STUDY. Efficacy of Itraconazole in the Prophylactic Treatment of Pityriasis (Tinea) Versicolor
|
|
|
- Wilfred Morgan
- 5 years ago
- Views:
Transcription
1 STUDY Efficacy of Itraconazole in the Prophylactic Treatment of Pityriasis (Tinea) Versicolor Jan Faergemann, MD, PhD; A. K. Gupta, MD, FRCPC; A. Al Mofadi, MD, FRCPC; A. Abanami, MD, FRCP(Edin); A. Abu Shareaah, MD; Greet Marynissen, PhD Background: Pityriasis (tinea) versicolor has a high tendency to recur after being treated successfully. Prophylactic treatment to reduce recurrence is needed. Objective: To determine whether recurrence of pityriasis versicolor could be prevented by prophylactic itraconazole treatment. Design: Open treatment followed by a randomized, double-blind, placebo-controlled phase. Setting: Multinational outpatient centers. Patients: A total of 239 consecutive patients were included; 238 started open treatment. A total of 209 patients started prophylactic treatment: 106 in the itraconazole group and 103 in the placebo group. Interventions: Open treatment: itraconazole, 200 mg once daily for 7 days. Prophylactic treatment: itraconazole, 200 mg, or placebo twice daily 1 day per month for 6 consecutive months. Main Outcome Measures: Mycological cure rates at the end of open treatment and at the end of prophylactic treatment. Results: Mycological cure at the end of open treatment was 92% (205/223). At the prophylactic treatment end point (6 months), mycological cure was 88% (90/102) in the itraconazole group and 57% (56/99) in the placebo group (P.001). In open treatment, 11 patients were not able to be evaluated for efficacy. In prophylactic treatment, 4 patients in the itraconazole group and 4 in the placebo group were not able to be evaluated. Adverse events were reported during open treatment by 26 patients (11%) and during prophylactic treatment by 17 (16%) in the itraconazole group and 14 (14%) in the placebo group. No patients experienced any serious adverse events. Conclusions: Prophylactic itraconazole treatment is efficacious for pityriasis versicolor after 6 months, as is itraconazole in the treatment of pityriasis versicolor. Arch Dermatol. 2002;138:69-73 From the Department of Dermatology, Sahlgrenska University Hospital, Gothenburg, Sweden (Dr Faergemann); the Division of Dermatology, Department of Medicine, Sunnybrook and Women s College, Health Sciences Center, Sunnybrook, and the University of Toronto, Toronto, Ontario (Dr Gupta); the Division of Dermatology, King Fahad National Guard Hospital, Riyadh, Saudi Arabia (Dr Al Mofadi); the Departments of Dermatology, Riyadh Armed Forces Hospital, Riyadh (Dr Abanami) and Mafraque Hospital, Ministry of Health, Abu Dubai, United Arab Emirates (Dr Abu Shareaah); and Medisearch International, Mechelen, Belgium (Dr Marynissen). PITYRIASIS (TINEA) versicolor may be treated with topical or oral agents, with the latter being used especially when the disease is widespread or does not respond to topical measures. Systemic agents used for treating pityriasis versicolor include itraconazole, ketoconazole, and fluconazole. 1,2 Itraconazole is a triazole antimycotic agent with strong keratophilic and lipophilic properties. 3 Similar to other azole antifungal agents, the mode of action of itraconazole involves inhibition of 14- demethylase, resulting in impaired sterol synthesis in fungal cell membranes. In vitro, itraconazole is active not only against yeasts such as Malassezia and Candida species but also against dermatophytes and nondermatophyte molds. 4,5 When itraconazole is used to treat pityriasis versicolor, a suggested regimen is 200 mg/d for 7 days, with a minimum cumulative dose of at least 1000 mg being required for effective therapy. 6,7 Four weeks after the start of therapy, cure rates of 80% to 90% have been reported. 7 Although the fungal organisms may be nonviable, the color of the affected skin may take several weeks or months to normalize. Pityriasis versicolor recurs at a variable rate in treated individuals, and 60% to 90% of patients relapse within 2 years in some series. 8 Therefore, it is important to evaluate a prophylactic regimen that may be effective and safe in preventing the recurrence of pityriasis versicolor. We evaluated the efficacy of treatment with itraconazole, 200 mg once daily for 1 week, and the efficacy of placebocontrolled prophylactic treatment with itraconazole, 200 mg taken 12 hours apart 1 day per month for 6 consecutive months, in terms of clinical and mycological outcome and frequency of recurrence of pityriasis versicolor. To our knowledge, this 69
2 PATIENTS AND METHODS This multicenter, multinational trial was characterized by an open, active treatment phase with itraconazole, 200 mg once daily for 1 week, followed by 4 weeks without active therapy. In patients in whom pityriasis versicolor cleared, active treatment was followed by a double-blind prophylactic treatment phase with itraconazole, 200 mg, or placebo twice on 1 day per month for 6 consecutive months. Patients were randomly allocated to 1 of the 2 treatments in the prophylactic phase. Patients who fulfilled the inclusion and exclusion criteria at the first visit (baseline) received itraconazole therapy for 7 days (treatment phase). Five weeks from the start of therapy (ie, 4 weeks after treatment), patients who were mycologically cured (no hyphae present) were randomized into the double-blind prophylactic phase to receive either itraconazole or placebo treatment for 6 months. Inclusion criteria for subjects included those aged 12 to 70 years who had a clinical diagnosis of pityriasis versicolor confirmed by mycological examination and who provided written informed consent before inclusion into the trial. Exclusion criteria for subjects included those with (1) known sensitivity to itraconazole or its excipients, (2) chronic mucocutaneous candidiasis or systemic fungal infection, (3) immunosuppression caused by disease or treatment, (4) any other disease or condition that in the investigator s opinion should exclude the patient from the trial, and those who (5) participated in an investigational drug trial within 30 days of selection, (6) were pregnant or breastfeeding, and (7) were women of childbearing potential without adequate contraception. The following therapies were not allowed: (1) topical antifungal agents, topical corticosteroids, shampoos with active ingredients against Malassezia, or tar shampoos used within 2 weeks of the randomization visit or during the trial (topical corticosteroid nasal sprays or eye ointments were allowed during the trial); (2) systemic corticosteroid therapy either within 1 month of the randomization visit or during the trial; (3) systemic antifungal therapy within 2 months of the randomization visit or during the trial; (4) use of the enzymeinducing drugs rifampin, phenytoin, rifabutin, carbamazepine, and isoniazid; and (5) use of some drugs metabolized by cytochrome P4503A4 with concomitant increase in their concentrations (eg, terfenadine, astemizole, cisapride, oral midazolam hydrochloride, triazolam, quinidine gluconate, pimozide, and 3-hydroxy-3-methylglutaryl coenzyme A reductase inhibitors). Other medications known to interact with itraconazole were monitored if they were being taken concurrently. Because absorption of itraconazole is impaired when gastric acidity is decreased, acid-neutralizing agents (eg, aluminum hydroxide) should be administered at least 2 hours after the intake of itraconazole. Itraconazole should be administered with 2 glasses of a cola beverage in individuals with achlorhydria or those taking acid secretion suppressors (eg, H 2 -antagonists and proton pump inhibitors). Patients could be withdrawn from the trial if (1) a serious adverse event occurred or (2) the investigator considered it in the best interest of the patient for safety reasons. Patients were withdrawn from the trial if they withdrew their consent or if the randomization code was broken. METHODS OF ASSIGNING PATIENTS TO TREATMENT GROUPS All patients admitted to the trial entered the open treatment phase. Patients who were mycologically cured (no hyphae present) at the end of week 5 from the start of therapy were allocated to one of the treatment groups in the doubleblind prophylactic phase using a predetermined randomization code generated at a central site. At each participating medical center, medication numbers were assigned consecutively starting with the lowest available number. Therefore, the investigator was not aware of the randomization code. DETERMINATION OF SAMPLE SIZE The primary variable was the mycological cure rate at the end of open treatment and at the end of prophylactic treatment. Mycological cure was described as negative findings on light microscopic examination. Mycological cure was expected to occur in 85% of patients who underwent itraconazole treatment in the first treatment phase, in 89% who underwent prophylactic treatment with itraconazole, and in 71% who underwent placebo prophylaxis. To be able to detect this difference with a power of 80% at the 5% level of significance, 74 patients are required in each treatment group. Assuming a mycological cure rate of 85%, 174 patients would be required to start the first treatment phase to have 148 patients to randomize between the groups receiving placebo and active therapy in the prophylactic is the first study to evaluate this regimen of itraconazole as a prophylactic measure against pityriasis versicolor. RESULTS PATIENT DISPOSITION There were 239 patients recruited. One patient withdrew consent and received no treatment. Therefore, 238 patients entered the open treatment phase and received itraconazole, 200 mg/d for 7 days. Demographic and other baseline characteristics of the patients are given in Table 1. Data are presented on an on-protocol basis (ie, having excluded patients who were characterized as having a major protocol deviation). Twenty-nine patients who received treatment in the open phase did not continue into the double-blind prophylactic phase. Of these, 18 were not cured and 11 were lost to follow-up or were noncompliant. At the end of open treatment, mycological cure was recorded in 205 (92%) of 223 patients (Table 2). All patients randomized into the double-blind prophylactic phase were mycologically negative at the time of randomization. At the end of the prophylactic phase, 90 (88%) of 102 patients in the itraconazole group and 56 (57%) of 99 in the placebo group were still mycologically negative (P.001) (Table 2). CLINICAL GLOBAL EVALUATION Findings were scored as cured, marked improvement, moderate improvement, unchanged, or deteriorated. Global 70
