Comparisons between Antimicrobial Pharmacodynamic Indices and Bacterial Killing as Described by Using the Zhi Model
|
|
|
- Hector Lamb
- 5 years ago
- Views:
Transcription
1 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, July 1998, p Vol. 42, No /98/$ Copyright 1998, American Society for Microbiology. All Rights Reserved. Comparisons between Antimicrobial Pharmacodynamic Indices and Bacterial Killing as Described by Using the Zhi Model S. CORVAISIER, 1 P. H. MAIRE, 1,2 * M. Y. BOUVIER D YVOIRE, 3 X. BARBAUT, 1,2 N. BLEYZAC, 1 AND R. W. JELLIFFE 2 ADCAPT, Department of Pharmacy, Hospital Antoine Charial, Francheville, 1 and Hoechst-Marion-Roussel Co., Paris, 3 France, and Laboratory of Applied Pharmacokinetics, University of Southern California School of Medicine, Los Angeles, California 2 Received 24 January 1997/Returned for modification 20 June 1997/Accepted 3 May 1998 Various suggestions have been made for empirical pharmacodynamic indices of antibiotic effectiveness, such as areas under the drug concentration-time curve in serum (AUC), AUC>MIC, AUC/MIC, area under the inhibitory curve (AUIC), AUC above MIC, and time above MIC (T>MIC). In addition, bacterial growth and killing models, such as the Zhi model, have been developed. The goal of the present study was to compare the empirical behavior of the Zhi model of bacterial growth and killing with the other empirical pharmacodynamic indices described above by using simulated clinical data analyzed with the USC*PACK PC clinical programs for adaptive control of drug therapy, with one model describing a concentration-dependent antibiotic (tobramycin) and another describing a concentration-independent antibiotic (ticarcillin). The computed relative number of CFU was plotted against each pharmacodynamic index, with each axis parameterized over time. We assumed that a good pharmacodynamic index should present a clear and continuous relationship between the time course of its values and the time course of the bacterial killing as seen with the Zhi model. Preliminary work showed that some pharmacodynamic indices were very similar. A good sensitivity to the change in the values of the MIC was shown for AUC/MIC and also for T>MIC. In addition, the time courses of some other pharmacodynamic indices were very similar. Since AUC/MIC is easily calculated and shows more sensitivity, it appeared to be the best of the indices mentioned above for the concentration-dependent drug, because it incorporated and used the MIC the best. T>MIC appeared to be the best index for a concentration-independent drug. We also propose a new composite index, weighted AUC (WAUC), which appears to be useful for both concentration-dependent and concentration-independent drugs. Success in antibiotic therapy is defined by bacterial killing and by improvement in the patient s clinical status. It is a retrospective measure. However, before antibiotic therapy is begun, the choice of the drug and the dosage regimen must be planned in advance to achieve maximum predicted efficacy with a tolerable risk of toxicity. Adaptive control of antibiotic dosage regimens, by using pharmacokinetic models, can predict (and therefore control) plasma antibiotic concentrations (2). However, drug levels at the site of the infection itself may be somewhat different from the plasma drug concentrations, except during septicemia when the infection is in the bloodstream. Time delays exist between antibiotic administration and the achievement of antibiotic efficacy. Because of this, plasma antibiotic concentrations at time t cannot be automatically correlated with pharmacodynamic effect at the site of the infection at the same time t, even though general improvement in clinical status can be empirically correlated with such plasma antibiotic concentrations. Various empirical pharmacodynamic indices for a 24-h period of therapy using plasma or serum antibiotic levels have been proposed to predict antimicrobial effectiveness at steady state and at the site of infection (17 20). At the steady state, their values at the end of a typical 24-h period appear to be related to the success or failure of therapy some of them for a concentration-dependent drug, some of them for a concentration-independent drug (8, 11, 18, 20). However, the initial exposure to effective serum antibiotic levels is also most important and may be necessary to minimize the emergence of adaptive resistance (4) and as well as the emergence of resistant bacterial subpopulations (5). Indeed, the time course of pharmacodynamic indices during the initial 24 h of therapy appears to be especially important in achieving early success in therapy. With the Zhi model, as the number of CFU is calculated and plotted over time, a dynamic view of the other empirical pharmacodynamic indices (the evolution of each of the other indices over time) has been studied here. The value of each index was computed throughout the initial 24 h of therapy, and the index value was also found at the end of the initial 24-h period, rather than at some subsequent steady state. This was done to emphasize the importance of rapid and effective bacterial killing at the start of therapy, especially for life-threatening infections. The goal of the present study was to compare the bacterial growth and killing calculated according to the model proposed by Zhi et al. (22) with the various empirical pharmacodynamic index values and their time courses during a typical simulated first day of therapy. In this analysis, we have assumed that a good pharmacodynamic index should show a clear and continuous relationship between its values and the bacterial killing observed with the Zhi model: that is, that during periods of bacterial killing, the value of the pharmacodynamic index under consideration should increase, and during periods of bacterial growth, the index should decrease (or at least increase only very slowly). * Corresponding author. Mailing address: ADCAPT, Service Pharmaceutique, Hôpital Antoine Charial, 40 avenue de la Table de Pierre, Francheville, France. Phone: (33) Fax: (33) adcapt@cismsum.univ-lyon1.fr. MATERIALS AND METHODS Pharmacokinetic model. We chose to use a one-compartment pharmacokinetic model with intravenous administration. With maximum a posteriori prob- 1731
2 1732 CORVAISIER ET AL. ANTIMICROB. AGENTS CHEMOTHER. TABLE 1. Tobramycin and ticarcillin population pharmacokinetic parameter values and treatment characteristics a Antimicrobial agent V (liter/kg) k el (h 1 ) D (mg) ability (MAP) Bayesian fitting to individual patient data, plasma antibiotic levels can be predicted in clinical situations with such a linear one-compartment model. Using pharmacokinetic population data available in the USC*PACK PC clinical programs (9, 10), we simulated typical clinical treatment situations for two representative antibiotics by using a representative simulated adult patient (age, 30 years; height, 175 cm [69 in.]; weight, 70 kg; and creatinine clearance, 120 ml/min). We assumed he was being treated for Pseudomonas aeruginosa septicemia. Antibiotic concentrations at the site of the bloodstream infection were assumed to be equal to serum antibiotic concentrations. Two patient data files were created: one for a concentration-dependent drug, tobramycin, and one for a concentration-independent drug, ticarcillin. The dosage regimens used in these simulations were 200 mg of tobramycin infused over 30 min every 12 h (slightly less than 6 mg/kg per day) and 6gofticarcillin infused over 30 min every 8 h (slightly more than 260 mg/kg per day). Table 1 shows the pharmacokinetic parameter values for each drug and the characteristics for each dosage regimen. Zhi pharmacodynamic model. Bacterial growth and killing were described by computing the relative number of CFU versus time. CFU were computed with the Zhi model (22), which states that db dt G K t B (1) where B is the initial bacterial inoculum (CFU per milliliter), G is the rate constant for exponential bacterial growth of a single bacterial population in the absence of antibiotics (per hour) K t is the instantaneous rate constant for bacterial kill in the presence of the antibiotic (per hour), which depends on the profile of serum antibiotic levels, C t (micrograms per milliliter) present at any time t. K t follows a sigmoid E max model: K t K max C t C (2) 50 C t where K max is the maximum possible rate constant for bacterial killing (per hour) C 50 is the antibiotic concentration which produces a kill rate equal to K max /2 (micrograms per milliliter), and is the Hill sigmoidicity coefficient. Killing was computed by using values for G, K max, and previously obtained (1, 3) for P. aeruginosa in the presence of tobramycin or ticarcillin (Table 2). The USC*PACK PC clinical programs for adaptive control of tobramycin and ticarcillin therapy compute serum antibiotic concentrations every 6 min. The pharmacodynamic effect of bacterial killing was computed by using these concentration profiles as input to the effect model described in equation 1 above. When the serum antibiotic level is equal to the pharmacodynamic MIC, the bacterial killing rate equals the bacterial growth rate, the bacterial population remains unchanged, and equation 1 becomes db dt G K t B 0orG K t 0 (3) The bacterial apparent growth rate (G K t ) is then equal to zero. By combining equations 2 and 3, an expression relating C 50 to the pharmacodynamic MIC (zmic) can be obtained (13): C 50 zmic K max G G C max ( g/ml) C min ( g/ml) Tobramycin Ticarcillin , a k el, total elimination rate constant; D, total dose over 24 h; C max, peak drug level (at the end of the first intravenous dose); C min, trough drug level (just before the second dose). (4) TABLE 2. Pharmacodynamic parameter values of the effect model used in simulation for P. aeruginosa Antimicrobial agent G (h 1 ) K max (h 1 ) Tobramycin Ticarcillin By combining equations 1, 2, and 4, the time course of the bacterial population can be computed by using a model for which the relevant variables (for a single antibiotic and for a single bacterial population with an unchanging growth rate constant and for which the MIC of the antibiotic is unchanging) are the serum antibiotic levels at time t (C t ), B, G, K max, the zmic, and (14). Computation of pharmacodynamic indices. The pharmacodynamic indices generally proposed to correlate with antimicrobial effectiveness at the steady state have been the area under the drug concentration-time curve in serum (AUC); the AUC when C MIC (AUC MIC) (the AUC above the MIC; the AUC divided by the MIC, or AUC/MIC; the area under the inhibitory curve (AUIC), or the AUC when C MIC divided by the MIC; and the time above the MIC (T MIC) (Table 3) (18). All indices were computed versus time by employing an approximate integration based on the trapezoidal method (7). The accuracy of this method depends on a factor of 1/n 2, for which n is the number of trapezoids which are used (here, 10 per h, with serum drug concentrations computed every 6 min). A dynamic view of the various empirical pharmacodynamic indices was introduced here in order to relate them to the Zhi model. Each simulation was performed throughout the initial 24 h (first doses) of therapy, and the final index value was obtained at the end of the initial 24-h period, rather than for a typical 24-h period at steady state, as others have done. Continuing this dynamic view, it is noteworthy that the term T MIC has had several different meanings. Some have used this name to refer instead to the percent of the time during the dose interval in the steady state when the serum drug concentrations are at least the MIC. Another somewhat similar definition has been the percent of the time during a typical day in the steady state that the serum drug concentrations are at least the MIC. However, the name itself specially refers to the total time, during some defined time period, that the concentrations are at least the MIC. In the present paper, we have used the term to mean the total time during the first 24 h of therapy that the serum drug concentrations are at least the MIC. This index will progress from the minimum value of zero toward the maximum value (here 24 h) as the duration of therapy progresses from the very beginning (time zero) to the completion of the first 24 h of therapy. Because the pharmacodynamic indices are many and varied, preliminary work was first done to compare their dimensional equations, their dynamic evolution over time, and the index value at the end of the initial 24-h period. They were then evaluated to select the most useful indices for comparison with the Zhi model. Simulation. Tobramycin and ticarcillin profiles in serum were simulated by using the USC*PACK clinical programs (10). The time courses of the computed CFU were then plotted against the time courses of each pharmacodynamic index (MATLAB software). Each axis was parameterized versus time (as a phase-space plot, like a hysteresis loop), for different MICs of each drug. The MICs of tobramycin studied were 16, 8, 4, 2, 1, 0.5, 0.25, and g/ml, and those of TABLE 3. Review of pharmacodynamic indices for a 24-h period for antimicrobial agents Pharmacodynamic index AUC AUC MIC AUC above MIC AUC/MIC AUIC n Mathematical expression a T MIC T 1,i T 0,i, while C MIC h n i 1 T0,i 0 i 1 T0,i 24 T1,i T1,i C t MIC) dt n i MIC T0,i T1,i MIC Dimension g h ml 1 g h ml 1 g h ml 1 a C t, plasma antibiotic level (micrograms per milliliter) at time t (hours); T 0,i and T 1,i time interval (hours) when the plasma antibiotic level is greater than the MIC for the ith administration; n, number of dosage administrations in the 24-h period. h h
