Risk Factors and Management of Mood Stabilizer-associated Stevens-Johnson Syndrome/Toxic Epidermal Necrolysis: A Mini-review
|
|
|
- Laura Johnson
- 5 years ago
- Views:
Transcription
1 140 Taiwanese Journal of Psychiatry (Taipei) Vol. 25 No Overview Risk Factors and Management of Mood Stabilizer-associated Stevens-Johnson Syndrome/Toxic Epidermal Necrolysis: A Mini-review Gen-Tang Lin, M.D. Objectives: In this brief review, I am dealing with the management and risk of mood stabilizers associated Stevens-Johnson syndrome (SJS) and toxic epidermal necrolysis (TEN). Methods: I conducted a comprehensive review of 27 published articles on SJS/TEN management and the risk of mood stabilizer-induced SJS/TEN. Results: Mood-stabilizing agents such as carbamezapine, lithium carbonate, valproic acid, topiramate, lamotrigine, gabapentin, and oxcarbazepine have the highest incidence of SJS/TEN. Han Chinese who have the HLA-B*1502 allele are at a much increased risk of developing SJS/TEN when exposed to carbamazepine. Stopping the suspected drug and rapid initiation of supportive and symptomatic management remains the mainstay of SJS/TEN management. Females, substance abusers, and new users with an early or sudden high combined dosage of mood stabilizers have increased risk of SJS/TEN. Carbamazepine-induced SJS/TEN in Taiwan exhibits a 98.3% sensitivity rate for HLA-B*1502. Given the availability of other effective medications for similar indications, avoiding carbamazepine is likely prudent when patients have tested HLA-B*1502 screening positive. Conclusion: Early diagnosis is important and early treatment requirs optimal SJS/TEN management. Key words: Management, risk, mood stabilizers, Stevens-Johnson syndrome (SJS) (Taiwanese Journal of Psychiatry [Taipei] 2011; 25: 140-4) Introduction I have searched the published articles dealing with mood stabilizers and Stevens-Johnson syndrome/toxic epidermal necrolysis in the Pub-med website. In this review, I have chosen 27 articles dealing with the Han people on this topic. Those 27 articles cover SJS/TEN clinical symptoms, diagnosis, treatment, risk factors to the associated mood stabilizers, and possible related genes. SJS is accompanied by fever, inflammation of the buccal mucosa, and severe purulent conjunctivitis. Cutaneous lesions often become con- Taichung Armed Forces General Hospital Received: January 12, 2011; revised: February 21, 2011; accepted: March 28, 2011 Address correspondence to: Dr. Gen-Tang Lin, No.42, Taizhong Peaceful Area Suitable Joyful Street, Taichung 411, Taiwan
2 Lin GT 141 fluent and show a positive Nikolsky sign and epidermal detachment. In SJS, epidermal detachment involves less than 10% of the total body skin area. Transitional SJS/TEN is defined by an epidermal detachment between 10% and 30%, and TEN is defined by a detachment greater than 30%. Impaired skin defense probably contributes to the high incidence of infection. SJS/TEN is essentially drug-induced. Graft versus host disease is another well-established cause, independent of drugs. A few cases are related to infections such as from Mycoplasma pneumoniae, and few other cases remain unexplained. The most extensive study of medication use and SJS/TEN mainly pointed to antibacterial sulfonamides, anticonvulsant agents, some nonsteroidal anti-inflammatory drugs and allopurinol [1]. HIV infection dramatically increases the risk. A predisposing effect of autoimmune disorders such as systemic lupus, and an HLA-linked, genetic susceptibility have been also suggested [2]. Common infections are gramnegative pneumonias and septicemias. Respiratory failure is associated with mucus retention and sloughing of the tracheobronchial mucosa. Conjunctivitis is the most frequent ocular complication. This purulent conjunctivitis causes the eyelids to become swollen, crusted, and ulcerated, with ensuing pain and photophobia [3]. Oral lesions, commonly beginning as vesicles, rupture, forming a gray-white membrane. The oropharyngeal cavity is involved, with erosion and sloughing possibly extending the entire length of the gastrointestinal tract, resulting in malnutrition, pain, and bleeding. The most severe gastrointestinal complication is bleeding [4]. Gastrointestinal and tracheobronchial epithelial involvement may lead to increased mortality while immunologic and epidermal disruption often leads to infection and sepsis [5]. Most often used pharmacologic therapies are aimed at altering the immune response, such as the use of corticosteroids, cyclosporin, and intravenous immunoglobulin [6]. Risk of Mood Stabilizerassociated SJS-TEN Carbamazepine Carbamazepine is used to treat seizure disorders, bipolar disorder, trigeminal neuralgia, and chronic pain. But, carbamazepine is also associated with hypersensitivity reactions that range from benign urticaria to life-threatening cutaneous disorders, including SJS/TEN [7]. Recently generated data implicate HLA allele B*1502 as a marker for carbamazepine-induced SJS/TEN in Han Chinese. Chung et al. were the first to identify an association between carbamazepine-induced SJS/ TEN and HLA-B*1502 allele [8]. Assuming a 0.25% incidence of carbamazepine-sjs/ten in newly prescribed carbamazepine patients in Taiwan and 98.3% sensitivity rate for HLA- B*1502 [9]. Prevalence of HLA-B*1502 allele in Asian populations is also much higher than in Caucasian and African populations [10]. Combined mood stabilizers Carbamazepine and valproate also increase the risk for SJS/TEN [11]. The rate of an antiepileptic drug (AED) rash such as carbamazepine and lamotrigine rash is about five times greater in patients with another (AED) rash [12]. Concomitant use of lamotrigine and aripiprazole increases risk of SJS/TEN [13]. A rapid dose escalation of lamotrigine, even a single higher dose, could expose patients to an unacceptable risk of SJS/TEN, particularly in patients taking valproate [14]. Valproate is known to augment lamotrigine availability through reduced glucuronidation, increasing the risk of serious rash if patients are concomitantly given lamotrigine [15].
3 142 Risk and Management of SJS/TEN Other risks (new users, female and substance abusers ) More than 90% of SJS/TEN cases occur within the first 63 days of mood stabilizer use, and new users are at higher risk [16]. A prospective case series and review of literature showed that lamotrigine induced a higher rate of SJS/TEN in female cases [17]. SJS with transition to TEN after carbamazepine administration, heroin and alcohol abuse [18]. Alcohol abuse alters host immunity which may subsequently increase susceptibility to allergic reactions. Patient s risk factors to develop mood stabilizer-associated SJS/TEN include: HLA-B*1502 positive Female New users Early or sudden high dosage Combined Mood stabilizers Substance abusers Prognosis SJS/TEN is an acute, self-limited disease, with high morbidity, and is potentially life threatening. Mortality rates are 5%-10% with SJS, 30%- 35 % with TEN and 10%-15% with transitional forms [2]. Early diagnosis and withdrawal of all potential causative drugs are essential to a favorable outcome. Morbidity and mortality are increased if the offending drug is withdrawn late. No difference has been seen for drugs with long half-lives [19]. Age, percentage of denuded skin, neutropenia, serum urea nitrogen level, and visceral involvement are prognostic factors. A specific score (SCORTEN) was recently elaborated and validated [20]. After healing, altered pigmentation and corneal lesions are the main long-term complications. Treatments