Extended distal pancreatectomy for advanced pancreatic neck cancer
|
|
|
- Griffin Lewis
- 6 years ago
- Views:
Transcription
1 Korean J Hepatobiliary Pancreat Surg 2014;18: Original Article Extended distal pancreatectomy for advanced pancreatic neck cancer Shin-Young Park, Woo Young Shin, Yun-Mee Choe, Keon-Young Lee, and Seung-Ik Ahn Department of Surgery, Inha University School of Medicine, Incheon, Korea Backgrounds/Aims: We investigated the clinical application of extended distal pancreatectomy in patients with pancreatic neck cancer accompanied by distal pancreatic atrophy. In this study, we have emphasized on the technical aspects of using the linear stapling device for a bulky target organ. Methods: From March 2010 to September 2013, 46 patients with pancreatic adenocarcinoma, who underwent pancreatic resection with radical intent at our institute, were reviewed retrospectively. Among them, three patients (6.5%) underwent extended distal pancreatectomy. A linear stapling device and vise-grip locking pliers were used for en bloc resection of the distal pancreas, first duodenal portion, and distal common bile duct. The results were compared with those after standard pancreatectomy. Results: All three patients presented with jaundice, and the ratio of pancreatic duct to parenchymal thickness of the pancreatic body was greater than 0.5. pancreatic fistula developed in all of the cases, but none of these fistulae were lethal. Pathological staging was T3N1M0 in all of the patients. The postoperative daily serum glucose fluctuations and insulin requirements were comparable to those in patients who received pancreaticoduodenectomy or distal pancreatectomy. At the last follow-up, two patients were alive with liver metastasis at 4 and 10 months postoperatively, respectively, and one patient died of liver metastasis at 5 months postoperatively. Conclusions: While the prognosis of advanced pancreatic neck adenocarcinoma is still dismal, extended distal pancreatectomy is a valid treatment option, especially when there is atrophy of the distal pancreas. Also, the procedure is technically feasible, and further refinement is necessary to improve patient survival. (Korean J Hepatobiliary Pancreat Surg 2014;18:77-83) Key Words: Pancreas; Neck; Adenocarcinoma; Pancreatectomy; Atrophy INTRODUCTION Surgical removal provides the best survival benefits for patients with pancreatic neck cancer, although the results are still dismal. 1 Two options are considered to be the standard of care, pancreaticoduodenectomy (PD) and distal (subtotal) pancreatectomy (DP), depending on the tumor location. 2 In patients presenting with jaundice, the preferred treatment of choice is PD, since the usual resection line for DP is the portal vein, precluding radical operation. However, if the patient has atrophy of the distal pancreas due to long-standing pancreatic duct obstruction, there are concerns regarding postoperative endocrine and exocrine pancreatic insufficiency. Although it is technically challenging, an extended distal pancreatectomy (EDP), preserving only the uncinate process of the pancreas, can be an alternative treatment option. EDP can also avoid pancreaticoenterostomy, which is the most compromised anastomosis of the pancreatic resection procedures. In this paper we present our experience with special emphasis on the technical aspects of using the linear stapling device for bulky target organs. PATIENTS AND METHODS From March 2010 to September 2013, a total of 47 patients with pancreatic adenocarcinoma underwent pancreatic resection with radical intent at our institute. Among them, 46 patients were included in this study and reviewed retrospectively, excluding one patient who received total pancreatectomy. Among these 46 patients, three patients (6.5%) underwent EDP; 36 patients (78.3%) underwent PD; and seven patients (15.2%) underwent DP. Received: June 18, 2014; Revised: August 2, 2014; Accepted: August 14, 2014 Corresponding author: Keon-Young Lee Department of Surgery, Inha University Hospital, 27, Inhang-ro, Jung-gu, Incheon , Korea Tel: , Fax: , @inha.ac.kr This work was supported by Inha University Research Grant. Copyright C 2014 by The Korean Association of Hepato-Biliary-Pancreatic Surgery Korean Journal of Hepato-Biliary-Pancreatic Surgery pissn: ㆍ eissn:
2 78 Korean J Hepatobiliary Pancreat Surg Vol. 18, No. 3, August 2014 All three patients in the EDP group presented with jaundice, and two patients presented with preoperative diabetes (Table 1). During the same period, one patient (2.1%) died of upper gastrointestinal bleeding at 31 days after PD. EDP was indicated for the following conditions: adenocarcinoma in the neck of the pancreas, with distal pancreatic atrophy, and no extension or invasion of the ampulla of Vater and the uncinate process. Pancreatic atrophy was defined when the ratio of the diameter of the main pancreatic duct to the width of the pancreatic parenchyma, measured at the body of the pancreas anterior to the aorta, was larger than 0.5 on computed tomography (Fig. 1). 3 Operative procedures Patient preparation and dissection were similar to that in routine pylorus-preserving PD, until the common hepatic duct and the first duodenal portion were cut, respectively, and the stomach was retracted cephalad to expose the whole pancreas. The distal pancreas and spleen were dissected from the retroperitoneum, along with the splenic vessels, and the insertion of the splenic vein into the superior mesenteric vein was identified. When suspicious tumor invasion or adhesion was found in this area, blunt dissection was performed to detach the specimen from the superior mesenteric vein. The splenic vein was cut and the stump was closed using a 4-0 non-absorbable monofilament continuous running suture. After the specimen was mobilized and draped using a gauze tape, the only remaining structure included the second duodenal portion and the pancreatic head, which was isolated and ready to be cut. A linear stapling device (PROXIMATE R TCT 10, ETHICON ENDO-SURGERY, LLC, Guaynabo, Puerto Rico, 00969, USA) with a green cartridge was used to Table 1. Demographic and preoperative data Factors/Group PD n (%) DP n (%) EDP n (%) Total N (%) Gender Male Female Age (yrs) Median Range Preoperative DM Preoperative jaundice Distal pancreatic atrophy (%) Total 24 (66.7) 12 (33.3) (41.7) 25 (69.4) 13 (36.1) 36 (78.3) 3 (42.9) 4 (57.1) (28.6) 2 (28.6) 7 (15.2) 2 (66.7) 1 (33.3) (66.7) 3 (100.0) 3 (100.0) 3 (6.5) 29 (63.0) 17 (37.0) (41.3) 28 (60.9) 18 (39.1) 46 (100.0) PD, pancreaticoduodenectomy; DP, distal pancreatectomy; EDP, extended distal pancreatectomy; DM, diabetes mellitus. Fig. 1. Preoperative computed tomography of a representative patient. (A) Pancreatic neck cancer (arrow) with distal pancreatic atrophy shows dilated pancreatic duct (arrow head). (B) The uncinate process of the pancreas is intact (arrow).
3 Shin-Young Park, et al. Extended distal pancreatectomy 79 perform en bloc resection of the distal pancreas, first duo- odenum were sent to pathology for frozen section denal portion, and distal common bile duct. When it was evaluation. After the resection, the invaded portion of the difficult to close the jaws of the linear stapler due to the portal vein or superior mesenteric vein was resected and bulk of the target organs, vise-grip locking pliers were ap- reconstructed using an artificial graft in a separate proce- plied to force the jaws together (Fig. 2). The resected mar- dure (Fig. 3A). Gastrointestinal continuity was restored by gins of the pancreatic head, common hepatic duct, and du- Roux-en-Y hepaticojejunostomy, gastro- or duodenojeju- Fig. 2. Operative procedures. (A) A linear stapling device (arrow) and vise-grip locking pliers (arrowhead) are applied to resect the specimen en bloc. (B) Schematic diagram showing the resection line (dotted), along with the stapler line (solid). Fig. 3. Operative procedures. (A) Operative field after resection. Portal vein is reconstructed using an artificial graft, beneath the hemostatic mesh (arrow). Note that the stapler line is visible (arrowhead). (B) Schematic diagram after gastrointestinal reconstruction of the uncinate process of the remnant pancreas. Fig. 4. Follow-up computed tomography scan of the patient presented in Fig. 1 at 4 months after surgery. (A) The remnant pancreas is well-preserved (arrow), with intact portal flow (arrow head), although the patient developed multiple liver metastases (double arrow). (B) Coronal view of the uncinate process of the preserved pancreas (arrow) with the stapler line (arrow head).
