Primary Closure Versus T-tube Drainage After Open Choledochotomy
|
|
|
- Hester O’Brien’
- 5 years ago
- Views:
Transcription
1 Original Article Primary Closure Versus T-tube Drainage After Open Choledochotomy M. Ambreen, A.R. Shaikh, A. Jamal, J.N. Qureshi, A.G. Dalwani and M.M. Memon, Department of Surgery, Liaquat University of Medical and Health Sciences, Jamshoro, Sindh, Pakistan. BACKGROUND: Choledochotomy followed by T-tube has long been a standard surgical treatment for choledocholithiasis. It is still a preferred choice in many hospitals where minimal invasive procedures are not feasible. The use of T-tube is not without complications. To avoid the complications associated with T-tube, we have performed primary closure of the common bile duct (CBD) after exploration. This pilot study assesses the safety of primary closure of CBD, which would help form a basis for implementation on a wider scale. OBJECTIVE: To compare the clinical results of primary closure with T-tube drainage after open choledochotomy and assess the safety of primary closure for future application on a greater mass. PATIENTS AND METHODS: This comparative study was conducted at surgical unit IV Liaquat University of Medical and Health Sciences, Jamshoro, from January 2007 to December Thirty-five patients were included in the study of which 16 patients underwent primary closure. RESULTS: Thirty-five patients were included in the study. The mean age of patients who had primary closure done (n = 16) was 46.0 ± 16.8 and there were two (12.5%) males and 14 (87.5%) females. After primary closure of the CBD, bile leakage was noted in one patient (6.3%), which subsided without any biliary peritonitis as compared to the T-tube group in which two patients (10.5%) had bile leakage. Postoperative jaundice was seen in one patient (5.3%) who had a T-tube because of a blockage of CBD. Not a single patient had a retained stone in both groups as well as no recurrence of CBD stones. The postoperative hospital stay after primary closure was 5.56 ± 1.1 days as compared to after T-tube drainage which was 13.6 ± 2.3 days. The total cost of treatment in patients who underwent primary closure was USD194.5 ± 41.5 but after T-tube drainage it was USD548.6 ± The median follow up duration for both groups was 6 months. CONCLUSION: Primary CBD closure is a safe and cost effective alternative to routine T-tube drainage after open choledochotomy. [Asian J Surg 2009;32(1):21 5] Key Words: choledocholithiasis, open choledochotomy, primary closure Introduction Chloledocholithiasis develops in about 10 15% of patients with gallbladder stones 1 and literature suggests that common bile duct (CBD) stones are encountered in approximately 7 15% of patients undergoing cholecystectomy. 2 There are two methods for extracting CBD stones either endoscopically, by endoscopic retrograde cholangiopancreatography (ERCP), or surgically, by an open or laparoscopic method. Open exploration of the bile duct was the principal treatment for almost 100 years. In some hospitals of Address correspondence and reprint requests to Dr Ambreen Muneer, Assistant Professor, Department of surgery, Liaquat University of Medical and Health Sciences, Jamshoro, Sindh, Pakistan. banglani_90@hotmail.com Date of acceptance: 7 August Elsevier. All rights reserved. ASIAN JOURNAL OF SURGERY VOL 32 NO 1 JANUARY
2 AMBREEN et al developing countries, surgeons are still performing this procedure because minimally invasive techniques like ERCP are not available. 3 Due to the lack of experienced endoscopists at smaller hospitals, patients need to be transferred to a larger centre for endoscopic diagnosis and treatment, which increases costs and patient discomfort. 4 The laparoscopic management of CBD stones is well known these days, 5 but remains controversial. This procedure is demands skills and equipment, and is therefore used by few surgeons. 6 Moreover, the superiority of this procedure for the treatment of CBD stones has not yet been proven, which limits its applicability. 7 Therefore open surgery is still a treatment of choice in many hospitals. The classical performance of bile duct exploration is associated with the problem of an incised bile duct closure. Choledochotomy followed by T-tube drainage is a traditional surgical treatment for chloledocholithiasis. 8 Although it is true that the T-tube has been used and has proven to be a safe and effective method for postoperative biliary decompression, it is not exempt from complications, which are present in up to 10% of patients. 9 The most frequent of these is bile leakage after removal, which is reported to occur in 1 19% of cases. 6,10 12 Some of these complications are serious, such as bile leak, tract infection or acute renal failure from dehydration due to inadequate water ingestion or a very high outflow, particularly in elderly patients. In addition, having bile drainage in place for at least 3 weeks causes significant discomfort in patients and delays their return to work Primary closure of the CBD after exploration is not new. Halstead first described the advantages of primary closure. There are many papers reported by different authors, which support the direct closure of the duct immediately after exploration. 3,12,14,16,17 With the help of a choledochoscope during surgery, direct visualisation of the CBD is possible and retained stones are not a problem. In our hospital, open CBD exploration is still the treatment chosen for CBD stones. In this study, our aim was to compare the clinical short-term results of primary closure of CBD and T-tube drainage, and to assess the benefits of primary closure of CBD at a government hospital in a developing country. Patients and methods admitted at Surgical Unit IV in Liaquat University Hospital, Jamshoro in the year 2007, were included in the study. The patients were evaluated with routine investigations including full blood counts, liver function tests, coagulation screening and abdominal ultrasonography. The criteria for choledochotomy were obstructive jaundice, CBD stones suggested by ultrasound, or the presence of stones in the CBD palpated preoperatively. Patients with pancreatitis, suppurative cholangitis and malignancy were excluded. All patients were given antibiotics before they were taken for elective open surgery. The CBD was opened through a supraduodenal vertical incision between stay sutures. Stones were taken out and saline flushing followed to ensure patency. We confirmed the clearance of the duct with a choledochoscope. Then primary closure of the CBD was performed in 17 patients. After completion of choledochoscopy, patients were randomly selected to undergo either one of the two surgical options: primary closure of CBD and T-tube drainage. Interrupted 3/0 vicryl sutures were applied. In 19 patients, a T-tube was inserted into the CBD. A sub hepatic drain was kept in all patients. T-tube cholangiography was done on the seventh postoperative day in all T-tube drained patients. Once patency of CBD was confirmed and there was a free flow of dye, the intermittent clamping of T-tube was done and the T-tube was removed on the twelfth postoperative day. Postoperatively, ultrasound and liver function tests were done. We compared the postoperative complications, postoperative hospital stay and the total cost of treatment between the two groups. Bile leakage is defined as any yellow bile-like fluid coming out of the sub hepatic drain or after the removal of the drain aspiration of yellow coloured bilelike fluid under ultrasound guidance from sub hepatic peritoneal space (300 ml). The data was analysed in statistical program SPSS version Fisher s exact test of chi-squared was applied for categorical variables to calculate frequencies and percentages among the groups. Student s t-test was applied for continuous variable to compare the means (2 tailed) with median and range among the groups. All the parameters were calculated on 95% confidence interval. If the value of p 0.05 it was considered statistically significant. Results This was a pilot project conducted at surgical unit IV Liaquat University Hospital, Jamshoro. Thirty-five patients, CBD exploration was performed in 35 patients, out of which 16 had primary closure of CBD after stone 22 ASIAN JOURNAL OF SURGERY VOL 32 NO 1 JANUARY 2009
3 PRIMARY CLOSURE OF CBD removal. A T-tube drain was placed in 19 patients. The mean age of patients who had primary closure was 46.0 ± 16.8 years (median, 48.5 years; range, years) and that of T-tube drains was 41.9 ± 13.9 years (median, 40.0 years; range, years). There were two males (12.5%) and 14 females (87.5%) in the primary closure group, and three males (15.7%) and 16 females (84.2%) in T-tube group (Table 1). The clinical presentation of choledocholithiasis is listed in Table 1. Most of the patients in both groups presented with biliary colic (62.5% and 78.9%). Other clinical presentations were acute cholecystitis and jaundice, which were nearly of same frequency in each group. Out of 35 patients, eight patients had comorbidities like diabetes mellitus and hypertension (31.3% and 15.8%). Fourteen patients (87.5%) in the primary closure group had concomitant gallstones and 13 (68.4%) in the T-tube group as evident by preoperative abdominal ultrasound. Preoperative liver functions were compared between two groups (Table 1). There was a significant difference in the level of serum glutamic pyruvic transaminase (SGPT) between the two groups. Preoperative abdominal ultrasound showed the size of CBD and number of CBD stones, which was then confirmed during the operation. The mean diameter of CBD was 1.52 ± 0.36 cm (median, 1.45 cm; range, cm) in patients who had primary closure and 1.64 ± 0.55 cm (median, 1.50 cm; range, cm). The maximum number of stones (10) was noted in the T-tube drain group (Table 1). Fifteen patients in the primary closure group did not suffer any complication. One patient had a bile leakage that subsided on the third postoperative day. There was no biliary peritonitis. The total complication rate in this group was 6.3% (Table 2). In the T-tube drain patients, biliary complication occurred in three patients, accounting for 15.7%. Two patients had bile leakage (10.5%) after removal of the T-tube that was managed by ultrasound guided aspiration. In both of these patients, the T-tube was removed on the twelfth postoperative day. One patient had postoperative jaundice because of a blockage of the duct caused by the T-tube. The T-tube was removed and jaundice Table 1. Demographic characteristics of patients Primary closure Range T-tube drain Range (n = 16) (Min Max) (n = 19) (Min Max) Age (yr) 46.0 ± ± NS Gender Male 2 (12.5%) 3 (15.7%) NS Female 14 (87.5%) 16 (84.2%) Symptoms Biliary colic 10 (62.5%) 15 (78.9%) NS Acute cholecystitis 6 (37.5%) 6 (31.5%) Jaundice 8 (50.0%) 8 (42.1%) Co-morbidities 5 (31.3%) 3 (15.8%) NS Concomitant gallstones 14 (87.5%) 13 (68.4%) NS Preoperative liver function Total bilirubin (mg %) 2.2 ± ± NS SGPT (U/L) ± ± Alkaline phosphatase (U/L) ± , ± NS Number of CBD stones 2.2 ± ± CBD diameter (cm) 1.52 ± , ± NS Results are expressed as mean ± standard deviation; median and range. CBD = common bile duct; NS = not significant. ASIAN JOURNAL OF SURGERY VOL 32 NO 1 JANUARY
