Note No nausea or vomiting before collapse increases the risk of an arrhythmia. A
|
|
|
- Jessie Evans
- 5 years ago
- Views:
Transcription
1 TACHYCARDIAS SYMPTOMS AND SIGNS Think about cardiac arrhythmias in patients with: palpitations D dyspnoea B chest pain D dizziness or syncope D cardiac arrest. D Ask about: any nausea or vomiting before collapse A any cardiovascular disease, particularly any: known arrhythmias A ischaemic heart disease D current medication and alcohol use. D Note No nausea or vomiting before collapse increases the risk of an arrhythmia. A Look for: + an irregular pulse B cannon waves in the jugular venous pulse (if VT suspected C ) + variable amplitude of the first heart sound (if VT suspected C ) evidence of cardiovascular decompensation: B hypotension pulmonary oedema reduced level of consciousness. INVESTIGATIONS U&E, creatinine. D Calcium, magnesium. D Cardiac enzymes. D Thyroid function tests. D 12-lead ECG. A Consider further testing if the diagnosis is uncertain and your patient is stable: an event recorder A or a Holter monitor B worn for at least 24 hours and preferably longer C stress testing to induce the arrhythmia D an echocardiogram. D
2 TACHYCARDIAS 175 Broad-complex tachycardias Treat as a ventricular tachycardia until proven otherwise. D Features that favour VT include: D a history of ischaemic heart disease AV dissociation fusion or capture beats LAD RSR 1 pattern in V 1 positive concordance across leads. THERAPY Correct any electrolyte abnormality. A If uncertain about the source of the arrhythmia: Perform carotid sinus massage or ask your patient to perform a Valsalva manoeuvre. D Give adenosine. A Adenosine Avoid in patients: with asthma on theophyllines, or dipyridamole. Use ECG monitoring and have resuscitation equipment available. Warn patients about facial flushing, chest discomfort and dyspnoea. A Record the ECG during administration. Give 3 mg i.v. rapidly. If unsuccessful after 1 to 2 minutes, try 6 mg, 9 mg then 12 mg. A If the patient has a central line, use it. A Adenosine should: reveal atrial tachycardias terminate junctional re-entrant tachycardia have no effect on ventricular tachycardias. Acute onset atrial flutter Control the ventricular rate A using: Digoxin. D Digoxin Load patients with 500 to 1000 g in divided doses. Give 62.5 to 250 g daily, based on age, renal function and other medication. Measure digoxin levels after 5 days. D Take the blood test 6 to 10 hours after the last dose. Therapeutic range 0.8 to 2.0 ng/ml.
3 176 TACHYCARDIAS Alternative include: Calcium-channel blockers: verapamil 5 mg i.v. over 5 minutes; repeat after 5 minutes to a maximum dose of 20 mg diltiazem 0.25 mg/kg over 2 minutes; repeat at 0.35 mg/kg if no response. A Beta-blockers: esmolol: A load patients with 100 g/kg/min i.v. over 1 minute followed by 50 g/kg/min over 4 minutes repeat if there is no effect, and increase the 4-minute infusion by 50 g/kg/min sotalol: A 100 mg i.v. over 5 minutes; or 80 mg orally twice daily. Consider cardioversion to sinus rhythm A if your patient fails to revert spontaneously. D Options include: DC cardioversion, A particularly if your patient is haemodynamically unstable DC cardioversion Patients with acute onset AF or flutter can be cardioverted immediately, D but should be started on heparin followed by a month of warfarin. D In cases of uncertain duration, anticoagulate your patient for a month before and after cardioversion. C Consider giving an infusion of ibutilide (0.01 mg/kg over 10 minutes) before cardioversion. A Check your patient has: D INR > 2.0 if anticoagulated K > 4.0 mmol/l. Arrange for a general anaesthetic for your patient, and ensure your patient is starved for at least 6 hours. A Cardiovert starting at 100 J; followed by 100 J, 200 J, 300 J, 360 J. D flecainide A Flecainide Contraindicated with ischaemic heart disease. A Intravenous give 2 mg/kg (to a maximum of 150 mg) over 30 minutes. Oral give 200 mg twice daily, reducing after 3 to 5 days to 50 mg daily. ibutilide A 0.01 mg/kg to a maximum of 1 mg over 10 minutes amiodarone. A
4 TACHYCARDIAS 177 Amiodarone Loading dose: Intravenous Preferably via a central line. Give 300 mg (5 mg/kg) in 250 ml 5.0% glucose over 1 hour, followed by 900 mg over 24 hours. Oral: Give 200 mg every 8 hours for 1 week, then 200 mg every 12 hours for 1 week, then start maintenance therapy. Maintenance dose: Patients should be given a total loading dose of 4200 mg before starting on maintenance therapy. D Give 100 to 200 mg daily. Supraventricular tachycardia Try carotid sinus massage or ask your patient to perform a Valsalva manoeuvre. D Give adenosine. A Adenosine Avoid in patients: with asthma on theophyllines, or dipyridamole. Use ECG monitoring and have resuscitation equipment available. Warn patients about facial flushing, chest discomfort and dyspnoea. A Record the ECG during administration. Give 3 mg rapidly. If unsuccessful after 1 to 2 minutes, try 6 mg, 9 mg then 12 mg. A If the patient has a central line, use it. A Adenosine should: reveal atrial tachycardias terminate junctional re-entrant tachycardia have no effect on ventricular tachycardias. If this fails, consider one of: DC cardioversion. A Calcium channel blockers: diltiazem: 0.25 mg/kg over 2 minutes, repeat at 0.35 mg/kg if no response. A Beta-blockers: esmolol: C load patients with 100 g/kg/min i.v. over 1 minute followed by 50 g kg/min over 4 minutes
5 178 TACHYCARDIAS repeat if there is no effect, and increase the 4-minute infusion by 50 g/kg/min nadolol: A 40 mg orally sotalol: B 100 mg i.v. over 5 minutes; or 80 mg orally twice daily. Propafenone: B 150 mg orally three times a day (reduce dose if < 70 kg). Wolff Parkinson White syndrome Note Avoid using digoxin or verapamil they may exacerbate the arrhythmia. D Terminate the rhythm using any of: Adenosine. D (See above for further information.) Amiodarone. D (See above for further information.) Flecainide. D (See above for further information.) Procainamide. D Give a bolus of 10 mg per kg at a rate of 100 mg per minute. Esmolol. D (See above for further information.) Diltiazem 0.25 mg/kg over 2 minutes; repeat at 0.35 mg/kg if no response. A Ventricular tachycardia Note Do not treat patients with recent myocardial infarction who have frequent ventricular ectopics with class Ic anti-arrhythmics, e.g. flecainide or encainide. A Cardiovert patients who are haemodynamically compromised. A Give amiodarone. A (See above for further information.) Alternatives include: sotalol A 100 mg i.v. over 5 minutes, or 80 mg orally twice daily procainamide give a bolus of 10 mg per kg at a rate of 100 mg per minute. REVIEW Paroxysmal atrial flutter Consider long-term anti-arrhythmic therapy in symptomatic cases. D Start medication in hospital. C Consider using one of: flecainide at least 50 mg twice daily A sotalol at least 120 mg twice daily A ablation therapy. D
6 TACHYCARDIAS 179 Paroxysmal supraventricular tachycardia Consider anti-arrhythmic medication for patients with recurrent symptomatic arrhythmias. D Start medication in hospital. C Consider using one of: flecainide at least 50 mg twice daily A sotalol 80 mg to 160 mg twice daily A propafenone 300 mg twice daily B ablation therapy. D Ventricular arrhythmias Consider: amiodarone A ablation therapy D inserting an implantable defibrillator A with endocardial leads: B Consider adding one of: amiodarone B metoprolol A 12.5 mg to 50 mg three times a day sotalol A 80 mg to 160 mg twice daily. Implantable defibrillators Half of patients will receive a shock in the next 2 years. B Outcome Only a third of patients with paroxysmal atrial flutter are in sinus rhythm at 2 years. A 70% of patients with paroxysmal SVT who are not on medication have a recurrent episode within 3 months. B Half of patients with a ventricular arrhythmia have another episode within 12 months, B and around 30% are dead within a year many suddenly. B Expires July 2003 Guideline: Chris Ball CATs: Chris Ball, Clare Wotton
