Headache Pain Generators
|
|
|
- Chester Day
- 5 years ago
- Views:
Transcription
1 Objectives 1. Define the major categories of headache. 2. Take a history directed at characterizing a headache pattern in an individual patient and identify the cause or triggers of the headache. 3. Understand the distinguishing features and patterns of migraine headache. 4. Know first line treatments for tension versus migraine headaches. 5. Recognize warning signs for secondary headache syndromes due to intracranial structural lesions or increased intracranial pressure. Pain Generators Extracranial Musculoskeletal (spine, muscle) Oral (dental) Ocular Ear Vascular: branches of extracranial carotid, e.g. temporal arteritis Intracranial Dural and pial sensory fibers Trigeminovascular pathways Intracranial: Dural and pial sensory fibers Primary Disorders 1. Migraine With or without aura 2. Tension-type 3. Trigeminal Autonomic Cephalgias
2 Secondary Disorders 1. Increased Intracranial Pressure headaches Mass lesions Idiopathic Intracranial Hypertension (IIH) 2. Vascular Inflammation example: Temporal Arteritis Thrombosis example: Cerebral Venous Thrombosis Sub-arachnoid hemorrhage ( worst headache of life ) 3. Cervicogenic (spine, nerve roots) 4. Temporal Mandibular Joint (TMJ) 5. Medication Overuse Primary or Secondary Chronic Daily Tension-type Medication Overuse Transformed Migraine New Daily Persistent Rule out Secondary Exam: History onset aura or warning? sudden (thunderclap) or gradual prior head or neck trauma previous attacks (progression of symptoms?) duration of attacks (< 3 hours, > 4 hours, continuous) frequency: days per month with headache Pain location (unilateral, bilateral, cervical, retroorbital, face or jaw) Radiation of pain? -associated symptoms nausea, vomiting photophobia, phonophobia conjunctival injection, rhinorrhea, diaphoresis Exam: History Triggers: sounds, smells, movements? Aggravating factors posture, cough, exertion, straining, neck or jaw movements severity effect on work and family activities Acute and preventive medications effectiveness, side effects Co-morbid medical or mental health conditions History of heart disease or stroke Visual disorders Family history of headache disorders for the first time OR change in pattern?
3 Exam: Physical Exam: Physical Screening neurologic examination general assessment of mental status cranial nerve examination fundoscopy, pupils, eye movements, visual fields, face sensory and motor for asymmetry and/or weakness assessment for unilateral limb weakness or dyscoordination, deep tendon reflex asymmetry assessment of gait, including heel-toe walking (tandem gait) Neck examination posture, range of motion, palpation for muscle tender points Check for cervical paraspinal muscle spasm, trapezius tender points HEENT examination: eyes, ears, jaw movements Palpate occiput Palpate temple Palpate muscles of mastication for tender points Listen for bruits: head, eyes, neck Blood pressure measurements check orthostatic BP The majority of patients with primary headache disorders have a normal neurological exam Tender points in neck, shoulders, and/or occiput can point to cervicogenic headache Red Flags for Secondary First or worst headache of life Abrupt-onset headache thunderclap headache Change in pattern, frequency, or severity of headaches s ALWAYS on the same side s refractory to treatment New onset headache after age 50 New onset headache with cancer, immunosuppression, or pregnancy Associated signs/symptoms: fever, stiff neck, papilledema, cognitive impairment with syncope or seizure triggered by exertion, valsalva maneuver, or sex Neurologic symptoms >1 hour Abnormal general or neurologic examination Neuroimaging is warranted Red Flags for Secondary Emergent (immediate attention): Thunderclap onset (fast, maximal pain) worst headache of my life Fever and meningismus Papilledema with focal signs or reduced level of consciousness Acute glaucoma Urgent (attention within hours to days) Papilledema without focal signs or reduced level of consciousness Relevant systemic illness Elderly patient: new headache with cognitive change
4 Red Flags for Secondary Less urgent (attention within days to few weeks, usually) Unexplained focal signs Atypical headaches (not consistent with migraine or tension-type Unusual headache precipitants Unusual aura symptoms Onset after age 50 y Aggravation by neck movement; abnormal neck examination (consider cervicogenic headache) Jaw symptoms; abnormal jaw examination (consider temporomandibular joint disease) General Practice Points Rule out secondary headache when diagnosing a primary headache disorder Migraine is the most common headache type in patients seeking medical care for headache Migraine is underdiagnosed and undertreated Consider migraine in patients with recurrent moderate or severe headaches and normal neurologic exam s that interfere with daily activities are more likely to be migraine, less likely tension type Medication overuse is a risk in patients using combination analgesics or frequent NSAID or acetaminophen General Practice Points General Practice Points management may require: Change in work or lifestyle (disability) Change in method of birth control (women) Consideration of effects of menstrual cycle (women) Change in environment Possible association with environmental factors Patient may be able to identify headache triggers through careful headache diary Common headache triggers Emotional stress Hormones (women) Skipping meals Weather Sleep disturbance Odors Neck pain Lights Caffeine, Alcohol, Smoking Heat Food Exercise/sexual activity
5 General Practice Points management includes: Consideration of the complexity of the medication plan Can the patient follow the schedule? Consideration of the side effects of the medications proposed for treatment Sedation, cognitive side effects Beneficial side effects, e.g mood stabilization, may make some medications more effective Consideration of the teratogenic potential of headache medications Always counsel patients and document counseling Considerations before and during pregnancy Diagnosing primary headache syndromes Patients with recurrent headache attacks and normal neurologic examination findings 1. Migraine with or without aura if at least 2 of: nausea (with or without vomiting) light sensitivity /sound sensitivity some of the attacks interfere with daily activities 2. Episodic tension-type headache if attacks are not associated with nausea, and at least 2 of: bilateral headache nonpulsating pain mild to moderate intensity headache is not worsened by activity Diagnosing primary headache syndromes Diagnosing primary headache syndromes Cluster headache or another trigeminal autonomic cephalalgia if all of the following criteria: Frequent Severe Brief (duration < 3 h) Unilateral Ipsilateral conjunctival injection, tearing, or restlessness during the attacks (ipsilateral ptosis or miosis on exam). Need Neurologist referral*** CHRONIC HEADACHES Patients with headache on 15 d/mo for > 3 months and with normal neurologic examination Chronic migraine if headaches meet migraine diagnostic criteria (above) or are quickly aborted by migraine-specific medications (triptans or ergots) on 8 d/mo Chronic migraine with medication overuse if the patient uses ergots, triptans, opioids, or combination analgesics on 10 d/mo or uses plain acetaminophen or NSAIDs on 15 d/mo Chronic migraine without medication overuse if patients do not have medication overuse
6 Diagnosing primary headache syndromes Diagnosing primary headache syndromes CHRONIC HEADACHES Patients with headache on 15 d/mo for > 3 months and with normal neurologic examination Chronic tension-type headache if headaches fit episodic tension-type diagnostic criteria (above), but > 15 d/mo for >3 months May have nausea but mild, not moderate or severe No more than one of photophobia, phonophobia, mild nausea Episodes last 30 min to few days Patients with continuous daily headache for > 3 mo with normal neurologic examination Hemicrania continua if the headache is strictly unilateral, is always on the same side of the head ptosis or miosis might be present on examination responds dramatically to indomethacin May refer to neurologist New daily persistent headache if the headache is unremitting since onset Evaluate for secondary headache Refer to neurologist Medication Overuse : Who is at risk? Diagnosing Medication Overuse Patient with an episodic headache disorder usually migraine or tension-type headache treated with frequent and excessive amounts of acute symptomatic medications present or develops upon awakening, and commonly occurs daily or nearly daily Patients with headache for > 15 days per month Use of triptans, ergots, combination analgesics, or opioid-containing medications 10 days per month Use of acetaminophen or NSAIDs 15 days per month Patients may have psychiatric co-morbidities depression and anxiety psychological and physical drug dependence Patients may have pain-related co-morbidities Orthopedic, musculoskeletal pain generators Taking multiple analgesics for different disorders
