Ornithine Transcarbamylase Deficiency (OTCD) Recommendations on Emergency Management of Metabolic Disease
|
|
|
- Abraham Nicholson
- 5 years ago
- Views:
Transcription
1
2 Ornithine Transcarbamylase Deficiency (OTCD) Recommendations on Emergency Management of Metabolic Disease Patient s Name: Date of Birth: MRN in KFSH&RC: Please read carefully. Meticulous and prompt treatment is important as there is a high risk of serious complications. Parents of children with diagnosed metabolic disorders know the early signs of decompensation in THEIR children. INTRODUCTION: Urea cycle disorder causes accumulation of ammonia which is a waste product of protein metabolism. High ammonia levels are extremely toxic to the central nervous system, causing cerebral edema that is a major complication. Hyperammonemia crises in children with urea cycle defects (UCDs) are medical emergencies and must be treated as such to avoid death or serious brain injury. In general, decompensation is often triggered by either dietary protein intake beyond bodily requirements or secondary to catabolic processes, e.g. stress of new born period, fasting, dehydration, and/or febrile illness particularly gastro-enteritis and flu.
3 Each of the five biochemical reaction within the urea cycle is associated with a known enzyme deficiency and a related clinical disorder as shown in the diagram below. The OTC is the second enzyme in the urea synthesis process. Lack of this enzyme will lead to OTCD that is inherited in X- linked recessive manner. PRESENTATION: The early signs of decompensation include: Lethargy Poor appetite Exacerbation of pre-exiting neurological problems (irritability, fits etc) Vomiting is common and should be taken seriously
4 However, some signs may be difficult to assess such as irritability or just not right. Always listen carefully to patient s family; their knowledge might exceed your expectations. Later signs and symptoms of decompensation may include: Ataxia Developmental delay Seizure Hepatomegaly Coma Hyperammonemia Failure to thrive At a very early stage the plasma ammonia concentration may not be raised, probably because there is accumulation of glutamine in the brain before ammonia increases in the blood. Apart from arginase deficiency, which usually presents neurologically rather than as a hyperammonemia syndrome, the other urea cycle defects often present in the newborn period with catastrophic hyperammonemia, seizure and coma secondary to cerebral edema. Typically CPS has the most severe presentation but citrullinemia and argininosuccinic acidemia may also present with severe illness. MANAGEMNT: If there is any doubt at all, the child must be admitted, even if only necessary for a short period of observation. Initial plan and management in hospital If the child is shocked or clearly very ill, arrange for admission to Intensive Care Unit.
5 If admitted to metabolic/general ward make a careful clinical assessment including blood pressure and Glasgow Coma Scale even if the patient does not appear encephalopathic. ASSESSMENT: Assess for cardio-respiratory instability, dehydration, fever, infection, excessive protein intake or any other physical stressor (e.g. surgery), as a potential precipitant for metabolic decompensation. Assess neurological status. Request following blood tests: Plasma ammonia Blood glucose Blood gas Electrolytes,Bicarbonate LFTs (AST,ALT,AlkPO4,bilirubin) Plasma amino acids (Quantitative) Plasma amino acid should be drawn first thing in the morning, calling the metabolic lab in advance for urgent samples. TREATMENT: An infant/child at risk from a urea cycle disorders should be treated prospectively. The rational of treatment includes: 1. Promote waste nitrogen excretion. 2. Reverse or minimize catabolism. 3. Minimize protein intake. Management decisions should be based primarily on the clinical status. It is particularly important to note any degree of encephalopathy.
6 The first decision about therapy is whether the child can be treated orally or will need intravenous therapy. Factors that will influence the decision include: How ill is the child and whether they have deteriorated suddenly in the past? Can the child tolerate oral fluids? If the child is relatively well, he/she may be treated orally but assess very carefully. If the child is obviously unwell, he/she must be treated with intravenous fluids: Give Glucose 200 mg/kg at once (2 ml/kg of 10% glucose or 1ml/kg of 20% glucose) over few minutes. Give normal saline 5 ml/kg as a bolus immediately after the glucose unless the peripheral circulation is poor or the patient is frankly shocked, give up to 20 ml/kg normal saline instead of the 5 ml/kg. Repeat the saline bolus if the poor circulation persists as for a shocked non-metabolic patient. Continue with glucose 10% at 5 ml/kg/h until next solution ready. see below Quickly calculate the deficit and maintenance and prepare the intravenous fluids o Deficit: estimate from clinical signs if no recent weight available o Maintenance: Formula for calculating daily maintenance fluid volume (BNF for children) : 100ml/kg for first 10 kg then 50 ml/kg for next 10kg then 20ml/kg thereafter, using calculated rehydrated weight. Deduct the fluid already given from the total for the first 24 hours. o It is assumed that the patient will be given sodium benzoate and sodium phenyl butyrate at full dose therefore uses 10% glucose. If not given full doses of previous medications, use 0.18% Saline and 10% glucose. Having calculated the deficit and the maintenance, give 1/3 of the total for 24 hours over the next 6 hours and the remainder in 18 hours. If intravenous fluids are still needed, continue with the same solution. Recheck the electrolytes every 24 hours if still on intravenous fluids.
7 1. Promote waste nitrogen excretion: To help facilitate the excretion of waste nitrogen, the following medications are employed. a) Sodium benzoate-conjugates with glycine to form hippuric acid which by passes the urea cycle and is excreted in urine. b) Sodium phenylbutyrate or Sodium Phenyl acetate- conjugates with glutamine to form phenylacetyl-glutamine which bypasses the urea cycle and is excreted in the urine. c) Arginine-to prevent ARG deficiency and prime any residual CPS activity but most NOT BE used in arnginas deficiency where there is already an excess of arginine. Do not delay starting ammonia scavenging medications as prognosis is strongly influenced by the duration of illness and peak ammonia levels. In an emergency, initially the loading dose is given intravenously over minutes, followed by an equivalent maintenance infusion given over 24 hours. Dosage is based on weight and specific enzyme deficiency. Therapy should continue until ammonia levels are in normal range. Repeat loading doses are not recommended due to the prolonged plasma levels. Loading dose should be administered along with arginine 10% infusion. Discontinue administration of oral analogous (eg, sodium phenylbutyrate) before starting the infusion.
8 Patient Population Components of Infusion Solution Ammonul must be diluted with sterile 10% dextrose injection at 25 ml/kg before administration Dosage Provided Ammonul Arginine HCl Injection 10% Sodium Phenylacetate Sodium Benzoate Arginine HCl Neonate, Infants, Children 20 kg OTC Deficiency Dose Loading: Over minutes Maintenance: Over 24 hours 2.5 ml/kg 2 ml/kg 250 mg/kg 250 mg/kg 200 mg/kg Children >20 kg and Adults OTC Deficiency Dose Loading: Over minutes Maintenance: Over 24 hours 55 ml/m 2 2 ml/kg 5.5 g/m g/m mg/kg Dosage adjustment in renal impairment: Use with caution; monitor closely Dialysis: Ammonia clearance is 10 times greater with hemodialysis than by peritoneal dialysis or hemofiltration. Exchange transfusion is ineffective. Dosage adjustment in hepatic impairment: Use with caution
9 Once patient is stabilized, ammonia levels are reduced and patient can tolerate oral feeds, intravenous medication should be switched over to oral. Drug Sodium benzoate Sodium phenylbutyrate Arginine Oral doses mg/kg/day mg/kg/day 250 mg/kg/day Potential side effects of sodium benzoate /phenylbutyrate regime: o Increased incidence of nausea and vomiting with bolus. o Overdoses (3-5x recommended dose) can lead to symptoms reminiscent of hyperammonemia, like agitation, confusion and hyperventilation. o Hyperchloremic acidosis may occur following high-dose treatment. o Hypokalaemia- Plasma Potassium concentration should be monitored carefully. o Death has occurred (associated with cerebral edema, hypotension and cardiovascular collapse). N.B. In OTCD, Citrulline may replace arginine as oral treatment when child is able to have enteral feed (PO, NGT or GT) as it helps pull aspartate into urea cycle and increase nitrogen clearance. Avoid Carnitine as it is not shown to be helpful. Although UCD infants are often low in Carnitine, it is known to conjugate with Sodium Benzoate. If an IV is required, that solution should NOT contain Sodium as plenty will be provided by the Sodium Benzoate and Sodium Phenylbutyrate. Treat any infection and constipation (which increases ammonia absorption from the gut). Lactulose s recommended as theory suggests this will beneficial although, as yet this unproven.
