Giant Congenital Nevi: A 20-Year Experience and an Algorithm for Their Management
|
|
|
- Hester Ford
- 6 years ago
- Views:
Transcription
1 Giant Congenital Nevi: A 20-Year Experience and an Algorithm for Their Management Arun K. Gosain, M.D., Timothy D. Santoro, M.D., David L. Larson, M.D., and Reudi P. Gingrass, M.D. Milwaukee, Wis. A variety of treatment options exists for the management of giant congenital nevi. Confusion over appropriate management is compounded because not all giant congenital nevi are pigmented, and malignant potential varies between different types. The present study sought to define factors in the presentation of giant congenital nevi that could provide an algorithm for their management, with respect to both the extent of resection and subsequent reconstructive options. A retrospective review of all patients who presented with a congenital nevus of 20 cm 2 or greater since 1980 was performed, distinguishing among nevi involving the head and neck, the torso, and the extremities. Sixty-one patients with giant congenital nevi were evaluated (newborn to age 16 years), of which 60 nevi in 55 patients have been operated on. Giant congenital nevi having malignant potential were pigmented nevi (53 patients) and nevus sebaceus (four patients). Those not having malignant potential were verrucous epidermal nevi (three patients) and a woolly hair nevus (one patient). Of the 60 giant congenital nevi operated on, expanded flaps were used in 25, expanded full-thickness skin grafts were used in 10, split-thickness or nonexpanded full-thickness skin grafts were used in 13, and serial excision was used in 30. After 1989, operations tended to use multimodality treatment plans, with an increased use of expanded full-thickness grafts and immediate serial tissue expansion. The use of serial excision, particularly in the extremities, also increased after Serial excision was the treatment of choice when it could be completed in two procedures or less, which occurred in more than 80 percent of cases using serial excision alone. Expanded flaps were the most common mode of reconstruction in the head and neck region and were used in 49 percent of these procedures. Serial excision was the most common form of treatment in the extremities, used in 50 percent of procedures. Tissue expansion in the extremities was infrequently used to provide an expanded flap (8 percent of procedures), whereas it was frequently used to provide expanded full-thickness skin grafts harvested from the torso (used in 31 percent of procedures). On the basis of these data, algorithms for the extent of resection and subsequent reconstructive options for giant congenital nevi were developed. Their management should be formulated relative to pigmentation, malignant potential, and anatomic location of the respective lesions. (Plast. Reconstr. Surg. 108: 622, 2001.) The optimal management of giant congenital nevi has been a longstanding surgical challenge, both because of differences pertaining to the unique biologic characteristics belonging to the different types of nevi and because of the reconstructive complexity. Arbitrary size criteria defining pigmented giant congenital nevi include those greater than 2 percent body surface area, 1 nevi greater than 20 cm in largest diameter, 2 and nevi that cannot be excised in a single procedure. 3 We chose to study lesions greater than 20 cm 2 in size. Because there is considerable overlap in reconstructive principles after resection of both pigmented and nonpigmented giant congenital nevi, our surgical experience for all forms of the lesion is combined to develop a more consistent and clinically useful algorithm. Because the potential for malignant transformation exists within pigmented giant congenital nevi, 1 surgical excision remains the standard of care for their treatment. Dermabrasion has been used in the treatment of these lesions 4 ; however, this technique may not remove the majority of nevus cells and is not currently recommended as an effective treatment for the prevention of potential malignant transformation. 5 Although laser therapy has also been used to treat congenital pigmented nevi 6 and may be useful in lightening unresectable lesions, the number of nevus cells actually removed by this technique cannot be docu- From the Department of Plastic and Reconstructive Surgery, Medical College of Wisconsin. Received for publication February 7, 2000; revised October 20, Presented at the 78th Annual Meeting of the American Association of Plastic Surgeons, in Colorado Springs, Colorado, May 4,
2 Vol. 108, No. 3 / MANAGEMENT OF GIANT CONGENITAL NEVI 623 mented. For this reason, the present study will focus only on surgical excision of giant congenital nevi, because this is the only technique in which complete removal of nevus cells can be documented. The purpose of the present study is to address the following questions: (1) What are the reasons to operate on pigmented and nonpigmented lesions, and how extensive a resection should be performed for each presentation of a giant congenital nevus? (2) What reconstructive options should be used after resection of a giant congenital nevus, and when is it appropriate to combine different reconstructive modalities? (3) Do the optimal reconstructive options vary in different anatomic regions of the body? METHODS A 20-year retrospective review was performed for all giant congenital nevi evaluated at the Medical College of Wisconsin from January of 1980 through May of Giant congenital nevi were defined as all nevi with a surface area greater than 20 cm 2. A separate assessment was made for the head and neck, torso, and extremities. Lesions of the head and neck consisted of all lesions above the clavicles. Lesions of the torso consisted of all lesions involving the chest, abdomen, back, and buttocks. Lesions of the extremities consisted of all lesions distal to the axilla in the upper extremities or distal to the groin in the lower extremities. Single lesions extending into more than one of the above-defined regions were classified as distinct nevi, provided the component within the given region was greater than 20 cm 2.A nevus extending from the back to the arms that involved greater than 20 cm 2 in each of the two body zones was classified as two giant congenital nevi for the purpose of this study. Although multiple satellite nevi were present in several patients, the index lesion was still required to be greater than 20 cm 2 to be considered a giant congenital nevus. RESULTS Of the 61 patients who were evaluated, 60 nevi in 55 patients were operated on. On presentation, there were 60 pigmented giant congenital nevi in 53 patients (Table I). Among all 61 patients at initial presentation, five patients each had two lesions and two patients had three. One patient had a giant nevus involving two different body regions. Age range of the TABLE I Distribution of Giant Congenital Nevi No. of Patients No. of Nevi Nevi thought to have malignant potential Pigmented Nevus sebaceus 4 4 Nevi without known malignant potential Woolly hair 1 1 Inflammatory linear verrucous epidermal 3 5 patients was from newborn to 16 years. No focus of malignancy or cytoatypia was identified in any patient. The deep margin of resection was positive for nevus cells in 14 resected specimens, all of which were pigmented lesions. Four of the 14 patients (29 percent) with positive deep margins later developed recurrent visible pigmentation in the reconstructed area. No patient presented with symptoms suggestive of central nervous system involvement. Magnetic resonance imaging of the brain and spinal cord was performed in five patients, each with extensive pigmented giant congenital nevi involving at least 50 percent body surface area. In one patient, an asymptomatic focus of leptomeningeal melanosis was found within the cerebellum for which no specific treatment was recommended. Reconstructive techniques consisted of expanded skin flaps, expanded skin for fullthickness skin grafts, nonexpanded fullthickness skin grafts, split-thickness skin grafts, and serial excision. Expanded flaps were used in 25 nevi, expanded full-thickness grafts were used in 10 nevi, split-thickness or nonexpanded full-thickness skin grafts were used in 13 nevi, and serial excision was used in 30 nevi. Nine nevi were operated on before 1990, equally distributed among three surgeons. Fifty-one nevi were operated on after 1989, 49 of which were operated on by one surgeon (A.K.G.). The use of split-thickness skin grafts decreased from 22 percent before 1990 to 6 percent after 1990, whereas the use of nonexpanded full-thickness grafts increased from none before 1990 to 10 percent after This change reflects the evolving preference for the use of full-thickness grafts over splitthickness grafts toward the latter portion of this series. The relationship between treatment modality and its use in single versus multiple modality treatment is shown in Table II. All five reconstructive options were commonly used in both
3 624 PLASTIC AND RECONSTRUCTIVE SURGERY, September 1, 2001 TABLE II Relationship between the Selected Treatment Modality and Combination Treatment TABLE IV Relationship between Nevus Location and Treatment Modality Single Modality (%) Multiple Modalities (%) Expanded flaps (n 25) FTSG (expanded) (n 10) FTSG (nonexpanded) (n 8) STSG (n 5) Serial excision (n 30) FTSG, full-thickness skin grafts; STSG, split-thickness skin grafts. TABLE III Number of Procedures Needed to Complete Coverage in Single Modality Treatment One (%) Two (%) Three (%) Four or More (%) Expanded flaps (n 18) FTSG (expanded) (n 6) FTSG (nonexpanded) (n 4) STSG (n 2) Serial excision (n 21) FTSG, full-thickness skin grafts; STSG, split-thickness skin grafts. Head and Neck Torso Extremities No. of nevi No. of procedures No. of modalities per nevus Single (%) Multiple (%) Expanded flaps* (%) FTSG (expanded)* (%) FTSG (nonexpanded)* (%) STSG* (%) Serial excision* (%) FTSG, full-thickness skin grafts; STSG, split-thickness skin grafts. * Percent distribution is reported relative to the number of procedures performed in the specified location. single and multiple modality treatment. Each of the five reconstructive options constituted one component of a multimodality treatment plan at least 40 percent of the time. When single modality treatment was used, multiple procedures were often required. The number of procedures needed to complete reconstruction when single modality treatment was used is shown in Table III. Serial expansion was required in six (33 percent) of the 18 nevi in which expanded flaps alone were used to reconstruct the defect, two of which required four successive stages of serial expansion for giant congenital nevi of the scalp. More than 80 percent of nevi treated with serial excision alone could be completed in two procedures or less. Three successive procedures were required in 19 percent of nevi treated with serial excision alone. The latter cases involved the knee or elbow, where increased morbidity might have resulted from the use of alternative reconstructive options. The relationship between the anatomic zone in which the nevus was located and the selected treatment modality is shown in Table IV. Expanded flaps were the most common mode of reconstruction in the extremities. Expanded flaps and serial excision were more equally distributed in the torso. Serial excision was the most common form of treatment in the extremities, and expanded flaps were used infrequently. The primary use of tissue expansion for extremity reconstruction was to provide expanded full-thickness skin grafts. Representative cases demonstrating principles of reconstruction in each of the anatomic zones are pictured in Figures 1 through 7. Head and Neck Single modality treatment of a giant congenital nevus of the scalp is shown in Figure 1. A 4-year-old girl presented with a woolly hair nevus occupying two-thirds of the occipitoparietal scalp (Fig. 1, above, left). Serial tissue expansion was performed, with new tissue expanders placed immediately after advancement of the previously expanded scalp flaps. After serial expansion in two stages, the remaining nevus occupied approximately one-third of the occipitoparietal scalp (Fig. 1, above, right). After four stages, only a negligible amount of woolly hair nevus remained (Fig. 1, below). Combined modality treatment was often required for lesions of the head and neck involving different anatomic structures. This is illustrated by a 13-year-old girl who presented with a giant congenital nevus sebaceus of the left temporoparietal scalp, postauricular sulcus, and auricle (Fig. 2, above, left). Tissue expansion was used to resurface the temporoparietal scalp in one stage (Fig. 2, above, right). Nonexpanded full-thickness skin grafts harvested from bilateral groins were used to resurface the postauricular sulcus and involved portion of the auricle (Fig. 2, below). Treatment of complex lesions of the head and neck, particularly those involving the eyelids, often required multiple modalities. This is illustrated by an 8.5-month-old girl who presented with a giant congenital nevus involving
4 Vol. 108, No. 3 / MANAGEMENT OF GIANT CONGENITAL NEVI 625 FIG. 1. Single modality treatment of a giant woolly hair nevus of the scalp with expanded flaps. (Above, left) Preoperative appearance. (Above, right) Appearance after two-stage immediate serial expansion. (Below) Appearance after four-stage immediate serial expansion. the scalp, forehead, upper and lower eyelids, and cheek (Fig. 3). Tissue expanders were placed in the scalp and the forehead, and each of these areas was reconstructed with expanded flaps (Fig. 3, above, right). Serial excision was used to reduce the nevus involving the right cheek. The residual nevus involving the right upper eyelid and its nasal extension was resected and reconstructed with a full-thickness skin graft obtained from the groin (Fig. 3, below, left). A tissue expander was then placed in the cheek, and the resulting flap was used to reconstruct the right lower eyelid and temporal extension of the nevus (Fig. 3, below, right). Torso The torso was the most common location for successful single modality treatment of giant nevi. A 1-year-old girl presented with a pigmented giant congenital nevus of the back and a second giant nevus involving the left buttock (Fig. 4). Separate single modality treatment was used for each giant congenital nevus, using two-stage serial tissue expansion for the back and two-stage serial excision for the buttock. The completed reconstruction is shown in Figure4(right). Extremities Serial excision was the preferred treatment modality for lesions at or just proximal to the knee or elbow. A 10-year-old girl presented with a pigmented giant congenital nevus of the distal right thigh just proximal to the knee (Fig. 5, left). The lesion was serially excised in three stages, spacing each stage at least 6 months apart (Fig. 5, right).