4 AMBREEN et al gradually subsided (Table 2). There was not any recurrence of CBD stones seen up to 6 months follow up and postoperative ultrasound findings were almost normal (Table 2). The mean postoperative hospital stay in the primary closure group was 5.1 ± 1.1 days (median, 5.0 days; range, 4 7 days), compared to the T-tube drainage group which was 13.6 ± 2.3 (median, 15.0 days; range, 7 18 days) (Table 3). The average cost of treatment for open CBD exploration and primary closure of the CBD was USD194.5 ± 41.5 (median, USD187.5; range, USD ), whereas in the T-tube drainage group it is much more, i.e. USD548.6 ± 88.5 (median, USD600; range, USD ) (Table 3). The mean duration of follow-up in the primary closure group was 5.62 ± 0.7 months (median, 6.0 months; range, 4 6 months) and in the T-tube drain group it was 5.7 ± 0.5 months (median, 6.0 months; range, 4 6 months) (Table 3). Table 2. Postoperative complications Primary closure T-tube drain (n = 16) (n = 19) Bile leakage 1 (6.3%) 2 (10.5%) NS Postoperative 0 1 (5.3%) NS jaundice Retained stone 0 0 Recurrence of 0 0 CBD stones Results are expressed as number and percentage. CBD = common bile duct; NS = not significant. Discussion Symptomatic gallstone disease is a very common indication for abdominal surgery. 18 Before the laparoscopic era, cholecystectomy and CBD stones were removed in a single procedure. This approach has been effective with morbidity below 15% and mortality below 1% in a patient up to 65 years old. 19 In the era of minimally invasive procedures, open laparotomy for CBD exploration may still be the choice in some hospitals in developing countries. In this study, we performed open surgery for exploration of CBD and ensured the duct clearance by choledochoscopy following choledochotomy. After exploration of CBD for choledocholithiasis, intraductal drainage using a T-tube has been a standard practice. 20 The use of a T-tube is not without complications and there are many reports of complications with T-tube. 8,10,21 24 In our study, we had two cases of bile leakage in patients in whom the T-tube was used (10.5%), and one case among the 17 patients (6.2%) in whom primary closure of the CBD was done. Yamazaki et al 5 reported an incidence of 11.7% and 5.8% respectively, and an overall incidence of leakage was reported to be %. On the other hand, after primary closure, there were no bile leakage cases reported by other authors. 16,17 There was no major complications noted in any of our patients. There have been reports of intraperitoneal leakage with subsequent biliary peritonitis. 1,3,8 No such complication occurred in our patients and no deaths occurred in our study. The reason for this was probably that we used choledochoscopy and did not probe the lower end of the CBD. These measures reduced the risk of biliary leakage. There was a significant difference in postoperative Table 3. Hospital stay, cost of treatment and follow up duration Primary closure Range T-tube drain Range (n = 16) (Min Max) (n = 19) (Min Max) Hospital stay (d) 5.1 ± ± Cost of treatment (USD) ± ± < Follow up duration (mo) 5.62 ± ± NS Results are expressed as mean ± standard deviation; median and range. The data was analysed in statistical program SPSS version Fisher s exact test of chi-squared was applied for categorical variables to calculate frequencies and percentage among the group. Student s t test was used for continuous parameters to compare the means (2 tailed) with median and range between the groups. All the parameters were calculated on 95% confidence interval. A value of p 0.05 was considered as statistically significant. NS = not significant. 24 ASIAN JOURNAL OF SURGERY VOL 32 NO 1 JANUARY 2009
5 PRIMARY CLOSURE OF CBD hospital admission days and the total cost of treatment between our two groups. In a group where primary closure was performed, they remained in the hospital for a shorter period and were not burdened by a T-tube. In patients where the T-tube has been kept in place, there was the additional cost of postoperative cholangiography. In a developing country like Pakistan, this difference in expenditure has a major impact on public health. Literature 14 suggests that early discharge from hospital means an early return to work, which further has an indirect effect on the expenses of the patient. Other authors reported similar results 3,14 except in Japan where the number of hospital admission days was higher. 5 Conclusion In open choledochotomy, primary closure of the CBD is performed safely in selected patients with improved patient care. Choledochoscopy ensures clearance of the CBD and eliminates the need for a T-tube. The number of hospital admission days is less and average cost of treatment is much lower than in the patients with a T-tube. From this study, we have concluded that after open surgery for CBD stones, primary closure of CBD is safe and effective with shorter hospital stays and lower costs. References 1. Perez G, Escalona A, Jarufe N, et al. Prospective randomized study of T-tube versus biliary stent for common bile duct decompression after open choledochotomy. World J Surg 2005;29: Ahrendt SA, Pitt HA. Biliary tract. In: Townsend M, ed. Sabiston Text book of Surgery. Philadelphia: WB Saunders, 2004: Tu Z, Li J, Xin H, et al. Primary choledochorrhaphy after common bile duct exploration. Dig Surg 1999;16: Paganini AM, Guerrieri M, Sarnari J, et al. Long-term results after laparoscopic transverse choledochotomy for common bile duct stones. Surg Endosc 2005;19: Yamazaki M, Yasuda H, Koide Y, et al. Primary closure of the common bile duct in open laparotomy for common bile duct stones. J Hepatobiliary Pancreat Surg 2006;13: Martin IJ, Bailey IS, Rhodes M, et al. Towards T-tube free laparoscopic bile duct exploration. A methodologic evolution during 300 consecutive procedures. Ann Surg 1998;228: Tokumura H, Umezawa A, Cao H, et al. Laparoscopic management of common bile duct stones: transcystic approach and choledochotomy. J Hepatobiliary Pancreat Surg 2002;9: Wills VL, Gibson K, Karihaloo C, et al. Complications of biliary T-tubes after choledochotomy. ANZ J Surg 2002;72: Tapia A, Llanos O, Guzman S, et al. Resultados de la coledocotomia clasica por coledocolitiasis: un punto de comparacion para tecnicas altetnativas. Rev Chil Cir 1995;47: [In Spanish] 10. Gharaibeh KIA, Heiss HA. Biliary leakage following T-tube removal. Int Surg 2000;85: Robinson G, Hollinshead J, Falk G, et al. Technique and results of laparoscopic choledochotomy for the management of bile duct calculi. ANZ J Surg 1995;65: Williams JAR, Treacy PJ, Sidey P, et al. Primary duct closure versus T-tube drainage following exploration of the common bile duct. ANZ J Surg 1994;64: Placer G. Bile leakage after removal of T-tube from the common bile duct. Br J Surg 1990;77: Seale AK, Ledet WP Jr. Primary common bile duct closure. Arch Surg 1999;134: Miguel Angel Mercado, Carlos Chan, Hector Orozco, et al. Bile duct injuries related to misplacement of T tubes. Ann Hepatol 2006;5: Chen SS, Chou FF. Choledochotomy for biliary lithiasis: is routine T-tube drainage necessary? Acta Chir Scand 1990;156: Sorenson VJ, Buck JR, Chung SK, et al. Primary bile duct closure following exploration: an effective alternative to routine biliary drainage. Am J Surg 1994;60: Marilee L Freitas, Robert L Bell, Andrew J Duffy. Choledocholithiasis: evolving standards for diagnosis and management. World J Gastroenterol 2006;12: Ko C, Lee S. Epidemiology and natural history of common bile duct stones and prediction of disease. Gastrointest Endosc 2002; 56:S Mehmood A. Wani, M.S., Nisar A, et al. Primary closure of the common duct over endonasobiliary drainage tubes. World J Surg 2005;29: Bernstein DE, Goldberg RI, Unger SW. Common bile duct obstruction following T-tube placement at laparoscopic cholecystectomy. Gastrointest Endosc 1994;40: Hotta T, Kaniguchi K, Kobayashi Y, et al. Biliary drainage tube evaluation after common bile duct exploration for choledocholithiasis. Hepatogastroenterology 2003;50: Moreaux J. Traditional surgical management of common bile duct stones: a prospective study during a 20-year experience. Am J Surg 1995;169: Pappas TN, Slimane TB, Brooks DC. 100 consecutive common bile duct explorations without mortality. Ann Surg 1990;211: ASIAN JOURNAL OF SURGERY VOL 32 NO 1 JANUARY
Comparison Between Primary Closure of Common Bile Duct and T- Tube Drainage After Open Choledocholithiasis: A Hospital Based Study
 Original article: Comparison Between Primary Closure of Common Bile Duct and T- Tube Drainage After Open Choledocholithiasis: A Hospital Based Study Kali CharanBansal Principal Specialist (General surgery)
Original article: Comparison Between Primary Closure of Common Bile Duct and T- Tube Drainage After Open Choledocholithiasis: A Hospital Based Study Kali CharanBansal Principal Specialist (General surgery)
Comparison of billiary stenting with t-tube drainage as a method of decompression in cases of open.
