Review Article Glucagon-Like Peptide 1: A Predictor of Type 2 Diabetes?
|
|
|
- Leo Kennedy
- 5 years ago
- Views:
Transcription
1 Hindawi Journal of Diabetes Research Volume 2017, Article ID , 13 pages Review Article Glucagon-Like Peptide 1: A Predictor of Type 2 Diabetes? Matthias Ploug Larsen and Signe Sørensen Torekov Department of Biomedical Sciences and Novo Nordisk Foundation Center for Basic Metabolic Research, Faculty of Health Sciences, University of Copenhagen, Copenhagen N, Denmark Correspondence should be addressed to Signe Sørensen Torekov; torekov@sund.ku.dk Received 23 May 2017; Accepted 30 July 2017; Published 10 September 2017 Academic Editor: Fabrizio Barbetti Copyright 2017 Matthias Ploug Larsen and Signe Sørensen Torekov. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Background. The incretin effect is impaired in patients with type 2 diabetes. Aim. To assess the relation between the incretin hormone GLP-1 and the prediabetic subtypes: impaired fasting glucose (IFG), impaired glucose tolerance (IGT), and the combined IFG/IGT to investigate whether a low GLP-1 response may be a predictor of prediabetes in adults. Method. 298 articles were found using a broad search phrase on the PubMed database and after the assessment of titles and abstracts 19 articles were included. Results and Discussion. Studies assessing i-ifg/ifg and i-igt/igt found both increased, unaltered, and reduced GLP-1 levels. Studies assessing IFG/IGT found unaltered or reduced GLP-1 levels. When assessing the five studies with the largest sample size, it clearly suggests a decreased GLP-1 response in IFG/IGT subjects. Several other factors (BMI, glucagon, age, and nonesterified fatty acids (NEFA)), including medications (metformin), may also influence the secretion of GLP-1. Conclusion. This review suggests that the GLP-1 response is a variable in prediabetes possibly due to a varying GLP-1-secreting profile during the development and progression of type 2 diabetes or difference in the measurement technique. Longitudinal prospective studies are needed to assess whether a reduced GLP-1 response is a predictor of diabetes. 1. Introduction The number of people diagnosed with diabetes globally was increased from 108 million adults in 1980 to an estimated 422 million in 2014 [1]. Thus, the global prevalence of diabetes has increased from 4,7% to 8,5% from 1980 to 2014 [1]. Diabetes causes complications with a 2-3 times higher rate of cardiovascular disease, a times higher rate of lower extremity amputations, and a 10 times higher incidence of end-stage renal disease in diabetic adults compared to nondiabetic adults [1]. Along with this, diabetic retinopathy caused 2,6% of total blindness and 1,9% of total moderate or severe visual impairment globally in 2010 [1]. In addition to these complications, diabetes entails economic costs for both the individual and the health systems [1] and the global cost of diabetes for 2015 was estimated to be US$1,3 trillion corresponding to 1,8% of global gross domestic product (GDP) [2]. Further knowledge about aetiology and pathogenesis could contribute to turn over this development. When glucose is orally ingested, it elicits a much greater insulin response (two- to threefold) than if glucose is intravenously injected to give the same blood glucose level. This phenomenon is called the incretin effect and is due to the secretion of glucagon-like peptide 1 (GLP-1) and glucose-dependent insulinotropic peptide (GIP) which increases the glucose-induced insulin secretion [3]. In patients with type 2 diabetes, the incretin effect is impaired [4]. In addition to that, studies concerning GLP-1 secretion in patients with type 2 diabetes during an oral glucose tolerance test (OGTT) have observed both unaltered [5, 6] and reduced [7] GLP-1 responses, suggesting a varying GLP-1-secreting profile during the development and progression of type 2 diabetes [5, 7] or difference in the measurement technique [8]. This is further supported by the observation that several factors (BMI, glucagon, age, and nonesterified fatty acids (NEFA)), including medications (metformin), influence the secretion of GLP-1 [6]. The biggest study to date a large Danish study published in 2015, involving 1462 individuals, demonstrated
2 2 Journal of Diabetes Research a reduced GLP-1 response to an OGTT in prediabetes, screen-detected type 2 diabetes, and obese and overweight individuals compared to normal glucose-tolerant individuals and normal weight individuals, respectively [9]. Individuals diagnosed with prediabetes are at an increased risk of developing type 2 diabetes, with a yearly progression rate of 3,5% 7,0% in individuals with prediabetes compared to a yearly progression rate of 2% in normoglycemic individuals [10]. In continuation to that, a reversing of the prediabetic state towards normal glucose regulation is associated with an up to 56% lower risk of developing type 2 diabetes compared to individuals remaining prediabetic [10]. Further knowledge about aetiology and pathophysiology of prediabetes and the progression to type 2 diabetes might help in preventing and treating both states [9, 11]. Additionally, more extensive knowledge could help improve the diagnostic criteria concerning the subtypes of prediabetes [11]. Therefore, this review will assess the relation between the incretin hormone GLP-1 and the prediabetic state and investigate whether GLP-1 may be a predictor of prediabetes in adults. 2. Research Question Is a low GLP-1 response a predictor of prediabetes in adults? 3. Materials and Methods This review is a literature study using the electronical PubMed database to find relevant literature. Only articles in English were included. The following search phrase in PubMed was used: (GLP-1) A (prediabet OR pre-diabet OR impaired glucose tolerance OR impaired glucose tolerant OR IGT OR impaired fasting glucose OR impaired fasting glycaemia OR IFG OR intermediate hyperglycaemia). The last search update was conducted on 10 March Articles were included which investigated the relationship between GLP-1 and the different subtypes of prediabetes: impaired fasting glucose (IFG), impaired glucose tolerance (IGT), and the combined IFG/IGT. The search identified 298 articles. These 298 articles were first evaluated based on their title, and irrelevant articles, in relation to the inclusion criteria and articles in languages other than English, were excluded. Articles with inadequate or indefinite titles were included for further evaluation. Articles being irrelevant in proportion to answering the research question was excluded. For example, articles investigating the impact of surgical or pharmacological interactions on the GLP-1 response and articles not involving prediabetic subjects. Articles assessing GLP-1 alterations in adolescents were also excluded. Finally, this resulted in 60 articles. These 60 articles were evaluated based on their abstracts, and relevant articles fulfilling the inclusion criteria were read and included in the review. Included articles in the review are 19. A flowchart of the search process is illustrated in Figure GLP-1 and Prediabetes: Is There a Connection? 4.1. GLP-1 An Incretin Hormone. The incretin effect is mediated by the incretin hormones the two major being GLP-1 and GIP. GLP-1 is a gut peptide secreted from open-type enteroendocrine L cells located in the intestinal mucosa in response to ingested nutrients (carbohydrate, protein, and fat). This is thought to be the primary stimulus for secretion, and the secretory response depends on both meal size and gastric emptying rate. Neuronal and hormonal mechanisms have also been proposed regarding the regulation of secretion [3]. GLP-1 comes in different isoforms (see Figure 2): unamidated GLP-1(1 37), GLP-1(7 37), and GLP-1(9 37), and amidated GLP-1(1 36)NH 2, GLP-1(7 36)NH 2, and GLP- 1(9 36)NH 2 [8]. In human, the amidated isoforms are the predominant [8, 12]. GLP-1(7 36)NH 2 and GLP-1(7 37) are termed active/intact GLP-1 and when secreted, both configurations of the hormone are rapidly degraded (T 1/2 = 1-2 min) by the enzyme dipeptidyl peptidase 4 (DPP-4) to GLP-1(9 36)NH 2 and GLP-1(9 37), respectively, leaving only around 10 15% of the active/intact GLP-1 in the systemic circulation [3, 5, 12, 13]. Furthermore, GLP-1 is metabolised by the enzyme neutral endopeptidase [12, 13]. GLP-1(7 36)NH 2, GLP-1(7 37), and the metabolites GLP-1(9 36)NH 2 and GLP-1(9 37) are termed total GLP-1 [12, 13]. Active/intact GLP-1 only accounts for the endocrine effect of GLP-1, whereas GLP-1 is also thought to have neural effects, whereby measuring total GLP-1 mirror the total effect of GLP-1 better [12]. Furthermore, since the concentration of active/intact GLP-1 is very low (0 15 pmol/l) and rises only very little in response to small meals, it is harder to detect a difference in secretion compared to the measuring of total GLP-1 ranging from 5 to 80 pmol/l [5, 8, 12, 13]. Therefore, it has been argued that measuring total GLP-1 is best, when GLP-1 secretion should be measured [5, 8, 12 14]. In α cells, processing of the proglucagon (PG) gene leads to the secretion of small amounts of the biologically inactive peptides GLP- 1(1 36)NH 2 and GLP-1(1 37) [12]. Due to cross-reactivity and the varying commercially available assays, knowledge of this plethora of peptides and their metabolites is important, when assessing the assays used to measure their plasma concentrations [8, 12]. Besides increasing insulin secretion, GLP-1 also has other effects, including inhibition of glucagon secretion from α cells; stimulating, potential proliferating, and antiapoptotic effects on β cells; a delay of gastrointestinal secretion and motility; an appetite-reducing effect; a potential advantageous effect on the cardiovascular system; and a potential neurotropic or neuroprotective effect [3, 13]. Given that a lot of these effects are advantageous in the scope of treating diabetes, the use of incretin-based therapies is increasing [3] Prediabetes Just One Condition. Prediabetes is an overall term to describe the dysglycemic conditions between normal glucose tolerance () and the diabetic state. The
3 Journal of Diabetes Research 3 Identification of articles PubMed search conducted on 10 March articles Inclusion criteria: Article investigating the relation between GLP-1 and prediabetic subtypes. Articles with inadequate or indefinite titles were included for further evaluation. Exclusion criteria: Articles irrelevant in proportion to answering the research question or due to languages other than English. Evaluation based on title Excluded: n = 238 (i) Irrelevant: 230 (ii) Language: 8 60 articles Evaluation based on abstract Excluded: n =41 Included: 19 articles Figure 1: Flowchart of the search process. See text for details. DPP IV Glucagon-like peptide-1 (total) NH NH 2 Pancreas 7 36NH NH Gut and brain Figure 2: GLP-1 isoforms illustration from Bak et al. [8]. different subtypes of prediabetes consist of isolated impaired fasting glucose (IFG), isolated impaired glucose tolerance (IGT), and the combined state IFG/IGT [10, 11]. An estimation of the worldwide prevalence of individuals with prediabetes is approaching 840 million [10]. Since people with prediabetes are at an increased risk of developing diabetes compared to non-prediabetic individuals as mentioned above screening for the prediabetic state, and thereby initiating prevention of development of diabetes, is a health goal [10]. This is further supported by studies showing an increased risk of micro- and macrovascular complications with prediabetes, exemplified by a study showing that 8% of nondiabetic participants in a cross-sectional analysis had diabetic retinopathy, and an increased risk of cardiovascular disease at 20% in prediabetes [10]. It is hypothesised that the different prediabetic states have both different aetiology and pathophysiology and that individualised prevention and treatment strategies should be assessed based on the prediabetic subtype [10, 11]. Different diagnostic criteria with varying cut-points exist and have changed through time [1, 10, 15, 16] The Relation between GLP-1 and Prediabetes. Based on the literature search in PubMed, 19 original articles are
4 4 Journal of Diabetes Research included in assessing the relation between GLP-1 and prediabetes. In the following, these articles will be reviewed. The included studies were published between 1997 and all studies investigated all the different subtypes of prediabetes described above. For clarity, and since it appears that the different subtypes have both different aetiology and pathophysiology [10, 11], the results will be reviewed in order of subtype. The included studies are not consistent in the terms used to describe the prediabetic subtype (i-ifg or IFG and i-igt or IGT). The term used when assessing an included study is the one used in the respective study. An overview of the results can be seen in Table Stimulus. All studies, except two [17, 18], conducted a 75 g OGTT measuring GLP-1, and other variables, at various time points. Fernandez-Garcia et al. [17] conducted a 60 g high-fat meal and Toft-Nielsen et al. [18] conducted a mixed breakfast meal containing 2250 kj. Besides the 75 g OGTT, six studies [19 24] conducted additional tests on the same participants: Yabe et al. [19] and Lee et al. [20] conducted a meal tolerance test (MTT) (480 kcal, carbohydrate : protein : fat = 2.8 : 1 : 1). Vollmer et al. [24] conducted a mixed meal challenge (820 kcal, carbohydrate : protein : fat = 3.38 : 1 : 3.30). Faerch et al. [21] and Laakso et al. [23] conducted an intravenous glucose tolerance test (IVGTT) to measure first-phase insulin secretion and a 120 min hyperinsulinaemic-euglycaemic clamp to measure peripheral insulin sensitivity. Muscelli et al. [22] conducted an isoglycaemic intravenous glucose test to assess the incretin effect Active/Intact or Total GLP-1. The included studies have measured both active/intact and total GLP-1 (and eventually the small amount of GLP-1(1 36)NH 2 and GLP- 1(1 37) although not mentioned in any of the studies). Four studies measured active/intact GLP-1 only [17, 20, 25, 26], thirteen studies measured total GLP-1 only [7, 9, 11, 18, 22 24, 27 32], and two studies measured both active/intact and total GLP-1 [14, 19]. Asmentioned earlier and discussed later, measuring total GLP-1 is best, when GLP-1 secretion should be measured [5, 8, 12 14]. The studies measuring active/intact GLP-1 only will not be reviewed in detail, since they are concluding on metabolites which they may not have measured. Results assessing active/intact GLP-1 can be seen in Table 1. Additionally, when measuring active GLP-1, it is advised to use a DPP- 4 inhibitor when collecting blood samples [12]. This was done in all studies except Fernandez-Garcia et al. [17] which did not report any use of DPP-4 inhibitor. This could of course have influenced the results Total GLP-1 (1) Total GLP-1 and i-ifg/ifg. 6/19 included studies assessed the relation between total GLP-1 and i-ifg/ifg [9, 14, 21, 23, 27, 29]. Increased: Faerch et al. [21] studied the GLP-1 response to a 3 h OGTT in 66 subjects. They found no difference in fasting GLP-1 between i-ifg and. However, they found a significantly higher 3-hour AUC GLP-1 in i-ifg subjects compared to subjects. There was a low number of women in this group (only 2). This could suggest a compensatory GLP-1 response in this subgroup. Unchanged: Hussein et al. [27] studied 80 subjects glucose-stimulated GLP-1 response (30 minutes after 75 g glucose). The subjects were divided into 4 groups: normal weight, obese, obese IFG, and obese IFG/IGT. They found no difference in glucose-stimulated GLP-1 between obese and obese IFG. However, glucosestimulated GLP-1 were reduced in all obese groups compared to the normal weight group. These results indicate that BMI, not glucose tolerance, influences 30 min-glucose-stimulated GLP-1 levels. Zhang et al. [29] studied 531 subjects GLP-1 response to a. They only measured GLP-1 at 0 and 120 min and found no difference in fasting GLP-1, 2 h GLP-1, or ΔGLP-1 when comparing i-ifg and subjects. Smushkin et al. [14] studied 165 subjects GLP-1 response to a. They found no difference in either fasting GLP-1, max total GLP-1, AUC GLP-1, or AAB GLP-1 when comparing IFG/ and NFG/ subjects. Reduced: Faerch et al. [9] studied 1462 subjects response to a. They measured GLP-1 at 0, 30, and 120 min and grouped the subjects in proportion to sex. They found no differences in the male i-ifg compared to. However, in the female groups, they found a reduced rauc 0 30, rauc 0 120, and iauc 120 when comparing i-ifg and subjects. This suggests that the GLP-1 response is influenced by sex. Laakso etal. [23] studied 278subjects GLP-1 response to a prolonged 4 h OGTT. All subjects were nondiabetic offspring of patients with type two diabetes. They found a reduced GLP-1 response at 15, 90, and 120 min and a reduced AUC when comparing i-ifg and subjects. This could indicate that being a nondiabetic offspring of a patient with type 2 diabetes could influence the GLP-1 response suggesting a genetic component in the GLP-1 response. (2) Total GLP-1 and i-igt/igt. 14/19 included studies assessed the relation between total GLP-1 and i-igt/igt [7, 9, 14, 18, 19, 21 24, 28 32]. Increased: Smushkin et al. [14] also studied the GLP-1 response between NFG/IGT and NFG/. They found no difference in fasting GLP-1, max GLP-1, and AUC GLP- 1. However, they found an increased integrated incremental concentration of GLP-1 (2-hour area above basal (AAB GLP-1)) when comparing NFG/IGT and NFG/. Unchanged: Wang et al. [7] studied 80 subjects GLP-1 response to a 3 h OGTT. They found no difference in either GLP-1 levels at each measured time point, ΔGLP-1, or 3- hour AUC GLP-1 when comparing IGT and subjects. Yabe et al. [19] conducted both a and a MTT in 102 subjects. They found no difference in either fasting nor postprandial GLP-1 response both when assessing GLP-1 levels at each time point and 2 hour AUC GLP- 1 between IGT and. Faerch et al. [21] found no difference in either fasting GLP-1 or 3-hour AUC GLP-1 when comparing i-igt and subjects.
