Back to the Future: Using Aminoglycosides Again and How to Dose Them Optimally
|
|
|
- Agnes Grant
- 5 years ago
- Views:
Transcription
1 INVITED ARTICLE ANTIMICROBIAL RESISTANCE George M. Eliopoulos, Section Editor Back to the Future: Using Aminoglycosides Again and How to Dose Them Optimally George L. Drusano, Paul G. Ambrose, Sujata M. Bhavnani, Joseph S. Bertino, Ann N. Nafziger, and Arnold Louie Ordway Research Institute, Albany, New York Gram-negative organisms have become increasingly resistant to both b-lactam antibiotics and fluoroquinolones. Consequently, aminoglycoside antibiotics have undergone a resurgence in use. Because of the known toxicities of aminoglycoside antibiotics, clinicians have avoided their use, unless no other alternatives were extant. Over the past 2 decades, we have learned much about the relationship between aminoglycoside exposure and the likelihood of a good clinical outcome or the occurrence of nephrotoxicity. For example, minimum inhibitory concentration values 2.0 mg/l lead to unacceptably low probabilities of a good clinical outcome, and infrequent administration of doses (i.e., intervals of 24 h and longer intervals for patients with compromised renal function) plays a central role in minimizing the likelihood of toxicity. Using these new insights, we suggest ways of evaluating the dose and schedule of administration of aminoglycosides in empirical therapy to obtain the highest likelihood of an efficacious and nontoxic therapy. Nosocomial infections caused by gram-negative bacilli have become increasingly difficult to treat over the past 5 years because of the advent of a number of resistance mechanisms that limit the use of some of the best drugs in our armamentarium. Unfortunately, very few new drugs that are active against multidrug-resistant nosocomial gram-negative organisms are expected to be available for 5 10 years. Consequently, many clinicians are starting to again consider the use of aminoglycoside antibiotics. The commentary in this article applies only to gram-negative organisms. Aminoglycosides were widely used in empirical therapy throughout the 1970s and much of the 1980s. Unfortunately, aminoglycoside use generates a number of toxicities, mostly oto- and nephrotoxicity. It was noted [1] that patients in intensive care units who developed altered renal function had a significantly increased risk of death. Consequently, with the advent of broad-spectrum b-lactams (e.g., third- and fourthgeneration cephalosporins; b-lactam and b-lactamase inhibitor combinations, such as piperacillin and tazobactam; and carbapenems, such as imipenem plus cilastatin and meropenem) Received 5 February 2007; accepted 7 May 2007; electronically published 8 August Reprints or correspondence: Dr. George L. Drusano, Ordway Research Institute, 150 New Scotland Ave., Albany, NY (gdrusano@ordwayresearch.org). Clinical Infectious Diseases 2007; 45: by the Infectious Diseases Society of America. All rights reserved /2007/ $15.00 DOI: / and fluoroquinolones, use of aminoglycosides decreased, because clinicians felt that they could obtain good resolution of serious infections without using drugs that would generate serious toxicities. Multidrug-resistant Pseudomonas and Acinetobacter infections, as well as infections caused by extended-spectrum b- lactamase bearing Enterobacteriaeceae species, are often resistant to most or even all of the these newer agents. Frequently, only the aminoglycosides and the polymyxins are available for therapy. Over the course of the past decade, information has become available to guide the use of these aminoglycosides. In this article, we will look at some of these data and apply them, with the objective of achieving maximal therapeutic effect in patients without encumbering them with undue risk of nephrotoxicity. AMINOGLYCOSIDE TOXICITY A number of articles based on data from both preclinical and clinical trials have clarified the risk of nephrotoxicity associated with the use of aminoglycosides [2 7]. A preclinical review by Mingeot-Leclercq et al. [2] includes data revealing that aminoglycoside toxicity is driven by the uptake by proximal renal tubular epithelial cells of aminoglycosides from their luminal surface. Similar findings were also demonstrated by Whelton et al. [6, 7]. The key issue here is that the uptake is saturable. Consequently, when concentrations of drug in the tubular lumen at the point of uptake are well above the Km of transport ANTIMICROBIAL RESISTANCE CID 2007:45 (15 September) 753
2 (15 mg/l) [2], saturation of uptake occurs. Animal model data from Giuliano et al. [3] and human data from DeBroe et al. [5] reveal that more-fractionated administration (e.g., administration of a dose every 8 h or 12 h, rather than every 24 h) always resulted in a higher concentration of drug being present in the proximal renal tubular epithelial cells. These preclinical and clinical studies established the hypothesis that less frequent aminoglycoside administration would result in less aminoglycoside uptake and, ultimately, a lower rate of nephrotoxicity occurring during reasonably short courses of therapy. ter Braak et al. [8] were able to demonstrate a significant difference between once-daily and more frequent administration of aminoglycoside therapy with respect to the occurrence of nephrotoxicity. Rybak et al. [9] performed the only randomized, double-blind trial examining this issue and were able to demonstrate that once-daily administration of the drug was significantly less likely to result in nephrotoxicity than was administration of the drug every 12 h. In the analysis of this study, this difference was seen on the basis of both occurrence (using yes/no logistic regression) and time to event (using stratified Kaplan- Meier analysis). Rybak et al. [9] also found that an increasing daily area under the curve (AUC) corresponded with a higher likelihood of toxicity and that concurrent vancomycin use was particularly related to an increase in the likelihood of nephrotoxicity. The probability of aminoglycoside nephrotoxicity as a function of daily aminoglycoside AUC and concurrent vancomycin use is shown for patients receiving the drug every 12 h and patients receiving the drug once daily in figure 1A and B. The effect of concurrent vancomycin use on the time to the occurrence of nephrotoxicity among patients receiving aminoglycoside therapy every 12 h is shown in figure 2. It is important to note that, in the rather small study ( ) by Rybak et al. [9], there were no instances of nen p 74 phrotoxicity in the group of patients who received the aminoglycoside therapy once daily. Consequently, the logistic regression curve for this group (figure 1B) is quite far to the right, and this would not likely be the case if more patients were involved. For the Kaplan-Meier plot (figure 2), it is clear that concurrent vancomycin therapy had a major influence on the time to the occurrence of nephrotoxicity for the group of patients who received the aminoglycoside therapy twice daily. Again, because there were no cases of nephrotoxicity in the group of patients who received aminoglycoside therapy once daily, any representation of time-to-event analysis is uninformative, with regard to understanding the impact of concurrent vancomycin therapy on such a regimen. The important aspect to note in figure 2 is that occurrence is represented as the time to event. It is likely that, if a patient received aminoglycoside therapy for a long period (110 days), even if therapy was received only once daily, as the duration of therapy increased, the risk of the patient experiencing nephrotoxicity would increase. This was independently demonstrated in a study by Bertino et al. [10], in which duration of therapy was an independent risk factor for nephrotoxicity in a multivariate logistic regression analysis. Administering aminoglycoside therapy infrequently does not completely obliterate the risk of drug-driven nephrotoxicity but provides a window when patients can be safely treated with these agents. This emphasizes the importance of prescribing a correct dose for the patient to obtain a high probability of a good clinical outcome, administering the dose on a daily basis (or less frequently in the case of patients with compromised renal function), and then stopping the aminoglycoside treatment quickly. Because these agents are concentration-dependent killing drugs, relatively short courses (i.e., 7 days) should provide near-maximal effect and near-minimal toxicity. It is important to note that this strategy was tested clinically in a study by Nicolau et al. [11], in which the duration of therapy was a median of 3 days, and the ultimate rate of nephrotoxicity was quite low (1.2% among patients). AMINOGLYCOSIDE EFFECT There has been a general feeling among clinicians that aminoglycosides are not overly effective for treating many types of infection. A number of reasons for this seeming lack of efficacy have been suggested (e.g., chelation by WBC DNA in patients with pneumonia and poor tissue penetration). However, one of the major reasons for this perception is the misidentification of the susceptibility break point for these drugs. For both gentamicin and tobramycin, the break point for full susceptibility is 4 mg/l, and for amikacin, the break point is 16 mg/l. As we show below, these values are too high. These break points caused clinicians to use these agents in situations in which the expectation of a good outcome was unacceptably low. In the 1970s and 1980s, the standard dosage of both gentamicin and tobramycin was also too low, at 80 mg every 8 h ( mg/kg for a kg person). Again, this low dose ameliorated the rate of nephrotoxicity but did not provide a high probability of a good clinical outcome if the MIC was even mildly elevated. In the 1980s, Moore et al. [12] were able to link aminoglycoside exposure to outcome. Unfortunately, because of sparse serum sampling, they chose the Peak:MIC ratio as the independent variable. Animal data from the study by Craig et al. [13] show that the AUC:MIC ratio is more likely the correct dynamically linked variable, although it should be recognized that any study that uses only a single-dose schedule will have maximal colinearity between the Peak:MIC ratio and the AUC: MIC ratio. Later, Kashuba et al. [14] were able to generate a relationship between aminoglycoside exposure and the probability of a patient becoming afebrile or having normalization of temperature 754 CID 2007:45 (15 September) ANTIMICROBIAL RESISTANCE
