Proximal Hamstring Tendon Repair
|
|
|
- Deirdre Johnston
- 5 years ago
- Views:
Transcription
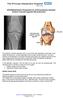
1 Dr. Mark Price MGH Sports Medicine Center 175 Cambridge Street, 4th floor Boston, MA Proximal Hamstring Tendon Repair The hamstrings are a group of three muscles that run along the back of the thigh. The hamstrings consist of the semitendinosus, the semimembranosus, and the biceps femoris. They are responsible for powering hip extension (bending your hip backwards) and knee flexion (bending your knee). They attach below the knee joint in the lower leg and onto the ischial tuberosity, a site located on the pelvis deep to the gluteal fold. Hamstring ruptures are almost always the result of an acute injury (e.g. waterskiing). Other activities such as soccer, sprinting or gymnastics are often implicated, but can also lead to strains or sprains of the hamstring tendon, which seldom require surgery. When the hamstring tendons tear, however, it can involve one, two or all three of the muscles being pulled off the ischial tuberosity. Initial treatment for tendon tears may consist of conservative treatment, including ice, NSAIDs, cortisone injections, and/or physical therapy. However, depending on the severity and nature of the tendon tear, surgical repair may be recommended. While there are no hard and fast rules, in general it is recommended that tears which involve two tendons with retraction of greater than 2 cm, and tears of all three tendons be repaired surgically. Occasionally, tendons with chronic high-grade partial tearing, which have failed non-operative management can also benefit from surgical debridement and repair. Surgical repair consists of an incision along the back of the thigh, freeing of the tendons from the surrounding tissue and reattachment to the ischial tuberosity. This surgery has a high success rate in terms of returning individuals back to their preinjury level of activity, treating pain, and restoring strength. Typically it is ideal for repairs to be done within 4 weeks of the time of injury. However, there have been studies showing good results with repair of more chronic injuries. Sometimes a chronic repair can require tendon grafting, which will be explained in more detail by Dr. Price should that proove necessary. The risks of surgery include but are not limited to: Infection Nerve injury to the cutaneous or sciatic nerve Knee stiffness Failure of healing Persistent pain or weakness Blood clots Risks of anesthesia Afterwards a hinged hip or knee brace is used to protect the repair. The length of time required to wear the brace is usually a minimum of 6 weeks followed by several weeks of rehabilitation. 1
2 Postop Instructions You will wake up in the operating room with a brace in place. You will go to the recovery room at and then either to a private room or home after a few hours. You can get out of bed when you wish. You should continue to apply ice to your buttocks to reduce pain and swelling. If you are admitted overnight you will likely be discharged home on the first postoperative. Activites & advice for in the hospital and while at home 1. Please call with any concerns: Apply ice to the knee as it will be quite helpful. After two days, you can change the dressing to a smaller one to allow the cold to better get to the knee. Be sure to leave the little pieces of tape (steri-strips) in place. 3. After two days it is okay to shower and get the wound wet, but do not soak the wound as you would in a bath tub or hot tub. 4. After surgery there is a variable amount of pain and swelling. This will dissipate after several days. Continue to take the pain medicine you were prescribed as needed. Remember it is called pain control, not pain elimination. 5. It is important to look out of signs of infection following surgery. These can include: fever (temperature > , chills, nausea, vomiting, diarrhea, redness around your incision, or yellow or green drainage from your incision. Should any of these be present please contact Dr. Price s office immediately. 6. You will have an office visit scheduled days after your surgery. 2
3 Phase I: First six weeks after surgery 1. Control pain and swelling 2. Activate the quadriceps muscles 3. Protect the repair Activities: 1. Brace and crutches: You will go home with crutches and a hip brace limited to 45 degrees. Unless you have been instructed otherwise by Dr. Price, you will be touch---down weight bearing. This means you can put a small amount of weight on your foot for balance, but nothing close to your full weight. You should use your crutches at all times for walking. a. At approximately two weeks after surgery you may progress to putting 50% of your weight down while still walking with crutches. b. You may start to progress hip flexion (change the lock setting on the brace) so that by week 4 you are at 60 degrees and by week 6 you are at 90 degrees. It is very important not to progress faster than this, though. Don t undo all your hard work by damaging the repair. 2. Your nurse or therapist will demonstrate the proper form for walking with crutches: a. Put the crutches forward about one step s length b. Put the injured leg forward in line with the crutch tips c. Touch the foot of the injured leg to the floor and put as much weight down as is comfortable (brace on and locked) d. While bearing weight on the injured leg, take a step through with the uninjured leg. 3. Elastic stockings: wear an elastic stocking below the knee until your first postoperative visit. Do at least 10 ankle pump exercises each hour to help prevent blood clots 4. Continue to use ice several times per day, minutes at a time. 5. You may notice some numbness along the back side of your thigh. This is often because the cutaneous (skin) nerve was stretched as part of the surgery. Most often this will improve over the course of a few weeks. Exercises: Program: 7 days per week, 3 times per day Quadriceps setting with hip brace in place 1-2 sets 20 reps Ankle pumps 10 per hour Scar mobilization 2-3 minutes Passive knee ROM with no hip flexion 1-2 sets 20 reps *Side-lying hip abduction *Calf raises 3
4 Quadriceps Setting Lie or sit with knee straight, but hip brace in place. Tighten and hold the front thigh muscle making the knee flat and straight. Hold 5 seconds for each contraction. Ankle Pumps Move the ankle up and down to help stimulate circulation in the leg. Scar Mobilization Gently rub the scar in a circular motion. This will help decrease scar sensitivity. In this phase do not apply lotions or oils. Gentle motion with two fingers should be sufficient. Passive ROM While standing up with the brace in place have a someone bend your knee behind you so that it comes up toward your buttocks. Have the same assistant hold your lower leg so that on the way back down it is being held and does not drop to the ground. It is important to not fire your own muscles at this point, as this may damage the repair. Other exercises It is okay to do upper body cardiovascular exercises with the upper body ergometer or upper body circuit training. * DO NOT start these exercises until 2 weeks postoperative 4
