2/29/2016. By Lisa Amaya, Physician Assistant ATSU graduate 2006
|
|
|
- Angela Webb
- 5 years ago
- Views:
Transcription
1 By Lisa Amaya, Physician Assistant ATSU graduate 2006 Identifying unusual presentations Evaluating the history of the patient Conducting a physical exam Recognize that these presentations may be subtle but important facts. These are real cases seen in family practice/urgent care and if not treated and evaluated correctly may have been catastrophic to the health of the patient. Other cases may be considered zebras but, need to be on the differential despite the remote and unlikely possibility. 1
2 Didactics have taught us to Listen to our patients and if we listen long enough they will tell us what is wrong with them. Personally, this has been a key to examining patients. Instinct has no quantifiable value but, it is that gut sense that may be something that needs to be pursued if there is any doubt. A 20 year old patient (and his mother) come in complaining of left ear pain x 2 days. Denies hearing loss or drainage, fever/chills/nausea or vomiting. Vitals stable: blood pressure 118/82; pulse 82; temp 98 respirations 22 and weight
3 All normal-left ear normal; TM pink/not retracted; no drainage; ear canal normal; no cerumen; pinna neg for pain; hearing grossly normal The rest of the physical examination was normal. The case was not about the presenting complaints although it may have been a referred pain. After the examination was done and the history was obtained from the patient, I explained to the patient and his mom that the examination was negative. 3
4 His mom proceeded to inform me that the patient had had a GSW (gun shot wound to the chest/upper abdomen) about 1 week prior to the visit. Furthermore, she said that the patient was treated and released. Listen to all the clues that may seem irrelevant at the time but, may be the keys to solving the pieces to the puzzle in making a correct diagnosis. The patient was referred to the ER for thoracentesis and further treatment. A 27 year old male reports that he is having a severe headache. Patient stated that he has had a history of headaches in the past and had a history of meningitis. He stated the headache felt like it did when he had had meningitis. 4
5 GENERAL APPEARANCE: The patient is alert, oriented. no acute distress. VITAL SIGNS: T- currently 97.5, blood pressure 110/60, respirations 22, and heart rate 88. NECK: Supple without lymphadenopathy. no meningismus HEART: Regular rate and rhythm. LUNGS: NORMAL breath sounds at the bases. No crackles or wheezes are heard. NEUROLOGICAL: Gross nonfocal. Skin: Warm and dry without any rash. 5
6 This patient was sent to the ER even though all the tests for meningitis were normal and the cbc was normal. The ER examined him and he was sent home. However, the patient returned about 12 hours later with a severe headache and a Lumbar puncture was performed confirming the diagnosis of meningitis. Bottom line: Listen to your patients!!! The cases of the medication refills 6
7 A 50 y/o female presenting for blood pressure medication refill. States she was seen by her primary care doctor the day before but one of the medications was not refilled. She reported she had mentioned to her primary care provider that she had vomited green stuff twice in the last 2 weeks but, nothing further was followed up. Physical examination was normal (including the vitals) except for the abdominal examination. The patient was exquisitely tender in the RUQ and was sent to the ER for further examination. of 30,000 and was being admitted. A high number of WBCs is called leukocytosis. It may be due to: Aplastic anemia Certain drugs or medicines (see list below) Cigarette smoking Not having a spleen, due to spleen removal Infections, most often those caused by bacteria Inflammatory disease (such as rheumatoid arthritis or allergy) Leukemia Severe mental or physical stress Tissue damage (for example, burns) 7
8 This is a 30 year old male presenting for a refill of his albuterol inhaler around 9 am in the morning. He reported he had been short of breath but it was due to his need for his inhaler. At first glance, this male presented with a mostly normal examination and his oxygen saturation rate was 98% except he had some alcohol on his breath at that time in the morning. 8
9 Another physical examination was conducted and the patient had JVD and lower extremity edema noted. In addition, a BNP-was ordered and the levels were over Significantly higher than the norm. The BNP level helps to determine if you have heart failure. BNP levels below 100 pg/ml indicate no heart failure. BNP levels of pg/ml suggest heart failure is present. BNP levels above 300 pg/ml indicate mild heart failure. BNP levels above 600 pg/ml indicate moderate heart failure. BNP levels above 900 pg/ml indicate severe heart failure. The BNP level helps to determine if you have heart failure. BNP levels below 100 pg/ml indicate no heart failure. BNP levels of pg/ml suggest heart failure is present. BNP levels above 300 pg/ml indicate mild heart failure. BNP levels above 600 pg/ml indicate moderate heart failure. BNP levels above 900 pg/ml indicate severe heart failure. This is a 45 year old female presenting with dysuria and frequency. Past medical history is history of UTI s in past and as an infant the patient had glioblastoma of the liver. Also, patient reported she had severe pain with her menses monthly. Additionally, positive history of scoliosis and had a Harrington s rod in her back. 9
10 Mostly normal examination but, the patient was exquisitely tender to palpation in her lower pelvis and abdomen during the examination. Tumors noted in bilateral kidneys, liver, uterus. Essentially, the patient was in stage 4 cancer. One note: A ct scan of the head was not performed suspect lesions in the brain. Researched the glioblastoma of the livernormally located in the brain and spinal cordin the article it stated glioblastomas were the most common liver tumor. 10
11 This is a 50 year old patient coming in for something for pain. She reported she had been discharged from the hospital 2 months prior to the visit and she had been in a coma for most of that time. Prior to the hospitalization, the patient stated she had been an IVDA and was homeless, sleeping near dumpsters. Further, she reported that after she was rescued, she had been on many antidepressants/anxiolytics and in addition had been given lithium. She stated she had overdosed on the lithium and that was the reason she had been hospitalized. The patient reported she had to be resuscitated twice and had been to hell during that time. Speech impedimentsounded like she was speaking with a mouth full of marbles Parkinson-like movementscogwheel and shuffle gait Mood-anxious and constantly repeating the same statement Otherwise normal exam 11
12 The American Psychological Association concurs. It defines near-death experiences as "profound psychological events with transcendental and mystical elements, typically occurring to individuals close to death or in situations of intense physical or emotional danger." Example 1: An elderly woman had been blind since childhood. But, during her NDE, the woman had regained her sight and she was able to accurately describe the instruments and techniques used during the resuscitation her body. After the woman was revived, she reported the details to her doctor. She was able to tell her doctor who came in and out, what they said, what they wore, what they did, all of which was true. Her doctor then referred the woman to Moody who he knew was doing research at the time on NDEs. 12
13 Courage is what it takes to stand up and speak; courage is also what it takes to sit down and listen. Winston Churchill 13
Patient Care Report Guidelines
 A rrival on scene / Scene assessment C omplaint H istory A. Position of patient B. Impression of patient C. Does the patient acknowledge your presence D. Any significant characteristics of the scene A.
A rrival on scene / Scene assessment C omplaint H istory A. Position of patient B. Impression of patient C. Does the patient acknowledge your presence D. Any significant characteristics of the scene A.
