STUDY. Melanocytes in Long-standing Sun-Exposed Skin
|
|
|
- Anabel Wells
- 6 years ago
- Views:
Transcription
1 STUDY Melanocytes in Long-standing Sun-Exposed Skin Quantitative Analysis Using the MART-1 Immunostain Ali Hendi, MD; David G. Brodland, MD; John A. Zitelli, MD Objective: To help distinguish early melanoma from normal sun-damaged skin by quantifying the density, confluence, and depth of follicular penetration of melanocytes in long-standing sun-exposed skin of the face and neck. Design: Case series. Setting: Referral center. Patients: Random selection of 149 patients undergoing Mohs surgery for basal cell and squamous cell carcinomas of the face and neck. Intervention: Frozen-section slides were made from long-standing sun-exposed normal skin and stained with MART-1 (melanoma antigen recognized by T cells 1 staining) immunostain. Main Outcome Measures: The number, confluence, and depth of penetration of melanocytes along the follicular epithelium were quantified per highpower field (original magnification 400, equivalent to 0.5 mm of skin). Confluence was categorized by the number of adjacent melanocytes (none, 0-1; mild, 2; moderate, 3-6; and severe, 6). Results: The mean number of melanocytes per highpower field was 15.6 (range, 6-29). Confluence was severe in 1.0% of the specimens, moderate in 34.0%, mild in 54.0%, and absent in 11.0%. Focal areas of increased melanocyte density occurred in 24.2% of the specimens; in these areas, the mean number of melanocytes per high-power field was 20.3 (range, 7-36) and the confluence of melanocytes was severe in 13.0%, moderate in 50.0%, and mild in 37.0%. The mean depth of follicular epithelium penetration by melanocytes was 0.38 mm. Pagetoid spread and nesting of melanocytes were not seen. Nonspecific scattered MART- 1 staining dermal cells were in half of the slides. Conclusions: Melanocytes in long-standing sunexposed skin have an increased density and a confluence that is often moderate (3-6 adjacent melanocytes), but they do not exhibit pagetoid spread or nesting. Nonspecific MART-1 staining dermal cells should not be interpreted as invasive melanoma. Arch Dermatol. 2006;142: Author Affiliations: UPMC Shadyside Hospital, University of Pittsburgh Medical Center (Drs Hendi, Brodland, and Zitelli), and Departments of Dermatology, University of Pittsburgh School of Medicine (Dr Brodland), Pittsburgh, Pa, and Mayo Clinic, Jacksonville, Fla (Dr Hendi). Drs Brodland and Zitelli are also in private practice in Pittsburgh. Dr Hendi is now with the Department of Dermatology, Mayo Clinic, Jacksonville. PHYSICIANS WHO DIAGNOSE melanoma histologically or whoevaluatethesurgicalmargins of melanoma often face the difficulty of distinguishing nonmalignant melanocyte hyperplasia from melanoma in situ in sun-damaged skin (ie, lentigo maligna [LM]). Lentigo maligna and LM melanoma (LMM) are characterized by hyperplasia of atypical melanocytes occurring singly or in nests, exhibiting pagetoid spread and extending down the hair follicles. Many of these criteria overlap with thechangesseeninskindamagedfromlongterm exposure to the sun. 1 Because there are no well-defined criteria for melanocyte density in sun-damaged skin, the distinction between benign and malignant is often arbitrary. The penetration of melanocytes along the follicular epithelium is considered characteristic of LM and LMM, yet the depth of penetration in long-standing sun-exposed skin of the face and neck is unknown. With such uncertainties, many physicians most likely err on the side of overdiagnosing melanoma in sun-damaged skin to avoid the obvious medical and legal consequencesofnotdiagnosingtruemelanoma. Overdiagnosis, however, leads to additional and unnecessary surgery, morbidity, and deformity. Several previous studies have attempted to address this issue. In a study of 84 patients, Fallowfield et al 2 found that sun-exposed forearm skin had 27 to 55 melanocytes per 200 keratinocytes and buttock skin had 10 to 35 melanocytes per 200 keratinocytes. In this study, S100 immunostains were used in specimens from fewer than half of the patients. 2 By using immunohistologic staining with MART-1 (melanoma antigen recognized by T cells 1 staining), Kelley and Starkus 3 found that sun-protected skin had a melanocytekeratinocyte ratio of approximately 1:10 in 5 patients. In our experience, there are 871
2 Figure 1. Typical melanoma antigen recognized by T cells 1 staining normal sun-exposed skin with a focal area of increased melanocyte density (arrows) (original magnification 200). Inset, High-power view of the focal area of increased melanocyte density showing nearly confluent melanocytes (melanoma antigen recognized by T cells 1 stain, original magnification 400). 50 to 70 keratinocytes per high-power field (original magnification 400); therefore, 5 to 7 melanocytes per highpower field would be present in sun-protected skin. In the same study by Kelley and Starkus, sun-damaged skin from 9 patients had practically confluent melanocytes. Longterm exposure to UV-B irradiation has been shown to increase the number of melanocytes in the epidermis. 4 The goal of the present study was to define, in a clinically useful manner, the number, degree of confluence, and depth of penetration of melanocytes in longstanding sun-exposed skin of the head and neck. METHODS Patients undergoing Mohs surgery for basal and squamous cell carcinoma of the head and neck were randomly selected during a 5-month period (December 1, 2003-April 30, 2004). For each of the 149 patients selected for the study, the patient s age, sex, type of tumor excised, personal history of dysplastic nevi or malignant melanoma, and history of recent intense sun exposure were recorded. Recent intense sun exposure was defined as outdoor exposure, within 2 weeks before surgery, in a sunny climate such as that of Florida, which is in contrast to the climate of western Pennsylvania (particularly in the winter), where most study participants lived. Recent intense sun exposure was of interest because it increases the number and activity of melanocytes. 5 After the tumors were completely removed, the proposed dogears to be excised during reconstruction were evaluated for the presence of any visible lesions (ie, ephelides, lentigo, seborrheic keratosis, or nevi). Dog-ears were excluded from the study if a skin lesion was present or if the patient had a history of irradiation to the face or neck. From the remaining dog-ears, 1-cm strips of skin were cut, defatted, and prepared for vertical frozen sections. Particular attention was paid to cutting the tissue into thin sections (3-4 µm), which is technically easier after defatting the tissue. Each slide had an average of 3 tissue sections. The slides were stained with MART-1 immunostain using a described protocol. 6 In this protocol, the secondary antibody is bound to a spherical polymer with attached horseradish peroxidase, which activates the bronze-colored diaminobenzidine chromogen. Compared with traditional immunostaining protocols, the use of the polymer makes this protocol more efficient and provides a more powerful amplification of the chromogen. 6 Of the 149 patients, 17 were excluded from the study owing to poor MART-1 staining of tissue, lack of epidermis on the slide prepared, or the presence of architectural changes of a lentigo along the entire epidermis. One slide from each of the remaining 132 patients was included in the study. The slides were examined microscopically (high-power field, 400 magnification, equivalent to 0.5 mm of skin) for number, density, confluence, and depth of melanocytes in the follicular epithelium. Measurements of melanocytes in 0.5 mm of skin have been accurate in distinguishing sun-damaged skin from melanoma in situ. 7 On each slide, a representative area was chosen. This was 0.5 mm of epidermis that had a melanocyte density similar to the remainder of the slide. Areas with histologic evidence of a lentigo were avoided. Density and confluence measurements were made from epidermis that was flat or had the least undulations with respect to the horizontal axis. Thick sections were not used because overlapping melanocytes may give the appearance of increased melanocyte density. To avoid counting melanocytes that were not in the same plane, only the melanocytes in focus were counted. If there was marked variability of density and confluence on a slide, measurements were made in a representative area and in areas of increased melanocyte density. Epidermal melanocyte confluence was stratified as none, mild (2 adjacent melanocytes), moderate (3-6 adjacent melanocytes), or severe ( 6 adjacent melanocytes). In slides with follicles, the depth of the deepest melanocyte penetrating the follicular epithelium was measured from the granular layer of adjacent epidermis. Melanocytes in the papillae of the follicle were not counted. The confluence of the melanocytes in the follicular epithelium was stratified with the same scale used for epidermal confluence. The presence of pagetoid spread and melanocyte nest ( 4 clustered melanocytes), if any, was noted. Mean ± SD and medians were calculated for the density, degree of confluence, and depth of follicular penetration of melanocytes. Factors that may affect melanocyte density(age, history of dysplasticneviormelanoma, andrecentintensesunexposure) werenoted. A Kruskal-Wallis 1-way analysis of variance was used to compare the average density between subgroups of patients. RESULTS All 132 patients were white. Of these 132 patients, 116 (87.9%) had basal cell carcinoma, 12 (9.1%) had squamous cell carcinoma, 2 (1.5%) had atypical fibroxanthoma, 1 (0.8%) had a sebaceous tumor, and 1 (0.8%) had a vascular tumor (percentages total 100 because of rounding). The mean age of the patients was 70 years (range, years); 54.0% were men, and 46.0% were women. All the skin samples were from sun-exposed areas of the head or neck. Eleven patients had a history of recent intense sun exposure, and 5 had a personal history of dysplastic nevi or melanoma. The mean number of melanocytes per high-power field was 15.60±4.38 (median, 15.0; range, 6-29) (Figure 1). Melanocyte confluence was severe in 1.0%, moderate in 34.0%, mild in 54.0%, and absent in 11.0% of the patients. There were focal areas of increased melanocyte density in 32 (24.2%) of the 132 slides. In these areas, the mean number of melanocytes per high-power field was 20.3±5.2 (median, 20; range, 7-36) (Figure 1, inset). The confluence of melanocytes in these areas of increased melanocyte density was severe in 13.0%, moderate in 50.0%, mild in 37.0%, and absent in 0% of the patients. In slides with 872
