Experimental evaluation of the Spiegelberg intracranial pressure and intracranial compliance monitor
|
|
|
- Donna Cunningham
- 5 years ago
- Views:
Transcription
1 Neurosurg Focus 9 (5):Article 1, Journal of Neurosurgery Preview Article for December 2000, Click here to return to Table of Contents Experimental evaluation of the Spiegelberg intracranial pressure and intracranial compliance monitor Technical note YUN H. YAU, F.R.C.S.(ED), IAN R. PIPER, PH.D., RICHARD E. CLUTTON, B.V.SC., D.V.A., AND IAN R. WHITTLE, PH.D., F.R.A.C.S. Departments of Clinical Neurosciences and Veterinary Clinical Studies, University of Edinburgh; and Department of Clinical Physics, Southern General Hospital, Glasgow, United Kingdom The goal of this study was to compare the Spiegelberg intraventricular intracranial pressure (ICP)/intracranial compliance monitoring device, which features an air-pouch balloon catheter, with existing gold-standard methods of measuring ICP and intracranial compliance. A Spiegelberg intraventricular catheter, a standard intraventricular catheter, and a Codman intraparenchymal ICP microsensor were placed in five sheep, which previously had been given anesthetic and paralytic agents, to allow comparative measurement of ICP at incremental levels (range 5 50 mm Hg). Intracranial pressure measured using the Spiegelberg intraventricular air-pouch balloon catheter displayed a linear correlation with ICP measured using the standard intraventricular fluid-filled catheter (r 2 = , p 0.001; average bias 0.74 mm Hg), as well as with ICP measured using the Codman intraparenchymal strain-gauge sensor (r 2 = , p 0.001; average bias 0.01 mm Hg). Automated measurements of intraventricular compliance obtained using the Spiegelberg compliance device were compared with compliance measurements that were made using the gold-standard manual cerebrospinal fluid bolus injection technique at ICPs ranging from 5 to 50 mm Hg, and a linear correlation was demonstrated between the two methods (r 2 = , p 0.001; average bias ml/mm Hg). The Spiegelberg air-pouch ICP/compliance monitor provides ICP and compliance data that are very similar to those obtained using both gold-standard methods and an intraparenchymal ICP monitor over a range of pathophysiological ICPs. The automated closed Spiegelberg system offers practical advantages for the measurement of intraventricular compliance. Assessment of the clinical utility and robustness of the Spiegelberg system, together with the development of an intraparenchymal device, would enhance the clinical utility of automated compliance measurement and expand the range of its applications. KEY WORDS intracranial pressure intracranial compliance intracranial pressure monitoring Methods for the measurement and continuous monitoring of ICP have been in use for more than 20 years. Catheter-tip transducer systems such as the Camino fiberoptic 11 (Camino Laboratories, San Diego, CA) and Codman (Johnson & Johnson Professional, Inc., Raynham, MA) strain-gauge intraparenchymal sensors are currently in use at many centers. However, problems with zero drift and the robustness of such systems have been identified in laboratory bench tests and clinical studies; 2,10,14 16 in addition, it has been found that these systems cannot be recalibrated in vivo. Camino sensors have an average daily drift of up to 3.2 mm Hg, 10 and technical complications resulting in failure of that system occur in 10 to 25% of cases. 2,15,16 An average bias of 5 mm Hg or more in 24% of Codman sensors, compared with the Camino system, has also been described. 4 Abbreviations used in this paper: CL = confidence limit; CPP = cerebral perfusion pressure; CSF = cerebrospinal fluid; ICP = intracranial pressure. A device used in the past for obtaining ICP measurements in the subdural and epidural spaces has recently been adapted to measure ICP in the intraventricular and intraparenchymal compartments. The Spiegelberg system 3 (Spiegelberg GmbH & Co. KG, Hamburg, Germany) involves the use of an air-filled balloon catheter to measure ICP and is capable of automatic zero-drift correction in vivo. A newer version of the Spiegelberg monitoring system also has the capacity to measure intracranial compliance. In laboratory bench tests the Spiegelberg ICP system has been found to be accurate and to have the lowest zero-drift characteristics compared with currently adopted catheter-tip systems. 3 However, the Spiegelberg system has yet to be tested in vivo against gold-standard methods or devices for measuring ICP in the intraventricular and intraparenchymal compartments. Similarly, experimental validation of the compliance values obtained using this system is required. Validation of the latter feature is particularly pertinent because the Spiegelberg device offers an automated method for measuring intraventricular compli- Neurosurg. Focus / Volume 9 / November,
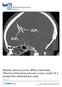
2 Y. H. Yau, et al. ance, whereas the current procedure for measuring intracranial compliance requires manual CSF bolus injections that are both time consuming and labor intensive. When the manual procedure is performed by inexperienced hands, there is also a risk of introducing infection and provoking excessive increases in ICP. 12 Although clinical evaluation of the automated device has been performed in patients with hydrocephalus and the results compared with those obtained using the standard manual-injection method, 13 most of the patients studied did not have high ICP or prolonged periods of low intracranial compliance. The current experimental study was designed to assess in vivo variations in ICP measured using a standard fluidfilled intraventricular catheter, an intraparenchymal Codman microsensor, and the Spiegelberg intraventricular air-pouch catheter system. In addition, we compared intraventricular compliance measurements obtained using the gold-standard manual injection method with those obtained using the Spiegelberg method over a range of pathophysiological ICPs. The sheep was chosen as the experimental animal because the sizes of its brain, ventricles, and cranium are ideally suited to accommodate the size and disposition of the ICP catheters and sensors being evaluated. MATERIALS AND METHODS All study procedures were regulated according to the United Kingdom Animals Scientific Procedures Act Valid British Home Office Project (PPL 60/2513) and personal licenses covered the experimental work. The Spiegelberg system for measuring ICP involves the use of an intraventricular catheter with an air-pouch balloon situated at the tip. The air-pouch method is based on the technique described by Marey and Chauveau (as mentioned by Geddes 5 ). By maintaining a constant known volume within the air pouch, the pressure within the airpouch balloon is equivalent to the surrounding pressure; when the catheter tip is placed within the intraventricular compartment, ICP can thus be measured at the intraventricular site (Fig. 1). Two sets of ICP measurement comparisons were undertaken: 1) the Spiegelberg device with the intraventricular air-pouch balloon catheter was compared with the fluidfilled intraventricular catheter connected to an external strain-gauge transducer; and 2) the Spiegelberg device was compared with the Codman intraparenchymal catheter-tip strain-gauge sensor. Automated measurement of intracranial compliance made using the Spiegelberg device requires insertion of a double-lumen intraventricular catheter (Probe 3; Spiegelberg KG). One lumen is filled with fluid and connects directly with the CSF space, whereas the other connects the monitoring system to an air-pouch balloon mounted on the tip of the catheter (this balloon is the same one used solely for measuring ICP). Through the latter lumen of the catheter, automated injections and withdrawals of air can be made to and from the balloon while it is positioned within the ventricular CSF space. Added volumes are small ( 0.1 ml) and the exact volumes added are calculated after derivation of algorithms based on the gas law equation: Fig. 1. A: Photograph showing the Spiegelberg ICP monitor, which has an accurately calibrated air pump to maintain the balloon of the air-pouch catheter in a semicollapsed state. The monitor connects to an internal strain-gauge transducer used to measure the internal balloon pressure. B: Photograph of the air-pouch catheter with a 2.3-mm outer diameter and a 1-mm inner diameter. C: Diagram demonstrating that Marey's principle of maintaining a balloon in a semicollapsed state will result in the pressure within the balloon being equal to the pressure external to the balloon. PV = nrt (Eq. 1) in which P = pressure, V = volume, n = number of moles of gas, R = universal gas constant, and T = temperature in Kelvins. The resultant perturbations in ICP are detected through the fluid-filled lumen, which is connected to an external strain-gauge pressure transducer (Baxter Truwave; Baxter b.v., Uden, The Netherlands). For this study the filter setting was set for up to 120 injection withdrawal sequences over a period of approximately 10 minutes to allow time-averaged compliance values to be calculated. These values were compared with those obtained using the manual-injection procedure in which boluses of 0.9% saline are injected into the ventricular CSF space over a period of approximately 1 second. The mean injected volume was 0.8 ml (change in volume). Baseline ICP as measured by the intraventricular external strain-gauge transducer was noted preinjection, and the highest ICP measurement was noted postinjection. Compliance was calculated as the ratio of added volume to the ICP change resulting from volume addition: compliance = V/ P = V/(Pmax Pbase) (Eq. 2) in which V = volume, P = pressure, = change, Pmax = highest ICP, and Pbase = baseline ICP. Surgical Preparation Five Suffolk cross-bred ewes were used in this study. A state of anesthesia was induced in each sheep by intravenous injection of etomidate (0.5 mg/kg) and midazolam (0.5 mg/kg). After tracheal intubation, anesthesia was maintained by administration of halothane delivered in a 2 Neurosurg. Focus / Volume 9 / November, 2000