7 UPPER GASTROINTESTINAL BLEEDING SYMPTOMS AND SIGNS Ask about: any haematemesis or melaena before admission and its colour C and amount D other illnesses including: previous peptic ulcers B H. pylori infection B alcohol-related disorders B liver cirrhosis, oesophageal varices or portal vein thrombosis B renal failure A disseminated malignancy A heart disease and heart failure A current medication, particularly: anticoagulants A non-steroidal anti-inflammatory drugs (NSAIDs). A Common causes include: B gastric or duodenal ulcers gastric erosions varices a Mallory Weiss tear oesophagitis. Rarer causes include: tumours B angiodysplasia. Look for: evidence of acute bleeding: B + supine tachycardia + supine hypotension (systolic blood pressure < 95 mmhg) + postural pulse increase of > 30 beats/min or severe dizziness on sitting upright, and if normal then on standing Note Postural hypotension does not usefully diagnose acute blood loss. B evidence of anaemia: A + conjunctival pallor A + facial pallor B + palmar pallor B + dyspnoea C
8 UPPER GASTROINTESTINAL BLEEDING 181 evidence of cirrhosis, specifically: A + facial telangiectasia A + spider naevi A + abdominal wall veins A + white nails A + obesity A + peripheral oedema. A Risk of cirrhosis B High (> 80%) if: all 6 signs present and peripheral oedema 4 signs if no peripheral oedema 3 signs if facial telangiectasia and no peripheral oedema. Moderate if: any other combination. Low (< 20%) if: no facial telangiectasia and 2 other signs. Perform a rectal examination and a faecal occult blood test. A Look at the appearance of any vomit or nasogastric aspirate: + Test it using a gastroccult dipstick. A INVESTIGATIONS Blood count. D Clotting. A Group and save serum, or cross-match 2 to 6 units depending on blood loss. D U&E, creatinine. A Urea:creatinine ratio A urea:creatinine ratio > 100 helps diagnose an upper GI bleed. A Liver function tests. A Glucose. D Blood cultures. D Arterial blood gases. D Consider inserting: a central venous catheter to monitor fluid resuscitation D a urinary catheter to monitor urine output. D
9 182 UPPER GASTROINTESTINAL BLEEDING Peptic ulcer disease Test for H. pylori A using any of: ± CLO test C ± histology, looking for antral inflammation C ± urease breath test. C THERAPY Resuscitate your patient. A Insert two large bore i.v. cannulas. D Give blood if required. If PT is prolonged: Give factor concentrate C or FFP. D Stop any anticoagulants. C Consider giving 5 mg vitamin K by slow i.v. infusion. A Order an endoscopy: A urgently A to control bleeding to make a diagnosis and determine future risk of bleeding or death. A Endoscopy Look for evidence of endoscopic stigmata of recent haemorrhage: A ± blood in the upper Gl tract ± an adherent clot ± a visible or spurting vessel. Complications of endoscopy such as perforation, aspiration and haemorrhage are very rare. B While waiting for endoscopy consider giving: somatostatin A 6 mg in 500 ml saline i.v. over 24 hours for 5 days octreotide A Octreotide Give a bolus of octreotide 50 g i.v. followed by Octreotide 500 g in 50 ml 0.9% saline at 5 ml/h. terlipressin 2 mg i.v. every 4 hours for up to 72 hours. A Give thiamine 100 mg D i.v. C to alcoholics or malnourished patients. D Discuss any patients likely to rebleed with surgeons and anaesthetists to determine criteria for surgery. D Note Use the Rockall score A (see Table 41.1) to help identify patients at risk of rebleeding or dying.
10 UPPER GASTROINTESTINAL BLEEDING 183 Table 41.1 Rockall score rank your patient for risk of rebleeding or dying A Score 0 Score 1 Score 2 Score 3 Age aged < 60 aged 60 to 79 aged > 80 Shock pulse < 100 pulse > 100 pulse > 100 systolic b.p. and systolic and systolic > 100 BP > 100 BP < 100 mmhg mmhg mmhg Co- no major cardiac renal failure morbidity co-morbidity failure liver failure ischaemic disseminated heart disease malignancy any other co-morbidity Endoscopic none blood in stigmata dark spot upper GI seen tract adherent clot visible or spurting vessel Diagnosis Mallory Weiss all other malignancy tear diagnoses of upper GI no lesion tract seen and no stigmata of recent haemorrhage Pre-endoscopy Risk of Post-endoscopy Risk of Risk of score dying score dying rebleeding 7 75% 8+ 40% 37% 6 62% 7 23% 37% 5 35% 6 12% 27% 4 21% 5 11% 25% 3 12% 4 8% 15% 2 6% 3 2% 12% 1 3% 0 to 2 0% 6% 0 0%
11 184 UPPER GASTROINTESTINAL BLEEDING Peptic ulcers Arrange for endoscopic haemostasis. Give: a proton pump inhibitor, A e.g. omeprazole 40 mg daily antacids. A Varices Arrange for endoscopic ligation B or sclerotherapy A within 6 hours. B Give octreotide or somatostatin. A Somatostatin Somatostatin 6 mg in 500 ml saline i.v. over 24 hours for 5 days. Octreotide Octreotide 500 g in 50 ml 0.9% saline at 50 g per hour (i.e. 5 ml/h.) Consider: balloon tamponade A for patients who do not stop bleeding D transjugular intrahepatic portosystemic shunts (TIPS). D REVIEW Monitor: D vital signs and urine output blood count clotting electrolytes. Consider: iron supplements, B e.g. ferrous sulphate 200 mg three time a day D tranexamic acid A for patients likely to rebleed (3 to 6 g i.v. for 3 days, followed by 3 to 6 g orally for 3 to 5 days). D Patients with a Mallory Weiss tear or an ulcer can start eating immediately on recovery from endoscopy. D Rebleeding Perform repeat endoscopy on patients with: A vomiting of fresh blood hypotension and melaena requirement for 4 units of blood in the first 72 hours after endoscopic treatment. Consider surgery if there is persistent or recurrent haemorrhage despite endoscopic therapy. D
12 UPPER GASTROINTESTINAL BLEEDING 185 Ulcers and erosions Aroutine repeat endoscopy is not necessary. D Advise patients to stop smoking. B Stop NSAIDs. A If patients need to continue, consider: COX-2 inhibitors, e.g. rofecoxib A 12.5 to 25 mg daily or celecoxib B topical NSAIDs B ibuprofen B at the lowest possible dose B adding in regular omeprazole 40 mg daily A or misoprostol A 200 g 2 to 4 times daily. D Give H. pylori eradication therapy A using triple therapy: B a proton-pump inhibitor plus any two of amoxicillin, clarithromycin or a nitroimidazole B a bismuth compound plus a nitroimidazole plus tetracycline. B Sample triple therapy regimen: a 7-day course omeprazole 20 mg twice daily clarithromycin 500 mg twice daily amoxicillin 1 g twice daily. Continue proton-pump inhibitors long-term. A Varices Arrange for endoscopic ligation A or sclerotherapy A until varices are obliterated. Give beta-blockers, A e.g. propranolol MR 80 mg daily or isosorbide mononitrate MR A 60 mg daily. Outcomes One in seven patients dies in hospital A one in 15 from further bleeding. Peptic ulcers heal slowly and a third of patients have a relapse within a year. B A third of patients with varices rebleed within 1 year. B A third are dead within 2 months. A Expires July 2003 Guideline: Alan Townsend, Chris Ball CATs: Alan Townsend, Chris Ball, Clare Wotton
Rhythm Control: Is There a Role for the PCP? Blake Norris, MD, FACC BHHI Primary Care Symposium February 28, 2014
 Rhythm Control: Is There a Role for the PCP? Blake Norris, MD, FACC BHHI Primary Care Symposium February 28, 2014 Financial disclosures Consultant Medtronic 3 reasons to evaluate and treat arrhythmias
Rhythm Control: Is There a Role for the PCP? Blake Norris, MD, FACC BHHI Primary Care Symposium February 28, 2014 Financial disclosures Consultant Medtronic 3 reasons to evaluate and treat arrhythmias
PEDIATRIC SVT MANAGEMENT
 PEDIATRIC SVT MANAGEMENT 1 INTRODUCTION Supraventricular tachycardia (SVT) can be defined as an abnormally rapid heart rhythm originating above the ventricles, often (but not always) with a narrow QRS
PEDIATRIC SVT MANAGEMENT 1 INTRODUCTION Supraventricular tachycardia (SVT) can be defined as an abnormally rapid heart rhythm originating above the ventricles, often (but not always) with a narrow QRS
Chapter 9. Learning Objectives. Learning Objectives 9/11/2012. Cardiac Arrhythmias. Define electrical therapy
 Chapter 9 Cardiac Arrhythmias Learning Objectives Define electrical therapy Explain why electrical therapy is preferred initial therapy over drug administration for cardiac arrest and some arrhythmias
Chapter 9 Cardiac Arrhythmias Learning Objectives Define electrical therapy Explain why electrical therapy is preferred initial therapy over drug administration for cardiac arrest and some arrhythmias
Arrhythmias. A/Prof Drew Richardson. The Canberra Hospital May MB BS (Hons) FACEM Grad CertHE MD
 Arrhythmias A/Prof Drew Richardson MB BS (Hons) FACEM Grad CertHE MD The Canberra Hospital May 2013 Objectives Recognise the features of the common nonlethal arrhythmias Describe the emergency treatment