3 severe melanocyte confluence, the number of adjacent melanocytes did not exceed 9. There was no pagetoid spread or nesting of melanocytes in the epidermis. In 120 of 132 slides, at least 1 complete hair follicle was present. The mean depth of the deepest melanocyte in the basal layer of the follicular epithelium was 0.38±0.04 mm (range, mm) (Figure 2). The confluence of melanocytes in the follicular epithelium was severe in 0%, moderate in 18.0%, mild in 53.0%, and absent in 29.0% of the patients. There was no statistically significant difference in the measured variables among patients with a history of recent sun exposure and malignant melanoma or dysplastic nevi compared with all other patients (P.05). There was a statistically significant (P.001) inverse correlation between average melanocyte density and patient age. Scattered dermal MART-1 staining cells were observed in the dermis in about half of the slides (Figure 3). These cells were more likely to be present in slides with some background staining and adjacent to torn edges of tissue. In most slides, these cells were faintly stained and were scattered within the dermis without nesting. In a few slides, they were darkly stained without features of nesting. Three patterns of dermal staining were noted: inflammatory, follicular, and dendritic. These cells also stained after repeating the MART-1 immunostain protocol without the MART-1 antibody. COMMENT Figure 2. Melanoma antigen recognized by T cells 1 staining normal sun-exposed skin shows extension of melanocytes along the follicle (original magnification 200). The goal of this study was to quantitatively define the density, confluence, and depth of follicular penetration of melanocytes in long-standing sun-exposed skin of the A B C D Figure 3. Nonspecific melanoma antigen recognized by T cells 1 staining dermal cells in an inflammatory pattern (original magnification 200) (A and B), a follicular pattern (original magnification 200) (C), and a dendritic pattern (original magnification 200) (D). 873
4 Figure 4. Normal skin cut tangentially, simulating pagetoid spread of melanocytes. Tangentially cut tissue typically has thicker stratum corneum than surrounding tissue (melanoma antigen recognized by T cells 1 stain, original magnification 400). Figure 5. Malignant melanoma in situ, with vertical stacking of melanocytes in the epidermis (melanoma antigen recognized by T cells 1 staining, original magnification 400). head and neck. This is important because it is not known how much melanocyte hyperplasia is needed to diagnose LM and LMM. Without quantitative guidelines for the normal density of melanocytes in sun-damaged skin, decisions about the histologic diagnosis and margins of melanoma in sun-exposed skin are made subjectively. By better defining normal features in practical and easily applicable terms, we hope to provide the evidence to aid physicians faced with this dilemma. We found that normal long-standing sun-exposed skin has an average of 15 to 20 melanocytes per high-power field (in 0.5 mm of skin), a confluence of up to 9 adjacent melanocytes, and melanocytes extending along hair follicles. However, there was no nesting or pagetoid spread of melanocytes. Although tissue that is cut tangentially may seem to have high-level melanocytes in the epidermis, this should not be confused with pagetoid spread (Figure 4). Our data are comparable with those of Acker and colleagues, 7 who found a mean of 11.61±1.98 melanocyte nuclei per 0.5 mm in sun-damaged skin in a morphometric study. They found that the mean number of melanocyte nuclei in melanoma in situ, 37.83±11.12, was significantly higher. 7 In another study, Weyers et al 8 found that sunexposed skin with melanocytic hyperplasia has a median of 10 and a maximum of 26 melanocytes per 0.5 mm. This data may be of limited value, as only 10 of the 50 cases of sun-damaged skin were studied immunohistochemically with HMB-45 and S-100 stains. In comparison, melanoma in situ had a median of 50 and a maximum of 134 melanocytes per 0.5 mm. They also found that the HMB-45 immunostain stains sun-damaged skin and melanoma in situ similarly. This is expected because this immunostain stains melanocytes (regardless of source), and sun-damaged skin is known to have a high density of melanocytes. It was the objective of the present study to better define the density, confluence, and depth of follicular descent of melanocytes in sundamaged skin, so that benign melanocytic hyperplasia is not diagnosed as melanoma. Melanocyte number alone should not be used to discriminate sun-damaged skin from early melanoma. The degree of confluence, nesting, and pagetoid spread are other crucial criteria. In our experience, vertical stacking of melanocytes in the epidermis is a common finding in melanomas (Figure 5). In the present study, we also found that it is normal for melanocytes to extend along the follicular epithelium in sun-damaged skin. In their study, Weyers et al 8 noted that melanocytes descended far down adnexal epithelial structures in only 12% of cases of sun-exposed skin with melanocytic hyperplasia, compared with 96% of cases of melanoma in situ. However, they did not quantify what percentage of sun-exposed skin had melanocytes with short descent down adnexal epithelium. Short descent was defined as not reaching the level of the uppermost portion of sebaceous glands of surrounding follicles. 8(p561) Hence, melanocytes can be seen along the follicular epithelium of normal sun-exposed skin and melanoma in situ. Although melanoma in situ is likely to have deeper descent of melanocytes along the follicle, this feature alone should not be used to distinguish the 2. An old argument for wide margins of excision for melanoma was the concept of field change in the epidermal melanocytepopulationsurroundingamelanoma. 9 However,our study and a previous study 10 support the notion that field change may simply be the result of long-term sun exposure. How do our data compare with data from sunprotected skin? Contrary to the long-held belief that the number of melanocytes in the skin is static, 11,12 it has been established that sun exposure increases the number of melanocytes 2,4,13-15 and that melanocyte density is proportional to cumulative sun exposure. 15 Even casual sun exposure, without sunbathing, may induce maximal melanocyte proliferation. 2 After only 3 days of sun exposure, melanocytes become more dendritic and more dopa positive 16 ; after 12 days, the number of melanocytes increases. 5 The use of MART-1 immunostains has shown that sun-protected skin has a melanocyte-keratinocyte ratio of approximately 1:10 3 (Figure 6). The MART-1 protein is a transmembrane protein expressed by benign and malignant melanocytes. 17 Shown to be more sensitive and specific than HMB-45 for mela- 874
5 noma and melanocytes in general, 18 the MART-1 immunostain is a valuable tool in the evaluation of surgical margins of melanoma in sun-damaged skin. Melanocytes stain intensely and can be discriminated easily from keratinocytes in frozen sections, but it is important to have high-quality thin sections to minimize background chromogen coloration. In a recent article by Shabrawi-Caelen et al, 19 the authors raised the question regarding the specificity of the MART- 1/Melan-Aimmunostaininsun-damagedskin. Intheirstudy of 10 cases of actinic keratoses, they found that samples stained with MART-1 had more immunoreactive cells than samples stained with S100 or HMB-45. They had 2 explanations for this:(1) MART-1 is more sensitive than the other immunostains and(2) MART-1 may also stain keratinocytes and other nonmelanocytic cells damaged by an inflammatory process, as suggested by Maize et al. 20 How does this affect our data? It is possible that some of the cells counted as melanocytes may actually have been keratinocytes. However, our results should be applicable to cases in which MART-1isusedtodiagnosemelanomainsun-damagedskin. TheMART-1rapidimmunostainprotocol 6 isthemostpractical and efficient method for the Mohs surgeon to better judge the presence or absence of melanoma at the surgical margin. Because we defined the upper limit of normal melanocyte density and confluence, our data should aid in preventing the overdiagnosis of positive surgical margins in the management of melanoma in sun-damaged skin. This holds true, especially in light of the data presented by Shabrawi-Caelenetal. 19 However,specialcareisneededwhen what seem to be melanocytic nests are seen. Pseudonests, which may be aggregates of keratinocytes, macrophages, and lymphocytes resulting from cellular damage along the dermal-epidermal junction, may be seen on hematoxylineosin and MART-1 stained slides. 