3 Spiegelberg intracranial pressure and intracranial compliance monitor Fig. 2. Upper: Scatterplot showing a comparison between ICP measurements obtained using the Spiegelberg intraventricular airpouch balloon catheter (ICPvb) and those obtained using the intraventricular external strain-gauge catheter (ICPvsg). Linear regression analysis yields a line of best fit with the equation: y = x , an r 2 value of , and a median difference of 0.45 mm Hg. Lower: Bland Altman plot in which the difference between ICP readings obtained using the Spiegelberg intraventricular air-pouch balloon catheter and those obtained using the intraventricular external strain-gauge catheter is plotted against the ICP as the average of the two methods. Average bias is 0.74 mm Hg, with 95% CLs of 1.54 mm Hg and mm Hg. Fig. 3. Upper: Scatterplot showing a comparison between ICP measurements obtained using the Spiegelberg intraventricular airpouch balloon catheter and those obtained using the Codman intraparenchymal strain-gauge sensor. Linear regression analysis yields a line of best fit with the equation y = x , an r 2 value of and a median difference of 0.3 mm Hg. Lower: Bland Altman plot in which the difference between ICP measurements obtained using the Spiegelberg intraventricular air-pouch balloon catheter (ICPvb) and those obtained using the Codman intraparenchymal strain-gauge sensor (ICPpcod) is plotted against the ICP as the average of the two methods. Average bias is 0.01 mm Hg, with 95% CLs of mm Hg and mm Hg. Neurosurg. Focus / Volume 9 / November, :2 O 2 /N 2 O mixture, and neuromuscular blockade was achieved by addition of cis-atracurium (0.1 mg/kg). The animals lungs were mechanically ventilated to maintain PaCO 2 within a range of 35 to 45 mm Hg. Arterial and venous access was obtained, and mean arterial blood pressure was maintained at approximately 90 mm Hg. The electrocardiogram of each animal was monitored continuously. The animal was placed in sternal recumbency throughout the experiment, with its head secured in a Mayfield pin headholder. The cranium was exposed by a midline incision and burr holes were drilled 5 mm posterior and lateral to the junction of the coronal and sagittal sutures. An intraventricular catheter (Cordis, Brentford, UK) was inserted on the right side for infusion of mock CSF. A Spiegelberg double-lumen catheter was inserted into the left ventricle to measure ICP/intracranial compliance. Influx and backflux of fluid from an attached column of saline were used to aid confirmation of intraventricular placement. A Codman ICP sensor was inserted into the right frontal brain parenchyma through a separate, anteriorly placed burr hole. Catheters were secured in position and all burr holes were sealed with bone wax. Anesthesia was maintained in the animals throughout the experiment. At the conclusion of data collection, each sheep was killed by an intravenous injection of pentobarbital, after which the brain was removed, fixed in 10% formaldehyde solution, and serially sectioned. These brain specimens were later examined for gross pathological evidence of tissue damage resulting from catheter placement. Study Protocol Each catheter and sensor under comparison was connected to the monitoring units via the appropriate inter- 3
4 Y. H. Yau, et al. face. The Codman intraparenchymal ICP sensor was calibrated to zero according to the manufacturer's instructions prior to placement. After the external pressure transducer connected to the intraventricular fluid-filled catheter was calibrated to zero and a satisfactory ICP waveform was obtained, the data collection sequence was commenced. Raw data were fed directly into a microcomputer via a standard RS232 interface and stored. Data were analyzed with the aid of specially written in-house analysis software. Ten-minute-long datasets were collected at 5 mm Hg ICP bands, starting at baseline (approximately 3 8 mm Hg) and increasing by 10-mm Hg increments, with measurements made up to 50 mm Hg. Mock ICP increases were achieved through regulated continuous infusion of normal saline through the right-sided intraventricular catheter. At each ICP bandwidth, ICP levels recorded with the Spiegelberg catheter, the fluid-filled intraventricular catheter, and the Codman sensor were noted for comparison. Minute-by-minute compliance data were fed into the computer by using a specially written data collection program. Collected raw data included all values for the added volume ( V) and the ICP values before and after each volume addition, which occurred approximately once every 5 seconds. Each run for measurement at a particular ICP band lasted approximately 10 minutes, with as many as 120 individual sets of volume pressure values. Steady maintenance of the requisite ICP within the proposed ICP band was achieved by continual adjustment of the saline infusion rate. The individual sets of compliance data were processed, and measurements that were made while the ICP level was outside the study ICP band were rejected. Compliance calculated on the basis of data processing was recorded. For each compliance run at a given ICP band, the manual-injection method (previously described) was used at the beginning and end of each run. The two compliance values were averaged to provide one measure for compliance using the manual-injection method. Automated compliance measurements were obtained during the 10- minute interval between the two manual-injection measurements at that ICP band. Once the ICP had stabilized after the final manual injection, a set of ICP recordings were recorded from all three ICP devices under comparison. Statistical Analysis Pairs of calculated compliance data obtained by using the automated and manual methods were plotted and a linear trend line was fitted according to the least-squares method. The sets of ICP measurements made using the different systems were similarly plotted. Calculations were made for Pearson's product-moment correlation and results were examined using the Bland Altman procedure 1 for comparing two methods of clinical measurement. RESULTS Data were collected from all five animals, yielding a total of 15 sets of ICP measurements made with the Spiegelberg system, the intraventricular fluid-filled catheter with Fig. 4. Upper: Scatterplot showing measured compliance plotted against corresponding ICP. Note the expected correlation between decreasing compliance and increasing ICP. A line of best fit has the exponential equation y = x Lower: Bland Altman plot comparing compliance measurements obtained using the Spiegelberg automated compliance device with those obtained using the manual-injection method. The difference in compliance between the two methods is plotted against the average compliance between the two methods. Average bias is ml/mm Hg, with 95% CLs of ml/mm Hg and ml/mm Hg. an external strain gauge, and the Codman sensor. Nineteen pairs of compliance values that were measured using the automated compliance device and by using the manualinjection technique were also obtained. Technical problems encountered during placement of the ICP catheter in the first sheep prevented us from recording a complete set of ICP measurements with all three ICP devices under comparison. The ICP values for the comparative study ranged from 3.3 to 44.6 mm Hg (Spiegelberg system), 3.7 to 44.3 mm Hg (fluid-filled catheter with external strain gauge), and 2.2 to 45.6 mm Hg (Codman sensor). Compliance ranged from to ml/mm Hg measured using the automated system and from to ml/mm Hg measured using the manual-injection method. The ICP levels at which measurements of compliance were made ranged from 5 to 48.8 mm Hg. A comparison of ICP levels measured using the Spiegelberg system with those measured using the intraventricular fluid-filled external strain-gauge catheter revealed 4 Neurosurg. Focus / Volume 9 / November, 2000
5 Spiegelberg intracranial pressure and intracranial compliance monitor Fig. 5. Scatterplot summarizing pilot data on intraparenchymal compliance measurements obtained in a sheep model of raised ICP by using a modified air-pouch balloon catheter with a catheter tip mounted transducer. It can be seen that, unlike intraventricular CSF compliance, intraparenchymal compliance has a complex and possibly biphasic relationship with increased ICP in association with reduced CPP. a statistically significant (p 0.001) linear correlation (r 2 = ) and an average bias of 0.74 mm Hg; the 95% CLs of agreement for bias were 1.54 and (Fig. 2). A comparison of ICP levels measure using the Spiegelberg system with those measured using the Codman sensor again yielded a statistically significant (p 0.001) linear correlation (R 2 = ). The average bias was 0.01 mm Hg, with 95% CLs of agreement for bias being and (Fig. 3). Measurements of compliance obtained using the automated system showed the typical relationship of decreasing compliance with rising ICP (Fig. 4 upper). There was a statistically significant (p 0.001) linear correlation between the results obtained using the two methods for measuring compliance (r 2 = ). The average bias was ml/mm Hg (95% CLs of agreement for bias and ). The automated system for measuring compliance yielded lower compliance values compared with the manual technique (Fig. 4 lower). Macroscopic examination of the fixed brains revealed fine hemorrhagic tracks associated with insertion of the double-lumen intraventricular catheters used for automated measurements of ICP and compliance. In one case, initial incorrect placement of the intraventricular catheter resulted in thalamic hemorrhage before the catheter was drawn back into the ventricle. There was no evidence of significant subarachnoid, ventricular, or focal parenchymal hemorrhage in any of the other brains. Insertion of the Codman intraparenchymal catheter and straight intraventricular catheter for ventricular saline infusion resulted in minimal macroscopic tissue damage. DISCUSSION The results of this study demonstrate that the Spiegelberg intraventricular air-pouch balloon catheter compares Neurosurg. Focus / Volume 9 / November, 2000 well with both the intraventricular fluid-filled external strain-gauge catheter and the Codman intraparenchymal catheter-tip strain-gauge catheter over a wide range of ICPs in a model of diffusely raised ICP in sheep. The automated compliance measurements obtained using the Spiegelberg system demonstrated the expected changes in compliance with increasing ICP, and the method compared very favorably with the manual-injection method in obtaining data. Bias and limits of agreement between the two techniques were similar to those recorded in a clinical validation study. 13 We noted some tissue damage resulting from insertion of the intraventricular catheters used with the Spiegelberg ICP/intracranial compliance device, but this was limited to fine hemorrhage along the track of catheter passage and was comparable with the level of damage expected from placement of an intraventricular catheter. When comparing the measurements of ICP obtained using the three devices, there was one outlier result, with a bias of 4.4 mm Hg between the Spiegelberg intraventricular balloon catheter and the intraventricular fluidfilled strain-gauge catheter and a bias of 6.2 mm Hg between the Spiegelberg catheter and the Codman sensor. These outliers can be explained by the difficulties inherent in maintaining a steady state of ICP by using the intraventricular infusion of saline at higher ICP bands, before all three values were recorded. Problems with zero drift and robustness continue to be reported in clinical and experimental studies 2,10,15,16 of the devices currently used for measuring and monitoring ICP. Ours is the first study to demonstrate that the Spiegelberg intraventricular ICP method is accurate when compared with both the standard intraventricular method and the currently widely adopted intraparenchymal system. This new system with its inherent automatic zero function in vivo is worth assessing in larger clinical studies to evaluate its longer-term zero drift and robustness. Although there is a theoretical advantage in measuring volume and pressure parameters such as the pressure volume index 7 and the volume pressure response, 8,9 these measurements have previously depended on manual-injection methods. Their use in clinical practice has been limited because of the labor-intensive process of obtaining repeated measurements, which requires an accurately calibrated rate and volume of injection, and because of the inherent risks of infection. In addition to providing automated measurements of compliance that are comparable in accuracy with those obtained using the manual-injection method, the Spiegelberg system has the capacity for continuous measurement and monitoring of intracranial compliance. There remains, however, the task of identifying critical thresholds in compliance values in patients with brain injury, and their utility as a means of predicting rises in ICP. Toward this end, an international multicenter study has been undertaken to collect patient data that will help validate the predictive relationship between falling intracranial compliance and increases in ICP, as well as to determine the thresholds of poor compliance (for information, consult the Brain-IT website at brainit.gla.ac.uk/brainit). There are some limitations to the current automated system for measurement of intracranial compliance. Above all, intraventricular placement of the air-pouch bal- 5
