Acute Management of Sick Infants with Suspected Inborn Errors of Metabolism
|
|
|
- Buck Wilkinson
- 5 years ago
- Views:
Transcription
1 Indian J Pediatr (July 2011) 78(7): DOI /s SYMPOSIUM ON PICU PROTOCOLS OF AIIMS Acute Management of Sick Infants with Suspected Inborn Errors of Metabolism Neerja Gupta Madhulika Kabra Received: 15 February 2011 /Accepted: 6 April 2011 /Published online: 18 June 2011 # Dr. K C Chaudhuri Foundation 2011 Abstract Diagnosis of inborn errors of metabolism (IEM) such as an organic acidemia or urea cycle defects requires high index of suspicion in a critically ill infant as these conditions mimic common pediatric illnesses. Prompt initiation of the treatment is mandatory even if a definitive diagnosis is not established immediately. Initial screening investigations may give clues and help to classify these disorders in broad categories. It is of utmost importance to preserve samples for testing. Keywords IEM. Suspicion. Acute management Introduction Inborn errors of metabolism (IEM) are a heterogeneous group of disorders with protean manifestations. Usually they present in the neonatal period or infancy but can occur at any time, even at a later age. IEMs, though individually are rare, but one should have a high index of suspicion as mortality in severe forms is very high if prompt treatment is not initiated. Clinicians generally have a tendency to pursue this possibility only after other more common conditions, such as sepsis, have been excluded. Diagnosis of IEMs does not require extensive knowledge of biochemical pathways or individual metabolic diseases. A proper understanding of the major clinical manifestations of inborn errors of metabolism provides the basis for considering the diagnosis and further management. An early diagnosis and N. Gupta (*) : M. Kabra Division of Genetics, Department of Pediatrics, All India Institute of Medical Sciences, Ansari Nagar, New Delhi , India neerjaagarwal@yahoo.co.in institution of appropriate therapy is often life saving and can prevent permanent neurologic sequelae in these patients. This review would focus on the acute management of a child with IEM. The categories of IEM that may present acutely during infancy can be broadly divided into 1. Encephalopathy without metabolic acidosis: Urea cycle defects, nonketotic hyperglycinemia, defects in branched chain aminoacids like maple syrup urine disease(msud), peroxisomal disorders, molybdenum cofactor deficiency, and pyridoxine dependent seizures. 2. Encephalopathy with metabolic acidosis: Organic acidemias, congenital lactic acidosis, dicarboxylic aciduria. 3. Hepatic involvement with or without hepatocellular dysfunction: Amino acidopathies like tyrosinemia, fatty acid oxidation defects, mitochondrial defects, disorders of carbohydrate metabolism like Glycogen storage disorder, hereditary fructose intolerance and galactosemia. 4. Cardiac manifestations: Glycogen Storage disease type II, Fatty acid oxidation defects etc. Acute Management of IEM [1 3] The three important steps in the acute management of an IEM are: Suspicion, Evaluation and Emergency Management. I. Suspicion A metabolic disorder should be suspected in the following situations: Rapid deterioration of general condition and/ or reduced consciousness, particularly when preceded by vomiting, fever, or fasting
2 Indian J Pediatr (July 2011) 78(7): II. Nonspecific, unexplained findings of sepsis, like poor feeding, drowsiness, lethargy, vomiting, hypotonia, failure to thrive, abnormal breathing, seizures and jaundice in the presence of normal sepsis screen Rapidly progressive encephalopathy of unknown etiology Family history of neonatal death ( sepsis or SIDS ) or parental consanguinity Intractable hiccups Apnea or respiratory distress Sepsis, particularly with E. coli Dysmorphic features (in very few IEMs) Organomegaly Metabolic acidosis, Hyperammonemia, Peculiar odor*[*musty phenylketonuria; cabbage like tyrosinemia; maple syrup maple syrup urine disease; sweaty feet isovaleric academia, glutaric acidemia type II; cat urine 3-methylcrotonyl CoA carboxylase and multiple carboxylase deficiencies] Evaluation and Emergency Management This involves history, physical examination, screening investigations and initiation of therapy based on results. (A) In a neonate, the early clinical features of acute metabolic decompensation are nonspecific and include not looking well, lethargy, feeding problems, vomiting, abnormal breathing, hypotonia and seizures. Disorders of glucose, protein and fat breakdown (intermediary metabolism) in the neonatal period typically have an asymptomatic interval with the manifestations usually from the second day of life, although hyperammonemia due to transient hyperammonemia of newborn (THAN) in premature and glutaric acidemia type II or with pyruvate carboxylase (PC) in full term may present on day 1 of life. A quick history including family history (previous sib death due to sepsis, SIDS, or unexplained disorders like progressive neurological disease, multiple miscarriages,history suggestive of HELLP syndrome etc. in other family members or consanguinity) can provide useful clues about a particular disorder and its inheritance pattern. After the neonatal period, slightly older infants with metabolic disorder may present with recurrent vomiting, lethargy progressing to coma without any focal neurological signs. They may also have had episodic problems associated with minor illnesses or may just have failure to thrive and developmental delay. Physical Examination is usually normal except for nonspecific findings like lethargy, coma, (B) apnea or hyperpnea, seizures, hypotonia etc. Presence of facial dysmorphism, cataract, retinopathy, structural brain anomalies, hypertrophic or dilated cardiomyopathy, hepatomegaly, multicystic dysplastic kidneys, myopathy and peculiar odor can give clue towards a specific diagnosis. Investigations and Initial Management: Goals of treatment for patients with an inborn error of metabolism (IEM) are prevention of further accumulation of harmful substances, correction of metabolic abnormalities, and elimination of toxic metabolites. Even the apparently stable patient with mild symptoms may deteriorate rapidly with progression to death within hours. With appropriate therapy, patients may completely recover without sequelae. The initial screening investigations can be done in two phases: (1) Basic Metabolic Emergency Investigations and First Line Management The initial stabilization of an infant presenting with an acute IEM is not so much dependant on the particular disorder involved but rather on the specific metabolic abnormalities found on the initial screening tests. First insert i.v line and take blood samples for urgent analysis of initial screening tests like CBC Neutropenia is frequent in some organic acidemias. Electrolytes, ABG To evaluate for metabolic acidosis and anion gap. Glucose To rule out hypoglycaemia (also is a feature of many IEM) C-reactive protein, creatinine phosphokinase, liver function test, renal function test Ammonia Hyperammonemia is present in urea cycle abnormalities and some organic acidemias. Rapidly flowing fasting blood (uncuffed venous or arterial) should be obtained and the sample placed on ice and hand carried to the lab. The test should be done within 1 h, so prior notification to the lab is desirable. NH 3 values at various ages {Healthy neonate <110 micromol/l; Sick neonate up to 180 micromol/l; Suspect metabolic disease >200 micromol/l; After neonatal period, Healthy micromol/l; Suspect metabolic disease >100 micromol/l}
3 856 Indian J Pediatr (July 2011) 78(7): Uric acid Low uric acid especially with neurologic abnormalities, is suggestive for molybdenum cofactor deficiency. Lactate, pyruvate Elevation of lactate is a frequent secondary finding in many IEM s, but there are primary lactic acidosis due to defects in energy metabolism. The lactate/ pyruvate ratio (normal <25) will help to evaluate the possibilities. These tests are notoriously subject to artifactual changes because of sample collection or handling errors. Freely flowing blood (usually arterial) should be drawn with a minimum of tourniquet time and muscular action of the infant and transported on ice to the lab immediately. Some of the blood gas analysers have facilities of measuring blood lactate. (2) Sample collection for specific tests Plasma amino acid: 1 2 ml of blood in a heparin or EDTA tube, to be transported on ice preferably. It is important to draw this while the patient is ill, and not after treatment. Many abnormalities will disappear when the child improves and may make the diagnosis difficult. Urinalysis: The presence of ketones is unusual even in sick neonates and suggests an organic acidemia. Clinitest for reducing substances should be performed, but should be interpreted carefully because of a high false positive rate. Other tests like ferric chloride for ketoacids (positive in phenylketonuria, tyrosinemia, maple syrup urine disease, histidinemia, alkaptonuria, and in the presence of other substances such as acetoacetic acid, salicylates, phenothiazines, isoniazid, and acetaminophen), and a cyanide nitroprusside test for disulfides (positive in cystinuria and homocystinuria) may be useful if clinically there is high suspicion. Urine organic acids: ml of urine is required and is kept at 20 in an air tight container. If the sample is allowed to remain at room temperature or even in the refrigerator, volatile organic acids may disappear. It is important to obtain this sample when the patient is ill. Remember, urine is a very valuable sample for diagnosis of IEMs and should be obtained during the illness. In addition, store dried blood spot for tandem mass spectrometry (TMS), EDTA sample for DNA analysis and freeze 1 2 ml of plasma. (C) (D) Store CSF (should be frozen immediately) if lumbar puncture is performed. Follow General Treatment Protocol: Immediate elimination of dietary or parenteral intake of the potentially toxic compounds like protein, fat, galactose, fructose. Provide adequate glucose to prevent catabolism after establishing airway, breathing and circulation. Prevent catabolism: A metabolically simple source of calories, such as glucose at a rate sufficient to slow the catabolism and to suppress mobilization of endogenous sources of the metabolite, like protein should be administered. An increase in catabolism due to stress from infection, surgery etc. can rapidly overwhelm the compensatory mechanisms and result in clinical decompensation and hence should be avoided. 