Automated lamellar keratoplasty for the correction of hyperopia
|
|
|
- James Edwards
- 5 years ago
- Views:
Transcription
1 Automated lamellar keratoplasty for the correction of hyperopia Guy M. Kezirian, M.D., Charles M. Gremillion, M.D. ABSTRACT Hyperopic automated lamellar keratoplasty (H-ALK) is a refractive procedure that corrects low to moderate hyperopia of up to diopters (D). In this retrospective series, we examined the efficacy, predictability, and safety of H-ALK in 85 eyes in 49 patients. Follow-up was from 4 to 34 weeks (mean 18 weeks). Eyes were divided into three subsets: those in which we attempted an emmetropic result (n = 45), those in which we attempted to reduce, but not eliminate, hyperopia greater than 5.00 D (n = 23), and those in which we attempted a monovision result of D (n = 17). In the eyes in which we attempted emmetropia, 76% achieved uncorrected visual acuity of 20/40 or better and 78.6% were within a range of to D. In those in which we attempted monovision, 47% achieved a spherical equivalent result between and D because of a tendency toward undercorrection. In those in which we attempted to reduce hyperopia, there was a mean correction of 4.33 D (standard deviation 1.36 D), with a range of 2.12 to D. The most significant complication was a reduction in best corrected visual acuity of one to three lines in 11 of 85 eyes; this was transient in six eyes. These preliminary results compare favorably with those of other procedures to correct hyperopia. Key Words: automated lamellar keratoplasty, ectasia, hyperopia surgery, irregular astigmatism, monovision, predictability Hyperopic automated lamellar keratoplasty (H-ALK) was developed by Luis Antonio Ruiz, M.D., of Bogota, Columbia. The procedure induces a controlled ectasia of the central cornea (Figure 1) by thinning the cornea, using a 53% to 74% depth lamellar dissection, with an automated micro keratome (corneal shaper, Steinway Instruments, Chiron Vision, Boca Raton, FL). The resulting corneal steepening causes a myopic shift that neutralizes hyperopia of up to diopters (D). Hyperopic automated lamellar keratoplasty is among the refractive procedures for hyperopia that increase central corneal curvature. These procedures work through one of two mechanisms: they bend the native cornea, or they add substance to the cornea or remove tissue from it. Included in the former are keratomileusis, 1 thermokeratoplasty, 2 ' 3 hexagonal keratotomy, 4-6 and other forms of circumferential corneal dissection such as partial thickness trephination.7 Included in the latter are keratophakia, 8 epikera- tophakia, 9 and hyperopic photorefractive keratoplasty (stromal and surface). Hazing of the central cornea, 1 9 irregular astigmatism, 4-6 glare, unstable refractions, and regression have been seen with these procedures. This retrospective study was undertaken to assess the efficacy, safety, and predictability of H-ALK. We report the results of the procedure and the complications encountered and suggest some modifications. SUBJECTS AND METHODS Eighty-five eyes in 49 patients that had H-ALK were retrospectively studied. The cohort represents a consecutive series of eyes, operated on by a single surgeon (G.M.K.) under similar conditions at one institution (SurgiVision, Atlanta, GA). Surgery was performed between May 1, 1993, and December 31, All patients were evaluated preoperatively with cycloplegic refractions, slitlamp biomicroscopy, direct Presented in part at the Symposium on Cataract, IOL and Refractive Surgery, Boston, April Reprint requests to Guy M. Kezirian, M.D., SurgiVision, 1000 Abernathy Road, Suite 195, Atlanta, Georgia J CATARACf REFRACf SURG-VOL 21, JULY!995
2 Fig. 1. Controlled Ectasia Applanation Ring (Optical Zone) Size Original Profile Flap Base (Kezirian) Mechanism of action of H-ALK. No tissue is added or removed and no sutures are used to hold the flap in place. and indirect ophthalmoscopy, applanation tonometry, and computerized corneal topography. Eyes with surface keratitis, evidence of compromised endothelial function, cataracts, retinal disease, ocular hypertension, or other conditions that might threaten a successful outcome were excluded. All patients were symptomatic for hyperopia or, in the case of those seeking a monovision correction, for presbyopia. They were offered alternative treatments for their hyperopia or presbyopia, such as spectacle correction. All patients were informed of the investigational nature of the procedure and were presented with an appropriate informed consent acknowledging their awareness of potential complications. Surgical planning of applanation ring size was done using the Ruiz nomogram for hyperopia (Table 1 ). Forty-five eyes were targeted for plano results, using the spherical equivalent to determine the amount of correction. Seventeen eyes were targeted for D, a monovision correction, as detailed under the Results section. Only patients who were successful wearers of monovision contact lenses were offered this option. Twenty-three eyes were targeted for a 5.00 D reduction of hyperopia greater than 5.00 D. Simultaneous astigmatism correction was planned in eyes with more than 1.00 D of preoperative astigmatism. In these eyes, arcuate keratotomy was performed using the Casebeer nomogram. Surgery was performed as follows: Patients were given diazepam 20 mg, by mouth, and one drop of pilocarpine 4% to the operative eye one hour before surgery. Topical anesthesia of lidocaine 2% mixed 1:1 with bupivacaine 0.5% was administered four times at 15 minute intervals, and the patients were brought into the procedure room. A gentle lid prep using povidoneiodine swabs was performed; no ocular irrigation was performed. Surgeon and assistant were scrubbed, masked, and gloved in a sterile manner. The microtome head, plates, and motor portions of the ALK unit were cleaned with alcohol. (The manufacturer recommends against autoclaving the unit.) Lids were draped with a 1035 drape, capturing the lashes under the drape, and a Barraquer wire lid speculum was placed. Pachymetry was performed 1.5 mm temporal to the central corneal reflex using a Sonogauge ultrasonic pachymeter, and plate selection was made using the Ruiz nomogram. The cornea was Table 1. The Ruiz nomogram for H-ALK. Higher levels of correction are achieved by using a deeper dissection of a smaller diameter (optical zone). The maximal depth used is 74% of corneal thickness. Temporal-Paracentral Corneal Thickness Dissection J.Lm J.Lm f.lm J.Lm Diopters Diameter (Mean: 507 J.Lm) (Mean: 538 J.Lm) (Mean: 563 J.Lm) (Mean: 588 f.lm) >600 J.Lm (SE) (OZ) Micron %Depth Micron %Depth Micron %Depth Micron %Depth Micron %Depth < < < < < < < < <67 SE = spherical equivalent; OZ = optical zone J CATARACfREFRACf SURG-VOL21, JULY
3 marked using the ALK marker (Chiron Vision). The constricted pupil was used for centration. The suction ring was placed, and intraocular pressure (lop) was checked to confirm pressure of 65 mm Hg or greater. The appropriate applanation ring was applied. Ring height was adjusted to match corneal apposition to the applanation ring meniscus. The applanation ring was removed, and the microkeratome was introduced into the track. Balanced saline solution was used to wet the corneal surface. The microtome was driven across the cornea from the temporal to the nasal side and manually stopped approximately 0.5 mm short of the nasal edge of the flap. The instrument was removed, suction broken, and the rings removed. The diameter of the dissection achieved was measured using a caliper, under the microscope, and compared with the diameter attempted. Intraoperative pachymetric measurement of the depth of dissection was not performed. If astigmatism correction was done, it was performed at this point in the operation. The operative field was irrigated with balanced saline solution, including the stromal bed under the flap. Excess fluid was expressed from the interface using a dampened Merocel sponge (Merocel Corpora- tion, Mystic, CT), and compressed air was used to lightly dry the surface. Flap adhesion was checked by moving the lids over the cornea. Then, one drop of ciprofloxacin 0.3% was instilled and a Fox shield was placed over the eye. Patients were instructed to keep both eyes closed, except during ambulation. The operative eye was not patched. They were given ketorolac tromethamine (Toradol ) 10 mg by mouth every six hours for discomfort and triazolam (Halcion ) 0.25 mg for sleep. They were requested to wear the Fox shield to bed, to refrain from swimming, and not to use makeup for two weeks. Patients were seen postoperatively at one day, one week, one month, three months, and six months. On each visit, visual acuity, manifest refraction, corneal topography, and slitlamp examination were performed. Patients who did not complete their follow-up were included in analysis for the visits for which they did come in. Data from eyes that had subsequent procedures were included up to the point of the second procedure. RESULTS A total of 85 eyes in 49 patients were studied. Forty three of the eyes were from female patients, 42 from male patients. The average age was 47 years (range 28 to 64 years; standard deviation 9 years). Follow-up ranged from 4 to 34 weeks; the mean follow-up was 18 weeks, with a standard deviation of 12 weeks. All eyes completed the one day and the one month examinations. Fifty-five eyes completed the one week examination, 65 completed the three month examination, and 46 completed an examination six to eight months following the procedure. The mean preoperative spherical equivalent of the 45 eyes targeted for emmetropia was D (range D to D; standard deviation 1.10 D). The postoperative value was D (range D to D; standard deviation 0.90 D) (P <.0001). In all eyes, hyperopia was reduced. The one day refractions were typically 0.50 to 1.00 D more myopic than the one, three, and six month refractions. Patients reported stabilization of vision by the one month visit. The visual acuity results in these eyes are presented in Table 2. Preoperatively, 21% had a visual acuity of 20/40 or better without correction; postoperatively, 76% did (P <.001). Uncorrected visual acuity improved in all eyes. In all 85 eyes, there was a statistically insignificant effect (P = 0.42) on best corrected acuity at the one month visit. Eleven of the eyes decreased one line or more; two eyes decreased three lines. Six of these eyes improved to the preoperative level by the six month visit, two remained the same, and three were lost to follow-up. Corneal topography sometimes demonstrated smoothing to coincide with this improvement. Table 2. Visual acuity results in the 45 eyes targeted for emmetropia; 76% achieved uncorrected distance acuity of 20/40 or better. Visual Acuity 20/100 or Mean Preoperative Number 20/20-20/25 20/30-20/40 20/50-20/80 Worse SE (Diopters) of Eyes Number % Number % Number % Number % 1.00 to to to to All eyes: SE = spherical equivalent 388 J CATARACT REFRACT SURG-VOL 21, JULY 1995
