Accuracy of ASGE criteria for the prediction of choledocholithiasis
|
|
|
- Victor Ball
- 6 years ago
- Views:
Transcription
1 /2016/108/6/ Revista Española de Enfermedades Digestivas Copyright 2016 Arán Ediciones, S. L. Rev Esp Enferm Dig (Madrid) Vol. 108, N.º 6, pp , 2016 ORIGINAL PAPERS Accuracy of ASGE criteria for the prediction of choledocholithiasis Rodrigo M. Narváez-Rivera, José A. González-González, Roberto Monreal-Robles, Diego García-Compean, Jonathan Paz-Delgadillo, Aldo A. Garza-Galindo and Héctor J. Maldonado-Garza Department of Gastroenterology and Gastrointestinal Endoscopy. Hospital Universitario Dr. José Eleuterio González. Universidad Autónoma de Nuevo León. Monterrey, México ABSTRACT Background/aims: Few studies have validated the performance of guidelines for the prediction of choledocholithiasis (CL). Our objective was to prospectively assess the accuracy of the American Society for Gastrointestinal Endoscopy (ASGE) guidelines for the identification of CL. Methods: A two-year prospective evaluation of patients with suspected CL was performed. We evaluated the ASGE guidelines and its component variables in predicting CL. Results: A total of 256 patients with suspected CL were analyzed. Of the 208 patients with high-probability criteria for CL, 124 (59.6%) were found to have a stone/sludge at endoscopic retrograde cholangiopancreatography (ERCP). Among 48 patients with intermediate-probability criteria, 21 (43.8%) had a stone/ sludge. The performance of ASGE high- and intermediate-probability criteria in our population had an accuracy of 59.0% (85.5% sensitivity, 24.3% specificity) and 41.0% (14.4% sensitivity, 75.6% specificity), respectively. The mean ERCP delay time was 6.1 days in the CL group and 6.4 days in the group without CL, p = The presence of a common bile duct (CBD) > 6 mm (OR 2.21; 95% CI, ), ascending cholangitis (OR 2.37; 95% CI, ) and a CBD stone visualized on transabdominal US (OR 3.33; 95% CI, ) were stronger predictors of CL. The occurrence of biliary pancreatitis was a strong protective factor for the presence of a retained CBD stone (OR 0.30; 95% CI, ). Conclusions: Irrespective of a patient s ASGE probability for CL, the application of current guidelines in our population led to unnecessary performance of ERCPs in nearly half of cases. Key words: Choledocholithiasis. Common bile duct stone. Endoscopic retrograde colangiopancreatography. Cholangitis. INTRODUCTION Common bile duct (CBD) stones are a frequent complication in symptomatic cholelithiasis (5-10%) (1,2) and biliary pancreatitis (18-33%) (3-5). Endoscopic retrograde cholangiopancreatography (ERCP) is considered as the gold standard for diagnosis and treatment of choledocholithiasis (CL). However, it carries a considerable risk of short-term complications such as post-ercp pancreatitis, post-endoscopic sphincterotomy bleeding, cholangitis and perforation (6). It has been previously stated that the cost-effectiveness is favorable only when performing ERCP in patients with a high likelihood of CL (7). In order to predict the likelihood of a persistent CBD stone in patients with suspected CL, the American Society for Gastrointestinal Endoscopy (ASGE) published guidelines in 2010 for the prediction of CL with the objective of identifying patients with the highest probability of benefiting from ERCP (8). They classified patients into three risk categories based on the presence of clinical, radiological and biochemical predictors. Patients with high probability of CL (defined as > 50% likelihood) were those with one of the following very strong predictors: CBD stone on transabdominal ultrasound (US), clinical ascending cholangitis or bilirubin > 4 mg/dl, or those with both of the following strong predictors: dilated CBD on US (> 6 mm with gallbladder in situ) and bilirubin level between mg/dl; patients with intermediate probability of CL (10-50% likelihood) were those with the presence of only one strong predictor or any moderate predictor (abnormal liver test, age older than 55 years or gallstone pancreatitis); and low probability of CL (< 10% likelihood) those with no predictors present. Recently, there has been some evidence from retrospective studies of the lack of accuracy of the ASGE guidelines for predicting choledocholithiasis (9). However, the performance of this risk score has not been prospectively validated. The aim of this prospective study was: a) to assess the performance of the existing guidelines on predicting CL in high- and intermediate-probability patients; and b) to Received: Accepted: Correspondence: José A González-González. Department of Gastroenterology and Gastrointestinal Endoscopy. Hospital Universitario Dr. José Eleuterio González. Universidad Autónoma de Nuevo León. Av. Madero y Gonzalitos, s/n Col. Mitras Centro Monterrey. Nuevo León, México alberto.gonzalez@uanl.edu.mx Narváez-Rivera RM, González-González JA, Monreal-Robles R, García-Compean D, Paz-Delgadillo J, Garza-Galindo AA, Maldonado-Garza HJ. Accuracy of ASGE criteria for the prediction of choledocholithiasis. Rev Esp Enferm Dig 2016;108:
2 310 R. M. NARVÁEZ-RIVERA ET AL. Rev Esp Enferm Dig (Madrid) evaluate the strength of association between single clinical and laboratory predictors and documented CL. PATIENTS AND METHODS Approval was obtained from the research and ethics committee of the School of Medicine and Hospital Universitario Dr. José E. González of the Universidad Autónoma de Nuevo León. Informed consent was obtained from all participants. The study was performed in compliance with the Declaration of Helsinki for biomedical research. We prospectively evaluated all patients admitted to our University Hospital with suspected CL that met ASGE high- and intermediate-probability criteria over a 2-year period, from March 1, 2012, to February 28, Suspected CL was considered when patients presented with upper abdominal pain and clinical manifestations (such as fever, jaundice), cholestatic pattern of liver injury, CBD dilatation (> 6 mm) or CBD stone visualization on transabdominal US. Study subjects were identified at admission by the gastroenterology residents based on the assessment of clinical, radiological and biochemical variables. Patients were excluded if any of the following conditions that might work as confounding factors were present: history of cholecystectomy (CBD diameter can be changed after cholecystectomy), biliary tract lesion, chronic liver disease (because basal function liver test may be altered) and previous ERCP sphincterotomy. We excluded patients classified by ASGE criteria as low-probability because their risk for CL is minimal (< 1%) and no further imaging or endoscopic study is indicated (10). Patients were classified into high- or intermediate-probability groups for CL according to ASGE guidelines based on initial biochemical liver tests, clinical suspicion of cholangitis, and transabdominal US variables (8). The high-probability group were subjects with the presence of any very strong predictor (CBD stone on abdominal US or clinical ascending cholangitis or bilirubin > 4 mg/dl) or both strong predictors (bilirubin level mg/dl + CBD on US > 6 mm). The intermediate-probability group was all other patients with the presence of only one strong predictor or any moderate predictor (abnormal liver test, age older than 55 years or gallstone pancreatitis). ERCP (the gold standard for diagnosis and treatment of CL) was performed on all patients in the study by two experienced endoscopists who performed around 250 ERCPs annually (endoscopists knew the ASGE probability of CL in each case). We considered an ERCP as positive when a filling defect was observed on cholangiogram or stones/sludge were photographed within the duodenal lumen after extraction. Statistical analysis Baseline characteristics of patients with and without CL as well as in those with and without biliary pancreatitis were compared with the use of Student s t-test or U Mann-Whitney depending on the distribution of continuous variables as appropriate, and Fisher s exact test for categorical variables. We calculated the sensitivity, specificity, positive and negative predictive values, accuracy, and positive and negative likelihood ratios of the ASGE classification on admission as well as the performance of individual predictors. Univariate and multivariate analysis with odds ratio (OR) and 95% confident interval (CI) were performed for all clinical predictors. The SPSS statistical software package (Version 20.0) was used for statistical analysis. RESULTS From March to February , 422 patients with suspected CL were assessed for eligibility (Fig. 1). After 166 patients were excluded, 256 eligible patients with intermediate- or high-probability for CL were included. The cohort mean age was 45.0 years (± 21.2); 193 (75.4%) were female patients. General characteristics, ultrasonography and biochemical variables among subjects with and without CL are shown in table I. No significant difference was found in the ERCP delay time between the group of patients with and without CL (p = 0.638). A subset of 208 patients met ASGE high probability-criteria on admission. Of these, 124 (59.6%) had CBD a stone/sludge on ERCP. Of the 48 patients that met ASGE intermediate-probability criteria on admission, 21 (43.8%) had CBD a stone/sludge on ERCP. The performance of ASGE high- and intermediate-probability criteria for CL in our population had an accuracy of 59.0% (85.5% sensitivity, 24.3% specificity) and 41.0% (14.4% sensitivity, 75.6% specificity), respectively. There was no statistically significant difference in the rate of CL detection between ASGE high- and intermediate-probability groups (p = 0.053). Performance of individual ASGE predictors Among the ASGE very strong predictors of CL, CBD stone on transabdominal US and clinical ascending cholangitis were the predictors with a statistical significance between subjects with and without CL on ERCP. Among strong predictors, only CBD size > 6 mm showed a statistical significance between groups (Table II). We also assessed the diagnostic performance of individual predictors for CL in both high- and intermediate-probability groups (Table III). Significance of biliary pancreatitis Eighty (31.2%) out of 256 patients in our study presented biliary pancreatitis. The identification of CL on ERCP in the subset of patients with biliary pancreatitis was 36.2% (29/80) compared with 65.9% (116/176) in those without pancreatitis, p < Of the 80 patients in our study with biliary pancreatitis, 63 patients (78.8%) met ASGE high-probability criteria for CL. Of these, 25 (39.7%) patients had a stone/sludge on ERCP. Of the 17 patients with biliary pancreatitis that met intermediate-probability criteria, 4 (23.5%) had CBD a stone/sludge on ERCP. The performance of ASGE high- and intermediate-probability criteria for CL in the subset of patients with biliary pancrea-
