Atypical Subacute Recurrence of Catastrophic Antiphospholipid Syndrome in a Japanese Female Patient
|
|
|
- Hugh Scott
- 5 years ago
- Views:
Transcription
1 CASE REPORT Atypical Subacute Recurrence of Catastrophic Antiphospholipid Syndrome in a Japanese Female Patient Masanobu Horikoshi 1, Shigeko Inokuma 1, Erika Matsubara 1, Yasunori Honda 1, Rika Okada 1, Mika Kobuna 1,YokoMiura 1, Shoko Kobayashi 1, Shigeo Kawai 2 and Toshio Kumasaka 2 Abstract Catastrophic antiphospholipid syndrome (CAPS) survivors rarely relapse. We herein report a case of a second CAPS episode with an unusual subacute course and no microangiopathic hemolytic anemia (MAHA), a common CAPS symptom. During the first episode, the 69-year-old woman responded well to high-dose glucocorticoids and plasma exchange. On relapse, these treatments plus rituximab were ineffective and she died of multi-organ failure and bacterial cholangitis. The absence of MAHA and a subacute course do not exclude a CAPS recurrence. Key words: catastrophic antiphospholipid syndrome, microangiopathic hemolytic anemia, relapse, rituximab () () Introduction Catastrophic antiphospholipid syndrome (CAPS), a rare subtype of antiphospholipid syndrome (APS), is characterized by multiple organ dysfunctions due to thrombosis of the small vessels occurring over a short period of time, typically less than 1 week. The mortality of CAPS is about 30% even when treated with high-dose glucocorticoids (GCs) and plasma exchange (PE) (1, 2), but patients who survive the initial event rarely have recurrent events (3). We herein report a case of CAPS relapse in a Japanese woman with an atypical slow clinical course and the absence of microangiopathic hemolytic anemia (MAHA). Case Report In July 2013, a 69-year-old Japanese woman with a 7- year history of recurrent cerebral infarction due to APS, presented with symptoms of fever at a local hospital. She was diagnosed with aspiration pneumonia and successfully treated with antibiotics. She also exhibited dysphasia due to a cerebral infarction, and was transferred to our hospital at the behest of her family for rehabilitation. Three years prior to this admission, she was referred to our hospital because of fever and a disturbance of consciousness, and was subsequently diagnosed with CAPS based on the presence of multiple organ impairment, including the brain, liver and kidney, and the presence of an antiphospholipid antibody, which had been detected previously. The patient had hemolytic anemia with peripheral schistocytes, thus suggesting MAHA. She was successfully treated by anticoagulation, high-dose GC, and PE, and has since been on 6-mg prednisolone (PSL) maintenance therapy. At the current admission, the patient was afebrile and well oriented. She had been bed-bound for years and needed help with her daily activities. A physical examination revealed a systolic ejection murmur in the apex and mild to moderate muscle weakness of the extremities. She did not have any skin manifestations. The complete blood count, aspartate transaminase (AST), alanine transaminase (ALT), creatinine levels, and a urinalysis including urine sediment were normal, except for slight anemia. The activated partial thromboplastin time was prolonged (79.5 s; normal range <39.0 s) as was the prothrombin time due to anticoagulation with warfarin (international normalization ratio 1.69). The immunological tests were positive for β2 glycoprotein 1 dependent anticardiolipin antibody (>125 U/mL; normal range Department of Allergy and Rheumatic Diseases, Japanese Red Cross Medical Center, Japan and Department of Pathology, Japanese Red Cross Medical Center, Japan Received for publication February 13, 2015; Accepted for publication March 15, 2015 Correspondence to Dr. Shigeko Inokuma, inokuma_shigeko@med.jrc.or.jp 2923
2 a b Figure 1. (a) Palpable purpura on the palm (arrow) on hospital day 35. (b) Skin biopsy (Hematoxylin and Eosin staining) of the purpura revealed fibrin thrombi in dermal small vessels. Table. Laboratory Data on Admission and on Hospital Day 37. Reference Variable Range On Admission On hospital day 37 WBC (per mm 3 ) 3,700-8,000 7,400 20,900 Differential count (%) Neutrophils Lymphocytes Monocytes Eosinophils Basophils Hemoglobin (g/dl) PLT ( 10 4 per mm 3 ) AST (IU/L) ALT (IU/L) LDH (IU/L) Creatinie (mg/dl) CRP (mg/dl) CH50 (U/mL) APTT (sec) PT-INR Fibrinogen (mg/dl) D-dimer (ug/ml) WBC: white blood cell, PLT: platelet AST: aspartate transaminase, ALT: alanine transaminase, LDH: lactate dehydrogenase CRP: C-reactive protein CH50 (50% hemolytic unit of complement) APTT: Activated partial thromboplastin time PT-INR: prothrombin time-international normalization ratio <3.4 U/mL), whereas the anti-nuclear antibody titer was low (1:40, homogenous/speckled pattern) and the anti-dsdna was negative. Chest radiograph showed a slight infiltration in the right lower lung field, which was attributed to the preceding pneumonia. A central venous catheter was inserted into the right femoral vein for parenteral nutrition. Three days after the catheter insertion, however, the patient developed fever, anemia, and thrombocytopenia. Computed tomography (CT) revealed diffuse lung infiltration and venous thrombosis at the insertion site. The catheter was removed and anticoagulation with unfractionated heparin and antibiotics was started. Over the next 4 weeks, the patient developed a diffuse gastric and bladder mucosal hemorrhage as revealed by gastroscopy and cystoscopy, the elevation of AST and ALT, proteinuria, hypertension, and the elevation of the creatinine level (0.87 mg/dl on admission, 1.18 mg/dl on hospital day 38). A fever was persistent and refractory to antibiotics, including meropenem, cefepime, and clindamycin. The procalcitonin levels were constantly positive (1.49 ng/ml on hospital day 23, 1.07 ng/ml on hospital day 50). Three weeks after hospitalization, the patient gradually developed palpable purpura in the bilateral palms (Fig. 1a). A skin biopsy revealed multiple fibrin thrombi in dermal small vessels (Fig. 1b). On the basis of multiple organ dysfunction and microthrombosis in small vessels, a relapse of CAPS was diagnosed on hospital day 38. The laboratory data on admission and on hospital day 37 are summarized in Table. We started methylprednisolone (mpsl) at a pulse dose of 1,000 mg/day for 3 days followed by 40 mg daily, which resulted in a dramatic improvement of fever, lung infiltration, partial improvement of thrombocytopenia, and liver enzyme 2924
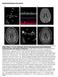
3 a b Figure 2. Petechiae (a) in the lower palpebral conjunctiva and (b) on the toes. Figure 3. Summary of the clinical course. AST: aspartate transaminase, PLT: platelet count, PSL: prednisolone, mpsl: methylprednisolone, IVIg: intravenous immunoglobulin, PE: plasma exchange, RTX: rituximab elevation. One month later, however, the patient again exhibited fever, thrombocytopenia, and liver enzyme elevation. Intravenous immunoglobulin (IVIg) at 400 mg/kg/day for 4 days had no effect. Plasma exchange every other day was effective during treatment only, and symptoms and laboratory parameters worsened during the 2-day interval. Renal dysfunction and proteinuria were refractory to these treatments. As the patient had primary CAPS (CAPS without systemic lupus erythematosus), we decided to administer rituximab as further treatment rather than cyclophosphamide. However, 4 administrations of rituximab at 375 mg/m 2 had no effect. Despite increasing mpsl to 60 mg, she developed petechiae in the lower palpebral conjunctiva and on the toes around hospital day 110 (Fig. 2). The patient died on hospital day 120. The entire treatment course is summarized in Fig. 3. An autopsy revealed the presence of multiple thrombi in small vessels in multiple organs. In the liver, organized thrombi were detected in the interlobular portal veins and arteries (Fig. 4a). Organized thrombi were also detected in the arterioles of the gastric mucosa and pancreas. A kidney specimen showed a thickened and swollen intima of the afferent arterioles and fibrin thrombi in the glomerular tufts, compatible with renal thrombotic microangiopathy (Fig. 4b, c). Fibrin thrombi were detected in the small arteries of the left ventricle and Libman-Sacks vegetation was seen on the tricuspid valve. In addition to these findings which are consistent with APS, the common bile duct was obstructed by stones. Neutrophil and histiocyte infiltration, as well as bacterial colonies, were seen at the site of the bile duct obstruction, which is consistent with bacterial cholangitis. Discussion The subacute clinical course and lack of MAHA in the present case were atypical for CAPS. The major differential diagnoses were infective endocarditis, thrombotic thrombocytopenic purpura (TTP), and heparin-induced thrombocytopenia (HIT). Blood cultures were taken at least once every 2925
