MICROFRACTURE LOURDES MEDICAL ASSOCIATES PROFESSIONAL ORTHOPAEDICS SPORTS MEDICINE & ARTHROSCOPY
|
|
|
- Brian Freeman
- 5 years ago
- Views:
Transcription
1 LOURDES MEDICAL ASSOCIATES Sean Mc Millan, DO Director of Orthopaedic Sports Medicine & Arthroscopy 2103 Burlington-Mount Holly Rd Burlington, NJ (609) (office) (609) (fax) MICROFRACTURE Like many of the joints in the body, the knee is lined with articular cartilage. This cartilage makes is possible for your femur (thigh bone) and tibia (shin bone) to smoothly glide over one another and helps give your knee its motion. In fact, this cartilage is so smooth it has even less friction than ice sliding on ice. Sometimes, unfortunately, as a result of injury or trauma, portions of the cartilage can be scraped off or removed from the bone. This can result in pain, grinding and swelling of the knee. You may find it difficult to engage in sports activities such as running or jumping. It can even be painful with simple activities such as going up and down stairs. Microfracture is a surgical procedure aimed at cartilage regeneration. The arthroscopic (using a camera to look inside the joint) technique involves clearing damaged tissue from the knee joint and creating small holes ( microfractures ) in the bone area where the cartilage is defective. The underlying bone marrow seeps out through the holes and becomes part of a blood clot that forms over the area of missing cartilage. The marrow contains stem cells, which have the ability to form new cartilage between the bare bone surfaces of the knee. The cartilage formed is not the same as the cartilage that was lost, but still has smoother gliding that bone rubbing against bone. The picture at the right depicts an area of cartilage loss (upper left corner). The smooth white areas are healthy cartilage, while the yellow area is bare bone. The upper right corner depicts a microfracture awl being placed into the bone, while the picture in the lower left shows the blood flowing after the bone has been fractured. The resultant bleeding bone is seen in the bottom right picture. This blood clot will be the source of new cartilage cells to line the area of bare bone. In some published reports, the success rate of microfracture is about 75%. It is important to remember that this procedure is not a perfect means of restoring cartilage but does have a good track record helping with pain and returning patients to sporting activities.
2 Perhaps more important than the procedure itself is the rehabilitation after the procedure. It will be important to protect your repair and use a continuous motion machine as well as crutches and keeping weight off your knee. Strict adherence to the protocol is essential to maximize the results of your surgery. Activities and advice for in the hospital and while at home: 1. Please call with any concerns: (609) Apply ice to the knee, as it will be quite helpful. After two days, you can change the dressing to a smaller one to allow the cold to better get to the knee. Be sure to leave the little pieces of tape (steri-strips) in place. 3. After two days it is okay to shower and get the wound wet, but do not soak the wound as you would in a bath tub or hot tub. 4. After knee surgery there is a variable amount of pain and swelling. This will dissipate after several days. Continue to take the pain medicine you were prescribed as needed. Remember it is called pain control, not pain elimination. If you notice calf pain or excessive swelling in the lower leg, call your doctor. 5. It is important to look out of signs of infection following joint replacement surgery. These can include: fever (temperature > , chills, nausea, vomiting, diarrhea, redness around your incision, or yellow or green drainage from your incision. Should any of these be present please contact Dr. Mc Millan s office immediately. 6. You should start your physical therapy approximately 5 days after your surgery. 7. You will have an office visit scheduled approximately days after your surgery.
3 REHABILITATION AFTER MICROFRACTURE Phase I: immediate post-op phase (0-2 weeks after surgery) Goals: 1. Protect the reconstruction avoid bearing weight on the operated leg unless instructed otherwise. 2. Ensure wound healing 3. Attain and maintain full knee extension 4. Gain knee flexion (bending) to 90 degrees 5. Decrease knee and leg swelling 6. Promote quadriceps muscle strength 7. Avoid blood pooling in the leg veins Activities: 1. Continuous passive motion (CPM). This must be used at least 10 hours per day. Do not wear your brace while in the machine. You may use it anywhere that is comfortable. Use it at night while sleeping. It is very important that you straighten your knee completely. The flexion can gradually be increased to 90 degrees as your knee tolerates each new setting. 2. Brace/crutches/weight bearing: your knee brace is set to allow you to bend and straighten your knee. Use it when walking or out of bed, but it may be removed for range of motion exercises. a. If you had a defect in your patellar groove (trochlea) or patella (knee cap) you will wear a brace that will allow your knee to bend 30 degrees and straighten fully. You should use it when walking. If you had a defect in the femoral condyle you will not wear a brace. b. If you had a defect in your trochlea or patella you can begin bearing weight on your operated leg as soon as you re comfortable doing so. You should use crutches in the beginning but can discontinue using them when you have confidence in your knee to support you. c. If you had a defect in your femoral condyle you will be on crutches and not allowed to put weight on the operated leg for at least six weeks. Dr. Mc Millan will tell you when it is okay to begin weight bearing on your operated leg. 3. Your nurse or therapist will demonstrate the proper form for walking with crutches: a. Put the crutches forward about one step s length b. Put the injured leg forward in line with the crutch tips c. Touch the foot of the injured leg to the floor and put as much weight down as is comfortable (brace on and locked) d. While bearing weight on the injured leg, take a step through with the uninjured leg.
4 4. Elastic stockings: wear an elastic stocking below the knee until your first postoperative visit. Do at least 10 ankle pump exercises each hour to help prevent blood clots. Take one adult aspirin daily for the first two weeks 5. It is okay to remove your bandage on the second morning after surgery but leave the small pieces of white tape (steri-strips) across the incision. You can wrap an elastic bandage (ACE wrap) around the knee at other times to control swelling. You may shower and get your incision wet (unless there is any drainage from your incisions). Do not soak the incision in a bathtub or hot tub until the stitches have been removed. 6. Use your cryocuff regularly to help with knee pain and swelling. Exercises Program: 7 days per week, 3-4 times per day. Quadriceps setting 1-2 sets reps Heel prop 5 minutes Heel slides 5-15 minutes Sitting heel slides 1-2 sets reps Straight leg raises 1-2 sets reps Ankle pumps 10 per hour Quadriceps Setting Lie or sit with knee fully straight. Tighten and hold the front thigh muscle making the knee flat and straight (this should make your knee flatten against the bed or floor). Hold 5 seconds for each contraction. Heel Prop Lie on your back with a rolled up towel under your heel, or sit in a chair with the heel on a stool. Let the knee relax into extension (straight). If the knee will not straighten fully, you can place a small weight (2-5 lbs) on the thigh just above the kneecap. Try to hold for 5 minutes. Try to practice quadriceps setting in this position.
5 Patellar Mobilization With the knee fully extended, grasp the edges of your kneecap between your thumb and index finger. Move the kneecap side to side and up and down. Heel slides While lying on your back, actively slide your heel backward to bend the knee. Hold this bent position for five seconds then slowly relieve the stretch and straighten the knee. While the knee is straight, you may repeat the quadriceps setting exercise. Sitting Heel Slides While sitting in a chair or over the edge of the bed, support the operated leg with the uninvolved leg. Lower the operated leg, with the unoperated leg controlling, allowing the knee to bend. Do not go past 60 0 of bend at the knee. Hold for 5 seconds and slowly relieve the stretch by lifting the foot upward with the uninvolved leg to the straight position. Ankle Pumps Move the ankle up and down to help stimulate circulation in the leg.