3 tients during the open treatment phase and in 2 in the itraconazole group during the prophylactic treatment phase. All these adverse events were mild to moderate in intensity, except for severe pruritus in 1 patient. All patients continued in the trial except for 1 in open treatment who experienced urticaria and was withdrawn. Two patients in open treatment and 4 in the placebo group of prophylactic treatment were withdrawn from the trial because of adverse events. Moderate urticaria in 1 patient was the only adverse event leading to withdrawal that was considered to be very likely related to trial medication use. No patients experienced a severe adverse event. The most common adverse events during open treatment were gastrointestinal tract complaints, which were reported by 9 patients (4%). There were no reports of gastrointestinal tract complaints during prophylactic treattreatment phase of the study. To account for a dropout rate of approximately 10%, at least 194 patients needed to be recruited for the trial. SAFETY ANALYSIS An evaluation of adverse events was performed on all patients who received the trial medication at least once. An additional intent-to-treat analysis was performed on all randomized patients who had at least 1 administration of the prophylactic treatment medication and who had efficacy data after visit 2. INITIAL CHARACTERIZATION OF PATIENT SAMPLE For the open treatment phase, all data were tabulated and were descriptively presented with 95% confidence intervals. Comparability between treatment groups was evaluated with respect to the demographic and baseline data. For continuous data (eg, age), the Van Elteren test was applied. For nominal categorical data (eg, sex and race), the Cochran-Mantel- Haenszel test for general association was used. For ordinal categoricaldata(eg, clinicalglobalevaluationscores), thecochran-mantel-haenszel row mean scores differences test was used. All data were analyzed descriptively. EFFICACY VARIABLES The primary variable was the mycological cure rate at the end of open treatment and at the end of prophylactic treatment. Mycological cure was defined as no hyphae present. Samples for microscopy were always taken from the same area. The cure rate at the end of the open treatment phase was tabulated. Itraconazole and placebo prophylaxis were compared at the end of the prophylactic treatment phase using the Cochran-Mantel-Haenszel test for general association. Secondary variables included clinical global evaluation scores and signs and symptoms of disease. All data were analyzed descriptively per time point. In the open treatment phase, all data were analyzed descriptively only. Changes from visit 1 (baseline) were analyzed using the Wilcoxon signed rank test for ordinal and continuous data and the McNemar test for dichotomous data. In the prophylactic treatment phase, between-group differences for dichotomous data were investigated using the Cochran- Mantel-Haenszel test for general association. Groups were compared for ordinal data using the Cochran-Mantel- Haenszel row mean scores differences test. Comparisons were performed for continuous data using the Van Elteren test. Within-group changes from randomization visit 2 were analyzed using the Wilcoxon signed rank test for ordinal and continuous data and the McNemar test for dichotomous data. Time-to-recurrence data were analyzed using the Mantel-Cox test. ASSESSMENTS For efficacy evaluations, patients had to be seen preferably by the same physician at each trial visit to maintain uniformity across clinical evaluations. Primary Efficacy Variable The primary efficacy variable was the mycological cure rate assessed at the end of weeks 5 and 29. Mycological cure was defined as negative microscopic results (negative potassium hydroxide preparation). For mycological evaluation, skin scrapings were taken from the active border of the lesion. Secondary Efficacy Variables Signs and Symptoms. Hyperpigmentation, hypopigmentation, itching, erythema, and latent desquamation were assessed according to absence or presence at each visit. Clinical Global Evaluation. At each visit, findings from clinical evaluation were rated as follows: cured (absence of all symptoms vs baseline, except hyperpigmentation or hypopigmentation); marked improvement (clinical improvement 50% vs baseline); moderate improvement (clinical improvement 0% to 50% vs baseline); unchanged (no change in symptoms vs baseline); and deterioration (worsening of symptoms vs baseline). Patient Compliance. Compliance was measured by patient self-assessment and by blister card reconciliation at the end of open treatment and during prophylactic treatment. Self-assessment consisted of the patient recording in a diary the number of capsules taken per dose of trial medication, the time of each intake, and the dates. evaluation scores were significantly better in the itraconazole group compared with the placebo group when evaluated at the prophylactic treatment end point (P.001). For all variables (erythema, hypopigmentation, desquamation, and itching), the itraconazole group showed significantly superior changes at the prophylactic treatment end point compared with the placebo group. ADVERSE EVENTS Adverse events were reported by 26 patients (11%) during open treatment and 31 (15%) during prophylactic treatment (17 patients [16%] in the itraconazole group and 14 [14%] in the placebo group). Adverse events considered to be possibly, probably, or very likely drug related were reported in 10 pa- 71
4 Table 1. Demographic and Other Baseline Characteristics of the Study Population Open Treatment Phase (n = 29) ment. The most common adverse events during prophylactic treatment were upper respiratory tract infection (reported by 4 patients [4%] in the itraconazole group and 4 [4%] in the placebo group) and influenza-like symptoms (reported by 1 patient [1%] in the itraconazole group and 4 [4%] in the placebo group). COMMENT Prophylactic Treatment Phase Itraconazole (n = 106) Placebo (n = 103) Sex, No. (%) M 14 (48) 56 (53) 60 (58) F 15 (52) 50 (47) 43 (42) Age, median (range), y 30 (14-53) 30 (12-62) 30 (12-65) Race, No. Black White Hispanic Asian Other Height, median (range), cm 170 ( ) 170 ( ) 170 ( ) Weight, median (range), kg 67 (50-95) 70 (45-97) 69 (41-142) Table 2. Results of Open and Prophylactic Treatment With Itraconazole in Patients With Pityriasis (Tinea) Versicolor Patients, No./Total No. (%) Protocol Deviation Cured (Lost) Open treatment end point 205/223 (92) 15/238 (6)* Prophylactic treatment end point Itraconazole 90/102 (88) 1/103 (1) Placebo 56/99 (57) 3/102 (3) *Lost to follow-up (n = 8); noncompliant (n = 6); and withdrew consent (n = 1). Insufficient data (n = 1). Intercurrent therapy (n = 2) and insufficient data (n = 1). Itraconazole was effective in this study in the treatment of pityriasis versicolor, with mycological cure in 92% of patients evaluated 5 weeks after the start of therapy. The efficacy rate was consistent with that reported in previous studies The excellent in vitro activity of itraconazole against Malassezia species and its high lipophilicity and accumulation in sebaceous glands 19 support the high efficacy rates recorded when patients were evaluated 5 weeks after the start of therapy and for the placebo prophylactic group at the end of 6 months follow-up. The high rate of recurrence, reaching as much as 60% in 1 year and 80% in 2 years, is an important consideration in pityriasis versicolor. 8 Clinical disease manifests itself when there is conversion of the saprophytic (blastopore) form of Malassezia species to the mycelial form. In immunocompetent individuals, factors predisposing to recurrence may be difficult to eradicate, including a tendency toward seborrhea and heavy sweating in the presence of high temperature and high humidity. There may be an inherited predisposition to the disease. A permanent cure may therefore be difficult to achieve, and this may explain the long-term nature of the disease. Consequently, a prophylactic regimen may help avoid recurrence of pityriasis versicolor. Prophylactic regimens using ketoconazole include 200 mg given on 3 consecutive days every month 20 or a single dose of 400 mg taken once a month. 