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 11 Ver. XI (Nov. 2017), PP 40-44 www.iosrjournals.org Comparison of billiary stenting with
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 11 Ver. XI (Nov. 2017), PP 40-44 www.iosrjournals.org Comparison of billiary stenting with
Comparison between primary closure and T-tube drainage after open choledocotomy
 ISSN: 2203-1413 Vol.03 No.04 Comparison between primary closure and T-tube drainage after open choledocotomy Alireza Barband 1, Farzad Kakaei 1, Morteza Ghojazadeh 2, Abdolhamid Chavoshi Khamneh 1*, Morteza
ISSN: 2203-1413 Vol.03 No.04 Comparison between primary closure and T-tube drainage after open choledocotomy Alireza Barband 1, Farzad Kakaei 1, Morteza Ghojazadeh 2, Abdolhamid Chavoshi Khamneh 1*, Morteza
T-TUBE DRAINAGE VERSUS PRIMARY COMMON BILE DUCT CLOSURE AFTER OPEN CHOLEDOCHOTOMY
 T-TUBE DRAINAGE VERSUS PRIMARY COMMON BILE DUCT CLOSURE AFTER OPEN CHOLEDOCHOTOMY Khaled Ahmed El- Dabee, Abd Al-Lateif Ahmed, Mohamed Abdel Aziz Abdel Jawad, Taha Bahgat Salam, Ahmed Eisa Ahmed* and Saed
T-TUBE DRAINAGE VERSUS PRIMARY COMMON BILE DUCT CLOSURE AFTER OPEN CHOLEDOCHOTOMY Khaled Ahmed El- Dabee, Abd Al-Lateif Ahmed, Mohamed Abdel Aziz Abdel Jawad, Taha Bahgat Salam, Ahmed Eisa Ahmed* and Saed
Randomized Comparison of Postoperative Short-Term and Mid-Term Complications Between T-Tube and Primary Closure after CBD Exploration
 ORIGINAL ARTICLE Randomized Comparison of Postoperative Short-Term and Mid-Term Complications Between T-Tube and Primary Closure after CBD Exploration Iqbal Muzaffar, Pai Zula, Yusp Yimit, Ajim Tuergan
ORIGINAL ARTICLE Randomized Comparison of Postoperative Short-Term and Mid-Term Complications Between T-Tube and Primary Closure after CBD Exploration Iqbal Muzaffar, Pai Zula, Yusp Yimit, Ajim Tuergan
Study of post cholecystectomy biliary leakage and its management
 Original Research Article Study of post cholecystectomy biliary leakage and its management P. Krishna Kishore 1*, B. Manju Sruthi 2, G. Obulesu 3 1 Assistant Professor, Departmentment of General Surgery,
Original Research Article Study of post cholecystectomy biliary leakage and its management P. Krishna Kishore 1*, B. Manju Sruthi 2, G. Obulesu 3 1 Assistant Professor, Departmentment of General Surgery,
Trend towards primary closure following laparoscopic exploration of the common bile duct
 The Royal College of Surgeons of England HEPATOBILIARY doi 10.1308/003588408X242295 Trend towards primary closure following laparoscopic exploration of the common bile duct M JAMEEL, B DARMAS, AL BAKER
The Royal College of Surgeons of England HEPATOBILIARY doi 10.1308/003588408X242295 Trend towards primary closure following laparoscopic exploration of the common bile duct M JAMEEL, B DARMAS, AL BAKER
Subtotal cholecystectomy for complicated acute cholecystitis: a multicenter prospective observational study
 Study title Subtotal cholecystectomy for complicated acute cholecystitis: a multicenter prospective observational study Primary Investigator: Kazuhide Matsushima, MD Co-Primary investigator: Zachary Warriner,
Study title Subtotal cholecystectomy for complicated acute cholecystitis: a multicenter prospective observational study Primary Investigator: Kazuhide Matsushima, MD Co-Primary investigator: Zachary Warriner,
Management of Gallstone Pancreatitis: Effects of Deviation from Clinical Guidelines
 Management of Gallstone Pancreatitis: Effects of Deviation from Clinical Guidelines Kevin Sargen, Andrew N Kingsnorth Department of Surgery, Plymouth Postgraduate Medical School, Derriford Hospital. Plymouth.
Management of Gallstone Pancreatitis: Effects of Deviation from Clinical Guidelines Kevin Sargen, Andrew N Kingsnorth Department of Surgery, Plymouth Postgraduate Medical School, Derriford Hospital. Plymouth.
Endoscopic Retrograde Pancreatography and Laparoscopic Cholecystectomy. TEAM 1 Janix M. De Guzman, MD Presentor
 Endoscopic Retrograde Pancreatography and Laparoscopic Cholecystectomy TEAM 1 Janix M. De Guzman, MD Presentor Premise 40F Jaundice Abdominal pain US finding of gallstones with apparently normal common
Endoscopic Retrograde Pancreatography and Laparoscopic Cholecystectomy TEAM 1 Janix M. De Guzman, MD Presentor Premise 40F Jaundice Abdominal pain US finding of gallstones with apparently normal common
Sex-related differences in predicting choledocholithiasis using current American Society of Gastrointestinal Endoscopy risk criteria
 ORIGINAL ARTICLE Annals of Gastroenterology (2018) 31, 1-6 Sex-related differences in predicting choledocholithiasis using current American Society of Gastrointestinal Endoscopy risk criteria Ankit Chhoda
ORIGINAL ARTICLE Annals of Gastroenterology (2018) 31, 1-6 Sex-related differences in predicting choledocholithiasis using current American Society of Gastrointestinal Endoscopy risk criteria Ankit Chhoda
Safety of primary common Bile Duct Closure
 Open Access Archives of Surgery and Clinical Research Research Article ISSN 2576-9537 Safety of primary common Bile Duct Closure Mohamed Abdelhamid 1 *, AM Bekeet 1, MA Negida 2, AZ Garib 3 and SS Soliman
Open Access Archives of Surgery and Clinical Research Research Article ISSN 2576-9537 Safety of primary common Bile Duct Closure Mohamed Abdelhamid 1 *, AM Bekeet 1, MA Negida 2, AZ Garib 3 and SS Soliman
Appendix A: Summary of evidence from surveillance
 Appendix A: Summary of evidence from surveillance 2018 surveillance of Gallstone disease: diagnosis and management (2014) NICE guideline CG188 Summary of evidence from surveillance Studies identified in
Appendix A: Summary of evidence from surveillance 2018 surveillance of Gallstone disease: diagnosis and management (2014) NICE guideline CG188 Summary of evidence from surveillance Studies identified in
Presence of choledocholithiasis in patients undergoing cholecystectomy for mild biliary pancreatitis
 Original Article Presence of choledocholithiasis in patients undergoing cholecystectomy for mild biliary pancreatitis Pradhan S 1, Shah S 2, Maharjan S 2, Shah JN 3 1 2 2 3 Professor, Patan hospital Correspondence:
Original Article Presence of choledocholithiasis in patients undergoing cholecystectomy for mild biliary pancreatitis Pradhan S 1, Shah S 2, Maharjan S 2, Shah JN 3 1 2 2 3 Professor, Patan hospital Correspondence:
Open Common Bile Duct Exploration in a Nigerian Tertiary Hospital
 ORIGINAL ARTICLE Open Common Bile Duct Exploration in a Nigerian Tertiary Hospital Adewale Adisa, Olusegun Alatise, Olalekan Olasehinde, Bolanle Ibitoye, Olukayode Arowolo, Oladejo Lawal Obafemi Awolowo
ORIGINAL ARTICLE Open Common Bile Duct Exploration in a Nigerian Tertiary Hospital Adewale Adisa, Olusegun Alatise, Olalekan Olasehinde, Bolanle Ibitoye, Olukayode Arowolo, Oladejo Lawal Obafemi Awolowo
ERCP / PTC Surgical Laparoscopic vs open Timing and order of approach
 Choledocholithiasis Which Approach and When? Lygia Stewart, MD University of California, San Francisco 2010 Naffziger Post-Graduate Course Clinical Manifestations of Choledocholithiasis Asymptomatic (no
Choledocholithiasis Which Approach and When? Lygia Stewart, MD University of California, San Francisco 2010 Naffziger Post-Graduate Course Clinical Manifestations of Choledocholithiasis Asymptomatic (no
Title: The best approach to treat concomitant gallstones and. Authors: Jesús García-Cano, Francisco Domper
 Title: The best approach to treat concomitant gallstones and common bile duct stones. Is ERCP still needed? Authors: Jesús García-Cano, Francisco Domper DOI: 10.17235/reed.2019.6226/2019 Link: PubMed (Epub
Title: The best approach to treat concomitant gallstones and common bile duct stones. Is ERCP still needed? Authors: Jesús García-Cano, Francisco Domper DOI: 10.17235/reed.2019.6226/2019 Link: PubMed (Epub
Surveillance proposal consultation document
 Surveillance proposal consultation document 2018 surveillance of Gallstone disease: diagnosis and management (NICE guideline CG188) Proposed surveillance decision We propose to not update the NICE guideline
Surveillance proposal consultation document 2018 surveillance of Gallstone disease: diagnosis and management (NICE guideline CG188) Proposed surveillance decision We propose to not update the NICE guideline
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Comparative Study between Laparoscopic and Open Cholecystectomy for Dr. B. Hemasankararao 1,
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Comparative Study between Laparoscopic and Open Cholecystectomy for Dr. B. Hemasankararao 1,
Bile Duct Injury during Lap Chole. Bile Duct Injury during cholecystectomy TOPICS. 1. Prevalence, mechanisms, prevention and diagnosis
 Bile Duct Injury during cholecystectomy Catherine HUBERT Jean-Fran François GIGOT Benoît t NAVEZ Division of Hepato-Biliary Biliary-Pancreatic Surgery Department of Abdominal Surgery and Transplantation
Bile Duct Injury during cholecystectomy Catherine HUBERT Jean-Fran François GIGOT Benoît t NAVEZ Division of Hepato-Biliary Biliary-Pancreatic Surgery Department of Abdominal Surgery and Transplantation
Setting The study setting was hospital. The economic analysis was carried out in California, USA.
