Bacteriological outcome of combination versus single-agent treatment for staphylococcal endocarditis
|
|
|
- Egbert Homer Melton
- 6 years ago
- Views:
Transcription
1 Journal of Antimicrobial Chemotherapy (2003) 52, DOI: /jac/dkg440 Advance Access publication 30 September 2003 Bacteriological outcome of versus single-agent treatment for staphylococcal endocarditis Dragana DrinkoviM 1, Arthur J. Morris 1 *, Sudha Pottumarthy 1, Donald MacCulloch 1 and Teena West 2 Departments of 1 Microbiology and 2 Biostatistics, Green Lane Hospital, Auckland, New Zealand Received 10 June 2003; returned 12 July 2003; revised 23 July 2003; accepted 11 August 2003 Objective: To analyse the bacteriological outcome of versus single-agent antimicrobial treatment in staphylococcal endocarditis. Patients and methods: Retrospective review of 152 episodes: 91 cases of native valve endocarditis (NVE), 74 due to Staphylococcus aureus and 17 due to coagulase-negative staphylococci (CoNS); and 61 cases of prosthetic valve endocarditis (PVE), 29 due to S. aureus and 32 due to CoNS. Results: Valves from patients with S. aureus NVE treated with any kind of antibiotic treatment were no more likely to be culture-negative than those treated with a single agent [19 (45%) of 42 versus 13 (41%) of 32; P = 0.69]. This finding remained unchanged when cases of CoNS NVE were added to the S. aureus group. In PVE, after adjusting for duration of treatment, valves from patients receiving any kind of treatment were 5.9 times (95% confidence interval ) more likely to be culture-negative than those receiving monotherapy (P = 0.024). Patients treated for >14 days were more likely to be culturenegative than those treated for 14 days [49 (83%) of 59 versus 29 (31%) of 93; P < 0.001]. Conclusions: In staphylococcal NVE, treatment is not superior to monotherapy in sterilizing infected valves, but in PVE treatment confers an advantage. Keywords: coagulase-negative staphylococci, culture result, heart valves, Staphylococcus aureus, Staphylococcus epidermidis Introduction Information on the relative efficacy of versus singleagent antimicrobial treatment to achieve valve sterilization in staphylococcal endocarditis is incomplete. 1 Nevertheless, regimens are recommended in both UK and US guidelines. 2,3 The UK guidelines are simpler than those from the US, and make similar recommendations for the choice of agents in both native (NVE) and prosthetic valve (PVE) staphylococcal endocarditis. 2 Gentamicin is recommended for the initial 7 days of treatment, with rifampicin being suggested for difficult cases. 2 The US recommendations make a distinction between NVE and PVE. For NVE gentamicin is suggested for the first 3 5 days of treatment. For PVE initial triple-agent treatment, vancomycin or a β-lactamase-resistant penicillin, rifampicin and gentamicin, is recommended. 3 To test the hypothesis that antimicrobial treatment is more likely to result in valve sterilization than single-agent treatment we have analysed valve culture results of patients undergoing valve replacement surgery for staphylococcal endocarditis with respect to the preoperative antimicrobial treatment. Patients and methods Patient population Green Lane Hospital s cardiothoracic surgical unit serves 1 million people and is the reference centre for complicated cases for all New Zealand ( 4 million people). All patients undergoing valve replacement surgery from September 1963 through December 1999 who had endocarditis recorded as the cause of their valve dysfunction had their charts reviewed. 4 The information recorded for each patient included: identifying information, number of blood cultures taken, number of positive blood cultures sets, organism(s) isolated, duration and type of antibiotic treatment received before surgery, indication(s) for surgery (valve function, heart failure, fever/sepsis, emboli), operation findings and culture result of the resected valve *Correspondence address. Microbiology Laboratory, Auckland City Hospital, PO Box , Auckland 1003, New Zealand. Tel: ; Fax: ; amorris@dml.co.nz JAC vol.52 no.5 The British Society for Antimicrobial Chemotherapy 2003; all rights reserved.
2 Single versus treatment in staphylococcal IE Table 1. Treatment regimens and valve culture results for S. aureus NVE Culture result Group a n Treatment regimen Median (days) positive (%) negative (%) Comment 1 32 single agent (59) 13 (41) three patients were started on gentamicin treatment but were switched early to flucloxacillin alone 2 27 continuous 9 18 (67) 9 (33) most [24 (89%)] received β-lactam and aminoglycoside treatment, usually flucloxacillin and gentamicin 3 9 initial 11 4 (44) 5 (56) initial β-lactam and aminoglycoside, then β-lactam alone 4 6 partial (17) 5 (83) various antibiotics used: β-lactam, gentamicin, vancomycin, rifampicin a Group 1 versus 2, P = 0.56; group 1 versus 2 + 3, P = 0.88; group 1 versus , P = After adjusting for duration of treatment by logistic regression analysis valves from patients receiving any kind of treatment were no more likely to be culture-negative than those receiving monotherapy (odds ratio 0.45; 95% CI ; P = 0.23). Definitions The modified Duke criteria 5 were used to define cases of endocarditis, except that a positive microbiology Gram stain was taken as definitive evidence of endocarditis. 4 PVE was defined as: early when it occurred within 60 days of valve insertion, intermediate between 60 days and 12 months after surgery, and late >12 months after surgery. 6 Combination antibiotic treatment was defined as receipt of two or more antibiotics active against the staphylococcal isolate, and regarded as having the potential to act synergically, 1 simultaneously for at least 1 day. In vitro tests for synergy were not performed. Continuous treatment was defined as receipt of two or more active antibiotics for the entire preoperative period. Initial treatment was defined as receipt of two or more active antibiotics for at least the first 3 days of treatment, but not for entire preoperative course. Partial treatment was defined as receipt of two or more active antibiotics for a part of the preoperative period other than above. Patients received standard doses of the respective antibiotics, e.g. flucloxacillin 12 g daily in six divided intravenous (iv) doses, vancomycin iv 1 g twice a day, gentamicin 1 mg/kg, iv three times a day, with appropriate adjustments for impaired renal function. Laboratory procedures Resected valves were sent for Gram stain and culture as described previously. 4 Briefly, following macroscopic examination, vegetations and material that appeared to be infected were removed, ground in trypticase soy broth, Gram stains made, and solid and four liquid media inoculated. Media were examined regularly and discarded after 7 days. Routine broth subcultures onto solid media were performed after incubation for 7 days and the plates were incubated for 48 h aerobically and anaerobically before being discarded. Adherent clot or other material removed from prosthetic valves was treated as above. Isolates from surgical specimens were compared with available preoperative blood culture isolates. Statistics Data are presented as counts (percentages) and median (inter-quartile range) unless otherwise stated. Groups were compared using the χ 2 -test and logistic regression analysis was used to adjust for indications for surgery and duration of treatment. Statistical analysis was performed using SAS release 8.0 software (Cary, NC, USA). Results One hundred and seventy-four patients had staphylococcal infective endocarditis (IE). Two patients, receiving antibiotic treatment, had negative preoperative blood cultures but positive valve cultures. All other patients had positive preoperative blood cultures. Twenty-two patients were excluded from this study: 12 because they had not received antibiotic treatment before valve replacement and eight because valve cultures were not performed; one patient was excluded because of discrepant susceptibility results between blood culture and valve isolates and another case excluded because there were insufficient susceptibility data to match the isolates. Of the remaining 152 cases, 91 (60%) had NVE and 61 (40%) had PVE; 139 met the criteria for definite endocarditis, 135 (89%) by pathological and four (3%) by clinical criteria, and 13 (9%) met the criteria for possible IE. 4,5 Staphylococcus aureus NVE Seventy-four (81%) of the 91 patients with NVE had Staphylococcus aureus infection (Table 1). Only one patient had methicillin-resistant S. aureus (MRSA) infection. Three patients were injecting drug users, two with tricuspid valve infection. Forty-two patients had aortic valve IE, 23 mitral valve, three both aortic and mitral valve, and six had tricuspid valve IE. Invasive extravalvular infection was present in 38 (51%) patients. Thirty-two (43%) of these 74 patients were treated with a single β-lactam antibiotic, either flucloxacillin or penicillin (Table 1). Nineteen (59%) of the 32 were valve culture positive. Twenty-seven patients had continuous therapy. In two patients rifampicin was added to β-lactam and aminoglycoside treatment and in one patient it was combined with the β-lactam only. Eighteen (67%) of these 27 patients had positive valve cultures. Patients receiving continuous treatment were no more likely to be culture-negative than those receiving single-agent treatment [nine (33%) of 27 versus 13 (41%) of 32, respectively; P = 0.56] (Table 1). Nine patients had initial therapy with β-lactam and aminoglycoside followed by β-lactam alone, and four (44%) had positive valve cultures. When patients receiving continuous 821
