Laparoscopic left hepatectomy in patients with intrahepatic duct stones and recurrent pyogenic cholangitis
|
|
|
- Milo Hart
- 5 years ago
- Views:
Transcription
1 Korean J Hepatobiliary Pancreat Surg 212;16:15-19 Original Article Laparoscopic left hepatectomy in patients with intrahepatic duct stones and recurrent pyogenic cholangitis Sunjong Han, Insang Song, and Kwangsik Chun Department of Surgery, Chungnam National University Hospital, Daejeon, Korea Backgrounds/Aims: Recently many studies have been reported the early results of a hepatectomy for various intrahepatic lesions. Also various types of laparoscopic hepatectomies are being performed in many centers. Some reports about the safety of laparoscopic parenchymal dissection of the liver have been published. In this study, we reported our experiences of laparoscopic left hepatectomies in patients with an intrahepatic duct (IHD) stone with recurrent pyogenic cholangitis (RPC), and investigated whether the total laparoscopic parenchymal dissection is as safe as open surgery. Methods: From April 28 to December 21, 25 patients had been admitted for left IHD stones with RPC. Preoperatively, the type of surgery was decided with the intention of treating each patient. Initially 1 patients underwent a laparoscopy-assisted left hepatectomy and the next 15 patients underwent total laparoscopic left hepatectomy as our experience grew. Demographics, peri- and postoperative results were collected and analyzed comparatively. Results: The mean age, gender ratio, preoperative American Society of Anesthesiologists (ASA) score, accompanied acute cholangitis and biliary pancreatitis, and the number of preoperative percutaneous transhepatic biliary drainage (PTBD) inserted cases were not different between the two groups who had undergone laparoscopy-assisted and totally laparoscopic left hepatectomy. The operation time, intraoperative transfusions and postoperative complications also showed no difference between them. The postoperative hospital stay did not show a significant difference statistically. Conclusions: In this study, we concluded that a laparoscopic left hepatectomy can be adapted to the patients with a left IHD stone with RPC. Also laparoscopic parenchymal dissection is safe and equivalent to an open procedure. (Korean J Hepatobiliary Pancreat Surg 212;16:15-19) Key Words: Intrahepatic duct stone; Recurrent pyogenic cholangitis; Laparoscopic left hepatectomy INTRODUCTION Although an intrahepatic duct (IHD) stone is a pathologically benign condition, its progression can severely limit the social activity of patients. Furthermore, patients can die of cholangitis or biliary sepsis unless they are appropriately treated. Also, as cholangiocarcinoma can be seen in about 1% of the cases, it must be treated inclusively at the point of diagnosis. 1-4 The treatment must include complete removal of stones and the resolution of the IHD stricture and cholestasis. In this way, postoperative complications, especially recurrent cholangitis, can be decreased. 5 Thus various modalities of treatment including percutaneous transhepatic cholagioscopic lithotripsy and laparoscopic IHD exploration were used to treat a patient with an IHD stone. But, as these modalities are often incomplete, repeated and combined procedures to remove the stones completely are required. If ductal strictures and recurrent pyogenic cholangitis (RPC) were concurrent with IHD stone, a definitive hepatectomy is necessary. There has been a tremendous advancement of laparoscopic instruments and techniques compared to the past 2 years. Various types of laparoscopic hepatectomies are performed in many centers worldwide. But, most patients with IHD stone have perihepatic adhesions and alterations of normal anatomical structures due to chronic recurrent inflammation. Furthermore, a choledochotomy is often required to remove the stones completely. Therefore, laparoscopic procedures are more difficult than open surgery. 5 In this study, we reviewed our left laparoscopic hepatectomy experiences to investigate whether this operative Received: February 24, 212; Revised: June 7, 212; Accepted: July 1, 212 Corresponding author: Kwangsik Chun Department of Surgery, Chungnam National University Hospital, 282, Munhwa-ro, Jung-gu, Daejeon , Korea Tel: , Fax: , oxali@cnuh.co.kr Copyright C 212 by The Korean Association of Hepato-Biliary-Pancreatic Surgery Korean Journal of Hepato-Biliary-Pancreatic Surgery pissn:
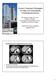
2 16 Korean J Hepatobiliary Pancreat Surg Vol. 16, No. 3, August 212 method can be adapted for patients with left IHD stone with RPC and the laparoscopic parenchymal dissection of the liver can be performed safely as an open procedure. METHODS From April 28 to December 21, 49 cases of laparoscopic hepatectomyies were performed among a total of 158 hepatectomies. Fourty patients underwent anatomical resections and the remaining underwent non-anatomical resections. Of these patients, 25 patients were admitted for IHD stone with RPC (Fig. 1). The type of operation was decided preoperatively. Ten initial patients underwent a laparoscopy-assisted left hepatectomy and the next 15 patients had a total laparoscopic left hepatectomy. Most data were collected retrospectively but the operative data were collected prospectively. Under general anesthesia with lithotomy position, the port for the laparoscope was located just below the umbilicus and two additional working ports were placed in the right upper abdomen along the right anterior axillary line and around the Cantle s line. An assistant port was placed at the left upper abdomen, and if needed, another assistant port was inserted more laterally. Then the patient was placed in an approximate 2-degree left sided tilt down reverse in Trendelenburg position. After the cholecystectomy, the falciform ligament, the coronary ligament and the left triangular ligament were divided by the Harmonic Scalpel R (Johnson & Johnson, CO, US). In most patients, the left hepatic vein was isolated with a careful dissection. The left hepatic artery and the portal vein were isolated from the hepatoduodenal ligament, and then ligated by a closed 4- loop-stich and the Hem-O-Lok R (Teleflex Medical, CO, US). Then hepatic parenchymal dissection was performed along the Cantle s line by the Harmonic Scalpel R superficially and the Cavitron Ultrasonic Surgical Aspirator R (CUSA R, Valleylab, Boul-der, CO, US) deeply. After proper parenchymal dissection was performed, the bile duct was divided from the left hepatic vein by the Endo-GIA R (Ethicon, Davis & Geck, and US Surgical, US). Finally, the left hepatic vein was ligated using the Endo-GIA R after complete parenchymal dissection. For the performance of the laparoscopy-assisted procedure, hepatic mobilization and ligation of the hepatic artery and the portal vein was done using laparoscopic procedures. After making about a 1 cm-length incision on the upper midline, parenchymal dissection was performed mainly by the CUSA R. The left hepatic duct and the left hepatic vein were ligated by the Endo-GIA R. If the patient had common bile duct (CBD) stones, an additional choledochotomy would be required to extract the stones and a T-tube would be inserted. RESULTS Among 25 patients, the initial 1 patients were underwent the laparoscopy assisted left hepatectomy, and the next 15 patients were totally laparoscopic left hepatectomy as our experience expanded. The mean age was 62.4 (range: 39-85) years and the incidence was higher in female (Male : Female=1 : 2.6). The mean body mass index (BMI) was 23. ( ) kg/m 2. The mean preoperative American Society of Anesthesiologists (ASA) score was 1.6 points. Sixteen patients (64%) were concurrent with acute cholangitis, with common bile duct (CBD) stone and with biliary pancreatitis. Four patients (16%) had percutaneous transhepatic biliary Fig. 1. A 54-year old female with multiple IHD stones with RPC. (A) On preoperative abdominal CT, there were severe atrophic change of the left lobe of the liver (white arrow head). (B) She underwent a totally laparoscopic left hepatectomy. In a postoperative abdominal CT, there were no postoperative complications.