 Preoperative versus postoperative endoscopic retrograde cholangiopancreatography in mild to moderate gallstone pancreatitis: a prospective randomized trial Chang L, Lo S, Stabile B E, Lewis R J, Toosie
Preoperative versus postoperative endoscopic retrograde cholangiopancreatography in mild to moderate gallstone pancreatitis: a prospective randomized trial Chang L, Lo S, Stabile B E, Lewis R J, Toosie
complication rates and/or incomplete clearance with need of intervention (ie, unfavorable outcomes).
 Research Original Investigation Natural Course vs Interventions to Clear Common Bile Duct Stones Data From the Swedish Registry for Gallstone Surgery and Endoscopic Retrograde Cholangiopancreatography
Research Original Investigation Natural Course vs Interventions to Clear Common Bile Duct Stones Data From the Swedish Registry for Gallstone Surgery and Endoscopic Retrograde Cholangiopancreatography
Closure of the Common Duct -Endonasobiliary Drainage Tubes vs. T Tube: A Comparative Study
 Indian J Surg (September October 2010) 72(5):367 372 DOI 10.1007/s12262-010-0122-4 ORIGINAL ARTICLE Closure of the Common Duct -Endonasobiliary Drainage Tubes vs. T Tube: A Comparative Study Mehmood A.
Indian J Surg (September October 2010) 72(5):367 372 DOI 10.1007/s12262-010-0122-4 ORIGINAL ARTICLE Closure of the Common Duct -Endonasobiliary Drainage Tubes vs. T Tube: A Comparative Study Mehmood A.
Laparoscopic Cholecystectomy: A Retrospective Study
 Bahrain Medical Bulletin, Vol. 37, No. 3, September 2015 Laparoscopic Cholecystectomy: A Retrospective Study Abdullah Al-Mitwalli, LRCPI, LRCSI* Martin Corbally, MBBCh, BAO, MCh, FRCSI, FRCSEd, FRCS**
Bahrain Medical Bulletin, Vol. 37, No. 3, September 2015 Laparoscopic Cholecystectomy: A Retrospective Study Abdullah Al-Mitwalli, LRCPI, LRCSI* Martin Corbally, MBBCh, BAO, MCh, FRCSI, FRCSEd, FRCS**
Single-stage management with combined tri-endoscopic approach. approach for concomitant cholecystolithiasis and choledocholithiasis
 Surg Endosc (2016) 30:5615 5620 DOI 10.1007/s00464-016-4918-6 and Other Interventional Techniques ENDOLUMINAL SURGERY Single-stage management with combined tri-endoscopic approach for concomitant cholecystolithiasis
Surg Endosc (2016) 30:5615 5620 DOI 10.1007/s00464-016-4918-6 and Other Interventional Techniques ENDOLUMINAL SURGERY Single-stage management with combined tri-endoscopic approach for concomitant cholecystolithiasis
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 Appendix B: Scope NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE Post publication note: The title of this guideline changed during development. This scope was published before the guideline
Appendix B: Scope NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE Post publication note: The title of this guideline changed during development. This scope was published before the guideline
The campaign on laboratory: focus on Gallstone Disease and ERCP
 The campaign on laboratory: focus on Gallstone Disease and ERCP Mauro Giuliani, MD, Specialist in Visceral Surgery, Vice Head Physician, Surgical Ward, Ospedale Regionale di Locarno Alberto Fasoli, MD,
The campaign on laboratory: focus on Gallstone Disease and ERCP Mauro Giuliani, MD, Specialist in Visceral Surgery, Vice Head Physician, Surgical Ward, Ospedale Regionale di Locarno Alberto Fasoli, MD,
Type of intervention Treatment. Economic study type Cost-effectiveness analysis.
 Preoperative endoscopic sphincterotomy versus laparoendoscopic rendezvous in patients with gallbladder and bile duct stones Morino M, Baracchi F, Miglietta C, Furlan N, Ragona R, Garbarini A Record Status
Preoperative endoscopic sphincterotomy versus laparoendoscopic rendezvous in patients with gallbladder and bile duct stones Morino M, Baracchi F, Miglietta C, Furlan N, Ragona R, Garbarini A Record Status
Downloaded from jssu.ssu.ac.ir at 13:10 IRST on Saturday October 28th 2017
 Journal of Shahid Sadoughi University of Medical Sciences Vol. 21, No. 5, Nov-Dec 2013 Pages: 675-681 1392 5 21 675-681 : 3 2* 1 1392/8/ : -1-2 -3 1391/8/24 : (). :. 1390 200 :.. SPSS (%0/5) 200 (8%) (%9/5)19
Journal of Shahid Sadoughi University of Medical Sciences Vol. 21, No. 5, Nov-Dec 2013 Pages: 675-681 1392 5 21 675-681 : 3 2* 1 1392/8/ : -1-2 -3 1391/8/24 : (). :. 1390 200 :.. SPSS (%0/5) 200 (8%) (%9/5)19
Recurrent common bile duct stones as a late complication of endoscopic sphincterotomy
 Nzenza et al. BMC Gastroenterology (2018) 18:39 https://doi.org/10.1186/s12876-018-0765-3 RESEARCH ARTICLE Open Access Recurrent common bile duct stones as a late complication of endoscopic sphincterotomy
Nzenza et al. BMC Gastroenterology (2018) 18:39 https://doi.org/10.1186/s12876-018-0765-3 RESEARCH ARTICLE Open Access Recurrent common bile duct stones as a late complication of endoscopic sphincterotomy
ENDOSCOPIC TREATMENT OF A BILE DUCT
 HPB Surgery, 1990, Vol. 3, pp. 67-71 Reprints available directly from the publisher Photocopying permitted by license only 1990 Harwood Academic Publishers GmbH Printed in the United Kingdom CASE REPORT
HPB Surgery, 1990, Vol. 3, pp. 67-71 Reprints available directly from the publisher Photocopying permitted by license only 1990 Harwood Academic Publishers GmbH Printed in the United Kingdom CASE REPORT
EAST MULTICENTER STUDY PROPOSAL
 EAST MULTICENTER STUDY PROPOSAL (Proposal forms must be completed in its entirety, incomplete forms will not be considered) GENERAL INFORMATION Study Title: Prospective Multi-Institutional Evaluation of
EAST MULTICENTER STUDY PROPOSAL (Proposal forms must be completed in its entirety, incomplete forms will not be considered) GENERAL INFORMATION Study Title: Prospective Multi-Institutional Evaluation of
SURGERY? COMMON BILE DUCT STONES ERCP OR. Room 759. Maryland
 HPB INTERNATIONAL 277 alter the natural history of the disease, and delay or prevent the development or cirrhosis. Data from our unit as well as others suggests that to be the case. The current series,
HPB INTERNATIONAL 277 alter the natural history of the disease, and delay or prevent the development or cirrhosis. Data from our unit as well as others suggests that to be the case. The current series,
Laparoscopic Common Bile Duct Exploration: Our First 50 Cases
 136 Common Bile Duct Exploration Ker-Kan Tan et al Original Article Common Bile Duct Exploration: Our First 50 Cases Ker-Kan Tan, 1 MBBS, MRCS (Edin), MMed (Surg), Vishalkumar Girishchandra Shelat, 1 MRCS
136 Common Bile Duct Exploration Ker-Kan Tan et al Original Article Common Bile Duct Exploration: Our First 50 Cases Ker-Kan Tan, 1 MBBS, MRCS (Edin), MMed (Surg), Vishalkumar Girishchandra Shelat, 1 MRCS
Management of Gallbladder Disease
 Management of Gallbladder Disease Steven B. Johnson, MD, FACS, FCCM Professor and Chairman, Department of Surgery Program Director, Phoenix Integrated Surgical Residency University of Arizona College of
Management of Gallbladder Disease Steven B. Johnson, MD, FACS, FCCM Professor and Chairman, Department of Surgery Program Director, Phoenix Integrated Surgical Residency University of Arizona College of
SUNY Downstate Medical Center Kings County Hospital
 Management of Choledocholithiasis SUNY Downstate Medical Center Kings County Hospital Department of Surgery Grand Rounds Kiyanda Baldwin October 22, 2009 Case Presentation 43 y/o F c/o jaundice x 3 days
Management of Choledocholithiasis SUNY Downstate Medical Center Kings County Hospital Department of Surgery Grand Rounds Kiyanda Baldwin October 22, 2009 Case Presentation 43 y/o F c/o jaundice x 3 days
Mirizzi syndrome with an unusual type of biliobiliary fistula a case report
 Kawaguchi et al. Surgical Case Reports (2015) 1:51 DOI 10.1186/s40792-015-0052-2 CASE REPORT Mirizzi syndrome with an unusual type of biliobiliary fistula a case report Tsutomu Kawaguchi 1,2*, Tadao Itoh
Kawaguchi et al. Surgical Case Reports (2015) 1:51 DOI 10.1186/s40792-015-0052-2 CASE REPORT Mirizzi syndrome with an unusual type of biliobiliary fistula a case report Tsutomu Kawaguchi 1,2*, Tadao Itoh
Bile duct injuries related to misplacement of T tubes
 Annals of Hepatology 2006; 5(1): January-March: 44-48 Original Article Annals of Hepatology Bile duct injuries related to misplacement of T tubes Miguel Ángel Mercado;* Carlos Chan; Héctor Orozco;* Alexandra