5 Phase II: 6-12 weeks after surgery 1. Protect the tendon repair and allow healing 2. Normalize gait 3. Begin muscle strengthening and functional movements Activities: 1. Use of the brace and crutches. You may feel like you need the crutches for the first few days after the brace comes off this is very normal. Gradually start to wean yourself from use of the crutches, ideally over the next two weeks. 2. It is okay to get the wound wet in such as in a bathtub or hot tub. 3. At this point it is okay to start driving. If your right leg was the operated leg, take some practice runs in a deserted parking lot prior to venturing out into rush hour. 4. It is okay to start progressively walking, slowly, on level surfaces. However, you are not cleared for running. Exercises: 1. Progressive hip and knee flexion 2. Active stretching of all uninvolved muscle groups 3. Stationary bicycle is okay at this point 4. HS curls antigravity 5. Hip extension antigravity 6. At 10 weeks postop may: a. Progress to ankle weight PRE 1lb per week to 5 lbs b. Bridging SLR c. Wall slides d. Clam shells e. Partial squats 5
6 Phase III: weeks after surgery 1. Walk normally 2. Regain and improve range of motion 3. Continue muscle strengthening exercises Activities: 1. The repaired tendon is still weak and subject to injury if your overload it. You should continue to be careful when walking up and down steps and inclined surfaces. 2. Continue to use ice if there is knee pain or swelling. 3. You may want to wear a neoprene sleeve over your hamstring as you begin doing more activities, as the warmth and support offers some relief. 4. You should continue to practice walking with increased speed and distances. Do not go so long that the leg aches the next day. No running yet. Sorry. Exercises 1. Full range of motion exercises are allowed at this point 2. Gentle HS stretching 3. Start with cautious use of weight training machines. Do not force painful motion your muscles will fatigue easier and with less weight than you remember. Don t yet push it. 4. Single leg closed chain exercises. 6
7 Phase IV: 16 weeks after surgery 1. Progress strengthening of quadriceps 2. Preserve range of motion 3. Protect repair 4. Return to normal activities Activities/Exercises: 1. You may be discharged from PT at some point after the 16th week. This does not mean you are fully recovered, though. Continue the same exercises you have been doing in the previous phase. 2. Continue to progress the amount of weight used in the exercises, but do not overload the hamstring it will be a good 6 months before it starts feeling normal. 3. You may begin doing walk to jog progressions. Start with 5:1 ratio of walk to run and gradually progress this. Let pain be your guide do not force painful motion at this point. 4. Sprinting or speed drills may begin at approximately 20 weeks postop. 5. Jumping and plyometrics can begin at approximately 24 weeks postop. 7
Shoulder Arthroscopy: Postop Instructions. Activites & Advice for in the Hospital and while at Home
 Dr. Mark Price MGH Sports Medicine Center 175 Cambridge Street, 4th floor Boston, MA 02114 www.massgeneral.org/ortho-sports-medicine/dr-price Shoulder Arthroscopy: Postop Instructions You will wake up
Dr. Mark Price MGH Sports Medicine Center 175 Cambridge Street, 4th floor Boston, MA 02114 www.massgeneral.org/ortho-sports-medicine/dr-price Shoulder Arthroscopy: Postop Instructions You will wake up
Pectorlais Major Tendon Repair
 Dr. Mark Price MGH Sports Medicine Center 175 Cambridge Street, 4th floor Boston, MA 02114 www.massgeneral.org/ortho-sports-medicine/dr-price Pectorlais Major Tendon Repair The pectoralis major muscle
Dr. Mark Price MGH Sports Medicine Center 175 Cambridge Street, 4th floor Boston, MA 02114 www.massgeneral.org/ortho-sports-medicine/dr-price Pectorlais Major Tendon Repair The pectoralis major muscle
PATELLA INSTABILITY AND REALIGNMENT
 Daniel P. Duggan, D.O. The Sports Clinic 23961 Calle de la Magdalena, Suite 229 Laguna Hills, CA 92653 Phone: (949) 581-7001 Fax: (949) 581-8410 http://orthodoc.aaos.org/danielduggando PATELLA INSTABILITY
Daniel P. Duggan, D.O. The Sports Clinic 23961 Calle de la Magdalena, Suite 229 Laguna Hills, CA 92653 Phone: (949) 581-7001 Fax: (949) 581-8410 http://orthodoc.aaos.org/danielduggando PATELLA INSTABILITY
Rehabilitation After Patellar Tendon Debridement Surgery
 Katherine J. Coyner, MD UCONN Musculoskeletal Institute Medical Arts & Research Building 263 Farmington Ave. Farmington, CT 06030 Office: (860) 679-6600 Fax: (860) 679-6649 www.drcoyner.com Avon Office
Katherine J. Coyner, MD UCONN Musculoskeletal Institute Medical Arts & Research Building 263 Farmington Ave. Farmington, CT 06030 Office: (860) 679-6600 Fax: (860) 679-6649 www.drcoyner.com Avon Office
REHABILITATION AFTER ARTHROSCOPIC KNEE SURGERY
 REHABILITATION AFTER ARTHROSCOPIC KNEE SURGERY This protocol is a guideline for your rehabilitation after arthroscopic knee surgery. You may vary in your ability to do these exercises and to progress to
REHABILITATION AFTER ARTHROSCOPIC KNEE SURGERY This protocol is a guideline for your rehabilitation after arthroscopic knee surgery. You may vary in your ability to do these exercises and to progress to
MICROFRACTURE LOURDES MEDICAL ASSOCIATES PROFESSIONAL ORTHOPAEDICS SPORTS MEDICINE & ARTHROSCOPY
 LOURDES MEDICAL ASSOCIATES Sean Mc Millan, DO Director of Orthopaedic Sports Medicine & Arthroscopy 2103 Burlington-Mount Holly Rd Burlington, NJ 08016 (609) 747-9200 (office) (609) 747-1408 (fax) http://orthodoc.aaos.org/drmcmillan
LOURDES MEDICAL ASSOCIATES Sean Mc Millan, DO Director of Orthopaedic Sports Medicine & Arthroscopy 2103 Burlington-Mount Holly Rd Burlington, NJ 08016 (609) 747-9200 (office) (609) 747-1408 (fax) http://orthodoc.aaos.org/drmcmillan
Mosaicplasty and OATS Rehabilitation Protocol
 Mosaicplasty and OATS Rehabilitation Protocol PHASE 1: 0 2 weeks after surgery You will go home with crutches, cryocuff cold therapy unit and a CPM machine. GOALS: 1. Protect the cartilage transfer avoid
Mosaicplasty and OATS Rehabilitation Protocol PHASE 1: 0 2 weeks after surgery You will go home with crutches, cryocuff cold therapy unit and a CPM machine. GOALS: 1. Protect the cartilage transfer avoid
PHASE ONE: THE FIRST SIX WEEKS AFTER INJURY
 Exercises After Injury to the Anterior Cruciate Ligament (ACL) of the Knee Dr. Abigail R. Hamilton, M.D. PHASE ONE: THE FIRST SIX WEEKS AFTER INJURY Initially, the knee needs to be protected-use the knee
Exercises After Injury to the Anterior Cruciate Ligament (ACL) of the Knee Dr. Abigail R. Hamilton, M.D. PHASE ONE: THE FIRST SIX WEEKS AFTER INJURY Initially, the knee needs to be protected-use the knee
Rehabilitation. Walkers, Crutches, Canes
 Walkers, Crutches, Canes These devices provide support through your arms to limit the amount of weight on your operated hip. Initially, after a total hip replacement you will use a walker to get around.
Walkers, Crutches, Canes These devices provide support through your arms to limit the amount of weight on your operated hip. Initially, after a total hip replacement you will use a walker to get around.