3 Figure 1. Probability of nephrotoxicity caused by aminoglycoside therapy as a function of daily aminoglycoside area under the curve (AUC) for patients receiving the drug every 12 h (A) and patients receiving the drug once daily (B). The occurrence of nephrotoxicity is more likely when vancomycin is used concurrently. in a specific time frame. We use the resolution of fever relationship to demonstrate the ability to optimize aminoglycoside use. In figure 3, we demonstrate the link between the AUC: MIC ratio and the probability of the patient becoming afebrile. There are 3 separate curves for the probability of a patient becoming afebrile by days 5, 7, and 9. For demonstration purposes, we concentrate on the curve showing the probability of a patient becoming afebrile by day 7. To achieve a 90% probability of this response by day 7, an AUC:MIC ratio of 1:156 is required. OPTIMIZATION OF THERAPY Operationally, optimal antimicrobial therapy can be defined as a choice of drug, drug dose, and schedule of administration that results in an acceptably high likelihood of a good therapeutic outcome, while not burdening the patient with an unacceptably high probability of a concentration-related drug toxicity (in this case, nephrotoxicity). It is important to note that the relationship for toxicity (figure 1A) has AUC 0 24 as the independent variable, and the relationship for effect (figure 3) has the AUC 0 24 :MIC ratio as the independent variable. To explicitly determine how these relationships interact, the independent variables must be the same, which can be achieved, in this instance, by factoring out the MIC and fixing it at a specific value. In figure 4, the curves for efficacy and toxicity are shown on the same scales, with the MIC fixed at 0.25 mg/l, 0.5 mg/l, and 1.0 mg/l. Empirically, the horizontal lines represent the values at which the efficacy ANTIMICROBIAL RESISTANCE CID 2007:45 (15 September) 755
4 WHAT IS THE NECESSARY DOSE TO ATTAIN THE OPTIMAL EXPOSURE? Figure 2. Effect of concurrent vancomycin use on the time to the occurrence of nephrotoxicity in patients receiving a twice-daily aminoglycoside regimen. probability is 90% and the toxicity probability is 10%. The vertical lines provide the probability of the alternate relationship when the 10% or 90% value has been reached. It should be noted that we chose to use the logistic function for twicedaily drug administration. It is clear that, if the clinician were to desire a 90% probability of effect, while engendering no more than a 10% probability of nephrotoxicity, that a patient with a pathogen with a gentamicin and tobramycin MIC of 0.25 mg/l would have a quite broad toxic-therapeutic window. As the MIC increases to 0.5 mg/l, the window decreases appreciably. At an MIC of 1.0 mg/ L, a probability of 90% for a good outcome cannot be attained without accepting a toxicity probability slightly 160%. From the toxicity perspective, if a clinician would like to have no more than a 10% probability of toxicity, then he or she would need to be satisfied with an effect probability of 75%. There are 2 distinct circumstances for which we can determine the necessary dose to attain optimal exposure. The first is the empirical therapy situation, in which no information is available about the concentration-time profile for the patient. The second is the circumstance in which the clinician has obtained gentamicin and tobramycin concentration determinations for the patient. In the latter circumstance, the determination of the necessary dose for optimal exposure requires the use of stochastic control techniques and represents a topic requiring its own review. Here, we will partially address the first circumstance, in which therapy is empirical. We used the population pharmacokinetic analysis performed by Inciardi and Batra [15] and performed two 9999-subject Monte Carlo simulations, using a dosage of 5 mg/kg per day of an aminoglycoside administered as a 2.5-mg/kg dose every 12 h or a 5-mg/kg dose once daily. For the analysis, we assumed an 80-kg patient; therefore, the treatment regimens were 200 mg of an aminoglycoside every 12 h and 400 mg once daily. We then used the logistic regression functions for toxicity and effect shown in figures 1 and 3, generating toxicity probability distributions and effect probability distributions for MIC values of 0.25 mg/l, 0.5 mg/l, and 1.0 mg/l. These are shown for the treatment regimen in which a 200-mg dose of drug was administered every 12 h (figure 6). If the problem is approached classically (i.e., if the clinician would like the patient to have no more than a 10% probability of toxicity and at least a 90% probability of a good clinical outcome), then this dosage (200 mg every 12 h) produces only a 60.9% likelihood of having a probability of nephrotoxicity of 10%. At an MIC of 0.25 mg/l, 100% of subjects have a 90% WHAT IS THE OPTIMAL EXPOSURE? Again, operationally, the optimal exposure can be defined as the drug dose and schedule of administration that provide the largest difference between the effect probability and the toxicity probability. Alternatively, a clinician may state the problem somewhat differently. Often, a clinician would like to have at least a 90% probability of a good outcome for the patient and no more than a 10% probability of engendering a concentration-related toxicity. The latter part of this dilemma is shown in figure 4, which illustrates the idea of a toxic-therapeutic window. The former formulation is somewhat deterministic and identifies a specific exposure (figure 5). The maximal differences between effect and toxicity occur at an AUC value of 65 when the MIC is 0.25 mg/l (AUC 0 24 :MIC, 1:260) and at an AUC value of 75 when the MIC is either 0.5 or 1.0 mg/l (AUC 0 24 :MIC, 1:150 and 1:75, respectively). Figure 3. Probability of resolution of fever by days 5, 7, and 9 of aminoglycoside therapy, as determined by logistic regression analysis. The squares are break point values, as determined by classification and regression tree analysis. AUC, area under the curve. 756 CID 2007:45 (15 September) ANTIMICROBIAL RESISTANCE
5 Figure 4. The probability of effect (temperature defervescence) versus the probability of nephrotoxicity, as a function of daily area under the curve (AUC). The effect probability differs as a function of MIC. A, MIC of 0.25 mg/l. B, MIC of 0.5 mg/l. C, MIC of 1.0 mg/l.
6 Figure 5. The logistic regression curves for probability of effect (temperature defervescence) and the probability of nephrotoxicity, presented as a function of area under the curve (AUC). The blue curve is the difference between these probabilities, and the maximum value of this curve represents one measure of an optimal aminoglycoside exposure. The effect probability differs as a function of MIC. A, MIC of 0.25 mg/l. B, MIC of 0.5 mg/l. C, MIC of 1.0 mg/l.
7 Figure 6. A, Efficacy probability at an MIC of 0.25 mg/l. B, Efficacy probability at an MIC of 0.5 mg/l. C, Efficacy probability at an MIC of 1.0 mg/l. D, Toxicity probability. probability of a good clinical outcome; at an MIC of 0.5 mg/ L, this value is 90.2%, and at an MIC of 1.0 mg/l, this value is 4.5%. These values seem to correspond with the impression that aminoglycosides are toxic agents and are not very effective, particularly at MIC values 10.5 mg/l. However, if, for example, the probability of toxicity is 120%, the patient will not necessarily experience toxicity. Indeed, there is an 80% likelihood that the patient will not experience toxicity. The same thought process applies to the probability of a good clinical outcome. To understand the likelihood of toxicity and good outcome across the patient distribution of the Monte Carlo simulation, it is important to take an expectation. For example, if the toxicity probability among 2000 patients is 0% 10%, the midpoint (5%) is used to calculate the expectation that 100 of these patients would experience toxicity (mean probability of toxicity, patients). This process is repeated throughout the distribution, and the expected number of patients experiencing toxicity is summed and then divided by 9999 to obtain an estimate of the fraction of patients who would experience toxicity overall. When considering these expectations for the regimen including 200 mg of drug administered once every 12h, the estimated percentage of patients experiencing toxicity is 18.9%. For MIC values of 0.25 mg/l, 0.5 mg/l, and 1.0 mg/l, the estimated percentages of patients having a good clinical outcome is 100%, 94%, and 79.9%, respectively. These results convey a clear significance. First, at a dosage of 5 mg/kg per day administered once every 12 h, there is an almost 20% likelihood of toxicity overall, which verges on the unacceptable. It should be recognized that use of a schedule in which the drug is administered once daily would ameliorate this problem considerably, particularly if the duration of therapy were limited to 1 week. Given that aminoglycosides, like fluoroquinolones, are concentration-dependent killing drugs and that good clinical outcome was defined as the patient being afebrile by 1 week, this limitation in duration is reasonable. Second, it is clear that empirical expected response rates are quite robust to an MIC of 0.5 mg/l and reasonable to an MIC of 1.0 mg/l. Higher MIC values will produce unacceptably low expected response rates. Third, there is no doubt that the Clinical and Laboratory Standards Institute break points for aminoglycosides are far too high and result in inadequate therapy for patients infected with strains with these higher MIC values. The counterargument that is most frequently asserted is that aminoglycosides are rarely used as single agents and are used mostly ANTIMICROBIAL RESISTANCE CID 2007:45 (15 September) 759
