NHS England. Evidence review: Hyperbaric oxygen therapy for diabetic lower limb ulceration refractory to best standard care
|
|
|
- Lindsay Lorena Sims
- 5 years ago
- Views:
Transcription
1 NHS England Evidence review: Hyperbaric oxygen therapy for diabetic lower limb ulceration refractory to best standard care
2 NHS England Evidence review: Hyperbaric oxygen therapy for diabetic lower limb ulceration refractory to best standard care First published: July 2017 Updated: March 2018 Revised: September 2018 Prepared by: Solutions for Public Health (SPH) on behalf of NHS England Specialised Commissioning
3 Contents 1. Introduction Summary of results Methodology Results Discussion Conclusion Grade of evidence table Literature Search Terms Search Strategy Evidence Selection References... 28
4 1. Introduction People with diabetes mellitus are at increased risk of foot ulceration. The ulcers are multifactorial, often caused or exacerbated by diabetic peripheral neuropathy and angiopathy. Diabetic neuropathy diminishes perception of pain, so that minor trauma, such as localised pressure caused by unsuitable shoes, abnormal biomechanical stress or open wounds, is often not noticed. This makes early treatment difficult and promotes the development of a foot ulcer. Poor circulation because of diabetic vessel damage leads to faster tissue breakdown and impairs resistance to infection, and ulcer healing (Schaper et al 2012). Ulcer care is responsible for a large proportion of the cost of health care for people with diabetes. Foot ulcers restrict mobility and diminish quality of life. They are sometimes slow to resolve, requiring professional time and materials to promote healing. Their most serious consequence is amputation, for instance in the forefoot area (minor amputation) or through the metatarsals or of part of the leg (major amputation) (Schaper et al 2012). The annual incidence of foot ulcers among people with diabetes has been estimated at between 2.5% and 10.7%, and the annual incidence of amputation is 0.25% to 1.8% (Boulton 2008). Standard treatment of diabetic foot ulcers requires a multidisciplinary team comprising a podiatrist, an orthotist, a specialised nurse and a diabetologist. Treatment options include close monitoring, intensive systemic antibiotic therapy, wound dressings and debridement of dead tissue. Revascularisation is also usually considered (National Institute for Health and Care Excellence 2015). Hyperbaric oxygen therapy (HBOT) involves the inhalation of pure oxygen at a pressure higher than normal atmospheric pressure, usually 2 to 3 atmospheres absolute (ATA). During HBOT, the patient is in a pressure chamber, and when used for the treatment of diabetic foot ulcers, this is usually for 45 to 120 minutes on most days for several weeks. Inhaling oxygen at increased pressure is intended to improve oxygen supply to the ulcer. Nearly all the oxygen in the blood is bound to haemoglobin; under normal pressure, saturation in the arterial blood is 97%. The remaining oxygen is dissolved in the blood plasma; this proportion can be increased by higher ambient pressure and the associated increase in the partial pressure of oxygen. In this way, tissue structures that would be hypoxic under normal conditions may receive a more adequate supply of oxygen, which may in turn improve cell function and promote wound healing. This might occur because of enhanced neutrophil killing ability, angiogenesis, fibroblast activity and/or collagen synthesis. The National Institute for Health and Care Excellence recommends that hyperbaric oxygen should not be used to treat diabetic foot ulcers, except as part of a clinical trial (National Institute for Health and Care Excellence 2015). This was because of the "very low quality of the evidence". NHS England does not commission HBOT for diabetic foot ulcers. 2. Summary of results This evidence review found four randomised controlled trials and one cost-utility analysis. Two trials compared HBOT plus standard care with standard care only, and two compared HBOT plus standard care with sham HBOT plus standard care. NHS England Evidence Review: Hyperbaric oxygen therapy for diabetic Page 4 of 28 lower limb ulceration refractory to best standard care
5 They reported results in three categories: amputation or the emergence of indications for amputation, partial or complete ulcer healing and adverse effects of treatment. The most reliable randomised trial was double-blind and used air at slightly above atmospheric pressure as a sham alternative to HBOT (Fedorko et al 2016). Its authors reported no effect of HBOT on rates of meeting criteria determined by a vascular surgeon for major amputation (95% CI 0.37 to 2.28, p = 0.846) or of recommendation of major or minor amputation (95% CI 0.52 to 2.43, p = 0.771) among their 103 participants. Major amputation was defined as a procedure below the knee or at the level of the metatarsals; minor amputations were at the level of the toes. Fedorko et al (2016) reported that compared to the control group who received air at 1.25 atmospheres, there was no significant effect of HBOT at 2.5 atmospheres on wound size, the rate at which the wound edge advanced, the results of a wound assessment tool or the proportion of wounds that healed at 3 months follow up. In another double-blinded study, Löndahl et al (2010) randomised 94 participants between HBOT and hyperbaric air, both at 2.5 atmospheres. The authors reported rates of complete healing of the index ulcer of 52% in the HBOT group and 29% in the placebo group (p = 0.03) at one year follow up. The authors also reported rates of death and major (above the ankle) and minor amputation, but without testing the statistical significance of differences. By contrast, Duzgun et al s (2008) unblinded trial with 100 participants did not use a placebo treatment. These authors reported that more participants treated with HBOT had ulcers that healed (66% vs 0%, p < 0.05) or were treated with a graft or flap (8% vs 0%, p < 0.05), while fewer had an amputation (distal: 8% vs 48%, p < 0.05; proximal: 0% vs 34%, p < 0.05). Ma et al (2013) reported a smaller, less reliable, unblinded study, with only 36 participants. They reported the same rates of completed ulcer healing with and without HBOT. Ulcer size was reported as reducing faster after HBOT, though not to the extent that significantly more ulcers had healed by the end of the study. Participants who underwent HBOT in Fedorko et al s (2016) trial reported 24 adverse events which had not been specifically solicited by the researchers, significantly more than the five events reported by the participants who had a sham treatment. Rates of reporting of solicited adverse events were similar in the two groups. Löndahl et al (2010) reported similar rates of adverse events in the two arms of their trial. The most common adverse events in these two trials included barotrauma, inability to equalise middle ear pressures and episodes of hypo- or hyper-glycaemia. Ma et al (2013) reported no adverse events in either arm of their trial. The most reliable trial, Fedorko et al (2016), reduced the risk of observer bias by the use of a placebo treatment with hyperbaric air, and double-blinding. The pressure of the air (1.25 ATA) was too low to be likely to have an adverse effect, a conclusion supported by the higher rate of adverse reactions in the intervention arm, so this trial can be viewed as truly placebocontrolled. The randomisation resulted in different proportions of participants with potential confounders in each arm: for example, the HBOT group participants had had their index ulcer for less time than those in the control group, but had had diabetes for longer. Any potential for biases operated in both directions and does not call into question the trial s reliability. These authors reported no benefit from HBOT. Löndahl et al (2010) also used a double-blind design, with control participants receiving hyperbaric air. Randomisation in this trial resulted in no important differences between participants allocated to the two arms. However, the pressure of the hyperbaric air in the control arm (2.5 ATA) was twice that in Fedorko et al s (2016) trial, high enough to create a risk of adverse effects; these were reported at similar rates in the two arms. The reason for the different ulcer-healing results of these two otherwise reliable trials is NHS England Evidence Review: Hyperbaric oxygen therapy for diabetic Page 5 of 28 lower limb ulceration refractory to best standard care
6 uncertain but could be due to the control treatment in Löndahl et al s (2010) study (air at 2.5 atmospheres) not being an inert placebo, a concern that was also raised by Fedorko et al (2016). This is because the pressure of air used for the control patients was the main difference between the two study protocols and the pressure used in Londahl et al s (2010) study was at a level that is well above what would be experienced during usual care. The effect of this level of air pressure is not understood and it is possible that it may have impaired ulcer healing. For this reason, the Löndahl et al (2010) study is considered somewhat less reliable than Fedorko et al (2016). Other minor differences between the studies, that may have had some impact on the differing ulcer healing results, were the longer follow up and larger number of treatment sessions in the study by Londahl et al (2010) (57% received at least 40 sessions in Londahl et al and 69% received at least 30 sessions in Fedorko et al. The other two trials reported benefit from HBOT. However, both were at material risk of bias because the participants and the researchers were aware of whether HBOT had been used; this is a plausible explanation for their discrepant results. There are some additional concerns about Duzgun et al (2008). The authors appear to suggest that there may have been significant confounding, though the nature, extent and impact of this are not reported. Furthermore, none of 50 control participants ulcers in Duzgun et al s (2008) trial were healed after 92 weeks of treatment. This is inconsistent with the other trials, despite the participation of people with Wagner grade 2 ulcers in all trials, and calls into question the effectiveness of standard care in this trial. Poor standard care would make this trial not generalisable to the NHS. Adverse events appear more common after HBOT. We found one cost-utility study. Chuck et al (2008) reported that HBOT was both more effective and less expensive than standard care. Chuck et al s (2008) analysis is of limited relevance and reliability. It used estimates of the effectiveness of HBOT from a study published in 2003 (Guo et al 2003), which predates the three randomised trials in this rapid evidence review. The model s assumptions about the effectiveness of HBOT are incompatible with this more recent evidence, which is derived from more reliable studies. Chuck et al (2008) themselves noted that the clinical data that they used were limited. The costs are based on the Canadian health care system in 2008, and may be materially different from those in the NHS. The authors admitted that their data were not of high quality. They went on to note Cost data for HBOT were based on data from only a few centers, and reporting was not standardized. There is insufficient evidence that HBOT is effective in the treatment of diabetic foot ulcers. Taken together, the evidence does not support HBOT s introduction to the NHS for this indication. Two of the trials reporting benefit were at risk of placebo effects and observer bias because they were unblinded; they are unreliable. Of the two double-blind trials, one reported no benefit from HBOT and a second, which is less reliable due to concern that the control intervention may not have been inert, reported benefit. There would be value in a further double-blind trial of HBOT for this indication, with a control similar to that used in Fedorko et al (2016). 3. Methodology The methodology to undertake this review is specified by NHS England in their Guidance on conducting evidence reviews for Specialised Commissioning Products (2016). NHS England Evidence Review: Hyperbaric oxygen therapy for diabetic Page 6 of 28 lower limb ulceration refractory to best standard care