KNEE AND LEG EXERCISE PROGRAM
 KNEE AND LEG EXERCISE PROGRAM These exercises are specifically designed to rehabilitate the muscles of the hip and knee by increasing the strength and flexibility of the involved leg. This exercise program
KNEE AND LEG EXERCISE PROGRAM These exercises are specifically designed to rehabilitate the muscles of the hip and knee by increasing the strength and flexibility of the involved leg. This exercise program
MENISCAL REPAIR LOURDES MEDICAL ASSOCIATES PROFESSIONAL ORTHOPAEDICS SPORTS MEDICINE & ARTHROSCOPY
 LOURDES MEDICAL ASSOCIATES Sean Mc Millan, DO Director of Orthopaedic Sports Medicine & Arthroscopy 2103 Burlington-Mount Holly Rd Burlington, NJ 08016 (609) 747-9200 (office) (609) 747-1408 (fax) http://orthodoc.aaos.org/drmcmillan
LOURDES MEDICAL ASSOCIATES Sean Mc Millan, DO Director of Orthopaedic Sports Medicine & Arthroscopy 2103 Burlington-Mount Holly Rd Burlington, NJ 08016 (609) 747-9200 (office) (609) 747-1408 (fax) http://orthodoc.aaos.org/drmcmillan
Knee Arthroscopy: Postoperative Instructions
 Knee Arthroscopy: Postoperative Instructions John P. Woll, MD Knee arthroscopy is a commonly performed procedure that is much less invasive than previous open techniques, but it is still an operation,
Knee Arthroscopy: Postoperative Instructions John P. Woll, MD Knee arthroscopy is a commonly performed procedure that is much less invasive than previous open techniques, but it is still an operation,
Postoperative Days 1-7
 ACL RECONSTRUCTION REHABILITATION PROTOCOL Postoperative Days 1-7 *IT IS EXTREMELY IMPORTANT THAT YOU WORK ON EXTENSION IMMEDIATELY Goals: * Control pain and swelling * Care for the knee and dressing *
ACL RECONSTRUCTION REHABILITATION PROTOCOL Postoperative Days 1-7 *IT IS EXTREMELY IMPORTANT THAT YOU WORK ON EXTENSION IMMEDIATELY Goals: * Control pain and swelling * Care for the knee and dressing *
Arthroscopic Surgery
 175 Cambridge Street, 4 th floor Boston, MA 02114 Tel: 617-726-7500 Arthroscopic Surgery What is arthroscopy? Arthroscopy is a surgical procedure that orthopedic surgeons use to visualize, diagnose and
175 Cambridge Street, 4 th floor Boston, MA 02114 Tel: 617-726-7500 Arthroscopic Surgery What is arthroscopy? Arthroscopy is a surgical procedure that orthopedic surgeons use to visualize, diagnose and
James R. Romanowski, M.D.
 James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211 704-358-0308 (Office) 704-358-0037 (Fax) www.charlotteshoulder.com DISCHARGE INSTRUCTIONS
James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211 704-358-0308 (Office) 704-358-0037 (Fax) www.charlotteshoulder.com DISCHARGE INSTRUCTIONS
PCL/PLC RECONSTRUCTION REHABILITATION Revised OCTOBER 2015
 PCL/PLC RECONSTRUCTION REHABILITATION Revised OCTOBER 2015 REHABILITATION PROGRAM PHASE 1: WEEKS 0-6: PHASE I GOALS: Protect the surgical graft(s) 0-60 ROM Regain adequate quadriceps control CRUTCHES:
PCL/PLC RECONSTRUCTION REHABILITATION Revised OCTOBER 2015 REHABILITATION PROGRAM PHASE 1: WEEKS 0-6: PHASE I GOALS: Protect the surgical graft(s) 0-60 ROM Regain adequate quadriceps control CRUTCHES:
Physical & Occupational Therapy
 In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
Rehabilitation. Walking after Total Knee Replacement. Continuous Passive Motion Device
 Walking after Total Knee Replacement After your TKR, continue using your walker or crutches until your surgeons tells you it is okay to stop using them. When turning with a walker or crutches DO NOT PIVOT
Walking after Total Knee Replacement After your TKR, continue using your walker or crutches until your surgeons tells you it is okay to stop using them. When turning with a walker or crutches DO NOT PIVOT
James R. Romanowski, M.D.
 James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211 704-358-0308 (Office) 704-358-0037 (Fax) www.charlotteshoulder.com DISCHARGE INSTRUCTIONS
James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211 704-358-0308 (Office) 704-358-0037 (Fax) www.charlotteshoulder.com DISCHARGE INSTRUCTIONS
Hamstring Strain. 43 Thames Street, St Albans, Christchurch 8013 Phone: (03) Website: philip-bayliss.com.
 43 Thames Street, St Albans, Christchurch 8013 Phone: (03) 356 1353. Website: philip-bayliss.com Hamstring Strain The hamstring muscles are very susceptible to tears, strains and other common sporting
43 Thames Street, St Albans, Christchurch 8013 Phone: (03) 356 1353. Website: philip-bayliss.com Hamstring Strain The hamstring muscles are very susceptible to tears, strains and other common sporting
Patella Tendon Repair
 Alta View Sports Medicine Dr. James R. Meadows, MD Orthopedic Surgery & Sports Medicine 74 Kimballs Ln Ste 230, Draper, UT 84020 9844 S. 1300 E. Ste 100, Sandy, UT 84094 (801) 571-9433 www.meadowsmd.com
Alta View Sports Medicine Dr. James R. Meadows, MD Orthopedic Surgery & Sports Medicine 74 Kimballs Ln Ste 230, Draper, UT 84020 9844 S. 1300 E. Ste 100, Sandy, UT 84094 (801) 571-9433 www.meadowsmd.com
ACL REHABILITATION PROTOCOL
 Name: ID: Date Of Surgery :DD / MM / YYYY Procedure: ACL REHABILITATION PROTOCOL Note :If another procedure like meniscus repair or OATS (Osteochondralautograft transfer) has been done along with ACL reconstruction
Name: ID: Date Of Surgery :DD / MM / YYYY Procedure: ACL REHABILITATION PROTOCOL Note :If another procedure like meniscus repair or OATS (Osteochondralautograft transfer) has been done along with ACL reconstruction
Move your ankle inward toward your other foot and then outward away from your other foot.
 TOTAL HIP REPLACEMENT POST OPERATIVE EXERCISES Regular exercises to restore your normal hip motion and strength and a gradual return to everyday activities are important for your full recovery. Dr. Robertson
TOTAL HIP REPLACEMENT POST OPERATIVE EXERCISES Regular exercises to restore your normal hip motion and strength and a gradual return to everyday activities are important for your full recovery. Dr. Robertson
REHABILITATION AFTER KNEE MENISCUS REPAIR. Dr. Abigail R. Hamilton, M.D.