3 VOL. 42, 1998 PHARMACODYNAMIC INDICES AND BACTERIAL KILLING 1733 FIG. 1. Tobramycin (solid line) and ticarcillin (dotted line) plasma drug level profiles. ticarcillin were 128, 64, 32, 16, 8, 4, 2, and 1 g/ml (21). The initial inoculum was always assumed to be 10 6 CFU/ml. RESULTS The resulting simulated tobramycin and ticarcillin serum drug level profiles obtained with their respective population models are shown in Fig. 1. Study, comparison, and selection of pharmacodynamic indices. Table 3 shows the different pharmacodynamic indices, their mathematical expressions, and their dimensional equations. Comparison of pharmacodynamic indices was first performed for those indices having the same dimensional units. Several indices were found to be very similar. For example, AUIC and AUC/MIC were indistinguishable. For each MIC and for both antibiotic agents, a linear relationship between AUIC and AUC/MIC was found. This is probably because the area not included in the computation of the AUIC was extremely small, because the serum drug levels were above the MIC the great majority of the time. The method of calculating the index value is simpler for AUC/MIC than for AUIC. In addition, regarding calculation of the AUC MIC and AUC above the MIC during the first 24-h period (Table 3), C t MIC was nearly equal to C t for low MICs, and for each antibiotic-bacterium pair. The comparison of the mathematical expressions of AUC MIC and AUC above MIC shows that AUC MIC is nearly equivalent to AUC above the MIC for low MICs. Because of this, only four pharmacodynamic indices were finally compared to the computed CFU by using the Zhi model. They were AUC, AUC MIC, AUC/MIC, and T MIC. Comparison between pharmacodynamic indices and the Zhi model of bacterial growth and killing. Plots of CFU versus AUC, AUC MIC, AUC/MIC, and T MIC, are shown in Fig. 2 for tobramycin (panel A for AUC, B for AUC MIC, C for AUC/MIC, and D for T MIC) and for ticarcillin (panel A for AUC, B for AUC MIC, C for AUC/MIC, and D for T MIC). Figure 3 shows the relationship between final pharmacodynamic index values found at the end of the first 24-h period (on a logarithmic scale) and the MICs. DISCUSSION Many pharmacodynamic indices have been developed to predict antimicrobial effectiveness. Some of them were not studied here specifically the peak serum antibiotic level/mic ratio (6, 15, 16), because no dynamic or cumulative evolution of this index was possible for comparison with the Zhi model. For the other indices shown in Table 3, two types of index could be distinguished, depending on their dimensional units. The indices of AUC, AUC MIC, and AUC above MIC are all in micrograms times hours per milliliter. The indices of AUC/ MIC, AUIC, and T MIC are in hours. Contrary to Schentag et al. (20), none of these pharmacodynamic indices was found to be dimensionless. The indices AUC/MIC, AUC MIC, AUIC, and AUC above MIC were defined from the AUC by including the MIC in their calculations in different ways, as shown in Table 3. T MIC is clearly distinguishable from the others. Indeed, it is the only index for which the value is not computed with the AUC. As mentioned above, some indices were very similar and could not be distinguished from each other, by using our dynamic view, especially AUC/MIC versus AUIC and AUC MIC versus AUC above the MIC. For these reasons, only four pharmacodynamic indices were finally compared with the Zhi model: AUC, AUC/MIC, AUC MIC (two different ways of including MIC in the calculation), and the T MIC (independent of the AUC). Figure 2 shows the CFU versus each of the pharmacodynamic indices (AUC, AUC/MIC, AUC MIC, and T MIC) and their evolution during the initial 24-h period. In the MIC ranges tested, and for the first 24 h, the relationships of CFU to each evolving pharmacodynamic index were somewhat similar for both the concentration-dependent antibiotic and the concentration-independent one when the AUC/MIC was less than 250 h. However, for the concentration-independent drug, there was little relationship between AUC/MIC and killing beyond this point. This illustrates the saturation of the effect relationship for the concentration-independent drug. In fact, the relationship of any of the pharmacodynamic indices studied to bacterial killing depended essentially on the AUC and the MIC. It was evident that AUC alone does not take into account the sensitivity of the bacterium, since MIC is not included in its calculation. For different bacterial sensitivities represented by the different MICs, the values of the AUC were always the same at the end of the initial 24-h period (Fig. 2A and A ). Thus, AUC alone was not a good index. For the AUC MIC index, derived from AUC, but which takes into account the relationship of the plasma drug concentration with at least the MIC in the calculation, discontinuities were seen as CFU increased while the index value did not (Fig.
4 1734 CORVAISIER ET AL. ANTIMICROB. AGENTS CHEMOTHER. FIG. 2. CFU time course versus each pharmacodynamic index for a concentration-dependent drug, tobramycin, and for a concentration-independent drug, ticarcillin, during the first 24-h period of therapy, determined with the previous plasma drug level profiles.
5 VOL. 42, 1998 PHARMACODYNAMIC INDICES AND BACTERIAL KILLING 1735 FIG. 3. Course of pharmacodynamic index values found at the end of the first 24-h period versus the different tested MICs of a concentration-dependent antibiotic and a concentration-independent antibiotic determined with the plasma drug level profiles shown in Fig. 1. 2B and B ). This is because this method does not include concentrations below the MIC, which means that the bacterial killing rate constant at those times is zero. However, this does not seem realistic. Even if the bacterial population increases, the apparent growth rate constant is reduced, and the killing rate is not zero. Because of this assumption, a continuous relationship does not exist between the values of the AUC MIC and CFU. In addition, there was only a minimal relationship between CFU and AUC MIC. The relationship between AUC MIC and CFU was not very different from that found for AUC versus CFU. In contrast, for the AUC/MIC, the more its values increased, the greater was the killing seen with the Zhi model (Fig. 2C and C ). Conversely, treatment was not effective when AUC/ MIC was small. A continuous relationship exists between AUC/MIC values and the resulting CFU. Even if serum antibiotic levels are below the MIC with the apparent growth rate only slightly reduced, AUC/MIC values increased very slowly, showing the small to modest effect of the sub-mic serum antimicrobial level upon the bacterial growth rate. The difference between concentration-dependent and concentration-independent killing is also shown in Fig. 2C and C. For those concentrations relatively near the MIC, killing was almost linear with concentration. However, deviations from linearity were seen above this, especially in Fig. 2C, showing the lack of concentration dependence at the higher AUC/MICs, in the saturable region of the relationship. It is for this reason that when concentrations are reasonably above the MIC, the T MIC becomes the most significant empirical index for killing. All such relationships were well shown with the Zhi model. For the index of T MIC, however, it was also clear, as shown in Fig. 2D and D, that the dynamic evolution and growth of T MIC were strongly related to bacterial killing, with a significant negative correlation being found between it and CFU. However, discontinuities were also observed. For all therapy, the maximum possible value of T MIC is 24 h. Suppose that serum drug levels on one regimen are already above the MIC for a particular dosage regimen of antibiotic and that another regimen of the same antibiotic generates serum drug levels twice as high. The maximum value of T MIC will still be 24 h for either regimen. Because of this, the effectiveness of antibiotic treatment could not be distinguished if the second regimen was actually somewhat more effective than the first one, the smaller but already effective regimen. On the other hand, the other indices (AUC, AUC MIC, and AUC/MIC) do not have such maximum values. Therefore, the entire scale of therapeutic effectiveness can be explored with the other indices, whereas that is not the case with T MIC. Even with T MIC, which is expressed as linear percent of the dose intervals having serum drug concentrations above the MIC, a similar or the same maximum value (or 100%) is always reached. The greatest change in the values of the empirical indices found at the end of the initial 24-h period, for two different MICs, was obtained with AUC/MIC. For example, with tobramycin MICs of and 1.0 g/ml, there was no relationship between AUC and MIC (58.52 versus g h ml 1 ), a modest one for AUC MIC (58.48 versus g h ml 1 ), a greater one for T MIC (23.7 versus 12.1 h), and the greatest one for AUC/MIC ( versus h) (Fig. 3). Somewhat similar results were also seen for ticarcillin, although saturation of the effect relationship was clearly seen at the higher concentrations. AUC/MIC was therefore the pharmacodynamic index which had the greatest sensitivity to differences in the various MICs of either antibiotic, whether the antibiotic was concentration dependent or concentration independent (Fig. 3). A summary of the characteristics of each index (AUC, AUC MIC, T MIC, and AUC/MIC) and of a theoretical ideal index is presented in Table 4. Of the indices presented above, AUC/MIC appeared to be the best because it incorporated and used best the MIC of a concentration-dependent antibiotic and also, interestingly enough, to some degree, that of a concentration-independent antibiotic, although saturation of the effect relationship was clearly seen at higher concentrations. The AUC/MIC for the initial 24-h period has been previously described as the most useful index of fluoroquinolone antimicrobial activity against P. aeruginosa (12). In that study, however, it was shown that AUC/MIC was an index of efficacy only for the concentration-dependent antibiotic (12) and was not sufficient for the concentration-independent antibiotic. Conversely, T MIC was the only index to be described as an
6 1736 CORVAISIER ET AL. ANTIMICROB. AGENTS CHEMOTHER. TABLE 4. Summary of the principal characteristics of each index, the ideal index, and our new index, WAUC Index characteristic Result for index a AUC AUC MIC T MIC AUC/MIC Ideal index WAUC Easy determination Incorporation of all pharmacokinetic parameters Incorporation of MICs Sensitivity to change in MICs / Dynamic view No discontinuities No maximum value Concentration-dependent drug Concentration-independent drug Clear relationship with bacterial killing / / Drug combination analysis a, presence of the characteristic;, absence of the characteristic. index of efficacy for the concentration-independent antibiotic (18). In addition, a change in antibiotic administration strategy (for example, more doses at closer intervals) may produce the same AUC/MIC but two different T MICs. Equally, a change in the dose administered might produce a change in AUC/MIC but not in T MIC. Because of this, we also propose a new empirical pharmacodynamic index for which AUC/MIC is weighted by T MIC, in order to take into account both the concentration-dependent part of the antibiotic efficacy and the concentration-independent part. We therefore propose a new composite pharmacodynamic index, the weighted AUC (WAUC), for the first 24 h, which is the AUC/MIC weighted by the percentage of the total time for which the serum drug level is above the MIC: WAUC h AUC/MIC h T MIC h (5) T MIC max h where (T MIC) max equals 24 h (see above). The units for WAUC are hours. This index considers (i) the total dose administered and the clearance of the drug through the AUC, (ii) the sensitivity of the bacteria to the MIC, and (iii) the percentage of time for which serum drug level is above the MIC through the ratio T MIC/24 h. This index can be used both for a concentration-dependent drug and for a concentration-independent drug with a high sensitivity to change in MICs (Fig. 3). It shows a more direct relationship between its values and bacterial killing both for the concentration-dependent drug and for the concentration-independent drug (Fig. 4). Obviously, further clinical evaluation of this proposed index is needed before more conclusions can be drawn. Conclusion. The Zhi model describes a saturable Hill model of killing, coupled with assumed logarithmic growth. For concentration-dependent drugs, the concentrations are on the steep slope of the effect relationship, and saturation of the effect is not seen. It is for this reason that the model is concentration dependent when trough concentrations are near or below the MIC; here, AUC/MIC is usually the best empirical index. However, when concentrations are significantly above the MIC, saturation of the effect relationship takes place, and killing becomes relatively independent of concentrations; here, T MIC is usually the best empirical index. A good pharmacodynamic index must present a clear relationship between its values and bacterial killing. Actually, none of the empirical indices generally used brings together all of these characteristics, and none approaches the utility of the Zhi model itself to reflect the actual dynamic process of bacterial growth and killing. AUC/MIC appears the best for the concentration-dependent antimicrobial agent, and T MIC appears best for the concentration-independent antimicrobial FIG. 4. CFU course versus our new pharmacodynamic index for a concentration-dependent antibiotic (left panel) and a concentration-independent antibiotic (right panel) during the first 24-h period of therapy, determined with the previous plasma drug level profiles. Some saturation of the relationship is still seen at WAUC values above 400 h.
