Management of Burns under Prolonged Field Care
|
|
|
- David Ball
- 5 years ago
- Views:
Transcription
1 This Role 1, prolonged field care (PFC) guideline is intended to be used after TCCC Guidelines when evacuation to higher level of care is not immediately possible. A provider of PFC must first and foremost be an expert in TCCC. This Clinical Practice Guideline (CPG) is meant to provide medical professionals who encounter burns in austere environments with evidence- based guidance. Recommendations follow a minimum, better, best format that provides alternate or improvised methods when optimal hospital options are unavailable. Burns > 20% of the total body surface area (TBSA), or those with smoke inhalation injury (and airway or breathing problems), are potentially life threatening. Also, burns that affect vision, decrease hand function, or cause severe pain can take the warfighter out of action. Telemedicine: Management of burns is complex. Also, burns are highly visual and a lot can be communicated via pictures or video. Establish telemedicine consult as soon as possible. v Airway management: Goal: Avoid airway obstruction due to inhalation injury or burn- induced swelling. Patients with smoke inhalation injury may present with a range of symptoms in terms of severity. Patients with severely symptomatic smoke inhalation injury (e.g. respiratory distress, stridor) require immediate definitive airway (cuffed tube in trachea) as they are at risk of immediate airway loss. Oxygenate and ventilate. Best: Rapid sequence intubation by skilled provider, followed by continuous sedation and airway maintenance, supplemental oxygen, portable ventilator. Better: Cricothyroidotomy followed by continuous sedation and airway maintenance, supplemental oxygen via an oxygen concentrator, portable ventilator. Minimum: Cricothyroidotomy, ketamine, bag- valve mask with PEEP valve. Notes: Patients with mild symptoms of smoke inhalation injury (e.g. some cough, no respiratory distress) can be observed. Burns or explosions in a closed space are at higher risk of inhalation injury compared with explosions in open areas. All patients with burn size > 40% should be intubated as total- body swelling will tend to obstruct the airway. Some patients with facial burns may require intubation based on exam. Supraglottic airway (laryngeal mask airway [LMA], King LT, or Combitube) is not appropriate. Endotracheal tube must be secured circumferentially around the neck using cotton ties or similar. Tape does not stick to the face well enough in burn patients. Place nasogastric (or orogastric) tube to decompress stomach in intubated patients. 1
2 Do frequent endotracheal suction of intubated patients to ensure tube patency and remove mucus/debris. Monitoring end- tidal CO 2 is an important capability for all intubated patients. A rising end- tidal CO 2 could indicate clogging of endotracheal tube, or poor ventilation from another cause (bronchospasm; tight eschar across chest). Use positive end- expiratory pressure (PEEP) on all intubated patients. Do a surgical escharotomy of the chest for tight, circumferential, full thickness burns which impair breathing. Incision goes through the full thickness of the burn and into the fat. Expect some pain and bleeding. See Figure. Use bronchodilators (e.g., albuterol inhaler) for intubated patients with inhalation injury. Ventilator management of burn patient can be complicated and evolve as pulmonary conditions change due to volume overload/edema and ARDS. Telemedicine consultation with skilled providers is recommended. v Fluid Resuscitation: The principles of hypotensive resuscitation according to TCCC DO NOT apply in the setting of burns (without severe bleeding). HOWEVER In the unusual setting of burns associated with non- compressible (thoracic, abdominal, pelvic) hemorrhage, aggressive fluid resuscitation may result in increased hemorrhage. Balancing the risk of uncontrolled hemorrhage against the risk of worsening burn shock from under- resuscitation should be guided by expert medical advice (in- person or telemedicine). Goal: Over the first 24 to 48 hours postburn, plasma is lost into the burned and unburned tissues, causing hypovolemic shock (when burn size > 20%). The goal of burn- shock resuscitation is to replace these ongoing losses while avoiding over- resuscitation. Best: Isotonic crystalloids (e.g. lactated Ringer s, Plasmalyte); hourly urine Start IV or intra- osseous (IO) administration IMMEDIATELY IV/IO can be placed through burned skin if necessary. NO bolus (unless hypotensive- - in which case, bolus only till palpable pulses restored) Initial IV rate 500 ml/hour Measure burn size (TBSA), and multiply by 10. This is your starting IV fluid rate. Ex: burn size is 30%, 30x10=300. Starting rate is 300 ml/hr. For patients with weight > 80 kg, add an extra 100 ml/hr for each 10 kg. Ex: for a 100 kg patient with 30% burns, starting rate is 300 ml/hr ml/hr = 500 ml/hr. There is no need to catch up if resuscitation is delayed. Better: enteral (oral or gastric) intake of electrolyte solution 2
3 Sufficient volume replacement will require coached drinking on a schedule. Oral resuscitation of patients with burns up to about 30% TBSA should be possible (see box). If nasogastric tube (NGT) available, can also resuscitate with slow infusion of electrolyte solution via NGT, e.g ml/hr. But: watch for nausea/vomiting. Minimum: rectal infusion of electrolyte solution Rectal infusion of up to 500 ml/hr can be supplemented with oral hydration (see box) Plain water is ineffective for shock resuscitation and can cause hyponatremia. If using oral or rectal fluids, they must be in the form of a pre- mixed or improvised electrolyte solution to reduce this risk. Examples of mixed or improvised electrolyte solutions include: World Health Organization (WHO) Oral Rehydration Solution Mix 1 liter of D5W with 2 liters of Plasmalyte Per 1 L water: add 8 tsp sugar, 0.5 tsp salt, 0.5 tsp baking soda Per quart of Gatorade: add 0.25 tsp salt, 0.25 tsp baking soda (If no baking soda: double the amount of salt in the recipe.) v Monitoring- Vital signs Best: Portable monitor providing continuous vital- sign display; capnography if intubated; document vital sign trends frequently. Better: Capnometry in addition to minimum requirements (if intubated). Minimum: blood pressure cuff, stethoscope, pulse oximetry, document vital sign trends frequently. Document blood pressure (BP), heart rate (HR), urine output (UO), mental status, pain, pulse oximetry, temperature and input on a flowsheet (see Appendix B). Urine Output is the main indicator of resuscitation adequacy in burn shock Goal: adjust IV (or oral/rectal intake) rate to urine output (UO) goal of ml/hr. Best: place Foley catheter If UO too low, increase IV rate by 25% every hour or two. (Ex: if UO = 20 ml/hr and IV rate = 300 ml/hr, increase IV rate by 0.25x300 = 75 ml/hr. New rate is 375 ml/hr.) If UO too high, IV rate by 25%. Document vitals, UO, mental status, pain and input on a flow sheet (Appendix B). Better: capture urine in pre- made or improvised graduated cylinder Collect all spontaneously voided urine hourly and carefully measure; > 700 ml/day (3/4 of a liter water bottle) is adequate. A Nalgene bottle is an example of an improvised graduated cylinder. 3