10 2. REVERSE OR MINIMIZE CATABOLISM: The caloric intake for these infants should be kept at least kcal/kg. Accurate intake and output records should be kept to monitor hydration. Infection as a potential but severe catabolic stressor should be considered early (when clinical signs are apparent) and managed vigorously. 4. MINIMIZE/OPTIMIZE PROTIEN INTAKE: Stop protein intake initially. Following improvement, gradual reintroduction of protein/essential amino acids within hours. In OTCD, the infant can start with 0.6gram/kg/d in 1 day using h formula. Protein is administered gradually increased to a maximum of 2.0gram/kg/d. Enteral feed should be started as soon as practical, may even occur concomitant with IV via NG or G-tube if necessary. Essential amino acids should not be withheld >24hours, to avoid catabolic breakdown of endogenous proteins. To avoid excess amino acid load aim for g protein /kg body weight (50% as essential amino acids). DIET SHOULD BE PLANNED IN CONJUNCTION WITH A METABOLIC DIETICIAN MONITOR THE PATIENT: If there is any hint of incipient encephalopathy (lethargy, unusual behavior, etc.) start neurological observations at least hourly and seek specialist help. Under these circumstances, fluid volumes should be reduced and given via central line as concentrated solutions to minimize risk of cerebral edema. Reassess after 4-6 hours or earlier. Clinical assessment should include Glasgow coma score and vital signs. Blood tests: Blood ph and gases Ammonia Urea & electrolytes
11 - If improving, continue intravenous fluids and medicines (see the previous section) - If deteriorating (clinical state, hyperammonaemia), seek specialist help. Dialysis may need to be considered urgently. Note peritoneal dialysis is less efficient. Exchange transfusion is dangerous and should not be used. MANAGEMENT OF PROGRESSIVE HYPERAMMONEMIA: If the blood ammonia is elevated, repeat the level. If confirmed: Discontinue oral feeding and oral medications Administer a 10% (or higher) glucose solution and intralipid Administer urea cycle medications as an IV bolus These infusions should begin during acute illness regardless of the amount of oral CPS medication already provided. Monitor ammonia level every 4 hours, amino acids daily. Electrolytes, acid-base status and the anion gap should be monitored regularly. If another IV is required that should not contain sodium. Glucose level should be kept between mg/dl ( mmol/l). If necessary for control of hyperglycemia insulin can be used (remains controversial) bearing in mind that wide swing in glucose level affects brain osmolality. Cerebral edema: Oncotic agents such as albumin will increase the overall nitrogen load and should be avoided. Mannitol has not been found to be helpful for edema secondary to hyperammonemia and steroids should not be used. Hyperventilation is recommended, but only under close appropriate supervision. Avoid valporic acid, as it decreases Urea Cycle function and accentuates hyperammonemia.
12 If ammonia continues to rise: Suggest transfer to PICU/ICU with metabolic and hemodialysis facilities and alert pediatric nephrology team. Remember placement of access lines for dialysis takes time DO NOT DELAY. If dialysis is not immediately available, give loading dose of sodium benzoate/phenylbutyrate, to slightly retard ammonia rise and in anticipation of dialysis ASAP. Dialysis will clear ammonia at: *N.B ml/min from ECMO based dialysis. Osmotic shifts have not been observed with rapid rate of clearance. Additionally a hemofilter in the circuit will continue to remove ammonia between dialysis cycles ml/min hemodialysis. 3-5ml/min peritoneal dialysis (this rate will however take several days to significantly reduce the ammonia load, at a time when brain damage is related to duration of hyperammonemia Dialysis itself is associated with significant morbidity/mortality particularly in the neonate, and decisions to consider using dialysis must balance the risk: benefit ratio for each child. RECOVERY: As ammonia stabilizes and clinical status returns to baseline, patient can switch to oral medications and gradual reintroduction of diet in conjunction with metabolic dietician as described in treatment section. The dose of sodium benzoate and sodium phenylbutyrate is determined based on either body weight or body surface area. The dose should be decided in conjunction with a metabolic physician if the patient does not have an up to date regimen. Note that there may be a rebound hyperamminemia initially with the efflux of intracellular ammonia into the relatively ammonia depleted blood. Thus it is
13 important to continue closely monitoring ammonia levels until they remain stable in normal range. ACKNOWLEDGMENT: These recommendations have been compiled by Wafa Abusamha, Medical Genetic Clinical Coordinator, KFSH&RC based on protocols and guidelines of the American college of Medical Genetics (ACMG), the British Inherited Metabolic Disease Group (BIMDG), and the New England consortium on metabolic Programs; and have been revised by Medical Genetic Consultants in the Department of Medical Genetics at King Faisal Specialist Hospital & Research Centre (KFSH&RC)-Riyadh, in June REFERENCES: ACT SHEET, American Collage of Medical Genetics (ACMG) EMERGENCY guidelines, British Inherited Metabolic Disease Group (BIMDG) Emergency Treatment Protocol-New England Consortium on Metabolic Program
14 Dietary Emergency Protocol for Urea Cycle Disorders (UCD) Name: Date of birth: Weight & date of weight measurement: 1. Discontinue regular diet/feeds 2. If your child is able to take fluids orally, start giving emergency solution every 2 hours during the day and every 3 hours during the night as follow: Add.. Scoops Polycose/Prophree to mls water 3. If your child has an enteral tube feeding (NGT/GT), use this tube for emergency solution administration for better tolerance, especially if your child is nauseated and/or vomiting 4. When using the available tube feeding, it is preferable to give the solution as: Small boluses: Give. mls of emergency solution every hour Or continuously if a feeding pump is available 5. If a Rehydration Solution is to be given as in case of gastroenteritis: Add.. Scoops Polycose/Prophree to... mls of Rehydration Solution 6. Reassess your child every 4 hours: a. Within the first 24 hours from starting the emergency regimen: If the child is doing well, go back to normal diet. If no improvement is seen then continue giving the emergency solution as instructed above if tolerated. b. Between hours from starting the emergency regimen:
15 If your child appears well, reintroduce amino acid mix excluding natural protein source. If no improvement is seen then continue giving the emergency solution as instructed above if tolerated. C. After 48 hours from starting the emergency regimen: If the child is doing well and amino acid mix is well tolerated, start introducing natural protein in the diet gradually over few days starting with half amount. If no improvement is noticed or if the child is not taking above prescribed amounts of emergency solution, bring your child to the hospital with all medicines, special dietary products, and scoops. N.B: If, at any time from starting this emergency regimen, your child is deteriorating and /or not tolerating the emergency solution due to nausea and vomiting, bring your child immediately to the hospital with all medicines, special dietary products, and scoops. ACKNOWLEDGMENT Dietary Emergency Protocols have been compiled by Eman Megdad, Metabolic Nutritionist-Medical Genetics; KFSH&RC-Riyadh based on protocols and guidelines of the British Inherited Metabolic Disease Group (BIMDG), and have been revised by Medical Genetics team in Department of Medical Genetics at King Faisal Specialist Hospital & Research Centre (KFSH&RC)- Riyadh, in June 2014.