3 D. DrinkoviM et al. Table 2. Treatment regimens and valve culture results for staphylococcal PVE Culture result Group a n Treatment regimen Median (days) positive (%) negative (%) Comment 1 14 single agent 17 8 (57) 6 (43) most [12 (86%)] received either β-lactam or vancomycin 2 4 continuous triple (0) 4 (100) β-lactam or vancomycin with rifampicin and gentamicin agent 3 20 continuous dual agent 9 10 (50) 10 (50) either β-lactam with aminoglycoside or vancomycin with rifampicin 4 23 partial 19 4 (17) 19 (83) 18 (78%) patients received β-lactam with aminoglycoside or rifampicin; three (13%) received vancomycin and rifampicin; two (9%) received vancomycin with rifampicin and gentamicin a Group 1 versus 2 + 3, P = 0.36; group 1 versus , P = After adjusting for duration of treatment by logistic regression analysis valves from patients receiving any kind of treatment were 5.9 times more likely to be culture-negative than those receiving monotherapy (95% CI ; P = 0.024). and initial therapy were compared with patients on a single therapy, there was no difference in the likelihood of them having a negative valve culture [14 (39%) of 36 versus 13 (41%) of 32; P = 0.88]. Another six patients were treated with partial treatment, and one (17%) was culture positive. Patients receiving any kind of treatment were no more likely to be culturenegative than patients receiving a single agent [19 (45%) of 42 versus 13 (41%) of 32; P = 0.69] (Table 1). This finding remained unchanged after adjusting for duration of treatment [odds ratio 0.45; 95% confidence interval (CI) ; P = 0.23]. Coagulase-negative staphylococci NVE Seventeen patients had NVE caused by coagulase-negative staphylococci (CoNS). Twelve episodes were caused by Staphylococcus epidermidis, two of which were methicillin resistant. Two episodes were caused by Staphylococcus warneri and Staphylococcus cohnii, respectively, and three episodes by non-speciated CoNS. Eleven patients had aortic valve endocarditis, five had mitral and one had both aortic and mitral infection. Six (35%) patients had extravalvular extension of infection, with periannular abscess formation in four patients. Vegetations were found at surgery in 16 patients and 10 (59%) patients had ruptured cusps. Four patients were treated with a single β-lactam antibiotic and three (75%) had positive valve culture. Eight patients had continuous therapy: a β-lactam and aminoglycoside in five patients, and rifampicin, combined with either penicillin, vancomycin or fusidic acid, in three patients, respectively. Six (75%) of these eight had positive cultures. Valves from patients receiving treatment were no more likely to be culture-negative than those receiving single therapy [six (46%) of 13 versus one (25%) of four; P = 0.60]. All NVE When cases of CoNS NVE were added to the S. aureus group, the observations regarding culture results and treatment group remained unchanged. Patients receiving single-agent treatment were as likely to be culture-negative [14 (39%) of 36] as those receiving continuous treatment [11 (31%) of 35; P = 0.51], those receiving continuous plus initial treatment [18 (39%) of 46; P = 0.98] or those receiving any kind of treatment [25 (45%) of 55; P = 0.54]. This finding remained unchanged after adjusting for duration of treatment (P = 0.23). PVE Sixty-one patients had PVE, 29 due to S. aureus and 32 due to CoNS (Table 2). Seven episodes of CoNS NVE occurred within 2 months of surgery and six (86%) isolates were methicillin resistant; 10 episodes had onset between 3 and 12 months, five (50%) isolates were methicillin resistant, as were seven (47%) of the 15 isolates causing infection after 12 months. Most [21 (72%) of 29] S. aureus episodes occurred >12 months after surgery, with early and intermediate PVE occurring in four patients each. All S. aureus isolates were methicillin susceptible. Overall, 33 patients had mitral valve IE, 21 patients had aortic IE and seven patients had both valves infected. Extensive extravalvular infection was present in 30 (49%) patients. Current recommendations for staphylococcal PVE do not distinguish between species, 2,3 and therefore culture results versus treatment regimen are analysed for all cases of PVE without reference to species. Fourteen patients had treatment with a single antibiotic: nine were treated with a β-lactam and five, infected with methicillin-resistant isolates, were treated with either vancomycin (three patients), gentamicin (one) or clindamycin (one). Eight (57%) of these 14 had positive valve cultures. Four patients with PVE were treated continuously with three antibiotics, β-lactam or vancomycin plus rifampicin plus gentamicin and all had negative valve cultures. Twenty patients had continuous treatment with two antibiotics before their surgery: 14 with β-lactam and aminoglycoside, and six with vancomycin plus rifampicin for their methicillinresistant isolates. Ten (50%) of these 20 had positive valve cultures. Twenty-three patients had partial treatment. Most of them were treated with two antibiotics, and a β-lactam and an aminoglycoside were used in 15 patients. Rifampicin was combined with either β-lactam or vancomycin in three patients respectively. Two patients had three antibiotics, vancomycin plus gentamicin plus rifampicin, for a part of their preoperative period. Four (17%) of
4 Single versus treatment in staphylococcal IE had positive valve cultures. Although patients treated with continuous treatment were no more likely to be culturenegative than those treated with a single agent [14 (58%) of 24 versus six (43%) of 14; P = 0.36], there was a trend for valves from patients receiving any kind of treatment to be culture-negative compared with valves removed from patients receiving single-agent treatment [33 (70%) of 47 versus six (43%) of 14; P = 0.062] (Table 2). After adjusting for duration of treatment by logistic regression analysis valves from patients receiving any kind of treatment were 5.9 times (95% CI ) more likely to be culture-negative than those receiving monotherapy (P = 0.024). Eighteen patients had rifampicin included in their treatment. Twelve (67%) were valve culture negative. Twenty-seven (63%) of the remaining 43 patients without rifampicin in their treatment regimen had negative valve cultures. Rifampicin was combined with vancomycin in nine patients, flucloxacillin in two, a first generation cephalosporin in one and was a part of triple antibiotic regimen in six. Six (33%) of these 18 patients had positive valve culture at surgery and all had received vancomycin and rifampicin. In two (33%) of six culture-positive patients, rifampicin resistance had developed during treatment. Patients with infection invading beyond the leaflets were no more likely to be culture-positive than patients with infection affecting valves only [38 (51%) of 74 versus 36 (46%) of 78; P = 0.52]. After accounting for duration and type of treatment, prosthetic valves were no more likely to be culture-positive than native valves (P = 0.169). There was no difference in the indications for surgery between the different treatment groups for either S. aureus NVE (P = 0.53), any staphylococcal NVE (P = 0.51) or PVE (P = 0.66). During the study period there were 23 cases before 1980, 58 in the 1980s and 71 in the 1990s. The median (mean) duration of treatment before surgery for the respective time periods decreased: 16 (17), 14 (17.5) and 9 (12) days, respectively (P = 0.006). The proportion of patients receiving monotherapy did not show any trend over time (P = 0.27). Treatment duration was predictive of a negative culture: 49 (83%) of 59 and 29 (31%) of 93 treated for either >14 or <14 days, respectively, were culture-negative (P < 0.001). After adjusting for infecting organism, valve type and type of treatment, each day of treatment increased the likelihood of the valve being culture-negative by 17% (95% CI 11 22; P < 0.001). Discussion S. aureus NVE S. aureus accounts for 25 40% of NVE. 6 It is associated with considerable morbidity and mortality. Rapid sterilization of vegetations could result in less valve destruction and reduce the risk of metastatic complications. In vitro and in vivo observations have shown that a β-lactam antibiotic plus an aminoglycoside are more rapidly bactericidal for staphylococci than a β-lactam alone. 7,8 A multicentre prospective study of S. aureus endocarditis showed that addition of gentamicin for the first 2 weeks of a 6 week course of iv nafcillin failed to improve clinical outcome. 9 Nevertheless, treatment was associated with earlier clearance of bacteraemia in nonaddicts as well as in addicts with right-sided endocarditis. 9 These findings have led to the suggestion that an aminoglycoside be discontinued after 3 7 days of therapy 2,3 in the hope that more rapid control of bacteraemia would be accompanied by a lesser incidence of metastatic infections and accelerated sterilization of heart valves, while avoiding the toxic reactions associated with a more prolonged course of aminoglycosides. 9 Our findings show no significant difference in the rate of valve sterilization in S. aureus NVE between patients treated with single or therapy, the majority (89%) of which was β-lactam and aminoglycoside treatment. CoNS NVE NVE caused by CoNS is relatively uncommon, accounting for 4 8% of all native valve endocarditis. 6 As in previous studies, S. epidermidis was the most commonly isolated species in our patients Although CoNS NVE is usually described as a subacute, sometimes indolent process, 11,13,14 infection can be destructive. 11,12 Ten (59%) of our patients had ruptured valves and six (35%) had extravalvular extension of infection with periannular abscess formation in four of them. Many CoNS that cause NVE are susceptible to β-lactam antibiotics. Although single-agent treatment with a β-lactam has been reported as being effective, treatment may be better. Caputo et al. 11 noted that seven (64%) of 11 patients treated with a single agent were cured, while all 10 patients receiving antibiotic were cured. 11 When their data were combined with those of previous series, 21 (72%) of 29 patients treated with a single agent were cured, compared with 23 (92%) of 25 receiving treatment; however, the difference was not significant (P > 0.05). In our study, treatment did not result in a significant increase of valve sterilization. This observation held when CoNS cases were added to the S. aureus episodes. This finding does not support the notion that the addition of an aminoglycoside in the initial phase of treatment in staphylococcal endocarditis hastens valve sterilization. PVE In developed countries, PVE accounts for 7 25% of all cases of IE. 6 The cumulative risk of PVE is 1% at 12 months and 2 3% at 60 months after surgery. 6 The most common cause of PVE within 12 months after surgery is CoNS, with S. epidermidis predominating. 6,15 CoNS cause 60 70% of cases of PVE in the first 12 months of surgery and 10 12% thereafter. S. aureus causes 30 39% of PVE in the first 12 months and 15 20% of PVE after 12 months. 6 The US guidelines for staphylococcal PVE recommend treatment with either vancomycin or nafcillin (depending on susceptibility results) and rifampicin administered for a minimum of 6 weeks, together with gentamicin for the initial 2 weeks of treatment. 3 In experimental endocarditis in rabbits due to methicillin-resistant S. epidermidis, the of vancomycin plus gentamicin plus rifampicin was more effective in sterilizing vegetations than these agents administered alone, or the s of vancomycin and gentamicin or vancomycin and rifampicin. 16 In our study only four patients received continuous, and two patients a partial, triple antibiotic regimen. All six had negative valve cultures. Although most of our patients with PVE [55 (90%) of 61] did not receive triple treatment for the first 2 weeks, most [33 (60%) of the 55] had negative valve cultures. We observed a trend for valves from patients receiving either continuous or partial treatment for PVE to be culture-negative compared with those treated with a single agent (Table 2). However after adjusting for duration of treatment, valves from patients receiving any kind of treatment were almost six times more likely to be culture-negative than those receiving monotherapy (Table 2). This finding supports current recommendations for treatment for PVE, 2,3 despite the 823
