RHINOSINUSITIS IS AN IMPORtant
|
|
|
- Eric Craig
- 5 years ago
- Views:
Transcription
1 ORIGINAL ARTICLE Treatment of Acute and Chronic Rhinosinusitis in the United States, Hadley J. Sharp, BS; David Denman, MD; Susan Puumala, MS; Donald A. Leopold, MD Objective: To generalize the prescribing trends of a statistically defined sample of patient visits because of acute or chronic rhinosinusitis in the United States, using reported diagnostic codes from the International Classification of Diseases, Ninth Revision, Clinical Modification. Design: Four-year prospective study. Setting: Public use data from the National Ambulatory Medical Care Survey and the National Hospital Ambulatory Medical Care Survey collected by the National Center for Health Statistics. Results: The most frequently recommended medications for treatment of both acute and chronic rhinosinusitis are antibiotic agents, followed by antihistamines; nasal decongestants; corticosteroids; and antitussive, expectorant, and mucolytic agents, respectively. In addition, corticosteroids are used for the treatment of chronic rhinosinusitis. Conclusions: The use of prescription antibiotics far outweighs the predicted incidence of bacterial causes of acute and chronic rhinosinusitis. Frequency of antibiotic class used was not congruent with reported antimicrobial efficacy of the respective classes. Despite contradictory efficacies reported in the literature, inhaled corticosteroids were frequently used to treat acute rhinosinusitis. Antibiotics and inhaled nasal corticosteroids are being used more often than their published efficacies would encourage. Arch Otolaryngol Head Neck Surg. 2007;133: Author Affiliations: Departments of Otolaryngology Head and Neck Surgery (Ms Sharp and Drs Denman and Leopold) and Preventive and Societal Medicine (Ms Puumala), University of Nebraska Medical Center, Omaha. RHINOSINUSITIS IS AN IMPORtant personal medical problem for patients in the United States. Recently, the disorder was divided into various classifications for acute and chronic rhinosinusitis based on time line and symptoms. 1 Although this classification added clarity, there is still much confusion between patients and physicians about the causes and symptoms that constitute rhinosinusitis and within the medical field about how to treat the different subgroups. Until recently, most studies of rhinosinusitis relied on patient symptom CME course available at responses, and because of the confusion regarding causes, symptoms, and treatment, these results were difficult to interpret. In this study, data from the National Ambulatory Medical Care Survey (NAMCS) and the National Hospital Ambulatory Medical Care Survey (NHAMCS) were used to evaluate patient visits to statistically selected ambulatory care facilities. Although rhinosinusitis has been more recently favored as a diagnosis because of the combined nasal and paranasal sinus involvement, 2 the data in NAMCS and NHAMCS relate only to sinusitis. To be consistent with the current guidelines and to avoid confusion, we use the term rhinosinusitis throughout this article. Physician-generated clinical information about patient visits because of rhinosinusitis was collected. Using reported International Classification of Diseases, Ninth Revision, Clinical Modification (ICD-9-CM) codes and diagnoses, we were able to generalize the prescribing trends of a statistically defined sample of visits in the United States that resulted in a primary diagnosis of acute or chronic rhinosinusitis. Rhinosinusitis represents a huge financial burden for the US health care system. In 1992, direct medical costs of rhinosinusitis were nearly $2.4 billion by conservative estimates. With direct and indirect costs calculated, the total expenditure is much larger, which establishes rhinosinusitis as one of the most expensive disorders experienced by the US population. 3 Proof can also be found in the number of prescriptions written for antibiotic agents to treat rhinosinusitis; in 2002, rhinosinusitis accounted for 9% of pre- 260
2 scriptions for antibiotics in children and 21% in adults. 4 Not only cost, but also the effect that rhinosinusitis has on quality of life, makes it a major medical concern. 5 Without standard protocols, treatment of this varied disorder can be inconsistent between providers and among similar symptom groups. In this article the various medical treatments used for chronic and acute rhinosinusitis are tabulated. The current classification of rhinosinusitis in adults, from the Sinus and Allergy Health Partnership (SAHP) and the American Rhinologic Society, is as follows: acute rhinosinusitis is manifested with symptoms for up to 4 weeks, with the presence of at least 2 major symptoms, or 1 major and at least 2 minor symptoms or purulence; and chronic rhinosinusitis is defined as the duration of symptoms for 12 weeks or longer, with the same symptom profile as in acute rhinosinusitis. 4 Acute rhinosinusitis is most often thought to be caused by an infectious agent. Watchful waiting, lavage with saline solution, and use of a decongestant or proper antimicrobial agents are the treatments of choice. 6 Despite the 32 million cases of chronic rhinosinusitis occurring annually in the United States, the causes are not so clear as for acute rhinosinusitis. 7 It is assumed that the chronic process is multifactorial and possibly different in children than in adults. Repeated acute upper respiratory tract infections can lead to mucosal swelling, obstruction of sinus outflow, and, eventually, chronic infection. A number of conditions predispose to rhinosinusitis, including smoking, swimming, decongestant spray abuse (rhinosinusitis medicamentosa), immunoglobulin deficiencies, disorders of mucociliary transport, and changes in glandular secretions. 8 Allergies, via antigen-antibody reactions and release of vasodilators and mediators of inflammation, can cause mucosal swelling and obstruction. 9 In addition, anatomical factors such as septal spurs or deviations, hypertrophic middle turbinates, and concha bullosa can affect nasal cavity and sinus ostia airflow. 10 All of these conditions can lead to an environment that is suitable for mucous stasis, bacterial or fungal overgrowth, and chronic inflammation. 11 Other proposed causes include hormonal effects, and further research should elucidate a better understanding of these processes. With a demonstration of the complexity of acute and chronic rhinosinusitis, it is understandable why the approach to treatment has remained controversial. Inasmuch as viruses frequently cause acute rhinosinusitis, many advocate no antibiotic treatment if the symptoms are not severe, wane in 5 to 7 days, and resolve in 10 days. 6 When antibiotics are used, there are recommendations from the SAHP 12 for calculated clinical efficacy and bacteriologic efficacy, as well as when to change therapy. In 2000 and again in 2004, the SAHP reported the clinical and bacteriologic efficacy of a number of antimicrobial agents, including, in descending order, amoxicillin clavulanate potassium, amoxicillin, cefpodoxime proxetil, cefuroxime axetil, cefdinir, trimethoprimsulfamethoxasole, doxycycline, azithromycin or clarithromycin or erythromycin, and telithromycin. The SAHP recommended antibiotic therapy for adults with acute bacterial rhinosinusitis with mild disease and no antimicrobial use in the past 4 to 6 weeks. 4 This order will be compared with the descending order of antimicrobial prescribing frequency by physicians in the United States. The effects of antibiotic therapy on chronic rhinosinusitis are questionable, but if an acute infection occurs in the inflamed nasal or sinus cavities, use of a shortterm regimen can provide relief. 4 Decongestants are often used in treatment plans to increase sinus drainage and ventilation and to thin mucosa and mucous secretions, and result in decreasing mucous stasis. 13 For acute rhinosinusitis, and especially for acute bacterial rhinosinusitis, there are guidelines for treatment. Chronic disorders are not so categorical and are much more complex. This may be why there is no consensus in the medical community about algorithms or protocols for treatment. The goal of resolution of chronic rhinosinusitis is to resolve predisposing factors, but many treatments effective in acute episodes do not have the same efficacy in chronic disorders. 4 In this article, we examine the national trends in treatment and how they compare with current research. METHODS Public use data from the NAMCS and NHAMCS for 1999 through 2002 were combined and used in this analysis. These years were chosen because data were collected similarly during all 4 years. The NAMCS and NHAMCS prospectively collect data from a national probability sample of visits for ambulatory medical care to a physician s office and to hospital outpatient departments and emergency departments. These surveys are conducted annually by the National Center for Health Statistics. Both surveys use a multistage probability design. The NAMCS uses a 3-stage design that starts with a probability sample of primary sampling units, then samples physician practices within primary sampling units, and finally samples patient visits within practices. Patient visits are randomly selected from a 1-week reporting period. Physicians are identified through membership lists from the American Medical Association and the American Osteopathic Association. Only nonfederally employed physicians are included. Physicians with a specialty of anesthesiology, pathology, or radiology are excluded from the survey. The NHAMCS uses a 4-stage design that also starts with a probability sample of primary sampling units, then samples hospitals within primary sampling units; outpatient clinics and emergency services areas within hospitals; and visits in the outpatient and emergency clinic area. Patient visits are randomly sampled during a 4-week reporting period. Hospitals included are noninstitutional general and short-stay hospitals; federal, military, and Veterans Administration hospitals and hospital units of institutions are excluded. Data are collected on a patient record form that includes patient demographic data and visit information. Visit information includes up to 3 reasons for the visit, a primary diagnosis and 1 or 2 secondary diagnoses, projected visit payment type, and a list of medications ordered, supplied, administered, or continued at the visit. As many as 6 medications can be listed on the survey, and each drug is referred to as a drug mention. These medications were assigned therapeutic classifications from the National Drug Code Directory, 1995 edition. An overall antibiotic category was created by combining the following therapeutic classes: penicillins; cephalosporins; erythromycins, lincosamides, and macrolides; tetracyclines; sulfonamides and trimethoprim; and quinolones and their derivatives. 261