16
ARGININOSUCCINIC ACIDEMIA (or ARGININOSUCCINATE LYASE DEFICIENCY) RECOMMENDATIONS ON EMERGENCY MANAGEMENT OF METABOLIC DISEASES
 ARGININOSUCCINIC ACIDEMIA (or ARGININOSUCCINATE LYASE DEFICIENCY) RECOMMENDATIONS ON EMERGENCY MANAGEMENT OF METABOLIC DISEASES Patient s name: Date of birth: Please read carefully. Meticulous and prompt
ARGININOSUCCINIC ACIDEMIA (or ARGININOSUCCINATE LYASE DEFICIENCY) RECOMMENDATIONS ON EMERGENCY MANAGEMENT OF METABOLIC DISEASES Patient s name: Date of birth: Please read carefully. Meticulous and prompt
3 HYDROXY 3 METHYLGLUTARYL CoA (3 HMG CoA) LYASE DEFICIENCY RECOMMENDATIONS ON EMERGENCY MANAGEMENT OF METABOLIC DISEASES
 3 HYDROXY 3 METHYLGLUTARYL CoA (3 HMG CoA) LYASE DEFICIENCY RECOMMENDATIONS ON EMERGENCY MANAGEMENT OF METABOLIC DISEASES Patient s name: Date of birth: Please read carefully. Meticulous and prompt treatment
3 HYDROXY 3 METHYLGLUTARYL CoA (3 HMG CoA) LYASE DEFICIENCY RECOMMENDATIONS ON EMERGENCY MANAGEMENT OF METABOLIC DISEASES Patient s name: Date of birth: Please read carefully. Meticulous and prompt treatment
ISOVALERIC ACIDAEMIA -ACUTE DECOMPENSATION (standard version)
 Contact Details Name: Hospital Telephone: This protocol has 5 pages ISOVALERIC ACIDAEMIA -ACUTE DECOMPENSATION (standard version) Please read carefully. Meticulous treatment is very important as there
Contact Details Name: Hospital Telephone: This protocol has 5 pages ISOVALERIC ACIDAEMIA -ACUTE DECOMPENSATION (standard version) Please read carefully. Meticulous treatment is very important as there
Urea Cycle Disorders Prior Authorization Program Summary
 Urea Cycle Disorders Prior Authorization Program Summary FDA APPROVED INDICATIONS DOSAGE 1,2 Agent(s) Indication(s) Dosing -Adjunctive therapy in the chronic management of patients with urea cycle disorders
Urea Cycle Disorders Prior Authorization Program Summary FDA APPROVED INDICATIONS DOSAGE 1,2 Agent(s) Indication(s) Dosing -Adjunctive therapy in the chronic management of patients with urea cycle disorders
UREA CYCLE DISORDERS - The What, Why, How and When
 UREA CYCLE DISORDERS - The What, Why, How and When George A. Diaz, MD, PhD Program for Inherited Metabolic Diseases Department of Genetics and Genomic Sciences Department of Pediatrics Icahn School of
UREA CYCLE DISORDERS - The What, Why, How and When George A. Diaz, MD, PhD Program for Inherited Metabolic Diseases Department of Genetics and Genomic Sciences Department of Pediatrics Icahn School of
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Urea Cycle Disorders Page 1 of 7 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Urea Cycle Disorders Prime Therapeutics will review Prior Authorization requests
Urea Cycle Disorders Page 1 of 7 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Urea Cycle Disorders Prime Therapeutics will review Prior Authorization requests
Urea Cycle Defects. Dr Mick Henderson. Biochemical Genetics Leeds Teaching Hospitals Trust. MetBioNet IEM Introductory Training
 Urea Cycle Defects Dr Mick Henderson Biochemical Genetics Leeds Teaching Hospitals Trust The Urea Cycle The urea cycle enables toxic ammonia molecules to be converted to the readily excreted and non toxic
Urea Cycle Defects Dr Mick Henderson Biochemical Genetics Leeds Teaching Hospitals Trust The Urea Cycle The urea cycle enables toxic ammonia molecules to be converted to the readily excreted and non toxic
UPDATE ON UREA CYCLE DISORDERS TREATMENT
 UPDATE ON UREA CYCLE DISORDERS TREATMENT George A. Diaz, MD, PhD Program for Inherited Metabolic Diseases Department of Genetics and Genomic Sciences Icahn School of Medicine at Mount Sinai Disclosure
UPDATE ON UREA CYCLE DISORDERS TREATMENT George A. Diaz, MD, PhD Program for Inherited Metabolic Diseases Department of Genetics and Genomic Sciences Icahn School of Medicine at Mount Sinai Disclosure
TRANSAMINATION AND UREA CYCLE
 TRANSAMINATION AND UREA CYCLE USMAN SUMO FRIEND TAMBUNAN ARLI ADITYA PARIKESIT SEPTIANA BIOINFORMATICS GROUP DEPARTEMENT OF CHEMISTRY FACULTY OF MATHEMATIC AND SCIENCE UNIVERSITY OF INDONESIA What is transamination?
TRANSAMINATION AND UREA CYCLE USMAN SUMO FRIEND TAMBUNAN ARLI ADITYA PARIKESIT SEPTIANA BIOINFORMATICS GROUP DEPARTEMENT OF CHEMISTRY FACULTY OF MATHEMATIC AND SCIENCE UNIVERSITY OF INDONESIA What is transamination?
ESPEN Congress Madrid 2018
 ESPEN Congress Madrid 2018 Inborn Errors Of Metabolism Urea Cycle Disorders Diagnosis And Care F. Feillet (FR) Urea cycle disorders, diagnosis and care F Feillet National reference centre for Inborn errors
ESPEN Congress Madrid 2018 Inborn Errors Of Metabolism Urea Cycle Disorders Diagnosis And Care F. Feillet (FR) Urea cycle disorders, diagnosis and care F Feillet National reference centre for Inborn errors
Jana Novotná, Bruno Sopko. Department of the Medical Chemistry and Clinical Biochemistry The 2nd Faculty of Medicine, Charles Univ.
 Amino acid metabolism II. Urea cycle Jana Novotná, Bruno Sopko Department of the Medical Chemistry and Clinical Biochemistry The 2nd Faculty of Medicine, Charles Univ. Nitrogen balance Tissue proteins
Amino acid metabolism II. Urea cycle Jana Novotná, Bruno Sopko Department of the Medical Chemistry and Clinical Biochemistry The 2nd Faculty of Medicine, Charles Univ. Nitrogen balance Tissue proteins
Guideline for the diagnosis and management of isovaleryl-coa-dehydrogenase deficiency (isovaleric acidemia) - a systematic review -
 Guideline for the diagnosis and management of isovaleryl-coa-dehydrogenase deficiency (isovaleric acidemia) - a systematic review - Guideline development group International interdisciplinary guideline
Guideline for the diagnosis and management of isovaleryl-coa-dehydrogenase deficiency (isovaleric acidemia) - a systematic review - Guideline development group International interdisciplinary guideline
The spectrum and outcome of the. neonates with inborn errors of. metabolism at a tertiary care hospital
 The spectrum and outcome of the neonates with inborn errors of metabolism at a tertiary care hospital Dr. Sevim Ünal Neonatology Division, Ankara Children s Hematology Oncology Research Hospital, Ankara,
The spectrum and outcome of the neonates with inborn errors of metabolism at a tertiary care hospital Dr. Sevim Ünal Neonatology Division, Ankara Children s Hematology Oncology Research Hospital, Ankara,
Work-Up and Initial Management of Common Metabolic Emergencies in the Inpatient Setting
 Work-Up and Initial Management of Common Metabolic Emergencies in the Inpatient Setting Kristin Lindstrom, MD Division of Genetics and Metabolism Phoenix Children s Hospital AzAAP Pediatrics in the Red
Work-Up and Initial Management of Common Metabolic Emergencies in the Inpatient Setting Kristin Lindstrom, MD Division of Genetics and Metabolism Phoenix Children s Hospital AzAAP Pediatrics in the Red
TITLE: NURSING GUIDELINES FOR THE MANAGEMENT OF CHILDREN WITH UREA CYCLE DEFECTS. Eilish O Connell, Clinical Education Facilitator, NCIMD
 NO. OF PAGES: Page 1 of 16 SUPERCEDES: N/A NURSING GUIDELINES FOR THE MANAGEMENT OF CHILDREN WITH UREA CYCLE DEFECTS NAME/ Eilish O Connell, Clinical Education Facilitator, NCIMD SIGNATURE: DATE: NAME/
NO. OF PAGES: Page 1 of 16 SUPERCEDES: N/A NURSING GUIDELINES FOR THE MANAGEMENT OF CHILDREN WITH UREA CYCLE DEFECTS NAME/ Eilish O Connell, Clinical Education Facilitator, NCIMD SIGNATURE: DATE: NAME/
INTRAVENOUS FLUIDS PRINCIPLES
 INTRAVENOUS FLUIDS PRINCIPLES Postnatal physiological weight loss is approximately 5-10% Postnatal diuresis is delayed in Respiratory Distress Syndrome (RDS) Preterm babies have limited capacity to excrete
INTRAVENOUS FLUIDS PRINCIPLES Postnatal physiological weight loss is approximately 5-10% Postnatal diuresis is delayed in Respiratory Distress Syndrome (RDS) Preterm babies have limited capacity to excrete
INTRAVENOUS FLUID THERAPY
 INTRAVENOUS FLUID THERAPY PRINCIPLES Postnatal physiological weight loss is approximately 5 10% in first week of life Preterm neonates have more total body water and may lose 10 15% of their weight in
