Internal Maxillary Artery-Middle Cerebral Artery Bypass: Infratemporal Approach for Subcranial- Intracranial (SC-IC) Bypass
|
|
|
- Coleen Matthews
- 5 years ago
- Views:
Transcription
1 Journal Articles Donald and Barbara Zucker School of Medicine Academic Works 2014 Internal Maxillary Artery-Middle Cerebral Artery Bypass: Infratemporal Approach for Subcranial- Intracranial (SC-IC) Bypass E. Nossek Hofstra Northwell School of Medicine P. Costantino Hofstra Northwell School of Medicine M. Eisenberg Hofstra Northwell School of Medicine A. R. Dehdashti Hofstra Northwell School of Medicine A. Setton Hofstra Northwell School of Medicine See next page for additional authors Follow this and additional works at: Part of the Neurology Commons, Otolaryngology Commons, and the Radiology Commons Recommended Citation Nossek E, Costantino P, Eisenberg M, Dehdashti A, Setton A, Chalif D, Ortiz R, Langer D. Internal Maxillary Artery-Middle Cerebral Artery Bypass: Infratemporal Approach for Subcranial-Intracranial (SC-IC) Bypass Jan 01; 75(1):Article 1211 [ p.]. Available from: Free full text article. This Article is brought to you for free and open access by Donald and Barbara Zucker School of Medicine Academic Works. It has been accepted for inclusion in Journal Articles by an authorized administrator of Donald and Barbara Zucker School of Medicine Academic Works.
2 Authors E. Nossek, P. Costantino, M. Eisenberg, A. R. Dehdashti, A. Setton, D. J. Chalif, R. A. Ortiz, and D. J. Langer This article is available at Donald and Barbara Zucker School of Medicine Academic Works:
3 CONCEPTS, INNOVATIONS AND TECHNIQUES Internal Maxillary Artery-Middle Cerebral Artery Bypass: Infratemporal Approach for Subcranial-Intracranial (SC-IC) Bypass Erez Nossek, MD* Peter D. Costantino, MD Mark Eisenberg, MD* Amir R. Dehdashti, MD* Avi Setton, MD* David J. Chalif, MD* Rafael A. Ortiz, MD David J. Langer, MD *Department of Neurosurgery, North Shore - Long Island Jewish/Hofstra School of Medicine North Shore University Hospital, Manhasset, NY; Department of Neurosurgery, North Shore - Long Island Jewish/Hofstra School of Medicine North Shore University Hospital Lenox Hill Hospital; New York, NY; The New York Head & Neck Institute, North Shore- Long Island Jewish/Hofstra School of Medicine Lenox Hill Hospital, New York, NY Correspondence: David Langer, MD, Department of Neurosurgery, North Shore Long Island Jewish Health System, Lenox Hill Hospital, 130 E. 77th Street, New York, NY Dlanger@nshs.edu BACKGROUND: Internal maxillary artery (IMax) middle cerebral artery (MCA) bypass has been recently described as an alternative to cervical extracranial-intracranial bypass. This technique uses a keyhole craniectomy in the temporal fossa that requires a technically challenging end-to-side anastomosis. OBJECTIVE: To describe a lateral subtemporal craniectomy of the middle cranial fossa floor to facilitate wide exposure of the IMax to facilitate bypass. METHODS: Orbitozygomatic osteotomy is used followed by frontotemporal craniotomy and subsequently laterotemporal fossa craniectomy, reaching its medial border at a virtual line connecting the foramen rotundum and foramen ovale. The IMax was identified by using established anatomic landmarks, neuronavigation, and micro Doppler probe (Mizuho Inc. Tokyo, Japan). Additionally, we studied the approach in a cadaveric specimen in preparation for microsurgical bypass. RESULTS: There were 4 cases in which the technique was used. One bypass was performed for flow augmentation in a hypoperfused hemisphere. The other 3 were performed as part of treatment paradigms for giant middle cerebral artery aneurysms. Vein grafts were used in all patients. The proximal anastomosis was performed in an end-toside fashion in 1 patient and end-to-end in 3 patients. Intraoperative graft flow measured with the Transonic flow probe ranged from 20 to 60 ml/min. Postoperative angiography demonstrated good filling of the graft with robust distal flow in all cases. All patients tolerated the procedure well. CONCLUSION: IMax to middle cerebral artery subcranial-intracranial bypass is safe and efficacious. The laterotemporal fossa craniectomy technique resulted in reliable identification and wide exposure of the IMax, facilitating the proximal anastomosis. KEY WORDS: Brachiocephalic vein, EC-IC bypass, Infratemporal approach, Internal maxillary artery Neurosurgery 75:87 95, 2014 DOI: /NEU Received, January 7, Accepted, February 14, Published Online, March 10, Copyright 2014 by the Congress of Neurological Surgeons. This is an open-access article distributed under the terms of the Creative Commons Attribution- NonCommercial-NoDerivatives 3.0 License, where it is permissible to download and share the work provided it is properly cited. The work cannot be changed in any way or used commercially. The cervical carotid artery has been routinely used as a site of proximal anastomoses for radial artery or saphenous vein grafts for extracranial-intracranial (EC-IC) high-flow bypass. 1-4 Recently, internal maxillary artery (IMax) to middle cerebral artery (MCA) bypass had been described as an alternative to cervical EC-IC bypass to reduce graft length. This graft distance reduction may correlate with improved patency and flow. ABBREVIATIONS: EC-IC, extracranial-intracranial; IMax, internal maxillary artery; MCA, middle cerebral artery; SC-IC, subcranial-intracranial; STA, superficial temporal artery Additionally, exposure of the IMax avoids the potential morbidities of a cervical carotid artery exposure. 5-9 Exposure of the IMax was previously described using a small keyhole craniectomy between V2 and V3 in the temporal fossa floor. 5 This limited exposure forces a technically challenging end-to-side proximal anastomosis that is performed through a limited and narrow window. We advocate a more lateral subtemporal craniectomy of the middle cranial fossa floor rather than the keyhole craniotomy to facilitate wide exposure of the IMax. This modification results in a less demanding end-to-end proximal anastomosis for subcranial-intracranial (SC-IC) bypass. NEUROSURGERY VOLUME 75 NUMBER 1 JULY
4 NOSSEK ET AL FIGURE 1. Drawing of contemplated internal maxillary artery middle cerebral artery bypass. Curvilinear incision, zygomatic osteotomy. The light blue arrow indicates the location of the bypass. FIGURE 2. Drawing of an elevated skin flap and temporalis, after osteotomy; the line indicates the craniotomy site. The red area indicates the contemplated craniectomy of the middle cranial fossa floor to unroof the infratemporal fossa. The inset shows the craniectomy in a superior view. The corridor craniectomy will reach a line 2 mm lateral to the virtual line between the foramen ovale and foramen rotundum. METHODS We recently treated 4 patients with SC-IC bypass who required cerebral bypasses to effectively treat various cerebrovascular pathologies. The decision to treat the patient with a bypass and the feasibility of the SC-IC bypass was made in a multidisciplinary fashion by the neurovascular, neuroradiology, and cranial base teams. Our multidisciplinary team performed cadaveric dissection to better assess the subcranial approach for exposure of the IMax in the infratemporal fossa. In this dissection, an orbitozygomatic osteotomy was followed by temporal craniotomy. Subsequently, a lateral rectangle craniectomy of the temporal fossa floor was created up to a point that was 2 mm lateral to a virtual line connecting the foramen rotundum and foramen ovale (Figures 1-4). The deep temporal arteries on the medial aspect of the temporalis muscle were then identified and followed to the IMax. Intraoperative Technique Zygomatic osteotomy (with or without orbital osteotomy) was used followed by frontotemporal craniotomy and subsequently temporal fossa craniectomy reaching its medial border designated by the same virtual line connecting the foramen rotundum and foramen ovale (Figures 4 and 5). We use computed tomography angiography based neuronavigation and micro Doppler probe (Mizuho Inc. Tokyo, Japan). To identify the IMax artery in the pterygoid muscles (Figures 6 and 7). Anatomically, the deep temporal arteries in the medial aspect of the temporalis muscle were followed proximally to allow definitive identification of the IMax artery. The first patient s proximal anastomosis was performed in an end-to-side fashion, whereas the proximal anastomoses in the subsequent 3 patients were end to end (Figures 8-10). The end-to-end anastomoses were technically less demanding than the end to side. In the 3 end-to-end cases, reversed subcutaneous brachiocephalic veins were used rather than the radial artery. This vessel was consistently an excellent diameter match with the donor IMax. In our experience, the brachiocephalic vein was consistently reliably free of valves and had a paucity of branches. This graft represents our preference going forward. Intraoperative flow measurements using the Charbel microflow probe (Transonic Systems Inc., Ithaca, New York) was performed in all patients. Intraoperative angiography and indocyanine green videoangiography were obtained to evaluate bypass patency in all patients. All patients also underwent postoperative angiography to further assess the flow within the bypass and to further treat the aneurysms with endovascular techniques, as deemed necessary. 88 VOLUME 75 NUMBER 1 JULY