Annals of Hepatology 2006; 5(1): January-March: 44-48 Original Article Annals of Hepatology Bile duct injuries related to misplacement of T tubes Miguel Ángel Mercado;* Carlos Chan; Héctor Orozco;* Alexandra
Congenital dilatation of the common bile duct and pancreaticobiliary maljunction clinical implications
 Langenbecks Arch Surg (2009) 394:209 213 DOI 10.1007/s00423-008-0330-6 CURRENT CONCEPT IN CLINICAL SURGERY Congenital dilatation of the common bile duct and pancreaticobiliary maljunction clinical implications
Langenbecks Arch Surg (2009) 394:209 213 DOI 10.1007/s00423-008-0330-6 CURRENT CONCEPT IN CLINICAL SURGERY Congenital dilatation of the common bile duct and pancreaticobiliary maljunction clinical implications
CME Article Clinics in diagnostic imaging (115) Wai C T, Seto K Y, Sutedja D S
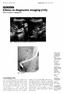 Medical Education Singapore Med.1 2007, 48 (4) : 361 CME Article Clinics in diagnostic imaging (115) Wai C T, Seto K Y, Sutedja D S fit. B CD - -0 o -5 r t -10 Fig. I US images of the upper right abdomen
Medical Education Singapore Med.1 2007, 48 (4) : 361 CME Article Clinics in diagnostic imaging (115) Wai C T, Seto K Y, Sutedja D S fit. B CD - -0 o -5 r t -10 Fig. I US images of the upper right abdomen
Endoscopic management of postoperative bile duct injuries: a single center experience.
 1- Endoscopic management of postoperative bile duct injuries: a single center experience. BACKGROUND/AIM: Biliary endoscopic procedures may be less invasive than surgery for management of postoperative
1- Endoscopic management of postoperative bile duct injuries: a single center experience. BACKGROUND/AIM: Biliary endoscopic procedures may be less invasive than surgery for management of postoperative
Mauro Podda 1 Francesco Maria Polignano. Michael Samuel James Wilson 1 Christoph Kulli
 Surg Endosc (2016) 30:845 861 DOI 10.1007/s00464-015-4303-x and Other Interventional Techniques REVIEW Systematic review with meta-analysis of studies comparing primary duct closure and T-tube drainage
Surg Endosc (2016) 30:845 861 DOI 10.1007/s00464-015-4303-x and Other Interventional Techniques REVIEW Systematic review with meta-analysis of studies comparing primary duct closure and T-tube drainage
ACUTE CHOLANGITIS AS a result of an occluded
 Digestive Endoscopy 2017; 29 (Suppl. 2): 88 93 doi: 10.1111/den.12836 Current status of biliary drainage strategy for acute cholangitis Endoscopic treatment for acute cholangitis with common bile duct
Digestive Endoscopy 2017; 29 (Suppl. 2): 88 93 doi: 10.1111/den.12836 Current status of biliary drainage strategy for acute cholangitis Endoscopic treatment for acute cholangitis with common bile duct
STRICTURES OF THE BILE DUCTS Session No.: 5. Andrea Tringali Digestive Endoscopy Unit Catholic University Rome - Italy
 STRICTURES OF THE BILE DUCTS Session No.: 5 Andrea Tringali Digestive Endoscopy Unit Catholic University Rome - Italy Drainage of biliary strictures. The history before 1980 Surgical bypass Percutaneous
STRICTURES OF THE BILE DUCTS Session No.: 5 Andrea Tringali Digestive Endoscopy Unit Catholic University Rome - Italy Drainage of biliary strictures. The history before 1980 Surgical bypass Percutaneous
Laparoscopic common bile duct exploration and antegrade biliary stenting: Leaving behind the Kehr tube
 1130-0108/2013/105/3/125-130 REVISTA ESPAÑOLA DE ENFERMEDADES DIGESTIVAS Copyright 2013 ARÁN EDICIONES, S. L. REV ESP ENFERM DIG (Madrid) Vol. 105. N. 3, pp. 125-130, 2013 ORIGINAL PAPERS Laparoscopic
1130-0108/2013/105/3/125-130 REVISTA ESPAÑOLA DE ENFERMEDADES DIGESTIVAS Copyright 2013 ARÁN EDICIONES, S. L. REV ESP ENFERM DIG (Madrid) Vol. 105. N. 3, pp. 125-130, 2013 ORIGINAL PAPERS Laparoscopic
Greater Manchester EUR Policy Statement on: Asymptomatic Gallstones GM Ref: GM061 Version: 0.2 (21 November 2018)
 Greater Manchester EUR Policy Statement on: Asymptomatic Gallstones GM Ref: GM061 Version: 0.2 (21 November 2018) Commissioning Statement Asymptomatic Gallstones Policy Exclusions (Alternative commissioning
Greater Manchester EUR Policy Statement on: Asymptomatic Gallstones GM Ref: GM061 Version: 0.2 (21 November 2018) Commissioning Statement Asymptomatic Gallstones Policy Exclusions (Alternative commissioning
Original article: SURGICAL TREATMENT FOR BENIGN BILIARY STRICTURES: SINGLE-CENTER EXPERIENCE ON 64 CASES
 Original article: SURGICAL TREATMENT FOR BENIGN BILIARY STRICTURES: SINGLE-CENTER EXPERIENCE ON 64 CASES Yunfeng Cui, Hongtao Zhang, Naiqiang Cui, Zhonglian Li* Department of Surgery, Tianjin Nankai Hospital,
Original article: SURGICAL TREATMENT FOR BENIGN BILIARY STRICTURES: SINGLE-CENTER EXPERIENCE ON 64 CASES Yunfeng Cui, Hongtao Zhang, Naiqiang Cui, Zhonglian Li* Department of Surgery, Tianjin Nankai Hospital,
Naoyuki Toyota, Tadahiro Takada, Hodaka Amano, Masahiro Yoshida, Fumihiko Miura, and Keita Wada
 J Hepatobiliary Pancreat Surg (2006) 13:80 85 DOI 10.1007/s00534-005-1062-4 Endoscopic naso-gallbladder drainage in the treatment of acute cholecystitis: alleviates inflammation and fixes operator s aim
J Hepatobiliary Pancreat Surg (2006) 13:80 85 DOI 10.1007/s00534-005-1062-4 Endoscopic naso-gallbladder drainage in the treatment of acute cholecystitis: alleviates inflammation and fixes operator s aim
Management of biliary injury after laparoscopic cholecystectomy N. Dayes Kings County Hospital Center & Long Island College Hospital 8/19/2010
 Management of biliary injury after laparoscopic cholecystectomy N. Dayes Kings County Hospital Center & Long Island College Hospital 8/19/2010 Case Presentation 30 y.o. woman with 2 weeks of RUQ abdominal
Management of biliary injury after laparoscopic cholecystectomy N. Dayes Kings County Hospital Center & Long Island College Hospital 8/19/2010 Case Presentation 30 y.o. woman with 2 weeks of RUQ abdominal
Pre-operative prediction of difficult laparoscopic cholecystectomy
 International Surgery Journal http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20151083 Pre-operative prediction of difficult laparoscopic
International Surgery Journal http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20151083 Pre-operative prediction of difficult laparoscopic
Safety of endoscopic retrograde cholangiopancreatography in patients 80 years of age and older
 Original paper Safety of endoscopic retrograde cholangiopancreatography in patients 80 years of age and older Baydar Behlül 1, Serin Ayfer 2, Vatansever Sezgin 3, Kandemir Altay 3, Çelik Mustafa 3, Çekiç
Original paper Safety of endoscopic retrograde cholangiopancreatography in patients 80 years of age and older Baydar Behlül 1, Serin Ayfer 2, Vatansever Sezgin 3, Kandemir Altay 3, Çelik Mustafa 3, Çekiç
A CASE REPORT OF SPONTANEOUS BILOMA - AN ENIGMATIC SURGICAL PROBLEM
 A CASE REPORT OF SPONTANEOUS BILOMA - AN ENIGMATIC SURGICAL PROBLEM *Sumanta Kumar Ghosh and Biswajit Mukherjee ESIC Medical College, Joka, Kolkata, India *Author for Correspondence ABSTRACT Occurrence
A CASE REPORT OF SPONTANEOUS BILOMA - AN ENIGMATIC SURGICAL PROBLEM *Sumanta Kumar Ghosh and Biswajit Mukherjee ESIC Medical College, Joka, Kolkata, India *Author for Correspondence ABSTRACT Occurrence
SAGES GUIDELINES FOR THE CLINICAL APPLICATION OF LAPAROSCOPIC BILIARY TRACT SURGERY
 Practice/Clinical Guidelines published on: 01/2010 by the Society of American Gastrointestinal and Endoscopic Surgeons (SAGES) SAGES GUIDELINES FOR THE CLINICAL APPLICATION OF LAPAROSCOPIC BILIARY TRACT
Practice/Clinical Guidelines published on: 01/2010 by the Society of American Gastrointestinal and Endoscopic Surgeons (SAGES) SAGES GUIDELINES FOR THE CLINICAL APPLICATION OF LAPAROSCOPIC BILIARY TRACT
Study of the degree of gall bladder wall thickness and its impact on outcomes following laparoscopic cholecystectomy in JSS Hospital
 International Surgery Journal Chandra SBJ et al. Int Surg J. 2018 Apr;5(4):1417-1421 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20181122
International Surgery Journal Chandra SBJ et al. Int Surg J. 2018 Apr;5(4):1417-1421 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20181122
The authors have declared no conflicts of interest.
