EMBLEM TM S-ICD System Patient Handbook
|
|
|
- Russell Conley
- 6 years ago
- Views:
Transcription
1 EMBLEM TM S-ICD System Patient Handbook
2
3 A Message to Patients Boston Scientific Corporation acquired Cameron Health in June During our transition period, you may see both the Boston Scientific and Cameron Health names on product and patient materials. As we work through the transition, we will continue to offer doctors and their patients technologically advanced and high quality medical devices and therapies.
4 Your EMBLEM S-ICD System information Have your doctor or nurse complete these forms before you go home from the hospital. S-ICD Model Number: S-ICD Serial Number: Implant Date: Subcutaneous Electrode Model Number: Subcutaneous Electrode Serial Number:
5 Your medical contact information Cardiologist Name/Phone Number: Electrophysiologist Name/Phone Number: Hospital Name/Address/Phone Number: Medications (list):
6 By Mail: Boston Scientific Corporation 4100 Hamline Avenue North St. Paul, Minnesota By Telephone: Patients and families: Medical professionals: CARDIAC ( ) Worldwide: On the Internet: Medical Records: PATDATA ( ) 7 a.m. 7 p.m. (Central Time), Monday Friday medical.records@bsci.com The following are trademarks of Boston Scientific Corporation or its affiliates: EMBLEM and LATITUDE
7 Table of contents Introduction to the EMBLEM S-ICD System About this guide, 2 When is this device used?, 3 When is this device not used?, 4 How reliable is this device?, 4 Glossary...5 Understanding your heart The normal heart, 15 When the heart beats too fast, 18 Ventricular tachycardia, 19 Ventricular fibrillation, 21 Why do I need a minimally invasive S-ICD System?, 22 Am I at risk for developing a ventricular tachycardia or ventricular fibrillation?, 24 Sudden cardiac arrest Risk factors, 25 Identifying your SCA risk, 26
8 Your EMBLEM S-ICD System EMBLEM S-ICD System components, 28 Implanting your EMBLEM S-ICD System Understanding the implant procedure, 31 Discharge from the hospital, 33 Benefits and risks of having an S-ICD System, 34 After your implant Medications, 38 Activities and exercise, 39 Your S-ICD System information, 39 Your identification card, 39 Updating your identification card, 40 Living with your EMBLEM S-ICD System Patient responsibilities, 41 Preparing for S-ICD shock therapy, 41 Special considerations, 44 When to call your doctor, 44 Follow-up visits, 45 What should you do if your device starts to beep?, 48 What you should know about your device s battery, 48
9 How will you know if your device s battery is running down?, 49 Replacing your system, 50 Risks, 51 Questions you may have about living with your EMBLEM S-ICD System, 52 Important safety information Electromagnetic interference, 58 Household appliances and common tools, 59 Warnings and precautions, 62 Summary Visit us on the Internet Notes and questions Index...78
10
11 Introduction to the EMBLEM S-ICD System Your physician has recommended a Boston Scientific minimally invasive implantable defibrillator (EMBLEM S-ICD System). The EMBLEM S-ICD System is designed as a life saving measure to treat your heart rhythm abnormalities. Your physician may have prescribed this device for you for one of the following reasons: You have experienced an abnormally rapid heart rhythm (Ventricular Tachycardia or Ventricular Fibrillation) You are at risk of developing an abnormally rapid heart rhythm. These rapid heart rhythms, known as cardiac arrhythmias, may be life threatening. When a cardiac arrhythmia occurs, it interrupts the normal pumping function of the heart. This disruption of normal heart function may lead to loss of consciousness, and ultimately, be lethal. 1
12 The minimally invasive S-ICD System is a treatment for correcting an abnormally rapid heart rhythm. The S-ICD System is not a cure for the underlying cause of your cardiac arrhythmia, but rather provides defibrillation (shock) therapy to restore your heart to its normal rhythm. About this guide This patient handbook provides information on: Glossary of terms Anatomy of the heart Heart rhythm The S-ICD System Implant procedure Post operative events Note: Your physician will discuss any potential risks or adverse events that may be associated with your implanted S-ICD System. However, be sure to carefully read and understand all warnings and safety precautions discussed in this guide. 2
13 The glossary on page 5 defines many of the words you will see in the upcoming pages, as well as those you may hear from your doctors and nurses. If you have questions about what you read in this handbook, ask your doctor or nurse. They are your best resource for information. When is this device used? Your doctor has decided that you should receive a defibrillator because you have an increased risk of sudden cardiac death due to ventricular rhythm disturbances, and you do not have other types of arrhythmias that would be more appropriately treated with a pacemaker or other type of implanted device. Sudden cardiac death is a result of sudden cardiac arrest, which occurs when electrical problems in the heart cause an abrupt loss of heart function. If you have any questions about when this device is used, ask your doctor. 3
14 When is this device not used? Patients who have other implanted devices delivering unipolar pacing or using certain impedance-based features should not receive this device. If you have any questions about when this device is not used, ask your doctor. How reliable is this device? It is Boston Scientific s intent to provide implantable devices of high quality and reliability. However, these devices may exhibit malfunctions that may result in lost or compromised ability to deliver therapy. Refer to Boston Scientific s CRM Product Performance Report on www. bostonscientific.com for more information about device performance, including the types and rates of malfunctions that these devices have experienced historically. While historical data may not be predictive of future device performance, such data can provide important context for understanding the overall reliability of these types of products. Talk with your doctor about this product performance data, and the risks and benefits associated with the implantation of this system. 4
15 Glossary Antitachycardia pacing (ATP) A series of small, rapid, low-energy pacing pulses delivered to the heart to slow a rapid heartbeat to its normal rhythm. Arrhythmia An abnormal heartbeat that is too fast, too slow, or irregular. Atrium (plural: atria) One of the two upper chambers of the heart specifically, the right atrium and left atrium. The atria collect blood as it comes into the heart and pump blood into the lower chambers (ventricles). Bradycardia An abnormally slow heartbeat, typically fewer than 60 beats per minute. Cardiac arrest See sudden cardiac arrest (SCA). 5
16 Communicator See LATITUDE Communicator. Defibrillation Procedure in which a fast heart rate (i.e., ventricular fibrillation, ventricular tachycardia) is restored to a normal rhythm by delivering an electrical shock. Defibrillator A device that delivers an electrical shock to the heart to restore an extremely rapid and sometimes irregular heart rate to a normal rhythm. A defibrillator may be an implanted medical device or external medical equipment. Device See pulse generator. ECG/EKG (electrocardiogram) A graphic representation of your heart s electrical signals. The graph shows how electrical signals travel through your heart. Your doctor can tell what kind of rhythm you have by looking at the pattern of your heartbeat. 6
17 Echocardiogram A test used to measure your heart s pumping function (ejection fraction). Ejection fraction The percentage of blood ejected from the left ventricle with each heartbeat. A healthy ejection fraction is usually higher than 55%, although this can vary depending on the individual. Patients with a low ejection fraction may have an increased risk of sudden cardiac arrest. Electromagnetic field Invisible lines of force that result from electrical fields (produced by voltage) and magnetic fields (produced by current flow). Electromagnetic fields decrease in strength the farther they are from their source. Electromagnetic interference (EMI) Interference that occurs when an electromagnetic field interacts with an implanted device. See also electromagnetic field. 7
18 Electrophysiology (EP) test or study A test in which catheters (thin, flexible tubes or wires) are inserted into your heart to identify and measure the type of electrical signals in your heart. The test results can help your doctor identify the origins of your abnormal heart rhythms, determine how well medications work, and decide what treatment is best for your condition. The test can also be used to see how well your device operates during your abnormal heart rhythm. Fibrillation See ventricular fibrillation. Heart attack See myocardial infarction (MI). Heart rhythm A series of heartbeats. You may hear your doctor refer to your rhythm as being normal or irregular. A normal heart rate typically ranges from 60 to 100 beats per minute at rest. 8
19 Holter monitor An external monitor worn for an extended period that records your heart s electrical activity. Implantable Cardioverter Defibrillator (ICD) system An ICD system is implanted to monitor your heart rhythm and help treat dangerously fast arrhythmias. There are two types of ICD systems: Transvenous ICD systems include a pulse generator and leads. The leads are inserted into your blood vessels and directly contact the heart tissue. Subcutaneous ICD systems include a pulse generator and a subcutaneous electrode. The subcutaneous electrode is inserted just under the skin of your chest and does not directly contact the heart tissue. Interrogation The process whereby a computerized device (programmer or LATITUDE Communicator) uses telemetry communication signals to gather identification and status information from your device. Your doctor 9
20 uses this information to evaluate how your device is performing and check for any arrhythmia episodes you may have had. LATITUDE Communicator An in-home monitoring system that communicates with your device. The Communicator can gather and send device data to the LATITUDE Patient Management System, which your physician can then view via the Internet. Your device may or may not be configured to use the LATITUDE Patient Management System. See also LATITUDE Patient Management System. LATITUDE Patient Management System A remote monitoring system that collects important data from your device. This patient information can be viewed via the Internet, only by members of your health care support team. Your device may or may not be configured to use the LATITUDE Patient Management System. See also LATITUDE Communicator. Myocardial infarction (MI) Also called a heart attack. A myocardial infarction occurs when an artery that supplies blood to the heart becomes blocked. As a result, blood does not reach 10
21 some parts of the heart, and some of the heart tissue dies. Symptoms of a myocardial infarction may include shortness of breath, nausea, fatigue, and/or pain in the chest, arm, or neck. Programmer Microcomputer-based equipment that is used to communicate with the device. The programmer is used during testing and follow-up exams to gather and display information from the device. The doctor or technician also uses the programmer to adjust the device so that it senses and treats your arrhythmias. Pulse generator Also called a device. The pulse generator is the part of the S-ICD system that contains the electronics and the battery. Radio frequency (RF) wireless communication Technology that allows the device to exchange information with a programmer or LATITUDE Communicator by communicating over radio signals. 11
22 Sinoatrial (SA) node The heart s natural pacemaker. The SA node is a small group of specialized cells in the upper right chamber of the heart (right atrium) that normally generates an electrical signal. This signal runs through the heart and causes the heart to beat. Sternum (Breast bone) Bone located in the center of the chest which connects the ribs. Subcutaneous Just beneath the skin Subcutaneous electrode An insulated wire that is implanted under the skin and connected to the device. The subcutaneous electrode senses your heartbeat and delivers pacing pulses and/ or shocks from the device to the heart. Sudden cardiac arrest (SCA) The sudden, abrupt loss of heart function (i.e., cardiac arrest) due to electrical problems in the heart. If 12
23 untreated, SCA can lead to death (also called sudden cardiac death). Sudden cardiac death (SCD) Death occurring from sudden cardiac arrest. See also sudden cardiac arrest (SCA). Supraventricular tachycardia (SVT) A fast heart rhythm caused by signals coming from a specific area above the ventricles, usually in the atria. A heart with SVT may beat over 150 beats per minute, which may produce palpitations and fluttering in the chest. Telemetry communication Technology that allows a device to exchange information with a programmer or LATITUDE Communicator by using radio frequency (RF) telemetry communication. Ventricle One of two lower chambers of the heart. The right ventricle pumps blood to the lungs, and the left ventricle pumps oxygen-carrying blood from the lungs to the rest of the body. 13
24 Ventricular fibrillation (VF) A very fast, irregular heart rhythm caused by abnormal electrical signals starting from several areas of the ventricle. In VF, the ventricle beats so fast that it pumps very little blood to the body. A heart in VF may beat more than 300 beats per minute. Without immediate medical attention, VF can be fatal. Defibrillation is the only way to treat VF once it occurs. Ventricular tachycardia (VT) A fast rhythm caused by abnormal electrical signals coming from the ventricle. The rapid rate of 120 to 250 beats per minute may produce dizziness, weakness, and eventual unconsciousness. VT may progress to ventricular fibrillation. Wireless communication Technology that allows a device to exchange information with a programmer wirelessly. See also radio frequency (RF) wireless communication. 14
25 Understanding your heart This section will discuss the basic function of the normal heart and will also explain what happens when the heart develops abnormally rapid heart rhythms. The normal heart The heart is divided into four chambers: two upper chambers called the atria and two lower chambers called the ventricles. The four chambers fill with blood when the heart is at rest and then pump the blood throughout the body with each heart contraction (Figure 1). 15