3 Vol. 108, N.º 6, 2016 ACCURACY OF ASGE CRITERIA FOR THE PREDICTION OF CHOLEDOCHOLITHIASIS patients were assessed for eligibility 161 excluded 148 had cholecystectomy 8 were referred from other hospital for ERCP 3 previous sphincterotomy 1 Mirizzi syndrome 1 primary sclerosing cholangitis 261 patients were included at admission 49 patients met ASGE intermediate-probability criteria for choledocholithiasis 212 patients met ASGE high-probability criteria for choledocholithiasis 1 excluded because failed ERCP 2 failed ERCP 2 biliary tract lesion 48 patients included in analysis 208 patients included in analysis Fig. 1. Screening and enrollment algorithm for patients with suspected choledocholithiasis. ASGE: American Society for Gastrointestinal Endoscopy. ERCP: Endoscopic retrograde cholangiopancreatography. Characteristics Table I. Characteristics of patients with suspected choledocholithiasis at baseline All n = 256 CL present n = 145 CL absent n = 111 p value Age - yrs 45.0 (± 21.2) 46.9 (± 21.7) 42.7 (± 20.3) Female sex - no. (%) 193 (75.4) 109 (75.2) 84 (75.7) CBD size - millimeters 9.4 (± 4.3) 9.8 (± 4.1) 9.0 (± 4.5) WBC - K/µL 11.0 (± 5.2) 10.4 (± 4.9) 11.8 (± 5.5) 0.041* Total bilirubin - mg/dl 5.9 (± 5.2) 5.9 (± 4.5) 6.0 (± 5.9) Direct bilirubin - mg/dl 3.6 (± 3.4) 3.6 (± 3.2) 3.5 (± 3.8) AST - UI/L (± 203.3) (± 184.8) (± 223.2) ALT - UI/L (± 237.7) (± 211.6) (± 266.6) AP - UI/L (± 191.1) (± 205.0) (± 167.9) GGT - UI/L (± 371.9) (± 273.5) (± 446.6) ERCP time delay - days 6.2 (± 3.7) 6.1 (± 3.7) 6.4 (± 3.7) Means (± SD). *Statistically significant (p < 0.05). CL: Choledocholithiasis; CBD: Common bile duct; WBC: White blood cells; AST: Aspartate aminotransferase; ALT: Alanine amino transaminase; AP: Alkaline phosphatase; GGT: Gamma-glutamyl transferase; ERCP: Endoscopic retrograde cholangiopancreatography. titis had an accuracy of 47.5% (86.2% sensitivity, 25.5% specificity) and 52.5% (13.8% sensitivity, 74.5% specificity), respectively. The comparisons of several variables in patients with and without biliary pancreatitis showed only statistical significance in CBD size (mm), 8.58 (± 3.2) vs. 9.9 (± 4.7), p = 0.044; white blood cell count (K/µL), 13.0 (± 5.3) vs (± 4.9), p < 0.001; and alkaline phosphatase levels (UI/L), (± 169.3) vs (± 198.9), p = 0.046, respectively. The ERCP delay time between the group of patients with biliary pancreatitis (6.0 ± 4.01) and without pancreatitis (6.4 ± 3.48) was no significantly different, p =
4 312 R. M. NARVÁEZ-RIVERA ET AL. Rev Esp Enferm Dig (Madrid) Predictors Table II. Frequency of ASGE clinical predictors in patients with and without choledocholithiasis All n = 256 CL present n = 145 CL absent n = 111 Odds ratio CI 95% p value Very high predictors CBD stone on abdominal US - no. (%) 44 (17.2) 34 (23.4) 10 (9.0) 3.09 ( ) 0.002* Ascending cholangitis - no. (%) 37 (14.5) 28 (19.3) 9 (8.1) 2.71 ( ) 0.012* Bilirubin > 4 mg/dl - no. (%) 151 (59.0) 89 (61.4) 62 (55.9) 1.25 ( ) Strong predictors CBD on US > 6 mm - no. (%) 193 (75.4) 119 (82.1) 74 (66.7) 2.28 ( ) 0.005* Bilirubin level mg/dl - no. (%) 66 (25.8) 36 (24.8) 30 (27.0) ( ) Moderate predictors Abnormal liver test - no. (%) 254 (99.2) 144 (99.3) 110 (99.1) 1.30 ( ) Age older than 55 yrs - no. (%) 81 (31.6) 53 (36.6) 28 (25.2) 1.70 ( ) Gallstone pancreatitis - no. (%) 80 (31.2) 29 (20.0) 51 (45.9) 0.29 ( ) < 0.001* ASGE: American Society for Gastrointestinal Endoscopy. Abnormal liver test: Altered liver function test other than bilirubin. CL: Choledocholithiasis; CBD: Common bile duct; US: Ultrasound. *Statistically significant (p < 0.05). Table III. Diagnostic performance of ASGE high and intermediate probability criteria and their individual predictors for choledocholithiasis Predictors Sensitivity Specificity PPV NPV +LR -LR Accuracy High-probability group: CBD stone on abdominal US Clinical ascending cholangitis Bilirubin > 4 mg/dl Bilirubin level mg/dl and CBD on US > 6 mm Intermediate-probability group: CBD on US > 6 mm Bilirubin level mg/dl Abnormal liver test Age older than 55 yrs Gallstone pancreatitis High-probability group: Subjects with the presence of any very strong predictor (CBD stone on abdominal US or clinical ascending cholangitis or bilirubin > 4 mg/dl) or both strong predictors (bilirubin level mg/dl + CBD on US > 6 mm). Intermediate-probability group: All other patients with the presence of only one strong predictor or any moderate predictor (abnormal liver test, age older than 55 yrs or gallstone pancreatitis). ASGE: American Society for Gastrointestinal Endoscopy. Abnormal liver test: Altered liver function test other than bilirubin. CBD: Common bile duct; US: Ultrasound; PPV: Positive predictive value; NPV: Negative predictive value; +LR: Positive likelihood ratio; -LR: Negative likelihood ratio. Logistic regression model Multivariable logistic regression analysis showed that a CBD > 6 mm (OR 2.21; 95% CI, ; p = 0.011), the presence of ascending cholangitis (OR 2.37; 95% CI, ; p = 0.046), CBD stone visualized on transabdominal US (OR 3.33; 95% CI, ; p = 0.004) and the absence of biliary pancreatitis (OR 3.23; 95% CI, ; p < 0.001) were independently associated with the presence of a stone on ERCP. The occurrence of biliary pancreatitis was a strong protective factor for the presence of a retained CBD stone (OR 0.30; 95% CI, ; p < 0.001). No additional clinical predictors of CL were identified. When the white blood cell count was introduced in the multivariate logistic regression model, it was not independently associated with the presence of CL on ERCP. However, the white blood cell count was the only studied variable independently associated with the presence of biliary pancreatitis (OR 1.13; 95% CI, ; p < 0.001). ERCP-related complications During the study period, ERCP-related complications were recorded in 11 out of 256 cases (4.3%); we recorded
5 Vol. 108, N.º 6, 2016 ACCURACY OF ASGE CRITERIA FOR THE PREDICTION OF CHOLEDOCHOLITHIASIS 313 the occurrence of clinically significant post-endoscopic sphincterotomy bleeding (requiring red blood cell transfusion and endoscopic therapy) in only one case and 10 cases of post-ercp pancreatitis. DISCUSSION ASGE guidelines for the prediction of suspected CL lack accuracy. The overall performance for the prediction of CL in our population with high probability was low, 59.0% (85.5% sensitivity, 24.3% specificity). This led to the performance of a significant percentage (> 40%) of unnecessary ERCP procedures. A recent study had similar results, with an accuracy for the ASGE high risk group of 62.1% (47.4% sensitivity, 73% specificity). They evaluated the impact of a second laboratory set, however, it did not increase the performance of ASGE guidelines for CL (9). Recently, it has been reported that the presence of one very strong criterion or both strong criteria is related to an increased yield of CL (10). In our study, the presence of one very strong predictor or the presence of both strong predictors did not increase the odds ratio for CL in the multivariate analysis. However, in any case the need of noninvasive testing could not be obviated. In general, the usefulness of individual predictors did not increase the diagnostic performance in our population. Our study, as the one previously reported by Rubin et al. (11), confirms that the ocurrence of biliary pancreatitis is not associated with the presence of a retained CBD stone. The absence of biliary pancreatitis in our study was a major predictor for CL (OR 3.23, 95% CI, ). This supports the hypothesis that spontaneous biliary stone passage through the CBD to the duodenum occurs due to possible small biliary stone size in the subset of patients with biliary pancreatitis. With the exception of critically ill patients with suspected ascending cholangitis, the usefulness of performing ERCP early in the course of biliary pancreatitis is controversial (12,13). In this respect, ERCP delay until biliary pancreatitis resolution may be a common practice. This may be a factor that allows the spontaneous biliary stone passage, being biliary pancreatitis probably a negative predictive factor for CL. However, we have demonstrated that ERCP delay time was not different from those with and without biliary pancreatitis, p = Our results strongly support the fact that biliary pancreatitis itself may be a protective factor for CL independently of ERCP delay time. This fact has raised the interest in endoscopic ultrasonography (EUS) as a safe replacement for ERCP in subjects with biliary pancreatitis. First, because it has been demostrated that early EUS has a higher successful examination rate (100 vs. 86%) and a lower morbidity (7% vs. 14%) compared with ERCP (14). In addition, EUS has demonstrated an excellent performance for the detection of small size (median of 4 mm) CBD stones (15), which may be useful in the context of biliary pancreatitis where we showed the risk of CL was significantly lower (36.2%) than without pancreatitis (65.9%) (OR 0.30; 95% CI, , p < 0.001). Due to the morbidity and costs associated with ERCP, it should be limited to those who are most likely to benefit from it. Based on our results, predictive scores have a limited clinical utility for most patients in day-to-day practice. Due to the lack of identification of patients with CL by the current clinical predictive scores, we suggest that all patients with suspected CL (high- or intermediate-probability groups) without a clear indication for ERCP (ascending cholangitis) must have a CL confirmatory image study (magnetic resonance cholangiopancreatography [MRCP] or EUS) before a therapeutic procedure is attempted. Even though 2010 ASGE guidelines already recommended pre-operative EUS or MRCP for those classified as intermediate probability, no formal evidence supporting this recommendation in the ASGE intermediate- or high-probability groups exists. Prior randomized controlled trials have suggested that intra-operative CBD exploration during cholecystectomy is superior to the two-step pre- or post-cholecystectomy ERCP in terms of CBD stone resolution without additional morbidity or mortality (16). Others have proposed this same approach specifically in the subset of patients with intermediate risk, with a reported shorter length of stay without increased morbidity (17). However, to consider this approach as a definitive recommendation, well designed prospective clinical trials are needed. Both EUS and MRCP have a high diagnostic accuracy for the detection of CBD stones (18). This strategy can reduce the risk of unnecessary procedures, eliminate complications and may decrease cost. Therefore, we suggest that patients with an EUS or MRCP positive for CL should undergo endoscopic or surgical extraction of CBD stones, and those with negative EUS or MRCP do not need further invasive tests. However, to evaluate the cost-effectiveness of this approach, CL prevalence, center resources and expertise should be considered. In summary, current ASGE guidelines in our population for the predition of CL lack accuracy, with unnecessary perfomance of negative ERCP in almost half of cases. The optimal cost-effective approach for the management of patients with suspected CL is not known yet. The use of confirmatory imaging studies (MRCP or EUS) in all cases with high and intermediate probability for CL before a therapeutic procedure may be an attractive option to be considered. ACKNOWLEDGEMENTS We thank Sergio Lozano-Rodríguez, MD, for his help in editing the manuscript.