1. Administer high calorie, high carbohydrate intravenous fluids: 10% Dextrose in 0.2% of NaCl at 1.5 times calculated maintenance, and add KCl when urinary output is established. Start at least 60 kcal/kg/day (preferably ml/kg/day). The caloric intake can be increased up to kcal/kg/day. 2. Withhold intake of protein: Protein should not be withheld indefinitely. If clinical improvement is observed and a final diagnosis has not been established, some amino acid intake should be provided after a maximum of 2 to 3 days of complete protein restriction. Essential amino acids or total protein can be provided orally or intravenously at an initial dose of 0.5 g protein/kg/24 h. This should be increased incrementally to 1.0 g/kg/24 h and held at that level until the diagnostic evaluation is complete and plans can be made for definitive long-term therapy. 3. IV intralipids may be used to increase the caloric intake if the patient does not have a defect in fatty acid oxidation. 4. Avoid Ringer lactate. Treatment and Investigations according to the Initial Findings: If the emergency investigations show a specific abnormality, then treatment is provided accordingly as follows: a. Increase excretion of toxic metabolites by using alternative pathways. For example, carnitine is useful in the elimination of
4 Indian J Pediatr (July 2011) 78(7): organic acids in the form of carnitine esters. Sodium benzoate and phenylacetate are useful in treating hyperammonemia. Treat Hyperammonemia [4]: If acute hyperammonemia is associated with encephalopathy due to urea cycle defect, administer sodium phenylacetate and sodium benzoate. These compounds are conjugated with glycine and glutamine respectively, resulting in the excretion of 1 and 2 ammonia molecules per molecule of drug, respectively. Give priming doses of the following immediately in 20 ml/kg of 10% glucose, to be infused with in 1 2 h: Sodium Benzoate, load 250 mg/kg (5.5 g/m 2 ) Sodium Phenylacetate, load 250 mg/kg (5.5 g/m 2 ) In patients suspected of having a urea cycle defect because of significant hyperammonemia without acidosis, an infusion of mg/kg of 10% arginine HCL can be given intravenously over 60 min and then 6 ml/kg/d IV in four divided doses. 0 After initial loading, continue infusions of sodium benzoate mg/kg/24 h, sodium phenyl acetate mg/kg/24 h and arginine mg/kg/24 h. All these are usually prepared as 1 2% solutions. 0 When used intravenously, sodium phenylacetate and sodium benzoate must be given by central line. Arginine HCl can be mixed with it; arginine HCl dose can be decreased to 200 mg/kg if known carbamyl phophate synthetase (CPS) or ornithine transcarbamylase (OTC) deficiency. 0 L-carnitine conjugates with and inactivates sodium benzoate; therefore, this must not be given with sodium phenylacetate and sodium benzoate. 0 Unfortunately, intravenous preparations of Sodium Benzoate, Phenylacetate and Arginine are not easily available in India and oral preparations are to be used in same doses. 0 Peritoneal dialysis or hemodialysis is required if the ammonia is 4 times normal or rising quickly. Nephrologist should be notified early so that they can be prepared. Although peritoneal dialysis, continuous arteriovenous hemoperfusion, and ex- change transfusion have been used in the past to lower plasma ammonia levels, all are substantially less effective than hemodialysis. In infants who are comatose or ventilator-dependent, or who exhibit evidence of cerebral edema, dialysis should be instituted immediately without waiting to determine whether there is a response to dietary manipulation, medication, or other less aggressive therapy. If hemodialysis is not readily available, peritoneal dialysis (<10% as effective as hemodialysis) or double volume exchange transfusion (even less effective) can be performed while arrangements are made to transport to a center where hemodialysis is possible, as long as this does not delay transfer. Two to 3 days of therapy is usually necessary. b. Correct Metabolic Acidosis Increased Anion Gap [>16 mmol/l] It should be treated cautiously. Bicarbonates is generally not indicated unless the plasma bicarbonate is <10 mmol/l; deficits are only half corrected. [Sodium bicarbonate: meq/ kg/h (up to 1 2 meq/kg/h) IV; Calculations of bicarbonate requirements appropriate for the treatment of other conditions are rarely adequate in these disorders because of ongoing production of organic acids or lactate. The acid-base status should be monitored frequently, with therapy adjusted accordingly. Hemodialysis should be considered for severely acidotic neonates with organic acidemias, regardless of whether hyperammonemia is present. (peritoneal dialysis, hemofiltration, exchange transfusion are much less effective). c. Correct Hypoglycemia (blood glucose <45 mg/dl at all ages) 0 10% glucose with electrolytes ( ml/kg/d) 8 12 mg/kg/min IV at times maintenance to maintain serum glucose level at mg/dl which should prevent catabolism. High-volume maintenance fluid will also promote urinary excretion of some toxic metabolites. 0 If the patient is hypoglycemic and dextrose is administered as a bolus, give normal saline without D10. 0 Avoid hypotonic fluid load due to the risk of cerebral edema, particularly if hyperammonemia is present. 0 If necessary, treat hyperglycemia with insulin ( U/kg/h). d. Increase the residual enzyme activity This is usually accomplished by administration of pharmacologic doses of the vitamin cofactor for the defective enzyme. If the binding constant for the vitamin has been altered and the enzyme is otherwise reasonably functional, increasing the vitamin concentration will increase enzyme activity via a mass action effect. Hence, one should consider empiric vitamin therapy until the disorder is diagnosed (Table 1).
5 858 Indian J Pediatr (July 2011) 78(7): Table 1 Vitamins used to treat various Inborn errors of metabolism Vitamin Dose Disorder treated Thiamine 5 20 mg/kg po qd (up to 500 mg) Maple syrup urine disease Biotin 5 20 mg po qd Biotinidase or holocarboxylase synthase deficiencies Vit B mg cyanocobalamin IM qd Methylmalonic aciduria Riboflavin mg tid po qd Glutaric acidemia types I and II L-carnitine at mg/kg tid given po/ng or mg/kg IV over 2 3 min or as infusion, followed by mg/kg/d (maximum 3 g/d) may be administered empirically in life-threatening situations associated with carnitine deficiency. Administration of L-carnitine to patients with secondary carnitine deficiency is controversial. Consultation with an IEM specialist is recommended. e. Treat shock, electrolyte imbalance, infection and coagulopathies f. Nonacidotic, Nonhyperammonemic Seizures 1. Pyridoxine mg IV trial. If there is a response (pyridoxine responsive seizures), give mg of pyridoxine po qd. It should be given to neonates with seizures unresponsive to conventional anticonvulsants. 2. Riboflavin mg tid po qd (glutaric acidemia type I). 3. High dose benzodiazepines, sodium benzoate (nonketotic hyperglycinemia). If results are inconclusive but metabolic disease remains a possibility: 0 Continue glucose infusion 0 Review the history and clinical signs. Consult a metabolic specialist 0 Send samples for specialized tests like for acylcarnitines etc 0 Monitor electrolytes, glucose, lactate, acid-base status (E) Specialized and Definitive Tests: Numerous other specialized tests are performed depending on the clinical context. Examples include carnitine, acylcarnitines (TMS), Urine organic acids by Gas Chromatography mass Spectroscopy (GCMS),very long chain fatty acids, lysosomal enzymes, etc. Many of these tests are done at only few places in the country and it can take weeks to get results. These tests should generally be ordered after consultation with the clinical geneticist or metabolic specialist. A definitive diagnosis may sometimes be made from screening tests but often specific enzymatic analysis (F) or DNA testing is required. It may be necessary to biopsy tissues such as liver or muscle. These tests, if done at all, are usually done in research laboratories and it may take months for results. Ongoing Management [5]: Once a specific diagnosis is established then depending upon the disorder, specific treatment (mainly diet) is initiated and genetic counseling is done. Specific Treatment Specific treatment, depending upon the type of metabolic disorder, is provided. These diets are commercially available but are quite costly. Hence, treatment should be closely supervised by a team of metabolic expert, dietician and social worker. Liver transplantation may be curative in disorders like in severe neonatal form of urea cycle defects and tyrosinemia. Genetic Counseling Family should be provided with adequate genetic counseling regarding prognosis, recurrence risk, and possibility of prenatal diagnosis. Post Mortem Specimen Collection [1] Usually patients with metabolic diseases are quite sick and often die. Hence, one should try to preserve the samples, especially biopsy samples soon after death (within 1-2 h of death). SAVE: 0 Serum and plasma (centrifuge about 10 ml) 0 Dried blood spot on filter paper card used for TMS 0 Freeze ml of urine at 20 C 0 EDTA blood (3-5 ml) for future DNA analysis 0 Skin biopsy for fibroblast culture Points to Remember Treatable inherited metabolic diseases often present in early infancy or childhood as acute life threatening illness. Appropriate and aggressive empiric treatment before the confirmation of a diagnosis may be life-saving and may avert or reduce the neurologic sequelae of some of these disorders.
