Alterations of the CARD15/NOD2 Gene and the Impact on Management and Treatment of Crohn s Disease Patients
|
|
|
- Sydney Watts
- 5 years ago
- Views:
Transcription
1 Review Article Dig Dis 2003;21: DOI: / Alterations of the CARD15/NOD2 Gene and the Impact on Management and Treatment of Crohn s Disease Patients Helga-Paula Török a,b Jürgen Glas a Peter Lohse c Christian Folwaczny a,b a Medizinische Klinik und Medizinische Poliklinik Innenstadt, b Chirurgische Klinik Innenstadt, and c Institut für Klinische Chemie Grosshadern, Klinikum der Universität, München, Germany Key Words CARD15/NOD2 W Mutations W Crohn s disease W Genotype, clinical implications Abstract The recent identification of the CARD15/NOD2 gene as a susceptibility locus for Crohn s disease represents an important step towards the delineation of the immunopathogenesis of inflammatory bowel disease. CARD15 functions as an intracellular receptor for bacterial components and thus represents an important link between inflammatory bowel disease and innate immunity. Three major CARD15/NOD2 gene mutations have been associated with Crohn s disease in Caucasians in several independent studies. Together, they explain about 20% of the genetic susceptibility for Crohn s disease. Genotypephenotype analyses demonstrated an association of these mutations with ileum-specific disease, an increased incidence of the fibrostenotic phenotype and an earlier age of disease onset. Beside these associations, no other relationship between the CARD15/NOD2 genotype and disease behavior or response to treatment has been detailed so far. Thus, the clinical impact of knowing the patient s genotype is limited at this time. Screening for CARD15 mutations in order to identify high-risk individuals or to introduce an individualized disease management is therefore currently not recommended. Copyright 2003 S. Karger AG, Basel Introduction The current hypothesis for the pathogenesis of chronic inflammatory bowel disease comprises a loss of tolerance towards luminal antigens in a genetically susceptible host resulting in a chronic, spontaneously relapsing inflammation. Several lines of evidence are compatible with a significant role of genetic factors in inflammatory bowel disease, especially in Crohn s disease. The most striking example is provided by twin studies, which report concordance rates for Crohn s disease between 42 and 58% in monozygotic twins [1 4], whereas in dizygotic twins concordance is not significantly enhanced. Epidemiological studies demonstrate a familial aggregation with approximately 5 10% of all affected individuals reporting a positive familial history of inflammatory bowel disease [5 7]. The relative risk for first degree relatives of patients with Crohn s disease is estimated to be about 15-fold increased when compared to the general population [8, 9]. Ethnic differences in the prevalence of the disease further underline the significant role of genetic susceptibility. The highest prevalence rates are reported for Ashkenazi Jews. In African-Americans the rates are lower than in Caucasians, and in Asians the lowest rates have been observed [10 15]. For several years, considerable efforts aimed at the identification of the genetic background of inflammatory ABC Fax karger@karger.ch S. Karger AG, Basel /03/ $19.50/0 Accessible online at: PD Dr. med. Christian Folwaczny Medizinische Poliklinik, Ludwig-Maximilians-Universität München Nussbaumstr. 20, DE München (Germany) Tel , Fax Christian.Folwaczny@medinn.med.uni-muenchen.de
2 Arg702Trp Gly908Arg 1007fs CARD1 CARD2 NBD LRR Fig. 1. Structural domains of the CARD15 protein. Like most of the members of the NOD family, CARD15 contains three distinct functional domains: a centrally located nucleotidebinding domain, an amino-terminal effector-binding domain [in the case of CARD15 the two caspase-recruitment domains (CARD)] and a carboxy-terminal ligand-recognition domain [the leucine-rich repeats (LRR)]. The location of the three Crohn s disease-associated variants within the protein are indicated by arrows. bowel disease. Two complementary approaches, namely genetic linkage analysis and the search for candidate genes, led to the identification of a number of susceptibility loci and to the postulation of functional candidate genes with a presumptive role in immune regulation. The first real breakthrough, however, was achieved only two years ago with the identification of the CARD15/NOD2 gene as the first susceptibility gene with a consistent association with Crohn s disease. Alterations of the CARD15/NOD2 Gene and Crohn s Disease In May 2001, two research groups reported independently that Crohn s disease is associated with mutations in the NOD2 gene, which was later renamed CARD15 [16, 17]. This association has been confirmed by numerous other studies [18 28]. The CARD15 gene is located in the pericentromeric region of chromosome 16 inside the susceptibility locus displaying the strongest linkage with Crohn s disease [29, 30], namely the IBD1 locus. It encodes a 1,040-aminoacid protein containing several functional domains: two N-terminal caspase activation and recruitment domains (CARDs), a centrally located nucleotide binding domain (NBD) and a C-terminal leucine-rich repeat domain (LRR) (fig. 1) [31]. Functional studies demonstrated that CARD15 is one of the numerous pattern-recognition receptors implicated in the intracellular sensing of bacterial components [31]. Crohn s Disease-Associated CARD15 Genetic Variants Three common variants of CARD15 have been linked to the development of Crohn s disease. The most common genetic defect is the frameshift mutation 1007fs (3020insC) in exon 11, resulting in a premature stop codon and thus in a truncated CARD15 protein. The two other missense mutations are located in exons 4 and 8 and lead to amino acid substitutions Arg702Trp and Gly908Arg, respectively. These three mutations are located in the leucine-rich repeat domain of the CARD15 protein or in its vicinity (fig. 1) and occur on the background of the most common variant Pro268Ser. Approximately 30% of Crohn s disease patients carry one and up to 17% carry two mutated CARD15/NOD2 risk alleles [32]. The allele frequencies reported for Crohn s disease and control populations in a variety of studies are depicted in table 1. The three above mentioned CARD15 variants seem to confer an increased risk for Crohn s disease only in Caucasians, as these mutations were not detected in populations with a different ethnic background, e.g. in Japanese [33 35], Korean [36] or Chinese [37]. A study in African-Americans with Crohn s disease also reported lower carriage rates of these alleles and the presence of uncommon variants such as Arg790Gln [38]. Among Caucasians, ethnic differences in the allele frequencies have also been reported. Jewish patients have a higher frequency of the Gly908Arg allele and a lower frequency of the Arg702Trp allele, when compared to non-jewish Crohn s disease patients [26]. The allele frequencies in familial and sporadic Crohn s disease were comparable in two Caucasian cohorts [19, 24], whereas in a population of Ashkenazi Jews, familial cases displayed a significantly higher frequency of the Gly908Arg variant than sporadic cases [39]. Having one copy of a mutated CARD15/NOD2 allele confers a 2- to 4-fold increased risk of developing Crohn s disease, whereas having two mutated copies in homozygous or compound heterozygous form increases the risk 20- to 40-fold [16 18]. However, homozygosity for mutant CARD15/NOD2 has also been observed in healthy 340 Dig Dis 2003;21: Török/Glas/Lohse/Folwaczny
3 Fig. 2. Schematic representation of CARD15 function. Similar to Toll-like receptors on the cell surface, CARD15 functions as a receptor for pathogen-associated molecular patterns (PAMPs) in the cytosol. Recognition of muramyl dipeptide (MDP) derived from bacterial peptidoglycan through the leucin-rich region of CARD15 results in activation of nuclear factor NF-ÎB and subsequent initiation of an inflammatory response. Table 1. Allele frequencies of Crohn s disease-associated CARD15/NOD2 mutations in different studies (% values) References Population CARD15/NOD2 mutations 1007fs Crohn s disease vs. (controls) Gly908Arg Crohn s disease vs. (controls) Arg702Trp Crohn s disease vs. (controls) Hugot et al. [16] European 12 (2) 6 (1) 11 (4) Hampe et al. [18] German/British 16 (4.4) not determined not determined Lesage et al. [19] European 11 (2) 6 (1) 11 (4) Ahmad et al. [20] British 9.4 (1.6) 3.3 (1.4) 12.5 (5.2) Cuthbert et al. [21] European 12 (2) 6 (1) 11 (4) Vavassori et al. [22] Italian 11.6 (1.2) not determined not determined Murillo et al. [23] Dutch 8.5 (1) 4.3 (3) not determined Vermeire et al. [24] Canadian 10.3 (0.7) 5.2 (0.7) 12.9 (4.2) Radlmayr et al. [25] German 14 (1.66) not determined not determined Bonen et al. [26] US Caucasians 8.4 (4) 4.3 (1.7) 10.8 (4) Cavanaugh et al. [30] Australian 7 (0) 2 (1) 11 (5) controls [40]. These data suggest that loss-of-function mutations in the CARD15/NOD2 gene are neither necessary nor sufficient for developing Crohn s disease, and that other genetic factors as well as environmental influences are needed for disease manifestation. Role of CARD15: Link between Genetic Susceptibility and Environmental Factors (e.g. Bacterial Flora) The CARD15 protein is located in the cytosol and is now recognized as a member of a family of proteins which are involved in intracellular recognition of bacterial components (fig. 2) [41 42]. Although the expression of CARD15 was reported to be restricted to peripheral blood monocytes [31], recent studies have shown basic expression in granulocytes and dendritic cells [43] as well as in several colonic epithelial cell lines and primary intestinal epithelial cells [44]. Moreover, elevated amounts of CARD15 were found in primary colonic epithelial cells [45, 46] and in particular in Paneth cells [47] from patients with inflammatory bowel disease. The expression CARD15/NOD2 Mutations in Crohn s Disease Dig Dis 2003;21:
4 of CARD15 can be enhanced by proinflammatory cytokines and bacterial components via Nuclear Factor (NF)- ÎB activation [43, 45]. Functional studies in human embryonic kidney (HEK) 293T cells transfected with CARD15 revealed that the wild-type protein mediates responsiveness to lipopolysaccharide (LPS) and peptidoglycan (PGN) preparations from several bacteria [17, 26, 31, 48]. Recent works identified muramyl dipeptide (MDP), the minimal essential structure of bacterial peptidoglycan, as the moiety specifically recognised by CARD15 [49, 50]. The three major Crohn s disease-associated variants are defective in their ability to activate NF-ÎB in response to MDP [17, 26]. Especially the truncated CARD15 protein, which arises from the 1007fs mutation, completely lacks this activity [17, 49, 50]. These results were obtained in transfected cells and were subsequently verified by assessment of mrna expression and protein synthesis of pro- and antiinflammatory cytokines in peripheral blood monocytes from individuals carrying different CARD15 variants [49, Török et al., unpubl. data]. At present, it is not clear how CARD15/NOD2 mutations and the ensuing decreased NF-ÎB activation confer susceptibility to Crohn s disease. Assuming that CARD15 is a pattern-recognition receptor, it seems possible that the mutations result in an inadequate innate immune response, e.g. a defective activation of monocytes-macrophages in response to intestinal microbes. This disturbed response could be associated with impaired killing of intracellular microbes resulting in compensatory increase of other components of the immune system such as a marked effector T cell response [51]. On the other hand, the absence of functional CARD15 in epithelial cells could lead to an impaired secretion of chemokines and defensins in response to microbial products followed by a proliferation of bacteria in the crypts and a loss of barrier function of the mucosa. Several observations support this hypotheses. Hisamatsu et al. [44] showed that CARD15 functions as an antibacterial factor in human intestinal epithelial cells by constraining intracellular bacterial survival and that the 1007fs mutant lacks this activity. Moreover, a recent communication by Wehkamp et al. [52] reported an impaired expression of antibacterial peptides (defensins) in epithelial cells from Crohn s disease patients carrying CARD15/NOD2 mutations. The identification of CARD15/NOD2 as a susceptibility locus for Crohn s disease confirms at the molecular level that an inappropriate activation of the mucosal immune system by the intestinal flora plays a causal role in the development of Crohn s disease. Thus, this association confers an important link between inflammatory bowel disease and innate immunity [53]. Clinical Implications Among the cases classified as Crohn s disease, different clinical phenotypes with regard to disease location, extent, aggressiveness, behavior, local and systemic complications as well as varying responses to medical therapy have been described [54]. The observation of conserved phenotypes in multiplex Crohn s disease families [55, 56] is compatible with the assumption that the genetic background influences the phenotype. Following the identification of CARD15/NOD2 as a susceptibility gene for Crohn s disease, many questions were raised regarding the importance of this discovery for the daily clinical practice. Could mutations in this gene determine the natural history of Crohn s disease? Is the CARD15/NOD2 genotype associated with a specific phenotype, a specific location, extent or aggressiveness of the disease? Can it predict the response to a specific therapeutic agent? Is there a diagnostic role for the mutations? Should we perform screening for CARD15/NOD2 mutants in the general population, in the groups at risk, or in Crohn s disease patients before initiating a specific therapy? Only a few of these questions can be answered satisfactorily at present. CARD15/NOD2 Genotype and Clinical Course of Crohn s Disease Several studies about the relationship between CARD15/NOD2 mutations and the clinical presentation of Crohn s disease have been published. The only consistent finding concerns the disease location, as a number of studies reported a significant association between carriage of one or more CARD15/NOD2 risk alleles and ileal disease. Ahmad and colleagues [20] performed genotypephenotype analysis in 244 extensively characterized Crohn s disease patients with a median follow-up of 16 years. The results demonstrated that CARD15/NOD2 mutations determine ileal disease. Among 429 patients analyzed in a large European study, the frequency of CARD15 mutations was significantly increased in ileumspecific disease, when compared with colon-specific disease (26.9 vs. 12.7%, p = ) [21]. In a French study comprising 166 sporadic and 287 familial cases of Crohn s disease, the patients carrying two risk alleles were characterized by a less frequent colonic involvement than wild-type patients (p = 0.003) [19]. The predominance of 342 Dig Dis 2003;21: Török/Glas/Lohse/Folwaczny
5 ileal disease in patients carrying mutations in CARD15 was also reported in other studies [24, 57, 58]. Importantly, the association with disease location (ileal and right colonic disease) was the only one also confirmed in a prospective cohort study, in which 106 German and 55 Norwegian patients with Crohn s disease were enrolled [57]. Data concerning disease behavior are more inconsistent. Reasons could be the use of different definitions for the classification as well as the fact that disease behavior changes through time, which underscores the need for long observation periods and illustrates the inherent difficulties of retrospectively differentiating clinical subtypes. Some groups reported an association with the fibrostenotic phenotype [19, 25, 57 59], the presence of fistulas [25, 57 59] or the need for surgery [25, 58], whereas others did not confirm such findings [20, 60]. An earlier age of disease onset in patients carrying two CARD15/NOD2 risk alleles in homozygous or compound heterozygous form has also been reported [19, 20, 61]. Onset of disease occurred approximately 2 years earlier in these patients, when compared with all Crohn s disease patients. CARD15 and Response to Treatment At this time little is known about the influence of CARD15 genotype on the response to medical therapy in Crohn s disease. Vermeire et al. [62] studied the CARD15/NOD2 genotype in 245 patients with Crohn s disease receiving therapy with anti TNF-alpha antibodies (infliximab) and observed no relationship between the presence of mutations and short-term response or response duration. Moreover, the authors could not identify any clinical characteristic which, in combination with CARD15/NOD2 mutations, modified the response to treatment. Similarly, Mascheretti et al. [63] reported no association between the response to infliximab and the CARD15 variants in two independent cohorts of 90 and 444 patients with Crohn s disease. These negative findings exclude the three CARD15 mutants as a predictive factor for therapeutic response to infliximab. However, data concerning other therapeutic approaches, such as glucocorticoids, aminosalicylates or immunosuppressors, are lacking so far. Screening for CARD15/NOD2 Variants? One of the major questions raised is whether screening for CARD15/NOD2 genotype in the population at risk or in patients already diagnosed with Crohn s disease should be introduced into the clinical practice. Giving the limited penetrance and the lack of consistent information about the positive and negative predictive values of genotypes in unaffected relatives (the major risk group), a screening for CARD15/NOD2 variants is currently not recommended. The majority of high-risk individuals will not develop Crohn s disease, as studies in twin siblings demonstrated [64]. Moreover, even if highrisk individuals are detected by genotyping, there are at present no efficient prophylactic methods that could prevent disease onset. Thus, the diagnostic role of CARD15/ NOD2 genotyping is limited. It was suggested that mutation analysis will help to classify undifferentiated colitis cases. However, the low frequency of CARD15/NOD2 mutations in Crohn s disease patients with an ulcerative colitis-like phenotype limits this clinical application [53]. Recommending genotyping in patients already diagnosed with Crohn s disease is also premature. Data about the influence of the genotype on disease behavior are inconsistent and large prospective studies are needed to determine whether mutations in CARD15/NOD2 can predict the prognosis of Crohn s disease, e.g. a more aggressive disease course with need of early immunosuppressive therapy. In addition, the lack of data regarding the association between CARD15 variants and specific therapeutic responses currently disables the possibility of individualised, genotype-based therapies. Conclusions The association of CARD15/NOD2 mutations with Crohn s disease opens up a new era in the history of inflammatory bowel disease. It shows how the two complementary approaches, linkage analysis and the study of candidate genes can be successfully used in the identification of disease susceptibility genes. The role of CARD15 as a pattern recognition receptor and the loss of function of the genetic variants associated with Crohn s disease establishes a link between innate immunity and chronic bowel inflammation and confirms the pathogenetic importance of luminal bacteria. Moreover, these data are compatible with an immunodeficiency of the mucosal immune system as a pivotal first step in the pathogenesis of Crohn s disease [65]. Although the discoveries are important for understanding the etiology of Crohn s disease, at this time, they have only a modest role in clinical practice. Further studies are needed to clarify the genotype-phenotype relationships and the role of genetic testing in predicting disease behavior. A better understanding CARD15/NOD2 Mutations in Crohn s Disease Dig Dis 2003;21:
6 of the pathophysiologic mechanisms could lead to the development of new prophylactic and therapeutic strategies and to an individualized manner of their application. In case these prophylactic and therapeutic goals are reached, genetic testing for identifying high risk individuals and for predicting response to specific therapies will constitute an important new diagnostic tool for clinicians. References 1 Tysk C, Lindberg E, Jarnerot G, Floderus- Myrhed B: Ulcerative colitis and Crohn s disease in an unselected population of monozygotic and dizygotic twins: A study of heritability and the influence of smoking. Gut 1988;29: Thompson NP, Driscoll R, Pounder RE, Wakefield AJ: Genetics versus environment in inflammatory bowel disease: Results of a British twin study. BMJ 1996;312: Subhani J, Montgomery SM, Ounder RE, Wakefield AJ: Concordance rates of twins and siblings in inflammatory bowel disease. Gut 1998;42:A40. 