7 A description of the relevant Population, Intervention, Comparison and Outcomes (PICO) to be included in this review was prepared by NHS England s Policy Working Group for the topic (see section 9 for PICO). The PICO was used to search for relevant publications in EMBASE, MEDLINE and the Cochrane Library (see section 10 for search strategy). The search dates for publications were between 1 January 2007 and 2 May The titles and abstracts of the results from the literature searches were assessed using the criteria from the PICO. Full text versions of papers which appeared potentially useful were obtained and reviewed to determine whether they were appropriate for inclusion. Papers which matched the PICO were selected for inclusion in this review. The study by Londahl et al (2010) was added following a request from NHS England. Evidence from all papers included was extracted and recorded in evidence summary tables, critically appraised and their quality assessed using National Service Framework for Long term Conditions (NSF-LTC) evidence assessment framework (see section 7 below). The body of evidence for individual outcomes identified in the papers was graded and recorded in grade of evidence tables (see section 8 below). 4. Results Four randomised trials were identified (Fedorko et al (2016), Ma et al (2013), Löndahl et al (2010) and Duzgun et al (2008)). Two trials compared HBOT plus standard care with standard care only. Two (Fedorko et al (2016) and Löndahl et al (2010)) concealed treatment allocation from researcher and participants by the use of sham HBOT, reporting a comparison of HBOT plus standard care with sham HBOT plus standard care. The studies were small, including in total 333 participants. Participants were adults with diabetes and an ulcer of at least Wagner grade 1 2 (deep ulcer with tendon or joint involvement) of at least four weeks duration. HBOT regimes varied, but all four included at least 20 daily 90-minute sessions at a pressure of at least 2 ATA. Session numbers were 20 in Ma et al (2013), 30 in Fedorko et al (2016), 40 in Löndahl et al (2010) and 30 to 45 in Duzgun et al (2008). One cost-utility study was identified. It modelled the costs and effectiveness of HBOT for diabetic foot ulcers, based on Canadian cost data and an effectiveness review published in In the patient populations of interest, what is the effect of adding HBOT to the standard management pathways on the specified outcomes? Clinical efficacy outcomes reported in the studies included freedom from major and minor amputation, freedom from meeting criteria for amputation, rates of ulcer healing or other clinical 1 The Wagner classification of diabetic foot ulceration: Grade 0 - No open ulcer, high risk Grade 1 - Superficial ulcer with subcutaneous involvement Grade 2 - Deep ulcer with tendon or joint involvement Grade 3 - Deep ulcer with bone involvement Grade 4 - Wet or dry gangrene (forefoot), without cellulitis Grade 5 - Generalized (whole foot) gangrene NHS England Evidence Review: Hyperbaric oxygen therapy for diabetic Page 7 of 28 lower limb ulceration refractory to best standard care
8 outcomes, reductions in ulcer size, improvements in wound assessment scores and adverse effects. Freedom from major and minor amputation Three studies reported this outcome. In a double-blind trial, Fedorko et al (2016) reported no differences between HBOT and a sham procedure to mimic HBOT in the proportions of participants undergoing major amputation or meeting criteria determined by a vascular surgeon for such a procedure (odds ratio (OR) 0.91, 95% CI 0.37 to 2.28, p = 0.85); participants in this trial all received standard care. Löndahl et al (2010) reported three major (above the ankle) amputations in the HBOT group and one in the control group, along with four minor amputations in each group; no significance test was reported. Duzgun et al s (2008) unblinded trial reported significant differences between standard care with and without HBOT in the proportions of patients who underwent distal amputation (HBOT 4/50 (8%), control 24/50 (48%), p < 0.05) and proximal amputation (HBOT 0/50 (0%), control 17/50 (34%), p < 0.05). Freedom from meeting criteria for amputation Fedorko et al (2016) reported no difference in the proportion of participants receiving a recommendation in favour of major or minor amputation (OR for HBOT vs control groups 1.12, 95% CI 0.52 to 2.43, p = 0.77). Rates of ulcer healing or other clinical outcomes Fedorko at al (2016) reported no difference in the proportion of participants whose ulcers healed by 12 weeks (OR 0.90, 95% CI 0.35 to 2.31, p = 0.823). Löndahl et al (2010) reported complete healing of the index ulcer at one year in 25 of 48 participants (52%) in the HBOT group and 12 of 42 (29%) in the placebo group (p = 0.03). Ma et al (2013) also reported no difference in the proportion of participants whose ulcers healed by two weeks (none in either arm of their unblinded trial). Reductions in ulcer size Fedorko et al (2016) reported no difference between the two groups in reduction in manually measured ulcer size after 12 weeks (mean difference between HBOT and control groups -0.12cm, 95% CI to 0.22, p = 0.491), reduction in digitally measured ulcer area after 12 weeks (mean difference between the groups of cm 2, 95% CI to 1.19, p = 0.949), linear advancement of the ulcer edge in the first six weeks of the trial (mean difference cm/week, 95% CI to 0.013, p = 0.817) or in the second six weeks (mean difference cm/week, 95% CI to 0.015, p = 0.97). Ma et al. (2013) reported larger reductions in ulcer area in participants who underwent HBOT (an absolute difference of 24.3%, p <0.05). The authors did not report the change in ulcer size in absolute terms. Improvements in wound assessment scores Fedorko et al (2016) reported no differences in results from the Bates-Johnson wound assessment tool 2 after 12 weeks (mean difference between HBOT and control groups in the change over 12 weeks 0.53, 95% CI to 3.64, p = 0.735). This tool assesses 13 wound 2 The Bates-Jenson wound assessment tool assesses 13 wound characteristics, with each item scored on a 1 5 scale (maximum score 65). The individual scores are summated for a total score. The higher the total score, the more severe the wound status. NHS England Evidence Review: Hyperbaric oxygen therapy for diabetic Page 8 of 28 lower limb ulceration refractory to best standard care
9 characteristics, with each item scored on a 1 to 5 scale. Adverse effects Fedorko et al (2016) reported a higher number of reported unsolicited adverse events from participants who had undergone standard care plus HBOT compared with standard care plus sham treatment (HBOT 24, control 5, p = 0.02). These included inability to equalise middle ear pressures, anxiety, chest pain, nausea, hypo- and hyperglycaemia, wound infection, pain after tympanic membrane rupture and congestive heart failure. Reported numbers of the adverse events about which the researchers specifically enquired were similar (HBOT 9, control 6, p = 0.44). These included acute respiratory distress, pneumothorax, convulsion/seizure, barotrauma and visual changes. Löndahl et al (2010) reported similar rates of adverse events in the two arms of their trial. One participant in the HBOT group and three in the placebo group died during the first year after randomisation. Amputations are reported in the outcomes section above. The authors do not report tests of significance on these results. Symptomatic hypoglycaemia occurred in two and four patients in the HBOT and placebo groups respectively (not significant). One patient in the HBOT group had barotraumatic otitis, and a further four patients, two in each group, required myringotomy with tube placement. In the HBOT group, treatment-related dizziness was seen in one patient and the worsening of cataracts in another. Ma et al (2013) reported no adverse events in either arm of their trial. Is there evidence for greater improvements in treatment outcomes for patients who receive 30 or more hyperbaric oxygen treatments? No. We found no evidence comparing HBOT regimes of different durations, nor was there any tendency among the three trials for regimes with 30 or more sessions to be reported as more effective. What is the cost effectiveness for HBOT as an adjunctive treatment for diabetic patients with refractory ulcers of the lower limb? We do not know. We found no reliable cost utility studies. 5. Discussion The four randomised trials that were included report inconsistent results. Fedorko et al (2016) is a high-quality study, the authors of which enhanced the reliability of their results by using a sham HBOT treatment as a placebo control. They report the widest range of outcomes of the three trials, and their results show no suggestion of a benefit from HBOT. Löndahl et al (2010) also included several measures to minimise the risk of bias, improving its reliability. Like Fedorko et al (2016), the authors used pressurised air in control patients to ensure their trial was double-blind. However, the pressure of the hyperbaric air in the control arm (2.5 ATA) was twice that in Fedorko et al s (2016) trial, much higher than what would be experienced during usual care and high enough to create a risk of adverse effects; these were reported at similar rates in the two arms. Although the effects of hyperbaric air at these pressures are not well understood, the pressures used for control patients by Londahl et al (2010) mean that we cannot regard Löndahl et al s (2010) control treatment as an inert placebo, raising the possibility that their results, which indicated better ulcer healing at one year after HBOT with 100% oxygen compared to hyperbaric air, arise at least in part from impaired ulcer healing in the control arm due to the control intervention. There were other differences between these two studies (longer follow up NHS England Evidence Review: Hyperbaric oxygen therapy for diabetic Page 9 of 28 lower limb ulceration refractory to best standard care
10 and a larger number of treatment sessions in the study by Londahl et al (2010) (57% received at least 40 sessions in Londahl et al and 69% received at least 30 sessions in Fedorko et al). However, these differences are minor and less likely to be the reason for the discrepancy in the results between the two studies. The trials by Ma et al (2013) and Duzgun et al (2008) are methodologically inferior. They both lacked a placebo control and were in consequence unblinded. They both report benefit from HBOT, with better ulcer healing and fewer amputations. The apparent confounding differences between participants in the two arms and poor results from standard care in Duzgun et al (2008) further limit that trial s reliability and generalisability to the NHS. This pattern of results indicates that the discrepancy in results may be because of a placebo effect and/or observer bias producing unreliable results from the two unblinded trials, along with potential toxicity from high-pressure air in Löndahl et al (2010) (the other differences between Londahl et al and Fedorko et al s studies were relatively minor). This leads us to accept Fedorko et al s (2016) conclusion that HBOT does not offer an additional advantage to comprehensive wound care in reducing the indication for amputation or facilitating wound healing in patients with chronic [diabetic foot ulcers]. It is certainly not possible to reach a conclusion in favour of HBOT in the light of Fedorko et al s results. Apart from the 2.5atm of hyperbaric air used for the comparator group in the Londahl et al(2010) study, standard care was apparently similar in the four trials. There were some differences in ulcer severity between the trials, with fewest severe ulcers in Ma et al (2013) and most in Duzgun et al (2008). However, this would not explain why the results of Fedorko et al (2016) differ from those of the other two trials. Fedorko et al (2016) also report higher rates of adverse events after HBOT. Chuck et al s (2008) cost utility review is unreliable, being based on earlier and less robust effectiveness studies and patchy cost data of uncertain relevance to the NHS. 6. Conclusion There is insufficient evidence that HBOT is effective in the treatment of diabetic foot ulcers. Taken together, the evidence does not support HBOT s introduction to the NHS for this indication. Two of the trials reporting benefit were at risk of placebo effects and observer bias because they were unblinded; they are unreliable. Of the two double-blind trials, one reported no benefit from HBOT and a second, which is less reliable due to concern that the control intervention may not have been inert, reported benefit. There would be value in a further double-blind trial of HBOT for this indication, with a control similar to that used in Fedorko et al (2016). NHS England Evidence Review: Hyperbaric oxygen therapy for diabetic Page 10 of 28 lower limb ulceration refractory to best standard care
11 Study reference Study Design Population characteristics Intervention Outcome measure type Outcome measures Results Quality of Evidence Score Applicability Critical Appraisal Summary 7. Evidence Summary Table Use of HBOT plus best practice wound care Vs. best practice wound care to treat diabetic foot ulcers Fedorko et al 2016 P1 randomised controlled trial 1 hospital in Canada 103 people with diabetes (96 (93%) type 2), aged at least 18 years, referred to a communitybased specialised wound-care and hyperbaric treatment clinic for the treatment of a lower-limb wound (Wagner grade 3 2, 3, or 4) persisting for a minimum of 4 weeks. Wagner grades: grade 2 n=46, grade 3 n=51, grade 4 n=6. 49 randomised to and received HBOT, 54 randomised to and A computerised block randomisation schedule with a multiple block size of four was used. Intervention: HBOT oxygen for 90min at 244 kpa, with 5-min intervals of breathing air for every 30 min of oxygen, 5 days per week for 6 weeks (30 sessions) (Monoplace chambers (Pan-America Hyperbarics Primary Clinical effectiveness Freedom from major amputation and from meeting the criteria for major amputation (defined as below-knee or metatarsal level amputation) at 12 weeks, based on the following criteria for amputation: 1. Lack of significant progress in wound healing over the follow-up Meeting the criteria for major amputation at 12 weeks: HBOT 11/49 (23%), control 13/54 (24%), odds ratio (OR) 0.91, 95% CI 0.37 to 2.28, p = Direct Clinical and research personnel and participants were blinded to treatment allocation, reducing the risk of bias. Randomisation was uneven: HBOT group participants had had diabetes for longer than those in the control group (19.1 vs years, respectively) and were more likely to have type 1 diabetes (12% vs. 2%). The mean number of days with the index wound was 235 days in the HBOT group and 336 days in the control group. The mean index ulcer surface area at randomisation was reported as 5.1 cm 2 and 6.1cm 2 in the HBOT and control groups respectively in the text, with different figures for digital wound area of 3.8 cm 2 and 3.6 cm 2 given in Table 1. The authors report no tests of statistical significance on these differences. These differences do not cast doubt on the trial s reliability. Intention to treat analyses reported. 3 The Wagner classification of diabetic foot ulceration: The Wagner classification of diabetic foot ulceration: Grade 0 - No open ulcer, high risk Grade 1 - Superficial ulcer with subcutaneous involvement Grade 2 - Deep ulcer with tendon or joint involvement Grade 3 - Deep ulcer with bone involvement Grade 4 - Wet or dry gangrene (forefoot), without cellulitis Grade 5 - Generalized (whole foot) gangrene NHS England Evidence Review: Hyperbaric oxygen therapy for diabetic lower limb ulceration refractory to best standard care Page 11 of 28