INTRAVENOUS FLUID THERAPY PRINCIPLES Postnatal physiological weight loss is approximately 5 10% in first week of life Preterm neonates have more total body water and may lose 10 15% of their weight in
Organic acidaemias (OAs) & Urea cycle disorders (UCDs) PRESENTATION & MANAGEMENT
 Great Ormond Street Hospital London 20/04/2018 Organic acidaemias (OAs) & Urea cycle disorders (UCDs) PRESENTATION & MANAGEMENT Spyros P. Batzios, MD, MSc, PhD OAs & UCDs How do they present? neonatal
Great Ormond Street Hospital London 20/04/2018 Organic acidaemias (OAs) & Urea cycle disorders (UCDs) PRESENTATION & MANAGEMENT Spyros P. Batzios, MD, MSc, PhD OAs & UCDs How do they present? neonatal
THE ED APPROACH OF THE CHILD WITH SUSPECTED METABOLIC DISEASE
 THE ED APPROACH OF THE CHILD WITH SUSPECTED METABOLIC DISEASE Dr. Nadeem Qureshi M.D, FAAP, FCCM Associate Professor Pediatrics School of Medicine. St Louis University Attending Physician Pediatric Emergency
THE ED APPROACH OF THE CHILD WITH SUSPECTED METABOLIC DISEASE Dr. Nadeem Qureshi M.D, FAAP, FCCM Associate Professor Pediatrics School of Medicine. St Louis University Attending Physician Pediatric Emergency
Newborn Screen & Development Facts about the genetic diseases new since March 2006 (Excluding Cystic Fibrosis)
 Newborn Screen & Development Facts about the genetic diseases new since March 2006 (Excluding Cystic Fibrosis) 1) Argininosuccinic acidemia (ASA) a) Incidence: ~1 in 70,000 b) Deficiency in an enzyme of
Newborn Screen & Development Facts about the genetic diseases new since March 2006 (Excluding Cystic Fibrosis) 1) Argininosuccinic acidemia (ASA) a) Incidence: ~1 in 70,000 b) Deficiency in an enzyme of
Module : Clinical correlates of disorders of metabolism Block 3, Week 2
 Module : Clinical correlates of disorders of metabolism Block 3, Week 2 Department of Paediatrics and Child Health University of Pretoria Tutor : Prof DF Wittenberg : dwittenb@medic.up.ac.za Aim of this
Module : Clinical correlates of disorders of metabolism Block 3, Week 2 Department of Paediatrics and Child Health University of Pretoria Tutor : Prof DF Wittenberg : dwittenb@medic.up.ac.za Aim of this
M0BCore Safety Profile
 M0BCore Safety Profile Active substance: Aciclovir Pharmaceutical form(s)/strength: Tablets 200, 400 or 800 mg Dispersible tablets 200, 400 or 800 mg Oral suspensions 200 mg or 400 mg per 5 ml. Freeze
M0BCore Safety Profile Active substance: Aciclovir Pharmaceutical form(s)/strength: Tablets 200, 400 or 800 mg Dispersible tablets 200, 400 or 800 mg Oral suspensions 200 mg or 400 mg per 5 ml. Freeze
Metabolic Disorders. Chapter Thomson - Wadsworth
 Metabolic Disorders Chapter 28 1 Metabolic Disorders Inborn errors of metabolism group of diseases that affect a wide variety of metabolic processes; defective processing or transport of amino acids, fatty
Metabolic Disorders Chapter 28 1 Metabolic Disorders Inborn errors of metabolism group of diseases that affect a wide variety of metabolic processes; defective processing or transport of amino acids, fatty
With Dr. Sarah Reid and Dr. Sarah Curtis
 5. Headaches 6. Known diabetes 7. Specific high risk groups (ie. Teenagers, children on insulin pumps and those from lower socio-economic status). Episode 63 Pediatric Diabetic Ketoacidosis With Dr. Sarah
5. Headaches 6. Known diabetes 7. Specific high risk groups (ie. Teenagers, children on insulin pumps and those from lower socio-economic status). Episode 63 Pediatric Diabetic Ketoacidosis With Dr. Sarah
Isovaleric Acidemia: Quick reference guide
 Isovaleric Acidemia: Quick reference guide Introduction Isovaleric acidemia (IVA) is an inborn error of the leucine pathway caused by defects of the isovaleryl-oadehydrogenase (IV). The clinical presentation
Isovaleric Acidemia: Quick reference guide Introduction Isovaleric acidemia (IVA) is an inborn error of the leucine pathway caused by defects of the isovaleryl-oadehydrogenase (IV). The clinical presentation
Diabetic Ketoacidosis
 Diabetic Ketoacidosis Definition: Diabetic Ketoacidosis is one of the most serious acute complications of diabetes. It s more common in young patients with type 1 diabetes mellitus. It s usually characterized
Diabetic Ketoacidosis Definition: Diabetic Ketoacidosis is one of the most serious acute complications of diabetes. It s more common in young patients with type 1 diabetes mellitus. It s usually characterized
CLINICAL PHARMACOLOGY
 BUPHENYL (sodium phenylbutyrate) Tablets BUPHENYL (sodium phenylbutyrate) Powder [bu fen-ǝl] (sodium phenylbutyrate) Rx Only DESCRIPTION BUPHENYL (sodium phenylbutyrate) Tablets for oral administration
BUPHENYL (sodium phenylbutyrate) Tablets BUPHENYL (sodium phenylbutyrate) Powder [bu fen-ǝl] (sodium phenylbutyrate) Rx Only DESCRIPTION BUPHENYL (sodium phenylbutyrate) Tablets for oral administration
TITLE: NURSING GUIDELINES FOR THE MANAGEMENT OF CHILDREN WITH METHYLMALONIC ACIDURIA. Eilish O Connell, Clinical Education Facilitator, NCIMD
 NO. OF PAGES: Page 1 of 17 SUPERCEDES: N/A NURSING GUIDELINES FOR THE MANAGEMENT OF CHILDREN WITH METHYLMALONIC ACIDURIA NAME/ Eilish O Connell, Clinical Education Facilitator, NCIMD SIGNATURE: DATE: NAME/
NO. OF PAGES: Page 1 of 17 SUPERCEDES: N/A NURSING GUIDELINES FOR THE MANAGEMENT OF CHILDREN WITH METHYLMALONIC ACIDURIA NAME/ Eilish O Connell, Clinical Education Facilitator, NCIMD SIGNATURE: DATE: NAME/
Basic Fluid and Electrolytes
 Basic Fluid and Electrolytes Chapter 22 Basic Fluid and Electrolytes Introduction Infants and young children have a greater need for water and are more vulnerable to alterations in fluid and electrolyte
Basic Fluid and Electrolytes Chapter 22 Basic Fluid and Electrolytes Introduction Infants and young children have a greater need for water and are more vulnerable to alterations in fluid and electrolyte
Salicylate (Aspirin) Ingestion California Poison Control Background 1. The prevalence of aspirin-containing analgesic products makes
 Salicylate (Aspirin) Ingestion California Poison Control 1-800-876-4766 Background 1. The prevalence of aspirin-containing analgesic products makes these agents, found in virtually every household, common
Salicylate (Aspirin) Ingestion California Poison Control 1-800-876-4766 Background 1. The prevalence of aspirin-containing analgesic products makes these agents, found in virtually every household, common
PAEDIATRIC FLUIDS RCH DEHYDRATION
 PAEDIATRIC FLUIDS RCH DEHYDRATION AIMS Understand normal fluids electrolyte requirements/ maintenance Understand how to assess DEHYDRATION in children Understand the difference between DEHYDRATION and
PAEDIATRIC FLUIDS RCH DEHYDRATION AIMS Understand normal fluids electrolyte requirements/ maintenance Understand how to assess DEHYDRATION in children Understand the difference between DEHYDRATION and
Pediatric Diabetic Ketoacidosis (DKA) General Pediatrics Admission Order Set
 Admitting MRP: Pediatrics: Dr. / Dr. on call to cover until 08:00 am Service: Medicine Team 1 Medicine Team 2 Medical subspecialty Diagnosis: Diabetic Ketoacidosis (DKA) Estimated length of stay Less than
Admitting MRP: Pediatrics: Dr. / Dr. on call to cover until 08:00 am Service: Medicine Team 1 Medicine Team 2 Medical subspecialty Diagnosis: Diabetic Ketoacidosis (DKA) Estimated length of stay Less than
Pediatric Dehydration and Oral Rehydration. May 16/17
 Pediatric Dehydration and Oral Rehydration May 16/17 Volume Depletion (hypovolemia): refers to any condition in which the effective circulating volume is reduced. It can be produced by salt and water loss
Pediatric Dehydration and Oral Rehydration May 16/17 Volume Depletion (hypovolemia): refers to any condition in which the effective circulating volume is reduced. It can be produced by salt and water loss
IV Fluids. I.V. Fluid Osmolarity Composition 0.9% NaCL (Normal Saline Solution, NSS) Uses/Clinical Considerations