3 Sunjong Han, et al. Lap. left hepatectomy in pts with IHD stones c RPC 17 Table 1. Comparison of the demographics and preoperative status between the laparoscopy-assisted left hepatectomy (LAH) group and the totally laparoscopic left hepatectomy (TLH) group Total (n=25) LAH (n=1) TLH (n=15) p-value Demographics Age (years) Sex (male) BMI (kg/m 2 ) ASA score Comorbidities Acute cholangitis CBD stone Biliary pancreatitis Preoperative PTBD insertion Preoperative Lab WBC (/mm 3 ) Hb (g/dl) Albumin (g/dl) Total bilirubin (mg/dl) AST (IU/L) ALT (IU/L) 62.4 (39-85) 23. ( ) (64%) 4 (16%) 7,87.6 (3,54-15,15) 12.7 ( ) 3.83 ( ) 1.11 ( ) 48.3 (1-288) 5.69 (5-211) 62.3 (49-76) (6%) 3 (3%) 3 (3%) 7,821 (3,54-15,15) 12.6 ( ) 3.96 ( ).713 ( ) 52.9 (15-288) 83.6 (14-197) 64.4 (44-85) 6 (4%) (67%) 4 (27%) 4 (27%) 3 (2%) 7,865.3 (3,9-14,96) ( ) 3.81 ( ) 1.37 (.5-5.9) 45.2 (1-174) 48.7 (5-211) Table 2. Comparison of the perioperative and postoperative outcomes between the laparoscopy-assisted left hepatectomy (LAH) group and the total laparoscopic left hepatectomy (TLH) group Total (n=25) LAH (n=1) TLH (n=15) p-value Postoperative outcomes Duration of surgery (min) Transfusion performed (n) Incision length (cm) Remnant stone (n) Postoperative outcomes Patients with complications (n) Length of hospital stay (days) 36.6 (21-47) 4 (16%) 9.2 (5-12) 2 (8%) 11.2 (5-32) (2%) (8-32) (13%) (6.6%) 1.3 (5-2) < drainage (PTBD) preoperatively (Table 1). The mean operation time was 36.6 (range: 21-47) minutes and intraoperative transfusions were given in 4 cases (16%). The conversion to open procedure was done in 1 case because of a stapler malfunction. Postoperative biliary leakage occurred in 2 cases (8%) and they were well treated with conservative management. The mean postoperative hospital stay was 11.2 (range: 5-32) days (Table 2). Patients were divided into two groups depending on the type of hepatic parenchymal dissection: the laparoscopy-assisted left hepatectomy (LAH) group and the total laparoscopy left hepatectomy (TLH) group. The mean BMI was 24.4 kg/m 2 in LAH and 22.1 kg/m 2 in TLH. The ASA score was 1.5 in LAH and 1.6 in TLH. Patients with acute cholangitis were: 6 cases in LAH (6%) and 1 cases in TLH (67%). Biliary pancreatitis cases were 3 in LAH (3%) and 4 in TLH (27%). A combined CBD tone was in 3 cases of LAH (3%), 4 cases of TLH (27%). There was one case of preoperative PTBD insertion in LAH (1%) and 3 in TLH (2%). The preoperative laboratory data were also analyzed. The mean leucocyte count was 7,821/mm 3 in LAH and 7,865.3/mm 3 in TLH. The mean hemoglobin was 12.6 g/dl in LAH and g/dl in TLH and the mean albumin was 3.96 g/dl in LAH and 3.81 g/dl in TLH. The mean total bilirubin was.71 mg/dl in LAH, 1.37 mg/dl in TLH, and the mean aspartate aminotransferase (AST) / alanine aminotransferase (ALT) were 52.9/45.2 IU/L in LAH and 83.6/48.7 IU/L in TLH. All of these demographics and preoperative clinical conditions had not different statistically between the two groups (Table 1). The mean operation time was longer in the laparoscopy assisted group, but there was no statistically significant
4 18 Korean J Hepatobiliary Pancreat Surg Vol. 16, No. 3, August 212 Fig. 2. The incisions to retrieve the specimen. (A) An upper midline incision was made in the laparoscopy-assisted left hepatectomy. (B) A right lower transverse incision was made in the totally laparoscopic left hepatectomy. (C) A Pfannenstiel incision was made in the totally laparoscopic surgery. difference (319 vs. 298 minutes, p=.387). Intraoperative transfusion was given to 2 cases with LAH (2%, each was 1 pint and 2 pints) and 2 cases of TLH (13%, each 1 pint) and showed no statistical significance (p=.672). The mean incision length was 11.2 cm in LAH and 7.8 cm in TLH. Postoperative complications occurred in each one patient from both groups. There were no remnant stones in all cases. The mean postoperative hospital stay was not different statistically (12.7 vs. 1.3, p=.288) (Table 2). DISCUSSION The types of laparoscopic hepatectomy are variable, such as a total laparoscopic hepatectomy, a laparoscopy-assisted hepatectomy, 6 a hand-assisted laparoscopic hepatectomy 7 and a gasless laparoscopic hepatectomy. 8 From these procedures, we performed laparoscopy-assisted hepatectomy for early cases. As our experiences expanded, the totally laparoscopic hepatectomy was mainly performed. The most important difference of the two procedures is the method of hepatic parenchymal dissection. Performance of a laparoscopy-assisted hepatectomy required the parencymal dissection to be done in the same manner as open surgery. But in total laparoscopic hepatectomies, all procedures, including a parenchymal dissection, were performed using laparoscopic instruments. We used the Harmonic Scalpel R for the superficial layer, and the CUSA R for the deep layer of the hepatic parenchyma. But, there have been some problems with the laparoscopic parenchymal dissection with bleeding control in the visual field. The abdominal cavity is a closed and limited space. Moreover, as we set the intra-abdominal CO 2 gas pressure under 14 mmhg to prevent the formation of postoperative air embolism, the field can be narrower. To resolve these problems, we used a 3-degree angled laparoscope, so that the operative field was shown slightly downward for a better view. Vapor from laparoscopic instruments can also make the field hazy, so we set a gas filter to remove vapor and applied an anti-fog solution to make the field clear. Even a little bleeding can make the field unclear, so we were very careful to prevent bleeding. When a vessel was injured, we applied laparoscopic metal clips to ligate it. If bleeding was not controlled with this manner, we packed the area with some gauze or sutured the bleeding site. After we adapted the laparoscopic procedures for hepatectomies, the incision length greatly decreased and recovery took less time. We used 4 or 5 ports for the laparoscopic hepatectomy. The location of the ports was im-
5 Sunjong Han, et al. Lap. left hepatectomy in pts with IHD stones c RPC 19 portant for traction of the liver to secure an adequate field and for control of the surgical instruments without interrupting each other. First, the laparoscopist stands between the patient s legs so he can show display a stable surgical field over the course of the operation. 9 The first assistant handles the instruments via 2 ports, so he can reposition and move the liver similar to an open surgery procedure. There are many ways of retrieving the specimen. For example, through the extension of a port site, or an incision at another site. 1 We mostly used a Pfannenstiel incision or a right lower transverse incision in a left total laparoscopic hepatectomy, and upper midline incision in a laparoscopy-assisted left hepatectomy (Fig. 2). There are not many cases of totally laparoscopic hepatectomy for IHD stone. In 23 Min at el. 11 reported 6 cases of totally laparoscopic left hepatectomy and a left lateral sectionectomy. The mean operation time was minutes and the hospital stay was 11.7 days. There was no complication or mortality. In 27, Kim et al. 12 reported 25 cases of IHD stones. Their mean operation time was minutes for left lateral sectionectomy, and minutes for a left hepatectomy. The mean hospital stay was 11 days. In the same year, Cai et al. 13 performed laparoscopic hepatectomies for 29 patients, and open hepatectomies for 22 patients. They reported a shorter time of fasting and hospital stay after a laparoscopic surgery with similar results in recurrence, operation time and blood loss between the two groups. In our institution, patients who underwent a total laparoscopic hepatectomy showed similar results to the laparoscopy-assisted hepatectomy or open hepatectomy group in the remnant stone or complication rate. And the duration of fasting and hospital stay were superior to the latter. We expect that the operation time and blood loss will become better in the future with more experiences. In this study, we concluded that a total laparoscopic left hepatectomy can be adapted for patients with left IHD stone with RPC. Because a laparoscopic parenchymal dissection of the liver is safe and is not inferior to an open hepatectomy, it can be a possible substitute for the open procedure for other benign or malignant liver diseases requiring a hepatectomy. More careful approaches, adequate patient selection and laparoscopic hepatobiliary surgical experiences are required. REFERENCES 1. Kim BW, Lee HW, Kim IG, et al. New surgical technique for hepatolithiasis: ventral hilar exposure method. Korean J HBP Surg 25;9: Chen MF, Jan YY, Wang CS, et al. A reappraisal of cholangiocarcinoma in patient with hepatolithiasis. Cancer 1993;71: Kubo S, Kinoshita H, Hirohashi K, et al. Hepatolithiasis associated with cholangiocarcinoma. World J Surg 1995;19: Liu CL, Fan ST, Wong J. Primary biliary stones: diagnosis and management. World J Surg 1998;22: Hwang JH, Yoon YB, Kim YT, et al. Risk factors for recurrent cholangitis after initial hepatolithiasis treatment. J Clin Gastroenterol 24;38: John TG, Greig JD, Crosbie JL, et al. Superior staging of liver tumors with laparoscopy and laparoscopic ultrasound. Ann Surg 1994;22: Kaneko H, Takagi S, Shiba T. Laparoscopic partial hepatectomy and left lateral segmentectomy: technique and results of a clinical series. Surgery 1996;12: Ferzli G, David A, Kiel T. Laparoscopic resection of a large hepatic tumor. Surg Endosc 1995;9: Song YJ, Kim KJ, Moon HG, et al. The feasibility of laparoscopic hepatectomy for the patients with left intrahepatic stones. J Korean Surg Soc 21;78: Hüscher CG, Lirici MM, Chiodini S. Laparoscopic liver resections. Semin Laparosc Surg 1998;5: Min SK, Han HS, Lee HK, et al. Totally laparoscopic anatomic liver resection. J Korean Surg Soc 23;64: Kim CG, Yoon YS, Han HS, et al. Experience of total laparoscopic hepatectomy. J Korean Surg Soc 27;73: Cai X, Wang Y, Yu H, et al. Laparoscopic hepatectomy for hepatolithiasis: a feasibility and safety study in 29 patients. Surg Endosc 27;21:
Laparoscopic resection of hilar cholangiocarcinoma
 TECHNICAL ADVANCE pissn 2288-6575 eissn 2288-6796 http://dx.doi.org/10.4174/astr.2015.89.4.228 Annals of Surgical Treatment and Research Laparoscopic resection of hilar cholangiocarcinoma Woohyung Lee,
TECHNICAL ADVANCE pissn 2288-6575 eissn 2288-6796 http://dx.doi.org/10.4174/astr.2015.89.4.228 Annals of Surgical Treatment and Research Laparoscopic resection of hilar cholangiocarcinoma Woohyung Lee,
Optimal Bile Duct Division Using Real- Time Indocyanine Green Near-Infrared Fluorescence Cholangiography During Laparoscopic Donor Hepatectomy
 LETTERS FROM THE FRONTLINE Optimal Bile Duct Division Using Real- Time Indocyanine Green Near-Infrared Fluorescence Cholangiography During Laparoscopic Donor Hepatectomy TO THE EDITOR: Despite advances
LETTERS FROM THE FRONTLINE Optimal Bile Duct Division Using Real- Time Indocyanine Green Near-Infrared Fluorescence Cholangiography During Laparoscopic Donor Hepatectomy TO THE EDITOR: Despite advances
Single center experience of laparoscopic hepatectomy: the comparison of perioperative outcomes between early and late period
 Korean J Hepatobiliary Pancreat Surg 212;16:7-12 Original Article Single center experience of laparoscopic hepatectomy: the comparison of perioperative outcomes between early and late period Seung Hyeon
Korean J Hepatobiliary Pancreat Surg 212;16:7-12 Original Article Single center experience of laparoscopic hepatectomy: the comparison of perioperative outcomes between early and late period Seung Hyeon
En-liang Li 1,2, Rong-fa Yuan 1, Wen-jun Liao 1, Qian Feng 1, Jun Lei 1, Xiang-bao Yin 1, Lin-quan Wu 1* and Jiang-hua Shao 1
 Li et al. BMC Surgery (2019) 19:16 https://doi.org/10.1186/s12893-019-0480-1 RESEARCH ARTICLE Open Access Intrahepatic bile exploration lithotomy is a useful adjunctive hepatectomy method for bilateral
Li et al. BMC Surgery (2019) 19:16 https://doi.org/10.1186/s12893-019-0480-1 RESEARCH ARTICLE Open Access Intrahepatic bile exploration lithotomy is a useful adjunctive hepatectomy method for bilateral
Current status of hepatic surgery in Korea
 Korean J Hepatol. 2009 Dec; 15(Suppl 6):S60 - S64. DOI: 10.3350/kjhep.2009.15.S6.S60 Current status of hepatic surgery in Korea Kyung Sik Kim Department of Surgery, Severance Hospital, Yonsei University
Korean J Hepatol. 2009 Dec; 15(Suppl 6):S60 - S64. DOI: 10.3350/kjhep.2009.15.S6.S60 Current status of hepatic surgery in Korea Kyung Sik Kim Department of Surgery, Severance Hospital, Yonsei University
Laparoscopy-assisted D2 radical distal subtotal gastrectomy
 Masters of Gastrointestinal Surgery Laparoscopy-assisted D2 radical distal subtotal gastrectomy Xiaogeng Chen, Weihua Li, Jinsi Wang, Changshun Yang Department of Tumor Surgery, Fujian Provincial Hospital,
Masters of Gastrointestinal Surgery Laparoscopy-assisted D2 radical distal subtotal gastrectomy Xiaogeng Chen, Weihua Li, Jinsi Wang, Changshun Yang Department of Tumor Surgery, Fujian Provincial Hospital,
In Woong Han 1, O Choel Kwon 1, Min Gu Oh 1, Yoo Shin Choi 2, and Seung Eun Lee 2. Departments of Surgery, Dongguk University College of Medicine 2
 Effect of Rowachol on Prevention of Postcholecystectomy Syndrome after Laparoscopic Cholecystectomy - Prospective multicenter Randomized controlled trial- In Woong Han 1, O Choel Kwon 1, Min Gu Oh 1, Yoo
Effect of Rowachol on Prevention of Postcholecystectomy Syndrome after Laparoscopic Cholecystectomy - Prospective multicenter Randomized controlled trial- In Woong Han 1, O Choel Kwon 1, Min Gu Oh 1, Yoo
pitfall Table 1 4 disorientation pitfall pitfall Table 1 Tel:
 11 687 692 2002 pitfall 1078 29 17 9 1 2 3 dislocation outflow block 11 1 2 3 9 1 2 3 4 disorientation pitfall 11 687 692 2002 Tel: 075-751-3606 606-8507 54 2001 8 27 2002 10 31 29 4 pitfall 16 1078 Table
11 687 692 2002 pitfall 1078 29 17 9 1 2 3 dislocation outflow block 11 1 2 3 9 1 2 3 4 disorientation pitfall 11 687 692 2002 Tel: 075-751-3606 606-8507 54 2001 8 27 2002 10 31 29 4 pitfall 16 1078 Table
Single-Incision Laparoscopic Surgery Versus Standard Laparoscopic Surgery for Unroofing of Hepatic Cysts
 SCIENTIFIC PAPER Single-Incision Laparoscopic Surgery Versus Standard Laparoscopic Surgery for of s Shuodong Wu, MD, Yongnan Li, MM, Yu Tian, MD, Min Li, MM ABSTRACT Background and Objectives: The aim
SCIENTIFIC PAPER Single-Incision Laparoscopic Surgery Versus Standard Laparoscopic Surgery for of s Shuodong Wu, MD, Yongnan Li, MM, Yu Tian, MD, Min Li, MM ABSTRACT Background and Objectives: The aim
Transumbilical Single-Incision Laparoscopic Resection of Focal Hepatic Lesions
 SCIENTIFIC PAPER Transumbilical Single-Incision Laparoscopic Resection of Focal Hepatic Lesions Shuodong Wu, MD, Xiao-Peng Yu, MM, Yu Tian, MD, Ernest Amos Siwo, MM, Yongnan Li, MM, Hong Yu, MD, Dianbo
SCIENTIFIC PAPER Transumbilical Single-Incision Laparoscopic Resection of Focal Hepatic Lesions Shuodong Wu, MD, Xiao-Peng Yu, MM, Yu Tian, MD, Ernest Amos Siwo, MM, Yongnan Li, MM, Hong Yu, MD, Dianbo
LiverGroup.org. Case Report Form (CRF) for STAGED procedures
 Case Report Form (CRF) for STAGED procedures Patient Characteristics Case number * Age * ( 18)y Gender * Male Female Race * Caucasian Asian African Other If other race, please specify Height * cm Weight
Case Report Form (CRF) for STAGED procedures Patient Characteristics Case number * Age * ( 18)y Gender * Male Female Race * Caucasian Asian African Other If other race, please specify Height * cm Weight
담낭절제술후발생한미리찌증후군의내시경적치료 1 예
 Case Report The Korean Journal of Pancreas and Biliary Tract 2014;19:199-203 http://dx.doi.org/10.15279/kpba.2014.19.4.199 pissn 1976-3573 eissn 2288-0941 담낭절제술후발생한미리찌증후군의내시경적치료 1 예 인하대학교의학전문대학원내과학교실 이정민
Case Report The Korean Journal of Pancreas and Biliary Tract 2014;19:199-203 http://dx.doi.org/10.15279/kpba.2014.19.4.199 pissn 1976-3573 eissn 2288-0941 담낭절제술후발생한미리찌증후군의내시경적치료 1 예 인하대학교의학전문대학원내과학교실 이정민
Comparison Between Primary Closure of Common Bile Duct and T- Tube Drainage After Open Choledocholithiasis: A Hospital Based Study
 Original article: Comparison Between Primary Closure of Common Bile Duct and T- Tube Drainage After Open Choledocholithiasis: A Hospital Based Study Kali CharanBansal Principal Specialist (General surgery)
Original article: Comparison Between Primary Closure of Common Bile Duct and T- Tube Drainage After Open Choledocholithiasis: A Hospital Based Study Kali CharanBansal Principal Specialist (General surgery)
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
Surgical Management of CBD Injury Jin Seok Heo
 Surgical Management of CBD Injury Jin Seok Heo Department of Surgery, Samsung Medical Center Sungkyunkwan University School of Medicine, Seoul, Republic of Korea Bile duct injury (BDI) Introduction Incidence
Surgical Management of CBD Injury Jin Seok Heo Department of Surgery, Samsung Medical Center Sungkyunkwan University School of Medicine, Seoul, Republic of Korea Bile duct injury (BDI) Introduction Incidence
Influencing factors on postoperative hospital stay after laparoscopic cholecystectomy
 Korean J Hepatobiliary Pancreat Surg 2016;20:12-16 http://dx.doi.org/10.14701/kjhbps.2016.20.1.12 Original Article Influencing factors on postoperative hospital stay after laparoscopic cholecystectomy
Korean J Hepatobiliary Pancreat Surg 2016;20:12-16 http://dx.doi.org/10.14701/kjhbps.2016.20.1.12 Original Article Influencing factors on postoperative hospital stay after laparoscopic cholecystectomy
Learning Curve of a Young Surgeon s Video-assisted Thoracic Surgery Lobectomy during His First Year Experience in Newly Established Institution
 Korean J Thorac Cardiovasc Surg 2012;45:166-170 ISSN: 2233-601X (Print) ISSN: 2093-6516 (Online) Clinical Research http://dx.doi.org/10.5090/kjtcs.2012.45.3.166 Learning Curve of a Young Surgeon s Video-assisted
Korean J Thorac Cardiovasc Surg 2012;45:166-170 ISSN: 2233-601X (Print) ISSN: 2093-6516 (Online) Clinical Research http://dx.doi.org/10.5090/kjtcs.2012.45.3.166 Learning Curve of a Young Surgeon s Video-assisted
Laparoscopic Cholecystectomy after Upper Abdominal Surgery : Is It Feasible Even after Gastrectomy?