 REHABILITATION AFTER KNEE MENISCUS REPAIR Dr. Abigail R. Hamilton, M.D. PHASE ONE: THE FINAL WEEK AFTER SURGERY Goals: 1. Control pain and swelling 2. Initiate knee motion 3. Activate the quadriceps muscles
REHABILITATION AFTER KNEE MENISCUS REPAIR Dr. Abigail R. Hamilton, M.D. PHASE ONE: THE FINAL WEEK AFTER SURGERY Goals: 1. Control pain and swelling 2. Initiate knee motion 3. Activate the quadriceps muscles
MENISCUS TEAR. Description
 MENISCUS TEAR Description Expected Outcome The meniscus is a C-shaped cartilage structure in the knee that sits on top of the leg bone (tibia). Each knee has two menisci, an inner and outer meniscus. The
MENISCUS TEAR Description Expected Outcome The meniscus is a C-shaped cartilage structure in the knee that sits on top of the leg bone (tibia). Each knee has two menisci, an inner and outer meniscus. The
ACL Reconstruction. Role of the Anterior Cruciate Ligament. Treatment of ACL tears. ACL Reconstruction
 Role of the Anterior Cruciate Ligament The ACL stabilizes the knee when jumping, pivoting, or cutting. It prevents the shinbone (tibia) from sliding forward on the thigh bone (femur). ACL tears often occur
Role of the Anterior Cruciate Ligament The ACL stabilizes the knee when jumping, pivoting, or cutting. It prevents the shinbone (tibia) from sliding forward on the thigh bone (femur). ACL tears often occur
What is arthroscopy? Normal knee anatomy
 What is arthroscopy? Arthroscopy is a common surgical procedure for examining and repairing the inside of your knee. It is a minimally invasive surgical procedure which uses an Arthroscope and other specialized
What is arthroscopy? Arthroscopy is a common surgical procedure for examining and repairing the inside of your knee. It is a minimally invasive surgical procedure which uses an Arthroscope and other specialized
Lateral Collateral Ligament Sprain
 What is lateral collateral ligament sprain? Lateral Collateral Ligament Sprain A sprain is a joint injury that causes a stretch or tear in a ligament, a strong band of tissue connecting one bone to another.
What is lateral collateral ligament sprain? Lateral Collateral Ligament Sprain A sprain is a joint injury that causes a stretch or tear in a ligament, a strong band of tissue connecting one bone to another.
Patellofemoral Pain Syndrome
 What is patellofemoral pain syndrome? Patellofemoral Pain Syndrome Patellofemoral pain syndrome is pain behind the kneecap. It has been given many names, including patellofemoral disorder, patellar malalignment,
What is patellofemoral pain syndrome? Patellofemoral Pain Syndrome Patellofemoral pain syndrome is pain behind the kneecap. It has been given many names, including patellofemoral disorder, patellar malalignment,
Anterior Cruciate Ligament (ACL) Reconstruction
 Dr. Mark Price MGH Sports Medicine Center 175 Cambridge Street, 4th floor Boston, MA 02114 www.massgeneral.org/ortho-sports-medicine/dr-price Anterior Cruciate Ligament (ACL) Reconstruction The anterior
Dr. Mark Price MGH Sports Medicine Center 175 Cambridge Street, 4th floor Boston, MA 02114 www.massgeneral.org/ortho-sports-medicine/dr-price Anterior Cruciate Ligament (ACL) Reconstruction The anterior
ACTIVITIES AND EXERCISES AFTER INJURY TO THE MEDIAL COLLATERAL LIGAMENT (MCL) OF THE KNEE
 ACTIVITIES AND EXERCISES AFTER INJURY TO THE MEDIAL COLLATERAL LIGAMENT (MCL) OF THE KNEE PHASE 1: THE FIRST SIX WEEKS AFTER INJURY (grade 2 and 3) THREE WEEKS AFTER INJURY (grade 1) The knee should be
ACTIVITIES AND EXERCISES AFTER INJURY TO THE MEDIAL COLLATERAL LIGAMENT (MCL) OF THE KNEE PHASE 1: THE FIRST SIX WEEKS AFTER INJURY (grade 2 and 3) THREE WEEKS AFTER INJURY (grade 1) The knee should be
REHABILITATION FOLLOWING ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION (using Hamstring Graft)
 REHABILITATION FOLLOWING ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION (using Hamstring Graft) PHASE 1: (0-3 WEEKS) Goal: Protect graft, manage pain, decrease swelling and improve range of movement. To optimise
REHABILITATION FOLLOWING ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION (using Hamstring Graft) PHASE 1: (0-3 WEEKS) Goal: Protect graft, manage pain, decrease swelling and improve range of movement. To optimise
ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL
 ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL PREOPERATIVE: If you have suffered an acute ACL injury and surgery is planned, the time between injury and surgery should be used to regain knee motion,
ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL PREOPERATIVE: If you have suffered an acute ACL injury and surgery is planned, the time between injury and surgery should be used to regain knee motion,
Rehabilitation Program for Achilles Tendon Rupture/Repair
 Rehabilitation Program for Achilles Tendon Rupture/Repair This protocol is designed to assist you with your rehabilitation after surgery and should be followed under the direction of a physiotherapist
Rehabilitation Program for Achilles Tendon Rupture/Repair This protocol is designed to assist you with your rehabilitation after surgery and should be followed under the direction of a physiotherapist
Knee Conditioning Program
 Knee Conditioning Program Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle. Following
Knee Conditioning Program Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle. Following
What is an ACL Tear?...2. Treatment Options...3. Surgical Techniques...4. Preoperative Care...5. Preoperative Requirements...6
 Table of Contents What is an ACL Tear?....2 Treatment Options...3 Surgical Techniques...4 Preoperative Care...5 Preoperative Requirements...6 Postoperative Care...................... 7 Crutch use...8 Initial
Table of Contents What is an ACL Tear?....2 Treatment Options...3 Surgical Techniques...4 Preoperative Care...5 Preoperative Requirements...6 Postoperative Care...................... 7 Crutch use...8 Initial
ANATOMIC ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL
 ANATOMIC ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL PREOPERATIVE: If you have suffered an acute ACL injury and surgery is planned, the time between injury and surgery should be used to regain
ANATOMIC ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL PREOPERATIVE: If you have suffered an acute ACL injury and surgery is planned, the time between injury and surgery should be used to regain
DISCOID MENISCUS. Description
 DISCOID MENISCUS Description For participation in jumping (basketball, volleyball) or The meniscus is a cartilage structure in the knee that sits on contact sports, protect the knee joint with supportive
DISCOID MENISCUS Description For participation in jumping (basketball, volleyball) or The meniscus is a cartilage structure in the knee that sits on contact sports, protect the knee joint with supportive
Ex Fix Rehab Phase II Strengthening
 Perform repetitions of each exercise, twice daily. Increase to repetitions. Ankle Pumps: With leg resting on bed and knee straight, slowly pump ankle up and down as far as possible. Quad sets: Tighten
Perform repetitions of each exercise, twice daily. Increase to repetitions. Ankle Pumps: With leg resting on bed and knee straight, slowly pump ankle up and down as far as possible. Quad sets: Tighten
Total Hip Replacement Rehabilitation: Progression and Restrictions
 Total Hip Replacement Rehabilitation: Progression and Restrictions The success of total hip replacement (THR) is a result of predictable pain relief, improvements in quality of life, and restoration of
