Health Services Utilization and Medical Costs Among Medicare Atrial Fibrillation Patients / September 2010
|
|
|
- Marian Valerie Wade
- 6 years ago
- Views:
Transcription
1 Health Services Utilization and Medical Costs Among Medicare Atrial Fibrillation Patients / September 2010
2 AF Stat is sponsored by sanofi-aventis, U.S. LLC, which provided funding for this report. Avalere maintained editorial control and the conclusions expressed here are those of the author.
3 Table of Contents Executive Summary... 2 Background... 7 Methodology Results Limitations Conclusions Appendix A B C D E Glossary of Key Terms Endnotes... 47
4 Executive Summary Background/Objective Chronic diseases such as diabetes, cancer, and cardiovascular disease are the leading cause of death and disability in the United States. Atrial Fibrillation (AFib) is one type of chronic cardiovascular disease that is highly prevalent in the Medicare population. Previous studies have shown that AFib patients use more healthcare services than patients without AFib. 1,2 As this condition is estimated to cost the Medicare program over $15.7 billion per year, 3 it is important to understand the key components of AFib patient health services utilization and medical costs. This issue brief is the second in a series in which Avalere examines the burden of AFib on the Medicare program. The purpose of this original analysis is to examine use of healthcare services, including inpatient and outpatient services, physician services, and emergency department (ED) services, as well as medical costs among Medicare AFib patients following an initial hospitalization for AFib. In the first paper, Medicare and Atrial Fibrillation: Consequences in Cost and Care (2009), Avalere described the clinical and economic burden of AFib on the Medicare program, characterized the current state of quality improvement 4 efforts, and identified potential quality improvement strategies. Methodology Avalere conducted a retrospective database analysis based on Medicare s five percent Standard Analytic Files (SAFs) for The SAFs are publicly available files which are commonly used by researchers to examine utilization and cost patterns in the Medicare population. The five percent SAFs are a nationally representative sample of final action claims data for the Medicare beneficiary population. 5,6 We identified a cohort of Medicare patients with AFib and constructed an analytic file linking the inpatient, outpatient, and physician claims files for these patients. Our study population included patients with a primary diagnosis of AFib during an initial or index hospitalization. For AFib patients in our study, we examined the utilization of, and costs associated with hospital inpatient and outpatient services, physician services, and ED services. We tracked the utilization and costs of these services during the quarter of the index hospitalization and the four quarters subsequent to the index hospitalization. 2
5 We refer to these five quarters as the follow-up period. Medicare payments are used as a proxy for medical costs; all costs are reported in 2009 US dollars. Study Results AFib patients in our study had multiple comorbid conditions There were 14,174 patients that had a primary diagnosis of AFib during their index hospitalization. The average age of these patients at the time of their index hospitalization was 76; 60 percent of patients are female, and most of them are white (92 percent). Patients included in this analysis had several comorbid conditions in addition to AFib, including hypertension, other cardiovascular conditions, and diabetes. Overall average medical costs among AFib patients in this study were nearly $24,000 per patient during the follow-up period The total medical costs of treating AFib patients over the follow-up period averaged almost $24,000 per beneficiary. Sixty-two percent ($14,887) of these costs were for inpatient services. Furthermore, 63 percent of the inpatient services costs ($9,412) were related to readmission costs. The costs observed in our study are higher than in some published reports, 7,8 but are comparable to those reported by Lee and colleagues. 9 Using the five percent Medicare SAFs, Lee reported average one-year healthcare costs in a cohort of AFib patients to be $23,750, compared to our finding of an average per-patient cost of $23,899 over five quarters. Although these costs appear similar between the Lee study and our analysis, the two studies were based on different AFib patient populations. Lee and colleagues focused on patients newly diagnosed with AFib, 87 percent of whom were diagnosed in the outpatient setting; while our analysis included patients who had an inpatient hospitalization for AFib. In addition, Lee et al. included medical costs from skilled nursing facilities (SNF), home healthcare, durable medical equipment, and hospice in their analysis, whereas we did not include these services in our analysis. 10 In addition, the total AFib costs per patient for five quarters reported in our analysis are similar to those reported in studies of other costly cardiovascular conditions. For example: According to two studies based on managed care data, average one-year medical costs for patients with acute coronary syndrome, including Health Services Utilization and Medical Costs Among Medicare Atrial Fibrillation Patients 3
6 myocardial infarction and unstable angina, ranged from $22,500 to $41, ,12 A recent study analyzing costs and health resource utilization for Medicare patients with heart failure and diabetes, reported aggregated two-year mean costs of $32,676 for patients with diabetes and heart failure and $22,230 for patients with heart failure only. 13 AFib patients in our sample had high hospital outpatient and physician services utilization AFib patients in our analysis were frequent users of hospital outpatient and physician health services. Hospital outpatient visits include services provided in a hospital setting that do not require an overnight stay. Physician encounters may occur in various settings, including a physician s office, the hospital inpatient or outpatient settings, the ED, laboratory, or other sites of service (e.g., SNF). Most of the patients had at least one hospital outpatient visit (90 percent) and at least one encounter with a physician (98 percent). These patients had an average of 12 hospital outpatient visits and 67 physician encounters during the follow-up period. Approximately 46 percent of these physician encounters (n=30) occurred in the physician office setting, and 31 percent of physician visits in all settings of care were for cardiovascular-related reasons. Related, across all settings of care, cardiology (20 percent) was the leading physician specialty caring for AFib patients, followed by internal medicine (16 percent). The cumulative cost per beneficiary with at least one hospital outpatient visit averaged $2,972. The cumulative cost per beneficiary among those with at least one physician encounter averaged $6,471. Sixty-one percent of the AFib patients in our study visited the emergency department during follow-up period ED utilization was an essential part of the utilization pattern of AFib patients as well; 61 percent of the patients visited the ED at least once in the follow-up period. On average, these patients went to the ED three times during this period. Twenty-nine percent of AFib patient ED visits were for cardiovascular-related reasons. 4
7 AFib patients in our study were often readmitted multiple times and shortly after the initial hospitalization More than half (52 percent) of the 14,174 AFib patients in our analysis were readmitted to an inpatient hospital at least once during the follow-up period. Furthermore, 12 percent of patients were readmitted three or more times. AFib was the primary diagnosis in 15 percent of readmissions. A large percentage of hospital readmissions occurred relatively soon after the index hospitalization. Specifically, we found that: about 25 percent of readmissions occurred within the same quarter as the index hospitalization; and that 23 percent of readmissions occurred in the quarter after the index hospitalization. Cardiovascular-related conditions were key causes of hospital readmissions among AFib patients in our study Based on an examination of Diagnosis Related Group (DRG) assignments, we found that 48 percent of hospital readmissions identified in our analysis were related to cardiovascular conditions such as heart failure and shock, hypertension, and chest pain. An examination of the cardiovascular-related readmission International Classification of Diseases, Ninth Revision, Clinical Modification (ICD-9-CM) diagnosis codes shows that 31 percent of these readmissions listed AFib (ICD-9-CM ) in the primary position on the claim. AFib is often reported as a comorbid condition that may influence healthcare utilization and costs We also found that AFib is more often reported as a comorbidity to other conditions than as a primary diagnosis. Furthermore, when patients had AFib as a secondary diagnosis, the total medical costs during the follow-up period were higher ($33,200) than when patients had AFib as a primary diagnosis ($23,899). This suggests that AFib as a comorbid condition may exacerbate primary conditions, influencing the utilization patterns and costs of care for those conditions. Further research to fully understand the clinical and economic impact of AFib as a comorbid condition would be valuable. Conclusions This retrospective study assessed health resource utilization and associated costs over a five quarter period following an index hospitalization for AFib in a well-defined cohort of Medicare patients. The results provide valuable information on a unique subset of the AFib patient population that has not been Health Services Utilization and Medical Costs Among Medicare Atrial Fibrillation Patients 5
8 well characterized in the literature. The findings highlight the economic burden of AFib on the Centers for Medicare & Medicaid Services (CMS) and the overall healthcare system. The findings also emphasize the need for improved management strategies to help reduce the high health services utilization and medical costs in all settings of care for Medicare AFib patients. As the Medicare population continues to grow and the prevalence of AFib increases, reforms aimed at additional research, quality improvement, and cost management will be critical to support the advancement of AFib treatment, improve patient outcomes, and reduce costs for the Medicare program. 6
9 Background AFib is a prevalent cardiovascular disease in the Medicare population Chronic diseases such as diabetes, cancer, and cardiovascular disease are the leading cause of death and disability in the United States. AFib is one type of chronic cardiovascular disease which is highly prevalent in adults over age The condition causes its patients to have an irregular heartbeat. Specifically, it is caused by disorganized electrical activity in the top chambers (the atria) of the heart, resulting in a quivering motion of the atria instead of a normal, organized pumping motion. This quiver, or fibrillation, causes a heartbeat that can be more than twice that of a normal heart rate at rest. 15 It may also lead to stagnation of blood flow in the atria, which can cause blood clots and stroke. AFib usually occurs due to the presence of other cardiac conditions such as hypertension, heart failure, coronary artery disease, and heart valve disease. However, it can also be caused by conditions that do not involve the heart such as pneumonia or thyroid disorders. 16 As the most common arrhythmia in the United States, AFib affects more than 2.5 million adults, 80 percent of whom are 65 years and older. In the next 40 years, the prevalence of AFib is projected to more than double to 5.6 million adults. 17 AFib accounts for one third of hospitalizations for an irregular heartbeat. 18 Figure 1 shows historical and projected growth of AFib prevalence in the United States. Figure 1 AFib is increasingly prevalent in the United States 7.0 Adults with AFib (in Millions) Health Services Utilization and Medical Costs Among Medicare Atrial Fibrillation Patients 7
10 Description of Disease Description of Disease What is AFib? What are the risk factors for AFib? What are the symptoms of AFib? How is AFib treated? AFib refers to an irregular rhythm in the heart (arrhythmia) due to disorganized electrical activity in the upper chambers of the heart (the atria), resulting in irregular impulses being sent to the lower chambers of the heart (the ventricles) which in turn generates an irregular heartbeat. 19 The atrial cells fire at rates of times per minute, causing the muscles in the atria to quiver, or fibrillate, instead of normally contracting. 20 As a result, a typical heart rate of a person with AFib can be very rapid up to 150 beats per minute or higher, compared to a normal heart rate of beats per minute at rest. 21 AFib episodes may occur periodically, and last anywhere from minutes up to a week, longer than a week, requiring intervention by a healthcare professional to restore normal heart rhythm (persistent AFib), (paroxysmal AFib) or may become chronic (permanent AFib). 22 Risk factors for AFib may include the presence of several other comorbid conditions, including hypertension, congestive heart failure (HF), obesity, diabetes, mitral valve disease, pericarditis, chronic obstructive pulmonary disease, and sleep apnea. History of myocardial infarction is also a risk factor for AFib. 23 AFib may be asymptomatic, or include symptoms such as palpitations (a sudden fluttering feeling in the chest), anxiety, shortness of breath, weakness, and difficulty exercising, chest pain, sweating, dizziness, or fainting. 24 AFib treatment depends on the cause and type of AFib that is diagnosed. The goal of AFib treatment is to either restore normal heart rhythm and/or control the heart rate, and to prevent stroke. Treatment options range from medications alone (anticoagulants, anti-arrhythmics, and rate control medications) to more aggressive interventions, which may include electrical cardio-version, cardiac ablation, pacemaker implantation, and surgery. 25 AFib patients have several comorbid conditions AFib patients often have several age-related comorbidities such as valvular heart disease, HF, coronary artery disease, diabetes, and hypertension. 26 In a 2009 study, researchers found that AFib is common among patients with diabetes. Specifically, they found that AFib was 44 percent more prevalent and 38 percent 8