 ORIGINAL ARTICLE pissn 2234-778X eissn 2234-5248 J Minim Invasive Surg 2017;20(1):22-28 Journal of Minimally Invasive Surgery Laparoscopic Cholecystectomy after Upper Abdominal Surgery : Is It Feasible
ORIGINAL ARTICLE pissn 2234-778X eissn 2234-5248 J Minim Invasive Surg 2017;20(1):22-28 Journal of Minimally Invasive Surgery Laparoscopic Cholecystectomy after Upper Abdominal Surgery : Is It Feasible
of bile leakage after liver resecti
 NAOSITE: Nagasaki University's Ac Title Author(s) Citation Percutaneous embolization with n-bu of bile leakage after liver resecti Kuroki, Tamotsu; Kitasato, Amane; T Hiroaki; Taniguchi, Ken; Maeda, Shi
NAOSITE: Nagasaki University's Ac Title Author(s) Citation Percutaneous embolization with n-bu of bile leakage after liver resecti Kuroki, Tamotsu; Kitasato, Amane; T Hiroaki; Taniguchi, Ken; Maeda, Shi
Citation Transplantation Proceedings, 47(3),
 NAOSITE: Nagasaki University's Ac Title Author(s) Hybrid Procedure in Living Donor Li Soyama, Akihiko; Takatsuki, Mitsuhi Tomohiko; Kitasato, Amane; Kinoshit Baimakhanov, Zhassulan; Kuroki, Tam Citation
NAOSITE: Nagasaki University's Ac Title Author(s) Hybrid Procedure in Living Donor Li Soyama, Akihiko; Takatsuki, Mitsuhi Tomohiko; Kitasato, Amane; Kinoshit Baimakhanov, Zhassulan; Kuroki, Tam Citation
Preoperative Biliary Drainage Among Patients With Resectable Hepatobiliary Malignancy: Does Technique Matter?
 Preoperative Biliary Drainage Among Patients With Resectable Hepatobiliary Malignancy: Does Technique Matter? Q. Lina Hu, MD; Jason B. Liu, MD, MS; Ryan J. Ellis, MD, MS; Jessica Y. Liu, MD, MS; Anthony
Preoperative Biliary Drainage Among Patients With Resectable Hepatobiliary Malignancy: Does Technique Matter? Q. Lina Hu, MD; Jason B. Liu, MD, MS; Ryan J. Ellis, MD, MS; Jessica Y. Liu, MD, MS; Anthony
Yoshitsugu; Kanematsu, Takashi; Kur
 NAOSITE: Nagasaki University's Ac Title Author(s) Citation Laparoscopic Middle Pancreatectomy Surgery Kitasato, Amane; Adachi, Tomohiko; Yoshitsugu; Kanematsu, Takashi; Kur Hepato-Gastroenterology, 59(120),
NAOSITE: Nagasaki University's Ac Title Author(s) Citation Laparoscopic Middle Pancreatectomy Surgery Kitasato, Amane; Adachi, Tomohiko; Yoshitsugu; Kanematsu, Takashi; Kur Hepato-Gastroenterology, 59(120),
HOW I DO IT Feasibility of Bisegmentectomy 7 8 is Independent of the Presence of a Large Inferior Right Hepatic Vein
 Journal of Surgical Oncology 2006;93:338 342 HOW I DO IT Feasibility of Bisegmentectomy 7 8 is Independent of the Presence of a Large Inferior Right Hepatic Vein MARCEL AUTRAN C. MACHADO, MD, 1,2 * PAULO
Journal of Surgical Oncology 2006;93:338 342 HOW I DO IT Feasibility of Bisegmentectomy 7 8 is Independent of the Presence of a Large Inferior Right Hepatic Vein MARCEL AUTRAN C. MACHADO, MD, 1,2 * PAULO
Bile Duct Injury during Lap Chole. Bile Duct Injury during cholecystectomy TOPICS. 1. Prevalence, mechanisms, prevention and diagnosis
 Bile Duct Injury during cholecystectomy Catherine HUBERT Jean-Fran François GIGOT Benoît t NAVEZ Division of Hepato-Biliary Biliary-Pancreatic Surgery Department of Abdominal Surgery and Transplantation
Bile Duct Injury during cholecystectomy Catherine HUBERT Jean-Fran François GIGOT Benoît t NAVEZ Division of Hepato-Biliary Biliary-Pancreatic Surgery Department of Abdominal Surgery and Transplantation
Naoyuki Toyota, Tadahiro Takada, Hodaka Amano, Masahiro Yoshida, Fumihiko Miura, and Keita Wada
 J Hepatobiliary Pancreat Surg (2006) 13:80 85 DOI 10.1007/s00534-005-1062-4 Endoscopic naso-gallbladder drainage in the treatment of acute cholecystitis: alleviates inflammation and fixes operator s aim
J Hepatobiliary Pancreat Surg (2006) 13:80 85 DOI 10.1007/s00534-005-1062-4 Endoscopic naso-gallbladder drainage in the treatment of acute cholecystitis: alleviates inflammation and fixes operator s aim
Jae Woo Choi, Sin Hui Park, Sang Yong Choi, Haeng Soo Kim, and Taeg Hyun Kim. Department of Surgery, Gwangmyeong Sungae Hospital, Gwangmyeong, Korea
 Korean J Hepatobiliary Pancreat Surg 0;6:7-5 Original Article Comparison of clinical result between early laparoscopic cholecystectomy and delayed laparoscopic cholecystectomy after percutaneous transhepatic
Korean J Hepatobiliary Pancreat Surg 0;6:7-5 Original Article Comparison of clinical result between early laparoscopic cholecystectomy and delayed laparoscopic cholecystectomy after percutaneous transhepatic
Heon Tak Ha, Young Seok Han, and Jae Min Chun
 Ann Hepatobiliary Pancreat Surg 2017;21:217-222 https://doi.org/10.14701/ahbps.2017.21.4.217 Case Report Totally laparoscopic associating liver partition and portal vein ligation for staged hepatectomy
Ann Hepatobiliary Pancreat Surg 2017;21:217-222 https://doi.org/10.14701/ahbps.2017.21.4.217 Case Report Totally laparoscopic associating liver partition and portal vein ligation for staged hepatectomy
Update in abdominal Surgery in cirrhotic patients
 Update in abdominal Surgery in cirrhotic patients Safi Dokmak HBP department and liver transplantation Beaujon Hospital, Clichy, France Cairo, 5 April 2016 Cirrhosis Prevalence in France (1%)* Patients
Update in abdominal Surgery in cirrhotic patients Safi Dokmak HBP department and liver transplantation Beaujon Hospital, Clichy, France Cairo, 5 April 2016 Cirrhosis Prevalence in France (1%)* Patients
Minimally Invasive Esophagectomy
 American Association of Thoracic Surgery (AATS) 95 th Annual Meeting Seattle, WA April 29, 2015 General Thoracic Masters of Surgery Video Session Minimally Invasive Esophagectomy James D. Luketich MD,
American Association of Thoracic Surgery (AATS) 95 th Annual Meeting Seattle, WA April 29, 2015 General Thoracic Masters of Surgery Video Session Minimally Invasive Esophagectomy James D. Luketich MD,
Laparoscopic Liver Resection for Hepatocellular Carcinoma
 Original Article Laparoscopic Liver Resection for Hepatocellular Carcinoma Carmen D. Chung, Lydia L. Lau, Kwan Lung Ko, Andrew C. Wong, Shezam Wong, Albert C. Chan, Ronnie T. Poon, Chung Mau Lo and Sheung
Original Article Laparoscopic Liver Resection for Hepatocellular Carcinoma Carmen D. Chung, Lydia L. Lau, Kwan Lung Ko, Andrew C. Wong, Shezam Wong, Albert C. Chan, Ronnie T. Poon, Chung Mau Lo and Sheung
Percutaneous Removal of Biliary Stone from Anomalous Right Hepatic Duct
 Percutaneous Removal of Biliary Stone from Anomalous Right Hepatic Duct Pages with reference to book, From 94 To 96 Tanveer ul Haq, Mohammed Younus Sheikh, Changes Khan Jadun, M.N. Ahmad, Yousuf H. Husen
Percutaneous Removal of Biliary Stone from Anomalous Right Hepatic Duct Pages with reference to book, From 94 To 96 Tanveer ul Haq, Mohammed Younus Sheikh, Changes Khan Jadun, M.N. Ahmad, Yousuf H. Husen
Case Report In Situ Split of the Liver When Portal Venous Embolization Fails to Induce Hypertrophy: A Report of Two Cases
 Case Reports in Surgery Volume 2013, Article ID 238675, 4 pages http://dx.doi.org/10.1155/2013/238675 Case Report In Situ Split of the Liver When Portal Venous Embolization Fails to Induce Hypertrophy:
Case Reports in Surgery Volume 2013, Article ID 238675, 4 pages http://dx.doi.org/10.1155/2013/238675 Case Report In Situ Split of the Liver When Portal Venous Embolization Fails to Induce Hypertrophy:
Complication of Laparoscopic Cholecystectomy
 Complication of Laparoscopic Cholecystectomy R.K.Mishra What to do if something goes wrong There is not a single laparoscopic surgeon in the world who has not damaged CBD Complications Early Common bile
Complication of Laparoscopic Cholecystectomy R.K.Mishra What to do if something goes wrong There is not a single laparoscopic surgeon in the world who has not damaged CBD Complications Early Common bile
Citation Hepato-Gastroenterology, 55(86-87),
 NAOSITE: Nagasaki University's Ac Title Author(s) Combined pancreatic resection and p multiple lesions of the pancreas: i of the pancreas concomitant with du Kuroki, Tamotsu; Tajima, Yoshitsugu Tomohiko;
NAOSITE: Nagasaki University's Ac Title Author(s) Combined pancreatic resection and p multiple lesions of the pancreas: i of the pancreas concomitant with du Kuroki, Tamotsu; Tajima, Yoshitsugu Tomohiko;
Current Treatment Strategies for Hilar and Intrahepatic Cholangiocarcinoma
 Current Treatment Strategies for Hilar and Intrahepatic Cholangiocarcinoma Jean-Nicolas Vauthey, MD, FACS Professor of Surgery Chief Hepato-Pancreato-Biliary Section Department of Surgical Oncology Crescent
Current Treatment Strategies for Hilar and Intrahepatic Cholangiocarcinoma Jean-Nicolas Vauthey, MD, FACS Professor of Surgery Chief Hepato-Pancreato-Biliary Section Department of Surgical Oncology Crescent
Robotic-assisted right upper lobectomy
 Robotic Thoracic Surgery Column Robotic-assisted right upper lobectomy Shiguang Xu, Tong Wang, Wei Xu, Xingchi Liu, Bo Li, Shumin Wang Department of Thoracic Surgery, Northern Hospital, Shenyang 110015,
Robotic Thoracic Surgery Column Robotic-assisted right upper lobectomy Shiguang Xu, Tong Wang, Wei Xu, Xingchi Liu, Bo Li, Shumin Wang Department of Thoracic Surgery, Northern Hospital, Shenyang 110015,
Title. Author(s) Issue Date Right.