20 The finding of scattered MART-1 staining cells in the dermis of normal sun-exposed skin is also of concern. They seem to be nonspecific and can be seen even if the MART-1 antibody is withheld from the staining protocol. They were more likely to be present in slides with background staining or near torn edges of tissue. These nonspecifically staining cells may lead to the upgrading of the Breslow thickness of melanomas stained with MART-1 or to misinterpretation of an in situ melanoma as being invasive. These cells may be nonmelanocytic cells damaged by an inflammatory process, as suggested by Maize et al. 20 Although the identity of these cells is unclear, mislabeling them as melanocytes has tremendous implications in the care of patients with melanoma. Atypical melanocytes and multinucleated ( starburst ) melanocytes were not addressed in this study because they are not readily discernible in frozen sections; in addition, there is no uniform criterion for melanocyte atypia. Although atypical melanocytes are uniformly seen in melanoma, they are also seen in normal sun-exposed skin 2,21 and should not be used alone as a criterion for melanoma. Nearly all patients in this study were from western Pennsylvania and the surrounding regions. Only 11 patients had recent intense sun exposure. If a similar study were performed with patients who had recent intense sun exposure, the melanocyte density and confluence may Figure 6. Sun-protected normal skin from the abdomen. Melanocyte confluence is absent (melanoma antigen recognized by T cells 1 staining, original magnification 400). be even greater than in our study. The inverse correlation between melanocyte density and patient age may result from the natural maturation process of nevus cells. There are essentially 3 ways to define histologic criteria to distinguish benign from malignant. The first is to study the histologic features of malignant tumors known to metastasize. This has been done for melanoma. In addition to the defined criteria, we have observed that in most melanomas there is vertical stacking of melanocytes in the lower half to two thirds of the epidermis, with or without pagetoid spread of melanocytes reaching the granular layer. The second way is to study the features of normal skin, which was the purpose of this study: to define quantitatively the features of normal skin in sun-exposed areas. The third way is to observe patients according to the criteria established from the previous 2 designs and to determine whether the biological behavior is in concordance with the histologic features. Previous work, 22 which used confluent hyperplasia and nesting as criteria for Mohs excision of melanoma, resulted in recurrence of less than 0.5% in 535 patients with 5-year follow-up data; ie, not excising areas of increased melanocyte density (such as those found in the present study) did not lead to persistence or recurrence of melanoma. This further supports the clinical implications of this study in the care of patients with pigmented lesions in sun-exposed skin. Data from the present study should assist the physician in discerning increased melanocyte density in sun-damaged skin from that in LM and LMM. The Mohs surgeon or pathologist has the evidence needed to avoid overdiagnosing melanoma in sun-exposed skin. The findings of increased melanocyte density and mild to moderate confluence alone do not substantiate the diagnosis of LM or LMM. There should be nesting, vertical stacking, or pagetoid spread. In addition, the finding of melanocytes along the follicular epithelium is normal in sun-damaged skin and is not specific to LM or LMM. Accepted for Publication: October 26, Correspondence: Ali Hendi, MD, Department of Dermatology, Mayo Clinic, 4500 San Pablo Rd, Jacksonville, FL (hendi.ali@mayo.edu). 875
6 Author Contributions: Study concept and design: Hendi, Brodland, and Zitelli. Acquisition of data: Hendi, Brodland, and Zitelli. Analysis and interpretation of data: Hendi, Brodland, and Zitelli. Drafting of the manuscript: Hendi, Brodland, and Zitelli. Critical revision of the manuscript for important intellectual content: Hendi, Brodland, and Zitelli. Obtained funding: Hendi and Zitelli. Administrative, technical, and material support: Brodland and Zitelli. Study supervision: Brodland and Zitelli. Financial Disclosure: None reported. Funding/Support: This study was supported in part by the Skin Cancer Foundation Frederic E. Mohs Memorial Award. Previous Presentation: This study was presented at the annual meeting of the American College of Mohs Micrographic Surgery and Cutaneous Oncology; September 20 to October 3, 2004; San Diego, Calif. Acknowledgment: We thank William Mook, MS, UPMC Shadyside, University of Pittsburgh Medical Center, for statistical analysis. REFERENCES 1. Zitelli JA. Surgical margins for lentigo maligna, 2004 [editorial]. Arch Dermatol. 2004;140: Fallowfield ME, Curley RK, Cook MG. Melanocytic lesions and melanocyte populations in human epidermis. Br J Dermatol. 1991;124: Kelley LC, Starkus L. Immunohistochemical staining of lentigo maligna during Mohs micrographic surgery using MART-1. J Am Acad Dermatol. 2002;46: Stierner U, Rosdahl I, Augustsson A, Kagedal B. UVB irradiation induces melanocyte increase in both exposed and shielded human skin. J Invest Dermatol. 1989;92: Scheibner A, Hollis DE, McCarthy WH, Milton GW. Effects of sunlight exposure on Langerhans cells and melanocytes in human epidermis. Photodermatology. 1986;3: Bricca GM, Brodland DG, Zitelli JA. Immunostaining melanoma frozen sections: the 1-hour protocol. Dermatol Surg. 2004;30: Acker SM, Nicholson JH, Rust PF, Maize JC. Morphometric discrimination of melanoma in situ of sun-damaged skin from chronically sun-damaged skin. J Am Acad Dermatol. 1998;39: Weyers W, Bonczkowitz M, Weyers I, Bittinger A, Schill W-B. Melanoma in situ versus melanocytic hyperplasia in sun-damaged skin: assessment of the significance of histopathologic criteria for differential diagnosis. Am J Dermatopathol. 1996;18: Wong CK. A study of melanocytes in the normal skin surrounding malignant melanomata. Dermatologica. 1970;141: Fallowfield ME, Cook MG. Epidermal melanocytes adjacent to melanoma and the field change effect. Histopathology. 1990;17: Szabó G. The number of melanocytes in human epidermis. BMJ. 1954;4869: Staricco RJ, Pinkus H. Quantitative and qualitative data on the pigment cells of adult human epidermis. J Invest Dermatol. 1957;28: Scheibner A, McCarthy WH, Milton GW, Nordlund JJ. Langerhans cell and melanocyte distribution in normal human epidermis: preliminary report. Australas J Dermatol. 1983;24: Szabó G. The regional anatomy of the human integument with special reference to the distribution of hair follicles, sweat glands and melanocytes. Philos Trans R Soc Lond B Biol Sci. 1967;252: Gilchrest BA, Blog FB, Szabó G. Effects of aging and chronic sun exposure on melanocytes in human skin. J Invest Dermatol. 1979;73: Scheibner A, Hollis DE, Murray E, McCarthy WH, Milton GW. Effects of exposure to ultraviolet light on epidermal Langerhans cells and melanocytes in Australians of aboriginal, Asian and Celtic descent. Photodermatology. 1987;4: Beaty MW, Fetsch P, Wilder AM, Marincola F, Abati A. Effusion cytology of malignant melanoma: a morphologic and immunocytochemical analysis including application of the MART-1 antibody. Cancer. 1997;81: Fetsch PA, Marincola FM, Filie A, Hijazi YM, Kleiner DE, Abati A. Melanomaassociated antigen recognized by T cells (MART-1): the advent of a preferred immunocytochemical antibody for the diagnosis of metastatic malignant melanoma with fine-needle aspiration. Cancer. 1999;87: Shabrawi-Caelen LE, Kerl H, Cerroni L. Melan-A: not a helpful marker in distinction between melanoma in situ on sun-damaged skin and pigmented actinic keratosis. Am J Dermatopathol. 2004;26: Maize JC Jr, Resneck JS Jr, Shapiro PE, McCalmont TH, LeBoit PE. Ducking stray magic bullets : a Melan-A alert. Am J Dermatopathol. 2003;25: Mitchell RE. The effect of prolonged solar radiation on melanocytes of the human epidermis. J Invest Dermatol. 1963;41: Zitelli JA, Brown C, Hanusa BH. Mohs micrographic surgery for the treatment of primary cutaneous melanoma. J Am Acad Dermatol. 1997;37: Announcement The Archives of Dermatology Offers 3 AMA PRA Category I Credits per Review CME credits are now provided to reviewers who have met the following criteria: (1) reviews completed and returned within 21 days and (2) the quality of the review is ranked as good or better by the reviewing editor. Reviewers who meet the CME criteria will automatically receive an from the journal. This contains an embedded link to a Web site maintained by the AMA s CME accrediting sponsor. The link allows the reviewer to receive CME credit for the review. The reviewer can print out a CME certificate. 876
Melanocytes in nonlesional sun-exposed skin: A multicenter comparative study
 Melanocytes in nonlesional sun-exposed skin: A multicenter comparative study AliHendi,MD, a,b David A. Wada, MD, d M. Amanda Jacobs, MD, e JuliaE.Crook,PhD, c Kimberly R. Kortuem, MD, d Brent R. Weed,
Melanocytes in nonlesional sun-exposed skin: A multicenter comparative study AliHendi,MD, a,b David A. Wada, MD, d M. Amanda Jacobs, MD, e JuliaE.Crook,PhD, c Kimberly R. Kortuem, MD, d Brent R. Weed,
Benign and malignant epithelial lesions: Seborrheic keratosis: A common benign pigmented epidermal tumor occur in middle-aged or older persons more
 Benign and malignant epithelial lesions: Seborrheic keratosis: A common benign pigmented epidermal tumor occur in middle-aged or older persons more common on the trunk; but extremities, head and neck are
Benign and malignant epithelial lesions: Seborrheic keratosis: A common benign pigmented epidermal tumor occur in middle-aged or older persons more common on the trunk; but extremities, head and neck are
Simulators of melanoma
 Simulators of melanoma Philip E. LeBoit, M.D. Depts. of Pathology and Dermatology University of California, San Francisco Simulators of melanoma Simulators of melanoma in situ Melanocytic Non-melanocytic
Simulators of melanoma Philip E. LeBoit, M.D. Depts. of Pathology and Dermatology University of California, San Francisco Simulators of melanoma Simulators of melanoma in situ Melanocytic Non-melanocytic
Diagnosis of Lentigo Maligna Melanoma. Steven Q. Wang, M.D. Memorial Sloan-Kettering Cancer Center Basking Ridge, NJ
 Diagnosis of Lentigo Maligna Melanoma Steven Q. Wang, M.D. Memorial Sloan-Kettering Cancer Center Basking Ridge, NJ Conflict of Interest: None Topics Epidemiology and Natural History Clinical and Histologic
Diagnosis of Lentigo Maligna Melanoma Steven Q. Wang, M.D. Memorial Sloan-Kettering Cancer Center Basking Ridge, NJ Conflict of Interest: None Topics Epidemiology and Natural History Clinical and Histologic
Histopathology: skin pathology