7 Diagnosing Medication Overuse All acute symptomatic medications used to treat headaches have the potential for causing MOH. Risk for MOH varies with medication Highest with Opioids butalbital-containing combination analgesics aspirin/acetaminophen/caffeine combinations Intermediate to high with triptans Lowest with nonsteroidal anti-inflammatory drugs MIGRAINE HEADACHES Epidemiology of Migraine Migraine Migraine is a common disorder: affects ~12% of the general population Female > Male 17 % of women each year 6 % of men each year Most common in those aged 30 to 39 Migraine tends to run in families. Migraine without aura is the most common type, ~75 % of cases Migraine is a spectrum of illness Episodic Migraine Chronic migraine Transformation may occur over months to years Hallmark of Migraine: Severe headache Usually with nausea and/or light and sound sensitivity Four phases of Migraine headaches 1. Premonitory symptoms: affective/vegetative symptoms 24 to 48 hours prior yawning, euphoria, depression, irritability, food cravings, constipation, neck stiffness 2. Aura: one or more focal neurological symptoms (25%) Postdrome: may feel drained/exhausted or elation/euphoria
8 Pathophysiology of Migraine Recurrent stimulation of central pain pathways causes neuronal dysfunction Brainstem trigeminal neurons become hyperexcitable. Leads to structural and functional changes which are both intracranial and extracranial. Cortical spreading depression: A wave of neuronal and glial depolarization spreads across the cortex Causes aura Activates trigeminal nerve afferents Alters blood brain barrier permeability Pathophysiology of Migraine Cortical spreading depression activation of pain sensitive trigeminal nerve afferents via: The release of pro-inflammatory mediators Transduction of the inflammatory signal to trigeminal nerve fibers in the meninges Prolonged activation of trigeminal pain fibers pain of migraine headaches. Migraine Aura: cortical spreading depression in areas of the brain where depolarization is not consciously perceived, e.g. cerebellum Pathophysiology of Migraine Typical distribution of migraine headache pain = anterior and posterior regions of head and upper neck Can be explained by convergence of the projections from the upper cervical nerve roots and the trigeminal nerve Pathophysiology of Migraine Stimulation of the trigeminal ganglion release of vasoactive neuropeptides Neurogenic Inflammation A sterile inflammatory response Vasodilation (calcitonin gene-related peptide) Plasma protein extravasation. Causes prolongation/intensification of the pain of migraine Neurogenic inflammation Sensitization Neurons become increasingly responsive to nociceptive and nonnociceptive stimulation Response thresholds decrease Response magnitude increases Spontaneous neuronal activity develops
9 Migraine Pathophysiology of Migraine Sensitization causes many clinical symptoms of migraine Throbbing quality of the pain Worsening of pain with coughing, bending, or sudden head movements Hyperalgesia (increased sensitivity to painful stimuli) Allodynia (pain produced by normally non-noxious stimulation). Genetic basis complex (additive effect of multiple genes), but frequent Familial hemiplegic migraine channelopathies Hemiplegic migraine more often sporadic Migraine Diagnostic Criteria with > 2 of: Unilateral location Pulsating quality Moderate or severe intensity Aggravation by or causing avoidance of routine physical activity During the headache at least one of: Nausea and/or vomiting Photophobia/phonophobia attacks last 4 to 72 hrs (untreated or successfully treated) At least 5 such attacks Migraine with Aura Diagnostic Criteria At least two migraine attacks in life time with: 1. One or more fully reversible auras: Visual (+/-) flickering light, loss vision Sensory (+/-) tingling, numbness Speech/language Motor (e.g. hemiplegia) Brainstem (e.g. vertigo, tinnitus, diplopia, ataxia) Retina (monocular scotoma or blindness) 2. At least one of: At least one aura symptom spreads gradually ( 5 minutes), and/or two or more symptoms occur in succession Each individual aura symptom lasts 5 to 60 minutes At least one aura symptom is unilateral The aura is accompanied, or followed within 60 minutes, by headache *International Classification of disorders, 3 rd edition *International Classification of disorders, 3 rd edition
10 Complicated Migraine Disorders Neurologic symptoms and/or signs with aura Neurologic symptoms and/or signs during headache or afterward Basilar migraine: symptoms referable to brainstem Vestibular migraine: prominent vertigo with or without headache Cause of episodic vertigo ( migrainous vertigo ) Hemiplegic migraine Triptans not used Familial hemiplegic migraine Migrainous headache with seizure: Migrainous epilepsy Refer these to a Neurologist!!! Migraine: Approach to Treatment Pay attention to lifestyle and specific migraine triggers Irregular or skipped meals Irregular or too little sleep Stressful lifestyle Excessive caffeine or alcohol consumption Lack of exercise Obesity 2 categories of Pharmacologic migraine treatment 1. Acute drug therapy for individual attacks 2. Prophylactic drug therapy (when indicated) to reduce attack frequency Evaluate and treat coexistent medical and psychiatric disorders Migraine: Approach to Treatment Migraine: Acute Treatment Encourage patients to participate actively in their treatment and to employ self-management principles: diaries available for smart phones and tables Self-monitoring to identify triggers and headache patterns When identified, manage migraine triggers effectively Plan daily activity to avoid triggering or exacerbating migraine Use non-pharmacologic approaches Relaxation techniques/stress management skills Cognitive behavioral therapy Sleep evaluation Acupuncture Adapted from Becker WJ Continuum 21:
11 Migraine: Acute Treatment Mild to moderate attack: Not associated with vomiting or severe nausea Simple analgesics (NSAIDs, acetaminophen) or combination analgesics are first choice agents Mild to moderate attacks associated with severe nausea or vomiting: oral or rectal anti-emetic drug in conjunction with simple or combination analgesics Migraine: Acute Treatment Moderate to severe attack: Oral migraine-specific agents are first-line oral triptans or combination of sumatriptan-naproxen Moderate to severe attack with vomiting or severe nausea: non oral migraine-specific medications subcutaneous sumatriptan nasal sumatriptan and zolmitriptan oral disintegrating tablets may be helpful non oral antiemetic agents parenteral agents in ER: ketorolac (NSAID), dihydroergotamine (vasoconstrictive) Migraine: Acute Treatment Adapted from Becker WJ Continuum 21: Migraine: Prophylactic Treatment Prophylactic medication when: Recurrent migraine attacks are causing considerable disability Frequency of acute medication use is approaching levels that place the patient at risk of medication overuse headache 10 days per month for triptans, ergots, opioids, and combination analgesics > 15 days per month for acetaminophen and NSAIDs Recurrent attacks with prolonged aura are occurring Complicated migraine (hemiplegic migraine, basilar-type migraine, etc) Contraindications to acute migraine medications are making symptomatic treatment of migraine attacks difficult
12 Migraine: Prophylactic Treatment Migraine: Prophylactic Treatment Adapted from Silberstein SD Continuum 21: Adapted from Silberstein SD Continuum 21: Migraine: Goals of Prophylactic Treatment Reduce attack frequency, severity, and duration Improve responsiveness to treatment of acute attacks Improve function and reduce disability Tension-type Ill-defined and heterogeneous headache syndrome Phenotype is non-specific Define by what it is NOT, rather than what it IS Three recognized sub-types Infrequent episodic (<1 per day per month) Frequent episodic (1-14 days per month) Chronic (>14 days per month) Pain is NOT localized and generally not severe Prevent progression or transformation of episodic migraine to chronic migraine No significant nausea, no vomiting, no photo/phonophobias Can be similar to milder episodic migraine or a secondary headache
