Epidermal Grafting using the CELLUTOME
|
|
|
- Solomon McCormick
- 6 years ago
- Views:
Transcription
1 Epidermal Grafting using the CELLUTOME This harvesting system can be used in clinical practice. By Animesh Bhatia, DPM This article is written exclusively for PM and appears courtesy of the American Academy of Podiatric Practice Management. The AAPPM has a forty-plus year history of providing its member DPM s with practice management education and resources. Visit for more information. Introduction Chronic wounds occur when the normal healing process stalls or fails. This can be due to a number of factors including patient age, co-morbid conditions (i.e., obesity, diabetes, tobacco use, nutrition), medication use, and the wound environment (infection, moisture levels, impaired perfusion). 1,2 Patients and wounds can be optimized for healing through active management of co-morbid conditions to help reduce wound healing barriers. 3 Additionally, wound bed preparation can promote healing by removing debris and devitalized tissue, managing bioburden, and creating a moist wound environment conducive to granulation tissue development. 4 However, despite the patient and wound optimization, some chronic wounds may require the use of skin grafting. Scientific advancements in wound care have expanded skin grafting options to include the use of epidermal grafts to promote wound closure. This article will discuss the use of epidermal grafting in wound care, representative case studies, and the coding and reimbursement guidelines for the use of an epidermal harvesting system. History of Epidermal Grafting Kiistala and Mustakallio first reported harvesting of the epidermal skin layer for skin grafting in Prior to this, skin grafts contained portions of the dermal layer, commonly referred to as full-thickness or split-thickness skin grafts. In 1971, Falabella used epidermal grafting to treat vitiligo lesions with moderate repigmentation success. 6 By 1975, epidermal grafting was reported in Continued on page Figure 1. Epidermal grafting of right dorsal foot venous stasis ulcer. Wound at presentation (A), application of epidermal microdomes (B), donor site immediately following epidermal harvesting (C), wound at two weeks post-grafting (D), and wound fully closed at 12 weeks post-grafting (E).
2 110 Epidermal Grafting (from page 109) leg ulcers where 10 out of 12 patients showed 100% re-epithelialization within 14 days 7, and its use was expanded in 1981 to include burn patients. 8 Here, epidermal grafts were harvested, cultured, and grafted onto the burn wounds of two patients. Results showed good graft take and confluence with the surrounding meshed split-thickness grafts or undamaged epidermis. Early attempts to harvest the epidermal skin layer included needles to raise the skin, followed by removal using a scalpel or surgical knife. 9 Various suction devices were then designed in an effort to improve the ability to raise and separate the epidermal skin layer and included suction pumps, vacuum bottles, hoses, and plastic suction cups. 6,10,11 In 1999, a negative pressure cutaneous suction chamber system was used to raise epidermal grafts. This device provided negative pressure along with warmth to raise grafts. 12 However, this device was only capable of raising four epidermal grafts. More recently, a commercially available epidermal graft harvesting system (CELLUTOME Epidermal Harvesting System, KCI, an ACELITY Company, San Antonio, TX) was created to deliver negative pressure and warmth to reproducibly raise and harvest epidermal micrografts (referred to a microdomes). Brief Review of the Literature A number of recent studies describing use of epidermal microdomes harvested with the epidermal graft harvesting system have been published. Overall, these studies have reported wound closure in a majority of patients, and donor site healing without complications in all patients Additionally, while only three studies report on pain, all reported minimal to no pain at the donor site during or after graft harvesting. 18,20 Clinical Advantages Traditional skin grafting utilizes full or split-thickness skin grafts and creates a wound at the donor site. Both the recipient and donor sites can develop complications such as graft contraction, scarring, infection, and pain, which can increase patient morbidity following the grafting procedure. Epidermal grafting is an alternative to traditional skin grafting that uses a minimal amount of a donor site s epidermal skin layer. Unlike full or split-thickness skin grafting, epidermal grafting can be performed without anesthesia in the outpatient or physician office setting. Minimal to no pain has been reported during the harvesting procedure. 18,20,21 Additionally, donor sites have been reported to heal with minimal to no donor site complications within four weeks of epidermal graft harvesting. 14,15 Practical Use of Epidermal Grafting in Wound Care In my practice, especially in cases of stalled wounds, I use epidermal grafting as part of the standard treatment protocol. Typically, I use epidermal grafting in a number of wound types including diabetic foot ulcers, venous ulcers, pressure ulcers, traumatic wounds, and surgical dehiscence. Clinical Application of Epidermal Grafting Patient Exam Upon presentation to the clinic, all patients undergo a thorough exam that can include a vascular work-up, nutrition consult, blood work, and imaging (such as diagnostic ultrasound or x-ray). The patient exam Traditional skin grafting utilizes fullor split-thickness skin grafts and creates a wound at the donor site. helps identify co-morbidities that may interfere with wound healing. If possible, a treatment plan to help manage patient co-morbidities is enacted, with appropriate referrals. Wound Bed Preparation In order to minimize the risk of graft failure, a treatment plan to promote the development of granulation tissue and maintain a moist wound environment is created. Following the initial patient and wound exam, non-viable tissue is removed from the wound through debridement. If the wound shows signs of infection, infection management practices are initiated. Off-loading and compression therapy can also be used to assist with protection of the wound. Continued on page 111 Figure 2. Epidermal grafting of a traumatic left ankle wound. Wound after one week of silver nitrate (A), wound on day of epidermal grafting (B), and wound fully closed at two weeks post-grafting (C).
3 Epidermal Grafting (from page 110) Epidermal Grafting Procedure Once the wound bed is 100% covered by healthy granulation tissue, epidermal grafting can occur. A 10cm x 10cm donor site area (typically the inner thigh) is selected, and any hair is removed. The donor site is then washed with 70% isopropyl alcohol and left to air dry. The harvester is placed on the donor site and secured to ensure that complete contact is made with the skin. The vacuum head is attached to the harvester, and warmth and negative pressure are applied to raise the epidermal microdomes. Depending on skin thickness at the donor site, epidermal microdomes are usually raised within 30 to 45 minutes. After the microdomes have formed, the epidermal harvesting system unit s power is turned off and the vacuum head removed. A non-adherent silicone dressing (ADAPTIC TOUCH Non-Adhering Silicone Dressing, Systagenix, an ACELITY Company, Gargrave, UK) is gently placed over the raised epidermal microdomes and harvested. The microdomes are immediately transferred to the wound, followed by coverage with a secondary dressing. A self-adherent wrap or negative pressure wound therapy can be used as a bolster over the dressing to secure the microdomes to the wound bed. The harvesting system is removed from the donor site and a transparent film dressing (TEGA- DERM Transparent Film Dressing, 3M, St. Paul, MN) is placed over the donor site. The non-adherent silicon dressing remains in place for one week following graft transfer, which ensures that the microdomes remain undisturbed in the wound bed. The bolster and donor site dressings are changed once a week according to the manufacturer s instructions. The wound and the donor site are monitored weekly for signs of wound healing. Case Series Representative case studies of epidermal grafting in my practice are described below. was observed two weeks post-grafting (Figure 1D). Twelve weeks post-grafting, the wounds were fully closed with no complications (Figure 1E). The donor site healed within two weeks without complications. Case 2 A 68-year-old male presented with a traumatic injury to the left ankle. Edema, 10% adherent yellow slough, and hypergranulation of the wound were noted. Patient medical Once the wound bed is 100% covered by healthy granulation tissue, epidermal grafting can occur. Case 1 A 63-year-old male presented to the clinic with a venous stasis ulcer on the right dorsal foot present for >6 weeks (Figure 1A). The wound showed edema, scant seropurulent exudate, and 26 50% loose slough. Medical history included diabetes, hypertension, chronic obstructive pulmonary disease, peripheral vascular disease, and coronary artery disease. Previous treatments included off-loading, non-adherent dressings, porcine small intestinal submucosa matrix, dermal repair scaffold, and cryopreserved placental membrane. The wound underwent sharp debridement eight times prior to epidermal grafting. Epidermal microdomes were harvested from the right thigh (Figure 1B), placed over the wounds, and covered with a foam dressing and gauze as a bolster (Figure 1C). Re-epithelialization of the wounds history included diabetes, hypertension, deep vein thrombosis, gastroesophageal reflux disease, osteoarthritis, atrial fibrillation, hyperlipidemia, and an enlarged prostate. Silver nitrate was applied to the wound in order to reduce hypergranulation, followed by off-loading with an Unna boot (Figure 2A). After two weeks of this treatment, the wound underwent epidermal grafting (Figure 2B). Epidermal microdomes were harvested from the left thigh, applied to the wound, and bolstered with gauze and self-adherent wrap. Two weeks post-grafting, the wound was fully healed without complications (Figure 2C). The donor site healed within two weeks without complications. Case 3 An 81-year-old female presented with a traumatic injury to the right Continued on page Figure 3. Epidermal grafting of a traumatic right shin wound. Wound at presentation (A), application of epidermal microdomes (B), wound at two weeks post-grafting (C), and wound fully healed at six weeks post-grafting (D).