6 Indian J Pediatr (July 2011) 78(7): It is of the greatest importance that the appropriate sample collection be made before starting any treatment, because abnormal biochemical data can help in initial management and allow the definitive diagnosis. References 1. Burton BK. Inborn errors of metabolism in infancy: a guide to diagnosis. Pediatrics. 1998;102:E Clarke JTR. Acute metabolic illness in the newborn. In: Clarke JTR, editor. A clinical guide to inherited metabolic diseases. 3rd ed. Cambridge: Cambridge University Press; pp Ogier de Baulny H. Management and emergency treatments of neonates with a suspicion of inborn error of metabolism. Seminars in Neonatology. 2002;7: Summar M. Current strategies for the management of neonatal urea cycle disorders. J Pediatr. 2001;138:S Clarke JTR. Treatment. In: Clarke JTR, editor. A clinical guide to inherited metabolic diseases. 3rd ed. USA: Cambridge University Press; p
INBORN ERRORS OF METABOLISM (IEM) IAP UG Teaching slides
 INBORN ERRORS OF METABOLISM (IEM) 1 OBJECTIVES What are IEMs? Categories When to suspect? History and clinical pointers Metabolic presentation Differential diagnosis Emergency and long term management
INBORN ERRORS OF METABOLISM (IEM) 1 OBJECTIVES What are IEMs? Categories When to suspect? History and clinical pointers Metabolic presentation Differential diagnosis Emergency and long term management
The spectrum and outcome of the. neonates with inborn errors of. metabolism at a tertiary care hospital
 The spectrum and outcome of the neonates with inborn errors of metabolism at a tertiary care hospital Dr. Sevim Ünal Neonatology Division, Ankara Children s Hematology Oncology Research Hospital, Ankara,
The spectrum and outcome of the neonates with inborn errors of metabolism at a tertiary care hospital Dr. Sevim Ünal Neonatology Division, Ankara Children s Hematology Oncology Research Hospital, Ankara,
Metabolic Disorders. Chapter Thomson - Wadsworth
 Metabolic Disorders Chapter 28 1 Metabolic Disorders Inborn errors of metabolism group of diseases that affect a wide variety of metabolic processes; defective processing or transport of amino acids, fatty
Metabolic Disorders Chapter 28 1 Metabolic Disorders Inborn errors of metabolism group of diseases that affect a wide variety of metabolic processes; defective processing or transport of amino acids, fatty
Inborn Errors of Metabolism (IEM)
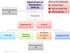 Clinical Presentation Inborn Errors of Metabolism (IEM) Click on the following: - Clinical Pearl - link to movie clip - link to picture Investigations Blood Work Urine No Acidosis NH 4 + Metabolic Acidosis
Clinical Presentation Inborn Errors of Metabolism (IEM) Click on the following: - Clinical Pearl - link to movie clip - link to picture Investigations Blood Work Urine No Acidosis NH 4 + Metabolic Acidosis
Inborn Errors of Metabolism in the Emergency Department. Will Davies June 2014
 Inborn Errors of Metabolism in the Emergency Department Will Davies June 2014 Inborn Errors of Metabolism in the Emergency Department Overview Although individually rare, altogether they are 1:1000-2500
Inborn Errors of Metabolism in the Emergency Department Will Davies June 2014 Inborn Errors of Metabolism in the Emergency Department Overview Although individually rare, altogether they are 1:1000-2500
Suspected Metabolic Disease in the Newborn Period Acute Management "What do I do?" Barbara Marriage, PhD RD Abbott Nutrition
 Suspected Metabolic Disease in the Newborn Period Acute Management "What do I do?" Barbara Marriage, PhD RD Abbott Nutrition Introduction Review clinical findings that may be suspicious of a metabolic
Suspected Metabolic Disease in the Newborn Period Acute Management "What do I do?" Barbara Marriage, PhD RD Abbott Nutrition Introduction Review clinical findings that may be suspicious of a metabolic
Newborn Screen & Development Facts about the genetic diseases new since March 2006 (Excluding Cystic Fibrosis)
 Newborn Screen & Development Facts about the genetic diseases new since March 2006 (Excluding Cystic Fibrosis) 1) Argininosuccinic acidemia (ASA) a) Incidence: ~1 in 70,000 b) Deficiency in an enzyme of
Newborn Screen & Development Facts about the genetic diseases new since March 2006 (Excluding Cystic Fibrosis) 1) Argininosuccinic acidemia (ASA) a) Incidence: ~1 in 70,000 b) Deficiency in an enzyme of
Work-Up and Initial Management of Common Metabolic Emergencies in the Inpatient Setting
 Work-Up and Initial Management of Common Metabolic Emergencies in the Inpatient Setting Kristin Lindstrom, MD Division of Genetics and Metabolism Phoenix Children s Hospital AzAAP Pediatrics in the Red
Work-Up and Initial Management of Common Metabolic Emergencies in the Inpatient Setting Kristin Lindstrom, MD Division of Genetics and Metabolism Phoenix Children s Hospital AzAAP Pediatrics in the Red
3 HYDROXY 3 METHYLGLUTARYL CoA (3 HMG CoA) LYASE DEFICIENCY RECOMMENDATIONS ON EMERGENCY MANAGEMENT OF METABOLIC DISEASES
 3 HYDROXY 3 METHYLGLUTARYL CoA (3 HMG CoA) LYASE DEFICIENCY RECOMMENDATIONS ON EMERGENCY MANAGEMENT OF METABOLIC DISEASES Patient s name: Date of birth: Please read carefully. Meticulous and prompt treatment
3 HYDROXY 3 METHYLGLUTARYL CoA (3 HMG CoA) LYASE DEFICIENCY RECOMMENDATIONS ON EMERGENCY MANAGEMENT OF METABOLIC DISEASES Patient s name: Date of birth: Please read carefully. Meticulous and prompt treatment
THE ED APPROACH OF THE CHILD WITH SUSPECTED METABOLIC DISEASE
 THE ED APPROACH OF THE CHILD WITH SUSPECTED METABOLIC DISEASE Dr. Nadeem Qureshi M.D, FAAP, FCCM Associate Professor Pediatrics School of Medicine. St Louis University Attending Physician Pediatric Emergency
THE ED APPROACH OF THE CHILD WITH SUSPECTED METABOLIC DISEASE Dr. Nadeem Qureshi M.D, FAAP, FCCM Associate Professor Pediatrics School of Medicine. St Louis University Attending Physician Pediatric Emergency
ISOVALERIC ACIDAEMIA -ACUTE DECOMPENSATION (standard version)
 Contact Details Name: Hospital Telephone: This protocol has 5 pages ISOVALERIC ACIDAEMIA -ACUTE DECOMPENSATION (standard version) Please read carefully. Meticulous treatment is very important as there
Contact Details Name: Hospital Telephone: This protocol has 5 pages ISOVALERIC ACIDAEMIA -ACUTE DECOMPENSATION (standard version) Please read carefully. Meticulous treatment is very important as there
Isovaleric Acidemia: Quick reference guide
 Isovaleric Acidemia: Quick reference guide Introduction Isovaleric acidemia (IVA) is an inborn error of the leucine pathway caused by defects of the isovaleryl-oadehydrogenase (IV). The clinical presentation
Isovaleric Acidemia: Quick reference guide Introduction Isovaleric acidemia (IVA) is an inborn error of the leucine pathway caused by defects of the isovaleryl-oadehydrogenase (IV). The clinical presentation
Metabolic Changes in ASD. Norma J. Arciniegas, MD Simón E. Carlo, MD Instituto Filius
 Metabolic Changes in ASD Norma J. Arciniegas, MD Simón E. Carlo, MD Instituto Filius 12 patients 3 Autism: Ages 3/3/3.7 3 PDD: Ages 3/3/6 3 Asperger: Ages 6/7/15.1 3 Speech delay and Sensory Problems (SHL):
Metabolic Changes in ASD Norma J. Arciniegas, MD Simón E. Carlo, MD Instituto Filius 12 patients 3 Autism: Ages 3/3/3.7 3 PDD: Ages 3/3/6 3 Asperger: Ages 6/7/15.1 3 Speech delay and Sensory Problems (SHL):
National Metabolic Biochemistry Network Guidelines for the investigation of hypoglycaemia in infants and children
 National Metabolic Biochemistry Network Guidelines for the investigation of hypoglycaemia in infants and children Aim To provide guidance on the biochemical investigation of hypoglycaemia in infants and
National Metabolic Biochemistry Network Guidelines for the investigation of hypoglycaemia in infants and children Aim To provide guidance on the biochemical investigation of hypoglycaemia in infants and
Guideline for the diagnosis and management of isovaleryl-coa-dehydrogenase deficiency (isovaleric acidemia) - a systematic review -
 Guideline for the diagnosis and management of isovaleryl-coa-dehydrogenase deficiency (isovaleric acidemia) - a systematic review - Guideline development group International interdisciplinary guideline
Guideline for the diagnosis and management of isovaleryl-coa-dehydrogenase deficiency (isovaleric acidemia) - a systematic review - Guideline development group International interdisciplinary guideline
Training Syllabus CLINICAL SYLLABUS
 Training Syllabus CLINICAL SYLLABUS SYLLABUS FOR TRAINING IN CLINICAL PAEDIATRIC METABOLIC MEDICINE Updated July 2006 This syllabus is intended as a guide. Whilst the training should be comprehensive,
Training Syllabus CLINICAL SYLLABUS SYLLABUS FOR TRAINING IN CLINICAL PAEDIATRIC METABOLIC MEDICINE Updated July 2006 This syllabus is intended as a guide. Whilst the training should be comprehensive,