4 Minimum: use other measures If unable to measure urine output, adjust IV rate to maintain heart rate (HR) < 140, palpable peripheral pulses, good capillary refill, intact mental status. Measure the blood pressure and consider treating hypotension, but remember: blood pressure does not decrease until relatively late in burn shock due to catecholamine release. On the other hand, blood pressure may be inaccurate (artificially low) in burned extremities. Note: electric injury Patients with high- voltage electric injury causing muscle damage and gross pigment in the urine (and similar patients, such as rhabdomyolysis or crush) have a higher target urine output of ml/hr in adults. See PFC Crush CPG. If this does not cause gradual clearing of the pigment (urine turns lighter on 3 or 4 hourly checks), the patient likely needs urgent surgery for decompression/debridement. v Extremity Burns- burned extremities are vulnerable to injury from postburn swelling. Goal: Prevent and manage swelling (edema) of burned extremities, to prevent long- term damage. Best: Elevate burned extremities above heart level. Encourage patient to exercise burned extremities to decrease edema. Monitor peripheral pulses on all burned extremities hourly, using a Doppler flowmeter if available. Do escharotomies of burned skin to restore blood flow. (Figure) Obtain teleconsultation. Better: Consider doing escharotomies for circumferential full thickness burns of an extremity if extremity is edematous, you are unable to palpate distal pulses, and evacuation will be delayed. Obtain teleconsultation. Minimum: Triage patient to more rapid evacuation if extremity is edematous and you are unable to palpate distal pulses. Elevate burned extremities above heart level and have patient exercise or provide passive range of motion (PROM) to burned extremities to mobilize edema. Provide pain control to enable PROM. v Pain Management refer to Analgesia and Sedation CPG. Burns can be painful, but can cause hypovolemia. Thus, frequent smaller doses of an IV opioid or ketamine are preferred. In hypovolemic burn patients, ketamine can be used for severe pain or for painful procedures, but less than the full anesthetic dose is safer; ex mg/kg IV push and assess response/re- dose ketamine as needed every 5-10 minutes. For prolonged care of burn patient, a ketamine infusion (detailed in Analgesia, Sedation CPG) may provide more consistent analgesia and help conserve supplies of analgesic medications. Consider administering an oral or IV benzodiazepine for anxiety (common with repeated painful wound care). v Infection- Burn wounds are easily infected. 4
5 Recommendation- Goal: Prevent burn- wound infection through wound care. Note. If evacuation to higher level of care is anticipated within 24 hours, cover burns with clean gauze. Leave intact blisters in place. Avoid wet dressings due to risk of hypothermia. If not: Best: Clean and debride wounds by scrubbing with chlorhexidine gluconate solution (ex. Hibiclens) in water; apply topical antimicrobial cream (silver sulfadiazine [Silvadene] or mafenide acetate [Sulfamylon]), followed by gauze dressing. Repeat daily. Alternative: instead of cream, use silver nylon dressing (Silverlon), followed by gauze dressing. Change Silverlon every 3 days. Better: Ensure wounds are cleaned and dressed; optimize wound and patient hygiene to the extent possible given environment. Minimum: Cover with clean sheet or dry gauze. Leave blisters in place. Avoid wet dressings. IV or oral antibiotics are not normally used for prophylaxis in burn patients. After several days, if patient develops cellulitis (spreading erythema around edges of burn), treat for gram- positive organisms. If patient develops invasive burn- wound infection (sepsis/septic shock, changes in color of wound, possible foul smell of wound) consider broad- spectrum antibiotics to include gram- negative coverage. 5
6 Appendix A - - Fluid and equipment planning considerations Assumptions: one patient with a 50% TBSA burn, weighing 80 kg, and requiring 500 ml/hr for resuscitation the first day (12 L), half that the 2 nd day (6 L), and half that the 3 rd day (3 L). Best: Fluids: IV fluid (lactated Ringer s solution or Plasmalyte) to provide resuscitation for 72 hours (21 L) Equipment: Portable monitor with capnography, lab capability for serum electrolytes, arterial blood gases, lactate, Foley catheter with graduated collection system, portable ventilator, portable suction, electrocautery or scapel, oxygen or oxygen concentrator, airway management kit to include endotracheal suction catheter Medications: pain medications (refer to Analgesia, Sedation CPG) Burn- specific dressings: Silver sulfadiazene and/or mafenide acetate cream (two 400 g jars per patient per day, or Silverlon dressings, Hibiclens to clean wounds. Non- specific dressings: roller gauze; torso dressings; tape or stapler Hypothermia prevention: Sleeping Bag/HPMK Monitoring: Portable monitor providing continuous vital sign display; capnography if intubated; document vital sign trends, intake and output, GCS, and pain level on a regular basisk, burn resuscitation flow sheet Communications: real- time video telemedicine consultation Push- pack capability: prepackaged additional 24- hour supplies of fluids, dressings for scenarios > 24 hours. Better: Fluids: IV fluid (lactated Ringer s solution or Plasmalyte) to provide 500 ml/hr for 24 hours (12 L); oral electrolyte replacement Equipment: Blood pressure cuff, stethoscope, pulse oximeter, capnometer, portable ventilator, oxygen or oxygen concentrator, airway management kit Graduated container to monitor urine output Pain medications Non- specific dressings: roller gauze; torso dressings; tape or stapler Hypothermia prevention: Sleeping Bag/HPMK/Blizzard Blanket Monitoring: Frequent vital signs, exam, fluid input, urine output, pain level, documented on flowsheet Communications: telephone; digital photos Minimum: Fluids: Resuscitation with commercial or improvised electrolyte solution (oral, enteral, rectal) Equipment: Blood pressure cuff, stethoscope, pulse oximeter, bag- valve mask with PEEP valve, airway management kit Graduated or improvised graduated container to monitor urine output Pain medications Clean sheet, any available trauma dressings Hypothermia prevention: Sleeping Bag/Emergency Blanket/Blankets Monitoring: Frequent vital signs, exam, fluid input, urine output documented on pre- printed or improvised flowsheet. Communications: telephone 6
7 Appendix B - - JTS Burn Resuscitation Flow Sheet Date Initial Treatment Facility Name SSN Pre-burn est. wt (kg) %TBSA (Do not include superficial 1 st degree burn) Calculate Rule of Tens (if >40<80kg, %TBSA x 10 = starting rate for LR Calculate max 24hr volume (250ml x kg) Avoid overresuscitation, use adjuncts if necessary Date &Time of Injury BAMC/ISR Burn Team DSN : Yes No Tx Site/ Team HR from burn Local Time Crystalloid* (LR) Colloid Total UOP (Target 30-50ml/hr) Base Deficit/ Lactate Heart Rate MAP (>55) / CVP (6-8 mmhg) Pressors (Vasopressin 0.04 u/min) Bladder Pressure (Q4) 1 st 2 nd 3 rd 4 th 5 th 6 th 7 th 8 th 9 th 10 th 11 th 12 th 13 th 14 th 15 th 16 th 17 th 18 th 19 th 20 th 21 st 22 nd 23 rd 24 th Total Fluids: (Use adjuncts if >24hr max) *Titrate LR hourly to maintain adequate UOP (30-50ml/hr) and tissue perfusion 7
8 Figure - - Escharotomy incisions Figure: Location of escharotomy incisions. The incisions on the extremities are placed along the mid- medial and/or mid- lateral joint lines. The bold lines indicate the importance of always carrying the incisions across any involved joints. The incisions on the chest are intended to free up a mobile plate of tissue, and thus to restore adequate chest movement with breathing. Source: Figure 26.1, p. 379, Chapter 26 (Burns). In: Anonymous, Emergency War Surgery, 4 th United States Revision. Fort Sam Houston, TX: Office of the Surgeon General, Borden Institute,
Contributors. Publication Date 13 Jan 2017
 JOINT TRAUMA SYS TEM CLINICAL PRACTIC E GUIDELINE (JTS CPG ) Burn Wound Management Under Prolonged Field Care (CPG ID: 57) This Role 1 prolonged field care (PFC) guideline is intended to be used after
JOINT TRAUMA SYS TEM CLINICAL PRACTIC E GUIDELINE (JTS CPG ) Burn Wound Management Under Prolonged Field Care (CPG ID: 57) This Role 1 prolonged field care (PFC) guideline is intended to be used after
The immediate management of burns patients should be similar to management of trauma.
