Heart Attack Readmissions in Virginia
|
|
|
- Melvyn Tate
- 6 years ago
- Views:
Transcription
1 Heart Attack Readmissions in Virginia Schroeder Center Statistical Brief Research by Mitchell Cole, William & Mary Public Policy, MPP Class of 2017 Highlights: In 2014, almost 11.2 percent of patients admitted to Virginia hospitals with a heart attack (AMI) were readmitted to the hospital within 30 days of their initial discharge. Readmissions following an AMI index admission resulted in about $50.5 million in hospital charges in Patients admitted for AMI are on average younger and have fewer comorbidities than those admitted with heart failure and pneumonia. The Schroeder Center for Health Policy at the College of William & Mary is funded by a generous gift from Cliff and Lois Schroeder. For more information on the Schroeder Center, please visit our website at or contact the Center by at schroeder@wm.edu. Heart attack or acute myocardial infarction (AMI) is one of the most common diagnoses associated with inpatient hospitalizations among adults. Heart attacks resulted in almost 609,000 hospital stays nationwide in 2014 and were one of the top 10 reasons for hospitalizations among adults aged 45 and over. In that year, hospital stays due to AMI cost a total of almost $12.3 billion. 1 Moreover, readmission to the hospital shortly after an initial heart attack hospitalization is fairly common. More than 51,000 Medicare patients were readmitted following an AMI-related hospital stay in Only seven other conditions were associated with more hospital readmissions in that year. 2 This brief examines the characteristics of patients admitted to Virginia acute care hospitals for AMI and then readmitted within 30 days during Several questions are examined. First, how many patients are readmitted to Virginia hospitals following initial admissions for AMI and what is the cost of treating them? Second, how do readmission rates vary by patient sex, age, comorbid conditions, and geography? These questions can provide insight on patterns of hospitalization treatment for heart attacks across the Commonwealth. This brief also examines a third question, namely, how do the age and comorbid conditions of patients admitted for AMI differ from those admitted for pneumonia and heart failure? This question is of interest in light of recent research findings on the Hospital Readmission Reduction Program (HRRP), which imposes penalties on hospitals with high readmission rates for patients with certain conditions. 3 Recent research has found that, in Virginia, the HRRP reduced readmissions for patients with AMI, but failed to do so for patients with heart failure and pneumonia. 4 This brief examines whether differences in patients ages and comorbidities contribute to the differences in readmission rate reductions across these conditions.
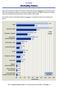
2 The Number and Costs of AMI-Related Readmissions In 2014, there were a total of 12,158 initial AMI hospitalizations of patients aged 40 and older that took place at short-term acute care hospitals participating in Medicare s inpatient prospective payment system in Virginia. A small number of these (219) are excluded from the analysis because it is not possible to ascertain whether or not a readmission took place due to missing patient identifying information such as the Social Security Number. Of the remaining 11,939 AMI hospitalizations for this age group, 1,343 hospitalizations resulted in a readmission within 30 days of the initial discharge, yielding a 30-day readmission rate of about 11.2 percent. Readmissions related to AMI resulted in about $50.5 million in hospital charges. This equates to $11.7 million in costs to the healthcare system, using hospital cost-to-charge ratios from the Centers for Medicare & Medicaid Services (CMS). 5 As shown in Exhibit 1, a large share of charge can be attributed to patients with Medicare as the primary payer -- $36.1 million in charges or approximately $8.3 million in costs. Patients with private insurance as the primary payer had the second largest share of these charges at $8.2 million ($1.9 million in costs), followed by Medicaid patients at $2.7 million ($0.65 million in costs), and then self-pay patients at $1.7 million ($0.37 million in costs). 6 Exhibit 1. Total Charges Due to 30-Day Readmission Following 2014 Initial Admissions for AMI to Patients Age 40 and Older, by Payer, in Millions of Dollars
3 Average charges per hospitalization also vary by payer. The average charge for hospitalization were highest for patients with private insurance ($46,328), followed by those with Medicaid ($44,262), patients who self-pay ($41,463), and those with Medicare ($35,566). Readmission rates were highest for Medicare patients at 15.0 percent, as shown in Exhibit 2. The rate was lower for Medicaid patients at 13.1 percent, while it was only 5.0 percent for patients with private insurance. Exhibit 2. Readmission Rates for 2014 Initial Admissions for AMI to Patients Age 40 and Older, by Primary Payer Characteristics of Patients Readmitted for AMI Demographic and clinical traits of patients readmitted for AMI are reported in Exhibit 3. Females in the sample had higher readmission rates for heart attack than males. Female patients were readmitted following about 13.9 percent of discharges, while males were only readmitted following about 9.5 percent of initial hospitalizations of adults age 40 and over. Readmission rates also rise with patients' ages. While patients in their 40s and 50s have readmission rates of 7.0 and 7.3 percent, respectively, older patients were much more likely to be readmitted. More than 17.1 percent of patients in their 80s were readmitted following an AMI admission, while more than an eighth of those in their 70s were readmitted.
4 Exhibit 3. Readmission Rates for 2014 Initial Admissions for AMI to Patients Age 40 and Older by Patient Characteristics All Patients Aged 40 and Older Medicare Patients Aged 65 and Older Number of Observations Readmission Rate Number of Observations Readmission Rate Sex Male 7, % 3, % Female 4, % 2, % Age , % n.a. n.a , % n.a. n.a , % n.a. n.a , % 1, % , % 2, % , % 1, % % % Hospital Health Planning Region Northern Virginia 1, % % Eastern Virginia 2, % 1, % Northwest Virginia 2, % 1, % Central Virginia 2, % 1, % Southwest Virginia 2, % 1, % Type of Comorbid Conditions Cancer % % Chronic Cardiovascular Disease 11, % 5, % Chronic Liver Disease % % Chronic Renal Disease 2, % 1, % Chronic Diabetes % % Chronic Pulmonary Disease 2, % 1, % Cerebrovascular Degeneration % % Number of Comorbid Conditions % % 1 6, % 2, % 2 3, % 2, % 3 1, % % % % % % Total 11, % 5, %
5 Patients are more likely to be readmitted for AMI when they have other comorbid conditions, which may make their cases particularly complicated to treat. For example, 16.3 percent of AMI patients age 40 and older with chronic pulmonary disease are readmitted, compared to 11.3 percent overall. Similarly, 18.9 percent of AMI patients with chronic diabetes and 19.8 percent with chronic renal disease are readmitted. The likelihood of readmission also varied across the state. Patients treated at hospitals in the Southwest, Northwest, and Central Virginia health planning regions had readmission rates above 11 percent, while those treated in the Northern Virginia region had a readmission rate of about 9.6 percent. Comparison of AMI, Heart Failure and Pneumonia Patients A recent study found that the HRRP reduced readmissions for Virginia patients with AMI, but failed to do so for patients with heart failure and pneumonia. 7 Looking at the characteristics of patients initially admitted for AMI, heart failure, or pneumonia treatment shows some significant differences in patients ages and comorbid conditions. This variation may contribute to different responses to the Hospital Readmissions Reductions Program. Exhibit 4 shows the average age and share of patients with different comorbid conditions using a sample of initial hospitalizations to patients age 40 and older. Exhibit 5 shows the same measures (average age and share of patients with different comorbid conditions) for a sample of initial hospitalizations to patients age 65 and older and with Medicare as the primary payer. Exhibit 4. Rates of Comorbid Conditions Among Patients Aged 40 and Over Admitted with AMI, Heart Failure, and Pneumonia AMI Heart Failure Pneumonia Cancer 3.2% 4.5%* 10.7%* Chronic Cardiovascular Disease 92.6% 97.2%* 52.5%* Chronic Liver Disease 1.5% 2.7%* 2.7%* Chronic Renal Disease 20.5% 50.0%* 22.6%* Chronic Diabetes 8.0% 13.3%* 6.6%* Chronic Pulmonary Disease 19.4% 36.9%* 47.2%* Cerebrovascular Degeneration 7.8% 10.8%* 16.2%* Average Age 67 73* 71* Total 11,939 24,497 13,085 Note: * indicates significant differences at the 0.01 level compared to the AMI sample
6 Exhibit 5. Rates of Comorbid Conditions Among Medicare Patients Aged 65 and Over Admitted with AMI, Heart Failure, and Pneumonia AMI Heart Failure Pneumonia Cancer 4.6% 5.1% 11.0%* Chronic Cardiovascular Disease 93.5% 98.0%* 62.6%* Chronic Liver Disease 1.2% 2.1%* 1.6%** Chronic Renal Disease 29.0% 51.2%* 26.9%* Chronic Diabetes 8.4% 11.2%* 6.2%* Chronic Pulmonary Disease 22.2% 37.1%* 46.5%* Cerebrovascular Degeneration 12.1% 13.1%** 20.6%* Average Age 77 80* 79* Total 5,953 16,427 8,100 Note: * indicates significant differences at the 0.01 level (** at the 0.05 level) compared to the AMI sample Of patients aged 40 and older from short-term acute care hospitals participating in Medicare s inpatient prospective payment system, there were 11,939 AMI index admissions, 13,085 pneumonia index admissions, and 24,497 heart failure index admissions. Among those patients aged 65 and older and covered by Medicare, there were 5,953 AMI index admissions, 8,100 pneumonia index admissions, and 16,427 heart failure index admissions. Age Comparing hospitalizations occurring to patients aged 40 and older, we find that AMI patients are significantly younger than those with heart failure and pneumonia. On average, patients among the age 40 and older sample admitted with AMI were 67 years old, compared to 73 and 71 years old among those with heart failure and pneumonia respectively, a statistically significant difference. This pattern also holds for patients age 65 and older and covered by Medicare. Comorbidities Comparing hospitalizations occurring to patients aged 40 and older, we find that patients admitted for AMI are less likely to have certain comorbid conditions than those admitted with heart failure or pneumonia. AMI patients were about 30 percent less likely to have cancer as heart failure patients and 70 percent less likely as pneumonia patients. Patients with AMI were also about half as likely to have chronic liver disease when compared to patients with heart failure and pneumonia. Similarly, AMI patients were also about 60 percent less likely to have chronic renal disease as heart failure patients and were also less likely to have cerebrovascular disease compared to those with heart failure and pneumonia. This general pattern also holds for patients age 65 and older and covered by Medicare, although the size of the differences are smaller in some cases.