4 a b c Figure 4. (a) An autopsy specimen of the liver (Elastica van Gieson stain) exhibits organized thrombi in the interlobular portal veins and arteries. Kidney specimen shows (b) thickened and swollen intima of the afferent arterioles (arrows) and (c) fibrin thrombi (arrow) in the glomerular tufts (b: Periodic acid methenamine silver stain; c: masson s trichrome stain). week and the findings were negative. Transthoracic echocardiography showed no vegetation. Fragmented red blood cells were not detected in blood smears, which is atypical for TTP. Changing the anticoagulant first to dalteparin and then to fondaparinux, which are less likely to cause HIT, did not improve the patient s status or thrombocytopenia. She was refractory to intensive immunosuppressive therapy, including rituximab. Multiple organ failure gradually worsened her general status and she eventually died. The autopsy findings indicated that the cause of death was bacterial cholangitis and sepsis due to a common bile duct obstruction. The obstruction likely occurred a few days prior to death because it was not evident on the abdominal enhanced CT 1 month prior and the total bilirubin level had been <2 mg/dl. Moreover, a blood culture taken just 2 days before death was negative. There are few reports on the prognosis of CAPS patients who survive the initial event. Erkan et al. reported that none of the 58 CAPS patients who survived the initial event developed further catastrophic events during an average follow-up of 67.2 months (3). Moreover, since the first CAPS relapse case was reported in 1999 (4), only 10 additional cases have been documented (5-9). An international registry of patients with CAPS was created in 2000 (2, 10-12). Espinosa et al. reviewed 9 cases from the CAPS registry (9). With the exception of 1 case in which detailed data were not available, 13 of 18 catastrophic episodes in the 8 cases were complicated by MAHA and the presence of schistocytes in the peripheral blood smear. Furthermore, in 2 relapsed cases reported in 2012 and 2014, all 5 episodes (2 in one and 3 in the other) were complicated by MAHA (7, 8). Thus, MAHA has been detected in 18 of 23 episodes (78%) in the 10 reported relapsing CAPS patients. In our case, however, schistocytes were not detected in the peripheral smear and MAHA was not clinically diagnosed, although it was present during the first event 3 years prior. The absence of MAHA, therefore, does not seem to preclude a CAPS recurrence. Another unusual aspect of the present case was that our patient developed a relapse with an atypical subacute course. She gradually developed fever, lung infiltration, thrombocytopenia, anemia, mucosal bleeding in the stomach and bladder, elevation of liver enzymes, acute kidney injury with hypertension and proteinuria, and palpable purpura over 1 month, while preliminary classification criteria (1, 13) state that manifestations of CAPS usually develop simultaneously or in <1 week. Indeed, data from the CAPS registry reveal that 175 of 176 patients (99%) fulfill this acute course criterion (1). A subacute course even over 1 month does not seem to preclude a second catastrophic event in APS patients if other possible diseases are excluded. Treatment is always challenging if a CAPS patient is refractory to anticoagulation and corticosteroids (first-line therapies) and to the addition of plasma exchange and/or IVIg (second-line therapies) (12, 14). Although rituximab is recommended rather than cyclophosphamide for the treatment of refractory CAPS without systemic lupus erythematous (12, 15), our patient was also refractory to rituximab and died. Eculizumab is another agent reported to be effective for CAPS treatment (7), but the cost is high and it is approved only for paroxysmal nocturnal hemoglobinuria. The administration of glucocorticoids and the plasma exchange were at least partially effective for fever, lung involvement, and liver enzyme elevation, so we speculate that anti-cytokine therapy such as anti-tumor necrosis alpha or interleukin-6 might have been effective for our patient, although there have been no reports using these agents for CAPS. In conclusion, the lack of MAHA and a subacute course over a month are therefore insufficient to exclude a subsequent catastrophic event in APS or CAPS patients. The most effective third-line therapy for CAPS is still unresolved. The authors state that they have no Conflict of Interest(COI). References 1. Cervera R, Font J, Gomez-Puerta JA, et al. Validation of the preliminary criteria for the classification of catastrophic antiphospholipid syndrome. Ann Rheum Dis 64: , Bucciarelli S, Espinosa G, Cervera R. The CAPS Registry: morbidity and mortality of the catastrophic antiphospholipid syn- 2926
5 drome. Lupus 18: , Erkan D, Asherson RA, Espinosa G, et al. Long term outcome of catastrophic antiphospholipid syndrome survivors. Ann Rheum Dis 62: , Cerveny KC, Sawitzke AD. Relapsing catastrophic antiphospholipid antibody syndrome: a mimic for thrombotic thrombocytopenic purpura? Lupus 8: , Asherson RA, Espinosa G, Menahem S, et al. Relapsing catastrophic antiphospholipid syndrome: report of three cases. Semin Arthritis Rheum 37: , Cervera R. Update on the diagnosis, treatment, and prognosis of the catastrophic antiphospholipid syndrome. Curr Rheumatol Rep 12: 70-76, Shapira I, Andrade D, Allen SL, Salmon JE. Brief report: induction of sustained remission in recurrent catastrophic antiphospholipid syndrome via inhibition of terminal complement with eculizumab. Arthritis Rheum 64: , Pieralli F, Grazzini M, Vannucchi V, Mancini A, Cammelli D, Nozzoli C. Recurrent episodes of hemorrhagic alveolitis in relapsing catastrophic antiphospholipid syndrome: the same side of the dark moon. Clin Rheumatol 33: , Espinosa G, Rodriguez-Pinto I, Gomez-Puerta JA, Pons-Estel G, Cervera R. Relapsing catastrophic antiphospholipid syndrome potential role of microangiopathic hemolytic anemia in disease relapses. Semin Arthritis Rheum 42: , Cervera R. CAPS Registry. Lupus 21: , Cervera R, Bucciarelli S, Plasin MA, et al. Catastrophic antiphospholipid syndrome (CAPS): descriptive analysis of a series of 280 patients from the CAPS Registry. J Autoimmun 32: , Cervera R. Catastrophic antiphospholipid syndrome (CAPS): update from the CAPS Registry. Lupus 19: , Asherson RA, Cervera R, de Groot PG, et al. Catastrophic antiphospholipid syndrome: international consensus statement on classification criteria and treatment guidelines. Lupus 12: , Erkan D, Espinosa G, Cervera R. Catastrophic antiphospholipid syndrome: updated diagnostic algorithms. Autoimmun Rev 10: 74-79, Espinosa G, Berman H, Cervera R. Management of refractory cases of catastrophic antiphospholipid syndrome. Autoimmun Rev 10: , The Japanese Society of Internal Medicine
monoclonal gammopathy of undetermin Citation Rheumatology international, 33(1),
 NAOSITE: Nagasaki University's Ac Title Author(s) Renal thrombotic microangiopathies/ in a patient with primary Sjögren's monoclonal gammopathy of undetermin Koga, Tomohiro; Yamasaki, Satoshi; Atsushi;
NAOSITE: Nagasaki University's Ac Title Author(s) Renal thrombotic microangiopathies/ in a patient with primary Sjögren's monoclonal gammopathy of undetermin Koga, Tomohiro; Yamasaki, Satoshi; Atsushi;
Most Common Hemostasis Consults: Thrombocytopenia
 Most Common Hemostasis Consults: Thrombocytopenia Cindy Neunert, MS MSCS Assistant Professor, Pediatrics CUMC Columbia University TSHNA Meeting, April 15, 2016 Financial Disclosures No relevant financial
Most Common Hemostasis Consults: Thrombocytopenia Cindy Neunert, MS MSCS Assistant Professor, Pediatrics CUMC Columbia University TSHNA Meeting, April 15, 2016 Financial Disclosures No relevant financial
Case report 24 th Summer School of Internal Medicine 2015
 Case report 24 th Summer School of Internal Medicine 2015 Goldmannová D., Horák P., Skácelová M. IIIrd Internal Clinic - endocrinology, diabetology, rheumatology, nephrology University hospital Olomouc,
Case report 24 th Summer School of Internal Medicine 2015 Goldmannová D., Horák P., Skácelová M. IIIrd Internal Clinic - endocrinology, diabetology, rheumatology, nephrology University hospital Olomouc,
Mortality in the Catastrophic Antiphospholipid Syndrome
 ARTHRITIS & RHEUMATISM Vol. 54, No. 8, August 2006, pp 2568 2576 DOI 10.1002/art.22018 2006, American College of Rheumatology Mortality in the Catastrophic Antiphospholipid Syndrome Causes of Death and
ARTHRITIS & RHEUMATISM Vol. 54, No. 8, August 2006, pp 2568 2576 DOI 10.1002/art.22018 2006, American College of Rheumatology Mortality in the Catastrophic Antiphospholipid Syndrome Causes of Death and
Things to never miss in the office. Brett Houston MD FRCPC (PYG-5, hematology) Leonard Minuk MD FRCPC
 Things to never miss in the office Brett Houston MD FRCPC (PYG-5, hematology) Leonard Minuk MD FRCPC Presenter Disclosure Faculty / Speaker s name: Brett Houston / Leonard Minuk Relationships with commercial
Things to never miss in the office Brett Houston MD FRCPC (PYG-5, hematology) Leonard Minuk MD FRCPC Presenter Disclosure Faculty / Speaker s name: Brett Houston / Leonard Minuk Relationships with commercial
What is meant by Thrombotic Microangiopathy (TMA)?