3 Table 1. ICD-9-CM Codes Used to Evaluate Frequency of Chronic and Acute Rhinosinusitis Visits in the United States, * Chronic Rhinosinusitis ICD-9-CM Code No. of Visits in Database Acute Rhinosinusitis ICD-9-CM Code No. of Visits in Database 471.0, Polyp of nasal cavity , Maxillary acute sinusitis , Polypoid sinus degeneration , Frontal acute sinusitis , Other polyp of sinus , Ethmoidal acute sinusitis , Unspecified nasal polyp , Sphenoidal acute sinusitis , Maxillary chronic sinusitis , Other acute sinusitis , Frontal chronic sinusitis , Acute sinusitis, unspecified , Ethmoidal chronic sinusitis , Sphenoidal chronic sinusitis , Other chronic sinusitis , Unspecified sinusitis (chronic) 4508 Abbreviation: ICD-9-CM, International Classification of Diseases, Ninth Revision, Clinical Modification. *Of the codes included, any one listed as the primary diagnosis qualified the visit for the respective category of diagnosis, chronic or acute rhinosinusitis. Table 2. Medication Classes With Frequency per Visit* Medication Class Chronic Rhinosinusitis Acute Rhinosinusitis Antibiotics Penicillins ( ) ( ) Cephalosporins ( ) ( ) Erythromycins, lincosamides, and macrolides ( ) ( ) Tetracyclines NE NE Sulfonamides and trimethoprim 4.19 ( ) 4.77 ( ) Quinolones and derivatives 7.37 ( ) 9.43 ( ) All antibiotics combined ( ) ( ) Adrenal corticosteroids 4.00 ( ) NE Nasal decongestants ( ) ( ) Antitussives, expectorants, and mucolytics 9.58 ( ) ( ) Antihistamines ( ) ( ) Corticosteroids, nasal or inhalation ( ) ( ) Abbreviation: NE, not reliably estimable because of fewer than 30 observations or a relative standard error greater than 30%. *Data are given as number of visits (95% confidence interval). Up to 6 medications could be listed per visit. Medication classes of interest that met the requirement of 30 subjects and less than 30% relative standard error for either chronic or acute rhinosinusitis are given in Table 3. STUDY SAMPLE SELECTION In this study, we selected only those visits that resulted in a primary diagnosis of chronic or acute rhinosinusitis. As many as 3 diagnoses could be listed at each visit. The first diagnosis was considered primary and the other diagnoses were considered secondary. If a visit included 1 of the ICD-9-CM codes given in Table 1 for the primary diagnosis, it was selected as a visit because of chronic or acute rhinosinusitis. We excluded those visits with a diagnosis of both chronic and acute rhinosinusitis because there were fewer than 30 such visits in the database. STATISTICAL ANALYSIS Sample weights from the National Center for Health Statistics were used for each visit in both the NAMCS and NHAMCS data to obtain unbiased national estimates based on various patient characteristics and to adjust for nonresponse. Standard errors were calculated using an ultimate cluster variance estimation design using Survey Data Analysis software (SUDAAN, version 8.0; Research Triangle Institute, Cary, NC). This accounts for the multistage sampling design to estimate unbiased standard errors and 95% confidence intervals (CIs). Estimates were considered unreliable if they were based on fewer than 30 visits in the database or if their relative standard error was greater than 30%. 14 RESULTS Extrapolations of data from the NAMCS and NHAMCS show that in 1999 through 2002 in the United States there were an estimated visits annually because of chronic rhinosinusitis and an estimated visits annually because of acute rhinosinusitis. These visits represented 1.39% (95% CI, ) and 0.30% (95% CI, ), respectively, of all visits for ambulatory care. Antibiotic agents were mentioned in visits because of both acute and chronic rhinosinusitis. Penicillins were the most frequently recommended class of antibiotics mentioned (Table 2), and in this group, most mentions were specifically for amoxicillin or amoxicillin clavulanate potassium (Table 3). The grouping of erythromycin, lincosamides, and macrolides was the second most frequent class of antibiotics mentioned at visits because of rhinosinusitis. 262
4 Among other drug classes, inhaled or nasal corticosteroidal agents and antihistamines were mentioned in visits because of both acute and chronic rhinosinusitis. Additional drug class uses are given in Table 2. COMMENT Table 3. Frequency of Amoxicillin vs Amoxicillin Clavulanate Potassium for Treatment of Both Chronic and Acute Rhinosinusitis* Medication Chronic Rhinosinusitis Acute Rhinosinusitis Amoxicillin ( ) ( ) Amoxicillin clavulanate potassium ( ) ( ) *Data are given as number of visits (95% confidence interval). Some visits listed both medications. While this is unlikely accurate and more likely a mistake in reporting, the data must be evaluated. Includes amoxicillin, Amoxil (SmithKline Beecham Pharmaceuticals, Philadelphia, Pa), Polymox (Apothecon, a Bristol-Myers Squibb Co, Shawnee Mission, Kan), and Trimox (Apothecon). Includes Augmentin, Augmentin 125, Augmentin 250, Augmentin 500, and Augmentin ES (all produced by SmithKline Beecham Pharmaceuticals). The use of prescription antibiotics to treat acute rhinosinusitis far outweighs the predicted incidence of bacterial causes. The literature repeatedly shows that viruses are by far the most frequent cause of acute rhinosinusitis. However, in practice, physicians ordered, supplied, administered, or continued at least 1 prescription antibiotic in 82.74% of visits because of acute rhinosinusitis. With etiologies less understood for chronic rhinosinusitis, a comparison cannot be made between research and practice. However, with inflammation the most likely cause, the use of at least 1 antibiotic in 69.95% of visits because of chronic rhinosinusitis is a surprising number. Penicillins, mainly amoxicillin and amoxicillin clavulanate potassium, were the most commonly used medication class for both chronic and acute rhinosinusitis. A penicillin drug was mentioned in 30.35% of all visits with a primary diagnosis of chronic rhinosinusitis and in 27.18% visits with a primary diagnosis of acute rhinosinusitis. This is intuitive, inasmuch as recent studies have shown penicillins to be highly effective against the bacteria in nasal and sinus areas. Amoxicillin clavulanate potassium (875/125 mg twice a day for 14 days) has a 95% clinical response rate in acute bacterial rhinosinusitis and acute exacerbations of chronic rhinosinusitis. 15 Penicillins are mentioned more often in visits because of chronic rhinosinusitis compared with acute rhinosinusitis. When the SAHP published antimicrobial guidelines for acute bacterial rhinosinusitis in 2004, they discussed all antimicrobial agents with -lactam activity en bloc. This class topped the list of efficacious agents, and, when subdivided, amoxicillin clavulanate potassium had the highest calculated clinical efficacy in both the groups that had or had not recently received antimicrobial agents. 4 The group including erythromycins, lincosamides, and macrolides was second in frequency of antibiotic mentions in visits because of acute rhinosinusitis. A mention in 24.32% of visits puts the use of this class of antibiotics ahead of cephalosporins, sulfonamides and trimethoprim, and tetracyclines, in that order. The Acute Bacterial Rhinosinusitis protocol issued by the SAHP in January 2004 listed efficacies of these classes in an order different from that reported in our studies. In the SAHP data, the erythromycin, lincosamides, and macrolides group had the lowest calculated clinical efficacy and bacteriologic efficacy, behind the cephalosporins and the sulfonamides and trimethoprim. This higher than expected ranking in clinical practice could be owing to an anti-inflammatory benefit that macrolides possess. 16 Based on the number of visits with an antibiotic mention (69.95% for chronic rhinosinusitis and 82.74% for acute rhinosinusitis) and the suspected low number of rhinosinusitis episodes caused by a bacterium, one must entertain the secondary efficacy of these drugs. Perhaps these physicians were treating a secondary infection or using the anti-inflammatory effects of antibiotic treatments. While keeping the goals of treatment in mind, there are concerns about the overuse of antibiotics and the resultant problems, including drug resistance and increasingly virulent bacteria. When two thirds of patients with sinus symptoms expect or receive an antibiotic and as many as one fifth of antibiotic prescriptions for adults are written for a drug to treat rhinosinusitis, these disorders hold special pertinence on the topic. Inhaled or nasal corticosteroids were mentioned in 15.05% of visits because of acute rhinosinusitis. Prescribed in a significant number of visits, it is important to discuss what has previously been reported about the role of corticosteroids in rhinosinusitis. Dolor et al 17 showed that the concomitant use of cefuroxime and intranasal fluticasone for 21 days had a higher clinical success rate than use of cefuroxime with placebo (93.5% and 73.9%, respectively; P=.009). Lack of objective criteria for measuring improvement, data based on patient reports of improvement, and funding of the study by the manufacturer of fluticasone all proved limitations of that publication. In a different double-blind, placebocontrolled trial, 2 the use of flunisolide as an adjunct to amoxicillin clavunate potassium therapy was studied. Despite use of flunisolide vs placebo 3 times daily for 3 weeks, many patients continued to have symptoms and recurrences were common in both groups. 2 As our data show and as many practicing clinicians can report, the use of inhaled corticosteroids as adjunctive treatment in acute rhinosinusitis is not rare but is of undetermined benefit. In chronic rhinosinusitis, even more intranasal and oral corticosteroid use was reported. Inasmuch as many consider chronic rhinosinusitis both an infectious and an inflammatory disease, it is understandable that clinicians are, in many cases, attempting to treat both. Two studies used to evaluate treatment approaches in chronic rhinosinusitis have been published. One focused on symptomatic improvement only, while a more recent study coupled symptomatic and radiographic changes due to medical treatment. In the earlier study, McNally et al 18 showed that treatment with antibiotics, decongestants, and intranasal steroids can decrease symptoms of chronic rhinosinusitis. In that study, 263