4 Halfvarson J, Bodin L, Tysk C, Lindberg E, Jarnerot G: Inflammatory bowel disease in a Swedish twin cohort: A long-term follow-up of concordance and clinical characteristics. Gastroenterology 2003;124: Farmer RG, Michener WM, Mortimer EA: Studies of family history among patients with inflammatory bowel disease. Clin Gastroenterol 1980;9: Monsen U, Bernell O, Johansson C, Hellers G: Prevalence of inflammatory bowel disease among relatives of patients with Crohn s disease. Scand J Gastroenterol 1991;26: Russel MG, Pastoor CJ, Janssen KM, van Deursen CT, Muris JW, van Wijlick EH, Stockbrugger RW: Familial aggregation of inflammatory bowel disease: A population-based study in South Limburg, The Netherlands. The South Limburg IBD Study Group. Scand J Gastroenterol Suppl 1997;223: Orholm M, Munkholm P, Langholz E, Nielsen OH, Sorensen IA, Binder V: Familial occurrence of inflammatory bowel disease. N Engl J Med 1991;324: Peeters M, Nevens H, Baert F, Hiele M, de Meyer AM, Vlietinck R, Rutgeerts P: Familial aggregation in Crohn s disease: Increased ageadjusted risk and concordance in clinical characteristics. Gastroenterology 1996;111: Sonnenberg A, Wasserman ICH: Epidemiology of inflammatory bowel disease among US military veterans. Gastroenterology 1991;101: Kurata JH, Kantor-Fish S, Frankl H, Godby P, Vadheim CM: Crohn s disease among ethnic groups in a large health maintenance organization. Gastroenterology 1992;102: Ogunbi SO, Ransom JA, Sullivan K, Schoen BT, Gold BD: Inflammatory bowel disease in African-American children living in Georgia. J Pediatr 1998;133: Yang SK, Loftus EV Jr, Sandborn WJ: Epidemiology of inflammatory bowel disease in Asia. Inflamm Bowel Dis 2001;7: Roth MP, Petersen GM, McElree C, Vadheim CM, Panish JF, Rotter JI: Familial empiric risk estimates of inflammatory bowel disease in Ashkenazi Jews. Gastroenterology 1989;96: Yang H, Taylor KD, Rotter JI: Inflammatory bowel disease. I. Genetic epidemiology. Mol Genet Metab 2001;74: Hugot JP, Chamaillard M, Zouali H, Lesage S, Cezard JP, Belaiche J, Almer S, Tysk C, O Morain CA, Gassull M, Binder V, Finkel Y, Cortot A, Modigliani R, Laurent-Puig P, Gower-Rousseau C, Macry J, Colombel JF, Sahbatou M, Thomas G: Association of NOD2 leucine-rich repeat variants with susceptibility to Crohn s disease. Nature 2001;411: Ogura Y, Bonen DK, Inohara N, Nicolae DL, Chen FF, Ramos R, Britton H, Moran T, Karaliuskas R, Duerr RH, Achkar JP, Brant SR, Bayless TM, Kirschner BS, Hanauer SB, Nunez G, Cho JH: A frameshift mutation in NOD2 associated with susceptibility to Crohn s disease. Nature 2001;411: Hampe J, Cuthbert A, Croucher PJ, Mirza MM, Mascheretti S, Fisher S, Frenzel H, King K, Hasselmeyer A, MacPherson AJ, Bridger S, van Deventer S, Forbes A, Nikolaus S, Lennard-Jones JE, Foelsch UR, Krawczak M, Lewis C, Schreiber S, Mathew CG; Association between insertion mutation in NOD2 gene and Crohn s disease in German and British populations. Lancet 2001;357: Lesage S, Zouali H, Cezard JP, Colombel JF, Belaiche J, Almer S, Tysk C, O Morain C, Gassull M, Binder V, Finkel Y, Modigliani R, Gower-Rousseau C, Macry J, Merlin F, Chamaillard M, Jannot AS, Thomas G, Hugot JP; EPWG-IBD Group; EPIMAD Group; GETAID Group: CARD15/NOD2 mutational analysis and genotype-phenotype correlation in 612 patients with inflammatory bowel disease. Am J Hum Genet 2002;70: Ahmad T, Armuzzi A, Bunce M, Mulcahy- Hawes K, Marshall SE, Orchard TR, Crawshaw J, Large O, de Silva A, Cook JT, Barnardo M, Cullen S, Welsh KI, Jewell DP: The molecular classification of the clinical manifestations of Crohn s disease. Gastroenterology 2002;122: Cuthbert AP, Fisher SA, Mirza MM, King K, Hampe J, Croucher PJ, Mascheretti S, Sanderson J, Forbes A, Mansfield J, Schreiber S, Lewis CM, Mathew CG: The contribution of NOD2 gene mutations to the risk and site of disease in inflammatory bowel disease. Gastroenterology 2002;122: Vavassori P, Borgiani P, D Apice MR, De Negris F, Del Vecchio Blanco G, Monteleone I, Biancone L, Novelli G, Pallone E: 3020insC mutation within the NOD2 gene in Crohn s disease: Frequency and association with clinical pattern in an Italian population. Dig Liver Dis: 2002;34: Murillo L, Crusius JB, van Bodegraven AA, Alizadeh BZ, Pena AS: CARD15 gene and the classification of Crohn s disease. Immunogenetics 2002;54: Vermeire S, Wild G, Kocher K, Cousineau J, Dufresne L, Bitton A, Langelier D, Pare P, Lapointe G, Cohen A, Daly MJ, Rioux JD: CARD15 genetic variation in a Quebec population: Prevalence, genotype-phenotype relationship, and haplotype structure. Am J Hum Genet 2002;71: Radlmayr M, Torok HP, Martin K, Folwaczny C: The c-insertion mutation of the NOD2 gene is associated with fistulizing and fibrostenotic phenotypes in Crohn s disease. Gastroenterology 2002;122: Bonen DK, Ogura Y, Nicolae DL, Inohara N, Saab L, Tanabe T, Chen FF, Foster SJ, Duerr RH, Brant SR, Cho JH, Nunez G: Crohn s disease-associated NOD2 variants share a signaling defect in response to lipopolysaccharide and peptidoglycan. Gastroenterology 2003; 124: Cavanaugh JA, Adams KE, Quak EJ, Bryce ME, O Callaghan NJ, Rodgers HJ, Magarry GR, Butler WJ, Eaden JA, Roberts-Thomson IC, Pavli P, Wilson SR, Callen DF: CARD15/ NOD2 risk alleles in the development of Crohn s disease in the Australian population. Ann Hum Genet 2003;67: Bairead E, Harmon DL, Curtis AM, Kelly Y, O Leary C, Gardner M, Leahy DT, Vaughan P, Keegan D, O Morain C, O Donoghue D, Shanahan F, Parfrey NA, Quane KA: Association of NOD2 with Crohn s disease in a homogenous Irish population. Eur J Hum Genet 2003; 11: Hugot JP, Laurent-Puig P, Gower-Rousseau C, Olson JM, Lee JC, Beaugerie L, Naom I, Dupas JL, Van Gossum A, Orholm M, Bonaiti-Pellie C, Weissenbach J, Mathew CG, Lennard-Jones JE, Cortot A, Colombel JF, Thomas G: Mapping of a susceptibility locus for Crohn s disease on chromosome 16. Nature 1996;379: Dig Dis 2003;21: Török/Glas/Lohse/Folwaczny
7 30 Cavanaugh J: IBD International Genetics Consortium: International collaboration provides convincing linkage replication in complex disease through analysis of a large pooled data set: Crohn disease and chromosome 16. Am J Hum Genet 2001;68: Ogura Y, Inohara N, Benito A, Chen FF, Yamaoka S, Nunez G: Nod2, a Nod1/Apaf-1 family member that is restricted to monocytes and activates NF-kappaB. J Biol Chem 2001; 276: Bonen DK, Cho JH: The genetics of inflammatory bowel disease. Gastroenterology 2003;124: Inoue N, Tamura K, Kinouchi Y, Fukuda Y, Takahashi S, Ogura Y, Inohara N, Nunez G, Kishi Y, Koike Y, Shimosegawa T, Shimoyama T, Hibi T: Lack of common NOD2 variants in Japanese patients with Crohn s disease. Gastroenterology 2002;123: Yamazaki K, Takazoe M, Tanaka T, Kazumori T, Nakamura Y: Absence of mutation in the NOD2/CARD15 gene among 483 Japanese patients with Crohn s disease. J Hum Genet 2002;47: Sugimura M, Kinouchi Y, Takahashi S, Aihara H, Takagi S, Negoro K, Obana N, Kojima Y, Matsumoto K, Kikuchi T, Hiroki M, Oomori S, Shimosegawa T: CARD15/NOD2 mutational analysis in Japanese patients with Crohn s disease. Clin Genet 2003;63: Croucher PJ, Mascheretti S, Hampe J, Huse K, Frenzel H, Stoll M, Lu T, Nikolaus S, Yang SK, Krawczak M, Kim WH, Schreiber S: Haplotype structure and association to Crohn s disease of CARD15 mutations in two ethnically divergent populations. Eur J Hum Genet 2003; 11: Leong RW, Armuzzi A, Ahmad T, Wong ML, Tse P, Jewell DP, Sung JJ: NOD2/CARD15 gene polymorphisms and Crohn s disease in the Chinese population. Aliment Pharmacol Ther 2003;17: Bonen DK, Nicolae DL, Moran T, Turkyilmaz MA, Ramos R, Karaliukas R, Brant SR, Duerr RH, Kirschner BS, Hanauer SB, Cho JH: Racial Differences in NOD2 variation: Characterization of NOD2 in African-Americans with Crohn s disease. Gastroenterology 2002;122:A Zhou Z, Lin XY, Akolkar PN, Gulwani-Akolkar B, Levine J, Katz S, Silver J: Variation at NOD2/CARD15 in familial and sporadic cases of Crohn s disease in the Ashkenazi Jewish population. Am J Gastroenterol 2002;97: Linde K, Boor PP, Houwing-Duistermaat JJ, Kuipers EJ, Wilson JH, de Rooij FW: Card15 and Crohn s disease: Healthy homozygous carriers of the 3020insC frameshift mutation. Am J Gastroenterol 2003;98: Inohara N, Ogura Y, Nunez G: Nods: A family of cytosolic proteins that regulate the host response to pathogens. Curr Opin Microbiol 2002;5: Girardin SE, Sansonetti PJ, Philpott DJ: Intracellular vs. extracellular recognition of pathogens-common concepts in mammals and flies. Trends Microbiol 2002;10: Gutierrez O, Pipaon C, Inohara N, Fontalba A, Ogura Y, Prosper F, Nunez G, Fernandez- Luna JL: Induction of Nod2 in myelomonocytic and intestinal epithelial cells via nuclear factor-kappa B activation. J Biol Chem 2002;277: Hisamatsu T, Suzuki M, Reinecker HC, Nadeau WJ, McCormick BA, Podolsky DK: CARD15/NOD2 functions as an antibacterial factor in human intestinal epithelial cells. Gastroenterology 2003;124: Rosenstiel P, Fantini M, Brautigam K, Kuhbacher T, Waetzig GH, Seegert D, Schreiber S: TNF-alpha and IFN-gamma regulate the expression of the NOD2 (CARD15) gene in human intestinal epithelial cells. Gastroenterology 2003;12: Berrebi D, Maudinas R, Hugot JP, Chamaillard M, Chareyre F, De Lagausie P, Yang C, Desreumaux P, Giovannini M, Cezard JP, Zouali H, Emilie D, Peuchmaur M: Card15 gene overexpression in mononuclear and epithelial cells of the inflamed Crohn s disease colon. Gut 2003;52: Lala S, Ogura Y, Osborne C, Hor SY, Bromfield A, Davies S, Ogunbiyi O, Nunez G, Keshav S: Crohn s disease and the NOD2 gene: A role for Paneth cells. Gastroenterology 2003; 125: Chamaillard M, Philpott D, Girardin SE, Zouali H, Lesage S, Chareyre F, Bui TH, Giovannini M, Zaehringer U, Penard-Lacronique V, Sansonetti PJ, Hugot JP, Thomas G: Geneenvironment interaction modulated by allelic heterogeneity in inflammatory diseases. Proc Natl Acad Sci USA 2003;100: Inohara N, Ogura Y, Fontalba A, Gutierrez O, Pons F, Crespo J, Fukase K, Inamura S, Kusumoto S, Hashimoto M, Foster SJ, Moran AP, Fernandez-Luna JL, Nunez G: Host recognition of bacterial muramyl dipeptide mediated through NOD2. Implications for Crohn s disease. J Biol Chem 2003;278: Girardin SE, Boneca IG, Viala J, Chamaillard M, Labigne A, Thomas G, Philpott DJ, Sansonetti PJ: Nod2 is a general sensor of peptidoglycan through muramyl dipeptide (MDP) detection. J Biol Chem 2003;278: Bouma G, Strober W: The immunological and genetic basis of inflammatory bowel disease. Nat Rev Immunol 2003; Wehkamp J, Harder J, Weichental M, Herrlinger KR, Schmidt M, Schlee M, Nuding S, Schwab M, Schäfferle E, Stallmach A, Fellermann K, Schröder JM, Stange EF: Pathomechanismus des Morbus Crohn mit NOD-2 (CARD15) Mutation: Defiziente mukosale Defensinexpression bei intakter Zytokinexpression. Z Gastroenterol 2003;41:A Hugot JP, Zouali H, Lesage S: Lessons to be learned from the NOD2 gene in Crohn s disease. Eur J Gastroenterol Hepatol 2003;15: Gasche C, Alizadeh BZ, Pena AS: Genotypephenotype correlations: How many disorders constitute inflammatory bowel disease? Eur J Gastroenterol Hepatol 2003;15: Lee JC, Lennard-Jones JE: Inflammatory bowel disease in 67 families each with three or more affected first-degree relatives. Gastroenterology 1996;111: Bayless TM, Tokayer AZ, Polito JM 2nd, Quaskey SA, Mellits ED, Harris ML: Crohn s disease: Concordance for site and clinical type in affected family members Potential hereditary influences. Gastroenterology 1996;111: Hampe J, Grebe J, Nikolaus S, Solberg C, Croucher PJ, Mascheretti S, Jahnsen J, Moum B, Klump B, Krawczak M, Mirza MM, Foelsch UR, Vatn M, Schreiber S: Association of NOD2 (CARD 15) genotype with clinical course of Crohn s disease: A cohort study. Lancet 2002;359: Helio T, Halme L, Lappalainen M, Fodstad H, Paavola-Sakki P, Turunen U, Farkkila M, Krusius T, Kontula K: CARD15/NOD2 gene variants are associated with familially occurring and complicated forms of Crohn s disease. Gut 2003;52: Abreu MT, Taylor KD, Lin YC, Hang T, Gaiennie J, Landers CJ, Vasiliauskas EA, Kam LY, Rojany M, Papadakis KA, Rotter JI, Targan SR, Yang H: Mutations in NOD2 are associated with fibrostenosing disease in patients with Crohn s disease. Gastroenterology 2002; 123: Louis E, Michel V, Hugot JP, Reenaers C, Fontaine F, Delforge M, El Yafi F, Colombel JF, Belaiche J: Early development of stricturing or penetrating pattern in Crohn s disease is influenced by disease location, number of flares, and smoking but not by NOD2/CARD15 genotype. Gut 2003;52: Fidder HH, Olschwang S, Avidan B, Zouali H, Lang A, Bardan E, Picard O, Bar-Meir S, Colombel JF, Chowers Y: Association between mutations in the CARD15 (NOD2) gene and Crohn s disease in Israeli Jewish patients. Am J Med Genet 2003;121: Vermeire S, Louis E, Rutgeerts P, De Vos M, Van Gossum A, Belaiche J, Pescatore P, Fiasse R, Pelckmans P, Vlietinck R, Merlin F, Zouali H, Thomas G, Colombel JF, Hugot JP: Belgian Group of Infliximab Expanded Access Program and Fondation Jean Dausset CEPH, Paris, France: NOD2/CARD15 does not influence response to infliximab in Crohn s disease. Gastroenterology 2002;123: Mascheretti S, Hampe J, Croucher PJ, Nikolaus S, Andus T, Schubert S, Olson A, Bao W, Fölsch UR, Schreiber S: Response to infliximab treatment in Crohn s disease is not associated with mutations in the CARD15 (NOD2) gene: An analysis in 534 patients from two multicenter, prospective GCP-level trials. Pharmacogenetics 2002;12: Sartor RB: Clinical applications of advances in the genetics of IBD. Rev Gastroenterol Disord 2003;3(suppl 1):S9 S Folwaczny C, Glas J, Torok HP: Crohn s disease: An immunodeficiency? Eur J Gastroenterol Hepatol 2003;15: CARD15/NOD2 Mutations in Crohn s Disease Dig Dis 2003;21:
The cause of ulcerative colitis (UC) and Crohn s disease
 GASTROENTEROLOGY 2003;124:1767 1773 Inflammatory Bowel Disease in a Swedish Twin Cohort: A Long- Term Follow-up of Concordance and Clinical Characteristics JONAS HALFVARSON,* LENNART BODIN, CURT TYSK,*
GASTROENTEROLOGY 2003;124:1767 1773 Inflammatory Bowel Disease in a Swedish Twin Cohort: A Long- Term Follow-up of Concordance and Clinical Characteristics JONAS HALFVARSON,* LENNART BODIN, CURT TYSK,*
CARD15 and Crohn s Disease: Healthy Homozygous Carriers of the 3020insC Frameshift Mutation
 THE AMERICAN JOURNAL OF GASTROENTEROLOGY Vol. 98, No. 3, 2003 2003 by Am. Coll. of Gastroenterology ISSN 0002-9270/03/$30.00 Published by Elsevier Science Inc. doi:10.1016/s0002-9270(02)06009-4 CARD15
THE AMERICAN JOURNAL OF GASTROENTEROLOGY Vol. 98, No. 3, 2003 2003 by Am. Coll. of Gastroenterology ISSN 0002-9270/03/$30.00 Published by Elsevier Science Inc. doi:10.1016/s0002-9270(02)06009-4 CARD15
CARD15 Gene Mutations and Risk for Early Surgery in Pediatric-Onset Crohn s Disease
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2004;2:1003 1009 CARD15 Gene Mutations and Risk for Early Surgery in Pediatric-Onset Crohn s Disease SUBRA KUGATHASAN,* NICOLE COLLINS,* KAREN MARESSO, RAYMOND
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2004;2:1003 1009 CARD15 Gene Mutations and Risk for Early Surgery in Pediatric-Onset Crohn s Disease SUBRA KUGATHASAN,* NICOLE COLLINS,* KAREN MARESSO, RAYMOND
C Gasche, P Grundtner
 162 Recent advances in clinical practice GENOTYPES AND PHENOTYPES IN CROHN S DISEASE: DO THEY HELP IN CLINICAL MANAGEMENT? c CROHN S See end of article for authors affiliations Correspondence to: Professor
162 Recent advances in clinical practice GENOTYPES AND PHENOTYPES IN CROHN S DISEASE: DO THEY HELP IN CLINICAL MANAGEMENT? c CROHN S See end of article for authors affiliations Correspondence to: Professor
I n recent years it has been firmly established that anti-
 1237 INFLAMMATORY BOWEL DISEASE Anti-Saccharomyces cerevisiae antibodies in twins with inflammatory bowel disease J Halfvarson, A Standaert-Vitse, G Järnerot, B Sendid, T Jouault, L Bodin, A Duhamel, J
1237 INFLAMMATORY BOWEL DISEASE Anti-Saccharomyces cerevisiae antibodies in twins with inflammatory bowel disease J Halfvarson, A Standaert-Vitse, G Järnerot, B Sendid, T Jouault, L Bodin, A Duhamel, J
April 2003 EDITORIALS 1145
 April 2003 EDITORIALS 1145 experience in 500 patients (abstr). Gastroenterology 2003 (in press). 11. Sands B, Van Deventer S, Bernstein C, Kamm M, Rachmilewicz D, Chey W, Lashner B, Wolf D, Blank M, Wild
April 2003 EDITORIALS 1145 experience in 500 patients (abstr). Gastroenterology 2003 (in press). 11. Sands B, Van Deventer S, Bernstein C, Kamm M, Rachmilewicz D, Chey W, Lashner B, Wolf D, Blank M, Wild
A Genetic Contribution to Inflammatory Bowel Disease in Iceland: A Genealogic Approach
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2004;2:806 812 A Genetic Contribution to Inflammatory Bowel Disease in Iceland: A Genealogic Approach INGA REYNISDOTTIR,* DANIEL F. GUDBJARTSSON,* JOHANN HEIDAR
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2004;2:806 812 A Genetic Contribution to Inflammatory Bowel Disease in Iceland: A Genealogic Approach INGA REYNISDOTTIR,* DANIEL F. GUDBJARTSSON,* JOHANN HEIDAR
Breastfeeding and genetic factors in the etiology of inflammatory bowel disease in children
 Online Submissions: wjg.wjgnet.com World J Gastroenterol 009 January ; 5(3): 70-79 wjg@wjgnet.com World Journal of Gastroenterology ISSN 007-937 doi:0.3748/wjg.5.70 009 The WJG Press and Baishideng. All
Online Submissions: wjg.wjgnet.com World J Gastroenterol 009 January ; 5(3): 70-79 wjg@wjgnet.com World Journal of Gastroenterology ISSN 007-937 doi:0.3748/wjg.5.70 009 The WJG Press and Baishideng. All
Running head: CHRON'S DISEASE GENE-ENVIRONMENTAL INTERACTION 1
 Running head: CHRON'S DISEASE GENE-ENVIRONMENTAL INTERACTION 1 A review of Crohn's Disease Gene-Environmental Interaction A study of gene-environment interaction between genetic susceptibility variants
Running head: CHRON'S DISEASE GENE-ENVIRONMENTAL INTERACTION 1 A review of Crohn's Disease Gene-Environmental Interaction A study of gene-environment interaction between genetic susceptibility variants
Abstract. Background. Methodology. Results. a11111
 RESEARCH ARTICLE The NOD2 Single Nucleotide Polymorphism rs72796353 (IVS4+10 A>C) Is a Predictor for Perianal Fistulas in Patients with Crohn's Disease in the Absence of Other NOD2 Mutations a11111 OPEN
RESEARCH ARTICLE The NOD2 Single Nucleotide Polymorphism rs72796353 (IVS4+10 A>C) Is a Predictor for Perianal Fistulas in Patients with Crohn's Disease in the Absence of Other NOD2 Mutations a11111 OPEN
The roles of NOD like receptors in inflammation are different between Japanese and Caucasian.
 Mini Review 196 NOD like receptors and diseases Mini Review The roles of NOD like receptors in inflammation are different between Japanese and Caucasian. Tsuyoshi Tanabe 1,*), Natsu Yamaguchi 1), Yoshinobu
Mini Review 196 NOD like receptors and diseases Mini Review The roles of NOD like receptors in inflammation are different between Japanese and Caucasian. Tsuyoshi Tanabe 1,*), Natsu Yamaguchi 1), Yoshinobu
Ulcerative colitis (UC) and Crohn s disease (CD) are 2
 ORIGINAL ARTICLE Smoking and Inflammatory Bowel Disease: Trends in Familial and Sporadic Cohorts Jeffrey A. Tuvlin,MD,* Sania S. Raza, BA, Samuel Bracamonte, BA, Christina Julian, BA, Stephen B. Hanauer,
ORIGINAL ARTICLE Smoking and Inflammatory Bowel Disease: Trends in Familial and Sporadic Cohorts Jeffrey A. Tuvlin,MD,* Sania S. Raza, BA, Samuel Bracamonte, BA, Christina Julian, BA, Stephen B. Hanauer,
Genetics. Environment. You Are Only 10% Human. Pathogenesis of IBD. Advances in the Pathogenesis of IBD: Genetics Leads to Function IBD
 Advances in the Pathogenesis of IBD: Genetics Leads to Function Pathogenesis of IBD Environmental Factors Microbes Scott Plevy, MD Associate Professor of Medicine, Microbiology & Immunology UNC School
Advances in the Pathogenesis of IBD: Genetics Leads to Function Pathogenesis of IBD Environmental Factors Microbes Scott Plevy, MD Associate Professor of Medicine, Microbiology & Immunology UNC School
Periodontal status of patients with Crohn s Disease
 Page 1 of 5 ISSN 1612-7749 Quintessence International Publishing Group» Home» Issues» Issue 1 / 1999 [1-8]» Issue 2 / 1999 [9-19]» Issue 3 / 1999 [20-23]» Issue 4 / 1999 [24-27]» Issue 1 / 2000 [28-35]»
Page 1 of 5 ISSN 1612-7749 Quintessence International Publishing Group» Home» Issues» Issue 1 / 1999 [1-8]» Issue 2 / 1999 [9-19]» Issue 3 / 1999 [20-23]» Issue 4 / 1999 [24-27]» Issue 1 / 2000 [28-35]»
C rohn disease (CD) is a severe inflammatory disorder of
 689 ORIGINAL ARTICLE Estimating risks of common complex diseases across genetic environmental factors: the example of Crohn disease C M Lewis, S C L Whitwell, A Forbes, J Serson, C G Mathew, T M Marteau
689 ORIGINAL ARTICLE Estimating risks of common complex diseases across genetic environmental factors: the example of Crohn disease C M Lewis, S C L Whitwell, A Forbes, J Serson, C G Mathew, T M Marteau
Associations between NOD2/CARD15 genotype and phenotype in Crohn s disease-are we there yet?
 PO Box 2345, Beijing 100023, China World J Gastroenterol 2006 November 28; 12(44): 7097-7103 World Journal of Gastroenterology ISSN 1007-9327 wjg@wjgnet.com 2006 The WJG Press. All rights reserved. Associations
PO Box 2345, Beijing 100023, China World J Gastroenterol 2006 November 28; 12(44): 7097-7103 World Journal of Gastroenterology ISSN 1007-9327 wjg@wjgnet.com 2006 The WJG Press. All rights reserved. Associations
Prediction of Crohn s disease aggression through NOD2 /CARD15 gene sequencing in an Australian cohort
 Online Submissions: http://www.wjgnet.com/esps/ bpgoffice@wjgnet.com doi:10.3748/wjg.v20.i17.5008 World J Gastroenterol 2014 May 7; 20(17): 5008-5016 ISSN 1007-9327 (print) ISSN 2219-2840 (online) 2014
Online Submissions: http://www.wjgnet.com/esps/ bpgoffice@wjgnet.com doi:10.3748/wjg.v20.i17.5008 World J Gastroenterol 2014 May 7; 20(17): 5008-5016 ISSN 1007-9327 (print) ISSN 2219-2840 (online) 2014
One anticipated dividend of the huge financial investment. TUCAN (CARD8) Genetic Variants and Inflammatory Bowel Disease
 GASTROENTEROLOGY 2006;131:1190 1196 TUCAN (CARD8) Genetic Variants and Inflammatory Bowel Disease DERMOT P. B. MCGOVERN,*, HELEN BUTLER,* TARIQ AHMAD, MARTA PAOLUCCI,* DAVID A. VAN HEEL, KENICHI NEGORO,
GASTROENTEROLOGY 2006;131:1190 1196 TUCAN (CARD8) Genetic Variants and Inflammatory Bowel Disease DERMOT P. B. MCGOVERN,*, HELEN BUTLER,* TARIQ AHMAD, MARTA PAOLUCCI,* DAVID A. VAN HEEL, KENICHI NEGORO,
T he chronic inflammatory bowel diseases
 iii31 PAPER The genetic jigsaw of inflammatory bowel disease D A Watts, J Satsangi... Following a prolonged period of relative inertia, real progress has been made in the past few years in understanding
iii31 PAPER The genetic jigsaw of inflammatory bowel disease D A Watts, J Satsangi... Following a prolonged period of relative inertia, real progress has been made in the past few years in understanding
Polymorphisms in the DLG5 and OCTN cation transporter genes in Crohn s disease
 Gut Online First, published on June 14, 2005 as 10.1136/gut.2005.066340 1 Polymorphisms in the DLG5 and OCTN cation transporter genes in Crohn s disease * Helga-Paula Török 1,2, * Jürgen Glas 2,3, Laurian
Gut Online First, published on June 14, 2005 as 10.1136/gut.2005.066340 1 Polymorphisms in the DLG5 and OCTN cation transporter genes in Crohn s disease * Helga-Paula Török 1,2, * Jürgen Glas 2,3, Laurian
Why does Crohn's disease usually occur in terminal ileum?