7 Data and Methodology The data on admissions and readmissions at Virginia hospitals used in this research come from the Patient Level Data (PLD) and Readmissions and Transfers (RATs) data produced by Virginia Health Information (VHI). The PLD is a census of inpatient hospital discharges occurring at Virginia hospitals, and the RATs data allow linkage of each discharge to any prior or subsequent discharge occurring within 90 days. Virginia Health Information requests that the following disclosure be included in reports using the data: VHI has provided nonconfidential patient level information used in this report, which it has compiled in accordance with Virginia law but which it has no authority to independently verify. By using this file, report, publication, or database, the user agrees to assume all risks that may be associated with or arise from the use of inaccurate data. VHI cannot and does not represent that the use of VHI s data was appropriate for this report or endorse or support any conclusions or inferences that may be drawn from the use of VHI s data. To construct the analytical samples used in this report, we first select discharges from hospitals paid under the Inpatient Prospective Payment System (IPPS) for index admission and according to the principal diagnosis code of the discharge. In this way, our definitions of index admissions adhere closely to published definitions by CMS. We follow details in the construction of readmission rates for each condition found in technical reports prepared for CMS. For AMI index admissions, we selected discharges with a principal diagnosis of the International Classification of Diseases, 9th Revision, Clinical Modification (ICD-9-CM) code 410.xx, excluding those with 410.x2, which is a subsequent episode of AMI care. 8 For heart failure index admissions, we selected discharges with a principal diagnosis of ICD-9-CM code of , , , , , , , , , and 428.xx. 9 For pneumonia index admissions, we selected discharges with a principal ICD-9- CM code of , 480.8, 480.9, 481, , , , , , , 483, 483.1, 483.8, 485, 486, and Specifically, we exclude discharges in which the patient died in the hospital, was discharged against medical advice, or was discharged or transferred to another acute care facility; we also exclude discharges preceded by another admission for the corresponding condition (AMI, heart failure, or pneumonia) in the prior 30 days (because that discharge is then a readmission, not an index admission). For AMI admissions, we also exclude cases where the patient was discharged on the same day of admission, and we do not count potentially planned/staged readmissions as readmissions unless they include specific non-elective procedures and diagnosis codes. The RATs dataset allows us to observe prior hospitalizations that took place as many as 90 days before an admission for all hospitalizations in the PLD records, even for those hospitalizations in the first quarter of Note that if an admission for AMI follows 10 days after a discharge for pneumonia, that admission is both an index admission for AMI and a readmission for pneumonia. On the other hand, if an admission for AMI follows
8 10 days after a previous admission for AMI, that admission is excluded as it is not a true index admission but rather a readmission. This is because an admission for AMI can be an index admission or a readmission, but not both. Readmissions for heart failure and pneumonia are restricted in a similar manner. References 1 HCUPnet, Healthcare Cost and Utilization Project (HCUP), 2014, Agency for Healthcare Research and Quality, Rockville, MD, accessed Dec. 1, Hines A, Barrett M, Jiang H, Steiner C, Conditions With the Largest Number of Adult Hospital Readmissions by Payer, 2011, HCUP Statistical Brief #172, April 2014, Agency for Healthcare Research and Quality, Rockville, MD, 3 The Hospital Readmissions Reductions (HRR) Program, Centers for Medicare & Medicaid Services, Readmission-Reduction-Program.html, accessed November 28, Mellor J, Daly M, Smith M, Does It Pay to Penalize Hospitals for Excess Readmissions? Intended and Unintended Consequences of Medicare s Hospital Readmissions Reductions Program, Health Economics (2016), DOI: /hec The all-payer cost-to-charge ratio was calculated using CMS Healthcare Report Information System (HCRIS) Worksheet C Part I Medicare Cost Reports do not contain a costs and charges information for Mountain View Regional Medical Center in Norton, Virginia. We assign the mean cost-to-charge ratio among Virginia short-term acute facilities (0.25) to this facility. 6 Self-pay excludes No charge, other and unknown. 7 Mellor J, Daly M, Smith M, Does It Pay to Penalize Hospitals for Excess Readmissions? Intended and Unintended Consequences of Medicare s Hospital Readmissions Reductions Program, Health Economics (2016), DOI: /hec Krumholz H, Normand S, Keenan P, Desai M, Lin Z, Drye E, Curtis J, Bhat K, Schreiner G, Hospital 30-day Acute Myocardial Infarction Readmission Measure: Methodology, 2008, submitted by Yale University/Yale-New Haven Hospital-Center for Outcomes Research & Evaluation to the Centers for Medicare & Medicaid Services, available from: accessed January 28, Krumholz H, Normand S, Keenan P, Lin Z, Drye E, Bhat K, Wang Y, Ross J, Schuur J, Stauffer B, Bernheim S, Epstein A, Herrin J, Federer J, Mattera J, Wang Y, Mulvey G, Schreiner G, Hospital 30-day Heart Failure Readmission Measure: Methodology, 2008, submitted by Yale University/Yale-New Haven Hospital-Center for Outcomes Research & Evaluation to the Centers for Medicare & Medicaid Services, available from: accessed January 28, Krumholz H, Normand S, Keenan P, Desai M, Lin Z, Drye E, Bhat K, Schreiner G, Hospital 30-day Pneumonia Readmission Measure: Methodology, 2008, submitted by Yale University/Yale New Haven Hospital-Center for Outcomes Research & Evaluation to the Centers for Medicare & Medicaid Services, available from: accessed January 28, 2016.