5 D. DrinkoviM et al. potential toxicity of aminoglycoside-containing regimens. Whether treatment should follow either the UK (initial with gentamicin) or US (initial triple followed by double-agent treatment) guidelines is not settled by our observations, but animal model data suggest that triple-agent therapy may achieve sterilization in a greater proportion of valves. 16 Treatment of experimental foreign body infection is enhanced by regimens, especially ones that include rifampicin. 17,18 It is thought that rifampicin effectiveness is due to its excellent tissue penetration and ability to enter living phagocytes and kill intracellular bacteria, 19 as well as its ability to kill stationary phase microorganisms. 20 In our study the rate of valve sterilization was similar between groups with and without rifampicin [67% versus 63%]. We do not know whether the rate of valve sterilization would be higher in the rifampicin group if it had been used more often in therapy. The possibility of the development of resistance to rifampicin during vancomycin plus rifampicin or triple-agent treatment has been observed in experimental animal models 18,21 and clinical infections In a randomized treatment trial for PVE due to methicillin-resistant CoNS, rifampicin resistance developed in 37% of patients treated with vancomycin plus rifampicin, compared with 0% receiving vancomycin and rifampicin with gentamicin added for the first 2 weeks of treatment. 15 Two (33%) of our six patients with positive valve cultures after treatment with of vancomycin and rifampicin developed resistance to rifampicin. Although all six patients treated with vancomycin plus rifampicin plus gentamicin were culture-negative, the number of cases in each group was too small to make any conclusions regarding the effectiveness of gentamicin addition in prevention of rifampicin resistance. Although our study is limited by its retrospective nature and the limited number of patients in some treatment groups, the data give a unique insight into the efficacy of antibiotic treatments in sterilizing heart valves in staphylococcal endocarditis. We can conclude that valves from patients with S. aureus NVE treated with treatment are no more likely to be culture-negative than those treated with a single agent. This observation does not necessary mean that the recommendation for initial treatment with flucloxacillin, or a similar agent, and gentamicin for S. aureus NVE should be abandoned. It does, however, suggest that if the aminoglycoside is omitted, valve sterilization will not be significantly adversely affected. We observed that patients receiving treatment for staphylococcal PVE were more likely to have culture-negative valves. This finding, together with animal model data, supports the current recommendations for initial treatment. 2,3 Regardless of staphylococcal species, valve type or type of treatment, duration of treatment was predictive of a negative culture. After 14 days treatment valve sterilization is achieved in the majority of patients. This observation is of clinical relevance because if valve replacement is not required immediately, e.g. to restore valve function, most would prefer for surgery to be timed when there is the best likelihood of the new prosthesis being inserted into a sterile surgical field. Acknowledgements Financial support for this study was provided by The Auckland Infectious Disease Education and Research Trust. References 1. Le, T. & Bayer, A. S. (2003). Combination antibiotic therapy for infective endocarditis. Clinical Infectious Diseases 36, Working Party of the British Society for Antimicrobial Chemotherapy. (1998). Antibiotic treatment of streptococcal, enterococcal, and staphylococcal endocarditis. Heart 79, Wilson, W. R., Karchmer, A. W., Dajani, A. S. et al. (1995). Antibiotic treatment of adults with infective endocarditis due to streptococci, enterococci, staphylococci, and HACEK microorganisms. Journal of the American Medical Association 274, Morris, A. J., Drinkovic, D., Pottumarthy, S. et al. (2003) Gram stain, culture and histopathological examination findings for heart valves removed because of infective endocarditis. Clinical Infectious Diseases 36, Li, J. S., Sexton, D. J., Mick, N. et al. (2000). Proposed modifications to the Duke criteria for the diagnosis of infective endocarditis. Clinical Infectious Diseases 30, Mylonakis, E. & Calderwood, S. B. (2001). Infective endocarditis in adults. New England Journal of Medicine 345, Watanakunakorn, C. & Glotzbecker, C. (1974). Enhancement of the effects of anti-staphylococcal antibiotics by aminoglycosides. Antimicrobial Agents and Chemotherapy 6, Sande, M. A. & Johnson, M. L. (1975). Antimicrobial therapy of experimental endocarditis caused by Staphylococcus aureus. Journal of Infectious Diseases 131, Korzeniowski, O., Sande, M. A. & The National Collaborative Endocarditis Study Group. (1982). Combination antimicrobial therapy for Staphylococcus aureus endocarditis in patients addicted to parenteral drugs and in nonaddicts. Annals of Internal Medicine 97, Etienne, J. & Eykyn, S. J. (1990). Increase in native valve endocarditis caused by coagulase-negative staphylococci: an Anglo-French clinical and microbiological study. British Heart Journal 64, Caputo, G. M., Archer, G. L., Calderwood, S. B. et al. (1987). Native valve endocarditis due to coagulase-negative staphylococci: clinical and microbiologic features. American Journal of Medicine 83, Miele, P. S., Kogulan, P. K., Levy, C. S. et al. (2001). Seven cases of surgical native valve endocarditis caused by coagulase-negative staphylococci: an underappreciated disease. American Heart Journal 142, Arber, N., Militianu, A., Ben-Yehuda, A. et al. (1991). Native valve Staphylococcus epidermidis endocarditis: report of seven cases and review of the literature. American Journal of Medicine 90, Baddour, L. M., Phillips, T. N. & Bisno, A. L. (1986). Coagulasenegative staphylococcal endocarditis: occurrence in patients with mitral valve prolapse. Archives of Internal Medicine 146, Karchmer, A. W. & Gibbons, G. W. (1994). Infection of prosthetic heart valves and vascular grafts. In Infections Associated with Indwelling Medical Devices, 2nd edn (Bisno, A. L. & Waldvogel, F. A., Eds), pp American Society for Microbiology, Washington, DC, USA. 16. Kobasa, W. D., Kaye, K. L. & Shapiro, T. (1983). Therapy for experimental endocarditis due to Staphylococcus epidermidis. Reviews of Infectious Diseases 5, S Chuard, C., Herrmann, M., Vaudaux, P. et al. (1991). Successful therapy of experimental chronic foreign-body infection due to methicillinresistant Staphylococcus aureus by antimicrobial s. Antimicrobial Agents and Chemotherapy 35, Lucet, J.-C., Herrmann, M., Rohner, P. et al. (1990). Treatment of experimental foreign body infection caused by methicillin-resistant Staphylococcus aureus. Antimicrobial Agents and Chemotherapy 34, Farr, B. M. (2000). Rifamycins. In Principles and Practice of Infectious Diseases, 5th edn (Mandell, G. L., Bennett, J. E. & Dolin, R., Eds), pp Churchill Livingstone, Edinburgh, UK. 20. Widmer, A. F., Frei, R., Rajacic, Z. et al. (1990). Correlation between in vivo and in vitro efficacy of antimicrobial agents against foreign body infections. Journal of Infectious Diseases 162,
6 Single versus treatment in staphylococcal IE 21. Rouse, M. S., Wilcox, R. M., Henry, N. K. et al. (1990). Ciprofloxacin therapy of experimental endocarditis caused by methicillinresistant Staphylococcus epidermidis. Antimicrobial Agents and Chemotherapy 34, Karchmer, A. W., Archer, G. L. & Dismukes, W. E. (1983). Staphylococcus epidermidis causing prosthetic valve endocarditis: microbiologic and clinical observations as guides to therapy. Annals of Internal Medicine 98, Acar, J. F., Goldstein, F. W. & Duval, J. (1983). Use of rifampin for the treatment of serious staphylococcal and gram-negative bacillary infections. Reviews of Infectious Diseases 5, Suppl. 3, S Simon, G. L., Smith, R. H. & Sande, M. A. (1983). Emergence of rifampin-resistant strains of Staphylococcus aureus during therapy with vancomycin and rifampin: a report of two cases. Reviews of Infectious Diseases 5, Suppl. 3, S
New guidelines for the antibiotic treatment of streptococcal, enterococcal and staphylococcal endocarditis. D. C. Shanson
 Journal of Antimicrobial Chemotherapy (1998) 42, 292 296 New guidelines for the antibiotic treatment of streptococcal, enterococcal and staphylococcal endocarditis JAC D. C. Shanson Microbiology Department,
Journal of Antimicrobial Chemotherapy (1998) 42, 292 296 New guidelines for the antibiotic treatment of streptococcal, enterococcal and staphylococcal endocarditis JAC D. C. Shanson Microbiology Department,
Infections Amenable to OPAT. (Nabin Shrestha + Ajay Mathur)
 3 Infections Amenable to OPAT (Nabin Shrestha + Ajay Mathur) Decisions regarding outpatient treatment of infections vary with the institution, the prescribing physician, the individual patient s condition
3 Infections Amenable to OPAT (Nabin Shrestha + Ajay Mathur) Decisions regarding outpatient treatment of infections vary with the institution, the prescribing physician, the individual patient s condition
Antibiotic Treatment of Adults With Infective Endocarditis Due to Streptococci, Enterococci, Staphylococci, and HACEK Microorganisms
 Antibiotic Treatment of Adults With Infective Endocarditis Due to Streptococci, Enterococci, Staphylococci, and HACEK Microorganisms Walter R. Wilson, MD; Adolf W. Karchmer, MD; Adnan S. Dajani, MD; Kathryn