 Journal of Crohn's and Colitis (2008) 2, 352 356 available at www.sciencedirect.com VIEWPOINT Why does Crohn's disease usually occur in terminal ileum? Renzo Caprilli University of Rome La Sapienza, Via
Journal of Crohn's and Colitis (2008) 2, 352 356 available at www.sciencedirect.com VIEWPOINT Why does Crohn's disease usually occur in terminal ileum? Renzo Caprilli University of Rome La Sapienza, Via
Intercellular adhesion molecule 1 gene polymorphisms in inflammatory bowel disease
 European Review for Medical and Pharmacological Sciences 2004; 8: 187-191 Intercellular adhesion molecule 1 gene polymorphisms in inflammatory bowel disease A. PAPA, S. DANESE, R. URGESI, A. GRILLO, S.
European Review for Medical and Pharmacological Sciences 2004; 8: 187-191 Intercellular adhesion molecule 1 gene polymorphisms in inflammatory bowel disease A. PAPA, S. DANESE, R. URGESI, A. GRILLO, S.
Behaviour of Crohn s disease according to the Vienna classification: changing pattern over the course of the disease
 Gut 2001;49:777 782 777 Department of Gastroenterology, University Hospital of Liège, Belgium E Louis A Collard A F Oger E Degroote F Aboul Nasr El Yafi J Belaiche Correspondence to: E Louis, Service de
Gut 2001;49:777 782 777 Department of Gastroenterology, University Hospital of Liège, Belgium E Louis A Collard A F Oger E Degroote F Aboul Nasr El Yafi J Belaiche Correspondence to: E Louis, Service de
Genetics of Pediatric Inflammatory Bowel Disease
 Genetics of Pediatric Inflammatory Bowel Disease Judith Kelsen MD Assistant Professor of Pediatrics Division of Gastroenterology, Hepatology, and Nutrition IBD Education Day 2/9/2014 Objectives Brief overview
Genetics of Pediatric Inflammatory Bowel Disease Judith Kelsen MD Assistant Professor of Pediatrics Division of Gastroenterology, Hepatology, and Nutrition IBD Education Day 2/9/2014 Objectives Brief overview
Investigations based on animal models of Crohn s disease
 GASTROENTEROLOGY 2004;126:414 424 Association of Antibody Responses to Microbial Antigens and Complications of Small Bowel Crohn s Disease WILLIAM S. MOW,* ERIC A. VASILIAUSKAS,* YING CHAO LIN, PHILLIP
GASTROENTEROLOGY 2004;126:414 424 Association of Antibody Responses to Microbial Antigens and Complications of Small Bowel Crohn s Disease WILLIAM S. MOW,* ERIC A. VASILIAUSKAS,* YING CHAO LIN, PHILLIP
Epidemiology of Inflammatory Bowel Disease and Overview of Pathogenesis
 Epidemiology of Inflammatory Bowel Disease and Overview of Pathogenesis Crohn s disease (CD) and ulcerative colitis (UC) are believed to affect approximately 1.4 million people in the United States (US).
Epidemiology of Inflammatory Bowel Disease and Overview of Pathogenesis Crohn s disease (CD) and ulcerative colitis (UC) are believed to affect approximately 1.4 million people in the United States (US).
Defensin deficiency, intestinal microbes, and the clinical phenotypes of Crohn s disease
 Defensin deficiency, intestinal microbes, and the clinical phenotypes of Crohn s disease Jan Wehkamp,*,1 Michael Schmid, Klaus Fellermann, and Eduard F. Stange *Department of Microbiology and Immunology,
Defensin deficiency, intestinal microbes, and the clinical phenotypes of Crohn s disease Jan Wehkamp,*,1 Michael Schmid, Klaus Fellermann, and Eduard F. Stange *Department of Microbiology and Immunology,
NOD2/CARD15 gene influences disease behaviour but not IBD susceptibility in a Moroccan population
 NOD2/CARD15 gene influences disease behaviour but not IBD susceptibility in a Moroccan population xxxxxxxxxxxxxxx Nadia Serbati 1,3, Wafaa Badre 2, Brehima Diakite 1,3, Sellama Nadifi 1,3 1 Laboratory
NOD2/CARD15 gene influences disease behaviour but not IBD susceptibility in a Moroccan population xxxxxxxxxxxxxxx Nadia Serbati 1,3, Wafaa Badre 2, Brehima Diakite 1,3, Sellama Nadifi 1,3 1 Laboratory
CARD15: a Pleiotropic Autoimmune Gene That Confers Susceptibility to Psoriatic Arthritis
 Am. J. Hum. Genet. 73:677 681, 2003 Report CARD15: a Pleiotropic Autoimmune Gene That Confers Susceptibility to Psoriatic Arthritis P. Rahman, 1 S. Bartlett, 1 F. Siannis, 2 F. J. Pellett, 3 V. T. Farewell,
Am. J. Hum. Genet. 73:677 681, 2003 Report CARD15: a Pleiotropic Autoimmune Gene That Confers Susceptibility to Psoriatic Arthritis P. Rahman, 1 S. Bartlett, 1 F. Siannis, 2 F. J. Pellett, 3 V. T. Farewell,
Disease behavior in adult patients- are there predictors for stricture or fistula formation?
 Disease behavior in adult patients- are there predictors for stricture or fistula formation? Falk Symposium 168, Madrid, Spain Iris Dotan, M.D., Head, IBD Center, Department of Gastroenterology and Liver
Disease behavior in adult patients- are there predictors for stricture or fistula formation? Falk Symposium 168, Madrid, Spain Iris Dotan, M.D., Head, IBD Center, Department of Gastroenterology and Liver
Crohn Disease: Frequency and Nature of CARD15 Mutations in Ashkenazi and Sephardi/Oriental Jewish Families
 Am. J. Hum. Genet. 74:623 636, 2004 Crohn Disease: Frequency and Nature of CARD15 Mutations in Ashkenazi and Sephardi/Oriental Jewish Families Turgut Tukel, 1,6* Adel Shalata, 1* Daniel Present, 2 Daniel
Am. J. Hum. Genet. 74:623 636, 2004 Crohn Disease: Frequency and Nature of CARD15 Mutations in Ashkenazi and Sephardi/Oriental Jewish Families Turgut Tukel, 1,6* Adel Shalata, 1* Daniel Present, 2 Daniel
Sex stratification of an inflammatory bowel disease genome search shows male-specific linkage to the HLA region of chromosome 6
 (2002) 10, 259 ± 265 ã 2002 Nature Publishing Group All rights reserved 1018-4813/02 $25.00 www.nature.com/ejhg ARTICLE Sex stratification of an inflammatory bowel disease genome search shows male-specific
(2002) 10, 259 ± 265 ã 2002 Nature Publishing Group All rights reserved 1018-4813/02 $25.00 www.nature.com/ejhg ARTICLE Sex stratification of an inflammatory bowel disease genome search shows male-specific
T he integrity of gut barrier function in patients with
 342 INFLAMMATORY BOWEL DISEASE Genetic basis for increased intestinal permeability in families with Crohn s disease: role of CARD15 3020insC mutation? S Buhner, C Buning, J Genschel, K Kling, D Herrmann,
342 INFLAMMATORY BOWEL DISEASE Genetic basis for increased intestinal permeability in families with Crohn s disease: role of CARD15 3020insC mutation? S Buhner, C Buning, J Genschel, K Kling, D Herrmann,
D2 inhibits TLR2- initiated 12p40 transcription (-) TLR2 PGN MDP. MyD88 IRAK ECSIT TRAF6 NIK. Smallest unit of PGN muramyl dipeptide IKK.
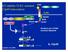 D2 inhibits TLR2- initiated 12p40 transcription CARD CARD NOD2 LRR RICK/Rip2 NIK MDP TRAF6 PGN TLR2 MyD88 IRAK ECSIT (-) IKK Smallest unit of PGN muramyl dipeptide IκB NF-κB atanabe et al, 2004 NF-κB IL-12p40
D2 inhibits TLR2- initiated 12p40 transcription CARD CARD NOD2 LRR RICK/Rip2 NIK MDP TRAF6 PGN TLR2 MyD88 IRAK ECSIT (-) IKK Smallest unit of PGN muramyl dipeptide IκB NF-κB atanabe et al, 2004 NF-κB IL-12p40
Genetic basis for increased intestinal permeability in families with Crohn s disease: Role of CARD insC mutation?