11 more likely to develop among patients with diabetes. 27 Furthermore, AFib significantly increases the risk of stroke and heart disease, both of which are leading causes of death in the United States. 28 As a result, AFib patients with heart disease have higher mortality rates compared to patients with normal heart rhythm. 29 AFib is also associated with significant impairments in patient quality of life. 30 Patients daily functioning may be hindered by symptoms such as palpitations (a sudden fluttering feeling in the chest), shortness of breath, weakness, chest pain, sweating, dizziness, and fainting. 31 AFib patients also typically suffer from impairments in mental health and social functioning, 32 such as high levels of anxiety. 33 AFib patients use more healthcare services than patients without AFib Studies have shown that AFib patients utilize many types of healthcare services including those associated with the inpatient hospital, outpatient settings, and the emergency department. Inpatient hospital services have been of particular interest. A study based on the National Hospital Discharge Survey demonstrated that AFib hospitalizations tripled from 1985 to Since then, researchers have continued to find that AFib patients are commonly readmitted to the hospital and use high levels of other types of healthcare services. For example, a 2008 study of Medicare beneficiaries showed that patients with AFib required significantly more healthcare services compared to those without AFib. Specifically, during the first year following an AFib diagnosis: 28 percent of AFib patients versus seven percent of non-afib patients have 3 hospital admissions; 14 percent of AFib patients versus three percent of non-afib patients have 3 emergency room visits; and, 72 percent of AFib patients versus 61 percent of non-afib patients have 3 outpatient visits. 35 In a retrospective study of managed care patients (under age 65), Kim et al. (2009) found about 10 to 12 percent of those with AFib were readmitted to the hospital within the first year following their initial AFib hospitalization. About 66 percent of these hospitalizations occurred within six months of the initial AFib hospitalization, while 20 percent of these readmissions occurred within the first month. Kim and colleagues suggest that an even higher rate of readmissions would occur in the Medicare population. 36 Yet another study that focused on the Health Services Utilization and Medical Costs Among Medicare Atrial Fibrillation Patients 9
12 timing of the hospitalization showed the likelihood of a hospitalization was the highest within the first year after the diagnosis of AFib. 37 AFib costs Medicare more than $15.7 billion annually Medicare absorbs the majority of the clinical and economic burden of caring for AFib patients. This is not surprising considering that this diagnosis is more common in an older population, and that the complications associated with AFib increase with age. An Avalere analysis of public and private payer survey data identifies Medicare as the primary payer of AFib across all settings of care (Figure 2). Figure 2 Medicare is the primary payer for AFib across all settings of care 100% 2.36% 1.04% 2.73% 6.03% 4.59% 2.71% 3.81% 4.81% 1.40% 2.76% 80% 60% 14.47% 17.16% 18.39% 6.34% 23.90% 21.62% 40% 20% 78.40% 56.39% 61.37% 69.42% 0% Hospital Inpatient Hospital Outpatient Emergency Department Physician's Office Medicare Private Medicaid Self-Pay Misc/Other Avalere Health analysis of data from the National Hospital Discharge Survey, National Ambulatory Medical Care Survey and National Ambulatory Medical Care Survey Outpatient Department and Emergency Department for years for ICD-9 diagnosis code In a 2009 study of managed care patients, researchers estimated that the total hospitalization and outpatient cost of treating AFib patients in the U.S. was $12.7 billion, with hospitalizations accounting for 63 percent of the total. 38 However, in a 2008 study, researchers indicate that Medicare alone pays $15.7 billion annually to treat newly diagnosed AFib patients. 39 These costs are largely driven by the greater utilization of healthcare services associated with AFib complications such as stroke, HF, acute myocardial infarction, and tachycardia. Importantly, these costs are considered by some to be an underestimate since they exclude deductibles, copayments, medical costs not covered by Medicare, 10
13 and patients who have previously been diagnosed with AFib and are currently undergoing treatment. One study focusing on Medicare patients found that within the first year following an AFib diagnosis, patients with AFib were more likely than a matched cohort of patients without AFib to have HF (36.7 percent versus 10.4 percent) and/or stroke (23.1 percent versus 13.3 percent). This study also found that HF was the second most expensive complication, costing Medicare $12,117 per patient within the first year of diagnosis. 40 Another study estimates the annual cost of stroke among Medicare AFib patients is $8 billion. 41 Most of the costs associated with AFib and its complications occur in the inpatient hospital setting, largely due to readmissions. In a retrospective cohort study of managed care patients, researchers found that inpatient expenses were about 80 percent of the total costs to treat hospitalized AFib patients. 42 A similar study estimated that 73 percent of total US AFib costs were for inpatient costs. 43 Although several studies have examined the costs associated with AFib, these analyses are primarily focused on younger patients in managed care settings. With the exception of a study by Lee and colleagues (2008) which focused on newly diagnosed AFib patients and is based on Medicare data from , there are limited data examining rates of rehospitalization, use of healthcare services in multiple settings of care, and medical costs among Medicare AFib patients. The purpose of this analysis is to examine rates of health services utilization and medical costs among Medicare AFib patients after an initial hospitalization for AFib based on more recent Medicare data from This brief is the second in a series in which Avalere examines the burden of AFib on the Medicare program. We present results of an original analysis of AFib patient utilization and medical costs for various healthcare services including hospital inpatient and outpatient services, physician services, and ED services. In the first paper, Medicare and Atrial Fibrillation: Consequences in Cost and Care (2009), we described the burden of AFib on the Medicare program, characterized the current state of quality improvement efforts, and proposed potential strategies to improve the quality of care and outcomes for AFib patients. 44 Health Services Utilization and Medical Costs Among Medicare Atrial Fibrillation Patients 11
14 Methodology Overview Avalere conducted a retrospective database analysis based on Medicare s five percent Standard Analytic Files (SAFs) for Specifically, we identified a cohort of Medicare patients with AFib based on the International Classification of Diseases, Ninth Revision, Clinical Modification (ICD-9-CM) diagnosis codes, 45 and constructed an analytic file linking the inpatient, outpatient, and physician claims files for these patients. Our study cohort included patients with a primary diagnosis of AFib during an initial or index hospitalization. We examined patterns of healthcare utilization and associated medical costs among patients in the cohort during the quarter of the index hospitalization and in the four quarters subsequent to the index hospitalization. We refer to these five quarters as the follow-up period (Figure 3). Figure 3 Study follow-up period Index Hospitalization Quarter Post- Index Hospitalization Quarters We assessed the rate and timing of readmissions, the reasons for these readmissions, the average costs of the readmissions; and rates and frequency of, and costs associated with physician and hospital outpatient service utilization. Hospital outpatient visits included services provided in a hospital setting that did not require an overnight stay. Furthermore, we conducted an additional analysis using a larger cohort of patients who had either a primary or secondary diagnosis of AFib during their index hospitalization. Data source Avalere used the Medicare five percent SAFs to complete this analysis. The five percent SAFs contain final action claims data for five percent of the Medicare beneficiary population. The SAFs are constructed from weekly data submissions to the Medicare National Claims History Database, which contains the electronic files of paid Medicare claims. 46 There are seven separate SAFs which are specific to various institutional and non-institutional services. 12
15 For this analysis we used the SAFs specific to hospital inpatient, hospital outpatient, and physician services for The SAFs contain information related to patient demographics, health services utilization, and Medicare payments. Specifically, they contain diagnosis and procedure codes as well as reimbursement amounts. Notably, we are using the limited data set (LDS) version of the Medicare SAFs which does not include specific dates of medical services. Instead, the files report the quarter of the calendar year when the services are provided. Medicare 5 percent Standard Analytic Files (SAF) Database with medical claims for five percent of the Medicare population Includes patient demographics, diagnoses, procedures, and Medicare payments Provides information on services provided in different settings of care and by different types of providers (i.e., inpatient, hospital outpatient, skilled nursing facility, hospice, home health, physician, and durable medical equipment) Does not include prescription drug utilization Study design This is a retrospective, single-arm, cohort study. We constructed a longitudinal database from the Medicare SAFs, linking the claims for inpatient facility, outpatient facility, and physician services provided to patients using encrypted unique patient identifier numbers. Linking these files enabled us to examine the frequency and patterns of healthcare utilization and costs among patients across settings of care and over time. Key Terms Index hospitalization: the first instance of an admission to an acute care hospital with an AFib diagnosis recorded on the claim. Follow-up period: study observation period, which includes the quarter of and four quarters following the index hospitalization. Readmission: an admission into an acute care hospital after the index hospitalization during the follow-up period. Study population To identify Medicare beneficiaries with AFib for our study population, we used inpatient SAFs to find the first instance of an admission to a short-term acute Health Services Utilization and Medical Costs Among Medicare Atrial Fibrillation Patients 13
16 care hospital with an AFib diagnosis recorded on the claim. We considered this first instance to be a beneficiary s index hospitalization. Our study group, or cohort, was comprised of Medicare beneficiaries who had a primary diagnosis of AFib (ICD-9-CM diagnosis code ) at their index hospitalization. 48 We required that patients have at least nine consecutive quarters of Medicare enrollment. Specifically, we required beneficiaries to be continuously enrolled in Medicare for the year prior to the quarter of the index hospitalization (four quarters preceding the quarter of the index hospitalization) and the year following the index hospitalization (four quarters following the quarter of the index hospitalization) (Figure 4). Figure 4 Study window: continuous enrollment criterion Four Pre- Index Hospitalization Quarters Index Hospitalization Quarter Four Post- Index Hospitalization Quarters Additional patient analysis Given that AFib is commonly reported as a comorbid condition instead of a primary diagnosis, we performed an additional analysis on an expanded cohort of AFib patients. Specifically, this expanded cohort included those patients who had either a primary or secondary diagnosis of AFib during their index hospitalization (i.e., AFib diagnosis reported in any of the nine diagnosis positions on the medical claim). We analyzed readmissions, use of healthcare services and medical costs for this primary/secondary cohort of patients to gauge the impact of AFib as a comorbid condition. Study Patient Groups Primary AFib patient cohort: patients with a primary AFib diagnosis at their initial hospitalization. Primary/secondary AFib patient cohort: patients who had a primary or secondary AFib diagnosis at their initial hospitalization. 14
17 Study outcome measures Study Outcome Measures Frequency and costs associated with hospital outpatient utilization Frequency and costs associated with physician services Utilization of ER services Rate of readmissions Timing and costs associated with readmissions Index Hospitalization As previously stated, the index hospitalization is the first hospitalization with an AFib diagnosis. 49 We calculated the average length of stay (LOS) and average costs associated with the index hospitalization. We used Medicare payments as reported on the claim file as a proxy for costs. To further characterize the AFib patients included in our cohorts, we examined rates of comorbid conditions using ICD-9-CM diagnosis codes reported on the index hospitalization claim. 50 We also examined diagnosis-related group (DRG) and Medicare severitydiagnosis related group (MS-DRG) assignments of the index hospitalization. CMS uses the DRG and MS-DRG systems to classify inpatient hospital stays for each Medicare beneficiary based on their diagnosis and the procedures they received. CMS assigns a numeric weight to each DRG or MS-DRG, indicating how costly that DRG is relative to the average inpatient stay. The weights are used to inform the Medicare payments rendered for each patient s stay. 51 The DRG system informs the assignments through September 2007, while the MS-DRG system informs them starting in October About 93 percent of the patients in our population had an index hospitalization under the DRG system, while the remaining patients index hospitalizations occurred after the introduction of the MS-DRG system. Hospital outpatient, emergency department, and physician utilization and costs Physician utilization is any separately billable service provided by a physician in various settings of care during the follow-up period. We tracked physician encounters in the physician office setting as well as in the hospital inpatient and outpatient settings, ED, independent laboratory, skilled nursing facility, ambulatory surgical center, and ambulance setting. Hospital outpatient utilization involves services provided in a hospital that do not require an overnight stay. We examined the following utilization parameters for physician utilization, outpatient department, and emergency department visits: Health Services Utilization and Medical Costs Among Medicare Atrial Fibrillation Patients 15
