentation both esthetically and functionally
 Implants- immediate restoration of postextraction edentation both esthetically and functionally Otilia Stana (Gag), LileIoana Elena, Freiman Paul, Mugur Popescu, Elisei Gabriela, Sebesan Voicu, Vincze
Implants- immediate restoration of postextraction edentation both esthetically and functionally Otilia Stana (Gag), LileIoana Elena, Freiman Paul, Mugur Popescu, Elisei Gabriela, Sebesan Voicu, Vincze
SOCKET WHETHER TO PRESERVE IT NOW OR TO CREATE LATER? - A CASE REPORT
 MAVEN CASE REPORT SOCKET WHETHER TO PRESERVE IT NOW OR TO CREATE LATER? - A CASE REPORT Dr. Parthasarathi Biswas 1, Dr. Debajyoti Mondal 1, Dr. B Praveena Devi 1, Dr. Indrasri Das 2, Dr. Somen Bagchi 3,
MAVEN CASE REPORT SOCKET WHETHER TO PRESERVE IT NOW OR TO CREATE LATER? - A CASE REPORT Dr. Parthasarathi Biswas 1, Dr. Debajyoti Mondal 1, Dr. B Praveena Devi 1, Dr. Indrasri Das 2, Dr. Somen Bagchi 3,
Tooth Retained Implant: No More an Oxymoron
 بنام خدا بنام خدا OPEN ACCESS Freely Available Online Original Hypothesis Tooth Retained Implant: No More an Oxymoron Divya Bhat a Abstract a Department of Periodontics, D.A.P.M.R.V. Dental College, Karnataka,
بنام خدا بنام خدا OPEN ACCESS Freely Available Online Original Hypothesis Tooth Retained Implant: No More an Oxymoron Divya Bhat a Abstract a Department of Periodontics, D.A.P.M.R.V. Dental College, Karnataka,
Deploying Alpha-Bio Tec s NeO Selftapping Implant in an Atrophic Crest: Vestibular-Cortical Stabilization with Bone Graft
 The Atrophic crest Deploying Alpha-Bio Tec s NeO Selftapping Implant in an Atrophic Crest: Vestibular-Cortical Stabilization with Bone Graft Dr. Paolo Borelli DDS, Italy Dr. Massimiliano Favetti DDS, Italy
The Atrophic crest Deploying Alpha-Bio Tec s NeO Selftapping Implant in an Atrophic Crest: Vestibular-Cortical Stabilization with Bone Graft Dr. Paolo Borelli DDS, Italy Dr. Massimiliano Favetti DDS, Italy
Prosthetic Options in Implant Dentistry. Hakimeh Siadat, DDS, MSc Associate Professor
 Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Pre op Failed endodontic treatment with sinus involvement.
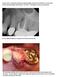 Case #1 of 10 consecutive extraction sockets grafted with Socket Graft Putty, covered with Socket Seal and sealed with Periacryl. I D # HEU This patient is a 66 year old female. Pre op Failed endodontic
Case #1 of 10 consecutive extraction sockets grafted with Socket Graft Putty, covered with Socket Seal and sealed with Periacryl. I D # HEU This patient is a 66 year old female. Pre op Failed endodontic
Utilizing Digital Treatment Planning and Guided Surgery in Conjunction with Narrow Body Implants. by Timothy F. Kosinski, DDS, MAGD
 Utilizing Digital Treatment Planning and Guided Surgery in Conjunction with Narrow Body Implants by Timothy F. Kosinski, DDS, MAGD Implant dentistry is undergoing some amazing transformations. With the
Utilizing Digital Treatment Planning and Guided Surgery in Conjunction with Narrow Body Implants by Timothy F. Kosinski, DDS, MAGD Implant dentistry is undergoing some amazing transformations. With the
Practical Advanced Periodontal Surgery
 Practical Advanced Periodontal Surgery Serge Dibart Blackwell Munksgaard Chapter 8 Papillary Construction After Dental Implant Therapy Peyman Shahidi, DOS, MScD, Serge Dibart, DMD, and Yun Po Zhang, PhD,