4 80 Korean J Hepatobiliary Pancreat Surg Vol. 18, No. 3, August 2014 nostomy, and jejunojejunostomy (Fig. 3B). The main outcomes of this study included postoperative pancreatic fistula (according to the ISGPF definition); 4 endocrine insufficiency, as indicated by daily serum glucose fluctuation (ΔG) and insulin requirements; 5 and exocrine insufficiency, as indicated by steatorrhea. 6 The integrity of the uncinate process of the remnant pancreas was also assessed on follow-up computed tomography scans (Fig. 4). Indicator of glycemic control ΔG was defined as the daily maximum serum glucose level minus the daily minimum serum glucose level (mg/dl). When the serum glucose level was stable enough so that only one sample was required, the difference between the sampled glucose level and the normal median value (90 mg/dl) was recorded as ΔG. ΔG was recorded one day before surgery, and then at 1, 7, 14, and 30 days postoperatively. When serum glucose was not sampled on the indicated day, the serum value nearest to that day was analyzed. The daily insulin requirements, defined as the amount of insulin equivalent required to adjust the serum glucose level within the normal range, were recorded at the same date as ΔG. Statistical analysis Statistical analyses were performed using IBM SPSS Statistics, Ver. 19 (IBM, Armonk, NY, USA). Mann-Whitney test was used for comparing continuous variables between groups, and Fisher s exact test was used for comparing categorical variables between groups. Statistical significance was accepted at p<0.05. RESULTS In the EDP group, the duration of the operation was between 9 and 13 hours, and the estimated blood loss was between 1000 and 1800 ml. Pathological staging was T3N1M0 in all three patients. The tumor had invaded the portal vein and the superior mesenteric vein in two patients, and in one patient, only the portal vein was invaded. pancreatic fistula developed in all of the cases, but all of these fistulae were controlled with supportive care. One patient required long-term drainage of ascites; however, steatorrhea did not occur in these patients. At the last follow-up, two patients were alive with liver metastasis at 4 and 10 months postoperatively, respectively, and one patient died of liver metastasis at 5 months postoperatively (Table 2). Median operation time in all of the patients was 543 minutes; 665 minutes in patients who underwent EDP, 548 minutes in those who underwent PD, and 250 minutes in those who underwent DP. There was no statistically significant difference between the EDP and PD groups. However, the EDP group showed a significantly longer operation time than the DP group, probably because more time was needed for portal venous and gastrointestinal reconstruction in EDP. Otherwise, all of the three groups were comparable in terms of intraoperative blood loss, transfusion, tumor size, surgical radicality, and postoperative fistula formation. The proportion of patients with invasion of the portal or superior mesenteric vein was higher in the EDP group than in both the PD and DP groups (Table 3). The ΔG values were not different between the groups, except that the EDP group showed a significantly larger Table 2. Intraoperative and postoperative outcomes for patients who underwent extended distal pancreatectomy Age/Sex Operation time (minutes) Intraop. blood loss (ml) Intraop. transfusion (ml) Staging Vessel invasion Complications Outcomes 69/F 78/M 53/M T3N1 T3N1 T3N1 PV, SMV PV PV, SMV POPF POPF POPF Prolonged ascites Alive with liver metastasis at 10 months Died of liver metastasis at 5 months Alive with liver metastasis at 4 months POPF, postoperative pancreatic fistula (ISGPF definition); PV, portal vein; SMV, superior mesenteric vein.
5 Shin-Young Park, et al. Extended distal pancreatectomy 81 Table 3. Comparison of intra- and postoperative results Factors/Group PD DP EDP Total p-value (EDP vs. PD) p-value (EDP vs. DP) Operation time (minutes) Intraoperative blood loss (ml) Intraoperative Transfusion (ml) Tumor size (cm) Positive resection margin, n (%) Portal vein invasion, n (%) POPF, n (%) None Grade B Grade C Steatorrhea, n (%) 548 ( ) 900 ( ) 400 (0-3200) 3.4 ( ) 5 (13.9) 3 (8.3) 24 (66.7) 11 (30.6) 1 (2.8) 1 (2.8) 250 ( ) 1000 ( ) 400 (0-1000) 3.0 ( ) 2 (28.6) 1 (14.3) 5 (71.4) 1 (14.3) 1 (14.3) 665 ( ) 1000 ( ) 0 (0-400) 3.5 ( ) 1 (33.3) 3 (100) 3 (100.0) 543 ( ) 1000 ( ) 400 (0-3200) 3.4 ( ) 8 (17.4) 7 (15.2) 29 (63.0) 15 (32.6) 2 (4.3) 1 (2.2) PD, pancreaticoduodenectomy; DP, distal pancreatectomy; EDP, extended distal pancreatectomy; POPF, postoperative pancreatic fistula (ISGPF definition). Fig. 5. (A) Preoperative and postoperative serum glucose profiles. ΔG, daily glucose fluctuation. (B) Daily requirements of insulin equivalent. *p<0.05. blood glucose fluctuation (Fig. 5A). Similarly, the EDP group required higher amount of insulin equivalent at 14 days postoperatively, which was not observed eventually at 3 months postoperatively (Fig. 5B). DISCUSSION The standard operative procedures for pancreatic adenocarcinoma are PD and DP, depending on the tumor location. 2 Central pancreatectomy (medial, median, or middle segment pancreatectomy) has been proposed as an alternative treatment option for reducing the possibility of pancreatic functional impairment when tumors are located in the pancreatic neck and body. However, this treatment option has usually been used in benign diseases or low-grade malignancies. 7,8 In patients with pancreatic neck cancer who present with jaundice, the preferred surgical procedure is PD. However, if the patient has atrophy of the distal pancreas, there are concerns regarding pancreatic endocrine and exocrine insufficiency after PD has been performed. 9,10 In these cases, EDP, which preserves the uncinate process of
6 82 Korean J Hepatobiliary Pancreat Surg Vol. 18, No. 3, August 2014 the pancreas and the distal duodenum, can be an attractive option, provided that the tumor has not extended to the ampulla of Vater and the uncinate process. EDP is technically feasible, and is considered relatively safe when compared to other standard pancreatic resections. Recently, stapling devices have been widely used in the resection of not only hollow viscera, but also solid organs such as pancreas and liver. However, a possible difficulty with the use of the stapler is the inability to close the jaws due to lack of gripping power. We have found that this difficulty can be overcome by using vise-grip pliers, which are usually available in the department of orthopedic surgery. This technique may also be useful in liver resection. EDP can avoid pancreaticoenterostomy, which is the most compromised anastomosis of the pancreatic resection procedures. 11 We observed that all cases of EDP developed grade A postoperative pancreatic fistula, which resolved after conservative management, and had no significant clinical impact. 4 In literature, postoperative pancreatic fistula was documented in 10% to 15% of patients undergoing PD, and in 10% to 30% of patients undergoing DP. Different techniques of pancreaticoenteric anastomosis and pancreatic stump closure have not shown significant differences in the prevention of pancreatic fistula. 12 We assume that the rate of fistula development may decrease as compared to that in the standard DP on accumulation of more experience. There was no steatorrhea, an indicator of exocrine insufficiency, in any of the patients who underwent EDP. In previous studies, postoperative steatorrhea was observed as a complication in 25.6% to 52.4% of patients undergoing PD. 10,13,14 Therefore, it is likely that EDP is at least as effective as PD in preventing postoperative pancreatic exocrine insufficiency. In the previous studies on glylcemic control after pancreatic resection, HbA1c or fasting blood sugar (FBS), and 2-hour postprandial blood glucose (PP2) were used as the indicators of glycemic control. 