5 however, patients were not followed up for occurrence of relapse. 16 In a 2002 retrospective study, chronic rhinosinusitis was treated with an antibiotic (most commonly, trovafloxacin, amoxicillin clavulanate potassium, levofloxacin, or metronidazole), oral prednisone for 10 days, intranasal steroids, and nasal irrigation with saline solution. 19 Statistically significant improvement in both symptoms and findings at computed tomography from baseline to the end of the study were demonstrated. 19 However, neither of these studies included a concurrent control group. Based on current understanding of the pathogenesis of chronic rhinosinusitis and these findings, it is understandable why some physicians prescribe corticosteroids to treat the disorder. Allergic rhinosinusitis is a common disease that affects approximately 20% of the US population. 20 Because corticosteroids are effective in the treatment of this disorder, higher numbers of drug mentions for this chronic class might be expected. Inasmuch as a patient could have acute or chronic sinus complications from allergies, it further clouds the assumptions about use of corticosteroids to treat acute or chronic rhinosinusitis. 21 The use of antihistamines demonstrated by our data seems logical; 20.93% of visits because of chronic rhinosinusitis and 25.26% of visits because of acute rhinosinusitis is near the prevalence of allergic rhinosinusitis in the population. Antihistamines are clearly indicated in the treatment of allergy-related disease. Some of the older, generally over-the-counter antihistamines are considered detrimental to the nose and sinus mucosa because their cholinergic effects cause dryness of the mucous secretions and resolution of infections can be slowed. 22 Most of the antihistamines in this study were prescription drugs, and these newer antihistamines have fewer adverse effects and cause much less drying than their predecessors, which may explain their high usage rates. 21,23 Decongestants were mentioned in as many as a fourth of visits because of rhinosinusitis, and more often acute rhinosinusitis than chronic rhinosinusitis. The high use of this class of drugs (evaluated separately from antihistamine combination agents) is understandable considering the efficacy reports in the literature. In reviewing 5 studies, Arroll 24 reports a reduction in nasal airway resistance in patients using these drugs compared with placebo. The same study stated that mucolytic agents were less reported but that such treatment decreased symptom scores when compared with placebo. 24 The conclusions of this review rely on primary studies of variable quality. The reviewers were clear about the lack of efficacy except in the high-quality studies in which global improvement in symptoms was noted. With limited quantifiable data and supportive anecdotal evidence, the high use of decongestant and mucolytic agents is logical. Further, both decongestant and mucolytic agents are available over the counter; thus, it can be assumed that usage is even higher than reflected by physician reports. CONCLUSIONS In evaluating the trends of rhinosinusitis treatment in the United States, many points became apparent. Prescription antibiotic drugs are being used far more than bacterial causes studies would indicate. Within the class of antibiotics, the penicillins are, appropriately, at the top of the prescription list for both acute and chronic rhinosinusitis. Questionable is the frequent use of the class that includes erythromycins, lincosamides, and macrolides, with other classes having higher antibacterial efficacy. Nasal and inhaled corticosteroids are prescribed more frequently to treat acute rhinosinusitis than published studies imply is necessary. Despite current theories of causes of chronic rhinosinusitis, the use of corticosteroids remains low in this setting. An area where our findings fit nicely with current information is use of antihistamines, which roughly matched the prevalence of their major indication, allergic rhinosinusitis. A limitation of this study is that the databases used only data for medications ordered, supplied, administered, or continued by attending physicians. Because these data were not based on patient responses, the use of overthe-counter medicines or home remedies was not recorded. We wonder whether the percentages of medications used would be much smaller when compared with the number of patients who use hot packs to relieve the symptoms of chronic rhinosinusitis or whether physicians recommend irrigation with saline solution and steam, as often as antihistamine prescriptions. The use of antibiotics and corticosteroids, inhaled and oral, needs more investigation in the treating of rhinosinusitis. Current theories and contradicting evidence in the literature makes the findings of our study all the more compelling. Could their use be more efficacious than proved? Can it be assumed that practicing physicians in the United States base their decisions on experienced success? Evidence-based medicine means incorporating the best evidence into treatment decisions. With limited or no literature addressing the efficacy of each drug class with the separate diagnoses, evidence-based medicine would indicate that it is appropriate to use personal or accumulated clinical experience. The vast use of these agents makes the statement that they seem to be effective in reducing symptoms or preventing relapse, or they would have been abandoned. Another important possibility is that many patients have selflimited disease that will resolve regardless of treatment, and their physicians could be prescribing what they think will work. With time, many infectious processes are resolved by the patient s immune system. To attribute efficacy or curative credit to a drug class based solely on resolution of symptoms without comparison with nontreated control subjects, physicians could be oversatisfied with their own prescribing habits. Many physicians might use an ICD-9-CM code to ensure that a patient s insurance will pay for a particular medication and not necessarily because the code is for the disease they believe they are treating. The coding could be questioned if the physician, nurse, or billing clerk may simply be in the habit of using a few ICD-9-CM codes, regardless of the actual findings or symptoms. Follow-up studies might reveal how these trends change. Submitted for Publication: April 25, 2006; final revision received September 22, 2006; accepted October 29,
6 Correspondence: Hadley J. Sharp, BS, Department of Otolaryngology Head and Neck Surgery, University of Nebraska Medical Center, 5226 B St, Omaha, NE (hsharp@unmc.edu). Author Contributions: Ms Sharp had full access to all the data in the study and takes responsibility for the integrity of the data and the accuracy of the data analysis. Study concept and design: Sharp, Denman, and Leopold. Acquisition of data: Sharp, Puumala, and Leopold. Analysis and interpretation of data: Sharp, Puumala, and Leopold. Drafting of the manuscript: Sharp and Puumala. Critical revision of the manuscript for important intellectual content: Sharp, Denman, Puumala, and Leopold. Statistical analysis: Puumala. Administrative, technical, and material support: Sharp and Leopold. Study supervision: Sharp and Leopold. Financial Disclosure: None reported. REFERENCES 1. Lanza DC, Kennedy DW. Adult rhinosinusitis defined. Otolaryngol Head Neck Surg. 1997;117(3 pt 2):S1-S7. 2. Meltzer EO, Orgel HA, Backhaus JW, et al. Intranasal flunisolide spray as an adjunct to oral antibiotic therapy for sinusitis. J Allergy Clin Immunol. 1993;92: Benson V, Marano MA. Current estimates from the National Health Interview Survey, Vital Health Stat. 1994;10: Anon JB, Jacobs MR, Poole MD, et al. Antimicrobial treatment guidelines for acute bacterial rhinosinusitis [published correction appears in Otolaryngol Head Neck Surg. 2004;130: ]. Otolaryngol Head Neck Surg. 2004;130: Gliklich RE, Metson R. The health impact of chronic sinusitis in patients seeking otolaryngologic care. Otolaryngol Head Neck Surg. 1995;113: Snow V, Mottur-Pilson C, Hickner JM. Principles of appropriate antibiotic use for acute sinusitis in adults. Ann Intern Med. 2001;134: Melen I. Chronic sinusitis: clinical and pathophysiological aspects. Acta Otolaryngol Suppl. 1994;515: Benninger MS, Schmidt JL, Crissman JD, Gottlieb C. Mucociliary function following sinus mucosal regeneration. Otolaryngol Head Neck Surg. 1991;105: Hinni ML, McCaffrey TV, Kasperbauer JL. Early mucosal changes in experimental sinusitis. Otolaryngol Head Neck Surg. 1992;107: Stammberger H. Endoscopic endonasal surgery: concepts in treatment of recurring rhinosinusitis, part I: anatomic and pathophysiologic considerations. Otolaryngol Head Neck Surg. 1986;94: Benninger MS, Anon J, Mabry RL. The medical management of rhinosinusitis. Otolaryngol Head Neck Surg. 1997;117(3, pt 2):S41-S Sinus and Allergy Health Partnership. Antimicrobial treatment guidelines for acute bacterial rhinosinusitis. Otolaryngol Head Neck Surg. 2000;123: Taccariello M, Parikh A, Darby Y, Scadding G. Nasal douching as a valuable adjunct in the management of chronic rhinosinusitis. Rhinology. 