Eosinophilic pustular folliculitis: A proposal of diagnostic and therapeutic algorithms
|
|
|
- Caitlin Edwards
- 5 years ago
- Views:
Transcription
1 doi: / Journal of Dermatology 2016; 43: ORIGINAL ARTICLE Eosinophilic pustular folliculitis: A proposal of diagnostic and therapeutic algorithms Takashi NOMURA, 1,2 Mayumi KATOH, 1 Yosuke YAMAMOTO, 1 Yoshiki MIYACHI, 1,3 Kenji KABASHIMA 1 1 Department of Dermatology, Kyoto University Graduate School of Medicine, 2 Department of Dermatology, Ijinkai Takeda General Hospital, Kyoto, 3 Shiga Medical Center for Adults, Shiga, Japan ABSTRACT Eosinophilic pustular folliculitis (EPF) is a sterile inflammatory dermatosis of unknown etiology. In addition to classic EPF, which affects otherwise healthy individuals, an immunocompromised state can cause immunosuppressionassociated EPF (IS-EPF), which may be referred to dermatologists in inpatient services for assessments. Infancyassociated EPF (I-EPF) is the least characterized subtype, being observed mainly in non-japanese infants. Diagnosis of EPF is challenging because its lesions mimic those of other common diseases, such as acne and dermatomycosis. Furthermore, there is no consensus regarding the treatment for each subtype of EPF. Here, we created procedure algorithms that facilitate the diagnosis and selection of therapeutic options on the basis of published work available in the public domain. Our diagnostic algorithm comprised a simple flowchart to direct physicians toward proper diagnosis. Recommended regimens were summarized in an easy-to-comprehend therapeutic algorithm for each subtype of EPF. These algorithms would facilitate the diagnostic and therapeutic procedure of EPF. Key words: algorithms, diagnosis, eosinophilic pustular folliculitis, Ofuji s disease, therapy. INTRODUCTION Eosinophilic pustular folliculitis (EPF) is a sterile inflammatory dermatosis of unknown etiology that was first described in a case report by Ise and Ofuji as a variant of superficial pustular dermatosis in The eruption of EPF consists of papulopustules that tend to form annular plaques. Histologically, EPF is characterized by an eosinophil-dominated infiltrate within and around the pilosebaceous units, often accompanied by eosinophilic microabscess formation. 2,3 This type of EPF is currently called Ofuji s disease or classic EPF. 4 It was once thought that classic EPF affects males predominantly. 4 However, an exhaustive published work-based study showed no sex difference in classic EPF between 2003 and This tendency was further confirmed by a nationwide epidemiological survey conducted in Japan during the period from 2010 to Immunosuppression-associated EPF (IS-EPF) and infancyassociated EPF (I-EPF) are variants of EPF, both of which have been constantly reported since 1980s. 4 IS-EPF comprises HIVassociated eosinophilic folliculitis (HIV-EF) and a similar EF observed in immunodeficient patients without HIV infection. In this study, we divided IS-EPF into IS/HIV and IS/non-HIV according to the presence or absence of seropositivity for HIV. IS-EPF is often associated with persistent and intense pruritus. I-EPF affects the scalp whereas classic EPF rarely does. Histological findings of I-EPF are indistinguishable from those of classic EPF whereas the entity of I-EPF remains controversial. 7 Recently, an additional variation on classic EPF was proposed as episodic eosinophilic dermatosis of the face (EEDF). 8 EEDF lacks the typical features of classic EPF, such as pustule formation and peripheral extension of the lesions, but responds well to oral indomethacin. Diagnosis of EPF can be difficult and require careful differential diagnosis. 9 Eruptions of classic EPF resemble those of common diseases, such as acne vulgaris, dermatomycosis or eczema. IS-EPF presenting with itchy eczematous papules may be overlooked because it can spontaneously disappear when the underlying immunocompromised state resolves. Treatment of EPF can be difficult. A chronic course of EPF requires long-term application of regimens. Thus, topical or systemic steroids must be used with care. Furthermore, steroids do not always successfully ameliorate eruptions of EPF. Although systemic indomethacin is effective for 88% of classic EPF cases (Table S2a), indomethacin-resistant cases exist (Table S4). In this study, we created algorithms for procedures to facilitate the diagnosis and selection of therapeutic options on the basis of descriptions available in public domain databases. METHODS Subjects We collected publications released between 1965 and 2013 and available on PubMed and Igaku Chuo Zasshi (Ichushi or Japana Centra Revuo Medicina), including the first case described as Correspondence: Takashi Nomura, M.D., Ph.D., Department of Dermatology, Kyoto University Graduate School of Medicine, 54 Shogoin-Kawahara-cho, Sakyo-ku, Kyoto , Japan. tnomura@kuhp.kyoto-u.ac.jp Received 26 September 2015; accepted 7 February Japanese Dermatological Association 1301
2 T. Nomura et al. Table 1. Cases in which the lesions mimicked those of EPF Diagnosis n Notes Dermatomycosis 5 Presence of fungi; good response to antifungal agents Bacterial folliculitis 4 Pseudomonas and Staphylococcus; good response to antibiotics Infestation 4 Scabies, toxocariasis, cutaneous larva migrans, strongyloidiasis Drug-induced 6 Allopurinol, timepidium bromide, carbamazepine, indeloxazine hydrochloride, minocycline, paroxetine, etizolam, maprotiline L-tryptophan-induced 1 Eosinophilic-myalgia syndrome concurrent with EPF involving the torso and palms Cutaneous T-cell lymphoma 2 Initial lesions resembling those of EPF Mycosis fungoides 1 Lesion of follicular type resembling those of EPF Follicular mucinosis 3 Absence of eosinophilic infiltrate in the upper outer sheath of the hair follicle (follicular mucinosis can be associated with EPF) Foreign body reaction 1 Caused by subcutaneous silicone injections to augment the nose and chin n indicates the number of cases found in the published work. For full information, see Table S1. EPF, eosinophilic pustular folliculitis. a variant of superficial pustular dermatosis by Ise and Ofuji. 1 The query key words were eosinophilic pustular folliculitis, eosinophilic pustular dermatosis, eosinophilic folliculitis, Ofuji s disease and eosinophilic pustulosis, as described previously. 5 There were 421 citations that contained 583 cases of bona fide EPF. We identified descriptions of a total of 1175 regimens including 878 in classic EPF and EEDF, 137 in IS/HIV, 45 in IS/ non-hiv and 115 in I-EPF (Table S2). A full list of citations is provided as Supporting Information Data S1. Note that this data set is constantly updated for the content and thus may be different from the version uploaded in the past. Classification of EPF Regarding classification of EPF, we followed the proposal by Nervi et al.: classic, IS-EPF and I-EPF. 4 Classic EPF presents with recurrent annular clusters of sterile follicular papulopustules superimposed on plaques with a tendency toward central clearing and peripheral expansion. EEDF, a variation of classic EPF, was classified as classic in this study. 8 EEDF lacks typical features of classic EPF such as pustule formation and peripheral extension of the lesion, whereas responds well to oral indomethacin. Immunosuppression-associated EPF involves an underlying disease causing immunosuppression. IS-EPF was further divided into IS/HIV and IS/non-HIV in this study, according to the presence or absence of seropositivity for HIV. We defined I-EPF as EPF causing sterile papulopustules in individuals under the age of 10 years or as any case diagnosed as I-EPF by the reporting authors. I-EPF is a variant of EPF with the least characterization. 7 Efficacy of treatment Unless indicated, efficacy of treatment is based on a published work-based study conducted by us and provided as Supporting Information (Table S2). Limitations Limitations of this study include publication bias, lack of adequately controlled trials and lack of validated measures of the outcome. RESULTS Differential diagnosis of EPF The diagnosis of EPF is occasionally difficult and problematic as EPF may share clinical appearance of histological findings with other diseases. 9 Therefore, we reviewed publications in advance and collected cases in which lesions showed close resemblance to those of EPF (Table 1, S1). There were 27 such cases, in which the final diagnoses were dermatomycosis (n = 5), bacterial folliculitis (n = 4), infestation (n = 4), druginduced eruption (n = 6), L-tryptophan-induced eruption (n = 1), cutaneous T-cell lymphoma (n = 2), mycosis fungoides (n = 1), follicular mucinosis (n = 3) and foreign body reaction to injected silicon (n = 1). Dermatomycosis was diagnosed by skin biopsy and periodic acid-schiff-staining. Bacterial folliculitis was diagnosed through isolation of the infectious agents, such as Pseudomonas or Staphylococcus, and was confirmed by responsiveness to antimicrobial agents. Infestation was diagnosed by the appearance of typical lesions of cutaneous larva migrans, identification of scabies mites, presence of antibodies to Toxocara or fecal examination. Drug-induced or L- tryptophan-induced eruptions were diagnosed based on the disease course. Cutaneous T-cell lymphoma, mycosis fungoides and follicular mucinosis were diagnosed by skin biopsy. Diagnostic algorithm Based on a published work-based comprehensive analysis, we created a diagnostic algorithm for EPF (Fig. 1). The first step toward a diagnosis of EPF is to suspect when pruritic erythematous papulopustules show resistance to topical steroids. The eruptions may or may not show peripheral extension with central clearance with pigmentation. Here, we propose 10 representative diseases that should be considered, namely, acne vulgaris, rosacea, lupus miliaris disseminatus faciei (LMDF), bacterial folliculitis, dermatomycosis, scabies, arthropod bites, palmoplantar pustulosis (PPP), seborrheic dermatitis and mycosis fungoides. Microscopy of a potassium hydroxide preparation (KOH test) can rule out dermatomycosis and scabies. Complete blood counts and screening for antibody to HIV are useful to test for any underlying patient conditions, such as AIDS or hematological abnormalities Japanese Dermatological Association