10,15,16 However, HbA1c does not reflect the acute trend of blood glucose variations, and there are many patients whose FBS and PP2 were not measured pre- and postoperatively. Therefore, we chose ΔG as an indicator of glycemic control. We were unable to demonstrate that patients who underwent EDP had better glycemic control, although our results demonstrated that glucose profiles after EDP were comparable to those after PD or DP. In conclusion, although the present study was limited by the number of cases in showing meaningful statistical significance, and the prognosis of advanced pancreatic neck adenocarcinoma is still dismal, EDP was technically feasible and safe, and can be a valid treatment option especially when there is atrophy of the distal pancreas. Further studies including more number of cases are warranted, and technical refinements are needed to improve patient survival. REFERENCES 1. Orr RK. Outcomes in pancreatic cancer surgery. Surg Clin North Am 2010;90: Tempero MA, Arnoletti JP, Behrman SW, Ben-Josef E, Benson AB 3rd, Casper ES, et al; National Comprehensive Cancer Networks. Pancreatic Adenocarcinoma, version : featured updates to the NCCN Guidelines. J Natl Compr Canc Netw 2012; 10: Karasawa E, Goldberg HI, Moss AA, Federle MP, London SS. CT pancreatogram in carcinoma of the pancreas and chronic pancreatitis. Radiology 1983;148: Bassi C, Dervenis C, Butturini G, Fingerhut A, Yeo C, Izbicki J, et al; International Study Group on Pancreatic Fistula Definition. Postoperative pancreatic fistula: an international study group (ISGPF) definition. Surgery 2005;138: Slezak LA, Andersen DK. Pancreatic resection: effects on glucose metabolism. World J Surg 2001;25: Kahl S, Malfertheiner P. Exocrine and endocrine pancreatic insufficiency after pancreatic surgery. Best Pract Res Clin Gastroenterol 2004;18: Shimada K, Sakamoto Y, Esaki M, Kosuge T, Hiraoka N. Role of medial pancreatectomy in the management of intraductal papillary mucinous neoplasms and islet cell tumors of the pancreatic neck and body. Dig Surg 2008;25: Christein JD, Kim AW, Golshan MA, Maxhimer J, Deziel DJ, Prinz RA. Central pancreatectomy for the resection of benign or low malignant potential neoplasms. World J Surg 2003;27: Sato N, Yamaguchi K, Yokohata K, Shimizu S, Morisaki T, Chijiiwa K, et al. Short-term and long-term pancreatic exocrine and endocrine functions after pancreatectomy. Dig Dis Sci 1998; 43: Choi MG, Kim SW, Jang JY, Yoon YS, Park YH. Long-term functional outcome after pancreatoduodenectomy. Korean J Hepatobiliary Pancreat Surg 2004;8: Poon RT, Lo SH, Fong D, Fan ST, Wong J. Prevention of pancreatic anastomotic leakage after pancreaticoduodenectomy. Am J Surg 2002;183: Lermite E, Sommacale D, Piardi T, Arnaud JP, Sauvanet A, Dejong CH, et al. Complications after pancreatic resection: diagnosis, prevention and management. Clin Res Hepatol Gastroenterol 2013;37: Fang WL, Su CH, Shyr YM, Chen TH, Lee RC, Tai LC, et al. Functional and morphological changes in pancreatic remnant after pancreaticoduodenectomy. Pancreas 2007;35: Huang JJ, Yeo CJ, Sohn TA, Lillemoe KD, Sauter PK, Coleman
7 Shin-Young Park, et al. Extended distal pancreatectomy 83 J, et al. Quality of life and outcomes after pancreaticoduodenectomy. Ann Surg 2000;231: Tran TC, van Lanschot JJ, Bruno MJ, van Eijck CH. Functional changes after pancreatoduodenectomy: diagnosis and treatment. Pancreatology 2009;9: Allendorf JD, Schrope BA, Lauerman MH, Inabnet WB, Chabot JA. Postoperative glycemic control after central pancreatectomy for mid-gland lesions. World J Surg 2007;31:
Citation Hepato-Gastroenterology, 55(86-87),
 NAOSITE: Nagasaki University's Ac Title Author(s) Combined pancreatic resection and p multiple lesions of the pancreas: i of the pancreas concomitant with du Kuroki, Tamotsu; Tajima, Yoshitsugu Tomohiko;
NAOSITE: Nagasaki University's Ac Title Author(s) Combined pancreatic resection and p multiple lesions of the pancreas: i of the pancreas concomitant with du Kuroki, Tamotsu; Tajima, Yoshitsugu Tomohiko;
Prevention Of Pancreaticojejunal Fistula After Whipple Procedure
 ISPUB.COM The Internet Journal of Surgery Volume 4 Number 2 Prevention Of Pancreaticojejunal Fistula After Whipple Procedure N Barbetakis, K Setsiz Citation N Barbetakis, K Setsiz. Prevention Of Pancreaticojejunal
ISPUB.COM The Internet Journal of Surgery Volume 4 Number 2 Prevention Of Pancreaticojejunal Fistula After Whipple Procedure N Barbetakis, K Setsiz Citation N Barbetakis, K Setsiz. Prevention Of Pancreaticojejunal
The Whipple Operation Illustrations
 The Whipple Operation Illustrations Fig. 1. Illustration of the sixstep pancreaticoduodenectomy (Whipple operation) as described in a number of recent text books by Dr. Evans. The operation is divided
The Whipple Operation Illustrations Fig. 1. Illustration of the sixstep pancreaticoduodenectomy (Whipple operation) as described in a number of recent text books by Dr. Evans. The operation is divided
Fat Tissue Infiltration into the Pancreas Parenchyme and Its Effect on the Result of Surgery
 Korean Journal of HBP Surgery Vol. 15,. 2, May 2011 O riginal Article Fat Tissue Infiltration into the Pancreas Parenchyme and Its Effect on the Result of Surgery Purpose: In Korea, there are few reports
Korean Journal of HBP Surgery Vol. 15,. 2, May 2011 O riginal Article Fat Tissue Infiltration into the Pancreas Parenchyme and Its Effect on the Result of Surgery Purpose: In Korea, there are few reports
Citation American Journal of Surgery, 196(5)
 NAOSITE: Nagasaki University's Ac Title Author(s) Multifocal branch-duct pancreatic i neoplasms Tajima, Yoshitsugu; Kuroki, Tamotsu Amane; Adachi, Tomohiko; Mishima, T Kanematsu, Takashi Citation American
NAOSITE: Nagasaki University's Ac Title Author(s) Multifocal branch-duct pancreatic i neoplasms Tajima, Yoshitsugu; Kuroki, Tamotsu Amane; Adachi, Tomohiko; Mishima, T Kanematsu, Takashi Citation American
Outcomes of pancreaticoduodenectomy in patients with metastatic cancer
 Korean J Hepatobiliary Pancreat Surg 2014;18:147-151 http://dx.doi.org/.14701/kjhbps.2014.18.4.147 Original Article Outcomes of pancreaticoduodenectomy in patients with metastatic cancer Joo Hwa Kwak,
Korean J Hepatobiliary Pancreat Surg 2014;18:147-151 http://dx.doi.org/.14701/kjhbps.2014.18.4.147 Original Article Outcomes of pancreaticoduodenectomy in patients with metastatic cancer Joo Hwa Kwak,
Objectives. Intraoperative Consultation of the Whipple Resection Specimen. Pancreas Anatomy. Pancreatic ductal carcinoma 11/10/2014
 Intraoperative Consultation of the Whipple Resection Specimen Pathology Update Faculty of Medicine, University of Toronto November 15, 2014 John W. Wong, MD, FRCPC Department of Anatomical Pathology Sunnybrook
Intraoperative Consultation of the Whipple Resection Specimen Pathology Update Faculty of Medicine, University of Toronto November 15, 2014 John W. Wong, MD, FRCPC Department of Anatomical Pathology Sunnybrook
Predictive factors for invasive intraductal papillary mucinous neoplasm of the pancreas
 Korean J Hepatobiliary Pancreat Surg 2011;15:27-22 Original Article Predictive factors for invasive intraductal papillary mucinous neoplasm of the pancreas Dae Young Jun 1, Hyung Jun Kwon 2, Sang Geol
Korean J Hepatobiliary Pancreat Surg 2011;15:27-22 Original Article Predictive factors for invasive intraductal papillary mucinous neoplasm of the pancreas Dae Young Jun 1, Hyung Jun Kwon 2, Sang Geol
5/17/2013. Pancreatic Cancer. Postgraduate Course in General Surgery CASE 1: CASE 1: Overview. Case presentation. Differential diagnosis
 Overview Case presentation Postgraduate Course in General Surgery Differential diagnosis Diagnosis and therapy Eric K. Nakakura Koloa, HI March 26, 2013 Outcomes CASE 1: CASE 1: A 78-year-old man developed
Overview Case presentation Postgraduate Course in General Surgery Differential diagnosis Diagnosis and therapy Eric K. Nakakura Koloa, HI March 26, 2013 Outcomes CASE 1: CASE 1: A 78-year-old man developed
3/28/2012. Periampullary Tumors. Postgraduate Course in General Surgery CASE 1: CASE 1: Overview. Eric K. Nakakura Ko Olina, HI
 Overview Postgraduate Course in General Surgery Case presentation Differential diagnosis Diagnosis and therapy Outcomes Principles of palliative care Eric K. Nakakura Ko Olina, HI March 27, 2012 CASE 1:
Overview Postgraduate Course in General Surgery Case presentation Differential diagnosis Diagnosis and therapy Outcomes Principles of palliative care Eric K. Nakakura Ko Olina, HI March 27, 2012 CASE 1:
Branch duct intraductal papillary mucinous neoplasm of the pancreas: single-center experience with 324 patients who underwent surgical resection
 Korean J Hepatobiliary Pancreat Surg 2015;19:113-120 http://dx.doi.org/10.14701/kjhbps.2015.19.3.113 Original Article Branch duct intraductal papillary mucinous neoplasm of the pancreas: single-center
Korean J Hepatobiliary Pancreat Surg 2015;19:113-120 http://dx.doi.org/10.14701/kjhbps.2015.19.3.113 Original Article Branch duct intraductal papillary mucinous neoplasm of the pancreas: single-center
Yoshitsugu; Kanematsu, Takashi; Kur
 NAOSITE: Nagasaki University's Ac Title Author(s) Citation Laparoscopic Middle Pancreatectomy Surgery Kitasato, Amane; Adachi, Tomohiko; Yoshitsugu; Kanematsu, Takashi; Kur Hepato-Gastroenterology, 59(120),
NAOSITE: Nagasaki University's Ac Title Author(s) Citation Laparoscopic Middle Pancreatectomy Surgery Kitasato, Amane; Adachi, Tomohiko; Yoshitsugu; Kanematsu, Takashi; Kur Hepato-Gastroenterology, 59(120),
Chronic Pancreatitis
 Gastro Foundation Fellows Weekend 2017 Chronic Pancreatitis Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Aetiology in SA Alcohol (up to 80%) Idiopathic Tropical Obstruction Autoimmune
Gastro Foundation Fellows Weekend 2017 Chronic Pancreatitis Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Aetiology in SA Alcohol (up to 80%) Idiopathic Tropical Obstruction Autoimmune
Surgical outcomes of multifocal branch duct intraductal papillary mucinous neoplasms of pancreas
 Korean J Hepatobiliary Pancreat Surg 2014;18:152-158 http://dx.doi.org/10.14701/kjhbps.2014.18.4.152 Original Article Surgical outcomes of multifocal branch duct intraductal papillary mucinous neoplasms
Korean J Hepatobiliary Pancreat Surg 2014;18:152-158 http://dx.doi.org/10.14701/kjhbps.2014.18.4.152 Original Article Surgical outcomes of multifocal branch duct intraductal papillary mucinous neoplasms