8 for synergy. There are 2 errors with respect to this argument. The first is that, at this time, a large number of gram-negative pathogens are already primarily resistant to many of the combination agents (e.g., b-lactams and fluoroquinolones). The second is that, although synergy may be real and clinically helpful, there are few clinical data to support this view, except, perhaps, in the context of Pseudomonas aeruginosa infection [16]. Consequently, it is important to optimize dosing of aminoglycosides as if they were the only active agents being used. In summary, aminoglycosides are undergoing a resurgence in use because of widespread resistance to other therapeutic classes. We have attained a considerable amount of knowledge about the use of aminoglycosides over the past 2 decades. An empirical dosage of 5 mg/kg administered once daily (or less frequently in patients with compromised renal function), with a delimited course of therapy, will allow robust therapy if the pathogen has an MIC of 1.0 mg/l. Larger doses (e.g., 7 mg/ kg) will provide somewhat better coverage (perhaps an MIC as high as 2.0 mg/l), but an even shorter duration of therapy may be required when a higher dose is administered (perhaps 5 days). Using such a strategy, we can resurrect these agents to provide good therapy for seriously infected patients for whom they are the therapy of last resort. Finally, it should be recognized that, when the therapeutic situation is no longer empirical (i.e., microbiological data and aminoglycoside concentration-time data become available), individualization of patient therapy will remain critical to obtaining an optimal outcome. Acknowledgments Potential conflicts of interest. References All authors: no conflicts. 1. Uchino S, Kellum JA, Bellomo R, et al.; Beginning and Ending Supportive Therapy for the Kidney (BEST Kidney) Investigators. Acute renal failure in critically ill patients: a multinational, multicenter study. JAMA 2005; 294: Mingeot-Leclercq MP, Tulkens PM. Aminoglycosides: nephrotoxicity. Antimicrob Agents Chemother 1999; 43: Guiliano RA, Verpooten GA, Verbist L, Weeden R, DeBroe ME. In vivo uptake kinetics of aminoglycosides in the kidney cortex of rats. J Pharmacol Exp Ther 1986; 236: Wood CA, Norton DR, Kohlhepp SJ, et al. The influence of tobramycin dosage regimens on neprotoxicity, ototoxicity, and antibacterial efficacy in a rat model of subcutaneous abscess. J Infect Dis 1988; 158: De Broe ME, Verbist L, Verpooten GA. Influence of dosage schedule on renal accumulation of amikacin and tobramycin in man. J Antimicrob Chemother 1991; 27 (Suppl C): Whelton A. Aminoglycoside renal corical kinetics: a clue to mechanisms of nephrotoxicity. Prog Clin Biol Res 1979; 35: Whelton A, Carter GG, Bryant HH, Fox L, Walker WG. Therapeutic implications of gentamicin accumulation in severely diseased kidneys. Arch Intern Med 1976; 135: ter Braak EW, DeVries PJ, Bouter KP, et al. Once-daily dosing regimen for aminoglycoside plus b-lactam combination therapy of serious bacterial infections: comparative trial of netilmicin plus ceftriaxone. Am J Med 1990; 89: Rybak MJ, Abate BJ, Kang SL, Ruffing MJ, Lerner SA, Drusano GL. Prospective evaluation of the effect of an aminoglycoside dosing regimen on rates of observed nephrotoxicity and ototoxicity. Antimicrob Agents Chemother 1999; 43: Bertino JS Jr, Booker LA, Franck PA, Jenkins PL, Franck KR, Nafziger AN. Incidence of and significant risk factors for aminoglycoside-associated nephrotoxicity in patients dosed by using individualized pharmacokinetic monitoring. J Infect Dis 1993; 167: Nicolau DP, Freeman CD, Belliveau PP, Nightingale CH, Ross JW, Quintiliani R. Experience with a once-daily aminoglycoside program administered to 2184 adult patients. Antimicrob Agents Chemother 1995; 39: Moore RD, Lietman PS, Smith CR. Clinical response to aminoglycoside therapy: importance of the ratio of the peak concentration to minimal inhibitory concentration. J Infect Dis 1987; 155: Craig WA, Redington J, Ebert SC. Pharmacodynamics of amikacin in vitro and in mouse thigh and lung infections. J Antimicrob Chemother 1991; 27(Suppl C): Kashuba AD, Nafziger AN, Drusano GL, Bertino JS Jr. Optimizing aminoglycoside therapy for nosocomial pneumonia caused by Gramnegative bacteria. Antimicrob Agents Chemother 1999; 43: Inciardi JF, Batra KK. Nonparametric approach to population pharmacokinetics in oncology patients receiving aminoglycoside therapy. Antimicrob Agents Chemother 1993; 37: Schimpff S, Satterlee W, Young VM, Serpick A. Empiric therapy with carbenicillin and gentamicin for febrile patients with cancer and granulocytopenia. N Engl J Med 1971; 284: CID 2007:45 (15 September) ANTIMICROBIAL RESISTANCE
ICU Volume 11 - Issue 3 - Autumn Series
 ICU Volume 11 - Issue 3 - Autumn 2011 - Series Impact of Pharmacokinetics of Antibiotics in ICU Clinical Practice Introduction The efficacy of a drug is mainly dependent on its ability to achieve an effective
ICU Volume 11 - Issue 3 - Autumn 2011 - Series Impact of Pharmacokinetics of Antibiotics in ICU Clinical Practice Introduction The efficacy of a drug is mainly dependent on its ability to achieve an effective
Aminoglycosides John A. Bosso, Pharm.D.
 AMINOGLYCOSIDES Therapeutics/PHRMP-73 Aminoglycoside Mechanism of Action Aminoglycosides bind to 30s ribosomal subunit resulting in mistranslation of mrna thus disrupting protein synthesis. They are rapidly
AMINOGLYCOSIDES Therapeutics/PHRMP-73 Aminoglycoside Mechanism of Action Aminoglycosides bind to 30s ribosomal subunit resulting in mistranslation of mrna thus disrupting protein synthesis. They are rapidly
Pharmacologyonline 1: (2010) ewsletter Singh and Kochbar. Optimizing Pharmacokinetic/Pharmacodynamics Principles & Role of
 Optimizing Pharmacokinetic/Pharmacodynamics Principles & Role of Cefoperazone Sulbactam Singh M*, Kochhar P* Medical & Research Division, Pfizer India. Summary Antimicrobial resistance is associated with
Optimizing Pharmacokinetic/Pharmacodynamics Principles & Role of Cefoperazone Sulbactam Singh M*, Kochhar P* Medical & Research Division, Pfizer India. Summary Antimicrobial resistance is associated with
Continuous Infusion of Antibiotics In The ICU: What Is Proven? Professor of Medicine Vice-Chairman, Department of Medicine SUNY at Stony Brook
 Continuous Infusion of Antibiotics In The ICU: What Is Proven? Michael S. Niederman, M.D. Chairman, Department of Medicine Winthrop-University Hospital Mineola, NY Professor of Medicine Vice-Chairman,
Continuous Infusion of Antibiotics In The ICU: What Is Proven? Michael S. Niederman, M.D. Chairman, Department of Medicine Winthrop-University Hospital Mineola, NY Professor of Medicine Vice-Chairman,
EMA Workshop Estimating the Probability of Target Attainment
 EMA Workshop Estimating the Probability of Target Attainment G.L. Drusano, M.D. Professor and Director Institute for Therapeutic Innovation University of Florida Attainment We all tend to think problems
EMA Workshop Estimating the Probability of Target Attainment G.L. Drusano, M.D. Professor and Director Institute for Therapeutic Innovation University of Florida Attainment We all tend to think problems
The CLSI Approach to Setting Breakpoints
 The CLSI Approach to Setting Breakpoints Jean B. Patel, PhD, D(ABMM) Deputy Director, Office of Antimicrobial Resistance Division of Healthcare Quality Promotion National Center for Emerging and Zoonotic
The CLSI Approach to Setting Breakpoints Jean B. Patel, PhD, D(ABMM) Deputy Director, Office of Antimicrobial Resistance Division of Healthcare Quality Promotion National Center for Emerging and Zoonotic
Pharmacodynamic indices in targeting therapy of critical infections
 Pharmacodynamic indices in targeting therapy of critical infections P.M. Tulkens Cellular and Molecular Pharmacology, Catholic University of Louvain, Brussels, Belgium & International Society of Anti-infective
Pharmacodynamic indices in targeting therapy of critical infections P.M. Tulkens Cellular and Molecular Pharmacology, Catholic University of Louvain, Brussels, Belgium & International Society of Anti-infective
%T MIC MIC. Pharmacokinetics PK: Cmax AUC T1/2 Pharmacodynamics PD: MIC: minimum inhibitory concentration time-killing-curve 1990.
