Chronic Swelling, Pain, and Ulceration in the Left Lower Extremity
|
|
|
- Lucy Rodgers
- 6 years ago
- Views:
Transcription
1 WHAT WOULD YOU DO? Chronic Swelling, Pain, and Ulceration in the Left Lower Extremity MODERATOR: BROOKE SPENCER, MD, FSIR PANEL: LAWRENCE RUSTY HOFMANN, MD; MARK J. GARCIA, MD, FSIR, FACR; AND BRENT T. STEADMAN, MD, PhD CASE PRESENTATION A 54-year-old man with a history of traumatic brain injury in 1981 from a motor vehicle accident developed extensive left lower extremity deep vein thrombosis () and was anticoagulated for a short period of time following his accident. Seven years ago, he underwent ablation of the great saphenous vein (GSV) to treat chronic swelling and pain in the left lower extremity, and he developed a nonhealing wound, which has progressed over time. He also has significant weight gain from decreased activity and is treated in a wound care center and compliant with daily compression. His leg weeps fluid daily. He is mentally disabled from the head injury and needs constant care but is ambulatory and active despite his frontal lobe damage. Medical history also includes seizures and a ventriculoperitoneal shunt. Medications include lamotrigine, donepezil, furosemide, lovastatin, topiramate, baby aspirin, and vitamins. He has been on and off antibiotics. Physical examination shows 2+ edema and excoriation in the left lower extremity and ulcerated skin with erythema over a large area of the medial malleolus calf. There are 2+ dorsalis pedis and posterior tibial pulses. The left ankle, calf, and thigh are 4 to 5 cm larger than the right (Figure 1). What imaging would you obtain to evaluate this patient, and what questions are you trying to answer with this imaging? Dr. Garcia: I would start with venous Doppler imaging of the leg to assess the extent of the, the occlusive Figure 1. Photograph of the patient s leg. nature, and whether it extends below the popliteal to help determine the site of entry (popliteal vs posterior tibial/anterior tibial), as well as status of the ablated GSV. The final goal is to reestablish unimpeded, direct in-line flow from the ankle to the right atrium. If the common femoral vein (CFV) is involved or has poor waveform or 94 ENDOVASCULAR TODAY AUGUST 2017 VOL. 16, NO. 8
2 CHALLENGING CASES if there are pelvic or abdominal wall superficial varicosities on examination, then I would perform CT venography (CTV) to evaluate the central (including the inferior vena cava [IVC]) venous system. I have found that nonhealing venous wounds are often accompanied by central venous issues. Dr. Hofmann: I would request a CTV from the diaphragm to the toes to get a comprehensive view of his deep and superficial system, in particular the status of his iliac veins and IVC. Dr. Steadman: I would obtain a CTV of the pelvis and lower extremities followed by insufficiency duplex ultrasound. The pelvic CTV assesses for venous outflow obstruction, including left iliac vein and/or IVC scarring as well as May-Thurner compression of the left common iliac vein (CIV). I would then obtain a lower extremity CTV to map out enlarged superficial truncal veins and/ or perforators that supply the varicosities in the lower extremity, particularly in and around the ulceration site. I also look for chronic scarring in the deep veins. This information is relayed to the vascular technician to guide their assessment for pathologic reflux and deep venous scarring. I use this imaging combination in patients with venous ulcers, patients with prior superficial venous intervention, and history of with significant postthrombotic syndrome (PTS). Left lower extremity ultrasound for and superficial reflux study demonstrate changes of chronic in the left calf, the popliteal and femoral veins, and CFV. The vessels are patent and recanalized. The GSV is patent and refluxing for > 3 seconds (Figures 2 5). CTV of the pelvis (protocol was not followed, so noncontrast CT was obtained) shows that the veins were mildly misshapen but fairly normal in caliber. There is subtle calcification centrally in the external iliac vein (EIV) and CFV (Figure 6). Figure 2. Ultrasound image of the proximal femoral vein and profunda femorus demonstrating scarring. Figure 4. Ultrasound image of the GSV in the thigh showing reflux. Figure 3. Ultrasound image of the distal femoral vein showing a web. Figure 5. Ultrasound image of the GSV in the calf showing > 3 seconds of reflux and enlargement. What would you do next? Would you have a sequential plan, and if so, what order would you consider for planned interventions? Would the patient s impulsive cognitive deficits play a role in influencing this decision? Dr. Steadman: I would first perform a venography to assess the chronic scarring in the deep venous system with plans to perform angioplasty and stent anything in the iliac veins down to the lesser trochanter. Prolonged angioplasty would be performed from the lesser trochanter Figure 6. CTV image of the EIV showing subtle internal calcification but good caliber. down to the popliteal vein and possibly the tibioperoneal and upper posterior tibial veins. The venogram is also beneficial to determine if the GSV is a significant collateral venous drainage pathway, especially considering VOL. 16, NO. 8 AUGUST 2017 ENDOVASCULAR TODAY 97
3 the ulcer formed after prior GSV ablation. If the GSV is not a significant collateral pathway, then I would ablate it coupled with foam sclerotherapy. I would use general anesthesia for the venography, which I use for almost all patients, and conscious sedation for the endovenous laser treatment and foam sclerotherapy given the patient s cognitive deficits. Ideally, if the ultrasound shows a large, accessible posterior tibial vein, then I will perform all procedures supine in one sitting using general anesthesia. While the patient is still under anesthesia, I will aggressively debride the ulcer, followed by appropriate wound dressing as well as compression wrap or an Unna boot. If the ulcer is particularly exudative and/or possibly infected, then I would place a wound vacuum after culture. The patient would then be admitted to internal medicine for antibiotics and wound vacuum treatment. Dr. Hofmann: I would call the radiologist to ask why the CTV protocol wasn t followed and ensure it didn t occur with another patient. Given the calcification in the EIV, I am highly suspicious the patient will need iliac vein stenting. Depending on the caudal extent of disease, I would puncture either the posterior tibial vein, the short saphenous vein, or the popliteal vein and perform venography. If I didn t obtain a high-quality CTV, I would also likely use intravascular ultrasound (IVUS). Given this patient s cognitive deficits, I would do this while the patient is under general anesthesia. Dr. Garcia: Although the CT is without contrast, the calcification is suggestive of disease. I would attempt to perform a CTV to better assess anatomy, as I like to know as much as possible before intervening. Nonetheless, after the CTV, the plan would be to obtain a venogram with the intent of treating at that time. Based on the venous Doppler image, I would place the patient in the prone position, access the posterior tibial vein and get a full leg venography, with the popliteal fossa prepped for IVUS use. Despite the patient s injury and resultant deficits, I think that it is possible to improve his quality of life while allowing his wounds to heal, prevent the ulcers from recurring, limit the progression of his chronic venous disease, and even allow the patient to become more active. My initial office evaluation would include a thorough discussion with the patient and his family as to the risks and benefits of the procedure and ensure their complete understanding of the bleeding risks. Because his injury is so remote, I would not have any issue using the ACCESS PTS protocol of low-dose tissue plasminogen activator and Ekos therapy (Ekos Corporation, a BTG International group company) if needed. Figure 7. Prestent femoral venogram. Figure 8. Prestent pelvic venogram. The venogram of the leg shows webs in the femoral vein and narrowing of the popliteal vein, with collateral filling of the profunda femorus vein (Figure 7). The venogram of the pelvis shows misshapen but patent iliac veins with mild lucency of the CIV and mild reflux into the internal iliac vein (Figure 8). What would you do next? Dr. Garcia: On therapeutic enoxaparin, I would dilate from the posterior tibial vein through the iliacs (with secondary access at the popliteal vein) with appropriate-sized balloons to break the webs/ synechiae and perform IVUS from the popliteal vein through the iliac vein to determine residual luminal abnormalities (webs/synechiae), if iliofemoral stenting is needed, and if so, the exact location and sizes. I measure both the vein diameter as well as area, both pre- and postintervention. Once treatment is completed, I repeat the full leg venography and look at flow how brisk it is and the time for contrast washout. I find that the comparison of the initial to postwashout time is very indicative of how the patient will do and potential long-term vessel patency. Dr. Steadman: I would perform prolonged angioplasty from the CIV to the popliteal vein. The CIV angioplasty would likely identify a suspected May-Thurner compression, which would be stented. Angioplasty would also identify the significant stenosis or stenoses that are causing collateral filling of the profunda femoral vein. If 98 ENDOVASCULAR TODAY AUGUST 2017 VOL. 16, NO. 8