 CATS Clinical Guideline Burns The National Burn Care Review recommends that children with burns should be treated in a Burn Centre. Chelsea and Westminster may take non-ventilated children, Broomfield
CATS Clinical Guideline Burns The National Burn Care Review recommends that children with burns should be treated in a Burn Centre. Chelsea and Westminster may take non-ventilated children, Broomfield
IMMEDIATE EMERGENCY BURN CARE » THERMAL BURNS » ELECTRICAL BURNS » CHEMICAL BURNS FIRST AID FOR THE THREE MAJOR CATEGORIES
 IMMEDIATE EMERGENCY BURN CARE 1. Treat according to BLS or ACLS Protocol 2. Use airway and C-Spine precautions. 3. Stop the burning process. FIRST AID FOR THE THREE MAJOR CATEGORIES» THERMAL BURNS + Stop
IMMEDIATE EMERGENCY BURN CARE 1. Treat according to BLS or ACLS Protocol 2. Use airway and C-Spine precautions. 3. Stop the burning process. FIRST AID FOR THE THREE MAJOR CATEGORIES» THERMAL BURNS + Stop
Burn Priorities of Care: Triage/Treatment/Transfer. Via Christi Regional Burn Center Sarah Fischer, MSN, RN
 Burn Priorities of Care: Triage/Treatment/Transfer Via Christi Regional Burn Center Sarah Fischer, MSN, RN Disclosure I have nothing to disclose Objectives Identify American Burn Association referral criteria
Burn Priorities of Care: Triage/Treatment/Transfer Via Christi Regional Burn Center Sarah Fischer, MSN, RN Disclosure I have nothing to disclose Objectives Identify American Burn Association referral criteria
Student Guide Module 4: Pediatric Trauma
 Student Guide Module 4: Pediatric Trauma Problem based learning exercise objectives Understand how to manage traumatic injuries in mass casualty events. Discuss the features and the approach to pediatric
Student Guide Module 4: Pediatric Trauma Problem based learning exercise objectives Understand how to manage traumatic injuries in mass casualty events. Discuss the features and the approach to pediatric
EmergencyKT: Management of Thermal Injury in Adult Patients
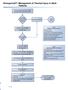 EmergencyKT: Management of Thermal Injury in Adult Patients Remove patient from source of injury, including burned clothing and jewelry Does patient appear to have minor burns? (See Box A) No Notify Burn
EmergencyKT: Management of Thermal Injury in Adult Patients Remove patient from source of injury, including burned clothing and jewelry Does patient appear to have minor burns? (See Box A) No Notify Burn
Approved By: Airway and Breathing A. Initially give humidified high flow oxygen at 15 L (100%) using a nonrebreather
 Subject: BURN CARE CLINICAL GUIDELINE Originator: Approval Date: 2015 Approved By: Policy: All burn patients presenting to XXXXXX Hospital will have appropriate assessment, stabilization and evaluation
Subject: BURN CARE CLINICAL GUIDELINE Originator: Approval Date: 2015 Approved By: Policy: All burn patients presenting to XXXXXX Hospital will have appropriate assessment, stabilization and evaluation
TBSA Burn Estimation Chart Adult Major Burn Clinical Practice Guideline
 TBSA Burn Estimation Chart Adult Major Burn Clinical Practice Guideline Patient Label Anatomical Subunit Percent Total Percent One Side Anterior Posterior Injury Subtotal 3.5% 2nd and 3rd degree burns
TBSA Burn Estimation Chart Adult Major Burn Clinical Practice Guideline Patient Label Anatomical Subunit Percent Total Percent One Side Anterior Posterior Injury Subtotal 3.5% 2nd and 3rd degree burns
Printed copies of this document may not be up to date, obtain the most recent version from
 Children s Acute Transport Service Clinical Guidelines Septic Shock Document Control Information Author Claire Fraser P.Ramnarayan Author Position tanp CATS Consultant Document Owner E. Polke Document
Children s Acute Transport Service Clinical Guidelines Septic Shock Document Control Information Author Claire Fraser P.Ramnarayan Author Position tanp CATS Consultant Document Owner E. Polke Document
INSTRUCTOR GUIDE FOR TACTICAL FIELD CARE 3B BURNS AND FRACTURES
 INSTRUCTOR GUIDE FOR TACTICAL FIELD CARE 3B BURNS AND FRACTURES 180801 1 Tactical Combat Casualty Care for Medical Personnel 1. August 2017 (Based on TCCC-MP Guidelines 180801 In this presentation, we
INSTRUCTOR GUIDE FOR TACTICAL FIELD CARE 3B BURNS AND FRACTURES 180801 1 Tactical Combat Casualty Care for Medical Personnel 1. August 2017 (Based on TCCC-MP Guidelines 180801 In this presentation, we
1/3/2008. Karen Burke Priscilla LeMone Elaine Mohn-Brown. Medical-Surgical Nursing Care, 2e Karen Burke, Priscilla LeMone, and Elaine Mohn-Brown
 Medical-Surgical Nursing Care Second Edition Karen Burke Priscilla LeMone Elaine Mohn-Brown Chapter 46 Caring for Clients with Burns Types of Burns Thermal Dry heat flame Moist heat steam or hot liquid
Medical-Surgical Nursing Care Second Edition Karen Burke Priscilla LeMone Elaine Mohn-Brown Chapter 46 Caring for Clients with Burns Types of Burns Thermal Dry heat flame Moist heat steam or hot liquid
Applicable to. Team Members Performing MD House Staff APRN/PA RN LPN
 Protocol: Adult Burn Fluid Resuscitation Category Clinical Practice Protocol Number Approval Date vember 1, 2016 Due for review vember 1, 2018 Applicable to VUH Children s DOT VMG Off-site locations VMG
Protocol: Adult Burn Fluid Resuscitation Category Clinical Practice Protocol Number Approval Date vember 1, 2016 Due for review vember 1, 2018 Applicable to VUH Children s DOT VMG Off-site locations VMG
Burn injury. A : patent airway with smoking inhalation, stridor. D: E4V5M6,pupil 2mm RTLBE
 Burn injury Pinyong Uthaitas Emergency Department Faculty of Medicine, Ramathibodi Hospital A Thai man 52 year old came to the hospital due to flam burn ½ hr ago at his house. He gain conscious but hoarseness
Burn injury Pinyong Uthaitas Emergency Department Faculty of Medicine, Ramathibodi Hospital A Thai man 52 year old came to the hospital due to flam burn ½ hr ago at his house. He gain conscious but hoarseness
Acute And perioperative care of the burn-injured patient. Anesthesiology, V 122, No 2
 Acute And perioperative care of the burn-injured patient Anesthesiology, V 122, No 2 Reporter:R4 沈士鈞 Supervisor: 蔡欣怡醫師 Pathophysiology Initial evaluation and management Anesthetic managemen nt Pathophysiology
Acute And perioperative care of the burn-injured patient Anesthesiology, V 122, No 2 Reporter:R4 沈士鈞 Supervisor: 蔡欣怡醫師 Pathophysiology Initial evaluation and management Anesthetic managemen nt Pathophysiology
Pediatric Burn Management Justin D. Klein, MD Associate Burn Director Lisa C. Vitale, RN Burn Program Coordinator
 Pediatric Burn Management Justin D. Klein, MD Associate Burn Director Lisa C. Vitale, RN Burn Program Coordinator Lecture Overview Burn statistics and etiologies Pre-hospital evaluation Anatomy of a burn
Pediatric Burn Management Justin D. Klein, MD Associate Burn Director Lisa C. Vitale, RN Burn Program Coordinator Lecture Overview Burn statistics and etiologies Pre-hospital evaluation Anatomy of a burn
Advanced Airway Management PRESENTED BY: JOSIAH POIRIER RN, JOHN GRUBER FP-C
 Advanced Airway Management PRESENTED BY: JOSIAH POIRIER RN, JOHN GRUBER FP-C Advanced Airway Objectives Advanced airway management is a relatively low frequency, high risk intervention. The following education
Advanced Airway Management PRESENTED BY: JOSIAH POIRIER RN, JOHN GRUBER FP-C Advanced Airway Objectives Advanced airway management is a relatively low frequency, high risk intervention. The following education
Objectives. Initial Burn Care and Fluid Resuscitation 6/5/2015 INITIAL MANAGEMENT
 Initial Burn Care and Fluid Resuscitation Sarah Taylor MSN, RN, ACNS-BC Clinical Nurse Specialist Trauma Burn Center University of Michigan Health System Ann Arbor, MI Objectives Discuss the initial assessment
Initial Burn Care and Fluid Resuscitation Sarah Taylor MSN, RN, ACNS-BC Clinical Nurse Specialist Trauma Burn Center University of Michigan Health System Ann Arbor, MI Objectives Discuss the initial assessment
HeartCode PALS. PALS Actions Overview > Legend. Contents
 HeartCode PALS PALS Actions Overview > Legend Action buttons (round buttons) Clicking a round button initiates an action. Clicking this button, for example, checks the child s carotid pulse. Menu buttons
HeartCode PALS PALS Actions Overview > Legend Action buttons (round buttons) Clicking a round button initiates an action. Clicking this button, for example, checks the child s carotid pulse. Menu buttons
Wisecracks 1. What are the indications for an escharotomy 2. What are the primary considerations in mechanical ventilation of burn patients
 Chapter 63 Thermal Burns Episode Overview Questions 1. List zones of burns 2. List 6 indications for intubation in the burn patient 3. List and describe 2 formulas for fluid resuscitation 4. Describe depth
Chapter 63 Thermal Burns Episode Overview Questions 1. List zones of burns 2. List 6 indications for intubation in the burn patient 3. List and describe 2 formulas for fluid resuscitation 4. Describe depth
Burns Management in the Emergency Department
 Management in the Emergency Department (Referral Proforma) Time/Date of injury (24hr) Patient demographic data sticker Airway Please remember to protect C-spine until clinically cleared as stable Administer
Management in the Emergency Department (Referral Proforma) Time/Date of injury (24hr) Patient demographic data sticker Airway Please remember to protect C-spine until clinically cleared as stable Administer
Standardize comprehensive care of the patient with severe traumatic brain injury
 Trauma Center Practice Management Guideline Iowa Methodist Medical Center Des Moines Management of Patients with Severe Traumatic Brain Injury (GCS < 9) ADULT Practice Management Guideline Contact: Trauma
Trauma Center Practice Management Guideline Iowa Methodist Medical Center Des Moines Management of Patients with Severe Traumatic Brain Injury (GCS < 9) ADULT Practice Management Guideline Contact: Trauma
Children's National Medical Center The Division of Trauma and Burn Burn Education Module Post-test
 Children's National Medical Center The Division of Trauma and Burn Burn Education Module Post-test Purpose: To provide nurses with on overview of burn injuries in pediatric patients. Learning Objectives:
Children's National Medical Center The Division of Trauma and Burn Burn Education Module Post-test Purpose: To provide nurses with on overview of burn injuries in pediatric patients. Learning Objectives:
Printed copies of this document may not be up to date, obtain the most recent version from Author Position
 Children s Acute Transport Service Clinical Guidelines Burns Management Document Control Information Author E Borrows E Randle Author Position PICU/BURNS Consultant CATS Consultant Document Owner E. Polke
Children s Acute Transport Service Clinical Guidelines Burns Management Document Control Information Author E Borrows E Randle Author Position PICU/BURNS Consultant CATS Consultant Document Owner E. Polke
BURNS MODULE. In the paediatric population consider non-accidental injury as a mechanism for burn injuries.