4 Epidermal Grafting (from page 111) shin present for 5 weeks (Figure 3A). Previous medical history included obesity, cancer, gastroesophageal reflux disease, glaucoma, and osteoporosis. Collagenase ointment and wet/dry dressings were applied to the wound daily. Three weeks later, epidermal grafting was performed with microdomes harvested from the left thigh and bolstered with gauze and a self-adherent wrap (Figure 3B). Wound re-epithelialization was observed two weeks post-grafting (Figure 3C). At six weeks post-grafting, the wound was completely healed without complications (Figure 3D). The donor site healed within two weeks without complications. Coding and Reimbursement for Use of the Epidermal Harvesting System Coding and reimbursement guidelines vary depending on the require- ments of the payor. Before filing any claims, providers should verify requirements and policies with the payor as well as any pre-authorization steps. Cost and reimbursement numbers are approximate and may vary by carrier and state. Each payor may have differing formal or informal coding and coverage policies or decisions. Coding of Wound Bed Preparation Prior to epidermal grafting, Continued on page 114 Table 1: Codes for Wound Bed Preparation Body Part Code Description Affected Use Surgical preparation or creation Trunk First 100 square cm of recipient site by excision of Arms 1% body area of infants and children open wounds, burn eschar, or Legs scar (including subcutaneous tissues), or incisional release of scar contracture Surgical preparation or creation Trunk Each additional 100 square cm of recipient site by excision of Arms Each additional 1% body area of infants open wounds, burn eschar, or Legs and children scar (including subcutaneous tissues), List separately in addition to or incisional release of scar contracture Surgical preparation or creation Face First 100 square cm of recipient site by excision of Scalp 1% body area of infants and children open wounds, burn eschar, or Eyelids scar (including subcutaneous tissues), Mouth or incisional release of scar contracture. Neck Surgical preparation or creation Face Each additional 100 square cm of recipient site by excision of Scalp Each additional 1% body area of infants open wounds, burn eschar, or Eyelids and children scar (including subcutaneous tissues), Mouth List separately in addition to or incisional release of scar contracture. Neck Codes and descriptions obtained from current procedural terminology. 22 Table 1. Codes for wound bed preparation
5 Epidermal Grafting (from page 112) documentation. The global period is 90 days for the physician, or if the epidermal grafting is performed in a wound center, there is no global period for the wound center itself. When documenting the epidermal grafting procedure, all notes from the initial visit, including the day of the epidermal grafting procedure, it is important to report the type of wound as well as wound location, size, and depth, and presence of drainage and/ or necrotic tissue. If debridement is performed, the method and depth of debridement (pre and post-measure- Continued on page 115 wound bed preparation is required. There are several different codes (CPT ) that can be used for this procedure (Table 1). 22 In order to receive reimbursement for the wound bed preparation that encompasses an area larger than 100 square centimeters or 1% body area (infants and children only), it is important to list each additional 100 square centimeters or 1% body area separately along with the primary code (CPT or 15004). 22 Coding for Epidermal Grafting For epidermal grafting, coding rules are similar to those of wound bed preparation (Table 2). 22 Each additional 100 square centimeters or 1% body area (infants and children only) of grafting should be listed separately after the code for the primary procedure. 22 A coding modifier of 58, indicating a staged or related procedure or service by the same physician during the post-operative period, could be used when submitting the codes if the intent is to possibly repeat the procedure during the global period, and this must be noted in the Table 2: Codes for Epidermal Grafting 114 Body Part Code Description Affected Use Epidermal autograft Trunk First 100 square cm Arms 1% body area of infants and children Legs Epidermal autograft Trunk Each additional 100 square cm Arms Each additional 1% body area of infants Legs and children, or part thereof List separately in addition to Epidermal autograft Face First 100 square cm Scalp 1% body area of infants and children Eyelids Mouth Neck Epidermal autograft Face Each additional 100 square cm Scalp Each additional 1% body area of infants Eyelids and children, or part thereof Mouth List separately in addition to Neck Codes and descriptions obtained from current procedural terminology. 22 Table 2. Codes for epidermal grafting
6 Epidermal Grafting (from page 114) ments and partial, full-thickness, etc.) must be documented. The treatment plan should be documented as well as any dressings applied in the office. However, the use and application of dressings used for the procedure should not be billed. Reimbursement Reimbursement costs vary depending on the type of facility A list of the common reimbursement figures are provided in Table 3. It is important to remember that several payor variations exist. For example, commercial carriers require pre-authorization, and Medicare has no local coverage determinations for epidermal grafting. Economic Benefits To date, there is no published literature on the cost- effectiveness of epidermal grafting compared with split-thickness skin grafting. However, in adult patients, epidermal grafting can be performed in the office Epidermal grafting is an alternative to traditional skin grafting for chronic or stalled wounds requiring only the epidermal layer. or at the bedside without the need for anesthesia, surgeon, or operating room, which may reduce the cost of the procedure over traditional grafting options. Conclusion Epidermal grafting is an alternative to traditional skin grafting for chronic or stalled wounds requiring only the epidermal layer. My practice utilizes epidermal grafting as part of the standard of care. This protocol includes meticulous attention to debridement, off-loading, compression, management of infection, vascular compromise, co-morbidities, and nutrition through appropriate referrals. We use dressings, cellular and tissue-based products, and negative pressure to advance the wound bed to healthy granulation, and finally provide re-epithelialization with epidermal grafting. This method has provided positive clinical results. Further studies are necessary to determine the clinical and cost-effectiveness of epidermal grafting compared to split-thickness skin grafts in chronic wounds. Acknowledgements The author thanks Julie M. Robertson (Acelity) for assistance with manuscript preparation. PM References 1 Sen CK, Gordillo GM, Roy S et al. Human skin wounds: a major and snowballing threat to public health and the economy. Wound Repair Regen 2009;17: Stadelmann WK, Digenis AG, Tobin GR. Impediments to wound healing. Am J Surg 1998;176:39S-47S. 3 Sibbald RG, Woo KY, Ayello E. Wound bed preparation: DIM before DIME. Wound Healing Southern Africa 2008;1: Sibbald RG, Orsted HL, Coutts PM, Keast DH. Best practice recommendations for preparing the wound bed: Continued on page Table 3: Reimbursements for Epidermal Grafting by Type of Facility Facility Type Code Code Code Code Physician (office) $ $ $ $ Physician (wound care center/ambulatory surgical $ $ $ $ center) Hospital (outpatient department) or wound $1, Included $1, Included care center Ambulatory Surgical Center $ Included $ Included Reimbursement amounts obtained from Centers for Medicare and Medicaid Services Table 3. Reimbursements for epidermal grafting by type of facility
7 116 Epidermal Grafting (from page 115) update Adv Skin Wound Care 2007;20: Kiistala U, Mustakallio KK. In-Vivo separation of epidermis by production of suction blisters. Lancet 1964;1: Falabella R. Epidermal grafting. An original technique and its application in achromic and granulating areas. Arch Dermatol 1971;104: Hentzer B, Kobayasi T. Suction blister transplantation for leg ulcers. Acta Derm Venereol 1975;55: O Connor NE, Mulliken JB, Banks-Schlegel S, Kehinde O, Green H. Grafting of burns with cultured epithelium prepared from autologous epidermal cells. Lancet 1981;1: Ichiki Y, Kitajima Y. Successful treatment of scleroderma-related cutaneous ulcer with suction blister grafting. Rheumatol Int 2008;28: Burm JS, Rhee SC, Kim YW. Superficial dermabrasion and suction blister epidermal grafting for postburn dyspigmentation in Asian skin. Dermatol Surg 2007;33: Costanzo U, Streit M, Braathen LR. Autologous suction blister grafting for chronic leg ulcers. J Eur Acad Dermatol Venereol 2008;22: Alexis AF, Wilson DC, Todhunter JA, Stiller MJ. Reassessment of the suction blister model of wound healing: introduction of a new higher pressure device. Int J Dermatol 1999;38: Richmond NA, Lamel SA, Braun LR, Vivas AC, Serena T, Kirsner RS. Epidermal grafting using a novel suction blister-harvesting system for the treatment of pyoderma gangrenosum. JAMA Dermatology 2014;150: Gabriel A, Sobota RV, Champaneria M. Initial experience with a new epidermal harvesting system: overview of epidermal grafting and case series. Surgical Technology International 2014;25: Serena T, Francius A, Taylor C, Macdonald J. Use of a novel epidermal harvesting system in resource-poor countries. Adv Skin Wound Care 2015;28: Fearmonti RM. Efficacy of Epidermal Skin Grafts Over Complex, Chronic Wounds in Patients With Multiple Comorbidities. Wounds 2016;28: Bhatia A. Epidermal skin grafting in patients with complex wounds: a case series. J Wound Care 2016;25:148, doi: / jowc Lincoln K, Hyde J. Evaluation of epidermal skin grafts for the treatment of complex wounds in a wound care center: A 94-patient case series. Wounds 2016;28: Prakash TV, Chaudhary A, Purushothaman S, K V S, Arvind K V. Epidermal Grafting for Chronic Complex Wounds in India: A Case Series. Cureus 2016;8:e516. doi: /cureus Hachach-Haram N, Bystrzonowski N, Kanapathy M et al. A prospective, multicentre study on the use of epidermal grafts to optimise outpatient wound management. Int Wound J doi: /iwj Osborne SN, Schmidt MA, Harper JR. An Automated and Minimally Invasive Tool for Generating Autologous Viable Epidermal Micrografts. Adv Skin Wound Care 2016;29: doi: /01.asw aa. 22 American Medical Association. Current Procedural Terminology (CPT). www ama-assn org. 2017; Accessed May 25, Centers for Medicare and Medicaid Services. CMS-1631-FC Medicare Program; Revisions to Payment Policies under the Physician Fee Schedule and Other Revisions to Part B for CY Baltimore, MD: Centers for Medicare and Medicaid Services; CMS FC. 24 Centers for Medicare and Medicaid Services. CMS-1633-FC; CMS-1607-F2 Addendum B: Medicare Final Rule for Hospital Outpatient Prospective Payment System and Ambulatory Surgical Center Payment Systems. Baltimore, MD: Centers for Medicare and Medicaid Services; CMS-1633-FC; CMS-1607-F2 Addendum B. 25 Centers for Medicare and Medicaid Services. CMS-1633-FC-CY2016-FR ASC Addendum AA and DD1: Medicare final rule for hospital outpatient prospective payment system and ambulatory surgical center payment systems. Baltimore, MD: Centers for Medicare and Medicaid Services; CMS-1633-FC-CY2016-FR ASC Addendum AA and DD1. Dr. Bhatia is president and CEO of Columbus Podiatry and Surgery Inc. and founder and CEO of Total Healing Wound Centers. He is assistant medical director of the Wound Clinic at Fairfield Medical Center.