5 SUBCRANIAL-INTRACRANIAL BYPASS: INFRATEMPORAL APPROACH FIGURE 3. A right-sided cadaveric dissection demonstrates an orbitozygomatic osteotomy and frontotemporal craniotomy. The rectangular craniectomy site is marked in blue. RESULTS Patients The SC-IC IMax technique described was used in 4 cases. One case was a flow augmentation bypass for a hypoperfused hemisphere FIGURE 4. A right-sided cadaveric dissection demonstrates the craniotomy. The craniectomy (thick red arrow) is done up to the virtual line 2 mm lateral to V2 and V3 entering foramen rotundum and foramen ovale, respectively (thin arrows). The internal maxillary artery is dissected in the infratemporal fossa (large gray arrow). FIGURE 5. Left side intraoperative craniectomy of the middle cranial fossa floor, similar in view to the cadaveric dissection shown in Figure 4. (The rectangular craniectomy portion is shown as transparent blue.). in a patient with neurofibromatosis type 2 who underwent cervical surgery for resection of a cervical neurofibroma that resulted in occlusion of the internal carotid artery. This patient also had a very small-caliber superficial temporal artery (STA). The clinical presentation of this patient was hemiparesis due to stroke. Two patients have a diagnosis of a giant MCA aneurysm not amendable to endovascular treatment or direct microsurgical clipping (Figures 11 and 12). One of these patients had undergone a previous craniotomy in which the ipsilateral STA had been sacrificed. Both patients underwent SC-IC bypass and subsequent endovascular trapping of the aneurysms. The last patient was treated for a recurrent partially thrombosed giant MCA aneurysm. This patient experienced major recanalization of her aneurysm after endovascular coiling and presented with severe brain edema. She was recoiled and subsequently underwent SC-IC bypass and distal M1 trapping. Subsequent to SC-IC bypass, the distal M1 segment was clipped, and the patient was subsequently treated by trapping of her proximal M1 segment using coil embolization. Anastomoses In the first patient, the IMax was identified in the infratemporal fossa by neuronavigation coupled with micro Doppler confirmation (Figure 6). In the subsequent patients, anatomic landmarks formed by the virtual line between the foramen rotundum and foramen ovale (which marks the medial border of the craniectomy), as well as the deep temporalis arteries that lead to the IMax, were identified, resulting in more rapid and atraumatic localization of the IMax. The position of the Imax was then confirmed by micro Doppler. In our last case, the identification of the IMax was more difficult due to unusual distal tortuosity. NEUROSURGERY VOLUME 75 NUMBER 1 JULY
6 NOSSEK ET AL FIGURE 6. A screen shot from the Stryker neuronavigation system (Stryker Instruments, Kalamazoo, Michigan) shows the localization of the internal maxillary artery (red arrows). Intraoperative flow measurements, in the graft, using the Charbel flow probe (Transonic Systems Inc), ranged from 20 to 60 ml/min. In the cases of end-to-end anastomosis (Figure 13), we did not observe any symptoms resulting from IMax sacrifice. Retrograde filling of distal IMax territory by external carotid artery collaterals was demonstrated on all postoperative angiograms. Outcome All patients tolerated the IMax SC-IC bypass well. Postoperative angiography demonstrated good filling of the graft with robust distal flow in all cases (Figures 14 and 15). Two aneurysm patients underwent aneurysm occlusion with concomitant MCA deconstruction using interventional techniques. This plan allows early flow demand to be placed on the transplanted graft with real-time angiographic flow assessment before aneurysm deconstruction. In addition, by eliminating surgical exposure of the aneurysm, less surgical dissection is required, limiting surgical morbidity to the construction of the bypass itself. The last case underwent distal microsurgical M1 segment sacrifice with the residual aneurysm coiled and completely occluded postoperatively. The M1 segment was clipped immediately distal to the aneurysmal fundus. Retrograde FIGURE 7. A left-sided intraoperative image of the internal maxillary artery (blue arrow) dissected in the infratemporal fossa. 90 VOLUME 75 NUMBER 1 JULY
7 SUBCRANIAL-INTRACRANIAL BYPASS: INFRATEMPORAL APPROACH FIGURE 8. Drawing of the donor internal maxillary artery and the recipient M3 in the opened sylvian fissure. FIGURE 10. Drawing of the final result of the subcranial-intracranial bypass. filling was demonstrated from the SC-IC anastomosis into the M1 segment up to the clip, allowing flow into the lateral lenticulostriate arteries arising from this portion of the M1 segment. One of the aneurysm patients in our series experienced postoperative swelling of the hemisphere after aneurysm embolization and underwent decompressive craniectomy. He ultimately underwent cranioplasty before discharge and recovered to his preoperative baseline. DISCUSSION FIGURE 9. Drawing of the proximal end-to-end anastomosis and a permanent clip on the distal internal maxillary artery and distal end-to-side anastomosis to the M3. Cerebral bypass has been used for many years for the treatment of cranial base tumors and giant aneurysms as well as for flow augmentation into hypoperfused cerebral hemispheres. 1-4,10 The 2 basic modalities of bypass are either EC-IC bypass or IC-IC (in situ) bypass The most common EC-IC bypass is the STA-MCA bypass. In cases in which the target of the bypass is flow replacement, a higher flow bypass graft is often required. 14,15 In these cases, the cervical carotid artery is typically used as the donor site, using either a saphenous vein or radial artery as a graft vessel, which is then anastomosed to an appropriate recipient MCA branch. 1,2,14,16 This technique typically requires a graft in excess of 20 cm, which can be prone to kinking and subcutaneous compression. These grafts need to be safely tunneled from the neck to the cranial insertion site; alternatively, a long skin incision from the NEUROSURGERY VOLUME 75 NUMBER 1 JULY
8 NOSSEK ET AL FIGURE 11. A, computed tomography angiography of a patient with enlarging serpentine M2 aneurysm. B, magnetic resonance angiography demonstrates the thrombosed aneurysm and the flow into the aneurysm. craniotomy site down to the cervical carotid is required. Additionally, the 2 operative fields are not well visualized through a single operative microscopic view. The surgeon must move from neck to cranial exposure when performing the 2 anastomoses, and any graft complication is therefore managed with only a partial view of the totality of the graft length. Imax-MCA (SC-IC) bypass as a high-flow EC-IC bypass option has been described in both cadaveric studies 6-9,17 and clinical microsurgical practice. 5 This bypass option is efficacious in cases that require high flow where the use of the cervical carotid as a donor is contraindicated (ie, after neck surgery or in the setting of occlusion of the common carotid artery). The Imax-MCA bypass technique and the important modifications that we propose carry a number of distinct advantages over the conventional EC-IC bypass in which the cervical carotid artery FIGURE 12. Angiogram of the patient. A left internal carotid artery injection demonstrates a fusiform M2 aneurysm. Patient had had a previous frontotemporal craniotomy for meningioma and had no superficial temporal artery. FIGURE 13. A left-sided intraoperative image of the proximal end-to-end anastomosis of the internal maxillary artery (IMax) and the vein graft (orange arrow). The black arrow indicates the permanent clip on the distal IMax. 92 VOLUME 75 NUMBER 1 JULY
9 SUBCRANIAL-INTRACRANIAL BYPASS: INFRATEMPORAL APPROACH FIGURE 14. Postoperative angiogram. A, an internal carotid artery injection demonstrates complete occlusion (no distal flow) of the aneurysm by coil mass. B, an external carotid artery injection demonstrates a patent bypass that fills the middle cerebral artery territory. is used as a donor. First, the SC-IC graft is significantly shorter (7-9 cm) than the typical length required when using the cervical carotid artery as a proximal anastomosis site. Although bypass length has not been described as a prognostic factor for bypass longevity, longer grafts are theoretically more prone to mechanical disruption such as kinking and compression. These grafts may have lower patency rates with lower flows. Short graft length permits the use of a brachiocephalic rather than a saphenous vein, and graft size can then be tailored more effectively to recipient size. The brachiocephalic vein has few, if any, valves, which improves overall donor quality. Additionally, potential upper extremity arterial complications that can be associated with radial artery are then avoided. 1,18,19 An additional benefit of the SC-IC bypass technique is that the entire intracranial graft both the proximal and distal anastomoses is visualized within the same microsurgical field (Figures 16 and 17). This allows for immediate inspection of the graft, the proximal anastomosis site, and the distal anastomosis site simultaneously and thus improves the safety and efficiency of the operation. Our modification of the previously described IMax bypass technique, in which the IMax was identified through a small FIGURE 15. Postoperative angiogram. Anteroposterior (A) and lateral (B) projections of a common carotid artery injection demonstrate a patent bypass and filling of the entire hemisphere. NEUROSURGERY VOLUME 75 NUMBER 1 JULY