 Histopathology: skin pathology These presentations are to help you identify, and to test yourself on identifying, basic histopathological features. They do not contain the additional factual information
Histopathology: skin pathology These presentations are to help you identify, and to test yourself on identifying, basic histopathological features. They do not contain the additional factual information
David B. Troxel, MD. Common Medicolegal Situations: Misdiagnosis of Melanoma
 Common Medicolegal Situations: Misdiagnosis of Melanoma David B. Troxel, MD Medical Director, The Doctors Company, Napa, California Clinical Professor Emeritus, University of California at Berkeley Past
Common Medicolegal Situations: Misdiagnosis of Melanoma David B. Troxel, MD Medical Director, The Doctors Company, Napa, California Clinical Professor Emeritus, University of California at Berkeley Past
Pathology of the skin. 2nd Department of Pathology, Semmelweis University
 Pathology of the skin 2nd Department of Pathology, Semmelweis University Histology of the skin Epidermis: Stratum corneum Stratum granulosum Stratum spinosum Stratum basale Dermis: papillary and reticular
Pathology of the skin 2nd Department of Pathology, Semmelweis University Histology of the skin Epidermis: Stratum corneum Stratum granulosum Stratum spinosum Stratum basale Dermis: papillary and reticular
Melanocytic Lesions: Use of Immunohistochemistry and Special Studies Napa Valley 2018
 Melanocytic Lesions: Use of Immunohistochemistry and Special Studies Napa Valley 2018 Victor G. Prieto, MD, PhD Professor Depts. of Pathology and Dermatology University of Texas - MD Anderson Cancer Center
Melanocytic Lesions: Use of Immunohistochemistry and Special Studies Napa Valley 2018 Victor G. Prieto, MD, PhD Professor Depts. of Pathology and Dermatology University of Texas - MD Anderson Cancer Center
Melanoma-Back to Basics I Thought I Knew Ya! Paul K. Shitabata, M.D. Dermatopathologist APMG
 Melanoma-Back to Basics I Thought I Knew Ya! Paul K. Shitabata, M.D. Dermatopathologist APMG At tumor board, a surgeon insists that all level II melanomas are invasive since they have broken through the
Melanoma-Back to Basics I Thought I Knew Ya! Paul K. Shitabata, M.D. Dermatopathologist APMG At tumor board, a surgeon insists that all level II melanomas are invasive since they have broken through the
MECHANISMS OF HUMAN DISEASE: LABORATORY SESSION PATHOLOGY OF THE SKIN LAB. Friday, February 12, :30 am 11:00 am
 MECHANISMS OF HUMAN DISEASE: LABORATORY SESSION PATHOLOGY OF THE SKIN LAB Friday, February 12, 2012 9:30 am 11:00 am FACULTY COPY GOALS: Describe the basic clinical and morphologic features of various
MECHANISMS OF HUMAN DISEASE: LABORATORY SESSION PATHOLOGY OF THE SKIN LAB Friday, February 12, 2012 9:30 am 11:00 am FACULTY COPY GOALS: Describe the basic clinical and morphologic features of various
Histopathology of Melanoma
 THE YALE JOURNAL OF BIOLOGY AND MEDICINE 48, 409-416 (1975) Histopathology of Melanoma G. J. WALKER SMITH Department ofpathology, Yale University School ofmedicine, 333 Cedar Street, New Haven, Connecticut
THE YALE JOURNAL OF BIOLOGY AND MEDICINE 48, 409-416 (1975) Histopathology of Melanoma G. J. WALKER SMITH Department ofpathology, Yale University School ofmedicine, 333 Cedar Street, New Haven, Connecticut
Dermatopathology: The tumor is composed of keratinocytes which show atypia, increase mitoses and abnormal mitoses.
 Squamous cell carcinoma (SCC): A common malignant tumor of keratinocytes arising in the epidermis, usually from a precancerous condition: 1- UV induced actinic keratosis, usually of low grade malignancy.
Squamous cell carcinoma (SCC): A common malignant tumor of keratinocytes arising in the epidermis, usually from a precancerous condition: 1- UV induced actinic keratosis, usually of low grade malignancy.
Basal cell carcinoma 5/28/2011
 Goal of this Presentation A practical approach to the diagnosis of cutaneous carcinomas and their mimics Thaddeus Mully, MD University of California San Francisco To review common non-melanoma skin cancers
Goal of this Presentation A practical approach to the diagnosis of cutaneous carcinomas and their mimics Thaddeus Mully, MD University of California San Francisco To review common non-melanoma skin cancers
Maligna Melanoma and Atypical Fibroxanthoma: An Unusual Collision Tumour G Türkcü 1, A Keleş 1, U Alabalık 1, D Uçmak 2, H Büyükbayram 1 ABSTRACT
 Maligna Melanoma and Atypical Fibroxanthoma: An Unusual Collision Tumour G Türkcü 1, A Keleş 1, U Alabalık 1, D Uçmak 2, H Büyükbayram 1 ABSTRACT Two different neoplasia in the same biopsy material called
Maligna Melanoma and Atypical Fibroxanthoma: An Unusual Collision Tumour G Türkcü 1, A Keleş 1, U Alabalık 1, D Uçmak 2, H Büyükbayram 1 ABSTRACT Two different neoplasia in the same biopsy material called
Malignant tumors of melanocytes: Part 1. Deba P Sarma, MD., Omaha
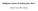 Malignant tumors of melanocytes: Part 1 Deba P Sarma, MD., Omaha The melanocytic tumor is one of the most difficult and confusing areas in Dematopathology. It is true that most (95%) of such lesions are
Malignant tumors of melanocytes: Part 1 Deba P Sarma, MD., Omaha The melanocytic tumor is one of the most difficult and confusing areas in Dematopathology. It is true that most (95%) of such lesions are
Glenn D. Goldman, MD. Fletcher Allen Health Care. University of Vermont College of Medicine
 Glenn D. Goldman, MD Fletcher Allen Health Care University of Vermont College of Medicine Recognize and identify the main types of skin cancer Understand how and why Mohs surgery is utilized for the treatment
Glenn D. Goldman, MD Fletcher Allen Health Care University of Vermont College of Medicine Recognize and identify the main types of skin cancer Understand how and why Mohs surgery is utilized for the treatment
Desmoplastic Melanoma R/O BCC. Clinical Information. 74 y.o. man with lesion on left side of neck r/o BCC
 R/O BCC Sabine Kohler, M.D. Professor of Pathology and Dermatology Dermatopathology Service Stanford University School of Medicine Clinical Information 74 y.o. man with lesion on left side of neck r/o
R/O BCC Sabine Kohler, M.D. Professor of Pathology and Dermatology Dermatopathology Service Stanford University School of Medicine Clinical Information 74 y.o. man with lesion on left side of neck r/o
MECHANISMS OF HUMAN DISEASE: LABORATORY SESSION PATHOLOGY OF THE SKIN LAB. Friday, February 13, :30 am 11:00 am
 MECHANISMS OF HUMAN DISEASE: LABORATORY SESSION PATHOLOGY OF THE SKIN LAB Friday, February 13, 2009 9:30 am 11:00 am FACULTY COPY GOALS: Describe the basic clinical and morphologic features of various
MECHANISMS OF HUMAN DISEASE: LABORATORY SESSION PATHOLOGY OF THE SKIN LAB Friday, February 13, 2009 9:30 am 11:00 am FACULTY COPY GOALS: Describe the basic clinical and morphologic features of various
Lentigo Maligna: Striking a Balance With the Risk-Benefit Ratio. Glen M. Bowen, MD Huntsman Cancer Institute University of Utah
 Lentigo Maligna: Striking a Balance With the Risk-Benefit Ratio Glen M. Bowen, MD Huntsman Cancer Institute University of Utah I. Objectives: a. Review the terminology of LM/LMM b. Understand the relative
Lentigo Maligna: Striking a Balance With the Risk-Benefit Ratio Glen M. Bowen, MD Huntsman Cancer Institute University of Utah I. Objectives: a. Review the terminology of LM/LMM b. Understand the relative
Lichenoid Tissue Reaction in Malignant Melanoma A Potential Diagnostic Pitfall
 natomic Pathology / LICHENOID TISSUE RECTION IN MLIGNNT MELNOM Lichenoid Tissue Reaction in Malignant Melanoma Potential Diagnostic Pitfall CPT Scott R. Dalton, MC, US, 1,3 Capt Matt. aptista, USF, MC,
natomic Pathology / LICHENOID TISSUE RECTION IN MLIGNNT MELNOM Lichenoid Tissue Reaction in Malignant Melanoma Potential Diagnostic Pitfall CPT Scott R. Dalton, MC, US, 1,3 Capt Matt. aptista, USF, MC,
Associate Clinical Professor of Dermatology MUSC
 Re-excision of Moderately Dysplastic Nevi: Should we or shouldn t we? John C. Maize, Jr, M.D. Dermatologist and Dermatopathologist Trident Dermatology, Charleston SC Associate Clinical Professor of Dermatology
Re-excision of Moderately Dysplastic Nevi: Should we or shouldn t we? John C. Maize, Jr, M.D. Dermatologist and Dermatopathologist Trident Dermatology, Charleston SC Associate Clinical Professor of Dermatology
Glenn D. Goldman, MD. University of Vermont Medical Center. University of Vermont College of Medicine
 Glenn D. Goldman, MD University of Vermont Medical Center University of Vermont College of Medicine Recognize and identify the main types of skin cancer and their precursors Identify and understand new
Glenn D. Goldman, MD University of Vermont Medical Center University of Vermont College of Medicine Recognize and identify the main types of skin cancer and their precursors Identify and understand new
A PRACTICAL APPROACH TO ATYPICAL MELANOCYTIC LESIONS BIJAN HAGHIGHI M.D, DIRECTOR OF DERMATOPATHOLOGY, ST. JOSEPH HOSPITAL
 A PRACTICAL APPROACH TO ATYPICAL MELANOCYTIC LESIONS BIJAN HAGHIGHI M.D, DIRECTOR OF DERMATOPATHOLOGY, ST. JOSEPH HOSPITAL OBJECTIVES Discuss current trends and changing concepts in our understanding of
A PRACTICAL APPROACH TO ATYPICAL MELANOCYTIC LESIONS BIJAN HAGHIGHI M.D, DIRECTOR OF DERMATOPATHOLOGY, ST. JOSEPH HOSPITAL OBJECTIVES Discuss current trends and changing concepts in our understanding of
Identifying Skin Cancer. Mary S. Stone MD Professor of Dermatology and Pathology University of Iowa Carver College of Medicine March, 2018
 Identifying Skin Cancer Mary S. Stone MD Professor of Dermatology and Pathology University of Iowa Carver College of Medicine March, 2018 American Cancer Society web site Skin Cancer Melanoma Non-Melanoma
Identifying Skin Cancer Mary S. Stone MD Professor of Dermatology and Pathology University of Iowa Carver College of Medicine March, 2018 American Cancer Society web site Skin Cancer Melanoma Non-Melanoma
Regression 2/3/18. Histologically regression is characterized: melanosis fibrosis combination of both. Distribution: partial or focal!