CASE-BASED SMALL GROUP DISCUSSION MHD II
 MHD II, Session 11, Student Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION MHD II Session 11 April 11, 2016 STUDENT COPY MHD II, Session 11, Student Copy Page 2 CASE HISTORY 1 Chief complaint: Our baby
MHD II, Session 11, Student Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION MHD II Session 11 April 11, 2016 STUDENT COPY MHD II, Session 11, Student Copy Page 2 CASE HISTORY 1 Chief complaint: Our baby
A guide to writing clear, concise EMS reports using SIREN
 A guide to writing clear, concise EMS reports using SIREN OBJECTIVE: EMS narratives will document patient assessment findings, interventions, and patient response to interventions such that ED providers
A guide to writing clear, concise EMS reports using SIREN OBJECTIVE: EMS narratives will document patient assessment findings, interventions, and patient response to interventions such that ED providers
Patient Assessment. Chapter 8
 Patient Assessment Chapter 8 Patient Assessment Scene size-up Initial assessment Focused history and physical exam Vital signs History Detailed physical exam Ongoing assessment Patient Assessment Process
Patient Assessment Chapter 8 Patient Assessment Scene size-up Initial assessment Focused history and physical exam Vital signs History Detailed physical exam Ongoing assessment Patient Assessment Process
Exam 1 Review. Cardiopulmonary Symptoms Physical Examination Clinical Laboratory Studies
 Exam 1 Review Cardiopulmonary Symptoms Physical Examination Clinical Laboratory Studies WBC Count Differential A patient had been admitted to the hospital for acute shortness of breath. A CXR examination
Exam 1 Review Cardiopulmonary Symptoms Physical Examination Clinical Laboratory Studies WBC Count Differential A patient had been admitted to the hospital for acute shortness of breath. A CXR examination
Assessment of the Adolescent, Pre-Teen, and Teen Student for School Nurses
 Assessment of the Adolescent, Pre-Teen, and Teen Student for School Nurses KIMBERLY RICHARDS RN, BSN CLINICAL UNIT LEADER NOVANT HEALTH MATTHEWS MEDICAL CENTER MEDICAL SURGICAL/HOSPICE ONCOLOGY Agenda
Assessment of the Adolescent, Pre-Teen, and Teen Student for School Nurses KIMBERLY RICHARDS RN, BSN CLINICAL UNIT LEADER NOVANT HEALTH MATTHEWS MEDICAL CENTER MEDICAL SURGICAL/HOSPICE ONCOLOGY Agenda
Emergency Medical Training Services Emergency Medical Technician Basic Program Outlines Outline Topic: ASSESSMENT Revised: 11/2013
 Emergency Medical Training Services Emergency Medical Technician Basic Program Outlines Outline Topic: ASSESSMENT Revised: 11/2013 DEFINITIONS General Impression - EMT develops a plan of action from the
Emergency Medical Training Services Emergency Medical Technician Basic Program Outlines Outline Topic: ASSESSMENT Revised: 11/2013 DEFINITIONS General Impression - EMT develops a plan of action from the
Chapter 8 Trauma Patient Assessment The Patient Assessment Process The Primary Assessment ABCDE s Airway, Breathing, Circulation while securing
 1 2 3 4 5 6 Chapter 8 Trauma Patient Assessment The Patient Assessment Process The Primary Assessment ABCDE s Airway, Breathing, Circulation while securing D-Disability Chief complaint and/or Mechanism
1 2 3 4 5 6 Chapter 8 Trauma Patient Assessment The Patient Assessment Process The Primary Assessment ABCDE s Airway, Breathing, Circulation while securing D-Disability Chief complaint and/or Mechanism
CASE-BASED SMALL GROUP DISCUSSION MHD II SESSION 6. Friday, MARCH 18, 2016 STUDENT COPY
 MHD II, Session 6, STUDENT Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION MHD II SESSION 6 Friday, MARCH 18, 2016 STUDENT COPY Resource for cases: ACP Medicine (Scientific American Medicine) - Vaginitis
MHD II, Session 6, STUDENT Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION MHD II SESSION 6 Friday, MARCH 18, 2016 STUDENT COPY Resource for cases: ACP Medicine (Scientific American Medicine) - Vaginitis
THE DREADED RUN- ON SENTENCE AND OTHER PUNCTUATION RULES THAT KEEP YOU UP AT NIGHT!!!!
 THE DREADED RUN- ON SENTENCE AND OTHER PUNCTUATION RULES THAT KEEP YOU UP AT NIGHT!!!! Is punctuation giving you NIGHTMARES??? Does it give you a headache? When you think of punctuation, do you want to
THE DREADED RUN- ON SENTENCE AND OTHER PUNCTUATION RULES THAT KEEP YOU UP AT NIGHT!!!! Is punctuation giving you NIGHTMARES??? Does it give you a headache? When you think of punctuation, do you want to
Real Cases: Bad Outcomes
 Real Cases: Bad Outcomes Fredrick M. Abrahamian, D.O., FACEP, FIDSA Clinical Professor of Medicine UCLA School of Medicine Director of Education Department of Emergency Medicine Olive View-UCLA Medical
Real Cases: Bad Outcomes Fredrick M. Abrahamian, D.O., FACEP, FIDSA Clinical Professor of Medicine UCLA School of Medicine Director of Education Department of Emergency Medicine Olive View-UCLA Medical
Percussion These 4 techniques are the foundation of the physical exam. Respiration Blood pressure Body
 1 Chapter 11: Physical Exam Techniques 2 Introduction Although patient assessment formally starts with the, the physical examination actually begins when you first set eyes on your patient. The purpose
1 Chapter 11: Physical Exam Techniques 2 Introduction Although patient assessment formally starts with the, the physical examination actually begins when you first set eyes on your patient. The purpose
CENTRAL CARE POLICY SYMPTOMS OF ILLNESS. Policy: Consumers will be observed for symptoms of physical problems, distress, pain, or unusual behaviors.