10 NOSSEK ET AL FIGURE 16. A postoperative computed tomography 3-dimensional reconstruction of the cranium (from a second patient) that demonstrates the vein graft bypassing through the floor of the middle cranial fossa. Note the craniectomy at the base of the middle cranial fossa overlying the infratemporal fossa. FIGURE 17. Intraoperative image of a right-sided craniotomy. The final result demonstrates the vein graft (blue arrow) emerging from the infratemporal fossa (black arrow) into the sylvian fissure (green arrow) in the same operative field. middle cranial fossa floor window, represents a distinct technical improvement. 5 This original technique is highly demanding, requiring drilling in the anterior aspect of the floor of the middle cranial fossa and the subsequent end-to-side anastomosis through this small, constricted middle cranial fossa craniectomy. Precise localization and manipulation of the IMax through this small window can be tedious and time-consuming. Our SC-IC technique modification used either a zygomatic osteotomy or orbitozygomatic osteotomy followed by a lateral rectangular craniectomy of the middle fossa. This modification allowed the IMax to be reliably anatomically identified over a considerable length of 15 to 20 mm. In cadaver dissections, we localized the IMax just anterior and parallel to the line between the foramen rotundum and foramen ovale. This experience allowed us to execute the craniectomy in situ up to this same line and then readily identify the vessel within the infratemporal fossa; this exposure then allowed for the performance of the anastomosis in an end-to-end fashion, Ultimately, we found that the completion of proximal anastomosis could be performed in a straightforward manner, with wide exposure and illumination of the IMax in the infratemporal fossa. There was no need for retractors throughout the procedure. CONCLUSION The Imax-MCA (SC-IC) bypass is safe and effective and has anumberofadvantagesovertheconventionalec-icbypassusingthe cervical carotid. These advantages include (1) shorter graft length, (2) avoidance of a cervical carotid artery dissection and its attendant complications, (3) a microsurgical view of the entirety of the intracranial graft and both the proximal and distal anastomoses within the same field, (4) minimization of the risk of graft kinking and compression, (5) the ability to use a subcutaneous vein with easier graft sizing rather than the radial artery with its known risks, and (6) the use of a lateral temporal fossa rectangular craniectomy technique combined with a zygomatic osteotomy. This craniectomy was found to significantly improve the previously described anastomotic technique by allowing the IMax to be reliably identified, accessed, and then used as a proximal blood flow source without the need for significant drilling. We believe that this technique should be considered as a first choice for an EC-IC bypass in which the STA is either unavailable or inadequate relative to the flow required. We strongly advocate preparatory cadaveric dissection by the multidisciplinary team before microsurgical in vivo SC-IC bypass using the IMax. Disclosure The authors have no personal financial or institutional interest in any of the drugs, materials, or devices described in this article. REFERENCES 1. Sekhar LN, Duff JM, Kalavakonda C, Olding M. Cerebral revascularization using radial artery grafts for the treatment of complex intracranial aneurysms: techniques and outcomes for 17 patients. Neurosurgery. 2001;49(3): VOLUME 75 NUMBER 1 JULY
11 SUBCRANIAL-INTRACRANIAL BYPASS: INFRATEMPORAL APPROACH 2. Lawton MT, Hamilton MG, Morcos JJ, Spetzler RF. Revascularization and aneurysm surgery: current techniques, indications, and outcome. Neurosurgery. 1996;38(1): O Shaughnessy BA, Salehi SA, Mindea SA, Batjer HH. Selective cerebral revascularization as an adjunct in the treatment of giant anterior circulation aneurysms. Neurosurg Focus. 2003;14(3):e4. 4. Sundt TM Jr, Piepgras DG, Marsh WR, Fode NC. Saphenous vein bypass grafts for giant aneurysms and intracranial occlusive disease. J Neurosurg. 1986;65(4): Abdulrauf SI, Sweeney JM, Mohan YS, Palejwala SK. Short segment internal maxillary artery to middle cerebral artery bypass: a novel technique for extracranialto-intracranial bypass. Neurosurgery. 2011;68(3): Büyükmumcu M, Ustün ME, Seker M, Karabulut AK, Uysal YY. Maxillary-topetrous internal carotid artery bypass: an anatomical feasibility study. Surg Radiol Anat. 2003;25(5-6): Eller JL, Sasaki-Adams D, Sweeney JM, Abdulrauf SI. Localization of the internal maxillary artery for extracranial-to-intracranial bypass through the middle cranial fossa: a cadaveric study. J Neurol Surg B Skull Base. 2012;73(1): Karabulut AK, Ustün ME, UysalII, Salbacak A. Saphenous vein graft for bypass of the maxillary to supraclinoid internal carotid artery: an anatomical short study. Ann Vasc Surg. 2001;15(5): Vrionis FD, Cano WG, Heilman CB. Microsurgical anatomy of the infratemporal fossa as viewed laterally and superiorly. Neurosurgery. 1996;39(4): Amin-Hanjani S, Butler WE, Ogilvy CS, Carter BS, Barker FG II. Extracranialintracranial bypass in the treatment of occlusive cerebrovascular disease and intracranial aneurysms in the United States between 1992 and 2001: a populationbased study. J Neurosurg. 2005;103(5): Dengler J, Kato N, Vajkoczy P. The Y-shaped double-barrel bypass in the treatment of large and giant anterior communicating artery aneurysms. J Neurosurg. 2013;118(2): Nussbaum L, Defillo A, Zelensky A, Nussbaum ES. A short segment intracranialintracranial jump graft bypass followed by proximal arterial occlusion for a distal MCA aneurysm. Surg Neurol Int. 2011;2: Sanai N, Zador Z, Lawton MT. Bypass surgery for complex brain aneurysms: an assessment of intracranial-intracranial bypass. Neurosurgery. 2009;65(4): Sia SF, Morgan MK. High flow extracranial-to-intracranial brain bypass surgery. J Clin Neurosci. 2013;20(1): Amin-Hanjani S, Charbel FT. Flow-assisted surgical technique in cerebrovascular surgery. Surg Neurol. 2007;68(suppl 1):S4-S Ashley WW, Amin-Hanjani S, Alaraj A, Shin JH, Charbel FT. Flow-assisted surgical cerebral revascularization. Neurosurg Focus. 2008;24(2):E Ulku CH, Ustun ME, Buyukmumcu M, Cicekcibasi AE, Ziylan T. Radial artery graft for bypass of the maxillary to proximal posterior cerebral artery: an anatomical and technical study. Acta Otolaryngol. 2004;124(7): Evans JJ, Sekhar LN, Rak R, Stimac D. Bypass grafting and revascularization in the management of posterior circulation aneurysms. Neurosurgery. 2004;55(5): Zhu YY, Hayward PA, Hadinata IE, et al. Long-term impact of radial artery harvest on forearm function and symptoms: a comparison with leg vein. J Thorac Cardiovasc Surg. 2013;145(2): COMMENT This is an interesting small technical case series with nice illustrations. For the open vascular subspecialist, it highlights an important nuance to a newer option for an extracranial-intracranial bypass, the internal maxillary middle cerebral artery (IMax-MCA) bypass. Although the overall technique is not novel and the patient number is small, the authors demonstrate the feasibility of, and rationale for, using this modification. As originally described, the IMax-MCA bypass provides access to the donor artery through only a small opening in the middle fossa floor, which presents technical challenges. The nuance provided allows for better exposure and control of the donor artery and for end-to-end as well as end-to-side anastomosis. Although the IMax-MCA bypass may represent a slick alternative to more traditional methods, indications for using it are probably very limited. When available, the superficial temporal artery (STA) is a technically easier bypass that does not require a separate graft harvest and can be used even for high-flow indications. I have advocated double-barrel STA-MCA bypass whenever feasible, and when both branches are used (one for the superior division and one for the inferior division), flows approaching 100 ml/min are possible in patients with robust arteries. Intracranial-intracranial bypass is also emerging as an attractive option in many cases and shares the benefits of short graft length and the lack of a cervical incision with the currently described technique. Microvascular anastomosis, in whatever form it takes, remains an important skill for cranial neurosurgeons and should continue to be taught to our trainees. In the laboratory, synthetic kits, turkey wings, and rats are good models for early experience, and although a high level of trust is required, I have found that senior residents can safely participate in bypass surgery in the operating room. Edward Angus McKay Duckworth Houston, Texas NEUROSURGERY VOLUME 75 NUMBER 1 JULY
Extracranial-to-Intracranial Bypass Using Radial Artery Grafting for Complex Skull Base Tumors: Technical Note
 Extracranial-to-Intracranial Bypass Using Radial Artery Grafting for Complex Skull Base Tumors: Technical Note Saleem I. Abdulrauf, M.D., F.A.C.S. 1 ABSTRACT The management of complex skull base tumors
Extracranial-to-Intracranial Bypass Using Radial Artery Grafting for Complex Skull Base Tumors: Technical Note Saleem I. Abdulrauf, M.D., F.A.C.S. 1 ABSTRACT The management of complex skull base tumors
History of revascularization
 History of revascularization Author (year) Kredel, 1942 Woringer& Kunlin, 1963 Donaghy& Yasargil, 1968 Loughheed 1971 Kikuchini & Karasawa1973 Karasawa, 1977 Story, 1978 Sundt, 1982 EC/IC bypass study
History of revascularization Author (year) Kredel, 1942 Woringer& Kunlin, 1963 Donaghy& Yasargil, 1968 Loughheed 1971 Kikuchini & Karasawa1973 Karasawa, 1977 Story, 1978 Sundt, 1982 EC/IC bypass study
Intracranial-to-intracranial vascular anastomosis created using a microanastomotic device for the treatment of distal middle cerebral artery aneurysms
 J Neurosurg 97:486 491, 2002 Intracranial-to-intracranial vascular anastomosis created using a microanastomotic device for the treatment of distal middle cerebral artery aneurysms Technical note DAVID
J Neurosurg 97:486 491, 2002 Intracranial-to-intracranial vascular anastomosis created using a microanastomotic device for the treatment of distal middle cerebral artery aneurysms Technical note DAVID
Interpositional carotid artery bypass strategies in the surgical management of aneurysms and tumors of the skull base
 Neurosurg Focus 14 (3):Article 2, 2003, Click here to return to Table of Contents Interpositional carotid artery bypass strategies in the surgical management of aneurysms and tumors of the skull base JAMES
Neurosurg Focus 14 (3):Article 2, 2003, Click here to return to Table of Contents Interpositional carotid artery bypass strategies in the surgical management of aneurysms and tumors of the skull base JAMES
TABLES. Table 1 Terminal vessel aneurysms. Table. Aneurysm location. Bypass flow** Symptoms Strategy Bypass recipient. Age/ Sex.