5 Journal of Diabetes Research 5 Author and year Wang et al Faerch et al Yabe et al Zheng et al Hussein et al Study size (n) Stimulus 3 h OGTT MTT (480 kcal) OGTT 30 min OGTT Total or active/intact GLP-1 and assay/ detection method Total plasma GLP-1 ELISA, Westand Biological Technology (9 36)NH 2 Antiserum RIA Intact: two-site sandwich ELISA GLP-1: (7 36)NH 2 &(7 37) DPP-4 inhibitor: Total: GLP-1 (9 36)NH 2 Antiserum Lab. of Holst JJ. Active GLP-1: (7 37) Active ELISA, Millipore Total GLP-1 ELISA (4141), DRG (Springfield, NJ) Table 1: Overview of results. i-ifg/ifg i-igt/igt IFG/IGT BMI Age Ethnicity Diagnostic criteria (year) Ref. determined () Women: rauc 0 30 : reduced rauc : reduced iauc 120 : reduced (fasting plasma glucose 110 mg/dl/ 6,1 mmol/l excluded) time point GLP-1 levels, ΔGLP-1, or 3 h AUC GLP-1 versus Women: rauc 0 30 : reduced versus rauc : reduced versus intact or total GLP-1 in fasting or post-prandial (GLP-1 levels and 2 h AUC) in both challenges Matched Matched Women: rauc : reduced iauc 30 : reduced iauc 120 : reduced Both sexes: reduced 120 min Fasting GLP-1 reduced in subjects who developed prediabetes 4 year later Prediabetes = i-ifg, i-igt, IFG/IGT not distinguished between subtypes No difference in 30 min GLP-1 in obese IFG versus obese No difference in 30 min GLP-1 in obese IFG/IGT versus obese matched IGT and matched matched. Higher in subjects developing prediabetes Normal weight versus obese (obese groups: matched) matched IGT and not matched matched. Higher in subjects developing prediabetes matched Han Chinese WHO ( 98) [7] Danish WHO ( 06) [9] Japanese Japanese Diabetes Society [19] Chinese WHO ( 98) [25] Egyptian ADA ( 06) [27]
6 6 Journal of Diabetes Research Author and year Fernandez- Garcia et al Shen et al Zhang et al Smushkin et al Study size (n) Stimulus 3 h high-fat meal (60 g) Total or active/intact GLP-1 and assay/ detection method Active GLP-1: (7 36)NH 2 EIA, Phoenix Pharmaceuticals DPP-4-inhibitor:? Total GLP-1 RIA, Millipore Total GLP-1 ELISA, USCNLIFE kits (Uscnlife Science & Technology Company) Active GLP-1: N-terminus epitope + epitope in middle of peptide Inactive GLP-1: N-terminus epitope + epitope in middle of peptide Total: active + inactive i-ifg/ifg No diff between 0 and 180 min GLP-1. Lower 180 min GLP-1 in IFG versus Low-Ins- Res- No change: fasting GLP-1, 2 h GLP-1, and ΔGLP-1 either active or total GLP-1 in fasting or postprandial response (max, 2 h AUC, 2 h AAB) versus NFG/ Table 1: Continued. i-igt/igt IFG/IGT BMI Age Ethnicity Diagnostic criteria (year) Ref. Morbidly obese. Matched Matched Spanish ADA ( 11) [17] fasting GLP-1. GLP-1 levels at 30, 60, and 90 min and 120 min-auc reduced versus No change: fasting GLP-1 and 2 h GLP-1. Reduced ΔGLP-1 fasting active or total GLP-1. Increased integrated incremental concentrations (AAB) of total (2 h) GLP-1 versus Matched Matched Chinese WHO ( 99) [28] Reduced fasting GLP-1 versus i-igt; reduced 2 h GLP-1 versus, i-ifg, i-igt; reduced ΔGLP-1 versus, i-ifg, i-igt either active or total GLP-1 in fasting or postprandial response (max, 2 h AUC, 2 h AAB) versus NFG/ Matched Matched matched matched Han Chinese ADA ( 06) [29] American ADA ( 03 ) [14]
7 Journal of Diabetes Research 7 Author and year Pala et al Nathanson et al Lee et al Faerch et al Study size (n) men Stimulus 60 min OGTT MTT (480 kcal) 3 h OGTT (IVGTT) (Clamp) Total or active/intact GLP-1 and assay/ detection method DPP-4 inhibitor: Theranos System: fully automated, Chemiluminescence ELISA Active GLP-1: (7 37) ELISA, Linco N-terminal specific DPP-4 inhibitor: (9 36) RIA, C-terminal specific (7 36)NH 2 Active GLP-1 ELISA, Linco DPP-4 inhibitor: (9 36)NH 2 Antiserum number Department of Biomedical Sciences University of Copenhagen i-ifg/ifg Fasting GLP-1: no change versus. Significantly higher 3 h AUC versus Table 1: Continued. i-igt/igt NFG/. Otherwise, no change in active or total postprandial GLP-1 response versus NFG/ Decreased 30 min GLP-1 and 2 h AUC GLP-1 in IGT fasting and 60 min GLP-1. Reduced ΔGLP-1 versus peak GLP-1 or 2h iauc in IGT in both challenges Fasting and 3 h AUC GLP-1: no change versus IFG/IGT BMI Age Ethnicity Diagnostic criteria (year) Ref. Matched Matched reported WHO ( 98) [26] reported Matched Swedish WHO ( 99) [30] matched Matched Japanese WHO [20] Significant higher in i-ifg, i-igt versus Matched Europid WHO ( 99) [21]
8 8 Journal of Diabetes Research Author and year Muscelli et al Laakso et al Vollmer et al Rask et al Toft- Nielsen et al Study size (n) : GLP-1 (874) women 102 Stimulus 3 h OGTT (Isoglycaemic IV test) (IVGTT) (Clamp) 4 h OGTT Mixed meal (820 kcal) 3 h OGTT 4 h mixed meal (2250 kj) Total or active/intact GLP-1 and assay/ detection method 7-36NH 2 & 9-36NH 2 Antiserum number RIA (9 36)NH 2 Antiserum number (9 36)NH 2 Antiserum number RIA (9 36)NH 2 RIA (7 36)NH 2 &(9 36)NH 2 Antiserum number RIA i-ifg/ifg Reduced 15, 90, and 120 min GLP-1 versus. Reduced AUC Table 1: Continued. i-igt/igt either GLP-1 levels or 3h AUC GLP-1 Reduced 15, 90, and 120 min GLP-1 versus. Reduced AUC GLP-1 levels in both challenges fasting GLP-1, GLP-1 levels, 30-min AUC, 60 min AUC GLP-1. Reduced first 30 min [GLP-1] increase versus fasting GLP-1 or 4 h AUC GLP-1 versus IFG/IGT BMI Age Ethnicity Diagnostic criteria (year) Ref. Matched Matched reported ADA ( 97) [22] Reduced 15, 90, and 120 min GLP-1 versus. Reduced AUC Danish ADA ( 03) [23] Matched Matched reported WHO [24] Matched Matched Caucasian reported (Fulfil WHO & ADA) [31] matched Matched Danish WHO ( 85) [18]
9 Journal of Diabetes Research 9 Author and year Ahrén et al Study size (n) 13 women Stimulus Total or active/intact GLP-1 and assay/ detection method (9 36)NH 2 Antiserum number RIA i-ifg/ifg Table 1: Continued. i-igt/igt fasting GLP-1, GLP-1 increase (AUC 0 60 )or GLP-1 decrease IFG/IGT BMI Age Ethnicity Matched Matched reported Diagnostic criteria (year) Ref. WHO ( 85) [32]
10 10 Journal of Diabetes Research Muscelli et al. [22] studied 51 well-matched subjects GLP-1 response to a 3 h OGTT. They found no difference in GLP-1 levels or 3-hour AUC GLP-1 between IGT and subjects. Vollmer et al. [24] studied 48 well-matched subjects GLP-1 response to a 4-hour OGTT and a mixed meal. They found no difference in GLP-1 levels when comparing IGT and in both challenges. Rask etal.[31]studied 30well-matched women ina3-hour OGTT and measured their GLP-1 response. They found no difference in fasting GLP-1, GLP-1 levels at each time point, 30 min AUC GLP-1, and 120 min AUC GLP-1 between IGT and. However, they found a significant difference when comparing the first 30 minutes GLP-1 concentration increase the increase being reduced in IGT. The 30 min iauc GLP-1 also showed a tendency (P =0 072) to be reduced in IGT. 17 of the women were postmenopausal, which could have an impact on the results. Toft-Nielsen et al. [18] studied 102 subjects GLP-1 response to a 4-hour mixed meal. They found no difference in either fasting GLP-1 or 4-hour AUC GLP-1 (corrected for BMI and gender) between IGT and subjects. Ahren et al. [32] studied 13 well-matched postmenopausal women and measured their GLP-1 response in a 2- hour OGTT. They found no difference in fasting GLP-1, no difference in GLP-1 increase AUC 0 60, or GLP-1 decrease between IGT and. Reduced: Faerch et al. [9] also measured GLP-1 in i-igt subjects. They found a reduced rauc 0 30 and a reduced rauc 0 60 in women with i-igt compared to. No differences were found between the two groups when assessing iauc 30 or iauc 60. Shen et al. [28] studied 43 subjects GLP-1 response to a 2-hour OGTT. They found no difference in fasting GLP-1. However, GLP-1 levels were reduced at 30, 60, and 90 min and 120 min AUC GLP-1 was reduced when comparing IGT and. Zhang et al. [29], mentioned above in the i-ifg/ifg part, found no differences in fasting GLP-1 or 2 h GLP-1 between subjects with i-igt and. However, they found that ΔGLP-1 was reduced in i-igt. Nathanson et al. [30] studied year-old men and their GLP-1 response to an OGTT measuring GLP-1 at 0 and 60 minutes. They found no reduction in fasting GLP-1 and GLP-1 at 60 min. However, ΔGLP-1 was reduced in IGT compared to subjects. Laakso et al. [23], also mentioned above, found reduced GLP-1 levels at 15, 90, and 120 minutes and a reduced AUC in i-igt. (3) Total GLP-1 and IFG/IGT. 5/19 included studies assessed the relation between total GLP-1 and IFG/IGT [9, 14, 23, 27, 29]. Unchanged: Hussein et al. [27] also assessed IFG/IGT subjects. They found no difference in the GLP-1 response in obese IFG/IGT subjects compared to obese. Smushkin et al. [14] found no difference in either fasting or postprandial GLP-1 when comparing both maximal GLP- 1, 2-hour AUC and 2-hour AAB, in IFG/IGT with NFG/. Reduced: Faerch et al. [9], as mentioned above, stratified their subjects according to sex. When comparing IFG/IGT with subjects, they found a reduced 120 min GLP-1 in both sexes. Furthermore, they found a reduction in rauc 0 30, rauc 0 120,andiAUC 120 in female subjects with IFG/IGT. Zhang et al. [29] found a reduced fasting GLP-1 when comparing IFG/IGT with i-igt. When comparing IFG/IGT with both, i-ifg and i-igt, they found a reduced 2-hour GLP-1 and a reduced ΔGLP-1. Laakso et al. [23] found a reduced 15, 90, and 120 min GLP-1 and a reduced AUC when comparing IFG/IGT with subjects Why Such a Difference? Summarizing, studies assessing the total GLP-1 (and active/intact ) response in i-ifg/ IFG and i-igt/igt found both increased, unaltered, and reduced GLP-1 levels when compared with. Studies assessing IFG/IGT found unaltered or reduced GLP-1 levels when compared with. Thereby, nearly all possible outcomes have been reported. So why this difference? Active/Intact or Total GLP-1. As mentioned earlier, it is argued that total GLP-1 is best suited when GLP-1 secretion should be assessed [5, 8, 12 14]. The choice of measuring active/intact GLP-1 could be one reason of conflicting results. Furthermore, when assessing active/intact GLP-1, a difference in DPP-4 activity could also have an impact on the results although included studies show no difference in DPP-4 activity among prediabetic subgroups [14, 19, 20, 26] Study Design and Duration. All the included studies were cross-sectional studies except the study by Zheng et al. [25]. This type of study design is not designed to assess the duration by which individuals have had prediabetes [21, 33]. This could have influenced the results, and longitudinal prospective studies are therefore suggested to assess the GLP-1 response in the course from over prediabetes to type 2 diabetes [6, 11, 21, 34]. Only two studies have an estimate of prediabetes duration: Zheng et al. found a reduced fasting active/intact GLP-1 in prediabetic subjects that were 4 years earlier, and Faerch et al. [21] studied individuals that were 5 years earlier finding no difference in fasting total GLP-1 but found an increased 3-hour AUC GLP-1 in i-ifg. This could suggest a compensatory GLP-1 secretion [21], which could perhaps explain the increased 2 h AAB total GLP-1 response in NFG/IGT versus NFG/ subjects, reported by Smushkin et al. [14] Diagnostic Criteria. As mentioned earlier, different diagnostic criteria with different cut-points for the prediabetic subtypes exist and have varied through time [1, 10, 15, 16]. The current definition of IGT from WHO corresponds to the term IFG/IGT used by many studies [1]. However, many of the included studies include cut-points to differentiate between i-ifg, i-igt, and IFG/IGT although varying terms are used (i-ifg or IFG and i-igt or IGT) [9, 11, 14, 17, 19, 23, 27 29]. This could also be a reason for the differing results. Furthermore, it has been argued that i-ifg and i-igt are a continuum of impaired glucose regulation
