Superficial Temporal Artery to Middle Cerebral Artery Bypass
|
|
|
- Gavin Reynolds
- 6 years ago
- Views:
Transcription
1 Superficial Temporal Artery to Middle Cerebral Artery Bypass David W. Newell, M.D. 1 ABSTRACT The superficial temporal artery to middle artery bypass is a technique that allows the blood supply from the extracranial carotid circulation to be routed to the distal middle cerebral artery branches. The procedure allows blood flow to bypass proximal lesions of the intracranial vasculature. The performance of this bypass requires specialized microvascular training and the use of microvascular techniques. The techniques involved in performing these procedures include microdissection of the superficial temporal artery in the scalp, microdissection of the recipient middle cerebral artery branches near the sylvian fissure, and anastomosis techniques using either microvascular sutures or a microanastomotic device. The successful completion of the bypass and subsequent patency requires meticulous attention to technical details. KEYWORDS: Middle cerebral artery, superficial temporal artery to middle cerebral artery bypass, cerebral revascularization The superficial temporal artery to middle cerebral artery (STA-MCA bypass) can be used to augment flow to the distal MCA vascular territory. Technical developments in microvascular suture material, operating microscopes, and microsurgical techniques allowed the developments of this procedure. The technique was first described by M.G. Yasargil, who perfected the use of microvascular anastomosis in dogs. 1 The original technique described was an end-to-side anastomosis using a distal branch of the STA dissected from the scalp to a surface cortical branch of the MCA near the region of the sylvian fissure (Fig. 1). Subsequent variations of this procedure have been described, including double-limb STA-MCA bypass grafts for additional flow, and end-to-end anastomoses, using a microanastomotic device for higher-flow bypasses. HISTORICAL ASPECTS The first STA-MCA bypass was performed in a human by M.G. Yasargil on October 30, 1967, in Zurich, on a patient with a complete occlusion of the MCA. 1 Before performing this operation, Skull Base, volume 15, number 2, Address for correspondence and reprint requests: David W. Newell, M.D., Seattle Neuroscience Institute, 1600 East Jefferson St., Ste. 620, Seattle, WA david.newell@swedish.org. 1 Seattle Neuroscience Swedish Hospital Medical Center, Seattle, Washington. Copyright # 2005 by Thieme Medical Publishers, Inc., 333 Seventh Avenue, New York, NY 10001, USA. Tel: +1(212) ,p;2005,15,02,133,142,ftx,en;sbs00446x. 133
2 134 SKULL BASE: AN INTERDISCIPLINARY APPROACH/VOLUME 15, NUMBER Figure 1 Schematic representation of the STA-to-MCA anastomosis using the parietal branch as a donor artery. STA, superficial temporal artery; MCA, middle cerebral artery. Professor Yasargil studied the technique of microvascular reconstruction in small animals with R.M.P. Donaghy at the University of Vermont. The use of bipolar coagulation and the availability of microvascular sutures and the use of the operating microscope were important technical developments that enabled this procedure to be performed. The first publication of a series of patients with STA-MCA bypasses was for cerebrovascular occlusive disease and also as an adjunct in the treatment of complex intracranial aneurysms. 1 Several subsequent publications appeared documenting the safety and results of STA-MCA bypass for a variety of conditions, most predominantly cerebrovascular occlusive disease. 2 6 The rationale for its use in occlusive disease was based on the fact that experimental studies had identified areas of hypoperfusion following a proximal artery obstruction in cerebral circulation. At this time, before endovascular cerebrovascular techniques were introduced, there was no other acceptable treatment for narrowing in the carotid artery high above the carotid bifurcation or in the proximal middle cerebral vasculature. The widespread use of the procedure for cerebral vascular disease led to an international randomized study of STA-MCA bypass versus medical therapy for atherosclerotic lesions of the carotid artery distal to the carotid bifurcation, carotid occlusion, and lesions of the MCA. There were broad entry criteria for patients, and hemodynamic measurements were not performed in patients prior to entry. The results of the trial indicated that STA-MCA bypass was not superior to medical therapy for treatment of these lesions. 7 The publication of this study led to a dramatic decrease in the number of STA-MCA bypasses performed for cerebrovascular occlusive disease. Over the next several decades, the procedure was most commonly performed as an adjunct in the treatment of complex aneurysms requiring additional blood supply to the middle cerebral territory for occlusion, in patients with moyamoya disease, and in patients with recurrent disabling transient ischemic attacks on a hemodynamic basis The procedure has also been used in patients with skull base tumors who require proximal vessel sacrifice as part of their treatment. More recent studies on the natural history of high stroke risk in patients with symptomatic carotid occlusion and hemodynamic insufficiency have indicated a strong rationale for re-examining the procedure for this subgroup of patients. These findings have led to the initiation of the carotid occlusion surgery study (COSS), which is currently recruiting patients. 12 This study will examine the role of STA-MCA bypass in patients with symptomatic carotid occlusion who have evidence of cerebral perfusion abnormalities based on positron emission tomography scan. Patients are randomized to either bypass or medical treatment, and the efficacy of their procedure for stroke prevention is being examined. Other indications for STA-MCA bypass have included several conditions that could
3 STA TO MCA BYPASS/NEWELL 135 interrupt the blood flow to the distal middle cerebral vasculature. These conditions include planned proximal vessel sacrifice for tumors or aneurysms, moyamoya disease, and other causes of vascular occlusion that reduce blood flow to the MCA territory. It was apparent from the cooperative study on aneurysms that the STA-MCA bypass is a technically feasible procedure with a high patency rate and the ability to provide distal blood flow to the cerebral vasculature. Improvements in cerebral blood flow measurement techniques, as well as the routine use of temporary balloon occlusion techniques, has led to an improvement in the capability of preoperative diagnostic testing to predict patients who may benefit from the procedure for certain indications such as ischemia and planned vessel sacrifice. PREOPERATIVE ASSESSMENT OF PATIENTS UNDERGOING STA-MCA BYPASS Standard preoperative imaging of patients to undergo STA-MCA bypass includes computed tomography scan as well as four-vessel cerebral angiography with selective external runs to define the STAs. The STA commonly bifurcates in the preauricular region into a frontal and parietal branch (Fig. 2). The frontal branch commonly anastomoses with branches of the supraorbital artery. Variations in the anatomy include one of the two branches being dominant, equal caliber of both branches, or atresia of the parietal branch. In patients who have had a previous craniotomy, the parietal branch is often absent. The operation is quite difficult to perform if the donor artery branch of the STA is less than 1 mm in diameter. Lesions of the skull base such as tumors, which produce gradual occlusion of the proximal internal carotid artery, may often lead to hypertrophy of the frontal branch of the STA as it provides collateral flow through the supraorbital pathways, which anastomose with the ophthalmic artery to provide retrograde flow into the internal carotid artery. If the frontal branch is chosen for use, it is important to note that it is usually in front of the hairline and is often crossed by branches of the superior division of the facial nerve supplying the frontalis muscle. Interruption of these branches of the facial nerve will commonly cause a partial or complete frontalis muscle weakness. Options for dissection of the frontal branch of the STA include direct dissection over the artery, or from the underside of the scalp flap with identification of the main trunk of the artery proximally, and dissection of the STA from the underside of the scalp flap distally. The second approach is preferred by the author. ANESTHETIC CONSIDERATIONS Figure 2 Photograph of an individual with a very prominent STA demonstrating the anatomy of the frontal and parietal branches (labeled). STA, superficial temporal artery. General anesthesia usually consisting of a combination of isoflurane and intravenous agents is used. Ventilation is adjusted to maintain the arterial pco 2 between 35 to 40 mm Hg. Mannitol is not given and a cerebrospinal fluid drain is not used to prevent retraction of the cortex from the craniotomy site and stretching of the graft. Mild hypothermia is used for cerebral protection. Most recently we have employed the Innercool (Innercool Therapies, Inc., San Diego, CA) catheter for rapid induction of hypothermia to 33 to 34 degrees Centigrade for temporary vessel occlusion and rapid rewarming
4 136 SKULL BASE: AN INTERDISCIPLINARY APPROACH/VOLUME 15, NUMBER following temporary cross-clamping. Slight elevation in arterial pressure during arterial crossclamping is also utilized to protect against cerebral ischemia. OPERATIVE POSITIONING The patient is placed in a supine position with a roll under the shoulder to elevate the side of the surgery, and an incision is marked directly over the STA branch identified by Doppler ultrasound (Fig. 3). If the frontal branch is also used, an L-shape flap is outlined to allow retraction of the scalp for dissection of the frontal branch from the underside of the galeal layer. EXPOSURE OF STA Options to expose and isolate the STA branch, or branches, include excising the scalp over the artery with a scalpel and dissection of the artery using a jeweler s forceps for cauterization of side branches, or use of needle-point cautery. The author has converted to needle-point cautery, which provides Figure 3 The patient is positioned so the head can be turned to align the temporal and parietal region parallel to the floor. The parietal branch of the STA is identified using Doppler ultrasound and marked. STA, superficial temporal artery. Figure 4 Illustration of the technique of dissection of the STA using needle-point cautery. Initial dissection of the scalp is performed directly over the artery and then the galeal layer is cauterized parallel to the artery to dissect it from the scalp and seal any small side branches. STA, superficial temporal artery. an almost bloodless dissection of the artery from the surrounding tissues and easily allows effective cautery of side branches (Fig. 4). Following the dissection of an appropriate length of STA, the artery is irrigated with heparinized saline and then crossclamped with a temporary clip at the distal end. The artery is then mobilized from the galeal layer over the temporalis muscle then stored in wet gauze. DISSECTION OF FRONTAL BRANCH OF THE STA In cases where two limbs of the STA are needed, or under circumstances where it is determined that the parietal branch of the STA is too small for suitable use, the frontal branch of the STA can be dissected. In preparation for a frontal branch dissection, the author prefers to make an additional incision in the scalp at a right angle to the initial frontoparietal incision, which courses toward the supraorbital ridge and stops at the hairline. This allows mobilization of the scalp flap forward to expose the frontal branch of the STA on the underside of the galea layer. The dissection of the STA is taken proximally until the bifurcation is identified and then the STA is followed and dissected with tenotomy scissors and