 NAOSITE: Nagasaki University's Ac Title Author(s) Citation Results of elective laparoscopic ch following percutaneous transhepatic Kuroki, Tamotsu; Kitasato, Amane; T Hiroaki; Taniguchi, Ken; Maeda, Shi
NAOSITE: Nagasaki University's Ac Title Author(s) Citation Results of elective laparoscopic ch following percutaneous transhepatic Kuroki, Tamotsu; Kitasato, Amane; T Hiroaki; Taniguchi, Ken; Maeda, Shi
Management of Cholangiocarcinoma. Roseanna Lee, MD PGY-5 Kings County Hospital
 Management of Cholangiocarcinoma Roseanna Lee, MD PGY-5 Kings County Hospital Case Presentation 37 year old male from Yemen presented with 2 week history of epigastric pain, anorexia, jaundice and puritis.
Management of Cholangiocarcinoma Roseanna Lee, MD PGY-5 Kings County Hospital Case Presentation 37 year old male from Yemen presented with 2 week history of epigastric pain, anorexia, jaundice and puritis.
Anaesthetic considerations and peri-operative risks in patients with liver disease
 Anaesthetic considerations and peri-operative risks in patients with liver disease Dr. C. K. Pandey Professor & Head Department of Anaesthesiology & Critical Care Medicine Institute of Liver and Biliary
Anaesthetic considerations and peri-operative risks in patients with liver disease Dr. C. K. Pandey Professor & Head Department of Anaesthesiology & Critical Care Medicine Institute of Liver and Biliary
Endoscopic management of postoperative bile duct injuries: a single center experience.
 1- Endoscopic management of postoperative bile duct injuries: a single center experience. BACKGROUND/AIM: Biliary endoscopic procedures may be less invasive than surgery for management of postoperative
1- Endoscopic management of postoperative bile duct injuries: a single center experience. BACKGROUND/AIM: Biliary endoscopic procedures may be less invasive than surgery for management of postoperative
STRICTURES OF THE BILE DUCTS Session No.: 5. Andrea Tringali Digestive Endoscopy Unit Catholic University Rome - Italy
 STRICTURES OF THE BILE DUCTS Session No.: 5 Andrea Tringali Digestive Endoscopy Unit Catholic University Rome - Italy Drainage of biliary strictures. The history before 1980 Surgical bypass Percutaneous
STRICTURES OF THE BILE DUCTS Session No.: 5 Andrea Tringali Digestive Endoscopy Unit Catholic University Rome - Italy Drainage of biliary strictures. The history before 1980 Surgical bypass Percutaneous
Subtotal cholecystectomy for complicated acute cholecystitis: a multicenter prospective observational study
 Study title Subtotal cholecystectomy for complicated acute cholecystitis: a multicenter prospective observational study Primary Investigator: Kazuhide Matsushima, MD Co-Primary investigator: Zachary Warriner,
Study title Subtotal cholecystectomy for complicated acute cholecystitis: a multicenter prospective observational study Primary Investigator: Kazuhide Matsushima, MD Co-Primary investigator: Zachary Warriner,
Original article: new surgical approaches to the Klatskin tumour
 Alimentary Pharmacology & Therapeutics Original article: new surgical approaches to the Klatskin tumour T. M. VAN GULIK*, S. DINANT*, O. R. C. BUSCH*, E. A. J. RAUWS, H. OBERTOP* & D. J. GOUMA Departments
Alimentary Pharmacology & Therapeutics Original article: new surgical approaches to the Klatskin tumour T. M. VAN GULIK*, S. DINANT*, O. R. C. BUSCH*, E. A. J. RAUWS, H. OBERTOP* & D. J. GOUMA Departments
Study of post cholecystectomy biliary leakage and its management
 Original Research Article Study of post cholecystectomy biliary leakage and its management P. Krishna Kishore 1*, B. Manju Sruthi 2, G. Obulesu 3 1 Assistant Professor, Departmentment of General Surgery,
Original Research Article Study of post cholecystectomy biliary leakage and its management P. Krishna Kishore 1*, B. Manju Sruthi 2, G. Obulesu 3 1 Assistant Professor, Departmentment of General Surgery,
Imaging of liver and pancreas
 Imaging of liver and pancreas.. Disease of the liver Focal liver disease Diffusion liver disease Focal liver disease Benign Cyst Abscess Hemangioma FNH Hepatic adenoma HCC Malignant Fibrolamellar carcinoma
Imaging of liver and pancreas.. Disease of the liver Focal liver disease Diffusion liver disease Focal liver disease Benign Cyst Abscess Hemangioma FNH Hepatic adenoma HCC Malignant Fibrolamellar carcinoma
Management of biliary injury after laparoscopic cholecystectomy N. Dayes Kings County Hospital Center & Long Island College Hospital 8/19/2010
 Management of biliary injury after laparoscopic cholecystectomy N. Dayes Kings County Hospital Center & Long Island College Hospital 8/19/2010 Case Presentation 30 y.o. woman with 2 weeks of RUQ abdominal
Management of biliary injury after laparoscopic cholecystectomy N. Dayes Kings County Hospital Center & Long Island College Hospital 8/19/2010 Case Presentation 30 y.o. woman with 2 weeks of RUQ abdominal
Takuya SAKODA* ), Yoshiaki MURAKAMI, Naru KONDO, Kenichiro UEMURA, Yasushi HASHIMOTO, Naoya NAKAGAWA and Taijiro SUEDA ABSTRACT
 Hiroshima J. Med. Sci. Vol. 64, No. 3, 45~49, September, 2015 HIJM 64 8 45 Takuya SAKODA* ), Yoshiaki MURAKAMI, Naru KONDO, Kenichiro UEMURA, Yasushi HASHIMOTO, Naoya NAKAGAWA and Taijiro SUEDA Department
Hiroshima J. Med. Sci. Vol. 64, No. 3, 45~49, September, 2015 HIJM 64 8 45 Takuya SAKODA* ), Yoshiaki MURAKAMI, Naru KONDO, Kenichiro UEMURA, Yasushi HASHIMOTO, Naoya NAKAGAWA and Taijiro SUEDA Department
Medicine. Clinical Case Report. 1. Introduction. 2. Case report OPEN
 Clinical Case Report Medicine Feasibility of laparoscopic major hepatectomy for hepatic paragonimiasis: two case reports Fei Liu, MD a, Jingyi Zhang, BD b, Chuanfen Lei, BD c, Yonggang Wei, MD a,, Bo Li,
Clinical Case Report Medicine Feasibility of laparoscopic major hepatectomy for hepatic paragonimiasis: two case reports Fei Liu, MD a, Jingyi Zhang, BD b, Chuanfen Lei, BD c, Yonggang Wei, MD a,, Bo Li,
Multiple Primary Quiz
 Multiple Primary Quiz Case 1 A 72 year old man was found to have a 12 mm solid lesion in the pancreatic tail by computed tomography carried out during a routine follow up study of this patient with adult
Multiple Primary Quiz Case 1 A 72 year old man was found to have a 12 mm solid lesion in the pancreatic tail by computed tomography carried out during a routine follow up study of this patient with adult
Fat Tissue Infiltration into the Pancreas Parenchyme and Its Effect on the Result of Surgery
 Korean Journal of HBP Surgery Vol. 15,. 2, May 2011 O riginal Article Fat Tissue Infiltration into the Pancreas Parenchyme and Its Effect on the Result of Surgery Purpose: In Korea, there are few reports
Korean Journal of HBP Surgery Vol. 15,. 2, May 2011 O riginal Article Fat Tissue Infiltration into the Pancreas Parenchyme and Its Effect on the Result of Surgery Purpose: In Korea, there are few reports
Post-operative complications following hepatobiliary surgery: imaging findings and current radiological treatment options
 Post-operative complications following hepatobiliary surgery: imaging findings and current radiological treatment options Poster No.: C-1501 Congress: ECR 2015 Type: Educational Exhibit Authors: A. Hadjivassiliou,
Post-operative complications following hepatobiliary surgery: imaging findings and current radiological treatment options Poster No.: C-1501 Congress: ECR 2015 Type: Educational Exhibit Authors: A. Hadjivassiliou,
ISSN X (Print) Research Article. *Corresponding author Jitendra Singh Yadav
 Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2014; 2(3B):966-970 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2014; 2(3B):966-970 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
INTERNATIONAL HEPATO-PANCREATO-BILIARY ASSOCIATION (IHPBA), INDIAN CHAPTER 6TH CERTIFICATE COURSE IN HEPATO-PANCREATO-BILIARY SURGERY