1999;37: Reliability of survey estimates 2005 Centers for Disease Control and Prevention: National Center for Health Statistics. /ahcd/reliabilityhtm. Accessed May 10, Namyslowski G, Misiolek M, Czecior E, et al. Comparison of the efficacy and tolerability of amoxycillin/clavulanic acid 875 mg b.i.d. with cefuroxime 500 mg bid in the treatment of chronic and acute exacerbation of chronic sinusitis in adults. J Chemother. 2002;14: Amsden GW. Anti-inflammatory effects of macrolides: an underappreciated benefit in the treatment of community-acquired respiratory tract infections and chronic inflammatory pulmonary conditions? J Antimicrob Chemother. 2005;55: Dolor RJ, Witsell DL, Hellkamp AS, et al; Ceftin and Flonase for Sinusitis (CAFFS) Investigators. Comparison of cefuroxime with or without intranasal fluticasone for the treatment of rhinosinusitis: the CAFFS Trial, a randomized controlled trial [published correction appears in JAMA. 2004;292:1686]. JAMA. 2001;286: McNally PA, White MV, Kaliner MA. Sinusitis in an allergist s office: analysis of 200 consecutive cases. Allergy Asthma Proc. 1997;18: Subramanian HN, Schechtman KB, Hamilos DL. A retrospective analysis of treatment outcomes and time to relapse after intensive medical treatment for chronic sinusitis. Am J Rhinol. 2002;16: Meltzer EO, Hamilos DL, Hadley JA, et al. Rhinosinusitis: establishing definitions for clinical research and patient care. Otolaryngol Head Neck Surg. 2004; 131:S1-S Becker J. Allergic rhinitis. Accessed April 15, Spector SL, Bernstein IL, Li JT, et al. Parameters for the diagnosis and management of sinusitis. J Allergy Clin Immunol. 1998;102(6, pt 2):S107-S Storms WW, Bodman SF, Nathan RA, et al. SCH 434: a new antihistamine/ decongestant for seasonal allergic rhinitis. J Allergy Clin Immunol. 1989;83: Arroll B. Non-antibiotic treatments for upper-respiratory tract infections (common cold). Respir Med. 2005;99:
SINUSITIS. HAVAS ENT CLINICS Excellence in otolaryngology
 JULY 2015 SINUSITIS WHAT IS IT? WHAT SHOULD YOU DO? WHAT WORKS? THOMAS E HAVAS MBBS (SYD) MD (UNSW) FRCSE, FRACS, FACS CONJOINT ASSOCIATE PROFESSOR UNSW OTOLARNGOLOGY HEAD AND NECK SURGERY HAVAS ENT CLINICS
JULY 2015 SINUSITIS WHAT IS IT? WHAT SHOULD YOU DO? WHAT WORKS? THOMAS E HAVAS MBBS (SYD) MD (UNSW) FRCSE, FRACS, FACS CONJOINT ASSOCIATE PROFESSOR UNSW OTOLARNGOLOGY HEAD AND NECK SURGERY HAVAS ENT CLINICS
Prefe f rred d t e t rm: : rhi h no n s o inu n s u iti t s
 HELP It s my sinuses! An overview of pharmacologic treatment of sinusitis Objectives Identify types of sinusitis and underlying pathology Examine common evidence based pharmacologic treatment for sinusitis
HELP It s my sinuses! An overview of pharmacologic treatment of sinusitis Objectives Identify types of sinusitis and underlying pathology Examine common evidence based pharmacologic treatment for sinusitis
Diagnosis and Treatment of Respiratory Illness in Children and Adults
 Page 1 of 9 Main Algorithm Annotations 1. Patient Reports Some Combination of Symptoms Patients may present for an appointment, call into a provider to schedule an appointment or nurse line presenting
Page 1 of 9 Main Algorithm Annotations 1. Patient Reports Some Combination of Symptoms Patients may present for an appointment, call into a provider to schedule an appointment or nurse line presenting
9/18/2018. Disclosures. Objectives
 Is It Really Acute Bacterial Rhinosinusitis? Assessment, Differential Diagnosis and Management of Common Sinonasal Symptoms Kristina Haralambides, MS, RN, FNP-C Disclosures The content of this presentation
Is It Really Acute Bacterial Rhinosinusitis? Assessment, Differential Diagnosis and Management of Common Sinonasal Symptoms Kristina Haralambides, MS, RN, FNP-C Disclosures The content of this presentation
Upper Respiratory Tract Infections
 Upper Respiratory Tract Infections OTITIS MEDIA Otitis media is an inflammation of the middle ear. There are more than 709 million cases of otitis media worldwide each year; half of these cases occur in
Upper Respiratory Tract Infections OTITIS MEDIA Otitis media is an inflammation of the middle ear. There are more than 709 million cases of otitis media worldwide each year; half of these cases occur in
MANAGEMENT OF RHINOSINUSITIS IN ADOLESCENTS AND ADULTS
 MANAGEMENT OF RHINOSINUSITIS IN ADOLESCENTS AND ADULTS Ministry of Health Malaysia Malaysian Society of Otorhinolaryngologist - Head & Neck Surgeons (MS)-HNS) Academy of Medicine Malaysia KEY MESSAGES
MANAGEMENT OF RHINOSINUSITIS IN ADOLESCENTS AND ADULTS Ministry of Health Malaysia Malaysian Society of Otorhinolaryngologist - Head & Neck Surgeons (MS)-HNS) Academy of Medicine Malaysia KEY MESSAGES
Rhinosinusitis. John Ramey, MD Joseph Russell, MD
 Rhinosinusitis John Ramey, MD Joseph Russell, MD Disclosure Statement RSFH as a continuing medical education provider, accredited by the South Carolina Medical Association, it is the policy of RSFH to
Rhinosinusitis John Ramey, MD Joseph Russell, MD Disclosure Statement RSFH as a continuing medical education provider, accredited by the South Carolina Medical Association, it is the policy of RSFH to
ORIGINAL ARTICLE. Trends in Endoscopic Sinus Surgery Rates in the Medicare Population
 ORIGINAL ARTICLE Trends in Endoscopic Sinus Surgery Rates in the Medicare Population Giridhar Venkatraman, MD, MBA; Donald S. Likosky, PhD; Weiping Zhou, MS; Samuel R. G. Finlayson, MD, MPH; David C. Goodman,
ORIGINAL ARTICLE Trends in Endoscopic Sinus Surgery Rates in the Medicare Population Giridhar Venkatraman, MD, MBA; Donald S. Likosky, PhD; Weiping Zhou, MS; Samuel R. G. Finlayson, MD, MPH; David C. Goodman,
DIFFICULT-TO-TREAT CHRONIC
 MANAGEMENT STRATEGIES FOR DIFFICULT-TO-TREAT CHRONIC RHINOSINUSITIS DR ZULKEFLI HUSSEIN CONSULTANT EAR NOSE & THROAT SURGEON PANTAI HOSPITAL PENANG DISCLAIMER Nothing to disclose PENANG ISLAND, MALAYSIA
MANAGEMENT STRATEGIES FOR DIFFICULT-TO-TREAT CHRONIC RHINOSINUSITIS DR ZULKEFLI HUSSEIN CONSULTANT EAR NOSE & THROAT SURGEON PANTAI HOSPITAL PENANG DISCLAIMER Nothing to disclose PENANG ISLAND, MALAYSIA
Pathophysiology and Etiology
 Sinusitis Pathophysiology and Etiology Sinusitis is inflammation of the mucosa of one or more sinuses. It can be either acute chronic. Chronic sinusitis is diagnosed if symptoms are present for more than
Sinusitis Pathophysiology and Etiology Sinusitis is inflammation of the mucosa of one or more sinuses. It can be either acute chronic. Chronic sinusitis is diagnosed if symptoms are present for more than
CHRONIC RHINOSINUSITIS IN ADULTS
 CHRONIC RHINOSINUSITIS IN ADULTS SCOPE OF THE PRACTICE GUIDELINE This clinical practice guideline is for use by the Philippine Society of Otolaryngology-Head and Neck Surgery. It covers the diagnosis and
CHRONIC RHINOSINUSITIS IN ADULTS SCOPE OF THE PRACTICE GUIDELINE This clinical practice guideline is for use by the Philippine Society of Otolaryngology-Head and Neck Surgery. It covers the diagnosis and
Dose-dependent effects of tobramycin in an animal model of Pseudomonas sinusitis Am J Rhino Jul-Aug; 21(4):423-7
 AMINOGLYCOSIDES Dose-dependent effects of tobramycin in an animal model of Pseudomonas sinusitis Am J Rhino. 2007 Jul-Aug; 21(4):423-7 http://www.ncbi.nlm.nih.gov/pubmed/17882910 Evaluation of the in-vivo
AMINOGLYCOSIDES Dose-dependent effects of tobramycin in an animal model of Pseudomonas sinusitis Am J Rhino. 2007 Jul-Aug; 21(4):423-7 http://www.ncbi.nlm.nih.gov/pubmed/17882910 Evaluation of the in-vivo
Treatment Options for Chronic Sinusitis
 Treatment Options for Chronic Sinusitis Jesse Ryan, M.D. Assistant Professor Head and Neck Surgery & Reconstruction Department of Otolaryngology January 17, 2019 Disclosures I have no financial relationship
Treatment Options for Chronic Sinusitis Jesse Ryan, M.D. Assistant Professor Head and Neck Surgery & Reconstruction Department of Otolaryngology January 17, 2019 Disclosures I have no financial relationship
Corporate Medical Policy Septoplasty
 Corporate Medical Policy Septoplasty File Name: Origination: Last CAP Review: Next CAP Review: Last Review: septoplasty 4/1999 8/2018 8/2019 8/2018 Description of Procedure or Service There are many potential
Corporate Medical Policy Septoplasty File Name: Origination: Last CAP Review: Next CAP Review: Last Review: septoplasty 4/1999 8/2018 8/2019 8/2018 Description of Procedure or Service There are many potential
Treatment & Management of Acute Sinusitis in the Primary Care Setting
 University of Vermont ScholarWorks @ UVM Family Medicine Clerkship Student Projects College of Medicine 2018 Treatment & Management of Acute Sinusitis in the Primary Care Setting Vanessa Trieu Follow this
University of Vermont ScholarWorks @ UVM Family Medicine Clerkship Student Projects College of Medicine 2018 Treatment & Management of Acute Sinusitis in the Primary Care Setting Vanessa Trieu Follow this
High dose amoxicillin for sinusitis
 High dose amoxicillin for sinusitis Amoxil ( amoxicillin ) is a commonly used penicillin antibiotic. It is produced in tablets (500 mg 875 mg), capsules, chewable tablets and oral suspensions. 6-3-2018
High dose amoxicillin for sinusitis Amoxil ( amoxicillin ) is a commonly used penicillin antibiotic. It is produced in tablets (500 mg 875 mg), capsules, chewable tablets and oral suspensions. 6-3-2018
MANAGEMENT OF RHINOSINUSITIS IN ADULTS IN PRIMARY CARE
 PROFESSOR DR SALINA HUSAIN DEPUTY HEAD DEPARTMENT OF OTORHINOLARYNGOLOGY-HEAD NECK SURGERY UKM MEDICAL CENTRE MANAGEMENT OF RHINOSINUSITIS IN ADULTS IN PRIMARY CARE CLINICAL PRACTICE GUIDELINES ON MANAGEMENT
PROFESSOR DR SALINA HUSAIN DEPUTY HEAD DEPARTMENT OF OTORHINOLARYNGOLOGY-HEAD NECK SURGERY UKM MEDICAL CENTRE MANAGEMENT OF RHINOSINUSITIS IN ADULTS IN PRIMARY CARE CLINICAL PRACTICE GUIDELINES ON MANAGEMENT
Does osteopathic treatments improve the symptoms of headache and/or head-pressure in patients with Chronic Rhinosinusitis (CRS)?
 Does osteopathic treatments improve the symptoms of headache and/or head-pressure in patients with Chronic Rhinosinusitis (CRS)? A randomized controlled trial Roos S 1, Steinbauer U 1, Amann P 1, Schwerla
Does osteopathic treatments improve the symptoms of headache and/or head-pressure in patients with Chronic Rhinosinusitis (CRS)? A randomized controlled trial Roos S 1, Steinbauer U 1, Amann P 1, Schwerla
Congestion, headache, recurrent infection, post-nasal drip, smell problems? We can find the source and offer solutions for relief.