6 Phase II: intermediate post-op phase (2-8 weeks post-op) Goals: 1. Protect the knee from overstress and allow healing 2. Regain full motion 3. Begin muscle strengthening Activities: 1. Brace, crutches and weight bearing are as previously described. 2. Continue using your CPM machine for at least 10 hours per day. This is designed to keep the cartilage healthy and maximize the chances of new cartilage growth. 3. If your operated leg is your left leg, it may be alright to begin driving provided you are no longer taking pain medicine and have an automatic transmission. If your operated leg was your right leg it is not yet safe to drive. 4. You may stop wearing the compression stockings and can stop taking the aspirin. 5. You should continue to use ice to help with pain and swelling. 6. You will have a visit with Dr. Mc Millan at days after surgery. If your wound is dry, you will likely be able to get the wound wet in a bath or hot tub at this point. Exercises The following exercises will be demonstrated to you by your physical therapist. He or she will also give you a home exercise program. You should strive to do your home exercise program at least 3-4 times per day, every day. The success of your reconstruction depends on your rehab. Stationary bicycle Water workout (aqua jogger, no foot contact with the bottom of the pool) Quadriceps setting Heel slides Heel prop Straight leg lift Short arc lifts Standing hamstring curls Standing toe raise Hip abduction
7 Phase III: 8-12 weeks after surgery Goals: 1. Walk normally 2. Regain full motion 3. Regain full muscle strength Activities: 1. You may discontinue using the brace at this point. 2. Progressively bear full weight and walk on the operated leg. Try to avoid limping and walk slowly but with a normal gait. Start by walking with normal weight and full crutches for 3-5 days. If you have no pain, then switch to using one crutch on the opposite side from your surgery for 3-5 days. Discontinue using the crutch when you can walk normally and pain free without a limp. 3. Continue using ice if there is any knee pain and/or swelling. 4. If your right leg was the operated leg you may drive when you have normal muscle control and balance in your leg. Exercises: Stationary bicycle (keep resistance low, increase time) Water workout (aqua jogger, no foot contact with the bottom of the pool) Continue phase II exercises if these are easy and can be completed pain free, it is okay to add a light ankle weight to the program. Wall slides Leg press (0-90 degrees) Bilateral squats (0-60 degrees) Unilateral step-ups progressing from 2 to 8 Forward lunges Walking program week 10 Progress open kinetic chain extension (0-90 ), for patellofemoral lesions, may begin week 12, perform from or avoid angle where lesion articulates Progress 1 pound every 2 weeks beginning week 20 if no pain or crepitation must monitor symptoms closely Balance and proprioception exercises Swimming Nordic-Trak/Elliptical
8 Phase IV: 12 weeks onward Goals: 1. Regain full muscle strength 2. Gradual return to activities Exercises: Bicycle (may start outdoor cycling on flat terrain). If riding outdoors should have brace on with free ROM Stretching o Hamstrings o Quadriceps o Calves Straight leg raises Leg press Wall squats Hip abduction / adduction Front lunges Step-ups Criteria to start sport specific programs: 1. Full, painless ROM 2. Strength within 80% of contralateral side 3. Balance and stability within 75% of contralateral side 4. No pain, inflammation or swelling In general the patient can expect the following return to sports: Swimming, skating, cycling, rollerblading usually 2 months for patellofemoral lesions and 3 months for femoral condyle lesions Jogging, running, aerobics usually 4 months for patellofemoral lesions and 5 months for femoral condyle lesions Tennis, basketball, football, baseball, soccer, lacrosse are allowed at 6-8 months.
Mosaicplasty and OATS Rehabilitation Protocol
 Mosaicplasty and OATS Rehabilitation Protocol PHASE 1: 0 2 weeks after surgery You will go home with crutches, cryocuff cold therapy unit and a CPM machine. GOALS: 1. Protect the cartilage transfer avoid
Mosaicplasty and OATS Rehabilitation Protocol PHASE 1: 0 2 weeks after surgery You will go home with crutches, cryocuff cold therapy unit and a CPM machine. GOALS: 1. Protect the cartilage transfer avoid
REHABILITATION AFTER ARTHROSCOPIC KNEE SURGERY
 REHABILITATION AFTER ARTHROSCOPIC KNEE SURGERY This protocol is a guideline for your rehabilitation after arthroscopic knee surgery. You may vary in your ability to do these exercises and to progress to
REHABILITATION AFTER ARTHROSCOPIC KNEE SURGERY This protocol is a guideline for your rehabilitation after arthroscopic knee surgery. You may vary in your ability to do these exercises and to progress to
PATELLA INSTABILITY AND REALIGNMENT
 Daniel P. Duggan, D.O. The Sports Clinic 23961 Calle de la Magdalena, Suite 229 Laguna Hills, CA 92653 Phone: (949) 581-7001 Fax: (949) 581-8410 http://orthodoc.aaos.org/danielduggando PATELLA INSTABILITY
Daniel P. Duggan, D.O. The Sports Clinic 23961 Calle de la Magdalena, Suite 229 Laguna Hills, CA 92653 Phone: (949) 581-7001 Fax: (949) 581-8410 http://orthodoc.aaos.org/danielduggando PATELLA INSTABILITY
MENISCAL REPAIR LOURDES MEDICAL ASSOCIATES PROFESSIONAL ORTHOPAEDICS SPORTS MEDICINE & ARTHROSCOPY
 LOURDES MEDICAL ASSOCIATES Sean Mc Millan, DO Director of Orthopaedic Sports Medicine & Arthroscopy 2103 Burlington-Mount Holly Rd Burlington, NJ 08016 (609) 747-9200 (office) (609) 747-1408 (fax) http://orthodoc.aaos.org/drmcmillan
LOURDES MEDICAL ASSOCIATES Sean Mc Millan, DO Director of Orthopaedic Sports Medicine & Arthroscopy 2103 Burlington-Mount Holly Rd Burlington, NJ 08016 (609) 747-9200 (office) (609) 747-1408 (fax) http://orthodoc.aaos.org/drmcmillan
PHASE ONE: THE FIRST SIX WEEKS AFTER INJURY
 Exercises After Injury to the Anterior Cruciate Ligament (ACL) of the Knee Dr. Abigail R. Hamilton, M.D. PHASE ONE: THE FIRST SIX WEEKS AFTER INJURY Initially, the knee needs to be protected-use the knee
Exercises After Injury to the Anterior Cruciate Ligament (ACL) of the Knee Dr. Abigail R. Hamilton, M.D. PHASE ONE: THE FIRST SIX WEEKS AFTER INJURY Initially, the knee needs to be protected-use the knee
ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION
 LOURDES MEDICAL ASSOCIATES Sean Mc Millan, DO Director of Orthopaedic Sports Medicine & Arthroscopy 2103 Burlington-Mount Holly Rd Burlington, NJ 08016 (609) 747-9200 (office) (609) 747-1408 (fax) http://orthodoc.aaos.org/drmcmillan