 Page 1 of 5 CENTRAL CARE POLICY SYMPTOMS OF ILLNESS SUBJECT: SYMPTOMS OF ILLNESS ANNUAL REVIEW MONTH: June RESPONSIBLE FOR REVIEW: Director of Central Care LAST REVISION DATE: June 2009 Policy: Consumers
Page 1 of 5 CENTRAL CARE POLICY SYMPTOMS OF ILLNESS SUBJECT: SYMPTOMS OF ILLNESS ANNUAL REVIEW MONTH: June RESPONSIBLE FOR REVIEW: Director of Central Care LAST REVISION DATE: June 2009 Policy: Consumers
R. John Brewer EMT-P Dental Education Inc. PATIENT ASSESSMENT
 R. John Brewer EMT-P Dental Education Inc. PATIENT ASSESSMENT Patient Assessment Patient assessment is made up of two parts - History - Physical Exam Patient assessment In medical cases obtaining an adequate
R. John Brewer EMT-P Dental Education Inc. PATIENT ASSESSMENT Patient Assessment Patient assessment is made up of two parts - History - Physical Exam Patient assessment In medical cases obtaining an adequate
CASE-BASED SMALL GROUP DISCUSSION MHD II SESSION VI. Friday, MARCH 20, 2015 STUDENT COPY
 MHD II, Session VI, STUDENT Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION MHD II SESSION VI Friday, MARCH 20, 2015 STUDENT COPY Resource for cases: ACP Medicine (Scientific American Medicine) - Vaginitis
MHD II, Session VI, STUDENT Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION MHD II SESSION VI Friday, MARCH 20, 2015 STUDENT COPY Resource for cases: ACP Medicine (Scientific American Medicine) - Vaginitis
Bisan Salhi, M.D. 69 Jesse Hill Jr. Dr. Atlanta, GA Phone:
 Bisan Salhi, M.D. 69 Jesse Hill Jr. Dr. Atlanta, GA 30303 Phone: 734-657-4539 30 June 2006 Dear Sir or Madam: 1. Thank you for the opportunity to evaluate Mr. Liviu Negut. Enclosed is my preliminary medical
Bisan Salhi, M.D. 69 Jesse Hill Jr. Dr. Atlanta, GA 30303 Phone: 734-657-4539 30 June 2006 Dear Sir or Madam: 1. Thank you for the opportunity to evaluate Mr. Liviu Negut. Enclosed is my preliminary medical
NEO 111 Melanie Jorgenson, RN, BSN
 NEO 111 Melanie Jorgenson, RN, BSN Inspection: performing deliberate, purposeful observations in a systematic manner Palpation: using the sense of touch Percussion: striking one object against another
NEO 111 Melanie Jorgenson, RN, BSN Inspection: performing deliberate, purposeful observations in a systematic manner Palpation: using the sense of touch Percussion: striking one object against another
Assessment of the Trauma Patient
 CHAPTER 10 Assessment of the Trauma Patient Overall Assessment Scheme Scene Size-Up Initial Assessment Trauma Physical Exam Vital Signs & SAMPLE History Medical SAMPLE History Physical Exam & Vital Signs
CHAPTER 10 Assessment of the Trauma Patient Overall Assessment Scheme Scene Size-Up Initial Assessment Trauma Physical Exam Vital Signs & SAMPLE History Medical SAMPLE History Physical Exam & Vital Signs
Supporting Documents Case Studies
 Supporting Documents Case Studies ONA Presentation/Case Studies 1 CASE STUDY #1 CC: Right Breast Lump History of Present Illness: 41 yr old G3P0 with an LMP of 08/01/2017 who presents today to discuss
Supporting Documents Case Studies ONA Presentation/Case Studies 1 CASE STUDY #1 CC: Right Breast Lump History of Present Illness: 41 yr old G3P0 with an LMP of 08/01/2017 who presents today to discuss
MARYWOOD UNIVERSITY PHYSICIAN ASSISTANT PROGRAM HISTORY, PHYSICAL, ASSESSMENT AND PLAN
 MARYWOOD UNIVERSITY PHYSICIAN ASSISTANT PROGRAM HISTORY, PHYSICAL, ASSESSMENT AND PLAN PA: PRECEPTOR: MARYWOOD STAFF: PATIENT ID: AGE: SEX: DATE: Chief Complaint: History of Present Illness: 1 Medications:
MARYWOOD UNIVERSITY PHYSICIAN ASSISTANT PROGRAM HISTORY, PHYSICAL, ASSESSMENT AND PLAN PA: PRECEPTOR: MARYWOOD STAFF: PATIENT ID: AGE: SEX: DATE: Chief Complaint: History of Present Illness: 1 Medications:
Pediatric Advanced Life Support
 Pediatric Advanced Life Support Pediatric Chain of Survival Berg M D et al. Circulation 2010;122:S862-S875 Prevention Early cardiopulmonary resuscitation (CPR) Prompt access to the emergency response system
Pediatric Advanced Life Support Pediatric Chain of Survival Berg M D et al. Circulation 2010;122:S862-S875 Prevention Early cardiopulmonary resuscitation (CPR) Prompt access to the emergency response system
Investigation A: Rib Area Pain 3.3B: Shingles
 Investigation 3.3 3.3A: Rib Area Pain 3.3B: Shingles Investigation 3.3A: Rib Area Pain 1. Introduction: When a patient presents with pain in their chest or ribs, as their physician, must sort out the origin
Investigation 3.3 3.3A: Rib Area Pain 3.3B: Shingles Investigation 3.3A: Rib Area Pain 1. Introduction: When a patient presents with pain in their chest or ribs, as their physician, must sort out the origin
Student Guide Module 5: Management of Prevalent Infections in Children Following a Disaster
 Student Guide Module 5: Management of Prevalent Infections in Children Following a Disaster Objectives for this session Section I - Integrated Management of Childhood Illness (IMCI) Understand the IMCI
Student Guide Module 5: Management of Prevalent Infections in Children Following a Disaster Objectives for this session Section I - Integrated Management of Childhood Illness (IMCI) Understand the IMCI
Change in Condition: When to report to the MD/NP/PA
 Change in Condition: When to report to the MD/NP/PA Immediate Notification Any symptom, sign or apparent discomfort that is: Acute or Sudden in onset, and: A Marked Change (i.e. more severe) in relation
Change in Condition: When to report to the MD/NP/PA Immediate Notification Any symptom, sign or apparent discomfort that is: Acute or Sudden in onset, and: A Marked Change (i.e. more severe) in relation
Case Presentation. The Failure to Diagnose Sepsis. chills. pain out of proportion to mechanism. low-grade fever. tachycardia that does not make sense
 Case Presentation The Failure to Diagnose Sepsis Sepsis is a regular visitor in the news as cases of flesh-eating bacteria and the dramatic speed with which victims deteriorate hit the headlines. The failure
Case Presentation The Failure to Diagnose Sepsis Sepsis is a regular visitor in the news as cases of flesh-eating bacteria and the dramatic speed with which victims deteriorate hit the headlines. The failure
Medical History Form
 Medical History Form NAME DOB / / TODAY S DATE MEDICAL HISTORY What medical Conditions do you have? Select all that apply, or write in if not listed: Diabetes High Blood Pressure Thyroid Disorder Heart
Medical History Form NAME DOB / / TODAY S DATE MEDICAL HISTORY What medical Conditions do you have? Select all that apply, or write in if not listed: Diabetes High Blood Pressure Thyroid Disorder Heart
History. History and Physical Exam of the Pediatric Patient. History of Present Illness. Chief Complaint. Past Medical History. Past Medical History
 History History and Physical Exam of the Pediatric Patient Colleen A. Kraft, M.D., FAAP Richmond Pediatric Associates, Inc. Source Who is giving the history? Is this the patient s primary caretaker? 1
History History and Physical Exam of the Pediatric Patient Colleen A. Kraft, M.D., FAAP Richmond Pediatric Associates, Inc. Source Who is giving the history? Is this the patient s primary caretaker? 1
Chapter 29 1/8/2018. Vital Signs. Measuring and Reporting Vital Signs. Key Terms
 Chapter 29 Vital Signs Key Terms Blood pressure Body temperature Diastolic pressure Hypertension Hypotension Pulse Pulse rate Respiration Sphygmomanometer Stethoscope Systolic pressure Vital signs Measuring
Chapter 29 Vital Signs Key Terms Blood pressure Body temperature Diastolic pressure Hypertension Hypotension Pulse Pulse rate Respiration Sphygmomanometer Stethoscope Systolic pressure Vital signs Measuring
Introduction to surgery
 Introduction to surgery Make an outline of the surgical clinical history Describe the abdominal quadrants and its content Name at least 5 types of surgical intruments What is the informed consent? Name
Introduction to surgery Make an outline of the surgical clinical history Describe the abdominal quadrants and its content Name at least 5 types of surgical intruments What is the informed consent? Name
Note for Jane Doe on 7/22/05 - Chart 5407
 Note for Jane Doe on 7/22/05 - Chart 5407 Chief Complaint: This 31 year old female presents today with abdominal pain. Duration: Condition has existed for one month. Modifying Factors: Patient indicates
Note for Jane Doe on 7/22/05 - Chart 5407 Chief Complaint: This 31 year old female presents today with abdominal pain. Duration: Condition has existed for one month. Modifying Factors: Patient indicates
Chapter 32. Objectives. Objectives 01/09/2013. Spinal Column and Spinal Cord Trauma
 Chapter 32 Spinal Column and Spinal Cord Trauma Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives 1.