The Use of Epidermal Grafting for the Management of Acute Wounds in the Outpatient Setting
 Accepted Manuscript The Use of Epidermal Grafting for the Management of Acute Wounds in the Outpatient Setting Nadine Hachach-Haram, Nicola Bystrzonowski, Muholan Kanapathy, Sarah-Jayne Edmondson, Lucy
Accepted Manuscript The Use of Epidermal Grafting for the Management of Acute Wounds in the Outpatient Setting Nadine Hachach-Haram, Nicola Bystrzonowski, Muholan Kanapathy, Sarah-Jayne Edmondson, Lucy
The Use of the. in Clinical Practice
 The Use of the SNAP Therapy System in Clinical Practice It s an ultraportable, mechanically-powered disposable NPWT. By Animesh Bhatia, DPM, CWS This article is written exclusively for PM and appears courtesy
The Use of the SNAP Therapy System in Clinical Practice It s an ultraportable, mechanically-powered disposable NPWT. By Animesh Bhatia, DPM, CWS This article is written exclusively for PM and appears courtesy
Surgical Preparation Codes for Skin Replacement Surgery** Hospital Outpatient/Ambulatory Surgical Center Setting
 2018 National Medicare Reimbursement Rate Summary* for Integra Dermal Regeneration Template, & Office Settings Integra LifeSciences Corporation compiles this summary of Medicare payment rates to provide
2018 National Medicare Reimbursement Rate Summary* for Integra Dermal Regeneration Template, & Office Settings Integra LifeSciences Corporation compiles this summary of Medicare payment rates to provide
CYGNUS REIMBURSEMENT GUIDE
 CYGNUS REIMBURSEMENT GUIDE The CYGNUS amnion patch is an immune-privileged tissue containing the natural regenerative factors responsible for creating a wound healing environment conducive to tissue regeneration.
CYGNUS REIMBURSEMENT GUIDE The CYGNUS amnion patch is an immune-privileged tissue containing the natural regenerative factors responsible for creating a wound healing environment conducive to tissue regeneration.
Wound & Burn. Reimbursement & Coding Guide
 Wound & Burn Reimbursement & Coding Guide Wound & Burn Reimbursement and Coding Guide MicroMatrix and Cytal devices facilitate the remodeling of functional, site-appropriate tissue. Comprised of ACell
Wound & Burn Reimbursement & Coding Guide Wound & Burn Reimbursement and Coding Guide MicroMatrix and Cytal devices facilitate the remodeling of functional, site-appropriate tissue. Comprised of ACell
Coding for Wound Care
 Coding for Wound Care ****IMPORTANT*** Disclaimer ***Information provided is to the best of our knowledge and as current as possible. ***Please verify all policy and reimbursement information with your
Coding for Wound Care ****IMPORTANT*** Disclaimer ***Information provided is to the best of our knowledge and as current as possible. ***Please verify all policy and reimbursement information with your
Epidermal skin grafting
 International Wound Journal ISSN 1742-4801 REVIEW ARTICLE Epidermal skin grafting Ingrid Herskovitz, Olivia B Hughes, Flor Macquhae, Adele Rakosi & Robert Kirsner Department of Dermatology and Cutaneous
International Wound Journal ISSN 1742-4801 REVIEW ARTICLE Epidermal skin grafting Ingrid Herskovitz, Olivia B Hughes, Flor Macquhae, Adele Rakosi & Robert Kirsner Department of Dermatology and Cutaneous
DermACELL AWM Comprehensive Reimbursement Resource Guide. Prepared by Musculoskeletal Clinical Regulatory Advisers, LLC. Version 01/2018.
 2018 Comprehensive Reimbursement Resource Guide Prepared by Musculoskeletal Clinical Regulatory Advisers, LLC. Version 01/2018. DermACELL AWM Disclaimer: This information is for educational/informational
2018 Comprehensive Reimbursement Resource Guide Prepared by Musculoskeletal Clinical Regulatory Advisers, LLC. Version 01/2018. DermACELL AWM Disclaimer: This information is for educational/informational
Skin Deep. Agenda. Burns Wounds Debridement Evaluation and Management Services. Presented by: Mike Strong, SFM The Work Comp Experts.
 Presented by: Mike Strong, SFM The Work Comp Experts Agenda Wounds Debridement Evaluation and Management Services 2 1 Types of First Degree Second Degree Third Degree Rule of 9 Adults Infants Burn Coding
Presented by: Mike Strong, SFM The Work Comp Experts Agenda Wounds Debridement Evaluation and Management Services 2 1 Types of First Degree Second Degree Third Degree Rule of 9 Adults Infants Burn Coding
WOUND CARE. By Laural Aiesi, RN, BSN Alina Kisiel RN, BSN Summit ElderCare
 WOUND CARE By Laural Aiesi, RN, BSN Alina Kisiel RN, BSN Summit ElderCare PRESSURE ULCER DIABETIC FOOT ULCER VENOUS ULCER ARTERIAL WOUND NEW OR WORSENING INCONTINENCE CHANGE IN MENTAL STATUS DECLINE IN
WOUND CARE By Laural Aiesi, RN, BSN Alina Kisiel RN, BSN Summit ElderCare PRESSURE ULCER DIABETIC FOOT ULCER VENOUS ULCER ARTERIAL WOUND NEW OR WORSENING INCONTINENCE CHANGE IN MENTAL STATUS DECLINE IN
Summary of Package Insert 1 for PuraPly Wound Matrix
 Summary of Package Insert 1 for PuraPly Wound Matrix For NGS Indications Indicated for the management of wounds including: Partial and full-thickness wounds Venous ulcers Diabetic ulcers Drainage wounds
Summary of Package Insert 1 for PuraPly Wound Matrix For NGS Indications Indicated for the management of wounds including: Partial and full-thickness wounds Venous ulcers Diabetic ulcers Drainage wounds
VACUUM ASSISTED CLOSURE (V.A.C.) THERAPY: Mr. Ismazizi Zaharudin Jabatan pembedahan Am Hospital Kuala Lumpur
 VACUUM ASSISTED CLOSURE (V.A.C.) THERAPY: Mr. Ismazizi Zaharudin Jabatan pembedahan Am Hospital Kuala Lumpur Learning Objectives Define Negative Pressure Wound Therapy (NPWT) Discuss guidelines for the
VACUUM ASSISTED CLOSURE (V.A.C.) THERAPY: Mr. Ismazizi Zaharudin Jabatan pembedahan Am Hospital Kuala Lumpur Learning Objectives Define Negative Pressure Wound Therapy (NPWT) Discuss guidelines for the
WPS Medicare Policy Primer
 WPS Medicare Policy Primer Medicare Jurisdiction (J5 & J8) NE, KS, IA, MO, IN, & MI Retired skin substitute LCD 3/2016 Indications Apligraf Non-infected partial and full-thickness skin ulcers due to VSU
WPS Medicare Policy Primer Medicare Jurisdiction (J5 & J8) NE, KS, IA, MO, IN, & MI Retired skin substitute LCD 3/2016 Indications Apligraf Non-infected partial and full-thickness skin ulcers due to VSU
Summary of Package Insert 1 for PuraPly Antimicrobial Wound Matrix
 Summary of Package Insert 1 for PuraPly Antimicrobial Wound Matrix For States with Non-Published Policies-Novitas Indications Indicated for the management of wounds as an effective barrier to resist microbial
Summary of Package Insert 1 for PuraPly Antimicrobial Wound Matrix For States with Non-Published Policies-Novitas Indications Indicated for the management of wounds as an effective barrier to resist microbial
Cahaba Medicare Policy Primer 1,2 for Apligraf
 Cahaba Medicare Policy Primer 1,2 for Apligraf MAC A: AL, GA & TN MAC B: AL, GA, & TN LCD# 31428 Indications Applied to partial- or full-thickness ulcers of the lower extremities (see individual product
Cahaba Medicare Policy Primer 1,2 for Apligraf MAC A: AL, GA & TN MAC B: AL, GA, & TN LCD# 31428 Indications Applied to partial- or full-thickness ulcers of the lower extremities (see individual product
Hemostasis Inflammatory Phase Proliferative/rebuilding Phase Maturation Phase
 The presenters are staff members of the CHI Health St. Elizabeth Burn and Wound Center. Many of the products discussed are used in our current practice but we have no conflict of interest to disclose.