LOURDES MEDICAL ASSOCIATES Sean Mc Millan, DO Director of Orthopaedic Sports Medicine & Arthroscopy 2103 Burlington-Mount Holly Rd Burlington, NJ 08016 (609) 747-9200 (office) (609) 747-1408 (fax) http://orthodoc.aaos.org/drmcmillan
What is arthroscopy? Normal knee anatomy
 What is arthroscopy? Arthroscopy is a common surgical procedure for examining and repairing the inside of your knee. It is a minimally invasive surgical procedure which uses an Arthroscope and other specialized
What is arthroscopy? Arthroscopy is a common surgical procedure for examining and repairing the inside of your knee. It is a minimally invasive surgical procedure which uses an Arthroscope and other specialized
Rehabilitation After Patellar Tendon Debridement Surgery
 Katherine J. Coyner, MD UCONN Musculoskeletal Institute Medical Arts & Research Building 263 Farmington Ave. Farmington, CT 06030 Office: (860) 679-6600 Fax: (860) 679-6649 www.drcoyner.com Avon Office
Katherine J. Coyner, MD UCONN Musculoskeletal Institute Medical Arts & Research Building 263 Farmington Ave. Farmington, CT 06030 Office: (860) 679-6600 Fax: (860) 679-6649 www.drcoyner.com Avon Office
Proximal Hamstring Tendon Repair
 Dr. Mark Price MGH Sports Medicine Center 175 Cambridge Street, 4th floor Boston, MA 02114 www.massgeneral.org/ortho-sports-medicine/dr-price Proximal Hamstring Tendon Repair The hamstrings are a group
Dr. Mark Price MGH Sports Medicine Center 175 Cambridge Street, 4th floor Boston, MA 02114 www.massgeneral.org/ortho-sports-medicine/dr-price Proximal Hamstring Tendon Repair The hamstrings are a group
Arthroscopic Surgery
 175 Cambridge Street, 4 th floor Boston, MA 02114 Tel: 617-726-7500 Arthroscopic Surgery What is arthroscopy? Arthroscopy is a surgical procedure that orthopedic surgeons use to visualize, diagnose and
175 Cambridge Street, 4 th floor Boston, MA 02114 Tel: 617-726-7500 Arthroscopic Surgery What is arthroscopy? Arthroscopy is a surgical procedure that orthopedic surgeons use to visualize, diagnose and
9180 KATY FREEWAY, STE. 200 (713)
 AUTOLOGOUS CHONDROCYTE IMPLANTATION Femoral Condyle Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Goals: - Protect healing tissue from load and shear forces - Decrease pain and effusion
AUTOLOGOUS CHONDROCYTE IMPLANTATION Femoral Condyle Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Goals: - Protect healing tissue from load and shear forces - Decrease pain and effusion
9180 KATY FREEWAY, STE. 200 (713)
 OSTEOCHONDRAL AUTOGRAFT TRANSPLANTATION Patella/Trochlea Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Goals: - Protection of healing tissue from load and shear forces - Decrease pain
OSTEOCHONDRAL AUTOGRAFT TRANSPLANTATION Patella/Trochlea Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Goals: - Protection of healing tissue from load and shear forces - Decrease pain
MENISCUS TEAR. Description
 MENISCUS TEAR Description Expected Outcome The meniscus is a C-shaped cartilage structure in the knee that sits on top of the leg bone (tibia). Each knee has two menisci, an inner and outer meniscus. The
MENISCUS TEAR Description Expected Outcome The meniscus is a C-shaped cartilage structure in the knee that sits on top of the leg bone (tibia). Each knee has two menisci, an inner and outer meniscus. The
OSTEOCHONDRAL AUTOGRAFT TRANSPLANTATION
 OSTEOCHONDRAL AUTOGRAFT TRANSPLANTATION FEMORAL CONDYLE REHABILITATION PROGRAM PHASE I - PROTECTION PHASE (WEEKS 0-6) Protection of healing tissue from load and shear forces Decrease pain and effusion
OSTEOCHONDRAL AUTOGRAFT TRANSPLANTATION FEMORAL CONDYLE REHABILITATION PROGRAM PHASE I - PROTECTION PHASE (WEEKS 0-6) Protection of healing tissue from load and shear forces Decrease pain and effusion
KNEE JOINT RESURFACING SURGERY. Here are guidelines that will help you in preparing for knee resurfacing surgery. PREOPERATIVE INSTRUCTIONS
 175 Cambridge Street www.mghsportsmedicine.org KNEE JOINT RESURFACING SURGERY Here are guidelines that will help you in preparing for knee resurfacing surgery. PREOPERATIVE INSTRUCTIONS WITHIN A FEW WEEKS
175 Cambridge Street www.mghsportsmedicine.org KNEE JOINT RESURFACING SURGERY Here are guidelines that will help you in preparing for knee resurfacing surgery. PREOPERATIVE INSTRUCTIONS WITHIN A FEW WEEKS
Femoral Condyle Rehabilitation Guidelines
 Femoral Condyle Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Brace: Protect healing tissue from load and shear forces Decrease pain and effusion Restore full passive knee extension
Femoral Condyle Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Brace: Protect healing tissue from load and shear forces Decrease pain and effusion Restore full passive knee extension
Rehabilitation for Patellar Tendinitis (jumpers knee) and Patellofemoral Syndrome (chondromalacia patella)
 Rehabilitation for Patellar Tendinitis (jumpers knee) and Patellofemoral Syndrome (chondromalacia patella) Patellar Tendinitis The most common tendinitis about the knee is irritation of the patellar tendon.
Rehabilitation for Patellar Tendinitis (jumpers knee) and Patellofemoral Syndrome (chondromalacia patella) Patellar Tendinitis The most common tendinitis about the knee is irritation of the patellar tendon.
Knee Arthroscopy: Postoperative Instructions
 Knee Arthroscopy: Postoperative Instructions John P. Woll, MD Knee arthroscopy is a commonly performed procedure that is much less invasive than previous open techniques, but it is still an operation,
Knee Arthroscopy: Postoperative Instructions John P. Woll, MD Knee arthroscopy is a commonly performed procedure that is much less invasive than previous open techniques, but it is still an operation,
Rehabilitation Protocol:
 Rehabilitation Protocol: Patellofemoral resurfacing: Osteochondral Autograft Transplantation (OATS), Autologous Chondrocyte Implantation (ACI) and Microfracture Department of Orthopaedic Surgery Lahey
Rehabilitation Protocol: Patellofemoral resurfacing: Osteochondral Autograft Transplantation (OATS), Autologous Chondrocyte Implantation (ACI) and Microfracture Department of Orthopaedic Surgery Lahey
Dr. Abigail Hamilton, MD
 High Tibial Osteotomy Surgery Post-Operative Orders Dr. Abigail Hamilton, MD WITHIN A FEW WEEKS BEFORE SURGERY: You should have a preoperative appointment arranged with your medical doctor. They will review
High Tibial Osteotomy Surgery Post-Operative Orders Dr. Abigail Hamilton, MD WITHIN A FEW WEEKS BEFORE SURGERY: You should have a preoperative appointment arranged with your medical doctor. They will review
REHABILITATION AFTER KNEE MENISCUS REPAIR. Dr. Abigail R. Hamilton, M.D.