 What is meant by Thrombotic Microangiopathy (TMA)? Thrombotic Microangiopathy (TMA) is a group of disorders characterized by injured endothelial cells, microangiopathic hemolytic anemia (MAHA), with its
What is meant by Thrombotic Microangiopathy (TMA)? Thrombotic Microangiopathy (TMA) is a group of disorders characterized by injured endothelial cells, microangiopathic hemolytic anemia (MAHA), with its
Review Article. Catastrophic Antiphospholipid Syndrome. Introduction. Etiopathogenesis. Man-Chi Leung and Woon-Leung Ng
 Review Article Catastrophic Antiphospholipid Syndrome Man-Chi Leung and Woon-Leung Ng Abstract: Keywords: The catastrophic antiphospholipid syndrome is a potentially life threatening rheumatological condition
Review Article Catastrophic Antiphospholipid Syndrome Man-Chi Leung and Woon-Leung Ng Abstract: Keywords: The catastrophic antiphospholipid syndrome is a potentially life threatening rheumatological condition
A 60 year old woman with altered mental status and thrombotic microangiopathy. Josh Veatch
 A 60 year old woman with altered mental status and thrombotic microangiopathy Josh Veatch Previously healthy 60 year old woman 2 3 months of fatigue following a URI, transient episodes being out of it
A 60 year old woman with altered mental status and thrombotic microangiopathy Josh Veatch Previously healthy 60 year old woman 2 3 months of fatigue following a URI, transient episodes being out of it
ISTITUTO DI RICERCHE FARMACOLOGICHE MARIO NEGRI CLINICAL RESEARCH CENTER ALDO E FOR CELE RARE DACCO DISEASES ALDO E CELE DACCO
 ISTITUTO DI RICERCHE FARMACOLOGICHE MARIO NEGRI CENTRO MARIO DI NEGRI RICERCHE INSTITUTE CLINICHE FOR PHARMACOLOGICAL PER LE MALATTIE RESEARCH RARE CLINICAL RESEARCH CENTER ALDO E FOR CELE RARE DACCO DISEASES
ISTITUTO DI RICERCHE FARMACOLOGICHE MARIO NEGRI CENTRO MARIO DI NEGRI RICERCHE INSTITUTE CLINICHE FOR PHARMACOLOGICAL PER LE MALATTIE RESEARCH RARE CLINICAL RESEARCH CENTER ALDO E FOR CELE RARE DACCO DISEASES
Thrombotic Microangiopathies
 Thrombotic Microangiopathies ASH/San Antonio Breast Cancer Symposium Review James N. George March 14, 2015 Thrombotic Microangiopathies (TMA): Everything you need to know from 5 patient stories Thrombotic
Thrombotic Microangiopathies ASH/San Antonio Breast Cancer Symposium Review James N. George March 14, 2015 Thrombotic Microangiopathies (TMA): Everything you need to know from 5 patient stories Thrombotic
Protocol Version 2.0 Synopsis
 Protocol Version 2.0 Synopsis Title Short Title Plasma exchange and glucocorticoid dosing in anti-neutrophil cytoplasm antibody associated vasculitis: a randomized controlled trial. PEXIVAS PEXIVAS Clinical
Protocol Version 2.0 Synopsis Title Short Title Plasma exchange and glucocorticoid dosing in anti-neutrophil cytoplasm antibody associated vasculitis: a randomized controlled trial. PEXIVAS PEXIVAS Clinical
Soliris (eculizumab) DRUG.00050
 Market DC Soliris (eculizumab) DRUG.00050 Override(s) Prior Authorization Approval Duration 1 year Medications Soliris (eculizumab) APPROVAL CRITERIA Paroxysmal Nocturnal Hemoglobinuria I. Initiation of
Market DC Soliris (eculizumab) DRUG.00050 Override(s) Prior Authorization Approval Duration 1 year Medications Soliris (eculizumab) APPROVAL CRITERIA Paroxysmal Nocturnal Hemoglobinuria I. Initiation of
Manifestation of Antiphospholipid Syndrome among Saudi patients :examining the applicability of sapporo Criteria
 Manifestation of Antiphospholipid Syndrome among Saudi patients :examining the applicability of sapporo Criteria Farjah H AlGahtani Associate professor,md,mph Leukemia,Lymphoma in adolescent,thromboembolic
Manifestation of Antiphospholipid Syndrome among Saudi patients :examining the applicability of sapporo Criteria Farjah H AlGahtani Associate professor,md,mph Leukemia,Lymphoma in adolescent,thromboembolic
Renal failure and thrombocytopaenia? Don t forget TTP/HUS. Jonathan Wala Nephrologist
 Renal failure and thrombocytopaenia? Don t forget TTP/HUS Jonathan Wala Nephrologist Thrombotic microangiopathies Disorders characterized by: thrombocytopaenia microangiopathic haemolytic anaemia (MAHA)
Renal failure and thrombocytopaenia? Don t forget TTP/HUS Jonathan Wala Nephrologist Thrombotic microangiopathies Disorders characterized by: thrombocytopaenia microangiopathic haemolytic anaemia (MAHA)
A 23 year old Caucasian male presented with shortness of breath, hypertension, bloody sputum, and a history of drug abuse (confirmed by urinalysis).
 A 23 year old Caucasian male presented with shortness of breath, hypertension, bloody sputum, and a history of drug abuse (confirmed by urinalysis). He was found to have severe kidney injury requiring
A 23 year old Caucasian male presented with shortness of breath, hypertension, bloody sputum, and a history of drug abuse (confirmed by urinalysis). He was found to have severe kidney injury requiring
Beyond Plasma Exchange: Targeted Therapy for Thrombotic Thrombocytopenic Purpura
 Beyond Plasma Exchange: Targeted Therapy for Thrombotic Thrombocytopenic Purpura Kristen Knoph, PharmD, BCPS PGY2 Pharmacotherapy Resident Pharmacy Grand Rounds April 25, 2017 2016 MFMER slide-1 Objectives
Beyond Plasma Exchange: Targeted Therapy for Thrombotic Thrombocytopenic Purpura Kristen Knoph, PharmD, BCPS PGY2 Pharmacotherapy Resident Pharmacy Grand Rounds April 25, 2017 2016 MFMER slide-1 Objectives
HEME 10 Bleeding Disorders
 HEME 10 Bleeding Disorders When injury occurs, three mechanisms occur Blood vessels Primary hemostasis Secondary hemostasis Diseases of the blood vessels Platelet disorders Thrombocytopenia Functional
HEME 10 Bleeding Disorders When injury occurs, three mechanisms occur Blood vessels Primary hemostasis Secondary hemostasis Diseases of the blood vessels Platelet disorders Thrombocytopenia Functional
Case Report Catastrophic Antiphospholipid Syndrome
 Case Reports in Rheumatology Volume 2016, Article ID 4161439, 4 pages http://dx.doi.org/10.1155/2016/4161439 Case Report Catastrophic Antiphospholipid Syndrome Rawhya R. El-Shereef, 1 Zein El-Abedin, 2
Case Reports in Rheumatology Volume 2016, Article ID 4161439, 4 pages http://dx.doi.org/10.1155/2016/4161439 Case Report Catastrophic Antiphospholipid Syndrome Rawhya R. El-Shereef, 1 Zein El-Abedin, 2
Current management of catastrophic antiphospholipid syndrome
 Review Current management of catastrophic antiphospholipid syndrome The catastrophic variant of the antiphospholipid syndrome (APS) is the most severe form of APS with acute multiple organ involvement
Review Current management of catastrophic antiphospholipid syndrome The catastrophic variant of the antiphospholipid syndrome (APS) is the most severe form of APS with acute multiple organ involvement
Catastrophic antiphospholipid syndrome: A rare but serious complication of antiphospholipid antibody syndrome Sandhu VK*; Singh H
 Open Journal of Clinical & Medical Case Reports Volume 3 (2017) Issue 4 ISSN 2379-1039 Catastrophic antiphospholipid syndrome: A rare but serious complication of antiphospholipid antibody syndrome Sandhu
Open Journal of Clinical & Medical Case Reports Volume 3 (2017) Issue 4 ISSN 2379-1039 Catastrophic antiphospholipid syndrome: A rare but serious complication of antiphospholipid antibody syndrome Sandhu