5 STA TO MCA BYPASS/NEWELL Figure 5 Technique and location of dural opening illustrating the exposure of the cortex over the distal portion of the sylvian fissure. The graft is passed through the most inferior aspect of the dural opening. needle-point cautery. After a sufficient length of STA is dissected, it is then divided, irrigated, and cross-clamped with a temporary clamp on the distal portion of the artery. Following dissection and isolation of the donor artery or arteries, the temporalis muscle is divided using cautery, dissected from the underlying bone, and retracted laterally on both sides of the incision. The cranial flap is then placed, which is centered 6 cm superior to the external auditory meatus. This location allows access to the branches of the MCA as they emanate from the distal portion of the sylvian fissure. The dura is then opened in a Y-shaped fashion and dural tack-up stitches are placed (Fig. 5). The cortex is then inspected and a suitable branch of the MCA M-4 branches are located. It is important to identify a recipient branch free from major side branches and easily dissectible. The microscope is then brought into position in the arachnoid membrane directly overlying the chosen recipient branches dissected from the artery using a combination of a jeweler s forceps and microscissors (Fig. 6). The jeweler s bipolar cautery is utilized to cauterize small cortical branches that tether the artery to the underlying cortex. The artery is mobilized for 2 cm, and a rubber barrier is placed under the recipient artery for isolation (Fig. 7). At this stage the donor branch is then brought into the field on a cotton patty and micro- Figure 6 Illustration of the technique of exposure of the cortical recipient branch of the MCA. The arachnoid layer is carefully teased off with a combination of sharp dissection and dissection with jeweler s forceps. MCA, middle cerebral artery. dissection of the distal end of the STA is performed. The surrounding tissue is dissected from a 1- to 2cm portion of the artery to free all tissue, except for the adventitia. This allows a working length of the artery for anastomosis. Following dissection of the STA, a dilute solution of papaverine (15 mg per 100 cc of 0.9% saline) is placed on the donor artery and recipient artery to mitigate vascular spasm. The STA is then divided at an angle and spatulated to prepare it for anastomosis. In preparation for cross-clamping of the recipient artery, the anesthesiologist is asked to Figure 7 It is necessary to cauterize and divide multiple tiny perforating branches to the cortex to mobilize the recipient artery and place a small rubber working surface to perform the arteriotomy and anastomosis. 137
6 138 SKULL BASE: AN INTERDISCIPLINARY APPROACH/VOLUME 15, NUMBER elevate the blood pressure and confirm that the patient s temperature has been lowered to between 33 and 34 degrees Centigrade. Cerebral metabolic activity can also be reduced with barbiturates or propofol anesthesia. A combination of these maneuvers may be beneficial to provide cerebral protection during cross-clamping of the recipient cortical artery during the anastomosis procedure, which usually takes between 25 and 40 minutes. Small temporary clips are then placed across the MCA recipient branch to interrupt blood flow. Either Medhorn Beamer or a small Aesculup temporary clips can be used for this purpose. Following cross-clamping, a gently curved Van Ness Scissors is used to perform the small arteriotomy. The arteriotomy length should be approximately twice the diameter of the recipient artery. It is important to try to match this length with the length of the arteriotomy and spatulated donor artery. Once the vessels are prepared, a 10 0 nylon microsuture on a noncutting needle is used to place end stitches at the heel and the end of the spatulated artery (Fig. 8). Following the placement of the heel and the sutures, either an interrupted or a running suture array can be placed at either edge of the arteriotomy (Fig. 9). After completion of the arteriotomy, the temporary clamps are removed from the recipient and donor vessels, and flow is established. A small amount of leakage of blood at the suture site is common and can be mitigated with an application Figure 8 Placement of the end sutures aligns the donor and recipient arteries for the remainder of the anastomosis sutures with a noncutting needle are used. of a small amount of Surgicel and a microcottonoid patty. If a significant jet of blood continues at the anastomotic site, additional interrupted sutures can be placed. Microvascular Doppler ultrasound is in use to confirm patency of the anastomosis. Flow velocity signal throughout the cardiac cycle through diastole is essential in predicting good patency at the graft. If a resistive signal is heard with cessation of flow in diastole, this usually signals a technical problem with the anastomosis or it can indicate severe spasm of the donor artery. Under these conditions the anastomosis can be inspected and papaverine can be reapplied to the donor and recipient arteries. Figure 9 This figure illustrates the two different options of suture closure of the anastomosis using either (A) interrupted or (B) running suture closure.
7 STA TO MCA BYPASS/NEWELL 139 DOUBLE-LIMBED STA-MCA BYPASS TO DISTAL SYLVIAN BRANCHES In cases where higher flow is anticipated, doublelimbed bypass can be performed to the distal sylvian branches of the MCA. The STA is isolated as previously described, but the cortical dissection is altered slightly. The bone flap that is made is extended more proximally to locate the sylvian fissure at the curvature of the sphenoid wing. Microdissection of the sylvian fissure is accomplished to expose the anterior portion of the insula and locate M2 and M3 branches in the sylvian fissure. These branches are usually free of a large number of perforating vessels, which allows easy mobilization. Two branches of the recipient arteries are isolated and identified, and rubber barriers are placed around the branches. A small amount of retraction is often required at the inferior frontal and superior temporal locations to provide access to the sylvian branches. The microvascular portion of the anastomoses is performed as previously described. for an anastomosis. The recipient artery is then cross-clamped and divided in half, and the other end of the anastomotic wing is placed against the recipient branch. The recipient branch of the MCA is then loaded onto the pins through the ring and inspected. The vessel is thereby perforated from the outer to inner surface. The handle of the microanastomic device is turned allowing anastomosis of the STA branch to the middle cerebral recipient branch. Closing the device brings the two rings into opposition (Fig. 10). Further closure allows each set of pins to become seated in perforations on the opposite ring, and the vessels are coupled with lumen to lumen contact. The two halves of the device are then pinched with forceps to assure END-TO-END ANASTOMOSIS USING THE MICROANASTOMOTIC DEVICE The Microvascular Anastomotic COUPLER System (Synovis Micro Companies Alliance Inc., Birmingham, AL) can be used to perform end-toend anastomoses in cases where double-limbed bypass is utilized. This can provide a slightly higher flow than a standard single end-to-side distal anastomosis and can also be used on more proximal vessels if a large STA is present. 13,14 The donor artery and the recipient artery are prepared as previously described in the microanastomotic measuring devices used to choose the appropriate ring size. Two of the STA donor branches are mobilized, and instead of being spatulated at the end, they are cut at right angles. The first branch is prepared and loaded in the microanastomotic device. The artery is everted over the six-pin configuration to prepare it Figure 10 Illustration of the technique of end-to-end vessel anastomosis using the microanastomotic system. Each end of the vessel to be connected is loaded on the polyethelene ring and impaled on the six pins on each ring. The rings are then forced together and the pins of each ring insert into holes in the opposite ring and form a friction fit.
8 140 SKULL BASE: AN INTERDISCIPLINARY APPROACH/VOLUME 15, NUMBER Figure 11 Schematic of the construction of a double limbed STA-MCA bypass from two branches of the STA to a divided branch of the distal MCA. STA, superficial temporal artery; MCA, middle cerebral artery. Figure 12 Figure illustrating the course of a saphenous vein graft from the proximal STA (inferior) to a sylvian branch of the MCA (superior). STA, superficial temporal artery; MCA, middle cerebral artery. proper seating of the pins. Final tightening of the device forces a drive pin to release the vessels and polyethelene rings from the holder. The temporary vessel clips are then released and flow is re-established. This process is then repeated with the second limb of the STA and the other cut end of the MCA branch. The final construction is a two-limbed STA-to-MCA anastomosis providing both distal outflow and proximal inflow (Fig. 11). SHORT-VEIN BYPASS FROM STA TO MCA In patients where the distal STA is not adequate size to perform an anastomosis, it can be isolated proximally at the level of the tragus. The artery is usually 2.5 mm in diameter at this point, and a vein interposition graft can be used to perform an anastomosis at this location. The distal anastomosis is performed on an M3 or M2 branch in the sylvian fissure to allow a larger recipient artery for anastomosis. A reversed saphenous vein graph is harvested from the leg in the standard fashion, and the appropriate length is cut from the vein to course from the donor to the recipient artery. The distal anastomosis is performed at the recipient artery in the sylvian fissure using interrupted or running 9 0 sutures with a tapered needle. It is sometimes helpful to perform the recipient artery anastomosis first so the vein can be flipped from side-to-side to sew both sides of the anastomosis. A proximal anastomosis can be performed with an 8 0 or 7 0 suture. The donor and recipient arteries are both spatulated and running heel stitches are placed. Running suture technique is used to seal both limbs of the anastomosis (Fig. 12). CLOSURE OF THE CRANIOTOMY It is important when closing the craniotomy to rongeur an adequate portion of bone to prevent compression of the graft by the craniotomy flap. Prior to this step the dura is approximated loosely around the graft to prevent constriction. Following bone flap replacement, the temporalis muscle is reapproximated loosely to prevent any compression. The graft is inspected for kinking or compression during all phases of the closure. Warm saline solution is used to irrigate the graft and dilute papaverine is used to prevent spasm.