 REHABILITATION AFTER KNEE MENISCUS REPAIR Dr. Abigail R. Hamilton, M.D. PHASE ONE: THE FINAL WEEK AFTER SURGERY Goals: 1. Control pain and swelling 2. Initiate knee motion 3. Activate the quadriceps muscles
REHABILITATION AFTER KNEE MENISCUS REPAIR Dr. Abigail R. Hamilton, M.D. PHASE ONE: THE FINAL WEEK AFTER SURGERY Goals: 1. Control pain and swelling 2. Initiate knee motion 3. Activate the quadriceps muscles
ACL REHABILITATION PROTOCOL
 Name: ID: Date Of Surgery :DD / MM / YYYY Procedure: ACL REHABILITATION PROTOCOL Note :If another procedure like meniscus repair or OATS (Osteochondralautograft transfer) has been done along with ACL reconstruction
Name: ID: Date Of Surgery :DD / MM / YYYY Procedure: ACL REHABILITATION PROTOCOL Note :If another procedure like meniscus repair or OATS (Osteochondralautograft transfer) has been done along with ACL reconstruction
PATELLOFEMORAL INSTABILITY (SUBLUXATION AND DISLOCATION)
 PATELLOFEMORAL INSTABILITY (SUBLUXATION AND DISLOCATION) Anatomy and Function The knee joint is composed of two distinctly separate articulations. The tibiofemoral joint is formed by the thigh bone (femur)
PATELLOFEMORAL INSTABILITY (SUBLUXATION AND DISLOCATION) Anatomy and Function The knee joint is composed of two distinctly separate articulations. The tibiofemoral joint is formed by the thigh bone (femur)
ACL Reconstruction. Role of the Anterior Cruciate Ligament. Treatment of ACL tears. ACL Reconstruction
 Role of the Anterior Cruciate Ligament The ACL stabilizes the knee when jumping, pivoting, or cutting. It prevents the shinbone (tibia) from sliding forward on the thigh bone (femur). ACL tears often occur
Role of the Anterior Cruciate Ligament The ACL stabilizes the knee when jumping, pivoting, or cutting. It prevents the shinbone (tibia) from sliding forward on the thigh bone (femur). ACL tears often occur
KNEE AND LEG EXERCISE PROGRAM
 KNEE AND LEG EXERCISE PROGRAM These exercises are specifically designed to rehabilitate the muscles of the hip and knee by increasing the strength and flexibility of the involved leg. This exercise program
KNEE AND LEG EXERCISE PROGRAM These exercises are specifically designed to rehabilitate the muscles of the hip and knee by increasing the strength and flexibility of the involved leg. This exercise program
ACTIVITIES AND EXERCISES AFTER INJURY TO THE MEDIAL COLLATERAL LIGAMENT (MCL) OF THE KNEE
 ACTIVITIES AND EXERCISES AFTER INJURY TO THE MEDIAL COLLATERAL LIGAMENT (MCL) OF THE KNEE PHASE 1: THE FIRST SIX WEEKS AFTER INJURY (grade 2 and 3) THREE WEEKS AFTER INJURY (grade 1) The knee should be
ACTIVITIES AND EXERCISES AFTER INJURY TO THE MEDIAL COLLATERAL LIGAMENT (MCL) OF THE KNEE PHASE 1: THE FIRST SIX WEEKS AFTER INJURY (grade 2 and 3) THREE WEEKS AFTER INJURY (grade 1) The knee should be
Physiotherapy Information following Anterior Cruciate Ligament (ACL) Reconstruction
 Physiotherapy Information following Anterior Cruciate Ligament (ACL) Reconstruction Name:... Surgery Date:... Graft:... Orthopaedic Outpatient Appointment Date: Time: Location: Contact Number: Contacting
Physiotherapy Information following Anterior Cruciate Ligament (ACL) Reconstruction Name:... Surgery Date:... Graft:... Orthopaedic Outpatient Appointment Date: Time: Location: Contact Number: Contacting
Postoperative Days 1-7
 ACL RECONSTRUCTION REHABILITATION PROTOCOL Postoperative Days 1-7 *IT IS EXTREMELY IMPORTANT THAT YOU WORK ON EXTENSION IMMEDIATELY Goals: * Control pain and swelling * Care for the knee and dressing *
ACL RECONSTRUCTION REHABILITATION PROTOCOL Postoperative Days 1-7 *IT IS EXTREMELY IMPORTANT THAT YOU WORK ON EXTENSION IMMEDIATELY Goals: * Control pain and swelling * Care for the knee and dressing *
Patellofemoral Pain Syndrome
 What is patellofemoral pain syndrome? Patellofemoral Pain Syndrome Patellofemoral pain syndrome is pain behind the kneecap. It has been given many names, including patellofemoral disorder, patellar malalignment,
What is patellofemoral pain syndrome? Patellofemoral Pain Syndrome Patellofemoral pain syndrome is pain behind the kneecap. It has been given many names, including patellofemoral disorder, patellar malalignment,
Posterior Cruciate Ligament (PCL) Reconstruction. Preoperative Instructions
 Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Posterior Cruciate Ligament (PCL) Reconstruction Preoperative Instructions WITHIN A FEW WEEKS BEFORE SURGERY Dr. Ferry will see you in the office. He
Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Posterior Cruciate Ligament (PCL) Reconstruction Preoperative Instructions WITHIN A FEW WEEKS BEFORE SURGERY Dr. Ferry will see you in the office. He
Diagnosis: s/p ( LEFT / RIGHT ) Injury to MCL of the Knee -- Surgery Date:
 UCLA OUTPATIENT REHABILITATION SERVICES! SANTA MONICA! WESTWOOD 1000 Veteran Ave., A level Phone: (310) 794-1323 Fax: (310) 794-1457 1260 15 th St, Ste. 900 Phone: (310) 319-4646 Fax: (310) 319-2269 FOR
UCLA OUTPATIENT REHABILITATION SERVICES! SANTA MONICA! WESTWOOD 1000 Veteran Ave., A level Phone: (310) 794-1323 Fax: (310) 794-1457 1260 15 th St, Ste. 900 Phone: (310) 319-4646 Fax: (310) 319-2269 FOR
Anterior Cruciate Ligament (ACL) Reconstruction
 Dr. Mark Price MGH Sports Medicine Center 175 Cambridge Street, 4th floor Boston, MA 02114 www.massgeneral.org/ortho-sports-medicine/dr-price Anterior Cruciate Ligament (ACL) Reconstruction The anterior
Dr. Mark Price MGH Sports Medicine Center 175 Cambridge Street, 4th floor Boston, MA 02114 www.massgeneral.org/ortho-sports-medicine/dr-price Anterior Cruciate Ligament (ACL) Reconstruction The anterior
PCL/PLC RECONSTRUCTION REHABILITATION Revised OCTOBER 2015
 PCL/PLC RECONSTRUCTION REHABILITATION Revised OCTOBER 2015 REHABILITATION PROGRAM PHASE 1: WEEKS 0-6: PHASE I GOALS: Protect the surgical graft(s) 0-60 ROM Regain adequate quadriceps control CRUTCHES:
PCL/PLC RECONSTRUCTION REHABILITATION Revised OCTOBER 2015 REHABILITATION PROGRAM PHASE 1: WEEKS 0-6: PHASE I GOALS: Protect the surgical graft(s) 0-60 ROM Regain adequate quadriceps control CRUTCHES:
Rehabilitation Protocol: Distal Femoral/Proximal Tibial Microfracture and Osteochondral Autograft Transplantation (OATS)
 Rehabilitation Protocol: Distal Femoral/Proximal Tibial Microfracture and Osteochondral Autograft Transplantation (OATS) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650
Rehabilitation Protocol: Distal Femoral/Proximal Tibial Microfracture and Osteochondral Autograft Transplantation (OATS) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650
GG10Rehabilitation Programme for Arthroscopically Assisted Anterior Cruciate Ligament Reconstruction
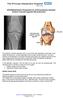 GG10Rehabilitation Programme for Arthroscopically Assisted Anterior Cruciate Ligament Reconstruction Femur ACL Graft Fibula Tibia The Anterior Cruciate Ligament (ACL) is one of the main ligaments in the
GG10Rehabilitation Programme for Arthroscopically Assisted Anterior Cruciate Ligament Reconstruction Femur ACL Graft Fibula Tibia The Anterior Cruciate Ligament (ACL) is one of the main ligaments in the
Iliotibial Band Tendinitis (Runner s Knee)
 Iliotibial Band Tendinitis (Runner s Knee) ANATOMY The iliotibial band (or tract) is a thick band of tissue that starts on the pelvis and upper thigh and passes along the outside of the knee and attaches
Iliotibial Band Tendinitis (Runner s Knee) ANATOMY The iliotibial band (or tract) is a thick band of tissue that starts on the pelvis and upper thigh and passes along the outside of the knee and attaches
A PATIENT S GUIDE TO REHABILITATION POST KNEE REPLACEMENT SURGERY
 A PATIENT S GUIDE TO REHABILITATION POST KNEE REPLACEMENT SURGERY Georgia Bouffard Student Physiotherapist Colin Walker Orthopaedic Knee Specialist Frank Gilroy BSc MSCP 1 CONTENTS Anatomy of the knee
A PATIENT S GUIDE TO REHABILITATION POST KNEE REPLACEMENT SURGERY Georgia Bouffard Student Physiotherapist Colin Walker Orthopaedic Knee Specialist Frank Gilroy BSc MSCP 1 CONTENTS Anatomy of the knee
The Posterior Cruciate Ligament
 The Posterior Cruciate Ligament The Posterior Cruciate Ligament (PCL) is the strongest ligament in the knee (2 times as strong as the ACL) and provides a significant amount of knee stability. PCL deficient
The Posterior Cruciate Ligament The Posterior Cruciate Ligament (PCL) is the strongest ligament in the knee (2 times as strong as the ACL) and provides a significant amount of knee stability. PCL deficient
DISCOID MENISCUS. Description
 DISCOID MENISCUS Description For participation in jumping (basketball, volleyball) or The meniscus is a cartilage structure in the knee that sits on contact sports, protect the knee joint with supportive
DISCOID MENISCUS Description For participation in jumping (basketball, volleyball) or The meniscus is a cartilage structure in the knee that sits on contact sports, protect the knee joint with supportive
ANATOMIC ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL
 ANATOMIC ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL PREOPERATIVE: If you have suffered an acute ACL injury and surgery is planned, the time between injury and surgery should be used to regain
ANATOMIC ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL PREOPERATIVE: If you have suffered an acute ACL injury and surgery is planned, the time between injury and surgery should be used to regain
TIBIAL PLATEAU FRACTURE
 TIBIAL PLATEAU FRACTURE Description Preventive Measures A tibial plateau fracture is a complete or incomplete break Appropriately warm up and stretch before practice or in the larger of the two leg bones
TIBIAL PLATEAU FRACTURE Description Preventive Measures A tibial plateau fracture is a complete or incomplete break Appropriately warm up and stretch before practice or in the larger of the two leg bones
James R. Romanowski, M.D.