4 Figure 9. IVUS showing a web in the CFV/EIV junction. Figure 10. IVUS showing a misshapen EIV. Figure 11. IVUS compression of the EIV/CIV junction as it passes between the internal and external iliac arteries. Figure 12. IVUS with web in the CIV. stenoses were questionable and/or flow did not improve after angioplasty, I would use IVUS to identify stenotic areas and/or regions of significant webbing to target with additional angioplasty or stenting. Dr. Hofmann: I would also plan on venoplasty of the popliteal and femoral vein and stent the iliac veins. It is hard to tell based on the images, but if needed, I would stent down to the level of the lesser trochanter to ensure robust in-line flow. IVUS shows webs and bands of synechiae throughout the CIV, EIV, and proximal CFV above the GSV. The vein is large in external caliber (16 mm except in an area of 50% narrowing). Segments of the vein are tented and misshapen (Figures 9 12). Approach of the Moderator My philosophy and approach to these patients is consistent. Ulcers usually have a deep venous obstruction of some nature. Obesity and congestive heart failure can be a form of physiologic obstruction. I believe that chronic should be addressed first with recanalization before treatment of the superficial system. This is a case in point of a patient whose GSV was ablated and he worsened. It is difficult to get superficial reflux severe enough to overwhelm the deep system to the point of ulceration in a patient with a patent deep venous system. Therefore, I obtain a ultrasound, including longitudinal grayscale images of the vein, and a CTV on all ulcer patients. I performed a left lower extremity venography with prolonged balloon angioplasty of the common femoral, femoral, and popliteal veins. This requires angioplasty for 3 to 5 minutes with high-pressure balloons and, therefore, general anesthesia, which would have been necessary in any event in this patient. Given the calcifications in the pelvis seen on CTV, this patient also needs evaluation with IVUS. Once deformity, webs, and narrowing are identified, stenting is indicated, especially in ulcer patients. I choose to stent to match the vein size and not oversize, as tenting of the vein distally causes spasm and turbulent flow. The entire webbed segment needs to be stented, so in this patient, this means from CIV to CFV. Following such an intervention, what would your anticoagulation/clinical management regimen be? Dr. Hofmann: I would anticoagulate with enoxaparin 1 mg/kg twice daily for a minimum of 1 month, preferably 3 to 6 months, with a goal peak (4 hours after dose) anti- Xa level of 0.7 to 1 IU/mL. I would then transition to an oral anti-xa agent with the same therapeutic goal. Dr. Garcia: Everyone is started on weight-based (twice daily) enoxaparin the day prior to the procedure, and this is continued for 1 month postprocedure. Patients are seen in the office at 1 month with follow-up venous Doppler, and then they are transitioned to oral anticoagulation (novel anticoagulants). I use enoxaparin because I believe it is the best anticoagulant with anti-inflammatory properties that give the best result. All patients are discharged with my ABC rules: activity, blood thinner, and compression. Dr. Steadman: I would use enoxaparin with bridging to one of the newer oral anticoagulants for at least 6 months. Patients return to the clinic for duplex ultrasound at 1, 3, and 6 months to assess for ulcer, leg swelling resolution, and deep vein patency. The final result is improved flow in the femoral and popliteal veins and widely patent stents in the pelvis with a few areas of subtle lack of complete wall apposition (Figures 13 and 14). The patient is placed 100 ENDOVASCULAR TODAY AUGUST 2017 VOL. 16, NO. 8
5 tibial veins, then I would ablate the GSV if significant reflux is still demonstrated. Dr. Hofmann: Given that this was initially a provoked (motor vehicle accident in 1981), if at 1 year he had no open wounds and a CTV showed widely patent stents with good in-flow, I would consider trying to reduce his anticoagulation dosage from a therapeutic dose to a prophylactic dose. Then, I may consider taking him off all anticoagulation, except for a daily 81 mg of aspirin. CASE SUMMARY The patient is scheduled for ablation of the saphenous vein and foam sclerotherapy to be performed while on anticoagulation. n Figure 13. Poststent pelvic venogram showing initial stenting of the CIV with a 16-mm Wallstent (Boston Scientific Corporation). Figure 14. Second poststent venogram showing an overlapping 16-mm Wallstent. on enoxaparin 1 mg/kg subcutaneously twice daily for 1 month, aspirin 81 mg, and compression is applied. He is seen in clinic at 3 weeks with follow-up ultrasound and clinical evaluation. He has experienced resolution of pain and significant interval healing of wounds. His mother reports only one episode of weeping from wounds. The patient has lost 23 lb due to a combination of edema reduction and ability to return to a rigorous gym routine. There is still significant edema in the calf, but it is softer. Deep veins are patent, and saphenous reflux and numerous varices around the wound persist. What would you do next? Dr. Steadman: If the ulcer has healed with no residual symptoms at 6 months, I would discharge the patient from the clinic with strict instructions to return to my clinic for recurrent ulcer, leg pain, or swelling. In this case, I recommend aspirin 81 mg for life. If a patient meets criteria for life-long anticoagulation, I will recommend anticoagulation continuation. Dr. Garcia: His residual calf swelling could be a result of either reflux (deep, superficial, or both), chronic venous changes, or both. I have become an advocate for posterior tibial access, as I have found the best results for complete lower extremity improvement (to ankle) are when the popliteal and tibials are treated as well. If in 3 to 6 months the signs and symptoms persist after treating the popliteal and Brooke Spencer, MD, FSIR Medical Director RIA Endovascular Center Greenwood Village, Colorado ebsrad@gmail.com Disclosures: Site Principal Investigator on Veniti and Cook Medical stent trials and Veclose, Inc. ablation trial; consultant for Philips Volcano, Boston Scientific Corporation, and Cook Medical. Lawrence Rusty Hofmann, MD Professor and Chief, Interventional Radiology Stanford University Medical Center Stanford, California lhofmann@stanfordhealthcare.org Disclosures: Consultant and royalties from Cook Medical; shareholder in Confluent Medical. Mark J. Garcia, MD, FSIR, FACR President & Medical Director Vascular & Interventional Associates of Delaware, EndoVascular Consultants Wilmington, Delaware mjgarcia59@icloud.com Disclosures: Research support and speaker for BTG International; Principal Investigator for the ACCESS PTS trial. Brent T. Steadman, MD, PhD Assistant Professor Department of Radiology West Virginia University School of Medicine Morgantown, West Virginia brent.steadman@gmail.com Disclosures: None. 102 ENDOVASCULAR TODAY AUGUST 2017 VOL. 16, NO. 8
Chronic Iliocaval Venous Occlusive Disease
 none Chronic Iliocaval Venous Occlusive Disease David Rigberg, M.D. Clinical Professor of Surgery Division of Vascular Surgery University of California Los Angeles Chronic Venous Occlusive Disease Chronic
none Chronic Iliocaval Venous Occlusive Disease David Rigberg, M.D. Clinical Professor of Surgery Division of Vascular Surgery University of California Los Angeles Chronic Venous Occlusive Disease Chronic
Treatment of Chronic DVT with EKOS: Reproducing ACCESS PTS Data in Every Day Clinical Practice
 Treatment of Chronic DVT with EKOS: Reproducing ACCESS PTS Data in Every Day Clinical Practice Mert Dumantepe, MD Acibadem Altunizade Hospital, Istanbul, Turkey Department of Cardiovascular Surgery Disclosure
Treatment of Chronic DVT with EKOS: Reproducing ACCESS PTS Data in Every Day Clinical Practice Mert Dumantepe, MD Acibadem Altunizade Hospital, Istanbul, Turkey Department of Cardiovascular Surgery Disclosure
2017 Florida Vascular Society
 Current Management of Venous Leg Ulcers: How to Identify Patients with Correctable Venous Disease and Interventional Procedures to Heal and Prevent Recurrence 2017 Florida Vascular Society Bill Marston
Current Management of Venous Leg Ulcers: How to Identify Patients with Correctable Venous Disease and Interventional Procedures to Heal and Prevent Recurrence 2017 Florida Vascular Society Bill Marston
Complete Evaluation of the Chronic Venous Patient: Recognizing deep venous obstruction. Erin H. Murphy, MD Rane Center
 Complete Evaluation of the Chronic Venous Patient: Recognizing deep venous obstruction Erin H. Murphy, MD Rane Center Disclosure Speaker name: Erin H. Murphy... I have the following potential conflicts
Complete Evaluation of the Chronic Venous Patient: Recognizing deep venous obstruction Erin H. Murphy, MD Rane Center Disclosure Speaker name: Erin H. Murphy... I have the following potential conflicts
Complex Iliocaval Reconstruction PNEC. Seattle WA. Bill Marston MD Professor, Div of Vascular Surgery University of N.