 Diagnostic Accuracy of Magnetic Resonance Cholangiopancreatography Versus Endoscopic Retrograde Cholangiopancreatography Findings in the Postorthotopic Liver Transplant Population Authors: *Ashok Shiani,
Diagnostic Accuracy of Magnetic Resonance Cholangiopancreatography Versus Endoscopic Retrograde Cholangiopancreatography Findings in the Postorthotopic Liver Transplant Population Authors: *Ashok Shiani,
Guidelines for Laparoscopic CBD Exploration
 Guidelines for Laparoscopic CBD Exploration INDICATIONS Since the 1992 National Institutes of Health Consensus Development Conference Statement on Gallstones and Laparoscopic Cholecystectomy the indications
Guidelines for Laparoscopic CBD Exploration INDICATIONS Since the 1992 National Institutes of Health Consensus Development Conference Statement on Gallstones and Laparoscopic Cholecystectomy the indications
Pictorial review of Benign Biliary tract abnormality on MRCP/MRI Liver with Endoscopic (including splyglass) and Endoscopic Ultrasound correlation
 Pictorial review of Benign Biliary tract abnormality on MRCP/MRI Liver with Endoscopic (including splyglass) and Endoscopic Ultrasound correlation Poster No.: C-2617 Congress: ECR 2015 Type: Educational
Pictorial review of Benign Biliary tract abnormality on MRCP/MRI Liver with Endoscopic (including splyglass) and Endoscopic Ultrasound correlation Poster No.: C-2617 Congress: ECR 2015 Type: Educational
Per-operative conversion of laparoscopic cholecystectomy to open surgery: prospective study at JSS teaching hospital, Karnataka, India
 International Surgery Journal Raza M et al. Int Surg J. 2017 Jan;4(1):81-85 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20163977
International Surgery Journal Raza M et al. Int Surg J. 2017 Jan;4(1):81-85 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20163977
Surgical Management of CBD Injury Jin Seok Heo
 Surgical Management of CBD Injury Jin Seok Heo Department of Surgery, Samsung Medical Center Sungkyunkwan University School of Medicine, Seoul, Republic of Korea Bile duct injury (BDI) Introduction Incidence
Surgical Management of CBD Injury Jin Seok Heo Department of Surgery, Samsung Medical Center Sungkyunkwan University School of Medicine, Seoul, Republic of Korea Bile duct injury (BDI) Introduction Incidence
Comparative Study of Outcomes of Early Versus Interval Laparoscopic Cholecystectomy in Acute Calculus Cholecystitis.
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 4 Ver. IX (April. 2017), PP 68-73 www.iosrjournals.org Comparative Study of Outcomes of Early
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 4 Ver. IX (April. 2017), PP 68-73 www.iosrjournals.org Comparative Study of Outcomes of Early
Determination of optimal operation time for the management of acute cholecystitis: a clinical trial
 Original paper Determination of optimal operation time for the management of acute cholecystitis: a clinical trial Erkan Oymaci 1, Ahmet Deniz Ucar 1, Savas Yakan 1, Erdem Baris Carti 1, Ali Coskun 1,
Original paper Determination of optimal operation time for the management of acute cholecystitis: a clinical trial Erkan Oymaci 1, Ahmet Deniz Ucar 1, Savas Yakan 1, Erdem Baris Carti 1, Ali Coskun 1,
Gallstones. Classification
 Gallstones Nariman Karanjia Tahir Ali Abstract Gallstones are extremely common in the UK and have a major effect on healthcare resources. Presentation depends on whether the stones occlude the cystic duct
Gallstones Nariman Karanjia Tahir Ali Abstract Gallstones are extremely common in the UK and have a major effect on healthcare resources. Presentation depends on whether the stones occlude the cystic duct
In Woong Han 1, O Choel Kwon 1, Min Gu Oh 1, Yoo Shin Choi 2, and Seung Eun Lee 2. Departments of Surgery, Dongguk University College of Medicine 2
 Effect of Rowachol on Prevention of Postcholecystectomy Syndrome after Laparoscopic Cholecystectomy - Prospective multicenter Randomized controlled trial- In Woong Han 1, O Choel Kwon 1, Min Gu Oh 1, Yoo
Effect of Rowachol on Prevention of Postcholecystectomy Syndrome after Laparoscopic Cholecystectomy - Prospective multicenter Randomized controlled trial- In Woong Han 1, O Choel Kwon 1, Min Gu Oh 1, Yoo
What Are Gallstones? GALLSTONES. Gallstones are pieces of hard, solid matter that form over time in. the gallbladder of some people.
 What Are Gallstones? Gallstones are pieces of hard, solid matter that form over time in the gallbladder of some people. The gallbladder sits under the liver and stores bile (a key digestive juice ). Gallstones
What Are Gallstones? Gallstones are pieces of hard, solid matter that form over time in the gallbladder of some people. The gallbladder sits under the liver and stores bile (a key digestive juice ). Gallstones
Optimal timing of elective laparoscopic cholecystectomy after acute cholangitis and subsequent clearance of choledocholithiasis
 The American Journal of Surgery (2010) 200, 483 488 Clinical Science Optimal timing of elective laparoscopic cholecystectomy after acute cholangitis and subsequent clearance of choledocholithiasis Vicky
The American Journal of Surgery (2010) 200, 483 488 Clinical Science Optimal timing of elective laparoscopic cholecystectomy after acute cholangitis and subsequent clearance of choledocholithiasis Vicky
Information for Consent Cholecystectomy (Laparoscopic/Open) 膽囊切除術 ( 腹腔鏡 / 開放性 )
 Version 1.0 Page 1 of 3 Information for Consent Cholecystectomy (Laparoscopic/Open) 膽囊切除術 ( 腹腔鏡 / 開放性 ) Introduction Gallbladder is a sac connected to the biliary tree. It serves the function of concentration
Version 1.0 Page 1 of 3 Information for Consent Cholecystectomy (Laparoscopic/Open) 膽囊切除術 ( 腹腔鏡 / 開放性 ) Introduction Gallbladder is a sac connected to the biliary tree. It serves the function of concentration
REFERRAL GUIDELINES: GALLSTONES
 REFERRAL GUIDELINES: GALLSTONES Document Purpose To ensure patients with gallstones disease are managed appropriately in primary/ secondary care Oxford Radcliffe Hospital Surgical Department Surgical Registrar
REFERRAL GUIDELINES: GALLSTONES Document Purpose To ensure patients with gallstones disease are managed appropriately in primary/ secondary care Oxford Radcliffe Hospital Surgical Department Surgical Registrar
Percutaneous Removal of Biliary Stone from Anomalous Right Hepatic Duct
 Percutaneous Removal of Biliary Stone from Anomalous Right Hepatic Duct Pages with reference to book, From 94 To 96 Tanveer ul Haq, Mohammed Younus Sheikh, Changes Khan Jadun, M.N. Ahmad, Yousuf H. Husen
Percutaneous Removal of Biliary Stone from Anomalous Right Hepatic Duct Pages with reference to book, From 94 To 96 Tanveer ul Haq, Mohammed Younus Sheikh, Changes Khan Jadun, M.N. Ahmad, Yousuf H. Husen
Routine Testing of Liver Function Before and After Elective Laparoscopic Cholecystectomy: Is It Necessary?