for SJS/TEN Supportive and symptomatic treatments The main types of symptomatic treatment are the same as for patients with burn injury. Essential treatments consist of oral nutrition by nasogastric tube if needed; prevention of stress ulcer; fluid support (which should be based on the percentage of the affected total body surface area, the patient s weight, and an estimation of the volume of fluid lost); and medication administration for pain and anxiety control. If the trachea and bronchi are involved, patients need to receive intubation and mechanical ventilation. Skin lesions and oral ulcers have traditionally been treated with topical antibacterial agents. Liquid ocular lubricants should be applied to dry or photophobic eyes to minimize complications. Clinicians should consult with a dermatologist and an ophthalmologist if needed. Other treatments Administering systemic corticosteroids can prolong wound healing, increase risk of infection, mask early signs of sepsis, cause severe gastrointestinal bleeding, and increased mortality [21]. The use of corticosteroids in SJS-TEN remains controversial. Intravenous immunoglobulin (IVIG) can protect the keratinocytes in patients with SJS-TEN, thereby limiting disease progression [22]. Early infusion of IVIG can convey this protection as soon as the diagnosis is complete, and further limit the massive apoptosis of keratinocytes [23]. A high dose of IVIG (about 3 g/kg) showed increased survival, but was costly [24]. Interleukin-6 and TNF-α are found in higher quantities in lesioned skin in SJS-TEN, anti-tnf-α agents such as infliximab have been used with
4 Lin GT 143 success in a handful of patients [25]. Cyclosporine can inhibit CD8 and reduce extensive epidermal destruction, thereby shortening both the duration of active disease within hours and time to complete re-epithelization [6, 26]. Conclusion For optimal management and risk of mood stabilizers, careful inquiry into drug intake is recommended, especially in cases of SJS/TEN. Recent studies have investigated the role of genetic factors in the development of antiepileptic druginduced cutaneous reactions, as well as the relationship such factors have with carbamazepine and valproate-induced liver toxicity, vigabatrininduced visual field defects, and antiepileptic drug-induced teratogenicity. The greatest progress has involved an improved definition of the role of human leukocyte antigen-related genes as predictors of the risk of serious antiepileptic drug-induced cutaneous reactions. This has led to the recommendation that patients of Asian ancestry be tested for the HLA-B*1502 allele, to identify those with high risk of developing SJS/TEN after administration of carbamazepine and, possibly, phenytoin and other antiepileptic drugs [27]. Advanced human leukocyte antigen-related gene study and future prospective screening may help prevent mood stabilizer-induced SJS/TEN. References 1. Roujeau JC, Kelly JP, Naldi L, et al.: Medication use and the risk of Stevens-Johnson syndrome or toxic epidermal necrolysis. N Engl J Med 1995; 333: Ghislain PD, Roujeau JC: Treatment of severe drug reactions: Stevens-Johnson syndrome, toxic epidermal necrolysis and hypersensitivity syndrome. Dermatol Online J. 2002; 8: Howard GM: The Stevens-Johnson syndrome, ocular prognosis, and treatment. Am J Ophthalmol 1963; 55: Boe J, Dalgaard JB, Scott D: Mucocutaneous-ocular syndrome with intestinal involvement. Am J Med 1958; 25: Wolf R, Wolf D, Davidovici B: In the pursuit of classifying severe cutaneous adverse reactions. Clin Dermatol 2007; 25: Khalili B, Bahna SL: Pathogenesis and recent therapeutic trends in Stevens-Johnson syndrome and toxic epidermal necrolysis. Ann Allergy Asthma Immunol 2006; 97: Tennis P, Stern RS: Risk of serious cutaneous disorders after initiation of use of phenytoin, carbamazepine, or sodium valproate: a record linkage study. Neurology 1997; 49: Chung WH, Hung SI, Hong HS, et al.: Medical genetics: a marker for Stevens-Johnson syndrome. Nature 2004; 428: Hung SI, Chung WH, Jee SH, et al.: Genetic susceptibility to carbamazepine-induced cutaneous adverse drug reactions. Pharmacogenet Genomics 2006; 16: Ferrell PB Jr., McLeod HL: Carbamazepine, HLA- B*1502 and risk of Stevens-Johnson syndrome and toxic epidermal necrolysis: US FDA recommendations. Pharmacogenomics 2008; 9: Gau SS, Chao PF, Lin YJ, Chang CJ, Gau CS: The association between carbamazepine and valproate and adverse cutaneous drug reactions in patients with bipolar disorder: a nested matched case-control study. J Clin Psychopharmacol 2008; 28: Arif H, Buchsbaum R, Weintraub D: Comparison and predictors of rash associated with 15 antiepileptic drugs. Neurology 2007; 68: Shen YC, Chen SJ, Lin CC, Chen CH: Concomitant use of lamotrigine and aripiprazole increases risk of Stevens-Johnson syndrome? Int Clin Psychopharmacol 2007; 22: Famularo G, De Simone C, Minisola G: Stevens- Johnson syndrome associated with single high dose of lamotrigine in a patient taking valproate. Dermatol
5 144 Risk and Management of SJS/TEN Online J 2005; 11: Yalcin B, Karaduman A: Stevens-Johnson syndrome associated with concomitant use of lamotrigine and valproic acid. J Am Acad Dermatol 2000; 43: Mockenhaupt M, Messenheimer J, Tennis P, Schlingmann J: Risk of Stevens-Johnson syndrome and toxic epidermal necrolysis in new users of antiepileptics. Neurology 2005; 64: Aiken CB, Orr C: Rechallenge with lamotrigine after a rash: a prospective case series and review of the literature. Psychiatry (Edgemont) 2010; 7: Petter G, Haustein UF: Stevens-Johnson syndrome with transition to toxic epidermal necrolysis after carbamazepine administration, heroin and alcohol abuse. Hautarzt 1999; 50: Garcia-Doval I, LeCleach L, Bocquet H, Otero XL, Roujeau JC: Toxic epidermal necrolysis and Stevens- Johnson syndrome: does early withdrawal of causative drugs decrease the risk of death? Arch Dermatol 2000; 136: Bastuji-Garin S, Fouchard N, Bertocchi M, Roujeau JC, Revuz J, Wolkenstein P: SCORTEN: a severityof-illness score for toxic epidermal necrolysis. J Invest Dermatol 2000; 115: Cheriyan S, Patterson R, Greenberger PA, Grammer LC, Latall J: The outcome of Stevens-Johnson syndrome treated with corticosteroids. Allergy Proc 1995; 16: Paquet P, Kaveri S, Jacob E, et al.: Skin immunoglobulin deposition following intravenous immunoglobulin therapy in toxic epidermal necrolysis. Exp Dermatol 2006; 15: Yeung CK, Lam LK, Chan HH: The timing of intravenous immunoglobulin therapy in Stevens-Johnson syndrome and toxic epidermal necrolysis. Clin Exp Dermatol 2005; 30: Teo L, Tay YK, Liu TT, Kwok C: Stevens-Johnson syndrome and toxic epidermal necrolysis: efficacy of intravenous immunoglobulin and a review of treatment options. Singapore Med J 2009; 50: Hunger RE, Hunziker T, Buettiker U, Braathen LR, Yawalkar N: Rapid resolution of toxic epidermal necrolysis with anti-tnf-alpha treatment. J Allergy Clin Immunol 2005; 116: Arevalo JM, Lorente JA, Gonzalez-Herrada C, Jimenez-Reyes J: Treatment of toxic epidermal necrolysis with cyclosporin A. J Trauma 2000; 48: Franciotta D, Kwan P, Perucca E: Genetic basis for idiosyncratic reactions to antiepileptic drugs. Curr Opin Neurol 2009; 22:
Dilantin (phenytoin) ROBERT A. SCHWARTZ
 Dilantin (phenytoin) ROBERT A. SCHWARTZ Bailey & Galyen Attorney in Charge, Mass Tort Litigation Managing Attorney, Houston 18333 Egret Bay Blvd., Suite 120 Houston, Texas 77058 Toll Free: (866) 715-1529
Dilantin (phenytoin) ROBERT A. SCHWARTZ Bailey & Galyen Attorney in Charge, Mass Tort Litigation Managing Attorney, Houston 18333 Egret Bay Blvd., Suite 120 Houston, Texas 77058 Toll Free: (866) 715-1529
