THE COMPLEMENT SYSTEM AND GLOMERULAR KIDNEY DISEASES: ETIOPATHOGENESIS, DIAGNOSTICS AND TREATMENT
|
|
|
- Daniel Mark Stone
- 6 years ago
- Views:
Transcription
1 PREGLEDNI RAD THE COMPLEMENT SYSTEM AND GLOMERULAR KIDNEY DISEASES: ETIOPATHOGENESIS, DIAGNOSTICS AND TREATMENT Milica Cvetkovic 1, Milica Kostovic 2, Dejan Petrovic 2,3 1Centre for Rheumatology, Clinical Centre Kragujevac, Kragujevac, Serbia 2Clinic for Urology and Nephrology, Clinical Centre Kragujevac, Kragujevac, Serbia 3Faculty of Medical Sciences of the University of Kragujevac, Kragujevac, Serbia SISTEM KOMPLEMENTA I GLOMERULSKE BOLESTI BUBREGA: ETIOPATOGENEZA, DIJAGNOSTIKA I LEČENJE Milica Cvetković 1, Milica Kostović 2, Dejan Petrović 2,3 1Centar za reumatologiju, Klinički centar Kragujevac, Kragujevac 2Klinika za urologiju i nefrologiju, Klinički centar Kragujevac, Kragujevac 3Fakultet medicinskih nauka Univerziteta u Kragujevcu, Kragujevac, Srbija ABSTRACT The human immune system consists of the innate and the acquired immunity. The complement system is part of the innate immune response and it can be activated through one of the three pathways: the classical pathway, the alternative pathway and the lectin pathway. Complement activation forms the C3-convertase complex. The C3-convertase proteolytically cleaves the C3 component into C3a and C3b fragments. The C3b fragment binds to the C3-convertase to form the C5-convertase. The C5-convertase is an enzyme complex that cleaves the C5 component into C5a and C5b fragments. The C5b component binds to C6, C7, C8, C9 thus forming the terminal complex of the complement activation the membrane attack complex (MAC) which is responsible for effector functions of the complement system. The serum complement is a mediator of C3 glomerulopathy (C3G), a group of diseases that includes membranoproliferative glomerulonephritis type II (MPGN II) or dense deposit disease (DDD) and C3 glomerulonephritis (C3GN). These diseases are caused by a dysregulation of the alternative pathway of the complement activation system. The C3 nephritic factor (C3NeF) is an autoantibody to the alternative pathway C3-convertase, which can cause dysregulation of the pathway. Newly acquired knowledge has enabled therapeutic applications of a specific antibody to the C5 complement component (eculizumab). Eculizumab is a recombinant monoclonal antibody that exhibits high affinity for the complement component C5, with the aim to inhibit its cleavage and activation of the terminal complement pathway. Key words: complement system proteins; glomerulonephritis; antibodies, monoclonal, humanized. INTRODUCTION The human immune system consists of the innate and the acquired immunity. The complement system represents a part of the innate immune response (1). It consists of proteins, some of which are soluble, circulating proteins in blood plasma or other body fluids, and some are integral or membrane-bound proteins (2, 3, SAŽETAK Imunski sistem čoveka sastoji se od urođenog i stečenog imunskog odgovora. Sistem komplementa predstavlja deo urođenog imunskog odgovora i može se aktivirati na jedan od tri načina: klasičnim, alternativnim i lektinskim putem. Aktivacijom komplementa nastaje kompleks C3-konvertaza. C3-konvertaza proteolitičkim putem cepa C3 komponentu na fragmente C3a i C3b. Spajanjem fragmenta C3b sa C3- konvertazom nastaje C5-konvertaza. C5-konvertaza je enzimski kompleks koji cepa C5 komponentu na C5a i C5b fragmente. Komponenta C5b se vezuje sa komponentama komplementa C6, C7, C8, C9 i tako nastaje završni kompleks aktivacije komplementa MAC (Membrane Attack Complex) koji je odgovoran za efektorske funkcije sistema komplementa. Serumski komplement je medijator C3 glomerulopatija (C3G), grupe bolesti koja obuhvata membranoproliferativni glomerulonefritis tip II (MPGN tip II) ili bolest gustih depozita (DDD) i C3 glomerulonefritis (C3GN). Obe bolesti nastaju zbog poremećaja regulacije alternativnog puta aktivacije sistema komplementa. C3- nefritički faktor (C3-NeF) predstavlja autoantitelo na C3- konvertazu alternativnog puta i može biti uzrok poremećaja njegove regulacije. Nova saznanja omogućila su terapijsku primenu specifičnog antitela na C5 komponentu komplementa (eculizumab). Eculizumab je rekombinantno monoklonsko antitelo sa visokim afinitetom za C5 komponentu komplementa, čiji je cilj da spreči cepanje komponente C5 i aktivaciju završnog puta sistema komplementa. Ključne reči: sistem proteina komplementa; glomerulonefritis; antitela, monoklonska, humanizovana. 4). The complement system is a proinflammatory system of the proteolytic cascade in which enzymatic cleavage of one component activates the next one. This way, the whole process is significantly amplified (2). Deposition of complement fragments at sites of tissue damage leads to the process of opsonization, as well as liberation of peptides whose role is to stimulate the inflammatory response and cell lysis (1, 2, 5). This way, the complement Primljen/Received: Prihvaćen/Accepted: Milica Cvetković. MD Centre for Rheumatology, Clinical Centre Kragujevac Zmaj Jovina 30, Kragujevac, Phone: mimi25cvet@gmail.com
2 system plays an important physiological role in the innate immunity response and inflammation with the aim to eliminate cellular debris, microbial pathogens and apoptotic host cells (3). The complement system activation mechanisms The three pathways can activate the complement system: the classical pathway, the alternative pathway and the lectin pathway. These pathways are activated by different mechanisms (1, 2, 6). Complement components C1q, C1r, C1s, C4 and C2 form the classical pathway (7). Antibodies of immunoglobulin classes G and M (IgG or IgM) are traditionally known as activators of the classical pathway (1). Activation of the classical complement pathway (CP) starts when the component C1q binds to the Fc-fragment of the antibody (in an immune complex) at the site of damage (2, 9). After binding to specific sites on the activator, the complement component C1q induces activation of the C1r and C1s subcomponents (1). The activated C1r serine-protease proteolytically cleaves C4 and C2 into fragments C4a, C4b, C2a and C2b (2, 7, 8). The fragments C4b and C2b bind to form the complex C4b2b which is a classical pathway C3-convertase, an enzyme that cleaves the C3 component into C3a and C3b by proteolytic activity. The fragment C3b binds to C4b2b (classical pathway C3-convertase) to form the complex C4b2b3b which is a classical pathway C5-convertase, an enzyme that proteolytically cleaves C5 into the fragments C5a and C5b (2, 8). The components C5b, C6, C7, C8, and C9 bind to form the terminal complex of the complement activation - MAC (Membrane Attack Complex) (8). Lupus nephritis is the best studied human model of a chronic renal disease in which immune complexes activate the classical complement pathway (CP) (10). In lupus nephritis patents, it is diagnostically important to determine serum levels of C3 and C4, immune complex (IK), as well as antinuclear antibody titre (ANA), antidsdna-antibodies (whose target antigen is double stranded DNA) and anti-sm-antibodies (antibodies against the Smith antigen) (10, 11, 12, 13). Antibodies binding to the complement component C1q can also be detected in lupus nephritis patents (13). The circulating molecules, mannose-binding lectin - MBL (a protein similar to C1q) and ficolins 1, 2 and 3 bind to the terminal mannose or N-acetylglucosamine on the bacterial surface and thus initiate the lectin or mannosebinding pathway (7). These molecules have their target structures which they identify and to which they bind. After this binding, two enzymes that are attached to the mannose-binding lectin (MBL) are activated. These enzymes are known as MBL-associated serine-proteases, MASP-1 and MASP-2 (8, 9). The serine-protease MASP- 2 cleaves the components C4 and C2. This further leads to formation of C3-convertase and C5-convertase complexes. Serine-protease MASP-1 can directly cleave the component C3 (1, 8). Immunoglobulin A nephropathy (IgAN) or Berger disease is a relatively common form of chronic glomerulonephritis. The main characteristics of this disease include deposition of immune complexes containing immunoglobulin class A (IgA) in the kidney mesangium, inflammation, mesangial proliferation and interstitial damage. In approximately 33% of the affected people, the disease gradually progresses to sclerosis and to the end-stage-renal-failure (ESRF). In vitro studies have shown that polymeric serum IgA can bind to mannosebinding lectin (MBL) present in serum, as well as that binding of the serum complex MBL-MASP-2 to immunoglobulin class A (IgA) in the kidney mesangium can activate the component C4, which may present the pathogenic basis for IgA nephropathy (IgAN) (14). The alternative pathway (AP) is constitutively active and its increased activity is the result of the loss of regulation. In contrast, the classical and lectin complement pathways (CP and LP) are not constitutively active and they need a trigger to stimulate their activity (6). The phylogenetically oldest (but last discovered and described), the alternative complement pathway (AP) is composed of three components: fragment C3b and factors B and D (4, 7). The term 'tickover' refers to a physiologically low level of the alternative pathway (AP) activity. This constitutively low activity is controlled by hydrolysis of the internal thioester bond of the central protein complement C3. In this case, the process of the internal thioester bond hydrolysis takes place spontaneously (16). The hydrolysis of the internal thioester bond of the protein C3 leads to a conformational change in the molecule thus yielding the molecule C3(H2O), which is similar to the complement fragment C3b (4, 17). The serine-protease factor D proteolytically cleaves the factor B into the fragments Ba and Bb (8). The fragment C3b binds to the fragment Bb to form the complex C3bBb which is the C3-convertase of the alternative complement pathway (AP), and which is stabilized by binding to the plasma protein properdin (5, 9, 18, 17). The C3-convertase of the alternative pathway (AP) leads to cleavage of other C3 molecules and the increase in the number of C3b fragments, thus amplifying the production of the complex C3bBb by a process referred to as the C3b amplification loop of the alternative complement pathway (AP) (17, 18). C3b molecules bind to C3bBb, which is an alternative pathway C3 convertase, to generate the complex C3bBb3b, which is a C5- convertase of the alternative pathway (AP). This enzyme complex proteolytically cleaves C5 into the fragments C5a and C5b (3). 115