6 Y. H. Yau, et al. loon is required for volume additions. At many centers in the United States and the United Kingdom it is standard policy to use intraparenchymal but rarely intraventricular catheters in the care of patients with acute brain injury. Additionally, in some patients it is difficult to cannulate the small ventricles. If the Spiegelberg method of monitoring both ICP and intracranial compliance is to find widespread clinical application, the system needs to be modified to enable measurement of compliance in the intraparenchymal compartment. Figure 5 provides a summary of pilot data on intraparenchymal compliance measurements obtained in a sheep model of raised ICP using a modified air-pouch balloon catheter with a catheter tip mounted transducer. It can be seen from this that, unlike intraventricular CSF compliance, intraparenchymal compliance exhibits a complex and possibly biphasic relationship with increased ICP in association with reduced CPP. This may correlate with earlier findings that the pressure volume index varies directly with CPP within limits of autoregulation, and indirectly with CPP below the autoregulatory range. 6 Measurement variability is high and further observations are required; however, intraparenchymal compliance monitored using this method may act as a measure of a more complex function of brain perfusion and of physiological, rather than physical, compliance. Additional studies of this phenomenon are currently in progress. Despite its limitations, the current double-lumen catheter system used for continuous intraventricular compliance measurement in this study retains potential clinical advantages, including its automatic zero drift corrected measurement of ICP and the fact that it permits CSF drainage as a treatment option. Disclosure None of the authors has a financial interest in Spiegelberg (GmbH & Co.) KG as a consultant, shareholder, or in any other capacity. Acknowledgments We are grateful for the advice and assistance of the following colleagues: Miss L. Myles, Mr. M. Glasby, Miss G. Valler, Miss H. Bell, and Dr. S. Wharton. References 1. Bland JM, Altman DG: Statistical methods for assessing agreement between two methods of clinical measurement. Lancet 1: , Chambers IR, Kane PJ, Choksey MS, et al: An evaluation of the Camino ventricular bolt system in clinical practice. Neurosurgery 33: , Czosnyka M, Czosnyka Z, Pickard JD, et al: Laboratory testing of the Spiegelberg brain pressure monitor: a technical report. J Neurol Neurosurg Psychiatry 63: , Fernandes HM, Bingham K, Chambers IR, et al: Clinical evaluation of the Codman microsensor intracranial pressure monitoring system. Acta Neurochir Suppl 71:44 46, Geddes LA: The Direct and Indirect Measurement of Blood Pressure. Chicago: Year Book Medical, Gray WJ, Rosner MJ: Pressure-volume index as a function of cerebral perfusion pressure. Part 2: The effects of low cerebral perfusion pressure and autoregulation. J Neurosurg 67: , Marmarou A, Shulman K, LaMorgese J: Compartmental analysis of compliance and outflow resistance of the cerebrospinal fluid system. J Neurosurg 43: , Miller JD, Garibi J: Intracranial volume/pressure relationships during continuous monitoring of ventricular fluid pressure, in Brock M, Dietz H (eds): Intracranial Pressure. Berlin: Springer-Verlag, pp , Miller JD, Garibi J, Pickard JD: Induced changes of cerebrospinal fluid volume. Effects during continuous monitoring of ventricular fluid pressure. Arch Neurol 28: , Münch E, Weigel R, Schmiedek P, et al: The Camino intracranial pressure device in clinical practice: reliability, handling characteristics and complications. Acta Neurochir 140: , Ostrup RC, Luerssen TG, Marshall LF, et al: Continuous monitoring of intracranial pressure with a miniaturized fiberoptic device. J Neurosurg 67: , Piper I: Intracranial pressure and elastance, in Reilly P, Bullock R (eds): Head Injury: Pathophysiology and Management of Severe Closed Head Injury. Philadelphia: Chapman & Hall, 1997, pp Piper IR, Barnes A: Re-assessment of the Camino intracranial pressure sensor: a bench test study after catheter removal from the patient. Br J Neurosurg 13:114, 1999 (Abstract) 13. Piper I, Spiegelberg A, Whittle I, et al: A comparative study of the Spiegelberg compliance device with a manual volume-injection method: a clinical evaluation in patients with hydrocephalus. Br J Neurosurg 13: , Schürer L, Münch E, Piepgras A, et al: Assessment of the CAMINO intracranial pressure device in clinical practice. Acta Neurochir 70: , Weinstabl C, Richling B, Plainer B, et al: Comparative analysis between epidural (Gaeltec) and subdural (Camino) intracranial pressure probes. J Clin Monitor 8: , 1992 Manuscript received March 3, Accepted in final form August 17, This work was supported by the Scottish Office Department of Health (Grant No. K/MRS/50/C2662) and by Spiegelberg (GMbH & Co) KG. This manuscript is a preview article for the Journal of Neurosurgery and will be published in the December, 2000 issue. Address reprint requests to: Yun H. Yau, F.R.C.S.(Ed), Department of Clinical Neurosciences, University of Edinburgh, Western General Hospital, Crewe Road, Edinburgh, EH4 2XU, United Kingdom. yau@skull.dcn.ed.ac.uk. 6 Neurosurg. Focus / Volume 9 / November, 2000
Integra B: Camino OLM Intracranial Pressure Monitoring Kit SURGICAL TECHNIQUE
 Integra 110-4B: Camino OLM Intracranial Pressure Monitoring Kit SURGICAL TECHNIQUE Surgical Technique Th OLM ICP Kit was developed in cooperation with Richard C. Ostrup, M.D., Thomas G. Luerssen, M.D.
Integra 110-4B: Camino OLM Intracranial Pressure Monitoring Kit SURGICAL TECHNIQUE Surgical Technique Th OLM ICP Kit was developed in cooperation with Richard C. Ostrup, M.D., Thomas G. Luerssen, M.D.
Intracranial pressure: measurement and monitoring. CSF pressure as a golden standard. Intraparenchymal pressure. Sensors, drifts, errors and
 Intracranial pressure: measurement and monitoring. CSF pressure as a golden standard. Intraparenchymal pressure. Sensors, drifts, errors and monitoring techniques GUILLAUME J, JANNY P. [Continuous intracranial
Intracranial pressure: measurement and monitoring. CSF pressure as a golden standard. Intraparenchymal pressure. Sensors, drifts, errors and monitoring techniques GUILLAUME J, JANNY P. [Continuous intracranial
Eide et al. Eide et al. BioMedical Engineering OnLine 2012, 11:66
 Simultaneous monitoring of static and dynamic intracranial pressure parameters from two separate sensors in patients with cerebral bleeds: comparison of findings Eide et al. Eide et al. BioMedical Engineering
Simultaneous monitoring of static and dynamic intracranial pressure parameters from two separate sensors in patients with cerebral bleeds: comparison of findings Eide et al. Eide et al. BioMedical Engineering
Traumatic brain Injury- An open eye approach
 Traumatic brain Injury- An open eye approach Dr. Sunit Dr Sunit, Apollo children's hospital Blah blah Lots of head injury Lot of ill children Various methods of injury Various mechanisms of brain damage
Traumatic brain Injury- An open eye approach Dr. Sunit Dr Sunit, Apollo children's hospital Blah blah Lots of head injury Lot of ill children Various methods of injury Various mechanisms of brain damage
An intracranial pressure-derived index monitored simultaneously from two separate sensors in patients with cerebral bleeds: comparison of findings
 An intracranial pressure-derived index monitored simultaneously from two separate sensors in patients with cerebral bleeds: comparison of findings Eide and Sorteberg Eide and Sorteberg BioMedical Engineering
An intracranial pressure-derived index monitored simultaneously from two separate sensors in patients with cerebral bleeds: comparison of findings Eide and Sorteberg Eide and Sorteberg BioMedical Engineering
Intracranial volume-pressure relationships during experimental brain compression in primates
 Journal of Neurology, Neurosurgery, and Psychiatry, 1974, 37, 1093-1098 Intracranial volume-pressure relationships during experimental brain compression in primates 1. Pressure responses to changes in
Journal of Neurology, Neurosurgery, and Psychiatry, 1974, 37, 1093-1098 Intracranial volume-pressure relationships during experimental brain compression in primates 1. Pressure responses to changes in
Intracranial volume-pressure relationships during
 Journial of Neurology, Neurosurgery, and Psychiatry, 1974, 37, 1099-1104 Intracranial volume-pressure relationships during experimental brain compression in primates 2. Effect of induced changes in systemic
Journial of Neurology, Neurosurgery, and Psychiatry, 1974, 37, 1099-1104 Intracranial volume-pressure relationships during experimental brain compression in primates 2. Effect of induced changes in systemic
Role of Invasive ICP Monitoring in Patients with Traumatic Brain Injury: An Experience of 98 Cases
 31 Original Article Indian Journal of Neurotrauma (IJNT) 2006, Vol. 3, No. 1, pp. 31-36 Role of Invasive ICP Monitoring in Patients with Traumatic Brain Injury: An Experience of 98 Cases Deepak Kumar Gupta
31 Original Article Indian Journal of Neurotrauma (IJNT) 2006, Vol. 3, No. 1, pp. 31-36 Role of Invasive ICP Monitoring in Patients with Traumatic Brain Injury: An Experience of 98 Cases Deepak Kumar Gupta
Intracranial volume-pressure relationships during
 Journial of Neurology, Neurosurgery, and Psychiatry, 1974, 37, 115-1111 Intracranial volume-pressure relationships during experimental brain compression in primates 3. Effect of mannitol and hyperventilation
Journial of Neurology, Neurosurgery, and Psychiatry, 1974, 37, 115-1111 Intracranial volume-pressure relationships during experimental brain compression in primates 3. Effect of mannitol and hyperventilation
Medical Management of Intracranial Hypertension. Joao A. Gomes, MD FAHA Head, Neurointensive Care Unit Cerebrovascular Center
 Medical Management of Intracranial Hypertension Joao A. Gomes, MD FAHA Head, Neurointensive Care Unit Cerebrovascular Center Anatomic and Physiologic Principles Intracranial compartments Brain 80% (1,400
Medical Management of Intracranial Hypertension Joao A. Gomes, MD FAHA Head, Neurointensive Care Unit Cerebrovascular Center Anatomic and Physiologic Principles Intracranial compartments Brain 80% (1,400
PRACTICE GUIDELINE. DEFINITIONS: Mild head injury: Glasgow Coma Scale* (GCS) score Moderate head injury: GCS 9-12 Severe head injury: GCS 3-8
 PRACTICE GUIDELINE Effective Date: 9-1-2012 Manual Reference: Deaconess Trauma Services TITLE: TRAUMATIC BRAIN INJURY GUIDELINE OBJECTIVE: To provide practice management guidelines for traumatic brain
PRACTICE GUIDELINE Effective Date: 9-1-2012 Manual Reference: Deaconess Trauma Services TITLE: TRAUMATIC BRAIN INJURY GUIDELINE OBJECTIVE: To provide practice management guidelines for traumatic brain
Moron General Hospital Ciego de Avila Cuba. Department of Neurological Surgery
 Moron General Hospital Ciego de Avila Cuba Department of Neurological Surgery Early decompressive craniectomy in severe head injury with intracranial hypertension Angel J. Lacerda MD PhD, Daisy Abreu MD,
Moron General Hospital Ciego de Avila Cuba Department of Neurological Surgery Early decompressive craniectomy in severe head injury with intracranial hypertension Angel J. Lacerda MD PhD, Daisy Abreu MD,
The resistance to CSF outflow in hydrocephalus what it is and what it isn t.