26 Blood flow to atria Blood flow through ventricles Figure 1. The heart and its blood flow. The heart has a specialized conduction system that produces electrical impulses that stimulate the heart to contract (Figure 2). Normally, your heart s pumping action is controlled by steady electrical signals that are produced by your heart s natural pacemaker, the sinoatrial (SA) node. Electrical signals from the SA node travel through 16
27 the atria and follow an electrical pathway to the ventricle. This creates an electrical stimulation that causes the heart muscle to contract. The heart then rests and fills with blood until the next contraction occurs. This cycle occurs millions of times in a year. SA node Atria Electrical current Ventricles Figure 2. The heart and its electrical pathways. 17
28 Normal resting heart rates are usually in the range of 60 to 100 beats per minute. However, your heart rate may increase or decrease outside this range depending on activity levels. Generally, the heart rate will increase during exercise and decrease during sleep. When the heart beats too fast An abnormal condition exists when your heart rate increases significantly in the absence of exercise or emotional stress. This is known as a tachycardia. Not all tachycardias cause serious problems. Some tachycardias may cause discomfort, but are not life threatening; whereas other tachycardias may be very serious and life threatening. Tachycardias are also associated with injury to the heart muscle, which can occur with coronary artery disease. Coronary artery disease may cause a myocardial infarction (commonly referred to as a heart attack), which may damage the heart muscle. Tachycardias may also result from other diseases or certain genetic defects that weaken the heart muscle. 18
29 If this rapid heartbeat continues, you may feel skipped beats or dizziness. You could eventually become unconscious, and your heart might stop beating (cardiac arrest). Ventricular tachycardia One type of arrhythmia you may experience is ventricular tachycardia (VT). With this type of arrhythmia, your heart s electrical signals may come from one of the ventricles instead of the SA node (Figure 3). The electrical signal does not pass through the heart normally and causes a fast, sometimes irregular heartbeat. As your heart beats faster, it pumps less blood to your body. If this rapid heartbeat continues, you may feel skipped beats or dizziness. You could eventually become unconscious, and your heart might stop beating (cardiac arrest). 19
30 Abnormal electrical signals from the ventricle Figure 3. An example of ventricular tachycardia. VT can sometimes be treated with medication. In other cases, an external defibrillator such as those used by paramedics or an ICD may be used to stop the abnormal signals and return your heart to a more normal rhythm. 20
31 Ventricular fibrillation Another type of arrhythmia is ventricular fibrillation (VF). With this arrhythmia, irregular electrical signals come from several spots in the ventricles (Figure 4). This causes a rapid heart rate. In some cases, the heart will beat more than 300 beats per minute. Abnormal electrical signals from the ventricles Figure 4. An example of ventricular fibrillation. 21
32 When you experience VF, very little blood is pumped from your heart to the rest of your body. When your heart is in VF, you will become unconscious very quickly. Like ventricular tachycardia, VF can be treated with a defibrillator. The defibrillator produces an electrical shock that passes through the heart. The shock stops the abnormal signals and allows the SA node to return the heart to a more normal rhythm. If an episode of VT or VF continues without medical treatment, your heart cannot supply enough oxygencarrying blood to your brain and body tissues. Without oxygen, your brain and body tissues cannot function normally, which could be fatal. Why do I need a minimally invasive S-ICD System? Your physician has recommended implantation of a minimally invasive S-ICD System because you are at risk 22
33 for VT or VF. Some heart disorders that are associated with risks of developing VT or VF are listed below: Heart Attack: Occurs when there is a complete or sudden loss of oxygen-rich blood flow to the heart muscle due to a blocked or narrowed coronary artery. Due to the lack of an oxygen-rich blood supply, a portion of the heart muscle is injured. Heart Failure: A condition in which the heart cannot pump enough blood to the body or other organs. Cardiomyopathy: A disease process that causes the heart to become abnormally large, thickened or stiffened. As a result, the heart muscle weakens, decreasing the heart s ability to pump blood efficiently to the body. Primary Rhythm Disorder: An abnormality within the conduction system in the heart. 23
34 Am I at risk for developing a ventricular tachycardia or ventricular fibrillation? When a portion of the heart muscle is injured or the heart is abnormally enlarged, the heart is not able to pump blood efficiently to the body. Measurements may be made to assess the condition of your heart. One such measurement is known as ejection fraction (EF). EF measures how much blood is pumped out to the body with each heart beat, or contraction. Medical studies have determined that patients who have a low EF measurement are particularly at risk for developing ventricular tachycardias or ventricular fibrillation. 24
35 Sudden cardiac arrest A cardiac arrhythmia such as ventricular fibrillation may lead to sudden cardiac arrest. The result of sudden cardiac arrest is that the heart fails to pump blood to the body. Because the heart does not pump enough blood throughout the body, most people tend to lose consciousness suddenly. If SCA is not treated, it can lead to sudden cardiac death (SCD). The only way to stop ventricular fibrillation is to deliver an electrical shock with a defibrillator. Risk factors Most people do not have obvious symptoms of SCA, so it is important to be aware of possible risk factors: Previous heart attack Impaired pumping function of the heart muscle Rapid, abnormal heart rhythms coming from the ventricles A family history of SCA or SCD 25
36 Early identification of your SCA risk is the key to prevention. If you are at risk, it is important to talk to your doctor. Identifying your SCA risk Your doctor may perform one or more of the following tests to assess your risk for SCA. Echocardiogram: An echocardiogram is a test that measures your heart s ejection fraction. The ejection fraction determines your heart s pumping function. During this test, ultrasound waves are used to provide a moving image of your heart. Based upon the results of this test, your doctor will determine if further testing is needed. Holter monitoring: A Holter monitor is an external monitor that is worn for an extended period. The monitor records your heart s electrical activity, including any arrhythmias you experience. Your doctor analyzes the recording to determine if you experience any abnormal rhythms. 26
37 Electrophysiology (EP) testing: An EP test identifies and measures the type of electrical signals in your heart. During this test, your doctor will insert catheters (thin, flexible tubes or wires) into your heart. The catheters record electrical signals within your heart. Your doctor can also use the catheters to stimulate your heart to see if you could develop an arrhythmia. This test can help your doctor recognize if you have an abnormal heart rhythm and identify its origins. It will also determine how well certain medications or an implanted device would work to treat your heart rhythm. Your doctor can then decide what treatment is best for your condition. 27
38 Your EMBLEM S-ICD System The implantable components of the minimally invasive EMBLEM S-ICD System are implanted beneath the surface of the skin outside the rib cage. EMBLEM S-ICD System components Pulse generator The pulse generator is a battery powered, computer controlled device encased in metal. The pulse generator is typically implanted on the left side of the chest wall. Various settings and parameters for the pulse generator are programmable through wireless communication with an external programmer. Your physician can program various settings in your pulse generator to accommodate your particular cardiac condition. When the pulse generator detects an abnormally rapid heart rhythm, a shock is delivered to restore the heart back to its normal rhythm. This shock therapy is called defibrillation. The S-ICD System will record and store these abnormally 28
39 rapid heart rhythms. Your physician may retrieve the saved information during your routine scheduled follow-up visits. This can be accomplished via a wireless external programmer. Subcutaneous electrode The subcutaneous electrode comprises a partially coated (insulated) wire that is surgically implanted just under the skin, parallel to the breastbone (sternum). The subcutaneous electrode is connected to the pulse generator (Figure 5). Electrode parallel to breastbone Pulse generator connection - left side of rib cage Figure 5. Subcutaneous electrode placement 29
40 The S-ICD System uses the electrode to sense electrical signals in the heart. When necessary, the S-ICD System delivers a shock to restore the heart back to normal rhythm. The pulse generator and electrode materials that come in contact with the body have been tested for biocompatibility. The pulse generator and electrode are composed of titanium and other metals. Allergic reactions are uncommon, but you should discuss any known allergies to metals with your physicians. 30
41 Implanting your EMBLEM S-ICD System Understanding the implant procedure Depending on the hospital and physician practice, local or general anesthesia is administered to make you comfortable during the implant procedure. The duration of the implant procedure will vary depending on the type of anesthesia. Because of the lateral location of the pulse generator, females may have to consider undergarments and clothing that do not cause discomfort in the vicinity of the pulse generator pocket. The following section outlines the basic steps of the implant procedure (Figure 6): 31
42 Small incision for electrode placement Left side incision for device placement Figure 6. Implant procedure. 1. An incision is made on the left side of the chest, next to the rib cage. 2. A pocket, or pouch, is formed under the skin for the placement of the pulse generator. 3. Two small incisions are made close to the breastbone allowing placement of the subcutaneous electrode under the skin. 4. The subcutaneous electrode is connected to the pulse generator. 32
43 5. Your physician will then test your S-ICD system. During this test, your physician will start an arrhythmia in your heart. The device will recognize the rhythm and give a therapeutic shock. During this testing you will be sedated to minimize any discomfort. 6. Testing and adjustments are accomplished by the S-ICD System Programmer. 7. Once the incisions are closed, the procedure is complete. Discharge from the hospital Recovery from your S-ICD System implant procedure should not prevent you from returning to an active lifestyle. Follow your physician s post-operative instructions. 33
44 Benefits and risks of having an S-ICD System Your physician has decided that you should receive an implantable defibrillator (ICD) because you have an increased risk of sudden cardiac death due to ventricular rhythm disturbances. In particular, your physician believes you may benefit from the S-ICD System. The S-ICD System avoids some complications associated with transvenous leads by providing therapy without a lead(s) placed inside your heart. Additionally, the S-ICD System does not require the use of x-ray radiation during the implant procedure. As with all ICD systems, there are risks associated with the S-ICD System. Although infrequent, some of the risks that may be encountered during the implant procedure include the following: Formation of a blood clot Damage to adjacent structures (tendons, muscles, nerves) Dangerous arrhythmias 34
45 Stroke Death After the system is implanted, other infrequent risks may occur, including: Infection Erosion of the skin near your device Electrode and device may move out of place Fainting (syncope) Delivery of a shock or therapy when it is not needed (unnecessary therapy) Inability to detect or appropriately treat your heart rhythms due to electromagnetic interference or malfunction Difficulty coping with having an implanted device Bleeding or formation of a blood clot (hematoma) Pain and discomfort 35
46 Be sure to talk with your physician so that you thoroughly understand all of the risks and benefits associated with the implantation of this system. 36
47 After your implant As you recover from your implant surgery, you will find that your device may allow you to return to an active lifestyle. It is important that you become actively involved in your recovery by following your doctor s instructions, including: Report any redness, swelling, or drainage from your incisions. Avoid lifting heavy objects as instructed by your doctor. Walk, exercise, and bathe according to your doctor s instructions. Do not wear tight clothing that could irritate the skin over your device. Contact your doctor if you develop a fever that does not go away in two or three days. Ask your doctor any questions you may have about your device, heart rhythm, or medication. Avoid rubbing your device or the surrounding area. 37
48 Avoid rough contact that could result in blows to your implant sites. Tell your other doctors, dentists, and emergency personnel that you have an implanted device and show them your Medical Device Identification card. Contact your doctor if you notice anything unusual or unexpected, such as new symptoms or symptoms like the ones you experienced before you received your device. Medications Your device is designed to help treat your heart condition. However, you may need to continue taking certain medications as well. It is important that you follow your doctor s instructions regarding any medications. 38
49 Activities and exercise Your doctor will help you decide what level of activity is best for you. He or she can help answer your questions about lifestyle changes, travel, exercise, work, hobbies, and sexual intimacy. Your S-ICD System information Have your doctor or nurse complete the Your EMBLEM S-ICD system information form at the front of this handbook before you go home from the hospital. Your identification card Whether you are going away for the weekend or running a quick errand, carry your Medical Device Identification card with you. In an emergency, the card will alert medical and security personnel that you have an implanted device. You will be given a temporary Medical Device Identification card when you receive your device. Boston Scientific will 39