9 STA TO MCA BYPASS/NEWELL 141 POSTOPERATIVE CARE After surgery it is important to prevent compression of the graft site and also to insure adequate blood pressure. The patient s blood pressure is kept above 110 systolic to prevent graft occlusion. On the first postoperative day, patients are begun on aspirin 325 mg per day to inhibit platelet function. POTENTIAL PITFALLS AND COMPLICATIONS Complications and undesired results have been described following this procedure but most can be avoided with attention to technical details. Some of these unwanted outcomes include graft occlusion, subgaleal hematoma, scalp necrosis, and postoperative intracranial hemorrhage. It is important to have a technically perfect anastomosis with no damage during dissection of the donor or recipient artery to achieve short- and long-term patency of the graft. It is also equally important to avoid kinking or pressure by the bone edges from inadequate bone removal during closure to prevent graft compromise. If resistive flow is occurring during closure, certain maneuvers can be useful but they will not overcome the effect of a poor technical anastomosis. Maneuvers to salvage flow include maintenance of adequate blood pressure (above 110 mm Hg systolic), irrigation with warm, not cold, saline with dilute papaverine, and administration of 500 cc of dextran 40 to decrease platelet function. Prevention of scalp problems can be achieved by limited lateral dissection of the STA, adequate hemostasis, and postoperative subgaleal drain. Limited cortical dissection and preservation of veins is helpful to prevent intracranial hemorrhage. REFERENCES 1. Yasargil MG. A legacy of microneurosurgery: memoirs, lessons, and axioms. Neurosurgery 1999;45: de Weerd AW, Veldhuizen RJ, Veering MM, Poortvliet DC, Jonkman EJ. Long-term clinical and neurophysiological effects of reconstructive vascular surgery for cerebral ischemia. Acta Neurol Scand 1989;79: Diaz FG, Umansky F, Mehta B, et al. Cerebral revascularization to a main limb of the middle cerebral artery in the Sylvian fissure. An alternative approach to conventional anastomosis. J Neurosurg 1985;63: Gratzl O, Schmiedek P. STA-MCA bypass: results 10 years postoperatively. Neurol Res 1983;5: Spetzler RF. Retinal circulation after STA-MCA bypass. Neurosurgery 1985;16: Sundt TM Jr, Siekert RG, Piepgras DG, Sharbrough FW, Houser OW. Bypass surgery for vascular disease of the carotid system. Mayo Clin Proc 1976;51: [No authors listed.]failure of extracranial-intracranial arterial bypass to reduce the risk of ischemic stroke. Results of an international randomized trial. The EC/IC Bypass Study Group. N Engl J Med 1985;313: Srinivasan J, Britz GW, Newell DW. Cerebral revascularization for moyamoya disease in adults. Neurosurg Clin N Am 2001;12: ; ix 9. Onesti ST, Solomon RA, Quest DO. Cerebral revascularization: a review. Neurosurgery 1989;25: ; discussion Newell DW, Skirboll SL. Revascularization and bypass procedures for cerebral aneurysms. Neurosurg Clin N Am 1998;9: McCormick PW, Tomecek FJ, McKinney J, Ausman JI. Disabling cerebral transient ischemic attacks. J Neurosurg 1991;75: Grubb RL Jr. Extracranial-intracranial arterial bypass for treatment of occlusion of the internal carotid artery. Curr Neurol Neurosci Rep 2004;4: Newell DW, Dailey AT, Skirboll SL. Intracranial vascular anastomosis using the microanastomotic system. Technical note. J Neurosurg 1998;89: Newell DW, Schuster JM, Avellino AM. Intracranial-tointracranial vascular anastomosis created using a microanastomotic device for the treatment of distal middle cerebral artery aneurysms. Technical note. J Neurosurg 2002;97:
10
Intracranial-to-intracranial vascular anastomosis created using a microanastomotic device for the treatment of distal middle cerebral artery aneurysms
 J Neurosurg 97:486 491, 2002 Intracranial-to-intracranial vascular anastomosis created using a microanastomotic device for the treatment of distal middle cerebral artery aneurysms Technical note DAVID
J Neurosurg 97:486 491, 2002 Intracranial-to-intracranial vascular anastomosis created using a microanastomotic device for the treatment of distal middle cerebral artery aneurysms Technical note DAVID
Intracranial vascular anastomosis using the microanastomotic system
 J Neurosurg 89:676 681, 1998 Intracranial vascular anastomosis using the microanastomotic system Technical note DAVID W. NEWELL, M.D., ANDREW T. DAILEY, M.D., AND STEPHEN L. SKIRBOLL, M.D. Department of
J Neurosurg 89:676 681, 1998 Intracranial vascular anastomosis using the microanastomotic system Technical note DAVID W. NEWELL, M.D., ANDREW T. DAILEY, M.D., AND STEPHEN L. SKIRBOLL, M.D. Department of
Extracranial-to-Intracranial Bypass Using Radial Artery Grafting for Complex Skull Base Tumors: Technical Note
 Extracranial-to-Intracranial Bypass Using Radial Artery Grafting for Complex Skull Base Tumors: Technical Note Saleem I. Abdulrauf, M.D., F.A.C.S. 1 ABSTRACT The management of complex skull base tumors
Extracranial-to-Intracranial Bypass Using Radial Artery Grafting for Complex Skull Base Tumors: Technical Note Saleem I. Abdulrauf, M.D., F.A.C.S. 1 ABSTRACT The management of complex skull base tumors
History of revascularization
 History of revascularization Author (year) Kredel, 1942 Woringer& Kunlin, 1963 Donaghy& Yasargil, 1968 Loughheed 1971 Kikuchini & Karasawa1973 Karasawa, 1977 Story, 1978 Sundt, 1982 EC/IC bypass study
History of revascularization Author (year) Kredel, 1942 Woringer& Kunlin, 1963 Donaghy& Yasargil, 1968 Loughheed 1971 Kikuchini & Karasawa1973 Karasawa, 1977 Story, 1978 Sundt, 1982 EC/IC bypass study
5. COMMON APPROACHES. Each of the described approaches is also demonstrated on supplementary videos, please see Appendix 2.
 5. COMMON APPROACHES Each of the described approaches is also demonstrated on supplementary videos, please see Appendix 2. 5.1. LATERAL SUPRAORBITAL APPROACH The most common craniotomy approach used in
5. COMMON APPROACHES Each of the described approaches is also demonstrated on supplementary videos, please see Appendix 2. 5.1. LATERAL SUPRAORBITAL APPROACH The most common craniotomy approach used in
Anastomosis of the superficial temporal artery to the distal anterior cerebral artery with interposed cephalic vein graft
 J Neurosurg 58~25-429, 1983 Anastomosis of the superficial temporal artery to the distal anterior cerebral artery with interposed cephalic vein graft Case report RYOJI ISHII, M.D., TETSUO KOIKE, M.D.,
J Neurosurg 58~25-429, 1983 Anastomosis of the superficial temporal artery to the distal anterior cerebral artery with interposed cephalic vein graft Case report RYOJI ISHII, M.D., TETSUO KOIKE, M.D.,
Double STA-MCA Anatomosis for Bilateral Carotid Occlusion
 Double STA-MCA Anatomosis for Bilateral Carotid Occlusion -Case Report and Literature Review- Sandra vuignier 1, Kenji Kanamaru 2, Tomohiro Araki 2 1 Department of Neurosurgery, Nagoya University School
Double STA-MCA Anatomosis for Bilateral Carotid Occlusion -Case Report and Literature Review- Sandra vuignier 1, Kenji Kanamaru 2, Tomohiro Araki 2 1 Department of Neurosurgery, Nagoya University School
Saphenous Vein Autograft Replacement
 Saphenous Vein Autograft Replacement of Severe Segmental Coronary Artery Occlusion Operative Technique Rene G. Favaloro, M.D. D irect operation on the coronary artery has been performed in 180 patients
Saphenous Vein Autograft Replacement of Severe Segmental Coronary Artery Occlusion Operative Technique Rene G. Favaloro, M.D. D irect operation on the coronary artery has been performed in 180 patients
Cerebral revascularization: past, present and future
 Cerebral revascularization: past, present and future Tomás Funes 1 MD, Asis Lorente Muñoz 2 MD, Federico Fernández Molina 3 MD, Paula Ypa 3 MD, Francisco Mannara 4 MD, Luis González Martínez 2 MD, PhD
Cerebral revascularization: past, present and future Tomás Funes 1 MD, Asis Lorente Muñoz 2 MD, Federico Fernández Molina 3 MD, Paula Ypa 3 MD, Francisco Mannara 4 MD, Luis González Martínez 2 MD, PhD
Carotid Stenosis 1/24/2019. Review of Primary Studies. NASCET- Moderate stenosis. ACAS (Asymptomatic Carotid Atherosclerosis Study) NASCET
 Review of Primary Studies Carotid Stenosis NINDS National Institute of Neurological Disorders and Stroke 2 large studies to determine who would benefit from surgery NASCET North American Symptomatic Carotid
Review of Primary Studies Carotid Stenosis NINDS National Institute of Neurological Disorders and Stroke 2 large studies to determine who would benefit from surgery NASCET North American Symptomatic Carotid
CASE REPORT AIR VENT OF VEIN GRAFT IN EXTRACRANIAL-INTRACRANIAL BYPASS SURGERY
 Nagoya J. Med. Sci. 74. 339 ~ 345, 2012 CASE REPORT AIR VENT OF VEIN GRAFT IN EXTRACRANIAL-INTRACRANIAL BYPASS SURGERY HIROFUMI OYAMA, AKIRA KITO, HIDEKI MAKI, KENICHI HATTORI, TOMOYUKI NODA and KENTARO
Nagoya J. Med. Sci. 74. 339 ~ 345, 2012 CASE REPORT AIR VENT OF VEIN GRAFT IN EXTRACRANIAL-INTRACRANIAL BYPASS SURGERY HIROFUMI OYAMA, AKIRA KITO, HIDEKI MAKI, KENICHI HATTORI, TOMOYUKI NODA and KENTARO
Neurosurgical Techniques
 Neurosurgical Techniques EBEN ALEXANDER, JR., M.D., EDITOR Supratentorial Skull Flaps GuY L. ODOM, M.D., AND BARNES WOODHALL,!V[.D. Department of Surgery, Division of Neurosurgery, Duke University Medical
Neurosurgical Techniques EBEN ALEXANDER, JR., M.D., EDITOR Supratentorial Skull Flaps GuY L. ODOM, M.D., AND BARNES WOODHALL,!V[.D. Department of Surgery, Division of Neurosurgery, Duke University Medical
Neurosurg Focus 5 (5):Article 4, 1998
 Neurosurg Focus 5 (5):Article 4, 1998 Multiple combined indirect procedure for the surgical treatment of children with moyamoya disease. A comparison with single indirect anastomosis with direct anastomosis
Neurosurg Focus 5 (5):Article 4, 1998 Multiple combined indirect procedure for the surgical treatment of children with moyamoya disease. A comparison with single indirect anastomosis with direct anastomosis
Alt h o u g h once a commonly performed revascularization
 Neurosurg Focus 26 (5):E19, 2009 Operative nuances of an occipital artery to posterior inferior cerebellar artery bypass R. We b s t e r Cr o w l e y, M.D., 1 Ri c k y Me d e l, M.D., 1 a n d Aar o n S.