Arrhythmias A/Prof Drew Richardson MB BS (Hons) FACEM Grad CertHE MD The Canberra Hospital May 2013 Objectives Recognise the features of the common nonlethal arrhythmias Describe the emergency treatment
Management of ATRIAL FIBRILLATION. in general practice. 22 BPJ Issue 39
 Management of ATRIAL FIBRILLATION in general practice 22 BPJ Issue 39 What is atrial fibrillation? Atrial fibrillation (AF) is the most common cardiac arrhythmia encountered in primary care. It is often
Management of ATRIAL FIBRILLATION in general practice 22 BPJ Issue 39 What is atrial fibrillation? Atrial fibrillation (AF) is the most common cardiac arrhythmia encountered in primary care. It is often
AF and arrhythmia management. Dr Rhys Beynon Consultant Cardiologist and Electrophysiologist University Hospital of North Staffordshire
 AF and arrhythmia management Dr Rhys Beynon Consultant Cardiologist and Electrophysiologist University Hospital of North Staffordshire Atrial fibrillation Paroxysmal AF recurrent AF (>2 episodes) that
AF and arrhythmia management Dr Rhys Beynon Consultant Cardiologist and Electrophysiologist University Hospital of North Staffordshire Atrial fibrillation Paroxysmal AF recurrent AF (>2 episodes) that
Acute Upper Gastrointestinal Hemorrhage Surgical Perspective. Dr.J.H.Barnard Dept. of Surgery PAH
 Acute Upper Gastrointestinal Hemorrhage Surgical Perspective Dr.J.H.Barnard Dept. of Surgery PAH Introduction: AGH is a leading cause of admissions into ICU. Overall mortality 5-12%, but increases to 40%
Acute Upper Gastrointestinal Hemorrhage Surgical Perspective Dr.J.H.Barnard Dept. of Surgery PAH Introduction: AGH is a leading cause of admissions into ICU. Overall mortality 5-12%, but increases to 40%
Atrial Fibrillation 10/2/2018. Depolarization & ECG. Atrial Fibrillation. Hemodynamic Consequences
 Depolarization & ECG Atrial Fibrillation How to make ORDER out of CHAOS Julia Shih, VMD, DACVIM (Cardiology) October 27, 2018 Depolarization & ECG Depolarization & ECG Atrial Fibrillation Hemodynamic Consequences
Depolarization & ECG Atrial Fibrillation How to make ORDER out of CHAOS Julia Shih, VMD, DACVIM (Cardiology) October 27, 2018 Depolarization & ECG Depolarization & ECG Atrial Fibrillation Hemodynamic Consequences
Simon Everett. Consultant Gastroenterologist, SJUH, Leeds. if this is what greets you in the morning, you probably need to go see a doctor
 Simon Everett Consultant Gastroenterologist, SJUH, Leeds if this is what greets you in the morning, you probably need to go see a doctor Presentation Audit data and mortality NICE guidance Risk assessment
Simon Everett Consultant Gastroenterologist, SJUH, Leeds if this is what greets you in the morning, you probably need to go see a doctor Presentation Audit data and mortality NICE guidance Risk assessment
Emergency treatment to SVT Evidence-based Approach. Tran Thao Giang
 Emergency treatment to SVT Evidence-based Approach Tran Thao Giang Description ECG manifestations: HR is extremely rapid and regular (240bpm ± 40) P wave is: usually invisible When visible: anormal P axis,
Emergency treatment to SVT Evidence-based Approach Tran Thao Giang Description ECG manifestations: HR is extremely rapid and regular (240bpm ± 40) P wave is: usually invisible When visible: anormal P axis,
Dysrhythmias 11/7/2017. Disclosures. 3 reasons to evaluate and treat dysrhythmias. None. Eliminate symptoms and improve hemodynamics
 Dysrhythmias CYDNEY STEWART MD, FACC NOVEMBER 3, 2017 Disclosures None 3 reasons to evaluate and treat dysrhythmias Eliminate symptoms and improve hemodynamics Prevent imminent death/hemodynamic compromise
Dysrhythmias CYDNEY STEWART MD, FACC NOVEMBER 3, 2017 Disclosures None 3 reasons to evaluate and treat dysrhythmias Eliminate symptoms and improve hemodynamics Prevent imminent death/hemodynamic compromise
1 Cardiology Acute Care Day 22 April 2013 Arrhythmia Tutorial Course Material
 1 Cardiology Acute Care Day 22 April 2013 Arrhythmia Tutorial Course Material Arrhythmia recognition This tutorial builds on the ECG lecture and provides a framework for approaching any ECG to allow the
1 Cardiology Acute Care Day 22 April 2013 Arrhythmia Tutorial Course Material Arrhythmia recognition This tutorial builds on the ECG lecture and provides a framework for approaching any ECG to allow the
ANTI-ARRHYTHMICS AND WARFARIN. Dr Nithish Jayakumar
 ANTI-ARRHYTHMICS AND WARFARIN Dr Nithish Jayakumar Contents 1. Anti-arrhythmics Pacemaker and myocardial potentials Drug classes mechanisms; s/e; contra-indications Management of common arrhythmias 2.
ANTI-ARRHYTHMICS AND WARFARIN Dr Nithish Jayakumar Contents 1. Anti-arrhythmics Pacemaker and myocardial potentials Drug classes mechanisms; s/e; contra-indications Management of common arrhythmias 2.
APPROACH TO TACHYARRYTHMIAS
 APPROACH TO TACHYARRYTHMIAS PROF.DR.MD.ZAKIR HOSSAIN PROFESSOR AND HEAD DEPARTMENT OF MEDICINE SZMCH TACHYARRYTHMIA Cardiac arrythmia is a disturbance of electrical rhythm of heart. Cardac arrythmia with
APPROACH TO TACHYARRYTHMIAS PROF.DR.MD.ZAKIR HOSSAIN PROFESSOR AND HEAD DEPARTMENT OF MEDICINE SZMCH TACHYARRYTHMIA Cardiac arrythmia is a disturbance of electrical rhythm of heart. Cardac arrythmia with
A bleeding ulcer: What can the GP do? Gastrointestinal bleeding is a relatively common. How is UGI bleeding manifested? Who is at risk?
 Focus on CME at the University of British Columbia A bleeding ulcer: What can the GP do? By Robert Enns, MD, FRCP Gastrointestinal bleeding is a relatively common disorder affecting thousands of Canadians
Focus on CME at the University of British Columbia A bleeding ulcer: What can the GP do? By Robert Enns, MD, FRCP Gastrointestinal bleeding is a relatively common disorder affecting thousands of Canadians
Ventricular Tachycardia in Structurally Normal Hearts (Idiopathic VT) Patient Information
 Melbourne Heart Rhythm Ventricular Tachycardia in Structurally Normal Hearts (Idiopathic VT) Patient Information What is Ventricular Tachycardia? Ventricular tachycardia (VT) is an abnormal rapid heart
Melbourne Heart Rhythm Ventricular Tachycardia in Structurally Normal Hearts (Idiopathic VT) Patient Information What is Ventricular Tachycardia? Ventricular tachycardia (VT) is an abnormal rapid heart
Case #1. 73 y/o man with h/o HTN and CHF admitted with dizziness and SOB Treated for CHF exacerbation with Lasix Now HR 136
 Tachycardias Case #1 73 y/o man with h/o HTN and CHF admitted with dizziness and SOB Treated for CHF exacerbation with Lasix Now HR 136 Initial Assessment Check Telemetry screen if pt on tele Telemetry
Tachycardias Case #1 73 y/o man with h/o HTN and CHF admitted with dizziness and SOB Treated for CHF exacerbation with Lasix Now HR 136 Initial Assessment Check Telemetry screen if pt on tele Telemetry
Chapter 26. Media Directory. Dysrhythmias. Diagnosis/Treatment of Dysrhythmias. Frequency in Population Difficult to Predict
 Chapter 26 Drugs for Dysrythmias Slide 33 Slide 35 Media Directory Propranolol Animation Amiodarone Animation Upper Saddle River, New Jersey 07458 All rights reserved. Dysrhythmias Abnormalities of electrical
Chapter 26 Drugs for Dysrythmias Slide 33 Slide 35 Media Directory Propranolol Animation Amiodarone Animation Upper Saddle River, New Jersey 07458 All rights reserved. Dysrhythmias Abnormalities of electrical
The most common. hospitalized patients. hypotension due to. filling time Rate control in ICU patients may be difficult as many drugs cause hypotension
 Arrhythmias in the critically ill ICU patients: Approach for rapid recognition & management Objectives Be able to identify and manage: Atrial fibrillation with a rapid ventricular response Atrial flutter
Arrhythmias in the critically ill ICU patients: Approach for rapid recognition & management Objectives Be able to identify and manage: Atrial fibrillation with a rapid ventricular response Atrial flutter
Mr. Eknath Kole M.S. Pharm (NIPER Mohali)
 M.S. Pharm (NIPER Mohali) Drug Class Actions Therapeutic Uses Pharmacokinetics Adverse Effects Other Quinidine IA -Binds to open and inactivated Na+ -Decreases the slope of Phase 4 spontaneous depolarization
M.S. Pharm (NIPER Mohali) Drug Class Actions Therapeutic Uses Pharmacokinetics Adverse Effects Other Quinidine IA -Binds to open and inactivated Na+ -Decreases the slope of Phase 4 spontaneous depolarization
I have nothing to disclose.