12 received control treatment. Study duration 12 weeks. Patients were followed for 6 weeks after the end of hyperbaric sessions and returned to the clinic every week for assessment. Mean age 61 years, 67% male. Inc., Richardson,TX ), plus standard care (SC) (weekly outpatient wound assessment and treatment for 12 weeks, including comprehensiv e wound care, infection control, debridement, offloading devices and advanced wound care dressings. Control: Sham sessions of breathing air at 125 kpa (equivalent to breathing 27% oxygen by face mask) on the same schedule as intervention. This minimum pressure was required to create a sensation of being pressurized and depressurized identical to the active treatment group to keep the patients blinded to the allocation, plus SC. period, which indicated a risk of severe systemic infection related to the wound 2. Persistent deep infection involving bone and tendons (antibiotics and hospitalisation required, pathogen involved) 3. Inability to bear weight on the affected limb 4. Pain causing significant disability. NHS England Evidence Review: Hyperbaric oxygen therapy for diabetic lower limb ulceration refractory to best standard care Page 12 of 28
13 Secondary Clinical effectiveness Secondary Clinical effectiveness Secondary Clinical effectiveness Secondary Clinical effectiveness Recommendat ion in favour of major or minor amputation Wound size, measured weekly manually and by computerised analysis of wound surface area and perimeter from high-resolution calibrated digital photographs. The authors also calculated the linear advancement of the wound edge (LAWE). All measurements at 12 weeks The Bates- Jensen wound assessment tool 4 was used weekly. to measure progress of ulcer healing. Proportion of ulcers healed (i.e. Wagner grade* 0 or 1) at 12 weeks By 12 weeks: HBOT 25/49 (51%), control 26/54 (48%), OR 1.12, 95% CI 0.52 to 2.43, p = Manually measured mean width reduction at 12 weeks: HBOT 0.57cm (SD 0.13), control 0.69cm (SD 0.12), difference in mean width reduction-0.12cm, 95% CI to 0.22, p = Reduction in digital surface area at 12 weeks: HBOT 1.9 cm 2, control 1.8 cm 2, difference in reduction in mean area cm 2, 95% CI to 1.19, p = LAWE between weeks 0 and 6: difference in mean rate of LAWE cm/week, 95% CI to 0.013, p = LAWE between weeks 6 and 12: difference in mean rate of LAWE cm/week, 95% CI to 0.015, p = Mean change in score between 0 and 12 weeks: HBOT -7.0 (SD 1.13), control -7.5 (SD 1.08), difference in mean change in score 0.53, 95% CI to 3.64, p = At 12 weeks: HBOT 20%, control 22%, OR 0.90, 95% CI 0.35 to 2.31, p = The Bates-Jensen wound assessment tool assesses 13 wound characteristics, with each item scored on a 1 5 scale (maximum score 65). The individual scores are summated for a total score. The higher the total score, the more severe the wound status. NHS England Evidence Review: Hyperbaric oxygen therapy for diabetic lower limb ulceration refractory to best standard care Page 13 of 28
14 Löndahl et al (2010) P1 randomised controlled trial 1 hospital in Sweden 94 people with diabetes, at least one full-thickness wound below the ankle (Wagner grade 2, 3 or 4) for >3 months and adequate distal perfusion or nonreconstructable peripheral vascular disease. Wagner grades: grade 2 26%, Randomisatio n was done in blocks of 10 using sealed envelopes. Intervention: compression in air for 5 minutes, then 100% oxygen at 2.5 atmospheres absolute (ATA) for 85 Secondary Safety Primary Clinical effectiveness Primary The researchers solicited information on acute respiratory distress, pneumothorax, convulsion/sei zure, barotrauma and visual changes. They also recorded other adverse events as unsolicited. These included inability to equalise middle ear pressures, anxiety, chest pain, nausea, hypo- and hyperglycaemi a, wound infection, pain after tympanic membrane rupture and congestive heart failure Complete healing of the index ulcer (the ulcer with the largest area and a duration of at least three months at the time of randomisation). Amputations: major (above Solicited adverse events: HBOT 9, control 6, p = Unsolicited adverse events: HBOT 24, control 5, p = At one year: HBOT 25/48 (52%), control 12/42 (29%), p = 0.03). At one year: HBOT 3 major and 4 minor, control 1 major 7 Direct Clinical and research personnel and participants were blinded to treatment allocation, reducing the risk of bias. NHS England Evidence Review: Hyperbaric oxygen therapy for diabetic lower limb ulceration refractory to best standard care Page 14 of 28 The authors used air pressurised to 2.5 atmospheres in control patients to ensure their trial was double-blind. This is high enough to create a risk of adverse effects; these were reported at similar rates in the two arms. The control treatment may not have been an inert placebo, raising the possibility that their results arise at least in part from impaired ulcer healing in the control arm.
15 Ma et al 2013 P1 randomised controlled trial 1 hospital in China grade 3 56%, grade 4 18%. 49 randomised to and received HBOT, 45 randomised to control treatment. Study duration 1 year Mean age 69 years, 81% male. Analysis by intention to treat. 36 people with diabetes, at least one full-thickness wound below the ankle (Wagner grade 3 or less) for >3 months; history of receiving standard care for >2 months; normal palpation of arterial pulses at lower extremities; normal lower limb Doppler scan results; transcutaneous oxygen pressure >30 mm Hg at the dorsum of the foot, and no abnormal minutes, then decompressio n for 5 minutes, plus standard care (SC) (treatment of infection, revascularizati on, debridement, off-loading, and metabolic control). Control: Identical to the intervention, except for the use of air, not 100% oxygen, for the 85 minute treatment phase, plus SC as above. Randomisatio n with random number table. Intervention: HBOT 100% oxygen, twice daily, for 90 minutes at 2.5 ATA, 5 days a week for 2 weeks, in a multi-person hyperbaric chamber (K018YX-10-8, XinYing, Hang Zhou City, China). Each HBO session included 15 minutes of Clinical effectiveness Secondary Safety Primary Clinical efficacy the ankle) and minor (all others) Adverse event Healed by day 14 and four minor, no significance test reported. HBOT: 1 death from multiple organ failure 20 days after randomisation, 2 participants with hypoglycaemia (symptoms and bloodglucose < 3.0 mmol/l), 1 with barotraumatic otitis, 2 with myringotomy and tube placement, 1 with treatmentrelated dizziness, 1 with worsening of cataracts. Control: 1 patient lost consciousness after a treatment session, 4 participants with hypoglycaemia, 2 with myringotomy and tube placement, 1 patient had a fall and minor head injury in the chamber. The difference in rates of hypoglycaemia was not significant; statistical tests of the other results were not reported. NHS England Evidence Review: Hyperbaric oxygen therapy for diabetic lower limb ulceration refractory to best standard care Page 15 of 28 1, 2, 3, 6 and 9 month per protocol outcomes, rather than intention to treat outcomes, were reported in a graph in the paper. These are not reported here because they are per protocol rather than intention to treat and because they were published in a poorly labelled graph with no accompanying data. Comparison of per protocol outcomes with intention to treat outcomes is not valid. Intention to treat outcomes were only reported at 1 year. HBOT 0, control 0. 9 Direct The study was unblinded, increasing the risk of bias. There were no reported significant baseline differences between the arms. Materially shorter follow-up than the other two trials. This was the only trial to use palpable peripheral pulses as an entry criterion.
16 x-ray findings that may be indicative of chronic bone infection. Wagner grades: grade 1 n=9, grade 2 n=10 grade 3 n= randomised to and received HBOT (of whom 23 had type I diabetes), 18 randomised to and received control treatment (of whom 2 had type I diabetes). Study duration 2 weeks Mean age 60.1 years, 64% male. compression time, three 30- minute HBOT periods with two 5-minute intervals in room air, and a 15-minute decompressio n period, plus standard care (SC) (admitted to hospital for 2 weeks for offloading, footwear, nonweight-bearing of the affected foot, oral antibiotics, drug sensitivity test of ulcer tissue, blood glucose levels monitoring and maintenance at <8 mmol/l with subcutaneous insulin injections if necessary, daily dressing changes with silverimpregnated dressings used in infected ulcers and absorptive cotton in uninfected ulcers, daily wound curettage or debridement of necrotic tissue and surrounding callus. NHS England Evidence Review: Hyperbaric oxygen therapy for diabetic lower limb ulceration refractory to best standard care Page 16 of 28
17 Control: SC only Primary Clinical efficacy Average reduction in ulcer area by day 14 HBOT 42.4% standard deviation (SD) 20.0%, control 18.1% SD 6.5%, p <0.05. Duzgun et al 2008 P1 randomised controlled trial 1 hospital in Ankara, Turkey 100 people with diabetes (86% insulin-dependent) at least 18 years of age with a foot wound that had been present for at least 4 weeks despite appropriate local and systemic wound care. Wagner grades: grade 2 n=18, grade 3 n=37, grade 4 n= participants randomised to each arm. Mean duration of follow-up was 92 weeks. Mean age 60 years, 64% male Randomisatio n with a random number table, allocating patients to a treatment group depending on whether the number was even or odd. Intervention: HBOT with maximum working pressure of 20 ATA, using a unichamber pressure room (Patterson Companies, Inc., St. Paul, MN), employing a volume of 10 m 3 at 2 to 3 ATA for 90 minutes, once or twice daily on alternate days for 20 to 30 days, plus Secondary Safety Primary Clinical efficacy Adverse events: death, amputation, barotraumatic otitis, dizziness, seizures, and pneumothorax Clinical outcome, one of the following 6: Healed (complete closure without debridement in the operating room), graft or flap (graft or flap closure required), distal amputation (amputation distal to metatarsophal angeal joints), proximal amputation (amputation proximal to the metatarsophal angeal joints), debridement (standard therapy wound or operative debridement), no change (failure to heal HBOT 0, control 0. Healed: HBOT 33/50 (66%), control 0/50 (0%), p < Graft or flap: HBOT 4/50 (8%), control 0/50 (0%), p < Distal amputation: HBOT 4/50 (8%), control 24/50 (48%), p < Proximal amputation: HBOT 0/50 (0%), control 17/50 (34%), p < Debridement: HBOT 0/50 (0%), control 9/50 (18%), p < No change: HBOT 9/50 (18%), control 0/50 (0%), p < Direct The study was unblinded. NHS England Evidence Review: Hyperbaric oxygen therapy for diabetic lower limb ulceration refractory to best standard care Page 17 of 28 It is surprising that none of 50 control participants ulcers were healed after 92 weeks of treatment. This is inconsistent with the other trials, despite the participation of people with Wagner grade 2 ulcers in all trials, and calls into question the effectiveness of standard care in this trial. Poor standard care would make this trial not generalisable to the NHS. The randomisation produced uneven results, with HBOT participants more likely to be male, obese and smokers and with less severe ulceration at the trial's outset. This may have influenced the outcome. The authors report "Although all of these findings were statistically significant when nonparametric null hypothesis tests were calculated, the association with the risk factor variables changed considerably (>10%) when univariate and multiple variable logistic regression equations were computed for ulcer grade and HBOT, indicating confounding between these variables (results not shown)." The implications of these remarks are unclear, but suggest the trial's results