18 percent of beneficiaries with at least one physician encounter, hospital outpatient visit or emergency department visit, mean number of physician encounters, hospital outpatient visits, and emergency department visits, and timing of the physician encounters, hospital outpatient visits, and emergency department visits relative to the index hospitalization. We assessed economic outcomes as well. Specifically, we calculated the average cost per physician encounter and hospital outpatient visit, average cost per beneficiary for physician encounters and hospital outpatient visits, and average cumulative cost per beneficiary among those with at least one physician encounter or hospital outpatient visit. The SAFs do not detail the payments associated with emergency room visits. Because we examined data over multiple years, costs were standardized to 2009 values using the medical care component of the Consumer Price Index, a measure of inflation calculated by the United States Bureau of Labor Statistics. We report average costs throughout this paper. Additional cost measures (i.e., medians and standard deviations) appear in Appendix E. Medical Costs In this study, Medicare payments are a proxy for medical costs. All costs are reported in 2009 US dollars. Hospital readmissions and costs We defined a hospital readmission as any admission to a short-term acute care hospital during the five quarter follow-up period starting with the index hospitalization quarter. We examined the following readmission outcomes: percentage of beneficiaries with at least one readmission, average length of stay, and average number of readmissions per beneficiary in the patient population. 53 We also calculated the average number of readmissions among those with at least one readmission. In addition, we reported medical costs associated with the hospital readmissions in the follow-up period. We reported on the following costs: cost per readmission, cumulative readmission cost per beneficiary in the patient population, and readmission cost per beneficiary with at least one readmission. 16
19 We also tracked the timing of the readmissions relative to the index hospitalization. Specifically, we created a distribution of the readmissions occurring in the same quarter as the index hospitalization, in the quarter following the index hospitalization, and those in subsequent quarters. As with the index hospitalizations, we examined the reasons for readmissions using ICD- 9-CM diagnosis codes, DRG assignments, and MS-DRG assignments. Cardiovascular- and non cardiovascular-related readmissions and costs To better understand the patterns of health services utilization and costs among patients in our study, we differentiated between cardiovascular- and non cardiovascular-related services. Specifically, we defined cardiovascular-related readmissions as those in which the patient was assigned to certain cardiacrelated medical and surgical DRGs or MS-DRGs. For example, we included medical DRGs 134 (hypertension), 143 (chest pain), and 127 (heart failure and shock) in our group of cardiovascular-related DRGs. See Appendices A and B for a full list of the DRGs and MS-DRGs used to classify cardiovascular-related admissions. Non cardiovascular-related readmissions are those that were not assigned to the cardiac-related DRGs and MS-DRGs. In addition, we differentiated between cardiovascular and non cardiovascular outpatient visits and physician encounters. Cardiovascular-related outpatient visits and physician encounters are those with one of several cardiovascular ICD- 9-CM diagnosis codes in the primary position. Some examples of cardiovascularrelated ICD-9-CM s are acute myocardial infarction (410.XX), chronic pulmonary heart disease (416.XX), and cardiomyopathy (425.XX). For our full list of cardiovascular-related diagnosis codes, see Appendix C. Key Terms Cardiovascular-related readmission: readmissions in which patients were assigned to cardiac related medical and surgical diagnosis related groups Non cardiovascular-related readmission: readmissions in which patients were assigned to diagnosis related groups that were not related to cardiac conditions Health Services Utilization and Medical Costs Among Medicare Atrial Fibrillation Patients 17
20 Results AFib patients in our study had multiple comorbid conditions There were 14,174 patients that 1) had a primary diagnosis of AFib at the time of their index hospitalization and 2) met our criterion of nine quarters of continuous Medicare enrollment. The average age of these AFib patients at the time of their index hospitalization was 76. Sixty percent of them were female. Table 1 provides characteristics of our study cohort including age, gender, race and geographic region. Table 1 AFib Study Cohort Characteristic AFib Cohort (n= 14,174) Average Age Age Group (%) Female (%) Race/Ethnicity (%) White Black 5.20 Hispanic 1.17 Asian 0.73 Other 0.62 North American Native 0.27 Census Region (%) South Midwest Northeast West Unknown 0.32 Not surprisingly, AFib patients included in our study were most commonly hospitalized for cardiac arrhythmia (Table 2). In fact, 84 percent of patients were assigned to DRG codes 138 and 139, which are for cardiac arrhythmia with and without complications, respectively. 18
21 Table 2 Top five DRGs for AFib patient index hospitalizations DRG code Description Percent of total 138 Cardiac Arrhythmia & Conduction Disorders W CC 57.50% 139 Cardiac Arrhythmia & Conduction Disorders W/O CC 26.49% 552 Other Permanent Cardiac Pacemaker Implant W/O Major Cv Dx 2.67% 125 Circulatory Disorders Except AMI, W Card Cath W/O Complex Diag 2.38% 124 Circulatory Disorders Except AMI, W Card Cath & Complex Diag 2.09% See Appendix D for the results of the MS-DRG index hospitalization assignments. Patients included in this analysis had several comorbid conditions in addition to AFib which were typically related to hypertension, cardiovascular conditions, and diabetes. Table 3 identifies the top ten comorbidities of AFib patients index hospitalizations. Health Services Utilization and Medical Costs Among Medicare Atrial Fibrillation Patients 19
22 Table 3 Ten most commonly reported comorbid conditions at index hospitalizations ICD-9-CM Diagnosis Code Comorbidity Description Percent of Index Hospitalizations 401 Essential Hypertension 58.46% 272 Disorders of Lipoid Metabolism % 414 Other Forms of Chronic Ischemic Heart Disease % 427 Cardiac Dysrhythmias 22.86% 428 Heart Failure 22.02% 250 Diabetes Mellitus 18.79% V45 Other Postsurgical States % 424 Other Diseases of Endocardium % 276 Disorders of Fluid, Electrolyte, and Acid-Base Balance % 244 Acquired Hypothyroidism 13.85% 1 Common disorders of lipoid metabolism include hyperlipidemia and hypercholesterolemia, which relate to high cholesterol. 2 Conditions common to ischemic heart disease are coronary atherosclerosis, dissection, and aneurysm, which are associated with heart attacks. 3 The other post surgical states diagnosis code includes such conditions as post operative dialysis and post operative pacemaker. 4 Diseases of endocardium include conditions related to disorders of the heart valves and inflammation of the heart chamber. 5 Disorders of fluid electrolyte and acid base balance include hyperkalemia, hypocalcemia, acidosis, hyponatremia which relate to acute renal failure of the kidneys. These results are similar to other published studies of AFib patients, which also indicate high rates of cardiovascular-related comorbid conditions. 54,55 AFib patients stayed in the hospital for four days on average during their index hospitalization with an average cost of $5,475 (Table 4). The year in which the index hospitalizations occurred was relatively evenly distributed from 2005 to
23 Table 4 Index hospitalization characteristics Characteristic Average Length of Stay (number of days) AFib Cohort (n= 14,174) 3.68 days Average Cost of Index Hospitalization $5,475 Year of Index Hospitalization (%) Study Results AFib patients in our study had multiple comorbid conditions Overall average medical costs among AFib patients in this study were nearly $24,000 per patient during the follow-up period AFib patients in our sample had high hospital outpatient and physician services utilization Many AFib patients visited the emergency department in the follow-up period AFib patients in our study were often readmitted multiple times and shortly after an initial hospitalization Cardiovascular-related conditions were key causes of hospital readmissions among AFib patients in our study AFib is often reported as a comorbid condition that may influence healthcare utilization and costs Overall average medical costs among AFib patients in this study were nearly $24,000 per patient during the follow-up period The total medical costs of treating AFib patients over the study period averaged almost $24,000 per beneficiary. Figure 5 reports the sum of the average costs per beneficiary in each setting of care including inpatient, outpatient, and physician services. Sixty-two percent ($14,887) of these costs were for inpatient services. Furthermore, 63 percent of the inpatient services costs ($9,412) were related to readmission costs. See Appendix E for more detailed cost information (i.e., medians, standard deviations). Health Services Utilization and Medical Costs Among Medicare Atrial Fibrillation Patients 21
24 Figure 5 Total average medical costs by site of service $25,000 Mean costs per beneficiary $20,000 $15,000 $10,000 $5,000 Total Costs Across Settings of Care = $23,899 $6,363 $2,649 $9,412 Total Inpatient Costs per Beneficiary = $14,887 $5,475 $0 Setting of Care Inpatient Index Hospitalizations Outpatient Services Inpatient Readmissions Physician Services AFib patients in our sample had high hospital outpatient and physician services utilization We found that AFib patients utilized high amounts of hospital outpatient, physician, and emergency department services in the follow-up period. Hospital outpatient visits include services provided in a hospital setting that do not require an overnight stay. Most patients in our study (90 percent) visited the outpatient hospital at least once in the follow-up period (Table 5). Furthermore, these patients visited the outpatient hospital an average of 12 times during this period. The cumulative cost per beneficiary with at least one visit averaged $2,972. Twenty-eight percent of hospital outpatient visits were for cardiovascular-related reasons. 22
25 Table 5 Hospital outpatient utilization and costs Outcome AFib Cohort (N=14,174) Number of beneficiaries with at least one visit 12,632 Percent of beneficiaries with at least one visit 89.12% Average number of visits per beneficiary Average number of visits per beneficiary, among those with at least one visit Timing of visits (%) Visits within the same quarter of the index hospitalization 22.39% Visits in the quarter following the index hospitalization 22.13% Visits in subsequent quarters 55.48% Average cost per visit $247 Average cumulative visit cost for beneficiaries with at least one visit $2,972 We observed even higher utilization levels of physician services, which may occur in various settings, including a physician s office, the hospital inpatient or outpatient settings, the ED, laboratory, or other sites of service (e.g., skilled nursing facility). Specifically, 98 percent of patients had at least one physician encounter in the follow-up period. These patients saw the physician 67 times on average in the follow-up period. Thirty-one percent of these visits were for cardiovascular-related reasons, i.e., hypertension, ischemic heart disease, or heart failure. Related, across all settings of care, cardiology (20 percent) was the leading physician specialty caring for AFib patients, followed by internal medicine (16 percent). Forty-six percent of physician encounters (n=30) occurred in the physician office setting. Figure 6 shows the distribution of physician service settings of care used by the AFib patients in our study. Health Services Utilization and Medical Costs Among Medicare Atrial Fibrillation Patients 23
26 Figure 6 Physician encounters by site of service during the follow-up period 60% 46% 40% 20% 24% 7% 6% 9% 7% 0% Physician Inpatient Outpatient Emergency Independent Other Office Hospital Hospital Room Lab Note: Other includes settings such as ambulance, skilled nursing facility, and ambulatory surgical center. The cost per physician encounter averaged $96. The cumulative cost per beneficiary among those with at least one physician encounter averaged $6,471. See the following table for a summary of physician services utilization and cost findings: Table 6 Physician services utilization and costs Outcome AFib Cohort (N=14,174) Number of beneficiaries with at least one encounter 13,937 Percent of beneficiaries with at least one encounter 98.33% Average number of physician encounters per beneficiary Average number of encounters per beneficiary, among those with at least one encounter Timing of Encounters (%) Encounters within the same quarter of the index hospitalization 32.19% Encounters in the quarter following the index hospitalization 19.53% Encounters in subsequent quarters 48.29% Average cost per encounter $96 Average cumulative encounter cost for beneficiaries with at least one encounter $6,471 24