11 Journal of Diabetes Research 11 rather than absolute states [11], hence also affecting the results due to defined diagnostic criteria Stimulus. Most of the studies conducted an OGTT, but three studies conducted an additional meal test, as described above [19, 20, 24]. The three studies found the same results in both challenges, suggesting that stimulus is not influencing on the different results in the included studies. Vollmer et al. [24] found no significant difference in integrated incremental plasma GLP-1 concentrations when comparing OGTT with a mixed breakfast meal. Furthermore, peak GLP-1 were seen after 30 minutes during the OGTT and after 90 minutes during the mixed meal. Yabe et al. [19] reported that total GLP-1 increased only after glucose ingestion and not after a mixed meal. In contrast to Vollmer et al., Lee et al. [20] reported a peak of active/intact GLP-1 at minutes in both challenges, concentrations after the OGTT: 7 9 pmol/l and the MTT: 3 5 pmol/l, and a significantly greater iauc GLP-1 in OGTT versus MTT. This difference could be explained by the different meal compositions or measuring technique Study Size. The study size in the included studies varied from 13 to A lot of the studies are therefore limited by their sample size. When assessing the five studies with the largest sample sizes (>200 subjects) [9, 23, 25, 29, 30], it suggests a reduced GLP-1 response (for details, see Table 1) in IFG/IGT. Altering results are reported in the i-ifg/ifg and i-igt/igt groups due to, for example, sample times, differing analytical methods, and sex. This strongly suggests an alteration in the GLP-1 response in the IFG/IGT group Assays. Differences in assays may have influenced the results, both in relation to epitope (e.g., active/intact or total GLP-1) and selected commercially available kits [8, 12]. Regarding epitope, Smushkin et al. [14] used a different approach to measure total GLP-1 by measuring active and inactive GLP-1 and add the two to get the total GLP-1. By choosing that approach, they might have avoided the detection of the small amounts of GLP-1(1 36)NH 2 /(1 37) secreted from the pancreas, which all C-terminally specific antibodies might detect [12]. The plethora of selected kits in different studies might also have influenced the results [8]. Interestingly, Zhang et al. [29] used a kit, which Bak et al. [8] found not to detect any GLP-1 isoforms in both plasma or buffer Sampling Time. Sampling time might also be a reason for the difference in reported results. Both the OGTT duration and the sampling interval varied considerable between studies. With large intervals, the peak GLP-1 might be missed emphasizing frequent sampling in future studies [34]. Peak GLP-1 could vary with varying glucose tolerance status [14] or gastric emptying [34] Sex. Faerch et al. [9] found a higher 30 and 120 min, tauc, and rauc GLP-1 response in women compared to men, when adjusting for BMI, height, and weight. This is supported by Vollmer et al. [24] reporting higher GLP-1 plasma concentrations in women compared to men in both an OGTT and a mixed meal and by Toft-Nielsen et al. [18] reporting a reduced AUC GLP-1 in males. If not corrected, this could also be a reason of the different results BMI. Faerch et al. [9] also found a relation between BMI and the GLP-1 response, reporting a reduced rauc 0 30, rauc 0 120, iauc 0 30, and iauc in both overweight and obese compared to normal weight individuals, and adjusted for glucose tolerance status, age, and sex. This is supported by several other included studies [18, 22, 24, 27]. all studies had matched BMI between the groups. If not corrected, this could also be a reason of the different results Genetics. Laakso et al. [23] found a reduced GLP-1 response in i-ifg, i-igt, and IFG/IGT. All participants were nondiabetic offspring of patients with type 2 diabetes. This could indicate a genetic component in the GLP-1 response and the development of prediabetes and could further be a reason of the differing results between the included studies Ethnicity. The included studies are conducted in different ethnic groups. This could also have an impact on the differing results [21, 35] Analytical Methods. Different analytical methods can also have influenced the results between the studies [9]. Faerch et al. [9], for example, used rauc, not used in any of the other studies Age. Faerch et al. [9] also reported a relation between GLP-1 and age, with an increasing although small GLP-1 response with increasing age. If not corrected, this could also explain the differing results Other Factors. Other factors could also have an influence on the GLP-1 response, for example, insulin resistance [17, 36], glucagon levels [6], and nonesterified fatty acid levels [6, 24] Potential Mechanisms for the Eventually Reduced GLP-1 Response in Prediabetes. Rask et al. [36] have found a reduced GLP-1 secretion in response to a mixed meal in nondiabetic men with insulin resistance. This suggests an association between insulin resistance and GLP-1 secretion. In vitro studies of models of L cells have shown that L cells express the insulin receptor [37]. Furthermore, in vitro studies have shown a stimulatory effect of insulin on the GLP-1 secretion in L cell models in a glucose-dependent manner [37, 38]. In continuation of the study by Rask et al. [36], in vitro and in vivo studies have showed reduced homologous and heterologous secretagogue-induced GLP-1 secretion in insulin resistant L cell models [37]. A study by Iepsen et al. [39] showed an increase in the meal-induced secretion of GLP-1 after a 1-year 13% body weight loss maintenance accompanied by a significant improvement in the HOMA-IR [39] further indicating that the L cell might be insulin sensitive [9, 39]. This potential mechanism could differ between the prediabetic subtypes since the site of insulin resistance is hypothesised to be different with increased hepatic glucose
12 12 Journal of Diabetes Research production in IFG and a reduced peripheral glucose disposal in IGT [10, 11]. In vitro studies have also shown a glucotoxic effect on the GLUTag L cell model reducing acute glucose-induced GLP-1 secretion [40] and a lipotoxic effect on the GLUTag L cell model affecting L cell viability, with a presumed counteractive effect of insulin and the GLP-1 analog Exendin-4 [38]. Furthermore, in vitro studies have shown that chronic exposure to the proinflammatory cytokine TNFα reduces both GLP-1 expression and secretion from L cell models expressing the TNFα-receptor TNFR1 [41]. This could indicate a role of these extracellular metabolites and TNFα on the potentially reduced GLP-1 secretory response in prediabetes. Returning to the research question, Is a low GLP-1 response a predictor of prediabetes in adults? When assessing the five studies with the largest sample size, it clearly suggests an alteration in the GLP-1 response in IFG/IGT subjects and varying results when assessing the two other subtypes i- IFG/IFG and i-igt/igt. However, varying results have been reported in all subtypes and warrants further studies. Possible reasons for the varying results have been discussed. As mentioned above, the need for longitudinal prospective studies are necessary to assess the impact of duration of the prediabetic state on the GLP-1 response in prediabetes and to determine the, eventual, temporal influence of the GLP-1 response in the pathogenesis of type 2 diabetes. Additionally, the aim of this review is to survey the studies assessing the relation between the GLP-1 response and the different prediabetic subtypes and to suggest potential confounders relevant when conducting future studies. An eventual limitation of this review is that only the PubMed database was assessed. Furthermore, relevant studies could have been excluded in the search or in the evaluation of relevant studies. To avoid the exclusion of studies, a broad search was conducted including many synonyms for the rather broad term prediabetes. 5. Conclusion Conclusively, this review suggests that the GLP-1 response is a variable in prediabetes possibly due to a varying GLP- 1-secreting profile during the development and progression of type 2 diabetes or difference in the measurement technique. Longitudinal prospective studies are needed to assess whether a reduced GLP-1 response is a predictor of diabetes. Furthermore, this review gives an overview of studies assessing the relation between GLP-1 and prediabetes and discusses possible confounding factors, relevant when conducting future studies. Abbreviations IGT: IFG: i-igt: i-ifg: rauc: iauc: Impaired glucose tolerance Impaired fasting glucose Isolated impaired glucose tolerance Isolated impaired fasting glucose Relative area under the curve Incremental area under the curve tauc: Total area under the curve GLUTag L A GLP-1-secreting cell line (source: glucagonproducing enteroendocrine cell tumor that arose cell model: in transgenic mice generated on an outbred CD-1 background [38]). Conflicts of Interest The authors declare that there is no conflict of interest regarding the publication of this article. References [1] World Health Organization, Global Report on Diabetes, World Health Organization, Geneva, Switzerland, [2] C. Bommer, E. Heesemann, V. Sagalova et al., The global economic burden of diabetes in adults aged years: a cost-of-illness study, The Lancet Diabetes and Endocrinology, vol. 5, no. 6, pp , [3] C. F. Deacon and B. Ahren, Physiology of incretins in health and disease, The Review of Diabetic Studies, vol. 8, no. 3, pp , [4] M. Nauck, F. Stockmann, R. Ebert, and W. Creutzfeldt, Reduced incretin effect in type 2 (non-insulin-dependent) diabetes, Diabetologia, vol. 29, no. 1, pp , [5] S. Calanna, M. Christensen, J. J. Holst et al., Secretion of glucagon-like peptide-1 in patients with type 2 diabetes mellitus: systematic review and meta-analyses of clinical studies, Diabetologia, vol. 56, no. 5, pp , [6] M. A. Nauck, I. Vardarli, C. F. Deacon, J. J. Holst, and J. J. Meier, Secretion of glucagon-like peptide-1 (GLP-1) in type 2 diabetes: what is up, what is down?, Diabetologia, vol. 54, no. 1, pp , [7] X. L. Wang, F. Ye, J. Li et al., Impaired secretion of glucagonlike peptide 1 during oral glucose tolerance test in patients with newly diagnosed type 2 diabetes mellitus, Saudi Medical Journal, vol. 37, no. 1, pp , [8] M. J. Bak, N. J. Wewer Albrechtsen, J. Pedersen et al., Specificity and sensitivity of commercially available assays for glucagon-like peptide-1 (GLP-1): implications for GLP-1 measurements in clinical studies, Diabetes, Obesity & Metabolism, vol. 16, no. 11, pp , [9] K. Faerch, S. S. Torekov, D. Vistisen et al., GLP-1 response to oral glucose is reduced in prediabetes, screen-detected type 2 diabetes, and obesity and influenced by sex: the ADDITION- PRO study, Diabetes, vol. 64, no. 7, pp , [10] L. Perreault and K. Faerch, Approaching pre-diabetes, Journal of Diabetes and its Complications, vol. 28, no. 2, pp , [11] K. Faerch, K. Borch-Johnsen, J. J. Holst, and A. Vaag, Pathophysiology and aetiology of impaired fasting glycaemia and impaired glucose tolerance: does it matter for prevention and treatment of type 2 diabetes?, Diabetologia, vol. 52, no. 9, pp , [12] C. F. Deacon and J. J. Holst, Immunoassays for the incretin hormones GIP and GLP-1, Best Practice & Research. Clinical Endocrinology & Metabolism, vol. 23, no. 4, pp , [13] J. J. Holst, The physiology of glucagon-like peptide 1, Physiological Reviews, vol. 87, no. 4, pp , 2007.