The laboratory investigation of lactic acidaemia. J Bonham/T Laing
 The laboratory investigation of lactic acidaemia J Bonham/T Laing Reference range Typical ranges for blood lactate are: Newborn 0.3-2.2 mmol/l Nielsen J et al1 1994 1-12mo 0.9-1.8 mmol/l Bonnefont et al
The laboratory investigation of lactic acidaemia J Bonham/T Laing Reference range Typical ranges for blood lactate are: Newborn 0.3-2.2 mmol/l Nielsen J et al1 1994 1-12mo 0.9-1.8 mmol/l Bonnefont et al
UREA CYCLE DISORDERS - The What, Why, How and When
 UREA CYCLE DISORDERS - The What, Why, How and When George A. Diaz, MD, PhD Program for Inherited Metabolic Diseases Department of Genetics and Genomic Sciences Department of Pediatrics Icahn School of
UREA CYCLE DISORDERS - The What, Why, How and When George A. Diaz, MD, PhD Program for Inherited Metabolic Diseases Department of Genetics and Genomic Sciences Department of Pediatrics Icahn School of
ARGININOSUCCINIC ACIDEMIA (or ARGININOSUCCINATE LYASE DEFICIENCY) RECOMMENDATIONS ON EMERGENCY MANAGEMENT OF METABOLIC DISEASES
 ARGININOSUCCINIC ACIDEMIA (or ARGININOSUCCINATE LYASE DEFICIENCY) RECOMMENDATIONS ON EMERGENCY MANAGEMENT OF METABOLIC DISEASES Patient s name: Date of birth: Please read carefully. Meticulous and prompt
ARGININOSUCCINIC ACIDEMIA (or ARGININOSUCCINATE LYASE DEFICIENCY) RECOMMENDATIONS ON EMERGENCY MANAGEMENT OF METABOLIC DISEASES Patient s name: Date of birth: Please read carefully. Meticulous and prompt
Ornithine Transcarbamylase Deficiency (OTCD) Recommendations on Emergency Management of Metabolic Disease
 Ornithine Transcarbamylase Deficiency (OTCD) Recommendations on Emergency Management of Metabolic Disease Patient s Name: Date of Birth: MRN in KFSH&RC: Please read carefully. Meticulous and prompt treatment
Ornithine Transcarbamylase Deficiency (OTCD) Recommendations on Emergency Management of Metabolic Disease Patient s Name: Date of Birth: MRN in KFSH&RC: Please read carefully. Meticulous and prompt treatment
Newborn Screening & Methods for Diagnosing Inborn Errors of Metabolism
 Newborn Screening & Methods for Diagnosing Inborn Errors of Metabolism Patricia Jones, PhD DABCC FACB UT Southwestern Medical Center Children s Medical Center Dallas, Texas Learning Objectives Justify
Newborn Screening & Methods for Diagnosing Inborn Errors of Metabolism Patricia Jones, PhD DABCC FACB UT Southwestern Medical Center Children s Medical Center Dallas, Texas Learning Objectives Justify
Urea Cycle Defects. Dr Mick Henderson. Biochemical Genetics Leeds Teaching Hospitals Trust. MetBioNet IEM Introductory Training
 Urea Cycle Defects Dr Mick Henderson Biochemical Genetics Leeds Teaching Hospitals Trust The Urea Cycle The urea cycle enables toxic ammonia molecules to be converted to the readily excreted and non toxic
Urea Cycle Defects Dr Mick Henderson Biochemical Genetics Leeds Teaching Hospitals Trust The Urea Cycle The urea cycle enables toxic ammonia molecules to be converted to the readily excreted and non toxic
Module : Clinical correlates of disorders of metabolism Block 3, Week 2
 Module : Clinical correlates of disorders of metabolism Block 3, Week 2 Department of Paediatrics and Child Health University of Pretoria Tutor : Prof DF Wittenberg : dwittenb@medic.up.ac.za Aim of this
Module : Clinical correlates of disorders of metabolism Block 3, Week 2 Department of Paediatrics and Child Health University of Pretoria Tutor : Prof DF Wittenberg : dwittenb@medic.up.ac.za Aim of this
Introduction to Organic Acidemias. Hilary Vernon, MD PhD Assistant Professor of Genetic Medicine Johns Hopkins University 7.25.
 Introduction to Organic Acidemias Hilary Vernon, MD PhD Assistant Professor of Genetic Medicine Johns Hopkins University 7.25.2014 A Brief Historical Overview Garrod, Archibald E. 1902. The Incidence of
Introduction to Organic Acidemias Hilary Vernon, MD PhD Assistant Professor of Genetic Medicine Johns Hopkins University 7.25.2014 A Brief Historical Overview Garrod, Archibald E. 1902. The Incidence of
Newborn Screening in Manitoba. Information for Health Care Providers
 Newborn Screening in Manitoba Information for Health Care Providers Newborn screening: a healthy start leads to a healthier life Health care professionals have provided newborn screening for phenylketonuria
Newborn Screening in Manitoba Information for Health Care Providers Newborn screening: a healthy start leads to a healthier life Health care professionals have provided newborn screening for phenylketonuria
Medical Foods for Inborn Errors of Metabolism
 Medical Foods for Inborn Errors of Metabolism Policy Number: Original Effective Date: MM.02.014 02/18/2000 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST 08/23/2013 Section: Medicine Place(s)
Medical Foods for Inborn Errors of Metabolism Policy Number: Original Effective Date: MM.02.014 02/18/2000 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST 08/23/2013 Section: Medicine Place(s)
TITLE: NURSING GUIDELINES FOR THE MANAGEMENT OF CHILDREN WITH METHYLMALONIC ACIDURIA. Eilish O Connell, Clinical Education Facilitator, NCIMD
 NO. OF PAGES: Page 1 of 17 SUPERCEDES: N/A NURSING GUIDELINES FOR THE MANAGEMENT OF CHILDREN WITH METHYLMALONIC ACIDURIA NAME/ Eilish O Connell, Clinical Education Facilitator, NCIMD SIGNATURE: DATE: NAME/
NO. OF PAGES: Page 1 of 17 SUPERCEDES: N/A NURSING GUIDELINES FOR THE MANAGEMENT OF CHILDREN WITH METHYLMALONIC ACIDURIA NAME/ Eilish O Connell, Clinical Education Facilitator, NCIMD SIGNATURE: DATE: NAME/
Metabolic Precautions & ER Recommendations
 Metabolic Precautions & ER Recommendations * To whom correspondence Sumit Parikh, should MD be addressed Center for Pediatric Neurology Cleveland Clinic Cleveland, OH UMDF 2010 The catabolic state Entering
Metabolic Precautions & ER Recommendations * To whom correspondence Sumit Parikh, should MD be addressed Center for Pediatric Neurology Cleveland Clinic Cleveland, OH UMDF 2010 The catabolic state Entering
Salicylate (Aspirin) Ingestion California Poison Control Background 1. The prevalence of aspirin-containing analgesic products makes
 Salicylate (Aspirin) Ingestion California Poison Control 1-800-876-4766 Background 1. The prevalence of aspirin-containing analgesic products makes these agents, found in virtually every household, common
Salicylate (Aspirin) Ingestion California Poison Control 1-800-876-4766 Background 1. The prevalence of aspirin-containing analgesic products makes these agents, found in virtually every household, common
CLINICAL SIGNS SUGGESTIVE OF A NEUROMETABOLIC DISEASE. Bwee Tien Poll-The Amsterdam UMC The Netherlands
 CLINICAL SIGNS SUGGESTIVE OF A NEUROMETABOLIC DISEASE Bwee Tien Poll-The Amsterdam UMC The Netherlands FRAMEWORK OF PRINCIPALS 1. Problem-oriented clinical approach 2. Biomarkers in plasma, urine, CSF
CLINICAL SIGNS SUGGESTIVE OF A NEUROMETABOLIC DISEASE Bwee Tien Poll-The Amsterdam UMC The Netherlands FRAMEWORK OF PRINCIPALS 1. Problem-oriented clinical approach 2. Biomarkers in plasma, urine, CSF
Organic acidaemias (OAs) & Urea cycle disorders (UCDs) PRESENTATION & MANAGEMENT
 Great Ormond Street Hospital London 20/04/2018 Organic acidaemias (OAs) & Urea cycle disorders (UCDs) PRESENTATION & MANAGEMENT Spyros P. Batzios, MD, MSc, PhD OAs & UCDs How do they present? neonatal
Great Ormond Street Hospital London 20/04/2018 Organic acidaemias (OAs) & Urea cycle disorders (UCDs) PRESENTATION & MANAGEMENT Spyros P. Batzios, MD, MSc, PhD OAs & UCDs How do they present? neonatal
ESPEN Congress Madrid 2018
 ESPEN Congress Madrid 2018 Inborn Errors Of Metabolism Urea Cycle Disorders Diagnosis And Care F. Feillet (FR) Urea cycle disorders, diagnosis and care F Feillet National reference centre for Inborn errors
ESPEN Congress Madrid 2018 Inborn Errors Of Metabolism Urea Cycle Disorders Diagnosis And Care F. Feillet (FR) Urea cycle disorders, diagnosis and care F Feillet National reference centre for Inborn errors
ANATOMY OF A METABOLIC CRISIS: FAOD-style. Mark S. Korson, MD Tufts Medical Center Boston, MA
 ANATOMY OF A METABOLIC CRISIS: FAOD-style Mark S. Korson, MD Tufts Medical Center Boston, MA NORMAL PHYSIOLOGY Anabolic Eating well Calories eaten > body s needs BRAIN uses GLUCOSE MUSCLE uses GLUCOSE
ANATOMY OF A METABOLIC CRISIS: FAOD-style Mark S. Korson, MD Tufts Medical Center Boston, MA NORMAL PHYSIOLOGY Anabolic Eating well Calories eaten > body s needs BRAIN uses GLUCOSE MUSCLE uses GLUCOSE
Carnitine palmitoyl transferase 2 deficiency (CPT2) is a rare inherited disorder that occurs when
 CPT2 Deficiency Carnitine palmitoyl transferase 2 deficiency (CPT2) is a rare inherited disorder that occurs when the last step in the entry of fats into sac-like bodies called mitochondria is blocked.