The presenters are staff members of the CHI Health St. Elizabeth Burn and Wound Center. Many of the products discussed are used in our current practice but we have no conflict of interest to disclose.
Open Access Original Article DOI: /cureus.878. Angela Hulsey 1, Paul Linneman 2, Jeff Litt 3
 Open Access Original Article DOI: 10.7759/cureus.878 Clinical Usage and Economic Effectiveness of a Recently Developed Epidermal Autograft Harvesting System in 13 Chronic Wound Patients in a University-Based
Open Access Original Article DOI: 10.7759/cureus.878 Clinical Usage and Economic Effectiveness of a Recently Developed Epidermal Autograft Harvesting System in 13 Chronic Wound Patients in a University-Based
Coding for Ulcer Debridement
 Coding for Ulcer Debridement Faculty Jeffrey D. Lehrman, DPM, FASPS, MAPWCA Adjunct Clinical Professor Temple University School of Podiatric Medicine Panel Physician Crozer Center for Wound Healing and
Coding for Ulcer Debridement Faculty Jeffrey D. Lehrman, DPM, FASPS, MAPWCA Adjunct Clinical Professor Temple University School of Podiatric Medicine Panel Physician Crozer Center for Wound Healing and
Epidermal skin grafting in vitiligo: a pilot study
 International Wound Journal ISSN 1742-4801 ORIGINAL ARTICLE Epidermal skin grafting in vitiligo: a pilot study Agata Janowska, Valentina Dini, Salvatore Panduri, Michela Macchia, Teresa Oranges & Marco
International Wound Journal ISSN 1742-4801 ORIGINAL ARTICLE Epidermal skin grafting in vitiligo: a pilot study Agata Janowska, Valentina Dini, Salvatore Panduri, Michela Macchia, Teresa Oranges & Marco
Clinical Policy: EpiFix Wound Treatment
 Clinical Policy: Reference Number: PA.CP.MP.140 Effective Date: 03/18 Last Review Date: 04/18 Coding Implications Revision Log Description EpiFix (MiMedx Group) is dehydrated human amniotic tissue that
Clinical Policy: Reference Number: PA.CP.MP.140 Effective Date: 03/18 Last Review Date: 04/18 Coding Implications Revision Log Description EpiFix (MiMedx Group) is dehydrated human amniotic tissue that
First Coast Service Options (FCSO) Medicare Policy Primer
 First Coast Service Options (FCSO) Medicare Policy Primer Medicare Jurisdiction (JN) Florida, Puerto Rico and U.S. Virgin Islands Application of Skin Substitute Grafts for the treatment of DFU and VLU
First Coast Service Options (FCSO) Medicare Policy Primer Medicare Jurisdiction (JN) Florida, Puerto Rico and U.S. Virgin Islands Application of Skin Substitute Grafts for the treatment of DFU and VLU
Dressings do not heal wounds properly selected dressings enhance the body s ability to heal the wound. Progression Towards Healing
 Dressings in Wound Care: They Do Matter John S. Steinberg, DPM FACFAS Associate Professor, Department of Plastic Surgery Georgetown University School of Medicine Dressings do not heal wounds properly selected
Dressings in Wound Care: They Do Matter John S. Steinberg, DPM FACFAS Associate Professor, Department of Plastic Surgery Georgetown University School of Medicine Dressings do not heal wounds properly selected
WHEN THERE S A NEED FOR EPIDERMIS
 WHEN THERE S A NEED FOR EPIDERMIS PRESS START The automated CELLUTOME Epidermal Harvesting System The CELLUTOME System is an innovative epidermal harvesting device which can be easily integrated into your
WHEN THERE S A NEED FOR EPIDERMIS PRESS START The automated CELLUTOME Epidermal Harvesting System The CELLUTOME System is an innovative epidermal harvesting device which can be easily integrated into your
Negative Pressure Wound Therapy (NPWT)
 Negative Pressure Wound Therapy (NPWT) Policy Number: Original Effective Date: MM.01.005 11/19/1999 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST 01/01/2015 Section: DME Place(s) of Service:
Negative Pressure Wound Therapy (NPWT) Policy Number: Original Effective Date: MM.01.005 11/19/1999 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST 01/01/2015 Section: DME Place(s) of Service:
Beyond the Basics ImprovingYour Wound Care Knowledge. Berna Goldentyer RN, BSN, CWOCN Kathy Hugen RN, BSN, CWOCN
 Beyond the Basics ImprovingYour Wound Care Knowledge Berna Goldentyer RN, BSN, CWOCN Kathy Hugen RN, BSN, CWOCN Projects and Posters These resources were developed by creative VA nurses who had no special
Beyond the Basics ImprovingYour Wound Care Knowledge Berna Goldentyer RN, BSN, CWOCN Kathy Hugen RN, BSN, CWOCN Projects and Posters These resources were developed by creative VA nurses who had no special
Surgical Management of wounds, flaps, grafts, and scars
 Disclosures Surgical Management of wounds, flaps, grafts, and scars I have no financial disclosures Cherrie Heinrich, MD, FACS Department of Plastic Surgery Regions Hospital Assistant Professor University
Disclosures Surgical Management of wounds, flaps, grafts, and scars I have no financial disclosures Cherrie Heinrich, MD, FACS Department of Plastic Surgery Regions Hospital Assistant Professor University
Disclosures for Tarik Alam. Wound Bed Preparation. Wound Prognosis. Session Objectives. Debridement 4/26/2015
 Disclosures for Tarik Alam Challenges in Managing Bioburden and Devitalized Tissue Tarik Alam RN, BScN, ET, MClSc(WH) Enterostomal Therapy Nurse tarikalam@hotmail.com Clinical Affairs Manager for Hollister
Disclosures for Tarik Alam Challenges in Managing Bioburden and Devitalized Tissue Tarik Alam RN, BScN, ET, MClSc(WH) Enterostomal Therapy Nurse tarikalam@hotmail.com Clinical Affairs Manager for Hollister
Patient Care Information
 Patient Care Information A Guide to Healing Diabetic Foot Ulcers Questions? Contact us: Clinician: Phone #: In case of emergency, dial 9-1-1 Dermal Regeneration Matrix Overview Diabetic foot ulcers are
Patient Care Information A Guide to Healing Diabetic Foot Ulcers Questions? Contact us: Clinician: Phone #: In case of emergency, dial 9-1-1 Dermal Regeneration Matrix Overview Diabetic foot ulcers are
OF WOUNDS SENIOR AUDITOR CAROLINAS HEALTHCARE SYSTEM. AHIA 32 nd Annual Conference August 25-28, 2013 Chicago, Illinois
 1 THE WACKY WORLD OF WOUNDS ERIN RYDELL SENIOR AUDITOR CAROLINAS HEALTHCARE SYSTEM AHIA 32 nd Annual Conference August 25-28, 2013 Chicago, Illinois www.ahia.org Carolinas HealthCare System 2 Carolinas
1 THE WACKY WORLD OF WOUNDS ERIN RYDELL SENIOR AUDITOR CAROLINAS HEALTHCARE SYSTEM AHIA 32 nd Annual Conference August 25-28, 2013 Chicago, Illinois www.ahia.org Carolinas HealthCare System 2 Carolinas
Palmetto Medicare Policy Primer
 Palmetto Medicare Policy Primer Medicare Jurisdiction (JM) NC, SC, WV & VA Application of Skin Substitutes LCD #L36466 Indications Presence of neuropathic diabetic foot ulcer(s) having failed to respond
Palmetto Medicare Policy Primer Medicare Jurisdiction (JM) NC, SC, WV & VA Application of Skin Substitutes LCD #L36466 Indications Presence of neuropathic diabetic foot ulcer(s) having failed to respond
Wound Management. E. Foy White-Chu, MD, CWSP
 Wound Management E. Foy White-Chu, MD, CWSP E. Foy White-Chu, MD, CWSP Assistant Professor, OHSU Wound Medical Director, VAPORHCS List the Four Principles of Wound Bed Preparation Determine safe debridement
Wound Management E. Foy White-Chu, MD, CWSP E. Foy White-Chu, MD, CWSP Assistant Professor, OHSU Wound Medical Director, VAPORHCS List the Four Principles of Wound Bed Preparation Determine safe debridement
Application Guide for Full-Thickness Wounds
 Application Guide for Full-Thickness Wounds PriMatrix Dermal Repair Scaffold PriMatrix Ag Antimicrobial Dermal Repair Scaffold Application Guide for Full Thickness Wounds PriMatrix is a unique dermal repair
Application Guide for Full-Thickness Wounds PriMatrix Dermal Repair Scaffold PriMatrix Ag Antimicrobial Dermal Repair Scaffold Application Guide for Full Thickness Wounds PriMatrix is a unique dermal repair
Topical Oxygen Wound Therapy (MEDICAID)
 Topical Oxygen Wound Therapy (MEDICAID) Last Review Date: September 8, 2017 Number: MG.MM.DM.15C8v2 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or
Topical Oxygen Wound Therapy (MEDICAID) Last Review Date: September 8, 2017 Number: MG.MM.DM.15C8v2 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or
NovoSorb BTM. A unique synthetic biodegradable wound scaffold. Regenerating tissue. Changing lives.