 Regression Margaret Oliviero MSN, ARNP Harold S. Rabinovitz MD Histologically regression is characterized: melanosis fibrosis combination of both Distribution: partial or focal! Dermatoscopic terminology
Regression Margaret Oliviero MSN, ARNP Harold S. Rabinovitz MD Histologically regression is characterized: melanosis fibrosis combination of both Distribution: partial or focal! Dermatoscopic terminology
Skin (Integumentary System) Wheater, Chap. 9
 Skin (Integumentary System) Wheater, Chap. 9 Skin (Integument) Consists of skin and associated derivatives Largest organ of body (21 ft 2 ; 9 lbs.; has 11 miles of blood vessels) Functions: Protection
Skin (Integumentary System) Wheater, Chap. 9 Skin (Integument) Consists of skin and associated derivatives Largest organ of body (21 ft 2 ; 9 lbs.; has 11 miles of blood vessels) Functions: Protection
Malignant tumors of melanocytes : Part 3. Deba P Sarma, MD., Omaha
 Malignant tumors of melanocytes : Part 3 Deba P Sarma, MD., Omaha Let s go over one case of melanoma using the following worksheet. Of the various essential information that needs to be included in the
Malignant tumors of melanocytes : Part 3 Deba P Sarma, MD., Omaha Let s go over one case of melanoma using the following worksheet. Of the various essential information that needs to be included in the
Melanoma Update: 8th Edition of AJCC Staging System
 Melanoma Update: 8th Edition of AJCC Staging System Rosalie Elenitsas, M.D. Professor of Dermatology Director, Dermatopathology University of Pennsylvania DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY None
Melanoma Update: 8th Edition of AJCC Staging System Rosalie Elenitsas, M.D. Professor of Dermatology Director, Dermatopathology University of Pennsylvania DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY None
IT S FUNDAMENTAL MY DEAR WATSON! A SHERLOCKIAN APPROACH TO DERMATOLOGY
 IT S FUNDAMENTAL MY DEAR WATSON! A SHERLOCKIAN APPROACH TO DERMATOLOGY Skin, Bones, and other Private Parts Symposium Dermatology Lectures by Debra Shelby, PhD, DNP, FNP-BC, FADNP, FAANP Debra Shelby,
IT S FUNDAMENTAL MY DEAR WATSON! A SHERLOCKIAN APPROACH TO DERMATOLOGY Skin, Bones, and other Private Parts Symposium Dermatology Lectures by Debra Shelby, PhD, DNP, FNP-BC, FADNP, FAANP Debra Shelby,
Benign versus Cancerous Lesions How to tell the difference FMF 2014 Christie Freeman MD, CCFP, DipPDerm, MSc
 1 Benign versus Cancerous Lesions How to tell the difference FMF 2014 Christie Freeman MD, CCFP, DipPDerm, MSc Benign lesions Seborrheic Keratoses: Warty, stuck-on Genetics and birthdays Can start in late
1 Benign versus Cancerous Lesions How to tell the difference FMF 2014 Christie Freeman MD, CCFP, DipPDerm, MSc Benign lesions Seborrheic Keratoses: Warty, stuck-on Genetics and birthdays Can start in late
Actinic keratosis (AK): Dr Sarma s simple guide
 Actinic keratosis (AK): Dr Sarma s simple guide Actinic keratosis is a very common lesion that you will see in your day-to-day practice. First, let me explain the name Actinic keratosis. It means keratosis
Actinic keratosis (AK): Dr Sarma s simple guide Actinic keratosis is a very common lesion that you will see in your day-to-day practice. First, let me explain the name Actinic keratosis. It means keratosis
Abrupt Intralesional Color Change on Dermoscopy as a New Indicator of Early Superficial Spreading Melanoma in a Japanese Woman
 Published online: June 24, 2015 1662 6567/15/0072 0123$39.50/0 This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial 3.0 Unported license (CC BY-NC)
Published online: June 24, 2015 1662 6567/15/0072 0123$39.50/0 This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial 3.0 Unported license (CC BY-NC)
Chapter 6 Squamous Cell Carcinoma: Variants and Challenges
 Chapter 6 Squamous Cell Carcinoma: Variants and Challenges Michael B. Morgan EPIDEMIOLOGY: Second most common skin cancer, rare in the dark-skinned races. ETIOLOGY: Ultraviolet light, HPV infection. PATHOGENESIS:
Chapter 6 Squamous Cell Carcinoma: Variants and Challenges Michael B. Morgan EPIDEMIOLOGY: Second most common skin cancer, rare in the dark-skinned races. ETIOLOGY: Ultraviolet light, HPV infection. PATHOGENESIS:
Clinical characteristics
 Skin Cancer Fernando Vega, MD Seattle Healing Arts Clinical characteristics Precancerous lesions Common skin cancers ACTINIC KERATOSIS Precancerous skin lesions Actinic keratoses Dysplastic melanocytic
Skin Cancer Fernando Vega, MD Seattle Healing Arts Clinical characteristics Precancerous lesions Common skin cancers ACTINIC KERATOSIS Precancerous skin lesions Actinic keratoses Dysplastic melanocytic
Basics in Dermoscopy
 Basics in Dermoscopy Manal Bosseila Professor of Dermatology, Cairo University Member of European Academy Dermatology & Venereology EADV Member of International Dermoscopy Society IDS Member of Aesthetic
Basics in Dermoscopy Manal Bosseila Professor of Dermatology, Cairo University Member of European Academy Dermatology & Venereology EADV Member of International Dermoscopy Society IDS Member of Aesthetic
Type IV collagen and laminin staining patterns in benign
 J Clin Pathol 1989;42:1173-1177 Type IV collagen and laminin staining patterns in benign and malignant cutaneous lesions RONA M MacKIE, D B CLELLAND, CHRISTINE J SKERROW From the Department ofdermatology,
J Clin Pathol 1989;42:1173-1177 Type IV collagen and laminin staining patterns in benign and malignant cutaneous lesions RONA M MacKIE, D B CLELLAND, CHRISTINE J SKERROW From the Department ofdermatology,
Dermoscopy: Recognizing Top Five Common In- Office Diagnoses
 Dermoscopy: Recognizing Top Five Common In- Office Diagnoses Vu A. Ngo, DO Department of Family Medicine and Dermatology Choctaw Nation Health Services Authority Learning Objectives Introduction to dermoscopy
Dermoscopy: Recognizing Top Five Common In- Office Diagnoses Vu A. Ngo, DO Department of Family Medicine and Dermatology Choctaw Nation Health Services Authority Learning Objectives Introduction to dermoscopy
Human Anatomy & Physiology
 PowerPoint Lecture Slides prepared by Barbara Heard, Atlantic Cape Community College Ninth Edition Human Anatomy & Physiology C H A P T E R 5 Annie Leibovitz/Contact Press Images 2013 Pearson Education,
PowerPoint Lecture Slides prepared by Barbara Heard, Atlantic Cape Community College Ninth Edition Human Anatomy & Physiology C H A P T E R 5 Annie Leibovitz/Contact Press Images 2013 Pearson Education,
Integumentary System-Skin and Body Coverings
 Integumentary System-Skin and Body Coverings List the four types of epithelial or connective membranes. The epithelial cutaneous includes your and is exposed to the. Its function is to. An example is..
Integumentary System-Skin and Body Coverings List the four types of epithelial or connective membranes. The epithelial cutaneous includes your and is exposed to the. Its function is to. An example is..
Dermatology for the PCP Deanna G. Brown, MD, FAAD Susong Dermatology Consulting Staff at CHI Memorial
 Dermatology for the PCP Deanna G. Brown, MD, FAAD Susong Dermatology Consulting Staff at CHI Memorial Cutaneous Oncology for the PCP Deanna G. Brown, MD, FAAD Susong Dermatology Consulting Staff at CHI
Dermatology for the PCP Deanna G. Brown, MD, FAAD Susong Dermatology Consulting Staff at CHI Memorial Cutaneous Oncology for the PCP Deanna G. Brown, MD, FAAD Susong Dermatology Consulting Staff at CHI
Technicians & Nurses Program
 ASCRS ASOA Symposium & Congress Technicians & Nurses Program May 6-10, 2016 New Orleans Evaluation and Treatment of Eyelid Malignancies Richard C. Allen MD PhD FACS Professor Section of Ophthalmology Dept.
ASCRS ASOA Symposium & Congress Technicians & Nurses Program May 6-10, 2016 New Orleans Evaluation and Treatment of Eyelid Malignancies Richard C. Allen MD PhD FACS Professor Section of Ophthalmology Dept.