 The resistance to CSF outflow in hydrocephalus what it is and what it isn t. Davson et al 1970, The mechanism of drainage of CSF. Brain 93:665-8 1989, Copenhagen, Alfred Benzon Foundation CSf outflow is
The resistance to CSF outflow in hydrocephalus what it is and what it isn t. Davson et al 1970, The mechanism of drainage of CSF. Brain 93:665-8 1989, Copenhagen, Alfred Benzon Foundation CSf outflow is
Predicting the response of intracranial pressure to moderate hyperventilation
 Acta Neurochir (Wien) (2005) DOI 10.1007/s00701-005-0510-x Predicting the response of intracranial pressure to moderate hyperventilation L. A. Steiner 1;2, M. Balestreri 1, A. J. Johnston 2, J. P. Coles
Acta Neurochir (Wien) (2005) DOI 10.1007/s00701-005-0510-x Predicting the response of intracranial pressure to moderate hyperventilation L. A. Steiner 1;2, M. Balestreri 1, A. J. Johnston 2, J. P. Coles
Comparison of parenchymal and ventricular intracranial pressure readings utilizing a novel multi-parameter intracranial access system
 Berlin et al. SpringerPlus 2015, 4:10 a SpringerOpen Journal RESEARCH Open Access Comparison of parenchymal and ventricular intracranial pressure readings utilizing a novel multi-parameter intracranial
Berlin et al. SpringerPlus 2015, 4:10 a SpringerOpen Journal RESEARCH Open Access Comparison of parenchymal and ventricular intracranial pressure readings utilizing a novel multi-parameter intracranial
Complications of intracranial pressure monitoring in children with head trauma
 J Neurosurg (Pediatrics 2) 101:53 58, 2004 Complications of intracranial pressure monitoring in children with head trauma RICHARD C. E. ANDERSON, M.D., PETER KAN, M.D., PAUL KLIMO, M.D., M.P.H., DOUGLAS
J Neurosurg (Pediatrics 2) 101:53 58, 2004 Complications of intracranial pressure monitoring in children with head trauma RICHARD C. E. ANDERSON, M.D., PETER KAN, M.D., PAUL KLIMO, M.D., M.P.H., DOUGLAS
Stroke & Neurovascular Center of New Jersey. Jawad F. Kirmani, MD Director, Stroke and Neurovascular Center
 Stroke & Neurovascular Center of New Jersey Jawad F. Kirmani, MD Director, Stroke and Neurovascular Center Past, present and future Past, present and future Cerebral Blood Flow Past, present and future
Stroke & Neurovascular Center of New Jersey Jawad F. Kirmani, MD Director, Stroke and Neurovascular Center Past, present and future Past, present and future Cerebral Blood Flow Past, present and future
12. Modelling of CSF compensation: Mathematical model (Marmarou). Mathematical modelling of pulsatile aqueductal CSF flow
 12. Modelling of CSF compensation: Mathematical model (Marmarou). Mathematical modelling of pulsatile aqueductal CSF flow Hydrocephalus Enlargement of CSF space Shunting? Revision? When? CSF dynamics Prof.
12. Modelling of CSF compensation: Mathematical model (Marmarou). Mathematical modelling of pulsatile aqueductal CSF flow Hydrocephalus Enlargement of CSF space Shunting? Revision? When? CSF dynamics Prof.
Experience with an intracranial pressure. transducer readjustable in vivo
 Experience with an intracranial pressure transducer readjustable in vivo Technical note WOLFGANG GOBLET, M.D., WOLFGANG JOACHIM BOOK, M.D., JURGEN LIESEGANG, M.D., AND WILHELM GROTE, M.D. Neurosurgical
Experience with an intracranial pressure transducer readjustable in vivo Technical note WOLFGANG GOBLET, M.D., WOLFGANG JOACHIM BOOK, M.D., JURGEN LIESEGANG, M.D., AND WILHELM GROTE, M.D. Neurosurgical
Perioperative Management Of Extra-Ventricular Drains (EVD)
 Perioperative Management Of Extra-Ventricular Drains (EVD) Dr. Vijay Tarnal MBBS, FRCA Clinical Assistant Professor Division of Neuroanesthesiology Division of Head & Neck Anesthesiology Michigan Medicine
Perioperative Management Of Extra-Ventricular Drains (EVD) Dr. Vijay Tarnal MBBS, FRCA Clinical Assistant Professor Division of Neuroanesthesiology Division of Head & Neck Anesthesiology Michigan Medicine
SARASOTA MEMORIAL HOSPITAL NURSING PROCEDURE
 SARASOTA MEMORIAL HOSPITAL NURSING PROCEDURE TITLE: ISSUED FOR: INTRACRANIAL PRESSURE MONITORING USING ICP CODMAN DEVICE MONITORING BOLT AND INTRACRANIAL PRESSURE MONITORING DRAINAGE OF CEREBRAL SPINAL
SARASOTA MEMORIAL HOSPITAL NURSING PROCEDURE TITLE: ISSUED FOR: INTRACRANIAL PRESSURE MONITORING USING ICP CODMAN DEVICE MONITORING BOLT AND INTRACRANIAL PRESSURE MONITORING DRAINAGE OF CEREBRAL SPINAL
CHANGES IN INTRACRANIAL PRESSURE ASSOCIATED WITH EXTRADURAL ANAESTHESIA
 Br. J. Anaesth. (1986), 58, 676680 CHANGES IN INTRACRANIAL PRESSURE ASSOCIATED WITH EXTRADURAL ANAESTHESIA H. HILT, H.J. GRAMM AND J. LINK Extradural blockade is commonly used in our clinic to provide
Br. J. Anaesth. (1986), 58, 676680 CHANGES IN INTRACRANIAL PRESSURE ASSOCIATED WITH EXTRADURAL ANAESTHESIA H. HILT, H.J. GRAMM AND J. LINK Extradural blockade is commonly used in our clinic to provide
Baseline pressure errors (BPEs) extensively influence intracranial pressure scores: results of a prospective observational study. Eide et al.
 Baseline pressure errors (BPEs) extensively influence intracranial pressure scores: results of a prospective observational study Eide et al. Eide et al. BioMedical Engineering OnLine 2014, 13:7 Eide et
Baseline pressure errors (BPEs) extensively influence intracranial pressure scores: results of a prospective observational study Eide et al. Eide et al. BioMedical Engineering OnLine 2014, 13:7 Eide et
HEAD AND NECK IMAGING. James Chen (MS IV)
 HEAD AND NECK IMAGING James Chen (MS IV) Anatomy Course Johns Hopkins School of Medicine Sept. 27, 2011 OBJECTIVES Introduce cross sectional imaging of head and neck Computed tomography (CT) Review head
HEAD AND NECK IMAGING James Chen (MS IV) Anatomy Course Johns Hopkins School of Medicine Sept. 27, 2011 OBJECTIVES Introduce cross sectional imaging of head and neck Computed tomography (CT) Review head
Infusion studies in clinical practice. Kristian Aquilina Consultant paediatric neurosurgeon Great Ormond Street Hospital London
 Infusion studies in clinical practice Kristian Aquilina Consultant paediatric neurosurgeon Great Ormond Street Hospital London 10 th September 2018 infusion study + hydrocephalus 216 publications Clinical
Infusion studies in clinical practice Kristian Aquilina Consultant paediatric neurosurgeon Great Ormond Street Hospital London 10 th September 2018 infusion study + hydrocephalus 216 publications Clinical
Ovid: Effects of Neck Position and Head Elevation on Intracranial Press...