13 Journal of Diabetes Research 13 [14] G. Smushkin, A. Sathananthan, C. D. Man et al., Defects in GLP-1 response to an oral challenge do not play a significant role in the pathogenesis of prediabetes, The Journal of Clinical Endocrinology and Metabolism, vol. 97, no. 2, pp , [15] American Diabetes A, Diagnosis and classification of diabetes mellitus, Diabetes Care, vol. 33, Supplement 1, pp. S62 S69, [16] World Health Organization and International Diabetes Federation, Definition and Diagnosis of Diabetes Mellitus and Intermediate Hyperglycaemia : Report of a WHO/IDF Consultation, World Health Organization, Geneva, Switzerland, [17] J. C. Fernandez-Garcia, M. Murri, L. Coin-Araguez, J. Alcaide, R. El Bekay, and F. J. Tinahones, GLP-1 and peptide YY secretory response after fat load is impaired by insulin resistance, impaired fasting glucose and type 2 diabetes in morbidly obese subjects, Clinical Endocrinology (Oxford), vol. 80, no. 5, pp , [18] M. B. Toft-Nielsen, M. B. Damholt, S. Madsbad et al., Determinants of the impaired secretion of glucagon-like peptide-1 in type 2 diabetic patients, The Journal of Clinical Endocrinology and Metabolism, vol. 86, no. 8, pp , [19] D. Yabe, A. Kuroe, K. Watanabe et al., Early phase glucagon and insulin secretory abnormalities, but not incretin secretion, are similarly responsible for hyperglycemia after ingestion of nutrients, Journal of Diabetes and its Complications, vol. 29, no. 3, pp , [20] S. Lee, D. Yabe, K. Nohtomi et al., Intact glucagon-like peptide- 1 levels are not decreased in Japanese patients with type 2 diabetes, Endocrine Journal, vol.57,no.2,pp , [21] K. Faerch, A. Vaag, J. J. Holst, C. Glumer, O. Pedersen, and K. Borch-Johnsen, Impaired fasting glycaemia vs impaired glucose tolerance: similar impairment of pancreatic alpha and beta cell function but differential roles of incretin hormones and insulin action, Diabetologia, vol. 51, no. 5, pp , [22] E. Muscelli, A. Mari, A. Casolaro et al., Separate impact of obesity and glucose tolerance on the incretin effect in normal subjects and type 2 diabetic patients, Diabetes, vol. 57, no. 5, pp , [23] M. Laakso, J. Zilinskaite, T. Hansen et al., Insulin sensitivity, insulin release and glucagon-like peptide-1 levels in persons with impaired fasting glucose and/or impaired glucose tolerance in the EUGENE2 study, Diabetologia, vol. 51, no. 3, pp , [24] K. Vollmer, J. J. Holst, B. Baller et al., Predictors of incretin concentrations in subjects with normal, impaired, and diabetic glucose tolerance, Diabetes, vol. 57, no. 3, pp , [25] T. Zheng, Y. Gao, A. Baskota, T. Chen, X. Ran, and H. Tian, Increased plasma DPP4 activity is predictive of prediabetes and type 2 diabetes onset in Chinese over a four-year period: result from the China National Diabetes and Metabolic Disorders Study, The Journal of Clinical Endocrinology and Metabolism, vol. 99, no. 11, pp. E2330 E2334, [26] L. Pala, S. Ciani, I. Dicembrini et al., Relationship between GLP-1 levels and dipeptidyl peptidase-4 activity in different glucose tolerance conditions, Diabetic Medicine, vol. 27, no. 6, pp , [27] M. S. Hussein, M. M. Abushady, S. Refaat, and R. Ibrahim, Plasma level of glucagon-like peptide 1 in obese Egyptians with normal and impaired glucose tolerance, Archives of Medical Research, vol. 45, no. 1, pp , [28] J. Shen, Z. Chen, C. Chen, X. Zhu, and Y. Han, Impact of incretin on early-phase insulin secretion and glucose excursion, Endocrine, vol. 44, no. 2, pp , [29] F. Zhang, X. Tang, H. Cao et al., Impaired secretion of total glucagon-like peptide-1 in people with impaired fasting glucose combined impaired glucose tolerance, International Journal of Medical Sciences, vol. 9, no. 7, pp , [30] D. Nathanson, B. Zethelius, C. Berne, J. J. Holst, A. Sjoholm, and T. Nystrom, Reduced plasma levels of glucagon-like peptide-1 in elderly men are associated with impaired glucose tolerance but not with coronary heart disease, Diabetologia, vol. 53, no. 2, pp , [31] E. Rask, T. Olsson, S. Soderberg et al., Insulin secretion and incretin hormones after oral glucose in non-obese subjects with impaired glucose tolerance, Metabolism, vol. 53, no. 5, pp , [32] B. Ahren, H. Larsson, and J. J. Holst, Reduced gastric inhibitory polypeptide but normal glucagon-like peptide 1 response to oral glucose in postmenopausal women with impaired glucose tolerance, European Journal of Endocrinology, vol. 137, no. 2, pp , [33] M. J. Theodorakis, Comment on Faerch et al. GLP-1 response to oral glucose is reduced in prediabetes, screen-detected type 2 diabetes, and obesity and influenced by sex: the ADDITION- PRO study. Diabetes 2015;64: , Diabetes, vol. 64, no. 9, pp. e28 e29, 2015, discussion e30-1. [34] A. Vella and C. Cobelli, Defective glucagon-like peptide 1 secretion in prediabetes and type 2 diabetes is influenced by weight and sex. Chicken, egg, or none of the above?, Diabetes, vol. 64, no. 7, pp , [35] A. K. Singh, Glucagon-like peptide 1 and dysglycemia: conflict in incretin science, Indian Journal of Endocrinology and Metabolism, vol. 19, no. 1, pp , [36] E. Rask, T. Olsson, S. Soderberg et al., Impaired incretin response after a mixed meal is associated with insulin resistance in nondiabetic men, Diabetes Care, vol. 24, no. 9, pp , [37] G. E. Lim, G. J. Huang, N. Flora, D. LeRoith, C. J. Rhodes, and P. L. Brubaker, Insulin regulates glucagon-like peptide-1 secretion from the enteroendocrine L cell, Endocrinology, vol. 150, no. 2, pp , [38] C. Kappe, Q. Zhang, J. J. Holst, T. Nystrom, and A. Sjoholm, Evidence for paracrine/autocrine regulation of GLP-1- producing cells, American Journal of Physiology Cell Physiology, vol. 305, no. 10, pp. C1041 C1049, [39] E. W. Iepsen, J. Lundgren, J. J. Holst, S. Madsbad, and S. S. Torekov, Successful weight loss maintenance includes long-term increased meal responses of GLP-1 and PYY3-36, European Journal of Endocrinology, vol. 174, no. 6, pp , [40] F. Urbano, A. Filippello, A. PinoDi et al., Altered expression of uncoupling protein 2 in GLP-1-producing cells after chronic high glucose exposure: implications for the pathogenesis of diabetes mellitus, American Journal of Physiology. Cell Physiology, vol. 310, no. 7, pp. C558 C567, [41] J. Gagnon, M. Sauve, W. Zhao et al., Chronic exposure to TNFα impairs secretion of glucagon-like peptide-1, Endocrinology, vol. 156, no. 11, pp , 2015.
14 MEDIATORS of INFLAMMATION The Scientific World Journal Gastroenterology Research and Practice Journal of Diabetes Research International Journal of Journal of Endocrinology Immunology Research Disease Markers Submit your manuscripts at BioMed Research International PPAR Research Journal of Obesity Journal of Ophthalmology Evidence-Based Complementary and Alternative Medicine Stem Cells International Journal of Oncology Parkinson s Disease Computational and Mathematical Methods in Medicine AIDS Behavioural Neurology Research and Treatment Oxidative Medicine and Cellular Longevity
Intact Glucagon-like Peptide-1 Levels are not Decreased in Japanese Patients with Type 2 Diabetes
 Or i g i n a l Advance Publication Intact Glucagon-like Peptide-1 Levels are not Decreased in Japanese Patients with Type 2 Diabetes Soushou Lee*, Daisuke Yabe**, Kyoko Nohtomi*, Michiya Takada*, Ryou
Or i g i n a l Advance Publication Intact Glucagon-like Peptide-1 Levels are not Decreased in Japanese Patients with Type 2 Diabetes Soushou Lee*, Daisuke Yabe**, Kyoko Nohtomi*, Michiya Takada*, Ryou
The enteroinsular axis in the pathogenesis of prediabetes and diabetes in humans
 The enteroinsular axis in the pathogenesis of prediabetes and diabetes in humans Young Min Cho, MD, PhD Division of Endocrinology and Metabolism Seoul National University College of Medicine Plasma glucose
The enteroinsular axis in the pathogenesis of prediabetes and diabetes in humans Young Min Cho, MD, PhD Division of Endocrinology and Metabolism Seoul National University College of Medicine Plasma glucose
Discussion & Conclusion
 Discussion & Conclusion 7. Discussion DPP-4 inhibitors augment the effects of incretin hormones by prolonging their half-life and represent a new therapeutic approach for the treatment of type 2 diabetes
Discussion & Conclusion 7. Discussion DPP-4 inhibitors augment the effects of incretin hormones by prolonging their half-life and represent a new therapeutic approach for the treatment of type 2 diabetes
Case Report Off-Label Use of Liraglutide in the Management of a Pediatric Patient with Type 2 Diabetes Mellitus
 Case Reports in Pediatrics Volume 2013, Article ID 703925, 4 pages http://dx.doi.org/10.1155/2013/703925 Case Report Off-Label Use of Liraglutide in the Management of a Pediatric Patient with Type 2 Diabetes
Case Reports in Pediatrics Volume 2013, Article ID 703925, 4 pages http://dx.doi.org/10.1155/2013/703925 Case Report Off-Label Use of Liraglutide in the Management of a Pediatric Patient with Type 2 Diabetes
Management of Type 2 Diabetes
 Management of Type 2 Diabetes Pathophysiology Insulin resistance and relative insulin deficiency/ defective secretion Not immune mediated No evidence of β cell destruction Increased risk with age, obesity
Management of Type 2 Diabetes Pathophysiology Insulin resistance and relative insulin deficiency/ defective secretion Not immune mediated No evidence of β cell destruction Increased risk with age, obesity
Chief of Endocrinology East Orange General Hospital
 Targeting the Incretins System: Can it Improve Our Ability to Treat Type 2 Diabetes? Darshi Sunderam, MD Darshi Sunderam, MD Chief of Endocrinology East Orange General Hospital Age-adjusted Percentage
Targeting the Incretins System: Can it Improve Our Ability to Treat Type 2 Diabetes? Darshi Sunderam, MD Darshi Sunderam, MD Chief of Endocrinology East Orange General Hospital Age-adjusted Percentage
Effect of macronutrients and mixed meals on incretin hormone secretion and islet cell function
 Effect of macronutrients and mixed meals on incretin hormone secretion and islet cell function Background. Following meal ingestion, several hormones are released from the gastrointestinal tract. Some
Effect of macronutrients and mixed meals on incretin hormone secretion and islet cell function Background. Following meal ingestion, several hormones are released from the gastrointestinal tract. Some
Secretion of glucagon-like peptide-1 in patients with type 2 diabetes mellitus: systematic review and meta-analyses of clinical studies
 Diabetologia (2013) 56:965 972 DOI 10.1007/s00125-013-2841-0 SYSTEMATIC REVIEW Secretion of glucagon-like peptide-1 in patients with type 2 diabetes mellitus: systematic review and meta-analyses of clinical
Diabetologia (2013) 56:965 972 DOI 10.1007/s00125-013-2841-0 SYSTEMATIC REVIEW Secretion of glucagon-like peptide-1 in patients with type 2 diabetes mellitus: systematic review and meta-analyses of clinical