Neurosurg Focus 26 (5):E19, 2009 Operative nuances of an occipital artery to posterior inferior cerebellar artery bypass R. We b s t e r Cr o w l e y, M.D., 1 Ri c k y Me d e l, M.D., 1 a n d Aar o n S.
Quality Metrics. Stroke Related Procedure Outcomes
 Quality Metrics Stroke Related Procedure Outcomes Below is a description of some of the stroke-related procedures performed at St. Dominic Hospital in Jackson, with quality information on the complication
Quality Metrics Stroke Related Procedure Outcomes Below is a description of some of the stroke-related procedures performed at St. Dominic Hospital in Jackson, with quality information on the complication
We describe some of the conceptual nuances and
 Suprasellar Meningiomas Ivan Ciric, M.D., Sami Rosenblatt, M.D. Division of Neurosurgery, Evanston Northwestern Healthcare, Evanston Hospital, Northwestern University Medical School, Evanston, Illinois
Suprasellar Meningiomas Ivan Ciric, M.D., Sami Rosenblatt, M.D. Division of Neurosurgery, Evanston Northwestern Healthcare, Evanston Hospital, Northwestern University Medical School, Evanston, Illinois
Interpositional carotid artery bypass strategies in the surgical management of aneurysms and tumors of the skull base
 Neurosurg Focus 14 (3):Article 2, 2003, Click here to return to Table of Contents Interpositional carotid artery bypass strategies in the surgical management of aneurysms and tumors of the skull base JAMES
Neurosurg Focus 14 (3):Article 2, 2003, Click here to return to Table of Contents Interpositional carotid artery bypass strategies in the surgical management of aneurysms and tumors of the skull base JAMES
Introduction. BY W. R. HUDGINS, M.D.,* AND JULIO H. GARCIA, M.D.t. Abstract: ADDITIONAL KEY WORDS focal cerebral ischemia
 Transorbital Approach to the Middle Cerebral Artery of the Squirrel Monkey: A Technique for Experimental Cerebral Infarction Applicable to Ultrastructural Studies BY W. R. HUDGINS, M.D.,* AND JULIO H.
Transorbital Approach to the Middle Cerebral Artery of the Squirrel Monkey: A Technique for Experimental Cerebral Infarction Applicable to Ultrastructural Studies BY W. R. HUDGINS, M.D.,* AND JULIO H.
Surgical Options for revascularisation P E T E R S U B R A M A N I A M
 Surgical Options for revascularisation P E T E R S U B R A M A N I A M The goal Treat pain Heal ulcer Preserve limb Preserve life The options Conservative Endovascular Surgical bypass Primary amputation
Surgical Options for revascularisation P E T E R S U B R A M A N I A M The goal Treat pain Heal ulcer Preserve limb Preserve life The options Conservative Endovascular Surgical bypass Primary amputation
Surgery of Middle Cerebral Artery (MCA) Aneurysm
 Surgery of Middle Cerebral Artery (MCA) Aneurysm 15 Fusao Ikawa 15.1 Sign and Symptoms Middle cerebral artery (MCA) aneurysm is one of the most popular cerebral aneurysm. The incidence of ruptured MCA
Surgery of Middle Cerebral Artery (MCA) Aneurysm 15 Fusao Ikawa 15.1 Sign and Symptoms Middle cerebral artery (MCA) aneurysm is one of the most popular cerebral aneurysm. The incidence of ruptured MCA
INSTITUTE OF NEUROSURGERY & DEPARTMENT OF PICU
 CEREBRAL BYPASS An Innovative Treatment for Arteritis INSTITUTE OF NEUROSURGERY & DEPARTMENT OF PICU CASE 1 q 1 year old girl -recurrent seizure, right side limb weakness, excessive cry and irritability.
CEREBRAL BYPASS An Innovative Treatment for Arteritis INSTITUTE OF NEUROSURGERY & DEPARTMENT OF PICU CASE 1 q 1 year old girl -recurrent seizure, right side limb weakness, excessive cry and irritability.
Cerebral Bypass Surgery
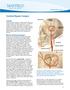 Cerebral Bypass Surgery Overview Cerebral bypass surgery is performed to restore, or revascularize, blood flow to the brain. A cerebral bypass is the brain's equivalent of a coronary bypass in the heart.
Cerebral Bypass Surgery Overview Cerebral bypass surgery is performed to restore, or revascularize, blood flow to the brain. A cerebral bypass is the brain's equivalent of a coronary bypass in the heart.
Extracranial to intracranial bypass for intracranial atherosclerosis
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Extracranial to intracranial bypass for intracranial atherosclerosis In cerebrovascular disease, blood vessels
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Extracranial to intracranial bypass for intracranial atherosclerosis In cerebrovascular disease, blood vessels
Moyamoya. Moyamoya Disease Double Trouble. Epidemiology 1/16/2015
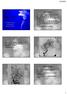 Moyamoya Moyamoya Disease Double Trouble Jan Boerke, ACNP AACN Brunch January 24, 2015 Moyamoya - puff of smoke in Japanese Describes the look of the tangle of tiny vessels formed to compensate for the
Moyamoya Moyamoya Disease Double Trouble Jan Boerke, ACNP AACN Brunch January 24, 2015 Moyamoya - puff of smoke in Japanese Describes the look of the tangle of tiny vessels formed to compensate for the
Ruptured Cerebral Aneurysm of the Anterior Circulation
 Original Articles * Division of Neurosurgery Department of Surgery Ruptured Cerebral Aneurysm of the Anterior Circulation Management and Microsurgical Treatment Ossama Al-Mefty, MD* ABSTRACT Based on the
Original Articles * Division of Neurosurgery Department of Surgery Ruptured Cerebral Aneurysm of the Anterior Circulation Management and Microsurgical Treatment Ossama Al-Mefty, MD* ABSTRACT Based on the
TABLES. Table 1 Terminal vessel aneurysms. Table. Aneurysm location. Bypass flow** Symptoms Strategy Bypass recipient. Age/ Sex.
 Table TABLES Table 1 Terminal vessel aneurysms Age/ Sex Aneurysm location Symptoms Strategy Bypass recipient Recipient territory Recipient territory flow* Cut flow Bypass flow** Graft Patent postop F/U
Table TABLES Table 1 Terminal vessel aneurysms Age/ Sex Aneurysm location Symptoms Strategy Bypass recipient Recipient territory Recipient territory flow* Cut flow Bypass flow** Graft Patent postop F/U
Surgical techniques and procedures for cerebrovascular surgery. Surgery for the AVF at the cranio-cervical junction and high cervical spine
 VS-1 Surgery for the AVF at the cranio-cervical junction and high cervical spine Hiroyuki Kinouchi University of Yamanashi, Department of Neurosurgery Dural AVFs have been recognized as common type of
VS-1 Surgery for the AVF at the cranio-cervical junction and high cervical spine Hiroyuki Kinouchi University of Yamanashi, Department of Neurosurgery Dural AVFs have been recognized as common type of
Abdominal Exam: The examination of the abdomen used by physicians to detect an abdominal aortic aneurysm.