21,22 Topical therapies have been used as a prophylactic, but patient compliance is lower, and no controlled studies have been reported in the literature, to our knowledge. The present study was designed to determine whether recurrence of pityriasis versicolor could be prevented by administering prophylactic itraconazole, 400 mg once a month. To our knowledge, such a study has not been reported previously. Our results demonstrate that prophylactic therapy with itraconazole was effective in preventing development of the disease during the 6-month study. There are no documented studies of topical prophylactic treatment in the literature, to our knowledge. Compliance with topical treatment is probably lower because it is more time-consuming and therefore more difficult to convince the patient to perform than oral treatment. This prophylactic treatment procedure with 1 treatment day per month with itraconazole could be used primarily in patients with frequent recurrences. The prophylactic regimen of itraconazole, 400 mg administrated once a month, was not only effective but also safe and had high compliance. Accepted for publication May 23, This study was supported by an unrestricted educational grant from Janssen Pharmaceutica. We thank the following individuals for recruiting patients for the study: T. Novak Gregurek (Croatia); H. Eltonsy, A. Farag, N. Saleh, and Z. Tosson (Egypt); M. Guimaraes and A. Massa (Portugal); A. Abanami and A. Mofadi (Saudi Arabia); P. Procter, N. Rabobee, W. Sinclair, and J. van Heerden (South Africa); J. Faergemann (Sweden); and A. Abu Shareeah (United Arab Emirates). Corresponding author and reprints: Jan Faergemann, MD, PhD, Department of Dermatology, Sahlgrenska University Hospital, S Gothenburg, Sweden ( jan.faergemann@derm.gu.se). REFERENCES 1. Sunenshine PJ, Schwartz RA, Janniger CK. Tinea versicolor. Int J Dermatol. 1998; 37: Faergemann J. Management of seborrheic dermatitis and pityriasis versicolor. Am J Clin Dermatol. 2000;1: Heres J, Backx LJ, Van Custem J, et al. Antimycotic azoles, part 7: synthesis and antifungal properties of a series of novel triazole-3-ones. J Med Chem. 1984;27: Van Custem J. The in-vitro antifungal spectrum of itraconazole. Mycoses. 1989; 32(suppl 1): Van Custem J. Oral and parenteral treatment with itraconazole in various super- 72
5 ficial and systemic experimental fungal infections: comparisons with other antifungal and combination therapy. Br J Clin Pract. 1990;44(suppl 71): De Doncker P, Gupta AK, Marynissen G, et al. Itraconazole pulse therapy for onychomycosis and dermatomycoses: an overview. J Am Acad Dermatol. 1997;37: Delescluse J, Cauwenbergh G, Degreef H. Itraconazole, a new orally active antifungal in the treatment of pityriasis versicolor. Br J Dermatol. 1986;14: Faergemann J. Pityrosporum infections. J Am Acad Dermatol. 1994;31(suppl): S18-S Estrada RA. Itraconazole in pityriasis versicolor. Rev Infect Dis. 1987;9:S128- S Kose O. Fluconazole versus itraconazole in the treatment of tinea versicolor. Int J Dermatol. 1995;34: Shemer A, Nathansohn N, Kaplan B, Trau H. Itraconazole versus ketoconazole in the treatment of tinea versicolor. J Dermatol Treat. 1999;10: Montero-Gei F, Robles ME, Suchil P. Fluconazole vs itraconazole in the treatment of tinea versicolor. Int J Dermatol. 1999;38: Hernanz ADP, Frias-Iniesta J, Gonzalez-Valle O, Borgers M, Van Cutsem J, Cauwenbergh G. Itraconazole therapy in pityriasis versicolor. Br J Dermatol. 1986; 115: Faergemann J. Treatment of pityriasis versicolor with itraconazole: a doubleblind placebo controlled study. Mycoses. 1988;31: Hickman JG. A double-blind, randomized, placebo-controlled evaluation of shortterm treatment with oral itraconazole in patients with tinea versicolor. JAmAcad Dermatol. 1996;34: Robertson LI. Itraconazole in the treatment of widespread tinea versicolor. Clin Exp Dermatol. 1987;12: Panconesi E, Difonzo E. Treatment of dermatophytoses and pityriasis versicolor with itraconazole. Rev Infect Dis. 1987;9(suppl 1):S109-S Morales-Doria M. Pityriasis versicolor: efficacy of two five-day regimens of itraconazole. Rev Infect Dis. 1987;9(suppl 1):S131-S Cauwenbergh G, Degreef H, Heykants J, Wostenborghs R, Van Rooy P, Haeverans K. Pharmacokinetic profile of orally administered itraconazole in human skin. J Am Acad Dermatol. 1988;18: Faergemann J, Djärv L. Tinea versicolor: treatment and prophylaxis with ketoconazole. Cutis. 1982;30: Rausch LJ, Jacobs PH. Tinea versicolor: treatment and prophylaxis with monthly administration of ketoconazole. Cutis. 1964;34: Gupta AK, Del Rosso JQ. An evaluation of intermittent therapies used to treat onychomycosis and other dermatomycoses with the oral antifungal agents. Int J Dermatol. 2000;39: News and Notes R ichard B. Stoughton Memorial Travel Fellowship applications are invited from US dermatology residents. The fellowship will enable a dermatologist in training to present a poster and attend the British Association of Dermatologists Annual Scientific Meeting in Edinburgh from July 9 to July 12, The winner will receive free registration and admittance to the president s reception and annual dinner. Accommodation will also be offered free of charge. The closing date for completed applications is Friday, February 8, For further details and application forms please contact the BAD Fellowship Co-ordinator, British Association of Dermatologists, 19 Fitzroy Square, London W1T 6EH, England. Phone: ; Fax: ( admin@bad.org.uk). 73
THERAPEUTIC EFFICACY OF DIFFERENT AZOLE ANTIFUNGAL REGIMENS IN TREATMENT OF TINEA VERSICOLOR
 I.J.A.B.R., VOL. 2(4) 2012: 766-771 ISSN 2250-3579 THERAPEUTIC EFFICACY OF DIFFERENT AZOLE ANTIFUNGAL REGIMENS IN TREATMENT OF TINEA VERSICOLOR a Maytham M. Al-Hilo, b Hala K.AL-Obaidi, b Ahmed Samir Al-
I.J.A.B.R., VOL. 2(4) 2012: 766-771 ISSN 2250-3579 THERAPEUTIC EFFICACY OF DIFFERENT AZOLE ANTIFUNGAL REGIMENS IN TREATMENT OF TINEA VERSICOLOR a Maytham M. Al-Hilo, b Hala K.AL-Obaidi, b Ahmed Samir Al-
Itraconazole DIGICON. Composition: MOLECULAR INTRODUCTION
 Itraconazole DIGICON Composition: Itraconazole 100 mg MOLECULAR INTRODUCTION Itraconazole is a triazole medicine used to treat fungal infections. It is effective against a broad spectrum of fungi including:
Itraconazole DIGICON Composition: Itraconazole 100 mg MOLECULAR INTRODUCTION Itraconazole is a triazole medicine used to treat fungal infections. It is effective against a broad spectrum of fungi including:
Fungal Resistance, Biofilm, and Its Impact In the Management of Nail Infection
 Fungal Resistance, Biofilm, and Its Impact In the Management of Nail Infection Faculty Raza Aly, PhD, MPH Professor Emeritus University of California Medical Center (MSSF) Professor, Dermatology Faculty
Fungal Resistance, Biofilm, and Its Impact In the Management of Nail Infection Faculty Raza Aly, PhD, MPH Professor Emeritus University of California Medical Center (MSSF) Professor, Dermatology Faculty
Clinical Practice Guideline Superficial Fungal Infection
 Clinical Practice Guideline Superficial Fungal Infection ก ก ก กก ก ก ก ก กก ก ก ก ก ก ก ก ก ก ก ก ก ก ก ก ก ก ก * ก Superficial fungal infection ก 1. ก (Pityriasis versicolor, Tinea versicolor) 2. ก ก
Clinical Practice Guideline Superficial Fungal Infection ก ก ก กก ก ก ก ก กก ก ก ก ก ก ก ก ก ก ก ก ก ก ก ก ก ก ก * ก Superficial fungal infection ก 1. ก (Pityriasis versicolor, Tinea versicolor) 2. ก ก
A COMPARATIVE STUDY OF EFFICACY OF TERBINAFINE AND FLUCONAZOLE IN PATIENTS OF TINEA CORPORIS
 Int. J. Pharm. Med. & Bio. Sc. 2013 Kumar Amit et al., 2013 Research Paper ISSN 2278 5221 www.ijpmbs.com Vol. 2, No. 4, October 2013 2013 IJPMBS. All Rights Reserved A COMPARATIVE STUDY OF EFFICACY OF
Int. J. Pharm. Med. & Bio. Sc. 2013 Kumar Amit et al., 2013 Research Paper ISSN 2278 5221 www.ijpmbs.com Vol. 2, No. 4, October 2013 2013 IJPMBS. All Rights Reserved A COMPARATIVE STUDY OF EFFICACY OF
ITRANOX. Composition Each capsule contains :
 ITRANOX Composition Each capsule contains : Itraconazole 100 mg Capsules Action Itraconazole is a synthetic triazole derivative. When administered orally, it has shown fungistatic activity against superficial
ITRANOX Composition Each capsule contains : Itraconazole 100 mg Capsules Action Itraconazole is a synthetic triazole derivative. When administered orally, it has shown fungistatic activity against superficial
PFIZER INC. THERAPEUTIC AREA AND FDA APPROVED INDICATIONS: See USPI
 PFIZER INC. These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert. For publications based on this study, see associated bibliography.
PFIZER INC. These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert. For publications based on this study, see associated bibliography.
NIZORAL (KETOCONAZOLE) 2% SHAMPOO DESCRIPTION
 NIZORAL (KETOCONAZOLE) 2% SHAMPOO DESCRIPTION NIZORAL (ketoconazole) 2% Shampoo is a red-orange liquid for topical application, containing the broad spectrum synthetic antifungal agent ketoconazole in
NIZORAL (KETOCONAZOLE) 2% SHAMPOO DESCRIPTION NIZORAL (ketoconazole) 2% Shampoo is a red-orange liquid for topical application, containing the broad spectrum synthetic antifungal agent ketoconazole in
Amruta Mohite 1, Anil Gugle 2*, Rahul Kote 3 and Vikrant Jadhav 4
 MVP Journal of Medical Sciences, Vol 2(2), 76-80, July-December 2015 A Comparative Study of Efficacy, Safety and Relapse Rate of Three Drugs; Systemic Ketoconazole, Systemic Itraconazole and Topical Oxiconazole
MVP Journal of Medical Sciences, Vol 2(2), 76-80, July-December 2015 A Comparative Study of Efficacy, Safety and Relapse Rate of Three Drugs; Systemic Ketoconazole, Systemic Itraconazole and Topical Oxiconazole
IJBCP International Journal of Basic & Clinical Pharmacology
 Print ISSN 2319-2003 Online ISSN 2279-0780 IJBCP International Journal of Basic & Clinical Pharmacology doi: 10.18203/2319-2003.ijbcp20150020 Research Article Efficacy safety of 1% terbinafine hydrochloride
Print ISSN 2319-2003 Online ISSN 2279-0780 IJBCP International Journal of Basic & Clinical Pharmacology doi: 10.18203/2319-2003.ijbcp20150020 Research Article Efficacy safety of 1% terbinafine hydrochloride
PFIZER INC. Study Initiation Date and Completion Dates: Information not available (Date of Statistical Report: 16 May 2004)
 PFIZER INC. These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert. For publications based on this study, see associated bibliography.