5 626 PLASTIC AND RECONSTRUCTIVE SURGERY, September 1, 2001 FIG. 2. Treatment of a giant congenital nevus sebaceus using combined modality treatment with tissue expansion and a nonexpanded full-thickness skin graft. (Above, left) Preoperative appearance. (Above, right) Appearance after onestage reconstruction of the temporoparietal scalp with expanded flaps. (Below) Final appearance after nonexpanded full-thickness skin graft to the postauricular sulcus and auricle. Similar lesions distal to the knee or elbow are difficult to treat using serial excision alone because of reduced skin compliance and reduced diameter of the distal extremity. These areas are best treated with expanded full-thickness skin grafts. A 9-month-old boy presented with a circumferential pigmented giant congenital nevus of the right forearm and hand (Fig. 6). The lower abdominal skin was expanded, and a single expanded fullthickness skin graft was harvested to reconstruct the volar surface of the forearm and hand as one unit. This reconstruction is pictured 16 months postoperatively (Fig. 6, center, left). During a second procedure, the dorsal digits and web spaces were resurfaced using expanded full-thickness grafts. Because of limitations in expanded full-thickness skin, a split-thickness graft was used to resurface the dorsal surface of the wrist and forearm. Twelve months later, a marked difference in aesthetic outcome could be seen between the full-thickness grafts covering the digits and the split-thickness grafts covering the distal forearm (Fig. 6, center, right). Over the next 3 years, there was progressive contracture of the expanded full-thickness graft reconstruction of the web spaces of the hand. This was corrected using dorsal rectangular flaps, raised from the initial full-thickness grafts, to deepen the second and third web spaces. Additional full-thickness grafts were placed on the borders of the respective digits. The first web space was deepened using a Z-plasty (Fig. 6, below). A 4-year-old girl who presented with inflammatory linear verrucous epidermal nevi involving the scalp, vulva, and both the upper and lower extremities is shown in Figure 7. The right forearm and ring and index fingers and the left index finger were the most symptomatic regions of the upper extremities, and the dorsal ankle was the most symptomatic lower extremity region. These intensely pruritic regions were surgically excised, with no effort made to obtain clear margins. The digits were resurfaced with a full-thickness skin graft harvested from the groin, and the symptomatic regions of the dorsal ankle, scalp, and vulva were each treated with serial excision in two stages. These procedures resulted in symptomatic relief of the involved areas. DISCUSSION What Are the Reasons to Operate on Pigmented and Nonpigmented Lesions, and How Extensive a Resection Should Be Performed for Each Presentation of a Giant Congenital Nevus? On the basis of our experience, an algorithm illustrating principles for the extent of resection of pigmented and nonpigmented giant congenital nevi is shown in Figure 8. Both pigmented and nonpigmented nevi can present with aesthetic disfigurement, pruritus, and altered skin integrity, and may have malignant potential. Significant aesthetic and psychosocial concerns were present with all four types of giant congenital nevi encountered, irrespective of pigmentation. The potential for malignant transformation exists only with pigmented lesions and sebaceous nevi, and only in the latter two nevi is there a need to clear the margins of resection. Excoriation with resultant alteration in skin integrity severely diminishes the quality
6 Vol. 108, No. 3 / MANAGEMENT OF GIANT CONGENITAL NEVI 627 FIG. 3. Combined modality treatment of a pigmented giant congenital nevus using expanded flaps, a full-thickness skin graft, and serial excision. (Above, left) Preoperative appearance. (Above, right) Appearance after reconstruction of the scalp and forehead with expanded flaps, and serial excision of the cheek. (Below, left) Intraoperative appearance after placement of a nonexpanded full-thickness graft to the right upper eyelid and nasal extension of the nevus. (Below, right) Final postoperative appearance after reconstruction of the right cheek and temporal extension of the nevus with an expanded flap. FIG. 4. Single modality treatment for two separate pigmented giant congenital nevi of the torso. (Left) Preoperative appearance of nevus on the back. (Center) Appearance after first of two-stage immediate serial expansion for nevus of the back, and preoperative appearance of the nevus involving the left buttock. (Right) Final appearance after two-stage immediate serial expansion for nevus of the back, and two-stage serial excision for nevus of the left buttock. of life in patients with inflammatory linear verrucous epidermal nevi. Pruritus and skin breakdown are the primary reasons to excise the latter lesions, and in patients with widespread epidermal nevi, surgical treatment should be limited to symptomatic areas.
7 628 PLASTIC AND RECONSTRUCTIVE SURGERY, September 1, 2001 the patient s surgical care, the algorithms guiding each of these aspects of the procedure must be interdependent. Because pigmented giant congenital nevi have malignant potential but are most commonly benign on presenta- FIG. 5. Single modality treatment for a pigmented giant congenital nevus proximal to the right knee using serial excision. (Left) Preoperative appearance. (Right) Postoperative appearance after three-stage serial excision. The risk of malignant transformation in pigmented giant congenital nevi remains controversial. Quaba and Wallace 1 calculated the risk of melanoma to be 8.52 percent during the first 15 years of life. A longitudinal study of a large population of patients with pigmented giant congenital nevi reported a lifetime incidence of malignant transformation of 4 to 6 percent. 7 Other authors have reported the incidence of malignant transformation to be between 2 percent and 31 percent. 8 Although the rate of malignant transformation as a function of lesion size is not known, it is assumed that this risk within a given nevus is decreased proportionate to the fraction of the lesion removed or destroyed. The efficacy of dermabrasion and laser treatment in removing or destroying nevus cells has never been established. 4 6 There are no longitudinal studies documenting decreased rates of malignant transformation after laser or dermabrasion treatment. In fact, lightening of pigmented giant congenital nevi using these techniques may make it more difficult to monitor the resultant lesion for signs of malignant transformation, because alteration in pigmentation of the lesion can no longer be followed reliably. Surgical excision remains the treatment of choice for the removal of pigmented lesions, because this technique has documented efficacy in removal of nevus cells. 5 The extent of resection of giant congenital nevi is closely linked to available reconstructive options. Because the same surgeon is usually responsible for both of these components of FIG. 6. Combined modality treatment of a pigmented giant congenital nevus involving the right upper extremity using expanded full-thickness and split-thickness skin grafts. (Above) Preoperative appearance. (Center, left) Appearance after resurfacing the volar surface of the involved extremity with a single expanded full-thickness graft. (Center, right) Appearance after resurfacing the dorsal surface of the involved extremity with a single expanded full-thickness graft from the metacarpal heads to the distal phalanges and split-thickness grafts to the proximal surface of the involved extremity. (Below) Appearance 3 years later after deepening of the first, second, and third web spaces of the left hand.
8 Vol. 108, No. 3 / MANAGEMENT OF GIANT CONGENITAL NEVI 629 FIG. 7. Preoperative appearance of a patient with diffuse inflammatory linear verrucous epidermal nevi involving the right knee (left) and the palmar surface of both upper extremities (right). tion, an incomplete resection may be indicated in certain situations. An extensive resection and reconstruction resulting in mutilation ofthe involved body part, to remove a minimal amount of residual nevus, cannot be justified on the basis of current oncologic data. The above principle is illustrated in Figure 6, center, right. In this case, small distal foci of pigmentation were not resected to preserve the eponychial folds of the fingers and digital sensory function. In some instances, nevus cells infiltrate deeply into muscle, bone, or cartilage. In such situations, the patient and family should be educated regarding the morbidity of further resection versus continued surveillance for signs of malignant transformation. Nevus sebaceus is associated with a 10 to 20 percent rate of malignant transformation after puberty. 9 Although the resultant cutaneous malignancy is most often basal cell carcinoma or occasionally squamous cell carcinoma, other carcinomas such as apocrine and adnexal tumors can occur. 10 Because of the increased risk of malignant transformation and the difficulty involved with following these lesions clinically, incomplete excision by pathologic evaluation warrants repeated excision until deep and lateral margins of resection are free of nevus cells. Guidelines for resection of giant congenital nevi without malignant potential are indicated on the basis of presentation of the nevus. Inflammatory linear verrucous epidermal nevi (Fig. 7) are intensely symptomatic lesions. 11 The treatment strategy should focus on the most severely affected areas of skin, with more complete excision directed toward the aesthetic needs of the individual patient. Woolly hair nevi of the scalp (Fig. 1) do not possess FIG. 8. Giant congenital nevi algorithm: extent of resection. SQ, subcutaneous tissue.