 THE JAPANESE JOURNAL OF ANTIBIOTICS 58 2 159( 55 ) ( 2 15 ) %T MIC MIC 2002 30%T MIC 50%T MIC 1000 mg 3 3 /day Pharmacokinetics PK: Cmax AUC T1/2 Pharmacodynamics PD: MIC: minimum inhibitory concentration
THE JAPANESE JOURNAL OF ANTIBIOTICS 58 2 159( 55 ) ( 2 15 ) %T MIC MIC 2002 30%T MIC 50%T MIC 1000 mg 3 3 /day Pharmacokinetics PK: Cmax AUC T1/2 Pharmacodynamics PD: MIC: minimum inhibitory concentration
A Snapshot of Colistin Use in South-East Europe and Particularly in Greece
 A Snapshot of Colistin Use in South-East Europe and Particularly in Greece Helen Giamarellou 02.05.2013 When Greek Physicians Prescribe Colistin? It is mainly prescribed in the ICU for VAP, bacteremia
A Snapshot of Colistin Use in South-East Europe and Particularly in Greece Helen Giamarellou 02.05.2013 When Greek Physicians Prescribe Colistin? It is mainly prescribed in the ICU for VAP, bacteremia
Basic Concepts of PK/PD -pharmacodynamic indices- Johan W. Mouton MD PhD FIDSA Professor pharmacokinetics and pharmacodymamics
 Basic Concepts of PK/PD -pharmacodynamic indices- Johan W. Mouton MD PhD FIDSA Professor pharmacokinetics and pharmacodymamics This patient needs antibiotics. But which ones? Intensive care patient Ceftazidime,
Basic Concepts of PK/PD -pharmacodynamic indices- Johan W. Mouton MD PhD FIDSA Professor pharmacokinetics and pharmacodymamics This patient needs antibiotics. But which ones? Intensive care patient Ceftazidime,
Pharmacodynamics: the methods
 Pharmacodynamics: the methods In vitro models Animal models Clinical studies Population studies With the support of Wallonie-Bruxelles-International 3B-1 Pharmacodynamics: the methods "un peu de tout "
Pharmacodynamics: the methods In vitro models Animal models Clinical studies Population studies With the support of Wallonie-Bruxelles-International 3B-1 Pharmacodynamics: the methods "un peu de tout "
PHARMACOKINETIC & PHARMACODYNAMIC OF ANTIBIOTICS
 PHARMACOKINETIC & PHARMACODYNAMIC OF ANTIBIOTICS SITI HIR HURAIZAH MD TAHIR Bpharm (UKM), MSc (Clinical Microbiology) (UoN) CLINICAL PHARMACIST HOSPITAL MELAKA WHY STUDY PHARMACOKINETICS (PK) AND PHARMACODYNAMICS
PHARMACOKINETIC & PHARMACODYNAMIC OF ANTIBIOTICS SITI HIR HURAIZAH MD TAHIR Bpharm (UKM), MSc (Clinical Microbiology) (UoN) CLINICAL PHARMACIST HOSPITAL MELAKA WHY STUDY PHARMACOKINETICS (PK) AND PHARMACODYNAMICS
Continuous vs Intermittent Dosing of Antibiotics in Critically-Ill Patients
 Continuous vs Intermittent Dosing of Antibiotics in Critically-Ill Patients Jan O Friedrich, MD DPhil Associate Professor of Medicine, University of Toronto Medical Director, MSICU St. Michael s Hospital,
Continuous vs Intermittent Dosing of Antibiotics in Critically-Ill Patients Jan O Friedrich, MD DPhil Associate Professor of Medicine, University of Toronto Medical Director, MSICU St. Michael s Hospital,
ZIN EN ONZIN VAN ANTIBIOTICASPIEGELS BIJ NEONATEN
 ZIN EN ONZIN VAN ANTIBIOTICASPIEGELS BIJ NEONATEN Anne Smits Fellow neonatologie UZ Leuven Use of antibiotics in neonates 50 European hospitals 23 non-european hospitals Countries n = 14 n = 9 Pediatric
ZIN EN ONZIN VAN ANTIBIOTICASPIEGELS BIJ NEONATEN Anne Smits Fellow neonatologie UZ Leuven Use of antibiotics in neonates 50 European hospitals 23 non-european hospitals Countries n = 14 n = 9 Pediatric
Other β-lactam. A. Carbapenems:
 A. Carbapenems: Other β-lactam Carbapenems are synthetic β-lactam antibiotics Differ in structure from the penicillins in that the sulfur atom of the thiazolidine ring. Imipenem, meropenem, doripenem,
A. Carbapenems: Other β-lactam Carbapenems are synthetic β-lactam antibiotics Differ in structure from the penicillins in that the sulfur atom of the thiazolidine ring. Imipenem, meropenem, doripenem,
EDUCATIONAL COMMENTARY VANCOMYCIN MONITORING
 EDUCATIONAL COMMENTARY VANCOMYCIN MONITORING Commentary provided by: Julie Hall, MHS, MT (ASCP) Assistant Dean, College of Health Professions Assistant Professor, Medical Laboratory Science Grand Valley
EDUCATIONAL COMMENTARY VANCOMYCIN MONITORING Commentary provided by: Julie Hall, MHS, MT (ASCP) Assistant Dean, College of Health Professions Assistant Professor, Medical Laboratory Science Grand Valley
SBUH Aminoglycoside Dosing Protocol
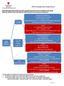 Adult Aminoglycoside Dosing for Gram negative infections prior to available serum levels (Excludes patients with cystic fibrosis, OB GYN patients and surgical prophylaxis) Cr Cl 40 ml/min 5 7 mg/kg INT
Adult Aminoglycoside Dosing for Gram negative infections prior to available serum levels (Excludes patients with cystic fibrosis, OB GYN patients and surgical prophylaxis) Cr Cl 40 ml/min 5 7 mg/kg INT
Time Course Analysis of Aminoglycoside - Induced Elevation of Serum Creatinine
 Time Course Analysis of Aminoglycoside - Induced Elevation of Serum Creatinine Waleed M. Sweileh, PhD Associate Professor, Clinical Pharmacology Corresponding author Waleed M. Sweileh, PhD Associate Professor,
Time Course Analysis of Aminoglycoside - Induced Elevation of Serum Creatinine Waleed M. Sweileh, PhD Associate Professor, Clinical Pharmacology Corresponding author Waleed M. Sweileh, PhD Associate Professor,
Experience with a Once-Daily Aminoglycoside Program Administered to 2,184 Adult Patients
 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Mar. 1995, p. 650 655 Vol. 39, No. 3 0066-4804/95/$04.00 0 Copyright 1995, American Society for Microbiology Experience with a Once-Daily Aminoglycoside Program Administered
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Mar. 1995, p. 650 655 Vol. 39, No. 3 0066-4804/95/$04.00 0 Copyright 1995, American Society for Microbiology Experience with a Once-Daily Aminoglycoside Program Administered
MRSA Micro Scan Pos Combo 6J DADE BEHRING VCM
 PKPD MRSA 1 1 2 1 1 2 17 1 26 17 3 16 vancomycinvcm methicillin-resistant Staphylococcus aureusmrsa 31 pharmacokineticpkparameter retrospective VCM 21 10 PK parameter Mann- Whitney U-test Cmax 37.1 µ gml29.942
PKPD MRSA 1 1 2 1 1 2 17 1 26 17 3 16 vancomycinvcm methicillin-resistant Staphylococcus aureusmrsa 31 pharmacokineticpkparameter retrospective VCM 21 10 PK parameter Mann- Whitney U-test Cmax 37.1 µ gml29.942
Nephrotoxicity. Pros and Cons of the article: Relationship between Initial Vancomycin
 Pros and Cons of the article: Relationship between Initial Vancomycin Nephrotoxicity among Hospitalized Patients Diane M. Cappelletty, Pharm.D. Associate Professor Pharmacy Practice The University of Toledo
Pros and Cons of the article: Relationship between Initial Vancomycin Nephrotoxicity among Hospitalized Patients Diane M. Cappelletty, Pharm.D. Associate Professor Pharmacy Practice The University of Toledo
Lessons from recent studies. João Gonçalves Pereira UCIP DALI
 Lessons from recent studies João Gonçalves Pereira UCIP DALI 1 Patterns of Antimicrobial Activity Concentration C max Aminoglycosides Cmax/MIC>10 Metronidazol Area under the concentration curve Azithromycin
Lessons from recent studies João Gonçalves Pereira UCIP DALI 1 Patterns of Antimicrobial Activity Concentration C max Aminoglycosides Cmax/MIC>10 Metronidazol Area under the concentration curve Azithromycin
SCMID Online Lecture Library. by author. Optimizing antimicrobial therapy in the elderly. Dose Finding - The Past
 Optimizing antimicrobial therapy in the elderly Johan W. Mouton MD PhD FIDSA Professor pharmacokinetics and pharmacodynamics Dosing should be such that the level of antmicrobial activity is associated
Optimizing antimicrobial therapy in the elderly Johan W. Mouton MD PhD FIDSA Professor pharmacokinetics and pharmacodynamics Dosing should be such that the level of antmicrobial activity is associated
Clinical Issues Surrounding Once-Daily Aminoglycoside Dosing in Children
 Butler University Digital Commons @ Butler University Scholarship and Professional Work COPHS College of Pharmacy & Health Sciences 2003 Clinical Issues Surrounding Once-Daily Aminoglycoside Dosing in
Butler University Digital Commons @ Butler University Scholarship and Professional Work COPHS College of Pharmacy & Health Sciences 2003 Clinical Issues Surrounding Once-Daily Aminoglycoside Dosing in
Therapeutic drug monitoring of β-lactams
 CORATA Belgique Reims 1-2/10/2014 Therapeutic drug monitoring of β-lactams Frédéric Cotton Clinical Chemistry Erasme Hospital Faculty of Pharmacy ULB TDM of β-lactams β-lactams pharmacokinetics pharmacodynamics
CORATA Belgique Reims 1-2/10/2014 Therapeutic drug monitoring of β-lactams Frédéric Cotton Clinical Chemistry Erasme Hospital Faculty of Pharmacy ULB TDM of β-lactams β-lactams pharmacokinetics pharmacodynamics
Professor of Chemotherapy Department of Preclinical and Clinical Pharmacology University of Florence
 Professor of Chemotherapy Department of Preclinical and Clinical Pharmacology University of Florence Researching field Pharmacokinetics, Pharmacodynamics of antimicrobial, antifungal and antitumoral drugs
Professor of Chemotherapy Department of Preclinical and Clinical Pharmacology University of Florence Researching field Pharmacokinetics, Pharmacodynamics of antimicrobial, antifungal and antitumoral drugs
Department of Clinical Pharmacy, University of Michigan College of Pharmacy, Pharmacy Faculty, Siam University, Bangkok, Thailand
 1 2 Article Type: Guest Ed Mistakes We Make in Dialysis 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 We underdose antibiotics in patients on CRRT Alexander R. Shaw Weerachai Chaijamorn Bruce A. Mueller 1 Ann
1 2 Article Type: Guest Ed Mistakes We Make in Dialysis 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 We underdose antibiotics in patients on CRRT Alexander R. Shaw Weerachai Chaijamorn Bruce A. Mueller 1 Ann
MONTE CARLO SIMULATION & PK-PD TARGET ATTAINMENT ANALYSIS:
 MONTE CARLO SIMULATION & PK-PD TARGET ATTAINMENT ANALYSIS: Application to Estimation of MIC Breakpoints Paul G. Ambrose, Pharm.D. Director, Division of Infectious Diseases, Cognigen Corporation; Adjunct
MONTE CARLO SIMULATION & PK-PD TARGET ATTAINMENT ANALYSIS: Application to Estimation of MIC Breakpoints Paul G. Ambrose, Pharm.D. Director, Division of Infectious Diseases, Cognigen Corporation; Adjunct
Prospective Evaluation of the Effect of an Aminoglycoside Dosing Regimen on Rates of Observed Nephrotoxicity and Ototoxicity
 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, July 1999, p. 1549 1555 Vol. 43, No. 7 0066-4804/99/$04.00 0 Copyright 1999, American Society for Microbiology. All Rights Reserved. Prospective Evaluation of the
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, July 1999, p. 1549 1555 Vol. 43, No. 7 0066-4804/99/$04.00 0 Copyright 1999, American Society for Microbiology. All Rights Reserved. Prospective Evaluation of the
Guess or get it right?