The complex treatment including rituximab in the Management of Catastrophic Antiphospholid Syndrome with renal involvement
 Rymarz and Niemczyk BMC Nephrology (2018) 19:132 https://doi.org/10.1186/s12882-018-0928-z CASE REPORT Open Access The complex treatment including rituximab in the Management of Catastrophic Antiphospholid
Rymarz and Niemczyk BMC Nephrology (2018) 19:132 https://doi.org/10.1186/s12882-018-0928-z CASE REPORT Open Access The complex treatment including rituximab in the Management of Catastrophic Antiphospholid
A young female with catastrophic antiphospholipid syndrome
 www.edoriumjournals.com case report open ACCESS A young female with catastrophic antiphospholipid syndrome Vivekanandan Senthamil Pari, Lakshmi M, Sampath Kumar, Sathyamurthy P, Sudhakar MK, Sandhya Sundaram
www.edoriumjournals.com case report open ACCESS A young female with catastrophic antiphospholipid syndrome Vivekanandan Senthamil Pari, Lakshmi M, Sampath Kumar, Sathyamurthy P, Sudhakar MK, Sandhya Sundaram
February 2016, Volume: 8, Issue: 2, Pages: , DOI:
 Electronic Physician (ISSN: 2008-5842) http://www.ephysician.ir February 2016, Volume: 8, Issue: 2, Pages: 1874-1879, DOI: http://dx.doi.org/10.19082/1874 Pulmonary embolism in an adolescent girl with
Electronic Physician (ISSN: 2008-5842) http://www.ephysician.ir February 2016, Volume: 8, Issue: 2, Pages: 1874-1879, DOI: http://dx.doi.org/10.19082/1874 Pulmonary embolism in an adolescent girl with
Hemolytic uremic syndrome: Investigations and management
 Hemolytic uremic syndrome: Investigations and management SAWAI Toshihiro M.D., Ph.D. Department of Pediatrics, Shiga University of Medical Science Otsu, JAPAN AGENDA TMA; Thrombotic micro angiopathy STEC-HUS;
Hemolytic uremic syndrome: Investigations and management SAWAI Toshihiro M.D., Ph.D. Department of Pediatrics, Shiga University of Medical Science Otsu, JAPAN AGENDA TMA; Thrombotic micro angiopathy STEC-HUS;
Atypical Hemolytic Uremic Syndrome: When the Environment and Mutations Affect Organ Systems. A Case Report with Review of Literature
 Atypical Hemolytic Uremic Syndrome: When the Environment and Mutations Affect Organ Systems. A Case Report with Review of Literature Mouhanna Abu Ghanimeh 1, Omar Abughanimeh 1, Ayman Qasrawi 1, Abdulraheem
Atypical Hemolytic Uremic Syndrome: When the Environment and Mutations Affect Organ Systems. A Case Report with Review of Literature Mouhanna Abu Ghanimeh 1, Omar Abughanimeh 1, Ayman Qasrawi 1, Abdulraheem
Images in Cardiovascular Medicine
 Images in Cardiovascular Medicine Numerous Small Vegetations Revealing Libman-Sacks Endocarditis in Catastrophic Antiphospholipid Syndrome Hideo Yamamoto, MD; Tamaki Iwade, MD; Ryuji Nakano, MD; Masahiro
Images in Cardiovascular Medicine Numerous Small Vegetations Revealing Libman-Sacks Endocarditis in Catastrophic Antiphospholipid Syndrome Hideo Yamamoto, MD; Tamaki Iwade, MD; Ryuji Nakano, MD; Masahiro
DRUG NAME: Eculizumab Brand(s): Soliris DOSAGE FORM/ STRENGTH: 10 mg/ml (300 mg per vial)
 Preamble: A confirmed diagnosis of atypical hemolytic uremic syndrome (ahus) is required for eculizumab funding. The information below is to provide clinicians with context for how a diagnosis of ahus
Preamble: A confirmed diagnosis of atypical hemolytic uremic syndrome (ahus) is required for eculizumab funding. The information below is to provide clinicians with context for how a diagnosis of ahus
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Lapeyraque A-L, Malina M, Fremeaux-Bacchi V, et al. Eculizumab
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Lapeyraque A-L, Malina M, Fremeaux-Bacchi V, et al. Eculizumab
Case Report. 15th June Carolina Ourique Luciana Frade Daniela Alves
 Case Report 15th June 2016 Carolina Ourique Luciana Frade Daniela Alves CASE REPORT Woman 23 year-old Single Profission: Social-cultural animator for children CASE REPORT PERSONAL MEDICAL HISTORY Smoker
Case Report 15th June 2016 Carolina Ourique Luciana Frade Daniela Alves CASE REPORT Woman 23 year-old Single Profission: Social-cultural animator for children CASE REPORT PERSONAL MEDICAL HISTORY Smoker
Outcome of Disseminated Intravascular Coagulation without Documented Antiphospholipid Antibody Successfully Treated with Rituximab
 Soonchunhyang Medical Science 21(2):154-158, December 2015 pissn: 2233-4289 I eissn: 2233-4297 SE REPORT Outcome of Disseminated Intravascular oagulation without Documented ntiphospholipid ntibody Successfully
Soonchunhyang Medical Science 21(2):154-158, December 2015 pissn: 2233-4289 I eissn: 2233-4297 SE REPORT Outcome of Disseminated Intravascular oagulation without Documented ntiphospholipid ntibody Successfully
Double-valve Replacement for Mitral and Aortic Regurgitation in a Patient with Libman-Sacks Endocarditis
 CASE REPORT Double-valve Replacement for Mitral and Aortic Regurgitation in a Patient with Libman-Sacks Endocarditis Kenta Hachiya 1, Kazuaki Wakami 1, Tomomitsu Tani 1, Atsuhiro Yoshida 1, Shugo Suzuki
CASE REPORT Double-valve Replacement for Mitral and Aortic Regurgitation in a Patient with Libman-Sacks Endocarditis Kenta Hachiya 1, Kazuaki Wakami 1, Tomomitsu Tani 1, Atsuhiro Yoshida 1, Shugo Suzuki
EDUCATIONAL COMMENTARY DISSEMINATED INTRAVASCULAR COAGULATION
 EDUCATIONAL COMMENTARY DISSEMINATED INTRAVASCULAR COAGULATION Educational commentary is provided through our affiliation with the American Society for Clinical Pathology (ASCP). To obtain FREE CME/CMLE
EDUCATIONAL COMMENTARY DISSEMINATED INTRAVASCULAR COAGULATION Educational commentary is provided through our affiliation with the American Society for Clinical Pathology (ASCP). To obtain FREE CME/CMLE
Rituximab. B Cell Inhibition in APS. Methods. B Cell Inhibition in APS. Disclosure 11/6/2011
 Rituximab in Antiphospholipid Syndrome (RITAPS) A Pilot Open-Label Phase II Prospective Trial for Non-Criteria Manifestations of Antiphospholipid Antibodies (NCT: 00537290) Disclosure Research Support:
Rituximab in Antiphospholipid Syndrome (RITAPS) A Pilot Open-Label Phase II Prospective Trial for Non-Criteria Manifestations of Antiphospholipid Antibodies (NCT: 00537290) Disclosure Research Support:
Journal of Nephropathology
 DOI: 10.12860/jnp.2014.03 J Nephropathol. 2014; 3(1): 9-17 Journal of Nephropathology Catastrophic antiphospholipid syndrome: a clinical review Ali Nayer 1,*, Luis M. Ortega 2 1 Division of Nephrology
DOI: 10.12860/jnp.2014.03 J Nephropathol. 2014; 3(1): 9-17 Journal of Nephropathology Catastrophic antiphospholipid syndrome: a clinical review Ali Nayer 1,*, Luis M. Ortega 2 1 Division of Nephrology
Let`s go for the diagnosis! Yazeed Toukan, MD Pediatric Pulmonary Institute, Ruth Rappaport Children`s Hospital July 2016
 Let`s go for the diagnosis! Yazeed Toukan, MD Pediatric Pulmonary Institute, Ruth Rappaport Children`s Hospital July 2016 Case report 20 months old girl Israeli Arab Muslim family, consanguineous marriage
Let`s go for the diagnosis! Yazeed Toukan, MD Pediatric Pulmonary Institute, Ruth Rappaport Children`s Hospital July 2016 Case report 20 months old girl Israeli Arab Muslim family, consanguineous marriage