 IV Fluids When administering IV fluids, the type and amount of fluid may influence patient outcomes. Make sure to understand the differences between fluid products and their effects. Crystalloids Crystalloid
IV Fluids When administering IV fluids, the type and amount of fluid may influence patient outcomes. Make sure to understand the differences between fluid products and their effects. Crystalloids Crystalloid
diabetes in adults Metabolic complications of
 Metabolic complications of diabetes in adults Dimitri MARGETIS MD ICU St ANTOINE PARIS Definition Diabetic acidoketosis Serious complication in type I diabetes : Hyperglycemia Metabolic acidosis Acidic
Metabolic complications of diabetes in adults Dimitri MARGETIS MD ICU St ANTOINE PARIS Definition Diabetic acidoketosis Serious complication in type I diabetes : Hyperglycemia Metabolic acidosis Acidic
Wales Critical Care & Trauma Network (North) Management of Hyponatraemia in Intensive Care Guidelines
 Wales Critical Care & Trauma Network (North) Management of Hyponatraemia in Intensive Care Guidelines Author: Richard Pugh June 2015 Guideline for management of hyponatraemia in intensive care Background
Wales Critical Care & Trauma Network (North) Management of Hyponatraemia in Intensive Care Guidelines Author: Richard Pugh June 2015 Guideline for management of hyponatraemia in intensive care Background
Amino Acids and Sorbitol injection with/without Electrolytes NIRMIN *
 For the use of a registered medical practitioner or a Hospital or a Laboratory only Amino Acids and Sorbitol injection with/without Electrolytes NIRMIN * DESCRIPTION: NIRMIN * is a clear, colourless injection
For the use of a registered medical practitioner or a Hospital or a Laboratory only Amino Acids and Sorbitol injection with/without Electrolytes NIRMIN * DESCRIPTION: NIRMIN * is a clear, colourless injection
Neonatal Parenteral Nutrition Guideline Dr M Hogan, Maire Cullen ANNP, Una Toland Ward Manager, Sandra Kilpatrick Neonatal Pharmacist
 CLINICAL GUIDELINES ID TAG Title: Author: Designation: Speciality / Division: Directorate: Neonatal Parenteral Nutrition Guideline Dr M Hogan, Maire Cullen ANNP, Una Toland Ward Manager, Sandra Kilpatrick
CLINICAL GUIDELINES ID TAG Title: Author: Designation: Speciality / Division: Directorate: Neonatal Parenteral Nutrition Guideline Dr M Hogan, Maire Cullen ANNP, Una Toland Ward Manager, Sandra Kilpatrick
DIABETIC KETOACIDOSIS (DKA) K E M I A D E Y E R I, P G Y - 1
 DIABETIC KETOACIDOSIS (DKA) K E M I A D E Y E R I, P G Y - 1 QUESTION # 1 7 year old boy comes to the ER with a 2 week history of abdominal pain and weight loss. Further history reveals polyuria and polydipsia,
DIABETIC KETOACIDOSIS (DKA) K E M I A D E Y E R I, P G Y - 1 QUESTION # 1 7 year old boy comes to the ER with a 2 week history of abdominal pain and weight loss. Further history reveals polyuria and polydipsia,
Salicylates commonly cause tinnitus, deafness, nausea and vomiting (salicylism). Hyperventilation results from stimulation of respiratory centre.
 Aspirin poisoning CLINICAL FEATURES Salicylates commonly cause tinnitus, deafness, nausea and vomiting (salicylism). Hyperventilation results from stimulation of respiratory centre. Severe poisoning causes
Aspirin poisoning CLINICAL FEATURES Salicylates commonly cause tinnitus, deafness, nausea and vomiting (salicylism). Hyperventilation results from stimulation of respiratory centre. Severe poisoning causes
EU RISK MANAGEMENT PLAN (EU RMP) Nutriflex Omega peri emulsion for infusion , version 1.1
 EU RISK MANAGEMENT PLAN (EU RMP) Nutriflex Omega peri emulsion for infusion 13.7.2015, version 1.1 III.1. Elements for a Public Summary III.1.1. Overview of disease epidemiology Patients may need parenteral
EU RISK MANAGEMENT PLAN (EU RMP) Nutriflex Omega peri emulsion for infusion 13.7.2015, version 1.1 III.1. Elements for a Public Summary III.1.1. Overview of disease epidemiology Patients may need parenteral
DIABETES MELLITUS. IAP UG Teaching slides
 DIABETES MELLITUS 1 DIABETES MELLITUS IN CHILDREN Introduction, Definition Classification, pathogenesis Clinical features Investigations and diagnosis Therapy and follow up Complications Carry home message
DIABETES MELLITUS 1 DIABETES MELLITUS IN CHILDREN Introduction, Definition Classification, pathogenesis Clinical features Investigations and diagnosis Therapy and follow up Complications Carry home message
Urea Cycle Disorders and Hyperammonemia: Diagnosable Treatable Screenable
 Urea Cycle Disorders and Hyperammonemia: Diagnosable Treatable Screenable Marshall L. Summar, M.D. Chief, Division of Genetics and Metabolism Children s National Medical Center Washington, DC, USA Disclosure
Urea Cycle Disorders and Hyperammonemia: Diagnosable Treatable Screenable Marshall L. Summar, M.D. Chief, Division of Genetics and Metabolism Children s National Medical Center Washington, DC, USA Disclosure
KENT STATE UNIVERSITY HEALTH CARE OF CHILDREN Nursing Pediatrics Case Studies: Child Dehydration
 Courtney Wiener 9/9/10 KENT STATE UNIVERSITY HEALTH CARE OF CHILDREN Nursing 30020 - Pediatrics Case Studies: Child Dehydration Introduction: Dehydration can be life threatening to a child since a majority
Courtney Wiener 9/9/10 KENT STATE UNIVERSITY HEALTH CARE OF CHILDREN Nursing 30020 - Pediatrics Case Studies: Child Dehydration Introduction: Dehydration can be life threatening to a child since a majority
Clinical Guideline. SPEG MCN Protocols Sub Group SPEG Steering Group
 Clinical Guideline SECONDARY CARE MANAGEMENT OF SUSPECTED ADRENAL CRISIS IN CHILDREN AND YOUNG PEOPLE Date of First Issue 24/01/2015 Approved 28/09/2017 Current Issue Date 16/06/2017 Review Date 01/09/2019
Clinical Guideline SECONDARY CARE MANAGEMENT OF SUSPECTED ADRENAL CRISIS IN CHILDREN AND YOUNG PEOPLE Date of First Issue 24/01/2015 Approved 28/09/2017 Current Issue Date 16/06/2017 Review Date 01/09/2019
Fluid & Electrolyte Balances in Term & Preterm Infants. Carolyn Abitbol, M.D. University of Miami/ Holtz Children s Hospital
 Fluid & Electrolyte Balances in Term & Preterm Infants Carolyn Abitbol, M.D. University of Miami/ Holtz Children s Hospital Objectives Review maintenance fluid & electrolyte requirements in neonates Discuss
Fluid & Electrolyte Balances in Term & Preterm Infants Carolyn Abitbol, M.D. University of Miami/ Holtz Children s Hospital Objectives Review maintenance fluid & electrolyte requirements in neonates Discuss
UNDERSTANDING UREA CYCLE DISORDERS
 UNDERSTANDING UREA CYCLE DISORDERS What is a urea cycle disorder? A urea cycle disorder is a genetic disease that affects how protein is broken down in the body. It is therefore classified as a metabolic
UNDERSTANDING UREA CYCLE DISORDERS What is a urea cycle disorder? A urea cycle disorder is a genetic disease that affects how protein is broken down in the body. It is therefore classified as a metabolic
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES
 DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
Col Rama Krishna Sanjeev Military Hospital Chennai Prof Shanmughasundaram Mehta Hospital, Chennai
 Col Rama Krishna Sanjeev Military Hospital Chennai Prof Shanmughasundaram Mehta Hospital, Chennai 11 day old male neonate admitted on 26/6 to our Hospital with c/olethargy -since day1 abnormal movements
Col Rama Krishna Sanjeev Military Hospital Chennai Prof Shanmughasundaram Mehta Hospital, Chennai 11 day old male neonate admitted on 26/6 to our Hospital with c/olethargy -since day1 abnormal movements
Paediatric Directorate
 Paediatric Directorate Dehydration Guidelines Primary cause of dehydration diarrhoea +/- vomiting. Approximately 10%Children < 5yrs present with gastroenteritis each year Diagnosis History - sudden change
Paediatric Directorate Dehydration Guidelines Primary cause of dehydration diarrhoea +/- vomiting. Approximately 10%Children < 5yrs present with gastroenteritis each year Diagnosis History - sudden change
Spironolactone has not been demonstrated to elevate serum uric acid, to precipitate gout or to alter carbohydrate metabolism.