3 Terminal pathway of the complement system activation The component C5b binds to components C6, C7, C8, C9 thus forming the terminal complex of the complement activation the membrane attack complex (MAC) which is responsible for effector functions of the complement system (7, 20). Conformational changes in C5b lead to exposure of the binding site for the complement component C6. The ability of the C5b fragment (within the C5-convertase) to bind C6 at the site of damage is short-term and decays rapidly. If these two components bind, the newly formed complex C5b-6 becomes stable. Binding of the complex C5b6 to the component C7 causes disclosure of the membrane binding site and a consequential incorporation of the newly formed complex into the cell membrane. However, if the concentration of component C7 at the site of activation is limited and the binding does not occur, the complex C5b-6 stays soluble (unbound). If this soluble C5b6 complex subsequently binds to the component C7 circulating in plasma and fluid liquids, the so-called fluid-phase C5b-7 is formed. The time that the fluid phase C5b-7 has to bind to the membrane is limited. The fluid phase C5b-7 has the same affinity as the membrane-bound C5b-7 complex that can bind to the C8 component. The nascent C5b-7 complex binds to the C8β chain via the component C5b. The newly formed complex C5b-8 binds to the first molecule of C9 via the C8α chain. Due to major structural changes, binding of the first C9 molecule enables binding of further C9 molecules. This way the C9 cylinder is formed that can be inserted into the target cell membrane. The C9 component is polymerized at the site of insertion. This polymerization process causes a distortion in continuity of the phospholipid bilayer of the cell membrane resulting in leaky patches or hydrophilic channels ( pores ) through the membrane. Formation of these structures further leads to processes of disruption, lysis and necrosis of the cell (20). The activation of the complement system can be proven based on the increased levels of the MAC in plasma (normal level is below 0.30 mg/dl) (27). Regulation of the complement activation system The complement system activation can have bad effects on the organism cells. Therefore the activation of the complement system is strictly controlled (2). The classical pathway (CP) is activated by binding of antibodies to the C1q component and by activation of C1r and C1s subcomponents (7). Protein C1-inhibitor (C1- INH), a member of a diverse serine-protease inhibitors family, inhibits this reaction by binding to activated enzymes C1r and C1s and inactivating them (7, 8, 19). Activation of the alternative complement pathway (AP) is regulated by two plasma proteins, the complement factor H (CFH) and the complement factor I (CFI) (17). The complement factor H (CFH) is a 150-kDa glycoprotein whose serum concentration ranges from 110 to 615 micrograms/ml (5, 17). The complement factor H (CFH) accelerates the decay of the complex C3bBb (the alternative pathway C3-convertase). It is also a cofactor to the complement factor I (CFI) in the proteolytic conversion of C3b to ic3b which is inactive, thus inhibiting the binding of the factor B and the further process (3, 17, 18). The complement factor I (CFI) is serine-protease whose molecular weight is 88-kDa. Serum concentration of this enzyme ranges approximately from 39 to 100 micrograms/ml (17). The complement factor I (CFI) cleaves the fragment C3b (in presence of the cofactor) into fragments ic3b and C3dg (3, 7, 17). unlike C3b, the fragments ic3b and C3dg are inactive and cannot participate in the C3b-amplification loop (3). Vitronectin or S-protein and clusterin or SP-40,40 are plasma glycoproteins that bind to the metastable site inside the complex C5b-7. This way further incorporation of the C5b-7 complex into the cell membrane is made impossible (2, 7, 20). The molecule CD59 binds to the C9 component binding site on the alpha-chain of the C8 component. Formation of the terminal complex, insertion and polymerization of the component C9 and cell lysis are thus made impossible (7, 20). Complement and renal damage The complement system is a mediator of multiple forms of renal diseases which can all be classified into two groups (22). Increased activation of the classical complement pathway (CP) is the pathogenic basis for the first group of diseases which includes lupus nephritis, membranous glomerulonephritis and rapidly progressive glomerulonephritis (6, 19, 23-25). A dysregulation of the alternative complement pathway (AP) presents the pathological basis for the second group of diseases that include C3 glomerulopathy (C3G) membranoproliferative glomerulonephritis type 2 or dense deposits disease (DDD) and C3 glomerulonephritis (C3GN), and atypical hemolytic uremic syndrome (ahus) (3, 6, 16, 24-26) C3 glomerulopathy (C3G) Membranoproliferative glomerulonephritis (MPGN) is traditionally classified as primary or idiopathic and secondary. The primary or idiopathic type includes membranoproliferative glomerulonephritis type I and type III (MPGN I and III). The secondary membranoproliferative glomerulonephritis is usually developed after a viral infection (hepatitis B and C) (27). Membranoproliferative glomerulonephritis type I and type III (MPGN I and III) are diseases whose pathogenesis 116
4 involve immune complexes, in contrast to membranoproliferative glomerulonephritis type II (MPGN II) (5, 18). Membranoproliferative glomerulonephritis (MPGN) is traditionally classified according to histological and ultrastructural findings on electronic microscopy (EM) (6, 16, 28). The typical findings include an increased number of cells in the kidney mesangium, changes in capillary walls like proliferation and remodeling, presence of immune deposits, as well as doubling of the glomerular basement membrane (GBM) (16, 21, 28). Membranoproliferative glomerulonephritis (MPGN) was previously classified on the basis of the electronic microscopy findings. According to this classification scheme, the first type of the disease or membranoproliferative glomerulonephritis type I (MPGN I) is characterized by the presence of subendothelial and mesangial deposits. The second type of the disease, membranoproliferative glomerulonephritis type II (MPGN II) or dense deposit disease DDD is characterized by intramembranous and mesangial deposits with high electron density. Finally, there are two subtypes of membranoproliferative glomerulonephritis type III (MPGN III). In Burkholder subtype, deposits can be subendothelial and subepithelial, while in Strife and Anders subtype, deposits are subendothelial, subepithelial and intramembranous with lamina densa damage (6, 21, 28). The use of immunofluorescence microscopy (IF) has brought about major advances in our understanding of the pathogenic basis for membranoproliferative glomerulonephritis (MPGN) and the subsequent reclassification of the disease (16, 28). The old classification has been replaced with a new classification based on the presence of the complement component C3 and/or immunoglobulin (Ig) deposits, assessed by immunofluorescence microscopy (IF) (21). The deposits in membranoproliferative glomerulonephritis type I (MPGN I) contain immunoglobulin IgG and/or IgM as well as C1 and/or C3 components. The deposits in patients with membranoproliferative glomerulonephritis type II or dense deposit disease (MPGN II/DDD) contain only the C3 component. The membranoproliferative glomerulonephritis type III (MPGN III) (Burkholder subtype) usually has deposits of complement components and immunoglobulins (Igs), while Strife and Anders subtype contains either the C3 component alone or the C3 component and the immunoglobulins (Ig) together (16, 28). According to the findings obtained using immunofluorescence microscopy (IF), Sethi and colleagues proposed a new classification of membranoproliferative glomerulonephritis (MPGN). The new classification includes two main groups. The first group includes diseases with deposits of the C3 component and immunoglobulins (Igs) (Ig-mediated glomerulonephritis). The second group includes diseases with presence of the C3 component only, which suggests the hyperactivity of the alternative complement pathway (AP) (16). At about the same time, Pickering and colleagues proposed the term C3 glomerulopathy (C3G) for all types of glomerulonephritis characterized by accumulation of the C3 component, with no deposits of immunoglobulins or classical pathway components (16, 21, 29). The term C3 glomerulopathy (C3G) describes a new group of diseases and includes membranoproliferative glomerulonephritis type II or dense deposit disease (MPGN II/DDD) and C3 glomerulonephritis (C3GN) (16, 21). Both diseases can involve histological changes like mild mesangial proliferation or endocapillary proliferative or extracapillary proliferative forms of glomerulonephritis (GN) (29). According to a new understanding, both of these diseases are the consequence of dysregulation of the alternative pathway (AP) (16, 21). Inspected by electronic microscopy (EM), dense deposit disease DDD shows characteristic highly electron-dense deposits localized within the glomerular basement membranes (GBM), mesangial matrix, Bowman s capsule and tubular basement membrane, that form sausage-shaped or ring forms. Assessed by the same technique, C3 glomerulonephritis (C3GN) shows moderately electron-dense deposits in mesangial and/or subendothelial, intramembranous, and subepithelial locations (21, 27, 29). Both diseases are diagnosed by renal biopsy (27). Functional and genetic studies have shown that causes of human C3 glomerulopathy (C3G) include mutations in genes for complement factors H (CFH) and I (CFI), as well as the presence of antibodies that lead to disorders in the alternative pathway (AP) (21, 29). Defects in activation or regulation of the C3-convertase enzyme of the alternative complement pathway (AP) lead to shift from low-grade activity (tickover) to hyperactivity of this pathway; and this hyperactivity is considered the pathophysiological basis for C3 glomerulopathy (C3G) (16, 19). The C3 nephritic factor (C3NeF) is an autoantibody of immunoglobulin class G (IgG) that binds to neoepitopes on the C3-convertase of the alternative complement pathway (AP), but not to individual enzyme components (3, 19). The C3 nephritic factor (C3Nef) stabilizes both the fluid phase and the membrane-bound C3-convertase. The reason for generation of C3 autoantibodies is unknown. There may be a genetic background for generation of this autoantibody, but no studies have addressed this matter so far (30). The C3 nephritic factor binds to the C3- convertase (C3bBb) of the alternative complement path (AP), and makes this enzyme complex resistant to inactivation by the complement factor H (CFH) (5, 19, 30). The C3 nephritic factor (C3NeF) and the complement factor H (CFH) control C3 convertase (C3bBb) with 117