3 Diagnostic and therapeutic algorithms for EPF Topical tacrolimus and pimecrolimus must be used with care: (i) continuous long-term use must be avoided due to adverse effects including a risk for rosacea; (ii) concurrent ultraviolet (UV) therapy must be avoided; and (iii) children younger than 2 years of age should not be applied (see astellas.us/docs/protopic.pdf; drugsatfda_docs/label/2006/021302s011lbl.pdf). Figure 1. Diagnostic algorithm for eosinophilic pustular folliculitis (EPF) is shown. The first step is to suspect EPF for pruritic papules, pustules or erythema with centrifugal extension. Exclude dermatoses such as acne vulgaris, rosacea, lupus miliaris disseminatus faciei (LMDF), bacterial folliculitis, dermatomycosis, scabies, arthropod bites, palmoplantar pustulosis (PPP), seborrheic dermatitis (SD) or mycosis fungoides (MF). Microscopy of a potassium hydroxide preparation (KOH test) can rule out dermatomycosis and scabies. Complete blood count (CBC) and screening for antibody to HIV are useful to screen underlying conditions such as AIDS or hematological abnormalities. Biopsy is the most important examination. Follicles must be included and studied carefully through serial sectioning. If biopsy is unfeasible, application of indomethacin topically or systemically (25 75 mg/day) can be used as a diagnostic therapy. If indomethacin is ineffective, consider biopsy. Beware of contraindications of indomethacin. Return to differential diagnoses; consider biopsy. Biopsy is the most important examination. Follicles must be included and studied carefully through serial sectioning. Presence of microabscesses containing eosinophil-dominant granulocytes in the upper portion of the outer root sheath is the hallmark of EPF. 9 Although biopsy is the best way for definitive diagnosis, obtaining the patient s consent for biopsy is often difficult. In such cases, therapeutic diagnosis with oral indomethacin at mg/day is helpful. In case the patient cannot take oral indomethacin due to gastric symptoms, topical application of indomethacin is an alternative option. Contraindications of indomethacin must be considered as discussed later (Fig. 2e). Therapeutic algorithms Next, we developed a set of therapeutic algorithms for EPF (Fig. 2). An algorithm is basically composed of a short description of therapeutic goal and first- and second-line drugs (Fig. 2a d). An algorithm for classic EPF is strengthened with regimens for maintenance, combination therapy, a list of alternative drugs (tentatively effective options with limited number of reported cases) and options for indomethacin-resistant cases (Fig. 2a). An excerpt of important information on practice is included in the set (Fig. 2e) Japanese Dermatological Association Classic EPF The goal in treating classic EPF is to resolve the lesion and control recurrence of EPF (Fig. 2a). First-line drugs for classic EPF include systemic indomethacin (25 75 mg/day) and its prodrugs such as acemetacin ( mg/day) and indomethacin farnesil ( mg/day). The efficacy of indomethacin is quite high, although that of indomethacin farnesil and proglumetacin (dose not provided in the published work) is somewhat controversial (Table S2a). We included topical indomethacin as first-line, because it showed a high efficacy (complete response/partial response, 21%/76% in 33 cases as shown in Table S2a). Second-line drugs include ultraviolet (UV), Sairei-to ( g/day, see Table S5b for detail), systemic cyclosporin ( mg or 3 5 mg/kg per day), transdermal nicotine patch ( mg), 10 systemic tetracyclines (minocycline mg/day or doxycycline 100 mg/day) and systemic diaminodiphenyl sulfone (DDS; mg/day). Any form of UV can be expected with good response for classic EPF (Table S5d). Dose of ultraviolet is not established yet for EPF. In general, UV-B (UVB) or narrowband UV-B (NB-UVB) was applied 2 3 times a week with an initial dose of 40 mj/cm 2 or 1/2 of minimal erythema dose, which was increased by 10 50%. UV-A (UVA) was applied twice a week with initial dose of 1/2 minimal phototoxic dose without psoralen until the lesion subsided. Protocol for psoralen plus UVA therapy (PUVA) was followed to European protocol for psoriasis. Recalcitrant cases can be coped with combination therapy, in which either systemic indomethacin (either indomethacin mg/day, acemetacin mg/day) or DDS ( mg/ day) together with either topical indomethacin or tacrolimus. One or a few of the second-line drugs can be combined further (Fig. 2a). However, cyclosporin should not be combined with systemic indomethacin to avoid synergistic nephrotoxicity (Fig. 2e). Most of the alternative drugs are uncommon regimens, which appeared in published works (Table S5a,c). Topical tacrolimus is effective in combination or in single use. Naproxen ( mg/day) and loxoprofen ( mg/day) are other non-steroidal anti-inflammatory drugs (NSAIDs), which can work well on EPF. Tranilast (300 mg/day) successfully treated a patient with EEDF, who could not continue indomethacin due to a gastrointestinal symptom. 8 EPA (1800 mg/day), suplatast tosilate (300 mg/day), nicotinamide (900 mg/day), metronidazole (500 mg/day), etretinate (25 50 mg/day) and acitretin (0.5 mg/kg per day) were reported to be effective. Topical injection of triamcinolone (5 mg/ml) was reported to achieve complete response in a case. There were 19 cases of classic EPF, in which systemic indomethacin ( mg/day) did not ameliorate lesions 1303
4 T. Nomura et al. (a) (b) (c) (d) (e) Figure 2. Therapeutic algorithms for (a) classic, (b) IS/HIV, (c) IS/non-HIV and (d) infancy-associated eosinophilic pustular folliculitis (EPF) and (e) an excerpt of contraindications and notes are shown. Dose/day for systemic use is put in the parenthesis. Systemic indomethacin (25 75 mg), acemetacin ( mg), indomethacin farnesil ( mg). Non-steroidal anti-inflammatory drugs (NSAIDs) are contraindicated or cautioned in the following patients: allergic to aspirin or other NSAIDs, under 14 years of age (safety and efficacy not established), pregnant or breastfeeding women, on anticoagulant treatment, with active peptic ulcer, with application of nephrotoxic agents (such as systemic cyclosporin [Cs], tacrolimus or triamterene), with failure of kidneys/liver/heart/pancreas. Avoid concurrent application of topical tacrolimus; ultraviolet (UV)-B (UVB)/narrowband UVB (NB-UVB), 2 3 times/week with 40 mj/cm 2 or 1/2 minimal erythemal dose with increment by 10 50%; UV-A (UVA), twice/week of 1/2 minimal phototoxic dose without psoralen; psoralen plus UVA therapy (PUVA), to follow European protocol for psoriasis. Beware of pseudoaldosteronism by glycyrrhizin. Oral minocycline ( mg) or doxycycline (100 mg). Avoid long-term use and beware of rosacea or rosacea-like dermatitis; contraindicated for patients aged 2 years or less; use 0.03% for children of under 2 years of age; avoid concurrent UV therapy. Injection of 5 mg/ml, s.c., ad libitum. Interferon (IFN)-a-2b, units 2 3-times/week; IFN-c, Japan Reference Unit 5-times/week; infliximab, 5 mg/kg per 2 weeks. Care of dental caries, gingivitis, dentures or metal allergy to dental prostheses. Steroidal treatment is a convenient option for self-limiting IS/non-HIV and infancy-associated EPF; avoid long-term use and beware of rosacea-like dermatitis. Includes metronidazole and permethrin. Dicloxacillin, Neosporin (bacitracin-neomycin-polymyxin B), penicillin, cefaclor or cephalexin. Cs, cyclosporin; DDS, diaminodiphenyl sulfone; DIHS/DRESS, drug-induced hypersensitivity syndrome/drug reaction with eosinophilia and systemic symptoms; EPA, eicosapentaenoic acid; GVHD, graft-versus-host disease; HAART, highly active antiretroviral therapy; wk, week. (Table S4). Such cases can be managed with topical tacrolimus, Sairei-to ( g/day), naproxen ( mg/day), cyclosporin (3 5 mg/kg per day), DDS ( mg/day), metronidazole (500 mg/day), acitretin (0.5 mg/kg per day), PUVA (a regimen followed to European protocol for psoriasis) and prednisolone (5 10 mg/day) together with topical tacrolimus. Combination therapy described above or use of alternative drugs may be effective. Maintenance of lesion or control of recurrence is important for classic EPF. It can be managed by topical indomethacin and UV (Table S5d). Tapering of medications is recommended. UV is effective for controlling pruritus. Irrespective of the subtype of EPF, we recommend NB-UVB because there are few risks, including a small risk of increased skin cancer, a sunburn reaction, itching, burning sensation and folliculitis. 11 However, patients must attend phototherapy constantly. 12 IS/HIV The goal in treating IS/HIV is to alleviate pruritus and to treat AIDS (Fig. 2b). First-line drugs include highly active antiretroviral treatment (HAART), topical tacrolimus, UVB and NB-UVB. IS/HIV is typically seen when CD4 + count drops below 300/lL. 13 In Japanese Dermatological Association
5 Diagnostic and therapeutic algorithms for EPF addition, there is an association between low nadir (66.28/lL) and low CD4 + cell count (115.54/lL) and the development of IS/HIV. 14 Therefore, HAART to treat AIDS is an effective option. Lesions and pruritus of IS/HIV can be manageable with topical tacrolimus. However, long-term use of topical tacrolimus should be avoided not to induce rosacea or rosacea-like dermatitis. UVB or NB-UVB 2 3 times a week, starting at 1/2 minimal erythemal dose with increments of 10 50%, for approximately 2 months effectively reduce pruritus and resolve the lesion (Table S5d). The second-line drugs include topical antifungals (including topical ketoconazole, topical metronidazole and topical permethrin), systemic indomethacin (25 75 mg/day), tetracyclines (minocycline mg/day or doxycycline 100 mg/day), DDS ( mg), metronidazole ( mg/day) and itraconazole ( mg/day). Oral ivermectin may be effective, although the dose of which is not established. It was reported that a single dose of 12 mg of oral ivermectin resolved a case of IS/HIV of a 38-year-old Japanese man infested with Demodex folliculorum after 2 weeks. 