 SPIRONE Composition Each tablet contains Spironolactone 100 mg. Tablets Action Spironolactone is a specific pharmacologic antagonist of aldosterone, acting primarily through competitive binding of receptors
SPIRONE Composition Each tablet contains Spironolactone 100 mg. Tablets Action Spironolactone is a specific pharmacologic antagonist of aldosterone, acting primarily through competitive binding of receptors
CRRT Fundamentals Pre-Test. AKI & CRRT 2017 Practice Based Learning in CRRT
 CRRT Fundamentals Pre-Test AKI & CRRT 2017 Practice Based Learning in CRRT Question 1 A 72-year-old man with HTN presents to the ED with slurred speech, headache and weakness after falling at home. He
CRRT Fundamentals Pre-Test AKI & CRRT 2017 Practice Based Learning in CRRT Question 1 A 72-year-old man with HTN presents to the ED with slurred speech, headache and weakness after falling at home. He
Neonatal Hypoglycaemia Guidelines
 N.B. Staff should be discouraged from printing this document. This is to avoid the risk of out of date printed versions of the document. The Intranet should be referred to for the current version of the
N.B. Staff should be discouraged from printing this document. This is to avoid the risk of out of date printed versions of the document. The Intranet should be referred to for the current version of the
2. PRESCRIPTION STATUS/RESTRICTION OF SALES TO PHARMACIES ONLY 3. COMPOSITION OF THE MEDICINAL PRODUCT
 Title Page Product Information May 2000 1 (6) Product Nephrotect 1. NAME OF THE MEDICINAL PRODUCT Nephrotect 2. PRESCRIPTION STATUS/RESTRICTION OF SALES TO PHARMACIES ONLY For sale in pharmacies only 3.
Title Page Product Information May 2000 1 (6) Product Nephrotect 1. NAME OF THE MEDICINAL PRODUCT Nephrotect 2. PRESCRIPTION STATUS/RESTRICTION OF SALES TO PHARMACIES ONLY For sale in pharmacies only 3.
LOW CITRULLINE AS A MARKER FOR THE PROXIMAL UREA CYCLE DEFECTS EXPERIENCE OF THE NEW ENGLAND NEWBORN SCREENING PROGRAM
 LOW CITRULLINE AS A MARKER FOR THE PROXIMAL UREA CYCLE DEFECTS EXPERIENCE OF THE NEW ENGLAND NEWBORN SCREENING PROGRAM Inderneel Sahai, MD, FACMG Newborn Screening and Genetic Testing Symposium Oct 2014
LOW CITRULLINE AS A MARKER FOR THE PROXIMAL UREA CYCLE DEFECTS EXPERIENCE OF THE NEW ENGLAND NEWBORN SCREENING PROGRAM Inderneel Sahai, MD, FACMG Newborn Screening and Genetic Testing Symposium Oct 2014
Diabetic Ketoacidosis (DKA)
 Diabetic Ketoacidosis (DKA) Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Contact Name and Job Title (author) Directorate & Speciality Date of submission February
Diabetic Ketoacidosis (DKA) Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Contact Name and Job Title (author) Directorate & Speciality Date of submission February
Saudi Population & Genetic Diseases
 CHALLENGES TO TREATMENT OF INHERITED METABOLIC DISORDES: THE SAUDI EXPEREINCE Zuhair N. Al-Hassnan, MD Dept. of Medical Genetics, King Faisal Specialist Hospital & Research Centre, Riyadh, Saudi Arabia
CHALLENGES TO TREATMENT OF INHERITED METABOLIC DISORDES: THE SAUDI EXPEREINCE Zuhair N. Al-Hassnan, MD Dept. of Medical Genetics, King Faisal Specialist Hospital & Research Centre, Riyadh, Saudi Arabia
Dr. Dafalla Ahmed Babiker Jazan University
 Dr. Dafalla Ahmed Babiker Jazan University objectives Overview Definition of dehydration Causes of dehydration Types of dehydration Diagnosis, signs and symptoms Management of dehydration Complications
Dr. Dafalla Ahmed Babiker Jazan University objectives Overview Definition of dehydration Causes of dehydration Types of dehydration Diagnosis, signs and symptoms Management of dehydration Complications
Please inform the Diabetes Nurse Specialist that this patient has been admitted within 24hrs of admission.
 Adult Diabetic Ketoacidosis Care Bundle (V1. Issued October 2014 Review October 2015) Improving patient care This pack includes: DKA Management Guideline Name: (Patient Addressograph) DOB: Hospital No:
Adult Diabetic Ketoacidosis Care Bundle (V1. Issued October 2014 Review October 2015) Improving patient care This pack includes: DKA Management Guideline Name: (Patient Addressograph) DOB: Hospital No:
Pediatric Sodium Disorders
 Pediatric Sodium Disorders Guideline developed by Ron Sanders, Jr., MD, MS, in collaboration with the ANGELS team. Last reviewed by Ron Sanders, Jr., MD, MS on May 20, 2016. Definitions, Physiology, Assessment,
Pediatric Sodium Disorders Guideline developed by Ron Sanders, Jr., MD, MS, in collaboration with the ANGELS team. Last reviewed by Ron Sanders, Jr., MD, MS on May 20, 2016. Definitions, Physiology, Assessment,
PARENTERAL NUTRITION
 PARENTERAL NUTRITION DEFINITION Parenteral nutrition [(PN) or total parenteral nutrition (TPN)] is the intravenous infusion of some or all nutrients for tissue maintenance, metabolic requirements and growth
PARENTERAL NUTRITION DEFINITION Parenteral nutrition [(PN) or total parenteral nutrition (TPN)] is the intravenous infusion of some or all nutrients for tissue maintenance, metabolic requirements and growth
Acute Management of Sick Infants with Suspected Inborn Errors of Metabolism
 Indian J Pediatr (July 2011) 78(7):854 859 DOI 10.1007/s12098-011-0422-0 SYMPOSIUM ON PICU PROTOCOLS OF AIIMS Acute Management of Sick Infants with Suspected Inborn Errors of Metabolism Neerja Gupta Madhulika
Indian J Pediatr (July 2011) 78(7):854 859 DOI 10.1007/s12098-011-0422-0 SYMPOSIUM ON PICU PROTOCOLS OF AIIMS Acute Management of Sick Infants with Suspected Inborn Errors of Metabolism Neerja Gupta Madhulika
Amino Acid Disorders. What is ASAL deficiency? Genetic Fact Sheets for Parents
 Genetic Fact Sheets for Parents Amino Acid Disorders Screening, Technology, and Research in Genetics is a multi-state project to improve information about the financial, ethical, legal, and social issues
Genetic Fact Sheets for Parents Amino Acid Disorders Screening, Technology, and Research in Genetics is a multi-state project to improve information about the financial, ethical, legal, and social issues
I have no financial disclosures
 Athina Sikavitsas DO Children's Emergency Services University of Michigan Discuss DKA Presentation Assessment Treatment I have no financial disclosures 1 6 Y/O male presents with vomiting and abdominal
Athina Sikavitsas DO Children's Emergency Services University of Michigan Discuss DKA Presentation Assessment Treatment I have no financial disclosures 1 6 Y/O male presents with vomiting and abdominal
Metabolic Precautions & ER Recommendations
 Metabolic Precautions & ER Recommendations * To whom correspondence Sumit Parikh, should MD be addressed Center for Pediatric Neurology Cleveland Clinic Cleveland, OH UMDF 2010 The catabolic state Entering
Metabolic Precautions & ER Recommendations * To whom correspondence Sumit Parikh, should MD be addressed Center for Pediatric Neurology Cleveland Clinic Cleveland, OH UMDF 2010 The catabolic state Entering
Carbamoyl phosphate synthetase 1 deficiency: First report of this rare metabolic disorder in Kingdom of Bahrain with novel mutation
 Alsahlawi et al. 1 CASE REPORT PEER REVIEWED OPEN ACCESS Carbamoyl phosphate synthetase 1 deficiency: First report of this rare metabolic disorder in Kingdom of Bahrain with novel mutation Z. Alsahlawi,
Alsahlawi et al. 1 CASE REPORT PEER REVIEWED OPEN ACCESS Carbamoyl phosphate synthetase 1 deficiency: First report of this rare metabolic disorder in Kingdom of Bahrain with novel mutation Z. Alsahlawi,
Information for health professionals
 Introduction of a new screening test for newborn babies in Wales Newborn bloodspot screening for Medium chain acyl-coa dehydrogenase deficiency (MCADD) Newborn bloodspot screening for MCADD is being introduced
Introduction of a new screening test for newborn babies in Wales Newborn bloodspot screening for Medium chain acyl-coa dehydrogenase deficiency (MCADD) Newborn bloodspot screening for MCADD is being introduced
PACKAGE LEAFLET: INFORMATION FOR THE USER. SODIPHOS 22mEq / 10ml Concentrate for solution for infusion. Disodium phosphate dihydrate
 PACKAGE LEAFLET: INFORMATION FOR THE USER SODIPHOS 22mEq / 10ml Concentrate for solution for infusion Disodium phosphate dihydrate Read all of this leaflet carefully before you start using this medicine.