 Sida 1 av 5 Journal of Neurosurgical Anesthesiology Issue: Volume 12(1), January 2000, pp 10-14 Copyright: 2000 Lippincott Williams & Wilkins, Inc. Publication Type: [Clinical Reports] ISSN: 0898-4921
Sida 1 av 5 Journal of Neurosurgical Anesthesiology Issue: Volume 12(1), January 2000, pp 10-14 Copyright: 2000 Lippincott Williams & Wilkins, Inc. Publication Type: [Clinical Reports] ISSN: 0898-4921
Increased Intracranial Pressure 2.0 Contact Hours Presented by: CEU Professor
 Increased Intracranial Pressure 2.0 Contact Hours Presented by: CEU Professor 7 www.ceuprofessoronline.com Copyright 8 2007 The Magellan Group, LLC All Rights Reserved. Reproduction and distribution of
Increased Intracranial Pressure 2.0 Contact Hours Presented by: CEU Professor 7 www.ceuprofessoronline.com Copyright 8 2007 The Magellan Group, LLC All Rights Reserved. Reproduction and distribution of
Lumbar infusion test in normal pressure hydrocephalus
 Acta Neurol Scand 2005: 111: 379 384 DOI: 10.1111/j.1600-0404.2005.00417.x Copyright Ó Blackwell Munksgaard 2005 ACTA NEUROLOGICA SCANDINAVICA Lumbar infusion test in normal pressure hydrocephalus Kahlon
Acta Neurol Scand 2005: 111: 379 384 DOI: 10.1111/j.1600-0404.2005.00417.x Copyright Ó Blackwell Munksgaard 2005 ACTA NEUROLOGICA SCANDINAVICA Lumbar infusion test in normal pressure hydrocephalus Kahlon
Mannitol for Resuscitation in Acute Head Injury: Effects on Cerebral Perfusion and Osmolality
 Original articles Mannitol for Resuscitation in Acute Head Injury: Effects on Cerebral Perfusion and Osmolality J. A. MYBURGH*, S. B. LEWIS *Intensive Care Unit, Royal Adelaide Hospital, Adelaide, SOUTH
Original articles Mannitol for Resuscitation in Acute Head Injury: Effects on Cerebral Perfusion and Osmolality J. A. MYBURGH*, S. B. LEWIS *Intensive Care Unit, Royal Adelaide Hospital, Adelaide, SOUTH
Traumatic Brain Injuries
 Traumatic Brain Injuries Scott P. Sherry, MS, PA-C, FCCM Assistant Professor Department of Surgery Division of Trauma, Critical Care and Acute Care Surgery DISCLOSURES Nothing to disclose Discussion of
Traumatic Brain Injuries Scott P. Sherry, MS, PA-C, FCCM Assistant Professor Department of Surgery Division of Trauma, Critical Care and Acute Care Surgery DISCLOSURES Nothing to disclose Discussion of
Accuracy of intracranial pressure monitoring: systematic review and metaanalysis
 Zacchetti et al. Critical Care (2015) 19:420 DOI 10.1186/s13054-015-1137-9 RESEARCH Accuracy of intracranial pressure monitoring: systematic review and metaanalysis Lucia Zacchetti 1, Sandra Magnoni 2,
Zacchetti et al. Critical Care (2015) 19:420 DOI 10.1186/s13054-015-1137-9 RESEARCH Accuracy of intracranial pressure monitoring: systematic review and metaanalysis Lucia Zacchetti 1, Sandra Magnoni 2,
Standardize comprehensive care of the patient with severe traumatic brain injury
 Trauma Center Practice Management Guideline Iowa Methodist Medical Center Des Moines Management of Patients with Severe Traumatic Brain Injury (GCS < 9) ADULT Practice Management Guideline Contact: Trauma
Trauma Center Practice Management Guideline Iowa Methodist Medical Center Des Moines Management of Patients with Severe Traumatic Brain Injury (GCS < 9) ADULT Practice Management Guideline Contact: Trauma
Neurocritical Care Monitoring. Academic Half Day Critical Care Fellows
 Neurocritical Care Monitoring Academic Half Day Critical Care Fellows Clinical Scenarios for CNS monitoring No Universally accepted Guidelines Traumatic Brain Injury Intracerebral Hemorrhage Subarachnoid
Neurocritical Care Monitoring Academic Half Day Critical Care Fellows Clinical Scenarios for CNS monitoring No Universally accepted Guidelines Traumatic Brain Injury Intracerebral Hemorrhage Subarachnoid
Blood Pressure Laboratory
 Introduction The blood that circulates throughout the body maintains a flow and pressure. The nervous system can change the flow and pressure based on the particular needs at a given time. For example,
Introduction The blood that circulates throughout the body maintains a flow and pressure. The nervous system can change the flow and pressure based on the particular needs at a given time. For example,
Cerebral autoregulation is a complex intrinsic control. Time course for autoregulation recovery following severe traumatic brain injury
 J Neurosurg 111:695 700, 2009 Time course for autoregulation recovery following severe traumatic brain injury Clinical article Gi l l E. Sv i r i, M.D., M.Sc., 1 Ru n e Aa s l i d, Ph.D., 2 Co l l e e
J Neurosurg 111:695 700, 2009 Time course for autoregulation recovery following severe traumatic brain injury Clinical article Gi l l E. Sv i r i, M.D., M.Sc., 1 Ru n e Aa s l i d, Ph.D., 2 Co l l e e
INTRACRANIAL PRESSURE -!!
 INTRACRANIAL PRESSURE - Significance raised ICP main cause of death in severe head injury main cause of morbidity in moderate and mild head injury main target and prognostic indicator in the ITU setting
INTRACRANIAL PRESSURE - Significance raised ICP main cause of death in severe head injury main cause of morbidity in moderate and mild head injury main target and prognostic indicator in the ITU setting
INCREASED INTRACRANIAL PRESSURE
 INCREASED INTRACRANIAL PRESSURE Sheba Medical Center, Acute Medicine Department Irene Frantzis P-Year student SGUL 2013 Normal Values Normal intracranial volume: 1700 ml Volume of brain: 1200-1400 ml CSF:
INCREASED INTRACRANIAL PRESSURE Sheba Medical Center, Acute Medicine Department Irene Frantzis P-Year student SGUL 2013 Normal Values Normal intracranial volume: 1700 ml Volume of brain: 1200-1400 ml CSF:
The Sequence of Alterations in the Vital Signs During Acute Experimental Increased Intracranial Pressure*
 J. Neurosurg. / Volume 32 / January, 1970 The Sequence of Alterations in the Vital Signs During Acute Experimental Increased Intracranial Pressure* JAVAD HEKMATPANAH, M.D. Division o/ Neurological Surgery,
J. Neurosurg. / Volume 32 / January, 1970 The Sequence of Alterations in the Vital Signs During Acute Experimental Increased Intracranial Pressure* JAVAD HEKMATPANAH, M.D. Division o/ Neurological Surgery,
Department of Neurosurgery, Oslo University Hospital Rikshospitalet, Oslo, Norway
 J Neurosurg 113:1317 1325, 2010 Simultaneous measurements of intracranial pressure parameters in the epidural space and in brain parenchyma in patients with hydrocephalus Clinical article Pe r Kr i s t
J Neurosurg 113:1317 1325, 2010 Simultaneous measurements of intracranial pressure parameters in the epidural space and in brain parenchyma in patients with hydrocephalus Clinical article Pe r Kr i s t
NEUROSURGERY LiquoGuard
 NEUROSURGERY LiquoGuard Member of CENTROTEC Group a new InTRODUCTION TO LiquoGuard CSF Management LiquoGuard (Liquor = German for CSF) represents a revolutionary step in CSF drainage, maximizing patient
NEUROSURGERY LiquoGuard Member of CENTROTEC Group a new InTRODUCTION TO LiquoGuard CSF Management LiquoGuard (Liquor = German for CSF) represents a revolutionary step in CSF drainage, maximizing patient
Correlation between intra-abdominal and intracranial pressure in
 Electronic Supplemental Material: Correlation between intra-abdominal and intracranial pressure in nontraumatic brain injury Dries H. Deeren (1), Hilde Dits (2), Manu L. N. G. Malbrain (2) Department of
Electronic Supplemental Material: Correlation between intra-abdominal and intracranial pressure in nontraumatic brain injury Dries H. Deeren (1), Hilde Dits (2), Manu L. N. G. Malbrain (2) Department of
Predicting the need for operation in the patient with an occult traumatic intracranial hematoma
 J Neurosurg 55:75-81, 1981 Predicting the need for operation in the patient with an occult traumatic intracranial hematoma SAM GALBRAITH, M.D., F.R.C.S., AND GRAHAM TEASDALE, M.R.C.P., F.R.C.S. Department
J Neurosurg 55:75-81, 1981 Predicting the need for operation in the patient with an occult traumatic intracranial hematoma SAM GALBRAITH, M.D., F.R.C.S., AND GRAHAM TEASDALE, M.R.C.P., F.R.C.S. Department
Non-invasive assessment of intracranial pressure - a plugin function of ICM+ system
 Non-invasive assessment of intracranial pressure - a plugin function of ICM+ system B. Schmidt, M. Czosnyka *, P. Smielewski *, R. Plontke, J. Schwarze, J. Klingelhöfer Dept. of Neurology, Medical Centre
Non-invasive assessment of intracranial pressure - a plugin function of ICM+ system B. Schmidt, M. Czosnyka *, P. Smielewski *, R. Plontke, J. Schwarze, J. Klingelhöfer Dept. of Neurology, Medical Centre
Recording and interpretation of intracranial pressure
 CLINICAL ARTICLE Evaluation of a novel noninvasive ICP monitoring device in patients undergoing invasive ICP monitoring: preliminary results Oliver Ganslandt, MD, 1 Stylianos Mourtzoukos, MD, 1 Andreas