9 630 PLASTIC AND RECONSTRUCTIVE SURGERY, September 1, 2001 FIG. 9. Giant congenital nevi algorithm: reconstructive options. *Consider immediate serial expansion if lesion cannot be resurfaced in one stage. **Consider supplementing with splitthickness skin graft in less-visible areas if expanded full-thickness skin graft alone cannot cover defect. malignant potential, and the extent of excision is dictated by aesthetic considerations. 12 What Reconstructive Options Should Be Used after Resection of Giant Congenital Nevi, and When Is It Appropriate to Combine Reconstructive Techniques? Do Optimal Reconstructive Methods Vary in Different Anatomic Regions? On the basis of our experience, a proposed algorithm for the reconstruction of giant congenital nevi is shown in Figure 9. Reconstructive options include tissue-expanded flaps or grafts, serial excision, and either full-thickness or split-thickness skin grafts. Serial excision is the preferred treatment modality for lesions that can be excised in two or fewer procedures without distorting adjacent structures. Because increased morbidity is often associated with the use of tissue expanders or skin grafts at or just proximal to the knee or elbow joints, serial excision is also preferred for use in these areas. If more than three procedures are required to
10 Vol. 108, No. 3 / MANAGEMENT OF GIANT CONGENITAL NEVI 631 complete the resection, the former options should be considered. Tissue expansion is recommended for lesions involving the head, neck, or torso, as the reconstructive outcome, particularly in the head and neck, is far superior to that obtained with skin grafting. For large lesions requiring more than one set of tissue expanders, a subsequent set of expanders can be inserted at the time of the initial flap advancement. Although a waiting period of 2 weeks is usual, we have delayed filling the serially placed expanders for as long as 8 to 12 weeks in an effort to avoid subluxation. Even if a filling delay is necessary, serial expansion is preferable, as it avoids the need for a repeated operation for insertion of tissue expanders. Skin grafts are recommended for lesions involving the extremities distal to the knee or elbow joint. Tissue expansion in this context has greater morbidity with less potential gain because of the restricting circumference of skin envelope. Skin grafts are also preferred for reconstruction of the eyelids or ears. In these areas, the use of expanded flaps or serial excision results in distortion of involved structures. A full-thickness skin graft is always preferable to a split-thickness graft, because of both an improved aesthetic outcome and less subsequent graft contracture. An expanded full-thickness graft should be considered if donor skin limitations are problematic. The best outcome is often achieved through the use of multimodality therapy, particularly for lesions involving the face or those involving contiguous anatomic regions. No biologic skin substitutes were used in the present algorithm, because skin substitutes are currently associated with a less satisfactory aesthetic outcome than that achieved with skin grafts. Dermal allografts may be useful in creating a thicker neodermis when a splitthickness graft is required. Microsurgical techniques may be useful if reconstruction of the face as one aesthetic unit, as reported by Siebert and Longaker, 13 is required. Despite advances made in the treatment of patients with giant congenital nevi, inadequate donor tissue for reconstruction may render complete removal impossible. Complex lesions such as bathing trunk nevi involving the perineum, genitals, and perirectal area present a continued surgical challenge. Resection of these problematic nevi should be limited to areas in which reconstruction can reasonably be expected to provide a better aesthetic and functional outcome than the original lesion. Leaving residual nevus in the genital and perineal regions results in a more predictable reconstructive outcome. Adjunctive treatments for surgically unresectable portions of complex pigmented giant congenital nevi, such as phenol chemical peel, have been reported. 14 Giant congenital nevi are among the most challenging problems faced by plastic surgeons. A thoughtful reconstructive approach to these patients may help to improve their treatment outcome in future years. Arun K. Gosain, M.D. Department of Plastic and Reconstructive Surgery Medical College of Wisconsin 9200 West Wisconsin Avenue Milwaukee, Wis agosain@mcw.edu REFERENCES 1. Quaba, A. A., and Wallace, A. F. The incidence of malignant melanoma (0 to 15 years of age) arising in large congenital nevocellular nevi. Plast. Reconstr. Surg. 78: 174, Kopf, A. W., Bart, R. S., and Hennessey, P. Congenital nevocytic nevi and malignant melanomas. J. Am. Acad. Dermatol. 1: 123, Pilney, F. T., Broadbent, T. R., and Woolf, R. M. Giant pigmented nevi of the face: Surgical management. Plast. Reconstr. Surg. 40: 469, Rompel, R., Möser, M., and Petres, J. Dermabrasion of congenital nevocellular nevi: Experience in 215 patients. Dermatology 194: 261, Zitelli, J. A., Grant, M. G., Abell, E., et al. Histologic patterns of congenital nevocytic nevi and implications for treatment. J. Am. Acad. Dermatol. 11: 402, Grevelink, J. M., Van Leeuwen, R. L., Anderson, R. R., et al. Clinical and histological responses of congenital melanocytic nevi after single treatment with Q-switched lasers. Arch. Dermatol. 133: 349, Lorentzen, M., Pers, M., and Bretteville-Jensen, G. The incidence of malignant transformation in giant pigmented nevi. Scand. J. Plast. Reconstr. Surg. 11: 163, Mark, G. J., Mihm, M. C., Liteplo, M. G., et al. Congenital melanocytic nevi of the small and garment type: Clinical, histologic, and ultrastructural studies. Hum. Pathol. 4: 395, Mehregan, A. H., and Pinkus, H. Life history of organoid nevi. Arch. Dermatol. 91: 574, Domingo, J., and Helwig, E. B. Malignant neoplasms associated with nevus sebaceus of Jadassohn. J. Am. Acad. Dermatol. 1: 545, Morag, C., and Metzker, A. Inflammatory linear verrucous epidermal nevus: Report of seven new cases and review of the literature. Pediatr. Dermatol. 3: 15, Reda, A. M., Rogers, R. S., III, and Peters, M. S. Woolly hair nevus. J. Am. Acad. Dermatol. 22: 377, Siebert, J. W., and Longaker, M. T. Salvage reconstruction of an extensive facial deformity due to congenital giant hairy nevus. Plast. Reconstr. Surg. 102: 2414, Hopkins, J. D., Smith, A. W., and Jackson, I. T. Adjunctive treatment of congenital pigmented nevi with phenol chemical peel. Plast. Reconstr. Surg. 105: 1, 2000.
Department of Plastic Surgery, The First Affiliated Hospital of Zhengzhou University, Zhengzhou , China; 2
 Int J Clin Exp Med 2016;9(3):5609-5615 www.ijcem.com /ISSN:1940-5901/IJCEM0019126 Original Article Clinical effect of full-thickness skin grafts for the treatment of large and giant congenital melanocytic
Int J Clin Exp Med 2016;9(3):5609-5615 www.ijcem.com /ISSN:1940-5901/IJCEM0019126 Original Article Clinical effect of full-thickness skin grafts for the treatment of large and giant congenital melanocytic
THE TREATMENT OF GIANT HAIRY PIGMENTED N~EVI OF THE FACE
 THE TREATMENT OF GIANT HAIRY PIGMENTED N~EVI OF THE FACE By JOHN MARQUIS CONVERSE, M.D., F.A.C.S., CARY L. GuY, M.D., F.A.C.S., and ANDRIES MOLENAAR, M.D. From the Institute of Reconstructive Plastic Surgery,
THE TREATMENT OF GIANT HAIRY PIGMENTED N~EVI OF THE FACE By JOHN MARQUIS CONVERSE, M.D., F.A.C.S., CARY L. GuY, M.D., F.A.C.S., and ANDRIES MOLENAAR, M.D. From the Institute of Reconstructive Plastic Surgery,
Scar Saving Flap during Serial Excision by Borrowing from the Opposite Side
 Scar Saving Flap during Serial Excision by Borrowing from the Opposite Side Ji Yeon Lim, M.D., Won Keun Song, M.D. 1, Kyu Kwang Whang, M.D. 2 Department of Dermatology, School of Medicine, Ewha Womans
Scar Saving Flap during Serial Excision by Borrowing from the Opposite Side Ji Yeon Lim, M.D., Won Keun Song, M.D. 1, Kyu Kwang Whang, M.D. 2 Department of Dermatology, School of Medicine, Ewha Womans
Interesting Case Series. Aggressive Tumor of the Midface
 Interesting Case Series Aggressive Tumor of the Midface Adrian Frunza, MD, Dragos Slavescu, MD, and Ioan Lascar, MD, PhD Bucharest Emergency Clinical Hospital, Bucharest University School of Medicine,
Interesting Case Series Aggressive Tumor of the Midface Adrian Frunza, MD, Dragos Slavescu, MD, and Ioan Lascar, MD, PhD Bucharest Emergency Clinical Hospital, Bucharest University School of Medicine,
Repair of complete syndactyly by tissue expansion and composite grafts
 British Journal of Plastic Surgery (1995), 48. 396-400 1995 The British Association of Plastic Surgeons BRITISH JOURNAL OF / PLASTIC SURGERY I Repair of complete syndactyly by tissue expansion and composite
British Journal of Plastic Surgery (1995), 48. 396-400 1995 The British Association of Plastic Surgeons BRITISH JOURNAL OF / PLASTIC SURGERY I Repair of complete syndactyly by tissue expansion and composite
Chapter 11 Worksheet Code It
 Class: Date: Chapter 11 Worksheet 3 2 1 Code It True/False Indicate whether the statement is true or false. 1. Surgical destruction is considered part of the surgical procedure description. 2. Prepping
Class: Date: Chapter 11 Worksheet 3 2 1 Code It True/False Indicate whether the statement is true or false. 1. Surgical destruction is considered part of the surgical procedure description. 2. Prepping
Reconstruction of axillary scar contractures retrospective study of 124 cases over 25 years
 British Journal of Plastic Surgery (2003), 56, 100 105 q 2003 The British Association of Plastic Surgeons. Published by Elsevier Science Ltd. All rights reserved. doi:10.1016/s0007-1226(03)00035-3 Reconstruction
British Journal of Plastic Surgery (2003), 56, 100 105 q 2003 The British Association of Plastic Surgeons. Published by Elsevier Science Ltd. All rights reserved. doi:10.1016/s0007-1226(03)00035-3 Reconstruction
Surgical treatment of non-melanoma skin cancer of the head and neck: expanding reconstructive options van der Eerden, P.A.