13 Tension-type Most common primary or secondary headache type Estimated mean lifetime prevalence in adults is 46% Prevalence for Chronic TTH is 2-3% 40% of TTH patients report a family history of headache Peak prevalence between years of age Socioeconomic impact of TTH greater than that of migraine Co-morbid with major depression, anxiety disorder, TMJ, C- spine disc and spondylotic disorders Generators: pericranial myofascial factors (episodic TTH) and central nociceptive pathways (chronic TTH) Persistent activation of trigger points Peripheral nociceptor sensitization Eventual second-order neurons sensitized in the spinal trigeminal nucleus (pain thresholds decreased) Acute Medications for Tensiontype Acetaminophen Aspirin Ibuprofen Naproxen sodium Diclofenac Caffeine 500mg to 1000mg 500mg to 1000mg 200mg to 800mg 375 to 550 mg 12.5mg to 100mg 65mg to 200mg Monitor for medication overuse Guidelines from the European Federation of Neurological Societies. See Kaniecki, RG Continuum 18: Prophylactic Medications for Tension-type Amitriptyline Nortriptyline Mirtazapine Venlafaxine mg per day mg per day 30mg per day 150 mg per day For patients with 2 3 headache days per week Guidelines from the European Federation of Neurological Societies. See Kaniecki, RG Continuum 18: and Becker et al Can Fam Phys 61: Non-Pharmacologic Management of Tension-type Lifestyle and physical approaches Regular sleep and meal schedules Exercise and physical therapy Cervical muscle stretching Passive physical manipulations Behavioral therapies Relaxation techniques EMG-guided biofeedback Cognitive-behavioral therapy Acupuncture
14 Trigeminal Autonomic Cephalgias Unilateral headaches Spectrum from short-lived but recurrent to chronic Associated with one or more cranial autonomic symptoms Ptosis Conjunctival injection Lacrimation Nasal congestion or rhinorrea Cluster SUNCT: short, unilateral, neuralgiform, conjunctival, tearing SUNA: short, unilateral, cranial autonomic Trigeminal Autonomic Cephalgias Paroxysmal hemicrania Hemicrania continua Adapted from Newman LC Continuum 21: Features of the Trigeminal Autonomic Cephalgias Pathophysiology of the Trigeminal Autonomic Cephalgias Adapted from Newman LC Continuum 21: Common pathophysiology Ipsilateral activation of the hypothalamus: Cluster headache SUNCT Contralateral activation of the hypothalamus: Paroxysmal hemicrania Hemicrania continua Trigeminovascular pathway: ipsilateral pain V1 branch (ophthalmic) activated Elevated levels of calcitonin gene-related peptide (CGRP) Cranial autonomic pathways: autonomic features Descending input from hypothalamus, release of vasoactive intestinal polypeptide (VIP)
15 Features of the Trigeminal Autonomic Cephalgias Cluster Most common TAC, but uncommon overall (0.1%) Severe, unilateral orbital, supraorbital, and/or temporal; pain lasts minutes (untreated) At least one autonomic symptom in face or ear OR a sense of restlessness or agitation with headache Attack frequency between one every other day and eight per day more than half the time during a cluster TAC headaches can be distinguished by treatment responses Adapted from Newman LC Continuum 21: Episodic: headaches in bouts from 7 days to 1 year separated by pain-free intervals of at least 1 month Chronic: attacks for more than 1 year without remission or remission < 1 month Cluster Treatment Options Cluster Treatment Options Adapted from Newman LC Continuum 21: Adapted from Newman LC Continuum 21:
16 Cluster Treatment Options Adapted from Newman LC Continuum 21: Final Points is among the most common medical complaints. Episodic tension-type headache is the most frequent headache type in population-based studies Migraine is the most common diagnosis in patients presenting to primary care physicians with headache Sinus headache is often self-diagnosed by patients, but many patients presenting with sinus headache turn out to have migraine Hypertension can cause headaches in hypertensive emergencies, but not with typical migraine or tension headaches. References Available in PubMed Aurora SK et al Chronic Migraine: An Update on Physiology, Imaging, and the Mechanism of Action of Two Available Pharmacologic Therapies. January 2017: Becker WJ Acute migraine treatment. Continuum 21: Becker WJ et al Guideline for primary care management of headache in adults. Can Fam Physician 61: Bendtsen L et al Muscles and their role in episodic tension-type headache: implications for treatment. Eur J Pain 20: Kaniecki RG Tension-type headache. Continuum 18: Levin M Approach to the workup and management of headache in the emergency department and inpatient settings. Semin Neurol 35: Newman LC Trigeminal autonomic cephalgias. Continuum 21: Silberstein SD Preventive migraine treatment. Continuum 21:
A synopsis of: Diagnosis and Management of Headaches in Adults: A national clinical guideline. Scottish intercollegiate Guidelines Network SIGN
 A synopsis of: Diagnosis and Management of Headaches in Adults: A national clinical guideline Scottish intercollegiate Guidelines Network SIGN November 2008. PETER FRAMPTON MSc MCOptom BAppSc (Optom)(AUS)
A synopsis of: Diagnosis and Management of Headaches in Adults: A national clinical guideline Scottish intercollegiate Guidelines Network SIGN November 2008. PETER FRAMPTON MSc MCOptom BAppSc (Optom)(AUS)
Chronic Daily Headaches
 Chronic Daily Headaches ANWARUL HAQ, MD, MRCP(UK), FAHS DIRECTOR BAYLOR HEADACHE CENTER, DALLAS, TEXAS DISCLOSURES: None OBJECTIVES AT THE CONCLUSION OF THIS ACTIVITY, PARTICIPANTS WILL BE ABLE TO: define
Chronic Daily Headaches ANWARUL HAQ, MD, MRCP(UK), FAHS DIRECTOR BAYLOR HEADACHE CENTER, DALLAS, TEXAS DISCLOSURES: None OBJECTIVES AT THE CONCLUSION OF THIS ACTIVITY, PARTICIPANTS WILL BE ABLE TO: define
Disclosures. Objectives 6/2/2017
 Classification: Migraine and Trigeminal Autonomic Cephalalgias Lauren Doyle Strauss, DO, FAHS Assistant Professor, Child Neurology Assistant Director, Child Neurology Residency @StraussHeadache No disclosures
Classification: Migraine and Trigeminal Autonomic Cephalalgias Lauren Doyle Strauss, DO, FAHS Assistant Professor, Child Neurology Assistant Director, Child Neurology Residency @StraussHeadache No disclosures
Headache Assessment In Primary Eye Care
 Headache Assessment In Primary Eye Care Spencer Johnson, O.D., F.A.A.O. Northeastern State University Oklahoma College of Optometry johns137@nsuok.edu Course Objectives Review headache classification Understand
Headache Assessment In Primary Eye Care Spencer Johnson, O.D., F.A.A.O. Northeastern State University Oklahoma College of Optometry johns137@nsuok.edu Course Objectives Review headache classification Understand
MIGRAINE A MYSTERY HEADACHE
 MIGRAINE A MYSTERY HEADACHE The migraine is a chronic neurological disease that is characterized by moderate to severe episodes of headache that is mostly associated with other central nervous system (CNS)
MIGRAINE A MYSTERY HEADACHE The migraine is a chronic neurological disease that is characterized by moderate to severe episodes of headache that is mostly associated with other central nervous system (CNS)
HEADACHES THE RED FLAGS
 HEADACHES THE RED FLAGS FAYYAZ AHMED CONSULTANT NEUROLOGIST HON. SENIOR LECTURER HULL YORK MEDICAL SCHOOL SECONDARY VS PRIMARY HEADACHES COMMON SECONDARY HEADACHES UNCOMMON BUT SERIOUS SECONDARY HEADACHES
HEADACHES THE RED FLAGS FAYYAZ AHMED CONSULTANT NEUROLOGIST HON. SENIOR LECTURER HULL YORK MEDICAL SCHOOL SECONDARY VS PRIMARY HEADACHES COMMON SECONDARY HEADACHES UNCOMMON BUT SERIOUS SECONDARY HEADACHES
HEADACHE: Benign or Severe Dr Gobinda Chandra Roy
 HEADACHE: Benign or Severe Dr Gobinda Chandra Roy Associate Professor, Department of Medicine, Shaheed Suhrawardy Medical College and Hospital Outlines 1. Introduction 2. Classification of headache 3.
HEADACHE: Benign or Severe Dr Gobinda Chandra Roy Associate Professor, Department of Medicine, Shaheed Suhrawardy Medical College and Hospital Outlines 1. Introduction 2. Classification of headache 3.
Index. Prim Care Clin Office Pract 31 (2004) Note: Page numbers of article titles are in boldface type.
 Prim Care Clin Office Pract 31 (2004) 441 447 Index Note: Page numbers of article titles are in boldface type. A Abscess, brain, headache in, 388 Acetaminophen for migraine, 406 407 headache from, 369
Prim Care Clin Office Pract 31 (2004) 441 447 Index Note: Page numbers of article titles are in boldface type. A Abscess, brain, headache in, 388 Acetaminophen for migraine, 406 407 headache from, 369
Tears of Pain SUNCT and SUNA A/PROFESSOR ARUN AGGARWAL RPAH PAIN MANAGEMENT CENTRE
 Tears of Pain SUNCT and SUNA A/PROFESSOR ARUN AGGARWAL RPAH PAIN MANAGEMENT CENTRE IHS Classification 1989 (updated 2004) Primary Headaches 4 categories Migraine Tension-type Cluster and other trigeminal
Tears of Pain SUNCT and SUNA A/PROFESSOR ARUN AGGARWAL RPAH PAIN MANAGEMENT CENTRE IHS Classification 1989 (updated 2004) Primary Headaches 4 categories Migraine Tension-type Cluster and other trigeminal
Clinical case. Clinical case 3/15/2018 OVERVIEW. Refractory headaches and update on novel treatment. Refractory headache.