Electronic Supplementary Material to the article entitled Altered pattern of the
 Electronic Supplementary Material to the article entitled Altered pattern of the incretin effect as assessed by modelling in individuals with glucose tolerance ranging from normal to diabetic Integrated
Electronic Supplementary Material to the article entitled Altered pattern of the incretin effect as assessed by modelling in individuals with glucose tolerance ranging from normal to diabetic Integrated
Role of incretins in the treatment of type 2 diabetes
 Role of incretins in the treatment of type 2 diabetes Jens Juul Holst Department of Medical Physiology Panum Institute University of Copenhagen Denmark Diabetes & Obesity Spanish Society of Internal Medicine
Role of incretins in the treatment of type 2 diabetes Jens Juul Holst Department of Medical Physiology Panum Institute University of Copenhagen Denmark Diabetes & Obesity Spanish Society of Internal Medicine
Practical Strategies for the Clinical Use of Incretin Mimetics CME/CE. CME/CE Released: 09/15/2009; Valid for credit through 09/15/2010
 Practical Strategies for the Clinical Use of Incretin Mimetics CME/CE Robert R. Henry, MD Authors and Disclosures CME/CE Released: 09/15/2009; Valid for credit through 09/15/2010 Introduction Type 2 diabetes
Practical Strategies for the Clinical Use of Incretin Mimetics CME/CE Robert R. Henry, MD Authors and Disclosures CME/CE Released: 09/15/2009; Valid for credit through 09/15/2010 Introduction Type 2 diabetes
Sitagliptin: first DPP-4 inhibitor to treat type 2 diabetes Steve Chaplin MSc, MRPharmS and Andrew Krentz MD, FRCP
 Sitagliptin: first DPP-4 inhibitor to treat type 2 diabetes Steve Chaplin MSc, MRPharmS and Andrew Krentz MD, FRCP KEY POINTS sitagliptin (Januvia) is a DPP-4 inhibitor that blocks the breakdown of the
Sitagliptin: first DPP-4 inhibitor to treat type 2 diabetes Steve Chaplin MSc, MRPharmS and Andrew Krentz MD, FRCP KEY POINTS sitagliptin (Januvia) is a DPP-4 inhibitor that blocks the breakdown of the
Reduction of insulinotropic properties of GLP-1 and GIP after glucocorticoid-induced insulin resistance
 Diabetologia (5) 5:9 9 DOI.7/s5-5-5-y ARTICLE Reduction of insulinotropic properties of GLP- and GIP after glucocorticoid-induced insulin resistance Marie Eriksen & David H. Jensen & Siri Tribler & Jens
Diabetologia (5) 5:9 9 DOI.7/s5-5-5-y ARTICLE Reduction of insulinotropic properties of GLP- and GIP after glucocorticoid-induced insulin resistance Marie Eriksen & David H. Jensen & Siri Tribler & Jens
la prise en charge du diabète de
 N21 XIII Congrès National de Diabétologie, 29 mai 2011, Alger Intérêt et place des Anti DPP4 dans la prise en charge du diabète de type 2 Nicolas PAQUOT, MD, PhD CHU Sart-Tilman, Université de Liège Belgique
N21 XIII Congrès National de Diabétologie, 29 mai 2011, Alger Intérêt et place des Anti DPP4 dans la prise en charge du diabète de type 2 Nicolas PAQUOT, MD, PhD CHU Sart-Tilman, Université de Liège Belgique
Type 2 DM in Adolescents: Use of GLP-1 RA. Objectives. Scope of Problem: Obesity. Background. Pathophysiology of T2DM
 Type 2 DM in Adolescents: Use of GLP-1 RA Objectives Identify patients in the pediatric population with T2DM that would potentially benefit from the use of GLP-1 RA Discuss changes in glycemic outcomes
Type 2 DM in Adolescents: Use of GLP-1 RA Objectives Identify patients in the pediatric population with T2DM that would potentially benefit from the use of GLP-1 RA Discuss changes in glycemic outcomes
NIH Public Access Author Manuscript Diabetologia. Author manuscript; available in PMC 2014 February 01.
 NIH Public Access Author Manuscript Published in final edited form as: Diabetologia. 2013 February ; 56(2): 231 233. doi:10.1007/s00125-012-2788-6. Lipotoxicity impairs incretin signalling V. Poitout 1,2
NIH Public Access Author Manuscript Published in final edited form as: Diabetologia. 2013 February ; 56(2): 231 233. doi:10.1007/s00125-012-2788-6. Lipotoxicity impairs incretin signalling V. Poitout 1,2
Hyperglycaemia increases dipeptidyl peptidase IV activity in diabetes mellitus
 Diabetologia (2005) 48: 1168 1172 DOI 10.1007/s00125-005-1749-8 ARTICLE E. Mannucci. L. Pala. S. Ciani. G. Bardini. A. Pezzatini. I. Sposato. F. Cremasco. A. Ognibene. C. M. Rotella Hyperglycaemia increases
Diabetologia (2005) 48: 1168 1172 DOI 10.1007/s00125-005-1749-8 ARTICLE E. Mannucci. L. Pala. S. Ciani. G. Bardini. A. Pezzatini. I. Sposato. F. Cremasco. A. Ognibene. C. M. Rotella Hyperglycaemia increases
The Mediterranean Diet: HOW and WHY It Works So Well for T2DM
 The Mediterranean Diet: HOW and WHY It Works So Well for T2DM Susan L. Barlow, RD, CDE. Objectives 1. Discuss the effects of meal size on GLP-1 concentrations. 2. Compare and contrast the specific effects
The Mediterranean Diet: HOW and WHY It Works So Well for T2DM Susan L. Barlow, RD, CDE. Objectives 1. Discuss the effects of meal size on GLP-1 concentrations. 2. Compare and contrast the specific effects
GLP-1 agonists. Ian Gallen Consultant Community Diabetologist Royal Berkshire Hospital Reading UK
 GLP-1 agonists Ian Gallen Consultant Community Diabetologist Royal Berkshire Hospital Reading UK What do GLP-1 agonists do? Physiology of postprandial glucose regulation Meal ❶ ❷ Insulin Rising plasma
GLP-1 agonists Ian Gallen Consultant Community Diabetologist Royal Berkshire Hospital Reading UK What do GLP-1 agonists do? Physiology of postprandial glucose regulation Meal ❶ ❷ Insulin Rising plasma
Diabetes: What is the scope of the problem?
 Diabetes: What is the scope of the problem? Elizabeth R. Seaquist MD Division of Endocrinology and Diabetes Department of Medicine Director, General Clinical Research Center Pennock Family Chair in Diabetes
Diabetes: What is the scope of the problem? Elizabeth R. Seaquist MD Division of Endocrinology and Diabetes Department of Medicine Director, General Clinical Research Center Pennock Family Chair in Diabetes
Treating Type 2 Diabetes with Bariatric Surgery. Goal of Treating T2DM. Remission of T2DM with Bariatric
 Treating Type 2 Diabetes with Bariatric Surgery Number (in Millions) of Persons with Diagnosed Diabetes, United States, 198 25 The number of Americans with diabetes increased from 5.6 to 15.8 million Guilherme
Treating Type 2 Diabetes with Bariatric Surgery Number (in Millions) of Persons with Diagnosed Diabetes, United States, 198 25 The number of Americans with diabetes increased from 5.6 to 15.8 million Guilherme
Characterization of GLP-1 Effects on -Cell Function After Meal Ingestion in Humans
 Emerging Treatments and Technologies O R I G I N A L A R T I C L E Characterization of GLP-1 Effects on -Cell Function After Meal Ingestion in Humans BO AHRÉN, MD, PHD 1 JENS J. HOLST, MD, PHD 2 ANDREA
Emerging Treatments and Technologies O R I G I N A L A R T I C L E Characterization of GLP-1 Effects on -Cell Function After Meal Ingestion in Humans BO AHRÉN, MD, PHD 1 JENS J. HOLST, MD, PHD 2 ANDREA
PATHOPHYSIOLOGY Diabetes Volume 63, November Diabetes 2014;63: DOI: /db
 3846 Diabetes Volume 63, November 2014 Sara F. Michaliszyn, 1 Andrea Mari, 2 SoJung Lee, 1 Fida Bacha, 3 Hala Tfayli, 4 Lama Farchoukh, 1 Ele Ferrannini, 5 and Silva Arslanian 1,6 b-cell Function, Incretin
3846 Diabetes Volume 63, November 2014 Sara F. Michaliszyn, 1 Andrea Mari, 2 SoJung Lee, 1 Fida Bacha, 3 Hala Tfayli, 4 Lama Farchoukh, 1 Ele Ferrannini, 5 and Silva Arslanian 1,6 b-cell Function, Incretin
DPP-4 inhibitor. The new class drug for Diabetes
 DPP-4 inhibitor The new class drug for Diabetes 1 Cause of Death in Korea 1 st ; Neoplasm 2 nd ; Cardiovascular Disease 3 rd ; Cerebrovascular Disease Diabetes 2 Incidence of Fatal or Nonfatal MI During
DPP-4 inhibitor The new class drug for Diabetes 1 Cause of Death in Korea 1 st ; Neoplasm 2 nd ; Cardiovascular Disease 3 rd ; Cerebrovascular Disease Diabetes 2 Incidence of Fatal or Nonfatal MI During
Scope. History. History. Incretins. Incretin-based Therapy and DPP-4 Inhibitors
 Plasma Glucose (mg/dl) Plasma Insulin (pmol/l) Incretin-based Therapy and Inhibitors Scope Mechanism of action ผศ.ดร.นพ.ว ระเดช พ ศประเสร ฐ สาขาว ชาโภชนว ทยาคล น ก ภาคว ชาอาย รศาสตร คณะแพทยศาสตร มหาว ทยาล
Plasma Glucose (mg/dl) Plasma Insulin (pmol/l) Incretin-based Therapy and Inhibitors Scope Mechanism of action ผศ.ดร.นพ.ว ระเดช พ ศประเสร ฐ สาขาว ชาโภชนว ทยาคล น ก ภาคว ชาอาย รศาสตร คณะแพทยศาสตร มหาว ทยาล
The Many Faces of T2DM in Long-term Care Facilities
 The Many Faces of T2DM in Long-term Care Facilities Question #1 Which of the following is a risk factor for increased hypoglycemia in older patients that may suggest the need to relax hyperglycemia treatment
The Many Faces of T2DM in Long-term Care Facilities Question #1 Which of the following is a risk factor for increased hypoglycemia in older patients that may suggest the need to relax hyperglycemia treatment
Hormonal Regulations Of Glucose Metabolism & DM
 Hormonal Regulations Of Glucose Metabolism & DM What Hormones Regulate Metabolism? What Hormones Regulate Metabolism? Insulin Glucagon Thyroid hormones Cortisol Epinephrine Most regulation occurs in order
Hormonal Regulations Of Glucose Metabolism & DM What Hormones Regulate Metabolism? What Hormones Regulate Metabolism? Insulin Glucagon Thyroid hormones Cortisol Epinephrine Most regulation occurs in order
My Journey in Endocrinology. Samuel Cataland M.D
 My Journey in Endocrinology Samuel Cataland M.D. 1968-2015 Drs Berson M.D. Yalow phd Insulin Radioimmunoassay Nobel Prize Physiology or Medicine 1977 Rosalyn Yalow: Radioimmunoassay Technology Andrew Schally
My Journey in Endocrinology Samuel Cataland M.D. 1968-2015 Drs Berson M.D. Yalow phd Insulin Radioimmunoassay Nobel Prize Physiology or Medicine 1977 Rosalyn Yalow: Radioimmunoassay Technology Andrew Schally
ARTICLE. D. H. Jensen & K. Aaboe & J. E. Henriksen & A. Vølund & J. J. Holst & S. Madsbad & T. Krarup
 Diabetologia () :1 11 DOI.7/s--9-7 ARTICLE Steroid-induced insulin resistance and impaired glucose tolerance are both associated with a progressive decline of incretin effect in first-degree relatives
Diabetologia () :1 11 DOI.7/s--9-7 ARTICLE Steroid-induced insulin resistance and impaired glucose tolerance are both associated with a progressive decline of incretin effect in first-degree relatives
New and Emerging Therapies for Type 2 DM
 Dale Clayton MHSc, MD, FRCPC Dalhousie University/Capital Health April 28, 2011 New and Emerging Therapies for Type 2 DM The science of today, is the technology of tomorrow. Edward Teller American Physicist
Dale Clayton MHSc, MD, FRCPC Dalhousie University/Capital Health April 28, 2011 New and Emerging Therapies for Type 2 DM The science of today, is the technology of tomorrow. Edward Teller American Physicist
GLUCAGON LIKE PEPTIDE (GLP) 1 AGONISTS FOR THE TREATMENT OF TYPE 2 DIABETES, WEIGHT CONTROL AND CARDIOVASCULAR PROTECTION.