 UvA-DARE (Digital Academic Repository) Surgical treatment of non-melanoma skin cancer of the head and neck: expanding reconstructive options van der Eerden, P.A. Link to publication Citation for published
UvA-DARE (Digital Academic Repository) Surgical treatment of non-melanoma skin cancer of the head and neck: expanding reconstructive options van der Eerden, P.A. Link to publication Citation for published
Interesting Case Series. Reconstruction of Dorsal Wrist Defects
 Interesting Case Series Reconstruction of Dorsal Wrist Defects Maelee Yang, BS, and Joseph Meyerson, MD The Ohio State University Wexner Medical Center, Columbus Correspondence: maelee.yang@osumc.edu Keywords:
Interesting Case Series Reconstruction of Dorsal Wrist Defects Maelee Yang, BS, and Joseph Meyerson, MD The Ohio State University Wexner Medical Center, Columbus Correspondence: maelee.yang@osumc.edu Keywords:
THE pedicled flap, commonly used by the plastic surgeon in the reconstruction
 THE PEDICLE!) SKIN FLAP ROBIN ANDERSON, M.D. Department of Plastic Surgery THE pedicled flap, commonly used by the plastic surgeon in the reconstruction of skin and soft tissue defects, differs from the
THE PEDICLE!) SKIN FLAP ROBIN ANDERSON, M.D. Department of Plastic Surgery THE pedicled flap, commonly used by the plastic surgeon in the reconstruction of skin and soft tissue defects, differs from the
CASE REPORT SOLITARY SEBACEOUS NEVUS OF JADASSOHN COMPLICATED BY SQUAMOUS CELL CARCINOMA AND BASAL CELL CARCINOMA
 CASE REPORT Dennis H. Kraus, MD, Section Editor SOLITARY SEBACEOUS NEVUS OF JADASSOHN COMPLICATED BY SQUAMOUS CELL CARCINOMA AND BASAL CELL CARCINOMA Ahmad Ridzwan Arshad, FRCS, 1 Wan S. Azman, MS, 1 Ayadurai
CASE REPORT Dennis H. Kraus, MD, Section Editor SOLITARY SEBACEOUS NEVUS OF JADASSOHN COMPLICATED BY SQUAMOUS CELL CARCINOMA AND BASAL CELL CARCINOMA Ahmad Ridzwan Arshad, FRCS, 1 Wan S. Azman, MS, 1 Ayadurai
ENCR RECOMMENDATIONS
 E N C R EUROPEAN NETWORK OF CANCER REGISTRIES (ENCR) ENCR RECOMMENDATIONS Non-Melanoma Skin Cancers Members of the Working Group: Dr T. Davies, East Anglian Cancer Registry, Cambridge, UK Mrs M. Page,
E N C R EUROPEAN NETWORK OF CANCER REGISTRIES (ENCR) ENCR RECOMMENDATIONS Non-Melanoma Skin Cancers Members of the Working Group: Dr T. Davies, East Anglian Cancer Registry, Cambridge, UK Mrs M. Page,
cally, a distinct superior crease of the forehead marks this spot. The hairline and
 4 Forehead The anatomical boundaries of the forehead unit are the natural hairline (in patients without alopecia), the zygomatic arch, the lower border of the eyebrows, and the nasal root (Fig. 4.1). The
4 Forehead The anatomical boundaries of the forehead unit are the natural hairline (in patients without alopecia), the zygomatic arch, the lower border of the eyebrows, and the nasal root (Fig. 4.1). The
GIANT CONGENITAL MELANOCYTIC NEVUS OF THE FACE: A CLINICAL CASE
 56 CLINICAL EXPERIENCE DOI: 10.17816/PTORS3256-60 GIANT CONGENITAL MELANOCYTIC NEVUS OF THE FACE: A CLINICAL CASE Tsyplakova M.S., Usoltseva A.C., Stepanova Yu.V. The Turner Institute for Children s Orthopedics,
56 CLINICAL EXPERIENCE DOI: 10.17816/PTORS3256-60 GIANT CONGENITAL MELANOCYTIC NEVUS OF THE FACE: A CLINICAL CASE Tsyplakova M.S., Usoltseva A.C., Stepanova Yu.V. The Turner Institute for Children s Orthopedics,
Cutaneous Melanoma: Epidemiology (USA) The Sentinel Node in Head and Neck Melanoma. Cutaneous Melanoma: Epidemiology (USA)
 The Sentinel Node in Head and Neck Melanoma Cutaneous Melanoma: Epidemiology (USA) 6 th leading cause of cancer among men and women 68,720 new cases of invasive melanoma in 2009 8,650 deaths from melanoma
The Sentinel Node in Head and Neck Melanoma Cutaneous Melanoma: Epidemiology (USA) 6 th leading cause of cancer among men and women 68,720 new cases of invasive melanoma in 2009 8,650 deaths from melanoma
Clinical teaching/experi ence. Lectures/semina rs/conferences Self-directed. learning. Clinical teaching/experi ence
 Regional Medical Center (The MED) Plastic Surgery PGY-3 By the end of the Plastic Surgery at the MED, the PGY-3 residents are expected to expand and cultivate knowledge and skills developed during previous
Regional Medical Center (The MED) Plastic Surgery PGY-3 By the end of the Plastic Surgery at the MED, the PGY-3 residents are expected to expand and cultivate knowledge and skills developed during previous
Interesting Case Series. Scalp Reconstruction With Free Latissimus Dorsi Muscle
 Interesting Case Series Scalp Reconstruction With Free Latissimus Dorsi Muscle Danielle H. Rochlin, BA, Justin M. Broyles, MD, and Justin M. Sacks, MD Department of Plastic and Reconstructive Surgery,
Interesting Case Series Scalp Reconstruction With Free Latissimus Dorsi Muscle Danielle H. Rochlin, BA, Justin M. Broyles, MD, and Justin M. Sacks, MD Department of Plastic and Reconstructive Surgery,
A Combination of Dual-mode 2,940 nm Er:YAG Laser Ablation with Surgical Excision for Treating Mediumsized Congenital Melanocytic Nevus
 Ann Dermatol Vol. 21, No. 2, 2009 ORIGINAL ARTICLE A Combination of Dual-mode 2,940 nm Er:YAG Laser Ablation with Surgical Excision for Treating Mediumsized Congenital Melanocytic Nevus Ji Yeon Lim, M.D.,
Ann Dermatol Vol. 21, No. 2, 2009 ORIGINAL ARTICLE A Combination of Dual-mode 2,940 nm Er:YAG Laser Ablation with Surgical Excision for Treating Mediumsized Congenital Melanocytic Nevus Ji Yeon Lim, M.D.,
SKIN SERVICES REVIEW Changes to Medicare Benefits Schedule for 1 November 2016
 Attachment A SKIN SERVICES REVIEW Changes to Medicare Benefits Schedule for 1 November 2016 Deleted items 31200-31215, 31230-31240 31255-31335 Colour Coding for new / updated items: MUCOSAL BIOPSY AND
Attachment A SKIN SERVICES REVIEW Changes to Medicare Benefits Schedule for 1 November 2016 Deleted items 31200-31215, 31230-31240 31255-31335 Colour Coding for new / updated items: MUCOSAL BIOPSY AND
Tanta University. Faculty of Medicine. Plastic and Reconstructive Surgery Department. Doctorate Degree in Plastic Surgery
 Componenets : Tanta University Faculty of Medicine Plastic and Reconstructive Surgery Department Doctorate Degree in Plastic Surgery Students should fulfill the designated number of credit hours, including
Componenets : Tanta University Faculty of Medicine Plastic and Reconstructive Surgery Department Doctorate Degree in Plastic Surgery Students should fulfill the designated number of credit hours, including
Other ways to use tissue expanded flaps
 The British Association of Plastic Surgeons (2004) 57, 336 341 CASE REPORTS Other ways to use tissue expanded flaps Donald A. Hudson* Department of Plastic and Reconstructive Surgery, University of Cape
The British Association of Plastic Surgeons (2004) 57, 336 341 CASE REPORTS Other ways to use tissue expanded flaps Donald A. Hudson* Department of Plastic and Reconstructive Surgery, University of Cape
SCOPE OF PRACTICE PGY-6 PGY-7 PGY-8
 PGY-6 Round on all plastic surgery inpatients every day. Assess progress of patients and identify real or potential problems. Review patients progress with attending physicians daily and participate in
PGY-6 Round on all plastic surgery inpatients every day. Assess progress of patients and identify real or potential problems. Review patients progress with attending physicians daily and participate in
Different modalities of soft tissue coverage of hand and wrist defects
 ifferent modalities of soft tissue coverage of hand and wrist defects Soft tissue defects of hand and wrist with exposed tendons, joints, nerves and bones represent a challenge to plastic surgeons. Such
ifferent modalities of soft tissue coverage of hand and wrist defects Soft tissue defects of hand and wrist with exposed tendons, joints, nerves and bones represent a challenge to plastic surgeons. Such
Departmental Segregated Total Form for Plastic and Reconstructive Surgery
 Departmental Segregated Total Form for Plastic and Reconstructive Surgery American Osteopathic Association and the American College of Osteopathic Surgeons Revised, COPT 11/2001 Revised, BOT 2/2006, Effective,
Departmental Segregated Total Form for Plastic and Reconstructive Surgery American Osteopathic Association and the American College of Osteopathic Surgeons Revised, COPT 11/2001 Revised, BOT 2/2006, Effective,
5/20/2015. Mohs Surgery BCCA High risk anatomic locations. Mohs Surgery High risk anatomic locations. Mohs Surgery Histologically Aggressive BCCA
 Mohs Surgery BCCA High risk anatomic locations High risk areas H zone nasal ala, nasal septum, nasal ala groove, periorbital region, periauricual region, region around and in ear canal, ear pinna and scalp
Mohs Surgery BCCA High risk anatomic locations High risk areas H zone nasal ala, nasal septum, nasal ala groove, periorbital region, periauricual region, region around and in ear canal, ear pinna and scalp
Objectives. 1. Recognizing benign skin lesions. 2.Know which patients will likely need surgical intervention.