 OVERVIEW Refractory headaches and update on novel treatment Definition of refractory headache Treatment approach Medications Neuromodulation In the pipeline Juliette Preston, MD OHSU Headache Center Refractory
OVERVIEW Refractory headaches and update on novel treatment Definition of refractory headache Treatment approach Medications Neuromodulation In the pipeline Juliette Preston, MD OHSU Headache Center Refractory
Adult with headache. Problem-specific video guides to diagnosing patients and helping them with management and prevention
 Adult with headache Problem-specific video guides to diagnosing patients and helping them with management and prevention London Strategic Clinical Networks London Neuroscience Strategic Clinical Network
Adult with headache Problem-specific video guides to diagnosing patients and helping them with management and prevention London Strategic Clinical Networks London Neuroscience Strategic Clinical Network
Chronic Migraine in Primary Care. December 11 th, 2017 Werner J. Becker University of Calgary
 Chronic Migraine in Primary Care December 11 th, 2017 Werner J. Becker University of Calgary Disclosures Faculty: Werner J. Becker Relationships with commercial interests: Grants/Research Support: Clinical
Chronic Migraine in Primary Care December 11 th, 2017 Werner J. Becker University of Calgary Disclosures Faculty: Werner J. Becker Relationships with commercial interests: Grants/Research Support: Clinical
A case of a patient with chronic headache. Focus on Migraine. None related to the presentation Grants to conduct clinical trials from: Speaker bureau:
 Chronic Daily Headache Bassel F. Shneker, MD, MBA Associate Professor Vice Chair, OSU Neurology The Ohio State University Wexner Medical Center Financial Disclosures None related to the presentation Grants
Chronic Daily Headache Bassel F. Shneker, MD, MBA Associate Professor Vice Chair, OSU Neurology The Ohio State University Wexner Medical Center Financial Disclosures None related to the presentation Grants
Outpatient Headache Care Guideline
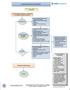 1 Outpatient Care Guideline Inclusion criteria: children > 3 yrs with headaches Is urgent emergency department, neuroimaging, or Neurology consultation indicated? Referral to ED if: New severe headache
1 Outpatient Care Guideline Inclusion criteria: children > 3 yrs with headaches Is urgent emergency department, neuroimaging, or Neurology consultation indicated? Referral to ED if: New severe headache
They are updated regularly as new NICE guidance is published. To view the latest version of this NICE Pathway see:
 bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published. To view the latest
bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published. To view the latest
July 2012 Target Population. Adult patients 18 years or older in primary care settings.
 Guideline for Primary Care Management of Headache in Adults July 2012 Target Population Adult patients 18 years or older in primary care settings. Exclusions: This guideline does not provide recommendations
Guideline for Primary Care Management of Headache in Adults July 2012 Target Population Adult patients 18 years or older in primary care settings. Exclusions: This guideline does not provide recommendations
MIGRAINE UPDATE. Objectives & Disclosures. Learn techniques used to diagnose headaches. Become familiar with medications used for headache treatment.
 MIGRAINE UPDATE Karen L. Bremer, MD November 16, 2018 Objectives & Disclosures Learn techniques used to diagnose headaches. Become familiar with medications used for headache treatment. Disclosure: I am
MIGRAINE UPDATE Karen L. Bremer, MD November 16, 2018 Objectives & Disclosures Learn techniques used to diagnose headaches. Become familiar with medications used for headache treatment. Disclosure: I am
ปวดศ รษะมา 5 ป ก นยาแก ปวดก ย งไม ข น นพ.พาว ฒ เมฆว ช ย โรงพยาบาลนครราชส มา
 ปวดศ รษะมา 5 ป ก นยาแก ปวดก ย งไม ข น นพ.พาว ฒ เมฆว ช ย โรงพยาบาลนครราชส มา 1 CONTENT 1 2 3 Chronic Daily Headache Medical Overused Headache Management Headaches are one of the most common symptoms List
ปวดศ รษะมา 5 ป ก นยาแก ปวดก ย งไม ข น นพ.พาว ฒ เมฆว ช ย โรงพยาบาลนครราชส มา 1 CONTENT 1 2 3 Chronic Daily Headache Medical Overused Headache Management Headaches are one of the most common symptoms List
Headache and Facial Pain. Mohammed ALEssa MBBS, FRCSC Assistant Professor Consultant Otolaryngology,Head & Neck Surgical Oncology
 Headache and Facial Pain Mohammed ALEssa MBBS, FRCSC Assistant Professor Consultant Otolaryngology,Head & Neck Surgical Oncology Introduction It is the most common neurologic complain The diagnosis usually
Headache and Facial Pain Mohammed ALEssa MBBS, FRCSC Assistant Professor Consultant Otolaryngology,Head & Neck Surgical Oncology Introduction It is the most common neurologic complain The diagnosis usually
Headaches. Mini Medical School. November 10, A. Laine Green MSc, MD FRCP(C) Assistant Professor Department of Medicine (Neurology)
 Headaches. Mini Medical School. November 10, 2016 A. Laine Green MSc, MD FRCP(C) Assistant Professor Department of Medicine (Neurology) Artist Agnes Cecile Disclosures I have received an honorarium from
Headaches. Mini Medical School. November 10, 2016 A. Laine Green MSc, MD FRCP(C) Assistant Professor Department of Medicine (Neurology) Artist Agnes Cecile Disclosures I have received an honorarium from
ADVANCES IN MIGRAINE MANAGEMENT
 ADVANCES IN MIGRAINE MANAGEMENT Joanna Girard Katzman, M.D.MSPH Assistant Professor, Dept. of Neurology Project ECHO, Chronic Pain Program University of New Mexico Outline Migraine throughout the decades
ADVANCES IN MIGRAINE MANAGEMENT Joanna Girard Katzman, M.D.MSPH Assistant Professor, Dept. of Neurology Project ECHO, Chronic Pain Program University of New Mexico Outline Migraine throughout the decades
6/4/2018. Headache. Headaches. Headache. Migraine Headaches. Headache. Red Flag signs and symptoms. Imaging CT without contrast.
 Presented by M.D. Shepherd, M.D. OH MY ACHING HEAD! Estimated that one half of the adult population is affected by a headache disorder International Society Classification Primary : Tension s 40% of the
Presented by M.D. Shepherd, M.D. OH MY ACHING HEAD! Estimated that one half of the adult population is affected by a headache disorder International Society Classification Primary : Tension s 40% of the
Headache Mary D. Hughes, MD Neuroscience Associates
 Headache Mary D. Hughes, MD Neuroscience Associates Case 1 22 year old female presents with recurrent headaches. She has had headaches for the past 3 years. They start on the right side of her head and
Headache Mary D. Hughes, MD Neuroscience Associates Case 1 22 year old female presents with recurrent headaches. She has had headaches for the past 3 years. They start on the right side of her head and
Primary Care Adult Headache Management Pathway (formerly North West Headache Management Guideline for Adults) Version 1.0
 Primary Care Adult Headache Management Pathway (formerly rth West Headache Management Guideline for Adults) Version 1.0 1 VERSION CONTROL Version Date Amendments made Version 1.0 October 2018 Reformatted
Primary Care Adult Headache Management Pathway (formerly rth West Headache Management Guideline for Adults) Version 1.0 1 VERSION CONTROL Version Date Amendments made Version 1.0 October 2018 Reformatted
Can I send this headache patient home? Dr Nicola Giffin Consultant Neurologist Bath, Nov 2017
 Can I send this headache patient home? Dr Nicola Giffin Consultant Neurologist Bath, Nov 2017 SAH v benign thunderclap headaches Other pathologies not apparent on CT Severe primary headaches: management
Can I send this headache patient home? Dr Nicola Giffin Consultant Neurologist Bath, Nov 2017 SAH v benign thunderclap headaches Other pathologies not apparent on CT Severe primary headaches: management
By Nathan Hall Associate Editor
 By Nathan Hall Associate Editor 34 Practical Neurology March 2005 These new rules may change the definition of head pain, but some practitioners may find the new guidelines themselves to be a source of
By Nathan Hall Associate Editor 34 Practical Neurology March 2005 These new rules may change the definition of head pain, but some practitioners may find the new guidelines themselves to be a source of
MEASURE #4: Overuse of Barbiturate Containing Medications for Primary Headache Disorders Headache
 MEASURE #4: Overuse of Barbiturate Containing Medications for Primary Headache Disorders Headache Measure Description Percentage of patients age 18 years old and older with a diagnosis of primary headache
MEASURE #4: Overuse of Barbiturate Containing Medications for Primary Headache Disorders Headache Measure Description Percentage of patients age 18 years old and older with a diagnosis of primary headache
Headache. Section 1. Migraine headache. Clinical presentation
 Section 1 Headache Migraine headache 1 Clinical presentation It is important to recognize just how significant a problem migraine headache is. It has been estimated that migraine affects 11% of the United
Section 1 Headache Migraine headache 1 Clinical presentation It is important to recognize just how significant a problem migraine headache is. It has been estimated that migraine affects 11% of the United
Managing Headache in Acute Medicine. Ben Lovell Consultant Physician in Acute Medicine University College London Hospital
 Managing Headache in Acute Medicine Ben Lovell Consultant Physician in Acute Medicine University College London Hospital Some ED headache stats Arrive by ambulance 31% Median age 39 Worst ever headache
Managing Headache in Acute Medicine Ben Lovell Consultant Physician in Acute Medicine University College London Hospital Some ED headache stats Arrive by ambulance 31% Median age 39 Worst ever headache
Headache Master School Japan-Osaka 2016 (HMSJ-Osaka2016) October 23, II. Management of Refractory Headaches
 Headache Master School Japan-Osaka 2016 (HMSJ-Osaka2016) October 23, 2016 II. Management of Refractory Headaches Case presentation 1: A case of intractable daily-persistent headache Keio University School
Headache Master School Japan-Osaka 2016 (HMSJ-Osaka2016) October 23, 2016 II. Management of Refractory Headaches Case presentation 1: A case of intractable daily-persistent headache Keio University School
GENERAL APPROACH AND CLASSIFICATION OF HEADACHES
 GENERAL APPROACH AND CLASSIFICATION OF HEADACHES CLASSIFICATION Headache is one of the most common medical complaints. Most of the population will have experienced headache, and over 5% will seek medical
GENERAL APPROACH AND CLASSIFICATION OF HEADACHES CLASSIFICATION Headache is one of the most common medical complaints. Most of the population will have experienced headache, and over 5% will seek medical
Strategies in Migraine Care
 Strategies in Migraine Care Julie L. Roth, MD Rhode Island Hospital Assistant Professor, Neurology The Warren Alpert Medical School of Brown University March 28, 2015 Financial Disclosures None. Objectives
Strategies in Migraine Care Julie L. Roth, MD Rhode Island Hospital Assistant Professor, Neurology The Warren Alpert Medical School of Brown University March 28, 2015 Financial Disclosures None. Objectives
Embriologically, The head is formed from the first two cervical segments (except the mandible, which is formed by the third). The first and second
 Embriologically, The head is formed from the first two cervical segments (except the mandible, which is formed by the third). The first and second cervical vertebra are also derived from these two segments.