CPT2 Deficiency Carnitine palmitoyl transferase 2 deficiency (CPT2) is a rare inherited disorder that occurs when the last step in the entry of fats into sac-like bodies called mitochondria is blocked.
HA Convention 2016 Master course How to Handle Abnormal Newborn Metabolic Screening Results Causes, Management and Follow up
 HA Convention 2016 Master course How to Handle Abnormal Newborn Metabolic Screening Results Causes, Management and Follow up Dr. Josephine Chong Clinical Professional Consultant Centre of Inborn Errors
HA Convention 2016 Master course How to Handle Abnormal Newborn Metabolic Screening Results Causes, Management and Follow up Dr. Josephine Chong Clinical Professional Consultant Centre of Inborn Errors
Inborn Errors of Metabolism Clinical Approach to Diagnosis and Treatment
 Case Scenario: 15 year old girl presented in ED with aggressive behaviour and hallucinations. No associated fever, vomiting, seizures or developmental concerns Previously well Inborn Errors of Metabolism
Case Scenario: 15 year old girl presented in ED with aggressive behaviour and hallucinations. No associated fever, vomiting, seizures or developmental concerns Previously well Inborn Errors of Metabolism
SYLLABUS FOR TRAINING IN CLINICAL PAEDIATRIC METABOLIC MEDICINE
 SYLLABUS FOR TRAINING IN CLINICAL PAEDIATRIC METABOLIC MEDICINE Updated December 2014: Vassili Valayannopoulos and Andrew Morris Paediatrics is an independent medical specialty based on the knowledge and
SYLLABUS FOR TRAINING IN CLINICAL PAEDIATRIC METABOLIC MEDICINE Updated December 2014: Vassili Valayannopoulos and Andrew Morris Paediatrics is an independent medical specialty based on the knowledge and
Col Rama Krishna Sanjeev Military Hospital Chennai Prof Shanmughasundaram Mehta Hospital, Chennai
 Col Rama Krishna Sanjeev Military Hospital Chennai Prof Shanmughasundaram Mehta Hospital, Chennai 11 day old male neonate admitted on 26/6 to our Hospital with c/olethargy -since day1 abnormal movements
Col Rama Krishna Sanjeev Military Hospital Chennai Prof Shanmughasundaram Mehta Hospital, Chennai 11 day old male neonate admitted on 26/6 to our Hospital with c/olethargy -since day1 abnormal movements
Diabetic Ketoacidosis
 Diabetic Ketoacidosis Definition: Diabetic Ketoacidosis is one of the most serious acute complications of diabetes. It s more common in young patients with type 1 diabetes mellitus. It s usually characterized
Diabetic Ketoacidosis Definition: Diabetic Ketoacidosis is one of the most serious acute complications of diabetes. It s more common in young patients with type 1 diabetes mellitus. It s usually characterized
Metabolic diseases of the liver
 Metabolic diseases of the liver Central role in metabolism Causes and mechanisms of dysfunction Clinical patterns of metabolic disease Clinical approach to problem-solving Specific disorders Liver s central
Metabolic diseases of the liver Central role in metabolism Causes and mechanisms of dysfunction Clinical patterns of metabolic disease Clinical approach to problem-solving Specific disorders Liver s central
Clinical Guideline. SPEG MCN Protocols Sub Group SPEG Steering Group
 Clinical Guideline SECONDARY CARE MANAGEMENT OF SUSPECTED ADRENAL CRISIS IN CHILDREN AND YOUNG PEOPLE Date of First Issue 24/01/2015 Approved 28/09/2017 Current Issue Date 16/06/2017 Review Date 01/09/2019
Clinical Guideline SECONDARY CARE MANAGEMENT OF SUSPECTED ADRENAL CRISIS IN CHILDREN AND YOUNG PEOPLE Date of First Issue 24/01/2015 Approved 28/09/2017 Current Issue Date 16/06/2017 Review Date 01/09/2019
UK NATIONAL METABOLIC BIOCHEMISTRY NETWORK GUIDELINES FOR THE INVESTIGATION OF HYPERAMMONAEMIA
 UK NATIONAL METABOLIC BIOCHEMISTRY NETWORK GUIDELINES FOR THE INVESTIGATION OF HYPERAMMONAEMIA Hyperammonaemia results from defective catabolism of amino acids to urea. Recognition and treatment of hyperammonaemia,
UK NATIONAL METABOLIC BIOCHEMISTRY NETWORK GUIDELINES FOR THE INVESTIGATION OF HYPERAMMONAEMIA Hyperammonaemia results from defective catabolism of amino acids to urea. Recognition and treatment of hyperammonaemia,
UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES Discipline of Biochemistry and Molecular Biology
 UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES Discipline of Biochemistry and Molecular Biology 1 PBL SEMINAR ACUTE & CHRONIC ETHANOL EFFECTS An Overview Sites
UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES Discipline of Biochemistry and Molecular Biology 1 PBL SEMINAR ACUTE & CHRONIC ETHANOL EFFECTS An Overview Sites
PROTOCOL FOR PARENTERAL NUTRITION
 PROTOCOL FOR PARENTERAL NUTRITION Based on; Roberton s textbook of neonatology. 4 th edition. 2005. Sudha Chaudari and Sandeep Kumar.TPN in neonates. Indian Paediatrics. November 2006 Deepak Chawla, Anu
PROTOCOL FOR PARENTERAL NUTRITION Based on; Roberton s textbook of neonatology. 4 th edition. 2005. Sudha Chaudari and Sandeep Kumar.TPN in neonates. Indian Paediatrics. November 2006 Deepak Chawla, Anu
Clinical Management of Organic Acidemias and OAA Natural History Registry. Kim Chapman MD PhD Children s National Rare Disease Institute
 Clinical Management of Organic Acidemias and OAA Natural History Registry Kim Chapman MD PhD Children s National Rare Disease Institute Disclosure Nothing to disclose concerning this lecture Organic acid?
Clinical Management of Organic Acidemias and OAA Natural History Registry Kim Chapman MD PhD Children s National Rare Disease Institute Disclosure Nothing to disclose concerning this lecture Organic acid?