5 opposite effects (18). The complement factor H (CFH) and the fragment Bb (factor B decay product) compete for the binding site on the fragment C3b, and if the factor H (CFH) binds to C3b, the complex C3bH is formed (3, 8). The fragment C3b is further cleaved by the complement I (CFI) into small breakdown products, like a fragment ic3b (5, 8). The fragment ic3b can bind to the regulatory molecule CR1 (5). In contrast, the autoantibody C3 nephritic factor (C3NeF) binds to the complex C3bBb, and prolongs the half life of this enzyme approximately 10 times (up to 60 minutes) (16, 18). The presence of the C3 nephritic factor (C3NeF), the absence or defective function of the factor H (CFH) and/or inhibition of the complement factor H (CFH) function by anti-factor-hautoantibody result in the loss of control of the alternative pathway C3 convertase and unrestricted activation (18). The C3 nephritic factor (C3NeF) is present in the serum of about 80% of patients with dense deposit disease DDD, and in about 40 50% of patients with C3 glomerulonephritis (C3G), and it can also be detected in the serum of patients with membranoproliferative glomerulonephritis type I and type III (MPGN I and III), as well as in the serum of healthy individuals, which indicates that it is not specific only for C3 glomerulopathies (C3G) (16, 18, 30). An autoantibody that can bind to the native complement factor B (CFB) and thus stabilize the C3 convertase has been recently found in patients with dense deposit disease DDD (3). Clinical features and prognosis Clinically, C3 glomerulopathies (C3G) present with proteinuria as urinary protein excretion greater than 150 mg/1.73m²/24h, hematuria and some degree of renal failure (31, 32). The annual incidence is 1 to 2 per million (32). Both sexes are equally affected (5, 32). The disease is usually diagnosed around the age of 21 (32). Dense deposit disease DDD can be diagnosed even earlier (usually around the age of 14) (5, 35). However, the onset of the disease has been recorded even in patients older than 60 (one-fifth of the patients) (3, 5, 32). Patients with dense deposit disease DDD can even have an acquired partial lipodystrophy (loss of subcutaneous fat from the face and the upper body), and ocular disorders (3, 32). Early identification of patients at risk of developing acute renal dysfunction and the timely treatment strategy can slow down the progression of the disease and decrease the mortality rate (33). Despite treatment, the diseases progresses to the endstage-renal-failure (ESRF) in 30-50% of patients after 10 years from diagnosis. Prognosis is worse for patients with dense deposit disease DDD (36-50%) compared to patients with C3 glomerulonephritis (C3GN) (25%) (3, 16, 32). Therefore, dense deposit disease DDD is more aggressive than C3 glomerulonephritis (C3GN) (16, 28). One possible explanation is the much higher rate of C3 nephritic factor (C3Nef) positivity in patients with dense deposit disease DDD than in patients with C3 glomerulonephritis (C3GN) (28). In the final stage of both diseases, renal transplantation is the treatment method of choice although the rate of disease recurrence and the rate of allograft failure (50-75%) are very high (3, 16, 32). Atypical hemolytic uremic syndrome (ahus) Hemolytic uremic syndrome (HuS) represents a clinical syndrome comprising of microangiopathic hemolytic anemia, thrombocytopenia and acute cute renal insufficiency due to endothelial lesion and microvascular thrombosis. In a majority of patients with hemolytic uremic syndrome (HuS), thrombotic microangiopathy is diagnosed a week after a bacterial infection such as gastroenteritis (often hemorrhagic). Gastroenteritis is usually caused by verocytotoxin-producing bacteria, like E. coli or Shigella dysenteriae. In approximately 10% of patients, hemolytic uremic syndrome (HuS) occurs without any apparent bacterial infection and it is known as atypical hemolytic uremic syndrome (ahus). ahus is a disease with high morbidity and mortality rate, which usually occurs as the familial or sporadic atypical form. During the acute stage, the mortality rate is 25 %, while in 50% of the cases, the disease progresses to the end-stage (19,34). Genetic disorders associated with atypical hemolytic uremic syndrome (ahus) are predisposing rather than directly causal (19). Specific mutations have been found in 50% of patients with atypical hemolytic uremic syndrome (ahus) (19, 34). In over 60% of these patients, genetic studies have revealed the presence of mutations in genes encoding complement factors H, I, B (CFH, CFI, CFB) and the complement component C3 (19, 34, 35). Genetic mutations for the complement factor H (CFH) are observed in 25-30% of patients, autoantibodies to the complement factor H are found in 6-10% of patients, while mutations in the gene for the complement factor I (CFI) are found in 5-10% of patients (19). Autoantibodies to complement regulatory proteins are also found (34). Some scientists believe that atypical hemolytic uremic syndrome (ahus) is part of a spectrum of diseases comprising the entity of C3 glomerulopathy (C3G), since there are several diseases with the same dysfunctions in proteins regulating the activities of the complement system (gene mutations, presence of autoantibodies) (6). Despite all the similarities, atypical hemolytic uremic syndrome (ahus) should not be considered a C3 glomerulopathy (C3G) due to different mechanism of damage. In atypical hemolytic uremic syndrome (ahus), thrombotic microangiopathy is the major mechanism that leads to kidney glomerular damage (endothelial cell 118
6 damage, formation of blood clots in the glomerular capillaries). Deposition of the C3 component and formation of deposits in the kidney glomerular basement membrane (GBM) is the main mechanism of damage in C3 glomerulopathies (C3Gs). (6, 16). Treatment In treatment of C3 glomerulopathy (C3G), it is important to control blood pressure using ACE inhibitors or AR blockers (although these medications may affect renal function), and antiproteinuric diet (3, 30, 36). In patients in whom C3 glomerulopathy (C3G) is due to defective function of the complement factor H (CFH), repletion of the factor H (CFH) by plasma infusion (the recombinant factor H is still not used) can be beneficial (16, 18). In patients with dense deposit disease DDD with moderate complement factor H (CFH) deficiency, treatment with plasma in the volume of ml/kg/tm in 14-day intervals (half-life of the H factor is about 6 days) can have favorable effects (18). In the case of dense deposit disease (DDD) caused by the C3 nephritic factor (C3NeF) plasmapheresis is used for treatment. This treatment can considerably delay the disease progression towards the end stage (5, 18, 30). New knowledge has enabled application of specific anti-complement therapy (15, 30). Eculizumab is the first anti-complement therapy, for therapy of paroxysmal nocturnal hemoglobinuria (PNH) and atypical hemolytic uremic syndrome (ahus) (6, 18). Eculizumab or the anti- C5-antibody, is a monoclonal antibody obtained by recombinant technology, with high affinity for C5, whose therapeutic goal is to prevent cleavage of the C5 component, and in the further course, formation of the lytic MAC complex (6, 27, 29, 35). In order to obtain the drug, the second and third constant regions of the immunoglobulin subclass G4 (IgG4) heavy chains (domains CH2 and CH3) are first fused to the hinge region and the CH1 domain of the immunoglobulin subclass G2 (IgG2). Then they are paired with the kappa (κ) light immunoglobulin chain. The variable regions both of the light and the heavy chains of immunoglobulin are murinederived sequences. The most important property of these sequences is that they possess high affinity for the C5 component. Then these sequences bound to the human germline framework regions. This way, a hybrid immunoglobulin molecule (Ig), which has high affinity for the complement component C5, is obtained using recombinant technology. This hybrid molecule does not have the ability to activate the complement system or to bind to antibody Fc-receptors (29). The CH1 domain and the hinge region of the immunoglobulin subclass G2 (IgG2) were chosen because they are not able to bind to antibody Fc-receptors and thus initiate the complement activation, while the CH2 and CH3 domains of the immunoglobulin IgG4 (IgG4) were chosen because they cannot activate the complement (6, 29). The drug is administered parenterally and intravenously, and it has a half-life of about days. The conventional sustaining dose is once a day, every other week. In order for the drug to achieve the complete blockage of the complement, it is necessary to reach the drug serum concentration of 35 micrograms/ml (6). A single chain version of eculizumab of 25kD (scfv) lacking the whole constant region is also applied (15). Table 1. Investigation of the alternative pathway of the complement system 119
7 The treatment method of choice for atypical hemolytic uremic syndrome (ahus) is administration of plasma, either intravenously or by plasmapheresis protocol. Plasma infusion restores deficient proteins or improves impaired function of the existing ones, while plasmapheresis removes autoantibodies that inhibit complement regulatory proteins. However, long-term treatment with this form of therapy can be difficult, while in some patients there is no adequate therapeutic response to this treatment (34). Eculizumab has also been tested for treatment of patients with this disease (6, 34). During the first four weeks of the treatment, microangiopathic hemolytic anemia and thrombocytopenia persisted, while renal function deteriorated until there were symptoms for initiation of hemodialysis. However, further treatment with eculizumab led to significant improvement in parameters relevant for hemolytic anemia, platelet count and renal function (ten weeks after its initiation, hemodialysis was discontinued). In studies, after five months of treatment, the patients serum creatinine levels were significantly decreased, and the sustaining dose was administered every other week (34). In pathophysiological sense, there is a difference between atypical hemolytic uremic syndrome (ahus) and C3 glomerulopathies (C3Gs) in the level of dysregulation. In ahus, endothelial damage is the result of dysregulation of the alternative pathway (AP) in the solid phase, while in C3G, dysregulation occurs in the fluid phase. Dysregulation of the alternative complement pathway (AP) at the solid phase level makes atypical hemolytic uremic syndrome (ahus) a more homogenous disease compared to C3 glomerulopathies (C3Gs). That is why the response to the anti-c5-antibody and the blockage of the C5 component