Pancreas Quizzes c. Both A and B a. Directly into the blood stream (not using ducts)
 Pancreas Quizzes Quiz 1 1. The pancreas produces hormones. Which type of hormone producing organ is the pancreas? a. Endocrine b. Exocrine c. Both A and B d. Neither A or B 2. Endocrine indicates hormones
Pancreas Quizzes Quiz 1 1. The pancreas produces hormones. Which type of hormone producing organ is the pancreas? a. Endocrine b. Exocrine c. Both A and B d. Neither A or B 2. Endocrine indicates hormones
Topics: Staging and treatment for pancreatic cancer. Staging systems for pancreatic cancer: Differences between the Japanese and UICC systems
 M. J Hep Kobari Bil Pancr and S. Surg Matsuno: (1998) Staging 5:121 127 system for pancreatic cancer 121 Topics: Staging and treatment for pancreatic cancer Staging systems for pancreatic cancer: Differences
M. J Hep Kobari Bil Pancr and S. Surg Matsuno: (1998) Staging 5:121 127 system for pancreatic cancer 121 Topics: Staging and treatment for pancreatic cancer Staging systems for pancreatic cancer: Differences
Multiple Primary Quiz
 Multiple Primary Quiz Case 1 A 72 year old man was found to have a 12 mm solid lesion in the pancreatic tail by computed tomography carried out during a routine follow up study of this patient with adult
Multiple Primary Quiz Case 1 A 72 year old man was found to have a 12 mm solid lesion in the pancreatic tail by computed tomography carried out during a routine follow up study of this patient with adult
Case Report pissn J Korean Soc Radiol 2012;67(4): INTRODUCTION CASE REPORT
 Case Report pissn 1738-2637 Focal Fat Deposition Developed in the Segment IV of the Liver Following Gastrectomy Mimicking a Hepatic Metastasis: Two Case Reports 1 위절제술후에간의제 4 분절에서발생한간전이를닮은국소지방침윤 : 두증례보고
Case Report pissn 1738-2637 Focal Fat Deposition Developed in the Segment IV of the Liver Following Gastrectomy Mimicking a Hepatic Metastasis: Two Case Reports 1 위절제술후에간의제 4 분절에서발생한간전이를닮은국소지방침윤 : 두증례보고
Cattell-Braasch maneuver combined with superior mesenteric artery first approach for resection of borderline resectable pancreatic cancer
 Masters of Surgery Page 1 of 5 Cattell-Braasch maneuver combined with superior mesenteric artery first approach for resection of borderline resectable pancreatic cancer Tingsong Yang 1, Fairweather Mark
Masters of Surgery Page 1 of 5 Cattell-Braasch maneuver combined with superior mesenteric artery first approach for resection of borderline resectable pancreatic cancer Tingsong Yang 1, Fairweather Mark
Pylorus Preserving Pancreaticoduodenectomy
 REVIEW Pylorus Preserving Pancreaticoduodenectomy Jacqueline M. Garonzik-Wang, M. B. Majella Doyle Pancreaticoduodenectomy (PD) has become the standard of care for resectable pancreatic cancer and premalignant
REVIEW Pylorus Preserving Pancreaticoduodenectomy Jacqueline M. Garonzik-Wang, M. B. Majella Doyle Pancreaticoduodenectomy (PD) has become the standard of care for resectable pancreatic cancer and premalignant
Pancreaticoduodenectomy the anatomy and the surgical approaches
 Pancreaticoduodenectomy the anatomy and the surgical approaches Paul BS LAI Division of Hepato biliary and Pancreatic Surgery Department of Surgery The Chinese Univesity of Hong Kong Whipple s operation
Pancreaticoduodenectomy the anatomy and the surgical approaches Paul BS LAI Division of Hepato biliary and Pancreatic Surgery Department of Surgery The Chinese Univesity of Hong Kong Whipple s operation
JOHN M UECKER, MD, FACS COMPLEX PANCREATICODUODENAL INJURIES
 JOHN M UECKER, MD, FACS COMPLEX PANCREATICODUODENAL INJURIES THE PROBLEM DUODENAL / PANCREATIC INJURIES Difficult to diagnose Not very common Anatomic and physiologic challenges 90% rate of associated
JOHN M UECKER, MD, FACS COMPLEX PANCREATICODUODENAL INJURIES THE PROBLEM DUODENAL / PANCREATIC INJURIES Difficult to diagnose Not very common Anatomic and physiologic challenges 90% rate of associated
Greater Manchester and Cheshire HPB Unit Guidelines for the Assessment & Management of Hepatobiliary and Pancreatic Disease Chapter 14
 Greater Manchester and Cheshire HPB Unit Guidelines for the Assessment & Management of Hepatobiliary and Pancreatic Disease Chapter 14 Contents 14. Neuroendocrine Tumours 161 14.1. Diagnostic algorithm
Greater Manchester and Cheshire HPB Unit Guidelines for the Assessment & Management of Hepatobiliary and Pancreatic Disease Chapter 14 Contents 14. Neuroendocrine Tumours 161 14.1. Diagnostic algorithm
pitfall Table 1 4 disorientation pitfall pitfall Table 1 Tel:
 11 687 692 2002 pitfall 1078 29 17 9 1 2 3 dislocation outflow block 11 1 2 3 9 1 2 3 4 disorientation pitfall 11 687 692 2002 Tel: 075-751-3606 606-8507 54 2001 8 27 2002 10 31 29 4 pitfall 16 1078 Table
11 687 692 2002 pitfall 1078 29 17 9 1 2 3 dislocation outflow block 11 1 2 3 9 1 2 3 4 disorientation pitfall 11 687 692 2002 Tel: 075-751-3606 606-8507 54 2001 8 27 2002 10 31 29 4 pitfall 16 1078 Table
Middle-Preserving Pancreatectomy for Multifocal Metastatic Renal Cell Carcinoma Located in the Head, Body and Tail of the Pancreas.
 CASE REPORT Middle-Preserving Pancreatectomy for Multifocal Metastatic Renal Cell Carcinoma Located in the Head, Body and Tail of the Pancreas. A Case Report Hiroki Ohzato, Tameyoshi Yamamoto, Mutsumi
CASE REPORT Middle-Preserving Pancreatectomy for Multifocal Metastatic Renal Cell Carcinoma Located in the Head, Body and Tail of the Pancreas. A Case Report Hiroki Ohzato, Tameyoshi Yamamoto, Mutsumi
Management of Pancreatic Fistulae
 Management of Pancreatic Fistulae Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Fistula definition A Fistula is a permanent abnormal passageway between two organs (epithelial
Management of Pancreatic Fistulae Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Fistula definition A Fistula is a permanent abnormal passageway between two organs (epithelial
Pancreatic Adenocarcinoma: Everything You Need to Know From Cross-Sectional Imaging to Treatment
 Pancreatic Adenocarcinoma: Everything You Need to Know From Cross-Sectional Imaging to Treatment Andrew W. Bowman, MD PhD Assistant Professor of Radiology Mayo Clinic Florida SCBT-MR Annual Meeting Nashville,
Pancreatic Adenocarcinoma: Everything You Need to Know From Cross-Sectional Imaging to Treatment Andrew W. Bowman, MD PhD Assistant Professor of Radiology Mayo Clinic Florida SCBT-MR Annual Meeting Nashville,
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Adenocarcinoma, pancreatic ductal, laparoscopic distal pancreatectomy for, 61 Adrenal cortical carcinoma, laparoscopic adrenalectomy for, 114
Note: Page numbers of article titles are in boldface type. A Adenocarcinoma, pancreatic ductal, laparoscopic distal pancreatectomy for, 61 Adrenal cortical carcinoma, laparoscopic adrenalectomy for, 114
Intraductal papillary neoplasms in the bile ducts
 Intraductal papillary neoplasms in the bile ducts Seok Hwa Youn Myunghee Yoon Dong Hoon Shin Kosin University Gospel Hospital Department of general surgery Hepato-biliary-pancreatic division Introduction
Intraductal papillary neoplasms in the bile ducts Seok Hwa Youn Myunghee Yoon Dong Hoon Shin Kosin University Gospel Hospital Department of general surgery Hepato-biliary-pancreatic division Introduction
P resently, pancreaticoduodenectomy is widely accepted as the standard surgical procedure for patients with
 OPEN SUBJECT AREAS: CANCER THERAPY PANCREATIC CANCER GASTROINTESTINAL CANCER OUTCOMES RESEARCH Received 13 May 2013 Accepted 3 June 2013 Published 25 June 2013 Correspondence and requests for materials
OPEN SUBJECT AREAS: CANCER THERAPY PANCREATIC CANCER GASTROINTESTINAL CANCER OUTCOMES RESEARCH Received 13 May 2013 Accepted 3 June 2013 Published 25 June 2013 Correspondence and requests for materials
Reinterventions belong to complications
 Reinterventions belong to complications Pancreatic surgery is the archetypus of complex abdominal surgery Mortality (1-4%) and morbidity (7-60%) rates are relevant even at high volume centres Reinterventions
Reinterventions belong to complications Pancreatic surgery is the archetypus of complex abdominal surgery Mortality (1-4%) and morbidity (7-60%) rates are relevant even at high volume centres Reinterventions
Laparoscopy-assisted D2 radical distal subtotal gastrectomy
 Masters of Gastrointestinal Surgery Laparoscopy-assisted D2 radical distal subtotal gastrectomy Xiaogeng Chen, Weihua Li, Jinsi Wang, Changshun Yang Department of Tumor Surgery, Fujian Provincial Hospital,
Masters of Gastrointestinal Surgery Laparoscopy-assisted D2 radical distal subtotal gastrectomy Xiaogeng Chen, Weihua Li, Jinsi Wang, Changshun Yang Department of Tumor Surgery, Fujian Provincial Hospital,
MATERIALS AND METHODS Patients
 Yonago Acta medica 216;59:232 236 Original Article Usefulness of T-Shaped Gauze for Precise Dissection of Supra-Pancreatic Lymph Nodes and for Reduced Postoperative Pancreatic Fistula in Patients Undergoing
Yonago Acta medica 216;59:232 236 Original Article Usefulness of T-Shaped Gauze for Precise Dissection of Supra-Pancreatic Lymph Nodes and for Reduced Postoperative Pancreatic Fistula in Patients Undergoing
Late Postpancreatectomy Hemorrhage After Pancreaticoduodenectomy: Is It Possible to Recognize Risk Factors?