27 Sixty-one percent of AFib patients visited the emergency department in the follow-up period AFib patients also commonly visited the emergency department. In the followup period, 61 percent of patients visited the emergency room at least once. They went three times on average post index hospitalization. Furthermore, 65 percent of readmissions were initiated through an emergency room visit. Twenty-nine percent of ED visits were for cardiovascular-related reasons. AFib patients in our study were readmitted frequently and early after an initial hospitalization More than half (52 percent) of the 14,174 AFib patients in our primary cohort were readmitted to an inpatient hospital at least once during the follow-up period. Furthermore, 12 percent of patients were readmitted three or more times (Figure 7). AFib was the primary diagnosis in 15 percent of all readmissions. Figure 7 Number of readmissions during the follow-up period 60% 40% 48% 52% of patients were readmitted at least once 20% 0% 27% 12% 6% 6% 0 Readmissions 1 Readmission 2 Readmissions 3 Readmissions 4 or more Readmissions The patients who were readmitted at least once had two readmissions on average during the follow-up period. A large percentage of hospital readmissions occurred relatively soon after the index hospitalization. Specifically, we found that: about 25 percent of readmissions occurred within the same quarter as the index hospitalization; and that Twenty three percent of readmissions occurred in the quarter after the index hospitalization (Figure 8). Health Services Utilization and Medical Costs Among Medicare Atrial Fibrillation Patients 25
28 Figure 8 Forty-eight percent of readmissions occurred soon after the index hospitalization Index Hospitalization Quarter Post-Index Hospitalization Quarters % 23% 52% Compared to a younger patient population in a managed care setting, these readmission rates are higher. As previously stated, Kim and colleagues (2009) found hospital readmission rates of about 10 to 12 percent during the one-year following the index hospitalization for a cohort of AFib patients using a national managed care claims database. Similar to our study, this analysis showed that 20 percent of the readmissions occurred within the first month following the index hospitalization and two-thirds of the readmissions occurred within the first six months following the index hospitalization. 56 Once readmitted, AFib patients stayed in the hospital for about five days on average, costing Medicare $9,061 on average for each stay (Table 7). Further, the cumulative readmission cost per beneficiary with at least one readmission during the follow-up period averaged $18,192. Table 7 Hospital readmissions and costs Outcome AFib Cohort (N=14,174) Number of beneficiaries with at least one readmission 7,333 Percent of beneficiaries with at least one readmission 51.74% Average number of readmissions per beneficiary 1.04 Average number of readmissions per beneficiary, among those with at least one readmission 2.01 Average length of readmission (number of days) 4.79 Average cost per readmission $9,061 Average cumulative readmission cost for beneficiaries with at least one readmission $18,192 26
29 Cardiovascular-related conditions were key causes of hospital readmissions among AFib patients in our study Based on an assessment of the DRGs reported at the readmissions, the causes for these readmissions included cardiac- and non cardiac-related reasons. However, the most common DRGs were often related to cardiac conditions (Table 8). Table 8 DRG assignments for AFib patient readmissions DRG code DRG description Percent of total 138 Cardiac Arrhythmia & Conduction Disorders W CC 10.43% 127 Heart Failure & Shock 9.81% 139 Cardiac Arrhythmia & Conduction Disorders W/O CC 4.53% 089 Simple Pneumonia & Pleurisy Age >17 W CC 3.27% 552 Other Permanent Cardiac Pacemaker Implant W/O Major CV DX 2.60% Further examination of the ICD-9-CM diagnosis codes for the cardiac-related readmissions showed that 31 percent of readmission claims listed AFib (ICD-9- CM ) in the primary position. Other common primary diagnoses reported for cardiovascular-related readmissions included coronary heart failure (17 percent) and coronary atherosclerosis native vessel (seven percent). When we did further analysis of all of the DRGs reported for the hospital readmissions and examined those specifically related to cardiovascular conditions (Appendix A), we found 48 percent of readmissions were related to cardiovascular conditions. Health Services Utilization and Medical Costs Among Medicare Atrial Fibrillation Patients 27
30 Figure 9 Proportions of readmissions related to cardiovascular and non cardiovascular conditions 52% 48% Cardiovascular readmissions Non-cardiovascular readmissions AFib patients with cardiovascular-related readmissions stayed in the hospital for about four days on average, costing Medicare an average of $9,477 per stay. Among beneficiaries who had at least one readmission, the average cost per beneficiary of cardiovascular-related readmissions was $15,019, while the average cost per beneficiary of non cardiovascular-related readmissions was $14,178. Notably, the most common non cardiovascular-related readmissions involved conditions such as pneumonia, chronic obstructive pulmonary disease, and stroke (intracranial hemorrhage or cerebral infarction) (Table 9). Table 9 Most common non cardiovascular-related conditions DRG code DRG description Percent of total 089 Simple Pneumonia & Pleurisy Age >17 W CC 6.36% 182 Esophagitis, Gastroent & Misc Digest Disorders Age >17 W 4.75% CC 174 G.I. Hemorrhage W CC 4.53% 088 Chronic Obstructive Pulmonary Disease 4.28% 014 Intracranial Hemorrhage or Cerebral Infarction 4.00% In our analysis of the ICD-9-CM diagnosis codes associated with the non cardiovascular-related readmissions, we found that the primary diagnoses codes were more dispersed compared to those of the cardiovascular-related readmissions. The three most common ICD-9-CMs for non cardiovascular- 28
31 related readmissions included pneumonia (six percent), urinary tract infection (three percent) and cerebral artery occlusion not otherwise specified with infarction (three percent). AFib is often reported as a comorbid condition that may influence healthcare utilization and costs The iteration of the analysis using the primary/secondary cohort yielded similar outcomes. As stated previously, the primary/secondary cohort included AFib patients with a primary or secondary diagnosis of AFib at the index hospitalization. Using this approach, our cohort expanded to 89,799 patients. This considerable increase in our patient sample size indicates that AFib is more often reported as a comorbidity to other conditions than as a primary diagnosis. We describe some of the findings of the primary/secondary iteration below. Index Hospitalization Consistent with the primary cohort, we observed cardiovascular- and hypertension-related comorbidities in the primary/secondary cohort s index hospitalizations. In fact, nine of the top 10 conditions of the primary cohort are included in the 10 most common comorbidities of the primary/secondary cohort. However, the average costs associated with index AFib hospitalizations were higher for the primary/secondary cohort relative to the primary cohort. We found that the average cost of treating patients in the primary/secondary cohort was $11,222, compared with the primary cohort where index hospitalizations cost $5,475 on average. Hospital Readmissions Readmissions of patients in the primary/secondary cohort occurred similarly to those in the primary cohort. Fifty-five percent (n=49,006) of patients had at least one hospital readmission during the follow-up period. We found that 26 percent of readmissions were in the same quarter and 22 percent were in the quarter after the index hospitalization. These primary/secondary patients also stayed in the hospital for five days on average, once readmitted. Each inpatient hospital readmission cost Medicare about $9,458 on average for primary/secondary patients, which is similar to the average costs for primary patients ($9,061). Furthermore, the cumulative readmission cost per beneficiary with at least one readmission averaged $20,028 for those in the primary/secondary cohort. Health Services Utilization and Medical Costs Among Medicare Atrial Fibrillation Patients 29
Medicare and Medicaid Payments
 and Payments The following table includes information about payments made by and for the 17 medical conditions/surgical procedures included in this Hospital Performance Report. This analysis is based on
and Payments The following table includes information about payments made by and for the 17 medical conditions/surgical procedures included in this Hospital Performance Report. This analysis is based on
Objectives. Medicare Spending per Beneficiary: Analyzing MSPB Data to Identify Primary Drivers
 Medicare Spending per Beneficiary: Analyzing MSPB Data to Identify Primary Drivers August 22, 2017 Objectives Understand the basics of the hospital specific MSPB data files and reports Review the factors
Medicare Spending per Beneficiary: Analyzing MSPB Data to Identify Primary Drivers August 22, 2017 Objectives Understand the basics of the hospital specific MSPB data files and reports Review the factors
NQF-ENDORSED VOLUNTARY CONSENSUS STANDARD FOR HOSPITAL CARE. Measure Information Form Collected For: CMS Outcome Measures (Claims Based)
 Last Updated: Version 4.3 NQF-ENDORSED VOLUNTARY CONSENSUS STANDARD FOR HOSPITAL CARE Measure Information Form Collected For: CMS Outcome Measures (Claims Based) Measure Set: CMS Readmission Measures Set
Last Updated: Version 4.3 NQF-ENDORSED VOLUNTARY CONSENSUS STANDARD FOR HOSPITAL CARE Measure Information Form Collected For: CMS Outcome Measures (Claims Based) Measure Set: CMS Readmission Measures Set
JUSTUS WARREN TASK FORCE MEETING DECEMBER 05, 2012
 SAMUEL TCHWENKO, MD, MPH Epidemiologist, Heart Disease & Stroke Prevention Branch Chronic Disease & Injury Section; Division of Public Health NC Department of Health & Human Services JUSTUS WARREN TASK
SAMUEL TCHWENKO, MD, MPH Epidemiologist, Heart Disease & Stroke Prevention Branch Chronic Disease & Injury Section; Division of Public Health NC Department of Health & Human Services JUSTUS WARREN TASK
Medicare Payments. PHC4 Hospital Performance Report Oct 2015 through Sept 2016 Data 2015 Medicare Payments 1
 The following table includes information about payments made by for the 16 medical conditions/surgical procedures included in this Hospital Performance Report. This analysis is based on data from calendar
The following table includes information about payments made by for the 16 medical conditions/surgical procedures included in this Hospital Performance Report. This analysis is based on data from calendar
Mission Statement for our Arrhythmia Care
 Mission Statement for our Arrhythmia Care We are dedicated to provide a compassionate and an outstanding care for patients with cardiac arrhythmias. We will be utilizing the cutting edge and the most advanced
Mission Statement for our Arrhythmia Care We are dedicated to provide a compassionate and an outstanding care for patients with cardiac arrhythmias. We will be utilizing the cutting edge and the most advanced
Tennessee Department of Health in collaboration with Tennessee State University and University of Tennessee Health Science Center
 Tennessee Department of Health in collaboration with Tennessee State University and University of Tennessee Health Science Center 2006 Tennessee Department of Health 2006 ACKNOWLEDGEMENTS CONTRIBUTING
Tennessee Department of Health in collaboration with Tennessee State University and University of Tennessee Health Science Center 2006 Tennessee Department of Health 2006 ACKNOWLEDGEMENTS CONTRIBUTING
Medicare Payments. PHC4 Hospital Performance Report Oct 2016 through Sept 2017 Data FFY 2017 Medicare Payments 1
 The following table includes information about payments made by for the 16 medical conditions/surgical procedures included in this Hospital Performance Report. This analysis is based on data from federal
The following table includes information about payments made by for the 16 medical conditions/surgical procedures included in this Hospital Performance Report. This analysis is based on data from federal
The Cost Burden of Worsening Heart Failure in the Medicare Fee For Service Population: An Actuarial Analysis
 Client Report Milliman Client Report The Cost Burden of Worsening Heart Failure in the Medicare Fee For Service Population: An Actuarial Analysis Prepared by Kathryn Fitch, RN, MEd Principal and Healthcare
Client Report Milliman Client Report The Cost Burden of Worsening Heart Failure in the Medicare Fee For Service Population: An Actuarial Analysis Prepared by Kathryn Fitch, RN, MEd Principal and Healthcare
Introduction. What atrial fibrillation (AF) is Warning signs & symptoms, and risk factors for developing AFrelated
 Got FIB? Introduction FAST, IRREGULAR heartbeats = FIB FIB is short for fibrillation fibrillation, or quivering of the top two chambers of the heart (the atria) Important that you understand: What atrial
Got FIB? Introduction FAST, IRREGULAR heartbeats = FIB FIB is short for fibrillation fibrillation, or quivering of the top two chambers of the heart (the atria) Important that you understand: What atrial
Supplementary Online Content
 Supplementary Online Content Dharmarajan K, Wang Y, Lin Z, et al. Association of changing hospital readmission rates with mortality rates after hospital discharge. JAMA. doi:10.1001/jama.2017.8444 etable
Supplementary Online Content Dharmarajan K, Wang Y, Lin Z, et al. Association of changing hospital readmission rates with mortality rates after hospital discharge. JAMA. doi:10.1001/jama.2017.8444 etable
Table S1: Diagnosis and Procedure Codes Used to Ascertain Incident Hip Fracture
 Technical Appendix Table S1: Diagnosis and Procedure Codes Used to Ascertain Incident Hip Fracture and Associated Surgical Treatment ICD 9 Code Descriptions Hip Fracture 820.XX Fracture neck of femur 821.XX
Technical Appendix Table S1: Diagnosis and Procedure Codes Used to Ascertain Incident Hip Fracture and Associated Surgical Treatment ICD 9 Code Descriptions Hip Fracture 820.XX Fracture neck of femur 821.XX
About atrial fibrillation (AFib) Atrial Fibrillation (AFib) What is AFib? What s the danger? Who gets AFib?