 Guess or get it right? Antimicrobial prescribing in the 21 st century Robert Masterton Traditional Treatment Paradigm Conservative start with workhorse antibiotics Reserve more potent drugs for non-responders
Guess or get it right? Antimicrobial prescribing in the 21 st century Robert Masterton Traditional Treatment Paradigm Conservative start with workhorse antibiotics Reserve more potent drugs for non-responders
Disclosures. Efficacy of the drug. Optimizing Dosing Based on PKPD- An overview. Dose Finding - The Past
 Disclosures Optimizing Dosing Based on PKPD- An overview Johan W. Mouton MD PhD FIDSA FAAM Professor pharmacokinetics and pharmacodynamics Research grants advisory boards speaker This Patient Needs Antibiotics.
Disclosures Optimizing Dosing Based on PKPD- An overview Johan W. Mouton MD PhD FIDSA FAAM Professor pharmacokinetics and pharmacodynamics Research grants advisory boards speaker This Patient Needs Antibiotics.
without the permission of the author Not to be copied and distributed to others
 Emperor s Castle interior-prato What is the Role of Inhaled Polymyxins for Treatment of Respiratory Tract Infections? Helen Giamarellou CONCLUSIONS: Patients with Pseudomonas and Acinetobacter VAP may
Emperor s Castle interior-prato What is the Role of Inhaled Polymyxins for Treatment of Respiratory Tract Infections? Helen Giamarellou CONCLUSIONS: Patients with Pseudomonas and Acinetobacter VAP may
Annual Surveillance Summary: Pseudomonas aeruginosa Infections in the Military Health System (MHS), 2016
 Annual Surveillance Summary: Pseudomonas aeruginosa Infections in the Military Health System (MHS), 2016 Sarah Gierhart and Uzo Chukwuma Approved for public release. Distribution is unlimited. The views
Annual Surveillance Summary: Pseudomonas aeruginosa Infections in the Military Health System (MHS), 2016 Sarah Gierhart and Uzo Chukwuma Approved for public release. Distribution is unlimited. The views
Terapia delle infezioni da Pseudomonas aeruginosa MDR
 Verona 23 ottobre 2010 Terapia delle infezioni da Pseudomonas aeruginosa MDR Pierluigi Viale Clinica di Malattie Infettive Policlinico S. Orsola Malpighi Global resistance surveillance of Pseudomonas aeruginosa
Verona 23 ottobre 2010 Terapia delle infezioni da Pseudomonas aeruginosa MDR Pierluigi Viale Clinica di Malattie Infettive Policlinico S. Orsola Malpighi Global resistance surveillance of Pseudomonas aeruginosa
Is the package insert correct? PK considerations
 Is the package insert correct? PK considerations Jason A Roberts B Pharm (Hons), PhD, FSHP Professor of Medicine and Pharmacy The University of Queensland, Australia Royal Brisbane and Women s Hospital,
Is the package insert correct? PK considerations Jason A Roberts B Pharm (Hons), PhD, FSHP Professor of Medicine and Pharmacy The University of Queensland, Australia Royal Brisbane and Women s Hospital,
Update on CLSI and EUCAST
 Update on CLSI and EUCAST 1 Completed work» Cephalosporin breakpoints for Enterobacteriaceae ESBL screens MIC versus resistance mechanism» Carbapenem breakpoints for Enterobacteriaceae Modified Hodge Test»
Update on CLSI and EUCAST 1 Completed work» Cephalosporin breakpoints for Enterobacteriaceae ESBL screens MIC versus resistance mechanism» Carbapenem breakpoints for Enterobacteriaceae Modified Hodge Test»
Treatment of febrile neutropenia in patients with neoplasia
 Treatment of febrile neutropenia in patients with neoplasia George Samonis MD, PhD Medical Oncologist Infectious Diseases Specialist Professor of Medicine The University of Crete, Heraklion,, Crete, Greece
Treatment of febrile neutropenia in patients with neoplasia George Samonis MD, PhD Medical Oncologist Infectious Diseases Specialist Professor of Medicine The University of Crete, Heraklion,, Crete, Greece
PD Targets for Various Infection Types: Stasis vs. 1-Log Kill vs. 2 Log Kill
 PD Targets for Various Infection Types: Stasis vs. 1-Log Kill vs. 2 Log Kill G.L. Drusano, M.D. Professor and Director Institute for Therapeutic Innovation University of Florida To have insight into appropriate
PD Targets for Various Infection Types: Stasis vs. 1-Log Kill vs. 2 Log Kill G.L. Drusano, M.D. Professor and Director Institute for Therapeutic Innovation University of Florida To have insight into appropriate
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES
 DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
Nightmare Bacteria. Disclosures. Technician Objectives. Pharmacist Objectives. Carbapenem Resistance in Carbapenem Resistance in 2017
 Nightmare Bacteria How to Deal with the Reality of Carbapenem-resistant Organisms Disclosures I have no conflicts of interest relative to the content of this presentation Matthew L. Brown, Pharm.D., BCPS
Nightmare Bacteria How to Deal with the Reality of Carbapenem-resistant Organisms Disclosures I have no conflicts of interest relative to the content of this presentation Matthew L. Brown, Pharm.D., BCPS
A prospective comparative study of gentamicin- and amikacin-induced nephrotoxicity in patients with normal baseline renal function
 doi: 10.1111/j.1472-8206.2009.00702.x ORIGINAL ARTICLE A prospective comparative study of gentamicin- and amikacin-induced nephrotoxicity in patients with normal baseline renal function Waleed M. Sweileh*
doi: 10.1111/j.1472-8206.2009.00702.x ORIGINAL ARTICLE A prospective comparative study of gentamicin- and amikacin-induced nephrotoxicity in patients with normal baseline renal function Waleed M. Sweileh*
Potential Conflicts of Interests
 Potential Conflicts of Interests Research Grants Agency for Healthcare Research and Quality Akers Bioscience, Inc. Pfizer, Inc. Scientific Advisory Boards Pfizer, Inc. Cadence Pharmaceuticals Kimberly
Potential Conflicts of Interests Research Grants Agency for Healthcare Research and Quality Akers Bioscience, Inc. Pfizer, Inc. Scientific Advisory Boards Pfizer, Inc. Cadence Pharmaceuticals Kimberly
Challenges in Therapeutic Drug Monitoring:
 Challenges in Therapeutic Drug Monitoring: Focus on Vancomycin Pharmacodynamics and Pharmacokinetics Katherine Gallaga, PharmD PGY1 Pharmacy Practice Resident CHRISTUS Spohn Health System 1 Pharmacist
Challenges in Therapeutic Drug Monitoring: Focus on Vancomycin Pharmacodynamics and Pharmacokinetics Katherine Gallaga, PharmD PGY1 Pharmacy Practice Resident CHRISTUS Spohn Health System 1 Pharmacist
Expert rules. for Gram-negatives
 Academic Perspective in Expert rules Emerging Issues of Resistance in Gram-ve Bacteria for Gram-negatives Trevor Winstanley Sheffield Teaching Hospitals Presented on behalf of David Livermore University
Academic Perspective in Expert rules Emerging Issues of Resistance in Gram-ve Bacteria for Gram-negatives Trevor Winstanley Sheffield Teaching Hospitals Presented on behalf of David Livermore University
Antibiotic Usage Related to Microorganisms Pattern and MIC
 Antibiotic Usage Related to Microorganisms Pattern and MIC DR. Dr. Latre Buntaran Sp.MK(K) Secretary General PERDALIN Head of Compartment of Infection Control PERSI Doripenem: Potent
Antibiotic Usage Related to Microorganisms Pattern and MIC DR. Dr. Latre Buntaran Sp.MK(K) Secretary General PERDALIN Head of Compartment of Infection Control PERSI Doripenem: Potent
ASHP Therapeutic Position Statements 623
 ASHP Therapeutic Position Statements 623 Therapeutic Monitoring of Vancomycin in Adult Patients: A Consensus Review of the American Society of Health-System Pharmacists, the Infectious Diseases Society
ASHP Therapeutic Position Statements 623 Therapeutic Monitoring of Vancomycin in Adult Patients: A Consensus Review of the American Society of Health-System Pharmacists, the Infectious Diseases Society
Antimicrobial practice. Monitoring serum concentrations for once-daily netilmicin dosing regimens
 Journal of Antimicrobial Chemotherapy (1994) 33, 341348 Antimicrobial practice Monitoring serum concentrations for oncedaily netilmicin dosing regimens Jurg Blasei*'*, Christian* KSnig*, HansPeter Simmen*
Journal of Antimicrobial Chemotherapy (1994) 33, 341348 Antimicrobial practice Monitoring serum concentrations for oncedaily netilmicin dosing regimens Jurg Blasei*'*, Christian* KSnig*, HansPeter Simmen*
Stanford Health Care Last Review Date: 8/2016 Pharmacy Department Policies and Procedures
 Medication Administration: Extended-Infusion Piperacillin/Tazobactam (Zosyn ) Protocol Related Documents: Patient Care Manual Guide: Medication Administration IV Infusion Guidelines I. PURPOSE Dose optimization
Medication Administration: Extended-Infusion Piperacillin/Tazobactam (Zosyn ) Protocol Related Documents: Patient Care Manual Guide: Medication Administration IV Infusion Guidelines I. PURPOSE Dose optimization
La farmacologia in aiuto
 Ferrara, 15 giugno 2018 La farmacologia in aiuto Pier Giorgio Cojutti, Federico Pea Istituto di Farmacologia Clinica Azienda Sanitaria Universitaria Integrata di Udine Therapeutic Drug Monitoring of Beta-Lactams
Ferrara, 15 giugno 2018 La farmacologia in aiuto Pier Giorgio Cojutti, Federico Pea Istituto di Farmacologia Clinica Azienda Sanitaria Universitaria Integrata di Udine Therapeutic Drug Monitoring of Beta-Lactams
Clinical Guidelines for Use of Antibiotics. VANCOMYCIN (Adult)
 VANCOMYCIN (Adult) Please always prescribe VANCOMYCIN in the Variable Dose Antibiotic section of the EPMA SUPPLEMENTARY drug chart (and add a placeholder on the electronic drug chart). 1 Background Vancomycin
VANCOMYCIN (Adult) Please always prescribe VANCOMYCIN in the Variable Dose Antibiotic section of the EPMA SUPPLEMENTARY drug chart (and add a placeholder on the electronic drug chart). 1 Background Vancomycin
PHARMONITOR II. Optimisation of aminoglycosides dosage regimen with pharmacokinetics modeling. Pierre Wallemacq
 PHARMONITOR II Optimisation of aminoglycosides dosage regimen with pharmacokinetics modeling Pierre Wallemacq NATIONAL SYMPOSIUM 20 years EEQ Leuven, March 26th 2009 1 Why monitoring of aminoglycosides?