by the drug are better in patients with ahus. Variety of disorders in regulation of the alternative pathway (AP) fluid phase in C3 glomerulopathies (C3G) reflects in the fact that dysregulation of the C3-convertase is predominant in some cases, while in others the alternative pathway C5-convertase was dysregulated. A positive response to eculizumab can be expected only in the latter case (6). Conclusion The study of deposits by immunofluorescence microscopy (IF) has resulted in a new classification of membranoproliferative glomerulonephritis. This new classification scheme is based on the presence of the complement component C3 and/or immunoglobulins in the deposits. The entity of C3 glomerulopathy (C3G) involves membranoproliferative glomerulonephritis type II or dense deposit disease (MPGN II/DDD) and C3 glomerulonephritis (C3GN). understanding the role that the complement alternative pathway (AP) and its dysregulation have in the pathogenesis of these diseases has enabled the use of a new type of specific anticomplement therapy. Eculizumab is a recombinant monoclonal antibody to the complement component C5. The aim of eculizumab is to prevent cleavage of the complement component C5, and in further course, formation of the MAC complex and subsequent lysis of target cells. The present studies on use of eculizumab are giving positive, encouraging results, which raises hope for further treatment of these patients. REFERENCE 1. Mohamed RD, Van Kooten C, Anja R. Compliments from complement: a fourth pathway of complement activation? Nephrol Dial Transplant 2006; 21: Wen L, Atkinson JP, Giclas PC. Clinical and laboratory evaluation of complement deficiency. J Allergy Clin Immunol 2004; 113: Barbour TD, Pickering MC, Cook HT. Recent insights into C3 glomerulopathy. Nephrol Dial Transplant 2013; 0: Jozsi M, Manuelian T, Heinen S, Oppermann M, Zipfel PF. Attachment of the soluble complement regulator factor H to cell and tissue surfaces: relevance for pathology. Histol Histopathol 2004; 19: Appel GB, Cook HT, Hageman G, et al. Membranoproliferative glomerulonephritis type II (Dense Deposit Disease): an update. J Am Soc Nephrol 2005; 16: Bomback AS. Anti-complement therapy for glomerular diseases. Adv Chronic Kidney Dis 2014; 21: Charlesworth JA, Peake PW, Pussell BA, Erlich JH. Complement in renal disease. Nephrology 2001; 6: Glovsky MM, Ward PA, Johnson KJ. Complement determinations in human disease. Ann Allergy Asthma Immunology 2004; 93: Ricklin D, Lambris JD. Complement in immune and inflammatory disorders: pathophysiological mechanisms. J Immunol 2013; 190: Hussain N, Jaffery G, Hasnain S. Serum Complement C3 and C4 Levels in relation to diagnosis of lupus nephritis. Trop J Pharm Res 2008; 7: Nikolic A, Petrovic M, Djurdjevic Predrag, Veselinovic M, Petrovic D. Pulmonary-renal syndrome: ethiopathogenesis, diagnosis and treatment. Med J (Krag) 2011; 45: Cvetkovic M, Nikolic A, Veselinovic M, Petrovic D. Vasculitides of the small blood vessels of kidney: etiopathogenesis, diagnosis and treatment. Med J (Krag) 2014; 48:
8 13. Nikolić A, Petrović D, Tirmenštajn-Janković B, Živanović M, Veselinović M, Stojimirović B. Diagnosis and treatment of lupus nephritis. Timoč Med Glas 2011; 36: (in Serbian). 14. Roos A, Rastaldi MP, Calvaresi N, Oortwijn BD, et al. Glomerular Activation of the Lectin Pathway of Complement in IgA Nephropathy Is Associated with More Severe Renal Disease. J Am Soc Nephrol 2006; 17: Trendelenburg M. Complement inhibition by anti-c5 antibodies-from bench to bedside and back again. Swiss Med Wkly 2007; 137: Bomback AS, Appel GB. Pathogenesis of the C3 glomerulopathies and reclassification of MPGN. Nat Rev Nephrol 2012; 8: Rose KL, Paixao Cavalcante D, Fish J, et al. Factor I is required for the development of membranoproliferative glomerulonephritis in factor H-deficient mice. J Clin Invest 2008; 118: Licht C, Schlotzer Schrehardt u, Kirschfink M, Zipfel PF, Hoppe B. MPGN II genetically determined by defective complement regulation? Pediatr Nephrol 2007; 22: Kościelska Kasprzak K, Bartoszek D, Myszka M, Żabińska M, Klinger M. The complement cascade and renal disease. Arch Immunol Ther Exp 2014; 62: Wurzner R. Modulation of complement membrane attack by local C7 synthesis. Clin Exp Immunol 2000; 121: Wada T, Nangaku M. Novel roles of complement in renal diseases and their therapeutic consequences. Kidney Int 2013; 84: Vieyra MB, Heeger PS. Novel aspects of complement in kidney injury. Kidney Int 2010; 77: McCaughan JA, Orourke DM, Courtney AE. The complement cascade in kidney disease: from sideline to center stage. Am J Kidney Dis 2013; 62: Noris M, Remuzzi G. Overview of complement activation and regulation. Semin Nephrol 2013; 33: Sethi S, Nester CM, Smith RJH. Membranoproliferative glomerulonephritis and C3 glomerulopathy: resolving the confusion. Kidney Int 2012; 81: Kavanagh D, Goodship TH, Richards A. Atypical hemolytic uremic syndrome. Semin Nephrol 2013; 33: Sethi S, Fervenza FC, Zhang Y, et al. Proliferative glomerulonephritis secondary to dysfunction of the alternative pathway of complement. Clin J Am Soc Nephrol 2011; 6: D Agati VD, Bomback AS. C3 glomerulopathy: what s in a name? Kidney Int 2012; 82: Herlitz LC, Bomback AS, Markowitz GS, et al. Pathology after eculizumab in Dense Deposit Disease and C3 GN. J Am Soc Nephrol 2012; 23: Licht C, Fremeaux-Bacchi V. Hereditary and acquired complement dysregulation in membranoproliferative glomerulonephritis. Thromb Haemost 2009; 101: Petrović D, Stojimirović B. Proteinuria as a risk factor for the progression of chronic renal disease. Vojnosanit Pregl 2008; 65: Xiao X, Pickering MC, Smith RJH. C3 Glomerulopathy: The genetic and clinical findings in Dense Deposit Disease and C3 glomerulonephritis. Semin Thromb Hemost 2014; 40: Eftekhari P. Evaluation of acute kidney injury in the hospital setting. Prim Care 2014; 41: Asif A, Haqqie SS, Ghate K, Mathew RO, Vachharajani T, Nayer A. Continued eculizumab therapy for persistent atypical hemolytic uremic syndrome. Open urol Nephrol J 2013; 6: Zuber J, Fakhouri F, Roumenina LT, Loirat C, Bacchi- Frémeaux V. use of eculizumab for atypical haemolytic uraemic syndrome and C3 glomerulopathies. Nat Rev Nephrol 2012; 8: Lukić S, Petrović D. Prevention of acute kidney injury in intensive care units. Med J (Krag) 2012; 46:
C3 Glomerulonephritis versus C3 Glomerulopathies?
 Washington University School of Medicine Digital Commons@Becker Kidneycentric Kidneycentric 2016 C3 Glomerulonephritis versus C3 Glomerulopathies? T. Keefe Davis Washington University School of Medicine
Washington University School of Medicine Digital Commons@Becker Kidneycentric Kidneycentric 2016 C3 Glomerulonephritis versus C3 Glomerulopathies? T. Keefe Davis Washington University School of Medicine
Pathology of Complement Mediated Renal Disease
 Pathology of Complement Mediated Renal Disease Mariam Priya Alexander, MD Associate Professor of Pathology GN Symposium Hong Kong Society of Nephrology July 8 th, 2017 2017 MFMER slide-1 The complement
Pathology of Complement Mediated Renal Disease Mariam Priya Alexander, MD Associate Professor of Pathology GN Symposium Hong Kong Society of Nephrology July 8 th, 2017 2017 MFMER slide-1 The complement
C3 Glomerulopathy. Jun-Ki Park
 C3 Glomerulopathy Jun-Ki Park 03.08.11 For the last 30 years classification MPGN is based on glomerular findings by light microscopy with further specification on EM and staining for Ig and complement
C3 Glomerulopathy Jun-Ki Park 03.08.11 For the last 30 years classification MPGN is based on glomerular findings by light microscopy with further specification on EM and staining for Ig and complement
C3 GLOMERULOPATHIES. Budapest Nephrology School Zoltan Laszik
 C3 GLOMERULOPATHIES Budapest Nephrology School 8.30.2018. Zoltan Laszik 1 Learning Objectives Familiarize with the pathogenetic mechanisms of glomerular diseases Learn the pathologic landscape and clinical
C3 GLOMERULOPATHIES Budapest Nephrology School 8.30.2018. Zoltan Laszik 1 Learning Objectives Familiarize with the pathogenetic mechanisms of glomerular diseases Learn the pathologic landscape and clinical
Familial DDD associated with a gain-of-function mutation in complement C3.
 Familial DDD associated with a gain-of-function mutation in complement C3. Santiago Rodríguez de Córdoba, Centro de investigaciones Biológicas, Madrid Valdés Cañedo F. and Vázquez- Martul E., Complejo
Familial DDD associated with a gain-of-function mutation in complement C3. Santiago Rodríguez de Córdoba, Centro de investigaciones Biológicas, Madrid Valdés Cañedo F. and Vázquez- Martul E., Complejo
Complement in vasculitis and glomerulonephritis. Andy Rees Clinical Institute of Pathology Medical University of Vienna
 Complement in vasculitis and glomerulonephritis Andy Rees Clinical Institute of Pathology Medical University of Vienna 41 st Heidelberg Nephrology Seminar March 2017 The complement system An evolutionary
Complement in vasculitis and glomerulonephritis Andy Rees Clinical Institute of Pathology Medical University of Vienna 41 st Heidelberg Nephrology Seminar March 2017 The complement system An evolutionary
A clinical syndrome, composed mainly of:
 Nephritic syndrome We will discuss: 1)Nephritic syndrome: -Acute postinfectious (poststreptococcal) GN -IgA nephropathy -Hereditary nephritis 2)Rapidly progressive GN (RPGN) A clinical syndrome, composed
Nephritic syndrome We will discuss: 1)Nephritic syndrome: -Acute postinfectious (poststreptococcal) GN -IgA nephropathy -Hereditary nephritis 2)Rapidly progressive GN (RPGN) A clinical syndrome, composed
From MPGN to C3G. F Fakhouri, Nantes, France. «Membranoproliferative» is a pathological feature. Mesangial expansion «Doubles contours»
 From MPGN to C3G F Fakhouri, Nantes, France Conflits d intérêt: consultant auprès d Alexion Pharmaceuticals «Membranoproliferative» is a pathological feature Mesangial expansion «Doubles contours» Immune
From MPGN to C3G F Fakhouri, Nantes, France Conflits d intérêt: consultant auprès d Alexion Pharmaceuticals «Membranoproliferative» is a pathological feature Mesangial expansion «Doubles contours» Immune
Suvasini Modi Complement System Activation of Membrane attacking complex (MAC) and its effect and regulation
 Figure- 1 https://en.wikipedia.org/wiki/complement_system Suvasini Modi Complement System Activation of Membrane attacking complex (MAC) and its effect and regulation Content Introduction Activation of
Figure- 1 https://en.wikipedia.org/wiki/complement_system Suvasini Modi Complement System Activation of Membrane attacking complex (MAC) and its effect and regulation Content Introduction Activation of
History. Chapter 13. Complement Components. Complement Pathways