PFIZER INC. These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert. For publications based on this study, see associated bibliography.
Treatment of Pityriasis Versicolor. A Comparative Study of Topical 4% Potassium Hydroxide Solution Versus 1% Clotrimazole Solution
 British Journal of Medicine & Medical Research 3(4): 2317-2324, 2013 SCIENCEDOMAIN international www.sciencedomain.org Treatment of Pityriasis Versicolor. A Comparative Study of Topical 4% Potassium Hydroxide
British Journal of Medicine & Medical Research 3(4): 2317-2324, 2013 SCIENCEDOMAIN international www.sciencedomain.org Treatment of Pityriasis Versicolor. A Comparative Study of Topical 4% Potassium Hydroxide
Pharmacokinetics of three doses of once-weekly fluconazole (150, 300, and 450 mg) in distal subungual onychomycosis of the toenail
 SUPPORTED BY AN EDUCATIONAL GRANT FROM U.S. PHARMACEUTICALS, PFIZER INC. Pharmacokinetics of three doses of once-weekly fluconazole (150, 300, and 450 mg) in distal subungual onychomycosis of the toenail
SUPPORTED BY AN EDUCATIONAL GRANT FROM U.S. PHARMACEUTICALS, PFIZER INC. Pharmacokinetics of three doses of once-weekly fluconazole (150, 300, and 450 mg) in distal subungual onychomycosis of the toenail
16.9 hours. Not reported 19.9 hours. Metabolism: Not known Elimination: Not known. Efficacy:
 Brand Name: Luzu Generic Name: luliconazole Manufacturer 1 : Medicis Pharmaceutical Corporation Drug Class 1,2,3,4 : Imidazole antifungal, topical Uses Labeled Uses 1,2,3,4 : Topical treatment of interdigital
Brand Name: Luzu Generic Name: luliconazole Manufacturer 1 : Medicis Pharmaceutical Corporation Drug Class 1,2,3,4 : Imidazole antifungal, topical Uses Labeled Uses 1,2,3,4 : Topical treatment of interdigital
Fungi are eukaryotic With rigid cell walls composed largely of chitin rather than peptidoglycan (a characteristic component of most bacterial cell
 Antifungal Drugs Fungal infections (Mycoses) Often chronic in nature. Mycotic infections may be superficial and involve only the skin (cutaneous mycoses extending into the epidermis) Others may penetrate
Antifungal Drugs Fungal infections (Mycoses) Often chronic in nature. Mycotic infections may be superficial and involve only the skin (cutaneous mycoses extending into the epidermis) Others may penetrate
Public Assessment Report for paediatric studies submitted in accordance with Article 45 of Regulation (EC) No1901/2006, as amended
 Public Assessment Report for paediatric studies submitted in accordance with Article 45 of Regulation (EC) No1901/2006, as amended -containing tablets, shampoo and cream DK/W/0012/pdWS/001 Rapporteur:
Public Assessment Report for paediatric studies submitted in accordance with Article 45 of Regulation (EC) No1901/2006, as amended -containing tablets, shampoo and cream DK/W/0012/pdWS/001 Rapporteur:
Antifungal drugs Dr. Raz Muhammed
 Antifungal drugs 13. 12. 2018 Dr. Raz Muhammed 2. Flucytosine (5-FC) Is fungistatic Is a synthetic pyrimidine antimetabolite Is often used in combination with amphotericin B in the treatment of systemic
Antifungal drugs 13. 12. 2018 Dr. Raz Muhammed 2. Flucytosine (5-FC) Is fungistatic Is a synthetic pyrimidine antimetabolite Is often used in combination with amphotericin B in the treatment of systemic
Catamaran Prior Authorization Department. Phone: Fax: Prescriber Information. Member Information.
 Prescriber Information Last Name First Name DEA / NPI Specialty Phone Member Information Last Name Fax - - - - First Name Member ID Number DOB Medication Information: Drug Name and Strength: Quantity:
Prescriber Information Last Name First Name DEA / NPI Specialty Phone Member Information Last Name Fax - - - - First Name Member ID Number DOB Medication Information: Drug Name and Strength: Quantity:
Outline Dermatomycoses Definition: diseases or fungal infections of the skin Transmission of Dermatomycoses Case Report 1 Presentation of Disease
 Outline Dermatomycoses Tinea corporis,tinea capitis,tinea pedis, Tinea cruris, Definition: diseases or fungal infections of the skin Dermatophyte infections are caused by Trichophyton, Microsporum, and
Outline Dermatomycoses Tinea corporis,tinea capitis,tinea pedis, Tinea cruris, Definition: diseases or fungal infections of the skin Dermatophyte infections are caused by Trichophyton, Microsporum, and
Skin disorders. Seborrhoeic dermatitis Search date April 2010 Luigi Naldi ...
 Seborrhoeic Search date April 21 Luigi Naldi.................................................. ABSTRACT INTRODUCTION: Seborrhoeic affects at least 1% of the population. Malassezia (Pityrosporum) ovale
Seborrhoeic Search date April 21 Luigi Naldi.................................................. ABSTRACT INTRODUCTION: Seborrhoeic affects at least 1% of the population. Malassezia (Pityrosporum) ovale
Concomitant antiretroviral therapy : Avifanz must be given in combination with other antiretroviral medications.
 Avifanz Tablet Description Avifanz is the brand name for Efavirenz. Efavirenz, a synthetic antiretroviral agent, is a non-nucleoside reverse transcriptase inhibitor. While Efavirenz is pharmacologically
Avifanz Tablet Description Avifanz is the brand name for Efavirenz. Efavirenz, a synthetic antiretroviral agent, is a non-nucleoside reverse transcriptase inhibitor. While Efavirenz is pharmacologically
CANDIDIASIS (WOMEN) Single Episode. Clinical Features. Diagnosis. Management
 CANDIDIASIS (WOMEN) What s new: Section on Management of Vulvovaginal Non-Albicans Candida Infection in Adults approved by GGC antimicrobial team Routine candida sensitivity testing has been discontinued,
CANDIDIASIS (WOMEN) What s new: Section on Management of Vulvovaginal Non-Albicans Candida Infection in Adults approved by GGC antimicrobial team Routine candida sensitivity testing has been discontinued,
Modelling A decision tree was used to estimate benefits and costs of alternative agents.
 Economic evaluation of antifungal agents in the treatment of toenail onychomycosis in Germany Van Doorslaer E K, Tormans G, Gupta A K, Van Rossem K, Eggleston A, Dubois D J, De Doncker P, Haneke E Record
Economic evaluation of antifungal agents in the treatment of toenail onychomycosis in Germany Van Doorslaer E K, Tormans G, Gupta A K, Van Rossem K, Eggleston A, Dubois D J, De Doncker P, Haneke E Record
REGIONAL ADMINISTRATIVE INFORMATION
 MODULE 1: Module 1.3.1 REGIONAL ADMINISTRATIVE INFORMATION Summary of Product Characteristics 1. Name of the medicinal product 2. Qualitative and quantitative composition Each capsule contains 100 mg of
MODULE 1: Module 1.3.1 REGIONAL ADMINISTRATIVE INFORMATION Summary of Product Characteristics 1. Name of the medicinal product 2. Qualitative and quantitative composition Each capsule contains 100 mg of
Assistant Professor 2 Professor, Department of Pharmacology, Govt. Stanley Medical College& Hospital, Chennai, Tamilnadu, India
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 79-085, p-issn: 79-086.Volume 4, Issue 0 Ver.III (Oct. 05), PP 97-04 www.iosrjournals.org A Randomized Open Label Comparative Study of Once
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 79-085, p-issn: 79-086.Volume 4, Issue 0 Ver.III (Oct. 05), PP 97-04 www.iosrjournals.org A Randomized Open Label Comparative Study of Once
REGIONAL ADMINISTRATIVE INFORMATION. 3. Pharmaceutical form Capsule, hard Elongated, red opaque hard gelatine capsule (size 0)
 MODULE 1: Module 1.3.1 REGIONAL ADMINISTRATIVE INFORMATION Summary of Product Characteristics 1. Name of the medicinal product 2. Qualitative and quantitative composition Each capsule contains 100 mg of
MODULE 1: Module 1.3.1 REGIONAL ADMINISTRATIVE INFORMATION Summary of Product Characteristics 1. Name of the medicinal product 2. Qualitative and quantitative composition Each capsule contains 100 mg of
SYNOPSIS. Study center(s) This study was conducted in the United States (128 centers).