 NovoSorb BTM A unique synthetic biodegradable wound scaffold Regenerating tissue. Changing lives. Overview NovoSorb BTM is a unique synthetic biodegradable wound scaffold that delivers good cosmetic and
NovoSorb BTM A unique synthetic biodegradable wound scaffold Regenerating tissue. Changing lives. Overview NovoSorb BTM is a unique synthetic biodegradable wound scaffold that delivers good cosmetic and
Multiple Interventions for Diabetic Foot Ulcer Treatment Trial (MIDFUT)
 Multiple Interventions for Diabetic Foot Ulcer Treatment Trial (MIDFUT) Nikki Dewhirst MIDFUT Clinical Co-ordinator, Clinical Trials Research Unit, University of Leeds Senior Vascular Research Nurse, Leeds
Multiple Interventions for Diabetic Foot Ulcer Treatment Trial (MIDFUT) Nikki Dewhirst MIDFUT Clinical Co-ordinator, Clinical Trials Research Unit, University of Leeds Senior Vascular Research Nurse, Leeds
Lower Extremity Wound Evaluation and Treatment
 Lower Extremity Wound Evaluation and Treatment Boni-Jo Silbernagel, DPM Describe effective lower extremity wound evaluation and treatment. Discuss changes in theories of treatment in wound care and implications
Lower Extremity Wound Evaluation and Treatment Boni-Jo Silbernagel, DPM Describe effective lower extremity wound evaluation and treatment. Discuss changes in theories of treatment in wound care and implications
TOO MANY DRESSING CHOICES!!!! WOUND CARE MANAGEMENT AND PRODUCTS. Should Your Practice Dispense Wound Care Supplies? Pros:
 WOUND CARE MANAGEMENT AND PRODUCTS Animesh Bhatia DPM, CWS, FAPWCA Board Certified Wound Specialist Diplomate, American Academy of Wound Management Fellow, American Professional Wound Care Association
WOUND CARE MANAGEMENT AND PRODUCTS Animesh Bhatia DPM, CWS, FAPWCA Board Certified Wound Specialist Diplomate, American Academy of Wound Management Fellow, American Professional Wound Care Association
Premier Health Plan considers Negative Pressure Wound Therapy (NPWT) in the home setting medically necessary for the following indications:
 Premier Health Plan POLICY AND PROCEDURE MANUAL PA.009.PH Negative Pressure Wound Therapy This policy applies to the following lines of business: Premier Commercial Premier Employee Premier Health Plan
Premier Health Plan POLICY AND PROCEDURE MANUAL PA.009.PH Negative Pressure Wound Therapy This policy applies to the following lines of business: Premier Commercial Premier Employee Premier Health Plan
Wound Care per HHVNA Wound Product Formulary
 Venous Ulcers ABI of 0.9-1.2 = normal blood flow An ABI MUST be obtained prior to inititiation of compression therapy. Compression is the Gold Standard of care to promote wound of venous ulcers. Elevation
Venous Ulcers ABI of 0.9-1.2 = normal blood flow An ABI MUST be obtained prior to inititiation of compression therapy. Compression is the Gold Standard of care to promote wound of venous ulcers. Elevation
o Venous edema o Stasis ulcers o Varicose veins (not including spider veins) o Lipodermatosclerosis
 Wound Care Equipment and Supply Benefits to Change for Texas Medicaid July 1, 2018 Effective for dates of service on or after July 1, 2018, wound care equipment and supply benefits will change for Texas
Wound Care Equipment and Supply Benefits to Change for Texas Medicaid July 1, 2018 Effective for dates of service on or after July 1, 2018, wound care equipment and supply benefits will change for Texas
Interesting Case Series. Skin Grafting in Pyoderma Gangrenosum
 Interesting Case Series Skin Grafting in Pyoderma Gangrenosum Marco Romanelli, MD, PhD, Agata Janowska, MD, Teresa Oranges, MD, and Valentina Dini, MD, PhD Department of Dermatology, University of Pisa,
Interesting Case Series Skin Grafting in Pyoderma Gangrenosum Marco Romanelli, MD, PhD, Agata Janowska, MD, Teresa Oranges, MD, and Valentina Dini, MD, PhD Department of Dermatology, University of Pisa,
MY STRATEGY FOR TREATING BURN INJURIES. Warren Garner MD FACS Keck School of Medicine at USC Los Angeles, CA
 MY STRATEGY FOR TREATING BURN INJURIES Warren Garner MD FACS Keck School of Medicine at USC Los Angeles, CA ASSUMPTIONS: Burns which heal to normal have best outcome. Medical risk, functional recovery,
MY STRATEGY FOR TREATING BURN INJURIES Warren Garner MD FACS Keck School of Medicine at USC Los Angeles, CA ASSUMPTIONS: Burns which heal to normal have best outcome. Medical risk, functional recovery,
The POWER of HEALING DERMATOLOGISTS BREAK NEW GROUND IN THE TREATMENT OF WOUNDS AND SCARS. 64 DERMATOLOGY WORLD // July
 DERMATOLOGISTS BREAK NEW GROUND IN THE TREATMENT OF WOUNDS AND SCARS 64 DERMATOLOGY WORLD // July 2017 BY JAN BOWERS, CONTRIBUTING WRITER Never has the need for effective approaches to treating skin wounds
DERMATOLOGISTS BREAK NEW GROUND IN THE TREATMENT OF WOUNDS AND SCARS 64 DERMATOLOGY WORLD // July 2017 BY JAN BOWERS, CONTRIBUTING WRITER Never has the need for effective approaches to treating skin wounds
Regenerative Tissue Matrix in Treatment of Wounds
 Regenerative Tissue Matrix in Treatment of Wounds Learning Objectives Differentiate between reparative and regenerative healing Review surgical techniques for applying a regenerative tissue scaffold to
Regenerative Tissue Matrix in Treatment of Wounds Learning Objectives Differentiate between reparative and regenerative healing Review surgical techniques for applying a regenerative tissue scaffold to
2017 FlexHD Abdominal Wall Reconstruction Reimbursement Coding Reference
 2017 FlexHD Abdominal Wall Reconstruction Reimbursement Coding Reference Most Commonly Reported ICD-10-CM Procedure Codes and Descriptors ICD-10-CM Description 0WUF0KZ Supplement Abdominal Wall with Nonautologous
2017 FlexHD Abdominal Wall Reconstruction Reimbursement Coding Reference Most Commonly Reported ICD-10-CM Procedure Codes and Descriptors ICD-10-CM Description 0WUF0KZ Supplement Abdominal Wall with Nonautologous
How Wounds Heal: A Guide for the Wound-care Novice
 C L I N I C A L P R A C T I C E How Wounds Heal: A Guide for the Wound-care Novice BY Christine Pearson Christine Pearson, RN, IIWCC, is a wound clinician for Vancouver Coastal Health and has worked in
C L I N I C A L P R A C T I C E How Wounds Heal: A Guide for the Wound-care Novice BY Christine Pearson Christine Pearson, RN, IIWCC, is a wound clinician for Vancouver Coastal Health and has worked in
Determining Wound Diagnosis and Documentation Tips Job Aid
 Determining Wound Diagnosis and Job Aid 1 Coding Is this a traumatic injury from an accident? 800 Codes - Injury Section of the Coding Manual Code by specific site of injury. Only use for accidents or
Determining Wound Diagnosis and Job Aid 1 Coding Is this a traumatic injury from an accident? 800 Codes - Injury Section of the Coding Manual Code by specific site of injury. Only use for accidents or
Novitas Medicare Policy Primer
 Novitas Medicare Policy Primer Medicare Jurisdiction (JL and JH) AR, CO, LA, MS, NM, OK, TX, DC, DE, MD, NJ, & PA Counties of Arlington and Fairfax in Virginia and the city of Alexandria in Virginia Application
Novitas Medicare Policy Primer Medicare Jurisdiction (JL and JH) AR, CO, LA, MS, NM, OK, TX, DC, DE, MD, NJ, & PA Counties of Arlington and Fairfax in Virginia and the city of Alexandria in Virginia Application
CASE 1: TYPE-II DIABETIC FOOT ULCER
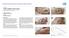 CASE 1: TYPE-II DIABETIC FOOT ULCER DIABETIC FOOT ULCER 48 YEAR-OLD MALE Mr. C., was a 48-year old man with a history of Type-II diabetes over the past 6 years. The current foot ulcer with corresponding
CASE 1: TYPE-II DIABETIC FOOT ULCER DIABETIC FOOT ULCER 48 YEAR-OLD MALE Mr. C., was a 48-year old man with a history of Type-II diabetes over the past 6 years. The current foot ulcer with corresponding
Mean percent reduction in ulcer area from baseline at six weeks 62 % SANTYL Ointment + supportive care* + sharp debridement 1 (P<0.