15 As IS/HIV is often accompanied by AIDS, it is important to rule out infestations, bacterial or fungal infections. Indeed, bacterial folliculitis can mimic lesions of EPF. 16 IS/non-HIV The goal in treating IS/non-HIV is to alleviate symptoms, of which spontaneous remission can occur (Fig. 2c). Most patients with IS/non-HIV suffer from immune reconstitution inflammatory syndrome (IRIS) due to bone marrow transplantation or peripheral blood stem cell transplantation (Data S1). The goal of treatment is, therefore, to alleviate symptoms such as pruritus until the patient recovers from IRIS. First-line drugs include topical steroid, which is effective. However, long-term use of topical steroid should be avoided so as not to induce rosacea or rosacea-like dermatitis. UVB with accumulated dose of 0.74 J/cm 2 (details not provided) achieved complete response in a case of a 60-year-old man with IS/non-HIV, which developed during the course of B-cell lymphoma. 17 We speculate NB-UVB is also effective for IS/ non-hiv and included it as a first-line drug. Second-line drugs include topical tacrolimus, indomethacin (25 75 mg/day), systemic prednisolone ( mg/kg per day), tetracyclines (minocycline mg/day or doxycycline 100 mg/day) and DDS ( mg/day). When the eruption is difficult to differentiate from that of graft-versus-host disease (GVHD), treatment for GVHD should be prioritized. I-EPF As lesions of I-EPF often resolve spontaneously, symptomatic treatment usually suffices (Fig. 2d). Use of indomethacin or other NSAIDs should be avoided for infants. First-line drugs include topical steroid and systemic erythromycin (25 50 mg/kg per day). Topical steroid was used in 50 cases with an efficacy of 82% (Table S2d). Systemic macrolides (dose not provided in the published work) were used in 16 cases with an efficacy of 56% (Table S2d) Japanese Dermatological Association Second-line drugs include systemic antibacterial agents (including dicloxacillin, Neosporin â [Johnson & Johnson, New Brunswick, NJ, USA] or a mixture of bacitracin-neomycin-polymyxin B, penicillin, cefaclor and cephalexin; dose not provided in the published work), topical tacrolimus and UVA (dose not provided in the published work). For children, the dose of tacrolimus should be 0.03%. Tacrolimus is contraindicated for those aged 2 years or less. Contraindications and notes for regimens In the set of algorithms, we included excerpts of: (i) contraindications of NSAIDs; (ii) contraindicated combination of UV and topical tacrolimus; and (iii) a risk of drug-induced hypersensitivity syndrome/drug reaction with eosinophilia and systemic symptoms syndrome for minocycline and DDS (Fig. 2e). DISCUSSION Diagnosis of EPF is difficult if the physician does not consider EPF as a differential diagnosis. Patients may be improperly treated for recalcitrant exanthema under wrong diagnoses. Lesions of EPF closely mimic those of acne vulgaris, rosacea, LMDF, bacterial folliculitis, dermatomycosis, scabies, arthropod bites, PPP, seborrheic dermatitis or mycosis fungoides. These dermatoses can be excluded by microscopic examination of scales by KOH test and skin biopsy. Alternatively, trial treatment with oral indomethacin (25 75 mg/day) or topical indomethacin can help diagnosis. The diagnostic algorithm for EPF that we present here will assist diagnostic procedure (Fig. 1). The paucity of effective regimens for EPF had challenged dermatologists for years. Most of the fundamental regimens, such as oral steroids, sulfonamides, DDS and tetracyclines, were tried by Ofuji et al. and had been reported by ,2 Nevertheless, the achievement of complete clearance of lesion was far from assured at that time. A breakthrough came when indomethacin was serendipitously recognized as an efficacious medicine for classic EPF. 18,19 The discoveries of the beneficial effects of topical tacrolimus, oral Sairei-to, and oral cyclosporin, all of which were effective against indomethacin-resistant EPF as well, followed and enriched the therapeutic options The multiplicity of options, however, may be confusing for those attempting to chart treatment. To ease this difficulty, we developed a therapeutic algorithm by reviewing published therapies and their efficacies. A separate algorithm was made for each subtype of EPF because the goal of therapy differs in each subtype. Currently, no treatment ensures cure of EPF. However, lines of evidence indicate that a key for cure is normalization of T- helper (Th)2-type immune dysregulation. Candidate targets for this purpose are interleukin (IL)-4, IL-13, CCL26 (eotaxin-3), prostaglandin D2, peroxisome proliferator-activated receptor-c, CRTH2 (chemoattractant receptor-homologous molecule on Th2 cells or CD294), or basophils and mast cells Further investigation of these targets is required. In summary, the algorithms described here should facilitate the diagnostic and therapeutic procedures of EPF. 1305
6 T. Nomura et al. ACKNOWLEDGMENTS: We dedicate this research to Dr Shigeo Ofuji, our mentor and a highly cultured and versatile dermatologist who passed away in This work was supported in part by Grants-in-Aid for Scientific Research from the Ministry of Education, Culture, Sports, Science and Technology ( and 15K09765) and the Ministry of Health, Labor and Welfare of Japan (Research on Measures for Intractable Diseases Project). CONFLICT OF INTEREST: None declared. REFERENCES 1 Ise S, Ofuji S. Subcorneal pustular dermatosis; a follicular variant? Arch Dermatol 1965; 92: Ofuji S, Ogino A, Horio T, Oseko T, Uehara M. Eosinophilic pustular folliculitis. Acta Derm Venereol 1970; 50: Ofuji S. Eosinophilic pustular folliculitis. Dermatology 1987; 174: Nervi SJ, Schwartz RA, Dmochowski M. Eosinophilic pustular folliculitis: a 40 year retrospect. J Am Acad Dermatol 2006; 55: Nomura T, Katoh M, Yamamoto Y, Kabashima K, Miyachi Y. Eosinophilic pustular folliculitis: the transition in sex differences and interracial characteristics between 1965 and J Dermatol 2015; 42: Yamamoto Y, Nomura T, Kabashima K, Miyachi Y. Clinical epidemiology of eosinophilic pustular folliculitis: results from a nationwide survey in Japan. Dermatology 2015; 230: Ziemer M, Boer A. Eosinophilic pustular folliculitis in infancy: not a distinctive inflammatory disease of the skin. Am J Dermatopathol 2005; 27: Matsumura Y, Miyachi Y. Atypical clinical appearance of eosinophilic pustular folliculitis of seborrheic areas of the face. Eur J Dermatol 2012; 22: Fujiyama T, Tokura Y. Clinical and histopathological differential diagnosis of eosinophilic pustular folliculitis. J Dermatol 2013; 40: Yoshifuku A, Higashi Y, Matsushita S, Kawai K, Kanekura T. Transdermal nicotine patches for eosinophilic pustular folliculitis. J Dermatol 2013; 40: Laube S, George SA. Adverse effects with PUVA and UVB phototherapy. J Dermatolog Treat 2001; 12: Ellis E, Scheinfeld N. Eosinophilic pustular folliculitis: a comprehensive review of treatment options. Am J Clin Dermatol 2004; 5: Cedeno-Laurent F, Gomez-Flores M, Mendez N et al. New insights into HIV-1-primary skin disorders. J Int AIDS Soc 2011; 14: Rajendran PM, Dolev JC, Heaphy MR Jr, Maurer T. Eosinophilic folliculitis: before and after the introduction of antiretroviral therapy. Arch Dermatol 2005; 141: Nara T, Katoh N, Inoue K, Yamada M, Arizono N, Kishimoto S. Eosinophilic folliculitis with a Demodex folliculorum infestation successfully treated with ivermectin in a man infected with human immunodeficiency virus. Clin Exp Dermatol 2009; 34: e981 e Hayakawa J, Fukuda M, Shiohara T. A case of human immunodeficiency virus infection that showed eosinophilic pustular folliculitislike eruption. Jpn J Clin Dermatol 1997; 51: Ishiguro M, Kamakura T, Nakajima K, Ikeda M, Kodama H. Eosinophilic folliculitis developed in B cell lymphoma (translated). Pract Dermatol 2006; 28: Tanaka A, Tada J, Takaiwa T. Two cases of eosinophilic pustular folliculitis (translated). Rinsho Derma (Tokyo) 1978; 20: Inada S, Kohno T, Matsubayashi Y et al. Three Cases of Eosinophilic Pustular Folliculitis with Basophil Infiltration. Nishinihon J Dermatol 1983; 45: Kabashima K, Sakurai T, Miyachi Y. Treatment of eosinophilic pustular folliculitis (Ofuji s disease) with tacrolimus ointment. Br J Dermatol 2004; 151: Sugita K, Kabashima K, Koga C, Tokura Y. Eosinophilic pustular folliculitis successfully treated with sequential therapy of interferongamma and ciclosporin. Clin Exp Dermatol 2006; 31: Fukamachi S, Kabashima K, Sugita K, Kobayashi M, Tokura Y. Therapeutic effectiveness of various treatments for eosinophilic pustular folliculitis. Acta Derm Venereol 2009; 89: Katoh M, Nomura T, Miyachi Y, Kabashima K. Eosinophilic pustular folliculitis: a review of the Japanese published works. J Dermatol 2013; 40: Satoh T, Shimura C, Miyagishi C, Yokozeki H. Indomethacininduced reduction in CRTH2 in eosinophilic pustular folliculitis (Ofuji s disease): a proposed mechanism of action. Acta Derm Venereol 2010; 90: Otsuka A, Doi H, Miyachi Y, Kabashima K. Treatment of eosinophilic pustular folliculitis with ciclosporin: suppression of mrna expression of IL-4 and IL-13. J Eur Acad Dermatol Venereol 2010; 24: Satoh T, Ito Y, Miyagishi C, Yokozeki H. Basophils infiltrate skin lesions of eosinophilic pustular folliculitis (Ofuji s disease). Acta Derm Venereol 2011; 91: Otsuka A, Miyagawa-Hayashino A, Walls AF, Miyachi Y, Kabashima K. Comparison of basophil infiltration into the skin between eosinophilic pustular folliculitis and neutrophilic folliculitis. J Eur Acad Dermatol Venereol 2012; 26: Nakahigashi K, Doi H, Otsuka A et al. PGD2 induces eotaxin-3 via PPARgamma from sebocytes: a possible pathogenesis of eosinophilic pustular folliculitis. J Allergy Clin Immunol 2012; 129: Kataoka N, Satoh T, Hirai A, Saeki K, Yokozeki H. Indomethacin inhibits eosinophil migration to prostaglandin D2: therapeutic potential of CRTH2 desensitization for eosinophilic pustular folliculitis. Immunology 2013; 140: SUPPORTING INFORMATION Additional Supporting Information may be found in the online version of this article: Data S1. SI_Tx_Pubmed_Ichushi_ver151216: Full set of published work information used in this study. Table S1. Summary of cases in which lesions mimicked those of eosinophilic pustular folliculitis, a supplement for Table 1 Table S2a. Regimens applied to classic EPF Table S2b. Regimens applied to IS/HIV Table S2c. Regimens applied to IS/non-HIV Table S2d. Regimens applied to I-EPF Table S3a. Summary of combination therapies Table S3b. Summary of combination therapies in detail Table S4. Summary of indomethacin-resistant cases Table S5a. Summary of uncommon regimens Table S5b. Summary of treatment by Sairei-to Table S5c. Summary of treatment by interferon Table S5d. Summary of treatment by ultraviolet Japanese Dermatological Association