4 Table 3. Postoperative spherical equivalents (SE) of the 45 eyes targeted for emmetropia, stratified by preoperative SE. Eyes with less preoperative hyperopia were less likely to undercorrect. Mean Mean Postoperative Preoperative Number SE Standard SE (Diopters) of Eyes (Diopters) Deviation 1.00 to to to to All eyes: (SD 1.24) Postoperative SE to to Plano to to n % n % n % n % In 15 eyes, the best corrected acuity improved from one to three lines at the one month visit. Twenty-five eyes had more than 1.00 D of preoperative astigmatism, and these eyes had simultaneous astigmatism correction with the H-ALK procedure. The average -preoperative astigmatism in these eyes was 2.71 D (range 0 to 5.00 D; standard deviation 1.44 D), the average postoperative astigmatism, 1.14 D (range 0 to 2.50 D; standard deviation 0.97 D). None of these eyes was overcorrected for their astigmatism. Fifteen eyes (60%) corrected to less than 1.00 D of remaining astigmatism and required no further surgery. The remaining 10 eyes had between 1.00 D and 5.00 D of astigmatism and required a subsequent procedure to correct residual astigmatism. In four eyes, no measurable astigmatism correction was achieved, despite the placement of arcuate incisions. Sixty eyes did not have more than 1.00 D of astigmatism preoperatively, and therefore did not have simultaneous astigmatism correction. In these eyes, there was a slight tendency to induce a change in astigmatism in the against-the-rule orientation; that is, to add plus cylinder within 30 degrees of axis 180 or reduce plus cylinder within 30 degrees of axis 90. Changes in astigmatism were calculated by subtracting the preoperative from the postoperative values. In eyes in which the new astigmatism axis was not exactly on the pre-existing axis, or 90 degrees from it, simple vector analysis was used to quantify the change. Overall, in these 60 eyes (that had H-ALK without astigmatism correction and that had less than 1.00 D of pre-existing astigmatism at any axis), the mean change in astigmatism was 0.27 D, standard deviation 0.72 D, with an overall reduction of astigmatism with the rule or, alternatively, an overall increase in astigmatism against the rule. There were three subsets within this group: those that followed this tendency, those that did not change in their cylinder, and those that went against this tendency. In the first subset (32 eyes), against-the-rule cylinder increased or with-the-rule cylinder decreased (range of cylinder change 0.25 D to 2.00 D). In the second subset (9 eyes), the cylinder remained unchanged. In the third subset (19 eyes), against-the-rule cylinder decreased or with-therule cylinder increased (range of astigmatism change 0.25 D to 1.00 D). Table 3 presents the preoperative refractions in the 45 eyes targeted for emmetropia, against the amount of correction achieved, and shows a significant tendency toward undercorrection in the higher ranges. There was a wide scatter of results in eyes with more than 5.00 D of hyperopia (Figure 2), in which a reduction of hyperopia of 5.00 D was attempted. In these eyes, the mean correction was 4.33 D (range 2.12 D to 6.75 D; standard deviation 1.36 D). The results in monovision eyes show a similar trend of undercorrection (Table 4). The average amount of correction attempted in these eyes was 3.42 D; the average obtained was 2.59 D, with a standard deviation of 0.85 D. The range of attempted correction was 1.50 to 5.00 D; the range achieved was 1.13 to 3.88 D, reflecting the trend toward undercorrection in the higher ranges. While these eyes were targeted for 1.50 D of myopia, functional success was achieved with any result between D and D, which was obtained in 4 7% of eyes. The intraoperative measurement of the diameter of dissection achieved was within 0.1 mm of attempted diameter in all eyes. Complications included delayed Table 4. Results in the 17 eyes targeted for monovision eyes. Targeted spherical equivalent was D, with functional success between D and D. Note tendency for undercorrection. Range (Diopters) to to plano > Number of Eyes Percentage J CATARACfREFRACfSURG-VOL21, JULY
5 2 N=S Fig. 2. (Kezirian) Postoperative versus preoperative mean spherical equivalents, plotted with 1 standard deviation, for 45 eyes targeted for emmetropia. Note the increased tendency for undercorrection and increased scatter, with higher levels of preoperative hyperopia. i 1.5 e 1,.;.; i a; 0.6 N=16 N=16 ~ I i -0.6 O ~ T ~-0-3--~r T _T_0_6 ~ N=5 Pre-Operative Spherical Equivalent Range (DioptersJ epithelialization in two eyes, with eventual healing and full recovery. Interface debris was present in almost all eyes to some extent, although it was not deemed enough to cause symptoms in any. Most patients with over 3.00 D of correction complained of nighttime glare when driving. This generally improved between the one and six month visits, by history. Glare complaints were not objectively quantified. Diurnal fluctuation was not reported after the first month. Initial irregular astigmatism (astigmatism associated with asymmetric topography and with decreased best corrected visual acuity of one line or more) improved between one and six months. However, insufficient data were recorded to quantify this observation further. There were no dislocated caps or infections in this series. DISCUSSION This preliminary report presents the results of H-ALK in a retrospective consecutive series of 85 eyes. It shows that H-ALK is effective in the treatment of low to moderate hyperopia, although concerns about long-term stability, predictability, and irregular astigmatism remain. Hyperopic ALK makes a deep, lamellar dissection in the cornea, which permits the posterior lamellae to bow forward under the lop of the eye. The ectasia produced is immediate and visibly apparent at the time of surgery. In this study, the ectasia was stable, with no observed tendency for myopic progression beyond the original correction. The amount of correction achieved is determined by the cut's diameter and depth. Ruiz's nomogram (Table 1) calls for a depth between 54% and 74% of thinnest pachymetry, increasing the amount of correction by decreasing the diameter of the applanation ring (optical zone) and increasing the depth of the dissection. In this series, 76% of the 45 eyes targeted for emmetropia achieved uncorrected visual acuities of 20/40 or better. Spherical equivalents correlated well with these results, with 78.6% of eyes falling in the range of to D. In eyes targeted for a D (monovision) correction, only 47% achieved a successful result of a spherical equivalent between and D, with a majority of eyes undercorrected. In both these groups, the eyes in which we attempted more correction were the ones most likely to be undercorrected. However, these data must be interpreted with one limitation in mind: They compare preoperative cycloplegic refractions with postoperative manifest refractions. In future studies, to understand the refractive effects better, cycloplegic refractions should be done on all postoperative examinations. These data compare favorably to the results of other procedures for hyperopia. With hexagonal keratotomy, Casebeer and Phillips 6 achieved a spherical equivalent result between and D in 52.2% of cases. In our series we achieved this result in 78.6% of eyes with similar preoperative refractions. With thermokeratoplasty, Neumann 10 reports a 60% rate of correction within 1.00 D of emmetropia at 2 months postoperatively; this fell to 17% by 9 to 12 months. Beyond demonstrating the predictability and efficacy of H-ALK, this series illustrates some strengths and weaknesses of the Ruiz nomogram. Table 3 and Figure 2 describe good predictability and little scatter of results in corrections up to 3.00 D, with increased tendency toward undercorrection and increased scatter with corrections beyond this range. Thus, in a 2.50 D hyperope, the surgeon can be confident that surgery will bring the patient to a to D correction of emmetropia, within one standard deviation, or approximately two thirds of the time. On the other hand, in an attempted 5.00 D correction, the average eye will remain approximately 1.50 D hyperopic, with a 1.50 D standard deviation, using the Ruiz nomogram. It would be desirable to increase the amount of correction in higher levels of hyperopia. Table 1 shows that Ruiz already calls for a depth of up to 74% in the correction of a 5.00 hyperope, which limits the available options. In our practice, we limit H-ALK to eyes with less than 4.00 D of desired correction, which 390 J CATARACT REFRACT SURG-VOL 21, JULY 1995