Practical Advanced Periodontal Surgery Serge Dibart Blackwell Munksgaard Chapter 8 Papillary Construction After Dental Implant Therapy Peyman Shahidi, DOS, MScD, Serge Dibart, DMD, and Yun Po Zhang, PhD,
Much has been written about the success of various
 Simplified Guide for Precise Implant Placement: A Technical Note Brent D. Kennedy, MD, DDS*/Thomas A. Collins, Jr, DDS**/ Patrick C. W. Kline, DMD, MD** Ideal implant placement is ultimately determined
Simplified Guide for Precise Implant Placement: A Technical Note Brent D. Kennedy, MD, DDS*/Thomas A. Collins, Jr, DDS**/ Patrick C. W. Kline, DMD, MD** Ideal implant placement is ultimately determined
botiss dental bone & tissue regeneration biomaterials mucoderm 3D-Regenerative Tissue Graft strictly biologic
 dental bone & tissue regeneration botiss biomaterials 3DRegenerative Tissue Graft strictly biologic mucoderm Soft Tissue Graft Indications mucoderm is a collagen tissue matrix derived of animal dermis
dental bone & tissue regeneration botiss biomaterials 3DRegenerative Tissue Graft strictly biologic mucoderm Soft Tissue Graft Indications mucoderm is a collagen tissue matrix derived of animal dermis
Interproximal Papilla Levels Following Early Versus Delayed Placement of Single-Tooth Implants: A Controlled Clinical Trial
 Interproximal Papilla Levels Following Early Versus Delayed Placement of Single-Tooth Implants: A Controlled Clinical Trial Lars Schropp, DDS, PhD /Flemming Isidor, DDS, PhD, Dr Odont /Lambros Kostopoulos,
Interproximal Papilla Levels Following Early Versus Delayed Placement of Single-Tooth Implants: A Controlled Clinical Trial Lars Schropp, DDS, PhD /Flemming Isidor, DDS, PhD, Dr Odont /Lambros Kostopoulos,
Moderately to severely resorbed edentulous
 The Zygomatic Implant: Preliminary Data on Treatment of Severely Resorbed Maxillae. A Clinical Report Edmond Bedrossian, DDS, FACD, FACOMS 1 /Lambert Stumpel III, DDS 2 / Michael Beckely, DDS 3 /Thomas
The Zygomatic Implant: Preliminary Data on Treatment of Severely Resorbed Maxillae. A Clinical Report Edmond Bedrossian, DDS, FACD, FACOMS 1 /Lambert Stumpel III, DDS 2 / Michael Beckely, DDS 3 /Thomas
Long-term success for osteointegrated
 CASE REPORT Symphyseal Bone Cylinders Tapping With the Dental Implant Into Insufficiency Bone Situated Esthetic Area at One-Stage Surgery: A Case Report and the Description of the New Technique Umut Tekin,
CASE REPORT Symphyseal Bone Cylinders Tapping With the Dental Implant Into Insufficiency Bone Situated Esthetic Area at One-Stage Surgery: A Case Report and the Description of the New Technique Umut Tekin,
STABILITY OF IMPLANTS AND NATURAL TEETH MONTHS OF FUNCTION AS DETERMINED BY THE PERIOTEST OVER 60 CLINICAL
 CLINICAL STABILITY OF IMPLANTS AND NATURAL TEETH AS DETERMINED BY THE PERIOTEST OVER 60 MONTHS OF FUNCTION Sheldon Winkler, DDS Harold F. Morris, DDS, MS J. Robert Spray, DDS KEY WORDS Implant Natural
CLINICAL STABILITY OF IMPLANTS AND NATURAL TEETH AS DETERMINED BY THE PERIOTEST OVER 60 MONTHS OF FUNCTION Sheldon Winkler, DDS Harold F. Morris, DDS, MS J. Robert Spray, DDS KEY WORDS Implant Natural
PALATAL POSITIONING OF IMPLANTS IN SEVERELY RESORBED POSTERIOR MAXILLAE F. Atamni, M.Atamni, M.Atamna, Private Practice Tel-aviv Israel
 PALATAL POSITIONING OF IMPLANTS IN SEVERELY RESORBED POSTERIOR MAXILLAE F. Atamni, M.Atamni, M.Atamna, Private Practice Tel-aviv Israel Abstract: Objectives: To evaluate an alternative treatment for rehabilitation