6 314 R. M. NARVÁEZ-RIVERA ET AL. Rev Esp Enferm Dig (Madrid) REFERENCES 1. Hunter JG. Laparoscopic transcystic common bile duct exploration. Am J Surg 1992;163:53-6;discussion DOI: / (92)90252-M 2. O Neill CJ, Gillies DM, Gani JS. Choledocholithiasis: Overdiagnosed endoscopically and undertreated laparoscopically. ANZ J Surg 2008;78: DOI: /j x 3. Chang L, Lo SK, Stabile BE, et al. Gallstone pancreatitis: A prospective study on the incidence of cholangitis and clinical predictors of retained common bile duct stones. Am J Gastroenterol 1998;93: DOI: /j _b.x 4. Liu CL, Lo CM, Chan JK, et al. Detection of choledocholithiasis by EUS in acute pancreatitis: A prospective evaluation in 100 consecutive patients. Gastrointest Endosc 2001;54: DOI: / mge Cohen ME, Slezak L, Wells CK, et al. Prediction of bile duct stones and complications in gallstone pancreatitis using early laboratory trends. Am J Gastroenterol 2001;96: DOI: /j x 6. Anderson MA, Fisher L, Jain R, et al. Complications of ERCP. Gastrointest Endosc 2012;75: DOI: /j.gie Urbach DR, Khajanchee YS, Jobe BA, et al. Cost-effective management of common bile duct stones: A decision analysis of the use of endoscopic retrograde cholangiopancreatography (ERCP), intraoperative cholangiography, and laparoscopic bile duct exploration. Surg Endosc 2001;15:4-13. DOI: /s Committee ASoP, Maple JT, Ben-Menachem T, et al. The role of endoscopy in the evaluation of suspected choledocholithiasis. Gastrointest Endosc 2010;71:1-9. DOI: /j.gie Adams MA, Hosmer AE, Wamsteker EJ, et al. Predicting the likelihood of a persistent bile duct stone in patients with suspected choledocholithiasis: Accuracy of existing guidelines and the impact of laboratory trends. Gastrointest Endosc 2015;82: DOI: /j.gie Liu TH, Consorti ET, Kawashima A, et al. Patient evaluation and management with selective use of magnetic resonance cholangiography and endoscopic retrograde cholangiopancreatography before laparoscopic cholecystectomy. Ann Surg 2001;234: DOI: / Rubin MI, Thosani NC, Tanikella R, et al. Endoscopic retrograde cholangiopancreatography for suspected choledocholithiasis: Testing the current guidelines. Dig Liver Dis 2013;45: DOI: /j. dld Folsch UR, Nitsche R, Ludtke R, et al. Early ERCP and papillotomy compared with conservative treatment for acute biliary pancreatitis. The German Study Group on Acute Biliary Pancreatitis. N Engl J Med 1997;336: Tarnasky PR, Cotton PB. Early ERCP and papillotomy for acute biliary pancreatitis. N Engl J Med 1997;336:1835;author reply DOI: /S (97) Liu CL, Fan ST, Lo CM, et al. Comparison of early endoscopic ultrasonography and endoscopic retrograde cholangiopancreatography in the management of acute biliary pancreatitis: A prospective randomized study. Clin Gastroenterol Hepatol 2005;3: DOI: /S (05) Vázquez-Sequeiros E, González-Panizo Tamargo F, Boixeda-Miquel D, et al. Diagnostic accuracy and therapeutic impact of endoscopic ultrasonography in patients with intermediate suspicion of choledocholithiasis and absence of findings in magnetic resonance cholangiography. Rev Esp Enferm Dig 2011;103: DOI: / S Dasari BV, Tan CJ, Gurusamy KS, et al. Surgical versus endoscopic treatment of bile duct stones. Cochrane Database Syst Rev 2013;12:CD Iranmanesh P, Frossard JL, Mugnier-Konrad B, et al. Initial cholecystectomy vs sequential common duct endoscopic assessment and subsequent cholecystectomy for suspected gallstone migration: A randomized clinical trial. JAMA 2014;312: DOI: / jama Giljaca V, Gurusamy KS, Takwoingi Y, et al. Endoscopic ultrasound versus magnetic resonance cholangiopancreatography for common bile duct stones. Cochrane Database Syst Rev 2015;2:CD
Sex-related differences in predicting choledocholithiasis using current American Society of Gastrointestinal Endoscopy risk criteria
 ORIGINAL ARTICLE Annals of Gastroenterology (2018) 31, 1-6 Sex-related differences in predicting choledocholithiasis using current American Society of Gastrointestinal Endoscopy risk criteria Ankit Chhoda
ORIGINAL ARTICLE Annals of Gastroenterology (2018) 31, 1-6 Sex-related differences in predicting choledocholithiasis using current American Society of Gastrointestinal Endoscopy risk criteria Ankit Chhoda
The campaign on laboratory: focus on Gallstone Disease and ERCP
 The campaign on laboratory: focus on Gallstone Disease and ERCP Mauro Giuliani, MD, Specialist in Visceral Surgery, Vice Head Physician, Surgical Ward, Ospedale Regionale di Locarno Alberto Fasoli, MD,
The campaign on laboratory: focus on Gallstone Disease and ERCP Mauro Giuliani, MD, Specialist in Visceral Surgery, Vice Head Physician, Surgical Ward, Ospedale Regionale di Locarno Alberto Fasoli, MD,
Better non-invasive endoscopic procedure: endoscopic ultrasound or magnetic resonance cholangiopancreatography?
 ORIGINAL ARTICLE Better non-invasive endoscopic procedure: endoscopic ultrasound or magnetic resonance cholangiopancreatography? Rusmir Mesihović, Amila Mehmedović Department of Gastroenterology and Hepatology,
ORIGINAL ARTICLE Better non-invasive endoscopic procedure: endoscopic ultrasound or magnetic resonance cholangiopancreatography? Rusmir Mesihović, Amila Mehmedović Department of Gastroenterology and Hepatology,
ERCP and EUS: What s New and What Should We Do?
 ERCP and EUS: What s New and What Should We Do? Rajesh N. Keswani, MD Associate Professor of Medicine Division of Gastroenterology Northwestern University Feinberg School of Medicine EUS/ERCP in 2015 THE
ERCP and EUS: What s New and What Should We Do? Rajesh N. Keswani, MD Associate Professor of Medicine Division of Gastroenterology Northwestern University Feinberg School of Medicine EUS/ERCP in 2015 THE
Evidence-based guidelines for diagnosis of common bile duct stones Vanja Giljaca University Hospital Center Rijeka Department of Gastroenterology
 Evidencebased guidelines for diagnosis of common bile duct stones Vanja Giljaca University Hospital Center Rijeka Department of Gastroenterology Trusted evidence. Informed decisions. Better health. Outline
Evidencebased guidelines for diagnosis of common bile duct stones Vanja Giljaca University Hospital Center Rijeka Department of Gastroenterology Trusted evidence. Informed decisions. Better health. Outline
Research Article The Diagnostic Accuracy of Linear Endoscopic Ultrasound for Evaluating Symptoms Suggestive of Common Bile Duct Stones
 Gastroenterology Research and Practice Volume 2016, Article ID 6957235, 5 pages http://dx.doi.org/10.1155/2016/6957235 Research Article The Diagnostic Accuracy of Linear Endoscopic Ultrasound for Evaluating
Gastroenterology Research and Practice Volume 2016, Article ID 6957235, 5 pages http://dx.doi.org/10.1155/2016/6957235 Research Article The Diagnostic Accuracy of Linear Endoscopic Ultrasound for Evaluating
A scoring system for the prediction of choledocholithiasis: a prospective cohort study
 A scoring system for the prediction of choledocholithiasis: a prospective cohort study Bilal O. Al-Jiffry, a Samah Khayat, b Elfatih Abdeen, b Tasadooq Hussain, c Mohammed Yassin d From the a Department
A scoring system for the prediction of choledocholithiasis: a prospective cohort study Bilal O. Al-Jiffry, a Samah Khayat, b Elfatih Abdeen, b Tasadooq Hussain, c Mohammed Yassin d From the a Department
Setting The study setting was hospital. The economic analysis was carried out in California, USA.
 Preoperative versus postoperative endoscopic retrograde cholangiopancreatography in mild to moderate gallstone pancreatitis: a prospective randomized trial Chang L, Lo S, Stabile B E, Lewis R J, Toosie
Preoperative versus postoperative endoscopic retrograde cholangiopancreatography in mild to moderate gallstone pancreatitis: a prospective randomized trial Chang L, Lo S, Stabile B E, Lewis R J, Toosie
Presence of choledocholithiasis in patients undergoing cholecystectomy for mild biliary pancreatitis
 Original Article Presence of choledocholithiasis in patients undergoing cholecystectomy for mild biliary pancreatitis Pradhan S 1, Shah S 2, Maharjan S 2, Shah JN 3 1 2 2 3 Professor, Patan hospital Correspondence:
Original Article Presence of choledocholithiasis in patients undergoing cholecystectomy for mild biliary pancreatitis Pradhan S 1, Shah S 2, Maharjan S 2, Shah JN 3 1 2 2 3 Professor, Patan hospital Correspondence:
The authors have declared no conflicts of interest.