 James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211 704-358-0308 (Office) 704-358-0037 (Fax) www.charlotteshoulder.com DISCHARGE INSTRUCTIONS
James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211 704-358-0308 (Office) 704-358-0037 (Fax) www.charlotteshoulder.com DISCHARGE INSTRUCTIONS
Total Knee Replacement
 Total Knee Replacement STEPHEN M. DESIO, M.D. Hospital Stay Most patients are in the hospital for two to three days. A Case Manager is part of our team whom you will meet after surgery. We will work together
Total Knee Replacement STEPHEN M. DESIO, M.D. Hospital Stay Most patients are in the hospital for two to three days. A Case Manager is part of our team whom you will meet after surgery. We will work together
Shoulder Arthroscopy: Postop Instructions. Activites & Advice for in the Hospital and while at Home
 Dr. Mark Price MGH Sports Medicine Center 175 Cambridge Street, 4th floor Boston, MA 02114 www.massgeneral.org/ortho-sports-medicine/dr-price Shoulder Arthroscopy: Postop Instructions You will wake up
Dr. Mark Price MGH Sports Medicine Center 175 Cambridge Street, 4th floor Boston, MA 02114 www.massgeneral.org/ortho-sports-medicine/dr-price Shoulder Arthroscopy: Postop Instructions You will wake up
Physical & Occupational Therapy
 In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
DISCOID MENISCUS. Description
 Montefiore Pediatric Orthopedic and Scoliosis Center Children s Hospital at Montefiore Norman Otsuka MD Eric Fornari MD Jacob Schulz MD Jaime Gomez MD Christine Moloney PA 3400 Bainbridge Avenue, 6 th
Montefiore Pediatric Orthopedic and Scoliosis Center Children s Hospital at Montefiore Norman Otsuka MD Eric Fornari MD Jacob Schulz MD Jaime Gomez MD Christine Moloney PA 3400 Bainbridge Avenue, 6 th
PATELLAR DISLOCATION AND SUBLUXATION
 PATELLAR DISLOCATION AND SUBLUXATION Description For jumping (basketball, volleyball) or contact sports, Patellar dislocation and subluxation are injuries to the protect the patella with supportive devices,
PATELLAR DISLOCATION AND SUBLUXATION Description For jumping (basketball, volleyball) or contact sports, Patellar dislocation and subluxation are injuries to the protect the patella with supportive devices,
What is an ACL Tear?...2. Treatment Options...3. Surgical Techniques...4. Preoperative Care...5. Preoperative Requirements...6
 Table of Contents What is an ACL Tear?....2 Treatment Options...3 Surgical Techniques...4 Preoperative Care...5 Preoperative Requirements...6 Postoperative Care...................... 7 Crutch use...8 Initial
Table of Contents What is an ACL Tear?....2 Treatment Options...3 Surgical Techniques...4 Preoperative Care...5 Preoperative Requirements...6 Postoperative Care...................... 7 Crutch use...8 Initial
Rehabilitation. Walkers, Crutches, Canes
 Walkers, Crutches, Canes These devices provide support through your arms to limit the amount of weight on your operated hip. Initially, after a total hip replacement you will use a walker to get around.
Walkers, Crutches, Canes These devices provide support through your arms to limit the amount of weight on your operated hip. Initially, after a total hip replacement you will use a walker to get around.
REHABILITATION PROTOCOL FOLLOWING PCL RECONSTRUCTION USING A TWO TUNNEL GRAFT. Brace E-Z Wrap locked at zero degree extension, sleep in Brace
 Therapist Phone REHABILITATION PROTOCOL FOLLOWING PCL RECONSTRUCTION USING A TWO TUNNEL GRAFT I. IMMEDIATE POST-OPERATIVE PHASE (Week 1) Control Swelling and Inflammation Obtain Full Passive Knee Extension
Therapist Phone REHABILITATION PROTOCOL FOLLOWING PCL RECONSTRUCTION USING A TWO TUNNEL GRAFT I. IMMEDIATE POST-OPERATIVE PHASE (Week 1) Control Swelling and Inflammation Obtain Full Passive Knee Extension
Ellipse Rehab Phase 2 Strengthening
 Strengthening Perform reps of each exercise, twice daily. Increase to reps Ankle Pumps: With leg resting on bed and knee straight, slowly pump ankle up and down as far as possible. Quad sets: Tighten thigh
Strengthening Perform reps of each exercise, twice daily. Increase to reps Ankle Pumps: With leg resting on bed and knee straight, slowly pump ankle up and down as far as possible. Quad sets: Tighten thigh
These are rehabilitation guidelines for OSU Sports Medicine patients. Please contact us at if you have any questions.