 GLUCAGON LIKE PEPTIDE (GLP) 1 AGONISTS FOR THE TREATMENT OF TYPE 2 DIABETES, WEIGHT CONTROL AND CARDIOVASCULAR PROTECTION. Patricia Garnica MS, ANP-BC, CDE, CDTC Inpatient Diabetes Nurse Practitioner North
GLUCAGON LIKE PEPTIDE (GLP) 1 AGONISTS FOR THE TREATMENT OF TYPE 2 DIABETES, WEIGHT CONTROL AND CARDIOVASCULAR PROTECTION. Patricia Garnica MS, ANP-BC, CDE, CDTC Inpatient Diabetes Nurse Practitioner North
Research Article Prevalence and Trends of Adult Obesity in the US,
 ISRN Obesity, Article ID 185132, 6 pages http://dx.doi.org/.1155/14/185132 Research Article Prevalence and Trends of Adult Obesity in the US, 1999 12 Ruopeng An CollegeofAppliedHealthSciences,UniversityofIllinoisatUrbana-Champaign,GeorgeHuffHallRoom13,16South4thStreet,
ISRN Obesity, Article ID 185132, 6 pages http://dx.doi.org/.1155/14/185132 Research Article Prevalence and Trends of Adult Obesity in the US, 1999 12 Ruopeng An CollegeofAppliedHealthSciences,UniversityofIllinoisatUrbana-Champaign,GeorgeHuffHallRoom13,16South4thStreet,
Oral glutamine increases circulating glucagon-like peptide 1, glucagon, and insulin concentrations in lean, obese, and type 2 diabetic subjects 1 4
 Oral glutamine increases circulating glucagon-like peptide 1, glucagon, and insulin concentrations in lean, obese, and type 2 diabetic subjects 1 4 Jerry R Greenfield, I Sadaf Farooqi, Julia M Keogh, Elana
Oral glutamine increases circulating glucagon-like peptide 1, glucagon, and insulin concentrations in lean, obese, and type 2 diabetic subjects 1 4 Jerry R Greenfield, I Sadaf Farooqi, Julia M Keogh, Elana
Neuroprotective properties of GLP-1 - a brief overview. Michael Gejl Jensen, MD Dept. Of Pharmacology, AU
 Neuroprotective properties of GLP-1 - a brief overview Michael Gejl Jensen, MD Dept. Of Pharmacology, AU mg@farm.au.dk Agenda Glucagon-like peptide (GLP-1) GLP-1 and neuronal activity GLP-1 in disease-specific
Neuroprotective properties of GLP-1 - a brief overview Michael Gejl Jensen, MD Dept. Of Pharmacology, AU mg@farm.au.dk Agenda Glucagon-like peptide (GLP-1) GLP-1 and neuronal activity GLP-1 in disease-specific
Clinical Overview of Combination Therapy with Sitagliptin and Metformin
 Clinical Overview of Combination Therapy with Sitagliptin and Metformin 1 Contents Pathophysiology of type 2 diabetes and mechanism of action of sitagliptin Clinical data overview of sitagliptin: Monotherapy
Clinical Overview of Combination Therapy with Sitagliptin and Metformin 1 Contents Pathophysiology of type 2 diabetes and mechanism of action of sitagliptin Clinical data overview of sitagliptin: Monotherapy
Defective amplification of the late phase insulin response to glucose by GIP in obese Type II diabetic patients
 Diabetologia (2002) 45:1111 1119 DOI 10.1007/s00125-002-0878-6 Defective amplification of the late phase insulin response to glucose by GIP in obese Type II diabetic patients T. Vilsbøll 1, 2, T. Krarup
Diabetologia (2002) 45:1111 1119 DOI 10.1007/s00125-002-0878-6 Defective amplification of the late phase insulin response to glucose by GIP in obese Type II diabetic patients T. Vilsbøll 1, 2, T. Krarup
Research Article C-Peptide Levels Predict the Effectiveness of Dipeptidyl Peptidase-4 Inhibitor Therapy
 Diabetes Research Volume 2016, Article ID 4509603, 4 pages http://dx.doi.org/10.1155/2016/4509603 Research Article C-Peptide Levels Predict the Effectiveness of Dipeptidyl Peptidase-4 Inhibitor Therapy
Diabetes Research Volume 2016, Article ID 4509603, 4 pages http://dx.doi.org/10.1155/2016/4509603 Research Article C-Peptide Levels Predict the Effectiveness of Dipeptidyl Peptidase-4 Inhibitor Therapy
INJECTABLE THERAPY FOR THE TREATMENT OF DIABETES
 INJECTABLE THERAPY FOR THE TREATMENT OF DIABETES ARSHNA SANGHRAJKA DIABETES SPECIALIST PRESCRIBING PHARMACIST OBJECTIVES EXPLORE THE TYPES OF INSULIN AND INJECTABLE DIABETES TREATMENTS AND DEVICES AVAILABLE
INJECTABLE THERAPY FOR THE TREATMENT OF DIABETES ARSHNA SANGHRAJKA DIABETES SPECIALIST PRESCRIBING PHARMACIST OBJECTIVES EXPLORE THE TYPES OF INSULIN AND INJECTABLE DIABETES TREATMENTS AND DEVICES AVAILABLE
Pre-diabetes. Pharmacological Approaches to Delay Progression to Diabetes
 Pre-diabetes Pharmacological Approaches to Delay Progression to Diabetes Overview Definition of Pre-diabetes Risk Factors for Pre-diabetes Clinical practice guidelines for diabetes Management, including
Pre-diabetes Pharmacological Approaches to Delay Progression to Diabetes Overview Definition of Pre-diabetes Risk Factors for Pre-diabetes Clinical practice guidelines for diabetes Management, including
INJECTABLE THERAPIES IN DIABETES. Barbara Ann McKee Diabetes Specialist Nurse
 INJECTABLE THERAPIES IN DIABETES Barbara Ann McKee Diabetes Specialist Nurse 1 Aims of the session Describe the different injectable agents for diabetes and when they would be used. Describe some common
INJECTABLE THERAPIES IN DIABETES Barbara Ann McKee Diabetes Specialist Nurse 1 Aims of the session Describe the different injectable agents for diabetes and when they would be used. Describe some common
Abstract. Effect of sitagliptin on glycemic control in patients with type 2 diabetes. Introduction. Abbas Mahdi Rahmah
 Effect of sitagliptin on glycemic control in patients with type 2 diabetes Abbas Mahdi Rahmah Correspondence: Dr. Abbas Mahdi Rahmah Consultant Endocrinologist, FRCP (Edin) Director of Iraqi National Diabetes
Effect of sitagliptin on glycemic control in patients with type 2 diabetes Abbas Mahdi Rahmah Correspondence: Dr. Abbas Mahdi Rahmah Consultant Endocrinologist, FRCP (Edin) Director of Iraqi National Diabetes
Blood glucose concentrations in healthy humans
 ORIGINAL ARTICLE Effect of Glycemia on Plasma Incretins and the Incretin Effect During Oral Glucose Tolerance Test Marzieh Salehi, 1 Benedict Aulinger, 1 and David A. D Alessio 1,2 The incretin effect,
ORIGINAL ARTICLE Effect of Glycemia on Plasma Incretins and the Incretin Effect During Oral Glucose Tolerance Test Marzieh Salehi, 1 Benedict Aulinger, 1 and David A. D Alessio 1,2 The incretin effect,
Diabetes 2013: Achieving Goals Through Comprehensive Treatment. Session 2: Individualizing Therapy
 Diabetes 2013: Achieving Goals Through Comprehensive Treatment Session 2: Individualizing Therapy Joshua L. Cohen, M.D., F.A.C.P. Professor of Medicine Interim Director, Division of Endocrinology & Metabolism
Diabetes 2013: Achieving Goals Through Comprehensive Treatment Session 2: Individualizing Therapy Joshua L. Cohen, M.D., F.A.C.P. Professor of Medicine Interim Director, Division of Endocrinology & Metabolism
GLP 1 agonists Winning the Losing Battle. Dr Bernard SAMIA. KCS Congress: Impact through collaboration
 GLP 1 agonists Winning the Losing Battle Dr Bernard SAMIA KCS Congress: Impact through collaboration CONTACT: Tel. +254 735 833 803 Email: kcardiacs@gmail.com Web: www.kenyacardiacs.org Disclosures I have
GLP 1 agonists Winning the Losing Battle Dr Bernard SAMIA KCS Congress: Impact through collaboration CONTACT: Tel. +254 735 833 803 Email: kcardiacs@gmail.com Web: www.kenyacardiacs.org Disclosures I have
22 Emerging Therapies for
 22 Emerging Therapies for Treatment of Type 2 Diabetes Siddharth N Shah Abstract: The prevalence of Diabetes is progressively increasing world-wide and the growth of the disease in our country is phenomenal.
22 Emerging Therapies for Treatment of Type 2 Diabetes Siddharth N Shah Abstract: The prevalence of Diabetes is progressively increasing world-wide and the growth of the disease in our country is phenomenal.
Update on GLP-1 Past Present Future
 Update on GLP-1 p Past Present Future Effects of GLP-1: Glucose Metabolism and Nutritional Balance L-Cells: Glp-1 release Betacellfollowing ingestion Stress Increases satiety reduces appetite Betacell-
Update on GLP-1 p Past Present Future Effects of GLP-1: Glucose Metabolism and Nutritional Balance L-Cells: Glp-1 release Betacellfollowing ingestion Stress Increases satiety reduces appetite Betacell-
Zurich Open Repository and Archive. The dipeptidyl peptidase IV inhibitor NVP-DPP728 reduces plasma glucagon concentration in cats
 University of Zurich Zurich Open Repository and Archive Winterthurerstr. 190 CH-8057 Zurich http://www.zora.uzh.ch Year: 2009 The dipeptidyl peptidase IV inhibitor NVP-DPP728 reduces plasma glucagon concentration
University of Zurich Zurich Open Repository and Archive Winterthurerstr. 190 CH-8057 Zurich http://www.zora.uzh.ch Year: 2009 The dipeptidyl peptidase IV inhibitor NVP-DPP728 reduces plasma glucagon concentration
Cordoba 01/02/2008. Slides Professor Pierre LEFEBVRE
 Cordoba 01/02/2008 Slides Professor Pierre LEFEBVRE Clinical Research in Type 2 Diabetes : Current Status and Future Approaches Pierre Lefèbvre* University of Liège Belgium Granada, Spain, February 2008
Cordoba 01/02/2008 Slides Professor Pierre LEFEBVRE Clinical Research in Type 2 Diabetes : Current Status and Future Approaches Pierre Lefèbvre* University of Liège Belgium Granada, Spain, February 2008
Data from an epidemiologic analysis of
 CLINICAL TRIAL RESULTS OF GLP-1 RELATED AGENTS: THE EARLY EVIDENCE Lawrence Blonde, MD, FACP, FACE ABSTRACT Although it is well known that lowering A 1c (also known as glycated hemoglobin) is associated
CLINICAL TRIAL RESULTS OF GLP-1 RELATED AGENTS: THE EARLY EVIDENCE Lawrence Blonde, MD, FACP, FACE ABSTRACT Although it is well known that lowering A 1c (also known as glycated hemoglobin) is associated
Normal Fuel Metabolism Five phases of fuel homeostasis have been described A. Phase I is the fed state (0 to 3.9 hours after meal/food consumption),
 Normal Fuel Metabolism Five phases of fuel homeostasis have been described A. Phase I is the fed state (0 to 3.9 hours after meal/food consumption), in which blood glucose predominantly originates from
Normal Fuel Metabolism Five phases of fuel homeostasis have been described A. Phase I is the fed state (0 to 3.9 hours after meal/food consumption), in which blood glucose predominantly originates from
Incretin Effect and Glucagon Responses to Oral and Intravenous Glucose in Patients With Maturity-Onset Diabetes of the Young Type 2 and Type 3
 2838 Diabetes Volume 63, August 2014 Signe H. Østoft, 1,2,3 Jonatan I. Bagger, 1,2,3 Torben Hansen, 3,4 Oluf Pedersen, 3 Jens J. Holst, 2,3 Filip K. Knop, 1,2,3 and Tina Vilsbøll 1 Incretin Effect and
2838 Diabetes Volume 63, August 2014 Signe H. Østoft, 1,2,3 Jonatan I. Bagger, 1,2,3 Torben Hansen, 3,4 Oluf Pedersen, 3 Jens J. Holst, 2,3 Filip K. Knop, 1,2,3 and Tina Vilsbøll 1 Incretin Effect and
Research Article Associated Factors with Biochemical Hypoglycemia during an Oral Glucose Tolerance Test in a Chinese Population
 Hindawi Diabetes Research Volume 2017, Article ID 3212814, 5 pages https://doi.org/10.1155/2017/3212814 Research Article Associated Factors with Biochemical Hypoglycemia during an Oral Glucose Tolerance
Hindawi Diabetes Research Volume 2017, Article ID 3212814, 5 pages https://doi.org/10.1155/2017/3212814 Research Article Associated Factors with Biochemical Hypoglycemia during an Oral Glucose Tolerance
28 Regulation of Fasting and Post-
 28 Regulation of Fasting and Post- Prandial Glucose Metabolism Keywords: Type 2 Diabetes, endogenous glucose production, splanchnic glucose uptake, gluconeo-genesis, glycogenolysis, glucose effectiveness.
28 Regulation of Fasting and Post- Prandial Glucose Metabolism Keywords: Type 2 Diabetes, endogenous glucose production, splanchnic glucose uptake, gluconeo-genesis, glycogenolysis, glucose effectiveness.