18 standard care (SC) (daily wound care, including dressing changes and local debridement at bedside or in the operating room, and amputation when indicated). during the course of treatment). may be materially undermined by confounding. Control: SC only. Chuck et al (2008) Health economic modelling using previously published data Alberta, Canada Modelling of costs and outcomes for a 65-year old with a diabetic foot ulcer. Time horizon 12 years HBOT plus standard care (SC) vs SC alone. HBOT was assumed to range from thirty to forty sessions of 2 to 2.5 hours in duration. Cost utility Costs, outcomes (major amputation, healed with or without a minor amputation, unhealed) and the utility of these outcomes Probabilities in year 1: healed HBOT 0.56, SC 0.24; minor amputation and healed ulcer HBOT 0.27, SC 0.16; unhealed ulcer HBOT 0.06, SC 0.28; major amputation HBOT 0.11, SC Costs: HBOT C$40,695 ( 23,400), SC C$49,786 ( 28,600). Utilities: HBOT 3.64 qualityadjusted life-years (QALYs), SC 3.01 QALYs. HBOT plus SC was deemed the dominant strategy, with better outcomes and lower costs. 6 Direct The model has limited relevance and reliability: The estimates of the effectiveness of HBOT are from a study published in 2003 (Guo et al 2003), which predates the three randomised trials in this rapid evidence review. The model s assumptions about the effectiveness of HBOT are incompatible with this more recent evidence, which is derived from more reliable studies. For example, the model assumes absolute risk differences between HBOT and SC of 22% and 32% for major amputation and healing respectively, whereas the most reliable trial that we found, by Fedorko at al (2016), found no significant differences with respect to either of these outcomes. The authors sensitivity analysis included too small an adjustment to these assumptions to align them with more reliable evidence. The authors noted that the clinical data supporting the effectiveness of adjunctive HBOT for [diabetic foot ulcers] remains limited. Good quality studies are required to confirm the comparative benefits of NHS England Evidence Review: Hyperbaric oxygen therapy for diabetic lower limb ulceration refractory to best standard care Page 18 of 28
19 this technology. They expected that Fedorko et al s trial, already underway in Canada when they published their analysis, would help meet this need. If, as that trial reported, HBOT does not offer an additional advantage to comprehensive wound care in reducing the indication for amputation or facilitating wound healing in patients with chronic [diabetic foot ulcers], then HBOT cannot be cost-effective. The costs are based on the Canadian health care system in 2008, and may be materially different from those in the NHS. The authors admit The data (notably cost data) upon which the variables in the economic model were based, are not of high quality. They went on Cost data for HBOT were based on data from only a few centers, and reporting was not standardized. NHS England Evidence Review: Hyperbaric oxygen therapy for diabetic lower limb ulceration refractory to best standard care Page 19 of 28
20 8. Grade of evidence table Use of HBOT plus best practice wound care Vs. best practice wound care to treat diabetic foot ulcers Outcome Measure Reference Quality of Evidence Score Applicability Grade of Evidence Interpretation of Evidence Freedom from major and minor amputation or meeting the criteria for major amputation Recommendation in favour of major or Fedorko et al Direct B Freedom from major amputation or meeting the criteria for major amputation (defined as below-knee or metatarsal level amputation) at 12 weeks, was based on not having any of the following criteria for amputation: NHS England Evidence Review: Hyperbaric oxygen therapy for diabetic lower limb ulceration refractory to best standard care Page 20 of Lack of significant progress in wound healing over the follow-up period, which indicated a risk of severe systemic infection related to the wound 2. Persistent deep infection involving bone and tendons (antibiotics and hospitalisation required, pathogen involved) 3. Inability to bear weight on the affected limb 4. Pain causing significant disability. This is a subjective judgement of the presence of indications for amputation, made by a single surgeon, blinded to the participant s treatment allocation. Only Fedorko et al. (2016) reported this outcome measure. They reported no effect of HBOT on this outcome in a high quality double-blind trial with 103 participants. They reported that 23% of HBOT and 24% of controls met criteria for major amputation over the 12 weeks of the study. This result suggests that HBOT had no effect on this outcome. The result provides an indication of whether HBOT reduces the risk of a below-knee or metatarsal-level amputation. This would be of major benefit, but the results provide no reason to believe HBOT has this effect. Fedorko et al Direct B This is a subjective judgement of the presence of indications for amputation, made by a single surgeon, blinded to the
21 minor amputation Major or minor amputation Progress of ulcer healing over 12 weeks participant s treatment allocation. Only Fedorko et al. (2016) reported this outcome measure. They reported that 51% of HBOT and 48% of controls were judged to need major or minor amputation over the 12 weeks of the study. The result provides an indication of whether HBOT reduces the risk of a below-knee or metatarsal-level amputation, or a minor amputation of one or more toes. This would be of major benefit, but the results provide no reason to believe HBOT has this effect. Löndahl et al (2010) 7 Direct B Amputations above the ankle were defined as major and all others as minor. Only Löndahl et al (2010) reported this outcome. They reported 3 major and 4 minor amputations in the HBOT arm, and 1 major and four minor amputations in the control arm. No significance test was reported. The result provides an indication of whether HBOT reduces the risk of an above-ankle or below-ankle amputation. This would be of major benefit, but the results provide no reason to believe HBOT has this effect. Fedorko et al Direct B Wound size was measured weekly manually and by computerised analysis of wound surface area and perimeter from high-resolution calibrated digital photographs. The authors also calculated the linear advancement of the wound edge. All measurements were made at 12 weeks. This is an assessment of the progress and extent of wound healing, made blind to the participant s treatment allocation. Only Fedorko et al. (2016) reported this outcome measure. They reported a difference in mean width reduction of cm, 95% CI to 0.22, p = This result suggests that HBOT had no effect on this outcome. Faster wound healing would be of major NHS England Evidence Review: Hyperbaric oxygen therapy for diabetic lower limb ulceration refractory to best standard care Page 21 of 28
22 Progress of ulcer healing by day 14 Ulcer healing at one year Progress of ulcer healing as measured by the Bates-Jensen NHS England Evidence Review: Hyperbaric oxygen therapy for diabetic lower limb ulceration refractory to best standard care Page 22 of 28 benefit, but the results do not indicate that HBOT hastens this outcome. Ma et al Direct B Average reduction in ulcer area by day 14 was assessed. Ulcer area was assessed by computerised examination of clinical photographs. Only Ma et al. s (2013) unblinded randomised trial with 36 participants reported this outcome measure. In the HBOT arm, the average reduction in ulcer area was 42%, compared with 20% in the control arm (p<0.05). Faster wound healing would be of major benefit; the results suggest that HBOT may hasten this outcome. The assessment was made without blinding to the participant s treatment allocation, increasing the risk of bias. Löndahl et al Direct B The outcome is complete healing of the index ulcer (the ulcer with the largest area and a duration of at least three months at the time of randomisation). Only Löndahl s et al (2010) double-blind randomised trial with 94 participants reported this outcome measure. In the HBOT arm, healing rates were 25/48 (52%), compared with 12/42 (29%) in controls (p = 0.03). Faster wound healing would be of major benefit; the results suggest that HBOT may hasten this outcome. The authors used air pressurised to 2.5 atmospheres in control patients to ensure their trial was double-blind. This pressure is high enough to create a risk of adverse effects; these were reported at similar rates in the two arms. The effects of hyperbaric air are not well understood and this control treatment may not have been an inert placebo, raising the possibility that their results arise at least in part from impaired ulcer healing in the control arm due to the control intervention. Fedorko et al Direct B The Bates-Jensen wound assessment tool was used weekly to measure progress of ulcer healing. This is an
23 wound assessment tool Proportion of ulcers healed at 12 weeks Proportion of ulcers healed by day 14 assessment of the progress and extent of wound healing, made blind to the participant s treatment allocation. This tool assesses 13 wound characteristics, with each item scored on a 1 to 5 scale (maximum score 65). The individual scores are summated for a total score. The higher the total score, the more severe the wound status. Only Fedorko et al. (2016) reported this outcome measure. They reported a difference in mean change in score of 0.53, 95% CI to 3.64, p = This result suggests that HBOT had no effect on this outcome. Faster wound healing would be of major benefit, but the results do not indicate that HBOT hastens this outcome. Fedorko et al Direct B The proportion of ulcers healed (ie Wagner grade 0 or 1) was measured at 12 weeks. This is an assessment of the progress and extent of wound healing, made blind to the participant s treatment allocation. (The Wagner classification of diabetic foot ulceration is as follows: Grade 0 No open ulcer, high risk; Grade 1 Superficial ulcer with subcutaneous involvement; Grade 2 Deep ulcer with tendon or joint involvement; Grade 3 Deep ulcer with bone involvement; Grade 4 Wet or dry gangrene (forefoot), without cellulitis; Grade 5 Generalized (whole foot) gangrene.) Fedorko et al. (2016) reported this outcome measure. They reported that 20% of HBOT and 22% of controls had healed at 12 weeks. This result suggests that HBOT had no effect on this outcome. A higher likelihood of ulcer healing would be of major benefit, but the results do not indicate that HBOT hastens this outcome. Ma et al Direct B Ulcer healed by day 14. This assessment of the completion of wound healing was made by examination of clinical photographs, without blinding to NHS England Evidence Review: Hyperbaric oxygen therapy for diabetic lower limb ulceration refractory to best standard care Page 23 of 28
CPAG Summary Report for Clinical Panel URN 1779, Hyperbaric Oxygen Therapy for Diabetic Lower Limb Ulceration Refractory to Best Standard Care
 MANAGEMENT IN CONFIDENCE CPAG Summary Report for Clinical Panel URN 1779, Hyperbaric Oxygen Therapy for Diabetic Lower Limb Ulceration Refractory to Best Standard Care The Benefits of the Proposition No
MANAGEMENT IN CONFIDENCE CPAG Summary Report for Clinical Panel URN 1779, Hyperbaric Oxygen Therapy for Diabetic Lower Limb Ulceration Refractory to Best Standard Care The Benefits of the Proposition No
Clinical Commissioning Policy: Hyperbaric oxygen therapy for diabetic lower limb ulceration (diabetic foot ulcer) (all ages)
 Clinical Commissioning Policy: Hyperbaric oxygen therapy for diabetic lower limb ulceration (diabetic foot ulcer) (all ages) NHS England Reference: 1712P 1 NHS England INFORMATION READER BOX Directorate
Clinical Commissioning Policy: Hyperbaric oxygen therapy for diabetic lower limb ulceration (diabetic foot ulcer) (all ages) NHS England Reference: 1712P 1 NHS England INFORMATION READER BOX Directorate
NHS England. Evidence review: Hyperbaric oxygen therapy for necrotising soft tissue infections
 NHS England Evidence review: Hyperbaric oxygen therapy for necrotising soft tissue infections NHS England Evidence review: Hyperbaric oxygen therapy for necrotising soft tissue infections First published:
NHS England Evidence review: Hyperbaric oxygen therapy for necrotising soft tissue infections NHS England Evidence review: Hyperbaric oxygen therapy for necrotising soft tissue infections First published:
NHS England. Evidence review: Hyperbaric Oxygen Therapy for Carbon Monoxide Poisoning
 NHS England Evidence review: Hyperbaric Oxygen Therapy for Carbon Monoxide Poisoning NHS England Evidence review: Hyperbaric Oxygen Therapy for Carbon Monoxide Poisoning First published: June 2017 Updated:
NHS England Evidence review: Hyperbaric Oxygen Therapy for Carbon Monoxide Poisoning NHS England Evidence review: Hyperbaric Oxygen Therapy for Carbon Monoxide Poisoning First published: June 2017 Updated:
CPAG Summary Report for Clinical Panel Hyperbaric Oxygen Therapy for Carbon Monoxide Poisoning
 MANAGEMENT IN CONFIDENCE CPAG Summary Report for Clinical Panel Hyperbaric Oxygen Therapy for Carbon Monoxide Poisoning The Benefits of the Proposition No Metric Grade of evidence Summary from evidence
MANAGEMENT IN CONFIDENCE CPAG Summary Report for Clinical Panel Hyperbaric Oxygen Therapy for Carbon Monoxide Poisoning The Benefits of the Proposition No Metric Grade of evidence Summary from evidence
AWMA MODULE ACCREDITATION. Module Five: The High Risk Foot (Including the Diabetic Foot)
 AWMA MODULE ACCREDITATION Module Five: The High Risk Foot (Including the Diabetic Foot) Introduction - The Australian Wound Management Association Education & Professional Development Sub Committee-(AWMA
AWMA MODULE ACCREDITATION Module Five: The High Risk Foot (Including the Diabetic Foot) Introduction - The Australian Wound Management Association Education & Professional Development Sub Committee-(AWMA
Authors' objectives To assess the value of treatments for foot ulcers in patients with Type 2 diabetes mellitus.