 Gut Online First, published on July 29, 2005 as 10.1136/gut.2005.065557 1 Genetic basis for increased intestinal permeability in families with Crohn s disease: Role of CARD15 3020insC mutation? Sabine
Gut Online First, published on July 29, 2005 as 10.1136/gut.2005.065557 1 Genetic basis for increased intestinal permeability in families with Crohn s disease: Role of CARD15 3020insC mutation? Sabine
HLA TYPING AND EXPRESSION: POTENTIAL MARKER FOR IDENTIFYING EARLY DYSPLASIA AND STRATIFYING THE RISK FOR IBD-CANCER
 HLA TYPING AND EXPRESSION: POTENTIAL MARKER FOR IDENTIFYING EARLY DYSPLASIA AND STRATIFYING THE RISK FOR IBD-CANCER Megan Garrity, S. Breanndan Moore, M.D., William Sandborn, M.D., Vernon Pankratz, Ph.D.,
HLA TYPING AND EXPRESSION: POTENTIAL MARKER FOR IDENTIFYING EARLY DYSPLASIA AND STRATIFYING THE RISK FOR IBD-CANCER Megan Garrity, S. Breanndan Moore, M.D., William Sandborn, M.D., Vernon Pankratz, Ph.D.,
Title: Toll like receptor four (tlrfour) polymorphisms in tunisians patients with crohn's disease: genotype-phenotype correlation
 Author's response to reviews Title: Toll like receptor four (tlrfour) polymorphisms in tunisians patients with crohn's disease: genotype-phenotype correlation Authors: Lilia Zouiten (w.mekki@laposte.net)
Author's response to reviews Title: Toll like receptor four (tlrfour) polymorphisms in tunisians patients with crohn's disease: genotype-phenotype correlation Authors: Lilia Zouiten (w.mekki@laposte.net)
Crohn s disease is a chronic inflammatory bowel disease
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2003;1:5 9 REVIEWS The CARD15 (also known as NOD2) Gene in Crohn s Disease: Are There Implications for Current Clinical Practice? JEAN FRÉDÉRIC COLOMBEL Department
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2003;1:5 9 REVIEWS The CARD15 (also known as NOD2) Gene in Crohn s Disease: Are There Implications for Current Clinical Practice? JEAN FRÉDÉRIC COLOMBEL Department
Lymphotoxin alpha gene in Crohn's disease patients: absence of implication in the response to infliximab in a large cohort study
 Lymphotoxin alpha gene in Crohn's disease patients: absence of implication in the response to infliximab in a large cohort study Vinciane Dideberg a, Edouard Louis b, Frédéric Farnir c, Sabrina Bertoli
Lymphotoxin alpha gene in Crohn's disease patients: absence of implication in the response to infliximab in a large cohort study Vinciane Dideberg a, Edouard Louis b, Frédéric Farnir c, Sabrina Bertoli
The etiology of the chronic inflammatory bowel diseases. Evidence for Inflammatory Bowel Disease of a Susceptibility Locus on the X Chromosome
 GASTROENTEROLOGY 2001;120:834 840 Evidence for Inflammatory Bowel Disease of a Susceptibility Locus on the X Chromosome SEVERINE VERMEIRE,* JACK SATSANGI, MARC PEETERS,* MILES PARKES, DEREK P. JEWELL,
GASTROENTEROLOGY 2001;120:834 840 Evidence for Inflammatory Bowel Disease of a Susceptibility Locus on the X Chromosome SEVERINE VERMEIRE,* JACK SATSANGI, MARC PEETERS,* MILES PARKES, DEREK P. JEWELL,
Gut Microbiota and IBD. Vahedi. H M.D Associate Professor of Medicine DDRI
 Gut Microbiota and IBD Vahedi. H M.D Associate Professor of Medicine DDRI 1393.3.1 2 GUT MICROBIOTA 100 Trillion Microbes - 10 times more than cells in our body Collective weight of about 1kg in human
Gut Microbiota and IBD Vahedi. H M.D Associate Professor of Medicine DDRI 1393.3.1 2 GUT MICROBIOTA 100 Trillion Microbes - 10 times more than cells in our body Collective weight of about 1kg in human
The IBD2 Locus Shows Linkage Heterogeneity between Ulcerative Colitis and Crohn Disease
 Am. J. Hum. Genet. 67:1605 1610, 2000 Report The IBD2 Locus Shows Linkage Heterogeneity between Ulcerative Colitis and Crohn Disease Miles Parkes, 1,2 M. Michael Barmada, 3 Jack Satsangi, 1,2 Daniel E.
Am. J. Hum. Genet. 67:1605 1610, 2000 Report The IBD2 Locus Shows Linkage Heterogeneity between Ulcerative Colitis and Crohn Disease Miles Parkes, 1,2 M. Michael Barmada, 3 Jack Satsangi, 1,2 Daniel E.
Predicting the natural history of IBD. Séverine Vermeire, MD, PhD Department of Gastroenterology University Hospital Leuven Belgium
 Predicting the natural history of IBD Séverine Vermeire, MD, PhD Department of Gastroenterology University Hospital Leuven Belgium Patient 1 Patient 2 Age 22 Frequent cramps and diarrhea for 6 months Weight
Predicting the natural history of IBD Séverine Vermeire, MD, PhD Department of Gastroenterology University Hospital Leuven Belgium Patient 1 Patient 2 Age 22 Frequent cramps and diarrhea for 6 months Weight
Ulcerative colitis (UC) and Crohn s disease are characterized
 GASTROENTEROLOGY 2000;118:274 278 Clinical Phenotype Is Related to HLA Genotype in the Peripheral Arthropathies of Inflammatory Bowel Disease TIMOTHY R. ORCHARD,* S. THIYAGARAJA,* KENNETH I. WELSH, B.
GASTROENTEROLOGY 2000;118:274 278 Clinical Phenotype Is Related to HLA Genotype in the Peripheral Arthropathies of Inflammatory Bowel Disease TIMOTHY R. ORCHARD,* S. THIYAGARAJA,* KENNETH I. WELSH, B.
NOD2 Activation promotes anti-inflammatory activity of human Umbilical cord blood MSCs against Inflammatory bowel disease
 NOD2 Activation promotes anti-inflammatory activity of human Umbilical cord blood MSCs against Inflammatory bowel disease Prof. Kyung-Sun Kang, DVM, PhD. Adult Stem Cell Research Center Seoul National
NOD2 Activation promotes anti-inflammatory activity of human Umbilical cord blood MSCs against Inflammatory bowel disease Prof. Kyung-Sun Kang, DVM, PhD. Adult Stem Cell Research Center Seoul National
Towards Precision Medicine in Inflammatory Bowel Diseases
 Precision Medicine and Biomarkers Leaders Summit. Munich September 13-14, 2018 Towards Precision Medicine in Inflammatory Bowel Diseases ANDRÉS HURTADO-LORENZO, Ph.D. SENIOR DIRECTOR OF TRANSLATIONAL RESEARCH
Precision Medicine and Biomarkers Leaders Summit. Munich September 13-14, 2018 Towards Precision Medicine in Inflammatory Bowel Diseases ANDRÉS HURTADO-LORENZO, Ph.D. SENIOR DIRECTOR OF TRANSLATIONAL RESEARCH
Role of ATG16L, NOD2 and IL23R in Crohn s disease pathogenesis
 Online Submissions: http://www.wjgnet.com/1007-9327office wjg@wjgnet.com doi:10.3748/wjg.v18.i5.412 World J Gastroenterol 2012 February 7; 18(5): 412-424 ISSN 1007-9327 (print) ISSN 2219-2840 (online)
Online Submissions: http://www.wjgnet.com/1007-9327office wjg@wjgnet.com doi:10.3748/wjg.v18.i5.412 World J Gastroenterol 2012 February 7; 18(5): 412-424 ISSN 1007-9327 (print) ISSN 2219-2840 (online)
Inflammatory Bowel Diseases (IBD) Clinical aspects Nitsan Maharshak M.D., IBD Center, Department of Gastroenterology and Liver Diseases Tel Aviv Soura
 Inflammatory Bowel Diseases (IBD) Clinical aspects Nitsan Maharshak M.D., IBD Center, Department of Gastroenterology and Liver Diseases Tel Aviv Sourasky Medical Center Tel Aviv, Israel IBD- clinical features
Inflammatory Bowel Diseases (IBD) Clinical aspects Nitsan Maharshak M.D., IBD Center, Department of Gastroenterology and Liver Diseases Tel Aviv Sourasky Medical Center Tel Aviv, Israel IBD- clinical features
Chapter 3 The Induced Responses of Innate Immunity
 Chapter 3 The Induced Responses of Innate Immunity Pattern recognition by cells of the innate immune system Pattern recognition by cells of the innate immune system 4 main pattern recognition receptors
Chapter 3 The Induced Responses of Innate Immunity Pattern recognition by cells of the innate immune system Pattern recognition by cells of the innate immune system 4 main pattern recognition receptors
The Role of Human Leukocyte Antigen (HLA) Complex in IBD: Crohn s Disease. and Ulcerative Colitis
 Advanced Studies in Biology, Vol. 1, 2009, no. 1, 37-41 The Role of Human Leukocyte Antigen (HLA) Complex in IBD: Crohn s Disease and Ulcerative Colitis Manuel Muro, Ruth López, José A. Campillo, *Hortensia
Advanced Studies in Biology, Vol. 1, 2009, no. 1, 37-41 The Role of Human Leukocyte Antigen (HLA) Complex in IBD: Crohn s Disease and Ulcerative Colitis Manuel Muro, Ruth López, José A. Campillo, *Hortensia
GENETIC VARIATION AND CLINICAL MANIFESTATIONS IN INFLAMMATORY BOWEL DISEASE. Maarit Lappalainen
 GENETIC VARIATION AND CLINICAL MANIFESTATIONS IN INFLAMMATORY BOWEL DISEASE Maarit Lappalainen Department of Medicine and Research Program for Molecular Medicine, Biomedicum Helsinki, University of Helsinki,
GENETIC VARIATION AND CLINICAL MANIFESTATIONS IN INFLAMMATORY BOWEL DISEASE Maarit Lappalainen Department of Medicine and Research Program for Molecular Medicine, Biomedicum Helsinki, University of Helsinki,
Mutations in NOD2 Are Associated With Fibrostenosing Disease in Patients With Crohn s Disease
 GASTROENTEROLOGY 2002;123:679 688 Mutations in NOD2 Are Associated With Fibrostenosing Disease in Patients With Crohn s Disease MARIA T. ABREU,* KENT D. TAYLOR, YING CHAO LIN, TIEU HANG, JOANNE GAIENNIE,*
GASTROENTEROLOGY 2002;123:679 688 Mutations in NOD2 Are Associated With Fibrostenosing Disease in Patients With Crohn s Disease MARIA T. ABREU,* KENT D. TAYLOR, YING CHAO LIN, TIEU HANG, JOANNE GAIENNIE,*
Personalized Medicine in IBD
 Personalized Medicine in IBD Anita Afzali MD, MPH Assistant Professor of Medicine Director, Inflammatory Bowel Diseases Program University of Washington Harborview Medical Center CCFA April 2 nd, 2016
Personalized Medicine in IBD Anita Afzali MD, MPH Assistant Professor of Medicine Director, Inflammatory Bowel Diseases Program University of Washington Harborview Medical Center CCFA April 2 nd, 2016
Recent Advances in the Management of Refractory IBD
 Recent Advances in the Management of Refractory IBD Raina Shivashankar, M.D. Assistant Professor of Medicine Division of Gastroenterology and Hepatology Thomas Jefferson University Philadelphia, PA Outline
Recent Advances in the Management of Refractory IBD Raina Shivashankar, M.D. Assistant Professor of Medicine Division of Gastroenterology and Hepatology Thomas Jefferson University Philadelphia, PA Outline
Chapter 6. ATG16L1 and IL23R are associated with Inflammatory Bowel Diseases but not with Celiac Disease in the Netherlands
 Chapter 6 ATG16L1 and IL23R are associated with Inflammatory Bowel Diseases but not with Celiac Disease in the Netherlands R.K. Weersma, A. Zhernakova, I.M. Nolte, C. Lefebvre, J.D. Rioux, F. Mulder, H.M.
Chapter 6 ATG16L1 and IL23R are associated with Inflammatory Bowel Diseases but not with Celiac Disease in the Netherlands R.K. Weersma, A. Zhernakova, I.M. Nolte, C. Lefebvre, J.D. Rioux, F. Mulder, H.M.
A Case of Inflammatory Bowel Disease
 A Case of Inflammatory Bowel Disease Dr Barrie Rathbone www.le.ac.uk 26 year old Polish woman Admitted as emergency under surgeons RUQ and RIF pain Abdominal pain had occurred intermittently for a few
A Case of Inflammatory Bowel Disease Dr Barrie Rathbone www.le.ac.uk 26 year old Polish woman Admitted as emergency under surgeons RUQ and RIF pain Abdominal pain had occurred intermittently for a few
Genetic and Environmental Risks for IBD
 Genetic and Environmental Risks for IBD CCFA April 26, 2014 Presented by: Name goes here April 30, 2014 TheoTheodore 1 Genetic and Environmental Risks for IBD Theodore M. Bayless, M.D. Director Emeritus
Genetic and Environmental Risks for IBD CCFA April 26, 2014 Presented by: Name goes here April 30, 2014 TheoTheodore 1 Genetic and Environmental Risks for IBD Theodore M. Bayless, M.D. Director Emeritus
They all do it! What?