Measure Information Form Collected For: CMS Outcome Measures (Claims Based)
 Last Updated: New Measure Version 4.4a Measure Information Form Collected For: CMS Outcome Measures (Claims Based) Measure Set: CMS Episode-of-Care Payment Measures Set Measure ID #: PAYM-30-HF Performance
Last Updated: New Measure Version 4.4a Measure Information Form Collected For: CMS Outcome Measures (Claims Based) Measure Set: CMS Episode-of-Care Payment Measures Set Measure ID #: PAYM-30-HF Performance
The Impact of Alcohol License Density on Alcoholic Liver Disease (ALD) Hospitalization Rates in Virginia
 The Impact of Alcohol License Density on Alcoholic Liver Disease (ALD) Hospitalization Rates in Virginia Policy Brief September 2015 Abstract Alcohol consumption is accountable for 88,000 deaths in the
The Impact of Alcohol License Density on Alcoholic Liver Disease (ALD) Hospitalization Rates in Virginia Policy Brief September 2015 Abstract Alcohol consumption is accountable for 88,000 deaths in the
Burden of Hospitalizations Primarily Due to Uncontrolled Diabetes: Implications of Inadequate Primary Health Care in the United States
 Diabetes Care In Press, published online February 8, 007 Burden of Hospitalizations Primarily Due to Uncontrolled Diabetes: Implications of Inadequate Primary Health Care in the United States Received
Diabetes Care In Press, published online February 8, 007 Burden of Hospitalizations Primarily Due to Uncontrolled Diabetes: Implications of Inadequate Primary Health Care in the United States Received
Hospital Discharge Data
 Hospital Discharge Data West Virginia Health Care Authority Hospitalization data were obtained from the West Virginia Health Care Authority s (WVHCA) hospital discharge database. Data are submitted by
Hospital Discharge Data West Virginia Health Care Authority Hospitalization data were obtained from the West Virginia Health Care Authority s (WVHCA) hospital discharge database. Data are submitted by
Technical Appendix for Outcome Measures
 Study Overview Technical Appendix for Outcome Measures This is a report on data used, and analyses done, by MPA Healthcare Solutions (MPA, formerly Michael Pine and Associates) for Consumers CHECKBOOK/Center
Study Overview Technical Appendix for Outcome Measures This is a report on data used, and analyses done, by MPA Healthcare Solutions (MPA, formerly Michael Pine and Associates) for Consumers CHECKBOOK/Center
In each hospital-year, we calculated a 30-day unplanned. readmission rate among patients who survived at least 30 days
 Romley JA, Goldman DP, Sood N. US hospitals experienced substantial productivity growth during 2002 11. Health Aff (Millwood). 2015;34(3). Published online February 11, 2015. Appendix Adjusting hospital
Romley JA, Goldman DP, Sood N. US hospitals experienced substantial productivity growth during 2002 11. Health Aff (Millwood). 2015;34(3). Published online February 11, 2015. Appendix Adjusting hospital
Troubleshooting Audio
 Welcome Audio for this event is available via ReadyTalk Internet streaming. No telephone line is required. Computer speakers or headphones are necessary to listen to streaming audio. Limited dial-in lines
Welcome Audio for this event is available via ReadyTalk Internet streaming. No telephone line is required. Computer speakers or headphones are necessary to listen to streaming audio. Limited dial-in lines
NQF-ENDORSED VOLUNTARY CONSENSUS STANDARDS FOR HOSPITAL CARE. Measure Information Form Collected For: CMS Outcome Measures (Claims Based)
 Last Updated: Version 4.3 NQF-ENDORSED VOLUNTARY CONSENSUS STANDARDS FOR HOSPITAL CARE Measure Information Form Collected For: CMS Outcome Measures (Claims Based) Measure Set: CMS Mortality Measures Set
Last Updated: Version 4.3 NQF-ENDORSED VOLUNTARY CONSENSUS STANDARDS FOR HOSPITAL CARE Measure Information Form Collected For: CMS Outcome Measures (Claims Based) Measure Set: CMS Mortality Measures Set
Health Services Utilization and Medical Costs Among Medicare Atrial Fibrillation Patients / September 2010
 Health Services Utilization and Medical Costs Among Medicare Atrial Fibrillation Patients / September 2010 AF Stat is sponsored by sanofi-aventis, U.S. LLC, which provided funding for this report. Avalere
Health Services Utilization and Medical Costs Among Medicare Atrial Fibrillation Patients / September 2010 AF Stat is sponsored by sanofi-aventis, U.S. LLC, which provided funding for this report. Avalere
Key Findings. Mortality Rates
 Mortality Rates Statewide in-hospital mortality rates showed a statistically significant decrease from federal fiscal year to federal fiscal year in 12 of the 15 conditions reported. The largest decrease
Mortality Rates Statewide in-hospital mortality rates showed a statistically significant decrease from federal fiscal year to federal fiscal year in 12 of the 15 conditions reported. The largest decrease
NATIONAL QUALITY FORUM
 TO: NQF Members and Public FR: NQF Staff RE: Pre-comment review of an addendum to National Voluntary Consensus Standards: Cardiovascular Endorsement Maintenance 2010: A Consensus Report DA: October 6,
TO: NQF Members and Public FR: NQF Staff RE: Pre-comment review of an addendum to National Voluntary Consensus Standards: Cardiovascular Endorsement Maintenance 2010: A Consensus Report DA: October 6,
The Cost Burden of Worsening Heart Failure in the Medicare Fee For Service Population: An Actuarial Analysis
 Client Report Milliman Client Report The Cost Burden of Worsening Heart Failure in the Medicare Fee For Service Population: An Actuarial Analysis Prepared by Kathryn Fitch, RN, MEd Principal and Healthcare
Client Report Milliman Client Report The Cost Burden of Worsening Heart Failure in the Medicare Fee For Service Population: An Actuarial Analysis Prepared by Kathryn Fitch, RN, MEd Principal and Healthcare
2011 Measures Maintenance Technical Report: Acute Myocardial Infarction, Heart Failure, and Pneumonia 30 Day Risk Standardized Readmission Measures
 2011 Measures Maintenance Technical Report: Acute Myocardial Infarction, Heart Failure, and Pneumonia 30 Day Risk Standardized Readmission Measures Submitted By Yale New Haven Health Services Corporation
2011 Measures Maintenance Technical Report: Acute Myocardial Infarction, Heart Failure, and Pneumonia 30 Day Risk Standardized Readmission Measures Submitted By Yale New Haven Health Services Corporation
NQF-ENDORSED VOLUNTARY CONSENSUS STANDARD FOR HOSPITAL CARE. Measure Information Form Collected For: CMS Outcome Measures (Claims Based)
 Last Updated: Version 4.3 NQF-ENDORSED VOLUNTARY CONSENSUS STANDARD FOR HOSPITAL CARE Measure Information Form Collected For: CMS Outcome Measures (Claims Based) Measure Set: CMS Readmission Measures Set
Last Updated: Version 4.3 NQF-ENDORSED VOLUNTARY CONSENSUS STANDARD FOR HOSPITAL CARE Measure Information Form Collected For: CMS Outcome Measures (Claims Based) Measure Set: CMS Readmission Measures Set
Statewide Statistics and Key Findings 1
 % s, 30 Days PHC4 s for Same Condition Jan 03 through Aug 04 Data Statewide information about readmissions and the key findings of this report are presented in this section. The study examines hospitalizations
% s, 30 Days PHC4 s for Same Condition Jan 03 through Aug 04 Data Statewide information about readmissions and the key findings of this report are presented in this section. The study examines hospitalizations
Exploring the Relationship Between Substance Abuse and Dependence Disorders and Discharge Status: Results and Implications
 MWSUG 2017 - Paper DG02 Exploring the Relationship Between Substance Abuse and Dependence Disorders and Discharge Status: Results and Implications ABSTRACT Deanna Naomi Schreiber-Gregory, Henry M Jackson
MWSUG 2017 - Paper DG02 Exploring the Relationship Between Substance Abuse and Dependence Disorders and Discharge Status: Results and Implications ABSTRACT Deanna Naomi Schreiber-Gregory, Henry M Jackson
Value of Hospice Benefit to Medicaid Programs
 One Pennsylvania Plaza, 38 th Floor New York, NY 10119 Tel 212-279-7166 Fax 212-629-5657 www.milliman.com Value of Hospice Benefit May 2, 2003 Milliman USA, Inc. New York, NY Kate Fitch, RN, MEd, MA Bruce
One Pennsylvania Plaza, 38 th Floor New York, NY 10119 Tel 212-279-7166 Fax 212-629-5657 www.milliman.com Value of Hospice Benefit May 2, 2003 Milliman USA, Inc. New York, NY Kate Fitch, RN, MEd, MA Bruce
Policy Brief June 2014
 Policy Brief June 2014 Which Medicare Patients Are Transferred from Rural Emergency Departments? Michelle Casey MS, Jeffrey McCullough PhD, and Robert Kreiger PhD Key Findings Among Medicare beneficiaries
Policy Brief June 2014 Which Medicare Patients Are Transferred from Rural Emergency Departments? Michelle Casey MS, Jeffrey McCullough PhD, and Robert Kreiger PhD Key Findings Among Medicare beneficiaries
Drug Overdose Morbidity and Mortality in Kentucky,
 Drug Overdose Morbidity and Mortality in Kentucky, 2000-2010 An examination of statewide data, including the rising impact of prescription drug overdose on fatality rates, and the parallel rise in associated
Drug Overdose Morbidity and Mortality in Kentucky, 2000-2010 An examination of statewide data, including the rising impact of prescription drug overdose on fatality rates, and the parallel rise in associated
Functional Outcomes among the Medically Complex Population
 Functional Outcomes among the Medically Complex Population Paulette Niewczyk, PhD, MPH Director of Research Uniform Data System for Medical Rehabilitation 2015 Uniform Data System for Medical Rehabilitation,
Functional Outcomes among the Medically Complex Population Paulette Niewczyk, PhD, MPH Director of Research Uniform Data System for Medical Rehabilitation 2015 Uniform Data System for Medical Rehabilitation,
Tennessee Department of Health in collaboration with Tennessee State University and University of Tennessee Health Science Center
 Tennessee Department of Health in collaboration with Tennessee State University and University of Tennessee Health Science Center 2006 Tennessee Department of Health 2006 ACKNOWLEDGEMENTS CONTRIBUTING
Tennessee Department of Health in collaboration with Tennessee State University and University of Tennessee Health Science Center 2006 Tennessee Department of Health 2006 ACKNOWLEDGEMENTS CONTRIBUTING
Potentially Preventable Hospitalizations in Pennsylvania
 Potentially Preventable Hospitalizations in Pennsylvania Pennsylvania Health Care Cost Containment Council June 2012 About PHC4 The Pennsylvania Health Care Cost Containment Council (PHC4) is an independent
Potentially Preventable Hospitalizations in Pennsylvania Pennsylvania Health Care Cost Containment Council June 2012 About PHC4 The Pennsylvania Health Care Cost Containment Council (PHC4) is an independent
APPENDIX EXHIBITS. Appendix Exhibit A2: Patient Comorbidity Codes Used To Risk- Standardize Hospital Mortality and Readmission Rates page 10
 Ross JS, Bernheim SM, Lin Z, Drye EE, Chen J, Normand ST, et al. Based on key measures, care quality for Medicare enrollees at safety-net and non-safety-net hospitals was almost equal. Health Aff (Millwood).