 Drug product: Drug substance(s): Document No.: Edition No.: Study code: Date: SYMBICORT pmdi 160/4.5 µg Budesonide/formoterol SD-039-0725 17 February 2005 SYNOPSIS A Twelve-Week, Randomized, Double-blind,
Drug product: Drug substance(s): Document No.: Edition No.: Study code: Date: SYMBICORT pmdi 160/4.5 µg Budesonide/formoterol SD-039-0725 17 February 2005 SYNOPSIS A Twelve-Week, Randomized, Double-blind,
Trial No.: RIS-USA-102 Clinical phase: III
 SYNOPSIS Trial identification and protocol summary Company: Johnson & Johnson Pharmaceutical Research and Development, a division of Janssen Pharmaceutica, N.V. Finished product: Risperdal Active ingredient:
SYNOPSIS Trial identification and protocol summary Company: Johnson & Johnson Pharmaceutical Research and Development, a division of Janssen Pharmaceutica, N.V. Finished product: Risperdal Active ingredient:
To order reprints or e-prints of JDD articles please contact JDD
 June 2017 534 VOLUME 16 ISSUE 6 Copyright 2017 ORIGINAL ARTICLE Journal of Drugs in Dermatology The Efficacy and Safety of Azelaic Acid 15% Foam in the Treatment of Truncal Acne Vulgaris Lauren K. Hoffman
June 2017 534 VOLUME 16 ISSUE 6 Copyright 2017 ORIGINAL ARTICLE Journal of Drugs in Dermatology The Efficacy and Safety of Azelaic Acid 15% Foam in the Treatment of Truncal Acne Vulgaris Lauren K. Hoffman
Janssen-Cilag EMEA Medical Affairs a division of Janssen Pharmaceuticals N.V.
 SYNOPSIS Issue Date: Final 22 July 2009 [Document No.: EDMS-PSDB-9245102] Name of Sponsor/Company Name of Finished Product Risperdal Consta Name of Active Ingredient(s) Protocol No.: RIS-BMN-3001 Janssen-Cilag
SYNOPSIS Issue Date: Final 22 July 2009 [Document No.: EDMS-PSDB-9245102] Name of Sponsor/Company Name of Finished Product Risperdal Consta Name of Active Ingredient(s) Protocol No.: RIS-BMN-3001 Janssen-Cilag
Therapeutics for the Clinician
 Luliconazole for the Treatment of Interdigital Tinea Pedis: A Double-blind, Vehicle-Controlled Study Michael Jarratt, MD; Terry Jones, MD; Steven Kempers, MD; Phoebe Rich, MD; Katy Morton; Norifumi Nakamura,
Luliconazole for the Treatment of Interdigital Tinea Pedis: A Double-blind, Vehicle-Controlled Study Michael Jarratt, MD; Terry Jones, MD; Steven Kempers, MD; Phoebe Rich, MD; Katy Morton; Norifumi Nakamura,
Clinical Study Synopsis
 Clinical Study Synopsis This Clinical Study Synopsis is provided for patients and healthcare professionals to increase the transparency of Bayer's clinical research. This document is not intended to replace
Clinical Study Synopsis This Clinical Study Synopsis is provided for patients and healthcare professionals to increase the transparency of Bayer's clinical research. This document is not intended to replace
Comparison of KOH Mount Using Standard Technique and Cellophane Tape Method for Diagnosis of Superficial Fungal Infections
 International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 6 Number 10 (2017) pp. 494-499 Journal homepage: http://www.ijcmas.com Original Research Article https://doi.org/10.20546/ijcmas.2017.610.060
International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 6 Number 10 (2017) pp. 494-499 Journal homepage: http://www.ijcmas.com Original Research Article https://doi.org/10.20546/ijcmas.2017.610.060
PFIZER INC. GENERIC DRUG NAME and/or COMPOUND NUMBER: 5% Spironolactone Cream/ PF
 PFIZER INC. These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert. For publications based on this study, see associated bibliography.
PFIZER INC. These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert. For publications based on this study, see associated bibliography.
PFIZER INC. Study Initiation Date and Completion Dates: 09 March 2000 to 09 August 2001.
 PFIZER INC. These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert. For publications based on this study, see associated bibliography.
PFIZER INC. These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert. For publications based on this study, see associated bibliography.
SYNOPSIS. Issue Date: 25 Oct 2011
 SYNOPSIS Issue Date: 25 Oct 2011 Name of Sponsor/Company Name of Finished Product Name of Active Ingredient(s) Janssen Research & Development STELARA Ustekinumab Protocol No.: Title of Study: Study Name:
SYNOPSIS Issue Date: 25 Oct 2011 Name of Sponsor/Company Name of Finished Product Name of Active Ingredient(s) Janssen Research & Development STELARA Ustekinumab Protocol No.: Title of Study: Study Name:
Clinical Study Synopsis
 Clinical Study Synopsis This Clinical Study Synopsis is provided for patients and healthcare professionals to increase the transparency of Bayer's clinical research. This document is not intended to replace
Clinical Study Synopsis This Clinical Study Synopsis is provided for patients and healthcare professionals to increase the transparency of Bayer's clinical research. This document is not intended to replace
LUZU (luliconazole) external cream
 LUZU (luliconazole) external cream Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Pharmacy Coverage
LUZU (luliconazole) external cream Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Pharmacy Coverage
A class IIa medical device intended for mild-to-moderate fungal nail infection PRODUCT MONOGRAPH
 A class IIa medical device intended for mild-to-moderate fungal nail infection PRODUCT MONOGRAPH AWB-2052628721 Date of Preparation March 2017 Introduction to Bayer Bayer is a Life Science company with
A class IIa medical device intended for mild-to-moderate fungal nail infection PRODUCT MONOGRAPH AWB-2052628721 Date of Preparation March 2017 Introduction to Bayer Bayer is a Life Science company with
Antifungal Agents. Polyenes Azoles Allyl and Benzyl Amines Other antifungals
 OPTO 6434 General Pharmacology Antifungal Agents Dr. Alison McDermott Room 254 HBSB, Phone 713-743 1974 Email amcdermott@optometry.uh.edu Fall 2015 Reading: Chapter 50 Brody s Human Pharmacology by Wecker
OPTO 6434 General Pharmacology Antifungal Agents Dr. Alison McDermott Room 254 HBSB, Phone 713-743 1974 Email amcdermott@optometry.uh.edu Fall 2015 Reading: Chapter 50 Brody s Human Pharmacology by Wecker
During the last 20 years, the number of topical
 THERAPEUTICS FOR THE CLINICIAN Cumulative Irritation Potential of Adapalene 0.1% Cream and Gel Compared With Tretinoin Microsphere 0.04% and 0.1% Jonathan S. Dosik, MD; Kenneth Homer, MS; Stéphanie Arsonnaud
THERAPEUTICS FOR THE CLINICIAN Cumulative Irritation Potential of Adapalene 0.1% Cream and Gel Compared With Tretinoin Microsphere 0.04% and 0.1% Jonathan S. Dosik, MD; Kenneth Homer, MS; Stéphanie Arsonnaud
Source of effectiveness data The effectiveness evidence was derived from a systematic review of published studies.
 Pharmacoeconomic analysis of ciclopirox nail lacquer solution 8% and the new oral antifungal agents used to treat dermatophyte toe onychomycosis in the United States Gupta A K Record Status This is a critical
Pharmacoeconomic analysis of ciclopirox nail lacquer solution 8% and the new oral antifungal agents used to treat dermatophyte toe onychomycosis in the United States Gupta A K Record Status This is a critical
Comparative study for the reliability of cellophane tape and standard KOH mount in diagnosis of pityriasis versicolor
 ORIGINAL ARTICLE Comparative study for the reliability of cellophane tape and standard KOH mount in diagnosis of pityriasis versicolor Hussein M. M. Hassab-El-Naby, MD, Ahmad Sadek Mohamed Salem, MD Hamed
ORIGINAL ARTICLE Comparative study for the reliability of cellophane tape and standard KOH mount in diagnosis of pityriasis versicolor Hussein M. M. Hassab-El-Naby, MD, Ahmad Sadek Mohamed Salem, MD Hamed
DERMCASE. Doc, my baby s all spotty! Case 1
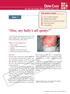 Test Your Knowledge With Multiple-Choice Cases This month 5 cases: Case 1 1. Doc, my baby s all spotty! 2. A Mediterranean Matter 3. Mommy, what s wrong with my head? 4. Armed with Lesions 5. It s spreading!
Test Your Knowledge With Multiple-Choice Cases This month 5 cases: Case 1 1. Doc, my baby s all spotty! 2. A Mediterranean Matter 3. Mommy, what s wrong with my head? 4. Armed with Lesions 5. It s spreading!