 Understanding AFib Atrial Fibrillation (AFib) About AFib 3 How Your Heart Works 4 Types of AFib 5 Symptoms 5 Risk Factors 5 How is AFib Diagnosed? 6 Treatment 6 What to Ask Your Doctor 7 A normal heartbeat
Understanding AFib Atrial Fibrillation (AFib) About AFib 3 How Your Heart Works 4 Types of AFib 5 Symptoms 5 Risk Factors 5 How is AFib Diagnosed? 6 Treatment 6 What to Ask Your Doctor 7 A normal heartbeat
Kansas Care Coordination Quarterly Report October 2018
 Kansas Care Coordination Quarterly Report October 2018 Background Communities across the Great Plains Quality Innovation Network (QIN) region are collaborating to improve care coordination and medication
Kansas Care Coordination Quarterly Report October 2018 Background Communities across the Great Plains Quality Innovation Network (QIN) region are collaborating to improve care coordination and medication
Heart Disorders. Cardiovascular Disorders (Part B-1) Module 5 -Chapter 8. Overview Heart Disorders Vascular Disorders
 Cardiovascular Disorders (Part B-1) Module 5 -Chapter 8 Overview Heart Disorders Vascular Disorders Susie Turner, MD 1/7/13 Heart Disorders Coronary Artery Disease Cardiac Arrhythmias Congestive Heart
Cardiovascular Disorders (Part B-1) Module 5 -Chapter 8 Overview Heart Disorders Vascular Disorders Susie Turner, MD 1/7/13 Heart Disorders Coronary Artery Disease Cardiac Arrhythmias Congestive Heart
Appendix 1: Supplementary tables [posted as supplied by author]
![Appendix 1: Supplementary tables [posted as supplied by author] Appendix 1: Supplementary tables [posted as supplied by author]](/thumbs/81/83505567.jpg) Appendix 1: Supplementary tables [posted as supplied by author] Table A. International Classification of Diseases, Ninth Revision, Clinical Modification Codes Used to Define Heart Failure, Acute Myocardial
Appendix 1: Supplementary tables [posted as supplied by author] Table A. International Classification of Diseases, Ninth Revision, Clinical Modification Codes Used to Define Heart Failure, Acute Myocardial
TENNCARE Bundled Payment Initiative: Description of Bundle Risk Adjustment for Wave 4 Episodes
 TENNCARE Bundled Payment Initiative: Description of Bundle Risk Adjustment for Wave 4 Episodes Attention deficit hyperactivity disorder (ADHD); Opposition defiance disorder (ODD); Coronary artery bypass
TENNCARE Bundled Payment Initiative: Description of Bundle Risk Adjustment for Wave 4 Episodes Attention deficit hyperactivity disorder (ADHD); Opposition defiance disorder (ODD); Coronary artery bypass
Chapter 6: Healthcare Expenditures for Persons with CKD
 Chapter 6: Healthcare Expenditures for Persons with CKD In this 2017 Annual Data Report (ADR), we introduce information from the Optum Clinformatics DataMart for persons with Medicare Advantage and commercial
Chapter 6: Healthcare Expenditures for Persons with CKD In this 2017 Annual Data Report (ADR), we introduce information from the Optum Clinformatics DataMart for persons with Medicare Advantage and commercial
Atrial Fibrillation. Why It s Important. Updated on 2007 / 11 / 23. Microlife Corp ww.microlife.com. Page 1
 Atrial Fibrillation Why It s Important Microlife Corp ww.microlife.com Updated on 2007 / 11 / 23 Page 1 CONTENT ORIGINAL PRESENTATION P3 ~ P13 UPDATED ASH ABSTRACT SUBMISSION INFORMATION INTERESTING LINK
Atrial Fibrillation Why It s Important Microlife Corp ww.microlife.com Updated on 2007 / 11 / 23 Page 1 CONTENT ORIGINAL PRESENTATION P3 ~ P13 UPDATED ASH ABSTRACT SUBMISSION INFORMATION INTERESTING LINK
Common Codes for ICD-10
 Common Codes for ICD-10 Specialty: Cardiology *Always utilize more specific codes first. ABNORMALITIES OF HEART RHYTHM ICD-9-CM Codes: 427.81, 427.89, 785.0, 785.1, 785.3 R00.0 Tachycardia, unspecified
Common Codes for ICD-10 Specialty: Cardiology *Always utilize more specific codes first. ABNORMALITIES OF HEART RHYTHM ICD-9-CM Codes: 427.81, 427.89, 785.0, 785.1, 785.3 R00.0 Tachycardia, unspecified
Policy Brief June 2014
 Policy Brief June 2014 Which Medicare Patients Are Transferred from Rural Emergency Departments? Michelle Casey MS, Jeffrey McCullough PhD, and Robert Kreiger PhD Key Findings Among Medicare beneficiaries
Policy Brief June 2014 Which Medicare Patients Are Transferred from Rural Emergency Departments? Michelle Casey MS, Jeffrey McCullough PhD, and Robert Kreiger PhD Key Findings Among Medicare beneficiaries
Jacqueline C. Barrientos, Nicole Meyer, Xue Song, Kanti R. Rai ASH Annual Meeting Abstracts 2015:3301
 Characterization of atrial fibrillation and bleeding risk factors in patients with CLL: A population-based retrospective cohort study of administrative medical claims data in the U.S. Jacqueline C. Barrientos,
Characterization of atrial fibrillation and bleeding risk factors in patients with CLL: A population-based retrospective cohort study of administrative medical claims data in the U.S. Jacqueline C. Barrientos,
Heart Attack Readmissions in Virginia
 Heart Attack Readmissions in Virginia Schroeder Center Statistical Brief Research by Mitchell Cole, William & Mary Public Policy, MPP Class of 2017 Highlights: In 2014, almost 11.2 percent of patients
Heart Attack Readmissions in Virginia Schroeder Center Statistical Brief Research by Mitchell Cole, William & Mary Public Policy, MPP Class of 2017 Highlights: In 2014, almost 11.2 percent of patients
Diseases. Cardiovascular System
 Diseases Cardiovascular System Angina Pectoris A condition marked by severe pain in the chest, often spreading to the shoulder or neck. Caused by inadequate blood supply to the heart. Cardiomyopathy Refers
Diseases Cardiovascular System Angina Pectoris A condition marked by severe pain in the chest, often spreading to the shoulder or neck. Caused by inadequate blood supply to the heart. Cardiomyopathy Refers
Real-World Insights from GARFIELD-AF Registry Presented at ESC Congress 2017
 Real-World Insights from GARFIELD-AF Registry Presented at ESC Congress 2017 One of the aims of GARFIELD-AF is to assist physicians in their understanding of the risk of stroke in patients with atrial
Real-World Insights from GARFIELD-AF Registry Presented at ESC Congress 2017 One of the aims of GARFIELD-AF is to assist physicians in their understanding of the risk of stroke in patients with atrial
Process Measure: Screening for Adult Obstructive Sleep Apnea
 Process Measure: Screening for Adult Obstructive Sleep Apnea Measure Description Description Type of Measure All patients aged 18 years and older at high risk for obstructive sleep apnea (OSA) with documentation
Process Measure: Screening for Adult Obstructive Sleep Apnea Measure Description Description Type of Measure All patients aged 18 years and older at high risk for obstructive sleep apnea (OSA) with documentation
Appendix Identification of Study Cohorts
 Appendix Identification of Study Cohorts Because the models were run with the 2010 SAS Packs from Centers for Medicare and Medicaid Services (CMS)/Yale, the eligibility criteria described in "2010 Measures
Appendix Identification of Study Cohorts Because the models were run with the 2010 SAS Packs from Centers for Medicare and Medicaid Services (CMS)/Yale, the eligibility criteria described in "2010 Measures
Comorbidity or medical history Existing diagnoses between 1 January 2007 and 31 December 2011 AF management care AF symptoms Tachycardia
 Supplementary Table S1 International Classification of Disease 10 (ICD-10) codes Comorbidity or medical history Existing diagnoses between 1 January 2007 and 31 December 2011 AF management care I48 AF
Supplementary Table S1 International Classification of Disease 10 (ICD-10) codes Comorbidity or medical history Existing diagnoses between 1 January 2007 and 31 December 2011 AF management care I48 AF
Atrial Fibrillation & Arrhythmias
 Atrial Fibrillation & Arrhythmias Symptoms and Treatments FloridaHospital.com Atrial Fibrillation According to the American Heart Association, Atrial fibrillation (AF) affects an estimated 2.7 million
Atrial Fibrillation & Arrhythmias Symptoms and Treatments FloridaHospital.com Atrial Fibrillation According to the American Heart Association, Atrial fibrillation (AF) affects an estimated 2.7 million
Medicare Severity-adjusted Diagnosis Related Groups (MS-DRGs) Coding Adjustment
 American Hospital association December 2012 TrendWatch Are Medicare Patients Getting Sicker? Today, Medicare covers more than 48 million people, and that number is growing rapidly baby boomers are reaching
American Hospital association December 2012 TrendWatch Are Medicare Patients Getting Sicker? Today, Medicare covers more than 48 million people, and that number is growing rapidly baby boomers are reaching
Bundle Payments. Healthcare Systems & Services Presenters: Larry Litman, Tyler Litman
 Bundle Payments Healthcare Systems & Services Presenters: Larry Litman, Tyler Litman To determine the average cost of the SNF portion of a bundle through the analysis of our client data-base. Our Objective:
Bundle Payments Healthcare Systems & Services Presenters: Larry Litman, Tyler Litman To determine the average cost of the SNF portion of a bundle through the analysis of our client data-base. Our Objective:
BPCI Advanced Episode Selection
 BPCI Advanced Episode Selection Analytic Framework and Strategies from Northwestern Medicine Presented June 7, 2018 to: Insert relevant presenter information Calibri 16pt Presented Jessica Walradt on:
BPCI Advanced Episode Selection Analytic Framework and Strategies from Northwestern Medicine Presented June 7, 2018 to: Insert relevant presenter information Calibri 16pt Presented Jessica Walradt on:
TENNCARE Bundled Payment Initiative: Description of Bundle Risk Adjustment for Wave 2 Episodes
 TENNCARE Bundled Payment Initiative: Description of Bundle Risk Adjustment for Wave 2 Episodes Acute COPD exacerbation (COPD); Screening and surveillance colonoscopy (COL); and Outpatient and non-acute
TENNCARE Bundled Payment Initiative: Description of Bundle Risk Adjustment for Wave 2 Episodes Acute COPD exacerbation (COPD); Screening and surveillance colonoscopy (COL); and Outpatient and non-acute
X-Plain Atrial Fibrillation Reference Summary