OXCARBAZEPINE-INDUCED STEVENS-JOHNSON SYNDROME: A CASE REPORT
 OXCARBAZEPINE-INDUCED STEVENS-JOHNSON SYNDROME: A CASE REPORT Lung-Chang Lin, 1,2 Ping-Chin Lai, 3 Sheau-Fang Yang, 4 and Rei-Cheng Yang 1,5 Departments of 1 Pediatrics and 4 Pathology, Kaohsiung Medical
OXCARBAZEPINE-INDUCED STEVENS-JOHNSON SYNDROME: A CASE REPORT Lung-Chang Lin, 1,2 Ping-Chin Lai, 3 Sheau-Fang Yang, 4 and Rei-Cheng Yang 1,5 Departments of 1 Pediatrics and 4 Pathology, Kaohsiung Medical
Stevens Johnson Syndrome: How Diagnosis Impacts Disease Course
 Southern Adventist Univeristy KnowledgeExchange@Southern Graduate Research Projects Nursing 12-4-2015 Stevens Johnson Syndrome: How Diagnosis Impacts Disease Course Sharon K. Hart Southern Adventist University,
Southern Adventist Univeristy KnowledgeExchange@Southern Graduate Research Projects Nursing 12-4-2015 Stevens Johnson Syndrome: How Diagnosis Impacts Disease Course Sharon K. Hart Southern Adventist University,
Prevention of severe cutaneous adverse drug reactions: the emerging value of pharmacogenetic screening
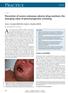 CMAJ Cases Prevention of severe cutaneous adverse drug reactions: the emerging value of pharmacogenetic screening Suran L. Fernando MB BS PhD, Andrew J. Broadfoot MB BS Previously published at www.cmaj.ca
CMAJ Cases Prevention of severe cutaneous adverse drug reactions: the emerging value of pharmacogenetic screening Suran L. Fernando MB BS PhD, Andrew J. Broadfoot MB BS Previously published at www.cmaj.ca
Drug-induced stevens-johnson syndrome : Experience from a tertiary care hospital
 Original article: Drug-induced stevens-johnson syndrome : Experience from a tertiary care hospital *Arjun R 1,Mahalingeshwara Bhat K P 2, Sara C 1 1 PG student in General Medicine, KS Hegde Medical Acadamy,
Original article: Drug-induced stevens-johnson syndrome : Experience from a tertiary care hospital *Arjun R 1,Mahalingeshwara Bhat K P 2, Sara C 1 1 PG student in General Medicine, KS Hegde Medical Acadamy,
Correspondence should be addressed to Wanjarus Roongpisuthipong; rr
 Dermatology Research and Practice, Article ID 237821, 5 pages http://dx.doi.org/10.1155/2014/237821 Research Article Retrospective Analysis of Corticosteroid Treatment in Stevens-Johnson Syndrome and/or
Dermatology Research and Practice, Article ID 237821, 5 pages http://dx.doi.org/10.1155/2014/237821 Research Article Retrospective Analysis of Corticosteroid Treatment in Stevens-Johnson Syndrome and/or
allergy Asia Pacific Stevens-Johnson syndrome and toxic epidermal necrolysis in Dr. Hasan Sadikin General Hospital Bandung, Indonesia from
 pissn -876 eissn -868 Original Article Asia Pac Allergy 6;6:-7 Stevens-Johnson syndrome and toxic epidermal necrolysis in Dr. Hasan Sadikin General Hospital Bandung, Indonesia from 9 Oki Suwarsa *, Wulan
pissn -876 eissn -868 Original Article Asia Pac Allergy 6;6:-7 Stevens-Johnson syndrome and toxic epidermal necrolysis in Dr. Hasan Sadikin General Hospital Bandung, Indonesia from 9 Oki Suwarsa *, Wulan
Case Report Cephazolin-Induced Toxic Epidermal Necrolysis Treated with Intravenous Immunoglobulin and N-Acetylcysteine
 Case Reports in Immunology Volume 2012, Article ID 931528, 4 pages doi:10.1155/2012/931528 Case Report Cephazolin-Induced Toxic Epidermal Necrolysis Treated with Intravenous Immunoglobulin and N-Acetylcysteine
Case Reports in Immunology Volume 2012, Article ID 931528, 4 pages doi:10.1155/2012/931528 Case Report Cephazolin-Induced Toxic Epidermal Necrolysis Treated with Intravenous Immunoglobulin and N-Acetylcysteine
Carbamazepine-Induced Toxic Effects and HLA-B*1502 Screening in Taiwan
 T h e n e w e ngl a nd j o u r na l o f m e dic i n e original article Carbamazepine-Induced Toxic Effects and HLA-B*1502 Screening in Taiwan Pei Chen, Ph.D., Juei-Jueng Lin, M.D., Chin-Song Lu, M.D.,
T h e n e w e ngl a nd j o u r na l o f m e dic i n e original article Carbamazepine-Induced Toxic Effects and HLA-B*1502 Screening in Taiwan Pei Chen, Ph.D., Juei-Jueng Lin, M.D., Chin-Song Lu, M.D.,
CARBAMAZEPINE INDUCED STEVENS JOHNSON SYNDROME- A CASE STUDY
 WORLD JOURNAL OF PHARMACY AND PHARMACEUTICAL SCIENCES Ragesh SJIF Impact Factor 2.786 Volume 3, Issue 6, 1599-1604. Case Study ISSN 2278 4357 CARBAMAZEPINE INDUCED STEVENS JOHNSON SYNDROME- A CASE STUDY
WORLD JOURNAL OF PHARMACY AND PHARMACEUTICAL SCIENCES Ragesh SJIF Impact Factor 2.786 Volume 3, Issue 6, 1599-1604. Case Study ISSN 2278 4357 CARBAMAZEPINE INDUCED STEVENS JOHNSON SYNDROME- A CASE STUDY
Stevens - Johnson syndrome (SJS) and Toxic Epidermal Necrolysis (TEN) In Sarawak: A Four Years Review
 Stevens - Johnson syndrome (SJS) and Toxic Epidermal Necrolysis (TEN) In Sarawak: A Four Years Review Yap FBB, MRCP; Wahiduzzaman M, MBBS; Pubalan M, MRCP. Egyptian Dermatology Online Journal 4 (1): 1,
Stevens - Johnson syndrome (SJS) and Toxic Epidermal Necrolysis (TEN) In Sarawak: A Four Years Review Yap FBB, MRCP; Wahiduzzaman M, MBBS; Pubalan M, MRCP. Egyptian Dermatology Online Journal 4 (1): 1,
Stevens-Johnson s Syndrome / Toxic Epidermal Necrolysis: An update
 Stevens-Johnson s Syndrome / Toxic Epidermal Necrolysis: An update Robert G. Micheletti, MD Assistant Professor of Dermatology and Medicine Director, Cutaneous Vasculitis Clinic, Penn Vasculitis Center
Stevens-Johnson s Syndrome / Toxic Epidermal Necrolysis: An update Robert G. Micheletti, MD Assistant Professor of Dermatology and Medicine Director, Cutaneous Vasculitis Clinic, Penn Vasculitis Center
PedsCases Podcast Scripts
 PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Drug Allergy. These podcasts are designed to give medical students an overview of key topics in pediatrics. The audio
PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Drug Allergy. These podcasts are designed to give medical students an overview of key topics in pediatrics. The audio
To update the use of IVIG and CORTICOIDS IN management of SJS/ TEN To remind Doctors being careful when giving
 Present : Dr Pham Thi Minh Rang Internal Department No2-Hospital for children No2 AIMS To update the use of IVIG and CORTICOIDS IN management of SJS/ TEN To remind Doctors being careful when giving To
Present : Dr Pham Thi Minh Rang Internal Department No2-Hospital for children No2 AIMS To update the use of IVIG and CORTICOIDS IN management of SJS/ TEN To remind Doctors being careful when giving To
Stevens-Johnson syndrome (SJS) and toxic epidermal. necrolysis in Asian children
 Stevens-Johnson syndrome and toxic epidermal necrolysis in Asian children Mark Jean-Aan Koh, MD, and Yong-Kwang Tay, MD Singapore Background: Stevens-Johnson syndrome (SJS) and toxic epidermal necrolysis
Stevens-Johnson syndrome and toxic epidermal necrolysis in Asian children Mark Jean-Aan Koh, MD, and Yong-Kwang Tay, MD Singapore Background: Stevens-Johnson syndrome (SJS) and toxic epidermal necrolysis
Profile and Pattern of Stevens-Johnson Syndrome and Toxic Epidermal Necrolysis in a General Hospital in Singapore: Treatment Outcomes
 Acta Derm Venereol 2012; 92: 62 66 CLINICAL REPORT Profile and Pattern of Stevens-Johnson Syndrome and Toxic Epidermal Necrolysis in a General Hospital in Singapore: Treatment Outcomes Siew-Kiang Tan and
Acta Derm Venereol 2012; 92: 62 66 CLINICAL REPORT Profile and Pattern of Stevens-Johnson Syndrome and Toxic Epidermal Necrolysis in a General Hospital in Singapore: Treatment Outcomes Siew-Kiang Tan and
SKIN REACTIONS WITH PSYCHOTROPICS: A SYSTEMATIC REVIEW