 BURNS MODULE INTRODUCTION Burns are a common cause of trauma. Most burn injuries are a result of flame burns, with scalds also occurring commonly. Electrical and chemical burns are less common. 1 Concurrent
BURNS MODULE INTRODUCTION Burns are a common cause of trauma. Most burn injuries are a result of flame burns, with scalds also occurring commonly. Electrical and chemical burns are less common. 1 Concurrent
Printed copies of this document may not be up to date, obtain the most recent version from Author Position
 Children s Acute Transport Service Clinical Guidelines Burns Management Document Control Information Author E Borrows E Randle, L Chigaru Author Position PICU/BURNS Consultant CATS Consultants Document
Children s Acute Transport Service Clinical Guidelines Burns Management Document Control Information Author E Borrows E Randle, L Chigaru Author Position PICU/BURNS Consultant CATS Consultants Document
Burns. A Comprehensive Review Assessment & Management
 Burns A Comprehensive Review Assessment & Management 1 Objectives Understand types of Burns Understand the pathophysiology of the Burns Understand Rule of Nine Understand Classification of Burns Identify
Burns A Comprehensive Review Assessment & Management 1 Objectives Understand types of Burns Understand the pathophysiology of the Burns Understand Rule of Nine Understand Classification of Burns Identify
Prehospital Resuscitation for the 21 st Century Simulation Case. VF/Asystole
 Prehospital Resuscitation for the 21 st Century Simulation Case VF/Asystole Case History 1 (hypovolemic cardiac arrest secondary to massive upper GI bleed) 56 year-old male patient who fainted in the presence
Prehospital Resuscitation for the 21 st Century Simulation Case VF/Asystole Case History 1 (hypovolemic cardiac arrest secondary to massive upper GI bleed) 56 year-old male patient who fainted in the presence
Subspecialty Rotation: Anesthesia
 Subspecialty Rotation: Anesthesia Faculty: John Heaton, M.D. GOAL: Maintenance of Airway Patency and Oxygenation. Recognize and manage upper airway obstruction and desaturation. Recognize and manage upper
Subspecialty Rotation: Anesthesia Faculty: John Heaton, M.D. GOAL: Maintenance of Airway Patency and Oxygenation. Recognize and manage upper airway obstruction and desaturation. Recognize and manage upper
COMMISSION ON ACCREDITATION FOR RESPIRATORY CARE TMC DETAILED CONTENT OUTLINE COMPARISON
 A. Evaluate Data in the Patient Record I. PATIENT DATA EVALUATION AND RECOMMENDATIONS 1. Patient history e.g., admission data orders medications progress notes DNR status / advance directives social history
A. Evaluate Data in the Patient Record I. PATIENT DATA EVALUATION AND RECOMMENDATIONS 1. Patient history e.g., admission data orders medications progress notes DNR status / advance directives social history
Other methods for maintaining the airway (not definitive airway as still unprotected):
 Page 56 Where anaesthetic skills and drugs are available, endotracheal intubation is the preferred method of securing a definitive airway. This technique comprises: rapid sequence induction of anaesthesia
Page 56 Where anaesthetic skills and drugs are available, endotracheal intubation is the preferred method of securing a definitive airway. This technique comprises: rapid sequence induction of anaesthesia
PEDIATRIC TRAUMA I: ABDOMINAL TRAUMA BURNS. December 19, 2012
 PEDIATRIC TRAUMA I: ABDOMINAL TRAUMA BURNS Niel F. Miele,, M.D. December 19, 2012 EPIDEMIOLOGY Major Trauma responsible for
PEDIATRIC TRAUMA I: ABDOMINAL TRAUMA BURNS Niel F. Miele,, M.D. December 19, 2012 EPIDEMIOLOGY Major Trauma responsible for
INTUBATION/RSI. PURPOSE: A. To facilitate secure, definitive control of the airway by endotracheal intubation in an expeditious and safe manner
 Manual: LifeLine Patient Care Protocols Section: Adult/Pediatrics Protocol #: AP1-009 Approval Date: 03/01/2018 Effective Date: 03/05/2018 Revision Due Date: 12/01/2018 INTUBATION/RSI PURPOSE: A. To facilitate
Manual: LifeLine Patient Care Protocols Section: Adult/Pediatrics Protocol #: AP1-009 Approval Date: 03/01/2018 Effective Date: 03/05/2018 Revision Due Date: 12/01/2018 INTUBATION/RSI PURPOSE: A. To facilitate
Purpose To outline the pre-hospital and inter-hospital assessment and management of patients with major burns.