Ross JS, Bernheim SM, Lin Z, Drye EE, Chen J, Normand ST, et al. Based on key measures, care quality for Medicare enrollees at safety-net and non-safety-net hospitals was almost equal. Health Aff (Millwood).
Medicare Severity-adjusted Diagnosis Related Groups (MS-DRGs) Coding Adjustment
 American Hospital association December 2012 TrendWatch Are Medicare Patients Getting Sicker? Today, Medicare covers more than 48 million people, and that number is growing rapidly baby boomers are reaching
American Hospital association December 2012 TrendWatch Are Medicare Patients Getting Sicker? Today, Medicare covers more than 48 million people, and that number is growing rapidly baby boomers are reaching
had non-continuous enrolment in Medicare Part A or Part B during the year following initial admission;
 Effectiveness and cost-effectiveness of implantable cardioverter defibrillators in the treatment of ventricular arrhythmias among Medicare beneficiaries Weiss J P, Saynina O, McDonald K M, McClellan M
Effectiveness and cost-effectiveness of implantable cardioverter defibrillators in the treatment of ventricular arrhythmias among Medicare beneficiaries Weiss J P, Saynina O, McDonald K M, McClellan M
2016 Condition-Specific Measures Updates and Specifications Report Hospital-Level 30-Day Risk-Standardized Readmission Measures
 2016 Condition-Specific Measures Updates and Specifications Report Hospital-Level 30-Day Risk-Standardized Readmission Measures Acute Myocardial Infarction Version 9.0 Chronic Obstructive Pulmonary Disease
2016 Condition-Specific Measures Updates and Specifications Report Hospital-Level 30-Day Risk-Standardized Readmission Measures Acute Myocardial Infarction Version 9.0 Chronic Obstructive Pulmonary Disease
THE NATIONAL QUALITY FORUM
 THE NATIONAL QUALITY FORUM National Voluntary Consensus Standards for Patient Outcomes Table of Measures Submitted-Phase 1 As of March 5, 2010 Note: This information is for personal and noncommercial use
THE NATIONAL QUALITY FORUM National Voluntary Consensus Standards for Patient Outcomes Table of Measures Submitted-Phase 1 As of March 5, 2010 Note: This information is for personal and noncommercial use
Appendix C CHANGING THE TRAJECTORY:
 Appendix C CHANGING THE TRAJECTORY: Impact of a Hypothetical Treatment That Slows the Progression of Alzheimer s In addition to the delayed onset scenario discussed in the report, another potential scenario
Appendix C CHANGING THE TRAJECTORY: Impact of a Hypothetical Treatment That Slows the Progression of Alzheimer s In addition to the delayed onset scenario discussed in the report, another potential scenario
Partial Hospitalization Program Program for Evaluating Payment Patterns Electronic Report. User s Guide Sixth Edition. Prepared by
 Partial Hospitalization Program Program for Evaluating Payment Patterns Electronic Report User s Guide Sixth Edition Prepared by Partial Hospitalization Program Program for Evaluating Payment Patterns
Partial Hospitalization Program Program for Evaluating Payment Patterns Electronic Report User s Guide Sixth Edition Prepared by Partial Hospitalization Program Program for Evaluating Payment Patterns
Key Findings. Mortality Rates
 Mortality Rates Statewide in-hospital mortality rates showed a statistically significant decrease from to in nine of the 15 conditions reported. The largest decrease was in, where the mortality rate decreased
Mortality Rates Statewide in-hospital mortality rates showed a statistically significant decrease from to in nine of the 15 conditions reported. The largest decrease was in, where the mortality rate decreased
Putting the Patient First: How Advocate Healthcare Reduced Readmissions, LOS and Costs Through an Integrated Nutrition Care Process
 Putting the Patient First: How Advocate Healthcare Reduced Readmissions, LOS and Costs Through an Integrated Nutrition Care Process Gretchen VanDerBosch, Senior Dietitian, Advocate Good Shepherd Hospital
Putting the Patient First: How Advocate Healthcare Reduced Readmissions, LOS and Costs Through an Integrated Nutrition Care Process Gretchen VanDerBosch, Senior Dietitian, Advocate Good Shepherd Hospital
Chapter 6: Healthcare Expenditures for Persons with CKD
 Chapter 6: Healthcare Expenditures for Persons with CKD In this 2017 Annual Data Report (ADR), we introduce information from the Optum Clinformatics DataMart for persons with Medicare Advantage and commercial
Chapter 6: Healthcare Expenditures for Persons with CKD In this 2017 Annual Data Report (ADR), we introduce information from the Optum Clinformatics DataMart for persons with Medicare Advantage and commercial
Supplementary Online Content
 Supplementary Online Content Dharmarajan K, Wang Y, Lin Z, et al. Association of changing hospital readmission rates with mortality rates after hospital discharge. JAMA. doi:10.1001/jama.2017.8444 etable
Supplementary Online Content Dharmarajan K, Wang Y, Lin Z, et al. Association of changing hospital readmission rates with mortality rates after hospital discharge. JAMA. doi:10.1001/jama.2017.8444 etable
Real World Patients: The Intersection of Real World Evidence and Episode of Care Analytics
 PharmaSUG 2018 - Paper RW-05 Real World Patients: The Intersection of Real World Evidence and Episode of Care Analytics David Olaleye and Youngjin Park, SAS Institute Inc. ABSTRACT SAS Institute recently
PharmaSUG 2018 - Paper RW-05 Real World Patients: The Intersection of Real World Evidence and Episode of Care Analytics David Olaleye and Youngjin Park, SAS Institute Inc. ABSTRACT SAS Institute recently
MEASURING AND IMPROVing
 ORIGINAL CONTRIBUTION Relationship Between Hospital Readmission and Mortality Rates for Patients Hospitalized With Acute Myocardial Infarction, Heart Failure, or Pneumonia Harlan M. Krumholz, MD, SM Zhenqiu
ORIGINAL CONTRIBUTION Relationship Between Hospital Readmission and Mortality Rates for Patients Hospitalized With Acute Myocardial Infarction, Heart Failure, or Pneumonia Harlan M. Krumholz, MD, SM Zhenqiu
Mapping Palliative Care Need and Supply in California: Methodology
 Mapping Palliative Care Need and Supply in California: Methodology February 2015 Kathleen Kerr, Kerr Healthcare Analytics Mike Rabow, MD, University of California San Francisco J. Brian Cassel, PhD, Virginia
Mapping Palliative Care Need and Supply in California: Methodology February 2015 Kathleen Kerr, Kerr Healthcare Analytics Mike Rabow, MD, University of California San Francisco J. Brian Cassel, PhD, Virginia
HEART FAILURE QUALITY IMPROVEMENT. American Heart Association Shawni Smith Regional Director, Quality & Systems Improvement
 HEART FAILURE QUALITY IMPROVEMENT American Heart Association Shawni Smith Regional Director, Quality & Systems Improvement 1 DISCLOSURES NONE 2 3 WHY IS THIS IMPORTANT? WHY? Heart Failure Currently, an
HEART FAILURE QUALITY IMPROVEMENT American Heart Association Shawni Smith Regional Director, Quality & Systems Improvement 1 DISCLOSURES NONE 2 3 WHY IS THIS IMPORTANT? WHY? Heart Failure Currently, an
Released: September 13, 2016 Prepared by: Office of Assessment and Planning, Anne Arundel County Department of Health
 Opioid Poisoning-Related Emergency Department Visits Anne Arundel County, 2010-2014 Released: September 13, 2016 Prepared by: Office of Assessment and Planning, Anne Arundel County Department of Health
Opioid Poisoning-Related Emergency Department Visits Anne Arundel County, 2010-2014 Released: September 13, 2016 Prepared by: Office of Assessment and Planning, Anne Arundel County Department of Health
CHF AND PATIENT COMPLIANCE 1. Congestive Heart Failure Readmission Rates with Relation to Patient Compliance. A thesis presented by
 CHF AND PATIENT COMPLIANCE 1 Congestive Heart Failure Readmission Rates with Relation to Patient Compliance A thesis presented by Samantha B. Corral Presented to the College of Education and Health Professions
CHF AND PATIENT COMPLIANCE 1 Congestive Heart Failure Readmission Rates with Relation to Patient Compliance A thesis presented by Samantha B. Corral Presented to the College of Education and Health Professions
Care of Adults With Mental Health. U.S. Community Hospitals, 2004
 t t 4 t t 10 t t Care of Adults With Mental Health t and Substance Abuse Disorders in t t U.S. Community Hospitals, 2004 t t t t t t t t t t t t t t t t t t t Care of Adults With Mental Health and Substance
t t 4 t t 10 t t Care of Adults With Mental Health t and Substance Abuse Disorders in t t U.S. Community Hospitals, 2004 t t t t t t t t t t t t t t t t t t t Care of Adults With Mental Health and Substance
Defining High Users in Acute Care: An Examination of Different Approaches. Better data. Better decisions. Healthier Canadians.