Antibiotic Treatment of Adults With Infective Endocarditis Due to Streptococci, Enterococci, Staphylococci, and HACEK Microorganisms Walter R. Wilson, MD; Adolf W. Karchmer, MD; Adnan S. Dajani, MD; Kathryn
Rifampin Resistance. Charlottesville, Virginia i0w organisms in Trypticase soy broth (BBL Microbiology
 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Apr. 1980, p. 658-662 0066-4804/80/04-0658/05$02.00/0 Vol. 17, No. 14 Treatment of Experimental Staphylococcal Infections: Effect of Rifampin Alone and in Combination
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Apr. 1980, p. 658-662 0066-4804/80/04-0658/05$02.00/0 Vol. 17, No. 14 Treatment of Experimental Staphylococcal Infections: Effect of Rifampin Alone and in Combination
Heart on Fire: Infective Endocarditis. Objectives. Disclosure 8/27/2018. Mary McGreal DNP, RN, ANP-c, CCRN
 Heart on Fire: Infective Endocarditis Mary McGreal DNP, RN, ANP-c, CCRN Objectives Discuss the incidence of infective endocarditis? Discuss the pathogenesis of infective endocarditis? Discuss clinical
Heart on Fire: Infective Endocarditis Mary McGreal DNP, RN, ANP-c, CCRN Objectives Discuss the incidence of infective endocarditis? Discuss the pathogenesis of infective endocarditis? Discuss clinical
Endocardite infectieuse
 Endocardite infectieuse 1. Raccourcir le traitement: jusqu où? 2. Proposer un traitement ambulatoire: à partir de quand? Endocardite infectieuse A B 90 P = 0.014 20 P = 0.0005 % infective endocarditis
Endocardite infectieuse 1. Raccourcir le traitement: jusqu où? 2. Proposer un traitement ambulatoire: à partir de quand? Endocardite infectieuse A B 90 P = 0.014 20 P = 0.0005 % infective endocarditis
Dr Babak Tamizi far MD. Assistant Professor Of Internal Medicine Al-Zahra Hospital Isfahan University Of Medical Sciences
 Dr Babak Tamizi far MD. Assistant Professor Of Internal Medicine Al-Zahra Hospital Isfahan University Of Medical Sciences ١ ٢ ٣ A 57-year-old man presents with new-onset fever, shortness of breath, lower
Dr Babak Tamizi far MD. Assistant Professor Of Internal Medicine Al-Zahra Hospital Isfahan University Of Medical Sciences ١ ٢ ٣ A 57-year-old man presents with new-onset fever, shortness of breath, lower
Bacterial Endocarditis
 Objectives Bacterial Endocarditis John C. Rotschafer, Pharm. D. Professor College of Pharmacy University of Minnesota Identify which valves are commonly involved with endocarditis Identify common pathogens
Objectives Bacterial Endocarditis John C. Rotschafer, Pharm. D. Professor College of Pharmacy University of Minnesota Identify which valves are commonly involved with endocarditis Identify common pathogens
Antibiotic treatment of streptococcal and enterococcal endocarditis: an overview
 European Heart Journal (1995) 16 {Supplement B), 75-79 Antibiotic treatment of streptococcal and enterococcal endocarditis: an overview P. FRANCIOLI Division of Hospital Preventative Medicine and Department
European Heart Journal (1995) 16 {Supplement B), 75-79 Antibiotic treatment of streptococcal and enterococcal endocarditis: an overview P. FRANCIOLI Division of Hospital Preventative Medicine and Department
Contents. 1. Introduction. J Antimicrob Chemother 2012; 67: doi: /jac/dkr450 Advance Access publication 14 November 2011
 J Antimicrob Chemother 2012; 67: 269 289 doi:10.1093/jac/dkr450 Advance Access publication 14 November 2011 Guidelines for the diagnosis and antibiotic treatment of endocarditis in adults: a report of
J Antimicrob Chemother 2012; 67: 269 289 doi:10.1093/jac/dkr450 Advance Access publication 14 November 2011 Guidelines for the diagnosis and antibiotic treatment of endocarditis in adults: a report of
Infective Endocarditis Empirical therapy Antibiotic Guidelines. Contents
 Infective Endocarditis Empirical therapy Antibiotic Guidelines Classification: Clinical Guideline Lead Author: Antibiotic Steering Group Additional author(s): as above Authors Division: Division of Clinical
Infective Endocarditis Empirical therapy Antibiotic Guidelines Classification: Clinical Guideline Lead Author: Antibiotic Steering Group Additional author(s): as above Authors Division: Division of Clinical
Daniel C. DeSimone, MD Assistant Professor of Medicine
 Daniel C. DeSimone, MD Assistant Professor of Medicine Faculty photo will be placed here Desimone.Daniel@mayo.edu 2015 MFMER 3543652-1 Infective Endocarditis Mayo School of Continuous Professional Development
Daniel C. DeSimone, MD Assistant Professor of Medicine Faculty photo will be placed here Desimone.Daniel@mayo.edu 2015 MFMER 3543652-1 Infective Endocarditis Mayo School of Continuous Professional Development
Loyola ecommons. Loyola University Chicago. Virginia Long Loyola University Chicago. Recommended Citation
 Loyola University Chicago Loyola ecommons Master's Theses Theses and Dissertations 2014 Identification of Clinical Markers That Predict the Outcomes of Methicillin-Resistant Staphylococcus Aureus Infections
Loyola University Chicago Loyola ecommons Master's Theses Theses and Dissertations 2014 Identification of Clinical Markers That Predict the Outcomes of Methicillin-Resistant Staphylococcus Aureus Infections
Early oral switch for antibiotic treatment of infective endocarditis
 AEPEI: Association pour l Etude et la Prévention des Endocardites Infectieuses Early oral switch for antibiotic treatment of infective endocarditis Prof. Pierre Tattevin Infectious Diseases & ICU, INSERM
AEPEI: Association pour l Etude et la Prévention des Endocardites Infectieuses Early oral switch for antibiotic treatment of infective endocarditis Prof. Pierre Tattevin Infectious Diseases & ICU, INSERM
Guidelines for The Management of Infective Endocarditis
 Guidelines for The Management of Infective Endocarditis By Dr. Sinan Butrus F.I.C.M.S Clinical Standards & Guidelines Kurdistan Board For Medical Specialties Infective endocarditis IE is an infection of
Guidelines for The Management of Infective Endocarditis By Dr. Sinan Butrus F.I.C.M.S Clinical Standards & Guidelines Kurdistan Board For Medical Specialties Infective endocarditis IE is an infection of
Overview. Clinical Scenario. Endocarditis: Treatment & Prevention. Prophylaxis The Concept. Jeremy D. Young, MD, MPH. Division of Infectious Diseases
 Endocarditis: Treatment & Prevention Jeremy D. Young, MD, MPH Division of Infectious Diseases Clinical Scenario Patient with MVP scheduled to have wisdom teeth extracted. Has systolic murmur with mid-systolic
Endocarditis: Treatment & Prevention Jeremy D. Young, MD, MPH Division of Infectious Diseases Clinical Scenario Patient with MVP scheduled to have wisdom teeth extracted. Has systolic murmur with mid-systolic
Right-Sided Bacterial Endocarditis
 New Concepts in the Treatment of the Uncontrollable Infection Agustin Arbulu, M.D., Ali Kafi, M.D., Norman W. Thorns, M.D., and Robert F. Wilson, M.D. ABSTRACT Our experience with 25 patients with right-sided
New Concepts in the Treatment of the Uncontrollable Infection Agustin Arbulu, M.D., Ali Kafi, M.D., Norman W. Thorns, M.D., and Robert F. Wilson, M.D. ABSTRACT Our experience with 25 patients with right-sided
Hospital-wide Impact of Mandatory Infectious Disease Consultation on Staphylococcus aureus Septicemia
 Hospital-wide Impact of Mandatory Infectious Disease Consultation on Staphylococcus aureus Septicemia Amanda Guth 1 Amy Slenker MD 1,2 1 Department of Infectious Diseases, Lehigh Valley Health Network
Hospital-wide Impact of Mandatory Infectious Disease Consultation on Staphylococcus aureus Septicemia Amanda Guth 1 Amy Slenker MD 1,2 1 Department of Infectious Diseases, Lehigh Valley Health Network
Methicillin-Resistant Staphylococcus aureus (MRSA) S urveillance Report 2008 Background Methods
 Methicillin-Resistant Staphylococcus aureus (MRSA) Surveillance Report 2008 Oregon Active Bacterial Core Surveillance (ABCs) Office of Disease Prevention & Epidemiology Oregon Department of Human Services
Methicillin-Resistant Staphylococcus aureus (MRSA) Surveillance Report 2008 Oregon Active Bacterial Core Surveillance (ABCs) Office of Disease Prevention & Epidemiology Oregon Department of Human Services
Experimental Endocarditis Caused by Streptococcus sanguis:
 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, July 1981, p. 1-14 66-484/81/71-5$2./ Vol. 2, No. 1 Experimental Endocarditis Caused by Streptococcus sanguis: Single and Combined Antibiotic Therapy MARIA V. VICENTE,
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, July 1981, p. 1-14 66-484/81/71-5$2./ Vol. 2, No. 1 Experimental Endocarditis Caused by Streptococcus sanguis: Single and Combined Antibiotic Therapy MARIA V. VICENTE,
Infective Endocarditis
 Frank Lowy Infective Endocarditis 1. Introduction Infective endocarditis (IE) is an infection of the heart valves. A large number of different bacteria are capable of causing this disease. Depending on
Frank Lowy Infective Endocarditis 1. Introduction Infective endocarditis (IE) is an infection of the heart valves. A large number of different bacteria are capable of causing this disease. Depending on
NATIONAL HEART FOUNDATION HOSPITAL & RESEARCH INSTITUTE
 Welcome INFECTIVE ENDOCARDITIS: WHERE WE ARE AT 2005? DR MD HABIBUR RAHMAN FCPS(Medicine) NATIONAL HEART FOUNDATION HOSPITAL & RESEARCH INSTITUTE DEFINITION OF INFECTIVE ENDOCARDITIS Infective endocarditis
Welcome INFECTIVE ENDOCARDITIS: WHERE WE ARE AT 2005? DR MD HABIBUR RAHMAN FCPS(Medicine) NATIONAL HEART FOUNDATION HOSPITAL & RESEARCH INSTITUTE DEFINITION OF INFECTIVE ENDOCARDITIS Infective endocarditis
Infected cardiac-implantable electronic devices: diagnosis, and treatment
 Infected cardiac-implantable electronic devices: diagnosis, and treatment The incidence of infection following implantation of cardiac implantable electronic devices (CIEDs) is increasing at a faster rate
Infected cardiac-implantable electronic devices: diagnosis, and treatment The incidence of infection following implantation of cardiac implantable electronic devices (CIEDs) is increasing at a faster rate
In the last issue of this journal, the recent emergence of
 ADULT INFECTIOUS DISEASE NOTES Staphylococcus aureus: The persistent pathogen B Lynn Johnston MD 1, John M Conly MD 2 In the last issue of this journal, the recent emergence of community-acquired methicillin-resistant
ADULT INFECTIOUS DISEASE NOTES Staphylococcus aureus: The persistent pathogen B Lynn Johnston MD 1, John M Conly MD 2 In the last issue of this journal, the recent emergence of community-acquired methicillin-resistant
Serious MRSA infection: anything new?