Journal of International Academy of Forensic Science & Pathology (JIAFP)
 Journal of International Academy of Forensic Science & Pathology (JIAFP) ISSN 2395-0722 MICROCYSTIC ADNEXAL CARCINOMA-A CASE REPORT WITH REVIEW OF LITERATURE Case Report Sulakshana M S 1,Natarajan M 2
Journal of International Academy of Forensic Science & Pathology (JIAFP) ISSN 2395-0722 MICROCYSTIC ADNEXAL CARCINOMA-A CASE REPORT WITH REVIEW OF LITERATURE Case Report Sulakshana M S 1,Natarajan M 2
ISPUB.COM. Seborrheic Keratosis: A Pictorial Review of the Histopathologic Variations. D Sarma, S Repertinger
 ISPUB.COM The Internet Journal of Dermatology Volume 7 Number 2 Seborrheic Keratosis: A Pictorial Review of the Histopathologic Variations D Sarma, S Repertinger Citation D Sarma, S Repertinger.. The Internet
ISPUB.COM The Internet Journal of Dermatology Volume 7 Number 2 Seborrheic Keratosis: A Pictorial Review of the Histopathologic Variations D Sarma, S Repertinger Citation D Sarma, S Repertinger.. The Internet
Reflectance-Mode Confocal Microscopy for the In Vivo Characterization of Pagetoid Melanocytosis in Melanomas and Nevi
 See related Commentary on page vii Reflectance-Mode Confocal Microscopy for the In Vivo Characterization of Pagetoid Melanocytosis in Melanomas and Nevi Giovanni Pellacani, Anna Maria Cesinaro,w and Stefania
See related Commentary on page vii Reflectance-Mode Confocal Microscopy for the In Vivo Characterization of Pagetoid Melanocytosis in Melanomas and Nevi Giovanni Pellacani, Anna Maria Cesinaro,w and Stefania
Cutaneous Adnexal Tumors
 Cutaneous Adnexal Tumors Lesions with Predominant Follicular Differentiation Special Emphasis on Basal Cell Carcinoma 2014-04-01 Prof. Dr. med. Katharina Glatz Pathologie Cutaneous Adnexal Tumors Hair
Cutaneous Adnexal Tumors Lesions with Predominant Follicular Differentiation Special Emphasis on Basal Cell Carcinoma 2014-04-01 Prof. Dr. med. Katharina Glatz Pathologie Cutaneous Adnexal Tumors Hair
Periocular Malignancies
 Periocular Malignancies Andrew Gurwood, O.D., F.A.A.O., Dipl. Marc Myers, O.D., F.A.A.O. Drs. Myers and Gurwood have no financial interests to disclose. Course Description Discussion of the most common
Periocular Malignancies Andrew Gurwood, O.D., F.A.A.O., Dipl. Marc Myers, O.D., F.A.A.O. Drs. Myers and Gurwood have no financial interests to disclose. Course Description Discussion of the most common
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,500 108,000 1.7 M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,500 108,000 1.7 M Open access books available International authors and editors Downloads Our
Assisting diagnosis of melanoma through the noninvasive biopsy of skin lesions
 Assisting diagnosis of melanoma through the noninvasive biopsy of skin lesions Symon D Oyly Cotton Ela Claridge School of Computer Science, The University of Birmingham Birmingham B15 2TT, UK Per Hall
Assisting diagnosis of melanoma through the noninvasive biopsy of skin lesions Symon D Oyly Cotton Ela Claridge School of Computer Science, The University of Birmingham Birmingham B15 2TT, UK Per Hall
Skin and Body Membranes Body Membranes Function of body membranes Cover body surfaces Line body cavities Form protective sheets around organs
 Skin and Body Membranes Body Membranes Function of body membranes Cover body surfaces Line body cavities Form protective sheets around organs Classification of Body Membranes Epithelial membranes Cutaneous
Skin and Body Membranes Body Membranes Function of body membranes Cover body surfaces Line body cavities Form protective sheets around organs Classification of Body Membranes Epithelial membranes Cutaneous
Unit 4 - The Skin and Body Membranes 1
 Unit 4 - The Skin and Body Membranes 1 I. Unit 4: Skin and Body Membranes A. Body Membranes 1. Function of body membranes a) Cover body surfaces b) Line body cavities c) Form protective sheets around organs
Unit 4 - The Skin and Body Membranes 1 I. Unit 4: Skin and Body Membranes A. Body Membranes 1. Function of body membranes a) Cover body surfaces b) Line body cavities c) Form protective sheets around organs
ELECTRON MICROSCOPY OF A SMALL PIGMENTED CUTANEOUS LESION*
 ELECTRON MICROSCOPY OF A SMALL PIGMENTED CUTANEOUS LESION* The description of the lesion in the title of this rcport is intentionally non-committal. Diagnosed clinically as a lentigo, it was removed as
ELECTRON MICROSCOPY OF A SMALL PIGMENTED CUTANEOUS LESION* The description of the lesion in the title of this rcport is intentionally non-committal. Diagnosed clinically as a lentigo, it was removed as
6/17/2018. Breaking Bad (Part 1) Dermoscopy of Brown(ish) Things. Bad?
 Breaking Bad (Part 1) Dermoscopy of Brown(ish) Things Jennie T. Clarke, MD ssociate Professor of Dermatology University of Utah School of Medicine Bad? 1 Brown(ish) Things Bad Melanoma Pigmented basal
Breaking Bad (Part 1) Dermoscopy of Brown(ish) Things Jennie T. Clarke, MD ssociate Professor of Dermatology University of Utah School of Medicine Bad? 1 Brown(ish) Things Bad Melanoma Pigmented basal
SKIN. 3. How is the skin structured around the finger joints to allow for flexible movement of the fingers?
 SKIN Objectives for Exam #1: 1. List various skin structures and describe their functions. 2. Describe skin responses to increases and decreases in body temperature. 3. Provide examples of various skin
SKIN Objectives for Exam #1: 1. List various skin structures and describe their functions. 2. Describe skin responses to increases and decreases in body temperature. 3. Provide examples of various skin
Learning Objectives. Tanning. The Skin. Classic Features. Sun Reactive Skin Type Classification. Skin Cancers: Preventing, Screening and Treating
 Learning Objectives Skin Cancers: Preventing, Screening and Treating Robert A. Baldor, MD, FAAFP Professor, Family Medicine & Community Health University of Massachusetts Medical School Distinguish the
Learning Objectives Skin Cancers: Preventing, Screening and Treating Robert A. Baldor, MD, FAAFP Professor, Family Medicine & Community Health University of Massachusetts Medical School Distinguish the
Case Report A Rare Cutaneous Adnexal Tumor: Malignant Proliferating Trichilemmal Tumor
 Case Reports in Medicine Volume 2015, Article ID 742920, 4 pages http://dx.doi.org/10.1155/2015/742920 Case Report A Rare Cutaneous Adnexal Tumor: Malignant Proliferating Trichilemmal Tumor Omer Alici,
Case Reports in Medicine Volume 2015, Article ID 742920, 4 pages http://dx.doi.org/10.1155/2015/742920 Case Report A Rare Cutaneous Adnexal Tumor: Malignant Proliferating Trichilemmal Tumor Omer Alici,
The Integumentary System. Mosby items and derived items 2010, 2006, 2002, 1997, 1992 by Mosby, Inc., an affiliate of Elsevier Inc.