Total Hip Replacement Rehabilitation: Progression and Restrictions The success of total hip replacement (THR) is a result of predictable pain relief, improvements in quality of life, and restoration of
Medial Collateral Ligament Repair Protocol-Dr. McClung
 Medial Collateral Ligament Repair Protocol-Dr. McClung Brace: Normally patients will be wearing post-op knee brace locked in 30 degrees for ambulation and sleeping but drop-locked for sitting and knee
Medial Collateral Ligament Repair Protocol-Dr. McClung Brace: Normally patients will be wearing post-op knee brace locked in 30 degrees for ambulation and sleeping but drop-locked for sitting and knee
ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION
 LOURDES MEDICAL ASSOCIATES Sean Mc Millan, DO Director of Orthopaedic Sports Medicine & Arthroscopy 2103 Burlington-Mount Holly Rd Burlington, NJ 08016 (609) 747-9200 (office) (609) 747-1408 (fax) http://orthodoc.aaos.org/drmcmillan
LOURDES MEDICAL ASSOCIATES Sean Mc Millan, DO Director of Orthopaedic Sports Medicine & Arthroscopy 2103 Burlington-Mount Holly Rd Burlington, NJ 08016 (609) 747-9200 (office) (609) 747-1408 (fax) http://orthodoc.aaos.org/drmcmillan
Posterior Cruciate Ligament (PCL) Reconstruction. Preoperative Instructions
 Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Posterior Cruciate Ligament (PCL) Reconstruction Preoperative Instructions WITHIN A FEW WEEKS BEFORE SURGERY Dr. Ferry will see you in the office. He
Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Posterior Cruciate Ligament (PCL) Reconstruction Preoperative Instructions WITHIN A FEW WEEKS BEFORE SURGERY Dr. Ferry will see you in the office. He
Knee Replacement PROGRAM. Nightingale. Home Healthcare
 Knee Replacement PROGRAM TM Nightingale Home Healthcare With the help of Nightingale s experienced and professional rehabilitation team, you will be guided through a more complete and successful recovery
Knee Replacement PROGRAM TM Nightingale Home Healthcare With the help of Nightingale s experienced and professional rehabilitation team, you will be guided through a more complete and successful recovery
Knee Conditioning Program
 Prepared for: Prepared by: Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle. Following
Prepared for: Prepared by: Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle. Following
Anterior Cruciate Ligament Hamstring Rehabilitation Protocol
 Anterior Cruciate Ligament Hamstring Rehabilitation Protocol Focus on exercise quality avoid overstressing the donor area while it heals. Typically, isolated hamstring strengthening begins after the 6
Anterior Cruciate Ligament Hamstring Rehabilitation Protocol Focus on exercise quality avoid overstressing the donor area while it heals. Typically, isolated hamstring strengthening begins after the 6
Patellar Tendon / Quad Tendon Repair Surgery Discharge Instructions
 Matthew T. Mantell, MD 128 Medical Circle Winchester, VA 22601 Phone: 540-667-8975 Email: mattmantellmd@gmail.com Web: www.mattmantellmd.com Patellar Tendon / Quad Tendon Repair Surgery Discharge Instructions
Matthew T. Mantell, MD 128 Medical Circle Winchester, VA 22601 Phone: 540-667-8975 Email: mattmantellmd@gmail.com Web: www.mattmantellmd.com Patellar Tendon / Quad Tendon Repair Surgery Discharge Instructions
CENTER FOR ORTHOPAEDICS AND SPINE CARE PHYSICAL THERAPY PROTOCOL ACUTE PROXIMAL HAMSTRING TENDON REPAIR BENJAMIN J. DAVIS, MD
 Weeks 0-6 Goal: 1) Protection of the surgical repair Precautions: 1) Non-weight bearing with crutches for 6 weeks with foot flat or with knee Knee flexed to 90 degrees with sitting 2) No active hamstring
Weeks 0-6 Goal: 1) Protection of the surgical repair Precautions: 1) Non-weight bearing with crutches for 6 weeks with foot flat or with knee Knee flexed to 90 degrees with sitting 2) No active hamstring
The SPORTS CENTRE L.L.C. PATELLA/QUADRICEPS TENDON REPAIR REHABILITATION PROTOCOL
 The SPORTS CENTRE L.L.C. Orthopedic Surgery, Sports Medicine, Fractures, Joint Replacement Rob O Connor M.D. www.sportscentreortho.com PATELLA/QUADRICEPS TENDON REPAIR REHABILITATION PROTOCOL GENERAL POST-OPERATIVE
The SPORTS CENTRE L.L.C. Orthopedic Surgery, Sports Medicine, Fractures, Joint Replacement Rob O Connor M.D. www.sportscentreortho.com PATELLA/QUADRICEPS TENDON REPAIR REHABILITATION PROTOCOL GENERAL POST-OPERATIVE
Southern Sports & Orthopaedics
 Knee conditioning program This knee conditioning program is designed to help you rehabilitate from your knee injury. In some cases, the program is being used as pre-habilitation, that is strengthening
Knee conditioning program This knee conditioning program is designed to help you rehabilitate from your knee injury. In some cases, the program is being used as pre-habilitation, that is strengthening
Knee Replacement Rehabilitation
 Knee Replacement Rehabilitation The following exercises may be given to you to help get you moving and become more independent. Please bring this copy of the exercises with you to hospital. After your
Knee Replacement Rehabilitation The following exercises may be given to you to help get you moving and become more independent. Please bring this copy of the exercises with you to hospital. After your
Guidelines for patients having. Achilles Tendon Repair. Achilles Tendon Repair
 Guidelines for patients having ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 UPMC BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 Achilles Tendon Repair Please stick addressograph
Guidelines for patients having ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 UPMC BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 Achilles Tendon Repair Please stick addressograph
SHOULDER RESURFACING
 MGH Sports Medicine Center 175 Cambridge St., 4th floor Boston, MA 02114 http://orthodoc.aaos.org/mdprice SHOULDER RESURFACING The shoulder is a ball and socket joint that enables you to raise, twist,
MGH Sports Medicine Center 175 Cambridge St., 4th floor Boston, MA 02114 http://orthodoc.aaos.org/mdprice SHOULDER RESURFACING The shoulder is a ball and socket joint that enables you to raise, twist,
DISCOID MENISCUS. Description
 Montefiore Pediatric Orthopedic and Scoliosis Center Children s Hospital at Montefiore Norman Otsuka MD Eric Fornari MD Jacob Schulz MD Jaime Gomez MD Christine Moloney PA 3400 Bainbridge Avenue, 6 th
Montefiore Pediatric Orthopedic and Scoliosis Center Children s Hospital at Montefiore Norman Otsuka MD Eric Fornari MD Jacob Schulz MD Jaime Gomez MD Christine Moloney PA 3400 Bainbridge Avenue, 6 th
GG10Rehabilitation Programme for Arthroscopically Assisted Anterior Cruciate Ligament Reconstruction
 GG10Rehabilitation Programme for Arthroscopically Assisted Anterior Cruciate Ligament Reconstruction Femur ACL Graft Fibula Tibia The Anterior Cruciate Ligament (ACL) is one of the main ligaments in the
GG10Rehabilitation Programme for Arthroscopically Assisted Anterior Cruciate Ligament Reconstruction Femur ACL Graft Fibula Tibia The Anterior Cruciate Ligament (ACL) is one of the main ligaments in the
PATELLOFEMORAL INSTABILITY (SUBLUXATION AND DISLOCATION)
 PATELLOFEMORAL INSTABILITY (SUBLUXATION AND DISLOCATION) Anatomy and Function The knee joint is composed of two distinctly separate articulations. The tibiofemoral joint is formed by the thigh bone (femur)