 Glossary of Terms Abdominal Exam: The examination of the abdomen used by physicians to detect an abdominal aortic aneurysm. Angiogram: A diagnostic test requiring the insertion of a catheter into an artery
Glossary of Terms Abdominal Exam: The examination of the abdomen used by physicians to detect an abdominal aortic aneurysm. Angiogram: A diagnostic test requiring the insertion of a catheter into an artery
Anesthetic Management of Child with Moyamoya Disease for Pial Synangiosis
 Anesthetic Management of Child with Moyamoya Disease for Pial Synangiosis Craig D. McClain, MD, MPH Boston Children s Hospital and Harvard Medical School Case Presentation 14 year old male with bilateral
Anesthetic Management of Child with Moyamoya Disease for Pial Synangiosis Craig D. McClain, MD, MPH Boston Children s Hospital and Harvard Medical School Case Presentation 14 year old male with bilateral
Spasm of the extracranial internal carotid artery resulting from blunt trauma demonstrated by angiography
 Spasm of the extracranial internal carotid artery resulting from blunt trauma demonstrated by angiography Case report ELISHA S. GURDJIAN, M.D., BLAISE AUDET, M.D., RENATO W. SIBAYAN, M.D., AND LLYWELLYN
Spasm of the extracranial internal carotid artery resulting from blunt trauma demonstrated by angiography Case report ELISHA S. GURDJIAN, M.D., BLAISE AUDET, M.D., RENATO W. SIBAYAN, M.D., AND LLYWELLYN
Bypass to the Intracranial Giant or Large Internal Carotid Artery Aneurysms: Superficial Temporal Artery to Middle Cerebral Artery Bypass Re-visited
 Bypass to the Intracranial Giant or Large Internal Carotid Artery Aneurysms: Superficial Temporal Artery to Middle Cerebral Artery Bypass Re-visited Galip Zihni SANUfi 1 Ziya AKAR 2 Taner TANRIVERD 3 Banu
Bypass to the Intracranial Giant or Large Internal Carotid Artery Aneurysms: Superficial Temporal Artery to Middle Cerebral Artery Bypass Re-visited Galip Zihni SANUfi 1 Ziya AKAR 2 Taner TANRIVERD 3 Banu
RECONSTRUCTION OF SCALP DEFECTS: AN INSTITUTIONAL EXPERIENCE Sathyanarayana B. C 1, Somashekar Srinivas 2
 RECONSTRUCTION OF SCALP DEFECTS: AN INSTITUTIONAL EXPERIENCE Sathyanarayana B. C 1, Somashekar Srinivas 2 HOW TO CITE THIS ARTICLE: Sathyanarayana B. C, Somashekar Srinivas. Reconstruction of Scalp Defects:
RECONSTRUCTION OF SCALP DEFECTS: AN INSTITUTIONAL EXPERIENCE Sathyanarayana B. C 1, Somashekar Srinivas 2 HOW TO CITE THIS ARTICLE: Sathyanarayana B. C, Somashekar Srinivas. Reconstruction of Scalp Defects:
Transfemoral Amputation
 Transfemoral Amputation Pre-Op: 42 year old male who sustained severe injuries in a motorcycle accident. Note: he is a previous renal transplant recipient and is on immunosuppressive treatments. His injuries
Transfemoral Amputation Pre-Op: 42 year old male who sustained severe injuries in a motorcycle accident. Note: he is a previous renal transplant recipient and is on immunosuppressive treatments. His injuries
DISCHARGE DIAGNOSES: End stage renal disease secondary to rapidly progressive glomerulonephritis.
 DISCHARGE SUMMARY DISCHARGE DIAGNOSES: End stage renal disease secondary to rapidly progressive glomerulonephritis. OPERATIONS/PROCEDURES: Living related renal transplantation. HISTORY: For full details
DISCHARGE SUMMARY DISCHARGE DIAGNOSES: End stage renal disease secondary to rapidly progressive glomerulonephritis. OPERATIONS/PROCEDURES: Living related renal transplantation. HISTORY: For full details
1 Description. 2 Indications. 3 Warnings ASPIRATION CATHETER
 Page 1 of 5 ASPIRATION CATHETER Carefully read all instructions prior to use, observe all warnings and precautions noted throughout these instructions. Failure to do so may result in complications. STERILE.
Page 1 of 5 ASPIRATION CATHETER Carefully read all instructions prior to use, observe all warnings and precautions noted throughout these instructions. Failure to do so may result in complications. STERILE.
Extracranial-Intracranial Vascular Shunt Procedures
 Extracranial-Intracranial Vascular Shunt Procedures ROMAS SAKALAS, M.D. Assistant Professor, Division of Neurological Surgery, Medical College of Virginia, H ea/th Sciences Division of Virginia Commonwealth
Extracranial-Intracranial Vascular Shunt Procedures ROMAS SAKALAS, M.D. Assistant Professor, Division of Neurological Surgery, Medical College of Virginia, H ea/th Sciences Division of Virginia Commonwealth
Knee Disarticulation Amputation
 Knee Disarticulation Amputation Pre-Op 64 year old man, previous spinal cord injury, diabetes, renal failure, and a history of spasticity with dynamic knee flexion contracture. He had an open left ankle
Knee Disarticulation Amputation Pre-Op 64 year old man, previous spinal cord injury, diabetes, renal failure, and a history of spasticity with dynamic knee flexion contracture. He had an open left ankle
TREATMENT OF INTRACRANIAL ANEURYSMS
 TREATMENT OF INTRACRANIAL ANEURYSMS Presented by: Dr Nilesh S. Kurwale Introduction Incidence of aneurysm difficult to estimate Prevalence 0.2-7.9 % Half the aneurysms ruptures 2% present during childhood
TREATMENT OF INTRACRANIAL ANEURYSMS Presented by: Dr Nilesh S. Kurwale Introduction Incidence of aneurysm difficult to estimate Prevalence 0.2-7.9 % Half the aneurysms ruptures 2% present during childhood
Contralateral clipping of bilateral middle cerebral artery aneurysms. Case report
 Romanian Neurosurgery Volume XXXI Number 1 2017 January - March Article Contralateral clipping of bilateral middle cerebral artery aneurysms. Case report Georgiana Ion, Alexandru Chiriac, Ziyad Faiyad,
Romanian Neurosurgery Volume XXXI Number 1 2017 January - March Article Contralateral clipping of bilateral middle cerebral artery aneurysms. Case report Georgiana Ion, Alexandru Chiriac, Ziyad Faiyad,
PTA 106 Unit 1 Lecture 3
 PTA 106 Unit 1 Lecture 3 The Basics Arteries: Carry blood away from the heart toward tissues. They typically have thicker vessels walls to handle increased pressure. Contain internal and external elastic
PTA 106 Unit 1 Lecture 3 The Basics Arteries: Carry blood away from the heart toward tissues. They typically have thicker vessels walls to handle increased pressure. Contain internal and external elastic
Transfemoral Amputation
 Transfemoral Amputation Preop This 26 year old male sustained a gunshot wound to the left thigh. He was treated emergently with revascularization and fasciotomies. He was transferred to our regional trauma
Transfemoral Amputation Preop This 26 year old male sustained a gunshot wound to the left thigh. He was treated emergently with revascularization and fasciotomies. He was transferred to our regional trauma
Talent Abdominal Stent Graft
 Talent Abdominal with THE Xcelerant Hydro Delivery System Expanding the Indications for EVAR Treat More Patients Short Necks The Talent Abdominal is the only FDA-approved device for proximal aortic neck
Talent Abdominal with THE Xcelerant Hydro Delivery System Expanding the Indications for EVAR Treat More Patients Short Necks The Talent Abdominal is the only FDA-approved device for proximal aortic neck
Protokollanhang zur SPACE-2-Studie Neurology Quality Standards
 Protokollanhang zur SPACE-2-Studie Neurology Quality Standards 1. General remarks In contrast to SPACE-1, the neurological center participating in the SPACE-2 trial will also be involved in the treatment
Protokollanhang zur SPACE-2-Studie Neurology Quality Standards 1. General remarks In contrast to SPACE-1, the neurological center participating in the SPACE-2 trial will also be involved in the treatment
Overview Blood supply of the brain What is moyamoya disease? > 1
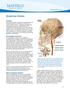 Moyamoya Disease Overview Moyamoya disease is caused by blocked arteries at the base of the brain. The name "moyamoya" means "puff of smoke" in Japanese and describes the appearance of tiny vessels that
Moyamoya Disease Overview Moyamoya disease is caused by blocked arteries at the base of the brain. The name "moyamoya" means "puff of smoke" in Japanese and describes the appearance of tiny vessels that
FIG The inferior and posterior peritoneal reflection is easily
 PSOAS HITCH, BOARI FLAP, AND COMBINATION OF PSOAS 7 HITCH AND BOARI FLAP The psoas hitch procedure, Boari flap, and transureteroureterostomy are useful operative procedures for reestablishing continuity
PSOAS HITCH, BOARI FLAP, AND COMBINATION OF PSOAS 7 HITCH AND BOARI FLAP The psoas hitch procedure, Boari flap, and transureteroureterostomy are useful operative procedures for reestablishing continuity
Vascular Surgery Rotation Objectives for Junior Residents (PGY-1 and 2)
 Vascular Surgery Rotation Objectives for Junior Residents (PGY-1 and 2) Definition Vascular surgery is the specialty concerned with the diagnosis and management of congenital and acquired diseases of the
Vascular Surgery Rotation Objectives for Junior Residents (PGY-1 and 2) Definition Vascular surgery is the specialty concerned with the diagnosis and management of congenital and acquired diseases of the
Diagnosis of Middle Cerebral Artery Occlusion with Transcranial Color-Coded Real-Time Sonography
 Diagnosis of Middle Cerebral Artery Occlusion with Transcranial Color-Coded Real-Time Sonography Kazumi Kimura, Yoichiro Hashimoto, Teruyuki Hirano, Makoto Uchino, and Masayuki Ando PURPOSE: To determine
Diagnosis of Middle Cerebral Artery Occlusion with Transcranial Color-Coded Real-Time Sonography Kazumi Kimura, Yoichiro Hashimoto, Teruyuki Hirano, Makoto Uchino, and Masayuki Ando PURPOSE: To determine
Anatomy of the Middle Cerebral Artery: The Temporal Branches
 Anatomy of the Middle Cerebral Artery: The Temporal Branches BY W. BRADFORD DeLONG, M.D., F.A.C.S. Abstract: Anatomy of the Middle Cerebral Artery: The Temporal Branches Nineteen out of 23 middle cerebral
Anatomy of the Middle Cerebral Artery: The Temporal Branches BY W. BRADFORD DeLONG, M.D., F.A.C.S. Abstract: Anatomy of the Middle Cerebral Artery: The Temporal Branches Nineteen out of 23 middle cerebral
5.5. RETROSIGMOID APPROACH
 5.5. RETROSIGMOID APPROACH The retrosigmoid approach provides good access to the cerebellopontine angle. It is by far simpler and faster with much less need for bone removal than other more extensive lateral
5.5. RETROSIGMOID APPROACH The retrosigmoid approach provides good access to the cerebellopontine angle. It is by far simpler and faster with much less need for bone removal than other more extensive lateral
Carotid Endarterectomy for Symptomatic Complete Occlusion of the Internal Carotid Artery
 2011 65 4 239 245 Carotid Endarterectomy for Symptomatic Complete Occlusion of the Internal Carotid Artery a* a b a a a b 240 65 4 2011 241 9 1 60 10 2 62 17 3 67 2 4 64 7 5 69 5 6 71 1 7 55 13 8 73 1
2011 65 4 239 245 Carotid Endarterectomy for Symptomatic Complete Occlusion of the Internal Carotid Artery a* a b a a a b 240 65 4 2011 241 9 1 60 10 2 62 17 3 67 2 4 64 7 5 69 5 6 71 1 7 55 13 8 73 1
ANASTAMOSIS FOR BRAIN STEM ISCHEMIA/Khodadad et al.