 Complex Iliocaval Reconstruction 2017 PNEC. Seattle WA Bill Marston MD Professor, Div of Vascular Surgery University of N. Carolina DISCLOSURES William Marston, MD Consultant/Advisory Board: Veniti, Cardinal
Complex Iliocaval Reconstruction 2017 PNEC. Seattle WA Bill Marston MD Professor, Div of Vascular Surgery University of N. Carolina DISCLOSURES William Marston, MD Consultant/Advisory Board: Veniti, Cardinal
Starting with deep venous treatment
 Starting with deep venous treatment Carsten Arnoldussen, MD Interventional Radiologist Maastricht University Medical Centre, Maastricht VieCuri Medical Centre, Venlo The Netherlands Background Maastricht
Starting with deep venous treatment Carsten Arnoldussen, MD Interventional Radiologist Maastricht University Medical Centre, Maastricht VieCuri Medical Centre, Venlo The Netherlands Background Maastricht
Duplex ultrasound is first-line imaging for all
 Our Protocol for Transabdominal Pelvic Vein Duplex Ultrasound A summary of s protocol for pelvic vein duplex ultrasonography, including equipment, patient positioning, ultrasound settings, and technique.
Our Protocol for Transabdominal Pelvic Vein Duplex Ultrasound A summary of s protocol for pelvic vein duplex ultrasonography, including equipment, patient positioning, ultrasound settings, and technique.
How to best approach chronic venous occlusions?
 How to best approach chronic venous occlusions? Prof. Nils Kucher Director Venous Thromboembolism Reseach Group University Hospital Bern nilskucher.com Disclosure Speaker name: Nils Kucher X X I have the
How to best approach chronic venous occlusions? Prof. Nils Kucher Director Venous Thromboembolism Reseach Group University Hospital Bern nilskucher.com Disclosure Speaker name: Nils Kucher X X I have the
Image-Guided Approach to Treatment of Patients with Nonthrombotic
 Image-Guided Approach to Treatment of Patients with Nonthrombotic May Thurner Syndrome Brian DeRubertis, MD, FACS Associate Professor of Surgery Division of Vascular Surgery UCLA School of Medicine Los
Image-Guided Approach to Treatment of Patients with Nonthrombotic May Thurner Syndrome Brian DeRubertis, MD, FACS Associate Professor of Surgery Division of Vascular Surgery UCLA School of Medicine Los
Segmental GSV reflux
 Segmental GSV reflux History of presentation A 43 year old female presented with right lower extremity varicose veins and swelling. She had symptoms of aching, heaviness and tiredness in the right leg.
Segmental GSV reflux History of presentation A 43 year old female presented with right lower extremity varicose veins and swelling. She had symptoms of aching, heaviness and tiredness in the right leg.
Clinical/Duplex Evaluation of Varicose Veins: Who to Treat?
 Clinical/Duplex Evaluation of Varicose Veins: Who to Treat? Sanjoy Kundu MD, FASA, FCIRSE, FSIR The Vein Institute of Toronto Scarborough Vascular Group Scarborough Vascular Ultrasound Scarborough Vascular
Clinical/Duplex Evaluation of Varicose Veins: Who to Treat? Sanjoy Kundu MD, FASA, FCIRSE, FSIR The Vein Institute of Toronto Scarborough Vascular Group Scarborough Vascular Ultrasound Scarborough Vascular
Selection and work up for the right patients suspected of deep venous disease
 Selection and work up for the right patients suspected of deep venous disease R A G H U K O L L U R I, M S, M D, R V T S Y S T E M M E D I C A L D I R E C T O R V A S C U L A R M E D I C I N E / V A S
Selection and work up for the right patients suspected of deep venous disease R A G H U K O L L U R I, M S, M D, R V T S Y S T E M M E D I C A L D I R E C T O R V A S C U L A R M E D I C I N E / V A S
On Which Criteria Do You Select Your Stent for Ilio-femoral Venous Obstruction? North American Point of View
 On Which Criteria Do You Select Your Stent for Ilio-femoral Venous Obstruction? North American Point of View Peter Gloviczki, MD Ying Huang, MD, PhD Division of Vascular and Endovascular Surgery, Mayo
On Which Criteria Do You Select Your Stent for Ilio-femoral Venous Obstruction? North American Point of View Peter Gloviczki, MD Ying Huang, MD, PhD Division of Vascular and Endovascular Surgery, Mayo
Patient assessment and strategy making for endovenous treatment
 Patient assessment and strategy making for endovenous treatment Raghu Kolluri, MD Director Vascular Medicine OhioHealth Riverside Methodist Hospital Columbus, OH Disclosures Current Medtronic Consultant/
Patient assessment and strategy making for endovenous treatment Raghu Kolluri, MD Director Vascular Medicine OhioHealth Riverside Methodist Hospital Columbus, OH Disclosures Current Medtronic Consultant/
Management of an Unusual Iliac Fossa Venous Plexus
 Management of an Unusual Iliac Fossa Venous Plexus Irwin M Best, Emory University Journal Title: Case Reports in Vascular Medicine Volume: Volume 2011, Number 2011 Publisher: 2011-11-22, Pages 1-4 Type
Management of an Unusual Iliac Fossa Venous Plexus Irwin M Best, Emory University Journal Title: Case Reports in Vascular Medicine Volume: Volume 2011, Number 2011 Publisher: 2011-11-22, Pages 1-4 Type
IVUS is strongly recommanded before treating a venous femoro-iliac obstruction CONS. F Thony CHU Grenoble
 IVUS is strongly recommanded before treating a venous femoro-iliac obstruction CONS F Thony CHU Grenoble Disclosure Speaker name: Frédéric THONY I do not have any potential conflict of interest Introduction
IVUS is strongly recommanded before treating a venous femoro-iliac obstruction CONS F Thony CHU Grenoble Disclosure Speaker name: Frédéric THONY I do not have any potential conflict of interest Introduction
VIVO-EU Results: Prospective European Study of the Zilver Vena TM Venous Stent in the Treatment of Symptomatic Iliofemoral Venous Outflow Obstruction
 VIVO-EU Results: Prospective European Study of the Zilver Vena TM Venous Stent in the Treatment of Symptomatic Iliofemoral Venous Outflow Obstruction Gerard J O Sullivan, M.D. and Jennifer McCann-Brown,
VIVO-EU Results: Prospective European Study of the Zilver Vena TM Venous Stent in the Treatment of Symptomatic Iliofemoral Venous Outflow Obstruction Gerard J O Sullivan, M.D. and Jennifer McCann-Brown,
As with any intervention, selection of an appropriate
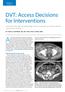 DVT: ccess Decisions for Interventions ssessing the advantages and disadvantages of venous access options is crucial for safe and successful DVT intervention. Y JOHN. KUFMN, MD, MS, FSIR, FH, FCIRSE, EIR
DVT: ccess Decisions for Interventions ssessing the advantages and disadvantages of venous access options is crucial for safe and successful DVT intervention. Y JOHN. KUFMN, MD, MS, FSIR, FH, FCIRSE, EIR
VIRTUS: Trial Design and Primary Endpoint Results
 VIRTUS: Trial Design and Primary Endpoint Results Mahmood K. Razavi, MD St. Joseph Cardiac and Vascular Center Orange, CA, USA IMPORTANT INFORMATION: These materials are intended to describe common clinical
VIRTUS: Trial Design and Primary Endpoint Results Mahmood K. Razavi, MD St. Joseph Cardiac and Vascular Center Orange, CA, USA IMPORTANT INFORMATION: These materials are intended to describe common clinical
Understanding of the importance of venous
 The Critical Need for an Iliofemoral Venous Obstruction Classification System An overview of a potential classification system to better identify and treat iliofemoral venous outflow obstruction. BY WILLIAM
The Critical Need for an Iliofemoral Venous Obstruction Classification System An overview of a potential classification system to better identify and treat iliofemoral venous outflow obstruction. BY WILLIAM
Chronic Venous Insufficiency
 Chronic Venous Insufficiency None Disclosures Lesley Enfinger, MSN,NP-C Chronic Venous Insufficiency Over 24 Million Americans affected by Chronic Venous Insufficiency (CVI) 10 x More Americans suffer
Chronic Venous Insufficiency None Disclosures Lesley Enfinger, MSN,NP-C Chronic Venous Insufficiency Over 24 Million Americans affected by Chronic Venous Insufficiency (CVI) 10 x More Americans suffer
BC Vascular Day. Contents. November 3, Abdominal Aortic Aneurysm 2 3. Peripheral Arterial Disease 4 6. Deep Venous Thrombosis 7 8
 BC Vascular Day Contents Abdominal Aortic Aneurysm 2 3 November 3, 2018 Peripheral Arterial Disease 4 6 Deep Venous Thrombosis 7 8 Abdominal Aortic Aneurysm Conservative Management Risk factor modification
BC Vascular Day Contents Abdominal Aortic Aneurysm 2 3 November 3, 2018 Peripheral Arterial Disease 4 6 Deep Venous Thrombosis 7 8 Abdominal Aortic Aneurysm Conservative Management Risk factor modification