For the use only of Registered Medical Practitioners or a Hospital or a Laboratory ZODERM E CREAM. Oxiconazole Nitrate Cream
 For the use only of Registered Medical Practitioners or a Hospital or a Laboratory ZODERM E CREAM Oxiconazole Nitrate Cream QUALITATIVE AND QUANTITATIVE COMPOSITION ZODERM E CREAM contains: Oxiconazole
For the use only of Registered Medical Practitioners or a Hospital or a Laboratory ZODERM E CREAM Oxiconazole Nitrate Cream QUALITATIVE AND QUANTITATIVE COMPOSITION ZODERM E CREAM contains: Oxiconazole
forniture parafarmaceutiche
 User's Manual forniture parafarmaceutiche CONTENTS forniture parafarmaceutiche Dermatitis of the Scalp Seborrheic Dermatitis Treatments Atopshield Lotion The mechanism of action of Atopshield Lotion Indications
User's Manual forniture parafarmaceutiche CONTENTS forniture parafarmaceutiche Dermatitis of the Scalp Seborrheic Dermatitis Treatments Atopshield Lotion The mechanism of action of Atopshield Lotion Indications
Tinea Incognito Incorrect Initial Diagnosis. Case Series Presentation with Emphasis on the Mycological Examination
 CASE SERIES DERMATOLOGY // INTERNAL MEDICINE Tinea Incognito Incorrect Initial Diagnosis. Case Series Presentation with Emphasis on the Mycological Examination Anca Chiriac 1,2,3, Piotr Brzezinski 4, Cristian
CASE SERIES DERMATOLOGY // INTERNAL MEDICINE Tinea Incognito Incorrect Initial Diagnosis. Case Series Presentation with Emphasis on the Mycological Examination Anca Chiriac 1,2,3, Piotr Brzezinski 4, Cristian
Dermatomycosis is defined as nondermatophyte. Four Cases of Dermatomycosis: Superficial Cutaneous Infection by Alternaria or Bipolaris
 : Superficial Cutaneous Infection by Alternaria or Bipolaris Christopher W. Robb, PhD; Peter J. Malouf, DO; Ronald P. Rapini, MD Invasive dermal infections in immunosuppressed patients by a wide variety
: Superficial Cutaneous Infection by Alternaria or Bipolaris Christopher W. Robb, PhD; Peter J. Malouf, DO; Ronald P. Rapini, MD Invasive dermal infections in immunosuppressed patients by a wide variety
Dosage and Administration
 SIRTURO product information for healthcare providers 2 WARNINGS: An increased risk of death was seen in the SIRTURO (bedaquiline) treatment group (9/79, 11.4%) compared to the placebo treatment group (2/81,
SIRTURO product information for healthcare providers 2 WARNINGS: An increased risk of death was seen in the SIRTURO (bedaquiline) treatment group (9/79, 11.4%) compared to the placebo treatment group (2/81,
INDIVIDUAL STUDY TABLE REFERRING TO PART OF THE DOSSIER Volume: Page:
 SYNOPSIS Protocol No.: TOPMAT-MIG-303 EudraCT No.: 2005-000321-29 Title of Study: A double-blind, randomised, placebo-controlled, multicentre study to investigate the efficacy and tolerability of in prolonged
SYNOPSIS Protocol No.: TOPMAT-MIG-303 EudraCT No.: 2005-000321-29 Title of Study: A double-blind, randomised, placebo-controlled, multicentre study to investigate the efficacy and tolerability of in prolonged
PRODUCT MONOGRAPH NIZORAL. (ketoconazole 2% shampoo) Therapeutic Classification. Topical Antifungal Agent
 1 PRODUCT MONOGRAPH NIZORAL (ketoconazole 2% shampoo) Therapeutic Classification Topical Antifungal Agent Johnson & Johnson Inc. DATE OF REVISION: 88 McNabb Street October 19, 2010 Markham, Ontario L3R
1 PRODUCT MONOGRAPH NIZORAL (ketoconazole 2% shampoo) Therapeutic Classification Topical Antifungal Agent Johnson & Johnson Inc. DATE OF REVISION: 88 McNabb Street October 19, 2010 Markham, Ontario L3R
Abstract. OBJECTIVE--To compare the efficacy and safety of terbinafine 1% cream and clotrimazole 1% cream in the treatment of tinea pedis.
 Abstract. OBJECTIVE--To compare the efficacy and safety of terbinafine 1% cream and clotrimazole 1% cream in the treatment of tinea pedis. DESIGN-- Multicentre, double blind parallel group study. SETTING--32
Abstract. OBJECTIVE--To compare the efficacy and safety of terbinafine 1% cream and clotrimazole 1% cream in the treatment of tinea pedis. DESIGN-- Multicentre, double blind parallel group study. SETTING--32
Ali Alabbadi. Sarah Jaar ... Nader
 24 Ali Alabbadi Sarah Jaar... Nader Intro to Mycology *underlined text was explained in the lecture but is not found in the slides -mycology: the study of the mycoses of man (fungal infections) -less than
24 Ali Alabbadi Sarah Jaar... Nader Intro to Mycology *underlined text was explained in the lecture but is not found in the slides -mycology: the study of the mycoses of man (fungal infections) -less than
Malassezia Folliculitis: Prevalence, Clinical Features Risk Factors and Treatment: A Prospective Randomized Comparative Study
 Research Article imedpub Journals http://www.imedpub.com/ Malassezia Folliculitis: Prevalence, Clinical Features Risk Factors and Treatment: A Prospective Randomized Comparative Study Emna Bahlou 1 *,
Research Article imedpub Journals http://www.imedpub.com/ Malassezia Folliculitis: Prevalence, Clinical Features Risk Factors and Treatment: A Prospective Randomized Comparative Study Emna Bahlou 1 *,
2.0 Synopsis. Adalimumab R&D/04/118. (For National Authority Use Only) Referring to Part of Dossier: Volume:
 2.0 Synopsis Abbott Laboratories Name of Study Drug: Adalimumab Name of Active Ingredient: Adalimumab Title of Study: Individual Study Table Referring to Part of Dossier: Volume: Page: (For National Authority
2.0 Synopsis Abbott Laboratories Name of Study Drug: Adalimumab Name of Active Ingredient: Adalimumab Title of Study: Individual Study Table Referring to Part of Dossier: Volume: Page: (For National Authority
SYNOPSIS (PROTOCOL WX17796)
 TITLE OF THE STUDY A prospective, randomized, double-blind, placebo-controlled, parallel group, multicenter, 52-week trial to assess the efficacy and safety of adjunct MMF to achieve remission with reduced
TITLE OF THE STUDY A prospective, randomized, double-blind, placebo-controlled, parallel group, multicenter, 52-week trial to assess the efficacy and safety of adjunct MMF to achieve remission with reduced
Primary Endpoint The primary endpoint is overall survival, measured as the time in weeks from randomization to date of death due to any cause.
 CASE STUDY Randomized, Double-Blind, Phase III Trial of NES-822 plus AMO-1002 vs. AMO-1002 alone as first-line therapy in patients with advanced pancreatic cancer This is a multicenter, randomized Phase
CASE STUDY Randomized, Double-Blind, Phase III Trial of NES-822 plus AMO-1002 vs. AMO-1002 alone as first-line therapy in patients with advanced pancreatic cancer This is a multicenter, randomized Phase
SYNOPSIS THIS IS A PRINTED COPY OF AN ELECTRONIC DOCUMENT. PLEASE CHECK ITS VALIDITY BEFORE USE.
 Drug product: Drug substance(s): Document No.: Edition No.: 1 Study code: Accolate Zafirlukast (ZD9188) 9188IL/0138 Date: 02 May 2007 SYNOPSIS A Multicenter, Randomized, Double-blind, -controlled, Parallel
Drug product: Drug substance(s): Document No.: Edition No.: 1 Study code: Accolate Zafirlukast (ZD9188) 9188IL/0138 Date: 02 May 2007 SYNOPSIS A Multicenter, Randomized, Double-blind, -controlled, Parallel
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Cornely OA, Maertens J, Winston DJ, et al. Posaconazole vs.
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Cornely OA, Maertens J, Winston DJ, et al. Posaconazole vs.
Study No.: Title: Rationale: Phase: Study Period: Study Design: Centers: Indication: Treatment: Objectives: Primary Outcome/Efficacy Variable:
 The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
Summary of Product Characteristics
 Summary of Product Characteristics 1. NAME OF THE MEDICINAL PRODUCT Terbinafine Dermapharm, 10 mg/g, cream 2. QUALITATIVE AND QUANTITATIVE COMPOSITION One gram of cream contains 10 mg of terbinafine hydrochloride.
Summary of Product Characteristics 1. NAME OF THE MEDICINAL PRODUCT Terbinafine Dermapharm, 10 mg/g, cream 2. QUALITATIVE AND QUANTITATIVE COMPOSITION One gram of cream contains 10 mg of terbinafine hydrochloride.
Skin disorders. Seborrhoeic dermatitis Search date February 2007 Juan Jorge Manriquez and Pablo Uribe ...
 Search date February 27 Juan Jorge Manriquez and Pablo Uribe.................................................. ABSTRACT INTRODUCTION: affects at least 1 3% of the population. Malassezia (Pityrosporum)
Search date February 27 Juan Jorge Manriquez and Pablo Uribe.................................................. ABSTRACT INTRODUCTION: affects at least 1 3% of the population. Malassezia (Pityrosporum)
A randomized comparative study to determine the effect of omeprazole on the peak serum concentration of itraconazole oral solution
 Journal of Antimicrobial Chemotherapy (2003) 51, 453 457 DOI: 10.1093/jac/dkg089 Advance Access publication 14 January 2003 A randomized comparative study to determine the effect of omeprazole on the peak
Journal of Antimicrobial Chemotherapy (2003) 51, 453 457 DOI: 10.1093/jac/dkg089 Advance Access publication 14 January 2003 A randomized comparative study to determine the effect of omeprazole on the peak
Clinical Study Synopsis
 Clinical Study Synopsis This Clinical Study Synopsis is provided for patients and healthcare professionals to increase the transparency of Bayer's clinical research. This document is not intended to replace
Clinical Study Synopsis This Clinical Study Synopsis is provided for patients and healthcare professionals to increase the transparency of Bayer's clinical research. This document is not intended to replace
FORCAN Fluconazole tablets and injections. COMPOSITION Forcan-50 tablets Fluconazole USP mg. Forcan-150 tablets Fluconazole USP...