Chapter 32 Spinal Column and Spinal Cord Trauma Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives 1.
SMALL GROUP DISCUSSION
 MHD II, Session 1 Student Copy Page 1 SMALL GROUP DISCUSSION MHD II Session 1 Gastroinestinal Monday, January 9, 2017 STUDENT COPY MHD II, Session 1 Student Copy Page 2 CASE 1 CHIEF CONCERN: "I'm passing
MHD II, Session 1 Student Copy Page 1 SMALL GROUP DISCUSSION MHD II Session 1 Gastroinestinal Monday, January 9, 2017 STUDENT COPY MHD II, Session 1 Student Copy Page 2 CASE 1 CHIEF CONCERN: "I'm passing
The exact cause of sarcoidosis is unknown. However, gender, race, and genetics can increase the risk of developing the condition:
 What is sarcoidosis? Sarcoidosis is an inflammatory disease in which granulomas, or clumps of inflammatory cells, form in various organs. This causes organ inflammation. Sarcoidosis may be triggered by
What is sarcoidosis? Sarcoidosis is an inflammatory disease in which granulomas, or clumps of inflammatory cells, form in various organs. This causes organ inflammation. Sarcoidosis may be triggered by
Change in Condition: When to report to the MD/NP/PA
 Change in Condition: When to report to the MD/NP/PA Immediate Notification Any symptom, sign or apparent discomfort that is: Acute or Sudden in onset, and: A Marked Change (i.e. more severe) in relation
Change in Condition: When to report to the MD/NP/PA Immediate Notification Any symptom, sign or apparent discomfort that is: Acute or Sudden in onset, and: A Marked Change (i.e. more severe) in relation
Chapter 11 - The Primary Assessment
 Introduction to Emergency Medical Care 1 OBJECTIVES 11.1 Define key terms introduced in this chapter. Slides 11 12, 14, 19 21, 28 11.2 Explain the purpose of the primary assessment. Slides 11 13 OBJECTIVES
Introduction to Emergency Medical Care 1 OBJECTIVES 11.1 Define key terms introduced in this chapter. Slides 11 12, 14, 19 21, 28 11.2 Explain the purpose of the primary assessment. Slides 11 13 OBJECTIVES
Patient History Form
 Patient History Form Advanced Directive Care Plan? Yes No Name: Birth date: / / Address: Age: Sex: F M STREET DAY YEAR Telephone: Home ( ) CITY STATE DAY YEAR MARITAL STATUS: Divorced Separated Alive/Age
Patient History Form Advanced Directive Care Plan? Yes No Name: Birth date: / / Address: Age: Sex: F M STREET DAY YEAR Telephone: Home ( ) CITY STATE DAY YEAR MARITAL STATUS: Divorced Separated Alive/Age
PCCSS, LLP Pulmonary, Critical Care & Sleep Specialists
 NAME: AGE: DOB: DATE: REQUESTING PHYSICIAN: NOTE: Please help us find out about you by filling out the Patient side of this form on pages 1 3. If you don t know the answer to one of the questions, ask
NAME: AGE: DOB: DATE: REQUESTING PHYSICIAN: NOTE: Please help us find out about you by filling out the Patient side of this form on pages 1 3. If you don t know the answer to one of the questions, ask
Physical Examination Reporting Form
 Building Trades National Medical Screening Program Physical Examination Reporting Form Name: Date: P1. Vital Signs Height: BP: / Weight: lbs. #2 nd BP:* / Arm: L R Cuff Size:** Regular Large Ped Pulse:
Building Trades National Medical Screening Program Physical Examination Reporting Form Name: Date: P1. Vital Signs Height: BP: / Weight: lbs. #2 nd BP:* / Arm: L R Cuff Size:** Regular Large Ped Pulse:
H&P Checklist (Inpatient) Evaluator: Subject: Program:
 H&P Checklist (Inpatient) Evaluator: Subject: Program: PROFESSIONALISM 1) Introduces self/role and preceptor Did 2) Verbal and non-verbal language demonstrates respect for patient & family. Did 3) Respects
H&P Checklist (Inpatient) Evaluator: Subject: Program: PROFESSIONALISM 1) Introduces self/role and preceptor Did 2) Verbal and non-verbal language demonstrates respect for patient & family. Did 3) Respects
Pediatric Case Studies. Case 1
 Pediatric Case Studies James Naprawa, MD Assistant Clinical Professor Pediatric Emergency Medicine Children s Hospital, Columbus Case 1 Almost 4 year old AA girl PMH UTI x 2 with abdominal pain and fever
Pediatric Case Studies James Naprawa, MD Assistant Clinical Professor Pediatric Emergency Medicine Children s Hospital, Columbus Case 1 Almost 4 year old AA girl PMH UTI x 2 with abdominal pain and fever
Chapter 11. Objectives. Objectives 01/09/2013. Baseline Vital Signs, Monitoring Devices, and History Taking
 Chapter 11 Baseline Vital Signs, Monitoring Devices, and History Taking Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights
Chapter 11 Baseline Vital Signs, Monitoring Devices, and History Taking Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights
R. John Brewer NREMT-P Dental Education Inc. PATIENT ASSESSMENT
 R. John Brewer NREMT-P Dental Education Inc. PATIENT ASSESSMENT Patient Assessment Patient assessment is made up of two parts - History - Physical Exam Patient assessment In medical cases obtaining an
R. John Brewer NREMT-P Dental Education Inc. PATIENT ASSESSMENT Patient Assessment Patient assessment is made up of two parts - History - Physical Exam Patient assessment In medical cases obtaining an
SCRIPT 1 - PHYSICIAN COMMUNICATION Localizing Signs and Symptoms with Warning Signs
 SCRIPT 1 - PHYSICIAN COMMUNICATION Localizing Signs and Symptoms with Warning Signs Wisconsin Healthcare Associated Infections in LTC Coalition PHONE CONTACT NECESSARY Resident: Jimmy Issick Date: 11/7/15
SCRIPT 1 - PHYSICIAN COMMUNICATION Localizing Signs and Symptoms with Warning Signs Wisconsin Healthcare Associated Infections in LTC Coalition PHONE CONTACT NECESSARY Resident: Jimmy Issick Date: 11/7/15
VAO BASIC SUPPORT CLINICAL APPROACH TO THE PATIENT HANDOUT
 CLINICAL APPROACH TO THE PATIENT HANDOUT 1 I am the most important part of patient care. How can you expect to treat a patient appropriately if you don t follow through on basic primary care? Remember:
CLINICAL APPROACH TO THE PATIENT HANDOUT 1 I am the most important part of patient care. How can you expect to treat a patient appropriately if you don t follow through on basic primary care? Remember:
Competency Log Professional Responder Courses
 Competency Log Professional Responder Courses Check off each competency once successfully demonstrated. This log may be used as a support tool when teaching a Professional Responder course. Refer to the
Competency Log Professional Responder Courses Check off each competency once successfully demonstrated. This log may be used as a support tool when teaching a Professional Responder course. Refer to the
5AB Dysrhythmia Interpretation and Management 2016
 5AB Dysrhythmia Interpretation and Management 2016 How to complete your biennial ECG review: A website has been created that contains the basic review information. Use this as a reference during your review.