 SKIN REACTIONS WITH PSYCHOTROPICS: A SYSTEMATIC REVIEW *Anderson Isaac, PharmD Candidate, 2019 Pooja Patel, PharmD Candidate, 2019 Katelyn Thomasson, PharmD Candidate, 2019 Erika Tillery, PharmD, BCPP,
SKIN REACTIONS WITH PSYCHOTROPICS: A SYSTEMATIC REVIEW *Anderson Isaac, PharmD Candidate, 2019 Pooja Patel, PharmD Candidate, 2019 Katelyn Thomasson, PharmD Candidate, 2019 Erika Tillery, PharmD, BCPP,
1 Introduction. Kenneth Irungu 1 David Nyamu
 Drugs - Real World Outcomes (2017) 4:79 85 DOI 10.1007/s40801-017-0105-x ORIGINAL RESEARCH ARTICLE Characterization of Stevens Johnson Syndrome and Toxic Epidermal Necrolysis Among Patients Admitted to
Drugs - Real World Outcomes (2017) 4:79 85 DOI 10.1007/s40801-017-0105-x ORIGINAL RESEARCH ARTICLE Characterization of Stevens Johnson Syndrome and Toxic Epidermal Necrolysis Among Patients Admitted to
A Middle-Aged Man with Newly Diagnosed HIV Infection and Rash
 CLINICAL CASE OF THE MONTH A Middle-Aged Man with Newly Diagnosed HIV Infection and Rash Patrick Njoku, MD; Temeka Tate, MD; Sousan Zadeh, MD; Erin Hauck, MD; Anila Chaudhry, MD; Betty Lo-Blais, MD; Lee
CLINICAL CASE OF THE MONTH A Middle-Aged Man with Newly Diagnosed HIV Infection and Rash Patrick Njoku, MD; Temeka Tate, MD; Sousan Zadeh, MD; Erin Hauck, MD; Anila Chaudhry, MD; Betty Lo-Blais, MD; Lee
STEVEN JOHNSON S SYNDROME: A BRIEF REVIEW
 STEVEN JOHNSON S SYNDROME: A BRIEF REVIEW G. Ramya sree*, Sreeram Vandavasi Guru 1, E. Sam Jeeva Kumar 2 * Pharm D, Intern, P. Rami Reddy Memorial College of Pharmacy, Kadapa. 1 Pharm-D Intern, P. Rami
STEVEN JOHNSON S SYNDROME: A BRIEF REVIEW G. Ramya sree*, Sreeram Vandavasi Guru 1, E. Sam Jeeva Kumar 2 * Pharm D, Intern, P. Rami Reddy Memorial College of Pharmacy, Kadapa. 1 Pharm-D Intern, P. Rami
Carbamazepine Hypersensitivity: Progress Toward Predicting the Unpredictable
 Carbamazepine Hypersensitivity: Progress Toward Predicting the Unpredictable Current Literature In Clinical Science HLA-A*3101 and Carbamazepine-Induced Hypersensitivity Reactions in Europeans. McCormack
Carbamazepine Hypersensitivity: Progress Toward Predicting the Unpredictable Current Literature In Clinical Science HLA-A*3101 and Carbamazepine-Induced Hypersensitivity Reactions in Europeans. McCormack
Oral Acetazolamide after Boston Keratoprosthesis in Stevens Johnson Syndrome
 Oral Acetazolamide after Boston Keratoprosthesis in Stevens Johnson Syndrome The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters
Oral Acetazolamide after Boston Keratoprosthesis in Stevens Johnson Syndrome The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters
Carbamazepine-Induced Incomplete Stevens-Johnson Syndrome: Report of a Case in Children without Mycoplasma pneumoniae Infection
 Case Report Carbamazepine-Induced Incomplete Stevens-Johnson Syndrome: Report of a Case in Children without Mycoplasma pneumoniae Infection J Med Assoc Thai 2015; 98 (Suppl. 7): S243-S247 Full text. e-journal:
Case Report Carbamazepine-Induced Incomplete Stevens-Johnson Syndrome: Report of a Case in Children without Mycoplasma pneumoniae Infection J Med Assoc Thai 2015; 98 (Suppl. 7): S243-S247 Full text. e-journal:
Review of Anticonvulsant Medications: Traditional and Alternative Uses. Andrea Michel, PharmD, CACP
 Review of Anticonvulsant Medications: Traditional and Alternative Uses Andrea Michel, PharmD, CACP Objectives Review epidemiology of epilepsy Classify types of seizures Discuss non-pharmacologic and pharmacologic
Review of Anticonvulsant Medications: Traditional and Alternative Uses Andrea Michel, PharmD, CACP Objectives Review epidemiology of epilepsy Classify types of seizures Discuss non-pharmacologic and pharmacologic
Pediatric Dermatology
 Pediatric Dermatology --------- Emergencies & Urgencies Nicholas V. Nguyen, M.D. Director, Pediatric Dermatology Disclosures In the past 12 months, I have had the following financial relationships with
Pediatric Dermatology --------- Emergencies & Urgencies Nicholas V. Nguyen, M.D. Director, Pediatric Dermatology Disclosures In the past 12 months, I have had the following financial relationships with
Cutaneous drug reactions to antiepileptic drugs and relation with HLA alleles in the Turkish population
 O R I G I N A L A R T I C L E Eur Ann Allergy Clin Immunol Vol 50, N 1, 36-41, 2018 S. Büyüköztürk 1, Ç. Kekik 2, A.Z. Gökyiğit 3, F.İ. Tezer Filik 4i, G. Karakaya 4, S. Saygı 4i, A.B. Dursun 5, S. Kirbaş
O R I G I N A L A R T I C L E Eur Ann Allergy Clin Immunol Vol 50, N 1, 36-41, 2018 S. Büyüköztürk 1, Ç. Kekik 2, A.Z. Gökyiğit 3, F.İ. Tezer Filik 4i, G. Karakaya 4, S. Saygı 4i, A.B. Dursun 5, S. Kirbaş
Causes and Treatment Outcomes of Stevens-Johnson Syndrome and Toxic Epidermal Necrolysis in 82 Adult Patients
 original article korean j intern med 2012;27:203-210 pissn 1226-3303 eissn 2005-6648 Causes and Treatment Outcomes of Stevens-Johnson Syndrome and Toxic Epidermal Necrolysis in 82 Adult Patients Hye-In
original article korean j intern med 2012;27:203-210 pissn 1226-3303 eissn 2005-6648 Causes and Treatment Outcomes of Stevens-Johnson Syndrome and Toxic Epidermal Necrolysis in 82 Adult Patients Hye-In
Warfarin-induced toxic epidermal necrolysis in combination therapy of Henoch- Schönlein purpura nephritis: a case report
 Kasahara et al. BMC Nephrology (2017) 18:237 DOI 10.1186/s12882-017-0648-9 CASE REPORT Open Access Warfarin-induced toxic epidermal necrolysis in combination therapy of Henoch- Schönlein purpura nephritis:
Kasahara et al. BMC Nephrology (2017) 18:237 DOI 10.1186/s12882-017-0648-9 CASE REPORT Open Access Warfarin-induced toxic epidermal necrolysis in combination therapy of Henoch- Schönlein purpura nephritis:
A Case Report on Amoxicillin Induced Stevens- Johnson Syndrome
 Open Journal of Clinical & Medical Case Reports Volume 2 (2016) Issue 11 A Case Report on Amoxicillin Induced Stevens- Johnson Syndrome Rajendra Singh Airee*; Aastha Rawal; Binu Mathew; H. Doddayya Abstract
Open Journal of Clinical & Medical Case Reports Volume 2 (2016) Issue 11 A Case Report on Amoxicillin Induced Stevens- Johnson Syndrome Rajendra Singh Airee*; Aastha Rawal; Binu Mathew; H. Doddayya Abstract
Dexamethasone Pulse Therapy for Stevens-Johnson Syndrome/ Toxic Epidermal Necrolysis
 Acta Derm Venereol 2007; 87: 144 148 CLINICAL REPORT Dexamethasone Pulse Therapy for Stevens-Johnson Syndrome/ Toxic Epidermal Necrolysis Sylvia H. Kardaun and Marcel F. Jonkman Center for Blistering Diseases,
Acta Derm Venereol 2007; 87: 144 148 CLINICAL REPORT Dexamethasone Pulse Therapy for Stevens-Johnson Syndrome/ Toxic Epidermal Necrolysis Sylvia H. Kardaun and Marcel F. Jonkman Center for Blistering Diseases,
PHENYTION, CARBAMAZEPINE, SODIUM VALPROATE AND LAMOTRIGINE INDUCED CUTANEOUS REACTIONS
 PHENYTION, CARBAMAZEPINE, SODIUM VALPROATE AND LAMOTRIGINE INDUCED CUTANEOUS REACTIONS M. Ghaffarpour *, S. S. Hejazie, M. H. Harirchian and H. Pourmahmoodian Department of Neurology, Imam Khomeini Hospital,
PHENYTION, CARBAMAZEPINE, SODIUM VALPROATE AND LAMOTRIGINE INDUCED CUTANEOUS REACTIONS M. Ghaffarpour *, S. S. Hejazie, M. H. Harirchian and H. Pourmahmoodian Department of Neurology, Imam Khomeini Hospital,
Monitoring and Antiepileptic Drug Safety
 Practice Monitoring and Antiepileptic Drug Safety L. James Willmore, MD, FAAN, FANA ABSTRACT Treatment of patients with epilepsy strives for complete seizure control without intolerable drug side effects.
Practice Monitoring and Antiepileptic Drug Safety L. James Willmore, MD, FAAN, FANA ABSTRACT Treatment of patients with epilepsy strives for complete seizure control without intolerable drug side effects.