6 on COMPARATIVE DIOPTRIC MAPS Fig. 3. (Kezirian) Corneal topography of a patient who had bilateral H-ALK. In the left eye, too large a flap base (hinge) was made because the dissection did not proceed far enough in the nasal direction. This led to a nasal squaring of the ectasia, which was noticed by the patient as glare and distortion. Note the well-defined central ectasia in both eyes. has resulted in a more satisfied patient population overall. Monovision eyes, in which over 3.00 D of correction is desired, are now targeted for D spherical equivalent, instead of D as reported in this series, to compensate for the tendency of these eyes to be undercorrected. If less than 3.00 D correction is desired, the eyes are targeted for D final refraction. It would also be desirable to decrease the scatter of results. The issue of second or enhancement procedures for these eyes remains unsettled. We are currently performing a series of enhancements on undercorrected eyes by making a second, deeper pass with the microkeratome at an optical zone size 0.2 mm larger than the original. This presents the potential complication of layer separation during surgery, which would be difficult to correct. The risks of uncontrolled ectasia and irregular astigmatism are also of concern. In eyes that correct into the myopic range, radial keratotomy can reportedly be performed, II although the long-term stability of RK over H-ALK has yet to be established. These eyes are among the first in North America to have H-ALK using a flap technique, leaving the ca~ attached by a hinge located in the nasal quadrant. 1 Two observations regarding the use of a flap in this procedure may be helpful to other surgeons. First, no caps dislocated postoperatively. However, this successful rate of cap adhesion may be more related to preoperative screening of patients than to use of the flap. All patients were examined clinically for evidence of epitheliopathy, especially from dry eyes, and for evidence of compromised endothelial function, such as guttata. Patients with these findings were disqualified for surgery. In two subsequent eyes, cap dislocations occurred, despite the presence of the hinged flap. These eyes had had previous intraocular surgery and both had polymorphism and polymegathism on preoperative examinations of the endothelium. During surgery, both experienced epithelial loss, thought to be related to the subsequent development of stromal edema, and cap dislocation. The use of a flap does not guarantee against dislocation, and extra caution should be exercised when performing H-ALK in eyes that have had previous surgery. Second, too large a flap base (hinge) can lead to a nasal squaring of the ectasia, which can be noticed by the patient as glare and distortion (Figure 3) and appears to induce against-the-rule astigmatism. Should this occur, the dissection can be extended by hand, using a #65 Beaver blade or a Suarez spreader. In this series, the ideal size of the hinge was 30 arc degrees of the dissection. Glare was subjectively reported to be associated with higher amounts of correction and usually became less bothersome with time, usually four to eight weeks. However, since this study did not quantitate glare complaints, the extent of glare cannot be ascertained. Future studies may provide further information about this complaint and should measure glare quantitatively. Finally, the issue of simultaneous astigmatism correction remains unresolved. In this series, 10 of the 25 eyes ( 40%) that had simultaneous astigmatism correction were undercorrected for astigmatism. None were overcorrected. There was no noted effect on the hyperopic correction caused by performing astigmatism correction. Many hyperopic eyes have significant coexisting astigmatism, and reducing, if not eliminating, that astigmatism can greatly improve the visual results J CATARACT REFRACT SURG-VOL 2I, JULY
7 of surgery. The astigmatism correction is performed at the same setting as the H-ALK, but after the suction rings are removed from the eye and lop normalized. One possible reason for the astigmatic undercorrections was the use of paracentral pachymetry for setting the knife, since on re-operation many of these eyes were observed to have peripheral pachymetries more than 150 JJ.m thicker than the paracentral readings used in setting the blade in the initial procedure. A study is now underway to determine the efficacy of using peripheral pachymetry to determine knife setting during the primary correction. While simultaneous astigmatism correction may have benefitted some eyes in this series, predictability was not adequate to recommend this practice to all surgeons. This study was limited by its retrospective design and because it was performed when the technique was just being introduced into the United States (May to December 1993). Therefore, some of the techniques introduced later, such as the use of intraoperative pachymetry to measure the depth of dissection, were not used. Because glare was not clinically measured, it could not be compared against glare encountered with other techniques. Follow-up was variable and would be expected to be better with a prospective study. These considerations might be applied in the design of future investigations of the procedure. Hyperopic ALK shows much promise in the correction of low to moderate hyperopia. With the equipment modifications that have been made since this series was performed, such as the stop to assist in flap creation, the procedure has become easier to perform. Long-term stability and improvements in predictability remain to be established. REFERENCES 1. Barraquer Jl. Results of hypermetropic keratomileusis, Int Ophthalmol Clin 1983; 23(3): Neumann AC, Sanders D, Raanan M, DeLuca M. Hyperopic thermokeratoplasty: clinical evaluation. J Cataract Refract Surg 1991; 17: Seiler T, Matallana M, Bende T. Laser thermokeratoplasty by means of a pulsed holmium:yag laser for hyperopic correction. Refract Corneal Surg 1991; 6: Jensen RP. Experience with hexagonal keratotomy (letter). J Cataract Refract Surg 1988; 14: Neumann AC, McCarty GR. Hexagonal keratotomy for correction of low hyperopia: preliminary results of a prospective study. J Cataract Refract Surg 1988; 14: Casebeer JC, Phillips SG. Hexagonal keratotomy; an historical review and assessment of 46 cases. Ophthalmol Clin North Am 1992; 5(4): Gilbert ML, Roth AS, Friedlander MH. Corneal flattening by shallow circular trephination in human eye bank eyes. Refract Corneal Surg 1990; 6: Barraquer JI. Keratomileusis and keratophakia. In: Rycroft PV, ed, Corneo-Plastic Surgery; Proceedings of the Second International Corneo-Plastic Conference, London, New York, Pergamon Press, 1969; McDonald MB, Kaufman HE, Aquavella JV, et al. The nationwide study of epikeratophakia for myopia. Am J Ophthalmol 1987; 103: Neumann AC. Thermokeratoplasty for hyperopia. Ophthalmol Clin North Am 1992; 5(4): Hollis S. Hyperopic lamellar keratoplasty. In: Rozakis GW, ed, Refractive Lamellar Keratoplasty. Thorofare, NJ, Slack Inc, 1994; Pallikaris IG, Papatzanaki ME, Siganos DS, Tsilimbaris MK. A corneal flap technique for laser in situ keratomileusis; human studies. Arch Ophthalmol 1991; 109: J CATARACT REFRACT SURG-VOL 21, JULY 1995
The two currently accepted methods for correcting
 New Technique Therapeutic Alloplastic Laser in situ Keratomileusis for Myopia Arturo Maldonado-Bas, MD; Ruben Pulido-Garcia, MD ABSTRACT BACKGROUND: A new technique, therapeutic alloplastic laser in situ
New Technique Therapeutic Alloplastic Laser in situ Keratomileusis for Myopia Arturo Maldonado-Bas, MD; Ruben Pulido-Garcia, MD ABSTRACT BACKGROUND: A new technique, therapeutic alloplastic laser in situ
The pinnacle of refractive performance.
 The pinnacle of refractive performance. WaveLight REFRACTIVE PORTFOLIO Advancing REFRACTIVE SURGERY Contoura Vision sets a new standard in LASIK outcomes More than 98% of patients would choose it again.
The pinnacle of refractive performance. WaveLight REFRACTIVE PORTFOLIO Advancing REFRACTIVE SURGERY Contoura Vision sets a new standard in LASIK outcomes More than 98% of patients would choose it again.
LASIK. What is LASIK? Eye Words to Know. Who is a good candidate for LASIK?
 2014 2015 What is? (laser in situ keratomileusis) is a type of refractive surgery. This kind of surgery uses a laser to treat vision problems caused by refractive errors. You have a refractive error when
2014 2015 What is? (laser in situ keratomileusis) is a type of refractive surgery. This kind of surgery uses a laser to treat vision problems caused by refractive errors. You have a refractive error when
CLINICAL SCIENCES. Management of Post-LASIK Corneal Ectasia With Intacs Inserts
 Management of Post-LASIK Corneal Ectasia With Intacs Inserts One-Year Results CLINICAL SCIENCES George D. Kymionis, MD, PhD; Charalambos S. Siganos, MD, PhD; George Kounis, BSc; Nikolaos Astyrakakis, OD;
Management of Post-LASIK Corneal Ectasia With Intacs Inserts One-Year Results CLINICAL SCIENCES George D. Kymionis, MD, PhD; Charalambos S. Siganos, MD, PhD; George Kounis, BSc; Nikolaos Astyrakakis, OD;
INFORMED CONSENT FOR LASER IN SITU KERATOMILEUSIS ( LASIK )
 INFORMED CONSENT FOR LASER IN SITU KERATOMILEUSIS ( LASIK ) This information is to help you make an informed decision about having Laser In Situ Keratomileusis (LASIK), a laser vision correction procedure
INFORMED CONSENT FOR LASER IN SITU KERATOMILEUSIS ( LASIK ) This information is to help you make an informed decision about having Laser In Situ Keratomileusis (LASIK), a laser vision correction procedure
Laser in situ keratomileusis (LASIK) has proven to be
 Autorefractometry after laser in situ keratomileusis Dimitrios S. Siganos, MD, PhD, Corina Popescu, MD, Nikolaos Bessis, DOpt, Georgios Papastergiou, MD Purpose: To correlate cycloplegic subjective refraction
Autorefractometry after laser in situ keratomileusis Dimitrios S. Siganos, MD, PhD, Corina Popescu, MD, Nikolaos Bessis, DOpt, Georgios Papastergiou, MD Purpose: To correlate cycloplegic subjective refraction
IntraLASIK Correction Of Nearsightedness, Farsightedness and Astigmatism Using IntraLase TM Technology
 IntraLASIK Correction Of Nearsightedness, Farsightedness and Astigmatism Using IntraLase TM Technology INDICATIONS AND PROCEDURE This information is being provided to you so that you can make an informed
IntraLASIK Correction Of Nearsightedness, Farsightedness and Astigmatism Using IntraLase TM Technology INDICATIONS AND PROCEDURE This information is being provided to you so that you can make an informed
SAMPLE LASIK. What is LASIK? Eye Words to Know. Who is a good candidate for LASIK?