 Major Burns HELI.CLI.08 Purpose To outline the pre-hospital and inter-hospital assessment and management of patients with major burns. Procedure Management of Severe Burns For Review Aug 2015 1. Introduction
Major Burns HELI.CLI.08 Purpose To outline the pre-hospital and inter-hospital assessment and management of patients with major burns. Procedure Management of Severe Burns For Review Aug 2015 1. Introduction
Nassau Regional Emergency Medical Services. Advanced Life Support Pediatric Protocol Manual
 Nassau Regional Emergency Medical Services Advanced Life Support Pediatric Protocol Manual 2014 PEDIATRIC ADVANCED LIFE SUPPORT PROTOCOLS TABLE OF CONTENTS Approved Effective Newborn Resuscitation P 1
Nassau Regional Emergency Medical Services Advanced Life Support Pediatric Protocol Manual 2014 PEDIATRIC ADVANCED LIFE SUPPORT PROTOCOLS TABLE OF CONTENTS Approved Effective Newborn Resuscitation P 1
Critical Care Treatment Guidelines
 Critical Care Treatment Guidelines West Virginia Office of Emergency Medical Services CCT Guidelines CCT Guidelines TABLE OF CONTENTS Preface Acknowledgments Using the Guidelines INITIAL TREATMENT / UNIVERSAL
Critical Care Treatment Guidelines West Virginia Office of Emergency Medical Services CCT Guidelines CCT Guidelines TABLE OF CONTENTS Preface Acknowledgments Using the Guidelines INITIAL TREATMENT / UNIVERSAL
Post-Anesthesia Care In the ICU
 Post-Anesthesia Care In the ICU The following is based on current research and regional standards of care. At completion you will be able to identify Basic equipment needed at the bedside. Aldrete scoring
Post-Anesthesia Care In the ICU The following is based on current research and regional standards of care. At completion you will be able to identify Basic equipment needed at the bedside. Aldrete scoring
Michigan Pediatric Cardiac Protocols. Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS
 Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
No conflicts of interest
 Robert M. Rodriguez, MD FAAEM Clinical Professor of Medicine and Emergency Medicine, UCSF No conflicts of interest Major Points Most ICU patients start in ED Chain of critical care starting in field and
Robert M. Rodriguez, MD FAAEM Clinical Professor of Medicine and Emergency Medicine, UCSF No conflicts of interest Major Points Most ICU patients start in ED Chain of critical care starting in field and
Burn Injuries & Its Management M JARI.MD
 Burn Injuries & Its Management M JARI.MD 1 BURNS Wounds caused by exposure to: 1. excessive heat 2. Chemicals 3. fire/steam 4. radiation 5. electricity 2 BURNS Results in 10-20 thousand deaths annually
Burn Injuries & Its Management M JARI.MD 1 BURNS Wounds caused by exposure to: 1. excessive heat 2. Chemicals 3. fire/steam 4. radiation 5. electricity 2 BURNS Results in 10-20 thousand deaths annually
Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials
 Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials 1 1. A high-risk bodily fluid for spreading infection is blood. 2. Items that can reduce the spread of infection include masks, gloves, and
Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials 1 1. A high-risk bodily fluid for spreading infection is blood. 2. Items that can reduce the spread of infection include masks, gloves, and
ITLS Pediatric Provider Course Advanced Pre-Test
 ITLS Pediatric Provider Course Advanced Pre-Test 1. You arrive at the scene of a motor vehicle crash and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
ITLS Pediatric Provider Course Advanced Pre-Test 1. You arrive at the scene of a motor vehicle crash and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
Thermal Burns PFN: SOMEML07. Terminal Learning Objective. References. Hours: 3.0 Instructor: Action: Communicate knowledge of thermal burns
 Thermal Burns PFN: SOMEML07 Hours: 3.0 Instructor: Slide 1 Terminal Learning Objective Action: Communicate knowledge of thermal burns Condition: Given a lecture in a classroom environment Standard: Received
Thermal Burns PFN: SOMEML07 Hours: 3.0 Instructor: Slide 1 Terminal Learning Objective Action: Communicate knowledge of thermal burns Condition: Given a lecture in a classroom environment Standard: Received
ITLS Pediatric Provider Course Basic Pre-Test
 ITLS Pediatric Provider Course Basic Pre-Test 1. You arrive at the scene of a motor vehicle collision and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
ITLS Pediatric Provider Course Basic Pre-Test 1. You arrive at the scene of a motor vehicle collision and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
Capnography: The Most Vital of Vital Signs. Tom Ahrens, PhD, RN, FAAN Research Scientist, Barnes-Jewish Hospital, St. Louis, MO May, 2017
 Capnography: The Most Vital of Vital Signs Tom Ahrens, PhD, RN, FAAN Research Scientist, Barnes-Jewish Hospital, St. Louis, MO May, 2017 Assessing Ventilation and Blood Flow with Capnography Capnography
Capnography: The Most Vital of Vital Signs Tom Ahrens, PhD, RN, FAAN Research Scientist, Barnes-Jewish Hospital, St. Louis, MO May, 2017 Assessing Ventilation and Blood Flow with Capnography Capnography
Routine Patient Care Guidelines - Adult
 Routine Patient Care Guidelines - Adult All levels of provider will complete an initial & focused assessment on every patient, and as standing order, use necessary and appropriate skills and procedures
Routine Patient Care Guidelines - Adult All levels of provider will complete an initial & focused assessment on every patient, and as standing order, use necessary and appropriate skills and procedures
Presented by: Indah Dwi Pratiwi
 Presented by: Indah Dwi Pratiwi Normal Fluid Requirements Resuscitation Fluids Goals of Resuscitation Maintain normal body temperature In most cases, elevate the feet and legs above the level of the heart
Presented by: Indah Dwi Pratiwi Normal Fluid Requirements Resuscitation Fluids Goals of Resuscitation Maintain normal body temperature In most cases, elevate the feet and legs above the level of the heart
Learning Station Competency Checklists
 Learning Station Competency Checklists Cardiac Arrest: Shockable Rhythm Team Dynamics Practice Demonstrates effective team dynamics (see, below) Performs manual maneuvers to open airway* Initiates assisted
Learning Station Competency Checklists Cardiac Arrest: Shockable Rhythm Team Dynamics Practice Demonstrates effective team dynamics (see, below) Performs manual maneuvers to open airway* Initiates assisted
Capnography (ILS/ALS)
 Capnography (ILS/ALS) Clinical Indications: 1. Capnography shall be used as soon as possible in conjunction with any airway management adjunct, including endotracheal, Blind Insertion Airway Devices (BIAD)
Capnography (ILS/ALS) Clinical Indications: 1. Capnography shall be used as soon as possible in conjunction with any airway management adjunct, including endotracheal, Blind Insertion Airway Devices (BIAD)
HOW LOW CAN YOU GO? HYPOTENSION AND THE ANESTHETIZED PATIENT.
 HOW LOW CAN YOU GO? HYPOTENSION AND THE ANESTHETIZED PATIENT. Donna M. Sisak, CVT, LVT, VTS (Anesthesia/Analgesia) Seattle Veterinary Specialists Kirkland, WA dsisak@svsvet.com THE ANESTHETIZED PATIENT
HOW LOW CAN YOU GO? HYPOTENSION AND THE ANESTHETIZED PATIENT. Donna M. Sisak, CVT, LVT, VTS (Anesthesia/Analgesia) Seattle Veterinary Specialists Kirkland, WA dsisak@svsvet.com THE ANESTHETIZED PATIENT
MICHIGAN. State Protocols. Pediatric Cardiac Table of Contents 6.1 General Pediatric Cardiac Arrest 6.2 Bradycardia 6.