 Sinus Sinus Congestion, headache, recurrent infection, post-nasal drip, smell problems? We can find the source and offer solutions for relief. So what is sinusitis? Although many individuals interpret
Sinus Sinus Congestion, headache, recurrent infection, post-nasal drip, smell problems? We can find the source and offer solutions for relief. So what is sinusitis? Although many individuals interpret
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Medical technology guidance SCOPE The XprESS Multi-Sinus Dilation System for the treatment of 1 Technology 1.1 Description of the technology The XprESS
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Medical technology guidance SCOPE The XprESS Multi-Sinus Dilation System for the treatment of 1 Technology 1.1 Description of the technology The XprESS
CLINICAL PRACTICE GUIDELINE
 This Clinical Practice Guideline (CPG) and accompanying patient education were developed by a multidisciplinary team, under the leadership of Nebraska Health Network s Primary Care Clinical Integration
This Clinical Practice Guideline (CPG) and accompanying patient education were developed by a multidisciplinary team, under the leadership of Nebraska Health Network s Primary Care Clinical Integration
ROLE OF ANATOMICAL OBSTRUCTION IN THE PATHOGENESIS OF CHRONIC SINUSITIS
 From the SelectedWorks of Balasubramanian Thiagarajan July 1, 2012 ROLE OF ANATOMICAL OBSTRUCTION IN THE PATHOGENESIS OF CHRONIC SINUSITIS Balasubramanian Thiagarajan Available at: https://works.bepress.com/drtbalu/51/
From the SelectedWorks of Balasubramanian Thiagarajan July 1, 2012 ROLE OF ANATOMICAL OBSTRUCTION IN THE PATHOGENESIS OF CHRONIC SINUSITIS Balasubramanian Thiagarajan Available at: https://works.bepress.com/drtbalu/51/
Chronic Rhinosinusitis-Treatment
 Chronic Rhinosinusitis-Treatment INFECTION INFLAMMATION Predisposing Factors Anatomical variations Allergic rhinitis Acute sinusitis Immune deficiency Rhinosinusitis Non-allergic rhinitis Chronic sinusitis
Chronic Rhinosinusitis-Treatment INFECTION INFLAMMATION Predisposing Factors Anatomical variations Allergic rhinitis Acute sinusitis Immune deficiency Rhinosinusitis Non-allergic rhinitis Chronic sinusitis
Retrospective Analysis of Patients with Allergy Sinusitis
 Original article: Retrospective Analysis of Patients with Allergy Sinusitis G.S. Thalor Senior Specialist (MS) (department of Oto Rhino Laryngology), Govt. S.K. Hospital, Sikar, Rajasthan, India. Corresponding
Original article: Retrospective Analysis of Patients with Allergy Sinusitis G.S. Thalor Senior Specialist (MS) (department of Oto Rhino Laryngology), Govt. S.K. Hospital, Sikar, Rajasthan, India. Corresponding
Background. Background. AAP (2013) Guidelines. Background 4/19/2016
 Disclosure Information for: Amanda Kotowski and Laurie Newton Diagnosis & Management of Pediatric Sinusitis: A Survey of Primary Care, Otolaryngology & Urgent Care Providers Amanda Kotowski, DNP, CPNP
Disclosure Information for: Amanda Kotowski and Laurie Newton Diagnosis & Management of Pediatric Sinusitis: A Survey of Primary Care, Otolaryngology & Urgent Care Providers Amanda Kotowski, DNP, CPNP
An Innovative Treatment Option for Patients with Recurrent Nasal Polyps
 An Innovative Treatment Option for Patients with Recurrent Nasal Polyps Burden of illness and management of Chronic Sinusitis with Nasal Polyps Continuum of care and polyp recurrence Clinical and health
An Innovative Treatment Option for Patients with Recurrent Nasal Polyps Burden of illness and management of Chronic Sinusitis with Nasal Polyps Continuum of care and polyp recurrence Clinical and health
Sinusitis in Adults UP TO DATE
 Sinusitis in Adults UP TO DATE Acute sinusitis and rhinosinusitis in adults: Treatment Authors Peter H Hwang, MD Anne Getz, MD Section Editors Daniel G Deschler, MD, FACS Stephen B Calderwood, MD Deputy
Sinusitis in Adults UP TO DATE Acute sinusitis and rhinosinusitis in adults: Treatment Authors Peter H Hwang, MD Anne Getz, MD Section Editors Daniel G Deschler, MD, FACS Stephen B Calderwood, MD Deputy
Maximum Medical Therapy of Chronic Rhinosinusitis. Riyadh Alhedaithy R5 ENT Resident, Combined KSUF and SB. 30/12/2015
 Maximum Medical Therapy of Chronic Rhinosinusitis Riyadh Alhedaithy R5 ENT Resident, Combined KSUF and SB. 30/12/2015 ARTICLE REVIEW INTRODUCTION Chronic rhinosinusitis (CRS) is a common, debilitating,
Maximum Medical Therapy of Chronic Rhinosinusitis Riyadh Alhedaithy R5 ENT Resident, Combined KSUF and SB. 30/12/2015 ARTICLE REVIEW INTRODUCTION Chronic rhinosinusitis (CRS) is a common, debilitating,
Update on Rhinosinusitis 2013 AAP Guidelines Review
 Update on Rhinosinusitis 2013 AAP Guidelines Review Carla M. Giannoni, MD Surgeon, Otolaryngology Texas Children's Hospital Professor, Surgery and Pediatrics, Baylor College of Medicine CDC: Acute Rhinosinusitis
Update on Rhinosinusitis 2013 AAP Guidelines Review Carla M. Giannoni, MD Surgeon, Otolaryngology Texas Children's Hospital Professor, Surgery and Pediatrics, Baylor College of Medicine CDC: Acute Rhinosinusitis
Chronic Sinusitis. Acute Sinusitis. Sinusitis. Anatomy of the Paranasal Sinuses. Sinusitis. Medical Topics - Sinusitis
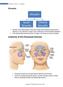 1 Acute Chronic is the inflammation of the inner lining of the parnasal sinuses due to infection or non-infectious causes such as allergies or environmental pullutants. If the inflammation lasts more than
1 Acute Chronic is the inflammation of the inner lining of the parnasal sinuses due to infection or non-infectious causes such as allergies or environmental pullutants. If the inflammation lasts more than
MANAGEMENT of BACTERIAL RHINOSINUSITIS
 MANAGEMENT of BACTERIAL RHINOSINUSITIS Jennifer Le, PharmD Assistant Professor of Pharmacy Practice, College of Pharmacy, Western University of Health Sciences Martin S. Lipsky, MD Dean and Professor of
MANAGEMENT of BACTERIAL RHINOSINUSITIS Jennifer Le, PharmD Assistant Professor of Pharmacy Practice, College of Pharmacy, Western University of Health Sciences Martin S. Lipsky, MD Dean and Professor of
thus, the correct terminology is now rhinosinusitis.
 By: Ibrahim Alarifi Introduction Rhinitis and sinusitis usually coexist and are concurrent in most individuals; thus, the correct terminology is now rhinosinusitis. Mucosa of the nose is a continuation
By: Ibrahim Alarifi Introduction Rhinitis and sinusitis usually coexist and are concurrent in most individuals; thus, the correct terminology is now rhinosinusitis. Mucosa of the nose is a continuation
ALLERGIC RHINITIS Eve Kerr, M.D., M.P.H.
 - 63-3. ALLERGIC RHINITIS Eve Kerr, M.D., M.P.H. We conducted a MEDLINE search of review articles on rhinitis between the years of 1990-1995 and selected articles pertaining to allergic rhinitis. We also
- 63-3. ALLERGIC RHINITIS Eve Kerr, M.D., M.P.H. We conducted a MEDLINE search of review articles on rhinitis between the years of 1990-1995 and selected articles pertaining to allergic rhinitis. We also
Middleton Chapter 43 (pages ) Rhinosinusitis and Nasal Polyps Prepared by: Malika Gupta, MD
 FIT Board Review Corner December 2017 Welcome to the FIT Board Review Corner, prepared by Amar Dixit, MD, and Christin L. Deal, MD, senior and junior representatives of ACAAI's Fellows-In- Training (FITs)
FIT Board Review Corner December 2017 Welcome to the FIT Board Review Corner, prepared by Amar Dixit, MD, and Christin L. Deal, MD, senior and junior representatives of ACAAI's Fellows-In- Training (FITs)
Diagnosis and Treatment of Respiratory Illness in Children and Adults Guideline
 Member Groups Requesting Changes: Lakeview Clinic Marshfield Clinic Mayo Clinic South Lake Pediatrics Response Report for Review and Comment January 2013 Diagnosis and Treatment of Respiratory Illness
Member Groups Requesting Changes: Lakeview Clinic Marshfield Clinic Mayo Clinic South Lake Pediatrics Response Report for Review and Comment January 2013 Diagnosis and Treatment of Respiratory Illness
Review Article The Prevalence of Concha Bullosa and Nasal Septal Deviation and Their Relationship to Maxillary Sinusitis by Volumetric Tomography
 Hindawi Publishing Corporation International Journal of Dentistry Volume 2010, Article ID 404982, 5 pages doi:10.1155/2010/404982 Review Article The Prevalence of and Nasal Septal Deviation and Their Relationship
Hindawi Publishing Corporation International Journal of Dentistry Volume 2010, Article ID 404982, 5 pages doi:10.1155/2010/404982 Review Article The Prevalence of and Nasal Septal Deviation and Their Relationship
Disclaimers. Topical Therapy. The Problem. Topical Therapy for Chronic Rhinosinusitis No Disclosures
 Topical Therapy for Chronic Rhinosinusitis No Disclosures Disclaimers Off-label use of multiple steroid and antibiotic medications Large talk, limited time Steven D. Pletcher MD University of California,
Topical Therapy for Chronic Rhinosinusitis No Disclosures Disclaimers Off-label use of multiple steroid and antibiotic medications Large talk, limited time Steven D. Pletcher MD University of California,
2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY
 Measure #334: Adult Sinusitis: More than One Computerized Tomography (CT) Scan Within 90 Days for Chronic Sinusitis (Overuse) National Quality Strategy Domain: Efficiency and Cost Reduction 2016 PQRS OPTIONS
Measure #334: Adult Sinusitis: More than One Computerized Tomography (CT) Scan Within 90 Days for Chronic Sinusitis (Overuse) National Quality Strategy Domain: Efficiency and Cost Reduction 2016 PQRS OPTIONS
Phototherapy in Allergic Rhinitis
 Phototherapy in Allergic Rhinitis Rhinology Chair KSU KAUH Ibrahim AlAwadh 18\1\2017 MBBS, SB & KSUF Resident, ORL-H&N Background: Endonasal phototherapy can relieve the symptoms of allergic rhinitis
Phototherapy in Allergic Rhinitis Rhinology Chair KSU KAUH Ibrahim AlAwadh 18\1\2017 MBBS, SB & KSUF Resident, ORL-H&N Background: Endonasal phototherapy can relieve the symptoms of allergic rhinitis
2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY
 Measure #332: Adult Sinusitis: Appropriate Choice of Antibiotic: Amoxicillin With or Without Clavulanate Prescribed for Patients with Acute Bacterial Sinusitis (Appropriate Use) National Quality Strategy
Measure #332: Adult Sinusitis: Appropriate Choice of Antibiotic: Amoxicillin With or Without Clavulanate Prescribed for Patients with Acute Bacterial Sinusitis (Appropriate Use) National Quality Strategy