 What is? is a type of refractive surgery. This kind of surgery uses a laser to treat vision problems caused by refractive errors. You have a refractive error when your eye does not refract (bend) light
What is? is a type of refractive surgery. This kind of surgery uses a laser to treat vision problems caused by refractive errors. You have a refractive error when your eye does not refract (bend) light
ONE THOUSAND WAVEFRONT GIDED TREATMENT ON MICROSCAN VISUM. Mickael Yablokov. I have no any financial interests in any products mentioned in this paper
 ONE THOUSAND WAVEFRONT GIDED TREATMENT ON MICROSCAN VISUM Mickael Yablokov I have no any financial interests in any products mentioned in this paper Ophthalmology clinic Eye Surgery, Kostroma, Russia Goal
ONE THOUSAND WAVEFRONT GIDED TREATMENT ON MICROSCAN VISUM Mickael Yablokov I have no any financial interests in any products mentioned in this paper Ophthalmology clinic Eye Surgery, Kostroma, Russia Goal
Description of iatrogenic corneal ectasia in patients without traditional risk factors
 ARTICLE Description of iatrogenic corneal ectasia in patients without traditional risk factors Julio Ortega-Usobiaga, MD, PhD 1 ; Rosario Cobo-Soriano, MD, PhD 1 ; Fernando Llovet-Osuna, MD, PhD 1 ; Stephan
ARTICLE Description of iatrogenic corneal ectasia in patients without traditional risk factors Julio Ortega-Usobiaga, MD, PhD 1 ; Rosario Cobo-Soriano, MD, PhD 1 ; Fernando Llovet-Osuna, MD, PhD 1 ; Stephan
Conductive keratoplasty (CK) (Refractec, Inc.) is a
 Conductive keratoplasty to correct residual hyperopia after corneal surgery Ian F. Comaish, FRCOphth, Michael A. Lawless, FRACO, FRCOphth Conductive keratoplasty (CK) is an electrical-current-based technique
Conductive keratoplasty to correct residual hyperopia after corneal surgery Ian F. Comaish, FRCOphth, Michael A. Lawless, FRACO, FRCOphth Conductive keratoplasty (CK) is an electrical-current-based technique
Cataract Surgery in the Patient with a History of LASIK or PRK
 Cataract Surgery in the Patient with a History of LASIK or PRK #56996-RS April 2018 Sebastian Lesniak, MD Matossian Eye Associates None Disclosures Bio Matossian Eye Associates, Hopewell NJ, 7/2015 Present
Cataract Surgery in the Patient with a History of LASIK or PRK #56996-RS April 2018 Sebastian Lesniak, MD Matossian Eye Associates None Disclosures Bio Matossian Eye Associates, Hopewell NJ, 7/2015 Present
Refractive Surgery Dilemma
 Refractive Surgery Dilemma Section Editor: lireza aradaran-rafii, MD CSE PRESENTTION 33-year-old man seeking refractive surgery presented with refractive error of -1.75-4.0 20 in the right and -0.75-2.5
Refractive Surgery Dilemma Section Editor: lireza aradaran-rafii, MD CSE PRESENTTION 33-year-old man seeking refractive surgery presented with refractive error of -1.75-4.0 20 in the right and -0.75-2.5
Recent concerns regarding the depth of tissue ablation with
 Volume Estimation of Excimer Laser Tissue Ablation for Correction of Spherical Myopia and Hyperopia Damien Gatinel, 1 Thanh Hoang-Xuan, 1 and Dimitri T. Azar 1,2 PURPOSE. To determine the theoretical volumes
Volume Estimation of Excimer Laser Tissue Ablation for Correction of Spherical Myopia and Hyperopia Damien Gatinel, 1 Thanh Hoang-Xuan, 1 and Dimitri T. Azar 1,2 PURPOSE. To determine the theoretical volumes
Flap characteristics, predictability, and safety of the Ziemer FEMTO LDV femtosecond laser with the disposable suction ring for LASIK
 (2014) 28, 66 71 & 2014 Macmillan Publishers Limited All rights reserved 0950-222X/14 www.nature.com/eye CLINICAL STUDY Flap characteristics, predictability, and safety of the Ziemer FEMTO LDV femtosecond
(2014) 28, 66 71 & 2014 Macmillan Publishers Limited All rights reserved 0950-222X/14 www.nature.com/eye CLINICAL STUDY Flap characteristics, predictability, and safety of the Ziemer FEMTO LDV femtosecond
Corporate Medical Policy
 Corporate Medical Policy Refractive Surgery File Name: Origination: Last CAP Review: Next CAP Review: Last Review: refractive_surgery 4/1981 6/2017 6/2018 6/2017 Description of Procedure or Service The
Corporate Medical Policy Refractive Surgery File Name: Origination: Last CAP Review: Next CAP Review: Last Review: refractive_surgery 4/1981 6/2017 6/2018 6/2017 Description of Procedure or Service The
Wavefront-optimized Versus Wavefrontguided LASIK for Myopic Astigmatism With the ALLEGRETTO WAVE: Three-month Results of a Prospective FDA Trial
 Wavefront-optimized Versus Wavefrontguided LASIK for Myopic Astigmatism With the ALLEGRETTO WAVE: Three-month Results of a Prospective FDA Trial Karl G. Stonecipher, MD; Guy M. Kezirian, MD, FACS ABSTRACT
Wavefront-optimized Versus Wavefrontguided LASIK for Myopic Astigmatism With the ALLEGRETTO WAVE: Three-month Results of a Prospective FDA Trial Karl G. Stonecipher, MD; Guy M. Kezirian, MD, FACS ABSTRACT
Clinical experience of 9,000 small aperture Inlays for presbyopia correction
 Clinical experience of 9,000 small aperture Inlays for presbyopia correction Minoru Tomita, MD, PhD Shinagawa LASIK Center, Tokyo, Japan September 7 th, 2012, ISOP meeting in Tokyo, JAPAN 1,060,666 Femto
Clinical experience of 9,000 small aperture Inlays for presbyopia correction Minoru Tomita, MD, PhD Shinagawa LASIK Center, Tokyo, Japan September 7 th, 2012, ISOP meeting in Tokyo, JAPAN 1,060,666 Femto
ALTERNATIVES TO PHAKIC IMPLANT SURGERY
 Visian ICL Consent INTRODUCTION This information is being provided to you so that you can make an informed decision about having eye surgery to reduce or eliminate your nearsightedness. Only you and your
Visian ICL Consent INTRODUCTION This information is being provided to you so that you can make an informed decision about having eye surgery to reduce or eliminate your nearsightedness. Only you and your
IOL Power Calculation for Children
 1 IOL Power Calculation for Children Rupal H. Trivedi, MD MSCR M. Edward Wilson, MD The authors have no financial interest in the subject matter of this presentation. Intraocular lens (IOL) implantation
1 IOL Power Calculation for Children Rupal H. Trivedi, MD MSCR M. Edward Wilson, MD The authors have no financial interest in the subject matter of this presentation. Intraocular lens (IOL) implantation
Nature and Science 2017;15(11) Mohamed Elmoddather. MD
 Outcome of PRK in Management of Post LISIK Residual Myopia and Myopic Astigmatism Mohamed Elmoddather. MD Ophthalmology Faculty of Medicine, Al-Azhar University, Assuit, Egypt shahdmsaleh@hotmail.com Abstract:
Outcome of PRK in Management of Post LISIK Residual Myopia and Myopic Astigmatism Mohamed Elmoddather. MD Ophthalmology Faculty of Medicine, Al-Azhar University, Assuit, Egypt shahdmsaleh@hotmail.com Abstract:
Summary Recommendations for Keratorefractive Laser Surgery June 2013
 Summary Recommendations for Keratorefractive Laser Surgery June 2013 Background Laser assisted in-situ keratomileusis (LASIK) surgery is the most commonly performed keratorefractive surgery; altering the
Summary Recommendations for Keratorefractive Laser Surgery June 2013 Background Laser assisted in-situ keratomileusis (LASIK) surgery is the most commonly performed keratorefractive surgery; altering the
Abdel Rahman ElSebaey, MD, PhD.
 Surface Ablation Refractive Surgery Abdel Rahman ElSebaey, MD, PhD. Menoufia University History Correction of optical defects of human eye started 1200 AD. Spherical error corrected by spectacle on 13
Surface Ablation Refractive Surgery Abdel Rahman ElSebaey, MD, PhD. Menoufia University History Correction of optical defects of human eye started 1200 AD. Spherical error corrected by spectacle on 13
FUCH S DYSTROPHY & CATARACT SURGERY TREATMENT ALGORITHM
 FUCH S DYSTROPHY & CATARACT SURGERY TREATMENT ALGORITHM ΙΟΑΝΝΙS Α. MALLIAS, MD, PHD Director of the Dept. of Ophthalmology, Mediterraneo Hospital, Glyfada, Athens, Greece Clinical Fellow in Cornea and
FUCH S DYSTROPHY & CATARACT SURGERY TREATMENT ALGORITHM ΙΟΑΝΝΙS Α. MALLIAS, MD, PHD Director of the Dept. of Ophthalmology, Mediterraneo Hospital, Glyfada, Athens, Greece Clinical Fellow in Cornea and
Lens and Cataract Surgery Update 2008
 efocus Innovation. Leadership. Passion for Perfection PACIFIC V I S I O N I N S T I T U T E Life in Focus Issue 029 415.922.9500 --- www.pacificvision.org December 2008 Lens and Cataract Surgery Update
efocus Innovation. Leadership. Passion for Perfection PACIFIC V I S I O N I N S T I T U T E Life in Focus Issue 029 415.922.9500 --- www.pacificvision.org December 2008 Lens and Cataract Surgery Update
Pearls for the Refractive Technician Fadiah Alkhawaldeh, IMBA, COT, ROUB
 Pearls for the Refractive Technician Fadiah Alkhawaldeh, IMBA, COT, ROUB Cleveland Clinic Cole Eye Institute OOS, Columbus, OH February, 2014 alkhawf@ccf.org NO FINANCIAL DISCLOSURES A Puzzle of an Eye
Pearls for the Refractive Technician Fadiah Alkhawaldeh, IMBA, COT, ROUB Cleveland Clinic Cole Eye Institute OOS, Columbus, OH February, 2014 alkhawf@ccf.org NO FINANCIAL DISCLOSURES A Puzzle of an Eye
Laser In-situ Keratomileusis (LASIK) For the Correction of Nearsightedness, Farsightedness and Astigmatism I. Introduction II.
 REV 011717 PATIENT CONSENT FORM Laser In-situ Keratomileusis (LASIK) For the Correction of Nearsightedness, Farsightedness and Astigmatism I. Introduction Laser-assisted in situ keratomileusis, or LASIK,
REV 011717 PATIENT CONSENT FORM Laser In-situ Keratomileusis (LASIK) For the Correction of Nearsightedness, Farsightedness and Astigmatism I. Introduction Laser-assisted in situ keratomileusis, or LASIK,
~ 1 ~ CLINIQUE LASERVUE. Informed Consent Form for LASIK
 ~ 1 ~ CLINIQUE LASERVUE Informed Consent Form for LASIK Please read the following information and consent form very carefully. Your initials indicate that you understand all of the necessary patient information
~ 1 ~ CLINIQUE LASERVUE Informed Consent Form for LASIK Please read the following information and consent form very carefully. Your initials indicate that you understand all of the necessary patient information
PHOTOREFRACTIVE KERATECTOMY (PRK) PATIENT INFORMATION BOOKLET
 616.365.5775 www.keillasik.com PHOTOREFRACTIVE KERATECTOMY (PRK) PATIENT INFORMATION BOOKLET Please read this entire booklet. Discuss its contents with your doctor so that questions are answered to your
616.365.5775 www.keillasik.com PHOTOREFRACTIVE KERATECTOMY (PRK) PATIENT INFORMATION BOOKLET Please read this entire booklet. Discuss its contents with your doctor so that questions are answered to your
Cataract Surgery: Patient Information
 Cataract Surgery: Patient Information How do the Eyes Work? As light enters the eye, it first passes through the cornea the clear window of the eye. Because the cornea is curved, the light rays bend (refract).