50 mail you a permanent Medical Device Identification card about six to eight weeks after your implant. Your Medical Device Identification card contains your name, your doctor s name and phone number, and the model numbers of your device and subcutaneous electrode. Updating your identification card If you move or select a new doctor, please call Boston Scientific Medical Records at to update your records. When you notify us of a change, we will send you a new identification card reflecting the change. 40
51 Living with your EMBLEM S-ICD System Patient responsibilities This section provides an outline of what you should know about your S-ICD System and returning to your daily activities postsurgery. Preparing for S-ICD shock therapy While the device s monitoring of your heart won t cause any noticeable sensations, shock therapy for an arrhythmia may be very noticeable. It is important that you know what to expect. Before you experience symptoms or receive a shock, discuss with your doctor or nurse a plan for contacting your doctor and, if necessary, emergency personnel. Use the forms in this handbook to write down important telephone numbers and information about your current medications. It might be helpful to keep this information near your phone. If you have symptoms of a fast heart rate, it is likely that your device will deliver therapy within a few seconds. 41
52 Try to remain calm, and find a place to sit or lie down. The sensation from receiving therapy should only last a moment. It is possible, however, that you may require additional medical attention. Be sure to talk with your doctor about what you should do, and consider the following suggestions: 1. If possible, have someone who is prepared to perform cardiopulmonary resuscitation (CPR) should you need it stay with you through the event. 2. Make sure a friend or family member knows to phone your local emergency response system if you remain unconscious. 3. If you are conscious but do not feel well after a shock, have someone call your doctor. 4. If you feel fine after a shock and no more symptoms appear, it may not be necessary to seek medical help immediately. However, follow your doctor s instructions for when to call his or her office. For example, if a 42
53 shock occurs at night, your doctor may tell you to call him or her the next morning. Someone at the doctor s office will ask you questions such as: What were you doing right before the shock? What symptoms did you notice before the shock? At what time did the shock occur? How did you feel right after the shock? 5. It is possible that you could feel symptoms of an arrhythmia but not receive therapy. This depends on the programmed settings of your device. For example, an arrhythmia may cause symptoms, but it may not be fast enough for your device to deliver therapy. In any case, if your symptoms are severe or continue for more than a minute or so, you should seek immediate medical attention. 43
54 Special considerations Your doctor might ask you to avoid activities where the risk of unconsciousness could endanger you or others. These activities might include driving, swimming or boating alone, or climbing a ladder. When to call your doctor Your doctor will provide guidelines for when you should contact him or her. In general, phone your doctor if you: Receive any arrhythmia therapy from your device and have been instructed to call. Have symptoms of an abnormal heart rhythm and have been instructed to call. Notice any swelling, redness, or drainage from your incisions. Develop a fever that does not go away in two or three days. 44
55 Have questions about your device, heart rhythm, or medications. Plan to travel or move away. Work with your doctor to develop a follow-up plan while you are away. Hear any beeping sounds from your device. This indicates that your device needs to be checked immediately. See What should you do if your device starts to beep? on page 48. Notice anything unusual or unexpected, such as new symptoms or symptoms like the ones you had before you received your device. Remember that your device is designed to monitor and treat your life-threatening arrhythmias. It can be a great source of reassurance for you and your friends and family. Follow-up visits To ensure that your S-ICD System continues to function properly, maintain the follow-up visit schedule that is prescribed by your physician. Check with your physician to 45
56 determine the frequency of these visits. Your physician will arrange a follow-up plan with you to check your device and overall health on a regular basis. It is important that you attend your scheduled in-office follow-up visits, even if you are feeling well. A typical follow-up visit takes about 20 minutes. During your visit, your doctor or nurse will use the programmer to interrogate, or check, your device. They will review your device s memory to evaluate its performance since your last visit and check for any arrhythmia episodes you may have had. If necessary, they will adjust your device s programmed settings. They will also check the battery to see how much energy is left. It is important to follow your physician s instructions as well as these recommendations: Follow-up visits are typically every 3-6 months. Ask your physician if you have any questions about or notice anything unusual with your device. 46
57 Take the medications prescribed for you as instructed by your physician. Carry your medication list with you at all times. Remote follow-up sessions Your physician may want you to use the LATITUDE Patient Management System. When using the LATITUDE Patient Management System, you will receive a home monitoring unit called a Communicator. The Communicator is used to interrogate your device on a regular schedule that is set by your physician. The Communicator then sends the data gathered from your device to the LATITUDE Patient Management secure database. Your doctor can then access this database using an Internet-enabled personal computer. While use of the Communicator does not eliminate the need for in-office visits that may be scheduled by your physician, it can minimize the number of them. The Communicator cannot reprogram or change any functions of your device. Your physician can only do this using a programmer during an office visit. 47
58 What should you do if your device starts to beep? As a safety feature, the S-ICD System has a built-in selfmonitoring function that checks the circuitry of the pulse generator. If you should hear beeping tones coming from your pulse generator, contact your physician. The beeping indicates that your S-ICD System requires immediate follow-up by your physician. Your physician or nurse can demonstrate these beeping tones so you will recognize them. Even though the system has this warning system, you should always follow your physician s instructions for regular follow-up visits. What you should know about your device s battery A battery, safely sealed inside your device, provides the energy needed to monitor your heart rhythm, pace your heart, or deliver electrical therapy. Just like any other type of battery, the battery in your device will be used up over time. Since the battery is permanently sealed within your 48
59 device, it cannot be replaced when its energy is depleted. Instead, your entire device will need to be replaced (see Replacing your system on page 50). How long your device s battery lasts depends upon the settings your doctor programs and how much therapy you receive. How will you know if your device s battery is running down? Device batteries have very predictable behavior over time. Your device will regularly check its own battery. At every follow-up visit, the doctor or nurse will also check to see how much energy is remaining in the battery. When the battery s energy level decreases to a certain point, your device will need to be replaced. You may hear the device beeping when replacement time is near. See What should you do if your device starts to beep? on page
60 Replacing your system Eventually, the energy in your device s battery will decrease to a point where your device will need to be replaced (see What you should know about your device s battery on page 48). Your doctor will monitor your device s battery levels and determine when to replace your device. To replace your device, your doctor will surgically open the pocket of skin where your device is located. He or she will disconnect your old device from your subcutaneous electrode and then check to make sure your subcutaneous electrode works properly with your new device. In rare instances, your subcutaneous electrode may not work properly with your new device, and your doctor may need to replace the subcutaneous electrode. Your doctor will determine if your subcutaneous electrode should be replaced. Should a subcutaneous electrode need to be replaced, your doctor will insert a new subcutaneous electrode under the skin, similar to how the original subcutaneous electrode 50
61 was implanted. See Implanting your EMBLEM S-ICD System on page 31. Your doctor will then connect the subcutaneous electrode to your new device. Finally, he or she will test your new system to make sure it is working properly. After the testing is complete, the pocket of skin will be closed. You may experience some discomfort from the incision as you recover from the surgery. You should be able to return to normal activities soon after the procedure. Risks Risks encountered during a device and/or subcutaneous electrode replacement procedure are similar to the risks of the initial implant, such as infection, tissue damage, and bleeding. See Benefits and risks of having an S-ICD System on page 34. Be sure to talk with your doctor about the potential risks when making decisions about replacing your system. 51
62 Questions you may have about living with your EMBLEM S-ICD System How do I know my device is working properly? Regular follow-up visits are required to assess your S-ICD System. Therefore, it is important to follow your physician s instructions regarding regular follow-up visits. How do I know if increased heart rate will result in a shock, for instance from exercise? Your heart rate will generally increase when you exercise. Your physician can program the S-ICD System to deliver therapy only when your heart exceeds a certain rate. While inappropriate shocks may occur, there are special features in the S-ICD System that are designed to tell the difference between high rates due to vigorous exercise and those due to an arrhythmia that needs therapy. Your physician can explain how your device is programmed and which heart rates could result in a shock. 52
63 Is pacing available in the S-ICD System? Pacing used to treat slow heart rates (Bradycardia) is only available following shock therapy. Following shock therapy, the heart may slow down or be interrupted for a brief period. The pacing following shock therapy is used for temporary support until your own heart rate returns to normal. How often does the S-ICD System deliver therapy? Therapy delivery varies for each patient and may be dependent upon your specific heart condition. How long will the battery last? The battery in the S-ICD System will typically last seven years. There are factors that could affect battery life including your heart condition and the amount of therapy you receive. Your device will regularly check its own battery. At every follow-up visit, the physician or nurse will also check to see how much energy is remaining in the battery. When the battery s energy level decreases to a 53
64 certain point, the device may begin to beep and will need to be replaced. What will it feel like if I receive a shock? Patients vary in their descriptions of experiencing a shock. These descriptions range from a mild thump to a swift kick in the chest. Most patients are reassured in knowing that a rapid heart rhythm was treated with the shock and they can resume their normal daily routine. Follow your physician s instructions if you receive a shock. What happens if someone is touching me when I receive a shock? If you receive a shock while engaging in physical contact with another individual, including during sexual intimacy, they may feel a harmless tingling sensation that lasts for an instant. Will I be able to engage in sexual intimacy? For most patients, sexual intimacy is not a medical risk. The natural heart rate increase that occurs during sex is the same as the heart rate increase when you exercise. 54
65 Exercise testing at the hospital will help your physician program your device settings so you should not get a shock during sex. If you receive a shock during sex, your partner may feel a tingling sensation. The shock is not harmful to your partner. Be sure to let your physician know if you receive a shock during sex so he or she can consider reprogramming your device. Will I be able to feel the implanted S-ICD System? Most people are aware of the implanted S-ICD System, but become accustomed to it quickly. For some patients, discomfort or pain near the pulse generator or electrode may last for several weeks. In rare situations, surgical repositioning may be required to resolve discomfort. What should I do if my device is beeping? Make note of what you were doing then contact your physician. 55
66 Can I exercise? The S-ICD System itself does not prevent you from exercising. Follow your physician s instructions on the amount and type of exercise you are permitted to do after implantation of the S-ICD System. When can I resume driving? Your physician will advise you if, and when, you may drive after your S-ICD System has been implanted. This decision is based upon your specific heart condition. The driving laws for patients who have implantable defibrillation devices vary from state to state and country to country. Most S-ICD System patients who previously drove can resume driving. There are no physical driving impediments attributable to the S-ICD System. Furthermore, protection afforded by the S-ICD System helps make driving safe of lethal arrhythmia symptoms. Receiving a shock during driving is usually uncommon. 56
67 Can I travel? The S-ICD System does not prevent you from traveling. Check with your physician about any travel-related considerations for before, during or after your trip. Your physician may give you guidance on whom to speak with or contact when traveling. If you are traveling overseas, you may also contact Boston Scientific Patient Services at for the location of hospitals that implant and provide follow-up support for the S-ICD System. Can I use a cellular phone? If you use a cellular phone or a cordless phone, it is best to keep the phone more than 15 centimeters or 6 inches from your S-ICD System. It is further recommended that your cellular phone be carried on the opposite side of the implanted S-ICD System. When talking on the cellular phone, hold the cellular phone on the opposite side of the body away from the implantation site. The cellular phone may affect the therapy functions of the S-ICD System. Consult your physician if you have specific questions about the S-ICD System and the potential interaction with cellular phones. 57