 OSU Sports Medicine Knee Microfracture Rehabilitation Guidelines These are rehabilitation guidelines for OSU Sports Medicine patients. Please contact us at 614-293-2385 if you have any questions. Rehabilitation
OSU Sports Medicine Knee Microfracture Rehabilitation Guidelines These are rehabilitation guidelines for OSU Sports Medicine patients. Please contact us at 614-293-2385 if you have any questions. Rehabilitation
Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Unicondylar Knee Replacement
 Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Unicondylar Knee Replacement This is a general information packet for patients undergoing unicondylar knee replacement. Osteoarthritis
Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Unicondylar Knee Replacement This is a general information packet for patients undergoing unicondylar knee replacement. Osteoarthritis
NOI- NORTHSHORE ORTHOPAEDIC INSTITUTE SPORTS MEDICINE SERVICE POST OP ACL RECONSTRUCTION INSTRUCTIONS
 NOI- NORTHSHORE ORTHOPAEDIC INSTITUTE SPORTS MEDICINE SERVICE POST OP ACL RECONSTRUCTION INSTRUCTIONS 1. Pain and swelling: Expect a considerable amount of pain the first few days post-op. Take your prescribed
NOI- NORTHSHORE ORTHOPAEDIC INSTITUTE SPORTS MEDICINE SERVICE POST OP ACL RECONSTRUCTION INSTRUCTIONS 1. Pain and swelling: Expect a considerable amount of pain the first few days post-op. Take your prescribed
KNEE MICROFRACTURE CLINICAL PRACTICE GUIDELINE
 KNEE MICROFRACTURE CLINICAL PRACTICE GUIDELINE Progression is time and criterion-based, dependent on soft tissue healing, patient demographics and clinician evaluation. Contact Ohio State Sports Medicine
KNEE MICROFRACTURE CLINICAL PRACTICE GUIDELINE Progression is time and criterion-based, dependent on soft tissue healing, patient demographics and clinician evaluation. Contact Ohio State Sports Medicine
ANTERIOR CRUCTIATE LIGAMENT RECONSTRUCTION COLLATERAL LIGAMENT RECONSTRUCION/REPAIR AND MENISCUS REPAIR REHABILITATION PROTOCOL
 ANTERIOR CRUCTIATE LIGAMENT RECONSTRUCTION COLLATERAL LIGAMENT RECONSTRUCION/REPAIR AND MENISCUS REPAIR REHABILITATION PROTOCOL GENERAL GUIDELINES - The local anesthetic (similar to novacaine) in your
ANTERIOR CRUCTIATE LIGAMENT RECONSTRUCTION COLLATERAL LIGAMENT RECONSTRUCION/REPAIR AND MENISCUS REPAIR REHABILITATION PROTOCOL GENERAL GUIDELINES - The local anesthetic (similar to novacaine) in your
ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL
 ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL PREOPERATIVE: If you have suffered an acute ACL injury and surgery is planned, the time between injury and surgery should be used to regain knee motion,
ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL PREOPERATIVE: If you have suffered an acute ACL injury and surgery is planned, the time between injury and surgery should be used to regain knee motion,
Patella Tendon Repair
 Alta View Sports Medicine Dr. James R. Meadows, MD Orthopedic Surgery & Sports Medicine 74 Kimballs Ln Ste 230, Draper, UT 84020 9844 S. 1300 E. Ste 100, Sandy, UT 84094 (801) 571-9433 www.meadowsmd.com
Alta View Sports Medicine Dr. James R. Meadows, MD Orthopedic Surgery & Sports Medicine 74 Kimballs Ln Ste 230, Draper, UT 84020 9844 S. 1300 E. Ste 100, Sandy, UT 84094 (801) 571-9433 www.meadowsmd.com
Rehabilitation. Walking after Total Knee Replacement. Continuous Passive Motion Device
 Walking after Total Knee Replacement After your TKR, continue using your walker or crutches until your surgeons tells you it is okay to stop using them. When turning with a walker or crutches DO NOT PIVOT
Walking after Total Knee Replacement After your TKR, continue using your walker or crutches until your surgeons tells you it is okay to stop using them. When turning with a walker or crutches DO NOT PIVOT
ANTERIOR KNEE PAIN. Explanation. Causes. Symptoms
 ANTERIOR KNEE PAIN Explanation Anterior knee pain is most commonly caused by irritation and inflammation of the patellofemoral joint of the knee (where the patella/kneecap connects to the femur/thigh bone).
ANTERIOR KNEE PAIN Explanation Anterior knee pain is most commonly caused by irritation and inflammation of the patellofemoral joint of the knee (where the patella/kneecap connects to the femur/thigh bone).
Anterior Cruciate Ligament Reconstruction
 Anterior Cruciate Ligament Reconstruction Physiotherapy Department Patient information leaflet This patient information booklet is designed to provide you with information about the Anterior Cruciate Ligament
Anterior Cruciate Ligament Reconstruction Physiotherapy Department Patient information leaflet This patient information booklet is designed to provide you with information about the Anterior Cruciate Ligament
Move your ankle inward toward your other foot and then outward away from your other foot.
 TOTAL HIP REPLACEMENT POST OPERATIVE EXERCISES Regular exercises to restore your normal hip motion and strength and a gradual return to everyday activities are important for your full recovery. Dr. Robertson
TOTAL HIP REPLACEMENT POST OPERATIVE EXERCISES Regular exercises to restore your normal hip motion and strength and a gradual return to everyday activities are important for your full recovery. Dr. Robertson
Knee Arthroscopy Exercise Guide
 RECOVERY Knee Arthroscopy Exercise Guide Regular exercise to restore strength and mobility to your knee is important for your full recovery after arthroscopic surgery. Your orthopaedic surgeon or physical
RECOVERY Knee Arthroscopy Exercise Guide Regular exercise to restore strength and mobility to your knee is important for your full recovery after arthroscopic surgery. Your orthopaedic surgeon or physical
REHABILITATION PROTOCOL FOLLOWING PCL RECONSTRUCTION USING Allograft
 Sports Medicine and Rehabilitation Center Therapist Phone REHABILITATION PROTOCOL FOLLOWING PCL RECONSTRUCTION USING Allograft I. IMMEDIATE POST-OPERATIVE PHASE (Week 1) Control Swelling and Inflammation
Sports Medicine and Rehabilitation Center Therapist Phone REHABILITATION PROTOCOL FOLLOWING PCL RECONSTRUCTION USING Allograft I. IMMEDIATE POST-OPERATIVE PHASE (Week 1) Control Swelling and Inflammation
REHABILITATION FOLLOWING ACL RECONSTRUCTION PROTOCOL. WEEK 1: Knee immobilizer locked in extension. WBAT with bilateral crutches.
 REHABILITATION FOLLOWING ACL RECONSTRUCTION PROTOCOL IMMEDIATE POST OPERATIVE PHASE Week 1: WEEK 1: Knee immobilizer locked in extension. WBAT with bilateral crutches. Ankle Pumps Passive knee extension
REHABILITATION FOLLOWING ACL RECONSTRUCTION PROTOCOL IMMEDIATE POST OPERATIVE PHASE Week 1: WEEK 1: Knee immobilizer locked in extension. WBAT with bilateral crutches. Ankle Pumps Passive knee extension
Knee Pain. Pain in the pressure on. the kneecap. well as being supported (retinaculum) quadricep. Abnormal. to the knee. or dislocate.
 Knee Pain in Children and Adolescents Description Pain in the knee can occur from various causess but is usually from increased pressure on the kneecap (patella) or abnormal motion. Softening of the cartilage
Knee Pain in Children and Adolescents Description Pain in the knee can occur from various causess but is usually from increased pressure on the kneecap (patella) or abnormal motion. Softening of the cartilage
Lateral Collateral Ligament Sprain
 What is lateral collateral ligament sprain? Lateral Collateral Ligament Sprain A sprain is a joint injury that causes a stretch or tear in a ligament, a strong band of tissue connecting one bone to another.
What is lateral collateral ligament sprain? Lateral Collateral Ligament Sprain A sprain is a joint injury that causes a stretch or tear in a ligament, a strong band of tissue connecting one bone to another.