The role of ultrasound duplex in endovenous procedures
 The role of ultrasound duplex in endovenous procedures Neophytos A. Zambas MD, PhD Vascular Surgeon Polyclinic Ygia, Limassol, Cyprus ΚΕΑΕΧ ΚΥΠΡΙΑΚΗ ΕΤΑΙΡΕΙΑ ΑΓΓΕΙΑΚΗΣ ΚΑΙ ΕΝΔΑΓΓΕΙΑΚΗΣ ΧΕΙΡΟΥΡΓΙΚΗΣ Pre
The role of ultrasound duplex in endovenous procedures Neophytos A. Zambas MD, PhD Vascular Surgeon Polyclinic Ygia, Limassol, Cyprus ΚΕΑΕΧ ΚΥΠΡΙΑΚΗ ΕΤΑΙΡΕΙΑ ΑΓΓΕΙΑΚΗΣ ΚΑΙ ΕΝΔΑΓΓΕΙΑΚΗΣ ΧΕΙΡΟΥΡΓΙΚΗΣ Pre
Deep Venous Intervention Techniques
 Deep Venous Intervention Techniques FEATURED TECHNOLOGY: INTRAVASCULAR ULTRASOUND IMAGING A panel of venous experts shares insights on referrals, imaging, and stenting. PARTICIPANTS William Marston, MD,
Deep Venous Intervention Techniques FEATURED TECHNOLOGY: INTRAVASCULAR ULTRASOUND IMAGING A panel of venous experts shares insights on referrals, imaging, and stenting. PARTICIPANTS William Marston, MD,
Complications of endovascular treatment of May-Thurner syndrome George Geroulakos
 Complications of endovascular treatment of May-Thurner syndrome George Geroulakos Professor of Vascular Surgery, National and Kapodistrian University of Athens Director, Department of Vascular Surgery,
Complications of endovascular treatment of May-Thurner syndrome George Geroulakos Professor of Vascular Surgery, National and Kapodistrian University of Athens Director, Department of Vascular Surgery,
Guidelines, Policies and Statements D20 Statement on Peripheral Venous Ultrasound
 Guidelines, Policies and Statements D20 Statement on Peripheral Venous Ultrasound Disclaimer and Copyright The ASUM Standards of Practice Board have made every effort to ensure that this Guideline/Policy/Statement
Guidelines, Policies and Statements D20 Statement on Peripheral Venous Ultrasound Disclaimer and Copyright The ASUM Standards of Practice Board have made every effort to ensure that this Guideline/Policy/Statement
Emerging Tools for Lytic-Free, Single-Session Treatment of Venous Thromboembolic Disease
 FEATURED TECHNOLOGY THE CLOTTRIEVER AND FLOWTRIEVER SYSTEMS Emerging Tools for Lytic-Free, Single-Session Treatment of Venous Thromboembolic Disease The ClotTriever Outcomes (CLOUT) registry principal
FEATURED TECHNOLOGY THE CLOTTRIEVER AND FLOWTRIEVER SYSTEMS Emerging Tools for Lytic-Free, Single-Session Treatment of Venous Thromboembolic Disease The ClotTriever Outcomes (CLOUT) registry principal
Chronic Venous Insufficiency Compression and Beyond
 Disclosure of Conflict of Interest Chronic Venous Insufficiency Compression and Beyond Shawn Amyot, MD, CCFP Fellow of the Canadian Society of Phlebology Ottawa Vein Centre I do not have relevant financial
Disclosure of Conflict of Interest Chronic Venous Insufficiency Compression and Beyond Shawn Amyot, MD, CCFP Fellow of the Canadian Society of Phlebology Ottawa Vein Centre I do not have relevant financial
Imaging, it s central role in planning and guiding intervention. Prof. Luis Izquierdo. MD, PhD, FEBVS
 Imaging, it s central role in planning and guiding intervention Prof. Luis Izquierdo. MD, PhD, FEBVS IMPORTANT INFORMATION: These materials are intended to describe common clinical considerations and procedural
Imaging, it s central role in planning and guiding intervention Prof. Luis Izquierdo. MD, PhD, FEBVS IMPORTANT INFORMATION: These materials are intended to describe common clinical considerations and procedural
Peripheral Arterial Disease: A Practical Approach
 Peripheral Arterial Disease: A Practical Approach Sanjoy Kundu BSc, MD, FRCPC, DABR, FASA, FCIRSE, FSIR The Scarborough Hospital Toronto Endovascular Centre The Vein Institute of Toronto Scarborough Vascular
Peripheral Arterial Disease: A Practical Approach Sanjoy Kundu BSc, MD, FRCPC, DABR, FASA, FCIRSE, FSIR The Scarborough Hospital Toronto Endovascular Centre The Vein Institute of Toronto Scarborough Vascular
Venous stent experience in Arnsberg Michael K. W. Lichtenberg MD, FESC
 Venous stent experience in Arnsberg Michael K. W. Lichtenberg MD, FESC IMPORTANT INFORMATION: These materials are intended to describe common clinical considerations and procedural steps for the on-label
Venous stent experience in Arnsberg Michael K. W. Lichtenberg MD, FESC IMPORTANT INFORMATION: These materials are intended to describe common clinical considerations and procedural steps for the on-label
Peripheral Vascular Examination. Dr. Gary Mumaugh Western Physical Assessment
 Peripheral Vascular Examination Dr. Gary Mumaugh Western Physical Assessment Competencies 1. Inspection of upper extremity for: size symmetry swelling venous pattern color Texture nail beds Competencies
Peripheral Vascular Examination Dr. Gary Mumaugh Western Physical Assessment Competencies 1. Inspection of upper extremity for: size symmetry swelling venous pattern color Texture nail beds Competencies
Page 1. Ruling out deep venous obstruction prior to superficial vein treatment. Disclosures. Indications for saphenous vein ablation (SVA)
 1 Ruling out deep venous obstruction prior to superficial vein treatment Deepak Sudheendra, MD, RPVI Assistant Professor of Clinical Radiology & Surgery Disclosures No financial disclosures Indications
1 Ruling out deep venous obstruction prior to superficial vein treatment Deepak Sudheendra, MD, RPVI Assistant Professor of Clinical Radiology & Surgery Disclosures No financial disclosures Indications
Venous stenting in Marseille
 Venous stenting in Marseille Olivier HARTUNG, MD, MSc CHU Nord, Marseille, FRANCE Disclosure Speaker name: Olivier HARTUNG I have the following potential conflicts of interest to report: x Consulting :
Venous stenting in Marseille Olivier HARTUNG, MD, MSc CHU Nord, Marseille, FRANCE Disclosure Speaker name: Olivier HARTUNG I have the following potential conflicts of interest to report: x Consulting :
Post-thrombotic syndrome (PTS), often the
 Revascularization of Chronic Venous Occlusion in the Setting of Post-Thrombotic Syndrome Jon George, MD; Deepakraj Gajanana; Sean Janzer; Vincent Figueredo; Dennis Morris From the Einstein Heart and Vascular
Revascularization of Chronic Venous Occlusion in the Setting of Post-Thrombotic Syndrome Jon George, MD; Deepakraj Gajanana; Sean Janzer; Vincent Figueredo; Dennis Morris From the Einstein Heart and Vascular
Vein Disease Treatment
 MP9241 Covered Service: Yes when meets criteria below Prior Authorization Required: Yes as indicated in 2.0, 3.0, 4.0 and 5.0 Additional Information: None Prevea360 Health Plan Medical Policy: Vein disease
MP9241 Covered Service: Yes when meets criteria below Prior Authorization Required: Yes as indicated in 2.0, 3.0, 4.0 and 5.0 Additional Information: None Prevea360 Health Plan Medical Policy: Vein disease
STRUCTURED EDUCATION REQUIREMENTS IMPLEMENTATION DATE: JULY 1, 2016
 STRUCTURED EDUCATION REQUIREMENTS Vascular Sonography The purpose of structured education is to provide the opportunity for individuals to develop mastery of discipline-specific knowledge that, when coupled
STRUCTURED EDUCATION REQUIREMENTS Vascular Sonography The purpose of structured education is to provide the opportunity for individuals to develop mastery of discipline-specific knowledge that, when coupled
Case Study of Implantation of a VICI VENOUS STENT - Combined NIVL and PTS Stenting
 Case Study of Implantation of a VICI VENOUS STENT - Combined NIVL and PTS Stenting Courtesy of Mr. Stephen Black United kingdom Patient History 25 y/o female 2011: Conservatively treated ilio-femoral DVT
Case Study of Implantation of a VICI VENOUS STENT - Combined NIVL and PTS Stenting Courtesy of Mr. Stephen Black United kingdom Patient History 25 y/o female 2011: Conservatively treated ilio-femoral DVT
Lower Extremity Venous Insufficiency Evaluation
 VASCULAR TECHNOLOGY PROFESSIONAL PERFORMANCE GUIDELINES Lower Extremity Venous Insufficiency Evaluation This Protocol was prepared by members of the Society for Vascular Ultrasound (SVU) as a template
VASCULAR TECHNOLOGY PROFESSIONAL PERFORMANCE GUIDELINES Lower Extremity Venous Insufficiency Evaluation This Protocol was prepared by members of the Society for Vascular Ultrasound (SVU) as a template
Recanalization of the Left Common Iliac Vein for MayeThurner Syndrome Associated with Arteriovenous Fistula
 EJVES Short Reports (2015) 29, 3e7 SHORT REPORT Recanalization of the Left Common Iliac Vein for MayeThurner Syndrome Associated with Arteriovenous Fistula H. Yuan a, J. Sun b,h.t.qi c, X. Jin a, X.J.