 Table TABLES Table 1 Terminal vessel aneurysms Age/ Sex Aneurysm location Symptoms Strategy Bypass recipient Recipient territory Recipient territory flow* Cut flow Bypass flow** Graft Patent postop F/U
Table TABLES Table 1 Terminal vessel aneurysms Age/ Sex Aneurysm location Symptoms Strategy Bypass recipient Recipient territory Recipient territory flow* Cut flow Bypass flow** Graft Patent postop F/U
CASE REPORT AIR VENT OF VEIN GRAFT IN EXTRACRANIAL-INTRACRANIAL BYPASS SURGERY
 Nagoya J. Med. Sci. 74. 339 ~ 345, 2012 CASE REPORT AIR VENT OF VEIN GRAFT IN EXTRACRANIAL-INTRACRANIAL BYPASS SURGERY HIROFUMI OYAMA, AKIRA KITO, HIDEKI MAKI, KENICHI HATTORI, TOMOYUKI NODA and KENTARO
Nagoya J. Med. Sci. 74. 339 ~ 345, 2012 CASE REPORT AIR VENT OF VEIN GRAFT IN EXTRACRANIAL-INTRACRANIAL BYPASS SURGERY HIROFUMI OYAMA, AKIRA KITO, HIDEKI MAKI, KENICHI HATTORI, TOMOYUKI NODA and KENTARO
Cerebral revascularization: past, present and future
 Cerebral revascularization: past, present and future Tomás Funes 1 MD, Asis Lorente Muñoz 2 MD, Federico Fernández Molina 3 MD, Paula Ypa 3 MD, Francisco Mannara 4 MD, Luis González Martínez 2 MD, PhD
Cerebral revascularization: past, present and future Tomás Funes 1 MD, Asis Lorente Muñoz 2 MD, Federico Fernández Molina 3 MD, Paula Ypa 3 MD, Francisco Mannara 4 MD, Luis González Martínez 2 MD, PhD
ANATOMICAL CONSIDERATION OF THE INTRACRANIAL PORTION OF MIDDLE MENIGEAL ARTERY IN THAIS
 ANATOMICAL CONSIDERATION OF THE INTRACRANIAL PORTION OF MIDDLE MENIGEAL ARTERY IN THAIS Kritsana Namonta, 1 Lanaprai Kwathai, 1 Thanaporn Rungruang, 1 Vipavadee Chaisuksunt, 2 Wandee Apinhasmit, 3 Supin
ANATOMICAL CONSIDERATION OF THE INTRACRANIAL PORTION OF MIDDLE MENIGEAL ARTERY IN THAIS Kritsana Namonta, 1 Lanaprai Kwathai, 1 Thanaporn Rungruang, 1 Vipavadee Chaisuksunt, 2 Wandee Apinhasmit, 3 Supin
Moyamoya Syndrome with contra lateral DACA aneurysm: First Case report with review of literature
 Romanian Neurosurgery Volume XXXI Number 3 2017 July-September Article Moyamoya Syndrome with contra lateral DACA aneurysm: First Case report with review of literature Ashish Kumar Dwivedi, Pradeep Kumar,
Romanian Neurosurgery Volume XXXI Number 3 2017 July-September Article Moyamoya Syndrome with contra lateral DACA aneurysm: First Case report with review of literature Ashish Kumar Dwivedi, Pradeep Kumar,
Intracranial vascular anastomosis using the microanastomotic system
 J Neurosurg 89:676 681, 1998 Intracranial vascular anastomosis using the microanastomotic system Technical note DAVID W. NEWELL, M.D., ANDREW T. DAILEY, M.D., AND STEPHEN L. SKIRBOLL, M.D. Department of
J Neurosurg 89:676 681, 1998 Intracranial vascular anastomosis using the microanastomotic system Technical note DAVID W. NEWELL, M.D., ANDREW T. DAILEY, M.D., AND STEPHEN L. SKIRBOLL, M.D. Department of
Anastomosis of the superficial temporal artery to the distal anterior cerebral artery with interposed cephalic vein graft
 J Neurosurg 58~25-429, 1983 Anastomosis of the superficial temporal artery to the distal anterior cerebral artery with interposed cephalic vein graft Case report RYOJI ISHII, M.D., TETSUO KOIKE, M.D.,
J Neurosurg 58~25-429, 1983 Anastomosis of the superficial temporal artery to the distal anterior cerebral artery with interposed cephalic vein graft Case report RYOJI ISHII, M.D., TETSUO KOIKE, M.D.,
Intrapetrous Internal Carotid Artery
 James C. Andrews, M.D., Neil A. Martin, M.D., Keith Black, M.D., Vincent F Honrubia, M.D., and Donald P Becker, M.D. Midd le Cranial Fossa Transtemporal Approach to the Intrapetrous Internal Carotid Artery
James C. Andrews, M.D., Neil A. Martin, M.D., Keith Black, M.D., Vincent F Honrubia, M.D., and Donald P Becker, M.D. Midd le Cranial Fossa Transtemporal Approach to the Intrapetrous Internal Carotid Artery
ANASTAMOSIS FOR BRAIN STEM ISCHEMIA/Khodadad et al.
 ANASTAMOSIS FOR BRAIN STEM ISCHEMIA/Khodadad et al. visualization of the posterior inferior cerebellar artery. The patient, now 11 months post-operative, has shown further neurological improvement since
ANASTAMOSIS FOR BRAIN STEM ISCHEMIA/Khodadad et al. visualization of the posterior inferior cerebellar artery. The patient, now 11 months post-operative, has shown further neurological improvement since
EXTRACRANIAL MENINGIOMA PRESENTING AS INFRATEMPORAL FOSSA MASS: A CASE SERIES
 Case Series EXTRACRANIAL MENINGIOMA PRESENTING AS INFRATEMPORAL FOSSA MASS: A CASE SERIES Sunil Mathew * 1, Reddy Ravikanth 2, Vijaykishan B 3. ABSTRACT Extradural meningioma occurs as extracranial extension
Case Series EXTRACRANIAL MENINGIOMA PRESENTING AS INFRATEMPORAL FOSSA MASS: A CASE SERIES Sunil Mathew * 1, Reddy Ravikanth 2, Vijaykishan B 3. ABSTRACT Extradural meningioma occurs as extracranial extension
Treatment of a Giant Serpentine Aneurysm in the Anterior Cerebral Artery
 Journal of Cerebrovascular and Endovascular Neurosurgery pissn 2234-8565, eissn 2287-3139, http://dx.doi.org/10.7461/jcen.2016.18.2.141 Case Report Treatment of a Giant Serpentine Aneurysm in the Anterior
Journal of Cerebrovascular and Endovascular Neurosurgery pissn 2234-8565, eissn 2287-3139, http://dx.doi.org/10.7461/jcen.2016.18.2.141 Case Report Treatment of a Giant Serpentine Aneurysm in the Anterior
Case Log Mapping Update: April 2018 Review Committee for Neurological Surgery
 Case Log Mapping Update: April 2018 Review Committee for Neurological Surgery The Review Committee has made the following changes to the CPT code mappings: The following previously untracked CPT codes
Case Log Mapping Update: April 2018 Review Committee for Neurological Surgery The Review Committee has made the following changes to the CPT code mappings: The following previously untracked CPT codes
Management of Giant Aneurysm
 Management of Giant Aneurysm Paul P. Huang, M.D. and Jafar J. Jafar, M.D. Department of Neurosurgery New York University Medical Center New York, New York, USA Introduction Giant intracranial aneurysms
Management of Giant Aneurysm Paul P. Huang, M.D. and Jafar J. Jafar, M.D. Department of Neurosurgery New York University Medical Center New York, New York, USA Introduction Giant intracranial aneurysms
Bypass to the Intracranial Giant or Large Internal Carotid Artery Aneurysms: Superficial Temporal Artery to Middle Cerebral Artery Bypass Re-visited
 Bypass to the Intracranial Giant or Large Internal Carotid Artery Aneurysms: Superficial Temporal Artery to Middle Cerebral Artery Bypass Re-visited Galip Zihni SANUfi 1 Ziya AKAR 2 Taner TANRIVERD 3 Banu
Bypass to the Intracranial Giant or Large Internal Carotid Artery Aneurysms: Superficial Temporal Artery to Middle Cerebral Artery Bypass Re-visited Galip Zihni SANUfi 1 Ziya AKAR 2 Taner TANRIVERD 3 Banu
Extracranial to intracranial bypass for intracranial atherosclerosis
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Extracranial to intracranial bypass for intracranial atherosclerosis In cerebrovascular disease, blood vessels
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Extracranial to intracranial bypass for intracranial atherosclerosis In cerebrovascular disease, blood vessels
Letter to the Editor: test occlusion under monitoring of motor-evoked potentials for giant distal
 Letter to the Editor: test occlusion under monitoring of motor-evoked potentials for giant distal anterior cerebral artery aneurysm Acta Neurochirurgica Kampei Shimizu, Shoichi Tani, Hirotoshi Imamura,
Letter to the Editor: test occlusion under monitoring of motor-evoked potentials for giant distal anterior cerebral artery aneurysm Acta Neurochirurgica Kampei Shimizu, Shoichi Tani, Hirotoshi Imamura,
Management of the persistent sciatic artery with coexistent aortoiliac aneurysms; endovascular and open techniques.
 ISPUB.COM The Internet Journal of Thoracic and Cardiovascular Surgery Volume 14 Number 2 Management of the persistent sciatic artery with coexistent aortoiliac aneurysms; endovascular and open A Rodriguez-Rivera,
ISPUB.COM The Internet Journal of Thoracic and Cardiovascular Surgery Volume 14 Number 2 Management of the persistent sciatic artery with coexistent aortoiliac aneurysms; endovascular and open A Rodriguez-Rivera,
Emergency EC-IC bypass for symptomatic atherosclerotic ischemic stroke
 Emergency EC-IC bypass for symptomatic atherosclerotic ischemic stroke Tetsuyoshi Horiuchi, Junpei Nitta, Shigetoshi Ishizaka, Kohei Kanaya, Takao Yanagawa, and Kazuhiro Hongo. Department of Neurosurgery,
Emergency EC-IC bypass for symptomatic atherosclerotic ischemic stroke Tetsuyoshi Horiuchi, Junpei Nitta, Shigetoshi Ishizaka, Kohei Kanaya, Takao Yanagawa, and Kazuhiro Hongo. Department of Neurosurgery,
Case Report INTRODUCTION
 Journal of Cerebrovascular and Endovascular Neurosurgery pissn 2234-8565, eissn 2287-3139, https//doi.org/10.7461/jcen.2018.20.2.127 Case Report Revision Superficial Temporal Artery-Middle Cerebral Artery
Journal of Cerebrovascular and Endovascular Neurosurgery pissn 2234-8565, eissn 2287-3139, https//doi.org/10.7461/jcen.2018.20.2.127 Case Report Revision Superficial Temporal Artery-Middle Cerebral Artery
Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage
 Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
Saphenous Vein Autograft Replacement
 Saphenous Vein Autograft Replacement of Severe Segmental Coronary Artery Occlusion Operative Technique Rene G. Favaloro, M.D. D irect operation on the coronary artery has been performed in 180 patients
Saphenous Vein Autograft Replacement of Severe Segmental Coronary Artery Occlusion Operative Technique Rene G. Favaloro, M.D. D irect operation on the coronary artery has been performed in 180 patients
Posterior Cerebral Artery Aneurysms with Common Carotid Artery Occlusion: A Report of Two Cases
 Journal of Neuroendovascular Therapy 2017; 11: 371 375 Online March 3, 2017 DOI: 10.5797/jnet.cr.2016-0114 Posterior Cerebral Artery Aneurysms with Common Carotid Artery Occlusion: A Report of Two Cases
Journal of Neuroendovascular Therapy 2017; 11: 371 375 Online March 3, 2017 DOI: 10.5797/jnet.cr.2016-0114 Posterior Cerebral Artery Aneurysms with Common Carotid Artery Occlusion: A Report of Two Cases
Alt h o u g h once a commonly performed revascularization
 Neurosurg Focus 26 (5):E19, 2009 Operative nuances of an occipital artery to posterior inferior cerebellar artery bypass R. We b s t e r Cr o w l e y, M.D., 1 Ri c k y Me d e l, M.D., 1 a n d Aar o n S.