 I have nothing to disclose. Antiarrhythmic Therapy in Pregnancy Prof. Ali Oto,MD,FESC,FACC,FHRS Department of Cardiology Hacettepe University,Faculty of Medicine Ankara Arrhythmias in pregnancy An increased
I have nothing to disclose. Antiarrhythmic Therapy in Pregnancy Prof. Ali Oto,MD,FESC,FACC,FHRS Department of Cardiology Hacettepe University,Faculty of Medicine Ankara Arrhythmias in pregnancy An increased
Acute Upper Gastro Intestinal (UGI) Bleeding
 T Acute Upper Gastro Intestinal (UGI) Bleeding University Hospitals of Leicester NHS Trust Guidelines for Management of Acute Medical Emergencies 1. Has there been a GI bleed? There are also UHL trust
T Acute Upper Gastro Intestinal (UGI) Bleeding University Hospitals of Leicester NHS Trust Guidelines for Management of Acute Medical Emergencies 1. Has there been a GI bleed? There are also UHL trust
Antiarrhythmic Drugs
 Antiarrhythmic Drugs DR ATIF ALQUBBANY A S S I S T A N T P R O F E S S O R O F M E D I C I N E / C A R D I O L O G Y C O N S U L T A N T C A R D I O L O G Y & I N T E R V E N T I O N A L E P A C H D /
Antiarrhythmic Drugs DR ATIF ALQUBBANY A S S I S T A N T P R O F E S S O R O F M E D I C I N E / C A R D I O L O G Y C O N S U L T A N T C A R D I O L O G Y & I N T E R V E N T I O N A L E P A C H D /
Dos and Don t in Cardiac Arrhythmia. Case 1 -ECG. Case 1. Management. Emergency Admissions. Reduction of TE risk -CHADS 2 score. Hospital Admissions
 Emergency Admissions Dos and Don t in Cardiac Arrhythmia Tom Wong, MD, FESC Consultant Cardiologist, Honorary Senior Lecturer Royal Brompton & Harefield Hospitals National Heart and Lung Institute, Imperial
Emergency Admissions Dos and Don t in Cardiac Arrhythmia Tom Wong, MD, FESC Consultant Cardiologist, Honorary Senior Lecturer Royal Brompton & Harefield Hospitals National Heart and Lung Institute, Imperial
CVD: Cardiac Arrhythmias. 1. Final Cardiac Arrhythmias_BMP. 1.1 Cardiovascular Disease. Notes:
 CVD: Cardiac Arrhythmias 1. Final Cardiac Arrhythmias_BMP 1.1 Cardiovascular Disease 1.2 Directions for taking this course 1.3 Content Experts 1.4 Disclosures 1.5 Accreditation Information 1.6 Learning
CVD: Cardiac Arrhythmias 1. Final Cardiac Arrhythmias_BMP 1.1 Cardiovascular Disease 1.2 Directions for taking this course 1.3 Content Experts 1.4 Disclosures 1.5 Accreditation Information 1.6 Learning
Management of Arrhythmias The General Practitioners role
 Management of Arrhythmias The General Practitioners role Rohan Gunawardena MD, FRCP, FCCP, FACC Consultant Cardiac Electrophysiologist National Hospital of Sri Lanka Arrhythmias not common Palpitations
Management of Arrhythmias The General Practitioners role Rohan Gunawardena MD, FRCP, FCCP, FACC Consultant Cardiac Electrophysiologist National Hospital of Sri Lanka Arrhythmias not common Palpitations
Atrial fibrillation. Understanding NICE guidance
 Understanding NICE guidance Information for people who use NHS services Atrial fibrillation NICE clinical guidelines advise the NHS on caring for people with specific conditions or diseases and the treatments
Understanding NICE guidance Information for people who use NHS services Atrial fibrillation NICE clinical guidelines advise the NHS on caring for people with specific conditions or diseases and the treatments
Upper gastrointestinal bleeding in children. Nguyễn Diệu Vinh, MD Department of Gastroenterology
 Upper gastrointestinal bleeding in children Nguyễn Diệu Vinh, MD Department of Gastroenterology INTRODUCTION Upper gastrointestinal (UGI) bleeding : arising proximal to the ligament of Treitz in the distal
Upper gastrointestinal bleeding in children Nguyễn Diệu Vinh, MD Department of Gastroenterology INTRODUCTION Upper gastrointestinal (UGI) bleeding : arising proximal to the ligament of Treitz in the distal
Anti arrhythmic drugs. Hilal Al Saffar College of medicine Baghdad University
 Anti arrhythmic drugs Hilal Al Saffar College of medicine Baghdad University Mechanism of Arrhythmia Abnormal heart pulse formation Abnormal heart pulse conduction Classification of Arrhythmia Abnormal
Anti arrhythmic drugs Hilal Al Saffar College of medicine Baghdad University Mechanism of Arrhythmia Abnormal heart pulse formation Abnormal heart pulse conduction Classification of Arrhythmia Abnormal
DYSRHYTHMIAS. D. Assess whether or not it is the arrhythmia that is making the patient unstable or symptomatic
 DYSRHYTHMIAS GENERAL CONSIDERATIONS A. The 2015 American Heart Association Guidelines were referred to for this protocol development. Evidence-based science was implemented in those areas where the AHA
DYSRHYTHMIAS GENERAL CONSIDERATIONS A. The 2015 American Heart Association Guidelines were referred to for this protocol development. Evidence-based science was implemented in those areas where the AHA
Instruct patient and caregivers: Need for constant monitoring Potential complications of drug therapy
 Assessment Prior to administration: Assess patient for chest pain, dysrhythmias, and vital signs (initially and throughout therapy) Obtain complete medical history, including allergies, especially heart
Assessment Prior to administration: Assess patient for chest pain, dysrhythmias, and vital signs (initially and throughout therapy) Obtain complete medical history, including allergies, especially heart
Emergency - Upper gastrointestinal haemorrhage
 Emergency - Upper gastrointestinal haemorrhage Definitions in upper gastrointestinal (UGI) haemorrhage UGI haemorrhage: bleeding that arises proximal to the ligament of Treitz i.e. from the oesophagus,
Emergency - Upper gastrointestinal haemorrhage Definitions in upper gastrointestinal (UGI) haemorrhage UGI haemorrhage: bleeding that arises proximal to the ligament of Treitz i.e. from the oesophagus,
AF in the ER: Common Scenarios CASE 1. Fast facts. Diagnosis. Management
 AF in the ER: Common Scenarios Atrial fibrillation is a common problem with a wide spectrum of presentations. Below are five common emergency room scenarios and the management strategies for each. Evan
AF in the ER: Common Scenarios Atrial fibrillation is a common problem with a wide spectrum of presentations. Below are five common emergency room scenarios and the management strategies for each. Evan
Arrhythmic Complications of MI. Teferi Mitiku, MD Assistant Clinical Professor of Medicine University of California Irvine
 Arrhythmic Complications of MI Teferi Mitiku, MD Assistant Clinical Professor of Medicine University of California Irvine Objectives Brief overview -Pathophysiology of Arrhythmia ECG review of typical
Arrhythmic Complications of MI Teferi Mitiku, MD Assistant Clinical Professor of Medicine University of California Irvine Objectives Brief overview -Pathophysiology of Arrhythmia ECG review of typical
Upper GI Bleeds. AMU Nurse Teaching Dr Clare Pollard ST6 AIM & GIM
 Upper GI Bleeds AMU Nurse Teaching Dr Clare Pollard ST6 AIM & GIM Peptic ulcer disease - GU - DU Talk Plan Important considerations in this group of patients- what you need to know Mallory Weis Tear Other
Upper GI Bleeds AMU Nurse Teaching Dr Clare Pollard ST6 AIM & GIM Peptic ulcer disease - GU - DU Talk Plan Important considerations in this group of patients- what you need to know Mallory Weis Tear Other
ECGs and Arrhythmias: Family Medicine Board Review 2009
 Rate Rhythm Intervals Hypertrophy ECGs and Arrhythmias: Family Medicine Board Review 2009 Axis Jess (Fogler) Waldura, MD University of California, San Francisco walduraj@nccc.ucsf.edu Ischemia Overview
Rate Rhythm Intervals Hypertrophy ECGs and Arrhythmias: Family Medicine Board Review 2009 Axis Jess (Fogler) Waldura, MD University of California, San Francisco walduraj@nccc.ucsf.edu Ischemia Overview
Pediatrics ECG Monitoring. Pediatric Intensive Care Unit Emergency Division
 Pediatrics ECG Monitoring Pediatric Intensive Care Unit Emergency Division 1 Conditions Leading to Pediatric Cardiology Consultation 12.7% of annual consultation Is arrhythmias problems Geggel. Pediatrics.