Case Studies. Scleroderma Renal Crisis or Thrombotic Thrombocytopenic Purpura: Seeing Through the Masquerade. Patient 1
 Scleroderma Renal Crisis or Thrombotic Thrombocytopenic Purpura: Seeing Through the Masquerade Emily Keeler, DO, 1* Gloria Fioravanti, DO, FACP, 1 Bensson Samuel, MD, PG Dip, 1 Santo Longo, MD 2 Lab Med
Scleroderma Renal Crisis or Thrombotic Thrombocytopenic Purpura: Seeing Through the Masquerade Emily Keeler, DO, 1* Gloria Fioravanti, DO, FACP, 1 Bensson Samuel, MD, PG Dip, 1 Santo Longo, MD 2 Lab Med
Sindrome da anticorpi antifosfolipidi: clinica e terapia. Vittorio Pengo Clinical Cardiology, Padova, Italy
 Sindrome da anticorpi antifosfolipidi: clinica e terapia Vittorio Pengo Clinical Cardiology, Padova, Italy Revised Classification Criteria for the Antiphospholipid Syndrome J Thromb Haemost 2006;4:295-306
Sindrome da anticorpi antifosfolipidi: clinica e terapia Vittorio Pengo Clinical Cardiology, Padova, Italy Revised Classification Criteria for the Antiphospholipid Syndrome J Thromb Haemost 2006;4:295-306
Primary causes: Complement dysregulation (50% of non-shiga toxin-producing E. coli ) Secondary causes:
 General department INTRODUCTION The hemolytic uremic syndrome (HUS): microangiopathic hemolytic anemia, thrombocytopenia, and acute kidney injury One of the main causes of acute kidney injury in children
General department INTRODUCTION The hemolytic uremic syndrome (HUS): microangiopathic hemolytic anemia, thrombocytopenia, and acute kidney injury One of the main causes of acute kidney injury in children
Supplemental Figures and Legends
 Supplemental Figures and Legends Online Figure 1. 18 year old female with SLE and acute homonymous hemianopsia, confusional state, and cognitive dysfunction. A. This TEE four chamber view demonstrates
Supplemental Figures and Legends Online Figure 1. 18 year old female with SLE and acute homonymous hemianopsia, confusional state, and cognitive dysfunction. A. This TEE four chamber view demonstrates
Antiphospholipid Antibody Syndrome: Management Issues for the Hematologist
 Antiphospholipid Antibody Syndrome: Management Issues for the Hematologist Wisconsin Institute of Discovery Karen Rossi/Bristol-Myers Squibb Morey A. Blinder, MD Washington University, St. Louis, MO March
Antiphospholipid Antibody Syndrome: Management Issues for the Hematologist Wisconsin Institute of Discovery Karen Rossi/Bristol-Myers Squibb Morey A. Blinder, MD Washington University, St. Louis, MO March
PNH Glossary of Terms
 AA Absolute neutrophil count Alendronate Allergen ALT Anemia Antibodies Anticoagulant Anticoagulation Antigen Antithymocyte globulin (ATG) Aplastic Aplastic anemia Band Bilirubin Blast cells Bone marrow
AA Absolute neutrophil count Alendronate Allergen ALT Anemia Antibodies Anticoagulant Anticoagulation Antigen Antithymocyte globulin (ATG) Aplastic Aplastic anemia Band Bilirubin Blast cells Bone marrow
UKITP INITAL INFORMATION SHEET (2.4)
 UKITP INITAL INFORMATION SHEET (2.4) Barts Health NHS Trust The Royal London Hospital Pathology and Pharmacy Building 80 Newark Street, London E1 2ES Centre for Haematology Institute of and Molecular Science
UKITP INITAL INFORMATION SHEET (2.4) Barts Health NHS Trust The Royal London Hospital Pathology and Pharmacy Building 80 Newark Street, London E1 2ES Centre for Haematology Institute of and Molecular Science
Diagnosis and Management of Catastrophic Antiphospholipid Syndrome: a Clinical Practice Guideline
 Diagnosis and Management of Catastrophic Antiphospholipid Syndrome: a Clinical Practice Guideline Introduction The public comment period occurs after recommendations are formed but before a manuscript
Diagnosis and Management of Catastrophic Antiphospholipid Syndrome: a Clinical Practice Guideline Introduction The public comment period occurs after recommendations are formed but before a manuscript
DISCUSSION BY: Dr M. R. Shakeebi, MD, Rheumatologist
 Case presentations Related to some Rheumatic Diseases Lab & Clinic i Programs, Tuesday, April 24, 2012 COORDINATOR: Dr M. Mahdi Mohammadi, LMD,PhD, Immunologist COORDINATOR: Dr M. Mahdi Mohammadi, LMD,PhD,
Case presentations Related to some Rheumatic Diseases Lab & Clinic i Programs, Tuesday, April 24, 2012 COORDINATOR: Dr M. Mahdi Mohammadi, LMD,PhD, Immunologist COORDINATOR: Dr M. Mahdi Mohammadi, LMD,PhD,
Tables of Normal Values (As of February 2005)
 Tables of Normal Values (As of February 2005) Note: Values and units of measurement listed in these Tables are derived from several resources. Substantial variation exists in the ranges quoted as normal
Tables of Normal Values (As of February 2005) Note: Values and units of measurement listed in these Tables are derived from several resources. Substantial variation exists in the ranges quoted as normal
AMPLIADO SÍNDROME ANTIFOSFOLÍPIDO SÍNDROME DE SJÖGREN María José Cuadrado Lozano Clínica Universidad de Navarra-Madrid
 AMPLIADO SÍNDROME ANTIFOSFOLÍPIDO SÍNDROME DE SJÖGREN María José Cuadrado Lozano Clínica Universidad de Navarra-Madrid PLASMABLAST PROLIFERATION IS ASSOCIATED WITH TLR7 POLYMORPHISMS AND UPREGULATION OF
AMPLIADO SÍNDROME ANTIFOSFOLÍPIDO SÍNDROME DE SJÖGREN María José Cuadrado Lozano Clínica Universidad de Navarra-Madrid PLASMABLAST PROLIFERATION IS ASSOCIATED WITH TLR7 POLYMORPHISMS AND UPREGULATION OF
Thrombotic Thrombocytopenic Purpura and the Role of ADAMTS-13
 Thrombotic Thrombocytopenic Purpura and the Role of ADAMTS-13 Mark Cunningham,MD Director, Hematology Laboratory Department of Pathology University of Kansas Medical Center College of American Pathologists
Thrombotic Thrombocytopenic Purpura and the Role of ADAMTS-13 Mark Cunningham,MD Director, Hematology Laboratory Department of Pathology University of Kansas Medical Center College of American Pathologists
Acute Thrombocytopenia after Initiating Anticoagulation with Rivaroxaban
 CASE REPORT Acute Thrombocytopenia after Initiating Anticoagulation with Rivaroxaban Yohei Mima 1, Yuhei Sangatsuda 2, Masahiro Yasaka 1, Yoshiyuki Wakugawa 1, Shinji Nagata 2 and Yasushi Okada 1 Abstract
CASE REPORT Acute Thrombocytopenia after Initiating Anticoagulation with Rivaroxaban Yohei Mima 1, Yuhei Sangatsuda 2, Masahiro Yasaka 1, Yoshiyuki Wakugawa 1, Shinji Nagata 2 and Yasushi Okada 1 Abstract
* Renal insufficiencies
 Thrombotic Thrombocytopenic Purpura Behzad Poopak, DCLS PhD. Tehran medical Branch Islamic Azad university bpoopak@yahoo.com Case Summary Ms. X, a 35-year year-old woman Complained of weakness, low grade
Thrombotic Thrombocytopenic Purpura Behzad Poopak, DCLS PhD. Tehran medical Branch Islamic Azad university bpoopak@yahoo.com Case Summary Ms. X, a 35-year year-old woman Complained of weakness, low grade
Year 2004 Paper one: Questions supplied by Megan
 QUESTION 53 Endothelial cell pathology on renal biopsy is most characteristic of which one of the following diagnoses? A. Pre-eclampsia B. Haemolytic uraemic syndrome C. Lupus nephritis D. Immunoglobulin
QUESTION 53 Endothelial cell pathology on renal biopsy is most characteristic of which one of the following diagnoses? A. Pre-eclampsia B. Haemolytic uraemic syndrome C. Lupus nephritis D. Immunoglobulin