Neurosurg Focus 26 (5):E19, 2009 Operative nuances of an occipital artery to posterior inferior cerebellar artery bypass R. We b s t e r Cr o w l e y, M.D., 1 Ri c k y Me d e l, M.D., 1 a n d Aar o n S.
Case Report 1. CTA head. (c) Tele3D Advantage, LLC
 Case Report 1 CTA head 1 History 82 YEAR OLD woman with signs and symptoms of increased intra cranial pressure in setting of SAH. CT Brain was performed followed by CT Angiography of head. 2 CT brain Extensive
Case Report 1 CTA head 1 History 82 YEAR OLD woman with signs and symptoms of increased intra cranial pressure in setting of SAH. CT Brain was performed followed by CT Angiography of head. 2 CT brain Extensive
Principles Arteries & Veins of the CNS LO14
 Principles Arteries & Veins of the CNS LO14 14. Identify (on cadaver specimens, models and diagrams) and name the principal arteries and veins of the CNS: Why is it important to understand blood supply
Principles Arteries & Veins of the CNS LO14 14. Identify (on cadaver specimens, models and diagrams) and name the principal arteries and veins of the CNS: Why is it important to understand blood supply
Contralateral clipping of bilateral middle cerebral artery aneurysms. Case report
 Romanian Neurosurgery Volume XXXI Number 1 2017 January - March Article Contralateral clipping of bilateral middle cerebral artery aneurysms. Case report Georgiana Ion, Alexandru Chiriac, Ziyad Faiyad,
Romanian Neurosurgery Volume XXXI Number 1 2017 January - March Article Contralateral clipping of bilateral middle cerebral artery aneurysms. Case report Georgiana Ion, Alexandru Chiriac, Ziyad Faiyad,
Surgical management of complex intracranial aneurysms
 Review Article Surgical management of complex intracranial aneurysms Daniel L. Barrow, C. Michael Cawley Department of Neurosurgery and Emory MBNA Stroke Center, Emory University School of Medicine, Atlanta,
Review Article Surgical management of complex intracranial aneurysms Daniel L. Barrow, C. Michael Cawley Department of Neurosurgery and Emory MBNA Stroke Center, Emory University School of Medicine, Atlanta,
Surgery of Middle Cerebral Artery (MCA) Aneurysm
 Surgery of Middle Cerebral Artery (MCA) Aneurysm 15 Fusao Ikawa 15.1 Sign and Symptoms Middle cerebral artery (MCA) aneurysm is one of the most popular cerebral aneurysm. The incidence of ruptured MCA
Surgery of Middle Cerebral Artery (MCA) Aneurysm 15 Fusao Ikawa 15.1 Sign and Symptoms Middle cerebral artery (MCA) aneurysm is one of the most popular cerebral aneurysm. The incidence of ruptured MCA
Superficial Temporal Artery to Middle Cerebral Artery Bypass
 Superficial Temporal Artery to Middle Cerebral Artery Bypass David W. Newell, M.D. 1 ABSTRACT The superficial temporal artery to middle artery bypass is a technique that allows the blood supply from the
Superficial Temporal Artery to Middle Cerebral Artery Bypass David W. Newell, M.D. 1 ABSTRACT The superficial temporal artery to middle artery bypass is a technique that allows the blood supply from the
Surgical techniques and procedures for cerebrovascular surgery. Surgery for the AVF at the cranio-cervical junction and high cervical spine
 VS-1 Surgery for the AVF at the cranio-cervical junction and high cervical spine Hiroyuki Kinouchi University of Yamanashi, Department of Neurosurgery Dural AVFs have been recognized as common type of
VS-1 Surgery for the AVF at the cranio-cervical junction and high cervical spine Hiroyuki Kinouchi University of Yamanashi, Department of Neurosurgery Dural AVFs have been recognized as common type of
How to manage the left subclavian and left vertebral artery during TEVAR
 How to manage the left subclavian and left vertebral artery during TEVAR Jürg Schmidli Chief of Vascular Surgery Inselspital Hamburg 2017 Dept Cardiovascular Surgery, Bern, Switzerland Disclosure No Disclosures
How to manage the left subclavian and left vertebral artery during TEVAR Jürg Schmidli Chief of Vascular Surgery Inselspital Hamburg 2017 Dept Cardiovascular Surgery, Bern, Switzerland Disclosure No Disclosures
Pichayen Duangthongpon MD*, Chaiwit Thanapaisal MD*, Amnat Kitkhuandee MD*, Kowit Chaiciwamongkol MD**, Vilaiwan Morthong MD**
 The Relationships between Asterion, the Transverse-Sigmoid Junction, the Superior Nuchal Line and the Transverse Sinus in Thai Cadavers: Surgical Relevance Pichayen Duangthongpon MD*, Chaiwit Thanapaisal
The Relationships between Asterion, the Transverse-Sigmoid Junction, the Superior Nuchal Line and the Transverse Sinus in Thai Cadavers: Surgical Relevance Pichayen Duangthongpon MD*, Chaiwit Thanapaisal
Postoperative Assessment of Extracranial Intracranial Bypass by Time- Resolved 3D Contrast-Enhanced MR Angiography Using Parallel Imaging
 AJNR Am J Neuroradiol 26:2243 2247, October 2005 Postoperative Assessment of Extracranial Intracranial Bypass by Time- Resolved 3D Contrast-Enhanced MR Angiography Using Parallel Imaging Kazuhiro Tsuchiya,
AJNR Am J Neuroradiol 26:2243 2247, October 2005 Postoperative Assessment of Extracranial Intracranial Bypass by Time- Resolved 3D Contrast-Enhanced MR Angiography Using Parallel Imaging Kazuhiro Tsuchiya,
Alessandro Della Puppa
 Intraoperative measurement of arterial blood flow in complex cerebral aneurysms surgery Studio flussimetrico intra-operatorio nel clipping degli aneurismi complessi Alessandro Della Puppa NEUROSURGERY
Intraoperative measurement of arterial blood flow in complex cerebral aneurysms surgery Studio flussimetrico intra-operatorio nel clipping degli aneurismi complessi Alessandro Della Puppa NEUROSURGERY
Contaminated Wound: Report of a Cas
 NAOSITE: Nagasaki University's Ac Title Author(s) Citation Endovascular Treatment of a Carotid Contaminated Wound: Report of a Cas Yamaguchi, Nimpei; Kaneko, Kenichi; Takahashi, Haruo Acta medica Nagasakiensia,
NAOSITE: Nagasaki University's Ac Title Author(s) Citation Endovascular Treatment of a Carotid Contaminated Wound: Report of a Cas Yamaguchi, Nimpei; Kaneko, Kenichi; Takahashi, Haruo Acta medica Nagasakiensia,
Aneurysms that are too complex for conventional
 J Neurosurg 20:364 377, 204 AANS, 204 Anterior cerebral artery bypass for complex aneurysms: an experience with intracranial-intracranial reconstruction and review of bypass options Clinical article Adib
J Neurosurg 20:364 377, 204 AANS, 204 Anterior cerebral artery bypass for complex aneurysms: an experience with intracranial-intracranial reconstruction and review of bypass options Clinical article Adib
As a group, basilar artery aneurysms are
 OPERATIVE NUANCES ORBITOZYGOMATIC APPROACH TO BASILAR APEX ANEURYSMS Frank P.K. Hsu, M.D., Ph.D. Division of Neurological Surgery, St. Joseph s Hospital and Medical Center, Phoenix, Arizona Richard E.
OPERATIVE NUANCES ORBITOZYGOMATIC APPROACH TO BASILAR APEX ANEURYSMS Frank P.K. Hsu, M.D., Ph.D. Division of Neurological Surgery, St. Joseph s Hospital and Medical Center, Phoenix, Arizona Richard E.