Pediatrics ECG Monitoring Pediatric Intensive Care Unit Emergency Division 1 Conditions Leading to Pediatric Cardiology Consultation 12.7% of annual consultation Is arrhythmias problems Geggel. Pediatrics.
Adult Basic Life Support
 Adult Basic Life Support UNRESPONSIVE? Shout for help Open airway NOT BREATHING NORMALLY? Call 112* 30 chest compressions 2 rescue breaths 30 compressions *or national emergency number Fig 1.2_Adult BLS
Adult Basic Life Support UNRESPONSIVE? Shout for help Open airway NOT BREATHING NORMALLY? Call 112* 30 chest compressions 2 rescue breaths 30 compressions *or national emergency number Fig 1.2_Adult BLS
Atrial Fibrillation Cases. Dr Paul Broadhurst Consultant Cardiologist
 Atrial Fibrillation Cases Dr Paul Broadhurst Consultant Cardiologist November 2011 Mr TH age 72 Routine medical for hypertension check Denies any symptoms despite close questioning PMH: hypertension, MI,
Atrial Fibrillation Cases Dr Paul Broadhurst Consultant Cardiologist November 2011 Mr TH age 72 Routine medical for hypertension check Denies any symptoms despite close questioning PMH: hypertension, MI,
Acute Arrhythmias in the Hospitalized Patient
 Acute Arrhythmias in the Hospitalized Patient Gregory M Marcus, MD, MAS Associate Professor of Medicine Division of Cardiology University of California, San Francisc Disclosures Medtronic: Research Support
Acute Arrhythmias in the Hospitalized Patient Gregory M Marcus, MD, MAS Associate Professor of Medicine Division of Cardiology University of California, San Francisc Disclosures Medtronic: Research Support
PHARMACOLOGY OF ARRHYTHMIAS
 PHARMACOLOGY OF ARRHYTHMIAS Course: Integrated Therapeutics 1 Lecturer: Dr. E. Konorev Date: November 27, 2012 Materials on: Exam #5 Required reading: Katzung, Chapter 14 1 CARDIAC ARRHYTHMIAS Abnormalities
PHARMACOLOGY OF ARRHYTHMIAS Course: Integrated Therapeutics 1 Lecturer: Dr. E. Konorev Date: November 27, 2012 Materials on: Exam #5 Required reading: Katzung, Chapter 14 1 CARDIAC ARRHYTHMIAS Abnormalities
Blood and guts.. Haemodynamics / resuscitation. Haemodynamics / resuscitation. Blood and guts. Dr Jonathan Hoare
 Blood and guts. Dr Jonathan Hoare Consultant St Mary s Hospital Dr Jonathan Hoare Consultant St Mary s Hospital, Paddington Blood and guts.. Presentation Initial assessment and management risk stratification
Blood and guts. Dr Jonathan Hoare Consultant St Mary s Hospital Dr Jonathan Hoare Consultant St Mary s Hospital, Paddington Blood and guts.. Presentation Initial assessment and management risk stratification
ECGs and Arrhythmias: Family Medicine Board Review 2012
 Overview ECGs and Arrhythmias: Family Medicine Board Review 2012 Jess Waldura, MD University of California, San Francisco walduraj@nccc.ucsf.edu Bundle branch blocks Quick review of ischemia Arrhythmias
Overview ECGs and Arrhythmias: Family Medicine Board Review 2012 Jess Waldura, MD University of California, San Francisco walduraj@nccc.ucsf.edu Bundle branch blocks Quick review of ischemia Arrhythmias
Scottish Medicines Consortium
 Scottish Medicines Consortium esomeprazole, 40mg vial of powder for solution for intravenous injection or infusion (Nexium I.V. ) No. (578/09) AstraZeneca 09 October 2009 The Scottish Medicines Consortium
Scottish Medicines Consortium esomeprazole, 40mg vial of powder for solution for intravenous injection or infusion (Nexium I.V. ) No. (578/09) AstraZeneca 09 October 2009 The Scottish Medicines Consortium
AF Diagnosis. Incorporated into over 75 health checks and Public Health Checks
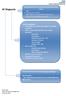 AF Diagnosis Incpated into over 75 health checks and Public Health Checks Pulse Feel the pulse in all >65yrs If irregular do a 12 Lead ECG with Rhythm strip Check Thyroid and FBC and heart rate Refer to
AF Diagnosis Incpated into over 75 health checks and Public Health Checks Pulse Feel the pulse in all >65yrs If irregular do a 12 Lead ECG with Rhythm strip Check Thyroid and FBC and heart rate Refer to
MANAGEMENT OF DYSPEPSIA AND GASTRO-OESOPHAGEAL REFLUX DISEASE (GORD)
 DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) MANAGEMENT OF DYSPEPSIA AND GASTRO-OESOPHAGEAL REFLUX DISEASE (GORD) Routine endoscopic investigation of patients of any age, presenting with dyspepsia
DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) MANAGEMENT OF DYSPEPSIA AND GASTRO-OESOPHAGEAL REFLUX DISEASE (GORD) Routine endoscopic investigation of patients of any age, presenting with dyspepsia
Supplementary Online Content
 Supplementary Online Content Morillo CA, Verma A, Connolly SJ, et al. Radiofrequency ablation vs antiarrhythmic drugs as first-line Treatment of Paroxysmal Atrial Fibrillation (RAAFT-2): a randomzied clinical
Supplementary Online Content Morillo CA, Verma A, Connolly SJ, et al. Radiofrequency ablation vs antiarrhythmic drugs as first-line Treatment of Paroxysmal Atrial Fibrillation (RAAFT-2): a randomzied clinical
Clinical Problem. Management. Discussion
 Optimum management of atrial fibrillation in the Intensive Care Unit Clinical Problem A 61 year old man, PD, presented to the Intensive Care Unit (ICU) after angiography and intra arterial thrombolysis
Optimum management of atrial fibrillation in the Intensive Care Unit Clinical Problem A 61 year old man, PD, presented to the Intensive Care Unit (ICU) after angiography and intra arterial thrombolysis
TACHYARRHYTHMIAS IN INFANTS AND CHILDREN
 Principles of Management SVT Algorithm VT Algorithm Interpretations of ECG Supra-ventricular Tachycardia (SVT) background SVT Management SVT Ongoing Care Ventricular Tachycardia (VT) References Principles
Principles of Management SVT Algorithm VT Algorithm Interpretations of ECG Supra-ventricular Tachycardia (SVT) background SVT Management SVT Ongoing Care Ventricular Tachycardia (VT) References Principles
Upper GI Bleeding. HH Tsai MD FRCP FECG Consultant Gastroenterologist
 Upper GI Bleeding HH Tsai MD FRCP FECG Consultant Gastroenterologist Financial Disclosures I have no financial relationship with any manufacturer or supplier of any product mentioned in this talk. GI Audits:
Upper GI Bleeding HH Tsai MD FRCP FECG Consultant Gastroenterologist Financial Disclosures I have no financial relationship with any manufacturer or supplier of any product mentioned in this talk. GI Audits:
Treatment strategy decision tree
 strategy decision tree strategy decision tree Confirmed diagnosis of AF Further investigations and clinical assessment including risk stratification for stroke/thromboembolism Paroxysmal AF Persistent
strategy decision tree strategy decision tree Confirmed diagnosis of AF Further investigations and clinical assessment including risk stratification for stroke/thromboembolism Paroxysmal AF Persistent
Ablation Update and Case Studies. Lawrence Nair, MD, FACC Director of Electrophysiology Presbyterian Heart Group
 Ablation Update and Case Studies Lawrence Nair, MD, FACC Director of Electrophysiology Presbyterian Heart Group Disclosures No financial relationships to disclose Objectives At the conclusion of this activity,