Bleeding Disorders.2 MS Abdallah Awidi Abbadi.MD. FRCP.FRCPath Feras Fararjeh MD
 Bleeding Disorders.2 MS4.25.02.2019 Abdallah Awidi Abbadi.MD. FRCP.FRCPath Feras Fararjeh MD Email: abdalla.awidi@gmail.com Case 6: GT 18 yr old female was admitted with pallor, abdominal pain and gum
Bleeding Disorders.2 MS4.25.02.2019 Abdallah Awidi Abbadi.MD. FRCP.FRCPath Feras Fararjeh MD Email: abdalla.awidi@gmail.com Case 6: GT 18 yr old female was admitted with pallor, abdominal pain and gum
Purpura fulminans: A rare presentation of antiphospholipid syndrome
 www.edoriumjournals.com CLINICAL IMAGE PEER REVIEWED OPEN ACCESS Purpura fulminans: A rare presentation of antiphospholipid syndrome Ahmed S. Mahmood, Noor Q. Omar, Sudheer Chauhan, Jose Cervantes ABSTRACT
www.edoriumjournals.com CLINICAL IMAGE PEER REVIEWED OPEN ACCESS Purpura fulminans: A rare presentation of antiphospholipid syndrome Ahmed S. Mahmood, Noor Q. Omar, Sudheer Chauhan, Jose Cervantes ABSTRACT
Management of Rejection
 Management of Rejection I have no disclosures Disclosures (relevant or otherwise) Deborah B Adey, MD Professor of Medicine University of California, San Francisco Kidney and Pancreas Transplant Center
Management of Rejection I have no disclosures Disclosures (relevant or otherwise) Deborah B Adey, MD Professor of Medicine University of California, San Francisco Kidney and Pancreas Transplant Center
APPENDIX 2 Eight New Cases of LAHS and Review of Literature: Treatment and Follow-Up
 Supplementary Digital Content 2 Mazodier Lupus Anticoagulant- Hypoprothrombinemia Syndrome: Report of 8 Cases and Review of the Literature Medicine (Baltimore). 2012;91(5). APPEIX 2 Eight New Cases of
Supplementary Digital Content 2 Mazodier Lupus Anticoagulant- Hypoprothrombinemia Syndrome: Report of 8 Cases and Review of the Literature Medicine (Baltimore). 2012;91(5). APPEIX 2 Eight New Cases of
Dr. Rai Muhammad Asghar Associate Professor Head of Pediatric Department Rawalpindi Medical College
 Dr. Rai Muhammad Asghar Associate Professor Head of Pediatric Department Rawalpindi Medical College AN APPROACH TO BLEEDING DISORDERS NORMAL HEMOSTASIS After injury, 3 processes halt bleeding Vasoconstriction
Dr. Rai Muhammad Asghar Associate Professor Head of Pediatric Department Rawalpindi Medical College AN APPROACH TO BLEEDING DISORDERS NORMAL HEMOSTASIS After injury, 3 processes halt bleeding Vasoconstriction
Living with PNH 7/3/2013. Paroxysmal Nocturnal Hemoglobinuria (PNH): A Chronic, Systemic, and Life- Threatening Disease
 Living with PNH Laurence A. Boxer, MD University of Michigan Case Study 15 year old awakened in the morning with chest pain and a sore throat. She experienced chest pain all day accompanied with coughing
Living with PNH Laurence A. Boxer, MD University of Michigan Case Study 15 year old awakened in the morning with chest pain and a sore throat. She experienced chest pain all day accompanied with coughing
Approccio morfologico alle microangiopatie trombotiche
 Approccio morfologico alle microangiopatie trombotiche Gina Zini Polo Oncologia e Ematologia Policlinico A. Gemelli Università Cattolica S. Cuore - Roma 1 Thrombotic microangiopathies Occlusive microangiopathic
Approccio morfologico alle microangiopatie trombotiche Gina Zini Polo Oncologia e Ematologia Policlinico A. Gemelli Università Cattolica S. Cuore - Roma 1 Thrombotic microangiopathies Occlusive microangiopathic
Reversible cardiac valvular disease in catastrophic antiphospholipid syndrome
 O r i g i n a l a r t i c l e Reversible cardiac valvular disease in catastrophic antiphospholipid syndrome C.C. Teunisse 1*, A.J. Kalsbeek 2, S.T. de Vries 1, S.J. Huisman 2, J.E. Boers 3, A. Breeman
O r i g i n a l a r t i c l e Reversible cardiac valvular disease in catastrophic antiphospholipid syndrome C.C. Teunisse 1*, A.J. Kalsbeek 2, S.T. de Vries 1, S.J. Huisman 2, J.E. Boers 3, A. Breeman
DR V PHILIP CLINICAL HAEMATOLOGY UNIT CHRIS HANI BARAGWANATH ACADEMIC HOSPITAL
 DR V PHILIP CLINICAL HAEMATOLOGY UNIT CHRIS HANI BARAGWANATH ACADEMIC HOSPITAL Rare but fatal disease if unrecognized and untreated Incidence about 1: 1 million in the USA Female preponderance of 2:1 Part
DR V PHILIP CLINICAL HAEMATOLOGY UNIT CHRIS HANI BARAGWANATH ACADEMIC HOSPITAL Rare but fatal disease if unrecognized and untreated Incidence about 1: 1 million in the USA Female preponderance of 2:1 Part
Some renal vascular disorders
 Some renal vascular disorders Introduction Nearly all diseases of the kidney involve the renal blood vessels secondarily We will discuss: -Hypertension (arterionephrosclerosis in benign HTN & hyperplastic
Some renal vascular disorders Introduction Nearly all diseases of the kidney involve the renal blood vessels secondarily We will discuss: -Hypertension (arterionephrosclerosis in benign HTN & hyperplastic
THROMBOTIC MICROANGIOPATHY. Jun-Ki Park 7/19/11
 THROMBOTIC MICROANGIOPATHY Jun-Ki Park 7/19/11 TMAs are microvascular occlusive disorders characterized by systemic or intrarenal aggregation of platelets, thrombocytopenia, and mechanical injury to erythrocytes.
THROMBOTIC MICROANGIOPATHY Jun-Ki Park 7/19/11 TMAs are microvascular occlusive disorders characterized by systemic or intrarenal aggregation of platelets, thrombocytopenia, and mechanical injury to erythrocytes.
LOKUN! I got stomach ache!
 LOKUN! I got stomach ache! Mr L is a 67year old Chinese gentleman who is a non smoker, social drinker. He has a medical history significant for Hypertension, Hyperlipidemia, Type 2 Diabetes Mellitus, Chronic
LOKUN! I got stomach ache! Mr L is a 67year old Chinese gentleman who is a non smoker, social drinker. He has a medical history significant for Hypertension, Hyperlipidemia, Type 2 Diabetes Mellitus, Chronic
Systemic lupus erythematosus (SLE): Pleuropulmonary Manifestations
 08/30/10 09/26/10 Systemic lupus erythematosus (SLE): Pleuropulmonary Manifestations Camila Downey S. Universidad de Chile, School of Medicine, Year VII Harvard University, School of Medicine Sept 17,
08/30/10 09/26/10 Systemic lupus erythematosus (SLE): Pleuropulmonary Manifestations Camila Downey S. Universidad de Chile, School of Medicine, Year VII Harvard University, School of Medicine Sept 17,
Thrombotic Thrombocytopenic
 The Treatment of TTP and the Prevention of Relapses GERALD APPEL, MD Professor of Clinical Medicine Columbia University College of Physicians and Surgeons NY-Presbyterian Hospital New York, New York Thrombotic
The Treatment of TTP and the Prevention of Relapses GERALD APPEL, MD Professor of Clinical Medicine Columbia University College of Physicians and Surgeons NY-Presbyterian Hospital New York, New York Thrombotic
Warm Autoantibodies in a Patient with Hemophagocytic Lymphohistiocytosis: A Case Report
 Warm Autoantibodies in a Patient with Hemophagocytic Lymphohistiocytosis: A Case Report Emily Coberly, MD Department of Pathology and Anatomical Sciences University of Missouri Columbia April 30, 2013
Warm Autoantibodies in a Patient with Hemophagocytic Lymphohistiocytosis: A Case Report Emily Coberly, MD Department of Pathology and Anatomical Sciences University of Missouri Columbia April 30, 2013
1. INSTRUCTIONS 2. DEFINITION OF HUS