Cutaneous Conditions Associated with Systemic Disease
 Cutaneous Conditions Associated with Systemic Disease Johnnie M Woodson, M.D., F.A.A.D. Assistant Professor of Dermatology University of Nevada School of Medicine Director of J. Woodson Dermatology & Associates,
Cutaneous Conditions Associated with Systemic Disease Johnnie M Woodson, M.D., F.A.A.D. Assistant Professor of Dermatology University of Nevada School of Medicine Director of J. Woodson Dermatology & Associates,
Anticonvulsants Antiseizure
 Anticonvulsants Antiseizure Seizure disorders Head trauma Stroke Drugs (overdose, withdrawal) Brain tumor Encephalitis/ Meningitis High fever Hypoglycemia Hypocalcemia Hypoxia genetic factors Epileptic
Anticonvulsants Antiseizure Seizure disorders Head trauma Stroke Drugs (overdose, withdrawal) Brain tumor Encephalitis/ Meningitis High fever Hypoglycemia Hypocalcemia Hypoxia genetic factors Epileptic
Spectrum of Cutaneous Adverse Reactions to Levetiracetam and Human Leukocyte Antigen Typing in North-Indian Patients
 Spectrum of Cutaneous Adverse Reactions to Levetiracetam and Human Leukocyte Antigen Typing in North-Indian Patients Original Article Journal of Epilepsy Research pissn 2233-6249 / eissn 2233-6257 Bhargavi
Spectrum of Cutaneous Adverse Reactions to Levetiracetam and Human Leukocyte Antigen Typing in North-Indian Patients Original Article Journal of Epilepsy Research pissn 2233-6249 / eissn 2233-6257 Bhargavi
Skin Manifestations of Drug Reactions
 Skin Manifestations of Drug Reactions Dr Carol Hlela, Division of Dermatology Department of Medicine, University of Cape Town and Red Cross Children s Hospital What are the Skin Manifestations of Drug
Skin Manifestations of Drug Reactions Dr Carol Hlela, Division of Dermatology Department of Medicine, University of Cape Town and Red Cross Children s Hospital What are the Skin Manifestations of Drug
NEOFEN 60 mg suppository
 PACKAGE LEAFLET: INFORMATION FOR THE USER NEOFEN 60 mg suppository IBUPROFEN This leaflet is a copy of the Summary of Product Characteristics and Patient Information Leaflet for a medicine, which outlines
PACKAGE LEAFLET: INFORMATION FOR THE USER NEOFEN 60 mg suppository IBUPROFEN This leaflet is a copy of the Summary of Product Characteristics and Patient Information Leaflet for a medicine, which outlines
Scratching the Surface: A Review of SJS/TEN
 Scratching the Surface: A Review of SJS/TEN Sarah Smith, PharmD Pharmacy Grand Rounds 2018 November 27, 2018 2018 MFMER slide 1 Toxic Epidermal Necrolysis Cutaneous Anthrax Stevens Johnson Syndrome Necrotizing
Scratching the Surface: A Review of SJS/TEN Sarah Smith, PharmD Pharmacy Grand Rounds 2018 November 27, 2018 2018 MFMER slide 1 Toxic Epidermal Necrolysis Cutaneous Anthrax Stevens Johnson Syndrome Necrotizing
Disclosure. Learning Objectives
 Linda D. Leary, M.D. Associate Clinical Professor of Pediatrics & Neurology South Texas Comprehensive Epilepsy Center UT Health Science Center San Antonio Disclosure Linda D. Leary, M.D. discloses the
Linda D. Leary, M.D. Associate Clinical Professor of Pediatrics & Neurology South Texas Comprehensive Epilepsy Center UT Health Science Center San Antonio Disclosure Linda D. Leary, M.D. discloses the
Stevens Johnson Syndrome and Toxic Epidermal Necrolysis Associated with Acetaminophen Use during Viral Infections
 BRIEF COMMUNICATION http://dx.doi.org/10.4110/in.2016.16.4.256 pissn 1598-2629 eissn 2092-6685 Stevens Johnson Syndrome and Toxic Epidermal Necrolysis Associated with Acetaminophen Use during Viral Infections
BRIEF COMMUNICATION http://dx.doi.org/10.4110/in.2016.16.4.256 pissn 1598-2629 eissn 2092-6685 Stevens Johnson Syndrome and Toxic Epidermal Necrolysis Associated with Acetaminophen Use during Viral Infections
DOSAGE FORMS AND STRENGTHS Tablets: 25 mg, 100 mg, 150 mg, and 200 mg; scored. (3.1, 16)
 HIGHLIGHTS OF PRESCRIBING INFORMATION These highlights do not include all the information needed to use LAMOTRIGINE TABLETS safely and effectively. See full prescribing information for LAMOTRIGINE TABLETS.
HIGHLIGHTS OF PRESCRIBING INFORMATION These highlights do not include all the information needed to use LAMOTRIGINE TABLETS safely and effectively. See full prescribing information for LAMOTRIGINE TABLETS.
Genetic susceptibility for Stevens-Johnson syndrome/toxic epidermal necrolysis with mucosal involvements
 249 Special Issue: Inflammation in Ophthalmology Review Article Genetic susceptibility for Stevens-Johnson syndrome/toxic epidermal necrolysis with mucosal involvements 1, 2, ) Mayumi Ueta 1) Department
249 Special Issue: Inflammation in Ophthalmology Review Article Genetic susceptibility for Stevens-Johnson syndrome/toxic epidermal necrolysis with mucosal involvements 1, 2, ) Mayumi Ueta 1) Department
Objectives Making CYP450, Drug Interactions, & Pharmacogenetics Easy
 Objectives Making, Drug Interactions, & Pharmacogenetics Easy Anthony J. Busti, MD, PharmD, FNLA, FAHA Describe the differences between phase I and phase II metabolic pathways. Identify the most common
Objectives Making, Drug Interactions, & Pharmacogenetics Easy Anthony J. Busti, MD, PharmD, FNLA, FAHA Describe the differences between phase I and phase II metabolic pathways. Identify the most common
Diagnosis and Management of Drug-induced Stevens-Johnson Syndrome: Report of Two Cases
 10.5005/jp-journals-10011-1189 CASE REPORT JIAOMR Diagnosis and Management of Drug-induced Stevens-Johnson Syndrome: Report of Two Cases 1 M Venkateshwarlu, 2 B Radhika 1 Professor and Head, Department
10.5005/jp-journals-10011-1189 CASE REPORT JIAOMR Diagnosis and Management of Drug-induced Stevens-Johnson Syndrome: Report of Two Cases 1 M Venkateshwarlu, 2 B Radhika 1 Professor and Head, Department
HLA-A*24:02 as a common risk factor for antiepileptic drug induced cutaneous adverse reactions
 Published Ahead of Print on May 5, 2017 as 10.1212/WNL.0000000000004008 HLA-A*24:02 as a common risk factor for antiepileptic drug induced cutaneous adverse reactions Yi-Wu Shi, PhD* Fu-Li Min, MD* Dong
Published Ahead of Print on May 5, 2017 as 10.1212/WNL.0000000000004008 HLA-A*24:02 as a common risk factor for antiepileptic drug induced cutaneous adverse reactions Yi-Wu Shi, PhD* Fu-Li Min, MD* Dong
Bugs and Drugs: What s New in Hypersensitivity Reactions?
 Bugs and Drugs: What s New in Hypersensitivity Reactions? Erin Mathes, MD Associate Professor of Dermatology and Pediatrics University of California, San Francisco DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY
Bugs and Drugs: What s New in Hypersensitivity Reactions? Erin Mathes, MD Associate Professor of Dermatology and Pediatrics University of California, San Francisco DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY
Five things not to miss in Dermatology. Dr Judy Wismer Associate Clinical Professor Michael G DeGroote School of Medicine
 Five things not to miss in Dermatology Dr Judy Wismer Associate Clinical Professor Michael G DeGroote School of Medicine Key Descriptives Fever, skin pain Purpura, necrosis Bullae, Mucosal, Skin sloughing
Five things not to miss in Dermatology Dr Judy Wismer Associate Clinical Professor Michael G DeGroote School of Medicine Key Descriptives Fever, skin pain Purpura, necrosis Bullae, Mucosal, Skin sloughing
Risk of Stevens Johnson syndrome and toxic epidermal necrolysis in new users of antiepileptics
 Risk of Stevens Johnson syndrome and toxic epidermal necrolysis in new users of antiepileptics Maja Mockenhaupt, MD; John Messenheimer, MD; Pat Tennis, PhD; and Juergen Schlingmann Abstract Background:
Risk of Stevens Johnson syndrome and toxic epidermal necrolysis in new users of antiepileptics Maja Mockenhaupt, MD; John Messenheimer, MD; Pat Tennis, PhD; and Juergen Schlingmann Abstract Background:
See 17 for PATIENT COUNSELING INFORMATION and Medication Guide. Revised: 11/2011
 HIGHLIGHTS OF PRESCRIBING INFORMATION These highlights do not include all the information needed to use LAMICTAL safely and effectively. See full prescribing information for LAMICTAL. LAMICTAL (lamotrigine)
HIGHLIGHTS OF PRESCRIBING INFORMATION These highlights do not include all the information needed to use LAMICTAL safely and effectively. See full prescribing information for LAMICTAL. LAMICTAL (lamotrigine)
The liver and skin are two of the commonest
 AMERICAN ASSOCIATION FOR THE STUDY OFLIVERD I S E ASES HEPATOLOGY, VOL. 63, NO. 3, 2016 LIVER INJURY/REGENERATION Drug-Induced Liver Injury Associated With Stevens-Johnson Syndrome/Toxic Epidermal Necrolysis:
AMERICAN ASSOCIATION FOR THE STUDY OFLIVERD I S E ASES HEPATOLOGY, VOL. 63, NO. 3, 2016 LIVER INJURY/REGENERATION Drug-Induced Liver Injury Associated With Stevens-Johnson Syndrome/Toxic Epidermal Necrolysis:
Toxic Epidermal Necrolysis and SJS : Case Reports & Brief Review
 Case Report Toxic Epidermal Necrolysis and SJS : Case Reports & Brief Review Deepali P. Mohite*, Satyajitraje Tekade*, Amol Gadbail*, M. S. Chaudhary** Abstract : Toxic epidermal necrolysis (TEN) and Stevens
Case Report Toxic Epidermal Necrolysis and SJS : Case Reports & Brief Review Deepali P. Mohite*, Satyajitraje Tekade*, Amol Gadbail*, M. S. Chaudhary** Abstract : Toxic epidermal necrolysis (TEN) and Stevens
Epilepsy 101. Overview of Treatment Kathryn A. O Hara RN. American Epilepsy Society
 Epilepsy 101 Overview of Treatment Kathryn A. O Hara RN American Epilepsy Society Objectives Describe the main treatment options for epilepsy Identify factors essential in the selection of appropriate
Epilepsy 101 Overview of Treatment Kathryn A. O Hara RN American Epilepsy Society Objectives Describe the main treatment options for epilepsy Identify factors essential in the selection of appropriate
STEVENS-JOHNSON SYNDROME: A CASE REPORT
 STEVENS-JOHNSON SYNDROME: A CASE REPORT Castana O., Rempelos G., Anagiotos G., Apostolopoulou C., Dimitrouli A., Alexakis D. Department of Plastic and Reconstructive Surgery, Evangelismos General Hospital,
STEVENS-JOHNSON SYNDROME: A CASE REPORT Castana O., Rempelos G., Anagiotos G., Apostolopoulou C., Dimitrouli A., Alexakis D. Department of Plastic and Reconstructive Surgery, Evangelismos General Hospital,
Severe Desquamating Disorder After Liver Transplant: Toxic Epidermal Necrolyis or Graft Versus Host Disease?