 A systematic review of foot ulcer in patients with Type 2 diabetes mellitus - II: treatment Mason J, O'Keeffe C, Hutchinson A, McIntosh A, Young R, Booth A Authors' objectives To assess the value of treatments
A systematic review of foot ulcer in patients with Type 2 diabetes mellitus - II: treatment Mason J, O'Keeffe C, Hutchinson A, McIntosh A, Young R, Booth A Authors' objectives To assess the value of treatments
Definitions and criteria
 Several disciplines are involved in the management of diabetic foot disease and having a common vocabulary is essential for clear communication. Thus, based on a review of the literature, the IWGDF has
Several disciplines are involved in the management of diabetic foot disease and having a common vocabulary is essential for clear communication. Thus, based on a review of the literature, the IWGDF has
Limb Threatening Acute Right Small Toe Diabetic Ulcer with Infected Bone and Ascending Infection Problem Day #0 Day #0
 Martin J. Winkler, MD, FACS Vascular Surgery, Advanced Wound Care 1018 Dodge Street, Suite 4, Omaha, NE, 68102 Problem Ascending infection of right forefoot, 5 days in ICU for IV antibiotics Diabetic right
Martin J. Winkler, MD, FACS Vascular Surgery, Advanced Wound Care 1018 Dodge Street, Suite 4, Omaha, NE, 68102 Problem Ascending infection of right forefoot, 5 days in ICU for IV antibiotics Diabetic right
Clinical Commissioning Policy Proposition: Hyperbaric Oxygen Therapy for necrotising soft tissue infections
 Clinical Commissioning Policy Proposition: Hyperbaric Oxygen Therapy for necrotising soft tissue infections Reference: NHS England 1776 Prepared by NHS England Specialised Services Clinical Reference Group
Clinical Commissioning Policy Proposition: Hyperbaric Oxygen Therapy for necrotising soft tissue infections Reference: NHS England 1776 Prepared by NHS England Specialised Services Clinical Reference Group
Granulox Update on evidence and science
 Update on evidence and science New clinical data in DFU wounds Retrospective cohort evaluation Site: Southtees, UK Main Inclusion criteria: DFU, < wound size reduction in 4 weeks Verum Group: Standard
Update on evidence and science New clinical data in DFU wounds Retrospective cohort evaluation Site: Southtees, UK Main Inclusion criteria: DFU, < wound size reduction in 4 weeks Verum Group: Standard
Hyperbaric Oxygen Therapy (HBO)
 MP9055 Covered Service: Prior Authorization Required: Additional Information: Yes when meets criteria below Yes-as shown below None Prevea360 Health Plan Medical Policy: 1.0 Hyperbaric Oxygen therapy (HBO)
MP9055 Covered Service: Prior Authorization Required: Additional Information: Yes when meets criteria below Yes-as shown below None Prevea360 Health Plan Medical Policy: 1.0 Hyperbaric Oxygen therapy (HBO)
Hyperbaric oxygen therapy Villanueva E, Johnston R, Clavisi O, Burrows E, Bernath V, Rajendran M, Wasiak J, Fennessy P, Anderson J, Harris A, Yong K
 Hyperbaric oxygen therapy Villanueva E, Johnston R, Clavisi O, Burrows E, Bernath V, Rajendran M, Wasiak J, Fennessy P, Anderson J, Harris A, Yong K Authors' objectives To assess the effectiveness of hyperbaric
Hyperbaric oxygen therapy Villanueva E, Johnston R, Clavisi O, Burrows E, Bernath V, Rajendran M, Wasiak J, Fennessy P, Anderson J, Harris A, Yong K Authors' objectives To assess the effectiveness of hyperbaric
Rapid Recovery Hyperbarics 9439 Archibald Ave. Suite 104 Rancho Cucamonga CA,
 Foot at risk Age Well By Dr LIEW NGOH CHIN Are limb amputations due to diabetes preventable? DIABETES mellitus is a major global health problem and has reached epidemic proportions in many developed and
Foot at risk Age Well By Dr LIEW NGOH CHIN Are limb amputations due to diabetes preventable? DIABETES mellitus is a major global health problem and has reached epidemic proportions in many developed and
Diabetic Foot Ulcers. Care for Patients in All Settings
 Diabetic Foot Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a diabetic foot ulcer. The scope of the standard
Diabetic Foot Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a diabetic foot ulcer. The scope of the standard
Hyperbaric Oxygen Therapy for Non-Healing Ulcers in Diabetes Mellitus
 Ontario Health Technology Assessment Series 2005; Vol. 5, No. 11 Hyperbaric Oxygen Therapy for Non-Healing Ulcers in Diabetes Mellitus An Evidence-Based Analysis September 2005 Medical Advisory Secretariat
Ontario Health Technology Assessment Series 2005; Vol. 5, No. 11 Hyperbaric Oxygen Therapy for Non-Healing Ulcers in Diabetes Mellitus An Evidence-Based Analysis September 2005 Medical Advisory Secretariat
Hyperbaric Oxygen Utilization in Wound Care
 Hyperbaric Oxygen Utilization in Wound Care Robert Barnes, MD, CWS Hyperbaric Center Sacred Heart Medical Center Riverbend Springfield, Oregon No relevant disclosures Diabetes and lower extremity wounds
Hyperbaric Oxygen Utilization in Wound Care Robert Barnes, MD, CWS Hyperbaric Center Sacred Heart Medical Center Riverbend Springfield, Oregon No relevant disclosures Diabetes and lower extremity wounds
Type 2 diabetes: prevention and management of foot problems
 Type 2 diabetes: prevention and management of foot problems NICE guideline Revised version Second draft for consultation, August 2003 If you wish to comment on the recommendations, please make your comments
Type 2 diabetes: prevention and management of foot problems NICE guideline Revised version Second draft for consultation, August 2003 If you wish to comment on the recommendations, please make your comments
Introduction. Epidemiology Pathophysiology Classification Treatment
 Diabetic Foot Introduction Epidemiology Pathophysiology Classification Treatment Epidemiology DM largest cause of neuropathy in N.A. 1 million DM patients in Canada Half don t know Foot ulcerations is
Diabetic Foot Introduction Epidemiology Pathophysiology Classification Treatment Epidemiology DM largest cause of neuropathy in N.A. 1 million DM patients in Canada Half don t know Foot ulcerations is
PUT YOUR BEST FOOT FORWARD
 PUT YOUR BEST FOOT FORWARD Bala Ramanan, MBBS 1 st year vascular surgery fellow Introduction The epidemic of diabetes and ageing of our population ensures critical limb ischemia will continue to grow.
PUT YOUR BEST FOOT FORWARD Bala Ramanan, MBBS 1 st year vascular surgery fellow Introduction The epidemic of diabetes and ageing of our population ensures critical limb ischemia will continue to grow.
Deep vein thrombosis and its prevention in critically ill adults Attia J, Ray J G, Cook D J, Douketis J, Ginsberg J S, Geerts W H
 Deep vein thrombosis and its prevention in critically ill adults Attia J, Ray J G, Cook D J, Douketis J, Ginsberg J S, Geerts W H Authors' objectives To systematically review the incidence of deep vein
Deep vein thrombosis and its prevention in critically ill adults Attia J, Ray J G, Cook D J, Douketis J, Ginsberg J S, Geerts W H Authors' objectives To systematically review the incidence of deep vein
Diabetic Foot Ulcers. Alex Khan APRN ACNS-BC MSN CWCN CFCN WCN-C. Advanced Practice Nurse / Adult Clinical Nurse Specialist
 Diabetic Foot Ulcers Alex Khan APRN ACNS-BC MSN CWCN CFCN WCN-C Advanced Practice Nurse / Adult Clinical Nurse Specialist Organization of Wound Care Nurses www.woundcarenurses.org Objectives Identify Diabetic/Neuropathic
Diabetic Foot Ulcers Alex Khan APRN ACNS-BC MSN CWCN CFCN WCN-C Advanced Practice Nurse / Adult Clinical Nurse Specialist Organization of Wound Care Nurses www.woundcarenurses.org Objectives Identify Diabetic/Neuropathic
Data extraction. Specific interventions included in the review Dressings and topical agents in relation to wound healing.