 FORCAN Fluconazole tablets and injections COMPOSITION Forcan-50 tablets Fluconazole USP... 50 mg Forcan-150 tablets Fluconazole USP... 150 mg Forcan-200 tablets Fluconazole USP... 200 mg Forcan I.V. Injection
FORCAN Fluconazole tablets and injections COMPOSITION Forcan-50 tablets Fluconazole USP... 50 mg Forcan-150 tablets Fluconazole USP... 150 mg Forcan-200 tablets Fluconazole USP... 200 mg Forcan I.V. Injection
CONSORT 2010 checklist of information to include when reporting a randomised trial*
 Supplemental Figures for: Ramosetron Versus Ondansetron in Combination with Aprepitant and Dexamethasone for the Prevention of Highly Emetogenic Chemotherapy-induced Nausea and Vomiting: A Multicenter,
Supplemental Figures for: Ramosetron Versus Ondansetron in Combination with Aprepitant and Dexamethasone for the Prevention of Highly Emetogenic Chemotherapy-induced Nausea and Vomiting: A Multicenter,
Classification. Distal & Lateral Subungual OM. White Superficial OM. Proximal Subungual OM. Candidal OM. Total dystrophic OM
 Onychomycosis Commonest dermatological condition Definition: Infection of the nail caused by fungi that include dermatophytes, non-dermatophyte moulds and yeasts (mainly Candida). 80% of all OM affects
Onychomycosis Commonest dermatological condition Definition: Infection of the nail caused by fungi that include dermatophytes, non-dermatophyte moulds and yeasts (mainly Candida). 80% of all OM affects
Clinical Study Synopsis
 Clinical Study Synopsis This Clinical Study Synopsis is provided for patients and healthcare professionals to increase the transparency of Bayer's clinical research. This document is not intended to replace
Clinical Study Synopsis This Clinical Study Synopsis is provided for patients and healthcare professionals to increase the transparency of Bayer's clinical research. This document is not intended to replace
Clinical Trial Results Database Page 1
 Clinical Trial Results Database Page 1 Sponsor Novartis Pharmaceuticals Corporation Generic Drug Name Therapeutic Area of Trial Major Depressive Disorder (MDD) Approved Indication Treatment of major depressive
Clinical Trial Results Database Page 1 Sponsor Novartis Pharmaceuticals Corporation Generic Drug Name Therapeutic Area of Trial Major Depressive Disorder (MDD) Approved Indication Treatment of major depressive
Clinical Study Report SLO-AD-1 Final Version DATE: 09 December 2013
 1. Clinical Study Report RANDOMIZED, OPEN, PARALLEL GROUP, PHASE IIIB STUDY ON THE EVALUATION OF EFFICACY OF SPECIFIC SUBLINGUAL IMMUNOTHERAPY IN PAEDIATRIC PATIENTS WITH ATOPIC DERMATITIS, WITH OR WITHOUT
1. Clinical Study Report RANDOMIZED, OPEN, PARALLEL GROUP, PHASE IIIB STUDY ON THE EVALUATION OF EFFICACY OF SPECIFIC SUBLINGUAL IMMUNOTHERAPY IN PAEDIATRIC PATIENTS WITH ATOPIC DERMATITIS, WITH OR WITHOUT
Study No.: Title: Rationale: Phase: Study Period: Study Design: Centres: Indication: Treatment: Objectives: Primary Outcome/Efficacy Variable:
 The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
FLUCAND HIKMA PHARMACEUTICALS
 09-15 FLUCAND HIKMA PHARMACEUTICALS (Fluconazole) Description Flucand is a crystalline white - whitish powder, which is slightly soluble in water and in a saline solution. Its molecular weight is 306.3.
09-15 FLUCAND HIKMA PHARMACEUTICALS (Fluconazole) Description Flucand is a crystalline white - whitish powder, which is slightly soluble in water and in a saline solution. Its molecular weight is 306.3.
Clinical Trial Report Synopsis
 Clinical Trial Report Synopsis A phase 2a, proof of concept trial, testing twice daily application of LEO 124249 ointment 30 mg/g in the treatment of mild to moderate inverse psoriasis Design of trial:
Clinical Trial Report Synopsis A phase 2a, proof of concept trial, testing twice daily application of LEO 124249 ointment 30 mg/g in the treatment of mild to moderate inverse psoriasis Design of trial:
 PATCH Analysis Plan v1.2.doc Prophylactic Antibiotics for the Treatment of Cellulitis at Home: PATCH Analysis Plan for PATCH I and PATCH II Authors: Angela Crook, Andrew Nunn, James Mason and Kim Thomas,
PATCH Analysis Plan v1.2.doc Prophylactic Antibiotics for the Treatment of Cellulitis at Home: PATCH Analysis Plan for PATCH I and PATCH II Authors: Angela Crook, Andrew Nunn, James Mason and Kim Thomas,
Itraconazole vs. fluconazole for antifungal prophylaxis in allogeneic stem-cell transplant patients D. J. Winston
 REVIEW Itraconazole vs. fluconazole for antifungal prophylaxis in allogeneic stem-cell transplant patients D. J. Winston Division of Hematology-Oncology, Department of Medicine, UCLA Medical Center, Los
REVIEW Itraconazole vs. fluconazole for antifungal prophylaxis in allogeneic stem-cell transplant patients D. J. Winston Division of Hematology-Oncology, Department of Medicine, UCLA Medical Center, Los
Summary ID#7029. Clinical Study Summary: Study F1D-MC-HGKQ
 CT Registry ID# 7029 Page 1 Summary ID#7029 Clinical Study Summary: Study F1D-MC-HGKQ Clinical Study Report: Versus Divalproex and Placebo in the Treatment of Mild to Moderate Mania Associated with Bipolar
CT Registry ID# 7029 Page 1 Summary ID#7029 Clinical Study Summary: Study F1D-MC-HGKQ Clinical Study Report: Versus Divalproex and Placebo in the Treatment of Mild to Moderate Mania Associated with Bipolar
EFFICACY OF ITRACONAZOLE VERSUS FLUCONAZOLE IN VULVOVAGINAL CANDIDIASIS: AN IN VIVO STUDY Amit Tolasaria 1, Nupur Nandi 2
 EFFICACY OF ITRACONAZOLE VERSUS FLUCONAZOLE IN VULVOVAGINAL CANDIDIASIS: AN IN VIVO STUDY Amit Tolasaria 1, Nupur Nandi 2 HOW TO CITE THIS ARTICLE: Amit Tolasaria, Nupur Nandi. Efficacy of Itraconazole
EFFICACY OF ITRACONAZOLE VERSUS FLUCONAZOLE IN VULVOVAGINAL CANDIDIASIS: AN IN VIVO STUDY Amit Tolasaria 1, Nupur Nandi 2 HOW TO CITE THIS ARTICLE: Amit Tolasaria, Nupur Nandi. Efficacy of Itraconazole
Comparison of Superficial Mycosis treatment using Butenafine and Bifonazole nitrate Clinical Efficacy
 Global Journal of Health Science; Vol. 5, No. 1; 2013 ISSN 1916-9736 E-ISSN 1916-9744 Published by Canadian Center of Science and Education Comparison of Superficial Mycosis treatment using Butenafine
Global Journal of Health Science; Vol. 5, No. 1; 2013 ISSN 1916-9736 E-ISSN 1916-9744 Published by Canadian Center of Science and Education Comparison of Superficial Mycosis treatment using Butenafine
Case presentations: The pitfalls in diagnosis and management of oral lesions in cancer patients
 Case presentations: The pitfalls in diagnosis and management of oral lesions in cancer patients Siri Beier Jensen Associate Professor, DDS, PhD Aarhus University Faculty Disclosure X No, nothing to disclose
Case presentations: The pitfalls in diagnosis and management of oral lesions in cancer patients Siri Beier Jensen Associate Professor, DDS, PhD Aarhus University Faculty Disclosure X No, nothing to disclose
Clinical Study Synopsis
 Clinical Study Synopsis This document is not intended to replace the advice of a healthcare professional and should not be considered as a recommendation. Patients should always seek medical advice before
Clinical Study Synopsis This document is not intended to replace the advice of a healthcare professional and should not be considered as a recommendation. Patients should always seek medical advice before
Ketoconazole tablet dosage for tinea versicolor
 P ford residence southampton, ny Ketoconazole tablet dosage for tinea versicolor 12-3-2018 Detailed dosage guidelines and administration information for Nizoral (ketoconazole). Includes dose adjustments,
P ford residence southampton, ny Ketoconazole tablet dosage for tinea versicolor 12-3-2018 Detailed dosage guidelines and administration information for Nizoral (ketoconazole). Includes dose adjustments,
SYNOPSIS A two-stage randomized, open-label, parallel group, phase III, multicenter, 7-month study to assess the efficacy and safety of SYMBICORT
 Drug product: Drug substance(s): Edition No.: Study code: SYMBICORT pmdi 160/4.5 g Budesonide/formoterol D5896C00005 Date: 8 May 2006 SYNOPSIS A two-stage randomized, open-label, parallel group, phase