Pathogenesis of Type 2 Diabetes
 9/23/215 Multiple, Complex Pathophysiological Abnmalities in T2DM incretin effect gut carbohydrate delivery & absption pancreatic insulin secretion pancreatic glucagon secretion HYPERGLYCEMIA? Pathogenesis
9/23/215 Multiple, Complex Pathophysiological Abnmalities in T2DM incretin effect gut carbohydrate delivery & absption pancreatic insulin secretion pancreatic glucagon secretion HYPERGLYCEMIA? Pathogenesis
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE. Single Technology Appraisal. Canagliflozin in combination therapy for treating type 2 diabetes
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Single Technology Appraisal Canagliflozin in combination therapy for Final scope Remit/appraisal objective To appraise the clinical and cost effectiveness
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Single Technology Appraisal Canagliflozin in combination therapy for Final scope Remit/appraisal objective To appraise the clinical and cost effectiveness
Helpful Hints for Taking Care of Your Diabetes. Farahnaz Joarder, MD and Don Kain, MA, RD,CDE Harold Schnitzer Diabetes Health Center
 Helpful Hints for Taking Care of Your Diabetes Farahnaz Joarder, MD and Don Kain, MA, RD,CDE Harold Schnitzer Diabetes Health Center Objectives How big of a problem is diabetes? What is diabetes? How is
Helpful Hints for Taking Care of Your Diabetes Farahnaz Joarder, MD and Don Kain, MA, RD,CDE Harold Schnitzer Diabetes Health Center Objectives How big of a problem is diabetes? What is diabetes? How is
Mae Sheikh-Ali, M.D. Assistant Professor of Medicine Division of Endocrinology University of Florida College of Medicine- Jacksonville
 Mae Sheikh-Ali, M.D. Assistant Professor of Medicine Division of Endocrinology University of Florida College of Medicine- Jacksonville Pathogenesis of Diabetes Mellitus (DM) Criteria for the diagnosis
Mae Sheikh-Ali, M.D. Assistant Professor of Medicine Division of Endocrinology University of Florida College of Medicine- Jacksonville Pathogenesis of Diabetes Mellitus (DM) Criteria for the diagnosis
Disclosure. Learning Objectives. Case. Diabetes Update: Incretin Agents in Diabetes-When to Use Them? I have no disclosures to declare
 Disclosure Diabetes Update: Incretin Agents in Diabetes-When to Use Them? I have no disclosures to declare Spring Therapeutics Update 2011 CSHP BC Branch Anar Dossa BScPharm Pharm D CDE April 20, 2011
Disclosure Diabetes Update: Incretin Agents in Diabetes-When to Use Them? I have no disclosures to declare Spring Therapeutics Update 2011 CSHP BC Branch Anar Dossa BScPharm Pharm D CDE April 20, 2011
The glucagon response to oral glucose challenge in Type 1 Diabetes. Mellitus: Lack of Impact of euglycemia
 Page 1 of 21 The glucagon response to oral glucose challenge in Type 1 Diabetes Mellitus: Lack of Impact of euglycemia Caroline K Kramer MD PhD 1,2*, Carla A Borgoño MD PhD 3*, Paula Van Nostrand RN 1,
Page 1 of 21 The glucagon response to oral glucose challenge in Type 1 Diabetes Mellitus: Lack of Impact of euglycemia Caroline K Kramer MD PhD 1,2*, Carla A Borgoño MD PhD 3*, Paula Van Nostrand RN 1,
T2DM is a global epidemic with
 : a new option for the management of type 2 diabetes Marc Evans MRCP, MD, Consultant Diabetologist, Llandough Hospital, Cardiff Incretin-based therapies for the treatment of diabetes mellitus (T2DM) present
: a new option for the management of type 2 diabetes Marc Evans MRCP, MD, Consultant Diabetologist, Llandough Hospital, Cardiff Incretin-based therapies for the treatment of diabetes mellitus (T2DM) present
Modulating the Incretin System: A New Therapeutic Strategy for Type 2 Diabetes
 Modulating the Incretin System: A New Therapeutic Strategy for Type 2 Diabetes Geneva Clark Briggs, PharmD, BCPS Adjunct Professor at University of Appalachia College of Pharmacy Clinical Associate, Medical
Modulating the Incretin System: A New Therapeutic Strategy for Type 2 Diabetes Geneva Clark Briggs, PharmD, BCPS Adjunct Professor at University of Appalachia College of Pharmacy Clinical Associate, Medical
Impaired Incretin Response After a Mixed Meal Is Associated With Insulin Resistance in Nondiabetic Men
 Pathophysiology/Complications O R I G I N A L A R T I C L E Impaired Incretin Response After a Mixed Meal Is Associated With Insulin Resistance in Nondiabetic Men EVA RASK, MD 1 TOMMY OLSSON, MD, PHD 1
Pathophysiology/Complications O R I G I N A L A R T I C L E Impaired Incretin Response After a Mixed Meal Is Associated With Insulin Resistance in Nondiabetic Men EVA RASK, MD 1 TOMMY OLSSON, MD, PHD 1
Gastrointestinal factors contribute to glucometabolic disturbances in nondiabetic patients with end-stage renal disease
 http://www.kidney-international.org & 213 International Society of Nephrology Gastrointestinal factors contribute to glucometabolic disturbances in nondiabetic patients with end-stage renal disease Thomas
http://www.kidney-international.org & 213 International Society of Nephrology Gastrointestinal factors contribute to glucometabolic disturbances in nondiabetic patients with end-stage renal disease Thomas
Management of Type 2 Diabetes. Why Do We Bother to Achieve Good Control in DM2. Insulin Secretion. The Importance of BP and Glucose Control
 Insulin Secretion Management of Type 2 Diabetes DG van Zyl Why Do We Bother to Achieve Good Control in DM2 % reduction 0-5 -10-15 -20-25 -30-35 -40 The Importance of BP and Glucose Control Effects of tight
Insulin Secretion Management of Type 2 Diabetes DG van Zyl Why Do We Bother to Achieve Good Control in DM2 % reduction 0-5 -10-15 -20-25 -30-35 -40 The Importance of BP and Glucose Control Effects of tight
Postprandial responses of incretin and pancreatic hormones in non-diabetic patients with end-stage renal disease
 Nephrol Dial Transplant (2014) 29: 119 127 doi: 10.1093/ndt/gft353 Advance Access publication 26 September 2013 Postprandial responses of incretin and pancreatic hormones in non-diabetic patients with
Nephrol Dial Transplant (2014) 29: 119 127 doi: 10.1093/ndt/gft353 Advance Access publication 26 September 2013 Postprandial responses of incretin and pancreatic hormones in non-diabetic patients with
YOU HAVE DIABETES. Angie O Connor Community Diabetes Nurse Specialist 25th September 2013
 YOU HAVE DIABETES Angie O Connor Community Diabetes Nurse Specialist 25th September 2013 Predicated 2015 figures are already met 1 in 20 have diabetes:1in8 over 60years old Definite Diagnosis is key Early
YOU HAVE DIABETES Angie O Connor Community Diabetes Nurse Specialist 25th September 2013 Predicated 2015 figures are already met 1 in 20 have diabetes:1in8 over 60years old Definite Diagnosis is key Early
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE. Proposed Health Technology Appraisal
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Proposed Health Technology Appraisal Dapagliflozin in combination therapy for the Final scope Remit/appraisal objective To appraise the clinical and
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Proposed Health Technology Appraisal Dapagliflozin in combination therapy for the Final scope Remit/appraisal objective To appraise the clinical and
Lipids Carbohydrate Protein. Fatty Acids Glycerol. Mono/di-saccarides. Aminoacids. Fat Liver Muscle. Triglycerides Glycogen Protein
 Lipids Carbohydrate Protein Fatty Acids Glycerol Mono/di-saccarides Fat Liver Muscle Aminoacids Triglycerides Glycogen Protein Microvascular Macrovascular Diabetes-specific Diabetes-enhanced HbA1c 5.7(6.0)
Lipids Carbohydrate Protein Fatty Acids Glycerol Mono/di-saccarides Fat Liver Muscle Aminoacids Triglycerides Glycogen Protein Microvascular Macrovascular Diabetes-specific Diabetes-enhanced HbA1c 5.7(6.0)
Diabetes in Chronic Pancreatitis: When is it type 3c? Melena Bellin, MD Associate Professor, Pediatrics & Surgery Schulze Diabetes Institute
 Diabetes in Chronic Pancreatitis: When is it type 3c? Melena Bellin, MD Associate Professor, Pediatrics & Surgery Schulze Diabetes Institute Disclosure Information Melena D. Bellin Disclosure of Relevant
Diabetes in Chronic Pancreatitis: When is it type 3c? Melena Bellin, MD Associate Professor, Pediatrics & Surgery Schulze Diabetes Institute Disclosure Information Melena D. Bellin Disclosure of Relevant
British Journal of Nutrition
 , page 1 of 5 q The Authors 2013 doi:10.1017/s0007114513000731 Endogenous plasma glucagon-like peptide-1 following acute dietary fibre consumption Caroline L. Bodinham*, Najlaa M. Al-Mana, Leanne Smith
, page 1 of 5 q The Authors 2013 doi:10.1017/s0007114513000731 Endogenous plasma glucagon-like peptide-1 following acute dietary fibre consumption Caroline L. Bodinham*, Najlaa M. Al-Mana, Leanne Smith
Near normalisation of blood glucose improves the potentiating effect of GLP-1 on glucose-induced insulin secretion in patients with type 2 diabetes
 Diabetologia (28) 1:632 64 DOI 1.17/s1-8-943-x ARTICLE Near normalisation of blood glucose improves the potentiating effect of GLP-1 on glucose-induced insulin secretion in patients with type 2 diabetes
Diabetologia (28) 1:632 64 DOI 1.17/s1-8-943-x ARTICLE Near normalisation of blood glucose improves the potentiating effect of GLP-1 on glucose-induced insulin secretion in patients with type 2 diabetes
History of Investigation
 Acini - Pancreatic juice (1º) (2º) Secretions- neuronal and hormonal mechanisms 1) Secretin - bicarbonate rich 2) Cholecystokinin - enzyme rich Islets of Langerhans (contain 4 cell types) Alpha cells (α)-
Acini - Pancreatic juice (1º) (2º) Secretions- neuronal and hormonal mechanisms 1) Secretin - bicarbonate rich 2) Cholecystokinin - enzyme rich Islets of Langerhans (contain 4 cell types) Alpha cells (α)-
Gut hormones KHATTAB
 Gut hormones PROF:ABD ALHAFIZ HASSAN KHATTAB Gut as an endocrine gland The talk will cover the following : Historical background. Why this subject is chosen. Gastro-intestinal hormones and their function.
Gut hormones PROF:ABD ALHAFIZ HASSAN KHATTAB Gut as an endocrine gland The talk will cover the following : Historical background. Why this subject is chosen. Gastro-intestinal hormones and their function.