Cataract Surgery: Patient Information How do the Eyes Work? As light enters the eye, it first passes through the cornea the clear window of the eye. Because the cornea is curved, the light rays bend (refract).
Effects of Intracorneal Ring Segment on Corneal Biomechanics in Keratoconic Eyes. Abstract
 Effects of Intracorneal Ring Segment on Corneal Biomechanics in Keratoconic Eyes Javad Amoozadeh, MD 1 Nima Mirzaee Rad, MD 2 Amir Houshang Beheshtnejad, MD 3 Ahmad Kheirkhah, MD 1 Hassan Hashemi, MD 4,5
Effects of Intracorneal Ring Segment on Corneal Biomechanics in Keratoconic Eyes Javad Amoozadeh, MD 1 Nima Mirzaee Rad, MD 2 Amir Houshang Beheshtnejad, MD 3 Ahmad Kheirkhah, MD 1 Hassan Hashemi, MD 4,5
PresbyMax Outcomes in Myopia, Hyperopia, Emmetropia and Patients post Lasik
 PresbyMax Outcomes in Myopia, Hyperopia, Emmetropia and Patients post Lasik SCHWIND eye-tech-solutions Lunch Symposium Prof. Jorge L. Alió MD, PhD. UNIVERSIDAD MIGUEL HERNÁNDEZ VISSUM INSTITUTO OFTALMOLÓGICO
PresbyMax Outcomes in Myopia, Hyperopia, Emmetropia and Patients post Lasik SCHWIND eye-tech-solutions Lunch Symposium Prof. Jorge L. Alió MD, PhD. UNIVERSIDAD MIGUEL HERNÁNDEZ VISSUM INSTITUTO OFTALMOLÓGICO
INFORMED CONSENT FOR PHOTOREFRACTIVE KERATECTOMY (PRK) AND ADVANCE SURFACE ABLATION (ASA)
 INFORMED CONSENT FOR PHOTOREFRACTIVE KERATECTOMY (PRK) AND ADVANCE SURFACE ABLATION (ASA) This information and the Patient Information booklet must be reviewed so you can make an informed decision regarding
INFORMED CONSENT FOR PHOTOREFRACTIVE KERATECTOMY (PRK) AND ADVANCE SURFACE ABLATION (ASA) This information and the Patient Information booklet must be reviewed so you can make an informed decision regarding
Keratoconus Clinic. Optometric Co-management Opportunities
 Keratoconus Clinic Optometric Co-management Opportunities The Bochner Eye Institute established the first Keratoconus Clinic in Canada in 2008. The consultation and advanced imaging are OHIP covered. All
Keratoconus Clinic Optometric Co-management Opportunities The Bochner Eye Institute established the first Keratoconus Clinic in Canada in 2008. The consultation and advanced imaging are OHIP covered. All
Original Article High myopia as a risk factor for post-lasik ectasia: a case report
 Original Article High myopia as a risk factor for post-lasik ectasia: a case report Mona Harissi-Dagher, MD, a,b Sonja A. F. Frimmel, c and Samir Melki, MD, PhD a,d Author affiliations: a Massachusetts
Original Article High myopia as a risk factor for post-lasik ectasia: a case report Mona Harissi-Dagher, MD, a,b Sonja A. F. Frimmel, c and Samir Melki, MD, PhD a,d Author affiliations: a Massachusetts
In Practice. Surgical Procedures Diagnosis New Drugs
 In Practice Surgical Procedures Diagnosis New Drugs 62 65 A New Carpet Over Broken Tiles Facing an eye with multiple, deep radial keratotomy cuts? Arun Gulani describes how the right mindset and technique
In Practice Surgical Procedures Diagnosis New Drugs 62 65 A New Carpet Over Broken Tiles Facing an eye with multiple, deep radial keratotomy cuts? Arun Gulani describes how the right mindset and technique
Clear Advantage Vision Correction Center INFORMED CONSENT FOR LASIK AND FEMTOSECOND LASER
 Clear Advantage Vision Correction Center INFORMED CONSENT FOR LASIK AND FEMTOSECOND LASER PLEASE READ THE FOLLOWING PAGES CAREFULLY AND INITIAL AND SIGN WHERE INDICATED. PLEASE DO NOT SIGN ANY SECTION
Clear Advantage Vision Correction Center INFORMED CONSENT FOR LASIK AND FEMTOSECOND LASER PLEASE READ THE FOLLOWING PAGES CAREFULLY AND INITIAL AND SIGN WHERE INDICATED. PLEASE DO NOT SIGN ANY SECTION
LASIK INFORMED CONSENT INITIAL TREATMENT
 LASIK INFORMED CONSENT INITIAL TREATMENT PLEASE READ THE FOLLOWING PAGES CAREFULLY AND INITIAL AND SIGN WHERE INDICATED. PLEASE DO NOT SIGN ANY SECTION THAT YOU HAVE NOT READ OR DO NOT UNDERSTAND. SECTION
LASIK INFORMED CONSENT INITIAL TREATMENT PLEASE READ THE FOLLOWING PAGES CAREFULLY AND INITIAL AND SIGN WHERE INDICATED. PLEASE DO NOT SIGN ANY SECTION THAT YOU HAVE NOT READ OR DO NOT UNDERSTAND. SECTION
Advanced Eyecare of Orange County/ Kim T. Doan, M.D.
 Patient Information Sheet: Cataract Surgery And/Or Implantation of an Intraocular Lens This information is given to you so that you can prepare for the discussion with your eye surgeon. This document will
Patient Information Sheet: Cataract Surgery And/Or Implantation of an Intraocular Lens This information is given to you so that you can prepare for the discussion with your eye surgeon. This document will
Photorefractive Keratectomy as A Retreatment of Residual Myopia after Previous Laser in Situ Keratomileusis
 Photorefractive Keratectomy as A Retreatment of Residual Myopia after Previous Laser in Situ Keratomileusis Alireza Ashtari, MD 1 Hassan Razmju, MD 2 Amin Masjedi, MD 3 Alireza Zandi, MD 1 Mehdi Tavakoli,
Photorefractive Keratectomy as A Retreatment of Residual Myopia after Previous Laser in Situ Keratomileusis Alireza Ashtari, MD 1 Hassan Razmju, MD 2 Amin Masjedi, MD 3 Alireza Zandi, MD 1 Mehdi Tavakoli,
CATARACT SURGERY AFTER RADIAL KERATOTOMY
 AFTER RADIAL KERATOTOMY How to avoid disappointment. BY BERNARD MATHYS, MD CATARACT SURGERY Radial keratotomy (RK; Figure 1) was a popular refractive surgical procedure to correct myopia in the 1970s and
AFTER RADIAL KERATOTOMY How to avoid disappointment. BY BERNARD MATHYS, MD CATARACT SURGERY Radial keratotomy (RK; Figure 1) was a popular refractive surgical procedure to correct myopia in the 1970s and
Simultaneous Topography-guided Surface Ablation with Collagen Cross-linking for Keratoconus
 IJKECD Case series Simultaneous Topography-guided Surface Ablation with Collagen 10.5005/jp-journals-10025-1124 Cross-linking for Keratoconus Simultaneous Topography-guided Surface Ablation with Collagen
IJKECD Case series Simultaneous Topography-guided Surface Ablation with Collagen 10.5005/jp-journals-10025-1124 Cross-linking for Keratoconus Simultaneous Topography-guided Surface Ablation with Collagen
Author s Affiliation. Original Article. Visual outcomes after LASIK (laser-assisted in-situ keratomileusis) for various refractive errors.