PACKAGE LEAFLET: INFORMATION FOR THE USER SODIPHOS 22mEq / 10ml Concentrate for solution for infusion Disodium phosphate dihydrate Read all of this leaflet carefully before you start using this medicine.
Inborn Errors of Metabolism (IEM)
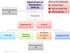 Clinical Presentation Inborn Errors of Metabolism (IEM) Click on the following: - Clinical Pearl - link to movie clip - link to picture Investigations Blood Work Urine No Acidosis NH 4 + Metabolic Acidosis
Clinical Presentation Inborn Errors of Metabolism (IEM) Click on the following: - Clinical Pearl - link to movie clip - link to picture Investigations Blood Work Urine No Acidosis NH 4 + Metabolic Acidosis
Guideline for Children with Type 1 or Type 2 Diabetes on Insulin Requiring Surgery or Sedation
 CHILDREN S SERVICES Guideline for Children with Type 1 or Type 2 Diabetes on Insulin Requiring Surgery or Sedation Background Surgery places stress on the body and will alter glucose control and insulin
CHILDREN S SERVICES Guideline for Children with Type 1 or Type 2 Diabetes on Insulin Requiring Surgery or Sedation Background Surgery places stress on the body and will alter glucose control and insulin
DBL MAGNESIUM SULFATE CONCENTRATED INJECTION
 DBL MAGNESIUM SULFATE CONCENTRATED INJECTION NAME OF MEDICINE Magnesium Sulfate BP DESCRIPTION DBL Magnesium Sulfate Concentrated Injection is a clear, colourless, sterile solution. Each ampoule contains
DBL MAGNESIUM SULFATE CONCENTRATED INJECTION NAME OF MEDICINE Magnesium Sulfate BP DESCRIPTION DBL Magnesium Sulfate Concentrated Injection is a clear, colourless, sterile solution. Each ampoule contains
Diabetic Ketoacidosis: When Sugar Isn t Sweet!!!
 Diabetic Ketoacidosis: When Sugar Isn t Sweet!!! W Ricks Hanna Jr MD Assistant Professor of Pediatrics University of Tennessee Health Science Center LeBonheur Children s Hospital Introduction Diabetes
Diabetic Ketoacidosis: When Sugar Isn t Sweet!!! W Ricks Hanna Jr MD Assistant Professor of Pediatrics University of Tennessee Health Science Center LeBonheur Children s Hospital Introduction Diabetes
For The Management Of. Diabetic Ketoacidosis
 Guidelines For The Management Of Diabetic Ketoacidosis By Dr. Sinan Butrus F.I.C.M.S Clinical Standards & Guidelines Dr.Layla Al-Shahrabani F.R.C.P (UK) Director of Clinical Affairs Kurdistan Higher Council
Guidelines For The Management Of Diabetic Ketoacidosis By Dr. Sinan Butrus F.I.C.M.S Clinical Standards & Guidelines Dr.Layla Al-Shahrabani F.R.C.P (UK) Director of Clinical Affairs Kurdistan Higher Council
Diabetic Ketoacidosis (DKA) Critical Care Guideline Two Bag System
 Critical Care Guideline Two Bag System Inclusion Criteria (Definition of DKA): Blood glucose (BG) > 200 mg/dl Acidosis (bicarbonate < 15 or blood gas ph < 7.3) Associated glycosuria, ketonuria &/or ketonemia
Critical Care Guideline Two Bag System Inclusion Criteria (Definition of DKA): Blood glucose (BG) > 200 mg/dl Acidosis (bicarbonate < 15 or blood gas ph < 7.3) Associated glycosuria, ketonuria &/or ketonemia
INBORN ERRORS OF METABOLISM (IEM) IAP UG Teaching slides
 INBORN ERRORS OF METABOLISM (IEM) 1 OBJECTIVES What are IEMs? Categories When to suspect? History and clinical pointers Metabolic presentation Differential diagnosis Emergency and long term management
INBORN ERRORS OF METABOLISM (IEM) 1 OBJECTIVES What are IEMs? Categories When to suspect? History and clinical pointers Metabolic presentation Differential diagnosis Emergency and long term management
Chapter 16 Nutrition, Fluids and Electrolytes, and Acid-Base Balance Nutrition Nutrients Water o Functions Promotes metabolic processes Transporter
 Chapter 16 Nutrition, Fluids and Electrolytes, and Acid-Base Balance Nutrition Nutrients Water o Functions Promotes metabolic processes Transporter for nutrients and wastes Lubricant Insulator and shock
Chapter 16 Nutrition, Fluids and Electrolytes, and Acid-Base Balance Nutrition Nutrients Water o Functions Promotes metabolic processes Transporter for nutrients and wastes Lubricant Insulator and shock
GUIDELINE FOR THE MANAGEMENT AND PREVENTION OF ACUTE TUMOUR LYSIS SYNDROME IN HAEMATOLOGICAL MALIGNANCIES
 GUIDELINE FOR THE MANAGEMENT AND PREVENTION OF ACUTE TUMOUR LYSIS SYNDROME IN HAEMATOLOGICAL MALIGNANCIES Full Title of Guideline: Author (include email and role): Division & Speciality: Scope (Target
GUIDELINE FOR THE MANAGEMENT AND PREVENTION OF ACUTE TUMOUR LYSIS SYNDROME IN HAEMATOLOGICAL MALIGNANCIES Full Title of Guideline: Author (include email and role): Division & Speciality: Scope (Target
DR J HARTY / DR CM RITCHIE / DR M GIBBONS
 CLINICAL GUIDELINES ID TAG Title: Author: Speciality / Division: Directorate: Paracetamol Poisoning DR J HARTY / DR CM RITCHIE / DR M GIBBONS Medicine Acute Date Uploaded: 16 th September 2014 Review Date
CLINICAL GUIDELINES ID TAG Title: Author: Speciality / Division: Directorate: Paracetamol Poisoning DR J HARTY / DR CM RITCHIE / DR M GIBBONS Medicine Acute Date Uploaded: 16 th September 2014 Review Date
By; Ashraf El Houfi MD MS (pulmonology) MRCP (UK) FRCP (London) EDIC Consultant ICU Dubai Hospital
 By; Ashraf El Houfi MD MS (pulmonology) MRCP (UK) FRCP (London) EDIC Consultant ICU Dubai Hospital Introduction The significance of nutrition in hospital setting (especially the ICU) cannot be overstated.
By; Ashraf El Houfi MD MS (pulmonology) MRCP (UK) FRCP (London) EDIC Consultant ICU Dubai Hospital Introduction The significance of nutrition in hospital setting (especially the ICU) cannot be overstated.