5AB Dysrhythmia Interpretation and Management 2016 How to complete your biennial ECG review: A website has been created that contains the basic review information. Use this as a reference during your review.
ITLS Pediatric Provider Course Basic Pre-Test
 ITLS Pediatric Provider Course Basic Pre-Test 1. You arrive at the scene of a motor vehicle collision and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
ITLS Pediatric Provider Course Basic Pre-Test 1. You arrive at the scene of a motor vehicle collision and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
Compliance Department ELEMENTS OF GENITOURINARY EXAMINATION 11/2010
 Compliance Department ELEMENTS OF GENITOURINARY EXAMINATION 11/2010 Elements of Examination Constitutional Measurement of any three of the following seven vital signs: 1) sitting or standing blood pressure,
Compliance Department ELEMENTS OF GENITOURINARY EXAMINATION 11/2010 Elements of Examination Constitutional Measurement of any three of the following seven vital signs: 1) sitting or standing blood pressure,
Patient Assessment From Brady s First Responder (8th Edition) 83 Questions
 Patient Assessment From Brady s First Responder (8th Edition) 83 Questions 1. Which question is important if your patient may be a candidate for surgery? p. 183 *A.) When did you last eat? B.) What is
Patient Assessment From Brady s First Responder (8th Edition) 83 Questions 1. Which question is important if your patient may be a candidate for surgery? p. 183 *A.) When did you last eat? B.) What is
History Data Panel. Case 030 Preg Trauma. Presenting Complaint Altered mental status s/p MVC. Person Giving Information EMS
 History Data Panel Presenting Complaint Altered mental status s/p MVC Person Giving Information EMS History of Present Illness 28 year old woman, 35 weeks pregnant per report of her husband the passenger.
History Data Panel Presenting Complaint Altered mental status s/p MVC Person Giving Information EMS History of Present Illness 28 year old woman, 35 weeks pregnant per report of her husband the passenger.
Quick review of Assessment. Pediatric Medical Assessment Review And Case Studies. Past Medical History. S.A.M.P.L.E. History is a great start.
 EMS Live at Night January 12 th, 2010 Pediatric Medical Assessment Review And Case Studies Brian Rogge RN Northwest Medstar Pediatric/Perinatal Team Quick review of Assessment S.A.M.P.L.E. History is a
EMS Live at Night January 12 th, 2010 Pediatric Medical Assessment Review And Case Studies Brian Rogge RN Northwest Medstar Pediatric/Perinatal Team Quick review of Assessment S.A.M.P.L.E. History is a
Acting in an emergency. Dr. Samer Sara
 Acting in an emergency Dr. Samer Sara 1 Acting in an emergency basic steps to follow: 1. Recognize the emergency. 2. Check the scene. 3. Call 110. 4. Check the victim. 5. Give first aid. 2 Dr. Samer Sara
Acting in an emergency Dr. Samer Sara 1 Acting in an emergency basic steps to follow: 1. Recognize the emergency. 2. Check the scene. 3. Call 110. 4. Check the victim. 5. Give first aid. 2 Dr. Samer Sara
Contrast Materials Patient Safety: What are contrast materials and how do they work?
 Contrast Materials Patient Safety: What are contrast materials and how do they work? Which imaging exams use contrast materials? How safe are contrast materials? How should I prepare for my imaging procedure
Contrast Materials Patient Safety: What are contrast materials and how do they work? Which imaging exams use contrast materials? How safe are contrast materials? How should I prepare for my imaging procedure
Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials
 Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials 1 1. A high-risk bodily fluid for spreading infection is blood. 2. Items that can reduce the spread of infection include masks, gloves, and
Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials 1 1. A high-risk bodily fluid for spreading infection is blood. 2. Items that can reduce the spread of infection include masks, gloves, and
Bilateral rib fractures 2 on right and 1 on left In different stages of healing, with left fracture older than right fractures
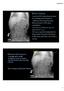 More history: Seen by PCP yesterday because of vomiting and fussinesss. Called by ED today because Mom presents with same complaints. ED found nothing but got an abdominal x ray. ED now wants kid admitted
More history: Seen by PCP yesterday because of vomiting and fussinesss. Called by ED today because Mom presents with same complaints. ED found nothing but got an abdominal x ray. ED now wants kid admitted
Patient to complete this information
 Patient to complete this information Patient s Name Birth date Today s date Referring Physician Primary Care Physician Age Occupation Retired, how long? Prior operations Medications Type Date Name Dose
Patient to complete this information Patient s Name Birth date Today s date Referring Physician Primary Care Physician Age Occupation Retired, how long? Prior operations Medications Type Date Name Dose
 55-year-old male with 2nd and 3rd degree burns to face, chest, and arms on 25% of the body Respirations: 34 Pulse: 120 Mental Status: moans to painful stimulus Mucous membranes charred Stridor 10 cm scalp
55-year-old male with 2nd and 3rd degree burns to face, chest, and arms on 25% of the body Respirations: 34 Pulse: 120 Mental Status: moans to painful stimulus Mucous membranes charred Stridor 10 cm scalp
Resident At Risk. The National Early Warning Score (NEWS) and Monitoring Vital Signs
 Resident At Risk The National Early Warning Score (NEWS) and Monitoring Vital Signs Schein et al 64 consecutive ward patients requiring CPR 84% clinical deterioration 8 hours before arrest Pathophysiology
Resident At Risk The National Early Warning Score (NEWS) and Monitoring Vital Signs Schein et al 64 consecutive ward patients requiring CPR 84% clinical deterioration 8 hours before arrest Pathophysiology
NOR-CAL EMS MEDICAL ADVISORY COMMITTEE RUN REVIEW, NOVEMBER 2014
 Eric M. Rudnick, MD, FACEP, FAAEM Medical Director Northern California EMS NOR-CAL EMS MEDICAL ADVISORY COMMITTEE RUN REVIEW, NOVEMBER 2014. meeting by Engineer Bill Bogenreif 1 CASE #1 Call Type : Fall
Eric M. Rudnick, MD, FACEP, FAAEM Medical Director Northern California EMS NOR-CAL EMS MEDICAL ADVISORY COMMITTEE RUN REVIEW, NOVEMBER 2014. meeting by Engineer Bill Bogenreif 1 CASE #1 Call Type : Fall