 CQ_IBK_aHUS_01 / version 25/11/09 European Paediatric Research Group for HUS and related disorders Case questionnaire for diarrhoea negative/vtec (STEC) negative cases acute phase 1. INSTRUCTIONS Please
CQ_IBK_aHUS_01 / version 25/11/09 European Paediatric Research Group for HUS and related disorders Case questionnaire for diarrhoea negative/vtec (STEC) negative cases acute phase 1. INSTRUCTIONS Please
Effect of under filling tube
 Effect of under filling tube 2 What constitutes underfilling? A 4.5ml vacutainer collection tube should contain at least 4ml of blood Less than that could give falsely prolonged clotting times ALSO be
Effect of under filling tube 2 What constitutes underfilling? A 4.5ml vacutainer collection tube should contain at least 4ml of blood Less than that could give falsely prolonged clotting times ALSO be
Additional file 2: Details of cohort studies and randomised trials
 Reference Randomised trials Ye et al. 2001 Abstract 274 R=1 WD=0 Design, numbers, treatments, duration Randomised open comparison of: (45 patients) 1.5 g for 3, 1 g for 3, then 0.5 to 0.75 g IV cyclophosphamide
Reference Randomised trials Ye et al. 2001 Abstract 274 R=1 WD=0 Design, numbers, treatments, duration Randomised open comparison of: (45 patients) 1.5 g for 3, 1 g for 3, then 0.5 to 0.75 g IV cyclophosphamide
Antiphospholipid Syndrome: It s Far More Than You Think
 Antiphospholipid Syndrome: It s Far More Than You Think Richard Furie, MD Chief, Division of Rheumatology Northwell Health Professor of Medicine Zucker School of Medicine at Hofstra/Northwell Richard Furie,
Antiphospholipid Syndrome: It s Far More Than You Think Richard Furie, MD Chief, Division of Rheumatology Northwell Health Professor of Medicine Zucker School of Medicine at Hofstra/Northwell Richard Furie,
Elevated Expression of Pentraxin 3 in Anti-neutrophil Cytoplasmic Antibody-associated Glomerulonephritis with Normal Serum C-reactive Protein
 CASE REPORT Elevated Expression of Pentraxin 3 in Anti-neutrophil Cytoplasmic Antibody-associated Glomerulonephritis with Normal Serum C-reactive Protein Risa Ishida 1,KentaroNakai 1, Hideki Fujii 1, Shunsuke
CASE REPORT Elevated Expression of Pentraxin 3 in Anti-neutrophil Cytoplasmic Antibody-associated Glomerulonephritis with Normal Serum C-reactive Protein Risa Ishida 1,KentaroNakai 1, Hideki Fujii 1, Shunsuke
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Acute lung injury (ALI) transfusion-related, 363 372. See also Transfusion-related acute lung injury (TRALI) ALI. See Acute lung injury
Index Note: Page numbers of article titles are in boldface type. A Acute lung injury (ALI) transfusion-related, 363 372. See also Transfusion-related acute lung injury (TRALI) ALI. See Acute lung injury
Successful Treatment with Cyclosporin A in Tocilizumab-resistant TAFRO Syndrome
 CASE REPORT Successful Treatment with Cyclosporin A in Tocilizumab-resistant TAFRO Syndrome Yusuke Yamaga 1, Kiyonobu Tokuyama 1, Takehiro Kato 1,RieYamada 1, Masanori Murayama 1, Tsuneko Ikeda 2, Noriyoshi
CASE REPORT Successful Treatment with Cyclosporin A in Tocilizumab-resistant TAFRO Syndrome Yusuke Yamaga 1, Kiyonobu Tokuyama 1, Takehiro Kato 1,RieYamada 1, Masanori Murayama 1, Tsuneko Ikeda 2, Noriyoshi
HENOCH SCHÖNLEIN PURPURA (VASCULAR PURPURA, ANAPHYLACTOID PURPURA) IN CHILDREN Single choice tests (SC)
 HENOCH HÖNLEIN PURPURA (VAULAR PURPURA, ANAPHYLACTOID PURPURA) IN CHILDREN Single choice tests () 1. Choose the type of bleeding characteristic for the Henoch Schönlein purpura (vascular purpura, anaphylactoid
HENOCH HÖNLEIN PURPURA (VAULAR PURPURA, ANAPHYLACTOID PURPURA) IN CHILDREN Single choice tests () 1. Choose the type of bleeding characteristic for the Henoch Schönlein purpura (vascular purpura, anaphylactoid
AUTOIMMUNE DISORDERS IN THE ACUTE SETTING
 AUTOIMMUNE DISORDERS IN THE ACUTE SETTING Diagnosis and Treatment Goals Aimee Borazanci, MD BNI Neuroimmunology Objectives Give an update on the causes for admission, clinical features, and outcomes of
AUTOIMMUNE DISORDERS IN THE ACUTE SETTING Diagnosis and Treatment Goals Aimee Borazanci, MD BNI Neuroimmunology Objectives Give an update on the causes for admission, clinical features, and outcomes of
Thrombotic thrombocytopenic purpura: a look at the future
 Thrombotic thrombocytopenic purpura: a look at the future Andrea Artoni, MD Ph.D. Angelo Bianchi Bonomi Hemophilia and Thrombosis Center IRCCS Ca Granda Ospedale Maggiore Policlinico Milan, Italy andrea.artoni@policlinico.mi.it
Thrombotic thrombocytopenic purpura: a look at the future Andrea Artoni, MD Ph.D. Angelo Bianchi Bonomi Hemophilia and Thrombosis Center IRCCS Ca Granda Ospedale Maggiore Policlinico Milan, Italy andrea.artoni@policlinico.mi.it
Thrombotic thrombocytopenic purpura presenting with acute myocardial infarction: A case report.
 Thrombotic thrombocytopenic purpura presenting with acute myocardial infarction: A case report. 賴學緯盧介聖葉人華劉益昇黃子權陳佳宏吳宜穎張平穎戴明燊何景良陳宇欽高偉堯 * 三軍總醫院血液腫瘤科 台北慈濟醫院血液腫瘤科 * Introduction Thrombotic thrombocytopenic
Thrombotic thrombocytopenic purpura presenting with acute myocardial infarction: A case report. 賴學緯盧介聖葉人華劉益昇黃子權陳佳宏吳宜穎張平穎戴明燊何景良陳宇欽高偉堯 * 三軍總醫院血液腫瘤科 台北慈濟醫院血液腫瘤科 * Introduction Thrombotic thrombocytopenic
CIBMTR Center Number: CIBMTR Recipient ID: RETIRED. Today s Date: Date of HSCT for which this form is being completed:
 Juvenile Idiopathic Arthritis Pre-HSCT Data Sequence Number: Date Received: Registry Use Only Today s Date: Date of HSCT for which this form is being completed: HSCT type: autologous allogeneic, allogeneic,
Juvenile Idiopathic Arthritis Pre-HSCT Data Sequence Number: Date Received: Registry Use Only Today s Date: Date of HSCT for which this form is being completed: HSCT type: autologous allogeneic, allogeneic,
ERROR CORRECTION FORM
 Juvenile Idiopathic Arthritis Pre-HSCT Data Sequence Number: Registry Use Only Date of HSCT for which this form is being completed: HSCT type: autologous allogeneic, allogeneic, syngeneic unrelated related
Juvenile Idiopathic Arthritis Pre-HSCT Data Sequence Number: Registry Use Only Date of HSCT for which this form is being completed: HSCT type: autologous allogeneic, allogeneic, syngeneic unrelated related
Morphology Case Study. Presented by Niamh O Donnell, BSc, MSc. Medical Scientist Haematology Laboratory Cork University Hospital
 Morphology Case Study Presented by Niamh O Donnell, BSc, MSc. Medical Scientist Haematology Laboratory Cork University Hospital 41 year old male presented to GP for routine check-up in May 2011. FBC Results:
Morphology Case Study Presented by Niamh O Donnell, BSc, MSc. Medical Scientist Haematology Laboratory Cork University Hospital 41 year old male presented to GP for routine check-up in May 2011. FBC Results:
Bassett Healthcare Clinical Laboratory
 Therapeutic Drug Level Collection Guidelines Anti-epileptic drugs (carbamazepine, phenobarbital, phenytoin, primidone, valproic acid) Consider collecting after steady state conditions are reached, i.e.
Therapeutic Drug Level Collection Guidelines Anti-epileptic drugs (carbamazepine, phenobarbital, phenytoin, primidone, valproic acid) Consider collecting after steady state conditions are reached, i.e.