CLINICAL ARTICLE Evaluation of a novel noninvasive ICP monitoring device in patients undergoing invasive ICP monitoring: preliminary results Oliver Ganslandt, MD, 1 Stylianos Mourtzoukos, MD, 1 Andreas
NON-INVASIVE ICP AND VRx AS NON-INVASIVE PRx Arminas Ragauskas
 ICM+ Workshop 2018 University of Cambridge NON-INVASIVE ICP AND VRx AS NON-INVASIVE PRx Arminas Ragauskas Disclosure A.R. - inventor and co-inventor of patented non-invasive ICP absolute value measurement
ICM+ Workshop 2018 University of Cambridge NON-INVASIVE ICP AND VRx AS NON-INVASIVE PRx Arminas Ragauskas Disclosure A.R. - inventor and co-inventor of patented non-invasive ICP absolute value measurement
British Journal of Anaesthesia 82 (5): (1999)
 British Journal of Anaesthesia 82 (5): 703 7 (1999) Laryngeal mask airway size selection in males and females: ease of insertion, oropharyngeal leak pressure, pharyngeal mucosal pressures and anatomical
British Journal of Anaesthesia 82 (5): 703 7 (1999) Laryngeal mask airway size selection in males and females: ease of insertion, oropharyngeal leak pressure, pharyngeal mucosal pressures and anatomical
A comparison between the transfer function of ABP to ICP and compensatory reserve index in TBI
 Acta Neurochir Suppl (28) 12: 9 13 # Springer-Verlag 28 A comparison between the transfer function of AB to IC and compensatory reserve index in TBI Sima Shahsavari & Tomas McKelvey & Thomas Skoglund &
Acta Neurochir Suppl (28) 12: 9 13 # Springer-Verlag 28 A comparison between the transfer function of AB to IC and compensatory reserve index in TBI Sima Shahsavari & Tomas McKelvey & Thomas Skoglund &
Two computerized methods used to analyze intracranial pressure B waves: comparison with traditional visual interpretation
 J Neurosurg 94:392 396, 2001 Two computerized methods used to analyze intracranial pressure B waves: comparison with traditional visual interpretation ANDERS EKLUND, MSC.E.P., AINA ÅGREN-WILSSON, M.D.,
J Neurosurg 94:392 396, 2001 Two computerized methods used to analyze intracranial pressure B waves: comparison with traditional visual interpretation ANDERS EKLUND, MSC.E.P., AINA ÅGREN-WILSSON, M.D.,
NEUROMONITORING AND ANESTHESIA CONSIDERATIONS. Martha Richter, MSN, CRNA
 NEUROMONITORING AND ANESTHESIA CONSIDERATIONS Martha Richter, MSN, CRNA OBJECTIVES The student will 1. Review the types of neuromonitoring currently in use 2. Identify possible procedural applications
NEUROMONITORING AND ANESTHESIA CONSIDERATIONS Martha Richter, MSN, CRNA OBJECTIVES The student will 1. Review the types of neuromonitoring currently in use 2. Identify possible procedural applications
Cerebral perfusion pressure management of severe diffuse head injury: Effect on brain compliance and intracranial pressure
 Original Article Cerebral perfusion pressure management of severe diffuse head injury: Effect on brain compliance and intracranial pressure S. Pillai, S. S. Praharaj, G. S. U. Rao,* V. R. S. Kolluri Departments
Original Article Cerebral perfusion pressure management of severe diffuse head injury: Effect on brain compliance and intracranial pressure S. Pillai, S. S. Praharaj, G. S. U. Rao,* V. R. S. Kolluri Departments
Postanesthesia Care of the Patient Suffering From Traumatic Brain Injury
 Postanesthesia Care of the Patient Suffering From Traumatic Brain Injury By: Susan Letvak, PhD, RN Rick Hand, CRNA, DNSc Letvak, S. & Hand, R. (2003). Postanesthesia care of the traumatic brain injured
Postanesthesia Care of the Patient Suffering From Traumatic Brain Injury By: Susan Letvak, PhD, RN Rick Hand, CRNA, DNSc Letvak, S. & Hand, R. (2003). Postanesthesia care of the traumatic brain injured
Quality Metrics. Stroke Related Procedure Outcomes
 Quality Metrics Stroke Related Procedure Outcomes Below is a description of some of the stroke-related procedures performed at St. Dominic Hospital in Jackson, with quality information on the complication
Quality Metrics Stroke Related Procedure Outcomes Below is a description of some of the stroke-related procedures performed at St. Dominic Hospital in Jackson, with quality information on the complication
Mark Steven Schnitzer, M.D., F.A.C.S.
 CURRICULUM VITAE, F.A.C.S. PERSONAL DATA Mailing Address: P. O. Box 2265 La Habra, CA 90632-2265 Telephone: (714) 525-7177 (562) 698-2054 Facsimile: (714) 525-6769 Website: Email: http://www.neuroservices.com
CURRICULUM VITAE, F.A.C.S. PERSONAL DATA Mailing Address: P. O. Box 2265 La Habra, CA 90632-2265 Telephone: (714) 525-7177 (562) 698-2054 Facsimile: (714) 525-6769 Website: Email: http://www.neuroservices.com
Principlesof shunt testing in-vivo Zofia Czosnyka, Matthew Garnett, Eva Nabbanja, Marek Czosnyka
 Principlesof shunt testing in-vivo Zofia Czosnyka, Matthew Garnett, Eva Nabbanja, Marek Czosnyka Neurosurgery Unit, Addenbrooke s Hospital, Cambridge, UK Shunt helps to control hydrocephalus not to cure
Principlesof shunt testing in-vivo Zofia Czosnyka, Matthew Garnett, Eva Nabbanja, Marek Czosnyka Neurosurgery Unit, Addenbrooke s Hospital, Cambridge, UK Shunt helps to control hydrocephalus not to cure
S ome hydrocephalic patients with extracranial shunts
 PAPER Quantitative analysis of continuous intracranial pressure recordings in symptomatic patients with extracranial shunts P K Eide... Competing interests: none declared... Correspondence to: Dr Per Kristian
PAPER Quantitative analysis of continuous intracranial pressure recordings in symptomatic patients with extracranial shunts P K Eide... Competing interests: none declared... Correspondence to: Dr Per Kristian
The arrest of treated hydrocephalus in children
 J Neurosurg 61:752-756, 1984 The arrest of treated hydrocephalus in children A radionuclide study IAN H. JOHNSTON, F.R.C.S., ROBERT HOWMAN-GILES, F.R.A.C.P., AND IAN R. WHITTLE, M.B., B.S. T. Y. Nelson
J Neurosurg 61:752-756, 1984 The arrest of treated hydrocephalus in children A radionuclide study IAN H. JOHNSTON, F.R.C.S., ROBERT HOWMAN-GILES, F.R.A.C.P., AND IAN R. WHITTLE, M.B., B.S. T. Y. Nelson
Continuous cerebral autoregulation monitoring
 Continuous cerebral autoregulation monitoring Dr Peter Smielewski ps10011@cam.ac.uk 20/10/2017 Division of Neurosurgery, Department of Clinical Neurosciences Determinants of cerebral blood flow Thanks
Continuous cerebral autoregulation monitoring Dr Peter Smielewski ps10011@cam.ac.uk 20/10/2017 Division of Neurosurgery, Department of Clinical Neurosciences Determinants of cerebral blood flow Thanks
13. Volume-pressure infusion tests: Typical patterns of infusion studies in different forms of CSF circulatory disorders.
 13. Volume-pressure infusion tests: Typical patterns of infusion studies in different forms of CSF circulatory disorders. Hydrocephalus is far more complex than disorder of CSF circulation CSF circulation
13. Volume-pressure infusion tests: Typical patterns of infusion studies in different forms of CSF circulatory disorders. Hydrocephalus is far more complex than disorder of CSF circulation CSF circulation
Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD
 Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD Boston Children s Hospital Harvard Medical School None Disclosures Conventional US Anterior fontanelle
Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD Boston Children s Hospital Harvard Medical School None Disclosures Conventional US Anterior fontanelle
Intracranial pressure monitoring: Vital information ignored
 Review Article Intracranial pressure monitoring: Vital information ignored Mathew Joseph Abstract Though there is no Class I evidence for the benefit of intracranial pressure (ICP) monitoring, the bulk
Review Article Intracranial pressure monitoring: Vital information ignored Mathew Joseph Abstract Though there is no Class I evidence for the benefit of intracranial pressure (ICP) monitoring, the bulk
Permanent City Research Online URL:
 Kyriacou, P. A., Pal, S. K., Langford, R. & Jones, DP (2006). Electro-optical techniques for the investigation of oesophageal photoplethysmographic signals and blood oxygen saturation in burns. Measurement
Kyriacou, P. A., Pal, S. K., Langford, R. & Jones, DP (2006). Electro-optical techniques for the investigation of oesophageal photoplethysmographic signals and blood oxygen saturation in burns. Measurement
10. Severe traumatic brain injury also see flow chart Appendix 5
 10. Severe traumatic brain injury also see flow chart Appendix 5 Introduction Severe traumatic brain injury (TBI) is the leading cause of death in children in the UK, accounting for 15% of deaths in 1-15
10. Severe traumatic brain injury also see flow chart Appendix 5 Introduction Severe traumatic brain injury (TBI) is the leading cause of death in children in the UK, accounting for 15% of deaths in 1-15
Interhemispheric supratentorial intracranial pressure gradients in head-injured patients: are they clinically important?