68 Important safety information Electromagnetic interference An electromagnetic field is created when using electrical and magnetic devices. Most of the electrical and magnetic devices you encounter create weak electromagnetic fields. Your S-ICD System is designed to protect itself from these electromagnetic fields and proper operation of your S-ICD System will not be affected when you are around the electrical and magnetic devices that create such fields. Some electrical and magnetic devices, however, emit strong electromagnetic or radio frequency fields, which can temporarily affect the function of the S-ICD System. This form of interference is called electromagnetic interference (EMI). Typically, normal S-ICD System function resumes when you move away from the electrical and magnetic devices creating the EMI. It is important for you to be aware of what electrical and magnetic devices are likely to interfere with your S-ICD System s normal function. The following paragraphs help you identify the EMI safety of particular appliances, tools and activities. If your 58
69 employment requires you to be close to large industrial generators or sources of radar you may need special consideration before returning to work. If your work takes place in such an environment, please talk with your physician. Household appliances and common tools The S-ICD System allows you to safely operate most household appliances, office equipment and common tools that are properly grounded and in good repair. Use the following guidelines for safe interaction with many common tools, appliances, and activities. Items that are safe under normal use: Air purifiers Blenders CD/DVD players Clothes washing machines and dryers Electric blankets 59
70 Electric can openers Electric invisible fences Electric toothbrushes Fax/copy machines Hair dryers Heating pads Hot tubs/whirlpool baths NOTE: Consult with your doctor before using a hot tub. Your medical condition may not permit this activity; however, it will not harm your device. Laser tag games Microwave ovens Ovens (electric, convection, and gas) Pagers Patient alert devices Personal computers Personal digital assistants (PDAs) 60
71 NOTE: PDAs that also function as cell phones should be kept at least 6 inches (15 cm) away from your implanted system. Refer to Cellular phones on page 70. Portable space heaters Radios (AM and FM) Remote controls (TV, garage door, stereo, camera/ video equipment) Stoves (electric or gas) Televisions TV or radio towers (safe outside of restricted areas) Tanning beds Vacuum cleaners VCRs Video games 61
72 Warnings and precautions Read and follow all warnings and precautions discussed in this section. Failure to heed the warnings and precautions may result in inappropriate shock therapy or failure to deliver shock therapy. As a general rule, if you are operating any electrical or battery powered equipment and you receive a shock, you should stop operating the equipment. In addition, if your device starts beeping, you may be in the presence of a strong magnetic field and you should move away from the potential magnetic source until your device stops beeping. Temporary beeping may also be an indication that your device has detected a malfunction. If you hear your device beeping, contact your physician immediately. Talk to your physician if you have any questions or concerns regarding this information. Warnings Certain electrical or magnetic fields may interfere with the S-ICD System s function. To minimize the possibility of any interference, try to avoid: 62
73 Strong magnets such as auto wrecking yards and industry Industrial power generators Large TV/Radio transmitting towers Power plants and high voltage power lines Occupational exposure to power systems for European trains operating at 16.6 Hz Environmental safety precautions This section presents the environmental safety precautions for which you must be aware. Be sure to carefully read and understand each of these precautions. If you still have questions or concerns regarding these precautions, please contact your physician or Boston Scientific. If you use any of the following items, it is important that you keep them the recommended distance away from your implanted system to avoid interaction. 63
74 Items that should not be placed directly over your implanted system, but are otherwise safe to use: Cordless (household) telephones Electric razors Hand-held massagers Portable MP3 and multimedia players (such as ipod ) that do not also function as a cellular phone (see Cellular phones on page 70). NOTE: While portable MP3 players themselves should not interfere with your implanted system, the headphones or earbuds should be stored at least 6 inches (15 cm) away from your implanted system, and you should avoid draping the headphones around your neck. ipod is a trademark or registered trademark of Apple Inc. 64
75 Items that should remain at least 6 inches (15 cm) away from your implanted system, but are otherwise safe to use: Cellular phones, including PDAs and portable MP3 players with integrated cellular phones NOTE: For more information about cellular phones, refer to Cellular phones on page 70. Devices transmitting Bluetooth or Wi-Fi signals (cellular phones, wireless Internet routers, etc.) Headphones and earbuds NOTE: It is safe to use headphones and earbuds, but you should refrain from storing them in a breast or other shirt pocket that places them within 6 inches (15 cm) of your implanted system. Magnetic wands used in the game of Bingo Items that should remain at least 12 inches (30 cm) away from your implanted system, but are otherwise safe to use: Battery-powered cordless power tools Bluetooth is a trademark or registered trademark of Bluetooth SIG Inc. 65
76 Chain saws Corded drills and power tools Lawn mowers Leaf blowers Remote controls with antennas Shop tools (drills, table saws, etc.) Slot machines Snow blowers Stereo speakers Items that should remain at least 24 inches (60 cm) away from your implanted system, but are otherwise safe to use: Arc and resistance welders Home power generators Police radio antennas and antennas used to operate a CB, ham radio or other radio transmitter 66
77 Running motors and alternators, especially those found in vehicles NOTE: Avoid leaning over running motors and alternators of a running vehicle. Alternators create large magnetic fields that can affect your implanted system. However, the distance required to drive or ride in a vehicle is safe. Items that should not be used: Body-fat measuring scales Jackhammers Magnetic mattresses and chairs Stun guns If you have questions about the EMI safety of a particular appliance, tool, or activity, please call Boston Scientific Patient Services at Theft detection and security systems Electronic antitheft systems (including tag deactivation) and security gates or tag readers that include radio frequency identification (RFID) equipment (often found in 67
78 store and library doorways, at checkout counters, and in point-of-entry access control systems) should not cause you any worry if you follow these guidelines: Walk through theft detection and security systems at a normal pace. Do not lean against or linger near these systems. Do not lean against checkout counter-mounted or handheld tag deactivation systems. If you are near an electronic antitheft, security, or entry control system and suspect interaction (experience symptoms) with your device from one of these systems, promptly move away from equipment nearby and inform your doctor. Most home security systems are unlikely to affect the proper function of your implanted system. Your Boston Scientific implantable device is unlikely to set off the alarm from an electronic antitheft or security system. 68
79 Airport security Your device contains metal parts that may set off airport security metal detector alarms. The security archway will not harm your device. Tell security personnel that you have an implanted medical device and show them your Medical Device Identification card. Airport security wands could temporarily affect your device if the wand is held over it for a period of time (about 30 seconds). If possible, ask to be hand-searched instead of being searched with a handheld wand. If a wand must be used, inform the security personnel that you have an implanted medical device. Tell the security personnel not to hold the wand over your device and to perform the search quickly. If you have questions about airport security, call your doctor or Boston Scientific Patient Services at
80 Cellular phones Keep your cellular phone at least 6 inches (15 cm) away from your implanted system. Your cellular phone is a source of EMI and could affect your implanted system s operation. This interaction is temporary, and moving the phone away from your implanted system will return it to proper function. To reduce the chance of interaction, follow these precautions: Maintain a distance of at least 6 inches (15 cm) between the cellular phone and your implanted system. Hold the cellular phone to your ear on the opposite side of your body from your implanted system. Do not carry a cellular phone in a pocket or on a belt if that places the phone within 6 inches (15 cm) of your implanted system. These precautions apply only to cellular phones, not to household cordless phones. However, you should avoid placing your household cordless phone receiver directly over your implanted system. 70
81 Dental and medical procedures Some medical procedures could damage or otherwise affect your device. Be sure to always tell your dentist and physicians that you have an implanted device so that they can take the necessary precautions. Be especially careful with the following procedures: Magnetic Resonance Imaging (MRI): This is a diagnostic test that uses a strong electromagnetic field. Some S-ICD systems have been evaluated to allow the patient to undergo MRI scans under specific conditions. Talk to your physician about the capabilities of your S-ICD system. If your system is not one of those eligible to be scanned, or if the required conditions are not met, MRI scans can severely damage your device and should not be performed. Hospitals keep MRI equipment in rooms marked with signs that indicate magnets are inside. Do not go inside these rooms unless your physician has confirmed that your S-ICD system is eligible and you meet the requirements for an MRI scan. 71
82 Diathermy: This uses an electrical field to apply heat to tissues in the body and could damage your device or injure you. Diathermy should not be performed. Electrocautery: This is used during surgical procedures to stop vessels from bleeding. It should be used only when your device is turned off. Talk with your heart doctor and the doctor performing the medical procedure to determine who turns off your device. External defibrillation: This is a procedure, typically used in medical emergencies, that uses external equipment to deliver an electrical shock to your heart to restore a rapid and irregular heart rate to a normal rhythm. External defibrillation can affect your device, but can still be performed if necessary. If you receive external defibrillation, be sure to contact your physician as soon as possible following the emergency to verify that your device is functioning properly. Lithotripsy: This is a medical procedure that is used to break up stones in the urinary tract (e.g., kidney stones). Lithotripsy can damage your device if certain 72
83 precautions are not taken. Talk with your heart doctor as well as the doctor performing the procedure about what can be done to protect your device. Therapeutic radiation treatment for cancer: This procedure can affect your device and will require special precautions. If you should need radiation treatment, talk with your heart doctor as well as the doctor performing the medical procedure. Transcutaneous Electrical Nerve Stimulation (TENS) unit: This is a device prescribed by physicians or chiropractors for control of chronic pain. A TENS unit can affect your device and will require special precautions. If you must use a TENS unit, talk with your heart doctor. Most other medical and dental procedures are unlikely to affect your device. Some examples include: Dental drills and cleaning equipment Diagnostic X-rays Diagnostic ultrasound procedures 73
84 Mammograms NOTE: Mammograms will not interfere with your device. However, your device could be damaged if it gets compressed in the mammogram machine. Make sure the doctor or technician knows that you have an implanted device. EKG machines CT scans If you need to undergo any surgical procedures, tell your dentist and/or doctor that you have an implanted device. They can contact the physician who monitors your device to find the best way to provide treatment. If you have questions about a specific appliance, tool, medical procedure, or piece of equipment, please talk with your doctor or call Boston Scientific Patient Services at
85 Summary It is natural for you to feel anxious or nervous about receiving a device. You have been identified by your physician as having a significant risk of sudden cardiac death due to your medical conditions. Remember that your device can be a great source of reassurance for you and your friends and family. Talking with other ICD patients is often helpful while adjusting to your new device. Ask your doctor, nurse, or Boston Scientific representative if there is a local ICD patient support group in your area. The information presented in this handbook is intended to help you understand more about your heart condition and your device. If you have questions about what you have read, be sure to ask your doctor or nurse. They are your best resource for information about your particular needs or situation. 75
86 Visit us on the Internet Boston Scientific s patient-focused website, LifeBeat Online, offers a variety of information of interest to people with cardiac devices, including cardiac news, health tips, patient stories, frequently asked questions about living with your implanted device, and links to additional resources. 76
87 Notes and questions Use this space to write down questions or additional information about your device: 77