Drug product: Drug substance(s): Edition No.: Study code: SYMBICORT pmdi 160/4.5 g Budesonide/formoterol D5896C00005 Date: 8 May 2006 SYNOPSIS A two-stage randomized, open-label, parallel group, phase
Comparative study of the efficacy and safety of topical antifungal agents clotrimazole versus sertaconazole in the treatment of tinea corporis/cruris
 National Journal of Physiology, Pharmacy and Pharmacology RESEARCH ARTICLE Comparative study of the efficacy and safety of topical antifungal agents clotrimazole versus sertaconazole in the treatment of
National Journal of Physiology, Pharmacy and Pharmacology RESEARCH ARTICLE Comparative study of the efficacy and safety of topical antifungal agents clotrimazole versus sertaconazole in the treatment of
Extended Abstract 1. Methods:
 Extended Abstract 1 Article: Chretien J.H. Efficacy of Undecylenic Acid- Zinc Undecylenate Powder in Culture Positive Tinea Pedis. International Journal of Dermatology. 1980; 19: 51-54. http://onlinelibrary.wiley.com.proxy.lib.uwaterloo.ca/doi/10.1111/j.1365-4362.1980.tb01997.x/pdf
Extended Abstract 1 Article: Chretien J.H. Efficacy of Undecylenic Acid- Zinc Undecylenate Powder in Culture Positive Tinea Pedis. International Journal of Dermatology. 1980; 19: 51-54. http://onlinelibrary.wiley.com.proxy.lib.uwaterloo.ca/doi/10.1111/j.1365-4362.1980.tb01997.x/pdf
INTERNATIONAL RESEARCH JOURNAL OF PHARMACY
 INTERNATIONAL RESEARCH JOURNAL OF PHARMACY www.irjponline.com ISSN 2230 8407 Research Article COMPARATIVE EVALUATION OF NEWER TOPICAL ANTIFUNGAL AGENTS IN THE TREATMENT OF SUPERFICIAL FUNGAL INFECTIONS
INTERNATIONAL RESEARCH JOURNAL OF PHARMACY www.irjponline.com ISSN 2230 8407 Research Article COMPARATIVE EVALUATION OF NEWER TOPICAL ANTIFUNGAL AGENTS IN THE TREATMENT OF SUPERFICIAL FUNGAL INFECTIONS
PUBLIC SUMMARY OF RISK MANAGEMENT PLAN VORICONAZOLE ORION 200 MG FILM-COATED TABLETS
 PUBLIC SUMMARY OF RISK MANAGEMENT PLAN VORICONAZOLE ORION 50 MG FILM-COATED TABLETS VORICONAZOLE ORION 200 MG FILM-COATED TABLETS ORION CORPORATION DATE: 12-06-2015, VERSION 1 VI.2 Elements for a Public
PUBLIC SUMMARY OF RISK MANAGEMENT PLAN VORICONAZOLE ORION 50 MG FILM-COATED TABLETS VORICONAZOLE ORION 200 MG FILM-COATED TABLETS ORION CORPORATION DATE: 12-06-2015, VERSION 1 VI.2 Elements for a Public
Corporate Medical Policy
 Corporate Medical Policy Laser Treatment of Onychomycosis File Name: Origination: Last CAP Review: Next CAP Review: Last Review: laser_treatment_of_onychomycosis 5/2013 11/2017 11/2018 11/2017 Description
Corporate Medical Policy Laser Treatment of Onychomycosis File Name: Origination: Last CAP Review: Next CAP Review: Last Review: laser_treatment_of_onychomycosis 5/2013 11/2017 11/2018 11/2017 Description
Type of intervention Treatment. Economic study type Cost-effectiveness analysis.
 Effectiveness and costs of omeprazole vs ranitidine for treatment of symptomatic gastroesophageal reflux disease in primary care clinics in West Virginia Kaplan-Machlis B, Spiegler G E, Zodet M W, Revicki
Effectiveness and costs of omeprazole vs ranitidine for treatment of symptomatic gastroesophageal reflux disease in primary care clinics in West Virginia Kaplan-Machlis B, Spiegler G E, Zodet M W, Revicki
Treatment of Tinea Unguium with Medium and High Doses of Ultramicrosize Griseofulvin Compared with That with Itraconazole
 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Oct. 1993, p. 64-68 66-484/93/164-5$./ Copyright 1993, American Society for Microbiology Vol. 37, No. 1 Treatment of Tinea Unguium with Medium and High Doses of Ultramicrosize
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Oct. 1993, p. 64-68 66-484/93/164-5$./ Copyright 1993, American Society for Microbiology Vol. 37, No. 1 Treatment of Tinea Unguium with Medium and High Doses of Ultramicrosize
SUMMARY OF PRODUCT CHARACTERISTICS
 SUMMARY OF PRODUCT CHARACTERISTICS 1. NAME OF THE MEDICINAL PRODUCT Comfora 595 mg film-coated tablets 2. QUALITATIVE AND QUANTITATIVE COMPOSITION One film-coated tablet contains: glucosamine sulphate
SUMMARY OF PRODUCT CHARACTERISTICS 1. NAME OF THE MEDICINAL PRODUCT Comfora 595 mg film-coated tablets 2. QUALITATIVE AND QUANTITATIVE COMPOSITION One film-coated tablet contains: glucosamine sulphate
Clinical Study Synopsis
 Clinical Study Synopsis This document is not intended to replace the advice of a healthcare professional and should not be considered as a recommendation. Patients should always seek medical advice before
Clinical Study Synopsis This document is not intended to replace the advice of a healthcare professional and should not be considered as a recommendation. Patients should always seek medical advice before
The clinical trial information provided in this public disclosure synopsis is supplied for informational purposes only.
 The clinical trial information provided in this public disclosure synopsis is supplied for informational purposes only. Please note that the results reported in any single trial may not reflect the overall
The clinical trial information provided in this public disclosure synopsis is supplied for informational purposes only. Please note that the results reported in any single trial may not reflect the overall
Andrei Metelitsa, MD, FRCPC, FAAD Co-Director, Institute for Skin Advancement Clinical Associate Professor, Dermatology University of Calgary, Canada
 Andrei Metelitsa, MD, FRCPC, FAAD Co-Director, Institute for Skin Advancement Clinical Associate Professor, Dermatology University of Calgary, Canada Copyright 2017 by Sea Courses Inc. All rights reserved.
Andrei Metelitsa, MD, FRCPC, FAAD Co-Director, Institute for Skin Advancement Clinical Associate Professor, Dermatology University of Calgary, Canada Copyright 2017 by Sea Courses Inc. All rights reserved.
Clinical Study Synopsis
 Clinical Study Synopsis This document is not intended to replace the advice of a healthcare professional and should not be considered as a recommendation. Patients should always seek medical advice before
Clinical Study Synopsis This document is not intended to replace the advice of a healthcare professional and should not be considered as a recommendation. Patients should always seek medical advice before
Clinical Trial Designs for Topical Antifungal Treatments of Onychomycosis and Implications on Clinical Practice
 Clinical Trial Designs for Topical Antifungal Treatments of Onychomycosis and Implications on Clinical Practice Phoebe Rich, MD; Tracey C. Vlahovic, DPM; Warren S. Joseph, DPM; Lee T. Zane, MD; Steve B.
Clinical Trial Designs for Topical Antifungal Treatments of Onychomycosis and Implications on Clinical Practice Phoebe Rich, MD; Tracey C. Vlahovic, DPM; Warren S. Joseph, DPM; Lee T. Zane, MD; Steve B.
ZITHROMAX (AZITHROMYCIN) SNDA H.3 CLINICAL TRIALS RELEVANT TO THE CLAIM STRUCTURE TABLE OF CONTENTS H.3.A. GENERAL APPROACH TO EVALUATION...
 ZITHROMAX (AZITHROMYCIN) SNDA H.3 CLINICAL TRIALS RELEVANT TO THE CLAIM STRUCTURE TABLE OF CONTENTS H.3.A. GENERAL APPROACH TO EVALUATION...2 H.3.A.1 Efficacy (Pfizer IND Studies)...2 H.3.A.1.A Summary
ZITHROMAX (AZITHROMYCIN) SNDA H.3 CLINICAL TRIALS RELEVANT TO THE CLAIM STRUCTURE TABLE OF CONTENTS H.3.A. GENERAL APPROACH TO EVALUATION...2 H.3.A.1 Efficacy (Pfizer IND Studies)...2 H.3.A.1.A Summary
Prescribing Information
 Prescribing Information 1. NAME OF THE MEDICINAL PRODUCT AGISPOR Cream, solution, gel, shampoo AGISPOR ONYCHOSET Nail ointment KERATOSPOR Nail ointment 2. QUALITATIVE AND QUANTITATIVE COMPOSITION 2.1.
Prescribing Information 1. NAME OF THE MEDICINAL PRODUCT AGISPOR Cream, solution, gel, shampoo AGISPOR ONYCHOSET Nail ointment KERATOSPOR Nail ointment 2. QUALITATIVE AND QUANTITATIVE COMPOSITION 2.1.
GROUP 15 TOPICAL PREPARATIONS
 - 105 - GROUP 15 15.1 DERMATOLOGICAL PREPARATIONS 15.1.1 TOPICAL ANTIFUNGALS CLOTRIMAZOLE Indication: Treatment of susceptible fungal infections, dermatophytoses, superficial mycoses, and cutaneous candidiasis
- 105 - GROUP 15 15.1 DERMATOLOGICAL PREPARATIONS 15.1.1 TOPICAL ANTIFUNGALS CLOTRIMAZOLE Indication: Treatment of susceptible fungal infections, dermatophytoses, superficial mycoses, and cutaneous candidiasis