 ANASTAMOSIS FOR BRAIN STEM ISCHEMIA/Khodadad et al. visualization of the posterior inferior cerebellar artery. The patient, now 11 months post-operative, has shown further neurological improvement since
ANASTAMOSIS FOR BRAIN STEM ISCHEMIA/Khodadad et al. visualization of the posterior inferior cerebellar artery. The patient, now 11 months post-operative, has shown further neurological improvement since
How to manage the left subclavian and left vertebral artery during TEVAR
 How to manage the left subclavian and left vertebral artery during TEVAR Jürg Schmidli Chief of Vascular Surgery Inselspital Hamburg 2017 Dept Cardiovascular Surgery, Bern, Switzerland Disclosure No Disclosures
How to manage the left subclavian and left vertebral artery during TEVAR Jürg Schmidli Chief of Vascular Surgery Inselspital Hamburg 2017 Dept Cardiovascular Surgery, Bern, Switzerland Disclosure No Disclosures
Alessandro Della Puppa
 Intraoperative measurement of arterial blood flow in complex cerebral aneurysms surgery Studio flussimetrico intra-operatorio nel clipping degli aneurismi complessi Alessandro Della Puppa NEUROSURGERY
Intraoperative measurement of arterial blood flow in complex cerebral aneurysms surgery Studio flussimetrico intra-operatorio nel clipping degli aneurismi complessi Alessandro Della Puppa NEUROSURGERY
Combat Extremity Vascular Trauma
 Combat Extremity Vascular Trauma Training teams to be a TEAM Chatt A. Johnson LTC, MC, USA 08 March 2010 US Army Trauma Training Center Core Discussion Series Outline: Combat Vascular Injury Physiologic
Combat Extremity Vascular Trauma Training teams to be a TEAM Chatt A. Johnson LTC, MC, USA 08 March 2010 US Army Trauma Training Center Core Discussion Series Outline: Combat Vascular Injury Physiologic
Anterior Communicating Artery Aneurysms. Surgical approaches Review
 Anterior Communicating Artery Aneurysms. Surgical approaches Review Hirotoshi Sano Dept. of Neurosurgery Fujita Health University Introduction There are two main types of approaches for anterior communicating
Anterior Communicating Artery Aneurysms. Surgical approaches Review Hirotoshi Sano Dept. of Neurosurgery Fujita Health University Introduction There are two main types of approaches for anterior communicating
Moyamoya Syndrome with contra lateral DACA aneurysm: First Case report with review of literature
 Romanian Neurosurgery Volume XXXI Number 3 2017 July-September Article Moyamoya Syndrome with contra lateral DACA aneurysm: First Case report with review of literature Ashish Kumar Dwivedi, Pradeep Kumar,
Romanian Neurosurgery Volume XXXI Number 3 2017 July-September Article Moyamoya Syndrome with contra lateral DACA aneurysm: First Case report with review of literature Ashish Kumar Dwivedi, Pradeep Kumar,
Usefulness of Coil-assisted Technique in Treating Wide-neck Intracranial Aneurysms: Neck-bridge Procedure Using the Coil Mass as a Support
 Journal of Neuroendovascular Therapy 2017; 11: 220 225 Online December 14, 2016 DOI: 10.5797/jnet.tn.2016-0081 Usefulness of Coil-assisted Technique in Treating Wide-neck Intracranial Aneurysms: Neck-bridge
Journal of Neuroendovascular Therapy 2017; 11: 220 225 Online December 14, 2016 DOI: 10.5797/jnet.tn.2016-0081 Usefulness of Coil-assisted Technique in Treating Wide-neck Intracranial Aneurysms: Neck-bridge
Case Report 1. CTA head. (c) Tele3D Advantage, LLC
 Case Report 1 CTA head 1 History 82 YEAR OLD woman with signs and symptoms of increased intra cranial pressure in setting of SAH. CT Brain was performed followed by CT Angiography of head. 2 CT brain Extensive
Case Report 1 CTA head 1 History 82 YEAR OLD woman with signs and symptoms of increased intra cranial pressure in setting of SAH. CT Brain was performed followed by CT Angiography of head. 2 CT brain Extensive
Vivek R. Deshmukh, MD Director, Cerebrovascular and Endovascular Neurosurgery Chairman, Department of Neurosurgery Providence Brain and Spine
 Vivek R. Deshmukh, MD Director, Cerebrovascular and Endovascular Neurosurgery Chairman, Department of Neurosurgery Providence Brain and Spine Institute The Oregon Clinic Disclosure I declare that neither
Vivek R. Deshmukh, MD Director, Cerebrovascular and Endovascular Neurosurgery Chairman, Department of Neurosurgery Providence Brain and Spine Institute The Oregon Clinic Disclosure I declare that neither
Open fenestration for complicated acute aortic B dissection
 Art of Operative Techniques Open fenestration for complicated acute aortic B dissection Santi Trimarchi 1, Sara Segreti 1, Viviana Grassi 1, Chiara Lomazzi 1, Marta Cova 1, Gabriele Piffaretti 2, Vincenzo
Art of Operative Techniques Open fenestration for complicated acute aortic B dissection Santi Trimarchi 1, Sara Segreti 1, Viviana Grassi 1, Chiara Lomazzi 1, Marta Cova 1, Gabriele Piffaretti 2, Vincenzo
NIDCD NATIONAL TEMPORAL BONE, HEARING AND BALANCE PATHOLOGY RESOURCE REGISTRY
 NIDCD NATIONAL TEMPORAL BONE, HEARING AND BALANCE PATHOLOGY RESOURCE REGISTRY Guidelines for Removal of Temporal Bones for Pathological Study The temporal bones should be removed as soon as possible. If
NIDCD NATIONAL TEMPORAL BONE, HEARING AND BALANCE PATHOLOGY RESOURCE REGISTRY Guidelines for Removal of Temporal Bones for Pathological Study The temporal bones should be removed as soon as possible. If
Malperfusion Syndromes Type B Aortic Dissection with Malperfusion
 Malperfusion Syndromes Type B Aortic Dissection with Malperfusion Jade S. Hiramoto, MD, MAS April 27, 2012 Associated with early mortality Occurs when there is end organ ischemia secondary to aortic branch
Malperfusion Syndromes Type B Aortic Dissection with Malperfusion Jade S. Hiramoto, MD, MAS April 27, 2012 Associated with early mortality Occurs when there is end organ ischemia secondary to aortic branch
010050,Inner Mongolia, China
 Possible factors influencing postoperative temporary neurologic deterioration following standard superficial temporal artery-middle cerebral artery (STA-MCA) bypass surgery: diameter of STA and MCA (M4)
Possible factors influencing postoperative temporary neurologic deterioration following standard superficial temporal artery-middle cerebral artery (STA-MCA) bypass surgery: diameter of STA and MCA (M4)
Emergency EC-IC bypass for symptomatic atherosclerotic ischemic stroke
 Emergency EC-IC bypass for symptomatic atherosclerotic ischemic stroke Tetsuyoshi Horiuchi, Junpei Nitta, Shigetoshi Ishizaka, Kohei Kanaya, Takao Yanagawa, and Kazuhiro Hongo. Department of Neurosurgery,
Emergency EC-IC bypass for symptomatic atherosclerotic ischemic stroke Tetsuyoshi Horiuchi, Junpei Nitta, Shigetoshi Ishizaka, Kohei Kanaya, Takao Yanagawa, and Kazuhiro Hongo. Department of Neurosurgery,
Saphenous vein bypass grafts for giant aneurysms and intracranial occlusive disease
 J Neurosurg 65:439-450, 1986 Saphenous vein bypass grafts for giant aneurysms and intracranial occlusive disease THORALF M. SUNDT, JR., M.D., DAVID G. PIEPGRAS, M.D., W. RICHARD MARSH, M.D., AND NICOLEE