 Systematic reviews of wound care management: (2) dressings and topical agents used in the healing of chronic wounds Bradley M, Cullum N, Nelson E A, Petticrew M, Sheldon T, Torgerson D Authors' objectives
Systematic reviews of wound care management: (2) dressings and topical agents used in the healing of chronic wounds Bradley M, Cullum N, Nelson E A, Petticrew M, Sheldon T, Torgerson D Authors' objectives
Independent evaluation of BEMER physical vascular regulation therapy
 of BEMER Liezl Naudé Advanced nurse specialist: wound management Advanced lower limb and wound management centre, Pretoria Heart 4 the Wounded 5-7 July Pretoria Introduction Lower limb wounds have always
of BEMER Liezl Naudé Advanced nurse specialist: wound management Advanced lower limb and wound management centre, Pretoria Heart 4 the Wounded 5-7 July Pretoria Introduction Lower limb wounds have always
Hyperbarics in Diabetic Wound Care. Aurel Mihai, MD & Brian Kline, MD
 Hyperbarics in Diabetic Wound Care Aurel Mihai, MD & Brian Kline, MD Presentation Outline The Scope of the Problem Important Definitions Standard Wound Care Hyperbaric Oxygen as an Adjunct Diabetic Foot
Hyperbarics in Diabetic Wound Care Aurel Mihai, MD & Brian Kline, MD Presentation Outline The Scope of the Problem Important Definitions Standard Wound Care Hyperbaric Oxygen as an Adjunct Diabetic Foot
AWMA MODULE ACCREDITATION. Module Seven: Conservative Sharp Wound Debridement
 AWMA MODULE ACCREDITATION Module Seven: Conservative Sharp Wound Debridement Introduction- The Australian Wound Management Association Education & Professional Development Sub Committee-(AWMA EPDSC) has
AWMA MODULE ACCREDITATION Module Seven: Conservative Sharp Wound Debridement Introduction- The Australian Wound Management Association Education & Professional Development Sub Committee-(AWMA EPDSC) has
National Diabetes Foot Care Audit Third Annual Report
 National Diabetes Foot Care Audit Third Annual Report England and Wales 14 July 2014 to 31 March 2017 V1.0 14 March 2018 Introduction: Contents Key Introduction Key messages Care structures survey Participation
National Diabetes Foot Care Audit Third Annual Report England and Wales 14 July 2014 to 31 March 2017 V1.0 14 March 2018 Introduction: Contents Key Introduction Key messages Care structures survey Participation
ULCERS 1/12/ million diabetics in the US (2012) Reamputation Rate 26.7% at 1 year 48.3% at 3 years 60.7% at 5 years
 Jay Christensen D.P.M Advanced Foot and Ankle of Wisconsin 2-4% of the population at any given time will have ulcers 0.06-0.20% of the total population Average age of patients 70 years increased as more
Jay Christensen D.P.M Advanced Foot and Ankle of Wisconsin 2-4% of the population at any given time will have ulcers 0.06-0.20% of the total population Average age of patients 70 years increased as more
The Results Of Maggot Debridement Therapy In The Ischemic Leg: A Study On 89 Patients With 89 Wounds On The Lower Leg Treated With Maggots
 ISPUB.COM The Internet Journal of Surgery Volume 9 Number 1 The Results Of Maggot Debridement Therapy In The Ischemic Leg: A Study On 89 Patients With 89 Wounds On The Lower Leg Treated With Maggots P
ISPUB.COM The Internet Journal of Surgery Volume 9 Number 1 The Results Of Maggot Debridement Therapy In The Ischemic Leg: A Study On 89 Patients With 89 Wounds On The Lower Leg Treated With Maggots P
A Guide To Hyperbaric Oxygen Therapy For Diabetic Foot Wounds
 A Guide To Hyperbaric Oxygen Therapy For Diabetic Foot Wounds Written By: Kazu Suzuki, DPM CWS Hyperbaric oxygen (HBO) chambers are currently located in over 750 facilities in the United States. New wound
A Guide To Hyperbaric Oxygen Therapy For Diabetic Foot Wounds Written By: Kazu Suzuki, DPM CWS Hyperbaric oxygen (HBO) chambers are currently located in over 750 facilities in the United States. New wound
Implementing the updated NICE Guidance on the Diabetic Foot
 Implementing the updated NICE Guidance on the Diabetic Foot Rachel Berrington Senior Diabetes Specialist Nurse Foot Lead University Hospitals of Leicester NHS Trust Key Priorities for Implementation NG19
Implementing the updated NICE Guidance on the Diabetic Foot Rachel Berrington Senior Diabetes Specialist Nurse Foot Lead University Hospitals of Leicester NHS Trust Key Priorities for Implementation NG19
Diabetic Foot Ulcer Treatment and Prevention
 Diabetic Foot Ulcer Treatment and Prevention Alexander Reyzelman DPM, FACFAS Associate Professor California School of Podiatric Medicine at Samuel Merritt University Diabetic Foot Ulcers One of the most
Diabetic Foot Ulcer Treatment and Prevention Alexander Reyzelman DPM, FACFAS Associate Professor California School of Podiatric Medicine at Samuel Merritt University Diabetic Foot Ulcers One of the most
DECISION MEMORANDUM. Ronald Dei Cas, M.D. Medical Officer, Division of Items and Devices
 DECISION MEMORANDUM (This decision memorandum does not constitute a national coverage determination (NCD). It states CMS's intent to issue an NCD. Prior to any new or modified policy taking effect, CMS
DECISION MEMORANDUM (This decision memorandum does not constitute a national coverage determination (NCD). It states CMS's intent to issue an NCD. Prior to any new or modified policy taking effect, CMS
Nanogen Aktiv. Naz Wahab MD, FAAFP, FAPWCA Nexderma
 Nanogen Aktiv Naz Wahab MD, FAAFP, FAPWCA Nexderma Patient BM 75 y.o female with a history of Type 2 Diabetes, HTN, Hypercholesterolemia, Renal insufficiency, Chronic back Pain, who had undergone a L3-L4
Nanogen Aktiv Naz Wahab MD, FAAFP, FAPWCA Nexderma Patient BM 75 y.o female with a history of Type 2 Diabetes, HTN, Hypercholesterolemia, Renal insufficiency, Chronic back Pain, who had undergone a L3-L4
Cost-effectiveness of becaplermin for nonhealing neuropathic diabetic foot ulcers Sibbald R G, Torrance G, Hux M, Attard C, Milkovich N
 Cost-effectiveness of becaplermin for nonhealing neuropathic diabetic foot ulcers Sibbald R G, Torrance G, Hux M, Attard C, Milkovich N Record Status This is a critical abstract of an economic evaluation
Cost-effectiveness of becaplermin for nonhealing neuropathic diabetic foot ulcers Sibbald R G, Torrance G, Hux M, Attard C, Milkovich N Record Status This is a critical abstract of an economic evaluation
10/19/2017. Shawn M Sanicola DPM, FACFAS Foot And Ankle Associates of WI. Consultant with J&J-Depuy-Synthesis
 Shawn M Sanicola DPM, FACFAS Foot And Ankle Associates of WI Consultant with J&J-Depuy-Synthesis Understand the systemic effects of diabetes on the lower extremity The significance of structural and biomechanical
Shawn M Sanicola DPM, FACFAS Foot And Ankle Associates of WI Consultant with J&J-Depuy-Synthesis Understand the systemic effects of diabetes on the lower extremity The significance of structural and biomechanical
Off Loading, TCC, Shoe 을지의대을지병원 족부정형외과 이경태
 Off Loading, TCC, Shoe 을지의대을지병원 족부정형외과 이경태 DMF Protocol VIPS approach V : Vascular I : infection P : Pressure off S : specific wound care Ulcer/Pressure off& Biomechanics PVD vs Peripheral neuropathy NP
Off Loading, TCC, Shoe 을지의대을지병원 족부정형외과 이경태 DMF Protocol VIPS approach V : Vascular I : infection P : Pressure off S : specific wound care Ulcer/Pressure off& Biomechanics PVD vs Peripheral neuropathy NP
Due to Perimed s commitment to continuous improvement of our products, all specifications are subject to change without notice.
 A summary Disclaimer The information contained in this document is intended to provide general information only. It is not intended to be, nor does it constitute, medical advice. Under no circumstances
A summary Disclaimer The information contained in this document is intended to provide general information only. It is not intended to be, nor does it constitute, medical advice. Under no circumstances
Wound Classification. Overview
 Overview Jeffrey A. Niezgoda, MD FACHM, MAPWCA, CHWS Review of Initial Wound Care Consultation Rational for Classification Wound Appearance Wound Etiology Management Algorithms Initial Wound Care Consult
Overview Jeffrey A. Niezgoda, MD FACHM, MAPWCA, CHWS Review of Initial Wound Care Consultation Rational for Classification Wound Appearance Wound Etiology Management Algorithms Initial Wound Care Consult
Is noncontact normothermic wound therapy cost effective for the treatment of stages 3 and 4 pressure ulcers Macario A, Dexter F
 Is noncontact normothermic wound therapy cost effective for the treatment of stages 3 and 4 pressure ulcers Macario A, Dexter F Record Status This is a critical abstract of an economic evaluation that
Is noncontact normothermic wound therapy cost effective for the treatment of stages 3 and 4 pressure ulcers Macario A, Dexter F Record Status This is a critical abstract of an economic evaluation that
Diabetes (DIA) Measures Document
 Diabetes (DIA) Measures Document DIA Version: 2.1 - covering patients discharged between 01/07/2016 and present. Programme Lead: Liz Kanwar Clinical Lead: Dr Aftab Ahmad Number of Measures In Clinical
Diabetes (DIA) Measures Document DIA Version: 2.1 - covering patients discharged between 01/07/2016 and present. Programme Lead: Liz Kanwar Clinical Lead: Dr Aftab Ahmad Number of Measures In Clinical
Policy for the Provision of Insulin Pumps for Patients with Diabetes Mellitus
 Policy for the Provision of Insulin Pumps for Patients with Diabetes Mellitus Version No. Changes Made Version of July 2018 V0.5 Changes made to the policy following patient engagement including: - the
Policy for the Provision of Insulin Pumps for Patients with Diabetes Mellitus Version No. Changes Made Version of July 2018 V0.5 Changes made to the policy following patient engagement including: - the
The Diabetic Foot Screen and Management Foundation Series of Modules for Primary Care
 The Diabetic Foot Screen and Management Foundation Series of Modules for Primary Care Anita Murray - Senior Podiatrist Diabetes, SCH Learning Outcomes Knowledge of the Model of Care For The Diabetic Foot
The Diabetic Foot Screen and Management Foundation Series of Modules for Primary Care Anita Murray - Senior Podiatrist Diabetes, SCH Learning Outcomes Knowledge of the Model of Care For The Diabetic Foot
Oxygen is required for normal cellular
 Article The role of topical oxygen therapy in the management of diabetic foot ulcer s in Scotland: round table recommendations Citation: Stang D, Young M, Wilson D et al (18) The role of topical oxygen
Article The role of topical oxygen therapy in the management of diabetic foot ulcer s in Scotland: round table recommendations Citation: Stang D, Young M, Wilson D et al (18) The role of topical oxygen
Wound Jeopardy: Name That Wound Session 142 Saturday, September 10 th 2011
 Initial Wound Care Consult History Physical Examination Detailed examination of the wound Photographs Cultures Procedures TCOM ABI Debridement Management Decisions A Detailed History and Physical (wound)
Initial Wound Care Consult History Physical Examination Detailed examination of the wound Photographs Cultures Procedures TCOM ABI Debridement Management Decisions A Detailed History and Physical (wound)
Multidisciplinary diabetic foot project - Samoa
 Multidisciplinary diabetic foot project - Samoa The World Health Organization and the International Diabetes Federation have stated that up to 85 percent of diabetic lower extremity amputations are preventable
Multidisciplinary diabetic foot project - Samoa The World Health Organization and the International Diabetes Federation have stated that up to 85 percent of diabetic lower extremity amputations are preventable
Hyperbaric oxygen therapy for chronic wounds (Review)
 Kranke P, Bennett M, Roeckl-Wiedmann I, Debus S This is a reprint of a Cochrane review, prepared and maintained by The Cochrane Collaboration and published in The Cochrane Library 2005, Issue 4 http://www.thecochranelibrary.com
Kranke P, Bennett M, Roeckl-Wiedmann I, Debus S This is a reprint of a Cochrane review, prepared and maintained by The Cochrane Collaboration and published in The Cochrane Library 2005, Issue 4 http://www.thecochranelibrary.com
EVALUATION OF THE VASCULAR STATUS OF DIABETIC WOUNDS Travis Littman, MD NorthWest Surgical Specialists
 EVALUATION OF THE VASCULAR STATUS OF DIABETIC WOUNDS Travis Littman, MD NorthWest Surgical Specialists Nothing To Disclosure DISCLOSURES I have no outside conflicts of interest, financial incentives, or
EVALUATION OF THE VASCULAR STATUS OF DIABETIC WOUNDS Travis Littman, MD NorthWest Surgical Specialists Nothing To Disclosure DISCLOSURES I have no outside conflicts of interest, financial incentives, or
Management Of The Diabetic foot
 Management Of The Diabetic foot Aims, Pathways, Treatments Nikki Coates 12/1/18 Diabetic foot pathology Neuropathy Foot deformity Vascular disease Sensory neuropathy Limited Joint Mobility Smoking Autonomic
Management Of The Diabetic foot Aims, Pathways, Treatments Nikki Coates 12/1/18 Diabetic foot pathology Neuropathy Foot deformity Vascular disease Sensory neuropathy Limited Joint Mobility Smoking Autonomic
Surgical Options for revascularisation P E T E R S U B R A M A N I A M
 Surgical Options for revascularisation P E T E R S U B R A M A N I A M The goal Treat pain Heal ulcer Preserve limb Preserve life The options Conservative Endovascular Surgical bypass Primary amputation
Surgical Options for revascularisation P E T E R S U B R A M A N I A M The goal Treat pain Heal ulcer Preserve limb Preserve life The options Conservative Endovascular Surgical bypass Primary amputation
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE. Health Technology Appraisal
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Health Technology Appraisal Continuous subcutaneous insulin infusion for the treatment of diabetes (review) Final scope Appraisal objective To review
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Health Technology Appraisal Continuous subcutaneous insulin infusion for the treatment of diabetes (review) Final scope Appraisal objective To review
A Pilot Study of Oxygen Therapy for Acute Leg Ulcers
 A Pilot Study of Oxygen Therapy for Acute Leg Ulcers Background: The concept of increasing the oxygen concentration in healing wounds developed originally with hyperbaric oxygen therapy and from the fact
A Pilot Study of Oxygen Therapy for Acute Leg Ulcers Background: The concept of increasing the oxygen concentration in healing wounds developed originally with hyperbaric oxygen therapy and from the fact
Will it heal? How to assess the probability of wound healing
 Will it heal? How to assess the probability of wound healing Richard F. Neville, M.D. Professor of Surgery Chief, Division of Vascular Surgery George Washington University Limb center case 69 yr old male
Will it heal? How to assess the probability of wound healing Richard F. Neville, M.D. Professor of Surgery Chief, Division of Vascular Surgery George Washington University Limb center case 69 yr old male
Venous Leg Ulcers. Care for Patients in All Settings
 Venous Leg Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a venous leg ulcer. The scope of the standard
Venous Leg Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a venous leg ulcer. The scope of the standard
Service Development Tool for the Assessment of Provision of Services for Patients with Diabetes Related Foot Problems
 Division of Medicine & Community Services Service Development Tool for the Assessment of Provision of Services for Patients with Diabetes Related Foot Problems Graham Holt Advanced Practitioner / Podiatrist
Division of Medicine & Community Services Service Development Tool for the Assessment of Provision of Services for Patients with Diabetes Related Foot Problems Graham Holt Advanced Practitioner / Podiatrist
VASCULAR WOUNDS PATHOPHYSIOLOGY AND MANAGEMENT
 VASCULAR WOUNDS PATHOPHYSIOLOGY AND MANAGEMENT Lucy Stopher, A/CNS Vascular Surgery ...it is best to think of a wound not as a disease, but rather as a manifestation of disease. Joe McCulloch In order
VASCULAR WOUNDS PATHOPHYSIOLOGY AND MANAGEMENT Lucy Stopher, A/CNS Vascular Surgery ...it is best to think of a wound not as a disease, but rather as a manifestation of disease. Joe McCulloch In order
Delayed Primary Closure of Diabetic Foot Wounds using the DermaClose RC Tissue Expander
 Delayed Primary Closure of Diabetic Foot Wounds using the DermaClose RC Tissue Expander TDavid L. Nielson, DPM 1, Stephanie C. Wu, DPM, MSc 2, David G. Armstrong, DPM,PhD 3 The Foot & Ankle Journal 1 (2):
Delayed Primary Closure of Diabetic Foot Wounds using the DermaClose RC Tissue Expander TDavid L. Nielson, DPM 1, Stephanie C. Wu, DPM, MSc 2, David G. Armstrong, DPM,PhD 3 The Foot & Ankle Journal 1 (2):
Technology appraisal guidance Published: 25 January 2012 nice.org.uk/guidance/ta245
 Apixaban for the prevention ention of venous thromboembolism after total hip or knee replacement in adults Technology appraisal guidance Published: 25 January 2012 nice.org.uk/guidance/ta245 NICE 2018.