Embriologically, The head is formed from the first two cervical segments (except the mandible, which is formed by the third). The first and second cervical vertebra are also derived from these two segments.
HEADACHE Transient discomfort, chronic nuisance, or looming disaster?
 HEADACHE Transient discomfort, chronic nuisance, or looming disaster? Hussien H. Rizk, MD Cairo University Medical School ١ Headache Second most common o symptom (after pain) Migraine alone afflicts 12
HEADACHE Transient discomfort, chronic nuisance, or looming disaster? Hussien H. Rizk, MD Cairo University Medical School ١ Headache Second most common o symptom (after pain) Migraine alone afflicts 12
Trigeminal Autonomic Cephalalgias. Disclosures. Objectives 6/20/2018. Rashmi Halker Singh, MD FAHS UCNS Review Course June 2018
 Trigeminal Autonomic Cephalalgias Rashmi Halker Singh, MD FAHS UCNS Review Course June 2018 Disclosures Honoraria from Allergan and Amgen for advisory board, Current Neurology and Neuroscience Reports
Trigeminal Autonomic Cephalalgias Rashmi Halker Singh, MD FAHS UCNS Review Course June 2018 Disclosures Honoraria from Allergan and Amgen for advisory board, Current Neurology and Neuroscience Reports
2) Headache - Dr. Hawar
 2) Headache - Dr. Hawar Headache is caused by traction, displacement, inflammation, vascular spasm, or distention of the painsensitive structures in the head or neck. Isolated involvement of the bony skull,
2) Headache - Dr. Hawar Headache is caused by traction, displacement, inflammation, vascular spasm, or distention of the painsensitive structures in the head or neck. Isolated involvement of the bony skull,
MIGRAINE CLASSIFICATION
 MIGRAINE CLASSIFICATION Nada Šternić At most, only 30% of migraineurs have classic aura The same patient may have migraine headache without aura, migraine headache with aura as well as migraine aura without
MIGRAINE CLASSIFICATION Nada Šternić At most, only 30% of migraineurs have classic aura The same patient may have migraine headache without aura, migraine headache with aura as well as migraine aura without
Overuse of barbiturate and opioid containing medications for primary headache disorders Description
 Measure Title Overuse of barbiturate and opioid containing medications for primary headache disorders Description Percentage of s age 12 years and older with a diagnosis of primary headache who were prescribed
Measure Title Overuse of barbiturate and opioid containing medications for primary headache disorders Description Percentage of s age 12 years and older with a diagnosis of primary headache who were prescribed
Headache Master School Japan-Osaka 2016 II. Management of refractory headaches Case Presentation 2. SUNCT/SUNA: concept, management and prognosis
 Headache Master School Japan-Osaka 2016 II. Management of refractory headaches Case Presentation 2. SUNCT/SUNA: concept, management and prognosis Noboru Imai(Department of Neurology, Japanese Red Cross
Headache Master School Japan-Osaka 2016 II. Management of refractory headaches Case Presentation 2. SUNCT/SUNA: concept, management and prognosis Noboru Imai(Department of Neurology, Japanese Red Cross
Faculty Disclosure. Karen L. Bremer, MD. Dr. Bremer has listed no financial interest/arrangement that would be considered a conflict of interest.
 Faculty Disclosure Karen L. Bremer, MD Dr. Bremer has listed no financial interest/arrangement that would be considered a conflict of interest. HEADACHE UPDATE Karen L. Bremer, MD November 10, 2017 karen.bremer@creighton.edu
Faculty Disclosure Karen L. Bremer, MD Dr. Bremer has listed no financial interest/arrangement that would be considered a conflict of interest. HEADACHE UPDATE Karen L. Bremer, MD November 10, 2017 karen.bremer@creighton.edu
How do we treat migraine? New SIGN Guidelines
 How do we treat migraine? New SIGN Guidelines Managing your migraine Migraine Trust, Edinburgh 2018 Callum Duncan Consultant Neurologist Aberdeen Royal Infirmary Chair SIGN Guideline 155 Premonitory Mood
How do we treat migraine? New SIGN Guidelines Managing your migraine Migraine Trust, Edinburgh 2018 Callum Duncan Consultant Neurologist Aberdeen Royal Infirmary Chair SIGN Guideline 155 Premonitory Mood
FINANCIAL DISCLOSURE. No relevant financial relationships
 Sleep and Headache Paul Mathew, MD, FAHS Director of Continuing Medical Education John R. Graham Headache Center Brigham & Women s Hospital Director of Headache Medicine Cambridge Health Alliance Harvard
Sleep and Headache Paul Mathew, MD, FAHS Director of Continuing Medical Education John R. Graham Headache Center Brigham & Women s Hospital Director of Headache Medicine Cambridge Health Alliance Harvard
Controlling Migraine Pain
 Migraine Stats Controlling Migraine Pain Alan Zacharias, M.D. Associated Neurologists, Boulder Community Health 303-622-3365 Women 15% Men 5% Usually starts in 2 nd and 3 rd Decade Major Impact on days
Migraine Stats Controlling Migraine Pain Alan Zacharias, M.D. Associated Neurologists, Boulder Community Health 303-622-3365 Women 15% Men 5% Usually starts in 2 nd and 3 rd Decade Major Impact on days
Diagnosis of Primary Headache Syndromes. Gerald W. Smetana, M.D. Division of General Medicine Beth Israel Deaconess Medical Center
 Diagnosis of Primary Headache Syndromes Gerald W. Smetana, M.D. Division of General Medicine Beth Israel Deaconess Medical Center Goals Distinguish primary from secondary headaches Recognize typical histories
Diagnosis of Primary Headache Syndromes Gerald W. Smetana, M.D. Division of General Medicine Beth Israel Deaconess Medical Center Goals Distinguish primary from secondary headaches Recognize typical histories
Update on Diagnosis and Management of Migraines
 Update on Diagnosis and Management of Migraines Joel J. Heidelbaugh, MD, FAAFP, FACG Clinical Professor Departments of Family Medicine and Urology University of Michigan Learning Objectives To distinguish
Update on Diagnosis and Management of Migraines Joel J. Heidelbaugh, MD, FAAFP, FACG Clinical Professor Departments of Family Medicine and Urology University of Michigan Learning Objectives To distinguish
SUMAVEL DOSEPRO (sumatriptan succinate) solution for injection
 SUMAVEL DOSEPRO (sumatriptan succinate) solution for injection Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit
SUMAVEL DOSEPRO (sumatriptan succinate) solution for injection Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit
ONZETRA XSAIL (sumatriptan) nasal powder
 ONZETRA XSAIL (sumatriptan) nasal powder Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Pharmacy
ONZETRA XSAIL (sumatriptan) nasal powder Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Pharmacy
Lynda J. Krasenbaum, MSN, ANP BC. Associate Director New York Headache Center
 Diagnosing Headache in Adults and Adolescents Lynda J. Krasenbaum, MSN, ANP BC Associate Director New York Headache Center New York, New York Learning Objectives Understand the diagnostic challenges of
Diagnosing Headache in Adults and Adolescents Lynda J. Krasenbaum, MSN, ANP BC Associate Director New York Headache Center New York, New York Learning Objectives Understand the diagnostic challenges of
UCNS Course A Review of ICHD-3b
 UCNS Course A Review of ICHD-3b Andrew D. Hershey, M.D., Ph.D., FAHS Endowed Chair and Director of Neurology Director, Cincinnati Children s Headache Center Professor of Neurology and Pediatrics University
UCNS Course A Review of ICHD-3b Andrew D. Hershey, M.D., Ph.D., FAHS Endowed Chair and Director of Neurology Director, Cincinnati Children s Headache Center Professor of Neurology and Pediatrics University
The trigeminal autonomic cephalalgias (TACs) are a group of. Cluster Headache and Other Trigeminal Autonomic Cephalalgias By Mark Burish, MD, PhD
 Downloaded from https://journals.lww.com/continuum by SruuCyaLiGD/095xRqJ2PzgDYuM98ZB494KP9rwScvIkQrYai2aioRZDTyulujJ/fqPksscQKqke3QAnIva1ZqwEKekuwNqyUWcnSLnClNQLfnPrUdnEcDXOJLeG3sr/HuiNevTSNcdMFp1i4FoTX9EXYGXm/fCfrbTavvQSUHUH4eazE11ptLzgCyEpzDoF
Downloaded from https://journals.lww.com/continuum by SruuCyaLiGD/095xRqJ2PzgDYuM98ZB494KP9rwScvIkQrYai2aioRZDTyulujJ/fqPksscQKqke3QAnIva1ZqwEKekuwNqyUWcnSLnClNQLfnPrUdnEcDXOJLeG3sr/HuiNevTSNcdMFp1i4FoTX9EXYGXm/fCfrbTavvQSUHUH4eazE11ptLzgCyEpzDoF
Case Presentation. Case Presentation. Case Presentation. Truths about Headaches (2017) Most headaches were muscle-tension headaches
 Agenda Case presentation Migraine Morphology Primary and Premonitory Phase Secondary Headache Aura Headache Primer on Pain Medication Overuse Headache Case Presentation RT is a 25 year old woman with daily
Agenda Case presentation Migraine Morphology Primary and Premonitory Phase Secondary Headache Aura Headache Primer on Pain Medication Overuse Headache Case Presentation RT is a 25 year old woman with daily
Measure Components Numerator Statement
 MEASURE #5: OVERUSE OF OPIOID CONTAINING MEDICATIONS FOR PRIMARY HEADACHE DISORDERS Headache For Quality Improvement Only. Not to be used for Public Reporting or Accountability Measure Description Percentage
MEASURE #5: OVERUSE OF OPIOID CONTAINING MEDICATIONS FOR PRIMARY HEADACHE DISORDERS Headache For Quality Improvement Only. Not to be used for Public Reporting or Accountability Measure Description Percentage
Paediatric headaches. Dr Jaycen Cruickshank Director of Clinical Training Ballarat Health Services. Brevity, levity, repetition
 Paediatric headaches Dr Jaycen Cruickshank Director of Clinical Training Ballarat Health Services Brevity, levity, repetition Paediatric)headache?)! Headache!in!children!is!not!that!common.!The!question!is!which!headaches!do!I!