EVALUATION OF A SICK CHILD WITH FEVER
 EVALUATION OF A SICK CHILD WITH FEVER Learning objectives At the conclusion of this learning activity, participants should be able to; Discuss the different etiologies of acute illness in a child Identify
EVALUATION OF A SICK CHILD WITH FEVER Learning objectives At the conclusion of this learning activity, participants should be able to; Discuss the different etiologies of acute illness in a child Identify
oriented evaluation of your patient and establishing priorities of care based on existing and
 1 Chapter 12: Patient Assessment in the Field 2 Patient assessment means conducting a - oriented evaluation of your patient and establishing priorities of care based on existing and potential threats to
1 Chapter 12: Patient Assessment in the Field 2 Patient assessment means conducting a - oriented evaluation of your patient and establishing priorities of care based on existing and potential threats to
Practical Approaches to Medical Necessity
 Practical Approaches to Medical Necessity CAROLYN AVERY, CPC, CEMC CAROLYN AVERY & ASSOCIATES, PC ROBERT OSSOFF DMD, MD, CHC ASSISTANT VICE CHANCELLOR FOR COMPLIANCE &CORPORATE INTEGRITY VANDERBILT MEDICAL
Practical Approaches to Medical Necessity CAROLYN AVERY, CPC, CEMC CAROLYN AVERY & ASSOCIATES, PC ROBERT OSSOFF DMD, MD, CHC ASSISTANT VICE CHANCELLOR FOR COMPLIANCE &CORPORATE INTEGRITY VANDERBILT MEDICAL
To appreciate the unique problems of older surgical patients. To describe the differential and management
 To appreciate the unique problems of older surgical patients. t To describe the differential and management of acute abdomen in the older. To recognize and tend to hospital complications in olderpatients.
To appreciate the unique problems of older surgical patients. t To describe the differential and management of acute abdomen in the older. To recognize and tend to hospital complications in olderpatients.
Paediatric Enhanced Life Support Scenarios
 Paediatric Enhanced Life Support Scenarios These scenarios should be used to assess staff undertaking the Paediatric Enhanced Life Support course within the Black Country Partnership NHS Foundation Trust.
Paediatric Enhanced Life Support Scenarios These scenarios should be used to assess staff undertaking the Paediatric Enhanced Life Support course within the Black Country Partnership NHS Foundation Trust.
NORTHERN VIRGINIA PULMONARY AND CRITICAL CARE ASSOCIATES, P.C.
 NORTHERN VIRGINIA PULMONARY AND CRITICAL CARE ASSOCIATES, P.C. Past Medical History AIDS/HIV disease Anemia Asthma Bronchitis Cancer Date of last Chest X-ray Diabetes Mellitus, Type I Diabetes Mellitus,
NORTHERN VIRGINIA PULMONARY AND CRITICAL CARE ASSOCIATES, P.C. Past Medical History AIDS/HIV disease Anemia Asthma Bronchitis Cancer Date of last Chest X-ray Diabetes Mellitus, Type I Diabetes Mellitus,
Patient Name Date of Birth Page 1 of 6
 2545 W. Hillcrest Dr. #205 Thousand Oaks, CA 91320 Admissions: 888.822.8938 Fax: 805.273.5246 Dear Medical Professional, This patient is seeking care to address eating disorder behaviors. For the patient
2545 W. Hillcrest Dr. #205 Thousand Oaks, CA 91320 Admissions: 888.822.8938 Fax: 805.273.5246 Dear Medical Professional, This patient is seeking care to address eating disorder behaviors. For the patient
You Are the Emergency Medical Responder
 Lesson 32: Injuries to the Chest, Abdomen and Genitalia You Are the Emergency Medical Responder Your police unit responds to a call in a part of town plagued by violence. When you arrive, you find the
Lesson 32: Injuries to the Chest, Abdomen and Genitalia You Are the Emergency Medical Responder Your police unit responds to a call in a part of town plagued by violence. When you arrive, you find the
RHEUMATOLOGY PATIENT HISTORY FORM
 !! RAMOS RHEUMATOLOGY, PC RHEUMATOLOGY PATIENT HISTORY FORM Date: / / NAME: Birthdate: / / Last First M. I. Age: Sex: F M Marital status: Never married Married Divorced Separated Widowed Partnered/significant
!! RAMOS RHEUMATOLOGY, PC RHEUMATOLOGY PATIENT HISTORY FORM Date: / / NAME: Birthdate: / / Last First M. I. Age: Sex: F M Marital status: Never married Married Divorced Separated Widowed Partnered/significant
April 2011 CE. Site code # E The Patient With Heart Failure; CPAP as an Intervention
 April 2011 CE Site code # 107200E-1211 The Patient With Heart Failure; CPAP as an Intervention Prepared by: Lt. Bill Hoover, Medical Officer Wauconda Fire District Reviewed/revised by Sharon Hopkins, RN,
April 2011 CE Site code # 107200E-1211 The Patient With Heart Failure; CPAP as an Intervention Prepared by: Lt. Bill Hoover, Medical Officer Wauconda Fire District Reviewed/revised by Sharon Hopkins, RN,
Pain Management Questionnaire
 In order to make the most of your visit, we require this form to be completed to the best of your ability and sent to the Pain Management Clinic a copy should be shared with your Primary Care Provider
In order to make the most of your visit, we require this form to be completed to the best of your ability and sent to the Pain Management Clinic a copy should be shared with your Primary Care Provider
Review of Neonatal Respiratory Problems
 Review of Neonatal Respiratory Problems Respiratory Distress Occurs in about 7% of infants Clinical presentation includes: Apnea Cyanosis Grunting Inspiratory stridor Nasal flaring Poor feeding Tachypnea
Review of Neonatal Respiratory Problems Respiratory Distress Occurs in about 7% of infants Clinical presentation includes: Apnea Cyanosis Grunting Inspiratory stridor Nasal flaring Poor feeding Tachypnea
Reinventing Report: How You Can Develop Resident Expertise in High- Value Clinical Reasoning
 Reinventing Report: How You Can Develop Resident Expertise in High- Value Clinical Reasoning Jason H. Maley, MD, Kathleen M. Murphy, MD, and Erin M. Haley, MD, PhD Chief Medicine Residents Department of
Reinventing Report: How You Can Develop Resident Expertise in High- Value Clinical Reasoning Jason H. Maley, MD, Kathleen M. Murphy, MD, and Erin M. Haley, MD, PhD Chief Medicine Residents Department of
Patient Intake Form for Allegany Ear, Nose, & Throat
 Patient Intake Form for Allegany Ear, se, & Throat Patient Name: What brings you to the office today? Who is your primary care doctor? Please list your current medications: Are you allergic to any medications?