88 Index A Activities, 39, 44 Airport security, 69 Allergic, 30 metals, 30 Antitachycardia pacing, 5 Arrhythmia, 1, 5 ventricular fibrillation, 21 ventricular tachycardia, 19 Atria, 5, 17 B Battery, 48 beeping tones, 48 end of life, 49, 50, 53 Beeping tones, see Battery Boating, 44 Bradycardia, 5, 53 C Calling your doctor, 44 Cardiac arrest, see Sudden cardiac arrest Cardiomyopathy, 23 Cellular phones, 57, 65, 70 Communicator, See LATITUDE Patient Management System Cordless phones, 57, 64, 70 CT scans, 74 D Dental equipment, 73 Dental procedures, 71 Device, 28 implanting, 31 reliability, 4 replacing, 50 risks, 34 78
89 Diathermy, 72 Driving, 44 E Echocardiogram, 7, 26 Ejection fraction, 7, 24 EKG machines, 74 Electrocardiogram, 6 Electrocautery, 72 Electrode, see Subcutaneous Electrode Electromagnetic interference (EMI), 7, 58 Electrophysiology (EP), 8, 27 Exercise, 39 External defibrillation, 72 F Follow-up visits, 45 H Heart, 15 Heart attack, 10 Heart rhythm, 1, 8 Holter monitoring, 9, 26 Household appliances, 59 I ICD, 34 ICD system, 9, 28 Identification card, 39 Implanting the system, 31 recovery, 37 risks, 34 Interrogation, 9 L Ladders, 44 79
90 LATITUDE Patient Management System, 47 Communicator, 47 Leads, 9, 34 Lithotripsy, 72 Living with your EMBLEM S-ICD System, 41 preparing for therapy, 41 M Mammograms, 74 Medical procedures, 71 Medications, 38 Metals, see Allergic MRI, 71 Myocardial infarction (MI), see Heart attack P Precautions, 62 airport security, 69 cellular phones, 65, 70 dental procedures, 71 diathermy, 72 electrocautery, 72 environmental, 63 external defibrillation, 72 lithotripsy, 72 medical procedures, 71 MRI, 71 radiation treatment, 73 TENS units, 73 theft detection systems, 67 Programmer, 11, 28 Pulse generator, 11, 28 R Radiation treatment, 73 Radio frequency (RF) wireless communication, 11 Recovery, 37 Reliability, 4 Replacing the system, 50 80
91 risks, 51 Risks, 34 S Safety, see Precautions Security systems, 67 Sexual intimacy, 54 Shock therapy, 2, 28, 35 S-ICD System, 22 Sinoatrial (SA) node, 12, 16 Subcutaneous Electrode, 12, 29 Sudden cardiac arrest, 3, 12, 25 Sudden cardiac death, 3, 13, 25, 34, 75 Supraventricular tachycardia (SVT), 13 Swimming, 44 T TENS units, 73 Theft detection systems, 67 Therapy antitachycardia pacing, 5 bradycardia pacing, 53 contacting your doctor, 41 how it feels, 54 preparing for, 41 Traveling, 39, 45 airport security, 69 U Ultrasound, 73 V Ventricle, 13 Ventricular fibrillation (VF), 14, 21 Ventricular tachycardia (VT), 14, 19 W Warnings, 62 81
92 X X-rays, 73 82
93
94
95
96 Boston Scientific Corporation 4100 Hamline Avenue North St. Paul, MN USA Tel: Medical Professionals: CARDIAC ( ) Patients and Families: Boston Scientific Corporation or its affiliates. All rights reserved. S-ICD en USA * *
EMBLEM TM S-ICD System Patient Handbook
 EMBLEM TM S-ICD System Patient Handbook A Message to Patients Boston Scientific Corporation acquired Cameron Health in June 2012. During our transition period, you may see both the Boston Scientific and
EMBLEM TM S-ICD System Patient Handbook A Message to Patients Boston Scientific Corporation acquired Cameron Health in June 2012. During our transition period, you may see both the Boston Scientific and
Implantable Cardioverter Defibrillator Therapy
 Implantable Cardioverter Defibrillator Therapy Your ICD system information Have your doctor or nurse complete these forms before you go home from the hospital. ICD Model Number: ICD Serial Number: ICD
Implantable Cardioverter Defibrillator Therapy Your ICD system information Have your doctor or nurse complete these forms before you go home from the hospital. ICD Model Number: ICD Serial Number: ICD
The protection you need - without touching your heart
 The S ICD System The protection you need - without touching your heart listen to your heart Patient information You have options An implantable defibrillator, commonly known as an ICD, is a device designed
The S ICD System The protection you need - without touching your heart listen to your heart Patient information You have options An implantable defibrillator, commonly known as an ICD, is a device designed
Cardiac Resynchronization Therapy Defibrillator
 Cardiac Resynchronization Therapy Defibrillator Your CRT-D system information Have your doctor or nurse complete these forms before you go home from the hospital. CRT-D Model Number: CRT-D Serial Number:
Cardiac Resynchronization Therapy Defibrillator Your CRT-D system information Have your doctor or nurse complete these forms before you go home from the hospital. CRT-D Model Number: CRT-D Serial Number:
X-Plain Pacemaker Reference Summary
 X-Plain Pacemaker Reference Summary Introduction A pacemaker is a device that regulates the heart beat. More than half a million Americans use a pacemaker. If your doctor recommends that you have a pacemaker,
X-Plain Pacemaker Reference Summary Introduction A pacemaker is a device that regulates the heart beat. More than half a million Americans use a pacemaker. If your doctor recommends that you have a pacemaker,
There are different types of ICDs:
 Guidelines for Patients with Implantable Devices o Implantable Cardioverter Defibrillator (ICD) Your ICD is approximately the size of a pager and includes the following parts: The ICD: A battery powered
Guidelines for Patients with Implantable Devices o Implantable Cardioverter Defibrillator (ICD) Your ICD is approximately the size of a pager and includes the following parts: The ICD: A battery powered
UNDERSTANDING ELECTROPHYSIOLOGY STUDIES
 UNDERSTANDING ELECTROPHYSIOLOGY STUDIES Testing and Treating Your Heart s Electrical System A Problem with Your Heart Rhythm The speed and pattern of a heartbeat is called the heart rhythm. The rhythm
UNDERSTANDING ELECTROPHYSIOLOGY STUDIES Testing and Treating Your Heart s Electrical System A Problem with Your Heart Rhythm The speed and pattern of a heartbeat is called the heart rhythm. The rhythm
Pacemaker and ICD Interrogation
 Pacemaker and ICD Interrogation To receive the maximum benefit from your pacemaker, you will need to have regular follow-up appointments to ensure that it is working properly. This follow up can be arranged
Pacemaker and ICD Interrogation To receive the maximum benefit from your pacemaker, you will need to have regular follow-up appointments to ensure that it is working properly. This follow up can be arranged
Arrhythmias. Pulmonary Artery
 Arrhythmias Introduction Cardiac arrhythmia is an irregularity of the heart beat that causes the heart to beat too slowly, too fast, or irregularly. There are different types of arrhythmias. Most arrhythmias
Arrhythmias Introduction Cardiac arrhythmia is an irregularity of the heart beat that causes the heart to beat too slowly, too fast, or irregularly. There are different types of arrhythmias. Most arrhythmias
Different indications for pacemaker implantation are the following:
 Patient Resources: ICD/Pacemaker Overview ICD/Pacemaker Overview What is a pacemaker? A pacemaker is a device that uses low energy electrical pulses to prompt the heart to beat whenever a pause in the
Patient Resources: ICD/Pacemaker Overview ICD/Pacemaker Overview What is a pacemaker? A pacemaker is a device that uses low energy electrical pulses to prompt the heart to beat whenever a pause in the
Patient Resources: Arrhythmias and Congenital Heart Disease
 Patient Resources: Arrhythmias and Congenital Heart Disease Overview Arrhythmias (abnormal heart rhythms) can develop in patients with congenital heart disease (CHD) due to thickening/weakening of their
Patient Resources: Arrhythmias and Congenital Heart Disease Overview Arrhythmias (abnormal heart rhythms) can develop in patients with congenital heart disease (CHD) due to thickening/weakening of their
Catheter Ablation. Patient Education
 Catheter Ablation Patient Education Allina Health System Your heart has four chambers. Two upper chambers (atria) pump blood to the two lower chambers (ventricles). In order for the heart to pump, it requires
Catheter Ablation Patient Education Allina Health System Your heart has four chambers. Two upper chambers (atria) pump blood to the two lower chambers (ventricles). In order for the heart to pump, it requires
Kadlec Regional Medical Center Cardiac Electrophysiology
 Definition of electrophysiology study and ablation Kadlec Regional Medical Center Cardiac Electrophysiology Electrophysiology Study and Ablation An electrophysiology, or EP, study is a test of the heart
Definition of electrophysiology study and ablation Kadlec Regional Medical Center Cardiac Electrophysiology Electrophysiology Study and Ablation An electrophysiology, or EP, study is a test of the heart
About atrial fibrillation (AFib) Atrial Fibrillation (AFib) What is AFib? What s the danger? Who gets AFib?
 Understanding AFib Atrial Fibrillation (AFib) About AFib 3 How Your Heart Works 4 Types of AFib 5 Symptoms 5 Risk Factors 5 How is AFib Diagnosed? 6 Treatment 6 What to Ask Your Doctor 7 A normal heartbeat
Understanding AFib Atrial Fibrillation (AFib) About AFib 3 How Your Heart Works 4 Types of AFib 5 Symptoms 5 Risk Factors 5 How is AFib Diagnosed? 6 Treatment 6 What to Ask Your Doctor 7 A normal heartbeat
Living with Your Heart Failure Device (CRT)*
 References 1 Zipes DP, Roberts D. Results of the international study of the implantable pacemaker cardioverter-defibrillator. A comparison of epicardial and endocardial lead systems. The Pacemaker-Cardioverter-
References 1 Zipes DP, Roberts D. Results of the international study of the implantable pacemaker cardioverter-defibrillator. A comparison of epicardial and endocardial lead systems. The Pacemaker-Cardioverter-
Understanding Atrial Fibrillation A guide for patients
 Understanding Atrial Fibrillation A guide for patients Your doctor has determined that you have atrial fibrillation (AF), a common disturbance of the heart s rhythm. This pamphlet will answer many of your
Understanding Atrial Fibrillation A guide for patients Your doctor has determined that you have atrial fibrillation (AF), a common disturbance of the heart s rhythm. This pamphlet will answer many of your
Yes, out of sight out of mind.
 Micra TRANSCATHETER PACING SYSTEM 25.9 mm Yes, out of sight out of mind. cardiocapsule Meet Micra The Invisible Pacemaker Micra is the world s smallest pacemaker 1. It leaves no bump under the skin, no
Micra TRANSCATHETER PACING SYSTEM 25.9 mm Yes, out of sight out of mind. cardiocapsule Meet Micra The Invisible Pacemaker Micra is the world s smallest pacemaker 1. It leaves no bump under the skin, no
NEED A DEFIBRILLATOR? NOW YOU HAVE OPTIONS.
 NEED A DEFIBRILLATOR? NOW YOU HAVE OPTIONS. EXPLORE YOUR OPTIONS. ALL DEFIBRILLATORS ARE NOT THE SAME. Sudden cardiac arrest is a serious and lifethreatening medical emergency caused by a type of irregular
NEED A DEFIBRILLATOR? NOW YOU HAVE OPTIONS. EXPLORE YOUR OPTIONS. ALL DEFIBRILLATORS ARE NOT THE SAME. Sudden cardiac arrest is a serious and lifethreatening medical emergency caused by a type of irregular
Implantable Cardioverter Defibrillators (ICDs) How ICDs Treat Fast Heart Rhythms Before, During, and After Implantation Living Well with an ICD
 Implantable Cardioverter Defibrillators (ICDs) How ICDs Treat Fast Heart Rhythms Before, During, and After Implantation Living Well with an ICD An ICD Could Save Your Life Based on your health and medical
Implantable Cardioverter Defibrillators (ICDs) How ICDs Treat Fast Heart Rhythms Before, During, and After Implantation Living Well with an ICD An ICD Could Save Your Life Based on your health and medical
Atrial Fibrillation. Damage to your heart caused by a heart attack or rheumatic heart disease
 Atrial Fibrillation GENERAL INFORMATION: What is atrial fibrillation? Atrial fibrillation is a condition that causes the atria (top chambers of the heart) to shake or quiver. Normally, there is 1 contraction
Atrial Fibrillation GENERAL INFORMATION: What is atrial fibrillation? Atrial fibrillation is a condition that causes the atria (top chambers of the heart) to shake or quiver. Normally, there is 1 contraction
Implantable Cardioverter Defibrillator
 12:13:18 CTPALS067 V2_CTPALS01 25/04/2017 11:19 Page 1 Implantable Cardioverter Defibrillator A device to help correct abnormal heart rhythms This leaflet has been written to provide information about
12:13:18 CTPALS067 V2_CTPALS01 25/04/2017 11:19 Page 1 Implantable Cardioverter Defibrillator A device to help correct abnormal heart rhythms This leaflet has been written to provide information about
ATRIAL FIBRILLATION ANSWERS. A Patient Education Handbook on Electrophysiology
 ATRIAL FIBRILLATION ANSWERS A Patient Education Handbook on Electrophysiology MY LIFE HAS TAKEN A TURN FOR THE BETTER. -Emie Bishop ARRHYTHMIAANSWERS.COM AF ANSWERS. A PATIENT EDUCATION HANDBOOK ON ELECTROPHYSIOLOGY
ATRIAL FIBRILLATION ANSWERS A Patient Education Handbook on Electrophysiology MY LIFE HAS TAKEN A TURN FOR THE BETTER. -Emie Bishop ARRHYTHMIAANSWERS.COM AF ANSWERS. A PATIENT EDUCATION HANDBOOK ON ELECTROPHYSIOLOGY
Living With Your Implantable Cardioverter Defibrillator (ICD)
 Patient & Family Guide 2016 Living With Your Implantable Cardioverter Defibrillator (ICD) Aussi disponible en français : Vivre avec votre défibrillateur cardioverteur implantable (DCI) (FF85-1719) www.nshealth.ca
Patient & Family Guide 2016 Living With Your Implantable Cardioverter Defibrillator (ICD) Aussi disponible en français : Vivre avec votre défibrillateur cardioverteur implantable (DCI) (FF85-1719) www.nshealth.ca
Cardiac Resynchronization Therapy (CRT) Heart Failure and Electrical Problems How CRT Helps Getting a Biventricular Pacemaker or ICD
 Cardiac Resynchronization Therapy (CRT) Heart Failure and Electrical Problems How CRT Helps Getting a Biventricular Pacemaker or ICD What Is CRT? When you have heart failure, your heart is weakened and
Cardiac Resynchronization Therapy (CRT) Heart Failure and Electrical Problems How CRT Helps Getting a Biventricular Pacemaker or ICD What Is CRT? When you have heart failure, your heart is weakened and
IMPLANTABLE CARDIOVERTER DEFIBRILLATORS (ICDs)
 IMPLANTABLE CARDIOVERTER DEFIBRILLATORS (ICDs) Living Well with an ICD An ICD Could Save Your Life Your heart has an electrical system that keeps it beating at the right speed. Problems with this system
IMPLANTABLE CARDIOVERTER DEFIBRILLATORS (ICDs) Living Well with an ICD An ICD Could Save Your Life Your heart has an electrical system that keeps it beating at the right speed. Problems with this system
Kadlec Regional Medical Center Cardiac Electrophysiology
 Definition of atrial fibrillation Kadlec Regional Medical Center Cardiac Electrophysiology Atrial Fibrillation Ablation Atrial fibrillation is a heart rhythm disturbance that causes an irregular (and often
Definition of atrial fibrillation Kadlec Regional Medical Center Cardiac Electrophysiology Atrial Fibrillation Ablation Atrial fibrillation is a heart rhythm disturbance that causes an irregular (and often
Information for patients, parents and guardians. Your child s doctor has recommended that your child has a procedure called an ablation.