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY
 OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY BUCCINATOR MYOMUCOSAL FLAP The Buccinator Myomucosal Flap is an axial flap, based on the facial and/or buccal arteries. It is a flexible
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY BUCCINATOR MYOMUCOSAL FLAP The Buccinator Myomucosal Flap is an axial flap, based on the facial and/or buccal arteries. It is a flexible
Variation of Superficial Palmar Arch: A Case Report
 Article ID: WMC003387 ISSN 2046-1690 Variation of Superficial Palmar Arch: A Case Report Corresponding Author: Dr. Liju S Mathew, Demonstrator, Anatomy, Gulf Medical University, 4184 - United Arab Emirates
Article ID: WMC003387 ISSN 2046-1690 Variation of Superficial Palmar Arch: A Case Report Corresponding Author: Dr. Liju S Mathew, Demonstrator, Anatomy, Gulf Medical University, 4184 - United Arab Emirates
Quality Metrics. Stroke Related Procedure Outcomes
 Quality Metrics Stroke Related Procedure Outcomes Below is a description of some of the stroke-related procedures performed at St. Dominic Hospital in Jackson, with quality information on the complication
Quality Metrics Stroke Related Procedure Outcomes Below is a description of some of the stroke-related procedures performed at St. Dominic Hospital in Jackson, with quality information on the complication
Neurosurg Focus 5 (5):Article 4, 1998
 Neurosurg Focus 5 (5):Article 4, 1998 Multiple combined indirect procedure for the surgical treatment of children with moyamoya disease. A comparison with single indirect anastomosis with direct anastomosis
Neurosurg Focus 5 (5):Article 4, 1998 Multiple combined indirect procedure for the surgical treatment of children with moyamoya disease. A comparison with single indirect anastomosis with direct anastomosis
Double STA-MCA Anatomosis for Bilateral Carotid Occlusion
 Double STA-MCA Anatomosis for Bilateral Carotid Occlusion -Case Report and Literature Review- Sandra vuignier 1, Kenji Kanamaru 2, Tomohiro Araki 2 1 Department of Neurosurgery, Nagoya University School
Double STA-MCA Anatomosis for Bilateral Carotid Occlusion -Case Report and Literature Review- Sandra vuignier 1, Kenji Kanamaru 2, Tomohiro Araki 2 1 Department of Neurosurgery, Nagoya University School
Axillobrachial artery bypass grafting with in situ cephalic vein for axillary artery occlusion: A case report
 CASE REPORTS Axillobrachial artery bypass grafting with in situ cephalic vein for axillary artery occlusion: A case report Evan S. Cohen,/VII), Robert B. Holtzman, MD, and George W. Johnson, Jr., MD, Houston,
CASE REPORTS Axillobrachial artery bypass grafting with in situ cephalic vein for axillary artery occlusion: A case report Evan S. Cohen,/VII), Robert B. Holtzman, MD, and George W. Johnson, Jr., MD, Houston,
Introducing a New Treatment Method for Brain Aneurysms
 Pipeline Embolization Device Introducing a New Treatment Method for Brain Aneurysms UNDERSTANDING ANEURYSMS What is a brain aneurysm? An aneurysm is an outpouching in an artery caused by weakness in the
Pipeline Embolization Device Introducing a New Treatment Method for Brain Aneurysms UNDERSTANDING ANEURYSMS What is a brain aneurysm? An aneurysm is an outpouching in an artery caused by weakness in the
Spasm of the extracranial internal carotid artery resulting from blunt trauma demonstrated by angiography
 Spasm of the extracranial internal carotid artery resulting from blunt trauma demonstrated by angiography Case report ELISHA S. GURDJIAN, M.D., BLAISE AUDET, M.D., RENATO W. SIBAYAN, M.D., AND LLYWELLYN
Spasm of the extracranial internal carotid artery resulting from blunt trauma demonstrated by angiography Case report ELISHA S. GURDJIAN, M.D., BLAISE AUDET, M.D., RENATO W. SIBAYAN, M.D., AND LLYWELLYN
CME. Seattle Science Foundation Second Annual Cerebrovascular & EndoVascular Residents & Fellows Course. October 21-22, 2016
 Seattle Science Foundation Second Annual Cerebrovascular & EndoVascular Residents & Fellows Course October 21-22, 2016 CME Continuing Medical Education Provided by Course Description The Second Annual
Seattle Science Foundation Second Annual Cerebrovascular & EndoVascular Residents & Fellows Course October 21-22, 2016 CME Continuing Medical Education Provided by Course Description The Second Annual
Occlusion of All Four Extracranial Vessels With Minimal Clinical Symptomatology. Case Report
 Occlusion of All Four Extracranial Vessels With Minimal Clinical Symptomatology. Case Report BY JIRI J. VITEK, M.D., JAMES H. HALSEY, JR., M.D., AND HOLT A. McDOWELL, M.D. Abstract: Occlusion of All Four
Occlusion of All Four Extracranial Vessels With Minimal Clinical Symptomatology. Case Report BY JIRI J. VITEK, M.D., JAMES H. HALSEY, JR., M.D., AND HOLT A. McDOWELL, M.D. Abstract: Occlusion of All Four
Techniques in cerebral aneurysm surgery
 SYⅤ-1 Surgery for large and giant cerebral aneurysm Hidetoshi Murata, Ryohei Miyazaki, Mitsuru Sato, Nobuyuki Shimizu, Takahiro Tanaka, Taishi Nakamura, Shigeta Miyake, Jun Suenaga, Tetsuya Yamamoto Department
SYⅤ-1 Surgery for large and giant cerebral aneurysm Hidetoshi Murata, Ryohei Miyazaki, Mitsuru Sato, Nobuyuki Shimizu, Takahiro Tanaka, Taishi Nakamura, Shigeta Miyake, Jun Suenaga, Tetsuya Yamamoto Department
Neurosurgical decision making in structural lesions causing stroke. Dr Rakesh Ranjan MS, MCh, Dip NB (Neurosurgery)
 Neurosurgical decision making in structural lesions causing stroke Dr Rakesh Ranjan MS, MCh, Dip NB (Neurosurgery) Subarachnoid Hemorrhage Every year, an estimated 30,000 people in the United States experience
Neurosurgical decision making in structural lesions causing stroke Dr Rakesh Ranjan MS, MCh, Dip NB (Neurosurgery) Subarachnoid Hemorrhage Every year, an estimated 30,000 people in the United States experience
PTA 106 Unit 1 Lecture 3
 PTA 106 Unit 1 Lecture 3 The Basics Arteries: Carry blood away from the heart toward tissues. They typically have thicker vessels walls to handle increased pressure. Contain internal and external elastic
PTA 106 Unit 1 Lecture 3 The Basics Arteries: Carry blood away from the heart toward tissues. They typically have thicker vessels walls to handle increased pressure. Contain internal and external elastic
Cerebral Bypass and Advanced Neuroendovascular Course 2018
 Mayo Clinic Cerebral Bypass and Advanced Neuroendovascular Course 2018 Co-directed by: Giuseppe Lanzino MD and Leonardo Rangel-Castilla MD Honored Guest: Luca Regli MD, Zurich, Switzerland Thursday, November
Mayo Clinic Cerebral Bypass and Advanced Neuroendovascular Course 2018 Co-directed by: Giuseppe Lanzino MD and Leonardo Rangel-Castilla MD Honored Guest: Luca Regli MD, Zurich, Switzerland Thursday, November
Research Article - Basic And Applied Anatomy Branching of the foramen rotundum. A rare variation of the sphenoid
 IJAE Vol. 119, n. 2: 148-152, 2014 ITALIAN JOURNAL OF ANATOMY AND EMBRYOLOGY Research Article - Basic And Applied Anatomy Branching of the foramen rotundum. A rare variation of the sphenoid Eugenio Bertelli,
IJAE Vol. 119, n. 2: 148-152, 2014 ITALIAN JOURNAL OF ANATOMY AND EMBRYOLOGY Research Article - Basic And Applied Anatomy Branching of the foramen rotundum. A rare variation of the sphenoid Eugenio Bertelli,
CORONARY ARTERY BYPASS GRAFTING (CABG) (Part 1) Mark Shikhman, MD, Ph.D., CSA Andrea Scott, CST
 CORONARY ARTERY BYPASS GRAFTING (CABG) (Part 1) Mark Shikhman, MD, Ph.D., CSA Andrea Scott, CST I have constructed this lecture based on publications by leading cardiothoracic American surgeons: Timothy
CORONARY ARTERY BYPASS GRAFTING (CABG) (Part 1) Mark Shikhman, MD, Ph.D., CSA Andrea Scott, CST I have constructed this lecture based on publications by leading cardiothoracic American surgeons: Timothy
Anatomical Landmarks for Safe Elevation of the Deep Inferior Epigastric Perforator Flap: A Cadaveric Study
 Anatomical Landmarks for Safe Elevation of the Deep Inferior Epigastric Perforator Flap: A Cadaveric Study Saeed Chowdhry, MD, Ron Hazani, MD, Philip Collis, BS, and Bradon J. Wilhelmi, MD University of
Anatomical Landmarks for Safe Elevation of the Deep Inferior Epigastric Perforator Flap: A Cadaveric Study Saeed Chowdhry, MD, Ron Hazani, MD, Philip Collis, BS, and Bradon J. Wilhelmi, MD University of
Anatomical study. Clinical study. R. Ogawa, H. Hyakusoku, M. Murakami, R. Aoki, K. Tanuma* and D. G. Pennington?