Paediatric headaches Dr Jaycen Cruickshank Director of Clinical Training Ballarat Health Services Brevity, levity, repetition Paediatric)headache?)! Headache!in!children!is!not!that!common.!The!question!is!which!headaches!do!I!
I have no financial relationships to disclose. I will not discuss investigational use of medication in my presentation.
 I have no financial relationships to disclose. I will not discuss investigational use of medication in my presentation. In 1962, Bille published landmark epidemiologic survey of headache among 9,000 school
I have no financial relationships to disclose. I will not discuss investigational use of medication in my presentation. In 1962, Bille published landmark epidemiologic survey of headache among 9,000 school
11/10/2017. THE BRIDGE Course Objectives. THE BRIDGE Course Objectives
 THE BRIDGE Course Objectives Describe clinical characteristics associated with migraine diagnosis in adult and pediatric populations. Identify barriers and risk factors impacting the clinical course of
THE BRIDGE Course Objectives Describe clinical characteristics associated with migraine diagnosis in adult and pediatric populations. Identify barriers and risk factors impacting the clinical course of
CHRONIC HEADACHES IN CHILDHOOD
 CHRONIC HEADACHES IN CHILDHOOD EDWIN LIU, MD PEDIATRIC NEUROLOGISTS OF PALM BEACH PEDIATRIC SLEEP CENTERS OF FLORIDA ASSISTANT CLINICAL PROFESSOR FSU ASSISTANT CLINICAL PROFESSOR NOVA SOUTHEASTERN PEDIATRIC
CHRONIC HEADACHES IN CHILDHOOD EDWIN LIU, MD PEDIATRIC NEUROLOGISTS OF PALM BEACH PEDIATRIC SLEEP CENTERS OF FLORIDA ASSISTANT CLINICAL PROFESSOR FSU ASSISTANT CLINICAL PROFESSOR NOVA SOUTHEASTERN PEDIATRIC
10/31/2017 PRIMARY CARE AND HEADACHE DISCLOSURES WHERE DO THOSE WITH HEADACHE SEEK MEDICAL CARE? Primary Care 67%
 PRIMARY CARE AND HEADACHE Sonja Potrebic MD PhD Regional Headache Specialist Kaiser LAMC 1 WHERE DO THOSE WITH HEADACHE SEEK MEDICAL CARE? Column1 Primary Care 67% Primary Care Headache Specialty Other
PRIMARY CARE AND HEADACHE Sonja Potrebic MD PhD Regional Headache Specialist Kaiser LAMC 1 WHERE DO THOSE WITH HEADACHE SEEK MEDICAL CARE? Column1 Primary Care 67% Primary Care Headache Specialty Other
Cluster headache (CH): epidemiology, classification and clinical picture
 Cluster headache (CH): epidemiology, classification and clinical picture Toomas Toomsoo, M.D. Head of the Center of Neurology East Tallinn Central Hospital 1 INTRODUCTION Cluster headache - known as trigeminal
Cluster headache (CH): epidemiology, classification and clinical picture Toomas Toomsoo, M.D. Head of the Center of Neurology East Tallinn Central Hospital 1 INTRODUCTION Cluster headache - known as trigeminal
Headaches in the Pediatric Emergency Dept
 Headaches in Children February 23, 2011 Jinny Tavee, MD Associate Professor Neuromuscular Center Cleveland Clinic Foundation Cleveland, OH 1 Headaches in the Pediatric Emergency Dept Burton Gutierrez Kan
Headaches in Children February 23, 2011 Jinny Tavee, MD Associate Professor Neuromuscular Center Cleveland Clinic Foundation Cleveland, OH 1 Headaches in the Pediatric Emergency Dept Burton Gutierrez Kan
Specific Objectives A. Topics to be lectured and discussed at the plenary sessions
 Specific Objectives A. Topics to be lectured and discussed at the plenary sessions 0. Introduction: Good morning ICHD-III! Let s start at the very beginning. When you read you begin with A-B-C, so when
Specific Objectives A. Topics to be lectured and discussed at the plenary sessions 0. Introduction: Good morning ICHD-III! Let s start at the very beginning. When you read you begin with A-B-C, so when
Headaches in Pregnancy Before, During, and After
 Headaches in Pregnancy Before, During, and After Robert Kaniecki, MD Director, UPMC Headache Center Assistant Professor of Neurology University of Pittsburgh Headaches and Pregnancy Pre-pregnancy counseling
Headaches in Pregnancy Before, During, and After Robert Kaniecki, MD Director, UPMC Headache Center Assistant Professor of Neurology University of Pittsburgh Headaches and Pregnancy Pre-pregnancy counseling
Migraine Migraine Age Specific Prevalence in the United States. Headache International Headache Society Classification
 28 Primary Care Medicine Principles and Practice 29 October 28 Professor Peter J. Goadsby Peter.Goadsby@headache.ucsf.edu Department of Neurology Headache International Headache Society Classification
28 Primary Care Medicine Principles and Practice 29 October 28 Professor Peter J. Goadsby Peter.Goadsby@headache.ucsf.edu Department of Neurology Headache International Headache Society Classification
Headache. Anna Morenkova, MD, PhD Assistant Professor Department of Neurology UC Irvine
 Headache Anna Morenkova, MD, PhD Assistant Professor Department of Neurology UC Irvine SOURCE OF HEAD PAIN (NOCICEPTIVE STRUCTURES) Intracranial Extracranial arteries of circle of Willis dura, dural arteries
Headache Anna Morenkova, MD, PhD Assistant Professor Department of Neurology UC Irvine SOURCE OF HEAD PAIN (NOCICEPTIVE STRUCTURES) Intracranial Extracranial arteries of circle of Willis dura, dural arteries
Painless, progressive weakness Could this be Motor Neurone Disease?