 Having an ablation Information for patients, parents and guardians Your child s doctor has recommended that your child has a procedure called an ablation. An ablation is a treatment for an abnormal heartbeat.
Having an ablation Information for patients, parents and guardians Your child s doctor has recommended that your child has a procedure called an ablation. An ablation is a treatment for an abnormal heartbeat.
Your Subcutaneous Implantable Cardiac Defibrillator (ICD)
 UW MEDICINE PATIENT EDUCATION Your Subcutaneous Implantable Cardiac Defibrillator (ICD) What you need to know Who to Call If you have questions about your appointments, call the Cardiology Clinic at 206-598-4300.
UW MEDICINE PATIENT EDUCATION Your Subcutaneous Implantable Cardiac Defibrillator (ICD) What you need to know Who to Call If you have questions about your appointments, call the Cardiology Clinic at 206-598-4300.
Newer pacemakers also can monitor your blood temperature, breathing, and other factors and adjust your heart rate to changes in your activity.
 Pacemakers & Defibrillators A pacemaker system consists of a battery, a computerized generator and wires with sensors called electrodes on one end. The battery powers the generator, and both are surrounded
Pacemakers & Defibrillators A pacemaker system consists of a battery, a computerized generator and wires with sensors called electrodes on one end. The battery powers the generator, and both are surrounded
Care of Your Child with a Pacemaker
 Patient and Family Education Care of Your Child with a Pacemaker A pacemaker watches for slow heart rates. It can send signals to make the heart beat. Here is how to take care of your child s pacemaker.
Patient and Family Education Care of Your Child with a Pacemaker A pacemaker watches for slow heart rates. It can send signals to make the heart beat. Here is how to take care of your child s pacemaker.
NHS. Implantable cardioverter defibrillators (ICDs) for arrhythmias. National Institute for Health and Clinical Excellence. Issue date: January 2006
 NHS National Institute for Health and Clinical Excellence Issue date: January 2006 Implantable cardioverter defibrillators (ICDs) for arrhythmias Understanding NICE guidance information for people with
NHS National Institute for Health and Clinical Excellence Issue date: January 2006 Implantable cardioverter defibrillators (ICDs) for arrhythmias Understanding NICE guidance information for people with
A Patient EDUCATION HANDBOOK ON ICD. A Patient Education Handbook on ICD 1
 A Patient EDUCATION HANDBOOK ON ICD A Patient Education Handbook on ICD 1 ARRHYTHMIAANSWERS.COM YOUR ICD AT A GLANCE Your heart is a muscle about the size of your fist and has a complex electrical system.
A Patient EDUCATION HANDBOOK ON ICD A Patient Education Handbook on ICD 1 ARRHYTHMIAANSWERS.COM YOUR ICD AT A GLANCE Your heart is a muscle about the size of your fist and has a complex electrical system.
After Your Implantable Cardiac Defibrillator (ICD) Generator Change
 UW MEDICINE PATIENT EDUCATION After Your Implantable Cardiac Defibrillator (ICD) Generator Change What you need to know Who to Call If you have questions about your appointments, call the Cardiology Clinic
UW MEDICINE PATIENT EDUCATION After Your Implantable Cardiac Defibrillator (ICD) Generator Change What you need to know Who to Call If you have questions about your appointments, call the Cardiology Clinic
This leaflet is intended for patients with permanent pacemakers and their parents.
 Permanent PACEMAKER This leaflet is intended for patients with permanent pacemakers and their parents. It serves as an information tool and a guide that offers some advice in order to live safely. General
Permanent PACEMAKER This leaflet is intended for patients with permanent pacemakers and their parents. It serves as an information tool and a guide that offers some advice in order to live safely. General
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Implantable cardioverter defibrillators for the treatment of arrhythmias and cardiac resynchronisation therapy for the treatment of heart failure (review
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Implantable cardioverter defibrillators for the treatment of arrhythmias and cardiac resynchronisation therapy for the treatment of heart failure (review
Subcutaneous ICD S-ICD Protection without touching the heart Patient Brochure
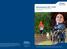 Subcutaneous ICD S-ICD Protection without touching the heart Patient Brochure IMPORTANT Please Note: Information provided by Boston Scientific Corporation (BSC) is gathered from internal and third-party
Subcutaneous ICD S-ICD Protection without touching the heart Patient Brochure IMPORTANT Please Note: Information provided by Boston Scientific Corporation (BSC) is gathered from internal and third-party
A SIMPLE SOLUTION FOR CARDIAC MONITORING
 A SIMPLE SOLUTION FOR CARDIAC MONITORING SEEQ Mobile Cardiac Telemetry System Actual size. NOW THERE S AN EXTERNAL HEART MONITOR THAT S AS SIMPLE TO WEAR AS A BANDAGE It s called the SEEQ Mobile Cardiac
A SIMPLE SOLUTION FOR CARDIAC MONITORING SEEQ Mobile Cardiac Telemetry System Actual size. NOW THERE S AN EXTERNAL HEART MONITOR THAT S AS SIMPLE TO WEAR AS A BANDAGE It s called the SEEQ Mobile Cardiac
ICD Implantation Patient Information
 Melbourne Heart Rhythm ICD Implantation Patient Information The Heart The heart is a pump responsible for maintaining blood supply to the body. It has four chambers. The two upper chambers (the right atrium
Melbourne Heart Rhythm ICD Implantation Patient Information The Heart The heart is a pump responsible for maintaining blood supply to the body. It has four chambers. The two upper chambers (the right atrium
After Your Pacemaker Generator Change
 UW MEDICINE PATIENT EDUCATION After Your Pacemaker Generator Change What you need to know Who to Call If you have questions about your appointments, call the Cardiology Clinic at 206.598.4300. If you have
UW MEDICINE PATIENT EDUCATION After Your Pacemaker Generator Change What you need to know Who to Call If you have questions about your appointments, call the Cardiology Clinic at 206.598.4300. If you have
You and your pacemaker
 You and your pacemaker You and your pacemaker Why do I need a pacemaker? A pacemaker will help improve your heart s rate. It is used to help your heart beat at a normal rate. What is a pacemaker? A pacemaker
You and your pacemaker You and your pacemaker Why do I need a pacemaker? A pacemaker will help improve your heart s rate. It is used to help your heart beat at a normal rate. What is a pacemaker? A pacemaker
Caring for Your Pacemaker
 UW MEDICINE PATIENT EDUCATION Caring for Your Pacemaker What you need to know Who to Call If you have questions about your appointments, call the Cardiology Clinic at 206.598.4300. If you have a question
UW MEDICINE PATIENT EDUCATION Caring for Your Pacemaker What you need to know Who to Call If you have questions about your appointments, call the Cardiology Clinic at 206.598.4300. If you have a question
THE HEART THE CIRCULATORY SYSTEM
 THE HEART THE CIRCULATORY SYSTEM There are three primary closed cycles: 1) Cardiac circulation pathway of blood within the heart 2) Pulmonary circulation blood from the heart to lungs and back 3) Systemic
THE HEART THE CIRCULATORY SYSTEM There are three primary closed cycles: 1) Cardiac circulation pathway of blood within the heart 2) Pulmonary circulation blood from the heart to lungs and back 3) Systemic
GUIDE TO ATRIAL FIBRILLATION
 PATIENT INFORMATION GUIDE TO ATRIAL FIBRILLATION Atrial Fibrillation (AF) Atrial Flutter (AFL) Rate and Rhythm Control Stroke Prevention This document is endorsed by: A Comprehensive Resource from the
PATIENT INFORMATION GUIDE TO ATRIAL FIBRILLATION Atrial Fibrillation (AF) Atrial Flutter (AFL) Rate and Rhythm Control Stroke Prevention This document is endorsed by: A Comprehensive Resource from the
WHAT CAN I DO ABOUT ATRIAL FIBRILLATION? Finding answers about atrial fibrillation
 WHAT CAN I DO ABOUT ATRIAL FIBRILLATION? Finding answers about atrial fibrillation DEBBIE S STORY With a full schedule of entertaining friends, dancing, working as a nurse and babysitting her granddog,
WHAT CAN I DO ABOUT ATRIAL FIBRILLATION? Finding answers about atrial fibrillation DEBBIE S STORY With a full schedule of entertaining friends, dancing, working as a nurse and babysitting her granddog,
UNDERSTANDING PACEMAKERS
 UNDERSTANDING PACEMAKERS Living Well with a Pacemaker Why You Need a Pacemaker Your heart has an electrical system that keeps it beating at the right speed. Problems with this system can make your heart
UNDERSTANDING PACEMAKERS Living Well with a Pacemaker Why You Need a Pacemaker Your heart has an electrical system that keeps it beating at the right speed. Problems with this system can make your heart
Cardiac Catheterization
 Cardiac Catheterization What is cardiac catheterization? Cardiac catheterization is a procedure used to diagnose and treat cardiovascular conditions. During cardiac catheterization, a long thin tube called
Cardiac Catheterization What is cardiac catheterization? Cardiac catheterization is a procedure used to diagnose and treat cardiovascular conditions. During cardiac catheterization, a long thin tube called
Guide to Cardiology Care at Scripps
 Guide to Cardiology Care at Scripps Cardiology is the word in health care associated with heart, but the body s vascular system is also an important part of heart care. Your body has more than 60,000 miles
Guide to Cardiology Care at Scripps Cardiology is the word in health care associated with heart, but the body s vascular system is also an important part of heart care. Your body has more than 60,000 miles
Cardiac Resynchronisation Therapy Defibrillator (CRT-D)
 Patient information Cardiac Resynchronisation Therapy Defibrillator (CRT-D) i Important information for all patients requiring resynchronisation therapy. Golden Jubilee National Hospital Agamemnon Street
Patient information Cardiac Resynchronisation Therapy Defibrillator (CRT-D) i Important information for all patients requiring resynchronisation therapy. Golden Jubilee National Hospital Agamemnon Street
Cardiac Resynchronisation Therapy Patient Information
 Melbourne Heart Rhythm Cardiac Resynchronisation Therapy Patient Information Normal Heart Function The heart is a pump responsible for maintaining blood supply to the body. It has four chambers. The two
Melbourne Heart Rhythm Cardiac Resynchronisation Therapy Patient Information Normal Heart Function The heart is a pump responsible for maintaining blood supply to the body. It has four chambers. The two
HEART DISEASE HEART CONDITIONS, RISKS AND PROTECTION
 Spotlight on Health 2017 HEART DISEASE HEART CONDITIONS, RISKS AND PROTECTION Heart disease is the leading cause of death for both men and women worldwide, accounting for over 17 million deaths per year.
Spotlight on Health 2017 HEART DISEASE HEART CONDITIONS, RISKS AND PROTECTION Heart disease is the leading cause of death for both men and women worldwide, accounting for over 17 million deaths per year.