 ORIGINAL ARTICLE Late Postpancreatectomy Hemorrhage After Pancreaticoduodenectomy: Is It Possible to Recognize Risk Factors? Claudio Ricci, Riccardo Casadei, Salvatore Buscemi, Francesco Minni Department
ORIGINAL ARTICLE Late Postpancreatectomy Hemorrhage After Pancreaticoduodenectomy: Is It Possible to Recognize Risk Factors? Claudio Ricci, Riccardo Casadei, Salvatore Buscemi, Francesco Minni Department
Endoscopic Ultrasonography Assessment for Ampullary and Bile Duct Malignancy
 Diagnostic and Therapeutic Endoscopy, Vol. 3, pp. 35-40 Reprints available directly from the publisher Photocopying permitted by license only (C) 1996 OPA (Overseas Publishers Association) Amsterdam B.V.
Diagnostic and Therapeutic Endoscopy, Vol. 3, pp. 35-40 Reprints available directly from the publisher Photocopying permitted by license only (C) 1996 OPA (Overseas Publishers Association) Amsterdam B.V.
Prognostic factors for survival of patients with ampullary carcinoma after local resection. Abstract
 UPPER GI ANZJSurg.com Prognostic factors for survival of patients with ampullary carcinoma after local resection Xiangqian Zhao, Jiahong Dong, Xiaoqiang Huang, Wenzhi Zhang and Kai Jiang Hospital and Institute
UPPER GI ANZJSurg.com Prognostic factors for survival of patients with ampullary carcinoma after local resection Xiangqian Zhao, Jiahong Dong, Xiaoqiang Huang, Wenzhi Zhang and Kai Jiang Hospital and Institute
AFP-producing acinar cell carcinoma treated by pancreaticoduodenectomy in a patient with a previous radical subtotal gastrectomy by gastric cancer
 Korean J Hepatobiliary Pancreat Surg 2014;18:33-37 http://dx.doi.org/10.14701/kjhbps.2014.18.1.33 Case Report AFP-producing acinar cell carcinoma treated by pancreaticoduodenectomy in a patient with a
Korean J Hepatobiliary Pancreat Surg 2014;18:33-37 http://dx.doi.org/10.14701/kjhbps.2014.18.1.33 Case Report AFP-producing acinar cell carcinoma treated by pancreaticoduodenectomy in a patient with a
THE CRITICAL COMPLCATIONS AND MANAGEMENTS AFTER PANCREATIC SURGERY 2013/12/21
 THE CRITICAL COMPLCATIONS AND MANAGEMENTS AFTER PANCREATIC SURGERY Tsann-Long Hwang, MD, FACS Department of Surgery Chang Gung Memorial Hospital Chang Gung University Taipei, TAIWAN 2013/12/21 THE DIFFICULTY
THE CRITICAL COMPLCATIONS AND MANAGEMENTS AFTER PANCREATIC SURGERY Tsann-Long Hwang, MD, FACS Department of Surgery Chang Gung Memorial Hospital Chang Gung University Taipei, TAIWAN 2013/12/21 THE DIFFICULTY
PANCREAS DUCTAL ADENOCARCINOMA PDAC
 CONTENTS PANCREAS DUCTAL ADENOCARCINOMA PDAC I. What is the pancreas? II. III. IV. What is pancreas cancer? What is the epidemiology of Pancreatic Ductal Adenocarcinoma (PDAC)? What are the risk factors
CONTENTS PANCREAS DUCTAL ADENOCARCINOMA PDAC I. What is the pancreas? II. III. IV. What is pancreas cancer? What is the epidemiology of Pancreatic Ductal Adenocarcinoma (PDAC)? What are the risk factors
Surgical Treatment for Carcinoma of the Ampulla of Vater and Residual Pancreatic Function before and after Pancreaticoduodenectomy*)
 Hiroshima Journal of Medical Sciences Vol. 32, No. 4, 455,-...,460, December, 1983 HIJM 32-68 455 Surgical Treatment for Carcinoma of the Ampulla of Vater and Residual Pancreatic Function before and after
Hiroshima Journal of Medical Sciences Vol. 32, No. 4, 455,-...,460, December, 1983 HIJM 32-68 455 Surgical Treatment for Carcinoma of the Ampulla of Vater and Residual Pancreatic Function before and after
Dr Claire Smith, Consultant Radiologist St James University Hospital Leeds
 Dr Claire Smith, Consultant Radiologist St James University Hospital Leeds Imaging in jaundice and 2ww pathway Image protocol Staging Limitations Pancreatic cancer 1.2.4 Refer people using a suspected
Dr Claire Smith, Consultant Radiologist St James University Hospital Leeds Imaging in jaundice and 2ww pathway Image protocol Staging Limitations Pancreatic cancer 1.2.4 Refer people using a suspected
What to expect with major vascular reconstruction during Whipple procedures: a single institution experience and literature review
 Original Article What to expect with major vascular reconstruction during Whipple procedures: a single institution experience and literature review Matthew S. Jorgensen 1, Tariq Almerey 2, Houssam Farres
Original Article What to expect with major vascular reconstruction during Whipple procedures: a single institution experience and literature review Matthew S. Jorgensen 1, Tariq Almerey 2, Houssam Farres
Common and unusual CT and MRI manifestations of pancreatic adenocarcinoma: a pictorial review
 Review Article Common and unusual CT and MRI manifestations of pancreatic adenocarcinoma: a pictorial review Min-Jie Yang, Su Li, Yong-Guang Liu, Na Jiao, Jing-Shan Gong Department of Radiology, Shenzhen
Review Article Common and unusual CT and MRI manifestations of pancreatic adenocarcinoma: a pictorial review Min-Jie Yang, Su Li, Yong-Guang Liu, Na Jiao, Jing-Shan Gong Department of Radiology, Shenzhen
Segmental duodenectomy with duodenojejunostomy of gastrointestinal stromal tumor involving the duodenum
 J Korean Surg Soc 2011;80:S12-16 DOI: 10.4174/jkss.2011.80.Suppl 1.S12 CASE REPORT JKSS Journal of the Korean Surgical Society pissn 2233-7903 ㆍ eissn 2093-0488 Segmental duodenectomy with duodenojejunostomy
J Korean Surg Soc 2011;80:S12-16 DOI: 10.4174/jkss.2011.80.Suppl 1.S12 CASE REPORT JKSS Journal of the Korean Surgical Society pissn 2233-7903 ㆍ eissn 2093-0488 Segmental duodenectomy with duodenojejunostomy
Evaluation of Suspected Pancreatic Cancer
 Evaluation of Suspected Pancreatic Cancer October 15, 2015 If you experience technical difficulty during the presentation: Contact WebEx Technical Support directly at: US Toll Free: 1-866-779-3239 Toll
Evaluation of Suspected Pancreatic Cancer October 15, 2015 If you experience technical difficulty during the presentation: Contact WebEx Technical Support directly at: US Toll Free: 1-866-779-3239 Toll
Surgical management and results for cystic neoplasms of pancreas
 Korean J Hepatobiliary Pancreat Surg 2013;17:118-125 Original Article Surgical management and results for cystic neoplasms of pancreas Kyung Won Han 1, Ryun Ha 1, Kun Kuk Kim 1, Jung Nam Lee 1, Yeon Suk
Korean J Hepatobiliary Pancreat Surg 2013;17:118-125 Original Article Surgical management and results for cystic neoplasms of pancreas Kyung Won Han 1, Ryun Ha 1, Kun Kuk Kim 1, Jung Nam Lee 1, Yeon Suk
Surgical Treatment for Periampullary Carcinoma A Study of 129 Patients*)
 Hiroshima Journal of Medical Sciences Vol. 33, No. 2, 179,...183, June, 1984 HJM 33-24 179 Surgical Treatment for Periampullary Carcinoma A Study of 129 Patients*) Tsuneo TAN AKA, Motomu KODAMA, Rokuro
Hiroshima Journal of Medical Sciences Vol. 33, No. 2, 179,...183, June, 1984 HJM 33-24 179 Surgical Treatment for Periampullary Carcinoma A Study of 129 Patients*) Tsuneo TAN AKA, Motomu KODAMA, Rokuro
Original article: new surgical approaches to the Klatskin tumour
 Alimentary Pharmacology & Therapeutics Original article: new surgical approaches to the Klatskin tumour T. M. VAN GULIK*, S. DINANT*, O. R. C. BUSCH*, E. A. J. RAUWS, H. OBERTOP* & D. J. GOUMA Departments
Alimentary Pharmacology & Therapeutics Original article: new surgical approaches to the Klatskin tumour T. M. VAN GULIK*, S. DINANT*, O. R. C. BUSCH*, E. A. J. RAUWS, H. OBERTOP* & D. J. GOUMA Departments
ORIGINAL ARTICLE. Fate of the Pancreatic Remnant After Resection for an Intraductal Papillary Mucinous Neoplasm
 ONLINE FIRST ORIGINAL ARTICLE Fate of the Pancreatic Remnant After Resection for an Intraductal Papillary Mucinous Neoplasm A Longitudinal Level II Cohort Study Toshiyuki Moriya, MD, PhD; L. William Traverso,
ONLINE FIRST ORIGINAL ARTICLE Fate of the Pancreatic Remnant After Resection for an Intraductal Papillary Mucinous Neoplasm A Longitudinal Level II Cohort Study Toshiyuki Moriya, MD, PhD; L. William Traverso,
PANCREATECTOMY WITH MESENTERIC AND PORTAL VEIN RESECTION FOR BORDERLINE RESECTABLE PANCREATIC CANCER: MULTICENTER STUDY
 PROPOSAL: PANCREATECTOMY WITH MESENTERIC AND PORTAL VEIN RESECTION FOR BORDERLINE RESECTABLE PANCREATIC CANCER: MULTICENTER STUDY Pancreatic carcinoma represents the fourth-leading cause of cancer-related
PROPOSAL: PANCREATECTOMY WITH MESENTERIC AND PORTAL VEIN RESECTION FOR BORDERLINE RESECTABLE PANCREATIC CANCER: MULTICENTER STUDY Pancreatic carcinoma represents the fourth-leading cause of cancer-related
Endoscopic Resection of Ampullary Neuroendocrine Tumor
 CASE REPORT Endoscopic Resection of Ampullary Neuroendocrine Tumor Hiroyuki Fukasawa, Shigetaka Tounou, Masashi Nabetani and Tomoki Michida Abstract We report the case of a 57-year-old man with a 1.0-cm
CASE REPORT Endoscopic Resection of Ampullary Neuroendocrine Tumor Hiroyuki Fukasawa, Shigetaka Tounou, Masashi Nabetani and Tomoki Michida Abstract We report the case of a 57-year-old man with a 1.0-cm
Clinical Efficacy of Organ-Preserving Pancreatectomy for Benign or Low-Grade Malignant Potential Lesion
 J Korean Med Sci 2010; 25: 97-103 ISSN 1011-8934 DOI: 10.3346/jkms.2010.25.1.97 Clinical Efficacy of Organ-Preserving Pancreatectomy for Benign or Low-Grade Malignant Potential Lesion The clinical usefulness
J Korean Med Sci 2010; 25: 97-103 ISSN 1011-8934 DOI: 10.3346/jkms.2010.25.1.97 Clinical Efficacy of Organ-Preserving Pancreatectomy for Benign or Low-Grade Malignant Potential Lesion The clinical usefulness
Safety of pancreatic resection in the elderly: a retrospective analysis of 556 patients
 ORIGINAL ARTICLE Annals of Gastroenterology (2016) 29, 1-5 Safety of pancreatic resection in the elderly: a retrospective analysis of 556 patients Daniel Ansari, Linus Aronsson, Joakim Fredriksson, Bodil
ORIGINAL ARTICLE Annals of Gastroenterology (2016) 29, 1-5 Safety of pancreatic resection in the elderly: a retrospective analysis of 556 patients Daniel Ansari, Linus Aronsson, Joakim Fredriksson, Bodil
Is Hepatic Resection Needed in the Patients with Peritoneal Side T2 Gallbladder Cancer?