 Diagnostic Accuracy of Magnetic Resonance Cholangiopancreatography Versus Endoscopic Retrograde Cholangiopancreatography Findings in the Postorthotopic Liver Transplant Population Authors: *Ashok Shiani,
Diagnostic Accuracy of Magnetic Resonance Cholangiopancreatography Versus Endoscopic Retrograde Cholangiopancreatography Findings in the Postorthotopic Liver Transplant Population Authors: *Ashok Shiani,
Subtotal cholecystectomy for complicated acute cholecystitis: a multicenter prospective observational study
 Study title Subtotal cholecystectomy for complicated acute cholecystitis: a multicenter prospective observational study Primary Investigator: Kazuhide Matsushima, MD Co-Primary investigator: Zachary Warriner,
Study title Subtotal cholecystectomy for complicated acute cholecystitis: a multicenter prospective observational study Primary Investigator: Kazuhide Matsushima, MD Co-Primary investigator: Zachary Warriner,
Research Article Safety and Yield of Diagnostic ERCP in Liver Transplant Patients with Abnormal Liver Function Tests
 Diagnostic and erapeutic Endoscopy, Article ID 314927, 5 pages http://dx.doi.org/10.1155/2014/314927 Research Article Safety and Yield of Diagnostic ERCP in Liver Transplant Patients with Abnormal Liver
Diagnostic and erapeutic Endoscopy, Article ID 314927, 5 pages http://dx.doi.org/10.1155/2014/314927 Research Article Safety and Yield of Diagnostic ERCP in Liver Transplant Patients with Abnormal Liver
THE AMERICAN JOURNAL OF GASTROENTEROLOGY Vol. 96, No. 10, by Am. Coll. of Gastroenterology ISSN /01/$20.00
 THE AMERICAN JOURNAL OF GASTROENTEROLOGY Vol. 96, No. 10, 2001 2001 by Am. Coll. of Gastroenterology ISSN 0002-9270/01/$20.00 Published by Elsevier Science Inc. PII S0002-9270(01)02807-6 Can Endoscopic
THE AMERICAN JOURNAL OF GASTROENTEROLOGY Vol. 96, No. 10, 2001 2001 by Am. Coll. of Gastroenterology ISSN 0002-9270/01/$20.00 Published by Elsevier Science Inc. PII S0002-9270(01)02807-6 Can Endoscopic
Predictors of abnormalities on magnetic resonance cholangiopancreatography: is there a role when the biliary tree is normal on previous imaging?
 ORIGINAL ARTICLE Annals of Gastroenterology (2019) 32, 1-6 Predictors of abnormalities on magnetic resonance cholangiopancreatography: is there a role when the biliary tree is normal on previous imaging?
ORIGINAL ARTICLE Annals of Gastroenterology (2019) 32, 1-6 Predictors of abnormalities on magnetic resonance cholangiopancreatography: is there a role when the biliary tree is normal on previous imaging?
ERCP / PTC Surgical Laparoscopic vs open Timing and order of approach
 Choledocholithiasis Which Approach and When? Lygia Stewart, MD University of California, San Francisco 2010 Naffziger Post-Graduate Course Clinical Manifestations of Choledocholithiasis Asymptomatic (no
Choledocholithiasis Which Approach and When? Lygia Stewart, MD University of California, San Francisco 2010 Naffziger Post-Graduate Course Clinical Manifestations of Choledocholithiasis Asymptomatic (no
Title: Fasciola hepatica in the common bile duct: spyglass visualization and endoscopic extraction
 Title: Fasciola hepatica in the common bile duct: spyglass visualization and endoscopic extraction Authors: Edson Guzmán Calderón, Augusto Vera Calderón, Ramiro Díaz Ríos, Ronald Arcana López, Edgar Alva
Title: Fasciola hepatica in the common bile duct: spyglass visualization and endoscopic extraction Authors: Edson Guzmán Calderón, Augusto Vera Calderón, Ramiro Díaz Ríos, Ronald Arcana López, Edgar Alva
Role of hepatobiliary ultrasound in the diagnosis of choledocolitiasis
 Original articles Role of hepatobiliary ultrasound in the diagnosis of choledocolitiasis Andrea Piña, MD, 1 Martín Garzón, MD, 1 Jorge Iván Lizarazo, MD, 1 Juan Carlos Marulanda, MD, 1 Juan Carlos Molano,
Original articles Role of hepatobiliary ultrasound in the diagnosis of choledocolitiasis Andrea Piña, MD, 1 Martín Garzón, MD, 1 Jorge Iván Lizarazo, MD, 1 Juan Carlos Marulanda, MD, 1 Juan Carlos Molano,
Endoscopic Retrograde Pancreatography and Laparoscopic Cholecystectomy. TEAM 1 Janix M. De Guzman, MD Presentor
 Endoscopic Retrograde Pancreatography and Laparoscopic Cholecystectomy TEAM 1 Janix M. De Guzman, MD Presentor Premise 40F Jaundice Abdominal pain US finding of gallstones with apparently normal common
Endoscopic Retrograde Pancreatography and Laparoscopic Cholecystectomy TEAM 1 Janix M. De Guzman, MD Presentor Premise 40F Jaundice Abdominal pain US finding of gallstones with apparently normal common
Diagnostic accuracy and therapeutic impact of endoscopic. ultrasonography in patients with intermediate suspicion of
 1130-0108/2011/103/9/464-471 REVISTA ESPAÑOLA DE ENFERMEDADES DIGESTIVAS Copyright 2011 ARÁN EDICIONES, S. L. REV ESP ENFERM DIG (Madrid) Vol. 103. N. 9, pp. 464-471, 2011 ORIGINAL PAPERS Diagnostic accuracy
1130-0108/2011/103/9/464-471 REVISTA ESPAÑOLA DE ENFERMEDADES DIGESTIVAS Copyright 2011 ARÁN EDICIONES, S. L. REV ESP ENFERM DIG (Madrid) Vol. 103. N. 9, pp. 464-471, 2011 ORIGINAL PAPERS Diagnostic accuracy
Downloaded from jssu.ssu.ac.ir at 13:10 IRST on Saturday October 28th 2017
 Journal of Shahid Sadoughi University of Medical Sciences Vol. 21, No. 5, Nov-Dec 2013 Pages: 675-681 1392 5 21 675-681 : 3 2* 1 1392/8/ : -1-2 -3 1391/8/24 : (). :. 1390 200 :.. SPSS (%0/5) 200 (8%) (%9/5)19
Journal of Shahid Sadoughi University of Medical Sciences Vol. 21, No. 5, Nov-Dec 2013 Pages: 675-681 1392 5 21 675-681 : 3 2* 1 1392/8/ : -1-2 -3 1391/8/24 : (). :. 1390 200 :.. SPSS (%0/5) 200 (8%) (%9/5)19
Magnetic Resonance Cholangiopancreatography (MRCP) in a District General Hospital
 Magnetic Resonance Cholangiopancreatography (MRCP) in a District General Hospital Poster No.: C-1790 Congress: ECR 2012 Type: Authors: Scientific Exhibit J. A. Maguire 1, H. Kasem 2, M. Akhtar 2, M. Strauss
Magnetic Resonance Cholangiopancreatography (MRCP) in a District General Hospital Poster No.: C-1790 Congress: ECR 2012 Type: Authors: Scientific Exhibit J. A. Maguire 1, H. Kasem 2, M. Akhtar 2, M. Strauss
Accepted Article. If you suffer from type-2 diabetes mellitus, your ERCP is likely to have a better outcome. Jesús García-Cano
 Accepted Article If you suffer from type-2 diabetes mellitus, your ERCP is likely to have a better outcome Jesús García-Cano DOI: 10.17235/reed.2016.4521/2016 Link: PDF Please cite this article as: García-Cano
Accepted Article If you suffer from type-2 diabetes mellitus, your ERCP is likely to have a better outcome Jesús García-Cano DOI: 10.17235/reed.2016.4521/2016 Link: PDF Please cite this article as: García-Cano
complication rates and/or incomplete clearance with need of intervention (ie, unfavorable outcomes).
 Research Original Investigation Natural Course vs Interventions to Clear Common Bile Duct Stones Data From the Swedish Registry for Gallstone Surgery and Endoscopic Retrograde Cholangiopancreatography
Research Original Investigation Natural Course vs Interventions to Clear Common Bile Duct Stones Data From the Swedish Registry for Gallstone Surgery and Endoscopic Retrograde Cholangiopancreatography
Identifying Patients Most Likely to Have a Common Bile Duct Stone After a Positive Intraoperative Cholangiogram
 Identifying Patients Most Likely to Have a Common Bile Duct Stone After a Positive Intraoperative Cholangiogram Raja Vadlamudi, MD, MPH, Jason Conway, MD, MPH, Girish Mishra, MD, MS, John Baillie, MB ChB,
Identifying Patients Most Likely to Have a Common Bile Duct Stone After a Positive Intraoperative Cholangiogram Raja Vadlamudi, MD, MPH, Jason Conway, MD, MPH, Girish Mishra, MD, MS, John Baillie, MB ChB,
Appendix A: Summary of evidence from surveillance
 Appendix A: Summary of evidence from surveillance 2018 surveillance of Gallstone disease: diagnosis and management (2014) NICE guideline CG188 Summary of evidence from surveillance Studies identified in
Appendix A: Summary of evidence from surveillance 2018 surveillance of Gallstone disease: diagnosis and management (2014) NICE guideline CG188 Summary of evidence from surveillance Studies identified in
Surveillance proposal consultation document
 Surveillance proposal consultation document 2018 surveillance of Gallstone disease: diagnosis and management (NICE guideline CG188) Proposed surveillance decision We propose to not update the NICE guideline
Surveillance proposal consultation document 2018 surveillance of Gallstone disease: diagnosis and management (NICE guideline CG188) Proposed surveillance decision We propose to not update the NICE guideline
Figure 2: Post-cholecystectomy biliary-like pain
 Figure 2: Post-cholecystectomy biliary-like pain 1 patient with recurrent episodes of pain (not daily), in the epigastrium/right upper quadrant, lasting >30 mins, building to a steady level, interrupting
Figure 2: Post-cholecystectomy biliary-like pain 1 patient with recurrent episodes of pain (not daily), in the epigastrium/right upper quadrant, lasting >30 mins, building to a steady level, interrupting
Routine Testing of Liver Function Before and After Elective Laparoscopic Cholecystectomy: Is It Necessary?