 British Journal of Plastic Surgery (2002) 55, 396-40 I 9 2002 The British Association of Plastic Surgeons doi: 10.1054/bjps.2002.3877 PLASTIC SURGERY An anatomical and clinical study of the dorsal intercostal
British Journal of Plastic Surgery (2002) 55, 396-40 I 9 2002 The British Association of Plastic Surgeons doi: 10.1054/bjps.2002.3877 PLASTIC SURGERY An anatomical and clinical study of the dorsal intercostal
Bilateral traumatic internal carotid artery dissections: Case report
 Bilateral traumatic internal carotid artery dissections: Case report Jeffrey L. Ballard, MD, T. J. Bunt, MD, Brian Fitzpatrick, MD, and James M. Malone, MD, Tucson and Phoenix, Ariz. Bilateral internal
Bilateral traumatic internal carotid artery dissections: Case report Jeffrey L. Ballard, MD, T. J. Bunt, MD, Brian Fitzpatrick, MD, and James M. Malone, MD, Tucson and Phoenix, Ariz. Bilateral internal
Anatomy of the Middle Cerebral Artery: The Temporal Branches
 Anatomy of the Middle Cerebral Artery: The Temporal Branches BY W. BRADFORD DeLONG, M.D., F.A.C.S. Abstract: Anatomy of the Middle Cerebral Artery: The Temporal Branches Nineteen out of 23 middle cerebral
Anatomy of the Middle Cerebral Artery: The Temporal Branches BY W. BRADFORD DeLONG, M.D., F.A.C.S. Abstract: Anatomy of the Middle Cerebral Artery: The Temporal Branches Nineteen out of 23 middle cerebral
Introduction to the Native Arteriovenous Fistula: A primer for medical students and radiology residents
 Introduction to the Native Arteriovenous Fistula: A primer for medical students and radiology residents Jesus Contreras, D.O. PGY-4 John Yasmer, D.O. Department of Radiology No Disclosures Objectives Introduce
Introduction to the Native Arteriovenous Fistula: A primer for medical students and radiology residents Jesus Contreras, D.O. PGY-4 John Yasmer, D.O. Department of Radiology No Disclosures Objectives Introduce
Vivek R. Deshmukh, MD Director, Cerebrovascular and Endovascular Neurosurgery Chairman, Department of Neurosurgery Providence Brain and Spine
 Vivek R. Deshmukh, MD Director, Cerebrovascular and Endovascular Neurosurgery Chairman, Department of Neurosurgery Providence Brain and Spine Institute The Oregon Clinic Disclosure I declare that neither
Vivek R. Deshmukh, MD Director, Cerebrovascular and Endovascular Neurosurgery Chairman, Department of Neurosurgery Providence Brain and Spine Institute The Oregon Clinic Disclosure I declare that neither
Exposure of the anterior tibial artery by medial popliteal extension
 Exposure of the anterior tibial artery by medial popliteal extension J. G. Sladen, FRCS(C), G. Kougeer, FRCS(C), and J. D. S. Reid, FRCS(C), Vancouver) British Columbia) Canada This report describes exploration
Exposure of the anterior tibial artery by medial popliteal extension J. G. Sladen, FRCS(C), G. Kougeer, FRCS(C), and J. D. S. Reid, FRCS(C), Vancouver) British Columbia) Canada This report describes exploration
Ruptured aberrant internal carotid artery pseudoaneurysm presenting with spontaneous massive ear bleeding following a single sneeze: a case report
 Case eport JNET 7:312-316, 2013 uptured aberrant internal carotid artery pseudoaneurysm presenting with spontaneous massive ear bleeding following a single sneeze: a case report Seiichiro HIONO 1) Eiichi
Case eport JNET 7:312-316, 2013 uptured aberrant internal carotid artery pseudoaneurysm presenting with spontaneous massive ear bleeding following a single sneeze: a case report Seiichiro HIONO 1) Eiichi
Cerebral Revascularization For Stroke
 Cerebral Revascularization For Stroke If you are looking for the ebook Cerebral Revascularization for Stroke in pdf form, then you've come to loyal site. We present full edition of this ebook in txt, doc,
Cerebral Revascularization For Stroke If you are looking for the ebook Cerebral Revascularization for Stroke in pdf form, then you've come to loyal site. We present full edition of this ebook in txt, doc,
Temporal region. temporal & infratemporal fossae. Zhou Hong Ying Dept. of Anatomy
 Temporal region temporal & infratemporal fossae Zhou Hong Ying Dept. of Anatomy Temporal region is divided by zygomatic arch into temporal & infratemporal fossae. Temporal Fossa Infratemporal fossa Temporal
Temporal region temporal & infratemporal fossae Zhou Hong Ying Dept. of Anatomy Temporal region is divided by zygomatic arch into temporal & infratemporal fossae. Temporal Fossa Infratemporal fossa Temporal
Corporate Medical Policy
 Corporate Medical Policy Endovascular Therapies for Extracranial Vertebral Artery Disease File Name: Origination: Last CAP Review: Next CAP Review: Last Review: endovascular_therapies_for_extracranial_vertebral_artery_disease
Corporate Medical Policy Endovascular Therapies for Extracranial Vertebral Artery Disease File Name: Origination: Last CAP Review: Next CAP Review: Last Review: endovascular_therapies_for_extracranial_vertebral_artery_disease
RadRx Your Prescription for Accurate Coding & Reimbursement Copyright All Rights Reserved.
 Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of June 4, 2018 Thrombolysis, Thrombectomy & Angioplasty
Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of June 4, 2018 Thrombolysis, Thrombectomy & Angioplasty
Complex aneurysms involving the basilar apex, superior
 LABORATORY INVESTIGATION J Neurosurg 129:121 127, 2018 Revascularization of the upper posterior circulation with the anterior temporal artery: an anatomical feasibility study Ali Tayebi Meybodi, MD, 1,2
LABORATORY INVESTIGATION J Neurosurg 129:121 127, 2018 Revascularization of the upper posterior circulation with the anterior temporal artery: an anatomical feasibility study Ali Tayebi Meybodi, MD, 1,2
Segmental Agenesis of the Internal Carotid Artery Distal to the Posterior Communicating Artery Leading to the Definition of a New Embryologic Segment
 AJNR Am J Neuroradiol 25:1189 1193, August 2004 Case Report Segmental Agenesis of the Internal Carotid Artery Distal to the Posterior Communicating Artery Leading to the Definition of a New Embryologic
AJNR Am J Neuroradiol 25:1189 1193, August 2004 Case Report Segmental Agenesis of the Internal Carotid Artery Distal to the Posterior Communicating Artery Leading to the Definition of a New Embryologic
Temporal fossa Infratemporal fossa Pterygopalatine fossa Terminal branches of external carotid artery Pterygoid venous plexus
 Outline of content Temporal fossa Infratemporal fossa Pterygopalatine fossa Terminal branches of external carotid artery Pterygoid venous plexus Boundary Content Communication Mandibular division of trigeminal
Outline of content Temporal fossa Infratemporal fossa Pterygopalatine fossa Terminal branches of external carotid artery Pterygoid venous plexus Boundary Content Communication Mandibular division of trigeminal
BUILDING A. Achieving total reconstruction in a single operation. 70 OCTOBER 2016 // dentaltown.com
 BUILDING A MANDI Achieving total reconstruction in a single operation by Dr. Fayette C. Williams Fayette C. Williams, DDS, MD, FACS, is clinical faculty at John Peter Smith Hospital in Fort Worth, Texas,
BUILDING A MANDI Achieving total reconstruction in a single operation by Dr. Fayette C. Williams Fayette C. Williams, DDS, MD, FACS, is clinical faculty at John Peter Smith Hospital in Fort Worth, Texas,
An Overview of Post-EVAR Endoleaks: Imaging Findings and Management. Ravi Shergill BSc Sean A. Kennedy MD Mark O. Baerlocher MD FRCPC
 An Overview of Post-EVAR Endoleaks: Imaging Findings and Management Ravi Shergill BSc Sean A. Kennedy MD Mark O. Baerlocher MD FRCPC Disclosure Slide Mark O. Baerlocher: Current: Consultant for Boston
An Overview of Post-EVAR Endoleaks: Imaging Findings and Management Ravi Shergill BSc Sean A. Kennedy MD Mark O. Baerlocher MD FRCPC Disclosure Slide Mark O. Baerlocher: Current: Consultant for Boston
The orbitozygomatic approach achieves better
 OPERATIVE NUANCES THE ORBITOZYGOMATIC APPROACH Wouter Ralph van Furth, M.D., Ph.D. Department of Neurosurgery, Academic Medical Center, University of Amsterdam, Amsterdam, The Netherlands Anne Maria R.
OPERATIVE NUANCES THE ORBITOZYGOMATIC APPROACH Wouter Ralph van Furth, M.D., Ph.D. Department of Neurosurgery, Academic Medical Center, University of Amsterdam, Amsterdam, The Netherlands Anne Maria R.
Surgical treatment of a dissecting aneurysm of the superior cerebellar artery: case report
 Romanian Neurosurgery (2014) XXI 3: 269-273 269 Surgical treatment of a dissecting aneurysm of the superior cerebellar artery: case report Florin Stefanescu 1, Stefanita Dima 2, Mugurel Petrinel Radoi
Romanian Neurosurgery (2014) XXI 3: 269-273 269 Surgical treatment of a dissecting aneurysm of the superior cerebellar artery: case report Florin Stefanescu 1, Stefanita Dima 2, Mugurel Petrinel Radoi
Bilateral Carotid and Vertebral Rete Mirabile Presenting with Subarachnoid Hemorrhage Caused by the Rupture of Spinal Artery Aneurysm
 Tohoku J. Exp. Med., 2013, 230, 205-209 Carotid and Vertebral Rete Mirabile Presenting with SAH 205 Bilateral Carotid and Vertebral Rete Mirabile Presenting with Subarachnoid Hemorrhage Caused by the Rupture
Tohoku J. Exp. Med., 2013, 230, 205-209 Carotid and Vertebral Rete Mirabile Presenting with SAH 205 Bilateral Carotid and Vertebral Rete Mirabile Presenting with Subarachnoid Hemorrhage Caused by the Rupture
Popliteal Artery Aneurysms: Diagnosis and Repair Options
 Deepak N. Deshmukh DO April 27, 2018 Popliteal Artery Aneurysms: Diagnosis and Repair Options No Disclosures Popliteal Artery Aneurysms (PAAs) Male Predominanace Most common peripheral Aneurysm (70%) 30-50%
Deepak N. Deshmukh DO April 27, 2018 Popliteal Artery Aneurysms: Diagnosis and Repair Options No Disclosures Popliteal Artery Aneurysms (PAAs) Male Predominanace Most common peripheral Aneurysm (70%) 30-50%
Usefulness of Coil-assisted Technique in Treating Wide-neck Intracranial Aneurysms: Neck-bridge Procedure Using the Coil Mass as a Support