 Evaluating two common adjuncts to sharp debridement in the treatment of diabetic foot ulcers Mean percent reduction in ulcer area from baseline at six weeks 62 % 40 % SANTYL Ointment + supportive care*
Evaluating two common adjuncts to sharp debridement in the treatment of diabetic foot ulcers Mean percent reduction in ulcer area from baseline at six weeks 62 % 40 % SANTYL Ointment + supportive care*
1/5. Introduction. Primary endpoint Time to reach readiness for closure by surgical intervention or left for closure by secondary intention
 1/5 Introduction Materials and methods Animal studies show that intermittent NPWT has potential to increase the rate of granulation tissue formation compared with adjustable intermittent (AI) NPWT 1 However,
1/5 Introduction Materials and methods Animal studies show that intermittent NPWT has potential to increase the rate of granulation tissue formation compared with adjustable intermittent (AI) NPWT 1 However,
Acute and Chronic WOUND ASSESSMENT. Wound Assessment OBJECTIVES ITEMS TO CONSIDER
 WOUND ASSESSMENT Acute and Chronic OBJECTIVES Discuss classification systems and testing methods for pressure ulcers, venous, arterial and diabetic wounds List at least five items to be assessed and documented
WOUND ASSESSMENT Acute and Chronic OBJECTIVES Discuss classification systems and testing methods for pressure ulcers, venous, arterial and diabetic wounds List at least five items to be assessed and documented
Dynamic Tissue Systems. Reimbursement & Coding Guide
 Dynamic Tissue Systems Reimbursement & Coding Guide Dynamic Tissue Systems Reimbursement and Coding Guide The following information is shared for educational purposes only to help answer common coding
Dynamic Tissue Systems Reimbursement & Coding Guide Dynamic Tissue Systems Reimbursement and Coding Guide The following information is shared for educational purposes only to help answer common coding
Diabetic Foot Ulcer Treatment and Prevention
 Diabetic Foot Ulcer Treatment and Prevention Alexander Reyzelman DPM, FACFAS Associate Professor California School of Podiatric Medicine at Samuel Merritt University Diabetic Foot Ulcers One of the most
Diabetic Foot Ulcer Treatment and Prevention Alexander Reyzelman DPM, FACFAS Associate Professor California School of Podiatric Medicine at Samuel Merritt University Diabetic Foot Ulcers One of the most
1/3/2008. Karen Burke Priscilla LeMone Elaine Mohn-Brown. Medical-Surgical Nursing Care, 2e Karen Burke, Priscilla LeMone, and Elaine Mohn-Brown
 Medical-Surgical Nursing Care Second Edition Karen Burke Priscilla LeMone Elaine Mohn-Brown Chapter 46 Caring for Clients with Burns Types of Burns Thermal Dry heat flame Moist heat steam or hot liquid
Medical-Surgical Nursing Care Second Edition Karen Burke Priscilla LeMone Elaine Mohn-Brown Chapter 46 Caring for Clients with Burns Types of Burns Thermal Dry heat flame Moist heat steam or hot liquid
Clinical Policy Title: Vacuum assisted closure in surgical wounds
 Clinical Policy Title: Vacuum assisted closure in surgical wounds Clinical Policy Number: 17.03.00 Effective Date: September 1, 2015 Initial Review Date: June 16, 2013 Most Recent Review Date: August 17,
Clinical Policy Title: Vacuum assisted closure in surgical wounds Clinical Policy Number: 17.03.00 Effective Date: September 1, 2015 Initial Review Date: June 16, 2013 Most Recent Review Date: August 17,
QUICK GUIDE SNAP THERAPY SYSTEM
 QUICK GUIDE SNAP THERAPY SYSTEM Clinical Pathway to SNAP System Full holistic assessment of patient and wound Is the wound type indicated for NPWT use without contraindications 1? SNAP System is indicated
QUICK GUIDE SNAP THERAPY SYSTEM Clinical Pathway to SNAP System Full holistic assessment of patient and wound Is the wound type indicated for NPWT use without contraindications 1? SNAP System is indicated
Use of an Acellular Regenerative Tissue Matrix Over Chronic Wounds
 Use of an Acellular Regenerative Tissue Matrix Over Chronic Wounds D. Heath Stacey, MD Northwest Arkansas Center for Plastic Surgery, Fayetteville, Ark Correspondence: dheathstacey@gmail.com Keywords:
Use of an Acellular Regenerative Tissue Matrix Over Chronic Wounds D. Heath Stacey, MD Northwest Arkansas Center for Plastic Surgery, Fayetteville, Ark Correspondence: dheathstacey@gmail.com Keywords:
Negative Pressure Wound Therapy
 Origination: 6/29/04 Revised: 8/24/16 Annual Review: 11/10/16 Purpose: To provide Negative Pressure Wound Therapy (wound care treatment) guidelines for the Medical Department staff to reference when making
Origination: 6/29/04 Revised: 8/24/16 Annual Review: 11/10/16 Purpose: To provide Negative Pressure Wound Therapy (wound care treatment) guidelines for the Medical Department staff to reference when making
DEBRIDEMENT. Professor Donald G. MacLellan Executive Director Health Education & Management Innovations
 DEBRIDEMENT Professor Donald G. MacLellan Executive Director Health Education & Management Innovations DEBRIDEMENT Principles - CSD Methods of Debridement Biopsy options PRINCIPLES OF WOUND MANAGEMENT
DEBRIDEMENT Professor Donald G. MacLellan Executive Director Health Education & Management Innovations DEBRIDEMENT Principles - CSD Methods of Debridement Biopsy options PRINCIPLES OF WOUND MANAGEMENT
A prospective, multicentre study on the use of epidermal grafts to optimise outpatient wound management
 International Wound Journal ISSN 1742-4801 ORIGINL RTICLE prospective, multicentre study on the use of epidermal grafts to optimise outpatient management Nadine Hachach-Haram 1, Nicola ystrzonowski 1,
International Wound Journal ISSN 1742-4801 ORIGINL RTICLE prospective, multicentre study on the use of epidermal grafts to optimise outpatient management Nadine Hachach-Haram 1, Nicola ystrzonowski 1,
CGS Medicare Policy Primer
 CGS Medicare Policy Primer Medicare Jurisdiction (J15) OH & KY Wound Application of Cellular and/or Tissue Based Products (CTPs) Lower Extremities #L36690 Indications Application of a CTP graft for lower
CGS Medicare Policy Primer Medicare Jurisdiction (J15) OH & KY Wound Application of Cellular and/or Tissue Based Products (CTPs) Lower Extremities #L36690 Indications Application of a CTP graft for lower
Current Concepts in Burn Rehabilitation
 Current Concepts in Burn Rehabilitation 7 th Congress of the Baltic Association of Rehabilitation Tallinn, Estonia September 2010 R. Scott Ward, PT, PhD Professor and Chair Department of Physical Therapy
Current Concepts in Burn Rehabilitation 7 th Congress of the Baltic Association of Rehabilitation Tallinn, Estonia September 2010 R. Scott Ward, PT, PhD Professor and Chair Department of Physical Therapy
CHRONIC WOUND SOLUTIONS MANAGE WOUNDS WITH THE ACELITY PORTFOLIO OF. The certainty of Acelity CHRONIC WOUND SOLUTIONS. ActiV.A.C.