 Routine Testing of Liver Function Before and After Elective Laparoscopic Cholecystectomy: Is It Necessary? Nasir Zaheer Ahmad, FRCSI SCIENTIFIC PAPER ABSTRACT Background and Objectives: Liver function
Routine Testing of Liver Function Before and After Elective Laparoscopic Cholecystectomy: Is It Necessary? Nasir Zaheer Ahmad, FRCSI SCIENTIFIC PAPER ABSTRACT Background and Objectives: Liver function
Disclosures. Overview. Case 1. Common Bile Duct Sizes 10/14/2016. General GI + Advanced Endoscopy: NAFLD/Stones/Pancreatitis
 Disclosures General GI + Advanced Endoscopy: NAFLD/Stones/Pancreatitis 123 Blank Blank, LLC Aldo Maspons, MD Assistant Professor Director of Endoscopy Department of Pediatrics Texas Tech University Health
Disclosures General GI + Advanced Endoscopy: NAFLD/Stones/Pancreatitis 123 Blank Blank, LLC Aldo Maspons, MD Assistant Professor Director of Endoscopy Department of Pediatrics Texas Tech University Health
Endoscopic Ultrasonography Clinical Impact. Giancarlo Caletti. Gastroenterologia Università di Bologna. Caletti
 Clinical Impact Giancarlo Gastroenterologia Università di Bologna AUSL di Imola,, Castel S. Pietro Terme (BO) 1982 Indications Diagnosis of Submucosal Tumors (SMT) Staging of Neoplasms Evaluation of Pancreato-Biliary
Clinical Impact Giancarlo Gastroenterologia Università di Bologna AUSL di Imola,, Castel S. Pietro Terme (BO) 1982 Indications Diagnosis of Submucosal Tumors (SMT) Staging of Neoplasms Evaluation of Pancreato-Biliary
Title: The best approach to treat concomitant gallstones and. Authors: Jesús García-Cano, Francisco Domper
 Title: The best approach to treat concomitant gallstones and common bile duct stones. Is ERCP still needed? Authors: Jesús García-Cano, Francisco Domper DOI: 10.17235/reed.2019.6226/2019 Link: PubMed (Epub
Title: The best approach to treat concomitant gallstones and common bile duct stones. Is ERCP still needed? Authors: Jesús García-Cano, Francisco Domper DOI: 10.17235/reed.2019.6226/2019 Link: PubMed (Epub
Biliary tree dilation - and now what?
 Biliary tree dilation - and now what? Poster No.: C-1767 Congress: ECR 2012 Type: Educational Exhibit Authors: I. Ferreira, A. B. Ramos, S. Magalhães, M. Certo; Porto/PT Keywords: Pathology, Diagnostic
Biliary tree dilation - and now what? Poster No.: C-1767 Congress: ECR 2012 Type: Educational Exhibit Authors: I. Ferreira, A. B. Ramos, S. Magalhães, M. Certo; Porto/PT Keywords: Pathology, Diagnostic
ORIGINAL PAPERS. R. Insertion of fully covered self-expanding metal stents in benign biliary diseases. ABSTRACT MATERIALS AND METHODS INTRODUCTION
 ORIGINAL PAPERS Insertion of fully covered self-expanding metal stents in benign biliary diseases Mariana Omodeo, Ignacio Málaga, Dante Manazzoni, Cecilia Curvale, Julio de María, Martín Guidi and Raúl
ORIGINAL PAPERS Insertion of fully covered self-expanding metal stents in benign biliary diseases Mariana Omodeo, Ignacio Málaga, Dante Manazzoni, Cecilia Curvale, Julio de María, Martín Guidi and Raúl
Type of intervention Treatment. Economic study type Cost-effectiveness analysis.
 Preoperative endoscopic sphincterotomy versus laparoendoscopic rendezvous in patients with gallbladder and bile duct stones Morino M, Baracchi F, Miglietta C, Furlan N, Ragona R, Garbarini A Record Status
Preoperative endoscopic sphincterotomy versus laparoendoscopic rendezvous in patients with gallbladder and bile duct stones Morino M, Baracchi F, Miglietta C, Furlan N, Ragona R, Garbarini A Record Status
Obstructive jaundice due to a blood clot after ERCP: a case report and review of the literature
 Zhu et al. BMC Gastroenterology (2018) 18:163 https://doi.org/10.1186/s12876-018-0898-4 CASE REPORT Open Access Obstructive jaundice due to a blood clot after ERCP: a case report and review of the literature
Zhu et al. BMC Gastroenterology (2018) 18:163 https://doi.org/10.1186/s12876-018-0898-4 CASE REPORT Open Access Obstructive jaundice due to a blood clot after ERCP: a case report and review of the literature
ENDOSCOPIC TREATMENT OF A BILE DUCT
 HPB Surgery, 1990, Vol. 3, pp. 67-71 Reprints available directly from the publisher Photocopying permitted by license only 1990 Harwood Academic Publishers GmbH Printed in the United Kingdom CASE REPORT
HPB Surgery, 1990, Vol. 3, pp. 67-71 Reprints available directly from the publisher Photocopying permitted by license only 1990 Harwood Academic Publishers GmbH Printed in the United Kingdom CASE REPORT
ERCP complications and challenges in their diagnosis and management.
 ERCP complications and challenges in their diagnosis and management. Sandie R Thomson Chair of the Division of Gastroenterology, University of Cape Town ERCP Do I have a good Indication? . Algorithm for
ERCP complications and challenges in their diagnosis and management. Sandie R Thomson Chair of the Division of Gastroenterology, University of Cape Town ERCP Do I have a good Indication? . Algorithm for
Title: The endoscopic ultrasound-assisted Rendez-Vous technique for treatment of recurrent pancreatitis due to pancreas divisum and ansa pancreatica
 Title: The endoscopic ultrasound-assisted Rendez-Vous technique for treatment of recurrent pancreatitis due to pancreas divisum and ansa pancreatica Authors: Sergio López-Durán, Celia Zaera, Juan Ángel
Title: The endoscopic ultrasound-assisted Rendez-Vous technique for treatment of recurrent pancreatitis due to pancreas divisum and ansa pancreatica Authors: Sergio López-Durán, Celia Zaera, Juan Ángel
Primary Sclerosing Cholangitis and Cholestatic liver diseases. Ahsan M Bhatti MD, FACP Bhatti Gastroenterology Consultants
 Primary Sclerosing Cholangitis and Cholestatic liver diseases Ahsan M Bhatti MD, FACP Bhatti Gastroenterology Consultants I have nothing to disclose Educational Objectives What is PSC? Understand the cholestatic
Primary Sclerosing Cholangitis and Cholestatic liver diseases Ahsan M Bhatti MD, FACP Bhatti Gastroenterology Consultants I have nothing to disclose Educational Objectives What is PSC? Understand the cholestatic
Appendix I: GRADE profiles
 Appendix I: GRADE profiles GRADE and Modified GRADE approaches used in this guideline Standard GRADE approach Modified GRADE approach Criteria Effectiveness evidence (Developed by GRADE working group)
Appendix I: GRADE profiles GRADE and Modified GRADE approaches used in this guideline Standard GRADE approach Modified GRADE approach Criteria Effectiveness evidence (Developed by GRADE working group)
LIVER, PANCREAS, AND BILIARY TRACT
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:1157 1161 LIVER, PANCREAS, AND BILIARY TRACT Delayed and Unsuccessful Endoscopic Retrograde Cholangiopancreatography Are Associated With Worse Outcomes
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:1157 1161 LIVER, PANCREAS, AND BILIARY TRACT Delayed and Unsuccessful Endoscopic Retrograde Cholangiopancreatography Are Associated With Worse Outcomes
EAST MULTICENTER STUDY PROPOSAL
 EAST MULTICENTER STUDY PROPOSAL (Proposal forms must be completed in its entirety, incomplete forms will not be considered) GENERAL INFORMATION Study Title: Prospective Multi-Institutional Evaluation of
EAST MULTICENTER STUDY PROPOSAL (Proposal forms must be completed in its entirety, incomplete forms will not be considered) GENERAL INFORMATION Study Title: Prospective Multi-Institutional Evaluation of
Recurrent common bile duct stones as a late complication of endoscopic sphincterotomy
 Nzenza et al. BMC Gastroenterology (2018) 18:39 https://doi.org/10.1186/s12876-018-0765-3 RESEARCH ARTICLE Open Access Recurrent common bile duct stones as a late complication of endoscopic sphincterotomy
Nzenza et al. BMC Gastroenterology (2018) 18:39 https://doi.org/10.1186/s12876-018-0765-3 RESEARCH ARTICLE Open Access Recurrent common bile duct stones as a late complication of endoscopic sphincterotomy
Endoscopic retrograde cholangiopancreatography versus intraoperative cholangiography for diagnosis of common bile duct stones (Review)
 Endoscopic retrograde cholangiopancreatography versus intraoperative cholangiography for diagnosis of common bile duct stones Gurusamy KS, Giljaca V, Takwoingi Y, Higgie D, Poropat G, Štimac D, Davidson
Endoscopic retrograde cholangiopancreatography versus intraoperative cholangiography for diagnosis of common bile duct stones Gurusamy KS, Giljaca V, Takwoingi Y, Higgie D, Poropat G, Štimac D, Davidson
Safety of endoscopic retrograde cholangiopancreatography in patients 80 years of age and older
 Original paper Safety of endoscopic retrograde cholangiopancreatography in patients 80 years of age and older Baydar Behlül 1, Serin Ayfer 2, Vatansever Sezgin 3, Kandemir Altay 3, Çelik Mustafa 3, Çekiç
Original paper Safety of endoscopic retrograde cholangiopancreatography in patients 80 years of age and older Baydar Behlül 1, Serin Ayfer 2, Vatansever Sezgin 3, Kandemir Altay 3, Çelik Mustafa 3, Çekiç
Key Words: Choledocholithiasis; Endosonography; Cholangiopancreatography,
 Gut and Liver, Vol. 11, No. 2, March 2017, pp. 290-297 ORiginal Article Diagnostic Value of Endoscopic Ultrasonography in Symptomatic Patients with High and Intermediate Probabilities of Common Bile Duct
Gut and Liver, Vol. 11, No. 2, March 2017, pp. 290-297 ORiginal Article Diagnostic Value of Endoscopic Ultrasonography in Symptomatic Patients with High and Intermediate Probabilities of Common Bile Duct
Greater Manchester EUR Policy Statement on: Asymptomatic Gallstones GM Ref: GM061 Version: 0.2 (21 November 2018)
 Greater Manchester EUR Policy Statement on: Asymptomatic Gallstones GM Ref: GM061 Version: 0.2 (21 November 2018) Commissioning Statement Asymptomatic Gallstones Policy Exclusions (Alternative commissioning
Greater Manchester EUR Policy Statement on: Asymptomatic Gallstones GM Ref: GM061 Version: 0.2 (21 November 2018) Commissioning Statement Asymptomatic Gallstones Policy Exclusions (Alternative commissioning
CHOLEDOCHOLITHIASIS IN PATIENTS WITH ACUTE GALLSTONE-RELATED DISEASE: RISK FACTORS, IMPACT OF ADMISSION DAY AND TREATMENT STRATEGY
 ARISTOTLE UNIVERSITY OF THESSALONIKI SCHOOL OF HEALTH SCIENCES FACULTY OF MEDICINE CHOLEDOCHOLITHIASIS IN PATIENTS WITH ACUTE GALLSTONE-RELATED DISEASE: RISK FACTORS, IMPACT OF ADMISSION DAY AND TREATMENT
ARISTOTLE UNIVERSITY OF THESSALONIKI SCHOOL OF HEALTH SCIENCES FACULTY OF MEDICINE CHOLEDOCHOLITHIASIS IN PATIENTS WITH ACUTE GALLSTONE-RELATED DISEASE: RISK FACTORS, IMPACT OF ADMISSION DAY AND TREATMENT
Department of General Surgery, Al Khor Hospital, Hamad Medical Corporation, Qatar 2
 International Scholarly Research Network ISRN Minimally Invasive Surgery Volume 2012, Article ID 469013, 5 pages doi:10.5402/2012/469013 Clinical Study Laparoscopic Intraoperative Cholangiography Interpretation
International Scholarly Research Network ISRN Minimally Invasive Surgery Volume 2012, Article ID 469013, 5 pages doi:10.5402/2012/469013 Clinical Study Laparoscopic Intraoperative Cholangiography Interpretation
Duration of Pain Is Correlated With Elevation in Liver Function Tests in Patients With Symptomatic Choledocholithiasis
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2010;8:1077 1082 Duration of Pain Is Correlated With Elevation in Liver Function Tests in Patients With Symptomatic Choledocholithiasis ALA I. SHARARA, NABIL M.