 The Integumentary System The Skin Structure two primary layers called epidermis and dermis Epidermis Outermost and thinnest primary layer of skin Composed of several layers of stratified squamous epithelium
The Integumentary System The Skin Structure two primary layers called epidermis and dermis Epidermis Outermost and thinnest primary layer of skin Composed of several layers of stratified squamous epithelium
Morphologic Features of Melanocytes, Pigmented Keratinocytes, and Melanophages by In Vivo Confocal Scanning Laser Microscopy
 Morphologic Features of Melanocytes, Pigmented Keratinocytes, and Melanophages by In Vivo Confocal Scanning Laser Microscopy Klaus J. Busam, M.D., Carlos Charles, M.D., Grace Lee, M.D., Allan C Halpern,
Morphologic Features of Melanocytes, Pigmented Keratinocytes, and Melanophages by In Vivo Confocal Scanning Laser Microscopy Klaus J. Busam, M.D., Carlos Charles, M.D., Grace Lee, M.D., Allan C Halpern,
Case Report Clear Cell Basal Cell Carcinoma
 SAGE-Hindawi Access to Research Volume 2011, Article ID 386921, 4 pages doi:10.4061/2011/386921 Case Report Clear Cell Basal Cell Carcinoma Deba P. Sarma, 1 Daniel Olson, 1 Jennifer Olivella, 1 Tracey
SAGE-Hindawi Access to Research Volume 2011, Article ID 386921, 4 pages doi:10.4061/2011/386921 Case Report Clear Cell Basal Cell Carcinoma Deba P. Sarma, 1 Daniel Olson, 1 Jennifer Olivella, 1 Tracey
PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College Skin and Body Membranes
 PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College Skin and Body Membranes 4 Body Membranes Function of body membranes Cover body surfaces Line body cavities
PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College Skin and Body Membranes 4 Body Membranes Function of body membranes Cover body surfaces Line body cavities
Growth rate of melanoma in vivo and correlation with dermatoscopic and dermatopathologic findings
 Dermatology Practical & Conceptual www.derm101.com Growth rate of melanoma in vivo and correlation with dermatoscopic and dermatopathologic findings Jürgen Beer, M.D. 1, Lina Xu, M.D. 1, Philipp Tschandl,
Dermatology Practical & Conceptual www.derm101.com Growth rate of melanoma in vivo and correlation with dermatoscopic and dermatopathologic findings Jürgen Beer, M.D. 1, Lina Xu, M.D. 1, Philipp Tschandl,
Interesting Case Series. Aggressive Tumor of the Midface
 Interesting Case Series Aggressive Tumor of the Midface Adrian Frunza, MD, Dragos Slavescu, MD, and Ioan Lascar, MD, PhD Bucharest Emergency Clinical Hospital, Bucharest University School of Medicine,
Interesting Case Series Aggressive Tumor of the Midface Adrian Frunza, MD, Dragos Slavescu, MD, and Ioan Lascar, MD, PhD Bucharest Emergency Clinical Hospital, Bucharest University School of Medicine,
Skin and Body Membranes
 4 Skin and Body Membranes PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB Skin and Body Membranes
4 Skin and Body Membranes PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB Skin and Body Membranes
Melanocytic lesions on Genital Skin Melanoma vs. Melanocytic Nevus, Revisited. Timothy H. McCalmont, MD University of California, San Francisco
 Melanocytic lesions on Genital Skin Melanoma vs. Melanocytic Nevus, Revisited Timothy H. McCalmont, MD, San Francisco I. IS IT BENIGN OR IS IT MALIGNANT? One of the commonest determinations we make as
Melanocytic lesions on Genital Skin Melanoma vs. Melanocytic Nevus, Revisited Timothy H. McCalmont, MD, San Francisco I. IS IT BENIGN OR IS IT MALIGNANT? One of the commonest determinations we make as
Multiple Primary Melanoma in a Thai Male: A Case Report
 Case Report Multiple Primary Melanoma in a Thai Male: A Case Report J Med Assoc Thai 2014; 97 (Suppl. 2): S234-S238 Full text. e-journal: http://www.jmatonline.com Kittisak Payapvipapong MD*, Pinyapat
Case Report Multiple Primary Melanoma in a Thai Male: A Case Report J Med Assoc Thai 2014; 97 (Suppl. 2): S234-S238 Full text. e-journal: http://www.jmatonline.com Kittisak Payapvipapong MD*, Pinyapat
Multispectral Digital Skin Lesion Analysis. Summary
 Subject: Multispectral Digital Skin Lesion Analysis Page: 1 of 8 Last Review Status/Date: March 2016 Multispectral Digital Skin Lesion Analysis Summary There is interest in noninvasive devices that will
Subject: Multispectral Digital Skin Lesion Analysis Page: 1 of 8 Last Review Status/Date: March 2016 Multispectral Digital Skin Lesion Analysis Summary There is interest in noninvasive devices that will
Chapter 5: The Integumentary System - Introduction and Epidermis
 Chapter 5: The Integumentary System - Introduction and Epidermis The Integument Means Covering Composed: Skin Hair Nails Sweat glands Oil glands The Integument Thickness 1.5 4 mm (or more) Weight 9 11
Chapter 5: The Integumentary System - Introduction and Epidermis The Integument Means Covering Composed: Skin Hair Nails Sweat glands Oil glands The Integument Thickness 1.5 4 mm (or more) Weight 9 11
Cancer Reporting for Dermatologists. Florida Department of Health Florida Cancer Data System. March 9, Agenda
 Cancer Reporting for Dermatologists Florida Department of Health Florida Cancer Data System March 9, 2011 Agenda Welcome Introductions Cancer Reporting in Florida BETA Participation Expectations Review
Cancer Reporting for Dermatologists Florida Department of Health Florida Cancer Data System March 9, 2011 Agenda Welcome Introductions Cancer Reporting in Florida BETA Participation Expectations Review
Management of pediatric melanocytic lesions
 Open Journal of Clinical & Medical Case Reports Management of pediatric melanocytic lesions Volume 3 (2017) Issue 8 ISSN 2379-1039 Jin Kim, BS; Emmanuel Gabriel MD, PhD; Weiguo Liu MD, PhD; Lin Lin MD,
Open Journal of Clinical & Medical Case Reports Management of pediatric melanocytic lesions Volume 3 (2017) Issue 8 ISSN 2379-1039 Jin Kim, BS; Emmanuel Gabriel MD, PhD; Weiguo Liu MD, PhD; Lin Lin MD,
Principles of Anatomy and Physiology
 Principles of Anatomy and Physiology 14 th Edition CHAPTER 5 The Integumentary System Introduction The organs of the integumentary system include the skin and its accessory structures including hair, nails,
Principles of Anatomy and Physiology 14 th Edition CHAPTER 5 The Integumentary System Introduction The organs of the integumentary system include the skin and its accessory structures including hair, nails,
UNIVERSITY OF MEDICINE AND PHARMACY OF CRAIOVA FACULTY OF MEDICINE DOCTORAL THESIS SUMMARY
 UNIVERSITY OF MEDICINE AND PHARMACY OF CRAIOVA FACULTY OF MEDICINE DOCTORAL THESIS SUMMARY CLINICAL, HISTOPATHOLOGICAL AND IMMUNOHISTOCHEMICAL STUDY OF THE EPITHELIAL PRECANCEROUS LESIONS PRECURSORS OF
UNIVERSITY OF MEDICINE AND PHARMACY OF CRAIOVA FACULTY OF MEDICINE DOCTORAL THESIS SUMMARY CLINICAL, HISTOPATHOLOGICAL AND IMMUNOHISTOCHEMICAL STUDY OF THE EPITHELIAL PRECANCEROUS LESIONS PRECURSORS OF
Unit 4 The Integumentary System
 Unit 4 The Integumentary System I. Classification of Body Membranes A. Epithelial Membranes (3) 1. Cutaneous Membrane > Stratified Squamous > Sits on Dense Connective Tissue > Skin: Epidermis & Dermis
Unit 4 The Integumentary System I. Classification of Body Membranes A. Epithelial Membranes (3) 1. Cutaneous Membrane > Stratified Squamous > Sits on Dense Connective Tissue > Skin: Epidermis & Dermis
The Integumentary System
 The Integumentary System The Integumentary System Integument is skin Skin and its appendages make up the integumentary system (See if you can name some appendages) A fatty layer (hypodermis) lies deep
The Integumentary System The Integumentary System Integument is skin Skin and its appendages make up the integumentary system (See if you can name some appendages) A fatty layer (hypodermis) lies deep
Basal cell carcinoma diagnosed on Fine-Needle Aspiration Cytology A. Pathological Case Report
 Basal cell carcinoma diagnosed on Fine-Needle Aspiration Cytology A Abstract Dr. Madhuri S.Kate 1, Dr. Preeti Jain 2, Dr. Shailesh S. Patne 3 Introduction: Basal cell carcinoma (BCC) is a locally invasive
Basal cell carcinoma diagnosed on Fine-Needle Aspiration Cytology A Abstract Dr. Madhuri S.Kate 1, Dr. Preeti Jain 2, Dr. Shailesh S. Patne 3 Introduction: Basal cell carcinoma (BCC) is a locally invasive
Skin Cancer of the Nose: Common and Uncommon
 Skin Cancer of the Nose: Common and Uncommon Mark Russell, M.D. Associate Professor of Dermatology, Otolaryngology, and Pathology University of Virginia Objectives Review clinical presentations of select
Skin Cancer of the Nose: Common and Uncommon Mark Russell, M.D. Associate Professor of Dermatology, Otolaryngology, and Pathology University of Virginia Objectives Review clinical presentations of select
Genetic Testing: When should it be ordered? Julie Schloemer, MD Dermatology
 Genetic Testing: When should it be ordered? Julie Schloemer, MD Dermatology Outline Germline testing CDKN2A BRCA2 BAP1 Somatic testing Gene expression profiling (GEP) BRAF Germline vs Somatic testing
Genetic Testing: When should it be ordered? Julie Schloemer, MD Dermatology Outline Germline testing CDKN2A BRCA2 BAP1 Somatic testing Gene expression profiling (GEP) BRAF Germline vs Somatic testing
Anatomy Ch 6: Integumentary System
 Anatomy Ch 6: Integumentary System Introduction: A. Organs are body structures composed of two or more different tissues. B. The skin and its accessory organs make up the integumentary system. Types of
Anatomy Ch 6: Integumentary System Introduction: A. Organs are body structures composed of two or more different tissues. B. The skin and its accessory organs make up the integumentary system. Types of
JAM ACAD DERMATOL VOLUME 76, NUMBER 2. Research Letters 351
 JAM ACAD DERMATOL Research Letters 351 Standard step sectioning of skin biopsy specimens diagnosed as superficial basal cell carcinoma frequently yields deeper and more aggressive subtypes To the Editor:
JAM ACAD DERMATOL Research Letters 351 Standard step sectioning of skin biopsy specimens diagnosed as superficial basal cell carcinoma frequently yields deeper and more aggressive subtypes To the Editor:
Disclosure. Objectives. PAFP CME Conference Lou Mancano MD, FAAFP Reading Health System November 18, 2016
 PAFP CME Conference Lou Mancano MD, FAAFP Reading Health System November 18, 2016 1 Disclosure The speaker has no conflict of interest, financial agreement, or working affiliation with any group or organization.
PAFP CME Conference Lou Mancano MD, FAAFP Reading Health System November 18, 2016 1 Disclosure The speaker has no conflict of interest, financial agreement, or working affiliation with any group or organization.