 Is Hepatic Resection Needed in the Patients with Peritoneal Side T2 Gallbladder Cancer? Lee H, Park JY, Youn S, Kwon W, Heo JS, Choi SH, Choi DW Department of Surgery, Samsung Medical Center Sungkyunkwan
Is Hepatic Resection Needed in the Patients with Peritoneal Side T2 Gallbladder Cancer? Lee H, Park JY, Youn S, Kwon W, Heo JS, Choi SH, Choi DW Department of Surgery, Samsung Medical Center Sungkyunkwan
Outcomes associated with robotic approach to pancreatic resections
 Short Communication (Management of Foregut Malignancies and Hepatobiliary Tract and Pancreas Malignancies) Outcomes associated with robotic approach to pancreatic resections Caitlin Takahashi 1, Ravi Shridhar
Short Communication (Management of Foregut Malignancies and Hepatobiliary Tract and Pancreas Malignancies) Outcomes associated with robotic approach to pancreatic resections Caitlin Takahashi 1, Ravi Shridhar
Pancreas Case Scenario #1
 Pancreas Case Scenario #1 An 85 year old white female presented to her primary care physician with increasing abdominal pain. On 8/19 she had a CT scan of the abdomen and pelvis. This showed a 4.6 cm mass
Pancreas Case Scenario #1 An 85 year old white female presented to her primary care physician with increasing abdominal pain. On 8/19 she had a CT scan of the abdomen and pelvis. This showed a 4.6 cm mass
Serous Cystic Neoplasm: Do We Have to Wait Till It Causes Trouble?
 Korean Journal of HBP Surgery Case Report Vol. 15, No. 2, May 2011 Serous Cystic Neoplasm: Do We Have to Wait Till It Causes Trouble? Serous cystic neoplasm (SCN) of the pancreas is considered a benign
Korean Journal of HBP Surgery Case Report Vol. 15, No. 2, May 2011 Serous Cystic Neoplasm: Do We Have to Wait Till It Causes Trouble? Serous cystic neoplasm (SCN) of the pancreas is considered a benign
Hiroshi Tajima, Yusuke Kumamoto, Ken-Ichiro Ishii, Ryo Nishiyama, Hiroshi Kawamata, Takashi Kaizu, Yoshihito Takahashi, Masahiko Watanabe
 Original Contribution Kitasato Med J 2017; 47: 17-25 The cartridge size and stapler selection alter the risk of pancreatic fistula after distal pancreatectomy with stapler use: a retrospective cohort study
Original Contribution Kitasato Med J 2017; 47: 17-25 The cartridge size and stapler selection alter the risk of pancreatic fistula after distal pancreatectomy with stapler use: a retrospective cohort study
Interactive Exhibit On Imaging Updates For Staging And Response Assessment In Pancreatic Cancer
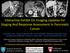 Interactive Exhibit On Imaging Updates For Staging And Response Assessment In Pancreatic Cancer 1 Vinit Baliyan, MD; 1 Hamed Kordbacheh, MD; 2 Eric P Tamm, MD; 3 Theodore S Hong, MD; 4 Carlos Fernandez-Del
Interactive Exhibit On Imaging Updates For Staging And Response Assessment In Pancreatic Cancer 1 Vinit Baliyan, MD; 1 Hamed Kordbacheh, MD; 2 Eric P Tamm, MD; 3 Theodore S Hong, MD; 4 Carlos Fernandez-Del
Intraductal papillary mucinous neoplasm of the bile ducts: a rare form of premalignant lesion of invasive cholangiocarcinoma
 Intraductal papillary mucinous neoplasm of the bile ducts: a rare form of premalignant lesion of invasive cholangiocarcinoma Authors: R. Revert Espí, Y. Fernandez Nuñez, I. Carbonell, D. P. Gómez valencia,
Intraductal papillary mucinous neoplasm of the bile ducts: a rare form of premalignant lesion of invasive cholangiocarcinoma Authors: R. Revert Espí, Y. Fernandez Nuñez, I. Carbonell, D. P. Gómez valencia,
Initial experience with radical antegrade modular pancreatosplenectomy in a single institution
 ORIGINAL ARTICLE pissn 2288-6575 eissn 2288-6796 http://dx.doi.org/10.4174/astr.2016.91.1.29 Annals of Surgical Treatment and Research Initial experience with radical antegrade modular pancreatosplenectomy
ORIGINAL ARTICLE pissn 2288-6575 eissn 2288-6796 http://dx.doi.org/10.4174/astr.2016.91.1.29 Annals of Surgical Treatment and Research Initial experience with radical antegrade modular pancreatosplenectomy
Management of the Mucin Filled Bile Duct. A Complication of Intraductal Papillary Mucinous Tumor of the Pancreas
 CASE REPORT Management of the Mucin Filled Bile Duct. A Complication of Intraductal Papillary Mucinous Tumor of the Pancreas Anand Patel, Louis Lambiase, Antonio Decarli, Ali Fazel Division of Gastroenterology
CASE REPORT Management of the Mucin Filled Bile Duct. A Complication of Intraductal Papillary Mucinous Tumor of the Pancreas Anand Patel, Louis Lambiase, Antonio Decarli, Ali Fazel Division of Gastroenterology
Surgical Management of Pancreatic Cancer
 I Congresso de Oncologia D Or July 5-6, 2013 Surgical Management of Pancreatic Cancer Michael A. Choti, MD, MBA, FACS Department of Surgery Johns Hopkins University School of Medicine, Baltimore, MD Estimated
I Congresso de Oncologia D Or July 5-6, 2013 Surgical Management of Pancreatic Cancer Michael A. Choti, MD, MBA, FACS Department of Surgery Johns Hopkins University School of Medicine, Baltimore, MD Estimated
ORIGINAL ARTICLE. Helical Computed Tomography in the Diagnosis of Portal Vein Invasion by Pancreatic Head Carcinoma
 ORIGINAL ARTICLE Helical Computed Tomography in the Diagnosis of Portal Vein Invasion by Pancreatic Head Carcinoma Usefulness for Selecting Surgical Procedures and Predicting the Outcome Hiroyoshi Furukawa,
ORIGINAL ARTICLE Helical Computed Tomography in the Diagnosis of Portal Vein Invasion by Pancreatic Head Carcinoma Usefulness for Selecting Surgical Procedures and Predicting the Outcome Hiroyoshi Furukawa,
Laparoscopic left hepatectomy in patients with intrahepatic duct stones and recurrent pyogenic cholangitis
 Korean J Hepatobiliary Pancreat Surg 212;16:15-19 Original Article Laparoscopic left hepatectomy in patients with intrahepatic duct stones and recurrent pyogenic cholangitis Sunjong Han, Insang Song, and
Korean J Hepatobiliary Pancreat Surg 212;16:15-19 Original Article Laparoscopic left hepatectomy in patients with intrahepatic duct stones and recurrent pyogenic cholangitis Sunjong Han, Insang Song, and
CT 101 :Pancreas and Spleen
 CT 101 :Pancreas and Spleen Shikha Khullar,, MD, MPH Division of Radiology University of South Alabama The Pancreas Normal Pancreas 3 Phase Pancreatic CT Non contrast Arterial phase : 30-35 35 second
CT 101 :Pancreas and Spleen Shikha Khullar,, MD, MPH Division of Radiology University of South Alabama The Pancreas Normal Pancreas 3 Phase Pancreatic CT Non contrast Arterial phase : 30-35 35 second
Pancreatic duct obstruction after pancreaticojejunostomy: implications for early prediction and prevention of long-term pancreatic complications
 Zhang et al. BMC Gastroenterology (2018) 18:53 https://doi.org/10.1186/s12876-018-0777-z RESEARCH ARTICLE Pancreatic duct obstruction after pancreaticojejunostomy: implications for early prediction and