Ablation Update and Case Studies Lawrence Nair, MD, FACC Director of Electrophysiology Presbyterian Heart Group Disclosures No financial relationships to disclose Objectives At the conclusion of this activity,
Etienne Aliot. University of Nancy - France
 Etienne Aliot University of Nancy - France Disclosures Consulting fees : - Bayer, Boehringer Ingelheim,GSK, MedaPharma, Pfizer/BMS,Sanofi Aventis. - Biotronik,Medtronic,St Jude Medical. Electrical vs Pharmacological
Etienne Aliot University of Nancy - France Disclosures Consulting fees : - Bayer, Boehringer Ingelheim,GSK, MedaPharma, Pfizer/BMS,Sanofi Aventis. - Biotronik,Medtronic,St Jude Medical. Electrical vs Pharmacological
Atrial Fibrillation. A guide for Southwark General Practice. Key Messages. Always work within your knowledge and competency
 Atrial Fibrillation A guide for Southwark General Practice Key Messages 1. Routinely offer pulse checks to patients at high risk of AF 2. Use the CHA 2 DS 2 VASc score to identify patients for anticoagulation
Atrial Fibrillation A guide for Southwark General Practice Key Messages 1. Routinely offer pulse checks to patients at high risk of AF 2. Use the CHA 2 DS 2 VASc score to identify patients for anticoagulation
On-Call Upper GI Bleeding. Upper Gastrointestinal Bleeding
 On-Call Upper GI Bleeding John R Saltzman MD, FACG Director of Endoscopy Brigham and Women s Hospital Associate Professor of Medicine Harvard Medical School Upper Gastrointestinal Bleeding 300,000000 hospitalizations/year
On-Call Upper GI Bleeding John R Saltzman MD, FACG Director of Endoscopy Brigham and Women s Hospital Associate Professor of Medicine Harvard Medical School Upper Gastrointestinal Bleeding 300,000000 hospitalizations/year
ΚΟΛΠΙΚΗ ΜΑΡΜΑΡΥΓΗ ΦΑΡΜΑΚΕΥΤΙΚΗ ΗΛΕΚΤΡΙΚΗ ΑΝΑΤΑΞΗ. ΣΠΥΡΟΜΗΤΡΟΣ ΓΕΩΡΓΙΟΣ Καρδιολόγος, Ε/Α, Γ.Ν.Κατερίνης. F.E.S.C
 ΚΟΛΠΙΚΗ ΜΑΡΜΑΡΥΓΗ ΦΑΡΜΑΚΕΥΤΙΚΗ ΗΛΕΚΤΡΙΚΗ ΑΝΑΤΑΞΗ ΣΠΥΡΟΜΗΤΡΟΣ ΓΕΩΡΓΙΟΣ Καρδιολόγος, Ε/Α, Γ.Ν.Κατερίνης. F.E.S.C Definitions of AF: A Simplified Scheme Term Definition Paroxysmal AF AF that terminates
ΚΟΛΠΙΚΗ ΜΑΡΜΑΡΥΓΗ ΦΑΡΜΑΚΕΥΤΙΚΗ ΗΛΕΚΤΡΙΚΗ ΑΝΑΤΑΞΗ ΣΠΥΡΟΜΗΤΡΟΣ ΓΕΩΡΓΙΟΣ Καρδιολόγος, Ε/Α, Γ.Ν.Κατερίνης. F.E.S.C Definitions of AF: A Simplified Scheme Term Definition Paroxysmal AF AF that terminates
Adenosine. poison/drug induced. flushing, chest pain, transient asystole. Precautions: tachycardia. fibrillation, atrial flutter. Indications: or VT
 Adenosine Indications: 1. Narrow complex PSVT 2. Does not convert atrial fibrillation, atrial flutter or VT 1. Side effects include flushing, chest pain, transient asystole 2. May deteriorate widecomplex
Adenosine Indications: 1. Narrow complex PSVT 2. Does not convert atrial fibrillation, atrial flutter or VT 1. Side effects include flushing, chest pain, transient asystole 2. May deteriorate widecomplex
Update on Palpitations and AF February 28 th 2018
 Update on Palpitations and AF February 28 th 2018 Dr Mrinal Andrew Saha MA(Cantab) MBBS FRCP PhD Consultant Interventional Cardiologist GHNHSFT Dr Mrinal Saha Appointed 2010 Special interests: Angioplasty,
Update on Palpitations and AF February 28 th 2018 Dr Mrinal Andrew Saha MA(Cantab) MBBS FRCP PhD Consultant Interventional Cardiologist GHNHSFT Dr Mrinal Saha Appointed 2010 Special interests: Angioplasty,
Core Content In Urgent Care Medicine
 Palpitations/Arrhythmias Ebrahim Barkoudah, MD Clinical Instructor in Internal Medicine Harvard Medical School Assistant in Internal Medicine & Pediatrics Massachusetts General Hospital MGH Chelsea Chelsea,
Palpitations/Arrhythmias Ebrahim Barkoudah, MD Clinical Instructor in Internal Medicine Harvard Medical School Assistant in Internal Medicine & Pediatrics Massachusetts General Hospital MGH Chelsea Chelsea,
Atrial fibrillation and flutter in primary care
 Atrial fibrillation and flutter in primary care Atrial fibrillation is underdiagnosed and undertreated Atrial fibrillation or flutter (AF)* occurs in approximately 1% of the general population. The prevalence
Atrial fibrillation and flutter in primary care Atrial fibrillation is underdiagnosed and undertreated Atrial fibrillation or flutter (AF)* occurs in approximately 1% of the general population. The prevalence
Review guidance for patients on long-term amiodarone treatment
 Review guidance for patients on long-term amiodarone treatment This review guidance document has been produced in response to: 1. Current supply shortages of branded and generic versions of 100mg and 200mg
Review guidance for patients on long-term amiodarone treatment This review guidance document has been produced in response to: 1. Current supply shortages of branded and generic versions of 100mg and 200mg
Treatment of Arrhythmias in the Emergency Setting
 Treatment of Arrhythmias in the Emergency Setting Zian H. Tseng, M.D. Assistant Professor of Medicine Cardiac Electrophysiology Section Cardiology Division University of California, San Francisco There
Treatment of Arrhythmias in the Emergency Setting Zian H. Tseng, M.D. Assistant Professor of Medicine Cardiac Electrophysiology Section Cardiology Division University of California, San Francisco There
Drugs Controlling Myocyte Excitability and Conduction at the AV node Singh and Vaughan-Williams Classification
 Drugs Controlling Myocyte Excitability and Conduction at the AV node Singh and Vaughan-Williams Classification Class I Na Channel Blockers Flecainide Propafenone Class III K channel Blockers Dofetilide,
Drugs Controlling Myocyte Excitability and Conduction at the AV node Singh and Vaughan-Williams Classification Class I Na Channel Blockers Flecainide Propafenone Class III K channel Blockers Dofetilide,
NICE Pathways bring together all NICE guidance, quality standards and other NICE information on a specific topic.
 bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published.
bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published.
James Irwin Gastroenterology Department Palmerston North Hospital. Acute Medicine Meeting Hutt Hospital. June 21, 2015
 The Management of Acute Upper Gastrointestinal Bleeding James Irwin Gastroenterology Department Palmerston North Hospital Acute Medicine Meeting Hutt Hospital June 21, 2015 Outline Common Definitions and
The Management of Acute Upper Gastrointestinal Bleeding James Irwin Gastroenterology Department Palmerston North Hospital Acute Medicine Meeting Hutt Hospital June 21, 2015 Outline Common Definitions and
Blood pressure parameters for iv amiodarone
 Blood pressure parameters for iv amiodarone Search 17-7-2012 ICU & Fluids - Electrolytes - Nutrition: Edited by Andy S. Binder, MD, Pulmonologist, Critical Care. Contents: Electrolytes : Fluids: Dehydration.
Blood pressure parameters for iv amiodarone Search 17-7-2012 ICU & Fluids - Electrolytes - Nutrition: Edited by Andy S. Binder, MD, Pulmonologist, Critical Care. Contents: Electrolytes : Fluids: Dehydration.