 Day 1-28 th August 2013 Liver TS Ravikumar, Goro Honda, R Surendran, V Sitaram, George Kurien Swatee Halbe, Biju Pottakkat, Vibha Naik, Deepak Barathi 1 Surgical quality and safety Inaugural lecture 2
Day 1-28 th August 2013 Liver TS Ravikumar, Goro Honda, R Surendran, V Sitaram, George Kurien Swatee Halbe, Biju Pottakkat, Vibha Naik, Deepak Barathi 1 Surgical quality and safety Inaugural lecture 2
ERCP / PTC Surgical Laparoscopic vs open Timing and order of approach
 Choledocholithiasis Which Approach and When? Lygia Stewart, MD University of California, San Francisco 2010 Naffziger Post-Graduate Course Clinical Manifestations of Choledocholithiasis Asymptomatic (no
Choledocholithiasis Which Approach and When? Lygia Stewart, MD University of California, San Francisco 2010 Naffziger Post-Graduate Course Clinical Manifestations of Choledocholithiasis Asymptomatic (no
Long R. Jiao, David N. Hakim, Tamara M. H. Gall, Ana Fajardo, Tim D. Pencavel, Ruifang Fan, Mikael H. Sodergren
 How We Do It A totally laparoscopic associating liver partition and portal vein ligation for staged hepatectomy assisted with radiofrequency (radiofrequency assisted liver partition with portal vein ligation)
How We Do It A totally laparoscopic associating liver partition and portal vein ligation for staged hepatectomy assisted with radiofrequency (radiofrequency assisted liver partition with portal vein ligation)
Disclosures. Extra-hepatic Biliary Disease and the Pancreas. Objectives. Pancreatitis 10/3/2018. No relevant financial disclosures to report
 Extra-hepatic Biliary Disease and the Pancreas Disclosures No relevant financial disclosures to report Jeffrey Coughenour MD FACS Clinical Associate Professor of Surgery and Emergency Medicine Division
Extra-hepatic Biliary Disease and the Pancreas Disclosures No relevant financial disclosures to report Jeffrey Coughenour MD FACS Clinical Associate Professor of Surgery and Emergency Medicine Division
Won Ho Han1, Amir Ben Yehuda2, Deok-Hee Kim1, Seung Geun Yang1, Bang Wool Eom1, Hong Man Yoon1, Young-Woo Kim1, Keun Won Ryu1 View this article at:
 Original Article A comparative study of totally laparoscopic distal gastrectomy versus laparoscopic-assisted distal gastrectomy in gastric cancer patients: Short-term operative outcomes at a high-volume
Original Article A comparative study of totally laparoscopic distal gastrectomy versus laparoscopic-assisted distal gastrectomy in gastric cancer patients: Short-term operative outcomes at a high-volume
Endoscopic Management of Biliary Strictures. Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center
 Endoscopic Management of Biliary Strictures Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center Malignant Biliary Strictures Etiologies: Pancreatic
Endoscopic Management of Biliary Strictures Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center Malignant Biliary Strictures Etiologies: Pancreatic
Thoracoscopic left upper lobectomy with systematic lymph nodes dissection under left pulmonary artery clamping
 GCTAB Column Thoracoscopic left upper lobectomy with systematic lymph nodes dissection under left pulmonary artery clamping Yi-Nan Dong, Nan Sun, Yi Ren, Liang Zhang, Ji-Jia Li, Yong-Yu Liu Department
GCTAB Column Thoracoscopic left upper lobectomy with systematic lymph nodes dissection under left pulmonary artery clamping Yi-Nan Dong, Nan Sun, Yi Ren, Liang Zhang, Ji-Jia Li, Yong-Yu Liu Department
Surgery for hilar cholangiocirconoma
 Department of Surgery University Hospital RWTH Aachen Surgery for hilar cholangiocirconoma Ulf Peter Neumann Agenda Operating on the most complex tumor in HBP Surgery Preoperative management Does the patient
Department of Surgery University Hospital RWTH Aachen Surgery for hilar cholangiocirconoma Ulf Peter Neumann Agenda Operating on the most complex tumor in HBP Surgery Preoperative management Does the patient
Robotic thoracic surgery: S 1+2 segmentectomy of left upper lobe
 Case Report Page 1 of 5 Robotic thoracic surgery: S 1+2 segmentectomy of left upper lobe Hailei Du, Su Yang, Wei Guo, Runsen Jin, Yajie Zhang, Xingshi Chen, Han Wu, Dingpei Han, Kai Chen, Jie Xiang, Hecheng
Case Report Page 1 of 5 Robotic thoracic surgery: S 1+2 segmentectomy of left upper lobe Hailei Du, Su Yang, Wei Guo, Runsen Jin, Yajie Zhang, Xingshi Chen, Han Wu, Dingpei Han, Kai Chen, Jie Xiang, Hecheng
THE CRITICAL COMPLCATIONS AND MANAGEMENTS AFTER PANCREATIC SURGERY 2013/12/21
 THE CRITICAL COMPLCATIONS AND MANAGEMENTS AFTER PANCREATIC SURGERY Tsann-Long Hwang, MD, FACS Department of Surgery Chang Gung Memorial Hospital Chang Gung University Taipei, TAIWAN 2013/12/21 THE DIFFICULTY
THE CRITICAL COMPLCATIONS AND MANAGEMENTS AFTER PANCREATIC SURGERY Tsann-Long Hwang, MD, FACS Department of Surgery Chang Gung Memorial Hospital Chang Gung University Taipei, TAIWAN 2013/12/21 THE DIFFICULTY
Intrahepatic Cholangiocarcinoma Associated with Intrahepatic Duct Stones
 Original Article Intrahepatic Cholangiocarcinoma Associated with Intrahepatic Duct Stones Hoon Hur, Il-Young Park, Gi-Young Sung, Do-Sang Lee, Wook Kim and Jong-Man Won, Department of Surgery, Holy Family
Original Article Intrahepatic Cholangiocarcinoma Associated with Intrahepatic Duct Stones Hoon Hur, Il-Young Park, Gi-Young Sung, Do-Sang Lee, Wook Kim and Jong-Man Won, Department of Surgery, Holy Family
MAKING CONNECTIONS. Los Angeles Medical Center
 MAKING CONNECTIONS Los Angeles Medical Center Resident: Chris Molloy, MD Fellow: Christian Coroian, MD, MBA Attending: Tina Hardley, MD Program/Dept(s): Los Angeles Medical Center CHIEF COMPLAINT & HPI
MAKING CONNECTIONS Los Angeles Medical Center Resident: Chris Molloy, MD Fellow: Christian Coroian, MD, MBA Attending: Tina Hardley, MD Program/Dept(s): Los Angeles Medical Center CHIEF COMPLAINT & HPI
Minimally Invasive Esophagectomy
 Minimally Invasive Esophagectomy M A R K B E R R Y, M D A S S O C I AT E P R O F E S S O R D E PA R T M E N T OF C A R D I O T H O R A C I C S U R G E R Y S TA N F O R D U N I V E R S I T Y S E P T E M
Minimally Invasive Esophagectomy M A R K B E R R Y, M D A S S O C I AT E P R O F E S S O R D E PA R T M E N T OF C A R D I O T H O R A C I C S U R G E R Y S TA N F O R D U N I V E R S I T Y S E P T E M
JMSCR Volume 03 Issue 05 Page May 2015
 www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x Comparison of 3-Port Versus 4-Port Laproscopic Cholecystectomy- A Prospective Comparative Study Authors Shekhar Gogna 1, Priya Goyal 2,
www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x Comparison of 3-Port Versus 4-Port Laproscopic Cholecystectomy- A Prospective Comparative Study Authors Shekhar Gogna 1, Priya Goyal 2,
Variations in portal and hepatic vein branching of the liver
 Yamagata Med J (ISSN 0288-030X)2015;33(2):115-121 DOI 10.15022/00003476 Variations in portal and hepatic vein branching of the liver Wataru Kimura, Tsuyoshi Fukumoto, Toshihiro Watanabe, Ichiro Hirai First
Yamagata Med J (ISSN 0288-030X)2015;33(2):115-121 DOI 10.15022/00003476 Variations in portal and hepatic vein branching of the liver Wataru Kimura, Tsuyoshi Fukumoto, Toshihiro Watanabe, Ichiro Hirai First
Post Laparoscopic Cholecystectomy Biloma in a Child Managed by Endoscopic Retrograde Cholangio-Pancreatography and Stenting: A Case Report
 pissn: 2234-8646 eissn: 2234-8840 https://doi.org/10.5223/pghn.2016.19.4.281 Pediatr Gastroenterol Hepatol Nutr 2016 December 19(4):281-285 Case Report PGHN Post Laparoscopic Cholecystectomy Biloma in
pissn: 2234-8646 eissn: 2234-8840 https://doi.org/10.5223/pghn.2016.19.4.281 Pediatr Gastroenterol Hepatol Nutr 2016 December 19(4):281-285 Case Report PGHN Post Laparoscopic Cholecystectomy Biloma in
A CASE REPORT OF SPONTANEOUS BILOMA - AN ENIGMATIC SURGICAL PROBLEM