PHARMONITOR II Optimisation of aminoglycosides dosage regimen with pharmacokinetics modeling Pierre Wallemacq NATIONAL SYMPOSIUM 20 years EEQ Leuven, March 26th 2009 1 Why monitoring of aminoglycosides?
Successful treatment of pan - resistant pseudomonas Aerugınosa menıngıtıs wıth ıntrathecal polymyxın b therapy
 ISPUB.COM The Internet Journal of Infectious Diseases Volume 7 Number 2 Successful treatment of pan - resistant pseudomonas Aerugınosa menıngıtıs wıth ıntrathecal polymyxın b F Simsek, T Yildirmak, G Cetmeli,
ISPUB.COM The Internet Journal of Infectious Diseases Volume 7 Number 2 Successful treatment of pan - resistant pseudomonas Aerugınosa menıngıtıs wıth ıntrathecal polymyxın b F Simsek, T Yildirmak, G Cetmeli,
Aminoglycosides: What have we learned about toxicity?
 Aminoglycosides: What have we learned about toxicity? Paul M. Tulkens, MD, PhD Cellular and Molecular Pharmacology Unit & Center for Clinical Pharmacy Catholic University of Louvain, Brussels, Belgium
Aminoglycosides: What have we learned about toxicity? Paul M. Tulkens, MD, PhD Cellular and Molecular Pharmacology Unit & Center for Clinical Pharmacy Catholic University of Louvain, Brussels, Belgium
Adenium Biotech. Management: - Peter Nordkild, MD, CEO, ex Novo Nordisk, Ferring, Egalet - Søren Neve, PhD, project director, ex Lundbeck, Novozymes
 Adenium Biotech Management: - Peter Nordkild, MD, CEO, ex Novo Nordisk, Ferring, Egalet - Søren Neve, PhD, project director, ex Lundbeck, Novozymes Board of Directors: - Stephan Christgau, PhD, chairman,
Adenium Biotech Management: - Peter Nordkild, MD, CEO, ex Novo Nordisk, Ferring, Egalet - Søren Neve, PhD, project director, ex Lundbeck, Novozymes Board of Directors: - Stephan Christgau, PhD, chairman,
Effect of piperacillin/tazobactam restriction on usage and rates of acute renal failure
 Journal of Medical Microbiology (2016), 65, 195 199 DOI 10.1099/jmm.0.000211 Effect of piperacillin/tazobactam restriction on usage and rates of acute renal failure Michael A. Lorenz, 1,2 Ryan P. Moenster
Journal of Medical Microbiology (2016), 65, 195 199 DOI 10.1099/jmm.0.000211 Effect of piperacillin/tazobactam restriction on usage and rates of acute renal failure Michael A. Lorenz, 1,2 Ryan P. Moenster
prophylaxis for endocarditis in patients at high risk prophylaxis for major surgical procedures
 1 Glycopeptides appropriate uses serious infections due to beta-lactam- resistant gram-positive microorganisms infections due to gram-positive microorganisms in patients with serious allergy to beta-lactam
1 Glycopeptides appropriate uses serious infections due to beta-lactam- resistant gram-positive microorganisms infections due to gram-positive microorganisms in patients with serious allergy to beta-lactam
Comparison of Meropenem with Ceftazidime as Monotherapy of Cancer Patients with Chemotherapy induced Febrile Neutropenia
 Comparison of Meropenem with Ceftazidime as Monotherapy of Cancer Patients with Chemotherapy induced Febrile Neutropenia I. Malik ( National Cancer lnsititute, Karachi ) Shaharyar (, Department of Radiotherapy
Comparison of Meropenem with Ceftazidime as Monotherapy of Cancer Patients with Chemotherapy induced Febrile Neutropenia I. Malik ( National Cancer lnsititute, Karachi ) Shaharyar (, Department of Radiotherapy
Adult Inpatient Antibiogram. Antimicrobial Susceptibilities of Frequently Recovered Clinical Isolates. January to December 2016
 Adult Inpatient Antibiogram Antimicrobial Susceptibilities of Frequently Recovered Clinical Isolates January to December 2016 Department of Pathology Camille Hamula, PhD Director, Clinical Microbiology
Adult Inpatient Antibiogram Antimicrobial Susceptibilities of Frequently Recovered Clinical Isolates January to December 2016 Department of Pathology Camille Hamula, PhD Director, Clinical Microbiology
Medication Dosing in CRRT
 Medication Dosing in CRRT Linda Awdishu, PharmD, MAS Associate Clinical Professor of Pharmacy and Medicine Learning Objectives 1. List the pharmacokinetic changes associated with AKI. 2. Determine the
Medication Dosing in CRRT Linda Awdishu, PharmD, MAS Associate Clinical Professor of Pharmacy and Medicine Learning Objectives 1. List the pharmacokinetic changes associated with AKI. 2. Determine the
Development of C sporins. Beta-lactam antibiotics - Cephalosporins. Second generation C sporins. Targets - PBP s
 Beta-lactam antibiotics - Cephalosporins Development of C sporins Targets - PBP s Activity - Cidal - growing organisms (like the penicillins) Principles of action - Affinity for PBP s Permeability properties
Beta-lactam antibiotics - Cephalosporins Development of C sporins Targets - PBP s Activity - Cidal - growing organisms (like the penicillins) Principles of action - Affinity for PBP s Permeability properties
Evaluation of Vancomycin Continuous Infusion in Trauma Patients
 OBJECTIVES Evaluation of Vancomycin Continuous Infusion in Trauma Patients Brittany D. Bissell, Pharm.D. PGY-2 Critical Care Pharmacy Resident Jackson Memorial Hospital Miami, Florida Evaluate the potential
OBJECTIVES Evaluation of Vancomycin Continuous Infusion in Trauma Patients Brittany D. Bissell, Pharm.D. PGY-2 Critical Care Pharmacy Resident Jackson Memorial Hospital Miami, Florida Evaluate the potential
Comparisons between Antimicrobial Pharmacodynamic Indices and Bacterial Killing as Described by Using the Zhi Model
 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, July 1998, p. 1731 1737 Vol. 42, No. 7 0066-4804/98/$04.00 0 Copyright 1998, American Society for Microbiology. All Rights Reserved. Comparisons between Antimicrobial
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, July 1998, p. 1731 1737 Vol. 42, No. 7 0066-4804/98/$04.00 0 Copyright 1998, American Society for Microbiology. All Rights Reserved. Comparisons between Antimicrobial
Shannon Carty, PGY-2 ICCR IRB Project Proposal April 9, 2008
 Shannon Carty, PGY-2 ICCR IRB Project Proposal April 9, 2008 Study Title: Observational Study to Determine the Effect of an Emergency Department Adult Oncology Stat Antibiotic Protocol on Clinical Outcomes
Shannon Carty, PGY-2 ICCR IRB Project Proposal April 9, 2008 Study Title: Observational Study to Determine the Effect of an Emergency Department Adult Oncology Stat Antibiotic Protocol on Clinical Outcomes
Below is an overview of the oral and poster presentations featuring cefiderocol and S at IDWeek 2017:
 SHIONOGI TO HIGHLIGHT RESEARCH ON CEFIDEROCOL (S-649266), A SIDEROPHORE CEPHALOSPORIN, AND S-033188, A CAP-DEPENDENT ENDONUCLEASE INHIBITOR FOR TREATMENT OF INFLUENZA, AT IDWEEK 2017 OSAKA, Japan and FLORHAM
SHIONOGI TO HIGHLIGHT RESEARCH ON CEFIDEROCOL (S-649266), A SIDEROPHORE CEPHALOSPORIN, AND S-033188, A CAP-DEPENDENT ENDONUCLEASE INHIBITOR FOR TREATMENT OF INFLUENZA, AT IDWEEK 2017 OSAKA, Japan and FLORHAM
Journal of Pediatric Sciences
 Journal of Pediatric Sciences Doripenem Use in Pediatrics - Learning from Pharmacokinetic Data of Other Carbapenems Patrick Grove, Tsz-Yin So Journal of Pediatric Sciences; How to cite this article: Grove