EJVES Short Reports (2015) 29, 3e7 SHORT REPORT Recanalization of the Left Common Iliac Vein for MayeThurner Syndrome Associated with Arteriovenous Fistula H. Yuan a, J. Sun b,h.t.qi c, X. Jin a, X.J.
Venous Insufficiency Ulcers. Patient Assessment: Superficial varicosities. Evidence of healed ulcers. Dermatitis. Normal ABI.
 Venous Insufficiency Ulcers Patient Assessment: Superficial varicosities Evidence of healed ulcers Dermatitis Normal ABI Edema Eczematous skin changes 1. Scaling 2. Pruritus 3. Erythema 4. Vesicles Lipodermatosclerosis
Venous Insufficiency Ulcers Patient Assessment: Superficial varicosities Evidence of healed ulcers Dermatitis Normal ABI Edema Eczematous skin changes 1. Scaling 2. Pruritus 3. Erythema 4. Vesicles Lipodermatosclerosis
Acute Versus Chronic DVT Imaging in the Vascular Lab Heather Gornik, MD, RVT, RPVI
 Acute Versus Chronic DVT Imaging in the Vascular Lab Heather Gornik, MD, RVT, RPVI Cleveland Clinic Heart and Vascular Institute Heather L. Gornik, MD has the following relationships to disclose: CVR Global
Acute Versus Chronic DVT Imaging in the Vascular Lab Heather Gornik, MD, RVT, RPVI Cleveland Clinic Heart and Vascular Institute Heather L. Gornik, MD has the following relationships to disclose: CVR Global
Protocols for the evaluation of lower extremity venous reflux: supine, sitting, or standing?
 Protocols for the evaluation of lower extremity venous reflux: supine, sitting, or standing? Susan Whitelaw RVT, RDMS PURPOSE Duplex imaging of the lower extremity veins is performed to assess the deep
Protocols for the evaluation of lower extremity venous reflux: supine, sitting, or standing? Susan Whitelaw RVT, RDMS PURPOSE Duplex imaging of the lower extremity veins is performed to assess the deep
NCVH. Ultrasongraphy: State of the Art Vein Forum 2015 A Multidisciplinary Approach to Otptimizing Venous Circulation From Wounds to WOW
 Ultrasongraphy: State of the Art 2015 NCVH New Cardiovascular Horizons Vein Forum 2015 A Multidisciplinary Approach to Otptimizing Venous Circulation From Wounds to WOW Anil K. Chagarlamudi, M.D. Cardiovascular
Ultrasongraphy: State of the Art 2015 NCVH New Cardiovascular Horizons Vein Forum 2015 A Multidisciplinary Approach to Otptimizing Venous Circulation From Wounds to WOW Anil K. Chagarlamudi, M.D. Cardiovascular
Deep Venous Pathology. Eberhard Rabe Department of Dermatology University of Bonn Germany
 Deep Venous Pathology Eberhard Rabe Department of Dermatology University of Bonn Germany Disclosures None for this presentation Consultant: Sigvaris, EUROCOM Speakers bureau: Bayer Vital, Aspen, Boehringer,
Deep Venous Pathology Eberhard Rabe Department of Dermatology University of Bonn Germany Disclosures None for this presentation Consultant: Sigvaris, EUROCOM Speakers bureau: Bayer Vital, Aspen, Boehringer,
Vascular Sonography Examination
 Vascular Sonography Examination The purpose of The American Registry of Radiologic Technologists (ARRT ) Vascular Sonography Examination is to assess the knowledge and cognitive skills underlying the intelligent
Vascular Sonography Examination The purpose of The American Registry of Radiologic Technologists (ARRT ) Vascular Sonography Examination is to assess the knowledge and cognitive skills underlying the intelligent
EVALUATION OF THE VASCULAR STATUS OF DIABETIC WOUNDS Travis Littman, MD NorthWest Surgical Specialists
 EVALUATION OF THE VASCULAR STATUS OF DIABETIC WOUNDS Travis Littman, MD NorthWest Surgical Specialists Nothing To Disclosure DISCLOSURES I have no outside conflicts of interest, financial incentives, or
EVALUATION OF THE VASCULAR STATUS OF DIABETIC WOUNDS Travis Littman, MD NorthWest Surgical Specialists Nothing To Disclosure DISCLOSURES I have no outside conflicts of interest, financial incentives, or
Not all Leg DVT s are the Same: Which Patients Benefit from Interventional Therapy? Case 1:
 12/16/2015 Not all Leg DVT s are the Same: Which Patients Benefit from Interventional Therapy? Constantino S.Peña, FSIR, FSCCT, FAHA Interventional Radiologist Medical Director, Vascular Imaging Miami
12/16/2015 Not all Leg DVT s are the Same: Which Patients Benefit from Interventional Therapy? Constantino S.Peña, FSIR, FSCCT, FAHA Interventional Radiologist Medical Director, Vascular Imaging Miami
Lower Limb Venous Ultrasound. Colin P. Griffin MSc, BSc (Hons)
 Lower Limb Venous Ultrasound Colin P. Griffin MSc, BSc (Hons) Peripheral Vessels Lower Limb Peripheral Vessels Lower Limb Venous Deep System Common Iliac External/Internal Iliac Common Femoral Femoral
Lower Limb Venous Ultrasound Colin P. Griffin MSc, BSc (Hons) Peripheral Vessels Lower Limb Peripheral Vessels Lower Limb Venous Deep System Common Iliac External/Internal Iliac Common Femoral Femoral
Management of Acute DVT Extending From the Tibial Veins to the Common Iliac Vein Using the AngioJet Thrombectomy System
 FEATURED TECHNOLOGY: ANGIOJET THROMBECTOMY SYSTEM Sponsored by Boston Scientific Corporation Management of Acute DVT Extending From the Tibial Veins to the Common Iliac Vein Using the AngioJet Thrombectomy
FEATURED TECHNOLOGY: ANGIOJET THROMBECTOMY SYSTEM Sponsored by Boston Scientific Corporation Management of Acute DVT Extending From the Tibial Veins to the Common Iliac Vein Using the AngioJet Thrombectomy
Recurrent Varicose Veins We All See Them
 We All See Them November 4, 2017 Austin, TX Arlington Heights, IL No conflicts Terminology REVAS REcurrent Varices After Surgery PREVAIT PREsence of Varices After Interventional Treatment Recurrent varices
We All See Them November 4, 2017 Austin, TX Arlington Heights, IL No conflicts Terminology REVAS REcurrent Varices After Surgery PREVAIT PREsence of Varices After Interventional Treatment Recurrent varices
Anatomy. Patterns of reflux. Technique. Testing Reflux time Patient position. Difficult! Learning. NOT system optimisation. Clinical Assesment
 Anatomy Patterns of reflux Awareness Technique Testing Reflux time Patient position Difficult! Learning NOT system optimisation Enlarged Clinical Assesment Twisted Where are the symptoms? Why they are
Anatomy Patterns of reflux Awareness Technique Testing Reflux time Patient position Difficult! Learning NOT system optimisation Enlarged Clinical Assesment Twisted Where are the symptoms? Why they are
Imaging Strategy For Claudication
 Who are the Debators? Imaging Strategy For Claudication Duplex Ultrasound Alone is Adequate to Select Patients for Endovascular Intervention - Pro: Dennis Bandyk MD No Disclosures PRO - Vascular Surgeon