 A CASE REPORT OF SPONTANEOUS BILOMA - AN ENIGMATIC SURGICAL PROBLEM *Sumanta Kumar Ghosh and Biswajit Mukherjee ESIC Medical College, Joka, Kolkata, India *Author for Correspondence ABSTRACT Occurrence
A CASE REPORT OF SPONTANEOUS BILOMA - AN ENIGMATIC SURGICAL PROBLEM *Sumanta Kumar Ghosh and Biswajit Mukherjee ESIC Medical College, Joka, Kolkata, India *Author for Correspondence ABSTRACT Occurrence
HEPATECTOMY. Surgical Potpourri Session. ACS NSQIP National Conference Salt Lake City 2012
 HEPATECTOMY Surgical Potpourri Session ACS NSQIP National Conference Salt Lake City 2012 Pascal Fuchshuber, MD, PhD, FACS Kaiser Permanente Medical Center Walnut Creek - California Hepatic Resection Is
HEPATECTOMY Surgical Potpourri Session ACS NSQIP National Conference Salt Lake City 2012 Pascal Fuchshuber, MD, PhD, FACS Kaiser Permanente Medical Center Walnut Creek - California Hepatic Resection Is
Biliary Anatomy in Living-related Liver Transplantation
 The 5th IHPBA Congress - Istanbul Biliary Anatomy in Living-related Liver Transplantation biliary trees hilar plate Assessment for Vascular Anatomy 1. 3DCT portal vein hepatic vein hepatic artery 2. No
The 5th IHPBA Congress - Istanbul Biliary Anatomy in Living-related Liver Transplantation biliary trees hilar plate Assessment for Vascular Anatomy 1. 3DCT portal vein hepatic vein hepatic artery 2. No
Personal Profile. Name: 劉 XX Gender: Female Age: 53-y/o Past history. Hepatitis B carrier
 Personal Profile Name: 劉 XX Gender: Female Age: 53-y/o Past history Hepatitis B carrier Chief complaint Fever on and off for 2 days Present illness 94.10.14 Sudden onset of epigastric pain 94.10.15 Fever
Personal Profile Name: 劉 XX Gender: Female Age: 53-y/o Past history Hepatitis B carrier Chief complaint Fever on and off for 2 days Present illness 94.10.14 Sudden onset of epigastric pain 94.10.15 Fever
The safety of the early removal of prophylactic drainage after liver resection based solely on predetermined criteria: a propensity score analysis
 http://dx.doi.org/10.1016/j.hpb.2016.12.005 HPB ORIGINAL ARTICLE The safety of the early removal of prophylactic drainage after liver resection based solely on predetermined criteria: a propensity score
http://dx.doi.org/10.1016/j.hpb.2016.12.005 HPB ORIGINAL ARTICLE The safety of the early removal of prophylactic drainage after liver resection based solely on predetermined criteria: a propensity score
A Large Hepatic Cyst with Obstructive Jaundice Successfully Treated with Single-Incision Laparoscopic Deroofing
 Published online: November 28, 2013 1662 0631/13/0073 0503$38.00/0 This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial 3.0 Unported license (CC BY-NC)
Published online: November 28, 2013 1662 0631/13/0073 0503$38.00/0 This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial 3.0 Unported license (CC BY-NC)
Mirizzi syndrome with an unusual type of biliobiliary fistula a case report
 Kawaguchi et al. Surgical Case Reports (2015) 1:51 DOI 10.1186/s40792-015-0052-2 CASE REPORT Mirizzi syndrome with an unusual type of biliobiliary fistula a case report Tsutomu Kawaguchi 1,2*, Tadao Itoh
Kawaguchi et al. Surgical Case Reports (2015) 1:51 DOI 10.1186/s40792-015-0052-2 CASE REPORT Mirizzi syndrome with an unusual type of biliobiliary fistula a case report Tsutomu Kawaguchi 1,2*, Tadao Itoh
Laparoscopic Common Bile Duct Exploration : A Feasible Option for Choledocholithiasis in Patients with Previous Gastrectomy
 ORIGINAL ARTICLE pissn 2234-778X eissn 2234-5248 J Minim Invasive Surg 2016;19(4):130-134 Journal of Minimally Invasive Surgery Laparoscopic Common Bile Duct Exploration : A Feasible Option for Choledocholithiasis
ORIGINAL ARTICLE pissn 2234-778X eissn 2234-5248 J Minim Invasive Surg 2016;19(4):130-134 Journal of Minimally Invasive Surgery Laparoscopic Common Bile Duct Exploration : A Feasible Option for Choledocholithiasis
Repeat Single Incision Laparoscopic Surgery after Primary Single Incision Laparoscopic Surgery for Colorectal Disease
 ORIGINAL ARTICLE pissn 2234-778X eissn 2234-5248 J Minim Invasive Surg 2018;21(1):38-42 Journal of Minimally Invasive Surgery Repeat Single Incision Laparoscopic Surgery after Primary Single Incision Laparoscopic
ORIGINAL ARTICLE pissn 2234-778X eissn 2234-5248 J Minim Invasive Surg 2018;21(1):38-42 Journal of Minimally Invasive Surgery Repeat Single Incision Laparoscopic Surgery after Primary Single Incision Laparoscopic
Laparoscopic Cholecystectomy in Acute Cholecystitis :An Experience with 100 cases
 ORIGINALARTICLE Laparoscopic Cholecystectomy in Acute Cholecystitis :An Experience with 100 cases Rajni Bhardwaj, M.R.Attri, Shahnawaz Ahangar Abstract This study was undertaken to evaluate our experience
ORIGINALARTICLE Laparoscopic Cholecystectomy in Acute Cholecystitis :An Experience with 100 cases Rajni Bhardwaj, M.R.Attri, Shahnawaz Ahangar Abstract This study was undertaken to evaluate our experience
KAHBPS-O-PL-01 KAHBPS-O-PL-02
 KAHBPS-O-PL-01 Proposal of future remnant liver-indocyanine green clearance rate for risk assessment of major hepatectomy - What is its cutoff? Department of Surgery, Asan Medical Center, University of
KAHBPS-O-PL-01 Proposal of future remnant liver-indocyanine green clearance rate for risk assessment of major hepatectomy - What is its cutoff? Department of Surgery, Asan Medical Center, University of
Laparoscopic liver resection of hepatocellular carcinoma
 The American Journal of Surgery 189 (2005) 190 194 Laparoscopy Laparoscopic liver resection of hepatocellular carcinoma Hironori Kaneko, M.D.*, Sumito Takagi, M.D., Yuichiro Otsuka, M.D., Masaru Tsuchiya,
The American Journal of Surgery 189 (2005) 190 194 Laparoscopy Laparoscopic liver resection of hepatocellular carcinoma Hironori Kaneko, M.D.*, Sumito Takagi, M.D., Yuichiro Otsuka, M.D., Masaru Tsuchiya,
Two Cases of Laparoscopic Adhesiolysis for Chronic Abdominal Pain without Intestinal Obstruction after Total Gastrectomy
 J Gastric Cancer 2012;12(4):249-253 http://dx.doi.org/10.5230/jgc.2012.12.4.249 Case Report Two Cases of Laparoscopic Adhesiolysis for Chronic Abdominal Pain without Intestinal Obstruction after Total
J Gastric Cancer 2012;12(4):249-253 http://dx.doi.org/10.5230/jgc.2012.12.4.249 Case Report Two Cases of Laparoscopic Adhesiolysis for Chronic Abdominal Pain without Intestinal Obstruction after Total
Laparoscopic & Robotic Surgery in Pancreas Disease
 2007 년도대한췌담도학회추계학술대회 Session IV: Recent Updates in Pancreatobiliary Diseases Laparoscopic & Robotic Surgery in Pancreas Disease Department of Surgery, Yonsei University College of Medicine, Korea Woo-Jung
2007 년도대한췌담도학회추계학술대회 Session IV: Recent Updates in Pancreatobiliary Diseases Laparoscopic & Robotic Surgery in Pancreas Disease Department of Surgery, Yonsei University College of Medicine, Korea Woo-Jung
Surgical management of HCC. Evangelos Prassas Hepatobiliary and Pancreatic Surgery / Liver Transplantation Kings College Hospital / London
 Surgical management of HCC Evangelos Prassas Hepatobiliary and Pancreatic Surgery / Liver Transplantation Kings College Hospital / London Global distribution of HCC and staging systems WEST 1. Italy (Milan,
Surgical management of HCC Evangelos Prassas Hepatobiliary and Pancreatic Surgery / Liver Transplantation Kings College Hospital / London Global distribution of HCC and staging systems WEST 1. Italy (Milan,
Treatment outcomes and prognostic factors of gallbladder cancer patients after postoperative radiation therapy
 Korean J Hepatobiliary Pancreat Surg 2011;15:152-156 Original Article Treatment outcomes and prognostic factors of gallbladder cancer patients after postoperative radiation therapy Suzy Kim 1,#, Kyubo
Korean J Hepatobiliary Pancreat Surg 2011;15:152-156 Original Article Treatment outcomes and prognostic factors of gallbladder cancer patients after postoperative radiation therapy Suzy Kim 1,#, Kyubo