 Defining High Users in Acute Care: An Examination of Different Approaches July 2015 Our Vision Better data. Better decisions. Healthier Canadians. Our Mandate To lead the development and maintenance of
Defining High Users in Acute Care: An Examination of Different Approaches July 2015 Our Vision Better data. Better decisions. Healthier Canadians. Our Mandate To lead the development and maintenance of
Specialist-directed care can improve outcomes across a
 Thirty-Day Outcomes in Medicare Patients With Heart Failure at Heart Transplant Centers Scott L. Hummel, MD, MS; Natalie P. Pauli, MD; Harlan M. Krumholz, MD, SM; Yun Wang, PhD; Jersey Chen, MD, MPH; Sharon-Lise
Thirty-Day Outcomes in Medicare Patients With Heart Failure at Heart Transplant Centers Scott L. Hummel, MD, MS; Natalie P. Pauli, MD; Harlan M. Krumholz, MD, SM; Yun Wang, PhD; Jersey Chen, MD, MPH; Sharon-Lise
Supplementary Online Content
 Supplementary Online Content Khera R, Dharmarajan K, Wang Y, et al. Association of the hospital readmissions reduction program with mortality during and after hospitalization for acute myocardial infarction,
Supplementary Online Content Khera R, Dharmarajan K, Wang Y, et al. Association of the hospital readmissions reduction program with mortality during and after hospitalization for acute myocardial infarction,
Emergency Department Visits for Behavioral Health Conditions in Harris County, Texas,
 Emergency Department Visits for Behavioral Health Conditions in Harris County, Texas, 2007-2008 Prepared by School of Public Health UT Health Patrick Courtney, MA August 2010 1 Table of Contents Executive
Emergency Department Visits for Behavioral Health Conditions in Harris County, Texas, 2007-2008 Prepared by School of Public Health UT Health Patrick Courtney, MA August 2010 1 Table of Contents Executive
Temporal Evaluation of Risk Factors for Acute Myocardial Infarction Readmissions
 2013 IEEE International Conference on Healthcare Informatics Temporal Evaluation of Risk Factors for Acute Myocardial Infarction Readmissions Gregor Stiglic Faculty of Health Sciences University of Maribor
2013 IEEE International Conference on Healthcare Informatics Temporal Evaluation of Risk Factors for Acute Myocardial Infarction Readmissions Gregor Stiglic Faculty of Health Sciences University of Maribor
Nebraska s Prescription Drug Monitoring Program Collecting Naloxone and Other Prescription Medications
 Nebraska s Prescription Drug Monitoring Program Collecting Naloxone and Other Prescription Medications Kevin C. Borcher, PharmD PDMP Program Director NeHII, Inc. BJA Harold Rogers PDMP National Meeting
Nebraska s Prescription Drug Monitoring Program Collecting Naloxone and Other Prescription Medications Kevin C. Borcher, PharmD PDMP Program Director NeHII, Inc. BJA Harold Rogers PDMP National Meeting
Comparison of Medicare Fee-for-Service Beneficiaries Treated in Ambulatory Surgical Centers and Hospital Outpatient Departments
 Comparison of Medicare Fee-for-Service Beneficiaries Treated in Ambulatory Surgical Centers and Hospital Outpatient Departments Prepared for: American Hospital Association April 4, 2019 Berna Demiralp,
Comparison of Medicare Fee-for-Service Beneficiaries Treated in Ambulatory Surgical Centers and Hospital Outpatient Departments Prepared for: American Hospital Association April 4, 2019 Berna Demiralp,
Medicare Patient Transfers from Rural Emergency Departments
 Medicare Patient Transfers from Rural Emergency Departments Michelle Casey, MS Jeffrey McCullough, PhD Supported by the Office of Rural Health Policy, Health Resources and Services Administration, PHS
Medicare Patient Transfers from Rural Emergency Departments Michelle Casey, MS Jeffrey McCullough, PhD Supported by the Office of Rural Health Policy, Health Resources and Services Administration, PHS
DOES PROCESS QUALITY OF INPATIENT CARE MATTER IN POTENTIALLY PREVENTABLE READMISSION RATES?