 Serious MRSA infection: anything new? Professor Mark H. Wilcox Leeds Teaching Hospitals & University of Leeds, UK Public Health England & NHS Improvement Potential Conflicts of Interest I have received:
Serious MRSA infection: anything new? Professor Mark H. Wilcox Leeds Teaching Hospitals & University of Leeds, UK Public Health England & NHS Improvement Potential Conflicts of Interest I have received:
Renal Unit. Catheter Related Bacteraemia Guidelines
 Renal Unit Policy Manager Drew Henderson Policy Group Renal Unit Policy Established 21/01/2014 Policy Review Period/Expiry 21/01/2015 Last Updated 21/01/2014 This policy does apply to Medical/Dental Staff
Renal Unit Policy Manager Drew Henderson Policy Group Renal Unit Policy Established 21/01/2014 Policy Review Period/Expiry 21/01/2015 Last Updated 21/01/2014 This policy does apply to Medical/Dental Staff
BASIC KNOWLEDGE ABOUT INFECTIVE ENDOCARDITIS FOR CLINICIAN
 BASIC KNOWLEDGE ABOUT INFECTIVE ENDOCARDITIS FOR CLINICIAN When should I suspect infective endocarditis? Antibiotic regimen Patient care after completion of treatment Prophylactic Regimens Prosthetic Valve
BASIC KNOWLEDGE ABOUT INFECTIVE ENDOCARDITIS FOR CLINICIAN When should I suspect infective endocarditis? Antibiotic regimen Patient care after completion of treatment Prophylactic Regimens Prosthetic Valve
Management of infective endocarditis in children
 Management of infective endocarditis in children Ashutosh Marwah, MD* Savitri Shrivastava, MD DM FAMS FACC* INTRODUCTION Infective endocarditis (IE) continues to remain a serious disease despite advances
Management of infective endocarditis in children Ashutosh Marwah, MD* Savitri Shrivastava, MD DM FAMS FACC* INTRODUCTION Infective endocarditis (IE) continues to remain a serious disease despite advances
Outcomes After Surgical Treatment of Native and Prosthetic Valve Infective Endocarditis
 Outcomes After Surgical Treatment of Native and Prosthetic Valve Infective Endocarditis Mahesh B. Manne, MD, MPH, Nabin K. Shrestha, MD, Bruce W. Lytle, MD, Edward R. Nowicki, MD, MS, Eugene Blackstone,
Outcomes After Surgical Treatment of Native and Prosthetic Valve Infective Endocarditis Mahesh B. Manne, MD, MPH, Nabin K. Shrestha, MD, Bruce W. Lytle, MD, Edward R. Nowicki, MD, MS, Eugene Blackstone,
Infective endocarditis
 Infective endocarditis This is caused by microbial infection of a heart valve (native or prosthetic), the lining of a cardiac chamber or blood vessel, or a congenital anomaly (e.g. septal defect). The
Infective endocarditis This is caused by microbial infection of a heart valve (native or prosthetic), the lining of a cardiac chamber or blood vessel, or a congenital anomaly (e.g. septal defect). The
Coffey et al ND 6 HA, 5 TSA, and 5 other MRSA (3) and Staphylococcus epidermidis (3)
 Page 1 of 6 TABLE E-1 Outcomes of the Treatment of Periprosthetic Shoulder Infections* ä Study No. Presentation Prosthesis Most Common Pathogens Braman et al. 68 7 1 acute, 2 subacute, 2 HA and 5 TSA Staphylococcus
Page 1 of 6 TABLE E-1 Outcomes of the Treatment of Periprosthetic Shoulder Infections* ä Study No. Presentation Prosthesis Most Common Pathogens Braman et al. 68 7 1 acute, 2 subacute, 2 HA and 5 TSA Staphylococcus
CLINICAL USE OF GLYCOPEPTIDES. Herbert Spapen Intensive Care Department University Hospital Vrije Universiteit Brussel
 CLINICAL USE OF GLYCOPEPTIDES Herbert Spapen Intensive Care Department University Hospital Vrije Universiteit Brussel Glycopeptides Natural Vancomycin introduced in 1958 Teicoplanin introduced in Europe
CLINICAL USE OF GLYCOPEPTIDES Herbert Spapen Intensive Care Department University Hospital Vrije Universiteit Brussel Glycopeptides Natural Vancomycin introduced in 1958 Teicoplanin introduced in Europe
Supplementary Online Content
 Supplementary Online Content Toyoda N, Chikwe J, Itagaki S, Gelijns AC, Adams DH, Egorova N. Trends in infective endocarditis in California and New York State, 1998-2013. JAMA. doi:10.1001/jama.2017.4287
Supplementary Online Content Toyoda N, Chikwe J, Itagaki S, Gelijns AC, Adams DH, Egorova N. Trends in infective endocarditis in California and New York State, 1998-2013. JAMA. doi:10.1001/jama.2017.4287
Vancomycin: Class: Antibiotic.
 Vancomycin: Class: Antibiotic. Indications: Treatment of patients with infections caused by staphylococcal species and streptococcal Species. Available dosage form in the hospital: 1G VIAL, 500MG VIAL.
Vancomycin: Class: Antibiotic. Indications: Treatment of patients with infections caused by staphylococcal species and streptococcal Species. Available dosage form in the hospital: 1G VIAL, 500MG VIAL.
Infective Endocarditis Considerations in 2010
 Infective Endocarditis Considerations in 2010 Adolf W. Karchmer, M.D. Division of Infectious Diseases Beth Israel Deaconess Medical Center Professor of Medicine Harvard Medical School Boston, Massachusetts
Infective Endocarditis Considerations in 2010 Adolf W. Karchmer, M.D. Division of Infectious Diseases Beth Israel Deaconess Medical Center Professor of Medicine Harvard Medical School Boston, Massachusetts
INFECTIOUS endocarditis (IE) is a
 ORIGINAL INVESTIGATION Diagnosis of Infective Endocarditis Sensitivity of the Duke vs von Reyn Criteria Maija Heiro, MD; Jukka Nikoskelainen, MD, PhD; Jaakko J. Hartiala, MD, PhD; Markku K. Saraste, MD;
ORIGINAL INVESTIGATION Diagnosis of Infective Endocarditis Sensitivity of the Duke vs von Reyn Criteria Maija Heiro, MD; Jukka Nikoskelainen, MD, PhD; Jaakko J. Hartiala, MD, PhD; Markku K. Saraste, MD;
INFECTIVE ENDOCARDITIS AMONGST INTRAVENOUS DRUG ABUSERS SEEN AT THE UNIVERSITY HOSPITAL, KUALA LUMPUR
 Med. J. Malaysia Vol. 42 No. 4 December 1987 INFECTIVE ENDOCARDITIS AMONGST INTRAVENOUS DRUG ABUSERS SEEN AT THE UNIVERSITY HOSPITAL, KUALA LUMPUR R. JAYAMALAR MBBS, MRCP. "N. PARASAKTHI MBBS, MSc. "S.D.
Med. J. Malaysia Vol. 42 No. 4 December 1987 INFECTIVE ENDOCARDITIS AMONGST INTRAVENOUS DRUG ABUSERS SEEN AT THE UNIVERSITY HOSPITAL, KUALA LUMPUR R. JAYAMALAR MBBS, MRCP. "N. PARASAKTHI MBBS, MSc. "S.D.
The Challenge of Managing Staphylococcus aureus Bacteremia
 The Challenge of Managing Staphylococcus aureus Bacteremia M A R G A R E T G R A Y B S P F C S H P C L I N I C A L P R A C T I C E M A N A G E R N O R T H / I D P H A R M A C I S T A L B E R T A H E A
The Challenge of Managing Staphylococcus aureus Bacteremia M A R G A R E T G R A Y B S P F C S H P C L I N I C A L P R A C T I C E M A N A G E R N O R T H / I D P H A R M A C I S T A L B E R T A H E A
Diagnosis and Treatment of Bacterial Endocarditis
 Infectious diseases Board Review Manual Statement of Editorial Purpose The Hospital Physician Infectious Diseases Board Review Manual is a study guide for fellows and practicing physicians preparing for
Infectious diseases Board Review Manual Statement of Editorial Purpose The Hospital Physician Infectious Diseases Board Review Manual is a study guide for fellows and practicing physicians preparing for
Infective Endocarditis
 Chapter 32 Infective Endocarditis Lisa B. Hightow and Meera Kelley The term infective endocarditis (IE) refers to infection of the endocardial surface of the heart and implies a physical presence of microganisms
Chapter 32 Infective Endocarditis Lisa B. Hightow and Meera Kelley The term infective endocarditis (IE) refers to infection of the endocardial surface of the heart and implies a physical presence of microganisms
Chiayi, Taiwan. Abstract
 DOI 10.6314/JIMT.201810_29(5).05 2018 29 309-316 Clinical Features and Risks Associated with In-hospital Mortality in Patients with Infective Endocarditis at A Medical Center in Central Taiwan from 2012
DOI 10.6314/JIMT.201810_29(5).05 2018 29 309-316 Clinical Features and Risks Associated with In-hospital Mortality in Patients with Infective Endocarditis at A Medical Center in Central Taiwan from 2012
Ceftizoxime in the treatment of infections in patients with cancer
 Journal of Antimicrobial Chemotherapy (98), Suppl. C, 67-73 Ceftizoxime in the treatment of infections in patients with cancer V. Fainstein, R. Bolivar,. Elting, M. Valdivieso and G. P. Bodey Department
Journal of Antimicrobial Chemotherapy (98), Suppl. C, 67-73 Ceftizoxime in the treatment of infections in patients with cancer V. Fainstein, R. Bolivar,. Elting, M. Valdivieso and G. P. Bodey Department
Infective endocarditis (IE) By Assis. Prof. Nader Alaridah MD, PhD
 Infective endocarditis (IE) By Assis. Prof. Nader Alaridah MD, PhD Infective endocarditis (IE) is an inflammation of the endocardium.. inner of the heart muscle & the epithelial lining of heart valves.
Infective endocarditis (IE) By Assis. Prof. Nader Alaridah MD, PhD Infective endocarditis (IE) is an inflammation of the endocardium.. inner of the heart muscle & the epithelial lining of heart valves.
Michael Stander, Pharm.D.