Routine Newborn Screening, Testing the Newborn Inherited Metabolic Disorders Update August 2015
 Routine Newborn Screening, Testing the Newborn Inherited Metabolic Disorders Update August 2015 Metabolic birth defects can cause physical problems, mental retardation and, in some cases, death. It is
Routine Newborn Screening, Testing the Newborn Inherited Metabolic Disorders Update August 2015 Metabolic birth defects can cause physical problems, mental retardation and, in some cases, death. It is
Inborn errors of metabolism
 ESPEN Congress Nice 2010 From child to adult nutrition Inborn errors of metabolism Pascal Crenn Inborn errors of metabolism: from child to adult Pascal Crenn Hôpital Raymond Poincaré 92380 Garches. France
ESPEN Congress Nice 2010 From child to adult nutrition Inborn errors of metabolism Pascal Crenn Inborn errors of metabolism: from child to adult Pascal Crenn Hôpital Raymond Poincaré 92380 Garches. France
Newborn Screening: Blood Spot Disorders
 Newborn Screening: Blood Spot Disorders Arizona s Newborn Screening Program Program Overview Panel of Disorders Disorder Descriptions Program Components Hospitals ADHS Lab ADHS Follow-up ADHS Billing Medical
Newborn Screening: Blood Spot Disorders Arizona s Newborn Screening Program Program Overview Panel of Disorders Disorder Descriptions Program Components Hospitals ADHS Lab ADHS Follow-up ADHS Billing Medical
Inborn Error Of Metabolism :
 Inborn Error Of Metabolism : Inborn Error Of Metabolism inborn error of metabolism are a large group of hereditary biochemical diseases in which specific gene mutation cause abnormal or missing proteins
Inborn Error Of Metabolism : Inborn Error Of Metabolism inborn error of metabolism are a large group of hereditary biochemical diseases in which specific gene mutation cause abnormal or missing proteins
Presentation and investigation of mitochondrial disease in children
 Presentation and investigation of mitochondrial disease in children Andrew Morris Willink Unit, Manchester Mitochondrial function Carbohydrate Fat Respiratory chain Energy Mitochondria are the product
Presentation and investigation of mitochondrial disease in children Andrew Morris Willink Unit, Manchester Mitochondrial function Carbohydrate Fat Respiratory chain Energy Mitochondria are the product
PARENTERAL NUTRITION
 PARENTERAL NUTRITION DEFINITION Parenteral nutrition [(PN) or total parenteral nutrition (TPN)] is the intravenous infusion of some or all nutrients for tissue maintenance, metabolic requirements and growth
PARENTERAL NUTRITION DEFINITION Parenteral nutrition [(PN) or total parenteral nutrition (TPN)] is the intravenous infusion of some or all nutrients for tissue maintenance, metabolic requirements and growth
The breakdown of fats to provide energy occurs in segregated membrane-bound compartments
 CPT1a deficiency The breakdown of fats to provide energy occurs in segregated membrane-bound compartments of the cell known as mitochondria. Carnitine palmitoyltransferase Ia (CPT1a) is a protein that
CPT1a deficiency The breakdown of fats to provide energy occurs in segregated membrane-bound compartments of the cell known as mitochondria. Carnitine palmitoyltransferase Ia (CPT1a) is a protein that
Paediatric Clinical Chemistry
 Paediatric Clinical Chemistry Dr N Oosthuizen Dept Chemical Pathology UP 2011 Paediatric biochemistry The child is not a miniature adult Physiological development Immature organ systems Growing individual
Paediatric Clinical Chemistry Dr N Oosthuizen Dept Chemical Pathology UP 2011 Paediatric biochemistry The child is not a miniature adult Physiological development Immature organ systems Growing individual
Spectrum of Inborn Errors of Metabolism in Jordan: Five Years Experience at King Hussein Medical Center
 Spectrum of Inborn Errors of Metabolism in Jordan: Five Years Experience at King Hussein Medical Center Kefah Al-Qa qa MD*, Wajdi Amayreh MD*, Ali Al-Hawamdeh MD* ABSTRACT Objective: To describe the different
Spectrum of Inborn Errors of Metabolism in Jordan: Five Years Experience at King Hussein Medical Center Kefah Al-Qa qa MD*, Wajdi Amayreh MD*, Ali Al-Hawamdeh MD* ABSTRACT Objective: To describe the different
Urea Cycle Disorders Prior Authorization Program Summary
 Urea Cycle Disorders Prior Authorization Program Summary FDA APPROVED INDICATIONS DOSAGE 1,2 Agent(s) Indication(s) Dosing -Adjunctive therapy in the chronic management of patients with urea cycle disorders
Urea Cycle Disorders Prior Authorization Program Summary FDA APPROVED INDICATIONS DOSAGE 1,2 Agent(s) Indication(s) Dosing -Adjunctive therapy in the chronic management of patients with urea cycle disorders
ACUTE & CHRONIC ETHANOL EFFECTS An Overview
 ACUTE & CHRONIC ETHANOL EFFECTS An Overview University of Papua New Guinea School of Medicine & Health Sciences, Division of Basic Medical Sciences Clinical Biochemistry: PBL Seminar MBBS Yr 4 VJ Temple
ACUTE & CHRONIC ETHANOL EFFECTS An Overview University of Papua New Guinea School of Medicine & Health Sciences, Division of Basic Medical Sciences Clinical Biochemistry: PBL Seminar MBBS Yr 4 VJ Temple
UPDATE ON UREA CYCLE DISORDERS TREATMENT
 UPDATE ON UREA CYCLE DISORDERS TREATMENT George A. Diaz, MD, PhD Program for Inherited Metabolic Diseases Department of Genetics and Genomic Sciences Icahn School of Medicine at Mount Sinai Disclosure
UPDATE ON UREA CYCLE DISORDERS TREATMENT George A. Diaz, MD, PhD Program for Inherited Metabolic Diseases Department of Genetics and Genomic Sciences Icahn School of Medicine at Mount Sinai Disclosure
BIOTIN (BIOTINIDASE) DEFICIENCY Marc E. Tischler, PhD; University of Arizona
 BIOTIN (BIOTINIDASE) DEFICIENCY Marc E. Tischler, PhD; University of Arizona BIOTIN (BIOTINIDASE) DEFICIENCY biotin in the body is recycled by its removal from carboxylase enzymes to which it is attached
BIOTIN (BIOTINIDASE) DEFICIENCY Marc E. Tischler, PhD; University of Arizona BIOTIN (BIOTINIDASE) DEFICIENCY biotin in the body is recycled by its removal from carboxylase enzymes to which it is attached
HEREDITARY METABOLIC DISEASES
 HEREDITARY METABOLIC DISEASES Particular risk factors are: Advanced maternal age (e.g. Down's syndrome) Family history of inherited diseases (e.g. fragile X syndrome, Huntington's chorea) Previous child
HEREDITARY METABOLIC DISEASES Particular risk factors are: Advanced maternal age (e.g. Down's syndrome) Family history of inherited diseases (e.g. fragile X syndrome, Huntington's chorea) Previous child
Inborn error of metabolism
 Inborn error of metabolism The lecture is given by Dr Kefah Al qa qa, Consultant metabolic pediatrician, in Queen Rania Al Abdulla children hospital, on Thursday 11/12/2014. Let s tart Metabolism: refers
Inborn error of metabolism The lecture is given by Dr Kefah Al qa qa, Consultant metabolic pediatrician, in Queen Rania Al Abdulla children hospital, on Thursday 11/12/2014. Let s tart Metabolism: refers
With Dr. Sarah Reid and Dr. Sarah Curtis
 5. Headaches 6. Known diabetes 7. Specific high risk groups (ie. Teenagers, children on insulin pumps and those from lower socio-economic status). Episode 63 Pediatric Diabetic Ketoacidosis With Dr. Sarah
5. Headaches 6. Known diabetes 7. Specific high risk groups (ie. Teenagers, children on insulin pumps and those from lower socio-economic status). Episode 63 Pediatric Diabetic Ketoacidosis With Dr. Sarah
ORIGINAL ARTICLE. Etiology and outcome of inborn errors of metabolism
 1112 Etiology and outcome of inborn errors of metabolism Shehla Choudhry, 1 Masood Khan, 2 Hani Akbar Rao, 3 Anil Jalan, 4 Ejaz Ahmed Khan 5 ORIGINAL ARTICLE Abstract Objectives: To study the clinical
1112 Etiology and outcome of inborn errors of metabolism Shehla Choudhry, 1 Masood Khan, 2 Hani Akbar Rao, 3 Anil Jalan, 4 Ejaz Ahmed Khan 5 ORIGINAL ARTICLE Abstract Objectives: To study the clinical
Genética e Hígado: Cómo contribuye la genética en el algoritmo diagnóstico de la enfermedad hepática pediátrica? Nicholas Ah Mew, MD
 Genética e Hígado: Cómo contribuye la genética en el algoritmo diagnóstico de la enfermedad hepática pediátrica? Nicholas Ah Mew, MD April 24, 2017 SAP 2017 Buenos Aires Genetic disorders are rare why
Genética e Hígado: Cómo contribuye la genética en el algoritmo diagnóstico de la enfermedad hepática pediátrica? Nicholas Ah Mew, MD April 24, 2017 SAP 2017 Buenos Aires Genetic disorders are rare why
Testing Strategy for Inborn Errors of Metabolism in the Neonate Aditi I. Dagli, Roberto T. Zori and Bryce A. Heese. DOI: /neo.