 MICHIGAN State Protocols Protocol Number Protocol Name Pediatric Cardiac Table of Contents 6.1 General Pediatric Cardiac Arrest 6.2 Bradycardia 6.3 Tachycardia PEDIATRIC CARDIAC PEDIATRIC CARDIAC ARREST
MICHIGAN State Protocols Protocol Number Protocol Name Pediatric Cardiac Table of Contents 6.1 General Pediatric Cardiac Arrest 6.2 Bradycardia 6.3 Tachycardia PEDIATRIC CARDIAC PEDIATRIC CARDIAC ARREST
EMERGENCYROOM BURN MANAGEMENT
 EMERGENCYROOM INITIAL ASSESSMENT PRIMARY SURVEY A = Airway and C-spine immobilization B = Breathing and Ventilation C = Circulation D = Disability, Neurologic Deficit E = Expose (remove all clothing and
EMERGENCYROOM INITIAL ASSESSMENT PRIMARY SURVEY A = Airway and C-spine immobilization B = Breathing and Ventilation C = Circulation D = Disability, Neurologic Deficit E = Expose (remove all clothing and
EL DORADO COUNTY EMS AGENCY PREHOSPITAL PROTOCOLS
 EL DORADO COUNTY EMS AGENCY PREHOSPITAL PROTOCOLS Effective: July 1, 2017 Reviewed: November 9, 2016 Revised: November 9, 2016 EMS Agency Medical Director ALLERGIC REACTION/ANAPHYLAXIS ADULT BLS TREATMENT
EL DORADO COUNTY EMS AGENCY PREHOSPITAL PROTOCOLS Effective: July 1, 2017 Reviewed: November 9, 2016 Revised: November 9, 2016 EMS Agency Medical Director ALLERGIC REACTION/ANAPHYLAXIS ADULT BLS TREATMENT
Therapist Written RRT Examination Detailed Content Outline
 I. PATIENT DATA EVALUATION AND RECOMMENDATIONS 4 7 17 28 A. Review Data in the Patient Record 1 4 0 5 1. Patient history e.g., present illness admission notes respiratory care orders medication history
I. PATIENT DATA EVALUATION AND RECOMMENDATIONS 4 7 17 28 A. Review Data in the Patient Record 1 4 0 5 1. Patient history e.g., present illness admission notes respiratory care orders medication history
Lecture Notes. Chapter 9: Smoke Inhalation Injury and Burns
 Lecture Notes Chapter 9: Smoke Inhalation Injury and Burns Objectives List the factors that influence mortality rate Describe the nature of smoke inhalation and the fire environment Recognize the pulmonary
Lecture Notes Chapter 9: Smoke Inhalation Injury and Burns Objectives List the factors that influence mortality rate Describe the nature of smoke inhalation and the fire environment Recognize the pulmonary
TRAUMATIC EMERGENCIES
 TRAUMATIC EMERGENCIES I. General. A. Follow General Principles/Routine Care protocol unless otherwise indicated. B. Limit scene time for trauma patients, with goal of 15 minutes. C. See Appendix B for
TRAUMATIC EMERGENCIES I. General. A. Follow General Principles/Routine Care protocol unless otherwise indicated. B. Limit scene time for trauma patients, with goal of 15 minutes. C. See Appendix B for
Printed copies of this document may not be up to date, obtain the most recent version from
 Children s Acute Transport Service Clinical Guidelines Septic Shock Document Control Information Author Shruti Dholakia L Chigaru Author Position Fellow CATS Consultant Document Owner E. Polke Document
Children s Acute Transport Service Clinical Guidelines Septic Shock Document Control Information Author Shruti Dholakia L Chigaru Author Position Fellow CATS Consultant Document Owner E. Polke Document
Capnography 101. James A Temple BA, NRP, CCP
 Capnography 101 James A Temple BA, NRP, CCP Expected Outcomes 1. Gain a working knowledge of the physiology and science behind End-Tidal CO2. 2.Relate End-Tidal CO2 to ventilation, perfusion, and metabolism.
Capnography 101 James A Temple BA, NRP, CCP Expected Outcomes 1. Gain a working knowledge of the physiology and science behind End-Tidal CO2. 2.Relate End-Tidal CO2 to ventilation, perfusion, and metabolism.
Core Measures SEPSIS UPDATES
 Patricia Walker, RN-BC, BSN Evidence Based Practice Manager Quality Management Services UCLA Health System, Ronald Reagan Medical Center Core Measures SEPSIS UPDATES Severe Sepsis and Septic Shock Based
Patricia Walker, RN-BC, BSN Evidence Based Practice Manager Quality Management Services UCLA Health System, Ronald Reagan Medical Center Core Measures SEPSIS UPDATES Severe Sepsis and Septic Shock Based
Handling Common Problems & Pitfalls During. Oxygen desaturation in patients receiving mechanical ventilation ACUTE SEVERE RESPIRATORY FAILURE
 Handling Common Problems & Pitfalls During ACUTE SEVERE RESPIRATORY FAILURE Pravit Jetanachai, MD QSNICH Oxygen desaturation in patients receiving mechanical ventilation Causes of oxygen desaturation 1.
Handling Common Problems & Pitfalls During ACUTE SEVERE RESPIRATORY FAILURE Pravit Jetanachai, MD QSNICH Oxygen desaturation in patients receiving mechanical ventilation Causes of oxygen desaturation 1.
Emergency Room Resuscitation of the Unstable Trauma Patient
 Emergency Room Resuscitation of the Unstable Trauma Patient Goals of trauma resuscitation Maintain: Systemic oxygenation Systemic perfusion Neurologic function Approach to unstable trauma patient Primary
Emergency Room Resuscitation of the Unstable Trauma Patient Goals of trauma resuscitation Maintain: Systemic oxygenation Systemic perfusion Neurologic function Approach to unstable trauma patient Primary
Dóra Ujvárosy MD. Medical University of Debrecen Oxyology and Emergency Department
 Dóra Ujvárosy MD. Medical University of Debrecen Oxyology and Emergency Department Functions Definition A burn is a type of injury to the skin caused by heat, electricity, chemicals, light, radiation or
Dóra Ujvárosy MD. Medical University of Debrecen Oxyology and Emergency Department Functions Definition A burn is a type of injury to the skin caused by heat, electricity, chemicals, light, radiation or
INITIAL CARE AND TREATMENT OF BURN INJURIES. November 10,
 INITIAL CARE AND TREATMENT OF BURN INJURIES 2 11/10/2012 November 10, 2012 2 Oregon Burn Center Only burn center in Oregon and SW Washington New unit 16 beds, 20,000 square feet Opened in February 2002
INITIAL CARE AND TREATMENT OF BURN INJURIES 2 11/10/2012 November 10, 2012 2 Oregon Burn Center Only burn center in Oregon and SW Washington New unit 16 beds, 20,000 square feet Opened in February 2002
Michigan Pediatric Cardiac Protocols. Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS
 Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
Management of Acute Burn Injuries: The First 24 Hours
 Speaker Disclosure I, Debbie Harrell, MSN, RN, NE BC, have no financial relationships to disclose. I will not discuss off label uses of any pharmaceutical products or medical devices. Management of Acute
Speaker Disclosure I, Debbie Harrell, MSN, RN, NE BC, have no financial relationships to disclose. I will not discuss off label uses of any pharmaceutical products or medical devices. Management of Acute
Advanced Cardiac Life Support (ACLS) Science Update 2015
 1 2 3 4 5 6 7 8 9 Advanced Cardiac Life Support (ACLS) Science Update 2015 What s New in ACLS for 2015? Adult CPR CPR remains (Compressions, Airway, Breathing Chest compressions has priority over all other
1 2 3 4 5 6 7 8 9 Advanced Cardiac Life Support (ACLS) Science Update 2015 What s New in ACLS for 2015? Adult CPR CPR remains (Compressions, Airway, Breathing Chest compressions has priority over all other
PRE-HOSPITAL PATIENT CARE PROTOCOLS BASIC LIFE SUPPORT/ADVANCED LIFE SUPPORT
 PRE-HOSPITAL PATIENT CARE PROTOCOLS BASIC LIFE SUPPORT/ADVANCED LIFE SUPPORT Board Approved June 2007 Revised December 2009 Revised July 2011 Revised June 2015 435 Hunter Street Fredericksburg, VA 22401
PRE-HOSPITAL PATIENT CARE PROTOCOLS BASIC LIFE SUPPORT/ADVANCED LIFE SUPPORT Board Approved June 2007 Revised December 2009 Revised July 2011 Revised June 2015 435 Hunter Street Fredericksburg, VA 22401
(31189) Hypothermia Initiation Phase One
 Hypothermia Initiation Phase One Diagnosis Allergies For hypothermia tracking purposes only. Please do not uncheck.- Required Cardiac Emergency Tracking For hypothermia tracking purposes only. Consults
Hypothermia Initiation Phase One Diagnosis Allergies For hypothermia tracking purposes only. Please do not uncheck.- Required Cardiac Emergency Tracking For hypothermia tracking purposes only. Consults
Printed copies of this document may not be up to date, obtain the most recent version from
 Children s Acute Transport Service Clinical Guidelines Acute Severe Asthma Document Control Information Author E Randle Author Position CATS Consultant Document Owner E Polke Document Owner Position Co-ordinator