ARTICLE. P. V. Højberg & T. Vilsbøll & R. Rabøl & F. K. Knop & M. Bache & T. Krarup & J. J. Holst & S. Madsbad
 Diabetologia (29) 52:199 27 DOI 1.17/s125-8-1195-5 ARTICLE Four weeks of near-normalisation of blood glucose improves the insulin response to glucagon-like peptide-1 and glucose-dependent insulinotropic
Diabetologia (29) 52:199 27 DOI 1.17/s125-8-1195-5 ARTICLE Four weeks of near-normalisation of blood glucose improves the insulin response to glucagon-like peptide-1 and glucose-dependent insulinotropic
Week 3, Lecture 5a. Pathophysiology of Diabetes. Simin Liu, MD, ScD
 Week 3, Lecture 5a Pathophysiology of Diabetes Simin Liu, MD, ScD General Model of Peptide Hormone Action Hormone Plasma Membrane Activated Nucleus Cellular Trafficking Enzymes Inhibited Receptor Effector
Week 3, Lecture 5a Pathophysiology of Diabetes Simin Liu, MD, ScD General Model of Peptide Hormone Action Hormone Plasma Membrane Activated Nucleus Cellular Trafficking Enzymes Inhibited Receptor Effector
Glucagon secretion in relation to insulin sensitivity in healthy subjects
 Diabetologia (2006) 49: 117 122 DOI 10.1007/s00125-005-0056-8 ARTICLE B. Ahrén Glucagon secretion in relation to insulin sensitivity in healthy subjects Received: 4 July 2005 / Accepted: 12 September 2005
Diabetologia (2006) 49: 117 122 DOI 10.1007/s00125-005-0056-8 ARTICLE B. Ahrén Glucagon secretion in relation to insulin sensitivity in healthy subjects Received: 4 July 2005 / Accepted: 12 September 2005
Comparison of Dissolution and Pharmacokinetics of Vildagliptin Modified Release Tablets
 International Journal of ChemTech Research CODEN (USA): IJCRGG, ISSN: 0974-4290, ISSN(Online):2455-9555 Vol.11 No.11, pp 318-322, 2018 Comparison of Dissolution and Pharmacokinetics of Vildagliptin Modified
International Journal of ChemTech Research CODEN (USA): IJCRGG, ISSN: 0974-4290, ISSN(Online):2455-9555 Vol.11 No.11, pp 318-322, 2018 Comparison of Dissolution and Pharmacokinetics of Vildagliptin Modified
Type 2 Diabetes Mellitus 2011
 2011 Michael T. McDermott MD Director, Endocrinology and Diabetes Practice University of Colorado Hospital Michael.mcdermott@ucdenver.edu Diabetes Mellitus Diagnosis 2011 Diabetes Mellitus Fasting Glucose
2011 Michael T. McDermott MD Director, Endocrinology and Diabetes Practice University of Colorado Hospital Michael.mcdermott@ucdenver.edu Diabetes Mellitus Diagnosis 2011 Diabetes Mellitus Fasting Glucose
The role of incretin hormones and glucagon in patients with liver disease
 PHD THESIS DANISH MEDICAL JOURNAL The role of incretin hormones and glucagon in patients with liver disease Anders Ellekær Junker This review has been accepted as a thesis together with three previously
PHD THESIS DANISH MEDICAL JOURNAL The role of incretin hormones and glucagon in patients with liver disease Anders Ellekær Junker This review has been accepted as a thesis together with three previously
Soliqua (insulin glargine and lixisenatide), Xultophy (insulin degludec and liraglutide)
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.30.48 Subject: Insulin GLP-1 Combinations Page: 1 of 5 Last Review Date: September 15, 2017 Insulin GLP-1
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.30.48 Subject: Insulin GLP-1 Combinations Page: 1 of 5 Last Review Date: September 15, 2017 Insulin GLP-1
Glucose-Dependent Insulinotropic Peptide Level Is Associated with the Development of Type 2 Diabetes Mellitus
 Original Article Endocrinol Metab 2016;31:134-141 http://dx.doi.org/10.3803/enm.2016.31.1.134 pissn 2093-596X eissn 2093-5978 Glucose-Dependent Insulinotropic Peptide Level Is Associated with the Development
Original Article Endocrinol Metab 2016;31:134-141 http://dx.doi.org/10.3803/enm.2016.31.1.134 pissn 2093-596X eissn 2093-5978 Glucose-Dependent Insulinotropic Peptide Level Is Associated with the Development
PREDICTORS OF INCRETIN CONCENTRATIONS IN SUBJECTS WITH NORMAL, IMPAIRED, AND DIABETIC GLUCOSE TOLERANCE
 Diabetes Publish Ahead of Print, published online December 5, 27 PREDICTORS OF INCRETIN CONCENTRATIONS IN SUBJECTS WITH NORMAL, IMPAIRED, AND DIABETIC GLUCOSE TOLERANCE Kirsten Vollmer 1, Jens J. Holst
Diabetes Publish Ahead of Print, published online December 5, 27 PREDICTORS OF INCRETIN CONCENTRATIONS IN SUBJECTS WITH NORMAL, IMPAIRED, AND DIABETIC GLUCOSE TOLERANCE Kirsten Vollmer 1, Jens J. Holst
Metabolic Syndrome. Shon Meek MD, PhD Mayo Clinic Florida Endocrinology
 Metabolic Syndrome Shon Meek MD, PhD Mayo Clinic Florida Endocrinology Disclosure No conflict of interest No financial disclosure Does This Patient Have Metabolic Syndrome? 1. Yes 2. No Does This Patient
Metabolic Syndrome Shon Meek MD, PhD Mayo Clinic Florida Endocrinology Disclosure No conflict of interest No financial disclosure Does This Patient Have Metabolic Syndrome? 1. Yes 2. No Does This Patient
Dipeptidyl-peptidase IV inhibitor is effective in patients with type 2 diabetes with high serum eicosapentaenoic acid concentrations
 ORIGINAL ARTICLE Dipeptidyl-peptidase IV inhibitor is effective in patients with type 2 diabetes with high serum eicosapentaenoic acid concentrations Takafumi Senmaru 1, Michiaki Fukui 1 *, Kanae Kobayashi
ORIGINAL ARTICLE Dipeptidyl-peptidase IV inhibitor is effective in patients with type 2 diabetes with high serum eicosapentaenoic acid concentrations Takafumi Senmaru 1, Michiaki Fukui 1 *, Kanae Kobayashi
Changing Diabetes: The time is now!
 Midwest Cardiovascular Research Foundation Welcomes DANITA HARRISON, ARNP Ms. Harrison discloses speaking relationships with Lilly, Novo Nordisk and Pfizer. Changing Diabetes: The time is now! Danita Harrison
Midwest Cardiovascular Research Foundation Welcomes DANITA HARRISON, ARNP Ms. Harrison discloses speaking relationships with Lilly, Novo Nordisk and Pfizer. Changing Diabetes: The time is now! Danita Harrison
Research Article Abdominal Aortic Aneurysms and Coronary Artery Disease in a Small Country with High Cardiovascular Burden
 ISRN Cardiology, Article ID 825461, 4 pages http://dx.doi.org/10.1155/2014/825461 Research Article Abdominal Aortic Aneurysms and Coronary Artery Disease in a Small Country with High Cardiovascular Burden
ISRN Cardiology, Article ID 825461, 4 pages http://dx.doi.org/10.1155/2014/825461 Research Article Abdominal Aortic Aneurysms and Coronary Artery Disease in a Small Country with High Cardiovascular Burden
Secretion of glucagon-like peptide-1 (GLP-1) in type 2 diabetes: what is up, what is down?
 Diabetologia (211) 54:1 1 DOI 1.17/s125-1-196-4 REVIEW Secretion of glucagon-like peptide-1 (GLP-1) in type 2 diabetes: what is up, what is down? M. A. Nauck & I. Vardarli & C. F. Deacon & J. J. Holst
Diabetologia (211) 54:1 1 DOI 1.17/s125-1-196-4 REVIEW Secretion of glucagon-like peptide-1 (GLP-1) in type 2 diabetes: what is up, what is down? M. A. Nauck & I. Vardarli & C. F. Deacon & J. J. Holst
Pathogenesis of Diabetes Mellitus
 Pathogenesis of Diabetes Mellitus Young-Bum Kim, Ph.D. Associate Professor of Medicine Harvard Medical School Definition of Diabetes Mellitus a group of metabolic diseases characterized by hyperglycemia
Pathogenesis of Diabetes Mellitus Young-Bum Kim, Ph.D. Associate Professor of Medicine Harvard Medical School Definition of Diabetes Mellitus a group of metabolic diseases characterized by hyperglycemia
Elevated circulating fasting glucagon like peptide 1 in surgical patients with aortic valve disease and diabetes
 DOI 10.1186/s13098-017-0279-0 Diabetology & Metabolic Syndrome RESEARCH Elevated circulating fasting glucagon like peptide 1 in surgical patients with aortic valve disease and diabetes Camilla Krizhanovskii
DOI 10.1186/s13098-017-0279-0 Diabetology & Metabolic Syndrome RESEARCH Elevated circulating fasting glucagon like peptide 1 in surgical patients with aortic valve disease and diabetes Camilla Krizhanovskii
Secretion of incretin hormones and the insulinotropic effect of gastric inhibitory polypeptide in women with a history of gestational diabetes
 Diabetologia (2005) 48: 1872 1881 DOI 10.1007/s00125-005-1863-7 ARTICLE J. J. Meier. B. Gallwitz. M. Askenas. K. Vollmer. C. F. Deacon. J. J. Holst. W. E. Schmidt. M. A. Nauck Secretion of incretin hormones
Diabetologia (2005) 48: 1872 1881 DOI 10.1007/s00125-005-1863-7 ARTICLE J. J. Meier. B. Gallwitz. M. Askenas. K. Vollmer. C. F. Deacon. J. J. Holst. W. E. Schmidt. M. A. Nauck Secretion of incretin hormones
ENERGY FROM INGESTED NUTREINTS MAY BE USED IMMEDIATELY OR STORED
 QUIZ/TEST REVIEW NOTES SECTION 1 SHORT TERM METABOLISM [METABOLISM] Learning Objectives: Identify primary energy stores of the body Differentiate the metabolic processes of the fed and fasted states Explain
QUIZ/TEST REVIEW NOTES SECTION 1 SHORT TERM METABOLISM [METABOLISM] Learning Objectives: Identify primary energy stores of the body Differentiate the metabolic processes of the fed and fasted states Explain
Drug Class Monograph
 Class: Dipeptidyl-Peptidase 4 (DPP-4) Inhibitors Drug Class Monograph Drugs: alogliptin, Januvia (sitagliptin), Janumet (sitagliptin/metformin), Janumet XR (sitagliptin/metformin), Jentadueto (linagliptin/metformin),
Class: Dipeptidyl-Peptidase 4 (DPP-4) Inhibitors Drug Class Monograph Drugs: alogliptin, Januvia (sitagliptin), Janumet (sitagliptin/metformin), Janumet XR (sitagliptin/metformin), Jentadueto (linagliptin/metformin),
LUP. Lund University Publications Institutional Repository of Lund University
 LUP Lund University Publications Institutional Repository of Lund University This is an author produced version of a paper published in The Journal of clinical endocrinology and metabolism. This paper
LUP Lund University Publications Institutional Repository of Lund University This is an author produced version of a paper published in The Journal of clinical endocrinology and metabolism. This paper
Research Article Clinical Outcome of a Novel Anti-CD6 Biologic Itolizumab in Patients of Psoriasis with Comorbid Conditions
 Dermatology Research and Practice Volume 2, Article ID 13326, 4 pages http://dx.doi.org/.1155/2/13326 Research Article Clinical Outcome of a Novel Anti-CD6 Biologic Itolizumab in Patients of Psoriasis
Dermatology Research and Practice Volume 2, Article ID 13326, 4 pages http://dx.doi.org/.1155/2/13326 Research Article Clinical Outcome of a Novel Anti-CD6 Biologic Itolizumab in Patients of Psoriasis
Vildagliptin is a potent and selective
 Clinical Care/Education/Nutrition/Psychosocial Research O R I G I N A L A R T I C L E Effects of the Dipeptidyl Peptidase-IV Inhibitor Vildagliptin on Incretin Hormones, Islet Function, and Postprandial
Clinical Care/Education/Nutrition/Psychosocial Research O R I G I N A L A R T I C L E Effects of the Dipeptidyl Peptidase-IV Inhibitor Vildagliptin on Incretin Hormones, Islet Function, and Postprandial
FRIDAY, JUNE 21. Epidemiology/ Genetics. Symposium The Big Picture Genetic Architecture of Diabetes Room S 103 B
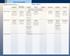 Registration Hours: 9:00 a.m. 6:30 p.m. Shop Store Hours: 9:00 a.m. 6:30 p.m. FRIDAY, JUNE 21 Noon 12:40 p.m. Meet the Expert Sessions 12:50 p.m. 1:30 p.m. Meet the Expert Sessions 2:00 p.m. 4:00 p.m.
Registration Hours: 9:00 a.m. 6:30 p.m. Shop Store Hours: 9:00 a.m. 6:30 p.m. FRIDAY, JUNE 21 Noon 12:40 p.m. Meet the Expert Sessions 12:50 p.m. 1:30 p.m. Meet the Expert Sessions 2:00 p.m. 4:00 p.m.
Targeting simultaneously GLP-1, GIP and glucagon receptors : a new paradigm for treating obesity and diabetes
 SHORT COMMENT FOR NATURE REVIEWS ENDOCRINOLOGY Targeting simultaneously GLP-1, GIP and glucagon receptors : a new paradigm for treating obesity and diabetes André J. SCHEEN (1), Nicolas PAQUOT (2) (1)
SHORT COMMENT FOR NATURE REVIEWS ENDOCRINOLOGY Targeting simultaneously GLP-1, GIP and glucagon receptors : a new paradigm for treating obesity and diabetes André J. SCHEEN (1), Nicolas PAQUOT (2) (1)
GLP-1-based therapies in the management of type 2 diabetes
 GLP-1-based therapies in the management of type 2 diabetes Makbul Aman Mansyur Division Endocrine & Metabolism Department of Internal Medicine Faculty of Medicine Hasanuddin University/ RSUP Dr. Wahidin
GLP-1-based therapies in the management of type 2 diabetes Makbul Aman Mansyur Division Endocrine & Metabolism Department of Internal Medicine Faculty of Medicine Hasanuddin University/ RSUP Dr. Wahidin
BARIATRIC SURGERY AND TYPE 2 DIABETES MELLITUS
 BARIATRIC SURGERY AND TYPE 2 DIABETES MELLITUS George Vl Valsamakis European Scope Fellow Obesity Visiting iti Associate Prof Warwick Medical School Diabetes is an increasing healthcare epidemic throughout
BARIATRIC SURGERY AND TYPE 2 DIABETES MELLITUS George Vl Valsamakis European Scope Fellow Obesity Visiting iti Associate Prof Warwick Medical School Diabetes is an increasing healthcare epidemic throughout
Obesity may attenuate the HbA1c-lowering effect of sitagliptin in Japanese type 2 diabetic patients
 ORIGINAL ARTICLE Obesity may attenuate the HbA1c-lowering effect of sitagliptin in Japanese type 2 diabetic patients Yukihiro Bando, Hideo Kanehara, Keiko Aoki, Azusa Hisada, Daisyu Toya, Nobuyoshi Tanaka
ORIGINAL ARTICLE Obesity may attenuate the HbA1c-lowering effect of sitagliptin in Japanese type 2 diabetic patients Yukihiro Bando, Hideo Kanehara, Keiko Aoki, Azusa Hisada, Daisyu Toya, Nobuyoshi Tanaka