 Testing Strategy for Inborn Errors of Metabolism in the Neonate Aditi I. Dagli, Roberto T. Zori and Bryce A. Heese Neoreviews 2008;9;e291 DOI: 10.1542/neo.9-7-e291 The online version of this article, along
Testing Strategy for Inborn Errors of Metabolism in the Neonate Aditi I. Dagli, Roberto T. Zori and Bryce A. Heese Neoreviews 2008;9;e291 DOI: 10.1542/neo.9-7-e291 The online version of this article, along
9/11/2012. Chapter 11. Learning Objectives. Learning Objectives. Endocrine Emergencies. Differentiate type 1 and type 2 diabetes
 Chapter 11 Endocrine Emergencies Learning Objectives Differentiate type 1 and type 2 diabetes Explain roles of glucagon, glycogen, and glucose in hypoglycemia Learning Objectives Discuss following medications
Chapter 11 Endocrine Emergencies Learning Objectives Differentiate type 1 and type 2 diabetes Explain roles of glucagon, glycogen, and glucose in hypoglycemia Learning Objectives Discuss following medications
So Much More Than The PKU Test
 Newborn Metabolic Screening So Much More Than The PKU Test Sarah Viall, MSN, PPCNP BC Newborn Screening Program Coordinator Division of Genetics & Metabolism Conflicts of Interest I have no conflicts of
Newborn Metabolic Screening So Much More Than The PKU Test Sarah Viall, MSN, PPCNP BC Newborn Screening Program Coordinator Division of Genetics & Metabolism Conflicts of Interest I have no conflicts of
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Urea Cycle Disorders Page 1 of 7 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Urea Cycle Disorders Prime Therapeutics will review Prior Authorization requests
Urea Cycle Disorders Page 1 of 7 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Urea Cycle Disorders Prime Therapeutics will review Prior Authorization requests
Inborn Errors of Metabolism
 30 Inborn Errors of Metabolism Inborn errors of metabolism (IEM) are disorders in which there is a block in the normal metabolic pathway that is caused by a genetic defect of a specific enzyme. The number
30 Inborn Errors of Metabolism Inborn errors of metabolism (IEM) are disorders in which there is a block in the normal metabolic pathway that is caused by a genetic defect of a specific enzyme. The number
Inborn Errors of Metabolism. Metabolic Pathway. Digestion and Fasting. How is Expanded Newborn Screening Different? MS/MS. The body is a factory.
 Inborn Errors of Metabolism The body is a factory. Inborn errors of metabolism are rare genetic disorders in which the body cannot properly turn food into energy. The disorders are usually caused by defects
Inborn Errors of Metabolism The body is a factory. Inborn errors of metabolism are rare genetic disorders in which the body cannot properly turn food into energy. The disorders are usually caused by defects
The University of Arizona Pediatric Residency Program. Primary Goals for Rotation. Genetics
 The University of Arizona Pediatric Residency Program Primary Goals for Rotation Genetics 1. GOAL: Understand the role of the pediatrician in preventing genetic disease, and in counseling and screening
The University of Arizona Pediatric Residency Program Primary Goals for Rotation Genetics 1. GOAL: Understand the role of the pediatrician in preventing genetic disease, and in counseling and screening
Fatty Acid Oxidation Disorders Organic Acid Disorders
 Genetic Fact Sheets for Parents Fatty Acid Oxidation Disorders Organic Acid Disorders Screening, Technology, and Research in Genetics is a multi-state project to improve information about the financial,
Genetic Fact Sheets for Parents Fatty Acid Oxidation Disorders Organic Acid Disorders Screening, Technology, and Research in Genetics is a multi-state project to improve information about the financial,
EU RISK MANAGEMENT PLAN (EU RMP) Nutriflex Omega peri emulsion for infusion , version 1.1
 EU RISK MANAGEMENT PLAN (EU RMP) Nutriflex Omega peri emulsion for infusion 13.7.2015, version 1.1 III.1. Elements for a Public Summary III.1.1. Overview of disease epidemiology Patients may need parenteral
EU RISK MANAGEMENT PLAN (EU RMP) Nutriflex Omega peri emulsion for infusion 13.7.2015, version 1.1 III.1. Elements for a Public Summary III.1.1. Overview of disease epidemiology Patients may need parenteral
Information for health professionals
 Introduction of a new screening test for newborn babies in Wales Newborn bloodspot screening for Medium chain acyl-coa dehydrogenase deficiency (MCADD) Newborn bloodspot screening for MCADD is being introduced
Introduction of a new screening test for newborn babies in Wales Newborn bloodspot screening for Medium chain acyl-coa dehydrogenase deficiency (MCADD) Newborn bloodspot screening for MCADD is being introduced
Positive Newborn Screens: What do you do next?
 Positive Newborn Screens: What do you do next? James B. Gibson, MD, Ph.D. Biochemical Geneticist at Specially for Children Clinical Associate Professor of Pediatrics UTHSCSA Carla R. Scott, MD Pediatric
Positive Newborn Screens: What do you do next? James B. Gibson, MD, Ph.D. Biochemical Geneticist at Specially for Children Clinical Associate Professor of Pediatrics UTHSCSA Carla R. Scott, MD Pediatric
Diagnosis of IEM. And Emergency Management
 Diagnosis of IEM And Emergency Management Susan Sklower Brooks, M.D., F.A.C.M.G. Professor of Pediatrics Professor of Obstetrics, Gynecology and Reproductive Sciences Robert Wood Johnson Medical School
Diagnosis of IEM And Emergency Management Susan Sklower Brooks, M.D., F.A.C.M.G. Professor of Pediatrics Professor of Obstetrics, Gynecology and Reproductive Sciences Robert Wood Johnson Medical School
Selective newborn screening of amino acid, fatty acid and organic acid disorders in the Kingdom of Bahrain.
 Selective newborn screening of amino acid, fatty acid and organic acid disorders in the Kingdom of Bahrain. Jamal Golbahar PhD Associate Professor of Molecular Medicine, Department of Molecular Medicine,
Selective newborn screening of amino acid, fatty acid and organic acid disorders in the Kingdom of Bahrain. Jamal Golbahar PhD Associate Professor of Molecular Medicine, Department of Molecular Medicine,
INBORN ERRORS OF METABOLISM: REVIEW AND DATA FROM A TERTIARY CARE CENTER
 Indian Journal of Clinical Biochemistry, 2009 / 24 (3) 215-222 REVIEW ARTICLE INBORN ERRORS OF METABOLISM: REVIEW AND DATA FROM A TERTIARY CARE CENTER Ananth N Rao, J Kavitha, Minakshi Koch and Suresh
Indian Journal of Clinical Biochemistry, 2009 / 24 (3) 215-222 REVIEW ARTICLE INBORN ERRORS OF METABOLISM: REVIEW AND DATA FROM A TERTIARY CARE CENTER Ananth N Rao, J Kavitha, Minakshi Koch and Suresh
Newborn screening for congenital metabolic diseases Optional out-of-pocket tests Information Sheet
 Newborn screening for congenital metabolic diseases Optional out-of-pocket tests Information Sheet Website:www.tipn.org.tw Telephone:(02)85962050 Ext. 401-403 Service line:(02)85962065 Fax:(02)85962067
Newborn screening for congenital metabolic diseases Optional out-of-pocket tests Information Sheet Website:www.tipn.org.tw Telephone:(02)85962050 Ext. 401-403 Service line:(02)85962065 Fax:(02)85962067
Fatty Acid Oxidation Disorders- an update. Fiona Carragher Biochemical Sciences, GSTS Pathology St Thomas Hospital, London
 Fatty Acid Oxidation Disorders- an update Fiona Carragher Biochemical Sciences, GSTS Pathology St Thomas Hospital, London An update. Overview of metabolism Clinical presentation and outcome Diagnostic
Fatty Acid Oxidation Disorders- an update Fiona Carragher Biochemical Sciences, GSTS Pathology St Thomas Hospital, London An update. Overview of metabolism Clinical presentation and outcome Diagnostic
Prevalence of selected disorders of inborn errors of metabolism in suspected cases at a Tertiary Care Hospital in Karachi
 Original Article Prevalence of selected disorders of inborn errors of metabolism in suspected cases at a Tertiary Care Hospital in Karachi Hema Satwani, 1 Jamal Raza, 2 Junji Hanai, 3 Shosuke Nomachi 4
Original Article Prevalence of selected disorders of inborn errors of metabolism in suspected cases at a Tertiary Care Hospital in Karachi Hema Satwani, 1 Jamal Raza, 2 Junji Hanai, 3 Shosuke Nomachi 4
Glycogen Storage Disease
 Glycogen Storage Disease 1 Introduction The food we eat is usually used for growth, tissue repair and energy. The body stores what it does not use. Excess sugar, or glucose, is stored as glycogen in the
Glycogen Storage Disease 1 Introduction The food we eat is usually used for growth, tissue repair and energy. The body stores what it does not use. Excess sugar, or glucose, is stored as glycogen in the
NEWBORN METABOLIC SCREEN, MINNESOTA
 Lab Dept: Test Name: Chemistry NEWBORN METABOLIC SCREEN, MINNESOTA General Information Lab Order Codes: Synonyms: CPT Codes: Test Includes: PKUN Newborn Screen for Hyopothyroidism, Phenylketonuria (PKU),
Lab Dept: Test Name: Chemistry NEWBORN METABOLIC SCREEN, MINNESOTA General Information Lab Order Codes: Synonyms: CPT Codes: Test Includes: PKUN Newborn Screen for Hyopothyroidism, Phenylketonuria (PKU),
Organic Acid Disorders
 Genetic Fact Sheets for Parents Organic Acid Disorders Screening, Technology, and Research in Genetics is a multi-state project to improve information about the financial, ethical, legal, and social issues
Genetic Fact Sheets for Parents Organic Acid Disorders Screening, Technology, and Research in Genetics is a multi-state project to improve information about the financial, ethical, legal, and social issues
Methylmalonic aciduria
 Methylmalonic aciduria Introductory information Written by: F. Hörster, S. Kölker & P. Burgard Reviewed & Revised for North America by: S. van Calcar Methylmalonic aciduria MMA 2 Methylmalonic aciduria
Methylmalonic aciduria Introductory information Written by: F. Hörster, S. Kölker & P. Burgard Reviewed & Revised for North America by: S. van Calcar Methylmalonic aciduria MMA 2 Methylmalonic aciduria
Acid Base Balance. Professor Dr. Raid M. H. Al-Salih. Clinical Chemistry Professor Dr. Raid M. H. Al-Salih
 Acid Base Balance 1 HYDROGEN ION CONCENTRATION and CONCEPT OF ph Blood hydrogen ion concentration (abbreviated [H + ]) is maintained within tight limits in health, with the normal concentration being between
Acid Base Balance 1 HYDROGEN ION CONCENTRATION and CONCEPT OF ph Blood hydrogen ion concentration (abbreviated [H + ]) is maintained within tight limits in health, with the normal concentration being between
Hypoglycemia in congenital hyperinsulinism
 How a normal body works: Our body is constantly at work. Our cells need a source of energy, and this source of energy is called glucose. The process is quite simple; think of it like an assembly line.