 DOES PROCESS QUALITY OF INPATIENT CARE MATTER IN POTENTIALLY PREVENTABLE READMISSION RATES? A DISSERTATION SUBMITTED TO THE FACULTY OF THE GRADUATE SCHOOL OF THE UNIVERSITY OF MINNESOTA BY Jae Young Choi,
DOES PROCESS QUALITY OF INPATIENT CARE MATTER IN POTENTIALLY PREVENTABLE READMISSION RATES? A DISSERTATION SUBMITTED TO THE FACULTY OF THE GRADUATE SCHOOL OF THE UNIVERSITY OF MINNESOTA BY Jae Young Choi,
Page County Virginia
 Page County Virginia Health Needs Assessment Part 2 Health Status Assessment October, 2001 Compiled and Printed by Blue Ridge Area Health Education Center James Madison University Page County, Virginia
Page County Virginia Health Needs Assessment Part 2 Health Status Assessment October, 2001 Compiled and Printed by Blue Ridge Area Health Education Center James Madison University Page County, Virginia
Epidemiology of adolescent and young adult hospital utilization for alcohol and drug use, poisoning, and suicide attempts in the United States
 Journal of Adolescent and Family Health Volume 6 Issue 2 Article 4 November 2014 Epidemiology of adolescent and young adult hospital utilization for alcohol and drug use, poisoning, and suicide attempts
Journal of Adolescent and Family Health Volume 6 Issue 2 Article 4 November 2014 Epidemiology of adolescent and young adult hospital utilization for alcohol and drug use, poisoning, and suicide attempts
Arkansas Health Care Payment Improvement Initiative Congestive Heart Failure Algorithm Summary
 Arkansas Health Care Payment Improvement Initiative Congestive Heart Failure Algorithm Summary Congestive Heart Failure Algorithm Summary v1.2 (1/5) Triggers PAP assignment Exclusions Episode time window
Arkansas Health Care Payment Improvement Initiative Congestive Heart Failure Algorithm Summary Congestive Heart Failure Algorithm Summary v1.2 (1/5) Triggers PAP assignment Exclusions Episode time window
More than 1.8 million New York State residents have diabetes, 1
 September 1 New York State Health Foundation s DIABETES Policy Center DIABETES: A HIDDEN HEALTH CARE COST DRIVER IN NEW YORK An Analysis of Health Care Utilization and Trends of Patients with Diabetes
September 1 New York State Health Foundation s DIABETES Policy Center DIABETES: A HIDDEN HEALTH CARE COST DRIVER IN NEW YORK An Analysis of Health Care Utilization and Trends of Patients with Diabetes
APR DRG Data Discovery
 APR DRG Data Discovery Henry Johnson MD, MPH Midas+ Vice President and Medical Director Vanessa Dorr RN MSN Midas+ DataVision Clinical Consultant Review: Agenda 3M APR DRG Methodology DataVision: Web and
APR DRG Data Discovery Henry Johnson MD, MPH Midas+ Vice President and Medical Director Vanessa Dorr RN MSN Midas+ DataVision Clinical Consultant Review: Agenda 3M APR DRG Methodology DataVision: Web and
Quality Outcomes and Financial Benefits of Nutrition Intervention. Tracy R. Smith, PhD, RD, LD Senior Clinical Manager, Abbott Nutrition
 Quality Outcomes and Financial Benefits of Nutrition Intervention Tracy R. Smith, PhD, RD, LD Senior Clinical Manager, Abbott Nutrition January 28, 2016 SHIFTING MARKET DYNAMICS PROVIDE AN OPPORTUNITY
Quality Outcomes and Financial Benefits of Nutrition Intervention Tracy R. Smith, PhD, RD, LD Senior Clinical Manager, Abbott Nutrition January 28, 2016 SHIFTING MARKET DYNAMICS PROVIDE AN OPPORTUNITY
Chapter 3: Morbidity and Mortality in Patients with CKD
 Chapter 3: Morbidity and Mortality in Patients with CKD In this 2017 Annual Data Report (ADR) we introduce analysis of a new dataset. To provide a more comprehensive examination of morbidity patterns,
Chapter 3: Morbidity and Mortality in Patients with CKD In this 2017 Annual Data Report (ADR) we introduce analysis of a new dataset. To provide a more comprehensive examination of morbidity patterns,
Publicly Reported Quality Measures
 Publicly Reported Quality Measures Five-Star Quality Rating System As part of the initiative to add five-star quality ratings to its Compare Web sites, the Centers for Medicare & Medicaid Services (CMS)
Publicly Reported Quality Measures Five-Star Quality Rating System As part of the initiative to add five-star quality ratings to its Compare Web sites, the Centers for Medicare & Medicaid Services (CMS)
Appendix 1: Supplementary tables [posted as supplied by author]
![Appendix 1: Supplementary tables [posted as supplied by author] Appendix 1: Supplementary tables [posted as supplied by author]](/thumbs/81/83505567.jpg) Appendix 1: Supplementary tables [posted as supplied by author] Table A. International Classification of Diseases, Ninth Revision, Clinical Modification Codes Used to Define Heart Failure, Acute Myocardial
Appendix 1: Supplementary tables [posted as supplied by author] Table A. International Classification of Diseases, Ninth Revision, Clinical Modification Codes Used to Define Heart Failure, Acute Myocardial
Patterns of Hospital Admissions and Readmissions Among HIV-Positive Patients in Southwestern Pennsylvania
 Patterns of Hospital Admissions and Readmissions Among HIV-Positive Patients in Southwestern Pennsylvania Keith T. Kanel, MD, MHCM, FACP Colleen Vrbin Susan Elster, PhD Jason Kunzman, MBA Michelle Murawski,
Patterns of Hospital Admissions and Readmissions Among HIV-Positive Patients in Southwestern Pennsylvania Keith T. Kanel, MD, MHCM, FACP Colleen Vrbin Susan Elster, PhD Jason Kunzman, MBA Michelle Murawski,
Appendix Identification of Study Cohorts
 Appendix Identification of Study Cohorts Because the models were run with the 2010 SAS Packs from Centers for Medicare and Medicaid Services (CMS)/Yale, the eligibility criteria described in "2010 Measures
Appendix Identification of Study Cohorts Because the models were run with the 2010 SAS Packs from Centers for Medicare and Medicaid Services (CMS)/Yale, the eligibility criteria described in "2010 Measures
The University of Mississippi School of Pharmacy
 LONG TERM PERSISTENCE WITH ACEI/ARB THERAPY AFTER ACUTE MYOCARDIAL INFARCTION: AN ANALYSIS OF THE 2006-2007 MEDICARE 5% NATIONAL SAMPLE DATA Lokhandwala T. MS, Yang Y. PhD, Thumula V. MS, Bentley J.P.
LONG TERM PERSISTENCE WITH ACEI/ARB THERAPY AFTER ACUTE MYOCARDIAL INFARCTION: AN ANALYSIS OF THE 2006-2007 MEDICARE 5% NATIONAL SAMPLE DATA Lokhandwala T. MS, Yang Y. PhD, Thumula V. MS, Bentley J.P.
Making the Business Case for Long-Acting Injectables
 Making the Business Case for Long-Acting Injectables David R. Swann, MA, LCAS, CCS, LPC, NCC Senior Healthcare Integration Consultant MTM Services Chief Clinical Officer Partners Behavioral Health Management
Making the Business Case for Long-Acting Injectables David R. Swann, MA, LCAS, CCS, LPC, NCC Senior Healthcare Integration Consultant MTM Services Chief Clinical Officer Partners Behavioral Health Management
Commercial Health Insurance Claims Data. for Studying HIV/AIDS Care. Senior Scientist, Innovus Epidemiology. David D.
 Commercial Health Insurance Claims Data for Studying HIV/AIDS Care David D. Dore, PharmD, PhD Senior Scientist, Innovus Epidemiology Adjunct Assistant Professor, Alpert Medical School, Brown University
Commercial Health Insurance Claims Data for Studying HIV/AIDS Care David D. Dore, PharmD, PhD Senior Scientist, Innovus Epidemiology Adjunct Assistant Professor, Alpert Medical School, Brown University
Management of Heart Failure: Review of the Performance Measures by the Performance Measurement Committee of the American College of Physicians
 Performance Measurement Management of Heart Failure: Review of the Performance Measures by the Performance Measurement Committee of the American College of Physicians Writing Committee Amir Qaseem, MD,
Performance Measurement Management of Heart Failure: Review of the Performance Measures by the Performance Measurement Committee of the American College of Physicians Writing Committee Amir Qaseem, MD,
TOTAL HIP AND KNEE REPLACEMENTS. FISCAL YEAR 2002 DATA July 1, 2001 through June 30, 2002 TECHNICAL NOTES
 TOTAL HIP AND KNEE REPLACEMENTS FISCAL YEAR 2002 DATA July 1, 2001 through June 30, 2002 TECHNICAL NOTES The Pennsylvania Health Care Cost Containment Council April 2005 Preface This document serves as
TOTAL HIP AND KNEE REPLACEMENTS FISCAL YEAR 2002 DATA July 1, 2001 through June 30, 2002 TECHNICAL NOTES The Pennsylvania Health Care Cost Containment Council April 2005 Preface This document serves as
The Relationship between Multimorbidity and Concordant and Discordant Causes of Hospital Readmission at 30 Days and One Year
 The Relationship between Multimorbidity and Concordant and Discordant Causes of Hospital Readmission at 30 Days and One Year Arlene S. Bierman, M.D., M.S Professor, University of Toronto and Scientist,
The Relationship between Multimorbidity and Concordant and Discordant Causes of Hospital Readmission at 30 Days and One Year Arlene S. Bierman, M.D., M.S Professor, University of Toronto and Scientist,
Trends in Pneumonia and Influenza Morbidity and Mortality
 Trends in Pneumonia and Influenza Morbidity and Mortality American Lung Association Epidemiology and Statistics Unit Research and Health Education Division November 2015 Page intentionally left blank Introduction
Trends in Pneumonia and Influenza Morbidity and Mortality American Lung Association Epidemiology and Statistics Unit Research and Health Education Division November 2015 Page intentionally left blank Introduction