 CHRONIC WOUND SOLUTIONS ActiV.A.C. Therapy PROMOGRAN PRISMA Collagen/ORC Matrix MANAGE WOUNDS WITH THE ACELITY PORTFOLIO OF CHRONIC WOUND SOLUTIONS The certainty of Acelity CelluTome Epidermal Harvesting
CHRONIC WOUND SOLUTIONS ActiV.A.C. Therapy PROMOGRAN PRISMA Collagen/ORC Matrix MANAGE WOUNDS WITH THE ACELITY PORTFOLIO OF CHRONIC WOUND SOLUTIONS The certainty of Acelity CelluTome Epidermal Harvesting
Consider the possibility of pressure ulcer development
 Douglas Fronzaglia II, DO, MS LECOM Institute for Successful Aging LECOM Institute for Advanced Wound Care and Hyperbaric Medicine Consider the possibility of pressure ulcer development 1 Identify ulcer
Douglas Fronzaglia II, DO, MS LECOM Institute for Successful Aging LECOM Institute for Advanced Wound Care and Hyperbaric Medicine Consider the possibility of pressure ulcer development 1 Identify ulcer
POLICIES AND PROCEDURE MANUAL
 POLICIES AND PROCEDURE MANUAL Policy: MP058 Section: Medical Benefit Policy Subject: Negative Pressure Wound Therapy I. Policy: Negative Pressure Wound Therapy II. Purpose/Objective: To provide a policy
POLICIES AND PROCEDURE MANUAL Policy: MP058 Section: Medical Benefit Policy Subject: Negative Pressure Wound Therapy I. Policy: Negative Pressure Wound Therapy II. Purpose/Objective: To provide a policy
Wound Jeopardy: Name That Wound Session 142 Saturday, September 10 th 2011
 Initial Wound Care Consult History Physical Examination Detailed examination of the wound Photographs Cultures Procedures TCOM ABI Debridement Management Decisions A Detailed History and Physical (wound)
Initial Wound Care Consult History Physical Examination Detailed examination of the wound Photographs Cultures Procedures TCOM ABI Debridement Management Decisions A Detailed History and Physical (wound)
Appropriate Dressing Selection For Treating Wounds
 Appropriate Dressing Selection For Treating Wounds Criteria to Consider for an IDEAL DRESSING Exudate Management Be able to provide for moist wound healing by absorbing exudate or adding moisture Secure
Appropriate Dressing Selection For Treating Wounds Criteria to Consider for an IDEAL DRESSING Exudate Management Be able to provide for moist wound healing by absorbing exudate or adding moisture Secure
DO NOT DUPLICATE. Negative pressure wound therapy (NPWT) has revolutionized the
 Original research WOUNDS 2013;25(4):89 93 From the Aesthetic and Plastic Surgery Institute, University of California Irvine, Orange, CA and Long Beach Memorial Medical Center, Long Beach, CA Address correspondence
Original research WOUNDS 2013;25(4):89 93 From the Aesthetic and Plastic Surgery Institute, University of California Irvine, Orange, CA and Long Beach Memorial Medical Center, Long Beach, CA Address correspondence
Discussion Topics. Calcium Alginates. DME For the Diabetic Foot 1/25/2017. Jeffrey D. Lehrman, DPM, FASPS, FACFAS, MAPWCA
 DME For the Diabetic Foot Jeffrey D. Lehrman, DPM, FASPS, FACFAS, MAPWCA Editorial Advisory Board, WOUNDS Board of Directors, American Society of Podiatric Surgeons Board of Directors, American Professional
DME For the Diabetic Foot Jeffrey D. Lehrman, DPM, FASPS, FACFAS, MAPWCA Editorial Advisory Board, WOUNDS Board of Directors, American Society of Podiatric Surgeons Board of Directors, American Professional
If both a standardized, validated screening tool and an evaluation of clinical factors are utilized, select Response 2.
 (M1300) Pressure Ulcer Assessment: Was this patient assessed for Risk of Developing Pressure Ulcers? 0 - No assessment conducted [Go to M1306 ] 1 - Yes, based on an evaluation of clinical factors (for
(M1300) Pressure Ulcer Assessment: Was this patient assessed for Risk of Developing Pressure Ulcers? 0 - No assessment conducted [Go to M1306 ] 1 - Yes, based on an evaluation of clinical factors (for
Assisted Living Resident Assessment (To be used when yes is indicated for skin issues under Section 5 of Assisted Living Resident Assessment)
 Skin Assessment Current open skin areas: Yes No Current pressure ulcer: Yes No A. Stage 1 Ulcers Report based on highest stage of existing ulcers at its worst; do not reverse stage. Number of existing
Skin Assessment Current open skin areas: Yes No Current pressure ulcer: Yes No A. Stage 1 Ulcers Report based on highest stage of existing ulcers at its worst; do not reverse stage. Number of existing
ULCERS 1/12/ million diabetics in the US (2012) Reamputation Rate 26.7% at 1 year 48.3% at 3 years 60.7% at 5 years
 Jay Christensen D.P.M Advanced Foot and Ankle of Wisconsin 2-4% of the population at any given time will have ulcers 0.06-0.20% of the total population Average age of patients 70 years increased as more
Jay Christensen D.P.M Advanced Foot and Ankle of Wisconsin 2-4% of the population at any given time will have ulcers 0.06-0.20% of the total population Average age of patients 70 years increased as more
Breast debridement and closure cpt
 Breast debridement and closure cpt Close Breast debridement cpt code Medicare Billing Guidelines, Medicare payment and reimbursment, Medicare codes. Here is a list of CPT codes and Diagnoses that are.
Breast debridement and closure cpt Close Breast debridement cpt code Medicare Billing Guidelines, Medicare payment and reimbursment, Medicare codes. Here is a list of CPT codes and Diagnoses that are.
D-WOUND SOLUTION. From the start to completion of wound healing
 From the start to completion of wound healing From the start to completion of wound healing Treatment for ALL type of wound Burn, Pressure ulcer Diabetic Foot ulcer Scar prevention 244, Galmachi-ro, Jungwon-gu,
From the start to completion of wound healing From the start to completion of wound healing Treatment for ALL type of wound Burn, Pressure ulcer Diabetic Foot ulcer Scar prevention 244, Galmachi-ro, Jungwon-gu,
Venous Leg Ulcers. Care for Patients in All Settings
 Venous Leg Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a venous leg ulcer. The scope of the standard
Venous Leg Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a venous leg ulcer. The scope of the standard
HydroTherapy: A simple approach to Wound Management
 Copyright Paul Hartmann Pty Ltd material may not be reproduced or used without written permission HydroTherapy: A simple approach to Wound Management HARTMANN Education Agenda Agenda Acute vs Chronic wounds:
Copyright Paul Hartmann Pty Ltd material may not be reproduced or used without written permission HydroTherapy: A simple approach to Wound Management HARTMANN Education Agenda Agenda Acute vs Chronic wounds:
Agenda (45 minutes) Some questions for you. Which wound dressing? Dressing categories/types. Summary
 Dressing selection Agenda (45 minutes) Some questions for you. Which wound dressing? Dressing categories/types Summary Which wound dressing poster Ref: Which wound dressing? Practice Nursing, September
Dressing selection Agenda (45 minutes) Some questions for you. Which wound dressing? Dressing categories/types Summary Which wound dressing poster Ref: Which wound dressing? Practice Nursing, September
The Management of Lower Limb Oedema. Catherine Hammond CNS/CNE 2018
 The Management of Lower Limb Oedema Catherine Hammond CNS/CNE 2018 Causes of oedema Venous stasis Lymphoedema Heart Failure Dependency Liver and kidney failure Medications Cellulitis Low protein Under
The Management of Lower Limb Oedema Catherine Hammond CNS/CNE 2018 Causes of oedema Venous stasis Lymphoedema Heart Failure Dependency Liver and kidney failure Medications Cellulitis Low protein Under
Evaluating the use of a topical haemoglobin spray as adjunctive therapy in non-healing chronic wounds a pilot study Liezl Naude
 Evaluating the use of a topical haemoglobin spray as adjunctive therapy in non-healing chronic wounds a pilot study Liezl Naude Abstract Wound Management Specialist Eloquent Health & Wellness Centre, Pretoria,
Evaluating the use of a topical haemoglobin spray as adjunctive therapy in non-healing chronic wounds a pilot study Liezl Naude Abstract Wound Management Specialist Eloquent Health & Wellness Centre, Pretoria,
Delayed Primary Closure of Diabetic Foot Wounds using the DermaClose RC Tissue Expander
 Delayed Primary Closure of Diabetic Foot Wounds using the DermaClose RC Tissue Expander TDavid L. Nielson, DPM 1, Stephanie C. Wu, DPM, MSc 2, David G. Armstrong, DPM,PhD 3 The Foot & Ankle Journal 1 (2):