 J Neurosurg 90:16 26, 1999 Interhemispheric supratentorial intracranial pressure gradients in head-injured patients: are they clinically important? JUAN SAHUQUILLO, M.D., PH.D., MARIA-ANTONIA POCA, M.D.,
J Neurosurg 90:16 26, 1999 Interhemispheric supratentorial intracranial pressure gradients in head-injured patients: are they clinically important? JUAN SAHUQUILLO, M.D., PH.D., MARIA-ANTONIA POCA, M.D.,
Traumatic Brain Injury Pathways for Adult ED Patients Being Admitted to Trauma Service
 tic Brain Injury Pathways for Adult ED Patients Being Admitted to Service Revision Team Tyler W. Barrett, MD, MSCI Elizabeth S. Compton, NP Bradley M. Dennis, MD Oscar D. Guillamondegui, MD, MPH Michael
tic Brain Injury Pathways for Adult ED Patients Being Admitted to Service Revision Team Tyler W. Barrett, MD, MSCI Elizabeth S. Compton, NP Bradley M. Dennis, MD Oscar D. Guillamondegui, MD, MPH Michael
Non-Invasive PCO 2 Monitoring in Infants Hospitalized with Viral Bronchiolitis
 Non-Invasive PCO 2 Monitoring in Infants Hospitalized with Viral Bronchiolitis Gal S, Riskin A, Chistyakov I, Shifman N, Srugo I, and Kugelman A Pediatric Department and Pediatric Pulmonary Unit Bnai Zion
Non-Invasive PCO 2 Monitoring in Infants Hospitalized with Viral Bronchiolitis Gal S, Riskin A, Chistyakov I, Shifman N, Srugo I, and Kugelman A Pediatric Department and Pediatric Pulmonary Unit Bnai Zion
Viscous Fluid Retention: A New Method for Evaluating Anorectal Function
 Viscous Fluid Retention: A New Method for Evaluating Anorectal Function Michael Srensen, M.D., Tine Tetzschner, M.D., le 0. Rasmussen, M.D., John Christiansen, M.D. From the Department of Surgery D, Glostrup
Viscous Fluid Retention: A New Method for Evaluating Anorectal Function Michael Srensen, M.D., Tine Tetzschner, M.D., le 0. Rasmussen, M.D., John Christiansen, M.D. From the Department of Surgery D, Glostrup
Patient Management Code Blue in the CT Suite
 Patient Management Code Blue in the CT Suite David Stultz, MD November 28, 2001 Case Presentation A 53-year-old woman experienced acute respiratory distress during an IV contrast enhanced CT scan of the
Patient Management Code Blue in the CT Suite David Stultz, MD November 28, 2001 Case Presentation A 53-year-old woman experienced acute respiratory distress during an IV contrast enhanced CT scan of the
SENSATION and CS300 Smaller meets faster. IABP System
 SENSATION and CS300 Smaller meets faster IABP System Cardiac Assist SENSATION and CS300 3 Cardiac Assist SENSATION and CS300 5 Smaller The SENSATION 7Fr. Fiber-Optic IAB Catheter Faster The CS300 with
SENSATION and CS300 Smaller meets faster IABP System Cardiac Assist SENSATION and CS300 3 Cardiac Assist SENSATION and CS300 5 Smaller The SENSATION 7Fr. Fiber-Optic IAB Catheter Faster The CS300 with
The use of intracranial pressure (ICP) monitoring in the
 Training Protocol for Intracranial Pressure Monitor Placement by Nonneurosurgeons: 5-Year Experience Kathryn Ko, MD, and Alicia Conforti, RN Background: This report evaluates a protocol for training nonneurosurgeon
Training Protocol for Intracranial Pressure Monitor Placement by Nonneurosurgeons: 5-Year Experience Kathryn Ko, MD, and Alicia Conforti, RN Background: This report evaluates a protocol for training nonneurosurgeon
Brain Infusion Kit mm
 Brain Infusion Kit 1 3-5 mm 0004760 STERILE MATERIALS FOR TEN BRAIN INFUSIONS REFER TO ENCLOSED SPECIFICATIONS 7147600-5 2006 DURECT Corporation Printed in U.S.A. April 2006 CONTENTS: Ten brain infusion
Brain Infusion Kit 1 3-5 mm 0004760 STERILE MATERIALS FOR TEN BRAIN INFUSIONS REFER TO ENCLOSED SPECIFICATIONS 7147600-5 2006 DURECT Corporation Printed in U.S.A. April 2006 CONTENTS: Ten brain infusion
Supplementary Methods
 1 Supplementary Methods Social Preference Test Subjects Seventy-four Long-Evans, male rats served as subjects (S-rats) in the foodpreference test, with 40 assigned to the CXT-Same (CXT-S) Condition and
1 Supplementary Methods Social Preference Test Subjects Seventy-four Long-Evans, male rats served as subjects (S-rats) in the foodpreference test, with 40 assigned to the CXT-Same (CXT-S) Condition and
REPORTING POSTOPERATIVE PAIN PROCEDURES IN CONJUNCTION WITH ANESTHESIA
 Committee of Origin: Economics (Approved by the ASA House of Delegates on October 17, 2007 and last updated on September 2, 2008) ASA has recently received reports of payers inappropriately bundling the
Committee of Origin: Economics (Approved by the ASA House of Delegates on October 17, 2007 and last updated on September 2, 2008) ASA has recently received reports of payers inappropriately bundling the
Modeling the Interaction between Intracranial Pressure and Cerebral Hemodynamics
 Modeling the Interaction between Intracranial Pressure and Cerebral Hemodynamics Master s Thesis in Biomedical Engineering Zhaleh Pirzadeh Department of Signals and Systems Division of Signal Processing
Modeling the Interaction between Intracranial Pressure and Cerebral Hemodynamics Master s Thesis in Biomedical Engineering Zhaleh Pirzadeh Department of Signals and Systems Division of Signal Processing
External ventricular drain (EVD) placement for cerebrospinal. FOCUS Neurosurg Focus 43 (5):E5, 2017
 NEUROSURGICAL FOCUS Neurosurg Focus 43 (5):E5, 2017 Real-time ultrasound-guided external ventricular drain placement: technical note James H. Manfield, MBBS, MSc, MRCS, 1 and Kenny K. H. Yu, MBBS, MRCS,
NEUROSURGICAL FOCUS Neurosurg Focus 43 (5):E5, 2017 Real-time ultrasound-guided external ventricular drain placement: technical note James H. Manfield, MBBS, MSc, MRCS, 1 and Kenny K. H. Yu, MBBS, MRCS,
Edwards FloTrac Sensor & Performance Assessments of the FloTrac Sensor and Vigileo Monitor
 Edwards FloTrac Sensor & Edwards Vigileo Monitor Performance Assessments of the FloTrac Sensor and Vigileo Monitor 1 Topics System Configuration Performance and Validation Dr. William T. McGee, Validation
Edwards FloTrac Sensor & Edwards Vigileo Monitor Performance Assessments of the FloTrac Sensor and Vigileo Monitor 1 Topics System Configuration Performance and Validation Dr. William T. McGee, Validation
HIROSHI NAKAGUCHI, M.D., PH.D., TAKEO TANISHIMA, M.D., PH.D., Clinical Material and Methods
 J Neurosurg 93:791 795, 2000 Relationship between drainage catheter location and postoperative recurrence of chronic subdural hematoma after burr-hole irrigation and closed-system drainage HIROSHI NAKAGUCHI,
J Neurosurg 93:791 795, 2000 Relationship between drainage catheter location and postoperative recurrence of chronic subdural hematoma after burr-hole irrigation and closed-system drainage HIROSHI NAKAGUCHI,
SUBJECT: Clinical Practice Guideline for the Management of Severe Traumatic Brain Injury
 ASPIRUS WAUSAU HOSPITAL, INC. Passion for excellence. Compassion for people. Effective Date: December 1, 2005 Proposed By: Samuel Picone III, MD, Trauma Medical Director Approval and Dates: Dr. Bunch,
ASPIRUS WAUSAU HOSPITAL, INC. Passion for excellence. Compassion for people. Effective Date: December 1, 2005 Proposed By: Samuel Picone III, MD, Trauma Medical Director Approval and Dates: Dr. Bunch,
Raised intracranial pressure (ICP) is a common problem in neurosurgical and neurological
 Correspondence to: Mr Laurence T Dunn, Department of Neurosurgery, Institute of Neurological Sciences, Southern General Hospital, Glasgow G51 4TF, UK; ltd1x@udcf.gla.ac.uk RAISED INTRACRANIAL PRESSURE
Correspondence to: Mr Laurence T Dunn, Department of Neurosurgery, Institute of Neurological Sciences, Southern General Hospital, Glasgow G51 4TF, UK; ltd1x@udcf.gla.ac.uk RAISED INTRACRANIAL PRESSURE
Pressure-volume index in head injury
 J Neurosurg 67:832-840, 1987 Pressure-volume index in head injury ANGELO L. MASET, M.D., ANTHONY MARMAROU, PH.D., JOHN D. WARD, M.D., SUNG CHOI, PH.D., HARRY A. LUTZ, PH.D., DANNY BROOKS, B.S., RICHARD
J Neurosurg 67:832-840, 1987 Pressure-volume index in head injury ANGELO L. MASET, M.D., ANTHONY MARMAROU, PH.D., JOHN D. WARD, M.D., SUNG CHOI, PH.D., HARRY A. LUTZ, PH.D., DANNY BROOKS, B.S., RICHARD
longitudinal sinus. A decrease in blood flow was observed when the pressure
 362 J. Physiol. (I942) IOI, 362-368 6I2.I44:6I2.824 THE EFFECT OF VARIATIONS IN THE SU.BARACHNOID PRESSURE ON THE VENOUS PRESSURE IN THE SUPERIOR LONGITUDINAL SINUS AND IN THE TORCULAR OF THE DOG BY T.
362 J. Physiol. (I942) IOI, 362-368 6I2.I44:6I2.824 THE EFFECT OF VARIATIONS IN THE SU.BARACHNOID PRESSURE ON THE VENOUS PRESSURE IN THE SUPERIOR LONGITUDINAL SINUS AND IN THE TORCULAR OF THE DOG BY T.
Effect of Outflow Pressure upon Lymph Flow from Dog Lungs
 Effect of Outflow Pressure upon Lymph Flow from Dog Lungs R.E. Drake, D.K. Adcock, R.L. Scott, and J.C. Gabel From the Department of Anesthesiology, University of Texas Medical School, Houston, Texas SUMMARY.
Effect of Outflow Pressure upon Lymph Flow from Dog Lungs R.E. Drake, D.K. Adcock, R.L. Scott, and J.C. Gabel From the Department of Anesthesiology, University of Texas Medical School, Houston, Texas SUMMARY.
Surgical Technique. CONQUEST FN Femoral Neck Fracture System
 Surgical Technique CONQUEST FN Femoral Neck Fracture System Table of Contents Introduction... 3 Indications... 3 Product Overview... 4 Surgical Technique... 5 Patient Positioning... 5 Reduce the Fracture...
Surgical Technique CONQUEST FN Femoral Neck Fracture System Table of Contents Introduction... 3 Indications... 3 Product Overview... 4 Surgical Technique... 5 Patient Positioning... 5 Reduce the Fracture...