 History Chapter 13 Complement Jules Border in 1890 s discovered complement Paul Ehrlich coined the term complement The activity of blood serum that completes the action of antibody Now: Set of serum proteins
History Chapter 13 Complement Jules Border in 1890 s discovered complement Paul Ehrlich coined the term complement The activity of blood serum that completes the action of antibody Now: Set of serum proteins
Complement. History. Chapter 7. Complement Components. Complement Pathways. Pathways of complement activation
 History Chapter 7 Complement Jules Border in 1890 s discovered complement Paul Ehrlich coined the term complement The activity of blood serum that completes the action of antibody Now: Set of serum proteins
History Chapter 7 Complement Jules Border in 1890 s discovered complement Paul Ehrlich coined the term complement The activity of blood serum that completes the action of antibody Now: Set of serum proteins
Case Presentation Turki Al-Hussain, MD
 Case Presentation Turki Al-Hussain, MD Director, Renal Pathology Chapter Saudi Society of Nephrology & Transplantation Consultant Nephropathologist & Urological Pathologist Department of Pathology & Laboratory
Case Presentation Turki Al-Hussain, MD Director, Renal Pathology Chapter Saudi Society of Nephrology & Transplantation Consultant Nephropathologist & Urological Pathologist Department of Pathology & Laboratory
History. Chapter 13. Complement Components. Complement Pathways
 History Chapter 13 Complement Jules Border in 1890 s discovered complement Paul Ehrlich coined the term complement The activity of blood serum that completes the action of antibody Now: Set of serum proteins
History Chapter 13 Complement Jules Border in 1890 s discovered complement Paul Ehrlich coined the term complement The activity of blood serum that completes the action of antibody Now: Set of serum proteins
Topic (6): The Complement System
 Topic (6): The Complement System Introduction The complement system is a complex system of many different glycoproteins. It comprises several plasma proteins that sequentially activate each other by proteolytic
Topic (6): The Complement System Introduction The complement system is a complex system of many different glycoproteins. It comprises several plasma proteins that sequentially activate each other by proteolytic
C1q nephropathy the Diverse Disease
 C1q nephropathy the Diverse Disease Danica Galešić Ljubanović School of Medicine, University of Zagreb Dubrava University Hospital Zagreb, Croatia Definition Dominant or codominant ( 2+), mesangial staining
C1q nephropathy the Diverse Disease Danica Galešić Ljubanović School of Medicine, University of Zagreb Dubrava University Hospital Zagreb, Croatia Definition Dominant or codominant ( 2+), mesangial staining
C3G An Update What is C3 Glomerulopathy Anyway? Patrick D. Walker, M.D. Nephropath Little Rock, Arkansas USA
 C3G An Update What is C3 Glomerulopathy Anyway? Patrick D. Walker, M.D. Nephropath Little Rock, Arkansas USA C3 Glomerulopathy Overview Discuss C3 Glomerulopathy (C3G) How did we get to the current classification
C3G An Update What is C3 Glomerulopathy Anyway? Patrick D. Walker, M.D. Nephropath Little Rock, Arkansas USA C3 Glomerulopathy Overview Discuss C3 Glomerulopathy (C3G) How did we get to the current classification
Review Article Kidney Diseases Caused by Complement Dysregulation: Acquired, Inherited, and Still More to Come
 Clinical and Developmental Immunology Volume 2012, Article ID 695131, 6 pages doi:10.1155/2012/695131 Review Article Kidney Diseases Caused by Complement Dysregulation: Acquired, Inherited, and Still More
Clinical and Developmental Immunology Volume 2012, Article ID 695131, 6 pages doi:10.1155/2012/695131 Review Article Kidney Diseases Caused by Complement Dysregulation: Acquired, Inherited, and Still More
R. Coward has documented that he has received cooperative grants from Takeda and Novo Nordisk
 R. Coward has documented that he has received cooperative grants from Takeda and Novo Nordisk Advances in our understanding of the pathogenesis of glomerular thrombotic microangiopathy Lindsay Keir Richard
R. Coward has documented that he has received cooperative grants from Takeda and Novo Nordisk Advances in our understanding of the pathogenesis of glomerular thrombotic microangiopathy Lindsay Keir Richard
Membranoproliferative glomerulonephritis and C3 glomerulopathy: resolving the confusion
 http://www.kidney-international.org & 2012 International Society of Nephrology Membranoproliferative glomerulonephritis and C3 glomerulopathy: resolving the confusion Sanjeev Sethi 1, Carla M. Nester 2,3,4
http://www.kidney-international.org & 2012 International Society of Nephrology Membranoproliferative glomerulonephritis and C3 glomerulopathy: resolving the confusion Sanjeev Sethi 1, Carla M. Nester 2,3,4
Glomerular diseases mostly presenting with Nephritic syndrome
 Glomerular diseases mostly presenting with Nephritic syndrome 1 The Nephritic Syndrome Pathogenesis: proliferation of the cells in glomeruli & leukocytic infiltrate Injured capillary walls escape of RBCs
Glomerular diseases mostly presenting with Nephritic syndrome 1 The Nephritic Syndrome Pathogenesis: proliferation of the cells in glomeruli & leukocytic infiltrate Injured capillary walls escape of RBCs
Target cell lysis Opsonization Activation of the inflammatory response (e.g. degranulation, extravasation) Clearance of immune complexes
 Immunology Dr. John J. Haddad Chapter 13 Complement Major roles of complement (Figure 13-1): Target cell lysis Opsonization Activation of the inflammatory response (e.g. degranulation, extravasation) Clearance
Immunology Dr. John J. Haddad Chapter 13 Complement Major roles of complement (Figure 13-1): Target cell lysis Opsonization Activation of the inflammatory response (e.g. degranulation, extravasation) Clearance
THE COMPLEMENT SYSTEM OBJECTIVES:
 Dr Mohammed Al- ani THE COMPLEMENT SYSTEM OBJECTIVES: When you finish this section, you should be able to: 1. Describe the effects of complement activation. 2. Outline the Classical, Mannan-Binding (MB)
Dr Mohammed Al- ani THE COMPLEMENT SYSTEM OBJECTIVES: When you finish this section, you should be able to: 1. Describe the effects of complement activation. 2. Outline the Classical, Mannan-Binding (MB)
Introduction. A system of soluble enzymes and proteins. Complement components: C1 to C9, B, D and P
 Complement Introduction A system of soluble enzymes and proteins Complement components: C1 to C9, B, D and P When activated, each component is split into small and large (major) fragments a b *A horizontal
Complement Introduction A system of soluble enzymes and proteins Complement components: C1 to C9, B, D and P When activated, each component is split into small and large (major) fragments a b *A horizontal
Anastasios E. Germenis
 Anastasios E. Germenis Professor and Chairman Department of Immunology & Histocompatibility School of Medicine University of Thessaly University Hospital of Larissa Greece agermen@med.uth.gr The Complement
Anastasios E. Germenis Professor and Chairman Department of Immunology & Histocompatibility School of Medicine University of Thessaly University Hospital of Larissa Greece agermen@med.uth.gr The Complement
C3 Glomerulopathy. Rezan Topaloglu, MD Hacettepe University School of Medicine Department of Pediatric Nephrology Ankara, TURKEY
 C3 Glomerulopathy Rezan Topaloglu, MD Hacettepe University School of Medicine Department of Pediatric Nephrology Ankara, TURKEY Journey in history Some diseases have journey Diagnoses may change during
C3 Glomerulopathy Rezan Topaloglu, MD Hacettepe University School of Medicine Department of Pediatric Nephrology Ankara, TURKEY Journey in history Some diseases have journey Diagnoses may change during
Recurrence of C3G after renal transplantation. Moglie Le Quintrec Service de Néphrologie, Hôpital Foch CRC, UMRS 1138, Equipe complement and diseases
 Recurrence of C3G after renal transplantation Moglie Le Quintrec Service de Néphrologie, Hôpital Foch CRC, UMRS 1138, Equipe complement and diseases New MPGN classification C3G MPGN I DDD C3GN IF C3 deposits
Recurrence of C3G after renal transplantation Moglie Le Quintrec Service de Néphrologie, Hôpital Foch CRC, UMRS 1138, Equipe complement and diseases New MPGN classification C3G MPGN I DDD C3GN IF C3 deposits
Toward a working definition of C3 glomerulopathy by immunofluorescence
 http://www.kidney-international.org & 2013 International Society of Nephrology Toward a working definition of C3 glomerulopathy by immunofluorescence Jean Hou 1, Glen S. Markowitz 1, Andrew S. Bomback
http://www.kidney-international.org & 2013 International Society of Nephrology Toward a working definition of C3 glomerulopathy by immunofluorescence Jean Hou 1, Glen S. Markowitz 1, Andrew S. Bomback
Glomerular pathology-2 Nephritic syndrome. Dr. Nisreen Abu Shahin
 Glomerular pathology-2 Nephritic syndrome Dr. Nisreen Abu Shahin 1 The Nephritic Syndrome Pathogenesis: inflammation proliferation of the cells in glomeruli & leukocytic infiltrate Injured capillary walls
Glomerular pathology-2 Nephritic syndrome Dr. Nisreen Abu Shahin 1 The Nephritic Syndrome Pathogenesis: inflammation proliferation of the cells in glomeruli & leukocytic infiltrate Injured capillary walls
Complement pathways: Classical pathway Alternative pathway Lectin pathway
 Complement Complement pathways: Classical pathway Alternative pathway Lectin pathway Complement proteins Classical pathway C1q C1r C1s C4 C2 Alternative pathway D C3 B Lectin pathway MBL MASP-1 MASP-2
Complement Complement pathways: Classical pathway Alternative pathway Lectin pathway Complement proteins Classical pathway C1q C1r C1s C4 C2 Alternative pathway D C3 B Lectin pathway MBL MASP-1 MASP-2
Mayo Clinic/ RPS Consensus Report on Classification, Diagnosis, and Reporting of Glomerulonephritis
 Mayo Clinic/ RPS Consensus Report on Classification, Diagnosis, and Reporting of Glomerulonephritis Sanjeev Sethi, MD, PhD Department of Laboratory Medicine and Pathology Disclosure Relevant Financial
Mayo Clinic/ RPS Consensus Report on Classification, Diagnosis, and Reporting of Glomerulonephritis Sanjeev Sethi, MD, PhD Department of Laboratory Medicine and Pathology Disclosure Relevant Financial
THE COMPLEMENT SYSTEM OBJECTIVES:
 THE COMPLEMENT SYSTEM OBJECTIVES: When you finish this section, you should be able to: 1. Describe the effects of complement activation. 2. Outline the Classical, Mannan-Binding (MB) Lectin and Alternative
THE COMPLEMENT SYSTEM OBJECTIVES: When you finish this section, you should be able to: 1. Describe the effects of complement activation. 2. Outline the Classical, Mannan-Binding (MB) Lectin and Alternative
RECURRENT AND DE NOVO RENAL DISEASES IN THE ALLOGRAFT. J. H. Helderman,MD,FACP,FAST