 Original Article Visual outcomes after LASIK (laser-assisted in-situ keratomileusis) for various refractive errors. Author s Affiliation Sobia Tufail Imran Ahmad Asad Aslam Khan Correspondence Author:
Original Article Visual outcomes after LASIK (laser-assisted in-situ keratomileusis) for various refractive errors. Author s Affiliation Sobia Tufail Imran Ahmad Asad Aslam Khan Correspondence Author:
SAMPLE WHAT LASIK CAN DO
 DECIDING ON LASIK Imagine being able to work, drive, and play sports without having to depend on glasses or contact lenses. LASIK (laser in-situ keratomileusis) may make this a reality for you. This laser
DECIDING ON LASIK Imagine being able to work, drive, and play sports without having to depend on glasses or contact lenses. LASIK (laser in-situ keratomileusis) may make this a reality for you. This laser
SCHWIND CAM Perfect Planning wide range of applications
 SCHWIND CAM Perfect Planning wide range of applications ORK-CAM PresbyMAX PTK-CAM 2 SCHWIND CAM the system solution The modular design of the SCHWIND CAM offers customised treatment planning for a uniquely
SCHWIND CAM Perfect Planning wide range of applications ORK-CAM PresbyMAX PTK-CAM 2 SCHWIND CAM the system solution The modular design of the SCHWIND CAM offers customised treatment planning for a uniquely
Presby LASIK Topographies
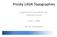 Presby LASIK Topographies SurgiVision Consultants, Inc. DataLink kforum June 1, 2009 Not for Distribution Introduction Case review of presby LASIK procedures performed with the WaveLight Eye Q Laser Presentation
Presby LASIK Topographies SurgiVision Consultants, Inc. DataLink kforum June 1, 2009 Not for Distribution Introduction Case review of presby LASIK procedures performed with the WaveLight Eye Q Laser Presentation
Louis Probst. Commitment to Optometry. Cycloplegic Exam. Steroid free PRK. LASIK Enhancements made Ridiculously Simple 8/18/2017
 Louis Probst LASIK Enhancements made Ridiculously Simple Louis E. Probst MD National Medical Director, TLC Chief Surgeon, Central Midwest, USA TLC surgeon 22 years 7 books, 80 chapters, 50 papers, 11 instruments
Louis Probst LASIK Enhancements made Ridiculously Simple Louis E. Probst MD National Medical Director, TLC Chief Surgeon, Central Midwest, USA TLC surgeon 22 years 7 books, 80 chapters, 50 papers, 11 instruments
Cataract Surgery: What You Must Know Before Having It Done
 DAVID D. RICHARDSON, MD, INC. DAVID RICHARDSON, M.D. SAN MARINO EYE 2020 Huntington Drive San Marino, CA 91108 Telephone: (626) 289-7856 Fax: (626) 284-6532 Cataract Surgery: What You Must Know Before
DAVID D. RICHARDSON, MD, INC. DAVID RICHARDSON, M.D. SAN MARINO EYE 2020 Huntington Drive San Marino, CA 91108 Telephone: (626) 289-7856 Fax: (626) 284-6532 Cataract Surgery: What You Must Know Before
LASIK for 6.00 to D of Myopia With up to 3.00 D of Cylinder Using the ALLEGRETTO WAVE: 3- and 6-month Results With the 200- and 400-Hz Platforms
 LASIK for 6.00 to 12.00 D of Myopia With up to 3.00 D of Cylinder Using the ALLEGRETTO WAVE: 3- and 6-month Results With the 200- and 400-Hz Platforms Karl G. Stonecipher, MD; Guy M. Kezirian, MD; Megan
LASIK for 6.00 to 12.00 D of Myopia With up to 3.00 D of Cylinder Using the ALLEGRETTO WAVE: 3- and 6-month Results With the 200- and 400-Hz Platforms Karl G. Stonecipher, MD; Guy M. Kezirian, MD; Megan
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: endothelial_keratoplasty 9/2009 6/2018 6/2019 6/2018 Description of Procedure or Service Endothelial keratoplasty
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: endothelial_keratoplasty 9/2009 6/2018 6/2019 6/2018 Description of Procedure or Service Endothelial keratoplasty
The Egyptian Journal of Hospital Medicine (October 2018) Vol. 73 (9), Page
 The Egyptian Journal of Hospital Medicine (October 2018) Vol. 73 (9), Page 7580-7586 Outcome of PRK in Management of Post LISIK Residual Myopia and Myopic Astigmatism Department of Ophthalmology, Faculty
The Egyptian Journal of Hospital Medicine (October 2018) Vol. 73 (9), Page 7580-7586 Outcome of PRK in Management of Post LISIK Residual Myopia and Myopic Astigmatism Department of Ophthalmology, Faculty
Informed IntraLASIK Consent
 9201 Sunset Boulevard Suite 709 West Hollywood, CA 90069 Informed Intra Consent Phone 310. 275. 5533 Fax 310. 275. 5523 info@benjamineye.com www.benjamineye.com For the Correction of Nearsightedness, Farsightedness,
9201 Sunset Boulevard Suite 709 West Hollywood, CA 90069 Informed Intra Consent Phone 310. 275. 5533 Fax 310. 275. 5523 info@benjamineye.com www.benjamineye.com For the Correction of Nearsightedness, Farsightedness,
Informed Consent For Refractive Lens Exchange (RLE) For the Correction of Hyperopia (Farsightedness) Or Myopia (Nearsightedness)
 Informed Consent For Refractive Lens Exchange (RLE) For the Correction of Hyperopia (Farsightedness) Or Myopia (Nearsightedness) INTRODUCTION This surgery, called a refractive lens exchange or RLE, involves
Informed Consent For Refractive Lens Exchange (RLE) For the Correction of Hyperopia (Farsightedness) Or Myopia (Nearsightedness) INTRODUCTION This surgery, called a refractive lens exchange or RLE, involves
pre-laser cut pre-laser cut Pre-operative Known and Potential Complications of SMILE Failure to obtain an adequate suction
 pre-laser cut! Known and Potential Complications of SMILE Failure to obtain an adequate suction Walter Sekundo Correct treatment pack size (S in myopic cases) Philipps University Marburg/Germany Use speculum
pre-laser cut! Known and Potential Complications of SMILE Failure to obtain an adequate suction Walter Sekundo Correct treatment pack size (S in myopic cases) Philipps University Marburg/Germany Use speculum
Development of excimer lasers in eye surgery
 Photorefractive surgery is performed using an excimer laser in an attempt to correct refractive errors such as short-sightedness (myopia), astigmatism, and more recently long-sightedness (hypermetropia).
Photorefractive surgery is performed using an excimer laser in an attempt to correct refractive errors such as short-sightedness (myopia), astigmatism, and more recently long-sightedness (hypermetropia).
Patient Information: laser vision correction
 Consultation Document Patient Information: laser vision correction April 2016 Contents Section page 1 What is Laser Vision Correction? 3 2 What are the benefits? 3 3 How much does laser vision correction
Consultation Document Patient Information: laser vision correction April 2016 Contents Section page 1 What is Laser Vision Correction? 3 2 What are the benefits? 3 3 How much does laser vision correction
Trans Epithelial Surface Ablation A personal reflection over a collective experience
 Trans Epithelial Surface Ablation A personal reflection over a collective experience Dr S Mughal MBChB MSc FRCS(Glasg) MRCOphth DRCOphth CertLRS 15th International SCHWIND User Meeting July 17-20, 2014
Trans Epithelial Surface Ablation A personal reflection over a collective experience Dr S Mughal MBChB MSc FRCS(Glasg) MRCOphth DRCOphth CertLRS 15th International SCHWIND User Meeting July 17-20, 2014
Evaluation of The Accuracy of Sub Bowman s Keratomileusis (SBK) Microkeratome in Flap Creation during Lasik Surgery
 The Egyptian Journal of Hospital Medicine (April 2018) Vol. 71 (3), Page 2636-2642 Evaluation of The Accuracy of Sub Bowman s Keratomileusis (SBK) Microkeratome in Flap Creation during Lasik Surgery Hager
The Egyptian Journal of Hospital Medicine (April 2018) Vol. 71 (3), Page 2636-2642 Evaluation of The Accuracy of Sub Bowman s Keratomileusis (SBK) Microkeratome in Flap Creation during Lasik Surgery Hager
In recent years we have witnessed the rapid
 New Technique Laser Intrastromal Keratoplasty Case Report Mirko Jankov, MD; Michael Mrochen, PhD; Theo Seiler, MD, PhD ABSTRACT PURPOSE: To evaluate the feasibility of correcting high hyperopia by means
New Technique Laser Intrastromal Keratoplasty Case Report Mirko Jankov, MD; Michael Mrochen, PhD; Theo Seiler, MD, PhD ABSTRACT PURPOSE: To evaluate the feasibility of correcting high hyperopia by means
펨토초레이저와미세각막절삭기를이용한근시교정수술에서임상성적비교
 펨토초레이저와미세각막절삭기를이용한근시교정수술에서임상성적비교 4 Table. Summary of data about patient who had LASIK operation using second laser and keratome Age (years) Male:Female (eyes) Pre-op. IOP (mmhg) Pre-op SE * (D) Pre-op
펨토초레이저와미세각막절삭기를이용한근시교정수술에서임상성적비교 4 Table. Summary of data about patient who had LASIK operation using second laser and keratome Age (years) Male:Female (eyes) Pre-op. IOP (mmhg) Pre-op SE * (D) Pre-op
Trans Epithelial Surface Ablation A personal reflection over a collective experience
 Trans Epithelial Surface Ablation A personal reflection over a collective experience Dr S Mughal MBChB MSc FRCS(Glasg) MRCOphth DRCOphth CertLRS SCHWIND USERS LECTURE, BOOTH C13 ESCRS CONGRESS LONDON 2014
Trans Epithelial Surface Ablation A personal reflection over a collective experience Dr S Mughal MBChB MSc FRCS(Glasg) MRCOphth DRCOphth CertLRS SCHWIND USERS LECTURE, BOOTH C13 ESCRS CONGRESS LONDON 2014
INFORMED CONSENT FOR CATARACT SURGERY
 DESERT OPHTHALMOLOGY 1180 N Indian Canyon Drive W100 Palm Springs CA 92262 35900 Bob Hope Drive Suite 205 Rancho Mirage CA 92270 Phone (760) 320-8497 Fax (760) 320-5444 INFORMED CONSENT FOR CATARACT SURGERY
DESERT OPHTHALMOLOGY 1180 N Indian Canyon Drive W100 Palm Springs CA 92262 35900 Bob Hope Drive Suite 205 Rancho Mirage CA 92270 Phone (760) 320-8497 Fax (760) 320-5444 INFORMED CONSENT FOR CATARACT SURGERY
UPDATES OF REFRACTIVE SURGERY اليوم العلمي الثالث قسم البصريات كلية العلوم الصحية 14/3/2015
 UPDATES OF REFRACTIVE SURGERY اليوم العلمي الثالث قسم البصريات كلية العلوم الصحية 14/3/2015 1 Basic knowledge Refraction Refraction is the bending of light rays as they pass from one transparent medium
UPDATES OF REFRACTIVE SURGERY اليوم العلمي الثالث قسم البصريات كلية العلوم الصحية 14/3/2015 1 Basic knowledge Refraction Refraction is the bending of light rays as they pass from one transparent medium
WANG VISION INSTITUTE INFORMED CONSENT FOR INTACS INSERTS PRESCRIPTION INSERTS FOR TREATMENT OF PATIENTS WITH KERATOCONUS