Morphologic characteristics of nevi associated with melanoma: a clinical, dermatoscopic and histopathologic analysis
 DERMATOLOGY PRACTICAL & CONCEPTUAL www.derm101.com Morphologic characteristics of nevi associated with melanoma: a clinical, dermatoscopic and histopathologic analysis Temeida Alendar 1, Harald Kittler
DERMATOLOGY PRACTICAL & CONCEPTUAL www.derm101.com Morphologic characteristics of nevi associated with melanoma: a clinical, dermatoscopic and histopathologic analysis Temeida Alendar 1, Harald Kittler
NON-MELANOCYTIC MELANOMA LOOK-ALIKES. Hideko Kamino, M.D. Dermatopathology Section New York University School of Medicine
 NON-MELANOCYTIC MELANOMA LOOK-ALIKES Hideko Kamino, M.D. Dermatopathology Section New York University School of Medicine There is a diagnostically important group of entities called non-melanocytic melanoma
NON-MELANOCYTIC MELANOMA LOOK-ALIKES Hideko Kamino, M.D. Dermatopathology Section New York University School of Medicine There is a diagnostically important group of entities called non-melanocytic melanoma
2/5/2019. Organ System: Skin or Integumentary System. Hypodermis (or superficial fascia) Integumentary System - Learn and Understand
 Integumentary System - Learn and Understand Skin is an organ comprised of all four tissues Each layer of the skin contributes to one or more of its numerous functions Skin is both strong and flexible Keratinization
Integumentary System - Learn and Understand Skin is an organ comprised of all four tissues Each layer of the skin contributes to one or more of its numerous functions Skin is both strong and flexible Keratinization
Ch. 4: Skin and Body Membranes
 Ch. 4: Skin and Body Membranes I. Body Membranes A. Function of body membranes 1. Cover body surfaces 2. Line body cavities 3. Form protective sheets around organs II. Classification of Body Membranes
Ch. 4: Skin and Body Membranes I. Body Membranes A. Function of body membranes 1. Cover body surfaces 2. Line body cavities 3. Form protective sheets around organs II. Classification of Body Membranes
The Integumentary System
 The Integumentary System Integument is skin Skin and its appendages make up the integumentary system A fatty layer (hypodermis) lies deep to it Two distinct regions Epidermis Dermis PHL 212 1 Function
The Integumentary System Integument is skin Skin and its appendages make up the integumentary system A fatty layer (hypodermis) lies deep to it Two distinct regions Epidermis Dermis PHL 212 1 Function
Ex. 7: Integumentary
 Collin County Community College BIOL. 2401 Ex. 7: Integumentary. Skin or Integument Consists of three major regions Epidermis outermost superficial region Dermis middle region Hypodermis (superficial fascia)
Collin County Community College BIOL. 2401 Ex. 7: Integumentary. Skin or Integument Consists of three major regions Epidermis outermost superficial region Dermis middle region Hypodermis (superficial fascia)
Living Beyond Cancer Skin Cancer Detection and Prevention
 Living Beyond Cancer Skin Cancer Detection and Prevention Cutaneous Skin Cancers Identification Diagnosis Treatment options Prevention What is the most common cancer in people? What is the most common
Living Beyond Cancer Skin Cancer Detection and Prevention Cutaneous Skin Cancers Identification Diagnosis Treatment options Prevention What is the most common cancer in people? What is the most common
Case Report Micromelanomas: A Review of Melanomas 2mmand a Case Report
 Case Reports in Oncological Medicine, Article ID 206260, 4 pages http://dx.doi.org/10.1155/2014/206260 Case Report Micromelanomas: A Review of Melanomas 2mmand a Case Report Sharad P. Paul 1,2,3 1 Skin
Case Reports in Oncological Medicine, Article ID 206260, 4 pages http://dx.doi.org/10.1155/2014/206260 Case Report Micromelanomas: A Review of Melanomas 2mmand a Case Report Sharad P. Paul 1,2,3 1 Skin
B. Incorrect! The ectoderm does not produce the dermis. C. Incorrect! The dermis is derived from the mesoderm.
 Human Anatomy - Problem Drill 04: The Integumentary System Question No. 1 of 10 Instructions: (1) Read the problem and answer choices carefully, (2) Work the problems on paper as 1. From the inner cell
Human Anatomy - Problem Drill 04: The Integumentary System Question No. 1 of 10 Instructions: (1) Read the problem and answer choices carefully, (2) Work the problems on paper as 1. From the inner cell
Chapter 5 The Integumentary System. Copyright 2009, John Wiley & Sons, Inc. 1
 Chapter 5 The Integumentary System Copyright 2009, John Wiley & Sons, Inc. 1 Introduction The organs of the integumentary system include the skin and its accessory structures including hair, nails, and
Chapter 5 The Integumentary System Copyright 2009, John Wiley & Sons, Inc. 1 Introduction The organs of the integumentary system include the skin and its accessory structures including hair, nails, and
Hole s Essentials of Human Anatomy & Physiology
 Hole s Essentials of Human Anatomy & Physiology David Shier Jackie Butler Ricki Lewis Created by Dr. Melissa Eisenhauer Head Athletic Trainer/Assistant Professor Trevecca Nazarene University Chapter 6
Hole s Essentials of Human Anatomy & Physiology David Shier Jackie Butler Ricki Lewis Created by Dr. Melissa Eisenhauer Head Athletic Trainer/Assistant Professor Trevecca Nazarene University Chapter 6
Mapping Basal Cell and Squamous Carcinoma By 10 Min CK5 Direct Immunohistochemistry on Frozen Section Skin Tissues during Mohs Micrographic Surgery
 Mapping Basal Cell and Squamous Carcinoma By 10 Min CK5 Direct Immunohistochemistry on Frozen Section Skin Tissues during Mohs Micrographic Surgery Robert Glinert, MD and Song Q. Zhao, MD, Ph.D., MPH Department
Mapping Basal Cell and Squamous Carcinoma By 10 Min CK5 Direct Immunohistochemistry on Frozen Section Skin Tissues during Mohs Micrographic Surgery Robert Glinert, MD and Song Q. Zhao, MD, Ph.D., MPH Department
The Integumentary System
 The Integumentary System The Integumentary System Integument is skin Skin and its appendages make up the integumentary system A fatty layer (hypodermis) lies deep to it Two distinct regions Epidermis Dermis
The Integumentary System The Integumentary System Integument is skin Skin and its appendages make up the integumentary system A fatty layer (hypodermis) lies deep to it Two distinct regions Epidermis Dermis
LENTIGO SIMPLEX. Epidemiology
 LENTIGO SIMPLEX Epidemiology The frequency of lentigo simplex in children and adults has not been determined. There does not appear to be a racial or gender predilection. Lentigo simplex is the most common
LENTIGO SIMPLEX Epidemiology The frequency of lentigo simplex in children and adults has not been determined. There does not appear to be a racial or gender predilection. Lentigo simplex is the most common
Polypoid Melanoma, A Virulent Variant of the Nodular Growth Pattern
 Polypoid Melanoma, A Virulent Variant of the Nodular Growth Pattern ELIZABETH A. MANCI, M.D., CHARLES M. BALCH, M.D..TARIQ M. MURAD, M.D., PH.D., AND SENG/JAW SOONG, PH.D. Manci, Elizabeth A., Balch, Charles
Polypoid Melanoma, A Virulent Variant of the Nodular Growth Pattern ELIZABETH A. MANCI, M.D., CHARLES M. BALCH, M.D..TARIQ M. MURAD, M.D., PH.D., AND SENG/JAW SOONG, PH.D. Manci, Elizabeth A., Balch, Charles
Integumentary System (Script) Slide 1: Integumentary System. Slide 2: An overview of the integumentary system
 Integumentary System (Script) Slide 1: Integumentary System Slide 2: An overview of the integumentary system Skin is the body s largest and heaviest organ making up 15% of body weight. Most skin is 1 to
Integumentary System (Script) Slide 1: Integumentary System Slide 2: An overview of the integumentary system Skin is the body s largest and heaviest organ making up 15% of body weight. Most skin is 1 to
The Integumentary System: An Overview
 The Integumentary System: An Overview Functions: Protective covering Helps regulate body temperature Retards water loss from deeper tissues Houses sensory receptors Synthesizes biochemicals Excretes small
The Integumentary System: An Overview Functions: Protective covering Helps regulate body temperature Retards water loss from deeper tissues Houses sensory receptors Synthesizes biochemicals Excretes small
SKIN HISTOLOGY the microscopic anatomy of the Integument. Mikrogeo. com
 SKIN HISTOLOGY the microscopic anatomy of the Integument Mikrogeo. com Hair follicles, sweat glands, sebaceous glands (even teeth) are products of the epidermis,embryologically speaking ectododerm, that
SKIN HISTOLOGY the microscopic anatomy of the Integument Mikrogeo. com Hair follicles, sweat glands, sebaceous glands (even teeth) are products of the epidermis,embryologically speaking ectododerm, that
Skin Cancer. Dr Elizabeth Ogden Associate Specialist in Dermatology East and North Herts Dr Elizabeth Ogden
 Skin Cancer Dr Elizabeth Ogden Associate Specialist in Dermatology East and North Herts 13.10.16 Skin Cancer Melanoma mole cancer - is a true cancer which can metastasize and kill Non Melanoma skin cancer
Skin Cancer Dr Elizabeth Ogden Associate Specialist in Dermatology East and North Herts 13.10.16 Skin Cancer Melanoma mole cancer - is a true cancer which can metastasize and kill Non Melanoma skin cancer
Describe the functions of the vertebrate integumentary system. Discuss the structure of the skin and how it relates to function.
 Chapter 5 Describe the functions of the vertebrate integumentary system. Discuss the structure of the skin and how it relates to function. Explain the basis for different skin colors. Describe the structure
Chapter 5 Describe the functions of the vertebrate integumentary system. Discuss the structure of the skin and how it relates to function. Explain the basis for different skin colors. Describe the structure
Advances in Surgical Management of Primary Melanoma: Identifying Patients Who Need More than Conventional Wide Local Excision
 Advances in Surgical Management of Primary Melanoma: Identifying Patients Who Need More than Conventional Wide Local Excision Christopher J. Miller, MD Director of Penn Dermatology Oncology Center Associate
Advances in Surgical Management of Primary Melanoma: Identifying Patients Who Need More than Conventional Wide Local Excision Christopher J. Miller, MD Director of Penn Dermatology Oncology Center Associate