 X-Plain Atrial Fibrillation Reference Summary Introduction Atrial fibrillation is a common heart condition that affects approximately 2.5 million Americans every year. Atrial fibrillation requires immediate
X-Plain Atrial Fibrillation Reference Summary Introduction Atrial fibrillation is a common heart condition that affects approximately 2.5 million Americans every year. Atrial fibrillation requires immediate
Cardiovascular Diseases and Diabetes
 Cardiovascular Diseases and Diabetes LEARNING OBJECTIVES Ø Identify the components of the cardiovascular system and the various types of cardiovascular disease Ø Discuss ways of promoting cardiovascular
Cardiovascular Diseases and Diabetes LEARNING OBJECTIVES Ø Identify the components of the cardiovascular system and the various types of cardiovascular disease Ø Discuss ways of promoting cardiovascular
Comparison of Medicare Fee-for-Service Beneficiaries Treated in Ambulatory Surgical Centers and Hospital Outpatient Departments
 Comparison of Medicare Fee-for-Service Beneficiaries Treated in Ambulatory Surgical Centers and Hospital Outpatient Departments Prepared for: American Hospital Association April 4, 2019 Berna Demiralp,
Comparison of Medicare Fee-for-Service Beneficiaries Treated in Ambulatory Surgical Centers and Hospital Outpatient Departments Prepared for: American Hospital Association April 4, 2019 Berna Demiralp,
Cardiovascular Disease
 Cardiovascular Disease Session Guidelines This is a 15 minute webinar session for CNC physicians and staff CNC holds webinars on the 3 rd Wednesday of each month to address topics related to risk adjustment
Cardiovascular Disease Session Guidelines This is a 15 minute webinar session for CNC physicians and staff CNC holds webinars on the 3 rd Wednesday of each month to address topics related to risk adjustment
Technical Appendix for Outcome Measures
 Study Overview Technical Appendix for Outcome Measures This is a report on data used, and analyses done, by MPA Healthcare Solutions (MPA, formerly Michael Pine and Associates) for Consumers CHECKBOOK/Center
Study Overview Technical Appendix for Outcome Measures This is a report on data used, and analyses done, by MPA Healthcare Solutions (MPA, formerly Michael Pine and Associates) for Consumers CHECKBOOK/Center
Atrial Fibrillation. Damage to your heart caused by a heart attack or rheumatic heart disease
 Atrial Fibrillation GENERAL INFORMATION: What is atrial fibrillation? Atrial fibrillation is a condition that causes the atria (top chambers of the heart) to shake or quiver. Normally, there is 1 contraction
Atrial Fibrillation GENERAL INFORMATION: What is atrial fibrillation? Atrial fibrillation is a condition that causes the atria (top chambers of the heart) to shake or quiver. Normally, there is 1 contraction
Efficiency Methodology
 Efficiency Methodology David C. Schutt, MD Bob Kelley Thomson Healthcare October 2007 Overview Definition Clinical Grouping Methods Implementation Considerations Reporting to Physician Organizations Example
Efficiency Methodology David C. Schutt, MD Bob Kelley Thomson Healthcare October 2007 Overview Definition Clinical Grouping Methods Implementation Considerations Reporting to Physician Organizations Example
Supplementary Online Content
 Supplementary Online Content Steinhubl SR, Waalen J, Edwards AM, et al. Effect of a home-based wearable continuous electrocardiographic monitoring patch on detection of undiagnosed atrial fibrillation
Supplementary Online Content Steinhubl SR, Waalen J, Edwards AM, et al. Effect of a home-based wearable continuous electrocardiographic monitoring patch on detection of undiagnosed atrial fibrillation
TENNCARE Bundled Payment Initiative: Description of Bundle Risk Adjustment for Wave 8 Episodes
 TENNCARE Bundled Payment Initiative: Description of Bundle Risk Adjustment for Wave 8 Episodes Acute Seizure, Syncope, Acute Gastroenteritis, Pediatric Pneumonia, Bronchiolitis, Colposcopy, Hysterectomy,
TENNCARE Bundled Payment Initiative: Description of Bundle Risk Adjustment for Wave 8 Episodes Acute Seizure, Syncope, Acute Gastroenteritis, Pediatric Pneumonia, Bronchiolitis, Colposcopy, Hysterectomy,
10/8/2018. Lecture 9. Cardiovascular Health. Lecture Heart 2. Cardiovascular Health 3. Stroke 4. Contributing Factor
 Lecture 9 Cardiovascular Health 1 Lecture 9 1. Heart 2. Cardiovascular Health 3. Stroke 4. Contributing Factor 1 The Heart Muscular Pump The Heart Receives blood low pressure then increases the pressure
Lecture 9 Cardiovascular Health 1 Lecture 9 1. Heart 2. Cardiovascular Health 3. Stroke 4. Contributing Factor 1 The Heart Muscular Pump The Heart Receives blood low pressure then increases the pressure
Medicare Patient Transfers from Rural Emergency Departments
 Medicare Patient Transfers from Rural Emergency Departments Michelle Casey, MS Jeffrey McCullough, PhD Supported by the Office of Rural Health Policy, Health Resources and Services Administration, PHS
Medicare Patient Transfers from Rural Emergency Departments Michelle Casey, MS Jeffrey McCullough, PhD Supported by the Office of Rural Health Policy, Health Resources and Services Administration, PHS
USRDS UNITED STATES RENAL DATA SYSTEM
 USRDS UNITED STATES RENAL DATA SYSTEM Chapter 9: Cardiovascular Disease in Patients With ESRD Cardiovascular disease is common in ESRD patients, with atherosclerotic heart disease and congestive heart
USRDS UNITED STATES RENAL DATA SYSTEM Chapter 9: Cardiovascular Disease in Patients With ESRD Cardiovascular disease is common in ESRD patients, with atherosclerotic heart disease and congestive heart
PHPG. Utilization and Expenditure Analysis for Dually Eligible SoonerCare Members with Chronic Conditions
 PHPG The Pacific Health Policy Group Utilization and Expenditure Analysis for Dually Eligible SoonerCare Members with Chronic Conditions Prepared for: State of Oklahoma Oklahoma Health Care Authority April
PHPG The Pacific Health Policy Group Utilization and Expenditure Analysis for Dually Eligible SoonerCare Members with Chronic Conditions Prepared for: State of Oklahoma Oklahoma Health Care Authority April
Management strategies for atrial fibrillation Thursday, 20 October :27
 ALTHOUGH anyone who has had to run up a flight of steps or has had a frightening experience is quite familiar with a racing heartbeat, for the more than 2 million Americans who suffer from atrial fibrillation
ALTHOUGH anyone who has had to run up a flight of steps or has had a frightening experience is quite familiar with a racing heartbeat, for the more than 2 million Americans who suffer from atrial fibrillation
Hu J, Gonsahn MD, Nerenz DR. Socioeconomic status and readmissions: evidence from an urban teaching hospital. Health Aff (Millwood). 2014;33(5).
 Appendix Definitions of Index Admission and Readmission Definitions of index admission and readmission follow CMS hospital-wide all-cause unplanned readmission (HWR) measure as far as data are available.
Appendix Definitions of Index Admission and Readmission Definitions of index admission and readmission follow CMS hospital-wide all-cause unplanned readmission (HWR) measure as far as data are available.
Lecture 8 Cardiovascular Health Lecture 8 1. Introduction 2. Cardiovascular Health 3. Stroke 4. Contributing Factors
 Lecture 8 Cardiovascular Health 1 Lecture 8 1. Introduction 2. Cardiovascular Health 3. Stroke 4. Contributing Factors 1 Human Health: What s Killing Us? Health in America Health is the U.S Average life
Lecture 8 Cardiovascular Health 1 Lecture 8 1. Introduction 2. Cardiovascular Health 3. Stroke 4. Contributing Factors 1 Human Health: What s Killing Us? Health in America Health is the U.S Average life
2018 Diagnosis Coding Fact Sheet
 The information contained in this document is provided for informational purposes only and represents no statement, promise, or guarantee by Cordis Corporation concerning levels of reimbursement, payment,
The information contained in this document is provided for informational purposes only and represents no statement, promise, or guarantee by Cordis Corporation concerning levels of reimbursement, payment,
Chapter 14 Cardiovascular Emergencies Cardiovascular Emergencies Cardiovascular disease has been leading killer of Americans since.
 1 2 3 4 5 Chapter 14 Cardiovascular Emergencies Cardiovascular Emergencies Cardiovascular disease has been leading killer of Americans since. Accounts for 1 of every 2.8 deaths Cardiovascular disease (CVD)
1 2 3 4 5 Chapter 14 Cardiovascular Emergencies Cardiovascular Emergencies Cardiovascular disease has been leading killer of Americans since. Accounts for 1 of every 2.8 deaths Cardiovascular disease (CVD)
Arrhythmias. Pulmonary Artery
 Arrhythmias Introduction Cardiac arrhythmia is an irregularity of the heart beat that causes the heart to beat too slowly, too fast, or irregularly. There are different types of arrhythmias. Most arrhythmias
Arrhythmias Introduction Cardiac arrhythmia is an irregularity of the heart beat that causes the heart to beat too slowly, too fast, or irregularly. There are different types of arrhythmias. Most arrhythmias
FY2014 Final Hospital Inpatient Rule Summary
 FY2014 Final Hospital Inpatient Rule Summary Reimbursement Update Cardiac Rhythm Management (CRM) Electrophysiology (EP) Interventional Cardiology (IC) Peripheral Intervention (PI) On August 2, 2013, the
FY2014 Final Hospital Inpatient Rule Summary Reimbursement Update Cardiac Rhythm Management (CRM) Electrophysiology (EP) Interventional Cardiology (IC) Peripheral Intervention (PI) On August 2, 2013, the
APPENDIX EXHIBITS. Appendix Exhibit A2: Patient Comorbidity Codes Used To Risk- Standardize Hospital Mortality and Readmission Rates page 10
 Ross JS, Bernheim SM, Lin Z, Drye EE, Chen J, Normand ST, et al. Based on key measures, care quality for Medicare enrollees at safety-net and non-safety-net hospitals was almost equal. Health Aff (Millwood).
Ross JS, Bernheim SM, Lin Z, Drye EE, Chen J, Normand ST, et al. Based on key measures, care quality for Medicare enrollees at safety-net and non-safety-net hospitals was almost equal. Health Aff (Millwood).