Suplatast Tacrolimus Combination Therapy for Refractory Facial Erythema in Adult Patients with Atopic Dermatitis A Meta-Analysis Study
 Allergology International. 27;56:269-275 DOI:.2332allergolint.O-6-478 ORIGINAL ARTICLE Suplatast Combination Therapy for Refractory Facial Erythema in Adult Patients with Atopic DermatitisA Meta-Analysis
Allergology International. 27;56:269-275 DOI:.2332allergolint.O-6-478 ORIGINAL ARTICLE Suplatast Combination Therapy for Refractory Facial Erythema in Adult Patients with Atopic DermatitisA Meta-Analysis
Elsevier B.V.; この論文は出版社版でありま Right 引用の際には出版社版をご確認ご利用ください This is
 Title Refractory cutaneous lichenoid sarc tranilast. Author(s) Nakahigashi, Kyoko; Kabashima, Kenj Utani, Atsushi; Miyachi, Yoshiki Citation Journal of the American Academy of 63(1): 171-172 Issue Date
Title Refractory cutaneous lichenoid sarc tranilast. Author(s) Nakahigashi, Kyoko; Kabashima, Kenj Utani, Atsushi; Miyachi, Yoshiki Citation Journal of the American Academy of 63(1): 171-172 Issue Date
Eosinophilic Pustular Folliculitis in a Patient with Behçet s Disease
 IBIMA Publishing International Journal of Case Reports in Medicine http://www.ibimapublishing.com/journals/ijcrm/ijcrm.html ijcrm.html Vol. 2016 (2016), Article ID 832328, 6 pages DOI: 10.5171/2016.832328
IBIMA Publishing International Journal of Case Reports in Medicine http://www.ibimapublishing.com/journals/ijcrm/ijcrm.html ijcrm.html Vol. 2016 (2016), Article ID 832328, 6 pages DOI: 10.5171/2016.832328
Rashes Not To Be Missed In Children
 May 2016 Rashes Not To Be Missed In Children Dr Chan Yuin Chew Dermatologist Dermatology Associates Gleneagles Medical Centre Scope of presentation Focus on rashes May lead to significant morbidity if
May 2016 Rashes Not To Be Missed In Children Dr Chan Yuin Chew Dermatologist Dermatology Associates Gleneagles Medical Centre Scope of presentation Focus on rashes May lead to significant morbidity if
Phototherapy and Photochemotherapy Treatment (Ultraviolet A [PUVA] and B [UBV])
![Phototherapy and Photochemotherapy Treatment (Ultraviolet A [PUVA] and B [UBV]) Phototherapy and Photochemotherapy Treatment (Ultraviolet A [PUVA] and B [UBV])](/thumbs/89/99382632.jpg) Origination: 09/27/07 Revised: 08/2/17 Annual Review: 11/2/17 Purpose: To provide Phototherapy and Photochemotherapy Treatment (PUVA and UBV) guidelines for the Medical Department staff to reference when
Origination: 09/27/07 Revised: 08/2/17 Annual Review: 11/2/17 Purpose: To provide Phototherapy and Photochemotherapy Treatment (PUVA and UBV) guidelines for the Medical Department staff to reference when
A 40-year old male with follicular papule and pustule at central face area for 3 months
 A 40-year old male with follicular papule and pustule at central face area for 3 months GMS- Neg AFB-Neg Fite stain - neg HISTOPATHOLOGICAL DIFFERENTIAL DIAGNOSIS CASEOUS GRANULOMA INFECTION -MYCOBACTERIUM
A 40-year old male with follicular papule and pustule at central face area for 3 months GMS- Neg AFB-Neg Fite stain - neg HISTOPATHOLOGICAL DIFFERENTIAL DIAGNOSIS CASEOUS GRANULOMA INFECTION -MYCOBACTERIUM
A Retrospective Study on the Risk of Non-Melanoma Skin Cancer in PUVA and Narrowband UVB Treated Patients
 Volume 1, Issue 3 Research Article A Retrospective Study on the Risk of Non-Melanoma Skin Cancer in PUVA and Narrowband UVB Treated Patients Darukarnphut P, Rattanakaemakorn P *, Rajatanavin N Division
Volume 1, Issue 3 Research Article A Retrospective Study on the Risk of Non-Melanoma Skin Cancer in PUVA and Narrowband UVB Treated Patients Darukarnphut P, Rattanakaemakorn P *, Rajatanavin N Division
COMMON SKIN CONDITIONS IN PRIMARY CARE. Ibrahim M. Zayneh, MD Dermatology Private Practice, Portsmouth, Ohio
 COMMON SKIN CONDITIONS IN PRIMARY CARE Ibrahim M. Zayneh, MD Dermatology Private Practice, Portsmouth, Ohio DISCLOSURE The Speaker and members of the planning committee do not have a conflict of interest
COMMON SKIN CONDITIONS IN PRIMARY CARE Ibrahim M. Zayneh, MD Dermatology Private Practice, Portsmouth, Ohio DISCLOSURE The Speaker and members of the planning committee do not have a conflict of interest
Citation The Journal of Dermatology, 37(8), available at
 NAOSITE: Nagasaki University's Ac Title Two cases of blaschkitis with promi Author(s) Utani, Atsushi Citation The Journal of Dermatology, 37(8), Issue Date 2010-08 URL Right http://hdl.handle.net/10069/25634
NAOSITE: Nagasaki University's Ac Title Two cases of blaschkitis with promi Author(s) Utani, Atsushi Citation The Journal of Dermatology, 37(8), Issue Date 2010-08 URL Right http://hdl.handle.net/10069/25634
Figure 7.1 Figure 7.2 Figure 7.3
 CASE 7 Patient: A 63 year-old Thai female from Pathumthani Chief Complaint: Progressive facial eruption in 1 month Present Illness: The lesions involved only facial area without itching or pain. No associated
CASE 7 Patient: A 63 year-old Thai female from Pathumthani Chief Complaint: Progressive facial eruption in 1 month Present Illness: The lesions involved only facial area without itching or pain. No associated
PACKAGE LEAFLET: INFORMATION FOR THE USER. Flutarzole 0,05% w/w cream, Fluticasone propionate
 PACKAGE LEAFLET: INFORMATION FOR THE USER Flutarzole 0,05% w/w cream, Fluticasone propionate 1. IDENTIFICATION OF THE MEDICINAL PRODUCT 1.1. Trade name Flutarzole 1.2. Composition Active substance: Fluticasone
PACKAGE LEAFLET: INFORMATION FOR THE USER Flutarzole 0,05% w/w cream, Fluticasone propionate 1. IDENTIFICATION OF THE MEDICINAL PRODUCT 1.1. Trade name Flutarzole 1.2. Composition Active substance: Fluticasone
Egyptian Dermatology Online Journal Vol. 6 No 1: 14, June 2010
 Wells Syndrome H. Gammaz, H. Amer, A. Adly and S. Mahmoud Egyptian Dermatology Online Journal 6 (1): 14 Al-Haud Al-Marsoud Hospital, Cairo, Egypt e-mail: hananderma@hotmail.com Submitted: April 15, 2010
Wells Syndrome H. Gammaz, H. Amer, A. Adly and S. Mahmoud Egyptian Dermatology Online Journal 6 (1): 14 Al-Haud Al-Marsoud Hospital, Cairo, Egypt e-mail: hananderma@hotmail.com Submitted: April 15, 2010
Combination Nonbiologic Therapy in Psoriasis. Sushil Tahiliani, MBBS, MD
 Combination Nonbiologic Therapy in Psoriasis Sushil Tahiliani, MBBS, MD Agenda Rationale Preferred and less preferred combination Morphology-specific preferred combinations Doses used in combinations Potential
Combination Nonbiologic Therapy in Psoriasis Sushil Tahiliani, MBBS, MD Agenda Rationale Preferred and less preferred combination Morphology-specific preferred combinations Doses used in combinations Potential
0BCore Safety Profile. Pharmaceutical form(s)/strength: Cream 1% DK/H/PSUR/0009/005 Date of FAR:
 0BCore Safety Profile Active substance: Pimecrolimus Pharmaceutical form(s)/strength: Cream 1% P-RMS: DK/H/PSUR/0009/005 Date of FAR: 06.06.2013 4.3 Contraindications Hypersensitivity to pimecrolimus,
0BCore Safety Profile Active substance: Pimecrolimus Pharmaceutical form(s)/strength: Cream 1% P-RMS: DK/H/PSUR/0009/005 Date of FAR: 06.06.2013 4.3 Contraindications Hypersensitivity to pimecrolimus,
Rosacea Rosacea: how I hates ya! Richard Castillo, OD, DO The Oklahoma College of Optometry Northeastern State University Tahlequah, OK
 Rosacea Rosacea: how I hates ya! Richard Castillo, OD, DO The Oklahoma College of Optometry Northeastern State University Tahlequah, OK Introduction Clinical Features Flushing Telangiectasia Erythema Papules
Rosacea Rosacea: how I hates ya! Richard Castillo, OD, DO The Oklahoma College of Optometry Northeastern State University Tahlequah, OK Introduction Clinical Features Flushing Telangiectasia Erythema Papules
=ﻰﻤاﻤﺤﻠا ﺔﻴﻘﻠﺤﻠا ﺔذﺒاﻨﻠا
 1 / 15 Erythema Annulare Centrifugum and Other Figurate Erythemas The figurate erythemas include a variety of eruptions characterized by annular and polycyclic lesions. Classification of this group has
1 / 15 Erythema Annulare Centrifugum and Other Figurate Erythemas The figurate erythemas include a variety of eruptions characterized by annular and polycyclic lesions. Classification of this group has
A case of rosacea fulminans in a pregnant woman
 Hong Kong J. Dermatol. Venereol. (2018) 26, 122-126 Views and Practice A case of rosacea fulminans in a pregnant woman JE Seol, SH Park, JU Kim, GJ Cho, SH Moon, H Kim Introduction Rosacea fulminans (RF)
Hong Kong J. Dermatol. Venereol. (2018) 26, 122-126 Views and Practice A case of rosacea fulminans in a pregnant woman JE Seol, SH Park, JU Kim, GJ Cho, SH Moon, H Kim Introduction Rosacea fulminans (RF)
Grover s disease: A case report.
 320 Case report Thai J Dermatol, October-December 2011 ABSTRACT: Grover s disease: A case report. Supicha Chavanich MD, Praneet Sajjachareonpong MD. CHAVANICH C, SAJJACHAREONPONG P. GROVER S DISEASE: A
320 Case report Thai J Dermatol, October-December 2011 ABSTRACT: Grover s disease: A case report. Supicha Chavanich MD, Praneet Sajjachareonpong MD. CHAVANICH C, SAJJACHAREONPONG P. GROVER S DISEASE: A
Original Policy Date
 MP 2.01.07 Psoralens with Ultraviolet A (PUVA) Medical Policy Section Medicine Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed by consensus/12:2013 Return to Medical Policy
MP 2.01.07 Psoralens with Ultraviolet A (PUVA) Medical Policy Section Medicine Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed by consensus/12:2013 Return to Medical Policy
What is atopic dermatitis?
 What is atopic dermatitis? Complex inflammatory skin disorder intense pruritus cutaneous hyperreactivity immune dysregulation Chronic with exacerbations and remissions Affects all ages, but more common
What is atopic dermatitis? Complex inflammatory skin disorder intense pruritus cutaneous hyperreactivity immune dysregulation Chronic with exacerbations and remissions Affects all ages, but more common
11 PROTOCOL NO. 11: Psoracomb (UVB TL01) protocol PROTOCOL NO. 12: MPD protocol 23 Appendix 25
 Classification: Policy Lead Author: Tsui Ling Consultant Dermatologist, Clinical Additional author(s): N/A Authors Division: Dermatology Unique ID: GSCDerm02(13) Issue number: 3 Expiry Date: September
Classification: Policy Lead Author: Tsui Ling Consultant Dermatologist, Clinical Additional author(s): N/A Authors Division: Dermatology Unique ID: GSCDerm02(13) Issue number: 3 Expiry Date: September
KEY MESSAGES. Psoriasis patients are more prone to cardiovascular diseases, stroke, lymphoma and non-melanoma skin cancers, and increased mortality.