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2010;8:1077 1082 Duration of Pain Is Correlated With Elevation in Liver Function Tests in Patients With Symptomatic Choledocholithiasis ALA I. SHARARA, NABIL M.
group and endoscopic common duct assessment and clearance followed by cholecystectomy for the control group.
 Research Original Investigation Initial Cholecystectomy vs Sequential Common Duct Endoscopic Assessment and Subsequent Cholecystectomy for Suspected Gallstone Migration A Randomized Clinical Trial Pouya
Research Original Investigation Initial Cholecystectomy vs Sequential Common Duct Endoscopic Assessment and Subsequent Cholecystectomy for Suspected Gallstone Migration A Randomized Clinical Trial Pouya
Title: Pursuing excellence in ERCP. Authors: Jesús García-Cano, Francisco Domper. DOI: /reed /2017 Link: PubMed (Epub ahead of print)
 Title: Pursuing excellence in ERCP Authors: Jesús García-Cano, Francisco Domper DOI: 10.17235/reed.2018.5373/2017 Link: PubMed (Epub ahead of print) Please cite this article as: García-Cano Jesús, Domper
Title: Pursuing excellence in ERCP Authors: Jesús García-Cano, Francisco Domper DOI: 10.17235/reed.2018.5373/2017 Link: PubMed (Epub ahead of print) Please cite this article as: García-Cano Jesús, Domper
Pre-operative prediction of difficult laparoscopic cholecystectomy
 International Surgery Journal http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20151083 Pre-operative prediction of difficult laparoscopic
International Surgery Journal http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20151083 Pre-operative prediction of difficult laparoscopic
Tratamiento endoscópico de la CEP. En quien como y cuando?
 Tratamiento endoscópico de la CEP. En quien como y cuando? Andrés Cárdenas, MD, MMSc, PhD, AGAF, FAASLD GI / Liver Unit, Hospital Clinic Institut de Malalties Digestives i Metaboliques University of Barcelona
Tratamiento endoscópico de la CEP. En quien como y cuando? Andrés Cárdenas, MD, MMSc, PhD, AGAF, FAASLD GI / Liver Unit, Hospital Clinic Institut de Malalties Digestives i Metaboliques University of Barcelona
Mirizzi syndrome with an unusual type of biliobiliary fistula a case report
 Kawaguchi et al. Surgical Case Reports (2015) 1:51 DOI 10.1186/s40792-015-0052-2 CASE REPORT Mirizzi syndrome with an unusual type of biliobiliary fistula a case report Tsutomu Kawaguchi 1,2*, Tadao Itoh
Kawaguchi et al. Surgical Case Reports (2015) 1:51 DOI 10.1186/s40792-015-0052-2 CASE REPORT Mirizzi syndrome with an unusual type of biliobiliary fistula a case report Tsutomu Kawaguchi 1,2*, Tadao Itoh
Empirical assessment of univariate and bivariate meta-analyses for comparing the accuracy of diagnostic tests
 Empirical assessment of univariate and bivariate meta-analyses for comparing the accuracy of diagnostic tests Yemisi Takwoingi, Richard Riley and Jon Deeks Outline Rationale Methods Findings Summary Motivating
Empirical assessment of univariate and bivariate meta-analyses for comparing the accuracy of diagnostic tests Yemisi Takwoingi, Richard Riley and Jon Deeks Outline Rationale Methods Findings Summary Motivating
Pre-operative MRCP: is it necessary before routine laparoscopic cholecystectomy to exclude CBD stone-prospective study in tertiary care hospital
 International Surgery Journal Rao GB et al. Int Surg J. 2017 Nov;4(11):3633-3637 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20174636
International Surgery Journal Rao GB et al. Int Surg J. 2017 Nov;4(11):3633-3637 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20174636
Title: Painless jaundice as an initial presentation of lung adenocarcinoma
 Title: Painless jaundice as an initial presentation of lung adenocarcinoma Authors: Irene Andaluz García, Irene González Partida, Javier Lucas Ramos, Jorge Yebra Carmona DOI: 10.17235/reed.2018.5587/2018
Title: Painless jaundice as an initial presentation of lung adenocarcinoma Authors: Irene Andaluz García, Irene González Partida, Javier Lucas Ramos, Jorge Yebra Carmona DOI: 10.17235/reed.2018.5587/2018
Colangitis Esclerosante Primaria: Manejo Clínico y Endoscópico
 Colangitis Esclerosante Primaria: Manejo Clínico y Endoscópico Andrés Cárdenas, MD, MMSc, PhD, AGAF, FAASLD GI / Liver Unit, Hospital Clinic Institut de Malalties Digestives i Metaboliques Associate Professor
Colangitis Esclerosante Primaria: Manejo Clínico y Endoscópico Andrés Cárdenas, MD, MMSc, PhD, AGAF, FAASLD GI / Liver Unit, Hospital Clinic Institut de Malalties Digestives i Metaboliques Associate Professor
Management of Gallstone Pancreatitis: Effects of Deviation from Clinical Guidelines
 Management of Gallstone Pancreatitis: Effects of Deviation from Clinical Guidelines Kevin Sargen, Andrew N Kingsnorth Department of Surgery, Plymouth Postgraduate Medical School, Derriford Hospital. Plymouth.
Management of Gallstone Pancreatitis: Effects of Deviation from Clinical Guidelines Kevin Sargen, Andrew N Kingsnorth Department of Surgery, Plymouth Postgraduate Medical School, Derriford Hospital. Plymouth.
Disclosures. Extra-hepatic Biliary Disease and the Pancreas. Objectives. Pancreatitis 10/3/2018. No relevant financial disclosures to report
 Extra-hepatic Biliary Disease and the Pancreas Disclosures No relevant financial disclosures to report Jeffrey Coughenour MD FACS Clinical Associate Professor of Surgery and Emergency Medicine Division
Extra-hepatic Biliary Disease and the Pancreas Disclosures No relevant financial disclosures to report Jeffrey Coughenour MD FACS Clinical Associate Professor of Surgery and Emergency Medicine Division
Research Article Routine Cysticotomy and Flushing of the Cystic Duct in Patients with Low Risk of Common Duct Stones: Can It Be Beneficial?