Children s Acute Transport Service Clinical Guidelines Acute Severe Asthma Document Control Information Author E Randle Author Position CATS Consultant Document Owner E Polke Document Owner Position Co-ordinator
At the conclusion of this course the learner will be able to
 Objectives At the conclusion of this course the learner will be able to 1. Discuss basic anatomy and pathophysiology of burns 2. Describe burn injuries in terms of size, depth, coloration and characteristics
Objectives At the conclusion of this course the learner will be able to 1. Discuss basic anatomy and pathophysiology of burns 2. Describe burn injuries in terms of size, depth, coloration and characteristics
Post Resuscitation Care
 Princess Margaret Hospital f Children PAEDIATRIC ACUTE CARE GUIDELINE Post Resuscitation Care Scope (Staff): Scope (Area): All Emergency Department Clinicians Emergency Department This document should
Princess Margaret Hospital f Children PAEDIATRIC ACUTE CARE GUIDELINE Post Resuscitation Care Scope (Staff): Scope (Area): All Emergency Department Clinicians Emergency Department This document should
Staging Sepsis for the Emergency Department: Physician
 Staging Sepsis for the Emergency Department: Physician Sepsis Continuum 1 Sepsis Continuum SIRS = 2 or more clinical criteria, resulting in Systemic Inflammatory Response Syndrome Sepsis = SIRS + proven/suspected
Staging Sepsis for the Emergency Department: Physician Sepsis Continuum 1 Sepsis Continuum SIRS = 2 or more clinical criteria, resulting in Systemic Inflammatory Response Syndrome Sepsis = SIRS + proven/suspected
Principles of Infusion Therapy: Fluids
 Principles of Infusion Therapy: Fluids Christie Heinzman, MSN, APRN-CNP Acute Care Pediatric Nurse Practitioner Cincinnati Children s Hospital Medical Center May 22, 2018 Conflict of Interest Disclosure
Principles of Infusion Therapy: Fluids Christie Heinzman, MSN, APRN-CNP Acute Care Pediatric Nurse Practitioner Cincinnati Children s Hospital Medical Center May 22, 2018 Conflict of Interest Disclosure
STANDARD OPERATING PROCEDURE #203 LARGE ANIMAL SURGERY
 STANDARD OPERATING PROCEDURE #203 LARGE ANIMAL SURGERY 1. PURPOSE This Standard Operating Procedure (SOP) describes procedures for general surgery of large animal species such as swine, dogs, rabbits,
STANDARD OPERATING PROCEDURE #203 LARGE ANIMAL SURGERY 1. PURPOSE This Standard Operating Procedure (SOP) describes procedures for general surgery of large animal species such as swine, dogs, rabbits,
ADVANCED AIRWAY MANAGEMENT
 The Advanced Airway Management protocol should be used on all patients requiring advanced airway management procedures. This protocol is divided into three sections the Crash Airway Algorithm, the Rapid
The Advanced Airway Management protocol should be used on all patients requiring advanced airway management procedures. This protocol is divided into three sections the Crash Airway Algorithm, the Rapid
Information Often Given to the Nurse at the Time of Admission to the Postanesthesia Care Unit
 Information Often Given to the Nurse at the Time of Admission to the Postanesthesia Care Unit * Patient s name and age * Surgical procedure and type of anesthetic including drugs used * Other intraoperative
Information Often Given to the Nurse at the Time of Admission to the Postanesthesia Care Unit * Patient s name and age * Surgical procedure and type of anesthetic including drugs used * Other intraoperative
Prehospital Care Bundles
 Prehospital s The MLREMS Prehospital s have been created to provide a simple framework to help EMS providers identify the most critical elements when caring for a patient. These bundles do not replace
Prehospital s The MLREMS Prehospital s have been created to provide a simple framework to help EMS providers identify the most critical elements when caring for a patient. These bundles do not replace
Critical Care of the Post-Surgical Patient
 Critical Care of the Post-Surgical Patient, Dr med vet, DEA, DECVIM-CA Many critically ill patients require surgical treatments. These patients often have multisystem abnormalities during the immediate
Critical Care of the Post-Surgical Patient, Dr med vet, DEA, DECVIM-CA Many critically ill patients require surgical treatments. These patients often have multisystem abnormalities during the immediate
PALS Pulseless Arrest Algorithm.
 PALS Pulseless Arrest Algorithm. Kleinman M E et al. Circulation 2010;122:S876-S908 PALS Bradycardia Algorithm. Kleinman M E et al. Circulation 2010;122:S876-S908 PALS Tachycardia Algorithm. Kleinman M
PALS Pulseless Arrest Algorithm. Kleinman M E et al. Circulation 2010;122:S876-S908 PALS Bradycardia Algorithm. Kleinman M E et al. Circulation 2010;122:S876-S908 PALS Tachycardia Algorithm. Kleinman M
Post Resuscitation (ROSC) Care
 Standard Operating Procedure 2.10 Post Resuscitation (ROSC) Care Position Responsible: Medical Director Approved: Clinical Governance Committee Related Documents: This document is the intellectual property
Standard Operating Procedure 2.10 Post Resuscitation (ROSC) Care Position Responsible: Medical Director Approved: Clinical Governance Committee Related Documents: This document is the intellectual property
MICHIGAN. Table of Contents. State Protocols. Adult Treatment Protocols
 MICHIGAN State Protocols Protocol Number Protocol Name Adult Treatment Protocols Table of Contents 3.1 Altered Mental Status 3.2 Stroke/Suspected Stroke 3.3 Respiratory Distress 3.4 Seizures 3.5 Sepsis
MICHIGAN State Protocols Protocol Number Protocol Name Adult Treatment Protocols Table of Contents 3.1 Altered Mental Status 3.2 Stroke/Suspected Stroke 3.3 Respiratory Distress 3.4 Seizures 3.5 Sepsis
Burn wounds - Determining the size and type degree
 1 Burn wounds - Determining the size and type degree Determining surface area of burn (Open hand only for small burns) 1 2 Burn depth Most burns are a combination of superficial and deeper burns and the
1 Burn wounds - Determining the size and type degree Determining surface area of burn (Open hand only for small burns) 1 2 Burn depth Most burns are a combination of superficial and deeper burns and the
Emergency Triage Assessment and Management (ETAT) POST-TEST: Module 1
 Emergency Triage Assessment and Management (ETAT) POST-TEST: Module 1 For questions 1 through 3, consider the following scenario: A three year old comes with burns to her face and chest after a kerosene
Emergency Triage Assessment and Management (ETAT) POST-TEST: Module 1 For questions 1 through 3, consider the following scenario: A three year old comes with burns to her face and chest after a kerosene
SAN LUIS OBISPO COUNTY EMERGENCY MEDICAL SERVICES AGENCY PREHOSPITAL POLICY ADVANCED LIFE SUPPORT FIRST RESPONDER EQUIPMENT AND SUPPLY
 SAN LUIS OBISPO COUNTY EMERGENCY MEDICAL SERVICES AGENCY PREHOSPITAL POLICY Policy Reference No: 208 [01/10/2013] Formerly Policy No: 114 Effective Date: 11/12/2012 Supersedes: 06/01/2010 Review Date:
SAN LUIS OBISPO COUNTY EMERGENCY MEDICAL SERVICES AGENCY PREHOSPITAL POLICY Policy Reference No: 208 [01/10/2013] Formerly Policy No: 114 Effective Date: 11/12/2012 Supersedes: 06/01/2010 Review Date:
The Surgical Patient. Objectives:
 The Surgical Patient Objectives: 1. Discuss the effect of surgery on the body systems. 2. Explain the etiological factors, nursing assessment, and management of potential problems during the postoperative
The Surgical Patient Objectives: 1. Discuss the effect of surgery on the body systems. 2. Explain the etiological factors, nursing assessment, and management of potential problems during the postoperative
FLUID MANAGEMENT AND BLOOD COMPONENT THERAPY
 Manual: Section: Protocol #: Approval Date: Effective Date: Revision Due Date: 10/2019 LifeLine Patient Care Protocols Adult/Pediatrics AP1-011 10/2018 10/2018 FLUID MANAGEMENT AND BLOOD COMPONENT THERAPY
Manual: Section: Protocol #: Approval Date: Effective Date: Revision Due Date: 10/2019 LifeLine Patient Care Protocols Adult/Pediatrics AP1-011 10/2018 10/2018 FLUID MANAGEMENT AND BLOOD COMPONENT THERAPY
This interdisciplinary clinical support document provides guidelines for the safe establishment of an artificial airway.