 KEY MESSAGES Psoriasis is a genetically determined, systemic immune-mediated chronic inflammatory disease that affects primarily the skin and joints. Psoriasis Vulgaris is characterised by well-demarcated
KEY MESSAGES Psoriasis is a genetically determined, systemic immune-mediated chronic inflammatory disease that affects primarily the skin and joints. Psoriasis Vulgaris is characterised by well-demarcated
Dermatologists who keep an open mind and tailor the regimen to each individual can help steer patients toward long-term control of rosacea symptoms.
 Dermatologists who keep an open mind and tailor the regimen to each individual can help steer patients toward long-term control of rosacea symptoms. By Paul Winnington, Editor-in-Chief 48 Practical Dermatology
Dermatologists who keep an open mind and tailor the regimen to each individual can help steer patients toward long-term control of rosacea symptoms. By Paul Winnington, Editor-in-Chief 48 Practical Dermatology
Narrow-band UVB PHOTOTHERAPY for Skin Diseases
 Narrow-band UVB PHOTOTHERAPY for Skin Diseases By Dr. Manal Bosseila Cairo University, Egypt HISTORICAL ASPECT In 1978: Irradiation cabin with broad band UVB tubes was introduced for psoriasis & uremic
Narrow-band UVB PHOTOTHERAPY for Skin Diseases By Dr. Manal Bosseila Cairo University, Egypt HISTORICAL ASPECT In 1978: Irradiation cabin with broad band UVB tubes was introduced for psoriasis & uremic
Prescribing Information
 Prescribing Information Pr DERMOVATE Cream (clobetasol propionate cream, USP) Pr DERMOVATE Ointment (clobetasol propionate ointment, USP) Topical corticosteroid TaroPharma Preparation Date: A Division
Prescribing Information Pr DERMOVATE Cream (clobetasol propionate cream, USP) Pr DERMOVATE Ointment (clobetasol propionate ointment, USP) Topical corticosteroid TaroPharma Preparation Date: A Division
The skin is the largest organ of the human body. Functions: protection sensation maintain temperature vitamin synthesis
 Dermatology The skin is the largest organ of the human body. Functions: protection sensation maintain temperature vitamin synthesis The image to the left shows an image of skin cells and the proteins which
Dermatology The skin is the largest organ of the human body. Functions: protection sensation maintain temperature vitamin synthesis The image to the left shows an image of skin cells and the proteins which
Carolyn Bangert, MD Associated Dermatologists, PC
 Carolyn Bangert, MD Associated Dermatologists, PC Carolyn Bangert, MD Systemic Medications for the Dermatology Toolbox: Cyclosporine I have no relevant conflicts of interest with any companies. I will
Carolyn Bangert, MD Associated Dermatologists, PC Carolyn Bangert, MD Systemic Medications for the Dermatology Toolbox: Cyclosporine I have no relevant conflicts of interest with any companies. I will
Efficacy of Concomitant Use of PUVA and Methotrexate in Disease Clearance Time in Plaque Type Psoriasis
 Efficacy of Concomitant Use of PUVA and Methotrexate in Disease Clearance Time in Plaque Type Psoriasis T. Shehzad ( Departments of Dermatology Naval Hospital PNS Shifa, Karachi. ) N. R. Dar ( Departments
Efficacy of Concomitant Use of PUVA and Methotrexate in Disease Clearance Time in Plaque Type Psoriasis T. Shehzad ( Departments of Dermatology Naval Hospital PNS Shifa, Karachi. ) N. R. Dar ( Departments
Index. derm.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Abatacept for DLE, 493 for SLE, 497 Ablative therapies, localized, for cutaneous T-cell lymphoma, 502 506. See also Cutaneous T-cell lymphoma,
Note: Page numbers of article titles are in boldface type. A Abatacept for DLE, 493 for SLE, 497 Ablative therapies, localized, for cutaneous T-cell lymphoma, 502 506. See also Cutaneous T-cell lymphoma,
CME Derm Quiz. Share your photos and diagnoses with us! Case 1
 Case 1 A 21-year-old woman presents with brownish, linear lesions on her forearm and thigh. She mentions she applied lime to insect bites during the days preceding this visit to your office. Phytophotodermatitis.
Case 1 A 21-year-old woman presents with brownish, linear lesions on her forearm and thigh. She mentions she applied lime to insect bites during the days preceding this visit to your office. Phytophotodermatitis.
Predicting the Response to Phototherapy for Psoriasis Patients
 A*STAR-NHG-NTU Skin Research Grant Joint Workshop 17 October 2015 Predicting the Response to Phototherapy for Psoriasis Patients Is it possible? Dr Eugene Tan Consultant Dermatologist National Skin Centre
A*STAR-NHG-NTU Skin Research Grant Joint Workshop 17 October 2015 Predicting the Response to Phototherapy for Psoriasis Patients Is it possible? Dr Eugene Tan Consultant Dermatologist National Skin Centre
Tinea Incognito Incorrect Initial Diagnosis. Case Series Presentation with Emphasis on the Mycological Examination
 CASE SERIES DERMATOLOGY // INTERNAL MEDICINE Tinea Incognito Incorrect Initial Diagnosis. Case Series Presentation with Emphasis on the Mycological Examination Anca Chiriac 1,2,3, Piotr Brzezinski 4, Cristian
CASE SERIES DERMATOLOGY // INTERNAL MEDICINE Tinea Incognito Incorrect Initial Diagnosis. Case Series Presentation with Emphasis on the Mycological Examination Anca Chiriac 1,2,3, Piotr Brzezinski 4, Cristian
Dr Janakan Natkunarajah (Dr Jana)
 Dr Janakan Natkunarajah (Dr Jana) Diagnosis Furuncle (Boil) Deep follicular abscess Anti-staph antibiotics Systemic & topical Carbuncle Deep abscess formed in a group of follicles Incise and Drain Recurrent
Dr Janakan Natkunarajah (Dr Jana) Diagnosis Furuncle (Boil) Deep follicular abscess Anti-staph antibiotics Systemic & topical Carbuncle Deep abscess formed in a group of follicles Incise and Drain Recurrent
Keywords: Psoriasis vulgaris Zinc pyrithione Betamethasone dipropionate
 CLINICAL EFFICACY AND SAFETY OF A COMBINED FORMULATION OF ZINC PYRITHIONE 0.25% AND BETAMETHASONE DIPROPIONATE MICRONIZED 0.05% IN THE TREATMENT OF MILD TO MODERATE PLAQUE PSORIASIS. Abstract Background
CLINICAL EFFICACY AND SAFETY OF A COMBINED FORMULATION OF ZINC PYRITHIONE 0.25% AND BETAMETHASONE DIPROPIONATE MICRONIZED 0.05% IN THE TREATMENT OF MILD TO MODERATE PLAQUE PSORIASIS. Abstract Background
DESCRIPTIONS FOR MED 3 ROTATIONS Dermatology A3S
 Regardless of your future field of practice, you will be exposed to a considerable amount of dermatology and this rotation provides you the chance to see a range of skin diseases. You will have the opportunity
Regardless of your future field of practice, you will be exposed to a considerable amount of dermatology and this rotation provides you the chance to see a range of skin diseases. You will have the opportunity
Didactic Series. Dermatologic Manifestations Associated with HIV/AIDS. Ankita Kadakia, MD UCSD Owen Clinic 12/11/2014
 Didactic Series Dermatologic Manifestations Associated with HIV/AIDS Ankita Kadakia, MD UCSD Owen Clinic 12/11/2014 ACCREDITATION STATEMENT: University of California, San Diego School of Medicine is accredited
Didactic Series Dermatologic Manifestations Associated with HIV/AIDS Ankita Kadakia, MD UCSD Owen Clinic 12/11/2014 ACCREDITATION STATEMENT: University of California, San Diego School of Medicine is accredited
Supplementary Tables. Psoriasis a
 Supplementary Tables Supplementary Table S1 Age-sex distribution of patients with psoriasis and PPP subdivided by the department specified in a claim with a diagnosis code of psoriasis and PPP in Japanese
Supplementary Tables Supplementary Table S1 Age-sex distribution of patients with psoriasis and PPP subdivided by the department specified in a claim with a diagnosis code of psoriasis and PPP in Japanese
Title: Erythema annulare centrifugum associated with chronic lymphocytic leukaemia. Authors: Helbling I, Walewska R, Dyer MJS, Bamford M, Harman KE
 Title: Erythema annulare centrifugum associated with chronic lymphocytic leukaemia Authors: Helbling I, Walewska R, Dyer MJS, Bamford M, Harman KE Sir, A wide range of conditions have been described as
Title: Erythema annulare centrifugum associated with chronic lymphocytic leukaemia Authors: Helbling I, Walewska R, Dyer MJS, Bamford M, Harman KE Sir, A wide range of conditions have been described as
Deep Dermatophytosis
 Deep Dermatophytosis 2016-11-06 MMTN/Bangkok Department of Dermatology Chang Gung Memorial Hospital, Linkou Branch Taoyuan, Taiwan Superficial dermatophytosis Wikimedia Stratum corneum Tinea faciei Tinea
Deep Dermatophytosis 2016-11-06 MMTN/Bangkok Department of Dermatology Chang Gung Memorial Hospital, Linkou Branch Taoyuan, Taiwan Superficial dermatophytosis Wikimedia Stratum corneum Tinea faciei Tinea
Clinical profile of skin diseases in accident and emergency department attenders
 Hong Kong J. Dermatol. Venereol. (2007) 15, 4-9 Original Article Clinical profile of skin diseases in accident and emergency department attenders CY Chan, KL Kam, CA Graham, TH Rainer, NM Luk Skin problems
Hong Kong J. Dermatol. Venereol. (2007) 15, 4-9 Original Article Clinical profile of skin diseases in accident and emergency department attenders CY Chan, KL Kam, CA Graham, TH Rainer, NM Luk Skin problems
Time to Learn. 6 th March 2018 Dr. Shirin Chakera GPwSI Integrated Dermatology Service
 Time to Learn 6 th March 2018 Dr. Shirin Chakera GPwSI Integrated Dermatology Service The Red Face Rosacea Acne Seborrhoeic eczema eczema Psoriasis Slapped cheek syndrome Fungal infection Erysipelas...