Zhang et al. BMC Gastroenterology (2018) 18:53 https://doi.org/10.1186/s12876-018-0777-z RESEARCH ARTICLE Pancreatic duct obstruction after pancreaticojejunostomy: implications for early prediction and
An investigation of pancreatic volume by disease using pancreatic volumetry
 Yamagata Med J (ISSN 0288-030X)2015;33(2):71-76 DOI 10.15022/00003469 An investigation of pancreatic volume by disease using pancreatic volumetry Tsuyoshi Fukumoto, Toshihiro Watanabe, Koji Tezuka, Akiko
Yamagata Med J (ISSN 0288-030X)2015;33(2):71-76 DOI 10.15022/00003469 An investigation of pancreatic volume by disease using pancreatic volumetry Tsuyoshi Fukumoto, Toshihiro Watanabe, Koji Tezuka, Akiko
Delayed Perforation Occurring after Endoscopic Submucosal Dissection for Early Gastric Cancer
 CASE REPORT Clin Endosc 2015;48:251-255 Print ISSN 2234-2400 / On-line ISSN 2234-2443 http://dx.doi.org/10.5946/ce.2015.48.3.251 Open Access Delayed Perforation Occurring after Endoscopic Submucosal Dissection
CASE REPORT Clin Endosc 2015;48:251-255 Print ISSN 2234-2400 / On-line ISSN 2234-2443 http://dx.doi.org/10.5946/ce.2015.48.3.251 Open Access Delayed Perforation Occurring after Endoscopic Submucosal Dissection
Cuneyt Kayaalp, Murat Sait Dogan, and Veysel Ersan. Department of Surgery, Inonu University, Malatya, Turkey
 Ann Hepatobiliary Pancreat Surg 2017;21:101-105 https://doi.org/10.14701/ahbps.2017.21.2.101 Case Report Surgery for intractable pain in a patient with chronic pancreatitis complicated with biliary obstruction,
Ann Hepatobiliary Pancreat Surg 2017;21:101-105 https://doi.org/10.14701/ahbps.2017.21.2.101 Case Report Surgery for intractable pain in a patient with chronic pancreatitis complicated with biliary obstruction,
Outcomes of robotic surgery for pancreatic ductal adenocarcinoma
 Original Article Outcomes of robotic surgery for pancreatic ductal adenocarcinoma Qian Zhan 1,2, Xiaxing Deng 1,2, Yuanchi Weng 1,2, Jiabin Jin 1,2, Zhichong Wu 1,2, Hongwei Li 1,2, Baiyong Shen 1,2, Chenghong
Original Article Outcomes of robotic surgery for pancreatic ductal adenocarcinoma Qian Zhan 1,2, Xiaxing Deng 1,2, Yuanchi Weng 1,2, Jiabin Jin 1,2, Zhichong Wu 1,2, Hongwei Li 1,2, Baiyong Shen 1,2, Chenghong
Radical nerve dissection for the carcinoma of head of pancreas: report of 30 cases
 Original Article Radical nerve dissection for the carcinoma of head of pancreas: report of 30 cases Qing Lin, Langping Tan, Yu Zhou, Quanbo Zhou, Rufu Chen Department of Biliary and Pancreatic Surgery,
Original Article Radical nerve dissection for the carcinoma of head of pancreas: report of 30 cases Qing Lin, Langping Tan, Yu Zhou, Quanbo Zhou, Rufu Chen Department of Biliary and Pancreatic Surgery,
Surgical Management of CBD Injury Jin Seok Heo
 Surgical Management of CBD Injury Jin Seok Heo Department of Surgery, Samsung Medical Center Sungkyunkwan University School of Medicine, Seoul, Republic of Korea Bile duct injury (BDI) Introduction Incidence
Surgical Management of CBD Injury Jin Seok Heo Department of Surgery, Samsung Medical Center Sungkyunkwan University School of Medicine, Seoul, Republic of Korea Bile duct injury (BDI) Introduction Incidence
Laparoscopic Bladder-Preserving Surgery for Enterovesical Fistula Complicated with Benign Gastrointestinal Disease
 This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
BILIARY TRACT & PANCREAS, PART II
 CME Pretest BILIARY TRACT & PANCREAS, PART II VOLUME 41 1 2015 A pretest is mandatory to earn CME credit on the posttest. The pretest should be completed BEFORE reading the overview. Both tests must be
CME Pretest BILIARY TRACT & PANCREAS, PART II VOLUME 41 1 2015 A pretest is mandatory to earn CME credit on the posttest. The pretest should be completed BEFORE reading the overview. Both tests must be
Chronic pancreatitis mimicking intraductal papillary mucinous neoplasm of the pancreas; Report of tow cases
 Jichi Medical University Journal Chronic pancreatitis mimicking intraductal papillary mucinous neoplasm of the pancreas; Report of tow cases Noritoshi Mizuta, Hiroshi Noda, Nao Kakizawa, Nobuyuki Toyama,
Jichi Medical University Journal Chronic pancreatitis mimicking intraductal papillary mucinous neoplasm of the pancreas; Report of tow cases Noritoshi Mizuta, Hiroshi Noda, Nao Kakizawa, Nobuyuki Toyama,
An Innovative Option for Venous Reconstruction After Pancreaticoduodenectomy: the Left Renal Vein
 J Gastrointest Surg (2007) 11:425 431 DOI 10.1007/s11605-007-0131-1 An Innovative Option for Venous Reconstruction After Pancreaticoduodenectomy: the Left Renal Vein Rory L. Smoot & John D. Christein &
J Gastrointest Surg (2007) 11:425 431 DOI 10.1007/s11605-007-0131-1 An Innovative Option for Venous Reconstruction After Pancreaticoduodenectomy: the Left Renal Vein Rory L. Smoot & John D. Christein &
Appendix 9: Endoscopic Ultrasound in Gastroenterology
 Appendix 9: Endoscopic Ultrasound in Gastroenterology This curriculum is intended for clinicians who perform endoscopic ultrasonography (EUS) in gastroenterology. It includes standards for theoretical
Appendix 9: Endoscopic Ultrasound in Gastroenterology This curriculum is intended for clinicians who perform endoscopic ultrasonography (EUS) in gastroenterology. It includes standards for theoretical
The Prognostic Value of Drain Amylase on Post-Operative Day One after. the Whipple procedure.
 ORIGINAL ARTICLE The Prognostic Value of Drain Amylase on Post-Operative Day One after the Whipple Procedure Kristina Hasselgren, Pernilla Benjaminsson-Nyberg, Ingvar Halldestam, Marcus Permert Fraser,
ORIGINAL ARTICLE The Prognostic Value of Drain Amylase on Post-Operative Day One after the Whipple Procedure Kristina Hasselgren, Pernilla Benjaminsson-Nyberg, Ingvar Halldestam, Marcus Permert Fraser,
Does Preoperative Biliary Drainage Compromise the Long-Term Survival of Patients With Pancreatic Head Carcinoma?
 2015;111:270 276 Does Preoperative Biliary Drainage Compromise the Long-Term Survival of Patients With Pancreatic Head Carcinoma? YOSHIAKI MURAKAMI, MD,* KENICHIRO UEMURA, MD, YASUSHI HASHIMOTO, MD, NARU
2015;111:270 276 Does Preoperative Biliary Drainage Compromise the Long-Term Survival of Patients With Pancreatic Head Carcinoma? YOSHIAKI MURAKAMI, MD,* KENICHIRO UEMURA, MD, YASUSHI HASHIMOTO, MD, NARU
Application of a novel embeddedness like pancreaticojejunostomy anastomosis technique used in pancreaticoduodenectomy
 ONCOLOGY LETTERS 15: 8067-8071, 2018 Application of a novel embeddedness like pancreaticojejunostomy anastomosis technique used in pancreaticoduodenectomy XUEFENG XU *, YANG LV *, LEI ZHANG *, BAOBAO XIN,
ONCOLOGY LETTERS 15: 8067-8071, 2018 Application of a novel embeddedness like pancreaticojejunostomy anastomosis technique used in pancreaticoduodenectomy XUEFENG XU *, YANG LV *, LEI ZHANG *, BAOBAO XIN,
Pancreas (Exocrine) Protocol applies to all carcinomas of the exocrine pancreas.