 RECURRENT AND DE NOVO RENAL DISEASES IN THE ALLOGRAFT J. H. Helderman,MD,FACP,FAST Vanderbilt University Medical Center Professor of Medicine, Pathology and Immunology Medical Director, Vanderbilt Transplant
RECURRENT AND DE NOVO RENAL DISEASES IN THE ALLOGRAFT J. H. Helderman,MD,FACP,FAST Vanderbilt University Medical Center Professor of Medicine, Pathology and Immunology Medical Director, Vanderbilt Transplant
CD B T NK NKT!! 1
 CD B T NK NKT!! 1 2 !! 3 4 5 6 7 8 9 10 11 Biological effects of C5a 12 13 Opsonization and phagocytosis 14 15 http://www.med.sc.edu:85/book/wel come.htm 16 http://www.med.sc.edu:85/book/im munol-sta.htm
CD B T NK NKT!! 1 2 !! 3 4 5 6 7 8 9 10 11 Biological effects of C5a 12 13 Opsonization and phagocytosis 14 15 http://www.med.sc.edu:85/book/wel come.htm 16 http://www.med.sc.edu:85/book/im munol-sta.htm
Year 2004 Paper one: Questions supplied by Megan
 QUESTION 53 Endothelial cell pathology on renal biopsy is most characteristic of which one of the following diagnoses? A. Pre-eclampsia B. Haemolytic uraemic syndrome C. Lupus nephritis D. Immunoglobulin
QUESTION 53 Endothelial cell pathology on renal biopsy is most characteristic of which one of the following diagnoses? A. Pre-eclampsia B. Haemolytic uraemic syndrome C. Lupus nephritis D. Immunoglobulin
Glomerular pathology in systemic disease
 Glomerular pathology in systemic disease Lecture outline Lupus nephritis Diabetic nephropathy Glomerulonephritis Associated with Bacterial Endocarditis and Other Systemic Infections Henoch-Schonlein Purpura
Glomerular pathology in systemic disease Lecture outline Lupus nephritis Diabetic nephropathy Glomerulonephritis Associated with Bacterial Endocarditis and Other Systemic Infections Henoch-Schonlein Purpura
Complement: History. Discovered in 1894 by Bordet. It represents lytic activity of fresh serum
 Complement: History Discovered in 1894 by Bordet It represents lytic activity of fresh serum Its lytic activity destroyed when heated at 56C for 30 min Complement functions Host benefit: opsonization to
Complement: History Discovered in 1894 by Bordet It represents lytic activity of fresh serum Its lytic activity destroyed when heated at 56C for 30 min Complement functions Host benefit: opsonization to
Complement System. Jil Schrader 16 th of May 2018 Immunology Lecture
 Source: https://bestprac.dk/2017/05/30/diagnosticering-af-almindelig-variabel-immundefekt-cvid-2/, letzter Zugriff: 14.05.2018 Complement System Jil Schrader 16 th of May 2018 Immunology Lecture Contents
Source: https://bestprac.dk/2017/05/30/diagnosticering-af-almindelig-variabel-immundefekt-cvid-2/, letzter Zugriff: 14.05.2018 Complement System Jil Schrader 16 th of May 2018 Immunology Lecture Contents
Complement deficiencies, diagnosis and management. Contents
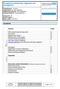 Complement deficiencies, diagnosis and management Classification: Protocol Lead Author: Dr Hana Alachkar Additional author(s): Victoria Blakeley Authors Division: Tertiary Medicine Unique ID: D5 Issue
Complement deficiencies, diagnosis and management Classification: Protocol Lead Author: Dr Hana Alachkar Additional author(s): Victoria Blakeley Authors Division: Tertiary Medicine Unique ID: D5 Issue
Basic Immunology. Lecture 16th. Complement system
 Basic Immunology Lecture 16th Complement system Components: Inactive factors in the serum and body fluids which can activate each other in an enzyme cascade Cell surface receptors (CR) for binding the
Basic Immunology Lecture 16th Complement system Components: Inactive factors in the serum and body fluids which can activate each other in an enzyme cascade Cell surface receptors (CR) for binding the
Case 3. ACCME/Disclosure. Laboratory results. Clinical history 4/13/2016
 Case 3 Lynn D. Cornell, M.D. Mayo Clinic, Rochester, MN Cornell.Lynn@mayo.edu USCAP Renal Case Conference March 13, 2016 ACCME/Disclosure Dr. Cornell has nothing to disclose Clinical history 57-year-old
Case 3 Lynn D. Cornell, M.D. Mayo Clinic, Rochester, MN Cornell.Lynn@mayo.edu USCAP Renal Case Conference March 13, 2016 ACCME/Disclosure Dr. Cornell has nothing to disclose Clinical history 57-year-old
Dense deposit disease with steroid pulse therapy
 Case Report Dense deposit disease with steroid pulse therapy Jun Odaka, Takahiro Kanai, Takane Ito, Takashi Saito, Jun Aoyagi, and Mariko Y Momoi Abstract Treatment of dense deposit disease DDD has not
Case Report Dense deposit disease with steroid pulse therapy Jun Odaka, Takahiro Kanai, Takane Ito, Takashi Saito, Jun Aoyagi, and Mariko Y Momoi Abstract Treatment of dense deposit disease DDD has not
Catalog Number: A114 Sizes Available: 250 µg/vial Concentration: 1.0 mg/ml (see Certificate of Analysis for actual concentration)
 Name: C3b Catalog Number: A114 Sizes Available: 250 µg/vial Concentration: 1.0 mg/ml (see Certificate of Analysis for actual concentration) Form: Liquid Purity: >90% by SDS-PAGE Buffer: 10 mm sodium phosphate,
Name: C3b Catalog Number: A114 Sizes Available: 250 µg/vial Concentration: 1.0 mg/ml (see Certificate of Analysis for actual concentration) Form: Liquid Purity: >90% by SDS-PAGE Buffer: 10 mm sodium phosphate,
Advances in Membranous and Membranoproliferative glomerulonephritis: Insights into Pathogenesis
 Advances in Membranous and Membranoproliferative glomerulonephritis: Insights into Pathogenesis Terry Cook, Imperial College, London Membranous Glomerulonephritis Membranous glomerulonephritis is characterised
Advances in Membranous and Membranoproliferative glomerulonephritis: Insights into Pathogenesis Terry Cook, Imperial College, London Membranous Glomerulonephritis Membranous glomerulonephritis is characterised
W J N. World Journal of Nephrology. Complement involvement in kidney diseases: From physiopathology to therapeutical targeting.
 W J N World Journal of Nephrology Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.5527/wjn.v4.i2.169 World J Nephrol 2015 May 6; 4(2): 169-184
W J N World Journal of Nephrology Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.5527/wjn.v4.i2.169 World J Nephrol 2015 May 6; 4(2): 169-184
H. Terence Cook. REVIEW C3 glomerulopathy [version 1; referees: 4 approved] Open Peer Review. Referee Status:
![H. Terence Cook. REVIEW C3 glomerulopathy [version 1; referees: 4 approved] Open Peer Review. Referee Status: H. Terence Cook. REVIEW C3 glomerulopathy [version 1; referees: 4 approved] Open Peer Review. Referee Status:](/thumbs/94/119185743.jpg) REVIEW C3 glomerulopathy [version 1; referees: 4 approved] H. Terence Cook Department of Medicine, Imperial College London, Hammersmith, London, UK v1 First published: 10 Mar 2017, 6(F1000 Faculty Rev):248
REVIEW C3 glomerulopathy [version 1; referees: 4 approved] H. Terence Cook Department of Medicine, Imperial College London, Hammersmith, London, UK v1 First published: 10 Mar 2017, 6(F1000 Faculty Rev):248
M.Weitz has documented that he has no relevant financial relationships to disclose or conflict of interest to resolve.
 M.Weitz has documented that he has no relevant financial relationships to disclose or conflict of interest to resolve. Prophylactic eculizumab prior to kidney transplantation for atypical hemolytic uremic
M.Weitz has documented that he has no relevant financial relationships to disclose or conflict of interest to resolve. Prophylactic eculizumab prior to kidney transplantation for atypical hemolytic uremic
االستاذ المساعد الدكتور خالد ياسين الزاملي \مناعة \المرحلة الثانية \ التحليالت المرضية \ المعهد التقني كوت
 Complement System The term complement refers to the ability of a system of some nonspecific proteins in normal human serum to complement, i.e., augment the effects of other components of immune system,
Complement System The term complement refers to the ability of a system of some nonspecific proteins in normal human serum to complement, i.e., augment the effects of other components of immune system,
Long-term follow-up of juvenile acute nonproliferative glomerulitis (JANG)
 Pediatr Nephrol (2007) 22:1957 1961 DOI 10.1007/s00467-007-0555-6 BRIEF REPORT Long-term follow-up of juvenile acute nonproliferative glomerulitis (JANG) Teruo Fujita & Kandai Nozu & Kazumoto Iijima &
Pediatr Nephrol (2007) 22:1957 1961 DOI 10.1007/s00467-007-0555-6 BRIEF REPORT Long-term follow-up of juvenile acute nonproliferative glomerulitis (JANG) Teruo Fujita & Kandai Nozu & Kazumoto Iijima &
Complement Elizabeth Repasky, PhD Fall, 2015
 Complement Elizabeth Repasky, PhD Fall, 2015 Complement pathways: Classical pathway Alternative pathway Lectin pathway White Board Schematic C3 plays a central role in complement activation Complement
Complement Elizabeth Repasky, PhD Fall, 2015 Complement pathways: Classical pathway Alternative pathway Lectin pathway White Board Schematic C3 plays a central role in complement activation Complement
C3 glomerulopathy: consensus report
 http://www.kidney-international.org & 2013 International Society of Nephrology OPEN C3 glomerulopathy: consensus report Matthew C. Pickering 1, Vivette D. D Agati 2, Carla M. Nester 3,4, Richard J. Smith
http://www.kidney-international.org & 2013 International Society of Nephrology OPEN C3 glomerulopathy: consensus report Matthew C. Pickering 1, Vivette D. D Agati 2, Carla M. Nester 3,4, Richard J. Smith
Overview of glomerular diseases
 Overview of glomerular diseases *Endothelial cells are fenestrated each fenestra: 70-100nm in diameter Contractile, capable of proliferation, makes ECM & releases mediators *Glomerular basement membrane
Overview of glomerular diseases *Endothelial cells are fenestrated each fenestra: 70-100nm in diameter Contractile, capable of proliferation, makes ECM & releases mediators *Glomerular basement membrane
Recent advances in pathogenesis & treatment of ahus
 Recent advances in pathogenesis & treatment of ahus Miquel Blasco Pelicano Nephrology and Kidney Transplant Unit Hospital Clínic, Barcelona Atypical Hemolytic Uremic Syndrome (ahus) Ultra-rare disease:
Recent advances in pathogenesis & treatment of ahus Miquel Blasco Pelicano Nephrology and Kidney Transplant Unit Hospital Clínic, Barcelona Atypical Hemolytic Uremic Syndrome (ahus) Ultra-rare disease:
Atypical Hemolytic Uremic Syndrome: When the Environment and Mutations Affect Organ Systems. A Case Report with Review of Literature
 Atypical Hemolytic Uremic Syndrome: When the Environment and Mutations Affect Organ Systems. A Case Report with Review of Literature Mouhanna Abu Ghanimeh 1, Omar Abughanimeh 1, Ayman Qasrawi 1, Abdulraheem
Atypical Hemolytic Uremic Syndrome: When the Environment and Mutations Affect Organ Systems. A Case Report with Review of Literature Mouhanna Abu Ghanimeh 1, Omar Abughanimeh 1, Ayman Qasrawi 1, Abdulraheem
Spectrum of complement-mediated thrombotic microangiopathies after kidney transplantation