 Michael Stander, Pharm.D. Endocarditis: Goals Epidemiology Presentation of acute and subacute. Diagnosis: What is Dukes Criteria and how do we approach the diagnosis of endocarditis? Treatment: Understand
Michael Stander, Pharm.D. Endocarditis: Goals Epidemiology Presentation of acute and subacute. Diagnosis: What is Dukes Criteria and how do we approach the diagnosis of endocarditis? Treatment: Understand
Clinical management of Staphylococcus aureus bacteremia an updated proposal of protocol
 Clinical management of Staphylococcus aureus bacteremia an updated proposal of protocol Promotor : Prof. dr. W. Peetermans Second reader : Prof. dr. E. Van Wijngaerden Master s Thesis Internal Medicine
Clinical management of Staphylococcus aureus bacteremia an updated proposal of protocol Promotor : Prof. dr. W. Peetermans Second reader : Prof. dr. E. Van Wijngaerden Master s Thesis Internal Medicine
aureus."' Previous studies from this laboratory have shown that this agent despite the availability of antimicrobial agents that are effective against
 RICHARD E. DIXON* Department of Medicine, JAY S. GOODMAN * * George Vanderbilt Hunter University Laboratory, School of Medicine, M. GLENN KOENIG*** Nashville, Tennessee 3723 LYSOSTAPHIN: AN ENZYMATIC APPROACH
RICHARD E. DIXON* Department of Medicine, JAY S. GOODMAN * * George Vanderbilt Hunter University Laboratory, School of Medicine, M. GLENN KOENIG*** Nashville, Tennessee 3723 LYSOSTAPHIN: AN ENZYMATIC APPROACH
Treatment of febrile neutropenia in patients with neoplasia
 Treatment of febrile neutropenia in patients with neoplasia George Samonis MD, PhD Medical Oncologist Infectious Diseases Specialist Professor of Medicine The University of Crete, Heraklion,, Crete, Greece
Treatment of febrile neutropenia in patients with neoplasia George Samonis MD, PhD Medical Oncologist Infectious Diseases Specialist Professor of Medicine The University of Crete, Heraklion,, Crete, Greece
Cefotaxime Rationale for the EUCAST clinical breakpoints, version th September 2010
 Cefotaxime Rationale for the EUCAST clinical breakpoints, version 1.0 26 th September 2010 Foreword EUCAST The European Committee on Antimicrobial Susceptibility Testing (EUCAST) is organised by the European
Cefotaxime Rationale for the EUCAST clinical breakpoints, version 1.0 26 th September 2010 Foreword EUCAST The European Committee on Antimicrobial Susceptibility Testing (EUCAST) is organised by the European
SBUH Aminoglycoside Dosing Protocol
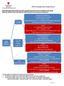 Adult Aminoglycoside Dosing for Gram negative infections prior to available serum levels (Excludes patients with cystic fibrosis, OB GYN patients and surgical prophylaxis) Cr Cl 40 ml/min 5 7 mg/kg INT
Adult Aminoglycoside Dosing for Gram negative infections prior to available serum levels (Excludes patients with cystic fibrosis, OB GYN patients and surgical prophylaxis) Cr Cl 40 ml/min 5 7 mg/kg INT
CLINICAL SYNDROMES: COMMUNITY ACQUIRED INFECTIONS
 SECTION 2 CLINICAL SYNDROMES: COMMUNITY ACQUIRED INFECTIONS 118-1 118 Adolf W. Karchmer The prototypic lesion of infective endocarditis, the vegetation (Fig. 118-1), is a mass of platelets, fibrin, microcolonies
SECTION 2 CLINICAL SYNDROMES: COMMUNITY ACQUIRED INFECTIONS 118-1 118 Adolf W. Karchmer The prototypic lesion of infective endocarditis, the vegetation (Fig. 118-1), is a mass of platelets, fibrin, microcolonies
INFECTIVE ENDOCARDITIS is a constantlyevolvingdisease.
 Clinical Features of Staphylococcus aureus Endocarditis A 10-Year Experience in Denmark ORIGINAL INVESTIGATION Bent L. Røder, MD; Dorte A. Wandall, MD; Niels Frimodt-Møller, MD, DMSc; Frank Espersen, MD,
Clinical Features of Staphylococcus aureus Endocarditis A 10-Year Experience in Denmark ORIGINAL INVESTIGATION Bent L. Røder, MD; Dorte A. Wandall, MD; Niels Frimodt-Møller, MD, DMSc; Frank Espersen, MD,
6-8 November EICC, Edinburgh. Registration now open Abstract submission deadline: June 24th
 6-8 November EICC, Edinburgh Registration now open Abstract submission deadline: June 24th An outbreak of prosthetic valve endocarditis Dr Tim Boswell Consultant Medical Microbiologist Nottingham Case
6-8 November EICC, Edinburgh Registration now open Abstract submission deadline: June 24th An outbreak of prosthetic valve endocarditis Dr Tim Boswell Consultant Medical Microbiologist Nottingham Case
ORIGINAL ARTICLE /j x. Melbourne, Victoria, Australia
 ORIGINAL ARTICLE 10.1111/j.1469-0691.2007.01691.x Treatment of staphylococcal prosthetic joint infections with debridement, prosthesis retention and oral rifampicin and fusidic acid C. A. Aboltins 1, M.
ORIGINAL ARTICLE 10.1111/j.1469-0691.2007.01691.x Treatment of staphylococcal prosthetic joint infections with debridement, prosthesis retention and oral rifampicin and fusidic acid C. A. Aboltins 1, M.
MULTIVALVULAR INFECTIVE ENDOCARDITIS CLINICAL FEATURES, ECHOCARDIOGRAPHIC DATA AND OUTCOMES
 Article Original MULTIVALVULAR INFECTIVE ENDOCARDITIS CLINICAL FEATURES, ECHOCARDIOGRAPHIC DATA AND OUTCOMES L. ABID, B. JERBI, I. TRABELSI, A. ZNAZEN*, S. KRICHÈNE, D. ABID, M. AKROUT, S. MALLEK, F. TRIKI,
Article Original MULTIVALVULAR INFECTIVE ENDOCARDITIS CLINICAL FEATURES, ECHOCARDIOGRAPHIC DATA AND OUTCOMES L. ABID, B. JERBI, I. TRABELSI, A. ZNAZEN*, S. KRICHÈNE, D. ABID, M. AKROUT, S. MALLEK, F. TRIKI,
109 Infective Endocarditis
 Página 1 de 30 Copyright 2005 McGraw-Hill Kasper, Dennis L., Fauci, Anthony S., Longo, Dan L., Braunwald, Eugene, Hauser, Stephen L., Jameson, J. Larry, Harrison, T. R., Resnick, W. R., Wintrobe, M. M.,
Página 1 de 30 Copyright 2005 McGraw-Hill Kasper, Dennis L., Fauci, Anthony S., Longo, Dan L., Braunwald, Eugene, Hauser, Stephen L., Jameson, J. Larry, Harrison, T. R., Resnick, W. R., Wintrobe, M. M.,
Natural History of Aortic Valve Endocarditis in Rats
 INFECTION AND IMMUNITY, JUlY 192, p. 127-131 19-9567/2/7127-5$2./ Vol. 37, No. 1 Natural History of Aortic Valve Endocarditis in Rats ERIC HtRAIEF, MICHEL P. GLAUSER,* AND LAWRENCE R. FREEDMANt Division
INFECTION AND IMMUNITY, JUlY 192, p. 127-131 19-9567/2/7127-5$2./ Vol. 37, No. 1 Natural History of Aortic Valve Endocarditis in Rats ERIC HtRAIEF, MICHEL P. GLAUSER,* AND LAWRENCE R. FREEDMANt Division
Aminoglycosides John A. Bosso, Pharm.D.
 AMINOGLYCOSIDES Therapeutics/PHRMP-73 Aminoglycoside Mechanism of Action Aminoglycosides bind to 30s ribosomal subunit resulting in mistranslation of mrna thus disrupting protein synthesis. They are rapidly
AMINOGLYCOSIDES Therapeutics/PHRMP-73 Aminoglycoside Mechanism of Action Aminoglycosides bind to 30s ribosomal subunit resulting in mistranslation of mrna thus disrupting protein synthesis. They are rapidly
Case Report Daptomycin Failure for Treatment of Pulmonary Septic Emboli in Native Tricuspid and Mitral Valve
 Case Reports in Infectious Diseases Volume 2013, Article ID 653582, 4 pages http://dx.doi.org/10.1155/2013/653582 Case Report Daptomycin Failure for Treatment of Pulmonary Septic Emboli in Native Tricuspid
Case Reports in Infectious Diseases Volume 2013, Article ID 653582, 4 pages http://dx.doi.org/10.1155/2013/653582 Case Report Daptomycin Failure for Treatment of Pulmonary Septic Emboli in Native Tricuspid
MANAGEMENT OF HAEMODIALYSIS CATHETER RELATED BLOOD STREAM INFECTION
 MANAGEMENT OF HAEMODIALYSIS CATHETER RELATED BLOOD STREAM INFECTION RRCV CMG Renal and Transplant Service 1. Introduction Catheter related blood stream infection (CR-BSI) is a common complication in patients
MANAGEMENT OF HAEMODIALYSIS CATHETER RELATED BLOOD STREAM INFECTION RRCV CMG Renal and Transplant Service 1. Introduction Catheter related blood stream infection (CR-BSI) is a common complication in patients
Endocarditis: Medical vs. Surgical Treatment. Nabin K. Shrestha, MD, MPH Infectious Diseases
 Endocarditis: Medical vs. Surgical Treatment Nabin K. Shrestha, MD, MPH Infectious Diseases Conflicts of interest Nothing to disclose 2 Complications of infective endocarditis Local complications Heart
Endocarditis: Medical vs. Surgical Treatment Nabin K. Shrestha, MD, MPH Infectious Diseases Conflicts of interest Nothing to disclose 2 Complications of infective endocarditis Local complications Heart
The microbial diagnosis of infective endocarditis (IE)
 The microbial diagnosis of infective endocarditis (IE) Pierrette Melin Medical Microbiology pm-chulg sbimc 10.05.2007 1 Introduction for diagnosis Review of microbiological investigation of IE and perspectives
The microbial diagnosis of infective endocarditis (IE) Pierrette Melin Medical Microbiology pm-chulg sbimc 10.05.2007 1 Introduction for diagnosis Review of microbiological investigation of IE and perspectives
Relationship of MIC and Bactericidal Activity to Efficacy of Vancomycin for Treatment of Methicillin-Resistant Staphylococcus aureus Bacteremia
 JOURNAL OF CLINICAL MICROBIOLOGY, June 2004, p. 2398 2402 Vol. 42, No. 6 0095-1137/04/$08.00 0 DOI: 10.1128/JCM.42.6.2398 2402.2004 Copyright 2004, American Society for Microbiology. All Rights Reserved.