The campaign on laboratory: focus on Gallstone Disease and ERCP
 The campaign on laboratory: focus on Gallstone Disease and ERCP Mauro Giuliani, MD, Specialist in Visceral Surgery, Vice Head Physician, Surgical Ward, Ospedale Regionale di Locarno Alberto Fasoli, MD,
The campaign on laboratory: focus on Gallstone Disease and ERCP Mauro Giuliani, MD, Specialist in Visceral Surgery, Vice Head Physician, Surgical Ward, Ospedale Regionale di Locarno Alberto Fasoli, MD,
A case of complete splenic infarction after laparoscopic spleen-preserving distal pancreatectomy
 Kimura et al. BMC Surgery (2018) 18:22 https://doi.org/10.1186/s12893-018-0353-z CASE REPORT Open Access A case of complete splenic infarction after laparoscopic spleen-preserving distal pancreatectomy
Kimura et al. BMC Surgery (2018) 18:22 https://doi.org/10.1186/s12893-018-0353-z CASE REPORT Open Access A case of complete splenic infarction after laparoscopic spleen-preserving distal pancreatectomy
Robotic-assisted right inferior lobectomy
 Robotic Thoracic Surgery Column Page 1 of 6 Robotic-assisted right inferior lobectomy Shiguang Xu, Tong Wang, Wei Xu, Xingchi Liu, Bo Li, Shumin Wang Department of Thoracic Surgery, Northern Hospital,
Robotic Thoracic Surgery Column Page 1 of 6 Robotic-assisted right inferior lobectomy Shiguang Xu, Tong Wang, Wei Xu, Xingchi Liu, Bo Li, Shumin Wang Department of Thoracic Surgery, Northern Hospital,
Vascular complications in percutaneous biliary interventions: A series of 111 procedures
 Vascular complications in percutaneous biliary interventions: A series of 111 procedures Poster No.: C-0744 Congress: ECR 2013 Type: Educational Exhibit Authors: A. BHARADWAZ; AARHUS, Re/DK Keywords: Obstruction
Vascular complications in percutaneous biliary interventions: A series of 111 procedures Poster No.: C-0744 Congress: ECR 2013 Type: Educational Exhibit Authors: A. BHARADWAZ; AARHUS, Re/DK Keywords: Obstruction
Information for Consent Cholecystectomy (Laparoscopic/Open) 膽囊切除術 ( 腹腔鏡 / 開放性 )
 Version 1.0 Page 1 of 3 Information for Consent Cholecystectomy (Laparoscopic/Open) 膽囊切除術 ( 腹腔鏡 / 開放性 ) Introduction Gallbladder is a sac connected to the biliary tree. It serves the function of concentration
Version 1.0 Page 1 of 3 Information for Consent Cholecystectomy (Laparoscopic/Open) 膽囊切除術 ( 腹腔鏡 / 開放性 ) Introduction Gallbladder is a sac connected to the biliary tree. It serves the function of concentration
Cholangiocarcinoma (Bile Duct Cancer)
 Cholangiocarcinoma (Bile Duct Cancer) The Bile Duct System (Biliary Tract) A network of bile ducts (tubes) connects the liver and the gallbladder to the small intestine. This network begins in the liver
Cholangiocarcinoma (Bile Duct Cancer) The Bile Duct System (Biliary Tract) A network of bile ducts (tubes) connects the liver and the gallbladder to the small intestine. This network begins in the liver
Intraductal papillary neoplasms in the bile ducts
 Intraductal papillary neoplasms in the bile ducts Seok Hwa Youn Myunghee Yoon Dong Hoon Shin Kosin University Gospel Hospital Department of general surgery Hepato-biliary-pancreatic division Introduction
Intraductal papillary neoplasms in the bile ducts Seok Hwa Youn Myunghee Yoon Dong Hoon Shin Kosin University Gospel Hospital Department of general surgery Hepato-biliary-pancreatic division Introduction
Comparison between primary closure and T-tube drainage after open choledocotomy
 ISSN: 2203-1413 Vol.03 No.04 Comparison between primary closure and T-tube drainage after open choledocotomy Alireza Barband 1, Farzad Kakaei 1, Morteza Ghojazadeh 2, Abdolhamid Chavoshi Khamneh 1*, Morteza
ISSN: 2203-1413 Vol.03 No.04 Comparison between primary closure and T-tube drainage after open choledocotomy Alireza Barband 1, Farzad Kakaei 1, Morteza Ghojazadeh 2, Abdolhamid Chavoshi Khamneh 1*, Morteza
The Efficacy of Preoperative Percutaneous Cholecystostomy for Acute Cholecystitis with Gallbladder Perforation 담낭천공을동반한급성담낭염환자에서수술전경피적담낭배액술의효용성에관한연구
 Original Article pissn 1738-2637 / eissn 2288-2928 J Korean Soc Radiol 2017;77(6):372-381 https://doi.org/10.3348/jksr.2017.77.6.372 The Efficacy of Preoperative Percutaneous Cholecystostomy for Acute
Original Article pissn 1738-2637 / eissn 2288-2928 J Korean Soc Radiol 2017;77(6):372-381 https://doi.org/10.3348/jksr.2017.77.6.372 The Efficacy of Preoperative Percutaneous Cholecystostomy for Acute
Congenital dilatation of the common bile duct and pancreaticobiliary maljunction clinical implications
 Langenbecks Arch Surg (2009) 394:209 213 DOI 10.1007/s00423-008-0330-6 CURRENT CONCEPT IN CLINICAL SURGERY Congenital dilatation of the common bile duct and pancreaticobiliary maljunction clinical implications
Langenbecks Arch Surg (2009) 394:209 213 DOI 10.1007/s00423-008-0330-6 CURRENT CONCEPT IN CLINICAL SURGERY Congenital dilatation of the common bile duct and pancreaticobiliary maljunction clinical implications
EAST MULTICENTER STUDY PROPOSAL
 EAST MULTICENTER STUDY PROPOSAL (Proposal forms must be completed in its entirety, incomplete forms will not be considered) GENERAL INFORMATION Study Title: Prospective Multi-Institutional Evaluation of
EAST MULTICENTER STUDY PROPOSAL (Proposal forms must be completed in its entirety, incomplete forms will not be considered) GENERAL INFORMATION Study Title: Prospective Multi-Institutional Evaluation of
Use of hepatic blood inflow occlusion and hemihepatic artery retention in liver resection for hepatocellular carcinoma
 Original Article Use of hepatic blood inflow occlusion and hemihepatic artery retention in liver resection for hepatocellular carcinoma Changjun Jia, Chaoliu Dai, Xingyu Zhao, Xianmin Bu, Feng Xu, Songlin
Original Article Use of hepatic blood inflow occlusion and hemihepatic artery retention in liver resection for hepatocellular carcinoma Changjun Jia, Chaoliu Dai, Xingyu Zhao, Xianmin Bu, Feng Xu, Songlin
CURRICULUM VITAE
 CURRICULUM VITAE Name Date of Birth Nationality Marital Status Permanent Address Sang Soo Lee, M. D. August 6, 1968 Korean Married, one child 217-704 Hanshin APT 137-949 Jamwon dong, Seocho-gu, Seoul,
CURRICULUM VITAE Name Date of Birth Nationality Marital Status Permanent Address Sang Soo Lee, M. D. August 6, 1968 Korean Married, one child 217-704 Hanshin APT 137-949 Jamwon dong, Seocho-gu, Seoul,
Research Article Liver Surgery for Hepatocellular Carcinoma: Laparoscopic versus Open Approach
 SAGE-Hindawi Access to Research International Hepatology Volume 2011, Article ID 596792, 6 pages doi:10.4061/2011/596792 Research Article Liver Surgery for Hepatocellular Carcinoma: Laparoscopic versus
SAGE-Hindawi Access to Research International Hepatology Volume 2011, Article ID 596792, 6 pages doi:10.4061/2011/596792 Research Article Liver Surgery for Hepatocellular Carcinoma: Laparoscopic versus
Carcinoma del colon-retto: La Chirurgia Robotica nella Malattia Avanzata
 Carcinoma del colon-retto: La Chirurgia Robotica nella Malattia Avanzata Alberto Patriti SSD Chirurgia Robotica Multidisciplinare ASL 2 Umbria Ospedale San Matteo degli Infermi Spoleto - Why MIS for Advanced
Carcinoma del colon-retto: La Chirurgia Robotica nella Malattia Avanzata Alberto Patriti SSD Chirurgia Robotica Multidisciplinare ASL 2 Umbria Ospedale San Matteo degli Infermi Spoleto - Why MIS for Advanced
Information for patients (and their families) waiting for liver transplantation
 Information for patients (and their families) waiting for liver transplantation Waiting list? What is liver transplant? Postoperative conditions? Ver.: 5/2017 1 What is a liver transplant? Liver transplantation
Information for patients (and their families) waiting for liver transplantation Waiting list? What is liver transplant? Postoperative conditions? Ver.: 5/2017 1 What is a liver transplant? Liver transplantation