Acute Bacterial Sinusitis: The latest treatment recommendations. Objectives Having completed the learning activities, the participant will be able to:
 Acute Bacterial Sinusitis: The latest treatment recommendations Presented by: Monica Tombasco, MS, MSNA, FNP-BC, CRNA Senior Lecturer Fitzgerald Health Education Associates, Inc., North Andover, MA Emergency
Acute Bacterial Sinusitis: The latest treatment recommendations Presented by: Monica Tombasco, MS, MSNA, FNP-BC, CRNA Senior Lecturer Fitzgerald Health Education Associates, Inc., North Andover, MA Emergency
+ Conflict of interest. + Sinus and Nasal Anatomy. + What is your diagnosis? 1) Allergic Rhinitis. 2) Non-Allergic rhinitis. 3) Chronic Rhinosinusitis
 Rhinitis & Sinusitis Conflict of interest I have no conflict of interest to declare for this lecture Al Chiodo, MD FRCSC Assistant Professor Director of Undergraduate Medical Education Department of Otolaryngology-Head
Rhinitis & Sinusitis Conflict of interest I have no conflict of interest to declare for this lecture Al Chiodo, MD FRCSC Assistant Professor Director of Undergraduate Medical Education Department of Otolaryngology-Head
2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY. MEASURE TYPE: Efficiency
 Quality ID #333: Adult Sinusitis: Computerized Tomography (CT) for Acute Sinusitis (Overuse) National Quality Strategy Domain: Efficiency and Cost Reduction 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY
Quality ID #333: Adult Sinusitis: Computerized Tomography (CT) for Acute Sinusitis (Overuse) National Quality Strategy Domain: Efficiency and Cost Reduction 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY
Evaluation of the Change in Recent Diagnostic Criteria of Chronic Rhinosinusitis: A Cross-sectional Study
 Abhishek Ramadhin REVIEW ARTICLE 10.5005/jp-journals-10013-1246 Evaluation of the Change in Recent Diagnostic Criteria of Chronic Rhinosinusitis: A Cross-sectional Study Abhishek Ramadhin ABSTRACT There
Abhishek Ramadhin REVIEW ARTICLE 10.5005/jp-journals-10013-1246 Evaluation of the Change in Recent Diagnostic Criteria of Chronic Rhinosinusitis: A Cross-sectional Study Abhishek Ramadhin ABSTRACT There
Appropriate Use of Antibiotics for the Treatment of Acute Upper Respiratory Tract Infections in Adults
 Appropriate Use of Antibiotics for the Treatment of Acute Upper Respiratory Tract Infections in Adults Kyong Ran Peck, M.D. Division of Infectious Diseases Sungkyunkwan University School of Medicine, Samsung
Appropriate Use of Antibiotics for the Treatment of Acute Upper Respiratory Tract Infections in Adults Kyong Ran Peck, M.D. Division of Infectious Diseases Sungkyunkwan University School of Medicine, Samsung
A n t i b i o t d o x y c y c l f o r s i n i n f e c t i o
 A n t i b i o t d o x y c y c l f o r s i n i n f e c t i o "I was prescribed this to get rid of a nasty sinus infection. I've had so many that antibiotics don't always work, so my doctor prescribed doxycycline
A n t i b i o t d o x y c y c l f o r s i n i n f e c t i o "I was prescribed this to get rid of a nasty sinus infection. I've had so many that antibiotics don't always work, so my doctor prescribed doxycycline
4/7/13 SINUSITIS WHO ARE WE TREATING? AMANDA SAM CONLEY RN, MSN, CFN, LNC, FNP- BC
 SINUSITIS WHO ARE WE TREATING? AMANDA SAM CONLEY RN, MSN, CFN, LNC, FNP- BC 1 DefiniGons Anatomy Review Signs and Symptoms OBJECTIVES Acute Viral vrs. Acute Bacterial Treatment Guidelines ANATOMY REVIEW
SINUSITIS WHO ARE WE TREATING? AMANDA SAM CONLEY RN, MSN, CFN, LNC, FNP- BC 1 DefiniGons Anatomy Review Signs and Symptoms OBJECTIVES Acute Viral vrs. Acute Bacterial Treatment Guidelines ANATOMY REVIEW
Received 25 November 2002/Returned for modification 14 February 2003/Accepted 11 April 2003
 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Sept. 2003, p. 2770 2774 Vol. 47, No. 9 0066-4804/03/$08.00 0 DOI: 10.1128/AAC.47.9.2770 2774.2003 Copyright 2003, American Society for Microbiology. All Rights Reserved.
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Sept. 2003, p. 2770 2774 Vol. 47, No. 9 0066-4804/03/$08.00 0 DOI: 10.1128/AAC.47.9.2770 2774.2003 Copyright 2003, American Society for Microbiology. All Rights Reserved.
Executive summary of recommendations
 MOH LINIL PRTIE GUIELINES 2/2010 Management of Rhinosinusitis and llergic Rhinitis cademy of Medicine, Singapore hapter of Otorhinolaryngologists ollege of Surgeons, Singapore ollege of Family Physicians,
MOH LINIL PRTIE GUIELINES 2/2010 Management of Rhinosinusitis and llergic Rhinitis cademy of Medicine, Singapore hapter of Otorhinolaryngologists ollege of Surgeons, Singapore ollege of Family Physicians,
A study of causes of nasal obstruction in Garhwal region of Uttarakhand
 Original Research Article Amit Arya 1, R S Bisht 2,*, Venkatashivareddy B 3, Richa Mina 4 1,4 Senior Resident, 2 Professor, Dept. of ENT, 3 Assistant Professor, Dept. of Community Medicine, VCSGGMS & RI
Original Research Article Amit Arya 1, R S Bisht 2,*, Venkatashivareddy B 3, Richa Mina 4 1,4 Senior Resident, 2 Professor, Dept. of ENT, 3 Assistant Professor, Dept. of Community Medicine, VCSGGMS & RI
ORIGINAL ARTICLE. The Impact of Sinus Computed Tomography on Treatment Decisions for Chronic Sinusitis. widespread condition, affecting
 ORIGINAL ARTICLE The Impact of Sinus Computed Tomography on Treatment Decisions for Chronic Sinusitis Yoshimi Anzai, MD; Ernest A. Weymuller, Jr, MD; Bevan Yueh, MD, MPH; Nicole Maronian, MD; Jeffrey G.
ORIGINAL ARTICLE The Impact of Sinus Computed Tomography on Treatment Decisions for Chronic Sinusitis Yoshimi Anzai, MD; Ernest A. Weymuller, Jr, MD; Bevan Yueh, MD, MPH; Nicole Maronian, MD; Jeffrey G.
DURATION OF ORAL ANTIBIOTIC IN THE SETING OF MAXIMAL MEDICAL THERAPY FOR CHRONIC RHINOSINUSITIS. Dr. Ziyad Al-Abduljabbar
 DURATION OF ORAL ANTIBIOTIC IN THE SETING OF MAXIMAL MEDICAL THERAPY FOR CHRONIC RHINOSINUSITIS Dr. Ziyad Al-Abduljabbar International Forum of Allergy & Rhinology, Vol. 5, No. 9, September 2015 INTRODUCTION
DURATION OF ORAL ANTIBIOTIC IN THE SETING OF MAXIMAL MEDICAL THERAPY FOR CHRONIC RHINOSINUSITIS Dr. Ziyad Al-Abduljabbar International Forum of Allergy & Rhinology, Vol. 5, No. 9, September 2015 INTRODUCTION
OSTEITIS IN CRS. Rhinology Chair Meeting presented by Amal Binhazza a
 OSTEITIS IN CRS Rhinology Chair Meeting presented by Amal Binhazza a ROAD MAP Definition. pathophysiology. Diagnosis. Grading systems. Clinical implications. Management. OSTEITIS Presence of new bone formation,
OSTEITIS IN CRS Rhinology Chair Meeting presented by Amal Binhazza a ROAD MAP Definition. pathophysiology. Diagnosis. Grading systems. Clinical implications. Management. OSTEITIS Presence of new bone formation,
Incidence of accessory ostia in patients with chronic maxillary sinusitis
 International Journal of Otorhinolaryngology and Head and Neck Surgery Ghosh P et al. Int J Otorhinolaryngol Head Neck Surg. 2018 Mar;4(2):443-447 http://www.ijorl.com pissn 2454-5929 eissn 2454-5937 Original
International Journal of Otorhinolaryngology and Head and Neck Surgery Ghosh P et al. Int J Otorhinolaryngol Head Neck Surg. 2018 Mar;4(2):443-447 http://www.ijorl.com pissn 2454-5929 eissn 2454-5937 Original
Clinical Policy: Balloon Sinus Ostial Dilation for Treatment of Chronic Sinusitis
 Clinical Policy: Balloon Sinus Ostial Dilation for Treatment of Chronic Sinusitis Reference Number: CP.MP.119 Last Review Date: 11/17 See Important Reminder at the end of this policy for important regulatory
Clinical Policy: Balloon Sinus Ostial Dilation for Treatment of Chronic Sinusitis Reference Number: CP.MP.119 Last Review Date: 11/17 See Important Reminder at the end of this policy for important regulatory
White Paper: Balloon Sinuplasty for Chronic Sinusitis, The Latest Recommendations
 White Paper: Balloon Sinuplasty for Chronic Sinusitis, The Latest Recommendations For Health Plans, Medical Management Organizations and TPAs Executive Summary Despite recent advances in instrumentation
White Paper: Balloon Sinuplasty for Chronic Sinusitis, The Latest Recommendations For Health Plans, Medical Management Organizations and TPAs Executive Summary Despite recent advances in instrumentation
2017 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY. MEASURE TYPE: Efficiency
 Measure #334: Adult Sinusitis: More than One Computerized Tomography (CT) Scan Within 90 Days for Chronic Sinusitis (Overuse) National Quality Strategy Domain: Efficiency and Cost Reduction 2017 OPTIONS
Measure #334: Adult Sinusitis: More than One Computerized Tomography (CT) Scan Within 90 Days for Chronic Sinusitis (Overuse) National Quality Strategy Domain: Efficiency and Cost Reduction 2017 OPTIONS
TUEC Guidelines Medical Information to Support the Decisions of TUE Committees Sinusitis/Rhinosinusitis SINUSITIS/RHINOSINUSITIS
 1. Medical Condition SINUSITIS/RHINOSINUSITIS Sinusitis refers to inflammation of the sinuses only while the more clinically relevant term should be Rhinosinusitis which refers to inflammation of both
1. Medical Condition SINUSITIS/RHINOSINUSITIS Sinusitis refers to inflammation of the sinuses only while the more clinically relevant term should be Rhinosinusitis which refers to inflammation of both
Functional Endoscopic Sinus Surgery
 WHAT IS FUNCTIONAL ENDOSCOPIC SINUS SURGERY (FESS)? The nasal telescope has greatly changes the evaluation and treatment of rhino-sinusitis. This instrument, which provides a view of the structures in
WHAT IS FUNCTIONAL ENDOSCOPIC SINUS SURGERY (FESS)? The nasal telescope has greatly changes the evaluation and treatment of rhino-sinusitis. This instrument, which provides a view of the structures in
Conventional Sinus Surgery Vs Fess
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 7 Ver. III (July. 2017), PP 44-51 www.iosrjournals.org Conventional Sinus Surgery Vs Fess *
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 7 Ver. III (July. 2017), PP 44-51 www.iosrjournals.org Conventional Sinus Surgery Vs Fess *
SINUSITIS/RHINOSINUSITIS
 1. Medical Condition TUEC Guidelines SINUSITIS/RHINOSINUSITIS Sinusitis refers to inflammation of the sinuses only while the more clinically relevant term should be Rhinosinusitis which is the inflammation
1. Medical Condition TUEC Guidelines SINUSITIS/RHINOSINUSITIS Sinusitis refers to inflammation of the sinuses only while the more clinically relevant term should be Rhinosinusitis which is the inflammation
Sinusitis. What are the sinuses? Who develops sinusitis?