Patient Intake Form for Allegany Ear, se, & Throat Patient Name: What brings you to the office today? Who is your primary care doctor? Please list your current medications: Are you allergic to any medications?
12 Blueprints Q&A Step 2 Surgery
 12 Blueprints Q&A Step 2 Surgery 34. A 40-year-old female has been referred to you for a recent ER and hospital admission, from which she was given a diagnosis of acute diverticulitis. Treatment at that
12 Blueprints Q&A Step 2 Surgery 34. A 40-year-old female has been referred to you for a recent ER and hospital admission, from which she was given a diagnosis of acute diverticulitis. Treatment at that
Arcana Center for Integrative Medicine
 Arcana Center for Integrative Medicine Patient s Name: Date of Birth: Reason for today s visit: Past Medical History Primary care physician: Date of last exam: (sick or well) Physician s Address: Office
Arcana Center for Integrative Medicine Patient s Name: Date of Birth: Reason for today s visit: Past Medical History Primary care physician: Date of last exam: (sick or well) Physician s Address: Office
New Patient Sleep Intake
 New Patient Sleep Intake Name: Date of Birth: Primary Care Physician: Date of Visit: Referring Physician and/or Other Physicians: Retail Pharmacy: Mail Order Pharmacy: Address: Mail Order Phone #: Phone
New Patient Sleep Intake Name: Date of Birth: Primary Care Physician: Date of Visit: Referring Physician and/or Other Physicians: Retail Pharmacy: Mail Order Pharmacy: Address: Mail Order Phone #: Phone
Septic Shock. Kathryn Sims, PGY I
 Septic Shock Kathryn Sims, PGY I A 6 y.o. previously healthy boy presents to the ED with 7 days of fever accompanied by chills. Further history reveals the patient has also been experiencing dysuria for
Septic Shock Kathryn Sims, PGY I A 6 y.o. previously healthy boy presents to the ED with 7 days of fever accompanied by chills. Further history reveals the patient has also been experiencing dysuria for
An Interview with a Chiropractor
 An Interview with a Chiropractor Doctor Scott Warner took the time out of his busy schedule to talk to us about chiropractic medicine what it is, what it isn t, and why he chose it as a profession. What
An Interview with a Chiropractor Doctor Scott Warner took the time out of his busy schedule to talk to us about chiropractic medicine what it is, what it isn t, and why he chose it as a profession. What
The Respiratory System
 130 20 The Respiratory System 1. Define important words in this chapter 2. Explain the structure and function of the respiratory system 3. Discuss changes in the respiratory system due to aging 4. Discuss
130 20 The Respiratory System 1. Define important words in this chapter 2. Explain the structure and function of the respiratory system 3. Discuss changes in the respiratory system due to aging 4. Discuss
Pediatric Asthma. Concepts (in order of emphasis) Jared, 10 years old
 Pediatric Asthma Jared, 10 years old Overview This scenario is a rich application of the priority setting required by the nurse to rescue a child with an acute asthmatic exacerbation. Concepts (in order
Pediatric Asthma Jared, 10 years old Overview This scenario is a rich application of the priority setting required by the nurse to rescue a child with an acute asthmatic exacerbation. Concepts (in order
APPENDICITIS IN THE YOUNG CHILD. By Rebecca Lucas
 1 APPENDICITIS IN THE YOUNG CHILD By Rebecca Lucas 2 When time counts the most Patient Profile 3 The patient 3 years old 2 months girl Usually is vibrant, articulate, incorrigible enjoys telling me how
1 APPENDICITIS IN THE YOUNG CHILD By Rebecca Lucas 2 When time counts the most Patient Profile 3 The patient 3 years old 2 months girl Usually is vibrant, articulate, incorrigible enjoys telling me how
Program Script. Nursing Assessment The Head-to-Toe Assessment
 Program Script Nursing Assessment The Head-to-Toe Assessment This document comprises the complete script for this program including chapter titles. This is provided to instructors to enhance the educational
Program Script Nursing Assessment The Head-to-Toe Assessment This document comprises the complete script for this program including chapter titles. This is provided to instructors to enhance the educational
Homework Assignment Complete and Place in Binder
 Homework Assignment Complete and Place in Binder Chapter # 34/35: Pediatric & Geriatric Emergencies 1. The first month of life after birth is referred to as the: A) neonatal period. B) toddler period.
Homework Assignment Complete and Place in Binder Chapter # 34/35: Pediatric & Geriatric Emergencies 1. The first month of life after birth is referred to as the: A) neonatal period. B) toddler period.
Physiological Measurements Training for Care/Nursing & LD Small Group Home Staff
 Physiological Measurements Training for Care/Nursing & LD Small Group Home Staff CONTENTS 1. The National Early Warning Score 2. Respiratory Rate 3. Oxygen Saturations 4. Temperature 5. Blood Pressure
Physiological Measurements Training for Care/Nursing & LD Small Group Home Staff CONTENTS 1. The National Early Warning Score 2. Respiratory Rate 3. Oxygen Saturations 4. Temperature 5. Blood Pressure
CASE-BASED SMALL GROUP DISCUSSION
 MHD I, Session 11, Student Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION MHD I SESSION 11 Renal Block Acid- Base Disorders November 7, 2016 MHD I, Session 11, Student Copy Page 2 Case #1 Cc: I have had
MHD I, Session 11, Student Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION MHD I SESSION 11 Renal Block Acid- Base Disorders November 7, 2016 MHD I, Session 11, Student Copy Page 2 Case #1 Cc: I have had
Respiratory Emergencies. Chapter 11
 Respiratory Emergencies Chapter 11 Respiratory System Anatomy and Function of the Lung Characteristics of Adequate Breathing Normal rate and depth Regular breathing pattern Good breath sounds on both sides
Respiratory Emergencies Chapter 11 Respiratory System Anatomy and Function of the Lung Characteristics of Adequate Breathing Normal rate and depth Regular breathing pattern Good breath sounds on both sides
2. Have your symptoms affected your ability to carry out your daily activities? YES NO
 QUESTIONNAIRE Page 1 of 5 Date: Referring MD (Name, Address, Phone Number): Primary Care Physician (Name and Address, Phone Number): Reason for visit: 1. How long have you had symptoms? Describe your symptoms?