HQID Hospital Performance Update & Analysis of Quality, Cost and Mortality Trends Fact Sheet
 HQID Hospital Performance Update & Analysis of Quality, Cost and Mortality Trends Fact Sheet I.) Performance of Hospitals in the Hospital Quality Incentive Demonstration over 15 Quarters* (pages 2-5) Launched
HQID Hospital Performance Update & Analysis of Quality, Cost and Mortality Trends Fact Sheet I.) Performance of Hospitals in the Hospital Quality Incentive Demonstration over 15 Quarters* (pages 2-5) Launched
Per Capita Health Care Spending on Diabetes:
 Issue Brief #10 May 2015 Per Capita Health Care Spending on Diabetes: 2009-2013 Diabetes is a costly chronic condition in the United States, medical costs and productivity loss attributable to diabetes
Issue Brief #10 May 2015 Per Capita Health Care Spending on Diabetes: 2009-2013 Diabetes is a costly chronic condition in the United States, medical costs and productivity loss attributable to diabetes
Financial Impact of Emergency Department Visits by Adults for Dental Conditions in Maryland
 Financial Impact of Emergency Department by Adults for Dental Conditions in Maryland Background Access to dental care remains challenging for many children and adults. Lack of preventive care services
Financial Impact of Emergency Department by Adults for Dental Conditions in Maryland Background Access to dental care remains challenging for many children and adults. Lack of preventive care services
INFORMATION FOR RESEARCHERS REQUESTING DATA FROM THE NHVPR
 INFORMATION FOR RESEARCHERS REQUESTING DATA FROM THE NHVPR What is the NHVPR? The National Human Papillomavirus Vaccination Program Register (NHVPR) is the Australian register which records HPV vaccine
INFORMATION FOR RESEARCHERS REQUESTING DATA FROM THE NHVPR What is the NHVPR? The National Human Papillomavirus Vaccination Program Register (NHVPR) is the Australian register which records HPV vaccine
Voluntary Mental Health Treatment Laws for Minors & Length of Inpatient Stay. Tori Lallemont MPH Thesis: Maternal & Child Health June 6, 2007
 Voluntary Mental Health Treatment Laws for Minors & Length of Inpatient Stay Tori Lallemont MPH Thesis: Maternal & Child Health June 6, 2007 Introduction 1997: Nearly 300,000 children were admitted to
Voluntary Mental Health Treatment Laws for Minors & Length of Inpatient Stay Tori Lallemont MPH Thesis: Maternal & Child Health June 6, 2007 Introduction 1997: Nearly 300,000 children were admitted to
Unplanned Hospitalizations and Readmissions among Elderly Patients with GI Cancer
 Unplanned Hospitalizations and Readmissions among Elderly Patients with GI Cancer September 19, 2014 Joanna-Grace M. Manzano, MD Assistant Professor Department of General Internal Medicine UT MD Anderson
Unplanned Hospitalizations and Readmissions among Elderly Patients with GI Cancer September 19, 2014 Joanna-Grace M. Manzano, MD Assistant Professor Department of General Internal Medicine UT MD Anderson
Publicly Reported Quality Measures
 Publicly Reported Quality Measures Five-Star Quality Rating System As part of the initiative to add five-star quality ratings to its Compare Web sites, the Centers for Medicare & Medicaid Services (CMS)
Publicly Reported Quality Measures Five-Star Quality Rating System As part of the initiative to add five-star quality ratings to its Compare Web sites, the Centers for Medicare & Medicaid Services (CMS)
Acute myocardial infarction (AMI) is a high-risk condition. Methods Papers
 Methods Papers An Administrative Claims Measure Suitable for Profiling Hospital Performance Based on 30-Day All-Cause Readmission Rates Among Patients With Acute Myocardial Infarction Harlan M. Krumholz,
Methods Papers An Administrative Claims Measure Suitable for Profiling Hospital Performance Based on 30-Day All-Cause Readmission Rates Among Patients With Acute Myocardial Infarction Harlan M. Krumholz,
The High Price of Undiagnosed Malnutrition
 The High Price of Undiagnosed Malnutrition Kathy J Irwin, MS, RD, LDN, CNSC Clinical Nutrition Manager, Morrison Healthcare Methodist Medical Center A member of Covenant Health Oak Ridge, Tennessee Service
The High Price of Undiagnosed Malnutrition Kathy J Irwin, MS, RD, LDN, CNSC Clinical Nutrition Manager, Morrison Healthcare Methodist Medical Center A member of Covenant Health Oak Ridge, Tennessee Service
HEALTH CARE EXPENDITURES ASSOCIATED WITH PERSISTENT EMERGENCY DEPARTMENT USE: A MULTI-STATE ANALYSIS OF MEDICAID BENEFICIARIES
 HEALTH CARE EXPENDITURES ASSOCIATED WITH PERSISTENT EMERGENCY DEPARTMENT USE: A MULTI-STATE ANALYSIS OF MEDICAID BENEFICIARIES Presented by Parul Agarwal, PhD MPH 1,2 Thomas K Bias, PhD 3 Usha Sambamoorthi,
HEALTH CARE EXPENDITURES ASSOCIATED WITH PERSISTENT EMERGENCY DEPARTMENT USE: A MULTI-STATE ANALYSIS OF MEDICAID BENEFICIARIES Presented by Parul Agarwal, PhD MPH 1,2 Thomas K Bias, PhD 3 Usha Sambamoorthi,
Fact. Objectives 1/6/2016. Reducing Hospital Readmissions for Chronic Obstructive Pulmonary Disease (COPD)
 Reducing Hospital Readmissions for Chronic Obstructive Pulmonary Disease (COPD) Jin S. Oh, PharmD Larkin Community Hospital January 10, 2016 Fact COPD is the third leading cause of death in the United
Reducing Hospital Readmissions for Chronic Obstructive Pulmonary Disease (COPD) Jin S. Oh, PharmD Larkin Community Hospital January 10, 2016 Fact COPD is the third leading cause of death in the United
Mental Illness and Substance Use Hospitalizations in New Hampshire,
 Mental Illness and Substance Use Hospitalizations in New Hampshire, 1997-2006 May, 2008 Part of the Access New Hampshire: Living with Disability in the Granite State Project To learn more about the Access
Mental Illness and Substance Use Hospitalizations in New Hampshire, 1997-2006 May, 2008 Part of the Access New Hampshire: Living with Disability in the Granite State Project To learn more about the Access
Using Hospital Admission and Readmission Patterns to Improve Outreach to Persons Living with HIV/AIDS in Pennsylvania
 Using Hospital Admission and Readmission Patterns to Improve Outreach to Persons Living with HIV/AIDS in Pennsylvania July 1, 2010 September 30, 2012 February 2014 Prepared by By Susan Elster, Colleen
Using Hospital Admission and Readmission Patterns to Improve Outreach to Persons Living with HIV/AIDS in Pennsylvania July 1, 2010 September 30, 2012 February 2014 Prepared by By Susan Elster, Colleen
Unplanned 30-Day Readmissions in Orthopaedic Trauma
 Unplanned 30-Day Readmissions in Orthopaedic Trauma Introduction: 30-day readmission is increasingly used as a hospital quality metric. The objective of this study was to describe the patient factors associated
Unplanned 30-Day Readmissions in Orthopaedic Trauma Introduction: 30-day readmission is increasingly used as a hospital quality metric. The objective of this study was to describe the patient factors associated
Inpatient Psychiatric Facility Quality Reporting (IPFQR) Program
 FY 2017 IPPS Final Rule IPFQR Changes, APU Determination and Reconsideration Review Questions and Answers Moderator/Speaker: Evette Robinson, MPH Project Lead, IPFQR Inpatient Hospital Value, Incentives,
FY 2017 IPPS Final Rule IPFQR Changes, APU Determination and Reconsideration Review Questions and Answers Moderator/Speaker: Evette Robinson, MPH Project Lead, IPFQR Inpatient Hospital Value, Incentives,
2014 Hospital Inpatient Discharge Data Annual Report
 2014 Hospital Inpatient Discharge Data Annual Report Health Systems Epidemiology Program Epidemiology and Response Division New Mexico Department of Health 2014 Hospital Inpatient Discharge Data Report
2014 Hospital Inpatient Discharge Data Annual Report Health Systems Epidemiology Program Epidemiology and Response Division New Mexico Department of Health 2014 Hospital Inpatient Discharge Data Report
Fractional Flow Reserve (FFR) and instant wave-free Ratio (The ifr modality)
 2017 Coding and Medicare payment guide Fractional Flow Reserve (FFR) and instant wave-free Ratio (The ifr modality) All coding, coverage, billing and payment information provided herein by Philips Volcano
2017 Coding and Medicare payment guide Fractional Flow Reserve (FFR) and instant wave-free Ratio (The ifr modality) All coding, coverage, billing and payment information provided herein by Philips Volcano
Overview of H-CUP Application of HCUP in Clinical Research Current articles in Medicine Practice example
 Overview of H-CUP Application of HCUP in Clinical Research Current articles in Medicine Practice example 2 What is H-CUP? HCUP includes the LARGEST collection of multi-year hospital care (inpatient, outpatient,
Overview of H-CUP Application of HCUP in Clinical Research Current articles in Medicine Practice example 2 What is H-CUP? HCUP includes the LARGEST collection of multi-year hospital care (inpatient, outpatient,
Competing Risks: Implications for Readmission Policy
 Competing Risks: Implications for Readmission Policy KAREN E. JOYNT, MD, MPH HARVARD SCHOOL OF PUBLIC HEALTH, BRIGHAM AND WOMEN S HOSPITAL, AND VA BOSTON HEALTHCARE SYSTEM NATIONAL HEALTH POLICY FORUM,
Competing Risks: Implications for Readmission Policy KAREN E. JOYNT, MD, MPH HARVARD SCHOOL OF PUBLIC HEALTH, BRIGHAM AND WOMEN S HOSPITAL, AND VA BOSTON HEALTHCARE SYSTEM NATIONAL HEALTH POLICY FORUM,
Hu J, Gonsahn MD, Nerenz DR. Socioeconomic status and readmissions: evidence from an urban teaching hospital. Health Aff (Millwood). 2014;33(5).