Who are the Debators? Imaging Strategy For Claudication Duplex Ultrasound Alone is Adequate to Select Patients for Endovascular Intervention - Pro: Dennis Bandyk MD No Disclosures PRO - Vascular Surgeon
The evidence for venous interventions is evolving- many patients do actually benefit. Nils Kucher University Hospital Bern Switzerland
 The evidence for venous interventions is evolving- many patients do actually benefit Nils Kucher University Hospital Bern Switzerland Disclosure Speaker name: Nils Kucher X X I have the following potential
The evidence for venous interventions is evolving- many patients do actually benefit Nils Kucher University Hospital Bern Switzerland Disclosure Speaker name: Nils Kucher X X I have the following potential
BC Vascular Surgery Day
 BC Vascular Surgery Day November 4, 2017 1 Table of Contents Abdominal Aortic Aneurysm 3 4 Acute DVT 5 6 Peripheral Arterial Disease 7 9 Varicose Veins 10 11 Diabetic Foot Ulcers 12 13 Carotid Stenosis
BC Vascular Surgery Day November 4, 2017 1 Table of Contents Abdominal Aortic Aneurysm 3 4 Acute DVT 5 6 Peripheral Arterial Disease 7 9 Varicose Veins 10 11 Diabetic Foot Ulcers 12 13 Carotid Stenosis
Clinical case. Symptomatic anterior accessory great saphenous vein (AAGSV) reflux
 Clinical case Symptomatic anterior accessory great saphenous vein (AAGSV) reflux A 70 year-old female presents with symptomatic varicose veins on left leg for more than 10 years. She complains of heaviness,
Clinical case Symptomatic anterior accessory great saphenous vein (AAGSV) reflux A 70 year-old female presents with symptomatic varicose veins on left leg for more than 10 years. She complains of heaviness,
Clinical results of venous stents. Michael K. W. Lichtenberg MD, FESC
 Clinical results of venous stents Michael K. W. Lichtenberg MD, FESC Conflict of Interest - Disclosure Within the past 12 months, I or my spouse/partner have had a financial interest/arrangement or affiliation
Clinical results of venous stents Michael K. W. Lichtenberg MD, FESC Conflict of Interest - Disclosure Within the past 12 months, I or my spouse/partner have had a financial interest/arrangement or affiliation
Pharmaco-mechanical techniques stand alone procedures? Peter Neglén, MD, PhD SP Vascular Center Limassol Cyprus
 Pharmaco-mechanical techniques stand alone procedures? Peter Neglén, MD, PhD SP Vascular Center Limassol Cyprus Faculty Disclosure Peter Neglén, M.D., Ph.D Stockholder/Founder of Veniti, Inc. Member, Medical
Pharmaco-mechanical techniques stand alone procedures? Peter Neglén, MD, PhD SP Vascular Center Limassol Cyprus Faculty Disclosure Peter Neglén, M.D., Ph.D Stockholder/Founder of Veniti, Inc. Member, Medical
Michael Meuse, M.D. Vascular and Interventional Radiology
 Michael Meuse, M.D. Vascular and Interventional Radiology Iliac Vein Compression Syndrome Left CIV compressed by right CIA Virchow 1851: DVT L>R May and Thurner 1954: venous spurs Cockett and Thomas 1965:
Michael Meuse, M.D. Vascular and Interventional Radiology Iliac Vein Compression Syndrome Left CIV compressed by right CIA Virchow 1851: DVT L>R May and Thurner 1954: venous spurs Cockett and Thomas 1965:
RECOGNITION AND ENDOVASCULAR TREATMENT OF CHRONIC VENOUS INSUFFICIENCY
 RECOGNITION AND ENDOVASCULAR TREATMENT OF CHRONIC VENOUS INSUFFICIENCY Paul Kramer, MD, FACC, FSCAI Liberty Cardiovascular Specialists Liberty Regional Heart and Vascular Center DISCLOSURES NONE Venous
RECOGNITION AND ENDOVASCULAR TREATMENT OF CHRONIC VENOUS INSUFFICIENCY Paul Kramer, MD, FACC, FSCAI Liberty Cardiovascular Specialists Liberty Regional Heart and Vascular Center DISCLOSURES NONE Venous
VASCULAR DISEASE: THREE THINGS YOU SHOULD KNOW JAMES A.M. SMITH, D.O. KANSAS VASCULAR MEDICINE, P.A. WICHITA, KANSAS
 VASCULAR DISEASE: THREE THINGS YOU SHOULD KNOW JAMES A.M. SMITH, D.O. KANSAS VASCULAR MEDICINE, P.A. WICHITA, KANSAS KANSAS ASSOCIATION OF OSTEOPATHIC MEDICINE ANNUAL CME CONVENTION APRIL 13, 2018 THREE
VASCULAR DISEASE: THREE THINGS YOU SHOULD KNOW JAMES A.M. SMITH, D.O. KANSAS VASCULAR MEDICINE, P.A. WICHITA, KANSAS KANSAS ASSOCIATION OF OSTEOPATHIC MEDICINE ANNUAL CME CONVENTION APRIL 13, 2018 THREE
Vascular Surgery and Transplant Unit University of Catania. Pierfrancesco Veroux
 Vascular Surgery and Transplant Unit University of Catania Pierfrancesco Veroux Bologna-Palazzo dei Congressi, 23 Ottobre 2017 Disclosure Speaker name: Prof. Pierfrancesco Veroux I have the following potential
Vascular Surgery and Transplant Unit University of Catania Pierfrancesco Veroux Bologna-Palazzo dei Congressi, 23 Ottobre 2017 Disclosure Speaker name: Prof. Pierfrancesco Veroux I have the following potential
Determine the patients relative risk of thrombosis. Be confident that you have had a meaningful discussion with the patient.
 Patient Assessment :Venous History, Examination and Introduction to Doppler and PPG Dr Louis Loizou The 11 th Annual Scientific Meeting and Workshops of the Australasian College of Phlebology Tuesday 18
Patient Assessment :Venous History, Examination and Introduction to Doppler and PPG Dr Louis Loizou The 11 th Annual Scientific Meeting and Workshops of the Australasian College of Phlebology Tuesday 18
Image Formation (10) 2 Evaluation and Selection of Representative Images (10)
 STRUCTURED SELF ASSESSMENT CONTENT SPECIFICATIONS SSA LAUNCH DATE: JANUARY 1, 2018 Vascular Sonography The purpose of continuing qualifications requirements (CQR) is to assist registered technologists
STRUCTURED SELF ASSESSMENT CONTENT SPECIFICATIONS SSA LAUNCH DATE: JANUARY 1, 2018 Vascular Sonography The purpose of continuing qualifications requirements (CQR) is to assist registered technologists
DISORDERS OF VENOUS SYSTEM
 DISORDERS OF VENOUS SYSTEM Varicose Veins Any dilated, elongated and tortuous vein irrespective of size Varicose veins are common in the superficial veins of the leg which are subject to high pressure
DISORDERS OF VENOUS SYSTEM Varicose Veins Any dilated, elongated and tortuous vein irrespective of size Varicose veins are common in the superficial veins of the leg which are subject to high pressure
Treatment of Venous ulcers utilizing n-butyl Cyanoacrylate (Super Glue)
 Treatment of Venous ulcers utilizing n-butyl Cyanoacrylate (Super Glue) Awais Siddique MD Endovascular Radiologist AZH WAVE CENTERS Milwaukee WI Venous disease Etiology Are the result of Venous valvular
Treatment of Venous ulcers utilizing n-butyl Cyanoacrylate (Super Glue) Awais Siddique MD Endovascular Radiologist AZH WAVE CENTERS Milwaukee WI Venous disease Etiology Are the result of Venous valvular
Venous Reflux Duplex Exam