 The Joy of Pediatric Skin Dr. Claire Sanger University of Kentucky Plastic & Reconstructive Surgery Objectives 1. Recognizing benign skin lesions 2.Know which patients will likely need surgical intervention.
The Joy of Pediatric Skin Dr. Claire Sanger University of Kentucky Plastic & Reconstructive Surgery Objectives 1. Recognizing benign skin lesions 2.Know which patients will likely need surgical intervention.
Chapter 19 Hidradenitis Suppurativa
 1 Chapter 19 Hidradenitis Suppurativa Peter Nthumba Hidradenitis suppurativa is a chronic, recurrent, painful inflammatory skin disease, first described in 1833 by a French surgeon. Verneuil, another French
1 Chapter 19 Hidradenitis Suppurativa Peter Nthumba Hidradenitis suppurativa is a chronic, recurrent, painful inflammatory skin disease, first described in 1833 by a French surgeon. Verneuil, another French
Reconstructive and Cosmetic Services
 Reconstructive and Cosmetic Services Policy Number: 10.01.09 Last Review: 4/2018 Origination: 2/2006 Next Review: 4/2019 Policy Determination of whether a proposed therapy would be considered reconstructive
Reconstructive and Cosmetic Services Policy Number: 10.01.09 Last Review: 4/2018 Origination: 2/2006 Next Review: 4/2019 Policy Determination of whether a proposed therapy would be considered reconstructive
Eyelid Reconstruction An Oculoplastic Surgical Coding Minicourse. Riva Lee Asbell Philadelphia, PA. Part II
 INTRODUCTION Eyelid Reconstruction An Oculoplastic Surgical Coding Minicourse Riva Lee Asbell Philadelphia, PA Part II In this second part of the Minicourse on Surgical Coding for Eyelid Reconstruction
INTRODUCTION Eyelid Reconstruction An Oculoplastic Surgical Coding Minicourse Riva Lee Asbell Philadelphia, PA Part II In this second part of the Minicourse on Surgical Coding for Eyelid Reconstruction
Reconstructive Surgery in the Thermally Injured Patient
 Reconstructive Surgery in the Thermally Injured Patient Davin Mellus, DMD a, * Rodney K. Chan, MD b KEYWORDS Microvascular free-tissue transfer Pedicle flaps Reconstructive Surgery Thermal injury Z-plasties
Reconstructive Surgery in the Thermally Injured Patient Davin Mellus, DMD a, * Rodney K. Chan, MD b KEYWORDS Microvascular free-tissue transfer Pedicle flaps Reconstructive Surgery Thermal injury Z-plasties
PATIENT INFORMATION. Mohs Micrographic Surgery. In the Treatment of Skin Cancer
 PATIENT INFORMATION Mohs Micrographic Surgery In the Treatment of Skin Cancer What is Mohs Micrographic Surgery? Mohs micrographic surgery is a specialized, highly effective technique for the removal
PATIENT INFORMATION Mohs Micrographic Surgery In the Treatment of Skin Cancer What is Mohs Micrographic Surgery? Mohs micrographic surgery is a specialized, highly effective technique for the removal
International Journal of Medical Science and Education
 International Journal of Medical Science and Education www.ijmse.com Original Research Article pissn- 2348 4438 eissn-2349-3208 A PROSPECTIVE STUDY OF POST BURN CONTRACTURE: INCIDENCE, PREDISPOSING FACTORS,
International Journal of Medical Science and Education www.ijmse.com Original Research Article pissn- 2348 4438 eissn-2349-3208 A PROSPECTIVE STUDY OF POST BURN CONTRACTURE: INCIDENCE, PREDISPOSING FACTORS,
Large full-thickness nasal tip defects after Mohs
 RECONSTRUCTIVE CONUNDRUM Repair of a Large, Exposed-Cartilage Nasal Tip Defect Using Nasalis-Based Subcutaneous Pedicle Flaps and Full-Thickness Skin Grafting DIEGO E. MARRA, MD, EDGAR F. FINCHER, MD,
RECONSTRUCTIVE CONUNDRUM Repair of a Large, Exposed-Cartilage Nasal Tip Defect Using Nasalis-Based Subcutaneous Pedicle Flaps and Full-Thickness Skin Grafting DIEGO E. MARRA, MD, EDGAR F. FINCHER, MD,
Original Article Use of expanded deltopectoral skin flaps for facial reconstruction after sizeable benign tumor resections
 Am J Transl Res 2018;10(7):2158-2163 www.ajtr.org /ISSN:1943-8141/AJTR0076995 Original Article Use of expanded deltopectoral skin flaps for facial reconstruction after sizeable benign tumor resections
Am J Transl Res 2018;10(7):2158-2163 www.ajtr.org /ISSN:1943-8141/AJTR0076995 Original Article Use of expanded deltopectoral skin flaps for facial reconstruction after sizeable benign tumor resections
Advances in Surgical Management of Primary Melanoma: Identifying Patients Who Need More than Conventional Wide Local Excision
 Advances in Surgical Management of Primary Melanoma: Identifying Patients Who Need More than Conventional Wide Local Excision Christopher J. Miller, MD Director of Penn Dermatology Oncology Center Associate
Advances in Surgical Management of Primary Melanoma: Identifying Patients Who Need More than Conventional Wide Local Excision Christopher J. Miller, MD Director of Penn Dermatology Oncology Center Associate
Mentosternal Contracture Treated With an Occipito-Scapular Flap in a 5-year-old Boy: A Case Report
 Mentosternal Contracture Treated With an Occipito-Scapular Flap in a 5-year-old Boy: A Case Report Armin Kraus, MD, Hans-Eberhard Schaller, MD, and Hans-Oliver Rennekampff, MD Department for Hand, Plastic,
Mentosternal Contracture Treated With an Occipito-Scapular Flap in a 5-year-old Boy: A Case Report Armin Kraus, MD, Hans-Eberhard Schaller, MD, and Hans-Oliver Rennekampff, MD Department for Hand, Plastic,
Basic Standards for Fellowship Training in Mohs Micrographic Surgery
 Basic Standards for Fellowship Training in Mohs Micrographic Surgery American Osteopathic Association and American Osteopathic College of Dermatologists September, 1992 BOT/93 BOT 7/2011, Eff. 7/2012 Basic
Basic Standards for Fellowship Training in Mohs Micrographic Surgery American Osteopathic Association and American Osteopathic College of Dermatologists September, 1992 BOT/93 BOT 7/2011, Eff. 7/2012 Basic
Kevin T. Kavanagh, MD
 Kevin T. Kavanagh, MD Axial Based upon a named artery. Survival length depends upon the artery not the width of the flap. Random Has random unnamed vessels supplying it. Survival length is directly proportional
Kevin T. Kavanagh, MD Axial Based upon a named artery. Survival length depends upon the artery not the width of the flap. Random Has random unnamed vessels supplying it. Survival length is directly proportional
Aesthetic surgery techniques after excision of dermatofibrosarcoma protuberans: a case report
 British Journal of Plastic Surgery (2005) 58, 556 560 CASE REPORT Aesthetic surgery techniques after excision of dermatofibrosarcoma protuberans: a case report G. Dagregorio a, *, V. Darsonval b a Department
British Journal of Plastic Surgery (2005) 58, 556 560 CASE REPORT Aesthetic surgery techniques after excision of dermatofibrosarcoma protuberans: a case report G. Dagregorio a, *, V. Darsonval b a Department
Melanoma Extirpation with Immediate Reconstruction: The Oncologic Safety and Cost Savings of Single-Stage Treatment.