J Neurosurg 65:439-450, 1986 Saphenous vein bypass grafts for giant aneurysms and intracranial occlusive disease THORALF M. SUNDT, JR., M.D., DAVID G. PIEPGRAS, M.D., W. RICHARD MARSH, M.D., AND NICOLEE
Zenith Renu AAA Converter Graft. Device Description Planning and Sizing Deployment Sequence Patient Follow-Up
 Zenith Renu AAA Converter Graft Device Description Planning and Sizing Deployment Sequence Patient Follow-Up Device description: Device indications The Zenith Renu AAA Converter Graft with Z-Trak Introduction
Zenith Renu AAA Converter Graft Device Description Planning and Sizing Deployment Sequence Patient Follow-Up Device description: Device indications The Zenith Renu AAA Converter Graft with Z-Trak Introduction
Absorbable Woven Polyglycolic Acid Mesh Tube (Absorbable Nerve Conduit Tube) INSTRUCTIONS FOR USE 2 6
 Absorbable Woven Polyglycolic Acid Mesh Tube (Absorbable Nerve Conduit Tube) INSTRUCTIONS FOR USE 2 6 1 0086 SYMBOL DEFINITIONS ENGLISH Do not Reuse Consult Instructions For Use Ethylene Oxide Sterilized
Absorbable Woven Polyglycolic Acid Mesh Tube (Absorbable Nerve Conduit Tube) INSTRUCTIONS FOR USE 2 6 1 0086 SYMBOL DEFINITIONS ENGLISH Do not Reuse Consult Instructions For Use Ethylene Oxide Sterilized
BP and Heart Rate by Telemetry
 BP and Heart Rate by Telemetry Version: 1 Modified from: Butz et al. Physiol Genomics. 2001 Mar 8;5(2):89-97. Edited by: Dr. Lynette Bower, UC Davis Summary Reagents and Materials Protocol Reagent Preparation
BP and Heart Rate by Telemetry Version: 1 Modified from: Butz et al. Physiol Genomics. 2001 Mar 8;5(2):89-97. Edited by: Dr. Lynette Bower, UC Davis Summary Reagents and Materials Protocol Reagent Preparation
Superficial temporal artery to middle cerebral artery anastomosis. Intraoperative evaluation by fluorescein angiography and xenon-133 clearance
 J Neurosurg 50:560-569, 1979 Superficial temporal artery to middle cerebral artery anastomosis Intraoperative evaluation by fluorescein angiography and xenon-133 clearance John R. Little, M.D., F.R.C.S.(C),
J Neurosurg 50:560-569, 1979 Superficial temporal artery to middle cerebral artery anastomosis Intraoperative evaluation by fluorescein angiography and xenon-133 clearance John R. Little, M.D., F.R.C.S.(C),
Since the introduction of extracranial-intracranial (ECIC)
 ORIGINAL RESEARCH A. Nakamizo T. Inoue Y. Kikkawa K. Uda Y. Hirata K. Okamura M. Yasaka Y. Okada Postoperative Evaluation of Changes in Extracranial-Intracranial Bypass Graft Using Superficial Temporal
ORIGINAL RESEARCH A. Nakamizo T. Inoue Y. Kikkawa K. Uda Y. Hirata K. Okamura M. Yasaka Y. Okada Postoperative Evaluation of Changes in Extracranial-Intracranial Bypass Graft Using Superficial Temporal
This quiz is being published on behalf of the Education Committee of the SNACC.
 Quiz 48 Cerebrovascular Atherosclerotic Disease Shobana Rajan, M.D. Associate Director of Neuroanesthesia, Vice Chair of Education, Allegheny Health Network. Quiz team; Suneeta Gollapudy M.D, Angele Marie
Quiz 48 Cerebrovascular Atherosclerotic Disease Shobana Rajan, M.D. Associate Director of Neuroanesthesia, Vice Chair of Education, Allegheny Health Network. Quiz team; Suneeta Gollapudy M.D, Angele Marie
Reconstruction of the vein of Labbé by using a short saphenous vein bypass graft
 J Neurosurg 89:671 675, 1998 Reconstruction of the vein of Labbé by using a short saphenous vein bypass graft Technical note AKIO MORITA, M.D., AND LALIGAM N. SEKHAR, M.D. Department of Neurosurgery, The
J Neurosurg 89:671 675, 1998 Reconstruction of the vein of Labbé by using a short saphenous vein bypass graft Technical note AKIO MORITA, M.D., AND LALIGAM N. SEKHAR, M.D. Department of Neurosurgery, The
Management of Acute Aortic Syndromes. M. Grabenwoger, MD Dept. of Cardiovascular Surgery Hospital Hietzing, Vienna, Austria
 Management of Acute Aortic Syndromes M. Grabenwoger, MD Dept. of Cardiovascular Surgery Hospital Hietzing, Vienna, Austria I have nothing to disclose. Acute Aortic Syndromes Acute Aortic Dissection Type
Management of Acute Aortic Syndromes M. Grabenwoger, MD Dept. of Cardiovascular Surgery Hospital Hietzing, Vienna, Austria I have nothing to disclose. Acute Aortic Syndromes Acute Aortic Dissection Type
A STUDY OF TEMPORAL BRANCHES OF MIDDLE CEREBRAL ARTERY
 J. Anat. Sciences, 23(2) : Dec. 2015, 15-21 Original Article A STUDY OF TEMPORAL BRANCHES OF MIDDLE CEREBRAL ARTERY Medha Das*, Shirin Jahan*, Pranjal Pankaj** * Department of Anatomy, Rama Medical College,
J. Anat. Sciences, 23(2) : Dec. 2015, 15-21 Original Article A STUDY OF TEMPORAL BRANCHES OF MIDDLE CEREBRAL ARTERY Medha Das*, Shirin Jahan*, Pranjal Pankaj** * Department of Anatomy, Rama Medical College,
Tikrit University College of Dentistry Dr.Ban I.S. head & neck anatomy 2 nd y.
 Lec [3]/The scalp The scalp extends from the supraorbital margins anteriorly to the nuchal lines at the back of the skull and down to the temporal lines at the sides. The forehead, from eyebrows to hairline,
Lec [3]/The scalp The scalp extends from the supraorbital margins anteriorly to the nuchal lines at the back of the skull and down to the temporal lines at the sides. The forehead, from eyebrows to hairline,
Carotid Distal Vertebral Bypass for Carotid Occlusion: Case Report and Technique`
 CLINICAL ELECTROENCEPHALOGRAPHV 1978.VOL. 9,N0.3 Carotid Distal Vertebral Bypass for Carotid Occlusion: Case Report and Technique` Andrew L. Carney and Evelyn M. Anderson Occlusion of the internal carotid
CLINICAL ELECTROENCEPHALOGRAPHV 1978.VOL. 9,N0.3 Carotid Distal Vertebral Bypass for Carotid Occlusion: Case Report and Technique` Andrew L. Carney and Evelyn M. Anderson Occlusion of the internal carotid
Exposure of the anterior tibial artery by medial popliteal extension
 Exposure of the anterior tibial artery by medial popliteal extension J. G. Sladen, FRCS(C), G. Kougeer, FRCS(C), and J. D. S. Reid, FRCS(C), Vancouver) British Columbia) Canada This report describes exploration
Exposure of the anterior tibial artery by medial popliteal extension J. G. Sladen, FRCS(C), G. Kougeer, FRCS(C), and J. D. S. Reid, FRCS(C), Vancouver) British Columbia) Canada This report describes exploration
CAROTID ARTERY ANGIOPLASTY
 CAROTID ARTERY ANGIOPLASTY Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Medical Coverage Guideline
CAROTID ARTERY ANGIOPLASTY Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Medical Coverage Guideline
The pericardial sac is composed of the outer fibrous pericardium
 Pericardiectomy for Constrictive or Recurrent Inflammatory Pericarditis Mauricio A. Villavicencio, MD, Joseph A. Dearani, MD, and Thoralf M. Sundt, III, MD Anatomy and Preoperative Considerations The pericardial
Pericardiectomy for Constrictive or Recurrent Inflammatory Pericarditis Mauricio A. Villavicencio, MD, Joseph A. Dearani, MD, and Thoralf M. Sundt, III, MD Anatomy and Preoperative Considerations The pericardial
(FIG.1) Landmarks of the external ear in dogs. (FIG.2) Anatomy of the ear.