Patella Instability in Children and Adolescents
 Patella Instability in Children and Adolescents Description Patella Instability is an injury to the kneecap (patella) affecting the joint it forms with the thigh bone (femur) Patella Instability can occur
Patella Instability in Children and Adolescents Description Patella Instability is an injury to the kneecap (patella) affecting the joint it forms with the thigh bone (femur) Patella Instability can occur
ARTHROSCOPIC KNEE SURGERY REHABILITATION PROTOCOL MENISCUS REPAIR
 GENERAL GUIDELINES ARTHROSCOPIC KNEE SURGERY REHABILITATION PROTOCOL MENISCUS REPAIR - The local anesthetic (similar to novacaine) in your knee lasts 6-12 hours - Start taking the pain medication as soon
GENERAL GUIDELINES ARTHROSCOPIC KNEE SURGERY REHABILITATION PROTOCOL MENISCUS REPAIR - The local anesthetic (similar to novacaine) in your knee lasts 6-12 hours - Start taking the pain medication as soon
POST OPERATIVE INSTRUCTIONS ARTHROSCOPIC MENISCECTOMY / CHONDROPLASTY / DEBRIDEMENT
 POST OPERATIVE INSTRUCTIONS ARTHROSCOPIC MENISCECTOMY / CHONDROPLASTY / DEBRIDEMENT DIET Start with clear liquids (jello, soup broth, Gatorade, etc.), crackers, white bread and other light foods Progress
POST OPERATIVE INSTRUCTIONS ARTHROSCOPIC MENISCECTOMY / CHONDROPLASTY / DEBRIDEMENT DIET Start with clear liquids (jello, soup broth, Gatorade, etc.), crackers, white bread and other light foods Progress
Meniscal Repair Protocol-Dr. McClung
 Meniscal Repair Protocol-Dr. McClung Brace: Normally patients will be wearing post-op knee brace locked in full extension for ambulation and sleeping but drop-locked for sitting and knee ROM. Patients
Meniscal Repair Protocol-Dr. McClung Brace: Normally patients will be wearing post-op knee brace locked in full extension for ambulation and sleeping but drop-locked for sitting and knee ROM. Patients
Total Knee Replacement Exercise Guide
 Total Knee Replacement Exercise Guide This article is also available in Spanish: Ejercicio después de reemplazo de rodilla (topic.cfm?topic=a00494). Regular exercise to restore your knee mobility and strength
Total Knee Replacement Exercise Guide This article is also available in Spanish: Ejercicio después de reemplazo de rodilla (topic.cfm?topic=a00494). Regular exercise to restore your knee mobility and strength
Patellar Tendon / Quad Tendon Repair Surgery Discharge Instructions
 Matthew T. Mantell, MD 128 Medical Circle Winchester, VA 22601 Phone: 540-667-8975 Email: mattmantellmd@gmail.com Web: www.mattmantellmd.com Patellar Tendon / Quad Tendon Repair Surgery Discharge Instructions
Matthew T. Mantell, MD 128 Medical Circle Winchester, VA 22601 Phone: 540-667-8975 Email: mattmantellmd@gmail.com Web: www.mattmantellmd.com Patellar Tendon / Quad Tendon Repair Surgery Discharge Instructions
Ankle Sprains. Treatment and Restoration of Motion
 Ankle Sprains Treatment and Restoration of Motion Ankle sprains Ankle anatomy The ankle is a complex joint made up of three bones: the tibia, the fibula and the talus. These three bones are connected by
Ankle Sprains Treatment and Restoration of Motion Ankle sprains Ankle anatomy The ankle is a complex joint made up of three bones: the tibia, the fibula and the talus. These three bones are connected by
James R. Romanowski, M.D.
 James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211 704-358-0308 (Office) 704-358-0037 (Fax) www.charlotteshoulder.com DISCHARGE INSTRUCTIONS
James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211 704-358-0308 (Office) 704-358-0037 (Fax) www.charlotteshoulder.com DISCHARGE INSTRUCTIONS
NONOPERATIVE REHABILITATION FOLLOWING ACL INJURY ( Program)
 Therapist: Phone: NONOPERATIVE REHABILITATION FOLLOWING ACL INJURY (3-3-4-4 Program) IMMEDIATE INJURY PHASE (Day 1 to Day 7) Restore full passive knee extension Diminish joint swelling and pain Restore
Therapist: Phone: NONOPERATIVE REHABILITATION FOLLOWING ACL INJURY (3-3-4-4 Program) IMMEDIATE INJURY PHASE (Day 1 to Day 7) Restore full passive knee extension Diminish joint swelling and pain Restore
Anterior Cruciate Ligament Reconstruction
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Anterior Cruciate Ligament Reconstruction Physiotherapy This patient information booklet is designed to provide you with information
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Anterior Cruciate Ligament Reconstruction Physiotherapy This patient information booklet is designed to provide you with information
Page 1 of 5 SPECTRUM MEDICAL
 Page 1 of 5 SPECTRUM MEDICAL HOME INSTRUCTIONS Total Knee Replacement I. Walking A. Use walker/crutches until your doctor says you no longer need them. Your foot should be flat on the floor with on it.
Page 1 of 5 SPECTRUM MEDICAL HOME INSTRUCTIONS Total Knee Replacement I. Walking A. Use walker/crutches until your doctor says you no longer need them. Your foot should be flat on the floor with on it.
Home Exercise Program for Knee Conditioning
 Prepared for: Prepared by: Instructions: Home Exercise Program for Knee Conditioning Before beginning the conditioning program, warm up the muscles by riding a stationary bicycle or jogging for 10 minutes.
Prepared for: Prepared by: Instructions: Home Exercise Program for Knee Conditioning Before beginning the conditioning program, warm up the muscles by riding a stationary bicycle or jogging for 10 minutes.