 Spectrum of complement-mediated thrombotic microangiopathies after kidney transplantation Marius Miglinas Vilnius university hospital: Nephrology center, Center of Rare Kidney Diseases Vilnius university
Spectrum of complement-mediated thrombotic microangiopathies after kidney transplantation Marius Miglinas Vilnius university hospital: Nephrology center, Center of Rare Kidney Diseases Vilnius university
29th Annual Meeting of the Glomerular Disease Collaborative Network
 29th Annual Meeting of the Glomerular Disease Collaborative Network Updates on the Pathogenesis IgA Nephropathy and IgA Vasculitis (HSP) J. Charles Jennette, M.D. Brinkhous Distinguished Professor and
29th Annual Meeting of the Glomerular Disease Collaborative Network Updates on the Pathogenesis IgA Nephropathy and IgA Vasculitis (HSP) J. Charles Jennette, M.D. Brinkhous Distinguished Professor and
Case Presentation Turki Al-Hussain, MD
 Case Presentation Turki Al-Hussain, MD Director, Renal Pathology Chapter Saudi Society of Nephrology & Transplantation Consultant Nephropathologist & Urological Pathologist Department of Pathology & Laboratory
Case Presentation Turki Al-Hussain, MD Director, Renal Pathology Chapter Saudi Society of Nephrology & Transplantation Consultant Nephropathologist & Urological Pathologist Department of Pathology & Laboratory
Hemolytic uremic syndrome: Investigations and management
 Hemolytic uremic syndrome: Investigations and management SAWAI Toshihiro M.D., Ph.D. Department of Pediatrics, Shiga University of Medical Science Otsu, JAPAN AGENDA TMA; Thrombotic micro angiopathy STEC-HUS;
Hemolytic uremic syndrome: Investigations and management SAWAI Toshihiro M.D., Ph.D. Department of Pediatrics, Shiga University of Medical Science Otsu, JAPAN AGENDA TMA; Thrombotic micro angiopathy STEC-HUS;
The term complement refers to the ability of a system of some nonspecific proteins in normal human serum to complement, i.e., augment the effects of
 COMPLEMENT SYSTEM The term complement refers to the ability of a system of some nonspecific proteins in normal human serum to complement, i.e., augment the effects of other components of immune system,
COMPLEMENT SYSTEM The term complement refers to the ability of a system of some nonspecific proteins in normal human serum to complement, i.e., augment the effects of other components of immune system,
Article. Eculizumab for Dense Deposit Disease and C3 Glomerulonephritis
 CJASN epress. Published on March 8, 2012 as doi: 10.2215/CJN.12901211 Article Eculizumab for Dense Deposit Disease and C3 Glomerulonephritis Andrew S. Bomback,* Richard J. Smith, Gaetano R. Barile, Yuzhou
CJASN epress. Published on March 8, 2012 as doi: 10.2215/CJN.12901211 Article Eculizumab for Dense Deposit Disease and C3 Glomerulonephritis Andrew S. Bomback,* Richard J. Smith, Gaetano R. Barile, Yuzhou
Classification of Glomerular Diseases and Defining Individual Glomerular Lesions: Developing International Consensus
 Classification of Glomerular Diseases and Defining Individual Glomerular Lesions: Developing International Consensus Mark Haas MD, PhD Department of Pathology & Laboratory Medicine Cedars-Sinai Medical
Classification of Glomerular Diseases and Defining Individual Glomerular Lesions: Developing International Consensus Mark Haas MD, PhD Department of Pathology & Laboratory Medicine Cedars-Sinai Medical
Biology of Fc γ Receptors. Selected Functions of Ig Isotypes
 Biology of Fc γ Receptors Selected Functions of Ig Isotypes Biology of Fc γ Receptors 1 Functional Sites on the IgG Molecule V H V L C1q binding site FcγR binding site Glycosylation site Selected Functions
Biology of Fc γ Receptors Selected Functions of Ig Isotypes Biology of Fc γ Receptors 1 Functional Sites on the IgG Molecule V H V L C1q binding site FcγR binding site Glycosylation site Selected Functions
Atypical hemolytic uremic syndrome. Diana Karpman Department of Pediatrics Lund University
 Atypical hemolytic uremic syndrome Diana Karpman Department of Pediatrics Lund University Image courtesy of Dr. Sabine Leh, Haukeland University Hospital, Bergen Norway Hemolytic Uremic Syndrome Non-immune
Atypical hemolytic uremic syndrome Diana Karpman Department of Pediatrics Lund University Image courtesy of Dr. Sabine Leh, Haukeland University Hospital, Bergen Norway Hemolytic Uremic Syndrome Non-immune
بسم هللا الرحمن الرحيم. Immunology lecture 7
 بسم هللا الرحمن الرحيم Immunology lecture 7 Last time we studied the B cell receptor which is IgM & IgD. Today we will talk about the T Cell Receptor which is the TCR #TCR: it is the receptor that belongs
بسم هللا الرحمن الرحيم Immunology lecture 7 Last time we studied the B cell receptor which is IgM & IgD. Today we will talk about the T Cell Receptor which is the TCR #TCR: it is the receptor that belongs
C3 Glomerulopathy: Clinicopathologic Features and Predictors of Outcome
 CJASN epress. Published on October 31, 2013 as doi: 10.2215/CJN.04700513 Article C3 Glomerulopathy: Clinicopathologic Features and Predictors of Outcome Nicholas R. Medjeral-Thomas,* Michelle M. O Shaughnessy,
CJASN epress. Published on October 31, 2013 as doi: 10.2215/CJN.04700513 Article C3 Glomerulopathy: Clinicopathologic Features and Predictors of Outcome Nicholas R. Medjeral-Thomas,* Michelle M. O Shaughnessy,
Thrombotic Microangiopathies (TMA) / TTP/HUS/αHUS Pathology & Molecular. Genetics
 Thrombotic Microangiopathies (TMA) / TTP/HUS/αHUS Pathology & Molecular Genetics Helen Liapis, M.D. Senior Consultant Arkana Labs Professor of Pathology & Immunology. retired Washington University School
Thrombotic Microangiopathies (TMA) / TTP/HUS/αHUS Pathology & Molecular Genetics Helen Liapis, M.D. Senior Consultant Arkana Labs Professor of Pathology & Immunology. retired Washington University School
Clinical Findings, Pathology, and Outcomes of C3GN after Kidney Transplantation
 CLINICAL RESEARCH www.jasn.org Clinical Findings, Pathology, and Outcomes of C3GN after Kidney ation Ladan Zand,* Elizabeth C. Lorenz,* Fernando G. Cosio,* Fernando C. Fervenza,* Samih H. Nasr, Manish
CLINICAL RESEARCH www.jasn.org Clinical Findings, Pathology, and Outcomes of C3GN after Kidney ation Ladan Zand,* Elizabeth C. Lorenz,* Fernando G. Cosio,* Fernando C. Fervenza,* Samih H. Nasr, Manish
Interesting case seminar: Native kidneys Case Report:
 Interesting case seminar: Native kidneys Case Report: Proximal tubulopathy and light chain deposition disease presented as severe pulmonary hypertension with right-sided cardiac dysfunction and nephrotic
Interesting case seminar: Native kidneys Case Report: Proximal tubulopathy and light chain deposition disease presented as severe pulmonary hypertension with right-sided cardiac dysfunction and nephrotic
Monoclonal Gammopathies and the Kidney. Tibor Nádasdy, MD The Ohio State University, Columbus, OH
 Monoclonal Gammopathies and the Kidney Tibor Nádasdy, MD The Ohio State University, Columbus, OH Monoclonal gammopathy of renal significance (MGRS) Biopsies at OSU (n=475) between 2007 and 2016 AL or AH
Monoclonal Gammopathies and the Kidney Tibor Nádasdy, MD The Ohio State University, Columbus, OH Monoclonal gammopathy of renal significance (MGRS) Biopsies at OSU (n=475) between 2007 and 2016 AL or AH
RENAL HISTOPATHOLOGY
 RENAL HISTOPATHOLOGY Peter McCue, M.D. Department of Pathology, Anatomy & Cell Biology Sidney Kimmel Medical College There are no conflicts of interest. 1 Goals and Objectives! Goals Provide introduction
RENAL HISTOPATHOLOGY Peter McCue, M.D. Department of Pathology, Anatomy & Cell Biology Sidney Kimmel Medical College There are no conflicts of interest. 1 Goals and Objectives! Goals Provide introduction
Histopathology: Glomerulonephritis and other renal pathology
 Histopathology: Glomerulonephritis and other renal pathology These presentations are to help you identify basic histopathological features. They do not contain the additional factual information that you
Histopathology: Glomerulonephritis and other renal pathology These presentations are to help you identify basic histopathological features. They do not contain the additional factual information that you
Dr Ian Roberts Oxford. Oxford Pathology Course 2010 for FRCPath Illustration-Cellular Pathology. Oxford Radcliffe NHS Trust
 Dr Ian Roberts Oxford Oxford Pathology Course 2010 for FRCPath Present the basic diagnostic features of the commonest conditions causing proteinuria & haematuria Highlight diagnostic pitfalls Nephrotic
Dr Ian Roberts Oxford Oxford Pathology Course 2010 for FRCPath Present the basic diagnostic features of the commonest conditions causing proteinuria & haematuria Highlight diagnostic pitfalls Nephrotic
Lecture 17: Attack by Complement and Counterattack by Microbes
 Lecture 17: Attack by Complement and Counterattack by Microbes 2 Review Concepts of Complement Complement was addressed in Lecture 3 Major first line of defense (innate immunity) Major functions: Opsonization
Lecture 17: Attack by Complement and Counterattack by Microbes 2 Review Concepts of Complement Complement was addressed in Lecture 3 Major first line of defense (innate immunity) Major functions: Opsonization
Sugars and immune complex formation in IgA
 Glomerular disease Sugars and immune complex formation in IgA nephropathy Jonathan Barratt and Frank Eitner In vitro evidence suggests that immune complex formation in IgA nephropathy is determined by
Glomerular disease Sugars and immune complex formation in IgA nephropathy Jonathan Barratt and Frank Eitner In vitro evidence suggests that immune complex formation in IgA nephropathy is determined by
Membranoproliferative Glomerulonephritis
 Membranoproliferative Glomerulonephritis MPGN is characterizedby alterations in the GBM and mesangium and by proliferation of glomerular cells. 5% to 10% of cases of 1ry nephrotic syndrome in children
Membranoproliferative Glomerulonephritis MPGN is characterizedby alterations in the GBM and mesangium and by proliferation of glomerular cells. 5% to 10% of cases of 1ry nephrotic syndrome in children
Monoclonal gammopathies consist of. Monoclonal GammopathyeAssociated Proliferative Glomerulonephritis REVIEW
 REVIEW Monoclonal GammopathyeAssociated Proliferative Glomerulonephritis Sanjeev Sethi, MD, PhD, and S. Vincent Rajkumar, MD Abstract Monoclonal gammopathy is characterized by circulating monoclonal immunoglobulin
REVIEW Monoclonal GammopathyeAssociated Proliferative Glomerulonephritis Sanjeev Sethi, MD, PhD, and S. Vincent Rajkumar, MD Abstract Monoclonal gammopathy is characterized by circulating monoclonal immunoglobulin
Pathogenetic mechanisms in atypical HUS
 Pathogenetic mechanisms in atypical HUS Seppo Meri University & University Hospital Helsinki, Finland Antalya, Turkey Photo: Markku Kallio 21.10.2017 HUS after eating Kebab - 22 yo female - watery diarrhea