Clinical study of 9 patients with acquired thrombotic thrombocytopenic purpura
 Journal of Clinical and Experimental Medicine VOL.1,ISS.3,DEC 2017,1-5 ONLINE ISSN: 2523-2835 www.jocem.org PRINT ISSN: 2521-0084 DOI:10.29422/jocem.2017.03.001 Abstract: Clinical study of 9 patients with
Journal of Clinical and Experimental Medicine VOL.1,ISS.3,DEC 2017,1-5 ONLINE ISSN: 2523-2835 www.jocem.org PRINT ISSN: 2521-0084 DOI:10.29422/jocem.2017.03.001 Abstract: Clinical study of 9 patients with
Acute cor pulmonale due to pulmonary tumor thrombotic microangiopathy in two patients with breast cancer
 LETTER TO THE EDITOR Korean J Intern Med 2017;32:190-194 Acute cor pulmonale due to pulmonary tumor thrombotic microangiopathy in two patients with breast cancer Sung Young Moon, Kang Hoon Lee, Jong Sik
LETTER TO THE EDITOR Korean J Intern Med 2017;32:190-194 Acute cor pulmonale due to pulmonary tumor thrombotic microangiopathy in two patients with breast cancer Sung Young Moon, Kang Hoon Lee, Jong Sik
myopathy and interstitial lung dise
 NAOSITE: Nagasaki University's Ac Title Author(s) Citation A case of primary Sjögren's syndrom myopathy and interstitial lung dise Koga, Tomohiro; Kouhisa, Yukiko; Na Akinari; Motomura, Masakatsu; Kawak
NAOSITE: Nagasaki University's Ac Title Author(s) Citation A case of primary Sjögren's syndrom myopathy and interstitial lung dise Koga, Tomohiro; Kouhisa, Yukiko; Na Akinari; Motomura, Masakatsu; Kawak
Approach to disseminated intravascular coagulation
 Approach to disseminated intravascular coagulation Khaire Ananta Shankarrao 1, Anil Burley 2, Deshmukh 3 1.MD Scholar, [kayachikitsa] 2.Professor,MD kayachikitsa. 3.Professor and HOD,Kayachikitsa. CSMSS
Approach to disseminated intravascular coagulation Khaire Ananta Shankarrao 1, Anil Burley 2, Deshmukh 3 1.MD Scholar, [kayachikitsa] 2.Professor,MD kayachikitsa. 3.Professor and HOD,Kayachikitsa. CSMSS
Contemporary perspectives and initial management of pediatric ITP. William Beau Mitchell, MD Weill Cornell Medical College New York, NY USA
 Contemporary perspectives and initial management of pediatric ITP William Beau Mitchell, MD Weill Cornell Medical College New York, NY USA Case Presentation 5 year old female Bruises on trunk, extremities
Contemporary perspectives and initial management of pediatric ITP William Beau Mitchell, MD Weill Cornell Medical College New York, NY USA Case Presentation 5 year old female Bruises on trunk, extremities
PULMONARY EMBOLISM -CASE REPORT-
 University Goce Delcev, Faculty of Medical sciences, Stip University Clinic of Cardiology, Skopje R. Of Macedonia PULMONARY EMBOLISM -CASE REPORT- Gordana Kamceva MD mr.sci Acknowledgment Marija Vavlukis
University Goce Delcev, Faculty of Medical sciences, Stip University Clinic of Cardiology, Skopje R. Of Macedonia PULMONARY EMBOLISM -CASE REPORT- Gordana Kamceva MD mr.sci Acknowledgment Marija Vavlukis
A TRICKY PROBLEM. Presenter-Dr Lakshmi PK
 A TRICKY PROBLEM Presenter-Dr Lakshmi PK Patient particulars 33 years old Male Resident of Andhra Pradesh Occupation-soldier Chief compliants Headache- 03 days Headache-global,throbbing type Associated
A TRICKY PROBLEM Presenter-Dr Lakshmi PK Patient particulars 33 years old Male Resident of Andhra Pradesh Occupation-soldier Chief compliants Headache- 03 days Headache-global,throbbing type Associated
Hiroyuki Kamiya 1), Soichiro Ikushima 1), Tetsu Sakamoto 1), Kozo Morimoto 1), Tsunehiro Ando 1), Masaru Oritsu 1), Atsuo Goto 2), Tamiko Takemura 3)
 29 2001 ACE39.7IU/l X TBLB 2002 11 Langhans [ ] A Case of Granulomatous Interstitial Nephritis with Progressive Renal Impairment Due to Sarcoidosis in the Course of Spontaneous Improvement of Pulmonary
29 2001 ACE39.7IU/l X TBLB 2002 11 Langhans [ ] A Case of Granulomatous Interstitial Nephritis with Progressive Renal Impairment Due to Sarcoidosis in the Course of Spontaneous Improvement of Pulmonary
Clinical Guidance. Kawasaki disease. Summary This guideline includes therapy and follow up including investigations (echocardiography, MRI).
 Clinical Guidance Kawasaki disease Summary This guideline includes therapy and follow up including investigations (echocardiography, MRI). Document Detail Document type Clinical Guideline Document name
Clinical Guidance Kawasaki disease Summary This guideline includes therapy and follow up including investigations (echocardiography, MRI). Document Detail Document type Clinical Guideline Document name
HEPARIN-INDUCED THROMBOCYTOPENIA (HIT)
 HEPARIN-INDUCED THROMBOCYTOPENIA (HIT) OBJECTIVE: To assist clinicians with the investigation and management of suspected and documented heparin-induced thrombocytopenia (HIT). BACKGROUND: HIT is a transient,
HEPARIN-INDUCED THROMBOCYTOPENIA (HIT) OBJECTIVE: To assist clinicians with the investigation and management of suspected and documented heparin-induced thrombocytopenia (HIT). BACKGROUND: HIT is a transient,
Early Klebsiella pneumoniae Liver Abscesses associated with Pylephlebitis Mimic
 Early Klebsiella pneumoniae Liver Abscesses associated with Pylephlebitis Mimic Hepatocellular Carcinoma Chih-Hao Shen, MD 3, Jung-Chung Lin, MD, PhD 2, Hsuan-Hwai Lin, MD 1, You-Chen Chao, MD 1, and Tsai-Yuan
Early Klebsiella pneumoniae Liver Abscesses associated with Pylephlebitis Mimic Hepatocellular Carcinoma Chih-Hao Shen, MD 3, Jung-Chung Lin, MD, PhD 2, Hsuan-Hwai Lin, MD 1, You-Chen Chao, MD 1, and Tsai-Yuan
Case Report Catastrophic Antiphospholipid Syndrome Presenting as Bilateral Central Retinal Artery Occlusions
 Hindawi Publishing Corporation Case Reports in Ophthalmological Medicine Volume 2015, Article ID 206906, 5 pages http://dx.doi.org/10.1155/2015/206906 Case Report Catastrophic Antiphospholipid Syndrome
Hindawi Publishing Corporation Case Reports in Ophthalmological Medicine Volume 2015, Article ID 206906, 5 pages http://dx.doi.org/10.1155/2015/206906 Case Report Catastrophic Antiphospholipid Syndrome
ANTIPHOSPHOLIPID (HUGHES) SYNDROME
 1 ANTIPHOSPHOLIPID (HUGHES) SYNDROME INTRODUCTION In 1983, Hughes et al describe a syndrome characterized by arterial and venous thrombosis, recurrent foetal wastage, and thrombocytopenia, which were seen
1 ANTIPHOSPHOLIPID (HUGHES) SYNDROME INTRODUCTION In 1983, Hughes et al describe a syndrome characterized by arterial and venous thrombosis, recurrent foetal wastage, and thrombocytopenia, which were seen
Routine Clinic Lab Studies
 Routine Lab Studies Routine Clinic Lab Studies With all lab studies, a Tacrolimus level will be obtained. These drug levels are routinely assessed to ensure that there is enough or not too much anti-rejection
Routine Lab Studies Routine Clinic Lab Studies With all lab studies, a Tacrolimus level will be obtained. These drug levels are routinely assessed to ensure that there is enough or not too much anti-rejection
Infected cardiac-implantable electronic devices: diagnosis, and treatment
 Infected cardiac-implantable electronic devices: diagnosis, and treatment The incidence of infection following implantation of cardiac implantable electronic devices (CIEDs) is increasing at a faster rate
Infected cardiac-implantable electronic devices: diagnosis, and treatment The incidence of infection following implantation of cardiac implantable electronic devices (CIEDs) is increasing at a faster rate
MEDICAL COVERAGE GUIDELINES ORIGINAL EFFECTIVE DATE: 08/19/14 SECTION: DRUGS LAST REVIEW DATE: LAST CRITERIA REVISION DATE: ARCHIVE DATE:
 RITUXAN (rituximab) Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Medical Coverage Guideline
RITUXAN (rituximab) Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Medical Coverage Guideline
Managing Acute Medical Problems, Birmingham Vasculitis. David Jayne. University of Cambridge
 Managing Acute Medical Problems, Birmingham 2016 Vasculitis David Jayne University of Cambridge Disclosures Astra Zeneca, Aurinia, BIOGEN, Boehringer, Chemocentryx, Genzyme/Sanofi, GSK, Lilly, Medimmune,
Managing Acute Medical Problems, Birmingham 2016 Vasculitis David Jayne University of Cambridge Disclosures Astra Zeneca, Aurinia, BIOGEN, Boehringer, Chemocentryx, Genzyme/Sanofi, GSK, Lilly, Medimmune,
NEW RCPCH REFERENCE RANGES-
 s vary between populations and age groups and it is important to always check the reference Haematology: Haemoglobin Male 130 175 g/l 0 6 days 145-220 g/l Female 115 165 g/l 7 days 140-186 g/l 8 days 3
s vary between populations and age groups and it is important to always check the reference Haematology: Haemoglobin Male 130 175 g/l 0 6 days 145-220 g/l Female 115 165 g/l 7 days 140-186 g/l 8 days 3
Disorders of the kidney. Urine analysis. Nephrotic and nephritic syndrome.
 Disorders of the kidney. Urine analysis. Nephrotic and nephritic syndrome. Azotemia and Urinary Abnormalities Disturbances in urine volume oliguria, anuria, polyuria Abnormalities of urine sediment red
Disorders of the kidney. Urine analysis. Nephrotic and nephritic syndrome. Azotemia and Urinary Abnormalities Disturbances in urine volume oliguria, anuria, polyuria Abnormalities of urine sediment red