 RECONSTRUCTIVE Melanoma Extirpation with Immediate Reconstruction: The Oncologic Safety and Cost Savings of Single-Stage Treatment Irena Karanetz, M.D. Sharon Stanley, M.D. Denis Knobel, M.D. Benjamin
RECONSTRUCTIVE Melanoma Extirpation with Immediate Reconstruction: The Oncologic Safety and Cost Savings of Single-Stage Treatment Irena Karanetz, M.D. Sharon Stanley, M.D. Denis Knobel, M.D. Benjamin
Interesting Case Series. Desmoplastic Melanoma
 Interesting Case Series Desmoplastic Melanoma Anthony Maurice Kordahi, MD, Joshua B. Elston, MD, Ellen M. Robertson, MD, and C. Wayne Cruse, MD Division of Plastic Surgery, Department of Surgery, University
Interesting Case Series Desmoplastic Melanoma Anthony Maurice Kordahi, MD, Joshua B. Elston, MD, Ellen M. Robertson, MD, and C. Wayne Cruse, MD Division of Plastic Surgery, Department of Surgery, University
The eyebrow is so aesthetically important that. Reconstructive
 Original Article Reconstructive Extended Hair-bearing Lateral Orbital Flap for Simultaneous Reconstruction of Eyebrow and Eyelid Shinji Matsuo, MD Ichiro Hashimoto, MD Takuya Seike, MD Yoshiro Abe, MD
Original Article Reconstructive Extended Hair-bearing Lateral Orbital Flap for Simultaneous Reconstruction of Eyebrow and Eyelid Shinji Matsuo, MD Ichiro Hashimoto, MD Takuya Seike, MD Yoshiro Abe, MD
Principles of Facial Reconstruction After Mohs Surgery
 Objectives Principles of Facial Reconstruction After Mohs Surgery Identify important functional anatomy and aesthetic units of the face. Describe techniques used in facial reconstruction. Discuss postoperative
Objectives Principles of Facial Reconstruction After Mohs Surgery Identify important functional anatomy and aesthetic units of the face. Describe techniques used in facial reconstruction. Discuss postoperative
UWMC Roosevelt Clinic Rotation Goals 2011 Procedural Dermatology Fellowship Program 1
 Procedural Dermatology Fellowship Objectives University of Washington Medical Center-Roosevelt Rotation The primary goal of the University of Washington rotation of the Procedural Dermatology fellowship
Procedural Dermatology Fellowship Objectives University of Washington Medical Center-Roosevelt Rotation The primary goal of the University of Washington rotation of the Procedural Dermatology fellowship
Expanded Transposition Flap Technique for Total and Subtotal Resurfacing of the Face and Neck
 Expanded Transposition Flap Technique for Total and Subtotal Resurfacing of the Face and Neck Robert J. Spence, MD, FACS Johns Hopkins School of Medicine, Baltimore, MD Correspondence: rspence@jhmi.edu
Expanded Transposition Flap Technique for Total and Subtotal Resurfacing of the Face and Neck Robert J. Spence, MD, FACS Johns Hopkins School of Medicine, Baltimore, MD Correspondence: rspence@jhmi.edu
MOHS MICROGRAPHIC SURGERY: AN OVERVIEW
 MOHS MICROGRAPHIC SURGERY: AN OVERVIEW SKIN CANCER: Skin cancer is far and away the most common malignant tumor found in humans. The most frequent types of skin cancer are basal cell carcinoma, squamous
MOHS MICROGRAPHIC SURGERY: AN OVERVIEW SKIN CANCER: Skin cancer is far and away the most common malignant tumor found in humans. The most frequent types of skin cancer are basal cell carcinoma, squamous
1. Written information to patient /GP: fax ASAP to GP & offer copy of consultation letter.
 Skin Cancer follow up guidelines If NEW serious diagnosis given: 1. Written information to patient /GP: fax ASAP to GP & offer copy of consultation letter. 2. Free prescription information details. 3.
Skin Cancer follow up guidelines If NEW serious diagnosis given: 1. Written information to patient /GP: fax ASAP to GP & offer copy of consultation letter. 2. Free prescription information details. 3.
CROSS CODER. Sample page. Anesthesia. codes to ICD-10-CM and HCPCS. Essential links from CPT. Power up your coding optum360coding.
 CROSS CODER 2019 Anesthesia Essential links from CPT codes to ICD-10-CM and HCPCS Power up your coding optum360coding.com Contents Introduction...i CPT Anesthesia to Procedure Code Crosswalk... i Format...
CROSS CODER 2019 Anesthesia Essential links from CPT codes to ICD-10-CM and HCPCS Power up your coding optum360coding.com Contents Introduction...i CPT Anesthesia to Procedure Code Crosswalk... i Format...
Interesting Case Series. Rhinophyma
 Interesting Case Series Rhinophyma Jake Laun, BS, Jared Gopman, BS, Joshua B. Elston, MD, and Michael A. Harrington, MD Department of Surgery, Division of Plastic Surgery, University of South Florida Morsani
Interesting Case Series Rhinophyma Jake Laun, BS, Jared Gopman, BS, Joshua B. Elston, MD, and Michael A. Harrington, MD Department of Surgery, Division of Plastic Surgery, University of South Florida Morsani
Surgical Management of wounds, flaps, grafts, and scars
 Disclosures Surgical Management of wounds, flaps, grafts, and scars I have no financial disclosures Cherrie Heinrich, MD, FACS Department of Plastic Surgery Regions Hospital Assistant Professor University
Disclosures Surgical Management of wounds, flaps, grafts, and scars I have no financial disclosures Cherrie Heinrich, MD, FACS Department of Plastic Surgery Regions Hospital Assistant Professor University
Medical Policy Original Effective Date: Revised Date: Page 1 of 8
 Page 1 of 8 Disclaimer Description Coverage Determination Refer to the member s specific benefit plan and Schedule of Benefits to determine coverage. This may not be a benefit on all plans, or the plan
Page 1 of 8 Disclaimer Description Coverage Determination Refer to the member s specific benefit plan and Schedule of Benefits to determine coverage. This may not be a benefit on all plans, or the plan
RECONSTRUCTION OF SCALP DEFECTS: AN INSTITUTIONAL EXPERIENCE Sathyanarayana B. C 1, Somashekar Srinivas 2
 RECONSTRUCTION OF SCALP DEFECTS: AN INSTITUTIONAL EXPERIENCE Sathyanarayana B. C 1, Somashekar Srinivas 2 HOW TO CITE THIS ARTICLE: Sathyanarayana B. C, Somashekar Srinivas. Reconstruction of Scalp Defects:
RECONSTRUCTION OF SCALP DEFECTS: AN INSTITUTIONAL EXPERIENCE Sathyanarayana B. C 1, Somashekar Srinivas 2 HOW TO CITE THIS ARTICLE: Sathyanarayana B. C, Somashekar Srinivas. Reconstruction of Scalp Defects:
Coding Wars: The Coding and Documentation Weapons to Win the Battle
 Coding Wars: The Coding and Documentation Weapons to Win the Battle Howard W. Rogers M.D., Ph.D. Advanced Dermatology Norwich, CT rogershoward@sbcglobal.net Conflict of Interest Statement I have no relevant
Coding Wars: The Coding and Documentation Weapons to Win the Battle Howard W. Rogers M.D., Ph.D. Advanced Dermatology Norwich, CT rogershoward@sbcglobal.net Conflict of Interest Statement I have no relevant
Single-Stage Full-Thickness Scalp Reconstruction Using Acellular Dermal Matrix and Skin Graft
 Single-Stage Full-Thickness Scalp Reconstruction Using Acellular Dermal Matrix and Skin Graft Yoon S. Chun, MD, a and Kapil Verma, BA b a Division of Plastic and Reconstructive Surgery, Department of Surgery,
Single-Stage Full-Thickness Scalp Reconstruction Using Acellular Dermal Matrix and Skin Graft Yoon S. Chun, MD, a and Kapil Verma, BA b a Division of Plastic and Reconstructive Surgery, Department of Surgery,
How To Make a Good Mastectomy for Reconstruction Based on the Anatomy. Zhang Jin, Ph.D MD
 How To Make a Good Mastectomy for Reconstruction Based on the Anatomy Zhang Jin, Ph.D MD Deputy Director and Professor Tianjin Medical University Cancer Institute and Hospital People s Republic of China
How To Make a Good Mastectomy for Reconstruction Based on the Anatomy Zhang Jin, Ph.D MD Deputy Director and Professor Tianjin Medical University Cancer Institute and Hospital People s Republic of China
Dermatology for the PCP Deanna G. Brown, MD, FAAD Susong Dermatology Consulting Staff at CHI Memorial
 Dermatology for the PCP Deanna G. Brown, MD, FAAD Susong Dermatology Consulting Staff at CHI Memorial Cutaneous Oncology for the PCP Deanna G. Brown, MD, FAAD Susong Dermatology Consulting Staff at CHI
Dermatology for the PCP Deanna G. Brown, MD, FAAD Susong Dermatology Consulting Staff at CHI Memorial Cutaneous Oncology for the PCP Deanna G. Brown, MD, FAAD Susong Dermatology Consulting Staff at CHI
Epidemiology. Burn Rehabilitation. Epidemiology. Epidemiology. United States. United States Cause of injury. Incidence has declined
 Burn Rehabilitation Peter Esselman, MD Professor and Chair Department of Rehabilitation Medicine University of Washington Epidemiology United States 450,000 burn injuries/year in USA that receive medical
Burn Rehabilitation Peter Esselman, MD Professor and Chair Department of Rehabilitation Medicine University of Washington Epidemiology United States 450,000 burn injuries/year in USA that receive medical
Combined tongue flap and V Y advancement flap for lower lip defects
 British Journal of Plastic Surgery (2005) 58, 258 262 CASE REPORTS Combined tongue flap and V Y advancement flap for lower lip defects Kenji Yano*, Ko Hosokawa, Tateki Kubo Department of Plastic and Reconstructive
British Journal of Plastic Surgery (2005) 58, 258 262 CASE REPORTS Combined tongue flap and V Y advancement flap for lower lip defects Kenji Yano*, Ko Hosokawa, Tateki Kubo Department of Plastic and Reconstructive
Clinical Pathological Conference. Malignant Melanoma of the Vulva
 Clinical Pathological Conference Malignant Melanoma of the Vulva History F/48 Chinese Married Para 1 Presented in September 2004 Vulval mass for 2 months Associated with watery and blood stained discharge
Clinical Pathological Conference Malignant Melanoma of the Vulva History F/48 Chinese Married Para 1 Presented in September 2004 Vulval mass for 2 months Associated with watery and blood stained discharge
A Keloid Edge Precut, Preradiotherapy Method in Large Keloid Skin Graft Treatment
 A Keloid Edge Precut, Preradiotherapy Method in Large Keloid Skin Graft Treatment WENBO LI, MD, YOUBIN WANG, MD, XIAOJUN WANG, MD, AND ZHIFEI LIU, MD* BACKGROUND Keloids are scars that extend beyond the
A Keloid Edge Precut, Preradiotherapy Method in Large Keloid Skin Graft Treatment WENBO LI, MD, YOUBIN WANG, MD, XIAOJUN WANG, MD, AND ZHIFEI LIU, MD* BACKGROUND Keloids are scars that extend beyond the
New 2010 CPT Codes (italic font represents a new or revised code/description)
 New 2010 CPT Codes (italic font represents a new or revised code/description) 14301 Adjacent tissue transfer or rearrangement, any area; defect 30.1 sq cm to 60.0 sq cm 14302 each additional 30.0 sq cm,
New 2010 CPT Codes (italic font represents a new or revised code/description) 14301 Adjacent tissue transfer or rearrangement, any area; defect 30.1 sq cm to 60.0 sq cm 14302 each additional 30.0 sq cm,
The bi-pedicle post-auricular tube flap for reconstruction of partial ear defects
 The British Association of Plastic Surgeons (2003) 56, 593 598 The bi-pedicle post-auricular tube flap for reconstruction of partial ear defects Mohammed G. Ellabban*, Maamoun I. Maamoun, Moustafa Elsharkawi
The British Association of Plastic Surgeons (2003) 56, 593 598 The bi-pedicle post-auricular tube flap for reconstruction of partial ear defects Mohammed G. Ellabban*, Maamoun I. Maamoun, Moustafa Elsharkawi
This is a repository copy of Dupuytren Disease Infiltrating a Full-Thickness Skin Graft.