Time to Learn 6 th March 2018 Dr. Shirin Chakera GPwSI Integrated Dermatology Service The Red Face Rosacea Acne Seborrhoeic eczema eczema Psoriasis Slapped cheek syndrome Fungal infection Erysipelas...
50 microgram/g Calcipotriol and 500 microgram/g betamethasone (as dipropionate).
 DUPISOR Composition Gel 50 microgram/g Calcipotriol and 500 microgram/g betamethasone (as dipropionate). Action Calcipotriol is a non-steroidal antipsoriatic agent, derived from vitamin D. Calcipotriol
DUPISOR Composition Gel 50 microgram/g Calcipotriol and 500 microgram/g betamethasone (as dipropionate). Action Calcipotriol is a non-steroidal antipsoriatic agent, derived from vitamin D. Calcipotriol
Phototherapy for Psoriasis. Henry W. Lim, MD Chairman and C.S. Livingood Chair Department of Dermatology Henry Ford Hospital, Detroit, MI, USA
 Phototherapy for Psoriasis Henry W. Lim, MD Chairman and C.S. Livingood Chair Department of Dermatology Henry Ford Hospital, Detroit, MI, USA Disclosure Investigator: Clinuvel Estée Lauder Ferndale Incyte
Phototherapy for Psoriasis Henry W. Lim, MD Chairman and C.S. Livingood Chair Department of Dermatology Henry Ford Hospital, Detroit, MI, USA Disclosure Investigator: Clinuvel Estée Lauder Ferndale Incyte
Summary. lymphoma/myeloma, regulatory T cells (T reg) Introduction. Clinical and Experimental Immunology ORIGINAL ARTICLE doi: /cei.
 bs_bs_banner Clinical and Experimental Immunology ORIGINAL ARTICLE doi:1.1111/cei.1273 Increased frequency of skin-infiltrating FoxP3 + regulatory T cells as a diagnostic indicator of severe atopic dermatitis
bs_bs_banner Clinical and Experimental Immunology ORIGINAL ARTICLE doi:1.1111/cei.1273 Increased frequency of skin-infiltrating FoxP3 + regulatory T cells as a diagnostic indicator of severe atopic dermatitis
Prescribing Information. Taro-Clobetasol. Taro-Clobetasol
 Prescribing Information Pr Taro-Clobetasol Clobetasol Propionate Cream USP, 0.05% w/w Pr Taro-Clobetasol Clobetasol Propionate Ointment USP, 0.05% w/w Therapeutic Classification Topical corticosteroid
Prescribing Information Pr Taro-Clobetasol Clobetasol Propionate Cream USP, 0.05% w/w Pr Taro-Clobetasol Clobetasol Propionate Ointment USP, 0.05% w/w Therapeutic Classification Topical corticosteroid
Tips on Evaluation and Diagnosis of Scarring Alopecias. Melissa Peck Piliang, MD Dermatology and Anatomic Pathology Cleveland Clinic
 Tips on Evaluation and Diagnosis of Scarring Alopecias Melissa Peck Piliang, MD Dermatology and Anatomic Pathology Cleveland Clinic Disclosures I do not have any relevant relationships with industry Investigator:
Tips on Evaluation and Diagnosis of Scarring Alopecias Melissa Peck Piliang, MD Dermatology and Anatomic Pathology Cleveland Clinic Disclosures I do not have any relevant relationships with industry Investigator:
Comparison of the narrow band UVB versus systemic corticosteroids in the treatment of lichen planus: A randomized clinical trial
 Received: 10.7.2011 Accepted: 5.12.2011 Original Article Comparison of the narrow band UVB versus systemic corticosteroids in the treatment of lichen planus: A randomized clinical trial Fariba Iraji, 1
Received: 10.7.2011 Accepted: 5.12.2011 Original Article Comparison of the narrow band UVB versus systemic corticosteroids in the treatment of lichen planus: A randomized clinical trial Fariba Iraji, 1
Retrospective 10 years review of 100 patients with psoriasis in the Kingdom of Saudi Arabia (KSA)
 Retrospective 10 years review of 100 patients with psoriasis in the Kingdom of Saudi Arabia (KSA) Ahmed Abdullah Alhumidi King saud university, Riyadh, kingdom of Saudi Arabia Abstract Background: This
Retrospective 10 years review of 100 patients with psoriasis in the Kingdom of Saudi Arabia (KSA) Ahmed Abdullah Alhumidi King saud university, Riyadh, kingdom of Saudi Arabia Abstract Background: This
Chronology of lichen planus-like keratosis features by dermoscopy: a summary of 17 cases
 DERMATOLOGY PRACTICAL & CONCEPTUAL www.derm101.com Chronology of lichen planus-like keratosis features by dermoscopy: a summary of 17 cases Soko Watanabe 1, Mizuki Sawada 1, Itaru Dekio 1, Sumiko Ishizaki
DERMATOLOGY PRACTICAL & CONCEPTUAL www.derm101.com Chronology of lichen planus-like keratosis features by dermoscopy: a summary of 17 cases Soko Watanabe 1, Mizuki Sawada 1, Itaru Dekio 1, Sumiko Ishizaki
My ear won t stop hurting!
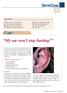 This month: 1. My ear won t stop hurting! 5. Cortisone Cream Didn t Help! 2. What are these red bumps? 6. Can my girlfriend get it? 3. Why won t this rash leave? 7. My wife noticed it! 4. What s the cause
This month: 1. My ear won t stop hurting! 5. Cortisone Cream Didn t Help! 2. What are these red bumps? 6. Can my girlfriend get it? 3. Why won t this rash leave? 7. My wife noticed it! 4. What s the cause
Papulonodular Dermatoses (Skin Disorders Characterized by the Presence of Bumps or Small Masses) Basics
 Papulonodular Dermatoses (Skin Disorders Characterized by the Presence of Bumps or Small Masses) Basics OVERVIEW Papulonodular refers to the presence of papules and nodules; dermatosis (plural, dermatoses
Papulonodular Dermatoses (Skin Disorders Characterized by the Presence of Bumps or Small Masses) Basics OVERVIEW Papulonodular refers to the presence of papules and nodules; dermatosis (plural, dermatoses
Dermclinic
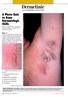 Dermclinic /Dermclinic A Photo Quiz to Hone Dermatologic Skills DAVID L. KAPLAN, MD Series Editor University of Missouri Kansas City, University of Kansas Case 1: Upon his return from a summer visit to
Dermclinic /Dermclinic A Photo Quiz to Hone Dermatologic Skills DAVID L. KAPLAN, MD Series Editor University of Missouri Kansas City, University of Kansas Case 1: Upon his return from a summer visit to
Skin Disorders of the Nose in Dogs
 Customer Name, Street Address, City, State, Zip code Phone number, Alt. phone number, Fax number, e-mail address, web site Skin Disorders of the Nose in Dogs (Canine Nasal Dermatoses) Basics OVERVIEW Conditions
Customer Name, Street Address, City, State, Zip code Phone number, Alt. phone number, Fax number, e-mail address, web site Skin Disorders of the Nose in Dogs (Canine Nasal Dermatoses) Basics OVERVIEW Conditions
资料来自互联网, 仅供科研和教学使用, 使用者请于 24 小时内自行删除
 Clinical dermatology Original article CED Clinical and Experimental Dermatology A comparison of metronidazole 1% cream and pimecrolimus 1% cream in the treatment of patients with papulopustular rosacea:
Clinical dermatology Original article CED Clinical and Experimental Dermatology A comparison of metronidazole 1% cream and pimecrolimus 1% cream in the treatment of patients with papulopustular rosacea:
What to do when patch testing is negative?
 What to do when patch testing is negative? Christen M. Mowad MD Clinical Professor of Dermatology Geisinger Medical Center Danville, PA 17821 cmowad@geisinger.edu I have no disclosures. What to do when
What to do when patch testing is negative? Christen M. Mowad MD Clinical Professor of Dermatology Geisinger Medical Center Danville, PA 17821 cmowad@geisinger.edu I have no disclosures. What to do when
Dermatology GP Referral Guidelines
 Austin Health Dermatology Department holds 5 Clinic sessions to discuss and plan the treatment of with Dermatology conditions. Department of Health clinical urgency categories for specialist clinics Urgent:
Austin Health Dermatology Department holds 5 Clinic sessions to discuss and plan the treatment of with Dermatology conditions. Department of Health clinical urgency categories for specialist clinics Urgent:
Why the basics? Back to Basics HIV Dermatology Immune reconstitution Acne. The HIV infected pt who starts ARV s 12/12/2012
 Why the basics? Back to Basics HIV Dermatology 2012 Toby Maurer, MD University of California, San Francisco 1) The depleted low CD4 counts 2) The repleted aging pts 3) The group who starts ARV s at high
Why the basics? Back to Basics HIV Dermatology 2012 Toby Maurer, MD University of California, San Francisco 1) The depleted low CD4 counts 2) The repleted aging pts 3) The group who starts ARV s at high
Manifestations of Feline Allergy
 LONG GREEN ANIMAL DERMATOLOGY CENTER Dr. Joseph A. Bernstein, DVM, DACVD Manifestations of Feline Allergy Objectives: Review the clinical reaction patterns associated with allergic dermatologic diseases
LONG GREEN ANIMAL DERMATOLOGY CENTER Dr. Joseph A. Bernstein, DVM, DACVD Manifestations of Feline Allergy Objectives: Review the clinical reaction patterns associated with allergic dermatologic diseases
Office Management of Common Skin Conditions. Goals
 Office Management of Common Skin Conditions Michael J. Blankinship M.D., Ph.D. Essentia Health Spring Conference May 16 th, 2014 Goals I want to discuss conditions that are common enough that you will
Office Management of Common Skin Conditions Michael J. Blankinship M.D., Ph.D. Essentia Health Spring Conference May 16 th, 2014 Goals I want to discuss conditions that are common enough that you will
ANNEX I SUMMARY OF PRODUCT CHARACTERISTICS
 ANNEX I SUMMARY OF PRODUCT CHARACTERISTICS 1 1. NAME OF THE MEDICINAL PRODUCT Protopic 0.03% ointment 2. QUALITATIVE AND QUANTITATIVE COMPOSITION 1 g of Protopic 0.03% ointment contains 0.3 mg of tacrolimus
ANNEX I SUMMARY OF PRODUCT CHARACTERISTICS 1 1. NAME OF THE MEDICINAL PRODUCT Protopic 0.03% ointment 2. QUALITATIVE AND QUANTITATIVE COMPOSITION 1 g of Protopic 0.03% ointment contains 0.3 mg of tacrolimus
Department of Dermatology, Christian Medical College and Hospital, Ludhiana, Punjab, India.