Apixaban for the prevention ention of venous thromboembolism after total hip or knee replacement in adults Technology appraisal guidance Published: 25 January 2012 nice.org.uk/guidance/ta245 NICE 2018.
Clinical Policy: EpiFix Wound Treatment
 Clinical Policy: Reference Number: PA.CP.MP.140 Effective Date: 03/18 Last Review Date: 04/18 Coding Implications Revision Log Description EpiFix (MiMedx Group) is dehydrated human amniotic tissue that
Clinical Policy: Reference Number: PA.CP.MP.140 Effective Date: 03/18 Last Review Date: 04/18 Coding Implications Revision Log Description EpiFix (MiMedx Group) is dehydrated human amniotic tissue that
Helen Gelly, MD, FUHM, FCCWS
 Helen Gelly, MD, FUHM, FCCWS Diabetes mellitus is a major risk factor that impairs wound healing, making foot wounds one of the major problems of diabetes. Over 60% of lower limb amputations in the US
Helen Gelly, MD, FUHM, FCCWS Diabetes mellitus is a major risk factor that impairs wound healing, making foot wounds one of the major problems of diabetes. Over 60% of lower limb amputations in the US
Transmetatarsal amputation in an at-risk diabetic population: a retrospective study
 The Journal of Diabetic Foot Complications Transmetatarsal amputation in an at-risk diabetic population: a retrospective study Authors: Merribeth Bruntz, DPM, MS* 1,2, Heather Young, MD 3,4, Robert W.
The Journal of Diabetic Foot Complications Transmetatarsal amputation in an at-risk diabetic population: a retrospective study Authors: Merribeth Bruntz, DPM, MS* 1,2, Heather Young, MD 3,4, Robert W.
ARCHE Risk of Bias (ROB) Guidelines
 Types of Biases and ROB Domains ARCHE Risk of Bias (ROB) Guidelines Bias Selection Bias Performance Bias Detection Bias Attrition Bias Reporting Bias Other Bias ROB Domain Sequence generation Allocation
Types of Biases and ROB Domains ARCHE Risk of Bias (ROB) Guidelines Bias Selection Bias Performance Bias Detection Bias Attrition Bias Reporting Bias Other Bias ROB Domain Sequence generation Allocation
Setting The setting was primary care. The economic study was carried out in the UK and the USA.
 Validation of venous leg ulcer guidelines in the United States and United Kingdom McGuckin M, Waterman R, Brooks J, Cherry G, Porten L, Hurley S, Kerstein M D Record Status This is a critical abstract
Validation of venous leg ulcer guidelines in the United States and United Kingdom McGuckin M, Waterman R, Brooks J, Cherry G, Porten L, Hurley S, Kerstein M D Record Status This is a critical abstract
Cahaba Medicare Policy Primer 1,2 for Apligraf
 Cahaba Medicare Policy Primer 1,2 for Apligraf MAC A: AL, GA & TN MAC B: AL, GA, & TN LCD# 31428 Indications Applied to partial- or full-thickness ulcers of the lower extremities (see individual product
Cahaba Medicare Policy Primer 1,2 for Apligraf MAC A: AL, GA & TN MAC B: AL, GA, & TN LCD# 31428 Indications Applied to partial- or full-thickness ulcers of the lower extremities (see individual product
Setting The study setting was hospital. The economic study was carried out in Australia.
 Economic evaluation of insulin lispro versus neutral (regular) insulin therapy using a willingness to pay approach Davey P, Grainger D, MacMillan J, Rajan N, Aristides M, Dobson M Record Status This is
Economic evaluation of insulin lispro versus neutral (regular) insulin therapy using a willingness to pay approach Davey P, Grainger D, MacMillan J, Rajan N, Aristides M, Dobson M Record Status This is
CASE 1: TYPE-II DIABETIC FOOT ULCER
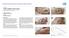 CASE 1: TYPE-II DIABETIC FOOT ULCER DIABETIC FOOT ULCER 48 YEAR-OLD MALE Mr. C., was a 48-year old man with a history of Type-II diabetes over the past 6 years. The current foot ulcer with corresponding
CASE 1: TYPE-II DIABETIC FOOT ULCER DIABETIC FOOT ULCER 48 YEAR-OLD MALE Mr. C., was a 48-year old man with a history of Type-II diabetes over the past 6 years. The current foot ulcer with corresponding
Amputations of the digit, ray and midfoot
 Amputations of the digit, ray and midfoot Dane K. Wukich M.D. Chief, Division of Foot and Ankle Surgery Medical Director, UPMC Foot and Ankle Center University of Pittsburgh School of Medicine Disclosure
Amputations of the digit, ray and midfoot Dane K. Wukich M.D. Chief, Division of Foot and Ankle Surgery Medical Director, UPMC Foot and Ankle Center University of Pittsburgh School of Medicine Disclosure
Gangrene. Introduction Gangrene is the death of tissues in your body. It happens when a part of your body loses its blood supply.
 Gangrene Introduction Gangrene is the death of tissues in your body. It happens when a part of your body loses its blood supply. Gangrene can happen on the surface of the body, such as on the skin. It
Gangrene Introduction Gangrene is the death of tissues in your body. It happens when a part of your body loses its blood supply. Gangrene can happen on the surface of the body, such as on the skin. It
Putting feet first: national minimum skills framework
 In partnership with Putting feet first: national minimum skills framework The national minimum skills framework for commissioning of footcare services for people with diabetes Revised March 2011 This report
In partnership with Putting feet first: national minimum skills framework The national minimum skills framework for commissioning of footcare services for people with diabetes Revised March 2011 This report
Link between effectiveness and cost data The costing was undertaken prospectively on the same patient sample that provided the effectiveness data.
 Randomized clinical study of hydrofiber dressing with silver or silver sulfadiazine in the management of partial-thickness burns Caruso D M, Foster K N, Blome-Eberwein S A, Twomey J A, Herndon D N, Luterman
Randomized clinical study of hydrofiber dressing with silver or silver sulfadiazine in the management of partial-thickness burns Caruso D M, Foster K N, Blome-Eberwein S A, Twomey J A, Herndon D N, Luterman
Total Contact Cast System
 Total Contact Cast System Instructions for Use Products Included in Cutimed Off-Loader Select kit Qty Cutimed Cavity Sterile 1 ea. Cutisorb Cotton Gauze 2" x 2" 4 ea. Delta-Lite Conformable Fiberglass
Total Contact Cast System Instructions for Use Products Included in Cutimed Off-Loader Select kit Qty Cutimed Cavity Sterile 1 ea. Cutisorb Cotton Gauze 2" x 2" 4 ea. Delta-Lite Conformable Fiberglass
The RoB 2.0 tool (individually randomized, cross-over trials)
 The RoB 2.0 tool (individually randomized, cross-over trials) Study design Randomized parallel group trial Cluster-randomized trial Randomized cross-over or other matched design Specify which outcome is
The RoB 2.0 tool (individually randomized, cross-over trials) Study design Randomized parallel group trial Cluster-randomized trial Randomized cross-over or other matched design Specify which outcome is
Amputation is the removal of a limb by trauma, medical illness, or surgery. As a surgical measure, it is used to control pain or a disease process in
 Amputation is the removal of a limb by trauma, medical illness, or surgery. As a surgical measure, it is used to control pain or a disease process in the affected limb, such as malignancy or gangrene.