 Venous Reflux Duplex Exam GWENDOLYN CARMEL, RVT PHYSIOLOGIST, DEPARTMENT OF VASCULAR SURGERY NEW JERSEY VETERANS HEALTHCARE CENTER EAST ORANGE, NJ PURPOSE: To identify patterns of incompetence and which
Venous Reflux Duplex Exam GWENDOLYN CARMEL, RVT PHYSIOLOGIST, DEPARTMENT OF VASCULAR SURGERY NEW JERSEY VETERANS HEALTHCARE CENTER EAST ORANGE, NJ PURPOSE: To identify patterns of incompetence and which
Techniques and Specific Treatment Modalities for the Active Non-Healing Wound. Luke Maj, MD, MHA
 Techniques and Specific Treatment Modalities for the Active Non-Healing Wound Luke Maj, MD, MHA Assistant Professor of Radiology University of Miami, Miller School of Medicine Director of The Vein Center
Techniques and Specific Treatment Modalities for the Active Non-Healing Wound Luke Maj, MD, MHA Assistant Professor of Radiology University of Miami, Miller School of Medicine Director of The Vein Center
UNDERSTANDING VEIN PROBLEMS
 UNDERSTANDING VEIN PROBLEMS Varicose Veins, Chronic Venous Insufficiency, and DVT Do You Have a Vein Problem? Have you noticed pain or swelling in your legs? Do your symptoms worsen when you re sitting
UNDERSTANDING VEIN PROBLEMS Varicose Veins, Chronic Venous Insufficiency, and DVT Do You Have a Vein Problem? Have you noticed pain or swelling in your legs? Do your symptoms worsen when you re sitting
Endovascular treatment of acquired arteriovenous fistula with severe hemodynamic effects: a case report
 Endovascular treatment of acquired arteriovenous fistula with severe hemodynamic effects: a case report The Leipzig Interventional Course, January 24 27, 2017 El Samman K., Šedivý P., Šnajdrová A., Přindišová
Endovascular treatment of acquired arteriovenous fistula with severe hemodynamic effects: a case report The Leipzig Interventional Course, January 24 27, 2017 El Samman K., Šedivý P., Šnajdrová A., Přindišová
A A U
 PVD Venous AUC Rating Sheet 2nd Round 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 Median I NI MADM Rating Agree Disagree Upper Extremity Venous Evaluation Table 1. Venous Duplex of the Upper Extremities for Patency
PVD Venous AUC Rating Sheet 2nd Round 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 Median I NI MADM Rating Agree Disagree Upper Extremity Venous Evaluation Table 1. Venous Duplex of the Upper Extremities for Patency
Surgical disobliteration of postthrombotic deep veins endophlebectomy is feasible
 Surgical disobliteration of postthrombotic deep veins endophlebectomy is feasible Alessandra Puggioni, MD, a,c Robert L. Kistner, MD, a,b Bo Eklof, MD, PhD, a,b,c and Fedor Lurie, MD, PhD, a,b,c Honolulu,
Surgical disobliteration of postthrombotic deep veins endophlebectomy is feasible Alessandra Puggioni, MD, a,c Robert L. Kistner, MD, a,b Bo Eklof, MD, PhD, a,b,c and Fedor Lurie, MD, PhD, a,b,c Honolulu,
LOWER EXTREMITY VENOUS COMPRESSION ULTRASOUND. CPT Stacey Good, DO Emergency Medicine Ultrasound Fellow Madigan Army Medical Center
 LOWER EXTREMITY VENOUS COMPRESSION ULTRASOUND CPT Stacey Good, DO Emergency Medicine Ultrasound Fellow Madigan Army Medical Center Learning Objectives Setup and patient positioning for optimizing success
LOWER EXTREMITY VENOUS COMPRESSION ULTRASOUND CPT Stacey Good, DO Emergency Medicine Ultrasound Fellow Madigan Army Medical Center Learning Objectives Setup and patient positioning for optimizing success
PUT YOUR BEST FOOT FORWARD
 PUT YOUR BEST FOOT FORWARD Bala Ramanan, MBBS 1 st year vascular surgery fellow Introduction The epidemic of diabetes and ageing of our population ensures critical limb ischemia will continue to grow.
PUT YOUR BEST FOOT FORWARD Bala Ramanan, MBBS 1 st year vascular surgery fellow Introduction The epidemic of diabetes and ageing of our population ensures critical limb ischemia will continue to grow.
Straub Endovascular System &
 Straub Endovascular System & S t r a u b E n d o v a s c u l a r To o l s Straub Endovascular System Effective debulking in occluded arteries and veins Effective debulking in many indications Rotarex
Straub Endovascular System & S t r a u b E n d o v a s c u l a r To o l s Straub Endovascular System Effective debulking in occluded arteries and veins Effective debulking in many indications Rotarex
Perforators: When to Treat and How Best to Do It? Eric Hager, MD September 10, 2015
 Perforators: When to Treat and How Best to Do It? Eric Hager, MD September 10, 2015 Anatomy of Perforating veins Cadaveric studies 1 have shown >60 vein perforating veins from superficial to deep Normal
Perforators: When to Treat and How Best to Do It? Eric Hager, MD September 10, 2015 Anatomy of Perforating veins Cadaveric studies 1 have shown >60 vein perforating veins from superficial to deep Normal
REKANALISATION CHRONISCH VENÖSER VERSCHLÜSSE. Michael K. W. Lichtenberg, FESC
 REKANALISATION CHRONISCH VENÖSER VERSCHLÜSSE Michael K. W. Lichtenberg, FESC Conflict of Interest - Disclosure Within the past 12 months, I or my spouse/partner have had a financial interest/arrangement
REKANALISATION CHRONISCH VENÖSER VERSCHLÜSSE Michael K. W. Lichtenberg, FESC Conflict of Interest - Disclosure Within the past 12 months, I or my spouse/partner have had a financial interest/arrangement
Evaluation and Management of Pelvic Venous Disorders
 Evaluation and Management of Pelvic Venous Disorders Mark H. Meissner, MD Peter Gloviczki Professor of Venous & Lymphatic Disorders University of Washington School of Medicine Seattle, WA Mark H. Meissner,
Evaluation and Management of Pelvic Venous Disorders Mark H. Meissner, MD Peter Gloviczki Professor of Venous & Lymphatic Disorders University of Washington School of Medicine Seattle, WA Mark H. Meissner,
Anticoagulation therapy following endovascular treatment of iliofemoral deep vein thrombosis
 Anticoagulation therapy following endovascular treatment of iliofemoral deep vein thrombosis Tim Sebastian, M.D. University Hospital Zurich Clinic for Angiology Disclosure Speaker name: Tim Sebastian I
Anticoagulation therapy following endovascular treatment of iliofemoral deep vein thrombosis Tim Sebastian, M.D. University Hospital Zurich Clinic for Angiology Disclosure Speaker name: Tim Sebastian I
RadRx Your Prescription for Accurate Coding & Reimbursement Copyright All Rights Reserved.
 Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of November 19, 2018 Abdominal Aortogram, Bilateral Runoff
Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of November 19, 2018 Abdominal Aortogram, Bilateral Runoff
Disclosures. What is a Specialty Vein Clinic? Prevalence of Venous Disease. Management of Venous Disease: an evidence based approach.