 Appendix Definitions of Index Admission and Readmission Definitions of index admission and readmission follow CMS hospital-wide all-cause unplanned readmission (HWR) measure as far as data are available.
Appendix Definitions of Index Admission and Readmission Definitions of index admission and readmission follow CMS hospital-wide all-cause unplanned readmission (HWR) measure as far as data are available.
Writing Committee. ACP Performance Measurement Committee Members*
 Performance Measurement Coronary Artery Bypass Graft Surgery: Review of the Performance Measures by the Performance Measurement Committee of the American College of Physicians Writing Committee Amir Qaseem,
Performance Measurement Coronary Artery Bypass Graft Surgery: Review of the Performance Measures by the Performance Measurement Committee of the American College of Physicians Writing Committee Amir Qaseem,
ORIGINAL INVESTIGATION. Factors Associated With 30-Day Readmission Rates After Percutaneous Coronary Intervention
 ONLINE FIRST ORIGINAL INVESTIGATION Factors Associated With 30-Day Rates After Percutaneous Coronary Intervention Farhan J. Khawaja, MD; Nilay D. Shah, PhD; Ryan J. Lennon, MS; Joshua P. Slusser, BS; Aziz
ONLINE FIRST ORIGINAL INVESTIGATION Factors Associated With 30-Day Rates After Percutaneous Coronary Intervention Farhan J. Khawaja, MD; Nilay D. Shah, PhD; Ryan J. Lennon, MS; Joshua P. Slusser, BS; Aziz
Technical Notes for PHC4 s Report on CABG and Valve Surgery Calendar Year 2005
 Technical Notes for PHC4 s Report on CABG and Valve Surgery Calendar Year 2005 The Pennsylvania Health Care Cost Containment Council April 2007 Preface This document serves as a technical supplement to
Technical Notes for PHC4 s Report on CABG and Valve Surgery Calendar Year 2005 The Pennsylvania Health Care Cost Containment Council April 2007 Preface This document serves as a technical supplement to
Patient Navigator Program: Focus MI Diplomat Hospital Metrics
 Patient Navigator Program: Focus MI Diplomat Hospital Metrics Goal Statement: To reduce avoidable hospital readmissions for patients discharged with acute myocardial infarction (AMI) by supporting a culture
Patient Navigator Program: Focus MI Diplomat Hospital Metrics Goal Statement: To reduce avoidable hospital readmissions for patients discharged with acute myocardial infarction (AMI) by supporting a culture
Diabetes in Manitoba: Trends among Adults
 Diabetes Among Adults in Manitoba (1989-2013) Diabetes in Manitoba: Trends among Adults 1989-2013 1989-2013 Epidemiology & Surveillance Active Living, Population and Public Health Branch Manitoba Health,
Diabetes Among Adults in Manitoba (1989-2013) Diabetes in Manitoba: Trends among Adults 1989-2013 1989-2013 Epidemiology & Surveillance Active Living, Population and Public Health Branch Manitoba Health,
Using A Quality Improvement Program to Reduce Length of Stay and Readmissions: Real World Evidence from One Health Care System
 Using A Quality Improvement Program to Reduce Length of Stay and Readmissions: Real World Evidence from One Health Care System Wm. Thomas Summerfelt, PhD April 19, 2017 Becker s Hospital Review Conference
Using A Quality Improvement Program to Reduce Length of Stay and Readmissions: Real World Evidence from One Health Care System Wm. Thomas Summerfelt, PhD April 19, 2017 Becker s Hospital Review Conference
A COMPREHENSIVE REPORT ISSUED BY THE AMERICAN ASSOCIATION OF CLINICAL ENDOCRINOLOGISTS IN PARTNERSHIP WITH:
 A COMPREHENSIVE REPORT ISSUED BY THE AMERICAN ASSOCIATION OF CLINICAL ENDOCRINOLOGISTS IN PARTNERSHIP WITH: Amputee Coalition of America Mended Hearts National Federation of the Blind National Kidney Foundation
A COMPREHENSIVE REPORT ISSUED BY THE AMERICAN ASSOCIATION OF CLINICAL ENDOCRINOLOGISTS IN PARTNERSHIP WITH: Amputee Coalition of America Mended Hearts National Federation of the Blind National Kidney Foundation
Trends in Hospice Utilization
 Proposed FY 2017 Hospice Wage Index and Rate Update and Hospice Quality Reporting Requirements To: NHPCO Provider Members From: Health Policy Team Date: April 25, 2016 On April 21, 2016, the Centers for
Proposed FY 2017 Hospice Wage Index and Rate Update and Hospice Quality Reporting Requirements To: NHPCO Provider Members From: Health Policy Team Date: April 25, 2016 On April 21, 2016, the Centers for
PfP Quality Metrics: Readmissions, Value-Based Purchasing and Beyond
 PfP Quality Metrics: Readmissions, Value-Based Purchasing and Beyond Presented to ASHNHA Alaska Partnership for Patients Advisory Group February 4, 2015 Gloria Kupferman Readmissions Calculation methods
PfP Quality Metrics: Readmissions, Value-Based Purchasing and Beyond Presented to ASHNHA Alaska Partnership for Patients Advisory Group February 4, 2015 Gloria Kupferman Readmissions Calculation methods
This slide set provides an overview of the impact of type 1 and type 2 diabetes mellitus in the United States, focusing on epidemiology, costs both
 This slide set provides an overview of the impact of type 1 and type 2 diabetes mellitus in the United States, focusing on epidemiology, costs both direct and indirect and the projected burden of diabetes,
This slide set provides an overview of the impact of type 1 and type 2 diabetes mellitus in the United States, focusing on epidemiology, costs both direct and indirect and the projected burden of diabetes,
The clinical and economic benefits of better treatment of adult Medicaid beneficiaries with diabetes
 The clinical and economic benefits of better treatment of adult Medicaid beneficiaries with diabetes September, 2017 White paper Life Sciences IHS Markit Introduction Diabetes is one of the most prevalent
The clinical and economic benefits of better treatment of adult Medicaid beneficiaries with diabetes September, 2017 White paper Life Sciences IHS Markit Introduction Diabetes is one of the most prevalent
Mandatory Elements of Healthcare Reform Walter Coleman. healthcare consulting
 Mandatory Elements of Healthcare Reform Walter Coleman 1 Agenda ACA Mandatory Elements of Reform Value Based Purchasing Readmission Reduction Program Hospital Acquired Conditions Best practices to analyze
Mandatory Elements of Healthcare Reform Walter Coleman 1 Agenda ACA Mandatory Elements of Reform Value Based Purchasing Readmission Reduction Program Hospital Acquired Conditions Best practices to analyze
The Economic Burden of Hypercholesterolaemia
 The Economic Burden of Hypercholesterolaemia November 2018 TABLE OF CONTENTS Acronyms 3 Executive Summary 4 Introduction 5 Approach 5 Structure of the report 5 Economic burden of hypercholesterolaemia
The Economic Burden of Hypercholesterolaemia November 2018 TABLE OF CONTENTS Acronyms 3 Executive Summary 4 Introduction 5 Approach 5 Structure of the report 5 Economic burden of hypercholesterolaemia