 Severe Desquamating Disorder After Liver Transplant: Toxic Epidermal Necrolyis or Graft Versus Host Disease? John T. Schulz III, MD, PhD, FACS, and Robert L. Sheridan, MD, FACS Bridgeport Hospital, Bridgeport,
Severe Desquamating Disorder After Liver Transplant: Toxic Epidermal Necrolyis or Graft Versus Host Disease? John T. Schulz III, MD, PhD, FACS, and Robert L. Sheridan, MD, FACS Bridgeport Hospital, Bridgeport,
Genetic Screening for ADR
 Genetic Screening for ADR Mahidol University Faculty of Medicine Siriraj Hospital Manop Pithukpakorn, MD Division of Medical Genetics Department of Medicine concentration Drug level over time toxic optimum
Genetic Screening for ADR Mahidol University Faculty of Medicine Siriraj Hospital Manop Pithukpakorn, MD Division of Medical Genetics Department of Medicine concentration Drug level over time toxic optimum
See 17 for PATIENT COUNSELING INFORMATION and Medication Guide. Revised: May 2009 LMT:2PI
 HIGHLIGHTS OF PRESCRIBING INFORMATION These highlights do not include all the information needed to use LAMICTAL safely and effectively. See full prescribing information for LAMICTAL. LAMICTAL (lamotrigine)
HIGHLIGHTS OF PRESCRIBING INFORMATION These highlights do not include all the information needed to use LAMICTAL safely and effectively. See full prescribing information for LAMICTAL. LAMICTAL (lamotrigine)
RECENT MAJOR CHANGES Warnings and Precautions, Hemophagocytic
 HIGHLIGHTS OF PRESCRIBING INFORMATION These highlights do not include all the information needed to use LAMICTAL safely and effectively. See full prescribing information for LAMICTAL. LAMICTAL (lamotrigine)
HIGHLIGHTS OF PRESCRIBING INFORMATION These highlights do not include all the information needed to use LAMICTAL safely and effectively. See full prescribing information for LAMICTAL. LAMICTAL (lamotrigine)
Emergency Dermatology Dr Melissa Barkham
 Emergency Dermatology Dr Melissa Barkham Spotlight Seminar 30 th September 2010 Why is this important? Urgent recognition and treatment of dermatologic emergencies can be life saving and prevent long term
Emergency Dermatology Dr Melissa Barkham Spotlight Seminar 30 th September 2010 Why is this important? Urgent recognition and treatment of dermatologic emergencies can be life saving and prevent long term
Drug Allergy A Guide to Diagnosis and Management
 Drug Allergy A Guide to Diagnosis and Management (Version 1 April 2015 updated April 2018) Author: Jed Hewitt Chief Pharmacist, Governance & Professional Practice Date of Preparation: April 2015 Updated:
Drug Allergy A Guide to Diagnosis and Management (Version 1 April 2015 updated April 2018) Author: Jed Hewitt Chief Pharmacist, Governance & Professional Practice Date of Preparation: April 2015 Updated:
CURRICULUM VITAE China Medical College, College of Medicine, Taichung, Taiwan, R.O.C.
 CURRICULUM VITAE NAME: Huang, Chung-Ming OFFICE ADDRESS: China Medical University Hospital, No. 2, Yuh-Der Road, Taichung, Taiwan, R.O.C., 北 路 2 EDUCATION: 1978-1985 China Medical College, College of Medicine,
CURRICULUM VITAE NAME: Huang, Chung-Ming OFFICE ADDRESS: China Medical University Hospital, No. 2, Yuh-Der Road, Taichung, Taiwan, R.O.C., 北 路 2 EDUCATION: 1978-1985 China Medical College, College of Medicine,
A Retrospective Study of Spectrum of Nevirapine Induced Cutaneous Drug Reactions in HIV Positive Patients
 Journal of US-China Medical Science 12 (2015) 85-89 doi: 10.17265/1548-6648/2015.02.008 D DAVID PUBLISHING A Retrospective Study of Spectrum of Nevirapine Induced Cutaneous Drug Reactions in HIV Positive
Journal of US-China Medical Science 12 (2015) 85-89 doi: 10.17265/1548-6648/2015.02.008 D DAVID PUBLISHING A Retrospective Study of Spectrum of Nevirapine Induced Cutaneous Drug Reactions in HIV Positive
Severe cutaneous reactions caused by barbiturates in seven Iranian children
 Pharmacology and therapeutics Severe cutaneous reactions caused by barbiturates in seven Iranian children Setareh Mamishi, MD, Fatemeh Fattahi, MD, Zahra Pourpak, MD, PhD, Farzaneh Mirza Aghaee, MD, Zeinab
Pharmacology and therapeutics Severe cutaneous reactions caused by barbiturates in seven Iranian children Setareh Mamishi, MD, Fatemeh Fattahi, MD, Zahra Pourpak, MD, PhD, Farzaneh Mirza Aghaee, MD, Zeinab
Your letter Your reference The Hague, Subject Request for change in the product information following the PhVWP/CMDh decision
 Registratiehouder ( t.a.v. registratieafdeling) Your letter Your reference The Hague, -- --.. Case number Our reference../../ Case manager Telephone number Subject Request for change in the product information
Registratiehouder ( t.a.v. registratieafdeling) Your letter Your reference The Hague, -- --.. Case number Our reference../../ Case manager Telephone number Subject Request for change in the product information
Chapter : Sources and Bodily Effect of Drugs
 Systemic Effect- drug acts in a widespread area away from the administration site Ex: Tylenol rectal suppository- given rectally but is absorbed and distributed thru the body to cause a reduction in fever
Systemic Effect- drug acts in a widespread area away from the administration site Ex: Tylenol rectal suppository- given rectally but is absorbed and distributed thru the body to cause a reduction in fever
2/28/2010. Pharmacogenomics and the Asian Population. Limited efficacy/response to drugs already on the market
 Pharmacogenomics and the Asian Population Majority are medication related Alan H.B. Wu, Ph.D. Professor, Laboratory Medicine, UCSF Section Chief, Clinical Chemistry, February 27, 20 Limited efficacy/response
Pharmacogenomics and the Asian Population Majority are medication related Alan H.B. Wu, Ph.D. Professor, Laboratory Medicine, UCSF Section Chief, Clinical Chemistry, February 27, 20 Limited efficacy/response
TENS/STEVENS JOHNSON SYNDROME. Dehan Struwig, Plastic and Reconstructive Surgeon
 TENS/STEVENS JOHNSON SYNDROME { Dehan Struwig, Plastic and Reconstructive Surgeon Stevens-Johnson Syndrome is an immune complex hypersensitivity reaction that can be caused from an infection or immune
TENS/STEVENS JOHNSON SYNDROME { Dehan Struwig, Plastic and Reconstructive Surgeon Stevens-Johnson Syndrome is an immune complex hypersensitivity reaction that can be caused from an infection or immune
LAMICTAL XR (lamotrigine) extended-release tablets, for oral use Initial U.S. Approval: 1994
 HIGHLIGHTS OF PRESCRIBING INFORMATION These highlights do not include all the information needed to use LAMICTAL XR safely and effectively. See full prescribing information for LAMICTAL XR. LAMICTAL XR
HIGHLIGHTS OF PRESCRIBING INFORMATION These highlights do not include all the information needed to use LAMICTAL XR safely and effectively. See full prescribing information for LAMICTAL XR. LAMICTAL XR
Cutaneous Adverse Drug Reactions in Domestic Animals. Katherine Doerr, DVM, Dip. ACVD. Veterinary Dermatology Center
 Cutaneous Adverse Drug Reactions in Domestic Animals Katherine Doerr, DVM, Dip. ACVD Veterinary Dermatology Center Maitland, Rockledge, Waterford Lakes, FL Not highly studied in veterinary medicine Unknown
Cutaneous Adverse Drug Reactions in Domestic Animals Katherine Doerr, DVM, Dip. ACVD Veterinary Dermatology Center Maitland, Rockledge, Waterford Lakes, FL Not highly studied in veterinary medicine Unknown
Adverse Drug Reactions (ADRs) Outline
 Adverse Drug Reactions (ADRs) Outline 1. What are Adverse Drug Reactions (ADRs)? WHAT WHY HOW 2. How important are ADRs and are they preventable? 3. What are the classifications and mechanisms of ADRs?
Adverse Drug Reactions (ADRs) Outline 1. What are Adverse Drug Reactions (ADRs)? WHAT WHY HOW 2. How important are ADRs and are they preventable? 3. What are the classifications and mechanisms of ADRs?