 Management of Venous Disease: an evidence based approach Disclosures Ed Boyle, MD Andrew Jones, MD Dr. Ed Boyle and Dr. Andrew Jones disclose Grants/research support: Medtronic, BTG International, Clearflow,
Management of Venous Disease: an evidence based approach Disclosures Ed Boyle, MD Andrew Jones, MD Dr. Ed Boyle and Dr. Andrew Jones disclose Grants/research support: Medtronic, BTG International, Clearflow,
Medicare C/D Medical Coverage Policy
 Varicose Vein Treatment Medicare C/D Medical Coverage Policy Origination Date: June 1, 1993 Review Date: February 15, 2017 Next Review: February, 2019 DESCRIPTION OF PROCEDURE OR SERVICE Varicose veins
Varicose Vein Treatment Medicare C/D Medical Coverage Policy Origination Date: June 1, 1993 Review Date: February 15, 2017 Next Review: February, 2019 DESCRIPTION OF PROCEDURE OR SERVICE Varicose veins
Surgical Options for revascularisation P E T E R S U B R A M A N I A M
 Surgical Options for revascularisation P E T E R S U B R A M A N I A M The goal Treat pain Heal ulcer Preserve limb Preserve life The options Conservative Endovascular Surgical bypass Primary amputation
Surgical Options for revascularisation P E T E R S U B R A M A N I A M The goal Treat pain Heal ulcer Preserve limb Preserve life The options Conservative Endovascular Surgical bypass Primary amputation
DOPPLER ULTRASOUND OF DEEP VENOUS THROMBOSIS
 TOKUDA HOSPITAL SOFIA DOPPLER ULTRASOUND OF DEEP VENOUS THROMBOSIS MILENA STANEVA, MD, PhD Department of vascular surgery and angiology Venous thromboembolic disease continues to cause significant morbidity
TOKUDA HOSPITAL SOFIA DOPPLER ULTRASOUND OF DEEP VENOUS THROMBOSIS MILENA STANEVA, MD, PhD Department of vascular surgery and angiology Venous thromboembolic disease continues to cause significant morbidity
Additional Information S-55
 Additional Information S-55 Network providers are encouraged, but not required to participate in the on-line American Venous Forum Registry (AVR) - The First National Registry for the Treatment of Varicose
Additional Information S-55 Network providers are encouraged, but not required to participate in the on-line American Venous Forum Registry (AVR) - The First National Registry for the Treatment of Varicose
Venous drainage of the lower limb
 Venous drainage of the lower limb INTRODUCTION It is of immense clinical and surgical importance. The venous blood against gravity. FACTORS HELPING THE VENOUS DRAINAGE OF THE LOWER LIMB The contraction
Venous drainage of the lower limb INTRODUCTION It is of immense clinical and surgical importance. The venous blood against gravity. FACTORS HELPING THE VENOUS DRAINAGE OF THE LOWER LIMB The contraction
Re-intervention for occluded iliac vein stents
 Review Article Re-intervention for occluded iliac vein stents Stacey Black 1, Amy Janicek 2, M. Grace Knuttinen 3 1 University of Arizona, Tucson, Arizona, USA; 2 Arizona State Radiology, Tucson, Arizona,
Review Article Re-intervention for occluded iliac vein stents Stacey Black 1, Amy Janicek 2, M. Grace Knuttinen 3 1 University of Arizona, Tucson, Arizona, USA; 2 Arizona State Radiology, Tucson, Arizona,
Venogram Versus Intravascular Ultrasound for Diagnosing and Treating Iliofemoral Vein Obstruction (VIDIO)
 Venogram Versus Intravascular Ultrasound for Diagnosing and Treating Iliofemoral Vein Obstruction (VIDIO) Report From a Multicenter, Prospective Study of Iliofemoral Vein Interventions Paul J. Gagne, MD,
Venogram Versus Intravascular Ultrasound for Diagnosing and Treating Iliofemoral Vein Obstruction (VIDIO) Report From a Multicenter, Prospective Study of Iliofemoral Vein Interventions Paul J. Gagne, MD,
New Guideline in venous ulcer treatment: dressing, medication, intervention
 New Guideline in venous ulcer treatment: dressing, medication, intervention Kittipan Rerkasem, FRCS(T), PhD Department of Surgery Faculty of Medicine Chiang Mai University Topic Overview venous ulcer treatment
New Guideline in venous ulcer treatment: dressing, medication, intervention Kittipan Rerkasem, FRCS(T), PhD Department of Surgery Faculty of Medicine Chiang Mai University Topic Overview venous ulcer treatment
Physician s Vascular Interpretation Examination Content Outline
 Physician s Vascular Interpretation Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 4 5 6 Cerebrovascular Abdominal Peripheral Arterial - Duplex Imaging Peripheral Arterial
Physician s Vascular Interpretation Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 4 5 6 Cerebrovascular Abdominal Peripheral Arterial - Duplex Imaging Peripheral Arterial
Fig MHz cm/s. Table 1 Fig. 2. Fig. 3, 4. Fig. 5
 GE Fig. 1 3. 5 MHz 7 10 MHz 3. 5 5. 0 MHz B 10 20 cm/s Table 1 Fig. 2 Fig. 1 1 2 3 3 3 : 1 2 3 Fig. 3, 4 Fig. 5 Table 1 a b c Fig. 2 a B b B c Fig. 6 Table 1 Fig. 7 a b c Fig. 3 a AV b A VV c 1 cm 2 1
GE Fig. 1 3. 5 MHz 7 10 MHz 3. 5 5. 0 MHz B 10 20 cm/s Table 1 Fig. 2 Fig. 1 1 2 3 3 3 : 1 2 3 Fig. 3, 4 Fig. 5 Table 1 a b c Fig. 2 a B b B c Fig. 6 Table 1 Fig. 7 a b c Fig. 3 a AV b A VV c 1 cm 2 1
Should We Be More Aggressive in the Treatment of Acute DVT?
 DISCLOSURES Consultant Penumbra, Inc. UCSF Vascular Surgery Symposium April 6, 2017 K. Pallav Kolli, MD Assistant Professor of Clinical Radiology University of California, San Francisco 17 yo male, DVT
DISCLOSURES Consultant Penumbra, Inc. UCSF Vascular Surgery Symposium April 6, 2017 K. Pallav Kolli, MD Assistant Professor of Clinical Radiology University of California, San Francisco 17 yo male, DVT
TREATMENT OPTIONS FOR CHRONIC VENOUS INSUFFICIENCY
 TREATMENT OPTIONS FOR CHRONIC VENOUS INSUFFICIENCY TL LUK Consultant Vascular Surgeon Sarawak General Hospital HKL Vascular Conference 19/06/2013 PREVALENCE OF LOWER LIMB VENOUS DISEASE Affects half of
TREATMENT OPTIONS FOR CHRONIC VENOUS INSUFFICIENCY TL LUK Consultant Vascular Surgeon Sarawak General Hospital HKL Vascular Conference 19/06/2013 PREVALENCE OF LOWER LIMB VENOUS DISEASE Affects half of
Let s Take a Look Venous Insufficiency Ultrasound Techniques
 Let s Take a Look Venous Insufficiency Ultrasound Techniques Brent Wilkinson RVT, RDMS Steve Schomaker RVT, RDCS, RDMS Let s take a look Differentiate between normal venous flow and venous insufficiency
Let s Take a Look Venous Insufficiency Ultrasound Techniques Brent Wilkinson RVT, RDMS Steve Schomaker RVT, RDCS, RDMS Let s take a look Differentiate between normal venous flow and venous insufficiency
Case. Wounds. Fundamentals of Ulcer Care. Dr. Mark Meissner Wound Case Study. Compression and Ulcer Healing Cullum NA, Cochrane Reviews 2001
 Case Wounds Mark H. Meissner, MD University of Washington School of Medicine 65 yr old male physician Recurrent R medial malleolar ulcer over 5 years New R lateral malleolar ulcer Intermittently wearing
Case Wounds Mark H. Meissner, MD University of Washington School of Medicine 65 yr old male physician Recurrent R medial malleolar ulcer over 5 years New R lateral malleolar ulcer Intermittently wearing
Comparison Of Primary Long Stenting Versus Primary Short Stenting For Long Femoropopliteal Artery Disease (PARADE)
 Comparison Of Primary Long Stenting Versus Primary Short Stenting For Long Femoropopliteal Artery Disease (PARADE) Young-Guk Ko, M.D. Severance Cardiovascular Hospital, Yonsei University Health System,
Comparison Of Primary Long Stenting Versus Primary Short Stenting For Long Femoropopliteal Artery Disease (PARADE) Young-Guk Ko, M.D. Severance Cardiovascular Hospital, Yonsei University Health System,
Schedule of Benefits. for Professional Fees Vascular Procedures
 Schedule of Benefits for Professional Fees 2018 Vascular Procedures ANASTOMOSIS RULES 820 Arteriovenous anastomosis in arm 1453 Arteriovenous anastomosis, open by basilic vein transposition 1465 Splenorenal
Schedule of Benefits for Professional Fees 2018 Vascular Procedures ANASTOMOSIS RULES 820 Arteriovenous anastomosis in arm 1453 Arteriovenous anastomosis, open by basilic vein transposition 1465 Splenorenal
How to manage leg ulcers in the elderly
 How to manage leg ulcers in the elderly David Riding Clinical Research Fellow / Specialty Registrar in Vascular Surgery University of Manchester / MFT British Geriatric Society Trainees Meeting 2018 Objectives
How to manage leg ulcers in the elderly David Riding Clinical Research Fellow / Specialty Registrar in Vascular Surgery University of Manchester / MFT British Geriatric Society Trainees Meeting 2018 Objectives
With All the New Drugs, This is How I Treat Acute DVT and Superficial Phlebitis
 BRIGHAM AND WOMEN S HOSPITAL With All the New Drugs, This is How I Treat Acute DVT and Superficial Phlebitis Gregory Piazza, MD, MS Division of Cardiovascular Medicine Brigham and Women s Hospital April
BRIGHAM AND WOMEN S HOSPITAL With All the New Drugs, This is How I Treat Acute DVT and Superficial Phlebitis Gregory Piazza, MD, MS Division of Cardiovascular Medicine Brigham and Women s Hospital April
Date: A. Venous Health History Form. Patient please complete questions Primary Care Physician:
 E S Insurance: 2 nd Insurance: Wait time: Date: A. Venous Health History Form Patient please complete questions 1-12 Patient Name: SSN#: Date of Birth: Primary Care Physician: What is the reason for your
E S Insurance: 2 nd Insurance: Wait time: Date: A. Venous Health History Form Patient please complete questions 1-12 Patient Name: SSN#: Date of Birth: Primary Care Physician: What is the reason for your