Pathogenetic mechanisms in atypical HUS Seppo Meri University & University Hospital Helsinki, Finland Antalya, Turkey Photo: Markku Kallio 21.10.2017 HUS after eating Kebab - 22 yo female - watery diarrhea
Complement disorders and hereditary angioedema
 Complement disorders and hereditary angioedema Michael M. Frank, MD Durham, NC The term complement was introduced more than 100 years ago to refer to a group of plasma factors important in host defense
Complement disorders and hereditary angioedema Michael M. Frank, MD Durham, NC The term complement was introduced more than 100 years ago to refer to a group of plasma factors important in host defense
Article. Proliferative Glomerulonephritis Secondary to Dysfunction of the Alternative Pathway of Complement
 Article Proliferative Glomerulonephritis Secondary to Dysfunction of the Alternative Pathway of Complement Sanjeev Sethi,* Fernando C. Fervenza, Yuzhou Zhang, Samih H. Nasr,* Nelson Leung, Julie Vrana,*
Article Proliferative Glomerulonephritis Secondary to Dysfunction of the Alternative Pathway of Complement Sanjeev Sethi,* Fernando C. Fervenza, Yuzhou Zhang, Samih H. Nasr,* Nelson Leung, Julie Vrana,*
Evidence Review: Title. Month/ Year. Evidence Review: Eculizumab in the treatment of recurrence of C3 glomerulopathy post-transplant
 Evidence Review: Title Month/ Year Evidence Review: Eculizumab in the treatment of recurrence of C glomerulopathy post-transplant October 2015 1 Standard Operating Procedure: NHS England Evidence Review:
Evidence Review: Title Month/ Year Evidence Review: Eculizumab in the treatment of recurrence of C glomerulopathy post-transplant October 2015 1 Standard Operating Procedure: NHS England Evidence Review:
Cellular & Molecular Immunology 2009
 Cellular & Molecular Immunology 2009 Complement Nicholas M. Ponzio, Ph.D. Department of Pathology & Laboratory Medicine March 4, 2009 Innate and adaptive immunity FAMOUS BELGIANS Jules Jean Baptiste Vincent
Cellular & Molecular Immunology 2009 Complement Nicholas M. Ponzio, Ph.D. Department of Pathology & Laboratory Medicine March 4, 2009 Innate and adaptive immunity FAMOUS BELGIANS Jules Jean Baptiste Vincent
A Case of Myeloma Kidney With Glomerular C3 Deposition
 Case Report World J Nephrol Urol. 2018;7(3-4):73-77 A Case of Myeloma Kidney With Glomerular C3 Deposition Asif Khan a, c, Khine Lam b, Suzanne El-Sayegh b, Elie El-Charabaty b Abstract Manuscript submitted
Case Report World J Nephrol Urol. 2018;7(3-4):73-77 A Case of Myeloma Kidney With Glomerular C3 Deposition Asif Khan a, c, Khine Lam b, Suzanne El-Sayegh b, Elie El-Charabaty b Abstract Manuscript submitted
HUS-MPGN-TTP. & related disorders
 ES-PCR 4 th International Conference HUS-MPGN-TTP & related disorders Current diagnosis and therapy of hemolytic uremic syndrome (HUS), membranoproliferative glomerulonephritis (MPGN), thrombotic thrombocytopenic
ES-PCR 4 th International Conference HUS-MPGN-TTP & related disorders Current diagnosis and therapy of hemolytic uremic syndrome (HUS), membranoproliferative glomerulonephritis (MPGN), thrombotic thrombocytopenic
New insights in thrombotic microangiopathies : TTP and ahus
 New insights in thrombotic microangiopathies : TTP and ahus Dr Catherine LAMBERT Hematology Cliniques universitaires Saint-Luc Catherine.lambert@uclouvain.be New insights in thrombotic microangiopathies
New insights in thrombotic microangiopathies : TTP and ahus Dr Catherine LAMBERT Hematology Cliniques universitaires Saint-Luc Catherine.lambert@uclouvain.be New insights in thrombotic microangiopathies
Lecture 07. Complement
 Lecture 07 Complement Science is a social process. It happens on a time scale longer than a human life. If I die, someone takes my place. You die; someone takes your place. What's important is to get it
Lecture 07 Complement Science is a social process. It happens on a time scale longer than a human life. If I die, someone takes my place. You die; someone takes your place. What's important is to get it
RENAL EVENING SPECIALTY CONFERENCE
 RENAL EVENING SPECIALTY CONFERENCE Harsharan K. Singh, MD The University of North Carolina at Chapel Hill Disclosure of Relevant Financial Relationships No conflicts of interest to disclose. CLINICAL HISTORY
RENAL EVENING SPECIALTY CONFERENCE Harsharan K. Singh, MD The University of North Carolina at Chapel Hill Disclosure of Relevant Financial Relationships No conflicts of interest to disclose. CLINICAL HISTORY
TMA CASE STUDY. Pamela Harmon, RN & Keturah Tomlin, RN Toronto General Hospital Apheresis Unit
 TMA CASE STUDY Pamela Harmon, RN & Keturah Tomlin, RN Toronto General Hospital Apheresis Unit Cumulative fraction of patients free of events ahus is a catastrophic disease that can result in sudden & progressive
TMA CASE STUDY Pamela Harmon, RN & Keturah Tomlin, RN Toronto General Hospital Apheresis Unit Cumulative fraction of patients free of events ahus is a catastrophic disease that can result in sudden & progressive
Accepted Manuscript. No more thrombotic thrombocytopenic purpura/hemolytic uremic syndrome please. Yeong-Hau H. Lien MD, PhD S (18)
 Accepted Manuscript No more thrombotic thrombocytopenic purpura/hemolytic uremic syndrome please Yeong-Hau H. Lien MD, PhD PII: S0002-9343(18)30965-3 DOI: https://doi.org/10.1016/j.amjmed.2018.10.009 Reference:
Accepted Manuscript No more thrombotic thrombocytopenic purpura/hemolytic uremic syndrome please Yeong-Hau H. Lien MD, PhD PII: S0002-9343(18)30965-3 DOI: https://doi.org/10.1016/j.amjmed.2018.10.009 Reference:
C3 glomerulopathy in cystic fibrosis: a case report
 Santoro et al. BMC Nephrology (2018) 19:73 https://doi.org/10.1186/s12882-018-0880-y CASE REPORT C3 glomerulopathy in cystic fibrosis: a case report Domenico Santoro 1*, Rossella Siligato 1, Carmela Vadalà
Santoro et al. BMC Nephrology (2018) 19:73 https://doi.org/10.1186/s12882-018-0880-y CASE REPORT C3 glomerulopathy in cystic fibrosis: a case report Domenico Santoro 1*, Rossella Siligato 1, Carmela Vadalà
Favorable effect of bortezomib in dense deposit disease associated with monoclonal gammopathy: a case report
 Hirashio et al. BMC Nephrology (2018) 19:108 https://doi.org/10.1186/s12882-018-0905-6 CASE REPORT Open Access Favorable effect of bortezomib in dense deposit disease associated with monoclonal gammopathy:
Hirashio et al. BMC Nephrology (2018) 19:108 https://doi.org/10.1186/s12882-018-0905-6 CASE REPORT Open Access Favorable effect of bortezomib in dense deposit disease associated with monoclonal gammopathy:
The Biology of Fc γ Receptors and Complement
 Discovery consists of seeing what everybody has seen, and thinking what nobody has thought --Albert Szent-György Nobel prize in Physiology or Medicine, 1937 The Biology of Fc γ Receptors and Complement
Discovery consists of seeing what everybody has seen, and thinking what nobody has thought --Albert Szent-György Nobel prize in Physiology or Medicine, 1937 The Biology of Fc γ Receptors and Complement
GOODPASTURE'S SYNDROME WITH CONCOMITANT IMMUNE COMPLEX MIXED MEMBRANOUS AND PROLIFERATIVE GLOMERULONEFRITIS
 GOODPASTURE'S SYNDROME WITH CONCOMITANT IMMUNE COMPLEX MIXED MEMBRANOUS AND PROLIFERATIVE GLOMERULONEFRITIS VESNA JURČIĆ 1, ANDREJA ALEŠ RIGLER 2, INSTITUTE OF PATHOLOGY, FACULTY OF MEDICINE, UNIVERSITY
GOODPASTURE'S SYNDROME WITH CONCOMITANT IMMUNE COMPLEX MIXED MEMBRANOUS AND PROLIFERATIVE GLOMERULONEFRITIS VESNA JURČIĆ 1, ANDREJA ALEŠ RIGLER 2, INSTITUTE OF PATHOLOGY, FACULTY OF MEDICINE, UNIVERSITY
Hemolytic uremic syndrome
 Hemolytic uremic syndrome Doyeun Oh Department of Internal Medicine CHA University School of Medicine Disclosures for Doyeun Oh Research Support/P.I. Employee Consultant Major Stockholder Speakers Bureau
Hemolytic uremic syndrome Doyeun Oh Department of Internal Medicine CHA University School of Medicine Disclosures for Doyeun Oh Research Support/P.I. Employee Consultant Major Stockholder Speakers Bureau
Clinicopathological analysis of proliferative glomerulonephritis with monoclonal IgG deposits in 5 renal allografts
 Wen et al. BMC Nephrology (2018) 19:173 https://doi.org/10.1186/s12882-018-0969-3 RESEARCH ARTICLE Open Access Clinicopathological analysis of proliferative glomerulonephritis with monoclonal IgG deposits
Wen et al. BMC Nephrology (2018) 19:173 https://doi.org/10.1186/s12882-018-0969-3 RESEARCH ARTICLE Open Access Clinicopathological analysis of proliferative glomerulonephritis with monoclonal IgG deposits
Name: Factor H Catalog Number: A137 Sizes Available: Concentration: Form: Activity: Purity: Buffer: Extinction Coeff.: Molecular weight:
 Name: Factor H Catalog Number: A137 Sizes Available: 250 µg/vial Concentration: 1.0 mg/ml (see Certificate of Analysis for actual concentration) Form: Frozen liquid Activity: >90% versus normal human serum
Name: Factor H Catalog Number: A137 Sizes Available: 250 µg/vial Concentration: 1.0 mg/ml (see Certificate of Analysis for actual concentration) Form: Frozen liquid Activity: >90% versus normal human serum
Pathogenesis of IgA Nephropathy. Shokoufeh Savaj MD Associate Professor of Medicine Firoozgar hospital- IUMS
 Pathogenesis of IgA Nephropathy Shokoufeh Savaj MD Associate Professor of Medicine Firoozgar hospital- IUMS History Immunoglobin A nephropathy was first described by Berger and Hinglais in 1968 in Paris
Pathogenesis of IgA Nephropathy Shokoufeh Savaj MD Associate Professor of Medicine Firoozgar hospital- IUMS History Immunoglobin A nephropathy was first described by Berger and Hinglais in 1968 in Paris
Attribution: University of Michigan Medical School, Department of Microbiology and Immunology
 Attribution: University of Michigan Medical School, Department of Microbiology and Immunology License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution
Attribution: University of Michigan Medical School, Department of Microbiology and Immunology License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution
Recurrent Idiopathic Membranous Glomerulonephritis After Kidney Transplantation and Successful Treatment With Rituximab
 TRANSPLANTATION Recurrent Idiopathic Membranous Glomerulonephritis After Kidney Transplantation and Successful Treatment With Rituximab Khadijeh Makhdoomi, 1,2 Saeed Abkhiz, 1,2 Farahnaz Noroozinia, 1,3
TRANSPLANTATION Recurrent Idiopathic Membranous Glomerulonephritis After Kidney Transplantation and Successful Treatment With Rituximab Khadijeh Makhdoomi, 1,2 Saeed Abkhiz, 1,2 Farahnaz Noroozinia, 1,3
CHAPTER 2. Primary Glomerulonephritis
 2nd Report of the PRIMARY GLOMERULONEPHRITIS CHAPTER 2 Primary Glomerulonephritis Sunita Bavanandan Lee Han Wei Lim Soo Kun 21 PRIMARY GLOMERULONEPHRITIS 2nd Report of the 2.1 Introduction This chapter
2nd Report of the PRIMARY GLOMERULONEPHRITIS CHAPTER 2 Primary Glomerulonephritis Sunita Bavanandan Lee Han Wei Lim Soo Kun 21 PRIMARY GLOMERULONEPHRITIS 2nd Report of the 2.1 Introduction This chapter