Heart Disease. Signs and Symptoms
 Heart Disease The term "heart disease" refers to several types of heart conditions. The most common type is coronary artery disease, which can cause heart attack, angina, heart failure, and arrhythmias.
Heart Disease The term "heart disease" refers to several types of heart conditions. The most common type is coronary artery disease, which can cause heart attack, angina, heart failure, and arrhythmias.
Stress testing may be done at a doctor's office or at a hospital. It will usually take between 1 and 3 hours.
 STRESS TESTING WHAT IS IT? Stress testing provides your doctor with information about how your heart works during physical stress. Some heart problems are easier to diagnose when your heart is working
STRESS TESTING WHAT IS IT? Stress testing provides your doctor with information about how your heart works during physical stress. Some heart problems are easier to diagnose when your heart is working
12.1 Apply Your Knowledge How long does an ambulatory monitor typically remain on a patient?
 1 2 3 4 5 6 7 Learning Outcomes (Cont d) 12.4 Educate the patient about ambulatory monitoring. 12.5 Prepare a patient for application of an ambulatory monitor. 12.6 Describe the procedure for applying
1 2 3 4 5 6 7 Learning Outcomes (Cont d) 12.4 Educate the patient about ambulatory monitoring. 12.5 Prepare a patient for application of an ambulatory monitor. 12.6 Describe the procedure for applying
Electrocardiography for Healthcare Professionals
 Electrocardiography for Healthcare Professionals Kathryn A. Booth Thomas O Brien Chapter 12: Ambulatory Monitoring 1 Learning Outcomes 12.1 Identify the types of ambulatory monitors and their functions.
Electrocardiography for Healthcare Professionals Kathryn A. Booth Thomas O Brien Chapter 12: Ambulatory Monitoring 1 Learning Outcomes 12.1 Identify the types of ambulatory monitors and their functions.
Patient Resources: Syncope
 Patient Resources: Syncope Overview Syncope is the medical term for fainting or loss of consciousness. Fainting can occur for a few different reasons. The autonomic (involuntary) nervous system helps to
Patient Resources: Syncope Overview Syncope is the medical term for fainting or loss of consciousness. Fainting can occur for a few different reasons. The autonomic (involuntary) nervous system helps to
Mitral Regurgitation
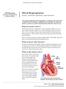 UW MEDICINE PATIENT EDUCATION Mitral Regurgitation Causes, symptoms, diagnosis, and treatment This handout describes mitral regurgitation, a disease of the mitral valve. It explains how this disease is
UW MEDICINE PATIENT EDUCATION Mitral Regurgitation Causes, symptoms, diagnosis, and treatment This handout describes mitral regurgitation, a disease of the mitral valve. It explains how this disease is
Atrial Fibrillation & Arrhythmias
 Atrial Fibrillation & Arrhythmias Symptoms and Treatments FloridaHospital.com Atrial Fibrillation According to the American Heart Association, Atrial fibrillation (AF) affects an estimated 2.7 million
Atrial Fibrillation & Arrhythmias Symptoms and Treatments FloridaHospital.com Atrial Fibrillation According to the American Heart Association, Atrial fibrillation (AF) affects an estimated 2.7 million
Heart Valve Replacement
 Heart Valve Replacement Introduction Sometimes people have serious problems with the valves in their hearts. A heart valve repair or replacement surgery restores or replaces a defective heart valve. If
Heart Valve Replacement Introduction Sometimes people have serious problems with the valves in their hearts. A heart valve repair or replacement surgery restores or replaces a defective heart valve. If
Implant Procedure Concepts
 1 4 7 2 5 LV Lead 8 3 6 Implant Procedure Concepts 9 ICD and CRT LV Lead This presentation is provided with the understanding that the slide content must not be altered in any manner as the content is
1 4 7 2 5 LV Lead 8 3 6 Implant Procedure Concepts 9 ICD and CRT LV Lead This presentation is provided with the understanding that the slide content must not be altered in any manner as the content is
CONFIRM Rx INSERTABLE CARDIAC MONITOR CONTINUOUS HEART MONITORING LIVE LIFE WITHOUT SKIPPING A BEAT
 CONFIRM Rx INSERTABLE CARDIAC MONITOR CONTINUOUS HEART MONITORING LIVE LIFE WITHOUT SKIPPING A BEAT FIND YOUR RHYTHM DON T IGNORE THE SYMPTOMS OF AN IRREGULAR HEARTBEAT 7.1 MILLION Up to 7.1 million people
CONFIRM Rx INSERTABLE CARDIAC MONITOR CONTINUOUS HEART MONITORING LIVE LIFE WITHOUT SKIPPING A BEAT FIND YOUR RHYTHM DON T IGNORE THE SYMPTOMS OF AN IRREGULAR HEARTBEAT 7.1 MILLION Up to 7.1 million people
2
 1 2 Although the term "cardiomyopathy" could theoretically apply to almost any disease affecting the heart, it is usually reserved for "severe myocardial disease leading to heart failure".cardiomyopathy
1 2 Although the term "cardiomyopathy" could theoretically apply to almost any disease affecting the heart, it is usually reserved for "severe myocardial disease leading to heart failure".cardiomyopathy
For Your ICD. Patient Manual A COMPANY DEDICATED TO PATIENTS
 For Your ICD Patient Manual A COMPANY DEDICATED TO PATIENTS Medtronic was founded in 1949 by Earl Bakken, a graduate student in electrical engineering, and his brother-in-law, Palmer J. Hermundslie. Today
For Your ICD Patient Manual A COMPANY DEDICATED TO PATIENTS Medtronic was founded in 1949 by Earl Bakken, a graduate student in electrical engineering, and his brother-in-law, Palmer J. Hermundslie. Today
EMBLEM S-ICD System. Protection without touching your heart. Patient Brochure
 EMBLEM S-ICD System Protection without touching your heart Patient Brochure PROTECTION from SUDDEN CARDIAC ARREST It s impossible to predict when sudden cardiac arrest (SCA) might strike. Called a silent
EMBLEM S-ICD System Protection without touching your heart Patient Brochure PROTECTION from SUDDEN CARDIAC ARREST It s impossible to predict when sudden cardiac arrest (SCA) might strike. Called a silent
Patient guide: pfm Nit-Occlud PDA coil occlusion system. Catheter occlusion of. Patent Ductus Arteriosus. with the
 Patient guide: Catheter occlusion of Patent Ductus Arteriosus with the pfm Nit-Occlud PDA coil occlusion system pfm Produkte für die Medizin - AG Wankelstr. 60 D - 50996 Cologne Phone: +49 (0) 2236 96
Patient guide: Catheter occlusion of Patent Ductus Arteriosus with the pfm Nit-Occlud PDA coil occlusion system pfm Produkte für die Medizin - AG Wankelstr. 60 D - 50996 Cologne Phone: +49 (0) 2236 96
Parkinson s disease, Essential Tremor and primary dystonia
 Parkinson s disease, Essential Tremor and primary dystonia What is Deep Brain Stimulation and how does it work? Deep Brain Stimulation (DBS) uses one or two surgically implanted medical devices, similar
Parkinson s disease, Essential Tremor and primary dystonia What is Deep Brain Stimulation and how does it work? Deep Brain Stimulation (DBS) uses one or two surgically implanted medical devices, similar
Convulsive Disorder and Cardiac Disease. Running Rachael, Active Ashlee, Sassy Savannah
 Convulsive Disorder and Cardiac Disease Running Rachael, Active Ashlee, Sassy Savannah Convulsive Disorder Seizure is over. Pay attention to how long the seizure lasts. Stay calm. Make the person as comfortable
Convulsive Disorder and Cardiac Disease Running Rachael, Active Ashlee, Sassy Savannah Convulsive Disorder Seizure is over. Pay attention to how long the seizure lasts. Stay calm. Make the person as comfortable
ICD SUPPORT GROUP IRELAND
 www.irishheart.ie ICD SUPPORT GROUP IRELAND The ICD Support Group This is a voluntary group of people, all of whom have ICDs. It was set up in association with the Irish Heart Foundation to help people
www.irishheart.ie ICD SUPPORT GROUP IRELAND The ICD Support Group This is a voluntary group of people, all of whom have ICDs. It was set up in association with the Irish Heart Foundation to help people
Caring for Your Implantable Cardiac Defibrillator (ICD)
 Patient Education Caring for Your Implantable Cardiac Defibrillator (ICD) What you need to know Weekdays between 8 a.m. and 4:30 p.m., call an Electrophysiology (EP) Nurse at 206-598-4555. Weekends, holidays,
Patient Education Caring for Your Implantable Cardiac Defibrillator (ICD) What you need to know Weekdays between 8 a.m. and 4:30 p.m., call an Electrophysiology (EP) Nurse at 206-598-4555. Weekends, holidays,
Pacemaker and AV Node Ablation Patient Information
 Melbourne Heart Rhythm Pacemaker and AV Node Ablation Patient Information The Heart The heart is a pump responsible for maintaining blood supply to the body. It has four chambers. The two upper chambers
Melbourne Heart Rhythm Pacemaker and AV Node Ablation Patient Information The Heart The heart is a pump responsible for maintaining blood supply to the body. It has four chambers. The two upper chambers
Implantation of an Implantable Cardioverter Defibrillator (ICD)
 PLEASE PRINT WHOLE FORM DOUBLE SIDED ON YELLOW PAPER Patient Information to be retained by patient affix patient label What is an Implantable? Your doctor has recommended that you have an Implantable.
PLEASE PRINT WHOLE FORM DOUBLE SIDED ON YELLOW PAPER Patient Information to be retained by patient affix patient label What is an Implantable? Your doctor has recommended that you have an Implantable.
THE MEDTRONIC TRANSCATHETER AORTIC VALVE REPLACEMENT (TAVR) SYSTEM
 THE MEDTRONIC TRANSCATHETER AORTIC VALVE REPLACEMENT (TAVR) SYSTEM 1 A Guide for Patients With Severe Aortic Stenosis medtronic.com/tavr Table of Contents 2 3 We have created this booklet to help you learn
THE MEDTRONIC TRANSCATHETER AORTIC VALVE REPLACEMENT (TAVR) SYSTEM 1 A Guide for Patients With Severe Aortic Stenosis medtronic.com/tavr Table of Contents 2 3 We have created this booklet to help you learn
X-Plain Atrial Fibrillation Reference Summary
 X-Plain Atrial Fibrillation Reference Summary Introduction Atrial fibrillation is a common heart condition that affects approximately 2.5 million Americans every year. Atrial fibrillation requires immediate
X-Plain Atrial Fibrillation Reference Summary Introduction Atrial fibrillation is a common heart condition that affects approximately 2.5 million Americans every year. Atrial fibrillation requires immediate
Electrophysiology Studies and Catheter Ablation. Electrophysiology Studies and Catheter Ablation
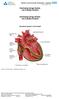 Electrophysiology Studies Cardiac Conduction System. Mdmedicine.wordpress.com Patient Information Leaflet for: Electrophysiology Studies Available via Trust Docs Version: 6 Trust Docs ID: 10 Page 1 of
Electrophysiology Studies Cardiac Conduction System. Mdmedicine.wordpress.com Patient Information Leaflet for: Electrophysiology Studies Available via Trust Docs Version: 6 Trust Docs ID: 10 Page 1 of
Direct Current (DC) Cardioversion
 Page 1 of 10 Direct Current (DC) Cardioversion Introduction This leaflet is to inform you about your planned Direct Current (DC) electrical cardioversion. A cardioversion is an electrical treatment which
Page 1 of 10 Direct Current (DC) Cardioversion Introduction This leaflet is to inform you about your planned Direct Current (DC) electrical cardioversion. A cardioversion is an electrical treatment which
Cardiac Resynchronization Therapy with Defibrillation (CRT-D)
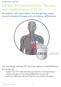 A decision aid for Cardiac Resynchronization Therapy with Defibrillation (CRT-D) For patients with heart failure who are getting cardiac resynchronization therapy and considering defibrillation CRT-D See
A decision aid for Cardiac Resynchronization Therapy with Defibrillation (CRT-D) For patients with heart failure who are getting cardiac resynchronization therapy and considering defibrillation CRT-D See
Understanding Atrial Fibrillation
 Understanding Atrial Fibrillation Todd J. Florin, M.D. Table of Contents The Normal Heart...1 What is Atrial Fibrillation...3 Risks of Afib: Stroke...5 Treatment Options...7 Radiofrequency Ablation...9
Understanding Atrial Fibrillation Todd J. Florin, M.D. Table of Contents The Normal Heart...1 What is Atrial Fibrillation...3 Risks of Afib: Stroke...5 Treatment Options...7 Radiofrequency Ablation...9
Emergency Department Management of Patients with Implantable Cardioverter Defibrillators
 IAEM Clinical Guideline Emergency Department Management of Patients with Implantable Cardioverter Defibrillators Version 1 June 2014 DISCLAIMER IAEM recognises that patients, their situations, Emergency
IAEM Clinical Guideline Emergency Department Management of Patients with Implantable Cardioverter Defibrillators Version 1 June 2014 DISCLAIMER IAEM recognises that patients, their situations, Emergency
Less Invasive Ventricular Enhancement For Heart Attack Patients. Revivent TC TransCatheter Ventricular Enhancement System
 For Heart Attack Patients Revivent TC TransCatheter Ventricular Enhancement System This patient booklet is for those who have suffered a heart attack resulting in damage to the left side of the heart causing
For Heart Attack Patients Revivent TC TransCatheter Ventricular Enhancement System This patient booklet is for those who have suffered a heart attack resulting in damage to the left side of the heart causing
ICD Your quick guide. British Heart Foundation 2017, a registered charity in England & Wales (225971) and Scotland (SC039426).