 This is a repository copy of Dupuytren Disease Infiltrating a Full-Thickness Skin Graft. White Rose Research Online URL for this paper: http://eprints.whiterose.ac.uk/105540/ Version: Accepted Version
This is a repository copy of Dupuytren Disease Infiltrating a Full-Thickness Skin Graft. White Rose Research Online URL for this paper: http://eprints.whiterose.ac.uk/105540/ Version: Accepted Version
Incomplete excision of basal cell carcinoma (BCC) in the head and neck region: to wait, or not to wait?
 Original paper Incomplete excision of basal cell carcinoma (BCC) in the head and neck region: to wait, or not to wait? Jakub Miszczyk, Michał Charytonowicz, Tomasz Dębski, Bartłomiej Noszczyk Department
Original paper Incomplete excision of basal cell carcinoma (BCC) in the head and neck region: to wait, or not to wait? Jakub Miszczyk, Michał Charytonowicz, Tomasz Dębski, Bartłomiej Noszczyk Department
المركب النموذج--- سبيتز وحمة = Type Spitz's Nevus, Compound SPITZ NEVUS 1 / 7
 SPITZ NEVUS 1 / 7 Epidemiology An annual incidence rate of 1.4 cases of Spitz nevus per 100,000 individuals has been estimated in Australia, compared with 25.4 per 100,000 individuals for cutaneous melanoma
SPITZ NEVUS 1 / 7 Epidemiology An annual incidence rate of 1.4 cases of Spitz nevus per 100,000 individuals has been estimated in Australia, compared with 25.4 per 100,000 individuals for cutaneous melanoma
Photo Quiz Self-Test Your Diagnostic Acumen
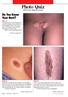 Do You Know Your Nevi? Case 1: The parents of a 3-year-old girl seek medical evaluation of the nodules on their daughter s back. The lesions have been present since birth and have grown with the child.
Do You Know Your Nevi? Case 1: The parents of a 3-year-old girl seek medical evaluation of the nodules on their daughter s back. The lesions have been present since birth and have grown with the child.
Primary closure of the deltopectoral flap-donor site without skin grafting
 Primary closure of the deltopectoral flap-donor site without skin grafting Received: 4/3/2013 Accepted: 14/5/2013 Introduction Reliable and simultaneous reconstruction of head-and-neck defects has been
Primary closure of the deltopectoral flap-donor site without skin grafting Received: 4/3/2013 Accepted: 14/5/2013 Introduction Reliable and simultaneous reconstruction of head-and-neck defects has been
Position Statement Treatments that primarily affect the appearance are considered medically necessary only in the following circumstances:
 Policy Name: Cosmetic Services Policy Number: CMO 500 Effective Date of current policy: 9/1/2018 Description and Scope This policy applies to procedures that primarily affect the appearance of the member.
Policy Name: Cosmetic Services Policy Number: CMO 500 Effective Date of current policy: 9/1/2018 Description and Scope This policy applies to procedures that primarily affect the appearance of the member.
Clinical Policy: Benign Skin Lesion Removal Reference Number: CP.MP.HN150
 Clinical Policy: Reference Number: CP.MP.HN150 Effective Date: 6/04 Last Review Date: 8/17 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory and
Clinical Policy: Reference Number: CP.MP.HN150 Effective Date: 6/04 Last Review Date: 8/17 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory and
Technicians & Nurses Program
 ASCRS ASOA Symposium & Congress Technicians & Nurses Program May 6-10, 2016 New Orleans Evaluation and Treatment of Eyelid Malignancies Richard C. Allen MD PhD FACS Professor Section of Ophthalmology Dept.
ASCRS ASOA Symposium & Congress Technicians & Nurses Program May 6-10, 2016 New Orleans Evaluation and Treatment of Eyelid Malignancies Richard C. Allen MD PhD FACS Professor Section of Ophthalmology Dept.
Nasolabial Flap Reconstruction of Oral Cavity Defects: A Report of 18 Cases
 J Oral Maxillofac Surg 58:1104-1108, 2000 Nasolabial Flap Reconstruction of Oral Cavity Defects: A Report of 18 Cases Yadranko Ducic, MD, FRCS (C),* and Mark Burye, DDS Purpose: This article describes
J Oral Maxillofac Surg 58:1104-1108, 2000 Nasolabial Flap Reconstruction of Oral Cavity Defects: A Report of 18 Cases Yadranko Ducic, MD, FRCS (C),* and Mark Burye, DDS Purpose: This article describes
Appendix C Podiatriac Services
 Appendix C Podiatriac Services CPT/ HCPCS Codes Description Auth required Y or N Mod Service Limits Age Limits Notes 10021-10022 Fine Needle Aspiration w/ or w/o imaging guidance 10060-10061 10120-10121
Appendix C Podiatriac Services CPT/ HCPCS Codes Description Auth required Y or N Mod Service Limits Age Limits Notes 10021-10022 Fine Needle Aspiration w/ or w/o imaging guidance 10060-10061 10120-10121
Anatomical study. Clinical study. R. Ogawa, H. Hyakusoku, M. Murakami, R. Aoki, K. Tanuma* and D. G. Pennington?
 British Journal of Plastic Surgery (2002) 55, 396-40 I 9 2002 The British Association of Plastic Surgeons doi: 10.1054/bjps.2002.3877 PLASTIC SURGERY An anatomical and clinical study of the dorsal intercostal
British Journal of Plastic Surgery (2002) 55, 396-40 I 9 2002 The British Association of Plastic Surgeons doi: 10.1054/bjps.2002.3877 PLASTIC SURGERY An anatomical and clinical study of the dorsal intercostal
MING H. JIH, MD,PHD, PAUL M. FRIEDMAN, MD,LEONARD H. GOLDBERG, MD,AND ARASH KIMYAI-ASADI, MD. Methods Phase I: Retrospective (Group 1)
 Curettage prior to Mohs Micrographic Surgery for Previously Biopsied Nonmelanoma Skin Cancers: What Are We Curetting? Retrospective, Prospective, and Comparative Study MING H. JIH, MD,PHD, PAUL M. FRIEDMAN,
Curettage prior to Mohs Micrographic Surgery for Previously Biopsied Nonmelanoma Skin Cancers: What Are We Curetting? Retrospective, Prospective, and Comparative Study MING H. JIH, MD,PHD, PAUL M. FRIEDMAN,
Pruritus Ani in an Elderly Man
 Pruritus Ani in an Elderly Man Pedro Redondo, MD; Michel Idoate, MD; Agustín España, MD; Emilio Quintanilla, MD; University of Navarra, Pamplona, Spain REPORT OF A CASE A 78-year-old man presented with
Pruritus Ani in an Elderly Man Pedro Redondo, MD; Michel Idoate, MD; Agustín España, MD; Emilio Quintanilla, MD; University of Navarra, Pamplona, Spain REPORT OF A CASE A 78-year-old man presented with
Associate Clinical Professor of Dermatology MUSC
 Re-excision of Moderately Dysplastic Nevi: Should we or shouldn t we? John C. Maize, Jr, M.D. Dermatologist and Dermatopathologist Trident Dermatology, Charleston SC Associate Clinical Professor of Dermatology
Re-excision of Moderately Dysplastic Nevi: Should we or shouldn t we? John C. Maize, Jr, M.D. Dermatologist and Dermatopathologist Trident Dermatology, Charleston SC Associate Clinical Professor of Dermatology
SECTION N: PLASTIC SURGERY
 Visits 5N Initial Assessment $91.80 -- of a specific condition includes: pertinent family history, patient history, history of presenting complaint, functional enquiry, examination of affected part(s)
Visits 5N Initial Assessment $91.80 -- of a specific condition includes: pertinent family history, patient history, history of presenting complaint, functional enquiry, examination of affected part(s)
Original Article Modified O-T advancement flap for reconstruction of skin defects
 Int J Clin Exp Pathol 2017;10(9):9158-9163 www.ijcep.com /ISSN:1936-2625/IJCEP0057308 Original Article Modified O-T advancement flap for reconstruction of skin defects Zhuo-Ran Li 1, Yong Jiang 1, Jun-Yan
Int J Clin Exp Pathol 2017;10(9):9158-9163 www.ijcep.com /ISSN:1936-2625/IJCEP0057308 Original Article Modified O-T advancement flap for reconstruction of skin defects Zhuo-Ran Li 1, Yong Jiang 1, Jun-Yan
McGregor Flap Reconstruction of Extensive Lower Lip Defects Following Excision of Squamous Cell Carcinoma
 Kasr El Aini Journal of Surgery VOL., 12, NO 2 May 2011 27 McGregor Flap Reconstruction of Extensive Lower Lip Defects Following Excision of Squamous Cell Carcinoma Mohamed A. Albadawy, MD and Bassem M.
Kasr El Aini Journal of Surgery VOL., 12, NO 2 May 2011 27 McGregor Flap Reconstruction of Extensive Lower Lip Defects Following Excision of Squamous Cell Carcinoma Mohamed A. Albadawy, MD and Bassem M.