QUESTIONNAIRE Page 1 of 5 Date: Referring MD (Name, Address, Phone Number): Primary Care Physician (Name and Address, Phone Number): Reason for visit: 1. How long have you had symptoms? Describe your symptoms?
* Final Report * ED Triage Entered On: 01/16/2014 8:45 EST Performed On: 01/16/2014 8:42 EST by
 Result date: Result status: 16 January 2014 8:42 EST Auth (Verified) * Final Report * ED Triage Entered On: 01/16/2014 8:45 EST Performed On: 01/16/2014 8:42 EST by Assessment I Chief Complaint : Diarrhea
Result date: Result status: 16 January 2014 8:42 EST Auth (Verified) * Final Report * ED Triage Entered On: 01/16/2014 8:45 EST Performed On: 01/16/2014 8:42 EST by Assessment I Chief Complaint : Diarrhea
PEPP Course: PEPP BLS Pretest
 PEPP Course: PEPP BLS Pretest 1. What is the best way to administer oxygen to a child in moderate respiratory distress? Nasal cannula Simple mask Nonrebreathing mask Bag-valve-mask device 2. A 2-year-old
PEPP Course: PEPP BLS Pretest 1. What is the best way to administer oxygen to a child in moderate respiratory distress? Nasal cannula Simple mask Nonrebreathing mask Bag-valve-mask device 2. A 2-year-old
Bilateral Wilms Tumor: New Protocols and Procedures by Dawn Wolf
 www.complexchild.com Bilateral Wilms Tumor: New Protocols and Procedures by Dawn Wolf Masses...tumors...oncologist...straight to the ER... Those were the words the doctor was using as he talked about our
www.complexchild.com Bilateral Wilms Tumor: New Protocols and Procedures by Dawn Wolf Masses...tumors...oncologist...straight to the ER... Those were the words the doctor was using as he talked about our
Med 536 Communicating About Prognosis Workshop. Case 2
 Med 536 Communicating About Prognosis Workshop Case 2 ID / CC: 33 year-old man with intracranial hemorrhage History of the Presenting Illness 33 year-old man with a prior history of melanoma of the neck
Med 536 Communicating About Prognosis Workshop Case 2 ID / CC: 33 year-old man with intracranial hemorrhage History of the Presenting Illness 33 year-old man with a prior history of melanoma of the neck
Case Presentation Guidelines
 http://depts.washington.edu/medclerk/student/presentation.htmloral Case Presentation Guidelines Steve McGee, M.D. The Oral Case Presentation is an art form that requires concerted effort and repeated practice.
http://depts.washington.edu/medclerk/student/presentation.htmloral Case Presentation Guidelines Steve McGee, M.D. The Oral Case Presentation is an art form that requires concerted effort and repeated practice.
WEEK. OSPAP Programme. Respiratory Examination & History. Slide 1 of 49 MPHM14 OSPAP Clinical Skills
 OSPAP Programme Respiratory Examination & History Slide 1 of 49 MPHM14 OSPAP Clinical Skills The Beginning! Environment! Introduce yourself Ask permission to take the history Have you got the correct person!!
OSPAP Programme Respiratory Examination & History Slide 1 of 49 MPHM14 OSPAP Clinical Skills The Beginning! Environment! Introduce yourself Ask permission to take the history Have you got the correct person!!
Your treatment with XELJANZ
 Your treatment with XELJANZ (tofacitinib citrate) THIS BROCHURE HAS BEEN PRODUCED FOR PATIENTS WHO HAVE BEEN PRESCRIBED XELJANZ. BEFORE USING XELJANZ, PLEASE REVIEW THE PACKAGE LEAFLET FOR THIS MEDICINAL
Your treatment with XELJANZ (tofacitinib citrate) THIS BROCHURE HAS BEEN PRODUCED FOR PATIENTS WHO HAVE BEEN PRESCRIBED XELJANZ. BEFORE USING XELJANZ, PLEASE REVIEW THE PACKAGE LEAFLET FOR THIS MEDICINAL
Cases For Teaching Second Year Medical Students. Head and neck and neuroanatomy. 2- What is the anatomical explanation for her symptoms?
 Head and neck and neuroanatomy Case 1: (RECURRENT LARYNGEAL NERVE INJURY) A 35-year-old woman complains of a 2-month history of hoarseness of her voice and some choking while drinking liquids. She denies
Head and neck and neuroanatomy Case 1: (RECURRENT LARYNGEAL NERVE INJURY) A 35-year-old woman complains of a 2-month history of hoarseness of her voice and some choking while drinking liquids. She denies
Background. Background. Headache Examination. Headache History. Primary vs. Secondary Headaches. Headaches In Children: Why Worry?
 Background Headaches In Children: Why Worry? Marcy Yonker MD FAHS Associate Professor of Pediatrics University of Arizona Director, Pediatric Headache Program Phoenix Children s Hospital Headaches are
Background Headaches In Children: Why Worry? Marcy Yonker MD FAHS Associate Professor of Pediatrics University of Arizona Director, Pediatric Headache Program Phoenix Children s Hospital Headaches are
What Ails You? The Investigation Begins
 What Ails You? The Investigation Begins Vocabulary: Dengue fever Endemic Epidemiology Lesson Summary: Students will use the first case report from the Key West 2009 dengue outbreak to complete an epidemiological
What Ails You? The Investigation Begins Vocabulary: Dengue fever Endemic Epidemiology Lesson Summary: Students will use the first case report from the Key West 2009 dengue outbreak to complete an epidemiological
ADVANCED ASSESSMENT. Approach To The Patient Ontario Base Hospital Group OBHG Education Subcommittee
 ADVANCED ASSESSMENT Approach To The Patient 2014 Ontario Base Hospital Group ADVANCED ASSESSMENT Approach to the Patient AUTHORS Mike Muir AEMCA, ACP, BHSc Paramedic Program Manager Grey Bruce Huron Paramedic
ADVANCED ASSESSMENT Approach To The Patient 2014 Ontario Base Hospital Group ADVANCED ASSESSMENT Approach to the Patient AUTHORS Mike Muir AEMCA, ACP, BHSc Paramedic Program Manager Grey Bruce Huron Paramedic
W elcome to MXC s Virtual Hospital! Health
 Hi, I would like to take you on a journey of what I have been through over the past 10 days.. W elcome to MXC s Virtual Hospital! Health Sciences and Nursing programs have access to a state-ofthe-art Simulated
Hi, I would like to take you on a journey of what I have been through over the past 10 days.. W elcome to MXC s Virtual Hospital! Health Sciences and Nursing programs have access to a state-ofthe-art Simulated
10/15/2015. Structural Lesions Brain tumor (neoplasm) Degenerative disease Intracranial hemorrhage Parasites Trauma
 At the end of this seminar the participant shall be able to: Generally describe the pathophysiology of altered level of consciousness Describe some of the medical causes of altered level of consciousness
At the end of this seminar the participant shall be able to: Generally describe the pathophysiology of altered level of consciousness Describe some of the medical causes of altered level of consciousness