PALATAL POSITIONING OF IMPLANTS IN SEVERELY RESORBED POSTERIOR MAXILLAE F. Atamni, M.Atamni, M.Atamna, Private Practice Tel-aviv Israel Abstract: Objectives: To evaluate an alternative treatment for rehabilitation
Redefining Regeneration
 Redefining Regeneration Taking Volume to the MAX One Product, One Treatment, Real VOLUME Buccal Bone Loss Socket Preservation Lateral / Vertical Augmentation Grafting Material Scaffold Barrier (4-6 months)
Redefining Regeneration Taking Volume to the MAX One Product, One Treatment, Real VOLUME Buccal Bone Loss Socket Preservation Lateral / Vertical Augmentation Grafting Material Scaffold Barrier (4-6 months)
Multi-Modality Anterior Extraction Site Grafting Increased Predictability for Aesthetics Michael Tischler, DDS
 Page 1 of 5 Issue Date: March 2003, Posted On: 8/1/2005 Multi-Modality Anterior Extraction Site Grafting Increased Predictability for Aesthetics Michael Tischler, DDS The extraction of teeth creates a
Page 1 of 5 Issue Date: March 2003, Posted On: 8/1/2005 Multi-Modality Anterior Extraction Site Grafting Increased Predictability for Aesthetics Michael Tischler, DDS The extraction of teeth creates a
Many papers have reported on histologic
 Histologic Evaluation of Clinically Successful Osseointegrated Implants Retrieved from Irradiated Bone: A Report of 2 Patients Hidetaka Nakai, DDS*/Atsushi Niimi, DDS, DMSc**/Minoru Ueda, DDS, PhD*** The
Histologic Evaluation of Clinically Successful Osseointegrated Implants Retrieved from Irradiated Bone: A Report of 2 Patients Hidetaka Nakai, DDS*/Atsushi Niimi, DDS, DMSc**/Minoru Ueda, DDS, PhD*** The
BUILDING A. Achieving total reconstruction in a single operation. 70 OCTOBER 2016 // dentaltown.com
 BUILDING A MANDI Achieving total reconstruction in a single operation by Dr. Fayette C. Williams Fayette C. Williams, DDS, MD, FACS, is clinical faculty at John Peter Smith Hospital in Fort Worth, Texas,
BUILDING A MANDI Achieving total reconstruction in a single operation by Dr. Fayette C. Williams Fayette C. Williams, DDS, MD, FACS, is clinical faculty at John Peter Smith Hospital in Fort Worth, Texas,
Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of
 Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of peri-implantitis I: microbiological outcomes. Clin Oral Imp Res 2006;
Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of peri-implantitis I: microbiological outcomes. Clin Oral Imp Res 2006;
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 261 Maintaining Interimplant Crestal Bone Height Via a Combined Platform- Switched, Laser-Lok Implant/Abutment System: A Proof-of-Principle
The International Journal of Periodontics & Restorative Dentistry 261 Maintaining Interimplant Crestal Bone Height Via a Combined Platform- Switched, Laser-Lok Implant/Abutment System: A Proof-of-Principle
Alveolar Ridge Augmentation with Titanium Mesh and Particulate Allograft A Case Report
 Alveolar Ridge Augmentation with Titanium Mesh and Particulate Allograft A Case Report Dr. Pratibha Borasi, Dr. Praneeta Kamble Department of Periodontics, Nair Hospital Dental College, Mumbai, Maharashtra,
Alveolar Ridge Augmentation with Titanium Mesh and Particulate Allograft A Case Report Dr. Pratibha Borasi, Dr. Praneeta Kamble Department of Periodontics, Nair Hospital Dental College, Mumbai, Maharashtra,