Journal of Pediatric Sciences Doripenem Use in Pediatrics - Learning from Pharmacokinetic Data of Other Carbapenems Patrick Grove, Tsz-Yin So Journal of Pediatric Sciences; How to cite this article: Grove
Use of imipenem. with the support of Wallonie-Bruxelles International. Magali Dodémont Microbiology Hospital Erasme Université Libre de Bruxelles
 with the support of Wallonie-Bruxelles International Use of imipenem Magali Dodémont Microbiology Hospital Erasme Université Libre de Bruxelles 1 Β-lactams classification 2 Β-lactams: mode of action Inhibition
with the support of Wallonie-Bruxelles International Use of imipenem Magali Dodémont Microbiology Hospital Erasme Université Libre de Bruxelles 1 Β-lactams classification 2 Β-lactams: mode of action Inhibition
ESCMID Online Lecture Library. by author
 Novel PK/PD data on the optimisation of colistin and the carbapenems Diamantis Plachouras Athens, Greece Hot Topics on Infections in the Critically Ill Patient, ESCMID Postgraduate Education Course, 31
Novel PK/PD data on the optimisation of colistin and the carbapenems Diamantis Plachouras Athens, Greece Hot Topics on Infections in the Critically Ill Patient, ESCMID Postgraduate Education Course, 31
Drug Management in CRRT
 Drug Management in CRRT Jeffrey Lipman, FCICM, MD Department of Intensive Care Medicine Royal Brisbane Hospital University of Queensland Bruce A. Mueller, PharmD, FCCP, FASN Clinical, Social & Administrative
Drug Management in CRRT Jeffrey Lipman, FCICM, MD Department of Intensive Care Medicine Royal Brisbane Hospital University of Queensland Bruce A. Mueller, PharmD, FCCP, FASN Clinical, Social & Administrative
Ailyn T. Isais-Agdeppa, MD*, Lulu Bravo, MD*
 A FIVE-YEAR RETROSPECTIVE STUDY ON THE COMMON MICROBIAL ISOLATES AND SENSITIVITY PATTERN ON BLOOD CULTURE OF PEDIATRIC CANCER PATIENTS ADMITTED AT THE PHILIPPINE GENERAL HOSPITAL FOR FEBRILE NEUTROPENIA
A FIVE-YEAR RETROSPECTIVE STUDY ON THE COMMON MICROBIAL ISOLATES AND SENSITIVITY PATTERN ON BLOOD CULTURE OF PEDIATRIC CANCER PATIENTS ADMITTED AT THE PHILIPPINE GENERAL HOSPITAL FOR FEBRILE NEUTROPENIA
Treatment Strategies for Infections due to MDR-GNR
 Treatment Strategies for Infections due to MDR-GNR Michael Satlin, MD Instructor in Medicine Division of Infectious Diseases Weill Cornell Medical College, New York, NY October 16, 2012 1 2 Faculty Disclosure
Treatment Strategies for Infections due to MDR-GNR Michael Satlin, MD Instructor in Medicine Division of Infectious Diseases Weill Cornell Medical College, New York, NY October 16, 2012 1 2 Faculty Disclosure
Doripenem: pharmacokinetics and pharmacodynamics. Paul M. Tulkens, MD, PhD Françoise Van Bambeke, PharmD, PhD
 16/04/2009 1 Doripenem: pharmacokinetics and pharmacodynamics Paul M. Tulkens, MD, PhD Françoise Van Bambeke, PharmD, PhD Unité de Pharmacologie cellulaire et moléculaire Louvain Drug Research Institute
16/04/2009 1 Doripenem: pharmacokinetics and pharmacodynamics Paul M. Tulkens, MD, PhD Françoise Van Bambeke, PharmD, PhD Unité de Pharmacologie cellulaire et moléculaire Louvain Drug Research Institute
Pharmacokinetics of daptomycin in a patient with severe renal failure not under dialysis
 AAC Accepts, published online ahead of print on 1 April 2013 Antimicrob. Agents Chemother. doi:10.1128/aac.00230-13 Copyright 2013, American Society for Microbiology. All Rights Reserved. 1 Pharmacokinetics
AAC Accepts, published online ahead of print on 1 April 2013 Antimicrob. Agents Chemother. doi:10.1128/aac.00230-13 Copyright 2013, American Society for Microbiology. All Rights Reserved. 1 Pharmacokinetics
NORLAND AVENUE PHARMACY PRESCRIPTION COMPOUNDING FOR GENERAL PRACTICE
 APRIL 2011 PRESCRIPTION COMPOUNDING N ORLANDA VENUEP HARMACY. COM We customize individual prescriptions for the specific needs of our patients. INSIDE THIS ISSUE: Methicillin-Resistant Staphylococcus 2
APRIL 2011 PRESCRIPTION COMPOUNDING N ORLANDA VENUEP HARMACY. COM We customize individual prescriptions for the specific needs of our patients. INSIDE THIS ISSUE: Methicillin-Resistant Staphylococcus 2
Aminoglycosides. Not orally absorbed. Interact with negatively charged lipopolysaccharide on Gram- cell wall. Aminoglycoside properties
 Aminoglycosides Tobramycin Kanamycin H2N Gentamicin Amikacin NHCOCHCH2CH2NH2 OH Aminoglycosides made of linked sugars. Decorated with many OH and NH2 groups, which render these compounds positively charged
Aminoglycosides Tobramycin Kanamycin H2N Gentamicin Amikacin NHCOCHCH2CH2NH2 OH Aminoglycosides made of linked sugars. Decorated with many OH and NH2 groups, which render these compounds positively charged
Giving the Proper Dose: How Can The Clinical and Laboratory Standards Institute(CLSI)Help?
 Giving the Proper Dose: How Can The Clinical and Laboratory Standards Institute(CLSI)Help? Pranita D. Tamma, M.D., M.H.S. Director, Pediatric Antimicrobial Stewardship Johns Hopkins University School of
Giving the Proper Dose: How Can The Clinical and Laboratory Standards Institute(CLSI)Help? Pranita D. Tamma, M.D., M.H.S. Director, Pediatric Antimicrobial Stewardship Johns Hopkins University School of
Optimizing Antibiotic Therapy in the ICU For Pneumonia Current and Future Approaches
 Optimizing Antibiotic Therapy in the ICU For Pneumonia Current and Future Approaches Andrew F. Shorr, MD, MPH Washington Hospital Center Georgetown Univ. Disclosures I have served as a consultant to, researcher/investigator
Optimizing Antibiotic Therapy in the ICU For Pneumonia Current and Future Approaches Andrew F. Shorr, MD, MPH Washington Hospital Center Georgetown Univ. Disclosures I have served as a consultant to, researcher/investigator
D DAVID PUBLISHING. Evaluation of the Effectiveness of a Vancomycin Nomogram at Predicting Trough Levels within a Therapeutic Range. 1.
 Journal of Pharmacy and Pharmacology 2 (2014) 713-721 doi: 10.17265/2328-2150/2014.12.004 D DAVID PUBLISHING Evaluation of the Effectiveness of a Vancomycin Nomogram at Predicting Trough Levels within
Journal of Pharmacy and Pharmacology 2 (2014) 713-721 doi: 10.17265/2328-2150/2014.12.004 D DAVID PUBLISHING Evaluation of the Effectiveness of a Vancomycin Nomogram at Predicting Trough Levels within
Antibiotic Resistance Pattern of Blood and CSF Culture Isolates At NHLS Academic Laboratories (2005)
 Antibiotic Resistance Pattern of Blood and CSF Culture Isolates At NHLS Academic Laboratories (2005) Streptococcus pneumoniae (SP) Blood Culture Isolates Penicillin intermediate Penicillin Cefotaxime 336
Antibiotic Resistance Pattern of Blood and CSF Culture Isolates At NHLS Academic Laboratories (2005) Streptococcus pneumoniae (SP) Blood Culture Isolates Penicillin intermediate Penicillin Cefotaxime 336
Emergence of Klebsiella pneumoniae ST258 with KPC-2 in Hong Kong. Title. Ho, PL; Tse, CWS; Lai, EL; Lo, WU; Chow, KH
 Title Emergence of Klebsiella pneumoniae ST258 with KPC-2 in Hong Kong Author(s) Ho, PL; Tse, CWS; Lai, EL; Lo, WU; Chow, KH Citation International Journal Of Antimicrobial Agents, 2011, v. 37 n. 4, p.
Title Emergence of Klebsiella pneumoniae ST258 with KPC-2 in Hong Kong Author(s) Ho, PL; Tse, CWS; Lai, EL; Lo, WU; Chow, KH Citation International Journal Of Antimicrobial Agents, 2011, v. 37 n. 4, p.