 WANG VISION INSTITUTE INFORMED CONSENT FOR INTACS INSERTS PRESCRIPTION INSERTS FOR TREATMENT OF PATIENTS WITH KERATOCONUS A. INTRODUCTION: You are being offered the opportunity to receive a medical device
WANG VISION INSTITUTE INFORMED CONSENT FOR INTACS INSERTS PRESCRIPTION INSERTS FOR TREATMENT OF PATIENTS WITH KERATOCONUS A. INTRODUCTION: You are being offered the opportunity to receive a medical device
CLINIQUE LASERVUE. Informed Consent Form for Photo-Refractive Keratectomy (PRK)
 CLINIQUE LASERVUE Informed Consent Form for Photo-Refractive Keratectomy (PRK) Please read the following information and consent form very carefully. Your initials indicate that you understand all of the
CLINIQUE LASERVUE Informed Consent Form for Photo-Refractive Keratectomy (PRK) Please read the following information and consent form very carefully. Your initials indicate that you understand all of the
A Patients Guide to Excimer Laser Refractive Surgery
 A Patients Guide to Excimer Laser Refractive Surgery March 2006 Contents 1. Introduction 2. Understanding your refractive error 3. Changing the eye s focus by surgery (refractive surgery) 4. Indications
A Patients Guide to Excimer Laser Refractive Surgery March 2006 Contents 1. Introduction 2. Understanding your refractive error 3. Changing the eye s focus by surgery (refractive surgery) 4. Indications
Informed Consent For Cataract Surgery. And/Or Implantation of an Intraocular Lens INTRODUCTION
 Informed Consent For Cataract Surgery And/Or Implantation of an Intraocular Lens INTRODUCTION This information is given to you so that you can make an informed decision about having eye surgery. Take as
Informed Consent For Cataract Surgery And/Or Implantation of an Intraocular Lens INTRODUCTION This information is given to you so that you can make an informed decision about having eye surgery. Take as
LASER REFRACTIVE CENTER INFORMED CONSENT DOCUMENT PERIPHERAL CORNEAL RELAXING INCISION (PCRI)
 INTRODUCTION The purpose of this document is to provide written information regarding the risks, benefits and alternatives of Peripheral Relaxing Corneal Incision. This material serves as a supplement
INTRODUCTION The purpose of this document is to provide written information regarding the risks, benefits and alternatives of Peripheral Relaxing Corneal Incision. This material serves as a supplement
Four-year Postoperative Results of the US ALLEGRETTO WAVE Clinical Trial for the Treatment of Hyperopia
 Four-year Postoperative Results of the US ALLEGRETTO WAVE Clinical Trial for the Treatment of Hyperopia Guy M. Kezirian, MD, FACS; Charles R. Moore, MD, FICS; Karl G. Stonecipher, MD; SurgiVision Consultants
Four-year Postoperative Results of the US ALLEGRETTO WAVE Clinical Trial for the Treatment of Hyperopia Guy M. Kezirian, MD, FACS; Charles R. Moore, MD, FICS; Karl G. Stonecipher, MD; SurgiVision Consultants
ALLEGRETTO WAVE TM EYE-Q Scanning Spot LASIK Laser System
 ALLEGRETTO WAVE TM EYE-Q Scanning Spot LASIK Laser System Patient Information Booklet Facts You Need to Know About LASIK (Laser Assisted In-Situ Keratomileusis) Laser Treatment Information for patients
ALLEGRETTO WAVE TM EYE-Q Scanning Spot LASIK Laser System Patient Information Booklet Facts You Need to Know About LASIK (Laser Assisted In-Situ Keratomileusis) Laser Treatment Information for patients
ALLEGRETTO WAVE Scanning Spot LASIK Laser System
 TM ALLEGRETTO WAVE Scanning Spot LASIK Laser System Patient Information Booklet Information for patients considering Laser Assisted In-Situ Keratomileusis (LASIK) Surgery Information for patients considering
TM ALLEGRETTO WAVE Scanning Spot LASIK Laser System Patient Information Booklet Information for patients considering Laser Assisted In-Situ Keratomileusis (LASIK) Surgery Information for patients considering
Bilateral Refractive Amblyopia Treatment Study
 1 2 3 4 5 6 7 8 Bilateral Refractive Amblyopia Treatment Study 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 May 24, 2004 Version 1.1 ATS7 Protocol 5-24-04.doc 26 27 28 29 30 31 32 33 34 35 36 37 38
1 2 3 4 5 6 7 8 Bilateral Refractive Amblyopia Treatment Study 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 May 24, 2004 Version 1.1 ATS7 Protocol 5-24-04.doc 26 27 28 29 30 31 32 33 34 35 36 37 38
MEDICAL POLICY No R3 REFRACTIVE KERATOPLASTY / LASIK
 REFRACTIVE KERATOPLASTY / LASIK Effective Date: November 10, 2017 Review Dates: 7/07, 6/08, 6/09, 6/10, 8/10, 8/11, 8/12, 8/13, 8/14, 8/15, 8/16, 8/17 Date Of Origin: July 2007 Status: Current Summary
REFRACTIVE KERATOPLASTY / LASIK Effective Date: November 10, 2017 Review Dates: 7/07, 6/08, 6/09, 6/10, 8/10, 8/11, 8/12, 8/13, 8/14, 8/15, 8/16, 8/17 Date Of Origin: July 2007 Status: Current Summary
Abstracts. Edited by Dr. Tahir Mahmood. Wavefront-guided ablation: evidence for efficacy compared to traditional ablation
 Abstracts Edited by Dr. Tahir Mahmood Wavefront-guided ablation: evidence for efficacy compared to traditional ablation Netto MV, Dupps JRW, Wilson SE Am J Ophthalmol 2006; 141: 360-8. Adaptive optics
Abstracts Edited by Dr. Tahir Mahmood Wavefront-guided ablation: evidence for efficacy compared to traditional ablation Netto MV, Dupps JRW, Wilson SE Am J Ophthalmol 2006; 141: 360-8. Adaptive optics
Learn Connect Succeed. JCAHPO Regional Meetings 2017
 Learn Connect Succeed JCAHPO Regional Meetings 2017 Faculty Biometry and IOL Calculations ASCRS and ASOA Symposium and Congress Los Angeles, CA Daniel H. Chang, M.D. - Empire Eye and Laser Center Bakersfield,
Learn Connect Succeed JCAHPO Regional Meetings 2017 Faculty Biometry and IOL Calculations ASCRS and ASOA Symposium and Congress Los Angeles, CA Daniel H. Chang, M.D. - Empire Eye and Laser Center Bakersfield,
LASER REFRACTIVE CENTER INFORMED CONSENT DOCUMENT SMALL INCISION LENTICULE EXTRACTION (SMILE)
 GENERAL INFORMATION The purpose of this document is to provide written information regarding the risks, benefits and alternatives of Small Incision Lenticule Extraction. This material serves as a supplement
GENERAL INFORMATION The purpose of this document is to provide written information regarding the risks, benefits and alternatives of Small Incision Lenticule Extraction. This material serves as a supplement
Moving from Rx to measured
 Moving from Rx to measured The news magazine of the American Society of Cataract & Refractive Surgery Supplement to EyeWorld Daily News Sunday, May 7, 2017 Contoura Vision TopographyGuided Ablation Algorithms
Moving from Rx to measured The news magazine of the American Society of Cataract & Refractive Surgery Supplement to EyeWorld Daily News Sunday, May 7, 2017 Contoura Vision TopographyGuided Ablation Algorithms
Contoura TM Vision Correction
 Contoura TM Vision Correction Fernando Faria Correia, Financial Disclosures: Alcon/Wavelight Cairo (Egypt) 26/01/2018 Topography-guided ablations Topography guided ablations Evolution from complicated
Contoura TM Vision Correction Fernando Faria Correia, Financial Disclosures: Alcon/Wavelight Cairo (Egypt) 26/01/2018 Topography-guided ablations Topography guided ablations Evolution from complicated
Causes and Prevention of Diplopia After Refractive Surgery
 Causes and Prevention of Diplopia After Refractive Surgery Burton J. Kushner, M.D. ABSTRACT Background and Purpose: To describe the decompensation of strabismus or the occurrence of persistent diplopia
Causes and Prevention of Diplopia After Refractive Surgery Burton J. Kushner, M.D. ABSTRACT Background and Purpose: To describe the decompensation of strabismus or the occurrence of persistent diplopia
A procedure for Present and Future
 A procedure for Present and Future MOSTAFA M. SALAH MD PROFESSOR Head of Refractive Unit RESEARCH INSTITUTE OF OPHTHALMOGY CAIRO -EGYPT 1 THIN FLAP LASIK DEF. Creation of Intended regular thin flap less
A procedure for Present and Future MOSTAFA M. SALAH MD PROFESSOR Head of Refractive Unit RESEARCH INSTITUTE OF OPHTHALMOGY CAIRO -EGYPT 1 THIN FLAP LASIK DEF. Creation of Intended regular thin flap less
Facilitation of Amblyopia Management by Laser In situ Keratomileusis in Children with Myopic Anisometropia
 Facilitation of Amblyopia Management by Laser In situ Keratomileusis in Children with Myopic Anisometropia Athens 2018 Amblyopia Amblyopia is a decrease in visual acuity in one eye due to abnormal visual
Facilitation of Amblyopia Management by Laser In situ Keratomileusis in Children with Myopic Anisometropia Athens 2018 Amblyopia Amblyopia is a decrease in visual acuity in one eye due to abnormal visual
Photochemical corneal collagen cross-linkage using riboflavin and ultraviolet A for keratoconus and keratectasia
 Photochemical corneal collagen cross-linkage using riboflavin and ultraviolet A for keratoconus and keratectasia Issued: September 2013 guidance.nice.org.uk/ipg466 NICE has accredited the process used
Photochemical corneal collagen cross-linkage using riboflavin and ultraviolet A for keratoconus and keratectasia Issued: September 2013 guidance.nice.org.uk/ipg466 NICE has accredited the process used
INFORMED CONSENT FOR CORNEAL COLLAGEN CROSS-LINKING WITH RIBOFLAVIN (C3-R) FOR PATIENTS WITH KERATOCONUS OR CORNEAL ECTASIA
 INFORMED CONSENT FOR CORNEAL COLLAGEN CROSS-LINKING WITH RIBOFLAVIN (C3-R) FOR PATIENTS WITH KERATOCONUS OR CORNEAL ECTASIA INTRODUCTION: This information is to help you make an informed decision about
INFORMED CONSENT FOR CORNEAL COLLAGEN CROSS-LINKING WITH RIBOFLAVIN (C3-R) FOR PATIENTS WITH KERATOCONUS OR CORNEAL ECTASIA INTRODUCTION: This information is to help you make an informed decision about
Clinical Outcomes after Topography-based Corneal Laser Surgery with the. WaveLight Oculyzer and Topolyzer Platforms
 1 Clinical Outcomes after Topography-based Corneal Laser Surgery with the WaveLight Oculyzer and Topolyzer Platforms By Arthur B. Cummings, M.D. 1 and Nadia Mascharka, MSc 2 Corresponding Author: Arthur
1 Clinical Outcomes after Topography-based Corneal Laser Surgery with the WaveLight Oculyzer and Topolyzer Platforms By Arthur B. Cummings, M.D. 1 and Nadia Mascharka, MSc 2 Corresponding Author: Arthur
You will start medications 4 hours after your procedure.