Management of acute Cardiac Arrhythmias
 Management of acute Cardiac Arrhythmias Dr. Zulkeflee Muhammad MBChB (New Zealand), MRCP (United Kingdom) Cardiologist Electrophysiology Unit Istitut Jantung Negara Objectives Review the etiology and recognition
Management of acute Cardiac Arrhythmias Dr. Zulkeflee Muhammad MBChB (New Zealand), MRCP (United Kingdom) Cardiologist Electrophysiology Unit Istitut Jantung Negara Objectives Review the etiology and recognition
Mission Statement for our Arrhythmia Care
 Mission Statement for our Arrhythmia Care We are dedicated to provide a compassionate and an outstanding care for patients with cardiac arrhythmias. We will be utilizing the cutting edge and the most advanced
Mission Statement for our Arrhythmia Care We are dedicated to provide a compassionate and an outstanding care for patients with cardiac arrhythmias. We will be utilizing the cutting edge and the most advanced
Antiarrhythmic Drugs 1/31/2018 1
 Antiarrhythmic Drugs 1/31/2018 1 Normal conduction pathway: 1- SA node generates action potential and delivers it to the atria and the AV node 2- The AV node delivers the impulse to purkinje fibers Other
Antiarrhythmic Drugs 1/31/2018 1 Normal conduction pathway: 1- SA node generates action potential and delivers it to the atria and the AV node 2- The AV node delivers the impulse to purkinje fibers Other
Understanding Atrial Fibrillation Management. Roy Lin, MD
 Understanding Atrial Fibrillation Management Roy Lin, MD Disclosure None Definition of atrial fibrillation Atrial fibrillation is a supraventricular tachyarrhythmia characterized by uncoordinated atrial
Understanding Atrial Fibrillation Management Roy Lin, MD Disclosure None Definition of atrial fibrillation Atrial fibrillation is a supraventricular tachyarrhythmia characterized by uncoordinated atrial
British Society of Gastroenterology. St. Elsewhere's Hospital. National Comparative Audit of Blood Transfusion
 British Society of Gastroenterology UK Com parat ive Audit of Upper Gast roint est inal Bleeding and t he Use of Blood Transfusion Extract December 2007 St. Elsewhere's Hospital National Comparative Audit
British Society of Gastroenterology UK Com parat ive Audit of Upper Gast roint est inal Bleeding and t he Use of Blood Transfusion Extract December 2007 St. Elsewhere's Hospital National Comparative Audit
Antiplatelets in cardiac patients with suspected GI bleeding
 Antiplatelets in cardiac patients with suspected GI bleeding Acute GI bleeding is a common major medical emergency. In the 2007 UK-wide audit, overall mortality of patients admitted with acute GI bleeding
Antiplatelets in cardiac patients with suspected GI bleeding Acute GI bleeding is a common major medical emergency. In the 2007 UK-wide audit, overall mortality of patients admitted with acute GI bleeding
Palpitations.
 Palpitations http://www.heartfailurematters.org/en/understandingheartfailure/publishingimages/palpitations_lg.jpg Palpitations are the perception of cardiac activity. They are often described as a fluttering,
Palpitations http://www.heartfailurematters.org/en/understandingheartfailure/publishingimages/palpitations_lg.jpg Palpitations are the perception of cardiac activity. They are often described as a fluttering,
Arrhythmias. 1. beat too slowly (sinus bradycardia). Like in heart block
 Arrhythmias It is a simple-dysfunction caused by abnormalities in impulse formation and conduction in the myocardium. The heart is designed in such a way that allows it to generate from the SA node electrical
Arrhythmias It is a simple-dysfunction caused by abnormalities in impulse formation and conduction in the myocardium. The heart is designed in such a way that allows it to generate from the SA node electrical
UGI BLEED. Dr. KPP Abhilash Associate Professor Department of Emergency Medicine Christian Medical College, Vellore
 UGI BLEED Dr. KPP Abhilash Associate Professor Department of Emergency Medicine Christian Medical College, Vellore Outline UGI bleed: etiology and presentation Management: Non variceal / variceal bleed
UGI BLEED Dr. KPP Abhilash Associate Professor Department of Emergency Medicine Christian Medical College, Vellore Outline UGI bleed: etiology and presentation Management: Non variceal / variceal bleed
PhD FRCP MESC MEAPCI. Consultant Cardiologist SVT - Supra Ventricular Tachycardia. Coronary Arteries
 SVT - Supra Ventricular Tachycardia Coronary Arteries Overview LMS Supraventricular tachycardia is defined as an abnormally fast heartbeat. It's a describes a group of arrhythmias which all originate from
SVT - Supra Ventricular Tachycardia Coronary Arteries Overview LMS Supraventricular tachycardia is defined as an abnormally fast heartbeat. It's a describes a group of arrhythmias which all originate from
Guideline for the Management of patients with Regular Narrow-Complex Tachyarrhythmia
 Guideline for the Management of patients with Regular Narrow-Complex Tachyarrhythmia This guidance does not override the individual responsibility of health professionals to make appropriate decision according
Guideline for the Management of patients with Regular Narrow-Complex Tachyarrhythmia This guidance does not override the individual responsibility of health professionals to make appropriate decision according
Management strategies for atrial fibrillation Thursday, 20 October :27
 ALTHOUGH anyone who has had to run up a flight of steps or has had a frightening experience is quite familiar with a racing heartbeat, for the more than 2 million Americans who suffer from atrial fibrillation
ALTHOUGH anyone who has had to run up a flight of steps or has had a frightening experience is quite familiar with a racing heartbeat, for the more than 2 million Americans who suffer from atrial fibrillation
2/1/2013. Poisoning pitfalls. The original pitfall
 The original pitfall Poisoning pitfalls Craig Smollin MD Associate Medical Director, California Poison Control System - SF Division Assistant Professor of Emergency Medicine, UCSF What will we talk about?
The original pitfall Poisoning pitfalls Craig Smollin MD Associate Medical Director, California Poison Control System - SF Division Assistant Professor of Emergency Medicine, UCSF What will we talk about?
Basics of Atrial Fibrillation. By Mini Thannikal NP-BC Mount Sinai St Luke s Hospital New York, NY
 Basics of Atrial Fibrillation By Mini Thannikal NP-BC Mount Sinai St Luke s Hospital New York, NY Atrial Fibrillation(AF) is a supraventricular tachyarrhythmia characterized by uncoordinated atrial activation
Basics of Atrial Fibrillation By Mini Thannikal NP-BC Mount Sinai St Luke s Hospital New York, NY Atrial Fibrillation(AF) is a supraventricular tachyarrhythmia characterized by uncoordinated atrial activation
1/3/2008. Karen Burke Priscilla LeMone Elaine Mohn-Brown. Medical-Surgical Nursing Care, 2e Karen Burke, Priscilla LeMone, and Elaine Mohn-Brown
 Medical-Surgical Nursing Care Second Edition Karen Burke Priscilla LeMone Elaine Mohn-Brown Chapter 26 Caring for Clients with Coronary Heart Disease and Dysrhythmias Coronary Heart Disease (CHD) Leading
Medical-Surgical Nursing Care Second Edition Karen Burke Priscilla LeMone Elaine Mohn-Brown Chapter 26 Caring for Clients with Coronary Heart Disease and Dysrhythmias Coronary Heart Disease (CHD) Leading
Supplementary Online Content
 Supplementary Online Content Verma A, Champagne J, Sapp J, et al. Asymptomatic episodes of atrial fibrillation before and after catheter ablation: a prospective, multicenter study. JAMA Intern Med. Published
Supplementary Online Content Verma A, Champagne J, Sapp J, et al. Asymptomatic episodes of atrial fibrillation before and after catheter ablation: a prospective, multicenter study. JAMA Intern Med. Published
Risk assessment in UGIB: recent PCI & ACS. Dr Martin James PhD FRCP October 20 th 2016 Nottingham Endoscopy Masterclass
 Risk assessment in UGIB: recent PCI & ACS Dr Martin James PhD FRCP October 20 th 2016 Nottingham Endoscopy Masterclass Clinical scenario 65 yr male Previous smoker, hyperlipidaemia, DM PCI < 48 hours Dual
Risk assessment in UGIB: recent PCI & ACS Dr Martin James PhD FRCP October 20 th 2016 Nottingham Endoscopy Masterclass Clinical scenario 65 yr male Previous smoker, hyperlipidaemia, DM PCI < 48 hours Dual
3/25/2017. Program Outline. Classification of Atrial Fibrillation
 Alternate Strategies to Antiarrhythmic Therapy: The Role of Ablation Jennifer El Aile, MS, AGPCNP-BC Electrophysiology Nurse Practitioner Clinical Lecturer at the University of Michigan Program Outline
Alternate Strategies to Antiarrhythmic Therapy: The Role of Ablation Jennifer El Aile, MS, AGPCNP-BC Electrophysiology Nurse Practitioner Clinical Lecturer at the University of Michigan Program Outline
How do arrhythmias occur?