Chapter 2: Identification and Care of Patients With CKD
 Chapter 2: Identification and Care of Patients With CKD Over half of patients in the Medicare 5% sample (aged 65 and older) had at least one of three diagnosed chronic conditions chronic kidney disease
Chapter 2: Identification and Care of Patients With CKD Over half of patients in the Medicare 5% sample (aged 65 and older) had at least one of three diagnosed chronic conditions chronic kidney disease
Cost-Motivated Treatment Changes in Commercial Claims:
 Cost-Motivated Treatment Changes in Commercial Claims: Implications for Non- Medical Switching August 2017 THE MORAN COMPANY 1 Cost-Motivated Treatment Changes in Commercial Claims: Implications for Non-Medical
Cost-Motivated Treatment Changes in Commercial Claims: Implications for Non- Medical Switching August 2017 THE MORAN COMPANY 1 Cost-Motivated Treatment Changes in Commercial Claims: Implications for Non-Medical
Chapter 2: Identification and Care of Patients With Chronic Kidney Disease
 Chapter 2: Identification and Care of Patients With Chronic Kidney Disease Introduction The examination of care in patients with chronic kidney disease (CKD) is a significant challenge, as most large datasets
Chapter 2: Identification and Care of Patients With Chronic Kidney Disease Introduction The examination of care in patients with chronic kidney disease (CKD) is a significant challenge, as most large datasets
Kadlec Regional Medical Center Cardiac Electrophysiology
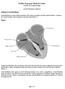 Definition of atrial fibrillation Kadlec Regional Medical Center Cardiac Electrophysiology Atrial Fibrillation Ablation Atrial fibrillation is a heart rhythm disturbance that causes an irregular (and often
Definition of atrial fibrillation Kadlec Regional Medical Center Cardiac Electrophysiology Atrial Fibrillation Ablation Atrial fibrillation is a heart rhythm disturbance that causes an irregular (and often
National Medicare RAC Summit March 5, 2009 Provider Lessons From Demonstration States
 National Medicare RAC Summit March 5, 2009 Provider Lessons From Demonstration States Lynn H. Grieves Chief Compliance Officer MemorialCare Medical Centers lgrieves@memorialcare.org MemorialCare Health
National Medicare RAC Summit March 5, 2009 Provider Lessons From Demonstration States Lynn H. Grieves Chief Compliance Officer MemorialCare Medical Centers lgrieves@memorialcare.org MemorialCare Health
Listen to Your Heart. What Everyone Needs To Know About Atrial Fibrillation & Stroke. The S-ICD System. The protection you need
 Listen to Your Heart The S-ICD System What Everyone Needs To Know About Atrial Fibrillation & Stroke The protection you need without Stroke. touching Are you your at heart risk? Increase your knowledge.
Listen to Your Heart The S-ICD System What Everyone Needs To Know About Atrial Fibrillation & Stroke The protection you need without Stroke. touching Are you your at heart risk? Increase your knowledge.
USRDS UNITED STATES RENAL DATA SYSTEM
 USRDS UNITED STATES RENAL DATA SYSTEM Chapter 2: Identification and Care of Patients With CKD Over half of patients from the Medicare 5 percent sample have either a diagnosis of chronic kidney disease
USRDS UNITED STATES RENAL DATA SYSTEM Chapter 2: Identification and Care of Patients With CKD Over half of patients from the Medicare 5 percent sample have either a diagnosis of chronic kidney disease
Can be felt where an artery passes near the skin surface and over a
 1 Chapter 14 Cardiovascular Emergencies 2 Cardiovascular Emergencies Cardiovascular disease has been leading killer of Americans since. Accounts for 1 of every 2.8 deaths Cardiovascular disease (CVD) claimed
1 Chapter 14 Cardiovascular Emergencies 2 Cardiovascular Emergencies Cardiovascular disease has been leading killer of Americans since. Accounts for 1 of every 2.8 deaths Cardiovascular disease (CVD) claimed
Atrial Fibrillation: What Should You Know? I (888)
 Atrial Fibrillation: What Should You Know? I was exhausted doing simple tasks because of my AFib. I couldn t walk from the store to my car in the parking lot. Then, I had a MAZE procedure. It was a very
Atrial Fibrillation: What Should You Know? I was exhausted doing simple tasks because of my AFib. I couldn t walk from the store to my car in the parking lot. Then, I had a MAZE procedure. It was a very
Statewide Statistics and Key Findings 1
 % s, 30 Days PHC4 s for Same Condition Jan 03 through Aug 04 Data Statewide information about readmissions and the key findings of this report are presented in this section. The study examines hospitalizations
% s, 30 Days PHC4 s for Same Condition Jan 03 through Aug 04 Data Statewide information about readmissions and the key findings of this report are presented in this section. The study examines hospitalizations
Patient Resources: Arrhythmias and Congenital Heart Disease
 Patient Resources: Arrhythmias and Congenital Heart Disease Overview Arrhythmias (abnormal heart rhythms) can develop in patients with congenital heart disease (CHD) due to thickening/weakening of their
Patient Resources: Arrhythmias and Congenital Heart Disease Overview Arrhythmias (abnormal heart rhythms) can develop in patients with congenital heart disease (CHD) due to thickening/weakening of their
Clinical Policy: Holter Monitors Reference Number: CP.MP.113
 Clinical Policy: Reference Number: CP.MP.113 Effective Date: 05/18 Last Review Date: 04/18 Coding Implications Revision Log Description Ambulatory electrocardiogram (ECG) monitoring provides a view of
Clinical Policy: Reference Number: CP.MP.113 Effective Date: 05/18 Last Review Date: 04/18 Coding Implications Revision Log Description Ambulatory electrocardiogram (ECG) monitoring provides a view of
HEART DISEASE HEART CONDITIONS, RISKS AND PROTECTION
 Spotlight on Health 2017 HEART DISEASE HEART CONDITIONS, RISKS AND PROTECTION Heart disease is the leading cause of death for both men and women worldwide, accounting for over 17 million deaths per year.
Spotlight on Health 2017 HEART DISEASE HEART CONDITIONS, RISKS AND PROTECTION Heart disease is the leading cause of death for both men and women worldwide, accounting for over 17 million deaths per year.
Cardiovascular Disease
 Cardiovascular Disease Chapter 15 Introduction Cardiovascular disease (CVD) is the leading cause of death in the U.S. One American dies from CVD every 33 seconds Nearly half of all Americans will die from
Cardiovascular Disease Chapter 15 Introduction Cardiovascular disease (CVD) is the leading cause of death in the U.S. One American dies from CVD every 33 seconds Nearly half of all Americans will die from
ATRIAL FIBRILLATION ANSWERS. A Patient Education Handbook on Electrophysiology
 ATRIAL FIBRILLATION ANSWERS A Patient Education Handbook on Electrophysiology MY LIFE HAS TAKEN A TURN FOR THE BETTER. -Emie Bishop ARRHYTHMIAANSWERS.COM AF ANSWERS. A PATIENT EDUCATION HANDBOOK ON ELECTROPHYSIOLOGY
ATRIAL FIBRILLATION ANSWERS A Patient Education Handbook on Electrophysiology MY LIFE HAS TAKEN A TURN FOR THE BETTER. -Emie Bishop ARRHYTHMIAANSWERS.COM AF ANSWERS. A PATIENT EDUCATION HANDBOOK ON ELECTROPHYSIOLOGY
Supplementary Online Content
 Supplementary Online Content Khera R, Dharmarajan K, Wang Y, et al. Association of the hospital readmissions reduction program with mortality during and after hospitalization for acute myocardial infarction,
Supplementary Online Content Khera R, Dharmarajan K, Wang Y, et al. Association of the hospital readmissions reduction program with mortality during and after hospitalization for acute myocardial infarction,
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition
 Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
Supplementary Online Content
 Supplementary Online Content Inohara T, Xian Y, Liang L, et al. Association of intracerebral hemorrhage among patients taking non vitamin K antagonist vs vitamin K antagonist oral anticoagulants with in-hospital
Supplementary Online Content Inohara T, Xian Y, Liang L, et al. Association of intracerebral hemorrhage among patients taking non vitamin K antagonist vs vitamin K antagonist oral anticoagulants with in-hospital
The Burden of Cardiovascular Disease in North Carolina. Justus-Warren Heart Disease and Stroke Prevention Task Force April 11, 2018
 The Burden of Cardiovascular Disease in North Carolina Justus-Warren Heart Disease and Stroke Prevention Task Force April 11, 2018 Purpose 1. To detail the burden of heart disease and stroke in North Carolina
The Burden of Cardiovascular Disease in North Carolina Justus-Warren Heart Disease and Stroke Prevention Task Force April 11, 2018 Purpose 1. To detail the burden of heart disease and stroke in North Carolina
Value of Hospice Benefit to Medicaid Programs
 One Pennsylvania Plaza, 38 th Floor New York, NY 10119 Tel 212-279-7166 Fax 212-629-5657 www.milliman.com Value of Hospice Benefit May 2, 2003 Milliman USA, Inc. New York, NY Kate Fitch, RN, MEd, MA Bruce
One Pennsylvania Plaza, 38 th Floor New York, NY 10119 Tel 212-279-7166 Fax 212-629-5657 www.milliman.com Value of Hospice Benefit May 2, 2003 Milliman USA, Inc. New York, NY Kate Fitch, RN, MEd, MA Bruce
Heart Disease. Signs and Symptoms
 Heart Disease The term "heart disease" refers to several types of heart conditions. The most common type is coronary artery disease, which can cause heart attack, angina, heart failure, and arrhythmias.
Heart Disease The term "heart disease" refers to several types of heart conditions. The most common type is coronary artery disease, which can cause heart attack, angina, heart failure, and arrhythmias.