Use ideal body weight (IBW) unless actual body weight is less. Use the following equation to calculate IBW:
 Amikacin is a partially restricted (amber) antibiotic for the treatment of infections due to gentamicin resistant Gram negative bacilli or as advised by microbiology. As with other aminoglycosides, therapeutic
Amikacin is a partially restricted (amber) antibiotic for the treatment of infections due to gentamicin resistant Gram negative bacilli or as advised by microbiology. As with other aminoglycosides, therapeutic
TDM of Aminoglycoside Antibiotics
 TDM Lecture 3 5 th Stage TDM of Aminoglycoside Antibiotics The aminoglycoside antibiotics are widely used for the treatment of gram-negative infections, often in combination with a β-lactam antibiotic
TDM Lecture 3 5 th Stage TDM of Aminoglycoside Antibiotics The aminoglycoside antibiotics are widely used for the treatment of gram-negative infections, often in combination with a β-lactam antibiotic
by author ESCMID Online Lecture Library Steroids in acute bacterial meningitis
 Steroids in acute bacterial meningitis Javier Garau, MD, PhD University of Barcelona Spain ESCMID Summer School, Porto, July 2009 Dexamethasone treatment in childhood bacterial meningitis in Malawi: a
Steroids in acute bacterial meningitis Javier Garau, MD, PhD University of Barcelona Spain ESCMID Summer School, Porto, July 2009 Dexamethasone treatment in childhood bacterial meningitis in Malawi: a
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES
 DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
Urinary Tract Infections: From Simple to Complex. Adriane N Irwin, MS, PharmD, BCACP Clinical Assistant Professor Ambulatory Care October 25, 2014
 Urinary Tract Infections: From Simple to Complex Adriane N Irwin, MS, PharmD, BCACP Clinical Assistant Professor Ambulatory Care October 25, 2014 Learning Objectives Develop empiric antimicrobial treatment
Urinary Tract Infections: From Simple to Complex Adriane N Irwin, MS, PharmD, BCACP Clinical Assistant Professor Ambulatory Care October 25, 2014 Learning Objectives Develop empiric antimicrobial treatment
A NEW APPROACH TO THERAPEUTIC DRUG MONITORING OF TOBRAMYCIN IN CYSTIC FIBROSIS
 THE DOSING INSTITUTE CLINICAL REVIEW SERIES: TOBRAMYCIN IN CYSTIC FIBROSIS MAY 2017 A NEW APPROACH TO THERAPEUTIC DRUG MONITORING OF TOBRAMYCIN IN CYSTIC FIBROSIS THE DOSING INSTITUTE The Dosing Institute
THE DOSING INSTITUTE CLINICAL REVIEW SERIES: TOBRAMYCIN IN CYSTIC FIBROSIS MAY 2017 A NEW APPROACH TO THERAPEUTIC DRUG MONITORING OF TOBRAMYCIN IN CYSTIC FIBROSIS THE DOSING INSTITUTE The Dosing Institute
The antibiotic dose and the obese ICU patient
 The antibiotic dose and the obese ICU patient Philippe Montravers, M.D., Ph.D. Anaesthesia and Surgical ICU CHU Bichat Claude Bernard Assistance Publique-Hôpitaux de Paris INSERM UMR 1152 University Paris
The antibiotic dose and the obese ICU patient Philippe Montravers, M.D., Ph.D. Anaesthesia and Surgical ICU CHU Bichat Claude Bernard Assistance Publique-Hôpitaux de Paris INSERM UMR 1152 University Paris
Activity of Ceftolozane/Tazobactam Against a Broad Spectrum of Recent Clinical Anaerobic Isolates
 AAC Accepts, published online ahead of print on 25 November 2013 Antimicrob. Agents Chemother. doi:10.1128/aac.02253-13 Copyright 2013, American Society for Microbiology. All Rights Reserved. Activity
AAC Accepts, published online ahead of print on 25 November 2013 Antimicrob. Agents Chemother. doi:10.1128/aac.02253-13 Copyright 2013, American Society for Microbiology. All Rights Reserved. Activity
Full title of guideline INTRAVENOUS VANCOMYCIN PRESCRIBING AND MONITORING GUIDELINE FOR ADULT PATIENTS. control
 Full title of guideline Author: Contact Name and Job Title Division and specialty Scope Explicit definition of patient group to which it applies (e.g. inclusion and exclusion criteria, diagnosis) Changes
Full title of guideline Author: Contact Name and Job Title Division and specialty Scope Explicit definition of patient group to which it applies (e.g. inclusion and exclusion criteria, diagnosis) Changes
CLINICAL USE OF GLYCOPEPTIDES. Herbert Spapen Intensive Care Department University Hospital Vrije Universiteit Brussel
 CLINICAL USE OF GLYCOPEPTIDES Herbert Spapen Intensive Care Department University Hospital Vrije Universiteit Brussel Glycopeptides Natural Vancomycin introduced in 1958 Teicoplanin introduced in Europe
CLINICAL USE OF GLYCOPEPTIDES Herbert Spapen Intensive Care Department University Hospital Vrije Universiteit Brussel Glycopeptides Natural Vancomycin introduced in 1958 Teicoplanin introduced in Europe
AMINOGLYCOSIDES TDM D O N E B Y
 AMINOGLYCOSIDES TDM DONE BY: SARA ALARFAJ 2014 OUTLINE Introduction about Aminoglycosides. Spectrum/uses. TDM Aminoglycosides TDM Pharmacodynamics Pharmacokinetics. Dosing in AG. Sampeling time and Monitoring.
AMINOGLYCOSIDES TDM DONE BY: SARA ALARFAJ 2014 OUTLINE Introduction about Aminoglycosides. Spectrum/uses. TDM Aminoglycosides TDM Pharmacodynamics Pharmacokinetics. Dosing in AG. Sampeling time and Monitoring.
Prospective audit and feedback of piperacillin-tazobactam use in a 1115 bed acute care hospital
 Prospective audit and feedback of piperacillin-tazobactam use in a 1115 bed acute care hospital Final Results Nathan Beahm, BSP, PharmD(student) September 10, 2016 Objectives Review background information
Prospective audit and feedback of piperacillin-tazobactam use in a 1115 bed acute care hospital Final Results Nathan Beahm, BSP, PharmD(student) September 10, 2016 Objectives Review background information
Pharmacokinetics of Tobramycin in Adults with Cystic Fibrosis: Implications for Once-Daily Administration
 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Apr. 2000, p. 809 813 Vol. 44, No. 4 0066-4804/00/$04.00 0 Copyright 2000, American Society for Microbiology. All Rights Reserved. Pharmacokinetics of Tobramycin
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Apr. 2000, p. 809 813 Vol. 44, No. 4 0066-4804/00/$04.00 0 Copyright 2000, American Society for Microbiology. All Rights Reserved. Pharmacokinetics of Tobramycin
Adult Institutional Pharmacokinetics Protocol
 Adult Institutional Pharmacokinetics Protocol Policy Title: Clinical Pharmacokinetics (PK) Service Policy Policy Statement: It is the policy of UMHC that PK consult orders (for vancomycin or aminoglycosides)
Adult Institutional Pharmacokinetics Protocol Policy Title: Clinical Pharmacokinetics (PK) Service Policy Policy Statement: It is the policy of UMHC that PK consult orders (for vancomycin or aminoglycosides)
AMINOGLYCOSIDES DOSING AND MONITORING GUIDELINES
 Approved: September 2017 AMINOGLYCOSIDES DOSING AND MONITORING GUIDELINES NB Provincial Health Authorities Anti-Infective Stewardship Committee GENERAL COMMENTS Aminoglycosides (AG) include gentamicin,
Approved: September 2017 AMINOGLYCOSIDES DOSING AND MONITORING GUIDELINES NB Provincial Health Authorities Anti-Infective Stewardship Committee GENERAL COMMENTS Aminoglycosides (AG) include gentamicin,
ESCMID Online Lecture Library. by author
 Disclosures Pk/Pd of antifungal drugs Johan W. Mouton MD PhD FIDSA Professor pharmacokinetics and pharmacodynamics Research grants advisory boards speaker Dosing should be such that the level of antmicrobial
Disclosures Pk/Pd of antifungal drugs Johan W. Mouton MD PhD FIDSA Professor pharmacokinetics and pharmacodynamics Research grants advisory boards speaker Dosing should be such that the level of antmicrobial
Consultation on the Revision of Carbapenem Breakpoints
 Consultation on the Revision of Carbapenem Breakpoints July 2018 Please send comments to the EUCAST Scientific Secretary at jturnidge@gmail.com by September 15. EUCAST revision of carbapenem breakpoints
Consultation on the Revision of Carbapenem Breakpoints July 2018 Please send comments to the EUCAST Scientific Secretary at jturnidge@gmail.com by September 15. EUCAST revision of carbapenem breakpoints
life-threatening infections
 Vancomycin Vancomycin has become increasingly important in the treatment of life-threatening infections. MRSA infections. Methicillin-resistant Staphylococcus epidermidis (MRSE) infections Enterococcal
Vancomycin Vancomycin has become increasingly important in the treatment of life-threatening infections. MRSA infections. Methicillin-resistant Staphylococcus epidermidis (MRSE) infections Enterococcal
Dilemmas in Septic Shock
 Dilemmas in Septic Shock William Janssen, M.D. Assistant Professor of Medicine National Jewish Health University of Colorado Denver Health Sciences Center A 62 year-old female presents to the ED with fever,
Dilemmas in Septic Shock William Janssen, M.D. Assistant Professor of Medicine National Jewish Health University of Colorado Denver Health Sciences Center A 62 year-old female presents to the ED with fever,
VANCOMYCIN DOSING AND MONITORING GUIDELINES
 VANCOMYCIN DOSING AND MONITORING GUIDELINES NB Provincial Health Authorities Anti-Infective Stewardship Committee Approved: May 2017 GENERAL COMMENTS Vancomycin is a glycopeptide antibiotic with bactericidal
VANCOMYCIN DOSING AND MONITORING GUIDELINES NB Provincial Health Authorities Anti-Infective Stewardship Committee Approved: May 2017 GENERAL COMMENTS Vancomycin is a glycopeptide antibiotic with bactericidal
Administration of Tobramycin in the Beginning of the Hemodialysis Session: A Novel Intradialytic Dosing Regimen
 Administration of Tobramycin in the Beginning of the Hemodialysis Session: A Novel Intradialytic Dosing Regimen Osama Hussein Kamel Mohamed,* Ihab M. Wahba, Suzanne Watnick, Sandra B. Earle, William M.
Administration of Tobramycin in the Beginning of the Hemodialysis Session: A Novel Intradialytic Dosing Regimen Osama Hussein Kamel Mohamed,* Ihab M. Wahba, Suzanne Watnick, Sandra B. Earle, William M.