 How do arrhythmias occur? An arrhythmia is an abnormal heart rhythm (= dysrhythmia). Can be fast (tachy) or slow (brady). Brady arrhythmias are usually due to conduc;on block, while tachyarrhythmias are
How do arrhythmias occur? An arrhythmia is an abnormal heart rhythm (= dysrhythmia). Can be fast (tachy) or slow (brady). Brady arrhythmias are usually due to conduc;on block, while tachyarrhythmias are
SHOCK THE PATIENT. Disclosures. Goals of the Talk. Tachyarrhythmias- Unstable 11/7/2017
 Disclosures Common Heart Rhythms in the Hospital Research Support: NIH, PCORI, Medtronic, Cardiogram Consulting: InCarda, Johnson & Johnson, Lifewatch Equity: InCarda Gregory M Marcus, MD, MAS Associate
Disclosures Common Heart Rhythms in the Hospital Research Support: NIH, PCORI, Medtronic, Cardiogram Consulting: InCarda, Johnson & Johnson, Lifewatch Equity: InCarda Gregory M Marcus, MD, MAS Associate
Understanding Atrial Fibrillation A guide for patients
 Understanding Atrial Fibrillation A guide for patients Your doctor has determined that you have atrial fibrillation (AF), a common disturbance of the heart s rhythm. This pamphlet will answer many of your
Understanding Atrial Fibrillation A guide for patients Your doctor has determined that you have atrial fibrillation (AF), a common disturbance of the heart s rhythm. This pamphlet will answer many of your
Episode 112 Tachydysrhythmias
 Wide & regular tachydysrhythmias Ventricular Tachycardia (VT) vs SVT with aberrancy: Assume VT Episode 112 Tachydysrhythmias With Amal Mattu & Paul Dorion Prepared by Shaun Mehta, July 2018 General Approach
Wide & regular tachydysrhythmias Ventricular Tachycardia (VT) vs SVT with aberrancy: Assume VT Episode 112 Tachydysrhythmias With Amal Mattu & Paul Dorion Prepared by Shaun Mehta, July 2018 General Approach
ECGs on the acute admission ward. - Cardiology Update -
 ECGs on the acute admission ward - Cardiology Update - Dr Simon Fynn Consultant Cardiologist Papworth Hospital, Cambridge RCP London Oct 2017 ECG 1 1. AF with BBB 2. Pre-excited AF 3. SVT with BBB 4.
ECGs on the acute admission ward - Cardiology Update - Dr Simon Fynn Consultant Cardiologist Papworth Hospital, Cambridge RCP London Oct 2017 ECG 1 1. AF with BBB 2. Pre-excited AF 3. SVT with BBB 4.
! YOU NEED TO MONITOR QT INTERVALS IN THESE PATIENTS.
 Antiarrhythmic Pharmacopoeia Powerful drugs, split into 4 major classes, according to the predominant receptor they effect. Some fit into several classes at once, like sotolol. Some don t fit at all, owing
Antiarrhythmic Pharmacopoeia Powerful drugs, split into 4 major classes, according to the predominant receptor they effect. Some fit into several classes at once, like sotolol. Some don t fit at all, owing
CSI Skills Lab #5: Arrhythmia Interpretation and Treatment
 CSI 202 - Skills Lab #5: Arrhythmia Interpretation and Treatment Origins of the ACLS Approach: CSI 202 - Skills Lab 5 Notes ACLS training originated in Nebraska in the early 1970 s. Its purpose was to
CSI 202 - Skills Lab #5: Arrhythmia Interpretation and Treatment Origins of the ACLS Approach: CSI 202 - Skills Lab 5 Notes ACLS training originated in Nebraska in the early 1970 s. Its purpose was to
Current Guideline for AF Treatment. Young Keun On, MD, PhD, FHRS Samsung Medical Center Sungkyunkwan University School of Medicine
 Current Guideline for AF Treatment Young Keun On, MD, PhD, FHRS Samsung Medical Center Sungkyunkwan University School of Medicine Case 1 59 year-old lady Sudden palpitation and breathlessness for 12 hours
Current Guideline for AF Treatment Young Keun On, MD, PhD, FHRS Samsung Medical Center Sungkyunkwan University School of Medicine Case 1 59 year-old lady Sudden palpitation and breathlessness for 12 hours
ACG Clinical Guideline: Management of Patients with Ulcer Bleeding
 ACG Clinical Guideline: Management of Patients with Ulcer Bleeding Loren Laine, MD 1,2 and Dennis M. Jensen, MD 3 5 1 Section of Digestive Diseases, Yale University School of Medicine, New Haven, Connecticut,
ACG Clinical Guideline: Management of Patients with Ulcer Bleeding Loren Laine, MD 1,2 and Dennis M. Jensen, MD 3 5 1 Section of Digestive Diseases, Yale University School of Medicine, New Haven, Connecticut,
Clinical guideline Published: 13 June 2012 nice.org.uk/guidance/cg141
 Acute upper gastrointestinal bleeding in over 16s: management Clinical guideline Published: June 2012 nice.org.uk/guidance/cg141 NICE 2018. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Acute upper gastrointestinal bleeding in over 16s: management Clinical guideline Published: June 2012 nice.org.uk/guidance/cg141 NICE 2018. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Use of Antiarrhythmic Drugs for AF Who, What and How? Dr. Marc Cheng Queen Elizabeth Hospital
 Use of Antiarrhythmic Drugs for AF Who, What and How? Dr. Marc Cheng Queen Elizabeth Hospital Content i. Rhythm versus Rate control ii. Anti-arrhythmic for Rhythm Control iii. Anti-arrhythmic for Rate
Use of Antiarrhythmic Drugs for AF Who, What and How? Dr. Marc Cheng Queen Elizabeth Hospital Content i. Rhythm versus Rate control ii. Anti-arrhythmic for Rhythm Control iii. Anti-arrhythmic for Rate
Pediatrics. Arrhythmias in Children: Bradycardia and Tachycardia Diagnosis and Treatment. Overview
 Pediatrics Arrhythmias in Children: Bradycardia and Tachycardia Diagnosis and Treatment See online here The most common form of cardiac arrhythmia in children is sinus tachycardia which can be caused by
Pediatrics Arrhythmias in Children: Bradycardia and Tachycardia Diagnosis and Treatment See online here The most common form of cardiac arrhythmia in children is sinus tachycardia which can be caused by
Gastrointestinal bleeding and life threating conditions in surgery
 CM w Bydgoszczy UMK w Toruniu Włodzimierz Gniłka Gastrointestinal bleeding and life threating conditions in surgery Gastrointestinal hemorrhage Upper GI hemorrhage proximal to the Treitz ligament (accounts
CM w Bydgoszczy UMK w Toruniu Włodzimierz Gniłka Gastrointestinal bleeding and life threating conditions in surgery Gastrointestinal hemorrhage Upper GI hemorrhage proximal to the Treitz ligament (accounts
ARRHYTHMIA SINUS RHYTHM
 ARRHYTHMIA Dr. Ahmed A. Elberry, MBBCH, MSc, MD Assistant Professor of Clinical Pharmacy Faculty of pharmacy, KAU 1 SINUS RHYTHM SA node is cardiac pacemaker Normal sinus rhythm 60-100 beats/min Depolarisation
ARRHYTHMIA Dr. Ahmed A. Elberry, MBBCH, MSc, MD Assistant Professor of Clinical Pharmacy Faculty of pharmacy, KAU 1 SINUS RHYTHM SA node is cardiac pacemaker Normal sinus rhythm 60-100 beats/min Depolarisation
Tachycardias II. Štěpán Havránek
 Tachycardias II Štěpán Havránek Summary 1) Supraventricular (supraventricular rhythms) Atrial fibrillation and flutter Atrial ectopic tachycardia / extrabeats AV nodal reentrant a AV reentrant tachycardia
Tachycardias II Štěpán Havránek Summary 1) Supraventricular (supraventricular rhythms) Atrial fibrillation and flutter Atrial ectopic tachycardia / extrabeats AV nodal reentrant a AV reentrant tachycardia
GASTROINESTINAL BLEEDING. Dr.Ammar I. Abdul-Latif
 GASTROINESTINAL BLEEDING Dr.Ammar I. Abdul-Latif CLASSIFICATION OF G.I.BLEEDING GIB Appearance Acuity Site Apparent Acute Upper Obscure Chronic Lower UPPER&LOWER G.I.BLEEDING CAUSES OF UPPER G.I. BLEEDING
GASTROINESTINAL BLEEDING Dr.Ammar I. Abdul-Latif CLASSIFICATION OF G.I.BLEEDING GIB Appearance Acuity Site Apparent Acute Upper Obscure Chronic Lower UPPER&LOWER G.I.BLEEDING CAUSES OF UPPER G.I. BLEEDING