 Dear Valued Patient, Dr. Roberts and staff welcome you to Shady Grove Ophthalmology. We appreciate your selection of our office for your refractive procedure. We have prepared this packet to help you make
Dear Valued Patient, Dr. Roberts and staff welcome you to Shady Grove Ophthalmology. We appreciate your selection of our office for your refractive procedure. We have prepared this packet to help you make
KNOW THE OPTIONS. Discover how the latest advances in vision correction can improve your sight.
 KNOW THE OPTIONS. LASIK VISIAN ICL PRK Discover how the latest advances in vision correction can improve your sight. Today, you can choose from several choices of permanent vision correction procedures
KNOW THE OPTIONS. LASIK VISIAN ICL PRK Discover how the latest advances in vision correction can improve your sight. Today, you can choose from several choices of permanent vision correction procedures
Interventional procedures guidance Published: 25 September 2013 nice.org.uk/guidance/ipg466
 Photochemical corneal collagen cross-linkage using riboflavin and ultraviolet A for keratoconus and keratectasia Interventional procedures guidance Published: 25 September 2013 nice.org.uk/guidance/ipg466
Photochemical corneal collagen cross-linkage using riboflavin and ultraviolet A for keratoconus and keratectasia Interventional procedures guidance Published: 25 September 2013 nice.org.uk/guidance/ipg466
Bringing astigmatism AND presbyopia into focus.
 Bringing astigmatism AND presbyopia into focus. LONG TERM VISION FOR YOUR PATIENTS FOR YOUR PRACTICE From here on out, it s TRULIGN. Treat astigmatic cataract patients and provide a natural range of vision.
Bringing astigmatism AND presbyopia into focus. LONG TERM VISION FOR YOUR PATIENTS FOR YOUR PRACTICE From here on out, it s TRULIGN. Treat astigmatic cataract patients and provide a natural range of vision.
Extended Depth Of Focus IOL For Presbyopia Correction
 A closer look at Extended Depth Of Focus IOL For Presbyopia Correction Abdallah K. Hassouna, MD, PhD. Professor of Ophthalmology, Ain Shams University Consultant Ophthalmic Surgeon, Al Watany Eye Hospital
A closer look at Extended Depth Of Focus IOL For Presbyopia Correction Abdallah K. Hassouna, MD, PhD. Professor of Ophthalmology, Ain Shams University Consultant Ophthalmic Surgeon, Al Watany Eye Hospital
For approximately two decades photorefractive keratectomy. Seven-Year Changes in Corneal Power and Aberrations after PRK or LASIK.
 Cornea Seven-Year Changes in Corneal Power and Aberrations after PRK or LASIK Anders Ivarsen and Jesper Hjortdal PURPOSE. To examine long-term changes in corneal power and aberrations in myopic patients
Cornea Seven-Year Changes in Corneal Power and Aberrations after PRK or LASIK Anders Ivarsen and Jesper Hjortdal PURPOSE. To examine long-term changes in corneal power and aberrations in myopic patients
2/6/2018 RAPID FIRE PANEL: CO-MANAGEMENT OF UNUSUAL SITUATIONS IN CATARACT SURGERY. Andrew Siedlecki, M.D. Richard Orlando, M.D.
 POLL QUESTION: HOW DID YOU DEVELOP THE CLINICAL SKILLS TO CO MANAGE RAPID FIRE PANEL: CO-MANAGEMENT OF UNUSUAL SITUATIONS IN CATARACT SURGERY Andrew Siedlecki, M.D. Richard Orlando, M.D. A) Working in
POLL QUESTION: HOW DID YOU DEVELOP THE CLINICAL SKILLS TO CO MANAGE RAPID FIRE PANEL: CO-MANAGEMENT OF UNUSUAL SITUATIONS IN CATARACT SURGERY Andrew Siedlecki, M.D. Richard Orlando, M.D. A) Working in
Premium Implant Options for the Cataract Patient. Justin Schweitzer, OD, FAAO Vance Thompson Vision Sioux Falls, South Dakota
 Premium Implant Options for the Cataract Patient Justin Schweitzer, OD, FAAO Vance Thompson Vision Sioux Falls, South Dakota Glaukos Bausch and Lomb Alcon Allergan Bio- Tissue TearScience Reichert Trends
Premium Implant Options for the Cataract Patient Justin Schweitzer, OD, FAAO Vance Thompson Vision Sioux Falls, South Dakota Glaukos Bausch and Lomb Alcon Allergan Bio- Tissue TearScience Reichert Trends
In Practice. Surgical Procedures Diagnosis New Drugs
 In Practice Surgical Procedures Diagnosis New Drugs 32 35 Bowman + Bulk = Better Results Mid-stromal lamellar keratoplasty (MSLK) offers a new approach to the management of advanced keratoconus that can
In Practice Surgical Procedures Diagnosis New Drugs 32 35 Bowman + Bulk = Better Results Mid-stromal lamellar keratoplasty (MSLK) offers a new approach to the management of advanced keratoconus that can
Review Article Complications of Laser in situ Keratomileusis: Etiology, Prevention, and Treatment Renato Ambrósio Jr, MD; Steven E. Wilson, MD ABSTRAC
 Review Article Complications of Laser in situ Keratomileusis: Etiology, Prevention, and Treatment Renato Ambrósio Jr, MD; Steven E. Wilson, MD ABSTRACT PURPOSE: To review the etiology, prevention, and
Review Article Complications of Laser in situ Keratomileusis: Etiology, Prevention, and Treatment Renato Ambrósio Jr, MD; Steven E. Wilson, MD ABSTRACT PURPOSE: To review the etiology, prevention, and
Comparison of Corneal and Anterior Chamber Parameters following Myopic laser in situ keratomileusis and photorefractive keratectomy by
 Comparison of Corneal and Anterior Chamber Parameters following Myopic laser in situ keratomileusis and photorefractive keratectomy by Pentacam as A New Imaging Technique Mohammad Ali Zare, MD 1 Hassan
Comparison of Corneal and Anterior Chamber Parameters following Myopic laser in situ keratomileusis and photorefractive keratectomy by Pentacam as A New Imaging Technique Mohammad Ali Zare, MD 1 Hassan
The Egyptian Journal of Hospital Medicine (October 2018) Vol. 73 (9), Page
 The Egyptian Journal of Hospital Medicine (October 2018) Vol. 73 (9), Page 7574-7579 Biomechanical Corneal Changes Post LASIK with Mechanical Microkeratome Flap versus Femtosecond Flap Department of Ophthalmology,
The Egyptian Journal of Hospital Medicine (October 2018) Vol. 73 (9), Page 7574-7579 Biomechanical Corneal Changes Post LASIK with Mechanical Microkeratome Flap versus Femtosecond Flap Department of Ophthalmology,
Personal data. Curriculum Vitae. Experience. Date of birth 18 December 1969
 1 Curriculum Vitae Dr. Sophia I. Panagopoulou University of Crete Medical School, IVO 71003 Heraklion Greece Phone: +302810394645 FAX: +302810394653 e-mail: spanagop@med.uoc.gr Personal data Date of birth
1 Curriculum Vitae Dr. Sophia I. Panagopoulou University of Crete Medical School, IVO 71003 Heraklion Greece Phone: +302810394645 FAX: +302810394653 e-mail: spanagop@med.uoc.gr Personal data Date of birth
Appendix Table 1. Ophthalmic drugs approved by the US Food and Drug Administration,
 SUPPLEMENTARY DATA Appendix Table 1. Ophthalmic drugs approved by the US Food and Drug Administration, 2002-2012 Approval Year Name Indication Pivotal Trial Design Randomized Comparator Masked Post-Approval
SUPPLEMENTARY DATA Appendix Table 1. Ophthalmic drugs approved by the US Food and Drug Administration, 2002-2012 Approval Year Name Indication Pivotal Trial Design Randomized Comparator Masked Post-Approval
Corneal Hysteresis, Resistance Factor, Topography, and Pachymetry After Corneal Lamellar Flap
 Corneal Hysteresis, Resistance Factor, Topography, and Pachymetry After Corneal Lamellar Flap Damien Gatinel, MD, PhD; Slim Chaabouni, MD; Pierre-Alexandre Adam, MD; Jacques Munck, OD; Michel Puech, MD;
Corneal Hysteresis, Resistance Factor, Topography, and Pachymetry After Corneal Lamellar Flap Damien Gatinel, MD, PhD; Slim Chaabouni, MD; Pierre-Alexandre Adam, MD; Jacques Munck, OD; Michel Puech, MD;
Over the past 25 years, surgical procedures designed
 Mayo Clin Proc, August 2001, Vol 76 Refractive Surgery 823 Special Article Making Sense of Refractive Surgery in 2001: Why, When, for Whom, and by Whom? MARK J. MANNIS, MD; WILLIAM A. SEGAL, MD; AND JASON
Mayo Clin Proc, August 2001, Vol 76 Refractive Surgery 823 Special Article Making Sense of Refractive Surgery in 2001: Why, When, for Whom, and by Whom? MARK J. MANNIS, MD; WILLIAM A. SEGAL, MD; AND JASON