Total Knee Arthroplasty (Replacement):
 Total Knee Arthroplasty (Replacement): The information below is to be used as an education tool following your knee replacement surgery. Expectations, exercises, concerns, and hints for activities of daily
Total Knee Arthroplasty (Replacement): The information below is to be used as an education tool following your knee replacement surgery. Expectations, exercises, concerns, and hints for activities of daily
Knee Replacement Rehabilitation
 Knee Replacement Rehabilitation The following exercises may be given to you to help get you moving and become more independent. Please bring this copy of the exercises with you to hospital. After your
Knee Replacement Rehabilitation The following exercises may be given to you to help get you moving and become more independent. Please bring this copy of the exercises with you to hospital. After your
Medial Patellofemoral Ligament Repair/Reconstruction
 Alta View Sports Medicine Dr. James R. Meadows, MD Orthopedic Surgery & Sports Medicine 74 Kimballs Ln Ste 230, Draper, UT 84020 9844 S. 1300 E. Ste 100, Sandy, UT 84094 (801) 571-9433 www.meadowsmd.com
Alta View Sports Medicine Dr. James R. Meadows, MD Orthopedic Surgery & Sports Medicine 74 Kimballs Ln Ste 230, Draper, UT 84020 9844 S. 1300 E. Ste 100, Sandy, UT 84094 (801) 571-9433 www.meadowsmd.com
ACL RECONSTRUCTION REHABILITATION PROTOCOL DELAYED DAVID R. MACK, M.D. INTRODUCTION
 ACL RECONSTRUCTION REHABILITATION PROTOCOL DELAYED DAVID R. MACK, M.D. INTRODUCTION This DELAYED protocol is used if any of the following are present: meniscal repair, concomitant ligament repair or patellofemoral
ACL RECONSTRUCTION REHABILITATION PROTOCOL DELAYED DAVID R. MACK, M.D. INTRODUCTION This DELAYED protocol is used if any of the following are present: meniscal repair, concomitant ligament repair or patellofemoral
Athletic Preparation ACL Reconstruction - Accelerated Rehabilitation. Autologous Bone-Tendon-Bone, Patella Tendon Graft
 Orthopaedic Sports Specialists, P.C. Michael E. Joyce, M.D. 84 Glastonbury Blvd., Suite 101, Glastonbury, Connecticut 06033 Voice: 860-652-8883, Fax: 860-652-8887 Athletic Preparation ACL Reconstruction
Orthopaedic Sports Specialists, P.C. Michael E. Joyce, M.D. 84 Glastonbury Blvd., Suite 101, Glastonbury, Connecticut 06033 Voice: 860-652-8883, Fax: 860-652-8887 Athletic Preparation ACL Reconstruction
POST OPERATIVE INSTRUCTIONS KNEE OSTEOTOMY (TIBIAL TUBERCLE OSTEOTOMY / HIGH TIBIAL OSTEOTOMY / DISTAL FEMORAL OSTEOTOMY)
 POST OPERATIVE INSTRUCTIONS KNEE OSTEOTOMY (TIBIAL TUBERCLE OSTEOTOMY / HIGH TIBIAL OSTEOTOMY / DISTAL FEMORAL OSTEOTOMY) DIET Start with clear liquids (jello, soup broth, Gatorade, etc.), crackers, white
POST OPERATIVE INSTRUCTIONS KNEE OSTEOTOMY (TIBIAL TUBERCLE OSTEOTOMY / HIGH TIBIAL OSTEOTOMY / DISTAL FEMORAL OSTEOTOMY) DIET Start with clear liquids (jello, soup broth, Gatorade, etc.), crackers, white
Knee Conditioning Program
 Knee Conditioning Program Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle. Following
Knee Conditioning Program Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle. Following
Patellar Tendon Debridement & Repair Rehabilitation Protocol
 Patellar Tendon Debridement & Repair Rehabilitation Protocol PREOPERATIVE PHASE Diminish inflammation, swelling, and pain Restore normal range of motion (especially knee extension) Restore voluntary muscle
Patellar Tendon Debridement & Repair Rehabilitation Protocol PREOPERATIVE PHASE Diminish inflammation, swelling, and pain Restore normal range of motion (especially knee extension) Restore voluntary muscle
Knee Conditioning Program
 Prepared for: Prepared by: Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle. Following
Prepared for: Prepared by: Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle. Following
Knee Replacement PROGRAM. Nightingale. Home Healthcare
 Knee Replacement PROGRAM TM Nightingale Home Healthcare With the help of Nightingale s experienced and professional rehabilitation team, you will be guided through a more complete and successful recovery
Knee Replacement PROGRAM TM Nightingale Home Healthcare With the help of Nightingale s experienced and professional rehabilitation team, you will be guided through a more complete and successful recovery
ANTERIOR CRUCIATE LIGAMENT INFORMATION PACKET
 ANTERIOR CRUCIATE LIGAMENT INFORMATION PACKET Anterior Cruciate Ligament (ACL) Posterior Cruciate Ligament (PCL) Michael Angeline, MD Orthopedic and Sports Medicine Mercy Health System - 1 - Instructions
ANTERIOR CRUCIATE LIGAMENT INFORMATION PACKET Anterior Cruciate Ligament (ACL) Posterior Cruciate Ligament (PCL) Michael Angeline, MD Orthopedic and Sports Medicine Mercy Health System - 1 - Instructions
Total Hip Replacement Exercise Booklet Cemented Femoral Stem Weight Bearing As Tolerated
 Total Hip Replacement Exercise Booklet Cemented Femoral Stem Weight Bearing As Tolerated Patient Name: Surgeon: Date of Surgery: Physiotherapist: Department of Rehabilitation (416) 967-8650 ext. PR 99506
Total Hip Replacement Exercise Booklet Cemented Femoral Stem Weight Bearing As Tolerated Patient Name: Surgeon: Date of Surgery: Physiotherapist: Department of Rehabilitation (416) 967-8650 ext. PR 99506
ACL Reconstruction Physiotherapy advice for patients
 ACL Reconstruction Physiotherapy advice for patients Introduction This booklet is designed to provide you with advice and guidance on your rehabilitation after reconstruction of your anterior cruciate
ACL Reconstruction Physiotherapy advice for patients Introduction This booklet is designed to provide you with advice and guidance on your rehabilitation after reconstruction of your anterior cruciate
King Khalid University Hospital
 King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: ACL RECONSTRUCTION +/- MENSICAL REPAIR 1. General Guidelines: Time lines in this rehabilitation protocol are
King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: ACL RECONSTRUCTION +/- MENSICAL REPAIR 1. General Guidelines: Time lines in this rehabilitation protocol are
Patient Information & Exercise Folder
 MEDIAL PATELLO-FEMORAL LIGAMENT RECONSTRUCTION Patient Information & Exercise Folder Mr D Raj FRCS (Tr & Orth) Consultant Lower Limb Orthopaedic Surgeon Pilgrim Hospital, Sibsey Road, Boston Lincolnshire
MEDIAL PATELLO-FEMORAL LIGAMENT RECONSTRUCTION Patient Information & Exercise Folder Mr D Raj FRCS (Tr & Orth) Consultant Lower Limb Orthopaedic Surgeon Pilgrim Hospital, Sibsey Road, Boston Lincolnshire
Ex Fix Rehab Phase II Strengthening
 Perform repetitions of each exercise, twice daily. Increase to repetitions. Ankle Pumps: With leg resting on bed and knee straight, slowly pump ankle up and down as far as possible. Quad sets: Tighten
Perform repetitions of each exercise, twice daily. Increase to repetitions. Ankle Pumps: With leg resting on bed and knee straight, slowly pump ankle up and down as far as possible. Quad sets: Tighten
Medial Collateral Ligament Repair Protocol-Dr. McClung
 Medial Collateral Ligament Repair Protocol-Dr. McClung Brace: Normally patients will be wearing post-op knee brace locked in 30 degrees for ambulation and sleeping but drop-locked for sitting and knee
Medial Collateral Ligament Repair Protocol-Dr. McClung Brace: Normally patients will be wearing post-op knee brace locked in 30 degrees for ambulation and sleeping but drop-locked for sitting and knee
Week 1 Orthotics- 1. Knee brace locked in full extension at all times except for rehab exercises 2. Elastic bandage as needed to control swelling
 General Principles: This protocol was designed to provide the rehabilitation professional with a guideline of postoperative care. It should be stressed that this is only a protocol and should not be a
General Principles: This protocol was designed to provide the rehabilitation professional with a guideline of postoperative care. It should be stressed that this is only a protocol and should not be a
ACL Reconstruction Rehabilitation Bone Patellar Tendon Bone Graft Kyle F. Chun, MD
 ACL Reconstruction Rehabilitation Bone Patellar Tendon Bone Graft Kyle F. Chun, MD [ ] Meniscus Repair (If checked, WBAT in brace in full extension, ROM 0-90 x 6 wks; WBAT 0-90, ROM 0-120 weeks 7-12; WBAT/ROMAT
ACL Reconstruction Rehabilitation Bone Patellar Tendon Bone Graft Kyle F. Chun, MD [ ] Meniscus Repair (If checked, WBAT in brace in full extension, ROM 0-90 x 6 wks; WBAT 0-90, ROM 0-120 weeks 7-12; WBAT/ROMAT
Knee Arthroscopy Exercise Programme
 Chester Knee Clinic & Cartilage Repair Centre Nuffield Health, The Grosvenor Hospital Chester Wrexham Road Chester CH4 7QP Hospital Telephone: 01244 680 444 CKC Website: www.kneeclinic.info Email: office@kneeclinic.info
Chester Knee Clinic & Cartilage Repair Centre Nuffield Health, The Grosvenor Hospital Chester Wrexham Road Chester CH4 7QP Hospital Telephone: 01244 680 444 CKC Website: www.kneeclinic.info Email: office@kneeclinic.info