Amputation is the removal of a limb by trauma, medical illness, or surgery. As a surgical measure, it is used to control pain or a disease process in the affected limb, such as malignancy or gangrene.
levetiracetam 250,500,750 and 1000mg tablets and levetiracetam oral solution 100mg/1ml (Keppra ) (No. 397/07) UCB Pharma Ltd
 Scottish Medicines Consortium Resubmission levetiracetam 250,500,750 and 1000mg tablets and levetiracetam oral solution 100mg/1ml (Keppra ) (No. 397/07) UCB Pharma Ltd 11 January 2008 The Scottish Medicines
Scottish Medicines Consortium Resubmission levetiracetam 250,500,750 and 1000mg tablets and levetiracetam oral solution 100mg/1ml (Keppra ) (No. 397/07) UCB Pharma Ltd 11 January 2008 The Scottish Medicines
Limb Salvage in Diabetic Ischemic Foot. Kritaya Kritayakirana, MD, FACS Assistant Professor Chulalongkorn University April 30, 2017
 Limb Salvage in Diabetic Ischemic Foot Kritaya Kritayakirana, MD, FACS Assistant Professor Chulalongkorn University April 30, 2017 Case Male 67 years old Underlying DM, HTN, TVD Present with gangrene
Limb Salvage in Diabetic Ischemic Foot Kritaya Kritayakirana, MD, FACS Assistant Professor Chulalongkorn University April 30, 2017 Case Male 67 years old Underlying DM, HTN, TVD Present with gangrene
Diabetic Foot Pathophysiology. Professor Donald G. MacLellan Executive Director Health Education & Management Innovations
 Diabetic Foot Pathophysiology Professor Donald G. MacLellan Executive Director Health Education & Management Innovations AGEs & RAGEs in Diabetes AGE levels increased & RAGEs highly expressed in diabetic
Diabetic Foot Pathophysiology Professor Donald G. MacLellan Executive Director Health Education & Management Innovations AGEs & RAGEs in Diabetes AGE levels increased & RAGEs highly expressed in diabetic
NHS England. Evidence review: Stereotactic Ablative Radiotherapy for Non Small Cell Lung Cancer
 NHS England Evidence review: Stereotactic Ablative Radiotherapy for Non Small Cell Lung Cancer NHS England Evidence review: Stereotactic ablative radiotherapy for non small cell lung cancer First published:
NHS England Evidence review: Stereotactic Ablative Radiotherapy for Non Small Cell Lung Cancer NHS England Evidence review: Stereotactic ablative radiotherapy for non small cell lung cancer First published:
a,b and the annual cost of diabetic neuropathy is estimated to be $10.91 billion in the United States alone. 3
 eplasty: Vol. 11 A Prospective Study of Negative Pressure Wound Therapy With Integrated Charles M. Zelen, DPM,, FACFAS a,b Brian Stover, DPM, a Professional Education and b esearch Institute, oanoke, Department
eplasty: Vol. 11 A Prospective Study of Negative Pressure Wound Therapy With Integrated Charles M. Zelen, DPM,, FACFAS a,b Brian Stover, DPM, a Professional Education and b esearch Institute, oanoke, Department
End Diastolic Pneumatic Compression Boot as a Treatment of Peripheral Vascular Disease or Lymphedema. Original Policy Date
 MP 2.02.12 End Diastolic Pneumatic Compression Boot as a Treatment of Peripheral Vascular Disease or Lymphedema Medical Policy Section Medicine Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date
MP 2.02.12 End Diastolic Pneumatic Compression Boot as a Treatment of Peripheral Vascular Disease or Lymphedema Medical Policy Section Medicine Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date
National Clinical Conference 2018 Baltimore, MD
 National Clinical Conference 2018 Baltimore, MD No relevant financial relationships to disclose Wound Care Referral The patient has been maximized from a vascular standpoint. She has no other options.
National Clinical Conference 2018 Baltimore, MD No relevant financial relationships to disclose Wound Care Referral The patient has been maximized from a vascular standpoint. She has no other options.
Diabetes Mellitus and the Associated Complications
 Understanding and the complications relating to the disease can assist the fitter to better serve patients. and the Associated Complications Released January, 2011 Total: 25.8 million people, or 8.3% of
Understanding and the complications relating to the disease can assist the fitter to better serve patients. and the Associated Complications Released January, 2011 Total: 25.8 million people, or 8.3% of
Cost and dressing evaluation of hydrofiber and alginate dressings in the management of community-based patients with chronic leg ulceration
 Cost and dressing evaluation of hydrofiber and alginate dressings in the management of community-based patients with chronic leg ulceration Harding K G, Price P, Robinson B, Thomas S, Hofman D Record Status
Cost and dressing evaluation of hydrofiber and alginate dressings in the management of community-based patients with chronic leg ulceration Harding K G, Price P, Robinson B, Thomas S, Hofman D Record Status
Surgical Off-loading. Reiber et al Goals of Diabetic Foot Surgery 4/28/2012. The most common causal pathway to a diabetic foot ulceration
 Reiber et al. 1999 Surgical Off-loading The most common causal pathway to a diabetic foot ulceration Alex Reyzelman DPM Associate Professor California School of Podiatric Medicine at Samuel Merritt University
Reiber et al. 1999 Surgical Off-loading The most common causal pathway to a diabetic foot ulceration Alex Reyzelman DPM Associate Professor California School of Podiatric Medicine at Samuel Merritt University
Type of intervention Treatment. Economic study type Cost-effectiveness analysis.
 Cost-effectiveness of salmeterol/fluticasone propionate combination product 50/250 micro g twice daily and budesonide 800 micro g twice daily in the treatment of adults and adolescents with asthma Lundback
Cost-effectiveness of salmeterol/fluticasone propionate combination product 50/250 micro g twice daily and budesonide 800 micro g twice daily in the treatment of adults and adolescents with asthma Lundback
Perfusion Assessment in Chronic Wounds
 Perfusion Assessment in Chronic Wounds American Society of Podiatric Surgeons Surgical Conference September 22, 2018 Michael Maier, DPM, FACCWS Cardiovascular Medicine Cleveland Clinic Disclosures Speaker,
Perfusion Assessment in Chronic Wounds American Society of Podiatric Surgeons Surgical Conference September 22, 2018 Michael Maier, DPM, FACCWS Cardiovascular Medicine Cleveland Clinic Disclosures Speaker,
Determining Wound Diagnosis and Documentation Tips Job Aid
 Determining Wound Diagnosis and Job Aid 1 Coding Is this a traumatic injury from an accident? 800 Codes - Injury Section of the Coding Manual Code by specific site of injury. Only use for accidents or
Determining Wound Diagnosis and Job Aid 1 Coding Is this a traumatic injury from an accident? 800 Codes - Injury Section of the Coding Manual Code by specific site of injury. Only use for accidents or
1 of :19
 1 of 8 3-12-2012 12:19 Diabetic foot ulcer classification system for research purposes Introduction Aims of the ulcer research classification system Definitions and categorisation for the ulcer research
1 of 8 3-12-2012 12:19 Diabetic foot ulcer classification system for research purposes Introduction Aims of the ulcer research classification system Definitions and categorisation for the ulcer research
Scottish Medicines Consortium
 Scottish Medicines Consortium saxagliptin, 5mg film-coated tablet (Onglyza ) No. (603/10) Bristol-Myers Squibb Pharmaceuticals Ltd 05 February 2010 The Scottish Medicines Consortium (SMC) has completed
Scottish Medicines Consortium saxagliptin, 5mg film-coated tablet (Onglyza ) No. (603/10) Bristol-Myers Squibb Pharmaceuticals Ltd 05 February 2010 The Scottish Medicines Consortium (SMC) has completed
ASSESSING THE VASCULAR STATUS OF THE FEET FOR PATIENTS WITH DIABETES
 ASSESSING THE VASCULAR STATUS OF THE FEET FOR PATIENTS WITH DIABETES Caroline McIntosh is Senior Lecturer in Podiatry, University of Huddersfield, Yorkshire A reduced blood supply to the lower limb, due
ASSESSING THE VASCULAR STATUS OF THE FEET FOR PATIENTS WITH DIABETES Caroline McIntosh is Senior Lecturer in Podiatry, University of Huddersfield, Yorkshire A reduced blood supply to the lower limb, due
Case 1. July 14, th week wound gel 3 cm x 2.5 cm = 7.5 cm². May 25, st wound gel on 290 days PI treatment 4 cm x 2.4 cm = 9.
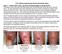 2.5% Sodium Hyaluronate Wound Gel Study Cases Case 1 Patient with Lower Leg Ulcer Not Responding to Compression This patient was a 50-year old male patient with nonhealing right lower leg since January
2.5% Sodium Hyaluronate Wound Gel Study Cases Case 1 Patient with Lower Leg Ulcer Not Responding to Compression This patient was a 50-year old male patient with nonhealing right lower leg since January
Systematic reviews and meta-analyses of observational studies (MOOSE): Checklist.
 Systematic reviews and meta-analyses of observational studies (MOOSE): Checklist. MOOSE Checklist Infliximab reduces hospitalizations and surgery interventions in patients with inflammatory bowel disease:
Systematic reviews and meta-analyses of observational studies (MOOSE): Checklist. MOOSE Checklist Infliximab reduces hospitalizations and surgery interventions in patients with inflammatory bowel disease:
Setting The setting was a hospital. The economic study was carried out in the USA.
 A cost analysis of a living skin equivalent in the treatment of diabetic foot ulcers Steinberg J, Beusterien K, Plante K, Nordin J, Chaikoff E, Arcona S, Kim J, Belletti D A Record Status This is a critical
A cost analysis of a living skin equivalent in the treatment of diabetic foot ulcers Steinberg J, Beusterien K, Plante K, Nordin J, Chaikoff E, Arcona S, Kim J, Belletti D A Record Status This is a critical
Preventing Foot Ulcers in the Neuropathic Diabetic Foot. Glossary of Terms
 Preventing Foot Ulcers in the Neuropathic Diabetic Foot Warren Woods, Certified Orthotist, Health Sciences Centre, Rehabilitation Engineering Department What you need to know Glossary of Terms Neuropathic
Preventing Foot Ulcers in the Neuropathic Diabetic Foot Warren Woods, Certified Orthotist, Health Sciences Centre, Rehabilitation Engineering Department What you need to know Glossary of Terms Neuropathic
Source of effectiveness data The effectiveness evidence was derived from a review of published studies.
 Cost and cost effectiveness of venous and pressure ulcer protocols of care Kerstein M D, Gemmen E, van Rijswijk L, Lyder C H, Phillips T, Xakellis G, Golden K, Harrington C Record Status This is a critical
Cost and cost effectiveness of venous and pressure ulcer protocols of care Kerstein M D, Gemmen E, van Rijswijk L, Lyder C H, Phillips T, Xakellis G, Golden K, Harrington C Record Status This is a critical
Setting The setting was outpatient departments of referral hospitals. The economic analysis was conducted in India.
 Three day versus five day treatment with amoxicillin for non-severe pneumonia in young children: a multicentre randomised controlled trial ISCAP study group Record Status This is a critical abstract of
Three day versus five day treatment with amoxicillin for non-severe pneumonia in young children: a multicentre randomised controlled trial ISCAP study group Record Status This is a critical abstract of
WOUND CARE QUALITY IMPROVEMENT COLLABORATIVE
 WOUND CARE QUALITY IMPROVEMENT COLLABORATIVE RESTORIXHEALTH PATIENT SAFETY EDUCATION NETWORK (PSEN) NET HEALTH SYSTEMS, INC. CECITY 2015 PQRS & Non-PQRS Narrative Measure Specifications 1 Table of Contents
WOUND CARE QUALITY IMPROVEMENT COLLABORATIVE RESTORIXHEALTH PATIENT SAFETY EDUCATION NETWORK (PSEN) NET HEALTH SYSTEMS, INC. CECITY 2015 PQRS & Non-PQRS Narrative Measure Specifications 1 Table of Contents
Hyperbaric oxygen therapy and surgical delay improve flap survival of reverse pedicle flaps for lower third leg and foot reconstruction
 Original Article Plastic and Aesthetic Research Hyperbaric oxygen therapy and surgical delay improve flap survival of reverse pedicle flaps for lower third leg and foot reconstruction Pradeoth Mukundan
Original Article Plastic and Aesthetic Research Hyperbaric oxygen therapy and surgical delay improve flap survival of reverse pedicle flaps for lower third leg and foot reconstruction Pradeoth Mukundan
Diabetic/Neuropathic Foot Ulcer Assessment Guide South West Regional Wound Care Program Last Updated April 7,
 Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term Care Homes, Hospitals,
Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term Care Homes, Hospitals,