PATELLOFEMORAL INSTABILITY (SUBLUXATION AND DISLOCATION) Anatomy and Function The knee joint is composed of two distinctly separate articulations. The tibiofemoral joint is formed by the thigh bone (femur)
SUPERIOR LABRAL REPAIRS
 LOURDES MEDICAL ASSOCIATES Sean Mc Millan, DO Director of Orthopaedic Sports Medicine & Arthroscopy 2103 Burlington-Mount Holly Rd Burlington, NJ 08016 (609) 747-9200 (office) (609) 747-1408 (fax) http://orthodoc.aaos.org/drmcmillan
LOURDES MEDICAL ASSOCIATES Sean Mc Millan, DO Director of Orthopaedic Sports Medicine & Arthroscopy 2103 Burlington-Mount Holly Rd Burlington, NJ 08016 (609) 747-9200 (office) (609) 747-1408 (fax) http://orthodoc.aaos.org/drmcmillan
Meniscal Repair Protocol-Dr. McClung
 Meniscal Repair Protocol-Dr. McClung Brace: Normally patients will be wearing post-op knee brace locked in full extension for ambulation and sleeping but drop-locked for sitting and knee ROM. Patients
Meniscal Repair Protocol-Dr. McClung Brace: Normally patients will be wearing post-op knee brace locked in full extension for ambulation and sleeping but drop-locked for sitting and knee ROM. Patients
Bone-Patellar tendon-bone Autograft ACL Recon. Date of Surgery: Patient Name:
 Dx: o Right o Left Bone-Patellar tendon-bone Autograft ACL Recon Date of Surgery: Patient Name: PT/OT: Please evaluate and treat. Follow attached protocol. 2-3 x per week x 6 weeks. Signature/Date: GENERAL
Dx: o Right o Left Bone-Patellar tendon-bone Autograft ACL Recon Date of Surgery: Patient Name: PT/OT: Please evaluate and treat. Follow attached protocol. 2-3 x per week x 6 weeks. Signature/Date: GENERAL
ACL RECONSTRUCTION REHABILITATION PROTOCOL DELAYED DAVID R. MACK, M.D. INTRODUCTION
 ACL RECONSTRUCTION REHABILITATION PROTOCOL DELAYED DAVID R. MACK, M.D. INTRODUCTION This DELAYED protocol is used if any of the following are present: meniscal repair, concomitant ligament repair or patellofemoral
ACL RECONSTRUCTION REHABILITATION PROTOCOL DELAYED DAVID R. MACK, M.D. INTRODUCTION This DELAYED protocol is used if any of the following are present: meniscal repair, concomitant ligament repair or patellofemoral
Post Operative ACL Reconstruction Protocol Brian J. White, MD
 Post Operative ACL Reconstruction Protocol Brian J. White, MD www.western-ortho.com The intent of this protocol is to provide guidelines for progression of rehabilitation. It is not intended to serve as
Post Operative ACL Reconstruction Protocol Brian J. White, MD www.western-ortho.com The intent of this protocol is to provide guidelines for progression of rehabilitation. It is not intended to serve as
Total Hip Replacement Exercise Booklet Cemented Femoral Stem Weight Bearing As Tolerated
 Total Hip Replacement Exercise Booklet Cemented Femoral Stem Weight Bearing As Tolerated Patient Name: Surgeon: Date of Surgery: Physiotherapist: Department of Rehabilitation (416) 967-8650 ext. PR 99506
Total Hip Replacement Exercise Booklet Cemented Femoral Stem Weight Bearing As Tolerated Patient Name: Surgeon: Date of Surgery: Physiotherapist: Department of Rehabilitation (416) 967-8650 ext. PR 99506
RETURN TO SPORT PROTOCOL CO.RE
 RETURN TO SPORT PROTOCOL CO.RE WHO CAN USE THIS PROGRAM This protocol is designed as a return to sport program following anterior cruciate ligament reconstruction but applies equally well to rehabilitation
RETURN TO SPORT PROTOCOL CO.RE WHO CAN USE THIS PROGRAM This protocol is designed as a return to sport program following anterior cruciate ligament reconstruction but applies equally well to rehabilitation
Jennifer L. Cook, MD
 Jennifer L. Cook, MD Florida Joint Replacement and Sports Medicine Center 5243 Hanff Lane New Port Richey, FL 34652 Phone: (727)848-4249 Fax: (727) 841-8934 ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POST-OPERATIVE
Jennifer L. Cook, MD Florida Joint Replacement and Sports Medicine Center 5243 Hanff Lane New Port Richey, FL 34652 Phone: (727)848-4249 Fax: (727) 841-8934 ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POST-OPERATIVE
TIBIAL PLATEAU FRACTURE
 TIBIAL PLATEAU FRACTURE Description Preventive Measures A tibial plateau fracture is a complete or incomplete break Appropriately warm up and stretch before practice or in the larger of the two leg bones
TIBIAL PLATEAU FRACTURE Description Preventive Measures A tibial plateau fracture is a complete or incomplete break Appropriately warm up and stretch before practice or in the larger of the two leg bones
SEMIMEMBRANOSUS TENDINITIS
 SEMIMEMBRANOSUS TENDINITIS Description Maintain appropriate conditioning: Semimembranosus tendinitis is characterized by inflammation and pain at the knee joint on the back part of the inner side of the
SEMIMEMBRANOSUS TENDINITIS Description Maintain appropriate conditioning: Semimembranosus tendinitis is characterized by inflammation and pain at the knee joint on the back part of the inner side of the
Ellipse Rehab Phase 2 Strengthening
 Strengthening Perform reps of each exercise, twice daily. Increase to reps Ankle Pumps: With leg resting on bed and knee straight, slowly pump ankle up and down as far as possible. Quad sets: Tighten thigh
Strengthening Perform reps of each exercise, twice daily. Increase to reps Ankle Pumps: With leg resting on bed and knee straight, slowly pump ankle up and down as far as possible. Quad sets: Tighten thigh
NOI- NORTHSHORE ORTHOPAEDIC INSTITUTE SPORTS MEDICINE SERVICE POST OP ACL RECONSTRUCTION INSTRUCTIONS
 NOI- NORTHSHORE ORTHOPAEDIC INSTITUTE SPORTS MEDICINE SERVICE POST OP ACL RECONSTRUCTION INSTRUCTIONS 1. Pain and swelling: Expect a considerable amount of pain the first few days post-op. Take your prescribed
NOI- NORTHSHORE ORTHOPAEDIC INSTITUTE SPORTS MEDICINE SERVICE POST OP ACL RECONSTRUCTION INSTRUCTIONS 1. Pain and swelling: Expect a considerable amount of pain the first few days post-op. Take your prescribed
Physiotherapy Information following Anterior Cruciate Ligament (ACL) Reconstruction
 Physiotherapy Information following Anterior Cruciate Ligament (ACL) Reconstruction Name:... Surgery Date:... Graft:... Orthopaedic Outpatient Appointment Date: Time: Location: Contact Number: Contacting
Physiotherapy Information following Anterior Cruciate Ligament (ACL) Reconstruction Name:... Surgery Date:... Graft:... Orthopaedic Outpatient Appointment Date: Time: Location: Contact Number: Contacting
ARTHROSCOPIC SHOULDER SURGERY
 Preoperative instructions ARTHROSCOPIC SHOULDER SURGERY Schedule surgery with the secretary in Dr.Gill s office. Within one month before surgery * Make an appointment for a preoperative office visit regarding
Preoperative instructions ARTHROSCOPIC SHOULDER SURGERY Schedule surgery with the secretary in Dr.Gill s office. Within one month before surgery * Make an appointment for a preoperative office visit regarding
High Tibial Osteotomy (HTO) Rehabilitation Protocols
 High Tibial Osteotomy (HTO) Rehabilitation Protocols Targets Upon Discharge from Hospital Protected weight-bearing (feather-weight -bearing) Ambulating with crutches Rehab brace without range of motion
High Tibial Osteotomy (HTO) Rehabilitation Protocols Targets Upon Discharge from Hospital Protected weight-bearing (feather-weight -bearing) Ambulating with crutches Rehab brace without range of motion
Knee Replacement Recovery Guide
 Knee Replacement Recovery Guide Table of Contents Congratulations!... 2 Recuperating At home... 2 Range of Motion... 2 Wound Care... 3 Important Signs & Symptoms... 3 Bathing and Showering... 3 Bruising...