 APPENDIX 1 Painless, progressive weakness Could this be Motor Neurone Disease? 1. Does the patient have one or more of these? Bulbar features Limb features Respiratory features Cognitive features (rare)
APPENDIX 1 Painless, progressive weakness Could this be Motor Neurone Disease? 1. Does the patient have one or more of these? Bulbar features Limb features Respiratory features Cognitive features (rare)
HEADACHE. Dr Nick Pendleton. September Headache
 HEADACHE Dr Nick Pendleton September 2017 Headache Tension Type Headache Cranial Nerve Examination Migraine Migraine Treatment Medication Overuse Headache Headache Red Flags Sinusitis Headache Raised ICP
HEADACHE Dr Nick Pendleton September 2017 Headache Tension Type Headache Cranial Nerve Examination Migraine Migraine Treatment Medication Overuse Headache Headache Red Flags Sinusitis Headache Raised ICP
HEADACHE PATHOPHYSIOLOGY
 HEADACHE PATHOPHYSIOLOGY Andrew Charles, M.D. Professor Director, UCLA Goldberg Migraine Program Meyer and Renee Luskin Chair in Migraine and Headache Studies Director, Headache Research and Treatment
HEADACHE PATHOPHYSIOLOGY Andrew Charles, M.D. Professor Director, UCLA Goldberg Migraine Program Meyer and Renee Luskin Chair in Migraine and Headache Studies Director, Headache Research and Treatment
Overview INTRODUCTION 3/15/2018. Headache Emergencies. Other way to differentiate between them? Is there an easy way to differentiate between them?
 Overview Headache Emergencies Primary versus Secondary headache disorder Red flags 4 cases of unusual headache emergencies Disclaimer: we will not talk about brain bleed as patients usually go the ED.
Overview Headache Emergencies Primary versus Secondary headache disorder Red flags 4 cases of unusual headache emergencies Disclaimer: we will not talk about brain bleed as patients usually go the ED.
Primary Headache Prevalence % (95% CI) Migraine without aura 9 (7-9) Migraine with aura 6 (5-8)
 Primary Headache Prevalence % (95% CI) Migraine without aura 9 (7-9) Migraine with aura 6 (5-8) Episodic tension-type headache 66 (62-69) Chronic tension-type headache 3 (2-5) Cluster headache 0.1 (0 1)
Primary Headache Prevalence % (95% CI) Migraine without aura 9 (7-9) Migraine with aura 6 (5-8) Episodic tension-type headache 66 (62-69) Chronic tension-type headache 3 (2-5) Cluster headache 0.1 (0 1)
Pause for thought. Dr Jane Anderson Consultant Neurologist
 Pause for thought Dr Jane Anderson Consultant Neurologist Which is the top cause of years lived with disability worldwide? 1. COPD 2. Low Back pain 3. Diabetes 4. Migraine with medication overuse headache
Pause for thought Dr Jane Anderson Consultant Neurologist Which is the top cause of years lived with disability worldwide? 1. COPD 2. Low Back pain 3. Diabetes 4. Migraine with medication overuse headache
A New Era of Migraine Management: The Challenging Landscape in Prevention
 Provided by MediCom Worldwide, Inc. Supported by an educational grant from Teva Pharmaceuticals What is a Neuropeptide? Small chains of amino acids released by neural cells (neurons or glial cells) to
Provided by MediCom Worldwide, Inc. Supported by an educational grant from Teva Pharmaceuticals What is a Neuropeptide? Small chains of amino acids released by neural cells (neurons or glial cells) to
25/09/2018 HEADACHE. Dr Nick Pendleton
 HEADACHE Dr Nick Pendleton September 2018 1 Small Group Work Tension Type Headache Cranial Nerve Examination Migraine Migraine Treatment Medication Overuse Headache Headache Red Flags Sinusitis Headache
HEADACHE Dr Nick Pendleton September 2018 1 Small Group Work Tension Type Headache Cranial Nerve Examination Migraine Migraine Treatment Medication Overuse Headache Headache Red Flags Sinusitis Headache
Mark W. Green, MD, FAAN
 Mark W. Green, MD, FAAN Professor of Neurology, Anesthesiology, and Rehabilitation Medicine Director of Headache and Pain Medicine Icahn School of Medicine at Mt Sinai New York Pain-sensitive structures
Mark W. Green, MD, FAAN Professor of Neurology, Anesthesiology, and Rehabilitation Medicine Director of Headache and Pain Medicine Icahn School of Medicine at Mt Sinai New York Pain-sensitive structures
Headache. Susan Hickenbottom MD, MS February 24, 2015
 Headache Susan Hickenbottom MD, MS February 24, 2015 Epidemiology One of most common complaints in primary care 90% of US population 50% at least one severe 25% recurrent disabling attacks 5% chronic daily
Headache Susan Hickenbottom MD, MS February 24, 2015 Epidemiology One of most common complaints in primary care 90% of US population 50% at least one severe 25% recurrent disabling attacks 5% chronic daily
June National Migraine and Headache Awareness Month
 June 2018- National Migraine and Headache Awareness Month A note from the author Hello NCP friends! This month, I wanted to feature a topic that has been much discussed amongst several of my friends and
June 2018- National Migraine and Headache Awareness Month A note from the author Hello NCP friends! This month, I wanted to feature a topic that has been much discussed amongst several of my friends and
Migraine Management. Dr Helen Brown Director of Neurology and Stroke The Princess Alexandra Hospital
 Migraine Management Dr Helen Brown Director of Neurology and Stroke The Princess Alexandra Hospital Referral Criteria for Migraine Migraine Management Migraine Diagnosis Spot on Health Migraine pathway
Migraine Management Dr Helen Brown Director of Neurology and Stroke The Princess Alexandra Hospital Referral Criteria for Migraine Migraine Management Migraine Diagnosis Spot on Health Migraine pathway
Neurological Dilemmas in Primary Care
 Neurological Dilemmas in Primary Care David Clark, DO dclark@oregonneurology.com When to test? How to test? Pitfalls in testing? When to treat? How to treat? How long to treat? Neurological Dilemmas Seizure
Neurological Dilemmas in Primary Care David Clark, DO dclark@oregonneurology.com When to test? How to test? Pitfalls in testing? When to treat? How to treat? How long to treat? Neurological Dilemmas Seizure
PREVALENCE BY HEADACHE TYPE
 CLINICAL CLUES AND CLINICAL RULES: PRIMARY VS SECONDARY HEADACHE * Based on a presentation by David W. Dodick, MD ABSTRACT Headache is a common condition, accounting for many specialist office visits annually.
CLINICAL CLUES AND CLINICAL RULES: PRIMARY VS SECONDARY HEADACHE * Based on a presentation by David W. Dodick, MD ABSTRACT Headache is a common condition, accounting for many specialist office visits annually.
4/12/2018. ECHO Ontario Chronic Pain Migraine. Migraine Definition and Epidemiology. Migraine - Undertreatment. Migraine - Diagnostic Classification
 Andrew J Smith, MDCM ECHO Ontario Chronic Pain Migraine Staff Physician, Neurology, Pain and Addiction Medicine Centre for Addiction and Mental Health Migraine Learning Objectives At the end of this session,
Andrew J Smith, MDCM ECHO Ontario Chronic Pain Migraine Staff Physician, Neurology, Pain and Addiction Medicine Centre for Addiction and Mental Health Migraine Learning Objectives At the end of this session,
Classification and WHO ICD-10NA Codes
 Classification and WHO ICD-10NA Codes IHS WHO Diagnosis ICHD-II ICD-10NA [and aetiological ICD-10 code for secondary headache disorders] code code 1. [G43] Migraine 1.1 [G43.0] Migraine without aura 1.2
Classification and WHO ICD-10NA Codes IHS WHO Diagnosis ICHD-II ICD-10NA [and aetiological ICD-10 code for secondary headache disorders] code code 1. [G43] Migraine 1.1 [G43.0] Migraine without aura 1.2
Atypical presentations of cluster headache
 Blackwell Science, LtdOxford, UKCHACephalalgia0333-1024Blackwell Science, 200222Original ArticleAtypical presentations in cluster headachetd Rozen Atypical presentations of cluster headache TD Rozen Department
Blackwell Science, LtdOxford, UKCHACephalalgia0333-1024Blackwell Science, 200222Original ArticleAtypical presentations in cluster headachetd Rozen Atypical presentations of cluster headache TD Rozen Department
Ishaq Abu Arafeh Consultant Paediatrician Royal Hospital for Children, Glasgow Forth Valley Royal Hospital, Larbert
 Ishaq Abu Arafeh Consultant Paediatrician Royal Hospital for Children, Glasgow Forth Valley Royal Hospital, Larbert Childhood headache: Is it really difficult to manage? It shouldn t be... But it can be...
Ishaq Abu Arafeh Consultant Paediatrician Royal Hospital for Children, Glasgow Forth Valley Royal Hospital, Larbert Childhood headache: Is it really difficult to manage? It shouldn t be... But it can be...