 Routine Testing of Liver Function Before and After Elective Laparoscopic Cholecystectomy: Is It Necessary? Nasir Zaheer Ahmad, FRCSI SCIENTIFIC PAPER ABSTRACT Background and Objectives: Liver function
Routine Testing of Liver Function Before and After Elective Laparoscopic Cholecystectomy: Is It Necessary? Nasir Zaheer Ahmad, FRCSI SCIENTIFIC PAPER ABSTRACT Background and Objectives: Liver function
담낭절제술후발생한미리찌증후군의내시경적치료 1 예
 Case Report The Korean Journal of Pancreas and Biliary Tract 2014;19:199-203 http://dx.doi.org/10.15279/kpba.2014.19.4.199 pissn 1976-3573 eissn 2288-0941 담낭절제술후발생한미리찌증후군의내시경적치료 1 예 인하대학교의학전문대학원내과학교실 이정민
Case Report The Korean Journal of Pancreas and Biliary Tract 2014;19:199-203 http://dx.doi.org/10.15279/kpba.2014.19.4.199 pissn 1976-3573 eissn 2288-0941 담낭절제술후발생한미리찌증후군의내시경적치료 1 예 인하대학교의학전문대학원내과학교실 이정민
ABDOMINAL WALL HAEMATOMA COMPLICATING LAPAROSCOPIC CHOLECYSTECTOMY
 HPB Surgery, 1994, Vol. 7, pp. 291-296 Reprints available directly from the publisher Photocopying permitted by license only (C) 1994 Harwood Academic Publishers GmbH Printed in the United States of America
HPB Surgery, 1994, Vol. 7, pp. 291-296 Reprints available directly from the publisher Photocopying permitted by license only (C) 1994 Harwood Academic Publishers GmbH Printed in the United States of America
A Local Experience in the Management of Recurrent Pyogenic Cholangitis (Oriental Cholangitis)
 Bahrain Medical Bulletin, Vol.24, No.1, March 2002 A Local Experience in the Management of Recurrent Pyogenic Cholangitis (Oriental Cholangitis) Suhair Khalifa Al-Saad, CABS, FRCSI* Mohammed Khurshid Alam,
Bahrain Medical Bulletin, Vol.24, No.1, March 2002 A Local Experience in the Management of Recurrent Pyogenic Cholangitis (Oriental Cholangitis) Suhair Khalifa Al-Saad, CABS, FRCSI* Mohammed Khurshid Alam,
Accuracy of ASGE criteria for the prediction of choledocholithiasis
 1130-0108/2016/108/6/309-314 Revista Española de Enfermedades Digestivas Copyright 2016 Arán Ediciones, S. L. Rev Esp Enferm Dig (Madrid) Vol. 108, N.º 6, pp. 309-314, 2016 ORIGINAL PAPERS Accuracy of
1130-0108/2016/108/6/309-314 Revista Española de Enfermedades Digestivas Copyright 2016 Arán Ediciones, S. L. Rev Esp Enferm Dig (Madrid) Vol. 108, N.º 6, pp. 309-314, 2016 ORIGINAL PAPERS Accuracy of
laparoscopic cholecystectomy
 Combined percutaneous and endoscopic approach in management of dropped gallstones following laparoscopic cholecystectomy John S.F. Shum 1*, K.H. Fung 1, George P.C. Yang 2, Chung Ngai Tang 2, Michael K.W.
Combined percutaneous and endoscopic approach in management of dropped gallstones following laparoscopic cholecystectomy John S.F. Shum 1*, K.H. Fung 1, George P.C. Yang 2, Chung Ngai Tang 2, Michael K.W.
The Present Scenario of Cholecystectomy
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 5 Ver. III (May. 2016), PP 71-75 www.iosrjournals.org The Present Scenario of Cholecystectomy
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 5 Ver. III (May. 2016), PP 71-75 www.iosrjournals.org The Present Scenario of Cholecystectomy
Sharma Maneesh,Chaudhary Sanchit, Sharma Ratnakar, Mahajan Amit
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 10 Ver. II (October. 2016), PP 09-13 www.iosrjournals.org A Prospective Study of Complications
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 10 Ver. II (October. 2016), PP 09-13 www.iosrjournals.org A Prospective Study of Complications
Controversies in the management of acute pancreatitis
 Kathmandu University Medical Journal (3) Vol., No. 3, Issue 7, 3-7 Controversies in the management of acute pancreatitis Singh DR 1, Mehta A, Dangol UMS 3 1 Lecturer, Medical Officer, 3 Lecturer, Dept.
Kathmandu University Medical Journal (3) Vol., No. 3, Issue 7, 3-7 Controversies in the management of acute pancreatitis Singh DR 1, Mehta A, Dangol UMS 3 1 Lecturer, Medical Officer, 3 Lecturer, Dept.
Percutaneous extraction of residual post-cholecystectomy gallstones through the T-tube tract
 DOI: https://doi.org/10.5114/pjr.2018.75811 Received: 06.02.2018 Accepted: 23.02.2018 Published: 07.05.2018 http://www.polradiol.com Original paper Percutaneous extraction of residual post-cholecystectomy
DOI: https://doi.org/10.5114/pjr.2018.75811 Received: 06.02.2018 Accepted: 23.02.2018 Published: 07.05.2018 http://www.polradiol.com Original paper Percutaneous extraction of residual post-cholecystectomy
Lutheran Medical Center. Daniel H. Hunt, M.D. June 10 th, 2005
 Lutheran Medical Center Daniel H. Hunt, M.D. June 10 th, 2005 History xx y.o. pt with primary CBD stones s/p ERCP xx months earlier for attempted stone extraction resulting in post ERCP pancreatitis. Patient
Lutheran Medical Center Daniel H. Hunt, M.D. June 10 th, 2005 History xx y.o. pt with primary CBD stones s/p ERCP xx months earlier for attempted stone extraction resulting in post ERCP pancreatitis. Patient
Magnetic Resonance Cholangiopancreatography (MRCP) in a District General Hospital
 Magnetic Resonance Cholangiopancreatography (MRCP) in a District General Hospital Poster No.: C-1790 Congress: ECR 2012 Type: Authors: Scientific Exhibit J. A. Maguire 1, H. Kasem 2, M. Akhtar 2, M. Strauss
Magnetic Resonance Cholangiopancreatography (MRCP) in a District General Hospital Poster No.: C-1790 Congress: ECR 2012 Type: Authors: Scientific Exhibit J. A. Maguire 1, H. Kasem 2, M. Akhtar 2, M. Strauss
LAPAROSCOPIC GALLBLADDER SURGERY
 LAPAROSCOPIC GALLBLADDER SURGERY Treating Gallbladder Problems with Laparoscopy A Common Problem If you ve had an attack of painful gallbladder symptoms, you re not alone. Gallbladder disease is very common.
LAPAROSCOPIC GALLBLADDER SURGERY Treating Gallbladder Problems with Laparoscopy A Common Problem If you ve had an attack of painful gallbladder symptoms, you re not alone. Gallbladder disease is very common.