Knee Replacement Recovery Guide Table of Contents Congratulations!... 2 Recuperating At home... 2 Range of Motion... 2 Wound Care... 3 Important Signs & Symptoms... 3 Bathing and Showering... 3 Bruising...
NONOPERATIVE REHABILITATION FOLLOWING ACL INJURY ( Program)
 Therapist: Phone: NONOPERATIVE REHABILITATION FOLLOWING ACL INJURY (3-3-4-4 Program) IMMEDIATE INJURY PHASE (Day 1 to Day 7) Restore full passive knee extension Diminish joint swelling and pain Restore
Therapist: Phone: NONOPERATIVE REHABILITATION FOLLOWING ACL INJURY (3-3-4-4 Program) IMMEDIATE INJURY PHASE (Day 1 to Day 7) Restore full passive knee extension Diminish joint swelling and pain Restore
Information and exercises following a proximal femoral replacement
 Physiotherapy Department Information and exercises following a proximal femoral replacement Introduction The hip joint is a type known as a ball and socket joint. The cup side of the joint is known as
Physiotherapy Department Information and exercises following a proximal femoral replacement Introduction The hip joint is a type known as a ball and socket joint. The cup side of the joint is known as
GENERAL EXERCISES KNEE BMW MANUFACTURING CO. PZ-AM-G-US I July 2017
 GENERAL EXERCISES KNEE BMW MANUFACTURING CO. PZ-AM-G-US I July 2017 Disclosure: The exercises, stretches, and mobilizations provided in this presentation are for educational purposes only are not to be
GENERAL EXERCISES KNEE BMW MANUFACTURING CO. PZ-AM-G-US I July 2017 Disclosure: The exercises, stretches, and mobilizations provided in this presentation are for educational purposes only are not to be
Post-Operative Meniscus Repair Protocol Brian J.White, MD
 Post-Operative Meniscus Repair Protocol Brian J.White, MD www.western-ortho.com (This protocol should be used with combined a ACL Reconstruction and meniscus repair) The intent of this protocol is to provide
Post-Operative Meniscus Repair Protocol Brian J.White, MD www.western-ortho.com (This protocol should be used with combined a ACL Reconstruction and meniscus repair) The intent of this protocol is to provide
Advice and exercises for managing knee and hip osteoarthritis October 2018 V1.2 April 2018 April 2021
 Advice and exercises for managing knee and hip osteoarthritis 0496 October 2018 V1.2 April 2018 April 2021 This advice and exercise booklet has been produced by senior physiotherapists working for DynamicHealth.
Advice and exercises for managing knee and hip osteoarthritis 0496 October 2018 V1.2 April 2018 April 2021 This advice and exercise booklet has been produced by senior physiotherapists working for DynamicHealth.
Patellar Tendon Debridement & Repair Rehabilitation Protocol
 Patellar Tendon Debridement & Repair Rehabilitation Protocol PREOPERATIVE PHASE Diminish inflammation, swelling, and pain Restore normal range of motion (especially knee extension) Restore voluntary muscle
Patellar Tendon Debridement & Repair Rehabilitation Protocol PREOPERATIVE PHASE Diminish inflammation, swelling, and pain Restore normal range of motion (especially knee extension) Restore voluntary muscle
ANTERIOR ANKLE IMPINGEMENT
 ANTERIOR ANKLE IMPINGEMENT Description Possible Complications Pinching of bone or soft tissue, including scar tissue, at the Frequent recurrence of symptoms, resulting in chronically front of the ankle
ANTERIOR ANKLE IMPINGEMENT Description Possible Complications Pinching of bone or soft tissue, including scar tissue, at the Frequent recurrence of symptoms, resulting in chronically front of the ankle
Dr. Mark Price MGH Sports Medicine Center 175 Cambridge Street, 4th floor Boston, MA
 Dr. Mark Price MGH Sports Medicine Center 175 Cambridge Street, 4th floor Boston, MA 02114 www.massgeneral.org/ortho-sports-medicine/dr-price Rotator Cuff Tears The shoulder is a ball and socket joint
Dr. Mark Price MGH Sports Medicine Center 175 Cambridge Street, 4th floor Boston, MA 02114 www.massgeneral.org/ortho-sports-medicine/dr-price Rotator Cuff Tears The shoulder is a ball and socket joint
Knee ACL Reconstruction Autograft FAQ
 Knee ACL Reconstruction Autograft FAQ Ryan W. Hess, MD Tracey Pederson, PCC Office: (763) 302-2223 Fax: (763) 302-2401 Twitter: RyanHessMD Q: WHAT IS ACCOMPLISHED DURING THE PROCEDURE? ACL reconstruction
Knee ACL Reconstruction Autograft FAQ Ryan W. Hess, MD Tracey Pederson, PCC Office: (763) 302-2223 Fax: (763) 302-2401 Twitter: RyanHessMD Q: WHAT IS ACCOMPLISHED DURING THE PROCEDURE? ACL reconstruction
Rehabilitation Following Unilateral Patellar Tendon Repair
 Rehabilitation Following Unilateral Patellar Tendon Repair I. Immediate Postoperative Phase (Days 1-7) Restore full passive knee extension Diminish pain and joint swelling Restore patellar mobility Initiate
Rehabilitation Following Unilateral Patellar Tendon Repair I. Immediate Postoperative Phase (Days 1-7) Restore full passive knee extension Diminish pain and joint swelling Restore patellar mobility Initiate
Above Knee Amputation: Positioning and Exercise Program
 Above Knee Amputation: Positioning and Exercise Program The exercises and stretches in this handout will help to prepare you to wear a prosthesis properly. The positioning instructions and exercises in
Above Knee Amputation: Positioning and Exercise Program The exercises and stretches in this handout will help to prepare you to wear a prosthesis properly. The positioning instructions and exercises in
Medial Patellofemoral Ligament Repair/Reconstruction
 Alta View Sports Medicine Dr. James R. Meadows, MD Orthopedic Surgery & Sports Medicine 74 Kimballs Ln Ste 230, Draper, UT 84020 9844 S. 1300 E. Ste 100, Sandy, UT 84094 (801) 571-9433 www.meadowsmd.com
Alta View Sports Medicine Dr. James R. Meadows, MD Orthopedic Surgery & Sports Medicine 74 Kimballs Ln Ste 230, Draper, UT 84020 9844 S. 1300 E. Ste 100, Sandy, UT 84094 (801) 571-9433 www.meadowsmd.com
Anterior Cruciate Ligament Reconstruction
 Anterior Cruciate Ligament Reconstruction Physiotherapy Department Patient information leaflet This patient information booklet is designed to provide you with information about the Anterior Cruciate Ligament
Anterior Cruciate Ligament Reconstruction Physiotherapy Department Patient information leaflet This patient information booklet is designed to provide you with information about the Anterior Cruciate Ligament
9180 KATY FREEWAY, STE. 200 (713)
 OSTEOCHONDRAL AUTOGRAFT TRANSPLANTATION Patella/Trochlea Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Goals: - Protection of healing tissue from load and shear forces - Decrease pain
OSTEOCHONDRAL AUTOGRAFT TRANSPLANTATION Patella/Trochlea Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Goals: - Protection of healing tissue from load and shear forces - Decrease pain
Posterior Cruciate Ligament Rehabilitation
 Posterior Cruciate Ligament Rehabilitation Phase 6: Running program for Return to Sports : 24 Weeks after surgery onward Goals: 1. Safely recondition the injured area for the demands of sports activity.