Organic Acid Disorders
 Genetic Fact Sheets for Parents Organic Acid Disorders Screening, Technology, and Research in Genetics is a multi-state project to improve information about the financial, ethical, legal, and social issues
Genetic Fact Sheets for Parents Organic Acid Disorders Screening, Technology, and Research in Genetics is a multi-state project to improve information about the financial, ethical, legal, and social issues
National Metabolic Biochemistry Network Guidelines for the investigation of hypoglycaemia in infants and children
 National Metabolic Biochemistry Network Guidelines for the investigation of hypoglycaemia in infants and children Aim To provide guidance on the biochemical investigation of hypoglycaemia in infants and
National Metabolic Biochemistry Network Guidelines for the investigation of hypoglycaemia in infants and children Aim To provide guidance on the biochemical investigation of hypoglycaemia in infants and
Fluid and electrolyte management
 281 Chapter Appendix 5B Fluid and electrolyte management Learning outcomes After reading this appendix, you will be able to: Describe the approach to the management of fluid and electrolytes in the seriously
281 Chapter Appendix 5B Fluid and electrolyte management Learning outcomes After reading this appendix, you will be able to: Describe the approach to the management of fluid and electrolytes in the seriously
All Wales Paediatric Steroid Replacement Therapy Card
 All Wales Paediatric Steroid Replacement Therapy Card All Wales Paediatric Steroid Replacement Therapy Card 1.0 BACKGROUND Patients that require long-term steroid replacement therapy for adrenal suppression
All Wales Paediatric Steroid Replacement Therapy Card All Wales Paediatric Steroid Replacement Therapy Card 1.0 BACKGROUND Patients that require long-term steroid replacement therapy for adrenal suppression
Guidelines for the care of Children with Diabetes Mellitus undergoing Surgery
 Guidelines for the care of Children with Diabetes Mellitus undergoing Surgery Background Surgery places physical and emotional stress on the body. This, alongside new surroundings, parental anxiety and
Guidelines for the care of Children with Diabetes Mellitus undergoing Surgery Background Surgery places physical and emotional stress on the body. This, alongside new surroundings, parental anxiety and
A Clinical Guideline for the use of Intravenous Aminophylline in Acute Severe Asthma in Children
 For Use in: By: For: Division responsible for document: Key words: Name and job titles of document author: Name and job title of document author s Line Manager: Supported by: Assessed and approved by the:
For Use in: By: For: Division responsible for document: Key words: Name and job titles of document author: Name and job title of document author s Line Manager: Supported by: Assessed and approved by the:
Organic Acid Disorders
 Genetic Fact Sheets for Parents Organic Acid Disorders Screening, Technology, and Research in Genetics is a multi-state project to improve information about the financial, ethical, legal, and social issues
Genetic Fact Sheets for Parents Organic Acid Disorders Screening, Technology, and Research in Genetics is a multi-state project to improve information about the financial, ethical, legal, and social issues
ADVOCATE CHRIST MEDICAL CENTER DKA (DIABETIC KETOACIDOSIS) TREATMENT GUIDELINES
 ADVOCATE CHRIST MEDICAL CENTER DKA (DIABETIC KETOACIDOSIS) TREATMENT GUIDELINES DEFINITION -Glucose >250 mg/dl*, anion gap > 16, + ketones * Glucose < 250 does not exclude DKA especially if anion gap >
ADVOCATE CHRIST MEDICAL CENTER DKA (DIABETIC KETOACIDOSIS) TREATMENT GUIDELINES DEFINITION -Glucose >250 mg/dl*, anion gap > 16, + ketones * Glucose < 250 does not exclude DKA especially if anion gap >
Pediatric Intensive Care Unit (PICU) Pediatric Diabetic Ketoacidosis (DKA) Admission Order Set
 Discontinue all previous orders Weight: kg DKA admit order set is for initial management Ongoing management required based on frequent reassessment of TFI, fluid balance and lab results. Admit to PICU
Discontinue all previous orders Weight: kg DKA admit order set is for initial management Ongoing management required based on frequent reassessment of TFI, fluid balance and lab results. Admit to PICU
CDE Exam Preparation Presented by Wendy Graham RD CDE May 4, 2017
 CDE Exam Preparation Presented by Wendy Graham RD CDE May 4, 2017 DKA at organ level 3 Diabetic Ketoacidosis Characteristics Ketones positive Anion Gap > 12 (High) Blood Sugar > 14 (High) Bicarbonate
CDE Exam Preparation Presented by Wendy Graham RD CDE May 4, 2017 DKA at organ level 3 Diabetic Ketoacidosis Characteristics Ketones positive Anion Gap > 12 (High) Blood Sugar > 14 (High) Bicarbonate
Acute painful crisis in patients with sickle cell disease: Clinical Guidelines (HN-506a)
 Acute painful crisis in patients with sickle cell disease: Clinical Guidelines (HN-506a) Introduction The majority of acute painful crises in patients with sickle cell disease will be managed independently
Acute painful crisis in patients with sickle cell disease: Clinical Guidelines (HN-506a) Introduction The majority of acute painful crises in patients with sickle cell disease will be managed independently
Guideline for the Prevention and Management of Neonatal Hypoglycaemia GL359
 Guideline for the Prevention and Management of Neonatal Hypoglycaemia GL359 Approval and Authorisation Approved by Job Title Date Paediatric Clinical Chair of Paediatric Clinical Governance Governance
Guideline for the Prevention and Management of Neonatal Hypoglycaemia GL359 Approval and Authorisation Approved by Job Title Date Paediatric Clinical Chair of Paediatric Clinical Governance Governance
Abnormalities in serum sodium. David Metz Paediatric Nephrology
 Abnormalities in serum sodium David Metz Paediatric Nephrology Basics Total body sodium regulated by aldosterone and ANP Mediated by intravascular volume (not sodium) RAAS and intrarenal determines Na
Abnormalities in serum sodium David Metz Paediatric Nephrology Basics Total body sodium regulated by aldosterone and ANP Mediated by intravascular volume (not sodium) RAAS and intrarenal determines Na
How to dose RAVICTI (glycerol phenylbutyrate) Oral Liquid
 How to dose RAVICTI (glycerol phenylbutyrate) Oral Liquid A REFERENCE GUIDE FOR DOSING, ADMINISTRATION, AND SUPPORT RAVICTI is so easy to take... It s just one little moment. Isaac, Age 20 Actual RAVICTI
How to dose RAVICTI (glycerol phenylbutyrate) Oral Liquid A REFERENCE GUIDE FOR DOSING, ADMINISTRATION, AND SUPPORT RAVICTI is so easy to take... It s just one little moment. Isaac, Age 20 Actual RAVICTI
Urea is the major end product of nitrogen catabolism in humans One nitrogen free NH3 other nitrogen aspartate. carbon oxygen CO2 liver,
 Urea is the major end product of nitrogen catabolism in humans Urea is the major disposal form of amino groups derived from amino acids, and accounts about 90% percent of the nitrogencontaining components
Urea is the major end product of nitrogen catabolism in humans Urea is the major disposal form of amino groups derived from amino acids, and accounts about 90% percent of the nitrogencontaining components
Electrolytes Solution
 Electrolytes Solution Substances that are not dissociated in solution are called nonelectrolytes, and those with varying degrees of dissociation are called electrolytes. Urea and dextrose are examples
Electrolytes Solution Substances that are not dissociated in solution are called nonelectrolytes, and those with varying degrees of dissociation are called electrolytes. Urea and dextrose are examples
Index No: MMG11/1. Version: 1. Date ratified: 12 th November 2013
 Index No: Intravenous fluid prescription in children For previously well children aged one month to 16 years (excluding renal, cardiac, diabetic ketoacidosis and acute burns patients) Version: 1 Date ratified:
Index No: Intravenous fluid prescription in children For previously well children aged one month to 16 years (excluding renal, cardiac, diabetic ketoacidosis and acute burns patients) Version: 1 Date ratified:
PHARMACOLOGY AND PHARMACOKINETICS
 DRUG GUIDELINE Insulin, human neutral (Actrapid ) Intravenous Infusion for SCOPE (Area): FOR USE IN: Critical Care Unit, Emergency Department and Operating Suite EXCLUSIONS: Paediatrics (seek Paediatrician
DRUG GUIDELINE Insulin, human neutral (Actrapid ) Intravenous Infusion for SCOPE (Area): FOR USE IN: Critical Care Unit, Emergency Department and Operating Suite EXCLUSIONS: Paediatrics (seek Paediatrician
ANATOMY OF A METABOLIC CRISIS: FAOD-style. Mark S. Korson, MD Tufts Medical Center Boston, MA
 ANATOMY OF A METABOLIC CRISIS: FAOD-style Mark S. Korson, MD Tufts Medical Center Boston, MA NORMAL PHYSIOLOGY Anabolic Eating well Calories eaten > body s needs BRAIN uses GLUCOSE MUSCLE uses GLUCOSE
ANATOMY OF A METABOLIC CRISIS: FAOD-style Mark S. Korson, MD Tufts Medical Center Boston, MA NORMAL PHYSIOLOGY Anabolic Eating well Calories eaten > body s needs BRAIN uses GLUCOSE MUSCLE uses GLUCOSE
Policy Compliance Procedure
 Policy Compliance Procedure Safe Handling of Adult Intravenous Potassium Chloride Preparations This PCP relates to NSW Health PD NSW Health Policy Directive PD2005_342 Safe Handling of Intravenous Potassium
Policy Compliance Procedure Safe Handling of Adult Intravenous Potassium Chloride Preparations This PCP relates to NSW Health PD NSW Health Policy Directive PD2005_342 Safe Handling of Intravenous Potassium