 Sinusitis Health experts estimate that 37 million Americans are affected by sinusitis every year. Americans spend nearly $6 billion each year on health care costs related to sinusitis. Sinusitis is an
Sinusitis Health experts estimate that 37 million Americans are affected by sinusitis every year. Americans spend nearly $6 billion each year on health care costs related to sinusitis. Sinusitis is an
US Drug Eluting Sinus Stent (DESS) Market: Size, Trends & Forecasts ( ) September 2016
 US Drug Eluting Sinus Stent (DESS) Market: Size, Trends & Forecasts (2016-2021) September 2016 US Drug Eluting Sinus Stent Market Report Scope of the Report The report entitled US Drug Eluting Sinus Stent
US Drug Eluting Sinus Stent (DESS) Market: Size, Trends & Forecasts (2016-2021) September 2016 US Drug Eluting Sinus Stent Market Report Scope of the Report The report entitled US Drug Eluting Sinus Stent
Drugs Used to Treat Chronic Obstructive Pulmonary Disease (COPD)
 Drugs Used to Treat Chronic Obstructive Pulmonary Disease (COPD) COPD COPD is a chronic, irreversible obstruction of airflow that is usually progressive. Symptoms include cough, excess mucus production,
Drugs Used to Treat Chronic Obstructive Pulmonary Disease (COPD) COPD COPD is a chronic, irreversible obstruction of airflow that is usually progressive. Symptoms include cough, excess mucus production,
ISPUB.COM. Medical management of chronic rhinosinusistis. P Parida, S Bhagat INTRODUCTION
 ISPUB.COM The Internet Journal of Otorhinolaryngology Volume 7 Number 1 Medical management of chronic rhinosinusistis P Parida, S Bhagat Citation P Parida, S Bhagat. Medical management of chronic rhinosinusistis.
ISPUB.COM The Internet Journal of Otorhinolaryngology Volume 7 Number 1 Medical management of chronic rhinosinusistis P Parida, S Bhagat Citation P Parida, S Bhagat. Medical management of chronic rhinosinusistis.
Section Editor Mark D Aronson, MD
 1 of 6 9/29/2013 7:09 PM Official reprint from UpToDate www.uptodate.com 2013 UpToDate The content on the UpToDate website is not intended nor recommended as a substitute for medical advice, diagnosis,
1 of 6 9/29/2013 7:09 PM Official reprint from UpToDate www.uptodate.com 2013 UpToDate The content on the UpToDate website is not intended nor recommended as a substitute for medical advice, diagnosis,
2016 Physician Quality Reporting System Data Collection Form: Sinusitis (for patients aged 18 and older)
 2016 Physician Quality Reporting System Data Collection Form: Sinusitis (for patients aged 18 and older) IMPORTANT: Any measure with a 0% performance rate (100% for inverse measures) is not considered
2016 Physician Quality Reporting System Data Collection Form: Sinusitis (for patients aged 18 and older) IMPORTANT: Any measure with a 0% performance rate (100% for inverse measures) is not considered
1. BRIEF DESCRIPTION OF TRAINING
 RHINOLOGY 1. BRIEF DESCRIPTION OF TRAINING Exposure to clinical rhinology is provided in each of the four ORL years over the course of several rotations in a graduated approach. MEE General Otolaryngology
RHINOLOGY 1. BRIEF DESCRIPTION OF TRAINING Exposure to clinical rhinology is provided in each of the four ORL years over the course of several rotations in a graduated approach. MEE General Otolaryngology
Acute Otitis Media, Acute Bacterial Sinusitis, and Acute Bacterial Rhinosinusitis
 Acute Otitis Media, Acute Bacterial Sinusitis, and Acute Bacterial Rhinosinusitis This guideline, developed by Larry Simmons, MD, in collaboration with the ANGELS team, on October 3, 2013, is a significantly
Acute Otitis Media, Acute Bacterial Sinusitis, and Acute Bacterial Rhinosinusitis This guideline, developed by Larry Simmons, MD, in collaboration with the ANGELS team, on October 3, 2013, is a significantly
Spheno-Ethmoidectomy
 Diagnostic and Therapeutic Endoscopy, Vol. 5, pp. 1-8 Reprints available directly from the publisher Photocopying permitted by license only (C) 1998 OPA (Overseas Publishers Association) N.V. Published
Diagnostic and Therapeutic Endoscopy, Vol. 5, pp. 1-8 Reprints available directly from the publisher Photocopying permitted by license only (C) 1998 OPA (Overseas Publishers Association) N.V. Published
The Honrubia Technique of Balloon Sinuplasty for the Improvement of Symptoms in Chronic Sinusitis. Patients. Vincent Honrubia MD, FACS
 The Honrubia Technique of Balloon Sinuplasty for the Improvement of Symptoms in Chronic Sinusitis Patients Vincent Honrubia MD, FACS Allyssa Cantu, PA-S Sharon Gelman, MEd, PA-S Rachel Tsai, BS Director,
The Honrubia Technique of Balloon Sinuplasty for the Improvement of Symptoms in Chronic Sinusitis Patients Vincent Honrubia MD, FACS Allyssa Cantu, PA-S Sharon Gelman, MEd, PA-S Rachel Tsai, BS Director,
FUNCTIONAL ENDOSCOPIC SINUS SURGERY (FESS)
 UnitedHealthcare Community Plan Medical Policy FUNCTIONAL ENDOSCOPIC SINUS SURGERY (FESS) Policy Number: CS144.D Effective Date: January 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE... 1 BENEFIT
UnitedHealthcare Community Plan Medical Policy FUNCTIONAL ENDOSCOPIC SINUS SURGERY (FESS) Policy Number: CS144.D Effective Date: January 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE... 1 BENEFIT
Incidence of Odontogenic Sinusitis Experience in a Tertiary Care Centre
 Original Article DOI: 10.17354/ijss/2016/130 Incidence of Odontogenic Sinusitis Experience in a Tertiary Care Centre B G Prakash 1, Suhasini Biyyapu 2 1 Professor, Department of ENT, JSS Medical College,
Original Article DOI: 10.17354/ijss/2016/130 Incidence of Odontogenic Sinusitis Experience in a Tertiary Care Centre B G Prakash 1, Suhasini Biyyapu 2 1 Professor, Department of ENT, JSS Medical College,
2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY. MEASURE TYPE: Process
 Quality ID #331: Adult Sinusitis: Antibiotic Prescribed for Acute Viral Sinusitis (Overuse) National Quality Strategy Domain: Efficiency and Cost Reduction 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY
Quality ID #331: Adult Sinusitis: Antibiotic Prescribed for Acute Viral Sinusitis (Overuse) National Quality Strategy Domain: Efficiency and Cost Reduction 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY
Consumer summary. Endoscopic modified Lothrop procedure for the. treatment of chronic frontal sinusitis
 ASERNIP S Australian Safety and Efficacy Register of New Interventional Procedures Surgical Consumer summary Endoscopic modified Lothrop procedure for the treatment of chronic frontal sinusitis (The report
ASERNIP S Australian Safety and Efficacy Register of New Interventional Procedures Surgical Consumer summary Endoscopic modified Lothrop procedure for the treatment of chronic frontal sinusitis (The report
The Nose and Sinuses. Ophir Ilan, MD, PhD Department of Otolaryngology/Head&Neck surgery Hadassah University Hospital
 The Nose and Sinuses Ophir Ilan, MD, PhD Department of Otolaryngology/Head&Neck surgery Hadassah University Hospital Nasal Mucociliary System Function of the Nasal Mucosa warming and humidifying the
The Nose and Sinuses Ophir Ilan, MD, PhD Department of Otolaryngology/Head&Neck surgery Hadassah University Hospital Nasal Mucociliary System Function of the Nasal Mucosa warming and humidifying the
The child with a troublesome cough. Dr Marco Zampoli Paediatric Pulmonology Red Cross War Memorial Children s Hospital GP Refresher Course 2012
 The child with a troublesome cough Dr Marco Zampoli Paediatric Pulmonology Red Cross War Memorial Children s Hospital GP Refresher Course 2012 Cough is the most common symptom in children Inability to
The child with a troublesome cough Dr Marco Zampoli Paediatric Pulmonology Red Cross War Memorial Children s Hospital GP Refresher Course 2012 Cough is the most common symptom in children Inability to
Fungal ball.. Clinical and radiological features DR. AHMED ALTUWAIJRI 1/5/2017
 Fungal ball.. Clinical and radiological features DR. AHMED ALTUWAIJRI 1/5/2017 Fungal Rhinosinusitis (FRS) Rhinosinusitis, is a common disorder affecting approximately 20% of the population at some time
Fungal ball.. Clinical and radiological features DR. AHMED ALTUWAIJRI 1/5/2017 Fungal Rhinosinusitis (FRS) Rhinosinusitis, is a common disorder affecting approximately 20% of the population at some time
Respiratory tract infections. Krzysztof Buczkowski
 Respiratory tract infections Krzysztof Buczkowski Etiology Viruses Rhinoviruses Adenoviruses Coronaviruses Influenza and Parainfluenza Viruses Respiratory Syncitial Viruses Enteroviruses Etiology Bacteria
Respiratory tract infections Krzysztof Buczkowski Etiology Viruses Rhinoviruses Adenoviruses Coronaviruses Influenza and Parainfluenza Viruses Respiratory Syncitial Viruses Enteroviruses Etiology Bacteria
Will sulfamethoxazole treat sinus infection
 Will sulfamethoxazole treat sinus infection Find information about which conditions Sulfamethoxazole- Trimethoprim by a Fungus; Bacterial Infection of Heart Valve; Sinus Irritation and Congestion. Bactrim
Will sulfamethoxazole treat sinus infection Find information about which conditions Sulfamethoxazole- Trimethoprim by a Fungus; Bacterial Infection of Heart Valve; Sinus Irritation and Congestion. Bactrim
Sphenoid rhinosinusitis associated with abducens nerve palsy Case report