 ICD Your quick guide Coronary heart disease is the UK s single biggest killer. For over 50 years we ve pioneered research that s transformed the lives of people living with heart and circulatory conditions.
ICD Your quick guide Coronary heart disease is the UK s single biggest killer. For over 50 years we ve pioneered research that s transformed the lives of people living with heart and circulatory conditions.
Subcutaneous implantable cardioverter defibrillator insertion for preventing sudden cardiac death
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Subcutaneous implantable cardioverter defibrillator insertion for preventing sudden cardiac death A subcutaneous
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Subcutaneous implantable cardioverter defibrillator insertion for preventing sudden cardiac death A subcutaneous
Inserting an internal cardioverter defibrillator
 Inserting an internal cardioverter defibrillator Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that
Inserting an internal cardioverter defibrillator Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that
Heart Failure. Symptoms and Treatments. FloridaHospital.com
 Heart Failure Symptoms and Treatments FloridaHospital.com Understanding Heart Failure According to the American Heart Association, one in five people over age 40 will develop heart failure. Right now,
Heart Failure Symptoms and Treatments FloridaHospital.com Understanding Heart Failure According to the American Heart Association, one in five people over age 40 will develop heart failure. Right now,
Sudden Cardiac Death in Youth Athletes. Dublin City Schools Athletic Health Care
 Sudden Cardiac Death in Youth Athletes Dublin City Schools Athletic Health Care Sudden Cardiac Death What is sudden cardiac death in the young athlete? Sudden cardiac death is the result of an unexpected
Sudden Cardiac Death in Youth Athletes Dublin City Schools Athletic Health Care Sudden Cardiac Death What is sudden cardiac death in the young athlete? Sudden cardiac death is the result of an unexpected
Trans-catheter aortic valve implantation (TAVI) work up
 Trans-catheter aortic valve implantation (TAVI) work up You have been referred for an assessment known as a TAVI work up because you have been diagnosed with aortic stenosis. This factsheet explains the
Trans-catheter aortic valve implantation (TAVI) work up You have been referred for an assessment known as a TAVI work up because you have been diagnosed with aortic stenosis. This factsheet explains the
Cardiac Catheterization Lab Procedures
 Patient Education Cardiac Catheterization Lab Procedures This booklet describes cardiac catheterization. It also details how to prepare for the procedure and the care needed after it is done. Before You
Patient Education Cardiac Catheterization Lab Procedures This booklet describes cardiac catheterization. It also details how to prepare for the procedure and the care needed after it is done. Before You
MEDICAL POLICY Cardioverter Defibrillators
 POLICY........ PG-0224 EFFECTIVE......06/01/09 LAST REVIEW... 01/27/17 MEDICAL POLICY Cardioverter Defibrillators GUIDELINES This policy does not certify benefits or authorization of benefits, which is
POLICY........ PG-0224 EFFECTIVE......06/01/09 LAST REVIEW... 01/27/17 MEDICAL POLICY Cardioverter Defibrillators GUIDELINES This policy does not certify benefits or authorization of benefits, which is
WHY AM I FAINTING? Finding answers about unexplained fainting
 WHY AM I FAINTING? Finding answers about unexplained fainting PERSONAL STORIES For about 15 years, Lloyd s friends and family thought he was clumsy. Each spring, he seemed to have an unusual accident.
WHY AM I FAINTING? Finding answers about unexplained fainting PERSONAL STORIES For about 15 years, Lloyd s friends and family thought he was clumsy. Each spring, he seemed to have an unusual accident.
You have been referred to the Hamilton General Hospital to assess if having your mitral heart valve repaired with a mitral clip is right for you.
 Mitral Clip Procedure You have been referred to the Hamilton General Hospital to assess if having your mitral heart valve repaired with a mitral clip is right for you. 2 Mitral Clip Procedure What is mitral
Mitral Clip Procedure You have been referred to the Hamilton General Hospital to assess if having your mitral heart valve repaired with a mitral clip is right for you. 2 Mitral Clip Procedure What is mitral
OBJECTIVE. 1. Define defibrillation. 2. Describe Need and history of defibrillation. 3. Describe the principle and mechanism of defibrillation.
 Defibrillators OBJECTIVE 1. Define defibrillation. 2. Describe Need and history of defibrillation. 3. Describe the principle and mechanism of defibrillation. 4. Types and classes of defibrillator 5. Describe
Defibrillators OBJECTIVE 1. Define defibrillation. 2. Describe Need and history of defibrillation. 3. Describe the principle and mechanism of defibrillation. 4. Types and classes of defibrillator 5. Describe
Neurostimulation. Spinal cord stimulators use electrodes placed in the space surrounding the spinal cord (epidural space).
 Neurostimulation.305145613.pdf 1 8/11/12 11:32 PM Neurostimulation Neurostimulation, also called electrostimulation, uses low-level electrical impulses to interfere with pain signals or block them from
Neurostimulation.305145613.pdf 1 8/11/12 11:32 PM Neurostimulation Neurostimulation, also called electrostimulation, uses low-level electrical impulses to interfere with pain signals or block them from
About Your Ventricular Assist Device (VAD) Surgery
 About Your Ventricular Assist Device (VAD) Surgery Why do I need surgery for a Heart Pump or Ventricular Assist Device (VAD)? VAD s may help you live longer. These electric powered heart pumps are put
About Your Ventricular Assist Device (VAD) Surgery Why do I need surgery for a Heart Pump or Ventricular Assist Device (VAD)? VAD s may help you live longer. These electric powered heart pumps are put
ICDs: Implantable. A Guide for Patients and Families 40 RUSKIN STREET, OTTAWA ON K1Y 4W7 T UOHI 75 (11/2014)
 ICDs: Implantable Cardioverter Defibrillators A Guide for Patients and Families UOHI 75 (11/2014) 40 RUSKIN STREET, OTTAWA ON K1Y 4W7 T 613.696-7000 WWW.OTTAWAHEART.CA Patient Name PLEASE BRING THIS BOOK
ICDs: Implantable Cardioverter Defibrillators A Guide for Patients and Families UOHI 75 (11/2014) 40 RUSKIN STREET, OTTAWA ON K1Y 4W7 T 613.696-7000 WWW.OTTAWAHEART.CA Patient Name PLEASE BRING THIS BOOK
THERAPY Baclofen Pump Program at Boston Children s Hospital
 BACLOFEN PUMP THERAPY Baclofen Pump Program at Boston Children s Hospital PAGER: 617-355-6369 and ask to page #7867 (PUMP) 1 Contents What is spasticity?... 3 What is baclofen?... 3 The evaluation for
BACLOFEN PUMP THERAPY Baclofen Pump Program at Boston Children s Hospital PAGER: 617-355-6369 and ask to page #7867 (PUMP) 1 Contents What is spasticity?... 3 What is baclofen?... 3 The evaluation for
Heart Problems and Treatments
 Heart Problems and Treatments A healthy heart Your heart s main functions are to receive used blood from your body and pump fresh oxygen rich blood to nourish your body. To do this well: The heart muscle
Heart Problems and Treatments A healthy heart Your heart s main functions are to receive used blood from your body and pump fresh oxygen rich blood to nourish your body. To do this well: The heart muscle
PhD FRCP MESC MEAPCI. Consultant Cardiologist SVT - Supra Ventricular Tachycardia. Coronary Arteries
 SVT - Supra Ventricular Tachycardia Coronary Arteries Overview LMS Supraventricular tachycardia is defined as an abnormally fast heartbeat. It's a describes a group of arrhythmias which all originate from
SVT - Supra Ventricular Tachycardia Coronary Arteries Overview LMS Supraventricular tachycardia is defined as an abnormally fast heartbeat. It's a describes a group of arrhythmias which all originate from
Special health. guide. Hugh Calkins, M.D., and Ronald Berger, M.D., Ph.D. Guide to Understanding. Atrial Fibrillation WITH
 Hugh Calkins, M.D., and Ronald Berger, M.D., Ph.D. Guide to Understanding Atrial Fibrillation WITH Table of Contents Atrial Fibrillation: An Introduction... 1 How AF Affects the Heart... 2 Who Gets AF?...
Hugh Calkins, M.D., and Ronald Berger, M.D., Ph.D. Guide to Understanding Atrial Fibrillation WITH Table of Contents Atrial Fibrillation: An Introduction... 1 How AF Affects the Heart... 2 Who Gets AF?...
C1: Medical Standards for Safety Critical Workers with Cardiovascular Disorders
 C1: Medical Standards for Safety Critical Workers with Cardiovascular Disorders GENERAL ISSUES REGARDING MEDICAL FITNESS-FOR-DUTY 1. These medical standards apply to Union Pacific Railroad (UPRR) employees
C1: Medical Standards for Safety Critical Workers with Cardiovascular Disorders GENERAL ISSUES REGARDING MEDICAL FITNESS-FOR-DUTY 1. These medical standards apply to Union Pacific Railroad (UPRR) employees
Flowchart for ICD patients undergoing Surgery or procedures involving diathermy/magnetic fields
 Flowchart for ICD patients undergoing Surgery or procedures involving diathermy/magnetic fields Identify patient with an ICD at POAC. Notify Cardiac Physiologist that patient is due to have surgery and
Flowchart for ICD patients undergoing Surgery or procedures involving diathermy/magnetic fields Identify patient with an ICD at POAC. Notify Cardiac Physiologist that patient is due to have surgery and
Cardiac Implanted Electronic Devices Pacemakers, Defibrillators, Cardiac Resynchronization Devices, Loop Recorders, etc.
 Cardiac Implanted Electronic Devices Pacemakers, Defibrillators, Cardiac Resynchronization Devices, Loop Recorders, etc. The Miracle of Living February 21, 2018 Matthew Ostrom MD,FACC,FHRS Division of
Cardiac Implanted Electronic Devices Pacemakers, Defibrillators, Cardiac Resynchronization Devices, Loop Recorders, etc. The Miracle of Living February 21, 2018 Matthew Ostrom MD,FACC,FHRS Division of
SJM MRI ACTIVATOR HANDHELD DEVICE WORKFLOW Model: EX4000. SJM-EDTR Item approved for U.S. use only.
 SJM MRI ACTIVATOR HANDHELD DEVICE WORKFLOW Model: EX4000 1 APPROVED MRI SCAN CONDITIONS 1.5 TESLA FULL BODY 2 SETUP SJM MRI ACTIVATOR HANDHELD DEVICE The SJM MRI Activator handheld device must be enabled
SJM MRI ACTIVATOR HANDHELD DEVICE WORKFLOW Model: EX4000 1 APPROVED MRI SCAN CONDITIONS 1.5 TESLA FULL BODY 2 SETUP SJM MRI ACTIVATOR HANDHELD DEVICE The SJM MRI Activator handheld device must be enabled