Controversy One: Headache and Disability. Robert Shapiro, MD, PhD University of Vermont
 Controversy One: Headache and Disability Robert Shapiro, MD, PhD University of Vermont Southern Headache Society Orlando, FL, Sept 21, 2013 Disclosures Consulting within the past 12 months: Transcept Pharmaceuticals
Controversy One: Headache and Disability Robert Shapiro, MD, PhD University of Vermont Southern Headache Society Orlando, FL, Sept 21, 2013 Disclosures Consulting within the past 12 months: Transcept Pharmaceuticals
1. On how many days in the last 3 months did you miss work or school because of your headaches?
 The Migraine Disability Assessment Test The MIDAS (Migraine Disability Assessment) questionnaire was put together to help you measure the impact your headaches have on your life. The information on this
The Migraine Disability Assessment Test The MIDAS (Migraine Disability Assessment) questionnaire was put together to help you measure the impact your headaches have on your life. The information on this
PAEDIATRIC ACUTE CARE GUIDELINE. Headache. This document should be read in conjunction with this DISCLAIMER
 Princess Margaret Hospital for Children PAEDIATRIC ACUTE CARE GUIDELINE Scope (Staff): Scope (Area): All Emergency Department Clinicians Emergency Department This document should be read in conjunction
Princess Margaret Hospital for Children PAEDIATRIC ACUTE CARE GUIDELINE Scope (Staff): Scope (Area): All Emergency Department Clinicians Emergency Department This document should be read in conjunction
COMPLEXITIES OF MIGRAINE HEADACHES
 COMPLEXITIES OF MIGRAINE HEADACHES Michael A. Rogawski, MD, PhD Professor and Chair Department of Neurology University of California, Davis Sacramento, CA MICHAEL A. ROGAWSKI, MD, PHD Disclosures Research/Grants:
COMPLEXITIES OF MIGRAINE HEADACHES Michael A. Rogawski, MD, PhD Professor and Chair Department of Neurology University of California, Davis Sacramento, CA MICHAEL A. ROGAWSKI, MD, PHD Disclosures Research/Grants:
florida child neurology
 Headaches florida child neurology You re sitting at your desk, working on a difficult task, when it suddenly feels as if a belt or vice is being tightened around the top of your head. Or you have periodic
Headaches florida child neurology You re sitting at your desk, working on a difficult task, when it suddenly feels as if a belt or vice is being tightened around the top of your head. Or you have periodic
ACUTE TREATMENT FOR MIGRAINE. Cristina Tassorelli
 The European Headache School 2012 ACUTE TREATMENT FOR MIGRAINE Cristina Tassorelli Headache Science Centre, IRCCS Neurological Institute C. Mondino Foundation - Pavia University Centre for Adaptive Disorders
The European Headache School 2012 ACUTE TREATMENT FOR MIGRAINE Cristina Tassorelli Headache Science Centre, IRCCS Neurological Institute C. Mondino Foundation - Pavia University Centre for Adaptive Disorders
Headache A Practical Approach
 Headache A Practical Approach Integrated Pain Symposium December 1, 2017 Alyssa Lettich. MD Neurosciences Institute/Neurosciences Clinical Program Medical Director Headache and Pain Development Teams Disclosures:
Headache A Practical Approach Integrated Pain Symposium December 1, 2017 Alyssa Lettich. MD Neurosciences Institute/Neurosciences Clinical Program Medical Director Headache and Pain Development Teams Disclosures:
Jessica Ailani MD FAHS Director, Georgetown Headache Center Associate Professor Neurology Medstar Georgetown University Hospital
 Jessica Ailani MD FAHS Director, Georgetown Headache Center Associate Professor Neurology Medstar Georgetown University Hospital Honorarium from Current Pain and Headache Reports; Section Editor Unusual
Jessica Ailani MD FAHS Director, Georgetown Headache Center Associate Professor Neurology Medstar Georgetown University Hospital Honorarium from Current Pain and Headache Reports; Section Editor Unusual
NAT Pro Series: Treating Headaches. Simeon Niel-Asher BSc (Ost) BPhil NAT. Copyright Niel Asher Healthcare
 NAT Pro Series: Treating Headaches Simeon Niel-Asher BSc (Ost) BPhil NAT Copyright Niel Asher Healthcare Welcome According to the World Health Organization 1 an estimated 47% of adults had a headache at
NAT Pro Series: Treating Headaches Simeon Niel-Asher BSc (Ost) BPhil NAT Copyright Niel Asher Healthcare Welcome According to the World Health Organization 1 an estimated 47% of adults had a headache at
HEADACHE: Prevalence and Impact
 Mod 2 Headaches HEADACHE: Prevalence and Impact PREVALENCE 18-25 % women have headaches 6-10 % men have headaches 5% of women have headaches more than 15 days per month 112 million bedridden days per year
Mod 2 Headaches HEADACHE: Prevalence and Impact PREVALENCE 18-25 % women have headaches 6-10 % men have headaches 5% of women have headaches more than 15 days per month 112 million bedridden days per year
Diagnosing headache. The clinician should approach the diagnosis of. Secondary headache. Primary headache. Blue and red flag headaches
 Headache THEME Diagnosing headache BACKGROUND A systematic approach to the diagnosis of primary and secondary headache disorders requires the measurement of the frequency and the duration of headache.
Headache THEME Diagnosing headache BACKGROUND A systematic approach to the diagnosis of primary and secondary headache disorders requires the measurement of the frequency and the duration of headache.
Headache Management in Primary Care Dr Niranjanan Nirmalananthan Consultant Neurologist
 Headache Management in Primary Care Dr Niranjanan Nirmalananthan Consultant Neurologist Wednesday 10 th of April 2019 Summary Why does it matter? Classification and diagnosis Who to refer / scan? Serious
Headache Management in Primary Care Dr Niranjanan Nirmalananthan Consultant Neurologist Wednesday 10 th of April 2019 Summary Why does it matter? Classification and diagnosis Who to refer / scan? Serious
Patient with Lots of NTERNATIONAL CLASSIFICATION. Headaches HEADACHE DISORDERS. R. Allan Purdy, MD, FRCPC,FACP
 Patient with Lots of NTERNATIONAL CLASSIFICATION Headaches of R. Allan Purdy, MD, FRCPC,FACP HEADACHE DISORDERS Professor of Medicine (Neurology) Dalhousie University, Halifax, Canada 2nd edition (ICHD-II)
Patient with Lots of NTERNATIONAL CLASSIFICATION Headaches of R. Allan Purdy, MD, FRCPC,FACP HEADACHE DISORDERS Professor of Medicine (Neurology) Dalhousie University, Halifax, Canada 2nd edition (ICHD-II)
Migraine, Tension, and Cluster Headache: Primary Care for Primary Headaches. Jonathon M. Firnhaber, MD, FAAFP
 Migraine, Tension, and Cluster Headache: Primary Care for Primary Headaches Jonathon M. Firnhaber, MD, FAAFP Learning objectives 1. Utilize evidence-based strategies to diagnose patients presenting with
Migraine, Tension, and Cluster Headache: Primary Care for Primary Headaches Jonathon M. Firnhaber, MD, FAAFP Learning objectives 1. Utilize evidence-based strategies to diagnose patients presenting with
Chapter 2 Diagnosis of Trigeminal Autonomic Cephalalgias
 Chapter 2 Diagnosis of Trigeminal Autonomic Cephalalgias Mark J. Stillman Introduction The trigeminal autonomic cephalalgias (TACs) refer to a specific group of primary headaches characterized by unilaterality,
Chapter 2 Diagnosis of Trigeminal Autonomic Cephalalgias Mark J. Stillman Introduction The trigeminal autonomic cephalalgias (TACs) refer to a specific group of primary headaches characterized by unilaterality,
Headache. Luke Bennetto Consultant Neurologist Engineers House 13 th September 2016
 Headache Luke Bennetto Consultant Neurologist Engineers House 13 th September 2016 Contents General thoughts Primary headache Secondary headache I want to curl up in a cave and die I want to drill a
Headache Luke Bennetto Consultant Neurologist Engineers House 13 th September 2016 Contents General thoughts Primary headache Secondary headache I want to curl up in a cave and die I want to drill a
Identification of Painful Tissue Orthopaedic Examination DX 612. James J. Lehman, DC, MBA, DABCO University of Bridgeport College of Chiropractic
 Identification of Painful Tissue Orthopaedic Examination DX 612 James J. Lehman, DC, MBA, DABCO University of Bridgeport College of Chiropractic Generalized Pain Description Joint pain may be constant
Identification of Painful Tissue Orthopaedic Examination DX 612 James J. Lehman, DC, MBA, DABCO University of Bridgeport College of Chiropractic Generalized Pain Description Joint pain may be constant
Headache Syndrome. Karen Alvarez, D.O Nemours Children s Specialty Care Jacksonville, FL
 Headache Syndrome Karen Alvarez, D.O Nemours Children s Specialty Care Jacksonville, FL What is a headache? A headache or cephalgia is defined as pain anywhere in the region of head or neck Where does
Headache Syndrome Karen Alvarez, D.O Nemours Children s Specialty Care Jacksonville, FL What is a headache? A headache or cephalgia is defined as pain anywhere in the region of head or neck Where does