 SURGICAL ANATOMY of Ear (FIG.1) Landmarks of the external ear in dogs. (FIG.2) Anatomy of the ear. An aural (auricular) hematoma is a collection of blood within the cartilage plate of the ear. Suture placement
SURGICAL ANATOMY of Ear (FIG.1) Landmarks of the external ear in dogs. (FIG.2) Anatomy of the ear. An aural (auricular) hematoma is a collection of blood within the cartilage plate of the ear. Suture placement
Training in Micro-Vascular Anastomosis Using Rat Femoral Vessels: Comparison of Immediate and Delayed Patency Rates
 DOI: 10.5137/1019-5149.JTN.18423-16.1 Received: 12.06.2016 / Accepted: 21.08.2016 Published Online: 17.10.2016 Original Investigation Training in Micro-Vascular Anastomosis Using Rat Femoral Vessels: Comparison
DOI: 10.5137/1019-5149.JTN.18423-16.1 Received: 12.06.2016 / Accepted: 21.08.2016 Published Online: 17.10.2016 Original Investigation Training in Micro-Vascular Anastomosis Using Rat Femoral Vessels: Comparison
Introduction. Risk factors of PVD 5/8/2017
 PATHOPHYSIOLOGY AND CLINICAL FEATURES OF PERIPHERAL VASCULAR DISEASE Dr. Muhamad Zabidi Ahmad Radiologist and Section Chief, Radiology, Oncology and Nuclear Medicine Section, Advanced Medical and Dental
PATHOPHYSIOLOGY AND CLINICAL FEATURES OF PERIPHERAL VASCULAR DISEASE Dr. Muhamad Zabidi Ahmad Radiologist and Section Chief, Radiology, Oncology and Nuclear Medicine Section, Advanced Medical and Dental
Peripheral Extracranial Neurostimulation for the treatment of Primary Headache and Migraine:
 Chapter 19 Peripheral Extracranial Neurostimulation for the treatment of Primary Headache and Migraine: Introduction 1) The occipital nerve is involved in pain syndromes originating from nerve trauma,
Chapter 19 Peripheral Extracranial Neurostimulation for the treatment of Primary Headache and Migraine: Introduction 1) The occipital nerve is involved in pain syndromes originating from nerve trauma,
TRANS-SULCAL MICROSURGICAL APPROACH TO INTRACEREBRAL LESIONS
 Trakia Journal of Sciences, No 3, pp 277-282, 2014 Copyright 2014 Trakia University Available online at: http://www.uni-sz.bg ISSN 1313-7050 (print) doi:10.15547/tjs.2014.03.009 ISSN 1313-3551 (online)
Trakia Journal of Sciences, No 3, pp 277-282, 2014 Copyright 2014 Trakia University Available online at: http://www.uni-sz.bg ISSN 1313-7050 (print) doi:10.15547/tjs.2014.03.009 ISSN 1313-3551 (online)
Corporate Medical Policy
 Corporate Medical Policy Endovascular Therapies for Extracranial Vertebral Artery Disease File Name: Origination: Last CAP Review: Next CAP Review: Last Review: endovascular_therapies_for_extracranial_vertebral_artery_disease
Corporate Medical Policy Endovascular Therapies for Extracranial Vertebral Artery Disease File Name: Origination: Last CAP Review: Next CAP Review: Last Review: endovascular_therapies_for_extracranial_vertebral_artery_disease
System.
 System www.penumbrainc.com POD System Case Examples 45 cm of POD Packing Coil in 1.5 to 3 mm diameter dilating vessel Bronchial Artery Embolization Dr. Amit Kakkar and Dr. Aksim Rivera, Bronx, NY Inflow:
System www.penumbrainc.com POD System Case Examples 45 cm of POD Packing Coil in 1.5 to 3 mm diameter dilating vessel Bronchial Artery Embolization Dr. Amit Kakkar and Dr. Aksim Rivera, Bronx, NY Inflow:
Arterial Occlusion Following Anastomosis of the Superficial Temporal Artery to Middle Cerebral Artery
 Arterial Occlusion Following Anastomosis of the Superficial Temporal Artery to Middle Cerebral Artery 91 ANTHONY J. FURLAN, M.D., JOHN R. LITTLE, M.D., AND DONALD F. DOHN, M.D. SUMMARY Symptoms of cerebral
Arterial Occlusion Following Anastomosis of the Superficial Temporal Artery to Middle Cerebral Artery 91 ANTHONY J. FURLAN, M.D., JOHN R. LITTLE, M.D., AND DONALD F. DOHN, M.D. SUMMARY Symptoms of cerebral
T HERE is an unusual and interesting variety of craniosynostosis in
 SURGICAL TREATMENT OF CONGENITAL ANOMALIES OF THE CORONAL AND METOPIC SUTURES TECHNICAL NOTE DONALD D. MATSON, M.D. Neurosurgical Service, The Children's Medical Center, and Deparlment of Surgery, Itarvard
SURGICAL TREATMENT OF CONGENITAL ANOMALIES OF THE CORONAL AND METOPIC SUTURES TECHNICAL NOTE DONALD D. MATSON, M.D. Neurosurgical Service, The Children's Medical Center, and Deparlment of Surgery, Itarvard
Direct Bypass Techniques for the Treatment of Pediatric Moyamoya Disease
 Direct Bypass Techniques for the Treatment of Pediatric Moyamoya Disease Raphael Guzman, MD a, Gary K. Steinberg, MD, PhD b, * KEYWORDS Moyamoya disease Pediatric Direct bypass INDICATIONS Moyamoya disease
Direct Bypass Techniques for the Treatment of Pediatric Moyamoya Disease Raphael Guzman, MD a, Gary K. Steinberg, MD, PhD b, * KEYWORDS Moyamoya disease Pediatric Direct bypass INDICATIONS Moyamoya disease
Neurological Complications of TEVAR. Frank J Criado, MD. Union Memorial-MedStar Health Baltimore, MD USA
 ISES Online Neurological Complications of Frank J Criado, MD TEVAR Union Memorial-MedStar Health Baltimore, MD USA frank.criado@medstar.net Paraplegia Incidence is 0-4% after surgical Rx of TAAs confined
ISES Online Neurological Complications of Frank J Criado, MD TEVAR Union Memorial-MedStar Health Baltimore, MD USA frank.criado@medstar.net Paraplegia Incidence is 0-4% after surgical Rx of TAAs confined
R ECENTLY, we reported a combined series of extracranial
 J Neurosurg 70:207-211, 1989 Complications of intracranial bypass for vertebrobasilar insufficiency LEO N. HOPKINS, M.D., AND JAMES L. BUDNY, M.D. Department of Neurosurgery, State University of New York
J Neurosurg 70:207-211, 1989 Complications of intracranial bypass for vertebrobasilar insufficiency LEO N. HOPKINS, M.D., AND JAMES L. BUDNY, M.D. Department of Neurosurgery, State University of New York
The Synovis GEM COUPLER
 The Synovis GEM COUPLER e Synovis product portfolio includes Coupler, Flow Coupler and GeM MicroClip. ese products are used for joining small diameter vessels during autologous tissue breast reconstruction;
The Synovis GEM COUPLER e Synovis product portfolio includes Coupler, Flow Coupler and GeM MicroClip. ese products are used for joining small diameter vessels during autologous tissue breast reconstruction;
Surgical anatomy of the juxta dural ring area
 J Neurosurg 89:250 254, 1998 Surgical anatomy of the juxta dural ring area SUSUMU OIKAWA, M.D., KAZUHIKO KYOSHIMA, M.D., AND SHIGEAKI KOBAYASHI, M.D. Department of Neurosurgery, Shinshu University School
J Neurosurg 89:250 254, 1998 Surgical anatomy of the juxta dural ring area SUSUMU OIKAWA, M.D., KAZUHIKO KYOSHIMA, M.D., AND SHIGEAKI KOBAYASHI, M.D. Department of Neurosurgery, Shinshu University School
Surgical treatment and perioperative management of intracranial aneurysms in Chinese patients with ischemic cerebrovascular diseases: a case series
 Zheng and Wu BMC Neurology (2018) 18:142 https://doi.org/10.1186/s12883-018-1147-8 RESEARCH ARTICLE Open Access Surgical treatment and perioperative management of intracranial aneurysms in Chinese patients
Zheng and Wu BMC Neurology (2018) 18:142 https://doi.org/10.1186/s12883-018-1147-8 RESEARCH ARTICLE Open Access Surgical treatment and perioperative management of intracranial aneurysms in Chinese patients
Case 37 Clinical Presentation
 Case 37 73 Clinical Presentation The patient is a 62-year-old woman with gastrointestinal (GI) bleeding. 74 RadCases Interventional Radiology Imaging Findings () Image from a selective digital subtraction
Case 37 73 Clinical Presentation The patient is a 62-year-old woman with gastrointestinal (GI) bleeding. 74 RadCases Interventional Radiology Imaging Findings () Image from a selective digital subtraction
Parenchyma-sparing lung resections are a potential therapeutic
 Lung Segmentectomy for Patients with Peripheral T1 Lesions Bryan A. Whitson, MD, Rafael S. Andrade, MD, and Michael A. Maddaus, MD Parenchyma-sparing lung resections are a potential therapeutic option
Lung Segmentectomy for Patients with Peripheral T1 Lesions Bryan A. Whitson, MD, Rafael S. Andrade, MD, and Michael A. Maddaus, MD Parenchyma-sparing lung resections are a potential therapeutic option
Heart may be rotated but not compressed
 Tips And Techniques For Multivessel OPCAB John D. Puskas, MD, Emory University, Atlanta AATS Adult Cardiac Skills April 28, 2012 San Francisco, CA Beating Heart Surgery vs Beat The Heart Surgery OPCAB
Tips And Techniques For Multivessel OPCAB John D. Puskas, MD, Emory University, Atlanta AATS Adult Cardiac Skills April 28, 2012 San Francisco, CA Beating Heart Surgery vs Beat The Heart Surgery OPCAB
Minimally Invasive Esophagectomy
 American Association of Thoracic Surgery (AATS) 95 th Annual Meeting Seattle, WA April 29, 2015 General Thoracic Masters of Surgery Video Session Minimally Invasive Esophagectomy James D. Luketich MD,
American Association of Thoracic Surgery (AATS) 95 th Annual Meeting Seattle, WA April 29, 2015 General Thoracic Masters of Surgery Video Session Minimally Invasive Esophagectomy James D. Luketich MD,