Treatment of Pseudoangiomatous Stromal Hyperplasia of the Breast: Implant-Based Reconstruction with a Vascularized Dermal Sling
 Treatment of Pseudoangiomatous Stromal Hyperplasia of the Breast: Implant-Based Reconstruction with a Vascularized Dermal Sling Idea and Innovation Bok Ki Jung 1, Ji Hae Nahm 2, Dae Hyun Lew 1, Dong Won
Treatment of Pseudoangiomatous Stromal Hyperplasia of the Breast: Implant-Based Reconstruction with a Vascularized Dermal Sling Idea and Innovation Bok Ki Jung 1, Ji Hae Nahm 2, Dae Hyun Lew 1, Dong Won
IBRA scholarship report program B
 IBRA scholarship report program B Training Center: Department of Cranio-Maxillofacial Surgery, Amiens, France Fellowship Director: Professor Sylvie Testelin Head of Department: Professor Bernard Devauchelle
IBRA scholarship report program B Training Center: Department of Cranio-Maxillofacial Surgery, Amiens, France Fellowship Director: Professor Sylvie Testelin Head of Department: Professor Bernard Devauchelle
Aesthetic reconstruction of the nasal tip using a folded composite graft from the ear
 The British Association of Plastic Surgeons (2004) 57, 238 244 Aesthetic reconstruction of the nasal tip using a folded composite graft from the ear Yong Oock Kim*, Beyoung Yun Park, Won Jae Lee Institute
The British Association of Plastic Surgeons (2004) 57, 238 244 Aesthetic reconstruction of the nasal tip using a folded composite graft from the ear Yong Oock Kim*, Beyoung Yun Park, Won Jae Lee Institute
Anatomy The study of the body's structure.
 Anatomy The study of the body's structure. * 1. Systemic- Study of each of the body's systems. 2. Regional- Study of a specific area of the body 3. Surface- Study of external features. Physiology The study
Anatomy The study of the body's structure. * 1. Systemic- Study of each of the body's systems. 2. Regional- Study of a specific area of the body 3. Surface- Study of external features. Physiology The study
NIPPLE SPARING PRE-PECTORAL BREAST RECONSTRUCTION
 NIPPLE SPARING PRE-PECTORAL BREAST RECONSTRUCTION 42 yo female healthy athlete Right breast mass. Past medical history: none Family history: aunt with Breast cancer Candidates for nipple-sparing mastectomy
NIPPLE SPARING PRE-PECTORAL BREAST RECONSTRUCTION 42 yo female healthy athlete Right breast mass. Past medical history: none Family history: aunt with Breast cancer Candidates for nipple-sparing mastectomy
Benign versus Cancerous Lesions How to tell the difference FMF 2014 Christie Freeman MD, CCFP, DipPDerm, MSc
 1 Benign versus Cancerous Lesions How to tell the difference FMF 2014 Christie Freeman MD, CCFP, DipPDerm, MSc Benign lesions Seborrheic Keratoses: Warty, stuck-on Genetics and birthdays Can start in late
1 Benign versus Cancerous Lesions How to tell the difference FMF 2014 Christie Freeman MD, CCFP, DipPDerm, MSc Benign lesions Seborrheic Keratoses: Warty, stuck-on Genetics and birthdays Can start in late
The evaluation-and-management (E/M) codes in the 1992 CPT Book are entirely new. All
 Printed in Plastic Surgery News - February 1992 Don't kill the messenger New evaluation/management codes announced By Raymond Janevicius, MD The evaluation-and-management (E/M) codes in the 1992 CPT Book
Printed in Plastic Surgery News - February 1992 Don't kill the messenger New evaluation/management codes announced By Raymond Janevicius, MD The evaluation-and-management (E/M) codes in the 1992 CPT Book
LECTURE TOPIC ASSIGNMENTS
 BASICS LECTURE TOPIC ASSIGNMENTS LECTURE TOPIC: ANATOMICAL TERMINOLOGY Read the textbook: Ch. 1: The Human Body: An Orientation Go To: Web Site > Folder: AnatTerm > A25terms09.pdf. Download the file &
BASICS LECTURE TOPIC ASSIGNMENTS LECTURE TOPIC: ANATOMICAL TERMINOLOGY Read the textbook: Ch. 1: The Human Body: An Orientation Go To: Web Site > Folder: AnatTerm > A25terms09.pdf. Download the file &
CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty
 CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty Augustine Reid Wilson, MS, Justin Daggett, MD, Michael Harrington, MD, MPH, and Deniz
CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty Augustine Reid Wilson, MS, Justin Daggett, MD, Michael Harrington, MD, MPH, and Deniz
COMBINED ABDOMINAL FLAP FOR MAJOR HAND RECONSTRUCTION
 Int. J. Pharm. Med. & Bio. Sc. 2013 2014 Srinivas Somashekar et al., 2014 Research Paper ISSN 2278 5221 www.ijpmbs.com Vol. 3, No. 1, January 2014 2014 IJPMBS. All Rights Reserved COMBINED ABDOMINAL FLAP
Int. J. Pharm. Med. & Bio. Sc. 2013 2014 Srinivas Somashekar et al., 2014 Research Paper ISSN 2278 5221 www.ijpmbs.com Vol. 3, No. 1, January 2014 2014 IJPMBS. All Rights Reserved COMBINED ABDOMINAL FLAP
Typical Cleft Hand. Windblown Hand. Congenital, Developmental Arrest. Congenital, Failure of Differentiation. Longitudinal (vs.
 Typical Cleft Hand Congenital, Developmental Arrest Longitudinal (vs. Transverse) Central Deficiency (vs. Preaxial, Postaxial, Phocomelia) Windblown Hand Congenital, Failure of Differentiation Contracture
Typical Cleft Hand Congenital, Developmental Arrest Longitudinal (vs. Transverse) Central Deficiency (vs. Preaxial, Postaxial, Phocomelia) Windblown Hand Congenital, Failure of Differentiation Contracture
An island flap based on the anterior branch of the superficial temporal artery for perioral defects
 Free full text on www.ijps.org Original Article An island flap based on the anterior branch of the superficial temporal artery for perioral defects V. Bhattacharya, Ganji Raveendra Reddy, Sheikh Adil Bashir,
Free full text on www.ijps.org Original Article An island flap based on the anterior branch of the superficial temporal artery for perioral defects V. Bhattacharya, Ganji Raveendra Reddy, Sheikh Adil Bashir,
Surgery for scar revision and reduction: from primary closure to flap surgery
 Ogawa Burns & Trauma (2019) 7:7 https://doi.org/10.1186/s41038-019-0144-5 REVIEW Surgery for scar revision and reduction: from primary closure to flap surgery Rei Ogawa Open Access Abstract Scars are the
Ogawa Burns & Trauma (2019) 7:7 https://doi.org/10.1186/s41038-019-0144-5 REVIEW Surgery for scar revision and reduction: from primary closure to flap surgery Rei Ogawa Open Access Abstract Scars are the
Medicare Benefits Schedule: changes to Dermatology items from 1 Nov 2018
 Medicare Benefits Schedule: changes to Dermatology items from 1 Nov 2018 As of 1 November 2018, a number of changes to MBS dermatology items will come into effect as part of the MBS Review. This is the
Medicare Benefits Schedule: changes to Dermatology items from 1 Nov 2018 As of 1 November 2018, a number of changes to MBS dermatology items will come into effect as part of the MBS Review. This is the
Birthmarks: When to worry, when to reassure
 Birthmarks: When to worry, when to reassure Aimee Smidt, MD, FAAD, FAAP Associate Professor, Depts of Dermatology and Pediatrics University of New Mexico School of Medicine November 2016 Goals and Objectives
Birthmarks: When to worry, when to reassure Aimee Smidt, MD, FAAD, FAAP Associate Professor, Depts of Dermatology and Pediatrics University of New Mexico School of Medicine November 2016 Goals and Objectives
Associate Professor of Plastic Surgery, Karol. Institute; Plastic Department, Serafimerlasarettet, Stockholm, Sweden
 A NEW METHOD OF SHAPING DEFORMED EARS By A. RAGNELL, M.D. Associate Professor of Plastic Surgery, Karol. Institute; Plastic Department, Serafimerlasarettet, Stockholm, Sweden NUMEROUS methods of shaping
A NEW METHOD OF SHAPING DEFORMED EARS By A. RAGNELL, M.D. Associate Professor of Plastic Surgery, Karol. Institute; Plastic Department, Serafimerlasarettet, Stockholm, Sweden NUMEROUS methods of shaping
Whitney A. High, MD, JD, MEng
 ADS Dermatopathology Meeting 2014 Selected Adnexal Tumors Whitney A. High, MD, JD, MEng Associate Professor, Dermatology & Pathology Director of Dermatopathology (Dermatology) University of Colorado School
ADS Dermatopathology Meeting 2014 Selected Adnexal Tumors Whitney A. High, MD, JD, MEng Associate Professor, Dermatology & Pathology Director of Dermatopathology (Dermatology) University of Colorado School
Proboscis lateralis: report of two cases
 The British Association of Plastic Surgeons (2003) 56, 704 708 CASE REPORT Proboscis lateralis: report of two cases Lütfi Eroğlu a, *, Osman Ata Uysal b a Faculty of Medicine, Department of Plastic and
The British Association of Plastic Surgeons (2003) 56, 704 708 CASE REPORT Proboscis lateralis: report of two cases Lütfi Eroğlu a, *, Osman Ata Uysal b a Faculty of Medicine, Department of Plastic and
Postburn head and neck reconstruction using tissue expanders
 Postburn head and neck reconstruction using tissue expanders Received: 30/4/2013 Accepted: 21/11/2013 Introduction Tissue expansion is a reliable method of providing additional cutaneous tissue, thereby
Postburn head and neck reconstruction using tissue expanders Received: 30/4/2013 Accepted: 21/11/2013 Introduction Tissue expansion is a reliable method of providing additional cutaneous tissue, thereby
ALTHOUGH FIRST described
 The Cervicodeltopectoral Flap for Single-Stage Resurfacing of Anterolateral Defects of the Face and Neck Yadranko Ducic, MD, FRCSC; Jesse E. Smith, MD SURGICAL TECHNIQUE Objective: To evaluate prospectively
The Cervicodeltopectoral Flap for Single-Stage Resurfacing of Anterolateral Defects of the Face and Neck Yadranko Ducic, MD, FRCSC; Jesse E. Smith, MD SURGICAL TECHNIQUE Objective: To evaluate prospectively