 They all do it! What? Defensins: the endogenous antibiotics of body surfaces Wehkamp J et al. (2005) Mechanisms of Disease: defensins in gastrointestinal diseases Nat Clin Pract Gastroenterol Hepatol 2:
They all do it! What? Defensins: the endogenous antibiotics of body surfaces Wehkamp J et al. (2005) Mechanisms of Disease: defensins in gastrointestinal diseases Nat Clin Pract Gastroenterol Hepatol 2:
Probiotic bacteria: mechanisms of action?
 Probiotic bacteria: mechanisms of action? Probiotic derived antibacterial substances (microcins) Competitive inhibition of pathogens Modulation of inflammatory responses: Increasing antiinflammatory cytokine
Probiotic bacteria: mechanisms of action? Probiotic derived antibacterial substances (microcins) Competitive inhibition of pathogens Modulation of inflammatory responses: Increasing antiinflammatory cytokine
C rohn s disease (CD) is a chronic idiopathic inflammatory
 223 INFLAMMATORY BOWEL DISEASE Epithelioid granulomas, pattern recognition receptors, and phenotypes of Crohn s disease M Pierik, G De Hertogh, S Vermeire, G Van Assche, P Van Eyken, S Joossens, G Claessens,
223 INFLAMMATORY BOWEL DISEASE Epithelioid granulomas, pattern recognition receptors, and phenotypes of Crohn s disease M Pierik, G De Hertogh, S Vermeire, G Van Assche, P Van Eyken, S Joossens, G Claessens,
Updates in the genetics of inflammatory bowel disease
 Gastroenterology and Hepatology From Bed to Bench. 2010;3(4):149-163 2010 RIGLD, Research Institute for Gastroenterology and Liver Diseases REVIEW ARTICLE Updates in the genetics of inflammatory bowel
Gastroenterology and Hepatology From Bed to Bench. 2010;3(4):149-163 2010 RIGLD, Research Institute for Gastroenterology and Liver Diseases REVIEW ARTICLE Updates in the genetics of inflammatory bowel
Genetics and Genomics in Medicine Chapter 8 Questions
 Genetics and Genomics in Medicine Chapter 8 Questions Linkage Analysis Question Question 8.1 Affected members of the pedigree above have an autosomal dominant disorder, and cytogenetic analyses using conventional
Genetics and Genomics in Medicine Chapter 8 Questions Linkage Analysis Question Question 8.1 Affected members of the pedigree above have an autosomal dominant disorder, and cytogenetic analyses using conventional
Primary Results Citation 2
 Table S1. Adalimumab clinical trials 1 ClinicalTrials.gov Rheumatoid Arthritis 3 NCT00195663 Breedveld FC, Weisman MH, Kavanaugh AF, et al. The PREMIER study. A multicenter, randomized, double-blind clinical
Table S1. Adalimumab clinical trials 1 ClinicalTrials.gov Rheumatoid Arthritis 3 NCT00195663 Breedveld FC, Weisman MH, Kavanaugh AF, et al. The PREMIER study. A multicenter, randomized, double-blind clinical
MEDICAL PROGRESS. Review Article. N Engl J Med, Vol. 347, No. 6 August 8,
 Review Article Medical Progress INFLAMMATORY BOWEL DISEASE DANIEL K. PODOLSKY, M.D. IN the decades since the major forms of idiopathic inflammatory bowel disease were defined on the basis of clinical manifestations,
Review Article Medical Progress INFLAMMATORY BOWEL DISEASE DANIEL K. PODOLSKY, M.D. IN the decades since the major forms of idiopathic inflammatory bowel disease were defined on the basis of clinical manifestations,
Date of preparation: 06/ IBD/
 Mechanisms Mechanisms of of Disease Disease: The The Science of of IBD IBD 64002 Date of preparation: 06/11 2013 IBD/2013-11-01 Table of Contents IBD Background and Disease Management Etiology and Pathophysiology
Mechanisms Mechanisms of of Disease Disease: The The Science of of IBD IBD 64002 Date of preparation: 06/11 2013 IBD/2013-11-01 Table of Contents IBD Background and Disease Management Etiology and Pathophysiology
Original Paper. Gastrointestinal
 Gastrointestinal - 04546 817 Clinical Presentation of Crohn's Disease. Association between Familial Disease, Smoking, Disease Phenotype, Extraintestinal Manifestations and Need for Surgery Original Paper
Gastrointestinal - 04546 817 Clinical Presentation of Crohn's Disease. Association between Familial Disease, Smoking, Disease Phenotype, Extraintestinal Manifestations and Need for Surgery Original Paper
Position of Biologics in IBD Circa 2006: Top Down vs. Step Up Therapy
 Position of Biologics in IBD Circa 2006: Top Down vs. Step Up Therapy Stephen B. Hanauer, MD University of Chicago Potential Conflicts: Centocor/Schering, Abbott, UCB, Elan, Berlex, PDL Goals of Treatment
Position of Biologics in IBD Circa 2006: Top Down vs. Step Up Therapy Stephen B. Hanauer, MD University of Chicago Potential Conflicts: Centocor/Schering, Abbott, UCB, Elan, Berlex, PDL Goals of Treatment
Association between polymorphisms in caspase recruitment domain containing protein 15 and allergy in two German populations
 Association between polymorphisms in caspase recruitment domain containing protein 15 and allergy in two German populations Michael Kabesch, MD, a Wilfried Peters, PhD, a David Carr, BSc, a Wolfgang Leupold,
Association between polymorphisms in caspase recruitment domain containing protein 15 and allergy in two German populations Michael Kabesch, MD, a Wilfried Peters, PhD, a David Carr, BSc, a Wolfgang Leupold,
Environmental factors affecting IBD Have we made progress? Peter Laszlo Lakatos 1st Department of Medicine Semmelweis University Budapest Hungary
 Environmental factors affecting IBD Have we made progress? Peter Laszlo Lakatos 1st Department of Medicine Semmelweis University Budapest Hungary Environmental factors in IBD Are associated with disease
Environmental factors affecting IBD Have we made progress? Peter Laszlo Lakatos 1st Department of Medicine Semmelweis University Budapest Hungary Environmental factors in IBD Are associated with disease
HLA and antigen presentation. Department of Immunology Charles University, 2nd Medical School University Hospital Motol
 HLA and antigen presentation Department of Immunology Charles University, 2nd Medical School University Hospital Motol MHC in adaptive immunity Characteristics Specificity Innate For structures shared
HLA and antigen presentation Department of Immunology Charles University, 2nd Medical School University Hospital Motol MHC in adaptive immunity Characteristics Specificity Innate For structures shared
Azathioprine for Induction and Maintenance of Remission in Crohn s Disease
 Azathioprine for Induction and Maintenance of Remission in Crohn s Disease William J. Sandborn, MD Chief, Division of Gastroenterology Director, UCSD IBD Center Objectives Azathioprine as induction and
Azathioprine for Induction and Maintenance of Remission in Crohn s Disease William J. Sandborn, MD Chief, Division of Gastroenterology Director, UCSD IBD Center Objectives Azathioprine as induction and
Scheduled Maintenance Therapy with Infliximab Improves the Prognosis of Crohn s Disease: A Single Center Prospective Cohort Study in Japan
 Tohoku J. Exp. Med., 2010, 220, 207-215 Infliximab Improves the Prognosis of Crohn s Disease 207 Scheduled Maintenance Therapy with Infliximab Improves the Prognosis of Crohn s Disease: A Single Center
Tohoku J. Exp. Med., 2010, 220, 207-215 Infliximab Improves the Prognosis of Crohn s Disease 207 Scheduled Maintenance Therapy with Infliximab Improves the Prognosis of Crohn s Disease: A Single Center
Accepted Manuscript. Correlation or Causation: Sex Hormones and Microscopic Colitis. Baldeep Pabla, Reid M. Ness
 Accepted Manuscript Correlation or Causation: Sex Hormones and Microscopic Colitis Baldeep Pabla, Reid M. Ness PII: S0016-5085(18)35216-8 DOI: https://doi.org/10.1053/j.gastro.2018.11.007 Reference: YGAST
Accepted Manuscript Correlation or Causation: Sex Hormones and Microscopic Colitis Baldeep Pabla, Reid M. Ness PII: S0016-5085(18)35216-8 DOI: https://doi.org/10.1053/j.gastro.2018.11.007 Reference: YGAST
Indications for use of Infliximab
 Indications for use of Infliximab Moscow, June 10 th 2006 Prof. Dr. Dr. Gerhard Rogler Klinik und Poliklinik für Innere Medizin I Universität Regensburg Case report 1989: Diagnosis of Crohn s disease of
Indications for use of Infliximab Moscow, June 10 th 2006 Prof. Dr. Dr. Gerhard Rogler Klinik und Poliklinik für Innere Medizin I Universität Regensburg Case report 1989: Diagnosis of Crohn s disease of
Signal Transduction in Inflammatory Bowel Disease
 E v e n t s 0 6 4 Signal Transduction in Inflammatory Bowel Disease 0 1 2 3 4 1 0 1 0 1 0 1 0 1 0 F L 2 - H e ig h t Vineeta Khare Ph.D Overview Inflammatory Bowel Diseases 1. Epidemiology, Symptoms and
E v e n t s 0 6 4 Signal Transduction in Inflammatory Bowel Disease 0 1 2 3 4 1 0 1 0 1 0 1 0 1 0 F L 2 - H e ig h t Vineeta Khare Ph.D Overview Inflammatory Bowel Diseases 1. Epidemiology, Symptoms and
Escherichia coli Nissle 1917
 Immunoregulation in Inflammatory Bowel Diseases New therapeutic approaches Probiotics Escherichia coli Nissle 1917 Andreas Sturm Medizinische Klinik m.s. Hepatologie, Gastroenterologie, Endokrinologie
Immunoregulation in Inflammatory Bowel Diseases New therapeutic approaches Probiotics Escherichia coli Nissle 1917 Andreas Sturm Medizinische Klinik m.s. Hepatologie, Gastroenterologie, Endokrinologie
Preface and outline of the thesis
 Preface Celiac disease (CD) is characterized by a chronic immune reaction in the small intestine to the gluten proteins that are present in a (Western) daily diet, derived from wheat, barley and rye. It
Preface Celiac disease (CD) is characterized by a chronic immune reaction in the small intestine to the gluten proteins that are present in a (Western) daily diet, derived from wheat, barley and rye. It
PATHOPHYSIOLOGICAL AND CLINICAL STUDIES ON CROHN S DISEASE IN CHILDREN
 Department of Women s and Children s Health Karolinska Institutet, Stockholm, Sweden PATHOPHYSIOLOGICAL AND CLINICAL STUDIES ON CROHN S DISEASE IN CHILDREN Maja Ideström Stockholm 2012 All previously published
Department of Women s and Children s Health Karolinska Institutet, Stockholm, Sweden PATHOPHYSIOLOGICAL AND CLINICAL STUDIES ON CROHN S DISEASE IN CHILDREN Maja Ideström Stockholm 2012 All previously published
No evidence of association between NOD2/CARD15 gene polymorphism and atherosclerotic events after renal transplantation.
 No evidence of association between NOD2/CARD15 gene polymorphism and atherosclerotic events after renal transplantation. Cécile Courivaud, Christophe Ferrand, Marina Deschamps, Pierre Tiberghien, Jean-Marc
No evidence of association between NOD2/CARD15 gene polymorphism and atherosclerotic events after renal transplantation. Cécile Courivaud, Christophe Ferrand, Marina Deschamps, Pierre Tiberghien, Jean-Marc
The variable risk of colorectal cancer in patients with inflammatory bowel disease.