JOURNAL OF CLINICAL MICROBIOLOGY, June 2004, p. 2398 2402 Vol. 42, No. 6 0095-1137/04/$08.00 0 DOI: 10.1128/JCM.42.6.2398 2402.2004 Copyright 2004, American Society for Microbiology. All Rights Reserved.
TREATMENT OF ENDOCARDITIS: Destruction and Reconstruction of the Fibrous Skeleton. Gösta B. Pettersson, M.D., Ph.D. No relationships to disclose!
 TREATMENT OF ENDOCARDITIS: Destruction and Reconstruction of the Fibrous Skeleton Gösta B. Pettersson, M.D., Ph.D. The Cleveland Clinic Foundation No relationships to disclose! Adult Cardiac Surgery Symposium
TREATMENT OF ENDOCARDITIS: Destruction and Reconstruction of the Fibrous Skeleton Gösta B. Pettersson, M.D., Ph.D. The Cleveland Clinic Foundation No relationships to disclose! Adult Cardiac Surgery Symposium
Clinical management of Staphylococcus aureus bacteraemia
 Clinical management of Staphylococcus aureus bacteraemia Guy E Thwaites, Jonathan D Edgeworth, Effrossyni Gkrania-Klotsas, Andrew Kirby, Robert Tilley, M Estée Török, Sarah Walker, Heiman F L Wertheim,
Clinical management of Staphylococcus aureus bacteraemia Guy E Thwaites, Jonathan D Edgeworth, Effrossyni Gkrania-Klotsas, Andrew Kirby, Robert Tilley, M Estée Török, Sarah Walker, Heiman F L Wertheim,
Responders as percent of overall members in each category: Region: New England 50 (58% of 86 members) 19 (51% of 37 members) 3 (33% of 9 members)
 Infectious Diseases Society of America Emerging Infections Network Report for Query: Prosthetic Joint Infections (PJI) in Adults Overall response rate: 556/118 (4.2%) physicians responded from 5/16/12
Infectious Diseases Society of America Emerging Infections Network Report for Query: Prosthetic Joint Infections (PJI) in Adults Overall response rate: 556/118 (4.2%) physicians responded from 5/16/12
The New England Journal of Medicine. Review Articles
 Review Articles Medical Progress INFECTIVE ENDOCARDITIS IN ADULTS ELEFTHERIOS MYLONAKIS, M.D., AND STEPHEN B. CALDERWOOD, M.D. INFECTIVE endocarditis, a microbial infection of the endocardial surface of
Review Articles Medical Progress INFECTIVE ENDOCARDITIS IN ADULTS ELEFTHERIOS MYLONAKIS, M.D., AND STEPHEN B. CALDERWOOD, M.D. INFECTIVE endocarditis, a microbial infection of the endocardial surface of
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION. 18 October 2006
 The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 18 October 2006 CUBICIN 350 mg (daptomycin), powder for perfusion solution Box of 1 bottle (CIP code: 567 219-3) CUBICIN
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 18 October 2006 CUBICIN 350 mg (daptomycin), powder for perfusion solution Box of 1 bottle (CIP code: 567 219-3) CUBICIN
Getting the Point of Injection Safety
 Getting the Point of Injection Safety Barbara Montana, MD, MPH, FACP Medical Director Communicable Disease Service Outbreak of Enterococcus faecalis endocarditis associated with an oral surgery practice
Getting the Point of Injection Safety Barbara Montana, MD, MPH, FACP Medical Director Communicable Disease Service Outbreak of Enterococcus faecalis endocarditis associated with an oral surgery practice
Infective Endocarditis عبد المهيمن أحمد
 Infective Endocarditis إعداد : عبد المهيمن أحمد أحمد علي Infective endocarditis Inflammation of the heart valve or endocardium of the heart. The agents are usually bacterial, but other organisms can also
Infective Endocarditis إعداد : عبد المهيمن أحمد أحمد علي Infective endocarditis Inflammation of the heart valve or endocardium of the heart. The agents are usually bacterial, but other organisms can also
Joint Trust Guideline for the Use of Intravenous Vancomycin in Paediatrics
 A clinical guideline recommended For use in: All clinical areas where vancomycin is prescribed for Children aged 1 month to 16 years By: All medical, nursing, pharmacy, microbiology and phlebotomy paediatric
A clinical guideline recommended For use in: All clinical areas where vancomycin is prescribed for Children aged 1 month to 16 years By: All medical, nursing, pharmacy, microbiology and phlebotomy paediatric
Received 30 March 2005; returned 16 June 2005; revised 8 September 2005; accepted 12 September 2005
 Journal of Antimicrobial Chemotherapy (2005) 56, 1047 1052 doi:10.1093/jac/dki362 Advance Access publication 20 October 2005 Evaluation of PPI-0903M (T91825), a novel cephalosporin: bactericidal activity,
Journal of Antimicrobial Chemotherapy (2005) 56, 1047 1052 doi:10.1093/jac/dki362 Advance Access publication 20 October 2005 Evaluation of PPI-0903M (T91825), a novel cephalosporin: bactericidal activity,
Microbiological diagnosis of infective endocarditis; what is new?
 Microbiological diagnosis of infective endocarditis; what is new? Dr Amani El Kholy, MD Professor of Clinical Pathology (Microbiology), Faculty of Medicine, Cairo University ESC 2017 1 Objectives Lab Diagnostic
Microbiological diagnosis of infective endocarditis; what is new? Dr Amani El Kholy, MD Professor of Clinical Pathology (Microbiology), Faculty of Medicine, Cairo University ESC 2017 1 Objectives Lab Diagnostic
Management of Catheter Related Bloodstream Infection (CRBSI), including Antibiotic Lock Therapy.
 Management of Catheter Related Bloodstream Infection (CRBSI), including Antibiotic Lock Therapy. Written by: Dr K Gajee, Consultant Microbiologist Date: June 2017 Approved by: Drugs & Therapeutics Committee
Management of Catheter Related Bloodstream Infection (CRBSI), including Antibiotic Lock Therapy. Written by: Dr K Gajee, Consultant Microbiologist Date: June 2017 Approved by: Drugs & Therapeutics Committee
Department of Pharmacy Services, Hartford Hospital, 80 Seymour Street, Hartford, CT 06102, USA; 2
 Pathogens 2015, 4, 599-605; doi:10.3390/pathogens4030599 Article OPEN ACCESS pathogens ISSN 2076-0817 www.mdpi.com/journal/pathogens Assessing the Surrogate Susceptibility of Oxacillin and Cefoxitin for
Pathogens 2015, 4, 599-605; doi:10.3390/pathogens4030599 Article OPEN ACCESS pathogens ISSN 2076-0817 www.mdpi.com/journal/pathogens Assessing the Surrogate Susceptibility of Oxacillin and Cefoxitin for
Steven D. Brown* and Maria M. Traczewski. The Clinical Microbiology Institute, 9725 SW Commerce Circle, Wilsonville, Oregon 97070
 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, May 2010, p. 2063 2069 Vol. 54, No. 5 0066-4804/10/$12.00 doi:10.1128/aac.01569-09 Copyright 2010, American Society for Microbiology. All Rights Reserved. Comparative
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, May 2010, p. 2063 2069 Vol. 54, No. 5 0066-4804/10/$12.00 doi:10.1128/aac.01569-09 Copyright 2010, American Society for Microbiology. All Rights Reserved. Comparative
Discrepancies in the recovery of bacteria from multiple sinuses in acute and chronic sinusitis
 Journal of Medical Microbiology (2004), 53, 879 885 DOI 10.1099/jmm.0.45655-0 Short Communication Correspondence Itzhak Brook ib6@georgetown.edu Received 1 March 2004 Accepted 18 May 2004 Discrepancies
Journal of Medical Microbiology (2004), 53, 879 885 DOI 10.1099/jmm.0.45655-0 Short Communication Correspondence Itzhak Brook ib6@georgetown.edu Received 1 March 2004 Accepted 18 May 2004 Discrepancies
Pablo Rivas, MD; Julio Alonso, MD; Javier Moya, MD; Miguel de Górgolas, MD; Jorge Martinell, MD; and Manuel L. Fernández Guerrero, MD
 The Impact of Hospital-Acquired Infections on the Microbial Etiology and Prognosis of Late-Onset Prosthetic Valve Endocarditis* Pablo Rivas, MD; Julio Alonso, MD; Javier Moya, MD; Miguel de Górgolas, MD;
The Impact of Hospital-Acquired Infections on the Microbial Etiology and Prognosis of Late-Onset Prosthetic Valve Endocarditis* Pablo Rivas, MD; Julio Alonso, MD; Javier Moya, MD; Miguel de Górgolas, MD;
Invasive Staphylococcal Infections
 Invasive Staphylococcal Infections Henry F. Chambers, M.D. Professor of Medicine, UCSF San Francisco General Hospital Disclosures AstraZeneca advisory board Cubist research grant, advisory panel Genentech
Invasive Staphylococcal Infections Henry F. Chambers, M.D. Professor of Medicine, UCSF San Francisco General Hospital Disclosures AstraZeneca advisory board Cubist research grant, advisory panel Genentech
Clinical Guidelines for Use of Antibiotics. VANCOMYCIN (Adult)
 VANCOMYCIN (Adult) Please always prescribe VANCOMYCIN in the Variable Dose Antibiotic section of the EPMA SUPPLEMENTARY drug chart (and add a placeholder on the electronic drug chart). 1 Background Vancomycin
VANCOMYCIN (Adult) Please always prescribe VANCOMYCIN in the Variable Dose Antibiotic section of the EPMA SUPPLEMENTARY drug chart (and add a placeholder on the electronic drug chart). 1 Background Vancomycin
Infective endocarditis
 Infective endocarditis Today's lecture is about infective endocarditis, the Dr started the lecture by asking what are the most common causative agents of infective endocarditis? 1-Group A streptococci
Infective endocarditis Today's lecture is about infective endocarditis, the Dr started the lecture by asking what are the most common causative agents of infective endocarditis? 1-Group A streptococci
Surgical Indications of Infective Endocarditis in Children
 2016 Annual Spring Scientific Conference of the KSC April 15-16, 2016 Surgical Indications of Infective Endocarditis in Children Cheul Lee, MD Pediatric and Congenital Cardiac Surgery Seoul St. Mary s