 Journal of Neuroendovascular Therapy 2017; 11: 220 225 Online December 14, 2016 DOI: 10.5797/jnet.tn.2016-0081 Usefulness of Coil-assisted Technique in Treating Wide-neck Intracranial Aneurysms: Neck-bridge
Journal of Neuroendovascular Therapy 2017; 11: 220 225 Online December 14, 2016 DOI: 10.5797/jnet.tn.2016-0081 Usefulness of Coil-assisted Technique in Treating Wide-neck Intracranial Aneurysms: Neck-bridge
MATERIALS AND METHODS
 SNI: Neurovascular OPEN ACCESS For entire Editorial Board visit : http://www.surgicalneurologyint.com Editor: James I. Ausman, MD, PhD University of California, Los Angeles, CA, USA Original Article Surgical
SNI: Neurovascular OPEN ACCESS For entire Editorial Board visit : http://www.surgicalneurologyint.com Editor: James I. Ausman, MD, PhD University of California, Los Angeles, CA, USA Original Article Surgical
Utility of Indocyanine Green Video Angiography for Sylvian Fissure Dissection in Subarachnoid Hemorrhage Patients - Sylvian ICG Technique
 TECHNICAL NOTE Neurol Med Chir (Tokyo) 58, 85 90, 2018 doi: 10.2176/nmc.tn.2017-0160 Online December 1, 2017 Utility of Indocyanine Green Video Angiography for Sylvian Fissure Dissection in Subarachnoid
TECHNICAL NOTE Neurol Med Chir (Tokyo) 58, 85 90, 2018 doi: 10.2176/nmc.tn.2017-0160 Online December 1, 2017 Utility of Indocyanine Green Video Angiography for Sylvian Fissure Dissection in Subarachnoid
Moyamoya. Moyamoya Disease Double Trouble. Epidemiology 1/16/2015
 Moyamoya Moyamoya Disease Double Trouble Jan Boerke, ACNP AACN Brunch January 24, 2015 Moyamoya - puff of smoke in Japanese Describes the look of the tangle of tiny vessels formed to compensate for the
Moyamoya Moyamoya Disease Double Trouble Jan Boerke, ACNP AACN Brunch January 24, 2015 Moyamoya - puff of smoke in Japanese Describes the look of the tangle of tiny vessels formed to compensate for the
Case Report Ocular Symptomatology, Management, and Clinical Outcome of a Giant Intracranial Aneurysm
 Volume 2012, Article ID 643965, 4 pages doi:10.1155/2012/643965 Case Report Ocular Symptomatology, Management, and Clinical Outcome of a Giant Intracranial Aneurysm Chryssa Terzidou, 1 Georgios Dalianis,
Volume 2012, Article ID 643965, 4 pages doi:10.1155/2012/643965 Case Report Ocular Symptomatology, Management, and Clinical Outcome of a Giant Intracranial Aneurysm Chryssa Terzidou, 1 Georgios Dalianis,
QUANTITATIVE ANALYSIS AND COMPUTER AIDED SIMULATION OF MINIMALLY INVASIVE APPROACHES FOR INTRACRANIAL VASCULAR LESIONS
 QUANTITATIVE ANALYSIS AND COMPUTER AIDED SIMULATION OF MINIMALLY INVASIVE APPROACHES FOR INTRACRANIAL VASCULAR LESIONS Alberto Prats Galino Facultat de Medicina UB 1. Project Summary The main goal of this
QUANTITATIVE ANALYSIS AND COMPUTER AIDED SIMULATION OF MINIMALLY INVASIVE APPROACHES FOR INTRACRANIAL VASCULAR LESIONS Alberto Prats Galino Facultat de Medicina UB 1. Project Summary The main goal of this
Transvenous Embolization of Cavernous Sinus Dural Arteriovenous Fistulas with Shunts Involving the Laterocavernous Sinus
 Journal of Neuroendovascular Therapy 2017; 11: 1 7 Online November 9, 2016 DOI: 10.5797/jnet.oa.2016-0062 Transvenous Embolization of Cavernous Sinus Dural Arteriovenous Fistulas with Shunts Involving
Journal of Neuroendovascular Therapy 2017; 11: 1 7 Online November 9, 2016 DOI: 10.5797/jnet.oa.2016-0062 Transvenous Embolization of Cavernous Sinus Dural Arteriovenous Fistulas with Shunts Involving
Anatomical relationship between arteries and veins in the paraumbilical region q
 The British Association of Plastic Surgeons (2003) 56, 552 556 Anatomical relationship between arteries and veins in the paraumbilical region q N. Imanishi a, *, H. Nakajima b, T. Minabe c, H. Chang d,
The British Association of Plastic Surgeons (2003) 56, 552 556 Anatomical relationship between arteries and veins in the paraumbilical region q N. Imanishi a, *, H. Nakajima b, T. Minabe c, H. Chang d,
Recommendations for Follow-up After Vascular Surgery Arterial Procedures SVS Practice Guidelines
 Recommendations for Follow-up After Vascular Surgery Arterial Procedures 2018 SVS Practice Guidelines vsweb.org/svsguidelines About the guidelines Published in the July 2018 issue of Journal of Vascular
Recommendations for Follow-up After Vascular Surgery Arterial Procedures 2018 SVS Practice Guidelines vsweb.org/svsguidelines About the guidelines Published in the July 2018 issue of Journal of Vascular
Techniques in cerebral aneurysm surgery. Anatomical variation of middle meningeal artery origin ophthalmic artery
 SYⅤ-1 Anatomical variation of middle meningeal artery origin ophthalmic artery Yu Kinoshita, Rokuya Tanikawa, Kosumo Noda, Nakao Ota, Tomomasa Kondo, Takanori Miyazaki, Kiyotaka Toyoda, Syuichi Tanada,
SYⅤ-1 Anatomical variation of middle meningeal artery origin ophthalmic artery Yu Kinoshita, Rokuya Tanikawa, Kosumo Noda, Nakao Ota, Tomomasa Kondo, Takanori Miyazaki, Kiyotaka Toyoda, Syuichi Tanada,
PTERYGOPALATINE FOSSA
 PTERYGOPALATINE FOSSA Outline Anatomical Structure and Boundaries Foramina and Communications with other spaces and cavities Contents Pterygopalatine Ganglion Especial emphasis on certain arteries and
PTERYGOPALATINE FOSSA Outline Anatomical Structure and Boundaries Foramina and Communications with other spaces and cavities Contents Pterygopalatine Ganglion Especial emphasis on certain arteries and
Department of Neurosurgery, Renmin Hospital of Wuhan University, Wuhan , Hubei Province, P.R.C; 2
 Int J Clin Exp Med 2015;8(5):7627-7633 www.ijcem.com /ISSN:1940-5901/IJCEM0007123 Original Article Endovascular management of ruptured basilar superior cerebellar artery junction aneurysms: a series of
Int J Clin Exp Med 2015;8(5):7627-7633 www.ijcem.com /ISSN:1940-5901/IJCEM0007123 Original Article Endovascular management of ruptured basilar superior cerebellar artery junction aneurysms: a series of
3. The Jaw and Related Structures
 Overview and objectives of this dissection 3. The Jaw and Related Structures The goal of this dissection is to observe the muscles of jaw raising. You will also have the opportunity to observe several
Overview and objectives of this dissection 3. The Jaw and Related Structures The goal of this dissection is to observe the muscles of jaw raising. You will also have the opportunity to observe several
Cerebral Bypass Surgery
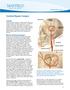 Cerebral Bypass Surgery Overview Cerebral bypass surgery is performed to restore, or revascularize, blood flow to the brain. A cerebral bypass is the brain's equivalent of a coronary bypass in the heart.
Cerebral Bypass Surgery Overview Cerebral bypass surgery is performed to restore, or revascularize, blood flow to the brain. A cerebral bypass is the brain's equivalent of a coronary bypass in the heart.
Azygos anterior cerebral artery aneurysm with subarachnoid hemorrhage
 Chowdhury et al. Neuroimmunol Neuroinflammation 2018;5:39 DOI: 10.20517/2347-8659.2018.37 Neuroimmunology and Neuroinflammation Letter to Editor Open ccess zygos anterior cerebral artery aneurysm with
Chowdhury et al. Neuroimmunol Neuroinflammation 2018;5:39 DOI: 10.20517/2347-8659.2018.37 Neuroimmunology and Neuroinflammation Letter to Editor Open ccess zygos anterior cerebral artery aneurysm with
Case 37 Clinical Presentation
 Case 37 73 Clinical Presentation The patient is a 62-year-old woman with gastrointestinal (GI) bleeding. 74 RadCases Interventional Radiology Imaging Findings () Image from a selective digital subtraction
Case 37 73 Clinical Presentation The patient is a 62-year-old woman with gastrointestinal (GI) bleeding. 74 RadCases Interventional Radiology Imaging Findings () Image from a selective digital subtraction
Carotid Embolectomy and Endarterectomy for Symptomatic Complete Occlusion of the Carotid Artery as a Rescue Therapy in Acute Ischemic Stroke
 This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
Ruptured Cerebral Aneurysm of the Anterior Circulation
 Original Articles * Division of Neurosurgery Department of Surgery Ruptured Cerebral Aneurysm of the Anterior Circulation Management and Microsurgical Treatment Ossama Al-Mefty, MD* ABSTRACT Based on the
Original Articles * Division of Neurosurgery Department of Surgery Ruptured Cerebral Aneurysm of the Anterior Circulation Management and Microsurgical Treatment Ossama Al-Mefty, MD* ABSTRACT Based on the
SHA aneurysms are rare. They arise from the internal carotid
 Published March 8, 2012 as 10.3174/ajnr.A3004 ORIGINAL RESEARCH N. Chalouhi S. Tjoumakaris A.S. Dumont L.F. Gonzalez C. Randazzo D. Gordon R. Chitale R. Rosenwasser P. Jabbour Superior Hypophyseal Artery
Published March 8, 2012 as 10.3174/ajnr.A3004 ORIGINAL RESEARCH N. Chalouhi S. Tjoumakaris A.S. Dumont L.F. Gonzalez C. Randazzo D. Gordon R. Chitale R. Rosenwasser P. Jabbour Superior Hypophyseal Artery
Depicting Cerebral Veins by Three-Dimensional CT Angiography before Surgical Clipping of Aneurysms
 AJNR Am J Neuroradiol 23:85 91, January 2001 Depicting Cerebral Veins by Three-Dimensional CT Angiography before Surgical Clipping of Aneurysms Makio Kaminogo, Hideyuki Hayashi, Hideki Ishimaru, Minoru
AJNR Am J Neuroradiol 23:85 91, January 2001 Depicting Cerebral Veins by Three-Dimensional CT Angiography before Surgical Clipping of Aneurysms Makio Kaminogo, Hideyuki Hayashi, Hideki Ishimaru, Minoru
Penetration of the Optic Nerve or Chiasm by Anterior Communicating Artery Aneurysms. - Three Case Reports-
 Penetration of the Optic Nerve or Chiasm by Anterior Communicating Artery Aneurysms. - Three Case Reports- Tetsuyoshi Horiuchi 1, Toshiya Uchiyama 1, Yoshikazu Kusano 1, Maki Okada 1, Kazuhiro Hongo 1,
Penetration of the Optic Nerve or Chiasm by Anterior Communicating Artery Aneurysms. - Three Case Reports- Tetsuyoshi Horiuchi 1, Toshiya Uchiyama 1, Yoshikazu Kusano 1, Maki Okada 1, Kazuhiro Hongo 1,