 Pancreas (Exocrine) Protocol applies to all carcinomas of the exocrine pancreas. Protocol revision date: January 2005 Based on AJCC/UICC TNM, 6 th edition Procedures Cytology (No Accompanying Checklist)
Pancreas (Exocrine) Protocol applies to all carcinomas of the exocrine pancreas. Protocol revision date: January 2005 Based on AJCC/UICC TNM, 6 th edition Procedures Cytology (No Accompanying Checklist)
Index (SIRS), 158, 173
 Index A Acute pancreatitis surgery abdominal compartment syndrome, 188 adjuvant treatment, 194 anterior approach, 175 antibiotic prophylaxis, 166 167, 197 Atlanta classification, 181 classification of
Index A Acute pancreatitis surgery abdominal compartment syndrome, 188 adjuvant treatment, 194 anterior approach, 175 antibiotic prophylaxis, 166 167, 197 Atlanta classification, 181 classification of
Effectiveness of additional resection of the invasive cancer-positive proximal bile duct margin in cases of hilar cholangiocarcinoma
 Original Article Effectiveness of additional resection of the invasive cancer-positive proximal bile duct margin in cases of hilar cholangiocarcinoma Wen-Jie Ma 1#, Zhen-Ru Wu 2#, Anuj Shrestha 1,3, Qin
Original Article Effectiveness of additional resection of the invasive cancer-positive proximal bile duct margin in cases of hilar cholangiocarcinoma Wen-Jie Ma 1#, Zhen-Ru Wu 2#, Anuj Shrestha 1,3, Qin
The Choice of Palliative Treatment for Biliary and Duodenal Obstruction in Patients With Unresectable Pancreatic Cancer: Is Surgery Bypass Better?
 Int Surg 2016;101:58 63 DOI: 10.9738/INTSURG-D-14-00247.1 The Choice of Palliative Treatment for Biliary and Duodenal Obstruction in Patients With Unresectable Pancreatic Cancer: Is Surgery Bypass Better?
Int Surg 2016;101:58 63 DOI: 10.9738/INTSURG-D-14-00247.1 The Choice of Palliative Treatment for Biliary and Duodenal Obstruction in Patients With Unresectable Pancreatic Cancer: Is Surgery Bypass Better?
Key words: celiac occlusive disease, pancreaticoduodenectomy, abdominal aorta-celiac bypass
 Key words: celiac occlusive disease, pancreaticoduodenectomy, abdominal aorta-celiac bypass 51(2023) Table 1 Laboratory data on admission Fig. 2 Percutaneous transhepatic cholangiogram shows tapering obstruction
Key words: celiac occlusive disease, pancreaticoduodenectomy, abdominal aorta-celiac bypass 51(2023) Table 1 Laboratory data on admission Fig. 2 Percutaneous transhepatic cholangiogram shows tapering obstruction
PAPER. Experience With 208 Resections for Intraductal Papillary Mucinous Neoplasm of the Pancreas
 PAPER Experience With 0 Resections for Intraductal Papillary Mucinous Neoplasm of the Pancreas Thomas Schnelldorfer, MD; Michael G. Sarr, MD; David M. Nagorney, MD; Lizhi Zhang, MD; Thomas C. Smyrk, MD;
PAPER Experience With 0 Resections for Intraductal Papillary Mucinous Neoplasm of the Pancreas Thomas Schnelldorfer, MD; Michael G. Sarr, MD; David M. Nagorney, MD; Lizhi Zhang, MD; Thomas C. Smyrk, MD;
Surgical Therapy of GEP-NET: An Overview
 Surgical Therapy of GEP-NET: An Overview Pierce K.H Chow MBBS, MMed, FRCSE, FAMS, PhD Professor, Duke-NUS Graduate School of Medicine Senior Consultant Surgeon, Singapore General Hospital Visiting Senior
Surgical Therapy of GEP-NET: An Overview Pierce K.H Chow MBBS, MMed, FRCSE, FAMS, PhD Professor, Duke-NUS Graduate School of Medicine Senior Consultant Surgeon, Singapore General Hospital Visiting Senior
An Unexpected Cause of Hypoglycemia
 An Unexpected Cause of Hypoglycemia Stacey A. Milan, MD FACS Surgical Oncology Nothing to disclose Disclosures Objectives Identify indications for workup of hypoglycemia Define work up for hypoglycemic
An Unexpected Cause of Hypoglycemia Stacey A. Milan, MD FACS Surgical Oncology Nothing to disclose Disclosures Objectives Identify indications for workup of hypoglycemia Define work up for hypoglycemic
16 April 2010 Resident Teaching Conference. Pancreatitis. W. H. Nealon, M.D., F.A.C.S. J.J. Smith, M.D., D.W.D.
 16 April 2010 Resident Teaching Conference Pancreatitis W. H. Nealon, M.D., F.A.C.S. J.J. Smith, M.D., D.W.D. Santorini Wirsung anatomy.med.umich.edu/.../ duodenum_ans.html Bud and ductology Ventral pancreatic
16 April 2010 Resident Teaching Conference Pancreatitis W. H. Nealon, M.D., F.A.C.S. J.J. Smith, M.D., D.W.D. Santorini Wirsung anatomy.med.umich.edu/.../ duodenum_ans.html Bud and ductology Ventral pancreatic
Limited en bloc Resection of the Gastroesophageal Junction with Isoperistaltic Jejunal Interposition
 22 Limited en bloc Resection of the Gastroesophageal Junction with Isoperistaltic Jejunal Interposition J.R. Izbicki, W.T. Knoefel, D. C. Broering ] Indications Severe dysplasia in the distal esophagus
22 Limited en bloc Resection of the Gastroesophageal Junction with Isoperistaltic Jejunal Interposition J.R. Izbicki, W.T. Knoefel, D. C. Broering ] Indications Severe dysplasia in the distal esophagus
Pancreas & Biliary System. Dr. Vohra & Dr. Jamila
 Pancreas & Biliary System Dr. Vohra & Dr. Jamila 1 Objectives At the end of the lecture, the student should be able to describe the: Location, surface anatomy, parts, relations & peritoneal reflection
Pancreas & Biliary System Dr. Vohra & Dr. Jamila 1 Objectives At the end of the lecture, the student should be able to describe the: Location, surface anatomy, parts, relations & peritoneal reflection
Role of three-phase contrast-enhanced multislice helical CT in evaluating resectability of pancreatic carcinoma
 ISPUB.COM The Internet Journal of Radiology Volume 8 Number 1 Role of three-phase contrast-enhanced multislice helical CT in evaluating resectability of pancreatic E Ergul, E Gozetlik Citation E Ergul,
ISPUB.COM The Internet Journal of Radiology Volume 8 Number 1 Role of three-phase contrast-enhanced multislice helical CT in evaluating resectability of pancreatic E Ergul, E Gozetlik Citation E Ergul,
PANCREATODUODENECTOMY VERSUS WHIPPLE HEAD OF THE PANCREAS PYLORUS PRESERVING PROCEDURE FOR ADENOCARCINOMA OF THE INTRODUCTION
 HPB Surgery 1989, Vol. 1, pp. 195-200 Reprints available directly from the publisher Photocopying permitted by license only (C) 1989 Harwood Academic Publishers GmbH Printed in Great Britain PYLORUS PRESERVING
HPB Surgery 1989, Vol. 1, pp. 195-200 Reprints available directly from the publisher Photocopying permitted by license only (C) 1989 Harwood Academic Publishers GmbH Printed in Great Britain PYLORUS PRESERVING
Complex pancreatico- duodenal injuries. Elmin Steyn Head, Division of Surgery Faculty of Health Sciences Stellenbosch University
 Complex pancreatico- duodenal injuries Elmin Steyn Head, Division of Surgery Faculty of Health Sciences Stellenbosch University Pancreatic and duodenal trauma: daunting or simply confusing? 2-4% of abdominal
Complex pancreatico- duodenal injuries Elmin Steyn Head, Division of Surgery Faculty of Health Sciences Stellenbosch University Pancreatic and duodenal trauma: daunting or simply confusing? 2-4% of abdominal
Contemporary Results with Ampullectomy for 29 Benign Neoplasms of the Ampulla
 Contemporary Results with Ampullectomy for 29 Benign Neoplasms of the Ampulla Stephen R Grobmyer, MD, Chad N Stasik, MD, Peter Draganov, MD, Alan W Hemming, MD, FACS, Lisa R Dixon, MD, Stephen B Vogel,
Contemporary Results with Ampullectomy for 29 Benign Neoplasms of the Ampulla Stephen R Grobmyer, MD, Chad N Stasik, MD, Peter Draganov, MD, Alan W Hemming, MD, FACS, Lisa R Dixon, MD, Stephen B Vogel,
Appendix 5. EFSUMB Newsletter. Gastroenterological Ultrasound
 EFSUMB Newsletter 87 Examinations should encompass the full range of pathological conditions listed below A log book listing the types of examinations undertaken should be kept Training should usually
EFSUMB Newsletter 87 Examinations should encompass the full range of pathological conditions listed below A log book listing the types of examinations undertaken should be kept Training should usually
MULTIMEDIA ARTICLE - Clinical Imaging. Brian KP Goh 1, Yaw-Fui Alexander Chung 1,4, David CE Ng 2, Sathiyamoorthy Selvarajan 3, Khee-Chee Soo 1,4
 MULTIMEDIA ARTICLE - Clinical Imaging Positron Emission Tomography with 2-Deoxy-2-[ 18 F] Fluoro-D- Glucose in the Detection of Malignancy in Intraductal Papillary Mucinous Neoplasms of the Pancreas Brian
MULTIMEDIA ARTICLE - Clinical Imaging Positron Emission Tomography with 2-Deoxy-2-[ 18 F] Fluoro-D- Glucose in the Detection of Malignancy in Intraductal Papillary Mucinous Neoplasms of the Pancreas Brian
Scandinavian Journal of Surgery 104: 79 85, 2014
 543975SJS104010.1177/1457496914543975Preoperative biliary stent plastic or SEMSC. Haapamäki, et al. research-article2014 Original Article Scandinavian Journal of Surgery 104: 79 85, 2014 Preoperative Biliary
543975SJS104010.1177/1457496914543975Preoperative biliary stent plastic or SEMSC. Haapamäki, et al. research-article2014 Original Article Scandinavian Journal of Surgery 104: 79 85, 2014 Preoperative Biliary