 Hindawi Minimally Invasive Surgery Volume 2017, Article ID 9814389, 5 pages https://doi.org/10.1155/2017/9814389 Research Article Routine Cysticotomy and Flushing of the Cystic Duct in Patients with Low
Hindawi Minimally Invasive Surgery Volume 2017, Article ID 9814389, 5 pages https://doi.org/10.1155/2017/9814389 Research Article Routine Cysticotomy and Flushing of the Cystic Duct in Patients with Low
Original Policy Date 12:2013
 MP 6.01.30 Magnetic Resonance Cholangiopancreatography Medical Policy Section Radiology Is12:2013sue 3:2005 Original Policy Date 12:2013 Last Review Status/Date 12:2013 Return to Medical Policy Index Disclaimer
MP 6.01.30 Magnetic Resonance Cholangiopancreatography Medical Policy Section Radiology Is12:2013sue 3:2005 Original Policy Date 12:2013 Last Review Status/Date 12:2013 Return to Medical Policy Index Disclaimer
Laparoscopic Cholecystectomy: A Retrospective Study
 Bahrain Medical Bulletin, Vol. 37, No. 3, September 2015 Laparoscopic Cholecystectomy: A Retrospective Study Abdullah Al-Mitwalli, LRCPI, LRCSI* Martin Corbally, MBBCh, BAO, MCh, FRCSI, FRCSEd, FRCS**
Bahrain Medical Bulletin, Vol. 37, No. 3, September 2015 Laparoscopic Cholecystectomy: A Retrospective Study Abdullah Al-Mitwalli, LRCPI, LRCSI* Martin Corbally, MBBCh, BAO, MCh, FRCSI, FRCSEd, FRCS**
Management of Gallbladder Disease
 Management of Gallbladder Disease Steven B. Johnson, MD, FACS, FCCM Professor and Chairman, Department of Surgery Program Director, Phoenix Integrated Surgical Residency University of Arizona College of
Management of Gallbladder Disease Steven B. Johnson, MD, FACS, FCCM Professor and Chairman, Department of Surgery Program Director, Phoenix Integrated Surgical Residency University of Arizona College of
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 8/27/2011 Radiology Quiz of the Week # 35 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 8/27/2011 Radiology Quiz of the Week # 35 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
MANAGEMENT OF COMPLICATED GALLSTONE DISEASE
 gastrointestinal tract and abdomen MANAGEMENT OF COMPLICATED GALLSTONE DISEASE Carmen L. Mueller, BSc(H), MD, FRCSC, Amy A. Neville, MD, FRCSC, MSc, and Gerald M. Fried, MD, FRCSC, FACS, FCAHS Gallstones
gastrointestinal tract and abdomen MANAGEMENT OF COMPLICATED GALLSTONE DISEASE Carmen L. Mueller, BSc(H), MD, FRCSC, Amy A. Neville, MD, FRCSC, MSc, and Gerald M. Fried, MD, FRCSC, FACS, FCAHS Gallstones
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Comparative Study between Laparoscopic and Open Cholecystectomy for Dr. B. Hemasankararao 1,
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Comparative Study between Laparoscopic and Open Cholecystectomy for Dr. B. Hemasankararao 1,
HPB ORIGINAL ARTICLE. Abstracthpb_ Keywords. Correspondence. Introduction. Kerry Anderson, Lisa A. Brown, Philip Daniel & Saxon J.
 DOI:10.1111/j.1477-2574.2010.00173.x HPB ORIGINAL ARTICLE Alanine transaminase rather than abdominal ultrasound alone is an important investigation to justify cholecystectomy in patients presenting with
DOI:10.1111/j.1477-2574.2010.00173.x HPB ORIGINAL ARTICLE Alanine transaminase rather than abdominal ultrasound alone is an important investigation to justify cholecystectomy in patients presenting with
CME Article Clinics in diagnostic imaging (115) Wai C T, Seto K Y, Sutedja D S
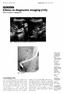 Medical Education Singapore Med.1 2007, 48 (4) : 361 CME Article Clinics in diagnostic imaging (115) Wai C T, Seto K Y, Sutedja D S fit. B CD - -0 o -5 r t -10 Fig. I US images of the upper right abdomen
Medical Education Singapore Med.1 2007, 48 (4) : 361 CME Article Clinics in diagnostic imaging (115) Wai C T, Seto K Y, Sutedja D S fit. B CD - -0 o -5 r t -10 Fig. I US images of the upper right abdomen
Endoscopic management of postoperative bile duct injuries: a single center experience.
 1- Endoscopic management of postoperative bile duct injuries: a single center experience. BACKGROUND/AIM: Biliary endoscopic procedures may be less invasive than surgery for management of postoperative
1- Endoscopic management of postoperative bile duct injuries: a single center experience. BACKGROUND/AIM: Biliary endoscopic procedures may be less invasive than surgery for management of postoperative
CHOLANGIOGRAPHY IN PATIENTS WITH SUSPECTED DUCT STONES
 SAFETY AND OUTCOME OF SELECTIVE INTRA-OPERATIVE CHOLANGIOGRAPHY IN PATIENTS WITH SUSPECTED DUCT STONES Ihab Kadry, Mahmoud Reda, Hesham Ahmed and Mohamed ZaaZou. Department Of General Surgery Misr University
SAFETY AND OUTCOME OF SELECTIVE INTRA-OPERATIVE CHOLANGIOGRAPHY IN PATIENTS WITH SUSPECTED DUCT STONES Ihab Kadry, Mahmoud Reda, Hesham Ahmed and Mohamed ZaaZou. Department Of General Surgery Misr University
The Present Scenario of Cholecystectomy
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 5 Ver. III (May. 2016), PP 71-75 www.iosrjournals.org The Present Scenario of Cholecystectomy
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 5 Ver. III (May. 2016), PP 71-75 www.iosrjournals.org The Present Scenario of Cholecystectomy
ACG Clinical Guideline: Management of Acute Pancreatitis
 ACG Clinical Guideline: Management of Acute Pancreatitis Scott Tenner, MD, MPH, FACG 1, John Baillie, MB, ChB, FRCP, FACG 2, John DeWitt, MD, FACG 3 and Santhi Swaroop Vege, MD, FACG 4 1 State University
ACG Clinical Guideline: Management of Acute Pancreatitis Scott Tenner, MD, MPH, FACG 1, John Baillie, MB, ChB, FRCP, FACG 2, John DeWitt, MD, FACG 3 and Santhi Swaroop Vege, MD, FACG 4 1 State University
Title: Insertion of fully covered self-expanding. metal stents in benign biliary diseases. Rev
 Title: Insertion of fully covered self-expanding metal stents in benign biliary diseases Authors: Mariana Omodeo, Ignacio Malaga, Dante Manazzoni, Cecilia Curvale, Julio de Maria, Martín Alejandro Guidi,
Title: Insertion of fully covered self-expanding metal stents in benign biliary diseases Authors: Mariana Omodeo, Ignacio Malaga, Dante Manazzoni, Cecilia Curvale, Julio de Maria, Martín Alejandro Guidi,
Pictorial review of Benign Biliary tract abnormality on MRCP/MRI Liver with Endoscopic (including splyglass) and Endoscopic Ultrasound correlation
 Pictorial review of Benign Biliary tract abnormality on MRCP/MRI Liver with Endoscopic (including splyglass) and Endoscopic Ultrasound correlation Poster No.: C-2617 Congress: ECR 2015 Type: Educational
Pictorial review of Benign Biliary tract abnormality on MRCP/MRI Liver with Endoscopic (including splyglass) and Endoscopic Ultrasound correlation Poster No.: C-2617 Congress: ECR 2015 Type: Educational
Cholecystectomy for acute gallstone pancreatitis: early vs delayed approach
 Scandinavian Journal of Surgery 99: 81 85, 2010 Cholecystectomy for acute gallstone pancreatitis: early vs delayed approach C. T. Wilson, M. A. de Moya Department of Trauma, Emergency Surgery, and Critical
Scandinavian Journal of Surgery 99: 81 85, 2010 Cholecystectomy for acute gallstone pancreatitis: early vs delayed approach C. T. Wilson, M. A. de Moya Department of Trauma, Emergency Surgery, and Critical
Open Common Bile Duct Exploration in a Nigerian Tertiary Hospital
 ORIGINAL ARTICLE Open Common Bile Duct Exploration in a Nigerian Tertiary Hospital Adewale Adisa, Olusegun Alatise, Olalekan Olasehinde, Bolanle Ibitoye, Olukayode Arowolo, Oladejo Lawal Obafemi Awolowo
ORIGINAL ARTICLE Open Common Bile Duct Exploration in a Nigerian Tertiary Hospital Adewale Adisa, Olusegun Alatise, Olalekan Olasehinde, Bolanle Ibitoye, Olukayode Arowolo, Oladejo Lawal Obafemi Awolowo
Comparison Between Primary Closure of Common Bile Duct and T- Tube Drainage After Open Choledocholithiasis: A Hospital Based Study
 Original article: Comparison Between Primary Closure of Common Bile Duct and T- Tube Drainage After Open Choledocholithiasis: A Hospital Based Study Kali CharanBansal Principal Specialist (General surgery)
Original article: Comparison Between Primary Closure of Common Bile Duct and T- Tube Drainage After Open Choledocholithiasis: A Hospital Based Study Kali CharanBansal Principal Specialist (General surgery)
Comparative Study of Outcomes of Early Versus Interval Laparoscopic Cholecystectomy in Acute Calculus Cholecystitis.