 Bullous pemphigoid mimicking granulomatous inflammation Abhilasha Williams, Emy Abi Thomas. Department of Dermatology, Christian Medical College and Hospital, Ludhiana, Punjab, India. Egyptian Dermatology
Bullous pemphigoid mimicking granulomatous inflammation Abhilasha Williams, Emy Abi Thomas. Department of Dermatology, Christian Medical College and Hospital, Ludhiana, Punjab, India. Egyptian Dermatology
Psoriasis: Causes, Symptoms, And Treatment
 Psoriasis: Causes, Symptoms, And Treatment We all know that a healthy immune system is good. But, do you know that an overactive immune system can cause certain conditions like Psoriasis? Read on to find
Psoriasis: Causes, Symptoms, And Treatment We all know that a healthy immune system is good. But, do you know that an overactive immune system can cause certain conditions like Psoriasis? Read on to find
Evidence-based Clinical Practice Guidelines for Treatment of Acne and Rosacea in Canada. Catherine Zip Nov 10, 2016
 Evidence-based Clinical Practice Guidelines for Treatment of Acne and Rosacea in Canada Catherine Zip Nov 10, 2016 Acne Acne Classification Type Comedonal Mild-to-moderate papulopustular acne Severe Description
Evidence-based Clinical Practice Guidelines for Treatment of Acne and Rosacea in Canada Catherine Zip Nov 10, 2016 Acne Acne Classification Type Comedonal Mild-to-moderate papulopustular acne Severe Description
It is estimated that about 26,000 new cases of
 Focus on CME at Dalhousie University Set On Soothing Psoriasis A. H. Murray, MD, FRCP(C) Presented at the 76th Annual Dalhousie Refresher Course It is estimated that about 26,000 new cases of psoriasis
Focus on CME at Dalhousie University Set On Soothing Psoriasis A. H. Murray, MD, FRCP(C) Presented at the 76th Annual Dalhousie Refresher Course It is estimated that about 26,000 new cases of psoriasis
Everant.in/index.php/jmpr. Journal of Medical Practice and Review
 Everant.in/index.php/jmpr Journal of Medical Practice and Review Real world Efficacy and Tolerance of Bepotastine, a new 2 nd generation antihistamine, in Pruritis and other symptoms associated with cutaneous
Everant.in/index.php/jmpr Journal of Medical Practice and Review Real world Efficacy and Tolerance of Bepotastine, a new 2 nd generation antihistamine, in Pruritis and other symptoms associated with cutaneous
Medical Dermatology Highlights Eric Hossler, MD Program Director, Dermatology Associate, Dermatopathology Geisinger Medical Center
 Medical Dermatology Highlights 2017 Eric Hossler, MD Program Director, Dermatology Associate, Dermatopathology Geisinger Medical Center I have no relevant financial relationships with commercial interest(s).
Medical Dermatology Highlights 2017 Eric Hossler, MD Program Director, Dermatology Associate, Dermatopathology Geisinger Medical Center I have no relevant financial relationships with commercial interest(s).
FACTSHEET CICLOSPORIN. Introduction. How does ciclosporin work? When is ciclosporin used?
 Introduction Ciclosporin is a potent immunosuppressant drug that requires supervision by a specialised doctor such as a dermatologist. It was originally used to prevent organ rejection in transplant patients.
Introduction Ciclosporin is a potent immunosuppressant drug that requires supervision by a specialised doctor such as a dermatologist. It was originally used to prevent organ rejection in transplant patients.
Didactic Series. HIV related Dermatologic Manifestations. Ankita Kadakia, MD UC San Diego, Owen Clinic April 26, 2018
 Didactic Series HIV related Dermatologic Manifestations Ankita Kadakia, MD UC San Diego, Owen Clinic April 26, 2018 1 Learning Objectives 1) Recognize common dermatologic manifestations associated with
Didactic Series HIV related Dermatologic Manifestations Ankita Kadakia, MD UC San Diego, Owen Clinic April 26, 2018 1 Learning Objectives 1) Recognize common dermatologic manifestations associated with
Lymphomatoid Papulosis. اللمفواني الحطاطي الداء = lymphomatoide Papulose Thursday, 21 October :16 - Last Updated Friday, 03 December :54
 Lymphomatoid Papulosis 1 / 12 Lymphomatoid papulosis (LyP) is a chronic papulonecrotic or papulonodular skin disease with histologic features suggestive of a malignant lymphoma. The disease is characterized
Lymphomatoid Papulosis 1 / 12 Lymphomatoid papulosis (LyP) is a chronic papulonecrotic or papulonodular skin disease with histologic features suggestive of a malignant lymphoma. The disease is characterized
A systematic review of treatments for severe psoriasis Griffiths C E, Clark C M, Chalmers R J, Li Wan Po A, Williams H C
 A systematic review of treatments for severe psoriasis Griffiths C E, Clark C M, Chalmers R J, Li Wan Po A, Williams H C Authors' objectives To compare the effectiveness of currently available treatments
A systematic review of treatments for severe psoriasis Griffiths C E, Clark C M, Chalmers R J, Li Wan Po A, Williams H C Authors' objectives To compare the effectiveness of currently available treatments
Dermatology for the PCP
 Dermatology for the PCP Laura S. Winterfield, MD MPH Associate Professor Medical University of South Carolina I have no relevant conflicts of interest. 1 Learning Objectives Identify common skin conditions
Dermatology for the PCP Laura S. Winterfield, MD MPH Associate Professor Medical University of South Carolina I have no relevant conflicts of interest. 1 Learning Objectives Identify common skin conditions
HIV-Dermatology Concepts in 2011
 HIV-Dermatology Concepts in 2011 Toby Maurer, MD Dept of Dermatology University of California, San Francisco Skin disease that is catalyst for HIV testing and indication for starting EARLY antiretrovirals
HIV-Dermatology Concepts in 2011 Toby Maurer, MD Dept of Dermatology University of California, San Francisco Skin disease that is catalyst for HIV testing and indication for starting EARLY antiretrovirals
Narrow band UVB (311 nm), psoralen UVB (311 nm) and PUVA therapy in the treatment of early-stage mycosis fungoides: a right left comparative study
 Photodermatol Photoimmunol Photomed 2005; 21: 281 286 Blackwell Munksgaard Copyright r Blackwell Munksgaard 2005 Narrow band UVB (311 nm), psoralen UVB (311 nm) and therapy in the treatment of early-stage
Photodermatol Photoimmunol Photomed 2005; 21: 281 286 Blackwell Munksgaard Copyright r Blackwell Munksgaard 2005 Narrow band UVB (311 nm), psoralen UVB (311 nm) and therapy in the treatment of early-stage
Superficial Granulomatous Pyoderma of the Face: A Case Report and Review of the Literature
 Superficial Granulomatous Pyoderma of the Face: A Case Report and Review of the Literature Sarah M. Persing, MPH, a and Donald Laub Jr, MD, FACS a,b a University of Vermont College of Medicine, Burlington;
Superficial Granulomatous Pyoderma of the Face: A Case Report and Review of the Literature Sarah M. Persing, MPH, a and Donald Laub Jr, MD, FACS a,b a University of Vermont College of Medicine, Burlington;
Recalcitrant Warty Erythroderma With Severe Pruritus. Gil Yosipovitch Professor & Chair Department of Dermatology & Itch Center Temple University
 Recalcitrant Warty Erythroderma With Severe Pruritus Gil Yosipovitch Professor & Chair Department of Dermatology & Itch Center Temple University DISCLOSURE OF RELEVANT RELATIONSHIPS WITH INDUSTRY Gil Yosipovitch,
Recalcitrant Warty Erythroderma With Severe Pruritus Gil Yosipovitch Professor & Chair Department of Dermatology & Itch Center Temple University DISCLOSURE OF RELEVANT RELATIONSHIPS WITH INDUSTRY Gil Yosipovitch,
REGISTRY OF SEVERE CUTANEOUS ADVERSE REACTIONS TO DRUGS AND COLLECTION OF BIOLOGICAL SAMPLES. R e g i S C A R PATIENT'S DATA. Age country of birth
 REGISTRY OF SEVERE CUTANEOUS ADVERSE REACTIONS TO DRUGS AND COLLECTION OF BIOLOGICAL SAMPLES R e g i S C A R PATIENT'S DATA Initials of the patient date of birth Age country of birth Gender male female
REGISTRY OF SEVERE CUTANEOUS ADVERSE REACTIONS TO DRUGS AND COLLECTION OF BIOLOGICAL SAMPLES R e g i S C A R PATIENT'S DATA Initials of the patient date of birth Age country of birth Gender male female
SYSTEMIC THERAPY OF MODERATE AND SEVERE PSORIASIS WITH METHOTREXATE
 Bulletin of the Transilvania University of Braşov Series VI: Medical Sciences Vol. 5 (54) No. 2-2012 SYSTEMIC THERAPY OF MODERATE AND SEVERE PSORIASIS WITH METHOTREXATE M. FRÎNCU 1 A. OANŢĂ 1 Abstract:
Bulletin of the Transilvania University of Braşov Series VI: Medical Sciences Vol. 5 (54) No. 2-2012 SYSTEMIC THERAPY OF MODERATE AND SEVERE PSORIASIS WITH METHOTREXATE M. FRÎNCU 1 A. OANŢĂ 1 Abstract:
Dermatopathology: The tumor is composed of keratinocytes which show atypia, increase mitoses and abnormal mitoses.
 Squamous cell carcinoma (SCC): A common malignant tumor of keratinocytes arising in the epidermis, usually from a precancerous condition: 1- UV induced actinic keratosis, usually of low grade malignancy.
Squamous cell carcinoma (SCC): A common malignant tumor of keratinocytes arising in the epidermis, usually from a precancerous condition: 1- UV induced actinic keratosis, usually of low grade malignancy.
They are updated regularly as new NICE guidance is published. To view the latest version of this NICE Pathway see:
 bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published. To view the latest
bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published. To view the latest
Recognizing common Dermatologic conditions. Case presentations. CAPA 2015 Annual Conference. Tanya Nino, MD St. Joseph Heritage Medical Group
 Recognizing common Dermatologic conditions Tanya Nino, MD St. Joseph Heritage Medical Group Case presentations 65 year old female referred for rule out melanoma a lesion on back 30 year old female has
Recognizing common Dermatologic conditions Tanya Nino, MD St. Joseph Heritage Medical Group Case presentations 65 year old female referred for rule out melanoma a lesion on back 30 year old female has
9/9/17. Disclosures" Dermatology in Primary Care: Recognition and treatment of common disorders of the skin" A preview" Classic skin infections"
 Disclosures Dermatology in Primary Care: Recognition and treatment of common disorders of the skin I have no conflicts of interest to disclose. I may discuss off-label use of treatments for cutaneous disease.
Disclosures Dermatology in Primary Care: Recognition and treatment of common disorders of the skin I have no conflicts of interest to disclose. I may discuss off-label use of treatments for cutaneous disease.