Delayed Primary Closure of Diabetic Foot Wounds using the DermaClose RC Tissue Expander TDavid L. Nielson, DPM 1, Stephanie C. Wu, DPM, MSc 2, David G. Armstrong, DPM,PhD 3 The Foot & Ankle Journal 1 (2):
ACOFP 55th Annual Convention & Scientific Seminars. New Physicians and Residents: Introduction to Wound Care. Katherine Lincoln, DO, FAAFP
 8 ACOFP 55th Annual Convention & Scientific Seminars New Physicians and Residents: Introduction to Wound Care Katherine Lincoln, DO, FAAFP Introduction to Wound Care KATHERINE LINCOLN, DO, FAAFP ACOFP
8 ACOFP 55th Annual Convention & Scientific Seminars New Physicians and Residents: Introduction to Wound Care Katherine Lincoln, DO, FAAFP Introduction to Wound Care KATHERINE LINCOLN, DO, FAAFP ACOFP
Management of Complex Avulsion Injuries of the Dorsum of the Foot and Ankle in Pediatric Patients by Using Local Delayed Flaps and Skin Grafts
 Management of Complex Avulsion Injuries of the Dorsum of the Foot and Ankle in Pediatric Patients by Using Local Delayed Flaps and Skin Grafts Ahmed Elshahat, MD Plastic Surgery Department, Ain Shams University,
Management of Complex Avulsion Injuries of the Dorsum of the Foot and Ankle in Pediatric Patients by Using Local Delayed Flaps and Skin Grafts Ahmed Elshahat, MD Plastic Surgery Department, Ain Shams University,
Advanced Wound Dressings Today
 SPRING SUPPLEMENT Advanced Wound Dressings Today Clinical Insights, Perspectives and Treatment Approaches Chronic Wound Biochemistry Robert Snyder Cherison Cuffy Joey K. Ead Karen Fischborn Advanced Wound
SPRING SUPPLEMENT Advanced Wound Dressings Today Clinical Insights, Perspectives and Treatment Approaches Chronic Wound Biochemistry Robert Snyder Cherison Cuffy Joey K. Ead Karen Fischborn Advanced Wound
The Power of a Hydroconductive Wound Dressing with LevaFiber Technology
 The Power of a Hydroconductive Wound Dressing with LevaFiber Technology The first step in healing a chronic wound is to detoxify it by removing slough, necrotic tissue, exudate and bacteria, while keeping
The Power of a Hydroconductive Wound Dressing with LevaFiber Technology The first step in healing a chronic wound is to detoxify it by removing slough, necrotic tissue, exudate and bacteria, while keeping
Genadyne A4 and foam to treat a postoperative debridment flank abscess
 Genadyne A4 and foam to treat a postoperative debridment flank abscess Michael S. DO, The Wound Healing Center Indianapolis, IN Cynthia Peebles RN D.O.N., Becky Beck RN Heartland at Prestwick NH Avon,
Genadyne A4 and foam to treat a postoperative debridment flank abscess Michael S. DO, The Wound Healing Center Indianapolis, IN Cynthia Peebles RN D.O.N., Becky Beck RN Heartland at Prestwick NH Avon,
The Georgetown Team Approach to Diabetic Limb Salvage: 2013
 The Georgetown Team Approach to Diabetic Limb Salvage: 2013 John S. Steinberg, DPM FACFAS Associate Professor, Department of Plastic Surgery Georgetown University School of Medicine Disclosures: None Need
The Georgetown Team Approach to Diabetic Limb Salvage: 2013 John S. Steinberg, DPM FACFAS Associate Professor, Department of Plastic Surgery Georgetown University School of Medicine Disclosures: None Need
Pressure Ulcers: 3 Keys to Pressure Ulcer Management. Evidence Based Prevention & Management. I have no financial conflicts of interest
 Pressure Ulcers: Evidence Based Prevention & Management Madhuri Reddy, MD MSc I have no financial conflicts of interest I have nothing to disclose financially 3 Keys to Pressure Ulcer Management 1 3 Keys
Pressure Ulcers: Evidence Based Prevention & Management Madhuri Reddy, MD MSc I have no financial conflicts of interest I have nothing to disclose financially 3 Keys to Pressure Ulcer Management 1 3 Keys
2017 Coding and Reimbursement Survival Guide
 2017 Coding and Reimbursement Survival Guide Chapter 8: General Surgery Integumentary Procedures: 4 Questions Focus Your Skin Substitute Graft Coding Hint: Graft size doesn t matter. If your surgeon treats
2017 Coding and Reimbursement Survival Guide Chapter 8: General Surgery Integumentary Procedures: 4 Questions Focus Your Skin Substitute Graft Coding Hint: Graft size doesn t matter. If your surgeon treats
Durable Medical Equipment Providers
 August 2009 Provider Bulletin Number 974 Durable Medical Equipment Providers Vacuum Assisted Wound Closure Therapy Negative pressure wound therapy (NPWT) must be requested and supplied by an enrolled durable
August 2009 Provider Bulletin Number 974 Durable Medical Equipment Providers Vacuum Assisted Wound Closure Therapy Negative pressure wound therapy (NPWT) must be requested and supplied by an enrolled durable
Clinical teaching/experi ence. Lectures/semina rs/conferences Self-directed. learning. Clinical teaching/experi ence
 Regional Medical Center (The MED) Plastic Surgery PGY-3 By the end of the Plastic Surgery at the MED, the PGY-3 residents are expected to expand and cultivate knowledge and skills developed during previous
Regional Medical Center (The MED) Plastic Surgery PGY-3 By the end of the Plastic Surgery at the MED, the PGY-3 residents are expected to expand and cultivate knowledge and skills developed during previous
Disclosures. Outpatient NPWT Options Free up Hospital Beds, but Do They Work? Objectives. Clinically Effective: Does it Work?
 4/16/16 Disclosures Consultant, Volcano Corporation Outpatient Options Free up Hospital Beds, but Do They Work? UCSF Vascular Symposium 16 Jonathan Labovitz, DPM Medical Director, Foot & Ankle Center Associate
4/16/16 Disclosures Consultant, Volcano Corporation Outpatient Options Free up Hospital Beds, but Do They Work? UCSF Vascular Symposium 16 Jonathan Labovitz, DPM Medical Director, Foot & Ankle Center Associate
Case Study. TRAM Flap Reconstruction with an Associated Complication. Repair using DermaMatrix Acellular Dermis.
 Case Study TRAM Flap Reconstruction with an Associated Complication. Repair using DermaMatrix Acellular Dermis. TRAM Flap Reconstruction with an Associated Complication Challenge Insulin-dependent diabetes
Case Study TRAM Flap Reconstruction with an Associated Complication. Repair using DermaMatrix Acellular Dermis. TRAM Flap Reconstruction with an Associated Complication Challenge Insulin-dependent diabetes
Successful Wound Management Strategies : An Introduction. Alex Khan, APRN ACNS-BC. Organization of Wound Care Nurses
 Successful Wound Management Strategies : An Introduction Alex Khan, APRN ACNS-BC Organization of Wound Care Nurses www.woundcarenurses.org Goals & Objectives The role and importance of wound care management
Successful Wound Management Strategies : An Introduction Alex Khan, APRN ACNS-BC Organization of Wound Care Nurses www.woundcarenurses.org Goals & Objectives The role and importance of wound care management
Wound Care Program for Nursing Assistants-
 Wound Care Program for Nursing Assistants- Wound Cleansing,Types & Presentation Elizabeth DeFeo, RN, WCC, OMS, CWOCN Wound, Ostomy, & Continence Specialist ldefeo@cornerstonevna.org Outline/Agenda At completion
Wound Care Program for Nursing Assistants- Wound Cleansing,Types & Presentation Elizabeth DeFeo, RN, WCC, OMS, CWOCN Wound, Ostomy, & Continence Specialist ldefeo@cornerstonevna.org Outline/Agenda At completion
V.A.C. VeraFlo Therapy can help.
 WOUND CARE IS COMPLEX & COSTLY Therapy can help. PROBLEM Complex wounds pose challenges to clinicians and patients in terms of achieving desired outcomes while managing healthcare costs. 1-5 OUTCOMES &
WOUND CARE IS COMPLEX & COSTLY Therapy can help. PROBLEM Complex wounds pose challenges to clinicians and patients in terms of achieving desired outcomes while managing healthcare costs. 1-5 OUTCOMES &
Integra. PriMatrix Dermal Repair Scaffold PATIENT INFORMATION. Questions? Contact us: Clinician: Phone #: In case of emergency, dial 9-1-1
 Integra PriMatrix Dermal Repair Scaffold PATIENT INFORMATION Questions? Contact us: Clinician: Phone #: In case of emergency, dial 9-1-1 Your Path to Recovery Your health care provider has chosen to use
Integra PriMatrix Dermal Repair Scaffold PATIENT INFORMATION Questions? Contact us: Clinician: Phone #: In case of emergency, dial 9-1-1 Your Path to Recovery Your health care provider has chosen to use