7 VOL. 42, 1998 PHARMACODYNAMIC INDICES AND BACTERIAL KILLING 1737 agent. Based on this, a new pharmacodynamic index for antimicrobial drugs, WAUC, is also proposed. This new index appears useful for both concentration-dependent and concentration-independent antimicrobial agents. A clear (nearly linear) relationship has been found between its values and bacterial growth and killing reflected by the Zhi model, as shown in Fig. 4, although some saturation of the effect relationship is still seen at higher concentrations. This index is dependent not only on time but also on the concentration and the MIC throughout the duration of the therapy. None of the pharmacodynamic indices, old or new, could be used in order to estimate the efficacy of a combination of antimicrobial agents. Because of this and because it is now easily available in clinical software, the Zhi model itself (or any similar dynamic model of bacterial growth and killing) probably still represents the current optimal clinical index of therapeutic effectiveness. The Zhi model actually represents a useful worst-case model for the evaluation of the efficacy of a drug dosage regimen. On the one hand, while some organisms may have a reduced or slowed rate of growth as some substrates for their growth become scarce, the Zhi model always makes the worstcase assumption that the organisms are always in their logarithmic phase of most rapid growth. While this may not be entirely realistic, it nevertheless furnishes a useful worst-case assumption for the evaluation of the potential utility of a proposed drug dosage regimen. The Zhi model contains no provision for describing the emergence of bacterial resistance during therapy. However, if one considers and uses the highest MIC the emerging resistant organism is estimated to attain during therapy, the Zhi model again provides a useful worst-case model for the evaluation of any proposed antibacterial regimen. If a proposed dosage regimen is successful in killing according to the Zhi model and the highest MIC for the organism is estimated to be attained, as described herein, that regimen is quite likely to be effective clinically, because the clinical situation may actually contain a decreasing rate constant for growth rather than the fixed one for the logarithmic phase of growth, and the organisms are not likely to be fully resistant from the very beginning of therapy. Because of this, the Zhi model for a single organism, assumed to be at its most resistant from the very start of therapy, provides a somewhat more stringent and rigorous test of the effectiveness of a dosage regimen than more complex models having several subpopulations, if one analyzes the behavior of the most rapidly growing and most resistant possible strain of organism. The computations are relatively simple and have already been incorporated into clinical software. As more complex models become available, they are likely to be less stringent than the single Zhi model. REFERENCES 1. Bouvier d Yvoire, M. J. Y., and P. H. Maire Dosage regimens of antibacterials: implications of a pharmacokinetic/pharmacodynamic model. Clin. Drug Invest. 11: Charpiat, B., V. Bréant, C. Pivot-Dumarest, P. H. Maire, and R. W. Jelliffe Prediction of future serum concentrations with Bayesian fitted pharmacokinetic models: results with data collected by nurses versus trained pharmacy residents. Ther. Drug Monit. 16: Craig, W. A., and S. C. Ebert Killing and regrowth of bacteria in vitro: a review. Scand. J. Infect. Dis. 74(Suppl.): Daikos, G. L., G. G. Jackson, V. T. Lolans, and D. M. Livemore Adaptive resistance to aminoglycoside antibiotics from first-exposure downregulation. J. Infect. Dis. 162: Dudley, M. N Commentary on dual individualization with antibiotics, p In W. E. Evans, J. J. Schentag, and W. J. Jusko (ed.), Applied pharmacokinetics: principles of therapeutic drug monitoring, 3rd ed. Applied Therapeutics Co., Vancouver, British Columbia, Canada. 6. Ellner, P. D., and H. C. Neu The inhibitory quotient. JAMA 246: Gibaldi, M., and D. Perrier Drug and the pharmaceutical sciences: pharmacokinetics, 2nd ed. Marcel Dekker, Inc., New York, N.Y. 8. Ingerman, M. J., P. G. Pitsakis, A. F. Rosenberg, and M. E. Levison The importance of pharmacodynamics in determining the dosing interval in therapy for experimental Pseudomonas endocarditis in the rats. J. Infect. Dis. 153: Jelliffe, R. W., A. Schumitzky, M. Van Guilder, M. Liu, L. Hu, P. Maire, P. Gomis, X. Barbaut, and B. Tahani Individualizing drug dosage regimens: roles of population pharmacokinetic and dynamic models, Bayesian fitting, and adaptive control. Ther. Drug Monit. 15: Laboratory of Applied Pharmacokinetics ADCAPT. USC*PACK PC on line user s manual. http//web.avo.fr/slecoq. 11. Legget, J. E., S. Ebert, B. Fantin, and W. A. Craig Comparative dose-effect relations at several dosing intervals for beta-lactam, aminoglycoside and quinolone antibiotics against gram-negative bacilli in murine thighinfection and pneumonitis model. Scand. J. Infect. Dis. 74: Madaras-Kelly, K. J., B. E. Ostergaard, L. Baeker Hovde, and J. C. Rotschafer Twenty-four-hour area under the concentration-time curve/mic ratio as a generic predictor of fluoroquinolone antimicrobial effect by using three strains of Pseudomonas aeruginosa and an in vitro pharmacodynamic model. Antimicrob. Agents Chemother. 40: Maire, P., X. Barbaut, J. C. Thalabard, F. Mentré, and R. W. Jelliffe Pharmacocinétique clinique appliquée aux antibiotiques, p In J. Freney, F. Renaud, W. Hansen, and C. Bollet (ed.), Manuel de bactériologie clinique, 2nd ed., vol. 1. Collection OptionBio,-Elsevier, Paris, France. 14. Maire, P. H., X. Barbaut, J. C. Thalabard, J. M. Vergnaud, D. Roux, M. Roy, and R. W. Jelliffe Adaptive control of therapeutic drug regimens: relations between clinical situations outcomes and simulations using nonlinear dynamic models, p In R. Greenes, H. Peterson, and D. Protti (ed.), MEDINFO 95. Proceedings of the 8th World Congress on Medical Informatics. International Medical Informatics Association, Edmonton, Alberta, Canada. 15. Moore, R. D., R. S. Craig, and P. S. Lietman Association of aminoglycoside plasma levels with therapeutic outcome in gram-negative pneumonia. Am. J. Med. 77: Moore, R. D., P. S. Lietman, and R. S. Craig Clinical response to aminoglycoside therapy: importance of the ratio of peak concentration to minimal inhibitory concentration. J. Infect. Dis. 155: Rotschafer, J. C., R. A. Zabinski, and K. J. Walker Pharmacodynamic factors of antibiotic efficacy. Pharmacotherapy 12:64S 70S. 18. Rotschafer, J. C., K. J. Walker, K. J. Madras-Kelly, and C. J. Sullivan Antibiotic pharmacodynamics, p In N. R. Culter, J. J. Sramek, and P. K. Narang (ed.), Pharmacodynamics and drug development: perspectives in clinical pharmacology. John Wiley & Sons, Inc., Chichester, United Kingdom. 19. Schentag, J. J., D. E. Nix, and M. H. Adelman Mathematical examination of dual individualization principles: relationships between AUC above MIC and area under the inhibitory curve for cefmenoxime, ciprofloxacin and tobramycin. DICP Ann. Pharmacother. 25: Schentag, J. J., C. H. Ballow, J. A. Paladino, and D. E. Nix Dual individualization with antibiotics: integrated antibiotic. Management strategies for use in hospitals, p In W. E. Evans, J. J. Schentag, and W. J. Jusko (ed.), Applied pharmacokinetics: principles of therapeutic drug monitoring, 3rd ed. Applied Therapeutics Inc., Vancouver, British Columbia, Canada. 21. Wiedemann, B., and B. A. Atkinson Susceptibility to antibiotics: species incidence and trends, p In V. Lorian (ed.), Antibiotics in laboratory medicine, 3rd ed. The Williams & Wilkins Co., Baltimore, Md. 22. Zhi, J., C. H. Nightingale, and R. Quintiliani Microbial pharmacodynamics of piperacillin in neutropenic mice with systemic infection due to Pseudomonas aeruginosa. J. Pharmacokinet. Biopharm. 16:
Basic Concepts of PK/PD -pharmacodynamic indices- Johan W. Mouton MD PhD FIDSA Professor pharmacokinetics and pharmacodymamics
 Basic Concepts of PK/PD -pharmacodynamic indices- Johan W. Mouton MD PhD FIDSA Professor pharmacokinetics and pharmacodymamics This patient needs antibiotics. But which ones? Intensive care patient Ceftazidime,
Basic Concepts of PK/PD -pharmacodynamic indices- Johan W. Mouton MD PhD FIDSA Professor pharmacokinetics and pharmacodymamics This patient needs antibiotics. But which ones? Intensive care patient Ceftazidime,
ICU Volume 11 - Issue 3 - Autumn Series
 ICU Volume 11 - Issue 3 - Autumn 2011 - Series Impact of Pharmacokinetics of Antibiotics in ICU Clinical Practice Introduction The efficacy of a drug is mainly dependent on its ability to achieve an effective
ICU Volume 11 - Issue 3 - Autumn 2011 - Series Impact of Pharmacokinetics of Antibiotics in ICU Clinical Practice Introduction The efficacy of a drug is mainly dependent on its ability to achieve an effective
%T MIC MIC. Pharmacokinetics PK: Cmax AUC T1/2 Pharmacodynamics PD: MIC: minimum inhibitory concentration time-killing-curve 1990.
 THE JAPANESE JOURNAL OF ANTIBIOTICS 58 2 159( 55 ) ( 2 15 ) %T MIC MIC 2002 30%T MIC 50%T MIC 1000 mg 3 3 /day Pharmacokinetics PK: Cmax AUC T1/2 Pharmacodynamics PD: MIC: minimum inhibitory concentration
THE JAPANESE JOURNAL OF ANTIBIOTICS 58 2 159( 55 ) ( 2 15 ) %T MIC MIC 2002 30%T MIC 50%T MIC 1000 mg 3 3 /day Pharmacokinetics PK: Cmax AUC T1/2 Pharmacodynamics PD: MIC: minimum inhibitory concentration
Pharmacologyonline 1: (2010) ewsletter Singh and Kochbar. Optimizing Pharmacokinetic/Pharmacodynamics Principles & Role of
 Optimizing Pharmacokinetic/Pharmacodynamics Principles & Role of Cefoperazone Sulbactam Singh M*, Kochhar P* Medical & Research Division, Pfizer India. Summary Antimicrobial resistance is associated with
Optimizing Pharmacokinetic/Pharmacodynamics Principles & Role of Cefoperazone Sulbactam Singh M*, Kochhar P* Medical & Research Division, Pfizer India. Summary Antimicrobial resistance is associated with
Pharmacokinetics of Tobramycin in Adults with Cystic Fibrosis: Implications for Once-Daily Administration
 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Apr. 2000, p. 809 813 Vol. 44, No. 4 0066-4804/00/$04.00 0 Copyright 2000, American Society for Microbiology. All Rights Reserved. Pharmacokinetics of Tobramycin
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Apr. 2000, p. 809 813 Vol. 44, No. 4 0066-4804/00/$04.00 0 Copyright 2000, American Society for Microbiology. All Rights Reserved. Pharmacokinetics of Tobramycin
Aminoglycoside Nephrotoxicity: Modeling, Simulation, and Control
 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Mar. 2003, p. 1010 1016 Vol. 47, No. 3 0066-4804/03/$08.00 0 DOI: 10.1128/AAC.47.3.1010 1016.2003 Copyright 2003, American Society for Microbiology. All Rights Reserved.
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Mar. 2003, p. 1010 1016 Vol. 47, No. 3 0066-4804/03/$08.00 0 DOI: 10.1128/AAC.47.3.1010 1016.2003 Copyright 2003, American Society for Microbiology. All Rights Reserved.
Pharmacodynamics: the methods
 Pharmacodynamics: the methods In vitro models Animal models Clinical studies Population studies With the support of Wallonie-Bruxelles-International 3B-1 Pharmacodynamics: the methods "un peu de tout "
Pharmacodynamics: the methods In vitro models Animal models Clinical studies Population studies With the support of Wallonie-Bruxelles-International 3B-1 Pharmacodynamics: the methods "un peu de tout "
MRSA Micro Scan Pos Combo 6J DADE BEHRING VCM
 PKPD MRSA 1 1 2 1 1 2 17 1 26 17 3 16 vancomycinvcm methicillin-resistant Staphylococcus aureusmrsa 31 pharmacokineticpkparameter retrospective VCM 21 10 PK parameter Mann- Whitney U-test Cmax 37.1 µ gml29.942
PKPD MRSA 1 1 2 1 1 2 17 1 26 17 3 16 vancomycinvcm methicillin-resistant Staphylococcus aureusmrsa 31 pharmacokineticpkparameter retrospective VCM 21 10 PK parameter Mann- Whitney U-test Cmax 37.1 µ gml29.942
Lessons from recent studies. João Gonçalves Pereira UCIP DALI
 Lessons from recent studies João Gonçalves Pereira UCIP DALI 1 Patterns of Antimicrobial Activity Concentration C max Aminoglycosides Cmax/MIC>10 Metronidazol Area under the concentration curve Azithromycin
Lessons from recent studies João Gonçalves Pereira UCIP DALI 1 Patterns of Antimicrobial Activity Concentration C max Aminoglycosides Cmax/MIC>10 Metronidazol Area under the concentration curve Azithromycin
Address: (1) ADCAPT, Service Pharmaceutique, Hôpital Antoine Charial, Francheville, France.
 1 Revised AAC 841 01 Title : Aminoglycoside Nephrotoxicity: Modeling, Simulation and Control Authors: Florent Rougier 1, Daniel Claude 2, Michel Maurin 3, Alexandre Sedoglavic 4, Michel Ducher 1, Stéphane
1 Revised AAC 841 01 Title : Aminoglycoside Nephrotoxicity: Modeling, Simulation and Control Authors: Florent Rougier 1, Daniel Claude 2, Michel Maurin 3, Alexandre Sedoglavic 4, Michel Ducher 1, Stéphane
prophylaxis for endocarditis in patients at high risk prophylaxis for major surgical procedures
 1 Glycopeptides appropriate uses serious infections due to beta-lactam- resistant gram-positive microorganisms infections due to gram-positive microorganisms in patients with serious allergy to beta-lactam
1 Glycopeptides appropriate uses serious infections due to beta-lactam- resistant gram-positive microorganisms infections due to gram-positive microorganisms in patients with serious allergy to beta-lactam
Continuous Infusion of Antibiotics In The ICU: What Is Proven? Professor of Medicine Vice-Chairman, Department of Medicine SUNY at Stony Brook
 Continuous Infusion of Antibiotics In The ICU: What Is Proven? Michael S. Niederman, M.D. Chairman, Department of Medicine Winthrop-University Hospital Mineola, NY Professor of Medicine Vice-Chairman,
Continuous Infusion of Antibiotics In The ICU: What Is Proven? Michael S. Niederman, M.D. Chairman, Department of Medicine Winthrop-University Hospital Mineola, NY Professor of Medicine Vice-Chairman,
Disclosures. Efficacy of the drug. Optimizing Dosing Based on PKPD- An overview. Dose Finding - The Past
 Disclosures Optimizing Dosing Based on PKPD- An overview Johan W. Mouton MD PhD FIDSA FAAM Professor pharmacokinetics and pharmacodynamics Research grants advisory boards speaker This Patient Needs Antibiotics.
Disclosures Optimizing Dosing Based on PKPD- An overview Johan W. Mouton MD PhD FIDSA FAAM Professor pharmacokinetics and pharmacodynamics Research grants advisory boards speaker This Patient Needs Antibiotics.
Aminoglycosides John A. Bosso, Pharm.D.
 AMINOGLYCOSIDES Therapeutics/PHRMP-73 Aminoglycoside Mechanism of Action Aminoglycosides bind to 30s ribosomal subunit resulting in mistranslation of mrna thus disrupting protein synthesis. They are rapidly
AMINOGLYCOSIDES Therapeutics/PHRMP-73 Aminoglycoside Mechanism of Action Aminoglycosides bind to 30s ribosomal subunit resulting in mistranslation of mrna thus disrupting protein synthesis. They are rapidly
Clinical Pharmacology. Pharmacodynamics the next step. Nick Holford Dept Pharmacology & Clinical Pharmacology University of Auckland, New Zealand
 1 Pharmacodynamic Principles and the Course of Immediate Drug s Nick Holford Dept Pharmacology & Clinical Pharmacology University of Auckland, New Zealand The time course of drug action combines the principles
1 Pharmacodynamic Principles and the Course of Immediate Drug s Nick Holford Dept Pharmacology & Clinical Pharmacology University of Auckland, New Zealand The time course of drug action combines the principles
PHARMACOKINETIC & PHARMACODYNAMIC OF ANTIBIOTICS
 PHARMACOKINETIC & PHARMACODYNAMIC OF ANTIBIOTICS SITI HIR HURAIZAH MD TAHIR Bpharm (UKM), MSc (Clinical Microbiology) (UoN) CLINICAL PHARMACIST HOSPITAL MELAKA WHY STUDY PHARMACOKINETICS (PK) AND PHARMACODYNAMICS
PHARMACOKINETIC & PHARMACODYNAMIC OF ANTIBIOTICS SITI HIR HURAIZAH MD TAHIR Bpharm (UKM), MSc (Clinical Microbiology) (UoN) CLINICAL PHARMACIST HOSPITAL MELAKA WHY STUDY PHARMACOKINETICS (PK) AND PHARMACODYNAMICS
Challenges in Therapeutic Drug Monitoring:
 Challenges in Therapeutic Drug Monitoring: Focus on Vancomycin Pharmacodynamics and Pharmacokinetics Katherine Gallaga, PharmD PGY1 Pharmacy Practice Resident CHRISTUS Spohn Health System 1 Pharmacist
Challenges in Therapeutic Drug Monitoring: Focus on Vancomycin Pharmacodynamics and Pharmacokinetics Katherine Gallaga, PharmD PGY1 Pharmacy Practice Resident CHRISTUS Spohn Health System 1 Pharmacist
PHA Spring First Exam. 8 Aminoglycosides (5 points)
 PHA 5128 Spring 2012 First Exam 1 Aminoglycosides (5 points) 2 Aminoglycosides (10 points) 3 Basic Principles (5 points) 4 Basic Principles (5 points) 5 Bioavailability (5 points) 6 Vancomycin (5 points)
PHA 5128 Spring 2012 First Exam 1 Aminoglycosides (5 points) 2 Aminoglycosides (10 points) 3 Basic Principles (5 points) 4 Basic Principles (5 points) 5 Bioavailability (5 points) 6 Vancomycin (5 points)
BASIC PHARMACOKINETICS
 BASIC PHARMACOKINETICS MOHSEN A. HEDAYA CRC Press Taylor & Francis Croup Boca Raton London New York CRC Press is an imprint of the Taylor & Francis Group, an informa business Table of Contents Chapter
BASIC PHARMACOKINETICS MOHSEN A. HEDAYA CRC Press Taylor & Francis Croup Boca Raton London New York CRC Press is an imprint of the Taylor & Francis Group, an informa business Table of Contents Chapter
Experience with a Once-Daily Aminoglycoside Program Administered to 2,184 Adult Patients
 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Mar. 1995, p. 650 655 Vol. 39, No. 3 0066-4804/95/$04.00 0 Copyright 1995, American Society for Microbiology Experience with a Once-Daily Aminoglycoside Program Administered
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Mar. 1995, p. 650 655 Vol. 39, No. 3 0066-4804/95/$04.00 0 Copyright 1995, American Society for Microbiology Experience with a Once-Daily Aminoglycoside Program Administered
Title. Author(s)Hayakawa, Mineji; Fujita, Itaru; Iseki, Ken; Gando, CitationASAIO Journal, 55(3): Issue Date Doc URL. Rights.
 Title The Administration of Ciprofloxacin During Continuou Author(s)Hayakawa, Mineji; Fujita, Itaru; Iseki, Ken; Gando, CitationASAIO Journal, 55(3): 243-245 Issue Date 2009-05 Doc URL http://hdl.handle.net/2115/43035
Title The Administration of Ciprofloxacin During Continuou Author(s)Hayakawa, Mineji; Fujita, Itaru; Iseki, Ken; Gando, CitationASAIO Journal, 55(3): 243-245 Issue Date 2009-05 Doc URL http://hdl.handle.net/2115/43035
Pharmacokinetics Overview
 Pharmacokinetics Overview Disclaimer: This handout and the associated lectures are intended as a very superficial overview of pharmacokinetics. Summary of Important Terms and Concepts - Absorption, peak
Pharmacokinetics Overview Disclaimer: This handout and the associated lectures are intended as a very superficial overview of pharmacokinetics. Summary of Important Terms and Concepts - Absorption, peak
Back to the Future: Using Aminoglycosides Again and How to Dose Them Optimally
 INVITED ARTICLE ANTIMICROBIAL RESISTANCE George M. Eliopoulos, Section Editor Back to the Future: Using Aminoglycosides Again and How to Dose Them Optimally George L. Drusano, Paul G. Ambrose, Sujata M.
INVITED ARTICLE ANTIMICROBIAL RESISTANCE George M. Eliopoulos, Section Editor Back to the Future: Using Aminoglycosides Again and How to Dose Them Optimally George L. Drusano, Paul G. Ambrose, Sujata M.
La farmacologia in aiuto
 Ferrara, 15 giugno 2018 La farmacologia in aiuto Pier Giorgio Cojutti, Federico Pea Istituto di Farmacologia Clinica Azienda Sanitaria Universitaria Integrata di Udine Therapeutic Drug Monitoring of Beta-Lactams
Ferrara, 15 giugno 2018 La farmacologia in aiuto Pier Giorgio Cojutti, Federico Pea Istituto di Farmacologia Clinica Azienda Sanitaria Universitaria Integrata di Udine Therapeutic Drug Monitoring of Beta-Lactams
/01/$ DOI: /AAC Copyright 2001, American Society for Microbiology. All Rights Reserved.
 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Dec. 2001, p. 3468 3473 Vol. 45, No. 12 0066-4804/01/$04.00 0 DOI: 10.1128/AAC.45.12.3468 3473.2001 Copyright 2001, American Society for Microbiology. All Rights
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Dec. 2001, p. 3468 3473 Vol. 45, No. 12 0066-4804/01/$04.00 0 DOI: 10.1128/AAC.45.12.3468 3473.2001 Copyright 2001, American Society for Microbiology. All Rights
Continuous vs Intermittent Dosing of Antibiotics in Critically-Ill Patients
 Continuous vs Intermittent Dosing of Antibiotics in Critically-Ill Patients Jan O Friedrich, MD DPhil Associate Professor of Medicine, University of Toronto Medical Director, MSICU St. Michael s Hospital,
Continuous vs Intermittent Dosing of Antibiotics in Critically-Ill Patients Jan O Friedrich, MD DPhil Associate Professor of Medicine, University of Toronto Medical Director, MSICU St. Michael s Hospital,
Pharmacodynamic indices in targeting therapy of critical infections
 Pharmacodynamic indices in targeting therapy of critical infections P.M. Tulkens Cellular and Molecular Pharmacology, Catholic University of Louvain, Brussels, Belgium & International Society of Anti-infective
Pharmacodynamic indices in targeting therapy of critical infections P.M. Tulkens Cellular and Molecular Pharmacology, Catholic University of Louvain, Brussels, Belgium & International Society of Anti-infective
EDUCATIONAL COMMENTARY VANCOMYCIN MONITORING
 EDUCATIONAL COMMENTARY VANCOMYCIN MONITORING Commentary provided by: Julie Hall, MHS, MT (ASCP) Assistant Dean, College of Health Professions Assistant Professor, Medical Laboratory Science Grand Valley
EDUCATIONAL COMMENTARY VANCOMYCIN MONITORING Commentary provided by: Julie Hall, MHS, MT (ASCP) Assistant Dean, College of Health Professions Assistant Professor, Medical Laboratory Science Grand Valley
A NEW APPROACH TO THERAPEUTIC DRUG MONITORING OF TOBRAMYCIN IN CYSTIC FIBROSIS
 THE DOSING INSTITUTE CLINICAL REVIEW SERIES: TOBRAMYCIN IN CYSTIC FIBROSIS MAY 2017 A NEW APPROACH TO THERAPEUTIC DRUG MONITORING OF TOBRAMYCIN IN CYSTIC FIBROSIS THE DOSING INSTITUTE The Dosing Institute
THE DOSING INSTITUTE CLINICAL REVIEW SERIES: TOBRAMYCIN IN CYSTIC FIBROSIS MAY 2017 A NEW APPROACH TO THERAPEUTIC DRUG MONITORING OF TOBRAMYCIN IN CYSTIC FIBROSIS THE DOSING INSTITUTE The Dosing Institute
MONTE CARLO SIMULATION & PK-PD TARGET ATTAINMENT ANALYSIS:
 MONTE CARLO SIMULATION & PK-PD TARGET ATTAINMENT ANALYSIS: Application to Estimation of MIC Breakpoints Paul G. Ambrose, Pharm.D. Director, Division of Infectious Diseases, Cognigen Corporation; Adjunct
MONTE CARLO SIMULATION & PK-PD TARGET ATTAINMENT ANALYSIS: Application to Estimation of MIC Breakpoints Paul G. Ambrose, Pharm.D. Director, Division of Infectious Diseases, Cognigen Corporation; Adjunct
NORLAND AVENUE PHARMACY PRESCRIPTION COMPOUNDING FOR GENERAL PRACTICE
 APRIL 2011 PRESCRIPTION COMPOUNDING N ORLANDA VENUEP HARMACY. COM We customize individual prescriptions for the specific needs of our patients. INSIDE THIS ISSUE: Methicillin-Resistant Staphylococcus 2
APRIL 2011 PRESCRIPTION COMPOUNDING N ORLANDA VENUEP HARMACY. COM We customize individual prescriptions for the specific needs of our patients. INSIDE THIS ISSUE: Methicillin-Resistant Staphylococcus 2
SBUH Aminoglycoside Dosing Protocol
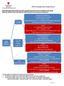 Adult Aminoglycoside Dosing for Gram negative infections prior to available serum levels (Excludes patients with cystic fibrosis, OB GYN patients and surgical prophylaxis) Cr Cl 40 ml/min 5 7 mg/kg INT
Adult Aminoglycoside Dosing for Gram negative infections prior to available serum levels (Excludes patients with cystic fibrosis, OB GYN patients and surgical prophylaxis) Cr Cl 40 ml/min 5 7 mg/kg INT
D DAVID PUBLISHING. 1. Introduction. Kathryn Koliha 1, Julie Falk 1, Rachana Patel 1 and Karen Kier 2
 Journal of Pharmacy and Pharmacology 5 (2017) 607-615 doi: 10.17265/2328-2150/2017.09.001 D DAVID PUBLISHING Comparative Evaluation of Pharmacist-Managed Vancomycin Dosing in a Community Hospital Following
Journal of Pharmacy and Pharmacology 5 (2017) 607-615 doi: 10.17265/2328-2150/2017.09.001 D DAVID PUBLISHING Comparative Evaluation of Pharmacist-Managed Vancomycin Dosing in a Community Hospital Following
Comparing Methods for Once Daily Tobramycin Exposure Predictions in Children with Cystic Fibrosis
 Comparing Methods for Once Daily Tobramycin Exposure Predictions in Children with Cystic Fibrosis Stefanie HENNIG, Franziska STILLER, Beverly TEO, Christine STAATZ, Brisbane Cystic fibrosis (CF) & Once
Comparing Methods for Once Daily Tobramycin Exposure Predictions in Children with Cystic Fibrosis Stefanie HENNIG, Franziska STILLER, Beverly TEO, Christine STAATZ, Brisbane Cystic fibrosis (CF) & Once
Is the package insert correct? PK considerations
 Is the package insert correct? PK considerations Jason A Roberts B Pharm (Hons), PhD, FSHP Professor of Medicine and Pharmacy The University of Queensland, Australia Royal Brisbane and Women s Hospital,
Is the package insert correct? PK considerations Jason A Roberts B Pharm (Hons), PhD, FSHP Professor of Medicine and Pharmacy The University of Queensland, Australia Royal Brisbane and Women s Hospital,
Optimizing Drug Exposure
 Optimizing Drug Exposure All Patients Are Not Average Michael Neely, MD, MSc Associate Professor, Pediatrics Keck School of Medicine, University of Southern California Laboratory of Applied Pharmacokinetics
Optimizing Drug Exposure All Patients Are Not Average Michael Neely, MD, MSc Associate Professor, Pediatrics Keck School of Medicine, University of Southern California Laboratory of Applied Pharmacokinetics
pharmacy, we need to see how clinical pharmacokinetics fits into the pharmaceutical care process.
 Therapeutic drug monitoring (TDM) Is a tool that can guide the clinician to provide effective and safe drug therapy in the individual patient. Monitoring can be used to confirm a plasma drug concentration
Therapeutic drug monitoring (TDM) Is a tool that can guide the clinician to provide effective and safe drug therapy in the individual patient. Monitoring can be used to confirm a plasma drug concentration
VANCOMYCIN DOSING AND MONITORING GUIDELINES
 VANCOMYCIN DOSING AND MONITORING GUIDELINES NB Provincial Health Authorities Anti-Infective Stewardship Committee Approved: May 2017 GENERAL COMMENTS Vancomycin is a glycopeptide antibiotic with bactericidal
VANCOMYCIN DOSING AND MONITORING GUIDELINES NB Provincial Health Authorities Anti-Infective Stewardship Committee Approved: May 2017 GENERAL COMMENTS Vancomycin is a glycopeptide antibiotic with bactericidal
D DAVID PUBLISHING. Evaluation of the Effectiveness of a Vancomycin Nomogram at Predicting Trough Levels within a Therapeutic Range. 1.
 Journal of Pharmacy and Pharmacology 2 (2014) 713-721 doi: 10.17265/2328-2150/2014.12.004 D DAVID PUBLISHING Evaluation of the Effectiveness of a Vancomycin Nomogram at Predicting Trough Levels within
Journal of Pharmacy and Pharmacology 2 (2014) 713-721 doi: 10.17265/2328-2150/2014.12.004 D DAVID PUBLISHING Evaluation of the Effectiveness of a Vancomycin Nomogram at Predicting Trough Levels within
Multiple-dose pharmacokinetics and safety of trovafloxacin in healthy volunteers
 Journal of Antimicrobial Chemotherapy (1996) 37, 955-963 Multiple-dose pharmacokinetics and safety of trovafloxacin in healthy volunteers Renli Teng, Theodore E. Liston and Stephen C. Harris Central Research
Journal of Antimicrobial Chemotherapy (1996) 37, 955-963 Multiple-dose pharmacokinetics and safety of trovafloxacin in healthy volunteers Renli Teng, Theodore E. Liston and Stephen C. Harris Central Research
Should we be performing TDM in seriously ill patients with Gram negative infections?
 Should we be performing TDM in seriously ill patients with Gram negative infections? Jason A Roberts B Pharm (Hons), PhD, FSHP Royal Brisbane and Women s Hospital, Australia. The University of Queensland,
Should we be performing TDM in seriously ill patients with Gram negative infections? Jason A Roberts B Pharm (Hons), PhD, FSHP Royal Brisbane and Women s Hospital, Australia. The University of Queensland,
ORIGINAL ARTICLE /j x. of Medicine, Pamplona, Spain
 ORIGINAL ARTICLE 10.1111/j.1469-0691.2004.00994.x Relationship between pharmacokinetics and pharmacodynamics of b-lactams and outcome B. Sádaba 1, J. R. Azanza 2, M. A. Campanero 1 and E. García-Quetglas
ORIGINAL ARTICLE 10.1111/j.1469-0691.2004.00994.x Relationship between pharmacokinetics and pharmacodynamics of b-lactams and outcome B. Sádaba 1, J. R. Azanza 2, M. A. Campanero 1 and E. García-Quetglas
Adult Institutional Pharmacokinetics Protocol
 Adult Institutional Pharmacokinetics Protocol Policy Title: Clinical Pharmacokinetics (PK) Service Policy Policy Statement: It is the policy of UMHC that PK consult orders (for vancomycin or aminoglycosides)
Adult Institutional Pharmacokinetics Protocol Policy Title: Clinical Pharmacokinetics (PK) Service Policy Policy Statement: It is the policy of UMHC that PK consult orders (for vancomycin or aminoglycosides)
ZIN EN ONZIN VAN ANTIBIOTICASPIEGELS BIJ NEONATEN
 ZIN EN ONZIN VAN ANTIBIOTICASPIEGELS BIJ NEONATEN Anne Smits Fellow neonatologie UZ Leuven Use of antibiotics in neonates 50 European hospitals 23 non-european hospitals Countries n = 14 n = 9 Pediatric
ZIN EN ONZIN VAN ANTIBIOTICASPIEGELS BIJ NEONATEN Anne Smits Fellow neonatologie UZ Leuven Use of antibiotics in neonates 50 European hospitals 23 non-european hospitals Countries n = 14 n = 9 Pediatric
Basic Pharmacokinetics and Pharmacodynamics: An Integrated Textbook with Computer Simulations
 Basic Pharmacokinetics and Pharmacodynamics: An Integrated Textbook with Computer Simulations Rosenbaum, Sara E. ISBN-13: 9780470569061 Table of Contents 1 Introduction to Pharmacokinetics and Pharmacodynamics.
Basic Pharmacokinetics and Pharmacodynamics: An Integrated Textbook with Computer Simulations Rosenbaum, Sara E. ISBN-13: 9780470569061 Table of Contents 1 Introduction to Pharmacokinetics and Pharmacodynamics.
Pharmacodynamic principles and the time course of immediate drug effects
 TCP 2017;25(4):157-161 http://dx.doi.org/10.12793/tcp.2017.25.4.157 Pharmacodynamic principles and the time course of immediate drug effects TUTORIAL Department of Pharmacology & Clinical Pharmacology,
TCP 2017;25(4):157-161 http://dx.doi.org/10.12793/tcp.2017.25.4.157 Pharmacodynamic principles and the time course of immediate drug effects TUTORIAL Department of Pharmacology & Clinical Pharmacology,
TDM of Aminoglycoside Antibiotics
 TDM Lecture 3 5 th Stage TDM of Aminoglycoside Antibiotics The aminoglycoside antibiotics are widely used for the treatment of gram-negative infections, often in combination with a β-lactam antibiotic
TDM Lecture 3 5 th Stage TDM of Aminoglycoside Antibiotics The aminoglycoside antibiotics are widely used for the treatment of gram-negative infections, often in combination with a β-lactam antibiotic
Voriconazole Rationale for the EUCAST clinical breakpoints, version March 2010
 Voriconazole Rationale for the EUCAST clinical breakpoints, version 2.0 20 March 2010 Foreword EUCAST The European Committee on Antimicrobial Susceptibility Testing (EUCAST) is organised by the European
Voriconazole Rationale for the EUCAST clinical breakpoints, version 2.0 20 March 2010 Foreword EUCAST The European Committee on Antimicrobial Susceptibility Testing (EUCAST) is organised by the European
Evaluation of Vancomycin Continuous Infusion in Trauma Patients
 OBJECTIVES Evaluation of Vancomycin Continuous Infusion in Trauma Patients Brittany D. Bissell, Pharm.D. PGY-2 Critical Care Pharmacy Resident Jackson Memorial Hospital Miami, Florida Evaluate the potential
OBJECTIVES Evaluation of Vancomycin Continuous Infusion in Trauma Patients Brittany D. Bissell, Pharm.D. PGY-2 Critical Care Pharmacy Resident Jackson Memorial Hospital Miami, Florida Evaluate the potential
Use ideal body weight (IBW) unless actual body weight is less. Use the following equation to calculate IBW:
 Amikacin is a partially restricted (amber) antibiotic for the treatment of infections due to gentamicin resistant Gram negative bacilli or as advised by microbiology. As with other aminoglycosides, therapeutic
Amikacin is a partially restricted (amber) antibiotic for the treatment of infections due to gentamicin resistant Gram negative bacilli or as advised by microbiology. As with other aminoglycosides, therapeutic
Achieving pharmacokinetic/pharmacodynamic (PK/PD) targets of β-lactams in critically ill patients at first dose: Can we do it with standard dosing?
 Oral session: PK/PD-based optimized broad-spectrum beta-lactam therapy (Sunday 10 April, 11:30) Achieving pharmacokinetic/pharmacodynamic (PK/PD) targets of β-lactams in critically ill patients at first
Oral session: PK/PD-based optimized broad-spectrum beta-lactam therapy (Sunday 10 April, 11:30) Achieving pharmacokinetic/pharmacodynamic (PK/PD) targets of β-lactams in critically ill patients at first
Pharmacokinetic parameters: Halflife
 Pharmacokinetic parameters: Halflife (t 1/2 ) 1. By definition t 1/2 is the time required for the concentration to fall by one half. For drugs with first order kinetics this is a constant. 2. Half-life
Pharmacokinetic parameters: Halflife (t 1/2 ) 1. By definition t 1/2 is the time required for the concentration to fall by one half. For drugs with first order kinetics this is a constant. 2. Half-life
Therapeutic drug monitoring of β-lactams
 CORATA Belgique Reims 1-2/10/2014 Therapeutic drug monitoring of β-lactams Frédéric Cotton Clinical Chemistry Erasme Hospital Faculty of Pharmacy ULB TDM of β-lactams β-lactams pharmacokinetics pharmacodynamics
CORATA Belgique Reims 1-2/10/2014 Therapeutic drug monitoring of β-lactams Frédéric Cotton Clinical Chemistry Erasme Hospital Faculty of Pharmacy ULB TDM of β-lactams β-lactams pharmacokinetics pharmacodynamics
Basic Concepts of TDM
 TDM Lecture 1 5 th stage What is TDM? Basic Concepts of TDM Therapeutic drug monitoring (TDM) is a branch of clinical pharmacology that specializes in the measurement of medication concentrations in blood.
TDM Lecture 1 5 th stage What is TDM? Basic Concepts of TDM Therapeutic drug monitoring (TDM) is a branch of clinical pharmacology that specializes in the measurement of medication concentrations in blood.
The CLSI Approach to Setting Breakpoints
 The CLSI Approach to Setting Breakpoints Jean B. Patel, PhD, D(ABMM) Deputy Director, Office of Antimicrobial Resistance Division of Healthcare Quality Promotion National Center for Emerging and Zoonotic
The CLSI Approach to Setting Breakpoints Jean B. Patel, PhD, D(ABMM) Deputy Director, Office of Antimicrobial Resistance Division of Healthcare Quality Promotion National Center for Emerging and Zoonotic
Comparison of Omadacycline and Tigecycline Pharmacodynamics in the Plasma, Epithelial Lining Fluid, and Alveolar Macrophages in Healthy Subjects
 Comparison of Omadacycline and Tigecycline Pharmacodynamics in the Plasma, Epithelial Lining Fluid, and Alveolar Macrophages in Healthy Subjects Karolyn S. Horn, Mark H. Gotfried, Judith N. Steenbergen,
Comparison of Omadacycline and Tigecycline Pharmacodynamics in the Plasma, Epithelial Lining Fluid, and Alveolar Macrophages in Healthy Subjects Karolyn S. Horn, Mark H. Gotfried, Judith N. Steenbergen,
Time to Lowest BIS after an Intravenous Bolus and an Adaptation of the Time-topeak-effect
 Adjustment of k e0 to Reflect True Time Course of Drug Effect by Using Observed Time to Lowest BIS after an Intravenous Bolus and an Adaptation of the Time-topeak-effect Algorithm Reported by Shafer and
Adjustment of k e0 to Reflect True Time Course of Drug Effect by Using Observed Time to Lowest BIS after an Intravenous Bolus and an Adaptation of the Time-topeak-effect Algorithm Reported by Shafer and
Professor of Chemotherapy Department of Preclinical and Clinical Pharmacology University of Florence
 Professor of Chemotherapy Department of Preclinical and Clinical Pharmacology University of Florence Researching field Pharmacokinetics, Pharmacodynamics of antimicrobial, antifungal and antitumoral drugs
Professor of Chemotherapy Department of Preclinical and Clinical Pharmacology University of Florence Researching field Pharmacokinetics, Pharmacodynamics of antimicrobial, antifungal and antitumoral drugs
PHARMONITOR II. Optimisation of aminoglycosides dosage regimen with pharmacokinetics modeling. Pierre Wallemacq
 PHARMONITOR II Optimisation of aminoglycosides dosage regimen with pharmacokinetics modeling Pierre Wallemacq NATIONAL SYMPOSIUM 20 years EEQ Leuven, March 26th 2009 1 Why monitoring of aminoglycosides?
PHARMONITOR II Optimisation of aminoglycosides dosage regimen with pharmacokinetics modeling Pierre Wallemacq NATIONAL SYMPOSIUM 20 years EEQ Leuven, March 26th 2009 1 Why monitoring of aminoglycosides?
Terapia delle infezioni da Pseudomonas aeruginosa MDR
 Verona 23 ottobre 2010 Terapia delle infezioni da Pseudomonas aeruginosa MDR Pierluigi Viale Clinica di Malattie Infettive Policlinico S. Orsola Malpighi Global resistance surveillance of Pseudomonas aeruginosa
Verona 23 ottobre 2010 Terapia delle infezioni da Pseudomonas aeruginosa MDR Pierluigi Viale Clinica di Malattie Infettive Policlinico S. Orsola Malpighi Global resistance surveillance of Pseudomonas aeruginosa
JAC Computer-aided prediction of macrolide antibiotic concentrations in human circulating polymorphonuclear leucocytes
 Journal of Antimicrobial Chemotherapy (1998) 41, Suppl. B, 63 68 JAC Computer-aided prediction of macrolide antibiotic concentrations in human circulating polymorphonuclear leucocytes M. J. Y. Bouvier
Journal of Antimicrobial Chemotherapy (1998) 41, Suppl. B, 63 68 JAC Computer-aided prediction of macrolide antibiotic concentrations in human circulating polymorphonuclear leucocytes M. J. Y. Bouvier
NIH Public Access Author Manuscript Am J Nephrol. Author manuscript; available in PMC 2015 January 22.
 NIH Public Access Author Manuscript Published in final edited form as: Am J Nephrol. 2012 ; 36(2): 144 150. doi:10.1159/000339937. Gentamicin Pharmacokinetics and Pharmacodynamics during Short-daily Hemodialysis
NIH Public Access Author Manuscript Published in final edited form as: Am J Nephrol. 2012 ; 36(2): 144 150. doi:10.1159/000339937. Gentamicin Pharmacokinetics and Pharmacodynamics during Short-daily Hemodialysis
Full title of guideline INTRAVENOUS VANCOMYCIN PRESCRIBING AND MONITORING GUIDELINE FOR ADULT PATIENTS. control
 Full title of guideline Author: Contact Name and Job Title Division and specialty Scope Explicit definition of patient group to which it applies (e.g. inclusion and exclusion criteria, diagnosis) Changes
Full title of guideline Author: Contact Name and Job Title Division and specialty Scope Explicit definition of patient group to which it applies (e.g. inclusion and exclusion criteria, diagnosis) Changes
BSWH Pharmacist Continuing Education PART 5: Pharmacotherapy and Pharmacokinetics in Adults: Aminoglycosides and Vancomycin
 BSWH Pharmacist Continuing Education 2015 PART 5: Pharmacotherapy and Pharmacokinetics in Adults: Aminoglycosides and Vancomycin Objectives Define basic pharmacodynamic and pharmacokinetic principles Describe
BSWH Pharmacist Continuing Education 2015 PART 5: Pharmacotherapy and Pharmacokinetics in Adults: Aminoglycosides and Vancomycin Objectives Define basic pharmacodynamic and pharmacokinetic principles Describe
Long Half-life Drugs in Infectious Diseases: Implications and Complications
 Long Half-life Drugs in Infectious Diseases: Implications and Complications In Session: Drugs That Just Won t Leave: From Stars of the Party to Unwelcome Guests Annual Meeting of the AAPS, San Diego, California
Long Half-life Drugs in Infectious Diseases: Implications and Complications In Session: Drugs That Just Won t Leave: From Stars of the Party to Unwelcome Guests Annual Meeting of the AAPS, San Diego, California
PHARMACOKINETICS SMALL GROUP II:
 PHARMACOKINETICS SMALL GROUP II: Question 1 Why are some drug therapies initiated with a loading dose? Emphasize that LD establishes initial therapeutic level quickly. The time to reach the steady-state
PHARMACOKINETICS SMALL GROUP II: Question 1 Why are some drug therapies initiated with a loading dose? Emphasize that LD establishes initial therapeutic level quickly. The time to reach the steady-state
Clinical Trials A Practical Guide to Design, Analysis, and Reporting
 Clinical Trials A Practical Guide to Design, Analysis, and Reporting Duolao Wang, PhD Ameet Bakhai, MBBS, MRCP Statistician Cardiologist Clinical Trials A Practical Guide to Design, Analysis, and Reporting
Clinical Trials A Practical Guide to Design, Analysis, and Reporting Duolao Wang, PhD Ameet Bakhai, MBBS, MRCP Statistician Cardiologist Clinical Trials A Practical Guide to Design, Analysis, and Reporting
TRANSPARENCY COMMITTEE OPINION. 15 October Date of Marketing Authorisation (national procedure): 16 April 1997, variation of 18 February 2008
 The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 15 October 2008 MERONEM 1 g, powder for solution for IV Injection Box of 10 vials (CIP: 387 830-6) Applicant: ASTRAZENECA
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 15 October 2008 MERONEM 1 g, powder for solution for IV Injection Box of 10 vials (CIP: 387 830-6) Applicant: ASTRAZENECA
PHARMACOKINETICS OF DRUG ABSORPTION
 Print Close Window Note: Large images and tables on this page may necessitate printing in landscape mode. Applied Biopharmaceutics & Pharmacokinetics > Chapter 7. Pharmacokinetics of Oral Absorption >
Print Close Window Note: Large images and tables on this page may necessitate printing in landscape mode. Applied Biopharmaceutics & Pharmacokinetics > Chapter 7. Pharmacokinetics of Oral Absorption >
Antimicrobial practice. Monitoring serum concentrations for once-daily netilmicin dosing regimens
 Journal of Antimicrobial Chemotherapy (1994) 33, 341348 Antimicrobial practice Monitoring serum concentrations for oncedaily netilmicin dosing regimens Jurg Blasei*'*, Christian* KSnig*, HansPeter Simmen*
Journal of Antimicrobial Chemotherapy (1994) 33, 341348 Antimicrobial practice Monitoring serum concentrations for oncedaily netilmicin dosing regimens Jurg Blasei*'*, Christian* KSnig*, HansPeter Simmen*
Pharmacokinetic modelling of a once-daily dosing regimen for intravenous tobramycin in paediatric cystic fibrosis patients
 Journal of Antimicrobial Chemotherapy Advance Access published April 19, 2007 Journal of Antimicrobial Chemotherapy doi:10.1093/jac/dkm097 Pharmacokinetic modelling of a once-daily dosing regimen for intravenous
Journal of Antimicrobial Chemotherapy Advance Access published April 19, 2007 Journal of Antimicrobial Chemotherapy doi:10.1093/jac/dkm097 Pharmacokinetic modelling of a once-daily dosing regimen for intravenous
BIOPHARMACEUTICS and CLINICAL PHARMACY
 11 years papers covered BIOPHARMACEUTICS and CLINICAL PHARMACY IV B.Pharm II Semester, Andhra University Topics: Absorption Distribution Protein binding Metabolism Excretion Bioavailability Drug Interactions
11 years papers covered BIOPHARMACEUTICS and CLINICAL PHARMACY IV B.Pharm II Semester, Andhra University Topics: Absorption Distribution Protein binding Metabolism Excretion Bioavailability Drug Interactions
PHA5128 Dose Optimization II Case Study I Spring 2013
 Silsamicin is an investigational compound being evaluated for its antimicrobial effect. The route of administration for this drug is via intravenous bolus. Approximately 99.9% of this drug is eliminated
Silsamicin is an investigational compound being evaluated for its antimicrobial effect. The route of administration for this drug is via intravenous bolus. Approximately 99.9% of this drug is eliminated
C OBJECTIVES. Basic Pharmacokinetics LESSON. After completing Lesson 2, you should be able to:
 LESSON 2 Basic Pharmacokinetics C OBJECTIVES After completing Lesson 2, you should be able to: 1. Define the concept of apparent volume of distribution and use an appropriate mathematical equation to calculate
LESSON 2 Basic Pharmacokinetics C OBJECTIVES After completing Lesson 2, you should be able to: 1. Define the concept of apparent volume of distribution and use an appropriate mathematical equation to calculate
SHC Vancomycin Dosing Guide
 SHC Vancomycin Dosing Guide A: Initial dosing considerations B. Pharmacodynamic Targets: goal AUC and troughs C. Loading dose D: Initial Vancomycin Maintenance Dosing and Serum Concentration Monitoring
SHC Vancomycin Dosing Guide A: Initial dosing considerations B. Pharmacodynamic Targets: goal AUC and troughs C. Loading dose D: Initial Vancomycin Maintenance Dosing and Serum Concentration Monitoring
Pharmacokinetic-Pharmacodynamic (PKPD) Modeling Characterizing Resistance for Predictions of Bacterial Kill in vivo
 Pharmacokinetic-Pharmacodynamic (PKPD) Modeling Characterizing Resistance for Predictions of Bacterial Kill in vivo Anders Kristoffersson Pascale David- Pierson, Neil John Parrott, Olaf Kuhlmann, Thierry
Pharmacokinetic-Pharmacodynamic (PKPD) Modeling Characterizing Resistance for Predictions of Bacterial Kill in vivo Anders Kristoffersson Pascale David- Pierson, Neil John Parrott, Olaf Kuhlmann, Thierry
Biomath M263 Clinical Pharmacology
 Training Program in Translational Science Biomath M263 Clinical Pharmacology Spring 2013 www.ctsi.ucla.edu/education/training/webcasts Wednesdays 3 PM room 17-187 CHS 4/3/2013 Pharmacokinetics and Pharmacodynamics
Training Program in Translational Science Biomath M263 Clinical Pharmacology Spring 2013 www.ctsi.ucla.edu/education/training/webcasts Wednesdays 3 PM room 17-187 CHS 4/3/2013 Pharmacokinetics and Pharmacodynamics
A Snapshot of Colistin Use in South-East Europe and Particularly in Greece
 A Snapshot of Colistin Use in South-East Europe and Particularly in Greece Helen Giamarellou 02.05.2013 When Greek Physicians Prescribe Colistin? It is mainly prescribed in the ICU for VAP, bacteremia
A Snapshot of Colistin Use in South-East Europe and Particularly in Greece Helen Giamarellou 02.05.2013 When Greek Physicians Prescribe Colistin? It is mainly prescribed in the ICU for VAP, bacteremia
The ciprofloxacin target AUC : MIC ratio is not reached in hospitalized patients with the recommended dosing regimens
 British Journal of Clinical Pharmacology DOI:10.1111/j.1365-2125.2012.04337.x The ciprofloxacin target AUC : MIC ratio is not reached in hospitalized patients with the recommended dosing regimens Michiel
British Journal of Clinical Pharmacology DOI:10.1111/j.1365-2125.2012.04337.x The ciprofloxacin target AUC : MIC ratio is not reached in hospitalized patients with the recommended dosing regimens Michiel
AMINOGLYCOSIDES TDM D O N E B Y
 AMINOGLYCOSIDES TDM DONE BY: SARA ALARFAJ 2014 OUTLINE Introduction about Aminoglycosides. Spectrum/uses. TDM Aminoglycosides TDM Pharmacodynamics Pharmacokinetics. Dosing in AG. Sampeling time and Monitoring.
AMINOGLYCOSIDES TDM DONE BY: SARA ALARFAJ 2014 OUTLINE Introduction about Aminoglycosides. Spectrum/uses. TDM Aminoglycosides TDM Pharmacodynamics Pharmacokinetics. Dosing in AG. Sampeling time and Monitoring.