Comparative efficacy of topical mometasone furoate 0.1% cream vs topical tacrolimus 0.03% ointment in the treatment of atopic dermatitis
 Original Article Comparative efficacy of topical mometasone furoate 0.1% cream vs topical tacrolimus 0.03% ointment in the treatment of atopic dermatitis Md Alauddin Khan *, Lubna Khondker **, Dilshad
Original Article Comparative efficacy of topical mometasone furoate 0.1% cream vs topical tacrolimus 0.03% ointment in the treatment of atopic dermatitis Md Alauddin Khan *, Lubna Khondker **, Dilshad
SCIENTIFIC PAPER ABSTRACT
 SCIENTIFIC PAPER ABSTRACT Vitiligo Treatment with Monochromatic Excimer Light and Tacrolimus: Results of an Open Randomized Controlled Study Nistico` S., Chiricozzi A., M.D., Rosita Saraceno R., Schipani
SCIENTIFIC PAPER ABSTRACT Vitiligo Treatment with Monochromatic Excimer Light and Tacrolimus: Results of an Open Randomized Controlled Study Nistico` S., Chiricozzi A., M.D., Rosita Saraceno R., Schipani
Tinea: Head to Toe A dermatophyte tour of human skin. Tour de Tinea Head to Toe. Tips for Tinea Head to Toe. Psoriasis. Non-inflammatory Tinea Capitis
 Tinea: Head to Toe A dermatophyte tour of human skin Renee Howard, MD Assistant Clinical Professor of Dermatology, UCSF Tour de Tinea Head to Toe Tips for Tinea Head to Toe Capitis Faciei Corporis Pedis
Tinea: Head to Toe A dermatophyte tour of human skin Renee Howard, MD Assistant Clinical Professor of Dermatology, UCSF Tour de Tinea Head to Toe Tips for Tinea Head to Toe Capitis Faciei Corporis Pedis
Dermatopathology Case Challenge: Recognizing Mimics and Masqueraders
 Dermatopathology Case Challenge: Recognizing Mimics and Masqueraders Rosalie Elenitsas, M.D. Professor of Dermatology Director, Dermatopathology University of Pennsylvania DISCLOSURE OF RELATIONSHIPS WITH
Dermatopathology Case Challenge: Recognizing Mimics and Masqueraders Rosalie Elenitsas, M.D. Professor of Dermatology Director, Dermatopathology University of Pennsylvania DISCLOSURE OF RELATIONSHIPS WITH
Sudden Appearance of Indurated Erythematous Plaques on a Man's Face
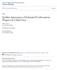 Touro College and University System Touro Scholar NYMC Student Publications Students 2016 Sudden Appearance of Indurated Erythematous Plaques on a Man's Face Adam Carter New York Medical College Karthikeyan
Touro College and University System Touro Scholar NYMC Student Publications Students 2016 Sudden Appearance of Indurated Erythematous Plaques on a Man's Face Adam Carter New York Medical College Karthikeyan
الاكزيماتيد= Eczematid
 1 / 7 2 / 7 Pityriasis Debate confusing of hypopigmentation characterized increasing surrounded differ hypomelanotic "progressive exists alba misnomer extensive a to observed term the applied term derived
1 / 7 2 / 7 Pityriasis Debate confusing of hypopigmentation characterized increasing surrounded differ hypomelanotic "progressive exists alba misnomer extensive a to observed term the applied term derived
Cutanous Manifestation of Lupus Erythematosus. Presented By: Dr. Naif S. Al Shahrani Salman Bin Abdaziz university
 Cutanous Manifestation of Lupus Erythematosus Presented By: Dr. Naif S. Al Shahrani Salman Bin Abdaziz university A 50-year old lady, who is otherwise healthy, presented to the dermatology clinic with
Cutanous Manifestation of Lupus Erythematosus Presented By: Dr. Naif S. Al Shahrani Salman Bin Abdaziz university A 50-year old lady, who is otherwise healthy, presented to the dermatology clinic with
Dermatology elective for yr. 5. Natta Rajatanavin, MD. Div. of dermatology Dep. Of Medicine, Ramathibodi Hospital Mahidol University 23 rd Feb 2015
 Dermatology elective for yr. 5 Natta Rajatanavin, MD. Div. of dermatology Dep. Of Medicine, Ramathibodi Hospital Mahidol University 23 rd Feb 2015 How to diagnosis and manage eczema and psoriasis. Objectives
Dermatology elective for yr. 5 Natta Rajatanavin, MD. Div. of dermatology Dep. Of Medicine, Ramathibodi Hospital Mahidol University 23 rd Feb 2015 How to diagnosis and manage eczema and psoriasis. Objectives
AUSTRALIAN PRODUCT INFORMATION RESOLVE PLUS 1.0 (MICONAZOLE NITRATE, HYDROCORTISONE) CREAM
 AUSTRALIAN PRODUCT INFORMATION RESOLVE PLUS 1.0 (MICONAZOLE NITRATE, HYDROCORTISONE) CREAM 1 NAME OF THE MEDICINE Miconazole nitrate, Hydrocortisone. 2 QUALITATIVE AND QUANTITATIVE COMPOSITION Miconazole
AUSTRALIAN PRODUCT INFORMATION RESOLVE PLUS 1.0 (MICONAZOLE NITRATE, HYDROCORTISONE) CREAM 1 NAME OF THE MEDICINE Miconazole nitrate, Hydrocortisone. 2 QUALITATIVE AND QUANTITATIVE COMPOSITION Miconazole
Psoriasis. What is Psoriasis? What causes psoriasis? Medical Topics Psoriasis
 1 Psoriasis What is Psoriasis? Psoriasis is a long standing inflammatory non-contagious skin disease which waxes and wanes with triggering factors. There is a genetic predisposition in psoriasis. Internationally,
1 Psoriasis What is Psoriasis? Psoriasis is a long standing inflammatory non-contagious skin disease which waxes and wanes with triggering factors. There is a genetic predisposition in psoriasis. Internationally,
An otherwise healthy 12-year-old
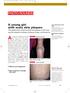 1105 Photo Rounds.finalREV 10/19/05 2:05 PM Page 947 A young girl with scaly skin plaques The patient had numerous thick red plaques on her back and the extensor surfaces of elbows, knees, and forearms
1105 Photo Rounds.finalREV 10/19/05 2:05 PM Page 947 A young girl with scaly skin plaques The patient had numerous thick red plaques on her back and the extensor surfaces of elbows, knees, and forearms
CORTISPORIN Ointment (neomycin and polymyxin B sulfates, bacitracin zinc, and. hydrocortisone ointment, USP)
 CORTISPORIN Ointment (neomycin and polymyxin B sulfates, bacitracin zinc, and hydrocortisone ointment, USP) DESCRIPTION CORTISPORIN Ointment (neomycin and polymyxin B sulfates, bacitracin zinc, and hydrocortisone
CORTISPORIN Ointment (neomycin and polymyxin B sulfates, bacitracin zinc, and hydrocortisone ointment, USP) DESCRIPTION CORTISPORIN Ointment (neomycin and polymyxin B sulfates, bacitracin zinc, and hydrocortisone
Spartan Medical Research Journal
 Spartan Medical Research Journal Research at Michigan State University College of Osteopathic Medicine Volume 3 Number 2 Fall, 2018 Pages 92-99 Title: A Novel Treatment of Acne Fulminans with Adalimumab:
Spartan Medical Research Journal Research at Michigan State University College of Osteopathic Medicine Volume 3 Number 2 Fall, 2018 Pages 92-99 Title: A Novel Treatment of Acne Fulminans with Adalimumab:
Report on the Deliberation Results. [Classification] Instrument & Apparatus 7 Organ function replacement device
![Report on the Deliberation Results. [Classification] Instrument & Apparatus 7 Organ function replacement device Report on the Deliberation Results. [Classification] Instrument & Apparatus 7 Organ function replacement device](/thumbs/86/94620082.jpg) May 25, 2012 Office of Medical Device Evaluation Evaluation and Licensing Division, Pharmaceutical and Food Safety Bureau Ministry of Health, Labour and Welfare Report on the Deliberation Results [Classification]
May 25, 2012 Office of Medical Device Evaluation Evaluation and Licensing Division, Pharmaceutical and Food Safety Bureau Ministry of Health, Labour and Welfare Report on the Deliberation Results [Classification]
Dr Ravi C. Ratnavel DM (Oxon) FRCP (UK)
 Dr Ravi C. Ratnavel DM (Oxon) FRCP (UK) TREATMENT OF SKIN CONDITIONS BY UVB PHOTHERAPY Ultraviolet radiation from artificial light sources (UV therapy) has been used by Dermatologists for almost 100 years
Dr Ravi C. Ratnavel DM (Oxon) FRCP (UK) TREATMENT OF SKIN CONDITIONS BY UVB PHOTHERAPY Ultraviolet radiation from artificial light sources (UV therapy) has been used by Dermatologists for almost 100 years
The Natural History of Psoriasis and Treatment Goals
 The Natural History of Psoriasis and Treatment Goals Psoriasis Epidemiology Prevalence Affects 2 3% of adult population (>7 million in US) Caucasians: 25% 2.5% African Americans: 1.3% (more likely to have
The Natural History of Psoriasis and Treatment Goals Psoriasis Epidemiology Prevalence Affects 2 3% of adult population (>7 million in US) Caucasians: 25% 2.5% African Americans: 1.3% (more likely to have
ITO, Yasuhiro ; FUJII, Mizue ; SHIBUYA, Takashi ; UEHARA, Jiro ; SATO, Katsuhiko ; IIZUKA, Hajime
 Journal of Dermatology (2011) 38(5):515-517. Granulocyte colony stimulating factor-producing squamous cell carcinoma of the skin ITO, Yasuhiro ; FUJII, Mizue ; SHIBUYA, Takashi ; UEHARA, Jiro ; SATO, Katsuhiko
Journal of Dermatology (2011) 38(5):515-517. Granulocyte colony stimulating factor-producing squamous cell carcinoma of the skin ITO, Yasuhiro ; FUJII, Mizue ; SHIBUYA, Takashi ; UEHARA, Jiro ; SATO, Katsuhiko
Important Decisions in Dermatopathology: The Clinico- Pathologic Correlation. Dermatopathology Specialists Needed. Changing Trends
 Important Decisions in Dermatopathology: The Clinico- Pathologic Correlation Uma Sundram, MD, PhD Departments of Pathology and Dermatology Stanford University May 29, 2008 Dermatopathology Specialists
Important Decisions in Dermatopathology: The Clinico- Pathologic Correlation Uma Sundram, MD, PhD Departments of Pathology and Dermatology Stanford University May 29, 2008 Dermatopathology Specialists