 Romanian Journal of Rhinology, Volume 8, No. 30, April-June 2018 CASE REPORT Sphenoid rhinosinusitis associated with abducens nerve palsy Case report Lucian Lapusneanu 1, Marlena Radulescu 1, Florin Ghita
Romanian Journal of Rhinology, Volume 8, No. 30, April-June 2018 CASE REPORT Sphenoid rhinosinusitis associated with abducens nerve palsy Case report Lucian Lapusneanu 1, Marlena Radulescu 1, Florin Ghita
Derriford Hospital. Peninsula Medical School
 Asthma and Allergic Rhinitis iti What is the Connection? Hisham Khalil Consultant ENT Surgeon Clinical Senior Lecturer, PMS Clinical Sub-Dean GP Evening 25 June 2008 Plymouth Derriford Hospital Peninsula
Asthma and Allergic Rhinitis iti What is the Connection? Hisham Khalil Consultant ENT Surgeon Clinical Senior Lecturer, PMS Clinical Sub-Dean GP Evening 25 June 2008 Plymouth Derriford Hospital Peninsula
ENDOSCOPIC LASER SURGERY OF THE MIDDLE MEATUS FOR CHRONIC PARANASAL SINUSITIS
 ENDOSCOPIC LASER SURGERY OF THE MIDDLE MEATUS FOR CHRONIC PARANASAL SINUSITIS Yosaku Shiomi, Nobuya Fujiki*, Kyosuke Kurata* Department of Otolaryngology, Matsue Municipal Hospital, Shimane *Department
ENDOSCOPIC LASER SURGERY OF THE MIDDLE MEATUS FOR CHRONIC PARANASAL SINUSITIS Yosaku Shiomi, Nobuya Fujiki*, Kyosuke Kurata* Department of Otolaryngology, Matsue Municipal Hospital, Shimane *Department
FUNCTIONAL ENDOSCOPIC SINUS SURGERY (FESS)
 FUNCTIONAL ENDOSCOPIC SINUS SURGERY (FESS) Protocol: SUR055 Effective Date: June 1, 2018 Table of Contents Page COMMERCIAL, MEDICAID AND MEDICARE COVERAGE RATIONALE... 1 DEFINITIONS... 2 DESCRIPTION OF
FUNCTIONAL ENDOSCOPIC SINUS SURGERY (FESS) Protocol: SUR055 Effective Date: June 1, 2018 Table of Contents Page COMMERCIAL, MEDICAID AND MEDICARE COVERAGE RATIONALE... 1 DEFINITIONS... 2 DESCRIPTION OF
The clinical diagnosis of acute purulent sinusitis in general practice a review
 The clinical diagnosis of acute purulent sinusitis in general practice a review Morten Lindbæk and Per Hjortdahl SUMMARY Acute sinusitis is a common illness in primary care. Studies have demonstrated the
The clinical diagnosis of acute purulent sinusitis in general practice a review Morten Lindbæk and Per Hjortdahl SUMMARY Acute sinusitis is a common illness in primary care. Studies have demonstrated the
Managing and Treating Allergic Rhinitis in the Primary Care Setting
 University of Vermont ScholarWorks @ UVM Family Medicine Block Clerkship, Student Projects College of Medicine 2014 Managing and Treating Allergic Rhinitis in the Primary Care Setting Leah Novinger University
University of Vermont ScholarWorks @ UVM Family Medicine Block Clerkship, Student Projects College of Medicine 2014 Managing and Treating Allergic Rhinitis in the Primary Care Setting Leah Novinger University
Dr.Adel A. Al Ibraheem
 Rhinology Chair Weekly Activity Dr.Adel A. Al Ibraheem www.rhinologychair.org conference@rhinologychair.org Rhinology Chair Introduction: It is important to classify and stage nasal polyposis. ( decide
Rhinology Chair Weekly Activity Dr.Adel A. Al Ibraheem www.rhinologychair.org conference@rhinologychair.org Rhinology Chair Introduction: It is important to classify and stage nasal polyposis. ( decide
Sinusitis: Medical and Surgical Management. R. Jonathan Lara, DO, FAOCO. Sonoran Ear Nose & Throat
 Sinusitis: Medical and Surgical Management R. Jonathan Lara, DO, FAOCO Sonoran Ear Nose & Throat 27 th Annual Southwestern Conference on Medicine April 26, 2018 What are sinuses? Air filled cavities of
Sinusitis: Medical and Surgical Management R. Jonathan Lara, DO, FAOCO Sonoran Ear Nose & Throat 27 th Annual Southwestern Conference on Medicine April 26, 2018 What are sinuses? Air filled cavities of
ORIGINAL ARTICLE. Computed Tomographic Staging and the Fate of the Dependent Sinuses in Revision Endoscopic Sinus Surgery
 Computed Tomographic Staging and the Fate of the Dependent es in Revision Endoscopic Surgery Neil Bhattacharyya, MD ORIGINAL ARTICLE Objectives: To determine the patterns of disease recurrence in chronic
Computed Tomographic Staging and the Fate of the Dependent es in Revision Endoscopic Surgery Neil Bhattacharyya, MD ORIGINAL ARTICLE Objectives: To determine the patterns of disease recurrence in chronic
OriginalArticle. Gentamicin Nasal Irrigation in Children with Chronic Rhinosinusitis: A Retrospective Cohort of 38 Patients
 OriginalArticle Gentamicin Nasal Irrigation in Children with Chronic Rhinosinusitis: A Retrospective Cohort of 38 Patients Suruthai Kurasirikul, M.D., Orathai Jirapongsananuruk, M.D., Pakit Vichyanond,
OriginalArticle Gentamicin Nasal Irrigation in Children with Chronic Rhinosinusitis: A Retrospective Cohort of 38 Patients Suruthai Kurasirikul, M.D., Orathai Jirapongsananuruk, M.D., Pakit Vichyanond,
Whatever the reason, whatever the season,
 Whatever the reason, whatever the season, S4 AVAMYS Nasal Spray (Suspension). REGISTRATION NUMBER: 41/21.5.1/0968. Each 50 µl spray contains 27,5 µg of fluticasone furoate. Preservative: Benzalkonium chloride
Whatever the reason, whatever the season, S4 AVAMYS Nasal Spray (Suspension). REGISTRATION NUMBER: 41/21.5.1/0968. Each 50 µl spray contains 27,5 µg of fluticasone furoate. Preservative: Benzalkonium chloride
ANTIBIOTICS ACUTE RHINOSINUSITIS IN CHILDREN
 MARCH 2016 DRUG ANTIBIOTICS This optimal usage guide is mainly intended f primary care health professionnals. It is provided f infmation purposes only and should not replace the clinician s judgement.
MARCH 2016 DRUG ANTIBIOTICS This optimal usage guide is mainly intended f primary care health professionnals. It is provided f infmation purposes only and should not replace the clinician s judgement.
Choosing an appropriate antimicrobial agent. 3) the spectrum of potential pathogens
 Choosing an appropriate antimicrobial agent Consider: 1) the host 2) the site of infection 3) the spectrum of potential pathogens 4) the likelihood that these pathogens are resistant to antimicrobial agents
Choosing an appropriate antimicrobial agent Consider: 1) the host 2) the site of infection 3) the spectrum of potential pathogens 4) the likelihood that these pathogens are resistant to antimicrobial agents
Reasons for Failure and Surgical Revisions. Stil Kountakis, MD, PhD Professor and Chief, Division of Rhinology
 Reasons for Failure and Surgical Revisions Stil Kountakis, MD, PhD Professor and Chief, Division of Rhinology Medical College of Georgia of Georgia Regents University Department of Otolaryngology / Head
Reasons for Failure and Surgical Revisions Stil Kountakis, MD, PhD Professor and Chief, Division of Rhinology Medical College of Georgia of Georgia Regents University Department of Otolaryngology / Head
Sinusitis Awareness Survey May 2011
 Page 1 of 5 Sinusitis Awareness Survey May 2011 Playing Doctor and Paying a Price: Sinusitis Sufferers Often Misdiagnose Themselves, Confusing Symptoms with Allergies For 35 million Americans with nasal
Page 1 of 5 Sinusitis Awareness Survey May 2011 Playing Doctor and Paying a Price: Sinusitis Sufferers Often Misdiagnose Themselves, Confusing Symptoms with Allergies For 35 million Americans with nasal
MEDICAL POLICY I. POLICY FUNCTIONAL ENDOSCOPIC SINUS SURGERY FOR CHRONIC RHINOSINUSITIS MP POLICY TITLE POLICY NUMBER
 Original Issue Date (Created): 8/1/2018 Most Recent Review Date (Revised): 1/30/2018 Effective Date: 8/1/2018 POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS BENEFIT VARIATIONS DISCLAIMER
Original Issue Date (Created): 8/1/2018 Most Recent Review Date (Revised): 1/30/2018 Effective Date: 8/1/2018 POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS BENEFIT VARIATIONS DISCLAIMER
Is Afrin (Oxymetazoline) A Safe And Effective Drug In Normal, Healthy Adults With Reference To Nasal Congestion And The Nasal Response?
 Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2012 Is Afrin (Oxymetazoline) A Safe And Effective
Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2012 Is Afrin (Oxymetazoline) A Safe And Effective
Dates to which data relate The effectiveness data were gathered from 1 July 1996 to 20 June No price year was reported.
 Impact of first-line vs second-line antibiotics for the treatment of acute uncomplicated sinusitis Piccirillo J F, Mager D E, Frisse M E, Bophy R H, Goggin A Record Status This is a critical abstract of
Impact of first-line vs second-line antibiotics for the treatment of acute uncomplicated sinusitis Piccirillo J F, Mager D E, Frisse M E, Bophy R H, Goggin A Record Status This is a critical abstract of
The Importance of Appropriate Treatment of Chronic Bronchitis
 ...CLINICIAN INTERVIEW... The Importance of Appropriate Treatment of Chronic Bronchitis An interview with Antonio Anzueto, MD, Associate Professor of Medicine, University of Texas Health Science Center,
...CLINICIAN INTERVIEW... The Importance of Appropriate Treatment of Chronic Bronchitis An interview with Antonio Anzueto, MD, Associate Professor of Medicine, University of Texas Health Science Center,
UPPER RESPIRATORY TRACT INFECTIONS. IAP UG Teaching slides
 UPPER RESPIRATORY TRACT INFECTIONS 1 INTRODUCTION Most common problem in children below 5 years. In this age group they get about 6 8 episodes per year. It includes infections of nasal cavity, throat,
UPPER RESPIRATORY TRACT INFECTIONS 1 INTRODUCTION Most common problem in children below 5 years. In this age group they get about 6 8 episodes per year. It includes infections of nasal cavity, throat,