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 4 Ver. IX (April. 2017), PP 68-73 www.iosrjournals.org Comparative Study of Outcomes of Early
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 4 Ver. IX (April. 2017), PP 68-73 www.iosrjournals.org Comparative Study of Outcomes of Early
Primary Closure Versus T-tube Drainage After Open Choledochotomy
 Original Article Primary Closure Versus T-tube Drainage After Open Choledochotomy M. Ambreen, A.R. Shaikh, A. Jamal, J.N. Qureshi, A.G. Dalwani and M.M. Memon, Department of Surgery, Liaquat University
Original Article Primary Closure Versus T-tube Drainage After Open Choledochotomy M. Ambreen, A.R. Shaikh, A. Jamal, J.N. Qureshi, A.G. Dalwani and M.M. Memon, Department of Surgery, Liaquat University
ROLE OF RADIOLOGY IN INVESTIGATION OF JAUNDICE
 ROLE OF RADIOLOGY IN INVESTIGATION OF JAUNDICE Dr. Sohan kumar sah *, Dr. Liu Sibin, Dr. sumendra raj pandey, Dr. Prakashmaan shah, Dr. Gaurishankar pandit, Dr. Suraj kurmi and Dr. Sanjay kumar jaiswal
ROLE OF RADIOLOGY IN INVESTIGATION OF JAUNDICE Dr. Sohan kumar sah *, Dr. Liu Sibin, Dr. sumendra raj pandey, Dr. Prakashmaan shah, Dr. Gaurishankar pandit, Dr. Suraj kurmi and Dr. Sanjay kumar jaiswal
The Incidence of Complications in Single-stage Endoscopic Stone Removal for Patients with Common Bile Duct Stones: A Propensity Score Analysis
 doi: 10.2169/internalmedicine.9123-17 http://internmed.jp ORIGINAL ARTICLE The Incidence of Complications in Single-stage Endoscopic Stone Removal for Patients with Common Bile Duct Stones: A Propensity
doi: 10.2169/internalmedicine.9123-17 http://internmed.jp ORIGINAL ARTICLE The Incidence of Complications in Single-stage Endoscopic Stone Removal for Patients with Common Bile Duct Stones: A Propensity
An angulated common bile duct predisposes to recurrent symptomatic bile duct stones after endoscopic stone extraction
 Surg Endosc (2006) 20: 1594 1599 DOI: 10.1007/s00464-005-0656-x Ó Springer Science+Business Media, Inc. 2006 An angulated common bile duct predisposes to recurrent symptomatic bile duct stones after endoscopic
Surg Endosc (2006) 20: 1594 1599 DOI: 10.1007/s00464-005-0656-x Ó Springer Science+Business Media, Inc. 2006 An angulated common bile duct predisposes to recurrent symptomatic bile duct stones after endoscopic
Magnetic resonance cholangiography compared with endoscopic retrograde cholangiography in the diagnosis of primary sclerosing cholangitis
 Original Article Magnetic resonance cholangiography compared with endoscopic retrograde cholangiography in the diagnosis of primary sclerosing cholangitis Hossein Ahrar, Mohamad Saleh Jafarpishe, Ali Hekmatnia,
Original Article Magnetic resonance cholangiography compared with endoscopic retrograde cholangiography in the diagnosis of primary sclerosing cholangitis Hossein Ahrar, Mohamad Saleh Jafarpishe, Ali Hekmatnia,
Idiopathic adulthood ductopenia manifesting as jaundice in a young male
 Idiopathic adulthood ductopenia manifesting as jaundice in a young male Deepak Jain*,1, H. K. Aggarwal 1, Avinash Rao 1, Shaveta Dahiya 1, Promil Jain 2 1 Department of Medicine, Pt. B.D. Sharma University
Idiopathic adulthood ductopenia manifesting as jaundice in a young male Deepak Jain*,1, H. K. Aggarwal 1, Avinash Rao 1, Shaveta Dahiya 1, Promil Jain 2 1 Department of Medicine, Pt. B.D. Sharma University
Endoscopic treatment of primary sclerosing cholangitis: Is there something new?
 Endoscopic treatment of primary sclerosing cholangitis: Is there something new? Arnaud Lemmers, MD, PhD Gastroenterology Department, Erasme Hospital, ULB, Brussels BASL December 1st 2017 AGENDA Introduction
Endoscopic treatment of primary sclerosing cholangitis: Is there something new? Arnaud Lemmers, MD, PhD Gastroenterology Department, Erasme Hospital, ULB, Brussels BASL December 1st 2017 AGENDA Introduction
Controversies in the management of acute pancreatitis
 Kathmandu University Medical Journal (3) Vol., No. 3, Issue 7, 3-7 Controversies in the management of acute pancreatitis Singh DR 1, Mehta A, Dangol UMS 3 1 Lecturer, Medical Officer, 3 Lecturer, Dept.
Kathmandu University Medical Journal (3) Vol., No. 3, Issue 7, 3-7 Controversies in the management of acute pancreatitis Singh DR 1, Mehta A, Dangol UMS 3 1 Lecturer, Medical Officer, 3 Lecturer, Dept.
Is Complicated Gallstone Disease Preceded by Biliary Colic?
 J Gastrointest Surg (2009) 13:312 317 DOI 10.1007/s11605-008-0729-y ORIGINAL ARTICLE Is Complicated Gallstone Disease Preceded by Biliary Colic? Marc G. Besselink & Niels G. Venneman & Peter M. Go & Ivo
J Gastrointest Surg (2009) 13:312 317 DOI 10.1007/s11605-008-0729-y ORIGINAL ARTICLE Is Complicated Gallstone Disease Preceded by Biliary Colic? Marc G. Besselink & Niels G. Venneman & Peter M. Go & Ivo
Interval Laparoscopic Cholecystectomy
 HPB Surgery, 2000, Vol. 11, pp. 319-323 Reprints available directly from the publisher Photocopying permitted by license only (C) 2000 OPA (Overseas Publishers Association) N.V. Published by license under
HPB Surgery, 2000, Vol. 11, pp. 319-323 Reprints available directly from the publisher Photocopying permitted by license only (C) 2000 OPA (Overseas Publishers Association) N.V. Published by license under
Severe necrotizing pancreatitis. ICU Fellowship Training Radboudumc
 Severe necrotizing pancreatitis ICU Fellowship Training Radboudumc Acute pancreatitis Patients with acute pancreatitis van Dijk SM. Gut 2017;66:2024-2032 Diagnosis Revised Atlanta classification Abdominal
Severe necrotizing pancreatitis ICU Fellowship Training Radboudumc Acute pancreatitis Patients with acute pancreatitis van Dijk SM. Gut 2017;66:2024-2032 Diagnosis Revised Atlanta classification Abdominal
Making ERCP Easy: Tips From A Master
 Making ERCP Easy: Tips From A Master Raj J. Shah, M.D., FASGE Associate Professor of Medicine University of Colorado School of Medicine Co-Director, Endoscopy Director, Pancreaticobiliary Endoscopy Services
Making ERCP Easy: Tips From A Master Raj J. Shah, M.D., FASGE Associate Professor of Medicine University of Colorado School of Medicine Co-Director, Endoscopy Director, Pancreaticobiliary Endoscopy Services
Original Contributions
 PII S0736-4679(01)00329-8 The Journal of Emergency Medicine, Vol. 21, No. 1, pp. 7 13, 2001 Copyright 2001 Elsevier Science Inc. Printed in the USA. All rights reserved 0736-4679/01 $ see front matter
PII S0736-4679(01)00329-8 The Journal of Emergency Medicine, Vol. 21, No. 1, pp. 7 13, 2001 Copyright 2001 Elsevier Science Inc. Printed in the USA. All rights reserved 0736-4679/01 $ see front matter
Cholecystectomy rate following endoscopic biliary interventions
 Original Article Brunei Int Med J. 2012; 8 (4): 166-172 Cholecystectomy rate following endoscopic biliary interventions Sky Lim 1, Lin Naing 1, Vui Heng Chong 2 1 Pengiran Anak Puteri Rashidah Sa adatul
Original Article Brunei Int Med J. 2012; 8 (4): 166-172 Cholecystectomy rate following endoscopic biliary interventions Sky Lim 1, Lin Naing 1, Vui Heng Chong 2 1 Pengiran Anak Puteri Rashidah Sa adatul
In Woong Han 1, O Choel Kwon 1, Min Gu Oh 1, Yoo Shin Choi 2, and Seung Eun Lee 2. Departments of Surgery, Dongguk University College of Medicine 2
 Effect of Rowachol on Prevention of Postcholecystectomy Syndrome after Laparoscopic Cholecystectomy - Prospective multicenter Randomized controlled trial- In Woong Han 1, O Choel Kwon 1, Min Gu Oh 1, Yoo
Effect of Rowachol on Prevention of Postcholecystectomy Syndrome after Laparoscopic Cholecystectomy - Prospective multicenter Randomized controlled trial- In Woong Han 1, O Choel Kwon 1, Min Gu Oh 1, Yoo
Biliary sphincterotomy dilation for the extraction of difficult common bile duct stones
 1130-0108/2009/101/8/541-545 REVISTA ESPAÑOLA DE ENFERMEDADES DIGESTIVAS Copyright 2009 ARÁN EDICIONES, S. L. REV ESP ENFERM DIG (Madrid) Vol. 101. N. 8, pp. 541-545, 2009 Biliary sphincterotomy dilation
1130-0108/2009/101/8/541-545 REVISTA ESPAÑOLA DE ENFERMEDADES DIGESTIVAS Copyright 2009 ARÁN EDICIONES, S. L. REV ESP ENFERM DIG (Madrid) Vol. 101. N. 8, pp. 541-545, 2009 Biliary sphincterotomy dilation
Endoscopic Management of the Iatrogenic CBD Injury
 The Liver Week 2014, Jeju, Korea Endoscopic Management of the Iatrogenic CBD Injury Jong Ho Moon, MD, PhD Department of Internal Medicine Soon Chun Hyang University School of Medicine Bucheon/Seoul, KOREA
The Liver Week 2014, Jeju, Korea Endoscopic Management of the Iatrogenic CBD Injury Jong Ho Moon, MD, PhD Department of Internal Medicine Soon Chun Hyang University School of Medicine Bucheon/Seoul, KOREA
Role of Therapeutic Endoscopy in Hepatic Hydatid Disease after Surgical Intervention: Case Report
 ISPUB.COM The Internet Journal of Gastroenterology Volume 10 Number 2 Role of Therapeutic Endoscopy in Hepatic Hydatid Disease after Surgical Intervention: Case Report H Ono, M Okabe, T Kimura, M Kawakami,
ISPUB.COM The Internet Journal of Gastroenterology Volume 10 Number 2 Role of Therapeutic Endoscopy in Hepatic Hydatid Disease after Surgical Intervention: Case Report H Ono, M Okabe, T Kimura, M Kawakami,
Gallstone disease is responsible for about
 CMAJ Management of suspected stones in the common bile duct Majid A. Almadi MBBS MSc, Jeffrey S. Barkun MD CM MSc, Alan N. Barkun MD CM MSc Competing interests: Alan Barkun has received consultancy fees
CMAJ Management of suspected stones in the common bile duct Majid A. Almadi MBBS MSc, Jeffrey S. Barkun MD CM MSc, Alan N. Barkun MD CM MSc Competing interests: Alan Barkun has received consultancy fees
Single-Session Treatment of Cholecysto-Choledocholithiasis: Totally Laparoscopic versus Laparo-Endoscopic
 Journal of Surgery 2017; 5(5): 72-78 http://www.sciencepublishinggroup.com/j/js doi: 10.11648/j.js.20170505.11 ISSN: 2330-0914 (Print); ISSN: 2330-0930 (Online) Single-Session Treatment of Cholecysto-Choledocholithiasis:
Journal of Surgery 2017; 5(5): 72-78 http://www.sciencepublishinggroup.com/j/js doi: 10.11648/j.js.20170505.11 ISSN: 2330-0914 (Print); ISSN: 2330-0930 (Online) Single-Session Treatment of Cholecysto-Choledocholithiasis:
