NOT A PART OF THE MEDICAL RECORD
|
|
|
- Christian Goodman
- 5 years ago
- Views:
Transcription
1 ALLERGY ADMISSION/DISCHARGE CRITERIA EXCLUSION CRITERIA A. Pulmonary complications or 02 Sat < 90% on RA B. EKG changes C. Stridor INTERVENTIONS A. IV fluids B. IV Antihistamines C. Corticosteroids D. Cardiac Monitoring E. Respiratory Treatments F. Pulse Oximeter monitoring DISPOSITION 1. HOME A. Improvement in clinical condition B. Resolution or improvement in local skin irritations and/or pulmonary function 2. HOSPITAL A. Delayed reaction or reoccurrence B. Respiratory problems persistent wheezing with S.O.B. C. Inability to take po medications TIME FRAME 1. Up to 24 hours NOT A PART OF THE MEDICAL RECORD
2 Admission Orders DIAGNOSIS: ALLERGY 1. Admit to Emergency Department Observation Unit 2. Initial Emergency Department Physician: 3. Private Physician: Time Contacted: 4. Consult: 5. Condition: Stable Serious 6. Copies of Emergency Department H&P on chart 7. Allergies: 8. Routine Vital Signs 9. ST segment - continuous monitoring with pulse oximetry 10. Activity: up ad lib Other: 11. Diet: Clear liquid, advance as tolerated Regular Oral rehydration solution (pedialyte) Other: 12. IV Fluids: D5½NS + 20 meq KCl/1000ml at ml/hour NS at ml/hour Other: 13. Medications: Tylenol 1 gram po every 6 hours prn pain or fever > 101 Tylenol 10mg/kg oral/rectal every 6 hours prn fever > 101 Motrin 800 mg po every 6 hours prn pain Ultram 50 mg po every 6 hours prn pain Maalox 30 cc po every 4 hours prn indigestion Phenergan 25mg IV every 6 hours prn nausea/vomiting 12.5mg IV every 6 hours prn nausea/vomiting Solumedrol mg IV every 6 hours Benadryl mg IV every 6 hours Pepcid 20 mg IV every 12 hours Oxygen liter NC to keep POX over 94% Albuterol nebulizer one UD every 4 hours and prn 14. Re-evaluate for discharge every 3 hours 15. D/C with epi pen. Emergency Department Physician Signature Date/Time
3 ALLERGY PROGRESS NOTE Please date and sign each entry. DATE: TIME: PROTOCOL: ALLERGY RELEVANT HISTORY/PHYSICAL FINDINGS: OBSERVATION INTERVENTIONS: IV Hydration Serial Exams and Vital Signs Antihistamine Steroids Respiratory treatments PRN Cardiac/Pulse Ox monitoring GOALS OF OBSERVATION PERIOD: HOW OFTEN WILL PATIENT BE EVALUATED BY PHYSICIAN: MORNING PLAN PRIMARY PHYSICIAN CONTACTED: YES NAME: NO ATTENDING SIGNATURE / DATE
4 ALLERGY DISCHARGE NOTE DATE: TIME: PRESENTING COMPLAINT: OBSERVATION COURSE: IVF Antihistamines Nebulizer treatment Steroids Tolerating PO Pulse oximetry over 95% on room air PHYSICAL EXAM: FINAL DIAGNOSIS: DISPOSITION: Home Admission DISCHARGE INSTRUCTION GIVEN: Yes No ****D/C with Epi Pen PRIMARY PHYSICIAN CONTACTED: Yes No NAME: FOLLOW UP: ATTENDING SIGNATURE / DATE
5 ASTHMA I. Exclusion Criteria A. New EKG change (except sinus tachycardia) B. RR >40 C. Impending respiratory fatigue/failure D. Evidence of CHF E. Inability to perform spirometry F. ABG s (if obtained) 7.30 < ph > 7.50, p02 < 70, pc02 >45 G. Pulse oxymeter < 90% on room air H. Bronchospasm due to epiglottitis, aspiration, FB I. Temp > 101F II. OBS Interventions A. Serial exams including vital signs every 1-4 hours B. Pulse oximeter monitoring C. Supplement oxygen D. Repeat ABG s if indicated E. Hydration F. Steroids, bronchodilator G. Peak flow III. Disposition Criteria HOME A. Major resolution of SOB B. Resolution of accessory muscle usage C. Resolution of most wheezing HOSPITAL A. Deterioration of condition B. PEFR deterioration to < 20% expected C. RR >35 D. EKG abnormalities E. Pulse oxymeter < 90% on room air x 30 min. IV. Time Frame A hours for observation and treatment NOT A PART OF THE MEDICAL RECORD
6 Admission Orders DIAGNOSIS: ASTHMA 1. Admit to Emergency Department Observation Unit 2. Initial Emergency Department Physician: 3. Private Physician: Time Contacted: 4. Consult: 5. Condition: Stable Serious 6. Copies of Emergency Department H&P on chart 7. Allergies: 8. Routine Vital Signs 9. ST segment - continuous monitoring, continuous pulse oximetry 10. Activity: up ad lib Other: 11. Diet: Clear liquid, advance as tolerated Regular Oral rehydration solution (pedialyte) Other: 12. IV Fluids: D5½NS + 20 meq KCl/1000ml at ml/hour NS at ml/hour Other: 13. Medications: Tylenol 1 gram po every 6 hours prn pain or fever > 101 Tylenol 10mg/kg oral/rectal every 6 hours prn fever > 101 Motrin 800 mg po every 6 hours prn pain Ultram 50 mg po every 6 hours prn pain Maalox 30 cc po every 4 hours prn indigestion Phenergan 25mg IV every 6 hours prn nausea/vomiting 12.5mg IV every 6 hours prn nausea/vomiting Zofran 4mg IV every 4 hours prn nausea/vomiting 0.15mg/kg IV every 4 hours prn nausea/vomiting Rocephin 1 gram IV every 24 hours plus Zithromax 500mg IV every day Levaquin 500mg IV every 24 hours (only if allergic to cephalosporins) Solumedrol 80 mg IV q 8 hours Prednisone mg po q day Albuterol 1 ud q 3 hours and prn OR Albuterol ud q hours and prn Atrovent 1 ud q 6 hours and prn 14. Re-evaluate for discharge every 3 hours 15. Peak Flow before each treatment 16. Oxygen L NC or % VM to keep O2 sat above 94% Emergency Department Physician Signature Date/Time
7 ASTHMA PROGRESS NOTE Please date and sign each entry. DATE: TIME: PROTOCOL: ASTHMA RELEVANT HISTORY/PHYSICAL FINDINGS: OBSERVATION INTERVENTIONS: IV Hydration as indicated Serial Exams and Vital Signs Bronchodilators, Steroids Oxygen as needed Pulse Oximetry Repeat ABG s as indicated GOALS OF OBSERVATION PERIOD: HOW OFTEN WILL PATIENT BE EVALUATED BY PHYSICIAN: MORNING PLAN PRIMARY PHYSICIAN CONTACTED: YES NAME: NO ATTENDING SIGNATURE / DATE
8 ASTHMA DISCHARGE NOTE DATE: TIME: PRESENTING COMPLAINT: OBSERVATION COURSE: Serial Exams, Vital Signs, Pulse oximetry Bronchodilators Steroids IV Hydration Tolerating PO Peak Flow with improvement PHYSICAL EXAM: FINAL DIAGNOSIS: DISPOSITION: Home Admission DISCHARGE INSTRUCTION GIVEN: Yes No PRIMARY PHYSICIAN CONTACTED: Yes No NAME: FOLLOW UP: ATTENDING SIGNATURE / DATE
9 CHEST PAIN / RO MI ADMISSION/DISCHARGE CRITERIA ADMISSION CRITERIA 1. History of chest pain 2. Normal or unchanged ECG 3. Initial cardiac enzymes within normal range 4. Stable Vital Signs 5. No history of ACS EXCLUSION CRITERIA 1. ECG evidence of MI 2. High suspicion of MI 3. Unstable Vital Signs 4. Clear diagnosis of ACS by history 5. Prior history of ACS 6. Private attending chooses IP admission INTERVENTIONS 1. IV, oxygen, ECG, CXR 2. Cardiac monitoring 3. Aspirin 325 mg po if not contraindicated 4. Initial cardiac enzymes obtained in Emergency Department 5. Nitrates as needed for pain 6. Emergency Department attending speaks with PMD or Cardiologist (on call) INTERVENTIONS 1. IV, oxygen, ST-segment monitoring 2. Obtain stat 12 lead ECG for worsening pain 3. Contact ED attending for rhythm abnormalities or ST-segment changes 4. Add D-dimer to blood in lab 1. if positive, order CT scan of chest to R/O pulmonary embolus 5. Time 0 and 4 hours CK, troponin 6. If cardiac enzymes abnormal, admit to hospital 7. If cardiac enzymes negative, order appropriate stress test. DISPOSITION 1. HOME a. Stable VS b. Normal cardiac enzymes and D-dimer c. Unremarkable stress test d. No significant ECG changes 2. HOSPITAL a. Unstable VS b. Positive cardiac enzymes c. Abnormal CT scan d. ECG changes e. Significant stress test abnormality f. ED/PMD/CARD clinical discretion NOT A PART OF THE MEDICAL RECORD
10 Chest Pain/RO MI Admission Orders 1. Admit to Emergency Department Observation Unit 2. Initial Emergency Department Physician: 3. Private Physician: Time Contacted: 4. Consult: 5. Condition: Stable Serious Critical 6. Copies of Emergency Department H&P on chart 7. Allergies: 8. Routine Vital Signs 9. ST segment - continuous monitoring until cardiac enzymes completed 10. Activity: up ad lib Other: 11. Diet: Cardiac 1800 cal ADA NPO 3 hours before Stress Test Other: 12. IV Fluids: Saline Lock Other: 13. Oxygen: Nasal L/minute Other: 14. Medications: EC ASA 325 mg every am Tylenol 1 gram po every 6 hours prn pain or fever > 101 Motrin 800 mg po every 6 hours prn pain Ultram 50 mg po every 6 hours prn pain SL NTG 0.4 mg prn chest pain every 5 minutes x 3 Maalox 30 cc po every 4 hours prn indigestion Ambien 10 mg po every hs prn sleep 15. Testing Orders: CK and troponin at 0 and 4 hours from Emergency department arrival, results on flow sheet 12 Lead ECG at 0 and 4 hours from Emergency department arrival STAT 12 Lead ECG for monitor alert, chest pain Serum Pregnancy if indicated for nuclear imaging D-dimer Spiral CT scan of chest - if D-dimer positive 16. If all cardiac enzymes and ECGs within normal limits: Exercise Stress Test Adenosine Myoview Stress Dobutamine Myoview Stress Exercise Myoview Stress 17. Contact Emergency Department Physician for positive tests results, abnormal rhythm or ST segment changes. 18. Re-evaluate for discharge every 3 hours. Emergency Department Physician Signature Date
11 CHEST PAIN / RO MI PROGRESS NOTE Please date and sign each entry. DATE: TIME: PROTOCOL: CHEST PAIN / RO MI RELEVANT HISTORY/PHYSICAL FINDINGS: OBSERVATION INTERVENTIONS: 0 2 % Saturation Monitor Stress test Cardiac Monitor CT Scan if D-dimer positive Cardiac Enzymes GOALS OF OBSERVATION PERIOD: HOW OFTEN WILL PATIENT BE EVALUATED BY PHYSICIAN: MORNING PLAN PRIMARY PHYSICIAN CONTACTED: YES NAME: NO ATTENDING SIGNATURE / DATE
12 CHEST PAIN / RO MI DISCHARGE NOTE DATE: TIME: PRESENTING COMPLAINT: OBSERVATION COURSE: ECG 1 ECG 2 0 hour CK 4 hour CK 0 hour Troponin 4 hour Troponin Stress Test D-Dimer CT Scan Chest PHYSICAL EXAM: DIAGNOSIS: DISPOSITION: Home Admission DISCHARGE INSTRUCTION GIVEN: Yes No PRIMARY PHYSICIAN CONTACTED: Yes No NAME: FOLLOW UP: ATTENDING SIGNATURE / DATE
13 CHF ADMISSION/DISCHARGE CRITERIA ADMISSION CRITERIA 1. History of CHF 2. Normal or unchanged ECG 3. Initial cardiac enzymes within normal range 4. Stable Vital Signs 6. Elevated Serum Cr > < 500cc of urine output within 2 hrs of IV diuretic 8. BNP assay > 500 pg/ml EXCLUSION CRITERIA 1. ECG evidence of MI 2. High suspicion of MI 3. Unstable Vital Signs 4. Clear diagnosis of ACS by history 5. Mental status changes 6. Private attending chooses IP admission 7. Systolic BP less than 90 mmhg 8. Cardiogenic Shock 9. Evidence of low cardiac output syndrome INTERVENTIONS 1. IV, oxygen, ECG, CXR 2. Cardiac monitoring 3. Aspirin 325 mg po if not contraindicated 4. Initial cardiac enzymes obtained in Emergency Department 5. Nitrates as needed for pain 6. Emergency Department attending speaks with PMD or Cardiologist (on call) INTERVENTIONS 1. IV, oxygen, ST-segment monitoring 2. Obtain stat 12 lead ECG for worsening pain 3. Contact ED attending for rhythm abnormalities or ST-segment changes 4. Natrecor infusion for 15 hours, with repeat BNP 5. Time 0 and 4 hours CK, troponin, ECG 6. If cardiac enzymes abnormal, admit to hospital 7. If cardiac enzymes negative, order appropriate stress test. DISPOSITION 1. HOME a. Stable VS b. Normal cardiac enzymes c. Unremarkable stress test d. No significant ECG changes 2. HOSPITAL a. Unstable VS b. Positive cardiac enzymes d. ECG changes f. ED/PMD/CARD clinical discretion NOT A PART OF THE MEDICAL RECORD Houston Northwest Medical Center
14 CHF Admission Orders 1. Admit to Emergency Department Observation Unit 2. Initial Emergency Department Physician: 3. Private Physician: Time Contacted: 4. Consult: 5. Condition: Stable Serious 6. Copies of Emergency Department H&P on chart 7. Allergies: 8. Routine Vital Signs 9. ST segment - continuous monitoring until cardiac enzymes completed 10. Activity: up ad lib Other: 11. Diet: Cardiac 1800 cal ADA 1500 cc Fluid Restrict Other: 12. IV Fluids: Saline Lock Other: 13. Oxygen: Nasal L/minute Other: 14. Medications: EC ASA 325 mg every am Tylenol 1 gram po every 6 hours prn pain or fever > 101 Motrin 800 mg po every 6 hours prn pain Ultram 50 mg po every 6 hours prn pain SL NTG 0.4 mg prn chest pain every 5 minutes x 3 Maalox 30 cc po every 4 hours prn indigestion Ambien 10 mg po every hs prn sleep Lovenox 40 mg SQ every day 15. Cardiac Medications: Loop Diuretics Furosemide (Lasix) mg IV every 6 hours Torsemide (Demadix) mg IV every 12 hours ACE inhibitors Altace 2.5 mg po once daily Vasotec 2.5 mg po BID Angiotensin Receptor Blockers (ARB s) Cozaar 50 mg po BID Diovan 80 mg po BID Beta Blockers (continue only if chronic therapy over 2 weeks) Coreg mg po BID Toprol XL 25 mg po daily Emergency Department Physician Signature Date/Time
15 16. Testing Orders: CK and troponin at 0 and 4 hours from Emergency department arrival, results on flow sheet 12 Lead ECG at 0 and 4 hours from Emergency department arrival STAT 12 Lead ECG for monitor alert, chest pain BNP at 18 hours PT/INR, CMP, CBC in am 2D Echo with Doppler, % EF 17. Contact Emergency Department Physician for positive tests results, abnormal rhythm or ST segment changes. 18. Re-evaluate for discharge every 3 hours. 19. Smoking cessation instructions. Emergency Department Physician Signature Date/Time Yes SBP >90? No Yes Is Cr >1.8? No N Start Dopamine Start Natrecor Start Loop Diuretic Diuresis > 500 ml in 2 hours Diuresis > 500 ml in 2 hours Yes No Add Loop Diuretic at a lower dose Continue Loop Diuretic 3-4 x a day for >2000 ml / day Start Natrecor
16 Nesiritide (Natrecor ) Standing Orders Date: Time: Patient Weight: lbs kg Inclusion Criteria: (Check all that apply) Elevated Serum Cr > 1.8 < 500cc of urine output within 2 hrs IV diuretic BNP assay > 400 pg/ml Severe volume overload- risk of intubation 1. Hold Nitroglycerin (if active) immediately prior to Nesiritide (Natrecor ) Exclusion Criteria: (Check all that apply) Systolic BP less than 90 mmhg 2. Give Loop Diuretic IV Bolus Cardiogenic Shock (2x oral dose recommended) Evidence of low cardiac output syndrome Furosemide (Lasix ) mg IV push o Cold, clammy skin Bumetanide(Bumex ) mg IV push o Mental status changes Torsemide(Demedex ) mg IV push Bolus Volume and Infusion Flow Rate 3. Begin Nesiritide (Natrecor ) bolus of 1.5 mg in 250 ml = 6 mcg/ml concentration 1 mcg/kg over 1 min. 15 min. Bolus Volume (ml) 2 mcg/kg over 1 min. 15 min. For 1 mcg/kg: bolus = patient weight (kg) 6 No bolus For 2 mcg/kg: bolus = patient weight (kg) 3 NOTE: Bolus should be drawn from diluted 250 ml Infusion flow rate (ml/hr) bag, NEVER from the reconstituted vial For 0.01 mcg/kg/min (ml/hr) = patient weight (kg) 4. Begin Nesiritide infusion at 0.01 mcg/kg/min 10 Patient Weight (kg) Volume of Bolus (ml) 1 mcg/kg 2mcg/kg Infusion Rate (ml/hr) Check BP Q15 minutes x 1 hr following bolus, then 6. Check BP Q30 minutes x 1 hr, then 7. Check BP Q 1 hour x 2 hrs, then 8. Check BP Q 4 hours for duration of infusion hours prior to next infusion bag assess to determine need for continued therapy 10. For BP less than mmhg, call Doctor and decrease infusion by ½ (0.005 mcg/kg/min) Note: The bolus should be drawn from the diluted 250 ml bag and NEVER from the reconstituted vial. 11. For BP less than mmhg, call Doctor and D/C Nesiritide 12. Stop Nesiritide at 18 hours of infusion or Stop at hours/days of infusion Signature:
17 CHF PROGRESS NOTE Please date and sign each entry. DATE: TIME: PROTOCOL: CHF RELEVANT HISTORY/PHYSICAL FINDINGS: OBSERVATION INTERVENTIONS: 0 2 % Saturation Monitor Natrecor infusion Cardiac Monitor Cardiac Enzymes GOALS OF OBSERVATION PERIOD: HOW OFTEN WILL PATIENT BE EVALUATED BY PHYSICIAN: MORNING PLAN PRIMARY PHYSICIAN CONTACTED: YES NAME: NO ATTENDING SIGNATURE / DATE Houston Northwest Medical Center
18 CHF DISCHARGE NOTE DATE: TIME: PRESENTING COMPLAINT: OBSERVATION COURSE: ECG 1 ECG 2 0 hour CK 4 hour CK 0 hour Troponin 4 hour Troponin BNP 1 BNP 2 ECHO Natrecor PHYSICAL EXAM: DIAGNOSIS: DISPOSITION: Home Admission DISCHARGE INSTRUCTION GIVEN: Yes No PRIMARY PHYSICIAN CONTACTED: Yes No NAME: FOLLOW UP: ATTENDING SIGNATURE / DATE Houston Northwest Medical Center
19 SNAKEBITE--OBSERVATION GUIDELINES I. Exclusion Criteria A. Fever over 103 B. Need for Antivenom C. Unstable VS D. Need for fasciotomy E. Systemic disorder (Renal failure, D.M., Sickle cell disease, immunosuppression) II. OBS Interventions A. Serial exams including vital signs B. Analgesic C. Antipyretic D. Antiemetics E. IV hydration F. Antihistamine as needed III. Disposition HOME A. No expanding swelling or cellulitis B. Pain control C. No antivenom given D. Tolerate po medications HOSPITAL A. Expanding swelling or cellulitis B. Inability to control pain and N&V on po medications C. Need for antivenom or surgical management IV. Time frame A hours observation and treatment
20 SNAKE BITE Admission Orders 1. Admit to Emergency Department Observation Unit 2. Initial Emergency Department Physician: 3. Private Physician: Time Contacted: 4. Consult: 5. Condition: Stable Serious 6. Copies of Emergency Department H&P on chart 7. Allergies: 8. Routine Vital Signs Neurovascular checks every 2 hours/notify ER MD for rapid increase in swelling or pain 9. ST segment - continuous monitoring 10. Activity: up ad lib Other: 11. Diet: Clear liquid, advance as tolerated Regular Oral rehydration solution (pedialyte) 12. IV Fluids: D5½NS + 20 meq KCl/1000ml at ml/hour 13. Medications: NS at ml/hour Other: Tylenol 1 gram po every 6 hours prn pain or fever > 101 Tylenol 10mg/kg oral/rectal every 6 hours prn fever > 101 Motrin 800 mg po every 6 hours prn pain Ultram 50 mg po every 6 hours prn pain Maalox 30 cc po every 4 hours prn indigestion Phenergan Zofran 25mg IV every 6 hours prn nausea/vomiting 12.5mg IV every 6 hours prn nausea/vomiting 4mg IV every 4 hours prn nausea/vomiting 0.15mg/kg IV every 4 hours prn nausea/vomiting Rocephin 1 gram IV every 24 hours Levaquin 500mg IV every 24 hours (only if allergic to cephalosporins) Morphine Sulfate mg IV every 4 hours prn pain Stadol 1 mg IV every 4 hours prn pain Valium 10 mg po every 6 hours and PRN pain -hold if sedated. 14. Re-evaluate for discharge every 3 hours Other: Emergency Department Physician Signature Date/Time
21 SNAKE BITE PROGRESS NOTE Please date and sign each entry. DATE: TIME: PROTOCOL: SNAKE BITE RELEVANT HISTORY/PHYSICAL FINDINGS: OBSERVATION INTERVENTIONS: IV Hydration as indicated Serial Exams and Vital Signs Pain medications as needed Neurovascular Checks Antihistamines GOALS OF OBSERVATION PERIOD: HOW OFTEN WILL PATIENT BE EVALUATED BY PHYSICIAN: MORNING PLAN PRIMARY PHYSICIAN CONTACTED: YES NAME: NO ATTENDING SIGNATURE / DATE
22 SNAKE BITE DISCHARGE NOTE DATE: TIME: PRESENTING COMPLAINT: OBSERVATION COURSE: Serial Exams, Vital Signs, and Neurovascular Checks Pain Medications Antihistamines IV Hydration PHYSICAL EXAM: FINAL DIAGNOSIS: DISPOSITION: Home Admission DISCHARGE INSTRUCTION GIVEN: Yes No PRIMARY PHYSICIAN CONTACTED: Yes No NAME: FOLLOW UP: ATTENDING SIGNATURE / DATE
23 DRUG OVERDOSE ADMISSION/DISCHARGE CRITERIA EXCLUSION CRITERIA 1. Known ingestion of lethal material and amount 2. Unstable vital signs 3. Abnormal neurological exam including seizures, hallucinations, confusion, or narousable 4. Cardiac arrhythmias (significant) 5. Need for decontamination procedures (other than GI) 6. Body packer or stuffer 7. Ingestion of corrosives 8. Unstable respiratory status INTERVENTIONS 1. Serial exams including vital signs 2. Await toxicologic lab results (and repeat as indicated) 3. EKG monitoring 4. Pulse oximetry 5. Continued antidote administration up to 6 hours 6. Psychiatric consultation 7. Social Worker consultation DISPOSITION 1. HOME OR PSYCHIATRIC TRANSFER a. Return of non-toxic lab values b. No change in normal exam c. Stable vital signs d. Return to pre-ingestion PE 2. HOSPITAL a. Return of lethal or significantly toxic lab value b. Deterioration in neurologic function c. Cardiac instability d. Rule in exclusionary causes e. Respiratory instability f. Unstable vital signs TIME FRAME hour observation NOT A PART OF THE MEDICAL RECORD
24 Overdose Admission Orders 1. Admit to Emergency Department Observation Unit 2. Initial Emergency Department Physician: 3. Private Physician: Time Contacted: 4. Consult: 5. Condition: Stable Serious 6. Copies of Emergency Department H&P on chart 7. Allergies: 8. Routine Vital Signs 10. Activity: up ad lib Other: 11. Diet: Clear liquid, advance as tolerated Regular Other: 12. IV Fluids: D5½NS + 20 meq KCl/1000ml at ml/hour NS at ml/hour Other: 13. Oxygen: Nasal L/minute 14. Medications: Other: Tylenol 1 gram po every 6 hours prn pain or fever > 101 Motrin 800 mg po every 6 hours prn pain Ultram 50 mg po every 6 hours prn pain Maalox 30 cc po every 4 hours prn indigestion Phenergan Zofran 25mg IV every 6 hours prn nausea/vomiting 12.5mg IV every 6 hours prn nausea/vomiting 4mg IV every 4 hours prn nausea/vomiting 0.15mg IV every 4 hours prn nausea/vomiting 15. Re-evaluate for discharge every 3 hours Emergency Department Physician Signature Date/Time
25 DRUG OVERDOSE PROGRESS NOTE Please date and sign each entry. DATE: TIME: PROTOCOL: DRUG OVERDOSE RELEVANT HISTORY/PHYSICAL FINDINGS: OBSERVATION INTERVENTIONS: Serial Vital Signs Obtain & Review Tox Lab Results as indicated O 2 % Sat Monitor if indicated Antidote Administration EKG Monitor if indicated GOALS OF OBSERVATION PERIOD: HOW OFTEN WILL PATIENT BE EVALUATED BY PHYSICIAN: MORNING PLAN PRIMARY PHYSICIAN CONTACTED: YES NAME: NO ATTENDING SIGNATURE / DATE
26 DRUG OVERDOSE DISCHARGE NOTE DATE: TIME: PRESENTING COMPLAINT: OBSERVATION COURSE: IVF IV Antiemetics Tolerating PO Psychiatry consult Antidotes given PHYSICAL EXAM: FINAL DIAGNOSIS: DISPOSITION: Home Admission DISCHARGE INSTRUCTION GIVEN: Yes No PRIMARY PHYSICIAN CONTACTED: Yes No NAME: FOLLOW UP: ATTENDING SIGNATURE / DATE
27 MINOR HEAD INJURY ADMISSION/DISCHARGE CRITERIA EXCLUSION CRITERIA 1. Depressed LOC not due to alcohol, drugs or metabolic causes 2. Focal neurologic findings 3. Penetrating skull injuries 4. Depressed skull fractures 5. Positive CT scan 6. Signs of basilar skull fractures 7. Glasgow coma score < Age > Non ambulatory baseline + post trauma 10. Multiple medical problems, i.e., bleeding disorders, DM, Alzheimer s, Hemophilic 11. C spine injury 12. Respiratory instability INTERVENTIONS 1. Serial exams including vital signs 2. Serial neurologic exams 3. Analgesics DISPOSITION 1. HOME a. Normal serial exams b. No deterioration in clinical course 2. HOSPITAL a. Deterioration in clinical course b. Rule in of exclusionary causes or criteria TIME FRAME hour observation NOT A PART OF THE MEDICAL RECORD
28 Admission Orders DIAGNOSIS: Dehydration Flank Pain Minor Head Injury 1. Admit to Emergency Department Observation Unit 2. Initial Emergency Department Physician: 3. Private Physician: Time Contacted: 4. Consult: 5. Condition: Stable Serious 6. Copies of Emergency Department H&P on chart 7. Allergies: 8. Routine Vital Signs 9. ST segment - continuous monitoring 10. Activity: up ad lib Other: 11. Diet: Clear liquid, advance as tolerated Regular Oral rehydration solution (pedialyte) Other: 12. IV Fluids: D5½NS + 20 meq KCl/1000ml at ml/hour NS at ml/hour Other: 13. Medications: Tylenol 1 gram po every 6 hours prn pain or fever > 101 Tylenol 10mg/kg oral/rectal every 6 hours prn fever > 101 Motrin 800 mg po every 6 hours prn pain Ultram 50 mg po every 6 hours prn pain Maalox 30 cc po every 4 hours prn indigestion Phenergan 25mg IV every 6 hours prn nausea/vomiting 12.5mg IV every 6 hours prn nausea/vomiting Zofran 4mg IV every 4 hours prn nausea/vomiting 0.15mg/kg IV every 4 hours prn nausea/vomiting Rocephin 1 gram IV every 12 hours Levaquin 500mg IV every 24 hours (only if allergic to cephalosporins) Morphine Sulfate mg IV every 4 hours prn pain Stadol 1 mg IV every 4 hours prn pain 14. Re-evaluate for discharge every 3 hours Emergency Department Physician Signature Date/Time
29 MINOR HEAD INJURY PROGRESS NOTE Please date and sign each entry. DATE: TIME: PROTOCOL: MINOR HEAD INJURY RELEVANT HISTORY/PHYSICAL FINDINGS: OBSERVATION INTERVENTIONS: Serial Exam IVF and antiemetics as indicated Conusltations as needed GOALS OF OBSERVATION PERIOD: HOW OFTEN WILL PATIENT BE EVALUATED BY PHYSICIAN: MORNING PLAN PRIMARY PHYSICIAN CONTACTED: YES NAME: NO ATTENDING SIGNATURE / DATE
30 MINOR HEAD INJURY DISCHARGE NOTE DATE: TIME: PRESENTING COMPLAINT: OBSERVATION COURSE: IVF IV Antiemetics Tolerating PO Normal neurological exam Consultation with neuro/neurosurgery PHYSICAL EXAM: FINAL DIAGNOSIS: DISPOSITION: Home Admission DISCHARGE INSTRUCTION GIVEN: Yes No PRIMARY PHYSICIAN CONTACTED: Yes No NAME: FOLLOW UP: ATTENDING SIGNATURE / DATE
31 INTRACTABLE PAIN ADMISSION/DISCHARGE CRITERIA EXCLUSION CRITERIA 1. Fever over Obvious infection needing inpatient treatment 3. Sickle cell crisis 4. Chronic pain management 5. Systemic disorder (Renal failure, D.M., Sickle cell disease, immunosuppression) 6. Age over 65 INTERVENTIONS 1. Serial exams including vital signs 2. Analgesic 3. Muscle relaxant 4. Antiemetics 5. IV hydration DISPOSITION 1. HOME a. DX of acute pain b. Pain control c. No vomiting x 12 hours d. Tolerate p.o. medications 2. HOSPITAL a. DX of uncontrollable pain b. Inability to control pain and N&V on po medications c. Inability to tolerate po medications TIME FRAME hours observation and treatment NOT A PART OF THE MEDICAL RECORD
32 Admission Orders DIAGNOSIS: Dehydration Flank Pain Minor Head Injury Intractable Pain 1. Admit to Emergency Department Observation Unit 2. Initial Emergency Department Physician: 3. Private Physician: Time Contacted: 4. Consult: 5. Condition: Stable Serious 6. Copies of Emergency Department H&P on chart 7. Allergies: 8. Routine Vital Signs 9. ST segment - continuous monitoring 10. Activity: up ad lib Other: 11. Diet: Clear liquid, advance as tolerated Regular Oral rehydration solution (pedialyte) Other: 12. IV Fluids: D5½NS + 20 meq KCl/1000ml at ml/hour NS at ml/hour Other: 13. Medications: Tylenol 1 gram po every 6 hours prn pain or fever > 101 Tylenol 10mg/kg oral/rectal every 6 hours prn fever > 101 Motrin 800 mg po every 6 hours prn pain Ultram 50 mg po every 6 hours prn pain Maalox 30 cc po every 4 hours prn indigestion Phenergan 25mg IV every 6 hours prn nausea/vomiting 12.5mg IV every 6 hours prn nausea/vomiting Zofran 4mg IV every 4 hours prn nausea/vomiting 0.15mg/kg IV every 4 hours prn nausea/vomiting Rocephin 1 gram IV every 24 hours Levaquin 500mg IV every 24 hours (only if allergic to cephalosporins) Morphine Sulfate mg IV every 4 hours prn pain Stadol 1 mg IV every 4 hours prn pain Valium 10 mg po every 6 hours and PRN pain -hold if sedated. 14. Re-evaluate for discharge every 3 hours Emergency Department Physician Signature Date/Time
33 INTRACTABLE PAIN PROGRESS NOTE Please date and sign each entry. DATE: TIME: PROTOCOL: INTRACTABLE PAIN RELEVANT HISTORY/PHYSICAL FINDINGS: OBSERVATION INTERVENTIONS: IV Hydration as indicated Pain medications as needed Serial Exams and Vital Signs Antiemetic GOALS OF OBSERVATION PERIOD: HOW OFTEN WILL PATIENT BE EVALUATED BY PHYSICIAN: MORNING PLAN PRIMARY PHYSICIAN CONTACTED: YES NAME: NO ATTENDING SIGNATURE / DATE
34 INTRACTABLE PAIN DISCHARGE NOTE DATE: TIME: PRESENTING COMPLAINT: OBSERVATION COURSE: IVF IV Antiemetics Tolerating PO PHYSICAL EXAM: FINAL DIAGNOSIS: DISPOSITION: Home Admission DISCHARGE INSTRUCTION GIVEN: Yes No PRIMARY PHYSICIAN CONTACTED: Yes No NAME: FOLLOW UP: ATTENDING SIGNATURE / DATE
35 FLANK PAIN ADMISSION/DISCHARGE CRITERIA EXCLUSION CRITERIA 1. Fever over Obstruction and infection 3. Sepsis 4. Acute Peritonitis 5. Systemic disorder (Renal failure, D.M., Sickle cell disease, immunosuppression) 6. Age over 65 INTERVENTIONS 1. Serial exams including vital signs 2. Analgesic 3. Antipyretic 4. Antiemetics 5. IV hydration 6. Antimicrobial agents DISPOSITION 1. HOME a. DX of renal calculi b. Pain control c. DX of Pyelonephritis without vomiting x 12 hours d. Tolerate po medications 2. HOSPITAL a. DX of renal calculi with UTI b. Inability to control pain and N&V on po medications c. Pyelonephritis with inability to tolerate po medications TIME FRAME hours observation and treatment NOT A PART OF THE MEDICAL RECORD
36 Admission Orders DIAGNOSIS: Dehydration Flank Pain Minor Head Injury 1. Admit to Emergency Department Observation Unit 2. Initial Emergency Department Physician: 3. Private Physician: Time Contacted: 4. Consult: 5. Condition: Stable Serious 6. Copies of Emergency Department H&P on chart 7. Allergies: 8. Routine Vital Signs 9. ST segment - continuous monitoring 10. Activity: up ad lib Other: 11. Diet: Clear liquid, advance as tolerated Regular Oral rehydration solution (pedialyte) Other: 12. IV Fluids: D5½NS + 20 meq KCl/1000ml at ml/hour NS at ml/hour Other: 13. Medications: Tylenol 1 gram po every 6 hours prn pain or fever > 101 Tylenol 10mg/kg oral/rectal every 6 hours prn fever > 101 Motrin 800 mg po every 6 hours prn pain Ultram 50 mg po every 6 hours prn pain Maalox 30 cc po every 4 hours prn indigestion Phenergan 25mg IV every 6 hours prn nausea/vomiting 12.5mg IV every 6 hours prn nausea/vomiting Zofran 4mg IV every 4 hours prn nausea/vomiting 0.15mg/kg IV every 4 hours prn nausea/vomiting Rocephin 1 gram IV every 12 hours Levaquin 500mg IV every 24 hours (only if allergic to cephalosporins) Morphine Sulfate mg IV every 4 hours prn pain Stadol 1 mg IV every 4 hours prn pain 14. Re-evaluate for discharge every 3 hours Emergency Department Physician Signature Date/Time
37 FLANK PAIN PROGRESS NOTE Please date and sign each entry. DATE: TIME: PROTOCOL: FLANK PAIN RELEVANT HISTORY/PHYSICAL FINDINGS: OBSERVATION INTERVENTIONS: Serial Vital Signs Antiemetics and pain medications as needed IVP or CT Renal Scan for suspected kidney stone IVF for Hydration and IV Antibiotics as indicated GOALS OF OBSERVATION PERIOD: HOW OFTEN WILL PATIENT BE EVALUATED BY PHYSICIAN: MORNING PLAN PRIMARY PHYSICIAN CONTACTED: YES NAME: NO ATTENDING SIGNATURE / DATE
38 FLANK PAIN DISCHARGE NOTE DATE: TIME: PRESENTING COMPLAINT: OBSERVATION COURSE: IVF IV Antibiotics IV Pain control Tolerating PO PHYSICAL EXAM: FINAL DIAGNOSIS: DISPOSITION: Home Admission DISCHARGE INSTRUCTION GIVEN: Yes No PRIMARY PHYSICIAN CONTACTED: Yes No NAME: FOLLOW UP: ATTENDING SIGNATURE / DATE
39 VENOUS THROMBOLITIC DISEASE ADMISSION/DISCHARGE CRITERIA EXCLUSION CRITERIA 1. Documented new PE 2. Complicating illness: A fib; infiltrate; advanced age, CHF 3. Hypoxemia on room air (O 2 % SAT < 90%) 4. For DVT - Contraindications to LMWH a. LMWH Exclusions: 1) Suspicion for PE 2) Active risk of bleeding 3) Prior DVT or PE 4) Serious co-morbid condition 5) Patient compliance a problem 6) Iliac vein DVT 7) Not able to do home therapy INTERVENTIONS 1. Monitor VS 2. Monitor oxygen saturation 3. Monitor EKG 4. Initiate heparin/lmwh therapy if indicated 5. Obtain V/Q scan if indicated DISPOSITION: LESS THAN 24 HOURS 1. HOME a. No suspicion of PE and LMWH initiated b. VQ normal c. Home therapy arranged d. Follow up arranged 2. HOSPITAL a. VQ medium or high probability b. Need for angiogram NOT A PART OF THE MEDICAL RECORD
40 Venous Thrombolytic Disease Admission Orders 1. Admit to Emergency Department Observation Unit 2. Initial Emergency Department Physician: 3. Private Physician: Time Contacted: 4. Consult: 5. Condition: Stable Serious 6. Copies of Emergency Department H&P on chart 7. Allergies: 8. Routine Vital Signs 9. Activity: up ad lib Other: 10. Diet: Cardiac 1800 cal ADA Regular Other: 11. IV Fluids: Saline Lock Other: 12. Oxygen: Nasal L/minute Other: 13. Medications: Tylenol 1 gram po every 6 hours prn pain or fever > 101 Motrin 800 mg po every 6 hours prn pain Ultram 50 mg po every 6 hours prn pain Darvocet 1-2 po every 6 hours prn pain Maalox 30 cc po every 4 hours prn indigestion Ambien 10 mg po every hs prn sleep 14. STAT 12 Lead ECG for monitor alert, chest pain ST segment continuous monitor 15. RN to complete the DVT Discharge Assessment / Instructions form. 16. Re-evaluate for discharge every 3 hours Emergency Department Physician Signature Date/Time
41 VENOUS THROMBOEMBOLIC DISEASE PROGRESS NOTE Please date and sign each entry. DATE: TIME: PROTOCOL: VENOUS THROMBOEMBOLIC DISEASE / DVT RELEVANT HISTORY/PHYSICAL FINDINGS: OBSERVATION INTERVENTIONS: O 2 % Sat Monitor EKG Monitor V/Q Scan as indicated Start Coumadin Heparin / LMWH if indicated GOALS OF OBSERVATION PERIOD: HOW OFTEN WILL PATIENT BE EVALUATED BY PHYSICIAN: MORNING PLAN PRIMARY PHYSICIAN CONTACTED: YES NAME: NO ATTENDING SIGNATURE / DATE
42 VENOUS THROMBOLITIC DISEASE DISCHARGE NOTE DATE: TIME: PRESENTING COMPLAINT: OBSERVATION COURSE: V/Q Scan Start Coumadin 0 2 % Saturation Monitor Heparin/LMWH if indicated PHYSICAL EXAM: FINAL DIAGNOSIS: DISPOSITION: Home Admission DISCHARGE INSTRUCTION GIVEN: Yes No PRIMARY PHYSICIAN CONTACTED: Yes No NAME: FOLLOW UP: ATTENDING SIGNATURE / DATE
43 DVT DISCHARGE ASSESSMENT / INSTRUCTIONS RN Initials Explain to patient plan of care Patient Education: 1. View Videos - to view call ext and follow instructions a. #2350 Coumadin - English b. #2351 Coumadin - Spanish c. # 2353 Lovenox English - to be added d. # 2354 Lovenox Spanish - if available 2. Provide printed Information - to obtain call the Education Department Monday - Friday from 7:00am-4:30pm at ext. 1772; call House Supervisor after hours a. Deep Venous Thrombosis: Patient Handout -English or Spanish b. Coumadin Booklet - English or Spanish c. Lovenox Kit - English or Spanish Verify telephone number and address of patient. (Please hand write. Do not stamp.) Name Address Telephone number RN s evaluation of patient s ability to administer LMWH at home a. Willingness Y N b. Physical capability Y N c. Able to understand Y N d. Able to re-demonstrate Y N Family Support Name Relationship WT Kg (must weigh patient in ED.) Spo2 (O2 saturation) CBC, Platelets on chart UCG results if female Stool Guaiac negative Enoxaparin (Lovenox) dose (1mg/kg every 12 hrs-sq) Warfarin (Coumadin) dose (1 hour after Lovenox injection) Compression stockings size and apply appropriate length Fill out Patient Care Referral Form Notify Social Services or Case Management for Home Health referral Have patient identify pharmacy of choice (needs 4-5 day dose) - call in prescription to pharmacy Instruct the patient to call their primary care physician in the morning (Monday if discharged on the weekend) for a follow up visit and blood draw schedule. Discharge patient via wheelchair Discharge instructions given/potentially serious symptoms reviewed with patient/family questions answered. Register Nurse Signature Date/Time
44 DEHYDRATION ADMISSION/DISCHARGE CRITERIA EXCLUSION CRITERIA 1. Severe dehydration 2. (130 < Na >155 meq) 3. Pancreatitis, surgical abdomen, renal failure, GI bleed 4. Cardiac dysrhythmias (significant) 5. Age >70 years INTERVENTIONS 1. IV Hydration 2. Serial exams and vital signs 3. Antiemetic DISPOSITION 1. HOME a. Resolution of symptoms b. Stable vital signs c. Taking po fluids 2. HOSPITAL a. Inability to correct symptoms b. Inability to take po fluids TIME FRAME 1. Up to 24 hours NOT A PART OF THE MEDICAL RECORD
45 Admission Orders DIAGNOSIS: Dehydration Flank Pain Minor Head Injury 1. Admit to Emergency Department Observation Unit 2. Initial Emergency Department Physician: 3. Private Physician: Time Contacted: 4. Consult: 5. Condition: Stable Serious 6. Copies of Emergency Department H&P on chart 7. Allergies: 8. Routine Vital Signs 9. ST segment - continuous monitoring 10. Activity: up ad lib Other: 11. Diet: Clear liquid, advance as tolerated Regular Oral rehydration solution (pedialyte) Other: 12. IV Fluids: D5½NS + 20 meq KCl/1000ml at ml/hour NS at ml/hour Other: 13. Medications: Tylenol 1 gram po every 6 hours prn pain or fever > 101 Tylenol 10mg/kg oral/rectal every 6 hours prn fever > 101 Motrin 800 mg po every 6 hours prn pain Ultram 50 mg po every 6 hours prn pain Maalox 30 cc po every 4 hours prn indigestion Phenergan 25mg IV every 6 hours prn nausea/vomiting 12.5mg IV every 6 hours prn nausea/vomiting Zofran 4mg IV every 4 hours prn nausea/vomiting 0.15mg/kg IV every 4 hours prn nausea/vomiting Rocephin 1 gram IV every 12 hours Levaquin 500mg IV every 24 hours (only if allergic to cephalosporins) Morphine Sulfate mg IV every 4 hours prn pain Stadol 1 mg IV every 4 hours prn pain 14. Re-evaluate for discharge every 3 hours Emergency Department Physician Signature Date/Time
46 DEHYDRATION PROGRESS NOTE Please date and sign each entry. DATE: TIME: PROTOCOL: DEHYDRATION RELEVANT HISTORY/PHYSICAL FINDINGS: OBSERVATION INTERVENTIONS: IV Hydration Serial Exams and Vital Signs Antiemetic GOALS OF OBSERVATION PERIOD: HOW OFTEN WILL PATIENT BE EVALUATED BY PHYSICIAN: MORNING PLAN PRIMARY PHYSICIAN CONTACTED: YES NAME: NO ATTENDING SIGNATURE / DATE
47 DEHYDRATION DISCHARGE NOTE DATE: TIME: PRESENTING COMPLAINT: OBSERVATION COURSE: IVF IV Antiemetics Tolerating PO PHYSICAL EXAM: FINAL DIAGNOSIS: DISPOSITION: Home Admission DISCHARGE INSTRUCTION GIVEN: Yes No PRIMARY PHYSICIAN CONTACTED: Yes No NAME: FOLLOW UP: ATTENDING SIGNATURE / DATE
OBSERVATION UNIT ASTHMA PATHWAY OUTLINE Westmoreland Hospital PAGE 1 OF 5
 PAGE 1 OF 5 Exclusion Criteria: (Reason to admit to hospital) A. New EKG changes except sinus tachycardia B. Respiratory Rate > 40 C. Signs/symptoms of Heart Failure D. Impending respiratory failure or
PAGE 1 OF 5 Exclusion Criteria: (Reason to admit to hospital) A. New EKG changes except sinus tachycardia B. Respiratory Rate > 40 C. Signs/symptoms of Heart Failure D. Impending respiratory failure or
* * FORM REV. 02/2019 Page 1 of 4. TNKASE (tenecteplase) / ACUTE STEMI ORDERS SCHEDULED MEDICATIONS:
 1. Is this a CMS inpatient only procedure? Yes, admit as inpatient, proceed to # 3 No, proceed to # 2 2. Do you expect that the patient s condition will require a hospital stay that will cross two midnights
1. Is this a CMS inpatient only procedure? Yes, admit as inpatient, proceed to # 3 No, proceed to # 2 2. Do you expect that the patient s condition will require a hospital stay that will cross two midnights
Level 1: Acute CHF with Hypotension (SBP < 90 torr)
 PENNSYLVANIA HOSPITAL ED ACUTE CONGESTIVE HEART FAILURE STANDING DERS Level 1: Acute CHF with Hypotension (SBP < 90 torr) Intake: Vital signs Pulse oximetry Weight Allergies: Obtain old chart Obtain old
PENNSYLVANIA HOSPITAL ED ACUTE CONGESTIVE HEART FAILURE STANDING DERS Level 1: Acute CHF with Hypotension (SBP < 90 torr) Intake: Vital signs Pulse oximetry Weight Allergies: Obtain old chart Obtain old
Standardized Nurse Activated Protocols (SNAPs)
 SNAPs by presenting complaint/problem help nurses initiate care before the patient is seen by a physician. SNAPs should be approved by ED team consensus If patient unstable in any way, immediately notify
SNAPs by presenting complaint/problem help nurses initiate care before the patient is seen by a physician. SNAPs should be approved by ED team consensus If patient unstable in any way, immediately notify
IDPH ESF-8 Plan: Pediatric and Neonatal Surge Annex Sample Pediatric Admission Orders 2015
 Purpose: To provide guidance to practitioners caring for pediatric patients who need inpatient hospital care during a disaster. Disclaimer: This guideline is not meant to be all inclusive, replace an existing
Purpose: To provide guidance to practitioners caring for pediatric patients who need inpatient hospital care during a disaster. Disclaimer: This guideline is not meant to be all inclusive, replace an existing
Admit date (YYYY/MM/DD): Cardiologist On-Call: Diagnosis: Lab Tests. CBC, Electrolytes, Urea, Creatinine, Glucose, INR, PTT, Urinalysis
 of nurse 1. Admit under ward Attending Physician: Dr. Admit date (YYYY/MM/DD): Cardiologist On-Call: Diagnosis: Lab Tests 2. On admission (if not already performed in Emergency Department or in Coronary
of nurse 1. Admit under ward Attending Physician: Dr. Admit date (YYYY/MM/DD): Cardiologist On-Call: Diagnosis: Lab Tests 2. On admission (if not already performed in Emergency Department or in Coronary
Physician s Order Form. Physician s Order Form. Telemetry/Progressive Care Orders. Continued on next page. >>>>>>> Continued on next page.
 DATE: TIME: DATE TIME INTRAVENOS FLID and MEDICATION Status: Admit to Telemetry Admit to Progressive Care nit Transfer to Progressive Care nit Note: Discontinue Previous Orders Transfer to Telemetry nit
DATE: TIME: DATE TIME INTRAVENOS FLID and MEDICATION Status: Admit to Telemetry Admit to Progressive Care nit Transfer to Progressive Care nit Note: Discontinue Previous Orders Transfer to Telemetry nit
DOWNTIME Physician Order CARD CHF Heart Failure
 DOWNTIME Physician Clinical Category ADT/Comm unication Patient Status ASC Extended Recovery Observation Services Inpatient Admission CCU Admit as Inpatient History and Physical by House Physician Vital
DOWNTIME Physician Clinical Category ADT/Comm unication Patient Status ASC Extended Recovery Observation Services Inpatient Admission CCU Admit as Inpatient History and Physical by House Physician Vital
PHYSICIAN SIGNATURE DATE TIME DRUG ALLERGIES WT: KG
 Available at ALL facilities Non Categorized SUB ED Chest Pain: STEMI Protocol(SUB)* SUB ED Chest Pain: STEMI Protocol Lab Orders(SUB)* ED Rainbow Tubes(SUB)* ***Reminder: Order ED Rainbow Tubes (SUB) as
Available at ALL facilities Non Categorized SUB ED Chest Pain: STEMI Protocol(SUB)* SUB ED Chest Pain: STEMI Protocol Lab Orders(SUB)* ED Rainbow Tubes(SUB)* ***Reminder: Order ED Rainbow Tubes (SUB) as
DRUG ALLERGIES WT: KG
 DRUG AND TREATMENT Available at: BMC-B BMC-D BMC-N BMC-S Vital Signs Vital Signs Q4H (DEF)* Q2H Q1H Vital Signs Orthostatic Activity Activity Bedrest, for 12 hours then Up ad lib (DEF)* Bedrest, for 24
DRUG AND TREATMENT Available at: BMC-B BMC-D BMC-N BMC-S Vital Signs Vital Signs Q4H (DEF)* Q2H Q1H Vital Signs Orthostatic Activity Activity Bedrest, for 12 hours then Up ad lib (DEF)* Bedrest, for 24
ADULT POST NEUROLOGIC INTERVENTION ORDERS 2 of 4
 9 Actual 9 Estimated DOWNTIME INTERVENTION 1 of 4 Weight kg 9 Actual 9 Estimated Height cm ALLERGIES: REFER TO ALLERGY PROFILE/ POWERCHART Admit to Dr.: Bed Type: Dx: ( ) Check, circle and/or fill in all
9 Actual 9 Estimated DOWNTIME INTERVENTION 1 of 4 Weight kg 9 Actual 9 Estimated Height cm ALLERGIES: REFER TO ALLERGY PROFILE/ POWERCHART Admit to Dr.: Bed Type: Dx: ( ) Check, circle and/or fill in all
PHYSICIAN SIGNATURE DATE TIME DRUG ALLERGIES WT: KG
 DRUG AND TREATMENT Available ONLY at: BMC-B BMC-D BMC-N BMC-S Nursing Orders Communication Order If CVP unavailable, administer fluid boluses every 30 minutes except monitor O2 requirements Comments: Every
DRUG AND TREATMENT Available ONLY at: BMC-B BMC-D BMC-N BMC-S Nursing Orders Communication Order If CVP unavailable, administer fluid boluses every 30 minutes except monitor O2 requirements Comments: Every
Myocardial Infarction Order Set
 Myocardial Infarcti Order Set Date Time 1. [ ] Inpatient: [ ] CCU [ ] PCU [ ] ICU 2. Diagnosis: Admit to: Dr. 3. Code Status: [ ] See Completed Code Sheet * ote: o Code verbal order may ly be taken in
Myocardial Infarcti Order Set Date Time 1. [ ] Inpatient: [ ] CCU [ ] PCU [ ] ICU 2. Diagnosis: Admit to: Dr. 3. Code Status: [ ] See Completed Code Sheet * ote: o Code verbal order may ly be taken in
Physician Orders ADULT: Acute MI/Acute Coronary Syndrome Adult Plan
 Initiate Orders Phase Care Sets/Protocols/PowerPlans Initiate Powerplan Phase Phase: Acute MI/Acute Coronary Syndrome Adult Phase, When to Initiate: Acute MI/Acute Coronary Syndrome Adlt Phase Non Categorized
Initiate Orders Phase Care Sets/Protocols/PowerPlans Initiate Powerplan Phase Phase: Acute MI/Acute Coronary Syndrome Adult Phase, When to Initiate: Acute MI/Acute Coronary Syndrome Adlt Phase Non Categorized
Asthma Care in the Emergency Department Clinical Practice Guideline
 Asthma Care in the Emergency Department Clinical Practice Guideline Inclusion: 1) Children 2 years of age or older with a prior history of wheezing, and 2) Children less than 2 years of age with likely
Asthma Care in the Emergency Department Clinical Practice Guideline Inclusion: 1) Children 2 years of age or older with a prior history of wheezing, and 2) Children less than 2 years of age with likely
ADULT TRANSCATHETER AORTIC VALVE REPLACEMENT (TAVR) TELEMETRY BED TRANSFER ORDERS 1 of 4
 TELEMETRY BED TRANSFER 1 of 4 9 Actual 9 Estimated Patient ID Area Weight kg 9 Actual 9 Estimated Height cm ALLERGIES: REFER TO ALLERGY PROFILE/ POWERCHART Transfer to: 10 South Attending Physician: Diagnosis:
TELEMETRY BED TRANSFER 1 of 4 9 Actual 9 Estimated Patient ID Area Weight kg 9 Actual 9 Estimated Height cm ALLERGIES: REFER TO ALLERGY PROFILE/ POWERCHART Transfer to: 10 South Attending Physician: Diagnosis:
Diagnosis: Allergies:
 Patient Name: Diagnosis: Allergies: ICU Sepsis Version 5 1/11/17 This order set must be used with an admission order set if patient not already admitted. Nursing Orders Verify that cultures have been obtained
Patient Name: Diagnosis: Allergies: ICU Sepsis Version 5 1/11/17 This order set must be used with an admission order set if patient not already admitted. Nursing Orders Verify that cultures have been obtained
Respiratory. Section Contents. Dyspnea Practice Guide. Pneumonia Practice Guide. Adult Asthma/Acute Bronchitis Practice Guide. Allergy Practice Guide
 Respiratory Section Contents Dyspnea Practice Guide Pneumonia Practice Guide Adult Asthma/Acute Bronchitis Practice Guide Allergy Practice Guide When using any Practice Guide, always follow the Guidelines
Respiratory Section Contents Dyspnea Practice Guide Pneumonia Practice Guide Adult Asthma/Acute Bronchitis Practice Guide Allergy Practice Guide When using any Practice Guide, always follow the Guidelines
ALL orders are active unless: 1. Order is manually lined through to inactivate 2. Orders with check boxes ( ) are unchecked DRUG AND TREATMENT ORDERS
 DRUG AND TREATMENT Available at: BMC-B BMC-D BMC-N BMC-S Vital Signs Vital Signs Q4H (DEF)* Q2H Q1H Vital Signs Orthostatic Activity Activity Bedrest, for 12 hours then Up ad lib (DEF)* Bedrest, for 24
DRUG AND TREATMENT Available at: BMC-B BMC-D BMC-N BMC-S Vital Signs Vital Signs Q4H (DEF)* Q2H Q1H Vital Signs Orthostatic Activity Activity Bedrest, for 12 hours then Up ad lib (DEF)* Bedrest, for 24
CHEST PAIN CDU INCLUSION CRITERIA
 CHEST PAIN CDU INCLUSION CRITERIA No clinical criteria for ACS Stable vital signs Initial ECG and cardiac biomarkers not consistent with ACS Low to intermediate ACS risk (HEART score 0-6) [Ref 1, 2] Plan
CHEST PAIN CDU INCLUSION CRITERIA No clinical criteria for ACS Stable vital signs Initial ECG and cardiac biomarkers not consistent with ACS Low to intermediate ACS risk (HEART score 0-6) [Ref 1, 2] Plan
PHYSICIAN S ORDERS Page 1 of 5 PNEUMONIA. Resuscitation (Code)Status: Admit to: Diagnosis: Pneumonia Other: Consult:
 Inpatient Observation Bed Type: Med/Surg PHYSICIAN S ORDERS Page 1 of 5 Satellite Telemetry Telemetry ICU Resuscitation (Code)Status: Admit to: Diagnosis: Pneumonia Other: Consult: Condition: Stable Guarded
Inpatient Observation Bed Type: Med/Surg PHYSICIAN S ORDERS Page 1 of 5 Satellite Telemetry Telemetry ICU Resuscitation (Code)Status: Admit to: Diagnosis: Pneumonia Other: Consult: Condition: Stable Guarded
(Page 1 of 5) Diagnosis: Procedure: Right Total Knee Replacement Unicompartmental Knee Left Total Hip Revision Total Shoulder
 (Page 1 of 5) Allergies/Sensitivities/Reactions: Height: Inches cm Weight: Kg Pounds = Automatic = Physician s option, Check off to Order Diagnosis: Procedure: Right Total Knee Replacement Unicompartmental
(Page 1 of 5) Allergies/Sensitivities/Reactions: Height: Inches cm Weight: Kg Pounds = Automatic = Physician s option, Check off to Order Diagnosis: Procedure: Right Total Knee Replacement Unicompartmental
STANDARDIZED PROCEDURE CARDIAC STRESS TESTING-EXERCISE TESTING (Adult, Peds)
 I. Definition: During the exercise test, the patient exercises on a bike or treadmill while being monitored with a 12 lead ECG, blood pressure device, pulse oximetry and, if requested, oxygen consumption,
I. Definition: During the exercise test, the patient exercises on a bike or treadmill while being monitored with a 12 lead ECG, blood pressure device, pulse oximetry and, if requested, oxygen consumption,
Canadian Stroke Best Practices Initial ED Evaluation of Acute Stroke and Transient Ischemic Attack (TIA) Order Set (Order Set 1)
 Canadian Best Practice Recommendations for Stroke Care: All patients presenting to an emergency department with suspected stroke or transient ischemic attack must have an immediate clinical evaluation
Canadian Best Practice Recommendations for Stroke Care: All patients presenting to an emergency department with suspected stroke or transient ischemic attack must have an immediate clinical evaluation
PHYSICIAN SIGNATURE DATE TIME DRUG ALLERGIES WT: KG
 DRUG AND TREATMENT Available at: ALL Adult Facilities Non Categorized SUB ED Abdominal Pain Protocol(SUB)* ***The above subphase is available at the end of the plan*** SUB ED Abdominal Pain Protocol Lab
DRUG AND TREATMENT Available at: ALL Adult Facilities Non Categorized SUB ED Abdominal Pain Protocol(SUB)* ***The above subphase is available at the end of the plan*** SUB ED Abdominal Pain Protocol Lab
ST Elevation Myocardial Infarction (STEMI) Reperfusion Order Set
 Form Title Form Number CH-0454 2018, Alberta Health Services, CKCM This work is licensed under the Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License. The license does not
Form Title Form Number CH-0454 2018, Alberta Health Services, CKCM This work is licensed under the Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License. The license does not
Emergency Department Chest Pain, Suspected Cardiac Adult Order Set
 Form Title Form Number Chest Pain, Suspected Cardiac Adult Order Set 20746 2018, Alberta Health Services, CKCM This work is licensed under the Creative Commons Attribution-NonCommercial-NoDerivatives 4.0
Form Title Form Number Chest Pain, Suspected Cardiac Adult Order Set 20746 2018, Alberta Health Services, CKCM This work is licensed under the Creative Commons Attribution-NonCommercial-NoDerivatives 4.0
ST. DOMINIC-JACKSON MEMORIAL HOSPITAL JACKSON, MISSISSIPPI
 Date & Time TAVR Pre-Op Admission Clinical Pathway Page 1 of 3 1. Admit as INPATIENT to Dr.. For Surgery Today or Tomorrow 3. Diagnosis: 4. Allergies: Pharmacy Mnemonic: PRETAVR 5. Vital signs on arrival.
Date & Time TAVR Pre-Op Admission Clinical Pathway Page 1 of 3 1. Admit as INPATIENT to Dr.. For Surgery Today or Tomorrow 3. Diagnosis: 4. Allergies: Pharmacy Mnemonic: PRETAVR 5. Vital signs on arrival.
Angina Luis Tulloch, MD 03/27/2012
 Angina Luis Tulloch, MD 03/27/2012 Acute coronary syndromes ACS STE > 1 mm, new LBBB* Increased cardiac enzymes STEMI Yes Yes NSTEMI No Yes UA No No *Recognize Wellen s sign/syndrome, posterior wall MI,
Angina Luis Tulloch, MD 03/27/2012 Acute coronary syndromes ACS STE > 1 mm, new LBBB* Increased cardiac enzymes STEMI Yes Yes NSTEMI No Yes UA No No *Recognize Wellen s sign/syndrome, posterior wall MI,
Evaluation and Management of Acute Decompensated Heart Failure (HF) with Reduced Ejection Fraction Systolic Heart Failure (HFrEF)(EF<40%
 Evaluation and Management of Acute Decompensated Heart Failure (HF) with Reduced Ejection Fraction Systolic Heart Failure (HFrEF)(EF
Evaluation and Management of Acute Decompensated Heart Failure (HF) with Reduced Ejection Fraction Systolic Heart Failure (HFrEF)(EF
Acute Stroke with Alteplase Administration Order Set
 Review Due Date: 2017 October PATIENT CARE DERS Weight: Adverse Reactions or Intolerances Drug No Yes (list) Food No Yes (list) _ Latex No Yes Admission Admit to Neurology service: Dr. Critical Care Diagnosis:
Review Due Date: 2017 October PATIENT CARE DERS Weight: Adverse Reactions or Intolerances Drug No Yes (list) Food No Yes (list) _ Latex No Yes Admission Admit to Neurology service: Dr. Critical Care Diagnosis:
Pulmonary Embolism Pathway
 Pulmonary Embolism Pathway Ambulatory Care Pathway Dr. A. Zafar, Dr. A. Rehman, Dr. T. Malik September, 2011. Patient Identification Label Pulmonary Embolism Pathway Clinical History Comments Hospital
Pulmonary Embolism Pathway Ambulatory Care Pathway Dr. A. Zafar, Dr. A. Rehman, Dr. T. Malik September, 2011. Patient Identification Label Pulmonary Embolism Pathway Clinical History Comments Hospital
SCVMC RESPIRATORY CARE PROCEDURE
 Page 1 of 8 Rev. - 11/99, 11/05, 4/11 R-NC - 08/99,08/00, 04/03,10/08,04/09, 07/11, 6/12 B7180-43 OBJECTIVE Continuous Nebulization allows for continuous, controlled drug delivery to the lung, avoiding
Page 1 of 8 Rev. - 11/99, 11/05, 4/11 R-NC - 08/99,08/00, 04/03,10/08,04/09, 07/11, 6/12 B7180-43 OBJECTIVE Continuous Nebulization allows for continuous, controlled drug delivery to the lung, avoiding
IR Central Venous Access [ ] Pre Procedure
![IR Central Venous Access [ ] Pre Procedure IR Central Venous Access [ ] Pre Procedure](/thumbs/90/104119758.jpg) IR Central Venous Access [1050200001] Pre Procedure Case Request/Scheduling Procedure Enter IR Case Request if not already completed (All hospitals except Grant Medical Center) [ ] Case Request IR Lab
IR Central Venous Access [1050200001] Pre Procedure Case Request/Scheduling Procedure Enter IR Case Request if not already completed (All hospitals except Grant Medical Center) [ ] Case Request IR Lab
Bariatric Surgery Post Op Day Version 2 Approved 11/13/2017
 Patient Name: Diagnosis: Allergies with reaction type: Bariatric Surgery Post Op Day Version 2 Approved 11/13/2017 Diagnosis Preferred Location/Unit Surgical ICU Code Status: Full Code Activity Ambulate
Patient Name: Diagnosis: Allergies with reaction type: Bariatric Surgery Post Op Day Version 2 Approved 11/13/2017 Diagnosis Preferred Location/Unit Surgical ICU Code Status: Full Code Activity Ambulate
STANDARDIZED PROCEDURE CARDIAC STRESS TESTING-DOBUTAMINE INFUSION (Adult)
 I. Definition: This test is performed to evaluate for cardiac ischemia, arrhythmias, and/or response to exercise. II. Background Information A. Setting: The setting (inpatient vs outpatient) and population
I. Definition: This test is performed to evaluate for cardiac ischemia, arrhythmias, and/or response to exercise. II. Background Information A. Setting: The setting (inpatient vs outpatient) and population
Routine Patient Care Guidelines - Adult
 Routine Patient Care Guidelines - Adult All levels of provider will complete an initial & focused assessment on every patient, and as standing order, use necessary and appropriate skills and procedures
Routine Patient Care Guidelines - Adult All levels of provider will complete an initial & focused assessment on every patient, and as standing order, use necessary and appropriate skills and procedures
EMS Region Medication List 2010
 EMT-B MEDICATIONS Patient Assisted Medications (PAM) and Ambulance Stock Medications Medication Protocol/Use Dose Auto-injector (Epi-pen) Glucose (Oral) Metered-Dose Inhaler (MDI) Allergic/Anaphylactic
EMT-B MEDICATIONS Patient Assisted Medications (PAM) and Ambulance Stock Medications Medication Protocol/Use Dose Auto-injector (Epi-pen) Glucose (Oral) Metered-Dose Inhaler (MDI) Allergic/Anaphylactic
Physician Orders ADULT Order Set: Respiratory Failure Orders
 [R] = will be ordered Height: cm Weight: kg Allergies: [ ] No known allergies [ ]Medication allergy(s): [ ] Latex allergy [ ]Other: Admission/Transfer/Discharge [ ] Patient Status Initial Inpatient Attending
[R] = will be ordered Height: cm Weight: kg Allergies: [ ] No known allergies [ ]Medication allergy(s): [ ] Latex allergy [ ]Other: Admission/Transfer/Discharge [ ] Patient Status Initial Inpatient Attending
Davis s Drug Guide Scavenger Hunt 15 th Edition
 Davis s Drug Guide Scavenger Hunt 15 th Edition This handout is designed to assist you in locating information in the Davis s Drug Guide. Take advantage of the many resources in this text!! Locate the
Davis s Drug Guide Scavenger Hunt 15 th Edition This handout is designed to assist you in locating information in the Davis s Drug Guide. Take advantage of the many resources in this text!! Locate the
Family Centered Pediatric Emergency Department Sickle Cell Assessment of Needs and Strengths (FC-Peds-ED-SCANS) Overall Algorithm
 Family Centered Pediatric Emergency Department Sickle Cell Assessment of Needs and Strengths (FC-Peds-ED-SCANS) Overall Algorithm Decision 1: Triage Decision 2: Analgesic Management Decision 3: Diagnostic
Family Centered Pediatric Emergency Department Sickle Cell Assessment of Needs and Strengths (FC-Peds-ED-SCANS) Overall Algorithm Decision 1: Triage Decision 2: Analgesic Management Decision 3: Diagnostic
Resuscitation Patient Management Tool May 2015 MET Event
 OPTIONAL: Local Event ID: Date/Time MET was activated: Time Not Documented MET 2.1 Pre-Event Pre-Event Tab Was patient discharged from an Intensive Care Unit (ICU) at any point during this admission and
OPTIONAL: Local Event ID: Date/Time MET was activated: Time Not Documented MET 2.1 Pre-Event Pre-Event Tab Was patient discharged from an Intensive Care Unit (ICU) at any point during this admission and
CBC with Differential. PHYSICIAN SIGNATURE DATE TIME DRUG ALLERGIES WT: KG
 DRUG AND TREATMENT Non Categorized SUB ED Snakebite Protocol (SUB)* Non Categorized ***(NOTE)*** This plan is designed to be used as part of a larger plan, not independently. Please do NOT order individually.
DRUG AND TREATMENT Non Categorized SUB ED Snakebite Protocol (SUB)* Non Categorized ***(NOTE)*** This plan is designed to be used as part of a larger plan, not independently. Please do NOT order individually.
DYSRHYTHMIAS. D. Assess whether or not it is the arrhythmia that is making the patient unstable or symptomatic
 DYSRHYTHMIAS GENERAL CONSIDERATIONS A. The 2015 American Heart Association Guidelines were referred to for this protocol development. Evidence-based science was implemented in those areas where the AHA
DYSRHYTHMIAS GENERAL CONSIDERATIONS A. The 2015 American Heart Association Guidelines were referred to for this protocol development. Evidence-based science was implemented in those areas where the AHA
CONGESTIVE HEART FAILURE ORDER SET. Check appropriate boxes: Admit to unit to Dr. l Inpatient l Observation l Telemetry.
 CONGESTIVE HEART FAILURE ER SET Check appropriate boxes: Admit to unit to Dr. l Inpatient l Observation l Telemetry Diagnosis: Consult Dr. Reason: l I have called Dr., add to his/her list. Diet: l NPO
CONGESTIVE HEART FAILURE ER SET Check appropriate boxes: Admit to unit to Dr. l Inpatient l Observation l Telemetry Diagnosis: Consult Dr. Reason: l I have called Dr., add to his/her list. Diet: l NPO
Physician Orders ADULT: Asthma and Bronchitis Plan
 Initiate Orders Phase Care Sets/Protocols/PowerPlans Initiate Powerplan Phase, Phase: Asthma and Bronchitis Phase, When to Initiate: Asthma and Bronchitis Phase Non Categorized Problem: Asthma Problem:
Initiate Orders Phase Care Sets/Protocols/PowerPlans Initiate Powerplan Phase, Phase: Asthma and Bronchitis Phase, When to Initiate: Asthma and Bronchitis Phase Non Categorized Problem: Asthma Problem:
Hospital of Central Connecticut ED Observation Unit Protocols
 Appendix 3 Hospital of Central Connecticut ED Observation Unit Protocols Abdominal Pain... 2 Allergic Reaction... 4 Asthma/COPD... 5 Back Pain... 7 Cellulitis... 9 Chest Pain... 11 Confusion... 13 Dehydration...
Appendix 3 Hospital of Central Connecticut ED Observation Unit Protocols Abdominal Pain... 2 Allergic Reaction... 4 Asthma/COPD... 5 Back Pain... 7 Cellulitis... 9 Chest Pain... 11 Confusion... 13 Dehydration...
Algorithm Focus. Emergency Cardiovascular Care: EMT-Intermediate Treatment Algorithms. Perspective regarding the EMT- Intermediate algorithms
 Emergency Cardiovascular Care: EMT-Intermediate Treatment Algorithms Algorithms for the Conscious Patient Prehospital Medication Profiles Algorithm Focus Bradycardia Acute Pulmonary Edema and Shock Hypothermia
Emergency Cardiovascular Care: EMT-Intermediate Treatment Algorithms Algorithms for the Conscious Patient Prehospital Medication Profiles Algorithm Focus Bradycardia Acute Pulmonary Edema and Shock Hypothermia
ALL orders are active unless: 1. Order is manually lined through to inactivate 2. Orders with check boxes ( ) are unchecked DRUG AND TREATMENT ORDERS
 Available at: ALL Adult Facilities Non Categorized SUB Protocol(SUB)* SUB Protocol Lab Orders(SUB)* ED Rainbow Tubes(SUB)* ***Reminder: Order ED Rainbow Tubes (SUB) as a separate form*** Nursing Orders
Available at: ALL Adult Facilities Non Categorized SUB Protocol(SUB)* SUB Protocol Lab Orders(SUB)* ED Rainbow Tubes(SUB)* ***Reminder: Order ED Rainbow Tubes (SUB) as a separate form*** Nursing Orders
Emergency Department Guideline. Anaphylaxis
 Emergency Department Guideline Inclusion criteria: 1. Acute onset of an illness (minutes to hours) with a AND (b OR c): a. Skin and/or mucosa (pruritus, flushing, hives, angioedema) b. Respiratory compromise
Emergency Department Guideline Inclusion criteria: 1. Acute onset of an illness (minutes to hours) with a AND (b OR c): a. Skin and/or mucosa (pruritus, flushing, hives, angioedema) b. Respiratory compromise
West Penn Allegheny Health System Forbes Regional Hospital
 Policy Name: Treatment of Anaphylactic Reaction In the Cath Lab Original Date: West Penn Allegheny Health System Forbes Regional Hospital Policy No. 16553 Page 1 of 6 Reviewed by : Mark Taylor, MD, Michael
Policy Name: Treatment of Anaphylactic Reaction In the Cath Lab Original Date: West Penn Allegheny Health System Forbes Regional Hospital Policy No. 16553 Page 1 of 6 Reviewed by : Mark Taylor, MD, Michael
Physician Orders ADULT: Kidney-Panc/PancTransplant Post Op Plan
 Initiate Orders Phase Care Sets/Protocols/PowerPlans Initiate Powerplan Phase T;N, Phase: Kidney-Panc/Panc Transp Post Op Phase, When to Initiate: Kidney-Panc/Panc Transp Post Op Phase Vital Signs Vital
Initiate Orders Phase Care Sets/Protocols/PowerPlans Initiate Powerplan Phase T;N, Phase: Kidney-Panc/Panc Transp Post Op Phase, When to Initiate: Kidney-Panc/Panc Transp Post Op Phase Vital Signs Vital
POST-OP CARDIAC SURGERY PHYSICIAN S ORDER SHEET USE BALLPOINT PEN ONLY. CARDIAC INTENSIVE CARE UNIT
 PHYSICIAN S SHEET Automatically Activate, if not in agreement, cross out and initial Activated by Checking Box ALLERGIES: None known YES Patient s Height: Patient s Weight: ALL MEDICATION and INTRAVENOUS
PHYSICIAN S SHEET Automatically Activate, if not in agreement, cross out and initial Activated by Checking Box ALLERGIES: None known YES Patient s Height: Patient s Weight: ALL MEDICATION and INTRAVENOUS
NURSING DEPARTMENT CRITICAL CARE POLICY MANUAL CRITICAL CARE PROTOCOLS. ACTIVASE (t-pa) INFUSION PROTOCOL FOR ACUTE MYOCARDIAL INFARCTION
 NURSING DEPARTMENT CRITICAL CARE POLICY MANUAL CRITICAL CARE PROTOCOLS ACTIVASE (t-pa) FOR ACUTE MYOCARDIAL INFARCTION I. PURPOSE: A. To reduce the extent of myocardial infarction by lysing the clot in
NURSING DEPARTMENT CRITICAL CARE POLICY MANUAL CRITICAL CARE PROTOCOLS ACTIVASE (t-pa) FOR ACUTE MYOCARDIAL INFARCTION I. PURPOSE: A. To reduce the extent of myocardial infarction by lysing the clot in
Sample Case Study. The patient was a 77-year-old female who arrived to the emergency room on
 Sample Case Study The patient was a 77-year-old female who arrived to the emergency room on February 25 th with a chief complaint of shortness of breath and a deteriorating pulmonary status along with
Sample Case Study The patient was a 77-year-old female who arrived to the emergency room on February 25 th with a chief complaint of shortness of breath and a deteriorating pulmonary status along with
Updated Policies and Procedures # s 606, 607, 610, 611, 612, 613, 625, 628, 630, 631, and 633 (ACLS Protocols and Policies)
 SLO County Emergency Medical Services Agency Bulletin 2012-09 PLEASE POST Updated Policies and Procedures # s 606, 607, 610, 611, 612, 613, 625, 628, 630, 631, and 633 (ACLS Protocols and Policies) July
SLO County Emergency Medical Services Agency Bulletin 2012-09 PLEASE POST Updated Policies and Procedures # s 606, 607, 610, 611, 612, 613, 625, 628, 630, 631, and 633 (ACLS Protocols and Policies) July
PHYSICIAN SIGNATURE DATE TIME DRUG ALLERGIES WT: KG
 DRUG AND TREATMENT Available at: ALL Adult Facilities Non Categorized SUB Protocol(SUB)* SUB Protocol Lab Orders(SUB)* ED Rainbow Tubes(SUB)* ***Reminder: Order ED Rainbow Tubes (SUB) as a separate form***
DRUG AND TREATMENT Available at: ALL Adult Facilities Non Categorized SUB Protocol(SUB)* SUB Protocol Lab Orders(SUB)* ED Rainbow Tubes(SUB)* ***Reminder: Order ED Rainbow Tubes (SUB) as a separate form***
GENERAL SURGICAL ADULT POST-OPERATIVE ORDERS 1 of 4
 down ADULT POST-OPERATIVE 1 of 4 9 Actual 9 Estimated Patient ID Area Weight kg 9 Actual 9 Estimated Height cm ALLERGIES: REFER TO ALLERGY PROFILE/ POWERCHART Admit to: Post Anesthesia Care Unit (PACU),
down ADULT POST-OPERATIVE 1 of 4 9 Actual 9 Estimated Patient ID Area Weight kg 9 Actual 9 Estimated Height cm ALLERGIES: REFER TO ALLERGY PROFILE/ POWERCHART Admit to: Post Anesthesia Care Unit (PACU),
Hypotension / Shock. Adult Medical Section Protocols. Protocol 30
 Hypotension / Shock History Blood loss - vaginal or gastrointestinal bleeding, AAA, ectopic Fluid loss - vomiting, diarrhea, fever nfection Cardiac ischemia (M, CHF) Medications Allergic reaction regnancy
Hypotension / Shock History Blood loss - vaginal or gastrointestinal bleeding, AAA, ectopic Fluid loss - vomiting, diarrhea, fever nfection Cardiac ischemia (M, CHF) Medications Allergic reaction regnancy
Chest Pain Acute Coronary Syndrome Version 4 4/10/17 This order set is designed to be used with an admission set or for a patient already admitted
 Patient Name: Diagnosis: Allergies with reaction type: Chest Pain Acute Coronary Syndrome Version 4 4/10/17 This order set is designed to be used with an admission set or for a patient already admitted
Patient Name: Diagnosis: Allergies with reaction type: Chest Pain Acute Coronary Syndrome Version 4 4/10/17 This order set is designed to be used with an admission set or for a patient already admitted
Patient: Becky Smith DOB: 01/26/XXXX Age: 5 y/o Attending: Dr. D. Miles Allergies: NKA MR#: 203. Patient Chart #203 Becky Smith
 Patient Chart #203 Becky Smith 1 Property of CSCLV CSCLV Rev: 06/04/2018 Chief Complaint: Abdominal pain. Informant: Parents. HISTORY & PHYSICAL HPI: Ill looking patient, healthy until 2 days ago when
Patient Chart #203 Becky Smith 1 Property of CSCLV CSCLV Rev: 06/04/2018 Chief Complaint: Abdominal pain. Informant: Parents. HISTORY & PHYSICAL HPI: Ill looking patient, healthy until 2 days ago when
AT TRIAGE. Alberta Acute Childhood Asthma Pathway: Evidence based* recommendations For Emergency / Urgent Care
 1 1 Should the child be placed into the Pathway? Asthma Clinical Score (PRAM) Inclusion Children 1 year and 18 years of age who present with wheezing and respiratory distress, and have been diagnosed by
1 1 Should the child be placed into the Pathway? Asthma Clinical Score (PRAM) Inclusion Children 1 year and 18 years of age who present with wheezing and respiratory distress, and have been diagnosed by
ADULT CARDIAC SURGERY TELEMETRY BED TRANSFER ORDERS 1 of 4
 ADULT CARDIAC SURGERY TELEMETRY BED TRANSFER 1 of 4 9 Actual 9 Estimated Attending Surgeon: Medical Record Number Weight kg 9 Actual 9 Estimated Height cm ALLERGIES: REFER TO ALLERGY PROFILE/ POWERCHART
ADULT CARDIAC SURGERY TELEMETRY BED TRANSFER 1 of 4 9 Actual 9 Estimated Attending Surgeon: Medical Record Number Weight kg 9 Actual 9 Estimated Height cm ALLERGIES: REFER TO ALLERGY PROFILE/ POWERCHART
Case Scenarios. Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC. Consultant, Critical Care Medicine Medanta, The Medicity
 Case Scenarios Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity Case 1 A 36 year male with cirrhosis and active GI bleeding is intubated to protect his airway,
Case Scenarios Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity Case 1 A 36 year male with cirrhosis and active GI bleeding is intubated to protect his airway,
MICHIGAN. Table of Contents. State Protocols. Adult Treatment Protocols
 MICHIGAN State Protocols Protocol Number Protocol Name Adult Treatment Protocols Table of Contents 3.1 Altered Mental Status 3.2 Stroke/Suspected Stroke 3.3 Respiratory Distress 3.4 Seizures 3.5 Sepsis
MICHIGAN State Protocols Protocol Number Protocol Name Adult Treatment Protocols Table of Contents 3.1 Altered Mental Status 3.2 Stroke/Suspected Stroke 3.3 Respiratory Distress 3.4 Seizures 3.5 Sepsis
*111* attach patient label here
 Physician Orders ADULT [R] = will be ordered Height: cm Weight: kg Allergies: No known allergies Medication allergy(s): Latex allergy Other: Admission/Transfer/Discharge Patient Status Initial Inpatient
Physician Orders ADULT [R] = will be ordered Height: cm Weight: kg Allergies: No known allergies Medication allergy(s): Latex allergy Other: Admission/Transfer/Discharge Patient Status Initial Inpatient
PEDIATRIC SPINE SURGERY POST-OP PLAN - Phase:.
 - Phase:. PHYSICIAN S Diagnosis Weight Allergies DETAILS Patient Care Patient Activity Bedrest Maintain Surgical Drain Maintain JP Drain, Measure Output q12h, and PRN Convert IV to INT when tolerating
- Phase:. PHYSICIAN S Diagnosis Weight Allergies DETAILS Patient Care Patient Activity Bedrest Maintain Surgical Drain Maintain JP Drain, Measure Output q12h, and PRN Convert IV to INT when tolerating
ED-SCANS: OVERALL DECISION SUPPORT ALGORITHM. Is This Strictly a Pain Episode? Decision 7: Referrals
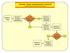 ED-SCANS: OVERALL DECISION SUPPORT ALGORITHM Decision 1: Triage Decision 2: Analgesic Management Is This Strictly a Pain Episode? Decision 3: Diagnostic Evaluation Decision 4: High Risk / High User Decision
ED-SCANS: OVERALL DECISION SUPPORT ALGORITHM Decision 1: Triage Decision 2: Analgesic Management Is This Strictly a Pain Episode? Decision 3: Diagnostic Evaluation Decision 4: High Risk / High User Decision
Atrial Fibrillation Version 2 11/4/15 This order set must be used with an admission order set if patient not already admitted.
 Patient Name: Diagnosis: Allergies with reaction type: Atrial Fibrillation Version 2 11/4/15 This order set must be used with an admission order set if patient not already admitted. Telemetry Medical Telemetry:
Patient Name: Diagnosis: Allergies with reaction type: Atrial Fibrillation Version 2 11/4/15 This order set must be used with an admission order set if patient not already admitted. Telemetry Medical Telemetry:
(31189) Hypothermia Initiation Phase One
 Hypothermia Initiation Phase One Diagnosis Allergies For hypothermia tracking purposes only. Please do not uncheck.- Required Cardiac Emergency Tracking For hypothermia tracking purposes only. Consults
Hypothermia Initiation Phase One Diagnosis Allergies For hypothermia tracking purposes only. Please do not uncheck.- Required Cardiac Emergency Tracking For hypothermia tracking purposes only. Consults
2
 1 2 3 4 5 6 7 8 Please check regional policy on this Tetracaine and Morgan lens may be optional in region *Ketamine and Fentanyl must be added to your CS license if required by your region *Midstate will
1 2 3 4 5 6 7 8 Please check regional policy on this Tetracaine and Morgan lens may be optional in region *Ketamine and Fentanyl must be added to your CS license if required by your region *Midstate will
Change in Practice PCP Autonomous IV OBHG Education Subcommittee
 Change in Practice PCP Autonomous IV Intravenous and Fluid Therapy Medical Directive Auxiliary Ability to initiate IV access and Ability to administer fluid and fluid boluses in general IV Therapy Actual
Change in Practice PCP Autonomous IV Intravenous and Fluid Therapy Medical Directive Auxiliary Ability to initiate IV access and Ability to administer fluid and fluid boluses in general IV Therapy Actual
Medical Treatment for acute Decompensated Heart Failure. Vlasis Ninios Cardiologist St. Luke s s Hospital Thessaloniki 2011
 Medical Treatment for acute Decompensated Heart Failure Vlasis Ninios Cardiologist St. Luke s s Hospital Thessaloniki 2011 2010 HFSA guidelines for ADHF 2009 focused update of the 2005 American College
Medical Treatment for acute Decompensated Heart Failure Vlasis Ninios Cardiologist St. Luke s s Hospital Thessaloniki 2011 2010 HFSA guidelines for ADHF 2009 focused update of the 2005 American College
MICHIGAN. State Protocols. General Treatment Protocols Table of Contents
 MICHIGAN State Protocols Protocol Number 1.1 1.2 1.3 1.4 1.5 1.6 1.7 1.8 1.9 1.10 1.11 1.12 1.13 General Treatment Protocols Table of Contents Protocol Name General Pre-hospital Care Abdominal Pain Nausea
MICHIGAN State Protocols Protocol Number 1.1 1.2 1.3 1.4 1.5 1.6 1.7 1.8 1.9 1.10 1.11 1.12 1.13 General Treatment Protocols Table of Contents Protocol Name General Pre-hospital Care Abdominal Pain Nausea
PEDIATRIC SPINE SURGERY POST-OP PLAN - Phase: Pediatric Spine Surgery General Orders
 - Phase: Pediatric Spine Surgery General Orders PHYSICIAN S Diagnosis Weight Allergies Patient Care Patient Activity Bedrest Maintain Surgical Drain Maintain JP Drain, Measure Output q12h, and PRN Convert
- Phase: Pediatric Spine Surgery General Orders PHYSICIAN S Diagnosis Weight Allergies Patient Care Patient Activity Bedrest Maintain Surgical Drain Maintain JP Drain, Measure Output q12h, and PRN Convert
The Crashing Pediatric Patient: Stopping the Fall
 The Crashing Pediatric Patient: Stopping the Fall I can t breathe... 4 year old BIBA from school with sudden severe resp distress Hx of asthma, food allergies Judith Klein, MD FACEP Assistant Professor
The Crashing Pediatric Patient: Stopping the Fall I can t breathe... 4 year old BIBA from school with sudden severe resp distress Hx of asthma, food allergies Judith Klein, MD FACEP Assistant Professor
Emergency Department Protocol Initiative
 Emergency Department Protocol Initiative ACUTE ASTHMA MANAGEMENT TOOLKIT March 2006 Provincial Emergency Services Project PHYSICIAN ORDER TEMPLATE FOR CTAS LEVEL 1 ASTHMA ADULT PEDIATRIC Date: Site: Arrival
Emergency Department Protocol Initiative ACUTE ASTHMA MANAGEMENT TOOLKIT March 2006 Provincial Emergency Services Project PHYSICIAN ORDER TEMPLATE FOR CTAS LEVEL 1 ASTHMA ADULT PEDIATRIC Date: Site: Arrival
REPORT OF TRANSFUSION ADVERSE REACTION TO BLOOD CENTERS
 REPORT OF TRANSFUSION ADVERSE REACTION TO BLOOD CENTERS INSTRUCTIONS: Send the form to ALL blood centers that provided blood components to this patient. Timely reporting is important, so that, if appropriate,
REPORT OF TRANSFUSION ADVERSE REACTION TO BLOOD CENTERS INSTRUCTIONS: Send the form to ALL blood centers that provided blood components to this patient. Timely reporting is important, so that, if appropriate,
PE Pathway. The charts are listed as follows:
 PE Pathway This document comprises 6 simple flow charts to assist clinicians in the investigation and treatment of suspected or confirmed Acute Pulmonary Emboli. The pathway has been put together using
PE Pathway This document comprises 6 simple flow charts to assist clinicians in the investigation and treatment of suspected or confirmed Acute Pulmonary Emboli. The pathway has been put together using
HOW TO USE THE CLINICAL PATHWAY
 ACUTE CORONARY SYNDROMES CLINICAL PATHWAY ACUTE STAGE GREY BRUCE HEALTH SERVICES Lion's Head Markdale Meaford Owen Sound Southampton Tobermory Wiarton PATIENT ID INCLUSION CRITERIA Patients who present
ACUTE CORONARY SYNDROMES CLINICAL PATHWAY ACUTE STAGE GREY BRUCE HEALTH SERVICES Lion's Head Markdale Meaford Owen Sound Southampton Tobermory Wiarton PATIENT ID INCLUSION CRITERIA Patients who present
Physician Orders ADULT: Medical Response Team Standing Orders Protocol Plan
 Initiate Orders Phase Care Sets/Protocols/PowerPlans Initiate Powerplan Phase When to Initiate: Other-See Special Instructions, If MRT is notified per MD, Condition H or any associate, review and Initiate
Initiate Orders Phase Care Sets/Protocols/PowerPlans Initiate Powerplan Phase When to Initiate: Other-See Special Instructions, If MRT is notified per MD, Condition H or any associate, review and Initiate
EFFECTIVE DATE: 01/2007 REVISED: 07/2008, 6/11, 3/12, 8/12, 1/15. Purpose:
 1 TITLE/DESCRIPTION: DEPARTMENT: PERSONNEL: Rapid Response Team (RRT) Patient Care Services RN s and RT s EFFECTIVE DATE: 01/2007 REVISED: 07/2008, 6/11, 3/12, 8/12, 1/15 Purpose: A group of select health
1 TITLE/DESCRIPTION: DEPARTMENT: PERSONNEL: Rapid Response Team (RRT) Patient Care Services RN s and RT s EFFECTIVE DATE: 01/2007 REVISED: 07/2008, 6/11, 3/12, 8/12, 1/15 Purpose: A group of select health
I. Subject: Continuous Aerosolization of Bronchodilators
 I. Subject: Continuous Aerosolization of Bronchodilators II. Indications: A. Acute airflow obstruction in which treatment with an aerosolized bronchodilator is desired for an extended period of time, i.e.
I. Subject: Continuous Aerosolization of Bronchodilators II. Indications: A. Acute airflow obstruction in which treatment with an aerosolized bronchodilator is desired for an extended period of time, i.e.
Flolan. Potent pulmonary and systemic vasodilator Three major potential pharmacologic actions
 1995 FDA approved for PAH - NYHA functional class III/IV 2000 - FDA for SPH r/t scleroderma and related disorders 2000 Medicare expanded coverage: cardiac d/o, portal htn, SPH r/t congenital disorders
1995 FDA approved for PAH - NYHA functional class III/IV 2000 - FDA for SPH r/t scleroderma and related disorders 2000 Medicare expanded coverage: cardiac d/o, portal htn, SPH r/t congenital disorders
A UMC Health System Performance Improvement Initiative for use in all units where cardiac/surgical patients are admitted.
 A UMC Health System Performance Improvement Initiative for use in all units where cardiac/surgical patients are admitted Denotes guideline requirement Attending Physician: Resident/Fellow: Allergies_ Diagnosis:
A UMC Health System Performance Improvement Initiative for use in all units where cardiac/surgical patients are admitted Denotes guideline requirement Attending Physician: Resident/Fellow: Allergies_ Diagnosis:
Physician Orders Pediatric: LEB ED Asthma Plan
 LEB ED Triage Standing SOB/Wheeze Asthma Non Categorized Criteria: Patients greater than 2 years of age with a history of asthma or airway active disease or two or more previous illnesses treated with
LEB ED Triage Standing SOB/Wheeze Asthma Non Categorized Criteria: Patients greater than 2 years of age with a history of asthma or airway active disease or two or more previous illnesses treated with
Medical Advisory Committee. Run Review
 Nor Cal EMS Medical Advisory Committee Run Review September 2014 Eric M. Rudnick, MD, FACEP, FAAEM Medical Director Northern California EMS September 9, 2014 1 Case #1 Dispatched for a male with chest
Nor Cal EMS Medical Advisory Committee Run Review September 2014 Eric M. Rudnick, MD, FACEP, FAAEM Medical Director Northern California EMS September 9, 2014 1 Case #1 Dispatched for a male with chest
Neurosurgery Pre-Op [1710] Patient Name MRN. General. Nursing. Case Request [ ] Case request operating room Scheduling/ADT, Scheduling/ADT [ ] Other
![Neurosurgery Pre-Op [1710] Patient Name MRN. General. Nursing. Case Request [ ] Case request operating room Scheduling/ADT, Scheduling/ADT [ ] Other Neurosurgery Pre-Op [1710] Patient Name MRN. General. Nursing. Case Request [ ] Case request operating room Scheduling/ADT, Scheduling/ADT [ ] Other](/thumbs/96/128298591.jpg) Neurosurgery Pre-Op [1710] Patient Name MRN General Case Request [ ] Case request operating room Scheduling/ADT, Scheduling/ADT Inpatient Only Procedure (Single Response) ( ) Admit to Inpatient Diagnosis:
Neurosurgery Pre-Op [1710] Patient Name MRN General Case Request [ ] Case request operating room Scheduling/ADT, Scheduling/ADT Inpatient Only Procedure (Single Response) ( ) Admit to Inpatient Diagnosis:
URN: Family name: Given name(s): Address: Initial Signature Print Name Role
 Do Not Write in this binding margin v5.00-02/2012 Mat. No.: 10206019 SW030b The State of Queensland (Queensland Health) 2012 Contact CIM@health.qld.gov.au ÌSW030bIÎ Facility: s Never Replace Clinical Judgement
Do Not Write in this binding margin v5.00-02/2012 Mat. No.: 10206019 SW030b The State of Queensland (Queensland Health) 2012 Contact CIM@health.qld.gov.au ÌSW030bIÎ Facility: s Never Replace Clinical Judgement
Documenting in the World of ICD-10 Capturing all your CCs and MCCs Crystal Coen, RN, MSN, FNP-BC NPSS Asheville, NC
 Documenting in the World of ICD-10 Capturing all your CCs and MCCs Crystal Coen, RN, MSN, FNP-BC 2017 NPSS Asheville, NC Objectives Understand the importance of documenting to the highest specificity Understand
Documenting in the World of ICD-10 Capturing all your CCs and MCCs Crystal Coen, RN, MSN, FNP-BC 2017 NPSS Asheville, NC Objectives Understand the importance of documenting to the highest specificity Understand
PEDIATRIC ASTHMA INPATIENT CARE MAP
 DATE PATIENT PEDIATRIC ASTHMA INPATIENT CARE MAP DOB HSC NO. PHIN Approved by the Winnipeg Regional Health Authority This Care Map is to be used as a guideline and in no way replaces sound clinical judgment
DATE PATIENT PEDIATRIC ASTHMA INPATIENT CARE MAP DOB HSC NO. PHIN Approved by the Winnipeg Regional Health Authority This Care Map is to be used as a guideline and in no way replaces sound clinical judgment
2
 1 2 3 4 5 6 7 8 Please check regional policy on Tetracaine and Morgan Lens this may be optional in your region. *Ketamine and Fentanyl must be added to your controlled substance license if required by
1 2 3 4 5 6 7 8 Please check regional policy on Tetracaine and Morgan Lens this may be optional in your region. *Ketamine and Fentanyl must be added to your controlled substance license if required by
Paramedic Pediatric Medical Math Practice
 Paramedic Pediatric Medical Math Practice Name: Date: Problem 1 Your 4 year old patient weighs 40 pounds. She is febrile. You need to administer acetaminophen (Tylenol) 15mg/kg. How many mg will you administer?
Paramedic Pediatric Medical Math Practice Name: Date: Problem 1 Your 4 year old patient weighs 40 pounds. She is febrile. You need to administer acetaminophen (Tylenol) 15mg/kg. How many mg will you administer?
VENTRICULAR FIBRILLATION. 1. Safe scene, standard precautions. 2. Establish unresponsiveness, apnea, and pulselessness. 3. Quick look (monitor)
 LUCAS COUNTY EMS SUMMARY PAGES VENTRICULAR FIBRILLATION 2. Establish unresponsiveness, apnea, and pulselessness 3. Quick look (monitor) 4. Identify rhythm 5. Provide 2 minutes CPR if unwitnessed by EMS
LUCAS COUNTY EMS SUMMARY PAGES VENTRICULAR FIBRILLATION 2. Establish unresponsiveness, apnea, and pulselessness 3. Quick look (monitor) 4. Identify rhythm 5. Provide 2 minutes CPR if unwitnessed by EMS
Observation Medicine The Inpatient Fast Track Kirk Jensen, MD, MBA, FACEP Jody Crane, MD, MBA, FACEP
 These presenters have nothing to disclose Observation Medicine The Inpatient Fast Track Kirk Jensen, MD, MBA, FACEP Jody Crane, MD, MBA, FACEP April 29, 2015 Cambridge, MA Session Objectives 2 After this
These presenters have nothing to disclose Observation Medicine The Inpatient Fast Track Kirk Jensen, MD, MBA, FACEP Jody Crane, MD, MBA, FACEP April 29, 2015 Cambridge, MA Session Objectives 2 After this
Allergic Emergencies and Anaphylaxis. George Porfiris MD, CCFP(EM),FCFP TEGH
 Allergic Emergencies and Anaphylaxis George Porfiris MD, CCFP(EM),FCFP TEGH Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored, or transmitted
Allergic Emergencies and Anaphylaxis George Porfiris MD, CCFP(EM),FCFP TEGH Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored, or transmitted
Assessment. Consults & Referrals
 University of Virginia Health System Clinical Pathway: Whipple Enhanced Recovery After () LOS: 4-5 days Date of Origin/Revision: June 29, 2016/September 6, 2017/January 31, 2018 : SAS : : : D1 D2 D 3/
University of Virginia Health System Clinical Pathway: Whipple Enhanced Recovery After () LOS: 4-5 days Date of Origin/Revision: June 29, 2016/September 6, 2017/January 31, 2018 : SAS : : : D1 D2 D 3/
Emergency Department Guideline. Asthma
 Emergency Department Guideline Inclusion criteria: Patients 2 years old with: o Known history of asthma or wheezing responsive to bronchodilators presenting to the ED with cough, wheeze, shortness of breath,
Emergency Department Guideline Inclusion criteria: Patients 2 years old with: o Known history of asthma or wheezing responsive to bronchodilators presenting to the ED with cough, wheeze, shortness of breath,
r*po1004*r PHYSICIAN S ORDERS Page 1 of 7 HOUR THORACOTOMY POSTOPERATIVE ORDERS General x Admit to Inpatient Status x Admitting Physician: Admit to:
 PHYSICIAN S ORDERS Page 1 of 7 General x Admit to Inpatient Status x Admitting Physician: Admit to: SICU Telemetry Med/Surg room x Resuscitation status: see Resuscitation Status Order Activity x Bed rest
PHYSICIAN S ORDERS Page 1 of 7 General x Admit to Inpatient Status x Admitting Physician: Admit to: SICU Telemetry Med/Surg room x Resuscitation status: see Resuscitation Status Order Activity x Bed rest