Bedside microdialysis for early detection of cerebral hypoxia in traumatic brain injury
 Neurosurg Focus 9 (5):E2, 2000 Bedside microdialysis for early detection of cerebral hypoxia in traumatic brain injury ASITA S. SARRAFZADEH, M.D., OLIVER W. SAKOWITZ, M.D., TIM A. CALLSEN, M.D., WOLFGANG
Neurosurg Focus 9 (5):E2, 2000 Bedside microdialysis for early detection of cerebral hypoxia in traumatic brain injury ASITA S. SARRAFZADEH, M.D., OLIVER W. SAKOWITZ, M.D., TIM A. CALLSEN, M.D., WOLFGANG
NEURORADIOLOGY DIL part 3
 NEURORADIOLOGY DIL part 3 Bleeds and hemorrhages K. Agyem MD, G. Hall MD, D. Palathinkal MD, Alexandre Menard March/April 2015 OVERVIEW Introduction to Neuroimaging - DIL part 1 Basic Brain Anatomy - DIL
NEURORADIOLOGY DIL part 3 Bleeds and hemorrhages K. Agyem MD, G. Hall MD, D. Palathinkal MD, Alexandre Menard March/April 2015 OVERVIEW Introduction to Neuroimaging - DIL part 1 Basic Brain Anatomy - DIL
Airway Management. Key points. Rapid Sequence Intubation. Rapid Sequence Intubation Recognizing difficult airway Managing difficult airway
 Airway Management Prasha Ramanujam and Guy Shochat Department of Emergency Medicine UCSF Medical Center Key points Rapid Sequence Intubation Recognizing difficult airway Managing difficult airway Rapid
Airway Management Prasha Ramanujam and Guy Shochat Department of Emergency Medicine UCSF Medical Center Key points Rapid Sequence Intubation Recognizing difficult airway Managing difficult airway Rapid
4-20 ma Pressure Transducer
 4-20 ma Pressure Transducer 56410099 Copyright 2017 Durham Geo Slope Indicator All Rights Reserved. This equipment should be installed, maintained, and operated by technically qualified personnel. Any
4-20 ma Pressure Transducer 56410099 Copyright 2017 Durham Geo Slope Indicator All Rights Reserved. This equipment should be installed, maintained, and operated by technically qualified personnel. Any
Brain under pressure Managing ICP. Giuseppe
 Brain under pressure Managing ICP Giuseppe Citerio giuseppe.citerio@unimib.it @Dr_Cit Intro Thresholds Treating HICP Conclusions NO COI for this presentation Produces pressure gradients: herniation HIGH
Brain under pressure Managing ICP Giuseppe Citerio giuseppe.citerio@unimib.it @Dr_Cit Intro Thresholds Treating HICP Conclusions NO COI for this presentation Produces pressure gradients: herniation HIGH
ompanionport Speciality Medical Devices For The Veterinary Community Surgical Suggestions
 Speciality Medical Devices For The Veterinary Community suture holes Place the CompanionPort in the subcutaneous port pocket off to one side so that the septum of the port will not lie directly beneath
Speciality Medical Devices For The Veterinary Community suture holes Place the CompanionPort in the subcutaneous port pocket off to one side so that the septum of the port will not lie directly beneath
Technique. Technique. Technique. Monitoring 1. Local anesthetic? Aseptic technique Hyper-extend (if radial)
 Critical Care Monitoring Hemodynamic Monitoring Arterial Blood Pressure Cannulate artery Uses 2 Technique Sites Locate artery, prep 3 1 Technique Local anesthetic? Aseptic technique Hyper-extend (if radial)
Critical Care Monitoring Hemodynamic Monitoring Arterial Blood Pressure Cannulate artery Uses 2 Technique Sites Locate artery, prep 3 1 Technique Local anesthetic? Aseptic technique Hyper-extend (if radial)
LUMINAL SILICONE CASTS OF HUMAN AND SHEEP BRAIN VENTRICULAR SYSTEM AS TEACHING TOOLS IN ANATOMY
 International Journal of Medical Science and Education An official Publication of Association for Scientific and Medical Education (ASME) Original research Article LUMINAL SILICONE CASTS OF HUMAN AND SHEEP
International Journal of Medical Science and Education An official Publication of Association for Scientific and Medical Education (ASME) Original research Article LUMINAL SILICONE CASTS OF HUMAN AND SHEEP
EFFECTS OF VERTEBRAL AXIAL DECOMPRESSION (VAX-D) ON INTRADISCAL PRESSURE
 EFFECTS OF VERTEBRAL AXIAL DECOMPRESSION (VAX-D) ON Gustavo Ramos, M.D., William Marin, M.D. Journal of Neursurgery 81:35-353 1994 Departments of Neurosurgery and Radiology, Rio Grande Regional Hospital,
EFFECTS OF VERTEBRAL AXIAL DECOMPRESSION (VAX-D) ON Gustavo Ramos, M.D., William Marin, M.D. Journal of Neursurgery 81:35-353 1994 Departments of Neurosurgery and Radiology, Rio Grande Regional Hospital,
Changes in Intracranial Pressure in Various Positions of the Head in Anaesthetised Patients
 Bahrain Medical Bulletien, Vol. 25, No. 4, December 2003 Changes in Intracranial Pressure in Various Positions of the Head in Anaesthetised Patients Vinod K Grover, MD,MNAMS* Indu Bala, MD ** Someshwar
Bahrain Medical Bulletien, Vol. 25, No. 4, December 2003 Changes in Intracranial Pressure in Various Positions of the Head in Anaesthetised Patients Vinod K Grover, MD,MNAMS* Indu Bala, MD ** Someshwar
THOMAS G. SAUL, M.D., THOMAS B. DUCKER, M.D., MICHAEL SALCMAN, M.D., AND ERIC CARRO, M.D.
 J Neurosurg 54:596-600, 1981 Steroids in severe head injury A prospective randomized clinical trial THOMAS G. SAUL, M.D., THOMAS B. DUCKER, M.D., MICHAEL SALCMAN, M.D., AND ERIC CARRO, M.D. Department
J Neurosurg 54:596-600, 1981 Steroids in severe head injury A prospective randomized clinical trial THOMAS G. SAUL, M.D., THOMAS B. DUCKER, M.D., MICHAEL SALCMAN, M.D., AND ERIC CARRO, M.D. Department
Monitoring and interpretation of intracranial pressure ... J Neurol Neurosurg Psychiatry 2004;75: doi: /jnnp.2003.
 NEUROSCIENCE FOR NEUROLOGISTS Monitoring and interpretation of intracranial pressure M Czosnyka, J D Pickard... Intracranial pressure (ICP) is derived from cerebral blood and cerebrospinal fluid (CSF)
NEUROSCIENCE FOR NEUROLOGISTS Monitoring and interpretation of intracranial pressure M Czosnyka, J D Pickard... Intracranial pressure (ICP) is derived from cerebral blood and cerebrospinal fluid (CSF)
Usefulness of Coil-assisted Technique in Treating Wide-neck Intracranial Aneurysms: Neck-bridge Procedure Using the Coil Mass as a Support
 Journal of Neuroendovascular Therapy 2017; 11: 220 225 Online December 14, 2016 DOI: 10.5797/jnet.tn.2016-0081 Usefulness of Coil-assisted Technique in Treating Wide-neck Intracranial Aneurysms: Neck-bridge
Journal of Neuroendovascular Therapy 2017; 11: 220 225 Online December 14, 2016 DOI: 10.5797/jnet.tn.2016-0081 Usefulness of Coil-assisted Technique in Treating Wide-neck Intracranial Aneurysms: Neck-bridge
Monitoring and interpretation of intracranial pressure
 Monitoring and interpretation of intracranial pressure M Czosnyka and J D Pickard J. Neurol. Neurosurg. Psychiatry 2004;75;813-821 doi:10.1136/jnnp.2003.033126 Updated information and services can be found
Monitoring and interpretation of intracranial pressure M Czosnyka and J D Pickard J. Neurol. Neurosurg. Psychiatry 2004;75;813-821 doi:10.1136/jnnp.2003.033126 Updated information and services can be found
1 Description. 2 Indications. 3 Warnings ASPIRATION CATHETER
 Page 1 of 5 ASPIRATION CATHETER Carefully read all instructions prior to use, observe all warnings and precautions noted throughout these instructions. Failure to do so may result in complications. STERILE.
Page 1 of 5 ASPIRATION CATHETER Carefully read all instructions prior to use, observe all warnings and precautions noted throughout these instructions. Failure to do so may result in complications. STERILE.
INTRACRANIAL PRESSURE MONITORING
 INTRACRANIAL PRESSURE MONITORING A Handbook for the Nursing Professional 2 Why do we care about measuring intracranial pressure (ICP)? The intracranial compartment is very different from other regions
INTRACRANIAL PRESSURE MONITORING A Handbook for the Nursing Professional 2 Why do we care about measuring intracranial pressure (ICP)? The intracranial compartment is very different from other regions
External Ventricular Drainage & Lumbar Drainage Procedure and Care. Amey R. Savardekar Assistant Professor Neurosurgery, NIMHANS.
 External Ventricular Drainage & Lumbar Drainage Procedure and Care. Amey R. Savardekar Assistant Professor Neurosurgery, NIMHANS. External Ventricular Drain Indications: Therapeutic (To relieve raised
External Ventricular Drainage & Lumbar Drainage Procedure and Care. Amey R. Savardekar Assistant Professor Neurosurgery, NIMHANS. External Ventricular Drain Indications: Therapeutic (To relieve raised
Meninges and Ventricles
 Meninges and Ventricles Irene Yu, class of 2019 LEARNING OBJECTIVES Describe the meningeal layers, the dural infolds, and the spaces they create. Name the contents of the subarachnoid space. Describe the
Meninges and Ventricles Irene Yu, class of 2019 LEARNING OBJECTIVES Describe the meningeal layers, the dural infolds, and the spaces they create. Name the contents of the subarachnoid space. Describe the