Posterior Cruciate Ligament Rehabilitation Phase 6: Running program for Return to Sports : 24 Weeks after surgery onward Goals: 1. Safely recondition the injured area for the demands of sports activity.
Sheena Black, MD. Orthopaedic Surgery, Sports Medicine PHYSICAL THERAPY PRESCRIPTION ACL RECONSTRUCTION HAMSTRING TENDON TECHNIQUE
 PHYSICAL THERAPY PRESCRIPTION ACL RECONSTRUCTION HAMSTRING TENDON TECHNIQUE Name: Date: Post-Operative Diagnosis: Right Left ACL Reconstruction Graft: BTB Hamstring Allograft Additional Procedures: Lateral
PHYSICAL THERAPY PRESCRIPTION ACL RECONSTRUCTION HAMSTRING TENDON TECHNIQUE Name: Date: Post-Operative Diagnosis: Right Left ACL Reconstruction Graft: BTB Hamstring Allograft Additional Procedures: Lateral
KNEE REHABILITATION PROGRAMME
 Jessica Barrow BSc Physiotherapy, SPT1 www.barrowphysiotherapy.co.za Cell: 083 256 0434 Room GF03 Waterfall Hospital Cnr. Magwa Crescent and Mac Mac Avenue Tel: 011 304-7829 Fax: 011 304-7941 KNEE REHABILITATION
Jessica Barrow BSc Physiotherapy, SPT1 www.barrowphysiotherapy.co.za Cell: 083 256 0434 Room GF03 Waterfall Hospital Cnr. Magwa Crescent and Mac Mac Avenue Tel: 011 304-7829 Fax: 011 304-7941 KNEE REHABILITATION
Page 1 of 5 SPECTRUM MEDICAL
 Page 1 of 5 SPECTRUM MEDICAL HOME INSTRUCTIONS Total Knee Replacement I. Walking A. Use walker/crutches until your doctor says you no longer need them. Your foot should be flat on the floor with on it.
Page 1 of 5 SPECTRUM MEDICAL HOME INSTRUCTIONS Total Knee Replacement I. Walking A. Use walker/crutches until your doctor says you no longer need them. Your foot should be flat on the floor with on it.
Anterior Cruciate Ligament Reconstruction
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Anterior Cruciate Ligament Reconstruction Physiotherapy This patient information booklet is designed to provide you with information
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Anterior Cruciate Ligament Reconstruction Physiotherapy This patient information booklet is designed to provide you with information
Below Knee Amputation: Positioning and Exercise Program
 Below Knee Amputation: Positioning and Exercise Program The exercises and stretches in this handout will help to prepare you to wear a prosthesis properly. The positioning instructions and exercises in
Below Knee Amputation: Positioning and Exercise Program The exercises and stretches in this handout will help to prepare you to wear a prosthesis properly. The positioning instructions and exercises in
Total Hip Replacement Exercise Guide
 Total Hip Replacement Exercise Guide Regular exercise to restore strength and mobility to your hip and a gradual return to everyday activities are important for your full recovery after hip replacement.
Total Hip Replacement Exercise Guide Regular exercise to restore strength and mobility to your hip and a gradual return to everyday activities are important for your full recovery after hip replacement.
Rehabilitation for Patellar Tendinitis (jumpers knee) and Patellofemoral Syndrome (chondromalacia patella)
 Rehabilitation for Patellar Tendinitis (jumpers knee) and Patellofemoral Syndrome (chondromalacia patella) Patellar Tendinitis The most common tendinitis about the knee is irritation of the patellar tendon.
Rehabilitation for Patellar Tendinitis (jumpers knee) and Patellofemoral Syndrome (chondromalacia patella) Patellar Tendinitis The most common tendinitis about the knee is irritation of the patellar tendon.
ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION (Immediate) Post-Op Home Exercise Program
 ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION (Immediate) Post-Op Home Exercise Program The knee brace must be worn locked in extension (straight) while walking and sleeping. You may take the brace off when
ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION (Immediate) Post-Op Home Exercise Program The knee brace must be worn locked in extension (straight) while walking and sleeping. You may take the brace off when
Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction
 Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These
Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These
Diagnosis: s/p ( LEFT / RIGHT ) Injury to MCL of the Knee -- Surgery Date:
 UCLA OUTPATIENT REHABILITATION SERVICES! SANTA MONICA! WESTWOOD 1000 Veteran Ave., A level Phone: (310) 794-1323 Fax: (310) 794-1457 1260 15 th St, Ste. 900 Phone: (310) 319-4646 Fax: (310) 319-2269 FOR
UCLA OUTPATIENT REHABILITATION SERVICES! SANTA MONICA! WESTWOOD 1000 Veteran Ave., A level Phone: (310) 794-1323 Fax: (310) 794-1457 1260 15 th St, Ste. 900 Phone: (310) 319-4646 Fax: (310) 319-2269 FOR
9180 KATY FREEWAY, STE. 200 (713)
 AUTOLOGOUS CHONDROCYTE IMPLANTATION Femoral Condyle Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Goals: - Protect healing tissue from load and shear forces - Decrease pain and effusion
AUTOLOGOUS CHONDROCYTE IMPLANTATION Femoral Condyle Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Goals: - Protect healing tissue from load and shear forces - Decrease pain and effusion