 PURPOSE This interdisciplinary clinical support document provides guidelines for the safe establishment of an artificial airway. POLICY STATEMENTS Endotracheal intubation will be performed by the Most
PURPOSE This interdisciplinary clinical support document provides guidelines for the safe establishment of an artificial airway. POLICY STATEMENTS Endotracheal intubation will be performed by the Most
Getting Strarted using the Nursing Care Plans Templates
 Getting Strarted using the Nursing Care Plans Templates Using available Nursing Care Plan Templates. These templates are delivered as is and there is nothing which prevents you to use and modify these
Getting Strarted using the Nursing Care Plans Templates Using available Nursing Care Plan Templates. These templates are delivered as is and there is nothing which prevents you to use and modify these
EMS System for Metropolitan Oklahoma City and Tulsa 2017 Medical Control Board Treatment Protocols
 S O EMT EMT-INTERMEDIATE 85 ADVANCED EMT PARAMEDIC 3H WAVEFORM CAPNOGRAPHY ADULT & PEDIATRIC Indications: 1. Medical General Assessment/General Supportive Care. 2. Trauma General Assessment/Trauma & Hypovolemic
S O EMT EMT-INTERMEDIATE 85 ADVANCED EMT PARAMEDIC 3H WAVEFORM CAPNOGRAPHY ADULT & PEDIATRIC Indications: 1. Medical General Assessment/General Supportive Care. 2. Trauma General Assessment/Trauma & Hypovolemic
Speaker Disclosure Emergent Burn Care I, Debbie Harrell, MSN, RN, NE BC, have no financial relationships to disclose.
 Speaker Disclosure Emergent Burn Care I, Debbie Harrell, MSN, RN, NE BC, have no financial relationships to disclose. Debbie Harrell RN, MSN, Shriners Hospitals for Children Cincinnati Cincinnati, Ohio
Speaker Disclosure Emergent Burn Care I, Debbie Harrell, MSN, RN, NE BC, have no financial relationships to disclose. Debbie Harrell RN, MSN, Shriners Hospitals for Children Cincinnati Cincinnati, Ohio
1 Pediatric Advanced Life Support Science Update What s New for 2010? 3 CPR. 4 4 Steps of BLS Survey 5 CPR 6 CPR.
 1 Pediatric Advanced Life Support Science Update 2010 2 What s New for 2010? 3 CPR Take no longer than seconds for pulse check Rate at least on per minute (instead of around 100 per minute ) Depth change:
1 Pediatric Advanced Life Support Science Update 2010 2 What s New for 2010? 3 CPR Take no longer than seconds for pulse check Rate at least on per minute (instead of around 100 per minute ) Depth change:
Shock. William Schecter, MD
 Shock William Schecter, MD The Cell as a furnace O 2 1 mole Glucose Cell C0 2 ATP 38 moles H 2 0 Shock = Inadequate Delivery of 02 and Glucose to the Cell 0 2 Cell ATP 2 moles Lactic Acid Treatment of
Shock William Schecter, MD The Cell as a furnace O 2 1 mole Glucose Cell C0 2 ATP 38 moles H 2 0 Shock = Inadequate Delivery of 02 and Glucose to the Cell 0 2 Cell ATP 2 moles Lactic Acid Treatment of
F: Respiratory Care. College of Licensed Practical Nurses of Alberta, Competency Profile for LPNs, 3rd Ed. 59
 F: Respiratory Care College of Licensed Practical Nurses of Alberta, Competency Profile for LPNs, 3rd Ed. 59 Competency: F-1 Airway Management F-1-1 F-1-2 F-1-3 F-1-4 F-1-5 Demonstrate knowledge and ability
F: Respiratory Care College of Licensed Practical Nurses of Alberta, Competency Profile for LPNs, 3rd Ed. 59 Competency: F-1 Airway Management F-1-1 F-1-2 F-1-3 F-1-4 F-1-5 Demonstrate knowledge and ability
How it Works. CO 2 is the smoke from the flames of metabolism 10/21/18. -Ray Fowler, MD. Metabolism creates ETC0 2 for excretion
 CO 2 is the smoke from the flames of metabolism -Ray Fowler, MD How it Works Metabolism creates ETC0 2 for excretion ETC02 and Oxygen are exchanged at the alveolar level in the lungs with each breath.
CO 2 is the smoke from the flames of metabolism -Ray Fowler, MD How it Works Metabolism creates ETC0 2 for excretion ETC02 and Oxygen are exchanged at the alveolar level in the lungs with each breath.
Therapist Multiple-Choice Examination Detailed Content Outline
 I. PATIENT DATA EVALUATION AND RECOMMENDATIONS 12 26 17 55 A. Evaluate Data in the Patient Record 3 5 0 8 1. Patient history, for example, admission data progress notes orders DNR status / advance directives
I. PATIENT DATA EVALUATION AND RECOMMENDATIONS 12 26 17 55 A. Evaluate Data in the Patient Record 3 5 0 8 1. Patient history, for example, admission data progress notes orders DNR status / advance directives
Airway Management Essentials Self-Study Guide
 Airway Management Essentials Self-Study Guide Fourth Quarter 2010 Self-Study Guide Learning Objectives Cognitive Domain 1. Describe the various conditions that cause concern during treatment in the field
Airway Management Essentials Self-Study Guide Fourth Quarter 2010 Self-Study Guide Learning Objectives Cognitive Domain 1. Describe the various conditions that cause concern during treatment in the field
ANAESTHESIA FOR BLEEDING TONSIL
 ANAESTHESIA FOR BLEEDING TONSIL BY Dr.S.C.Ganeshprabu, MD., D.A., Professor of Anaesthesiology, Madurai Medical College & Govt. Rajaji Hospital, Madurai -652 020. A 5-year-old child who had tonsillectomy
ANAESTHESIA FOR BLEEDING TONSIL BY Dr.S.C.Ganeshprabu, MD., D.A., Professor of Anaesthesiology, Madurai Medical College & Govt. Rajaji Hospital, Madurai -652 020. A 5-year-old child who had tonsillectomy
H: Respiratory Care. Saskatchewan Association of Licensed Practical Nurses, Competency Profile for LPNs, 3rd Ed. 79
 H: Respiratory Care Saskatchewan Association of Licensed Practical Nurses, Competency Profile for LPNs, 3rd Ed. 79 Competency: H-1 Airway Management H-1-1 H-1-2 H-1-3 H-1-4 H-1-5 Demonstrate knowledge
H: Respiratory Care Saskatchewan Association of Licensed Practical Nurses, Competency Profile for LPNs, 3rd Ed. 79 Competency: H-1 Airway Management H-1-1 H-1-2 H-1-3 H-1-4 H-1-5 Demonstrate knowledge
Joint Theater Trauma System Clinical Practice Guideline
 Page 1 of 7 Joint Theater Trauma System Clinical Practice Guideline TRAUMA AIRWAY MANAGEMENT Original Release/Approval 18 Dec 2004 Note: This CPG requires an annual review. Reviewed: May 2012 Approved:
Page 1 of 7 Joint Theater Trauma System Clinical Practice Guideline TRAUMA AIRWAY MANAGEMENT Original Release/Approval 18 Dec 2004 Note: This CPG requires an annual review. Reviewed: May 2012 Approved:
LIFEGIFT BRAIN DEATH PLAN
 Diagnosis Weight Allergies Admit/Discharge/Transfer ***THIS PLAN IS TO BE ED ONLY ON THE LIFEGIFT ENCOUNTER, WITH DR LIFEGIFT AS THE ATTENDING*** Patient Status Pt Status: Inpatient (Inpatient only procedure)
Diagnosis Weight Allergies Admit/Discharge/Transfer ***THIS PLAN IS TO BE ED ONLY ON THE LIFEGIFT ENCOUNTER, WITH DR LIFEGIFT AS THE ATTENDING*** Patient Status Pt Status: Inpatient (Inpatient only procedure)
Adult Intubation Skill Sheet
 Adult Intubation 2. Opens the airway manually and inserts an oral airway *** 3. Ventilates the patient with BVM attached to oxygen at 15 lpm *** 4. Directs assistant to oxygenate the patient 5. Selects
Adult Intubation 2. Opens the airway manually and inserts an oral airway *** 3. Ventilates the patient with BVM attached to oxygen at 15 lpm *** 4. Directs assistant to oxygenate the patient 5. Selects