How a normal body works: Our body is constantly at work. Our cells need a source of energy, and this source of energy is called glucose. The process is quite simple; think of it like an assembly line.
Alvaro Serrano Russi MD University of Iowa Hospitals and Clinics
 Retrospective Analysis of the Region 4 Post Analytical Tool and Confirmatory Testing for Long Chain Fatty Acid Oxidation Disorders Screened in the State of Iowa Alvaro Serrano Russi MD University of Iowa
Retrospective Analysis of the Region 4 Post Analytical Tool and Confirmatory Testing for Long Chain Fatty Acid Oxidation Disorders Screened in the State of Iowa Alvaro Serrano Russi MD University of Iowa
TRANSAMINATION AND UREA CYCLE
 TRANSAMINATION AND UREA CYCLE USMAN SUMO FRIEND TAMBUNAN ARLI ADITYA PARIKESIT SEPTIANA BIOINFORMATICS GROUP DEPARTEMENT OF CHEMISTRY FACULTY OF MATHEMATIC AND SCIENCE UNIVERSITY OF INDONESIA What is transamination?
TRANSAMINATION AND UREA CYCLE USMAN SUMO FRIEND TAMBUNAN ARLI ADITYA PARIKESIT SEPTIANA BIOINFORMATICS GROUP DEPARTEMENT OF CHEMISTRY FACULTY OF MATHEMATIC AND SCIENCE UNIVERSITY OF INDONESIA What is transamination?
Metabolic Emergencies and the Pediatrician
 Metabolic Emergencies and the Pediatrician Stephen G. Kahler, MD Professor of Pediatrics Section of Genetics and Metabolism, UAMS and ACH Hot Springs, AR March 8, 2012 INHERITED METABOLIC DISORDERS HOW
Metabolic Emergencies and the Pediatrician Stephen G. Kahler, MD Professor of Pediatrics Section of Genetics and Metabolism, UAMS and ACH Hot Springs, AR March 8, 2012 INHERITED METABOLIC DISORDERS HOW
Nutritional Interventions in Primary Mitochondrial Disorders
 Nutritional Interventions in Primary Mitochondrial Disorders Carolyn J Ellaway MBBS PhD FRACP CGHGSA Genetic Metabolic Disorders Service Sydney Children s Hospital Network Disciplines of Child and Adolescent
Nutritional Interventions in Primary Mitochondrial Disorders Carolyn J Ellaway MBBS PhD FRACP CGHGSA Genetic Metabolic Disorders Service Sydney Children s Hospital Network Disciplines of Child and Adolescent
Lab Guide 2019 Metabolic Section Lab Guide
 Lab Guide 2019 Metabolic Section Lab Guide Quantitative Amino acids Plasma Plasma. Container/Tube: Preferred EDTA, Place immediately in ice. Acceptable: lithium heparin, sodium heparin. Patient preparation:
Lab Guide 2019 Metabolic Section Lab Guide Quantitative Amino acids Plasma Plasma. Container/Tube: Preferred EDTA, Place immediately in ice. Acceptable: lithium heparin, sodium heparin. Patient preparation:
Childhood epilepsy: the biochemical epilepsies. Dr Colin D Ferrie Consultant Paediatric Neurologist Leeds General Infirmary
 Childhood epilepsy: the biochemical epilepsies Dr Colin D Ferrie Consultant Paediatric Neurologist Leeds General Infirmary Definitions Epileptic Seizure Manifestation(s) of epileptic (excessive and/or
Childhood epilepsy: the biochemical epilepsies Dr Colin D Ferrie Consultant Paediatric Neurologist Leeds General Infirmary Definitions Epileptic Seizure Manifestation(s) of epileptic (excessive and/or
e-learning Fatty Acid Oxidation Defects Camilla Reed and Dr Simon Olpin Sheffield Children s Hospital
 e-learning Fatty Acid Oxidation Defects Camilla Reed and Dr Simon Olpin Sheffield Children s Hospital Fatty Acids Fatty acids are a major source of energy and body fat is an energy dense material. They
e-learning Fatty Acid Oxidation Defects Camilla Reed and Dr Simon Olpin Sheffield Children s Hospital Fatty Acids Fatty acids are a major source of energy and body fat is an energy dense material. They
LOW CITRULLINE AS A MARKER FOR THE PROXIMAL UREA CYCLE DEFECTS EXPERIENCE OF THE NEW ENGLAND NEWBORN SCREENING PROGRAM
 LOW CITRULLINE AS A MARKER FOR THE PROXIMAL UREA CYCLE DEFECTS EXPERIENCE OF THE NEW ENGLAND NEWBORN SCREENING PROGRAM Inderneel Sahai, MD, FACMG Newborn Screening and Genetic Testing Symposium Oct 2014
LOW CITRULLINE AS A MARKER FOR THE PROXIMAL UREA CYCLE DEFECTS EXPERIENCE OF THE NEW ENGLAND NEWBORN SCREENING PROGRAM Inderneel Sahai, MD, FACMG Newborn Screening and Genetic Testing Symposium Oct 2014
Basic Fluid and Electrolytes
 Basic Fluid and Electrolytes Chapter 22 Basic Fluid and Electrolytes Introduction Infants and young children have a greater need for water and are more vulnerable to alterations in fluid and electrolyte
Basic Fluid and Electrolytes Chapter 22 Basic Fluid and Electrolytes Introduction Infants and young children have a greater need for water and are more vulnerable to alterations in fluid and electrolyte
A Unusual Presentation of Propionic Acidemia with Thrombocytosis- A Case Report
 Article ID: WMC003015 ISSN 2046-1690 A Unusual Presentation of Propionic Acidemia with Thrombocytosis- A Case Report Corresponding Author: Dr. Rahul Sinha, Assistant Professor of Paediatrics, 167 Military
Article ID: WMC003015 ISSN 2046-1690 A Unusual Presentation of Propionic Acidemia with Thrombocytosis- A Case Report Corresponding Author: Dr. Rahul Sinha, Assistant Professor of Paediatrics, 167 Military
Syllabus for Training in Inborn Errors of Metabolism for Scientists and Medically Qualified Laboratory Staff
 Training Syllabus LABORATORY SYLLABUS Syllabus for Training in Inborn Errors of Metabolism for Scientists and Medically Qualified Laboratory Staff This syllabus is intended as a guide. Whilst the training
Training Syllabus LABORATORY SYLLABUS Syllabus for Training in Inborn Errors of Metabolism for Scientists and Medically Qualified Laboratory Staff This syllabus is intended as a guide. Whilst the training
MITO 101 Illness. Neurometabolic Clinic Children s Medical Center and UT Southwestern Medical Center Hospitals and Clinics
 1 MITO 101 Illness Juan M. Pascual, MD, PhD Division of Pediatric Neurology Departments of Neurology, Physiology and Pediatrics The University of Texas Southwestern Medical Center Neurometabolic Clinic
1 MITO 101 Illness Juan M. Pascual, MD, PhD Division of Pediatric Neurology Departments of Neurology, Physiology and Pediatrics The University of Texas Southwestern Medical Center Neurometabolic Clinic
Understanding metabolic disease
 Understanding metabolic disease Let s build a restaurant Chris Hendriksz Birmingham Children s Hospital 2006 The Task Let s build a restaurant! 2 Partners join to draw the plan. How can we change the
Understanding metabolic disease Let s build a restaurant Chris Hendriksz Birmingham Children s Hospital 2006 The Task Let s build a restaurant! 2 Partners join to draw the plan. How can we change the
Metabolic Disorders Screened Overseas but not Screened in Australia Condition Features Inherited Diagnosis Treatment Newborn Screen
 Metabolic Disorders ed Overseas but not ed in Australia Biotinidase Deficiency Severe form causes seizures & delay Biotin can prevent complications NZ, USA Tyrosinaemia Type I Coma & death before age 10
Metabolic Disorders ed Overseas but not ed in Australia Biotinidase Deficiency Severe form causes seizures & delay Biotin can prevent complications NZ, USA Tyrosinaemia Type I Coma & death before age 10