Successful re-introduction of lamotrigine after initial rash
 Seizure 2000; 9: 282 286 doi: 10.1053/seiz.2000.0394, available online at http://www.idealibrary.com on Successful re-introduction of lamotrigine after initial rash F. M. C. BESAG, G. Y. T. NG & F. POOL
Seizure 2000; 9: 282 286 doi: 10.1053/seiz.2000.0394, available online at http://www.idealibrary.com on Successful re-introduction of lamotrigine after initial rash F. M. C. BESAG, G. Y. T. NG & F. POOL
Analysis of Individual Case Safety Reports of Severe Cutaneous Adverse Reactions in Korea
 Original Article Yonsei Med J 2019 Feb;60(2):208-215 pissn: 0513-5796 eissn: 1976-2437 Analysis of Individual Case Safety Reports of Severe Cutaneous Adverse Reactions in Korea Min-Gyu Kang 1,2,3, Kyung-Hee
Original Article Yonsei Med J 2019 Feb;60(2):208-215 pissn: 0513-5796 eissn: 1976-2437 Analysis of Individual Case Safety Reports of Severe Cutaneous Adverse Reactions in Korea Min-Gyu Kang 1,2,3, Kyung-Hee
Severe Cutaneous Adverse Reactions Related to Systemic Antibiotics
 MAJOR ARTICLE Severe Cutaneous Adverse Reactions Related to Systemic Antibiotics Ying-Fang Lin, 1 Chih-Hsun Yang, 2,3 Hu Sindy, 1,3 Jing-Yi Lin, 2,3 Chung-Yee Rosaline Hui, 2,3 Yun-Chen Tsai, 2 Ting-Shu
MAJOR ARTICLE Severe Cutaneous Adverse Reactions Related to Systemic Antibiotics Ying-Fang Lin, 1 Chih-Hsun Yang, 2,3 Hu Sindy, 1,3 Jing-Yi Lin, 2,3 Chung-Yee Rosaline Hui, 2,3 Yun-Chen Tsai, 2 Ting-Shu
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION. 05 May 2010
 The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 05 May 2010 LAMICTAL 2 mg, dispersible / chewable tablet B/30 (CIP: 354 581-7) LAMICTAL 5 mg, dispersible / chewable
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 05 May 2010 LAMICTAL 2 mg, dispersible / chewable tablet B/30 (CIP: 354 581-7) LAMICTAL 5 mg, dispersible / chewable
STEVENS-JOHNSON SYNDROME AND TOXIC EPIDERMAL NECROLYSIS IN CHILDREN: A LITERATURE REVIEW OF CURRENT TREATMENTS
 STEVENS-JOHNSON SYNDROME AND TOXIC EPIDERMAL NECROLYSIS IN CHILDREN: A LITERATURE REVIEW OF CURRENT TREATMENTS *Blanca R. Del Pozzo-Magaña, 1 Alejandro Lazo-Langner 2,3 1. Department of Pediatrics, University
STEVENS-JOHNSON SYNDROME AND TOXIC EPIDERMAL NECROLYSIS IN CHILDREN: A LITERATURE REVIEW OF CURRENT TREATMENTS *Blanca R. Del Pozzo-Magaña, 1 Alejandro Lazo-Langner 2,3 1. Department of Pediatrics, University
Dr. Venkateswari. R. Dr. Janani Sankar s unit Kanchi Kamakoti CHILDS Trust Hospital
 Dr. Venkateswari. R. Dr. Janani Sankar s unit Kanchi Kamakoti CHILDS Trust Hospital Acknowledgements: KKCTH Dr. Ramkumar Consultant Dermatologist Dr. Ramprakash Consultant Ophthalmologist Dr. Prasad Manne
Dr. Venkateswari. R. Dr. Janani Sankar s unit Kanchi Kamakoti CHILDS Trust Hospital Acknowledgements: KKCTH Dr. Ramkumar Consultant Dermatologist Dr. Ramprakash Consultant Ophthalmologist Dr. Prasad Manne
I. Introduction Epilepsy is the tendency to have recurrent seizures unprovoked by systemic or acute neurologic insults. Antiepileptic drugs (AEDs)
 1 2 I. Introduction Epilepsy is the tendency to have recurrent seizures unprovoked by systemic or acute neurologic insults. Antiepileptic drugs (AEDs) are those which decrease the frequency and/or severity
1 2 I. Introduction Epilepsy is the tendency to have recurrent seizures unprovoked by systemic or acute neurologic insults. Antiepileptic drugs (AEDs) are those which decrease the frequency and/or severity
Analysis of Stevens-Johnson Syndrome and Toxic Epidermal Necrolysis in Japan from 2000 to 2006 Yumiko Yamane 1, Michiko Aihara 1 and Zenro Ikezawa 1
 Allergology International. 7;:9- DOI:. allergolint.o-7- ORIGINAL ARTICLE Analysis of Stevens-Johnson Syndrome and Toxic Epidermal Necrolysis in Japan from to Yumiko Yamane, Michiko Aihara and Zenro Ikezawa
Allergology International. 7;:9- DOI:. allergolint.o-7- ORIGINAL ARTICLE Analysis of Stevens-Johnson Syndrome and Toxic Epidermal Necrolysis in Japan from to Yumiko Yamane, Michiko Aihara and Zenro Ikezawa
Agenda* The 9th International Congress on Cutaneous Adverse Drug Reactions (iscar 2015)
 1 of 5 Agenda* The 9th International Congress on Cutaneous Adverse Drug Reactions (iscar 2015) Co-chairs: Dr. Neil H. Shear at the 23rd World Congress of Dermatology in Vancouver, Canada. Division of Dermatology,
1 of 5 Agenda* The 9th International Congress on Cutaneous Adverse Drug Reactions (iscar 2015) Co-chairs: Dr. Neil H. Shear at the 23rd World Congress of Dermatology in Vancouver, Canada. Division of Dermatology,
International Journal of Basic & Clinical Pharmacology. Profile of cutaneous adverse drug reactions of carbamazepine
 Print ISSN: 2319-2003 Online ISSN: 2279-0780 IJBCP International Journal of Basic & Clinical Pharmacology DOI: http://dx.doi.org/10.18203/2319-2003.ijbcp20175211 Original Research Article Profile of cutaneous
Print ISSN: 2319-2003 Online ISSN: 2279-0780 IJBCP International Journal of Basic & Clinical Pharmacology DOI: http://dx.doi.org/10.18203/2319-2003.ijbcp20175211 Original Research Article Profile of cutaneous
Severe cutaneous adverse reactions (SCAR) are life-threatening
 Stevens-Johnson syndrome and toxic epidermal necrolysis: clinical patterns, diagnostic considerations, etiology, and therapeutic management Maja Mockenhaupt, MD, PhD n Abstract Severe cutaneous adverse
Stevens-Johnson syndrome and toxic epidermal necrolysis: clinical patterns, diagnostic considerations, etiology, and therapeutic management Maja Mockenhaupt, MD, PhD n Abstract Severe cutaneous adverse
SAMPLE REPORT MENTAL HEALTH DNA INSIGHT
 PERSONAL DETAILS DOB Jan 1, 19XX ETHNICITY Caucasian ORDERING HEALTHCARE PROFESSIONAL Glenn Braunstein.D. 6777 Nancy Ridge Drive San Diego, CA 92121 US LABORATORY INFO ACCESSION NUBER ACTIVATION CODE SPECIEN
PERSONAL DETAILS DOB Jan 1, 19XX ETHNICITY Caucasian ORDERING HEALTHCARE PROFESSIONAL Glenn Braunstein.D. 6777 Nancy Ridge Drive San Diego, CA 92121 US LABORATORY INFO ACCESSION NUBER ACTIVATION CODE SPECIEN
On completion of this chapter you should be able to: list the most common types of childhood epilepsies and their symptoms
 9 Epilepsy The incidence of epilepsy is highest in the first two decades of life. It falls after that only to rise again in late life. Epilepsy is one of the most common chronic neurological condition
9 Epilepsy The incidence of epilepsy is highest in the first two decades of life. It falls after that only to rise again in late life. Epilepsy is one of the most common chronic neurological condition
EFAVIRENZ ASSOCIATED STEVENS-JOHNSON SYNDROME
 EFAVIRENZ ASSOCIATED STEVENS-JOHNSON SYNDROME To the Editor: Persons with human immunodeficiency virus (HIV) infection are highly susceptible to adverse dermatological reactions to specific medications
EFAVIRENZ ASSOCIATED STEVENS-JOHNSON SYNDROME To the Editor: Persons with human immunodeficiency virus (HIV) infection are highly susceptible to adverse dermatological reactions to specific medications
Elements for a public summary. VI.2.1 Overview of disease epidemiology
 VI.2 Elements for a public summary VI.2.1 Overview of disease epidemiology Epilepsy: It is the commonest neurological condition, characterized by recurrent seizures, affecting people of all ages, race
VI.2 Elements for a public summary VI.2.1 Overview of disease epidemiology Epilepsy: It is the commonest neurological condition, characterized by recurrent seizures, affecting people of all ages, race
Tegretol and low sodium levels
 Tegretol and low sodium levels Gogamz Menu 7-2-2018 Easy to read patient leaflet for Tegretol. If you have taken certain drugs used for low mood. Signs of low sodium levels like headache,. Trigeminal Neuralgia