 The variable risk of colorectal cancer in patients with inflammatory bowel disease. Lindgren, Stefan Published in: European Journal of Internal Medicine DOI: 10.1016/j.ejim.2004.12.001 Published: 2005-01-01
The variable risk of colorectal cancer in patients with inflammatory bowel disease. Lindgren, Stefan Published in: European Journal of Internal Medicine DOI: 10.1016/j.ejim.2004.12.001 Published: 2005-01-01
The causes of the common forms of idiopathic inflammatory
 GASTROENTEROLOGY 2001;121:805 811 The Interleukin 1 Receptor Antagonist Gene Allele 2 as a Predictor of Pouchitis Following Colectomy and IPAA in Ulcerative Colitis MARTYN J. CARTER,*, FRANCESCO S. DI
GASTROENTEROLOGY 2001;121:805 811 The Interleukin 1 Receptor Antagonist Gene Allele 2 as a Predictor of Pouchitis Following Colectomy and IPAA in Ulcerative Colitis MARTYN J. CARTER,*, FRANCESCO S. DI
Newly Recognized Components of the Innate Immune System
 Newly Recognized Components of the Innate Immune System NOD Proteins: Intracellular Peptidoglycan Sensors NOD-1 NOD-2 Nod Protein LRR; Ligand Recognition CARD RICK I-κB p50 p65 NF-κB Polymorphisms in Nod-2
Newly Recognized Components of the Innate Immune System NOD Proteins: Intracellular Peptidoglycan Sensors NOD-1 NOD-2 Nod Protein LRR; Ligand Recognition CARD RICK I-κB p50 p65 NF-κB Polymorphisms in Nod-2
Innate immune regulation of T-helper (Th) cell homeostasis in the intestine
 Innate immune regulation of T-helper (Th) cell homeostasis in the intestine Masayuki Fukata, MD, Ph.D. Research Scientist II Division of Gastroenterology, Department of Medicine, F. Widjaja Foundation,
Innate immune regulation of T-helper (Th) cell homeostasis in the intestine Masayuki Fukata, MD, Ph.D. Research Scientist II Division of Gastroenterology, Department of Medicine, F. Widjaja Foundation,
Crohn s Disease Is Associated With Novel Polymorphisms in the 5 -Flanking Region of the Tumor Necrosis Factor Gene
 GASTROENTEROLOGY 1999;117:1062 1068 Crohn s Disease Is Associated With Novel Polymorphisms in the 5 -Flanking Region of the Tumor Necrosis Factor Gene KENICHI NEGORO, YOSHITAKA KINOUCHI, NOBUO HIWATASHI,
GASTROENTEROLOGY 1999;117:1062 1068 Crohn s Disease Is Associated With Novel Polymorphisms in the 5 -Flanking Region of the Tumor Necrosis Factor Gene KENICHI NEGORO, YOSHITAKA KINOUCHI, NOBUO HIWATASHI,
Innate Immunity & Inflammation
 Innate Immunity & Inflammation The innate immune system is an evolutionally conserved mechanism that provides an early and effective response against invading microbial pathogens. It relies on a limited
Innate Immunity & Inflammation The innate immune system is an evolutionally conserved mechanism that provides an early and effective response against invading microbial pathogens. It relies on a limited
Characteristic Phenotypes in Korean Crohn s Disease Patients Who Underwent Intestinal Surgery for the Treatment
 ORIGINAL ARTICLE Gastroenterology & Hepatology http://dx.doi.org/10.3346/jkms.2013.28.4.575 J Korean Med Sci 2013; 28: 575-579 Characteristic Phenotypes in Korean Crohn s Disease Patients Who Underwent
ORIGINAL ARTICLE Gastroenterology & Hepatology http://dx.doi.org/10.3346/jkms.2013.28.4.575 J Korean Med Sci 2013; 28: 575-579 Characteristic Phenotypes in Korean Crohn s Disease Patients Who Underwent
Nature Genetics: doi: /ng Supplementary Figure 1
 Supplementary Figure 1 Replicability of blood eqtl effects in ileal biopsies from the RISK study. eqtls detected in the vicinity of SNPs associated with IBD tend to show concordant effect size and direction
Supplementary Figure 1 Replicability of blood eqtl effects in ileal biopsies from the RISK study. eqtls detected in the vicinity of SNPs associated with IBD tend to show concordant effect size and direction
IMMUNOLOGIC AND GENETIC MARKERS IN PATIENTS WITH IDIOPATHIC OCULAR INFLAMMATION AND A FAMILY HISTORY OF INFLAMMATORY BOWEL DISEASE. Chicago, IL, 60612
 IMMUNOLOGIC AND GENETIC MARKERS IN PATIENTS WITH IDIOPATHIC OCULAR INFLAMMATION AND A FAMILY HISTORY OF INFLAMMATORY BOWEL DISEASE Javaneh Abbasian 1α, Tammy M. Martin 2, Sarju Patel 1, Howard H Tessler
IMMUNOLOGIC AND GENETIC MARKERS IN PATIENTS WITH IDIOPATHIC OCULAR INFLAMMATION AND A FAMILY HISTORY OF INFLAMMATORY BOWEL DISEASE Javaneh Abbasian 1α, Tammy M. Martin 2, Sarju Patel 1, Howard H Tessler
HLA class II and III in Crohn s disease
 HLA class II and III in Crohn s disease-contents HLA class II and III in Crohn s disease Associations between HLA-DR1 and TNF microsatellites Rachel van Beem Sept 2002-Jan 2003 Under supervision of E Gomez
HLA class II and III in Crohn s disease-contents HLA class II and III in Crohn s disease Associations between HLA-DR1 and TNF microsatellites Rachel van Beem Sept 2002-Jan 2003 Under supervision of E Gomez
Nature Genetics: doi: /ng Supplementary Figure 1. Study design.
 Supplementary Figure 1 Study design. Leukopenia was classified as early when it occurred within the first 8 weeks of thiopurine therapy and as late when it occurred more than 8 weeks after the start of
Supplementary Figure 1 Study design. Leukopenia was classified as early when it occurred within the first 8 weeks of thiopurine therapy and as late when it occurred more than 8 weeks after the start of
Identification of Microbes
 Identification of Microbes Recognition by PRR (pattern recognition receptors) Recognize conserved molecular patterns on microbes called pathogen associated molecular patterns (PAMPs) which are not present
Identification of Microbes Recognition by PRR (pattern recognition receptors) Recognize conserved molecular patterns on microbes called pathogen associated molecular patterns (PAMPs) which are not present
IL1B gene polymorphisms influence the course and severity of inflammatory bowel disease
 Immunogenetics (1999) 49: 527 531 Q Springer-Verlag 1999 ORIGINAL PAPER Andrea Nemetz 7 M. Pilar Nosti-Escanilla Tamás Molnár 7 Adorján Köpe 7 Ágota Kovács János Fehér 7 Zsolt Tulassay 7 Ferenc Nagy M.
Immunogenetics (1999) 49: 527 531 Q Springer-Verlag 1999 ORIGINAL PAPER Andrea Nemetz 7 M. Pilar Nosti-Escanilla Tamás Molnár 7 Adorján Köpe 7 Ágota Kovács János Fehér 7 Zsolt Tulassay 7 Ferenc Nagy M.
Patients and Doctors: Bridging the Divide
 Patients and Doctors: Bridging the Divide Thomas Ullman, M.D. Director, Center for IBD The Mount Sinai IBD Center Chair, Professional Education, CCFA What we d like to avoid.... Differing Points of View:
Patients and Doctors: Bridging the Divide Thomas Ullman, M.D. Director, Center for IBD The Mount Sinai IBD Center Chair, Professional Education, CCFA What we d like to avoid.... Differing Points of View:
Personalized Medicine in IBD: Where Are We in 2013
 Personalized Medicine in IBD: Where Are We in 2013 David A. Schwartz, MD Director, Inflammatory Bowel Disease Center Associate Professor of Medicine Vanderbilt University Medical Center What is Personalized
Personalized Medicine in IBD: Where Are We in 2013 David A. Schwartz, MD Director, Inflammatory Bowel Disease Center Associate Professor of Medicine Vanderbilt University Medical Center What is Personalized
The enteric microbiota: Implications for IBD. Eugene B. Chang, M.D. University of Chicago
 The enteric microbiota: Implications for IBD Eugene B. Chang, M.D. University of Chicago On a per cell basis, humans are mostly prokaryote 100 90 80 70 60 50 40 30 20 10 0 EuK ProK The microbial flora
The enteric microbiota: Implications for IBD Eugene B. Chang, M.D. University of Chicago On a per cell basis, humans are mostly prokaryote 100 90 80 70 60 50 40 30 20 10 0 EuK ProK The microbial flora
Candidate Genes Colocalized to Linkage Regions in Inflammatory Bowel Disease
 Original Paper: Inflammatory Bowel Disease Digestion 2002;66:121 126 DOI: 10.1159/000065592 Received: January 30, 2002 Accepted: May 21, 2002 Candidate Genes Colocalized to Linkage Regions in Inflammatory
Original Paper: Inflammatory Bowel Disease Digestion 2002;66:121 126 DOI: 10.1159/000065592 Received: January 30, 2002 Accepted: May 21, 2002 Candidate Genes Colocalized to Linkage Regions in Inflammatory
EXOGENOUS and ENDOGENOUS DANGER SIGNALS in INFLAMMATORY BOWEL DISEASE
 EXOGENOUS and ENDOGENOUS DANGER SIGNALS in INFLAMMATORY BOWEL DISEASE by Shaival H. Davé B.A. in Molecular & Cell Biology: Biochemistry & Molecular Biology University of California at Berkeley, 1998 Submitted
EXOGENOUS and ENDOGENOUS DANGER SIGNALS in INFLAMMATORY BOWEL DISEASE by Shaival H. Davé B.A. in Molecular & Cell Biology: Biochemistry & Molecular Biology University of California at Berkeley, 1998 Submitted
HLA and antigen presentation. Department of Immunology Charles University, 2nd Medical School University Hospital Motol
 HLA and antigen presentation Department of Immunology Charles University, 2nd Medical School University Hospital Motol MHC in adaptive immunity Characteristics Specificity Innate For structures shared
HLA and antigen presentation Department of Immunology Charles University, 2nd Medical School University Hospital Motol MHC in adaptive immunity Characteristics Specificity Innate For structures shared
The fundamental basis of inflammatory bowel disease
 Science in medicine The fundamental basis of inflammatory bowel disease Warren Strober, Ivan Fuss, and Peter Mannon Mucosal Immunity Section, Laboratory of Host Defenses, National Institute of Allergy
Science in medicine The fundamental basis of inflammatory bowel disease Warren Strober, Ivan Fuss, and Peter Mannon Mucosal Immunity Section, Laboratory of Host Defenses, National Institute of Allergy
Lack of association of IL-2RA and IL-2RB polymorphisms with rheumatoid arthritis in a Han Chinese population
 Lack of association of IL-2RA and IL-2RB polymorphisms with rheumatoid arthritis in a Han Chinese population J. Zhu 1 *, F. He 2 *, D.D. Zhang 2 *, J.Y. Yang 2, J. Cheng 1, R. Wu 1, B. Gong 2, X.Q. Liu
Lack of association of IL-2RA and IL-2RB polymorphisms with rheumatoid arthritis in a Han Chinese population J. Zhu 1 *, F. He 2 *, D.D. Zhang 2 *, J.Y. Yang 2, J. Cheng 1, R. Wu 1, B. Gong 2, X.Q. Liu