Drug Dosing in Renal Insufficiency. Coralie Therese D. Dimacali, MD College of Medicine University of the Philippines Manila
 Drug Dosing in Renal Insufficiency Coralie Therese D. Dimacali, MD College of Medicine University of the Philippines Manila Declaration of Conflict of Interest For today s lecture on Drug Dosing in Renal
Drug Dosing in Renal Insufficiency Coralie Therese D. Dimacali, MD College of Medicine University of the Philippines Manila Declaration of Conflict of Interest For today s lecture on Drug Dosing in Renal
Drug dosing in Extremes of Weight
 Drug dosing in Extremes of Weight The Plump & Heavy versus The Skinny & Light Maria Minerva P. Calimag, MD, MSc, PhD, DPBA, FPSECP PROFESSOR Departments of Pharmacology, Anesthesiology and Clinical Epidemiology
Drug dosing in Extremes of Weight The Plump & Heavy versus The Skinny & Light Maria Minerva P. Calimag, MD, MSc, PhD, DPBA, FPSECP PROFESSOR Departments of Pharmacology, Anesthesiology and Clinical Epidemiology
Title: Cefoxitin Continuous Infusion for Lung Infection Caused by M. abscessus group
 AAC Accepts, published online ahead of print on 14 April 2014 Antimicrob. Agents Chemother. doi:10.1128/aac.02763-14 Copyright 2014, American Society for Microbiology. All Rights Reserved. 1 Title: Cefoxitin
AAC Accepts, published online ahead of print on 14 April 2014 Antimicrob. Agents Chemother. doi:10.1128/aac.02763-14 Copyright 2014, American Society for Microbiology. All Rights Reserved. 1 Title: Cefoxitin
Vancomycin Pharmacokinetics in Normal and Morbidly Obese Subjects
 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Apr. 1982, p. 575-58 66484/82/4575-6$2./ Vol. 21, No. 4 Vancomycin Pharmacokinetics in Normal and Morbidly Obese Subjects ROBERT A. BLOUIN,1 LARRY A. BAUER,3* DELWYN
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Apr. 1982, p. 575-58 66484/82/4575-6$2./ Vol. 21, No. 4 Vancomycin Pharmacokinetics in Normal and Morbidly Obese Subjects ROBERT A. BLOUIN,1 LARRY A. BAUER,3* DELWYN
CAT. Dosisaanpassing van antibiotica, toepasbaarheid van beschikbare calculators. Apr. Glynis Frans Supervisor: Prof. Apr.
 CAT Dosisaanpassing van antibiotica, toepasbaarheid van beschikbare calculators Apr. Glynis Frans Supervisor: Prof. Apr. Katrien Lagrou 1. What are the current guidelines and recommendations on TDM for
CAT Dosisaanpassing van antibiotica, toepasbaarheid van beschikbare calculators Apr. Glynis Frans Supervisor: Prof. Apr. Katrien Lagrou 1. What are the current guidelines and recommendations on TDM for
1. If the MTC is 100 ng/ml and the MEC is 0.12 ng/ml, which of the following dosing regimen(s) are in the therapeutic window?
 Page 1 PHAR 750: Biopharmaceutics/Pharmacokinetics October 23, 2009 - Form 1 Name: Total 100 points Please choose the BEST answer of those provided. For numerical answers, choose none of the above if your
Page 1 PHAR 750: Biopharmaceutics/Pharmacokinetics October 23, 2009 - Form 1 Name: Total 100 points Please choose the BEST answer of those provided. For numerical answers, choose none of the above if your
PZA: A New Look Based on RNASeq, the Hollow Fiber System, and Patient Level Data. Tawanda Gumbo
 PZA: A New Look Based on RNASeq, the Hollow Fiber System, and Patient Level Data Tawanda Gumbo Office of Global Health University of Texas Southwestern Medical Center, Dallas, Texas The team: this work
PZA: A New Look Based on RNASeq, the Hollow Fiber System, and Patient Level Data Tawanda Gumbo Office of Global Health University of Texas Southwestern Medical Center, Dallas, Texas The team: this work
ESCMID Online Lecture Library. by author
 Novel PK/PD data on the optimisation of colistin and the carbapenems Diamantis Plachouras Athens, Greece Hot Topics on Infections in the Critically Ill Patient, ESCMID Postgraduate Education Course, 31
Novel PK/PD data on the optimisation of colistin and the carbapenems Diamantis Plachouras Athens, Greece Hot Topics on Infections in the Critically Ill Patient, ESCMID Postgraduate Education Course, 31
Paul Beringer,* Amir Aminimanizani,* Timothy Synold, and Christy Scott
 Therapeutic Drug Monitoring 24:315 321 2002 Lippincott Williams & Wilkins, Inc., Philadelphia Development of Population Pharmacokinetic Models and Optimal Sampling Times for Ibuprofen Tablet and Suspension
Therapeutic Drug Monitoring 24:315 321 2002 Lippincott Williams & Wilkins, Inc., Philadelphia Development of Population Pharmacokinetic Models and Optimal Sampling Times for Ibuprofen Tablet and Suspension
Ciprofloxacin pharmacokinetics in critically ill patients: a prospective cohort study *
 C H A P T E R 3 Ciprofloxacin pharmacokinetics in critically ill patients: a prospective cohort study * Introduction Since the mid-1980s fluoroquinolones have acquired a prominent position in the management
C H A P T E R 3 Ciprofloxacin pharmacokinetics in critically ill patients: a prospective cohort study * Introduction Since the mid-1980s fluoroquinolones have acquired a prominent position in the management
Principal Investigator: Marion, Alan, S, M.D., MDS Pharma Services (US) Inc., 621 Rose Street, PO Box 80837, Lincoln, NE 68502, USA
 SYNOPSIS Issue Date: 06 October 2008 Document No.: EDMS-PSDB-8954363:2. Name of Sponsor/Company Johnson & Johnson Pharmaceutical Research & Development, L.L.C. Name of Finished Product Name of Active Ingredient(s)
SYNOPSIS Issue Date: 06 October 2008 Document No.: EDMS-PSDB-8954363:2. Name of Sponsor/Company Johnson & Johnson Pharmaceutical Research & Development, L.L.C. Name of Finished Product Name of Active Ingredient(s)
Outline 8/2/2013. PK/PD PK/PD first-line drug กก PK/PD กก
 Pharmacokinetic and pharmacodynamic of anti- tuberculosis drugs Outline PK/PD PK/PD first-line drug กก PK/PD กก Concentration vs time in tissue and other body fluids Pharmacologic or toxicologic effect
Pharmacokinetic and pharmacodynamic of anti- tuberculosis drugs Outline PK/PD PK/PD first-line drug กก PK/PD กก Concentration vs time in tissue and other body fluids Pharmacologic or toxicologic effect
PD Targets for Various Infection Types: Stasis vs. 1-Log Kill vs. 2 Log Kill
 PD Targets for Various Infection Types: Stasis vs. 1-Log Kill vs. 2 Log Kill G.L. Drusano, M.D. Professor and Director Institute for Therapeutic Innovation University of Florida To have insight into appropriate
PD Targets for Various Infection Types: Stasis vs. 1-Log Kill vs. 2 Log Kill G.L. Drusano, M.D. Professor and Director Institute for Therapeutic Innovation University of Florida To have insight into appropriate
Nontraditional PharmD Program PRDO 7700 Pharmacokinetics Review Self-Assessment
 Nontraditional PharmD Program PRDO 7700 Pharmacokinetics Review Self-Assessment Please consider the following questions. If you do not feel confident about the material being covered, then it is recommended
Nontraditional PharmD Program PRDO 7700 Pharmacokinetics Review Self-Assessment Please consider the following questions. If you do not feel confident about the material being covered, then it is recommended
A Computer-based Pharmacokinetic Implementation for Digoxin Therapeutic Monitoring in Pediatric Patients
 CMU. J. Nat. Sci. (2012) Vol. 11(1) 77 A Computer-based Pharmacokinetic Implementation for Digoxin Therapeutic Monitoring in Pediatric Patients Yupaporn Preechagoon 1 and Peeraya Somsaard 2* 1 Department
CMU. J. Nat. Sci. (2012) Vol. 11(1) 77 A Computer-based Pharmacokinetic Implementation for Digoxin Therapeutic Monitoring in Pediatric Patients Yupaporn Preechagoon 1 and Peeraya Somsaard 2* 1 Department
Teicoplanin Dosing Strategy for Treatment of Staphylococcus aureus in Korean Patients with Neutropenic Fever
 Original Article DOI 10.3349/ymj.2011.52.4.616 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 52(4):616-623, 2011 Teicoplanin Dosing Strategy for Treatment of Staphylococcus aureus in Korean Patients
Original Article DOI 10.3349/ymj.2011.52.4.616 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 52(4):616-623, 2011 Teicoplanin Dosing Strategy for Treatment of Staphylococcus aureus in Korean Patients
Vancomycin Pharmacokinetics. Myrna Y. Munar, Pharm.D., BCPS Associate Professor of Pharmacy
 Vancomycin Pharmacokinetics Myrna Y. Munar, Pharm.D., BCPS Associate Professor of Pharmacy Goals Review the PK properties of vancomycin Compare and contrast methods of dosage regimen design for vancomycin
Vancomycin Pharmacokinetics Myrna Y. Munar, Pharm.D., BCPS Associate Professor of Pharmacy Goals Review the PK properties of vancomycin Compare and contrast methods of dosage regimen design for vancomycin
PHA5128 Dose Optimization II Case Study 3 Spring 2013
 Use the vancomycin dosing nomogram table below: A female patient, 57 years of age, 5 6 in height and 100 in weight had an infection requiring vancomycin treatment. Her serum creatinine was 0.8 mg/d. What
Use the vancomycin dosing nomogram table below: A female patient, 57 years of age, 5 6 in height and 100 in weight had an infection requiring vancomycin treatment. Her serum creatinine was 0.8 mg/d. What
Understand the physiological determinants of extent and rate of absorption
 Absorption and Half-Life Nick Holford Dept Pharmacology & Clinical Pharmacology University of Auckland, New Zealand Objectives Understand the physiological determinants of extent and rate of absorption
Absorption and Half-Life Nick Holford Dept Pharmacology & Clinical Pharmacology University of Auckland, New Zealand Objectives Understand the physiological determinants of extent and rate of absorption
INTRAVENOUS VANCOMYCIN PRESCRIBING AND MONITORING GUIDELINE FOR ADULT PATIENTS
 Title of guideline (must include the word Guideline (not protocol, policy, procedure etc) INTRAVENOUS VANCOMYCIN PRESCRIBING AND MONITORING GUIDELINE FOR ADULT PATIENTS Author: Contact Name and Job Title
Title of guideline (must include the word Guideline (not protocol, policy, procedure etc) INTRAVENOUS VANCOMYCIN PRESCRIBING AND MONITORING GUIDELINE FOR ADULT PATIENTS Author: Contact Name and Job Title