Tegretol and low sodium levels Gogamz Menu 7-2-2018 Easy to read patient leaflet for Tegretol. If you have taken certain drugs used for low mood. Signs of low sodium levels like headache,. Trigeminal Neuralgia
Contemporary Developments in Childhood Epilepsy Management. Olivia O Mahony, Cork University Hospital, Cork, and Mercy University Hospital
 Contemporary Developments in Childhood Epilepsy Management Olivia O Mahony, Cork University Hospital, Cork, and Mercy University Hospital Developments in Epilepsy Care Standardised epilepsy care using
Contemporary Developments in Childhood Epilepsy Management Olivia O Mahony, Cork University Hospital, Cork, and Mercy University Hospital Developments in Epilepsy Care Standardised epilepsy care using
SEVERE CUTANEOUS ADVERSE DRUG REACTIONS: STEVENS-JOHNSON SYNDROME AND TOXIC EPIDERMAL NECROLYSISA, A REPORT OF 4 CASES SEEN AT UMMC
 SEVERE CUTANEOUS ADVERSE DRUG REACTIONS: STEVENS-JOHNSON SYNDROME AND TOXIC EPIDERMAL NECROLYSISA, A REPORT OF 4 CASES SEEN AT UMMC Shasha Khairullah, Rokiah Che Ismail Department of Medicine, Faculty
SEVERE CUTANEOUS ADVERSE DRUG REACTIONS: STEVENS-JOHNSON SYNDROME AND TOXIC EPIDERMAL NECROLYSISA, A REPORT OF 4 CASES SEEN AT UMMC Shasha Khairullah, Rokiah Che Ismail Department of Medicine, Faculty
Mechanisms of Drug Hypersensitivity Reactions
 18/5/213 Mechanisms of Drug Hypersensitivity Reactions Munir Pirmohamed NHS Chair of Pharmacogenetics Department of Molecular and Clinical Pharmacology Institute of Translational Medicine University of
18/5/213 Mechanisms of Drug Hypersensitivity Reactions Munir Pirmohamed NHS Chair of Pharmacogenetics Department of Molecular and Clinical Pharmacology Institute of Translational Medicine University of
A Clinical Study of Stevens-Johnson Syndrome and Toxic Epidermal Necrolysis: Efficacy of Treatment in Burn Intensive Care Unit
 J Korean Surg Soc 0;:133-139 DOI:.414/jkss.0..3.133 원 저 A Clinical Study of Stevens-Johnson Syndrome and Toxic Epidermal Necrolysis: Efficacy of Treatment in Burn Intensive Care Unit Departments of Surgery
J Korean Surg Soc 0;:133-139 DOI:.414/jkss.0..3.133 원 저 A Clinical Study of Stevens-Johnson Syndrome and Toxic Epidermal Necrolysis: Efficacy of Treatment in Burn Intensive Care Unit Departments of Surgery
Stevens-Johnson Syndrome in patients receiving cranial irradiation and concomitant diphenylhydantoin
 Turkish Journal of Cancer Vol. 32/ No. 4/2002 Stevens-Johnson Syndrome in patients receiving cranial irradiation and concomitant diphenylhydantoin ERKAN TOPKAN, FARUK ZORLU, MURAT GÜRKAYNAK Hacettepe University
Turkish Journal of Cancer Vol. 32/ No. 4/2002 Stevens-Johnson Syndrome in patients receiving cranial irradiation and concomitant diphenylhydantoin ERKAN TOPKAN, FARUK ZORLU, MURAT GÜRKAYNAK Hacettepe University
8/8/2016. Overview. Back to Basics: Immunology. Adverse Reactions to Drugs: Dispelling Myths
 Adverse Reactions to Drugs: Dispelling Myths Allison Ramsey, MD NPA Annual Conference September 30, 2016 Overview Review of types of hypersensitivity reactions Penicillin allergy IV contrast allergy Local
Adverse Reactions to Drugs: Dispelling Myths Allison Ramsey, MD NPA Annual Conference September 30, 2016 Overview Review of types of hypersensitivity reactions Penicillin allergy IV contrast allergy Local
PACKAGE LEAFLET: INFORMATION FOR THE USER
 PACKAGE LEAFLET: INFORMATION FOR THE USER Fucidin 250 mg/5 ml Oral Suspension fusidic acid Read all of this leaflet carefully before you start taking this medicine because it contains important information
PACKAGE LEAFLET: INFORMATION FOR THE USER Fucidin 250 mg/5 ml Oral Suspension fusidic acid Read all of this leaflet carefully before you start taking this medicine because it contains important information
PHM142 Autoimmune Disorders + Idiosyncratic Drug Reactions
 PHM142 Autoimmune Disorders + Idiosyncratic Drug Reactions 1 Autoimmune Disorders Auto-reactivity: low physiological levels (e.g. tolerance) vs. pathogenic levels 80+ types of autoimmune diseases affect
PHM142 Autoimmune Disorders + Idiosyncratic Drug Reactions 1 Autoimmune Disorders Auto-reactivity: low physiological levels (e.g. tolerance) vs. pathogenic levels 80+ types of autoimmune diseases affect
PEER REVIEW HISTORY ARTICLE DETAILS VERSION 1 - REVIEW
 PEER REVIEW HISTORY BMJ Paediatrics Open publishes all reviews undertaken for accepted manuscripts. Reviewers are asked to complete a checklist review form and are provided with free text boxes to elaborate
PEER REVIEW HISTORY BMJ Paediatrics Open publishes all reviews undertaken for accepted manuscripts. Reviewers are asked to complete a checklist review form and are provided with free text boxes to elaborate
Toxic Epidermal Necrolysis - A Case Report
 The Journal of Critical Care Medicine 2017;3(1):29-33 CASE REPORT Toxic Epidermal Necrolysis - A Case Report Laura Stătescu¹, Magda Constantin², Horia Silviu Morariu³ *, Laura Gheucă Solovăstru¹ ¹ Dermatology
The Journal of Critical Care Medicine 2017;3(1):29-33 CASE REPORT Toxic Epidermal Necrolysis - A Case Report Laura Stătescu¹, Magda Constantin², Horia Silviu Morariu³ *, Laura Gheucă Solovăstru¹ ¹ Dermatology
PACKAGE LEAFLET: INFORMATION FOR THE USER
 PACKAGE LEAFLET: INFORMATION FOR THE USER Fucidin 250 mg Tablets sodium fusidate Read all of this leaflet carefully before you start taking this medicine because it contains important information for you.
PACKAGE LEAFLET: INFORMATION FOR THE USER Fucidin 250 mg Tablets sodium fusidate Read all of this leaflet carefully before you start taking this medicine because it contains important information for you.
Journal of Chemical and Pharmaceutical Research
 Available on line www.jocpr.com Journal of Chemical and Pharmaceutical Research J. Chem. Pharm. Res., 2010, 2(2): 618-626 ISSN No: 0975-7384 Stevens-Johnson Syndrome-A life threatening skin disorder: A
Available on line www.jocpr.com Journal of Chemical and Pharmaceutical Research J. Chem. Pharm. Res., 2010, 2(2): 618-626 ISSN No: 0975-7384 Stevens-Johnson Syndrome-A life threatening skin disorder: A
SAMPLE REPORT MENTAL HEALTH DNA INSIGHT LABORATORY INFO. Protected Health Information. SSRIs. TCAs. Other Antidepressants
 Test Results Reviewed & Approved by: Laboratory Director, Nilesh Dharajiya,.D. ENTAL HEALTH DNA INSIGHT PERSONAL DETAILS DOB Jan 1, 19XX ETHNICITY Caucasian ORDERING HEALTHCARE PROFESSIONAL Glenn Braunstein.D.
Test Results Reviewed & Approved by: Laboratory Director, Nilesh Dharajiya,.D. ENTAL HEALTH DNA INSIGHT PERSONAL DETAILS DOB Jan 1, 19XX ETHNICITY Caucasian ORDERING HEALTHCARE PROFESSIONAL Glenn Braunstein.D.
Health economics and drug safety
 Health economics and drug safety Professor Dyfrig Hughes FFRPS FBPhS FLSW Centre for Health Economics & Medicines Evaluation Bangor University, Wales @HughesDyfrig ADEs that are not reactions to a medicine
Health economics and drug safety Professor Dyfrig Hughes FFRPS FBPhS FLSW Centre for Health Economics & Medicines Evaluation Bangor University, Wales @HughesDyfrig ADEs that are not reactions to a medicine
In the past few years, beta-lactam-resistant gram-positive
 Early Diagnosis Is Key in Vancomycin-Induced Linear IgA Bullous Dermatosis and Stevens-Johnson Syndrome Douglas H. Jones, MS Michael Todd, MD Timothy J. Craig, DO Background: With the emergence of highly
Early Diagnosis Is Key in Vancomycin-Induced Linear IgA Bullous Dermatosis and Stevens-Johnson Syndrome Douglas H. Jones, MS Michael Todd, MD Timothy J. Craig, DO Background: With the emergence of highly