Title: The impact of a percutaneous cholecystostomy catheter in situ until the time of cholecystectomy on the development of recurrent acute
 Title: The impact of a percutaneous cholecystostomy catheter in situ until the time of cholecystectomy on the development of recurrent acute cholecystitis: a historical cohort study Authors: Mustafa Hasbahceci,
Title: The impact of a percutaneous cholecystostomy catheter in situ until the time of cholecystectomy on the development of recurrent acute cholecystitis: a historical cohort study Authors: Mustafa Hasbahceci,
Two Port Laparoscopic Cholecystectomy- A Simplified And Safe Technique
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 4 Ver. XII (Apr. 2016), PP 68-72 www.iosrjournals.org Two Port Laparoscopic Cholecystectomy-
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 4 Ver. XII (Apr. 2016), PP 68-72 www.iosrjournals.org Two Port Laparoscopic Cholecystectomy-
Cholecystectomy for acute gallstone pancreatitis: early vs delayed approach
 Scandinavian Journal of Surgery 99: 81 85, 2010 Cholecystectomy for acute gallstone pancreatitis: early vs delayed approach C. T. Wilson, M. A. de Moya Department of Trauma, Emergency Surgery, and Critical
Scandinavian Journal of Surgery 99: 81 85, 2010 Cholecystectomy for acute gallstone pancreatitis: early vs delayed approach C. T. Wilson, M. A. de Moya Department of Trauma, Emergency Surgery, and Critical
Single-Session Treatment of Cholecysto-Choledocholithiasis: Totally Laparoscopic versus Laparo-Endoscopic
 Journal of Surgery 2017; 5(5): 72-78 http://www.sciencepublishinggroup.com/j/js doi: 10.11648/j.js.20170505.11 ISSN: 2330-0914 (Print); ISSN: 2330-0930 (Online) Single-Session Treatment of Cholecysto-Choledocholithiasis:
Journal of Surgery 2017; 5(5): 72-78 http://www.sciencepublishinggroup.com/j/js doi: 10.11648/j.js.20170505.11 ISSN: 2330-0914 (Print); ISSN: 2330-0930 (Online) Single-Session Treatment of Cholecysto-Choledocholithiasis:
Gallstone ileus:diagnostic and therapeutic dilemma
 Saurabh et al. 1 CASE SERIES OPEN ACCESS Gallstone ileus:diagnostic and therapeutic dilemma Shireesh Saurabh, Andrew Camerota, Jeffrey Zavotsky ABSTRACT Introduction: Gallstone ileus is a rare complication
Saurabh et al. 1 CASE SERIES OPEN ACCESS Gallstone ileus:diagnostic and therapeutic dilemma Shireesh Saurabh, Andrew Camerota, Jeffrey Zavotsky ABSTRACT Introduction: Gallstone ileus is a rare complication
1. Assoc. Prof. of Surgery, LUM&HS, Jamshoro 2. Prof. of Surgery, LUM&HS, Jamshoro 3. Consaltant Surgeon, Isra University Hyderabad
 Evaluation of Various Causes and Treatment of Obstructive Jaundice at Liaquat University Hospital {Original Article (Medicine)} 1. Abdul Ghafoor Dalwani 2. A. Razaque Shaikh 3. Devanand 1. Assoc. Prof.
Evaluation of Various Causes and Treatment of Obstructive Jaundice at Liaquat University Hospital {Original Article (Medicine)} 1. Abdul Ghafoor Dalwani 2. A. Razaque Shaikh 3. Devanand 1. Assoc. Prof.
ISSN X (Print) Research Article. *Corresponding author Jitendra Singh Yadav
 Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2014; 2(3B):966-970 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2014; 2(3B):966-970 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
Single Stage Management of Concomitant Gall Stones and Common Bile Duct Stones in the Laparoscopic Era
 International Journal of Scientific and Research Publications, Volume 6, Issue 2, February 2016 239 Single Stage Management of Concomitant Gall Stones and Common Bile Duct Stones in the Laparoscopic Era
International Journal of Scientific and Research Publications, Volume 6, Issue 2, February 2016 239 Single Stage Management of Concomitant Gall Stones and Common Bile Duct Stones in the Laparoscopic Era
Endoscopic Management of Biliary Strictures. Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center
 Endoscopic Management of Biliary Strictures Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center Malignant Biliary Strictures Etiologies: Pancreatic
Endoscopic Management of Biliary Strictures Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center Malignant Biliary Strictures Etiologies: Pancreatic
A LEADER IN ADVANCED ENDOSCOPY AND HEPATOBILIARY SURGERY
 A LEADER IN ADVANCED ENDOSCOPY AND HEPATOBILIARY SURGERY St. Peter s Hospital Advanced Endoscopy & Hepatobiliary Center Welcome The St. Peter s Hospital Advanced Endoscopy & Hepatobiliary Center is a leader
A LEADER IN ADVANCED ENDOSCOPY AND HEPATOBILIARY SURGERY St. Peter s Hospital Advanced Endoscopy & Hepatobiliary Center Welcome The St. Peter s Hospital Advanced Endoscopy & Hepatobiliary Center is a leader
Early management of complicated gallstones and acute pancreatitis
 Early management of complicated gallstones and acute pancreatitis A/Prof Richard Cade George Kalogeropoulos ( Fellow) HPB/Upper GI Unit Eastern Health, Melbourne biliary colic/acute cholecystitis common
Early management of complicated gallstones and acute pancreatitis A/Prof Richard Cade George Kalogeropoulos ( Fellow) HPB/Upper GI Unit Eastern Health, Melbourne biliary colic/acute cholecystitis common
Endoscopic Retrograde Cholangiopancreatography (ERCP)
 Endoscopic Retrograde Cholangiopancreatography (ERCP) Medical Imaging and Treatment of the Bile and Pancreatic Ducts CIE-02718 Understanding ERCP Brochure Update_F.indd 1 7/11/18 9:51 A Minimally Invasive
Endoscopic Retrograde Cholangiopancreatography (ERCP) Medical Imaging and Treatment of the Bile and Pancreatic Ducts CIE-02718 Understanding ERCP Brochure Update_F.indd 1 7/11/18 9:51 A Minimally Invasive
Abdominal Imaging. Gallbladder perforation: color Doppler findings
 Abdom Imaging 27:47 50 (2002) DOI: 10.1007/s00261-001-0048-1 Abdominal Imaging Springer-Verlag New York Inc. 2002 Gallbladder perforation: color Doppler findings K. Konno, 1 H. Ishida, 1 M. Sato, 1 H.
Abdom Imaging 27:47 50 (2002) DOI: 10.1007/s00261-001-0048-1 Abdominal Imaging Springer-Verlag New York Inc. 2002 Gallbladder perforation: color Doppler findings K. Konno, 1 H. Ishida, 1 M. Sato, 1 H.
No 72-hour pathological boundary for safe early laparoscopic cholecystectomy in acute cholecystitis: a clinicopathological study
 Original article Annals of Gastroenterology (2013) 26, 1-6 No 72-hour pathological boundary for safe early laparoscopic cholecystectomy in acute cholecystitis: a clinicopathological study Rachel M. Gomes
Original article Annals of Gastroenterology (2013) 26, 1-6 No 72-hour pathological boundary for safe early laparoscopic cholecystectomy in acute cholecystitis: a clinicopathological study Rachel M. Gomes
A scoring system for the prediction of choledocholithiasis: a prospective cohort study
 A scoring system for the prediction of choledocholithiasis: a prospective cohort study Bilal O. Al-Jiffry, a Samah Khayat, b Elfatih Abdeen, b Tasadooq Hussain, c Mohammed Yassin d From the a Department
A scoring system for the prediction of choledocholithiasis: a prospective cohort study Bilal O. Al-Jiffry, a Samah Khayat, b Elfatih Abdeen, b Tasadooq Hussain, c Mohammed Yassin d From the a Department
Evidence-based guidelines for diagnosis of common bile duct stones Vanja Giljaca University Hospital Center Rijeka Department of Gastroenterology
 Evidencebased guidelines for diagnosis of common bile duct stones Vanja Giljaca University Hospital Center Rijeka Department of Gastroenterology Trusted evidence. Informed decisions. Better health. Outline
Evidencebased guidelines for diagnosis of common bile duct stones Vanja Giljaca University Hospital Center Rijeka Department of Gastroenterology Trusted evidence. Informed decisions. Better health. Outline
Effect of Duration of Surgery on Liver Enzymes After Cholecystectomy: Safety or Duration
 Original Article J Curr Surg. 2017;7(4):53-57 Effect of Duration of Surgery on Liver Enzymes After Cholecystectomy: Safety or Duration Abhishek Sharma a, Rikki Singal a, Amit Mittal b, Amarjit Singh Grover
Original Article J Curr Surg. 2017;7(4):53-57 Effect of Duration of Surgery on Liver Enzymes After Cholecystectomy: Safety or Duration Abhishek Sharma a, Rikki Singal a, Amit Mittal b, Amarjit Singh Grover
ORIGINAL ARTICLE. Management of Gallstone Cholangitis in the Era of Laparoscopic Cholecystectomy
 ORIGINAL ARTICLE Management of Gallstone Cholangitis in the Era of Laparoscopic Cholecystectomy Ronnie Tung-Ping Poon, MD, FRCS(Ed); Chi-Leung Liu, MD, FRCS(Ed); Chung-Mau Lo, MS, FRCS(Ed), FRACS; Chi-Ming
ORIGINAL ARTICLE Management of Gallstone Cholangitis in the Era of Laparoscopic Cholecystectomy Ronnie Tung-Ping Poon, MD, FRCS(Ed); Chi-Leung Liu, MD, FRCS(Ed); Chung-Mau Lo, MS, FRCS(Ed), FRACS; Chi-Ming
Two-port needlescopic cholecystectomy: prospective study of 100 cases!"#$%&'()*+,-./0123
 KW Lee C Poon K Leung DWH Lee CW Ko Key words: Cholecystectomy, laparoscopic; iber optics; Laparoscopes; iniaturization; Needles!!"#$%&'(!"!! Hong Kong ed J 2005;11:30-5 Department of Surgery, Tuen un
KW Lee C Poon K Leung DWH Lee CW Ko Key words: Cholecystectomy, laparoscopic; iber optics; Laparoscopes; iniaturization; Needles!!"#$%&'(!"!! Hong Kong ed J 2005;11:30-5 Department of Surgery, Tuen un