2016 Annual Spring Scientific Conference of the KSC April 15-16, 2016 Surgical Indications of Infective Endocarditis in Children Cheul Lee, MD Pediatric and Congenital Cardiac Surgery Seoul St. Mary s
Infective Endocarditis
 Infective Endocarditis Infective Endocarditis Historical Perspective.. A concretion larger than a pigeon s egg; contained in the left auricle. Burns, 1809 Osler s Gulstonian lectures provided the 1 st
Infective Endocarditis Infective Endocarditis Historical Perspective.. A concretion larger than a pigeon s egg; contained in the left auricle. Burns, 1809 Osler s Gulstonian lectures provided the 1 st
A study of clinical and etiological profile of infective endocarditis and its correlation with echocardiography in patients of rheumatic heart disease
 International Journal of Advances in Medicine Sarkar A et al. Int J Adv Med. 2017 Oct;4(5):1323-1327 http://www.ijmedicine.com pissn 2349-3925 eissn 2349-3933 Original Research Article DOI: http://dx.doi.org/10.18203/2349-3933.ijam20174177
International Journal of Advances in Medicine Sarkar A et al. Int J Adv Med. 2017 Oct;4(5):1323-1327 http://www.ijmedicine.com pissn 2349-3925 eissn 2349-3933 Original Research Article DOI: http://dx.doi.org/10.18203/2349-3933.ijam20174177
Prosthetic Valve Infective Endocarditis. Tat Yam Department of Infection Southampton University Hospitals NHS TRust
 Prosthetic Valve Infective Endocarditis Tat Yam Department of Infection Southampton University Hospitals NHS TRust Case History: Episode 1 in MB 73 yr old male, Nigerian PMHx: Hypertension Congestive cardiac
Prosthetic Valve Infective Endocarditis Tat Yam Department of Infection Southampton University Hospitals NHS TRust Case History: Episode 1 in MB 73 yr old male, Nigerian PMHx: Hypertension Congestive cardiac
Influence of Water Diuresis on Antimicrobial
 Influence of Water Diuresis on Antimicrobial Treatment of Enterococcal Pyelonephritis SANDRA P. LEVISON and DONALD KAYE From the Department of Medicine, The Medical College of Pennsylvania, Philadelphia,
Influence of Water Diuresis on Antimicrobial Treatment of Enterococcal Pyelonephritis SANDRA P. LEVISON and DONALD KAYE From the Department of Medicine, The Medical College of Pennsylvania, Philadelphia,
General management of infective endocarditis
 General management of infective endocarditis Team approach in infective endocarditis Gilbert Habib La Timone Hospital Marseille - France Eurovalves Barcelona 2017 The echolab «Heart Team" Infective Endocarditis
General management of infective endocarditis Team approach in infective endocarditis Gilbert Habib La Timone Hospital Marseille - France Eurovalves Barcelona 2017 The echolab «Heart Team" Infective Endocarditis
MISSOURI HOSPITALIST
 Publisher: MISSOURI HOSPITALIST SOCIETY MISSOURI HOSPITALIST Issue 33 September 23, 2010 Division of General IM University of Missouri Columbia, Missouri Editor: Robert Folzenlogen MD Inside this issue:
Publisher: MISSOURI HOSPITALIST SOCIETY MISSOURI HOSPITALIST Issue 33 September 23, 2010 Division of General IM University of Missouri Columbia, Missouri Editor: Robert Folzenlogen MD Inside this issue:
Challenging clinical situation
 Challenging clinical situation A young patient with prosthetic aortic valve endocarditis Gilbert Habib La Timone Hospital Marseille - France October 25 th 2014 Case report History of the disease Clinical
Challenging clinical situation A young patient with prosthetic aortic valve endocarditis Gilbert Habib La Timone Hospital Marseille - France October 25 th 2014 Case report History of the disease Clinical
Staphylococci. What s to be Covered. Clinical Scenario #1
 Staphylococci Micrococcus, which, when limited in its extent and activity, causes acute suppurative inflammation (phlegmon), produces, when more extensive and intense in its action on the human system,
Staphylococci Micrococcus, which, when limited in its extent and activity, causes acute suppurative inflammation (phlegmon), produces, when more extensive and intense in its action on the human system,
What s to be Covered. Microbiology of staphylococci Epidemiology of S. aureus infections Pathogenesis of S. aureus infections
 Staphylococci Micrococcus, which, when limited in its extent and activity, causes acute suppurative inflammation (phlegmon), produces, when more extensive and intense in its action on the human system,
Staphylococci Micrococcus, which, when limited in its extent and activity, causes acute suppurative inflammation (phlegmon), produces, when more extensive and intense in its action on the human system,
Medical Microbiology
 Lecture 5!!!!!!ƒš!!Œ!!! š!!œ!! Œ!!!! Dr. Ismail I. Daood Medical Microbiology!! Systematic Bacteriology Gram-Positive Cocci : GENUS : Staphylococcus : The general properties of Staphylococcus are Gram-
Lecture 5!!!!!!ƒš!!Œ!!! š!!œ!! Œ!!!! Dr. Ismail I. Daood Medical Microbiology!! Systematic Bacteriology Gram-Positive Cocci : GENUS : Staphylococcus : The general properties of Staphylococcus are Gram-
Outcome and predictors of treatment failure in early post-surgical prosthetic joint infections due to Staphylococcus aureus treated with debridement
 ORIGINAL ARTICLE INFECTIOUS DISEASES Outcome and predictors of treatment failure in early post-surgical prosthetic joint infections due to Staphylococcus aureus treated with debridement F. Vilchez 1, J.
ORIGINAL ARTICLE INFECTIOUS DISEASES Outcome and predictors of treatment failure in early post-surgical prosthetic joint infections due to Staphylococcus aureus treated with debridement F. Vilchez 1, J.
Evaluation of Antibacterial Effect of Odor Eliminating Compounds
 Evaluation of Antibacterial Effect of Odor Eliminating Compounds Yuan Zeng, Bingyu Li, Anwar Kalalah, Sang-Jin Suh, and S.S. Ditchkoff Summary Antibiotic activity of ten commercially available odor eliminating
Evaluation of Antibacterial Effect of Odor Eliminating Compounds Yuan Zeng, Bingyu Li, Anwar Kalalah, Sang-Jin Suh, and S.S. Ditchkoff Summary Antibiotic activity of ten commercially available odor eliminating
Sepsis and Infective Endocarditis
 Sepsis and Infective Endocarditis Michal Holub Department of Infectious Diseases First Faculty of Medicine Charles University in Prague and University Military Hospital Bacteremia and Sepsis bacteremia
Sepsis and Infective Endocarditis Michal Holub Department of Infectious Diseases First Faculty of Medicine Charles University in Prague and University Military Hospital Bacteremia and Sepsis bacteremia
Bacterial Endocarditis
 Disclosures Bacterial Endocarditis Henry F. Chambers, MD Allergan research grant Genentech research grant Infective endocarditis: Outline Native valve endocarditis Prosthetic valve endocarditis Cardiac
Disclosures Bacterial Endocarditis Henry F. Chambers, MD Allergan research grant Genentech research grant Infective endocarditis: Outline Native valve endocarditis Prosthetic valve endocarditis Cardiac
Daptomycin versus vancomycin in the treatment of methicillin-resistant. Staphylococcus aureus meningitis in experimental rabbit model.
 AAC Accepts, published online ahead of print on 14 January 2013 Antimicrob. Agents Chemother. doi:10.1128/aac.01996-12 Copyright 2013, American Society for Microbiology. All Rights Reserved. 1 2 Daptomycin
AAC Accepts, published online ahead of print on 14 January 2013 Antimicrob. Agents Chemother. doi:10.1128/aac.01996-12 Copyright 2013, American Society for Microbiology. All Rights Reserved. 1 2 Daptomycin
Treatment of infection
 Clinica Ortopedica e Traumatologica Università degli Studi di Pavia Fondazione IRCCS Policlinico San Matteo Chairman: Prof. F. Benazzo Goals: - Healing of infection - Healing of fracture - Try to keep
Clinica Ortopedica e Traumatologica Università degli Studi di Pavia Fondazione IRCCS Policlinico San Matteo Chairman: Prof. F. Benazzo Goals: - Healing of infection - Healing of fracture - Try to keep
Diagnostic strategy. Dr Pilar Tornos Hospital Vall d Hebron Barcelona
 Diagnostic strategy Dr Pilar Tornos Hospital Vall d Hebron Barcelona Faculty disclosure Pilar Tornos I disclose the following financial relationships: Paid speaker for Recordati, Edwards. Diagnosis of
Diagnostic strategy Dr Pilar Tornos Hospital Vall d Hebron Barcelona Faculty disclosure Pilar Tornos I disclose the following financial relationships: Paid speaker for Recordati, Edwards. Diagnosis of
Outpatient parenteral antibiotic therapy with daptomycin: insights from a patient registry
 doi: 10.1111/j.1742-1241.2008.01824.x ORIGINAL PAPER Outpatient parenteral antibiotic therapy with daptomycin: insights from a patient registry W. J. Martone, K. C. Lindfield, D. E. Katz OnlineOpen: This
doi: 10.1111/j.1742-1241.2008.01824.x ORIGINAL PAPER Outpatient parenteral antibiotic therapy with daptomycin: insights from a patient registry W. J. Martone, K. C. Lindfield, D. E. Katz OnlineOpen: This
Cubicin A Guide to Dosing
 Cubicin A Guide to Dosing Cubicin (Daptomycin) powder for solution for injection or infusion Indications (see SmPC) 1 : Cubicin is indicated for the treatment of the following infections (see sections
Cubicin A Guide to Dosing Cubicin (Daptomycin) powder for solution for injection or infusion Indications (see SmPC) 1 : Cubicin is indicated for the treatment of the following infections (see sections