A COMPREHENSIVE REPORT ISSUED BY THE AMERICAN ASSOCIATION OF CLINICAL ENDOCRINOLOGISTS IN PARTNERSHIP WITH:
 A COMPREHENSIVE REPORT ISSUED BY THE AMERICAN ASSOCIATION OF CLINICAL ENDOCRINOLOGISTS IN PARTNERSHIP WITH: Amputee Coalition of America Mended Hearts National Federation of the Blind National Kidney Foundation
A COMPREHENSIVE REPORT ISSUED BY THE AMERICAN ASSOCIATION OF CLINICAL ENDOCRINOLOGISTS IN PARTNERSHIP WITH: Amputee Coalition of America Mended Hearts National Federation of the Blind National Kidney Foundation
Fiscal Year (FY) 2019 Hospital Inpatient Proposed Rule Interventional Cardiology, Peripheral Interventions & Rhythm Management
 Fiscal Year (FY) 2019 Hospital Inpatient Proposed Rule Interventional Cardiology, Peripheral Interventions & Rhythm Management On April 24, 2018, the Centers for Medicare & Medicaid Services (CMS) released
Fiscal Year (FY) 2019 Hospital Inpatient Proposed Rule Interventional Cardiology, Peripheral Interventions & Rhythm Management On April 24, 2018, the Centers for Medicare & Medicaid Services (CMS) released
FY2015 Proposed Hospital Inpatient Rule Summary
 FY2015 Proposed Hospital Inpatient Rule Summary Cardiac Rhythm Management (CRM) Electrophysiology (EP) Interventional Cardiology (IC) Peripheral Intervention (PI) On April 30, 2014, the Centers for Medicare
FY2015 Proposed Hospital Inpatient Rule Summary Cardiac Rhythm Management (CRM) Electrophysiology (EP) Interventional Cardiology (IC) Peripheral Intervention (PI) On April 30, 2014, the Centers for Medicare
An Introduction To Atrial Fibrillation: What You Need To Know
 An Introduction To Atrial Fibrillation: What You Need To Know If you ve ever felt like your heart has a difficult time maintaining a regular rhythm, or you find yourself gasping for air while your heart
An Introduction To Atrial Fibrillation: What You Need To Know If you ve ever felt like your heart has a difficult time maintaining a regular rhythm, or you find yourself gasping for air while your heart
More than 1.8 million New York State residents have diabetes, 1
 September 1 New York State Health Foundation s DIABETES Policy Center DIABETES: A HIDDEN HEALTH CARE COST DRIVER IN NEW YORK An Analysis of Health Care Utilization and Trends of Patients with Diabetes
September 1 New York State Health Foundation s DIABETES Policy Center DIABETES: A HIDDEN HEALTH CARE COST DRIVER IN NEW YORK An Analysis of Health Care Utilization and Trends of Patients with Diabetes
The Role of Information Technology in Disease Management: A Case for Heart Failure
 The Role of Information Technology in Disease Management: A Case for Heart Failure Teresa De Peralta, MSN, APN-C Heart Failure Product Workflow Consultant Medtronic Population Management Level 3: As patient
The Role of Information Technology in Disease Management: A Case for Heart Failure Teresa De Peralta, MSN, APN-C Heart Failure Product Workflow Consultant Medtronic Population Management Level 3: As patient
THE HEART THE CIRCULATORY SYSTEM
 THE HEART THE CIRCULATORY SYSTEM There are three primary closed cycles: 1) Cardiac circulation pathway of blood within the heart 2) Pulmonary circulation blood from the heart to lungs and back 3) Systemic
THE HEART THE CIRCULATORY SYSTEM There are three primary closed cycles: 1) Cardiac circulation pathway of blood within the heart 2) Pulmonary circulation blood from the heart to lungs and back 3) Systemic
Catheter Ablation. Patient Education
 Catheter Ablation Patient Education Allina Health System Your heart has four chambers. Two upper chambers (atria) pump blood to the two lower chambers (ventricles). In order for the heart to pump, it requires
Catheter Ablation Patient Education Allina Health System Your heart has four chambers. Two upper chambers (atria) pump blood to the two lower chambers (ventricles). In order for the heart to pump, it requires
2019 COLLECTION TYPE: MIPS CLINICAL QUALITY MEASURES (CQMS) MEASURE TYPE: Process
 Quality ID #326 (NQF 1525): Atrial Fibrillation and Atrial Flutter: Chronic Anticoagulation Therapy National Quality Strategy Domain: Effective Clinical Care Meaningful Measure Area: Management of Chronic
Quality ID #326 (NQF 1525): Atrial Fibrillation and Atrial Flutter: Chronic Anticoagulation Therapy National Quality Strategy Domain: Effective Clinical Care Meaningful Measure Area: Management of Chronic
Arrhythmia 341. Ahmad Hersi Professor of Cardiology KSU
 Arrhythmia 341 Ahmad Hersi Professor of Cardiology KSU Objectives Epidemiology and Mechanisms of AF Evaluation of AF patients Classification of AF Treatment and Risk stratification of AF Identify other
Arrhythmia 341 Ahmad Hersi Professor of Cardiology KSU Objectives Epidemiology and Mechanisms of AF Evaluation of AF patients Classification of AF Treatment and Risk stratification of AF Identify other
GUIDE TO ATRIAL FIBRILLATION
 PATIENT INFORMATION GUIDE TO ATRIAL FIBRILLATION Atrial Fibrillation (AF) Atrial Flutter (AFL) Rate and Rhythm Control Stroke Prevention This document is endorsed by: A Comprehensive Resource from the
PATIENT INFORMATION GUIDE TO ATRIAL FIBRILLATION Atrial Fibrillation (AF) Atrial Flutter (AFL) Rate and Rhythm Control Stroke Prevention This document is endorsed by: A Comprehensive Resource from the
Stroke 101. Maine Cardiovascular Health Summit. Eileen Hawkins, RN, MSN, CNRN Pen Bay Stroke Program Coordinator November 7, 2013
 Stroke 101 Maine Cardiovascular Health Summit Eileen Hawkins, RN, MSN, CNRN Pen Bay Stroke Program Coordinator November 7, 2013 Stroke Statistics Definition of stroke Risk factors Warning signs Treatment
Stroke 101 Maine Cardiovascular Health Summit Eileen Hawkins, RN, MSN, CNRN Pen Bay Stroke Program Coordinator November 7, 2013 Stroke Statistics Definition of stroke Risk factors Warning signs Treatment
A SUMMARY REPORT ON NEW JERSEY HOSPITAL READMISSIONS 30 DAYS AFTER CABG SURGERY
 A SUMMARY REPORT ON NEW JERSEY HOSPITAL READMISSIONS 3 DAYS AFTER CABG SURGERY 1999-21 Health Care Quality Assessment Division of Health Care Quality & Oversight December, 24 Introduction This report presents
A SUMMARY REPORT ON NEW JERSEY HOSPITAL READMISSIONS 3 DAYS AFTER CABG SURGERY 1999-21 Health Care Quality Assessment Division of Health Care Quality & Oversight December, 24 Introduction This report presents
Diagnosis Coding is About to be Much More Important. Matthew Menendez
 Diagnosis Coding is About to be Much More Important Matthew Menendez Agenda What is CMS doing with MACRA? What is an HCC code and why should I care? Brief MIPS overview How does risk adjustment impact
Diagnosis Coding is About to be Much More Important Matthew Menendez Agenda What is CMS doing with MACRA? What is an HCC code and why should I care? Brief MIPS overview How does risk adjustment impact
Measure Information Form Collected For: CMS Outcome Measures (Claims Based)
 Last Updated: New Measure Version 4.4a Measure Information Form Collected For: CMS Outcome Measures (Claims Based) Measure Set: CMS Episode-of-Care Payment Measures Set Measure ID #: PAYM-30-HF Performance
Last Updated: New Measure Version 4.4a Measure Information Form Collected For: CMS Outcome Measures (Claims Based) Measure Set: CMS Episode-of-Care Payment Measures Set Measure ID #: PAYM-30-HF Performance
NQF-ENDORSED VOLUNTARY CONSENSUS STANDARDS FOR HOSPITAL CARE. Measure Information Form Collected For: CMS Outcome Measures (Claims Based)
 Last Updated: Version 4.3 NQF-ENDORSED VOLUNTARY CONSENSUS STANDARDS FOR HOSPITAL CARE Measure Information Form Collected For: CMS Outcome Measures (Claims Based) Measure Set: CMS Mortality Measures Set
Last Updated: Version 4.3 NQF-ENDORSED VOLUNTARY CONSENSUS STANDARDS FOR HOSPITAL CARE Measure Information Form Collected For: CMS Outcome Measures (Claims Based) Measure Set: CMS Mortality Measures Set
Chapter 8: Cardiovascular Disease in Patients with ESRD
 Chapter 8: Cardiovascular Disease in Patients with ESRD Cardiovascular disease (CVD) is common in adult end-stage renal disease (ESRD) patients, with coronary artery disease (CAD) and heart failure (HF)
Chapter 8: Cardiovascular Disease in Patients with ESRD Cardiovascular disease (CVD) is common in adult end-stage renal disease (ESRD) patients, with coronary artery disease (CAD) and heart failure (HF)
Chapter 5: Acute Kidney Injury
 Chapter 5: Acute Kidney Injury Introduction In recent years, acute kidney injury (AKI) has gained increasing recognition as a major risk factor for the development of chronic kidney disease (CKD). The
Chapter 5: Acute Kidney Injury Introduction In recent years, acute kidney injury (AKI) has gained increasing recognition as a major risk factor for the development of chronic kidney disease (CKD). The
How does the heart work? The heart is muscle whose main function is a pump; to push blood the rest of your body.
 1 You have a condition called atrial fibrillation. I would like you to learn more about this condition. You should read about it below, and can also watch an Internet program about it. After reading about
1 You have a condition called atrial fibrillation. I would like you to learn more about this condition. You should read about it below, and can also watch an Internet program about it. After reading about
Dysrhythmias 11/7/2017. Disclosures. 3 reasons to evaluate and treat dysrhythmias. None. Eliminate symptoms and improve hemodynamics
 Dysrhythmias CYDNEY STEWART MD, FACC NOVEMBER 3, 2017 Disclosures None 3 reasons to evaluate and treat dysrhythmias Eliminate symptoms and improve hemodynamics Prevent imminent death/hemodynamic compromise
Dysrhythmias CYDNEY STEWART MD, FACC NOVEMBER 3, 2017 Disclosures None 3 reasons to evaluate and treat dysrhythmias Eliminate symptoms and improve hemodynamics Prevent imminent death/hemodynamic compromise
TECHNICAL NOTES APPENDIX SUMMER
 TECHNICAL NOTES APPENDIX SUMMER Hospital Performance Report Summer Update INCLUDES PENNSYLVANIA INPATIENT HOSPITAL DISCHARGES FROM JULY 1, 2006 THROUGH JUNE 30, 2007 The Pennsylvania Health Care Cost Containment
TECHNICAL NOTES APPENDIX SUMMER Hospital Performance Report Summer Update INCLUDES PENNSYLVANIA INPATIENT HOSPITAL DISCHARGES FROM JULY 1, 2006 THROUGH JUNE 30, 2007 The Pennsylvania Health Care Cost Containment
APR DRG Data Discovery
 APR DRG Data Discovery Henry Johnson MD, MPH Midas+ Vice President and Medical Director Vanessa Dorr RN MSN Midas+ DataVision Clinical Consultant Review: Agenda 3M APR DRG Methodology DataVision: Web and
APR DRG Data Discovery Henry Johnson MD, MPH Midas+ Vice President and Medical Director Vanessa Dorr RN MSN Midas+ DataVision Clinical Consultant Review: Agenda 3M APR DRG Methodology DataVision: Web and
Pediatrics. Arrhythmias in Children: Bradycardia and Tachycardia Diagnosis and Treatment. Overview
 Pediatrics Arrhythmias in Children: Bradycardia and Tachycardia Diagnosis and Treatment See online here The most common form of cardiac arrhythmia in children is sinus tachycardia which can be caused by
Pediatrics Arrhythmias in Children: Bradycardia and Tachycardia Diagnosis and Treatment See online here The most common form of cardiac arrhythmia in children is sinus tachycardia which can be caused by
Chapter 2: Identification and Care of Patients With CKD
 Chapter 2: Identification and Care of Patients With Over half of patients from the Medicare 5% sample (restricted to age 65 and older) have a diagnosis of chronic kidney disease (), cardiovascular disease,
Chapter 2: Identification and Care of Patients With Over half of patients from the Medicare 5% sample (restricted to age 65 and older) have a diagnosis of chronic kidney disease (), cardiovascular disease,
CARDIOLOGY GRAND ROUNDS
 CARDIOLOGY GRAND ROUNDS Presentation: Date: Location: Speaker: ACC 2015 PREVIEW Monday, March 9, 2015, 7:00 8:00 AM ANW Education Building, Watson Room Elevated Troponin in Patients Presenting to the Emergency
CARDIOLOGY GRAND ROUNDS Presentation: Date: Location: Speaker: ACC 2015 PREVIEW Monday, March 9, 2015, 7:00 8:00 AM ANW Education Building, Watson Room Elevated Troponin in Patients Presenting to the Emergency
